Cells of the Human Body
Content
Cells of the Human Body
PDF generated using the open source mwlib toolkit. See http://code.pediapress.com/ for more information. PDF generated at: Wed, 24 Apr 2013 09:08:34 UTC
Contents
List of distinct cell types in the adult human body Salivary gland Von Ebner's gland Mammary gland Lacrimal gland Ceruminous gland Eccrine sweat gland Apocrine sweat gland Moll's gland Sebaceous gland Olfactory glands Brunner's glands Prostate Bulbourethral gland Bartholin's gland Endometrium Urethral gland Gastric chief cell Pepsin Parietal cell Hydrochloric acid Human gastrointestinal tract Goblet cell Respiratory tract Mucus Enzyme Paneth cell Intestine Bicarbonate Lysozyme Surfactant Clara cell Somatotropic cell Prolactin cell Thyrotropic cell Gonadotropic cell 1 7 10 11 16 19 20 21 24 25 29 30 31 41 43 45 48 49 51 57 60 67 73 76 77 79 97 99 102 105 110 117 119 120 121 122
Corticotropic cell Melanocyte-stimulating hormone Magnocellular neurosecretory cell Oxytocin Vasopressin Serotonin Endorphins Somatostatin Gastrin Secretin Cholecystokinin Insulin Glucagon Bombesin Follicular cell Parafollicular cell Parathyroid gland Parathyroid chief cell Oxyphil cell (parathyroid) Chromaffin cell Steroid hormone Mineralocorticoid Glucocorticoid Leydig cell Folliculogenesis Progesterone Corpus luteum cell Corpus luteum Juxtaglomerular cell Renin Macula densa Mesangial cell Keratinocyte Epidermis (skin) Stem cell Huxley's layer Henle's layer Trichocyte (human)
123 123 126 127 138 148 158 162 168 174 179 182 192 199 200 202 203 207 208 209 211 213 215 226 228 235 246 247 250 251 257 259 259 262 267 279 280 280
Epithelium Squamous epithelial cell Hair cell Sensory neuron Merkel cell Olfactory receptor neuron Photoreceptor cell Rod cell Cone cell Carotid body Taste bud Schwann cell Satellite glial cell Neuroglia Astrocyte Neuron Oligodendrocyte Spindle neuron Hepatocyte Adipocyte White adipose tissue Brown adipose tissue Hepatic stellate cell Podocyte Proximal convoluted tubule Thin segment Distal convoluted tubule Kidney collecting duct cell Pneumocyte Centroacinar cell Collecting duct system Microvillus Epididymis Ameloblast Organ of Corti Corneal keratocyte Tendon cell Bone marrow
281 287 288 292 296 298 300 308 312 316 319 321 324 330 336 344 357 361 365 369 371 372 375 377 380 384 385 387 387 388 389 393 396 399 401 403 405 406
Reticular connective tissue Fibroblast Pericyte Nucleus pulposus Cementoblast Odontoblast Hyaline cartilage Fibrocartilage Chondrocyte Osteoblast Osteocyte Stellate cell Skeletal striated muscle Nuclear bag fiber Nuclear chain cell Myosatellite cell Cardiac muscle Purkinje fibers Smooth muscle tissue Myoepithelial cell Red blood cell Megakaryocyte Monocyte Langerhans cell Platelet Osteoclast Dendritic cell Lymphatic system Microglia Neutrophil granulocyte Eosinophil granulocyte Basophil granulocyte Hybridoma technology Mast cell T helper cell Regulatory T cell Cytotoxic T cell Natural killer T cell
412 413 415 420 422 423 425 427 429 431 433 437 438 445 445 446 450 453 455 463 464 475 478 481 484 492 496 501 508 518 524 527 529 533 536 543 547 550
B cell Natural killer cell Reticulocyte Progenitor cell Ovum Oocyte Spermatid Sperm Spermatogonium Sertoli cell Kidney
552 558 565 567 569 572 577 579 583 585 589
References
Article Sources and Contributors Image Sources, Licenses and Contributors 601 617
Article Licenses
License 627
List of distinct cell types in the adult human body
1
List of distinct cell types in the adult human body
Cells that are derived primarily from endoderm
Exocrine secretory epithelial cells
300 different cell types in the human body • • • • • • • • • • • • • • • • • • • • • • • • • • • Salivary gland mucous cell (polysaccharide-rich secretion) Salivary gland serous cell (glycoprotein enzyme-rich secretion) Von Ebner's gland cell in tongue (washes taste buds) Mammary gland cell (milk secretion) Lacrimal gland cell (tear secretion) Ceruminous gland cell in ear (earwax secretion) Eccrine sweat gland dark cell (glycoprotein secretion) Eccrine sweat gland clear cell (small molecule secretion) Apocrine sweat gland cell (odoriferous secretion, sex-hormone sensitive) Gland of Moll cell in eyelid (specialized sweat gland) Sebaceous gland cell (lipid-rich sebum secretion) Bowman's gland cell in nose (washes olfactory epithelium) Brunner's gland cell in duodenum (enzymes and alkaline mucus) Seminal vesicle cell (secretes seminal fluid components, including fructose for swimming sperm) Prostate gland cell (secretes seminal fluid components) Bulbourethral gland cell (mucus secretion) Bartholin's gland cell (vaginal lubricant section) Gland of Littre cell (mucus secretion) Uterus endometrium cell (carbohydrate secretion) Isolated goblet cell of respiratory and digestive tracts (mucus secretion) Stomach lining mucous cell (mucus secretion) Gastric gland zymogenic cell (pepsinogen secretion) Gastric gland oxyntic cell (hydrochloric acid secretion) Pancreatic acinar cell (bicarbonate and digestive enzyme secretion Paneth cell of small intestine (lysozyme secretion) Type II pneumocyte of lung (surfactant secretion) Clara cell of lung
Hormone secreting cells
• Anterior pituitary cells • Somatotropes • Lactotropes • Thyrotropes • Gonadotropes • Corticotropes • Intermediate pituitary cell, secreting melanocyte-stimulating hormone • Magnocellular neurosecretory cells • secreting oxytocin • secreting vasopressin
List of distinct cell types in the adult human body • Gut and respiratory tract cells • secreting serotonin • secreting endorphin • secreting somatostatin • secreting gastrin • secreting secretin • secreting cholecystokinin • secreting insulin • secreting glucagon • secreting bombesin • Thyroid gland cells • thyroid epithelial cell • parafollicular cell • Parathyroid gland cells • Parathyroid chief cell • Oxyphil cell • Adrenal gland cells • chromaffin cells • secreting steroid hormones (mineralcorticoids and gluco corticoids) • Leydig cell of testes secreting testosterone • Theca interna cell of ovarian follicle secreting estrogen • Corpus luteum cell of ruptured ovarian follicle secreting progesterone • Granulosa lutein cells • Theca lutein cells Juxtaglomerular cell (renin secretion) Macula densa cell of kidney Peripolar cell of kidney Mesangial cell of kidney
2
• • • •
Derived primarily from ectoderm
Integumentary system
Keratinizing epithelial cells • • • • • • • • • • Epidermal keratinocyte (differentiating epidermal cell) Epidermal basal cell (stem cell) Keratinocyte of fingernails and toenails Nail bed basal cell (stem cell) Medullary hair shaft cell Cortical hair shaft cell Cuticular hair shaft cell Cuticular hair root sheath cell Hair root sheath cell of Huxley's layer Hair root sheath cell of Henle's layer
• External hair root sheath cell • Hair matrix cell (stem cell)
List of distinct cell types in the adult human body Wet stratified barrier epithelial cells • Surface epithelial cell of stratified squamous epithelium of cornea, tongue, oral cavity, esophagus, anal canal, distal urethra and vagina • basal cell (stem cell) of epithelia of cornea, tongue, oral cavity, esophagus, anal canal, distal urethra and vagina • Urinary epithelium cell (lining urinary bladder and urinary ducts)
3
Nervous system
Sensory transducer cells • • • • • • • • Auditory inner hair cell of organ of Corti Auditory outer hair cell of organ of Corti Basal cell of olfactory epithelium (stem cell for olfactory neurons) Cold-sensitive primary sensory neurons Heat-sensitive primary sensory neurons Merkel cell of epidermis (touch sensor) Olfactory receptor neuron Pain-sensitive primary sensory neurons (various types) • Photoreceptor rod cells • Photoreceptor blue-sensitive cone cell of eye • Photoreceptor green-sensitive cone cell of eye • Photoreceptor red-sensitive cone cell of eye Proprioceptive primary sensory neurons (various types) Touch-sensitive primary sensory neurons (various types) Type I carotid body cell (blood pH sensor) Type II carotid body cell (blood pH sensor) Type I hair cell of vestibular apparatus of ear (acceleration and gravity) Type II hair cell of vestibular apparatus of ear (acceleration and gravity) Type I taste bud cell
• Photoreceptor cells of retina in eye:
• • • • • • •
Autonomic neuron cells • Cholinergic neural cell (various types) • Adrenergic neural cell (various types) • Peptidergic neural cell (various types) Sense organ and peripheral neuron supporting cells • • • • • • • • • Inner pillar cell of organ of Corti Outer pillar cell of organ of Corti Inner phalangeal cell of organ of Corti Outer phalangeal cell of organ of Corti Border cell of organ of Corti Hensen cell of organ of Corti Vestibular apparatus supporting cell Taste bud supporting cell Olfactory epithelium supporting cell
• Schwann cell • Satellite glial cell (encapsulating peripheral nerve cell bodies)
List of distinct cell types in the adult human body • Enteric glial cell Central nervous system neurons and glial cells • • • • Astrocyte (various types) Neuron cells (large variety of types, still poorly classified) Oligodendrocyte Spindle neuron
4
Lens cells • Anterior lens epithelial cell • Crystallin-containing lens fiber cell
Derived primarily from mesoderm
Metabolism and storage cells
• Hepatocyte (liver cell) • Adipocytes: • White fat cell • Brown fat cell • Liver lipocyte
Barrier function cells (lung, gut, exocrine glands and urogenital tract)
Kidney • • • • • • • • • Kidney parietal cell Kidney glomerulus podocyte Kidney proximal tubule brush border cell Loop of Henle thin segment cell Kidney distal tubule cell Kidney collecting duct cell Type I pneumocyte (lining air space of lung cell) Pancreatic duct cell (centroacinar cell) Nonstriated duct cell (of sweat gland, salivary gland, mammary gland, etc.) • principal cell • Intercalated cell Duct cell (of seminal vesicle, prostate gland, etc.) Intestinal brush border cell (with microvilli) Exocrine gland striated duct cell Gall bladder epithelial cell Ductulus efferens nonciliated cell Epididymal principal cell Epididymal basal cell
• • • • • • •
List of distinct cell types in the adult human body
5
Extracellular matrix cells
• • • • • • • • • • • • • • • • • • • • • Ameloblast epithelial cell (tooth enamel secretion) Planum semilunatum epithelial cell of vestibular apparatus of ear (proteoglycan secretion) Organ of Corti interdental epithelial cell (secreting tectorial membrane covering hair cells) Loose connective tissue fibroblasts Corneal fibroblasts (corneal keratocytes) Tendon fibroblasts Bone marrow reticular tissue fibroblasts Other nonepithelial fibroblasts Pericyte Nucleus pulposus cell of intervertebral disc Cementoblast/cementocyte (tooth root bonelike cementum secretion) Odontoblast/odontocyte (tooth dentin secretion) Hyaline cartilage chondrocyte Fibrocartilage chondrocyte Elastic cartilage chondrocyte Osteoblast/osteocyte Osteoprogenitor cell (stem cell of osteoblasts) Hyalocyte of vitreous body of eye Stellate cell of perilymphatic space of ear Hepatic stellate cell (Ito cell) Pancreatic stelle cell
Contractile cells
• Skeletalex muscle cells • Red skeletal muscle cell (slow) • White skeletal muscle cell (fast) • Intermediate skeletal muscle cell • nuclear bag cell of muscle spindle • nuclear chain cell of muscle spindle • Satellite cell (stem cell) • Heart muscle cells • Ordinary heart muscle cell • Nodal heart muscle cell • Purkinje fiber cell • Smooth muscle cell (various types) • Myoepithelial cell of iris • Myoepithelial cell of exocrine glands
List of distinct cell types in the adult human body
6
Blood and immune system cells
• • • • • • • • • • • • • • • • • • • • • Erythrocyte (red blood cell) Megakaryocyte (platelet precursor) Monocyte Connective tissue macrophage (various types) Epidermal Langerhans cell Osteoclast (in bone) Dendritic cell (in lymphoid tissues) Microglial cell (in central nervous system) Neutrophil granulocyte Eosinophil granulocyte Basophil granulocyte Hybridoma cell Mast cell Helper T cell Suppressor T cell Cytotoxic T cell Natural Killer T cell B cell Natural killer cell Reticulocyte Stem cells and committed progenitors for the blood and immune system (various types)
Germ cells
• • • • • Oogonium/Oocyte Spermatid Spermatocyte Spermatogonium cell (stem cell for spermatocyte) Spermatozoon
Nurse cells
• Ovarian follicle cell • Sertoli cell (in testis) • Thymus epithelial cell
Interstitial cells
• Interstitial kidney cells
References External links
• Types of neurons from NeuroLex (http://neurolex.org/wiki/Cell_Types_With_Definitions) • Eukaryotic cell types in COPE database (http://www.copewithcytokines.de/cope.cgi?key=cell types).
Salivary gland
7
Salivary gland
Salivary gland
Salivary glands: #1 is Parotid gland, #2 is Submandibular gland, #3 is Sublingual gland Latin glandulae salivariae
The salivary glands in mammals are exocrine glands, glands with ducts, that produce saliva. They also secrete amylase, an enzyme that breaks down starch into maltose. In other organisms such as insects, salivary glands are often used to produce biologically important proteins like silk or glues, and fly salivary glands contain polytene chromosomes that have been useful in genetic research.
Histology
The gland is internally divided into lobules. Blood vessels and nerves enter the glands at the hilum and gradually branch out into the lobules.
Ducts
In the duct system, the lumina are formed by intercalated ducts, which in turn join to form striated ducts. These drain into ducts situated between the lobes of the gland (called interlobar ducts or secretory ducts). All of the human salivary glands terminate in the mouth, where the saliva proceeds to aid in digestion. The saliva that salivary glands release is quickly inactivated in the stomach by the acid that is present there but the saliva also contains enzymes that are actually activated by the acid.
Salivary gland
8
Anatomy
Parotid glands
The parotid gland is a salivary gland wrapped around the mandibular ramus in humans. It is one of a pair being the largest of the salivary glands, it secretes saliva through Stensen's ducts into the oral cavity, to facilitate mastication and swallowing and to begin the digestion of starches. The secretion produced is mainly serous in nature and enters the oral cavity via Stensen's duct. It is located posterior to the mandibular ramus and in front of the mastoid process of temporal bone. This gland is clinically relevant in dissections of facial nerve branches while exposing the different lobes of it since any iatrogenic lesion will result in either loss of action or strength of muscles involved in facial expression.
Submandibular glands
The submandibular glands are a pair of glands located beneath the The salivary glands are situated at the entrance to lower jaws, superior to the digastric muscles. The secretion produced is the gastrointestinal system to help begin the a mixture of both serous fluid and mucus, and enters the oral cavity via process of digestion. Wharton's ducts. Approximately 70% of saliva in the oral cavity is produced by the submandibular glands, even though they are much smaller than the parotid glands.You can usually feel this gland, as it is in the upper neck and feels like a rounded ball. It is located about two fingers above the Adam's apple (on a man) and about two inches apart under the chin.
Sublingual glands
The sublingual glands are a pair of glands located beneath the tongue, anterior to the submandibular glands. The secretion produced is mainly mucus in nature, however it is categorized as a mixed gland. Unlike the other two major glands, the ductal system of the sublingual glands do not have striated ducts, and exit from 8-20 excretory ducts. Approximately 5% of saliva entering the oral cavity come from these glands.
Minor salivary glands
There are 800-1000 minor salivary glands located throughout the oral cavity within the submucosa[1] of the oral mucosa, apart from areas including the anterior third of the hard palate, the attached gingivaand the anterior third of the dorsal surface of the tongue.[] They are 1-2mm in diameter and unlike the other glands, they are not encapsulated by connective tissue only surrounded by it. The gland is usually a number of acini connected in a tiny lobule. A minor salivary gland may have a common excretory duct with another gland, or may have its own excretory duct. Their secretion is mainly mucous in nature (except for Von Ebner's glands) and have many functions such as coating the oral cavity with saliva. Problems with dentures are sometimes associated with minor salivary glands.[1]
Salivary gland Von Ebner's glands Von Ebner's glands are glands found in circumvallate papillae of the tongue. They secrete a serous fluid that begin lipid hydrolysis. They facilitate the perception of taste.
9
Innervation
Salivary glands are innervated, either directly or indirectly, by the parasympathetic and sympathetic arms of the autonomic nervous system. Both result in increased amylase output and volume flow. • Parasympathetic innervation to the salivary glands is carried via cranial nerves. The parotid gland receives its parasympathetic input from the glossopharyngeal nerve (CN IX) via the otic ganglion, while the submandibular and sublingual glands receive their parasympathetic input from the facial nerve (CN VII) via the submandibular ganglion. These nerves release acetylcholine and substance P, which activate the IP3 and DAG pathways respectively. • Direct sympathetic innervation of the salivary glands takes place via preganglionic nerves in the thoracic segments T1-T3 which synapse in the superior cervical ganglion with postganglionic neurons that release norepinephrine, which is then received by β-adrenergic receptors on the acinar and ductal cells of the salivary glands, leading to an increase in cyclic adenosine monophosphate (cAMP) levels and the corresponding increase of saliva secretion. Note that in this regard both parasympathetic and sympathetic stimuli result in an increase in salivary gland secretions.[2] The sympathetic nervous system also affects salivary gland secretions indirectly by innervating the blood vessels that supply the glands.
Role in disease
See mumps (parotiditis epidemica), Sjögren's syndrome, Mucocele, Graft versus host disease and Salivary gland neoplasm. Salivary duct calculus may cause blockage of the ducts, causing pain and swelling of the gland because of cysts. Many anti-cancer treatments may impair salivary flow. Radiation therapy may cause permanent xerostomia, whereas chemotherapy may cause only temporary salivary impairment. Graft versus host disease after allogeneic bone marrow transplantation may manifest as dry mouth and many small mucoceles. Tumors of the salivary glands may occur. A sialogram is a radiocontrast study of a salivary duct. Saliva production may be pharmacologically stimulated by so-called sialagogues (e.g., pilocarpin, cevimeline). It can also be suppressed by so-called antisialagogues (e.g., tricyclic antidepressants, SSRI, antihypertensives, polypharmacy). [] The salivary glands of some species, however, are modified to produce enzymes; salivary amylase is found in many, but by no means all, bird and mammal species (including humans, as noted above). Furthermore, the venom glands of poisonous snakes, Gila monsters, and some shrews, are modified salivary glands.[]
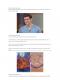
Micrograph of chronic inflammation of the salivary gland sialadenitis).
Salivary gland
10
References
[1] A.R TEN CATE, "Oral histology. Development, structure, and function".(1998), 2003, 2008|page=3|Edition=5thISBN=0-8151-2952-1
External links
• Salivary Gland Disorders at intelihealth.com (http://www.intelihealth.com/IH/ihtIH/WSIHW000/9339/9658. html) • Illustration at merck.com (http://www.merck.com/media/mmhe2/figures/fg111_1.gif) • Illustration at .washington.edu (http://www.orthop.washington.edu/_Rainbow/Album/ 10357m26b8e09e-6490-41ab-8955-725a7a75ec05.gif) • plastic/371 (http://www.emedicine.com/plastic/topic371.htm#) at eMedicine - "Parotid Tumors, Benign" • Medical Encyclopedia Medline Plus: Salivary gland (http://vsearch.nlm.nih.gov/vivisimo/cgi-bin/ query-meta?v:project=medlineplus&query=Salivary+Gland+&x=25&y=14)
Von Ebner's gland
Ebner's glands, also Von Ebner's glands are exocrine glands found in the mouth. More specifically, they are serous salivary glands which reside adjacent to the moats surrounding the circumvallate papillae in the posterior one-third of the tongue, anterior to the terminal sulcus. Von Ebner's glands (also called gustatory glands) are named after Anton Gilbert Victor von Ebner, Ritter von Rosenstein, who was an Austrian histologist. These glands are located around circumvallate and foliate papillae in the tongue, and they secrete lingual lipase, beginning the process of Human Von Ebner's Gland. lipid hydrolysis in the mouth. These glands empty their serous secretion into the base of the moats located around the foliate and circumvallate papillae. This secretion presumably flushes material from the moat to enable the taste buds to respond rapidly to changing stimuli. The Von Ebner glands are innervated by Cranial Nerve IX, the glossopharyngeal nerve. It secretes lingual lipase.[1]
References External links
• Anton Gilbert Viktor Ebner, Ritter von Rofenstein entry @ whonamedit.com (http://www.whonamedit.com/ doctor.cfm/2269.html) • pubmed/16859632 (http://www.ncbi.nlm.nih.gov/pubmed/16859632) • synd/2602 (http://www.whonamedit.com/synd.cfm/2602.html) at Who Named It? • BU Histology Learning System: 09503loa (http://www.bu.edu/histology/p/09503loa.htm) • Histology at OU 126_05 (http://w3.ouhsc.edu/histology/Glass slides/126_05.jpg) • Dental histology at usc.edu (http://www.usc.edu/hsc/dental/ohisto/Cards/muc/57_bb.html)
Mammary gland
11
Mammary gland
Mammary gland in a human female
Cross section of the breast of a human female
Dissection of a lactating breast. 1 – Fat 2 – Lactiferous duct/lobule 3 – Lobule 4 – Connective tissue 5 – Sinus of lactiferous duct 6 – Lactiferous duct Latin Gray's Artery glandula mammaria subject #271 1267
[1]
Internal thoracic artery [] Lateral thoracic artery Internal thoracic vein [] Axillary vein Supraclavicular nerves [1] Intercostal nerves (lateral and medial branches) Pectoral axillary lymph nodes
[]
Vein
Nerve
Lymph
Precursor Mesoderm (blood vessels and connective tissue) [2] Ectoderm (cellular elements) MeSH A01.236.249
[4]
Mammary gland A mammary gland is an organ in female mammals that produces milk to feed young offspring. Mammals get their name from the word "mammary." In humans, the mammary glands are situated in the breasts. In ruminants such as cows, goats, and deer, the mammary glands are contained in the udders. The mammary glands of mammals having more than two breasts, such as dogs and cats, are sometimes called dugs.
12
Humans
Histology
A mammary gland is a specific type of apocrine gland specialized for manufacture of colostrum when giving birth. Mammary glands can be identified as apocrine because they exhibit striking "decapitation" secretion. Many sources assert that mammary glands are modified sweat glands.[3][4][] Some authors dispute that and argue instead that they are sebaceous glands.[3]
Structure
The basic components of a mature mammary gland are the alveoli (hollow cavities, a few millimeters large) lined with milk-secreting cuboidal cells and surrounded by myoepithelial cells. These alveoli join to form groups known as lobules. Each lobule has a lactiferous duct that drains into openings in the nipple. The myoepithelial cells contract under the stimulation of oxytocin, excreting the milk secreted by alveolar units into the lobule lumen toward the nipple. As the infant begins to suck, the oxytocin-mediated "let down reflex" ensues and the mother's milk is secreted – not sucked from the gland – into the baby's mouth. All the milk-secreting tissue leading to a single lactiferous duct is called a "simple mammary gland"; in a "complex mammary gland" all the simple mammary glands serve one nipple. Humans normally have two complex mammary glands, one in each breast, and each complex mammary gland consists of 10–20 simple glands. The presence of more than two nipples is known as polythelia and the presence of more than two complex mammary glands as polymastia. Maintaining the correct polarized morphology of the lactiferous duct tree requires another essential component – mammary epithelial cells extracellular matrix (ECM) which, together with adipocytes, fibroblast, inflammatory cells, and others, constitute mammary stroma. [] Mammary epithelial ECM mainly contains myoepithelial basement membrane and the connective tissue. They not only help to support mammary basic structure, but also serve as a communicating bridge between mammary epithelia and their local and global environment throughout this organ's development.[][]
Development and hormonal control
Mammary glands develop during different growth cycles. They exist in both sexes during embryonic stage, forming only a rudimentary duct tree at birth. In this stage, mammary gland development depends on systemic (and maternal) hormones,[] but is also under the (local) regulation of paracrine communication between neighboring epithelial and mesenchymal cells by parathyroid hormone-related protein(PTHrP).[5] This locally secreted factor gives rise to a series of outside-in and inside-out positive feedback between these two types of cells, so that mammary bud epithelial cells can proliferate and sprout down into the mesenchymal layer until they reach the fat pad to begin the first round of branching.[] At the same time, the embryonic mesenchymal cells around the epithelial bud receive secreting factors activated by PTHrP, such as BMP4. These mesenchymal cells can transform into a dense, mammary-specific mesenchyme, which later develop into connective tissue with fibrous threads, forming blood vessels and the lymph system.[6] A basement membrane, mainly containing laminin and collagen, formed afterward by differentiated myoepithelial cells, keeps the polarity of this primary duct tree. Lactiferous duct development occurs in females in response to circulating hormones. First development is frequently seen during pre- and postnatal stages, and later during puberty. Estrogen promotes branching differentiation,[7]
Mammary gland whereas in males testosterone inhibits it. A mature duct tree reaching the limit of the fat pad of the mammary gland comes into being by bifurcation of duct terminal end buds (TEB), secondary branches sprouting from primary ducts[][8] and proper duct lumen formation. These processes are tightly modulated by components of mammary epithelial ECM interacting with systemic hormones and local secreting factors. However, for each mechanism the epithelial cells' "niche" can be delicately unique with different membrane receptor profiles and basement membrane thickness from specific branching area to area, so as to regulate cell growth or differentiation sub-locally.[9] Important players include beta-1 integrin, epidermal growth factor receptor (EGFR), laminin-1/5, collagen-IV, matrix metalloproteinase(MMPs), heparan sulfate proteoglycans, and others. Elevated circulating level of growth hormone and estrogen get to multipotent cap cells on TEB tips through a thin, leaky layer of basement membrane. These hormones promote specific gene expression. Hence cap cells can differentiate into myoepithelial and luminal (duct) epithelial cells, and the increased amount of activated MMPs can degrade surrounding ECM helping duct buds to reach further in the fat pads.[10][11] On the other hand, basement membrane along the mature mammary ducts is thicker, with strong adhesion to epithelial cells via binding to integrin and non-integrin receptors. When side branches develop, it is a much more “pushing-forward” working process including extending through myoepithelial cells, degrading basement membrane and then invading into a periductal layer of fibrous stromal tissue.[] Degraded basement membrane fragments (laminin-5) roles to lead the way of mammary epithelial cells migration.[12] Whereas, laminin-1 interacts with non-integrin receptor dystroglycan negatively regulates this side branching process in case of cancer.[13] These complex "Yin-yang" balancing crosstalks between mammary ECM and epithelial cells "instruct" healthy mammary gland development until adult. Secretory alveoli develop mainly in pregnancy, when rising levels of prolactin, estrogen, and progesterone cause further branching, together with an increase in adipose tissue and a richer blood flow. In gestation, serum progesterone remains at a stably high concentration so signaling through its receptor is continuously activated. As one of the transcribed genes, Wnts secreted from mammary epithelial cells act paracrinely to induce more neighboring cells' branching.[14][15] When the lactiferous duct tree is almost ready, "leaves" alveoli are differentiated from luminal epithelial cells and added at the end of each branch. In late pregnancy and for the first few days after giving birth, colostrum is secreted. Milk secretion (lactation) begins a few days later due to reduction in circulating progesterone and the presence of another important hormone prolactin, which mediates further alveologenesis, milk protein production, and regulates osmotic balance and tight junction function. Laminin and collagen in myoepithelial basement membrane interacting with beta-1 integrin on epithelial surface again, is essential in this process.[][] Their binding ensures correct placement of prolactin receptors on the basal lateral side of alveoli cells and directional secretion of milk into lactiferous ducts.[][] Suckling of the baby causes release of the hormone oxytocin, which stimulates contraction of the myoepithelial cells. In this combined control from ECM and systemic hormones, milk secretion can be reciprocally amplified so as to provide enough nutrition for the baby. During weaning, decreased prolactin, missing mechanical stimulation (baby suckling), and changes in osmotic balance caused by milk stasis and leaking of tight junctions cause cessation of milk production. In some species there is complete or partial involution of alveolar structures after weaning, in humans there is only partial involution and the level of involution in humans appears to be highly individual. In some other species (such as cows), all alveoli and secretory duct structures collapse by programmed cell death (apoptosis) and autophagy for lack of growth promoting factors either from the ECM or circulating hormones.[16][17] At the same time, apoptosis of blood capillary endothelial cells speeds up the regression of lactation ductal beds. Shrinkage of the mammary duct tree and ECM remodeling by various proteinase is under the control of somatostatin and other growth inhibiting hormones and local factors.[18] This major structural change leads loose fat tissue to fill the empty space afterward. But a functional lactiferous duct tree can be formed again when a female is pregnant again.
13
Mammary gland
14
Breast cancer
Tumorigenesis in mammary glands can be induced biochemically by abnormal expression level of circulating hormones or local ECM components,[19] or from a mechanical change in the tension of mammary stroma.[20] Under either of the two circumstances, mammary epithelial cells would grow out of control and eventually result in cancer. Almost all instances of breast cancer originate in the lobules or ducts of the mammary glands.
Other mammals
The constantly protruding breasts of the adult human female, unusually large relative to body size, are a unique evolutionary development whose purpose is not yet fully known (see breasts); other mammals tend to have less conspicuous mammary glands that protrude only while actually filling with milk. The number and positioning of complex and simple mammary glands varies widely in different mammals. The nipples and glands can occur anywhere along the two milk lines, two nearly parallel lines along the ventral aspect of the body. In general most mammals develop mammary glands in pairs along these lines, with a number approximating the number of young typically birthed at a time. The number of nipples varies from 2 (in most primates) to 18 (in pigs). The Virginia Opossum has 13, one of the few mammals with an odd number.[21][22] The following table lists the number and position of glands normally found in a range of mammals:
Species [23] Anterior Intermediate Posterior (thoracic) (abdominal) (inguinal) 0 0 2 Total
Goat, sheep, horse guinea pig Cattle Cat Dog [24]
2
0 2 4 6 6 6 2
0 2 2 0 2 6 0
4 4 2 or 4 4 4 6 0
4 8 8 or 10 10 12 18 2
Mouse Rat Pig proboscideans, primates
Male mammals typically have rudimentary mammary glands and nipples, with a few exceptions: male mice do not have nipples, and male horses lack nipples and mammary glands.[citation needed] The male Dayak fruit bat has lactating mammary glands.[25] Male lactation occurs infrequently in some species, including humans. Mammary glands are true protein factories, and several labs have constructed transgenic animals, mainly goats and cows, to produce proteins for pharmaceutical use.[26] Complex glycoproteins such as monoclonal antibodies or antithrombin cannot be produced by genetically engineered bacteria, and the production in live mammals is much cheaper than the use of mammalian cell cultures.
Evolution
The evolution of the mammary gland is difficult to explain; this is because mammary glands are typically required by mammals to feed their young. There are many theories on how mammary glands evolved, for example, it is believed that the mammary gland is a transformed sweat gland, more closely related to apocrine sweat glands.[27] Since mammary glands do not fossilize well, supporting such theories with fossil evidence is difficult. Many of the current theories are based on comparisons between lines of living mammals – monotremes, marsupials and eutherians. One theory proposes that mammary glands evolved from glands that were used to keep the eggs of early mammals moist[28][29] and free from infection[30][31] (monotremes still lay eggs). Other theories suggest that early
Mammary gland secretions were used directly by hatched young,[32] or that the secretions were used by young to help them orient to their mothers.[33] Lactation is assumed to have developed long before the evolution of the mammary gland and mammals; see evolution of lactation.
15
Gallery
Cattle
Cat
Pig
Sheep
Goat
Elephant
Human
References
[3] Ackerman (2005) ch.1 Apocrine Units (http:/ / www. derm101. com/ content/ 13501) [4] Moore (2010) ch.1 Thorax, p. 99 [22] Stockard, Mary (2005) Raising Orphaned Baby Opossums (http:/ / web. archive. org/ web/ 20100701012225/ http:/ / www. awrc. org/ Baby Opossums. htm). Alabama Wildlife Center. [24] Dog breeds vary in the number of mammary glands: larger breeds tend to have 5 pairs, smaller breeds have 4 pairs. [28] Lactating on Eggs (http:/ / web. archive. org/ web/ 20090419024229/ http:/ / nationalzoo. si. edu/ ConservationAndScience/ SpotlightOnScience/ oftedalolav20030714. cfm). Smithsonian National Zoo, July 14, 2003. [30] Breast beginnings (http:/ / web. archive. org/ web/ 20070312005054/ http:/ / scienceblogs. com/ pharyngula/ 2006/ 05/ breast_beginnings. php). scienceblogs.com
Bibliography
• Ackerman, A. Bernard; Almut Böer, Bruce Bennin, and Geoffrey J. Gottlieb (2005). Histologic Diagnosis of Inflammatory Skin Diseases An Algorithmic Method Based on Pattern Analysis (http://www.derm101.com/ content/13501). ISBN 978-1-893357-25-9. • Moore, Keith L. et al. (2010) Clinically Oriented Anatomy 6th Ed
External links
• Comparative Mammary Gland Anatomy (http://web.archive.org/web/20051201011719/http://classes.aces. uiuc.edu/AnSci308/anatomycompar.html) by W. L. Hurley • On the anatomy of the breast (http://jdc.jefferson.edu/cooper/61/) by Sir Astley Paston Cooper (1840). Numerous drawings, in the public domain. • mammary+gland (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=mammary+gland) at eMedicine Dictionary
Lacrimal gland
16
Lacrimal gland
Lacrimal gland
Lacrimal apparatus of the right eye. The lacrimal gland is to the upper left. The right side of the picture is towards the nose.
Tear system. a = lacrimal gland b = superior lacrimal punctum c = superior lacrimal canal d = lacrimal sac e = inferior lacrimal punctum f = inferior lacrimal canal g = nasolacrimal canal Latin Gray's Artery Nerve glandula lacrimalis subject #227 1028 lacrimal artery lacrimal nerve, Zygomatic nerve via Communicating branch
[1]
The lacrimal glands are paired almond-shaped glands, one for each eye, that secrete the aqueous layer of the tear film. They are situated in the upper, outer portion of each orbit, in the lacrimal fossa of the orbit formed by the frontal bone.[1] Inflammation of the lacrimal glands is called dacryoadenitis. The lacriminal gland produces tears which then flow into canals that lead to the lacriminal sac. From this sac, the tears drain through a passage into the nose. [citation needed] Anatomists divide the gland into two sections. The smaller palpebral portion, lies close to the eye, along the inner surface of the eyelid; if the upper eyelid is everted, the palpebral portion can be seen. The orbital portion contains fine interlobular ducts that unite to form 3 - 5 main excretory ducts, joining 5 - 7 ducts in the palpebral portion before the secreted fluid may enter on the surface of the eye. Tears secreted collect in the fornix conjunctiva of the upper lid, and pass over the eye surface to the lacrimal puncta, small holes found at the inner corner of the eyelids. These pass the tears on to the lacrimal sac, in turn to the nasolacrimal duct, which dumps them out into the nose.[2]
Lacrimal gland
17
Microanatomy
The lacrimal gland is a compound tubuloacinar gland, it is made up of many lobules separated by connective tissue, each lobule contains many acini. The acini contain only serous cells and produce a watery serous secretion. Each acinus consists of a grape-like mass of lacrimal gland cells with their apices pointed to a central lumen. The central lumen of many of the units converge to form intralobular ducts, and then unite to from interlobular ducts. The gland lacks striated ducts.
Innervation
The parasympathetic nerve supply originates from the lacrimal nucleus of the facial nerve in the pons. Just distal to the geniculate ganglion, the facial nerve gives off the greater petrosal nerve. This nerve carries the parasympathetic secretomotor fibers through the pterygoid canal, where it joins the deep petrosal nerve (containing postganglionic sympathetic fibers from the superior cervical ganglion) to form the nerve of the pterygoid canal (vidian nerve). This nerve travels through the pterygoid canal to the pterygopalatine ganglion. Here the fibers synapse and postganglionic fibers join the fibers of the maxillary nerve, which travels through the inferior orbital fissure. Once it has traversed this opening, the parasympathetic secretomotor fibers branch off with the zygomatic nerve and then branch off again, joining with the lacrimal branch of the ophthalmic division of CN V, which supplies sensory innervation to the lacrimal gland along with the eyelid and conjunctiva. The sympathetic postganglionic fibers originate from the superior cervical ganglion. They travel as a periarteriolar plexus with the middle meningeal artery, before they merge and form the deep petrosal nerve, which joins the greater petrosal nerve in the pterygoid canal. Together, greater petrosal and deep petrosal nerves form the nerve of the pterygoid canal (vidian nerve) and reach the pterygopalatine ganglion in the pterygopalatine fossa. In contrast to their parasympathetic counterparts, sympathetic fibers do not synapse in the pterygopalatine ganglion, having done so already in the sympathetic trunk. However, they continue to course with the parasympathetic fibers innervating the lacrimal gland.
Blood supply
The lacrimal artery, derived from the ophthalmic artery supplies the lacrimal gland. Venous blood returns via the superior ophthalmic vein.
Nerve supply
The lacrimal nerve, derived from the ophthalmic nerve supplies the lacrimal gland
Applied anatomy
• The upper part of the lacrimal sac is covered by the medial palpabral ligament. Hence the abscesses within the sac bulge below the medial palpabrel ligament, where it should be incised for letting out the pus. • The angular vein is in front of the sac and it should be take care during incising the sac. Between the lacrimal sac and the fascia coverning the sac there is the collection of venous plexus present hence the incising causes considerable bleeding. • Around the nasolacrimal duct there is the rich plexus of veins, in the form of an erectile tissue, which may engorge and cause obstruction to the duct.
Lacrimal gland
18
Pathology
• Dacryoadenitis • Sjögren's syndrome
Additional images
The ophthalmic artery and its branches.
Nerves of the orbit. Seen from above.
Sympathetic connections of the sphenopalatine and superior cervical ganglia.
The tarsal glands, etc., seen from the inner surface of the eyelids.
Alveoli of lacrimal gland.
Extrinsic eye muscle. Nerves of orbita. Deep dissection.
Extrinsic eye muscle. Nerves of orbita. Deep dissection.
Extrinsic eye muscle. Nerves of orbita. Deep dissection.
Extrinsic eye muscle. Nerves of orbita. Deep dissection.
Extrinsic eye muscle. Nerves of orbita. Deep dissection.
References
[1] Clinically Oriented Anatomy (http:/ / www. amazon. com/ dp/ 0781775256), Moore, Dalley & Agur. [2] "eye, human."Encyclopædia Britannica. 2010. Encyclopædia Britannica 2010 Ultimate Reference Suite DVD 2010
External links
• Lacrimal+gland (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=Lacrimal+gland) at eMedicine Dictionary • lesson3 (http://mywebpages.comcast.net/wnor/lesson3.htm) at The Anatomy Lesson (http://home.comcast. net/~wnor/homepage.htm) by Wesley Norman (Georgetown University) ( orbit2 (http://mywebpages.comcast. net/wnor/orbit2.jpg))
Ceruminous gland
19
Ceruminous gland
Ceruminous glands are specialized sudoriferous glands (sweat glands) located subcutaneously in the external auditory canal. Ceruminous glands are simple, coiled, tubular glands made up of an inner secretory layer of cells and an outer myoepithelial layer of cells.[1] The glands drain into larger ducts, which then drain into the guard hairs that reside in the external auditory canal.[2] Here they produce cerumen, or earwax, by mixing their secretion with sebum and dead epidermal cells. Cerumen keeps the eardrum pliable, lubricates and cleans the external auditory canal, waterproofs the canal, kills bacteria, and serves as a barrier to trap foreign particles (dust, fungal spores, etc.) by coating the guard hairs of the ear, making them sticky.[1] These glands are capable of developing both benign and malignant tumors. The benign tumors include ceruminous adenoma, ceruminous pleomorphic adenoma, and ceruminous syringocystadenoma papilliferum. The Malignant tumors include ceruminous adenocarcinoma, adenoid cystic carcinoma, and mucoepidermoid carcinoma.[2]
References
[1] Saladin,Kenneth. Anatomy & Physiology: The Unity of Form and Function, Fifth Edition. McGraw-Hill. 2010 [2] http:/ / emedicine. medscape. com/ article/ 1960501-overview
External links
• http://www.anatomyatlases.org/MicroscopicAnatomy/Section07/Plate07142.shtml • http://emedicine.medscape.com/article/1960501-overview
Eccrine sweat gland
20
Eccrine sweat gland
Eccrine sweat gland
A sectional view of the skin (magnified), with eccrine glands highlighted. Latin System Nerve Precursor MeSH Code Glandula sudorifera merocrina; Glandula sudorifera eccrina Integumentary
[] []
Cholinergic sympathetic nerves Ectoderm
[] [1]
Eccrine+Glands
TH H3.12.00.3.03009
Eccrine glands (/ˈɛkrən/, /ˈɛˌkraɪn/, or /ˈɛˌkrin/; from ekkrinein "secrete";[1] sometimes called merocrine glands) are the major sweat glands of the human body, found in virtually all skin.[1] They produce a clear, odorless substance, consisting primarily of water and NaCl (note that the odor from sweat is due to bacterial activity on the secretions of the apocrine glands). NaCl is reabsorbed in the duct to reduce salt loss.[2] They are active in thermoregulation and emotional sweating (induced by anxiety, fear, stress, and pain).[]:170 Eccrine glands are composed of an intreaepidermal spiral duct, the "acrosyringium"; a dermal duct, comprising a straight and coiled portion; and a secretory tubule, coiled deep in the dermis or hypodermis.[]:172 Eccrine glands are innervated by the sympathetic nervous system, primarily by cholinergic fibers, but by adrenergic fibers as well.[3] Dermcidin is a newly isolated antimicrobial peptide produced by the eccrine sweat glands.[4]
References External links
• American Academy of Dermatology – Eccrine and Apocrine Glands (http://www.aad.org/education/students/ glands.htm)
Apocrine sweat gland
21
Apocrine sweat gland
Apocrine sweat gland
Latin System Nerve Glandula sudorifera apocrina Integumentary system Adrenergic nerves
[1] [] []
Precursor Primary epithelial germ[2] MeSH Code Apocrine+Glands
[3]
TH H3.12.00.3.03002
An apocrine sweat gland (/ˈæpəkrən/, /ˈæpəˌkraɪn/, or /ˈæpəˌkrin/, from Greek apo– "away" and krinein "to separate")[3][4] is a sweat gland composed of a coiled secretory portion located at the junction of the dermis and subcutaneous fat, from which a straight portion inserts and secretes into the infundibular portion of the hair follicle.[1] In humans, apocrine sweat glands are found only in certain locations of the body: the axillae (armpits), areola and nipples of the breast, ear canal, eyelids, wings of the nostril, perianal region, and some parts of the external genitalia.[5] Modified apocrine glands include the ciliary glands in the eyelids; the ceruminous glands, which produce ear wax; and the mammary glands, which produce milk.[1] The rest of the body is covered by eccrine sweat glands.[] Most non-primate mammals, however, have apocrine sweat glands over the greater part of their body.[5] Domestic animals such as dogs and cats have apocrine glands at each hair follicle but eccrine glands only in foot pads and snout. Their apocrine glands, like those in humans, produce an odorless, oily, opaque secretion[] that gains its characteristic odor upon bacterial decomposition.[6] Eccrine glands on their paws increase friction and prevent them from slipping when fleeing from danger.[7]
Structure
The apocrine gland comprises a glomerulus of secretory tubules and an excretory duct that opens into hair follicle;[8] on occasion, an excretory duct opens to the skin surface next to the hair.[9] The gland is large and spongy, located in the subcutaneous fat deep in the dermis,[][10] and has a larger overall structure and lumen diameter than the eccrine sweat gland.[11][5] Unlike eccrine secretory tubules, secretory tubules of the apocrine gland are single-layered (lacking ductal cells),[10] vary in diameter from place to place, and sometimes branch off into multiple ducts. The tubules are wrapped in myoepithelial cells, which are more developed than their eccrine gland counterparts.[12][13]
Sweating
In hoofed animals and marsupials, apocrine glands act as the main thermoregulator, secreting watery sweat.[] For most mammals, however, apocrine sweat glands secrete an oily (and eventually smelly) compound that acts as a pheromone,[] territorial marker, and warning signal.[][14][15] Being sensitive to adrenaline, apocrine sweat glands are involved in emotional sweating in humans (induced by anxiety, stress, fear, sexual stimulation, and pain).[14] In a five-month-old human fetus, apocrine glands are distributed all over the body; after a few weeks, they exist in only restricted areas,[] including the armpits and external genitalia.[5] They are inactive until stimulated by hormonal changes in puberty.[14]
Apocrine sweat gland
22
Mechanism
The apocrine gland secretes an oily fluid with proteins, lipids, and steroids that is odorless before microbial activity. It appears on the skin surface mixed with sebum, as sebaceous glands open into the same hair follicle.[16] Unlike eccrine sweat glands, which secrete continuously, the apocrine glands secrete in periodic spurts.[] Apocrine sweat glands were originally thought use only apocrine secretion: vesicles pinch off the secretory cells, then degrade in the secretory lumen, releasing their product.[] More recent research has also shown that merocrine secretion takes place.[] Myoepithelial cells form a smooth muscle lining around the secretory cells; when the muscle contracts, they squeeze the secretory ducts and push out the accumulated fluid into the hair follicle.[][] Sweat and sebum are mixed in the hair follicle and arrive mixed at the epidermal surface.[] The apocrine sweat is cloudy, viscous, initially odorless, and at a pH of 6–7.5. It contains water, protein, carbohydrate waste material, and NaCl.[] The sweat only attains its characteristic odor upon being degraded by bacteria, which releases volatile odor molecules.[16] More bacteria (especially corynebacteria) leads to stronger odor. The presence of axillary hair also makes the odor worse, as secretions, debris, keratin, and bacteria accumulate on the hairs.[10]
Prevalence
Non-primate mammals have usually apocrine sweat glands over most of their bodies.[5] Horses use them as a thermoregulatory device, as they are regulated by adrenaline and more widely distributed on equines than on other groups.[] Skunks, on the other hand, use the glands to release a stench that acts as a defense mechanism.[] The "axillary organs", limited regions with equal numbers of apocrine and eccrine sweat glands, only exist in humans, gorillas, and chimpanzees.[] In humans, the apocrine glands in this region are the most developed (with the most complex glomeruli).[12] Men have fewer apocrine sweat glands than women in all axillary regions.[17][18] East Asians have fewer such glands than Europeans and people of African descent, which decreases their susceptibility to body odor.[17][19] Individuals of African ancestry have the largest and most active apocrine glands.[20] Racial differences also exist in the cerumen glands: apocrine sweat glands which produce earwax.[1] East Asians have predominantly dry earwax, as opposed to sticky; the gene encoding for this is strongly linked to reduced body odor, whereas those with wet, sticky earwax (Europeans and Africans) are prone to more body odor.[21]
Notes
[1] Krstic 2004, p. 466. [2] Tsai 2006, p. 496. [5] Kurosumi, Shibasaki & Ito 1984, p. 255. [6] Eroschenko 2008, pp. 228–229. [7] Wilke et al. 2007, p. 170. [8] Kurosumi, Shibasaki & Ito 1984, pp. 255–256. [9] Tsai 2006, pp. 496–497. [10] Tsai 2006, p. 497. [11] Krstic 2004, p. 468. [12] Kurosumi, Shibasaki & Ito 1984, p. 256. [13] Eroschenko 2008, p. 226. [14] Wilke et al. 2007, p. 171. [16] Wilke et al. 2007, p. 175. [17] Wilke et al. 2007, p. 174. [18] Stoddart 1990, p. 60. [19] Stoddart 1990, p. 61.
Apocrine sweat gland
23
References
• Eroschenko, Victor P. (2008). "Integumentary System". DiFiore's Atlas of Histology with Functional Correlations. Lippincott Williams & Wilkins. pp. 212–234. ISBN 9780781770576. • Krstic, Radivoj V. (18 March 2004). Human Microscopic Anatomy: An Atlas for Students of Medicine and Biology. Springer. pp. 464, 466–469. ISBN 9783540536666. • Kurosumi, Kazumasa; Shibasaki, Susumu; Ito, Toshiho (1984). "Cytology of the Secretion in Mammalian Sweat Glands". In Bourne, Geoffrey H.; Danielli, James F. Protein Diffusion in Cell Membranes: Some Biological Implications. Orlando, Florida: Academic Press. pp. 253–330. ISBN 9780123644879. • Stoddart, D. Michael (1990). The scented ape: The biology and culture of human odour. Cambridge: Cambridge University Press. pp. 60–61. ISBN 0521375118. • Tsai, Ren-Yu (1 January 2006). "Treatment of Excessive Axillary Sweat Syndrome (Hyperhidrosis, Osmidrosis, Bromhidrosis) with Liposuction". In Shiffman, Melvin A.; Di Giuseppe, Alberto. Liposuction: Non-Cosmetic Applications. Germany: Springer. pp. 496–497. ISBN 9783540280439. • Wilke, K.; Martin, A.; Terstegen, L.; Biel, S. S. (June 2007). "A short history of sweat gland biology" (http:// onlinelibrary.wiley.com/doi/10.1111/j.1467-2494.2007.00387.x/pdf) (pdf). International journal of cosmetic science 29 (3): 169–179. doi: 10.1111/j.1467-2494.2007.00387.x (http://dx.doi.org/10.1111/j. 1467-2494.2007.00387.x). ISSN 1468-2494 (http://www.worldcat.org/issn/1468-2494).
External links
• Diagram of eccrine and apocrine sweat glands (http://www.mayoclinic.com/health/medical/IM00027) from Mayo Clinic
Moll's gland
24
Moll's gland
Gland of Moll
Latin glandulae ciliares conjunctivales Gray's subject #227 1025 [1]
Glands of Moll, also known as ciliary glands, are modified apocrine sweat glands that are found on the margin of the eyelid. They are next to the base of the eyelashes, and anterior to the Meibomian glands within the distal eyelid margin. These glands are relatively large and tubular-shaped. The glands of Moll are named after Dutch oculist Jacob Anton Moll (1832–1914). Glands of Moll empty into the adjacent lashes. Glands of Moll and Zeis secrete lipid that adds to the superficial layer of the tear film, retarding evaporation. The glands of Moll are prone to infection and blockage of its duct with sebum and cell debris. Blockage of the gland's duct causes swelling which can manifest itself as a stye.
References
• American Family Physician, Eyelid Disorders: Diagnosis and Management [2] • Anatomy of the Human Eyelid [3]
Sebaceous gland
25
Sebaceous gland
Sebaceous gland
Schematic view of hair follicle & sebaceous gland.
Cross-section of all skin layers. A hair follicle with associated structures. (Sebaceous glands labeled at center left.) Latin Gray's MeSH glandula sebacea subject #234 1069
[1] [2]
Sebaceous+glands
The sebaceous glands are microscopic glands in the skin that secrete an oily/waxy matter, called sebum, to lubricate and waterproof the skin and hair of mammals.[1] In humans, they are found in greatest abundance on the face and scalp, though they are distributed throughout all skin sites except the palms and soles.[1] In the eyelids, meibomian sebaceous glands secrete a special type of sebum into tears. There are several related medical conditions, including acne, sebaceous cysts, hyperplasia, sebaceous adenoma and sebaceous gland carcinoma (see section below: Pathology).
Locations and morphology
A branched type of acinar gland, the sebaceous glands exist in humans throughout the skin except in the palms of the hands and soles of the feet. Sebaceous glands can usually be found in hair-covered areas, where they are connected to hair follicles (see image at top). The glands deposit sebum on the hairs, and bring it to the skin surface along the hair shaft. The structure consisting of hair, hair follicle, arrector pili muscle, and sebaceous gland is known as a pilosebaceous unit. Sebaceous glands are also found in non-haired areas (glabrous skin) of eyelids, nose, penis, labia minora and nipples. Here, the sebum traverses ducts that terminate in sweat pores on the surface of the skin.[citation needed] At the rim of the eyelids, meibomian glands are a specialized form of sebaceous gland. They secrete a form of sebum (called (meibum)) onto the eye, slowing the evaporation of tears.
Sebaceous gland
26
Sebum
Sebaceous glands secrete the oily, waxy substance called sebum (Latin, meaning fat or tallow) that is made of triglyceride oils, wax, squalene, and metabolytes of fat-producing cells.[2][3] In the glands, sebum is produced within specialized cells and is released as these cells burst; sebaceous glands are thus classified as holocrine glands. Seborrhoea is the name for the condition of greasy skin caused by excess sebum.[4] Sebum keeps hair and skin supple. Sebum is odorless, but its bacterial breakdown can produce odors. Sebum is the cause of some people's experiencing "oily" hair,[5] as in hot weather or if not washed for several days. Earwax is partly composed of sebum.
Function
All of the sebaceous glands in humans have been demonstrated to show similarity in structure and secrete sebum by a holocrine process. Sebum excreted by the sebaceous gland is primarily composed of tryglycerides, wax esters, and squalene.[6] Wax esters, like squalene, are unique to sebum and not produced anywhere else in the body.[7] Sebum also contains 45% water-insoluble fatty acids known to have broad antimicrobial activity.[][8] Additionally, sebaceous gland secretion provides Vitamin E to the upper layers of facial skin.[9] Sebaceous lipids contribute to maintaining the integrity of the skin barrier, and express pro-inflammatory and anti-inflammatory properties.[10][][] Recent research suggests that sebum may represent a delivery system for antioxidants, antimicrobial lipids, pheromones, and hydration of stratum corneum.[] During the last gestation trimester, it is known that sebaceous glands produce vernix caseosa which protects the embryonic skin from amniotic water.[11] Sebaceous secretions in conjunction with apocrine glands also play an important thermoregulatory role. In hot conditions, the secretions emulsify and foment formation of and prevent the loss of sweat drops from the skin. In colder conditions, sebum repels rain from skin and hair.[] Increased facial surface sebum secretion is also associated with the development of acne.[]
Composition
The composition of sebum varies across species. In humans, the lipid content is as follows:[12]
Percent composition Substance 25% 41% 16% 12% wax monoesters triglycerides free fatty acids squalene
Sapienic acid is a sebum fatty acid that is unique to humans.
Sebaceous gland
27
Control
The following treatments have been shown to reduce sebum secretion rates: • Isotretinoin[13] • SMT D002[14] • Spironolactone[15] (suitable for females only)
Changes during development
The sebaceous glands of a human fetus in utero secrete a substance called Vernix caseosa, a "waxy" or "cheesy" white substance coating the skin of newborns. The activity of the sebaceous glands increases during puberty because of heightened levels of androgens, producing smegma. In males, sebaceous glands begin to appear predominantly on the penis, on the shaft and around the rim of the penile head during and after puberty. This is however normal, not to be confused with an STD. In females, they appear predominantly in the labia minora.
Pathology
Sebaceous glands are involved in skin problems such as acne and keratosis pilaris. In the skin pores, sebum and keratin can create a hyperkeratotic plug called a "microcomedone". The prescription drug isotretinoin significantly reduces the amount of sebum produced by the sebaceous glands, and is used to treat acne. The extreme use (up to 10 times doctor-prescribed amounts) of anabolic steroids by bodybuilders, for muscle gain can cause acne. The sebaceous gland is stimulated due to some steroids conversion into dihydrotestosterone. This may cause serious acne on the face, neck, chest, back and shoulders. It is a common misconception that a blocked sebaceous gland is known as a sebaceous cyst. Cysts that are commonly called sebaceous cysts actually do not involve a sebaceous gland. Instead, they are collection of keratin and dead keratinocytes which develop within the epidermal skin layer. These cysts are called Epidermal Cysts. A condition involving enlarged sebaceous glands is known as sebaceous hyperplasia. Sebaceous gland carcinoma is a rare and aggressive form of cancer involving the sebaceous glands; sebaceous adenoma is a more benign neoplasm of the sebaceous glands. Sebum can also build up around body piercings.[16]
Importance to other animals
Certain species of Demodex mites feed on sebum and are commonly found in the sebaceous glands of mammals, including those of humans. The preputial glands of mice and rats are large modified sebaceous glands that produce pheromones.
Demodex mite
Sebaceous gland
28
Additional images
Pilosebaceous unit
Base of pilosebaceous unit
Insertion of sebaceous glands into hair shaft
Sagittal section through the upper eyelid.
A hair follicle with associated structures.
References
[1] Dellmann's textbook of veterinary histology (405 pages), Jo Ann Coers Eurell, Brian L. Frappier, 2006, p.29, weblink: Books-Google-RTOC (http:/ / books. google. com/ books?id=FnS4uiOlRT0C& pg=PA29& lpg=PA29). [2] "Exercise 15: Hair", VT.edu, 2008, webpage: Vetmed-lab15 (http:/ / education. vetmed. vt. edu/ Curriculum/ VM8054/ Labs/ Lab15/ Lab15. htm). [5] "Hair Care: An Illustrated Dermatologic Handbook", Zoe Diana Draelos, Zoe Kececioglu Draelos, 2005, p.26, web: Books-Google-5QC (http:/ / books. google. com/ books?id=Z2rHHGQc-5QC& pg=PA26& lpg=PA26): oily hair & detergents. [14] http:/ / www. summitplc. com/ uploads/ RNSSeborrhoeatrialFINAL. pdf
External links
• BU Histology Learning System: 08801loa (http://www.bu.edu/histology/p/08801loa.htm) - "Integument: scalp" • Sebaceous Glands (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Sebaceous+Glands) at the US National Library of Medicine Medical Subject Headings (MeSH)
Olfactory glands
29
Olfactory glands
Olfactory glands
Section of the olfactory mucous membrane. Latin Gray's Code glandulae olfactoriae subject #223 996
[1] [2]
TH H3.05.00.0.00026
Bowman's glands (a.k.a. olfactory glands, glands of Bowman) are situated in the olfactory mucosa, beneath the olfactory epithelium, in the lamina propria, a connective tissue also containing fibroblasts, blood vessels, and bundles of fine axons from the olfactory neurons.[1] The structure of the Bowman's glands consists of an acinus in the lamina propria and a secretory duct going out through the olfactory epithelium. Electron microscopy studies show that Bowman's glands contain cells with large secretory vesicles.[2] Bowman's glands might secrete proteins such as Lysozyme, amylase and IgA similarly to serous glands. The exact composition of the secretions from Bowman's glands is unclear, but there is evidence that Bowman's glands do not produce odorant binding protein.[3]
References External links
• Slide at ouhsc.edu (http://w3.ouhsc.edu/histology/Glass slides/11_07.jpg) This article incorporates text from a public domain edition of Gray's Anatomy.
Brunner's glands
30
Brunner's glands
Brunner's glands
Section of duodenum. (Duodenal glands in submucosa are labeled at right, fourth from the top.) Latin Gray's glandulae duodenales subject #248 1176
[1]
Brunner's glands (or duodenal glands) are compound tubular submucosal glands found in that portion of the duodenum which is above the hepatopancreatic sphincter (Sphincter of Oddi). The main function of these glands is to produce a mucus-rich alkaline secretion (containing bicarbonate) in order to: • protect the duodenum from the acidic content of chyme (which is introduced into the duodenum from the stomach); • provide an alkaline condition for the intestinal enzymes to be active, thus enabling absorption to take place; • lubricate the intestinal walls. They also secrete urogastrone, which inhibits parietal and chief cells of the stomach from secreting acid and their digestive enzymes. This is another form of protection for the duodenum. They are the distinguishing feature of the duodenum, and are named for the Swiss physician who first described them, Johann Conrad Brunner.
External links
• duodenal+glands [2] at eMedicine Dictionary • BU Histology Learning System: 11504loa [3] - "Digestive System: Alimentary Canal: pyloro/duodenal junction, duodenum" • BU Histology Learning System: 11513loa [4] - "Digestive System: Alimentary Canal: pyloro/duodenal junction" • BU Histology Learning System: 11609loa [5] - "Digestive System: Alimentary Canal: duodenum, plicae circularis"
Human brunner's gland
Prostate
31
Prostate
Prostate
Male Anatomy
Prostate with seminal vesicles and seminal ducts, viewed from in front and above. Latin Gray's Artery Vein Nerve Lymph Precursor MeSH prostata subject #263 1251
[1]
internal pudendal artery, inferior vesical artery, and middle rectal artery prostatic venous plexus, pudendal plexus, vesicle plexus, internal iliac vein inferior hypogastric plexus external iliac lymph nodes, internal iliac lymph nodes, sacral lymph nodes Endodermic evaginations of the urethra Prostate
[2]
Dorlands/Elsevier Prostate [3]
The prostate (from Greek προστάτης – prostates, literally "one who stands before", "protector", "guardian"[1]) is a compound tubuloalveolar exocrine gland of the male reproductive system in most mammals.[][2] It differs considerably among species anatomically, chemically, and physiologically. In 2002, female paraurethral glands, or Skene's glands, were officially renamed the female prostate by the Federative International Committee on Anatomical Terminology.[3]
Prostate
32
Function
The function of the prostate is to secrete a slightly alkaline fluid, milky or white in appearance,[] that usually constitutes 50–75% of the volume of the semen along with spermatozoa and seminal vesicle fluid.[] Semen is made alkaline overall with the secretions from the other contributing glands, including, at least, the seminal vesicle fluid. The alkalinity of semen helps neutralize the acidity of the vaginal tract, prolonging the lifespan of sperm. The alkalinization of semen is primarily accomplished through secretion from the seminal vesicles.[4] The prostatic fluid is expelled in the first ejaculate fractions, together with most of the spermatozoa. In comparison with the few spermatozoa expelled together with mainly seminal vesicular fluid, those expelled in prostatic fluid have better motility, longer survival and better protection of the genetic material. The prostate also contains some smooth muscles that help expel semen during ejaculation.
Secretions
Prostatic secretions vary among species. They are generally composed of simple sugars and are often slightly acidic. In human prostatic secretions, the protein content is less than 1% and includes proteolytic enzymes, prostatic acid phosphatase, beta-microseminoprotein, and prostate-specific antigen. The secretions also contain zinc with a concentration 500–1,000 times the concentration in blood.
Regulation
To work properly, the prostate needs male hormones (testosterones), which are responsible for male sex characteristics. The main male hormone is testosterone, which is produced mainly by the testicles. Some male hormones are produced in small amounts by the adrenal glands. However, it is dihydrotestosterone that regulates the prostate.
Development
The prostatic part of the urethra develops from the pelvic (middle) part of the urogenital sinus (endodermal origin). Endodermal outgrowths arise from the prostatic part of the urethra and grow into the surrounding mesenchyme. The glandular epithelium of the prostate differentiates from these endodermal cells, and the associated mesenchyme differentiates into the dense stroma and the smooth muscle of the prostate.[5] The prostate glands represent the modified wall of the proximal portion of the male urethra and arises by the 9th week of embryonic life in the development of the reproductive system. Condensation of mesenchyme, urethra and Wolffian ducts gives rise to the adult prostate gland, a composite organ made up of several glandular and non-glandular components tightly fused.
Female prostate gland
The Skene's gland, also known as the paraurethral gland, found in females, is homologous to the prostate gland in males. However, anatomically, the uterus is in the same position as the prostate gland. In 2002 the Skene's gland was officially renamed to female prostate by the Federative International Committee on Anatomical Terminology.[6] The female prostate, like the male prostate, secretes PSA and levels of this antigen rise in the presence of carcinoma of the gland. The gland also expels fluid, like the male prostate, during orgasm.[]
Prostate
33
Structure
A healthy human prostate is classically said to be slightly larger than a walnut. The mean weight of the "normal" prostate in adult males is about 11 grams, usually ranging between 7 and 16 grams.[7] It surrounds the urethra just below the urinary bladder and can be felt during a rectal exam. It is the only exocrine organ located in the midline in humans and similar animals. The secretory epithelium is mainly pseudostratified, comprising tall columnar cells and basal cells which are supported by a fibroelastic stroma containing randomly orientated smooth muscle bundles. The epithelium is highly variable and areas of low cuboidal or squamous epithelium are also present, with transitional epithelium in the distal regions of the longer ducts.[] Within the prostate, the urethra coming from the bladder is called the prostatic urethra and merges with the two ejaculatory ducts. The prostate can be divided in two ways: by zone, or by lobe.[] It does not have a capsule, rather an integral fibromuscular band surrounds it.[8] It is sheathed in the muscles of the pelvic floor, which contract during the ejaculatory process.
Micrograph of benign prostatic glands with corpora amylacea. H&E stain.
Zones
The "zone" classification is more often used in pathology. The idea of "zones" was first proposed by McNeal in 1968. McNeal found that the relatively homogeneous cut surface of an adult prostate in no way resembled "lobes" and thus led to the description of "zones."[9] The prostate gland has four distinct glandular regions, two of which arise from different segments of the prostatic urethra:
Urinary bladder (black butterfly-like shape) and hyperplastic prostate (BPH) visualized by Medical ultrasonography technique
Name Peripheral zone (PZ)
Fraction of gland
Description
Up to 70% in young The sub-capsular portion of the posterior aspect of the prostate gland that surrounds the distal [10][11] men urethra. It is from this portion of the gland that ~70–80% of prostatic cancers originate. Approximately 25% This zone surrounds the ejaculatory ducts. The central zone accounts for roughly 2.5% of prostate normally cancers although these cancers tend to be more aggressive and more likely to invade the seminal [] vesicles. 5% at puberty ~10–20% of prostate cancers originate in this zone. The transition zone surrounds the proximal urethra and is the region of the prostate gland that grows throughout life and is responsible for the [10][11] disease of benign prostatic enlargement. (2) This zone is usually devoid of glandular components, and composed only, as its name suggests, of muscle and fibrous tissue.
Central zone (CZ)
Transition zone (TZ)
Anterior fibro-muscular Approximately 5% zone (or stroma)
Prostate
34
Lobes
The "lobe" classification is more often used in anatomy.
Prostate with a large median lobe bulging upwards. A metal instrument is placed in the urethra which passes through the prostate. This specimen was almost 7 centimeters long with a volume of about 60 cubic centimetres on transrectal ultrasound and was removed during a Hryntschak procedure or transvesical prostatectomy (removal of the prostate through the bladder) for benign prostatic hyperplasia.
Anterior lobe (or isthmus) Posterior lobe Lateral lobes
roughly corresponds to part of transitional zone roughly corresponds to peripheral zone spans all zones
Median lobe (or middle lobe) roughly corresponds to part of central zone
Prostate
35
Prostate disorders
Prostatitis
Prostatitis is inflammation of the prostate gland. There are primarily four different forms of prostatitis, each with different causes and outcomes. Two relatively uncommon forms, acute prostatitis and chronic bacterial prostatitis, are treated with antibiotics (category I and II, respectively). Chronic non-bacterial prostatitis or male chronic pelvic pain syndrome (category III), which comprises about 95% of prostatitis diagnoses, is treated by a large variety of modalities including alpha blockers, phytotherapy, physical therapy, psychotherapy, antihistamines, anxiolytics, nerve modulators, surgery,[12] and more.[] More recently, a combination of trigger point and psychological therapy has proved effective for category III prostatitis as well.[] Category IV prostatitis, relatively uncommon in the general population, is a type of leukocytosis.
Micrograph showing an inflamed prostate gland, the histologic correlate of prostatitis. A normal non-inflamed prostatic gland is seen on the left of the image. H&E stain.
Benign prostatic hyperplasia
Benign prostatic hyperplasia (BPH) occurs in older men;[] the prostate often enlarges to the point where urination becomes difficult. Symptoms include needing to urinate often (frequency) or taking a while to get started (hesitancy). If the prostate grows too large, it may constrict the urethra and impede the flow of urine, making urination difficult and painful and, in extreme cases, completely impossible. BPH can be treated with medication, a minimally invasive procedure or, in extreme cases, surgery that removes the prostate. Minimally invasive procedures include transurethral needle ablation of the prostate (TUNA) and transurethral microwave thermotherapy (TUMT).[13] These outpatient procedures may be followed by the insertion of a temporary prostatic stent, to allow normal voluntary urination, without exacerbating irritative symptoms.[] The surgery most often used in such cases is called transurethral resection of the prostate (TURP or TUR). In TURP, an instrument is inserted through the urethra to remove prostate tissue that is pressing against the upper part of the urethra and restricting the flow of urine. TURP results in the removal of mostly transitional zone tissue in a patient with BPH. Older men often have corpora amylacea[14] (amyloid), dense accumulations of calcified proteinaceous material, in the ducts of their prostates. The corpora amylacea may obstruct the lumens of the prostatic ducts, and may underlie some cases of BPH. Urinary frequency due to bladder spasm, common in older men, may be confused with prostatic hyperplasia. Statistical observations suggest that a diet low in fat and red meat and high in protein and vegetables, as well as regular alcohol consumption, could protect against BPH.[]
Prostate
36
Prostate cancer
Prostate cancer is one of the most common cancers affecting older men in developed countries and a significant cause of death for elderly men (estimated by some specialists at 3%). Despite this, the American Cancer Society's position regarding early detection is "Research has not yet proven that the potential benefits of testing outweigh the harms of testing and treatment" and that they believe "that men should not be tested without learning about what we know and don’t know about the risks and possible benefits of testing and treatment. Starting at age 50 Micrograph showing normal prostatic glands and (age 45 if you are of Black race or if your father or brother acquired glands of prostate cancer (prostate prostate cancer before age 65), talk to your doctor about the pros and adenocarcinoma) – right upper aspect of image. cons of testing so you can decide if testing is the right choice for HPS stain. Prostate biopsy. you".[15] If checks are performed, they can be in the form of a physical rectal exam, measurement of prostate specific antigen (PSA) level in the blood, or checking for the presence of the protein Engrailed-2 (EN2) in the urine. Co-researchers Hardev Pandha and Richard Morgan published their findings regarding checking for EN2 in urine in the 1 March 2011 issue of the journal Clinical Cancer Research.[16] A laboratory test currently identifies EN2 in urine, and a home test kit is envisioned similar to a home pregnancy test strip. According to Morgan, "We are preparing several large studies in the UK and in the US and although the EN2 test is not yet available, several companies have expressed interest in taking it forward."[17]
Male sexual response
During male ejaculation, sperm is transmitted from the ductus deferens into the male urethra via the ejaculatory ducts, which lie within the prostate gland. It is possible for men to achieve orgasm solely through stimulation of the prostate gland, such as prostate massage or receptive anal intercourse.[][][]
Vasectomy and risk of prostate cancer
In 1983, the Journal of the American Medical Association reported a connection between vasectomy and an increased risk of prostate cancer. Reported studies of 48,000 and 29,000 men who had vasectomies showed 66 percent and 56 percent higher rates of prostate cancer, respectively. The risk increased with age and the number of years since the vasectomy was performed. However, in March of the same year, the National Institute of Child Health and Human Development held a conference cosponsored by the National Cancer Institute and others to review the available data and information on the link between prostate cancer and vasectomies. It was determined that an association between the two was very weak at best, and even if having a vasectomy increased one's risk, the risk was relatively small. In 1997, the NCI held a conference with the prostate cancer Progressive Review Group (a committee of scientists, medical personnel, and others). Their final report, published in 1998 stated that evidence that vasectomies help to develop prostate cancer was weak at best.[18]
Prostate
37
Unclogging a prostate
A surgeon can unclog a blocked prostate by inserting an artificial 'tube' called a stent. Stents can be temporary or permanent. They are inserted into the urethra. This is mostly done on an outpatient basis under local or spinal anesthesia and takes about 30 minutes.
Additional images
Urinary bladder
Structure of the penis
Lobes of prostate
Zones of prostate
Prostate
38
Prostate
Microscopic glands of the prostate
Male Anatomy
The deeper branches of the internal pudendal artery.
Prostate
39
Lymphatics of the prostate.
Fundus of the bladder with the vesiculæ seminales.
Vesiculae seminales and ampullae of ductus deferentes, front view.
Vertical section of bladder, penis, and urethra.
Prostate
40
Dissection of prostate showing prostatic urethra.
References
The text of this article was originally taken from NIH Publication No. 02-4806, a public domain resource.[19]
[5] Moore, Keith L.; Persaud, T. V. N. and Torchia, Mark G. (2008) Before We Are Born, Essentials of Embryology and Birth Defects, 7th edition, Saunders Elsevier, ISBN 978-1-4160-3705-7 [10] "Basic Principals: Prostate Anatomy" (http:/ / www. urologymatch. com/ ProstateAnatomy. htm). Urology Match. Www.urologymatch.com. Web. 14 June 2010. [11] "Prostate Cancer Information from the Foundation of the Prostate Gland." (http:/ / www. prostate-cancer. com/ prostate-cancer-treatment-overview/ overview-prostate-anatomy. html) Prostate Cancer Treatment Guide. Web. 14 June 2010. [15] American Cancer Society American Cancer Society Guidelines for the early detection of cancer Cited: September 2011 (http:/ / www. cancer. org/ Healthy/ FindCancerEarly/ CancerScreeningGuidelines/ american-cancer-society-guidelines-for-the-early-detection-of-cancer). Cancer.org. Retrieved on 2013-01-21. [17] New prostate cancer twice as effective as a PSA test could be available by next year (http:/ / www. medicinechest. co. uk/ index. php?option=com_content& view=article& id=543). medicinechest.co.uk (2 March 2011)
Bulbourethral gland
41
Bulbourethral gland
Bulbourethral gland
Male Anatomy
The deeper branches of the internal pudendal artery. (Bulbourethral gland labeled at center left.) Latin Gray's Artery Precursor MeSH glandulæ bulbourethrales subject #264 1253
[1]
Artery of the urethral bulb Urogenital sinus Bulbourethral+Glands
[2]
A bulbourethral gland, also called a Cowper's gland for anatomist William Cowper, is one of two small exocrine glands present in the reproductive system of male mammals (including humans). They are homologous to Bartholin's glands in females.
Bulbourethral gland
42
Location
Bulbourethral glands are located posterior and lateral to the membranous portion of the urethra at the base of the penis, between the two layers of the fascia of the urogenital diaphragm, in the deep perineal pouch. They are enclosed by transverse fibers of the sphincter urethrae membranaceae muscle.
Structure
The bulbourethral glands are compound tubulo-alveolar glands, each approximately the size of a pea. They are composed of several lobules held together by a fibrous covering. Each lobule consists of a number of acini, lined by columnar epithelial cells, opening into a duct that joins with the ducts of other lobules to form a single excretory duct. This duct is approximately 2.5 cm long and opens into the urethra at the base of the penis. The glands gradually diminish in size with advancing age.[1] Wikipedia:Identifying reliable sources
Function
During sexual arousal each gland produces a clear, salty, viscous secretion known as pre-ejaculate. This fluid helps to lubricate the urethra for spermatozoa to pass through, neutralizing traces of acidic urine in the urethra,[2] and helps flush out any residual urine or foreign matter. It is possible for this fluid to pick up sperm, remaining in the urethral bulb from previous ejaculations, and carry them out prior to the next ejaculation. The Dissection of prostate showing the bulbourethral glands within the fibers of the external urethral sphincter just underneath the prostate. Cowper's gland also produces some amount of prostate-specific antigen (PSA), and Cowper's tumors may increase PSA to a level that makes prostate cancer suspected.[citation needed]
Gallery
Structure of the penis
Male pelvic organs seen from right side.
Vertical section of bladder, penis, and urethra.
Bulbourethral gland
43
Notes
[1] Gray's Anatomy, 38th edn, p 1861.
Bartholin's gland
Bartholin's gland
Genital organs of female. Latin Gray's Artery Nerve Lymph Precursor MeSH glandula vestibularis major subject #270 1266
[1] [1]
external pudendal artery ilioinguinal nerve
[1]
superficial inguinal lymph nodes Urogenital sinus Bartholin's+Glands
[3]
Dorlands/Elsevier Bartholin gland [4]
The Bartholin's glands (also called Bartholin glands or greater vestibular glands) are two glands located slightly posterior and to the left and right of the opening of the vagina. They secrete mucus to lubricate the vagina and are homologous to bulbourethral glands in males. However, while Bartholin's glands are located in the superficial perineal pouch in females, bulbourethral glands are located in the deep perineal pouch in males.
Function
They secrete mucus to provide vaginal lubrication.[2][3] Bartholin's glands secrete relatively minute amounts (one or two drops) of fluid when a woman is sexually aroused.[] The minute droplets of fluid were once believed to be important for lubricating the vagina, but research from Masters and Johnson demonstrated that vaginal lubrication comes from deeper within the vagina.[] The fluid may slightly moisten the labial opening of the vagina, serving to make contact with this sensitive area more comfortable for the woman.[]
Bartholin's gland
44
Pathology
Although unusual, it is possible for the Bartholin's glands to become irritated or infected, resulting in pain.[] If the duct becomes obstructed, a Bartholin's cyst can develop, and a Bartholin's cyst in turn can become infected and form an abscess. Adenocarcinoma of the gland is rare, but benign tumors and hyperplasia are even more rare.[4]
Eponym
Bartholin's glands were first described in the 17th century by the Danish anatomist Caspar Bartholin the Younger (1655–1738).[5] Some sources mistakenly ascribe their discovery to his grandfather, theologian and anatomist Caspar Bartholin the Elder (1585–1629).[6]
References
[1] Greater Vestibular (Bartholin) gland (http:/ / summit. stanford. edu/ ourwork/ PROJECTS/ LUCY/ lucywebsite/ vestib_gl. html) [6] C. C. Gillispie (ed.): Dictionary of Scientific Biography, New York 1970. See the article on Thomas Bartholin.
External links
• SUNY Labs 41:11-0200 (http://ect.downstate.edu/courseware/haonline/labs/l41/110200.htm)—"The Female Perineum: Muscles of the Superficial Perineal Pouch" • SUNY Anatomy Image 9243 (http://ect.downstate.edu/courseware/haonline/imgs/00000/9000/200/9243. jpg) • SUNY Anatomy Image 9694 (http://ect.downstate.edu/courseware/haonline/imgs/00000/9000/600/9694. jpg)—opening • greater+vestibular+gland (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=greater+ vestibular+gland) at eMedicine Dictionary
Endometrium
45
Endometrium
Endometrium
Uterus and uterine tubes. (Endometrium labeled at center right.) Latin Gray's MeSH Dorlands/Elsevier tunica mucosa uteri subject #268 1262 Endometrium Endometrium
[2] [3] [1]
The endometrium is the inner mucous membrane of the mammalian uterus.
Function
The endometrium is the innermost glandular layer and functions as a lining for the uterus, preventing adhesions between the opposed walls of the myometrium, thereby maintaining the patency of the uterine cavity. During the menstrual cycle or estrous cycle, the endometrium grows to a thick, blood vessel-rich, glandular tissue layer. This represents an optimal environment for the implantation of a blastocyst upon its arrival in the uterus. The endometrium is central, echogenic (detectable using ultrasound scanners), and has an average thickness of 6.7 mm. During pregnancy, the glands and blood vessels in the endometrium further increase in size and number. Vascular spaces fuse and become interconnected, forming the placenta, which supplies oxygen and nutrition to the embryo and foetus.
Cycle
The endometrial lining undergoes cyclic regeneration. Humans and the great apes display the menstrual cycle, whereas most other mammals are subject to an estrous cycle. In both cases, the endometrium initially proliferates under the influence of estrogen. However, once ovulation occurs, in addition to estrogen, the ovary will also start to produce progesterone. This changes the proliferative pattern of the endometrium to a secretory lining. Eventually, the secretory lining provides a hospitable environment for one or more blastocysts. If a blastocyst implants, then the lining remains as decidua. The decidua becomes part of the placenta; it provides support and protection for the gestation. If there is inadequate stimulation of the lining, due to lack of hormones, the endometrium remains thin and inactive. In humans, this will result in amenorrhea, or the absence of a menstrual period. After menopause, the lining is often described as being atrophic. In contrast, endometrium that is chronically exposed to estrogens, but not to progesterone, may become hyperplastic. Long-term use of oral contraceptives with highly potent progestins can also induce endometrial atrophy.[1][2] In humans, the cycle of building and shedding the endometrial lining lasts an average of 28 days. The endometrium develops at different rates in different mammals. Its formation is sometimes affected by seasons, climate, stress, and other factors. The endometrium itself produces certain hormones at different points along the cycle. This affects
Endometrium other portions of the reproductive system.
46
Histology
The endometrium consists of a single layer of columnar epithelium resting on the stroma, a layer of connective tissue that varies in thickness according to hormonal influences. Simple tubular uterine glands reach from the endometrial surface through to the base of the stroma, which also carries a rich blood supply of spiral arteries. In a woman of reproductive age, two layers of endometrium can be distinguished. These two layers occur only in endometrium lining the cavity of the uterus, not in the lining of the Fallopian tubes:[3] • The functional layer is adjacent to the uterine cavity. This layer is built up after the end of menstruation during the first part of the previous menstrual cycle. Proliferation is induced by estrogen (follicular phase of menstrual cycle), and later changes in this layer are engendered by progestrone from the corpus luteum (luteal phase). It is adapted to provide an optimum environment for the implantation and growth of the embryo. This layer is completely shed during menstruation. • The basal layer, adjacent to the myometrium and below the functional layer, is not shed at any time during the menstrual cycle, and from it the functional layer develops. In the absence of progesterone, the arteries supplying blood to the functional layer constrict, so that cells in that layer become ischaemic and die, leading to menstruation. It is possible to identify the phase of the menstrual cycle by observing histological differences at each phase:
Phase Menstrual phase Days 1–4 Thickness Thin Absent Epithelium High magnification micrograph of decidualized endometrium due to exogenous progesterone (oral contraceptive pill). H&E stain.
Low magnification micrograph of decidualized endometrium. H&E stain.
Proliferative phase 4–14 Secretory phase
Intermediate Columnar Columnar. Also visible are helicine branches of uterine artery
15–28 Thick
Chorionic tissue can result in marked endometrial changes, known as an Arias-Stella reaction, that have an appearance similar to cancer.[] Historically, this change was diagnosed as endometrial cancer and it is important only in so far as it should not be misdiagnosed as cancer.
Endometrium
47
Pathological conditions
Adenomyosis is the growth of the endometrium into the muscle layer of the uterus (the myometrium). Endometriosis is the growth of endometrial tissue outside the uterus. Endometrial cancer is the most common cancer of the human female genital tract. Asherman's syndrome, also known as intrauterine adhesions occurs when the basal layer of the endometrium is damaged by instrumentation (e.g., D&C) or infection (e.g., endometrial tuberculosis) resulting in endometrial sclerosis and adhesion formation partially or completely obliterating the uterine cavity. Thin endometrium may be defined as an endometrial thickness of less than 8 mm. It usually occurs after menopause. Treatments that can improve endometrial thickness include Vitamin E, L-arginine and sildenafil citrate.[4] Gene expression profiling using cDNA microarray can be used for the diagnosis of endometrial disorders.[5]
Additional images
The initial stages of human embryogenesis
Vertical section of mucous membrane of human uterus.
Endometrioid adenocarcinoma from biopsy. H&E stain.
Micrograph of the endometrium.
Micrograph of decidualized endometrium due to exogenous progesterone. H&E stain.
Micrograph of decidualized endometrium due to exogenous progesterone. H&E stain.
Micrograph showing endometrial stromal condensation, a finding seen in menses.
References
[1] Effects of hormone therapy on the endometrium, http:/ / www. ncbi. nlm. nih. gov/ pubmed/ 8426860 [2] William's Gynecology, McGraw 2008, Chapter 8, Abnormal Uterine Bleeding [3] Blue Histology - Female Reproductive System. School of Anatomy and Human Biology - The University of Western Australia http:/ / www. lab. anhb. uwa. edu. au/ mb140/ CorePages/ FemaleRepro/ FemaleRepro. htm Accessed 20061228 20:35
External links
• SUNY Figs 43:05-15 (http://ect.downstate.edu/courseware/haonline/figs/l43/430515.htm) - "The uterus, uterine tubes and ovary with associated structures." • BU Histology Learning System: 18902loa (http://www.bu.edu/histology/p/18902loa.htm) - "Female Reproductive System uterus, endometrium" • Swiss embryology (from UL, UB, and UF) gnidation/role02 (http://www.embryology.ch/anglais/gnidation/ role02.html)
Endometrium • Histology at OU 20_01 (http://w3.ouhsc.edu/histology/Glass slides/20_01.jpg) • Histology at utah.edu. Slide is proliferative phase - click forward to see secretory phase (http://medlib.med. utah.edu/WebPath/FEMHTML/FEM017.html)
48
Urethral gland
Urethral gland
Latin glandulae urethrales urethrae masculinae Gray's subject #262 1250 [1]
The urethral or periurethral glands (also Littre glands after Alexis Littré)[] are glands that branch off the wall of the urethra of male mammals. The glands secrete mucus[1] and are most numerous in the section of the urethra that runs through the penis. Urethral glands produce a colloid secretion containing glycosaminoglycans; this secretion protects the epithelium against urine.[2] Unsafe sex can lead to urethritis. Untreated, this can lead to infection of the urethral glands, which can cause the urethra to be impeded by strictures.
References
[2] Human Microscopic Anatomy: An Atlas for Students of Medicine and Biology By Radivoj V. Krstić, page 382
External links
• Slide at uottawa.ca (http://courseweb.edteched.uottawa.ca/Medicine-histology/English/Reproduction/male/ fig22malerepro.htm) • glands+of+the+male+urethra (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=glands+ of+the+male+urethra) at eMedicine Dictionary
Gastric chief cell
49
Gastric chief cell
Chief cell
H&E stain of fundic gland polyp showing shortening of the gastric pits with cystic dilatation
A fundus gland. A. Transverse section of gland. Latin Code exocrinocytus principalis TH H3.04.02.1.00031
A gastric chief cell (or peptic cell, or gastric zymogenic cell) is a cell in the stomach that releases pepsinogen, gastric lipase and chymosin.[1] The cell stains basophilic upon H&E prep due to the large proportion of rough endoplasmic reticulum in its cytoplasm. Chief cells release the zymogen (enzyme precursor) pepsinogen when stimulated by a variety of factors including cholinergic activity from the vagus nerve and acidic condition in the stomach. Gastrin and secretin may also act as secretagogues.[2] It works in conjunction with the parietal cell, which releases gastric acid, converting the pepsinogen into pepsin.
Gastric chief cell
50
Nomenclature
The terms "chief cell" and "zymogenic cell" are often used without the word "gastric" to name this type of cell. However those terms can also be used to describe other cell types (for example, parathyroid chief cells.) Chief cells are also known as peptic cells.
References
[2] Johnson. Gastrointestinal Physiology 6th Edition. Mosby. 2001
External links
• Anatomy Atlases - Microscopic Anatomy, plate 01.05 (http:// www.anatomyatlases.org/MicroscopicAnatomy/Section01/ Plate0105.shtml) • BU Histology Learning System: 22201loa (http://www.bu. edu/histology/p/22201loa.htm) - "Ultrastructure of the Cell: chief cells and enteroendocrine cell"
human chief cells
• BU Histology Learning System: 11304loa (http://www.bu.edu/histology/p/11304loa.htm) - "Digestive System: Alimentary Canal: fundic stomach, gastric glands, base" • " chief cell (http://web.archive.org/web/20090616022448/http://www.mercksource.com/pp/us/cns/ cns_hl_dorlands_split.jsp?pg=/ppdocs/us/common/dorlands/dorland/two/000018589.htm)" at Dorland's Medical Dictionary • Physiology at MCG 6/6ch4/s6ch4_8 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section6/6ch4/s6ch4_8.htm)
Pepsin
51
Pepsin
pepsin B
Identifiers EC number CAS number 3.4.23.2 [1] [2]
9025-48-3
Databases IntEnz BRENDA ExPASy KEGG MetaCyc PRIAM PDB structures IntEnz view [3] [4] [5]
BRENDA entry NiceZyme view KEGG entry [6]
metabolic pathway profile [8] [9]
[7]
RCSB PDB
PDBe
[10]
PDBsum
[11]
Search PMC articles [12]
PubMed articles [13] NCBI proteins [14]
pepsin C (gastricsin)
Identifiers EC number CAS number 3.4.23.3 [15] [16]
9012-71-9
Databases IntEnz BRENDA ExPASy KEGG MetaCyc PRIAM PDB structures IntEnz view [17] [18] [19]
BRENDA entry NiceZyme view KEGG entry
[20] [21]
metabolic pathway profile [22] [23]
RCSB PDB
PDBe
[24]
PDBsum
[25]
Pepsin
52
Search PMC articles [26]
PubMed articles [27] NCBI proteins [28]
Pepsin is an enzyme whose zymogen (pepsinogen) is released by the chief cells in the stomach and that degrades food proteins into peptides. It was discovered in 1836 by Theodor Schwann who also coined its name from the Greek word pepsis, meaning digestion (peptein: to digest).[][] It was the first enzyme to be discovered, and, in 1929, it became one of the first enzymes to be crystallized, by John H. Northrop.[] Pepsin is a digestive protease, a member of the aspartate protease family.[1] Pepsin is one of three principal protein-degrading, or proteolytic, enzymes in the digestive system, the other two being chymotrypsin and trypsin. The three enzymes were among the first to be isolated in crystalline form. During the process of digestion, these enzymes, each of which is specialized in severing links between particular types of amino acids, collaborate to break down dietary proteins into their components, i.e., peptides and amino acids, which can be readily absorbed by the intestinal lining. Pepsin is most efficient in cleaving peptide bonds between hydrophobic and preferably aromatic amino acids such as phenylalanine, tryptophan, and tyrosine.[]
History
The term "pepsin" was first coined by Theodor Schwann in the early 19th century. Scientists around this time began discovering many biochemical compounds that play a significant role in biological processes and pepsin was one of them. It was with the identification of a chemical agent found in the stomachs of animals, that scientists began looking into the digestive properties of organisms. This acidic substance that was able to convert nitrogen based foods into water soluble material was determined to be pepsin.[]
Precursor
Pepsin is expressed as a pro-form zymogen, pepsinogen, whose primary structure has an additional 44 amino acids. In the stomach, chief cells release pepsinogen. This zymogen is activated by hydrochloric acid (HCl), which is released from parietal cells in the stomach lining. The hormone gastrin and the vagus nerve trigger the release of both pepsinogen and HCl from the stomach lining when food is ingested. Hydrochloric acid creates an acidic environment, which allows pepsinogen to unfold and cleave itself in an autocatalytic fashion, thereby generating pepsin (the active form). Pepsin cleaves the 44 amino acids from pepsinogen to create more pepsin. Pepsin will digest up to 20% of ingested amide bonds by cleaving preferentially after the N-terminal[]:96 of aromatic amino acids such as phenylalanine, tryptophan, and tyrosine.[]:675 Pepsin exhibits preferential cleavage for hydrophobic, preferably aromatic, residues in P1 and P1' positions. Increased susceptibility to hydrolysis occurs if there is a sulfur-containing amino acid close to the peptide bond, which has an aromatic amino acid. Pepsin cleaves Phe1Val, Gln4His, Glu13Ala, Ala14Leu, Leu15Tyr, Tyr16Leu, Gly23Phe, Phe24Phe and Phe25Tyr bonds in the B chain of insulin.[2] Peptides may be further digested by other proteases (in the duodenum) and eventually absorbed by the body. Pepsin is stored as pepsinogen so it will only be released when needed, and does not digest the body's own proteins in the stomach's lining.
Pepsin
53
Activity and stability
Pepsin is most active in acidic environments between 37°C and 42°C.[3][4] Accordingly, its primary site of synthesis and activity is the stomach (pH 1.5 to 2). Pepsin exhibits maximal activity at pH 2.0 and is inactive at pH 6.5 and above, however pepsin is not fully denatured or irreversibly inactivated until pH 8.0.[] Therefore pepsin in solution of up to pH 8.0 can be reactivated upon re-acidification. The stability of pepsin at high pH has significant implications on disease attributed to laryngopharyngeal reflux. Pepsin remains in the larynx following a gastric reflux event.[][] At the mean pH of the laryngopharynx (pH = 6.8) pepsin would be inactive but could be reactivated upon subsequent acid reflux events resulting in damage to local tissues.
In laryngopharyngeal reflux
Pepsin is one of the primary causes of mucosal damage during laryngopharyngeal reflux.[][] Pepsin remains in the larynx (pH 6.8) following a gastric reflux event.[][] While enzymatically inactive in this environment, pepsin would remain stable and could be reactivated upon subsequent acid reflux events.[] Exposure of laryngeal mucosa to enzymatically active pepsin, but not irreversibly inactivated pepsin or acid, results in reduced expression of protective proteins and thereby increases laryngeal susceptibility to damage.[][][] Pepsin may also cause mucosal damage during weakly acidic or non-acid gastric reflux. Weak or non-acid reflux is correlated with reflux symptoms and mucosal injury.[][][5][] Under non-acid conditions (neutral pH), pepsin is internalized by cells of the upper airways such as the larynx and hypopharynx by a process known as receptor-mediated endocytosis.[] The receptor by which pepsin is endocytosed is currently unknown. Upon cellular uptake, pepsin is stored in intracellular vesicles of low pH at which its enzymatic activity would be restored. Pepsin is retained within the cell for up to 24 hours.[] Such exposure to pepsin at neutral pH and endoyctosis of pepsin causes changes in gene expression associated with inflammation, which underlies signs and symptoms of reflux,[] and tumor progression.[] This and other research[] implicates pepsin in carcinogenesis attributed to gastric reflux. Pepsin in airway specimens is considered to be a sensitive and specific marker for laryngopharyngeal reflux.[][] Research to develop new pepsin-targeted therapeutic and diagnostic tools for gastric reflux is ongoing.
Storage
Pepsins should be stored at very cold temperatures (between −80 °C and −20 °C) to prevent autolysis (self-cleavage).
Inhibitors
Pepsin may be inhibited by high pH (see "Activity" and "Stability", above) or by inhibitor compounds. Pepstatin is a low molecular weight compound and potent inhibitor specific for acid proteases with a Ki of about 10−10 M for pepsin. The statyl residue of pepstatin is thought to be responsible for pepstatin inhibition of pepsin; statine is a potential analog of the transition state for catalysis by pepsin and other acid proteases. Pepstatin does not covalently bind pepsin and inhibition of pepsin by pepstatin is therefore reversible.[] 1-bis(diazoacetyl)-2-penylethane reversibly inactivates pepsin at pH 5, a reaction which is accelerated by the presence of Cu(II).[] Pepsin also undergoes feedback inhibition; a product of protein digestion slows down the reaction by inhibiting pepsin.[][]
Pepsin
54
Applications
Commercial pepsin is extracted from the glandular layer of hog stomachs. It is a component of rennet used to curdle milk during the manufacture of cheese. Pepsin is used for a variety of applications in food manufacturing: to modify and provide whipping qualities soy protein and gelatin,[] to modify vegetable proteins for use in nondairy snack items, to make precooked cereals into instant hot cereals[] and to prepare animal and vegetable protein hydrolysates for use in flavoring foods and beverages. It is used in the leather industry to remove hair and residual tissue from hides and in the recovery of silver from discarded photographic films by digesting the gelatin layer that holds the silver.[] Pepsin was historically an additive of Beemans gum brand chewing gum by Dr. Edward E. Beeman. It also gave name to Pepsi-Cola, originally formulated with pepsin and cola nuts. Pepsin is commonly used in the preparation of F(ab')2 fragments from antibodies. In some assays, it is preferable to use only the antigen-binding (Fab) portion of the antibody. For these applications, antibodies may be enzymatically digested to produce either an Fab or an F(ab')2 fragment of the antibody. To produce an F(ab')2 fragment, IgG is digested with pepsin, which cleaves the heavy chains near the hinge region. One or more of the disulfide bonds that join the heavy chains in the hinge region are preserved, so the two Fab regions of the antibody remain joined together, yielding a divalent molecule (containing two antibody binding sites), hence the designation F(ab')2. The light chains remain intact and attached to the heavy chain. The Fc fragment is digested into small peptides. Fab fragments are generated by cleavage of IgG with papain instead of pepsin. Papain cleaves IgG above the hinge region containing the disulfide bonds that join the heavy chains, but below the site of the disulfide bond between the light chain and heavy chain. This generates two separate monovalent (containing a single antibody binding site) Fab fragments and an intact Fc fragment. The fragments can be purified by gel filtration, ion exchange, or affinity chromatography.[] Fab and F(ab')2 antibody fragments are used in assay systems where the presence of the Fc region may cause problems. In tissues such as lymph nodes or spleen, or in peripheral blood preparations, cells with Fc receptors (macrophages, monocytes, B lymphocytes, and natural killer cells) are present which can bind the Fc region of intact antibodies, causing background staining in areas that do not contain the target antigen. Use of F(ab')2 or Fab fragments ensures that the antibodies are binding to the antigen and not Fc receptors. These fragments may also be desirable for staining cell preparations in the presence of plasma, because they are not able to bind complement, which could lyse the cells. F(ab')2, and to a greater extent Fab, fragments allow more exact localization of the target antigen, i.e., in staining tissue for electron microscopy. The divalency of the F(ab')2 fragment enables it to cross-link antigens, allowing use for precipitation assays, cellular aggregation via surface antigens, or rosetting assays.[]
Genes
The following three genes encode identical human pepsinogen A enyzmes:
pepsinogen 3, group I (pepsinogen A)
Identifiers Symbol Entrez HUGO OMIM RefSeq UniProt PGA3 643834 8885 [34]
[35] [36] [37]
169710
NM_001079807 P00790 [38]
Pepsin
55
Other data EC number Locus 3.4.23.1 [39] [40]
Chr. 11 q13
pepsinogen 4, group I (pepsinogen A)
Identifiers Symbol Entrez HUGO OMIM RefSeq UniProt PGA4 643847 8886 [41]
[42] [43] [44]
169720
NM_001079808 P00790 Other data [38]
EC number Locus
3.4.23.1
[39] [40]
Chr. 11 q13
pepsinogen 5, group I (pepsinogen A)
Identifiers Symbol Entrez HUGO OMIM RefSeq UniProt PGA5 5222 8887 [45] [46] [47] [48]
169730
NM_014224 P00790 Other data [38]
EC number Locus
3.4.23.1
[39] [40]
Chr. 11 q13
A fourth human gene encodes gastricsin also known as pepsinogen C:
Pepsin
56
progastricsin (pepsinogen C)
Identifiers Symbol Entrez HUGO OMIM RefSeq UniProt PGC 5225 8890 [49] [50] [51] [52]
169740
NM_001166424 P20142 [53]
Other data EC number 3.4.23.3 [54] Locus Chr. 6 pter-p21.1 [55]
References
[2] IUBMB Enzyme Nomenclature: http:/ / www. chem. qmul. ac. uk/ iubmb/ enzyme/ EC3/ 4/ 23/ 1. html [4] "Brenda-enzymes: Entry of pepsin A (EC-Number 3.4.23.1 )". Retrieved 2008-12-14 [5] Oelschlager BK, Quiroga E, Isch JA, et al. Gastroesophageal and pharyngeal reflux detection using impedance and 24-hour pH monitoring in asymptomatic subjects: defining the normal environment. J Gastrointest Surg 2006;10:54–62.
External links
• The MEROPS online database for peptidases and their inhibitors: Pepsin A A01.001 (http://merops.sanger.ac. uk/cgi-bin/merops.cgi?id=A01.001), Pepsin B A01.002 (http://merops.sanger.ac.uk/cgi-bin/merops. cgi?id=A01.002), Pepsin C (Gastricsin) A01.003 (http://merops.sanger.ac.uk/cgi-bin/merops.cgi?id=A01. 003) • Pepsin A (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Pepsin+A) at the US National Library of Medicine Medical Subject Headings (MeSH) • Pepsinogens (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Pepsinogens) at the US National Library of Medicine Medical Subject Headings (MeSH) • Pepsinogen A (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Pepsinogen+A) at the US National Library of Medicine Medical Subject Headings (MeSH) • Pepsinogen C (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Pepsinogen+C) at the US National Library of Medicine Medical Subject Headings (MeSH) • Beemans Gum (http://beemansgum.org) • Pepsin: Molecule of the Month (http://www.rcsb.org/pdb/101/motm.do?momID=12), by David Goodsell, RCSB Protein Data Bank
Parietal cell
57
Parietal cell
Parietal cell
Human parietal cells (pink staining) - stomach
Control of stomach acid Latin MeSH Code exocrinocytus parietalis Gastric+Parietal+Cells TH H3.04.02.1.00033
[1]
Parietal cells, or oxyntic cells, are the stomach epithelium cells that secrete gastric acid (HCl) and intrinsic factor in response to histamine (H2 receptor), acetylcholine (M3 receptors[]) and gastrin (CCK2 receptors). The histamine receptors act by increasing intracellular cAMP, whereas the muscarinic and gastrin receptors increase intracellular Ca2+ levels. Both cAMP and Ca2+ act via protein kinases to increase the transport of acid into the stomach. Gastrin is more important indirectly by increasing histamine synthesis in ECL cells,[1] as gastrin has no effect on the maximum histamine-stimulated gastric acid secretion.[2] Parietal cells contain an extensive secretory network (called canaliculi) from which the HCl is secreted by active transport into the stomach. The enzyme hydrogen potassium ATPase (H+/K+ ATPase) is unique to the parietal cells and transports the H+ against a concentration gradient of about 3 million to 1, which is the steepest ion gradient formed in the human body. Hydrochloric acid is formed in the following manner: • Hydrogen ions are formed from the dissociation of water molecules. The enzyme carbonic anhydrase converts one molecule of carbon dioxide and one molecule of water indirectly into a bicarbonate ion (HCO3-) and a hydrogen ion (H+). • The bicarbonate ion (HCO3-) is exchanged for a chloride ion (Cl-) on the basal side of the cell and the bicarbonate diffuses into the venous blood, leading to an alkaline tide. • Potassium (K+) and chloride (Cl-) ions diffuse into the canaliculi. • Hydrogen ions are pumped out of the cell into the canaliculi in exchange for potassium ions, via the H+/K+ ATPase.
Parietal cell The resulting highly-acidic environment causes proteins from food to unfold (or denature), exposing the peptide bonds that link together amino acids. HCl also activates pepsinogen, an endopeptidase, allowing it to help digestion by breaking specific peptide bonds, a process known as proteolysis. Furthermore, the sudden increase in gastric acid secretion following a meal can cause a physiological phenomenon called an alkaline tide, which is due to the production and export of bicarbonate from parietal cells. The alkaline tide is neutralized by the action of the pancreatic duct which produces a bicarbonate secretion that is deposited into the lumen of the duct while the byproduct, hydrogen ions, are pumped out the basal membrane into the portal blood stream, thereby neutralizing the bicarbonate from the stomach. Parietal cells secrete acid in response to three types of stimuli:[3] • H2 histamine receptors (most significant contribution) • Acetylcholine from parasympathetic activity via the vagus nerve and enteric nervous system • gastrin (least significant contribution, but note that histamine secretion by ECL cells is due in part to gastrin) Upon stimulation, adenylate cyclase is activated within the parietal cells. This increases intracellular cyclic AMP, which leads to activation of protein kinase A. Protein kinase A phosphorylates proteins involved in the transport of H+/K+ ATPase from the cytoplasm to the cell membrane. This causes resorption of K+ ions and secretion of H+ ions. The pH of the secreted fluid can fall by 0.8.
58
Intrinsic factor
Parietal cells also produce intrinsic factor. Intrinsic factor is required for the absorption of Vitamin B12 in the diet. A long-term deficiency in vitamin B12 can lead to megaloblastic anemia, characterized by large fragile erythrocytes. Pernicious anemia is a condition where intrinsic factor is not produced and leads to the same type of anemia. Atrophic gastritis, particularly in the elderly, will cause an inability to absorb B12 and can lead to deficiencies such as decreased DNA synthesis and nucleotide metabolism in the bone marrow.
Canaliculus
A canaliculus is an adaptation found on gastric parietal cells. It is a deep infolding, or little channel, which serves to increase the surface area, e.g. for secretion. The membrane of parietal cells is dynamic; the numbers of canaliculi rise and fall according to secretory need. This is accomplished by the fusion of canalicular precursors, or "tubulovesicles", with the membrane to increase surface area, and the reciprocal endocytosis of the canaliculi (reforming the tubulovesicles) to decrease it.
Diseases of parietal cells
• Peptic ulcers can result from over-acidity in the stomach. Antacids can be used to enhance the natural tolerance of the gastric lining. Antimuscarinic drugs such as pirenzepine or H2 antihistamines can reduce acid secretion. Proton pump inhibitors are more potent at reducing gastric acid production since that is the final common pathway of all stimulation of acid production. • In pernicious anemia, autoantibodies directed against parietal cells or intrinsic factor cause a reduction in vitamin B12 absorption. It can be treated with injections of replacement vitamin B12 (methylcobalamin, hydroxocobalamin or cyanocobalamin).
Immunofluorescence staining pattern of gastric parietal antibodies on a stomach section
• Achlorhydria is another autoimmune disease of the parietal cells. The damaged parietal cells are unable to produce the required amount of gastric acid. This leads to an increase in gastric pH, impaired digestion of food and increased risk of gastroenteritis.
Parietal cell
59
References
[1] Waldum, Helge L., Kleveland, Per M., et al. (2009)'Interactions between gastric acid secretagogues and the localization of the gastrin receptor',Scandinavian Journal of Gastroenterology,44:4,390 — 393 [2] Kleveland PM, Waldum HL, Larsson M. Gastric acid secretion in the totally isolated, vascularly perfused rat stomach. A selective muscarinic-1 agent does, whereas gastrin does not, augment maximal histamine-stimulated acid secretion. Scand J Gastroenterol 1987;/22:/705�13.
External links
• Illustration of Chief cells and Parietal cells at anatomyatlases.org (http://www.anatomyatlases.org/ MicroscopicAnatomy/Section01/Plate0105.shtml) • The Parietal Cell: Mechanism of Acid Secretion at vivo.colostate.edu (http://www.vivo.colostate.edu/hbooks/ pathphys/digestion/stomach/parietal.html) • BU Histology Learning System: 11303loa (http://www.bu.edu/histology/p/11303loa.htm) - Digestive System: Alimentary Canal: fundic stomach, gastric glands, lumen" • Physiology at MCG 6/6ch4/s6ch4_8 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section6/6ch4/s6ch4_8.htm) • Physiology at MCG 6/6ch4/s6ch4_14 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section6/6ch4/s6ch4_14.htm) • Parietal cell antibody (http://www.antibodypatterns.com/gpc.php) • Antibody to GPC (http://www.ii.bham.ac.uk/clinicalimmunology/CISimagelibrary/GPC.htm)
Hydrochloric acid
60
Hydrochloric acid
Hydrochloric acid
Identifiers CAS number ChemSpider UNII EC number ChEMBL ATC code 7647-01-0 10633809
[1] [2] [3]
QTT17582CB 231-595-7
[4]
CHEMBL1231821 A09 AB03 Properties
[6]
[5] [7]
,B05 XA13
Appearance
Colourless, transparent liquid Hazards
MSDS EU Index R-phrases S-phrases
External MSDS 017-002-01-X R34, R37 (S1/2), S26, S45 Related compounds
Related compounds
• • •
Hydrofluoric acid Hydrobromic acid Hydroiodic acid
Supplementary data page Structure and properties Thermodynamic data Spectral data
(verify) [8]
n, ε , etc.
r
Phase behaviour Solid, liquid, gas UV, IR, NMR, MS
(what is: / ?) Except where noted otherwise, data are given for materials in their standard state (at 25 °C, 100 kPa)
Infobox references
Hydrochloric acid Hydrochloric acid is a clear, colourless solution of hydrogen chloride (H Cl) in water. It is a highly corrosive, strong mineral acid with many industrial uses. Hydrochloric acid is found naturally in gastric acid. Historically called muriatic acid, and spirits of salt, hydrochloric acid was produced from vitriol (sulfuric acid) and common salt. It first appeared during the Renaissance, Wikipedia:Verifiability and then it was used by chemists such as Glauber, Priestley and Davy in their scientific research. With major production starting in the Industrial Revolution, hydrochloric acid is used in the chemical industry as a chemical reagent in the large-scale production of vinyl chloride for PVC plastic, and MDI/TDI for polyurethane. It has numerous smaller-scale applications, including household cleaning, production of gelatin and other food additives, descaling, and leather processing. About 20 million tonnes of hydrochloric acid are produced annually.
61
Etymology
Hydrochloric acid was known to European alchemists as spirits of salt or acidum salis (salt acid). Both names are still used, especially in non-English languages, such as German: Salzsäure and Dutch: Zoutzuur. Gaseous HCl was called marine acid air. The old (pre-systematic) name muriatic acid has the same origin (muriatic means "pertaining to brine or salt"), and this name is still sometimes used.[][1]
History
Aqua regia, a mixture consisting of hydrochloric acid and nitric acid, prepared by dissolving sal ammoniac in nitric acid, was described in the works of Pseudo-Geber, the 13th-century European alchemist.[2][][][3][4] Other references suggest that the first mention of aqua regia is in Byzantine manuscripts dating to the end of the thirteenth century.[][5][6][7] Free hydrochloric acid was first formally described in the 16th century by Libavius, who prepared it by heating salt in clay crucibles.[] Other authors claim that pure hydrochloric acid was first discovered by the German benedictine monk Basil Valentine in the 15th century,[8] by heating common salt and green vitriol,[9] whereas others claim that there is no clear reference to the preparation of pure hydrochloric acid until the end of the sixteenth century.[] In the seventeenth century, Johann Rudolf Glauber from Karlstadt am Main, Germany used sodium chloride salt and sulfuric acid for the preparation of sodium sulfate in the Mannheim process, releasing hydrogen chloride gas. Joseph Priestley of Leeds, England prepared pure hydrogen chloride in 1772, and in 1818 Humphry Davy of Penzance, England proved that the chemical composition included hydrogen and chlorine.[] During the Industrial Revolution in Europe, demand for alkaline substances increased. A new industrial process by Nicolas Leblanc (Issoundun, France) enabled cheap large-scale production of sodium carbonate (soda ash). In this Leblanc process, common salt is converted to soda ash, using sulfuric acid, limestone, and coal, releasing hydrogen chloride as a by-product. Until the British Alkali Act 1863 and similar legislation in other countries, the excess HCl was vented to air. After the passage of the act, soda ash producers were obliged to absorb the waste gas in water, producing hydrochloric acid on an industrial scale.[][] In the twentieth century, the Leblanc process was effectively replaced by the Solvay process without a hydrochloric acid by-product. Since hydrochloric acid was already fully settled as an important chemical in numerous applications, the commercial interest initiated other production methods, some of which are still used today. After the year 2000, hydrochloric acid is mostly made by absorbing by-product hydrogen chloride from industrial organic compounds production.[][][] Since 1988, hydrochloric acid has been listed as a Table II precursor under the 1988 United Nations Convention Against Illicit Traffic in Narcotic Drugs and Psychotropic Substances because of its use in the production of heroin, cocaine, and methamphetamine.[]
Hydrochloric acid
62
Chemical properties and reactions
Hydrogen chloride (HCl) is a monoprotic acid, which means it can dissociate (i.e., ionize) only once to give up one H+ ion (a single proton). In aqueous hydrochloric acid, the H+ joins a water molecule to form a hydronium ion, H3O+:[][] The other ion formed is Cl−, the chloride ion. Hydrochloric acid can therefore be used to prepare salts called chlorides, such as sodium chloride. Hydrochloric acid is a strong acid, since it is essentially completely dissociated in water.[][] Monoprotic acids have one acid dissociation constant, Ka, which indicates the level of dissociation in water. For a strong acid like HCl, the Ka is large. Theoretical attempts to assign a Ka to HCl have been made.[] When chloride salts such as NaCl are added to aqueous HCl they have practically no effect on pH, indicating that Cl− is an exceedingly weak conjugate base and that HCl is fully dissociated in aqueous solution. For intermediate to strong solutions of hydrochloric acid, the assumption that H+ molarity (a unit of concentration) equals HCl molarity is excellent, agreeing to four significant digits.[][] Of the six common strong mineral acids in chemistry, hydrochloric acid is the monoprotic acid least likely to undergo an interfering oxidation-reduction reaction. It is one of the least hazardous strong acids to handle; despite its acidity, it consists of the non-reactive and non-toxic chloride ion. Intermediate-strength hydrochloric acid solutions are quite stable upon storage, maintaining their concentrations over time. These attributes, plus the fact that it is available as a pure reagent, make hydrochloric acid an excellent acidifying reagent. Hydrochloric acid is the preferred acid in titration for determining the amount of bases. Strong acid titrants give more precise results due to a more distinct endpoint. Azeotropic or "constant-boiling" hydrochloric acid (roughly 20.2%) can be used as a primary standard in quantitative analysis, although its exact concentration depends on the atmospheric pressure when it is prepared.[10] Hydrochloric acid is frequently used in chemical analysis to prepare ("digest") samples for analysis. Concentrated hydrochloric acid dissolves many metals and forms oxidized metal chlorides and hydrogen gas, and it reacts with basic compounds such as calcium carbonate or copper(II) oxide, forming the dissolved chlorides that can be analyzed.[][] HCl + H2O → H3O+ + Cl−
Physical properties
Concentration Density Molarity pH Viscosity Specific heat kJ/(kg·K) 3.47 2.99 2.60 2.55 2.50 2.46 2.43 Vapour pressure kPa 1.95 1.40 2.13 3.73 7.24 14.5 28.3 Boiling point °C 103 108 90 84 71 61 48 Melting point °C −18 −59 −52 −43 −36 −30 −26
kg HCl/kg 10% 20% 30% 32% 34% 36% 38%
kg HCl/m3 Baumé 104.80 219.60 344.70 370.88 397.46 424.44 451.82 6.6 13 19 20 21 22 23
kg/L 1.048 1.098 1.149 1.159 1.169 1.179 1.189
mol/dm3 2.87 6.02 9.45 10.17 10.90 11.64 12.39 −0.5 −0.8 −1.0 −1.0 −1.0 −1.1 −1.1
mPa·s 1.16 1.37 1.70 1.80 1.90 1.99 2.10
The reference temperature and pressure for the above table are 20 °C and 1 atmosphere (101.325 kPa). Vapour pressure values are taken from the International Critical Tables, and refer to the total vapour pressure of the solution.
Hydrochloric acid
63
Physical properties of hydrochloric acid, such as boiling and melting points, density, and pH, depend on the concentration or molarity of HCl in the aqueous solution. They range from those of water at very low concentrations approaching 0% HCl to values for fuming hydrochloric acid at over 40% HCl.[][][] Hydrochloric acid as the binary (two-component) mixture of HCl and H2O has a constant-boiling azeotrope at 20.2% HCl and 108.6 °C (227 °F). There are four constant-crystallization eutectic points for hydrochloric acid, between the crystal form of HCl·H2O (68% HCl), HCl·2H2O (51% HCl), HCl·3H2O (41% HCl), HCl·6H2O (25% HCl), and ice (0% HCl). There is also a metastable eutectic point at 24.8% between ice and the HCl·3H2O crystallization.[]
Melting temperature as a function of HCl [11][12] concentration in water.
Production
Hydrochloric acid is prepared by dissolving hydrogen chloride in water. Hydrogen chloride can be generated in many ways, and thus several precursors to hydrochloric acid exist. The large-scale production of hydrochloric acid is almost always integrated with the industrial scale production of other chemicals.
Industrial market
Hydrochloric acid is produced in solutions up to 38% HCl (concentrated grade). Higher concentrations up to just over 40% are chemically possible, but the evaporation rate is then so high that storage and handling need extra precautions, such as pressure and low temperature. Bulk industrial-grade is therefore 30% to 34%, optimized for effective transport and limited product loss by HCl vapors. Solutions for household purposes in the US, mostly cleaning, are typically 10% to 12%, with strong recommendations to dilute before use. In the United Kingdom, where it is sold as "Spirits of Salt" for domestic cleaning, the potency is the same as the US industrial grade.[] Major producers worldwide include Dow Chemical at 2 million metric tons annually (2 Mt/year), calculated as HCl gas, and FMC, Georgia Gulf Corporation, Tosoh Corporation, Akzo Nobel, and Tessenderlo at 0.5 to 1.5 Mt/year each. Total world production, for comparison purposes expressed as HCl, is estimated at 20 Mt/year, with 3 Mt/year from direct synthesis, and the rest as secondary product from organic and similar syntheses. By far, most hydrochloric acid is consumed captively by the producer. The open world market size is estimated at 5 Mt/year.[]
Applications
Hydrochloric acid is a strong inorganic acid that is used in many industrial processes. The application often determines the required product quality.[]
Pickling of steel
One of the most important applications of hydrochloric acid is in the pickling of steel, to remove rust or iron oxide scale from iron or steel before subsequent processing, such as extrusion, rolling, galvanizing, and other techniques.[][] Technical quality HCl at typically 18% concentration is the most commonly used pickling agent for the pickling of carbon steel grades. Fe2O3 + Fe + 6 HCl → 3 FeCl2 + 3 H2O The spent acid has long been re-used as iron(II) chloride (also known as ferrous chloride) solutions, but high heavy-metal levels in the pickling liquor have decreased this practice.
Hydrochloric acid The steel pickling industry has developed hydrochloric acid regeneration processes, such as the spray roaster or the fluidized bed HCl regeneration process, which allow the recovery of HCl from spent pickling liquor. The most common regeneration process is the pyrohydrolysis process, applying the following formula:[] By recuperation of the spent acid, a closed acid loop is established.[] The iron(III) oxide by-product of the regeneration process is valuable, used in a variety of secondary industries.[] 4 FeCl2 + 4 H2O + O2 → 8 HCl+ 2 Fe2O3
64
Production of organic compounds
Another major use of hydrochloric acid is in the production of organic compounds, such as vinyl chloride and dichloroethane for PVC. This is often captive use, consuming locally produced hydrochloric acid that never actually reaches the open market. Other organic compounds produced with hydrochloric acid include bisphenol A for polycarbonate, activated carbon, and ascorbic acid, as well as numerous pharmaceutical products.[] 2 CH2=CH2 + 4 HCl + O2 → 2 ClCH2CH2Cl + 2 H2O (dichloroethane by oxychlorination) wood + HCl + heat → activated carbon (chemical activation)
Production of inorganic compounds
Numerous products can be produced with hydrochloric acid in normal acid-base reactions, resulting in inorganic compounds. These include water treatment chemicals such as iron(III) chloride and polyaluminium chloride (PAC). Fe2O3 + 6 HCl → 2 FeCl3 + 3 H2O (iron(III) chloride from magnetite) Both iron(III) chloride and PAC are used as flocculation and coagulation agents in sewage treatment, drinking water production, and paper production. Other inorganic compounds produced with hydrochloric acid include road application salt calcium chloride, nickel(II) chloride for electroplating, and zinc chloride for the galvanizing industry and battery production.[] CaCO3 + 2 HCl → CaCl2 + CO2 + H2O (calcium chloride from limestone)
pH Control and neutralization
Hydrochloric acid can be used to regulate the acidity (pH) of solutions. OH− + HCl → H2O + Cl− In industry demanding purity (food, pharmaceutical, drinking water), high-quality hydrochloric acid is used to control the pH of process water streams. In less-demanding industry, technical quality hydrochloric acid suffices for neutralizing waste streams and swimming pool treatment.[]
Regeneration of ion exchangers
High-quality hydrochloric acid is used in the regeneration of ion exchange resins. Cation exchange is widely used to remove ions such as Na+ and Ca2+ from aqueous solutions, producing demineralized water. The acid is used to rinse the cations from the resins.[] Na+ is replaced with H+ and Ca2+ with 2 H+. Ion exchangers and demineralized water are used in all chemical industries, drinking water production, and many food industries.[]
Hydrochloric acid
65
Other
Hydrochloric acid is used for a large number of small-scale applications, such as leather processing, purification of common salt, household cleaning,[13] and building construction.[] Oil production may be stimulated by injecting hydrochloric acid into the rock formation of an oil well, dissolving a portion of the rock, and creating a large-pore structure. Oil well acidizing is a common process in the North Sea oil production industry.[] Many chemical reactions involving hydrochloric acid are applied in the production of food, food ingredients, and food additives. Typical products include aspartame, fructose, citric acid, lysine, hydrolyzed vegetable protein as food enhancer, and in gelatin production. Food-grade (extra-pure) hydrochloric acid can be applied when needed for the final product.[][]
Presence in living organisms
Gastric acid is one of the main secretions of the stomach. It consists mainly of hydrochloric acid and acidifies the stomach content to a pH of 1 to 2.[] [14] Chloride (Cl−) and hydrogen (H+) ions are secreted separately in the stomach fundus region at the top of the stomach by parietal cells of the gastric mucosa into a secretory network called canaliculi before it enters the stomach lumen.[] Gastric acid acts as a barrier against microorganisms to prevent infections and is important for the digestion of food. Its low pH denatures proteins and thereby makes them susceptible to degradation by digestive enzymes such as pepsin. The low pH also activates the enzyme precursor pepsinogen into the active enzyme pepsin by self-cleavage. After leaving the stomach, the hydrochloric acid of the chyme is neutralized in the duodenum by sodium bicarbonate.[]
Diagram of alkaline mucous layer in stomach with mucosal defense mechanisms
The stomach itself is protected from the strong acid by the secretion of a thick mucus layer, and by secretin induced buffering with sodium bicarbonate. Heartburn or peptic ulcers can develop when these mechanisms fail. Drugs of the antihistaminic and proton pump inhibitor classes can inhibit the production of acid in the stomach, and antacids are used to neutralize existing acid.[][15]
Safety
Hydrochloric acid
66
Concentration Classification[] R-Phrases by weight 10–25% > 25% Irritant (Xi) Corrosive (C) R36/37/38 R34 R37
Concentrated hydrochloric acid (fuming hydrochloric acid) forms acidic mists. Both the mist and the solution have a corrosive effect on human tissue, with the potential to damage respiratory organs, eyes, skin, and intestines irreversibly. Upon mixing hydrochloric acid with common oxidizing chemicals, such as sodium hypochlorite (bleach, NaClO) or potassium permanganate (KMnO4), the toxic gas chlorine is produced. NaClO + 2 HCl → H2O + NaCl + Cl2 2 KMnO4 + 16 HCl → 2 MnCl2 + 8 H2O + 2 KCl + 5 Cl2 Personal protective equipment such as rubber or PVC gloves, protective eye goggles, and chemical-resistant clothing and shoes are used to minimize risks when handling hydrochloric acid. The United States Environmental Protection Agency rates and regulates hydrochloric acid as a toxic substance.[16] The UN number or DOT number is 1789. This number will be displayed on a placard on the container.
References External links
• NIST WebBook, general link (http://webbook.nist.gov/) • Hydrochloric Acid – Part One (http://www.periodicvideos.com/videos/mv_HCl1.htm) and Hydrochloric Acid – Part Two (http://www.periodicvideos.com/videos/mv_HCl2.htm) at The Periodic Table of Videos (University of Nottingham) General safety information • EPA Hazard Summary (http://www.epa.gov/ttn/atw/hlthef/hydrochl.html) • Hydrochloric acid MSDS by Georgia Institute of Technology (http://grover.mirc.gatech.edu/data/msds/50. html) • NIOSH Pocket Guide to Chemical Hazards (http://www.cdc.gov/niosh/npg/npgd0332.html) Pollution information • National Pollutant Inventory – Hydrochloric Acid Fact Sheet (http://www.npi.gov.au/substances/ hydrochloric-acid/index.html)
Human gastrointestinal tract
67
Human gastrointestinal tract
Human gastrointestinal tract (Digestive System)
Stomach colon rectum diagram Latin Tractus digestorius (mouth to anus), canalis alimentarius (esophagus to large Intestine), canalis gastrointestinales (stomach to large Intestine]
System Digestive system
The human gastrointestinal tract is the stomach and intestine,[1] sometimes including all the structures from the mouth to the anus.[2] (The "digestive system" is a broader term that includes other structures, including the accessory organs of digestion).[3] In an adult male human, the gastrointestinal (GI) tract is 5 metres (20 ft) long in a live subject, or up to 9 metres (30 ft) without the effect of muscle tone, and consists of the upper and lower GI tracts. The tract may also be divided into foregut, midgut, and hindgut, reflecting the embryological origin of each segment of the tract. The GI tract always releases hormones to help regulate the digestive process. These hormones, including gastrin, secretin, cholecystokinin, and grehlin, are mediated through either intracrine or autocrine mechanisms, indicating that the cells releasing these hormones are conserved structures throughout evolution.[4]
Human gastrointestinal tract
68
Upper gastrointestinal tract
The upper gastrointestinal tract consists of the esophagus, stomach, and duodenum.[5] The exact demarcation between "upper" and "lower" can vary. Upon dissection, the duodenum may appear to be a unified organ, but it is often divided into two parts based upon function, arterial supply, or embryology.
Lower gastrointestinal tract
The lower gastrointestinal tract includes most of the small intestine and all of the large intestine.[6] According to some sources, it also includes the anus.[citation needed] • Bowel or intestine • Small Intestine: Has three parts: • Duodenum: Here the digestive juices from the pancreas (digestive enzymes) and hormones and the gall bladder (bile) mix. The digestive enzymes break down proteins and bile and emulsify fats into micelles. The duodenum contains Brunner's glands which produce bicarbonate. In combination with bicarbonate from pancreatic juice, this neutralizes HCl of the stomach.
Upper and Lower human gastrointestinal tract
• Jejunum: This is the midsection of the intestine, connecting the duodenum to the ileum. It contains the plicae circulares, and villi to increase the surface area of that part of the GI Tract. Products of digestion (sugars, amino acids, fatty acids) are absorbed into the bloodstream. • Ileum: Has villi and absorbs mainly vitamin B12 and bile acids, as well as any other remaining nutrients. • Large Intestine: Has three parts: • Caecum: The Vermiform appendix is attached to the caecum. • Colon: Includes the ascending colon, transverse colon, descending colon and sigmoid Flexure: The main function of the Colon is to absorb water, but it also contains bacteria that produce beneficial vitamins like vitamin K. • Rectum • Anus: Passes fecal matter from the body. The Ligament of Treitz is sometimes used to divide the upper and lower GI tracts.[]
Human gastrointestinal tract
69
Embryology
The gut is an endoderm-derived structure. At approximately the sixteenth day of human development, the embryo begins to fold ventrally (with the embryo's ventral surface becoming concave) in two directions: the sides of the embryo fold in on each other and the head and tail fold toward one another. The result is that a piece of the yolk sac, an endoderm-lined structure in contact with the ventral aspect of the embryo, begins to be pinched off to become the primitive gut. The yolk sac remains connected to the gut tube via the vitelline duct. Usually this structure regresses during development; in cases where it does not, it is known as Meckel's diverticulum. During fetal life, the primitive gut can be divided into three segments: foregut, midgut, and hindgut. Although these terms are often used in reference to segments of the primitive gut, they are also used regularly to describe components of the definitive gut as well. Each segment of the gut gives rise to specific gut and gut-related structures in later development. Components derived from the gut proper, including the stomach and colon, develop as swellings or dilatations of the primitive gut. In contrast, gut-related derivatives — that is, those structures that derive from the primitive gut but are not part of the gut proper, in general develop as out-pouchings of the primitive gut. The blood vessels supplying these structures remain constant throughout development.[7]
Part Part in adult Gives rise to Esophagus, Stomach, Duodenum (1st and 2nd parts), Liver, Gallbladder, Pancreas, Superior portion of pancreas (Note that though the Spleen is supplied by the celiac trunk, it is derived from dorsal mesentery and therefore not a foregut derivative) lower duodenum, jejunum, ileum, cecum, appendix, ascending colon, and first two-third of the transverse colon last third of the transverse colon, descending colon, rectum, and upper part of the anal canal Arterial supply celiac trunk
Foregut Esophagus to first 2 sections of the duodenum
Midgut
lower duodenum, to the first two-thirds of the transverse colon
branches of the superior mesenteric artery branches of the inferior mesenteric artery
Hindgut last third of the transverse colon, to the upper part of the anal canal
Transit time
The time taken for food or other ingested objects to transit through the gastrointestinal tract varies depending on many factors, but roughly, it takes less than an hour after a meal for 50% of stomach contents to empty into the intestines and total emptying of the stomach takes around 2 hours. Subsequently, 50% emptying of the small intestine takes 1 to 2 hours. Finally, transit through the colon takes 12 to 50 hours with wide variation between individuals.[8] [9]
Pathology
There are a number of diseases and conditions affecting the gastrointestinal system, including: • • • • • • • • • • Appendicitis Cancer Celiac Disease Cholera Colorectal cancer Diarrhoea Diverticulitis Enteric duplication cyst Gastroenteritis, also known as "stomach flu"; an inflammation of the stomach and intestines Giardiasis
Human gastrointestinal tract • • • • • Inflammatory bowel disease (including Crohn's disease and ulcerative colitis) Irritable bowel syndrome Pancreatitis Peptic ulcer disease Yellow Fever
70
Immune function
The gastrointestinal tract is also a prominent part of the immune system.[10] The surface area of the digestive tract is estimated to be the surface area of a football field. With such a large exposure, the immune system must work hard to prevent pathogens from entering into blood and lymph.[11] The low pH (ranging from 1 to 4) of the stomach is fatal for many microorganisms that enter it. Similarly, mucus (containing IgA antibodies) neutralizes many of these microorganisms. Other factors in the GI tract help with immune function as well, including enzymes in saliva and bile. Enzymes such as Cyp3A4, along with the antiporter activities, also are instrumental in the intestine's role of detoxification of antigens and xenobiotics, such as drugs, involved in first pass metabolism. Health-enhancing intestinal bacteria serve to prevent the overgrowth of potentially harmful bacteria in the gut. These two types of bacteria compete for space and "food," as there are limited resources within the intestinal tract. A ratio of 80-85% beneficial to 15-20% potentially harmful bacteria generally is considered normal within the intestines. Microorganisms also are kept at bay by an extensive immune system comprising the gut-associated lymphoid tissue (GALT).
Histology
The gastrointestinal tract has a form of general histology with some differences that reflect the specialization in functional anatomy.[12] The GI tract can be divided into four concentric layers in the following order: • Mucosa • Submucosa • Muscularis externa (the external muscular layer) • Adventitia or serosa
Mucosa
General structure of the gut wall The mucosa is the innermost layer of the gastrointestinal tract. that is surrounding the lumen, or open space within the tube. This layer comes in direct contact with digested food (chyme),
The mucosa is made up of three layers: • Epithelium - innermost layer. Responsible for most digestive, absorptive and secretory processes. • Lamina propria - a layer of connective tissue. Unusually cellular compared to most connective tissue • Muscularis mucosae - a thin layer of smooth muscle. Function is still under debate The mucosae are highly specialized in each organ of the gastrointestinal tract to deal with the different conditions. The most variation is seen in the epithelium. In the esophagus, the epithelium is stratified, squamous and non-keratinising, for protective purposes.
Human gastrointestinal tract In the stomach it is simple columnar, and is organised into gastric pits and glands to deal with secretion. The gastro-oesophageal junction is extremely abrupt. The small intestine epithelium (particularly the ileum) is specialised for absorption; it is organised into plicae circulares and villi, and the enterocytes have microvilli. This creates a brush border which greatly increases the surface area for absoption. The epithelium is simple columnar with microvilli. In the ileum there are occasionally Peyer's patches in the lamina propria. The colon has simple columnar epithelium with no villi. There are goblet cells. The appendix has a mucosa resembling the colon but is heavily infiltrated with lymphocytes. The ano-rectal junction (at the pectinate line) is again very abrupt; there is a transition from simple columnar to stratified squamous non-keratinising epithelium (as in the oesophagus) for protective purposes.
71
Submucosa
The submucosa consists of a dense irregular layer of connective tissue with large blood vessels, lymphatics, and nerves branching into the mucosa and muscularis externa. It contains Meissner's plexus, an enteric nervous plexus, situated on the inner surface of the muscularis externa.
Muscularis externa
The muscularis externa consists of an inner circular layer and a longitudinal outer muscular layer. The circular muscle layer prevents food from traveling backward and the longitudinal layer shortens the tract. The layers are not truly longitudinal or circular, rather the layers of muscle are helical with different pitches. The inner circular is helical with a steep pitch and the outer longitudinal is helical with a much shallower pitch. The coordinated contractions of these layers is called peristalsis and propels the food through the tract. Food in the GI tract is called a bolus (ball of food) from the mouth down to the stomach. After the stomach, the food is partially digested and semi-liquid, and is referred to as chyme. In the large intestine the remaining semi-solid substance is referred to as faeces. Between the two muscle layers are the myenteric or Auerbach's plexus. This controls peristalsis. Activity is initiated by the pacemaker cells (interstitial cells of Cajal). The gut has intrinsic peristaltic activity (basal electrical rhythm) due to its self-contained enteric nervous system. The rate can of course be modulated by the rest of the autonomic nervous system. The thickness of muscularis externa varies in each part of the tract. In the colon, for example, the muscularis externa is much thicker because the faeces are large and heavy, and require more force to push along. The outer longitudinal layer of the colon thins out into 3 discontinuous longitudinal bands, known as tiniae coli (bands of the colon). This is one of the 3 features helping to distinguish between the large and small intestine. Occasionally in the large intestine (2-3 times a day) there will be mass contraction of certain segments, moving a lot of faeces along. This is generally when one gets the urge to defecate. The pylorus of the stomach has a thickened portion of the inner circular layer: the pyloric sphincter. Alone among the GI tract, the stomach has a third layer of muscularis externa. This is the inner oblique layer, and helps churn the chyme in the stomach.
Human gastrointestinal tract
72
Adventitia/serosa
The outermost layer of the GI tract consists of several layers of connective tissue. Intraperitoneal parts of the GI tract are covered with serosa. These include most of the stomach, first part of the duodenum, all of the small intestine, caecum and appendix, transverse colon, sigmoid colon and rectum. In these sections of the gut there is clear boundary between the gut and the surrounding tissue. These parts of the tract have a mesentery. Retroperitoneal parts are covered with adventitia. They blend in to the surrounding tissue and are fixed in position. For example, the retroperitoneal section of the duodenum usually passes through the transpyloric plane. These include the oesophagus, pylorus of the stomach, distal duodenum, ascending colon, descending colon and anal canal. In addition, the oral cavity has adventitia.
References
[4] Nelson RJ. 2005. Introduction to Behavioral Endocrinology. Sinauer Associates: Massachusetts. p 57. [8] Kim SK. Small intestine transit time in the normal small bowel study. American Journal of Roentgenology 1968; 104(3):522-524. [9] (http:/ / www. ncbi. nlm. nih. gov/ pmc/ articles/ PMC3325313/ ) Uday C Ghoshal, Vikas Sengar, and Deepakshi Srivastava. Colonic Transit Study Technique and Interpretation: Can These Be Uniform Globally in Different Populations With Non-uniform Colon Transit Time? J Neurogastroenterol Motil. 2012 April; 18(2): 227–228. [11] Animal Physiology textbook
External links
• • • • Pediatric Overview of Human Digestive System (http://www.pediatricfeeding.org/gi_anatomy.html) Anatomy atlas of the Digestive System (http://www.innerbody.com/image/digeov.html) Overview (http://www.vivo.colostate.edu/hbooks/pathphys/digestion/) at Colorado State University Your Digestive System and How It Works at National Institutes of Health (http://digestive.niddk.nih.gov/ ddiseases/pubs/yrdd/)
Goblet cell
73
Goblet cell
Goblet cell
Section of mucus membrane of human stomach, near the cardiac orifice. X 45. c. Cardiac glands. d. Their ducts. cr. Gland similar to the intestinal glands, with goblet cells. mm. Mucous membrane. m. Muscularis mucosae. m’. Muscular tissue within the mucous membrane.
Transverse section of a villus, from the human intestine. X 350. a. Basement membrane, here somewhat shrunken away from the epithelium. b. Lacteal. c. Columnar epithelium. d. Its striated border. e. Goblet cells. f. Leucocytes in epithelium. f’. Leucocytes below epithelium. g. Blood vessels. h. Muscle cells cut across. Latin Code exocrimohsinocytus caliciformis TH H3.04.03.0.00009; H3.04.03.0.00016 H3.05.00.0.00006
Goblet cells are glandular simple columnar epithelial cells whose function is to secrete mucin, which dissolves in water to form mucus. They use both apocrine and merocrine methods for secretion. The majority of the cell's cytoplasm is occupied by mucinogen granules, except at the bottom. Rough endoplasmic reticulum, mitochondria, the nucleus, and other organelles are concentrated in the basal portion. The apical plasma membrane projects microvilli to increase surface area for secretion. Recent study suggests that glycoprotein is
Goblet cell located inside goblet cells. It is an organ-specific antigen in the gut.
74
Locations
They are found scattered among the epithelial lining of organs, such as the intestinal and respiratory tracts.[1] They are found inside the trachea, bronchus, and larger bronchioles in respiratory tract, small intestines, the colon, and conjunctiva in the upper eyelid.(Goblet cells are the chief source of tear mucus. These occur throughout the conjunctiva, especially the plica semilunaris. These are most dense in nasal conjunctiva, least dense in upper temporal fornix and absent in palpebral mucocutaneous junction and limbus.) They may be an indication of metaplasia, such as in Barrett's esophagus.
Histology
In mucicarmine stains, deep red mucin found within goblet cell bodies. The nuclei of goblet cells tend to be displaced toward the basal end of the cell body, leading to intense basophilic staining.
Etymology
The term goblet refers to these cells' goblet-like shape. The apical portion is shaped like a cup, as it is distended by abundant mucinogen granules; its basal portion is shaped like a stem, as it is narrow for lack of these granules. There are other cells that secrete mucus (as in the foveolar cells of the stomach[2]), but they are not usually called "goblet cells" because they do not have this distinctive shape.
Basal secretion
This is the normal base level secretion of mucus, which is accomplished by cytoskeletal movement of secretory granules.
Stimulated secretion
Secretion may be stimulated by dust, smoke, etc. Other stimuli include viruses, bacteria, etc.
Role in Oral Tolerance
Oral tolerance is the proccess by which the immune system is prevented from responding to antigen derived from food products, as peptides from food may pass into the bloodstream via the gut, which would in theory lead to an immune response. A recent paper published in Nature, has shed some light on the process and implicated goblet cells as having a role in the process.[] It was known that CD103 expressing dendritic cells of the lamina propria had a role to play in the induction of oral tolerance (potentially by inducing the differentiation of regulatory T cells), and this paper suggests that the goblet cells act to preferentially deliver antigen to these CD103+ dendritic cells.[]
Goblet cell
75
References
[2] - Digestive System: Alimentary Canal: fundic stomach, gastric glands, lumen"
Additional images
An intestinal gland from the human intestine.
Goblet cell in ileum
section of mouse intestine. Mucus of goblet cells in blue.
External links
• Histology at KUMC epithel-epith08 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/epithel/ epith08.htm) "Slide 8: Trachea" • Goblet+cell (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=Goblet+cell) at eMedicine Dictionary • Goblet Cells at cvmbs.colostate.edu (http://arbl.cvmbs.colostate.edu/hbooks/pathphys/misc_topics/goblets. html) • Diagram at uwlax.edu (http://bioweb.uwlax.edu/) • Bioweb at UWLAX Zoolab (http://bioweb.uwlax.edu/zoolab/Table_of_Contents/Lab-1b/ Cross_section_of_the_small_int/Goblet_cells/goblet_cells.htm)
Respiratory tract
76
Respiratory tract
In humans the respiratory tract is the part of the anatomy involved with the process of respiration. The respiratory tract is divided into 3 segments: • Upper respiratory tract: nose and nasal passages, paranasal sinuses, and throat or pharynx • Respiratory airways: voice box or larynx, trachea, bronchi, and bronchioles • Lungs: respiratory bronchioles, alveolar ducts, alveolar sacs, and alveoli The respiratory tract is a common site for infections. Upper respiratory tract infections are probably the most common infections in the world. Most of the respiratory tract exists merely as a piping system for air to travel in the lungs, and alveoli are the only part of the lung that exchanges oxygen and carbon dioxide with the blood. Moving down the respiratory tract starting at the trachea, the tubes get smaller and divide into more and more tubes. There are estimated to be about 20 to 23 divisions, ending up at an alveolus. Even though the cross-sectional area of each bronchus or bronchiole is smaller, because there are so many, the total surface area is larger. This means there is less resistance at the terminal bronchioles. (Most resistance is around the 3-4 division from the trachea due to turbulence.)
General histology
The respiratory tract is covered in an epithelium, the type of which varies down the tract. There are glands and mucus produced by goblet cells in parts, as well as smooth muscle, elastin or cartilage. Most of the epithelium (from the nose to the bronchi) is covered in pseudostratified columnar ciliated epithelial cells, commonly called respiratory epithelium. The cilia beat in one direction, moving mucus towards the throat where it is swallowed. Moving down the bronchioles, the cells get more cuboidal in shape but are still ciliated. Cartilage is present until the small bronchi. In the trachea they are C-shaped rings, whereas in the bronchi they are interspersed plates.
This image compares the histological differences along the respiratory tract.
Glands are abundant in the upper respiratory tract, but there are fewer lower down and they are absent starting at the bronchioles. The same goes for goblet cells, although there are scattered ones in the first bronchioles. Smooth muscle starts in the trachea, where it joins the C-shaped rings of cartilage. It continues down the bronchi and bronchioles, which it completely encircles. Instead of hard cartilage, the bronchi and bronchioles are composed of elastic tissue.
Respiratory tract
77
References
• Syllabus: Infectious Diseases (http://www.kcom.edu/faculty/chamberlain/Website/lectures/syllabi3.htm) see Respiratory Tract Infections by Neal Chamberlain, PhD. Kirksville College of Osteopathic Medicine, Missouri, USA
Mucus
In vertebrates, mucus (adjectival form: "mucous") is a slippery secretion produced by, and covering, mucous membranes. Mucous fluid is typically produced from cells found in mucous glands. Mucous cells secrete products that are rich in glycoproteins and water. Mucous fluid may also originate from mixed glands, which contain both serous and mucous cells. It is a viscous colloid containing antiseptic enzymes (such as lysozyme), immunoglobulins, inorganic salts, proteins such as lactoferrin,[1] and glycoproteins known as mucins that are produced by goblet cells in the mucous membranes and submucosal glands. This mucus serves to protect epithelial cells (the lining of the tubes) in the respiratory, gastrointestinal, urogenital, visual, and auditory systems in mammals; the epidermis in amphibians; and the gills in fish. A major Mucous cells on the stomach lining function of this mucus is to protect against infectious agents such as fungi, bacteria and viruses. The average human body produces about a litre of mucus per day.[2] Bony fish, hagfish, snails, slugs, and some other invertebrates also produce external mucus. In addition to serving a protective function against infectious agents, such mucus provides protection against toxins produced by predators, can facilitate movement and may play a role in communication. The rest of this article is devoted entirely to mucus production and function in humans.
Respiratory system
In the human respiratory system, mucus aids in the protection of the lungs by trapping foreign particles that enter it, in particular, through the nose, during normal breathing. "Phlegm" is a specialized term for mucus that is restricted to the respiratory tract, whereas the term "nasal mucus" describes secretions of the nasal passages. Nasal mucus is produced by the nasal mucosa; and mucosal tissues lining the airways (trachea, bronchus, bronchioles) is produced by specialized airway epithelial cells (goblet cells) and submucosal glands. Small particles such as dust, particulate pollutants, and allergens, as well as infectious agents bacteria are caught in the viscous nasal or airway mucus and prevented from entering the system. This event along with the continual movement of the respiratory mucus layer toward the oropharynx, helps prevent foreign objects from entering the lungs during breathing. This explains why coughing often occurs in those who smoke filtered cigarettes. The body's natural reaction is to increase mucus production. In addition, mucus aids in moisturizing the inhaled air and prevents tissues such as the nasal and airway epithelia from drying out.[] Nasal and airway mucus is produced continuously, with most of it swallowed unconsciously, even when it is dried.[] Increased mucus production in the respiratory tract is a symptom of many common illnesses, such as the common cold and influenza. Hypersecretion of mucus can occur in inflammatory respiratory diseases such as respiratory allergies, asthma, and chronic bronchitis.[] The presence of mucus in the nose and throat is normal, but increased quantities can impede comfortable breathing and must be cleared by blowing the nose or expectorating phlegm from the throat.
Mucus
78
Diseases involving mucus
In general, nasal mucus is clear and thin, serving to filter air during inhalation. During times of infection, mucus can change color to yellow or green either as a result of trapped bacteria[3] or due to the body's reaction to viral infection.[4] The green color of mucus comes from the heme group in the iron-containing enzyme myeloperoxidase secreted by white blood cells as a cytotoxic defense during a respiratory burst. In the case of bacterial infection, the bacterium becomes trapped in already-clogged sinuses, breeding in the moist, nutrient-rich environment. Sinusitis is an uncomfortable condition which may include congestion of mucus. A bacterial infection in sinusitis will cause discolored mucus and would respond to antibiotic treatment; viral infections typically resolve without treatment.[5] Almost all sinusitis infections are viral and antibiotics are ineffective and not recommended for treating typical cases.[6] In the case of a viral infection such as cold or flu, the first stage and also the last stage of the infection cause the production of a clear, thin mucus in the nose or back of the throat. As the body begins to react to the virus (generally one to three days), mucus thickens and may turn yellow or green. Viral infections cannot be treated with antibiotics, and are a major avenue for their misuse. Treatment is generally symptom-based; often it is sufficient to allow the immune system to fight off the virus over time.[7] Cystic fibrosis Cystic fibrosis is an inherited disease that affects the entire body, but symptoms begin mostly in the lungs with extremely viscous (thick) production of mucus that is difficult to expel. Mucus as a medical symptom Increased mucus production in the upper respiratory tract is a symptom of many common ailments, such as the common cold. Nasal mucus may be removed by blowing the nose or by using nasal irrigation. Excess nasal mucus, as with a cold or allergies may be treated cautiously with decongestant medications. Excess mucus production in the bronchi and bronchioles, as may occur in asthma, bronchitis or influenza, may be treated with anti-inflammatory medications as a means of reducing the airway inflammation, which triggers mucus over-production. Thickening of mucus as a "rebound" effect following overuse of decongestants may produce nasal or sinus drainage problems and circumstances that promote infection.
Cold weather and mucus
During cold weather, the cilia, which normally sweep mucus away from the nostrils and toward the back of the throat (see respiratory epithelium), become sluggish or completely cease functioning. This results in mucus running down the nose and dripping (a runny nose).Template:Citation neeeded Mucus also thickens in cold weather; when an individual comes in from the cold, the mucus thaws and begins to run before the cilia begin to work again.Template:Citation neeeded
Mucus
79
Digestive system
In the human digestive system, mucus is used as a lubricant for materials that must pass over membranes, e.g., food passing down the esophagus. A layer of mucus along the inner walls of the stomach is vital to protect the cell linings of that organ from the highly acidic environment within it.[] Mucus is not digested in the intestinal tract. Mucus is also secreted from glands within the rectum due to stimulation of the mucous membrane within. [citation needed]
Reproductive system
In the human female reproductive system, cervical mucus prevents infection. The consistency of cervical mucus varies depending on the stage of a woman's menstrual cycle. At ovulation cervical mucus is clear, runny, and conducive to sperm; post-ovulation, mucus becomes thicker and is more likely to block sperm.[citation needed] In the human male reproductive system, the seminal vesicles contribute up to 100% of the total volume of the semen and contain mucus, amino acids, prostaglandins, vitamin C, and fructose as the main energy source for the sperm.[citation needed]
Notes References
Enzyme
Enzymes (pron.: /ˈɛnzaɪmz/) are large biological molecules responsible for the thousands of chemical interconversions that sustain life.[1][2] They are highly selective catalysts, greatly accelerating both the rate and specificity of metabolic reactions, from the digestion of food to the synthesis of DNA. Most enzymes are proteins, although some catalytic RNA molecules have been identified. Enzymes adopt a specific three-dimensional structure, and may employ organic (e.g. biotin) and inorganic (e.g. magnesium ion) cofactors to assist in catalysis. In enzymatic reactions, the molecules at the beginning of the process, called substrates, Human glyoxalase I. Two zinc ions that are needed for the enzyme to catalyze its are converted into different molecules, reaction are shown as purple spheres, and an enzyme inhibitor called called products. Almost all chemical S-hexylglutathione is shown as a space-filling model, filling the two active sites. reactions in a biological cell need enzymes in order to occur at rates sufficient for life. Since enzymes are selective for their substrates and speed up only a few reactions from among many possibilities, the set of enzymes made in a cell determines which metabolic pathways occur in that cell.
Enzyme Like all catalysts, enzymes work by lowering the activation energy (Ea‡) for a reaction, thus dramatically increasing the rate of the reaction. As a result, products are formed faster and reactions reach their equilibrium state more rapidly. Most enzyme reaction rates are millions of times faster than those of comparable un-catalyzed reactions. As with all catalysts, enzymes are not consumed by the reactions they catalyze, nor do they alter the equilibrium of these reactions. However, enzymes do differ from most other catalysts in that they are highly specific for their substrates. Enzymes are known to catalyze about 4,000 biochemical reactions.[3] A few RNA molecules called ribozymes also catalyze reactions, with an important example being some parts of the ribosome.[4][5] Synthetic molecules called artificial enzymes also display enzyme-like catalysis.[6] Enzyme activity can be affected by other molecules. Inhibitors are molecules that decrease enzyme activity; activators are molecules that increase activity. Many drugs and poisons are enzyme inhibitors. Activity is also affected by temperature, pressure, chemical environment (e.g., pH), and the concentration of substrate. Some enzymes are used commercially, for example, in the synthesis of antibiotics. In addition, some household products use enzymes to speed up biochemical reactions (e.g., enzymes in biological washing powders break down protein or fat stains on clothes; enzymes in meat tenderizers break down proteins into smaller molecules, making the meat easier to chew).
80
Etymology and history
As early as the late 17th and early 18th centuries, the digestion of meat by stomach secretions[] and the conversion of starch to sugars by plant extracts and saliva were known. However, the mechanism by which this occurred had not been identified.[7] In 1833, French chemist Anselme Payen discovered the first enzyme, diastase. A few decades later, when studying the fermentation of sugar to alcohol by yeast, Louis Pasteur came to the conclusion that this fermentation was catalyzed by a vital force contained within the yeast cells called "ferments", which were thought to function only within living organisms. He wrote that "alcoholic fermentation is an act correlated with the life and organization of the yeast cells, not with the death or putrefaction of the cells."[8] In 1877, German physiologist Wilhelm Kühne (1837–1900) first used the term enzyme, which comes from Greek ενζυμον, "in leaven", to describe this process.[9] The word enzyme was used later to refer to nonliving substances such as pepsin, and the word ferment was used to refer to chemical activity produced by living organisms. In 1897, Eduard Buchner submitted his first paper on the ability of yeast extracts that lacked any living yeast cells to ferment sugar. In a series of experiments at the University of Berlin, he found that the sugar was fermented even when there were no living yeast cells in the mixture.[10] He named the enzyme that brought about the fermentation of sucrose "zymase".[11] In 1907, he received the Nobel Prize in Chemistry "for his biochemical research and his discovery of cell-free fermentation". Following Buchner's example, enzymes are usually named according to the reaction they carry out. Typically, to generate the name of an enzyme, the suffix -ase is added to the name of its substrate (e.g., lactase is the enzyme that cleaves lactose) or the type of reaction (e.g., DNA polymerase forms DNA polymers).[12] Having shown that enzymes could function outside a living cell, the next step was to determine their biochemical nature. Many early workers noted that enzymatic activity was associated with proteins, but several scientists (such as Nobel laureate Richard Willstätter) argued that proteins were merely carriers for the true enzymes and that proteins per se were incapable of catalysis.[13] However, in 1926, James B. Sumner showed that the enzyme urease was a pure protein and crystallized it; Sumner did likewise for the enzyme catalase in 1937. The conclusion that pure proteins can be enzymes was definitively proved by Northrop and Stanley, who worked on the digestive enzymes pepsin (1930), trypsin and chymotrypsin. These three scientists were awarded the 1946 Nobel Prize in Chemistry.[14] This discovery that enzymes could be crystallized eventually allowed their structures to be solved by x-ray crystallography. This was first done for lysozyme, an enzyme found in tears, saliva and egg whites that digests the coating of some bacteria; the structure was solved by a group led by David Chilton Phillips and published in
Enzyme 1965.[15] This high-resolution structure of lysozyme marked the beginning of the field of structural biology and the effort to understand how enzymes work at an atomic level of detail.
81
Structures and mechanisms
Enzymes are in general globular proteins and range from just 62 amino acid residues in size, for the monomer of 4-oxalocrotonate tautomerase,[16] to over 2,500 residues in the animal fatty acid synthase.[17] A small number of RNA-based biological catalysts exist, with the most common being the ribosome; these are referred to as either RNA-enzymes or ribozymes. The activities of enzymes are determined by their three-dimensional structure.[18] However, although structure does determine function, predicting a novel enzyme's activity just from its structure is a very difficult problem that has not yet been solved.[19] Most enzymes are much larger than the substrates they act on, and only a small Ribbon diagram showing human carbonic anhydrase II. The grey sphere is the zinc [16] portion of the enzyme (around 2–4 amino cofactor in the active site. Diagram drawn from PDB 1MOO . [20] acids) is directly involved in catalysis. The region that contains these catalytic residues, binds the substrate, and then carries out the reaction is known as the active site. Enzymes can also contain sites that bind cofactors, which are needed for catalysis. Some enzymes also have binding sites for small molecules, which are often direct or indirect products or substrates of the reaction catalyzed. This binding can serve to increase or decrease the enzyme's activity, providing a means for feedback regulation. Like all proteins, enzymes are long, linear chains of amino acids that fold to produce a three-dimensional product. Each unique amino acid sequence produces a specific structure, which has unique properties. Individual protein chains may sometimes group together to form a protein complex. Most enzymes can be denatured—that is, unfolded and inactivated—by heating or chemical denaturants, which disrupt the three-dimensional structure of the protein. Depending on the enzyme, denaturation may be reversible or irreversible. Structures of enzymes with substrates or substrate analogs during a reaction may be obtained using Time resolved crystallography methods.
Enzyme
82
Specificity
Enzymes are usually very specific as to which reactions they catalyze and the substrates that are involved in these reactions. Complementary shape, charge and hydrophilic/hydrophobic characteristics of enzymes and substrates are responsible for this specificity. Enzymes can also show impressive levels of stereospecificity, regioselectivity and chemoselectivity.[21] Some of the enzymes showing the highest specificity and accuracy are involved in the copying and expression of the genome. These enzymes have "proof-reading" mechanisms. Here, an enzyme such as DNA polymerase catalyzes a reaction in a first step and then checks that the product is correct in a second step.[22] This two-step process results in average error rates of less than 1 error in 100 million reactions in high-fidelity mammalian polymerases.[23] Similar proofreading mechanisms are also found in RNA polymerase,[24] aminoacyl tRNA synthetases[25] and ribosomes.[26] Some enzymes that produce secondary metabolites are described as promiscuous, as they can act on a relatively broad range of different substrates. It has been suggested that this broad substrate specificity is important for the evolution of new biosynthetic pathways.[27] "Lock and key" model Enzymes are very specific, and it was suggested by the Nobel laureate organic chemist Emil Fischer in 1894 that this was because both the enzyme and the substrate possess specific complementary geometric shapes that fit exactly into one another.[28] This is often referred to as "the lock and key" model. However, while this model explains enzyme specificity, it fails to explain the stabilization of the transition state that enzymes achieve. In 1958, Daniel Koshland suggested a modification to the lock and key model: since enzymes are rather flexible structures, the active site is continuously reshaped by interactions with the substrate as the substrate interacts with the enzyme.[29] As a result, the substrate does not simply bind to a rigid active site; the amino Diagrams to show the induced fit hypothesis of enzyme action acid side-chains that make up the active site are molded into the precise positions that enable the enzyme to perform its catalytic function. In some cases, such as glycosidases, the substrate molecule also changes shape slightly as it enters the active site.[30] The active site continues to change until the substrate is completely bound, at which point the final shape and charge is determined.[31] Induced fit may enhance the fidelity of molecular recognition in the presence of competition and noise via the conformational proofreading mechanism.[32]
Mechanisms
Enzymes can act in several ways, all of which lower ΔG‡ (Gibbs energy):[33] • Lowering the activation energy by creating an environment in which the transition state is stabilized (e.g. straining the shape of a substrate—by binding the transition-state conformation of the substrate/product molecules, the enzyme distorts the bound substrate(s) into their transition state form, thereby reducing the amount of energy required to complete the transition). • Lowering the energy of the transition state, but without distorting the substrate, by creating an environment with the opposite charge distribution to that of the transition state. • Providing an alternative pathway. For example, temporarily reacting with the substrate to form an intermediate ES complex, which would be impossible in the absence of the enzyme.
Enzyme • Reducing the reaction entropy change by bringing substrates together in the correct orientation to react. Considering ΔH‡ alone overlooks this effect. • Increases in temperatures speed up reactions. Thus, temperature increases help the enzyme function and develop the end product even faster. However, if heated too much, the enzyme's shape deteriorates and the enzyme becomes denatured. Some enzymes like thermolabile enzymes work best at low temperatures. It is interesting that this entropic effect involves destabilization of the ground state,[34] and its contribution to catalysis is relatively small.[35] Transition state stabilization The understanding of the origin of the reduction of ΔG‡ requires one to find out how the enzymes can stabilize its transition state more than the transition state of the uncatalyzed reaction. It seems that the most effective way for reaching large stabilization is the use of electrostatic effects, in particular, when having a relatively fixed polar environment that is oriented toward the charge distribution of the transition state.[36] Such an environment does not exist in the uncatalyzed reaction in water. Dynamics and function The internal dynamics of enzymes has been suggested to be linked with their mechanism of catalysis.[37][38][39] Internal dynamics are the movement of parts of the enzyme's structure, such as individual amino acid residues, a group of amino acids, or even an entire protein domain. These movements occur at various time-scales ranging from femtoseconds to seconds. Networks of protein residues throughout an enzyme's structure can contribute to catalysis through dynamic motions.[40][41][42][43] This is simply seen in the kinetic scheme of the combined process, enzymatic activity and dynamics; this scheme can have several independent Michaelis-Menten-like reaction pathways that are connected through fluctuation rates.[][][] Protein motions are vital to many enzymes, but whether small and fast vibrations, or larger and slower conformational movements are more important depends on the type of reaction involved. However, although these movements are important in binding and releasing substrates and products, it is not clear if protein movements help to accelerate the chemical steps in enzymatic reactions.[44] These new insights also have implications in understanding allosteric effects and developing new medicines.
83
Allosteric modulation
Allosteric sites are sites on the enzyme that bind to molecules in the cellular environment. The sites form weak, noncovalent bonds with these molecules, causing a change in the conformation of the enzyme. This change in conformation translates to the active site, which then affects the reaction rate of the enzyme.[45] Allosteric interactions can both inhibit and activate enzymes and are a common way that enzymes are controlled in the body.[46]
Allosteric transition of an enzyme between R and T states, stabilized by an agonist, an inhibitor and a substrate (the MWC model)
Cofactors and coenzymes
Enzyme
84
Cofactors
Some enzymes do not need any additional components to show full activity. However, others require non-protein molecules called cofactors to be bound for activity.[47] Cofactors can be either inorganic (e.g., metal ions and iron-sulfur clusters) or organic compounds (e.g., flavin and heme). Organic cofactors can be either prosthetic groups, which are tightly bound to an enzyme, or coenzymes, which are released from the enzyme's active site during the reaction. Coenzymes include NADH, NADPH and adenosine triphosphate. These molecules transfer chemical groups between enzymes.[48] An example of an enzyme that contains a cofactor is carbonic anhydrase, and is shown in the ribbon diagram above with a zinc cofactor bound as part of its active site.[49] These tightly bound molecules are usually found in the active site and are involved in catalysis. For example, flavin and heme cofactors are often involved in redox reactions. Enzymes that require a cofactor but do not have one bound are called apoenzymes or apoproteins. An apoenzyme together with its cofactor(s) is called a holoenzyme (this is the active form). Most cofactors are not covalently attached to an enzyme, but are very tightly bound. However, organic prosthetic groups can be covalently bound (e.g., biotin in the enzyme pyruvate carboxylase). The term "holoenzyme" can also be applied to enzymes that contain multiple protein subunits, such as the DNA polymerases; here the holoenzyme is the complete complex containing all the subunits needed for activity.
Coenzymes
Coenzymes are small organic molecules that can be loosely or tightly bound to an enzyme. Tightly bound coenzymes can be called prosthetic groups. Coenzymes transport chemical groups from one enzyme to another.[50] Some of these chemicals such as riboflavin, thiamine and folic acid are vitamins (compounds that cannot be synthesized by the body and must be acquired from the diet). The chemical groups carried include the hydride ion (H-) carried by NAD or NADP+, the phosphate group carried by adenosine triphosphate, the acetyl group carried by coenzyme A, formyl, methenyl or methyl groups carried by folic acid and the methyl group carried by S-adenosylmethionine. Since coenzymes are chemically changed as a consequence of enzyme action, it is useful to consider coenzymes to be a special class of substrates, or second substrates, which are common to many different enzymes. For example, about 700 enzymes are known to use the coenzyme NADH.[51]
Space-filling model of the coenzyme NADH
Coenzymes are usually continuously regenerated and their concentrations maintained at a steady level inside the cell: for example, NADPH is regenerated through the pentose phosphate pathway and S-adenosylmethionine by methionine adenosyltransferase. This continuous regeneration means that even small amounts of coenzymes are used very intensively. For example, the human body turns over its own weight in ATP each day.[52]
Enzyme
85
Thermodynamics
As all catalysts, enzymes do not alter the position of the chemical equilibrium of the reaction. Usually, in the presence of an enzyme, the reaction runs in the same direction as it would without the enzyme, just more quickly. However, in the absence of the enzyme, other possible uncatalyzed, "spontaneous" reactions might lead to different products, because in those conditions this different product is formed faster. Furthermore, enzymes can couple two or more reactions, so that a thermodynamically favorable reaction can be used to "drive" a thermodynamically unfavorable one. For example, the hydrolysis of ATP is often used to drive other chemical reactions.[]
The energies of the stages of a chemical reaction. Substrates need a lot of potential energy to reach a transition state, which then decays into products. The enzyme stabilizes the transition state, reducing the energy needed to form products.
Enzymes catalyze the forward and backward reactions equally. They do not alter the equilibrium itself, but only the speed at which it is reached. For example, carbonic anhydrase catalyzes its reaction in either direction depending on the concentration of its reactants. (in tissues; high CO2 concentration) (in lungs; low CO2 concentration) Nevertheless, if the equilibrium is greatly displaced in one direction, that is, in a very exergonic reaction, the reaction is in effect irreversible. Under these conditions, the enzyme will, in fact, catalyze the reaction only in the thermodynamically allowed direction.
Kinetics
Enzyme kinetics is the investigation of how enzymes bind substrates and turn them into products. The rate data used in kinetic analyses are commonly obtained from enzyme assays, where since the 90s, the dynamics of many enzymes are studied on the level of individual molecules. In 1902 Victor Henri proposed a quantitative theory of enzyme kinetics,[53] but his experimental data were not useful because the significance of the hydrogen ion concentration was not yet appreciated. After Peter Lauritz Sørensen had defined the logarithmic pH-scale and introduced the concept of buffering in 1909[54] the German chemist Leonor Michaelis and his Canadian postdoc Maud Leonora Menten repeated Henri's experiments and confirmed his equation, which is referred to as Henri-Michaelis-Menten kinetics (termed also Michaelis-Menten kinetics).[55] Their work was further developed by G. E. Briggs and J. B. S. Haldane, who derived kinetic equations that are still widely considered today a starting point in solving enzymatic activity.[56]
Mechanism for a single substrate enzyme catalyzed reaction. The enzyme (E) binds a substrate (S) and produces a product (P).
Enzyme The major contribution of Henri was to think of enzyme reactions in two stages. In the first, the substrate binds reversibly to the enzyme, forming the enzyme-substrate complex. This is sometimes called the Michaelis complex. The enzyme then catalyzes the chemical step in the reaction and releases the product. Note that the simple Michaelis Menten mechanism for the enzymatic activity is considered today a basic idea, where many examples show that the enzymatic activity involves structural dynamics. This is incorporated in the enzymatic mechanism while introducing several Michaelis Menten pathways that are connected with fluctuating rates.[][][] Nevertheless, there is a mathematical relation connecting the behavior obtained from the basic Michaelis Menten mechanism (that was indeed proved correct in many experiments) with the generalized Michaelis Menten mechanisms involving dynamics and activity; [] this means that the measured activity of enzymes on the level of many enzymes may be explained with the simple Michaelis-Menten equation, yet, the actual activity of enzymes is richer and involves structural dynamics. Enzymes can catalyze up to several million reactions per second. For example, the uncatalyzed decarboxylation of orotidine 5'-monophosphate has a half life of 78 million years. However, when the enzyme orotidine 5'-phosphate decarboxylase is added, the same process takes just 25 milliseconds.[57] Enzyme rates depend on solution conditions and substrate concentration. Conditions that denature the protein abolish enzyme activity, such as high temperatures, extremes of pH or high salt concentrations, while raising substrate concentration tends to increase activity Saturation curve for an enzyme reaction showing the relation between the substrate concentration (S) and rate (v) when [S] is low. To find the maximum speed of an enzymatic reaction, the substrate concentration is increased until a constant rate of product formation is seen. This is shown in the saturation curve on the right. Saturation happens because, as substrate concentration increases, more and more of the free enzyme is converted into the substrate-bound ES form. At the maximum reaction rate (Vmax) of the enzyme, all the enzyme active sites are bound to substrate, and the amount of ES complex is the same as the total amount of enzyme. However, Vmax is only one kinetic constant of enzymes. The amount of substrate needed to achieve a given rate of reaction is also important. This is given by the Michaelis-Menten constant (Km), which is the substrate concentration required for an enzyme to reach one-half its maximum reaction rate. Each enzyme has a characteristic Km for a given substrate, and this can show how tight the binding of the substrate is to the enzyme. Another useful constant is kcat, which is the number of substrate molecules handled by one active site per second. The efficiency of an enzyme can be expressed in terms of kcat/Km. This is also called the specificity constant and incorporates the rate constants for all steps in the reaction. Because the specificity constant reflects both affinity and catalytic ability, it is useful for comparing different enzymes against each other, or the same enzyme with different substrates. The theoretical maximum for the specificity constant is called the diffusion limit and is about 108 to 109 (M−1 s−1). At this point every collision of the enzyme with its substrate will result in catalysis, and the rate of product formation is not limited by the reaction rate but by the diffusion rate. Enzymes with this property are called catalytically perfect or kinetically perfect. Example of such enzymes are triose-phosphate isomerase, carbonic anhydrase, acetylcholinesterase, catalase, fumarase, β-lactamase, and superoxide dismutase. Michaelis-Menten kinetics relies on the law of mass action, which is derived from the assumptions of free diffusion and thermodynamically driven random collision. However, many biochemical or cellular processes deviate
86
Enzyme significantly from these conditions, because of macromolecular crowding, phase-separation of the enzyme/substrate/product, or one or two-dimensional molecular movement.[58] In these situations, a fractal Michaelis-Menten kinetics may be applied.[59][60][61][62] Some enzymes operate with kinetics, which are faster than diffusion rates, which would seem to be impossible. Several mechanisms have been invoked to explain this phenomenon. Some proteins are believed to accelerate catalysis by drawing their substrate in and pre-orienting them by using dipolar electric fields. Other models invoke a quantum-mechanical tunneling explanation, whereby a proton or an electron can tunnel through activation barriers, although for proton tunneling this model remains somewhat controversial.[63][64] Quantum tunneling for protons has been observed in tryptamine.[65] This suggests that enzyme catalysis may be more accurately characterized as "through the barrier" rather than the traditional model, which requires substrates to go "over" a lowered energy barrier.
87
Inhibition
Enzyme reaction rates can be decreased by various types of enzyme inhibitors. Competitive inhibition In competitive inhibition, the inhibitor and substrate compete for the enzyme (i.e., they can not bind at the same time).[67] Often competitive inhibitors strongly resemble the real substrate of the enzyme. For example, methotrexate is a competitive inhibitor of the enzyme dihydrofolate reductase, which catalyzes the reduction of dihydrofolate to tetrahydrofolate. The Competitive inhibitors bind reversibly to the enzyme, preventing the binding of substrate. similarity between the structures of On the other hand, binding of substrate prevents binding of the inhibitor. Substrate and folic acid and this drug are shown in inhibitor compete for the enzyme. the figure to the right bottom. In some cases, the inhibitor can bind to a site other than the binding-site of the usual substrate and exert an allosteric effect to change the shape of the usual binding-site. For example, strychnine acts as an allosteric inhibitor of the glycine receptor in the mammalian spinal cord and brain stem. Glycine is a major post-synaptic inhibitory neurotransmitter with a specific receptor site. Strychnine binds to an alternate site that reduces the affinity of the glycine receptor for glycine, resulting in convulsions due to
Enzyme lessened inhibition by the glycine.[68] In competitive inhibition the maximal rate of the reaction is not changed, but higher substrate concentrations are required to reach a given maximum rate, increasing the apparent Km. Uncompetitive inhibition In uncompetitive inhibition, the inhibitor cannot bind to the free enzyme, only to the ES-complex. The EIS-complex thus formed is enzymatically inactive. This type of inhibition is rare, but may occur in multimeric enzymes. Non-competitive inhibition Non-competitive inhibitors can bind to the enzyme at the binding site at the same time as the substrate,but not to the active site. Both the EI and EIS complexes are enzymatically inactive. Because the inhibitor can not be driven from the enzyme by higher substrate concentration (in contrast to competitive inhibition), the apparent Vmax changes. But because the substrate can still bind to the enzyme, the Km stays the same.
88
Types of inhibition. This classification was introduced by W.W. Cleland.
[66]
Mixed inhibition This type of inhibition resembles the non-competitive, except that the EIS-complex has residual enzymatic activity.This type of inhibitor does not follow Michaelis-Menten equation. In many organisms, inhibitors may act as part of a feedback mechanism. If an enzyme produces too much of one substance in the organism, that substance may act as an inhibitor for the enzyme at the beginning of the pathway that produces it, causing production of the substance to slow down or stop when there is sufficient amount. This is a form of negative feedback. Enzymes that are subject to this form of regulation are often multimeric and have allosteric binding sites for regulatory substances. Their substrate/velocity plots are not hyperbolar, but sigmoidal (S-shaped). Irreversible inhibitors react with the enzyme and form a covalent adduct with the protein. The inactivation is irreversible. These compounds include eflornithine a drug used to treat the parasitic disease sleeping sickness.[] Penicillin and Aspirin also act in this The coenzyme folic acid (left) and the anti-cancer drug methotrexate (right) are very manner. With these drugs, the similar in structure. As a result, methotrexate is a competitive inhibitor of many enzymes that use folates. compound is bound in the active site and the enzyme then converts the inhibitor into an activated form that reacts irreversibly with one or more amino acid residues. Uses of inhibitors
Enzyme Since inhibitors modulate the function of enzymes they are often used as drugs. A common example of an inhibitor that is used as a drug is aspirin, which inhibits the COX-1 and COX-2 enzymes that produce the inflammation messenger prostaglandin, thus suppressing pain and inflammation. However, other enzyme inhibitors are poisons. For example, the poison cyanide is an irreversible enzyme inhibitor that combines with the copper and iron in the active site of the enzyme cytochrome c oxidase and blocks cellular respiration.[69]
89
Biological function
Enzymes serve a wide variety of functions inside living organisms. They are indispensable for signal transduction and cell regulation, often via kinases and phosphatases.[70] They also generate movement, with myosin hydrolyzing ATP to generate muscle contraction and also moving cargo around the cell as part of the cytoskeleton.[71] Other ATPases in the cell membrane are ion pumps involved in active transport. Enzymes are also involved in more exotic functions, such as luciferase generating light in fireflies.[72] Viruses can also contain enzymes for infecting cells, such as the HIV integrase and reverse transcriptase, or for viral release from cells, like the influenza virus neuraminidase. An important function of enzymes is in the digestive systems of animals. Enzymes such as amylases and proteases break down large molecules (starch or proteins, respectively) into smaller ones, so they can be absorbed by the intestines. Starch molecules, for example, are too large to be absorbed from the intestine, but enzymes hydrolyze the starch chains into smaller molecules such as maltose and eventually glucose, which can then be absorbed. Different enzymes digest different food substances. In ruminants, which have herbivorous diets, microorganisms in the gut produce another enzyme, cellulase, to break down the cellulose cell walls of plant fiber.[73] Several enzymes can work together in a specific order, creating metabolic pathways. In a metabolic pathway, one enzyme takes the product of another enzyme as a substrate. After the catalytic reaction, the product is then passed on to another enzyme. Sometimes more than one enzyme can catalyze the same reaction in parallel; this can allow more complex regulation: with, for example, a low constant activity provided by one
Glycolytic enzymes and their functions in the metabolic pathway of glycolysis
enzyme but an inducible high activity from a second enzyme. Enzymes determine what steps occur in these pathways. Without enzymes, metabolism would neither progress through the same steps nor be fast enough to serve the needs of the cell. Indeed, a metabolic pathway such as glycolysis could not exist independently of enzymes. Glucose, for example, can react directly with ATP to become phosphorylated at one or more of its carbons. In the absence of enzymes, this occurs so slowly as to be insignificant. However, if hexokinase is added, these slow reactions continue to take place except that phosphorylation at carbon 6 occurs so rapidly that, if the mixture is tested a short time later, glucose-6-phosphate is found to be the only significant product. As a consequence, the network of metabolic pathways within each cell depends on the set of functional enzymes that are present.
Enzyme
90
Control of activity
There are five main ways that enzyme activity is controlled in the cell. 1. Enzyme production (transcription and translation of enzyme genes) can be enhanced or diminished by a cell in response to changes in the cell's environment. This form of gene regulation is called enzyme induction and inhibition. For example, bacteria may become resistant to antibiotics such as penicillin because enzymes called beta-lactamases are induced that hydrolyze the crucial beta-lactam ring within the penicillin molecule. Another example are enzymes in the liver called cytochrome P450 oxidases, which are important in drug metabolism. Induction or inhibition of these enzymes can cause drug interactions. 2. Enzymes can be compartmentalized, with different metabolic pathways occurring in different cellular compartments. For example, fatty acids are synthesized by one set of enzymes in the cytosol, endoplasmic reticulum and the Golgi apparatus and used by a different set of enzymes as a source of energy in the mitochondrion, through β-oxidation.[74] 3. Enzymes can be regulated by inhibitors and activators. For example, the end product(s) of a metabolic pathway are often inhibitors for one of the first enzymes of the pathway (usually the first irreversible step, called committed step), thus regulating the amount of end product made by the pathways. Such a regulatory mechanism is called a negative feedback mechanism, because the amount of the end product produced is regulated by its own concentration. Negative feedback mechanism can effectively adjust the rate of synthesis of intermediate metabolites according to the demands of the cells. This helps allocate materials and energy economically, and prevents the manufacture of excess end products. The control of enzymatic action helps to maintain a stable internal environment in living organisms. 4. Enzymes can be regulated through post-translational modification. This can include phosphorylation, myristoylation and glycosylation. For example, in the response to insulin, the phosphorylation of multiple enzymes, including glycogen synthase, helps control the synthesis or degradation of glycogen and allows the cell to respond to changes in blood sugar.[75] Another example of post-translational modification is the cleavage of the polypeptide chain. Chymotrypsin, a digestive protease, is produced in inactive form as chymotrypsinogen in the pancreas and transported in this form to the stomach where it is activated. This stops the enzyme from digesting the pancreas or other tissues before it enters the gut. This type of inactive precursor to an enzyme is known as a zymogen. 5. Some enzymes may become activated when localized to a different environment (e.g., from a reducing (cytoplasm) to an oxidizing (periplasm) environment, high pH to low pH, etc.). For example, hemagglutinin in the influenza virus is activated by a conformational change caused by the acidic conditions, these occur when it is taken up inside its host cell and enters the lysosome.[76]
Enzyme
91
Involvement in disease
Since the tight control of enzyme activity is essential for homeostasis, any malfunction (mutation, overproduction, underproduction or deletion) of a single critical enzyme can lead to a genetic disease. The importance of enzymes is shown by the fact that a lethal illness can be caused by the malfunction of just one type of enzyme out of the thousands of types present in our bodies. One example is the most common type of phenylketonuria. A mutation of a single amino acid in the enzyme phenylalanine hydroxylase, which catalyzes the first step in the degradation of phenylalanine, results in build-up of phenylalanine and related products. This can lead to mental retardation if the disease is untreated.[77] Another example of enzyme deficiency is pseudocholinesterase, in which there is slow metabolic degradation of exogenous choline.[citation needed]
Phenylalanine hydroxylase. Created from PDB 1KW0 [78]
Another example is when germline mutations in genes coding for DNA repair enzymes cause hereditary cancer syndromes such as xeroderma pigmentosum. Defects in these enzymes cause cancer since the body is less able to repair mutations in the genome. This causes a slow accumulation of mutations and results in the development of many types of cancer in the sufferer. Oral administration of enzymes can be used to treat several diseases (e.g. pancreatic insufficiency and lactose intolerance). Since enzymes are proteins themselves they are potentially subject to inactivation and digestion in the gastrointestinal environment. Therefore a non-invasive imaging assay was developed to monitor gastrointestinal activity of exogenous enzymes (prolyl endopeptidase as potential adjuvant therapy for celiac disease) in vivo.[78]
Naming conventions
An enzyme's name is often derived from its substrate or the chemical reaction it catalyzes, with the word ending in -ase. Examples are lactase, alcohol dehydrogenase and DNA polymerase. This may result in different enzymes, called isozymes, with the same function having the same basic name. Isoenzymes have a different amino acid sequence and might be distinguished by their optimal pH, kinetic properties or immunologically. Isoenzyme and isozyme are homologous proteins. Furthermore, the normal physiological reaction an enzyme catalyzes may not be the same as under artificial conditions. This can result in the same enzyme being identified with two different names. For example, glucose isomerase, which is used industrially to convert glucose into the sweetener fructose, is a xylose isomerase in vivo (within the body). The International Union of Biochemistry and Molecular Biology have developed a nomenclature for enzymes, the EC numbers; each enzyme is described by a sequence of four numbers preceded by "EC". The first number broadly classifies the enzyme based on its mechanism. The top-level classification is[79] • EC 1 Oxidoreductases: catalyze oxidation/reduction reactions • EC 2 Transferases: transfer a functional group (e.g. a methyl or phosphate group) • EC 3 Hydrolases: catalyze the hydrolysis of various bonds • EC 4 Lyases: cleave various bonds by means other than hydrolysis and oxidation • EC 5 Isomerases: catalyze isomerization changes within a single molecule
Enzyme • EC 6 Ligases: join two molecules with covalent bonds. According to the naming conventions, enzymes are generally classified into six main family classes and many sub-family classes. Some web-servers, e.g., EzyPred [82] [80] and bioinformatics tools have been developed to predict which main family class [81] and sub-family class [82] [83] an enzyme molecule belongs to according to its sequence information alone via the pseudo amino acid composition.
92
Industrial applications
Enzymes are used in the chemical industry and other industrial applications when extremely specific catalysts are required. However, enzymes in general are limited in the number of reactions they have evolved to catalyze and also by their lack of stability in organic solvents and at high temperatures. As a consequence, protein engineering is an active area of research and involves attempts to create new enzymes with novel properties, either through rational design or in vitro evolution.[84][85] These efforts have begun to be successful, and a few enzymes have now been designed "from scratch" to catalyze reactions that do not occur in nature.[86]
Application Food processing Enzymes used Amylases from fungi and plants Uses Production of sugars from starch, such as in making [87] high-fructose corn syrup. In baking, catalyze breakdown of starch in the flour to sugar. Yeast fermentation of sugar produces the carbon dioxide that raises the dough.
Amylases catalyze the release of simple sugars from starch. Baby foods Brewing industry
Proteases
Biscuit manufacturers use them to lower the protein level of flour.
Trypsin Enzymes from barley are released during the mashing stage of beer production. Industrially produced barley enzymes Amylase, glucanases, proteases Betaglucanases and arabinoxylanases Amyloglucosidase and pullulanases
To predigest baby foods They degrade starch and proteins to produce simple sugar, amino acids and peptides that are used by yeast for fermentation. Widely used in the brewing process to substitute for the natural enzymes found in barley. Split polysaccharides and proteins in the malt. Improve the wort and beer filtration characteristics.
Low-calorie beer and adjustment of fermentability.
Germinating barley used for malt
Proteases Acetolactatedecarboxylase (ALDC)
Remove cloudiness produced during storage of beers. Increases fermentation efficiency by reducing diacetyl [88] formation. Clarify fruit juices.
Fruit juices
Cellulases, pectinases
Enzyme
93
Rennin, derived from the stomachs Manufacture of cheese, used to hydrolyze protein of young ruminant animals (like calves and lambs)
Dairy industry
Microbially produced enzyme
Now finding increasing use in the dairy industry
Lipases
Is implemented during the production of Roquefort cheese to enhance the ripening of the blue-mold cheese.
Roquefort cheese Meat tenderizers Starch industry
Lactases
Break down lactose to glucose and galactose.
Papain
To soften meat for cooking
Amylases, amyloglucosideases and Converts starch into glucose and various syrups. glucoamylases Glucose isomerase Converts glucose into fructose in production of high-fructose syrups from starchy materials. These syrups have enhanced sweetening properties and lower calorific values than sucrose for the same level of sweetness. Degrade starch to lower viscosity, aiding sizing and coating paper. Xylanases reduce bleach required for decolorizing; cellulases smooth fibers, enhance water drainage, and promote ink removal; lipases reduce pitch and lignin-degrading enzymes remove lignin to soften paper.
Glucose
Fructose
Paper industry
Amylases, Xylanases, Cellulases and ligninases
A paper mill in South Carolina Biofuel industry Cellulases Used to break down cellulose into sugars that can be fermented (see cellulosic ethanol)
Ligninases
Use of lignin waste
Cellulose in 3D Biological detergent Primarily proteases, produced in an Used for presoak conditions and direct liquid extracellular form from bacteria applications helping with removal of protein stains from clothes Amylases Detergents for machine dish washing to remove resistant starch residues Used to assist in the removal of fatty and oily stains Used in biological fabric conditioners
Lipases Cellulases
Enzyme
94
Proteases To remove proteins on contact lens to prevent infections To generate oxygen from peroxide to convert latex into foam rubber Dissolve gelatin off scrap film, allowing recovery of its silver content. Used to manipulate DNA in genetic engineering, important in pharmacology, agriculture and medicine. Essential for restriction digestion and the polymerase chain reaction. Molecular biology is also important in forensic science.
Contact lens cleaners
Rubber industry
Catalase
Photographic industry
Protease (ficin)
Molecular biology
Restriction enzymes, DNA ligase and polymerases
Part of the DNA double helix
References
[7] Williams, H. S. (1904) A History of Science: in Five Volumes. Volume IV: Modern Development of the Chemical and Biological Sciences (http:/ / etext. lib. virginia. edu/ toc/ modeng/ public/ Wil4Sci. html) Harper and Brothers (New York) Accessed 4 April 2007 [9] Kühne coined the word "enzyme" in: W. Kühne (1877) " Über das Verhalten verschiedener organisirter und sog. ungeformter Fermente (http:/ / books. google. com/ books?id=jzdMAAAAYAAJ& pg=PA190& ie=ISO-8859-1& output=html)" (On the behavior of various organized and so-called unformed ferments), Verhandlungen des naturhistorisch-medicinischen Vereins zu Heidelberg, new series, vol. 1, no. 3, pages 190–193. The relevant passage occurs on page 190: "Um Missverständnissen vorzubeugen und lästige Umschreibungen zu vermeiden schlägt Vortragender vor, die ungeformten oder nicht organisirten Fermente, deren Wirkung ohne Anwesenheit von Organismen und ausserhalb derselben erfolgen kann, als Enzyme zu bezeichnen." (Translation: In order to obviate misunderstandings and avoid cumbersome periphrases, [the author, a university lecturer] suggests designating as "enzymes" the unformed or not organized ferments, whose action can occur without the presence of organisms and outside of the same.) [10] Nobel Laureate Biography of Eduard Buchner at http:/ / nobelprize. org (http:/ / nobelprize. org/ nobel_prizes/ chemistry/ laureates/ 1907/ buchner-bio. html). Retrieved 4 April 2007. [11] Text of Eduard Buchner's 1907 Nobel lecture at http:/ / nobelprize. org (http:/ / nobelprize. org/ nobel_prizes/ chemistry/ laureates/ 1907/ buchner-lecture. html). Retrieved 4 April 2007. [12] The naming of enzymes by adding the suffix "-ase" to the substrate on which the enzyme acts, has been traced to French scientist Émile Duclaux (1840–1904), who intended to honor the discoverers of diastase – the first enzyme to be isolated – by introducing this practice in his book Traité de Microbiologie (http:/ / books. google. com/ books?id=Kp9EAAAAQAAJ& printsec=frontcover), vol. 2 (Paris, France: Masson and Co., 1899). See Chapter 1, especially page 9. [13] Willstätter, R. (1927). Problems and Methods in Enzyme Research. Cornell University Press, Ithaca. quoted in [14] 1946 Nobel prize for Chemistry laureates at http:/ / nobelprize. org (http:/ / nobelprize. org/ nobel_prizes/ chemistry/ laureates/ 1946/ ). Retrieved 4 April 2007. [20] The Catalytic Site Atlas at The European Bioinformatics Institute (http:/ / www. ebi. ac. uk/ thornton-srv/ databases/ CSA/ ). Retrieved 4 April 2007. [51] BRENDA The Comprehensive Enzyme Information System (http:/ / www. brenda. uni-koeln. de/ ). Retrieved 4 April 2007. [55] English translation (http:/ / web. lemoyne. edu/ ~giunta/ menten. html). Retrieved 6 April 2007. [77] Phenylketonuria: NCBI Genes and Disease (http:/ / www. ncbi. nlm. nih. gov/ books/ bv. fcgi?call=bv. View. . ShowSection& rid=gnd. section. 234). Retrieved 4 April 2007. [79] The complete nomenclature can be browsed at Enzyme Nomenclature (http:/ / www. chem. qmul. ac. uk/ iubmb/ enzyme/ ). Recommendations of the Nomenclature Committee of the International Union of Biochemistry and Molecular Biology on the Nomenclature and Classification of Enzymes by the Reactions they Catalyse. Nomenclature Committee of the International Union of Biochemistry and Molecular Biology (NC-IUBMB)
Enzyme
95
Further reading
Etymology and history • "New Beer in an Old Bottle: Eduard Buchner and the Growth of Biochemical Knowledge, edited by Athel Cornish-Bowden and published by Universitat de València (1997): ISBN 84-370-3328-4" (http:/ / web. archive. org/ web/ 20080207101706/ http:/ / bip. cnrs-mrs. fr/ bip10/ buchner. htm). Archived from the original (http:/ / bip. cnrs-mrs. fr/ bip10/ buchner. htm) on 7 February 2008., A history of early enzymology. Williams, Henry Smith, 1863–1943. A History of Science: in Five Volumes. Volume IV: Modern Development of the Chemical and Biological Sciences (http:/ / etext. lib. virginia. edu/ toc/ modeng/ public/ Wil4Sci. html), A textbook from the 19th century. Kleyn J, Hough J (1971). "The microbiology of brewing". Annu. Rev. Microbiol. 25: 583–608. doi: 10.1146/annurev.mi.25.100171.003055 (http:/ / dx. doi. org/ 10. 1146/ annurev. mi. 25. 100171. 003055). PMID 4949040 (http:/ / www. ncbi. nlm. nih. gov/ pubmed/ 4949040). Kinetics and inhibition • Cornish-Bowden, Athel. Fundamentals of Enzyme Kinetics. (3rd edition), Portland Press, 2004. ISBN 1-85578-158-1. Segel Irwin H. Enzyme Kinetics: Behavior and Analysis of Rapid Equilibrium and Steady-State Enzyme Systems. (New Ed edition), Wiley-Interscience, 1993. ISBN 0-471-30309-7. Baynes, John W. Medical Biochemistry. (2nd edition), Elsevier-Mosby, 2005. ISBN 0-7234-3341-0, p. 57.
•
•
•
•
Function and control of enzymes in the cell • Price, N. and Stevens, L. Fundamentals of Enzymology: Cell and Molecular Biology of Catalytic Proteins. Oxford University Press, 1999. ISBN 0-19-850229-X. "Nutritional and Metabolic Diseases" (http:/ / www. ncbi. nlm. nih. gov/ books/ bv. fcgi?rid=gnd. chapter. 86). Chapter of the on-line textbook Introduction to Genes and Disease from the NCBI.
Enzyme structure and mechanism • • • • • Fersht, Alan (1999). Structure and mechanism in protein science: a guide to enzyme catalysis and protein folding. San Francisco: W.H. Freeman. ISBN 0-7167-3268-8. Walsh C (1979). Enzymatic reaction mechanisms. San Francisco: W. H. Freeman. ISBN 0-7167-0070-0. Page, M. I., and Williams, A. (Eds.). Enzyme Mechanisms. Royal Society of Chemistry, 1987. ISBN 0-85186-947-5. Bugg, T. Introduction to Enzyme and Coenzyme Chemistry. (2nd edition), Blackwell Publishing Limited, 2004. ISBN 1-4051-1452-5. Warshel, A. Computer Modeling of Chemical Reactions in enzymes and Solutions. John Wiley & Sons Inc., 1991. ISBN 0-471-18440-3.
•
Enzyme-naming conventions • Enzyme Nomenclature (http:/ / www. chem. qmul. ac. uk/ iubmb/ enzyme/ ), Recommendations for enzyme names from the Nomenclature Committee of the International Union of Biochemistry and Molecular Biology. Koshland, D. The Enzymes, v. I, ch. 7. Acad. Press, New York, 1959.
Thermodynamics • "Reactions and Enzymes" (http:/ / www. emc. maricopa. edu/ faculty/ farabee/ BIOBK/ BioBookEnzym. html) Chapter 10 of on-line biology book at Estrella Mountain Community College. •
Industrial applications • "History of industrial enzymes" (http:/ / www. mapsenzymes. com/ History_of_Enzymes. asp), Article about the history of industrial enzymes from the late 1900s to the present times.
External links
• Structure/Function of Enzymes (http://mcdb-webarchive.mcdb.ucsb.edu/sears/biochemistry/), Web tutorial on enzyme structure and function. • Enzymes in diagnosis (http://www.science2day.info/2008/02/enzyme-test-or-cpk-test-what-is-it.html) Role of enzymes in diagnosis of diseases. • Enzyme spotlight (http://www.ebi.ac.uk/intenz/spotlight.jsp) Monthly feature at the European Bioinformatics Institute on a selected enzyme. • AMFEP (http://www.amfep.org/), Association of Manufacturers and Formulators of Enzyme Products • BRENDA (http://www.brenda-enzymes.org/) database, a comprehensive compilation of information and literature references about all known enzymes; requires payment by commercial users. • Enzyme Structures (http://pdbe.org/ec) Explore 3-D structure data of enzymes in the Protein Data Bank. • Enzyme Structures Database (http://www.ebi.ac.uk/thornton-srv/databases/enzymes/) links to the known 3-D structure data of enzymes in the Protein Data Bank.
Enzyme • ExPASy enzyme (http://us.expasy.org/enzyme/) database, links to Swiss-Prot sequence data, entries in other databases and to related literature searches. • KEGG: Kyoto Encyclopedia of Genes and Genomes (http://www.genome.jp/kegg/) Graphical and hypertext-based information on biochemical pathways and enzymes. • (http://www.enzyme-database.org/) enzyme database • MACiE (http://www.ebi.ac.uk/thornton-srv/databases/MACiE/) database of enzyme reaction mechanisms. • MetaCyc database of enzymes and metabolic pathways • Face-to-Face Interview with Sir John Cornforth who was awarded a Nobel Prize for work on stereochemistry of enzyme-catalyzed reactions (http://www.vega.org.uk/video/programme/19) Freeview video by the Vega Science Trust • Sigma Aldrich Enzyme Assays by Enzyme Name (http://www.sigmaaldrich.com/life-science/metabolomics/ enzyme-explorer.html)—Hundreds of assays sorted by enzyme name. • Bugg TD (2001). "The development of mechanistic enzymology in the 20th century". Nat Prod Rep 18 (5): 465–93. doi: 10.1039/b009205n (http://dx.doi.org/10.1039/b009205n). PMID 11699881 (http://www.ncbi. nlm.nih.gov/pubmed/11699881).
96
Paneth cell
97
Paneth cell
Paneth cell
Paneth cells Latin MeSH Code cellula panethensis Paneth+Cells
[1]
TH H3.04.03.0.00017
Paneth cells, along with goblet cells, enterocytes, and enteroendocrine cells, represent the principal cell types of the epithelium of the small intestine.[1] (A few may also be found sporadically in the cecum and appendix.) They are identified microscopically by their location just below the intestinal stem cells in the intestinal glands (AKA crypts of Lieberkühn) and the large eosinophilic refractile granules that occupy most of their cytoplasm. These granules consist of several anti-microbial compounds and other compounds that are known to be important in immunity and host-defense. When exposed to bacteria or bacterial antigens, Paneth cells secrete some of these compounds into the lumen of the intestinal gland, thereby contributing to maintenance of the gastrointestinal barrier. Paneth cells are named after Joseph Paneth (1857–1890), an Austrian physician.
Location
Paneth cells are found throughout the small intestine and the appendix at the base of the intestinal glands.[2] The Paneth cell numbers demonstrate an ascending trend with highest numbers towards the distal end of the small intestine. Like the other epithelial cell lineages in the small intestine, paneth cells originate at the stem cell region near the bottom of the gland.[3] However, unlike the other epithelial cell types, paneth cells migrate downward from the stem cell region and settle just adjacent to it.[3] This close relationship to the stem cell region is thought to suggest that Paneth cells are important in defending the gland stem cells from microbial damage,[3] although their function is not entirely known.[2] Furthermore, among the four aforementioned intestinal cell lineages, the Paneth cells live the longest (18-23 days).
Function
Small intestinal crypts house stem cells that serve to constantly replenish epithelial cells that die and are lost from the villi. Protection of these stem cells is essential for long-term maintenance of the intestinal epithelium, and the location of Paneth cells adjacent to stem cells suggests that they play a critical role in defending epithelial cell renewal.
Sensing microbiota
Paneth cells sense bacteria via MyD88-dependent toll-like receptor (TLR) activation which then triggers antimicrobial action.[4]
Paneth cell
98
Secretions
Defensins
The principal defense molecules secreted by Paneth cells are alpha-defensins, which are known as cryptdins in mice.[5] These peptides have hydrophobic and positively-charged domains that can interact with phospholipids in cell membranes. This structure allows defensins to insert into membranes, where they interact with one another to form pores that disrupt membrane function, leading to cell lysis. Due to the higher concentration of negatively-charged phospholipids in bacterial than vertebrate cell membranes, defensins preferentially bind to and disrupt bacterial cells, sparing the cells they are functioning to protect.[6] Paneth cells are stimulated to secrete defensins when exposed to bacteria (both Gram positive and negative types) or such bacterial products as lipopolysaccharide, muramyl dipeptide and lipid A.
Other secretions
In addition to defensins, Paneth cells secrete lysozyme,[] tumor necrosis factor-alpha,[] and phospholipase A2.[citation needed] Lysozyme and phospholipase A2 both have clear antimicrobial activity. This battery of secretory molecules gives Paneth cells a potent arsenal against a broad spectrum of agents, including bacteria, fungi and even some enveloped viruses.
References
[1] http:/ / www. copewithcytokines. org/ cope. cgi?key=Paneth%20cells [2] http:/ / www. britannica. com/ EBchecked/ topic/ 441200/ Paneths-cell [3] http:/ / books. google. com/ books?id=wSTISCdSIosC& pg=PA244& lpg=PA244& dq=paneth+ cell& source=vrt& ots=KZ4tH-wh4s& sig=mMRz3PETnVY9URDkCDyjoIGkLM8& hl=en& ei=fOR-TeW2BInagQeSyoGgCA& sa=X& oi=book_result& ct=result& resnum=13& ved=0CHkQ6AEwDA#v=onepage& q=paneth%20cell& f=false
Further reading
• Ganz T (1999). "Defensins and host defense.". Science 286 (5439): 420–1. doi: 10.1126/science.286.5439.420 (http://dx.doi.org/10.1126/science.286.5439.420). PMID 10577203 (http://www.ncbi.nlm.nih.gov/ pubmed/10577203). • Ganz T (2000). "Paneth cells--guardians of the gut cell hatchery.". Nat Immunol 1 (2): 99–100. doi: 10.1038/77884 (http://dx.doi.org/10.1038/77884). PMID 11248797 (http://www.ncbi.nlm.nih.gov/ pubmed/11248797).
External links
• BU Histology Learning System: 11604loa (http://www.bu.edu/histology/p/11604loa.htm) - "Endocrine System: duodenum, enteroendocrine cells" • BU Histology Learning System: 11606loa (http://www.bu.edu/histology/p/11606loa.htm) - "Digestive System: Alimentary Canal - duodenum, paneth cells" • Overview and diagram at colostate.edu (http://www.vivo.colostate.edu/hbooks/pathphys/digestion/smallgut/ paneth.html) • Histology at ucsd.edu (http://meded.ucsd.edu/hist-img-bank/chapter_6/Slide_94_crypts_duodenum/pages/b. 6.94.1.5.htm)
Intestine
99
Intestine
In human anatomy, the intestine (or bowel, hose or gut) is the segment of the alimentary canal extending from the pyloric sphincter of the stomach to the anus and, in humans and other mammals, consists of two segments, the small intestine and the large intestine. In humans, the small intestine is further subdivided into the duodenum, jejunum and ileum while the large intestine is subdivided into the cecum and colon.[1]
Structure and function
The structure and function can be described both as gross anatomy and at a microscopic level. The intestinal tract can be broadly divided into two different parts, the small and large intestine.[2] People will have different sized intestines according to their size and age. The intestine is divided into two parts: The Small Intestine and the Large Intestine. The lumen is the cavity where digested food passes through and from where nutrients are absorbed. Both intestines share a general structure with the whole gut, and are composed of several layers. Going from inside the lumen radially outwards, one passes the mucosa (glandular epithelium and muscularis mucosa), sub mucosa, muscularis externa (made up of inner circular and outer longitudinal), and lastly serosa.
• Along the whole length of the gut in the glandular epithelium are goblet cells. These secrete mucus which lubricates the passage of food along and protects it from digestive enzymes. In the small intestine, villi are vaginations (folds) of the mucosa and increase the overall surface area of the intestine while also containing a lacteal, which is connected to the lymph system and aids in the removal of lipids and tissue fluid from the blood supply. Micro villi are present on the epithelium of a villus and further increase the surface area over which The general structure of the intestinal wall absorption can take place. Pocket-like invaginations into the underlying tissue are termed Crypts of Lieberkühn. In the large intestines, villi are absent and a flat surface with thousands of crypts is observed. • Underlying the epithelium is the lamina propria, which contains myofibroblasts, blood vessels, nerves, and several different immune cells. • The next layer is the muscularis mucosa which is a layer of smooth muscle that aids in the action of continued peristalsis and catastalsis along the gut. The sub mucosa contains nerves (e.g. Meissner's plexus), blood vessels and elastic fibre with collagen that stretches with increased capacity but maintains the shape of the intestine.
Intestine • Surrounding this is the muscularis externa which comprises longitudinal and circular smooth muscle that again helps with continued peristalsis and the movement of digested material out of and along the gut. In between the two layers of muscle lies Auerbach's plexus. • Lastly there is the serosa which is made up of loose connective tissue and coated in mucus so as to prevent friction damage from the intestine rubbing against other tissue. Holding all this in place are the mesenteries which suspend the intestine in the abdominal cavity and stop it being disturbed when a person is physically active. The large intestine hosts several kinds of bacteria that deal with molecules the human body is not able to break down itself.[citation needed] This is an example of symbiosis. These bacteria also account for the production of gases inside our intestine (this gas is released as flatulence when eliminated through the anus). However the large intestine is mainly concerned with the absorption of water from digested material (which is regulated by the hypothalamus) and the re absorption of sodium, as well as any nutrients that may have escaped primary digestion in the ileum.
100
Diseases and disorders
• • • • Gastroenteritis is an inflammation of the intestines. It is the most common disease of all the intestines. Ileus is a blockage of the intestines. Ileitis is an inflammation of the ileum. Colitis is an inflammation of the large intestine.
• Appendicitis is inflammation of the vermiform appendix located at the caecum. This is a potentially fatal disease if left untreated; most cases of appendicitis require surgical intervention. • Coeliac disease is a common form of malabsorption, affecting up to 1% of people of northern European descent. An autoimmune response is triggered in intestinal cells by digestion of gluten proteins. Ingestion of proteins found in wheat, barley and rye, causes villous atrophy in the small intestine. Lifelong dietary avoidance of these foodstuffs in a gluten-free diet is the only treatment. • Crohn's disease and ulcerative colitis are examples of inflammatory bowel disease. While Crohn's can affect the entire gastrointestinal tract, ulcerative colitis is limited to the large intestine. Crohn's disease is widely regarded as an autoimmune disease. Although ulcerative colitis is often treated as though it were an autoimmune disease, there is no consensus that it actually is such. (See List of autoimmune diseases). • Enteroviruses are named by their transmission-route through the intestine (enteric meaning intestinal), but their symptoms aren't mainly associated with the intestine. • Irritable bowel syndrome (IBS) is the most common functional disorder of the intestine. Functional constipation and chronic functional abdominal pain are other disorders of the intestine that have physiological causes, but do not have identifiable structural, chemical, or infectious pathologies. They are aberrations of normal bowel function but not diseases.[3] • Diverticular disease is a condition that is very common in older people in industrialized countries. It usually affects the large intestine but has been known to affect the small intestine as well. Diverticulosis occurs when pouches form on the intestinal wall. Once the pouches become inflamed it is known as diverticulitis. • Endometriosis can affect the intestines, with similar symptoms to IBS. • Bowel twist (or similarly, bowel strangulation) is a comparatively rare event (usually developing sometime after major bowel surgery). It is, however, hard to diagnose correctly, and if left uncorrected can lead to bowel infarction and death. (The singer Maurice Gibb is understood to have died from this.) • Angiodysplasia of the colon • Chronic functional abdominal pain • Colorectal cancer • Constipation • Diarrhea • Hirschsprung's disease (aganglionosis) • Intussusception
Intestine • Polyp (medicine) (see also Colorectal polyp) • Pseudomembranous colitis • Ulcerative colitis and toxic megacolon
101
In non-human animals
Animal intestines have multiple uses. From each species of livestock that is a source of milk, a corresponding rennet is obtained from the intestines of milk-fed calves. Pig and calf intestines are eaten, and pig intestines are used as sausage casings. Calf intestines supply Calf Intestinal Alkaline Phosphatase (CIP), and are used to make Goldbeater's skin.
References
[3] http:/ / www. irregularbowelsyndrome. info
• Encyclopædia Britannica article on intestine (http://www.britannica.com/eb/article-9002491/intestine) retrieved on 2007-03-27
Bicarbonate
102
Bicarbonate
Bicarbonate
Identifiers CAS number PubChem ChemSpider KEGG ChEBI ChEMBL Beilstein Reference Gmelin Reference 3DMet Jmol-3D images 71-52-3 769 749
[2] [3] [4] [5] [6] [1]
C00288
CHEBI:17544
CHEMBL363707 3903504 49249 B00080
[7] [8]
Image 1 [9] Image 2 Properties
Molecular formula Molar mass log P Acidity (pK )
a
CHO− 3 61.0168 g mol-1 -0.82 10.3 3.7
Basicity (pK )
b
Except where noted otherwise, data are given for materials in their standard state (at 25 °C, 100 kPa) Infobox references
In inorganic chemistry, bicarbonate (IUPAC-recommended nomenclature: hydrogencarbonate[1]) is an intermediate form in the deprotonation of carbonic acid. It is an anion with the chemical formula HCO3−. Bicarbonate serves a crucial biochemical role in the physiological pH buffering system.[]
Bicarbonate
103
Chemical properties
The bicarbonate ion (hydrogen carbonate ion) is an anion with the empirical formula HCO3− and a molecular mass of 61.01 daltons; it consists of one central carbon atom surrounded by three oxygen atoms in a trigonal planar arrangement, with a hydrogen atom attached to one of the oxygens. It is isoelectronic with nitric acid HNO3. The bicarbonate ion carries a negative one formal charge and is the conjugate base of carbonic acid H2CO3; it is the conjugate acid of CO2− 3, the carbonate ion, as shown by these equilibrium reactions. CO32− + 2 H2O H2CO3 + 2 H2O HCO3− + H2O + OH− HCO3− + H3O+ + H2O H2CO3 +2 OH− CO32− + 2 H3O+
A bicarbonate salt forms when a positively charged ion attaches to the negatively charged oxygen atoms of the ion, forming an ionic compound. Many bicarbonates are soluble in water at standard temperature and pressure, in particular sodium bicarbonate contributes to total dissolved solids, a common parameter for assessing water quality.[citation needed]
Biochemical role
Bicarbonate is alkaline, and a vital component of the pH buffering system[] of the human body (maintaining acid-base homeostasis). 70-75% of CO2 in the body is converted into carbonic acid (H2CO3), which can quickly turn into bicarbonate (HCO3−). With carbonic acid as the central intermediate species, bicarbonate – in conjunction with water, hydrogen ions, and carbon dioxide – forms this buffering system, which is maintained at the volatile equilibrium[] required to provide prompt resistance to drastic pH changes in both the acidic and basic directions. This is especially important for protecting tissues of the central nervous system, where pH changes too far outside of the normal range in either direction could prove disastrous (see acidosis or alkalosis). Bicarbonate also acts to regulate pH in the small intestine. It is released from the pancreas in response to the hormone secretin to neutralize the acidic chyme entering the duodenum from the stomach.[2]
Bicarbonate
104
Bicarbonate in the environment
In freshwater ecology, strong photosynthetic activity by freshwater plants in daylight releases gaseous oxygen into the water and at the same time produces bicarbonate ions. These shift the pH upward until in certain circumstances the degree of alkalinity can become toxic to some organisms or can make other chemical constituents such as ammonia toxic. In darkness, when no photosynthesis occurs, respiration processes release carbon dioxide, and no new bicarbonate ions are produced, resulting in a rapid fall in pH.
Other uses
The most common salt of the bicarbonate ion is sodium bicarbonate, NaHCO3, which is commonly known as baking soda. When heated or exposed to an acid such as acetic acid (vinegar), sodium bicarbonate releases carbon dioxide. This is used as a leavening agent in baking. The flow of bicarbonate ions from rocks weathered by the carbonic acid in rainwater is an important part of the carbon cycle. Bicarbonate also serves much in the digestive system. It raises the internal pH of the stomach, after highly acidic digestive juices have finished in their digestion of food. Ammonium bicarbonate is used in digestive biscuit manufacture.
Diagnostics
In diagnostic medicine, the blood value of bicarbonate is one of several indicators of the state of acid-base physiology in the body. The parameter standard bicarbonate concentration (SBCe) is the bicarbonate concentration in the blood at a PaCO2 of 40 mmHg (5.33 kPa), full oxygen saturation and 36 °C.[3]
Reference ranges for blood tests, comparing blood content of bicarbonate (shown in blue at right) with other constituents.
Bicarbonate compounds
• • • • • Sodium bicarbonate Potassium bicarbonate Calcium bicarbonate Ammonium bicarbonate Carbonic acid
References
[2] Berne & Levy, Principles of Physiology [3] Acid Base Balance (page 3) (http:/ / www. nda. ox. ac. uk/ wfsa/ html/ u13/ u1312_03. htm)
External links
• Bicarbonates (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Bicarbonates) at the US National Library of Medicine Medical Subject Headings (MeSH)
Lysozyme
105
Lysozyme
Lysozyme
Lysozyme single crystal Identifiers EC number CAS number 3.2.1.17 [1] [2]
9001-63-2
Databases IntEnz BRENDA ExPASy KEGG MetaCyc PRIAM PDB structures Gene Ontology IntEnz view [3] [4] [5]
BRENDA entry NiceZyme view KEGG entry [6]
metabolic pathway profile [8] [9]
[7]
RCSB PDB AmiGO
PDBe
[10]
PDBsum
[11]
[12]
/ EGO
[13]
Search PMC articles [14]
PubMed articles [15] NCBI proteins [16]
Lysozyme
106
Lysozyme
PDB rendering based on 132l. Available structures PDB Ortholog search: PDBe [17], RCSB [18] List of PDB id codes 133L , 134L , 1B5U , 1B5V , 1B5W , 1B5X , 1B5Y , 1B5Z , 1B7L , 1B7M , 1B7N [29] [30] [31] [32] [33] [34] [35] [36] [37] [38] [39] , 1B7O , 1B7P , 1B7Q , 1B7R , 1B7S , 1BB3 , 1BB4 , 1BB5 , 1C43 , 1C45 , 1C46 [40] [41] [42] [43] [44] [45] [46] [47] [48] [49] [50] , 1C7P , 1CJ6 , 1CJ7 , 1CJ8 , 1CJ9 , 1CKC , 1CKD , 1CKF , 1CKG , 1CKH , [51] [52] [53] [54] [55] [56] [57] [58] [59] [60] 1D6P , 1D6Q , 1DI3 , 1DI4 , 1DI5 , 1EQ4 , 1EQ5 , 1EQE , 1GAY , 1GAZ , 1GB0 [61] [62] [63] [64] [65] [66] [67] [68] [69] [70] [71] , 1GB2 , 1GB3 , 1GB5 , 1GB6 , 1GB7 , 1GB8 , 1GB9 , 1GBO , 1GBW , 1GBX , [72] [73] [74] [75] [76] [77] [78] [79] [80] [81] 1GBY , 1GBZ , 1GDW , 1GDX , 1GE0 , 1GE1 , 1GE2 , 1GE3 , 1GE4 , 1GEV , 1GEZ [82] [83] [84] [85] [86] [87] [88] [89] [90] [91] [92] , 1GF0 , 1GF3 , 1GF4 , 1GF5 , 1GF6 , 1GF7 , 1GF8 , 1GF9 , 1GFA , 1GFE , [93] [94] [95] [96] [97] [98] [99] [100] [101] [102] 1GFG , 1GFH , 1GFJ , 1GFK , 1GFR , 1GFT , 1GFU , 1GFV , 1HNL , 1I1Z , 1I20 [103] [104] [105] [106] [107] [108] [109] [110] [111] [112] [113] , 1I22 , 1INU , 1IOC , 1IP1 , 1IP2 , 1IP3 , 1IP4 , 1IP5 , 1IP6 , 1IP7 , [114] [115] [116] [117] [118] [119] [120] [121] [122] 1IWT , 1IWU , 1IWV , 1IWW , 1IWX , 1IWY , 1IWZ , 1IX0 , 1IY3 , 1IY4 [123] [124] [125] [126] [127] [128] [129] [130] [131] [132] , 1JKA , 1JKB , 1JKC , 1JKD , 1JSF , 1JWR , 1LAA , 1LHH , 1LHI , [133] [134] [135] [136] [137] [138] [139] [140] [141] 1LHJ , 1LHK , 1LHL , 1LHM , 1LMT , 1LOZ , 1LYY , 1LZ1 , 1LZ4 , 1LZ5 [142] [143] [144] [145] [146] [147] [148] [149] [150] [151] , 1LZ6 , 1LZR , 1LZS , 1OP9 , 1OUA , 1OUB , 1OUC , 1OUD , 1OUE , [152] [153] [154] [155] [156] [157] [158] [159] [160] 1OUF , 1OUG , 1OUH , 1OUI , 1OUJ , 1QSW , 1RE2 , 1REM , 1REX , 1REY [161] [162] [163] [164] [165] [166] [167] [168] [169] , 1REZ , 1TAY , 1TBY , 1TCY , 1TDY , 1UBZ , 1W08 , 1WQM , 1WQN [170] [171] [172] [173] [174] [175] [176] [177] [178] , 1WQO , 1WQP , 1WQQ , 1WQR , 1YAM , 1YAN , 1YAO , 1YAP , 1YAQ [179] [180] [181] [182] [183] [184] [185] [186] [187] [188] , 207L , 208L , 2BQA , 2BQB , 2BQC , 2BQD , 2BQE , 2BQF , 2BQG , [189] [190] [191] [192] [193] [194] [195] [196] [197] 2BQH , 2BQI , 2BQJ , 2BQK , 2BQL , 2BQM , 2BQN , 2BQO , 2HEA , 2HEB [198] [199] [200] [201] [202] [203] [204] [205] [206] , 2HEC , 2HED , 2HEE , 2HEF , 2LHM , 2MEA , 2MEB , 2MEC , 2MED [207] [208] [209] [210] [211] [212] [213] [214] [215] [216] , 2MEE , 2MEF , 2MEG , 2MEH , 2MEI , 2NWD , 2ZIJ , 2ZIK , 2ZIL , [217] [218] [219] [220] [221] 2ZWB , 3EBA , 3FE0 , 3LHM , 3LN2
[19] [20] [21] [22] [23] [24] [25] [26] [27] [28]
Identifiers Symbols External IDs EC number LYZ
[222]
; LZM
[223]
OMIM: 153450 3.2.1.17
[227]
MGI: 96897
[224]
HomoloGene: 121490
[225]
GeneCards: LYZ Gene
[226]
Lysozyme
107
Gene Ontology Molecular function • lysozyme activity [228] Cellular component • extracellular region [229] [230] • extracellular space Biological process • inflammatory response • cell wall macromolecule catabolic process
[232] [231]
• cytolysis [234] • defense response to bacterium Sources: Amigo
[235]
[233]
/ QuickGO
[236]
RNA expression pattern
More reference expression data Orthologs Species Entrez Ensembl UniProt RefSeq (mRNA) RefSeq (protein) Location (UCSC) Human 4069
[238] [240]
[237]
Mouse 17105
[239] [241]
ENSG00000090382 P61626
[242] [244]
ENSMUSG00000069516 Q3TXG2
[243] [245]
NM_000239 NP_000230
NM_017372 NP_059068
[246]
[247]
Chr 12: [248] 69.74 – 69.75 Mb
[250]
Chr 10: [249] 116.68 – 116.69 Mb
[251]
PubMed search
Lysozymes, also known as muramidase or N-acetylmuramide glycanhydrolase, are glycoside hydrolases. These are enzymes (EC 3.2.1.17 [252]) that damage bacterial cell walls by catalyzing hydrolysis of 1,4-beta-linkages between N-acetylmuramic acid and N-acetyl-D-glucosamine residues in a peptidoglycan and between N-acetyl-D-glucosamine residues in chitodextrins. Lysozyme is abundant in a number of secretions, such as tears, saliva, human milk, and mucus. It is also present in cytoplasmic granules of the polymorphonuclear neutrophils (PMN). Large amounts of lysozyme can be found in egg white. C-type lysozymes are closely related to alpha-lactalbumin in sequence and structure, making them part of the same family. In humans, the lysozyme enzyme is encoded by the LYZ gene.[][]
Lysozyme
108
Function
The enzyme functions by attacking peptidoglycans (found in the cell walls of bacteria, especially Gram-positive bacteria) and hydrolyzing the glycosidic bond that connects N-acetylmuramic acid with the fourth carbon atom of N-acetylglucosamine. It does this by binding to the peptidoglycan molecule in the binding site within the prominent cleft between its two domains. This causes the substrate molecule to adopt a strained conformation similar to that of the transition state.[] According to Phillips-Mechanism, the lysozyme binds to a hexasaccharide. The lysozyme then distorts the fourth sugar in hexasaccharide (the D ring) into a half-chair conformation. In this stressed state, the glycosidic bond is easily broken.
Overview of the reaction
The amino acid side-chains glutamic acid 35 (Glu35) and aspartate 52 (Asp52) have been found to be critical to the activity of this enzyme. Glu35 acts as a proton donor to the glycosidic bond, cleaving the C-O bond in the substrate, whereas Asp52 acts as a nucleophile to generate a glycosyl enzyme intermediate. The glycosyl enzyme intermediate then reacts with a water molecule, to give the product of hydrolysis and leaving the enzyme unchanged.[]
Role in disease
Lysozyme is part of the innate immune system. Reduced lysozyme levels have been associated with bronchopulmonary dysplasia in newborns.[] Children fed infant formula lacking lysozyme in their diet have three times the rate of diarrheal disease.[] Since lysozyme is a natural form of protection from gram-positive pathogens like Bacillus and Streptococcus,[1] a deficiency due to infant formula feeding can lead to increased incidence of disease. Whereas the skin is a protective barrier due to its dryness and acidity, the conjunctiva (membrane covering the eye) is, instead, protected by secreted enzymes, mainly lysozyme and defensin. However, when these protective barriers fail, conjunctivitis results. In certain cancers (especially myelomonocytic leukemia) excessive production of lysozyme by cancer cells can lead to toxic levels of lysozyme in the blood. High lysozyme blood levels can lead to kidney failure and low blood potassium, conditions that may improve or resolve with treatment of the primary malignancy.
Lysozyme
109
History
The antibacterial property of hen egg white, due to the lysozyme it contains, was first observed by Laschtschenko in 1909,[] although it was not until 1922 that the name 'lysozyme' was coined, by Alexander Fleming (1881–1955), the discoverer of penicillin.[] Fleming first observed the antibacterial action of lysozyme when he treated bacterial cultures with nasal mucus from a patient suffering from a head cold.[] The three-dimensional structure of hen egg white lysozyme was described by David Chilton Phillips (1924–1999) in 1965, when he obtained the first 2-Ångström (200 pm) resolution model via X-ray crystallography.[2][3] The structure was publicly presented at a Royal Institution lecture in 1965.[] Lysozyme was the second protein structure and the first enzyme structure to be solved via X-ray diffraction methods, and the first enzyme to be fully sequenced that contains all twenty common amino acids.[] As a result of Phillips' elucidation of the structure of lysozyme, it was also the first enzyme to have a detailed, specific mechanism suggested for its method of catalytic action.[] This work led Phillips to provide an explanation for how enzymes speed up a chemical reaction in terms of its physical structures. The original mechanism proposed by Phillips was more recently revised.[4] Howard Florey (1898–1968) and Ernst B. Chain (1906–1979) also investigated lysozymes. Although they never made much progress in this field, they, along with Fleming, developed penicillin.
References
[1] Microbiology: A human perspective. Nester, Anderson, Roberts, Nester. 5th Ed. 2007
External links
• Muramidase (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Muramidase) at the US National Library of Medicine Medical Subject Headings (MeSH) • "Lysozyme: enzyme, sequence, crystallization, structure" (http://lysozyme.co.uk/). lysozyme.co.uk. Retrieved 2009-01-04. • Proteopedia.org HEW Lysozyme (http://www.proteopedia.org/wiki/index.php/ Hen_Egg-White_(HEW)_Lysozyme) • JBdirectory: Lysozyme chloride (http://health.jbdirectory.com/Lysozyme_chloride)
Surfactant
110
Surfactant
Surfactants are compounds that lower the surface tension of a liquid, the interfacial tension between two liquids, or that between a liquid and a solid. Surfactants may act as detergents, wetting agents, emulsifiers, foaming agents, and dispersants.
Etymology and definition
The term surfactant/surfactants is a blend of surface active agents.[] In Index Medicus and the United States National Library of Medicine, surfactant/surfactants is reserved for the meaning pulmonary surfactant. For the more general meaning, surface active agent/s is the heading.
Micelle in aqueous solution
Composition and structure
Surfactants are usually organic compounds that are amphiphilic, meaning they contain both hydrophobic groups (their tails) and hydrophilic groups (their heads).[] Therefore, a surfactant contains both a water insoluble (or oil soluble) component and a water soluble component. Surfactants will diffuse in water and adsorb at interfaces between air and water or at the interface between oil and water, in the case where water is mixed with oil. The insoluble hydrophobic group may extend out of the bulk water phase, into the air or into the oil phase, while the water soluble head group remains in the water phase. This alignment of surfactants at the surface modifies the surface properties of water at the water/air or water/oil interface. World production of surfactants is estimated at 15 Mton/y, of which about half are soaps. Other surfactants produced on a particularly large scale are linear alkylbenzenesulfonates (1700 kton/y), lignin sulfonates (600 kton/y), fatty alcohol ethoxylates (700 ktons/y), and alkylphenol ethoxylates (500 kton/y).[1]
A micelle—the lipophilic tails of the surfactant ions remain on the inside of the micelle due to unfavourable interactions. The polar "heads" of the micelle, due to favourable interactions with water, form a hydrophilic outer layer that in effect protects the hydrophobic core of the micelle. The compounds that make up a micelle are typically amphiphilic in nature, meaning that micelles are soluble not only in protic solvents such as water but also in aprotic solvents as a reverse micelle.
Structure of surfactant phases in water
In the bulk aqueous phase, surfactants form aggregates, such as micelles, where the hydrophobic tails form the core of the aggregate and the hydrophilic heads are in contact with the surrounding liquid. Other types of aggregates such as spherical or cylindrical micelles or bilayers can be formed. The shape of the aggregates depends on the chemical
Surfactant structure of the surfactants, depending on the balance of the sizes of the hydrophobic tail and hydrophilic head. This is known as the HLB, Hydrophilic-lipophilic balance. Surfactants reduce the surface tension of water by adsorbing at the liquid-gas interface. The relation that links the surface tension and the surface excess is known as the Gibbs isotherm.
111
Dynamics of surfactants at interfaces
The dynamics of adsorption of surfactants is of great importance for practical applications such as foaming, emulsifying or coating processes, where bubbles or drops are rapidly generated and need to be stabilized. The dynamics of adsorption depends on the diffusion coefficient of the surfactants. Indeed, as the interface is created, the adsorption is limited by the diffusion of the surfactants to the interface. In some cases, there exists a barrier of energy for the adsorption or the desorption of the surfactants, then the adsorption dynamics is known as ‘kinetically limited'. Such energy barrier can be due to steric or electrostatic repulsions. The surface rheology of surfactant layers, including the elasticity and viscosity of the surfactant layers plays a very important role in foam or emulsion stability.
Characterization of interfaces and surfactant layers
Interfacial and surface tension can be characterized by classical methods such as the -pendant or spinning drop method Dynamic surface tensions, i.e. surface tension as a function of time, can be obtained by the Maximum Bubble Pressure apparatus The structure of surfactant layers can be studied by ellipsometry or X-Ray reflectivity. Surface rheology can be characterized by the oscillating drop method or shear surface rheometers such as double-cone, double-ring or magnetic rod shear surface rheometer.
Detergents in biochemistry and biotechnology
In solution, detergents help solubilize a variety of chemical species by dissociating aggregates and unfolding proteins. Popular surfactants in the biochemistry laboratory are SDS and CTAB. Detergents are key reagents to extract protein by lysis of the cells and tissues: They disorganize the membrane's lipidic bilayer (SDS, Triton X-100, X-114, CHAPS, DOC, and NP-40), and solubilize proteins. Milder detergents such as (OctylThioGlucosides) are used to solubilize sensible proteins (enzymes, receptors). Non-solubilized material is harvested by centrifugation or other means. For electrophoresis, for example, proteins are classically treated with SDS to denature the native tertiary and quaternary structures, allowing the separation of proteins according to their molecular weight. Detergents have also been used to decellularise organs. This process maintains a matrix of proteins that preserves the structure of the organ and often the microvascular network. The process has been successfully used to prepare organs such as the liver and heart for transplant in rats.[2] Pulmonary surfactants are also naturally secreted by type II cells of the lung alveoli in mammals.
Classification of surfactants
The "tail" of most surfactants are fairly similar, consisting of a hydrocarbon chain, which can be branch, linear, or aromatic. Fluorosurfactants have fluorocarbon chains. Siloxane surfactants have siloxane chains. Many important surfactants include a polyether chain terminating in a highly polar anionic group. The polyether groups often comprise ethoxylated (polyethylene oxide-like) sequences inserted to increase the hydrophilic character of a surfactant. Polypropylene oxides conversely, may be inserted to increase the lipophilic character of a surfactant. Surfactant molecules have either one tail or two; those with two tails are said to be double-chained.
Surfactant
112
Most commonly, surfactants are classified according to polar head group. A non-ionic surfactant has no charge groups in its head. The head of an ionic surfactant carries a net charge. If the charge is negative, the surfactant is more specifically called anionic; if the charge is positive, it is called cationic. If a surfactant contains a head with two oppositely charged groups, it is termed zwitterionic. Commonly encountered surfactants of each type include:
Anionic
Sulfate, sulfonate, and phosphate esters
Surfactant classification according to the composition of their head: nonionic, anionic, cationic, amphoteric.
Anionic surfactants contain anionic functional groups at their head, such as sulfate, sulfonate, phosphate, and carboxylates. Prominent alkyl sulfates include ammonium lauryl sulfate, sodium lauryl sulfate (SDS, sodium dodecyl sulfate, another name for the compound) and the related alkyl-ether sulfates sodium laureth sulfate, also known as sodium lauryl ether sulfate (SLES), and sodium myreth sulfate. Docusates: dioctyl sodium sulfosuccinate, perfluorooctanesulfonate (PFOS), perfluorobutanesulfonate, linear alkylbenzene sulfonates (LABs). These include alkyl-aryl ether phosphates and the alkyl ether phosphate Carboxylates These are the most common surfactants and comprise the alkyl carboxylates (soaps), such as sodium stearate. More specialized species include sodium lauroyl sarcosinate and carboxylate-based fluorosurfactants such as perfluorononanoate, perfluorooctanoate (PFOA or PFO).
Cationic head groups
• pH-dependent primary, secondary, or tertiary amines: Primary and secondary amines become positively charged at pH < 10:[3] • Octenidine dihydrochloride; • Permanently charged quaternary ammonium cation: • Alkyltrimethylammonium salts: cetyl trimethylammonium bromide (CTAB) a.k.a. hexadecyl trimethyl ammonium bromide, cetyl trimethylammonium chloride (CTAC • Cetylpyridinium chloride (CPC) • Benzalkonium chloride (BAC) • Benzethonium chloride (BZT) • 5-Bromo-5-nitro-1,3-dioxane • Dimethyldioctadecylammonium chloride • Cetrimonium bromide • Dioctadecyldimethylammonium bromide (DODAB)
Surfactant
113
Zwitterionic surfactants
Zwitterionic (amphoteric) surfactants have both cationic and anionic centers attached to the same molecule. The cationic part is based on primary, secondary, or tertiary amines or quaternary ammonium cations. The anionic part can be more variable and include sulfonates, as in CHAPS (3-[(3-Cholamidopropyl)dimethylammonio]-1-propanesulfonate). Other anionic groups are sultaines illustrated by cocamidopropyl hydroxysultaine. Betaines, e.g., cocamidopropyl betaine. Phosphates: lecithin
Nonionic surfactant
Many long chain alcohols exhibit some surfactant properties. Prominent among these are the fatty alcohols cetyl alcohol, stearyl alcohol, and cetostearyl alcohol (consisting predominantly of cetyl and stearyl alcohols), and oleyl alcohol. • Polyoxyethylene glycol alkyl ethers (Brij): CH3–(CH2)10–16–(O-C2H4)1–25–OH: • Octaethylene glycol monododecyl ether • Pentaethylene glycol monododecyl ether • Polyoxypropylene glycol alkyl ethers: CH3–(CH2)10–16–(O-C3H6)1–25–O • Glucoside alkyl ethers: CH3–(CH2)10–16–(O-Glucoside)1–3–OH: • Decyl glucoside, • Lauryl glucoside • Octyl glucoside • Polyoxyethylene glycol octylphenol ethers: C8H17–(C6H4)–(O-C2H4)1–25–OH: • Triton X-100 • Polyoxyethylene glycol alkylphenol ethers: C9H19–(C6H4)–(O-C2H4)1–25–OH: • Nonoxynol-9 • Glycerol alkyl esters: • • • • • • • Glyceryl laurate Polyoxyethylene glycol sorbitan alkyl esters: Polysorbate Sorbitan alkyl esters: Spans Cocamide MEA, cocamide DEA Dodecyldimethylamine oxide Block copolymers of polyethylene glycol and polypropylene glycol: Poloxamers Polyethoxylated tallow amine (POEA).
According to the composition of their counter-ion
In the case of ionic surfactants, the counter-ion can be: • Monoatomic / Inorganic: • Cations: metals : alkali metal, alkaline earth metal, transition metal • Anions: halides: chloride (Cl−), bromide (Br−), iodide (I−) • Polyatomic / Organic: • Cations: ammonium, pyridinium, triethanolamine (TEA) • Anions: tosyls, trifluoromethanesulfonates, methylsulfate
Surfactant
114
Current market and forecast
The annual global production of surfactants was 13 million metric tons in 2008, and the annual turnover reached US$24.33 billion in 2009, nearly 2% up from the previous year. The market is expected to experience quite healthy growth by 2.8% annually to 2012 and by 3.5 – 4% thereafter.[4][] Specialists expect the global surfactant market to generate revenues of more than US$41 billion in 2018 – translating to an average annual growth of 4.5%[5]
Health and environmental controversy
Surfactants are routinely deposited in numerous ways on land and into water systems, whether as part of an intended process or as industrial and household waste. Some of them are known to be toxic to animals, ecosystems, and humans, and can increase the diffusion of other environmental contaminants.[][][] As a result, there are proposed or voluntary restrictions on the use of some surfactants. For example, PFOS is a persistent organic pollutant as judged by the Stockholm Convention. Additionally, PFOA has been subject to a voluntary agreement by the U.S. Environmental Protection Agency and eight chemical companies to reduce and eliminate emissions of the chemical and its precursors.[6] The two major surfactants used in the year 2000 were linear alkylbenzene sulfonates (LAS) and the alkyl phenol ethoxylates (APE). They break down in the aerobic conditions found in sewage treatment plants and in soil.[] Ordinary dishwashing detergent, for example, will promote water penetration in soil, but the effect would last only a few days (many standard laundry detergent powders contain levels of chemicals such as alkali and chelating agents that can be damaging to plants and should not be applied to soils). Commercial soil wetting agents will continue to work for a considerable period, but they will eventually be degraded by soil micro-organisms. Some can, however, interfere with the life-cycles of some aquatic organisms, so care should be taken to prevent run-off of these products into streams, and excess product should not be washed down.[citation needed] Anionic surfactants can be found in soils as the result of sludge application, wastewater irrigation, and remediation processes. Relatively high concentrations of surfactants together with multimetals can represent an environmental risk. At low concentrations, surfactant application is unlikely to have a significant effect on trace metal mobility.[7][8]
Biosurfactants
Biosurfactants are surface-active substances synthesised by living cells.[citation needed] Interest in microbial surfactants has been steadily increasing in recent years due to their diversity, environmentally friendly nature, possibility of large-scale production, selectivity, performance under extreme conditions, and potential applications in environmental protection.[][] Biosurfactants enhance the emulsification of hydrocarbons, have the potential to solubilise hydrocarbon contaminants and increase their availability for microbial degradation. The use of chemicals for the treatment of a hydrocarbon polluted site may contaminate the environment with their by-products, whereas biological treatment may efficiently destroy pollutants, while being biodegradable themselves. Hence, biosurfactant-producing microorganisms may play an important role in the accelerated bioremediation of hydrocarbon-contaminated sites.[9][10][] These compounds can also be used in enhanced oil recovery and may be considered for other potential applications in environmental protection.[][11] Other applications include herbicides and pesticides formulations, detergents, healthcare and cosmetics, pulp and paper, coal, textiles, ceramic processing and food industries, uranium ore-processing, and mechanical dewatering of peat.[][][12] Several microorganisms are known to synthesise surface-active agents; most of them are bacteria and yeasts.[13][14] When grown on hydrocarbon substrate as the carbon source, these microorganisms synthesise a wide range of chemicals with surface activity, such as glycolipid, phospholipid, and others.[15][16] These chemicals are synthesised to emulsify the hydrocarbon substrate and facilitate its transport into the cells. In some bacterial species such as Pseudomonas aeruginosa, biosurfactants are also involved in a group motility behavior called swarming motility.
Surfactant
115
Safety and environmental risks
Most anionic and nonionic surfactants are nontoxic, having LD50 comparable to sodium chloride. The situation for cationic surfactants is more diverse. Dialkyldimethylammonium chlorides have very low LD50's (5 g/kg) but alkylbenzyldimethylammonium chloride has an LD50 of 0.35 g/kg. Prolonged exposure of skin to surfactants can cause chaffing because surfactants (e.g., soap) disrupts the lipid coating that protects skin (and other) cells.[1]
Biosurfactants and Deepwater Horizon
The use of biosurfactants as a way to remove petroleum from contaminated sites has been questioned, and criticized as environmentally unsafe. Biosurfactants were not used by BP after the Deepwater Horizon oil spill. However, unprecedented amounts of Corexit (active ingredient: Tween-80), were sprayed directly into the ocean at the leak and on the sea-water's surface, the theory being that the surfactants isolate droplets of oil, making it easier for petroleum-consuming microbes to digest the oil.
Applications
Surfactants play an important role as cleaning, wetting, dispersing, emulsifying, foaming and anti-foaming agents in many practical applications and products, including: • • • • • • • • • • • Detergents Fabric softeners Emulsions Paints Adhesives Inks Anti-fogs Ski waxes, snowboard wax Deinking of recycled papers, in flotation, washing and enzymatic processes Laxatives Agrochemical formulations
• Herbicides (some) • Insecticides • Quantum dot coatings • Biocides (sanitizers) • Cosmetics: • Shampoos • Hair conditioners (after shampoo) • Toothpastes Spermicides (nonoxynol-9) Firefighting Pipelines, liquid drag reducing agent Alkali Surfactant Polymers (used to mobilize oil in oil wells) Ferrofluids Leak Detectors
• • • • • •
Surfactant
116
References
[1] Kurt Kosswig "Surfactants" in Ullmann's Encyclopedia of Industrial Chemistry, Wiley-VCH, 2005, Weinheim. [5] Market Study on Surfactants by Ceresana Research (http:/ / www. ceresana. com/ en/ market-studies/ chemicals/ surfactants) [6] USEPA: "2010/15 PFOA Stewardship Program" (http:/ / www. epa. gov/ opptintr/ pfoa/ pubs/ pfoastewardship. htm) Accessed October 26, 2008.
External links
• Surfactants explained for parents (http://www.curoservice.com/parents_visitors/surfactant/ surfactant_composition_action.asp) • Identification of Surfactants Using Liquid Chromatography-Mass Spectrometry (LC-MS) (http:// littlemsandsailing.wordpress.com/2011/05/01/ identification-of-surfactants-in-commercial-products-by-mass-spectrometry/)
Clara cell
117
Clara cell
Clara cell
Latin exocrinocytus bronchiolaris Code TH H3.05.02.0.00008 [2]
Clara cells are dome-shaped cells with short microvilli found in the small airways (bronchioles) of the lungs.[] Clara cells are found in the ciliated simple epithelium. These cells may secrete glycosaminoglycans to protect the bronchiole lining. Bronchiolar cells gradually increase in number as the number of goblet cells decrease. They are also known as "bronchiolar exocrine cells".[]
Name
"Clara cells" were originally described by their namesake, Max Clara in 1937. Clara was born in South Tyrol in 1899 and died in 1966. He was a Nazi doctor who used tissue from executed victims of the Third Reich for his research at Leipzig, including the work that led to his discovery of Clara cells.[1] Some scholars believe that the eponymous name of these cells should be changed because of the ethical controversy surrounding the discovery of the cells but other scholars disagree and think that the name should remain because it is a testament to a time when medicine crossed an ethical line.[2]
Function
One of the main functions of Clara cells is to protect the bronchiolar epithelium. They do this by secreting a small variety of products, including Clara cell secretory protein (CCSP) and a solution similar to the component of the lung surfactant. They are also responsible for detoxifying harmful substances inhaled into the lungs. Clara cells accomplish this with cytochrome P450 enzymes found in their smooth endoplasmic reticulum. Clara cells also act as a stem cell and multiply and differentiate into ciliated cells to regenerate the bronchiolar epithelium.[3]
Mechanism
The respiratory bronchioles represent the transition from the conducting portion to the respiratory portion of the respiratory system. The narrow channels are usually less than 2 mm in diameter and they are lined by a simple cuboidal epithelium, consisting of ciliated cells and non-ciliated Clara cells, which are unique to bronchioles. In addition to being structurally diverse, Clara cells are also functionally variable. One major function they carry out is the synthesis and secretion of the material lining the bronchiolar lumen. This material includes glycosaminoglycans, proteins such as lysozymes, and conjugation of the secretory portion of IgA antibodies. These play an important defensive role, and they also contribute to the degradation of the mucus produced by the upper airways. The heterogeneous nature of the dense granules within the Clara cell's cytoplasm suggests that they may not all have a secretory function. Some of them may contain lysosomal enzymes, which carry out a digestive role, either in defense: Clara cells engulf airborne toxins and break them down via their cytochrome P-450 enzymes (particularly CYP4B1, which is only present in the clara cells) present in their smooth endoplasmic reticulum; or in the recycling of secretory products. Clara cells are mitotically active cells. They divide and differentiate to form both ciliated and non-ciliated epithelial cells.
Clara cell
118
Role in disease
Clara cells contain Tryptase clara, which is believed to be responsible for cleaving the hemagglutinin surface protein of influenza A virus, thereby activating it and causing the symptoms of flu.[] When the l7Rn6 protein is disrupted in mice, these mice display severe emphysema at birth as a result of disorganization of the Golgi apparatus and formation of aberrant vesicular structures within clara cells.[]
References
[3] http:/ / medical-dictionary. thefreedictionary. com/ Clara+ cell
External links
• • • • BU Histology Learning System: 13805loa (http://www.bu.edu/histology/p/13805loa.htm) -415956935 (http://www.gpnotebook.co.uk/simplepage.cfm?ID=-415956935) at GPnotebook UIUC Histology Subject 1385 (https://histo.life.illinois.edu/histo/atlas/oimages.php?oid=1385) Histology at ucsf.edu (http://pathhsw5m54.ucsf.edu/case24/image245.html)
Somatotropic cell
119
Somatotropic cell
Somatotropic cell
Code TH H3.08.02.2.00021 [1]
Somatotropes are cells in the anterior pituitary that produce growth hormone.
Description
Somatotropic cells constitute 30-40% of anterior pituitary cells. They release growth hormone (GH) in response to Growth hormone releasing hormone (GHRH, or somatocrinin) or are inhibited by GHIH (somatostatin), both received from the hypothalamus via the hypophyseal portal system vein and the secondary plexus. Somatotrope cells are classified as acidophilic cells. These cells take years to grow and mature very slowly. If these cells grow large enough they can impair vision, cause headaches or damage other pituitary functions.
Hormone Deficiency
When levels of somatotropin are low in the body, a physican may prescribe human growth hormone as a drug—see Growth hormone treatment. Deficiency in somatotrope secretion before puberty, or before the end of new bone tissue growth, can lead to pituitary dwarfism. When growth hormone is deficient, blood sugar is low because insulin is not opposed by normal amount of growth hormone. Dwarfs are usually well proportioned, but sometimes have a large head compared to the body.
Hormone Excess
If there is an excess of growth hormone it is usually because of over-secretion of somatotrope cells in the anterior pituitary gland. A significant amount of excess somatotrope secretion before puberty, or before the end of new bone tissue growth, can lead to gigantism. Gigantism is a disease that causes excess growth of body (e.g. being over 7 ft. tall) and unusually long limbs. An excess of secretion of growth hormone after puberty can lead to acromegaly. This is a disease that causes abnormal growth in the hands, head, jaw, and tongue. Some symptoms associated with acromegaly include heavy sweating, oily skin, improper processing of sugars in the diet (diabetes), high blood pressure, increased calcium in urine and swelling of the thyroid gland and arthritis
Bovine
Bovine somatotropin occurs in the pituitary of cattle and differs in structure from human pituitary growth hormone and is biologically inactive in the human being. Bovine somatotropin aids in regulating the amount of milk produced. Recombinant bovine somatotropin (rBST) is a hormone that is injected in cows that increases milk production.
References
• "E-Study Guide For: Human Anatomy" by By Cram101 Reviews, Michael OLoughlin
Prolactin cell
120
Prolactin cell
Prolactin cell
Code TH H3.08.02.2.00022 [1]
Prolactin cell (also known as epsilon acidophil, lactotrope, lactotropic cell, lactotroph, mammatroph, mammotroph) is a cell in the anterior pituitary which produces prolactin in response to hormonal signals including dopamine which is inhibitory and thyrotropin-releasing hormone which is secretagogue. Other regulators include oxytocin, estrogen and progesterone. Prolactin is involved in the maturation of mammary glands and their secretion of milk in association with oxytocin, estrogen, progesterone, glucocorticoids, and others. Prolactin has numerous other effects in both sexes. Prolactin cell are acidophilic by H&E stains and comprise about 20% of all cells in the anterior pituitary gland. If these cells undergo neoplastic transformation, they will give rise to a prolactinoma, a prolactin-secreting pituitary adenoma.
External links
• "Lactotroph [1]" at Dorland's Medical Dictionary
Thyrotropic cell
121
Thyrotropic cell
Thyrotropic cell
Code TH H3.08.02.2.00005 [1]
Thyrotropes (also called thyrotrophs) are endocrine cells in the anterior pituitary which produce thyroid stimulating hormone (TSH) in response to thyrotropin releasing hormone (TRH). Thyrotropes appear basophilic in histological preparations.
Gonadotropic cell
122
Gonadotropic cell
Gonadotropic cell
Code TH H3.08.02.2.00004 [1]
Gonadotropes are endocrine cells in the anterior pituitary that produce the gonadotropins, such as the follicle-stimulating hormone (FSH) and luteinizing hormone (LH). Release of FSH and LH by gonadotrophs is regulated by gonadotropin-releasing hormone (GnRH) from the hypothalamus.[1] Gonadotropes appear basophilic in histological preparations. Gonadotropes have insulin receptors, which can be overstimulated by too high insulin levels. This may lead to infertility as hormone release levels are disrupted. [][2]
References
[1] Ganong, William F.: "Review of Medical Physiology", page 248. Lange, 2005.
Corticotropic cell
123
Corticotropic cell
Corticotropic cell
Code TH H3.08.02.2.00009 [1]
Corticotropes (or corticotrophs) are basophilic cells in the anterior pituitary that produce melanocyte-stimulating hormone, adrenocorticotropic hormone (ACTH) and lipotropin. The cells produce pro-opiomelanocortin (POMC) which undergoes cleavage to ACTH and β-lipotropin (β-LPH). These cells respond to corticotropin releasing hormone (CRH) and make up about 20% of the cells in the anterior pituitary.
Melanocyte-stimulating hormone
pro-opiomelanocortin
Identifiers Symbol POMC Entrez HUGO OMIM RefSeq 5443 9201 [1] [2] [3] [4]
176830
NM_000939
UniProt P01189 [5] Other data Locus Chr. 2 p23 [6]
Melanocyte-stimulating hormone
Clinical data Pregnancy cat. ? Legal status ? Identifiers ATC code ChEMBL ? CHEMBL214332 [7]
Chemical data Formula ? [8]
(what is this?) (verify)
The melanocyte-stimulating hormones (collectively referred to as MSH or intermedins) are a class of peptide hormones that are produced by cells in the intermediate lobe of the pituitary gland. Synthetic analogs of these naturally occurring hormones have also been developed and researched.
Melanocyte-stimulating hormone
124
Function
They stimulate the production and release of melanin (melanogenesis) by melanocytes in skin and hair. MSH signals to the brain have effects on appetite and sexual arousal.
In amphibians
In some animals (such as the claw-toed frog Xenopus laevis) production of MSH is increased when the animal is in a dark location. This causes pigment to be dispersed in pigment cells in the toad's skin, making it become darker, and harder for predators to spot. The pigment cells are called melanophores and therefore, in amphibians, the hormone is often called melanophore-stimulating hormone.
In humans
An increase in MSH will cause a darkening in humans too. Melanocyte-stimulating hormone increases in humans during pregnancy. This, along with increased estrogens, causes increased pigmentation in pregnant women. Cushing's syndrome due to excess adrenocorticotropic hormone (ACTH) may also result in hyperpigmentation, such as acanthosis nigricans in the axilla. Most people with primary Addison's have darkening (hyperpigmentation) of the skin, including areas not exposed to the sun; characteristic sites are skin creases (e.g. of the hands), nipple, and the inside of the cheek (buccal mucosa), new scars become hyperpigmented, whereas older ones do not darken. This occurs because melanocyte-stimulating hormone (MSH) and adrenocorticotropic hormone (ACTH) share the same precursor molecule, Pro-opiomelanocortin (POMC). Different levels of MSH are not the major cause of racial variation in skin colour. However, in many red headed people, and other people who do not tan well, there are variations in their hormone receptors, causing them to not respond to MSH in the blood. See melanocortin receptor for more information.
Structure of MSH
proopiomelanocortin derivatives POMC γ-MSH ACTH α-MSH CLIP β-lipotropin γ-lipotropin β-MSH β-endorphin
Melanocyte-stimulating hormone belongs to a group called the melanocortins. This group includes ACTH, alpha-melanocyte-stimulating hormone (α-MSH), beta-melanocyte-stimulating hormone (β-MSH) and gamma-melanocyte-stimulating hormone (γ-MSH); these peptides are all cleavage products of a large precursor peptide called pro-opiomelanocortin (POMC). α-MSH is the most important melanocortin for pigmentation. The different melanocyte-stimulating hormones have the following amino acid sequences:
Melanocyte-stimulating hormone
125
α-MSH: β-MSH (human):
Ac-Ser-Tyr-Ser-Met-Glu-His-Phe-Arg-Trp-Gly-Lys-Pro-Val Ala-Glu-Lys-Lys-Asp-Glu-Gly-Pro-Tyr-Arg-Met-Glu-His-Phe-Arg-Trp-Gly-Ser-Pro-Pro-Lys-Asp
β-MSH (porcine): Asp-Glu-Gly-Pro-Tyr-Lys-Met-Glu-His-Phe-Arg-Trp-Gly-Ser-Pro-Pro-Lys-Asp γ-MSH: Tyr-Val-Met-Gly-His-Phe-Arg-Trp-Asp-Arg-Phe-Gly
Synthetic MSH
Synthetic analogs of α-MSH have been developed for human use. Two of the better known are afamelanotide (melanotan-1) in testing by Clinuvel Pharmaceuticals in Australia and bremelanotide by Palatin Technologies, a New Jersey company. • Afamelanotide (formerly CUV1647) is being investigated as a method of photoprotection in patients with erythropoietic protoporphyria, polymorphous light eruption, actinic keratosis and squamous cell carcinoma (a form of skin cancer).[1] • An additional analog called Melanotan II causes enhanced libido and erections in most male test subject and arousal with corresponding genital involvement in most female test subjects.[] Bremelanotide (formerly PT-141) which stemmed from Melanotan II research was previously under development by the New Jersey company for its aphrodisiac effects. These effects are mediated by actions in the hypothalamus on neurons that express MC3R and MC4R receptors.
References
[1] Clinuvel FAQs (http:/ / www. clinuvel. com/ en/ faqs/ )
Further reading
• Millington GW (May 2006). "Proopiomelanocortin (POMC): the cutaneous roles of its melanocortin products and receptors". Clin. Exp. Dermatol. 31 (3): 407–12. doi: 10.1111/j.1365-2230.2006.02128.x (http://dx.doi.org/10. 1111/j.1365-2230.2006.02128.x). PMID 16681590 (http://www.ncbi.nlm.nih.gov/pubmed/16681590). • Millington GW (2007). "The role of proopiomelanocortin (POMC) neurones in feeding behaviour" (http://www. ncbi.nlm.nih.gov/pmc/articles/PMC2018708). Nutr Metab (Lond) 4: 18. doi: 10.1186/1743-7075-4-18 (http:// dx.doi.org/10.1186/1743-7075-4-18). PMC 2018708 (http://www.ncbi.nlm.nih.gov/pmc/articles/ PMC2018708). PMID 17764572 (http://www.ncbi.nlm.nih.gov/pubmed/17764572).
External links
• Melanocyte-Stimulating Hormones (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=& term=Melanocyte-Stimulating+Hormones) at the US National Library of Medicine Medical Subject Headings (MeSH) • Clinuvel Pharmaceuticals (http://www.clinuvel.com) • Palatin Technologies (http://www.palatin.com/)
Magnocellular neurosecretory cell
126
Magnocellular neurosecretory cell
Magnocellular neurosecretory cells are large neuroendocrine cells within the supraoptic nucleus and paraventricular nucleus of the hypothalamus. They are also found in smaller numbers in accessory cell groups between these two nuclei, the largest one being the nucleus circularis. There are two types of magnocellular neurosecretory cells, oxytocin-producing cells and vasopressin-producing cells, but a small number can produce both hormones. These cells are neuroendocrine neurons, are electrically excitable, and generate action potentials in response to afferent stimulation.[1] Magnocellular neurosecretory cells in the rat (where these neurons have been most extensively studied) in general have a single long varicose axon, which projects to the posterior pituitary. Each axon gives rise to about 10,000 neurosecretory terminals and many axon swellings that store very large numbers of hormone-containing vesicles.[2] These vesicles are released from the axon swellings and nerve terminals by exocytosis in response to calcium entry through voltage-gated channels, which occurs when action potentials are propagated down the axons.[3] The cells typically have two or three long dendrites, which also contain large dilations, and which also contain a very high density of hormone-containing vesicles. Oxytocin and vasopressin can, thus, be released within the brain from these dendrites, as well as into the blood from the terminals in the posterior pituitary gland.[4] However, the release of oxytocin and vasopressin from dendrites is not consistently accompanied by peripheral secretion, as dendritic release is regulated differently. Dendritic release can be triggered by depolarisation, but can also be triggered by the mobilisation of intracellular calcium stores. The dendrites receive most of the synaptic inputs from afferent neurons that regulate the magnocellular neurons; typically a magnocellular neuron receives about 10,000 synapses from afferent neurons.
References
Oxytocin
127
Oxytocin
Oxytocin
Systematic (IUPAC) name
1-({(4R,7S,10S,13S,16S,19R)-19-amino- 7-(2-amino-2-oxoethyl)- 10-(3-amino-3-oxopropyl)- 16-(4-hydroxybenzoyl)13-[(1S)-1-methylpropyl]- 6,9,12,15,18-pentaoxo- 1,2-dithia- 5,8,11,14,17-pentaazacycloicosan-4-yl}carbonyl)- L-prolylL-leucylglycinamide
Clinical data Trade names AHFS/Drugs.com Pregnancy cat. Legal status Routes Pitocin monograph A (AU) POM (UK) ℞-only (US) Intranasal, IV, IM Pharmacokinetic data Bioavailability Protein binding Metabolism Half-life Excretion nil 30% hepatic oxytocinases 1–6 min Biliary and renal Identifiers CAS number ATC code PubChem IUPHAR ligand 50-56-6 [2] [1]
H01BB02
[3] [4]
CID 439302 2174 [5]
Oxytocin
[6] [8]
128
DrugBank ChemSpider UNII KEGG ChEBI ChEMBL
DB00107 388434
[7]
1JQS135EYN D00089 [9]
CHEBI:7872
[10]
[11]
CHEMBL265640 Chemical data
Formula Mol. mass
C43H66N12O12S2 1007.19 g/mol
(what is this?) (verify)
[12]
Oxytocin (Oxt) (pron.: /ˌɒksɨˈtoʊsɪn/) is a mammalian neurohypophysial hormone that acts primarily as a neuromodulator in the brain. Oxytocin plays roles in sexual reproduction, in particular during and after childbirth. It is released in large amounts after distension of the cervix and uterus during labor, facilitating birth, maternal bonding, and, after stimulation of the nipples, breastfeeding. Both childbirth and milk ejection result from positive feedback mechanisms.[1] Recent studies have begun to investigate oxytocin's role in various behaviors, including orgasm, social recognition, pair bonding, anxiety, and maternal behaviors.[] For this reason, it is sometimes referred to as the "love hormone". There is some evidence that oxytocin promotes ethnocentric behavior, incorporating the trust and empathy of in-groups with their suspicion and rejection of outsiders.[] Furthermore, genetic differences in the oxytocin receptor gene (OXTR) have been associated with maladaptive social traits such as aggressive behaviour.[]
Discovery
The word oxytocin was derived from Greek ὀξύς, oxys, and τόκος, tokos, meaning "quick birth", after its uterine-contracting properties were discovered by British pharmacologist Sir Henry Hallett Dale in 1906.[] The milk ejection property of oxytocin was described by Ott and Scott in 1910[2] and by Schafer and Mackenzie in 1911.[] The nine amino acid sequence of oxytocin was elucidated by Vincent du Vigneaud et al. and by Tuppy in 1953[] and synthesized biochemically soon after by du Vigneaud et al. in 1953.[3][] Oxytocin was the first polypeptide hormone to be sequenced and synthesized.[]
Structure and relation to vasopressin
Oxytocin is a peptide of nine amino acids (a nonapeptide). Its systematic name is cysteine-tyrosine-isoleucine-glutamine-asparagine-cysteine-proline-leucine-glycine-amine (cys – tyr – ile – gln – asn – cys – pro – leu – gly – NH2, or CYIQNCPLG-NH2). Oxytocin has a molecular mass of 1007 daltons. One international unit (IU) of oxytocin is the equivalent of about 2 micrograms of pure peptide. While the structure of oxytocin is highly conserved in placental mammals, a novel structure of oxytocin was recently reported in marmosets, tamarins, and other new world primates. Genomic sequencing of the gene for oxytocin revealed a single in-frame mutation(thymine for cytosine) which results in a single amino acid substitution at the 8-position (proline for leucine).[] The biologically active form of oxytocin, commonly measured by RIA and/or HPLC techniques, is also known as the octapeptide "oxytocin disulfide" (oxidized form), but oxytocin also exists as a reduced dithiol nonapeptide called
Oxytocin oxytoceine.[4] It has been theorized that open chain oxytoceine (the reduced form of oxytocin) may also act as a free radical scavenger (by donating an electron to a free radical); oxytoceine may then be oxidized back to oxytocin via the redox potential of dehydroascorbate <---> ascorbate.[] The structure of oxytocin is very similar to that of vasopressin (cys – tyr – phe – gln – asn – cys – pro – arg – gly – NH2), also a nonapeptide with a sulfur bridge, whose sequence differs from oxytocin by two amino acids. A table showing the sequences of members of the vasopressin/oxytocin superfamily and the species expressing them is present in the vasopressin article. Oxytocin and vasopressin were isolated and synthesized by Vincent du Vigneaud in 1953, work for which he received the Nobel Prize in Chemistry in 1955. Oxytocin and vasopressin are the only known hormones released by the human posterior pituitary gland to act at a distance. However, oxytocin neurons make other Oxytocin (ball-and-stick) bound to its carrier protein neurophysin peptides, including corticotropin-releasing hormone and (ribbons) dynorphin, for example, that act locally. The magnocellular neurons that make oxytocin are adjacent to magnocellular neurons that make vasopressin, and are similar in many respects.
129
Actions
Oxytocin has peripheral (hormonal) actions, and also has actions in the brain. Its actions are mediated by specific, high-affinity oxytocin receptors. The oxytocin receptor is a G-protein-coupled receptor that requires Mg2+ and cholesterol. It belongs to the rhodopsin-type (class I) group of G-protein-coupled receptors.
Peripheral (hormonal) actions
The peripheral actions of oxytocin mainly reflect secretion from the pituitary gland. (See oxytocin receptor for more detail on its action.) • Letdown reflex: In lactating (breastfeeding) mothers, oxytocin acts at the mammary glands, causing milk to be 'let down' into subareolar sinuses, from where it can be excreted via the nipple.[5] Suckling by the infant at the nipple is relayed by spinal nerves to the hypothalamus. The stimulation causes neurons that make oxytocin to fire action potentials in intermittent bursts; these bursts result in the secretion of pulses of oxytocin from the neurosecretory nerve terminals of the pituitary gland. • Uterine contraction: Important for cervical dilation before birth, oxytocin causes contractions during the second and third stages of labor. Oxytocin release during breastfeeding causes mild but often painful contractions during the first few weeks of lactation. This also serves to assist the uterus in clotting the placental attachment point postpartum. However, in knockout mice lacking the oxytocin receptor, reproductive behavior and parturition are normal.[] • Social behavior and wound healing: Oxytocin is also thought to modulate inflammation by decreasing certain cytokines. Thus, the increased release in oxytocin following positive social interactions has the potential to improve wound healing. A study by Marazziti and colleagues used heterosexual couples to address this possibility. They found increases in plasma oxytocin following a social interaction were correlated with faster wound healing. They hypothesized this was due to oxytocin reducing inflammation, thus allowing the wound to heal faster. This study provides preliminary evidence that positive social interactions may directly impact aspects
Oxytocin of health.[6] • The relationship between oxytocin and human sexual response is unclear. At least two uncontrolled studies have found increases in plasma oxytocin at orgasm – in both men and women.[][] Plasma oxytocin levels are notably increased around the time of self-stimulated orgasm and are still higher than baseline when measured five minutes after self arousal.[] The authors of one of these studies speculated that oxytocin's effects on muscle contractibility may facilitate sperm and egg transport.[] In a study measuring oxytocin serum levels in women before and after sexual stimulation, the author suggests it serves an important role in sexual arousal. This study found genital tract stimulation resulted in increased oxytocin immediately after orgasm.[] Another study reported increases of oxytocin during sexual arousal could be in response to nipple/areola, genital, and/or genital tract stimulation as confirmed in other mammals.[] Murphy et al. (1987), studying men, found oxytocin levels were raised throughout sexual arousal with no acute increase at orgasm.[] A more recent study of men found an increase in plasma oxytocin immediately after orgasm, but only in a portion of their sample that did not reach statistical significance. The authors noted these changes "may simply reflect contractile properties on reproductive tissue".[] Oxytocin evokes feelings of contentment, reductions in anxiety, and feelings of calmness and security around the mate.[] This suggests oxytocin may be important for the inhibition of the brain regions associated with behavioral control, fear, and anxiety, thus allowing orgasm to occur. Oxytocin also functions to protect against stress. Meta-analyses conducted in 2003 demonstrated that oxytocin can alleviate mood and reduce stress with a good efficiency.[7] • Due to its similarity to vasopressin, it can reduce the excretion of urine slightly. In several species, oxytocin can stimulate sodium excretion from the kidneys (natriuresis), and, in humans, high doses can result in hyponatremia. • Oxytocin and oxytocin receptors are also found in the heart in some rodents, and the hormone may play a role in the embryonal development of the heart by promoting cardiomyocyte differentiation.[][] However, the absence of either oxytocin or its receptor in knockout mice has not been reported to produce cardiac insufficiencies.[] • Modulation of hypothalamic-pituitary-adrenal axis activity: Oxytocin, under certain circumstances, indirectly inhibits release of adrenocorticotropic hormone and cortisol and, in those situations, may be considered an antagonist of vasopressin.[] • Autism: Oxytocin may play a role in autism and may be an effective treatment for autism's repetitive and affiliative behaviors.[8] Oxytocin treatments also resulted in an increased retention of affective speech in adults with autism.[] Two related studies in adults, in 2003 and 2007, found oxytocin decreased repetitive behaviors and improved interpretation of emotions. More recently, intranasal administration of oxytocin was found to increase emotion recognition in children as young as 12 who are diagnosed with autism spectrum disorders [] Oxytocin has also been implicated in the etiology of autism, with one report suggesting autism is correlated with genomic deletion of the gene containing the oxytocin receptor gene (OXTR). Studies involving Caucasian and Finnish samples and Chinese Han families provide support for the relationship of OXTR with autism.[][] Autism may also be associated with an aberrant methylation of OXTR.[] After treatment with inhaled oxytocin, autistic patients exhibit more appropriate social behavior.[] While this research suggests some promise, further clinical trials of oxytocin are required to demonstrate potential benefit and side effects in the treatment of autism. As such, researchers do not recommend use of oxytocin as a treatment for autism outside of clinical trials. • Increasing trust and reducing fear: In a risky investment game, experimental subjects given nasally administered oxytocin displayed "the highest level of trust" twice as often as the control group. Subjects who were told they were interacting with a computer showed no such reaction, leading to the conclusion that oxytocin was not merely affecting risk-aversion.[] Nasally administered oxytocin has also been reported to reduce fear, possibly by inhibiting the amygdala (which is thought to be responsible for fear responses).[] Indeed, studies in rodents have shown oxytocin can efficiently inhibit fear responses by activating an inhibitory circuit within the amygdala. Some researchers have argued oxytocin has a general enhancing effect on all social emotions, since intranasal
130
Oxytocin administration of oxytocin also increases envy and Schadenfreude.[9] • Oxytocin effects social distance between adult males and females, and may be responsible at least in part for romantic attraction and subsequent monogamous pair bonding. An oxytocin nasal spray caused men in a monogamous relationship, but not single men, to increase the distance between themselves and an attractive woman during a first encounter by 10 to 15 centimeters. The researchers suggested that oxytocin may help promote fidelity within monogamous relationships.[] • Affecting generosity by increasing empathy during perspective taking: In a neuroeconomics experiment, intranasal oxytocin increased generosity in the Ultimatum Game by 80%, but has no effect in the Dictator Game that measures altruism. Perspective-taking is not required in the Dictator Game, but the researchers in this experiment explicitly induced perspective-taking in the Ultimatum Game by not identifying to participants into which role they would be placed.[] Serious methodological questions have arisen, however, with regard to the role of oxytocin in trust and generosity.[10] Empathy in healthy males has been shown to be increased after intranasal oxytocin[][] This is most likely due to the effect of oxytocin in enhancing eye gaze.[] There is some discussion about which aspect of empathy oxytocin might alter – for example, cognitive vs. emotional empathy.[] • Cognitive function: Certain learning and memory functions are impaired by centrally administered oxytocin.[] Also, systemic oxytocin administration can impair memory retrieval in certain aversive memory tasks.[] Interestingly, oxytocin does seem to facilitate learning and memory specifically for social information. Healthy males administered intranasal oxytocin show improved memory for human faces, in particular happy faces.[][] They also show improved recognition for positive social cues over threatening social cues [][] and improved recognition of fear.[11]
131
Actions within the brain
Oxytocin secreted from the pituitary gland cannot re-enter the brain because of the blood–brain barrier. Instead, the behavioral effects of oxytocin are thought to reflect release from centrally projecting oxytocin neurons, different from those that project to the pituitary gland, or that are collaterals from them.[] Oxytocin receptors are expressed by neurons in many parts of the brain and spinal cord, including the amygdala, ventromedial hypothalamus, septum, nucleus accumbens, and brainstem. • Sexual arousal: Oxytocin injected into the cerebrospinal fluid causes spontaneous erections in rats,[] reflecting actions in the hypothalamus and spinal cord. Centrally administrated oxytocin receptor antagonists can prevent noncontact erections, which is a measure of sexual arousal. Studies using oxytocin antagonists in female rats provide data that oxytocin increases lordosis behavior, indicating an increase in sexual receptivity.[] • Bonding: In the prairie vole, oxytocin released into the brain of the female during sexual activity is important for forming a monogamous pair bond with her sexual partner. Vasopressin appears to have a similar effect in males.[12] Oxytocin has a role in social behaviors in many species, so it likely also does in humans. In a 2003 study, both humans and dog oxytocin levels in the blood rose after five to 24 minutes of a petting session. This possibly plays a role in the emotional bonding between humans and dogs.[13] • Maternal behavior: Female rats given oxytocin antagonists after giving birth do not exhibit typical maternal behavior.[] By contrast, virgin female sheep show maternal behavior toward foreign lambs upon cerebrospinal fluid infusion of oxytocin, which they would not do otherwise.[] Oxytocin is involved in the initiation of maternal behavior, not its maintenance; for example, it is higher in mothers after they interact with unfamiliar children rather than their own.[] • Drug interactions: According to some studies in animals, oxytocin inhibits the development of tolerance to various addictive drugs (opiates, cocaine, alcohol), and reduces withdrawal symptoms.[] MDMA (ecstasy) may increase feelings of love, empathy, and connection to others by stimulating oxytocin activity via activation of
Oxytocin serotonin 5-HT1A receptors, if initial studies in animals apply to humans.[] The anxiolytic Buspar (buspirone) also appears to produce some or all of its effect via 5-HT1A receptor-induced oxytocin stimulation.[][] • Preparing fetal neurons for delivery: Crossing the placenta, maternal oxytocin reaches the fetal brain and induces a switch in the action of neurotransmitter GABA from excitatory to inhibitory on fetal cortical neurons. This silences the fetal brain for the period of delivery and reduces its vulnerability to hypoxic damage.[] • Romantic attachment: In some studies, high levels of plasma oxytocin have been correlated with romantic attachment. For example, if a couple is separated for a long period of time, anxiety can increase due to the lack of physical affection. Oxytocin may aid romantically attached couples by decreasing their feelings of anxiety when they are separated.[]
132
Drug forms
Synthetic oxytocin is sold as proprietary medication under the trade names Pitocin and Syntocinon, and as generic oxytocin. Oxytocin is destroyed in the gastrointestinal tract, so must be administered by injection or as nasal spray. It has a half-life of typically about three minutes in the blood, and given intravenously does not enter the brain in significant quantities – it is excluded from the brain by the blood–brain barrier. Evidence in rhesus macaques indicates oxytocin by nasal spray does enter the brain.[] Oxytocin nasal sprays have been used to stimulate breastfeeding, but the efficacy of this approach is doubtful.[] Injected oxytocin analogues are used for labor induction and to support labor in case of difficult parturition. It has largely replaced ergometrine as the principal agent to increase uterine tone in acute postpartum hemorrhage. Oxytocin is also used in veterinary medicine to facilitate birth and to stimulate milk release. The tocolytic agent atosiban (Tractocile) acts as an antagonist of oxytocin receptors; this drug is registered in many countries to suppress premature labor between 24 and 33 weeks of gestation. It has fewer side effects than drugs previously used for this purpose (ritodrine, salbutamol, and terbutaline). The trust-inducing property of oxytocin might help those who suffer from social anxieties and mood disorders,[] but with the potential for abuse with confidence tricks[][] and military applications.[]
Potential adverse reactions
Oxytocin is relatively safe when used at recommended doses, and side effects are uncommon.[] The following maternal events have been reported:[] • • • • • • • • • Subarachnoid hemorrhage Increased heart rate Decreased blood pressure Cardiac arrhythmia and premature ventricular contraction Impaired uterine blood flow Pelvic hematoma Afibrinogenonemia, which can lead to hemorrhage and death Anaphylaxis Nausea and vomiting
Excessive dosage or long-term administration (over a period of 24 hours or longer) have been known to result in tetanic uterine contractions, uterine rupture, postpartum hemorrhage, and water intoxication, sometimes fatal. Increased uterine motility has led to the following complications in the fetus/neonate:[] • Decreased heart rate or heart rate decelerations • Cardiac arrhythmia • Brain damage • Seizures
Oxytocin • Death
133
Synthesis, storage, and release
Oxytocin/neurophysin I prepropeptide
Identifiers Symbols External IDs OXT
[26]
; OT; OT-NPI; OXT-NPI
[27]
OMIM: 167050
MGI: 97453
[28]
HomoloGene: 55494
[29]
GeneCards: OXT Gene
[30]
Oxytocin
134
Gene Ontology Molecular function • neurohypophyseal hormone activity [31] [32] • oxytocin receptor binding Cellular component • extracellular region [229] [230] • extracellular space [33] • secretory granule [34] • terminal button Biological process • response to amphetamine [36] • regulation of heart rate [37] • maternal aggressive behavior [38] • signal transduction [39] • elevation of cytosolic calcium ion concentration [40] • heart development [41] • female pregnancy [42] • memory [43] • grooming behavior [44] • response to sucrose stimulus [45] • positive regulation of norepinephrine secretion [46] • response to activity [47] • sleep [48] • positive regulation of prostaglandin secretion [49] • response to estradiol stimulus [50] • response to retinoic acid [51] • response to progesterone stimulus [52] • response to prostaglandin E stimulus [53] • social behavior [54] • negative regulation of urine volume [55] • positive regulation of renal sodium excretion [56] • response to cocaine [57] • hyperosmotic salinity response [58] • maternal behavior [59] • sperm ejaculation [60] • eating behavior [61] • drinking behavior [62] • response to peptide hormone stimulus [63] • response to ether [64] • negative regulation of blood pressure [65] • positive regulation of blood pressure [66] • positive regulation of ossification [67] • positive regulation of female receptivity [68] • positive regulation of synaptic transmission [69] • response to glucocorticoid stimulus [70] • response to cAMP [71] • response to electrical stimulus [72] • regulation of sensory perception of pain [73] • positive regulation of synapse assembly [74] • male mating behavior [75] • positive regulation of penile erection [76] • positive regulation of hindgut contraction [77] • negative regulation of gastric acid secretion [78] • positive regulation of uterine smooth muscle contraction Sources: Amigo
[79] [35]
/ QuickGO
[80]
Orthologs
Oxytocin
135
Species Entrez Ensembl UniProt RefSeq (mRNA) RefSeq (protein) Human 5020
[81] [83]
Mouse 18429
[82] [84]
ENSG00000101405 P01178
[85] [87]
ENSMUSG00000027301 P35454
[86] [88]
NM_000915 NP_000906
NM_011025 NP_035155
[89]
[90]
Location (UCSC) Chr 20: [91] 3.05 – 3.05 Mb PubMed search
[93]
Chr 2: [92] 130.58 – 130.58 Mb
[94]
The oxytocin peptide is synthesized as an inactive precursor protein from the OXT gene.[][][] This precursor protein also includes the oxytocin carrier protein neurophysin I.[] The inactive precursor protein is progressively hydrolyzed into smaller fragments (one of which is neurophysin I) via a series of enzymes. The last hydrolysis that releases the active oxytocin nonapeptide is catalyzed by peptidylglycine alpha-amidating monooxygenase (PAM).[] The activity of the PAM enzyme system is dependent upon vitamin C (ascorbate), which is a necessary vitamin cofactor. By chance, sodium ascorbate by itself was found to stimulate the production of oxytocin from ovarian tissue over a range of concentrations in a dose-dependent manner.[] Many of the same tissues (e.g. ovaries, testes, eyes, adrenals, placenta, thymus, pancreas) where PAM (and oxytocin by default) is found are also known to store higher concentrations of vitamin C.[]
Neural sources
In the hypothalamus, oxytocin is made in magnocellular neurosecretory cells of the supraoptic and paraventricular nuclei, and is stored in Herring bodies at the axon terminals in the posterior pituitary. It is then released into the blood from the posterior lobe (neurohypophysis) of the pituitary gland. These axons (likely, but dendrites have not been ruled out) have collaterals that innervate oxytocin receptors in the nucleus accumbens.[] The peripheral hormonal and behavioral brain effects of oxytocin are thought to be coordinated through its common release through these collaterals.[] Oxytocin is also made by some neurons in the paraventricular nucleus that project to other parts of the brain and to the spinal cord.[14] Depending on the species, oxytocin receptor-expressing cells are located in other areas, including the amygdala and bed nucleus of the stria terminalis. In the pituitary gland, oxytocin is packaged in large, dense-core vesicles, where it is bound to neurophysin I as shown in the inset of the figure; neurophysin is a large peptide fragment of the larger precursor protein molecule from which oxytocin is derived by enzymatic cleavage. Secretion of oxytocin from the neurosecretory nerve endings is regulated by the electrical activity of the oxytocin cells in the hypothalamus. These cells generate action potentials that propagate down axons to the nerve endings in the pituitary; the endings contain large numbers of oxytocin-containing vesicles, which are released by exocytosis when the nerve terminals are depolarised.
Oxytocin
136
Non-neural sources
Outside the brain, oxytocin-containing cells have been identified in several diverse tissues, including the corpus luteum,[][] the interstitial cells of Leydig,[] the retina,[] the adrenal medulla,[] the placenta,[] the thymus[] and the pancreas.[] The finding of significant amounts of this classically "neurohypophysial" hormone outside the central nervous system raises many questions regarding its possible importance in these different tissues. Female Oxytocin is synthesized by corpora lutea of several species, including ruminants and primates. Along with estrogen, it is involved in inducing the endometrial synthesis of prostaglandin F2α to cause regression of the corpus luteum. Male The Leydig cells in some species have also been shown to possess the biosynthetic machinery to manufacture testicular oxytocin de novo, to be specific, in rats (which can synthesize vitamin C endogenously), and in guinea pigs, which, like humans, require an exogenous source of vitamin C (ascorbate) in their diets.[]
Oxytocin receptor polymorphism
The oxytocin receptor in humans has several alleles, which differ in their effectiveness. For example, at one particular marker, individuals homozygous for the "G" allele, when compared to carriers of the "A" allele, show higher empathy and lower stress response,[15] as well as lower prevalence of autism and of poor parenting skills.[16]
Evolution
Virtually all vertebrates have an oxytocin-like nonapeptide hormone that supports reproductive functions and a vasopressin-like nonapeptide hormone involved in water regulation. The two genes are usually located close to each other (less than 15,000 bases apart) on the same chromosome, and are transcribed in opposite directions (however, in fugu,[] the homologs are further apart and transcribed in the same direction). The two genes are believed to result from a gene duplication event; the ancestral gene is estimated to be about 500 million years old and is found in cyclostomata (modern members of the Agnatha).[]
References
[1] Marieb Human Anatomy & Physiology 9th edition, chapter:16, page:599 [2] Ott I, Scott JC. The Action of Infundibulum upon Mammary Secretion. Proc Soc Exp Biol. (1910) p.8:48–49. [5] http:/ / emedicine. medscape. com/ article/ 976504-overview [12] Vacek M, High on Fidelity. What can voles teach us about monogamy? (http:/ / www. americanscientist. org/ issues/ pub/ high-on-fidelity) [13] Kuchinskas Susan, The Chemistry of Connection: How the Oxytocin Response Can Help You Find Trust, Intimacy, and Love p65 (http:/ / books. google. com/ books?hl=en& lr=& id=VO6dp52RxnQC& oi=fnd& pg=PR5& dq=oxytocin+ petting+ dog& ots=mTRRd4zj_9& sig=5xIdHdfrvmOOmZJh0Eak_KgYl2w#v=onepage& q= petting dog& f=false)
Further reading
• Lee HJ, Macbeth AH, Pagani JH, Young WS (June 2009). "Oxytocin: the Great Facilitator of Life" (http://www. ncbi.nlm.nih.gov/pmc/articles/PMC2689929). Progress in Neurobiology 88 (2): 127–51. doi: 10.1016/j.pneurobio.2009.04.001 (http://dx.doi.org/10.1016/j.pneurobio.2009.04.001). PMC 2689929 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2689929). PMID 19482229 (http://www.ncbi.nlm.nih. gov/pubmed/19482229). • Caldwell HK, Young WS III (2006). "Oxytocin and Vasopressin: Genetics and Behavioral Implications" (http:// refworks.springer.com/mrw/fileadmin/pdf/Neurochemistry/0387303480C25.PDF). In Abel L, Lim R. Handbook of neurochemistry and molecular neurobiology. Berlin: Springer. pp. 573–607. ISBN 0-387-30348-0.
Oxytocin
137
External links
• Hug the Monkey (http://kuchinskas.typepad.com/hug_the_monkey/) – A weblog devoted entirely to oxytocin • The Soft Machine (http://tijmz.files.wordpress.com/2011/06/softmachine4.pdf) – Review of oxytocin and bonding in animal and human research (.pdf) • A Neurophysiologic Model of the Circuitry of Oxytocin in Arousal, Female Distress and Depression – Rainer K. Liedtke, MD (http://www.rkliedtke.de/oxytocin2_us.html) (2004) • Oxytocin.org (http://www.oxytocin.org/oxytoc/love-science.html) – 'I get a kick out of you: Scientists are finding that, after all, love really is down to a chemical addiction between people', The Economist (February 12, 2004) • NewScientist.com (http://www.newscientist.com/channel/sex/mg18925365.500) – 'Release of Oxytocin due to penetrative sex reduces stress and neurotic tendencies', New Scientist (January 26, 2006) • SMH.com.au (http://smh.com.au/news/mind-matters/to-sniff-at-danger/2006/01/12/1136956247384.html) – 'To sniff at danger: Inhalable oxytocin could become a cure for social fears', Boston Globe (January 12, 2006) • 'Cuddle chemical' could treat mental illness (http://www.newscientist.com/channel/being-human/ mg19826561.900-cuddle-chemical-could-treat-mental-illness.html) (14 May 2008) New Scientist • Molecular neurobiology of social bonding: Implications for autism spectrum disorders (http://videocast.nih. gov/Summary.asp?File=15521) a lecture by Prof. Larry Young, Jan. 4, 2010. • A TED talk by Prof.Paul Zak on Trust,Morality & Oxytocin (http://www.ted.com/talks/ paul_zak_trust_morality_and_oxytocin.html)
Vasopressin
138
Vasopressin
Arginine vasopressin
Space-filling model of arginine vasopressin Available structures PDB Ortholog search: PDBe [1], RCSB [2] List of PDB id codes 1jk4
[3]
, 1jk6
[4]
, 1npo
[5]
, 2bn2
[6]
Identifiers Symbols External IDs AVP
[7]
; ADH; ARVP; AVP-NPII; AVRP; VP
[8]
OMIM: 192340
MGI: 88121
[9]
HomoloGene: 417
[10]
GeneCards: AVP Gene
[11]
Vasopressin
139
Gene Ontology Molecular function • protein kinase activity [12] [13] • signal transducer activity [14] • receptor binding [15] • neuropeptide hormone activity [31] • neurohypophyseal hormone activity [16] • V1A vasopressin receptor binding [17] • V1B vasopressin receptor binding [18] • cysteine-type endopeptidase inhibitor activity involved in apoptotic process Cellular component • extracellular region [229] [230] • extracellular space [19] • cytosol [33] • secretory granule [20] • dendrite Biological process • maternal aggressive behavior [21] • positive regulation of systemic arterial blood pressure [22] • generation of precursor metabolites and energy [23] • protein phosphorylation [24] • water transport [38] • signal transduction [39] • elevation of cytosolic calcium ion concentration [25] • cell-cell signaling [26] • negative regulation of female receptivity [43] • grooming behavior [27] • locomotory behavior [28] • positive regulation of cell proliferation [29] • positive regulation of gene expression [30] • positive regulation of glutamate secretion [31] • positive regulation of cell growth [32] • positive regulation of cAMP biosynthetic process [33] • positive regulation of prostaglandin biosynthetic process [34] • positive regulation of cellular pH reduction [35] • positive regulation of peptidyl-serine phosphorylation [36] • response to nicotine [53] • social behavior [37] • regulation of renal sodium excretion [38] • vasoconstriction [57] • hyperosmotic salinity response [58] • maternal behavior [39] • negative regulation of apoptotic process [40] • penile erection • negative regulation of cysteine-type endopeptidase activity involved in apoptotic process
[41] [37]
• sodium-independent organic anion transport [43] • response to ethanol [44] • positive regulation of vasoconstriction [45] • multicellular organismal water homeostasis [46] • negative regulation of transmission of nerve impulse [47] • transmembrane transport [48] • ERK1 and ERK2 cascade [49] • protein kinase C signaling cascade [50] • negative regulation of release of cytochrome c from mitochondria Sources: Amigo
[51]
[42]
/ QuickGO
[52]
Vasopressin
140
RNA expression pattern
More reference expression data Orthologs Species Entrez Ensembl UniProt RefSeq (mRNA) RefSeq (protein) Location (UCSC) Human 551
[54] [56]
[53]
Mouse 11998
[55] [57]
ENSG00000101200 P01185
[58] [60]
ENSMUSG00000037727 P35455
[59] [61]
NM_000490 NP_000481
NM_009732 NP_033862
[62]
[63]
Chr 20: [64] 3.06 – 3.07 Mb
[66]
Chr 2: [65] 130.58 – 130.58 Mb
[67]
PubMed search
Arginine vasopressin (AVP), also known as vasopressin, argipressin or antidiuretic hormone (ADH), is a neurohypophysial hormone found in most mammals. Its two primary functions are to retain water in the body and to constrict blood vessels. Vasopressin regulates the body's retention of water by acting to increase water absorption in the collecting ducts of the kidney nephron.[] Vasopressin increases water permeability of the kidney's collecting duct and distal convoluted tubule by inducing translocation of aquaporin-CD water channels in the kidney nephron collecting duct plasma membrane.[] Vasopressin is a peptide hormone that controls the reabsorption of molecules in the tubules of the kidneys by affecting the tissue's permeability. It also increases peripheral vascular resistance, which in turn increases arterial blood pressure. It plays a key role in homeostasis, by the regulation of water, glucose, and salts in the blood. It is derived from a preprohormone precursor that is synthesized in the hypothalamus and stored in vesicles at the posterior pituitary. Most of it is stored in the posterior pituitary to be released into the bloodstream. However, some AVP may also be released directly into the brain, and accumulating evidence suggests it plays an important role in social behavior, sexual motivation and bonding, and maternal responses to stress.
Physiology
Function
One of the most important roles of AVP is to regulate the body's retention of water; it is released when the body is dehydrated and causes the kidneys to conserve water, thus concentrating the urine and reducing urine volume. At high concentrations, it also raises blood pressure by inducing moderate vasoconstriction. In addition, it has a variety of neurological effects on the brain, having been found, for example, to influence pair-bonding in voles. The high-density distributions of vasopressin receptor AVPr1a in prairie vole ventral forebrain regions have been shown to facilitate and coordinate reward circuits during partner preference formation, critical for pair bond formation.[] A very similar substance, lysine vasopressin (LVP) or lypressin, has the same function in pigs and is often used in human therapy.
Vasopressin Kidney Vasopressin has two effects by which it contributes to increased urine osmolarity (increased concentration) and decreased water excretion. These are: 1. Increasing the water permeability of distal tubule and collecting duct cells in the kidney, thus allowing water reabsorption and excretion of more concentrated urine, i.e., antidiuresis. This occurs through insertion of water channels (Aquaporin-2) into the apical membrane of distal tubule and collecting duct epithelial cells. Aquaporins allow water to move down their osmotic gradient and out of the nephron, increasing the amount of water re-absorbed from the filtrate (forming urine) back into the bloodstream. V2 receptors, which are G protein-coupled receptors on the basolateral plasma membrane of the epithelial cells, couple to the heterotrimeric G-protein Gs, which activates adenylyl cyclases III and VI to convert ATP into cAMP, plus 2 inorganic phosphates. The rise in cAMP then triggers the insertion of aquaporin-2 water channels by exocytosis of intracellular vesicles, recycling endosomes. Vasopressin also increases the concentration of calcium in the collecting duct cells, by episodic release from intracellular stores. Vasopressin, acting through cAMP, also increases transcription of the aquaporin-2 gene, thus increasing the total number of aquaporin-2 molecules in collecting duct cells. Cyclic-AMP activates protein kinase A (PKA) by binding to its regulatory subunits and allowing them to detach from the catalytic subunits. Detachment exposes the catalytic site in the enzyme, allowing it to add phosphate groups to proteins (including the aquaporin-2 protein), which alters their functions. 2. Increasing permeability of the inner medullary portion of the collecting duct to urea by regulating the cell surface expression of urea transporters,[] which facilitates its reabsorption into the medullary interstitium as it travels down the concentration gradient created by removing water from the connecting tubule, cortical collecting duct, and outer medullary collecting duct. Cardiovascular system Vasopressin increases peripheral vascular resistance (vasoconstriction) and thus increases arterial blood pressure. This effect appears small in healthy individuals; however it becomes an important compensatory mechanism for restoring blood pressure in hypovolemic shock such as that which occurs during hemorrhage. Central nervous system Vasopressin released within the brain has many actions: • It has been implicated in memory formation, including delayed reflexes, image, short- and long-term memory, though the mechanism remains unknown; these findings are controversial. However, the synthetic vasopressin analogue desmopressin has come to interest as a likely nootropic.
[68] Avp is expressed in the periventricular [] region of the hypothalamus in the adult mouse. Allen Brain Atlases
141
• Vasopressin is released into the brain in a circadian rhythm by neurons of the supraoptic nucleus. • Vasopressin released from centrally projecting hypothalamic neurons is involved in aggression, blood pressure regulation and
temperature regulation. • It is likely that vasopressin acts in conjunction with corticotropin-releasing hormone to modulate the release of corticosteroids from the adrenal gland in response to stress, particularly during pregnancy and lactation in mammals.[][][] • Selective AVPr1a blockade in the ventral pallidum has been shown to prevent partner preference in prairie voles, suggesting that these receptors in this ventral forebrain region are crucial for pair bonding.[]
Vasopressin • Recent evidence suggests that vasopressin may have analgesic effects. The analgesia effects of vasopressin were found to be dependent on both stress and gender.[] Evidence for this comes from experimental studies in several species, which indicate that the precise distribution of vasopressin and vasopressin receptors in the brain is associated with species-typical patterns of social behavior. In particular, there are consistent differences between monogamous species and promiscuous species in the distribution of AVP receptors, and sometimes in the distribution of vasopressin-containing axons, even when closely related species are compared.[] Moreover, studies involving either injecting AVP agonists into the brain or blocking the actions of AVP support the hypothesis that vasopressin is involved in aggression toward other males. There is also evidence that differences in the AVP receptor gene between individual members of a species might be predictive of differences in social behavior. One study has suggested that genetic variation in male humans affects pair-bonding behavior. The brain of males uses vasopressin as a reward for forming lasting bonds with a mate, and men with one or two of the genetic alleles are more likely to experience marital discord. The partners of the men with two of the alleles affecting vasopressin reception state disappointing levels of satisfaction, affection, and cohesion.[] Vasopressin receptors distributed along the reward circuit pathway, to be specific in the ventral pallidum, are activated when AVP is released during social interactions such as mating, in monogamous prairie voles. The activation of the reward circuitry reinforces this behavior, leading to conditioned partner preference, and thereby initiates the formation of a pair bond.[]
142
Control
Vasopressin is secreted from the posterior pituitary gland in response to reductions in plasma volume, in response to increases in the plasma osmolality, and in response to cholecystokinin (CCK) secreted by the small intestine: • Secretion in response to reduced plasma volume is activated by pressure receptors in the veins, atria, and carotids. • Secretion in response to increases in plasma osmotic pressure is mediated by osmoreceptors in the hypothalamus. • Secretion in response to increases in plasma CCK is mediated by an unknown pathway. The neurons that make AVP, in the hypothalamic supraoptic nuclei (SON) and paraventricular nuclei (PVN), are themselves osmoreceptors, but they also receive synaptic input from other osmoreceptors located in regions adjacent to the anterior wall of the third ventricle. These regions include the organum vasculosum of the lamina terminalis and the subfornical organ. Many factors influence the secretion of vasopressin: • Ethanol (alcohol) reduces the calcium-dependent secretion of AVP by blocking voltage-gated calcium channels in neurohypophyseal nerve terminals.[1] • Angiotensin II stimulates AVP secretion, in keeping with its general pressor and pro-volumic effects on the body.[] • Atrial natriuretic peptide inhibits AVP secretion, in part by inhibiting Angiotensin II-induced stimulation of AVP secretion.[]
Secretion
The main stimulus for secretion of vasopressin is increased osmolality of plasma. Reduced volume of extracellular fluid also has this effect, but is a less sensitive mechanism. The AVP that is measured in peripheral blood is almost all derived from secretion from the posterior pituitary gland (except in cases of AVP-secreting tumours). Vasopressin is produced by magnocellular neurosecretory neurons in the Paraventricular nucleus of hypothalamus (PVN) and Supraoptic nucleus (SON). It then travels down the axon through the infundibulum within neurosecretory granules that are found within Herring bodies, localized swellings of the axons and nerve terminals. These carry the peptide directly to the posterior pituitary gland, where it is stored until released into the blood. However there are two other sources of AVP with important local effects:
Vasopressin • AVP is also synthesized by parvocellular neurosecretory neurons at the PVN, transported and released at the median eminence, which then travels through the hypophyseal portal system to the anterior pituitary where it stimulates corticotropic cells synergistically with CRH to produce ACTH (by itself it is a weak secretagogue).[] • Vasopressin is also released into the brain by several different populations of smaller neurons.
143
Receptors
Below is a table summarizing some of the actions of AVP at its four receptors, differently expressed in different tissues and exerting different actions:
Type AVPR1A Second messenger system Locations Actions Vasoconstriction, gluconeogenesis, platelet aggregation, and release [] of factor VIII and von Willebrand factor; social recognition, [] circadian tau Adrenocorticotropic hormone secretion in response to stress; [] social interpretation of olfactory cues []
Phosphatidylinositol/calcium Liver, kidney, peripheral vasculature, brain
AVPR1B or AVPR3 AVPR2
Phosphatidylinositol/calcium Pituitary gland, brain
Adenylate cyclase/cAMP
Basolateral membrane of the cells lining the collecting ducts of the kidneys (especially the cortical and outer medullary collecting ducts)
Insertion of aquaporin-2 (AQP2) channels (water channels). This allows water to be reabsorbed down an osmotic gradient, and so the urine is more concentrated. Release of von Willebrand factor and surface expression of P-selectin through exocytosis of [][] Weibel-Palade bodies from endothelial cells Increases cytosolic calcium and acts as an inverse agonist of cAMP [] accumulation
VACM-1
Phosphatidylinositol/calcium Vascular endothelium and renal collecting tubules
Structure and relation to oxytocin
The vasopressins are peptides consisting of nine amino acids (nonapeptides). (NB: the value in the table above of 164 amino acids is that obtained before the hormone is activated by cleavage). The amino acid sequence of arginine vasopressin is Cys-Tyr-Phe-Gln-Asn-Cys-Pro-Arg-Gly, with the cysteine residues forming a disulfide bond. Lysine vasopressin has a lysine in place of the arginine. The structure of oxytocin is very similar to that of the vasopressins: It is also a nonapeptide with a disulfide bridge and its amino acid sequence differs at only two positions (see table below). The two genes are located on the same chromosome separated by a relatively small distance of less than 15,000 bases in most species. The magnocellular neurons that make vasopressin are adjacent to magnocellular neurons that make oxytocin, and are similar in many respects. The similarity of the two peptides can cause some cross-reactions: oxytocin has a slight antidiuretic function, and high levels of AVP can cause uterine contractions.[][] Below is a table showing the superfamily of vasopressin and oxytocin neuropeptides:
Chemical structure of the argipressin (indicating that this compound is of the vasopressin family with an arginine at the 8th amino acid position.
Chemical structure of oxytocin
Vasopressin
144
Vertebrate Vasopressin Family Cys-Tyr-Phe-Gln-Asn-Cys-Pro-Arg-Gly-NH2 Argipressin (AVP, ADH) Lypressin (LVP) Phenypressin Vasotocin† Most mammals
Cys-Tyr-Phe-Gln-Asn-Cys-Pro-Lys-Gly-NH2 Cys-Phe-Phe-Gln-Asn-Cys-Pro-Arg-Gly-NH2 Cys-Tyr-Ile-Gln-Asn-Cys-Pro-Arg-Gly-NH2
Pigs, hippos, warthogs, some marsupials Some marsupials Non-mammals
Vertebrate Oxytocin Family Cys-Tyr-Ile-Gln-Asn-Cys-Pro-Leu-Gly-NH2 Cys-Tyr-Ile-Gln-Asn-Cys-Pro-Pro-Gly-NH2 Cys-Tyr-Ile-Gln-Asn-Cys-Pro-Ile-Gly-NH2 Oxytocin (OXT) Prol-Oxytocin Mesotocin Most mammals, ratfish Some New World monkeys, northern tree shrews Most marsupials, all birds, reptiles, amphibians, lungfishes, coelacanths Frogs Bony fishes Skates Sharks
Cys-Tyr-Ile-Gln-Ser-Cys-Pro-Ile-Gly-NH2 Cys-Tyr-Ile-Ser-Asn-Cys-Pro-Ile-Gly-NH2 Cys-Tyr-Ile-Ser-Asn-Cys-Pro-Gln-Gly-NH2
Seritocin Isotocin Glumitocin
Cys-Tyr-Ile-Asn/Gln-Asn-Cys-Pro-Leu/Val-Gly-NH2 Various tocins
Invertebrate VP/OT Superfamily Cys-Leu-Ile-Thr-Asn-Cys-Pro-Arg-Gly-NH2 Cys-Phe-Val-Arg-Asn-Cys-Pro-Thr-Gly-NH2 Cys-Phe-Ile-Arg-Asn-Cys-Pro-Lys-Gly-NH2 Cys-Ile-Ile-Arg-Asn-Cys-Pro-Arg-Gly-NH2 Cys-Tyr-Phe-Arg-Asn-Cys-Pro-Ile-Gly-NH2 Cys-Phe-Trp-Thr-Ser-Cys-Pro-Ile-Gly-NH2 Diuretic Hormone Annetocin Lys-Connopressin Arg-Connopressin Cephalotocin Octopressin Locust Earthworm Geography & imperial cone snail, pond snail, sea hare, leech Striped cone snail Octopus Octopus [2]
†Vasotocin is the evolutionary progenitor of all the vertebrate neurohypophysial hormones.
Role in disease
Lack of AVP
Decreased AVP release or decreased renal sensitivity to AVP leads to diabetes insipidus, a condition featuring hypernatremia (increased blood sodium concentration), polyuria (excess urine production), and polydipsia (thirst).
Excess AVP
High levels of AVP secretion may lead to hyponatremia. In many cases, the AVP secretion is appropriate (due to severe hypovolemia), and the state is labelled "hypovolemic hyponatremia". In certain disease states (heart failure, nephrotic syndrome) the body fluid volume is increased but AVP production is not suppressed for various reasons; this state is labelled "hypervolemic hyponatremia". A proportion of cases of hyponatremia feature neither hyper- nor hypovolemia. In this group (labelled "euvolemic hyponatremia"), AVP secretion is either driven by a lack of cortisol or thyroxine (hypoadrenalism and hypothyroidism, respectively) or a very low level of urinary solute excretion (potomania, low-protein diet), or it is entirely inappropriate. This last category is classified as the syndrome of inappropriate antidiuretic hormone (SIADH).[] SIADH in turn can be caused by a number of problems. Some forms of cancer can cause SIADH, particularly small cell lung carcinoma but also a number of other tumors. A variety of diseases affecting the brain or the lung
Vasopressin (infections, bleeding) can be the driver behind SIADH. A number of drugs has been associated with SIADH, such as certain antidepressants (serotonin reuptake inhibitors and tricyclic antidepressants), the anticonvulsant carbamazepine, oxytocin (used to induce and stimulate labor), and the chemotherapy drug vincristine. Finally, it can occur without a clear explanation.[] Hyponatremia can be treated pharmaceutically through the use of vasopressin receptor antagonists.[]
145
Pharmacology
Vasopressin analogues
Vasopressin agonists are used therapeutically in various conditions, and its long-acting synthetic analogue desmopressin is used in conditions featuring low vasopressin secretion, as well as for control of bleeding (in some forms of von Willebrand disease and in mild haemophilia A) and in extreme cases of bedwetting by children. Terlipressin and related analogues are used as vasoconstrictors in certain conditions. Use of vasopressin analogues for esophageal varices commenced in 1970.[] Vasopressin infusion has also been used as a second line of management in septic shock patients not responding to high dose of inotropes (e.g., dopamine or norepinephrine).
The role of vasopressin analogues in cardiac arrest
Injection of vasopressors for the treatment of cardiac arrest was first suggested in the literature in 1896 when Austrian scientist Dr. R. Gottlieb described the vasopressor epinephrine as an "infusion of a solution of suprarenal extract [that] would restore circulation when the blood pressure had been lowered to unrecordable levels by chloral hydrate."[] Modern interest in vasopressors as a treatment for cardiac arrest stem mostly from canine studies performed in the 1960s by anesthesiologists Dr. John W. Pearson and Dr. Joseph Stafford Redding in which they demonstrated improved outcomes with the use of adjunct intracardiac epinephrine injection during resuscitation attempts after induced cardiac arrest.[] Also contributing to the idea that vasopressors may be useful treatments in cardiac arrest are studies performed in the early to mid 1990's that found significantly higher levels of endogenous serum vasopressin in adults after successful resuscitation from out-of-hospital cardiac arrest compared to those who did not live.[][] Results of animal models have supported the use of either vasopressin or epinephrine in cardiac arrest resuscitation attempts, showing improved coronary perfusion pressure[] and overall improvement in short-term survival as well as neurological outcomes.[] Vasopressin vs. epinephrine
Table 1. Meta-analysis of outcomes for patients treated with vasopressin versus epinephrine[]
RR (95% CI) Failure of ROSC Death before hospital admission Death within 24 hours Death before hospital discharge 0.81 (0.58-1.12) 0.72 (0.38-1.39) 0.74 (0.38-1.43) 0.96 (0.87-1.05)
Number of deaths and neurologically impaired survivors 1.00 (0.94-1.07)
Although both vasopressors, vasopressin and epinephrine differ in that vasopressin does not have direct effects on cardiac contractility as epinephrine does.[] Thus, vasopressin is theorized to be of increased benefit over epinephrine in cardiac arrest due to its properties of not increasing myocardial and cerebral oxygen demands.[] This idea has led
Vasopressin to the advent of several studies searching for the presence of a clinical difference in benefit of these two treatment choices. Initial small studies demonstrated improved outcomes with vasopressin in comparison to epinephrine.[] However, subsequent studies have not all been in agreement. Several randomized controlled trials have been unable to reproduce positive results with vasopressin treatment in both return of spontaneous circulation (ROSC) and survival to hospital discharge,[][][][] including a systematic review and meta-analysis completed in 2005 that found no evidence of a significant difference with vasopressin in five studied outcomes (see Table 1).[] Vasopressin and epinephrine vs. epinephrine alone
146
Table 2. Significant outcomes for combined vasopressin and epinephrine treatment
RR (95% CI) [] ROSC Survival to hospital admission [] In subgroup: PEA [] 1.42 (1.14-1.77) 1.42 (1.02-2.04) 0.05 1.30 (0.90-2.06) 0.02 p value
[] In subgroup: Collapse to ED arrival time of 15–30 minutes 1.22 (1.01-1.49) 0.05 [] In subgroup: Collapse to ED arrival time of 30–45 minutes 1.11 (1.00-1.24) 0.05 Survival to hospital discharge [] 3.69 (1.52-8.95)
There is no current evidence of significant survival benefit with improved neurological outcomes in patients given combinations of both epinephrine and vasopressin during cardiac arrest.[][][3][] A systematic review from 2008 did, however, find one study that showed a statistically significant improvement in ROSC and survival to hospital discharge with this combination treatment; unfortunately, those patients that survived to hospital discharge had overall poor outcomes and many suffered permanent, severe neurological damage.[][] A more recently published clinical trial out of Singapore has shown similar results, finding combination treatment to only improve the rate of survival to hospital admission, especially in the subgroup analysis of patients with longer "collapse to emergency department" arrival times of 15 to 45 minutes.[] Table 2 lists all statistically significant findings of a correlation between combined treatment and positive outcomes found in these two studies. 2010 American Heart Association Guidelines The 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care recommend the consideration of vasopressor treatment in the form of epinephrine in adults with cardiac arrest (Class IIb, LOE A recommendation).[] Due to the absence of evidence that vasopressin administered instead of or in addition to epinephrine has significant positive outcomes, the guidelines do not currently contain vasopressin as a part of the cardiac arrest algorithms.[] It does, however, allow for one dose of vasopressin to replace either the first or second dose of epinephrine in the treatment of cardiac arrest (Class IIb, LOE A recommendation).[]
Vasopressin
147
Vasopressin receptor inhibition
A vasopressin receptor antagonist is an agent that interferes with action at the vasopressin receptors. They can be used in the treatment of hyponatremia.[]
References Further reading
• Rector, Floyd C.; Brenner, Barry M. (2004). Brenner & Rector's the kidney (http://home.mdconsult.com/das/ search/openres/56203699-5?searchisbn=460046813) (7th ed.). Philadelphia: Saunders. ISBN 0-7216-0164-2.
External links
• Molecular neurobiology of social bonding: Implications for autism spectrum disorders (http://videocast.nih. gov/Summary.asp?File=15521) a lecture by Prof. Larry Young, Jan. 4, 2010.
Serotonin
148
Serotonin
Serotonin
Identifiers CAS number PubChem ChemSpider UNII KEGG MeSH ChEBI ChEMBL IUPHAR ligand Jmol-3D images 50-67-9 5202 5013
[2] [3] [4] [1]
333DO1RDJY C00780
[5]
Serotonin
[6] [7]
CHEBI:28790 CHEMBL39 5
[9] [10]
[8]
Image 1
Properties Molecular formula C H N O
10 12 2
Molar mass Appearance
176.215 g/mol White powder
Serotonin
[1] [2]
149
Melting point Boiling point
121–122°C (ligroin)
416 ±30.0°C (at 760 Torr)
Solubility in water slightly soluble Dipole moment 2.98 D Hazards MSDS LD50 External MSDS
[13] [] []
750 mg/kg (subcutaneous, rat), 4500 mg/kg (intraperitoneal, rat), 60 mg/kg (oral, rat)
(verify) [14]
(what is: / ?) Except where noted otherwise, data are given for materials in their standard state (at 25 °C, 100 kPa)
Infobox references
Serotonin (pron.: /ˌsɛrəˈtoʊnɨn/) or 5-hydroxytryptamine (5-HT) is a monoamine neurotransmitter. Biochemically derived from tryptophan, serotonin is primarily found in the gastrointestinal (GI) tract, platelets, and in the central nervous system (CNS) of animals including humans. It is popularly thought to be a contributor to feelings of well-being and happiness.[3] Approximately 90% of the human body's total serotonin is located in the enterochromaffin cells in the alimentary canal (gut), where it is used to regulate intestinal movements.[][] The remainder is synthesized in serotonergic neurons of the CNS, where it has various functions. These include the regulation of mood, appetite, and sleep. Serotonin also has some cognitive functions, including memory and learning. Modulation of serotonin at synapses is thought to be a major action of several classes of pharmacological antidepressants. Serotonin secreted from the enterochromaffin cells eventually finds its way out of tissues into the blood. There, it is actively taken up by blood platelets, which store it. When the platelets bind to a clot, they disgorge serotonin, where it serves as a vasoconstrictor and helps to regulate hemostasis and blood clotting. Serotonin also is a growth factor for some types of cells, which may give it a role in wound healing. Serotonin is mainly metabolized to 5-HIAA, chiefly by the liver. Metabolism involves first oxidation by monoamine oxidase to the corresponding aldehyde. This is followed by oxidation by aldehyde dehydrogenase to 5-HIAA, the indole acetic acid derivative. The latter is then excreted by the kidneys. One type of tumor, called carcinoid, sometimes secretes large amounts of serotonin into the blood, which causes various forms of the carcinoid syndrome of flushing, diarrhea, and heart problems. Because of serotonin's growth-promoting effect on cardiac myocytes, persons with serotonin-secreting carcinoid may suffer a right heart (tricuspid) valve disease syndrome, caused by proliferation of myocytes onto the valve. In addition to animals, serotonin is found in fungi and plants.[] Serotonin's presence in insect venoms and plant spines serves to cause pain, which is a side effect of serotonin injection. Serotonin is produced by pathogenic amoebae, and its effect on the gut causes diarrhea. Its widespread presence in many seeds and fruits may serve to stimulate the digestive tract into expelling the seeds.
Functions
Serotonin is a neurotransmitter, and is found in all bilateral animals [citation needed], where it mediates gut movements and the animals' perceptions of resource availability. In the simplest animals, resources are equivalent with food, but in advanced animals, such as arthropods and vertebrates, resources also can mean social dominance. In response to the perceived abundance or scarcity of resources, an animal's growth, reproduction or mood may be elevated or lowered[citation needed].
Serotonin
150
Gauge of food availability (appetite)
Serotonin functions as a neurotransmitter in the nervous systems of simple, as well as complex, animals. For example, in the roundworm Caenorhabditis elegans, which feeds on bacteria, serotonin is released as a signal in response to positive events, e.g., finding a new source of food or in male animals finding a female with which to mate[citation needed]. When a well-fed worm feels bacteria on its cuticle, dopamine is released, which slows it down; if it is starved, serotonin also is released, which slows the animal down further. This mechanism increases the amount of time animals spend in the presence of food.[] The released serotonin activates the muscles used for feeding, while octopamine suppresses them.[] Serotonin diffuses to serotonin-sensitive neurons, which control the animal's perception of nutrient availability. When humans smell food, dopamine is released to increase the appetite. But unlike in worms, serotonin does not increase anticipatory behaviour in humans; instead, the serotonin released while consuming activates 5-HT2C receptors on dopamine-producing cells. This halts their dopamine release, and thereby serotonin decreases appetite. Drugs which block 5-HT2C receptors make the body unable to shut off appetite, and are associated with increased weight gain,[] especially in people who have a low number of receptors.[] The expression of 5-HT2C receptors in the hippocampus follows a diurnal rhythm,[] just as the serotonin release in the ventromedial nucleus, which is characterised by a peak at morning when the motivation to eat is strongest.[] Effects of food content In humans, serotonin levels are affected by diet. An increase in the ratio of tryptophan to phenylalanine and leucine will increase serotonin levels. Fruits with a good ratio include dates, papayas and bananas. Foods with a lower ratio inhibit the production of serotonin. [citation needed] Research also suggests eating a diet rich in carbohydrates and low in protein will increase serotonin by secreting insulin, which helps in amino acid competition.[] However, increasing insulin for a long period may trigger the onset of insulin resistance, obesity, type 2 diabetes, and lower serotonin levels.[4][5] Muscles use many of the amino acids except tryptophan, allowing more muscular individuals to produce more serotonin.[] Myoinositol, a carbocyclic polyol present in many foods, is known to play a role in serotonin modulation.[] In the digestive tract (emetic) The gut is surrounded by enterochromaffin cells, which release serotonin in response to food in the lumen. This makes the gut contract around the food. Platelets in the veins draining the gut collect excess serotonin. If irritants are present in the food, the enterochromaffin cells release more serotonin to make the gut move faster, i.e., to cause diarrhea, so the gut is emptied of the noxious substance. If serotonin is released in the blood faster than the platelets can absorb it, the level of free serotonin in the blood is increased. This activates 5HT3 receptors in the chemoreceptor trigger zone that stimulate vomiting.[6] The enterochromaffin cells not only react to bad food, but they are also very sensitive to irradiation and cancer chemotherapy. Drugs that block 5HT3 are very effective in controlling the nausea and vomiting produced by cancer treatment, and are considered the gold standard for this purpose.[7] Gauge of social situation How much food an animal gets not only depends on the abundance of food, but also on the animal's ability to compete with others. This is especially true for social animals, where the stronger individuals might steal food from the weaker. Thus, serotonin is not only involved in the perception of food availability, but also of social rank. If a lobster is injected with serotonin, it behaves like a dominant animal, while octopamine causes subordinate behavior.[] A frightened crayfish flips its tail to flee, and the effect of serotonin on this behavior depends on the animal's social status. Serotonin inhibits the fleeing reaction in subordinates, but enhances it in socially dominant or isolated individuals. The reason for this is social experience alters the proportion between serotonin receptors (5-HT receptors) that have opposing effects on the fight-or-flight response.Wikipedia:Please clarify The effect of 5-HT1 receptors predominates in subordinate animals, while 5-HT2 receptors predominates in dominants.[] In humans,
Serotonin levels of 5-HT1A receptor activation in the brain show negative correlation with aggression,[8] and a mutation in the gene that codes for the 5-HT2A receptor may double the risk of suicide for those with that genotype.[] Most of the brain serotonin is not degraded after use, but is collected by serotonergic neurons by serotonin transporters on their cell surfaces. Studies have revealed nearly 10% of total variance in anxiety-related personality depends on variations in the description of where, when and how many serotonin transporters the neurons should deploy.[]
151
Growth and reproduction
In C. elegans, artificial depletion of serotonin or increase of octopamine cues behavior typical of a low-food environment: C. elegans becomes more active, and mating and egg-laying are suppressed, while the opposite occurs if serotonin is increased or octopamine is decreased in this animal.[] Serotonin is necessary for normal nematode male mating behavior,[] and the inclination to leave food to search for a mate.[] The serotonergic signaling used to adapt the worm's behaviour to fast changes in the environment affects insulin-like signaling and the TGF beta signaling pathway,[9] which control long-term adaption.
Aging and age-related phenotypes
Serotonin is known to regulate aging, learning and memory. The first evidence comes from the study of longevity in C. elegans.[10] During early phase of aging, the level of serotonin increases, which alters locomotory behaviors and associative memory.[11] The effect is restored by mutations and drugs (including mianserin and methiothepin) that inhibit serotonin receptors. The observation does not contradict with the notion that the serotonin level goes down in mammals and humans, which is typically seen in late but not early phase of aging.
Bone metabolism
In mice and humans, alterations in serotonin levels and signalling have been shown to regulate bone mass.[][][][] Mice that lack brain serotonin have osteopenia, while mice that lack gut serotonin have high bone density. In humans, increased blood serotonin levels have been shown to be significant negative predictor of low bone density. Serotonin can also be synthesized, albeit at very low levels, in the bone cells. It mediates its actions on bone cells using three different receptors. Through Htr1b receptors, it negatively regulates bone mass, while it does so positively through Htr2b and Htr2c. There is very delicate balance between physiological role of gut serotonin and its pathology. Increase in the extracellular content of serotonin results in a complex relay of signals in the osteoblasts culminating in FoxO1/ Creb and ATF4 dependent transcriptional events.[] These studies have opened a new area of research in bone metabolism that can be potentially harnessed to treat bone mass disorders.[]
Behavior
In the fruitfly, where insulin both regulates blood sugar and acts as a growth factor, serotonergic neurons regulate the adult body size by affecting insulin secretion.[][] Serotonin has also been identified as the trigger for swarm behavior in locusts.[] In humans, though insulin regulates blood sugar and IGF regulates growth, serotonin controls the release of both hormones, so serotonin suppresses insulin release from the beta cells in the pancreas,[] and exposure to SSRIs reduces fetal growth.[] Human serotonin can also act as a growth factor directly. Liver damage increases cellular expression of 5-HT2A and 5-HT2B receptors.[] Serotonin present in the blood then stimulates cellular growth to repair liver damage.[] 5HT2B receptors also activate osteocytes, which build up bone[] However, serotonin also inhibits osteoblasts, through 5-HT1B receptors.[]
Serotonin
152
Cardiovascular growth factor
Serotonin, in addition, evokes endothelial nitric oxide synthase activation and stimulates, through a 5-HT1B receptor-mediated mechanism, the phosphorylation of p44/p42 mitogen-activated protein kinase activation in bovine aortic endothelial cell cultures.[] In blood, serotonin is collected from plasma by platelets, which store it. It is thus active wherever platelets bind in damaged tissue, as a vasoconstrictor to stop bleeding, and also as a fibrocyte mitotic (growth factor), to aid healing.[] Some serotonergic agonist drugs also cause fibrosis anywhere in the body, particularly the syndrome of retroperitoneal fibrosis, as well as cardiac valve fibrosis.[] In the past, three groups of serotonergic drugs have been epidemiologically linked with these syndromes. They are the serotonergic vasoconstrictive antimigraine drugs (ergotamine and methysergide),[] the serotonergic appetite suppressant drugs (fenfluramine, chlorphentermine, and aminorex), and certain anti-Parkinsonian dopaminergic agonists, which also stimulate serotonergic 5-HT2B receptors. These include pergolide and cabergoline, but not the more dopamine-specific lisuride.[] As with fenfluramine, some of these drugs have been withdrawn from the market after groups taking them showed a statistical increase of one or more of the side effects described. An example is pergolide. The drug was declining in use since reported in 2003 to be associated with cardiac fibrosis.[12] Two independent studies published in the New England Journal of Medicine in January 2007, implicated pergolide, along with cabergoline, in causing valvular heart disease.[][] As a result of this, the FDA removed pergolide from the U.S. market in March, 2007.[13] (Since cabergoline is not approved in the U.S. for Parkinson's Disease, but for hyperprolactinemia, the drug remains on the market. Treatment for hyperprolactinemia requires lower doses than that for Parkinson's Disease, diminishing the risk of valvular heart disease).[] Local effects of injection: venoms and pain Since serotonin is an indicator of bleeding, a sudden large increase in peripheral levels causes pain. The reason wasps and deathstalker scorpions have serotonin in their venom [][] may be to increase the pain of their stings on large animals, and also to cause lethal vasoconstriction in smaller prey.
Deficiency
Genetically altered C. elegans worms that lack serotonin have an increased reproductive lifespan, may become obese, and sometimes present with arrested development at a dormant larval state.[][] Serotonin in mammals is made by two different tryptophan hydroxylases: TPH1 produces serotonin in the pineal gland[citation needed] and the enterochromaffin cells, while TPH2 produces it in the raphe nuclei and in the myenteric plexus. Genetically altered mice lacking TPH1 develop progressive loss of heart strength early on. They have pale skin and breathing difficulties, are easily tired, and eventually die of heart failure.[] Genetically altered mice that lack TPH2 are normal when they are born. However, after three days, they appear to be smaller and weaker, and have softer skin than their siblings. In a purebred strain, 50% of the mutants died during the first four weeks, but in a mixed strain, 90% survived. Normally, the mother weans the litter after three weeks, but the mutant animals needed five weeks. After that, they caught up in growth and had normal mortality rates. Subtle changes in the autonomic nervous system are present, but the most obvious difference from normal mice is the increased aggressiveness and impairment in maternal care of young.[] Despite the blood–brain barrier, the loss of serotonin production in the brain is partially compensated by intestinal serotonin. The behavioural changes become greatly enhanced if one crosses TPH1- with TPH2-lacking mice and gets animals that lack TPH entirely.[] In humans, defective signaling of serotonin in the brain may be the root cause of sudden infant death syndrome (SIDS). Scientists from the European Molecular Biology Laboratory in Monterotondo, Italy[14] genetically modified lab mice to produce low levels of the neurotransmitter serotonin. The results showed the mice suffered drops in heart rate and other symptoms of SIDS, and many of the animals died at an early age. Researchers now believe low levels of serotonin in the animals' brainstems, which control heartbeat and breathing, may have caused sudden death, they
Serotonin said in the July 4, 2008 issue of Science.[] If neurons that make serotonin — serotonergic neurons — are abnormal in infants, there is a risk of sudden infant death syndrome (SIDS).[] Recent research conducted at Rockefeller University shows, in both patients who suffer from depression and mice that model the disorder, levels of the p11 protein are decreased. This protein is related to serotonin transmission within the brain.[]
153
In the brain
Gross anatomy
The neurons of the raphe nuclei are the principal source of 5-HT release in the brain.[15] There are 7 or 8 raphe nuclei (some scientists chose to group the raphe linearis nuclei into one nucleus), all of which are located along the midline of the brainstem, and centered around the reticular formation.[16] Axons from the neurons of the raphe nuclei form a neurotransmitter system, reaching almost every part of the central nervous system. Axons of neurons in the lower raphe nuclei terminate in the cerebellum and spinal cord, while the axons of the higher nuclei spread out in the entire brain.
Serotonin system, contrasted with the dopamine system
Microanatomy
Serotonin is released into the space between neurons, and diffuses over a relatively wide gap (>20 µm) to activate 5-HT receptors located on the dendrites, cell bodies and presynaptic terminals of adjacent neurons. Receptors The 5-HT receptors, the receptors for serotonin, are located on the cell membrane of nerve cells and other cell types in animals, and mediate the effects of serotonin as the endogenous ligand and of a broad range of pharmaceutical and hallucinogenic drugs. With the exception of the 5-HT3 receptor, a ligand-gated ion channel, all other 5-HT receptors are G protein-coupled, seven transmembrane (or heptahelical) receptors that activate an intracellular second messenger cascade.[] Termination Serotonergic action is terminated primarily via uptake of 5-HT from the synapse. This is accomplished through the specific monoamine transporter for 5-HT, SERT, on the presynaptic neuron. Various agents can inhibit 5-HT reuptake, including MDMA (ecstasy), amphetamine, cocaine, dextromethorphan (an antitussive), tricyclic antidepressants and selective serotonin reuptake inhibitors (SSRIs). Interestingly, a 2006 study conducted by the University of Washington suggested a newly discovered monoamine transporter, known as PMAT, may account for "a significant percentage of 5-HT clearance".[] Contrasting with the high-affinity SERT, the PMAT has been identified as a low-affinity transporter, with an apparent Km of 114 micromoles/l for serotonin; approximately 230 times higher than that of SERT. However, the PMAT, despite its relatively low serotonergic affinity, has a considerably higher transport 'capacity' than SERT, "..resulting in roughly comparable uptake efficiencies to SERT in heterologous expression systems." The study also suggests some SSRIs, such as fluoxetine and sertraline, inhibit PMAT but at IC50 values which surpass the therapeutic plasma concentrations by up to four orders of magnitude; therefore, SSRI monotherapy is "ineffective" in PMAT inhibition. At present, no known pharmaceuticals are known to appreciably inhibit PMAT at normal therapeutic doses. The PMAT also suggestively transports dopamine and
Serotonin norepinephrine, albeit at Km values even higher than that of 5-HT (330–15,000 μmoles/L). Serotonylation Serotonin can also signal through a nonreceptor mechanism called serotonylation, in which serotonin modifies proteins.[] This process underlies serotonin effects upon platelet-forming cells (thrombocytes) in which it links to the modification of signaling enzymes called GTPases that then trigger the release of vesicle contents by exocytosis.[] A similar process underlies the pancreatic release of insulin.[] The effects of serotonin upon vascular smooth muscle "tone" (this is the biological function from which serotonin originally got its name) depend upon the serotonylation of proteins involved in the contractile apparatus of muscle cells.[]
154
Biosynthesis
In animals including humans, serotonin is synthesized from the amino acid L-tryptophan by a short metabolic pathway consisting of two enzymes: tryptophan hydroxylase (TPH) and amino acid decarboxylase (DDC). The TPH-mediated reaction is the rate-limiting step in the pathway. TPH has been shown to exist in two forms: TPH1, found in several tissues, and TPH2, which is a neuron-specific isoform.[] Serotonin can be synthesized from tryptophan in the lab using Aspergillus niger and Psilocybe coprophila as catalysts. The first phase to 5-hydroxytryptophan would require letting tryptophan sit in ethanol and water for 7 days, then mixing in enough HCl (or other acid) to bring the pH to 3, and then adding NaOH to make a pH of 13 for 1 hour. Asperigillus niger would be the catalyst for this first phase. The second phase to synthesizing tryptophan itself from the 5-hydroxytryptophan intermediate would require adding ethanol and water, and letting sit for 30 days this time. The next two steps would be the same as the first phase: adding HCl to make the pH = 3, and then adding NaOH to make the pH very basic at 13 for 1 hour. This phase uses the Psilocybe coprophila as the catalyst for the reaction. [17] Serotonin taken orally does not pass into the serotonergic The pathway for the synthesis of serotonin from pathways of the central nervous system, because it does not tryptophan. cross the blood–brain barrier. However, tryptophan and its metabolite 5-hydroxytryptophan (5-HTP), from which serotonin is synthesized, can and do cross the blood–brain barrier. These agents are available as dietary supplements, and may be effective serotonergic agents. One product of serotonin breakdown is 5-hydroxyindoleacetic acid (5-HIAA), which is excreted in the urine. Serotonin and 5-HIAA are sometimes produced in excess amounts by certain tumors or cancers, and levels of these substances may be measured in the urine to test for these tumors.
Serotonin
155
Drugs targeting the 5-HT system
Several classes of drugs target the 5-HT system, including some antidepressants, antipsychotics, anxiolytics, antiemetics, and antimigraine drugs, as well as the psychedelic drugs and empathogens.
Psychedelic drugs
The psychedelic drugs psilocin/psilocybin, DMT, mescaline, and LSD are agonists, primarily at 5HT2A/2C receptors.[][] The empathogen-entactogen MDMA releases serotonin from synaptic vesicles of neurons.[]
Antidepressants
Drugs which alter serotonin levels are used in depression, generalized anxiety disorder and social phobia. Monoamine oxidase inhibitors (MAOIs) prevent the breakdown of monoamine neurotransmitters (including serotonin), and therefore increase concentrations of the neurotransmitter in the brain. MAOI therapy is associated with many adverse drug reactions, and patients are at risk of hypertensive emergency triggered by foods with high tyramine content, and certain drugs. Some drugs inhibit the reuptake of serotonin, making it stay in the synaptic cleft longer. The tricyclic antidepressants (TCAs) inhibit the reuptake of both serotonin and norepinephrine. The newer selective serotonin reuptake inhibitors (SSRIs) have fewer side effects and fewer interactions with other drugs. The side effects that have become apparent recently include a decrease in bone mass in elderly and increased risk for osteoporosis. However, it is not yet clear whether it is due to SSRI action on peripheral serotonin production and or action in the gut or in the brain.[] Certain SSRI medications have been shown to lower serotonin levels below the baseline after chronic use, despite initial increases. This has been connected to the observation that the benefit of SSRIs may decrease in selected patients after a long-term treatment. A switch in medication will usually resolve this issue (up to 70% of the time).[] The novel antidepressant tianeptine, a selective serotonin reuptake "enhancer", has mood-elevating effects. This provides evidence for the theory that serotonin is most likely used to regulate the extent or intensity of moods, rather than level directly correlating with mood. In fact, the 5-HTTLPR gene codes for the number of serotonin transporters in the brain, with more serotonin transporters causing decreased duration and magnitude of serotonergic signaling.[18] The 5-HTTLPR polymorphism (l/l) causing more serotonin transporters to be formed is also found to be more resilient against depression and anxiety.[19][20] Therefore, increasing levels of extracellular serotonin may be associated with increased affect, for good or for worse. Although phobias and depression might be attenuated by serotonin-altering drugs, this does not mean the individual's situation has been improved, but only the individual's perception of the environment. Sometimes, a lower serotonin level might be beneficial, for example in the ultimatum game, where players with normal serotonin levels are more prone to accept unfair offers than participants whose serotonin levels have been artificially lowered.[] Serotonin syndrome Extremely high levels of serotonin can cause a condition known as serotonin syndrome, with toxic and potentially fatal effects. In practice, such toxic levels are essentially impossible to reach through an overdose of a single antidepressant drug, but require a combination of serotonergic agents, such as an SSRI with an MAOI.[21] The intensity of the symptoms of serotonin syndrome vary over a wide spectrum, and the milder forms are seen even at nontoxic levels.[]
Antiemetics
Some 5-HT3 antagonists, such as ondansetron, granisetron, and tropisetron, are important antiemetic agents. They are particularly important in treating the nausea and vomiting that occur during anticancer chemotherapy using cytotoxic drugs. Another application is in the treatment of postoperative nausea and vomiting.
Serotonin
156
In unicellular organisms
Serotonin is used by a variety of single-cell organisms for various purposes. SSRIs have been found to be toxic to algae.[] The gastrointestinal parasite Entamoeba histolytica secretes serotonin, causing a sustained secretory diarrhea in some patients.[][] Patients infected with E. histolytica have been found to have highly elevated serum serotonin levels which returned to normal following resolution of the infection.[] E. histolytica also responds to the presence of serotonin by becoming more virulent.[] This means serotonin secretion not only serves to increase the spread of enteamoebas by giving the host diarrhea, but also to coordinate their behaviour according to their population density, a phenomenon known as quorum sensing. Outside a host, the density of entoamoebas is low, hence also the serotonin concentration. Low serotonin signals to the entoamoebas they are outside a host and they become less virulent to conserve energy. When they enter a new host, they multiply in the gut, and become more virulent as the serotonin concentration increases.
In plants
In drying seeds, serotonin production is a way to get rid of the buildup of poisonous ammonia. The ammonia is collected and placed in the indole part of L-tryptophan, which is then decarboxylated by tryptophan decarboxylase to give tryptamine, which is then hydroxylated by a cytochrome P450 monooxygenase, yielding serotonin.[] However, since serotonin is a major gastrointestinal tract modulator, it may be produced by plants in fruits as a way of speeding the passage of seeds through the digestive tract, in the same way as many well-known seed and fruit associated laxatives. Serotonin is found in mushrooms, fruits and vegetables. The highest values of 25–400 mg/kg have been found in nuts of the walnut (Juglans) and hickory (Carya) genera. Serotonin concentrations of 3–30 mg/kg have been found in plantains, pineapples, banana, kiwifruit, plums, and tomatoes. Moderate levels from 0.1–3 mg/kg have been found in a wide range of tested vegetables.[22] Serotonin is one compound of the poison contained in stinging nettles (Urtica dioica), where it causes pain on injection in the same manner as its presence in insect venoms (see above). It is also naturally found in Paramuricea clavata, or the Red Sea Fan.[23] Serotonin and tryptophan have been found in chocolate with varying cocoa contents. The highest serotonin content (2.93 ug g-1) was found in chocolate with 85% cocoa, and the highest tryptophan content (13.27-13.34 ug g-1) was found in 70-85% cocoa. The intermediate in the synthesis from tryptophan to serotonin, 5-hydroxytryptophan, was not found.[24] Unlike its precursors, 5-HTP and tryptophan, serotonin does not cross the blood–brain barrier, which means ingesting serotonin in the diet has no effect on brain serotonin levels.
Methyl-tryptamines and hallucinogens
Several plants contain serotonin together with a family of related tryptamines that are methylated at the amino (NH2) and (OH) groups, are N-oxides, or miss the OH group. These compounds do reach the brain, although some portion of them are metabolized by MAO-B enzymes in the liver. Examples are plants from the Anadenanthera genus that are used in the hallucinogenic yopo snuff. These compounds are widely present in the leaves of many plants, and may serve as deterrents for animal ingestion. Serotonin occurs in several mushrooms of the genus Panaeolus.[25] Serotonin is also naturally occurring in toad venom.[26]
Serotonin
157
History
In 1935, Italian Vittorio Erspamer showed an extract from enterochromaffin cells made intestines contract. Some believed it contained adrenaline, but two years later, Erspamer was able to show it was a previously unknown amine, which he named "enteramine".[] In 1948, Maurice M. Rapport, Arda Green, and Irvine Page of the Cleveland Clinic discovered a vasoconstrictor substance in blood serum, and since it was a serum agent affecting vascular tone, they named it serotonin.[] In 1952, enteramine was shown to be the same substance as serotonin, and as the broad range of physiological roles was elucidated, the abbreviation 5-HT of the proper chemical name 5-hydroxytryptamine became the preferred name in the pharmacological field.[] Synonyms of serotonin include: 5-hydroxytriptamine, thrombotin, enteramin, substance DS, and 3-(β-Aminoethyl)-5-hydroxyindole.[27]
References
[1] Pietra, S.;Farmaco, Edizione Scientifica 1958, Vol. 13, pp. 75–9. [2] Calculated using Advanced Chemistry Development (ACD/Labs) Software V11.02 (©1994–2011 ACD/Labs) [9] Murakami H, Bessinger K, Hellmann J, Murakami S. Aging-dependent and -independent modulation of associative learning behavior by insulin/insulin-like growth factor-1 signal in Caenorhabditis elegans. J Neurosci. 2005 Nov 23;25(47):10894-904. PMID 16306402 (http:/ / www. ncbi. nlm. nih. gov/ pubmed/ 17559503) [12] Free full text (http:/ / www. tga. gov. au/ adr/ aadrb/ aadr0408. htm) from the Australian Therapeutic Goods Administration [16] The Raphe nuclei group of neurons are located along the brain stem from the labels 'Mid Brain' to 'Oblongata', centered on the pons. (See relevant image.) [17] Alarcon, J. Biotransformation of indole derivatives by mycelial cultures. Zeitschrift für Naturforschung.C, A journal of biosciences 2008, 63, 82. [23] Penez, N.; Culioli, G.; Briand, J.; Blache, Y.; Perez, T.; Thomas, O. P. Antifouling Properties of Simple Indole and Purine Alkaloids from the Mediterranean Gorgonian Paramuricea clavata. J. Nat. Prod. 2011, 74, 2304-2308. [24] Guillen-Casla, V.; Rosales-Conrado, N.; Leon-Gonzalez, M. E.; Perez-Arribas, L. V.; Polo-Diez, L. M. Determination ofserotonin and its precursors in chocolate samples by capillary liquid chromatography with mass spectrometry detection. J. Chromatogr. A. 2012, 1232, 158-165. [26] Zhang, P.; Cui, Z.; Liu, Y.; Wang, D.; Liu, N.; Yoshikawa, M. Quality Evaluation of Drug Toad Venom fromDifferent Origins through a Simultaneous Determination of Bufogeninsand Indole Alkaloids by HPLC. Chem. Pharm. Bull. 2005, 53, 1582-1586. [27] SciFinder – Serotonin Substance Detail. Accessed (4-11-2012).
External links
• Serotonin bound to proteins (http://www.ebi.ac.uk/pdbe-srv/PDBeXplore/ligand/?ligand=SRO) in the PDB • PsychoTropicalResearch (http://www.psychotropical.com/) Extensive reviews on serotonergic drugs and Serotonin Syndrome. • Molecule of the Month: Serotonin (http://www.chm.bris.ac.uk/motm/serotonin/home1.htm) at University of Bristol • 60-Second Psych: No Fair! My Serotonin Level Is Low (http://www.sciam.com/podcast/episode. cfm?id=68FC98F1-E48A-251D-8F65277181DB9A4E), Scientific American • Serotonin Test Interpretation on ClinLab Navigator (http://www.clinlabnavigator.com/Tests/Serotonin.html). • Tryptophan hydroxylase-2 gene variation influences personality traits and disorders related to emotional dysregulation (http://www.ncbi.nlm.nih.gov/pubmed/17176492) at the National Center for Biotechnology Information.
Endorphins
158
Endorphins
Endorphins ("endogenous morphine") are endogenous opioid peptides that function as neurotransmitters.[1] They are produced by the pituitary gland and the hypothalamus in vertebrates during exercise,[] excitement, pain, consumption of spicy food, love and orgasm,[][] and they resemble the opiates in their abilities to produce analgesia and a feeling of well-being.
Chemical structure of alpha-Neoendorphin (α-Neoendorphin)
The term implies a pharmacological activity (analogous to the activity of the corticosteroid category of biochemicals) as opposed to a specific chemical formulation. It consists of two parts: endo- and -orphin; these are short forms of the words endogenous and morphine, intended to mean "a morphine-like substance originating from within the body."[] The term "endorphin rush" has been adopted in popular speech to refer to feelings of exhilaration brought on by pain, danger, or other forms of stress,[] supposedly due to the influence of endorphins. When a nerve impulse reaches the spinal cord, endorphins that prevent nerve cells from releasing more pain signals are released.
History
Opioid neuropeptides were first discovered in 1974 by two independent groups of investigators: • John Hughes and Hans Kosterlitz of Scotland isolated — from the brain of a pig — what some called enkephalins (from the Greek εγκέφαλος, cerebrum).[][2] • Around the same time, in the calf brain, Rabi Simantov and Solomon H. Snyder of the United States found[3] what Eric Simon (who independently discovered opioid receptors in the brain) later termed "endorphin" by an abbreviation of "endogenous morphine", meaning "morphine produced naturally in the body".[] Importantly, recent studies have demonstrated that diverse animal and human tissues are in fact capable of producing morphine itself, which is not a peptide.[][]
Mechanism of action
Beta-endorphin (β-Endorphin) is released into blood from the pituitary gland and into the spinal cord and brain from hypothalamic neurons. The β-endorphin that is released into the blood cannot enter the brain in large quantities because of the blood–brain barrier, so the physiological Chemical structure of beta-endorphin importance of the β-endorphin that can be measured in the blood is far from clear. β-Endorphin is a cleavage product of pro-opiomelanocortin (POMC), which is also the precursor hormone for adrenocorticotrophic hormone (ACTH). The behavioural effects of β-endorphin are exerted by its actions in the brain and spinal cord, and it is presumed that the hypothalamic neurons are the major source of β-endorphin at these sites.
Endorphins In situations where the level of ACTH is increased (e.g., Cushing’s Syndrome), the level of endorphins also increases slightly. β-Endorphin has the highest affinity for the μ1 opioid receptor, slightly lower affinity for the μ2 and δ opioid receptors, and low affinity for the κ1 opioid receptors. μ-Opioid receptors are the main receptor through which morphine acts. In the classical sense, μ opioid receptors are presynaptic, and inhibit neurotransmitter release; through this mechanism, they inhibit the release of the inhibitory neurotransmitter GABA, and disinhibit the dopamine pathways, causing more dopamine to be released. By hijacking this process, exogenous opioids cause inappropriate dopamine release, and lead to aberrant synaptic plasticity, which causes dependency. Opioid receptors have many other and more important roles in the brain and periphery however, modulating pain, cardiac, gastric and vascular function as well as possibly panic and satiation, and receptors are often found at postsynaptic locations as well as presynaptically.
159
Activity
Scientists sometimes debate whether specific activities release measurable levels of endorphins. Much of the current data comes from animal models which may not be relevant to humans. The studies that do involve humans often measure endorphin plasma levels, which do not necessarily correlate with levels in the central nervous system. Other studies use a blanket opioid antagonist (usually naloxone) to indirectly measure the release of endorphins by observing the changes that occur when any endorphin activity that might be present is blocked.
Runner's high
A publicized effect of endorphin production is the so-called "runner's high", which is said to occur when strenuous exercise takes a person over a threshold that activates endorphin production. Endorphins are released during long, continuous workouts, when the level of intensity is between moderate and high, and breathing is difficult. This also corresponds with the time that muscles use up their stored glycogen. During a release of endorphins, the person may be exposed to bodily harm from strenuous bodily functions after going past his or her body's physical limit. This means that runners can keep running despite pain, continuously surpassing what they otherwise would consider to be their limit. Runner's high has also been known to create feelings of euphoria and happiness. Altough it is called runners high, the effect occurs to strenous exercise in general, and not just running. Runner's high has been suggested to have evolutionary roots based on the theory that it helped with the survival of early humans. Current African tribes make use of runner's high when conducting persistence hunting (a method in which tribesman hunt an animal and track it for miles, eventually killing the animal due to its vulnerability brought on by exhaustion[4]). In 2008, researchers in Germany reported on the mechanisms that cause the runner's high. Using PET scans combined with recently available chemicals that reveal endorphins in the brain, they were able to compare runners’ brains before and after a run.[] Previous research on the role of endorphins in producing runner's high questioned the mechanisms at work, their data possibly demonstrated that the "high" comes from completing a challenge rather than as a result of exertion.[5] Studies in the early 1980s cast doubt on the relationship between endorphins and the runner's high for several reasons: • The first was that when an antagonist (pharmacological agent that blocks the action for the substance under study) was infused (e.g., naloxone) or ingested (naltrexone) the same changes in mood state occurred as when the person exercised with no blocker. • A study in 2003 by the Georgia Institute of Technology found that runner's high might be caused by the release of another naturally produced chemical, anandamide.[][] The authors suggest that the body produces this chemical to deal with prolonged stress and pain from strenuous exercise, similar to the original theory involving endorphins.
Endorphins However, the release of anandamide was not reported with the cognitive effects of the runner's high; this suggests that anandamide release may not be significantly related to runner's high.[] • A study at the University of Arizona, published in April 2012, argues implicitly that endocannabinoids are, most likely, the causative agent in runner's high, while also arguing this to be a result of the evolutionary advantage endocannabinoids provide to endurance-based cursorial species. This largely refers to quadruped mammals, but also to biped hominids, such as humans. The study shows that both humans and dogs show significantly increased endocannabinoid signaling following high intensity running, but not low-intensity walking. The study does not, however, ever address the potential contribution of endorphins to runner's high.[6] However, in other research that has focused on the blood–brain barrier, it has been shown that endorphin molecules are too large to pass freely, thus very unlikely to be the cause of the runner's high feeling of euphoria.[7] It has been suggested that apart from endorphins, other chemicals can contribute to runner's high; candidates include epinephrine, serotonin, and dopamine.[citation needed]
160
Depersonalization disorder
Endorphins are known to play a role in depersonalization disorder. The opioid antagonists naloxone and naltrexone have both been proven to be successful in treating depersonalization.[][8] To quote a 2001 naloxone study, "In three of 14 patients, depersonalization symptoms disappeared entirely and seven patients showed a marked improvement. The therapeutic effect of naloxone provides evidence for the role of the endogenous opioid system in the pathogenesis of depersonalization."
Relaxation
In 2003, clinical researchers reported that profound relaxation in a float tank triggers the production of endorphins.[9] This explains the pain relief experienced during float sessions.[10]
Acupuncture
In 1999, clinical researchers reported that inserting acupuncture needles into specific body points triggers the production of endorphins.[][] In another study, higher levels of endorphins were found in cerebrospinal fluid after patients underwent acupuncture.[11] In addition, naloxone appeared to block acupuncture’s pain-relieving effects.
Pregnancy
A placental tissue of fetal origin — i.e., the syncytiotrophoblast — excretes beta-endorphins into the maternal blood system from the 3rd month of pregnancy. A recent study[] proposes an adaptive background for this phenomenon. The authors argue that fetuses make their mothers endorphin-dependent then manipulate them to increase nutrient allocation to the placenta. Their hypothesis predicts that: (1) anatomic position of endorphin production should mirror its presumed role in foetal-maternal conflict; (2) endorphin levels should co-vary positively with nutrient carrying capacity of maternal blood system; (3) postpartum psychological symptoms (such as postpartum blues, depression, and psychosis) in humans are side-effects of this mechanism that can be interpreted as endorphin-deprivation symptoms; (4) shortly after parturition, placentophagy could play an adaptive role in decreasing the negative side-effects of foetal manipulation; (5) later, breast-feeding-induced endorphin excretion of the maternal pituitary saves the mother from further deprivation symptoms. These predictions appear to be supported by empirical data.[]
Endorphins
161
Etymology
From the Greek: word endo ενδο meaning "within" (endogenous, Greek: ενδογενής, "proceeding from within") and morphine, from Morpheus, Greek: Μορφέας, the god of sleep in the Greek mythology, thus 'endo(genous) (mo)rphine’.
References
[1] Oswald Steward: Functional neuroscience (2000), page 116. Preview at: Google books. (http:/ / books. google. com/ books?id=nNH3p29wjK4C& pg=PA116& dq=endorphins+ neurotransmitter& hl=en& ei=IwwlTKfzHMr-_Aa-w6zGBA& sa=X& oi=book_result& ct=result& resnum=10& ved=0CFMQ6AEwCTgK#v=onepage& q=endorphins neurotransmitter& f=false) [4] http:/ / www. youtube. com/ watch?v=826HMLoiE_o [9] Anette Kjellgren, 2003, The experience of floatation REST (restricted Environmental stimulation technique), subjective stress and pain, Goteborg University Sweden,
External links
• Endorphins (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Endorphins) at the US National Library of Medicine Medical Subject Headings (MeSH) • "A genetic influence on alcohol addiction found - lack of endorphin" (http://www.news-medical.net/ ?id=33701#). News-Medical.Net. Dec-2007-12-21. Retrieved 2008-10-15.
Somatostatin
162
Somatostatin
Somatostatin
Available structures PDB Ortholog search: PDBe [1], RCSB [2] List of PDB id codes 1P2W
[3]
Identifiers Symbols External IDs SST
[4]
; SMST
[5]
OMIM: 182450
MGI: 98326
[6]
HomoloGene: 819
[7]
ChEMBL: 1795130
[8]
GeneCards: SST Gene
[9]
Gene Ontology Molecular function • hormone activity [10] Cellular component • extracellular region [229] [230] • extracellular space [11] • neuronal cell body Biological process • hyperosmotic response [13] • cell surface receptor signaling pathway [14] • G-protein coupled receptor signaling pathway [25] • cell-cell signaling [15] • synaptic transmission [16] • response to nutrient [17] • digestion [18] • negative regulation of cell proliferation • hormone-mediated apoptotic signaling pathway
[19] [12]
• response to heat [21] • regulation of cell migration [22] • response to drug [23] • response to amino acid stimulus [24] • response to steroid hormone stimulus Sources: Amigo
[25]
[20]
/ QuickGO
[26]
RNA expression pattern
Somatostatin
163
More reference expression data Orthologs Species Entrez Ensembl UniProt RefSeq (mRNA) RefSeq (protein) Human 6750
[28] [30]
[27]
Mouse 20604
[29] [31]
ENSG00000157005 P61278
[32] [34]
ENSMUSG00000004366 P60041
[33] [35]
NM_001048 NP_001039
NM_009215 NP_033241
[36]
[37]
Location (UCSC) Chr 3: [38] 187.39 – 187.39 Mb PubMed search
[40]
Chr 16: [39] 23.89 – 23.89 Mb
[41]
Somatostatin (also known as growth hormone-inhibiting hormone (GHIH) or somatotropin release-inhibiting factor (SRIF)) or somatotropin release-inhibiting hormone[citation needed] is a peptide hormone that regulates the endocrine system and affects neurotransmission and cell proliferation via interaction with G protein-coupled somatostatin receptors and inhibition of the release of numerous secondary hormones. Somatostatin has two active forms produced by alternative cleavage of a single preproprotein: one of 14 amino acids, the other of 28 amino acids.[] In all vertebrates, there exists six different somatostatin genes that have been named SS1, SS2, SS3, SS4, SS5, and SS6.[] The six different genes along with the five different somatostatin receptors allows somatostatin to possess a large range of functions.[] Humans have only one somatostatin gene, SST.[][][]
Somatostatin
164
Production
Digestive system
Somatostatin is secreted in several locations in the digestive system: • stomach • intestine • delta cells of the pancreas[]
Brain
[42] Sst is expressed in interneurons in the telencephalon of the embryonic day 15.5 mouse. Allen Brain Atlases Sst [43] expression in the adult mouse. Allen Brain Atlases
Somatostatin is produced by neuroendocrine neurons of the periventricular nucleus of the hypothalamus. These neurons project to the median eminence, where somatostatin is released from neurosecretory nerve endings into the hypothalamo-hypophysial system through neuron axons. Somatostatin is then carried to the anterior pituitary gland, where it inhibits the secretion of growth hormone from somatotrope cells. The somatostatin neurons in the periventricular nucleus mediate negative feedback effects of growth hormone on its own release; the somatostatin neurons respond to high circulating concentrations of growth hormone and somatomedins by increasing the release of somatostatin, so reducing the rate of secretion of growth hormone. Somatostatin is also produced by several other populations that project centrally, i.e., to other areas of the brain, and somatostatin receptors are expressed at many different sites in the brain. In particular, there are populations of somatostatin neurons in the arcuate nucleus,[citation needed] the hippocampus,[citation needed] and the brainstem nucleus of the solitary tract.[citation needed]
Somatostatin
165
Actions
Somatostatin is classified as an inhibitory hormone,[] whose actions are spread to different parts of the body:
Anterior pituitary
In the anterior pituitary gland, the effects of somatostatin are: • Inhibit the release of growth hormone (GH)[] (thus opposing the effects of Growth Hormone-Releasing Hormone (GHRH)) • Inhibit the release of thyroid-stimulating hormone (TSH)[1] • It is induced by low pH. • Inhibit adenylyl cyclase in parietal cells.
Gastrointestinal system
• Somatostatin is homologous with cortistatin (see somatostatin family) and suppresses the release of gastrointestinal hormones • Gastrin • Cholecystokinin (CCK) • Secretin • Motilin • Vasoactive intestinal peptide (VIP) • Gastric inhibitory polypeptide (GIP) • Enteroglucagon • Decrease rate of gastric emptying, and reduces smooth muscle contractions and blood flow within the intestine[] • Suppresses the release of pancreatic hormones • Inhibits insulin release when somatostatin is released from delta cells of pancreas[] • Inhibits the release of glucagon[] • Suppresses the exocrine secretory action of pancreas.
D cell is visible at upper-right, and somatostatin is represented by middle arrow pointing left
Synthetic substitutes
Octreotide (brand name Sandostatin, Novartis Pharmaceuticals) is an octapeptide that mimics natural somatostatin pharmacologically, though is a more potent inhibitor of growth hormone, glucagon, and insulin than the natural hormone and has a much longer half-life (approximately 90 minutes, compared to 2–3 minutes for somatostatin). Since it is absorbed poorly from the gut, it is administered parenterally (subcutaneously, intramuscularly, or intravenously). It is indicated for symptomatic treatment of carcinoid syndrome and acromegaly. It is also finding increased use in polycystic diseases of the liver and kidney. Lanreotide (INN) is a medication used in the management of acromegaly and symptoms caused by neuroendocrine tumors, most notably carcinoid syndrome. It is a long-acting analogue of somatostatin, like octreotide.
Somatostatin Lanreotide (as lanreotide acetate) is manufactured by Ipsen and marketed under the trade name Somatuline. It is available in several countries, including the United Kingdom, Australia, and Canada, and was approved for sale in the United States by the Food and Drug Administration (FDA) on August 30, 2007.
166
Evolutionary history
There are six somatostatin genes that have been discovered in vertebrates. The current proposed history as to how these six genes arose is based on the three whole-genome duplication events that took place in vertebrate evolution along with local duplications in teleost fish. An ancestral somatostatin gene was duplicated during the first whole-genome duplication event (1R) to create SS1 and SS2. These two genes were duplicated during the second whole-genome duplication event (2R) to create four new somatostatin genes: SS1, SS2, SS3, and one gene that was lost during the evolution of vertebrates. Tetrapods retained SS1 (also known as SS-14 and SS-28) and SS2 (also known as cortistatin) after the split in the sarcopterygii and actinopterygii lineage split. In teleost fish, SS1, SS2, and SS3 were duplicated during the third whole-genome duplication event (3R) to create SS1, SS2, SS4, SS5, and two genes that were lost during the evolution of teleost fish. SS1 and SS2 went through local duplications to give rise to SS6 and SS3.[]
References
[1] First Aid for the USMLE Step 1, 2010. Page 286.
Further reading
• Florio T, Schettini G (2002). "[Somatostatin and its receptors. Role in the control of cell proliferation]". Minerva Endocrinol. 26 (3): 91–102. PMID 11753230 (http://www.ncbi.nlm.nih.gov/pubmed/11753230). • Yamada Y, Reisine T, Law SF, et al. (1993). "Somatostatin receptors, an expanding gene family: cloning and functional characterization of human SSTR3, a protein coupled to adenylyl cyclase". Mol. Endocrinol. 6 (12): 2136–42. doi: 10.1210/me.6.12.2136 (http://dx.doi.org/10.1210/me.6.12.2136). PMID 1337145 (http:// www.ncbi.nlm.nih.gov/pubmed/1337145). • Yamada Y, Post SR, Wang K, et al. (1992). "Cloning and functional characterization of a family of human and mouse somatostatin receptors expressed in brain, gastrointestinal tract, and kidney" (http://www.ncbi.nlm.nih. gov/pmc/articles/PMC48214). Proc. Natl. Acad. Sci. U.S.A. 89 (1): 251–5. doi: 10.1073/pnas.89.1.251 (http:// dx.doi.org/10.1073/pnas.89.1.251). PMC 48214 (http://www.ncbi.nlm.nih.gov/pmc/articles/ PMC48214). PMID 1346068 (http://www.ncbi.nlm.nih.gov/pubmed/1346068). • Brazeau P, Vale W, Burgus R, et al. (1973). "Hypothalamic polypeptide that inhibits the secretion of immunoreactive pituitary growth hormone". Science 179 (4068): 77–9. doi: 10.1126/science.179.4068.77 (http:// dx.doi.org/10.1126/science.179.4068.77). PMID 4682131 (http://www.ncbi.nlm.nih.gov/pubmed/ 4682131). • Shen LP, Pictet RL, Rutter WJ (1982). "Human somatostatin I: sequence of the cDNA" (http://www.ncbi.nlm. nih.gov/pmc/articles/PMC346717). Proc. Natl. Acad. Sci. U.S.A. 79 (15): 4575–9. doi: 10.1073/pnas.79.15.4575 (http://dx.doi.org/10.1073/pnas.79.15.4575). PMC 346717 (http://www.ncbi. nlm.nih.gov/pmc/articles/PMC346717). PMID 6126875 (http://www.ncbi.nlm.nih.gov/pubmed/ 6126875). • Shen LP, Rutter WJ (1984). "Sequence of the human somatostatin I gene". Science 224 (4645): 168–71. doi: 10.1126/science.6142531 (http://dx.doi.org/10.1126/science.6142531). PMID 6142531 (http://www.ncbi. nlm.nih.gov/pubmed/6142531). • Montminy MR, Goodman RH, Horovitch SJ, Habener JF (1984). "Primary structure of the gene encoding rat preprosomatostatin" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC345502). Proc. Natl. Acad. Sci. U.S.A. 81 (11): 3337–40. doi: 10.1073/pnas.81.11.3337 (http://dx.doi.org/10.1073/pnas.81.11.3337). PMC
Somatostatin 345502 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC345502). PMID 6145156 (http://www.ncbi.nlm. nih.gov/pubmed/6145156). • Zabel BU, Naylor SL, Sakaguchi AY, et al. (1984). "High-resolution chromosomal localization of human genes for amylase, proopiomelanocortin, somatostatin, and a DNA fragment (D3S1) by in situ hybridization" (http:// www.ncbi.nlm.nih.gov/pmc/articles/PMC390100). Proc. Natl. Acad. Sci. U.S.A. 80 (22): 6932–6. doi: 10.1073/pnas.80.22.6932 (http://dx.doi.org/10.1073/pnas.80.22.6932). PMC 390100 (http://www.ncbi. nlm.nih.gov/pmc/articles/PMC390100). PMID 6196780 (http://www.ncbi.nlm.nih.gov/pubmed/ 6196780). • Panetta R, Greenwood MT, Warszynska A, et al. (1994). "Molecular cloning, functional characterization, and chromosomal localization of a human somatostatin receptor (somatostatin receptor type 5) with preferential affinity for somatostatin-28". Mol. Pharmacol. 45 (3): 417–27. PMID 7908405 (http://www.ncbi.nlm.nih. gov/pubmed/7908405). • Demchyshyn LL, Srikant CB, Sunahara RK, et al. (1993). "Cloning and expression of a human somatostatin-14-selective receptor variant (somatostatin receptor 4) located on chromosome 20". Mol. Pharmacol. 43 (6): 894–901. PMID 8100352 (http://www.ncbi.nlm.nih.gov/pubmed/8100352). • Kaupmann K, Bruns C, Hoyer D, et al. (1993). "Distribution and second messenger coupling of four somatostatin receptor subtypes expressed in brain". FEBS Lett. 331 (1–2): 53–9. doi: 10.1016/0014-5793(93)80296-7 (http:// dx.doi.org/10.1016/0014-5793(93)80296-7). PMID 8405411 (http://www.ncbi.nlm.nih.gov/pubmed/ 8405411). • Aguila MC, Rodriguez AM, Aguila-Mansilla HN, Lee WT (1996). "Somatostatin antisense oligodeoxynucleotide-mediated stimulation of lymphocyte proliferation in culture". Endocrinology 137 (5): 1585–90. doi: 10.1210/en.137.5.1585 (http://dx.doi.org/10.1210/en.137.5.1585). PMID 8612489 (http:// www.ncbi.nlm.nih.gov/pubmed/8612489). • Sharma K, Patel YC, Srikant CB (1997). "Subtype-selective induction of wild-type p53 and apoptosis, but not cell cycle arrest, by human somatostatin receptor 3". Mol. Endocrinol. 10 (12): 1688–96. doi: 10.1210/me.10.12.1688 (http://dx.doi.org/10.1210/me.10.12.1688). PMID 8961277 (http://www.ncbi.nlm.nih.gov/pubmed/ 8961277). • Dournaud P, Boudin H, Schonbrunn A, et al. (1998). "Interrelationships between somatostatin sst2A receptors and somatostatin-containing axons in rat brain: evidence for regulation of cell surface receptors by endogenous somatostatin". J. Neurosci. 18 (3): 1056–71. PMID 9437026 (http://www.ncbi.nlm.nih.gov/pubmed/ 9437026). • Barnea A, Roberts J, Ho RH (1999). "Evidence for a synergistic effect of the HIV-1 envelope protein gp120 and brain-derived neurotrophic factor (BDNF) leading to enhanced expression of somatostatin neurons in aggregate cultures derived from the human fetal cortex". Brain Res. 815 (2): 349–57. doi: 10.1016/S0006-8993(98)01098-1 (http://dx.doi.org/10.1016/S0006-8993(98)01098-1). PMID 9878821 (http://www.ncbi.nlm.nih.gov/ pubmed/9878821). • Ferone D, van Hagen PM, van Koetsveld PM, et al. (1999). "In vitro characterization of somatostatin receptors in the human thymus and effects of somatostatin and octreotide on cultured thymic epithelial cells". Endocrinology 140 (1): 373–80. doi: 10.1210/en.140.1.373 (http://dx.doi.org/10.1210/en.140.1.373). PMID 9886848 (http://www.ncbi.nlm.nih.gov/pubmed/9886848). • Brakch N, Lazar N, Panchal M, et al. (2002). "The somatostatin-28(1-12)-NPAMAP sequence: an essential helical-promoting motif governing prosomatostatin processing at mono- and dibasic sites". Biochemistry 41 (5): 1630–9. doi: 10.1021/bi011928m (http://dx.doi.org/10.1021/bi011928m). PMID 11814357 (http://www. ncbi.nlm.nih.gov/pubmed/11814357). • Oomen SP, van Hennik PB, Antonissen C, et al. (2002). "Somatostatin is a selective chemoattractant for primitive (CD34(+)) hematopoietic progenitor cells". Exp. Hematol. 30 (2): 116–25. doi: 10.1016/S0301-472X(01)00772-X (http://dx.doi.org/10.1016/S0301-472X(01)00772-X). PMID 11823046 (http://www.ncbi.nlm.nih.gov/
167
Somatostatin pubmed/11823046). • Simonetti M, Di BC (2002). "Structural motifs in the maturation process of peptide hormones. The somatostatin precursor. I. A CD conformational study". J. Pept. Sci. 8 (2): 66–79. doi: 10.1002/psc.370 (http://dx.doi.org/ 10.1002/psc.370). PMID 11860030 (http://www.ncbi.nlm.nih.gov/pubmed/11860030).
168
Gastrin
Gastrin
Identifiers Symbol Pfam InterPro PROSITE Gastrin PF00918 [1] [2] [3]
IPR001651
PDOC00232
Available protein structures: Pfam PDB structures [4] [5] ; PDBe [6]
RCSB PDB
PDBsum structure summary [7]
Gastrin
Identifiers Symbols External IDs GAST
[8]
; GAS
[9]
OMIM: 137250
MGI: 104768
[10]
HomoloGene: 628
[11]
GeneCards: GAST Gene
[12]
Gene Ontology Molecular function • hormone activity [10] Cellular component • extracellular region [229] Biological process • signal transduction [14] • G-protein coupled receptor signaling pathway
[13] [38]
Sources: Amigo
/ QuickGO
[14]
RNA expression pattern
More reference expression data
[15]
Gastrin
169
Orthologs Species Entrez Ensembl UniProt RefSeq (mRNA) RefSeq (protein) Human 2520
[16] [18]
Mouse 14459
[17] [19]
ENSG00000184502 P01350
[20] [22]
ENSMUSG00000017165 P48757
[21] [23]
NM_000805 NP_000796
NM_010257 NP_034387
[24]
[25]
Location (UCSC) Chr 17: [26] 39.87 – 39.87 Mb PubMed search
[28]
Chr 11: [27] 100.33 – 100.34 Mb
[29]
In humans, gastrin is a peptide hormone that stimulates secretion of gastric acid (HCl) by the parietal cells of the stomach and aids in gastric motility. It is released by G cells in the antrum of the stomach (the portion of the stomach adjacent the pyloric valve), duodenum, and the pancreas. It binds to cholecystokinin B receptors to stimulate the release of histamines in enterochromaffin-like cells, and it induces the insertion of K+/H+ ATPase pumps into the apical membrane of parietal cells (which in turn increases H+ release into the stomach cavity). Its release is stimulated by peptides in the lumen of the stomach.
History
Its existence was first suggested in 1905 by the British physiologist John Sydney Edkins,[1][2] and gastrins were isolated in 1964 by Roderic Alfred Gregory at the University of Liverpool.[3] In 1964 the structure of Gastrin was determined.[4]
G cell is visible near bottom left, and gastrin is labeled as the two black arrows leading from it. Note: this diagram does not illustrate gastrin's stimulatory effect on ECL cells.
Physiology
Genetics
The GAS gene is located on the long arm of the seventeenth chromosome (17q21).[5]
Gastrin
170
Synthesis
Gastrin is a linear peptide hormone produced by G cells of the duodenum and in the pyloric antrum of the stomach. It is secreted into the bloodstream. Gastrin is found primarily in three forms: • gastrin-34 ("big gastrin") • gastrin-17 ("little gastrin") • gastrin-14 ("minigastrin") Also, pentagastrin is an artificially synthesized, five amino acid sequence identical to the last five amino acid sequence at the C-terminus end of gastrin. The numbers refer to the amino acid count.
Release
Gastrin is released in response to certain stimuli. These include: • • • • stomach distension vagal stimulation (mediated by the neurocrine bombesin, or GRP in humans) the presence of partially digested proteins especially amino acids hypercalcemia
Gastrin release is inhibited by:[6][7] • The presence of acid (primarily the secreted HCl) in the stomach (a case of negative feedback). • Somatostatin also inhibits the release of gastrin, along with secretin, GIP (gastroinhibitory peptide), VIP (vasoactive intestinal peptide), glucagon and calcitonin.
Function
The presence of gastrin stimulates parietal cells of the stomach to secrete hydrochloric acid (HCl)/gastric acid. This is done both directly on the parietal cell and indirectly via binding onto CCK2/gastrin receptors on ECL cells in the stomach, which then responds by releasing histamine, which in turn acts in a paracrine manner on parietal cells stimulating them to secrete H+ ions. This is the major stimulus for acid secretion by parietal cells. Along with the above mentioned function, gastrin has been shown to have additional functions as well: • • • • Stimulates parietal cell maturation and fundal growth. Causes chief cells to secrete pepsinogen, the zymogen (inactive) form of the digestive enzyme pepsin. Increases antral muscle mobility and promotes stomach contractions. Strengthens antral contractions against the pylorus, and relaxes the pyloric sphincter, which stimulates gastric emptying. • Plays a role in the relaxation of the ileocecal valve.[] • Induces pancreatic secretions and gallbladder emptying.[] • Impacts lower esophageal sphincter (LES) tone, causing it to contract.[]
Gastrin
171
Factors influencing secretion
Gastric lumen • Stimulatory factors: dietary protein and amino acids (meat), hypercalcemia. (i.e. during the gastric phase) • Inhibitory factor: acidity (pH below 3) - a negative feedback mechanism, exerted via the release of somatostatin from δ cells in the stomach, which inhibits gastrin and histamine release. Paracrine • Stimulatory factor: bombesin • Inhibitory factor: somatostatin - acts on somatostatin-2 receptors on G cells. in a paracrine manner via local diffusion in the intercellular spaces, but also systemically through its release into the local mucosal blood circulation; it inhibits acid secretion by acting on parietal cells. Nervous • Stimulatory factors: Beta-adrenergic agents, cholinergic agents, gastrin-releasing peptide (GRP) • Inhibitory factor: Enterogastric reflex Circulation • Stimulatory factor: epinephrine • Inhibitory factors:gastric inhibitory peptide (GIP), secretin, somatostatin, glucagon, calcitonin
Role in disease
In the Zollinger-Ellison syndrome, gastrin is produced at excessive levels, often by a gastrinoma (gastrin-producing tumor, mostly benign) of the duodenum or the pancreas. To investigate for hypergastrinemia (high blood levels of gastrin), a "pentagastrin test" can be performed. In autoimmune gastritis, the immune system attacks the parietal cells leading to hypochlorhydria (low stomach acidity). This results in an elevated gastrin level in an attempt to compensate for increased pH in the stomach. Eventually, all the parietal cells are lost and achlorhydria results leading to a loss of negative feedback on gastrin secretion. Plasma gastrin concentration is elevated in virtually all individuals with mucolipidosis type IV (mean 1507 pg/mL; range 400-4100 pg/mL) (normal 0-200 pg/mL) secondary to a constitutive achlorhydria. This finding facilitates the diagnosis of patients with this neurogenetic disorder.[]
References Further reading
• Rozengurt E, Walsh JH (2001). "Gastrin, CCK, signaling, and cancer". Annu. Rev. Physiol. 63: 49–76. doi: 10.1146/annurev.physiol.63.1.49 (http://dx.doi.org/10.1146/annurev.physiol.63.1.49). PMID 11181948 (http://www.ncbi.nlm.nih.gov/pubmed/11181948). • Dockray GJ (2005). "Clinical endocrinology and metabolism. Gastrin". Best Pract. Res. Clin. Endocrinol. Metab. 18 (4): 555–68. doi: 10.1016/j.beem.2004.07.003 (http://dx.doi.org/10.1016/j.beem.2004.07.003). PMID 15533775 (http://www.ncbi.nlm.nih.gov/pubmed/15533775). • Anlauf M, Garbrecht N, Henopp T, et al. (2006). "Sporadic versus hereditary gastrinomas of the duodenum and pancreas: distinct clinico-pathological and epidemiological features". World J. Gastroenterol. 12 (34): 5440–6. PMID 17006979 (http://www.ncbi.nlm.nih.gov/pubmed/17006979). • Polosatov MV, Klimov PK, Masevich CG, et al. (1979). "Interaction of synthetic human big gastrin with blood proteins of man and animals". Acta hepato-gastroenterologica 26 (2): 154–9. PMID 463490 (http://www.ncbi.
Gastrin nlm.nih.gov/pubmed/463490). Fritsch WP, Hausamen TU, Scholten T (1977). "[Gastrointestinal hormones. I. Hormones of the gastrin group]". Zeitschrift für Gastroenterologie 15 (4): 264–76. PMID 871064 (http://www.ncbi.nlm.nih.gov/pubmed/ 871064). Higashimoto Y, Himeno S, Shinomura Y, et al. (1989). "Purification and structural determination of urinary NH2-terminal big gastrin fragments". Biochem. Biophys. Res. Commun. 160 (3): 1364–70. doi: 10.1016/S0006-291X(89)80154-8 (http://dx.doi.org/10.1016/S0006-291X(89)80154-8). PMID 2730647 (http://www.ncbi.nlm.nih.gov/pubmed/2730647). Pauwels S, Najdovski T, Dimaline R, et al. (1989). "Degradation of human gastrin and CCK by endopeptidase 24.11: differential behaviour of the sulphated and unsulphated peptides". Biochim. Biophys. Acta 996 (1–2): 82–8. doi: 10.1016/0167-4838(89)90098-8 (http://dx.doi.org/10.1016/0167-4838(89)90098-8). PMID 2736261 (http://www.ncbi.nlm.nih.gov/pubmed/2736261). Lund T, Geurts van Kessel AH, Haun S, Dixon JE (1986). "The genes for human gastrin and cholecystokinin are located on different chromosomes". Hum. Genet. 73 (1): 77–80. doi: 10.1007/BF00292669 (http://dx.doi.org/ 10.1007/BF00292669). PMID 3011648 (http://www.ncbi.nlm.nih.gov/pubmed/3011648).
172
•
•
•
•
• Kariya Y, Kato K, Hayashizaki Y, et al. (1987). "Expression of human gastrin gene in normal and gastrinoma tissues". Gene 50 (1–3): 345–52. doi: 10.1016/0378-1119(86)90338-0 (http://dx.doi.org/10.1016/ 0378-1119(86)90338-0). PMID 3034736 (http://www.ncbi.nlm.nih.gov/pubmed/3034736). • Gregory RA, Tracy HJ, Agarwal KL, Grossman MI (1969). "Aminoacid constitution of two gastrins isolated from Zollinger-Ellison tumour tissue" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1552899). Gut 10 (8): 603–8. doi: 10.1136/gut.10.8.603 (http://dx.doi.org/10.1136/gut.10.8.603). PMC 1552899 (http://www. ncbi.nlm.nih.gov/pmc/articles/PMC1552899). PMID 5822140 (http://www.ncbi.nlm.nih.gov/pubmed/ 5822140). • Bentley PH, Kenner GW, Sheppard RC (1967). "Structures of human gastrins I and II". Nature 209 (5023): 583–5. doi: 10.1038/209583b0 (http://dx.doi.org/10.1038/209583b0). PMID 5921183 (http://www.ncbi. nlm.nih.gov/pubmed/5921183). • Ito R, Sato K, Helmer T, et al. (1984). "Structural analysis of the gene encoding human gastrin: the large intron contains an Alu sequence" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC391550). Proc. Natl. Acad. Sci. U.S.A. 81 (15): 4662–6. doi: 10.1073/pnas.81.15.4662 (http://dx.doi.org/10.1073/pnas.81.15.4662). PMC 391550 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC391550). PMID 6087340 (http://www.ncbi.nlm. nih.gov/pubmed/6087340). • Wiborg O, Berglund L, Boel E, et al. (1984). "Structure of a human gastrin gene" (http://www.ncbi.nlm.nih. gov/pmc/articles/PMC344765). Proc. Natl. Acad. Sci. U.S.A. 81 (4): 1067–9. doi: 10.1073/pnas.81.4.1067 (http://dx.doi.org/10.1073/pnas.81.4.1067). PMC 344765 (http://www.ncbi.nlm.nih.gov/pmc/articles/ PMC344765). PMID 6322186 (http://www.ncbi.nlm.nih.gov/pubmed/6322186). • Kato K, Hayashizaki Y, Takahashi Y, et al. (1984). "Molecular cloning of the human gastrin gene" (http://www. ncbi.nlm.nih.gov/pmc/articles/PMC326575). Nucleic Acids Res. 11 (23): 8197–203. doi: 10.1093/nar/11.23.8197 (http://dx.doi.org/10.1093/nar/11.23.8197). PMC 326575 (http://www.ncbi.nlm. nih.gov/pmc/articles/PMC326575). PMID 6324077 (http://www.ncbi.nlm.nih.gov/pubmed/6324077). • Boel E, Vuust J, Norris F, et al. (1983). "Molecular cloning of human gastrin cDNA: evidence for evolution of gastrin by gene duplication" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC393933). Proc. Natl. Acad. Sci. U.S.A. 80 (10): 2866–9. doi: 10.1073/pnas.80.10.2866 (http://dx.doi.org/10.1073/pnas.80.10.2866). PMC 393933 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC393933). PMID 6574456 (http://www.ncbi.nlm. nih.gov/pubmed/6574456). • Kato K, Himeno S, Takahashi Y, et al. (1984). "Molecular cloning of human gastrin precursor cDNA". Gene 26 (1): 53–7. doi: 10.1016/0378-1119(83)90035-5 (http://dx.doi.org/10.1016/0378-1119(83)90035-5). PMID 6689486 (http://www.ncbi.nlm.nih.gov/pubmed/6689486).
Gastrin • Koh TJ, Wang TC (1995). "Molecular cloning and sequencing of the murine gastrin gene". Biochem. Biophys. Res. Commun. 216 (1): 34–41. doi: 10.1006/bbrc.1995.2588 (http://dx.doi.org/10.1006/bbrc.1995.2588). PMID 7488110 (http://www.ncbi.nlm.nih.gov/pubmed/7488110). • Rehfeld JF, Hansen CP, Johnsen AH (1995). "Post-poly(Glu) cleavage and degradation modified by O-sulfated tyrosine: a novel post-translational processing mechanism" (http://www.ncbi.nlm.nih.gov/pmc/articles/ PMC398093). EMBO J. 14 (2): 389–96. PMC 398093 (http://www.ncbi.nlm.nih.gov/pmc/articles/ PMC398093). PMID 7530658 (http://www.ncbi.nlm.nih.gov/pubmed/7530658). • Rehfeld JF, Johnsen AH (1994). "Identification of gastrin component I as gastrin-71. The largest possible bioactive progastrin product". Eur. J. Biochem. 223 (3): 765–73. doi: 10.1111/j.1432-1033.1994.tb19051.x (http:/ /dx.doi.org/10.1111/j.1432-1033.1994.tb19051.x). PMID 8055952 (http://www.ncbi.nlm.nih.gov/ pubmed/8055952). • Varro A, Dockray GJ (1993). "Post-translational processing of progastrin: inhibition of cleavage, phosphorylation and sulphation by brefeldin A" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1134634). Biochem. J. 295 (Pt 3): 813–9. PMC 1134634 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1134634). PMID 8240296 (http://www.ncbi.nlm.nih.gov/pubmed/8240296).
173
External links
• Overview at colostate.edu (http://www.vivo.colostate.edu/hbooks/pathphys/endocrine/gi/gastrin.html) • Physiology at MCG 6/6ch4/s6ch4_14 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section6/6ch4/s6ch4_14.htm)
Secretin
174
Secretin
Secretin
Identifiers Symbol External IDs SCT
[1] [2]
OMIM: 182099 Gene Ontology
MGI: 99466
[3]
HomoloGene: 7928
[4]
GeneCards: SCT Gene
[5]
Molecular function • hormone activity [10] Cellular component • cellular_component [6] [229] • extracellular region Biological process • pancreatic juice secretion
[8] [7]
Sources: Amigo
/ QuickGO
[9]
Orthologs Species Entrez Ensembl UniProt RefSeq (mRNA) RefSeq (protein) Human 6343
[10] [12]
Mouse 20287
[11] [13]
ENSG00000070031 P09683
[14] [16]
ENSMUSG00000038580 Q08535
[15] [17]
NM_021920 NP_068739
NM_011328 NP_035458
[18]
[19]
Location (UCSC) Chr 11: [20] 0.63 – 0.63 Mb PubMed search
[22]
Chr 7: [21] 141.28 – 141.28 Mb
[23]
Secretin is a hormone that both controls the environment in the duodenum by regulating secretions of the stomach and pancreas, and regulates water homeostasis throughout the body. It is produced in the S cells of the duodenum, which are located in the crypts of Lieberkühn.[] In humans, the secretin peptide is encoded by the SCT gene.[] Secretin was also the first hormone to be identified.[1] Secretin regulates the pH within the duodenum by inhibiting gastric acid secretion by the parietal cells of the stomach, and by stimulating bicarbonate production by the centroacinar cells and intercalated ducts of the pancreas.
[]
In 2007, secretin was discovered to play a role in osmoregulation by acting on the hypothalamus, pituitary, and kidney.[][]
Secretin
175
Discovery
In 1902, William Bayliss and Ernest Starling were studying how the nervous system controls the process of digestion.[] It was known that the pancreas secreted digestive juices in response to the passage of food (chyme) through the pyloric sphincter into the duodenum. They discovered (by cutting all the nerves to the pancreas in their experimental animals) that this process was not, in fact, governed by the nervous system. They determined that a substance secreted by the intestinal lining stimulates the pancreas after being transported via the bloodstream. They named this intestinal secretion secretin. Secretin was the first such "chemical messenger" identified. This type of substance is now called a hormone, a term coined by Bayliss in 1905.
Structure
Secretin is initially synthesized as a 120 amino acid precursor protein known as prosecretin. This precursor contains an N-terminal signal peptide, spacer, secretin itself (residues 28–54), and a 72-amino acid C-terminal peptide.[] The mature secretin peptide is a linear peptide hormone, which is composed of 27 amino acids and has a molecular weight of 3055. A helix is formed in the amino acids between positions 5 and 13. The amino acids sequences of secretin have some similarities to that of glucagon, vasoactive intestinal peptide (VIP), and gastric inhibitory peptide (GIP). Fourteen of 27 amino acids of secretin reside in the same positions as in glucagon, 7 the same as in VIP, and 10 the same as in GIP.[]
Secretin also has an amidated carboxyl-terminal amino acid which is valine.[] The sequence of amino acids in secretin is H2N–His-Ser-Asp-Gly-Thr-Phe-Thr-Ser-Glu-Leu-Ser-Arg-Leu-Arg-Asp-Ser-Ala-Arg-Leu-Gln-Arg-Leu-Leu-Gln-Gly-Leu-Val–CO
Physiology
Production
Secretin is synthesized in cytoplasmic secretory granules of S-cells, which are found mainly in the mucosa of the duodenum, and in smaller numbers in the jejunum of the small intestine.[]
Stimulus
Secretin is released into circulation and/or intestinal lumen in response to low duodenal pH that ranges between 2 and 4.5 depending on species.[] Also, the secretion of secretin is increased by the products of protein digestion bathing the mucosa of the upper small intestine.[] The acidity is due to hydrochloric acid in the chyme that enters the duodenum from the stomach via the pyloric sphincter. Secretin targets the pancreas, which causes the organ to secrete a bicarbonate-rich fluid that flows into the intestine. Bicarbonate ion is a base that neutralizes the acid, thus establishing a pH favorable to the action of other digestive enzymes in the small intestine and preventing acid burns.[2] Other factors are involved in the release of secretin such as bile salts and fatty acids, which result in additional bicarbonates being added to the small intestine.[] Secretin release is inhibited by H2 antagonists, which reduce gastric acid secretion. As a result, if the pH in the duodenum increases above 4.5, secretin cannot be released.[]
Function
Secretin increases watery bicarbonate solution from pancreatic and bile duct epithelium. Pancreatic centroacinar cells have secretin receptors in their plasma membrane. As secretin binds to these receptors, it stimulates adenylate cyclase activity and converts ATP to cyclic AMP.[] Cyclic AMP acts as second messenger in intracellular signal transduction and leads to increase in release of watery carbonate. It is known to promote the normal growth and maintenance of the pancreas.
Secretin Secretin increases water and bicarbonate secretion from duodenal Brunner's glands to buffer the incoming protons of the acidic chyme.[] It also enhances the effects of cholecystokinin to induce the secretion of digestive enzymes and bile from pancreas and gallbladder, respectively. It counteracts blood glucose concentration spikes by triggering increased insulin release from pancreas, following oral glucose intake.[] Although secretin releases gastrin from gastrinomas, it inhibits gastrin release from the normal stomach. It reduces acid secretion from the stomach by inhibiting gastrin release from G cells.[]:844 This helps neutralize the pH of the digestive products entering the duodenum from the stomach, as digestive enzymes from the pancreas (e.g., pancreatic amylase and pancreatic lipase) function optimally at slightly basic pH.[citation needed] In addition, secretin stimulates pepsin secretion from chief cells, which can help break down proteins in food digestion. It stimulates release of glucagon, pancreatic polypeptide and somatostatin.[]
176
Uses
Secretin has been widely used in medical field especially in pancreatic functioning test because it increases pancreatic secretions. Secretin is either injected[3] or given through a tube that is inserted through nose, stomach then duodenum.[] This test can provide information about whether there are any abnormalities in pancreas which can be gastrinoma, pancreatitis or pancreatic cancer. Secretin has been proposed as a possible treatment for autism based on a hypothetical gut-brain connection; as yet there is no evidence to support it as effective.[]
Osmoregulation
Secretin modulates water and electrolyte transport in pancreatic duct cells,[] liver cholangiocytes,[] and epididymis epithelial cells.[] It is found[] to play a role in the vasopressin-independent regulation of renal water reabsorption.[] Secretin is found in the magnocellular neurons of the paraventricular and supraoptic nuclei of the hypothalamus and along the neurohypophysial tract to neurohypophysis. During increased osmolality, it is released from the posterior pituitary. In the hypothalamus, it activates vasopressin release.[] It is also needed to carry out the central effects of angiotensin II. In the absence of secretin or its receptor in the gene knockout animals, central injection of angiotensin II was unable to stimulate water intake and vasopressin release.[] It has been suggested that abnormalities in such secretin release could explain the abnormalities underlying type D syndrome of inappropriate antidiuretic hormone hypersecretion (SIADH).[] In these individuals, vasopressin release and response are normal, although abnormal renal expression, translocation of aquaporin 2, or both are found.[] It has been suggested that "Secretin as a neurosecretory hormone from the posterior pituitary, therefore, could be the long-sought vasopressin independent mechanism to solve the riddle that has puzzled clinicians and physiologists for decades."[]
Secretin
177
Food intake
Secretin and its receptor are found in discrete nuclei of the hypothalamus, including the paraventricular nucleus and the arcuate nucleus, which are the primary brain sites for regulating body energy homeostasis. It was found that both central and peripheral injection of Sct reduce food intake in mouse, indicating a anorectic role of the peptide. This function of the peptide is mediated by the central melanocortin system.[]
References
[1] http:/ / www. ncbi. nlm. nih. gov/ pubmed/ 11816326 [2] http:/ / www. vivo. colostate. edu/ hbooks/ pathphys/ endocrine/ gi/ secretin. html
Further reading
• Saus E, Brunet A, Armengol L et al. (2010). "Comprehensive copy number variant (CNV) analysis of neuronal pathways genes in psychiatric disorders identifies rare variants within patients". Journal of Psychiatric Research 44 (14): 971–978. doi: 10.1016/j.jpsychires.2010.03.007 (http://dx.doi.org/10.1016/j.jpsychires.2010.03. 007). PMID 20398908 (http://www.ncbi.nlm.nih.gov/pubmed/20398908). • Bertenshaw GP, Turk BE, Hubbard SJ et al. (2001). "Marked differences between metalloproteases meprin A and B in substrate and peptide bond specificity". J. Biol. Chem. 276 (16): 13248–13255. doi: 10.1074/jbc.M011414200 (http://dx.doi.org/10.1074/jbc.M011414200). PMID 11278902 (http://www. ncbi.nlm.nih.gov/pubmed/11278902). • Lee LT, Lam IP, Chow BK (2008). "A functional variable number of tandem repeats is located at the 5' flanking region of the human secretin gene plays a downregulatory role in expression". J. Mol. Neurosci. 36 (1–3): 125–131. doi: 10.1007/s12031-008-9083-5 (http://dx.doi.org/10.1007/s12031-008-9083-5). PMID 18566919 (http://www.ncbi.nlm.nih.gov/pubmed/18566919). • Nussdorfer GG, Bahçelioglu M, Neri G, Malendowicz LK (2000). "Secretin, glucagon, gastric inhibitory polypeptide, parathyroid hormone, and related peptides in the regulation of the hypothalamus- pituitary-adrenal axis". Peptides 21 (2): 309–324. doi: 10.1016/S0196-9781(99)00193-X (http://dx.doi.org/10.1016/ S0196-9781(99)00193-X). PMID 10764961 (http://www.ncbi.nlm.nih.gov/pubmed/10764961). • Lossi L, Bottarelli L, Candusso ME et al. (2004). "Transient expression of secretin in serotoninergic neurons of mouse brain during development". Eur. J. Neurosci. 20 (12): 3259–3269. doi: 10.1111/j.1460-9568.2004.03816.x (http://dx.doi.org/10.1111/j.1460-9568.2004.03816.x). PMID 15610158 (http://www.ncbi.nlm.nih. gov/pubmed/15610158). • Lee SM, Yung WH, Chen L, Chow BK (2005). "Expression and spatial distribution of secretin and secretin receptor in human cerebellum". NeuroReport 16 (3): 219–222. doi: 10.1097/00001756-200502280-00003 (http:// dx.doi.org/10.1097/00001756-200502280-00003). PMID 15706223 (http://www.ncbi.nlm.nih.gov/ pubmed/15706223). • Lam IP, Lee LT, Choi HS et al. (2009). "Bile acids inhibit duodenal secretin expression via orphan nuclear receptor small heterodimer partner (SHP)" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2711755). Am. J. Physiol. Gastrointest. Liver Physiol. 297 (1): G90–G97. doi: 10.1152/ajpgi.00094.2009 (http://dx.doi.org/ 10.1152/ajpgi.00094.2009). PMC 2711755 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2711755). PMID 19372104 (http://www.ncbi.nlm.nih.gov/pubmed/19372104). • Yamagata T, Aradhya S, Mori M et al. (2002). "The human secretin gene: fine structure in 11p15.5 and sequence variation in patients with autism". Genomics 80 (2): 185–194. doi: 10.1006/geno.2002.6814 (http://dx.doi.org/ 10.1006/geno.2002.6814). PMID 12160732 (http://www.ncbi.nlm.nih.gov/pubmed/12160732). • Lee LT, Tan-Un KC, Chow BK (2006). "Retinoic acid-induced human secretin gene expression in neuronal cells is mediated by cyclin-dependent kinase 1". Ann. N. Y. Acad. Sci. 1070: 393–398. doi: 10.1196/annals.1317.051 (http://dx.doi.org/10.1196/annals.1317.051). PMID 16888198 (http://www.ncbi.nlm.nih.gov/pubmed/
Secretin 16888198). • Onori P, Wise C, Gaudio E et al. (2010). "Secretin inhibits cholangiocarcinoma growth via dysregulation of the cAMP-dependent signaling mechanisms of secretin receptor". Int. J. Cancer 127 (1): NA–NA. doi: 10.1002/ijc.25028 (http://dx.doi.org/10.1002/ijc.25028). PMID 19904746 (http://www.ncbi.nlm.nih.gov/ pubmed/19904746). • Lee LT, Tan-Un KC, Pang RT et al. (2004). "Regulation of the human secretin gene is controlled by the combined effects of CpG methylation, Sp1/Sp3 ratio, and the E-box element". Mol. Endocrinol. 18 (7): 1740–1755. doi: 10.1210/me.2003-0461 (http://dx.doi.org/10.1210/me.2003-0461). PMID 15118068 (http:/ /www.ncbi.nlm.nih.gov/pubmed/15118068). • Lu Y, Owyang C (2009). "Secretin-induced gastric relaxation is mediated by vasoactive intestinal polypeptide and prostaglandin pathways" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2743409). Neurogastroenterol. Motil. 21 (7): 754–e47. doi: 10.1111/j.1365-2982.2009.01271.x (http://dx.doi.org/10. 1111/j.1365-2982.2009.01271.x). PMC 2743409 (http://www.ncbi.nlm.nih.gov/pmc/articles/ PMC2743409). PMID 19239625 (http://www.ncbi.nlm.nih.gov/pubmed/19239625). • Gandhi S, Rubinstein I, Tsueshita T, Onyuksel H (2002). "Secretin self-assembles and interacts spontaneously with phospholipids in vitro". Peptides 23 (1): 201–204. doi: 10.1016/S0196-9781(01)00596-4 (http://dx.doi. org/10.1016/S0196-9781(01)00596-4). PMID 11814635 (http://www.ncbi.nlm.nih.gov/pubmed/ 11814635). • Love JW (2008). "Peptic ulceration may be a hormonal deficiency disease". Med. Hypotheses 70 (6): 1103–1107. doi: 10.1016/j.mehy.2007.12.011 (http://dx.doi.org/10.1016/j.mehy.2007.12.011). PMID 18280672 (http:/ /www.ncbi.nlm.nih.gov/pubmed/18280672). • Lam IP, Lee LT, Choi HS, Chow BK (2006). "Localization of small heterodimer partner (SHP) and secretin in mouse duodenal cells". Ann. N. Y. Acad. Sci. 1070: 371–375. doi: 10.1196/annals.1317.047 (http://dx.doi.org/ 10.1196/annals.1317.047). PMID 16888194 (http://www.ncbi.nlm.nih.gov/pubmed/16888194). • Luttrell LM (2008). "Reviews in molecular biology and biotechnology: transmembrane signaling by G protein-coupled receptors". Mol. Biotechnol. 39 (3): 239–264. doi: 10.1007/s12033-008-9031-1 (http://dx.doi. org/10.1007/s12033-008-9031-1). PMID 18240029 (http://www.ncbi.nlm.nih.gov/pubmed/18240029). • Du K, Couvineau A, Rouyer-Fessard C et al. (2002). "Human VPAC1 receptor selectivity filter. Identification of a critical domain for restricting secretin binding". J. Biol. Chem. 277 (40): 37016–37022. doi: 10.1074/jbc.M203049200 (http://dx.doi.org/10.1074/jbc.M203049200). PMID 12133828 (http://www. ncbi.nlm.nih.gov/pubmed/12133828). • Portela-Gomes GM, Johansson H, Olding L, Grimelius L (1999). "Co-localization of neuroendocrine hormones in the human fetal pancreas". Eur. J. Endocrinol. 141 (5): 526–533. doi: 10.1530/eje.0.1410526 (http://dx.doi.org/ 10.1530/eje.0.1410526). PMID 10576771 (http://www.ncbi.nlm.nih.gov/pubmed/10576771). • Mutoh H, Ratineau C, Ray S, Leiter AB (2000). "Review article: transcriptional events controlling the terminal differentiation of intestinal endocrine cells". Aliment. Pharmacol. Ther. 14 Suppl 1: 170–5. PMID 10807420 (http://www.ncbi.nlm.nih.gov/pubmed/10807420).
178
External links
• Overview at colostate.edu (http://www.vivo.colostate.edu/hbooks/pathphys/endocrine/gi/secretin.html) • Secretin (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Secretin) at the US National Library of Medicine Medical Subject Headings (MeSH) • Physiology at MCG 6/6ch2/s6ch2_17 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section6/6ch2/s6ch2_17.htm)
Cholecystokinin
179
Cholecystokinin
Cholecystokinin
Identifiers Symbols External IDs CCK
[1]
; MGC117187
[2]
OMIM: 118440
MGI: 88297
[3]
HomoloGene: 583
[4]
ChEMBL: 1649050
[5]
GeneCards: CCK Gene
[6]
Gene Ontology Molecular function • hormone activity [10] [15] • neuropeptide hormone activity Cellular component • extracellular region [229] [230] • extracellular space [7] • axon [20] • dendrite [8] • axon initial segment [34] • terminal button [9] • axon hillock [10] • perikaryon Biological process • behavioral fear response [12] • neuron migration [13] • release of cytochrome c from mitochondria • activation of cysteine-type endopeptidase activity involved in apoptotic process
[14] [11]
• signal transduction [15] • protein kinase C-activating G-protein coupled receptor signaling pathway [16] • axonogenesis [28] • positive regulation of cell proliferation [17] • negative regulation of appetite [18] • positive regulation of protein oligomerization [60] • eating behavior [19] • positive regulation of apoptotic process [20] • positive regulation of peptidyl-tyrosine phosphorylation [21] • positive regulation of mitochondrial depolarization [72] • regulation of sensory perception of pain Sources: Amigo
[22]
[38]
/ QuickGO
[23]
RNA expression pattern
More reference expression data Orthologs Species Entrez Human 885
[25]
[24]
Mouse 12424
[26]
Cholecystokinin
[27] [28]
180
Ensembl UniProt RefSeq (mRNA) RefSeq (protein)
ENSG00000187094 P06307
[29] [31]
ENSMUSG00000032532 P09240
[30] [32]
NM_000729 NP_000720
NM_031161 NP_112438
[33]
[34]
Location (UCSC) Chr 3: [35] 42.3 – 42.31 Mb PubMed search
[37]
Chr 9: [36] 121.49 – 121.5 Mb
[38]
Cholecystokinin (CCK or CCK-PZ; from Greek chole, "bile"; cysto, "sac"; kinin, "move"; hence, move the bile-sac (gallbladder)) is a peptide hormone of the gastrointestinal system responsible for stimulating the digestion of fat and protein. Cholecystokinin, previously called pancreozymin, is synthesized by I-cells in the mucosal epithelium of the small intestine and secreted in the duodenum, the first segment of the small intestine, and causes the release of digestive enzymes and bile from the pancreas and gallbladder, respectively. It also acts as a hunger suppressant. Recent evidence has suggested that it also plays a major role in inducing drug tolerance to opioids like morphine and heroin, and is partly implicated in experiences of pain hypersensitivity during opioid withdrawal.[][]
Structure
CCK identified at bottom right.
CCK is composed of varying numbers of amino acids depending on post-translational modification of the CCK gene product, preprocholecystokinin. Thus CCK is actually a family of hormones identified by number of amino acids, e.g., CCK58, CCK33, and CCK8. CCK58 assumes a helix-turn-helix configuration.[] Its existence was first suggested in 1905 by the British physiologist Joy Simcha Cohen. CCK is very similar in structure to gastrin, another of the gastrointestinal hormones. CCK and gastrin share the same five amino acids at their C-termini.
Functions
CCK mediates a number of physiological processes, including digestion and satiety. It is released by I cells located in the mucosal epithelium of the small intestine (mostly in the duodenum and jejunum), neurons of the enteric nervous system and neurons in the brain. Release of CCK is stimulated by monitor peptide released by pancreatic acinar cells as well as CCK-releasing protein, a paracrine factor secreted by enterocytes in the gastrointestinal mucosa. In addition, release of acetylcholine by the parasympathetic nerve fibers of the vagus nerve also stimulate its secretion. The presence of fatty acids and/or certain amino acids in the chyme entering the duodenum is the greatest stimulator of CCK release. CCK mediates digestion in the small intestine by inhibiting gastric emptying and gastric acid secretion. It stimulates the acinar cells of the pancreas to release digestive enzymes and stimulates the secretion of a juice rich in pancreatic digestive enzymes, hence the old name pancreozymin. Together these enzymes catalyze the digestion of fat, protein, and carbohydrates. Thus, as the levels of the substances that stimulated the release of CCK drop, the concentration of the hormone drops as well. The release of CCK is also inhibited by somatostatin. Trypsin, a protease released by pancreatic acinar cells hydrolyzes CCK-releasing peptide and monitor peptide effectively turning off the additional
Cholecystokinin signals to secrete CCK. CCK also causes the increased production of hepatic bile, and stimulates the contraction of the gall bladder and the relaxation of the Sphincter of Oddi (Glisson's sphincter), resulting in the delivery of bile into the duodenal part of the small intestine. Bile salts form amphipathic micelles that emulsify fats, aiding in their digestion and absorption.
181
Neurobiology
As a neuropeptide, CCK mediates satiety by acting on the CCK receptors distributed widely throughout the central nervous system. In humans, it has been suggested that CCK administration causes nausea and anxiety, and induces a satiating effect. CCK-4 is routinely used to induce anxiety in humans though certainly different forms of CCK are being shown to have highly variable effects.[] The mechanism for this hunger suppression is thought to be a decrease in the rate of gastric emptying.[] CCK also has stimulatory effects on the vagus nerve, effects that can be inhibited by capsaicin.[] The stimulatory effects of CCK oppose those of ghrelin, which has been shown to inhibit the vagus nerve.[] The CCK tetrapeptide fragment CCK-4 (Trp-Met-Asp-Phe-NH2) reliably causes anxiety when administered to humans, and is commonly used in scientific research to induce panic attacks for the purpose of testing new anxiolytic drugs.[] The effects of CCK vary between individuals. For example, in rats, CCK administration significantly reduces hunger in young males, but is slightly less effective in older subjects, and even slightly less effective in females. The hunger-suppressive effects of CCK also are reduced in obese rats.[]
Interactions
Cholecystokinin has been shown to interact with the Cholecystokinin A receptor located mainly on pancreatic acinar cells and Cholecystokinin B receptor mostly in the brain and stomach. CCKB receptor also binds gastrin, a gastrointestinal hormone involved in stimulating gastric acid release and growth of the gastric mucosa.[][][] CCK has also been shown to interact with calcineurin in the pancreas. Calcineurin will go on to activate the transcription factors NFAT 1–3, which will stimulate hypertrophy and growth of the pancreas. CCK can be stimulated by a diet high in protein, or by protease inhibitors.[] Cholecystokinin has been shown to interact with orexin neurons which control appetite and wakefulness (sleep).[] Cholecystokinin can have indirect effects on sleep regulation.[1] Cholecystokinin in the body cannot cross the blood brain barrier, but certain parts of the hypothalamus and brainstem aren't protected by the barrier. In the hypothalamus, CCK8 injection excites CRF neurosecretory neurons in par ventricular nucleus that is different cell responsive to pain stimulation:They show slow a 1 sec-hyperpolarizaiton with subsequent long (30min) depolarization to CCK8 injection (psychological stress), whereas tail pinch (physical stress), transient excitation. Consistently, in the cerebellum, Golgi cells express c-fos mRNA to CCK8 injection, whereas granule cells express junD mRNA to capsaicin injection to the limb skin. Thus, psychological and physical stress excite different neural path.
References External links
• Cholecystokinin (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Cholecystokinin) at the US National Library of Medicine Medical Subject Headings (MeSH)
Insulin
182
Insulin
WARNING: Article could not be rendered - ouputting plain text. Potential causes of the problem are: (a) a bug in the pdf-writer software (b) problematic Mediawiki markup (c) table is too wide InsulinComputer-generated image of six insulin molecules assembled in a hexamer, highlighting the threefold symmetry, the zinc ions holding it together, and the histidine residues involved in zinc binding. Insulin is stored in the body as a hexamer, while the active form is the monomer. ; Available structuresProtein Data BankPDB Ortholog search: PDBe, RCSBList of PDB id codes 1A7F, 1AI0, 1AIY, 1B9E, 1BEN, 1EFE, 1EV3, 1EV6, 1EVR, 1FU2, 1FUB, 1G7A, 1G7B, 1GUJ, 1HIQ, 1HIS, 1HIT, 1HLS, 1HTV, 1HUI, 1IOG, 1IOH, 1J73, 1JCA, 1JCO, 1K3M, 1KMF, 1LKQ, 1LPH, 1MHI, 1MHJ, 1MSO, 1OS3, 1OS4, 1Q4V, 1QIY, 1QIZ, 1QJ0, 1RWE, 1SF1, 1SJT, 1SJU, 1T0C, 1T1K, 1T1P, 1T1Q, 1TRZ, 1TYL, 1TYM, 1UZ9, 1VKT, 1W8P, 1XDA, 1XGL, 1XW7, 1ZEG, 1ZEH, 1ZNJ, 2AIY, 2C8Q, 2C8R, 2CEU, 2G54, 2G56, 2H67, 2HH4, 2HHO, 2HIU, 2JMN, 2JUM, 2JUU, 2JUV, 2JV1, 2JZQ, 2K91, 2K9R, 2KJJ, 2KJU, 2KQP, 2KQQ, 2KXK, 2L1Y, 2L1Z, 2LGB, 2M1D, 2M1E, 2M2M, 2M2N, 2M2O, 2M2P, 2OLY, 2OLZ, 2OM0, 2OM1, 2OMG, 2OMH, 2OMI, 2QIU, 2R34, 2R35, 2R36, 2RN5, 2VJZ, 2VK0, 2W44, 2WBY, 2WC0, 2WRU, 2WRV, 2WRW, 2WRX, 2WS0, 2WS1, 2WS4, 2WS6, 2WS7, 3AIY, 3BRR, 3BXQ, 3E7Y, 3E7Z, 3EXX, 3FQ9, 3HYD, 3I3Z, 3I40, 3ILG, 3INC, 3IR0, 3JSD, 3KQ6, 3P2X, 3P33, 3Q6E, 3ROV, 3TT8, 3U4N, 3UTQ, 3UTS, 3UTT, 3V19, 3V1G, 3W11, 3W12, 3W13, 3ZI3, 3ZQR, 3ZS2, 3ZU1, 4AIY, 4AJX, 4AJZ, 4AK0, 4AKJ, 4EFX, 4FKA, 4IUZ, 5AIYIdentifiersHuman Genome OrganisationSymbols INS; IDDM2; ILPR; IRDN; MODY10External IDsMendelian Inheritance in ManOMIM: 176730 Mouse Genome InformaticsMGI: 96573 HomoloGene: 173 ChEMBL: 5881 GeneCards: INS GeneGene OntologyMolecular function• protease binding• insulin receptor binding• insulin-like growth factor receptor binding• hormone activity• protein bindingCellular component• extracellular region• extracellular space• endoplasmic reticulum lumen• Golgi lumen• secretory granule• endosome lumenBiological process• MAPK cascade• negative regulation of acute inflammatory response• glucose metabolic process• energy reserve metabolic process• regulation of transcription, DNA-dependent• regulation of cellular amino acid metabolic process• acute-phase response• G-protein coupled receptor signaling pathway• cell-cell signaling• positive regulation of cell proliferation• insulin receptor signaling pathway• positive regulation of phosphatidylinositol 3-kinase cascade• glucose transport• regulation of transmembrane transporter activity• positive regulation of cell growth• positive regulation of cell migration• endocrine pancreas development• positive regulation of protein autophosphorylation• activation of protein kinase B activity• positive regulation of cellular protein metabolic process• negative regulation of protein oligomerization• regulation of protein localization• negative regulation of NAD(P)H oxidase activity• wound healing• negative regulation of protein catabolic process• glucose homeostasis• negative regulation of apoptotic process• positive regulation of MAPK cascade• small molecule metabolic process• positive regulation of nitric oxide biosynthetic process• positive regulation of cell differentiation• negative regulation of gluconeogenesis• positive regulation of glycogen biosynthetic process• positive regulation of DNA replication• negative regulation of glycogen catabolic process• positive regulation of glycolysis• positive regulation of mitosis• negative regulation of proteolysis• negative regulation of vasodilation• positive regulation of vasodilation• negative regulation of fatty acid metabolic process• positive regulation of glucose import• positive regulation of insulin receptor signaling pathway• alpha-beta T cell activation• positive regulation of lipid biosynthetic process• regulation of protein secretion• negative regulation of protein secretion• positive regulation of cytokine secretion• positive regulation of peptidyl-tyrosine phosphorylation• regulation of insulin secretion• negative regulation of lipid catabolic process• positive regulation of nitric-oxide synthase activity• positive regulation of
Insulin NF-kappaB transcription factor activity• positive regulation of protein kinase B signaling cascade• fatty acid homeostasis• negative regulation of respiratory burst involved in inflammatory response• positive regulation of respiratory burst• positive regulation of peptide hormone secretion• positive regulation of brown fat cell differentiation• negative regulation of feeding behaviorSources: Amigo / QuickGORNA expression pattern More reference expression dataOrthologsSpeciesHumanMouseEntrez 3630 16334Ensembl ENSG00000254647 ENSMUSG00000000215UniProt P01308 P01326RefSeq (mRNA) NM_000207 NM_001185083RefSeq (protein) NP_000198 NP_001172012Location (UCSC) Chr 11:2.18 – 2.18 Mb Chr 7:142.68 – 142.7 MbPubMed searchInsulin is a peptide hormone, produced by beta cells of the pancreas, and is central to regulating carbohydrate and fat metabolism in the body. Insulin causes cells in the liver, skeletal muscles, and fat cellfat tissue to absorb glucose from the blood. In the liver and skeletal muscles, glucose is stored as glycogen, and in fat cells (adipocytes) it is stored as triglycerides.Insulin stops the use of fat as an energy source by inhibiting the release of glucagon. With the exception of the metabolic disorder diabetes mellitus and metabolic syndrome, insulin is provided within the body in a constant proportion to remove excess glucose from the blood, which otherwise would be toxic. When blood glucose levels fall below a certain level, the body begins to use stored sugar as an energy source through glycogenolysis, which breaks down the glycogen stored in the liver and muscles into glucose, which can then be utilized as an energy source. As a central metabolic control mechanism, its status is also used as a control signal to other body systems (such as amino acid uptake by body cells). In addition, it has several other anabolismanabolic effects throughout the body. When control of insulin levels fails, diabetes mellitus can result. As a consequence, insulin is used medically to treat some forms of diabetes mellitus. Patients with Diabetes mellitus type 1type 1 diabetes depend on external insulin (most commonly Subcutaneous injectioninjected subcutaneously) for their survival because the hormone is no longer produced internally. Patients with Diabetes mellitus type 2type 2 diabetes are often insulin resistanceinsulin resistant and, because of such resistance, may suffer from a "relative" insulin deficiency. Some patients with type 2 diabetes may eventually require insulin if other medications fail to control blood glucose levels adequately. Over 40% of those with Type 2 diabetes require insulin as part of their diabetes management plan. The human insulin protein is composed of 51 amino acids, and has a molecular weight of 5808 Dalton (unit)Da. It is a protein dimerdimer of an A-chain and a B-chain, which are linked together by disulfide bonds. Insulin's name is derived from the Latin insula for "island". Insulin's structure varies slightly between species of animals. Insulin from animal sources differs somewhat in "strength" (in carbohydrate metabolism control effects) in humans because of those variations. pigPorcine insulin is especially close to the human version.Gene The preproinsulin precursor of insulin is encoded by the INS gene.Alleles A variety of mutant alleles with changes in the coding region have been identified. A Conjoined generead-through gene, INS-IGF2, overlaps with this gene at the 5' region and with the IGF2 gene at the 3' region.Regulation Several regulatory sequences in the Promoter (biology)promoter region of the human insulin gene bind to transcription factors. In general, the A-boxes bind to Pdx1 factors, E-boxes bind to NeuroD, C-boxes bind to MafA, and cAMP response elements to CREB. There are also silencer (genetics)silencers that inhibit transcription. Regulatory sequences and their transcription factors for the insulin gene.Regulatory sequence binding transcription factorsILPRDBP (gene)Par1A-box 5 of insulin geneA5Pdx1negative regulatory element (NRE)glucocorticoid receptor, POU2F1Oct1Z-box of insulin geneZ (overlapping NRE and C2) ISF (transcription factor)ISFC2 regulatory sequenceC2Pax4, MafA(?) E-box 2 of insulin geneE2USF1/USF2A-box 3 of insulin geneA3Pdx1CAMP response elementCREB RE - CAMP response elementCREB RECREB, CREMA-box 2 of insulin geneA2 - CAAT enhancer binding (CEB) (partly overlapping A2 and C1) - C-box 1 of insulin geneC1 - E-box 1 of insulin geneE1E2A, NeuroD1, TCF12HEBA-box 1 of insulin geneA1Pdx1G-box 1 of insulin geneG1 - Protein structure Within vertebrates, the amino acid sequence of insulin is conserved_sequencestrongly conserved. CowBovine insulin differs from human in only three amino acid residues, and Pigporcine insulin in one. Even insulin from some species of fish is similar enough to human to be clinically effective in humans. Insulin in some invertebrates is quite similar in sequence to human insulin, and has similar physiological effects. The strong homology seen in the insulin sequence of diverse species suggests that it has been conserved across much of animal evolutionary history. The C-peptide of proinsulin (discussed later), however,
183
Insulin differs much more among species; it is also a hormone, but a secondary one. The primary structure of bovine insulin was first determined by Frederick Sanger in 1951.; ; ; After that, this polypeptide was synthesized independently by several groups.Insulin is produced and stored in the body as a hexamer (a unit of six insulin molecules), while the active form is the monomer. The hexamer is an inactive form with long-term stability, which serves as a way to keep the highly reactive insulin protected, yet readily available. The hexamer-monomer conversion is one of the central aspects of insulin formulations for injection. The hexamer is far more stable than the monomer, which is desirable for practical reasons; however, the monomer is a much faster-reacting drug because diffusion rate is inversely related to particle size. A fast-reacting drug means insulin injections do not have to precede mealtimes by hours, which in turn gives diabetics more flexibility in their daily schedules. Insulin can aggregate and form fibrillar interdigitated beta-sheets. This can cause injection amyloidosis, and prevents the storage of insulin for long periods.Synthesis, physiological effects, and degradation Synthesis Insulin is produced in the pancreas and released when any of several stimuli are detected. These stimuli include ingested protein and glucose in the blood produced from digested food.[citation needed] Carbohydrates can be polymers of simple sugars or the simple sugars themselves. If the carbohydrates include glucose, then that glucose will be absorbed into the bloodstream and blood glucose level will begin to rise. In target cells, insulin initiates a signal transduction, which has the effect of increasing glucose uptake and storage. Finally, insulin is degraded, terminating the response. Insulin undergoes extensive posttranslational modification along the production pathway. Production and secretion are largely independent; prepared insulin is stored awaiting secretion. Both C-peptide and mature insulin are biologically active. Cell components and proteins in this image are not to scale.In mammals, insulin is synthesized in the pancreas within the beta cellβ-cells of the islets of Langerhans. One million to three million islets of Langerhans (pancreatic islets) form the endocrine part of the pancreas, which is primarily an exocrine gland. The endocrine portion accounts for only 2% of the total mass of the pancreas. Within the islets of Langerhans, beta cells constitute 65–80% of all the cells. Insulin consists of two polypeptide chains, the A- and B- chains, linked together by disulfide bonds. It is however first synthesized as a single polypeptide called preproinsulin in pancreatic beta cellβ-cells. Preproinsulin contains a 24-residue signal peptide which directs the nascent polypeptide chain to the rough endoplasmic reticulum (RER). The signal peptide is cleaved as the polypeptide is translocated into lumen of the RER, forming proinsulin. In the RER the proinsulin folds into the correct conformation and 3 disulfide bonds are formed. About 5–10 min after its assembly in the endoplasmic reticulum, proinsulin is transported to the trans-Golgi network (TGN) where immature granules are formed. Transport to the TGN may take about 30 min. Proinsulin undergoes maturation into active insulin through the action of cellular endopeptidases known as prohormone convertases (Proprotein convertase 1PC1 and proprotein convertase 2PC2), as well as the exoprotease carboxypeptidase E. The endopeptidases cleave at 2 positions, releasing a fragment called the C-peptide, and leaving 2 peptide chains, the B- and A- chains, linked by 2 disulfide bonds. The cleavage sites are each located after a pair of basic residues (lysine-64 and arginine-65, and arginine-31 and -32), and after cleavage these 2 pairs of basic residues are removed by the carboxypeptidase. The C-peptide is the central portion of proinsulin, and the primary sequence of proinsulin goes in the order "B-C-A" (the B and A chains were identified on the basis of mass and the C-peptide was discovered later). The resulting mature insulin is packaged inside mature granules waiting for metabolic signals (such as leucine, arginine, glucose and mannose) and vagal nerve stimulation to be exocytosed from the cell into the circulation.The endogenous production of insulin is regulated in several steps along the synthesis pathway: At DNA transcriptiontranscription from the insulin gene In mRNA stability At the mRNA translation In the posttranslational modifications Insulin and its related proteins have been shown to be produced inside the brain, and reduced levels of these proteins are linked to Alzheimer's disease.Release Beta CellBeta cells in the islets of Langerhans release insulin in two phases. The first phase release is rapidly triggered in response to increased blood glucose levels. The second phase is a sustained, slow release of newly formed vesicles triggered independently of sugar. The description of first phase release is as follows: Glucose enters the β-cells through the glucose transporter, GLUT2. Glucose goes into glycolysis and the respiratory cycle, where multiple, high-energy adenosine triphosphateATP molecules are produced by oxidation, leading to a rise in the ATP:ADP ratio within the cell. An increased intracellular ATP:ADP ratio closes the ATP-sensitive SUR1/Kir6.2
184
Insulin potassium channel (see sulfonylurea receptor). This prevents potassium ions (K+) from leaving the cell by facilitated diffusion, leading to a build up of potassium ions. As a result, the inside of the cell becomes more positive with respect to the outside, leading to the depolarisation of the cell surface membrane. On depolarizationdepolarisation, voltage-gated calcium channelscalcium ion (Ca2+) channels open which allows calcium ions to move into the cells by facilitated diffusion. An increased intracellular calcium ion concentration causes the activation of phospholipasephospholipase C, which cleaves the membrane phospholipid phosphatidyl inositol 4,5-bisphosphate into inositol 1,4,5-trisphosphate and diglyceridediacylglycerol. Inositol 1,4,5-trisphosphate (IP3) binds to receptor proteins in the plasma membrane of the endoplasmic reticulum (ER). This allows the release of Ca2+ ions from the ER via IP3-gated channels, and further raises the intracellular concentration of calcium ions. Significantly increased amounts of calcium ions in the cells causes the release of previously synthesized insulin, which has been stored in secretionsecretory vesicle (biology)vesicles. This is the primary mechanism for release of insulin. Other substances known to stimulate insulin release include the amino acids arginine and leucine, parasympathetic release of acetylcholine (via phospholipase C), sulfonylurea, cholecystokinin (CCK, via phospholipase C), and the gastrointestinally derived incretins glucagon-like peptide-1 (GLP-1) and glucose-dependent insulinotropic peptide (GIP). Release of insulin is strongly inhibited by the stress hormone norepinephrine (noradrenaline), which leads to increased blood glucose levels during stress. It appears that release of catecholamines by the sympathetic nervous system has conflicting influences on insulin release by beta cells, because insulin release is inhibited by α2-adrenergic receptors and stimulated by β2-adrenergic receptors. The net effect of norepinephrine from sympathetic nerves and epinephrine from adrenal glands on insulin release is inhibition due to dominance of the α-adrenergic receptors.When the glucose level comes down to the usual physiologic value, insulin release from the β-cells slows or stops. If blood glucose levels drop lower than this, especially to dangerously low levels, release of hyperglycemic hormones (most prominently glucagon from islet of Langerhans alpha cells) forces release of glucose into the blood from cellular stores, primarily liver cell stores of glycogen. By increasing blood glucose, the hyperglycemic hormones prevent or correct life-threatening hypoglycemia. Evidence of impaired first-phase insulin release can be seen in the glucose tolerance test, demonstrated by a substantially elevated blood glucose level at 30 minutes, a marked drop by 60 minutes, and a steady climb back to baseline levels over the following hourly time points. Oscillations Insulin release from pancreas oscillates with a period of 3–6 minutes.Even during digestion, in general, one or two hours following a meal, insulin release from the pancreas is not continuous, but oscillates with a period of 3–6 minutes, changing from generating a blood insulin concentration more than about 800 pico-punit molemol/l to less than 100 pmol/l. This is thought to avoid receptor downregulationdownregulation of insulin receptors in target cells, and to assist the liver in extracting insulin from the blood. This oscillation is important to consider when administering insulin-stimulating medication, since it is the oscillating blood concentration of insulin release, which should, ideally, be achieved, not a constant high concentration. This may be achieved by delivering insulin rhythmically to the portal vein or by islet cell transplantation to the liver. Future insulin pumps hope to address this characteristic. (See also Pulsatile Insulin.) Blood content The idealized diagram shows the fluctuation of blood sugar (red) and the sugar-lowering hormone insulin (blue) in humans during the course of a day containing three meals. In addition, the effect of a sucrosesugar-rich versus a starch-rich meal is highlighted. The blood content of insulin can be measured in international units, such as µIU/mL or in molar concentration, such as pmol/L, where 1 µIU/mL equals 6.945 pmol/L. A Dictionary of Units of Measurement By Russ Rowlett, the University of North Carolina at Chapel Hill. June 13, 2001 A typical blood level between meals is 8–11 μIU/mL (57–79 pmol/L).Signal transduction Special transporter proteins in cell membranes allow glucose from the blood to enter a cell. These transporters are, indirectly, under blood insulin's control in certain body cell types (e.g., muscle cells). Low levels of circulating insulin, or its absence, will prevent glucose from entering those cells (e.g., in type 1 diabetes). More commonly, however, there is a decrease in the sensitivity of cells to insulin (e.g., the reduced insulin sensitivity characteristic of type 2 diabetes), resulting in decreased glucose absorption. In either case, there is 'cell starvation' and weight loss, sometimes extreme. In a few cases, there is a defect in the release of insulin from the pancreas. Either way, the effect is the same: elevated blood glucose levels. Activation of insulin receptors leads to internal
185
Insulin cellular mechanisms that directly affect glucose uptake by regulating the number and operation of protein molecules in the cell membrane that transport glucose into the cell. The genes that specify the proteins that make up the insulin receptor in cell membranes have been identified, and the structures of the interior, transmembrane section, and the extra-membrane section of receptor have been solved. Two types of tissues are most strongly influenced by insulin, as far as the stimulation of glucose uptake is concerned: muscle cells (myocytes) and fat cells (adipocytes). The former are important because of their central role in movement, breathing, circulation, etc., and the latter because they accumulate excess food energy against future needs. Together, they account for about two-thirds of all cells in a typical human body. Insulin binds to the extracellular portion of the alpha subunits of the insulin receptor. This, in turn, causes a conformational change in the insulin receptor that activates the kinase domain residing on the intracellular portion of the beta subunits. The activated kinase domain autophosphorylates tyrosine residues on the C-terminus of the receptor as well as tyrosine residues in the IRS-1 protein. phosphorylated IRS-1, in turn, binds to and activates phosphoinositol 3 kinase (phosphoinositide 3-kinasePI3K) PI3K catalyzes the reaction phosphatidylinositol 4,5-bisphosphatePIP2 + Adenosine triphosphateATP → Phosphatidylinositol (3,4,5)-trisphosphatePIP3 + Adenosine diphosphateADP PIP3 activates protein kinase B (AKTPKB) PKB phosphorylates glycogen synthase kinase (GSK-3GSK) and thereby inactivates GSK GSK can no longer phosphorylate glycogen synthase (glycogen synthaseGS) unphosphorylated GS makes more glycogen PKB also facilitates vesicle fusion, resulting in an increase in GLUT4 transporters in the plasma membraneAfter the signal has been produced, termination of signaling is then needed. As mentioned below in the section on degradation, endocytosis and degradation of the receptor bound to insulin is a main mechanism to end signaling. In addition, signaling can be terminated by dephosphorylation of the tyrosine residues by tyrosine phosphatases. Serine/Threonine kinases are also known to reduce the activity of insulin. Finally, with insulin action being associated with the number of receptors on the plasma membrane, a decrease in the amount of receptors also leads to termination of insulin signaling.The structure of the insulin–insulin receptor complex has been determined using the techniques of X-ray crystallography.Physiological effects Effect of insulin on glucose uptake and metabolism. Insulin binds to its receptor (1), which starts many protein activation cascades (2). These include translocation of Glut-4 transporter to the plasma membrane and influx of glucose (3), glycogen synthesis (4), glycolysis (5) and triglyceride (6).The actions of insulin on the global human metabolism level include: Control of cellular intake of certain substances, most prominently glucose in muscle and adipose tissue (about two-thirds of body cells) Increase of DNA replication and protein synthesis via control of amino acid uptake Modification of the activity of numerous enzymes. The actions of insulin (indirect and direct) on cells include: Increased glycogen synthesis – insulin forces storage of glucose in liver (and muscle) cells in the form of glycogen; lowered levels of insulin cause liver cells to convert glycogen to glucose and excrete it into the blood. This is the clinical action of insulin, which is directly useful in reducing high blood glucose levels as in diabetes. Increased lipid synthesis – insulin forces fat cells to take in blood lipids, which are converted to triglycerides; lack of insulin causes the reverse. Increased esterification of fatty acids – forces adipose tissue to make fats (i.e., triglycerides) from fatty acid esters; lack of insulin causes the reverse. Decreased proteolysis – decreasing the breakdown of protein Decreased lipolysis – forces reduction in conversion of fat cell lipid stores into blood fatty acids; lack of insulin causes the reverse. Decreased gluconeogenesis – decreases production of glucose from nonsugar substrates, primarily in the liver (the vast majority of endogenous insulin arriving at the liver never leaves the liver); lack of insulin causes glucose production from assorted substrates in the liver and elsewhere. Decreased Autophagy (cellular)autophagy - decreased level of degradation of damaged organelles. Postprandial levels inhibit autophagy completely. Increased amino acid uptake – forces cells to absorb circulating amino acids; lack of insulin inhibits absorption. Increased potassium uptake – forces cells to absorb serum potassium; lack of insulin inhibits absorption. Insulin's increase in cellular potassium uptake lowers potassium levels in blood. This possibly occurs via insulin-induced translocation of the Na+/K+-ATPase to the surface of skeletal muscle cells. Arterial muscle tone – forces arterial wall muscle to relax, increasing blood flow, especially in microarteries; lack of insulin reduces flow by allowing these muscles to contract. Increase in the secretion of hydrochloric acid by parietal cells in the stomach Decreased renal sodium
186
Insulin excretion.Insulin also influences other body functions, such as compliance (physiology)#Blood vesselsvascular compliance and cognition. Once insulin enters the human brain, it enhances learning and memory and benefits verbal memory in particular. Enhancing brain insulin signaling by means of intranasal insulin administration also enhances the acute thermoregulatory and glucoregulatory response to food intake, suggesting that central nervous insulin contributes to the control of whole-body energy homeostasis in humans.Degradation Once an insulin molecule has docked onto the receptor and effected its action, it may be released back into the extracellular environment, or it may be degraded by the cell. The two primary sites for insulin clearance are the liver and the kidney. The liver clears most insulin during first-pass transit, whereas the kidney clears most of the insulin in systemic circulation. Degradation normally involves endocytosis of the insulin-receptor complex, followed by the action of insulin-degrading enzyme. An insulin molecule produced endogenously by the pancreatic beta cells is estimated to be degraded within about one hour after its initial release into circulation (insulin biological half-lifehalf-life ~ 4–6 minutes).Hypoglycemia Although other cells can use other fuels (most prominently fatty acids), neurons depend on glucose as a source of energy in the nonstarving human. They do not require insulin to absorb glucose, unlike muscle and adipose tissue, and they have very small internal stores of glycogen. Glycogen stored in liver cells (unlike glycogen stored in muscle cells) can be converted to glucose, and released into the blood, when glucose from digestion is low or absent, and the glycerol backbone in triglycerides can also be used to produce blood glucose. Sufficient lack of glucose and scarcity of these sources of glucose can dramatically make itself manifest in the impaired functioning of the central nervous system: dizziness, speech problems, and even loss of consciousness. Low blood glucose level is known as hypoglycemia or, in cases producing unconsciousness, "hypoglycemic coma" (sometimes termed "insulin shock" from the most common causative agent). Endogenous causes of insulin excess (such as an insulinoma) are very rare, and the overwhelming majority of insulin excess-induced hypoglycemia cases are Iatrogenesisiatrogenic and usually accidental. A few cases of murder, attempted murder, or suicide using insulin overdoses have been reported, but most insulin shocks appear to be due to errors in dosage of insulin (e.g., 20 units instead of 2) or other unanticipated factors (did not eat as much as anticipated, or exercised more than expected, or unpredicted kinetics of the subcutaneously injected insulin itself). Possible causes of hypoglycemia include: External insulin (usually injected subcutaneously) Oral hypoglycemic agents (e.g., any of the sulfonylureas, or similar drugs, which increase insulin release from β-cells in response to a particular blood glucose level) Ingestion of low-carbohydrate sugar substitutes in people without diabetes or with type 2 diabetes. Animal studies show these can trigger insulin release, albeit in much smaller quantities than sugar, according to a report in Discover magazine, August 2004, p 18. (This can never be a cause of hypoglycemia in patients with type 1 diabetes, since there is no endogenous insulin production to stimulate.)Diseases and syndromes There are several conditions in which insulin disturbance is pathologic: Diabetes mellitus – general term referring to all states characterized by hyperglycemia Diabetes mellitus type 1Type 1 – autoimmune-mediated destruction of insulin-producing β-cells in the pancreas, resulting in absolute insulin deficiency Diabetes mellitus type 2Type 2 – multifactoral syndrome with combined influence of genetic susceptibility and influence of environmental factors, the best known being obesity, age, and physical inactivity, resulting in insulin resistance in cells requiring insulin for glucose absorption. This form of diabetes is strongly inherited. Other types of impaired glucose tolerance (see the Diabetes) Insulinoma - a tumor of pancreatic β-cells producing excess insulin or reactive hypoglycemia. Metabolic syndrome – a poorly understood condition first called Syndrome X by Gerald Reaven, Reaven's Syndrome after Reaven, CHAOS in Australia (from the signs that seem to travel together). It is currently not clear whether these signs have a single, treatable cause, or are the result of body changes leading to type 2 diabetes. It is characterized by elevated blood pressure, dyslipidemia (disturbances in blood cholesterol forms and other blood lipids), and increased waist circumference (at least in populations in much of the developed world). The basic underlying cause may be the insulin resistance that precedes type 2 diabetes, which is a diminished capacity for Insulin#Physiological effectsinsulin response in some tissues (e.g., muscle, fat). It is common that morbidities, such as essential hypertension, obesity, type 2 diabetes, and cardiovascular disease (CVD) develop. Polycystic ovary syndrome – a complex syndrome in women in the reproductive years where anovulation and androgen excess are commonly displayed as hirsutism. In many cases of
187
Insulin PCOS, insulin resistance is present. As a medication Insulin vial Biosynthetic "human" insulin is now manufactured for widespread clinical use using Recombinant DNA#Synthetic insulin production using recombinant DNArecombinant DNA technology. More recently, researchers have succeeded in introducing the gene for human insulin into plants and in producing insulin in them, to be specific safflower. From SemBiosys, A New Kind Of Insulin INSIDE WALL STREET By Gene G. Marcial(AUGUST 13, 2007) This technique is anticipated to reduce production costs. Several of these slightly modified versions of human insulin, while having a clinical effect on blood glucose levels as though they were exact copies, have been designed to have somewhat different absorption or duration of action characteristics. They are usually referred to as "insulin analogues". For instance, the first one available, Humalog (insulin lispro), does not exhibit a delayed absorption effect found in regular insulin, and begins to have an effect in as little as 15 minutes. Other rapid-acting analogues are NovoRapid and Apidra, with similar profiles. All are rapidly absorbed due to a mutation in the sequence that prevents the insulin analogue from forming dimers and hexamers. Instead, the insulin molecule is a monomer, which is more rapidly absorbed. Using it, therefore, does not require the planning required for other insulins that begin to take effect much later (up to many hours) after administration. Another type is extended-release insulin; the first of these was Lantus (insulin glargine). These have a steady effect for the entire time they are active, without the peak and drop off effect in other insulins; typically, they continue to have an insulin effect for an extended period from 18 to 24 hours. Likewise, another protracted insulin analogue (Levemir) is based on a fatty acid acylation approach. A myristyric acid molecule is attached to this analogue, which in turn associates the insulin molecule to the abundant serum albumin, which in turn extends the effect and reduces the risk of hypoglycemia. Both protracted analogues need to be taken only once-daily, and are very much used in the type 1 diabetes market as the basal insulin. A combination of a rapid acting and a protracted insulin is also available for the patients, making it more likely for them to achieve an insulin profile that mimics that of the body´s own insulin release. Insulin is usually taken as subcutaneous Injection (medicine)injections by single-use syringes with hypodermic needleneedles, via an insulin pump, or by repeated-use insulin pens with needles. Unlike many medicines, insulin currently cannot be taken orally because, like nearly all other proteins introduced into the gastrointestinal tract, it is reduced to fragments (even single amino acid components), whereupon all activity is lost. There has been some research into ways to protect insulin from the digestive tract, so that it can be administered orally or sublingually. While experimental, several companies now have various formulations in human clinical trials, and one, the India-based Biocon, has formed an agreement with Bristol-MyersBMS to produce an oral-insulin alternative. NDTV Profit – November 16, 2012 – Biocon in pact with Bristol-Myers for oral insulin. Retrieved 2013-04-22.History Discovery In 1869 Paul Langerhans, a medical student in Berlin, was studying the structure of the pancreas under a microscope when he identified some previously unnoticed tissue clumps scattered throughout the bulk of the pancreas. The function of the "little heaps of cells", later eponymknown as the islets of Langerhans, was unknown, but Edouard Laguesse later suggested they might produce secretions that play a regulatory role in digestion. Paul Langerhans' son, Archibald, also helped to understand this regulatory role. The term "insulin" originates from insula, the Latin word for islet/island.In 1889, the Poles in GermanyPolish-German physician Oscar Minkowski, in collaboration with Joseph von Mering, removed the pancreas from a healthy dog to test its assumed role in digestion. Several days after the dog's pancreas was removed, Minkowski's animal keeper noticed a swarm of flies feeding on the dog's urine. On testing the urine, they found there was sugar in the dog's urine, establishing for the first time a relationship between the pancreas and diabetes. In 1901, another major step was taken by Eugene Opie, when he clearly established the link between the islets of Langerhans and diabetes: "Diabetes mellitus . . . is caused by destruction of the islets of Langerhans and occurs only when these bodies are in part or wholly destroyed." Before his work, the link between the pancreas and diabetes was clear, but not the specific role of the islets. The structure of insulin. The left side is a space-filling model of the insulin monomer, believed to be biologically active. Carbon is green, hydrogen white, oxygen red, and nitrogen blue. On the right side is a ribbon diagram of the insulin hexamer, believed to be the stored form. A monomer unit is highlighted with the A chain in blue and the B chain in cyan. Yellow denotes disulfide bonds, and magenta spheres are zinc ions.Over the next two decades, several attempts were made to isolate whatever it was the islets produced as a potential treatment. In 1906,
188
Insulin George Ludwig Zuelzer was partially successful treating dogs with pancreatic extract, but was unable to continue his work. Between 1911 and 1912, E.L. Scott at the University of Chicago used aqueous pancreatic extracts, and noted "a slight diminution of glycosuria", but was unable to convince his director of his work's value; it was shut down. Israel Kleiner (biochemist)Israel Kleiner demonstrated similar effects at Rockefeller University in 1915, but his work was interrupted by World War I, and he did not return to it.In 1916 Nicolae Paulescu, a RomaniansRomanian professor of physiology at the Carol Davila University of Medicine and PharmacyUniversity of Medicine and Pharmacy in Bucharest, developed an aqueous Pancreaspancreatic extract which, when injected into a Diabetesdiabetic dog, had a normalizing effect on blood sugar levels. He had to interrupt his experiments because of World War I, and in 1921 he wrote four papers about his work carried out in Bucharest and his tests on a diabetic dog. Later that year, he published "Research on the Role of the Pancreas in Food Assimilation".Extraction and purification In October 1920, Canadian Frederick Banting was reading one of Minkowski's papers and concluded that it was the very digestive secretions that Minkowski had originally studied that were breaking down the islet secretion(s), thereby making it impossible to extract successfully. He jotted a note to himself: "Ligate pancreatic ducts of the dog. Keep dogs alive till acini degenerate leaving islets. Try to isolate internal secretion of these and relieve glycosurea." The idea was the pancreas's internal secretion, which, it was supposed, regulates sugar in the bloodstream, might hold the key to the treatment of diabetes. A surgeon by training, Banting knew certain arteries could be tied off that would lead to atrophy of most of the pancreas, while leaving the islets of Langerhans intact. He theorized a relatively pure extract could be made from the islets once most of the rest of pancreas was gone. In the spring of 1921, Banting traveled to Toronto to explain his idea to John James Rickard MacleodJ.J.R. Macleod, who was Professor of Physiology at the University of Toronto, and asked Macleod if he could use his lab space to test the idea. Macleod was initially skeptical, but eventually agreed to let Banting use his lab space while he was on holiday for the summer. He also supplied Banting with ten dogs on which to experiment, and two medical students, Charles Herbert BestCharles Best and Clark Noble, to use as lab assistants, before leaving for Scotland. Since Banting required only one lab assistant, Best and Noble flipped a coin to see which would assist Banting for the first half of the summer. Best won the coin toss, and took the first shift as Banting's assistant. Loss of the coin toss may have proved unfortunate for Noble, given that Banting decided to keep Best for the entire summer, and eventually shared half his Nobel Prize money and a large part of the credit for the discovery of insulin with the winner of the toss. Had Noble won the toss, his career might have taken a different path. Banting's method was to tie a ligature (medicine)ligature around the pancreatic duct; when examined several weeks later, the pancreatic digestive cells had died and been absorbed by the immune system, leaving thousands of islets. They then isolated an extract from these islets, producing what they called "isletin" (what we now know as insulin), and tested this extract on the dogs starting July 27. Banting and Best were then able to keep a pancreatectomized dog named Marjorie alive for the rest of the summer by injecting her with the crude extract they had prepared. Removal of the pancreas in test animals in essence mimics diabetes, leading to elevated blood glucose levels. Marjorie was able to remain alive because the extracts, containing isletin, were able to lower her blood glucose levels. Banting and Best presented their results to Macleod on his return to Toronto in the fall of 1921, but Macleod pointed out flaws with the experimental design, and suggested the experiments be repeated with more dogs and better equipment. He then supplied Banting and Best with a better laboratory, and began paying Banting a salary from his research grants. Several weeks later, the second round of experiments was also a success; and Macleod helped publish their results privately in Toronto that November. However, they needed six weeks to extract the isletin, which forced considerable delays. Banting suggested they try to use fetal calf pancreas, which had not yet developed digestive glands; he was relieved to find this method worked well. With the supply problem solved, the next major effort was to purify the extract. In December 1921, Macleod invited the biochemist James Collip to help with this task, and, within a month, the team felt ready for a clinical test. On January 11, 1922, Leonard Thompson (diabetic)Leonard Thompson, a 14-year-old diabetic who lay dying at the Toronto General Hospital, was given the first injection of insulin. However, the extract was so impure, Thompson suffered a severe anaphylaxisallergic reaction, and further injections were canceled. Over the next 12 days, Collip worked day and night to improve the ox-pancreas extract, and a second dose was injected on
189
Insulin January 23. This was completely successful, not only in having no obvious side-effects but also in completely eliminating the glycosuria sign of diabetes. The first American patient was Elizabeth Hughes Gossett, the daughter of the governor of New York. The first patient treated in the U.S. was future woodcut artist James D. Havens; Dr. John Ralston Williams imported insulin from Toronto to Rochester, New York, to treat Havens.Children dying from diabetic ketoacidosis were kept in large wards, often with 50 or more patients in a ward, mostly comatose. Grieving family members were often in attendance, awaiting the (until then, inevitable) death. In one of medicine's more dramatic moments, Banting, Best, and Collip went from bed to bed, injecting an entire ward with the new purified extract. Before they had reached the last dying child, the first few were awakening from their coma, to the joyous exclamations of their families.Banting and Best never worked well with Collip, regarding him as something of an interloper, and Collip left the project soon after. Over the spring of 1922, Best managed to improve his techniques to the point where large quantities of insulin could be extracted on demand, but the preparation remained impure. The drug firm Eli Lilly and Company had offered assistance not long after the first publications in 1921, and they took Lilly up on the offer in April. In November, Lilly made a major breakthrough and was able to produce large quantities of highly refined insulin. Insulin was offered for sale shortly thereafter. Synthesis Purified animal-sourced insulin was the only type of insulin available to diabetics until genetic advances occurred later with medical research. The amino acid structure of insulin was characterized in the early 1950s by Frederick Sanger#Sequencing insulinFrederick Sanger, and the first synthetic insulin was produced simultaneously in the labs of Panayotis Katsoyannis at the University of Pittsburgh and Helmut Zahn at RWTH Aachen University in the early 1960s.The first genetically engineered, synthetic "human" insulin was produced in a laboratory in 1977 by Arthur Riggs, PhD, Keiichi Itakura, PhD, and Herbert Boyer using Escherichia coliE. coli. Partnering with Genentech founded by Swanson, Boyer and Eli Lilly and Company went on in 1982 to sell the first commercially available biosynthetic human insulin under the brand name Humulin. The vast majority of insulin currently used worldwide is now biosynthetic recombinant "human" insulin or its analogues.Recombinant insulin is produced either in yeast (usually baker's yeastsaccharomyces cerevisiae) or E. coli. In yeast, insulin may be engineered as a single-chain protein with a KexII endoprotease (a yeast homolog of PCI/PCII) site that separates the insulin A chain from a c-terminally truncated insulin B chain. A chemically synthesized c-terminal tail is then grafted onto insulin by reverse proteolysis using the inexpensive protease trypsin; typically the lysine on the c-terminal tail is protected with a chemical protecting group to prevent proteolysis. The ease of modular synthesis and the relative safety of modifications in that region accounts for common insulin analogs with c-terminal modifications (e.g. lispro, aspart, glulisine). The Genentech synthesis and completely chemical synthesis such as that by Bruce Merrifield are not preferred because the efficiency of recombining the two insulin chains is low, primarily due to competition with the precipitation of insulin B chain.Nobel Prizes Frederick Banting joined by Charles Best in office, 1924 The Nobel Prize committee in 1923 credited the practical extraction of insulin to a team at the University of Toronto and awarded the Nobel Prize to two men: Frederick Banting and John James Rickard MacleodJ.J.R. Macleod. They were awarded the Nobel Prize in Physiology or Medicine in 1923 for the discovery of insulin. Banting, insulted that Best was not mentioned, shared his prize with him, and Macleod immediately shared his with James Collip. The patent for insulin was sold to the University of Toronto for one half-dollar. The primary structure of insulin was determined by British molecular biologist Frederick Sanger. It was the first protein to have its sequence be determined. He was awarded the 1958 Nobel Prize in Chemistry for this work. In 1969, after decades of work, Dorothy Hodgkin determined the spatial conformation of the molecule, the so-called tertiary structure, by means of X-ray diffraction studies. She had been awarded a Nobel Prize in Chemistry in 1964 for the development of crystallography. Rosalyn Sussman Yalow received the 1977 Nobel Prize in Medicine for the development of the radioimmunoassay for insulin. George Minot, co-recipient of the 1934 Nobel Prize for the development of the first effective treatment for pernicious anemia, had diabetes mellitus. Dr. William Bosworth CastleWilliam Castle observed that the 1921 discovery of insulin, arriving in time to keep Minot alive, was therefore also responsible for the discovery of a cure for pernicious anemia.Nobel Prize controversy Nicolae PaulescuThe work published by Banting, Best, Collip and Macleod represented the preparation of purified insulin extract suitable for use on human patients. Although Paulescu discovered the
190
Insulin principles of the treatment his saline extract could not be used on humans, and he was not mentioned in the 1923 Nobel Prize. Professor Ian Murray was particularly active in working to correct "the historical wrong" against Nicolae Paulescu. Murray was a professor of physiology at the Anderson College of Medicine in Glasgow, Scotland, the head of the department of Metabolic Diseases at a leading Glasgow hospital, vice-president of the British Association of Diabetes, and a founding member of the International Diabetes Federation. Murray wrote: Insufficient recognition has been given to Paulesco, the distinguished RomaniaRoumanian scientist, who at the time when the Toronto team were commencing their research had already succeeded in extracting the antidiabetic hormone of the pancreas and proving its efficacy in reducing the hyperglycaemia in diabetic dogs.In a recent private communication Professor Arne TiseliusTiselius, head of the Nobel Institute, has expressed his personal opinion that Paulescu was equally worthy of the award in 1923.References Further reading Reaven, Gerald M.; Ami Laws (ed.) (1999--04-15). Insulin Resistance: The Metabolic Syndrome X (1st ed.). Totowa, New Jersey: Humana Press. Digital object identifierdoi: 10.1226/0896035883. International Standard Book NumberISBN 0-89603-588-3.Leahy, Jack L.; William T. Cefalu (ed.) (2002-03-22). Insulin Therapy (1st ed.). New York: Marcel Dekker. International Standard Book NumberISBN 0-8247-0711-7.Kumar, Sudhesh; Stephen O'Rahilly (ed.) (2005-01-14). Insulin Resistance: Insulin Action and Its Disturbances in Disease. Chichester, England: Wiley. International Standard Book NumberISBN 0-470-85008-6.Ehrlich, Ann; Carol L. Schroeder (2000-06-16). Medical Terminology for Health Professions (4th ed.). Thomson Delmar Learning. International Standard Book NumberISBN 0-7668-1297-9.Draznin, Boris; Derek LeRoith (September 1994). Molecular Biology of Diabetes: Autoimmunity and Genetics; Insulin Synthesis and Secretion. Totowa, New Jersey: Humana Press. Digital object identifierdoi: 10.1226/0896032868. International Standard Book NumberISBN 0-89603-286-8. Famous Canadian Physicians: Sir Frederick Banting at Library and Archives Canada McKeage K, Goa KL (2001). "Insulin glargine: a review of its therapeutic use as a long-acting agent for the management of type 1 and 2 diabetes mellitus". Drugs 61 (11): 1599–624. Digital object identifierdoi: 10.2165/00003495-200161110-00007. PubMed IdentifierPMID 11577797.External links The Insulin Protein Inspired by Insulin article by parent of a diabetic child Frederick Sanger, Nobel Prize for sequencing Insulin Freeview video with John Sanger and John Walker by the Vega Science Trust. Insulin: entry from protein databank The History of Insulin Insulin Lispro CBC Digital Archives - Banting, Best, Macleod, Collip: Chasing a Cure for Diabetes GeneReviews/NCBI/NIH/UW entry on Permanent Neonatal Diabetes Mellitus Cosmos Magazine: Insulin mystery cracked after 20 years National Diabetes Information Clearinghouse Discovery and Early Development of Insulin, 1920–1925 Secretion of Insulin and Glucagon Insulin Types Comparison Chart Insulin hormone dosage and side effects The True Discoverer of Insulin - Nicolae Paulescu Insulin signaling pathway Molecular Physiology of Signalling Proteins Animations of insulin's action in the body at AboutKidsHealth.ca
191
Glucagon
192
Glucagon
Glucagon
PDB rendering based on 1GCN. Available structures PDB Ortholog search: PDBe [1], RCSB [2] List of PDB id codes 1BH0
[3]
, 1D0R
[4]
, 1NAU
[5]
, 2G49
[6]
, 2L63
[7]
, 2L64
[8]
, 2M5P
[9]
, 2M5Q
[10]
, 3IOL
[11]
Identifiers Symbols External IDs GCG
[12]
; GLP1; GLP2; GRPP
[13]
OMIM: 138030 [17] Gene
MGI: 95674
[14]
HomoloGene: 1553
[15]
ChEMBL: 5736
[16]
GeneCards: GCG
Glucagon
193
Gene Ontology Molecular function • receptor binding [14] [10] • hormone activity [18] • glucagon receptor binding Cellular component • extracellular region [229] [230] • extracellular space [172] • endoplasmic reticulum lumen [19] • plasma membrane [33] • secretory granule Biological process • energy reserve metabolic process [38] • signal transduction [14] • G-protein coupled receptor signaling pathway [20] • adenylate cyclase-modulating G-protein coupled receptor signaling pathway [21] • feeding behavior [22] • cell proliferation [23] • protein kinase A signaling cascade [24] • positive regulation of peptidyl-threonine phosphorylation [32] • positive regulation of cAMP biosynthetic process [25] • positive regulation of protein binding [17] • negative regulation of appetite [35] • positive regulation of peptidyl-serine phosphorylation • positive regulation of insulin secretion involved in cellular response to glucose stimulus
[26] [178]
• negative regulation of apoptotic process [198] • small molecule metabolic process [27] • positive regulation of protein kinase activity [218] • regulation of insulin secretion [28] • positive regulation of ERK1 and ERK2 cascade [29] • cellular response to glucagon stimulus [30] • positive regulation of calcium ion import Sources: Amigo
[31]
[39]
/ QuickGO
[32]
RNA expression pattern
More reference expression data Orthologs Species Entrez Ensembl UniProt RefSeq (mRNA) RefSeq (protein) Human 2641
[34] [36]
[33]
Mouse 14526
[35] [37]
ENSG00000115263 P01275
[38] [40]
ENSMUSG00000000394 P55095
[39] [41]
NM_002054 NP_002045
NM_008100 NP_032126
[42]
[43]
Glucagon
194
Location (UCSC)
Chr 2: [44] 163 – 163.01 Mb
[46]
Chr 2: [45] 62.47 – 62.48 Mb
[47]
PubMed search
Glucagon, a peptide hormone secreted by the pancreas, raises blood glucose levels. Its effect is opposite that of insulin, which lowers blood glucose levels.[] The pancreas releases glucagon when blood sugar (glucose) levels fall too low. Glucagon causes the liver to convert stored glycogen into glucose, which is released into the bloodstream. High blood glucose levels stimulate the release of insulin. Insulin allows glucose to be taken up and used by insulin-dependent tissues. Thus, glucagon and insulin are part of a feedback system that keeps blood glucose levels at a stable level. Glucagon belongs to a family of several other related hormones.
Physiology
Production
The hormone is synthesized and secreted from alpha cells (α-cells) of the islets of Langerhans, which are located in the endocrine portion of the pancreas. In rodents, the alpha cells are located in the outer rim of the islet. Human islet structure is much less segregated, and alpha cells are distributed throughout the islet.
Regulation
Secretion of glucagon is stimulated by: • • • • • • Hypoglycemia Epinephrine (via β2, α2,[] and α1[] adrenergic receptors) Arginine Alanine (often from muscle-derived pyruvate/glutamate transamination (see alanine transaminase reaction). Acetylcholine[] Cholecystokinin
Secretion of glucagon is inhibited by: • • • • Somatostatin Insulin (via GABA)[] Increased free fatty acids and keto acids into the blood Increased urea production
Function
Glucagon generally elevates the amount of glucose in the blood by promoting gluconeogenesis and glycogenolysis.
A microscopic image stained for glucagon
Glucagon
195
Glucagon
Clinical data Pregnancy cat. Legal status ? ? Identifiers ATC code PubChem ? CID 16186314 [48]
IUPHAR ligand 1136 [49] ChemSpider UNII ChEMBL 10481928 [50]
76LA80IG2G
[51]
CHEMBL266481 Chemical data
[52]
Formula
? [53]
(what is this?) (verify)
Glucose is stored in the liver in the form of glycogen, which is a starch-like polymer chain made up of glucose molecules. Liver cells (hepatocytes) have glucagon receptors. When glucagon binds to the glucagon receptors, the liver cells convert the glycogen polymer into individual glucose molecules, and release them into the bloodstream, in a process known as glycogenolysis. As these stores become depleted, glucagon then encourages the liver and kidney to synthesize additional glucose by gluconeogenesis. Glucagon turns off glycolysis in the liver, causing glycolytic intermediates to be shuttled to gluconeogenesis. Glucagon also regulates the rate of glucose production through lipolysis. Glucagon has a minimal effect on lipolysis in humans. Glucagon production appears to be dependent on the central nervous system through pathways yet to be defined. In invertebrate animals, eyestalk removal has been reported to affect glucagon production. Excising the eyestalk in young crayfish produces glucagon-induced hyperglycemia.[]
Glucagon
196
Mechanism of action
Glucagon binds to the glucagon receptor, a G protein-coupled receptor, located in the plasma membrane. The conformation change in the receptor activates G proteins, a heterotrimeric protein with α, β, and γ subunits. When the G protein interacts with the receptor, it undergoes a conformational change that results in the replacement of the GDP molecule that was bound to the α subunit with a GTP molecule. This substitution results in the releasing of the α subunit from the β and γ subunits. The alpha subunit specifically activates the next enzyme in the cascade, adenylate cyclase. Adenylate cyclase manufactures cyclic adenosine monophosphate (cyclic AMP or cAMP), which activates protein kinase A (cAMP-dependent protein kinase). This enzyme, in turn, activates phosphorylase kinase, which, in turn, phosphorylates glycogen phosphorylase, converting into the active form called phosphorylase A. Phosphorylase A is the enzyme responsible for the release of glucose-1-phosphate from glycogen polymers.
History
In the 1920s, Kimball and Murlin studied pancreatic extracts, and found an additional substance with hyperglycemic properties. They described glucagon in 1923.[] The amino acid sequence of glucagon was described in the late 1950s.[] A more complete understanding of its role in physiology and disease was not established until the 1970s, when a specific radioimmunoassay was developed.
Etymology
Glucagon was named in 1923, probably from the Greek γλυκός sweet, and ἄγειν to lead.[1]
Structure
Glucagon is a 29-amino acid polypeptide. Its primary structure in humans is: NH2-His-Ser-Gln-Gly-Thr-Phe-Thr-Ser-Asp-Tyr-Ser-Lys-Tyr-Leu-Asp-Ser-Arg-Arg-Ala-Gln-Asp-Phe-Val-Gln-Trp-Leu-Met-Asn-T The polypeptide has a molecular weight of 3485 daltons. Glucagon is a peptide (nonsteroid) hormone. Glucagon is generated from the cleavage of proglucagon secreted by pancreatic islet α cells. In intestinal L cells, proglucagon is cleaved to the alternate products glicentin, GLP-1 (an incretin), IP-2, and GLP-2 (promotes intestinal growth).
Pathology
Abnormally elevated levels of glucagon may be caused by pancreatic tumors, such as glucagonoma, symptoms of which include necrolytic migratory erythema, reduced amino acids, and hyperglycemia. It may occur alone or in the context of multiple endocrine neoplasia type 1.
Uses and contraindications
Hypoglycemia
An injectable form of glucagon is vital first aid in cases of severe hypoglycemia when the victim is unconscious or for other reasons cannot take glucose orally. The dose for an adult is typically 1 milligram, and the glucagon is given by intramuscular, intravenous or subcutaneous injection, and quickly raises blood glucose levels. Glucagon can also be administered intravenously at 0.25 - 0.5 unit. To use the injectable form, it must be reconstituted prior to use, a step that requires a sterile diluent to be injected into a vial containing powdered glucagon, because the hormone is highly unstable when dissolved in solution. When dissolved in a fluid state, glucagon can form amyloid fibrils, or tightly woven chains of proteins made up of the individual glucagon peptides, and once glucagon begins to fibrilize,
Glucagon it becomes useless when injected, as the glucagon cannot be absorbed and used by the body. The reconstitution process makes using glucagon cumbersome, although there are a number of products now in development from a number of companies that aim to make the product easier to use.
197
Beta blocker overdose
Anecdotal evidence suggests a benefit of higher doses of glucagon in the treatment of overdose with beta blockers; the likely mechanism of action is the increase of cAMP in the myocardium, in effect bypassing the β-adrenergic second messenger system.[]
Impacted food bolus
Glucagon relaxes the lower esophageal sphincter and is used in emergencies involving an impacted food bolus in the esophagus.[]
Side-effects and interactions
Glucagon acts very quickly; common side-effects include headache and nausea. Drug interactions: Glucagon interacts only with oral anticoagulants, increasing the tendency to bleed.
Contraindications
While glucagon can be used clinically to treat various forms of hypoglycemia, it is severely contraindicated in patients with pheochromocytoma, as the drug interaction with elevated levels of adrenaline produced by the tumor may produce an exponential increase in blood sugar levels, leading to a hyperglycemic state, which may incur a fatal elevation in blood pressure.[] Likewise, glucagon is contraindicated in patients with an insulinoma, as its use may lead to rebound hypoglycemia.[]
Media References
[1] glucagon (http:/ / dictionary. reference. com/ browse/ glucagon) on dictionary.com
Further reading
• Kieffer TJ, Habener JF (2000). "The glucagon-like peptides". Endocr. Rev. 20 (6): 876–913. doi: 10.1210/er.20.6.876 (http://dx.doi.org/10.1210/er.20.6.876). PMID 10605628 (http://www.ncbi.nlm.nih. gov/pubmed/10605628). • Drucker DJ (2003). "Glucagon-like peptides: regulators of cell proliferation, differentiation, and apoptosis". Mol. Endocrinol. 17 (2): 161–71. doi: 10.1210/me.2002-0306 (http://dx.doi.org/10.1210/me.2002-0306). PMID 12554744 (http://www.ncbi.nlm.nih.gov/pubmed/12554744). • Jeppesen PB (2004). "Clinical significance of GLP-2 in short-bowel syndrome". J. Nutr. 133 (11): 3721–4. PMID 14608103 (http://www.ncbi.nlm.nih.gov/pubmed/14608103). • Brubaker PL, Anini Y (2004). "Direct and indirect mechanisms regulating secretion of glucagon-like peptide-1 and glucagon-like peptide-2". Can. J. Physiol. Pharmacol. 81 (11): 1005–12. doi: 10.1139/y03-107 (http://dx. doi.org/10.1139/y03-107). PMID 14719035 (http://www.ncbi.nlm.nih.gov/pubmed/14719035). • Baggio LL, Drucker DJ (2005). "Clinical endocrinology and metabolism. Glucagon-like peptide-1 and glucagon-like peptide-2". Best Pract. Res. Clin. Endocrinol. Metab. 18 (4): 531–54. doi: 10.1016/j.beem.2004.08.001 (http://dx.doi.org/10.1016/j.beem.2004.08.001). PMID 15533774 (http:// www.ncbi.nlm.nih.gov/pubmed/15533774).
Glucagon • Holz GG, Chepurny OG (2006). "Diabetes Outfoxed by GLP-1?" (http://www.ncbi.nlm.nih.gov/pmc/ articles/PMC2909599). Sci. STKE 2005 (268): pe2. doi: 10.1126/stke.2682005pe2 (http://dx.doi.org/10.1126/ stke.2682005pe2). PMC 2909599 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2909599). PMID 15671479 (http://www.ncbi.nlm.nih.gov/pubmed/15671479). • Dunning BE, Foley JE, Ahrén B (2006). "Alpha cell function in health and disease: influence of glucagon-like peptide-1". Diabetologia 48 (9): 1700–13. doi: 10.1007/s00125-005-1878-0 (http://dx.doi.org/10.1007/ s00125-005-1878-0). PMID 16132964 (http://www.ncbi.nlm.nih.gov/pubmed/16132964). • Gautier JF, Fetita S, Sobngwi E, Salaün-Martin C (2005). "Biological actions of the incretins GIP and GLP-1 and therapeutic perspectives in patients with type 2 diabetes". Diabetes Metab. 31 (3 Pt 1): 233–42. doi: 10.1016/S1262-3636(07)70190-8 (http://dx.doi.org/10.1016/S1262-3636(07)70190-8). PMID 16142014 (http://www.ncbi.nlm.nih.gov/pubmed/16142014). • De León DD, Crutchlow MF, Ham JY, Stoffers DA (2006). "Role of glucagon-like peptide-1 in the pathogenesis and treatment of diabetes mellitus". Int. J. Biochem. Cell Biol. 38 (5–6): 845–59. doi: 10.1016/j.biocel.2005.07.011 (http://dx.doi.org/10.1016/j.biocel.2005.07.011). PMID 16202636 (http:// www.ncbi.nlm.nih.gov/pubmed/16202636). • Beglinger C, Degen L (2007). "Gastrointestinal satiety signals in humans--physiologic roles for GLP-1 and PYY?". Physiol. Behav. 89 (4): 460–4. doi: 10.1016/j.physbeh.2006.05.048 (http://dx.doi.org/10.1016/j. physbeh.2006.05.048). PMID 16828127 (http://www.ncbi.nlm.nih.gov/pubmed/16828127). • Stephens JW, Bain SC (2007). "Safety and adverse effects associated with GLP-1 analogues". Expert opinion on drug safety 6 (4): 417–22. doi: 10.1517/14740338.6.4.417 (http://dx.doi.org/10.1517/14740338.6.4.417). PMID 17688385 (http://www.ncbi.nlm.nih.gov/pubmed/17688385). • Orskov C, Bersani M, Johnsen AH et al. (1989). "Complete sequences of glucagon-like peptide-1 from human and pig small intestine". J. Biol. Chem. 264 (22): 12826–9. PMID 2753890 (http://www.ncbi.nlm.nih.gov/ pubmed/2753890). • Drucker DJ, Asa S (1988). "Glucagon gene expression in vertebrate brain". J. Biol. Chem. 263 (27): 13475–8. PMID 2901414 (http://www.ncbi.nlm.nih.gov/pubmed/2901414). • Novak U, Wilks A, Buell G, McEwen S (1987). "Identical mRNA for preproglucagon in pancreas and gut". Eur. J. Biochem. 164 (3): 553–8. doi: 10.1111/j.1432-1033.1987.tb11162.x (http://dx.doi.org/10.1111/j. 1432-1033.1987.tb11162.x). PMID 3569278 (http://www.ncbi.nlm.nih.gov/pubmed/3569278). • White JW, Saunders GF (1986). "Structure of the human glucagon gene" (http://www.ncbi.nlm.nih.gov/pmc/ articles/PMC311486). Nucleic Acids Res. 14 (12): 4719–30. doi: 10.1093/nar/14.12.4719 (http://dx.doi.org/ 10.1093/nar/14.12.4719). PMC 311486 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC311486). PMID 3725587 (http://www.ncbi.nlm.nih.gov/pubmed/3725587). • Schroeder WT, Lopez LC, Harper ME, Saunders GF (1984). "Localization of the human glucagon gene (GCG) to chromosome segment 2q36----37". Cytogenet. Cell Genet. 38 (1): 76–9. doi: 10.1159/000132034 (http://dx.doi. org/10.1159/000132034). PMID 6546710 (http://www.ncbi.nlm.nih.gov/pubmed/6546710). • Bell GI, Sanchez-Pescador R, Laybourn PJ, Najarian RC (1983). "Exon duplication and divergence in the human preproglucagon gene". Nature 304 (5924): 368–71. doi: 10.1038/304368a0 (http://dx.doi.org/10.1038/ 304368a0). PMID 6877358 (http://www.ncbi.nlm.nih.gov/pubmed/6877358). • Kärgel HJ, Dettmer R, Etzold G et al. (1982). "Action of rat liver cathepsin L on glucagon". Acta Biol. Med. Ger. 40 (9): 1139–43. PMID 7340337 (http://www.ncbi.nlm.nih.gov/pubmed/7340337). • Wayman GA, Impey S, Wu Z et al. (1994). "Synergistic activation of the type I adenylyl cyclase by Ca2+ and Gs-coupled receptors in vivo". J. Biol. Chem. 269 (41): 25400–5. PMID 7929237 (http://www.ncbi.nlm.nih. gov/pubmed/7929237). • Unson CG, Macdonald D, Merrifield RB (1993). "The role of histidine-1 in glucagon action". Arch. Biochem. Biophys. 300 (2): 747–50. doi: 10.1006/abbi.1993.1103 (http://dx.doi.org/10.1006/abbi.1993.1103). PMID 8382034 (http://www.ncbi.nlm.nih.gov/pubmed/8382034).
198
Bombesin
199
Bombesin
Bombesin
Identifiers CAS number PubChem ChemSpider ChEMBL IUPHAR ligand Jmol-3D images 31362-50-2 16133891 26286924
[1]
[2] [3] [4]
CHEMBL437027 616
[5] [6]
Image 1 Properties
Molecular formula Molar mass
(verify) [7]
C71H110N24O18S 1619.85
(what is: / ?) Except where noted otherwise, data are given for materials in their standard state (at 25 °C, 100 kPa)
Infobox references
Bombesin is a 14-amino acid peptide[] originally isolated from the skin of the oriental fire-bellied toad (Bombina orientalis). It has two known homologs in mammals called neuromedin B and gastrin-releasing peptide. It stimulates gastrin release from G cells. It activates three different G-protein-coupled receptors known as BBR1, -2, and -3.[] It also activates these receptors in the brain. Together with cholecystokinin, it is the second major source of negative feedback signals that stop eating behaviour.[] Bombesin is also a tumor marker for small cell carcinoma of lung, gastric cancer, and neuroblastoma.[]
References
Follicular cell
200
Follicular cell
Follicular cell
Section of thyroid gland of sheep. X 160. ("Cubical epithelium" labeled at center left.) Code TH H3.08.02.4.00007
[1]
Thyroid epithelial cells (also called follicular cells or principal cells) are cells in the thyroid gland that are responsible for the production and secretion of thyroid hormones, that is, thyroxine (T4) and triiodothyronine (T3).
Function
The thyroid epithelial cells take up iodine and amino acids from the blood circulation on the basolateral side, synthesize thyroglobulin and thyroperoxidase from amino acids and secrete these into the thyroid follicles together with iodine. The thyroid epithelial cells can subsequently take up iodinated thyroglobulin from the follicles by endocytosis, extract thyroid hormones from it with the help of proteases and subsequently release thyroid hormones to the blood.
Thyroid hormone synthesis.
[1]
These thyroid hormones are transported throughout the body where they control metabolism (which is the conversion of oxygen and calories to energy). Every cell in the body depends upon thyroid hormones for regulation of their metabolism. The normal thyroid gland produces about 80% T4 and about 20% T3, however, T3 is about four times as potent as T4.
Follicular cell
201
Iodine transport
Iodine is taken up on the basolateral side of the thyroid epithelial cells by sodium-iodide symporters.[2] It is secreted into the follicle through the chloride/iodide transporter pendrin on the apical side.
Structure and development
They are simple cuboidal epithelium and are arranged in spherical follicles surrounding colloid. The interiors of one of these follicles is known as the follicular lumen. They have thyrotropin receptors on their surface, which respond to thyroid-stimulating hormone. Embryologic origin is from a median endodermal mass in the region of the tongue (foramen cecum) in contrast to the parafollicular (C) cells that arise from the 4th branchial pouch.
Relationship to other cell types
Calcitonin-producing parafollicular cells (C cells) can be found scattered along the basement membrane of the thyroid epithelium. Embryologic origin of these C-cells is neural crest, from the ultimobranchial body (4th pharyngeal pouch).
References External links
• Anatomy Atlases - Microscopic Anatomy, plate 15.287 (http://www.anatomyatlases.org/MicroscopicAnatomy/ Section15/Plate15287.shtml) • BU Histology Learning System: 14302loa (http://www.bu.edu/histology/p/14302loa.htm)
Parafollicular cell
202
Parafollicular cell
Parafollicular cell
Code TH H3.08.02.4.00009 [1]
Parafollicular cells (also called C cells) are neuroendocrine cells in the thyroid with primary function to secrete calcitonin. They are located adjacent to the thyroid follicles and reside in the connective tissue. These cells are large and have a pale stain compared with the follicular cells or colloid. In teleost and avian species these cells occupy a structure outside of the thyroid gland named the ultimobranchial body. Parafollicular cells themselves are derived from neural crest cells. Embryologically, they associate with the ultimobranchial body, which itself is a ventral derivative of the fourth (or fifth) pharyngeal pouch. In a series of experiments, Nicole LeDouarin transplanted neural crest cells from quail, with unique and easily identified nuclei, into non-quail neural crest. She subsequently demonstrated the presence of cells with quail nuclei populating the ultimobranchial body and concluded that C cells migrate during embryologic development from the neural crest.[1][2] They are not numerous in the thyroid and are typically situated basally in the epithelium, without direct contact with the follicular lumen. They are always situated within the basement membrane, which surrounds the entire follicle. Parafollicular cell are also known to secrete in smaller quantities several neuroendocrine peptides such as serotonin, somatostatin or CGRP.[3][4][5] They may also have a paracrine role in regulating thyroid hormones production, as they express TRH.[6][7] When parafollicular cells become cancerous, they lead to medullary carcinoma of the thyroid.
Literature
• Baber EC: Contributions to the minute anatomy of the thyroid gland of the dog. Phil Trans R Soc 166 (1876) 557-568 (full text)
References External links
• Histology at OU 42_04 (http://w3.ouhsc.edu/histology/Glass slides/42_04.jpg) • BU Histology Learning System: 14302loa (http://www.bu.edu/histology/p/14302loa.htm) • Histology at KUMC endo-/endo10 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/endo// endo10.htm) • Anatomy Atlases - Microscopic Anatomy, plate 15.287 (http://www.anatomyatlases.org/MicroscopicAnatomy/ Section15/Plate15287.shtml)
Parathyroid gland
203
Parathyroid gland
Parathyroid glands
Endocrine system. (Parathyroid gland not pictured, but are present on surface of thyroid gland, as shown below.)
Thyroid and parathyroid. Latin Gray's System Artery Vein Nerve Lymph Precursor MeSH glandula parathyroidea inferior, glandula parathyroidea superior subject #273 1271 Endocrine superior thyroid artery, inferior thyroid artery, superior thyroid vein, middle thyroid vein, inferior thyroid vein, middle cervical ganglion, inferior cervical ganglion pretracheal, prelaryngeal, jugulo-diagastric,and lympahtics of thymus neural crest mesenchyme and third and fourth pharyngeal pouch endoderm Parathyroid+Glands
[2] [1]
The parathyroid glands are small endocrine glands in the neck that produce parathyroid hormone. Humans usually have four parathyroid glands, which are usually located on the rear surface of the thyroid gland, or, in rare cases, within the thyroid gland itself or in the chest. Parathyroid glands control the amount of calcium in the blood and within the bones.
Parathyroid gland
204
Anatomy
The parathyroid glands are four or more small glands, about the size of a grain of rice, located on the posterior surface (back side) of the thyroid gland. The parathyroid glands usually weigh between 25 mg and 40 mg in humans. There are typically four parathyroid glands. The two parathyroid glands on each side which are positioned higher (closer to the head) are called the superior parathyroid glands, while the lower two are called the inferior parathyroid glands. Occasionally, some individuals may have six, eight, or even more parathyroid glands. The parathyroid glands are named for their proximity to the thyroid but serve a completely different role than the thyroid gland. The parathyroid glands are quite easily recognizable from the thyroid as they have densely packed cells, in contrast with the follicle structure of the thyroid.[1][2] However, at surgery, they are harder to differentiate from the thyroid or fat. Because the inferior thyroid arteries provide the primary blood supply to the posterior aspect of the thyroid gland where the parathyroid glands are located, branches of these arteries usually supply the parathyroid glands. However they may also be supplied by the branches of the superior thyroid arteries; the thyroid ima artery; or the laryngeal, tracheal and esophageal artery. Parathyroid veins drain into thyroid plexus of veins of the thyroid gland. Lymphatic vessels from the parathyroid glands drain into deep cervical lymph nodes and paratracheal lymph nodes. In the histological sense, they distinguish themselves from the thyroid gland, as they contain two types of cells:[3]
Name Staining Quantity Size many few Function Micrograph of a parathyroid gland. H&E stain.
parathyroid chief cells darker oxyphil cells lighter
smaller manufacture PTH (see below). larger function unknown. [4]
History
The parathyroid glands were first discovered in the Indian Rhinoceros by Richard Owen in 1850.[] The glands were first discovered in humans by Ivar Viktor Sandström (1852-1889), a Swedish medical student, in 1880 at Uppsala University.[] It is the last major organ to be recognized in humans so far.
Physiology
The major function of the parathyroid glands is to maintain the body's calcium level within a very narrow range, so that the nervous and muscular systems can function properly. Parathyroid hormone (PTH, also known as parathormone) is a small protein that takes part in the control of calcium and phosphate homeostasis, as well as bone physiology. Parathyroid hormone has effects antagonistic to those of calcitonin. Calcium PTH increases blood calcium levels by stimulating osteoclasts to break down bone and release calcium. PTH also increases gastrointestinal calcium absorption by activating vitamin D, and promotes calcium conservation (reabsorption) by the kidneys. Phosphate
Parathyroid gland PTH is the major regulator of serum phosphate concentrations via actions on the kidney. It is an inhibitor of proximal and also distal tubular reabsorption of phosphorus. Through activation of Vitamin D the absorption of Phosphate is increased.
205
Role in disease
Many conditions are associated with disorders of parathyroid function. These can be divided into those causing hyperparathyroidism, and those causing hypoparathyroidism.
Embryology and evolution
The parathyroid glands originate from the interaction of neural crest mesenchyme and third and fourth branchial pouch endoderm. Eya-1 (transcripitonal co-activator), Six-1 (a homeobox transcription factor), and Gcm-2 (a transcription factor) have been associated with the development of the parathyroid gland, and alterations in these genes alters parathyroid gland development. The superior parathyroids arise from the fourth pharyngeal pouch, and the inferior parathyroids arise from the third pharyngeal pouch. They are vertically transposed during embryogenesis. This is significant in function-preserving parathyroidectomy, because both the superior and the inferior parathyroids are supplied by the inferior thyroid artery. If the surgeon is to leave a single functional parathyroid for the patient, he/she must preserve the appropriate blood supply.
In other animals
Parathyroid glands are found in all adult tetrapods, although they vary in their number, and in their exact position. Mammals typically have four parathyroids, while other groups typically have six. Fish do not possess parathyroid glands, although the ultimobranchial glands, which are found close to the oesophagus, may have a similar function and could even be homologous with the tetrapod parathyroids. Even these glands are absent in the most primitive vertebrates, the jawless fish, but as these species have no bone in their skeletons, only cartilage, it may be that they have less need to regulate calcium metabolism. The conserved homology of genes and calcium-sensing receptors in fish gills with those in the parathryroid glands of birds and mammals is recognized by evolutionary developmental biology as evolution-using genes and gene networks in novel ways to generate new structures with some similar functions and novel functions.
Additional images
High magnification micrograph of a parathyroid gland. H&E stain.
Intermediate magnification micrograph of a parathyroid gland. H&E stain.
Low magnification micrograph of a parathyroid gland and parathyroid adenoma (bottom left). H&E stain.
Scheme showing development of branchial epithelial bodies. I, II, III, IV. Branchial pouches.
Parathyroid gland
206
Human parathyroid glands
References External links
• Endocrine Web at endocrineweb.com (http://www.endocrineweb.com/parathyroid.html) • The origin of the parathyroid gland at pnas.org (http://www.pnas.org/cgi/content/full/101/51/17716) • Parathyroid+gland (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=Parathyroid+ gland) at eMedicine Dictionary • Virtual Slidebox at Univ. Iowa Slide 149 (http://www.path.uiowa.edu/cgi-bin-pub/vs/fpx_gen. cgi?slide=149&viewer=java&view=0&lay=nlm)
Parathyroid chief cell
207
Parathyroid chief cell
Parathyroid chief cell
Micrograph of a parathyroid gland. H&E stain. Code TH H3.08.02.5.00002
[1]
Parathyroid chief cells (also called parathyroid principal cells or simply parathyroid cells) are cells in the parathyroid glands which produce parathyroid hormone. The end result of increased secretion by the chief cells of a parathyroid gland is an increase in the serum level of Calcium. Parathyroid chief cells constitute one of the few cell types of the body that regulate intracellular calcium levels as a consequence of extracellular (or serum) changes in calcium concentration. The calcium-sensing receptor (CaSR) is sensitive to an increase in serum calcium, and stimulates the uptake of calcium by the parathyroid chief cell. This mechanism is critically important, as it describes a physiological feed-back loop by which parathyroid hormone secretion is down-regulated in response to a restoration of serum calcium.
External links
• BU Histology Learning System: 15002loa [1]
Oxyphil cell (parathyroid)
208
Oxyphil cell (parathyroid)
Oxyphil cell (parathyroid)
Micrograph of a parathyroid gland. H&E stain. MeSH Code Oxyphil+Cells
[1] [1]
TH H3.08.02.5.00005
In the parathyroid gland, the parathyroid oxyphil cell is larger and paler than the parathyroid chief cell.[1] These cells can be found in clusters in the center of the section and at the periphery.[2][3][4][5] Oxyphil cells appear at the onset of puberty, but have no known function. With nuclear medicine scans, they selectively take up the Technetium-sestamibi complex radiotracer dye to allow delineation of glandular anatomy.[6] Oxyphil cells have been shown to express parathyroid-relevant genes found in the chief cells and have the potential to produce additional autocrine/paracrine factors, such as Parathyroid hormone-related protein (PTHrP) and calcitriol.[7] More work needs to be done to fully understand the functions of these cells and their secretions.
References
[2] [3] [4] [5] [6] Gartner, p. 208, Fig. 3 Ross, p. 628, Fig. 1 DiFiore, pp. 270 - 271 Wheater, pp. 312 - 313 "Minimally Invasive Radio-guided Surgery for Primary Hyperparathyroidism," Annals of Surgical Oncology 12/07 14(12) pp 3401-3402
Chromaffin cell
209
Chromaffin cell
Medullary chromaffin cell
Adrenal gland. (Medulla labeled at bottom right.) Latin Code endocrinocytus medullaris TH H3.08.02.6.00015
[1]
Chromaffin cells are neuroendocrine cells found mostly in the medulla of the adrenal glands (located above the kidneys) in mammals. They are in close proximity to pre-synaptic sympathetic ganglia of the sympathetic nervous system, with which they communicate, and structurally they are similar to post-synaptic sympathetic neurons. They release catecholamines: ~80% of Epinephrine (Adrenaline) and ~20% of Norepinephrine (Noradrenaline) into systemic circulation for systemic effects on multiple organs (similarly to secretory neurons of the hypothalamus), and can also send paracrine signals. Hence they are called neuroendocrine cells. In the mammalian fetal development (fourth to fifth week in humans), neuroblast cells migrate from the neural crest to form the sympathetic chain and preaortic ganglia. The cells migrate a second time to the adrenal medulla.[1] Chromaffin cells also settle near the sympathetic ganglia, vagus nerve, paraganglia, and carotid arteries. The largest extra-adrenal cluster of chromaffin cells in mammals is the organ of Zuckerkandl.[2] In lower concentrations, extra-adrenal chromaffin cells also reside in the bladder wall, prostate, and behind the liver. In non-mammals, chromaffin cells are found in a variety of places, generally not organized as an individual organ, and may be without innervation, relying only on endocrine or paracrine signals for secretion.[3][4]
Function
Chromaffin cells of the adrenal medulla are innervated by the splanchnic nerve and secrete adrenaline (epinephrine), noradrenaline (norepinephrine), a little dopamine, enkephalin and enkephalin-containing peptides, and a few other hormones into the blood stream. The secreted adrenaline and noradrenaline play an important role in the fight-or-flight response. The enkephalins and enkephalin-containing peptides are related to, but distinct from Epinephrine endogenous peptides named endorphins (which are secreted from the pituitary); all of these peptides bind to opioid receptors and produce analgesic (and other) responses. The hormones are secreted from chromaffin granules; this is where the enzyme dopamine
Chromaffin cell
210
β-hydroxylase catalyzes the conversion of dopamine to noradrenaline.[5] Distinct N and E cell forms exist (also Na and A cells in British nomenclature - noradrenaline and adrenaline); the former produce norepinephrine, the latter arise out of N cells through interaction with glucocorticoids, and convert norepinephrine into epinephrine.[6]
Nomenclature
Norepinephrine
The word 'Chromaffin' comes from a portmanteau of chromium and affinity. They are named as such because they can be visualized by staining with chromium salts. Chromium salts oxidize and polymerize catecholamines to form a brown color, most strongly in the cells secreting noradrenaline. Chromaffin cells are also called pheochromocytes. The enterochromaffin cells are so named because of their histological similarity to chromaffin cells (they also stain yellow when treated with chromium salts), but their function is quite different and they are not derivatives of the neural crest. Paraganglia are clusters of either chromaffin cells of glomus cells near sympathetic ganglia.
Pathology
Neoplasms arising from these cells are pheochromocytomas (also called chromaffin or sympathetic paragangliomas, in contrast to non-chromaffin or parasympathetic paragangliomas of glomus cells). Sometimes only neoplasms of adrenal origin are named pheochromocytomas, while others are named extra-adrenal paragangliomas.
References External links
• BU Histology Learning System: 14507loa (http://www.bu.edu/histology/p/14507loa.htm) - "Endocrine System: adrenal gland, reticularis and medulla" • Secretion Control in Adrenal Chromaffin Cells (http://www.mpibpc.gwdg.de/abteilungen/140/projects/ Chromaffin.html) • UC-San Diego Chromaffin Cell and Hypertension Research (http://hypertension.ucsd.edu) • A Primer on Chromaffin Cells (http://webpages.ull.es/users/isccb12/ChromaffinCell/Primer.html) • Rat Chromaffin cells primary cultures: Standardization and quality assessment for single-cell assays (a protocol) (http://www.natureprotocols.com/2006/09/29/rat_chromaffin_cells_primary_c.php)
Steroid hormone
211
Steroid hormone
A steroid hormone (abbreviated as sterone)[1] is a steroid that acts as a hormone. Steroid hormones can be grouped into five groups by the receptors to which they bind: glucocorticoids, mineralocorticoids, androgens, estrogens, and progestogens. Vitamin D derivatives are a sixth closely related hormone system with homologous receptors, though they are technically sterols rather than steroids. Steroid hormones help control metabolism, inflammation, immune functions, salt and water balance, development of sexual characteristics, and the ability to withstand illness and injury. The term steroid describes both hormones produced by the body and artificially produced medications that duplicate the action for the naturally occurring steroids.
Synthesis
The natural steroid hormones are generally synthesized from cholesterol in the gonads and adrenal glands. These forms of hormones are lipids. They can pass through the cell membrane[] as they are fat-soluble, and then bind to steroid hormone receptors which may be nuclear or cytosolic depending on the steroid hormone, to bring about changes within the cell. Steroid hormones are generally carried in the blood bound to specific carrier proteins such as sex hormone-binding globulin or corticosteroid-binding globulin. Further conversions and catabolism occurs in the liver, in other "peripheral" tissues, and in the target tissues.
Steroidogenesis with enzymes and intermediates
Synthetic steroids and sterols
A variety of synthetic steroids and sterols have also been contrived. Most are steroids, but some non-steroidal molecules can interact with the steroid receptors because of a similarity of shape. Some synthetic steroids are weaker, and some much stronger, than the natural steroids whose receptors they activate. Some examples of synthetic steroid hormones: • • • • • • Glucocorticoids: prednisone, dexamethasone, triamcinolone Mineralocorticoid: fludrocortisone Vitamin D: dihydrotachysterol Androgens: oxandrolone, testosterone, nandrolone (also known as anabolic steroids) Oestrogens: diethylstilbestrol (DES) Progestins: norethindrone, medroxyprogesterone acetate.
Steroid hormone
212
Effects
Steroids exert a wide variety of effects mediated by slow genomic as well as by rapid nongenomic mechanisms. They bind to nuclear receptors in the cell nucleus for genomic actions. Membrane-associated steroid receptors activate intracellular signaling cascades involved in nongenomic actions. Because steroids and sterols are lipid-soluble, they can diffuse fairly freely from the blood through the cell membrane and into the cytoplasm of target cells. In the cytoplasm, the steroid may or may not undergo an enzyme-mediated alteration such as reduction, hydroxylation, or aromatization. In the cytoplasm, the steroid binds to the specific receptor, a large metalloprotein. Upon steroid binding, many kinds of steroid receptor dimerize: Two receptor subunits join together to form one functional DNA-binding unit that can enter the cell nucleus. In some of the hormone systems known, the receptor is associated with a heat shock protein, which is released on the binding of the ligand, the hormone. Once in the nucleus, the steroid-receptor ligand complex binds to specific DNA sequences and induces transcription of its target genes.
References
[1] Definition @ Merriam-Webster online: -sterone (http:/ / mw1. m-w. com/ dictionary/ -sterone)
• Brook CG. Mechanism of puberty. Horm Res. 1999;51 Suppl 3:52–4. Review.PMID 10592444 • Holmes SJ, Shalet SM. Role of growth hormone and sex steroids in achieving and maintaining normal bone mass. Horm Res. 1996;45(1–2):86–93. Review. PMID 8742125 • Ottolenghi C, Uda M, Crisponi L, Omari S, Cao A, Forabosco A, Schlessinger D. Determination and stability of sex. Bioessays. 2007 Jan;29(1):15–25. Review. PMID 17187356 • Couse JF, Korach KS. Exploring the role of sex steroids through studies of receptor deficient mice. J Mol Med. 1998 Jun;76(7):497–511. Review. PMID 9660168 • McEwen BS. Steroid hormones: effect on brain development and function. Horm Res. 1992;37 Suppl 3:1–10. Review. PMID 1330863 • Simons SS Jr. What goes on behind closed doors: physiological versus pharmacological steroid hormone actions. Bioessays. 2008 Aug;30(8):744–56. PMID 18623071
External links
• An animated and narrated tutorial about nuclear receptor signaling (http://www.nursa.org/template. cfm?threadId=11320)
Mineralocorticoid
213
Mineralocorticoid
Mineralocorticoids are a class of steroid hormones characterized by their influence on salt and water balances. The primary mineralocorticoid is aldosterone.
Physiology
The name mineralocorticoid derives from early observations that these hormones were involved in the retention of sodium, a mineral. The primary endogenous mineralocorticoid is aldosterone, although a number of other endogenous hormones (including progesterone and deoxycorticosterone) have mineralocorticoid function. Aldosterone acts on the kidneys to provide active reabsorption of sodium and an associated passive reabsorption of water, as well as the active secretion of potassium in the principal cells of the cortical collecting tubule and active secretion of protons via proton ATPases in the lumenal membrane of the intercalated cells of the collecting tubule. This in turn results in an increase of blood pressure and blood volume. Aldosterone is produced in the cortex of the adrenal gland and its secretion is mediated principally by angiotensin II but also by adrenocorticotrophic hormone (ACTH) and local potassium levels.
Aldosterone
Deoxycorticosterone
Mode of action
The effects of mineralocorticoids are mediated by slow genomic mechanisms through nuclear receptors as well as by fast nongenomic mechanisms through membrane-associated receptors and signaling cascades.
Fludrocortisone
Mineralocorticoid
214
Genomic mechanisms
Mineralocorticoids bind to the cytosolic mineralocorticoid receptor. This type of receptor gets activated upon ligand binding. After a hormone binds to the corresponding receptor, the newly formed receptor-ligand complex translocates itself into the cell nucleus, where it binds to many hormone response elements (HREs) in the promoter region of the target genes in the DNA. The opposite mechanism is called transrepression. The hormone receptor without ligand binding interacts with heat shock proteins and prevents the transcription of targeted genes.
Steroidogenesis, showing mineralocorticoids in ellipse at top right. Note that it is not a
Aldosterone and cortisol (a strictly bounded group, but a continuum of structures with increasing mineralocorticoid effect, with the primary example aldosterone at top. glucosteroid) have similar affinity for the mineralocorticoid receptor; however, glucocorticoids circulate at roughly 100 times the level of mineralocorticoids. An enzyme exists in mineralocorticoid target tissues to prevent overstimulation by glucocorticoids. This enzyme, 11-beta hydroxysteroid dehydrogenase type II (Protein:HSD11B2), catalyzes the deactivation of glucocorticoids to 11-dehydro metabolites. Licorice is known to be an inhibitor of this enzyme and chronic consumption can result in a condition known as pseudohyperaldosteronism.
Pathophysiology
Hyperaldosteronism (the syndrome caused by elevated aldosterone) generally results from adrenal cancers. The two main resulting problems: 1. Hypertension and edema due to excessive Na+ and water retention. 2. Accelerated excretion of potassium ions (K+). With extreme K+ loss there is muscle weakness and eventually paralysis. Underproduction, or hypoaldosteronism, leads to the salt-wasting state associated with Addison's disease, although classical congenital adrenal hyperplasia and other disease states may also cause this situation.
Mineralocorticoid
215
Pharmacology
An example of a synthetic mineralocorticoid is fludrocortisone (Florinef). Important mineralocorticoid inhibitors are spironolactone and eplerenone.
References
• Stewart P (2008): "The Adrenal Cortex " In: Kronenberg, Melmed, Polonsky, Larsen (eds.) Williams Textbook of Endocrinology (11 ed)., Saunders Elsevier, Philadelphia, pp.445-504. • Bennett PN and Brown MJ (2008) “Adrenal corticosteroids, antagonists, corticotropin”, in Clinical Pharmacology (10ed), Churchill Livingstone Elsevier, Publ. pp. 593-607. • Hu X, Funder JW (2006) The evolution of mineralocorticoid receptors. Mol Endocrinol. 20(7):1471-8. • McKay L, Renoir JM, Weigel NL, Wilson EM, McDonnell DP, Cidlowski JA. (2006) International Union of Pharmacology. LXV. The pharmacology and classification of the nuclear receptor superfamily: glucocorticoid, mineralocorticoid, progesterone, and androgen receptors. Pharmacol Rev. Dec;58(4):782-97. • Pippal JB, Fuller PJ. (2008) Structure-function relationships in the mineralocorticoid receptor. J Mol Endocrinol. 41(6):405-13.
Glucocorticoid
Glucocorticoids (GC) are a class of steroid hormones that bind to the glucocorticoid receptor (GR), which is present in almost every vertebrate animal cell. The name glucocorticoid (pertaining to glucose + cortex ) derives from its role in the regulation of the metabolism of glucose, its synthesis in the adrenal cortex, and its steroidal structure (see structure to the right). GCs are part of the feedback mechanism in the immune system that turns immune activity (inflammation) down. They are therefore used in medicine to treat diseases caused by an overactive immune system, such Chemical structure of cortisol, a glucocorticoid as allergies, asthma, autoimmune diseases and sepsis. GCs have many diverse (pleiotropic) effects, including potentially harmful side effects, and as a result are rarely sold over the counter.[] They also interfere with some of the abnormal mechanisms in cancer cells, so they are used in high doses to treat cancer. This includes mainly inhibitory effects on lymphocyte proliferation (treatment of lymphomas and leukaemias) and mitigation of side effects of anticancer drugs. GCs cause their effects by binding to the glucocorticoid receptor (GR). The activated GR complex, in turn, up-regulates the expression of anti-inflammatory proteins in the nucleus (a process known as
Glucocorticoid
216
transactivation) and represses the expression of proinflammatory proteins in the cytosol by preventing the translocation of other transcription factors from the cytosol into the nucleus (transrepression).[] Glucocorticoids are distinguished from mineralocorticoids and sex steroids by their specific receptors, target cells, and effects. In technical terms, "corticosteroid" refers to both glucocorticoids and mineralocorticoids (as both are mimics of hormones produced by the adrenal cortex), but is often used as a synonym for "glucocorticoid". Cortisol (or hydrocortisone) is the most important Dexamethasone binds more powerfully to the glucocorticoid receptor human glucocorticoid. It is essential for life, and it than cortisol does. Dexamethasone is based on the cortisol structure regulates or supports a variety of important but differs in three positions (extra double bond in the A-ring cardiovascular, metabolic, immunologic, and between carbons 1 and 2 and addition of a 9-α-fluoro group and a 16-α-methyl substituent). homeostatic functions. Various synthetic glucocorticoids are available; these are used either as replacement therapy in glucocorticoid deficiency or to suppress the immune system.
Effects
Glucocorticoid effects may be broadly classified into two major categories: immunological and metabolic. In addition, glucocorticoids play important roles in fetal development and body fluid homeostasis.
Immune
As discussed in more detail below, glucocorticoids function through interaction with the glucocorticoid receptor: • up-regulate the expression of anti-inflammatory proteins. • down-regulate the expression of proinflammatory proteins. Glucocorticoids are also shown to play Steroidogenesis showing glucocorticoids in green ellipse at right - it is not a strictly a role in the development and bounded group, but a continuum of structures with increasing glucocorticoid effect, with homeostasis of T lymphocytes. This the primary example being cortisol. has been shown in transgenic mice with either increased or decreased sensitivity of T cell lineage to glucocorticoids.[]
Metabolic
Glucocorticoid The name "glucocorticoid" derives from early observations that these hormones were involved in glucose metabolism. In the fasted state, cortisol stimulates several processes that collectively serve to increase and maintain normal concentrations of glucose in blood. Metabolic effects: • Stimulation of gluconeogenesis, in particular, in the liver: This pathway results in the synthesis of glucose from nonhexose substrates, such as amino acids and glycerol from triglyceride breakdown, and is particularly important in carnivores and certain herbivores. Enhancing the expression of enzymes involved in gluconeogenesis is probably the best-known metabolic function of glucocorticoids. • Mobilization of amino acids from extrahepatic tissues: These serve as substrates for gluconeogenesis. • Inhibition of glucose uptake in muscle and adipose tissue: A mechanism to conserve glucose • Stimulation of fat breakdown in adipose tissue: The fatty acids released by lipolysis are used for production of energy in tissues like muscle, and the released glycerol provide another substrate for gluconeogenesis. Excessive glucocorticoid levels resulting from administration as a drug or hyperadrenocorticism have effects on many systems. Some examples include inhibition of bone formation, suppression of calcium absorption (both of which can lead to osteoporosis), delayed wound healing, muscle weakness, and increased risk of infection. These observations suggest a multitude of less-dramatic physiologic roles for glucocorticoids.[]
217
Developmental
Glucocorticoids have multiple effects on fetal development. An important example is their role in promoting maturation of the lung and production of the surfactant necessary for extrauterine lung function. Mice with homozygous disruptions in the corticotropin-releasing hormone gene (see below) die at birth due to pulmonary immaturity. In addition, glucocorticoids are necessary for normal brain development, by initiating terminal maturation, remodeling axons and dendrites, and affecting cell survival.[]
Arousal and cognition
Glucocorticoids act on the hippocampus, amygdala, and frontal lobes. Along with adrenaline, these enhance the formation of flashbulb memories of events associated with strong emotions, both positive and negative.[1] This has been confirmed in studies, whereby blockade of either glucocorticoids or noradrenaline activity impaired the recall of emotionally relevant information. Additional sources have shown subjects whose fear learning was accompanied by high cortisol levels had better consolidation of this memory (this effect was more important in men). Glucocorticoids have also been shown to have a significant impact on vigilance and cognitive performance. This A graphical representation of the Yerkes-Dodson curve appears to follow the Yerkes-Dodson curve, as studies have shown circulating levels of glucocorticoids vs. memory performance follow an upside-down U pattern, much like the Yerkes-Dodson curve. For example, long-term potentiation (the process of forming long-term memories) is optimal when glucocorticoid levels are mildly elevated, whereas significant decreases of LTP are observed after adrenalectomy (low-GC state) or after exogenous glucocorticoid administration (high-GC state). Elevated levels of glucocorticoids enhance memory for emotionally arousing events, but lead more often than not to poor memory for material unrelated to the source of stress/emotional arousal.[2] In contrast to the dose-dependent enhancing effects of glucocorticoids on memory consolidation, these stress hormones have been shown to inhibit the retrieval of already stored information.[3][4]
Glucocorticoid
218
Body fluid homeostasis
Glucocorticoids could act centrally, as well as peripherally, to assist in the normalization of extracellular fluid volume by regulating body’s action to atrial natriuretic peptide (ANP). Centrally, glucocorticoids could inhibit dehydration induced water intake;[] peripherally, glucocorticoids could induce a potent diuresis.[] The overall effect of glucocorticoids is to keep the body from volume overload.
Mechanism of action
Transactivation
Glucocorticoids bind to the cytosolic glucocorticoid receptor (GR). This type of receptor is activated by ligand binding. After a hormone binds to the corresponding receptor, the newly formed receptor-ligand complex translocates itself into the cell nucleus, where it binds to glucocorticoid response elements (GRE) in the promoter region of the target genes resulting in the regulation of gene expression. This process is commonly referred to as transactivation.[] The proteins encoded by these up-regulated genes have a wide range of effects, including, for example:[] • anti-inflammatory – lipocortin I, p11/calpactin binding protein and secretory leukoprotease inhibitor 1 (SLPI) • increased gluconeogenesis – glucose-6-phosphatase and tyrosine aminotransferase
Transrepression
The opposite mechanism is called transrepression. The activated hormone receptor interacts with specific transcription factors (such as AP-1 and NF-κB) and prevents the transcription of targeted genes. Glucocorticoids are able to prevent the transcription of proinflammatory genes, including interleukins IL-1B, IL-4, IL-5, and IL-8, chemokines, cytokines, GM-CSF, and TNFA genes.[]
Dissociation
The ordinary glucocorticoids do not distinguish among transactivation and transrepression and influence both the "wanted" immune and the "unwanted" genes regulating the metabolic and cardiovascular functions. Intensive research is aimed at discovering selectively acting glucocorticoids that will be able to repress only the immune system.[][] Genetically modified mice that express a modified GR incapable of DNA binding are still responsive to the anti-inflammatory effects of glucocorticoids, while the stimulation of gluconeogenesis by glucocorticoids is blocked.[] This result strongly suggests most of the desirable anti-inflammatory effects are due to transrepression, while the undesirable metabolic effects arise from transactivation, a hypothesis also underlying the development of selective glucocorticoid receptor agonists.
Nongenomic
Glucocorticoids have been shown to exert a number of rapid actions that are independent of the regulations of gene transcription. Binding of corticosteroids to the glucocorticoid receptor (GR) stimulates phosphatidylinositol 3-kinase and protein kinase AKT, leading to endothelial nitric oxide synthase (eNOS) activation and nitric oxide-dependent vasorelaxation.[] Membrane associated GR has been shown to mediate lymphocytolysis.[][][] In addition, some glucocorticoids have been shown to rapidly inhibit the release of the inflammatory prostaglandin PGE2, this effect is blocked by the glucocorticoid receptor antagonist mifepristone (RU-486) and is not affected by protein synthesis inhibitors. These data together suggest a nongenomic mechanism of action.[][]
Glucocorticoid
219
Glucocorticoid-induced neutrophilia
Acute or chronic administration of corticosteroids causes neutrophilia,[5] suggesting the enhanced release of PMNs from the bone marrow is an important mechanism of the glucocorticoid-induced granulocytosis. An alternative mechanism for the granulocytosis induced by glucocorticoids is an influx of PMNs from the intravascular marginated PMN pools.[6] The response is caused by a shift of cells from the marginal to the circulating pool; hence, it frequently is referred to as demargination.[7] Some of the immunosuppressive effects of glucocorticoids are mediated by nongenomic signalling involving the glucocortiocid receptor (GR). A multiprotein complex composed of the unliganded glucocorticoid receptor, Hsp90, and the tyrosine kinases LCK and FYN is recruited to the antigen-activated T cell receptor (TCR) in T cells. This GR complex is necessary for TCR signalling. On binding of glucocorticoids to GR, this complex dissociates, thus blocking TCR signalling.[]
Glucocorticoid-induced diuresis
Glucocorticoids could mediate the gene expression of ANP and its primary receptor, natriuretic peptide receptor A (NPR-A). It is well documented that glucocorticoids could up-regulate the expression of ANP gene in the cardiomyocytes in vitro and stimulated ANP release in vivo without negative effects on renal sodium and water excretion.[8][9] Additionally, glucocorticoids could up-regulate NPR-A expression in the kidney and hypothalamus. In the kidney, glucocorticoids improve renal responsiveness to ANP by upregulating NPR-A expression in the renal inner medullary collecting duct, inducing a potent diuresis.[] In hypothalamus, glucocorticoids inhibited dehydration or angiotensin II induced water intake by potentiating hypothalamic response to ANP.[] They work in concert to keep the body fluid volume in homeostasis.
Pharmacology
A variety of synthetic glucocorticoids, some far more potent than cortisol, have been created for therapeutic use. They differ in both pharmacokinetics (absorption factor, half-life, volume of distribution, clearance) and pharmacodynamics (for example the capacity of mineralocorticoid activity: retention of sodium (Na+) and water; renal physiology). Because they permeate the intestines easily, they are administered primarily per os (by mouth), but also by other methods, such as topically on skin. More than 90% of them bind different plasma proteins, though with a different binding specificity. Endogenous glucocorticoids and some synthetic corticoids have high affinity to the protein transcortin (also called corticosteroid-binding globulin), whereas all of them bind albumin. In the liver, they quickly metabolize by conjugation with a sulfate or glucuronic acid, and are secreted in the urine. Glucocorticoid potency, duration of effect, and overlapping mineralocorticoid potency varies. Cortisol (hydrocortisone) is the standard of comparison for glucocorticoid potency. Hydrocortisone is the name used for pharmaceutical preparations of cortisol. Data refer to oral dosing, except when mentioned. Oral potency may be less than parenteral potency because significant amounts (up to 50% in some cases) may not be absorbed from the intestine. Fludrocortisone, DOCA (Deoxycorticosterone acetate), and aldosterone are, by definition, not considered glucocorticoids, although they may have minor glucocorticoid potency, and are included in this table to provide perspective on mineralocorticoid potency.
Glucocorticoid
220
Comparative steroid potencies
Name Glucocorticoid potency Mineralocorticoid potency 1 0.8 0.8 0.8 0.5 0 0 0 Duration of action (t1/2 in hours) 8 oral 8, intramuscular 18+ 16-36 16-36 18-40 36-54 36-54 12-36 -
Hydrocortisone (cortisol) Cortisone Prednisone Prednisolone Methylprednisolone Dexamethasone Betamethasone Triamcinolone Beclometasone
1 0.8 3.5-5 4 5-7.5 25-80 25-30 5 8 puffs 4 times a day equals 14 mg oral prednisone once a dayWikipedia:Please clarify 15 0
Fludrocortisone acetate Deoxycorticosterone acetate (DOCA) Aldosterone
200 20
24 -
0.3
200-1000
-
Therapeutic use
Glucocorticoids may be used in low doses in adrenal insufficiency. In much higher doses, oral or inhaled glucocorticoids are used to suppress various allergic, inflammatory, and autoimmune disorders. Inhaled glucocorticoids are the second-line treatment for asthma. They are also administered as post-transplantory immunosuppressants to prevent the acute transplant rejection and the graft-versus-host disease. Nevertheless, they do not prevent an infection and also inhibit later reparative processes. Newly emerging evidence showed that glucocorticoids could be used in the treatment of heart failure to increase the renal responsiveness to diuretics and natriuretic peptides.
Physiological replacement
Any glucocorticoid can be given in a dose that provides approximately the same glucocorticoid effects as normal cortisol production; this is referred to as physiologic, replacement, or maintenance dosing. This is approximately 6–12 mg/m²/day (m² refers to body surface area (BSA), and is a measure of body size; an average man's BSA is 1.7 m²).
Therapeutic immunosuppression
Glucocorticoids cause immunosuppression, and the therapeutic component of this effect is mainly the decreases in the function and numbers of lymphocytes, including both B cells and T cells. The major mechanism for this immunosuppression through inhibition of nuclear factor kappa-light-chain-enhancer of activated B cells(NF-κB). NF-κB is a critical transcription factor involved in the synthesis of many mediators (i.e., cytokines) and proteins (i.e., adhesion proteins) that promote the immune response. Inhibition of this transcription factor, therefore, blunts the capacity of the immune system to mount a response.[]
Glucocorticoid Glucocorticoids suppress cell-mediated immunity by inhibiting genes that code for the cytokines IL-1, IL-2, IL-3, IL-4, IL-5, IL-6, IL-8 and IFN-γ, the most important of which is IL-2. Smaller cytokine production reduces the T cell proliferation.[] Glucocorticoids, however, not only reduce T cell proliferation, but also lead to another well known effect glucocorticoid-induced apoptosis. The effect is more prominent in immature T cells still inside in the thymus, but peripheral T cells are also affected. The exact mechanism underlying this glucocorticoid sensitivity still remains to be elucidated.[citation needed] Glucocorticoids also suppress the humoral immunity, thereby causing a humoral immune deficiency. Glucocorticoids cause B cells to express smaller amounts of IL-2 and of IL-2 receptors. This diminishes both B cell clone expansion and antibody synthesis. The diminished amounts of IL-2 also cause fewer T lymphocyte cells to be activated. Since glucocorticoid is a steroid, it regulates transcription factors; another factor it down-regulates is the expression of Fc receptors on macrophages, so there is a decreased phagocytosis of opsonised cells.[citation needed]
221
Anti-inflammatory
Glucocorticoids are potent anti-inflammatories, regardless of the inflammation's cause; their primary anti-inflammatory mechanism is lipocortin-1 (annexin-1) synthesis. Lipocortin-1 both suppresses phospholipase A2, thereby blocking eicosanoid production, and inhibits various leukocyte inflammatory events (epithelial adhesion, emigration, chemotaxis, phagocytosis, respiratory burst, etc.). In other words, glucocorticoids not only suppress immune response, but also inhibit the two main products of inflammation, prostaglandins and leukotrienes. They inhibit prostaglandin synthesis at the level of phospholipase A2 as well as at the level of cyclooxygenase/PGE isomerase (COX-1 and COX-2),[10] the latter effect being much like that of NSAIDs, potentiating the anti-inflammatory effect. In addition, glucocorticoids also suppress cyclooxygenase expression. Glucocorticoids marketed as anti-inflammatories are often topical formulations, such as nasal sprays for rhinitis or inhalers for asthma. These preparations have the advantage of only affecting the targeted area, thereby reducing side effects or potential interactions. In this case, the main compounds used are beclometasone, budesonide, fluticasone, mometasone and ciclesonide. In rhinitis, sprays are used. For asthma, glucocorticoids are administered as inhalants with a metered-dose or dry powder inhaler.[]
Hyperaldosteronism
Glucocorticoids can be used in the management of familial hyperaldosteronism type 1. They are not effective, however, for use in the type 2 condition.
Resistance
Resistance to the therapeutic uses of glucocorticoids can present difficulty; for instance, 25% of cases of severe asthma may be unresponsive to steroids. This may be the result of genetic predisposition, ongoing exposure to the cause of the inflammation (such as allergens), immunological phenomena that bypass glucocorticoids, and pharmacokinetic disturbances (incomplete absorption or accelerated excretion or metabolism).[]
Glucocorticoid
222
Heart failure
Glucocorticoids could be used in the treatment of decompensated heart failure to potentiate renal responsiveness to diuretics, especially in heart failure patients with refractory diuretic resistance with large dose of loop diuretics.[11][12][13][14][15][16][17]
Side effects
Glucocorticoid drugs currently being used act nonselectively, so in the long run they may impair many healthy anabolic processes. To prevent this, much research has been focused recently on the elaboration of selectively acting glucocorticoid drugs. Side effects include: • immunodeficiency (see separate section below) • hyperglycemia due to increased gluconeogenesis, insulin resistance, and impaired glucose tolerance ("steroid diabetes"); caution in those with diabetes mellitus • increased skin fragility, easy bruising • negative calcium balance due to reduced intestinal calcium absorption[18] • steroid-induced osteoporosis: reduced bone density (osteoporosis, osteonecrosis, higher fracture risk, slower fracture repair) • • • • • • • • • • weight gain due to increased visceral and truncal fat deposition (central obesity) and appetite stimulation adrenal insufficiency (if used for long time and stopped suddenly without a taper) muscle breakdown (proteolysis), weakness, reduced muscle mass and repair expansion of malar fat pads and dilation of small blood vessels in skin anovulation, irregularity of menstrual periods growth failure, delayed puberty increased plasma amino acids, increased urea formation, negative nitrogen balance excitatory effect on central nervous system (euphoria, psychosis) glaucoma due to increased cranial pressure cataracts
In high doses, hydrocortisone (cortisol) and those glucocorticoids with appreciable mineralocorticoid potency can exert a mineralocorticoid effect as well, although in physiologic doses this is prevented by rapid degradation of cortisol by 11β-hydroxysteroid dehydrogenase isoenzyme 2 (11β-HSD2) in mineralocorticoid target tissues. Mineralocorticoid effects can include salt and water retention, extracellular fluid volume expansion, hypertension, potassium depletion, and metabolic alkalosis. The combination of clinical problems produced by prolonged, excess glucocorticoids, whether synthetic or endogenous, is termed Cushing's syndrome.
Glucocorticoid
223
Immunodeficiency
Glucocorticoids cause immunosuppression, decreasing the function and/or numbers of neutrophils, lymphocytes (including both B cells and T cells), monocytes, macrophages, and the anatomical barrier function of the skin.[] This suppression, if large enough, can cause manifestations of immunodeficiency, including T cell deficiency, humoral immune deficiency and neutropenia.
Main pathogens of concern in glucocorticoid-induced immunodeficiency:[]
Bacteria • • • • • • • • • • Fungi • • • • • • • • • • Enterobacteriaceae Legionella micdadei Listeria monocytogenes Mycobacterium tuberculosis Nontuberculous mycobacteria Nocardia asteroides Rhodococcus equi Salmonella species Staphylococcus aureus Streptococci Aspergillus Blastomyces Candida albicans and nonalbicans species Coccidioides immitis Cryptococcus neoformans Fusarium species Histoplasma capsulatum Penicillium marneffei Pseudallescheria boydii Zygomycosis Adenovirus Cytomegalovirus Herpes simplex virus Human papillomavirus Influenza/parainfluenza Respiratory syncytial virus Varicella zoster Cryptosporidiosis/lsospora belli Pneumocystis carinii Strongyloides stercoralis Toxoplasma gondii
Viruses • • • • • • • Other • • • •
Withdrawal
In addition to the effects listed above, use of high-dose steroids for more than a week begins to produce suppression of the patient's adrenal glands because the exogenous glucocorticoids suppress hypothalamic corticotropin-releasing hormone and pituitary adrenocorticotropic hormone. With prolonged suppression, the adrenal glands atrophy (physically shrink), and can take months to recover full function after discontinuation of the exogenous glucocorticoid. During this recovery time, the patient is vulnerable to adrenal insufficiency during times of stress, such as illness. While suppressive dose and time for adrenal recovery vary widely, clinical guidelines have been devised to estimate potential adrenal suppression and recovery, to reduce risk to the patient. The following is one example, but many variations exist or may be appropriate in individual circumstances.[citation needed]
Glucocorticoid • If patients have been receiving daily high doses for five days or less, they can be abruptly stopped (or reduced to physiologic replacement if patients are adrenal-deficient). Full adrenal recovery can be assumed to occur by a week afterward. • If high doses were used for six to 10 days, reduce to replacement dose immediately and taper over four more days. Adrenal recovery can be assumed to occur within two to four weeks of completion of steroids. • If high doses were used for 11–30 days, cut immediately to twice replacement, and then by 25% every four days. Stop entirely when dose is less than half of replacement. Full adrenal recovery should occur within one to three months of completion of withdrawal. • If high doses were used more than 30 days, cut dose immediately to twice replacement, and reduce by 25% each week until replacement is reached. Then change to oral hydrocortisone or cortisone as a single morning dose, and gradually decrease by 2.5 mg each week. When the morning dose is less than replacement, the return of normal basal adrenal function may be documented by checking 0800 cortisol levels prior to the morning dose; stop drugs when 0800 cortisol is 10 μg/dl. Predicting the time to full adrenal recovery after prolonged suppressive exogenous steroids is difficult; some people may take nearly a year. • Flare-up of the underlying condition for which steroids are given may require a more gradual taper than outlined above.
224
Chemical synthesis
Hogg, J. A.; Beal, P. F.; Nathan, A. H.; Lincoln, F. H.; Schneider, W. P.; Magerlein, B. J.; Hanze, A. R.; Jackson, R. W. (1955). Journal of the American Chemical Society 77 (16): 4436. doi:10.1021/ja01621a092 [19].
Glucocorticoid
225
References
[3] de Quervain, D et al., Stress and glucocorticoids impair retrieval of long-term spatial memory. Nature, 394, 787-790 (1998) [4] de Quervain, D et al., Acute cortisone administration impairs retrieval of long-term declarative memory in humans. Nature Neuroscience, 3, 313-314 (2000) [5] http:/ / emedicine. medscape. com/ article/ 208576-overview#showall [6] http:/ / circ. ahajournals. org/ content/ 98/ 21/ 2307. full. pdf+ html [7] Williams Hematology, 8ed, Ch.65, Neutropenia and Neutrophylia
External links
• Glucocorticoids (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Glucocorticoids) at the US National Library of Medicine Medical Subject Headings (MeSH) • R. Bowen (2006-05-26). "Glucocorticoids" (http://www.vivo.colostate.edu/hbooks/pathphys/endocrine/ adrenal/gluco.html). Colorado State University. Retrieved 2008-05-11.
Leydig cell
226
Leydig cell
Leydig cell
Micrograph showing a cluster of Leydig cells (center of image). H&E stain.
Histological section through testicular parenchyma of a boar. 1 Lumen of convoluted part of the seminiferous tubules, 2 spermatids, 3 spermatocytes, 4 spermatogonia, 5 Sertoli cell, 6 myofibroblasts, 7 Leydig cells, 8 capillaries Gray's MeSH subject #258 1243 Leydig+cells
[2] [1]
Leydig cells, also known as interstitial cells of Leydig, are found adjacent to the seminiferous tubules in the testicle. They produce testosterone in the presence of luteinizing hormone (LH). Leydig cells are polyhedral in shape, display a large prominent nucleus, an eosinophilic cytoplasm and numerous lipid-filled vesicles.
Nomenclature
Leydig cells are named after the German anatomist Franz Leydig, who discovered them in 1850.[1]
Functions
Leydig cells release a class of hormones called androgens (19-carbon steroids). They secrete testosterone, androstenedione and dehydroepiandrosterone (DHEA), when stimulated by the pituitary hormone luteinizing hormone (LH). LH increases cholesterol desmolase activity (an enzyme associated with the conversion of cholesterol to pregnenolone), leading to testosterone synthesis and secretion by Leydig cells. Prolactin (PRL) increases the response of Leydig cells to LH by increasing the number of LH receptors expressed on Leydig cells.
Leydig cell
227
Ultrastructure
The mammalian Leydig cell is a polyhedral epithelioid cell with a single eccentrically located ovoid nucleus. The nucleus contains one to three prominent nucleoli and large amounts of dark-staining peripheral heterochromatin. The acidophilic cytoplasm usually contains numerous membrane-bound lipid droplets and large amounts of smooth endoplasmic reticulum (SER). Besides the obvious abundance of SER with scattered patches of rough endoplasmic reticulum, several mitochondria are also prominent within the cytoplasm. Frequently, lipofuscin pigment and rod-shaped crystal-like structures 3 to 20 micrometres in diameter (Reinke's crystals) are found. These inclusions have no known function.[][2] No other interstitial cell within the testes has a nucleus or cytoplasm with these characteristics, making identification relatively easy.
Development
'Adult'-type Leydig cells differentiate in the post-natal testis and are quiescent until puberty. They are preceded in the testis by a population of 'fetal'-type Leydig cells from the 8th to the 20th week of gestation, which produce enough testosterone for masculinisation of a male fetus.[]
Pathology
Leydig cells may grow uncontrollably and form a Leydig cell tumour. These tumours are usually benign. They may be hormonally active, i.e. secrete testosterone. Adrenomyeloneuropathy is another example of a disease affecting the Leydig cell: the patient's testosterone may fall despite higher-than-normal levels of LH and FSH. Electrostimulation therapy has been found to induce destruction of Leydig cells.[]
Micrograph of a Leydig cell tumour. H&E stain.
Additional images
Section of a genital cord of the testis of a human embryo 3.5 cm. long.
Intermediate magnification micrograph of a Leydig cell tumour. H&E stain.
High magnification micrograph of a Leydig cell tumour. H&E stain.
Cross-section of seminiferous tubules. Arrows indicate location of Leydig cells.
Leydig cell
228
References External links
• BU Histology Learning System: 16907loa (http://www.bu.edu/histology/p/16907loa.htm) • Reproductive Physiology (http://www2.ufp.pt/~pedros/qfisio/reproduction.htm) • Diagram at umassmed.edu (http://www.umassmed.edu/faculty/graphics/700/Leefig1.jpg)
Folliculogenesis
Note: Although the process is similar in many animals, this article will deal exclusively with human folliculogenesis. In biology, folliculogenesis is the maturation of the ovarian follicle, a densely-packed shell of somatic cells that contains an immature oocyte. Folliculogenesis describes the progression of a number of small primordial follicles into large preovulatory follicles that enter the menstrual cycle. Contrary to male spermatogenesis, which can last indefinitely, folliculogenesis ends when the remaining follicles in the ovaries are incapable of responding to the hormonal cues that previously recruited some follicles to mature. This depletion in follicle supply signals the beginning of menopause.
Overview
The primary role of the follicle is oocyte support. From birth, the ovaries of the human female contain a number of immature, primordial follicles. These follicles each contain a similarly immature primary oocyte. After puberty and commencing with the first menstruation, a clutch of follicles begins folliculogenesis, entering a growth pattern that will end in death or in ovulation (the process where the oocyte leaves the follicle). During post-pubescent follicular development, and over the course of roughly a year, primordial follicles that have begun development undergo a series of critical changes in character, both histologically and hormonally. Two-thirds of the way through this process, the follicles have transitioned to tertiary, or antral, follicles. At this stage in development, they become dependent on hormones emanating from the host body, causing a substantial increase in their growth rate. With a little more than ten days until the end of the period of follicular development, most of the original group of follicles have died (a process known as atresia). The remaining cohort of follicles enter the menstrual cycle,
Order of changes in ovary. 1 - Menstruation 2 - Developing follicle 3 - Mature follicle 4 - Ovulation 5 - Corpus luteum 6 - Deterioration of corpus luteum
Folliculogenesis competing with each other until only one follicle is left. This remaining follicle, the late tertiary or pre-ovulatory follicle, ruptures and discharges the oocyte (that has since grown into a secondary oocyte), ending folliculogenesis.
229
Diagram of folliculogenesis, starting from pre-antral (late secondary), courtesy NCBI
Phases of development
Folliculogenesis lasts for approximately 375 days. It coincides with thirteen menstrual cycles. The process begins continuously, meaning that at any time the ovary contains follicles in all stages of development, and ends when a mature oocyte departs from the preovulatory follicle in a process called ovulation. The growing follicle passes through the following distinct stages that are defined by certain structural characteristics (unfamiliar terms will be defined in their respective sections): In a larger perspective, the whole folliculogenesis, from primordial to preovulatory follicle, belongs to the stage of ootidogenesis of oogenesis.
Stage Primordial Description Dormant, small, only one layer of flat granulosa cells Mitotic cells, cuboidal granulosa cells Presence of theca cells, multiple layers of granulosa cells Size Primordial follicles are about 0.03-0.05 mm in diameter.
Primary Secondary
Almost 0.1 mm in diameter The follicle is now 0.2 mm in diameter
Early tertiary
The early tertiary follicle is arbitrarily divided into five classes. Class 1 follicles are 0.2 mm in diameter, class 2 about 0.4 mm, class 3 about 0.9 mm, class 4 about 2 mm, and class 5 about 5 mm. Fully formed antrum, no further cytodifferentiation, no novel progress Class 6 follicles are about 10 mm in diameter, class 7 about 16 mm, and class 8 about 20 mm. It is common for non-dominant follicles to grow beyond class 5, but rarely is there more than one class 8 follicle.
Late tertiary
Preovulatory Building growth in estrogen concentration, all other follicles atretic or dead
In addition, follicles that have formed an antrum are called antral follicles or Graafian follicles. Definitions differ in where this shift occurs in the staging given above, with some stating that it occurs when entering the secondary stage,[1] and others stating that it occurs when entering the tertiary stage.[2] Until the preovulatory stage, the follicle contains a primary oocyte that is arrested in prophase of meiosis I. During the late preovulatory stage, the oocyte continues meiosis and becomes a secondary oocyte, arrested in metaphase II.
Folliculogenesis
230
Primordial
At 18–22 weeks post-conception, the cortex of the female ovary contains its peak number of follicles (about 300,000 in the average case, but individual peak populations range from 35,000 to 2.5 million[3]). These primordial follicles contain immature oocytes surrounded by flat, squamous granulosa cells (the support cells) that are segregated from the oocyte's environment by the basal lamina. They are quiescent, showing little to no biological activity. Because primordial follicles can be dormant for up to 50 years in the human, the length of the ovarian cycle does not include this time. The supply of follicles decreases slightly before birth, and to 180,000 by puberty for the average case (populations at puberty range from 25,000 to 1.5 million).[3] By virtue of the "inefficient" nature of folliculogenesis (discussed later), only 400 of these follicles will ever reach the preovulatory stage. At menopause, only 1,000 follicles remain. It seems likely that early menopause occurs for women with low populations at birth, and late menopause occurs for women with high populations at birth, but there is as yet no clinical evidence for this.[3] The process by which primordial cells wake up is known as initial recruitment. Research has shown that initial recruitment is mediated by the counterbalance of various stimulatory and inhibitory hormones and locally produced growth factors.[4]
Primary
The granulosa cells of these primordial follicles change from a flat to a cuboidal structure, marking the beginning of the primary follicle. The oocyte genome is activated and genes become transcribed. Rudimentary paracrine signalling pathways that are vital for communication between the follicle and oocyte are formed. Both the oocyte and the follicle grow dramatically, increasing to almost 0.1 mm in diameter. Primary follicles develop receptors to follicle stimulating hormone (FSH) at this time, but they are gonadotropin-independent until the antral stage. Research has shown, however, that the presence of FSH accelerates follicle growth in vitro. A glycoprotein polymer capsule called the zona pellucida forms around the oocyte, separating it from the surrounding granulosa cells. The zona pellucida, which remains with the oocyte after ovulation, contains enzymes that catalyze with sperm to allow penetration.
Secondary
Stroma-like theca cells are recruited by oocyte-secreted signals. They surround the follicle's outermost layer, the basal lamina, and undergo cytodifferentiation to become the theca externa and theca interna. An intricate network of capillary vessels forms between these two thecal layers and begins to circulate blood to and from the follicle. The late-term secondary follicle is marked histologically by a fully grown oocyte surrounded by a zona pellucida, approximately nine layers of granulosa cells, a basal lamina, a theca interna, a capillary net, and a theca externa. 290 days have lapsed since recruitment.
Folliculogenesis
231
Antrum formation
The formation of a fluid-filled cavity adjacent to the oocyte called the antrum designates the follicle as an antral follicle, in contrast to so a called preantral follicle that still lacks an antrum. An antral follicle is also called a Graafian follicle. Definitions differ in which stage this shift occurs, with some designating follicles in the secondary stage as antral,[1] and others designating them as preantral.[2]
Early tertiary
In the tertiary follicle, the basic structure of the mature follicle has formed and no novel cells are detectable. Granulosa and theca cells continue to undergo mitotis concomitant with an increase in antrum volume. Tertiary follicles can attain a tremendous size that is hampered only by the availability of FSH, which it is now dependent on. Under action of an oocyte-secreted morphogenic gradient, the granulosa cells of the tertiary follicle undergo differentiation into four distinct subtypes: corona radiata, surrounding the zona pellucida; membrana, interior to the basal lamina; periantral, adjacent to the antrum and cumulus oophorous, which connects the membrana and corona radiata granulosa cells together. Each type of cell behaves differently in response to FSH. Theca cells express receptors for luteinizing hormone (LH). LH induces the production of androgens by the theca cells, most notably androstendione, which are aromatized by granulosa cells to produce estrogens, primarily estradiol. Consequently, estrogen levels begin to rise.
Late tertiary and preovulatory (the follicular phase of the menstrual cycle)
At this point, the majority of the group of follicles that started growth 360 days ago have already died. This process of follicle death is known as atresia, and it is characterized by radical apoptosis of all constituent cells and the oocyte. Although it is not known what causes atresia, the presence of high concentrations of FSH has been shown to prevent it. A rise in pituitary FSH caused by the disintegration of the corpus luteum at the conclusion of the twelfth menstrual cycle precipitates the selection of five to seven class 5 follicles to participate in the thirteenth. These follicles enter the end of the twelfth menstrual cycle and transition into the follicular phase of the thirteenth cycle. The selected follicles, called antral follicles, compete with each other for growth-inducing FSH. In response to the rise of FSH, the antral follicles begin to secrete estrogen and inhibin, which have a negative feedback effect on FSH.[5] Follicles that have fewer FSH-receptors will not be able to develop further; they will show retardation of their growth rate and become atretic. Eventually, only one follicle will be viable. This remaining follicle, called the dominant follicle, will grow quickly and dramatically—up to 20 mm in diameter—to become the preovulatory follicle. Note: Many sources misrepresent the pace of follicle growth, some even suggesting that it takes only fourteen days for a primordial follicle to become preovulatory. In all cases, the follicular phase of the menstrual cycle means the time between selection of a tertiary follicle and its subsequent growth into a preovulatory follicle.
Ovulation and the corpus luteum
By the end of the follicular, or proliferative, phase of the thirteenth day of the menstrual cycle, the cumulus oophorus layer of the preovulatory follicle will develop an opening, or stigma, and excrete the oocyte with a complement of cumulus cells in a process called ovulation. The oocyte is now called the ovum and is competent to undergo fertilization. The ovum will now travel down one of the fallopian tubes to eventually be discharged through menstruation, if not fertilized by a sperm cell, or implanted in the uterus, if previously fertilized. The fully developed oocyte (gamete) is now at the behest of the menstrual cycle.
Folliculogenesis The ruptured follicle will undergo a dramatic transformation into the corpus luteum, a steroidiogenic cluster of cells that maintains the endometrium of the uterus by the secretion of large amounts of progesterone and minor amounts of estrogen. These two steps, while not part of folliculogenesis, are included for completeness. They are discussed in their entirety by their respective articles, and placed into perspective by the menstrual cycle article. It is recommended that these three topics be reviewed.
232
Hormone function
As with most things related to the reproductive system, folliculogenesis is controlled by the endocrine system. Five hormones participate in an intricate process of positive and negative feedback to regulate folliculogenesis. They are: • gonadotropin-releasing hormone (GnRH) secreted by the hypothalamus • two gonadotropins: • follicle-stimulating hormone (FSH) • luteinizing hormone (LH) • estrogen • progesterone GnRH stimulates the release of FSH and LH from the anterior pituitary gland that will later have a stimulatory effect on follicle growth (not immediately, however, because only antral follicles are dependent on FSH and LH). When theca cells form in the tertiary follicle the amount of estrogen increases sharply (theca-derived androgen is aromatized into estrogen by the granulosa cells). At low concentration, estrogen inhibits gonadotropins, but high concentration of estrogen stimulates them. In addition, as more estrogen is secreted, more LH receptors are made by the theca cells, inciting theca cells to create more androgen that will become estrogen downstream. This positive feedback loop causes LH to spike sharply, and it is this spike that causes ovulation. Following ovulation, LH stimulates the formation of the corpus luteum. Estrogen has since dropped to negative stimulatory levels after ovulation and therefore serves to maintain the concentration of FSH and LH. Inhibin, which is also secreted by the corpus luteum, contributes to FSH inhibition. The endocrine system coincides with the menstrual cycle and goes through thirteen cycles (and thus thirteen LH spikes) during the course of normal folliculogenesis. However, coordinated enzyme signalling and the time-specific expression of hormonal receptors ensures that follicle growth does not become disregulated during these premature spikes.
Folliculogenesis
233
Number of follicles
Recently, two publications have challenged the idea that a finite number of follicles are set around the time of birth.[6][7] Renewal of ovarian follicles from germline stem cells (originating from bone marrow and peripheral blood) was reported in the postnatal mouse ovary. Studies attempting to replicate these results are underway, but a study of populations in 325 human ovaries found no supporting evidence for follicular replenishment.[3] In 2010, researchers at the University of Edinburgh determined that by the time women are 30 years old, only 10% of their non-growing follicles (NGFs) remain.[] At birth, women have all their follicles for folliculogenesis, and they steadily decline until menopause.
"Percentage of ovarian reserve related to increasing age. The curve describes the percentage of ovarian reserve remaining at ages from birth to 55 years, based on the ADC model. 100% is taken to be the maximum ovarian reserve, occurring at 18–22 weeks post-conception. The percentages apply to all women whose ovarian reserve declines in line with our model (i.e. late and early menopause are associated with high and low peak NGF populations, respectively). We estimate that for 95% of women by the age of 30 years only 12% of their maximum pre-birth NGF population is present and by the age of [6] [] 40 years only 3% remains. doi:10.1371/journal.pone.0008772.g005 "
Additional images
Section of the ovary. (#5 through #9 represent stages of folliculogenesis)
transitional primary follicle.
Folliculogenesis
234
References
[1] Page 769 (http:/ / books. google. com/ books?id=gOmpysGBC90C& pg=PT797), section "formation of the antrum" in: [2] Page 76 in: [3] Wallace WHB and Kelsey TW (2010) Human Ovarian Reserve from Conception to the Menopause. (http:/ / dx. plos. org/ 10. 1371/ journal. pone. 0008772) PLoS ONE 5(1):e8772. [5] de Ziegler D (2007), "Roles of FSH and LH during the follicular phase: insight into the natural cycle IVF", RBM Online volume 15 No. 5, page 508
• Caglar G, Asimakopoulos B, Nikolettos N, Diedrich K, Al-Hasani S (2005). "Recombinant LH in ovarian stimulation.". Reprod Biomed Online 10 (6): 774–85. doi: 10.1016/S1472-6483(10)61123-6 (http://dx.doi.org/ 10.1016/S1472-6483(10)61123-6). PMID 15970010 (http://www.ncbi.nlm.nih.gov/pubmed/15970010). • Gougeon A (1996). "Regulation of ovarian follicular development in primates: facts and hypotheses.". Endocr Rev 17 (2): 121–55. doi: 10.1210/er.17.2.121 (http://dx.doi.org/10.1210/er.17.2.121). PMID 8706629 (http://www.ncbi.nlm.nih.gov/pubmed/8706629). • Gougeon A (1986). "Dynamics of follicular growth in the human: a model from preliminary results.". Hum Reprod 1 (2): 81–7. PMID 3558758 (http://www.ncbi.nlm.nih.gov/pubmed/3558758). • van den Hurk R, Zhao J (2005). "Formation of mammalian oocytes and their growth, differentiation and maturation within ovarian follicles.". Theriogenology 63 (6): 1717–51. doi: 10.1016/j.theriogenology.2004.08.005 (http://dx.doi.org/10.1016/j.theriogenology.2004.08.005). PMID 15763114 (http://www.ncbi.nlm.nih. gov/pubmed/15763114).
External links
• Morphology and Physiology of the Ovary at endotext.org (http://www.endotext.org/female/female1/ femaleframe1.htm) • The ovary - folliculogenesis and oogenesis at nlm.nih.gov (http://www.ncbi.nlm.nih.gov/books/bv. fcgi?db=Books&rid=endocrin.section.1229) • Folliculogenesis and Ovulation at gfmer.ch (http://www.gfmer.ch/Books/Reproductive_health/ Folliculogenesis_and_ovulation.html) • Reproductive Physiology at ufp.pt (http://www2.ufp.pt/~pedros/qfisio/reproduction.htm)
Progesterone
235
Progesterone
Progesterone
Systematic (IUPAC) name
Pregn-4-ene-3,20-dione
Clinical data Trade names Crinone, Endometrin
AHFS/Drugs.com monograph [1] MedlinePlus Pregnancy cat. Legal status Routes a604017 B (USA) ? oral, implant, transdermal Pharmacokinetic data Bioavailability Protein binding Metabolism Half-life Excretion prolonged absorption, half-life approx 25-50 hours 96%-99% hepatic to pregnanediols and pregnanolones 34.8-55.13 hours renal Identifiers CAS number ATC code PubChem IUPHAR ligand DrugBank ChemSpider 57-83-0 [3] [2]
G03DA04 CID 5994 2377 [6]
[4] [5]
DB00396 5773 [8]
[7]
Progesterone
[9]
236
UNII KEGG ChEBI ChEMBL Synonyms
4G7DS2Q64Y D00066 [10]
CHEBI:17026 CHEMBL103
[11] [12]
4-pregnene-3,20-dione Chemical data
Formula Mol. mass
C21H30O2 314.46
Physical data Melt. point Spec. rot 126 °C (259 °F) [α]D (what is this?) (verify) [13]
Progesterone also known as P4 (pregn-4-ene-3,20-dione) is a C-21 steroid hormone involved in the female menstrual cycle, pregnancy (supports gestation) and embryogenesis of humans and other species. Progesterone belongs to a class of hormones called progestogens, and is the major naturally occurring human progestogen.
Chemistry
Progesterone was independently discovered by four research groups.[][][][] Willard Myron Allen co-discovered progesterone with his anatomy professor George Washington Corner at the University of Rochester Medical School in 1933. Allen first determined its melting point, molecular weight, and partial molecular structure. He also gave it the name Progesterone derived from Progestational Steroidal ketone.[] Like other steroids, progesterone consists of four interconnected cyclic hydrocarbons. Progesterone contains ketone and oxygenated functional groups, as well as two methyl branches. Like all steroid hormones, it is hydrophobic.
Sources
Animal
Progesterone is produced in the ovaries (by the corpus luteum), the adrenal glands (near the kidney), and, during pregnancy, in the placenta. Progesterone is also stored in adipose (fat) tissue. In humans, increasing amounts of progesterone are produced during pregnancy: • At first, the source is the corpus luteum that has been "rescued" by the presence of human chorionic gonadotropins (hCG) from the conceptus. • However, after the 8th week, production of progesterone shifts to the placenta. The placenta utilizes maternal cholesterol as the initial substrate, and most of the produced progesterone enters the maternal circulation, but some is picked up by the fetal circulation and used as substrate for fetal corticosteroids. At term the placenta produces about 250 mg progesterone per day. • An additional source of progesterone is milk products. After consumption of milk products the level of bioavailable progesterone goes up.[]
Progesterone
237
Plants
In at least one plant, Juglans regia, progesterone has been detected.[] In addition, progesterone-like steroids are found in Dioscorea mexicana. Dioscorea mexicana is a plant that is part of the yam family native to Mexico.[] It contains a steroid called diosgenin that is taken from the plant and is converted into progesterone.[] Diosgenin and progesterone are found in other Dioscorea species as well. Another plant that contains substances readily convertible to progesterone is Dioscorea pseudojaponica native to Taiwan. Research has shown that the Taiwanese yam contains saponins — steroids that can be converted to diosgenin and thence to progesterone.[] Many other Dioscorea species of the yam family contain steroidal substances from which progesterone can be produced. Among the more notable of these are Dioscorea villosa and Dioscorea polygonoides. One study showed that the Dioscorea villosa contains 3.5% diosgenin.[] Dioscorea polygonoides has been found to contain 2.64% diosgenin as shown by gas chromatography-mass spectrometry.[1] Many of the Dioscorea species that originate from the yam family grow in countries that have tropical and subtropical climates.[2]
Synthesis
Biosynthesis
In mammals, progesterone (6), like all other steroid hormones, is synthesized from pregnenolone (3), which in turn is derived from cholesterol (1) (see the upper half of the figure to the right). Cholesterol (1) undergoes double oxidation to produce 20,22-dihydroxycholesterol (2). This vicinal diol is then further oxidized with loss of the side chain starting at position C-22 to produce pregnenolone (3). This reaction is catalyzed by cytochrome P450scc. The conversion Top: Conversion of cholesterol (1) into pregnenolone (3) to progesterone (6). of pregnenolone to progesterone takes Bottom: Progesterone is important for aldosterone (mineralocorticoid) synthesis, as 17-hydroxyprogesterone is for cortisol (glucocorticoid), and androstenedione for sex place in two steps. First, the steroids. 3-hydroxyl group is oxidized to a keto group (4) and second, the double bond is moved to C-4, from C-5 through a keto/enol tautomerization reaction.[] This reaction is catalyzed by 3beta-hydroxysteroid dehydrogenase/delta(5)-delta(4)isomerase. Progesterone in turn (see lower half of figure to the right) is the precursor of the mineralocorticoid aldosterone, and after conversion to 17-hydroxyprogesterone (another natural progestogen) of cortisol and androstenedione. Androstenedione can be converted to testosterone, estrone and estradiol. Pregenolone and progesterone can also be synthesized by yeast.[]
Progesterone
238
Laboratory
An economical semisynthesis of progesterone from the plant steroid diosgenin isolated from yams was developed by Russell Marker in 1940 for the Parke-Davis pharmaceutical company (see figure to the right).[] This synthesis is known as the Marker degradation. Additional semisyntheses of progesterone have also been reported starting from a variety of [] The Marker semisynthesis of progesterone from diosgenin. steroids. For the example, cortisone can be simultaneously deoxygenated at the C-17 and C-21 position by treatment with iodotrimethylsilane in chloroform to produce 11-keto-progesterone (ketogestin), which in turn can be reduced at position-11 to yield progesterone.[] A total synthesis of progesterone was reported in 1971 by W.S. Johnson (see figure to the right).[] The synthesis begins with reacting the phosphonium salt 7 with phenyl lithium to produce the phosphonium ylide 8. The ylide 8 is reacted with an aldehyde to produce the alkene 9. The ketal protecting groups of 9 are hydrolyzed to produce the diketone 10, which in turn is cyclized to form the cyclopentenone 11. The ketone of 11 is reacted with methyl lithium to yield the tertiary alcohol 12, which in turn is treated with acid to produce the tertiary cation 13. The key step of the synthesis is the π-cation cyclization of 13 in which the B-, C-, and D-rings of the steroid are simultaneously formed to produce 14. This step resembles the cationic cyclization reaction used in the biosynthesis of steroids and hence is referred to as biomimetic. In the next step the enol orthoester is hydrolyzed to produce the ketone 15. The cyclopentene A-ring is then opened by oxidizing with ozone to produce 16. Finally, the diketone 17 undergoes an intramolecular aldol condensation by treating with aqueous potassium hydroxide to produce progesterone.[]
Levels
In women, progesterone levels are relatively low during the [] preovulatory phase of the menstrual cycle, rise after ovulation, and The Johnson total synthesis of progesterone. are elevated during the luteal phase, as shown in diagram below. Progesterone levels tend to be < 2 ng/ml prior to ovulation, and > 5 ng/ml after ovulation. If pregnancy occurs, human chorionic gonadotropin is released maintaining the corpus leuteum allowing it to maintain levels of progesterone. At around 12 weeks the placenta begins to produce progesterone in place of the corpus leuteum, this process is named the luteal-placental shift. After the luteal-placental shift progesterone levels start to rise further and may reach 100-200 ng/ml at term. Whether a decrease in progesterone levels is critical for the initiation of labor has been argued and may be species-specific. After delivery of the placenta and during lactation, progesterone levels are very low.
Progesterone Progesterone levels are relatively low in children and postmenopausal women.[] Adult males have levels similar to those in women during the follicular phase of the menstrual cycle.
Person type Reference range for blood test Lower limit Female - menstrual cycle Female - postmenopausal Upper limit Unit
239
(see diagram below) <0.2 <0,6 [3] [4] 1 3 [3] [4] [3] ng/mL nmol/L ng/mL nmol/L ng/mL nmol/L or 4.5 [3] ng/mL nmol/L
Female on oral contraceptives 0.34[3] 1.1 Males ≥16 years [4] [3] [4]
0.92 2.9 0.9 2.9 4.1 13
[4] [3] [4] [3]
0.27 0.86
Female or male 1–9 years
0.1 0.3
[3] [4]
[4]
[5] Progesterone levels during the menstrual cycle. - The ranges denoted By biological stage may be used in closely monitored menstrual cycles in regard to other markers of its biological progression, with the time scale being compressed or stretched to how much faster or slower, respectively, the cycle progresses compared to an average cycle.- The ranges denoted Inter-cycle variability are more appropriate to use in non-monitored cycles with only the beginning of menstruation known, but where the woman accurately knows her average cycle lengths and time of ovulation, and that they are somewhat averagely regular, with the time scale being compressed or stretched to how much a woman's average cycle length is shorter or longer, respectively, than the average of the population.- The ranges denoted Inter-woman variability are more appropriate to use when the average cycle lengths and time of ovulation are unknown, but only the beginning of menstruation is given.
Progesterone
240
Effects
Progesterone exerts its primary action through the intracellular progesterone receptor although a distinct, membrane bound progesterone receptor has also been postulated.[][] In addition, progesterone is a highly potent antagonist of the mineralocorticoid receptor (MR, the receptor for aldosterone and other mineralocorticosteroids). It prevents MR activation by binding to this receptor with an affinity exceeding even those of aldosterone and other corticosteroids such as cortisol and corticosterone.[] Progesterone has a number of physiological effects that are amplified Micrograph showing changes to the endometrium in the presence of estrogen. Estrogen through estrogen receptors due to progesterone (decidualization) H&E stain. upregulates the expression of progesterone receptors.[] Also, elevated levels of progesterone potently reduce the sodium-retaining activity of aldosterone, resulting in natriuresis and a reduction in extracellular fluid volume. Progesterone withdrawal, on the other hand, is associated with a temporary increase in sodium retention (reduced natriuresis, with an increase in extracellular fluid volume) due to the compensatory increase in aldosterone production, which combats the blockade of the mineralocorticoid receptor by the previously elevated level of progesterone.[]
Reproductive system
Progesterone has key effects via non-genomic signalling on human sperm as they migrate through the female tract before fertilization occurs, though the receptor(s) as yet remain unidentified.[] Detailed characterisation of the events occurring in sperm in response to progesterone has elucidated certain events including intracellular calcium transients and maintained changes,[] slow calcium oscillations,[] now thought to possibly regulate motility.[] Interestingly progesterone has also been shown to demonstrate effects on octopus spermatozoa.[] Progesterone modulates the activity of CatSper (cation channels of sperm) voltage-gated Ca2+ channels. Since eggs release progesterone, sperm may use progesterone as a homing signal to swim toward eggs (chemotaxis). Hence substances that block the progesterone binding site on CatSper channels could potentially be used in male contraception.[][] Progesterone is sometimes called the "hormone of pregnancy",[] and it has many roles relating to the development of the fetus: • Progesterone converts the endometrium to its secretory stage to prepare the uterus for implantation. At the same time progesterone affects the vaginal epithelium and cervical mucus, making it thick and impenetrable to sperm. If pregnancy does not occur, progesterone levels will decrease, leading, in the human, to menstruation. Normal menstrual bleeding is progesterone-withdrawal bleeding. If ovulation does not occur and the corpus luteum does not develop, levels of progesterone may be low, leading to anovulatory dysfunctional uterine bleeding. • During implantation and gestation, progesterone appears to decrease the maternal immune response to allow for the acceptance of the pregnancy. • Progesterone decreases contractility of the uterine smooth muscle.[] • In addition progesterone inhibits lactation during pregnancy. The fall in progesterone levels following delivery is one of the triggers for milk production. • A drop in progesterone levels is possibly one step that facilitates the onset of labor. The fetus metabolizes placental progesterone in the production of adrenal steroids.
Progesterone
241
Nervous system
Progesterone, like pregnenolone and dehydroepiandrosterone, belongs to the group of neurosteroids. It can be synthesized within the central nervous system and also serves as a precursor to another major neurosteroid, allopregnanolone. Neurosteroids affect synaptic functioning, are neuroprotective, and affect myelination.[] They are investigated for their potential to improve memory and cognitive ability. Progesterone affects regulation of apoptotic genes. Its effect as a neurosteroid works predominantly through the GSK-3 beta pathway, as an inhibitor. (Other GSK-3 beta inhibitors include bipolar mood stabilizers, lithium and valproic acid.)
Other effects
• It raises epidermal growth factor-1 levels, a factor often used to induce proliferation, and used to sustain cultures, of stem cells. • It increases core temperature (thermogenic function) during ovulation.[] • It reduces spasm and relaxes smooth muscle. Bronchi are widened and mucus regulated. (Progesterone receptors are widely present in submucosal tissue.) • It acts as an antiinflammatory agent and regulates the immune response. • It reduces gall-bladder activity.[] • It normalizes blood clotting and vascular tone, zinc and copper levels, cell oxygen levels, and use of fat stores for energy. • It may affect gum health, increasing risk of gingivitis (gum inflammation) and tooth decay.[citation needed] • It appears to prevent endometrial cancer (involving the uterine lining) by regulating the effects of estrogen. • Progesterone plays an important role in the signaling of insulin release and pancreatic function, and may affect the susceptibility to diabetes or gestational diabetes.[6][7]
Medical applications
The use of progesterone and its analogues have many medical applications, both to address acute situations and to address the long-term decline of natural progesterone levels. Because of the poor bioavailability of progesterone when taken orally, many synthetic progestins have been designed with improved oral bioavailability and have been used long before progesterone formulations became available.[] Progesterone was approved by the United States Food and Drug Administration as vaginal gel on July 31, 1997,[8] an oral capsule on May 14, 1998[9] in an injection form on April 25, 2001[10] and as a vaginal insert on June 21, 2007.[11] In Italy and Spain, Progesterone is sold under the trademark Progeffik.
Prometrium 100 mg Oral Capsule
Progesterone
242
Bioavailability
The route of administration impacts the effect of the drug. Given orally, progesterone has a wide person-to-person variability in absorption and bioavailability while synthetic progestins are rapidly absorbed with a longer half-life than progesterone and maintain stable levels in the blood.[12] Progesterone does not dissolve in water and is poorly absorbed when taken orally unless micronized in oil. Products are often sold as capsules containing micronised progesterone in oil. Progesterone can also be administered through vaginal or rectal suppositories or pessaries, transdermally through a gel or cream,[] or via injection (though the latter has a short half-life requiring daily administration). Transdermal "natural progesterone" products made with Progesterone USP do not require a prescription. Some of these products also contain "wild yam extract" derived from Dioscorea villosa, but there is no evidence that the human body can convert its active ingredient (diosgenin, the plant steroid that is chemically converted to produce progesterone industrially[]) into progesterone.[][]
Prevention of preterm birth
Vaginally dosed progesterone is being investigated as potentially beneficial in preventing preterm birth in women at risk for preterm birth. The initial study by Fonseca suggested that vaginal progesterone could prevent preterm birth in women with a history of preterm birth.[] According to a recent study, women with a short cervix that received hormonal treatment with a progesterone gel had their risk of prematurely giving birth reduced. The hormone treatment was administered vaginally every day during the second half of a pregnancy.[13] A subsequent and larger study showed that vaginal progesterone was no better than placebo in preventing recurrent preterm birth in women with a history of a previous preterm birth,[] but a planned secondary analysis of the data in this trial showed that women with a short cervix at baseline in the trial had benefit in two ways: a reduction in births less than 32 weeks and a reduction in both the frequency and the time their babies were in intensive care.[] In another trial, vaginal progesterone was shown to be better than placebo in reducing preterm birth prior to 34 weeks in women with an extremely short cervix at baseline.[] An editorial by Roberto Romero discusses the role of sonographic cervical length in identifying patients who may benefit from progesterone treatment.[] A meta-analysis published in 2011 found that vaginal progesterone cut the risk of premature births by 42 percent in women with short cervixes.[] The meta-analysis, which pooled published results of five large clinical trials, also found that the treatment cut the rate of breathing problems and reduced the need for placing a baby on a ventilator.[]
Other specific uses
• Progesterone is used for luteal support in Assisted Reproductive Technology (ART) cycles such as In-vitro Fertilization (IVF). • Progesterone is used to control persistent anovulatory bleeding. It is also used to prepare uterine lining in infertility therapy and to support early pregnancy. Patients with recurrent pregnancy loss due to inadequate progesterone production may receive progesterone. • Progesterone is also used in nonpregnant women with a delayed menstruation of one or more weeks, in order to allow the thickened endometrial lining to slough off. This process is termed a progesterone withdrawal bleed. The progesterone is taken orally for a short time (usually one week), after which the progesterone is discontinued and bleeding should occur.[citation needed] • Progesterone is being investigated as potentially beneficial in treating multiple sclerosis, since the characteristic deterioration of nerve myelin insulation halts during pregnancy, when progesterone levels are raised; deterioration commences again when the levels drop. • Progesterone also has a role in skin elasticity and bone strength, in respiration, in nerve tissue and in female sexuality, and the presence of progesterone receptors in certain muscle and fat tissue may hint at a role in sexually dimorphic proportions of those.[]WP:COPYLINK
Progesterone • Progesterone receptor antagonists, or selective progesterone receptor modulators (SPRM)s, such as RU-486 (Mifepristone), can be used to prevent conception or induce medical abortions (Note that methods of hormonal contraception do not contain progesterone but a progestin). • Progesterone may affect male behavior.[] • Progesterone is starting to be used in the treatment of the skin condition hidradenitis suppurativa.[citation needed]
243
Role in aging
Since most progesterone in males is created during testicular production of testosterone, and most in females by the ovaries, the shutting down (whether by natural or chemical means), or removal, of those inevitably causes a considerable reduction in progesterone levels. Previous concentration upon the role of progestogens (progesterone and molecules with similar effects) in female reproduction, when progesterone was simply considered a "female hormone", obscured the significance of progesterone elsewhere in both sexes. The tendency for progesterone to have a regulatory effect, the presence of progesterone receptors in many types of body tissue, and the pattern of deterioration (or tumor formation) in many of those increasing in later years when progesterone levels have dropped, is prompting widespread research into the potential value of maintaining progesterone levels in both males and females.
Role in brain damage
Studies as far back as 1987 show that female sex hormones have an effect on the recovery of traumatic brain injury.[] In these studies, it was first observed that pseudopregnant female rats had reduced edema after traumatic brain injury. Recent clinical trials have shown that among patients that have suffered moderate traumatic brain injury, those that have been treated with progesterone are more likely to have a better outcome than those who have not.[] Previous studies have shown that progesterone supports the normal development of neurons in the brain, and that the hormone has a protective effect on damaged brain tissue. It has been observed in animal models that females have reduced susceptibility to traumatic brain injury and this protective effect has been hypothesized to be caused by increased circulating levels of estrogen and progesterone in females.[] A number of additional animal studies have confirmed that progesterone has neuroprotective effects when administered shortly after traumatic brain injury.[] Encouraging results have also been reported in human clinical trials.[][]
Proposed mechanism
The mechanism of progesterone protective effects may be the reduction of inflammation that follows brain trauma.[] Damage incurred by traumatic brain injury is believed to be caused in part by mass depolarization leading to excitotoxicity. One way in which progesterone helps to alleviate some of this excitotoxicity is by blocking the voltage-dependent calcium channels that trigger neurotransmitter release.[] It does so by manipulating the signaling pathways of transcription factors involved in this release. Another method for reducing the excitotoxicity is by up-regulating the inhibitory neurotransmitter receptor, GABAA.[] Progesterone has also been shown to prevent apoptosis in neurons, a common consequence of brain injury.[] It does so by inhibiting enzymes involved in the apoptosis pathway specifically concerning the mitochondria, such as activated caspase 3 and cytochrome c. Not only does progesterone help prevent further damage, it has also been shown to aid in neuroregeneration. One of the serious effects of traumatic brain injury includes edema. Animal studies show that progesterone treatment leads to a decrease in edema levels by increasing the concentration of macrophages and microglia sent to the injured tissue.[][] This was observed in the form of reduced leakage from the blood brain barrier in secondary recovery in progesterone treated rats. In addition, progesterone was observed to have antioxidant properties, reducing the concentration of oxygen free radicals faster than without.[] There is also evidence that the addition of progesterone
Progesterone can also help remyelinate damaged axons due to trauma, restoring some lost neural signal conduction.[] Another way progesterone aids in regeneration includes increasing the circulation of endothelial progenitor cells in the brain.[] This helps new vasculature to grow around scar tissue which helps repair the area of insult.
244
Combination treatments
Vitamin D and progesterone separately have neuroprotective effects after traumatic brain injury, but when combined their effects are synergistic.[] When used at their optimal respective concentrations, the two combined have been shown to reduce cell death more than when alone. One study looks at a combination of progesterone with estrogen. Both progesterone and estrogen are known to have antioxidant-like qualities and are shown to reduce edema without injuring the blood-brain barrier. In this study, when the two hormones are administered alone it does reduce edema, but the combination of the two increases the water content, thereby increasing edema.[]
Clinical trials
The clinical trials for progesterone as a treatment for traumatic brain injury have only recently begun. ProTECT, a phase II trial conducted in Atlanta at Grady Memorial Hospital in 2007, the first to show that progesterone reduces edema in humans. Since then, trials have moved on to phase III. The National Institute of Health began conducting a nationwide phase III trial in 2011 led by Emory University.[] A global phase III initiative called SyNAPSe®, initiated in June 2010, is run by a U.S.-based private pharmaceutical company, BHR Pharma, and is being conducted in the United States, Argentina, Europe, Israel and Asia.[][14] Approximately 1,200 patients with severe (Glasgow Coma Scale scores of 3-8), closed-head TBI will be enrolled in the study at nearly 150 medical centers.
Progesterone
245
References
[3] Progesterone Reference Ranges (http:/ / cclnprod. cc. nih. gov/ dlm/ testguide. nsf/ 0/ CB26894E1EB28DEF85256BA5005B000E?OpenDocument), Performed at the Clinical Center at the National Institutes of Health, Bethesda MD, 03Feb09 [4] Converted from mass values using molar mass of 314.46 g/mol [5] References and further description of values are given in image page in Wikimedia Commons at Commons:File:Progesterone during menstrual cycle.png.
Additional images
Steroidogenesis, showing progesterone among the progestogens in yellow area.
Pregnenolone
Progesterone
246
Deoxycorticosterone
External links
• Progesterone (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Progesterone) at the US National Library of Medicine Medical Subject Headings (MeSH) • Kimball JW (2007-05-27). "Progesterone" (http://users.rcn.com/jkimball.ma.ultranet/BiologyPages/P/ Progesterone.html). Kimball's Biology Pages. Retrieved 2008-06-18. • "Progesterone Resource Center" (http://www.pms-menopause-progesterone.org/progesterone/). PMS, Menopause, and Progesterone Resource Center. Oasis Advanced Wellness, Inc. Retrieved 2008-06-18. • General discussion document on Progesterone, its uses and applications (http://www.lawleybasecamp.com/ media/pdf/condition-booklets/Progesterone_Booklet.pdf)
Corpus luteum cell
Corpus luteum cell may refer to: • Granulosa lutein cell • Theca lutein cell
Corpus luteum
247
Corpus luteum
Corpus luteum
Section of the ovary. 1. Outer covering. 1’. Attached border. 2. Central stroma. 3. Peripheral stroma. 4. Bloodvessels. 5. Vesicular follicles in their earliest stage. 6, 7, 8. More advanced follicles. 9. An almost mature follicle. 9’. Follicle from which the ovum has escaped. 10. Corpus luteum. Gray's subject #266 1256
[1]
The corpus luteum (Latin for "yellow body") (plural corpora lutea) is a temporary endocrine structure in female mammals that is involved in the production of relatively high levels of progesterone and moderate levels of estradiol and inhibin A. It is colored as a result of concentrating carotenoids from the diet and secretes a moderate amount of estrogen to inhibit further release of Gonadotropin-releasing hormone (GnRH) and thus secretion of Luteinizing hormone (LH) and Follicle-stimulating hormone (FSH).
Development and structure
The corpus luteum develops from an ovarian follicle during the luteal phase of the menstrual cycle or estrous cycle, following the release of a secondary oocyte from the follicle during ovulation. The follicle first forms a corpus hemorrhagicum before it becomes a corpus luteum, but the term refers to the visible collection of blood left after rupture of the follicle that secretes progesterone. While the oocyte (later the zygote if fertilization occurs) traverses the Fallopian tube into the uterus, the corpus luteum remains in the ovary. The corpus luteum is typically very large relative to the size of the ovary; in humans, the size of the structure ranges from under 2 cm to 5 cm in diameter.[][] Its cells develop from the follicular cells surrounding the ovarian follicle.[1] The follicular theca cells luteinize into small luteal cells, (thecal-lutein cells) and follicular granulosa cells (granulosal-lutein cells), luteinize into large luteal cells forming the corpus luteum. Progesterone is synthesized from cholesterol by both the large and small luteal cells upon luteal maturation. Cholesterol-LDL complexes bind to receptors on the plasma membrane of luteal cells and are internalized. Cholesterol is released and stored within the cell as cholesterol ester. LDL is recycled for further cholesterol transport. Large luteal cells produce more progesterone due to uninhibited/basal levels of PKA activity within the cell. Small luteal cells have LH receptors that regulate PKA activity within the cell. PKA actively phosphorylates StAR (steroidogenic acute regulatory protein) and PBR (peripheral benzodiazepine receptors) to transport cholesterol from the outer mitochondrial membrane to the inner mitochondrial membrane.[] The development of the corpus luteum is accompanied by an increase in the level of the steroidogenic enzyme P450scc that converts cholesterol to pregnenolone in the mitochondria.[] Pregnenolone is then converted to
Corpus luteum progesterone that is secreted out of the cell and into the blood stream. During the bovine estrous cycle, plasma levels of progesterone increase in parallel to the levels of P450scc and its electron donor adrenodoxin, indicating that progesterone secretion is a result of enhanced expression of P450scc in the corpus luteum.[] The mitochondrial P450 system electron transport chain including adrenodoxin reductase and adrenodoxin has been shown to leak electrons leading to the formation of superoxide radical.[][] Apparently to cope with the radicals produced by this system and by enhanced mitochondrial metabolism, the levels of antioxidant enzymes catalase and superoxide dismutase also increase in parallel with the enhanced steroidogenesis in the corpus luteum.[]
Follicular structure Luteal structure Theca cells Granulosa cells Theca lutein cells Secretion androgens, [2] estrogen [1] , and progesterone [2]
248
Granulosa lutein cells progesterone [1]), estrogen(majority),[1] and inhibin A[1][2]
Like the previous theca cells, the theca lutein cells lack the aromatase enzyme that is necessary to produce estrogen, so they can only perform steroidogenesis until formation of androgens.[3] The granulosa lutein cells do have aromatase, and use it to produce estrogens, using the androgens previously synthesized by the theca lutein cells, as the granulosa lutein cells in themselves do not have the 17α-hydroxylase or 17,20 lyase to produce androgens.[3] Once the corpus luteum regressed the remnant is known as corpus albicans.[4]
Function
The corpus luteum is essential for establishing and maintaining pregnancy in females. The corpus luteum secretes progesterone, which is a steroid hormone responsible for the decidualization of the endometrium (its development) and maintenance, respectively.
Steroidogenesis, with progesterone in yellow field at upper center. The androgens are shown in blue field, and aromatase at lower center - the enzyme present in granulosa lutein cells that convert androgens into estrogens (shown in pink triangle).
When egg is not fertilized
If the egg is not fertilized, the corpus luteum stops secreting progesterone and decays (after approximately 14 days in humans). It then degenerates into a corpus albicans, which is a mass of fibrous scar tissue. The uterine lining sloughs off without progesterone and is expelled through the vagina (in humans and some great apes, which go through a menstrual cycle). In an estrous cycle, the lining degenerates back to normal size.
When egg is fertilized
If the egg is fertilized and implantation occurs, the syncytiotrophoblast (derived from trophoblast) cells of the blastocyst secrete the hormone human chorionic gonadotropin (hCG, or a similar hormone in other species) by day 9 post-fertilization. Human chorionic gonadotropin signals the corpus luteum to continue progesterone secretion, thereby maintaining the thick lining (endometrium) of the uterus and providing an area rich in blood vessels in which the zygote(s) can develop. From this point on, the corpus luteum is called the corpus luteum graviditatis. The introduction of prostaglandins at this point causes the degeneration of the corpus luteum and the abortion of the fetus. However, in placental animals such as humans, the placenta eventually takes over progesterone production and the corpus luteum degrades into a corpus albicans without embryo/fetus loss.
Corpus luteum Luteal support refers to the administration of medication (generally progestins) for the purpose of increasing the success of implantation and early embryogenesis, thereby complementing the function of the corpus luteum.
249
Content of carotenoids
The yellow color and name of the corpus luteum, like that of the macula lutea of the retina, is due to its concentration of certain carotenoids, especially lutein. In 1968, a report indicated that beta-carotene was synthesized in laboratory conditions in slices of corpus luteum from cows. However, attempts have been made to replicate these findings, but have not succeeded. The idea is not presently accepted by the scientific community.[5] Rather, the corpus luteum concentrates carotenoids from the diet of the mammal.
Additional images
Order of changes in ovary
Human ovary with fully developed corpus luteum
Luteinized follicular cyst. H&E stain.
External links
• BU Histology Learning System: 18201loa [7] • SUNY Labs 43:05-0106 [8] – "The Female Pelvis: The Ovary"
References
[1] Page 1159 in: [2] The IUPS Physiome Project --> Female Reproductive System – Cells (http:/ / www. bioeng. auckland. ac. nz/ physiome/ ontologies/ female_repro_system/ cells. php) Retrieved on Nov 9, 2009 [3] Chapter 54, The Female Reproductive System > THE OVARIAN STEROIDS, in: [4] (http:/ / www. jstor. org/ pss/ 1563350) [5] Brian Davis. Carotenoid metabolism as a preparation for function. Pure & Applied Chemistry, Vol. 63, No. 1, pp. 131–140, 1991. available online. (http:/ / media. iupac. org/ publications/ pac/ 1991/ pdf/ 6301x0131. pdf) Accessed April 30, 2010.
Juxtaglomerular cell
250
Juxtaglomerular cell
The juxtaglomerular cells (JG cells, or granular cells) are cells in the kidney that synthesize, store, and secrete the enzyme renin. They are specialized smooth muscle cells in the wall of the afferent arteriole (and sometimes the efferent arteriole) that delivers blood to the glomerulus. In synthesizing renin, they play a critical role in the renin-angiotensin system and thus in renal autoregulation, the self-governance of the kidney. They secrete renin in response to the detection of low Na by the macula densa cells located on the distal convoluted tubule which has direct contact with its own afferent arterioles. In appropriately stained slides, juxtaglomerular cells are distinguished by their granulated cytoplasm. Similar to cardiac tissue, juxtaglomerular cells harbor β1 adrenergic receptors. When stimulated by epinephrine or norepinephrine, these receptors induce the secretion of renin. These cells also respond directly to a decrease in systemic blood pressure which is manifested as a lower renal perfusion pressure.
JG cells
Renal corpuscle. Juxtaglomerular cells are #6.
External links
• BU Histology Learning System: 16010loa [1] • juxtaglomerular+cells [2] at eMedicine Dictionary
Renin
251
Renin
Renin
PDB rendering based on 2ren Available structures PDB Ortholog search: PDBe [1], RCSB [2] List of PDB id codes 1BBS , 1BIL , 1BIM , 1HRN , 1RNE , 2BKS , 2BKT , 2FS4 , 2G1N , 2G1O , 2G1R , [14] [15] [16] [17] [18] [19] [20] [21] [22] [23] 2G1S , 2G1Y , 2G20 , 2G21 , 2G22 , 2G24 , 2G26 , 2G27 , 2I4Q , 2IKO , 2IKU [24] [25] [26] [27] [28] [29] [30] [31] [32] [33] [34] , 2IL2 , 2REN , 2V0Z , 2V10 , 2V11 , 2V12 , 2V13 , 2V16 , 2X0B , 3D91 , [35] [36] [37] [38] [39] [40] [41] [42] [43] [44] 3G6Z , 3G70 , 3G72 , 3GW5 , 3K1W , 3KM4 , 3O9L , 3OAD , 3OAG , 3OOT , [45] [46] [47] [48] [49] [50] [51] [52] [53] [54] 3OQF , 3OQK , 3OWN , 3Q3T , 3Q4B , 3Q5H , 3SFC , 3VCM , 3VSW , 3VSX , [55] [56] [57] [58] [59] [60] [61] [62] [63] [64] 3VYD , 3VYE , 3VYF , 4AMT , 4GJ5 , 4GJ6 , 4GJ7 , 4GJ8 , 4GJ9 , 4GJA , [65] [66] [67] 4GJB , 4GJC , 4GJD
[3] [4] [5] [6] [7] [8] [9] [10] [11] [12] [13]
Identifiers Symbols External IDs REN
[68]
; HNFJ2
[69]
OMIM: 179820 [73] Gene 3.4.23.15
[74]
MGI: 97898
[70]
HomoloGene: 20151
[71]
ChEMBL: 286
[72]
GeneCards: REN
EC number
Renin
252
Gene Ontology Molecular function • aspartic-type endopeptidase activity [75] [14] • receptor binding [170] • insulin-like growth factor receptor binding [76] • peptidase activity Cellular component • extracellular space [230] [77] • membrane [78] • cytoplasmic part Biological process • kidney development [80] • mesonephros development [81] • angiotensin maturation • renin-angiotensin regulation of aldosterone production
[82] [79]
• proteolysis [84] • response to stress [85] • regulation of blood pressure [86] • male gonad development [87] • hormone-mediated signaling pathway [22] • response to drug [61] • drinking behavior [88] • regulation of MAPK cascade [89] • cell maturation [70] • response to cAMP [90] • response to cGMP Sources: Amigo
[91]
[83]
/ QuickGO
[92]
Orthologs Species Entrez Ensembl UniProt RefSeq (mRNA) RefSeq (protein) Location (UCSC) Human 5972
[93] [95]
Mouse 19701
[94] [96]
ENSG00000143839 P00797
[97] [99]
ENSMUSG00000070645 P06281
[98] [100]
NM_000537 NP_000528
NM_031192 NP_112469
[101]
[102]
Chr 1: [103] 204.12 – 204.14 Mb
[105]
Chr 1: [104] 133.35 – 133.36 Mb
[106]
PubMed search
Renin
253
renin
Identifiers EC number CAS number 3.4.23.15 [107] [108]
9015-94-5
Databases IntEnz BRENDA ExPASy KEGG MetaCyc PRIAM PDB structures Gene Ontology IntEnz view [109] [110] [111]
BRENDA entry NiceZyme view KEGG entry
[112] [113]
metabolic pathway profile [114] [115]
RCSB PDB AmiGO
PDBe
[116]
PDBsum
[117]
[118]
/ EGO
[119]
Search PMC articles [120]
PubMed articles [121] NCBI proteins [122]
Renin (pron.: /ˈriːnɨn/ REE-nin), also known as an angiotensinogenase, is an enzyme that participates in the body's renin-angiotensin system (RAS)—also known as the renin-angiotensin-aldosterone axis—that mediates extracellular volume (i.e., that of the blood plasma, lymph and interstitial fluid), and arterial vasoconstriction. Thus, it regulates the body's mean arterial blood pressure.
Biochemistry and physiology
Structure
The primary structure of renin precursor consists of 406 amino acids with a pre- and a pro-segment carrying 20 and 46 amino acids, respectively. Mature renin contains 340 amino acids and has a mass of 37 kDa.[]
Secretion
The enzyme renin is secreted by the kidney from specialized cells called granular cells of the juxtaglomerular apparatus via 3 responses: 1. A decrease in arterial blood pressure (that could be related to a decrease in blood volume) as detected by baroreceptors (pressure-sensitive cells). This is the most direct causal link between blood pressure and renin secretion (the other two methods operate via longer pathways). 2. A decrease in sodium chloride levels in the ultra-filtrate of the nephron. This flow is measured by the macula densa of the juxtaglomerular apparatus.
Renin 3. Sympathetic nervous system activity, which also controls blood pressure, acting through the beta1 adrenergic receptors. Human renin is secreted by at least 2 cellular pathways: a constitutive pathway for the secretion of prorenin and a regulated pathway for the secretion of mature renin.[]
254
Renin-angiotensin system
The renin enzyme circulates in the blood stream and breaks down (hydrolyzes) angiotensinogen secreted from the liver into the peptide angiotensin I. Angiotensin I is further cleaved in the lungs by endothelial-bound angiotensin-converting enzyme (ACE) into angiotensin II, the most vasoactive peptide.[][2] Angiotensin II is a potent constrictor of all blood vessels. It acts on the smooth muscle and, therefore, raises the resistance posed by these arteries to the heart. The heart, trying to overcome this increase in its 'load', works more vigorously, causing the blood pressure to rise. Angiotensin II also acts on the adrenal glands and releases Aldosterone, which stimulates the epithelial cells in the distal tubule and collecting ducts of the kidneys to increase re-absorption of sodium and water, leading to raised blood volume and raised blood pressure. The RAS also acts on the CNS to increase water intake by stimulating thirst, as well as conserving blood volume, by reducing urinary loss through the secretion of Vasopressin from the posterior pituitary gland.
The renin-angiotensin system, showing role of renin at [1] bottom.
The normal concentration of renin in adult human plasma is 1.98-24.6 ng/L in the upright position.[3]
Function
Renin activates the renin-angiotensin system by cleaving angiotensinogen, produced by the liver, to yield angiotensin I, which is further converted into angiotensin II by ACE, the angiotensin-converting enzyme primarily within the capillaries of the lungs. Angiotensin II then constricts blood vessels, increases the secretion of ADH and aldosterone, and stimulates the hypothalamus to activate the thirst reflex, each leading to an increase in blood pressure. Renin is secreted from kidney cells, which are activated via signaling from the macula densa, which responds to the rate of fluid flow through the distal tubule, by decreases in renal perfusion pressure (through stretch receptors in the vascular wall), and by sympathetic nervous stimulation, mainly through beta-1 adrenoceptor activation. A drop in the rate of flow past the macula densa implies a drop in renal filtration pressure. Renin's primary function is therefore to eventually cause an increase in blood pressure, leading to restoration of perfusion pressure in the kidneys. Renin can bind to ATP6AP2, which results in a fourfold increase in the conversion of angiotensinogen to angiotensin I over that shown by soluble renin. In addition, renin binding results in phosphorylation of serine and tyrosine residues of ATP6AP2.[] The level of renin mRNA appears to be modulated by the binding of HADHB, HuR and CP1 to a regulatory region in the 3' UTR.[]
Renin
255
Genetics
The gene for renin, REN, spans 12 kb of DNA and contains 8 introns.[] It produces several mRNA that encode different REN isoforms.
Model organisms Ren1 knockout mouse phenotype
Characteristic Homozygote viability Fertility Body weight Anxiety Neurological assessment Grip strength Hot plate Dysmorphology Phenotype Normal Normal Normal Normal Normal Normal Normal Normal
Non-Invasive Blood Pressure Abnormal[] Indirect calorimetry Glucose tolerance test Normal Normal
Auditory brainstem response Normal DEXA Radiography Body temperature Eye morphology Clinical chemistry Haematology Micronucleus test Heart weight Skin Histopathology Brain histopathology Salmonella infection Citrobacter infection Normal Normal Normal Normal Normal Normal Normal Normal Normal Normal Normal [] []
Abnormal [][4]
All tests and analysis from
Model organisms have been used in the study of REN function. A knockout mouse line, called Ren1Ren-1c Enhancer KO was generated.[5] Male and female animals underwent a standardized phenotypic screen to determine the effects of deletion.[][6] Twenty four tests were carried out on mutant mice and two significant abnormalities were observed. Homozygous mutant animals had a decreased heart rate and an increased susceptibility to bacterial infection.[] A more detailed analysis of this line indicated plasma creatinine was also increased and males had lower mean arterial pressure than controls.[5]
Renin
256
Clinical applications
An over-active renin-angiotension system leads to vasoconstriction and retention of sodium and water. These effects lead to hypertension. Therefore, renin inhibitors can be used for the treatment of hypertension.[7][] This is measured by the plasma renin activity (PRA). In current medical practice, the renin-angiotensin-aldosterone-System's overactivity (and resultant hypertension) is more commonly reduced using either ACE inhibitors (such as ramipril and perindopril) or angiotensin II receptor blockers (ARBs, such as losartan, irbesartan or candesartan) rather than a direct oral renin inhibitor. ACE inhibitors or ARBs are also part of the standard treatment after a heart attack. The differential diagnosis of kidney cancer in a young patient with hypertension includes juxtaglomerular cell tumor (reninoma), Wilms' tumor, and renal cell carcinoma, all of which may produce renin.[]
Measurement
Renin is usually measured as the plasma renin activity (PRA). PRA is measured specially in case of certain diseases that present with hypertension or hypotension. PRA is also raised in certain tumors.[8] A PRA measurement may be compared to a plasma aldosterone concentration (PAC) as a PAC/PRA ratio.
Discovery
Renin was discovered, characterized, and named in 1898 by Robert Tigerstedt, Professor of Physiology and his student, Per Bergman, at the Karolinska Institute in Stockholm.[][9]
References
[1] Page 866-867 (Integration of Salt and Water Balance) and 1059 (The Adrenal Gland) in: [2] Brenner & Rector's The Kidney, 7th ed., Saunders, 2004. pp.2118-2119. Full Text with MDConsult subscription (http:/ / home. mdconsult. com/ das/ book/ 56203699-6/ view/ 1201?sid=460067115) [3] Hamilton Regional Laboratory Medicine Program - Laboratory Reference Centre Manual. [deadlink] [4] Mouse Resources Portal (http:/ / www. sanger. ac. uk/ mouseportal/ ), Wellcome Trust Sanger Institute. [7] Presentation on Direct Renin Inhibitors as Antihypertensive Drugs (http:/ / pharmaxchange. info/ presentations/ dri. html) [8] Hamilton Regional Laboratory Medicine Program - Laboratory Reference Centre Manual. Renin Direct.
External links
• GeneReviews/NCBI/NIH/UW entry on Familial Juvenile Hyperuricemic Nephropathy Type 2 (http://www. ncbi.nlm.nih.gov/books/NBK53700/) • OMIM entries on Familial Juvenile Hyperuricemic Nephropathy Type 2 (http://www.ncbi.nlm.nih.gov/omim/ 179820,613092) • The MEROPS online database for peptidases and their inhibitors: A01.007 (http://merops.sanger.ac.uk/ cgi-bin/merops.cgi?id=A01.007) • Renin (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Renin) at the US National Library of Medicine Medical Subject Headings (MeSH) • renin (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=renin) at eMedicine Dictionary
Macula densa
257
Macula densa
In the kidney, the macula densa is an area of closely packed specialized cells lining the wall of the distal tubule at the point of return of the nephron to the vascular pole of its parent glomerulus, (glomerular vascular pole). The cells of the macula densa are sensitive to the concentration of sodium chloride in the distal convoluted tubule. A decrease in sodium chloride concentration initiates a signal from the macula densa that has two effects: (1) it decreases resistance to blood flow in the afferent arterioles, which increases glomerular hydrostatic pressure Renal corpuscle. Macula densa is #7. and helps return glomerulus filtration rate (GFR) toward normal, and (2) it increases renin release from the juxtaglomerular cells of the afferent and efferent arterioles, which are the major storage sites for renin.[1] The release of renin is an essential component of the renin-angiotensin-aldosterone system (RAAS), which regulates blood pressure and volume.
Histology
The cells of the macula densa are taller and have more prominent nuclei than surrounding cells of the distal straight tubule (cortical thick ascending limb). The close proximity and prominence of the nuclei cause this segment of the distal tubule wall to appear darker in microscopic preparations,[2] hence the name macula densa.
Function
A decrease in blood pressure causes a decrease in the GFR (glomerular filtration rate) which causes more reabsorption, resulting in a decreased concentration of sodium and chloride ions in the filtrate and/or decreased filtrate flow rate. The macula densa can sense this decrease and trigger an autoregulatory response to further increase reabsorption of ions and water in order to return blood pressure to normal. Reduced blood pressure means
Schematic depicting how the RAAS works. Here, activation of the RAAS is initiated by a low perfusion pressure in the juxtaglomerular apparatus
Macula densa decreased venous pressure and hence a decreased peritubular capillary pressure. This causes a smaller capillary hydrostatic pressure which causes an increased absorption of sodium ions into the vasa recta at the proximal tubule. Because of this increased absorption, less NaCl is present at the distal tubule where the macula densa is located. The macula densa senses this drop in salt concentration and responds through two mechanisms: first, it triggers dilation of the renal afferent arteriole, decreasing afferent arteriole resistance and thus offsetting the decrease in glomerular hydrostatic pressure caused by the drop in blood pressure. Second, macula densa cells release prostaglandins, which triggers granular juxtaglomerular cells lining the afferent arterioles to release renin into the bloodstream. (The juxtaglomerular cells can also release renin independently of the macula densa, as they are also triggered by baroreceptors lining the arterioles, and release renin if a fall in blood pressure in the arterioles is detected.) Furthermore, activation of the sympathetic nervous system stimulates renin release through activation of beta-1 receptors. The process triggered by the Macula densa helps keep the glomerular filtration rate (GFR) fairly steady in response to varying artery pressure, due to dilation of the afferent arterioles and the action of Renin, which triggers constriction of the efferent arterioles, both of which increase hydrostatic pressure in the glomerulus.
258
References
[1] Guyton & Hall Textbook Of Physiology, 11th Edition 2006 - pg 324
External links
• Organology at UC Davis Urinary/mammal/cortex1/cortex5 (http://trc.ucdavis.edu/mjguinan/apc100/modules/ Urinary/mammal/cortex1/cortex5.html) - "Mammal, kidney cortex (LM, Medium)" • Physiology at MCG 7/7ch03/7ch03p17 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section7/7ch03/7ch03p17.htm) - "The Nephron: Juxtaglomerular Apparatus"
Mesangial cell
259
Mesangial cell
Mesangial cells are specialized cells around blood vessels in the kidneys, at the mesangium. They are specialized smooth muscle cells that function to regulate blood flow through the capillaries, usually divided into two types, each having a very distinct function and location: • Extraglomerular mesangial cells • Intraglomerular mesangial cells
Keratinocyte
Keratinocyte is the predominant cell type in the epidermis, the outermost layer of the skin, constituting 90% of the cells found there.[1] Those keratinocytes found in the basal layer (Stratum germinativum) of the skin are sometimes referred to as "basal cells" or "basal keratinocytes".[1]
Function
The primary function of keratinocytes is the formation of a barrier against environmental damage such as pathogens (bacteria, fungi, parasites, viruses), heat, UV radiation and water loss. Once pathogens start to invade the upper layers of the epidermis, keratinocytes can react with the production of proinflammatory mediators and in particular chemokines such as CXCL10, CCL2 which attract leukocytes to the site of pathogen invasion. [citation needed]
Structure
A number of structural proteins (filaggrin, keratin), enzymes (proteases), lipids and antimicrobial peptides (defensins) contribute to maintain the important barrier function of the skin. Keratinization is part of the physical barrier formation (cornification), in which the keratinocytes produce more and more keratin and eventually undergo programmed cell death. The fully cornified keratinocytes that form the outermost layer are constantly shed off and replaced by new cells. [citation needed]
Cell differentiation
Keratinocytes are formed first by differentiation from epidermal stem cells (transit amplifying cells), residing in the lower part of the stratum basale of the epidermis, attached to the basement membrane through hemidesmosomes.[2] Those stem cells and their differentiated progeny are organized into columns named epidermal proliferation units.[3][4] Keratinocytes in the stratum basale layer of the epidermis are attached together through desmosomes and will proliferate through a few rounds of cell divisions within the stratum basale before moving up through the epidermis as they differentiate. During this differentiation process, keratinocytes permanently withdraw from the cell cycle, initiate expression of epidermal differentiation markers, and move suprabasally as they become part of the stratum spinosum, stratum granulosum and eventually become corneocytes in the stratum corneum. Corneocytes are keratinocytes that have completed their differentiation program and have lost their nucleus and cytoplasmic organelles.[5] Corneocytes will eventually be shed off through desquamation as new one come in. At each stage of differentiation, keratinocytes express specific keratins, such as keratin 1, keratin 5, keratin 10 and keratin 14, but also other markers such as involucrin, loricrin, transglutaminase, filaggrin and caspase 14. In humans, it is estimated that keratinocytes turnover from stem cells to desquamation every 40–56 days[6] whereas in mice the estimated turnover time is 8–10 days.[7]
Keratinocyte Factors promoting keratinocyte differentiation: • A calcium gradient, with the lowest concentration in the stratum basale and increasing concentrations until the outer stratum granulosum, where it reaches its maximum. Calcium concentration in the stratum corneum is very low in part because those relatively dry cells are not able to dissolve the ions.[] Those elevations of extracellular calcium concentrations induces an increase in intracellular free calcium concentrations in keratinocyte.[8] Part of that intracellular calcium increase comes from calcium released from intracellular stores[9] and another part comes from transmembrane calcium influx,[10] through both calcium-sensitive chloride channels[11] and voltage-independent cation channels permeable to calcium.[12] Moreover, it has been suggested that an extracellular calcium-sensing receptor (CaSR) also contributes to the rise in intracellular calcium concentration.[13] • Vitamin D3 (cholecalciferol) regulates keratinocyte proliferation and differentiation mostly by modulating calcium concentrations and regulating the expression of genes involved in keratinocytes differentiation.[14][15] Keratinocytes are the only cells in the body with the entire vitamin D metabolic pathway from vitamin D production to catabolism and Vitamin D receptor expression.[16] • Cathepsin E.[17] • TALE homeodomain transcription factors.[18] • Hydrocortisone.[] Since keratinocyte differentiation stops keratinocyte proliferation, factors that promote keratinocyte proliferation should be considered as preventing differentiation, such as: • • • • • The transcription factor p63, by preventing epidermal stem cells to differentiate into keratinocytes.[19] Vitamin A and its analogues.[20] Epidermal growth factor.[21] Tumor growth factor alpha.[22] Cholera toxin[]
260
Interaction with other cells
Within the epidermis keratinocytes are associated with other cell types such as melanocytes and Langerhans cells. Keratinocytes form tight junctions with the nerves of the skin and hold the Langerhans cells and intra-dermal lymphocytes in position within the epidermis. Keratinocytes also modulate the immune system: apart from the above mentioned antimicrobial peptides and chemokines they are also potent producers of anti-inflammatory mediators such as IL-10 and TGF-β. When activated, they can stimulate cutaneous inflammation and Langerhans cell activation via TNFα and IL-1β secretion.[citation needed] Keratinocytes contribute to protecting the body from ultraviolet radiation (UVR) by taking up melanosomes, vesicles containing the endogenous photoprotectant melanin, from epidermal melanocytes. Each melanocyte in the epidermis has several dendrites that stretch out to connect it with many keratinocytes. The melanin is then stored within keratinocytes and melanocytes in the perinuclear area as supranuclear “caps”, where it protects the DNA from UVR-induced damage.[23]
Keratinocyte
261
Role in wound healing
Wounds to the skin will be repaired in part by the migration of keratinocytes to fill in the gap created by the wound. The first set of keratinocytes to participate in that repair come from the bulge region of the hair follicle and will only survive transiently. Within the healed epidermis they will be replaced by keratinocytes originating from the epidermis.[24][25] At the opposite, epidermal keratinocytes, can contribute to de novo hair follicle formation during the healing of large wounds.[26] Keratinocytes migrate with a rolling motion during the process of wound healing.[27][28] Functional keratinocytes are needed for tympanic perforation healing. [29]
Sunburn cells
A sunburn cell is a keratinocyte with a pyknotic nucleus and eosinophilic cytoplasm that appears after exposure to UVC or UVB radiation or UVA in the presence of psoralens. It shows premature and abnormal keratinization, and has been described as an example of apoptosis.[30][31]
References
[29] Y Shen, Y Guo, C Du, M Wilczynska, S Hellström, T Ny, Mice Deficient in Urokinase-Type Plasminogen Activator Have Delayed Healing of Tympanic Membrane Perforations, PLOS ONE, 2012
External links
• L. Tang1, J.J. Wu2, Q. Ma1, T. Cui1, F.M. Andreopoulos3, J. Gil1, J. Valdes1, S.C. Davis1, J. Li1,4 "Human lactoferrin stimulates skin keratinocyte function and wound re-epithelialization", British Journal of Dermatology Volume 163, Issue 1, pages 38–47 (July 2010). Article first published online: 6 MAR 2010. (http://www3. interscience.wiley.com/journal/123313996/abstract) doi: 10.1111/j.1365-2133.2010.09748.x (http://dx.doi. org/10.1111/j.1365-2133.2010.09748.x)
Epidermis (skin)
262
Epidermis (skin)
Epidermis
Histologic image of epidermis, delimited by white bar.
Histologic image detailing epidermal layers. Stratum corneum appears more compact in this image than above because of different sample preparation. Latin Code Epidermis TH H13.12.00.1.01001 TA A16.0.00.009
The epidermis is composed of the outermost layers of cells in the skin,[1] "epi" in Greek meaning "over" or "upon", which together with the dermis forms the cutis. The epidermis is a stratified squamous epithelium,[1] composed of proliferating basal and differentiated suprabasal keratinocytes which acts as the body's major barrier against an inhospitable environment, by preventing pathogens from entering, making the skin a natural barrier to infection.[] It also regulates the amount of water released from the body into the atmosphere through transepidermal water loss (TEWL).[] In humans, it is thinnest on the eyelids at 0.05 mm (0.0020 in) and thickest on the palms and soles at 1.5 mm (0.059 in).[] It is ectodermal in origin.
Structure
Cellular components
The epidermis is avascular, nourished by diffusion from the dermis, constituted at 95% of keratinocytes[1] but also containing melanocytes, Langerhans cells, Merkel cells,[1] and inflammatory cells. Rete ridges ("rete tips"[2]) are epidermal thickenings that extend downward between dermal papillae.[3] Blood capillaries are found beneath the epidermis, and are linked to an arteriole and a venule. Arterial shunt vessels may bypass the network in ears, the nose and fingertips.[citation needed]
Epidermis (skin)
263
Layers
The epidermis is composed of 4 or 5 layers depending on the region of skin being considered.[4] Those layers in descending order are[]: • cornified layer (stratum corneum) Composed of 10 to 30 layers of polyhedral, anucleated corneocytes (final step of keratinocyte differentiation), with the palms and soles having the most layers. Corneocytes are surrounded by a protein envelope (cornified envelope proteins), filled with water-retaining keratin proteins, attached together through corneodesmosomes and surrounded in the extracellular space by stacked layers of lipids.[5] Most of the barrier functions of the epidermis localize to this layer.[] • clear/translucent layer (stratum lucidum, only in palms and soles) • granular layer (stratum granulosum) Keratinocytes lose their nuclei and their cytoplasm appears granular. Lipids, contained into those keratinocytes within lamellar bodies, are released into the extracellular space through exocytosis to form a lipid barrier. Those polar lipids are then converted into non-polar lipids and arranged parallel to the cell surface. For example glycosphingolipids become ceramides and phospholipids become free fatty acids.[5] • spinous layer (stratum spinosum) Keratinocytes become connected through desmosomes and start produce lamellar bodies, from within the Golgi, enriched in polar lipids, glycosphingolipids, free sterols, phospholipids and catabolic enzymes.[] Langerhans cells, immunologically active cells, are located in the middle of this layer.[5] • basal/germinal layer (stratum basale/germinativum). Composed mainly of proliferating and non-proliferating keratinocytes, attached to the basement membrane by hemidesmosomes. Melanocytes are present, connected to numerous keratinocytes in this and other strata through dendrites. Merkel cells are also found in the stratum basale with large numbers in touch-sensitive sites such as the fingertips and lips. They are closely associated with cutaneous nerves and seem to be involved in light touch sensation.[5] The term Malpighian layer (stratum malpighi) is usually defined as both the stratum basale and stratum spinosum.[1] The epidermis is separated from the dermis, its underlying tissue, by a basement membrane.
Schematic image showing a section of epidermis with epidermal layers labeled.
Cellular kinyotics
Cell division The stratified squamous epithelium is maintained by cell division within the stratum basale. Differentiating cell delaminate from the basement membrane and are displaced outwards through the epidermal layers, undergoing multiple stages of differentiation until, in the stratum corneum, losing their nucleus and fusing to squamous sheets, which are eventually shed from the surface (desquamation). Differentiated keratinocytes secrete keratin proteins which contribute to the formation of an extracellular matrix and is an integral part of the skin barrier function. In normal skin, the rate of keratinocyte production equals the rate of loss,[1] taking about two weeks for a cell to journey from the stratum basale to the top of the stratum granulosum, and an additional four weeks to cross the stratum corneum.[] The entire epidermis is replaced by new cell growth over a period of about 48 days.[]
Epidermis (skin) Calcium concentration Keratinocyte differentiation throughout the epidermis is in part mediated by a calcium gradient, increasing from the stratum basale until the outer stratum granulosum, where it reaches its maximum, and decreasing in the stratum corneum. Calcium concentration in the stratum corneum is very low in part because those relatively dry cells are not able to dissolve the ions. This calcium gradient parallels keratinocyte differentiation and as such is considered a key regulator in the formation of the epidermal layers.[] Elevation of extracellular calcium concentrations induces an increase in intracellular free calcium concentrations.[6] Part of that intracellular increase comes from calcium released from intracellular stores[7] and another part comes from transmembrane calcium influx,[8] through both calcium-sensitive chloride channels[9] and voltage-independent cation channels permeable to calcium.[10] Moreover, it has been suggested that an extracellular calcium-sensing receptor (CaSR) also contributes to the rise in intracellular calcium concentration.[11]
264
Organogenesis
Epidermal organogenesis, the formation of the epidermis, begins in the cells covering the embryo after neurulation, the formation of the central nervous system. In most vertebrates, this original one-layered structure quickly transforms into a two-layered tissue; a temporary outer layer, the periderm, which is disposed once the inner basal layer or stratum germinativum has formed. [] This inner layer is a germinal epithelium that give rise to all epidermal cells. It divides to form the outer spinous layer (stratum spinosum). The cells of these two layers, together called the Malpighian layer(s) after Marcello Malpighi, divide to form the superficial granular layer (Stratum granulosum) of the epidermis. [] The cells in the stratum granulosum do not divide, but instead form skin cells called keratinocytes from the granules of keratin. These skin cells finally become the cornified layer (stratum corneum), the outermost epidermal layer, where the cells become flattened sacks with their nuclei located at one end of the cell. After birth these outermost cells are replaced by new cells from the stratum granulosum and throughout life they are shed at a rate of 1.5 g (0.053 oz) per day. [] Epidermal development is a product of several growth factors, two of which are:[] • Transforming growth factor Alpha (TGFα) is an autocrine growth factor by which basal cells stimulate their own division. • Keratinocyte growth factor (KGF or FGF7) is a paracrine growth factor produced by the underlying dermal fibroblasts in which the proliferation of basal cells is regulated.
Function
Barrier
The epidermis serves as a barrier to protect the body against microbial pathogens, oxidant stress (UV light) and chemical compounds and provides mechanical resistance. Most of that function is played by the stratum corneum.[] Characteristics of the barrier • Physical barrier through keratinocytes attached together via cell–cell junctions and associated to cytoskeletal proteins, which gives the epidermis its mechanical strength.[] • Chemical barrier through the presence of highly organized lipids, acids, hydrolytic enzymes and antimicrobial peptides.[] • Immunologically active barrier through humoral and cellular constituents of the immune system.[] • Water content of the stratum corneum drops towards the surface, creating hostile conditions for pathogenic microorganism growth.[]
Epidermis (skin) • An acidic pH (around 5.0) and low amounts of water make it hostile to many microorganic pathogens.[] • The presence of non-pathogenic microorganism on the epidermis surface help defend against pathogenic one by limiting food availability and through chemical secretions.[] Factors that will alter the barrier • Psychological stress, through an increase in glucocorticoids, compromises the stratum corneum and thus the barrier function.[12] • Sudden and large shifts in humidity alter stratum corneum hydration in a way that could allow entry of pathogenic microorganisms.[13]
265
Skin hydration
The ability of the skin to hold water is primarily due to the stratum corneum and is critical for maintaining healthy skin.[14] Lipids arranged through a gradient and in an organized manner between the cells of the stratum corneum form a barrier to transepidermal water loss.[15][16]
Skin color
The amount and distribution of melanin pigment in the epidermis is the main reason for variation in skin color in Homo sapiens. Melanin is found in the small melanosomes, particles formed in melanocytes from where they are transferred to the surrounding keratinocytes. The size, number, and arrangement of the melanosomes varies between racial groups, but while the number of melanocytes can vary between different body regions, their numbers remain the same in individual body regions in all human beings. In white and oriental skin the melanosomes are packed in "aggregates", but in black skin they are larger and distributed more evenly. The number of melanosomes in the keratinocytes increases with UV radiation exposure, while their distribution remain largely unaffected. [17]
Culture
Laboratory culture of keratinocytes to form a 3D structure (artificial skin) recapitulating most of the properties of the epidermis is routinely used as a tool for drug development and testing.
Additional images
Epidermis and dermis of human skin
Epidermis (skin)
266
Cross-section of all skin layers
Optical coherence tomography of fingertip
References
[1] James, William; Berger, Timothy; Elston, Dirk (2005) Andrews' Diseases of the Skin: Clinical Dermatology (10th ed.). Saunders. Page 2-3. ISBN 0-7216-2921-0. [2] http:/ / archderm. ama-assn. org/ cgi/ reprint/ 120/ 3/ 324. pdf [3] TheFreeDictionary > rete ridge (http:/ / medical-dictionary. thefreedictionary. com/ rete+ ridge) Citing: The American Heritage Medical Dictionary Copyright 2007, 2004 [4] The Ageing Skin - Structure (http:/ / pharmaxchange. info/ press/ 2011/ 03/ the-ageing-skin-part-1-structure-of-skin-and-introduction/ ) [5] http:/ / www. radcliffe-oxford. com/ books/ samplechapter/ 7750/ 01_bensouillah-241a6c80rdz. pdf [13] http:/ / onlinelibrary. wiley. com/ doi/ 10. 1021/ js950219p/ abstract
Stem cell
267
Stem cell
Stem cell
Mouse embryonic stem cells with fluorescent marker
Human embryonic stem cell colony on mouse embryonic fibroblast feeder layer Latin Code cellula precursoria TH H2.00.01.0.00001
Stem cells are biological cells found in all multicellular organisms, that can divide (through mitosis) and differentiate into diverse specialized cell types and can self-renew to produce more stem cells. In mammals, there are two broad types of stem cells: embryonic stem cells, which are isolated from the inner cell mass of blastocysts, and adult stem cells, which are found in various tissues. In adult organisms, stem cells and progenitor cells act as a repair system for the body, replenishing adult tissues. In a developing embryo, stem cells can differentiate into all the specialized cells (these are called pluripotent cells), but also maintain the normal turnover of regenerative organs, such as blood, skin, or intestinal tissues. There are three accessible sources of autologous adult stem cells in humans: 1. Bone marrow, which requires extraction by harvesting, that is, drilling into bone (typically the femur or iliac crest), 2. Adipose tissue (lipid cells), which requires extraction by liposuction, and 3. Blood, which requires extraction through pheresis, wherein blood is drawn from the donor (similar to a blood donation), passed through a machine that extracts the stem cells and returns other portions of the blood to the donor. Stem cells can also be taken from umbilical cord blood just after birth. Of all stem cell types, autologous harvesting involves the least risk. By definition, autologous cells are obtained from one's own body, just as one may bank his or her own blood for elective surgical procedures. Highly plastic adult stem cells are routinely used in medical therapies, for example in bone marrow transplantation. Stem cells can now be artificially grown and transformed (differentiated) into specialized cell types with
Stem cell characteristics consistent with cells of various tissues such as muscles or nerves through cell culture. Embryonic cell lines and autologous embryonic stem cells generated through therapeutic cloning have also been proposed as promising candidates for future therapies.[1] Research into stem cells grew out of findings by Ernest A. McCulloch and James E. Till at the University of Toronto in the 1960s.[2][3]
268
Properties
The classical definition of a stem cell requires that it possess two properties: • Self-renewal: the ability to go through numerous cycles of cell division while maintaining the undifferentiated state. • Potency: the capacity to differentiate into specialized cell types. In the strictest sense, this requires stem cells to be either totipotent or pluripotent—to be able to give rise to any mature cell type, although multipotent or unipotent progenitor cells are sometimes referred to as stem cells. Apart from this it is said that stem cell function is regulated in a feed back mechanism.
Self-renewal
Two mechanisms exist to ensure that a stem cell population is maintained: 1. Obligatory asymmetric replication: a stem cell divides into one father cell that is identical to the original stem cell, and another daughter cell that is differentiated 2. Stochastic differentiation: when one stem cell develops into two differentiated daughter cells, another stem cell undergoes mitosis and produces two stem cells identical to the original.
Potency definitions
Potency specifies the differentiation potential (the potential to differentiate into different cell types) of the stem cell.[] • Totipotent (a.k.a. omnipotent) stem cells can differentiate into embryonic and extraembryonic cell types. Such cells can construct a complete, viable organism.[] These cells are produced from the fusion of an egg and sperm cell. Cells produced by the first few divisions of the fertilized egg are also totipotent.[4] • Pluripotent stem cells are the descendants of totipotent cells and can differentiate into nearly all cells,[] i.e. cells derived from any of the three germ layers.[5] • Multipotent stem cells can differentiate into a number of cells, but only those of a closely related family of cells.[]
Pluripotent, embryonic stem cells originate as inner cell mass (ICM) cells within a blastocyst. These stem cells can become any tissue in the body, excluding a placenta. Only cells from an earlier stage of the embryo, known as the morula, are totipotent, able to become all tissues in the body and the extraembryonic placenta.
Stem cell • Oligopotent stem cells can differentiate into only a few cells, such as lymphoid or myeloid stem cells.[] • Unipotent cells can produce only one cell type, their own,[] but have the property of self-renewal, which distinguishes them from non-stem cells (e.g., muscle stem cells).
269
Identification
The practical definition of a stem cell is the functional definition—a cell that has the potential to regenerate tissue over a lifetime. For example, the defining test for a bone marrow or hematopoietic stem cell (HSC) is the ability to transplant one cell and save an individual without HSCs. In this case, a stem cell must be able to produce new blood cells and immune cells over a long term, demonstrating potency. It should also be possible to isolate stem cells from the transplanted individual, which can themselves be transplanted into another individual without HSCs, demonstrating that the stem cell was able to self-renew. Properties of stem cells can be illustrated in vitro, using methods such as clonogenic assays, in which single cells are assessed for their ability to differentiate and self-renew.[6][7] Stem cells can also be isolated by their possession of a distinctive set of cell surface markers. However, in vitro culture conditions can alter the behavior of cells, making it unclear whether the cells will behave in a similar manner in vivo. There is considerable debate as to whether some proposed adult cell populations are truly stem cells.
Human embryonic stem cells A: Cell colonies that are not yet differentiated. B: Nerve cell
Embryonic
Embryonic stem (ES) cell lines are cultures of cells derived from the epiblast tissue of the inner cell mass (ICM) of a blastocyst or earlier morula stage embryos.[8] A blastocyst is an early stage embryo—approximately four to five days old in humans and consisting of 50–150 cells. ES cells are pluripotent and give rise during development to all derivatives of the three primary germ layers: ectoderm, endoderm and mesoderm. In other words, they can develop into each of the more than 200 cell types of the adult body when given sufficient and necessary stimulation for a specific cell type. They do not contribute to the extra-embryonic membranes or the placenta. The endoderm is composed of the entire gut tube and the lungs, the ectoderm gives rise to the nervous system and skin, and the mesoderm gives rise to muscle, bone, blood—in essence, everything else that connects the endoderm to the ectoderm. Nearly all research to date has made use of mouse embryonic stem cells (mES) or human embryonic stem cells (hES). Both have the essential stem cell characteristics, yet they require very different environments in order to maintain an undifferentiated state. Mouse ES cells are grown on a layer of gelatin as an extracellular matrix (for support) and require the presence of leukemia inhibitory factor (LIF).[9] Human ES cells are grown on a feeder layer of mouse embryonic fibroblasts (MEFs) and require the presence of basic fibroblast growth factor (bFGF or FGF-2).[10] Without optimal culture conditions or genetic manipulation,[11] embryonic stem cells will rapidly differentiate. A human embryonic stem cell is also defined by the expression of several transcription factors and cell surface proteins. The transcription factors Oct-4, Nanog, and Sox2 form the core regulatory network that ensures the
Stem cell suppression of genes that lead to differentiation and the maintenance of pluripotency.[12] The cell surface antigens most commonly used to identify hES cells are the glycolipids stage specific embryonic antigen 3 and 4 and the keratan sulfate antigens Tra-1-60 and Tra-1-81. The molecular definition of a stem cell includes many more proteins and continues to be a topic of research.[13] There are currently no approved treatments using embryonic stem cells. The first human trial was approved by the US Food and Drug Administration in January 2009.[14] However, the human trial was not initiated until October 13, 2010 in Atlanta for spinal injury victims. On November 14, 2011 the company conducting the trial announced that it will discontinue further development of its stem cell programs.[15] ES cells, being pluripotent cells, require specific signals for correct differentiation—if injected directly into another body, ES cells will differentiate into many different types of cells, causing a teratoma. Differentiating ES cells into usable cells while avoiding transplant rejection are just a few of the hurdles that embryonic stem cell researchers still face.[16] Many nations currently have moratoria on either ES cell research or the production of new ES cell lines. Because of their combined abilities of unlimited expansion and pluripotency, embryonic stem cells remain a theoretically potential source for regenerative medicine and tissue replacement after injury or disease.
270
Fetal
The primitive stem cells located in the organs of fetuses are referred to as fetal stem cells.[]
Adult
Stem cell
271
Also known as somatic (from Greek Σωματικóς, "of the body") stem cells and germline (giving rise to gametes) stem cells, they can be found in children, as well as adults.[17] Pluripotent adult stem cells are rare and generally small in number but can be found in a number of tissues including umbilical cord blood.[18] Bone marrow has been found to be one of the rich sources of adult stem cells [19] which have been used in treating several conditions including Spinal cord injury,[20] Liver Cirrhosis,[21] Chronic Limb Ischemia [22] and Endstage heart failure.[23] The bone marrow stem cell quantity has been found to be declining with age and in reproductive age group of females it is relatively lesser than in males of same age group.[24] A great deal of adult stem cell research to date has had the aim of characterizing the capacity of the cells to divide or self-renew indefinitely and their differentiation potential.[25] In mice, pluripotent stem cells are directly generated from adult fibroblast cultures. Unfortunately, many mice do not live long with stem cell organs.[] Most adult stem cells are lineage-restricted (multipotent) and are generally referred to by their tissue origin (mesenchymal stem cell, adipose-derived stem cell, endothelial stem cell, dental pulp stem cell, etc.).[26][27] Adult stem cell treatments have been successfully used for many years to treat leukemia and related bone/blood cancers through bone marrow transplants.[28] Adult stem cells are also used in veterinary medicine to treat tendon and ligament injuries in horses.[29]
Stem cell division and differentiation. A: stem cell; B: progenitor cell; C: differentiated cell; 1: symmetric stem cell division; 2: asymmetric stem cell division; 3: progenitor division; 4: terminal differentiation
The use of adult stem cells in research and therapy is not as controversial as the use of embryonic stem cells, because the production of adult stem cells does not require the destruction of an embryo. Additionally, in instances where adult stem cells are obtained from the intended recipient (an autograft), the risk of rejection is essentially non-existent. Consequently, more US government funding is being provided for adult stem cell research.[30] An extremely rich source for adult mesenchymal stem cells is the developing tooth bud of the mandibular third molar.[31] The stem cells eventually form enamel (ectoderm), dentin, periodontal ligament, blood vessels, dental pulp, nervous tissues, and a minimum of 29 different end organs. Because of extreme ease in collection at 8–10 years of age before calcification and minimal to no morbidity, these will probably constitute a major source of cells for personal banking, research and current or future therapies. These stem cells have been shown capable of producing hepatocytes.[citation needed]
Amniotic
Multipotent stem cells are also found in amniotic fluid. These stem cells are very active, expand extensively without feeders and are not tumorigenic. Amniotic stem cells are multipotent and can differentiate in cells of adipogenic, osteogenic, myogenic, endothelial, hepatic and also neuronal lines.[32] All over the world, universities and research institutes are studying amniotic fluid to discover all the qualities of amniotic stem cells, and scientists such as Anthony Atala[33][34] and Giuseppe Simoni [35][36] have discovered important results. Use of stem cells from amniotic fluid overcomes the ethical objections to using human embryos as a source of cells. Roman Catholic teaching forbids the use of embryonic stem cells in experimentation; accordingly, the Vatican newspaper "Osservatore Romano" called amniotic stem cells "the future of medicine".[37]
Stem cell It is possible to collect amniotic stem cells for donors or for autologuous use: the first US amniotic stem cells bank [38][39] was opened in 2009 in Medford, MA, by Biocell Center Corporation[40][41][42] and collaborates with various hospitals and universities all over the world.[43]
272
Cord blood
A certain kind of cord blood stem cell (CB-SC) is multipotent and displays embryonic and hematopoietic characteristics. Phenotypic characterization demonstrates that (CB-SCs) display embryonic cell markers (e.g., transcription factors OCT-4 and Nanog, stage-specific embryonic antigen (SSEA)-3, and SSEA-4) and leukocyte common antigen CD45, but that they are negative for blood cell lineage markers (e.g., CD1a, CD3, CD4, CD8, CD11b, CD11c, CD13, CD14, CD19, CD20, CD34, CD41a, CD41b, CD83, CD90, CD105, and CD133).[44][] Additionally, CB-SCs display very low immunogenicity as indicated by expression of a very low level of major histocompatibility complex (MHC) antigens and failure to stimulate the proliferation of allogeneic lymphocytes.[44][45] They can give rise to three embryonic layer-derived cells in the presence of different inducers.[44][] More specifically, CB-SCs tightly adhere to culture dishes with a large rounded morphology and are resistant to common detaching methods (trypsin/EDTA).[44][45][] CB-SCs are the active agent in stem cell educator therapy, which has therapeutic potential against autoimmune diseases like type 1 diabetes according to studies by Yong Zhao et al.[][46][47][48]Wikipedia:Identifying reliable sources (medicine)
Induced pluripotent
These are not adult stem cells, but rather adult cells (e.g. epithelial cells) reprogrammed to give rise to pluripotent capabilities. Using genetic reprogramming with protein transcription factors, pluripotent stem cells equivalent to embryonic stem cells have been derived from human adult skin tissue.[][49][50] Shinya Yamanaka and his colleagues at Kyoto University used the transcription factors Oct3/4, Sox2, c-Myc, and Klf4[] in their experiments on cells from human faces. Junying Yu, James Thomson, and their colleagues at the University of Wisconsin–Madison used a different set of factors, Oct4, Sox2, Nanog and Lin28,[] and carried out their experiments using cells from human foreskin. As a result of the success of these experiments, Ian Wilmut, who helped create the first cloned animal Dolly the Sheep, has announced that he will abandon somatic cell nuclear transfer as an avenue of research.[51] Frozen blood samples can be used as a source of induced pluripotent stem cells, opening a new avenue for obtaining the valued cells.[52]
Lineage
To ensure self-renewal, stem cells undergo two types of cell division (see Stem cell division and differentiation diagram). Symmetric division gives rise to two identical daughter cells both endowed with stem cell properties. Asymmetric division, on the other hand, produces only one stem cell and a progenitor cell with limited self-renewal potential. Progenitors can go through several rounds of cell division before terminally differentiating into a mature cell. It is possible that the molecular distinction between symmetric and asymmetric divisions lies in differential segregation of cell membrane proteins (such as receptors) between the daughter cells.[53] An alternative theory is that stem cells remain undifferentiated due to environmental cues in their particular niche. Stem cells differentiate when they leave that niche or no longer receive those signals. Studies in Drosophila germarium have identified the signals decapentaplegic and adherens junctions that prevent germarium stem cells from differentiating.[54][55]
Stem cell The signals that lead to reprogramming of cells to an embryonic-like state are also being investigated. These signal pathways include several transcription factors including the oncogene c-Myc. Initial studies indicate that transformation of mice cells with a combination of these anti-differentiation signals can reverse differentiation and may allow adult cells to become pluripotent.[] However, the need to transform these cells with an oncogene may prevent the use of this approach in therapy. Challenging the terminal nature of cellular differentiation and the integrity of lineage commitment, it was recently determined that the somatic expression of combined transcription factors can directly induce other defined somatic cell fates; researchers identified three neural-lineage-specific transcription factors that could directly convert mouse fibroblasts (skin cells) into fully functional neurons. This "induced neurons" (iN) cell research inspires the researchers to induce other cell types. It implies that all cells are totipotent: with the proper tools, all cells may form all kinds of tissue.[56]
273
Treatments
Medical researchers believe that stem cell therapy has the potential to dramatically change the treatment of human disease. A number of adult stem cell therapies already exist, particularly bone marrow transplants that are used to treat leukemia.[58] In the future, medical researchers anticipate being able to use technologies derived from stem cell research to treat a wider variety of diseases including cancer, Parkinson's disease, spinal cord injuries, Amyotrophic lateral sclerosis, multiple sclerosis, and muscle damage, amongst a number of other impairments and conditions.[59][60] However, there still [57] Diseases and conditions where stem cell treatment is promising or emerging. Bone exists a great deal of social and marrow transplantation is, as of 2009, the only established use of stem cells. scientific uncertainty surrounding stem cell research, which could possibly be overcome through public debate and future research, and further education of the public. One concern of treatment is the risk that transplanted stem cells could form tumors and become cancerous if cell division continues uncontrollably.[61] Stem cells are widely studied, for their potential therapeutic use and for their inherent interest.[62] Supporters of embryonic stem cell research argue that such research should be pursued because the resultant treatments could have significant medical potential. It has been proposed that surplus embryos created for in vitro fertilization could be donated with consent and used for the research. The recent development of iPS cells has been called a bypass of the legal controversy. Laws limiting the destruction of human embryos have been credited for being the reason for development of iPS cells, but it is still not completely clear whether hiPS cells are equivalent to hES cells. Recent work demonstrates hotspots of aberrant epigenomic reprogramming in hiPS cells (Lister, R., et al., 2011).
Stem cell
274
Toxicity screening
Hepatotoxicity and drug-induced liver injury account for a substantial number of failures of new drugs in development and market withdrawal, highlighting the need for screening assays such as stem cell-derived hepatocyte-like cells, that are capable of detecting toxicity early in the drug development process.[]
Research patents
The patents covering a lot of work on human embryonic stem cells are owned by the Wisconsin Alumni Research Foundation (WARF). WARF does not charge academics to study human stem cells but does charge commercial users. WARF sold Geron Corp. exclusive rights to work on human stem cells but later sued Geron Corp. to recover some of the previously sold rights. The two sides agreed that Geron Corp. would keep the rights to only three cell types. In 2001, WARF came under public pressure to widen access to human stem-cell technology.[63] A request for reviewing the WARF patents 5,843,780; 6,200,806; 7,029,913 US Patent and Trademark Office were filed by non-profit patent-watchdogs The Foundation for Taxpayer & Consumer Rights [64], and the Public Patent Foundation as well as molecular biologist Jeanne Loring of the Burnham Institute. According to them, two of the patents granted to WARF are invalid because they cover a technique published in 1993 for which a patent had already been granted to an Australian researcher. Another part of the challenge states that these techniques, developed by James A. Thomson, are rendered obvious by a 1990 paper and two textbooks. Based on this challenge, patent 7,029,913 was rejected in 2010. The two remaining hES WARF patents are due to expire in 2015. The outcome of this legal challenge is particularly relevant to the Geron Corp. as it can only license patents that are upheld.[64]
Key research events
• 1908: The term "stem cell" was proposed for scientific use by the Russian histologist Alexander Maksimov (1874–1928) at congress of hematologic society in Berlin. It postulated existence of haematopoietic stem cells. • 1960s: Joseph Altman and Gopal Das present scientific evidence of adult neurogenesis, ongoing stem cell activity in the brain; their reports contradict Cajal's "no new neurons" dogma and are largely ignored. • 1963: McCulloch and Till illustrate the presence of self-renewing cells in mouse bone marrow. • 1968: Bone marrow transplant between two siblings successfully treats SCID. • 1978: Haematopoietic stem cells are discovered in human cord blood. • 1981: Mouse embryonic stem cells are derived from the inner cell mass by scientists Martin Evans, Matthew Kaufman, and Gail R. Martin. Gail Martin is attributed for coining the term "Embryonic Stem Cell". • 1992: Neural stem cells are cultured in vitro as neurospheres. • 1997: Leukemia is shown to originate from a haematopoietic stem cell, the first direct evidence for cancer stem cells. • 1998: James Thomson and coworkers derive the first human embryonic stem cell line at the University of Wisconsin–Madison.[] • 1998: John Gearhart (Johns Hopkins University) extracted germ cells from fetal gonadal tissue (primordial germ cells) before developing pluripotent stem cell lines from the original extract. • 2000s: Several reports of adult stem cell plasticity are published. • 2001: Scientists at Advanced Cell Technology clone first early (four- to six-cell stage) human embryos for the purpose of generating embryonic stem cells.[65] • 2003: Dr. Songtao Shi of NIH discovers new source of adult stem cells in children's primary teeth.[66] • 2004–2005: Korean researcher Hwang Woo-Suk claims to have created several human embryonic stem cell lines from unfertilised human oocytes. The lines were later shown to be fabricated.
Stem cell • 2005: Researchers at Kingston University in England claim to have discovered a third category of stem cell, dubbed cord-blood-derived embryonic-like stem cells (CBEs), derived from umbilical cord blood. The group claims these cells are able to differentiate into more types of tissue than adult stem cells. • 2005: Researchers at UC Irvine's Reeve-Irvine Research Center are able to partially restore the ability of rats with paralyzed spines to walk through the injection of human neural stem cells.[67] • April 2006 Scientists at the University of Illinois at Chicago identified novel stem cells from the umbilical cord blood with embryonic and hematopoietic characteristics.[44] • August 2006: Mouse Induced pluripotent stem cells: the journal Cell publishes Kazutoshi Takahashi and Shinya Yamanaka.[68] • November 2006: Yong Zhao et al. revealed the immune regulation of T lymphocytes by Cord Blood-Derived Multipotent Stem Cells (CB-SCs).[45] • October 2006: Scientists at Newcastle University in England create the first ever artificial liver cells using umbilical cord blood stem cells.[69][70]
275
• January 2007: Scientists at Wake Forest University led by Dr. Anthony Atala and Harvard University report discovery of a new type of stem cell in amniotic fluid.[71] This may potentially provide an alternative to embryonic stem cells for use in research and therapy.[72]
Yong Zhao, University of Illinois at Chicago
• June 2007: Research reported by three different groups shows that normal skin cells can be reprogrammed to an embryonic state in mice.[73] In the same month, scientist Shoukhrat Mitalipov reports the first successful creation of a primate stem cell line through somatic cell nuclear transfer[74] • October 2007: Mario Capecchi, Martin Evans, and Oliver Smithies win the 2007 Nobel Prize for Physiology or Medicine for their work on embryonic stem cells from mice using gene targeting strategies producing genetically engineered mice (known as knockout mice) for gene research.[] • November 2007: Human induced pluripotent stem cells: Two similar papers released by their respective journals prior to formal publication: in Cell by Kazutoshi Takahashi and Shinya Yamanaka, "Induction of pluripotent stem cells from adult human fibroblasts by defined factors",[75] and in Science by Junying Yu, et al., from the research group of James Thomson, "Induced pluripotent stem cell lines derived from human somatic cells":[76] pluripotent stem cells generated from mature human fibroblasts. It is possible now to produce a stem cell from almost any other human cell instead of using embryos as needed previously, albeit the risk of tumorigenesis due to c-myc and retroviral gene transfer remains to be determined. • January 2008: Robert Lanza and colleagues at Advanced Cell Technology and UCSF create the first human embryonic stem cells without destruction of the embryo[77]
Martin Evans, a co-winner of the Nobel Prize in recognition of his gene targeting work.
• January 2008: Development of human cloned blastocysts following somatic cell nuclear transfer with adult fibroblasts[78] • February 2008: Generation of pluripotent stem cells from adult mouse liver and stomach: these iPS cells seem to be more similar to embryonic stem cells than the previously developed iPS cells and not tumorigenic, moreover genes that are required for iPS cells do not need to be inserted into specific sites, which encourages the development of non-viral reprogramming techniques.[79]
Stem cell • March 2008-The first published study of successful cartilage regeneration in the human knee using autologous adult mesenchymal stem cells is published by clinicians from Regenerative Sciences[80] • October 2008: Sabine Conrad and colleagues at Tübingen, Germany generate pluripotent stem cells from spermatogonial cells of adult human testis by culturing the cells in vitro under leukemia inhibitory factor (LIF) supplementation.[81] • 30 October 2008: Embryonic-like stem cells from a single human hair.[82] • January 2009: Yong Zhao and colleagues confirmed the reversal of autoimmune-caused type 1 diabetes by Cord Blood-Derived Multipotent Stem Cells (CB-SCs) in an animal experiment.[][46] • 1 March 2009: Andras Nagy, Keisuke Kaji, et al. discover a way to produce embryonic-like stem cells from normal adult cells by using a novel "wrapping" procedure to deliver specific genes to adult cells to reprogram them into stem cells without the risks of using a virus to make the change.[83][84][85] The use of electroporation is said to allow for the temporary insertion of genes into the cell.[86][87][88][89] • 28 May 2009 Kim et al. announced that they had devised a way to manipulate skin cells to create patient specific "induced pluripotent stem cells" (iPS), claiming it to be the 'ultimate stem cell solution'.[90] • 11 October 2010 First trial of embryonic stem cells in humans.[91] • 25 October 2010: Ishikawa et al. write in the Journal of Experimental Medicine that research shows that transplanted cells that contain their new host's nuclear DNA could still be rejected by the invidual's immune system due to foreign mitochondrial DNA. Tissues made from a person's stem cells could therefore be rejected, because mitochondrial genomes tend to accumulate mutations.[92] • 2011: Israeli scientist Inbar Friedrich Ben-Nun led a team which produced the first stem cells from endangered species, a breakthrough that could save animals in danger of extinction.[93] • January 2012: The human clinical trial of treating type 1 diabetes with lymphocyte modification using Cord Blood-Derived Multipotent Stem Cells (CB-SCs) achieved an improvement of C-peptide levels, reduced the median glycated hemoglobin A1C (HbA1c) values, and decreased the median daily dose of insulin in both human patient groups with and without residual beta cell function.[47][48] Yong Zhao's Stem Cell Educator Therapy appears "so simple and so safe"[94] • 2012: Katsuhiko Hayashi et al. reported in the Journal Science that they used mouse skin cells to create stem cells and then used these stem cells to create mouse eggs. These eggs were then fertilized and produced healthy baby offspring. These latter mice were able to have their own babies.[95]
276
References
[51] "His inspiration comes from the research by Prof Shinya Yamanaka at Kyoto University, which suggests a way to create human embryo stem cells without the need for human eggs, which are in extremely short supply, and without the need to create and destroy human cloned embryos, which is bitterly opposed by the pro life movement." [52] Frozen blood a source of stem cells, study finds (http:/ / web. archive. org/ web/ 20100703175036/ http:/ / www. newsdaily. com/ stories/ tre6604si-us-stemcells-frozen/ ). newsdaily.com (2010-07-01) [57] Diabetes, rheumatoid arthritis, Parkinson's, Alzheimer's disease, osteoarthritis: • Cell Basics: What are the potential uses of human stem cells and the obstacles that must be overcome before these potential uses will be realized? (http:/ / stemcells. nih. gov/ info/ basics/ basics6Stem). In Stem Cell Information World Wide Web site. Bethesda, MD: National Institutes of Health, U.S. Department of Health and Human Services, 2009. cited Sunday, April 26, 2009
Stroke and traumatic brain injury repair:
• Stem Cells Tapped to Replenish Organs (http:/ / www. mult-sclerosis. org/ news/ Dec2000/ StemCellDebatePartII. html) thescientist.com, Nov 2000. By Douglas Steinberg
Learning defects:
• ISRAEL21c: Israeli scientists reverse brain birth defects using stem cells (http:/ / www. israel21c. org/ health/ israeli-scientists-reverse-brain-birth-defects-using-stem-cells) December 25, 2008. (Researchers from the Hebrew University of Jerusalem-Hadassah Medical led by Prof. Joseph Yanai)
Spinal cord injury repair:
Stem cell Heart infarction: Anti-cancer:
• thescientist.com, Nov 2000. By Douglas Steinberg
277
Baldness:
• Hair Cloning Nears Reality as Baldness Cure (http:/ / web. archive. org/ web/ 20080530042215rn_3/ www. webmd. com/ skin-problems-and-treatments/ hair-loss/ news/ 20041104/ hair-cloning-nears-reality-as-baldness-cure) WebMD November 2004
Replace missing teeth: Repair hearing:
• Gene therapy is first deafness 'cure' – health – 14 February 2005 – New Scientist (http:/ / www. newscientist. com/ article/ dn7003)
Restore vision:
• BBC NEWS | England | Southern Counties | Stem cells used to restore vision (http:/ / news. bbc. co. uk/ 1/ hi/ england/ southern_counties/ 4495419. stm)
Amyotrophic lateral sclerosis:
• Drs. Gearhart and Kerr of Johns Hopkins University. April 4, 2001 edition of JAMA (Vol. 285, 1691–1693)
Crohn's disease: Wound healing:
[61] "Stem-cell therapy: Promise and reality." Consumer Reports on Health 17.6 (2005): 8–9. Academic Search Premier. EBSCO. Web. 5 Apr. 2010. [63] Regalado, Antonio, David P. Hamilton (July 2006). "How a University's Patents May Limit Stem-Cell Researcher." (http:/ / www. geneticsandsociety. org/ article. php?id=1896) The Wall Street Journal. Retrieved on July 24, 2006. [64] Kintisch, Eli (2006-07-18) "Groups Target Stem Cell Patents." (http:/ / news. sciencemag. org/ sciencenow/ 2006/ 07/ 18-02. html) ScienceNOW Daily News. Retrieved August 15, 2006. [90] (cited in lay summary, not read) [93] Shtull-Trauring, Asaf (2011-09-06) Israeli scientist leads breakthrough stem cell research on endangered species (http:/ / www. haaretz. com/ print-edition/ news/ israeli-scientist-leads-breakthrough-stem-cell-research-on-endangered-species-1. 382754)
External links
General • Stem Cell Basics (http://stemcells.nih.gov/info/basics/) • Nature Reports Stem Cells: Introductory material, research advances and debates concerning stem cell research. (http://www.nature.com/stemcells) • Understanding Stem Cells: A View of the Science and Issues from the National Academies (http://dels.nas.edu/ bls/stemcells/booklet.shtml) • Scientific American Magazine (June 2004 Issue) The Stem Cell Challenge (http://www.scientificamerican. com/article.cfm?id=the-stem-cell-challenge) • Scientific American Magazine (July 2006 Issue) Stem Cells: The Real Culprits in Cancer? (http://www. scientificamerican.com/article.cfm?id=stem-cells-the-real-culpr-2006-07) • Ethics of Stem Cell Research (http://plato.stanford.edu/entries/stem-cells) entry by Andrew Siegel in the Stanford Encyclopedia of Philosophy • Isolation of amniotic stem cell lines with potential for therapy (http://www.nature.com/nbt/journal/v25/n1/ abs/nbt1274.html) • Children's Hospital Stem Cell Research (http://stemcell.childrenshospital.org) • Stem Cell Research and Industry Directory (http://stemcelllist.com) • Corneal endothelial and epithelial stem cell research and application (http://www.cesbank.org) • Stem Cell Consumer Progress and Research (http://www.stemcelltelevision.com) Peer-reviewed journals • Cytotherapy (http://www.tandf.co.uk/journals/titles/14653249.asp)
Stem cell • • • • • Cloning and Stem Cells (http://www.liebertpub.com/products/product.aspx?pid=9) Journal of Stem Cells and Regenerative Medicine (http://www.pubstemcell.com) Stem Cells and Development (http://www.liebertpub.com/products/product.aspx?pid=125) Regenerative Medicine (http://www.futuremedicine.com/loi/rme) Stem Cell Research (http://www.elsevier.com/wps/find/journaldescription.cws_home/711630/ description#description) • StemBook (http://www.stembook.org)
278
Huxley's layer
279
Huxley's layer
Huxley's layer
Transverse section of hair follicle. Gray's subject #234 1068
[1]
The second layer of the inner root sheath of the hair consists of one or two layers of horny, flattened, nucleated cells, known as Huxley's layer.
Henle's layer
280
Henle's layer
Henle's layer
Transverse section of hair follicle. Gray's subject #234 1068
[1]
Henle's layer is the third layer of the inner root sheath of the hair, consisting of a single layer of cubical cells with clear flattened nuclei. It is named after German physician, pathologist and anatomist Friedrich Gustav Jakob Henle.
External links
• synd/649 [1] at Who Named It? This article incorporates text from a public domain edition of Gray's Anatomy.
Trichocyte (human)
In mammals, trichocytes are the specialized epithelial cells from which the highly mechanically resilient tissues hair and nails are formed. They can be identified by the fact that they express "hard", "trichocyte" or "hair" keratin proteins.[1] These are modified keratins containing large amounts of the amino acid cysteine, which facilitates chemical cross-linking of these proteins to form the tough material from which hair and nail is composed. These cells give rise to non-hair non-keratinized IRSC (inner root sheath cell) as well.
References
Epithelium
281
Epithelium
Epithelium
Latin Epithelium Code TH H2.00.02.0.00001 [1]
Epithelium is one of the four basic types of animal tissue, along with connective tissue, muscle tissue and nervous tissue. Epithelial tissues line the cavities and surfaces of structures throughout the body, and also form many glands. Functions of epithelial cells include secretion, selective absorption, protection, transcellular transport and detection of sensation. In Greek "ἐπί" ("epi") means "on" or "upon", and "θηλή" ("thēlē") means "nipple".[1] Epithelial layers are avascular, so they must receive nourishment via diffusion of substances from the underlying connective tissue, through the basement membrane.[][2] Epithelia can also be organized into clusters of cells that function as exocrine and endocrine glands.
Structure
Cells in epithelium are very densely packed together like bricks in a wall, leaving very little intercellular space. The cells can form continuous sheets which are attached to each other at many locations by adherens junctions, tight junctions and desmosomes.[]
Basement membrane
All epithelial cells rest on a basement membrane, which acts as a scaffolding on which epithelium can grow and regenerate after injuries.[3] Epithelial tissue is innervated, but avascular. This epithelial tissue must be nourished by substances diffusing from the blood vessels in the underlying tissue, but they don't have their own blood supply. The basement membrane acts as a selectively permeable membrane that determines which substances will be able to enter the epithelium.[][2]
Cell junctions
Cell junctions are especially abundant in epithelial tissues. They consist of protein complexes and provide contact between neighbouring cells, between a cell and the extracellular matrix, or they build up the paracellular barrier of epithelia and control the paracellular transport.[citation needed] Cell junctions are the contact points between plasma membrane and tissue cells. There are mainly 5 different types of cell junctions. They are tight junctions, adherens junctions, desmosomes, hemidesmosomes, and gap junctions. Tight junctions are a pair of trans-membranar protein fused on outer plasma membrane. Adherens junctions are a plaque (protein layer on the inside plasma membrane) which attaches both cells' microfilaments. Desmosomes attach to the microfilaments of cytoskeleton made up of keratin protein. Hemidesmosomes resemble desmosomes on a section. They are made up of the integrin (a transmembraner protein) instead of cadherin. They attach the epithelial cell to the basement membrane. Gap junctions connect the cytoplasm of two cells and are made up of proteins called connexins (six of which come together to make a connexon).
Epithelium
282
Classification
Tissues are generally classified by the morphology of their cells, and the number of layers they are composed of.[][][4] Epithelial tissue that is only one cell thick is known as simple epithelium.[5] If it is two or more cells thick, it is known as stratified epithelium.[6] However, when taller simple epithelial cells (see columnar, Types of epithelium below) are viewed in cross section with several nuclei appearing at different heights, they can be confused with stratified epithelia. This kind of epithelium is therefore described as "pseudostratified" epithelium.[7] There are three principal morphologies associated with epithelial cells. Squamous epithelium has cells which are wider than they are tall (flat and scale-like). Cuboidal epithelium has cells whose height and width are approximately the same (cube shaped). Columnar epithelium has cells taller than they are wide (column shaped). In addition, the morphology of the cells in transitional epithelium may vary from squamous to cuboidal, depending on the amount of tension on the epithelium.[8]
Simple epithelium
Simple epithelium is one cell thick, that is, every cell is in direct contact with the underlying basement membrane. It is generally found where absorption and filtration occur. The thinness of the epithelial barrier facilitates these processes.[] Simple epithelial tissues are generally classified by the shape of their cells. The four major classes of simple epithelium are: (1) simple squamous; (2) simple cuboidal; (3) simple columnar; (4) pseudostratified.[] Simple squamous epithelium is found lining areas where passive diffusion of gases occur, including the walls of capillaries, the linings of the alveoli of the lungs, and the linings of the pericardial, pleural, and peritoneal cavities.
Functions
The primary functions of epithelial tissues are: (1) to protect the tissues that lie beneath it from radiation, desiccation, toxins, invasion by pathogens, and physical trauma; (2) the regulation and exchange of chemicals between the underlying tissues and a body cavity; (3) the secretion of hormones into the blood vascular system, and/or the secretion of sweat, mucus, enzymes, and other products that are delivered by ducts glandular epithelium;[9] (4) to provide sensation [11].
Secretory epithelia
As stated above, secretion is one major function of epithelial cells. Glands are formed from the invagination / infolding of epithelial cells and subsequent growth in the underlying connective tissue. There are two major classifications of glands: endocrine glands and exocrine glands. Endocrine glands secrete their product into the extracellular space where it is rapidly taken up by the blood vascular system. The exocrine glands secrete their products into a duct that then delivers the product to the lumen of an organ or onto the free surface of the epithelium. In arthropods, the integument, or external "skin", consists of a single layer of epithelial ectoderm from which arises the cuticle,[] an outer covering of chitin the rigidity of which varies as per its chemical composition.
Epithelium
283
Sensing the extracellular environment
"Some epithelial cells are ciliated, and they commonly exist as a sheet of polarised cells forming a tube or tubule with cilia projecting into the lumen." Primary cilia on epithelial cells provide chemosensation, thermosensation and mechanosensation of the extracellular environment by playing "a sensory role mediating specific signalling cues, including soluble factors in the external cell environment, a secretory role in which a soluble protein is released to have an effect downstream of the fluid flow, and mediation of fluid flow if the cilia are motile."[]
Embryological development
In general, there are epithelial tissues deriving from all of the embryological germ layers[citation needed]: • from ectoderm (e.g., the epidermis); • from endoderm (e.g., the lining of the gastrointestinal tract); • from mesoderm (e.g., the inner linings of body cavities). However, it is important to note that pathologists do not consider endothelium and mesothelium (both derived from mesoderm) to be true epithelium. This is because such tissues present very different pathology. For that reason, pathologists label cancers in endothelium and mesothelium sarcomas, whereas true epithelial cancers are called carcinomas. Also, the filaments that support these mesoderm-derived tissues are very distinct. Outside of the field of pathology, it is, in general, accepted that the epithelium arises from all three germ layers.[citation needed]
Growing in culture
When growing epithelium in culture, one can determine whether or not a particular cell is epithelial by examining its morphological characteristics. Epithelial cells tend to cluster together, and have a "characteristic tight pavementlike appearance". But this is not always the case, such as when the cells are derived from a tumor. In these cases, it is often necessary to use certain biochemical markers to make a positive identification. The intermediate filament proteins in the cytokeratin group are almost exclusively found in epithelial cells, and so are often used for this purpose.[10]
Location
Epithelium lines both the outside (skin) and the inside cavities and lumen of bodies. The outermost layer of our skin is composed of dead stratified squamous, keratinized epithelial cells.[citation needed] Tissues that line the inside of the mouth, the esophagus and part of the rectum are composed of nonkeratinized stratified squamous epithelium. Other surfaces that separate body cavities from the outside environment are lined by simple squamous, columnar, or pseudostratified epithelial cells. Other epithelial cells line the insides of the lungs, the gastrointestinal tract, the reproductive and urinary tracts, and make up the exocrine and endocrine glands. The outer surface of the cornea is covered with fast-growing, easily regenerated epithelial cells. Endothelium (the inner lining of blood vessels, the heart, and lymphatic vessels) is a specialized form of epithelium. Another type, mesothelium, forms the walls of the pericardium, pleurae, and peritoneum.[citation needed]
Epithelium
284
System circulatory digestive digestive digestive digestive digestive digestive digestive digestive digestive digestive
Tissue blood vessels ducts of submandibular glands attached gingiva dorsum of tongue hard palate oesophagus stomach small intestine large intestine rectum anus Simple squamous Stratified columnar
Epithelium
Subtype endothelium gastric epithelium intestinal epithelium intestinal epithelium -
Stratified squamous, keratinized Stratified squamous, keratinized Stratified squamous, keratinized Stratified squamous, non-keratinized Simple columnar, non-ciliated Simple columnar, non-ciliated Simple columnar, non-ciliated Simple columnar, non-ciliated Stratified squamous, non-keratinized superior to Hilton's white line Stratified squamous, keratinized inferior to Hilton's white line Simple columnar, non-ciliated Simple cuboidal Simple cuboidal Simple squamous Stratified squamous, keratinized Stratified cuboidal Simple squamous Simple cuboidal
digestive endocrine nervous lymphatic integumentary integumentary integumentary reproductive - female
gallbladder thyroid follicles ependyma lymph vessel skin - dead superficial layer sweat gland ducts mesothelium of body cavities ovaries
endothelium mesothelium germinal epithelium (female) germinal epithelium (male) -
reproductive - female reproductive - female reproductive - female reproductive - female reproductive - female reproductive - female reproductive - male
Fallopian tubes endometrium (uterus) cervix (endocervix) cervix (ectocervix) vagina labia majora tubuli recti
Simple columnar, ciliated Simple columnar, ciliated Simple columnar Stratified squamous, non-keratinized Stratified squamous, non-keratinized Stratified squamous, keratinized Simple cuboidal
reproductive - male reproductive - male reproductive - male reproductive - male reproductive - male reproductive - male (gland) reproductive - male (gland)
rete testis ductuli efferentes epididymis vas deferens ejaculatory duct bulbourethral glands
Simple cuboidal Pseudostratified columnar Pseudostratified columnar, with stereocilia Pseudostratified columnar Simple columnar Simple columnar
seminal vesicle
Pseudostratified columnar
-
Epithelium
285
oropharynx larynx larynx - True vocal cords trachea respiratory bronchioles cornea nose kidney - proximal convoluted tubule kidney - ascending thin limb Stratified squamous, non-keratinized Pseudostratified columnar, ciliated Stratified squamous, non-keratinized Pseudostratified columnar, ciliated Simple cuboidal Stratified squamous, non-keratinized Pseudostratified columnar Simple cuboidal, with microvilli respiratory epithelium respiratory epithelium corneal epithelium olfactory epithelium -
respiratory respiratory respiratory respiratory respiratory sensory sensory urinary
urinary urinary urinary urinary urinary urinary urinary urinary urinary urinary
Simple squamous
urothelium urothelium urothelium urothelium -
kidney - distal convoluted tubule Simple cuboidal, without microvilli kidney - collecting duct renal pelvis ureter urinary bladder prostatic urethra membranous urethra penile urethra external urethral orifice Simple cuboidal Transitional Transitional Transitional Transitional Pseudostratified columnar, non-ciliated Pseudostratified columnar, non-ciliated Stratified squamous
Additional images
Squamous Epithelium 100x
Human cheek cells (Nonkeratinized stratified squamous epithelium) 500x
Epithelium
286
References
Notes
[1] Epitheium at Wiktionary (http:/ / en. wiktionary. org/ wiki/ epithelium) [2] Freshney, 2002: p. 3 (http:/ / books. google. com/ books?id=KqKNxeWlU6MC& pg=PA3) [5] van Lommel, 2002: p. 94 (http:/ / books. google. com/ books?id=EvYjLNKLu9sC& pg=PA94) [6] van Lommel, 2002: p. 97 (http:/ / books. google. com/ books?id=EvYjLNKLu9sC& pg=PA97) [9] van Lommel, 2002: p. 91 (http:/ / books. google. com/ books?id=EvYjLNKLu9sC& pg=PA91) [10] Freshney, 2002: p. 9 (http:/ / books. google. com/ books?id=KqKNxeWlU6MC& pg=PA9)
Bibliography
• Freshney, R.I. (2002). "Introduction" (http://books.google.com/books?id=KqKNxeWlU6MC&pg=PA1). In Freshney, R. Ian & Freshney, Mary. Culture of epithelial cells. John Wiley & Sons. ISBN 978-0-471-40121-6. • van Lommel, Alfons T.L. (2002). From cells to organs: a histology textbook and atlas (http://books.google. com/books?id=EvYjLNKLu9sC). Springer. ISBN 978-1-4020-7257-4.
Further reading
• Green H (September 2008). "The birth of therapy with cultured cells". BioEssays 30 (9): 897–903. doi: 10.1002/bies.20797 (http://dx.doi.org/10.1002/bies.20797). PMID 18693268 (http://www.ncbi.nlm.nih. gov/pubmed/18693268). • Kefalides, Nicholas A. & Borel, Jacques P., ed. (2005). Basement membranes: cell and molecular biology (http:// books.google.com/books?id=RM-FVY47NEgC). Gulf Professional Publishing. ISBN 978-0-12-153356-4. • Nagpal R, Patel A, Gibson MC (March 2008). "Epithelial topology". BioEssays 30 (3): 260–6. doi: 10.1002/bies.20722 (http://dx.doi.org/10.1002/bies.20722). PMID 18293365 (http://www.ncbi.nlm.nih. gov/pubmed/18293365). • Yamaguchi Y, Brenner M, Hearing VJ (September 2007). "The regulation of skin pigmentation" (http://www. jbc.org/cgi/pmidlookup?view=long&pmid=17635904) (Review). J. Biol. Chem. 282 (38): 27557–61. doi: 10.1074/jbc.R700026200 (http://dx.doi.org/10.1074/jbc.R700026200). PMID 17635904 (http://www.ncbi. nlm.nih.gov/pubmed/17635904).
Squamous epithelial cell
287
Squamous epithelial cell
Squamous epithelial cell
Squamous epithelium is one of several types of epithelia. Code TH H2.00.02.0.01027
[1]
In anatomy, squamous epithelium (from Latin squama, "scale") is an epithelium characterised by its most superficial layer consisting of flat, scale-like cells called squamous epithelial cells. Epithelium may be composed of one layer of these cells, in which case it is referred to as simple squamous epithelium, or it may possess multiple layers, referred to then as stratified squamous epithelium. Both types perform differing functions, ranging from nutrient exchange to protection.[citation needed] Cancers of the squamous epithelium include squamous cell carcinoma, basal cell carcinoma, and other adnexal tumors.[citation needed] Squamous epithelial cells have a polygonal appearance when viewed from above.[1]
References External links
• Histology at KUMC epithel-epith02 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/epithel/ epith02.htm) Simple squamous epithelium of the glomerulus (kidney) • Diagrams of simple squamous epithelium (http://www.lima.ohio-state.edu/academics/biology/images/ anatomy/Simple Squamous Epithelium 400X.jpg) • Histology at KUMC epithel-epith12 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/epithel/ epith12.htm) Stratified squamous epithelium of the vagina • Histology at KUMC epithel-epith14 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/epithel/ epith14.htm) Stratified squamous epithelium of the skin (thin skin) • Histology at KUMC epithel-epith15 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/epithel/ epith15.htm) Stratified squamous epithelium of the skin (thick skin) • Stratified squamous epithelium of the esophagus (http://bioweb.uwlax.edu/zoolab/Table_of_Contents/ Lab-1b/Cross_section_of_the_esophagou/Stratified_squamous_epithelium/stratified_squamous_epithelium. htm) • Research News about Squamous Cell (http://www.ningishzida.com/classifieds/Squamous_Cell.html)
Hair cell
288
Hair cell
Neuron: PswiandfSW
Section through the spiral organ of Corti. Magnified. ("Outer hair cells" labeled near top; "inner hair cells" labeled near center). Location Function Morphology Presynaptic connections Postsynaptic connections Gray's NeuroLex ID Cochlea Amplify sound waves and transduce auditory information to the Brain Stem Unique (see text) None Via auditory nerve to vestibulocochlear nerve to inferior colliculus subject #232 1057 nifext_61 [2] [1]
Hair cells are the sensory receptors of both the auditory system and the vestibular system in all vertebrates. In mammals, the auditory hair cells are located within the organ of Corti on a thin basilar membrane in the cochlea of the inner ear. They derive their name from the tufts of stereocilia that protrude from the apical surface of the cell, a structure known as the hair bundle, into the scala media, a fluid-filled tube within the cochlea. Mammalian cochlear hair cells come in two anatomically and functionally distinct types: the outer and inner hair cells. Damage to these hair cells results in decreased hearing sensitivity, i.e. sensorineural hearing loss.
Hair bundles as sound detectors and amplifiers
Research of the past decades has shown that outer hair cells do not send neural signals to the brain, but that they mechanically amplify low-level sound that enters the cochlea. The amplification may be powered by movement of their hair bundles, or by an electrically driven motility of their cell bodies. The inner hair cells transform the sound vibrations in the fluids of the cochlea into electrical signals that are then relayed via the auditory nerve to the auditory brainstem and to the auditory cortex. Results in recent years further indicate that mammals apparently have conserved an evolutionarily earlier type of hair-cell motility. This so-called hair-bundle motility amplifies sound in all non-mammalian land vertebrates. It is affected by the closing mechanism of the mechanical sensory ion channels at the tips of the hair bundles. Thus, the same hair-bundle mechanism that detects sound vibrations also actively "vibrates back" and thereby mechanically amplifies weak incoming sound.
Hair cell
289
Inner hair cells – from sound to nerve signal
The deflection of the hair-cell stereocilia opens mechanically gated ion channels that allow any small, positively charged ions (primarily potassium and calcium) to enter the cell.[1] Unlike many other electrically active cells, the hair cell itself does not fire an action potential. Instead, the influx of positive ions from the endolymph in Scala media depolarizes the cell, resulting in a receptor potential. This receptor potential opens voltage gated calcium channels; calcium ions then enter the cell and trigger the release of neurotransmitters at the basal end of the cell. The neurotransmitters diffuse across the narrow space between the hair cell and a nerve terminal, where they then bind to receptors and thus trigger action Section through the organ of corti, showing inner and outer hair cells potentials in the nerve. In this way, the mechanical sound signal is converted into an electrical nerve signal. The repolarization in the hair cell is done in a special manner. The Perilymph in Scala tympani has a very low concentration of positive ions. The electrochemical gradient makes the positive ions flow through channels to the Perilymph. Hair cells chronically leak Ca2+. This leakage causes a tonic release of neurotransmitter to the synapses. It is thought that this tonic release is what allows the hair cells to respond so quickly in response to mechanical stimuli. The quickness of the hair cell response may also be due to that fact that it can increase the amount of neurotransmitter release in response to a change as little as 100 μV in membrane potential.[2]
Outer hair cells – acoustical pre-amplifiers
In mammalian outer hair cells, the receptor potential triggers active vibrations of the cell body. This mechanical response to electrical signals is termed somatic electromotility[3] and drives oscillations in the cell’s length, which occur at the frequency of the incoming sound and provide mechanical feedback amplification. A movie clip showing an isolated outer hair cell moving in response to electrical stimulation can be seen here. [6] Outer hair cells have evolved only in mammals. While hearing sensitivity of mammals is similar to that of other classes of vertebrates, without functioning outer hair cells, the sensitivity decreases by approximately 50 dB. Outer hair cells extend the hearing range to about 200 kHz in some marine mammals.[4] They have also improved frequency selectivity (frequency discrimination), which is of particular benefit for humans, because it enabled sophisticated speech and music. The effect of this system is to non-linearly amplify quiet sounds more than large ones, so that a wide range of sound pressures can be reduced to a much smaller range of hair displacements.[] This property of amplification is called the cochlear amplifier. The molecular biology of hair cells has seen considerable progress in recent years, with the identification of the motor protein (prestin) that underlies somatic electromotility in the outer hair cells. Santos-Sacchi et al. have shown that prestin's function is dependent on chloride channel signalling and that it is compromised by the common marine pesticide tributyltin (TBT). Because this class of pollutant bioconcentrates up the food chain, the effect is pronounced in top marine predators such as orcas and toothed whales.[5]
Hair cell
290
Neural connection
Neurons of the auditory or vestibulocochlear nerve (the VIIIth cranial nerve) innervate cochlear and vestibular hair cells.[6] The neurotransmitter released by hair cells to stimulate the dendrites of afferent neurons is thought to be glutamate. At the presynaptic juncture, there is a distinct presynaptic dense body or ribbon. This dense body is surrounded by synaptic vesicles and is thought to aid in the fast release of neurotransmitter. Nerve fiber innervation is much denser for inner hair cells than for outer hair cells. A single inner hair cell is innervated by numerous nerve fibers, whereas a single nerve fiber innervates many outer hair cells. Inner hair cell nerve fibers are also very heavily myelinated, which is in contrast to the unmyelinated outer hair cell nerve fibers. The region of the basilar membrane supplying the inputs to a particular afferent nerve fibre can be considered to be its receptive field. Efferent projections from the brain to the cochlea also play a role in the perception of sound. Efferent synapses occur on outer hair cells and on afferent (towards the brain) dendrites under inner hair cells. The presynaptic terminal bouton is filled with vesicles containing acetylcholine and a neuropeptide called Calcitonin gene-related peptide (CGRP). The effects of these compounds varies, in some hair cells the acetylcholine hyperpolarized the cell, which reduces the sensitivity of the cochlea locally.
Regrowth
Research on the regrowth of cochlea cells may lead to medical treatments that restore hearing. Unlike fish, birds, and reptiles, post-birth humans and other mammals are normally unable to regrow the cells of the inner ear that convert sound into neural signals when those cells are damaged by age or disease.[7] There is some contradictory information regarding the possibility of hair cell regeneration in mature mammals.[8][9][10] Researchers are making progress toward gene and stem-cell therapies that may allow the damaged cells to be regenerated.[11] Researchers have identified a mammalian gene that normally acts as a molecular switch to block the regrowth of cochlear hair cells in adults.[12] The Rb1 gene encodes the retinoblastoma protein that performs several physiological functions.[13] Not only do hair cells in a culture dish regenerate when the Rb1 gene is deleted, but mice bred to be missing the gene grow more hair cells than control mice that have the gene. The cell cycle inhibitor p27kip1 has also been shown to allow regrowth of cochlear hair cells in mice following genetic deletion or knock down with siRNA targeting p27.[14][15][16]
Additional images
The lamina reticularis and subjacent structures.
Inner ear illustration showing semicircular canal, hair cells, ampulla, cupula, vestibular nerve, & fluid
Stereocilia of frog inner ear
Hair cell
291
Notes
[14] (primary source) [15] (primary source)
References
• Coffin A, Kelley M, Manley GA, Popper AN. "Evolution of sensory hair cells". pp. 55–94. in Manley et al. (2004) • Fettiplace R, Hackney CM (2006). "The sensory and motor roles of auditory hair cells". Nature Reviews. Neuroscience 7 (1): 19–29. doi: 10.1038/nrn1828 (http://dx.doi.org/10.1038/nrn1828). PMID 16371947 (http://www.ncbi.nlm.nih.gov/pubmed/16371947). • Kandel ER, Schwartz JH, Jessell TM (2000). Principles of Neural Science (4th ed.). New York: McGraw-Hill. pp. 590–594. ISBN 0-8385-7701-6. • Manley GA, Popper AN, Fay RR (2004). Evolution of the Vertebrate Auditory System. New York: Springer-Verlag. ISBN 0-387-21093-8. • Manley GA. "Advances and perspectives in the study of the evolution of the vertebrate auditory system". pp. 360–368. in Manley et al. (2004) • Rabbitt RD, Boyle B, Highstein SM (1–5 February 2010). "Mechanical amplification by hair cells in the semicircular canals" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2840494). Proceedings of the National Academy of Sciences 107 (8): 3864–9. doi: 10.1073/pnas0906765107 (http://dx.doi.org/10.1073/ pnas0906765107). PMC 2840494 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2840494). PMID 20133682 (http://www.ncbi.nlm.nih.gov/pubmed/20133682). Lay summary (http://www.physorg.com/ news184935465.html). • Breneman KD, Brownell WE, Rabbitt RD (22 April 2009). "Hair cell bundles: flexoelectric motors of the inner ear" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2668172). In Brezina, Vladimir. PLOS One 4 (4): e5201. doi: 10.1371/journal.pone.0005201 (http://dx.doi.org/10.1371/journal.pone.0005201). PMC 2668172 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2668172). PMID 19384413 (http://www.ncbi. nlm.nih.gov/pubmed/19384413). Lay summary (http://www.physorg.com/news159599814.html).
External links
• Molecular Basis of Hearing (http://www.ks.uiuc.edu/Research/hearing/) • Hair Cells at the University of Montpellier (http://www.iurc.montp.inserm.fr/cric51/audition/english/corti/ hcells/fhcells.htm) • Dancing OHC (http://www.yaleearlab.org/) video Yale Ear Lab • NIF Search - Hair Cell (https://www.neuinfo.org/mynif/search.php?q=Hair Cell&t=data&s=cover&b=0& r=20) via the Neuroscience Information Framework • Hair-Tuning-Sound-Sensor (http://www.scribd.com/doc/96781099/Hair-Tuning-Sound-Sensor) A concise report on the recent development of sound sensors based on hair tuning by students of SMMEE, IIT Ropar (http:/ /www.iitrpr.ac.in/)
Sensory neuron
292
Sensory neuron
Sensory neurons are neurons responsible for converting various external stimuli that come from the environment into corresponding internal stimuli. They are activated by sensory input (vision, touch, hearing, etc.), and send projections to other elements of nervous system, ultimately conveying sensory information to the brain or spinal cord. Unlike neurons of the central nervous system, whose inputs come from other neurons, sensory neurons are activated by physical modalities such as light, sound, and temperature. In complex organisms, the central nervous system is the destination to which sensory neurons transmit their data; in the case of less complex organisms, such as the hydra, sensory neurons send their data to motor neurons and sensory neurons can also send data via electrical impulses to the brain. At the molecular level, sensory receptors located on the cell membrane of sensory neurons are responsible for the conversion of stimuli into electrical impulses. The type of receptor employed by a given sensory neuron determines the type of stimulus it will be sensitive to. For example, neurons containing mechanoreceptors are sensitive to tactile stimuli, while olfactory receptors make a cell sensitive to odors.[1]
Types and function
Somatic sensory system
The somatic sensory system includes the sensations of touch, pressure, vibration, limb position, heat, cold, and pain. The cell bodies of somatic sensory afferent fibers lie in ganglia throughout the spine. These neurons are responsible for relaying information about the body to the central nervous system. Neurons residing in ganglia of the head and body supply the central nervous system with information about the aforementioned external stimuli occurring to the body. Pseudounipolar neurons are located in the dorsal root ganglia (the head).[2] Mechanoreceptors Specialized receptor cells called mechanoreceptors often encapsulate afferent fibers to help tune the afferent fibers to the different types of somatic stimulation. Mechanoreceptors also help lower thresholds for action potential generation in afferent fibers and thus make them more likely to fire in the presence of sensory stimulation.[3] Proprioceptors are another type of mechanoreceptors which literally means "receptors for self." These receptors provide spatial information about limbs and other body parts.[4] Nociceptors are responsible for processing pain and temperature changes. The burning pain and irritation experienced after eating a chili pepper (due to its main ingredient, capsaicin), the cold sensation experienced after ingesting a chemical such as menthol or icillin, as well as the common sensation of pain are all a result of neurons with these receptors.[5] Problems with mechanoreceptors lead to disorders such as: • Neuropathic pain - a severe pain condition resulting from a damaged sensory nerve [6] • Hyperalgesia - an increased sensitivity to pain caused by sensory ion channel, TRPM8, which is typically responds to temperatures between 23 and 26 degrees, and provides the cooling sensation associated with menthol and icillin [7] • Phantom limb syndrome - a sensory system disorder where pain or movement is experienced in a limb that does not exist [8]
Sensory neuron
293
Vision
Vision is one of the most complex sensory systems. The eye has to first "see" via refraction of light. Then, light energy has to be converted to electrical signals by photoreceptor cells and finally these signals have to be refined and controlled by the synaptic interactions within the neurons of the retina. The five basic classes of neurons within the retina are photoreceptor cells, bipolar cells, ganglion cells, horizontal cells, and amacrine cells. The basic circuitry of the retina incorporates a three-neuron chain consisting of the photoreceptor (either a rod or cone), bipolar cell, and the ganglion cell. The first action potential occurs in the retinal ganglion cell. This pathway is the most direct way for transmitting visual information to the brain. Problems and decay of sensory neurons associated with vision lead to disorders such as: • Macular degeneration – degeneration of the central visual field due to either cellular debris or blood vessels accumulating between the retina and the choroid, thereby disturbing and/or destroying the complex interplay of neurons that are present there.[9] • Glaucoma – loss of retinal ganglion cells which causes some loss of vision to blindness.[10] • Diabetic retinopathy – poor blood sugar control due to diabetes damages the tiny blood vessels in the retina.[11]
Auditory
The auditory system is responsible for converting pressure waves generated by vibrating air molecules or sound into signals that can be interpreted by the brain. This mechanoelectrical transduction is mediated with hair cells within the ear. Depending on the movement, the hair cell can either hyperpolarize or depolarize. When the movement is towards the tallest stereocilia, the K+ cation channels open allowing K+ to flow into cell and the resulting depolarization causes the Ca2+ channels to open, thus releasing its neurotransmitter into the afferent auditory nerve. There are two types of hair cells: inner and outer. The inner hair cells are the sensory receptors while the outer hair cells are usually from efferent axons originating from cells in the superior olivary complex[12] Problems with sensory neurons associated with the auditory system leads to disorders such as: • Auditory Processing Disorder – auditory information in the brain is processed in an abnormal way. Patients with auditory processing disorder can usually gain the information normally, but their brain cannot process it properly, leading to hearing disability.[13] • Auditory verbal agnosia – comprehension of speech is lost but hearing, speaking, reading, and writing ability is retained. This is caused by damage to the posterior superior temporal lobes, again not allowing the brain to process auditory input correctly.[14]
Drugs
There are many drugs currently on the market that are used to manipulate or treat sensory system disorders. For instance, Gabapentin is a drug that is used to treat neuropathic pain by interacting with one of the voltage-dependent calcium channels present on non-receptive neurons.[15] Some drugs may be used to combat other health problems, but can have unintended side effects on the sensory system. Ototoxic drugs are drugs which affect the cochlea through the use of a toxin like aminoglycoside antibiotics, which poison hair cells. Through the use of these toxins, the K+ pumping hair cells cease their function. Thus, the energy generated by the endocochlear potential which drives the auditory signal transduction process is lost, leading to hearing loss.[16]
Sensory neuron
294
Plasticity (Neuroplasticity)
Ever since scientists observed cortical remapping in the brain of Taub’s Silver Spring monkeys, there has been a lot of research into sensory system plasticity. Huge strides have been made in treating disorders of the sensory system. Techniques such as constraint-induced movement therapy developed by Taub have helped patients with paralyzed limbs regain use of their limbs by forcing the sensory system to grow new neural pathways.[17] Phantom limb syndrome is a sensory system disorder in which amputees perceive that their amputated limb still exists and they may still be experiencing pain in it. The mirror box developed by V.S. Ramachandran, has enabled patients with phantom limb syndrome to realign their body map, the somatosensory system’s perception of where the body is in space with physical reality. It is a simple device which uses a mirror in a box to create an illusion in which the sensory system perceives that it is seeing two hands instead of one, therefore allowing the sensory system to control the "phantom limb". By doing this, the sensory system can gradually get acclimated to the amputated limb, and thus alleviate this syndrome.[18]
Fiber types
Peripheral nerve fibers can be classified based on axonal conduction velocity, mylenation, fiber size etc. For example, there are slow-conducting unmyelinated C fibers and faster-conducting myelinated Aδ fibers. These nerve fibers work with neurons to form the nervous system
Footnotes
[1] Purves et al., 207-392 [2] Purves et al., pg 207 [3] Purves et al., 209 [4] Purves et al., 215-216 [5] Lee 2005 [6] Lee 2005 [7] Lee 2005 [8] Halligan 1999 [9] de Jong 2006 [10] Alguire 1990 [11] Diabetic retinopathy 2005 [12] Purves et al., pg 327-330 [13] Auditory processing disorder, 2004 [14] Stefanatos et al., 2005 [15] Lee 2005 [16] Priuska and Schact 1997 [17] Schwartz and Begley 2002 [18] Ramachandran 1998
References
• Alguire P (1990). "The Eye Chapter 118 Tonometry>Basic Science". in Walker HK, Hall WD, Hurst JW. Clinical methods: the history, physical, and laboratory examinations (3rd ed.). London: Butterworths. ISBN 0-409-90077-X. http://www.ncbi.nlm.nih.gov/bookshelf/br.fcgi?book=cm&partid=222#A3607. • "Auditory Processing Disorder (APD). Pamphlet, (2004).". British Society of Audiology APD Special Interest Group. MRC Institute of Hearing Research. http://www.ihr.mrc.ac.uk/research/apd.php/apd. php?page=apd_docs. • De Jong, Ptvm. "Mechanisms of Disease: Age-Related Macular Degeneration." New England Journal of Medicine 355 14 (2006): 1474-85. Print. • Halligan, P. W., A. Zeman, and A. Berger. "Phantoms in the Brain - Question the Assumption That the Adult Brain Is "Hard Wired"." British Medical Journal 319 7210 (1999): 587-88. Print.
Sensory neuron • Lee, Y., Lee, C. H., & Oh, U. (2005). Painful channels in sensory neurons. [Review]. Molecules and Cells, 20(3), 315-324. Print. • "NIHSeniorHealth: Diabetic Retinopathy - Causes and Risk Factors". Diabetic Retinopathy. NIHSenior Health. 2005. http://nihseniorhealth.gov/diabeticretinopathy/causesandriskfactors/02.html. • Priuska, E.M. and J. Schact (1997) Mechanism and prevention of aminoglycoside ototoxicity: Outer hair cells as targets and tools. Ear, Nose, Throat J. 76: 164-171. • Purves, D., Augustine, G.J., Fitzpatrick, D., Hall, W.C., LaMantia, A., McNamara, J.O., White, L.E. Neuroscience. Fourth edition. (2008). Sinauer Associates, Sunderland, Mass. Print. • Ramachandran, V. S. and S. Blakeslee (1998), Phantoms in the brain: Probing the mysteries of the human mind., William Morrow & Company, ISBN 0-688-15247-3. Print. • Schwartz and Begley 2002, p. 160; "Constraint-Induced Movement Therapy", excerpted from "A Rehab Revolution," Stroke Connection Magazine, September/October 2004. Print. • Stefanatos GA, Gershkoff A, Madigan S (2005). "On pure word deafness, temporal processing, and the left hemisphere". Journal of the International Neuropsychological Society : JINS 11 (4): 456–70; discussion 455.
295
Merkel cell
296
Merkel cell
Neuron: Merkel cell
Diagram of human skin. In humans, Merkel cells (yellow dot) are found clustered beneath the epidermal ridges (aka fingerprints). NeuroLex ID nifext_87 [1]
Merkel cells or Merkel-Ranvier cells are oval receptor cells found in the skin of vertebrates that have synaptic contacts with somatosensory afferents. They are associated with the sense of light touch discrimination of shapes and textures. They can turn malignant and form the skin tumor known as Merkel cell carcinoma. There is evidence that they are derived from neural crest.[] More recent experiments in mammals have indicated that they are in fact epithelial in origin.[1]
Location
Merkel cells are found in the skin and some parts of the mucosa of all vertebrates. In mammalian skin, they are clear cells found in the stratum basale (at the bottom of sweat duct ridges) of the epidermis approximately 10 µm in diameter. They also occur in epidermal invaginations of the plantar foot surface called rete ridges.[2] Most often, they are associated with sensory nerve endings, when they are known as Merkel nerve endings (also called a Merkel cell-neurite complex). They are associated with slowly adapting (SA1) somatosensory nerve fibers.
Function
Friedrich Sigmund Merkel referred to these cells as Tastzellen or "touch cells" but this proposed function has been controversial as it has been hard to prove. However, genetic knockout mice have recently shown that Merkel cells are essential for the specialized coding by which afferent nerves resolve fine spatial details.[3] Merkel cells are sometimes considered APUD cells (an older definition. More commonly classified as a part of dispersed neuroendocrine system) because they contain dense core granules, and thus may also have a neuroendocrine function.
Merkel cell
297
Developmental origin
The origin of Merkel cells has been debated for over 20 years. Evidence from skin graft experiments in birds implies that they are neural crest derived, but experiments in mammals now demonstrate an epidermal origin.[4][5]
References External links
• MeSH A08.800.550.700.500.425 (http://www.nlm.nih.gov/cgi/mesh/2012/MB_cgi?mode=&term=Merkel+ Cells&field=entry#TreeA08.800.550.700.500.425) • NIF Search - Merckel Disc Cell (https://www.neuinfo.org/mynif/search.php?q=Merkel Cell&t=data& s=cover&b=0&r=20) via the Neuroscience Information Framework
Olfactory receptor neuron
298
Olfactory receptor neuron
Neuron: Olfactory receptor neuron
Labels in German. "Zellen" = "cell","riech" = "smell", "Riechnerv" = olfactory nerve, "cillien" = cilia. Location Function Neurotransmitter Morphology Presynaptic connections Postsynaptic connections Gray's NeuroLex ID Code olfactory epithelium in the nose Detect traces of chemicals in inhaled air (sense of smell) Glutamate Bipolar sensory receptor None Olfactory bulb subject #223 996 nifext_116 [1] [2] [1]
TH H3.11.07.0.01003
An olfactory receptor neuron (ORN), also called an olfactory sensory neuron (OSN), is a transduction cell within the olfactory system.[1]
Vertebrates
Humans have about 40 million olfactory receptors that detect up to 10,000 different odors. In vertebrates, ORNs are bipolar neurons with dendrites facing the inferior space of the nasal cavity and an axon that passes through the cribiform plate then travels along the olfactory nerve to the olfactory bulb. The ORNs are located in the olfactory epithelium in the nasal cavity. The cell bodies of the ORNs are distributed among all three of the stratified layers of the olfactory epithelium.[2]
Plan of olfactory neurons.
Structure
Many tiny hair-like cilia protrude from the olfactory receptor cell's dendrite into the mucus covering the surface of the olfactory epithelium. The surface of these cilia is covered with olfactory receptors, a type of G protein-coupled receptor. Each olfactory receptor cell expresses only one type of olfactory receptor (OR), but many separate olfactory receptor cells express ORs which bind the same set of odors. The axons of olfactory receptor cells which express the same OR converge to form glomeruli in the olfactory bulb.
Olfactory receptor neuron
299
Function
ORs, which are located on the membranes of the cilia have been classified as a complex type of ligand-gated metabotropic channels.[3] There are approximately 1000 different genes that code for the ORs, making them the largest gene family. An odorant will dissolve into the mucus of the olfactory epithelium and then bind to an OR. ORs can bind to a variety of odor molecules, with varying affinities. The difference in affinities causes differences in activation patterns resulting in unique odorant profiles.[4] [5] The activated OR in turn activates the intracellular G-protein, GOLF (GNAL), adenylate cyclase and production of cyclic AMP (cAMP) opens ion channels in the cell membrane, resulting in an influx of sodium and calcium ions into the cell, and an efflux of chloride ions. This influx of positive ions and efflux of negative ions causes the neuron to depolarize, generating an action potential.
Insects
In insects, olfactory receptor neurons typically reside on the antenna. Much like in vertebrates, axons from the sensory neurons converge into glomeruli in the antennal lobe.
References
[1] J. Rospars, (1998) Dendritic integration in olfactory sensory neurons: a steady-state analysis of how the neuron structure and neuron environment influence the coding of odor intensity. J Comput Neurosci. 5: 243-266. PMID 9663551 [2] A. Cunningham, P. Manis, P. Reed, G. Ronnett, (1999) Olfactory receptor neurons exist as distinct subclasses of immature and mature cells in primary culture. Neuroscience 93(4): 1301-1312. PMID 10501454 [3] K. Touhara, (2009) Insect olfactory receptor complex functions as a ligand-gated ionotropic channel 1170 International Symposium on Olfaction and Taste: Ann. N.Y. Acad. Sci. 177-180 PMID 19686133 [4] S. Bieri, K. Monastyrskaia, B. Schilling, (2004) Olfactory receptor neuron profiling using sandalwood odorants. Chem. Senses 29:483-487 PMID 15269120 [5] J. Fan and J. Ngai, (2001) Onset of odorant receptor gene expression during olfactory sensory neuron regeneration. Dev Biol. 229: 119-127 PMID 11133158
External links
• olfactory+receptor+cells (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=olfactory+ receptor+cells) at eMedicine Dictionary • NIF Search - Olfactory receptor neuron (https://www.neuinfo.org/mynif/search.php?q=Olfactory Receptor Neuron&t=data&s=cover&b=0&r=20) via the Neuroscience Information Framework • (http://www.olfacts.nl) Insect olfaction
Photoreceptor cell
300
Photoreceptor cell
Neuron: Photoreceptor Cell
NeuroLex ID sao1233810115 [1]
A photoreceptor cell is a specialized type of neuron found in the retina that is capable of phototransduction. The great biological importance of photoreceptors is that they convert light (visible electromagnetic radiation) into signals that can stimulate biological processes. To be more specific, photoreceptor proteins in the cell absorb photons, triggering a change in the cell's membrane potential. The two classic photoreceptor cells are rods and cones, each contributing information used by the visual system to form a representation of the visual world, sight. The rods are narrower than the cones and distributed differently across the retina, but the chemical process in each that supports phototransduction is similar.[1] A third class of photoreceptor cells was discovered during the 1990s:[] the photosensitive ganglion cells. These cells do not contribute to sight directly, but are thought to support circadian rhythms and pupillary reflex. There are major functional differences between the rods and cones. Rods are extremely sensitive, and can be triggered by as few as 6 photons.[] At very low light levels, visual experience is based solely on the rod signal. This explains why colors cannot be seen at low light levels: only one type of photoreceptor cell is active. Cones require significantly brighter light (i.e., a larger numbers of photons) in order to produce a signal. In humans, there are three different types of cone cell, distinguished by their pattern of response to different wavelengths of light. Color experience is calculated from these three distinct signals, perhaps via an opponent process.[] The three types of cone cell respond (roughly) to light of short, medium, and long wavelengths. Note that, due to the principle of univariance, the firing of the cell depends upon only the number of photons absorbed. The different responses of the three types of cone cells are determined by the likelihoods that their respective photoreceptor proteins will absorb photons of different wavelengths. So, for example, an L cone cell contains a photoreceptor protein that more readily absorbs long wavelengths of light (i.e., more "red"). Light of a shorter wavelength can also produce the same response, but it must be much brighter to do so. The human retina contains about 120 million rod cells and 6 million cone cells. The number and ratio of rods to cones varies among species, dependent on whether an animal is primarily diurnal or nocturnal. Certain owls, such as the tawny owl,[2] have a tremendous number of rods in their retinae. In addition, there are about 1.5 million ganglion cells in the human visual system, 1 to 2% of them photosensitive. Described here are vertebrate photoreceptors. Invertebrate photoreceptors in organisms such as insects and molluscs are different in both their morphological organization and their underlying biochemical pathways.
Photoreceptor cell
301
Histology
Rod and cone photoreceptors are found on the outermost layer of the retina; they both have the same basic structure. Closest to the visual field (and farthest from the brain) is the axon terminal, which releases a neurotransmitter called glutamate to bipolar cells. Farther back is the cell body, which contains the cell's organelles. Farther back still is the inner segment, a specialized part of the cell full of mitochondria. The chief function of the inner segment is to provide ATP (energy) for the sodium-potassium pump. Finally, closest to the brain (and farthest from the field of view) is the outer segment, the part of the photoreceptor that absorbs light. Outer segments are actually modified cilia [][] that contain disks filled with opsin, the molecule that absorbs photons, as well as voltage-gated sodium channels. The membranous photoreceptor protein opsin contains a pigment molecule called retinal. In rod cells, these together are called rhodopsin. In cone cells, there are different types of opsins that combine with retinal to form pigments called photopsins. Three different classes of photopsins in the cones react to different ranges of light frequency, a differentiation that allows the visual system to calculate color. The function of the photoreceptor cell is to convert the light energy of the photon into a form of energy communicable to the nervous system and readily usable to the organism: This conversion is called signal transduction.
Anatomy of a Rod Cell
[3]
The opsin found in the photosensitive ganglion cells of the retina that are involved in various reflexive responses of the brain and body to the presence of (day)light, such as the regulation of circadian rhythms, pupillary reflex and other non-visual responses to light, is called melanopsin. Atypical in vertebrates, melanopsin functionally resembles invertebrate opsins. In structure, it is an opsin, a retinylidene protein variety of G-protein-coupled receptor. When light activates the melanopsin signaling system, the melanopsin-containing ganglion cells discharge nerve impulses that are conducted through their axons to specific brain targets. These targets include the olivary pretectal nucleus (a center responsible for controlling the pupil of the eye), the LGN, and, through the retinohypothalamic tract (RHT), the suprachiasmatic nucleus of the hypothalamus (the master pacemaker of circadian rhythms). Melanopsin-containing ganglion cells are thought to influence these targets by releasing from their axon terminals the neurotransmitters glutamate and pituitary adenylate cyclase activating polypeptide (PACAP).
Photoreceptor cell
302
Humans
The human retina has approximately 6 million cones and 120 million rods.[] Signals from the rods and cones converge on ganglion and bipolar cells for preprocessing before they are sent to the lateral geniculate nucleus. At the "center" of the retina (the point directly behind the lens) is the fovea, which contains only cone photoreceptor cells; this is the region capable of producing the highest visual acuity. Across the rest of the retina, rods and cones are intermingled. No photoreceptors are found at the blind spot, the area where ganglion cell fibers are collected into the optic nerve and leave the eye.[]
Normalized human photoreceptor absorbances for different wavelengths of light
[4]
The photoreceptor proteins in the three types of cones differ in their sensitivity to photons of different wavelengths (see graph). Since cones respond to both the wavelength and intensity of light, the cone's sensitivity to wavelength is measured in terms of its relative rate of response if the intensity of a stimulus is held fixed, while the wavelength is varied. From this, in turn, is inferred the absorbance.[] The graph normalizes the degree of absorbance on a hundred point scale. For example, the S cone's relative response peaks around 420 nm (nanometers, a measure of wavelength). This tells us that an S cone is more likely to absorb a photon at 420 nm than at any other wavelength. If light of a different wavelength to which it is less sensitive, say 480 nm, is increased in brightness appropriately, however, it will produce exactly the same response in the S cone. So, the colors of the curves are misleading. Cones cannot detect color by themselves; rather, color vision requires comparison of the signal across different cone types.
Phototransduction
The process of phototransduction occurs in the retina.[5] The retina is thick with cells.[6] The photoreceptor cells (rods and cones) form the innermost layer.[7] The middle layer contains bipolar cells, which collect neural signals from the rods and the cones and then transmit them to the outermost layer of the retina[8] where the neurons called retinal ganglion cells (RGCs) organize the signals and send them to the brain.[9] The bundled RGC axons form the optic nerve, which leaves the eye through a hole in the retina creating the blind spot.[10] Activation of rods and cones is actually hyperpolarization; when they are not being stimulated, they depolarize and release glutamate continuously. In the dark, cells have a relatively high concentration of cyclic guanosine 3'-5' monophosphate (cGMP), which opens ion channels (largely sodium channels, though calcium can enter through these channels as well). The positive charges of the ions that enter the cell down its electrochemical gradient change the cell's membrane potential, cause depolarization, and lead to the release of the neurotransmitter glutamate. Glutamate can depolarize some neurons and hyperpolarize others. When light hits a photoreceptive pigment within the photoreceptor cell, the pigment changes shape. The pigment, called iodopsin or rhodopsin, consists of large proteins called opsin (situated in the plasma membrane), attached to a covalently bound prosthetic group: an organic molecule called retinal (a derivative of vitamin A). The retinal exists in the 11-cis-retinal form when in the dark, and stimulation by light causes its structure to change to all-trans-retinal. This structural change causes it to activate a regulatory protein called transducin, which leads to the activation of cGMP phosphodiesterase, which breaks cGMP down into 5'-GMP. Reduction in cGMP allows the ion channels to close, preventing the influx of positive ions, hyperpolarizing the cell, and stopping the release of neurotransmitters.[3]
Photoreceptor cell The entire process by which light initiates a sensory response is called visual phototransduction.
303
Dark current
Unstimulated (in the dark), cyclic-nucleotide gated channels in the outer segment are open because cyclic GMP (cGMP) is bound to them. Hence, positively charged ions (namely sodium ions) enter the photoreceptor, depolarizing it to about −40 mV (resting potential in other nerve cells is usually −65 mV). This depolarizing current is often known as dark current.
Signal transduction pathway
The signal transduction pathway is the mechanism by which the energy of a photon signals a mechanism in the cell that leads to its electrical polarization. This polarization ultimately leads to either the transmittance or inhibition of a neural signal that will be fed to the brain via the optic nerve. The steps, or signal transduction pathway, in the vertebrate eye's rod and cone photoreceptors are then: 1. The rhodopsin or iodopsin in the disc membrane of the outer segment absorbs a photon, changing the configuration of a retinal Schiff base cofactor inside the protein from the cis-form to the trans-form, causing the retinal to change shape. 2. This results in a series of unstable intermediates, the last of which binds stronger to the G protein in the membrane and activates transducin, a protein inside the cell. This is the first amplification step – each photoactivated rhodopsin triggers activation of about 100 transducins. (The shape change in the opsin activates a G protein called transducin.) 3. Each transducin then activates the enzyme cGMP-specific phosphodiesterase (PDE). 4. PDE then catalyzes the hydrolysis of cGMP to 5' GMP. This is the second amplification step, where a single PDE hydrolyses about 1000 cGMP molecules. 5. The net concentration of intracellular cGMP is reduced (due to its conversion to 5' GMP via PDE), resulting in the closure of cyclic nucleotide-gated Na+ ion channels located in the photoreceptor outer segment membrane. 6. As a result, sodium ions can no longer enter the cell, and the photoreceptor outer segment membrane becomes hyperpolarized, due to the charge inside the membrane becoming more negative. 7. This change in the cell's membrane potential causes voltage-gated calcium channels to close. This leads to a decrease in the influx of calcium ions into the cell and thus the intracellular calcium ion concentration falls. 8. A decrease in the intracellular calcium concentration means that less glutamate is released via calcium-induced exocytosis to the bipolar cell (see below). (The decreased calcium level slows the release of the neurotransmitter glutamate, which can either excite or inhibit the postsynaptic bipolar cells.) 9. Reduction in the release of glutamate means one population of bipolar cells will be depolarized and a separate population of bipolar cells will be hyperpolarized, depending on the nature of receptors (ionotropic or metabotropic) in the postsynaptic terminal (see receptive field). Thus, a rod or cone photoreceptor actually releases less neurotransmitter when stimulated by light. Less neurotransmitter could either stimulate (depolarize) or inhibit (hyperpolarize) the bi-polar cell it synapses with, dependent on the nature of the receptor on the bipolar cell. This ability is integral to the center on/off mapping of visual units.[citation needed] ATP provided by the inner segment powers the sodium-potassium pump. This pump is necessary to reset the initial state of the outer segment by taking the sodium ions that are entering the cell and pumping them back out. Although photoreceptors are neurons, they do not conduct action potentials with the exception of the photosensitive ganglion cell – which are involved mainly in the regulation of circadian rhythms, melatonin, and pupil dilation.
Photoreceptor cell
304
Advantages
Phototransduction in rods and cones is unique in that the stimulus (in this case, light) actually reduces the cell's response or firing rate, which is unusual for a sensory system where the stimulus usually increases the cell's response or firing rate. However, this system offers several key advantages. First, the classic (rod or cone) photoreceptor is depolarized in the dark, which means many sodium ions are flowing into the cell. Thus, the random opening or closing of sodium channels will not affect the membrane potential of the cell; only the closing of a large number of channels, through absorption of a photon, will affect it and signal that light is in the visual field. Hence, the system is noiseless. Second, there is a lot of amplification in two stages of classic phototransduction: one pigment will activate many molecules of transducin, and one PDE will cleave many cGMPs. This amplification means that even the absorption of one photon will affect membrane potential and signal to the brain that light is in the visual field. This is the main feature that differentiates rod photoreceptors from cone photoreceptors. Rods are extremely sensitive and have the capacity of registering a single photon of light, unlike cones. On the other hand, cones are known to have very fast kinetics in terms of rate of amplification of phototransduction, unlike rods.
Difference between rods and cones
Comparison of human rod and cone cells, from Eric Kandel et al. in Principles of Neural Science.[3]
Rods Used for scotopic vision (vision under low light conditions) Very light sensitive; sensitive to scattered light Loss causes night blindness Low visual acuity Not present in fovea Slow response to light, stimuli added over time Have more pigment than cones, so can detect lower light levels Cones Used for photopic vision (vision under high light conditions) Not very light sensitive; sensitive to only direct light Loss causes legal blindness High visual acuity; better spatial resolution Concentrated in fovea Fast response to light, can perceive more rapid changes in stimuli Have less pigment than rods, require more light to detect images
Stacks of membrane-enclosed disks are unattached to cell membrane directly Disks are attached to outer membrane About 120 million rods distributed around the retina One type of photosensitive pigment Confer achromatic vision [11] [12] About 6 million cones distributed in each retina Three types of photosensitive pigment in humans Confer color vision
Function
Photoreceptors do not signal color; they only signal the presence of light in the visual field. A given photoreceptor responds to both the wavelength and intensity of a light source. For example, red light at a certain intensity can produce the same exact response in a photoreceptor as green light of a different intensity. Therefore, the response of a single photoreceptor is ambiguous when it comes to color. To determine color, the visual system compares responses across a population of photoreceptors (specifically, the three different cones with differing absorption spectra). To determine intensity, the visual system computes how many photoreceptors are responding. This is the mechanism that allows trichromatic color vision in humans and some other animals.
Photoreceptor cell
305
Development
The key events mediating rod versus S cone versus M cone differentiation are induced by several transcription factors, including RORbeta, OTX2, NRL, CRX, NR2E3 and TRbeta2. The S cone fate represents the default photoreceptor program, however differential transcriptional activity can bring about rod or M cone generation. L cones are present in primates, however there is not much known for their developmental program due to use of rodents in research. There are five steps to developing photoreceptors: proliferation of multi-potent retinal progenitor cells (RPCs); restriction of competence of RPCs; cell fate specification; photoreceptor gene expression; and lastly axonal growth, synapse formation and outer segment growth. Early Notch signaling maintains progenitor cycling. Photoreceptor precursors come about through inhibition of Notch signaling and increased activity of various factors including achaete-scute homologue 1. OTX2 activity commits cells to the photoreceptor fate. CRX further defines the photoreceptor specific panel of genes being expressed. NRL expression leads to the rod fate. NR2E3 further restricts cells to the rod fate by repressing cone genes. RORbeta is needed for both rod and cone development. TRbeta2 mediates the M cone fate. If any of the previously mentioned factors' functions are ablated, the default photoreceptor is a S cone. These events take place at different time periods for different species and include a complex pattern of activities that bring about a spectrum of phenotypes. If these regulatory networks are disrupted, retinitis pigmentosa, macular degeneration or other visual deficits may result.[13]
Signaling
The rod and cone photoreceptors signal their absorption of photons via a decrease in the release of the neurotransmitter glutamate to bipolar cells at its axon terminal. Since the photoreceptor is depolarized in the dark, a high amount of glutamate is being released to bipolar cells in the dark. Absorption of a photon will hyperpolarize the photoreceptor and therefore result in the release of less glutamate at the presynaptic terminal to the bipolar cell. Every rod or cone photoreceptor releases the same neurotransmitter, glutamate. However, the effect of glutamate differs in the bipolar cells, depending upon the type of receptor imbedded in that cell's membrane. When glutamate binds to an ionotropic receptor, the bipolar cell will depolarize (and therefore will hyperpolarize with light as less glutamate is released). On the other hand, binding of glutamate to a metabotropic receptor results in a hyperpolarization, so this bipolar cell will depolarize to light as less glutamate is released. In essence, this property allows for one population of bipolar cells that gets excited by light and another population that gets inhibited by it, even though all photoreceptors show the same response to light. This complexity becomes both important and necessary for detecting color, contrast, edges, etc. Further complexity arises from the various interconnections among bipolar cells, horizontal cells, and amacrine cells in the retina. The final result is differing populations of ganglion cells in the retina, a sub-population of which is also intrinsically photosensitive, using the photopigment melanopsin.
Ganglion cell (non-rod non-cone) photoreceptors
A non-rod non-cone photoreceptor in the eyes of mice, which was shown to mediate circadian rhythms, was discovered in 1991 by Foster et al.[] These neuronal cells, called intrinsically photosensitive retinal ganglion cells (ipRGC), are a small subset (~1–3%) of the retinal ganglion cells located in the inner retina, that is, in front[14] of the rods and cones located in the outer retina. These light sensitive neurons contain a photopigment, melanopsin,[15][][16][17][] which has an absorption peak of the light at a different wavelength (~480 nm[]) than rods and cones. Beside circadian / behavioral functions, ipRGCs have a role in initiating the pupillary light reflex.[] Dennis Dacey with colleagues showed in a species of Old World monkey that giant ganglion cells expressing melanopsin projected to the lateral geniculate nucleus (LGN).[18] Previously only projections to the midbrain (pre-tectal nucleus) and hypothalamus (suprachiasmatic nucleus) had been shown. However a visual role for the
Photoreceptor cell receptor was still unsuspected and unproven. In 2007, Farhan H. Zaidi and colleagues published pioneering work using rodless coneless humans. Current Biology subsequently announced in their 2008 editorial, commentary and despatches to scientists and ophthalmologists, that the non-rod non-cone photoreceptor had been conclusively discovered in humans using landmark experiments on rodless coneless humans by Zaidi and colleagues[][19][20][21] As had been found in other mammals, the identity of the non-rod non-cone photoreceptor in humans was found to be a ganglion cell in the inner retina. The workers had tracked down patients with rare diseases wiping out classic rod and cone photoreceptor function but preserving ganglion cell function.[19][20][21] Despite having no rods or cones the patients continued to exhibit circadian photoentrainment, circadian behavioural patterns, melanopsin suppression, and pupil reactions, with peak spectral sensitivities to environmental and experimental light matching that for the melanopsin photopigment. Their brains could also associate vision with light of this frequency. In humans the retinal ganglion cell photoreceptor contributes to conscious sight as well as to non-image-forming functions like circadian rhythms, behaviour and pupil reactions.[] Since these cells respond mostly to blue light, it has been suggested that they have a role in mesopic vision.[citation needed] Zaidi and colleagues' work with rodless coneless human subjects hence also opened the door into image-forming (visual) roles for the ganglion cell photoreceptor. It was discovered that there are parallel pathways for vision – one classic rod and cone-based pathway arising from the outer retina, and the other a rudimentary visual brightness detector pathway arising from the inner retina, which seems to be activated by light before the other.[] Classic photoreceptors also feed into the novel photoreceptor system, and colour constancy may be an important role as suggested by Foster. The receptor could be instrumental in understanding many diseases including major causes of blindness worldwide like glaucoma, a disease that affects ganglion cells, and the study of the receptor offered potential as a new avenue to explore in trying to find treatments for blindness. It is in these discoveries of the novel photoreceptor in humans and in the receptors role in vision, rather than its non-image-forming functions, where the receptor may have the greatest impact on society as a whole, though the impact of disturbed circadian rhythms is another area of relevance to clinical medicine. Most work suggests that the peak spectral sensitivity of the receptor is between 460 and 482 nm. Steven Lockley et al. in 2003 showed that 460 nm wavelengths of light suppress melatonin twice as much as longer 555 nm light. However, in more recent work by Farhan Zaidi et al., using rodless coneless humans, it was found that what consciously led to light perception was a very intense 481 nm stimulus; this means that the receptor, in visual terms, enables some rudimentary vision maximally for blue light.[]
306
References
[1] "eye, human." Encyclopædia Britannica. Encyclopaedia Britannica Ultimate Reference Suite. Chicago: Encyclopædia Britannica, 2010. [2] "Owl Eyesight" (http:/ / www. owls. org/ Information/ eyesight. htm) at owls.org [3] Human Physiology and Mechanisms of Disease by Arthur C. Guyton (1992) ISBN 0-7216-3299-8 p. 373 [11] Schacter, Daniel L., Daniel T. Gilbert, and Daniel M. Wegner. "Sensation and Perception, Phototransduction in the Retina." Psychology. ; Second Edition. New York: Worth, Incorporated, 2011. 136-37. Print. [12] Schacter, Daniel L., Daniel T. Gilbert, and Daniel M. Wegner. "Sensation and Perception, Phototransduction in the Retina." Psychology. ; Second Edition. New York: Worth, Incorporated, 2011. 136-37. Print. [14] See retina for information on the retinal layer structure. [19] Genova, Cathleen, Blind humans lacking rods and cones retain normal responses to nonvisual effects of light (http:/ / www. eurekalert. org/ pub_releases/ 2007-12/ cp-bhl121307. php). Cell Press, December 13, 2007. [20] Coghlan A. Blind people 'see' sunrise and sunset (http:/ / www. newscientist. com/ article/ mg19626354. 100-blind-people-see-sunrise-and-sunset. html). New Scientist, 26 December 2007, issue 2635. [21] Medical News Today. Normal Responses To Non-visual Effects Of Light Retained By Blind Humans Lacking Rods And Cones (http:/ / www. medicalnewstoday. com/ articles/ 91836. php). 14 December 2007.
Photoreceptor cell
307
Bibliography
• Campbell, Neil A., and Reece, Jane B. (2002). Biology. San Francisco: Benjamin Cummings. pp. 1064–1067. ISBN 0-8053-6624-5. • Freeman, Scott (2002). Biological Science (2nd Edition). Englewood Cliffs, N.J: Prentice Hall. pp. 835–837. ISBN 0-13-140941-7.
External links
• NIF Search – Photoreceptor Cell (https://www.neuinfo.org/mynif/search.php?q=Photoreceptor Cell& t=data&s=cover&b=0&r=20) via the Neuroscience Information Framework
Rod cell
308
Rod cell
Neuron: Rod cell
Cross section of the retina. Rods are visible at far right. Location Function Morphology Presynaptic connections Retina Low light photoreceptor rod shaped None
Postsynaptic connections Bipolar Cells and Horizontal cells NeuroLex ID Code sao1458938856 [1] [2]
TH H3.11.08.3.01030
Rod cells, or rods, are photoreceptor cells in the retina of the eye that can function in less intense light than the other type of visual photoreceptor, cone cells. Rods are concentrated at the outer edges of the retina and are used in peripheral vision. On average, there are approximately 125 million rod cells in the human retina.[1] More sensitive than cone cells, rod cells are almost entirely responsible for night vision.
Structure and function
Rods are a little longer and leaner than cones but have the same structural basis. The pigment is on the outer side, lying on the pigment epithelium, completing the cell's homeostasis. This epithelium end contains many stacked disks. Rods have a high area for visual pigment and thus substantial efficiency of light absorption. Because they have only one type of light-sensitive pigment, rather than the three types that human cone cells have, rods have little, if any, role in colored vision. Like cones, rod cells have a synaptic terminal, an inner segment, and an outer segment. The synaptic terminal forms a synapse with another neuron, for example a bipolar cell. The inner and outer segments are connected by a cilium,[2] which lines the distal segment.[3] The inner segment contains organelles and the cell's nucleus, while the rod outer segment (abbreviated to ROS), which is pointed toward the back of the eye, contains the light-absorbing materials.[2]
Sensitivity
A rod cell is sensitive enough to respond to a single photon of light[] and is about 100 times more sensitive to a single photon than cones. Since rods require less light to function than cones, they are the primary source of visual information at night (scotopic vision). Cone cells, on the other hand, require tens to hundreds of photons to become activated. Additionally, multiple rod cells converge on a single interneuron, collecting and amplifying the signals. However, this convergence comes at a cost to visual acuity (or image resolution) because the pooled information from multiple cells is less distinct than it would be if the visual system received information from each rod cell individually.
Rod cell
309
Rod cells also respond slower to light than cones and the stimuli they receive are added over roughly 100 milliseconds. While this makes rods more sensitive to smaller amounts of light, it also means that their ability to sense temporal changes, such as quickly changing images, is less accurate than that of cones.[2] Experiments by George Wald and others showed that rods are most sensitive to wavelengths of light around 498 nm (green-blue), and insensitive to wavelengths Wavelength responsiveness of rods compared to that of three types of cones. The [4] longer than about 640 nm (red). This fact is dashed gray curve is for rods. responsible for the Purkinje effect: as intensity dims at twilight, the rods take over, and before color disappears completely, peak sensitivity of vision shifts towards the rods' peak sensitivity (blue-green).
Response to light
In vertebrates, activation of a photoreceptor cell is actually a hyperpolarization (inhibition) of the cell. When they are not being stimulated, such as in the dark, rod cells and cone cells depolarize and release a neurotransmitter spontaneously. This neurotransmitter hyperpolarizes the bipolar cell. Bipolar cells exist between photoreceptors and ganglion cells and act to transmit signals from the photoreceptors to the ganglion cells. As a result of the bipolar cell being hyperpolarized, it does not release its transmitter at the bipolar-ganglion synapse and the synapse is not excited. Activation of photopigments by light sends a signal by hyperpolarizing the rod cell, leading to the rod cell not sending its neurotransmitter, which leads to the bipolar cell then releasing its transmitter at the bipolar-ganglion synapse and exciting the synapse.
Anatomy of a Rod Cell
[5]
Depolarization of rod cells (causing release of their neurotransmitter) occurs because in the dark, cells have a relatively high concentration of cyclic guanosine 3'-5' monophosphate (cGMP), which opens ion channels (largely sodium channels, though calcium can enter through these channels as well). The positive charges of the ions that enter the cell down its electrochemical gradient change the cell's membrane potential, cause depolarization, and lead to the release of the neurotransmitter glutamate. Glutamate can depolarize some neurons and hyperpolarize others, allowing photoreceptors to interact in an antagonistic manner. When light hits photoreceptive pigments within the photoreceptor cell, the pigment changes shape. The pigment, called rhodopsin (photopsin is found in cone cells) comprises a large protein called opsin (situated in the plasma membrane), attached to which is a covalently bound prosthetic group: an organic molecule called retinal (a derivative of vitamin A). The retinal exists in the 11-cis-retinal form when in the dark, and stimulation by light causes its structure to change to all-trans-retinal. This structural change causes a series of changes in the opsin that
Rod cell ultimately lead it to activate a regulatory protein called transducin (a type of G protein), which leads to the activation of cGMP phosphodiesterase, which breaks cGMP down into 5'-GMP. Reduction in cGMP allows the ion channels to close, preventing the influx of positive ions, hyperpolarizing the cell, and stopping the release of neurotransmitters (Kandel et al., 2000). Though cone cells primarily use the neurotransmitter substance acetylcholine, rod cells use a variety. The entire process by which light initiates a sensory response is called visual phototransduction. Activation of a single unit of rhodopsin, the photosensitive pigment in rods, can lead to a large reaction in the cell because the signal is amplified. Once activated, rhodopsin can activate hundreds of transducin molecules, each of which in turn activates a phosphodiesterase molecule, which can break down over a thousand cGMP molecules per second (Kandel et al. 2000). Thus, rods can have a large response to a small amount of light. As the retinal component of rhodopsin is derived from vitamin A, a deficiency of vitamin A causes a deficit in the pigment needed by rod cells. Consequently, fewer rod cells are able to sufficiently respond in darker conditions, and as the cone cells are poorly adapted for sight in the dark, blindness can result. This is night-blindness.
310
Revert to the resting state
Rods make use of three inhibitory mechanisms (negative feedback mechanisms) to allow a rapid revert to the resting state after a flash of light. Firstly, there exists a rhodopsin kinase (RK) which would phosphorylate the cytosolic tail of the activated rhodopsin on the multiple serines, partially inhibiting the activation of transducin. Also, an inhibitory protein - arrestin then binds to the phosphorylated rhodopsins to further inhibit the rhodopsin's activity. While arrestin shuts off rhodopsin, an RGS protein (functioning as a GTPase-activating proteins(GAPs)) drives the transducin (G-protein) into an "off" state by increasing the rate of hydrolysis of the bounded GTP to GDP. Also as the cGMP sensitive channels allow not only the influx of sodium ions, but also calcium ions, with the decrease in concentration of cGMP, cGMP sensitive channels are then closed and reducing the normal influx of calcium ions. The decrease in the concentration of calcium ions stimulates the calcium ion-sensitive proteins, which would then activate the guanylyl cyclase to replenish the cGMP, rapidly restoring its original concentration. The restoration opens the cGMP sensitive channels and causes a depolarization of the plasma membrane.[6]
Desensitization
When the rods are exposed to a high concentration of photons for a prolonged period, they become desensitized (adapted) to the environment. As rhodopsin is phosphorylated by rhodopsin kinase (a member of the GPCR kinases(GRKs)), it binds with high affinity to the arrestin. The bound arrestin can contribute to the desensitization process in at least two ways. First, it prevents the interaction between the G protein and the activated receptor. Second, it serves as an adaptor protein to aid the receptor to the clathrin-dependent endocytosis machinery (to induce receptor-mediated endocytosis).[6]
Rod cell
311
References
[1] [2] [3] [5] [6] Curcio, C. A., K. R. Sloan, et al. (1990). "Human photoreceptor topography." The Journal of Comparative Neurology 292(4): 497-523. Kandel E.R., Schwartz, J.H., Jessell, T.M. (2000). Principles of Neural Science, 4th ed., pp.507-513. McGraw-Hill, New York. "Photoreception" McGraw-Hill Encyclopedia of Science & Technology, vol. 13, p.460 2007 Human Physiology and Mechanisms of Disease by Arthur C. Guyton (1992) p.373 Bruce Alberts, Alexander Johnson, Julian Lewis, Martin Raff, Keith Roberts, Peter Walter (2008). Molecular Biology of The Cell, 5th ed., pp.919-921. Garland Science.
External links
• NIF Search - Rod Cell (https://www.neuinfo.org/mynif/search.php?q=Rod Cell&t=data&s=cover&b=0& r=20) via the Neuroscience Information Framework
Cone cell
312
Cone cell
Neuron: Cone cell
Normalized responsivity spectra of human cone cells, S, M, and L types Function NeuroLex ID Code Color vision sao1103104164 [1] [2]
TH H3.11.08.3.01046
Cone cells, or cones, are one of the two types of photoreceptor cells that are in the retina of the eye which are responsible for color vision as well as eye color sensitivity; they function best in relatively bright light, as opposed to rod cells that work better in dim light. Cone cells are densely packed in the fovea centralis a 0.3 mm diameter rod-free area with very thin, densely packed cones, but quickly reduce in number towards the periphery of the retina. There are about six to seven million cones in a human eye and are most concentrated towards the macula. [1] A commonly cited figure of six million in the human eye was found by Osterberg in 1935.[2] Oyster's textbook (1999)[3] cites work by Curcio et al. (1990) indicating an average close to 4.5 million cone cells and 90 million rod cells in the human retina.[4] Cones are less sensitive to light than the rod cells in the retina (which support vision at low light levels), but allow the perception of colour. Cone cell structure They are also able to perceive finer detail and more rapid changes in images, because their response times to stimuli are faster than those of rods.[2] As opposed to rods, cones consist one of the three types of pigment namely: S-cones (absorbs blue), M-cones (absorbs green) and L-cones (absorbs red). Each cone is therefore sensitive to visible wavelengths of light that correspond to red (long-wavelength), green (medium-wavelength), or blue (short-wavelength) light.[5] Because humans usually have three kinds of cones with different photopsins, which have different response curves and thus respond to variation in colour in different ways, we have trichromatic vision. Being colour blind can change this, and there have been some unverified reports of people with four or more types of cones, giving them tetrachromatic vision.[6][7][8] Destruction to the cone cells from disease would result in blindness.
Cone cell
313
Types
Humans normally have three kinds of cones. The first responds the most to light of long wavelengths, peaking at a reddish colour; this type is sometimes designated L for long. The second type responds the most to light of medium-wavelength, peaking at a green colour, and is abbreviated M for medium. The third type responds the most to short-wavelength light, of a bluish colour, and is designated S for short. The three types have peak wavelengths near 564–580 nm, 534–545 nm, and 420–440 nm, respectively.[][9] The difference in the signals received from the three cone types allows the brain to perceive all possible colours, through the opponent process of colour vision. (Rod cells have a peak sensitivity at 498 nm, roughly halfway between the peak sensitivities of the S and M cones.) All of the receptors contain the pigment photopsin, with variations in its conformation causing differences in the optimum wavelengths absorbed. The colour yellow, for example, is perceived when the L cones are stimulated slightly more than the M cones, and the colour red is perceived when the L cones are stimulated significantly more than the M cones. Similarly, blue and violet hues are perceived when the S receptor is stimulated more than the other two. The S cones are most sensitive to light at wavelengths around 420 nm. However, the lens and cornea of the human eye are increasingly absorptive to shorter wavelengths, and this sets the short wavelength limit of human-visible light to approximately 380 nm, which is therefore called 'ultraviolet' light. People with aphakia, a condition where the eye lacks a lens, sometimes report the ability to see into the ultraviolet range.[10] At moderate to bright light levels where the cones function, the eye is more sensitive to yellowish-green light than other colors because this stimulates the two most common (M and L) of the three kinds of cones almost equally. At lower light levels, where only the rod cells function, the sensitivity is greatest at a blueish-green wavelength. Cones also tend to possess a significantly elevated visual acuity because each cone cell has a lone connection to the optic nerve, therefore, the cones have an easier time telling that two stimuli are isolated. Separate connectivity is established in the inner plexiform layer so that each connection is parallel. [11] While it has been discovered that there exists a mixed type of bipolar cells that bind to both rod and cone cells, bipolar cells still predominantly receive their input from cone cells.[12]
Structure
Cone cells are somewhat shorter than rods, but wider and tapered, and are much less numerous than rods in most parts of the retina, but greatly outnumber rods in the fovea. Structurally, cone cells have a cone-like shape at one end where a pigment filters incoming light, giving them their different response curves. They are typically 40–50 µm long, and their diameter varies from 0.5 to 4.0 µm, being smallest and most tightly packed at the center of the eye at the fovea. The S cones are a little larger than the others.[citation needed] Photobleaching can be used to determine cone arrangement. This is done by exposing dark-adapted retina to a certain wavelength of light that paralyzes the particular type of cone sensitive to that wavelength for up to thirty minutes from being able to dark-adapt making it appear white in contrast to the grey dark-adapted cones when a picture of the retina is taken. The results illustrate that S cones are randomly placed and appear much less frequently than the M and L cones. The ratio of M and L cones varies greatly among different people with regular
Bird, reptilian, and monotreme cone cells.
Cone cell vision (e.g. values of 75.8% L with 20.0% M versus 50.6% L with 44.2% M in two male subjects).[13] Like rods, each cone cell has a synaptic terminal, an inner segment, and an outer segment as well as an interior nucleus and various mitochondria. The synaptic terminal forms a synapse with a neuron such as a bipolar cell. The inner and outer segments are connected by a cilium.[2] The inner segment contains organelles and the cell's nucleus, while the outer segment, which is pointed toward the back of the eye, contains the light-absorbing materials.[2] Like rods, the outer segments of cones have invaginations of their cell membranes that create stacks of membranous disks. Photopigments exist as transmembrane proteins within these disks, which provide more surface area for light to affect the pigments. In cones, these disks are attached to the outer membrane, whereas they are pinched off and exist separately in rods. Neither rods nor cones divide, but their membranous disks wear out and are worn off at the end of the outer segment, to be consumed and recycled by phagocytic cells. The response of cone cells to light is also directionally nonuniform, peaking at a direction that receives light from the center of the pupil; this effect is known as the Stiles–Crawford effect.
314
Diseases
One of the diseases related to cone cells present in retina is retinoblastoma. Retinoblastoma is a rare cancer of the retina, caused by the mutation of both copies of retinoblastoma genes (RB1). Most cases of Retinablastoma occur during early childhood, because it is commonly found in children.[14] One or both eyes may be affected. The protein encoded by RB1 regulates a signal transduction pathway while controlling the cell cycle progression as normally. Retinoblastoma seems to originate in cone precursor cells present in the retina that consist of natural signalling networks which restrict cell death and promote cell survival after losing the RB1, or having both the RB1 copies mutated. It has been found that TRβ2 which is a transcription factor specifically affiliated with cones is essential for rapid reproduction and existence of the retinoblastoma cell.[] A drug that can be useful in the treatment of this disease is MDM2 (murine double minute 2) gene. Knockdown studies have shown that the MDM2 gene silences ARF-induced apoptosis in retinoblastoma cells and that MDM2 is necessary for the survival of cone cells.[] Although research and scientist have been able to discover a lot about this type of disease, there is still much to understand. It is unclear at this point why the retinoblastoma in humans is sensitive to RB1 inactivation. [15] The pupil may appear white or have white spots. A white glow in the eye is often seen in photographs taken with a flash, instead of the typical "red eye" from the flash, and the pupil may appear white or distorted. Other symptoms can include crossed eyes, double vision, eyes that do not align, eye pain and redness, poor vision or differing iris colours in each eye. If the cancer has spread, bone pain and other symptoms may occur.[][]
Color Afterimage
Sensitivity to a prolonged stimulation tends to decline over time, leading to neural adaptation. An interesting effect occurs when staring at a particular color for too long. Such action leads to an exhaustion of the cone cells that respond to that color - resulting in the afterimage. This vivid color aftereffect can last for a minute or more. [16]
References
[2] G. Osterberg (1935). “Topography of the layer of rods and cones in the human retina,” Acta Ophthalmol., Suppl. 13:6, pp. 1–102. [5] Schacter,Gilbert, Wegner, "Psychology", New York: Worth Publishers,2009. [10] Let the light shine in: You don't have to come from another planet to see ultraviolet light (http:/ / education. guardian. co. uk/ higher/ medicalscience/ story/ 0,9837,724257,00. html) EducationGuardian.co.uk, David Hambling (May 30, 2002) [11] Strettoi, E., et all; Complexity of retinal cone bipolar cells. Progress in Retinal and Eye Research (2010), 29 (4), pg. 272-283 [12] Strettoi et al. (2010), "Complexity of retinal cone bipolar cells", Progress in Retinal and Eye Research, 29 (4), pg. 272–283. [15] http:/ / www. nature. com. myaccess. library. utoronto. ca/ nrc/ index. html [16] Schacter, Daniel L. Psychology: the second edition. Chapter 4.9.
Cone cell
315
External links
• Cell Centered Database – Cone cell (http://ccdb.ucsd.edu/sand/main?stype=lite&keyword=cone& Submit=Go&event=display&start=1) • Webvision's Photoreceptors (http://webvision.umh.es/webvision/photo1.html) • NIF Search – Cone Cell (https://www.neuinfo.org/mynif/search.php?q=Cone Cell&t=data&s=cover&b=0& r=20) via the Neuroscience Information Framework • Model and image of cone cell (http://www.nanobotmodels.com/node/33)
Carotid body
316
Carotid body
Carotid body
Section of part of human glomus caroticum. Highly magnified. Numerous blood vessels are seen in section among the gland cells.
Diagram showing the origins of the main branches of the carotid arteries. Latin Gray's glomus caroticum subject #277 1281
[1]
The carotid body (carotid glomus or glomus caroticum) is a small cluster of chemoreceptors and supporting cells located near the fork (bifurcation) of the carotid artery (which runs along both sides of the throat). The carotid body detects changes in the composition of arterial blood flowing through it, mainly the partial pressure of oxygen, but also of carbon dioxide. Furthermore, it is also sensitive to changes in pH and temperature.
Composition
The carotid body is made up of two types of cells, called glomus cells: glomus type I (chief) cells, and glomus type II (sustentacular) cells. • Glomus type I/chief cells are derived from neural crest,[] which, in turn are derived from neuroectoderm. They release a variety of neurotransmitters, including acetylcholine, ATP, and dopamine that trigger EPSPs in synapsed neurons leading to the respiratory center. • Glomus type II/sustentacular cells resemble glia, express the glial marker S100 and act as supporting cells. The carotid body contains the most vascular tissue in the human body. The thyroid gland is very vascular, but not quite as much as the carotid body.
Carotid body
317
Function
The carotid body functions as a sensor: it responds to a stimulus, primarily O2 partial pressure, which is detected by the type I (glomus) cells, and triggers an action potential through the afferent fibers of the glossopharyngeal nerve, which relays the information to the central nervous system.
Stimulus
While the central chemoreceptors in the brainstem are highly sensitive to CO2 the carotid body is a peripheral chemoreceptor that mainly provides afferent input to the respiratory center that is highly O2 dependent. However, the carotid body also senses increases in CO2 partial pressure and decreases in arterial pH, but to a lesser degree than for O2 The output of the carotid bodies is low at an oxygen partial pressure above about 100 mmHg (13,3 kPa) (at normal physiological pH), but below this the activity of the type I (glomus) cells increases rapidly.
Detection
The mechanism for detecting reductions in PO2 has yet to be identified, there may be multiple mechanisms[] and could vary between species. Hypoxia detection has been shown to depend upon increased Hydrogen sulfide generation produced by cystathionine gamma-lyase as hypoxia detection is reduced in mice in which this enzyme is knocked out or pharmacologically inhibited. The process of detection involves the interaction of cystathionine gamma-lyase with hemeoxygenase-2 and the production of carbon monoxide.[1] Other theories suggest it may involve mitochondrial oxygen sensors and the haem-containing cytochromes that undergo reversible one-electron reduction during oxidative-phosphorylation. Haem reversibly binds O2 with an affinity similar to that of the carotid body, suggesting that haem containing proteins may have a role in O2, potentially this could be one of the complexes involved in oxidative-phosphorylation. This leads to increases in reactive oxygen species and rises in intracellular Ca2+. However, whether hypoxia leads to an increase or decrease in reactive oxygen species is unknown. The role of reactive oxygen species in hypoxia sensing is also under question.[] The oxygen dependent enzyme haem-oxidase has also been put forward as a hypoxia sensor. In normoxia, haem-oxygenase generates carbon monoxide (CO), CO activates the large conductance calcium-activated potassium channel, BK. Falls in CO that occur as a consequence of hypoxia would lead to closure of this potassium channel and this would lead to membrane depolarisation and consequence activation of the carotid body.[] A role for the "energy sensor" AMP-activated protein kinase (AMPK) has also been proposed in hypoxia sensing. This enzyme is activated during times of net energy usage and metabolic stress, including hypoxia. AMPK has a number of targets and it appears that, in the carotid body, when AMPK is activated by hypoxia, it leads to downstream potassium channel closure of both O2-sentive TASK-like and BK channels [] An increased PCO2 is detected because the CO2 diffuses into the cell, where it increases the concentration of carbonic acid and thus protons. The precise mechanism of CO2 sensing is unknown, however it has been demonstrated that CO2 and low pH inhibit a TASK-like potassium conductance, reducing potassium current. This leads to depolarisation of the cell membrane which leads to Ca2+ entry, excitation of glomus cells and consequent neurotransmitter release.[] Arterial acidosis (either metabolic or from altered PCO2) inhibits acid-base transporters (e.g. Na+-H+) which raise intracellular pH, and activates transporters (e.g. Cl--HCO3-) which decrease it. Changes in proton concentration caused by acidosis (or the opposite from alkalosis) inside the cell stimulates the same pathways involved in PCO2 sensing. Another mechanism is through oxygen sensitive potassium channels. A drop in dissolved oxygen lead to closing of these channels which results in depolarization. This leads to release of the neurotransmitter dopamine in the glossopharengeal and vagus afferente to the vasomotor area.
Carotid body
318
Action potential
The type I (glomus) cells in the carotid (and aortic bodies) are derived from neuroectoderm and are thus electrically excitable. A decrease in oxygen partial pressure, an increase in carbon dioxide partial pressure, and a decrease in arterial pH can all cause depolarization of the cell membrane, and they affect this by blocking potassium currents. This reduction in the membrane potential opens voltage-gated calcium channels, which causes a rise in intracellular calcium concentration. This causes exocytosis of vesicles containing a variety of neurotransmitters, including acetylcholine, noradrenaline, dopamine, adenosine, ATP, substance P, and met-enkephalin. These act on receptors on the afferent nerve fibres which lie in apposition to the glomus cell to cause an action potential.
Relay
The feedback from the carotid body is sent to the cardiorespiratory centers in the medulla oblongata via the afferent branches of the Glossopharyngeal nerve. The efferent fibres of the aortic body chemoreceptors are relayed by the Vagus nerve. These centers, in turn, regulate breathing and blood pressure.
Disorders
A paraganglioma is a tumor that may involve the carotid body and is usually benign. Rarely, a malignant neuroblastoma may originate from the carotid body.
References
[1] Peng Y-J, Nanduri J, Raghuraman G, Souvannakitti D, Gadalla M.M, Kumar GK, Snyder SH, Prabhakar NR. (2010). H2S mediates O2 sensing in the carotid body PNAS 107 (23) 10719-10724.
Micrograph of a carotid body tumor.
External links
• Carotid+body (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=Carotid+body) at eMedicine Dictionary
Taste bud
319
Taste bud
Taste buds
Semidiagrammatic view of a portion of the mucous membrane of the tongue. Two fungiform papillæ are shown. On some of the filiform papillæ the epithelial prolongations stand erect, in one they are spread out, and in three they are folded in. Latin Gray's MeSH Code caliculus gustatorius subject #222 991 Taste+Buds
[2] [3] [1]
TH H3.04.01.0.02116 [3] TH H3.04.01.0.03013
Taste buds contain the receptors for taste. They are located around the small structures on the upper surface of the tongue, soft palate, upper esophagus and epiglottis, which are called papillae.[1] These structures are involved in detecting the five (known) elements of taste perception: salty, sour, bitter, sweet, and umami. Via small openings in the tongue epithelium, called taste pores, parts of the food dissolved in saliva come into contact with taste receptors. These are located on top of the taste receptor cells that constitute the taste buds. The taste receptor cells send information detected by clusters of various receptors and ion channels to the gustatory areas of the brain via the seventh, ninth and tenth cranial nerves. On average, the human tongue has 2,000–8,000 taste buds.[2]
Types of papillae
The majority of taste buds on the tongue sit on raised protrusions of the tongue surface called papillae. There are four types of papillae present in the human tongue: • Fungiform papillae - as the name suggests, these are slightly mushroom-shaped if looked at in longitudinal section. These are present mostly at the dorsal surface of the tongue, as well as at the sides. Innervated by facial nerve. • Filiform papillae - these are thin, long papillae "V"-shaped cones that don't contain taste buds but are the most numerous. These papillae are mechanical and not involved in gustation. They are characterized by increased keratinization. • Foliate papillae - these are ridges and grooves towards the posterior part of the tongue found at the lateral borders. Innervated by facial nerve (anterior papillae) and glossopharyngeal nerve (posterior papillae). • Circumvallate papillae - there are only about 10 to 14 of these papillae on most people, and they are present at the back of the oral part of the tongue. They are arranged in a circular-shaped row just in front of the sulcus terminalis of the tongue. They are he associated with ducts of Von Ebner's glands, and are innervated by the glossopharyngeal nerve.
Taste bud Salts, sweet, sour and umami tastes causes depolarization of the taste cells, although different mechanisms are applied. Bitter causes an internal release of Ca2+, no external Ca2+ is required. The bud is formed by two kinds of cells: supporting cells and gustatory cells. The supporting (sustentacular) cells are mostly arranged like the staves of a cask, and form an outer envelope for the bud. Some, however, are found in the interior of the bud between the gustatory cells. The gustatory (taste) cells, a chemoreceptor, occupy the central portion of the bud; they are spindle-shaped, and each possesses a large spherical nucleus near the middle of the cell. The peripheral end of the cell terminates at the gustatory pore in a fine hair filament, the gustatory hair. The central process passes toward the deep extremity of the bud, and there ends in single or bifurcated varicosities. The nerve fibrils after losing their medullary sheaths enter the taste bud, and end in fine extremities between the gustatory cells; other nerve fibrils ramify between the supporting cells and terminate in fine extremities; these, however, are believed to be nerves of ordinary sensation and not gustatory. The average life of a taste bud is 10 days.
320
Additional images
schematic drawing of a taste bud
taste bud (nerve missing)
References
[1] Discovery News, October 26, 2010 (http:/ / news. discovery. com/ human/ taste-buds-found-in-lungs. ) [2] Encyclopædia Britannica. 2009. Encyclopædia Britannica Online. (http:/ / www. britannica. com/ EBchecked/ topic/ 584034/ taste-bud)
External links
• Taste Perception: Cracking the Code (http://biology.plosjournals.org/perlserv/?request=get-document& doi=10.1371/journal.pbio.0020064) • Scientists Explore the Workings of Taste Buds (http://www.npr.org/templates/story/story. php?storyId=4766647) from National Public Radio's Talk of the Nation, July 22, 2005 • http://kidshealth.org/kid/talk/qa/taste_buds.html For kids about taste buds! • http://www.newser.com/story/103744/your-lungs-have-their-own-taste-buds.html
Schwann cell
321
Schwann cell
Structure of a typical neuron
Schwann cells wrapped around an axon
Schwann cells (named after physiologist Theodor Schwann) or neurolemmocytes are the principal glia of the peripheral nervous system (PNS). Glial cells function to support neurons and in the PNS, also include satellite cells, olfactory ensheathing cells, enteric glia and glia that reside at sensory nerve endings, such as the Pacinian corpuscle. There are two types of Schwann cell, myelinating and nonmyelinating. Myelinating Schwann cells wrap around axons of motor and sensory neurons to form the myelin sheath. Schwann cells are involved in many important aspects of peripheral nerve biology—the conduction of nervous impulses along axons, nerve development and regeneration, trophic support for neurons, production of the nerve extracellular matrix, modulation of neuromuscular synaptic activity, and presentation of antigens to T-lymphocytes. Charcot-Marie-Tooth disease (CMT), Guillain-Barré syndrome (GBS), schwannomatosis and chronic inflammatory demyelinating polyneuropathy (CIDP) are all neuropathies involving Schwann cells.
Schwann cell
322
Description
Named after the German physiologist Theodor Schwann, Schwann cells are a variety of glial cell that keep peripheral nerve fibres (both myelinated and unmyelinated) alive. In myelinated axons, Schwann cells form the myelin sheath (see above). The sheath is not continuous. Individual myelinating Schwann cells cover about 100 micrometres of an axon—equating to approximately 10,000 Schwann cells along a 1 metre length of the axon—which can be up to a metre or more in length. The gaps between adjacent Schwann cells are called nodes of Ranvier (see above). The vertebrate nervous system relies on the myelin sheath for insulation and as a method of decreasing membrane capacitance in the axon. The action potential jumps from node to node, in a process called saltatory conduction, which can increase conduction velocity up to ten times, without an increase in axonal diameter. In this sense, Schwann cells are the peripheral nervous system's analogues of the central nervous system's oligodendrocytes. However, unlike oligodendrocytes, each myelinating Schwann cell provides insulation to only one axon (see image). This arrangement permits saltatory conduction of action potentials with repropagation at the nodes of Ranvier. In this way, myelination greatly increases speed of conduction and saves energy.[1] Non-myelinating Schwann cells are involved in maintenance of axons and are crucial for neuronal survival. Some group around smaller axons (External image here [2]) and form Remak bundles.[2] Myelinating Schwann cells begin to form the myelin sheath in mammals during fetal development and work by spiraling around the axon, sometimes with as many A Schwann cell in culture. as 100 revolutions. A well-developed Schwann cell is shaped like a rolled-up sheet of paper, with layers of myelin in between each coil. The inner layers of the wrapping, which are predominantly membrane material, form the myelin sheath while the outermost layer of nucleated cytoplasm forms the neurolemma. Only a small volume of residual cytoplasm communicates the inner from the outer layers. This is seen histologically as the Schmidt-Lantermann incisure. A number of experimental studies since 2001 have implanted Schwann cells in an attempt to induce remyelination in multiple sclerosis-afflicted patients.[3] In the past two decades, many studies have demonstrated positive results and potential for Schwann cell transplantation as a therapy for spinal cord injury, both in aiding regrowth and myelination of damaged CNS axons.[4] Indeed, Schwann cells are known for their roles in supporting nerve regeneration.[5] Nerves in the PNS consist of many axons myelinated by Schwann cells. If damage occurs to a nerve, the Schwann cells will aid in digestion of its axons (phagocytosis). Following this process, the Schwann cells can guide regeneration by forming a type of tunnel that leads toward the target neurons. The stump of the damaged axon is able to sprout, and those sprouts that grow through the Schwann-cell “tunnel” do so at the rate of approximately 1mm/day in good conditions. The rate of regeneration decreases with time. Successful axons can therefore reconnect with the muscles or organs they previously controlled with the help of Schwann cells, however, specificity is not maintained and errors are frequent, especially when long distances are involved.[6] If Schwann cells are prevented from associating with axons, the axons die. Regenerating axons will not reach any target unless Schwann cells are there to support them and guide them. They have been shown to be in advance of the growth cones. Schwann cells are essential for the maintenance of healthy axons. They produce a variety of factors, including neurotrophins, and also transfer essential molecules across to axons.
Schwann cell
323
Schwann cell lineage
Schwann cells are of neural crest origin. During mouse embryonic development, neural crest cells first differentiate into Schwann cell precursors (SCPs) at around embryonic day (E) 12–13. These precursor cells subsequently differentiate into immature Schwann cells at approximately E15–16, persisting until birth. The postnatal fate of the immature Schwann cell depends on its random association with axons. In a process called radial sorting, whereby Schwann cells segregate axons by extending processes into axon bundles, the Schwann cells that happen to associate with a large diameter axon (>1 μm) will develop into myelinating Schwann cells. Small diameter axons become entrenched in the invaginations of non-myelinating Schwann cells, also called Remak bundles. A key regulator of this process is the axonally-derived signal Neuregulin-1, which binds to cell surface receptors on the Schwann cell and promotes myelination of large diameter axons and sorting of small diameter axons in Remak bundles, dependent on the activity of the β-secretase BACE1 ([7][8][9][10][11]). A further class of non-myelinating Schwann cell, the terminal (or perisynaptic) Schwann cell, exists at the neuromuscular junction, in close proximity to the neuron-muscle synapse. The transition from immature Schwann cell to myelinating/non-myelinating Schwann cell is reversible. When the nerve is injured, Schwann cells can dedifferentiate to form a cell type resembling the immature Schwann cell, often referred to as a denervated or dedifferentiated Schwann cell. This allows them to re-enter the cell cycle in order to proliferate and aid nerve regeneration.[12]
Immunoreactivity
The different classes of Schwann cells express characteristic antigenic markers that can be targeted with antibodies. Myelinating Schwann cells can be visualised by immunohistochemistry using antibodies against the proteins S-100, Myelin protein zero (P-Zero) and Myelin basic protein (MBP). Non-myelinating Schwann cells such as those that form Remak bundles and terminal Schwann cells are positive for S-100 and Glial fibrillary acidic protein (GFAP).
References
[1] Kalat, James W. Biological Psychology, 9th ed. USA: Thompson Learning, 2007. [2] "Medical Student Named Rhodes Scholar" (http:/ / focus. hms. harvard. edu/ 2003/ Oct24_2003/ neurology. html) - FOCUS - News from Harvard Medical, Dental and Public Health Schools - Copyright © 2010 President and Fellows of Harvard College. [6] Carlson, Neil R. Physiology of Behavior, 9th ed. USA: Pearson Education, Inc., 2007.
External links
• Diagram at clc.uc.edu (http://biology.clc.uc.edu/courses/bio105/nervous.htm) • BU Histology Learning System: 21301loa (http://www.bu.edu/histology/p/21301loa.htm)—"Ultrastructure of the Cell: myelinated axon and Schwann cell" • Cell Centered Database - Schwann cell (http://ccdb.ucsd.edu/sand/main?stype=lite&keyword=schwann& Submit=Go&event=display&start=1)
Satellite glial cell
324
Satellite glial cell
Neuron: Satellite Cell
NeuroLex ID sao792373294 [1] Code Latin TH H2.00.06.2.02002 gliocytus ganglionicus [1]
Satellite glial cells are a type of glial cell that line the exterior surface of neurons in the peripheral nervous system (PNS). Satellite glial cells (SGCs) also surround neuron cell bodies within ganglia.[][] They are of a similar embryological origin to Schwann cells of the PNS, as they are both derived from the neural crest of the embryo during development.[] SGCs have been found to hold a variety of roles, including control over the microenvironment of sympathetic ganglia.[] They are thought to have a similar role to astrocytes in the central nervous system (CNS).[] They supply nutrients to the surrounding neurons and also have some structural function. Satellite cells also act as protective, cushioning cells. Additionally, they express a variety of receptors that allow for a range of interactions with neuroactive chemicals.[] Many of these receptors and other ion channels have recently been implicated in health issues including chronic pain[] and herpes simplex.[] There is much more to be learned about these cells, and research surrounding additional properties and roles of the SGCs is ongoing.[]
Anatomy
Satellite glial cells are the principle glial cells found in the peripheral nervous system, specifically in sensory,[] sympathetic, and parasympathetic ganglia.[] They compose the thin cellular sheaths that surround the individual neurons in these ganglia. In an SGC, the cell body is denoted by the region containing the single, relatively large nucleus. Each side of the cell body extends outward, forming perineuronal processes. The region containing the nucleus has the largest volume of cytoplasm, making this region of the SGC sheath thicker.[] The sheath can be even thicker if multiple SGCs are layered on top of one another, each measuring 0.1 micrometres (3.9×10−6 in).[] Despite their flattened shape, satellite glial cells contain all common organelles necessary to make cellular products and to maintain the homeostatic environment of the cell. The plasma membrane of SGCs is thin and not very dense,[] and it is associated with adhesion molecules,[] receptors for neurotransmitters and other molecules,[] and ion channels, specifically potassium ion channels.[] Within individual Satellite glial cells are expressed throughout the SGCs, there is both rough endoplasmic reticulum[] and smooth sympathetic and parasympathetic ganglia in their [] endoplasmic reticulum, but the latter is much less abundant.[] Most respective nervous system divisions. often the Golgi apparatus and the centrioles in an SGC are found in a region very close to the cell’s nucleus. On the other hand, mitochondria are found throughout the cytoplasm[] along with the organelles involved in autophagy and other forms of catabolic degradation, such as lysosomes, lipofuscin granules, and peroxisomes.[] Both microtubules and intermediate filaments can be seen throughout the cytoplasm, and most often they lie parallel to the SGC sheath. These filaments are found in greater concentrations at the axon
Satellite glial cell hillock and at the beginning portion of an axon in an SGC of the sympathetic ganglia.[] In some SGCs of the sensory ganglia researchers have seen a single cilium that extends outward from the cell surface near the nucleus and into the extracellular space of a deep indentation in the plasma membrane.[] The cilium, however, only has the nine pairs of peripheral microtubules while it lacks the axial pair of microtubules, making its structure very similar to the cilia of neurons, Schwann cells, and astrocytes of the CNS.[]
325
In sensory ganglia
Satellite glial cells in sensory ganglia are laminar cells that most often lack any true processes extending from the cell body. In general an envelope of multiple SGCs completely surrounds each sensory neuron.[] The number of SGCs that make up the sheath increases proportionately with the volume of the neuron which it surrounds. Additionally, the volume of the sheath itself increases proportionately with the volume and surface area of the neuron’s somata. The distance of extracellular space between the sheath and the neuronal plasma membrane measures 20 nanometres (7.9×10−7 in), allowing the neuron and its SGC sheath to form a single anatomical and functional unit.[] These individual units are separated by areas of connective tissue. However, there are some sensory neurons that occupy the same space within connective tissue and are therefore grouped together in a “cluster” of two or three neurons. Most often each individual neuron in a cluster is still surrounded by its own SGC sheath, but in some cases it is missing.[] Some sensory neurons have small projections called microvilli that extend outward from their cell surfaces. Due to their close proximity to the SGC sheath, these microvilli of the neuronal plasma membrane reach into the grooves of the sheath, allowing for possible exchange of materials between the cells.[]
In sympathetic ganglia
In the sympathetic ganglia, satellite glial cells are one of three main types of cells, the other two being the sympathetic ganglion neurons and small intensely fluorescent (SIF) cells.[] SIF cells of sympathetic ganglia are separated into groups, each of which is surrounded by an SGC sheath.[] The SGCs of the sympathetic ganglia come from the neural crest and do not proliferate during embryonic development until the neurons are present and mature, indicating that the neurons signal the division and maturation of the SGCs.[] The SGCs of sympathetic ganglia follow the same basic structure as the SGCs of sensory ganglia, except that sympathetic ganglia also receive synapses. Therefore, the SGC sheath of sympathetic neurons must extend even further to cover the axon hillock near the somata.[] Like the regions of the sheath near the glial nucleus, the regions of the sheath at the axon hillocks are thicker than those surrounding the rest of the neuron. This indicates that the SGCs play a role in the synaptic environment, thereby influencing synaptic transmission.
Differences from other glial cells
Many people liken SGCs to the astrocytes of the CNS because they share certain anatomical and physiological properties, such as the presence of neurotransmitter transporters and the expression of glutamine synthetase.[] However, there are distinguishing factors that put SGCs in their own distinct category of glial cells. SGCs most often surround individual sensory and parasympathetic neurons with a complete, unbroken sheath while most neurons of sympathetic ganglia lack a completely continuous SGC sheath, allowing for limited direct exchange of materials between the extracellular space of the neuron and the space within the connective tissue where the SGCs are situated.[] Furthermore, gap junctions exist between SGCs in the sheaths of adjacent neurons as well as between SGCs in the same sheath (reflexive gap junctions).[] These gap junctions have been identified through the use of electron microscopy and weight tracer markers, such as Lucifer yellow or neurobiotin. The degree to which SGCs are coupled to SGCs of another sheath or to SGCs of the same sheath is dependent on the pH of the cellular environment.[] From studies on rats and mice, researchers have found that satellite glial cells express many neurotransmitter receptors, such as muscarinic acetylcholine and erythropoietin receptors.[] In order to differentiate between SGCs
Satellite glial cell and other glial cells researchers have used markers to identify which proteins are found in different cells. Although SGCs express glial fibrillary acidic protein (GFAP)[]and different S-100 proteins,[] the most useful marker available today for SGC identification is glutamine synthetase (GS). The levels of GS are relatively low at rest, but they greatly increase if the neuron undergoes axonal damage.[] Furthermore, SGCs also possess mechanisms to release cytokines, adenosine triphosphate (ATP), and other chemical messengers.[]
326
Function
Research is currently ongoing in determining the physiological role of satellite glial cells. Current theories suggest that SGCs have a significant role in controlling the microenvironment of the sympathetic ganglia. This is based on the observation that SGCs almost completely envelop the neuron and can regulate the diffusion of molecules across the cell membrane.[] It has been previously shown that when fluorescent protein tracers are injected into the cervical ganglion in order to bypass the circulatory system, they are not found on the neuron surface. This suggests that the SGCs can regulate the extracellular space of individual neurons.[] Some speculate that SGCs in the autonomic ganglia have a similar role to the blood–brain barrier as a functional barrier to large molecules.[] SGCs role as a regulator of neuronal microenvironment is further characterized by its electrical properties which are very similar to that of astrocytes.[] Astrocytes have a well studied and defined role in controlling the microenvironment within the brain, therefore researchers are investigating any homologous role of SGCs within the sympathetic ganglia. An established mode of controlling the microenvironment in sensory ganglia is the uptake of substances by specialized transporters which carry neurotransmitters into cells when coupled with Na+ and Cl−.[] Transporters for glutamate and gamma-Aminobutyric acid (GABA)[] have been found in SGCs. They appear to be actively engaged in the control of the composition of the extracellular space of the ganglia. The enzyme glutamine synthetase, which catalyzes the conversion of glutamate into glutamine, is found in large amounts in SGCs.[] Additionally, SGCs contain the glutamate related enzymes glutamate dehydrogenase and pyruvate carboxylase, and thus can supply the neurons not only with glutamine, but also with malate and lactate.[]
Molecular properties
Unlike their adjacent neurons, SGCs do not have synapses but are equipped with receptors for a variety of neuroactive substances that are analogous to those found in neurons.[] Axon terminals as well as other parts of the neuron carry receptors to substances such as acetylcholine (ACh), GABA, glutamate, ATP, noradrenaline, substance P, and capsaicin that directly affect the physiology of these cells.[] Current research is revealing that SGCs are also able to respond to some of the same chemical stimuli as neurons. The research is ongoing and SGCs role in injury repair mechanisms is not yet fully understood. Molecular characteristics of SGCs
Molecule [] Type of Ganglia Method of Detection Comments
Glutamine synthetase Mouse TG GFAP Rat DRG, TG Rat DRG Rat, rabbit DRG Rat DRG
IHC IHC
Catalyzes the condensation of glutamate and ammonia to form glutamine Upregulated by nerve damage
S100 Endothelin ETB receptor Bradykinin B2 receptor P2Y receptor
IHC IHC, autoradiography
Upregulated by nerve damage Blockers of ETs are shown to alleviate pain in animal models
Electrophysiology
Involved in the inflammatory process
Mouse TG
Ca2+ imaging, IHC
Contributes to nociception
Satellite glial cell
327
Rat DRG IHC, mRNA (ISH) Role not well defined in sensory ganglia
ACh muscarinic receptor NGF trkA receptor TGFα Erythropoietin receptor TNF-α
Rat DRG Rat DRG Rat DRG
Immuno-EM mRNA (ISH), IHC IHC
May play a role in response to neuronal injury Stimulates neural proliferation after injury
Mouse DRG, IHC TG Mouse TG Rat DRG Rat DRG Rat DRG IHC IHC IHC IHC
Inflammatory mediator increased by nerve crush, herpes simplex activation
IL-6 ERK JAK2 Somatostatin sst1 receptor GABA transporter Glutamate transporter Guanylate cyclase
Cytokine released during inflammation, increased by UV irradiation Involved in functions including the regulation of meiosis, and mitosis Signaling protein apart of the type II cytokine receptor family Somatostatin inhibits the release of many hormones and other secretory proteins
Rat DRG Rat DRG
Autoradiography mRNA (ISH), IHC, Autoradiography IHC for cGMP Terminates the excitatory neurotransmitter signal by removal (uptake) of glutamate Second messenger that internalizes the message carried by intercellular messengers such as peptide hormones and NO Known to function as a neuromodulator as well as a trophic factor in the central nervous system
Rat DRG, TG Chick DRG
PGD synthase
IHC
Roles in health issues
Chronic pain
Glial cells, including SGCs, have long been recognized for their roles in response to neuronal damage and injury. SCGs have specifically been implicated in a new role involving the creation and persistence of chronic pain, which may involve hyperalgesia and other forms of spontaneous pain.[] Secretion of bioactive molecules SGCs have the ability to release cytokines and other bioactive molecules that transmit pain neuronally.[] Neurotrophins and tumor necrosis factor α (TNFα) are other cellular factors that work to sensitize neurons to pain.[] SGCs are present in the PNS in fewer numbers than other more well-known types of glial cells, like astrocytes, but have been determined to have an impact on nociception because of some of their physiological and pharmacological properties.[] In fact, just like astrocytes, SGCs have the ability to sense and regulate neighboring neuronal activity.[] First, after a period of nerve cell injury, SGCs are known to up-regulate GFAP and to undergo cell division. They have the ability to release chemoattractants, which are analogous to those released by Schwann cells and contribute to the recruitment and proliferation of macrophages. Additionally, several research groups have found that SGC coupling increases after nerve damage, which has an effect on the perception of pain, likely for several reasons. Normally, the gap junctions between SGCs are used in order to redistribute potassium ions between adjacent cells. However, in coupling of SGCs, the number of gap junctions greatly increases. This may possibly be to deal with larger amounts of ATP and glutamate, which eventually leads to increased recycling of the glutamate. The increased levels of glutamate lead to over excitation and an increase in nociception.[]
Satellite glial cell Expression of receptors and ion channels Various neuronal receptors present on SGCs have been named as participants in ATP-evoked pain signals, particularly the homomultimer P2X3 and the heteromultimer P2X2/3 purinoceptors. In general, the P2X family of receptors responds to neuronally released ATP. Each of the P2X subtypes are found in sensory neurons with the exception of the P2X7 receptor, which is selectively expressed by glial cells, including SGCs. The receptor has been implicated in the release of interleukin IL-1β from macrophages or microglia and astrocytes. The receptor likely has a part in the cascade of events that end with inflammation and neuropathic pain. It has been discovered that this receptor has an antagonist in the form of A-317491, which, when present, has the ability to reduce both the evoked and unprompted firing of various classes of spinal neurons, as well as to inhibit release of IL-1β. However, the outside influences of receptors P2X3 and P2Y1 are believed to complicate the interactions between P2X7 and its antagonist, making it a non-ideal target when using pharmacological strategy.[]
328
Representation of a typical P2X receptor subunit associated with the plasma membrane.
P2Y receptors are also found on both neurons and glial cells. Their role is less clear than that of the P2X receptors, but it has been noted they have several conflicting functions. In some cases, these receptors act as analgesics, as P2Y1 has the ability to inhibit the action of P2X3. In other cases, the receptors contribute to nociception through the modulation of the extracellular concentration of calcitonin gene related peptide (CGRP). These conflicting roles are being researched further so that they may serve as potential targets for the development of a variety of therapeutic drugs.[] SGCs also express a specific type of channel, the Kir4.1 channel, which works to maintain the desired low extracellular K+ concentration in order to control hyperexcitability, which is known to cause migraines. Additionally, extracellular K+ concentration has been found to be controlled by guanine nucleoside guanosine (Guo). Guo, which may be involved in neuron-to-SGC communication and interaction in sensory ganglia, is also a potential target that could control the alterations of extracellular K+ concentration associated with chronic pain.[]
Satellite glial cell
329
Herpes simplex
Sensory ganglia have been associated with infections from viruses like herpes simplex, which can exist in a dormant state within the ganglia for decades after the primary infection.[] When the virus becomes reactivated, blisters on the skin and mucous membranes appear. During the latent stage of the virus, the viruses are rarely located in the SGCs within the sensory ganglia, but the SGCs may still play an important role within the disease.[] It has been proposed that SGCs act to create walls to prevent the spread of the virus from infected to uninfected neurons.[][] If this wall of protection was to break down, then the infection could become more widespread.[] This property may be explained by looking at the location and arrangement of the SGCs, as they are centered on the neurons, allowing them to protect the neurons. It has also been proposed that SGCs may have a job in ridding the ganglia of the virus and in protecting and repairing the nervous system after the virus has left the dormant stage.[]
Herpes simplex virions.
Research directions
The majority of the information available on the subject of SGCs comes from research which was focused on the sensory neurons that the SGCs surround rather than the SGCs themselves. In the future, researchers plan to give more time and attention to the SGCs, which have many supportive and protective functions essential for life.[] Neurotransmitter and hormone receptors on SGCs in situ rather than in culture will likely be explored and definitively characterized.[] Changes in the receptors caused by various mutations and diseases will also be explored in order to determine the impact of these conditions.[] Additionally, the mechanisms behind neuronal-SGC communication is essentially unidentified, though it is likely that the various receptors both the neurons and SGCs have are used for chemical signaling, perhaps with P2Y.[] Ca2+ and NO and their impacts must also be observed to gain further understanding of interactions between the two types of cells.[] Finally, the possibility of an influence of SGCs on synaptic transmission within autonomic ganglia provides another direction for future research.[]
References
Neuroglia
330
Neuroglia
Glia
MeSH Glia [1] Code TA A14.0.00.005 [1] TH H2.00.06.2.00001
[2]
Glial cells, sometimes called neuroglia or simply glia (Greek γλία, γλοία "glue"; pronounced in English as either /ˈɡliːə/ or /ˈɡlaɪə/), are non-neuronal cells that maintain homeostasis, form myelin, and provide support and protection for neurons in the brain, and for neurons in other parts of the nervous system such as in the autonomic nervous system.[1] As the Greek name implies, glia are commonly known as the glue of the nervous system; however, this is not fully accurate. Neuroscience currently identifies four main functions of glial cells: 1. To surround neurons and hold them in place, 2. To supply nutrients and oxygen to neurons, 3. To insulate one neuron from another, 4. To destroy pathogens and remove dead neurons. For over a century, it was believed that they did not play any role in neurotransmission. That idea is now discredited;[] they do modulate neurotransmission, although the mechanisms are not yet well understood.[][][]
Neuroglia of the brain shown by Golgi's method.
Functions
Astrocytes can be identified in culture because, unlike other mature
glia, they express glial fibrillary acidic protein. Some glial cells function primarily as the physical support for neurons. Others regulate the internal environment of the brain, especially the fluid surrounding neurons and their synapses, and nutrify neurons. During early embryogenesis glial cells direct the migration of neurons and produce molecules that modify the growth of axons and dendrites. Recent researchWikipedia:Avoid weasel words indicates that glial cells of the hippocampus and cerebellum participate in synaptic transmission, regulate the clearance of neurotransmitters from the synaptic cleft, and release gliotransmitters such as ATP, which modulate synaptic function.
Neuroglia
331
Glial cells are known to be capable of mitosis. By contrast, scientific understanding of whether neurons are permanently post-mitotic,[2] or capable of mitosis,[3] is still developing. In the past, glia had been consideredWikipedia:Avoid weasel words to lack certain features of neurons. For example, glial cells were not believed to have chemical synapses or to release transmitters. They were considered to be the passive bystanders of neural transmission. However, recent studies have shown this to be untrue.[4] For example, astrocytes are crucial in clearance of neurotransmitters from within the synaptic cleft, which provides distinction between arrival of action potentials and prevents toxic build-up of certain neurotransmitters such as glutamate (excitotoxicity). It is also thought that glia play a role in many neurological diseases, including Alzheimer's disease. Furthermore, at least in vitro, astrocytes can release gliotransmitter glutamate in response to certain stimulation. Another unique type of glial cell, the oligodendrocyte precursor cells or OPCs, have very well-defined and functional synapses from at least two major groups of neurons.[citation needed] The only notable differences between neurons and glial cells are neurons' possession of axons and dendrites, and capacity to generate action potentials.
Glial cells in a rat brain stained with an antibody against GFAP.
23 week fetal brain culture astrocyte
Glia ought not to be regarded as "glue" in the nervous system as the name implies; rather, they are more of a partner to neurons.[5] They are also crucial in the development of the nervous system and in processes such as synaptic plasticity and synaptogenesis. Glia have a role in the regulation of repair of neurons after injury. In the CNS (Central Nervous System), glia suppress repair. Glial cells known as astrocytes enlarge and proliferate to form a scar and produce inhibitory molecules that inhibit regrowth of a damaged or Neoplastic glial cells stained with an antibody against GFAP severed axon. In the PNS (Peripheral Nervous System), (brown). Brain biopsy. glial cells known as Schwann cells promote repair. After axonal injury, Schwann cells regress to an earlier developmental state to encourage regrowth of the axon. This difference between PNS and CNS raises hopes for the regeneration of nervous tissue in the CNS. For example a spinal cord may be able to be repaired following injury or severance.
Neuroglia
332
Types
Microglia
Microglia are specialized macrophages capable of phagocytosis that protect neurons of the central nervous system.[6] They are derived from hematopoietic precursors rather than ectodermal tissue; they are commonly categorized as such because of their supportive role to neurons. These cells are found in all regions of the brain and spinal cord. Microglial cells are small relative to macroglial cells, with changing shapes and oblong nuclei. They are mobile within the brain and multiply when the brain is damaged. In the healthy central nervous system, microglia processes constantly sample all aspects of their environment (neurons, macroglia and blood vessels).
Macroglia
Location Name CNS Astrocytes Description The most abundant type of macroglial cell, astrocytes (also called astroglia) have numerous projections that anchor neurons to their blood supply. They regulate the external chemical environment of neurons by removing excess ions, notably potassium, and recycling neurotransmitters released during synaptic transmission. The current theory suggests that astrocytes may be the predominant "building blocks" of the blood–brain barrier. Astrocytes may regulate vasoconstriction and vasodilation by producing substances such as arachidonic acid, whose metabolites are vasoactive. Astrocytes signal each other using calcium. The gap junctions (also known as electrical synapses) between astrocytes allow the messenger molecule IP3 to diffuse from one astrocyte to another. IP3 activates calcium channels on cellular organelles, releasing calcium into the cytoplasm. This calcium may stimulate the production of more IP3. The net effect is a calcium wave that propagates from cell to cell. Extracellular release of ATP, and consequent activation of purinergic receptors on other astrocytes, may also mediate calcium waves in some cases. In general, there are two types of astrocytes, protoplasmic and fibrous, similar in function but distinct in morphology and distribution. Protoplasmic astrocytes have short, thick, highly branched processes and are typically found in gray matter. Fibrous astrocytes have long, thin, less branched processes and are more commonly found in white matter. It has recently been shown that astrocyte activity is linked to blood flow in the brain, and that this is what is actually [7] being measured in fMRI. They also have been involved in neuronal circuits playing an inhibitory role after [8] sensing changes in extracellular calcium. CNS Oligodendrocytes Oligodendrocytes are cells that coat axons in the central nervous system (CNS) with their cell membrane forming a specialized membrane differentiation called myelin, producing the so-called myelin sheath. The myelin sheath [9] provides insulation to the axon that allows electrical signals to propagate more efficiently. Ependymal cells Ependymal cells, also named ependymocytes, line the cavities of the CNS and make up the walls of the ventricles. These cells create and secrete cerebrospinal fluid(CSF) and beat their cilia to help circulate the CSF and make up the [10] Blood-CSF barrier. They are also thought to act as neural stem cells. Radial glia cells arise from neuroepithelial cells after the onset of neurogenesis. Their differentiation abilities are more restricted than those of neuroepithelial cells. In the developing nervous system, radial glia function both as neuronal progenitors and as a scaffold upon which newborn neurons migrate. In the mature brain, the cerebellum and retina retain characteristic radial glial cells. In the cerebellum, these are Bergmann glia, which regulate synaptic plasticity. In the retina, the radial Müller cell is the principal glial cell, and participates in a bidirectional [11] communication with neurons. Similar in function to oligodendrocytes, Schwann cells provide myelination to axons in the peripheral nervous system (PNS). They also have phagocytotic activity and clear cellular debris that allows for regrowth of PNS [12] neurons.
CNS
CNS
Radial glia
PNS
Schwann cells
Neuroglia
[13] Satellite glial cells are small cells that surround neurons in sensory, sympathetic and parasympathetic ganglia. These cells help regulate the external chemical environment. Like astrocytes, they are interconnected by gap junctions and respond to ATP by elevating intracellular concentration of calcium ions. They are highly sensitive to [14] injury and inflammation, and appear to contribute to pathological states, such as chronic pain.
333
Satellite cells
PNS
PNS
Enteric glial cells Are found in the intrinsic ganglia of the digestive system.They are thought to have many roles in the enteric system, [15] some related to homeostasis and muscular digestive processes.
Other
Pituicytes from the posterior pituitary are glia cells with characteristics in common to astrocytes.[16] Tanycytes from the hypothalamus descend from radial glia.[17]
Capacity to divide
Glia retain the ability to undergo cell division in adulthood, whereas most neurons cannot. The view is based on the general deficiency of the mature nervous system in replacing neurons after an injury, such as a stroke or trauma, while very often there is a profound proliferation of glia, or gliosis near or at the site of damage. However, detailed studies found no evidence that 'mature' glia, such as astrocytes or oligodendrocytes, retain the ability of mitosis. Only the resident oligodendrocyte precursor cells seem to keep this ability after the nervous system matures. On the other hand, there are a few regions in the mature nervous system, such as the dentate gyrus of the hippocampus and the subventricular zone, where generation of new neurons can be observed.[18]
Embryonic development
Most glia are derived from ectodermal tissue of the developing embryo, in particular the neural tube and crest. The exception is microglia, which are derived from hemopoietic stem cells. In the adult, microglia are largely a self-renewing population and are distinct from macrophages and monocytes, which infiltrate the injured and diseased CNS. In the central nervous system, glia develop from the ventricular zone of the neural tube. These glia include the oligodendrocytes, ependymal cells, and astrocytes. In the peripheral nervous system, glia derive from the neural crest. These PNS glia include Schwann cells in nerves and satellite glial cells in ganglia.
History
Glia were first described in 1856 by the pathologist Rudolf Virchow in a comment to his 1846 publication on connective tissue. In his 1858 publication `Cellularpathology´, he described glial cells in more detail. [19]
Numbers
Neuroglial cells are generally smaller than neurons and outnumber them by five to ten times; they comprise about half the total volume of the brain and spinal cord.(Clinical Neuro-Anatomy, Richard S. Snell, 7th edition) [] The ratio differs from one part of the brain to another. The glia/neuron ratio in the cerebral cortex is 3.72 (60.84 billion glia; 16.34 billion neurons) while that of the cerebellum is only 0.23 (16.04 billion glia; 69.03 billion neurons). The ratio in the cerebral cortex gray matter is 1.48 (the white matter part has few neurons). The ratio of the basal ganglia, diencephalon and brainstem combined is 11.35.[] Most cerebral cortex glia are oligodendrocytes (75.6%); astrocytes account for 17.3% and microglia (6.5%)[20] The amount of brain tissue that is made up of glial cells increases with brain size: the nematode brain contains only a few glia; a fruitfly's brain is 25% glia; that of a mouse, 65%; a human, 90%; and an elephant, 97%.Wikipedia:Please clarify[21]
Neuroglia
334
Additional images
Oligodendrocyte
Section of central canal of medulla spinalis, showing ependymal and neuroglial cells.
Transverse section of a cerebellar folium.
References
Notes
[1] Jessen, Kristjan R. & Mirsky, Rhona Glial cells in the enteric nervous system contain glial fibrillary acidic protein Nature 286, 736–737 (14 August 1980); [2] Nature Reviews Neuroscience 8, 368–378 (May 2007) | [3] ; ; . [4] The Other Brain, by R. Douglas Fields, Ph. D. Simon & Schuster, 2009 [5] The Root of Thought: Unlocking Glia, by Andrew Koob, FT Science Press, 2009 [6] Brodal, 2010: p. 19 (http:/ / books. google. com/ books?id=iJjI6yDNmr8C& pg=PA19) [9] Baumann, Nicole; Pham-Dinh, Danielle (2001), "Biology of Oligodendrocyte and Myelin in the Mammalian Central Nervous System", Physiological Reviews 18 (2): 871–927 [12] Jessen, K. R. & Mirsky, R. (2005), "The origin and development of glial cells in peripheral nerves", Nature Reviews Neuroscience 6 (9): 671–682 [13] Hanani, M. Satellite glial cells in sensory ganglia: from form to function. Brain Res. Rev. 48:457–476, 2005 [14] Ohara PT et al., Evidence for a role of connexin 43 in trigeminal pain using RNA interference in vivo. J Neurophysiol 2008;100:3064–3073 [15] Bassotti, G. et al, Laboratory Investigation (2007) 87, 628–632 [18] David R. Kornack*, Pasko Rakic (2008). Continuation of neurogenesis in the hippocampus of the adult macaque monkey Section of Neurobiology, Yale University School of Medicine, New Haven, CT 06510- (http:/ / www. pnas. org/ content/ 96/ 10/ 5768. abstract) [20] (figures given are those for females)
Bibliography
• Brodal, Per (2010). "Glia" (http://books.google.com/books?id=iJjI6yDNmr8C&pg=PA19). The central nervous system: structure and function. Oxford University Press. p. 19. ISBN 978-0-19-538115-3. • Kettenmann and Ransom, Neuroglia, Oxford University Press, 2012, ISBN13: 9780199794591 |http:// ukcatalogue.oup.com/product/9780199794591.do#.UVcswaD3Ay4|
Further reading
• "The Mystery and Magic of Glia: A Perspective on Their Roles in Health and Disease." (http://download.cell. com/images/edimages/neuron/pdf/barres.pdf) Neuron 60, November 6, 2008 by Ben Barres • Role of glia in synapse development (http://pfrieger.gmxhome.de/work/publications/pfrieger_2002.pdf) • Overstreet L (2005). "Quantal transmission: not just for neurons". Trends Neurosci 28 (2): 59–62. doi: 10.1016/j.tins.2004.11.010 (http://dx.doi.org/10.1016/j.tins.2004.11.010). PMID 15667925 (http://www. ncbi.nlm.nih.gov/pubmed/15667925). article (http://www.sciencedirect.com/science?_ob=ArticleURL&
Neuroglia _udi=B6T0V-4F05G3W-1&_coverDate=02/01/2005&_alid=242540802&_rdoc=1&_fmt=&_orig=search& _qd=1&_cdi=4872&_sort=d&view=c&_acct=C000006078&_version=1&_urlVersion=0&_userid=75682& md5=a6462b73c196ee912e6ea3407462f0b3) Peters A (2004). "A fourth type of neuroglial cell in the adult central nervous system". J Neurocytol 33 (3): 345–57. doi: 10.1023/B:NEUR.0000044195.64009.27 (http://dx.doi.org/10.1023/B:NEUR.0000044195. 64009.27). PMID 15475689 (http://www.ncbi.nlm.nih.gov/pubmed/15475689). Volterra A, Steinhäuser C (2004). "Glial modulation of synaptic transmission in the hippocampus". Glia 47 (3): 249–57. doi: 10.1002/glia.20080 (http://dx.doi.org/10.1002/glia.20080). PMID 15252814 (http://www. ncbi.nlm.nih.gov/pubmed/15252814). Huang Y, Bergles D (2004). "Glutamate transporters bring competition to the synapse". Curr Opin Neurobiol 14 (3): 346–52. doi: 10.1016/j.conb.2004.05.007 (http://dx.doi.org/10.1016/j.conb.2004.05.007). PMID 15194115 (http://www.ncbi.nlm.nih.gov/pubmed/15194115). Artist ADSkyler (http://www.anioman.com/Profile.php?viewedArtistID=1793201250&gallery=&page=1& back=1)(uses concepts of neuroscience and found inspiration from Glia)
335
•
•
•
•
External links
Audio • "The Other Brain" (http://www.wnyc.org/shows/lopate/2010/jan/22/the-other-brain/)—The Leonard Lopate Show (WNYC) "Neuroscientist Douglas Field, explains how glia, which make up approximately 85 percent of the cells in the brain, work. In The Other Brain: From Dementia to Schizophrenia, How New Discoveries about the Brain Are Revolutionizing Medicine and Science, he explains recent discoveries in glia research and looks at what breakthroughs in brain science and medicine are likely to come." • "Network Glia" (http://www.networkglia.eu/en/) A homepage devoted to glial cells
Astrocyte
336
Astrocyte
For the cell in the gastrointestinal tract, see Interstitial cell of Cajal.
Neuron: Astrocyte
Immunocytochemical staining of Astrocytes in culture using an antibody against glial fibrillary acidic protein. NeuroLex ID Dorlands/Elsevier sao1394521419 12165688 [2] [1]
Astrocytes (etymology: astron gk. star, cyte gk. cell), also known collectively as astroglia, are characteristic star-shaped glial cells in the brain and spinal cord. They are the most abundant cell of the human brain. They perform many functions, including biochemical support of endothelial cells that form the blood–brain barrier, provision of nutrients to the nervous tissue, maintenance of extracellular ion balance, and a role in the repair and scarring process of the brain and spinal cord following traumatic injuries. Research since the mid-1990s has shown that astrocytes propagate intercellular Ca2+ waves over long distances in response to stimulation, and, similar to neurons, release transmitters (called gliotransmitters) in a Ca2+-dependent manner. Data suggest that astrocytes also signal to neurons through Ca2+-dependent release of glutamate.[] Such discoveries have made astrocytes an important area of research within the field of neuroscience.
Description
Astrocytes are a sub-type of glial cells in the central nervous system. They are also known as astrocytic glial cells. Star-shaped, their many processes envelope synapses made by neurons. Astrocytes are classically identified using histological analysis; many of these cells express the intermediate filament glial fibrillary acidic protein (GFAP). Several forms of astrocytes exist in the Central Nervous System including fibrous (in white matter), protoplasmic (in grey matter), and radial. The fibrous glia are usually located within white matter, have relatively few organelles, and exhibit long unbranched cellular processes. This type often has "vascular feet" that physically connect the cells to the outside of capillary walls when they are in close proximity to them. The protoplasmic glia are the most prevalent and are found in grey matter tissue, possess a
Isolated Astrocyte shown with confocal microscopy. Image: Nathan S. Ivey and Andrew G. MacLean
Astrocyte
337
larger quantity of organelles, and exhibit short and highly branched tertiary processes. The radial glia are disposed in a plane perpendicular to axis of ventricles. One of their processes about the pia mater, while the other is deeply buried in gray matter. Radial glia are mostly present during development, playing a role in neuron migration. Mueller cells of retina and Bergmann glia cells of cerebellar cortex represent an exception, being present still during adulthood. When in proximity to the pia mater, all three forms of astrocytes send out processes to form the pia-glial membrane.
Astrocyte - rodent cell culture stained for GFAP (red)
23 weeks fetal brain culture human astrocyte
Astrocytes - rat spinal cord stained for GFAP (green)
Astrocytes (red) among neurons in the living cerebral cortex
Astrocyte
338
Functions
Previously in medical science, the neuronal network was considered the only important one, and astrocytes were looked upon as gap fillers. More recently, the function of astrocytes has been reconsidered,[1] and are now thought to play a number of active roles in the brain, including the secretion or absorption of neural transmitters and maintenance of the blood–brain barrier.[2] Following on this idea the concept of a "tripartite synapse" has been proposed, referring to the tight relationship occurring at synapses among a presynaptic element, a postsynaptic element and a glial element.[3]
• Structural: They are involved in the physical structuring of the brain. Astrocytes get their name because they are "star-shaped". They are the most abundant glial cells in the brain that are closely associated with neuronal synapses. They regulate the transmission of electrical impulses within the brain. • Glycogen fuel reserve buffer: Astrocytes contain glycogen and are capable of glycogenesis. The astrocytes next to neurons in the frontal cortex and hippocampus store and release glycogen. Thus, Astrocytes can fuel neurons with glucose during periods of high rate of glucose consumption and glucose shortage. Recent research suggests there may be a connection between this activity and exercise. [4] • Metabolic support: They provide neurons with nutrients such as lactate. • Blood–brain barrier: The astrocyte end-feet encircling endothelial cells were thought to aid in the maintenance of the blood–brain barrier, but recent research indicates that they do not play a substantial role; instead, it is the tight junctions and basal lamina of the cerebral endothelial cells that play the most substantial role in maintaining the barrier.[5] However, it has recently been shown that astrocyte activity is linked to blood flow in the brain, and that this is what is actually being measured in fMRI.[6] [7] • Transmitter uptake and release: Astrocytes express plasma membrane transporters such as glutamate transporters for several neurotransmitters, including glutamate, ATP, and GABA. More recently, astrocytes were shown to release glutamate or ATP in a vesicular, Ca2+-dependent manner.[8] (This has been disputed for hippocampal astrocytes.)[9] • Regulation of ion concentration in the extracellular space: Astrocytes express potassium channels at a high density. When neurons are active, they release potassium, increasing the local extracellular concentration. Because astrocytes are highly permeable to potassium, they rapidly clear the excess accumulation in the extracellular space.[10] If this function is interfered with, the extracellular concentration of potassium will rise, leading to neuronal depolarization by the Goldman equation. Abnormal accumulation of extracellular potassium is well known to result in epileptic neuronal activity.[citation needed] • Modulation of synaptic transmission: In the supraoptic nucleus of the hypothalamus, rapid changes in astrocyte morphology have been shown to affect heterosynaptic transmission between neurons.[11] In the hippocampus, astrocytes suppress synaptic transmission by releasing ATP, which is hydrolyzed by ectonucliotidases to yield adenosine. Adenosine acts on neuronal adenosine receptors to inhibit synaptic transmission, thereby increasing the dynamic range available for LTP.[12] • Vasomodulation: Astrocytes may serve as intermediaries in neuronal regulation of blood flow.[13]
Metabolic interactions between astrocytes and neurons. From a computational study by Çakιr et al., 2007.
Astrocyte • Promotion of the myelinating activity of oligodendrocytes: Electrical activity in neurons causes them to release ATP, which serves as an important stimulus for myelin to form. However, the ATP does not act directly on oligodendrocytes. Instead, it causes astrocytes to secrete cytokine leukemia inhibitory factor (LIF), a regulatory protein that promotes the myelinating activity of oligodendrocytes. This suggest that astrocytes have an executive-coordinating role in the brain.[14] • Nervous system repair: Upon injury to nerve cells within the central nervous system, astrocytes fill up the space to form a glial scar, repairing the area and replacing the CNS cells that cannot regenerate.[citation needed] • Long-term potentiation: Scientists continue to argue back and forth as to whether or not astrocytes integrate learning and memory in the hippocampus. It is known that glial cells are included in neuronal synapses, but many of the LTP studies are performed on slices, so scientists disagree on whether or not astrocytes have a direct role of modulating synaptic plasticity.
339
Recent studies
A recent study, done in November 2010 and published March 2011, was done by a team of scientists from the University of Rochester and University of Colorado School of Medicine They did an experiment to attempt to repair trauma to the Central Nervous System of an adult rat by replacing the glial cells. When the glial cells were injected into the injury of the adult rat’s spinal cord, astrocytes were generated by exposing human glial precursor cells to bone morphogenetic protein (Bone morphogenetic protein is important because it is considered to create tissue architecture throughout the body). So, with the bone protein and human glial cells combined, they promoted significant recovery of conscious foot placement, axonal growth, and obvious increases in neuronal survival in the spinal cord laminae. On the other hand, human glial precursor cells and astrocytes generated from these cells by being in contact with ciliary neurotrophic factors, failed to promote neuronal survival and support of axonal growth at the spot of the injury.[] One study done in Shanghai had two types of hippocampal neuronal cultures: In one culture, the neuron was grown from a layer of astrocytes and the other culture was not in contact with any astrocytes, but they were instead fed a Glial Conditioned Medium (GCM), which inhibits the rapid growth of cultured astrocytes in the brains of rats in most cases. In their results they were able to see that astrocytes had a direct role in Long-term potentiation with the mixed culture (which is the culture that was grown from a layer of astrocytes) but not in GCM cultures.[] Recent studies have shown that astrocytes play an important function in the regulation of neural stem cells. Research from the Schepens Eye Research Institute at Harvard shows the human brain to abound in neural stem cells, which are kept in a dormant state by chemical signals (ephrin-A2 and ephrin-A3) from the astrocytes. The astrocytes are able to activate the stem cells to transform into working neurons by dampening the release of ephrin-A2 and ephrin-A3.[citation needed] Furthermore, studies are underway to determine whether astroglia play an instrumental role in depression, based on the link between diabetes and depression. Altered CNS glucose metabolism is seen in both these conditions, and the astroglial cells are the only cells with insulin receptors in the brain. In a study published in a 2011 issue of Nature Biotechnology[15] and reported in lay science article,[16] a group of researchers from the University of Wisconsin reports that it has been able to direct embryonic and induced human stem cells to become astrocytes. A 2012 study[17] of the effects of marijuana on short term memories found that THC activates CB1 receptors of astrocytes which cause receptors for AMPA to be removed from the membranes of associated neurons.
Astrocyte
340
Calcium waves
Astrocytes are linked by gap junctions, creating an electrically coupled (functional) syncytium.[18] Because of this ability of astrocytes to communicate with their neighbors, changes in the activity of one astrocyte can have repercussions on the activities of others that are quite distant from the original astrocyte. An influx of Ca2+ ions into astrocytes is the essential change that ultimately generates calcium waves. Because this influx is directly caused by an increase in blood flow to the brain, calcium waves are said to be a kind of hemodynamic response function. An increase in intracellular calcium concentration can propagate outwards through this functional syncytium. Mechanisms of calcium wave propagation include diffusion of calcium ions and IP3 through gap junctions and extracellular ATP signalling.[19] Calcium elevations are the primary known axis of activation in astrocytes, and are necessary and sufficient for some types of astrocytic glutamate release.[20]
Development
Astrocytes are macroglial cells in the central nervous system. Astrocytes are derived from heterogeneous populations of progenitor cells in the neuroepithelium of the developing central nervous system. Recent works, summarized in a review by Rowitch and Kriegstein,[21] indicate that there is remarkable similarity between the well known genetic mechanisms that specify the lineage of diverse neuron subtypes and that of macroglial cells. Just as with neuronal cell specification, canonical signaling factors like Sonic hedgehog (SHH), Fibroblast growth factor (FGFs), WNTs and bone morphogenetic proteins (BMPs), provide positional information to developing macroglial cells through morphogen gradients along the dorsal–ventral, anterior–posterior and medial–lateral axes. The resultant patterning along the neuraxis leads to segmentation of the neuroepithelium into progenitor domains (p0, p1 p2, p3 and pMN) for distinct neuron types in the developing spinal cord. On the basis of several studies it is now believed that that this model also applies to macroglial cell specification. Studies carried out by Hochstim and colleagues have demonstrated that three distinct populations of astrocytes arise from the p1, p2 and p3 domains.[22] These subtypes of astrocytes can be identified on the basis of their expression of different transcription factors (PAX6, NKX6.1) and cell surface markers (reelin and SLIT1). The three populations of astrocyte subtypes which have been identified are 1) dorsally located VA1 astrocytes, derived from p1 domain, express PAX6 and reelin 2) ventrally located VA3 astrocytes, derived from p3, express NKX6.1 and SLIT1 and 3) and intermediate white-matter located VA2 astrocyte, derived from the p2 domain, which express PAX6, NKX6.1, reelin and SLIT1.[23] After astrocyte specification has occurred in the developing CNS, it is believed that astrocyte precursors migrate to their final positions within the nervous system before the process of terminal differentiation occurs.
Classification
There are several different ways to classify astrocytes.
Lineage and antigenic phenotype
These have been established by classic work by Raff et al. in early 1980s on Rat optic nerves. • Type 1: Antigenically Ran2+, GFAP+, FGFR3+, A2B5-, thus resembling the "type 1 astrocyte" of the postnatal day 7 rat optic nerve. These can arise from the tripotential glial restricted precursor cells (GRP), but not from the bipotential O2A/OPC (oligodendrocyte, type 2 astrocyte precursor, also called Oligodendrocyte progenitor cell) cells. • Type 2: Antigenically A2B5+, GFAP+, FGFR3-, Ran 2-. These cells can develop in vitro from the either tripotential GRP (probably via O2A stage) or from bipotential O2A cells (which some peopleWikipedia:Avoid weasel words think may in turn have been derived from the GRP) or in vivo when these progenitor cells are transplanted into lesion sites (but probably not in normal development, at least not in the rat optic nerve). Type-2 astrocytes are the major astrocytic component in postnatal optic nerve cultures that are generated by O2A
Astrocyte cells grown in the presence of fetal calf serum but are not thought to exist in vivo (Fulton et al., 1992).
341
Anatomical classification
• Protoplasmic: found in grey matter and have many branching processes whose end-feet envelop synapses. Some protoplasmic astrocytes are generated by multipotent subventricular zone progenitor cells.[][] • Gömöri-positive astrocytes. These are a subset of protoplasmic astrocytes that contain numerous cytoplasmic inclusions, or granules, that stain positively with Gömöri's chrome-alum hematoxylin stain. It is now known that these granules are formed from the remnants of degenerating mitochondria engulfed within lysosomes,[24] Some type of oxidative stress appears to be responsible for the mitochondrial damage within these specialized astrocytes. Gömöri-positive astrocytes are much more abundant within the arcuate nucleus of the hypothalamus and in the hippocampus than in other brain regions. They may have a role in regulating the response of the hypothalamus to glucose.[25][26] • Fibrous: found in white matter and have long thin unbranched processes whose end-feet envelop nodes of Ranvier.[27] Some fibrous astrocytes are generated by radial glia.[][][][][]
Transporter/receptor classification
• GluT type: express glutamate transporters (EAAT1/ SLC1A3 [30] and EAAT2/ SLC1A2 [31]) and respond to synaptic release of glutamate by transporter currents • GluR type: express glutamate receptors (mostly mGluR and AMPA type) and respond to synaptic release of glutamate by channel-mediated currents and IP3-dependent Ca2+ transients
Bergmann glia
Bergmann glia, a type of glia[28][29] also known as radial epithelial cells (as named by Camillo Golgi) or Golgi epithelial cells (GCEs; not to be mixed up with Golgi cells), are astrocytes in the cerebellum that have their cell bodies in the Purkinje cell layer and processes that extend into the molecular layer, terminating with bulbous endfeet at the pial surface. Bergmann glia express high densities of glutamate transporters that limit diffusion of the neurotransmitter glutamate during its release from synaptic terminals. Besides their role in early development of the cerebellum, Bergmann glia are also required for the pruning or addition of synapses.[citation needed]
Pathology
SLC1A3 expression highlights Bergmann glia in the brain of a mouse at 7th postnatal day, sagittal section.
Astrocytomas are primary intracranial tumors derived from astrocytes cells of the brain. It is also possible that glial progenitors or neural stem cells give rise to astrocytomas. Astrocytomas are brain tumors that develop from astrocytes. They may occur in many parts of the brain and sometimes in the spinal cord. They can occur at any age but they primarily occur in males. Astrocytomas are divided into two categories: Low grade (I and II) and High Grade (III and IV). Low grade tumors are more common in children and high grade tumors are more common in adults.[30] Pilocytic Astrocytoma are Grade I tumors. They are considered benign and slow growing tumors. Pilocytic Astrocytomas frequently have cystic portions filled with fluid and a nodule, which is the solid portion. Most are located in the cerebellum. Therefore, most symptoms are related to balance or coordination difficulties.[30] They also
Astrocyte occur more frequently in children and teens.[31] Grade II Tumors grow relatively slow but invade surrounding healthy tissue. Usually considered benign but can grow into malignant tumors. Other names that are used are Fibrillary or Protoplasmic astrocytomas. They are prevalent in younger people who are often present with seizures.[31] Anaplastic astrocytoma is classified as grade III and are malignant tumors. They grow more rapidly than lower grade tumors and tend to invade nearby healthy tissue. Anaplastic astrocytomas recur more frequently than lower grade tumors because of their tendency to spread into surrounding tissue makes them difficult to completely remove surgically.[30] Glioblastoma Multiforme is also a malignant tumor and classified as a grade IV. Glioblastomas can contain more than one cell type (i.e., astrocytes, oligondroctyes). Also, while one cell type may die off in response to a particular treatment, the other cell types may continue to multiply. Glioblastomas are the most invasive type of glial tumors. Grows rapidly and spreads to nearby tissue. Approximately 50% of astrocytomas are glioblastomas and are very difficult to treat.[30]
342
Tripartite synapse
Within the dorsal horn of the spinal cord, activated astrocytes have the ability to respond to almost all neurotransmitters (Haydon, 2001) and, upon activation, release a multitude of neuroactive molecules such as glutamate, ATP, nitric oxide (NO), prostaglandins (PG), and D-serine, which in turn influences neuronal excitability. The close association between astrocytes and presynaptic and postsynaptic terminals as well as their ability to integrate synaptic activity and release neuromodulators has been termed the "tripartite synapse" (Araque et al., 1999). Synaptic modulation by astrocytes takes place because of this 3-part association.
Astrocytes in chronic pain sensitization
Under normal conditions, pain conduction begins with some noxious signal followed by an action potential carried by nociceptive (pain sensing) afferent neurons, which elicit excitatory postsynaptic potentials (EPSP) in the dorsal horn of the spinal cord. That message is then relayed to the cerebral cortex, where we translate those EPSPs into "pain". Since the discovery of astrocytic influence, our understanding of the conduction of pain has been dramatically complicated. Pain processing is no longer seen as a repetitive relay of signals from body to brain, but as a complex system that can be up- and down-regulated by a number of different factors. One factor at the forefront of recent research is in the pain-potentiating synapse located in the dorsal horn of the spinal cord and the role of astrocytes in encapsulating these synapses. Garrison and co-workers (Garrison, 1991)Wikipedia:Citing sources#What information to include were the first to suggest association when they found a correlation between astrocyte hypertrophy in the dorsal horn of the spinal cord and hypersensitivity to pain after peripheral nerve injury, typically considered an indicator of glial activation after injury. Astrocytes detect neuronal activity and can release chemical transmitters, which in turn control synaptic activity (Volters and Meldolesi, 2005; Haydon, 2001; Fellin, et al., 2006). In the past, hyperalgesia was thought to be modulated by the release of substance P and excitatory amino acids (EAA), such as glutamate, from the presynaptic afferent nerve terminals in the spinal cord dorsal horn. Subsequent activation of AMPA (α-amino-3-hydroxy-5-methyl-4-isoxazole proprionic acid), NMDA (N-methyl-D-aspartate) and kainate subtypes of ionotropic glutamate receptors follows. It is the activation of these receptors that potentiates the pain signal up the spinal cord. This idea, although true, is an oversimplification of pain transduction. A litany of other neurotransmitter and neuromodulators, such as calcitonin gene-related peptide (CGRP), adenosine triphosphate (ATP), brain-derived neurotrophic factor (BDNF), somatostatin, vasoactive intestinal peptide (VIP), galanin, and vasopressin are all synthesized and released in response to noxious stimuli. In addition to each of these regulatory factors, several other interactions between pain-transmitting neurons and other neurons in the dorsal horn have added impact on pain pathways.
Astrocyte
343
Two states of persistent pain
After persistent peripheral tissue damage there is a release of several factors from the injured tissue as well as in the spinal dorsal horn. These factors increase the responsiveness of the dorsal horn pain-projection neurons to ensuing stimuli, termed "spinal sensitization," thus amplifying the pain impulse to the brain. Release of glutamate, substance P, and calcitonin gene-related peptide (CGRP) mediates NMDAR activation (originally silent because it is plugged by Mg2+), thus aiding in depolarization of the postsynaptic pain-transmitting neurons (PTN). In addition, activation of IP3 signaling and MAPKs (mitogen-activated protein kinases) such as ERK and JNK, bring about an increase in the synthesis of inflammatory factors that alter glutamate transporter function. ERK also further activates AMPARs and NMDARs in neurons. Nociception is further sensitized by the association of ATP and substance P with their respective receptors, P<sub>2</sub>X<sub>3</sub>, and neurokinin 1 receptor (NK1R), as well as activation of metabotropic glutamate receptors and release of BDNF. Persistent presence of glutamate in the synapse eventually results in dysregulation of GLT1 and GLAST, crucial transporters of glutamate into astrocytes. Ongoing excitation can also induce ERK and JNK activation, resulting in release of several inflammatory factors. As noxious pain is sustained, spinal sensitization creates transcriptional changes in the neurons of the dorsal horn that lead to altered function for extended periods. Mobilization of Ca2+ from internal stores results from persistent synaptic activity and leads to the release of glutamate, ATP, tumor necrosis factor-α (TNF-α), interleukin 1β (IL-1β), IL-6, nitric oxide (NO), and prostaglandin E2 (PGE2). Activated astrocytes are also a source of matrix metalloproteinase 2 (MMP2), which induces pro-IL-1β cleavage and sustains astrocyte activation. In this chronic signaling pathway, p38 is activated as a result of IL-1β signaling, and there is a presence of chemokines that trigger their receptors to become active. In response to nerve damage, heat shock proteins (HSP) are released and can bind to their respective TLRs, leading to further activation.
References
[2] Kolb & Whishaw: Fundamentals of Human Neuropsychology, 2008 [15] http:/ / www. nature. com/ nbt/ journal/ vaop/ ncurrent/ abs/ nbt. 1877. html [16] http:/ / www. sciencedebate. com/ science-blog/ human-astrocytes-cultivated-stem-cells-lab-dish-u-wisconsin-researchers [19] Newman, EA.(2001) "Propagation of intercellular calcium waves in retinal astrocytes and Müller cells." (http:/ / www. pubmedcentral. nih. gov/ articlerender. fcgi?tool=pubmed& pubmedid=11264297)J Neurosci. 21(7):2215-23 [25] Young JK, McKenzie JC (2004) " GLUT2 immunoreactivity in Gömöri-positive astrocytes of the hypothalamus (http:/ / www. jhc. org/ cgi/ content/ full/ 52/ 11/ 1519)."J. Histochemistry & Cytochemistry 52: 1519-1524 PMID [30] Astrocytomas. (2010). Retrieved 2011, from IRSA: http:/ / www. irsa. org/ astrocytoma. html [31] Astrocytoma Tumors (2005, August). Retrieved 2011, from American Association of Neurological Surgeons: http:/ / www. aans. org/ Patient%20Information/ Conditions%20and%20Treatments/ Astrocytoma%20Tumors. aspx.
• Halassa, M.M., Fellin, T., and Haydon, P.G. (2006). "The tripartite synapse: roles for gliotransmission in health and disease". Trends in Mol. Sci 13 (2): 54–63. doi: 10.1016/j.molmed.2006.12.005 (http://dx.doi.org/10. 1016/j.molmed.2006.12.005). PMID 17207662 (http://www.ncbi.nlm.nih.gov/pubmed/17207662). • White, F.A., Jung, H. and Miller, R.J. (2007). "Chemokines and the pathophysiology of neuropathic pain" (http:// www.ncbi.nlm.nih.gov/pmc/articles/PMC2154400). Proc. Natl Acad. Sci. USA 104 (51): 20151–20158. doi: 10.1073/pnas.0709250104 (http://dx.doi.org/10.1073/pnas.0709250104). PMC 2154400 (http://www.ncbi. nlm.nih.gov/pmc/articles/PMC2154400). PMID 18083844 (http://www.ncbi.nlm.nih.gov/pubmed/ 18083844). • Milligan, E.D. and Watson, L.R. (2009). "Pathological and protective roles of glia in chronic pain". Neuron-Glia Interactions 10: 23–36. • Watkins, L.R., Milligan, E.D. and Maier, S.F. (2001). "Glial activation: a driving force for pathological pain". Trends in Neurosci. 24 (8): 450–455. doi: 10.1016/S0166-2236(00)01854-3 (http://dx.doi.org/10.1016/ S0166-2236(00)01854-3). • Volterra, A. and Meldolesi, J. (2005). "Astrocytes, from brain glue to communication elements: the revolution continues". Nat. Rev Neurosci. 6 (8): 626–640. doi: 10.1038/nrn1722 (http://dx.doi.org/10.1038/nrn1722).
Astrocyte PMID 16025096 (http://www.ncbi.nlm.nih.gov/pubmed/16025096). • Freeman, M. R. (2010). "Specification and Morphogenesis of Astrocytes". Science 330 (6005): 774–8. doi: 10.1126/science.1190928 (http://dx.doi.org/10.1126/science.1190928). PMID 21051628 (http://www.ncbi. nlm.nih.gov/pubmed/21051628).
344
External links
• Cell Centered Database - Astrocyte (http://ccdb.ucsd.edu/sand/main?stype=lite&keyword=protoplasmic astrocyte&Submit=Go&event=display&start=1) • UIUC Histology Subject 57 (https://histo.life.illinois.edu/histo/atlas/oimages.php?oid=57) • "Astrocytes" (http://www.sfn.org/index.cfm?pagename=brainBriefings_astrocytes) at Society for Neuroscience • The Department of Neuroscience at Wikiversity • NIF Search - Astrocyte (https://www.neuinfo.org/mynif/search.php?q=Astrocyte&t=data&s=cover&b=0& r=20) via the Neuroscience Information Framework
Neuron
Neuron: nerve cell
Drawing by Santiago Ramón y Cajal of neurons in the pigeon cerebellum. (A) Denotes Purkinje cells, an example of a multipolar neuron. (B) Denotes granule cells, which are also multipolar. NeuroLex ID sao1417703748 [1]
A neuron (pron.: /ˈnjʊərɒn/ NYEWR-on or pron.: /ˈnʊərɒn/ NEWR-on; also known as a neurone or nerve cell) is an electrically excitable cell that processes and transmits information through electrical and chemical signals. A chemical signal occurs via a synapse, a specialized connection with other cells. Neurons connect to each other to form neural networks. Neurons are the core components of the nervous system, which includes the brain, spinal cord, and peripheral ganglia. A number of specialized types of neurons exist: sensory neurons respond to touch, sound, light and numerous other stimuli affecting cells of the sensory organs that then send signals to the spinal cord and brain. Motor neurons receive signals from the brain and spinal cord, cause muscle contractions, and affect glands. Interneurons connect neurons to other neurons within the same region of the brain or spinal cord. A typical neuron possesses a cell body (often called the soma), dendrites, and an axon. Dendrites are thin structures that arise from the cell body, often extending for hundreds of micrometres and branching multiple times, giving rise to a complex "dendritic tree". An axon is a special cellular extension that arises from the cell body at a site called the axon hillock and travels for a distance, as far as 1 meter in humans or even more in other species. The cell body of a neuron frequently gives rise to multiple dendrites, but never to more than one axon, although the axon may branch hundreds of times before it terminates. At the majority of synapses, signals are sent from the axon of one neuron to a
Neuron dendrite of another. There are, however, many exceptions to these rules: neurons that lack dendrites, neurons that have no axon, synapses that connect an axon to another axon or a dendrite to another dendrite, etc. All neurons are electrically excitable, maintaining voltage gradients across their membranes by means of metabolically driven ion pumps, which combine with ion channels embedded in the membrane to generate intracellular-versus-extracellular concentration differences of ions such as sodium, potassium, chloride, and calcium. Changes in the cross-membrane voltage can alter the function of voltage-dependent ion channels. If the voltage changes by a large enough amount, an all-or-none electrochemical pulse called an action potential is generated, which travels rapidly along the cell's axon, and activates synaptic connections with other cells when it arrives. Neurons do not undergo cell division. In most cases, neurons are generated by special types of stem cells. Astrocytes, a type of glial cell, have also been observed to turn into neurons by virtue of the stem cell characteristic pluripotency. In humans, neurogenesis largely ceases during adulthood—but in two brain areas, the hippocampus and olfactory bulb, there is strong evidence for generation of substantial numbers of new neurons.[1][]
345
Overview
Structure of a typical neuron
Neuron (peripheral nervous system)
A neuron is a specialized type of cell found in the bodies of most animals (all members of the group Eumetazoa). Only sponges and a few other simpler animals have no neurons. The features that define a neuron are electrical excitability and the presence of synapses, which are complex membrane junctions that transmit signals to other cells. The body's neurons, plus the glial cells that give them structural and metabolic support, together constitute the nervous system. In vertebrates, the majority of neurons belong to the central nervous system, but some reside in peripheral ganglia, and many sensory neurons are situated in sensory organs such as the retina and cochlea. Although neurons are very diverse and there are exceptions to nearly every rule, it is convenient to begin with a schematic description of the structure and function of a "typical" neuron. A typical neuron is divided into three parts: the soma or cell body, dendrites, and axon. The soma is usually compact; the axon and dendrites are filaments that extrude from it. Dendrites typically branch profusely, getting thinner with each branching, and extending their farthest branches a few hundred micrometres from the soma. The axon leaves the soma at a swelling called the axon hillock, and can extend for great distances, giving rise to hundreds of branches. Unlike dendrites, an axon usually maintains the same diameter as it extends. The soma may give rise to numerous dendrites, but never to more than one axon. Synaptic signals from other neurons are received by the soma and dendrites; signals to other neurons are transmitted by the axon. A typical synapse, then, is a contact between the axon of one neuron and a dendrite or soma of another. Synaptic signals may be excitatory or inhibitory. If the net excitation received by a neuron over a short
Neuron period of time is large enough, the neuron generates a brief pulse called an action potential, which originates at the soma and propagates rapidly along the axon, activating synapses onto other neurons as it goes. Many neurons fit the foregoing schema in every respect, but there are also exceptions to most parts of it. There are no neurons that lack a soma, but there are neurons that lack dendrites, and others that lack an axon. Furthermore, in addition to the typical axodendritic and axosomatic synapses, there are axoaxonic (axon-to-axon) and dendrodendritic (dendrite-to-dendrite) synapses. The key to neural function is the synaptic signaling process, which is partly electrical and partly chemical. The electrical aspect depends on properties of the neuron's membrane. Like all animal cells, every neuron is surrounded by a plasma membrane, a bilayer of lipid molecules with many types of protein structures embedded in it. A lipid bilayer is a powerful electrical insulator, but in neurons, many of the protein structures embedded in the membrane are electrically active. These include ion channels that permit electrically charged ions to flow across the membrane, and ion pumps that actively transport ions from one side of the membrane to the other. Most ion channels are permeable only to specific types of ions. Some ion channels are voltage gated, meaning that they can be switched between open and closed states by altering the voltage difference across the membrane. Others are chemically gated, meaning that they can be switched between open and closed states by interactions with chemicals that diffuse through the extracellular fluid. The interactions between ion channels and ion pumps produce a voltage difference across the membrane, typically a bit less than 1/10 of a volt at baseline. This voltage has two functions: first, it provides a power source for an assortment of voltage-dependent protein machinery that is embedded in the membrane; second, it provides a basis for electrical signal transmission between different parts of the membrane. Neurons communicate by chemical and electrical synapses in a process known as synaptic transmission. The fundamental process that triggers synaptic transmission is the action potential, a propagating electrical signal that is generated by exploiting the electrically excitable membrane of the neuron. This is also known as a wave of depolarization.
346
Anatomy and histology
Neurons are highly specialized for the processing and transmission of cellular signals. Given the diversity of functions performed by neurons in different parts of the nervous system, there is, as expected, a wide variety in the shape, size, and electrochemical properties of neurons. For instance, the soma of a neuron can vary from 4 to 100 micrometers in diameter.[2] • The soma is the central part of the neuron. It contains the nucleus of the cell, and therefore is where most protein synthesis occurs. The nucleus ranges from 3 to 18 micrometers in diameter.[3]
Diagram of a typical myelinated vertebrate motoneuron
• The dendrites of a neuron are cellular extensions with many branches, and metaphorically this overall shape and structure is referred to as a dendritic tree. This is where the majority of input to the neuron occurs via the dendritic spine.
Neuron • The axon is a finer, cable-like projection that can extend tens, hundreds, or even tens of thousands of times the diameter of the soma in length. The axon carries nerve signals away from the soma (and also carries some types of information back to it). Many neurons have only one axon, but this axon may—and usually will—undergo extensive branching, enabling communication with many target cells. The part of the axon where it emerges from the soma is called the axon hillock. Besides being an anatomical structure, the axon hillock is also the part of the neuron that has the greatest density of voltage-dependent sodium channels. This makes it the most easily excited part of the neuron and the spike initiation zone for the axon: in electrophysiological terms it has the most negative action potential threshold. While the axon and axon hillock are generally involved in information outflow, this region can also receive input from other neurons. • The axon terminal contains synapses, specialized structures where neurotransmitter chemicals are released to communicate with target neurons. Although the canonical view of the neuron attributes dedicated functions to its various anatomical components, dendrites and axons often act in ways contrary to their so-called main function. Axons and dendrites in the central nervous system are typically only about one micrometer thick, while some in the peripheral nervous system are much thicker. The soma is usually about 10–25 micrometers in diameter and often is not much larger than the cell nucleus it contains. The longest axon of a human motoneuron can be over a meter long, reaching from the base of the spine to the toes. Sensory neurons have axons that run from the toes to the dorsal columns, over 1.5 meters in adults. Giraffes have single axons several meters in length running along the entire length of their necks. Much of what is known about axonal function comes from studying the squid giant axon, an ideal experimental preparation because of its relatively immense size (0.5–1 millimeters thick, several centimeters long). Fully differentiated neurons are permanently postmitotic;[4] however, recent research shows that additional neurons throughout the brain can originate from neural stem cells found throughout the brain but in particularly high concentrations in the subventricular zone and subgranular zone through the process of neurogenesis.[5]
347
Histology and internal structure
Nerve cell bodies stained with basophilic dyes show numerous microscopic clumps of Nissl substance (named after German psychiatrist and neuropathologist Franz Nissl, 1860–1919), which consists of rough endoplasmic reticulum and associated ribosomal RNA. The prominence of the Nissl substance can be explained by the fact that nerve cells are metabolically very active, and hence are involved in large amounts of protein synthesis. The cell body of a neuron is supported by a complex meshwork of structural proteins called neurofilaments, which are assembled into larger neurofibrils. Some Golgi-stained neurons in human hippocampal tissue neurons also contain pigment granules, such as neuromelanin (a brownish-black pigment, byproduct of synthesis of catecholamines) and lipofuscin (yellowish-brown pigment that accumulates with age). There are different internal structural characteristics between axons and dendrites. Typical axons almost never contain ribosomes, except some in the initial segment. Dendrites contain granular endoplasmic reticulum or ribosomes, with diminishing amounts with distance from the cell body.
Neuron
348
Classes
Neurons exist in a number of different shapes and sizes and can be classified by their morphology and function. The anatomist Camillo Golgi grouped neurons into two types; type I with long axons used to move signals over long distances and type II with short axons, which can often be confused with dendrites. Type I cells can be further divided by where the cell body or soma is located. The basic morphology of type I neurons, represented by spinal motor neurons, consists of a cell body called the soma and a long thin axon covered by the myelin sheath. Around the cell body is a branching dendritic tree that receives signals from other neurons. The end of the axon has branching terminals (axon terminal) that release neurotransmitters into a gap called the synaptic cleft between the terminals and the dendrites of the next neuron.
Image of pyramidal neurons in mouse cerebral cortex expressing green fluorescent protein. The red staining indicates GABAergic [6] interneurons.
Structural classification
SMI32-stained pyramidal neurons in cerebral cortex
Neuron Polarity Most neurons can be anatomically characterized as: • Unipolar or pseudounipolar: dendrite and axon emerging from same process. • Bipolar: axon and single dendrite on opposite ends of the soma. • Multipolar: more than two dendrites: • Golgi I: neurons with long-projecting axonal processes; examples are pyramidal cells, Purkinje cells, and anterior horn cells. • Golgi II: neurons whose axonal process projects locally; the best example is the granule cell. Other Furthermore, some unique neuronal types can be identified according to their location in the nervous system and distinct shape. Some examples are: • Basket cells, interneurons that form a dense plexus of terminals around the soma of target cells, found in the cortex and cerebellum. • Betz cells, large motor neurons. • Medium spiny neurons, most neurons in the corpus striatum. • Purkinje cells, huge neurons in the cerebellum, a type of Golgi I multipolar neuron. • Pyramidal cells, neurons with triangular soma, a type of Golgi I. • Renshaw cells, neurons with both ends linked to alpha motor neurons. • Granule cells, a type of Golgi II neuron. • Anterior horn cells, motoneurons located in the spinal cord. • Spindle cells, interneurons that connect widely separated areas of the brain
Different kinds of neurons: 1 Unipolar neuron 2 Bipolar neuron 3 Multipolar neuron 4 Pseudounipolar neuron
349
Functional classification
Direction • Afferent neurons convey information from tissues and organs into the central nervous system and are sometimes also called sensory neurons. • Efferent neurons transmit signals from the central nervous system to the effector cells and are sometimes called motor neurons. • Interneurons connect neurons within specific regions of the central nervous system. Afferent and efferent also refer generally to neurons that, respectively, bring information to or send information from the brain region. Action on other neurons A neuron affects other neurons by releasing a neurotransmitter that binds to chemical receptors. The effect upon the postsynaptic neuron is determined not by the presynaptic neuron or by the neurotransmitter, but by the type of receptor that is activated. A neurotransmitter can be thought of as a key, and a receptor as a lock: the same type of key can here be used to open many different types of locks. Receptors can be classified broadly as excitatory (causing an increase in firing rate), inhibitory (causing a decrease in firing rate), or modulatory (causing long-lasting effects not directly related to firing rate).
Neuron The two most common neurotransmitters in the brain, glutamate and GABA, have actions that are largely consistent. Glutamate acts on several different types of receptors, and have effects that are excitatory at ionotropic receptors and a modulatory effect at metabotropic receptors. Similarly GABA acts on several different types of receptors, but all of them have effects (in adult animals, at least) that are inhibitory. Because of this consistency, it is common for neuroscientists to simplify the terminology by referring to cells that release glutamate as "excitatory neurons," and cells that release GABA as "inhibitory neurons." Since over 90% of the neurons in the brain release either glutamate or GABA, these labels encompass the great majority of neurons. There are also other types of neurons that have consistent effects on their targets, for example "excitatory" motor neurons in the spinal cord that release acetylcholine, and "inhibitory" spinal neurons that release glycine. The distinction between excitatory and inhibitory neurotransmitters is not absolute, however. Rather, it depends on the class of chemical receptors present on the postsynaptic neuron. In principle, a single neuron, releasing a single neurotransmitter, can have excitatory effects on some targets, inhibitory effects on others, and modulatory effects on others still. For example, photoreceptor cells in the retina constantly release the neurotransmitter glutamate in the absence of light. So-called OFF bipolar cells are, like most neurons, excited by the released glutamate. However, neighboring target neurons called ON bipolar cells are instead inhibited by glutamate, because they lack the typical ionotropic glutamate receptors and instead express a class of inhibitory metabotropic glutamate receptors.[7] When light is present, the photoreceptors cease releasing glutamate, which relieves the ON bipolar cells from inhibition, activating them; this simultaneously removes the excitation from the OFF bipolar cells, silencing them. It is possible to identify the type of inhibitory effect a presynaptic neuron will have on a postsynaptic neuron, based on the proteins the presynaptic neuron expresses. Parvalbumin-expressing neurons typically dampen the output signal of the postsynaptic neuron in the visual cortex, whereas somatostatin-expressing neurons typically block dendritic inputs to the postsynaptic neuron.[8] Discharge patterns Neurons can be classified according to their electrophysiological characteristics: • Tonic or regular spiking. Some neurons are typically constantly (or tonically) active. Example: interneurons in neurostriatum. • Phasic or bursting. Neurons that fire in bursts are called phasic. • Fast spiking. Some neurons are notable for their high firing rates, for example some types of cortical inhibitory interneurons, cells in globus pallidus, retinal ganglion cells.[9][10] Classification by neurotransmitter production Neurons differ in the type of neurotransmitter they manufacture. Some examples are: • Cholinergic neurons—acetylcholine. Acetylcholine is released from presynaptic neurons into the synaptic cleft. It acts as a ligand for both ligand-gated ion channels and metabotropic (GPCRs) muscarinic receptors. Nicotinic receptors, are pentameric ligand-gated ion channels composed of alpha and beta subunits that bind nicotine. Ligand binding opens the channel causing influx of Na+ depolarization and increases the probability of presynaptic neurotransmitter release. • GABAergic neurons—gamma aminobutyric acid. GABA is one of two neuroinhibitors in the CNS, the other being Glycine. GABA has a homologous function to ACh, gating anion channels that allow Cl- ions to enter the post synaptic neuron. Cl- causes hyperpolarization within the neuron, decreasing the probability of an action potential firing as the voltage becomes more negative (recall that for an action potential to fire, a positive voltage threshold must be reached). • Glutamatergic neurons—glutamate. Glutamate is one of two primary excitatory amino acids, the other being Aspartate. Glutamate receptors are one of four categories, three of which are ligand-gated ion channels and one of which is a G-protein coupled receptor (often referred to as GPCR).
350
Neuron 1. AMPA and Kainate receptors both function as cation channels permeable to Na+ cation channels mediating fast excitatory synaptic transmission 2. NMDA receptors are another cation channel that is more permeable to Ca2+. The function of NMDA receptors is dependant on Glycine receptor binding as a co-agonist within the channel pore. NMDA receptors do not function without both ligands present. 3. Metabotropic receptors, GPCRs modulate synaptic transmission and postsynaptic excitability. Glutamate can cause excitotoxicity when blood flow to the brain is interrupted, resulting in brain damage. When blood flow is suppressed, glutamate is released from presynaptic neurons causing NMDA and AMPA receptor activation moreso than would normally be the case outside of stress conditions, leading to elevated Ca2+ and Na+ entering the post synaptic neuron and cell damage. • Dopaminergic neurons—dopamine. Dopamine is a neurotransmitter that acts on D1 type (D1 and D5) Gs coupled receptors, which increase cAMP and PKA, and D2 type (D2, D3, and D4) receptors, which activate Gi-coupled receptors that decrease cAMP and PKA. Dopamine is connected to mood and behavior, and modulates both pre and post synaptic neurotransmission. Loss of dopamine neurons in the substantia nigra has been linked to Parkinson's disease. • Serotonergic neurons—serotonin. Serotonin,(5-Hydroxytryptamine, 5-HT), can act as excitatory or inhibitory. Of the four 5-HT receptor classes, 3 are GPCR and 1 is ligand gated cation channel. Serotonin is synthesized from tryptophan by tryptophan hydroxylase, and then further by aromatic acid decarboxylase. A lack of 5-HT at postsynaptic neurons has been linked to depression. Drugs that block the presynaptic serotonin transporter are used for treatment, such as Prozac and Zoloft.
351
Connectivity
Neurons communicate with one another via synapses, where the axon terminal or en passant boutons (terminals located along the length of the axon) of one cell impinges upon another neuron's dendrite, soma or, less commonly, axon. Neurons such as Purkinje cells in the cerebellum can have over 1000 dendritic branches, making connections with tens of thousands of other cells; other neurons, such as the magnocellular neurons of the supraoptic nucleus, have only one or two dendrites, each of which receives thousands of synapses. Synapses can be excitatory or inhibitory and either increase or decrease activity in the target neuron. Some neurons also communicate via electrical synapses, which are direct, electrically conductive junctions between cells. In a chemical synapse, the process of synaptic transmission is as follows: when an action potential reaches the axon terminal, it opens voltage-gated calcium channels, allowing calcium ions to enter the terminal. Calcium causes synaptic vesicles filled with neurotransmitter molecules to fuse with the membrane, releasing their contents into the synaptic cleft. The neurotransmitters diffuse across the synaptic cleft and activate receptors on the postsynaptic neuron. The human brain has a huge number of synapses. Each of the 1011 (one hundred billion) neurons has on average 7,000 synaptic connections to other neurons. It has been estimated that the brain of a three-year-old child has about 1015 synapses (1 quadrillion). This number declines with age, stabilizing by adulthood. Estimates vary for an adult, ranging from 1014 to 5 x 1014 synapses (100 to 500 trillion).[11]
Neuron
352
Mechanisms for propagating action potentials
In 1937, John Zachary Young suggested that the squid giant axon could be used to study neuronal electrical properties.[12] Being larger than but similar in nature to human neurons, squid cells were easier to study. By inserting electrodes into the giant squid axons, accurate measurements were made of the membrane potential. The cell membrane of the axon and soma contain voltage-gated ion channels that allow the neuron to generate and propagate an electrical signal (an action potential). These signals are generated and propagated by charge-carrying ions including sodium (Na+), potassium (K+), chloride (Cl-), and calcium (Ca2+). There are several stimuli that can activate a neuron leading to electrical activity, including pressure, stretch, chemical transmitters, and changes of the electric potential across the cell membrane.[13] Stimuli cause specific ion-channels within the cell membrane to open, leading to a flow of ions through the cell membrane, changing the membrane potential.
A signal propagating down an axon to the cell body and dendrites of the next cell
Thin neurons and axons require less metabolic expense to produce and carry action potentials, but thicker axons convey impulses more rapidly. To minimize metabolic expense while maintaining rapid conduction, many neurons have insulating sheaths of myelin around their axons. The sheaths are formed by glial cells: oligodendrocytes in the central nervous system and Schwann cells in the peripheral nervous system. The sheath enables action potentials to travel faster than in unmyelinated axons of the same diameter, whilst using less energy. The myelin sheath in peripheral nerves normally runs along the axon in sections about 1 mm long, punctuated by unsheathed nodes of Ranvier, which contain a high density of voltage-gated ion channels. Multiple sclerosis is a neurological disorder that results from demyelination of axons in the central nervous system. Some neurons do not generate action potentials, but instead generate a graded electrical signal, which in turn causes graded neurotransmitter release. Such nonspiking neurons tend to be sensory neurons or interneurons, because they cannot carry signals long distances.
Neuron
353
Neural coding
Neural coding is concerned with how sensory and other information is represented in the brain by neurons. The main goal of studying neural coding is to characterize the relationship between the stimulus and the individual or ensemble neuronal responses, and the relationships amongst the electrical activities of the neurons within the ensemble.[] It is thought that neurons can encode both digital and analog information.[14]
All-or-none principle
The conduction of nerve impulses is an example of an all-or-none response. In other words, if a neuron responds at all, then it must respond completely. Greater intensity of stimulation does not produce a stronger signal but can produce a higher frequency of firing. There are different types of receptor response to stimulus, slowly adapting or tonic receptors respond to steady stimulus and produce a steady rate of firing. These tonic receptors most often respond to increased intensity of stimulus by increasing their firing frequency, usually as a power function of stimulus plotted against impulses per second. This can be likened to an intrinsic property of light where to get greater intensity of a specific frequency (color) there have to be more photons, as the photons can't become "stronger" for a specific frequency. There are a number of other receptor types that are called quickly adapting or phasic receptors, where firing decreases or stops with steady stimulus; examples include: skin when touched by an object causes the neurons to fire, but if the object maintains even pressure against the skin, the neurons stop firing. The neurons of the skin and muscles that are responsive to pressure and vibration have filtering accessory structures that aid their function. The pacinian corpuscle is one such structure. It has concentric layers like an onion, which form around the axon terminal. When pressure is applied and the corpuscle is deformed, mechanical stimulus is transferred to the axon, which fires. If the pressure is steady, there is no more stimulus; thus, typically these neurons respond with a transient depolarization during the initial deformation and again when the pressure is removed, which causes the corpuscle to change shape again. Other types of adaptation are important in extending the function of a number of other neurons.[15]
History
The term neuron was coined by the German anatomist Heinrich Wilhelm Waldeyer. The neuron's place as the primary functional unit of the nervous system was first recognized in the early 20th century through the work of the Spanish anatomist Santiago Ramón y Cajal.[] Ramón y Cajal proposed that neurons were discrete cells that communicated with each other via specialized junctions, or spaces, between cells.[] This became known as the neuron doctrine, one of the central tenets of modern neuroscience.[] To observe the structure of individual neurons, Ramón y Cajal improved a silver staining process Drawing by Camillo Golgi of a hippocampus stained with the silver nitrate method known as Golgi's method, which had been developed by his rival, Camillo Golgi.[] Cajal's improvement, which involved a technique he called "double impregnation", is still in use. The silver impregnation stains are an extremely useful method for neuroanatomical investigations because, for reasons unknown, it stains a very small percentage of cells in a tissue, so one is able to see the complete micro structure of individual neurons without much overlap from other cells in the densely packed brain.[]
Neuron
354
The neuron doctrine
The neuron doctrine is the now fundamental idea that neurons are the basic structural and functional units of the nervous system. The theory was put forward by Santiago Ramón y Cajal in the late 19th century. It held that neurons are discrete cells (not connected in a meshwork), acting as metabolically distinct units. Later discoveries yielded a few refinements to the simplest form of the doctrine. For example, glial cells, which are not considered neurons, play an essential role in information processing.[16] Also, electrical synapses are more common than previously thought,[17] meaning that there are direct, cytoplasmic connections between neurons. In fact, there are examples of neurons forming even tighter coupling: the squid giant axon arises from the fusion of multiple axons.[18] Ramón y Cajal also postulated the Law of Dynamic Polarization, which states that a neuron receives signals at its dendrites and cell body and transmits them, as action potentials, along the axon in one direction: away from the cell body.[19] The Law of Dynamic Polarization has important exceptions; dendrites can serve as synaptic output sites of neurons[20] and axons can receive synaptic inputs.[21]
Drawing of a Purkinje cell in the cerebellar cortex done by Santiago Ramón y Cajal, demonstrating the ability of Golgi's staining method to reveal fine detail
Neurons in the brain
The number of neurons in the brain varies dramatically from species to species.[] One estimate puts the human brain at about 100 billion (1011) neurons and 100 trillion (1014) synapses.[] A lower 2012 estimate is 86 billion neurons, of which 16.3 billion are in the cerebral cortex, and 69 billion in the cerebellum.[] By contrast, the nematode worm Caenorhabditis elegans has just 302 neurons, making it an ideal experimental subject as scientists have been able to map all of the organism's neurons. The fruit fly Drosophila melanogaster, a common subject in biological experiments, has around 100,000 neurons and exhibits many complex behaviors. Many properties of neurons, from the type of neurotransmitters used to ion channel composition, are maintained across species, allowing scientists to study processes occurring in more complex organisms in much simpler experimental systems.
Neurological disorders
Charcot–Marie–Tooth disease (CMT), also known as hereditary motor and sensory neuropathy (HMSN), hereditary sensorimotor neuropathy and peroneal muscular atrophy, is a heterogeneous inherited disorder of nerves (neuropathy) that is characterized by loss of muscle tissue and touch sensation, predominantly in the feet and legs but also in the hands and arms in the advanced stages of disease. Presently incurable, this disease is one of the most common inherited neurological disorders, with 37 in 100,000 affected. Alzheimer's disease (AD), also known simply as Alzheimer's, is a neurodegenerative disease characterized by progressive cognitive deterioration together with declining activities of daily living and neuropsychiatric symptoms or behavioral changes. The most striking early symptom is loss of short-term memory (amnesia), which usually manifests as minor forgetfulness that becomes steadily more pronounced with illness progression, with relative preservation of older memories. As the disorder progresses, cognitive (intellectual) impairment extends to the domains of language (aphasia), skilled movements (apraxia), and recognition (agnosia), and functions such as decision-making and planning become impaired.
Neuron Parkinson's disease (PD), also known as Parkinson disease, is a degenerative disorder of the central nervous system that often impairs the sufferer's motor skills and speech. Parkinson's disease belongs to a group of conditions called movement disorders. It is characterized by muscle rigidity, tremor, a slowing of physical movement (bradykinesia), and in extreme cases, a loss of physical movement (akinesia). The primary symptoms are the results of decreased stimulation of the motor cortex by the basal ganglia, normally caused by the insufficient formation and action of dopamine, which is produced in the dopaminergic neurons of the brain. Secondary symptoms may include high level cognitive dysfunction and subtle language problems. PD is both chronic and progressive. Myasthenia gravis is a neuromuscular disease leading to fluctuating muscle weakness and fatigability during simple activities. Weakness is typically caused by circulating antibodies that block acetylcholine receptors at the post-synaptic neuromuscular junction, inhibiting the stimulative effect of the neurotransmitter acetylcholine. Myasthenia is treated with immunosuppressants, cholinesterase inhibitors and, in selected cases, thymectomy.
355
Demyelination
Demyelination is the act of demyelinating, or the loss of the myelin sheath insulating the nerves. When myelin degrades, conduction of signals along the nerve can be impaired or lost, and the nerve eventually withers. This leads to certain neurodegenerative disorders like multiple sclerosis and chronic inflammatory demyelinating polyneuropathy.
Axonal degeneration
Although most injury responses include a calcium influx signaling to promote resealing of severed parts, axonal injuries initially lead to acute axonal degeneration (AAD), which is rapid separation of the proximal and distal ends within 30 minutes of injury. Degeneration follows with swelling of the axolemma, and eventually leads to bead like formation. Granular disintegration of the axonal cytoskeleton and inner organelles occurs after axolemma degradation. Early changes include accumulation of mitochondria in the paranodal regions at the site of injury. Endoplasmic reticulum degrades and mitochondria swell up and eventually disintegrate. The disintegration is dependent on Ubiquitin and Calpain proteases (caused by influx of calcium ion), suggesting that axonal degeneration is an active process. Thus the axon undergoes complete fragmentation. The process takes about roughly 24 hrs in the PNS, and longer in the CNS. The signaling pathways leading to axolemma degeneration are currently unknown.
Nerve regeneration
It has been demonstrated that neurogenesis can sometimes occur in the adult vertebrate brain, a finding that led to controversy in 1999.[22] However, more recent studies of the age of human neurons suggest that this process occurs only for a minority of cells, and the overwhelming majority of neurons comprising the neocortex were formed before birth and persist without replacement.[] It is often possible for peripheral axons to regrow if they are severed. A report in Nature suggested that researchers had found a way to transform human skin cells into working nerve cells using a process called transdifferentiation in which "cells are forced to adopt new identities."[]
Neuron
356
References
[14] Thorpe, SJ (1990) Spike arrival times: A highly efficient coding scheme for neural networks (http:/ / web. archive. org/ web/ 20120215151304/ http:/ / pop. cerco. ups-tlse. fr/ fr_vers/ documents/ thorpe_sj_90_91. pdf). In R. Eckmiller, G. Hartmann, & G. Hauske (Eds.) Parallel processing in neural systems, Elsevier, pp. 91–94 ISBN 0444883908 [19] Sabbatini R.M.E. April–July 2003. Neurons and Synapses: The History of Its Discovery (http:/ / www. cerebromente. org. br/ n17/ history/ neurons3_i. htm). Brain & Mind Magazine, 17. Retrieved on March 19, 2007.
Further reading
• Kandel E.R., Schwartz, J.H., Jessell, T.M. 2000. Principles of Neural Science, 4th ed., McGraw-Hill, New York. • Bullock, T.H., Bennett, M.V.L., Johnston, D., Josephson, R., Marder, E., Fields R.D. 2005. The Neuron Doctrine, Redux, Science, V.310, p. 791–793. • Ramón y Cajal, S. 1933 Histology, 10th ed., Wood, Baltimore. • Richard S. Snell: Clinical neuroanatomy (Lippincott Williams & Wilkins, Ed.6th 2006) Philadelphia, Baltimore, New York, London. ISBN 978-963-226-293-2 • Roberts A., Bush B.M.H. 1981. Neurones Without Impulses. Cambridge University Press, Cambridge. • Peters, A., Palay, S.L., Webster, H, D., 1991 The Fine Structure of the Nervous System, 3rd ed., Oxford, New York
External links
• IBRO (International Brain Research Organization) (http://www.ibro.info). Fostering neuroscience research especially in less well-funded countries. • NeuronBank (http://NeuronBank.org) an online neuromics tool for cataloging neuronal types and synaptic connectivity. • High Resolution Neuroanatomical Images of Primate and Non-Primate Brains (http://brainmaps.org). • The Department of Neuroscience at Wikiversity, which presently offers two courses: Fundamentals of Neuroscience and Comparative Neuroscience. • NIF Search – Neuron (https://www.neuinfo.org/mynif/search.php?q=Neuron&t=data&s=cover&b=0& r=20) via the Neuroscience Information Framework • Cell Centered Database – Neuron (http://ccdb.ucsd.edu/sand/main?event=showMPByType&typeid=0& start=1&pl=y) • Complete list of neuron types (http://neurolex.org/wiki/Category:Neuron) according to the Petilla convention, at NeuroLex. • NeuroMorpho.Org (http://NeuroMorpho.org) an online database of digital reconstructions of neuronal morphology. • Immunohistochemistry Image Gallery: Neuron (http://www.immunoportal.com/modules. php?name=gallery2&g2_view=keyalbum.KeywordAlbum&g2_keyword=Neuron)
Oligodendrocyte
357
Oligodendrocyte
Oligodendrocyte
Oligodendrocyte
Oligodendrocytes form the electrical insulation around the axons of CNS nerve cells. Latin Code oligodendrocytus TH H2.00.06.2.01018
[1]
Oligodendrocytes (from Greek, meaning cells with a few branches), or oligodendroglia (Greek, few tree glue),[1] are a type of brain cell. They are a variety of neuroglia. Their main functions are to provide support and to insulate the axons (the long projection of nerve cells) in the central nervous system (the brain and spinal cord) of some vertebrates. (The same function is performed by Schwann cells in the peripheral nervous system.) Oligodendrocytes do this by creating the myelin sheath, which is 80% lipid and 20% protein.[2] A single oligodendrocyte can extend its processes to 50 axons, wrapping approximately 1 μm of myelin sheath around each axon; Schwann cells, on the other hand, can wrap around only 1 axon. Each oligodendrocyte forms one segment of myelin for several adjacent axons.[2]
Origin
Oligodendroglia, types of glial cells, arise during development from oligodendrocyte precursor cells, which can be identified by their expression of a number of antigens, including the ganglioside GD3,[3] the NG2 chondroitin sulfate proteoglycan,[4] and the platelet-derived growth factor-alpha receptor subunit PDGF-alphaR.[5] Most oligodendrocytes develop during embryogenesis and early postnatal life from restricted periventricular germinal regions.[6] They are the last cell type to be generated in the CNS.[7] Myelination is only prevalent in a few brain regions at birth and continues into adulthood. The entire process is not complete until about 25–30 years of age.[8] Oligodendrocyte formation in the adult brain is associated with glial-restricted progenitors cells, known as oligodendrocyte progenitor cells (OPCs).[9] SVZ cells migrate away from germinal[10] zones to populate both developing white and gray matter, where they differentiate and mature into myelin-forming oligodendroglia.[11]
Oligodendrocyte However, it is not clear whether all oligodendroglial progenitors undergo this sequence of events. It has been suggested that some undergo apoptosis [12] and others fail to differentiate into mature oligodendroglia but persist as adult oligodendroglial progenitors.[13]
358
Function
As part of the nervous system, oligodendrocytes are closely related to nerve cells, and, like all other glial cells, oligodendrocytes provide a supporting role for neurons. In addition, the nervous system of mammals depends crucially on myelin sheaths, which reduce ion leakage and decrease the capacitance of the cell membrane.[14] Myelin also increases impulse speed, as saltatory propagation of action potentials occurs at the nodes of Ranvier in between Schwann cells (of the PNS) and oligodendrocytes (of the CNS). Oligodendrocytes provide the same functionality as the insulation on a household electrical wire (with the rather large difference that, while household An oligodendrocyte seen myelinating several axons. electrical wires are in a non-conducting medium - air - the axons run in a solution of water and ions, which conducts electrical current well). Furthermore, impulse speed of myelinated axons increases linearly with the axon diameter, whereas the impulse speed of unmyelinated cells increases only with the square root of the diameter. The insulation must be proportional to the diameter of the fiber inside. The optimal ratio of axon diameter divided by the total fiber diameter (which includes the myelin) is 0.6.[8] In contrast, Satellite oligodendrocytes are functionally distinct from most oligodendrocytes. They are not attached to neurons and, therefore, do not serve an insulating role. They remain apposed to neurons and regulate the extracellular fluid.[15] Satellite oligodendrocytes are considered to be a part of the gray matter whereas myelinating oligodendrocytes are a part of the white matter. Myelination is an important component of intelligence. Neuroscientist Vincent J. Schmithorst found that there is a correlation with white matter and intelligence. People with greater white matter had higher IQ's.[8] A study done with rats by Janice M Juraska showed that rats that were raised in an enriched environment had more myelination in their corpus callosum.[16]
Pathology
Diseases that result in injury to the oligodendroglial cells include demyelinating diseases such as multiple sclerosis and leukodystrophies. Trauma to the body, e.g. spinal cord injury, can also cause demyelination. Cerebral palsy (periventricular leukomalacia) is caused by damage to developing oligodendrocytes in the brain areas around the cerebral ventricles. In cerebral palsy, spinal cord injury, stroke and possibly multiple sclerosis, oligodendrocytes are thought to be damaged by excessive release of the neurotransmitter glutamate.[17] Damage has also been shown to be mediated by N-methyl-d-aspartate receptors.[17] Oligodendrocyte dysfunction may also be implicated in the pathophysiology of schizophrenia and bipolar disorder.[18] Oligodendroglia are also susceptible to infection by the JC virus, which causes progressive multifocal leukoencephalopathy (PML), a condition that specifically affects white matter, typically in immunocompromised patients. Tumors of oligodendroglia are called oligodendrogliomas. The chemotherapy agent Fluorouracil (5-FU) causes damage to the oligodendrocytes in mice, leading to both acute central nervous system (CNS) damage and progressively worsening delayed degeneration of the CNS.[19]
Oligodendrocyte
359
Notes
[1] . [2] Carlson, Physiology of Behavior, 2010 [3] Curtis et al., 1988; LeVine and Goldman, 1988; Hardy and Reynolds, 1991; Levine et al., 1993 [4] Levine et al., 1993 [5] Pringle et al., 1992 [6] Vallstedt et al., 2004 [7] Thomas et al., Spatiotemporal development of oligodendrocytes in the embryonic brain., 2000 [8] Fields, 2008 [9] Menn, et al., Origin of Oligodendrocytes in the Subventricular Zone of the Adult Brain, 2006 [10] Menn, et al., 2006 [11] Hardy and Reynolds, 1991; Levison and Goldman, 1993 [12] Barres et al., 1992 [13] Wren et al., 1992 [14] Sokol, 2009 [15] Baumann and Pham-Dinh, 2001 [17] Káradóttir et al., 2007 [18] Tkachev et al., 2003 [19] "Chemotherapy-induced Damage to the CNS as a Precursor Cell Disease" (http:/ / www. urmc. rochester. edu/ biomedical-genetics/ faculty/ chemotherapy-induced-damage-to-cns. cfm) by Dr. Mark D. Noble, University of Rochester
References
• Baumann, N; Pham-Dinh, D (2001). "Biology of Oligodendrocyte and Myelin in the Mammalian Central Nervous System" (http://physrev.physiology.org/cgi/content/full/81/2/871). Physiological Reviews 18 (2): 871–927. PMID 11274346 (http://www.ncbi.nlm.nih.gov/pubmed/11274346). Retrieved 2007-07-13 More than one of |surname1= and |last1= specified (help); More than one of |given1= and |first1= specified (help); More than one of |surname2= and |last2= specified (help); More than one of |given2= and |first2= specified (help) • Ragheb, Fadi (1999). The M3 Muscarinic Acetylcholine Receptor Mediates p42mapk Activation and c-fos mRNA Expression in Oligodendrocyte Progenitors (http://www.collectionscanada.ca/obj/s4/f2/dsk1/tape9/ PQDD_0025/MQ50862.pdf). Ottawa: National Library of Canada. Retrieved 2006-03-07 • Raine, C.S. (1991). Oligodendrocytes and central nervous system myelin. In Textbook of Neuropathology, second edition, R.L. Davis and D.M. Robertson, eds. (Baltimore, Maryland: Williams and Wilkins), pp. 115–141. • Tkachev D, Mimmack ML, Ryan MM, et al. (September 2003). "Oligodendrocyte dysfunction in schizophrenia and bipolar disorder". Lancet 362 (9386): 798–805. doi: 10.1016/S0140-6736(03)14289-4 (http://dx.doi.org/ 10.1016/S0140-6736(03)14289-4). PMID 13678875 (http://www.ncbi.nlm.nih.gov/pubmed/13678875). • Káradóttir, R.; D. Attwell (14). "Neurotransmiter receptors in the life and death of oligodendrocytes" (http:// www.ncbi.nlm.nih.gov/pmc/articles/PMC2173944). Neuroscience 145 (4): 1426–1438. doi: 10.1038/bjc.1990.391 (http://dx.doi.org/10.1038/bjc.1990.391). PMC 2173944 (http://www.ncbi.nlm. nih.gov/pmc/articles/PMC2173944). PMID 2173944 (http://www.ncbi.nlm.nih.gov/pubmed/2173944). • Carlson, Neil (2010). Physiology of Behavior. Boston, MA: Allyn & Bacon. pp. 38–39. ISBN 0-205-66627-2. • Sokol, Stacey. "The Physiology and Pathophysiology of Multiple Sclerosis" (http://mylifehealthandprosperity. com/index.php?option=com_content&view=article&id=65&Itemid=160). Multiple Sclerosis: Physiological Tutorial. Retrieved 2012-04-29. • Fields, Douglas (18). "White Matter Matters" (http://www.scientificamerican.com/article. cfm?id=white-matter-matters). Scientific American 298 (March 2008): 54–61. Bibcode: 2008SciAm.298c..54D (http://adsabs.harvard.edu/abs/2008SciAm.298c..54D). doi: 10.1038/scientificamerican0308-54 (http://dx. doi.org/10.1038/scientificamerican0308-54). Retrieved 2012-04-29.
Oligodendrocyte • Menn, Benedicte; Jose Manuel Garcia-Verdugo, Cynthia Yaschine, Oscar Gonzalez-Perez, David Rowitch, Arturo Alvarez-Buylla (26). "Origin of Oligodendrocytes in the Subventricular Zone of the Adult Brain" (http:// www.jneurosci.org/content/26/30/7907.full). The Journal of Neuroscience 26 (30): 7907–7918. doi: 10.1523/JNEUROSCI.1299-06.2006 (http://dx.doi.org/10.1523/JNEUROSCI.1299-06.2006). PMID 16870736 (http://www.ncbi.nlm.nih.gov/pubmed/16870736). Retrieved 2012-04-29. • Vallstedt, A; Klos JM, Ericson F (6). "Multiple dorsoventral origins of oligodendrocyte generation in the spinal cord and hindbrain". Neuron. 1 45 (1): 55–67. doi: 10.1016/j.neuron.2004.12.026 (http://dx.doi.org/10.1016/j. neuron.2004.12.026). PMID 15629702 (http://www.ncbi.nlm.nih.gov/pubmed/15629702). • Thomas, JL; Spassky N, Perez Villegas EM, Olivier C, Cobos I, Goujet-Zalc C, Martínez S, Zalc B. (15). "Spatiotemporal development of oligodendrocytes in the embryonic brain" (http://www.ncbi.nlm.nih.gov/ pubmed/10679785). Journal of Neuroscience Research 59 (4): 471–476. doi: 10.1002/(SICI)1097-4547(20000215)59:4<471::AID-JNR1>3.0.CO;2-3 (http://dx.doi.org/10.1002/ (SICI)1097-4547(20000215)59:4<471::AID-JNR1>3.0.CO;2-3). PMID 10679785 (http://www.ncbi.nlm.nih. gov/pubmed/10679785). Retrieved 2012-04-29.
360
External links
• The Department of Neuroscience at Wikiversity • NIF Search - Oligodendrocyte (https://www.neuinfo.org/mynif/search.php?q="Oligodendrocyte"&t=data& s=cover&b=0&r=20) via the Neuroscience Information Framework
Spindle neuron
361
Spindle neuron
Neuron: Spindle neuron
Cartoon of a spindle cell (right) compared to a normal pyramidal cell (left). Location Function Morphology Presynaptic connections Anterior cingulate cortex and Fronto-insular cortex Global firing rate regulation and regulation of emotional state Unique spindle-shaped projection neuron Local input to ACC and FI
Postsynaptic connections Frontal and temporal cortex.
Spindle neurons, also called von Economo neurons (VENs), are a specific class of neurons that are characterized by a large spindle-shaped soma, gradually tapering into a single apical axon in one direction, with only a single dendrite facing opposite. Whereas other types of cells tend to have many dendrites, the polar shaped morphology of spindle neurons is unique. They are found in two very restricted regions in the brains of hominids – the family of species comprising humans and other great apes – the anterior cingulate cortex (ACC) and the fronto-insular cortex (FI). Recently they have been Micrograph showing a spindle neuron of the discovered in the dorsolateral prefrontal cortex of humans.[] Spindle cingulate. HE-LFB stain. cells are also found in the brains of the humpback whales, fin whales, killer whales, sperm whales,[1][] bottlenose dolphin, Risso’s dolphin, beluga whales,[] and the African and Asian elephants.[] The name von Economo neuron comes from their discoverer, Constantin von Economo (1876–1931) who described them in 1929.[2]
Function of spindle neurons
Spindle neurons are relatively enormous cells that may allow rapid communication across the relatively large brains of great apes, Elephantidaes, and Cetacea. Spindle neurons have been implicated by scientists as having an important role in many cognitive abilities and disabilities generally unique to humans, ranging from savant perceptiveness and perfect pitch to dyslexia and autism. While rare in comparison to other neurons, spindle neurons are abundant, and large, in humans. However, the concentration of spindle cells has been measured to be three times higher in Cetaceans in comparison to humans.[][3] They have only been found thus far in the anterior cingulate cortex (ACC), fronto-insular cortex (FI), and the dorsolateral prefrontal cortex.
Spindle neuron
362
Evolutionary significance
The observation that spindle neurons only occur in a highly significant group of animals (from a human point of view) has led to speculation that they are of great importance in human evolution and/or brain function. Their restriction (among the primates) to great apes leads to the hypothesis that they developed no earlier than 15-20 million years ago, prior to the divergence of orangutans from the African great apes. The discovery of spindle neurons in diverse whale species[][] has led to the suggestion that they are "a possible obligatory neuronal adaptation in very large brains, permitting fast information processing and transfer along highly specific projections and that evolved in relation to emerging social behaviors."[]p. 254 Their presence in the brains of these species supports this theory, pointing towards the existence of these specialized neurons only in highly intelligent mammals, and may be an example of convergent evolution.[4] Recently, primitive forms of spindle neurons have also been discovered in macaque monkey brains.[5]
ACC spindle neurons
In 1999, Professor John Allman, a neuroscientist, and colleagues at the California Institute of Technology first published a report on spindle neurons found in the anterior cingulate cortex (ACC) of hominids, but not in any other species. Neuronal volumes of ACC spindle neurons were larger in humans and the gracile (slender) chimpanzees than the spindle neurons of the robust gorillas and orangutans. Allman and his colleagues have delved beyond the level of brain infrastructure to investigate how spindle neurons function at the superstructural level, focusing on their role as 'air traffic controllers' for emotions. Allman's team reports that spindle neurons help channel neural signals from deep within the cortex to relatively distant parts of the brain. Specifically, Allman's team found signals from the ACC are received in Brodmann's area 10, in the frontal polar cortex, where regulation of cognitive dissonance (disambiguation between alternatives) is thought to occur. According to Allman, this neural relay appears to convey motivation to act, and concerns the recognition of error. Self-control – and avoidance of error – is thus facilitated by the executive gatekeeping function of the ACC, as it regulates the interference patterns of neural signals between these two brain regions. In humans, intense emotion activates the anterior cingulate cortex, as it relays neural signals transmitted from the amygdala (a primary processing center for emotions) to the frontal cortex, perhaps by functioning as a sort of lens to focus the complex texture of neural signal interference patterns. The ACC is also active during demanding tasks requiring judgment and discrimination, and when errors are detected by an individual. During difficult tasks, or when experiencing intense love, anger, or lust, activation of the ACC increases. In brain imaging studies, the ACC has specifically been found to be active when mothers hear infants cry, underscoring its role in affording a heightened degree of social sensitivity. The ACC is a relatively ancient cortical region, and is involved with many autonomic functions, including motor and digestive functions, while also playing a role in the regulation of blood pressure and heart rate. Significant olfactory and gustatory capabilities of the ACC and fronto-insular cortex appear to have been usurped, during recent evolution, to serve enhanced roles related to higher cognition – ranging from planning and self-awareness to role playing and deception. The diminished olfactory function of humans, compared to other primates, may be related to the fact that spindle cells located at crucial neural network hubs have only two dendrites rather than many, resulting in reduced neurological integration.
Spindle neuron
363
Fronto-insular spindle neurons
At a Society for Neuroscience meeting in 2003, Allman reported on spindle cells his team found in another brain region, the fronto-insular cortex, a region which appears to have undergone significant evolutionary adaptations in mankind – perhaps as recently as 100,000 years ago. This fronto-insular cortex is closely connected to the insula, a region that is roughly the size of a thumb in each hemisphere of the human brain. The insula and fronto-insular cortex are part of the orbitofrontal cortex, wherein the elaborate circuitry associated with spatial awareness and the sense of touch are found, and where self awareness and the complexities of emotion are thought to be generated and experienced. Moreover, this region of the right hemisphere is crucial to navigation and perception of three dimensional rotations.
Spindle neuron concentrations
ACC
The largest number of ACC spindle neurons are found in humans, fewer in the gracile great apes, and fewest in the robust great apes. In both humans and bonobos they are often found in clusters of 3 to 6 neurons. They are found in humans, bonobos, common chimpanzees, gorillas, orangutans, some cetaceans, and elephants.[6]:245 While total quantities of ACC spindle neurons were not reported by Allman in his seminal research report (as they were in a later report describing their presence in the frontoinsular cortex, below), his team's initial analysis of the ACC layer V in hominids revealed an average of ~9 spindle neurons per section for orangutans (rare, 0.6% of section cells), ~22 for gorillas (frequent, 2.3%), ~37 for chimpanzees (abundant, 3.8%), ~68 for bonobos (abundant/clusters, 4.8%), ~89 for humans (abundant/clusters, 5.6%).[7]
Fronto-insula
All of the primates examined had more spindle cells in the fronto-insula of the right hemisphere than in the left. In contrast to the higher number of spindle cells found in the ACC of the gracile bonobos and chimpanzees, the number of fronto-insular spindle cells was far higher in the cortex of robust gorillas (no data for Orangutans was given). An adult human had 82,855 such cells, a gorilla had 16,710, a bonobo had 2,159, and a chimpanzee had a mere 1,808 – despite the fact that chimpanzees and bonobos are great apes most closely related to humans.
Dorsolateral PFC
Von Economo neurons have been located in the Dorsolateral prefrontal cortex of humans[] and elephants.[] In humans they have been observed in higher concentration in Brodmann area 9 (BA9) – mostly isolated or in clusters of 2, while in Brodmann area 24 (BA24) they have been found mostly in clusters of 2-4.[]
Related pathologies
Abnormal spindle neuron development may be linked to several psychotic disorders, typically those characterized by distortions of reality, disturbances of thought, disturbances of language, and withdrawal from social contact. Altered spindle neuron states have been implicated in both schizophrenia and autism, but research into these correlations remains at a very early stage. An initial study suggested that Alzheimer's disease specifically targeted Von Economo neurons, however, this study was performed with end-stage Alzheimer brains in which cell destruction was widespread. Later, it was found that Alzheimer's disease doesn't affect the VENS, but behavioral variant frontotemporal lobe degeneration specifically targets these cell populations in the anterior cingulate cortex and the anterior insula early in the disease. [8]
Spindle neuron
364
References
[2] von Economo, C., & Koskinas, G. N. (1929). The cytoarchitectonics of the human cerebral cortex. London: Oxford University Press [5] http:/ / www. sciencedaily. com/ releases/ 2012/ 05/ 120521115353. htm
General References
• Allman J, Hakeem A, Watson K (Aug 2002). "Two phylogenetic specializations in the human brain" (http://nro. sagepub.com/cgi/pmidlookup?view=long&pmid=12194502). Neuroscientist 8 (4): 335–46. doi: 10.1177/107385840200800409 (http://dx.doi.org/10.1177/107385840200800409). PMID 12194502 (http:// www.ncbi.nlm.nih.gov/pubmed/12194502).
External links
• TaipeiTimes.com (http://www.taipeitimes.com/News/feat/archives/2003/12/10/2003079090/ print)Wikipedia:Link rot – Know Thyself and Others • "Well-wired whales" (http://sciencenow.sciencemag.org/cgi/content/full/2006/1127/1) Michael Balter (2006) ScienceNOW Daily News. 27 November • "Brain Cells for Socializing" (http://www.smithsonianmag.com/science-nature/The-Social-Brain.html?c=y& story=fullstory) Smithsonian, June 2009
Hepatocyte
365
Hepatocyte
Template:PAGE,n kgmkjNAME
Hepatocyte and sinusoid (blood vessel) in a rat liver with fenestrated endothelial cells. Fenestration are approx 100 nm diameter, and the sinusoidal width 5 µm.
Cross-section of the human liver. Latin Code hepatocytus TH H3.04.05.0.00006
A hepatocyte is a cell of the main tissue of the liver. Hepatocytes make up 70-85% of the liver's cytoplasmic mass. These cells are involved in: • • • • • Protein synthesis Protein storage Transformation of carbohydrates Synthesis of cholesterol, bile salts and phospholipids Detoxification, modification, and excretion of exogenous and endogenous substances
The hepatocyte also initiates formation and secretion of bile.
Hepatocyte
366
Structure
The typical hepatocyte forms a cubical cell of 15 µm sides (in comparison, a human hair has a diameter of 17 to 180 µm). The typical volume of a hepatocyte is 3.4 x 10-9 cm3. [1] The smooth endoplasmic reticulum (Smooth ER) is an abundant organelle in hepatocytes, whereas most cells in the body have small amounts of smooth ER. [2]
Histology
Hepatocytes display an eosinophilic cytoplasm, reflecting numerous mitochondria, and basophilic stippling due to large amounts of rough endoplasmic reticulum and free ribosomes. Brown lipofuscin granules are also observed (with increasing age) together with irregular unstained areas of cytoplasm; these correspond to cytoplasmic glycogen and lipid stores removed during histological preparation. The average life span of the hepatocyte is 5 months; they are able to regenerate. Hepatocyte nuclei are round with dispersed chromatin and prominent nucleoli. Anisokaryosis is common and often reflects tetraploidy and other degrees of polyploidy, a normal feature of 30-40% of hepatocytes in adult human liver.[3] Binucleate cells are also common. Hepatocytes are organised into plates separated by vascular channels (sinusoids), an arrangement supported by a reticulin (collagen type III) network. The hepatocyte plates are one cell thick in mammals and two cells thick in the chicken. Sinusoids display a discontinuous, fenestrated endothelial cell lining. The endothelial cells have no basement membrane and are separated from the hepatocytes by the space of Disse, which drains lymph into the portal tract lymphatics. Kupffer cells are scattered between endothelial cells; they are part of the reticuloendothelial system and phagocytose spent erythrocytes. Stellate (Ito) cells store vitamin A and produce extracellular matrix and collagen; they are also distributed amongst endothelial cells but are difficult to visualise by light microscopy. Hepatocytes are an important physiological example for evalutation of both biological and metabolic effects of xenobiotics. They are separated from the liver by collagenase digestion, which is a two step process. In the first step, the liver is placed in an isotonic solution, in which calcium is removed to disrupt cell-cell tight junctions by the use of a calcium chelating agent. Next, a solution containing collagenase is added to separate the hepatocytes from the liver stroma. This process creates a suspension of hepatocytes, which can be cultured and plated on 96 well plates for immediate use, or cryopreserved by freezing.[4] They do not proliferate in culture. Hepatocytes are intensely sensitive to damage during the cycles of cryopreservation including freezing and thawing. Even after the addition of classical cryoprotectants there is still damage done while being cryopreserved. [5]
Protein synthesis
The hepatocyte is a cell in the body that manufactures serum albumin, fibrinogen, and the prothrombin group of clotting factors (except for Factors 3 and 4). It is the main site for the synthesis of lipoproteins, ceruloplasmin, transferrin, complement, and glycoproteins. Hepatocytes manufacture their own structural proteins and intracellular enzymes. Synthesis of proteins is by the rough endoplasmic reticulum (RER), and both the rough and smooth endoplasmic reticulum (SER) are involved in secretion of the proteins formed. The endoplasmic reticulum (ER) is involved in conjugation of proteins to lipid and carbohydrate moieties synthesized by, or modified within, the hepatocytes.
Hepatocyte
367
Carbohydrate metabolism
The liver forms fatty acids from carbohydrates and synthesizes triglycerides from fatty acids and glycerol. Hepatocytes also synthesize apoproteins with which they then assemble and export lipoproteins (VLDL, HDL). The liver is also the main site in the body for gluconeogenesis, the formation of carbohydrates from precursors such as alanine, glycerol, and oxaloacetate.
Lipid metabolism
The liver receives many lipids from the systemic circulation and metabolizes chylomicron remnants. It also synthesizes cholesterol from acetate and further synthesizes bile salts. The liver is the sole site of bile salts formation.
Detoxification
Hepatocytes have the ability to metabolize, detoxify, and inactivate exogenous compounds such as drugs, (drug metabolism), and insecticides, and endogenous compounds such as steroids. The drainage of the intestinal venous blood into the liver requires efficient detoxification of miscellaneous absorbed substances to maintain homeostasis and protect the body against ingested toxins. One of the detoxifying functions of hepatocytes is to modify ammonia into urea for excretion. The most abundant organelle in liver cell is the smooth endoplasmic reticulum.
Additional images
Schemic diagram of Biliary system
Hepatocyte
368
References
[1] Lodish, H., Berk, A., Zipursky, S. L., Matsudaira, P., Baltimore, D., Darnell, J. E. Molecular Cell Biology (Fifth Edition). W. H. Freeman and Company. New York, 2000, pp 10. [2] Lodish, H., Berk, A., Zipursky, S. L., Matsudaira, P., Baltimore, D., Darnell, J. E. Molecular Cell Biology (Fifth Edition). W. H. Freeman and Company. New York, 2000, pp 168. [4] Li, Albert P.; "Screening for human ADME/Tox drug properties in Drug Discovery": Drug Discovery Today, Vol. 6, No. 7, April 2001, pp. 357-366 [5] Hamel et al.; "Wheat Extracts as an Efficient Cryoprotective Agent for Primary Cultures of Rat Hepatocytes": published online 21 Aug 2006 in Wiley Interscience www.interscience.wiley.com. Department des sciences bogiques, Montreal University.
External links
• BU Histology Learning System: 22101ooa (http://www.bu.edu/histology/p/22101ooa.htm) - "Ultrastructure of the Cell: hepatocytes and sinusoids" • Hepatic Histology: Hepatocytes (Colorado State University (http://www.vivo.colostate.edu/hbooks/pathphys/ digestion/liver/histo_hcytes.html) • The use of hepatocytes to measure clearance (http://www.cyprotex.com/admepk/in-vitro-metabolism/ hepatocyte-stability/) The performance of in vitro hepatic clearance studies including analysis of the data.
Adipocyte
369
Adipocyte
Adipocyte
Yellow adipose tissue in paraffin section Latin Code adipocytus TH H2.00.03.0.01005
[1]
Adipocytes, also known as lipocytes and fat cells, are the cells that primarily compose adipose tissue, specialized in storing energy as fat. There are two types of adipose tissue, white adipose tissue (WAT) and brown adipose tissue (BAT), which are also known as white fat and brown fat, respectively, and comprise two types of fat cells. Most recently presence of beige adipocytes with gene expression pattern distinct from either white or brown adipocytes has been described.[1]
White fat cells (unilocular cells)
White fat cells or monovacuolar cells contain a large lipid droplet surrounded by a layer of cytoplasm. The nucleus is flattened and located on the periphery. A typical fat cell is 0.1mm in diameter with some being twice that size and others half that size. The fat stored is in a semi-liquid state, and is composed primarily of triglycerides and cholesteryl ester. White fat cells secrete many proteins acting as adipokines such as resistin, adiponectin, leptin and Apelin. An average adult has 30 billion fat cells with a weight of 30 lbs or 13.5 kg. If excess weight is gained as an adult, fat cells increase in size about fourfold before dividing and increasing the absolute number of fat cells present.[2]
Brown fat cells (multilocular cells)
Brown fat cells or plurivacuolar cells are polygonal in shape. Unlike white fat cells, these cells have considerable cytoplasm, with lipid droplets scattered throughout. The nucleus is round, and, although eccentrically located, it is not in the periphery of the cell. The brown color comes from the large quantity of mitochondria. Brown fat, also known as "baby fat," is used to generate heat.
Lineage
Although the lineage of adipocytes is still unclear, pre-adipocytes are undifferentiated fibroblasts that can be stimulated to form adipocytes. Mesenchymal stem cells can differentiate into adipocytes, connective tissue, muscle or bone. Areolar connective tissue is composed of adipocytes. The term "lipoblast" is used to describe the precursor of the adult cell. The term "lipoblastoma" is used to describe a tumor of this cell type.[]
Adipocyte
370
Cell turnover
After marked weight loss the number of fat cells does not decrease (the cells contain less fat). Fat cells swell or shrink but remain constant in number. However, the number of fat cells may increase once existing fat cells are sufficiently full. Adult rats of various strains became obese when they were fed a highly palatable diet for several months. Analysis of their adipose tissue morphology revealed increases in both adipocyte size and number in most depots. Reintroduction of an ordinary chow diet to such animals precipitated a period of weight loss during which only mean adipocyte size returned to normal. Adipocyte number remained at the elevated level achieved during the period of weight gain.[3] However, in some reports and textbooks, the number of fat cell (adipocytes) increased in childhood and adolescence. The total number is constant in both obese and lean adult. Individuals who become obese as adults have no more fat cell than they had before.[] People who have been fat since childhood generally have an inflated number of fat cells. People who become fat as adults may have no more fat cells than their lean peers, but their fat cells are larger. In general, people with an excess of fat cells find it harder to lose weight and keep it off than the obese who simply have enlarged fat cells.[4] According to a research by Tchoukalova et al., 2010, it has been reported that the body fat cells could have regional responses to the overfeeding studied in adult subjects. In upper body, an increasing of the adipocyte size was correlated with upper-body fat gain; however, the total fat cells were not significantly changed. In contrast to the upper body fat cell responses, a number of lower-body adipocytes were significantly increased during the course of experiment but there was no change in the cell size.[5] Approximately 10% of fat cells are renewed annually at all adult ages and levels of body mass index without a significant increase in the overall number of adipocytes in adulthood.[]
Endocrine functions
Adipocytes can synthesize estrogens from androgens,[6] potentially being the reason why being underweight or overweight are risk factors for infertility.[7] Additionally, adipocytes are responsible for the production of the hormone leptin. Leptin is important in regulation of appetite and acts as a satiety factor.[8]
References
[1] Wu J, Bostrom P, Sparks LM, Ye L, Choi JH, Giang AH, et al. Beige adipocytes are a distinct type of thermogenic fat cell in mouse and human. Cell 2012; 150:366-76. [7] UNIQ-nowiki-0-b868a355cd8ea4cc-QINU FERTILITY FACT > Female Risks By the American Society for Reproductive Medicine (ASRM). Retrieved on Jan 4, 2009
External links
• BU Histology Learning System: 08201loa (http://www.bu.edu/histology/p/08201loa.htm) - "Connective Tissue: unilocular (white) adipocytes " • BU Histology Learning System: 04901lob (http://www.bu.edu/histology/p/04901lob.htm) - "Connective Tissue: multilocular (brown) adipocytes"
White adipose tissue
371
White adipose tissue
White adipose tissue
Latin textus adiposus albus Code TH H2.00.04.0.0002 [1]
White adipose tissue (WAT) or white fat is one of the two types of adipose tissue found in mammals. The other kind of adipose tissue is brown adipose tissue. In healthy, non-overweight humans, white adipose tissue composes as much as 20% of the body weight in men and 25% of the body weight in women. Its cells contain a single large fat droplet, which forces the nucleus to be squeezed into a thin rim at the periphery. They have receptors for insulin, growth hormones, norepinephrine and glucocorticoids. White adipose tissue is used as a store of energy. Upon release of insulin from the pancreas, white adipose cells' insulin receptors cause a Distribution of white adipose tissue in the human dephosphorylation cascade that lead to the inactivation of body. hormone-sensitive lipase. It was previously thought that upon release of glucagon from the pancreas, glucagon receptors cause a phosphorylation cascade that activates hormone-sensitive lipase, causing the breakdown of the stored fat to fatty acids, which are exported into the blood and bound to albumin, and glycerol, which is exported into the blood freely.There is actually no evidence at present that glucagon has any effect on white adipose tissue.[1] Glucagon is now thought to act exclusively on the liver to trigger glycogenolysis and gluconeogenesis.[] The trigger for this process in white adipose tissue is instead now thought to be adrenocorticotropic hormone (ACTH), adrenaline and noradrenaline[citation needed]. Fatty acids are taken up by muscle and cardiac tissue as a fuel source, and glycerol is taken up by the liver for gluconeogenesis. White adipose tissue also acts as a thermal insulator, helping to maintain body temperature. The hormone leptin is primarily manufactured in the adipocytes of white adipose tissue.
References
Brown adipose tissue
372
Brown adipose tissue
Brown adipose tissue
Brown adipose tissue in a woman shown in a PET/CT exam Latin Code textus adiposus fuscus TH H2.00.04.0.0004
[1]
Brown adipose tissue (BAT) or brown fat is one of two types of fat or adipose tissue (the other being white adipose tissue) found in mammals. It is especially abundant in newborns and in hibernating mammals.[] Its primary function is to generate body heat in animals or newborns that do not shiver. In contrast to white adipocytes (fat cells), which contain a single lipid droplet, brown adipocytes contain numerous smaller droplets and a much higher number of (iron containing) mitochondria, which make it brown.[] Brown fat also contains more capillaries than white fat, since it has a greater need for oxygen than most tissues.
Biochemistry
The mitochondria in a eukaryotic cell utilize fuels to produce energy (in the form of ATP). This process involves storing energy as a proton gradient, also known as the proton motive force (PMF), across the mitochondrial inner membrane. This energy is used to synthesize ATP when the protons flow across the membrane (down their concentration gradient) through the ATP synthase enzyme; this is known as chemiosmosis. In warm-blooded animals, body heat is maintained by signaling the mitochondria to allow protons to run back along the gradient without producing ATP.[citation needed] This can occur since an alternative return route for the protons exists through an uncoupling protein in the inner membrane. This protein, known as uncoupling protein 1 (thermogenin), facilitates the return of the protons after they have been actively pumped out of the mitochondria by the electron transport chain. This alternative route for protons uncouples oxidative phosphorylation and the energy in the PMF is instead released as heat. To some degree, all cells of endotherms give off heat, especially when body temperature is below a regulatory threshold. However, brown adipose tissue is highly specialized for this non-shivering thermogenesis. First, each cell has a higher number of mitochondria compared to more typical cells. Second, these mitochondria have a higher-than-normal concentration of thermogenin in the inner membrane.
Brown adipose tissue
373
Function in infants
In neonates (newborn infants), brown fat, which then makes up about 5% of the body mass and is located on the back, along the upper half of the spine and toward the shoulders, is of great importance to avoid lethal cold (hypothermia is a major death risk for premature neonates). Numerous factors make infants more susceptible to cold than adults: • • • • • • The higher ratio of body surface (proportional to heat loss) to body volume (proportional to heat production) The higher proportional surface area of the head The low amount of musculature and the inability or reluctance to shiver A lack of thermal insulation, e.g., subcutaneous fat and fine body hair (especially in prematurely born children) The inability to move away from cold areas, air currents or heat-draining materials The inability to use additional ways of keeping warm (e.g., drying their skin, putting on clothing, moving into warmer areas, or performing physical exercise) • The nervous system is not fully developed and does not respond quickly and/or properly to cold (e.g., by contracting blood vessels in and just below the skin; vasoconstriction). Heat production in brown fat provides an infant with an alternative means of heat regulation.
Presence in adults
It was believed that after infants grow up, most of the mitochondria (which are responsible for the brown color) in brown adipose tissue disappear, and the tissue becomes similar in function and appearance to white fat. However, more recent research has shown that brown fat is related not to white fat, but to skeletal muscle.[][1][2] Further, recent studies using Positron Emission Tomography scanning of adult humans have shown that it is still present in adults in the upper chest and neck. The remaining deposits become more visible Micrograph of a hibernoma, a benign tumour (increasing tracer uptake, that is, more metabolically active) with cold thought to arise from brown fat. H&E stain. exposure, and less visible if an adrenergic beta blocker is given before the scan. The recent study could lead to a new method of weight loss, since brown fat takes calories from normal fat and burns it. Scientists were able to stimulate brown fat growth in mice, but human trials have not yet begun.[3][4] In rare cases, brown fat continues to grow, rather than involuting; this leads to a tumour known as a hibernoma.
Embryology
Brown fat cells and muscle cells both seem to be derived from the same stem cells in the embryo. Both have the same marker on their surface (Myf5, myogenic factor), which white fat cells do not have.[] Brown fat cells and muscle cells both come from the middle embryo layer. The three layers of the embryo during the gastrulation stage are ectoderm, mesoderm, endoderm. Mesoderm is the source of myocytes (muscle cells), adipocytes, and chondrocytes (cartilage cells). Adipocytes give rise to white fat cells and brown fat cells. Researchers found that both muscle and brown fat cells expressed the same muscle factor Myf5, whereas white fat cells did not. This suggested that muscle cells and brown fat cells were both derived from the same stem cell. Furthermore, muscle cells that were cultured with the transcription factor PRDM16 were converted into brown fat cells, and brown fat cells without PRDM16 were converted into muscle cells.[] However, there may be two types of brown fat cells—with and without Myf5. The other type, without Myf5, may share the same origin as white fat cells. They both seem to be derived from pericytes, the cells which surround the blood vessels that run through white fat tissue.[]
Brown adipose tissue
374
References
[1] Brown adipose tissue -- when it pays to be inefficient, Francesco S. Celi, N Engl J Med, 360:1553, Apr. 9, 2009 [4] Scientists Create Energy-burning Brown Fat In Mice (http:/ / www. sciencedaily. com/ releases/ 2009/ 07/ 090729132109. htm) Science Daily, July 30, 2009
External links
• BU Histology Learning System: 04901lob (http://www.bu.edu/histology/p/04901lob.htm) - "Connective Tissue: multilocular (brown) adipocytes"
Hepatic stellate cell
375
Hepatic stellate cell
Hepatic stellate cell
Schematic presentation of hepatic stellate cells (HSC) located in the vicinity of adjacent hepatocytes (PC) beneath the sinusoidal endothelial cells (EC). S – liver sinusoids; KC – Kupffer cells. Down left shows cultured HSC at light-microscopy, whereas at down right electron microscopy (EM) illustrates numerous fat vacuoles (L) in a HSC, in which retinoids are stored.
Basic liver structure Latin Code cellula perisinusoidalis; cellula accumulans adipem TH H3.04.05.0.00013
Hepatic stellate cells (here HSC), also known as perisinusoidal cells or Ito cells (earlier lipocytes or fat-storing cells), are pericytes found in the perisinusoidal space (a small area between the sinusoids and hepatocytes) of the liver also known as the space of Disse. The stellate cell is the major cell type involved in liver fibrosis, which is the formation of scar tissue in response to liver damage.
Staining
Ito cells can be selectively stained with gold chloride, but their distinguishing feature in routine histological preparations is the presence of multiple lipid droplets in their cytoplasm.[] Reelin expressed by Ito cells has been shown to be a reliable marker in discerning them from other myofibroblasts.[1] The expression of reelin is increased after liver injury.
Function
In normal liver, stellate cells are described as being in a quiescent state. Quiescent stellate cells represent 5-8% of the total number of liver cells.[2] Each cell has several long protrusions that extend from the cell body and wrap around the sinusoids. The lipid droplets in the cell body store vitamin A as retinol ester. The function and role of quiescent hepatic stellate cells is unclear. Recent evidence suggests a role as a liver-resident antigen-presenting cell, presenting lipid antigens to and stimulating proliferation of NKT cells.[] When the liver is damaged, stellate cells can change into an activated state. The activated stellate cell is characterized by proliferation, contractility, and chemotaxis. The amount of stored vitamin A decreases progressively in liver injury.[] The activated stellate cell is also responsible for secreting collagen scar tissue, which can lead to cirrhosis. More recent studies have also shown that in vivo activation of hepatic stellate cells by agents
Hepatic stellate cell causing liver fibrosis can eventually lead to senescence of these cells, marked by increased SA-beta-galactosidase staining, as well as p53 accumulation and activation of Rb–hallmarks of cellular senescence. The senescent hepatic stellate cells have been demonstrated to limit liver fibrosis by activating the immune system by activating interactions with the NK cells.[]
376
Eponym
The cells of Ito were named for Toshio Ito, a twentieth century Japanese physician.[3]
References External links
• MedEd at Loyola orfpath/murali2.htm (http://www.meddean.luc.edu/Lumen/MedEd/orfpath/murali2.htm) • Liver Research at AU-KBC Stellate cell biology (http://bio.au-kbc.org/faculty/suvro/liver.php?go=hepatic)
Podocyte
377
Podocyte
Podocyte
Renal corpuscle structure Blood flows in the afferent arteriole (9) at the top, and out the efferent arteriole (11) at the bottom. Blood flows through the capillaries of the glomerulus (10), where it is filtered by pressure. The podocytes (3a and 3b, green) are wrapped around the capillaries. Blood is filtered through the slit diaphragm (or filtration slit), between the feet or processes of the podocytes. The filtered urine passes out the proximal tubule (B, yellow) on the right. A - Renal corpuscle B - Proximal tubule C - Distal convoluted tubule D - Juxtaglomerular apparatus 1. Basement membrane (Basal lamina) 2. Bowman's capsule - parietal layer) 3. Bowman's capsule - visceral layer 3a. Podocyte 3b. Pedicels (podocyte processes) 4. Bowman's space (urinary space) 5a. Mesangium - Intraglomerular cell 5b. Mesangium - Extraglomerular cell 6. Granular cells (Juxtaglomerular cells) 7. Macula densa 8. Myocytes (smooth muscle) 9. Afferent arteriole 10. Glomerulus capillaries 11. Efferent arteriole
Glomerulus. (Diagram in French, but "Membrane basale glomerulaire et ses podocytes" labeled near center.) Latin Dorlands/Elsevier podocytus Podocyte
[1]
Podocytes (or visceral epithelial cells) are cells in the Bowman's capsule in the kidneys that wrap around the capillaries of the glomerulus.[1] The Bowman's capsule filters blood, holding back large molecules such as proteins, and passing through small molecules such as water, salts, and sugar, as the first step in forming urine. The long processes, or "foot projections," of the podocytes wrap around the capillaries, and leave slits between them. Blood is filtered through these slits, each known as a slit diaphragm or filtration slit. Several proteins are required for the foot projections to wrap around the capillaries and function. When infants are born with certain defects in these proteins, such as nephrin and CD2AP, their kidneys cannot function. People have variations in these proteins, and
Podocyte some variations may predispose them to kidney failure later in life. Nephrin is a zipper-like protein that forms the slit diaphragm, with spaces between the teeth of the zipper, big enough to allow sugar and water through, but too small to allow proteins through. Nephron defects are responsible for congenital kidney failure. CD2AP regulates the podocyte cytoskeleton and stabilizes the slit diaphragm.[2][3]
378
Function
Adjacent podocytes interdigitate to cover the basal lamina which is intimately associated with the glomerular capillaries, but the podocytes leave gaps or thin filtration slits. The slits are covered by slit diaphragms which are composed of a number of cell-surface proteins including nephrin, podocalyxin, and P-cadherin, which ensure that large macromolecules such as serum albumin and gamma globulin remain in the bloodstream. Small molecules such as water, glucose, and ionic salts are able to pass through the slit diaphragms and form an ultrafiltrate[4] which is further processed by the nephron to produce urine. Podocytes are also involved in regulation of glomerular filtration rate (GFR). When podocytes contract, they cause closure of filtration slits. This decreases the GFR by reducing the surface area available for filtration.
Structure features
Structural features of podocytes indicate a high rate of vesicular traffic in these cells. Many coated vesicles and coated pits can be seen along the basolateral domain of the podocytes. In their cell bodies, podocytes possess a well-developed endoplasmic reticulum and a large Golgi apparatus, indicative of a high capacity for protein synthesis and post-translational modifications. There is also growing evidence of a large number of multivesicular bodies and other lysosomal components seen in these cells, indicating a high endocytic activity. "Pedicels" (or "foot processes") extend from the podocyte and increase the surface area which is crucial for the efficiency of ultrafiltration.[5]
Pathology
Disruption of the slit diaphragms or destruction of the podocytes can lead to massive proteinuria where large amounts of protein are lost from the blood. An example of this occurs in the congenital disorder Finnish-type nephrosis, which is characterised by neonatal proteinuria leading to end-stage renal failure. This disease has been found to be caused by a mutation in the nephrin gene.
Podocyte
379
Additional images
Filtration barrier
References
[2] First components found for key kidney filter, Ingrid Wickelgren, Science, 8 October 1999, 286:225
External links
• Organology at UC Davis Urinary/mammal/vasc1/vasc1 (http://trc.ucdavis.edu/mjguinan/apc100/modules/ Urinary/mammal/vasc1/vasc1.html) - "Mammal, renal vasculature (EM, High) • BU Histology Learning System: 22401loa (http://www.bu.edu/histology/p/22401loa.htm) - ". Ultrastructure of the Cell: podocytes and glomerular capillaries" • UIUC Histology Subject 1400 (https://histo.life.illinois.edu/histo/atlas/oimages.php?oid=1400) • podocyte.ca (http://www.podocyte.ca/) at Samuel Lunenfeld Research Institute
Proximal convoluted tubule
380
Proximal convoluted tubule
Proximal Convoluted Tubule
Scheme of renal tubule and its vascular supply. (1st convoluted tubule labeled at center top.)
1 Glomerulus, 2 proximal tubule, 3 distal tubule Latin Gray's Precursor tubulus contortus proximalis subject #253 1223
[1]
Metanephric blastema
The proximal tubule is the portion of the duct system of the nephron of the kidney which leads from Bowman's capsule to the loop of Henle.
Structure and appearance
The most distinctive characteristic of the proximal tubule is its brush border (or "striated border").
Brush border cell
The luminal surface of the epithelial cells of this segment of the nephron is covered with densely packed microvilli forming a border readily visible under the light microscope giving the brush border cell its name. The microvilli greatly increase the luminal surface area of the cells, presumably facilitating their resorptive function as well as putative flow sensing within the lumen.[1] The cytoplasm of the cells is densely packed with mitochondria, which are largely found in the basal region within the infoldings of the basal plasma membrane. The high quantity of mitochondria gives the cells an acidophilic appearance. The mitochondria are needed in order to supply the energy for the active transport of sodium ions out of the proximal tubule. Water passively follows the sodium out of the cell along its concentration gradient. Cuboidal epithelial cells lining the proximal tubule have extensive lateral interdigitations between neighboring cells, which lend an appearance of having no discrete cell margins when viewed with a light microscope.
Proximal convoluted tubule Agonal resorption of the proximal tubular contents after interruption of circulation in the capillaries surrounding the tubule often leads to disturbance of the cellular morphology of the proximal tubule cells, including the ejection of cell nuclei into the tubule lumen. This has led some observers to describe the lumen of proximal tubules as occluded or "dirty-looking," in contrast to the "clean" appearance of distal tubules, which have quite different properties.
381
Divisions
The proximal tubule as a part of the nephron can be divided into two sections, pars convoluta and pars recta. Differences in cell outlines exist between these segments, and therefore presumably in function too. Regarding ultrastructure, it can be divided into three segments, S1, S2, and S3:
Segment Gross divisions Ultrastructure divisions Description S1 S2 S3 [2] [2] [2] Lower cell complexity [2] Higher cell complexity [2]
Proximal tubule convoluted
straight
Pars convoluta
The "Pars convoluta" is the initial convoluted portion. In relation to the morphology of the kidney as a whole, the convoluted segments of the proximal tubules are confined entirely to the renal cortex. Some investigators on the basis of particular functional differences have divided the convoluted part into two segments designated S1 and S2.
Pars recta
The "Pars recta" is the following straight (descending) portion. Straight segments descend into the outer medulla. They terminate at a remarkably uniform level and it is their line of termination that establishes the boundary between the inner and outer stripes of the outer zone of the renal medulla. As a logical extension of the nomenclature described above, this segment is sometimes designated as S3.
Absorption
The proximal tubule regulates the pH of the filtrate by exchanging hydrogen ions in the interstitium for bicarbonate ions in the filtrate; it is also responsible for secreting organic acids, such as creatinine and other bases, into the filtrate. Fluid in the filtrate entering the proximal convoluted tubule is reabsorbed into the peritubular capillaries. This is driven by sodium transport from the lumen into the blood by the Na+/K+ ATPase in the basolateral membrane of the epithelial cells. Sodium reabsorption is primarily driven by this P-type ATPase. This is the most important transport mechanism in the PCT.
Proximal convoluted tubule
382
Substance
% of filtrate reabsorbed approximately two-thirds
Comments
salt and water
Much of the mass movement of water and solutes occurs through the cells, passively across the lumenal membrane via transcellular transport, which is then actively resorbed across the basolateral membrane via the Na/K/ATPase pump. The solutes are absorbed isotonically, in that the osmotic potential of the fluid leaving the proximal tubule is the same as that of the initial glomerular filtrate. Glucose, amino acids, inorganic phosphate, and some other solutes are reabsorbed via secondary active transport through cotransport channels driven by the sodium gradient out of the nephron.
organic solutes (primarily glucose and amino acids) potassium
100%
approximately 65% approximately 50% approximately 80%
Most of the filtered potassium is reabsorbed by two paracellular mechanisms - solvent drag and simple [3] diffusion. Paracellular fluid reabsorption sweeps some urea with it via solvent drag. As water leaves the lumen, the [4] concentration of urea increases, which facilitates diffusion in the late proximal tubule. Parathyroid hormone reduces reabsorption of phosphate in the proximal tubules, but, because it also enhances the uptake of phosphate from the intestine and bones into the blood, the responses to PTH cancel each other out, and the serum concentration of phosphate remains approximately the same. Acidosis increases absorption. Alkalosis decreases absorption.
urea
phosphate
citrate
70%–90%
[5]
Secretion
Many types of medications are secreted in the proximal tubule. Further reading: Table of medication secreted in kidney Most of the ammonium that is excreted in the urine is formed in the proximal tubule via the breakdown of glutamine to alpha-ketoglutarate.[] This takes place in two steps, each of which generates an ammonium anion: the conversion of glutamine to glutamate and the conversion of glutamate to alpha-ketoglutarate. [] The alpha-ketoglutarate generated in this process is then further broken down to form two bicarbonate anions,[] which are pumped out of the basolateral portion of the tubule cell by cotransport with sodium ions.
Pathophysiology in kidney disease
Proximal tubular epithelial cells (PTECs) have a pivotal role in kidney disease.
Malignant
Most renal cell carcinoma, the most common form of kidney cancer, arises from the convoluted tubules.[6]
Non-malignant
Acute tubular necrosis occurs when PTECs are directly damaged by Immunohistochemical staining of the convoluted toxins such as antibiotics (e.g., gentamicin), pigments (e.g., myoglobin tubules and glomeruli with CD10. and sepsis (e.g., mediated by lipopolysaccharide from gram-negative bacteria). Renal tubular acidosis (proximal type) (Fanconi syndrome) occurs when the PTECs are unable to properly reabsorb glomerular filtrate so that there is increased loss of bicarbonate, glucose, amino acids, and phosphate. PTECs also participate in the progression of tubulointerstitial injury due to glomerulonephritis, ischemia, interstitial nephritis, vascular injury, and diabetic nephropathy. In these situations, PTECs may be directly affected by protein
Proximal convoluted tubule (e.g., proteinuria in glomerulonephritis), glucose (in diabetes mellitus), or cytokines (e.g., interferon-γ and tumor necrosis factors). There are several ways in which PTECs may respond: producing cytokines, chemokines, and collagen; undergoing epithelial mesenchymal trans-differentiation; necrosis or apoptosis.
383
Additional images
Distribution of blood vessels in cortex of kidney.
Glomerulus.
TEM of negatively stained proximal convoluted tubule of Rat kidney tissue at a magnification of ~55,000x and 80KV with Tight junction.
Renal corpuscle
Diagram outlining movement of ions in nephron.
References
[2] Page 743 [3] Boron & Boulpaep. Medical Physiology. Updated Edition. 2005. [4] Boron & Boulpaep. Medical Physiology. Updated Edition. 2005.
External links
• 1771700264 (http://www.gpnotebook.co.uk/simplepage.cfm?ID=1771700264) at GPnotebook • Organology at UC Davis Urinary/mammal/cortex1/cortex6 (http://trc.ucdavis.edu/mjguinan/apc100/modules/ Urinary/mammal/cortex1/cortex6.html) - "Mammal, kidney cortex (LM, Medium)" • Physiology at MCG 7/7ch03/7ch03p14 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section7/7ch03/7ch03p14.htm) - "The Nephron: Proximal Tubule, Pars Convoluta & Pars Recta" • Swiss embryology (from UL, UB, and UF) turinary/urinhaute02 (http://www.embryology.ch/anglais/turinary/ urinhaute02.html) This article incorporates text from a public domain edition of Gray's Anatomy.
Thin segment
384
Thin segment
The thin segment is a segment of the nephron, which consists of: • thin descending limb of loop of Henle • thin ascending limb of loop of Henle
Histology
The basement membrane of the thin limb in humans has very uniform nodular thickenings that form a network that surrounds the tubule and acts as a support structure that is homologous to the collenchyma in plants. Smith, RA et al. (Arch Pathol Lab Med Vol 108, May 1984) have designated these nodules "Belliveau Bodies" after Robert Belliveau the pathologist who originally described these structures. The epithelium is Simple squamous epithelium.[1]
References
[1] - "University of Illinois College of Medicine"
Distal convoluted tubule
385
Distal convoluted tubule
Distal convoluted tubule
Kidney nephron ("1st proximal convoluted tubule", "2nd distal convoluted tubule")
Section of cortex of human kidney. Latin Gray's Precursor MeSH tubulus contortus distalis subject #253 1223
[1]
Metanephric blastema Distal+Kidney+Tubule
[1]
The distal convoluted tubule (DCT) is a portion of kidney nephron between the loop of Henle and the collecting duct system.
Physiology
It is partly responsible for the regulation of potassium, sodium, calcium, and pH. It is the primary site for the kidneys' hormone based regulation of calcium (Ca). On its apical surface (lumen side), cells of the DCT have a thiazide-sensitive Na-Cl cotransporter and are permeable to Ca, via TRPV5 channel. On the basolateral surface (blood) there is an ATP dependent Na/K antiport pump, a secondary active Na/Ca transporter-- antiport, and an ATP dependent Ca transporter. The basolateral ATP dependent Na/K pump produces the gradient for Na to be absorbed from the apical surface via the Na/Cl synport and for Ca to be reclaimed into the blood by the Na/Ca basolateral antiport. • It regulates pH by absorbing bicarbonate and secreting protons (H+) into the filtrate, or by absorbing protons and secreting bicarbonate into the filtrate. • Sodium and potassium levels are controlled by secreting K+ and absorbing Na+. Sodium absorption by the distal tubule is mediated by the hormone aldosterone. Aldosterone increases sodium reabsorption. Sodium and chloride (salt) reabsorption is also mediated by a group of kinases called WNK kinases. There are 4 different WNK
Distal convoluted tubule kinases, WNK1 [2], WNK2 [3], WNK3 [4], and WNK4 [5]. • It also participates in calcium regulation by reabsorbing Ca2+ in response to parathyroid hormone. [1] PTH effect is mediated through phosphorylation of regulatory proteins and enhancing the synthesis of all transporters within the distal convoluted tubule. • Arginine vasopressin receptor 2 is also expressed in the DCT.
386
Clinical significance
Thiazide diuretics inhibit Na+/Cl- reabsorption from the DCT by blocking the thiazide-sensitive Na-Cl cotransporter. By inhibiting the cotransporter, thiazide diuretics increase the gradient potential for Na. This increases the activity of the basolateral Na/Ca antiport and causes the increase in calcium reclamation associated with thiazide diuretics.
Histology
The DCT is lined with simple cuboidal cells that are shorter than those of the proximal convoluted tubule (PCT). The lumen appears larger in DCT than the PCT lumen because the PCT has a brush border (microvilli). DCT can be recognized by its numerous mitochondria, basal infoldings and lateral membrane interdigitations with neighboring cells. The point where DCT contacts afferent arteriole of renal corpuscle is called macula densa. It has tightly packed columnar cells which display reversed polarity and may monitor the osmolarity of blood. Histologically, cells of the DCT can be differentiated from cells of the proximal convoluted tubule:
Characteristic Apical brush border Eosinophilicity Cytoplasm PCT DCT
Usually present Not present More More Less Less More likely
Readily discernible nuclei Less likely
Additional images
1 Glomerulus, 2 proximal tubule, 3 distal tubule
Transverse section of pyramidal substance of kidney of pig, the bloodvessels of which are injected.
Renal corpuscle
Diagram outlining movement of ions in nephron.
Distal convoluted tubule
387
References External links
• Histology at OU 35_19 (http://w3.ouhsc.edu/histology/Glass slides/35_19.jpg) • Physiology at MCG 7/7ch03/7ch03p18 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section7/7ch03/7ch03p18.htm) • Physiology at MCG 7/7ch07/7ch07p14 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section7/7ch07/7ch07p14.htm) • BU Histology Learning System: 16004loa (http://www.bu.edu/histology/p/16004loa.htm) • BU Histology Learning System: 16007loa (http://www.bu.edu/histology/p/16007loa.htm)
Kidney collecting duct cell
A kidney collecting duct cell can be of two different cell types: • principal cells • Intercalated cells
Pneumocyte
Two types of pneumocytes (also named pneumonocyte) contribute to the maintenance of the alveoli of the lungs: Type I pneumocytes and Type II pneumocytes. These cells function to aid in gas exchange, secretion of pulmonary surfactant, and self-regeneration
External links
• Histology at KUMC resp-resp17 [1] • BU Histology Learning System: 13905loa [2] • Electron micrograph at luc.edu [3]
Centroacinar cell
388
Centroacinar cell
Centroacinar cell
Latin Gray's Code
cellula centroacinosa subject #251 1204
[1]
TH H3.04.07.0.00008
Centroacinar cells are spindle-shaped cells in the exocrine pancreas. Centroacinar cells are an extension of the intercalated duct cells into each pancreatic acinus.[] The intercalated ducts take the bicarbonate to intralobular ducts which become lobular ducts. These lobular ducts finally converge to form the main pancreatic duct.[] These cells are commonly known as duct cells, and secrete an aqueous bicarbonate solution under stimulation by the hormone secretin. They also secrete mucin.
References External links
• Anatomy Atlases - Microscopic Anatomy, plate 10.213 (http://www.anatomyatlases.org/MicroscopicAnatomy/ Section10/Plate10213.shtml) - "Pancreas" • BU Histology Learning System: 10406loa (http://www.bu.edu/histology/p/10406loa.htm) - "Liver, Gall Bladder, and Pancreas: pancreas, centroacinar cells" • UIUC Histology Subject 870 (https://histo.life.illinois.edu/histo/atlas/oimages.php?oid=870) This article incorporates text from a public domain edition of Gray's Anatomy.
Collecting duct system
389
Collecting duct system
Collecting duct system
Scheme of renal tubule and its vascular supply. Latin Gray's MeSH tubulus renalis colligens subject #253 1223
[1] [1]
Kidney+Collecting+Ducts
The collecting duct system of the kidney consists of a series of tubules and ducts that connect the nephrons to the ureter. It participates in electrolyte and fluid balance through reabsorption and excretion, processes regulated by the hormones aldosterone and antidiuretic hormone. There are several components of the collecting duct system, including the connecting tubules, cortical collecting ducts, and medullary collecting ducts.
Function
The collecting duct system is the final component of the kidney to influence the body's electrolyte and fluid balance. In humans, the system accounts for 4–5% of the kidney's reabsorption of sodium and 5% of the kidney's reabsorption of water. At times of extreme dehydration, over 24% of the filtered water may be reabsorbed in the collecting duct system. The wide variation in water reabsorption levels for the collecting duct system reflects its dependence on hormonal activation. The collecting ducts, in particular, the outer medullary and cortical collecting ducts, are largely impermeable to water without the presence of antidiuretic hormone (ADH, or vasopressin). • In the absence of ADH, water in the renal filtrate is left alone to enter the urine, promoting diuresis. • When ADH is present, aquaporins allow for the reabsorption of this water, thereby inhibiting diuresis. The collecting duct system participates in the regulation of other electrolytes, including chloride, potassium, hydrogen ions, and bicarbonate.
Anatomy
The segments of the system are as follows:
Collecting duct system
390
Segment connecting tubule initial collecting tubule cortical collecting ducts medullary collecting ducts papillary ducts, also known as duct of Bellini
Description
Before convergence of nephrons
Connecting tubule
With respect to the renal corpuscle, the "connecting tubule" is the most proximal part of the collecting duct system. It is adjacent to the distal convoluted tubule, the most distal segment of the renal tubule. Connecting tubules from several adjacent nephrons merge to form cortical collecting tubules, and these may join to form cortical collecting ducts. Connecting tubules of some juxtamedullary nephrons may arch upward, forming an arcade. The connecting tubule derives from the metanephric blastema, but the rest of the system derives from the ureteric bud. Because of this, some sources group the connecting tubule as part of the nephron, rather than grouping it with the collecting duct system.
Initial collecting tubule
The initial collecting tubule is a segment with a constitution similar as the collecting duct, but before the convergence with other tubules.[1]Wikipedia:Citing sources
Cortical collecting duct
The "cortical collecting ducts" receive filtrate from multiple initial collecting tubules and descend into the renal medulla to form medullary collecting ducts.
Medullary collecting duct
"Medullary collecting ducts" are divided into outer and inner segments, the latter reaching more deeply into the medulla. The variable reabsorption of water and, depending on fluid balances and hormonal influences, the reabsorption or secretion of sodium, potassium, hydrogen and bicarbonate ion continues here. Urea passively transports out of duct here and creates 500mOsm gradient. Outer segment The outer segment of the medullary collecting duct follows the cortical collecting duct. It reaches the level of the renal medulla where the thick ascending limb of loop of Henle borders with the thin ascending limb of loop of Henle[2] Inner segment The inner segment is the part of the collecting duct system between the outer segment and the papillary ducts.
Papillary duct
The terminal portions of the medullary collecting ducts are the "papillary ducts", which end at the renal papilla and empty into a minor calyx. It is also called duct of Bellini.
Collecting duct system
391
Cell types
Each component of the collecting duct system contains two cell types, intercalated cells and a segment-specific cell type: • For the connecting tubules, this specific cell type is the connecting tubule cell • For the collecting ducts, it is the principal cell. The inner medullary collecting ducts contain an additional cell type, called the inner medullary collecting duct cell.
Principal cells
The principal cell mediates the collecting duct's influence on sodium and potassium balance via sodium channels and potassium channels located on the cell's apical membrane. Aldosterone determines expression of sodium channels with increased aldosterone causing increased expression of luminal sodium channels[3]Wikipedia:Verifiability. Aldosterone increases the number of Na⁺/K⁺-ATPase pumps[4] that allow increased sodium reabsorption and potassium secretion.[5] Vasopressin determines the expression of aquaporin channels on the cell surface.[6] Together, aldosterone and vasopressin let the principal cell control the quantity of water that is reabsorbed.
Intercalated cells
Intercalated cells come in α and β varieties and participate in acid-base homeostasis.
Type of cell α-intercalated cells β-intercalated cells Secretes acid (via an apical H+-ATPase and H+/K+ exchanger) in the form of hydrogen ions bicarbonate (via pendrin a specialised apical Cl-/HCO3-) Reabsorbs bicarbonate (via band 3, a basolateral Cl-/HCO3[7] exchanger) acid (via a basal H+-ATPase)
For their contribution to acid-base homeostasis, the intercalated cells play important roles in the kidney's response to acidosis and alkalosis. Damage to the α-intercalated cell's ability to secrete acid can result in distal renal tubular acidosis (RTA type I, classical RTA).
Additional images
Transverse section of pyramidal substance of kidney of pig, the blood vessels of which are injected.
Alpha intercalated cell cartoon
Diagram outlining movement of ions in nephron.
Collecting duct system
392
References
[1] [2] [3] [4] [5] [7] Boron Boron, p. 837. – "The Nephron: Collecting Duct" Guyton 2006, p. 949. Guyton 2006, p. 336. – "Intercalated Cells"
• Boron, Walter F. (2005). Medical Physiology: A Cellular and Molecular Approach (updated ed.). Philadelphia: Elsevier/Saunders. ISBN 1-4160-2328-3. • Guyton, Arthur C.; John E. Hall (2006). Textbook of Medical Physiology (11 ed.). Philadelphia: Elsevier Saunders. ISBN 0-7216-0240-1.
External links
• Histology at KUMC epithel-epith04 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/epithel/ epith04.htm) "Collecting Duct (Kidney)" • BU Histology Learning System: 15803loa (http://www.bu.edu/histology/p/15803loa.htm) – "Urinary System: kidney, medulla, collecting duct and ascending tubule" • BU Histology Learning System: 16013loa (http://www.bu.edu/histology/p/16013loa.htm) – "Urinary System: kidney, H&E, collecting duct and ascending tubule"
Microvillus
393
Microvillus
Microvillus
Enterocytes with microvilli Code TH H1.00.01.1.01011
[1]
Microvilli (singular: microvillus) are microscopic cellular membrane protrusions that increase the surface area of cells,[] and are involved in a wide variety of functions, including absorption, secretion, cellular adhesion, and mechanotransduction.
Locations
Thousands of microvilli form a structure called the brush border that is found on the apical surface of some epithelial cells, such as the small intestinal. Microvilli are observed on the plasma surface of eggs, aiding in the anchoring of sperm cells that have penetrated the extracellular coat of egg cells. Clustering of elongated microtubules around a sperm allows for it to be drawn closer and held firmly so fusion can occur. Microvilli are also of importance on the cell surface of white blood cells, as they aid in the migration of white blood cells.
Structure
Microvilli are covered in plasma membrane, which encloses cytoplasm and microfilaments. Though these are cellular extensions, there are little or no cellular organelles present in the microvilli. Each microvillus has a dense bundle of cross-linked actin filaments, which serves as its structural core. 20 to 30 tightly bundled actin filaments are cross-linked by bundling proteins fimbrin and villin to form the core of the microvilli. In the enterocyte microvillus, the structural core is attached to the plasma membrane along its length by lateral arms made of myosin 1a and Ca2+ binding protein calmodulin. Myosin 1a functions through a binding site for filamentous actin on one end and a lipid binding domain on the other. The plus ends of the actin filaments are located at the tip of the microvillus and are capped, possibly by capZ proteins,[1] while the minus ends are anchored in the terminal web composed of a complicated set of proteins including spectrin and myosin II.
Microvillus
394
Function
Microvilli can act as mechanosensors in kidney proximal tubule.[2] They sense the fluid flow in the tubule lumen and convert this information via biochemical responses into reabsorption. Microvilli are also of importance on the cell surface of white blood cells, as they aid in the migration of white blood cells.[citation needed]
Relationship to cell
As mentioned, microvilli are formed as cell extensions from the plasma membrane surface. Actin filaments, present in the cytosol, are most abundant near the cell surface. These filaments are thought to determine the shape and movement of the plasma membrane. The nucleation of actin fibers occurs as a response to external stimuli, allowing a cell to alter its shape to suit a particular situation. This could account for the uniformity of the microvilli, which are observed to be of equal length and diameter. This nucleation process occurs from the minus end, allowing rapid growth from the plus end. Interestingly, though the length and composition of microvilli is consistent within a certain group of homogenous cells, it can differ slightly in a different part of the same organism. For example, the microvilli in the small and large intestines in mice are slightly different in length and amount of surface coat covering.[3] the microvilli of on the cell membrane differs in terms shape
Enzymes
Microvilli function as the primary surface of nutrient absorption in the gastrointestinal tract. Because of this vital function, the microvillar membrane is packed with enzymes that aid in the breakdown of complex nutrients into simpler compounds that are more easily absorbed. For example, enzymes that digest carbohydrates called glycosidases are present at high concentrations on the surface of enterocyte microvilli. Thus, microvilli not only increase the cellular surface area for absorption, they also increase the number of digestive enzymes that can be present on the cell surface.
Glycocalyx
The microvilli are covered with glycocalyx, consisting of peripheral glycoproteins that can attach themselves to a plasma membrane via transmembrane proteins. This layer may be used to aid binding of substances needed for uptake, to adhere nutrients or as protection against harmful elements. It can be another location for functional enzymes to be localized.
Destruction of microvilli
The destruction of microvilli can occur in certain diseases because of the rearrangement of cytoskeleton in host cells. This can lead to malabsorption of nutrients and persistent osmotic diarrhea, often accompanied by fever. This is seen in infections caused by EPEC subgroup Escherichia coli, in Celiac disease, and Microvillus Inclusion Disease[4] (an inherited disease characterized by defective microvilli and presence of cytoplasmic inclusions of the cell membrane other than the apical surface). The destruction of microvilli can actually be beneficial sometimes, as in the case of elimination of microvilli on white blood cells which can be used to combat auto immune diseases.[5] Congenital lack of microvilli in the intestinal tract causes microvillous atrophy, a rare, usually fatal condition found in new-born babies.
Microvillus
395
References
[1] The Cytoskeleton: Cytoskeleton in specialized tissues and in pathological states, edited by JE Hesketh and IF Pryme, Elsevier 1996 ,ISBN 1559386894, 9781559386890. Vol3, pp371, (http:/ / books. google. co. il/ books?id=lyrFRieEw-EC& pg=PA371& lpg=PA371& dq=actin+ filaments+ capping+ in+ microvilli+ tips& source=bl& ots=q7Pn83HgrA& sig=ZIOtFM0qPGS-ysoi0GQicqzYjQ8& hl=iw& ei=-VQeStPgNcTDsgbdpe3KCg& sa=X& oi=book_result& ct=result& resnum=4#PPP1,M1) [2] Guo P, Weinstein A, and Weinbaum S. A hydrodynamic mechanosensory hypothesis for brush border microvilli. Am. J. Physiol.: Renal Physiol., 279:F698-F712, 2000 [3] link (http:/ / www. jcb. org/ cgi/ reprint/ 34/ 2/ 447. pdf) [4] Malathy Kapali, MD, Ronald Jaffe, MD and Rocco M Agostini Jr. B.Sc. Final Diagnosis: Microvillus Inclusion Disease. http:/ / path. upmc. edu/ cases/ case163/ dx. html [5] Shattuck, T. (2004) Cells studied for immune function. http:/ / www. dartmouth. edu/ ~vox/ 0405/ 0927/ cells. html.
External links
• Organology at UC Davis TermsCells&Tissues/structures/microvilli (http://trc.ucdavis.edu/mjguinan/apc100/ modules/TermsCells&Tissues/structures/microvilli.html) • BU Histology Learning System: 21904loa (http://www.bu.edu/histology/p/21904loa.htm) - "Ultrastructure of the Cell: microvilli and basal enfoldings, endocytic vesicles" • BU Histology Learning System: 20601loa (http://www.bu.edu/histology/p/20601loa.htm) - "Ultrastructure of the Cell: microvillous border and Junctional Complex, oblique section" • Microvillus (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=Microvillus) at eMedicine Dictionary
Epididymis
396
Epididymis
Epididymis
Adult human testicle with epididymis: A. Head of epididymis, B. Body of epididymis, C. Tail of epididymis, and D. Vas deferens
The right testis, exposed by laying open the tunica vaginalis. Latin Gray's Vein Precursor MeSH Epididymis subject #258 1242
[1]
Pampiniform plexus Wolffian duct Epididymis
[2]
The epididymis (pron.: /ɛpɨˈdɪdɨmɪs/; plural: epididymides /ɛpɨˌdɪdɨˈmiːdiːz/) is part of the male reproductive system and is present in all male amniotes. It is a single, narrow, tightly-coiled tube (in adult humans, six to seven meters in length[1]) connecting the efferent ducts from the rear of each testicle to its vas deferens. A similar, but probably non-homologous, structure is found in cartilaginous fishes[citation needed].
Regions
The epididymis can be divided into three main regions: • The head (Caput). The head of the epididymis receives spermatozoa via the efferent ducts of the mediastinum of the testis. It is characterized histologically by a thin myoepithelium. The concentration of the sperm here is dilute. • The body (Corpus) • The tail (Cauda). This has a thicker myoepithelium than the head region, as it is involved in absorbing fluid to make the sperm more concentrated. In reptiles, there is an additional canal between the testis and the head of the epididymis and which receives the various efferent ducts. This is, however, absent in all birds and mammals.[]
Epididymis
397
Histology
The epididymis is covered by a two layered pseudostratified epithelium. The epithelium is separated by a basement membrane from the connective tissue wall which has smooth muscle cells. The major cell types in the epithelium are: • Principal cells: columnar cells that, with the basal cells, form the majority of the epithelium. These cells extend from the lumen to the basal lamina,[] They also have non-motile stereocilia, which are long and branching in the head region and shorter in the tail region.[] They also secrete carnitine, sialic acid, glycoproteins, and glycerylphosphorylcholine into the lumen. • Basal cells: shorter, pyramid-shaped cells which contact the basal lamina but taper off before their apical surfaces reach the lumen.[] These are thought to be undifferentiated precursors of principal cells.[] • Apical cells: predominantly found in the head region[] • Clear cells: predominant in the tail region[] • Intraepithelial lymphocytes: distributed throughout the tissue.[]
Role in storage of sperm and ejaculant
Spermatozoa formed in the testis enter the caput epididymis, progress to the corpus, and finally reach the cauda region, where they are stored. Sperm entering the caput epididymis are incomplete - they lack the ability to swim forward (motility) and to fertilize an egg. It stores the sperm for 2–3 months. During their transit in the epididymis, sperm undergo maturation processes necessary for them to acquire these functions.[2] Final maturation is completed in the female reproductive tract (capacitation). During ejaculation, sperm flow from the lower portion of the epididymis (which functions as a storage reservoir). They have not been activated by products from the prostate gland, and they are unable to swim, but are transported via the peristaltic action of muscle layers within the vas deferens, and are mixed with the diluting fluids of the seminal vesicles and other accessory glands prior to ejaculation (forming semen). The epithelial cells of the epididymis possess numerous apical modifications that are often referred to as stereocilia, as under the light microscope they look like cilia. However, as electron microscopy has revealed them to be structurally and functionally more similar to microvilli, some now refer to them as stereovilli.[3]
Pathology
An inflammation of the epididymis is called epididymitis. It is much more common than testicular inflammation, termed orchitis.
Embryology and vestigial structures
A Gartner's duct is a homologous remnant in the female. In the embryo, the epididymis develops from tissue that once formed the mesonephros, a primitive kidney found in many aquatic vertebrates. Persistence of the cranial end of the mesonephric duct will leave behind a remnant called the appendix of the epididymis. In addition, some mesonephric tubules can persist as the paradidymis, a small body caudal to the efferent ductules.
Epididymis
398
Epididymectomy
Epididymectomy is the surgical removal of the epididymis sometimes performed for post-vasectomy pain syndrome.
Gallery
Human Male reproductive system.
Testis
Schematic drawing of a cross-section through a testicle.
Micrograph of an epididymis. H&E stain.
Microscopic shot.
Notes
[2] abstract (http:/ / www. ingentaconnect. com/ search/ expand?pub=infobike:/ / bsc/ ija/ 1999/ 00000022/ 00000002/ art00151)
External links
• BU Histology Learning System: 16903loa (http://www.bu.edu/histology/p/16903loa.htm) • inguinalregion (http://mywebpages.comcast.net/wnor/inguinalregion.htm) at The Anatomy Lesson (http:// home.comcast.net/~wnor/homepage.htm) by Wesley Norman (Georgetown University) ( testes (http:// mywebpages.comcast.net/wnor/testes.jpg))
Ameloblast
399
Ameloblast
Ameloblast
A developing tooth with odontoblasts marked.
The cervical loop area: (1) dental follicle cells, (2) dental mesenchyme, (3) Odontoblasts, (4) Dentin, (5) stellate reticulum, (6) outer enamel epithelium, (7)inner enamel epithelium, (8) ameloblasts, (9) enamel. Latin Code ameloblastus TE E05.04.1.1.2.3.20
[1]
Ameloblasts are cells, present only during tooth development, that deposit tooth enamel, the hard outermost layer of the tooth that forms the chewing surface. Ameloblasts are cells which secrete the enamel proteins enamelin and amelogenin which will later mineralize to form enamel on teeth, the hardest substance in the human body.[1] Each ameloblast is approximately 4 micrometers in diameter, 40 micrometers in length and has a hexagonal cross section. The secretory end of the ameloblast ends in a six-sided pyramid-like projection known as the Tomes' process. The angulation of the Tomes' process is significant in the orientation of enamel rods. Ameloblasts are derived from oral epithelium tissue of ectodermal origin. Their differentiation from preameloblasts is a result of signaling from the ectomesenchymal cells of the dental papilla. The ameloblasts will only become fully functional after the first layer of dentine has been formed by odontoblasts. Ameloblasts control ionic and organic compositions of enamel. They adjust their secretory and resorptive activities to maintain favorable conditions for biomineralization. The murine ALC cell line is of ameloblastic origin.[2]
Ameloblast
400
Life cycle of ameloblasts
The life cycle of ameloblasts consists of six stages : 1. 2. 3. 4. 5. 6. Morphogenic stage Organizing stage Formative (secretory) stage (Tome's processes appear in secretory stage) Maturative stage Protective stage Desmolytic stage
References
Organ of Corti
401
Organ of Corti
Organ of Corti
A cross section of the cochlea illustrating the organ of Corti.
Section through the spiral organ of Corti. Magnified. Latin Gray's MeSH organum spirale subject #232 1056 Organ+of+Corti
[1]
[2]
The organ of Corti, found only in mammals, is part of the cochlea of the inner ear and is provided with hair cells or auditory sensory cells. [1] It evolved from the basilar papilla found in all tetrapods, except for a few derived species that have lost it. [2] The organ was named after the Italian anatomist Marquis Alfonso Giacomo Gaspare Corti (1822–1876), who conducted microscopic research of the mammalian auditory system.
Structure and functions
The organ of Corti has highly specialized structures that respond to fluid-borne vibrations in the cochlea with a shearing vector in the hairs of some cochlear hair cells. It contains between 15,000-20,000 auditory nerve receptors. Each receptor has its own hair cell. The shear on the hairs opens non-selective transduction ion channels that are permeable to potassium and calcium, leading to hair cell plasma membrane depolarization, activation of voltage-dependent calcium channels at the synaptic basolateral pole of the cells which triggers vesicle exocytosis and liberation of glutamate neurotransmitter to the synaptic cleft and electrical signaling to the auditory cortex via spiral ganglion neurons. The pinna and middle ear act as mechanical transformers and amplifiers, so that by the time sound waves reach the organ of Corti, their pressure amplitude is 22 times that of the air impinging on the pinna. The organ of Corti can be damaged by excessive sound levels, leading to noise-induced health effects. The organ of Corti is the structure that transduces pressure waves to action potentials. The organ of Corti sits inside the cochlear duct, between the scala vestibuli and the scala tympani. The basilar membrane on the scala tympani presses against the
Organ of Corti hair cells of the organ as perilymphatic pressure waves pass.
402
Hearing loss
The most common kind of hearing impairment, sensorineural hearing loss, includes as one major cause the reduction of function in the organ of Corti. Specifically, the active amplification function of the outer hair cells is very sensitive to damage from exposure to trauma from overly-loud sounds or to certain ototoxic drugs. Once outer hair cells are damaged, they do not regenerate, and the result is a loss of sensitivity and an abnormally large growth of loudness (known as recruitment) in the part of the spectrum that the damaged cells serve.[3] While hearing loss has always been considered irreversible in mammals, fish and birds routinely repair such damage. A recent study has shown that the use of particular drugs may reactivate genes normally expressed only during hair cell development. The research was carried out at Harvard Medical School, the Massachusetts Eye and Ear Infirmary, and the Keio University School of Medicine in Japan.[4]
Additional images
Transverse section of the cochlear duct of a fetal cat.
Diagrammatic longitudinal section of the cochlea.
Floor of ductus cochlearis.
Limbus laminæ spiralis and membrana basilaris.
Section through the spiral organ of Corti. Magnified.
Notes
[1] Definition of Organ of Corti (http:/ / www. merriam-webster. com/ medical/ organ of corti) - Merriam Webster - Retrieved 30 April 2012. [2] Dissecting the molecular basis of organ of Corti development (http:/ / pubmedcentralcanada. ca/ pmcc/ articles/ PMC3097286/ ) [4] Drug Induces Hearing Restoration in Rodents (http:/ / beyondthedish. wordpress. com/ tag/ cochlear-hair-cells/ )
References
• Corti A (1851) "Recherches sur l'organe de Corti de l'ouïe des mammifères". Z wiss Zool 3: 1-106. • Pritchard U. "On the organ of Corti in mammals". 2 March 1876, Proceedings of the Royal Society of London, volume 24, pp. 346–52 OCLC 1778190 (http://www.worldcat.org/oclc/1778190)
Organ of Corti
403
External links
• Dissecting the molecular basis of organ of Corti development (http://pubmedcentralcanada.ca/pmcc/articles/ PMC3097286/) • Organ of Corti 3D animation (http://www.youtube.com/watch?v=1JE8WduJKV4&feature=related) • http://lobe.ibme.utoronto.ca/presentations/OHC_Electromotility/sld005.htm Diagram at University of Toronto • http://mayoresearch.mayo.edu/mayo/research/ent_research/images/image02.gif Diagram at Mayo • http://www.iurc.montp.inserm.fr/cric51/audition/english/corti/fcorti.htm at University of Montpellier 1
Corneal keratocyte
Corneal keratocytes (corneal fibroblasts) are specialized fibroblasts residing in the stroma. This corneal layer, representing about 85-90% of corneal thickness, is built up from highly regular collagenous lamellae and extracellular matrix components. Keratocytes play the major role in keeping it transparent, healing its wounds, and synthesizing its components. In the unperturbed cornea keratocytes stay dormant, coming into action after any kind of injury or inflammation. Some keratocytes underlying the site of injury, even a light one, undergo apoptosis immediately after the injury.[] Any glitch in the precisely orchestrated process of healing may cloud the cornea, while excessive keratocyte apoptosis may be a part of the pathological process in the degenerative corneal disorders such as keratoconus, and these considerations prompt the ongoing research into the function of these cells.
Origin and functions
Keratocytes are developmentally derived from the cranial population of neural crest cells, from whence they migrate to settle in the mesenchyme. In some species the migration from neural crest comes in two waves, with the first giving birth to the corneal epithelium and the second invading the epithelium-secreted stromal anlage devoid of cells; in other species both populations come from a single wave of migration. Once settled in the stroma, keratocytes start synthesizing collagen molecules of different types (I, V, VI) and keratan sulfate. By the moment of eye opening after birth the proliferation of keratocytes is all but finished and most of them are in the quiescent state.[] By the end of eye development an interconnected keratocyte network is established in the cornea, with dendrites of neighbouring cells contacting each over.[] Quiescent keratocytes synthesize the so-called crystallins, known primarily for their role in the lens. Corneal crystallins, like the lens ones, are thought to help maintain the transparency and optimal refraction.[] They are also part of corneal antioxidant defense.[] Crystallins expressed by human keratocytes are ALDH1A1, ALDH3A1,[] ALDH2 and TKT. Different sets of crystallins are typical to distinct species.[] Keratan sulfate produced by keratocytes is thought to help maintain optimal corneal hydration;[] genetic disruption of its synthesis leads to the macular corneal dystrophy.[1] According to one study, average keratocyte density in the human stroma is about 20500 cells per mm3, or 9600 in a column of 1 mm2 in section. The highest density is observed in the upper 10% of the stroma. The number of keratocytes declines with age, at a rate approximately 0.45% per year.[] After an injury to the cornea, some keratocytes undergo apoptosis, prompted by the signaling molecules secreted by the upper layers, such as IL1 alpha and TNF-alpha. Other neighbouring keratocytes, when acted upon by the same molecules, become active, proliferate and start synthesizing matrix metalloproteinases that cause tissue remodeling. These activated cells are designated in different sources either as "active keratocytes" or "fibroblasts" or are said to assume a "repair phenotype". After heavier injuries or at the advanced stages of healing process a number of keratocytes transforms into myofibroblasts actively secreting ECM components; this transformation is thought to be caused by TGF-beta. As soon as the basement membrane of corneal epithelium is restored, TGF beta inflow into the stroma drastically decreases and myofibroblasts disappear, after which the remaining activated keratocytes continue
Corneal keratocyte for some time to reshape the extracellular matrix, secreting IL1-alpha in order to maintain their "repair phenotype".[] Apoptosis of keratocytes, either in quiescent or active state, is a process that attracts special attention. In a healthy cornea the programmed cell death is a rare occasion, but immediately after an injury to the uppermost layer keratocytes directly under the injury site commit apoptosis.[] One hypothesis explains such rapid reaction by the need to stem the possible infection from spreading into the cornea, because due to the limitations of ocular immune system the immune cells take up to several hours to arrive at the site of injury.[] In a normal course of events, the lack of keratocytes in gradually replenished by the mitosis of the adjacent cells.[] Apoptosis is observed after eye operations, including keratotomy and laser surgery,[] and may play a role in the development of post-surgery complications.
404
Clinical significance
Keratocytes may play a role in different corneal disorders. According to comparative research, their functions drastically diverge from the norm in keratoconus, the most frequent form of corneal dystrophy. In keratoconic corneas they have been shown to commit apoptosis far away from any epithelial injury; a hypothesis exists that presents excessive keratocyte apoptosis as a major pathological event in keratoconus.[] According to one study, patient's keratocytes have decreased levels of one of the alcohol dehydrogenase subforms,[] they secrete significantly less superoxide dismutase 3, according to another.[]
References
[1] MACULAR DYSTROPHY, CORNEAL, 1; MCDC1 (http:/ / www. ncbi. nlm. nih. gov/ entrez/ dispomim. cgi?id=217800) - OMIM.
External links
• Nigel Brookes (http://www.chimaera.co.nz/proto/pages/science. html) - researcher
Alcohol dehydrogenase immunoreactivity in a healthy cornea (top), in Fuchs' dystrophy and keratoconic cornea. Diaminobenzidine stains keratocytes in the cross-section of cornea. [] From Mootha et al., 2009.
Tendon cell
405
Tendon cell
Tendon cell
Latin Tendinocytus Code TH H3.03.00.0.00024 [1]
Vertebrates
Tendon cells, or tenocytes, are elongated fibroblast type cells. The cytoplasm is stretched between the collagen fibres of the tendon. They have a central cell nucleus with a prominent nucleolus. Tendon cells have a well-developed rough endoplasmic reticulum and they are responsible for synthesis and turnover of tendon fibres and ground substance.
Invertebrates
Tendon cells form a connecting epithelial layer between the muscle and shell in molluscs. In gastropods, for example, the retractor muscles connect to the shell via tendon cells. Muscle cells are attached to the collagenous myo-tendon space via hemidesmosomes. The myo-tendon space is then attached to the base of the tendon cells via basal hemidesmosomes, while apical hemidesmosomes, which sit atop microvilli, attach the tendon cells to a thin layer of collagen. This is in turn attached to the shell via organic fibres which insert into the shell. Molluscan tendon cells appear columnar and contain a large basal cell nucleus. The cytoplasm is filled with granular endoplasmic reticulum and sparse golgi. Dense bundles of microfilaments run the length of the cell connecting the basal to the apical hemidesmosomes.
References
Krstić, R. V. (1984) Illustrated Encyclopedia of Human Histology, Springer Verlag, Berlin Tompa, A. S. and Watabe, N. (1976). "Ultrastructural investigation of the mechanism of muscle attachment to the gastropod shell.". Journal of Morphology 149 (3): 339–351. doi:10.1002/jmor.1051490304 [2]. PMID 957445 [3].
Bone marrow
406
Bone marrow
Bone marrow
A simplified illustration of cells in bone marrow Latin MeSH Code Medulla ossium Bone+Marrow
[1] [2]
TA A13.1.01.001
Bone marrow is the flexible tissue found in the interior of bones. In humans, red blood cells are produced in the heads of long bones, in a process known as hematopoesis. On average, bone marrow constitutes 4% of the total body mass of humans; in an adult weighing 65 kilograms (140 lb), bone marrow accounts for approximately 2.6 kilograms (5.7 lb). The hematopoietic compartment of bone marrow produces approximately 500 billion blood cells per day, which use the bone marrow vasculature as a conduit to the body's systemic circulation.[1] Bone marrow is also a key component of the lymphatic system, producing the lymphocytes that support the body's immune system.[2] Bone marrow transplants can be conducted to treat severe diseases of the bone marrow, including certain forms of cancer. Additionally, bone marrow stem cells have been successfully transformed into functional neural cells,[] and can also potentially be used to treat illnesses such as inflammatory bowel disease.[3]
Marrow types
The two types of bone marrow are medulla ossium rubra (red marrow), which consists mainly of hematopoietic tissue, and medulla ossium flava (yellow marrow), which is mainly made up of fat cells. Red blood cells, platelets and most white blood cells arise in red marrow. Both types of bone marrow contain numerous blood vessels and capillaries. At birth, all bone marrow is red. With age, more and more of it is converted to the yellow type; only around half of adult bone marrow is red. Red marrow is found mainly in the flat bones, such as the pelvis, sternum, cranium, ribs, vertebrae and scapulae, and in the cancellous ("spongy") material at the epiphyseal ends of long bones such as the femur and humerus. Yellow marrow is found in the medullary cavity, the hollow interior of the middle portion of long bones. In cases of severe blood loss, the body can convert yellow marrow back to red marrow to increase blood cell production.
A femoral head with a cortex of cortical bone and medulla of trabecular bone. Both red bone marrow and a focus of yellow bone marrow are visible.
Stroma
Bone marrow The stroma of the bone marrow is all tissue not directly involved in the primary function of hematopoiesis. Yellow bone marrow makes up the majority of bone marrow stroma, in addition to smaller concentrations of stromal cells located in the red bone marrow. Though not as active as parenchymal red marrow, stroma is indirectly involved in hematopoiesis, since it provides the hematopoietic microenvironment that facilitates hematopoiesis by the parenchymal cells. For instance, they generate colony stimulating factors, which have a significant effect on hematopoiesis. Cells that constitute the bone marrow stroma are: • • • • • • fibroblasts (reticular connective tissue) macrophages adipocytes osteoblasts osteoclasts endothelial cells, which form the sinusoids. These derive from endothelial stem cells, which are also present in the bone marrow.[]
407
Macrophages contribute especially to red blood cell production, as they deliver iron for hemoglobin production.
Bone marrow barrier
The blood vessels of the bone marrow constitute a barrier, inhibiting immature blood cells from leaving the marrow. Only mature blood cells contain the membrane proteins required to attach to and pass the blood vessel endothelium. Hematopoietic stem cells may also cross the bone marrow barrier, and may thus be harvested from blood.
Mesenchymal stem cells
The bone marrow stroma contains mesenchymal stem cells (MSCs),[] also known as marrow stromal cells. These are multipotent stem cells that can differentiate into a variety of cell types. MSCs have been shown to differentiate, in vitro or in vivo, into osteoblasts, chondrocytes, myocytes, adipocytes and beta-pancreatic islets cells. MSCs can also transdifferentiate into neuronal cells.[]
Red marrow parenchyma
Cellular components
Hematopoietic precursor cells: promyelocyte in the center, two metamyelocytes next to it and band cells from a bone marrow aspirate.
Bone marrow
408
Cellular constitution of the red bone marrow parenchyma[4]
Group Cell type Average Reference fraction range 0.9% 3.3% 12.7% 0.8% 15.9% 1.2% 12.4% 0.9% 7.4% 0.5% 0.2-1.5 2.1-4.1 8.2-15.7 0.2-1.3 9.6-24.6 0.4-2.2 9.5-15.3 0.2-2.4 6.0-12.0 0.0-1.3 0.0-0.2 0.2-1.3 0.5-2.4 17.9-29.2 0.4-4.6 0.0-0.4 0.4-3.9 0.0-0.9 11.1-23.2 0.0-0.8
Cells of myelopoiesis
Myeloblasts Promyelocytes Neutrophilic myelocytes Eosinophilic myelocytes Neutrophilic metamyelocytes Eosinophilic metamyelocytes Neutrophilic band cells Eosinophilic band cells Segmented neutrophils Segmented eosinophils
Segmented basophils and mast cells 0.1% Cells of erythropoiesis Pronormoblasts Basophilic normoblasts Polychromatic normoblasts Orthochromatic normoblast Other cell types Megakaryocytes Plasma cells Reticular cells Lymphocytes Monocytes 0.6% 1.4% 21.6% 2.0% < 0.1% 1.3% 0.3% 16.2% 0.3%
In addition, the bone marrow contains hematopoietic stem cells, which give rise to the three classes of blood cells that are found in the circulation: white blood cells (leukocytes), red blood cells (erythrocytes), and platelets (thrombocytes).[]
Compartmentalization
Biological compartmentalization is evident within the bone marrow, in that certain cell types tend to aggregate in specific areas. For instance, erythrocytes, macrophages, and their precursors tend to gather around blood vessels, while granulocytes gather at the borders of the bone marrow.
Lymphatic role
The red bone marrow is a key element of the lymphatic system, being one of the primary lymphoid organs that generate lymphocytes from immature hematopoietic progenitor cells.[2] The bone marrow and thymus constitute the primary lymphoid tissues involved in the production and early selection of lymphocytes. Furthermore, bone marrow performs a valve-like function to prevent the backflow of lymphatic fluid in the lymphatic system.
Bone marrow
409
Diseases of the bone marrow
The normal bone marrow architecture can be damaged or displaced by aplastic anemia, malignancies such as multiple myeloma, or infections such as tuberculosis, leading to a decrease in the production of blood cells and blood platelets. The bone marrow can also be affected by various forms of leukemia, which attacks its hematologic progenitor cells.[5] Furthermore, exposure to radiation or chemotherapy will kill many of the rapidly dividing cells of the bone marrow, and will therefore result in a depressed immune system. Many of the symptoms of radiation sickness are due to damage sustained by the bone marrow cells. To diagnose diseases involving the bone marrow, a bone marrow aspiration is sometimes performed. This typically involves using a hollow needle to acquire a sample of red bone marrow from the crest of the ilium under general or local anesthesia.
Examination
Bone marrow examination is the pathologic analysis of samples of bone marrow obtained via biopsy and bone marrow aspiration. Bone marrow examination is used in the diagnosis of a number of conditions, including leukemia, multiple myeloma, anemia, and pancytopenia. The bone marrow produces the cellular elements of the blood, including platelets, red blood cells and white blood cells. While much information can be gleaned by testing the blood itself (drawn from a vein by phlebotomy), it is sometimes necessary to examine the source of the blood cells in the bone marrow to obtain more information on hematopoiesis; this is the role of bone marrow aspiration and biopsy. The ratio between myeloid series and erythroid cells is relevant to bone marrow function, and also to diseases of the bone marrow and peripheral blood, such as leukemia and anemia. The normal myeloid-to-erythroid ratio is around 3:1; this ratio may increase in myelogenous leukemias, decrease in polycythemias, and reverse in cases of thalassemia.[6]
A Wright's-stained bone marrow aspirate smear from a patient with leukemia.
Donation and transplantation
In a bone marrow transplant, hematopoietic stem cells are removed from a person and infused into another person (allogenic) or into the same person at a later time (autologous). If the donor and recipient are compatible, these infused cells will then travel to the bone marrow and initiate blood cell production. Transplantation from one person to another is conducted for the treatment of severe bone marrow diseases, such as congenital defects, autoimmune diseases or malignancies. The patient's own marrow is first killed off with drugs or radiation, and then A bone marrow harvest in progress. the new stem cells are introduced. Before radiation therapy or chemotherapy in cases of cancer, some of the patient's hematopoietic stem cells are sometimes harvested and later infused back when the therapy is finished to restore the immune system. In addition, bone marrow stem cells can be induced to become neural cells to treat neurological illnesses,[] and can also potentially be used for the treatment of other illnesses, such as inflammatory bowel disease.[7]
Bone marrow
410
Harvesting
The stem cells are typically harvested directly from the red marrow in the iliac crest, often under general anesthesia. The procedure is minimally invasive and does not require stitches afterwards. Depending on the donor's health and reaction to the procedure, the actual harvesting can be an outpatient procedure, or can require 1–2 days of recovery in the hospital.[8] Another option is to administer certain drugs that stimulate the release of stem cells from the bone marrow into circulating blood.[9] An IV is inserted into the donor's arm, and the stem cells are filtered out of the blood. This procedure is similar to donating blood or platelets. In adults, bone marrow may also be taken from the sternum, while the tibia is often used when taking samples from infants.[] In newborns, stem cells may be retrieved from the umbilical cord.[10]
Bone marrow in cuisine
Many cultures have used bone marrow as food throughout history. Some anthropologists believe that early humans were scavengers rather than hunters in some regions of the world. Marrow would have been a useful food source (largely due to its fat content) for tool-using hominids, who were able to crack open the bones of carcasses left by apex predators such as lions.[11] European diners in the 18th century often used a marrow scoop (or marrow spoon), often of silver and with a long, thin bowl, as a table implement for removing marrow from a bone. Bone marrow was also used in various preparations, such as pemmican. Bone marrow's popularity as a food is now relatively limited in the western world, but it remains in use in some gourmet restaurants, and is popular among food enthusiasts.[12]
In some parts of Germany, beef soup is served with Markklößchen (bone marrow balls).
In Vietnam, beef bone marrow is used as the soup base for the national staple dish, phở, while in the Philippines, the soup bulalo is made primarily of beef stock and marrow bones, seasoned with vegetables and boiled meat; a similar soup in the Philippines is called kansi.[13] In Indonesia, bone marrow is called sumsum and can be found especially in Minangkabau cuisine. Sumsum is often cooked as soup or as gulai (a curry-like dish). In India and Pakistan, slow-cooked marrow is the core ingredient of the dish nalli nihari. In Hungary, tibia is a main ingredient of beef soup; the bone is chopped into 10–15 cm pieces, and the ends are covered with salt to prevent the marrow from leaking from the bone while cooking. Upon serving the soup, the marrow is usually spread on toast. Beef bone marrow is also the main ingredient in Italian dish ossobuco (braised veal shanks), and beef marrow bones are often included in the French pot-au-feu broth, the cooked marrow being traditionally eaten on toasted bread with sprinkled coarse sea salt. In Iranian cuisine, lamb shanks are usually broken before cooking to allow diners to suck out and eat the marrow when the dish is served. Similar practices are also common in Pakistani cuisine. Some Native Alaskans eat the bone marrow of caribou and moose.
Bone marrow
411
References
[1] "Challenges in Cardiac Tissue Engineering"; Gordana Vunjak-Novakovic, Ph.D.,Nina Tandon, Ph.D., Amandine Godier, B.S.,1 Robert Maidhof, M.S.,Anna Marsano, Ph.D., Timothy P. Martens, M.D., Ph.D., and Milica Radisic, Ph.D. Tissue Engineering: Part B; Volume 16, Number 2 (2010). [2] The Lymphatic System (http:/ / allonhealth. com/ health-news/ par-lymphatic-system. htm). Allonhealth.com. Retrieved 5 December 2011. [4] Appendix A:IV (http:/ / www. msd. com. mx/ secure/ ebooks/ WintrobesClinicalHematology/ sid4266054. html) in Wintrobe's clinical hematology (9th edition). Philadelphia: Lea & Febiger (1993). [8] National Marrow Donor Program Donor Guide (http:/ / www. marrow. org/ DONOR/ When_You_re_Asked_to_Donate_fo/ index. html). Marrow.org. Retrieved 5 November 2012. [9] Mayo Clinic: Bone marrow donation: What to expect when you donate (http:/ / www. mayoclinic. com/ health/ bone-marrow/ CA00047). Mayo Clinic. Retrieved 16 February 2013. [10] "Production of stem cells with embryonic characteristics from human umbilical cord blood" (http:/ / www3. interscience. wiley. com/ journal/ 118705649/ abstract). Wiley Online Library. 11 August 2005. Retrieved 29 January 2012. [11] Bruce Bower. "Hunting ancient scavengers – some anthropologists say early humans were scavengers, not hunters" (http:/ / findarticles. com/ p/ articles/ mi_m1200/ is_v127/ ai_3677563). Science News. 9 March 1985. Retrieved 16 February 2013. [12] La Petite Bouche (Food Blog): Roasted Bone Marrow (http:/ / lapetitebouche. blogspot. com/ 2010/ 08/ roasted-bone-marrow. html). 30 August 2010. Retrieved 5 December 2011. [13] "Kansi" (http:/ / www. flickr. com/ photos/ kamums/ 4378949248/ ). Flickr. 22 February 2010. Retrieved 26 November 2012.
Further reading
• Nature Bone Marrow Transplantation (http://www.nature.com/bmt/index.html) (Nature Publishing Group) – specialist scientific journal with articles on bone marrow biology and clinical uses. • Cooper, B (2011). "The origins of bone marrow as the seedbed of our blood: from antiquity to the time of Osler" (http://baylorhealth.edu/proceedings/24_2/24_2_Cooper.pdf). Baylor University Medical Center Proceedings 24 (2): 115–8. PMC 3069519 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3069519). PMID 21566758 (http://www.ncbi.nlm.nih.gov/pubmed/21566758).
Reticular connective tissue
412
Reticular connective tissue
Reticular connective tissue is a type of connective tissue.[1] It has a network of reticular fibers, made of type III collagen.[] Reticular fibers are not unique to reticular connective tissue, but only in this type are they dominant.[] Reticular fibers are synthesized by special fibroblasts called reticular cells. The fibers are thin branching structures.
Location
Reticular connective tissue is found around the liver, the kidney, the spleen, and lymph nodes, as well as in bone marrow.[2]
Function
The fibers form a soft skeleton (stroma) to support the lymphoid organs (lymph nodes, red bone marrow, and spleen). Adipose tissue is held together by reticular fibers.
Staining
They can be identified in histology by staining with a heavy metal like silver or the PAS stain that stains carbohydrates.
Appearance
Reticular connective tissue resembles areolar connective tissue, but the only fibers in its matrix are reticular fibers, which form a delicate network along which fibroblasts called reticular cells lie scattered. Although reticular fibers are widely distributed in the body, reticular tissue is limited to certain sites. It forms a labyrinth-like stroma (literally, "bed or "mattress"), or internal framework, that can support many free blood cells (large lymphocytes) in lymph nodes, the spleen, and red bone marrow.
Classification
There are more than 20 types of reticular fibers. In Reticular Connective Tissue type III collagen/reticular fiber (100-150 nm in diameter) is the major fiber component. It forms the architectural framework of; liver, adipose tissue, bone marrow, spleen, basement membrane to name a few
References
Notes
[2] Martini, Frederic H. Fundamentals of Anatomy and Physiology. Seventh Edition. Pearson Benjamin Cummings. United States. 2006.
External links
• Organology at UC Davis TermsCells&Tissues/connective/reticular/reticular1 (http://trc.ucdavis.edu/mjguinan/ apc100/modules/TermsCells&Tissues/connective/reticular/reticular1.html) - "Connective tissue, reticular (LM, Medium)" • Histology at uwa.edu.au (http://www.lab.anhb.uwa.edu.au/mb140/CorePages/Connective/Connect. htm#labreticular)
Fibroblast
413
Fibroblast
Fibroblast
NIH/3T3 Fibroblasts in cell culture Latin Code fibroblastus TH H2.00.03.0.01002
[1]
A fibroblast is a type of cell that synthesizes the extracellular matrix and collagen,[1] the structural framework (stroma) for animal tissues, and plays a critical role in wound healing. Fibroblasts are the most common cells of connective tissue in animals.
Background information
Fibroblasts and fibrocytes are two states of the same cells, the former being the activated state, the latter the less active state, concerned with maintenance and tissue metabolism. Currently, there is a tendency to call both forms fibroblasts. The suffix "blast" is used in cellular biology to denote a stem cell or a cell in an activated state of metabolism. Fibroblasts are morphologically heterogeneous with diverse appearances depending on their location and activity. Though morphologically inconspicuous, ectopically transplanted fibroblasts can often retain positional memory of the location and tissue context where they had previously resided, at least over a few generations. This remarkable behavior may lead to discomfortWikipedia:Please clarify in the rare event that they stagnate there excessively.
Embryologic origin
The main function of fibroblasts is to maintain the structural integrity of connective tissues by continuously secreting precursors of the extracellular matrix. Fibroblasts secrete the precursors of all the components of the extracellular matrix, primarily the ground substance and a variety of fibers. The composition of the extracellular matrix determines the physical properties of connective tissues. Like other cells of connective tissue, fibroblasts are derived from primitive mesenchyme. Thus they express the intermediate filament protein vimentin, a feature used as a marker to distinguish their mesodermal origin. However, this test is not specific as epithelial cells cultured in vitro on adherent substratum may also express vimentin after some time. In certain situations epithelial cells can give rise to fibroblasts, a process called epithelial-mesenchymal transition (EMT). Conversely, fibroblasts in some situations may give rise to epithelia by undergoing a mesenchymal to epithelial transition (MET) and organizing into a condensed, polarized, laterally connected true epithelial sheet. This process is seen in many developmental situations (e.g. nephron and notocord development), as well as in wound healing and tumorigenesis.
Fibroblast
414
Structure and function
Fibroblasts have a branched cytoplasm surrounding an elliptical, speckled nucleus having two or more nucleoli. Active fibroblasts can be recognized by their abundant rough endoplasmic reticulum. Inactive fibroblasts, which are also called fibrocytes[citation needed], are smaller and spindle shaped. They have a reduced rough endoplasmic reticulum. Although disjointed and scattered when they have to cover a large space, fibroblasts when crowded often locally align in parallel clusters. Fibroblasts make collagens, glycosaminoglycans, reticular and elastic fibers, glycoproteins found in the extracellular matrix and cytokine TSLP. Growing individuals' fibroblasts are dividing and synthesizing ground substance. Tissue damage stimulates fibrocytes and induces the mitosis of fibroblasts. Unlike the epithelial cells lining the body structures, fibroblasts do not form flat monolayers and are not restricted by a polarizing attachment to a basal lamina on one side, although they may contribute to basal lamina components in some situations (e.g. subepithelial myofibroblasts in intestine may secrete the α-2 chain carrying component of the laminin which is absent only in regions of follicle associated epithelia which lack the myofibroblast lining). Fibroblasts can also migrate slowly over substratum as individual cells, again in contrast to epithelial cells. While epithelial cells form the lining of body structures, it is fibroblasts and related connective tissues which sculpt the "bulk" of an organism. The life span of a fibroblast, as measured in chick embryos, is 57 ± 3 days.[2]
Secondary actions
Mouse embryonic fibroblasts (MEFs) are often used as "feeder cells" in human embryonic stem cell research. However, many researchers are gradually phasing out MEFs in favor of culture media with precisely defined ingredients of exclusively human derivation[citation needed]. Further, the difficulty of exclusively using human derivation for media supplements is most often solved by the use of "defined media" where the supplements are synthetic and achieve the primary goal of eliminating the chance of contamination from derivative sources.
References
[1] http:/ / ghr. nlm. nih. gov/ glossary=fibroblast
External links
• UIUC Histology Subject 240 (https://histo.life.illinois.edu/histo/atlas/oimages.php?oid=240) • MedEd at Loyola Histo/practical/ctproper/hp3-15.html (http://www.meddean.luc.edu/Lumen/MedEd/Histo/ practical/ctproper/hp3-15.html)
Pericyte
415
Pericyte
Pericyte
Pericytes characteristically lining the outer surface of endothelial cells which encircle an erythrocyte (E). Latin Code pericytus TH H3.09.02.0.02006
[1]
Pericytes are contractile cells that wrap around the endothelial cells of capillaries and venules throughout the body. Also known as Rouget cells or mural cells, pericytes are embedded in basement membrane where they communicate with endothelial cells of the body's smallest blood vessels by means of both direct physical contact and paracrine signaling.[1] In the brain, pericytes help sustain the blood–brain barrier as well as several other homeostatic and hemostatic functions of the brain.[] These cells are also a key component of the neurovascular unit, which includes endothelial cells, astrocytes, and neurons.[] Pericytes regulate capillary blood flow, the clearance and phagocytosis of cellular debris, and the permeability of the blood–brain barrier. Pericytes stabilize and monitor the maturation of endothelial cells by means of direct communication between the cell membrane as well as through paracrine signaling.[] A deficiency of pericytes in the central nervous system can cause the blood–brain barrier to break down.[]
Morphology
In the central nervous system, pericytes wrap around the endothelial cells that line the outside of the capillary. These two types of cells can be easily distinguished from one another based on the presence of the prominent round nucleus of the pericyte compared to the flat elongated nucleus of the endothelial cells.[] Pericytes also project finger-like extensions that wrap around the capillary wall, allowing the cells to regulate capillary blood flow.[] Both pericytes and endothelial cells share a basement membrane where a variety of intercellular connections are made. Many types of integrin molecules facilitate Gap cell junction created between two neighboring cells by connexin. communication between pericytes and endothelial cells separated by [] the basement membrane. Pericytes can also form direct connections with neighboring cells by forming peg and socket arrangements in which parts of the cells interlock, similar to the gears of a clock. At these interlocking sites, gap junctions can be formed which allow the pericytes and neighboring cells to exchange ions and other small molecules.[] Important molecules in these intercellular connections include N-cadherin, fibronectin, connexin and various integrins.[] In some regions of the basement membrane, adhesion
Pericyte plaques composed of fibronectin can be found. These plaques facilitate the connection of the basement membrane to the cytoskeletal structure composed of actin, and the plasma membrane of the pericytes and endothelial cells.[]
416
Function
Blood–brain barrier
Pericytes play a crucial role in the formation and functionality of the selective permeable space between the circulatory system and central nervous system. This space is known as the blood–brain barrier. This barrier is composed of endothelial cells and assures the protection and functionality of the brain and central nervous system. Although it had been theorized that astrocytes were crucial to the postnatal formation of this barrier, it has been found that pericytes are now largely responsible for this role. Pericytes are responsible for tight junction formation and vesicle trafficking amongst endothelial cells. Furthermore, they allow the formation of the blood–brain barrier by inhibiting the effects of CNS immune cells (which can damage the formation of the barrier) and by reducing the expression of molecules that increase vascular permeability.[2] Aside from blood–brain barrier formation, pericytes also play an active role in its functionality by controlling the flow within blood vessels and between blood vessels and the brain. As contractile cells, they can open or close a given amount to allow (or disallow) certain sized particles to flow through the vessel. Such regulation of blood flow is beneficial to neuronal function because it prevents certain particles in the blood from entering the brain. When pericytes are not present, a process known as transcytosis occurs in the blood–brain barrier. This essentially allows particles of varying sizes, including large plasma proteins, to easily enter the brain with little to no regulation. This process is peculiar because the blood–brain barrier is highly regulatory under normal conditions. Therefore, such may confer a dysfunction of pericytes in the blood–brain barrier.[3] Thus, pericytes play a critical role in assuring that harmful chemicals do not enter the brain and disrupt neurological function. Pericyte functionality (or dysfunctionality) is also theorized to contribute to neurodegenerative diseases such as Alzheimer’s, Parkinson’s and ALS (Lou Gehrig's Disease). Furthermore, the elasticity of pericyte is beneficial because they can expand to reduce inflammation and allow harmful substances to diffuse out of the brain.[4] These cells also play a key role in increasing microcirculation and reducing the effects of brain aging. In a study involving adult pericyte-deficient mice, the absence of such cells in the brain had been found to lead to vascular damage from loss of microcirculation and cerebral blood flow. Such blood flow is imperative to mediate the effects caused by stress, hypoxia and several other conditions which may alter homeostasis. In addition, when pericytes are not present, the blood–brain barrier does not degrade certain neurotoxic and vasculotoxic serum proteins which thus bolsters degenerative changes. Such changes include inflammation as well as learning and memory impairment.[5]
Angiogenesis and the survival of endothelial cells
Pericytes are also associated with allowing endothelial cells to differentiate, multiply, form vascular branches (Angiogenesis), survive apoptotic signals and travel throughout the body. Certain pericytes, known as microvascular pericytes develop around the walls of capillaries and help to serve this function. Microvascular pericytes may not be contractile cells because they lack alpha-actin isoforms; structures that are common amongst other contractile cells. These cells communicate with endothelial cells via gap junctions and in turn cause endothelial cells to proliferate or be selectively inhibited. If this process did not occur, hyperplasia and abnormal vascular morphogenesis could occur. These types of pericyte can also phagocytose exogenous proteins. This suggests that the cell type might have been derived from microglia.[6] It is also important to note that pericytes maintain plasticity and thus can differentiate into various other cell types including, smooth muscle cells as well as fibroblasts and other mesenchymal stem cells. Such versatility is conducive because they actively remodel blood vessels throughout the body and can thereby blend homogeneously with the local tissue environment .[7]
Pericyte Aside from creating and remodeling blood vessels in a viable fashion, pericytes have been found to protect endothelial cells from death via apoptosis or cytotoxic elements. It has been studied in vivo that pericytes release a hormone known as pericytic aminopeptidase N/pAPN that may help to promote angiogenesis. When this hormone was mixed with cerebral endothelial cells as well as astrocytes, the pericytes grouped into structures that resembled capillaries. Furthermore, if experimental group contained all of the following with the exception of pericytes, the endothelial cells would undergo apoptosis. That being said, it was concluded that pericytes must be present to assure the proper function of endothelial cells and astrocytes must be present to assure that both remain in contact. If not, then proper angiogenesis cannot occur.[8] In addition, it has been found that pericytes contribute to the survival of endothelial cells because they secrete the protein Bcl-w during cellular crosstalk. Bcl-w is an instrumental protein in the pathway that enforces VEGF-A expression and discourages apoptosis.[9] Although there is some speculation as to why VEGF is directly responsible for preventing apoptosis, it is believed to be responsible for modulating apoptotic signal transduction pathways and inhibiting activation of apoptosis inducing enzymes. Two biochemical mechanisms utilized by VEGF to accomplish such would be phosphorylation of extracellular regulatory kinase 1 (ERK-1) which sustains cell survival over time and inhibition of stress-activated protein kinase/c-jun-NH2 kinase which also promotes apoptosis.[10]
417
Pathologies
Because of their crucial role in maintaining and regulating endothelial cell structure and blood flow, abnormalities in pericyte function are seen in many pathologies. They may either be present in excess, leading to diseases such as hypertension and tumor formation, or in deficiency, leading to neurodegenerative diseases.
Hemangiopericytoma
Hemangiopericytoma is a rare vascular neoplasm, or abnormal growth, that may either be benign or malignant. In its malignant form, metastasis to the lungs, liver, brain, and extremities may occur. It most commonly manifests itself in the femur and proximal tibia as a bone sarcoma, and is usually found in older individuals, though cases have been found in children. Hemangiopericytoma is caused by the excessive layering of sheets of pericytes around improperly formed blood vessels. Diagnosis of this tumor is difficult because of the inability to distinguish pericytes from other types of cells using light microscopy. Treatment may involve surgical removal and radiation therapy, depending on the level of bone penetration and stage in the tumor's development.[11]
Image of a solitary fibrous tumour that is most likely a hemangiopericytoma. It surrounds a staghorn-shaped blood vessel, which results from the arrangement of pericytes around the vessel
Diabetic retinopathy
The retina of diabetic individuals often exhibits loss of pericytes, and this loss is a characteristic factor of the early stages of diabetic retinopathy. Studies have found that pericytes are essential in diabetic individuals to protect the endothelial cells of retinal capillaries. With the loss of pericytes, microaneuryisms form in the capillaries. In response, the retina either increases its vascular permeability, leading to swelling of the eye through a macular edema, or forms new vessels that permeate into the vitreous membrane of the eye. The end result is reduction or loss of vision.[] While it is unclear why pericytes are lost in diabetic patients, one hypothesis is that toxic sorbitol and advanced glycation end products (AGE) accumulate in the pericytes. Because of the build-up of glucose, the polyol pathway increases its flux, and intracellular sorbitol and fructose accumulate. This leads to osmotic imbalance,which results in cellular damage. The presence of high glucose levels also leads to the buildup of AGE's, which also
Pericyte damage cells. []
418
Neurodegenerative diseases
Studies have found that pericyte loss in the adult and aging brain leads to the disruption of proper cerebral perfusion and maintenance of the blood–brain barrier, which causes neurodegeneration and neuroinflammation. The apoptosis of pericytes in the aging brain may be the result of a failure in communication between growth factors and receptors on pericytes. Platelet-derived growth factor B (PDGF-B)is released from endothelial cells in brain vasculature and binds to the receptor PDGFR-Beta on pericytes, initiating their proliferation and migration for proper vasculature maintenance. When this signalling is disrupted, pericytes undergo apoptosis, leading to many neurodegenerative diseases including Alzheimer's disease and Multiple Sclerosis.[12]
Current research
Endothelial and pericyte interactions
Endothelial cell and pericytes are interdependent, so failure of proper communication between the two cells can lead to numerous human pathologies, such as the ones listed above.[] There are several pathways of communication between the endothelial cells and pericytes. The first is transforming growth factor (TGF) signaling, which is mediated by endothelial cells. This is important for pericyte differentiation.[][] Angiopoietin 1 and Tie-2 signaling is essential for maturation and stabilization of endothelial cells.[] Platelet-derived growth factor (PDGF) pathway signaling from endothelial cells recruit pericytes, so that pericytes can migrate to growing vessels. If this pathway is blocked, it leads to pericyte deficiency.[] Sphingosine-1-phosphate (S1P) signaling also aides in pericyte recruitment by communication through G protein-coupled receptors. S1P signals through GTPases that promote N-cadherin trafficking to endothelial membranes. This trafficking strengthens contacts with pericytes.[] Communication between endothelial cells and pericytes are important. Inhibiting the PDGF pathway leads to pericyte deficiency. This causes endothelial hyperplasia, abnormal junctions, and diabetic retinotropy.[] A lack of pericytes also causes an upregulation of vascular endothelial growth factor (VEGF), leading to vascular leakage and hemorrhage.[] Also, angiopoietin 2 can act as an antagonist to Tie-2.[] This destabilizes the endothelial cells, which accounts for less endothelial cell and pericyte interaction. This can actually lead to the formation of tumors.[] Similar to the inhibition of the PDGF pathway, angiopoietin 2 reduces levels of pericyte, leading to diabetic retinopathy.[]
Scarring
After an injury in the CNS, scarring occurs to preserve the integrity of surrounding cells. Usually, astrocytes are associated with the scarring and are called glial scars. However, there is a stromal or nonglial component of the scarring, and there is evidence that perivascular pericytes play a critical role in assisting scar formation.[] An experiment was conducted on mice that have been genetically labeled using glutamate aspartate transporter (Glast). They found two different subtypes of pericytes and termed them subtype A and B. Subtype A accounts for about 10% of the pericytes in the adult spinal cord and plays a critical role in scarring. Subtype B accounts for the rest of the pericytes and has desmin and alpha smooth muscles. After the two subtypes were isolated and labeled, an incision was made to the dorsal part of the brain. Typically in an uninjured spinal cord there are ten times as many astrocytes than subtype A pericytes.[] However, two weeks after the injury, the number of pericytes were double that of the astrocytes. Subtype A were three times more prevalent than subtype B. The main difference in prevalence arises from the fact that subtype A is able to detach from blood vessel walls and can send tiny projections to nearby cells and deposit extracellular matrix proteins. The scarring is highly compartmentalized. The pericytes form the core of the scar, while ependymal cells form a second layer around the core, followed by another layer of astrocytes that originated through self-duplication.[]
Pericyte Inhibition of subtype A pericyte generation caused improper closing of spinal cord incisions, which supports the idea that pericytes are important for scarring.
419
References
[1] http:/ / www. ncbi. nlm. nih. gov/ pmc/ articles/ PMC1871727/ [2] Daneman, Richard et al. (2010) Pericytes are required for blood–brain barrier integrity during embryogenesis. "nature" 468, 562-566 [3] Investigators Reveal Key to Blood-Brain Barrier. This passage of particles can be adverse to brain function because many of such can are toxic or harmful to some extent."GEN" (2010)http:/ / www. genengnews. com/ gen-news-highlights/ investigators-reveal-key-to-blood-brain-barrier/ 81244067/ [4] Pericytes regulate blood–brain barrier (2010) (http:/ / www. news-medical. net/ news/ 20101015/ Pericytes-regulate-blood-brain-barrier. aspx) [5] Bell, Robert D. et al. Pericytes Control Key Neurovascular Functions and Neuronal Phenotype in the Adult Brain and during Brain Aging. "Cell" 68 Vol 3 409-427 (2010) http:/ / www. cell. com/ neuron/ abstract/ S0896-6273(10)00824-X [6] Pericyte, Astrocyte and Basal Lamina Association with the Blood Brain Barrier (BBB) http:/ / davislab. med. arizona. edu/ content/ pericyte-astrocyte-and-basal-lamina-association-blood-brain-barrier-bbb [7] Gerhardt H, Betsholtz C.(2003) Endothelial-pericyte interactions in angiogenesis. "Cell Tissue Res." 314(1), 15-23 http:/ / www. ncbi. nlm. nih. gov/ pubmed/ 12883993 [8] Ramsauer, Markus et. al. (2002) Angiogenesis of the blood–brain barrier in vitro and the function of cerebral pericytes "The FASEB Journal" 10.1096/fj.01-0814fje http:/ / www. fasebj. org/ content/ early/ 2002/ 08/ 02/ fj. 01-0814fje. full. pdf [9] Franco, Marcela et al. (2011) Pericytes promote endothelial cell survival through induction of autocrine VEGF-A signaling and Bcl-w expression "Blood" http:/ / bloodjournal. hematologylibrary. org/ content/ 118/ 10/ 2906 [10] VEGF prevents apoptosis of human microvascular endothelial cells via opposing effects on MAPK/ERK and SAPK/JNK signaling. Exp Cell Res. 1999 Mar 15;247(2):495-504. http:/ / www. ncbi. nlm. nih. gov/ pubmed/ 10066377 [12] http:/ / www. cell. com/ neuron/ abstract/ S0896-6273(10)00824-X
External links
• Pericytes (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Pericytes) at the US National Library of Medicine Medical Subject Headings (MeSH) • Diagram at udel.edu (http://www.udel.edu/Biology/Wags/histopage/illuspage/icv/icv17.gif)
Nucleus pulposus
420
Nucleus pulposus
Nucleus pulposus
Cervical vertebra with intervertebral disc. (Nucleus pulposus labeled at center right, and is visible at center in light blue.)
Stages of Spinal Disc Herniation Latin Gray's Precursor Nucleus pulposus subject #17 82 notochord
[1]
Nucleus pulposus is the jelly-like substance in the middle of the spinal disc. It is the remnant of the notochord.[1] It functions to distribute hydraulic pressure in all directions within each disc under compressive loads. The nucleus pulposus consists of chondrocyte-like cells, collagen fibrils, and proteoglycan aggrecans that aggregate through hyaluronic chains. Attached to each aggrecan molecule are the glycosaminoglycan (GAG) chains of chondroitin sulfate and keratan sulfate.[2] Aggrecan is negatively charged and hydrophilic. This property allows it to draw water into the Nucleus Pulposus.
Nucleus pulposus
421
Additional images
Sagittal section through an intervertebral fibrocartilage and adjacent parts of two vertebræ of an advanced sheep’s embryo.
References
[3] [2] See Figure 1 in US patent application 2007/0003525. [3] Link to referenced patent application. (http:/ / www. google. com/ patents?id=csSXAAAAEBAJ& printsec=abstract& zoom=4& dq=2007/ 0003525#PPA2,M1)
External links
• Image at spinesource.com (http://www.spinesource.com/images/Anatomy3.jpg) • Presentation on synthetic nucleus pulposus (http://www.campoly.com/documents/presentation/nucleus.pdf)
Cementoblast
422
Cementoblast
Cementoblast
Latin cementoblastus Code TE E05.041.1.2.3.36 [1]
A cementoblast is a biological cell that forms from the follicular cells around the root of a tooth, and whose biological function is cementogenesis, which is the creation of cementum (the hard tissue that covers the root of the tooth). Cementoblasts lay down the organic matrix of cementum which later gets mineralized by minerals from oral fluids. Thus the cementoblasts lay down collagen and secrete osteocalcin and sialoprotein. They possess all the organelles associated with protein synthesis such as RER and Golgi apparatus. The mechanism of differentiation of the cementoblasts is controversial but circumstantial evidence suggests that an epithelium or epithelial component may cause dental follicle cells to differentiate into cementoblasts, characterised by an increase in length. The initially formed cementum in coronal two-thirds of the root is acellular, but when the cementoblasts get trapped in lacunae in their own matrix like bone cells, the cementum is called cellular or secondary cementum and is present only in the apical third of the root. Once in this situation, the cementoblasts lose their secretory activity and become cementocytes.
Odontoblast
423
Odontoblast
Odontoblast
A developing tooth with odontoblasts marked.
The cervical loop area: (1) dental follicle cells, (2) dental mesenchyme, (3) Odontoblasts, (4) Dentin, (5) stellate reticulum, (6) outer enamel epithelium, (7)inner enamel epithelium, (8) ameloblasts, (9) enamel. Latin Code odontoblastus TE E04.0.3.3.1.0.13
[1]
In vertebrates, an odontoblast is a biological cell of neural crest origin that is part of the outer surface of the dental pulp, and whose biological function is dentinogenesis, which is the creation of dentin, the substance under the tooth enamel. Teeth in the molluscan radula are also produced by cells termed "odontoblasts".
Origin and differentiation
Odontoblasts first appear at sites of tooth development at 17–18 weeks in utero and remain present until death unless killed by bacterial or chemical attack, or indirectly through other means (e.g. being aspirated into dentinal tubules by the use of a turbine handpiece on tooth tissue above). The odontoblasts secrete dentin throughout life (secondary dentin, once root formation is complete), which may be an attempt to compensate for natural wear of the enamel. Odontoblasts also secrete tertiary dentin when irritated. Tertiary dentin secreted by odontoblasts is often due to chemical attack, either by chemicals diffusing through the dentin and insulting the odontoblasts, or by diffusion of toxic bacterial metabolites down the dentinal tubules in the instance of a carious attack. This tertiary dentin is called reactionary dentin. This is an attempt to slow down the progress of the caries so that it does not reach the pulp. In the case of an infection breaching the dentin to or very near the pulp, or in the instance of odontoblast death due to other attack (e.g. chemical or physical), Pulpal Stem Cells can differentiate into odontoblast-like cells which then secrete the other kind of tertiary dentin, reparative dentin, underneath the site of attack. This is not only to slow the progress of the attack, but also to prevent the diffusion of bacteria and their metabolites into the pulp, reducing the probability
Odontoblast of partial pulp necrosis. The distinction of the two kinds of tertiary dentin is important, because they are secreted by different cells for different reasons. Reactionary dentine is secreted at varying speeds, dependant on the speed of progression of caries above. Histologically, it is easily distinguishable by its disordered tube structure, its local secretion (causing it to protrude into the pulpal cavity) and its slightly lower degree of mineralisation than normal. The tooth is often able to be saved by a simple restoration. Reparative dentine is secreted when the tooth's situation is dire. The odontoblasts are dead, forcing the differentiation of pulpal stem cells into odontoblast-like cells that try desperately to avoid pulpitis.
424
Morphology
Odontoblasts are large columnar cells arranged in an epithelioid sheet along the junction between dentin and pulp, all the way down to the root apex. It is rich in endoplasmic reticulum and golgi apparatus, especially during primary dentin formation, to give it a high secretory capacity (firstly collagenous matrix to form predentine, then mineral to form the complete dentine). Its nucleus is aligned away from the dentine, with its golgi and ER above it (towards the dentine) reflecting its unidirectional secretion. On initial dentine formation it moves pulpally, away from the primitive amelodentinal junction (then Inner Enamel Epithelium/dental papillary junction) leaving behind a tubular structure known as the odontoblast process. This keeps its tapered structure with cytoskeletal fibres, mainly intermediate filaments. A pulpal A-delta (noxious, short sharp pain) nerve fibre is wrapped around the base of this process, or travels a short way into the dentinal tubule with the odontoblast process (max ~0.1mm) This process lies in a tubule, known simply as a dentinal tubule. In a complete tooth, this process rarely extends beyond 1/3 the depth of the dentine, which is why the odontoblast transduction theory of dentin sensitivity is unlikely. The functions of the odontoblast process are as follows: 1. To aid in the secretion of tubular dentin (dentin surrounding tubule) which further organises and strengthens the dentine as a whole tissue 2. General maintenance of the dentinal tubule and dentinal fluid (ion/protein content etc.) 3. To secrete sclerotic dentin upon carious attack to block off dentinal tubules, slowing the progress of the attack (air space above blockage is known as a dead tract) 4. To channel signals of attack to the odontoblast cell body, initiating reactionary dentin secretion 5. To channel hydrokinetic forces of water movement to the A delta fibre wrapped around its base, maintaining dentine sensitivity The biological tissue formed by odontoblasts is a type of hard tissue. It has been shown that odontoblasts secrete the extracellular matrix protein reelin.[][][]
References External links
• Odontoblasts (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Odontoblasts) at the US National Library of Medicine Medical Subject Headings (MeSH)
Hyaline cartilage
425
Hyaline cartilage
Hyaline cartilage
Hyaline cartilage showing microanatomy of chondrocytes and organelles, lacunae and matrix. Code TH H2.00.03.5.00015
[1]
Hyaline cartilage is a type of cartilage found on many joint surfaces. It is pearly bluish in color with firm consistency and considerable collagen. It contains no nerves or blood vessels, and its structure is relatively simple.
Description
Hyaline cartilage is covered externally by a fibrous membrane, called the perichondrium, except at the articular ends of bones and also where it is found directly under the skin, i.e. ears and nose. This membrane contains vessels that provide the cartilage with nutrition. If a thin slice is examined under the microscope, it will be found to consist of cells of a rounded or bluntly angular form, lying in groups of two or more in a granular or almost homogeneous matrix. The cells, when arranged in groups of two or more, have generally straight outlines where they are in contact with each other, and in the rest of their circumference are rounded. They consist of clear translucent protoplasm in which fine interlacing filaments and minute granules are sometimes present; embedded in this are one or two round nuclei, having the usual intranuclear network. The cells are contained in cavities in the matrix, called cartilage lacunae; these are actually artificial gaps formed by the shrinking of the cells during the staining and setting of the tissue for observation. The interterritorial space between the isogenous cell groups contains relatively more collagen fibers, causing it to maintain its shape while the actual cells shrink, creating the lacunae. This constitutes the so-called capsule of the space. Each lacuna is generally occupied by a single cell, but during the division of the cells it may contain two, four, or eight cells. (see isogenous group) Hyaline cartilage also contains chondrocytes which are cartilage cells that produce the matrix. Hyaline cartilage matrix is mostly made up of type II collagen and Chondroitin sulfate, both of which are also found in elastic cartilage. Hyaline cartilage exists on the ventral ends of ribs; in the larynx, trachea, and bronchi; and on the articular surface of bones.
Hyaline cartilage
426
Articular cartilage
Articular cartilage refers to hyaline cartilage on the articular[1] surfaces of bones.[1] Though it is often found in close contact with menisci and articular disks, articular cartilage is not considered a part of either of these structures, which are made entirely of fibrocartilage.
Images
Articular cartilage of the elbow joint as seen in dissection
A synovial joint with bone, articular cartilage, and articular disc shown.
Elbow joint. Deep dissection. Anterior view.
Elbow joint. Deep dissection. Anterior view.
External links
• Hyaline+cartilage [3] at eMedicine Dictionary • UIUC Histology Subject 331 [4] • BU Histology Learning System: 03301lba [5]
References
[1] http:/ / www. wheelessonline. com/ ortho/ articular_cartilage
Fibrocartilage
427
Fibrocartilage
Fibrocartilage
White fibrocartilage from an intervertebral fibrocartilage.
Symphysis pubis exposed by a coronal section. (Pubic symphysis visible at center left.) Gray's Code subject #68 281
[1] [1]
TH H2.00.03.5.00017
White fibrocartilage consists of a mixture of white fibrous tissue and cartilaginous tissue in various proportions. It owes its flexibility and toughness to the former of these constituents, and its elasticity to the latter. It is the only type of cartilage that contains type I collagen in addition to the normal type II. Fibrocartilage is found in the pubic symphysis, the annulus fibrosus of intervertebral discs, menisci, and the TMJ. During labor, relaxin loosens the pubic symphysis to aid in delivery, but this can lead to later joint problems.
Formation as a repair mechanism
If hyaline cartilage is torn all the way down to the bone, the blood supply from inside the bone is sometimes enough to start some healing inside the lesion. In cases like this, the body will form a scar in the area using a special type of cartilage called fibrocartilage. Fibrocartilage is a tough, dense, fibrous material that helps fill in the torn part of the cartilage; however, it is not an ideal replacement for the smooth, glassy articular cartilage that normally covers the surface of the knee joint.
Fibrocartilage
428
Pathology
Degeneration of fibrocartilage is seen in degenerative disc disease.
External links
• Fibrocartilage [2] at eMedicine Dictionary • BU Histology Learning System: 03201loa [3] This article incorporates text from a public domain edition of Gray's Anatomy.
Micrograph showing a fragment of an intervertebral disc demonstrating degenerative fibrocartilage with loss of nuclei and nests of chondrocytes, as seen in degenerative disc disease. HPS stain.
Chondrocyte
429
Chondrocyte
Chondrocyte
Chondrocytes of hyaline cartilage showing organelles, lacunae and matrix. Latin Code chondrocytus TH H2.00.03.5.00003
[1]
Chondrocytes (from Greek chondros cartilage + kytos cell) are the only cells found in healthy cartilage. They produce and maintain the cartilaginous matrix, which consists mainly of collagen and proteoglycans. Although chondroblast is still commonly used to describe an immature chondrocyte, use of the term is discouraged, for it is technically inaccurate since the progenitor of chondrocytes (which are mesenchymal stem cells) can also differentiate into several cell types including osteoblasts. The organization of chondrocytes within cartilage differs depending upon the type of cartilage and where in the tissue they are found.
Differentiation
From least- to terminally-differentiated, the chondrocytic lineage is: 1. 2. 3. 4. Colony-forming unit-fibroblast (CFU-F) Mesenchymal stem cell / marrow stromal cell (MSC) Chondrocyte Hypertrophic chondrocyte
When referring to bone or cartilage, mesenchymal stem cell (mesoderm origin) are undifferentiated meaning they can differentiate into different variance of generative cells (MSC) are commonly known as osteochondrogenic (or osteogenic, chondrogenic, osteoprogenitor, etc.) cell. Undifferentiated mesenchymal stem cell lose their process, proliferate and crowd together in a dense aggregate of chondrogenic cells(cartilage) at the center of chondrification. These condrogenic cells will then differentiate to chondroblasts which will then to synthesize the cartilage ECM(extra cellular matrix). Which consists of ground substance(proteoglycans, glycosaminoglycans for low osmotic potential) and fibers. The chondroblasts then trap themselves in a small space that is no longer in contact with the newly created matrix called lacunae which contain extracellular fluid. The chondroblast is now a chondrocyte, which is usually inactive but can still secrete and degrade matrix depending on the conditions. The majority of the cartilage that has been built has been synthesized from the chondroblast which are much more inactive at a late age (adult hood) compared to earlier years (pre-pubesence) BMP4 and FGF2 have been experimentally shown to increase chondrocyte differentiation.[1] Chondrocytes undergo terminal differentiation when they become hypertrophic during endochondral ossification. This last stage is characterized by major phenotypic changes in the cell.
Chondrocyte
430
Gallery
Chondrocytes in hyaline cartilage
Chondrocyte, stained for calcium, showing nucleus (N) and mitochondria (M)
References
• Dominici M, Hofmann T, Horwitz E (2001). "Bone marrow mesenchymal cells: biological properties and clinical applications". J Biol Regul Homeost Agents 15 (1): 28–37. PMID 11388742 (http://www.ncbi.nlm.nih.gov/ pubmed/11388742). • Bianco P, Riminucci M, Gronthos S, Robey P (2001). "Bone marrow stromal stem cells: nature, biology, and potential applications". Stem Cells 19 (3): 180–92. doi: 10.1634/stemcells.19-3-180 (http://dx.doi.org/10. 1634/stemcells.19-3-180). PMID 11359943 (http://www.ncbi.nlm.nih.gov/pubmed/11359943). • Stem cell information (http://stemcells.nih.gov/info/scireport/appendixE.asp)
External links
• BU Histology Learning System: 03317loa (http://www.bu.edu/histology/p/03317loa.htm) • Chondrocytes (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Chondrocytes) at the US National Library of Medicine Medical Subject Headings (MeSH)
Osteoblast
431
Osteoblast
Osteoblast
Osteoblasts (blue) rimming a bony spicule (pink - on diagonal of image). H&E stain. Latin Code osteoblastus TH H2.00.03.7.00002
[1]
Osteoblasts (from the Greek words for "bone" and "germ" or embryonic) are mononucleate cells that are responsible for bone formation; in essence, osteoblasts are specialized fibroblasts that in addition to fibroblastic products, express bone sialoprotein and osteocalcin.[1] Osteoblasts produce a matrix of osteoid, which is composed mainly of Type I collagen. Osteoblasts are also responsible for mineralization of this matrix. Zinc, copper and sodium are some of the minerals required in this process. Bone is a dynamic tissue that is constantly being reshaped by osteoblasts, which are in charge of production of matrix and mineral, and osteoclasts, which break down the tissue. The number of osteoblasts tends to decrease with age, affecting the balance of formation and resorption in the bone tissue,[] and potentially leading to osteoporosis.
Osteogenesis
Osteoblasts arise from osteoprogenitor cells located in the deeper layer of periosteum and the bone marrow. Osteoprogenitors are immature progenitor cells that express the master regulatory transcription factor Cbfa1/Runx2. Osteoprogenitors are induced to differentiate under the influence of growth factors, in particular the bone morphogenetic proteins (BMPs).[] Aside from BMPs, other growth factors including fibroblast growth factor (FGF),[] platelet-derived growth factor (PDGF) and transforming growth factor beta (TGF-β) may promote the division of osteoprogenitors and potentially increase osteogenesis.BMP4 and FGF2 have been experimentally shown to increase osteoblast differentiation.[2] Once osteoprogenitors start to differentiate into osteoblasts, they begin to express a range of genetic markers including Osterix, Col1,[] BSP, M-CSF, ALP,[3] osteocalcin,[] osteopontin, and osteonectin. Although the term osteoblast implies an immature cell type, osteoblasts are in fact the mature bone cells entirely responsible for generating bone tissue in animals and humans.
Osteoblast
432
Morphology and histological staining
Hematoxylin and eosin staining, or H&E staining, reveals that the cytoplasm of osteoblasts is basophilic due to the presence of a large amount of rough endoplasmic reticulum. The nucleus is spherical and large. An active osteoblast is characterized morphologically by a prominent Golgi apparatus that appears histologically as a clear zone adjacent to the nucleus. Active osteoblasts synthesize, and stain positively for, Type-I collagen and alkaline phosphatase.
Osteoblast (Wright Giemsa stain, 100x)
Osteoblasts lining bone (bottom) and actively synthesizing osteoid, containing two osteocytes.
Osteoblasts actively synthesizing osteoid (center).
Osteoblasts actively synthesizing rudimentary bone tissue (center).
Osteoblasts lining bone (H&E stain).
Osteoblasts (pointer) lining bone (H&E stain).
Osteoblasts and osteocytes
Osteoblasts that become trapped in the bone matrix and remain isolated in lacunae become osteocytes. They cease to generate osteoid and mineralized matrix, and instead act in a paracrine manner on active osteoblasts. They are believed to respond to mechanosensory stimuli.[][]
References
[1] Salentijn, L. Biology of Mineralized Tissues: Cartilage and Bone, Columbia University College of Dental Medicine post-graduate dental lecture series, 2007
Further reading
• Netter, Frank H. (1987). Musculoskeletal system: anatomy, physiology, and metabolic disorders. Summit, New Jersey: Ciba-Geigy Corporation ISBN 0-914168-88-6.
External links
• MedEd at Loyola Histo/practical/cartilage/hp9-49.html (http://www.meddean.luc.edu/Lumen/MedEd/Histo/ practical/cartilage/hp9-49.html)
Osteocyte
433
Osteocyte
Osteocyte
Transverse Section Of Bone Latin Code osteocytus TH H2.00.03.7.00003
[1]
An osteocyte, a star shaped cell, is the most commonly found cell in mature bone, and can live as long as the organism itself.[1] Osteocytes have an average half life of 25 years(Full life of 50 years), they do not divide, and they are derived from osteoprogenitors, some of which differentiate into active osteoblasts.[1] In mature bone, osteocytes and their processes reside inside spaces called lacunae and canaliculi, respectively.[1] Cells contain a nucleus and a thin ring piece of cytoplasm. When osteoblasts become trapped in the matrix that they secrete, they become osteocytes. Osteocytes are networked to each other via long cytoplasmic extensions that occupy tiny canals called canaliculi, which are used for exchange of nutrients and waste through gap junctions. The space that an osteocyte occupies is called a lacuna (Latin for a pit). Although osteocytes have reduced synthetic activity and, like osteoblasts are not capable of mitotic division, they are actively involved in the routine turnover of bony matrix, through various mechanosensory mechanisms. They destroy bone through a rapid, transient (relative to osteoclasts) mechanism called osteocytic osteolysis. Osteoblasts/osteocytes develop in mesenchyme. Hydroxyapatite, calcium carbonate and calcium phosphate is deposited around the cell.
Morphology
Osteocytes have a stellate shape, and in humans they are approximately 9 micrometers long in the short axis by 20 micrometers long in the long axis.[2] The cell body varies in size from 5-20micrometers in diameter and contain 40-60 cell processes per cell,[3] with a cell to cell distance between 20-30 micrometers.[4] A mature osteocyte contains a single nucleus that is located toward the vascular side and has one or two nucleoli and a membrane.[5] The cell also exhibits a reduced size endoplasmic reticulum, Golgi apparatus and mitochondria, and cell processes that radiate towards the mineralizing matrix.[5] Osteocytes form an extensive connecting syncitial network via small cytoplasmic/dendritic processes in canaliculi.[6]
Osteocyte
Osteocyte
434
Origin
Osteocytes are derived from Osteoblasts.[6] The fossil record shows that osteocytes were present in bones of jawless fish 400-250 million years ago, and dinosaurs 80 million years old.[7] Therefore, osteocytes have been used to estimate the size of the genome of extinct species.[6] During bone formation, an osteoblast is left behind and buried in the bone matrix as an "osteoid osteocyte", which maintains contact with the osteoblasts through extending cellular processes.[8] The process of osteocytogenesis is largely unknown, but the following molecules have been shown to play a crucial role in the production of healthy osteocytes, either in correct numbers or specific distributions: Matrix Metalloproteinases (MMPs), Dentin Matrix Protein 1 (DMP-1), Osteoblast/Osteocyte factor 45 (OF45), Klotho gene, TGF Beta inducile factor (TIEG), Lysophosphatidic acid (LPA), E11 antigen, and Oxygen.[6] The transformation from motile osteoblast to entraped osteocyte takes about three days, and during this time, the cell produces a volume of extracellular matrix three times its own cellular volume, which results in 70% volume reduction in the mature osteocyte cell body compared to the original osteoblast volume.[9] 10-20% of osteoblasts differentiate into osteocytes.[6] The cell undergoes a dramatic transformation from a polygonal shape to a cell that extends dendrites toward the mineralizing front, followed by dendrites that extend to either the vascular space or bone surface.[10] The embedded "osteoid-osteocyte" must do two functions simultaneously: regulate mineralization and form connective dendritic processes, which requires cleavage of collagen and other matrix molecules.[10] As the osteoblast transitions to an osteocyte, alkaline phosphatase is reduced, and casein kinase II is elevated, as is osteocalcin.[10] Those osteoblasts on the bone surface that are destined for burial as osteocytes slow down matrix production, and are buried by neighboring osteoblasts that continue to produce matrix actively.[11] Palumbo et al.(1990) distinguish three cell types from osteoblast to mature osteocyte: type I preosteocyte (osteoblastic osteocyte), type II preosteocyte (osteoid osteocyte), and type III preosteocyte (partially surrounded by mineral matrix.[11] Osteocytes appear to be enriched in proteins that are resistant to hypoxia, which appears to be due to their embedded location and restricted oxygen supply[12] Oxygen tension may regulate the differentiation of osteoblasts into osteocytes, and osteocyte hypoxia may play a role in disuse-mediated bone resorption.[12]
Function
Although osteocytes are relatively inert cells, they are capable of molecular synthesis and modification, as well as transmission of signals over long distances, in a way similar to the nervous system.[6] They are the most common cell type in bone (31,900 mm-3 in bovine bone to 93,200 mm-3 in rat bone).[6] Most of the receptor activities that play an important role in bone function are present in the mature osteocyte.[6] Osteocytes contain glutamate transporters that produce nerve growth factors after bone fracture, which provides evidence of a sensing and information transfer system.[6] When osteocytes were experimentally destroyed, the bones showed a significant increase in bone resorption, decreased bone formation, trabecular bone loss, and loss of response to unloading.[6] Osteocytes are thought to be mechanosensor cells that control the activity of osteoblasts and osteoclasts within a basic multicellular unit (BMU), a temporary anatomic structure where bone remodeling occurs.[13] Osteocytes generate an inhibitory signal that is passed through their cell processes to osteoblasts for recruitment to enable bone formation.[14] Osteocyte specific proteins such as sclerostin have been shown to function in mineral metabolism, as well as other molecules such as PHEX, DMP-1, MEPE, and FGF-23, which are highly expressed by osteocytes and regulate phosphate and biomineralization.[10] The osteocyte is an important regulator of bone mass and a key endocrine regulator of phosphate metabolism.[12]
Osteocyte
435
Sclerostin
Osteocytes synthesize sclerostin, a secreted protein that inhibits bone formation by binding to LRP5/LRP6 coreceptors and blunting Wnt signaling.[7] Sclerostin, the product of the SOST gene, is the first mediator of communication between osteocytes, bone forming osteoblasts and bone resorbing osteoclasts, critical for bone remodeling.[15] Only osteocytes express sclerostin, which acts in a paracrine fashion to inhibit bone formation.[15] Sclerostin is inhibited by parathyroid hormone (PTH) and mechanical loading.[15] Sclerostin anatagonizes the activity of BMP (bone morphogenetic protein),a citokine that induces bone and cartilage formation.[13]
Osteocyte Apoptosis and Associated Pathologies
Osteocytes die as a consequence of senescence, degeneration/necrosis, apoptosis(programmed cell death), and/or osteoclastic engulfment.[1] The percentage of dead osteocytes in bone increases with age from less than 1% at birth to 75% after age 80.[16] Osteocyte apoptosis is thought to be related to decreased mecanotransduction, which possibly leads to the development of osteoporosis.[17] Apoptotic osteocytes release apoptotic bodies expressing RANKL to recruit osteoclasts.[10] Mechanical loading increases osteocyte viability in vitro, and contributes to solute transport through the lacuno-canalicular system in bone, which enhances oxygen and nutrient exchange and diffusion to osteocytes.[17] Skeletal unloading has been shown to induce osteocyte hypoxia in vivo, this is when osteocytes undergo apoptosis and recruit osteoclasts to resorb bone.[17] Microdamage in bone occurs as the result of repetitive events of cycling loading, and appears to be associated with osteocyte death by apoptosis, which appear to secrete a signal to target osteoclasts to perform remodeling at a damaged site.[17] Under normal conditions, osteocytes express high amounts of TGF-β and thus repress bone resorption, but when bone grows old, the expression levels of TGF-β decrease, and the expression of osteoclast-stimulatory factors, such as RANKL and M-CSF increases, bone resorption is then enhanced, leading to net bone loss.[17] Mechanical stimulation of osteocytes results in opening of hemichannels to release PGE2 and ATP, among other biochemical signaling molecules, which play a crucial role in maintaining the balance between bone formation and resorption.[18] Osteocyte cell death can occur in association with pathologic conditions such as osteoporosis and osteoarthritis, which leads to increased skeletal fragility, linked to the loss of ability to sense microdamage and/or signal repair.[10][19] Oxygen deprivation that occurs as the result of immobilization (bed rest), glucocorticoid treatment, and withdrawal of oxygen have all been shown to promote osteocyte apoptosis.[10]
References
[1] Tate ML, Adamson JR, Tami AE, Bauer TW, (2004). "Cells in Focus, The osteocyte". The International Journal of Biochemistry and Cell Biology (36), 1-8. [2] Mullender,MG, van deer Meer, DD, Huiskes, R,Lips, P,(1996). Bone18(2):109-113. [3] Tanaka-Kamioka,K, Kamioka H, Ris, H, Lim, SS, (1998). "Osteocyte shape is dependant on actin filaments and osteocyte processes are unique actin-rich projections". J. Bone Miner. Res. 13(10):1555-68. [4] Sugawara, Y, Kamioka, H, Honjo, T, Tezuka, K, Takano-Yamamoto, T, (2005). "Three dimensional reconstruction of chick calvarial osteocytes and their cell processes using confocal microscopy". Bone 36(5):877-83. [5] Dudley, HR,and Spiro, D, (1961). "The fine structure of bone cells". The Journal of Biophysical and Biochemical Cytology 11, 627-649. [6] Noble,SN (2008). "The osteocyte lineage". Archives of Biochemistry and Biophysics 473, 106-111. [7] Divieti Pajevic P,(2009). "Regulation of Bone Resorption and Mineral Homeostasis by Osteocytes". IBMS BoneKEy 6(2):63-70. [8] Palumbo,C, Pallazini,D, Zaffe,D, Marotti,G, (1990). Acta Anat.(Basel) 137(4):350-358. [9] Palumbo,C (1986) "A three dimensional ultrastructural study of osteoid-osteocytes in the tibia of chick embryos." Cell Tissue Research, 246:125-131. [10] Bonewald L, (2011). "The Amazing Osteocyte" Journal of Bone and Mineral Research 26(2):229-238. [11] Franz-Odendaal T, Hall B, Witten PE, (2006). "Buried Alive: How Osteoblasts Become Osteocytes" Developmental Dynamics 235:176-190. [12] Dallas SL, Bonewald L, (2010). "Dynamics of the Transition from Osteoblast to Osteocyte" Ann N Y Acad. Sci. 1192:437-443. [13] ran Bezooijen Rl, Papapoulos SE, Hamdy NA, ten Dijke P, Lowik C (2005) "Control of Bone Formation by Osteocytes." BoneKEy-Osteovision, 2(12):33-38.
Osteocyte
[14] Marotti G, Ferretti M, Muglia MA, Palumbo C, Palazzani SA (1992) "A quantitative evaluation of osteoblast-osteocyte relationships on growing endosteal surface of rabbit tibiae." Bone, 13(5):363-368. [15] Bellido, T (2007) "Osteocyte Apoptosis Induces Bone Resorption and Impairs the Skeletal Response to Weighlessness." BoneKEy-Osteovision 4(9):252-256. [16] Tomkinson A, Reeve J, Shaw RW, Noble BS (1997) "The death of osteocytes via apoptosis accompanies estrogen withdrawal in human bone." The Journal of Clinical Endocrinology and Metabolism, 82(9):3128-3135. [17] Heino TJ, Kurata K, Higaki H, Vaananen K, (2009). "Evidence of the role of osteocytes in the initiation of targeted remodeling." Technology and Healthcare 17:49-56. [18] Burra S, Nicolella DP, Jiang JX, (2011). "Dark horse in osteocyte biology" Communicative and Integrative Biology 4(1)48-50. [19] Carpentier VT, Wong J, Yeap Y, Gan C, Sutton-Smith P, Badiei A, Fazzalari NL, Kuliwaba JS, (2012). "Increased proportion of hypermineralized osteocyte lacunae in osteoporotic and osteoarthritic human trabecular bone: Implications for bone remodeling" Bone 50 (3): 688–694
436
External links
• BU Histology Learning System: 02003loa (http://www.bu.edu/histology/p/02003loa.htm) - "Cartilage and Bone and Bone Histogenesis: cells of* BU Histology Learning System: 02705loa (http://www.bu.edu/ histology/p/02705loa.htm) - "Cartilage and Bone and Bone Histogenesis: compact bone"* =D Histology at ou.edu (http://casweb.cas.ou.edu/pbell/Histology/Captions/Bone/osteocyte.2.html)
Stellate cell
437
Stellate cell
Neuron: Stellate cell
Microcircuitry of the cerebellum. Excitatory synapses are denoted by (+) and inhibitory synapses by (-). MF: Mossy fiber. DCN: Deep cerebellar nuclei. IO: Inferior olive. CF: Climbing fiber. GC: Granule cell. PF: Parallel fiber. PC: Purkinje cell. GgC: Golgi cell. SC: Stellate cell. BC: Basket cell. NeuroLex ID Dorlands/Elsevier sao2046525601 12225156 [2] [1]
In neuroscience, stellate cells are neurons with several dendrites radiating from the cell body giving them a star shape. The three most common stellate cells are the inhibitory interneurons found within the molecular layer of the cerebellum, excitatory spiny stellate interneurons and inhibitory aspiny stellate interneurons. Cerebellar stellate cells synapse onto the dendritic arbors of Purkinje cells. Cortical spiny stellate cells are found in layer IVC of the V1 region in the visual cortex. They receive excitatory synaptic fibres from the thalamus and process feed forward excitation to 2/3 layer of V1 visual cortex to pyramidal cells. Cortical Spiny Stellate cells have a 'regular' firing pattern.
Golgi stained cortical neurons A) Layer II/IIIpyramidal cell B) layer IV spiny stellate cell
External links
• NIF Search - Stellate Cell [3] via the Neuroscience Information
Framework
Skeletal striated muscle
438
Skeletal striated muscle
Skeletal striated muscle
A top-down view of skeletal muscle Latin Code textus muscularis striatus skeletalis TH H2.00.05.2.00002
[1]
Skeletal muscle is a form of striated muscle tissue which is under the control of the somatic nervous system; that is to say, it is voluntarily controlled. It is one of three major muscle types, the others being cardiac and smooth muscle. As their name suggests, most skeletal muscles are attached to bones by bundles of collagen fibers known as tendons. Skeletal muscle is made up of individual components known as myocytes, or "muscle cells", sometimes colloquially called "muscle fibers". They are formed from the fusion of developmental myoblasts (a type of embryonic progenitor cell that gives rise to a muscle cell). These long, cylindrical, multinucleated cells are also called myofibers. The myofibers are in turn composed of myofibrils. The myofibrils are composed of actin and myosin filaments repeated as a sarcomere, the basic functional unit of the muscle fiber and responsible for skeletal muscle's striated appearance and forming the basic machinery necessary for muscle contraction. The term muscle refers to multiple bundles of muscle fibers held together by connective tissue.
Muscle fibers
Individual muscle fibers are formed during development from the fusion of several undifferentiated immature cells known as myoblasts into long, cylindrical, multi-nucleated cells. Differentiation into this state is primarily completed before birth with the cells continuing to grow in size thereafter. Skeletal muscle exhibits a distinctive banding pattern when viewed under the microscope due to the arrangement of cytoskeletal elements in the cytoplasm of the muscle fibers. The principal cytoplasmic proteins are myosin and actin (also known as "thick" and "thin" filaments, respectively) which are arranged in a repeating unit called a sarcomere. The interaction of myosin and actin is responsible for muscle contraction. There are two principal ways to categorize muscle fibers: the type of myosin (fast or slow) present, and the degree of oxidative phosphorylation that the fiber undergoes. Skeletal muscle can thus be broken down into two broad categories: Type I and Type II. Type I fibers appear red due to the presence of the oxygen binding protein myoglobin. These fibers are suited for endurance and are slow to fatigue because they use oxidative metabolism to generate ATP. Type II fibers are white due to the absence of myoglobin and a reliance on glycolytic enzymes. These fibers are efficient for short bursts of speed and power and use both oxidative metabolism and anaerobic metabolism depending on the particular sub-type. These fibers are quicker to fatigue.
Skeletal striated muscle
439
Type I fibers (red) Contraction time Size of motor neuron Resistance to fatigue Activity Used for Maximum duration of use Power produced Mitochondrial density Capillary density Oxidative capacity Glycolytic capacity Major storage fuel Slow Small High Aerobic Hours
Type II a fibers (red)
Type II x fibers
Type II b fibers (white)
Moderately Fast Medium Fairly high Long-term anaerobic <30 minutes
Fast Large Intermediate Short-term anaerobic <5 minutes
Very fast Very large Low Short-term anaerobic <1 minute
Low Very High High High Low Triglycerides
Medium High Intermediate High High Creatine phosphate, glycogen
High Medium Low Intermediate High
Very high Low Low Low High
ATP, Creatine phosphate, glycogen ATP, Creatine (little) phosphate Consume Creatine phosphate Consume Creatine phosphate MYH4 [1]
Note
Consume lactic acid MYH7
Produce lactic acid and Creatine phosphate MYH2
Myosin heavy chain, human genes
MYH1
Skeletal muscle fibers are not all the same. Traditionally, they were categorized depending on their varying color, which is a reflection of myoglobin content. Red Fibers: Those containing high levels of myoglobin and oxygen storing proteins had a red appearance. Red muscle fibers tend to have more mitochondria and greater local capillary density. White Fibers: Those with a low content had a white appearance. As more was learned about the functional differences between skeletal muscle fibers, they were also classified, depending on their twitch capabilities, into fast and slow twitch, traits that largely, but not completely, overlap the previous classification based on color. Fast Twitch: Some authors define a fast twitch fiber as one in which the myosin can split ATP very quickly. However, fast twitch fibers also demonstrate a higher capability for electrochemical transmission of action potentials and a rapid level of calcium release and uptake by the sarcoplasmic reticulum. The fast twitch fibers rely on a well-developed, short term, glycolytic system for energy transfer and can contract and develop tension at 2-3 times the rate of slow twitch fibers. Slow Twitch: The slow twitch fibers generate energy for ATP re-synthesis by means of a long term system of aerobic energy transfer. They tend to have a low activity level of ATPase, a slower speed of contraction with a less well developed glycolytic capacity. They contain large and numerous mitochondria and with the high levels of myoglobin that gives them a red pigmentation. They have been demonstrated to have high concentration of mitochondrial enzymes, thus they are fatigue resistant. The 2 main categories of muscle fibers become several, when further differentiating type II into several subtypes, based on myosin isoforms and denoted with letters of the alphabet. In humans the two subtypes are IIa and IIx; IIx is often referred to as IIb because earlier classification had clumped together two different types. Later on, further research recognized these subtypes as distinct, but the use of the name IIb remained entrenched.[1] Non human fiber types include true IIb fibers, IIc, IId and so on. Type I Red fibers. Slow oxidative (also called slow twitch or fatigue resistant fibers). Contain:
Skeletal striated muscle • • • • • • • • • Large amounts of myoglobin. Many mitochondria. Many blood capillaries. Generate ATP by the aerobic system, hence the term oxidative fibers. Split ATP at a slow rate. Slow contraction velocity. Resistant to fatigue. Found in large numbers in postural muscles. Needed for aerobic activities like long distance running.
440
Type IIa Red fibers. Fast oxidative (also called fast twitch A or fatigue resistant fibers). Contain: • • • • • Large amounts of myoglobin. Many mitochondria. Many blood capillaries. Large amount of glycogen. High capacity for generating ATP by oxidation. Split ATP at a very rapid rate and, hence, high contraction velocity • Resistant to fatigue but not as much as slow oxidative fibers. • Needed for sports such as middle distance running and swimming. Type IIx / IIb (dependent upon species) White. Fast glycolytic (also called fast twitch B or fatigable fibers). Contain: • • • • • • • Low myoglobin content. Few mitochondria. Few blood capillaries. Large amount of Creatine phosphate. Split ATP very quickly. Fatigue easily. Needed for sports like sprinting.
Individual muscles are a mixture of 3 types of muscle fibers (type 1, type 2a and type 2b), but their proportions vary depending on the action of that muscle. It must be remembered that skeletal muscles, although a mixture, can only have one type of muscle fiber within a motor unit. This is demonstrated if we look at contractions. E.g. If a weak contraction is needed only the type 1 motor units will be activated. These fibers are used mainly for endurance activities. If a stronger contraction is required the type 2a fibers will be activated or used to assist the type 1 fibers. Maximal contractions facilitate the use of type 2b fibers which are always activated last. These fibers are used during ballistic activities but tire easily. With advanced EMG techniques it is possible to look at which muscle fibers are recruited when performing an exercise/test. The total number of skeletal muscle fibers has traditionally been thought not to change. It is believed there are no sex or age differences in fiber distribution, however, relative fiber types vary considerably from muscle to muscle and person to person. Sedentary men and women (as well as young children) have 45% type 2 and 55% type 1 fibers.[citation needed] People at the higher end of any sport tend to demonstrate patterns of fiber distribution e.g. endurance athletes show a higher level of type 1 fibers. Sprint athletes, on the other hand, require large numbers of type 2 b fibers. Middle distance event athletes show approximately equal distribution of the 2 types. This is also often the case for power athletes such as throwers and jumpers. It has been suggested that various types of exercise can induce changes in the fibers of a skeletal muscle.[2] It is thought that if you perform endurance type events for a sustained period of time, some of the type 2b fibers transform into type 2a fibers. However, there is no consensus on the subject. It may well be that the type 2b fibers show enhancements of the oxidative capacity after high intensity endurance training which brings them to a level at which they are able to perform oxidative metabolism as effectively as slow twitch fibers of untrained subjects. This would be brought about
Skeletal striated muscle by an increase in mitochondrial size and number and the associated related changes not a change in fiber type.
441
Structure of skeletal muscle fiber
Every organelle and macromolecule of a muscle fiber are arranged to ensure form meets function. The plasma membrane is called the sarcolemma with the cytoplasm known as the sarcoplasm. In the sarcoplasm are the myofibrils. The myofibrils are long protein bundles about 1 micrometer in diameter each containing myofilaments. Pressed against the inside of the sarcolemma are the unusual flattened nuclei. Between the myofibrils are the mitochondria. While the muscle fiber does not have a smooth endoplasmic reticulum, it contains a sarcoplasmic reticulum. The sarcoplasmic reticulum surrounds the myofibrils and holds a reserve of the calcium ions needed to cause a muscle contraction. Periodically, it has dilated end sacs known as terminal cisternae. These cross the muscle fiber from one side to the other. In between two terminal cisternae is a tubular infoldings called a transverse tubule (T tubule). The T tubule are the pathway for the action potential to signal the sarcoplasmic reticulum to release calcium causing a muscle contraction. Together, two terminal cisternae and a transverse tubule form a triad.[3]
Organization of skeletal muscle fibers
While the muscle fibers of the fascicles lie parallel to one another, the fascicles themselves can vary in their relationship to one another and to their tendons.[] The different patterns of arrangement of the fasciles produce four different types of skeletal muscles: parallel muscles, convergent muscles, pennate muscles, and sphincter muscles.[] Parallel muscles The fascicles of parallel muscles run parallel to the direction of the muscle, thus these muscles on a whole function similarly to a single muscle fiber.[] Most skeletal muscles in the body are parallel muscles; although they can be seen in a variety of shapes such as flat bands, spindle shaped, and some can have large protrusions in their middle known as the belly of the muscle.[] ex: Triceps, biceps Convergent muscles The fibers in convergent muscles fan out from a common point of attachment.[] Covering a broad surface these fibers allow for more versatile types of movement.[] These muscles do not pull as hard on their corresponding tendons as their parallel muscle counterparts however due to the fibers not all pulling in the same direction, even pulling in different directions at opposite ends.[] ex: Pectoralis muscles Pennate muscles In a pennate muscle one or more tendons run through the body of the muscle with the fascicles forming an oblique angle to the tendons.[] Because the fascicles pull on the tendons at an angle they do not move the tendon as far as their parallel muscle counterparts. Despite this they generate greater tension due to their possessing a greater amount of muscle fibers than similarly sized parallel muscles.[] ex: Rectus femoris Sphincter muscles The fibers of the sphincter or circular muscles are arranged concentrically around an opening or recess.[] As the muscle contracts, the opening it circumvents gets smaller, for this reason these muscles are often found at the entrances and exits of external and internal passage ways.[] ex: Orbicularis oris
Skeletal striated muscle
442
Cellular physiology and contraction
In addition to the actin and myosin components that constitute the sarcomere, skeletal muscle fibers also contain two other important regulatory proteins, troponin and tropomyosin, that are necessary for muscle contraction to occur. These proteins are associated with actin and cooperate to prevent its interaction with myosin. Skeletal muscle cells are excitable and are subject to depolarization by the neurotransmitter acetylcholine, released at the neuromuscular junction by motor neurons.[4] Once a cell is sufficiently stimulated, the cell's sarcoplasmic reticulum releases ionic calcium (Ca2+), which then interacts with the regulatory protein troponin. Calcium-bound troponin undergoes a conformational change that leads to the movement of tropomyosin, subsequently exposing the myosin-binding sites on actin. This allows for myosin and actin ATP-dependent cross-bridge cycling and shortening of the muscle.
Physics
Muscle force is proportional to physiologic cross-sectional area (PCSA), and muscle velocity is proportional to muscle fiber length.[5] The strength of a joint, however, is determined by a number of biomechanical parameters, including the distance between muscle insertions and pivot points and muscle size. Muscles are normally arranged in opposition so that as one group of muscles contract, another group relaxes or lengthens. Antagonism in the transmission of nerve impulses to the muscles means that it is impossible to fully stimulate the contraction of two antagonistic muscles at any one time. During ballistic motions such as throwing, the antagonist muscles act to 'brake' the agonist muscles throughout the contraction, particularly at the end of the motion. In the example of throwing, the chest and front of the shoulder (anterior Deltoid) contract to pull the arm forward, while the muscles in the back and rear of the shoulder (posterior Deltoid) also contract and undergo eccentric contraction to slow the motion down to avoid injury. Part of the training process is learning to relax the antagonist muscles to increase the force input of the chest and anterior shoulder. Contracting muscles produce vibration and sound.[6] Slow twitch fibers produce 10 to 30 contractions per second (10 to 30 Hz). Fast twitch fibers produce 30 to 70 contractions per second (30 to 70 Hz).[7] The vibration can be witnessed and felt by highly tensing one's muscles, as when making a firm fist. The sound can be heard by pressing a highly tensed muscle against the ear, again a firm fist is a good example. The sound is usually described as a rumbling sound. Some individuals can voluntarily produce this rumbling sound by contracting the tensor tympani muscle of the middle ear. The rumbling sound can also be heard when the neck or jaw muscles are highly tensed.
Signal transduction pathways
Skeletal muscle fiber-type phenotype in adult animals is regulated by several independent signaling pathways. These include pathways involved with the Ras/mitogen-activated protein kinase (MAPK), calcineurin, calcium/calmodulin-dependent protein kinase IV, and the peroxisome proliferator γ coactivator 1 (PGC-1). The Ras/MAPK signaling pathway links the motor neurons and signaling systems, coupling excitation and transcription regulation to promote the nerve-dependent induction of the slow program in regenerating muscle. Calcineurin, a Ca2+/calmodulin-activated phosphatase implicated in nerve activity-dependent fiber-type specification in skeletal muscle, directly controls the phosphorylation state of the transcription factor NFAT, allowing for its translocation to the nucleus and leading to the activation of slow-type muscle proteins in cooperation with myocyte enhancer factor 2 (MEF2) proteins and other regulatory proteins. Calcium-dependent Ca2+/calmodulin kinase activity is also upregulated by slow motor neuron activity, possibly because it amplifies the slow-type calcineurin-generated responses by promoting MEF2 transactivator functions and enhancing oxidative capacity through stimulation of mitochondrial biogenesis. Contraction-induced changes in intracellular calcium or reactive oxygen species provide signals to diverse pathways that include the MAPKs, calcineurin and calcium/calmodulin-dependent protein kinase IV to activate transcription
Skeletal striated muscle factors that regulate gene expression and enzyme activity in skeletal muscle. PGC1-α (PPARGC1A), a transcriptional coactivator of nuclear receptors important to the regulation of a number of mitochondrial genes involved in oxidative metabolism, directly interacts with MEF2 to synergistically activate selective ST muscle genes and also serves as a target for calcineurin signaling. A peroxisome proliferator-activated receptor δ (PPARδ)-mediated Exercise-Included Signaling Pathways in Skeletal Muscle That Determine Specialized Characteristics of ST and FT Muscle Fibers transcriptional pathway is involved in the regulation of the skeletal musclefiber phenotype. Mice that harbor an activated form of PPARd display an “endurance” phenotype, with a coordinated increase in oxidative enzymes and mitochondrial biogenesis and an increased proportion of ST fibers. Thus—through functional genomics—calcineurin, calmodulin-dependent kinase, PGC-1α, and activated PPARδ form the basis of a signaling network that controls skeletal muscle fiber-type transformation and metabolic profiles that protect against insulin resistance and obesity. The transition from aerobic to anaerobic metabolism during intense work requires that several systems are rapidly activated to ensure a constant supply of ATP for the working muscles. These include a switch from fat-based to carbohydrate-based fuels, a redistribution of blood flow from nonworking to exercising muscles, and the removal of several of the by-products of anaerobic metabolism, such as carbon dioxide and lactic acid. Some of these responses are governed by transcriptional control of the FT glycolytic phenotype. For example, skeletal muscle reprogramming from an ST glycolytic phenotype to an FT glycolytic phenotype involves the Six1/Eya1 complex, composed of members of the Six protein family. Moreover, the Hypoxia Inducible Factor-1α (HIF-1α) has been identified as a master regulator for the expression of genes involved in essential hypoxic responses that maintain ATP levels in cells. Ablation of HIF-1α in skeletal muscle was associated with an increase in the activity of rate-limiting enzymes of the mitochondria, indicating that the citric acid cycle and increased fatty acid oxidation may be compensating for decreased flow through the glycolytic pathway in these animals. However, hypoxia-mediated HIF-1α responses are also linked to the regulation of mitochondrial dysfunction through the formation of excessive reactive oxygen species in mitochondria. Other pathways also influence adult muscle character. For example, physical force inside a muscle fiber may release the transcription factor Serum Response Factor (SRF) from the structural protein titin, leading to altered muscle growth.
443
Skeletal striated muscle
444
Research
Research on skeletal muscle properties uses many techniques. Electrical muscle stimulation is used to determine force and contraction speed at different stimulation frequencies, which are related to fiber-type composition and mix within an individual muscle group. In vitro muscle testing is used for more complete characterization of muscle properties.
References
[5] Quoted from National Skeletal Muscle Research Center; UCSD, Muscle Physiology Home Page - Skeletal Muscle Architecture (http:/ / muscle. ucsd. edu/ musintro/ arch. shtml), Effect of Muscle Architecture on Muscle Function [7] (http:/ / www. pponline. co. uk/ encyc/ endurance-training-understanding-your-slow-twitch-muscle-fibres-will-boost-performance-41374), Peak Performance - Endurance training: understanding your slow twitch muscle fibres will boost performance
Nuclear bag fiber
445
Nuclear bag fiber
Nuclear bag fiber
Latin myofibra sacculiformis Code TH H3.03.00.0.00013 [1]
A nuclear bag fiber is a type of intrafusal muscle fiber that lies in the center of a muscle spindle. Each has a large number of nuclei concentrated in bags and they cause excitation of both the primary and secondary nerve fibers. There are 2 kinds of bag fibers based upon contraction speed and motor innervation. 1) Bag2 fibers - are the largest. They have no striations in middle region and swell to enclose nuclei (hence their name) 2) Bag1 fibers - are smaller than bag2. Both bag types extend beyond the spindle capsule.
External links
• http://www.unmc.edu/Physiology/Mann/mann11.html
Nuclear chain cell
A nuclear chain cell is a type of cell that is found in the human body.
References
Myosatellite cell
446
Myosatellite cell
Myosatellite cell
Latin myosatellitocytus Code TH H2.00.05.2.01020 [1]
Myosatellite cells or satellite cells are small mononuclear progenitor cells with virtually no cytoplasm found in mature muscle. Satellite cells are precursors to skeletal muscle cells, able to give rise to satellite cells or differentiated skeletal muscle cells.[1] They have the potential to generate new muscle fibers, provide additional myonuclei to their parent muscle fiber, or return to a quiescent state.[2] More specifically, upon activation, satellite cells can re-enter the cell cycle to proliferate and differentiate into myoblasts.[3] Myosatellite cells are located between the basal lamina and sarcolemma of muscle fibers, and can lie in grooves either parallel or transversely to the longitudinal axis of the fiber. Their distribution across the fiber can vary significantly. Non-proliferative, quiescent myosatellite cells, which adjoin resting skeletal muscles, can be identified by their distinct location between sarcolemma and basal lamina, a high nuclear-to-cytoplasmic volume ratio, few organelles (e.g. ribosomes, endoplasmic reticulum, mitochondia, golgi complexes), small nuclear size, and a large quantity of nuclear heterochromatin relative to myonuclei. On the other hand, activated satellite cells have an increased number of caveolae, cytoplasmic organelles, and decreased levels of heterochromatin.[1] Satellite cells are able to differentiate and fuse to augment existing muscle fibers and to form new fibers. These cells represent the oldest known adult stem cell niche, and are involved in the normal growth of muscle, as well as regeneration following injury or disease. In undamaged muscle, the majority of satellite cells are quiescent; they neither differentiate nor undergo cell division. In response to mechanical strain, satellite cells become activated. Activated satellite cells initially proliferate as skeletal myoblasts before undergoing myogenic differentiation.
Genetic markers of satellite cells
Satellite cells express a number of distinctive genetic markers. Current thinking is that all satellite cells express PAX7 and PAX3[4] Moreover, both quiescent and activated human satellite cells can be identified by the membrane-bound neural cell adhesion molecule (N-CAM/CD56/Leu-19), a cell-surface glycoprotein. Myocyte nuclear factor (MNF), and c-met proto-oncogene (receptor for hepatocyte growth factor (HGF)) are less commonly used markers. [1] CD34 and Myf5 markers specifically define the majority of quiescent satellite cells.[5] Activated satellite cells prove problematic to identify, especially as their markers change with the degree of activation; for example, greater activation results in the progressive loss of Pax7 expression as the they enter the proliferative stage. However, Pax7 is expressed prominently after satellite cell differentiation.[6] Greater activation also results in increased expression of myogenic basic helix-loop-helix transcription factors MyoD, myogenin, and MRF4 - all responsible for the induction of myocyte-specific genes.[7] HGF testing is also used to identify active satellite cells.[1] Activated satellite cells also begin expressing muscle-specific filament proteins such as desmin as they differentiate. The field of satellite cell biology suffers from the same technical difficulties as other stem cell fields. Studies rely almost exclusively on Flow cytometry and Fluorescence Activated Cell Sorting (FACS) analysis, which gives no information about cell lineage or behaviour. As such, the satellite cell niche is relatively ill-defined and it is likely that it consists of multiple sub-populations.
Myosatellite cell
447
Function in muscle repair
When muscle cells undergo injury, quiescent satellite cells are released from beneath the basement membrane. They become activated and re-enter the cell cycle. These dividing cells are known as the "transit amplifying pool" before undergoing myogenic differentiation to form new (post-mitotic) myotubes. There is also evidence suggesting that these cells are capable of fusing with existing myofibers to facilitate growth and repair. The process of muscle regeneration involves considerable remodeling of extracellular matrix and, where extensive damage occurs, is incomplete. Fibroblasts within the muscle deposit scar tissue, which can impair muscle function, and is a significant part of the pathology of muscular dystrophies. Satellite cells proliferate following muscle trauma[8] and form new myofibers through a process similar to foetal muscle development.[] After several cell divisions, the satellite cells begin to fuse with the damaged myotubes and undergo further differentiations and maturation, with peripheral nuclei as in hallmark.[] One of the first roles described for IGF-1 was its involvement in the proliferation and differentiation of satellite cells. In addition, IGF-1 expression in skeletal muscle extends the capacity to activate satellite cell proliferation (Charkravarthy, et al., 2000), increasing and prolonging the beneficial effects to the aging muscle. [9] [10]
Effects of Exercise on Satellite Cell Activity
Satellite cell activation is measured by the extent of proliferation and differentiation. Typically, satellite cell content is expressed per muscle fiber or as a percentage of total nuclear content, the sum of satellite cell nuclei and myonuclei. While the adaptive response to exercise largely varies on an individual basis on factors such as genetics, age, diet, acclimatization to exercise, and exercise volume, human studies have demonstrated general trends.[1] It is suggested that exercise triggers the release of signaling molecules including inflammatory substances, cytokines and growth factors from surrounding connective tissues and active skeletal muscles.[1] Notably, HGF, a cytokine, is transferred from the extracellular matrix into muscles through the nitric-oxide dependent pathway. It is thought that HGF activates satellite cells, while insulin growth factor-I (IGF-1) and fibroblast growth factor (FGF) enhance satellite cell proliferation rate following activation.[11] Studies have demonstrated that intense exercise generally increases IGF-1 production, though individual responses vary significantly.[12] [13] More specifically, IGF-1 exists in two isoforms: mechano growth factor (MGF) and IGF-IEa.[14] While the former induces activation and proliferation, the latter causes differentiation of proliferating satellite cells.[14] Human studies have shown that both high resistance training and endurance training have yielded an increased number of satellite cells.[15] [6] These results suggest that a light, endurance training regimen may be useful to counteract the age-correlated satellite cell decrease.[1] In high-resistance training, activation and proliferation of satellite cells are evidenced by increased cyclinD1 mRNA, and p21 mRNA levels. This is consistent with the fact that cyclinD1 and p21 upregulation correlates to division and differentiation of cells. [2] Satellite cell activation has also been demonstrated on an ultrastructural level following exercise. Aerobic exercise has been shown to significantly increase granular endoplasmic reticulum, free ribosomes, and mitochondria of the stimulated muscle groups. Additionally, satellite cells have been shown to fuse with muscle fibers, developing new muscle fibers.[16] Other ultrastructural evidence for activated satellite cells include increased concentration of Golgi apparatus and pinocytotic vesicles.[17]
Myosatellite cell
448
Plasticity and therapeutic applications
Upon minimal stimulation, satellite cells in vitro or in vivo will undergo a myogenic differentiation program. Unfortunately, it seems that transplanted satellite cells have a limited capacity for migration, and are only able to regenerate muscle in the region of the delivery site. As such systemic treatments or even the treatment of an entire muscle in this way is not possible. However, other cells in the body such as pericytes and hematopoietic stem cells have all been shown to be able to contribute to muscle repair in a similar manner to the endogenous satellite cell. The advantage of using these cell types for therapy in muscle diseases is that they can be systemically delivered, autonomously migrating to the site of injury. Particularly successful recently has been the delivery of mesoangioblast cells into the Golden Retriever dog model of Duchenne muscular dystrophy, which effectively cured the disease.[18] However, the sample size used was relatively small and the study has since been criticized for a lack of appropriate controls for the use of immunosuppressive drugs. Recently, it has been reported that Pax7 expressing cells contribute to dermal wound repair by adopting a fibrotic phenotype through a Wnt/β-catenin mediated process.[19]
Regulation
Little is known of the regulation of satellite cells. Whilst together PAX3 and PAX7 currently form the definitive satellite markers, Pax genes are notoriously poor transcriptional activators. The dynamics of activation and quiesence and the induction of the myogenic program through the myogenic regulatory factors, Myf5, MyoD, myogenin, and MRF4 remains to be determined. There is some research indicating that satellite cells are negatively regulated by a protein called myostatin. Increased levels of myostatin up-regulate a cyclin-dependent kinase inhibitor called p21 and thereby induce the differentiation of satellite cells.[20]
References
[1] Kadi F, Charifi N, Denis C, Lexell J, Andersen JL, Schjerling P, Olsen S, Kjaer M. “The behaviour of satellite cells in response to exercise: what have we learned from human studies?” Pflugers Arch 2005; 451:319-27. [2] Kadi F, Schjerling P, Andersen LL, Charifi N, Madsen JL, Christensen LR, Andersen JL. “The effects of heavy resistance training and detraining on satellite cells in human skeletal muscles.” J Physiol 2004; 558:1005-12. [3] Siegel AL, Kuhlmann PK, Cornelison DD. “Muscle satellite cell proliferation and association: new insights from myofiber time-lapse imaging.” Skelet Muscle 2011; 1:7. [5] Beauchamp JR, Heslop L, Yu DS, Tajbakhsh S, Kelly RG, Wernig A, Buckingham ME, Partridge TA, Zammit PS. “Expression of CD34 and Myf5 defines the majority of quiescent adult skeletal muscle satellite cells.” J Cell Biol 2000; 151:1221-34 [6] Crameri R, Aagaard P, Qvortrup K, Kjaer M. “N-CAM and Pax7 immunoreactive cells are expressed differently in the human vastus lateralis after a single bout of exhaustive eccentric exercise.” J Physiol 2004; 565:165. [7] Marchildon F, Lala N, Li G, St-Louis C, Lamothe D, Keller C, Wiper-Bergeron N. “CCAAT/Enhancer Binding Protein Beta is Expressed in Satellite Cells and Controls Myogenesis.” Stem Cells 2012 [Epub ahead of print] [11] Anderson JE, Wozniak AC. “Satellite cell activation on fibers: modeling events in vivo—an invited review.” Can J Physiol Pharmacol 2004; 82:300–10. [12] Bamman MM, Shipp JR, Jiang J, Gower BA, Hunter GR, Goodman A, McLafferty CL, Urban RJ. “Mechanical load increases muscle IGF-I and androgen receptor mRNA concentrations in humans.” Am J Physiol 2001; 280:383–90. [13] Hellsten Y, Hansson HA, Johnson L, Frandsen U, Sjodin B. “Increased expression of xanthine oxidase and insulin-like growth factor I (IGF-I) immunoreactivity in skeletal muscle after strenuous exercise in humans.” Acta Physiol Scand 1996; 157:191–97. [14] Yang SY, Goldspink G. “Different roles of the IGF-I Ec peptide (MGF) and mature IGF-I in myoblast proliferation and differentiation.” FEBS Lett 2002; 522:156–60. [15] Charifi N, Kadi F, Feasson L, Denis C. “Effects of endurance training on satellite cell frequency in skeletal muscle of old men.” Muscle Nerve 2003; 28:87–92. [16] Appell HJ, Forsberg S, Hollmann W. “Satellite cell activation in human skeletal muscle after training: evidence for muscle fiber neoformation.” Int J Sports Med 1988; 9:297–99. [17] Roth SM, Martel GF, Ivey FM, Lemmer JT, Tracy BL, Metter EJ, Hurley BF, Rogers MA. “Skeletal muscle satellite cell characteristics in young and older men and women after heavy resistance strength training.” J Gerontol A Biol Sci Med Sci 2001; 56:240–47.
Myosatellite cell
449
External links
• Image at neuro.wustl.edu (http://www.neuro.wustl.edu/neuromuscular/mother/myogenesis.html#satcell) • Overview at brown.edu (http://www.brown.edu/Courses/BI0032/adltstem/sc.htm) • NIF Search - Satellite Cell (https://www.neuinfo.org/mynif/search.php?q=Satellite Cell&t=data&s=cover& b=0&r=20) via the Neuroscience Information Framework
Cardiac muscle
450
Cardiac muscle
Cardiac muscle
Cardiac muscle
Dog Cardiac Muscle 400X Latin Code textus muscularis striatus cardiacus TH H2.00.05.2.02001
[1]
Cardiac muscle (heart muscle) is a type of involuntary striated muscle found in the walls and histological foundation of the heart, specifically the myocardium. Cardiac muscle is one of three major types of muscle, the others being skeletal and smooth muscle. The cells that comprise cardiac muscle, called cardiomyocytes or myocardiocytes, only contain one, unique nucleus.[1][2] Coordinated contractions of cardiac muscle cells in the heart propel blood out of the atria and ventricles to the blood vessels of the left/body/systemic and right/lungs/pulmonary circulatory systems. This complex of actions makes up the systole of the heart.
An isolated cardiac muscle cell, beating.
Cardiac muscle cells, like all tissues in the body, rely on an ample blood supply to deliver oxygen and nutrients and to remove waste products such as carbon dioxide. The coronary arteries fulfill this function.
Metabolism
Cardiac muscle is adapted to be highly resistant to fatigue: it has a large number of mitochondria, enabling continuous aerobic respiration via oxidative phosphorylation, numerous myoglobins (oxygen-storing pigment) and a good blood supply, which provides nutrients and oxygen. The heart is so tuned to aerobic metabolism that it is unable to pump sufficiently in ischaemic conditions. At basal metabolic rates, about 1% of energy is derived from anaerobic metabolism. This can increase to 10% under moderately hypoxic conditions, but, under more severe hypoxic conditions, not enough energy can be liberated by lactate production to sustain ventricular contractions.[3]
Cardiac muscle Under basal aerobic conditions, 60% of energy comes from fat (free fatty acids and triglycerides), 35% from carbohydrates (primarily as glucose), and 5% from amino acids and ketone bodies. However, these proportions vary widely according to nutritional state. For example, during starvation, lactate can be recycled by the heart. This is very energy efficient, because one NAD+ is reduced to NADH and H+ (equal to 2.5 or 3 ATP) when lactate is oxidized to pyruvate, which can then be burned aerobically in the TCA cycle, liberating much more energy (ca 14 ATP per cycle). In the condition of diabetes, more fat and less carbohydrate is used due to the reduced induction of GLUT4 glucose transporters to the cell surfaces. However, contraction itself plays a part in bringing GLUT4 transporters to the surface.[4] This is true of skeletal muscle as well, but relevant in particular to cardiac muscle due to its continuous contractions.
451
Appearance
Striation
Cardiac muscle exhibits cross striations formed by alternating segments of thick and thin protein filaments. Like skeletal muscle, the primary structural proteins of cardiac muscle are actin and myosin. The actin filaments are thin causing the lighter appearance of the I bands in striated muscle, while the myosin filament is thicker lending a darker appearance to the alternating A bands as observed with electron microscopy. However, in contrast to skeletal muscle, cardiac muscle cells may be branched instead of linear and longitudinal.
T-Tubules
Another histological difference between cardiac muscle and skeletal muscle is that the T-tubules in the cardiac muscle are larger, broader and run along the Z-Discs. There are fewer T-tubules in comparison with skeletal muscle. Additionally, cardiac muscle forms diads instead of the triads formed between the T-tubules and the sarcoplasmic reticulum in skeletal muscle. T-tubules play critical role in excitation-contraction coupling (ECC). Recently, the action potentials of T-tubules were recorded optically by Guixue Bu et al.[5]
Intercalated discs
Intercalated discs (IDs) are complex adhering structures which connect single cardiac myocytes to an electrochemical syncytium (in contrast to the skeletal muscle, which becomes a multicellular syncytium during mammalian embryonic development) and are mainly responsible for force transmission during muscle contraction. Intercalated discs also support the rapid spread of action potentials and the synchronized contraction of the myocardium. IDs are described to consist of three different types of cell-cell junctions: the actin filament anchoring adherens junctions (fascia adherens), the intermediate filament anchoring desmosomes (macula adherens) and gap junctions. Gap junctions are responsible for electrochemical and metabolic coupling. They allow action potentials to spread between cardiac cells by permitting the passage of ions between cells, producing depolarization of the heart muscle. However, novel molecular biological and comprehensive studies unequivocally showed that IDs consist for the most part of mixed type adhering junctions named area composita (pl. areae compositae) representing an amalgamation of typical desmosomal and fascia adhaerens proteins (in contrast to various epithelia).[6][7][8] The authors discuss the high importance of these findings for the understanding of inherited cardiomyopathies (such as Arrhythmogenic Right Ventricular Cardiomyopathy, ARVC). Under light microscopy, intercalated discs appear as thin, typically dark-staining lines dividing adjacent cardiac muscle cells. The intercalated discs run perpendicular to the direction of muscle fibers. Under electron microscopy, an intercalated disc's path appears more complex. At low magnification, this may appear as a convoluted electron dense structure overlying the location of the obscured Z-line. At high magnification, the intercalated disc's path appears even more convoluted, with both longitudinal and transverse areas appearing in longitudinal section.[9]
Cardiac muscle
452
Role of calcium in contraction
In contrast to skeletal muscle, cardiac muscle requires extracellular calcium ions for contraction to occur. Like skeletal muscle, the initiation and upshoot of the action potential in ventricular muscle cells is derived from the entry of sodium ions across the sarcolemma in a regenerative process. However, an inward flux of extracellular calcium ions through L-type calcium channels sustains the depolarization of cardiac muscle cells for a longer duration. The reason for the calcium dependence is due to the mechanism of calcium-induced calcium release (CICR) from the sarcoplasmic reticulum that must occur under normal excitation-contraction (EC) coupling to cause contraction. Once the intracellular concentration of calcium increases, calcium ions bind to the protein troponin, which initiate extracellular fluid and intracellular stores, and skeletal muscle, which is only activated by calcium stored in the sarcoplasmic reticulum.
Regeneration of heart muscle cells
Until recently, it was commonly believed that cardiac muscle cells could not be regenerated. However, a study reported in the April 3, 2009 issue of Science contradicts that belief.[10] Olaf Bergmann and his colleagues at the Karolinska Institute in Stockholm tested samples of heart muscle from people born before 1955 when nuclear bomb testing caused elevated levels of radioactive carbon 14 in the Earth's atmosphere. They found that samples from people born before 1955 did have elevated carbon 14 in their heart muscle cell DNA, indicating that the cells had divided after the person's birth. By using DNA samples from many hearts, the researchers estimated that a 20-year-old renews about 1% of heart muscle cells per year and about 45 percent of the heart muscle cells of a 50-year-old were generated after he or she was born.
References
[1] Pollard, Thomas D. and Earnshaw, William. C., "Cell Biology". Philadelphia: Saunders. 2007. [3] Ganong, Review of Medical Physiology, 22nd Edition.Specialized form of muscle that is peculiar to the vertebrate heart.p81
External links
• Indiana State University, Muscle action (http://web.indstate.edu/thcme/mwking/muscle.html) • Physiology at MCG 2/2ch7/2ch7line (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section2/2ch7/2ch7line.htm)
Purkinje fibers
453
Purkinje fibers
Purkinje fibres
Isolated Heart conduction system showing purkinje fibers
The QRS complex is the large peak.
For the nervous cells, see Purkinje cell The Purkinje fibres (Purkyne tissue or subendocardial branches) are located in the inner ventricular walls of the heart, just beneath the endocardium. These fibers consist of specialized cardiomyocytes that are able to conduct cardiac action potentials more quickly and efficiently than any other cells in the heart. Purkinje fibres allow the heart's conduction system to create synchronized contractions of its ventricles, and are therefore essential for maintaining a consistent heart rhythm.
Histology
Purkinje fibers are a unique cardiac end-organ. Further histologic examination reveals that these fibers are split in atria and ventricles walls. The electrical origin of atrial Purkinje fibres arrives from the sinoatrial node. Given no aberrant channels, the atrial and ventricular Purkinje fibres are distinctly shielded from each other by collagen or the cardiac skeleton. The Purkinje fibres are further specialized to rapidly conduct impulses (numerous fast voltage-gated sodium channels and mitochondria, fewer myofibrils than the surrounding muscle tissue). Purkinje fibres take up stain differently from the surrounding muscle cells, and, on a slide, they often appear lighter and larger than their neighbors. They are binucleated.
Purkinje fibers
454
Function
Heart rate is governed by many influences from the Autonomic Nervous System. The Purkinje Fibers do not have any known role in setting heart rate, but are influenced by electrical discharge from the Sinoatrial node. During the ventricular contraction portion of the cardiac cycle, the Purkinje fibres carry the contraction impulse from both the left and right bundle branch to the myocardium of the ventricles. This causes the muscle tissue of the ventricles to contract, thus enabling a force to eject blood out of the heart; either to the Pulmonary circulation from the right ventricle or to the Systemic circulation from the left ventricle. Purkinje fibers also have the ability of automaticity,[1] firing at a rate of 15-40 beats per minute if left to their own devices. In contrast, the SA node in normal state can fire at 60-100 beats per minute. - in short, they generate action potentials, but at a slower rate than sinoatrial node. Thus they serve as the last resort when other pacemakers fail. When a Purkinje fibre does fire, it is called a premature ventricular contraction or PVC, or in other situations can be a ventricular escape. It plays a vital role in the circulatory system.
Etymology
They were discovered in 1839 by Jan Evangelista Purkyně, who gave them his name.
References
[1] [biomed.engr.sc.edu/bme_lab/lab%20reports/36)%20ECG%20I.pdf ]
External links
• subendocardial+branches+of+atrioventricular+bundles (http://www.emedicinehealth.com/script/main/ srchcont_dict.asp?src=subendocardial+branches+of+atrioventricular+bundles) at eMedicine Dictionary • Organology at UC Davis Circulatory/heart/purkinje/purkinje1 (http://trc.ucdavis.edu/mjguinan/apc100/ modules/Circulatory/heart/purkinje/purkinje1.html) - "Mammal heart, purkinje fibers (LM, Medium)" • Anatomy Atlases - Microscopic Anatomy, plate 05.78 (http://www.anatomyatlases.org/MicroscopicAnatomy/ Section05/Plate0578.shtml) • MedEd at Loyola Histo/practical/cardio/hp8-21.html (http://www.meddean.luc.edu/Lumen/MedEd/Histo/ practical/cardio/hp8-21.html) • Histology at ucsd.edu (http://meded.ucsd.edu/hist-img-bank/chapter_3/Slides_43_44_45_cardiac/pages/d.2. 44.1.2.htm) • Histology at nhmccd.edu (http://science.nhmccd.edu/Biol/cardio/purkinje.htm)
Smooth muscle tissue
455
Smooth muscle tissue
Smooth muscle tissue
Smooth muscle
Layers of Esophageal Wall: 1. Mucosa 2. Submucosa 3. Muscularis 4. Adventitia 5. Striated muscle 6. Striated and smooth 7. Smooth muscle 8. Lamina muscularis mucosae 9. Esophageal glands Latin textus muscularis levis; textus muscularis nonstriatus Code TH H2.00.05.1.00001 [1]
Smooth muscle is an involuntary non-striated muscle. It is divided into two sub-groups; the single-unit (unitary) and multiunit smooth muscle. Within single-unit smooth muscle tissues, the autonomic nervous system innervates a single cell within a sheet or bundle and the action potential is propagated by gap junctions to neighboring cells such that the whole bundle or sheet contracts as a syncytium (i.e., a multinucleate mass of cytoplasm that is not separated into cells). Multiunit smooth muscle tissues innervate individual cells; as such, they allow for fine control and gradual responses, much like motor unit recruitment in skeletal muscle. Smooth muscle is found within the walls of blood vessels (such smooth muscle specifically being termed vascular smooth muscle) such as in the tunica media layer of large (aorta) and small arteries, arterioles and veins. Smooth muscle is also found in lymphatic vessels, the urinary bladder, uterus (termed uterine smooth muscle), male and female reproductive tracts, gastrointestinal tract, respiratory tract, arrector pili of skin, the ciliary muscle, and iris of the eye. The structure and function is basically the same in smooth muscle cells in different organs, but the inducing stimuli differ substantially, in order to perform individual effects in the body at individual times. In addition, the
Smooth muscle tissue glomeruli of the kidneys contain smooth muscle-like cells called mesangial cells.
456
Structure
Most smooth muscle is of the single-unit variety, that is, either the whole muscle contracts or the whole muscle relaxes, but there is multiunit smooth muscle in the trachea, the large elastic arteries, and the iris of the eye. Single unit smooth muscle, however, is most common and lines blood vessels (except large elastic arteries), the urinary tract, and the digestive tract. Smooth muscle is fundamentally different from skeletal muscle and cardiac muscle in terms of structure, function, regulation of contraction, and excitation-contraction coupling. Smooth muscle fibers have a fusiform shape and, like striated muscle, can tense and relax. However, smooth muscle containing tissue tend to demonstrate greater elasticity and function within a larger length-tension curve than striated muscle. This ability to stretch and still maintain contractility is important in organs like the intestines and urinary bladder. In the relaxed state, each cell is spindle-shaped, 20-500 micrometers in length.
Molecular structure
A substantial portion of the volume of the cytoplasm of smooth muscle cells are taken up by the molecules myosin and actin,[1] which together have the capability to contract, and, through a chain of tensile structures, make the entire smooth muscle tissue contract with them. Myosin Myosin is primarily of class II in smooth muscle.[] • Myosin II contains two heavy chains which constitute the head and tail domains. Each of these heavy chains contains the N-terminal head domain, while the C-terminal tails take on a coiled-coil morphology, holding the two heavy chains together (imagine two snakes wrapped around each other, such as in a caduceus). Thus, myosin II has two heads. In smooth muscle, there is a single gene (MYH11[2]) that codes for the heavy chains myosin II, but there are splice variants of this gene that result in four distinct isoforms.[] Also, smooth muscle may contain MHC that is not involved in contraction, and that can arise from multiple genes.[] • Myosin II also contains 4 light chains, resulting in 2 per head, weighing 20 (MLC20) and 17 (MLC17) kDa.[] These bind the heavy chains in the "neck" region between the head and tail. • The MLC20 is also known as the regulatory light chain and actively participates in muscle contraction.[] Two MLC20 isoforms are found in smooth muscle, and they are encoded by different genes, but only one isoform participates in contractility.[] • The MLC17 is also known as the essential light chain.[] Its exact function is unclear, but it's believed that it contributes to the structural stability of the myosin head along with MLC20.[] Two variants of MLC17 (MLC17a/b) exist as a result of alternate splicing at the MLC17 gene.[] Different combinations of heavy and light chains allow for up to hundreds of different types of myosin structures, but it is unlikely that more than a few such combinations are actually used or permitted within a specific smooth muscle bed.[] In the uterus, a shift in myosin expression has been hypothesized to avail for changes in the directions
Smooth muscle tissue of uterine contractions that are seen during the menstrual cycle.[] Actin The thin filaments that form part of the contractile machinery are predominantly composed of α- and γ-actin.[] Smooth muscle α-actin (alpha actin) is the predominate isoform within smooth muscle. There are also lots of actin (mainly β-actin) that does not take part in contraction, but that polymerizes just below the plasma membrane in the presence of a contractile stimulant and may thereby assist in mechanical tension.[] Alpha actin is also expressed as distinct genetic isoforms such there is smooth muscle, cardiac muscle and skeletal muscle specific isoforms of alpha actin. (ref The actin gene family: function follows isoform.Perrin BJ, Ervasti JM.Cytoskeleton (Hoboken). 2010 Oct;67(10):630-4. Review.) The ratio of actin to myosin is between 2:1[] and 10:1[] in smooth muscle, compared to ~6:1 in skeletal muscle and 4:1 in cardiac muscle. Other proteins of the contractile apparatus Smooth muscle does not contain the protein troponin; instead calmodulin (which takes on the regulatory role in smooth muscle), caldesmon and calponin are significant proteins expressed within smooth muscle. • Tropomyosin is present in smooth muscle, spanning seven actin monomers and is laid out end to end over the entire length of the thin filaments. In striated muscle, tropomyosin serves to enhance actin–myosin interactions, but in smooth muscle, its function is unknown.[] • Calponin molecules may exist in equal number as actin, and has been proposed to be a load-bearing protein.[] • Caldesmon has been suggested to be involved in tethering actin, myosin and tropomyosin, and thereby enhance the ability of smooth muscle to maintain tension.[] Also, all three of these proteins may have a role in inhibiting the ATPase activity of the myosin complex that otherwise provides energy to fuel muscle contraction.[] Other tensile structures The myosin and actin are the contractile parts of continuous chains of tensile structures that stretch both across and between smooth muscle cells. The actin filaments of contractile units are attached to dense bodies. Dense bodies are rich in α-actinin,[] and also attach intermediate filaments (consisting largely of vimentin and desmin), and thereby appear to serve as anchors from which the thin filaments can exert force.[] Dense bodies also are associated with β-actin, which is the type found in the cytoskeleton, suggesting that dense bodies may coordinate tensions from both the contractile machinery and the cytoskeleton.[] The intermediate filaments are connected to other intermediate filaments via dense bodies, which eventually are attached to adherens junctions (also called focal adhesions) in the cell membrane of the smooth muscle cell, called the sarcolemma. The adherens junctions consist of large number of proteins including α-actinin, vinculin and cytoskeletal actin.[] The adherens junctions are scattered around dense bands that are circumfering the smooth muscle cell in a rib-like pattern.[1] The dense band (or dense plaques) areas alternate with regions of membrane containing numerous caveolae. When complexes of actin and myosin contract, force is transduced to the sarcolemma through intermediate filaments attaching to such dense bands. During contraction, there is a spatial reorganization of the contractile machinery to optimize force development.[] part of this reorganization consists of vimentin being phosphorylated at Ser56 by a p21 activated kinase, resulting in some disassembly of vimentin polymers.[] Also, the number of myosin filaments is dynamic between the relaxed and contracted state in some tissues as the ratio of actin to myosin changes, and the length and number of myosin filaments change.
457
Smooth muscle tissue Smooth muscle cells have been observed contracting in a spiral corkscrew fashion, and contractile proteins have been observed organizing into zones of actin and myosin along the axis of the cell. Smooth muscle-containing tissue needs to be stretched often, so elasticity is an important attribute of smooth muscle. Smooth muscle cells may secrete a complex extracellular matrix containing collagen (predominantly types I and III), elastin, glycoproteins, and proteoglycans. Smooth muscle also has specific elastin and collagen receptors to interact with these proteins of the extracellular matrix. These fibers with their extracellular matrices contribute to the viscoelasticity of these tissues. For example, the great arteries are viscolelastic vessels that act like a Windkessel, propagating ventricular contraction and smoothing out the pulsatile flow, and the smooth muscle within the tunica media contributes to this property. Caveolae The sarcolemma also contains caveolae, which are microdomains of lipid rafts specialized to cell-signaling events and ion channels. These invaginations in the sarcoplasma contain a host of receptors (prostacyclin, endothelin, serotonin, muscarinic receptors, adrenergic receptors), second messenger generators (adenylate cyclase, Phospholipase C), G proteins (RhoA, G alpha), kinases (rho kinase-ROCK, Protein kinase C, Protein Kinase A), ion channels (L type Calcium channels, ATP sensitive Potassium channels, Calcium sensitive Potassium channels) in close proximity. The caveolae are often close to sarcoplasmic reticulum or mitochondria, and have been proposed to organize signaling molecules in the membrane.
458
Excitation-contraction coupling
A smooth muscle is excited by external stimuli, which causes contraction. Each step is further detailed below.
Inducing stimuli and factors
Smooth muscle may contract spontaneously (via ionic channel dynamics) or as in the gut special pacemakers cells interstitial cells of Cajal produce rhythmic contractions. Also, contraction, as well as relaxation, can be induced by a number of physiochemical agents (e.g., hormones, drugs, neurotransmitters - particularly from the autonomic nervous system). Smooth muscle in various regions of the vascular tree, the airway and lungs, kidneys and vagina is different in their expression of ionic channels, hormone receptors, cell-signaling pathways, and other proteins that determine function. External substances For instance, most blood vessels respond to norepinephrine and epinephrine (from sympathetic stimulation or the adrenal medulla) by producing vasoconstriction (this response is mediated through alpha 1-adrenergic receptors). Blood vessels in skeletal muscle and cardiac muscle respond to these catecholamines producing vasodilation because the smooth muscle possess beta-adrenergic receptors. Generally, arterial smooth muscle responds to carbon dioxide by producing vasodilation, and responds to oxygen by producing vasoconstriction. Pulmonary blood vessels within the lung are unique as they vasodilate to high oxygen tension and vasoconstrict when it falls. Bronchiole, smooth muscle that line the airways of the lung, respond to high carbon dioxide producing vasodilation and vasoconstrict when carbon dioxide is low. These responses to carbon dioxide and oxygen by pulmonary blood vessels and bronchiole airway smooth muscle aid in matching perfusion and ventilation within the lungs. Further different smooth muscle tissues display extremes of abundant to little sarcoplasmic reticulum so excitation-contraction coupling varies with its dependence on intracellular or extracellular calcium. Recent research indicates that sphingosine-1-phosphate (S1P) signaling is an important regulator of vascular smooth muscle contraction. When transmural pressure increases, sphingosine kinase 1 phosphorylates sphingosine to S1P, which binds to the S1P2 receptor in plasma membrane of cells. This leads to a transient increase in intracellular
Smooth muscle tissue calcium, and activates Rac and Rhoa signaling pathways. Collectively, these serve to increase MLCK activity and decrease MLCP activity, promoting muscle contraction. This allows arterioles to increase resistance in response to increased blood pressure and thus maintain constant blood flow. The Rhoa and Rac portion of the signaling pathway provides a calcium-independent way to regulate resistance artery tone.[3]
459
Spread of impulse
To maintain organ dimensions against force, cells are fastened to one another by adherens junctions. As a consequence, cells are mechanically coupled to one another such that contraction of one cell invokes some degree of contraction in an adjoining cell. Gap junctions couple adjacent cells chemically and electrically, facilitating the spread of chemicals (e.g., calcium) or action potentials between smooth muscle cells. Single unit smooth muscle displays numerous gap junctions and these tissues often organize into sheets or bundles which contract in bulk.
Contraction
Smooth muscle contraction is caused by the sliding of myosin and actin filaments (a sliding filament mechanism) over each other. The energy for this to happen is provided by the hydrolysis of ATP. Myosin functions as an ATPase utilizing ATP to produce a molecular conformational change of part of the myosin and produces movement. Movement of the filaments over each other happens when the globular heads protruding from myosin filaments attach and interact with actin filaments to form crossbridges. The myosin heads tilt and drag along the actin filament a small distance (10-12 nm). The heads then release the actin filament and then changes angle to relocate to another site on the actin filament a further distance (10-12 nm) away. They can then re-bind to the actin molecule and drag it along further. This process is called crossbridge cycling and is the same for all muscles (see muscle contraction). Unlike cardiac and skeletal muscle, smooth muscle does not contain the calcium-binding protein troponin. Contraction is initiated by a calcium-regulated phosphorylation of myosin, rather than a calcium-activated troponin system. Crossbridge cycling causes contraction of myosin and actin complexes, in turn causing increased tension along the entire chains of tensile structures, ultimately resulting in contraction of the entire smooth muscle tissue. Phasic or tonic Smooth muscle may contract phasically with rapid contraction and relaxation, or tonically with slow and sustained contraction. The reproductive, digestive, respiratory, and urinary tracts, skin, eye, and vasculature all contain this tonic muscle type. This type of smooth muscle can maintain force for prolonged time with only little energy utilization. There are differences in the myosin heavy and light chains that also correlate with these differences in contractile patterns and kinetics of contraction between tonic and phasic smooth muscle. Activation of myosin heads Crossbridge cycling cannot occur until the myosin heads have been activated to allow crossbridges to form. When the light chains are phosphorylated, they become active and will allow contraction to occur. The enzyme that phosphorylates the light chains is called myosin light-chain kinase (MLCK), also called MLC20 kinase.[] In order to control contraction, MLCK will work only when the muscle is stimulated to contract. Stimulation will increase the intracellular concentration of calcium ions. These bind to a molecule called calmodulin, and form a calcium-calmodulin complex. It is this complex that will bind to MLCK to activate it, allowing the chain of reactions for contraction to occur. Activation consists of phosphorylation of a serine on position 19 (Ser19) on the MLC20 light chain, which causes a conformational change that increases the angle in the neck domain of the myosin heavy chain,[] which corresponds to the part of the cross-bridge cycle where the myosin head is unattached to the actin filament and relocates to another site on it. After attachment of the myosin head to the actin filament, this serine phosphorylation also activates the
Smooth muscle tissue ATPase activity of the myosin head region to provide the energy to fuel the subsequent contraction.[] Phosphorylation of a threonine on position 18 (Thr18) on MLC20 is also possible and may further increase the ATPase activity of the myosin complex.[] Sustained maintenance Phosphorylation of the MLC20 myosin light chains correlates well with the shortening velocity of smooth muscle. During this period there is a rapid burst of energy utilization as measured by oxygen consumption. Within a few minutes of initiation the calcium level markedly decrease, MLC20 myosin light chains phosphorylation decreases, and energy utilization decreases and the muscle can relax. Still, smooth muscle has the ability of sustained maintenance of force in this situation as well. This sustained phase has been attributed to certain myosin crossbridges, termed latch-bridges, that are cycling very slowly, notably slowing the progression to the cycle stage whereby dephosphorylated myosin detaches from the actin, thereby maintaining the force at low energy costs.[] This phenomenon is of great value especially for tonically active smooth muscle.[] Isolated preparations of vascular and visceral smooth muscle contract with depolarizing high potassium balanced saline generating a certain amount of contractile force. The same preparation stimulated in normal balanced saline with an agonist such as endothelin or serotonin will generate more contractile force. This increase in force is termed calcium sensitization. The myosin light chain phosphatase is inhibited to increase the gain or sensitivity of myosin light chain kinase to calcium. There are number of cell signalling pathways believed to regulate this decrease in myosin light chain phosphatase: a RhoA-Rock kinase pathway, a Protein kinase C-Protein kinase C potentiation inhibitor protein 17 (CPI-17) pathway, telokin, and a Zip kinase pathway. Further Rock kinase and Zip kinase have been implicated to directly phosphorylate the 20kd myosin light chains. Other contractile mechanisms Other cell signaling pathways and protein kinases (Protein kinase C, Rho kinase, Zip kinase, Focal adhesion kinases) have been implicated as well and actin polymerization dynamics plays a role in force maintenance. While myosin light chain phosphorylation correlates well with shortening velocity, other cell signaling pathways have been implicated in the development of force and maintenance of force. Notably the phosphorylation of specific tyrosine residues on the focal adhesion adapter protein-paxillin by specific tyrosine kinases has been demonstrated to be essential to force development and maintenance. For example, cyclic nucleotides can relax arterial smooth muscle without reductions in crossbridge phosphorylation, a process termed force suppression. This process is mediated by the phosphorylation of the small heat shock protein, hsp20, and may prevent phosphorylated myosin heads from interacting with actin.
460
Relaxation
The phosphorylation of the light chains by MLCK is countered by a myosin light-chain phosphatase, which dephosphorylates the MLC20 myosin light chains and thereby inhibits contraction.[] Other signaling pathways have also been implicated in the regulation actin and myosin dynamics. In general, the relaxation of smooth muscle is by cell-signaling pathways that increase the myosin phosphatase activity, decrease the intracellular calcium levels, hyperpolarize the smooth muscle, and/or regulate actin and myosin dynamics. Relaxation-inducing factors The relaxation of smooth muscle can be mediated by the endothelium-derived relaxing factor-nitric oxide, endothelial derived hyperpolarizing factor (either an endogenous cannabinoid, cytochrome P450 metabolite, or hydrogen peroxide), or prostacyclin (PGI2). Nitric oxide and PGI2 stimulate soluble guanylate cyclase and membrane bound adenylate cyclase, respectively. The cyclic nucleotides (cGMP and cAMP) produced by these cyclases activate Protein Kinase G and Proten Kinase A and phosphorylate a number of proteins. The phosphorylation events lead to a decrease in intracelluar calcium (inhibit L type Calcium channels, inhibits IP3
Smooth muscle tissue receptor channels, stimulates sarcoplasmic reticulum Calcium pump ATPase), a decrease in the 20kd myosin light chain phosphorylation by altering calcium sensitization and increasing myosin light chain phosphatase activity, a stimulation of calcium sensitive potassium channels which hyperpolarize the cell, and the phosphorylation of amino acid residue serine 16 on the small heat shock protein (hsp20)by Protein Kinases A and G. The phosphorylation of hsp20 appears to alter actin and focal adhesion dynamics and actin-myosin interaction, and recent evidence indicates that hsp20 binding to 14-3-3 protein is involved in this process. An alternative hypothesis is that phosphorylated Hsp20 may also alter the affinity of phosphorylated myosin with actin and inhibit contractility by interfering with crossbridge formation. The endothelium derived hyperpolarizing factor stimulates calcium sensitive potassium channels and/or ATP sensitive potassium channels and stimulate potassium efflux which hyperpolarizes the cell and produces relaxation.
461
Invertebrate smooth muscle
In invertebrate smooth muscle, contraction is initiated with the binding of calcium directly to myosin and then rapidly cycling cross-bridges, generating force. Similar to the mechanism of vertebrate smooth muscle, there is a low calcium and low energy utilization catch phase. This sustained phase or catch phase has been attributed to a catch protein that has similarities to myosin light-chain kinase and the elastic protein-titin called twitchin. Clams and other bivalve mollusks use this catch phase of smooth muscle to keep their shell closed for prolonged periods with little energy usage.
Specific effects
Although the structure and function is basically the same in smooth muscle cells in different organs, their specific effects or end-functions differ. Smooth muscle forms precapillary sphincters in blood vessels in metarterioles which regulates the blood flow in capillary beds of various organs and tissues. The contractile function of vascular smooth muscle also regulates the lumenal diameter of the small arteries-arterioles called resistance vessels, thereby contributing significantly to setting the level of blood pressure. Smooth muscle contracts slowly and may maintain the contraction (tonically) for prolonged periods in blood vessels, bronchioles, and some sphincters. Activating arteriole smooth muscle can decrease the lumenal diameter 1/3 of resting so it drastically alters blood flow and resistance. Activation of aortic smooth muscle doesn't significantly alter the lumenal diameter but serves to increase the viscoelasticity of the vascular wall. In the digestive tract, smooth muscle contracts in a rhythmic peristaltic fashion, rhythmically forcing foodstuffs through the digestive tract as the result of phasic contraction. A non-contractile function is seen in specialized smooth muscle within the afferent arteriole of the juxtaglomerular apparatus, which secretes renin in response to osmotic and pressure changes, and also it is believed to secrete ATP in tubuloglomerular regulation of glomerular filtration rate. Renin in turn activates the renin-angiotensin system to regulate blood pressure.
Smooth muscle tissue
462
Growth and rearrangement
The mechanism in which external factors stimulate growth and rearrangement is not yet fully understood. A number of growth factors and neurohumoral agents influence smooth muscle growth and differentiation. The Notch receptor and cell-signaling pathway have been demonstrated to be essential to vasculogenesis and the formation of arteries and veins. The proliferation is implicated in the pathogenesis of atherosclerosis and is inhibited by nitric oxide. The embryological origin of smooth muscle is usually of mesodermal origin. However, the smooth muscle within the Aorta and Pulmonary arteries (the Great Arteries of the heart) is derived from ectomesenchyme of neural crest origin, although coronary artery smooth muscle is of mesodermal origin.
Related diseases
"Smooth muscle condition" is a condition in which the body of a developing embryo does not create enough smooth muscle for the gastrointestinal system. This condition is fatal. Anti-smooth muscle antibodies (ASMA) can be a symptom of an auto-immune disorder, such as hepatitis, cirrhosis, or lupus. Vascular smooth muscle tumors are very rare. They can be malignant or benign, and morbidity can be significant with either type. Intravascular leiomyomatosis is a benign neoplasm that extends through the veins; angioleiomyoma is a benign neoplasm of the extremities; vascular leiomyosarcomas is a malignant neoplasm that can be found in the inferior vena cava, pulmonary arteries and veins, and other peripheral vessels. See Atherosclerosis.
References
[1] Page 174 (http:/ / books. google. com/ books?id=iOEQWGfiurYC& pg=PA175& lpg=PA174) in: The vascular smooth muscle cell: molecular and biological responses to the extracellular matrix. Authors: Stephen M. Schwartz, Robert P. Mecham. Editors: Stephen M. Schwartz, Robert P. Mecham. Contributors: Stephen M. Schwartz, Robert P. Mecham. Publisher: Academic Press, 1995. ISBN 0-12-632310-0, ISBN 978-0-12-632310-8 [3] Scherer EQ et al. Sphingosine-1-phosphate modulates spiral modiolar artery tone: A potential role in vascular-based inner ear pathologies? Cardiovasc Res. 2006 Apr 1;70(1):79–87.
External links
• BBC (http://news.bbc.co.uk/2/hi/health/3549285.stm) - baby born with smooth muscle condition has 8 organs transplanted • Smooth muscle antibody (http://www.ii.bham.ac.uk/clinicalimmunology/CISimagelibrary/smoothmuscle. htm) • Stomach smooth muscle identified using antibody (http://www.antibodypatterns.com/smoothmuscle.php) • UIUC Histology Subject 265 (https://histo.life.illinois.edu/histo/atlas/oimages.php?oid=265) • Histology at KUMC muscular-muscle08 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/ muscular/muscle08.htm) "Smooth Muscle" • BU Histology Learning System: 21701ooa (http://www.bu.edu/histology/p/21701ooa.htm)
Myoepithelial cell
463
Myoepithelial cell
Myoepithelial cell
Latin myoepitheliocytus Code TH H2.00.02.0.03059 [1]
Myoepithelial cells (sometimes referred to as myoepithelium) are cells usually found in glandular epithelium as a thin layer above the basement membrane but generally beneath the luminal cells. These may be positive for alpha smooth muscle actin and can contract and expel the secretions of exocrine glands. They are found in the sweat glands, mammary glands, lacrimal glands, and salivary glands. Myoepithelial cells in these cases constitute the basal cell layer of an epithelium that harbors the epithelial progenitor. In the case of wound healing, myoepithelial cells reactively proliferate. Presence of myoepithelial cells in a hyperplastic tissue proves the benignity of the gland and, when absent, indicates cancer. Only rare cancers like adenoid cystic carcinomas contains myoepithelial cells as one of the malignant components. It can be found in endoderm or ectoderm.[]
Markers
Myoepithelial cells are true epithelial cells positive for keratins, not to be confused with myofibroblasts which are true mesenchymal cells positive for vimentin. These cells are generally positive for alpha smooth muscle actin (αSMA), cytokeratin 5/6 and other high molecular weight cytokeratins, p63 and caldesmon. Myoepithelial cells are stellate in shape an are also known as basket cells. They lie between the basement membrane and glandular epithelium. Each cell consists of a cell body from which 4-8 processes radiate and embrace the secretory unit. Myoepithelial cells have contractile functions. They help in expelling secretions from the lumen of secretory units and facilitate the movement of saliva in salivary ducts.
References External links
• Myoepithelium (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=Myoepithelium) at eMedicine Dictionary • Anatomy Atlases - Microscopic Anatomy, plate 07.141 (http://www.anatomyatlases.org/MicroscopicAnatomy/ Section07/Plate07141.shtml) - "Axillary Sweat Gland: Myoepithelium" • Histology at OU 43_13 (http://w3.ouhsc.edu/histology/Glass slides/43_13.jpg) - "thick skin" • Histology at KUMC glands-glands09 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/ glands/glands09.htm) "Simple Tubular Coiled" • Physiology at MCG 6/6ch4/s6ch4_4 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section6/6ch4/s6ch4_4.htm)
Red blood cell
464
Red blood cell
Red blood cells, or erythrocytes, are the most common type of blood cell and the vertebrate organism's principal means of delivering oxygen (O2) to the body tissues via the blood flow through the circulatory system.[1] They take up oxygen in the lungs or gills and release it while squeezing through the body's capillaries. These cells' cytoplasm is rich in haemoglobin, an iron-containing biomolecule that can bind oxygen and is responsible for the blood's red color. In humans, mature red blood cells are oval and flexible biconcave disks. They lack a cell nucleus and most organelles to accommodate maximum space for haemoglobin. 2.4 million new erythrocytes are produced per second.[2] The cells develop in the bone marrow and circulate for about 100–120 days in the body before their components are recycled by macrophages. Each circulation takes about 20 seconds. Approximately a quarter of the cells in the human body are red blood cells.[3][]
Scanning electron micrograph of human red blood cells (size approximately 6-8 μm; artificial colors)
Red blood cells are also known as RBCs, red cells,[4] red blood corpuscles (an archaic term), haematids, erythroid cells or erythrocytes (from Greek erythros for "red" and kytos for "hollow vessel", with -cyte translated as "cell" in modern usage).
History
The first person to describe red blood cells was the young Dutch biologist Jan Swammerdam, who had used an early microscope in 1658 to study the blood of a frog.[5] Unaware of this work, Anton van Leeuwenhoek provided another microscopic description in 1674, this time providing a more precise description of red blood cells, even approximating their size, "25,000 times smaller than a fine grain of sand". In 1901, Karl Landsteiner published his discovery of the three main blood groups—A, B, and C (which he later renamed to O). Landsteiner described the regular patterns in which reactions occurred when serum was mixed with red blood cells, thus identifying compatible and conflicting combinations between these blood groups. A year later Alfred von Decastello and Adriano Sturli, two colleagues of Landsteiner, identified a fourth blood group—AB. In 1959, by use of X-ray crystallography, Dr. Max Perutz was able to unravel the structure of hemoglobin, the red blood cell protein that carries oxygen.[6] The oldest intact red blood cells ever discovered were found in Ötzi the Iceman, a natural mummy of a man who died around 3255 BCE. These cells were discovered in May 2012.[7]
Red blood cell
465
Vertebrate erythrocytes
Erythrocytes consist mainly of hemoglobin, a complex metalloprotein containing heme groups whose iron atoms temporarily bind to oxygen molecules (O2) in the lungs or gills and release them throughout the body. Oxygen can easily diffuse through the red blood cell's cell membrane. Hemoglobin in the erythrocytes also carries some of the waste product carbon dioxide back from the tissues; most waste carbon dioxide, however, is transported back to the pulmonary capillaries of the lungs as bicarbonate (HCO3-) dissolved in the blood plasma. Myoglobin, a compound related to hemoglobin, acts to store oxygen in muscle cells.[8] The color of erythrocytes is due to the heme group of hemoglobin. The blood plasma alone is straw-colored, but the red blood cells change color depending on the state of the hemoglobin: when combined with oxygen the resulting oxyhemoglobin is scarlet, and when oxygen has been released the resulting deoxyhemoglobin is of a dark red burgundy color, appearing bluish through the vessel wall and skin. Pulse oximetry takes advantage of this color change to directly measure the arterial blood oxygen saturation using colorimetric techniques. The sequestration of oxygen-carrying proteins inside specialized There is an immense size variation in vertebrate cells (rather than having them dissolved in body fluid) was an erythrocytes, as well as a correlation between cell and important step in the evolution of vertebrates as it allows for less nucleus size. Mammalian erythrocytes, which do not viscous blood, higher concentrations of oxygen, and better contain nuclei, are considerably smaller than those of [] most other vertebrates. diffusion of oxygen from the blood to the tissues. The size of erythrocytes varies widely among vertebrate species; erythrocyte width is on average about 25% larger than capillary diameter, and it has been hypothesized that this improves the oxygen transfer from erythrocytes to tissues.[] The only known vertebrates without erythrocytes are the crocodile icefishes (family Channichthyidae); they live in very oxygen-rich cold water and transport oxygen freely dissolved in their blood.[9] While they do not use hemoglobin anymore, remnants of hemoglobin genes can be found in their genome.[10]
Nucleus
Erythrocytes in mammals are anucleate when mature, meaning that they lack a cell nucleus. In comparison, the erythrocytes of other vertebrates have nuclei; the only known exceptions are salamanders of the Batrachoseps genus and fish of the Maurolicus genus with closely related species.[11][12]
Secondary functions
When erythrocytes undergo shear stress in constricted vessels, they release ATP, which causes the vessel walls to relax and dilate so as to promote normal blood flow.[13] When their hemoglobin molecules are deoxygenated, erythrocytes release S-nitrosothiols, which also acts to dilate vessels,[14] thus directing more blood to areas of the body depleted of oxygen.
Red blood cell It has been recently demonstrated that erythrocytes can also synthesize nitric oxide enzymatically, using L-arginine as substrate, just like endothelial cells.[15] Exposure of erythrocytes to physiological levels of shear stress activates nitric oxide synthase and export of nitric oxide,[16] which may contribute to the regulation of vascular tonus. Erythrocytes can also produce hydrogen sulfide, a signalling gas that acts to relax vessel walls. It is believed that the cardioprotective effects of garlic are due to erythrocytes converting its sulfur compounds into hydrogen sulfide.[17] Erythrocytes also play a part in the body's immune response: when lysed by pathogens such as bacteria, their hemoglobin releases free radicals, which break down the pathogen's cell wall and membrane, killing it.[18][19]
466
Mammalian erythrocytes
Mammalian erythrocytes are unique among the vertebrates as they are non-nucleated cells in their mature form. These cells have nuclei during early phases of erythropoiesis, but extrude them during development as they mature in order to provide more space for hemoglobin. In mammals, erythrocytes also lose all other cellular organelles such as their mitochondria, Golgi apparatus and endoplasmic reticulum. As a result of not containing mitochondria, these cells use none of the oxygen they transport; instead they produce the energy carrier ATP by the glycolysis of glucose and lactic acid fermentation on the resulting pyruvate.
Typical mammalian erythrocytes: (a) seen from surface; (b) in profile, forming rouleaux; (c) rendered spherical by water; (d) rendered crenate by salt. (c) and (d) do not normally occur in the body.
Because of the lack of nuclei and organelles, mature red blood cells do not contain DNA and cannot synthesize any RNA, and consequently cannot divide and have limited repair capabilities.[] This also ensures that no virus can evolve to target mammalian red blood cells.[20] Mammalian erythrocytes are typically shaped as biconcave disks: flattened and depressed in the center, with a dumbbell-shaped cross section, and a torus-shaped rim on the edge of the disk. This distinctive biconcave shape optimises the flow properties of blood in the large vessels, such as maximization of laminar flow and minimization of platelet scatter, which suppresses their atherogenic activity in those large vessels.[21] However, there are some exceptions concerning shape in the artiodactyl order (even-toed ungulates including cattle, deer, and their relatives), which displays a wide variety of bizarre erythrocyte morphologies: small and highly ovaloid cells in llamas and camels (family Camelidae), tiny spherical cells in mouse deer (family Tragulidae), and cells which assume fusiform, lanceolate, crescentic, and irregularly polygonal and other angular forms in red deer and wapiti (family Cervidae). Members of this order have clearly evolved a mode of red blood cell development substantially different from the mammalian norm.[][22] Overall, mammalian erythrocytes are remarkably flexible and deformable so as to squeeze through tiny capillaries, as well as to maximize their apposing surface by assuming a cigar shape, where they efficiently release their oxygen load.[23] In large blood vessels, red blood cells sometimes occur as a stack, flat side next to flat side. This is known as rouleaux formation, and it occurs more often if the levels of certain serum proteins are elevated, as for instance during inflammation. The spleen acts as a reservoir of red blood cells, but this effect is somewhat limited in humans. In some other mammals such as dogs and horses, the spleen sequesters large numbers of red blood cells which are dumped into the
Red blood cell blood during times of exertion stress, yielding a higher oxygen transport capacity.
467
Scanning electron micrograph of blood cells. From left to right: human erythrocyte, thrombocyte (platelet), leukocyte.
Human erythrocytes
A typical human erythrocyte has a disk diameter of approximately 6.2-8.2 µm[24] and a thickness at the thickest point of 2-2.5 µm and a minimum thickness in the centre of 0.8-1 µm, being much smaller than most other human cells. These cells have an average volume of about 90 fL[25] with a surface of about 136 μm2, and can swell up to a sphere shape containing 150 fL, without membrane distension. Adult humans have roughly 2–3 × 1013 (20-30 trillion) red blood cells at any given time, comprising approximately one quarter of the total human body cell number (women have about 4 to 5 million erythrocytes per microliter (cubic millimeter) of blood and men about 5 to 6 million; people living at high altitudes with low oxygen tension will have more). Red blood cells are thus much more common than the other blood particles: there are about 4,000–11,000 white blood cells and about 150,000–400,000 platelets in each microliter of human blood. Human red blood cells take on average 20 seconds to complete one cycle of circulation.[3][][26] As red blood cells contain no nucleus, protein biosynthesis is currently assumed to be absent in these cells, although a recent study indicates the presence of all the necessary biomachinery in the cells to do so.[]
Two drops of blood are shown with a bright red oxygenated drop on the left and a deoxygenated drop on the right.
The blood's red color is due to the spectral properties of the hemic iron ions in hemoglobin. Each human red blood cell contains approximately 270 million of these hemoglobin biomolecules, each carrying four heme groups; hemoglobin comprises about a third of the total cell volume. This protein is responsible for the transport of more than 98% of the oxygen (the remaining oxygen is carried dissolved in the blood plasma). The red blood cells of an average adult human male store collectively about 2.5 grams of iron, representing about 65% of the total iron contained in the body.[27][28] (See Human iron metabolism.)
An animation of a typical human red blood cell cycle in the circulatory system. This animation occurs at real time (20 seconds of cycle) and shows the red blood cell deform as it enters capillaries, as well as changing color as it alternates in states of oxygenation along the circulatory system.
Red blood cell
468
Life cycle
Human erythrocytes are produced through a process named erythropoiesis, developing from committed stem cells to mature erythrocytes in about 7 days. When matured, these cells live in blood circulation for about 100 to 120 days (and 80 to 90 days in a full term infant).[29] At the end of their lifespan, they become senescent, and are removed from circulation. Erythropoiesis Erythropoiesis is the development process by which new erythrocytes are produced; it lasts about 7 days. Through this process erythrocytes are continuously produced in the red bone marrow of large bones, at a rate of about 2 million per second in a healthy adult. (In the embryo, the liver is the main site of red blood cell production.) The production can be stimulated by the hormone erythropoietin (EPO), synthesised by the kidney. Just before and after leaving the bone marrow, the developing cells are known as reticulocytes; these comprise about 1% of circulating red blood cells. Functional lifetime The functional lifetime of an erythrocyte is about 100–120 days, during which time the erythrocytes are continually moved by the blood flow push (in arteries), pull (in veins) and a combination of the two as they squeeze through microvessels such as capillaries. Senescence The aging erythrocyte undergoes changes in its plasma membrane, making it susceptible to selective recognition by macrophages and subsequent phagocytosis in the reticuloendothelial system (spleen, liver and bone marrow), thus removing old and defective cells and continually purging the blood. This process is termed eryptosis, erythrocyte programmed cell death. This process normally occurs at the same rate of production by erythropoiesis, balancing the total circulating red blood cell count. Eryptosis is increased in a wide variety of diseases including sepsis, haemolytic uremic syndrome, malaria, sickle cell anemia, beta-thalassemia, glucose-6-phosphate dehydrogenase deficiency, phosphate depletion, iron deficiency and Wilson's disease. Eryptosis can be elicited by osmotic shock, oxidative stress, energy depletion as well as a wide variety of endogenous mediators and xenobiotics. Excessive eryptosis is observed in erythrocytes lacking the cGMP-dependent protein kinase type I or the AMP-activated protein kinase AMPK. Inhibitors of eryptosis include erythropoietin, nitric oxide, catecholamines and high concentrations of urea. Much of the resulting breakdown products are recirculated in the body. The heme constituent of hemoglobin are broken down into Fe3+ and biliverdin. The biliverdin is reduced to bilirubin, which is released into the plasma and recirculated to the liver bound to albumin. The iron is released into the plasma to be recirculated by a carrier protein called transferrin. Almost all erythrocytes are removed in this manner from the circulation before they are old enough to hemolyze. Hemolyzed hemoglobin is bound to a protein in plasma called haptoglobin which is not excreted by the kidney.[30]
Membrane composition
The membrane of the red blood cell plays many roles that aid in regulating their surface deformability, flexibility, adhesion to other cells and immune recognition. These functions are highly dependent on its composition, which defines its properties. The red blood cell membrane is composed of 3 layers: the glycocalyx on the exterior, which is rich in carbohydrates; the lipid bilayer which contains many transmembrane proteins, besides its lipidic main constituents; and the membrane skeleton, a structural network of proteins located on the inner surface of the lipid bilayer. Half of the membrane mass in human and most mammalian erythrocytes are proteins. The other half are lipids, namely phospholipids and cholesterol.[]
Red blood cell Membrane lipids The erythrocyte cell membrane comprises a typical lipid bilayer, similar to what can be found in virtually all human cells. Simply put, this lipid bilayer is composed of cholesterol and phospholipids in equal proportions by weight. The lipid composition is important as it defines many physical properties such as membrane permeability and fluidity. Additionally, the activity of many membrane proteins is regulated by interactions with lipids in the bilayer. Unlike cholesterol which is evenly distributed between the inner and outer leaflets, the 5 major phospholipids are asymmetrically disposed, as shown below: Outer monolayer • Phosphatidylcholine (PC); • Sphingomyelin (SM). Inner monolayer • Phosphatidylethanolamine (PE); • Phosphoinositol (PI) (small amounts). • Phosphatidylserine (PS); This asymmetric phospholipid distribution among the The most common erythrocyte cell membrane lipids, schematically bilayer is the result of the function of several disposed as they are distributed on the bilayer. Relative abundances energy-dependent and energy-independent are not at scale. phospholipid transport proteins. Proteins called “Flippases” move phospholipids from the outer to the inner monolayer while others called “floppases” do the opposite operation, against a concentration gradient in an energy dependent manner. Additionally, there are also “scramblase” proteins that move phospholipids in both directions at the same time, down their concentration gradients in an energy independent manner. There is still considerable debate ongoing regarding the identity of these membrane maintenance proteins in the red cell membrane. The maintenance of an asymmetric phospholipid distribution in the bilayer (such as an exclusive localization of PS and PIs in the inner monolayer) is critical for the cell integrity and function due to several reasons: • Macrophages recognize and phagocytose red cells that expose PS at their outer surface. Thus the confinement of PS in the inner monolayer is essential if the cell is to survive its frequent encounters with macrophages of the reticuloendothelial system, especially in the spleen. • Premature destruction of thallassemic and sickle red cells has been linked to disruptions of lipid asymmetry leading to exposure of PS on the outer monolayer. • An exposure of PS can potentiate adhesion of red cells to vascular endothelial cells, effectively preventing normal transit through the microvasculature. Thus it is important that PS is maintained only in the inner leaflet of the bilayer to ensure normal blood flow in microcirculation. • Both PS and phosphatidylinositol-4,5-bisphosphate (PIP2) can regulate membrane mechanical function, due to their interactions with skeletal proteins such as spectrin and protein 4.1R. Recent studies have shown that binding of spectrin to PS promotes membrane mechanical stability. PIP2 enhances the binding of protein band 4.1R to glycophorin C but decreases its interaction with protein band 3, and thereby may modulate the linkage of the
469
Red blood cell bilayer to the membrane skeleton. The presence of specialized structures named "lipid rafts" in the erythrocyte membrane have been described by recent studies. These are structures enriched in cholesterol and sphingolipids associated with specific membrane proteins, namely flotillins, stomatins (band 7), G-proteins, and β-adrenergic receptors. Lipid rafts that have been implicated in cell signaling events in nonerythroid cells have been shown in erythroid cells to mediate β2-adregenic receptor signaling and increase cAMP levels, and thus regulating entry of malarial parasites into normal red cells.[][31] Membrane proteins The proteins of the membrane skeleton are responsible for the deformability, flexibility and durability of the red blood cell, enabling it to squeeze through capillaries less than half the diameter of the erythrocyte (7-8 μm) and recovering the discoid shape as soon as these cells stop receiving compressive forces, in a similar fashion to an object made of rubber. There are currently more than 50 known membrane proteins, which can exist in a few hundred up to a million copies per erythrocyte. Approximately 25 of these membrane proteins carry the various blood group antigens, such as the A, B and Rh antigens, among many others. These membrane proteins can perform a wide diversity of functions, such as transporting ions and molecules across the red cell membrane, adhesion and interaction with other cells such as endothelial cells, as Red blood cell membrane proteins separated by signaling receptors, as well as other currently unknown functions. The [32] SDS-Page and silverstained blood types of humans are due to variations in surface glycoproteins of erythrocytes. Disorders of the proteins in these membranes are associated with many disorders, such as hereditary spherocytosis, hereditary elliptocytosis, hereditary stomatocytosis, and paroxysmal nocturnal hemoglobinuria.[][] The red blood cell membrane proteins organized according to their function: Transport • Band 3 - Anion transporter, also an important structural component of the erythrocyte cell membrane, makes up to 25% of the cell membrane surface, each red cell contains approximately one million copies. Defines the Diego Blood Group;[33] • Aquaporin 1 - water transporter, defines the Colton Blood Group; • Glut1 - glucose and L-dehydroascorbic acid transporter; • Kidd antigen protein - urea transporter; • RhAG - gas transporter, probably of carbon dioxide, defines Rh Blood Group and the associated unusual blood group phenotype Rhnull; • • • • • Na+/K+ - ATPase; Ca2+ - ATPase; Na+ K+ 2Cl- - cotransporter; Na+-Cl- - cotransporter; Na-H exchanger;
Red Blood Cell membrane major proteins
470
• K-Cl - cotransporter; • Gardos Channel.
Red blood cell Cell adhesion • ICAM-4 - interacts with integrins; • BCAM - a glycoprotein that defines the Lutheran blood group and also known as Lu or laminin-binding protein. Structural role - The following membrane proteins establish linkages with skeletal proteins and may play an important role in regulating cohesion between the lipid bilayer and membrane skeleton, likely enabling the red cell to maintain its favorable membrane surface area by preventing the membrane from collapsing (vesiculating). • Ankyrin-based macromolecular complex - proteins linking the bilayer to the membrane skeleton through the interaction of their cytoplasmic domains with Ankyrin. • Band 3 - also assembles various glycolytic enzymes, the presumptive CO2 transporter, and carbonic anhydrase into a macromolecular complex termed a “metabolon,” which may play a key role in regulating red cell metabolism and ion and gas transport function); • RhAG - also involved in transport, defines associated unusual blood group phenotype Rhmod. • Protein 4.1R-based macromolecular complex - proteins interacting with Protein 4.1R. • Protein 4.1R - weak expression of Gerbich antigens; • Glycophorin C and D - glycoprotein, defines Gerbich Blood Group; • XK - defines the Kell Blood Group and the Mcleod unusual phenotype (lack of Kx antigen and greatly reduced expression of Kell antigens); • RhD/RhCE - defines Rh Blood Group and the associated unusual blood group phenotype Rhnull; • Duffy protein - has been proposed to be associated with chemokine clearance;[34] • Adducin - interaction with band 3; • Dematin- interaction with the Glut1 glucose transporter.
[][]
471
Surface electrostatic potential
The zeta potential is an electrochemical property of cell surfaces that is determined by the net electrical charge of molecules exposed at the surface of cell membranes of the cell. The normal zeta potential of the erythrocyte is -15.7 millivolts (mV).[35] Much of this potential appears to be contributed by the exposed sialic acid residues in the membrane: their removal results in zeta potential of -6.06 mV.
Clinical notes
Separation and blood doping
Red blood cells can be obtained from whole blood by centrifugation, which separates the cells from the blood plasma in a process known as blood fractionation. Packed red blood cells, which are made in this way from whole blood with the plasma removed, are used in transfusion medicine.[36] During plasma donation, the red blood cells are pumped back into the body right away and only the plasma is collected. Some athletes have tried to improve their performance by blood doping: first about 1 litre of their blood is extracted, then the red blood cells are isolated, frozen and stored, to be reinjected shortly before the competition. (Red blood cells can be conserved for 5 weeks at −79 °C.) This practice is hard to detect but may endanger the human cardiovascular system which is not equipped to deal with blood of the resulting higher viscosity. Another method of blood doping involves injection with erythropoietin in order to stimulate production of red blood cells.
Red blood cell
472
Artificially grown red blood cells
In 2008 it was reported that human embryonic stem cells had been successfully coaxed into becoming erythrocytes in the lab. The difficult step was to induce the cells to eject their nucleus; this was achieved by growing the cells on stromal cells from the bone marrow. It is hoped that these artificial erythrocytes can eventually be used for blood transfusions.[37]
Diseases and diagnostic tools
Blood diseases involving the red blood cells include: • Anemias (or anaemias) are diseases characterized by low oxygen transport capacity of the blood, because of low red cell count or some abnormality of the red blood cells or the hemoglobin. • Iron deficiency anemia is the most common anemia; it occurs when the dietary intake or absorption of iron is insufficient, and hemoglobin, which contains iron, cannot be formed • Sickle-cell disease is a genetic disease that results in abnormal hemoglobin molecules. When these release their oxygen load in the tissues, they become insoluble, leading to mis-shaped red blood cells. These sickle shaped red cells are less deformable and viscoelastic meaning that they have become rigid and can cause blood vessel blockage, pain, strokes, and other tissue damage. • Thalassemia is a genetic disease that results in the production of an abnormal ratio of hemoglobin subunits. • Spherocytosis is a genetic disease that causes a defect in the red blood cell's cytoskeleton, causing the red blood cells to be small, sphere-shaped, and fragile instead of donut-shaped and flexible. • Pernicious anemia is an autoimmune disease wherein the body lacks intrinsic factor, required to absorb vitamin B12 from food. Vitamin B12 is needed for the production of hemoglobin. • Aplastic anemia is caused by the inability of the bone marrow to produce blood cells. • Pure red cell aplasia is caused by the inability of the bone marrow to produce only red blood cells. • Hemolysis is the general term for excessive breakdown of red blood cells. It can have several causes and can result in hemolytic anemia. • The malaria parasite spends part of its life-cycle in red blood cells, feeds on their hemoglobin and then breaks them apart, causing fever. Both sickle-cell disease and thalassemia are more common in malaria areas, because these mutations convey some protection against the parasite.
Affected by Sickle-cell disease, red blood cells alter shape and threaten to damage internal organs.
Effect of osmotic pressure on blood cells
• Polycythemias (or erythrocytoses) are diseases characterized by a surplus of red blood cells. The increased viscosity of the blood can cause a number of symptoms. • In polycythemia vera the increased number of red blood cells results from an abnormality in the bone marrow.
Red blood cell
473
• Several microangiopathic diseases, including disseminated intravascular coagulation and thrombotic microangiopathies, present with pathognomonic (diagnostic) red blood cell fragments called schistocytes. These pathologies generate fibrin strands that sever red blood cells as they try to move past a thrombus.
Micrographs of the effects of osmotic pressure
• Inherited hemolytic anemias caused by abnormalities of the erythrocyte membrane comprise an important group of inherited disorders. These disorders are characterized by clinical and biochemical heterogeneity and also genetic heterogeneity, as evidenced by recent molecular studies. • The Hereditary spherocytosis (HS) syndromes are a group of inherited disorders characterized by the presence of spherical-shaped erythrocytes on the peripheral blood smear. HS is found worldwide. It is the most common inherited anemia in individuals of northern European descent, affecting approximately 1 in 1000-2500 individuals depending on the diagnostic criteria. The primary defect in hereditary spherocytosis is a deficiency of membrane surface area. Decreased surface area may produced by two different mechanisms: 1) Defects of spectrin, ankyrin, or protein 4.2 lead to reduced density of the membrane skeleton, destabilizing the overlying lipid bilayer and releasing band 3-containing microvesicles. 2) Defects of band 3 lead to band 3 deficiency and loss of its lipid-stabilizing effect. This results in the loss of band 3-free microvesicles. Both pathways result in membrane loss, decreased surface area, and formation of spherocytes with decreased deformability. These deformed erythrocytes become trapped in the hostile environment of the spleen where splenic conditioning inflicts further membrane damage, amplifying the cycle of membrane injury. • Hereditary elliptocytosis • Hereditary pyropoikilocytosis • Hereditary stomatocytosis[38] • Hemolytic transfusion reaction is the destruction of donated red blood cells after a transfusion, mediated by host antibodies, often as a result of a blood type mismatch. Several blood tests involve red blood cells, including the RBC count (the number of red blood cells per volume of blood), the hematocrit (percentage of blood volume occupied by red blood cells), and the erythrocyte sedimentation rate. The blood type needs to be determined to prepare for a blood transfusion or an organ transplantation.
References
[2] Erich Sackmann, Biological Membranes Architecture and Function., Handbook of Biological Physics, (ed. R.Lipowsky and E.Sackmann, vol.1, Elsevier, 1995 [3] Laura Dean. Blood Groups and Red Cell Antigens (http:/ / www. ncbi. nlm. nih. gov/ books/ bv. fcgi?call=bv. View. . ShowTOC& rid=rbcantigen. TOC& depth=2) [5] "Swammerdam, Jan (1637–1680)", McGraw Hill AccessScience, 2007. Accessed 27 December 2007. [6] Red Gold - Blood History Timeline (http:/ / www. pbs. org/ wnet/ redgold), PBS 2002. Accessed 27 December 2007. [27] Iron Metabolism (http:/ / www. med-ed. virginia. edu/ courses/ path/ innes/ nh/ iron. cfm), University of Virginia Pathology. Accessed 22 September 2007. [28] Iron Transport and Cellular Uptake (http:/ / sickle. bwh. harvard. edu/ iron_transport. html) by Kenneth R. Bridges, Information Center for Sickle Cell and Thalassemic Disorders. Accessed 22 September 2007. [35] Tokumasu F, Ostera GR, Amaratunga C, Fairhurst RM (2012) Modifications in erythrocyte membrane zeta potential by Plasmodium falciparum infection. Exp Parasitol [37] First red blood cells grown in the lab (http:/ / www. newscientist. com/ article/ dn14565-first-red-blood-cells-grown-in-the-lab. html), New Scientist News, 19 August 2008
Red blood cell
474
External links
• Blood Groups and Red Cell Antigens (http://www.ncbi.nlm.nih.gov/books/bv.fcgi?call=bv.View.. ShowTOC&rid=rbcantigen.TOC&depth=2) by Laura Dean. Searchable and downloadable online textbook in the public domain. • Database of vertebrate erythrocyte sizes (http://www.genomesize.com/cellsize/). • Red Gold (http://www.pbs.org/wnet/redgold), PBS site containing facts and history
Megakaryocyte
475
Megakaryocyte
Megakaryocyte
two megakaryocytes in bone marrow, slightly below centre Latin Code megakaryocytus TH H2.00.04.3.05003
[1]
The megakaryocyte is a bone marrow cell responsible for the production of blood thrombocytes (platelets), which are necessary for normal blood clotting. Megakaryocytes normally account for 1 out of 10,000 bone marrow cells but can increase in number nearly 10-fold during the course of certain diseases.[]
Structure
In general, megakaryocytes are 10 to 15 times larger than a typical red blood cell, averaging 50-100 μm in diameter. During its maturation, the megakaryocyte grows in size and replicates its DNA without cytokinesis in a process called endomitosis. As a result, the nucleus of the megakaryocyte can become very large and lobulated, which, under a light microscope, can give the false impression that there are several nuclei. In some cases, the nucleus may contain up to 64N DNA, or 32 copies of the normal complement of DNA in a human cell. The cytoplasm, just as the platelets that bud off from it, contains α-granula and Dense bodies.
Megakaryocyte development
Megakaryocytes are derived from hematopoietic stem cell precursor cells in the bone marrow. They are primarily produced by the liver, kidney, spleen, and bone marrow. These multipotent stem cells live in the marrow sinusoids and are capable of producing all types of blood cells depending on the signals they receive. The primary signal for megakaryocyte production is thrombopoietin or TPO. TPO is sufficient but not absolutely necessary[] for inducing differentiation of progenitor cells in the bone marrow towards a final megakaryocyte phenotype. Other molecular signals for megakaryocyte differentiation include GM-CSF, IL-3, IL-6, IL-11, chemokines (SDF-1 ; FGF-4),[] and [] erythropoietin. The megakaryocyte develops through the following lineage: CFU-Me (pluripotential hemopoietic stem cell or hemocytoblast) -> megakaryoblast -> promegakaryocyte -> megakaryocyte. J
Megakaryocyte The cell eventually reaches megakaryocyte stage and loses its ability to divide. However, it is still able to replicate its DNA and continue development, becoming polyploid.[] The cytoplasm continues to expand and the DNA complement can increase up to 64N.
476
Platelet release
Once the cell has completed differentiation and become a mature megakaryocyte, it begins the process of producing platelets. The maturation process occurs via endomitotic synchronous replication whereby the cytoplasmic volume enlarges as the number of nuclei multiplies without cellular division. The cell ceases its growth at 4N, 8N or 16N, becomes granular, and begins to produce platelets.[1] Thrombopoietin plays a role in inducing the megakaryocyte to form small proto-platelet processes. Platelets are held within these internal membranes within the cytoplasm of megakaryocytes. There are two proposed mechanisms for platelet release. In one scenario, these proto-platelet processes break up explosively to become platelets.[] Alternatively, the cell may form platelet ribbons into blood vessels. The ribbons are formed via pseudopodia and they are able to continuously emit platelets into circulation. In either scenario, each of these proto-platelet processes can give rise to 2000-5000 new platelets upon breakup. Overall, 2/3 of these newly-produced platelets will remain in circulation while 1/3 will be sequestered by the spleen. After budding off platelets, what remains is mainly the cell nucleus. This crosses the bone marrow barrier to the blood and is consumed in the lung by alveolar macrophages.
Effects of cytokines
Cytokines are signals used in the immune system for intercellular communication. There are many cytokines which affect megakaryocytes. Certain cytokines such as IL-3, IL-6, IL-11, LIF, erythropoietin, and thrombopoietin all stimulate the maturation of megakaryocytic progenitor cells.[] Other signals such as PF4, CXCL5, CXCL7, and CCL5 inhibit platelet formation.[]
Thrombopoietin
Thrombopoietin (TPO) is a 353-amino acid protein located on chromosome 3p27. TPO is primarily synthesized in the liver[] but can be made by kidneys, testes, brain, and even bone marrow stromal cells. It has high homology with erythropoietin. It is essential for the formation of an adequate quantity of platelets. Mice lacking TPO or the TPO receptor (Mpl) have a 90% reduction in circulating platelet number, although the platelets are normal in morphology and function.[]
Disorders involving megakaryocytes
Megakaryocytes are directly responsible for producing platelets which are needed for the formation of a thrombus, or blood clot. There are several diseases which are directly attributable to abnormal megakaryocyte function or abnormal platelet function.[]
Essential Thrombocythemia
Essential thrombocytosis (ET-Also known as Essential thrombocythemia) is a disorder characterized by extremely high numbers of circulating platelets. The disease occurs in 1-2 per 100,000 people. The current WHO requirements for diagnosis include > 600,000 platelets/μL of blood (normal 150,000-400,000) and a bone marrow biopsy. Some of the consequences of having such high numbers of platelets include thrombosis or clots throughout the body. Thrombi form more frequently in arteries than veins. Ironically, having platelet counts above 1,000,000 platelets/μL can lead to hemorrhagic events.[] Recent evidence suggests that the majority of ET cases are due to a mutation in the JAK2 protein, a member of the JAK-STAT pathway.[] Evidence suggests this mutation renders the megakaryocyte hypersensitive to thrombopoietin and causes clonal proliferation of megakaryocytes. There is a significant risk of
Megakaryocyte transformation to leukemia with this disorder. The primary treatment consists of anagrelide or hydroxyurea to lower platelet levels.
477
Congenital amegakaryocytic thrombocytopenia (CAMT)
Congenital amegakaryocytic thrombocytopenia (CAMT) is a rare inherited disorder. The primary manifestations are thrombocytopenia and megakaryocytopenia, i.e. low numbers of platelets and megakaryocytes. There is an absence of megakaryocytes in the bone marrow with no associated physical abnormalities.[] The cause for this disorder appears to be a mutation in the gene for the TPO receptor, c-mpl, despite high levels of serum TPO.[][] In addition, there may be abnormalities with the central nervous system including the cerebrum and cerebellum which could cause symptoms.[] The primary treatment for CAMT is bone marrow transplantation. Bone marrow/stem cell transplant is the only remedy for this genetic disease. Frequent platelet transfusions are required to keep the patient from bleeding to death until transplant has been completed, although this is not always the case. One of the few non-medical research related sources on the web with some information on CAMT is: • CAMT Specific Infant Bone Marrow Transplant Journal [2] There appears to be no generic resource for CAMT patients on the web and this is potentially due to the rariety of the disease.
External links
• Megakaryocytes: Mature [3] Many microscopic images of mature megakaryocytes including in disease settings. • Cell size comparison [4] • CAMT Specific Infant Bone Marrow Transplant Journal [2]
References
Monocyte
478
Monocyte
Monocyte
Monocytes under a light microscope from a peripheral blood smear surrounded by red blood cells. Latin Code monocytus TH H2.00.04.1.02010
[1]
Monocytes are a type of white blood cell and are part of the innate immune system of vertebrates including all mammals (humans included), birds, reptiles, and fish. Monocytes play multiple roles in immune function. Such roles include: (1) replenish resident macrophages and dendritic cells under normal states, and (2) in response to inflammation signals, monocytes can move quickly (approx. 8–12 hours) to sites of infection in the tissues and divide/differentiate into macrophages and dendritic cells to elicit an immune response. Half of them are stored in the spleen.[1] Monocytes are usually identified in stained smears by their large kidney shaped or notched nucleus.
Physiology
Monocytes are produced by the bone marrow from hematopoietic stem cell precursors called monoblasts. Monocytes circulate in the bloodstream for about one to three days and then typically move into tissues throughout the body. They constitute between three to eight percent of the leukocytes in the blood. Half of them are stored as a reserve in the spleen in clusters in the red pulp's Cords of Billroth.[1] In the tissues, monocytes mature into different types of macrophages at different anatomical locations. Monocytes are the largest corpuscles in the blood. Monocytes which migrate from the bloodstream to other tissues will then differentiate into tissue resident macrophages or dendritic cells. Macrophages are responsible for protecting tissues from foreign substances, but are also suspected to be important in the formation of important organs like the heart and brain. They are cells that possess a large smooth nucleus, a large area of cytoplasm, and many internal vesicles for processing foreign material. Monocytes and their macrophage and dendritic-cell progeny serve three main functions in the immune system. These are phagocytosis, antigen presentation, and cytokine production. Phagocytosis is the process of uptake of microbes and particles followed by digestion and destruction of this material. Monocytes can perform phagocytosis using intermediary (opsonising) proteins such as antibodies or complement that coat the pathogen, as well as by binding to the microbe directly via pattern-recognition receptors that recognize pathogens. Monocytes are also capable of killing infected host cells via antibody, termed antibody-mediated cellular cytotoxicity. Vacuolization may be present in a cell that has recently phagocytized foreign matter. Microbial fragments that remain after such digestion can serve as antigen. The fragments can be incorporated into MHC molecules and then traffic to the cell surface of monocytes (and macrophages and dendritic cells). This process is called antigen presentation and it leads to activation of T lymphocytes, which then mount a specific immune response against the antigen.
Monocyte Other microbial products can directly activate monocytes and this leads to production of pro-inflammatory and with some delay of anti-inflammatory cytokines. Typical cytokines produced by monocytes are TNF, IL-1, and IL-12.
479
Monocyte subpopulations
There are at least three types of monocytes in human blood:[2] a) the classical monocyte is characterized by high level expression of the CD14 cell surface receptor (CD14++ CD16- monocyte) b) the non-classical monocyte shows low level expression of CD14 and with additional co-expression of the CD16 receptor (CD14+CD16++ monocyte).[3] c) the intermediate monocyte with high level expression of CD14 and low level expression of CD16 (CD14++CD16+ monocytes). There appears to be a developmental relationship in that the classical monocytes develop into the intermediate monocytes to then become the non-classical CD14+CD16++ monocytes. Hence the non-classical monocytes may represent a more mature version. After stimulation with microbial products the CD14+CD16++ monocytes produce high amounts of pro-inflammatory cytokines like tumor necrosis factor and interleukin-12. Said et al. showed that activated monocytes express high levels of PD-1 which might explain the higher expression of PD-1 in CD14+CD16++ monocytes as compared to CD14++CD16- monocytes. Triggering monocytes-expressed PD-1 by its ligand PD-L1 induces IL-10 production which activates CD4 Th2-cells and inhibits CD4 Th1-cell function.[4]
Diagnostic use
A monocyte count is part of a complete blood count and is expressed either as a ratio of monocytes to the total number of white blood cells counted, or by absolute numbers. Both may be useful in determining or refuting a possible diagnosis.
Monocytosis
Monocytosis is the state of excess monocytes in the peripheral blood. It may be indicative of various disease states. Examples of processes that can increase a monocyte count include: • chronic inflammation • stress response • • • • • hyperadrenocorticism immune-mediated disease pyogranulomatous disease necrosis red cell regeneration
• Viral Fever • sarcoidosis
A scanning electron microscope (SEM) image of normal circulating human blood. One can see red blood cells, several knobby white blood cells including lymphocytes, a monocyte, a neutrophil, and many small disc-shaped platelets.
A high count of CD14+CD16++ monocytes is found in severe infection (sepsis)[5] and a very low count of these cells is found after therapy with immuno-suppressive glucocorticoids[6]
Monocyte
480
Monocytopenia
Monocytopenia is a form of leukopenia associated with a deficiency of monocytes.
Dendritic cells
Monocytes can be used to generate dendritic cells in vitro by adding cytokines like Granulocyte Monocyte Colony Stimulating Factor (GMCSF) and IL-4.[]
Blood content
Reference ranges for blood tests of white blood cells, comparing monocyte amount (shown in green) with other cells.
References
[1] Swirski FK, Nahrendorf M, Etzrodt M, Wildgruber M, Cortez-Retamozo V, Panizzi P, Figueiredo J-L, Kohler RH, Chudnovskiy A, Waterman P, Aikawa E, Mempel TR, Libby P, Weissleder R, Pittet MJ. (2009). Identification of Splenic Reservoir Monocytes and Their Deployment to Inflammatory Sites. Science, 325: 612-616. PMID 19644120 [2] Ziegler-Heitbrock, L et al (2010): Nomenclature of monocytes and dendritic cells in blood. Blood,116 (16): e74-e80. PMID 20628149 [3] Ziegler-Heitbrock, L: The CD14+ CD16+ Blood Monocytes: their Role in Infection and Inflammation, Review. J Leukocyte Biology, 81:584, 2007 PMID 17135573 [4] Elias A. Said et al. 2009, PD-1 Induced IL10 Production by Monocytes Impairs T-cell Activation in a Reversible Fashion. Nature Medicine. 2010; 452-9. [5] Fingerle, G., Pforte, A., Passlick, B., Blumenstein, M., Ströbel, M., Ziegler-Heitbrock, H.W.L.: The novel subset of CD14+ CD16+ blood monocytes is expanded in sepsis patients. Blood, 82: 3170-3176, 1993 PMID 7693040 [6] Fingerle-Rowson, G., Angstwurm, M., Andreesen, R., Ziegler-Heitbrock, H.W.L.:Selective depletion of CD14+ CD16+ monocytes by glucocorticoid therapy.Clin. Exp. Immunol., 112: 501-506, 1998 PMID 9649222
External links
• BU Histology Learning System: 01702ooa (http://www.bu.edu/histology/p/01702ooa.htm) • Human Monocytes - Prof. Dr. Ziegler-Heitbrock (http://www.monocyte.eu/) • Circulation of Body Fluids (http://www.simplylearnt.com/topic/Circulation-of-Body-Fluids)
Langerhans cell
481
Langerhans cell
Not to be confused with the cells of the islets of Langerhans, found in the pancreas, or Langhans giant cell. Langerhans cells are dendritic cells (antigen-presenting immune cells) of the skin and mucosa, and contain large granules called Birbeck granules. They are present in all layers of the epidermis, but are most prominent in the stratum spinosum.[] They also occur in the papillary dermis, particularly around blood vessels,[] as well as in the mucosa of the mouth, foreskin, and vagina.[] They can be found in other tissues, such as lymph nodes, particularly in association with the condition Langerhans cell histiocytosis (LCH).
Section of skin showing large numbers of dendritic cells (Langerhans cells) in the epidermis. (M. ulcerans infection, S100 immunoperoxidase stain.)
History
The Langerhans cell is named after Paul Langerhans, a German physician and anatomist, who discovered the cells at the age of 21 while he was a medical student.[1] Because of their dendritic nature, he mistakenly identified the cells as part of the nervous system.[]
Function
In skin infections, the local Langerhans cells take up and process microbial antigens to become fully functional antigen-presenting cells. Generally, dendritic cells in tissue are active in the capture, uptake and processing of antigens. Once dendritic cells arrive in secondary lymphoid tissue, however, they lose these properties while gaining the capacity to interact with naive T-cells. Langerhans cells derive from the cellular differentiation of monocytes with the marker "Gr-1" (also known as "Ly-6G/Ly-6C"). This differentiation requires stimulation by colony stimulating factor (CSF)-1.[2] They are similar in morphology and function to macrophages.
Langerhans cell Langerin is a protein found in Langerhans cells,[] and other types of dendritic cells.[]
482
Clinical significance
LCH
In the rare disease Langerhans cell histiocytosis (LCH), an excess of these cells is produced. This can cause damage to skin, bone and other organs.
HIV
Langerhans cells may be initial cellular targets in the sexual transmission of HIV,[3] and may be a target, reservoir, and vector of dissemination.[4] Langerhans cells have been observed in foreskin, vaginal, and oral mucosa of humans; the lower concentrations in oral mucosa suggest that it is not a likely source of HIV infection relative to foreskin and vaginal mucosa.[]
The representation of Langerhans cells in the Cell Ontology. A portion of the Cell Ontology is shown with ovals corresponding to cell types defined in the ontology and arrows corresponding to relations between those cell types. Langerhans cell is represented by a yellow oval; blue arrows correspond to is_a relations, and orange arrows correspond to develops_from relations. Only a subset of [] Langerhans cell parent types are included in the figure.
On March 4, 2007 the online Nature Medicine magazine published the letter "Langerin is a natural barrier to HIV-1 transmission by Langerhans cells."[5] One of the authors of the study, Teunis Geijtenbeek, said that "Langerin is able to scavenge viruses from the surrounding environment, thereby preventing infection" and "since generally all tissues on the outside of our bodies have Langerhans cells, we think that the human body is equipped with an antiviral defense mechanism, destroying incoming viruses."[6]
Langerhans cell
483
References External links
• Langerhans Cell Histiocytosis (http://www.emedicine.com/derm/topic216.htm#) at eMedicine • http://www.trinity.edu/rblyston/MicroA/Lectures/L34-html/img018.jpgWikipedia:Link rot Illustration at trinity.edu • Brun, Scott C.; Rubin, Peter A. D. (1997). "25 year old kickboxer with progressive proptosis" (http://www.djo. harvard.edu/site.php?url=/physicians/gr/356). Digital Journal of Ophthalmology 3 (26). • Langerhans Cells (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Langerhans+Cells) at the US National Library of Medicine Medical Subject Headings (MeSH)
Platelet
484
Platelet
Platelet
Image from a light microscope (40×) from a peripheral blood smear surrounded by red blood cells. One normal platelet can be seen in the upper left side of the image (purple) and is significantly smaller in size than the red blood cells (stained pink). Two giant platelets (stained purple) are also visible. Latin Code thrombocytes TH H2.00.04.1.03001
[1]
Platelets, or thrombocytes (from Greek θρόμβος, "clot" and κύτος, "cell"), are small, disk shaped clear cell fragments (i.e. cells that do not have a nucleus), 2–3 µm in diameter,[1] which are derived from fragmentation of precursor megakaryocytes. The average lifespan of a platelet is normally just 5 to 9 days. Platelets are a natural source of growth factors. They circulate in the blood of mammals and are involved in hemostasis, leading to the formation of blood clots. If the number of platelets is too low, excessive bleeding can occur. However, if the number of platelets is too high, blood clots can form (thrombosis), which may obstruct blood vessels and result in such events as a stroke, myocardial infarction, pulmonary embolism or the blockage of blood vessels to other parts of the body, such as the extremities of the arms or legs. An abnormality or disease of the platelets is called a thrombocytopathy,[2] which could be either a low number of platelets (thrombocytopenia), a decrease in function of platelets (thrombasthenia), or an increase in the number of platelets (thrombocytosis). There are disorders that reduce the number of platelets, such as heparin-induced thrombocytopenia (HIT) or thrombotic thrombocytopenic purpura (TTP) that typically cause thromboses, or clots, instead of bleeding. Platelets release a multitude of growth factors including platelet-derived growth factor (PDGF), a potent chemotactic agent, and TGF beta, which stimulates the deposition of extracellular matrix. Both of these growth factors have been shown to play a significant role in the repair and regeneration of connective tissues. Other healing-associated growth factors produced by platelets include basic fibroblast growth factor, insulin-like growth factor 1, platelet-derived epidermal growth factor, and vascular endothelial growth factor. Local application of these factors in increased concentrations through Platelet-rich plasma (PRP) has been used as an adjunct to wound healing for several decades.[3][4][5][6][7][8][9]
Platelet
485
Kinetics
• The physiological range for platelets is (150 – 400) × 103 per mm3. • Platelets are produced in blood cell formation (thrombopoiesis) in bone marrow, by budding off from megakaryocytes. • Megakaryocyte and platelet production is regulated by thrombopoietin, a hormone usually produced by the liver and kidneys. • Each megakaryocyte produces between 5,000 and 10,000 platelets. • Around 1011 platelets are produced each day by an average healthy adult.
• Reserve platelets are stored in the spleen, and are released when needed by sympathetically induced splenic contraction. • The lifespan of circulating platelets is 5 to 9 days. • Old platelets are destroyed by phagocytosis in the spleen and by Kupffer cells in the liver.
HSC=hematopoietic stem cell, Progenitor=progenitor cell, L-blast=lymphoblast, lymphocyte, Mo-blast=monoblast, monocyte, myeloblast, Pro-M=promyelocyte, myelocyte, Meta-M=metamyelocyte, neutrophil, eosinophil, basophil, Pro-E=proerythroblast, Baso-E=basophilic erythroblast, poly-E=polychromatic erythroblast, Ortho-E=Orthochromatic erythroblast, erythrocyte, promegakaryocyte, megakaryocyte, platelet.
Thrombus formation
The function of platelets is the maintenance of hemostasis. This is achieved primarily by the formation of thrombi, when damage to the endothelium of blood vessels occurs. On the converse, thrombus formation must be inhibited at times when there is no damage to the endothelium.
Activation
The inner surface of blood vessels is lined with a thin layer of endothelial cells that, in normal hemostasis, acts to inhibit platelet activation by producing nitric oxide, endothelial-ADPase, and PGI2. Endothelial-ADPase clears away the platelet activator, ADP. Endothelial cells produce a protein called von Willebrand factor (vWF), a cell adhesion ligand, which helps endothelial cells adhere to collagen in the basement membrane. Under physiological conditions, collagen is not exposed to the bloodstream. vWF is secreted constitutively into the plasma by the endothelial cells, and is stored in granules within the endothelial cell and in platelets.
Aggregation of platelets. Platelet rich human blood plasma (left vial) is a turbid liquid. Upon addition of ADP, platelets are activated and start to aggregate, forming white flakes (right vial).
Platelet When the endothelial layer is injured, collagen, vWF and tissue factor from the subendothelium is exposed to the bloodstream. When the platelets contact collagen or vWF, they are activated (e.g. to clump together). They are also activated by thrombin (formed with the help of tissue factor). They can also be activated by a negatively charged surface, such as glass. Non-physiological flow conditions (especially high values of shear stress) caused by arterial stenosis or artificial devices (Mechanical Heart Valves, blood pumps etc) can also lead to platelet activation.[10] Platelet activation further results in the scramblase-mediated transport of negatively charged phospholipids to the platelet surface. These phospholipids provide a catalytic surface (with the charge provided by phosphatidylserine and phosphatidylethanolamine) for the tenase and prothrombinase complexes. Calcium ions are essential for binding of these coagulation factors. Shape change Activated platelets change in shape to become more spherical, and pseudopods form on their surface. Thus they assume a stellate shape. Granule secretion Platelets contain alpha and dense granules. Activated platelets excrete the contents of these granules into their canalicular systems and into surrounding blood. There are three types of granules: • dense (or delta) granules (containing ADP or ATP, calcium, and serotonin) • lambda granules – similar to lysosomes and contain several hydrolytic enzymes.
Scanning electron micrograph of blood cells. From left to right: human erythrocyte, activated thrombocyte (platelet), leukocyte.
486
• Alpha granules (containing P-selectin, platelet factor 4, transforming growth factor-β1, platelet-derived growth factor, fibronectin, B-thromboglobulin, vWF, fibrinogen, and coagulation factors V and XIII). Thromboxane A2 synthesis Platelet activation initiates the arachidonic acid pathway to produce TXA2. TXA2 is involved in activating other platelets and its formation is inhibited by COX inhibitors, such as aspirin.
Adhesion and aggregation
Platelets aggregate, or clump together, using fibrinogen and von Willebrand factor (vWF) as a connecting agent. The most abundant platelet aggregation receptor is glycoprotein IIb/IIIa (gpIIb/IIIa); this is a calcium-dependent receptor for fibrinogen, fibronectin, vitronectin, thrombospondin, and vWF. Other receptors include GPIb-V-IX complex (vWF) and GPVI (collagen). Activated platelets will adhere, via glycoprotein (GP) Ia, to the collagen that is exposed by endothelial damage. Aggregation and adhesion act together to form the platelet plug. Myosin and actin filaments in platelets are stimulated to contract during aggregation, further reinforcing the plug.
Platelets clumping from a blood smear. May Grunwald-Giemsa. Light Microscopy, oil immersion 100x.
Platelet aggregation is stimulated by ADP, thromboxane, and α2 receptor-activation, but inhibited by other inflammatory products like PGI2 and PGD2. Platelet aggregation is enhanced by exogenous administration of anabolic steroids.
Platelet
487
Wound repair
The blood clot is only a temporary solution to stop bleeding; vessel repair is therefore needed. The aggregated platelets help this process by secreting chemicals that promote the invasion of fibroblasts from surrounding connective tissue into the wounded area to completely heal the wound or form a scar. The obstructing clot is slowly dissolved by the fibrinolytic enzyme, plasmin, and the platelets are cleared by phagocytosis.
ADP (purinergic/P2) receptors
Human platelets have three types of P2 receptors: P2X(1), P2Y(1) and P2Y(12). Although abnormalities in all three genes have been documented, but clinical correlation is available only for P2Y(12).[11] Patients with P2Y(12) defects have a mild to moderate bleeding diathesis, characterized by mucocutaneous bleeding and excessive post-surgical and post-traumatic blood loss. A defects in P2Y(12) should be suspected when ADP, even at concentrations ≥10 micro molar, is unable to induce full, irreversible platelet aggregation. Confirmation of the diagnosis is with tests that evaluate the degree of inhibition of adenylyl cyclase by ADP.
Other functions
• Clot retraction • • • • Procoagulant Inflammation Cytokine signalling Phagocytosis[12]
Cytokine signaling
In addition to being the chief cellular effector of hemostasis, platelets are rapidly deployed to sites of injury or infection, and potentially modulate inflammatory processes by interacting with leukocytes and by secreting cytokines, chemokines, and other inflammatory mediators.[13][14][15][16] Platelets also secrete platelet-derived growth factor (PDGF).
Role in disease
High and low counts
A normal platelet count in a healthy individual is between 150,000 and 450,000 per μL (microlitre) of blood ((150–450)×109/L).[] Ninety-five percent of healthy people will have platelet counts in this range. Some will have statistically abnormal platelet counts while having no demonstrable abnormality. However, if it is either very low or very high, the likelihood of an abnormality being present is higher. Both thrombocytopenia and thrombocytosis may present with Diagram of the internal structure of a platelet coagulation problems. In general, low platelet counts increase bleeding risks; however there are exceptions (such as immune-mediated heparin-induced thrombocytopenia or paroxysmal nocturnal hemoglobinuria). High counts may lead to thrombosis, although this is mainly when the elevated count is due to myeloproliferative disorder. Transfusion is generally used only to correct unusually low platelet counts (typically below (10–15)×109/L). Transfusion is contraindicated in thrombotic thrombocytopenic purpura (TTP), as it fuels the coagulopathy. In patients undergoing surgery, a level below 50×109/L is associated with abnormal surgical bleeding, and regional
Platelet anaesthetic procedures such as epidurals are avoided for levels below 80×109/L.[17] Normal platelet counts are not a guarantee of adequate function. In some states, the platelets, while being adequate in number, are dysfunctional. For instance, aspirin irreversibly disrupts platelet function by inhibiting cyclooxygenase-1 (COX1), and hence normal hemostasis. The resulting platelets are unable to produce new cyclooxygenase because they have no DNA. Normal platelet function will not return until the use of aspirin has ceased and enough of the affected platelets have been replaced by new ones, which can take over a week. Ibuprofen, another NSAID, does not have such a long duration effect, with platelet function usually returning within 24 hours,[18] and taking ibuprofen before aspirin sometimes may prevent the irreversible effects of aspirin.[19] Uremia, a consequence of renal failure, leads to platelet dysfunction that may be ameliorated by the administration of desmopressin.
488
Medications
Oral agents often used to alter/suppress platelet function include aspirin, clopidogrel, cilostazol, ticlopidine, ticagrelor and prasugrel. Intravenous agents often used to alter/suppress platelet function include: abciximab, eptifibatide, tirofiban. In addition to platelet transfusion, hematopoetic agents such as Oprelvekin, Romiplostim, and Eltrombopag can be used to increase platelet counts.
Diseases
Disorders leading to a reduced platelet count: • Thrombocytopenia • Idiopathic thrombocytopenic purpura – also known as immune thrombocytopenic purpura (ITP) • Thrombotic thrombocytopenic purpura • Drug-induced thrombocytopenic purpura (for example heparin-induced thrombocytopenia (HIT)) • Gaucher's disease • Aplastic anemia • Onyalai Alloimmune disorders • Fetomaternal alloimmune thrombocytopenia • Some transfusion reactions Disorders leading to platelet dysfunction or reduced count: • • • • HELLP syndrome Hemolytic-uremic syndrome Chemotherapy Dengue
Disorders featuring an elevated count: • Thrombocytosis, including essential thrombocytosis (elevated counts, either reactive or as an expression of myeloproliferative disease); may feature dysfunctional platelets Disorders of platelet adhesion or aggregation: • Bernard-Soulier syndrome • Glanzmann thrombasthenia Disorders of platelet granule amount or release • Hermansky-Pudlak Syndrome • Gray platelet syndrome
Platelet Disorders of platelet metabolism • Decreased cyclooxygenase activity, induced or congenital • Storage pool defects, acquired or congenital Disorders that compromise platelet signaling: • Wiskott–Aldrich syndrome Disorders in which platelets play a key role: • • • • • • • • Atherosclerosis Coronary artery disease, CAD and myocardial infarction, MI Cerebrovascular disease and Stroke, CVA (cerebrovascular accident) Peripheral artery occlusive disease (PAOD) Cancer[20] Malaria[21] Asthma[22][23] Samter’s Triad (Aspirin Exacerbated Respiratory Disease/AERD)[24][25]
489
Laboratory findings in various platelet and coagulation disorders (V - T)
Condition Vitamin K deficiency or warfarin Disseminated intravascular coagulation Von Willebrand disease Hemophilia Aspirin Thrombocytopenia Liver failure, early Liver failure, end-stage Uremia Congenital afibrinogenemia Factor V deficiency Prothrombin time Partial thromboplastin time Bleeding time Prolonged Prolonged Unaffected Unaffected Unaffected Unaffected Prolonged Prolonged Unaffected Prolonged Prolonged Normal or mildly prolonged Unaffected Prolonged Prolonged Prolonged Unaffected Unaffected Unaffected Prolonged Unaffected Prolonged Prolonged Prolonged Unaffected Unaffected Prolonged Shortened Prolonged Prolonged Unaffected Prolonged Prolonged Unaffected Prolonged Prolonged Prolonged Unaffected Unaffected Prolonged Prolonged Unaffected Unaffected Platelet count Unaffected Decreased Unaffected Unaffected Unaffected Decreased Unaffected Decreased Unaffected Unaffected Unaffected Unaffected Unaffected Decreased or unaffected Unaffected Unaffected
Factor X deficiency as seen in amyloid purpura Prolonged Glanzmann's thrombasthenia Bernard-Soulier syndrome Factor XII deficiency C1INH deficiency Unaffected Unaffected Unaffected Unaffected
Platelet
490
Discovery
Although red blood cells had been known since van Leeuwenhoek (1632–1723), the German anatomist Max Schultze (1825–1874) was the first to describe platelets.[][] He described "spherules" that were much smaller than red blood cells and that occasionally clumped and were found in collections of fibrous material. Giulio Bizzozero (1846–1901), building on Schultze's findings, used "living circulation" to study blood cells of amphibians microscopically in vivo. He is especially noted for discovering that platelets clump at the site of blood vessel injury, a process that precedes the formation of a blood clot. This observation confirmed the role of platelets in coagulation.[]
In transfusion medicine
Platelets are either isolated from collected units of whole blood and pooled to make a therapeutic dose or collected by apheresis, sometimes concurrently with plasma or red blood cells. The industry standard is for platelets to be tested for bacteria before transfusion to avoid septic reactions, which can be fatal. Recently the AABB Industry Standards for Blood Banks and Transfusion Services (5.1.5.1) has allowed for use of pathogen reduction technology as an alternative to bacterial screenings in platelets.[26] Pooled whole-blood platelets, sometimes called “random” platelets, are made primarily by two methods.[27] In the US, a unit of whole blood is placed into a large centrifuge in what is referred to as a “soft spin.” At these settings, the platelets remain suspended in the plasma. The platelet-rich plasma (PRP) is removed from the RBCs, then centrifuged at a faster setting to harvest the platelets from the plasma. In other Platelet concentrate. regions of the world, the unit of whole blood is centrifuged using settings that cause the platelets to become suspended in the “buffy coat” layer, which includes the platelets and the white blood cells. The “buffy coat” is isolated in a sterile bag, suspended in a small amount of red blood cells and plasma, then centrifuged again to separate the platelets and plasma from the red and white blood cells. Regardless of the initial method of preparation, multiple donations may be combined into one container using a sterile connection device to manufacture a single product with the desired therapeutic dose. Apheresis platelets are collected using a mechanical device that draws blood from the donor and centrifuges the collected blood to separate out the platelets and other components to be collected. The remaining blood is returned to the donor. The advantage to this method is that a single donation provides at least one therapeutic dose, as opposed to the multiple donations for whole-blood platelets. This means that a recipient is not exposed to as many different donors and has less risk of transfusion-transmitted disease and other complications. Sometimes a person such as a cancer patient who requires routine transfusions of platelets will receive repeated donations from a specific donor to further minimize the risk. Pathogen reduction of platelets using for example, riboflavin and UV light treatments can also be carried out to reduce the infectious load of pathogens contained in donated blood products, thereby reducing the risk of transmission of transfusion transmitted diseases.[28][29] Platelets are not cross-matched unless they contain a significant amount of red blood cells (RBCs), which results in a reddish-orange color to the product. This is usually associated with whole-blood platelets, as apheresis methods are more efficient than “soft spin” centrifugation at isolating the specific components of blood. An effort is usually made to issue type specific platelets, but this is not as critical as it is with RBCs. Platelets collected by either method have a very short shelf life, typically five days. This results in frequent problems with short supply, as testing the donations often requires up to a full day. Since there are no effective preservative
Platelet solutions for platelets, they lose potency quickly and are best when fresh. Platelets are stored under constant agitation at 20–24 °C. Storage at room temperature provides an environment where any bacteria that are introduced to the blood component during the collection process may proliferate and subsequently cause bacteremia in the patient. Regulations are in place in the United States that require products to be tested for the presence of bacterial contamination before transfusion.[30] Platelets, either apheresis or random-donor platelets, can be processed through a volume reduction process. In this process, the platelets are spun in a centrifuge and the excess plasma is removed, leaving 10 to 100 mL of platelet concentrate. Volume-reduced platelets are normally transfused only to neonatal and pediatric patients when a large volume of plasma could overload the child's small circulatory system. The lower volume of plasma also reduces the chances of an adverse transfusion reaction to plasma proteins.[] Volume reduced platelets have a shelf life of only four hours.[31]
491
Other species
Nucleated thrombocytes of nonmammalian vertebrates differ from the mammalian thrombocytes not only in having a nucleus and resembling B lymphocytes, but also these nucleated thrombocytes do not aggregate in response to ADP, serotonin and adrenaline (although they do aggregate with thrombin).[citation needed]
References
[10] Kroll, M., J. Hellums, et al. (1996). "Platelets and shear stress." Blood 88(5): 1525-1541 [11] Cattaneo M (2011) Molecular defects of the platelet P2 receptors.Purinergic Signal [22] Kornerup KN, Page CP. The role of platelets in the pathophysiology of asthma. Platelets. 2007 Aug 18(5):319-28. [23] http:/ / www. ncbi. nlm. nih. gov/ pubmed/ 17654302 [24] Laidlaw TM, Kidder MS, Bhattacharyya N, Xing W, Shen S, Milne GL, Castells MC, Chhay H, Boyce JA. Cysteinyl leukotriene overproduction in aspirin exacerbated respiratory disease is driven by platelet-adherent leukocytes. Blood. 2012 Jan 18. [25] http:/ / www. ncbi. nlm. nih. gov/ pubmed/ 22262771 [26] American Association of Blood Banks Standards for Blood Banks and Transfusion Services, Bethesda, MD: 22rd ed, AABB, 2003, Section 5.1.5.1. [30] AABB Standards for Blood Banks and Transfusion Services 26th Edition Bethesda, MD: AABB, 2009. [31] CBBS: Washed and volume-reduced Plateletpheresis units (http:/ / www. cbbsweb. org/ enf/ 2001/ pltwashvol. html). Cbbsweb.org (2001-10-25). Retrieved on 2011-11-14.
Osteoclast
492
Osteoclast
Osteoclast
Osteoclast, with bone below it, showing typical distinguishing characteristics: a large cell with multiple nuclei and a "foamy" cytosol. Latin Code osteoclastus TH H2.00.03.7.00005
[1]
An osteoclast (from the Greek words for "bone" (Οστό) and "broken" (κλαστός)) is a type of bone cell that removes bone tissue by removing its mineralized matrix and breaking up the organic bone (organic dry weight is 90% collagen). This process is known as bone resorption. Osteoclasts were discovered by Kolliker in 1873.[] Osteoclasts and osteoblasts are instrumental in controlling the amount of bone tissue: osteoblasts form bone, osteoclasts resorb bone. Osteoclasts are formed by the fusion of cells of the monocyte-macrophage cell line.[1] Osteoclasts are characterized by high expression of tartrate resistant acid phosphatase (TRAP) and cathepsin K.
Morphology
An osteoclast is a large cell that is 40 micrometer in diameter. It contains 15-20 closely packed oval-shaped nuclei. Osteoclasts are found in pits in the bone surface which are called resorption bays, or Howship's Lacunae. Osteoclasts are characterized by a cytoplasm with a homogeneous, "foamy" appearance. This appearance is due to a high concentration of vesicles and vacuoles. These vacuoles are lysosomes filled with acid phophatase. Osteoclast rough endoplasmic reticulum is sparse, and the Golgi complex is extensive.[2][3][4] At a site of active bone resorption, the osteoclast forms a specialized cell membrane, the "ruffled border," that touches the surface of the bone tissue.[1] The ruffled border, which facilitates removal of the
Tartrate resistant acid phosphatase positive osteoclast in cell culture
bony
matrix,
Osteoclast
493
is a morphologic characteristic of an osteoclast that is actively resorbing bone. The ruffled border increases surface area interface for bone resorption. The mineral portion of the matrix (called hydroxyapatite) includes calcium and phosphate ions. These ions are absorbed into small vesicles (see endocytosis), which move across the cell and eventually are released into the extracellular fluid, thus increasing levels of the ions in the blood.
Illustrated cross-section of an activated osteoclast
Origin
Since their discovery in 1873 there has been considerable debate about their origin. Three theories were dominant: from 1949 to 1970 the connective tissue origin was popular, which stated that osteoclasts and osteoblasts are of the same lineage, and ostoblasts fuse together to form osteoclasts. At certain times osteoclasts dissociate into osteoblasts, which finally form osteocytes. In the 1970s the biphyletic theory became popular; it states that osteoblasts and osteoclasts are of different lineage. It was in the beginning of 1980 that the monocyte phagocytic system was recognized as precursor of osteoclasts.[] Osteoclast formation requires the presence of RANKL (receptor activator of nuclear factor κβ ligand) and M-CSF (Macrophage colony-stimulating factor). These membrane bound proteins are produced by neighbouring stromal cells and osteoblasts, thus requiring direct contact between these cells and osteoclast [Precursor (chemistry)[precursors. M-CSF acts through its receptor on the osteoclast, c-fms (colony-stimulating factor 1 receptor), a transmembrane tyrosine kinase-receptor, leading to secondary messenger activation of tyrosine kinase Src. Both of these molecules are necessary for osteoclastogenesis and are widely involved in the differentiation of monocyte/macrophage derived cells. RANKL is a member of the tumour necrosis family (TNF), and is essential in osteoclastogenesis. RANKL knockout mice exhibit a phenotype of osteopetrosis and defects of tooth eruption, along with an absence or deficiency of osteoclasts. RANKL activates NF-κβ (nuclear factor-κβ) and NFATc1 (nuclear factor of activated t cells, cytoplasmic, calcineurin-dependent 1) through RANK. NF-κβ activation is stimulated almost immediately after RANKL-RANK interaction occurs, and is not upregulated. NFATc1 stimulation, however, begins ~24–48 hours after binding occurs and its expression has been shown to be RANKL dependent. Osteoclast differentiation is inhibited by osteoprotegerin (OPG), which is produced by osteoblasts and binds to RANKL thereby preventing interaction with RANK.
Osteoclast
494
Function
Once activated, osteoclasts move to areas of microfracture in the bone by chemotaxis. Osteoclasts lie in a small cavity called Howship's lacunae, formed from the digestion of the underlying bone. The sealing zone is the attachment of the osteoclast's plasma membrane to the underlying bone. Sealing zones are bounded by belts of specialized adhesion structures called podosomes. Attachment to the bone matrix is facilitated by integrin receptors, such as αvβ3, via the specific amino acid motif Arg-Gly-Asp in bone matrix proteins, such as osteopontin. The osteoclast releases hydrogen ions through the action of carbonic anhydrase (H2O + CO2 → HCO3- + H+) through the ruffled border into the resorptive cavity, acidifying and aiding dissolution of the mineralized bone matrix into Ca2+, H3PO4, H2CO3, water and other substances. Dysfunction of the carbonic anhydrase has been documented to cause some forms of osteopetrosis. Hydrogen ions are pumped against a high concentration gradient by proton pumps, specifically a unique vacuolar-ATPase. This enzyme has been targeted in the prevention of osteoporosis. In addition, several hydrolytic enzymes, such as members of the cathepsin and matrix metalloprotease(MMP) groups, are released to digest the organic components of the matrix. These enzymes are released into the compartment by lysosomes. Of these hydrolytic enzymes, cathepsin K is of most importance.
Cathepsin K and other cathepsins
Cathepsin K is a collagenolytic, papain-like, cysteine protease that is mainly expressed in osteoclasts, and is secreted into the resorptive pit. Cathepsin K is the major protease involved in the degradation of type I collagen and other noncollagenous proteins. Mutations in the cathepsin K gene are associated with pycnodysostosis, a hereditary osteopetrotic disease, characterised by lack of functional cathepsin K expression. Knockout studies of cathepsin K in mice lead to an osteopetrotic phenotype, which, is partially compensated by increased expression of proteases other that cathepsin K and enhanced osteoclastogenesis. Cathepsin K has an optimal enzymatic activity in acidic conditions. It is synthesized as a proenzyme with a molecular weight of 37kDa, and upon activation by autocatalytic cleavage, is transformed into the mature, active form with a molecular weight of ~27kDa. Upon polarization of the osteoclast over the site of resorption, cathepsin K is secreted from the ruffled border into the resorptive pit. Cathepsin K transmigrates across the ruffled border by intercellular vesicles and is then released by the functional secretory domain. Within these intercellular vesicles, cathepsin K, along with reactive oxygen species generated by TRAP, further degrades the bone extracellular matrix. Numerous other cathepsins are expressed in osteoclasts. These include cathepsin B, C, D, E, G, and L. The function of these cysteine and aspartic proteases is generally unknown within bone, and they are expressed at much lower levels than cathepsin K. Studies on cathepsin L knockout mice have been mixed, with a report of reduced trabecular bone in homozygous and heterozygous cathepsin L knockout mice compared to wild-type and another report finding no skeletal abnormalities.
Matrix metalloproteinases
The matrix metalloproteinases (MMPs) comprise a family of more than 20 zinc-dependent endopeptidases. The role of matrix metalloproteinases (MMPs) in osteoclast biology is ill-defined, but in other tissue they have been linked with tumor promoting activities, such as activation of growth factors and are required for tumor metastasis and angiogenesis. MMP-9 is associated with the bone microenvironment. It is expressed by osteoclasts, and is known to be required for osteoclast migration and is a powerful gelatinase. Transgenic mice lacking MMP-9 develop defects in bone development, intraosseous angiogenesis, and fracture repair. MMP-13 is believed to be involved in bone resorption and in osteoclast differentiation, as knockout mice revealed decreased osteoclast numbers, osteopetrosis, and decreased bone resorption.
Osteoclast MMPs expressed by the osteoclast include MMP-9, -10, -12, and -14. apart from MMP-9, little is known about their relevance to the osteoclast, however, high levels of MMP-14 are found at the sealing zone.
495
Regulation
Osteoclasts are regulated by several hormones, including parathyroid hormone (PTH) from the parathyroid gland, calcitonin from the thyroid gland, and growth factor interleukin 6 (IL-6). This last hormone, IL-6, is one of the factors in the disease osteoporosis, which is an imbalance between bone resorption and bone formation. Osteoclast activity is also mediated by the interaction of two molecules produced by osteoblasts, namely osteoprotegerin and RANK ligand. Note that these molecules also regulate differentiation of the osteoclast.[5]
Alternate use of term
An osteoclast can also be an instrument used to fracture and reset bones (the origin is Greek osteon:bone and klastos:broken). To avoid confusion, the cell was originally termed osotoclast. When the surgical instrument went out of use, the cell became known by its present name.
References
[1] Netter, Frank H. (1987), Musculoskeletal system: anatomy, physiology, and metabolic disorders. Summit, New Jersey: Ciba-Geigy Corporation ISBN 0-914168-88-6, p. 169 [2] Standring S., Ed. Gray's Anatomy. 39th ed. 2005, Elsevier [4] p. 378
External links
• MedicineNet (http://www.medterms.com/script/main/art.asp?articlekey=11794) • Osteoclasts (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Osteoclasts) at the US National Library of Medicine Medical Subject Headings (MeSH) • The Life of Osteoclast (http://www.youtube.com/watch?v=6Cn4uusbGk8) • Animation by Random42 Medical Animation on the role of osteoclasts in bone remodeling (http://www. random42.com/bone-biology-osteoblasts-and-osteoclasts)
Dendritic cell
496
Dendritic cell
Dendritic cells (DCs) are immune cells forming part of the mammalian immune system. Their main function is to process antigen material and present it on the surface to other cells of the immune system. That is, dendritic cells function as antigen-presenting cells. They act as messengers between the innate and adaptive immunity. Dendritic cells are present in tissues in contact with the external environment, such as the skin (where there is a specialized dendritic cell type called Langerhans cells) and the inner lining of the nose, lungs, stomach and intestines. They can also be found in an immature state in the blood. Once activated, they migrate to the lymph nodes where they interact with T cells and B cells to initiate and shape the adaptive immune response. At certain development stages they grow branched projections, the dendrites that give the cell its name (δένδρον or déndron being Greek for "tree"). While similar in appearance, these are distinct structures from the dendrites of neurons. Immature dendritic cells are also called veiled cells, as they possess large cytoplasmic 'veils' rather than dendrites.
A dendritic cell
History
Dendritic cells were first described by Paul Langerhans (hence "Langerhans cells") in the late nineteenth century. It wasn't until 1973, however, that the term "dendritic cells" was coined by Ralph M. Steinman and Zanvil A. Cohn.[] For discovering the central role of dendritic cells in the adaptive immune response,[] Steinman was awarded the Albert Lasker Award for Basic Medical Research in 2007[] and the Nobel Prize in Physiology or Medicine in 2011.[]
Dendritic cells in skin
Types of dendritic cells
In all dendritic cells, the similar morphology results in a very large contact surface to their surroundings compared to overall cell volume.
In vivo – primate
The most common division of dendritic cells is "myeloid" vs. "plasmacytoid":
Dendritic cell
497
Name
Description
Secretion
Toll-like [1] receptors TLR 2, TLR 4
Myeloid dendritic cell (mDC)
Most similar to monocytes. mDC are IL-12 made up of at least two subsets: (1) the more common mDC-1, which is a major stimulator of T cells (2) the extremely rare mDC-2, which may have a function in fighting wound infection
[] Plasmacytoid Look like plasma cells, but have certain Can produce high amounts of interferon-alpha and thus became dendritic cell (pDC) characteristics similar to myeloid known as IPC (interferon-producing cells) before their dendritic [2] [3] dendritic cells. cell nature was revealed.
TLR 7, TLR 9
The markers BDCA-2, BDCA-3, and BDCA-4 can be used to discriminate among the types.[4] Lymphoid and myeloid DCs evolve from lymphoid or myeloid precursors respectively and thus are of hematopoietic origin. By contrast, follicular dendritic cells (FDC) are probably of mesenchymal rather than hematopoietic origin and do not express MHC class II, but are so named because they are located in lymphoid follicles and have long "dendritic" processes.
Dendritic cells in blood
The blood DCs are typically identified and enumerated in flow cytometry. Three types of DCs have been defined in human blood and these are the CD11c+ myeloid DCs, the CD141+ myeloid DCs and the CD303+ plasmacytoid DCs. This represents the nomenclature proposed by the respective IUIS nomenclature committee [5] Dendritic cells that circulate in blood do not have all the typical features of their counterparts in tissue, i.e. they are less mature and have no dendrites. Still, they can perform complex functions including chemokine-production in CD11c+ myeloid DCs, cross-presentation in CD141+ myeloid DCs and IFNalpha production in CD303+ plasmacytoid DCs.
In vitro
In some respects, dendritic cells cultured in vitro do not show the same behaviour or capability as dendritic cells isolated ex vivo. Nonetheless, they are often used for research as they are still much more readily available than genuine DCs. • Mo-DC or MDDC refers to cells matured from monocytes[6] • HP-DC refers to cells derived from hematopoietic progenitor cells.
Nonprimate
While humans and non-human primates such as Rhesus macaques appear to have DCs divided into these groups, other species (such as the mouse) have different subdivisions of DCs.
Life cycle
Formation of immature cells
Dendritic cells are derived from hematopoietic bone marrow progenitor cells. These progenitor cells initially transform into immature dendritic cells. These cells are characterized by high endocytic activity and low T-cell activation potential. Immature dendritic cells constantly sample the surrounding environment for pathogens such as viruses and bacteria. This is done through pattern recognition receptors (PRRs) such as the toll-like receptors (TLRs). TLRs recognize specific chemical signatures found on subsets of pathogens. Immature dendritic cells may
Dendritic cell also phagocytize small quantities of membrane from live own cells, in a process called nibbling. Once they have come into contact with a presentable antigen, they become activated into mature dendritic cells and begin to migrate to the lymph node. Immature dendritic cells phagocytose pathogens and degrade their proteins into small pieces and upon maturation present those fragments at their cell surface using MHC molecules. Simultaneously, they upregulate cell-surface receptors that act as co-receptors in T-cell activation such as CD80 (B7.1), CD86 (B7.2), and CD40 greatly enhancing their ability to activate T-cells. They also upregulate CCR7, a chemotactic receptor that induces the dendritic cell to travel through the blood stream to the spleen or through the lymphatic system to a lymph node. Here they act as antigen-presenting cells: they activate helper T-cells and killer T-cells as well as B-cells by presenting them with antigens derived from the pathogen, alongside non-antigen specific costimulatory signals Every helper T-cell is specific to one particular antigen. Only professional antigen-presenting cells (macrophages, B lymphocytes, and dendritic cells) are able to activate a resting helper T-cell when the matching antigen is presented. However, macrophages and B cells can only activate memory T cells[citation needed] whereas dendritic cells can activate both memory and naive T cells, and are the most potent of all the antigen-presenting cells. As mentioned above, mDC probably arise from monocytes, white blood cells which circulate in the body and, depending on the right signal, can turn into either dendritic cells or macrophages. The monocytes in turn are formed from stem cells in the bone marrow. Monocyte-derived dendritic cells can be generated in vitro from peripheral blood mononuclear cells (PBMCs). Plating of PBMCs in a tissue culture flask permits adherence of monocytes. Treatment of these monocytes with interleukin 4 (IL-4) and granulocyte-macrophage colony stimulating factor (GM-CSF) leads to differentiation to immature dendritic cells (iDCs) in about a week. Subsequent treatment with tumor necrosis factor (TNF) further differentiates the iDCs into mature dendritic cells.
498
Life span of dendritic cells
Activated macrophages have a lifespan of only a few days though new evidence suggest that it could be extended to weeks rather than days.[citation needed] The lifespan of activated dendritic cells, while somewhat varying according to type and origin, is of a similar order of magnitude, but immature dendritic cells seem to be able to exist in an inactivated state for much longer.
Research challenges
The exact genesis and development of the different types and subsets of dendritic cells and their interrelationship is only marginally understood at the moment, as dendritic cells are so rare and difficult to isolate that only in recent years they have become subject of focused research. Distinct surface antigens that characterize dendritic cells have only become known from 2000 on; before that, researchers had to work with a 'cocktail' of several antigens which, used in combination, result in isolation of cells with characteristics unique to DCs.
Dendritic cells and cytokines
The dendritic cells are constantly in communication with other cells in the body. This communication can take the form of direct cell–cell contact based on the interaction of cell-surface proteins. An example of this includes the interaction of the membrane proteins of the B7 family of the dendritic cell with CD28 present on the lymphocyte. However, the cell–cell interaction can also take place at a distance via cytokines. For example, stimulating dendritic cells in vivo with microbial extracts causes the dendritic cells to rapidly begin producing IL-12.[] IL-12 is a signal that helps send naive CD4 T cells towards a Th1 phenotype. The ultimate consequence is priming and activation of the immune system for attack against the antigens which the dendritic cell presents on its surface. However, there are differences in the cytokines produced depending on the type of dendritic cell. The plasmacytoid DC has the ability to produce huge amounts of type-1 IFN's, which recruit more activated macrophages to allow phagocytosis.[]
Dendritic cell
499
Disease
HIV infection
HIV, which causes AIDS, can bind to dendritic cells via various receptors expressed on the cell. The best studied example is DC-SIGN (usually on MDC subset 1, but also on other subsets under certain conditions; since not all dendritic cell subsets express DC-SIGN, its exact role in sexual HIV-1 transmission is not clear)[citation needed]. When the dendritic cell takes up HIV and then travels to the lymph node, the virus can be transferred to helper CD4+ T-cells, contributing to the developing infection. This infection of dendritic cells by HIV explains one mechanism by which the virus could persist after prolonged HAART[citation needed]. Many other viruses, such as the SARS virus seems to use DC-SIGN to 'hitchhike' to its target cells.[7] However, most work with virus binding to DC-SIGN expressing cells has been conducted using in vitro derived cells such as moDCs. The physiological role of DC-SIGN in vivo is more difficult to ascertain.
Autoimmunity
Altered function of dendritic cells is also known to play a major or even key role in allergy and autoimmune diseases like lupus erythematosus and inflammatory bowel diseases (Crohn's disease and ulcerative colitis).[][][]
Dendritic cells in animals other than humans
The above applies to humans. In other organisms, the function of dendritic cells can differ slightly. For example, in brown rats (but not mice), a subset of dendritic cells exists that displays pronounced killer cell-like activity, apparently through its entire lifespan[citation needed]. However, the principal function of dendritic cells as known to date is always to act as an immune sentinel. They survey the body and collect information relevant to the immune system, they are then able to instruct and direct the adaptive arms to respond to challenges. In addition, an immediate precursor to myeloid and lymphoid dendritic cells of the spleen has been identified.[] This precursor, termed pre-DC, lacks MHC class II surface expression, and is distinct from monocytes, which primarily give rise to DCs in non-lymphoid tissues. Although typically described in mammals, dendritic cells have also been found in chickens[8] and turtles.[9]
Dendritic cell
500
Media
A single dendritic cell can be seen here efficiently taking up at least four conidia in its vicinity.
References
[5] Ziegler-Heitbrock, L et al (2010): Nomenclature of monocytes and dendritic cells in blood. Blood,116 (16): e74-e80. PMID 20628149
External links
• (http://u1019.lille.inserm.fr/research-activities/?lang=en), Website of the Center for Infection and Immunity of Lille contains information on DCs and their study in research • Dendritic Cells (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Dendritic+Cells) at the US National Library of Medicine Medical Subject Headings (MeSH) • www.dc2007.eu : 5th International Meeting on Dendritic Cell Vaccination and other Strategies to tip the Balance of the Immune System (http://www.dc2007.eu) • Website of Dr. Ralph M. Steinman at The Rockefeller University (http://www.rockefeller.edu/labheads/ steinman/steinman-lab.php) contains information on DCs, links to articles, pictures and videos • Cancer 'danger receptor' found (http://news.bbc.co.uk/2/hi/health/7888042.stm), BBC News, 15 February 2009
Lymphatic system
501
Lymphatic system
Lymphatic System
Human lymphatic system Latin systema lymphoideum
The lymphatic system is part of the circulatory system, comprising a network of conduits called lymphatic vessels that carry a clear fluid called lymph (from Latin lympha "water goddess"[1]) directionally towards the heart. The lymphatic system was first described in the seventeenth century independently by Olaus Rudbeck and Thomas Bartholin. The lymph system is not a closed system. The circulatory system processes an average of 20 liters of blood per day through capillary filtration which removes plasma while leaving the blood cells. Roughly 17 liters of the filtered plasma actually get reabsorbed directly into the blood vessels, while the remaining 3 liters are left behind in the interstitial fluid. The primary function of the lymph system is to provide an accessory route for these excess 3 liters per day to get returned to the blood.[2] Lymph is essentially recycled blood plasma. Lymphatic organs play an important part in the immune system, having a considerable overlap with the lymphoid system. Lymphoid tissue is found in many organs, particularly the lymph nodes, and in the lymphoid follicles associated with the digestive system such as the tonsils. Lymphoid tissues contain lymphocytes, but they also contain other types of cells for support.[] The system also includes all the structures dedicated to the circulation and production of lymphocytes (the primary cellular component of lymph), which includes the spleen, thymus, bone marrow, and the lymphoid tissue associated with the digestive system.[] The blood does not directly come in contact with the parenchymal cells and tissues in the body, but constituents of the blood first exit the microvascular exchange blood vessels to become interstitial fluid, which comes into contact with the parenchymal cells of the body. Lymph is the fluid that is formed when interstitial fluid enters the initial lymphatic vessels of the lymphatic system. The lymph is then moved along the lymphatic vessel network by either intrinsic contractions of the lymphatic passages or by extrinsic compression of the lymphatic vessels via external tissue forces (e.g. the contractions of skeletal muscles). The organization of lymph nodes and drainage follows the organization of the body into external and internal regions; therefore, the lymphatic drainage of the head, limbs, and body cavity walls follows an external route, and the lymphatic drainage of the thorax, abdomen, and pelvic cavities follows an internal route.[3] Eventually, the lymph vessels empty into the lymphatic ducts, which drain into one of the two subclavian veins (near the junctions of the subclavian veins with the internal jugular veins).
Lymphatic system
502
Terminology
The adjective used for the lymph-transporting system is "lymphatic." The adjective used for the tissues where lymphocytes are formed is "lymphoid." Lymphatic comes from the Latin word lymphaticus, meaning "connected to water."
Functions
The lymphatic system has multiple interrelated functions:[4] • • • • It is responsible for the removal of interstitial fluid from tissues It absorbs and transports fatty acids and fats as chyle from the digestive system It transports white blood cells to and from the lymph nodes into the bones The lymph transports antigen-presenting cells (APCs), such as dendritic cells, to the lymph nodes where an immune response is stimulated.
Clinical significance
The study of lymphatic drainage of various organs is important in diagnosis, prognosis, and treatment of cancer. The lymphatic system, because of its physical proximity to many tissues of the body, is responsible for carrying cancerous cells between the various parts of the body in a process called metastasis. The intervening lymph nodes can trap the cancer cells. If they are not successful in destroying the cancer cells the nodes may become sites of secondary tumors.
Organization
The lymphatic system can be broadly divided into the conducting system and the lymphoid tissue. • The conducting system carries the lymph and consists of tubular vessels that include the lymph capillaries, the lymph vessels, and the right and left thoracic ducts. • The lymphoid tissue is primarily involved in immune responses and consists of lymphocytes[5] and other white blood cells enmeshed in connective tissue through which the lymph passes. Regions of the lymphoid tissue that are densely packed with lymphocytes are known as lymphoid follicles. Lymphoid tissue can either be structurally well organized as lymph nodes or may consist of loosely organized lymphoid follicles known as the mucosa-associated lymphoid tissue (MALT).
Lymphoid tissue
Lymphoid tissue associated with the lymphatic system is concerned with immune functions in defending the body against the infections and spread of tumors. It consists of connective tissue with various types of white blood cells enmeshed in it, most numerous being the lymphocytes. The lymphoid tissue may be primary, secondary, or tertiary depending upon the stage of lymphocyte development and maturation it is involved in. (The tertiary lymphoid tissue typically contains far fewer lymphocytes, and assumes an immune role only when challenged with antigens that result in inflammation. It achieves this by importing the lymphocytes from blood and lymph.[])
Lymphatic system
503
Primary lymphoid organs
The central or primary lymphoid organs generate lymphocytes from immature progenitor cells. The thymus and the bone marrow constitute the primary lymphoid tissues involved in the production and early selection of lymphocytes.
Secondary lymphoid organs
Secondary or peripheral lymphoid organs maintain mature naive lymphocytes and initiate an adaptive immune response. The peripheral lymphoid organs are the sites of lymphocyte activation by antigen. Activation leads to clonal expansion and affinity maturation. Mature lymphocytes recirculate between the blood and the peripheral lymphoid organs until they encounter their specific antigen. Secondary lymphoid tissue provides the environment for the foreign or altered native molecules (antigens) to interact with the lymphocytes. It is exemplified by the lymph nodes, and the lymphoid follicles in tonsils, Peyer's patches, spleen, adenoids, skin, etc. that are associated with the mucosa-associated lymphoid tissue (MALT). Lymph nodes A lymph node is an organized collection of lymphoid tissue, through which the lymph passes on its way to returning to the blood. Lymph nodes are located at intervals along the lymphatic system. Several afferent lymph vessels bring in lymph, which percolates through the substance of the lymph node, and is drained out by an efferent lymph vessel. The substance of a lymph node consists of lymphoid follicles in the A lymph node showing afferent and efferent lymphatic vessels outer portion called the "cortex," which contains the lymphoid follicles, and an inner portion called "medulla," which is surrounded by the cortex on all sides except for a portion known as the "hilum." The hilum presents as a depression on the surface of the lymph node, which makes the otherwise spherical or ovoid lymph node bean-shaped. The efferent lymph vessel directly emerges from the lymph node here. The arteries and veins supplying the lymph node with blood enter and exit through the hilum. Lymph follicles are a dense collection of lymphocytes, the number, size and configuration of which change in accordance with the functional state of the lymph node. For example, the follicles expand significantly upon encountering a foreign antigen. The selection of B cells occurs in the germinal center of the lymph nodes. Lymph nodes are particularly numerous in the mediastinum in the chest, neck, pelvis, axilla (armpit), inguinal (groin) region, and in association with the blood vessels of the intestines.[]
Lymphatic system
504
Lymphatics
Tubular vessels transport back lymph to the blood ultimately replacing the volume lost from the blood during the formation of the interstitial fluid. These channels are the lymphatic channels or simply called lymphatics.[6]
Function of the fatty acid transport system
Lymph vessels called lacteals are present in the lining of the gastrointestinal tract, predominantly in the small intestine. While most lymphatic system other nutrients absorbed by the small intestine are passed on to the portal venous system to drain via the portal vein into the liver for processing, fats (lipids) are passed on to the lymphatic system to be transported to the blood circulation via the thoracic duct. (There are exceptions, for example medium-chain triglycerides (MCTs) are fatty acid esters of glycerol that passively diffuse from the GI tract to the portal system.) The enriched lymph originating in the lymphatics of the small intestine is called chyle. The nutrients that are released to the circulatory system are processed by the liver, having passed through the systemic circulation.
Diseases of the lymphatic system
Lymphedema is the swelling caused by the accumulation of lymph fluid, which may occur if the lymphatic system is damaged or has malformations. It usually affects limbs, though face, neck and abdomen may also be affected. In an extreme state the edema progresses. Skin becomes thicken with an appearance similar to elephant limbs. Is called elephantiasis.[7] Causes are unknown in most of cases but sometimes the patient have a previous history of severe infection most commonly caused by a parasitic disease, like the lymphatic filariasis for example. Some common causes of swollen lymph nodes include infections, infectious mononucleosis, and cancer, e.g. Hodgkin's and non-Hodgkin lymphoma, and metastasis of cancerous cells via the lymphatic system. Hodgkin's lymphoma is a type of cancer. This type of cancer usually results from the white blood cells in the body becoming diseased or damaged. Nowadays, this kind of cancer is easily controlled [8] Lymphangiomatosis is a disease involving multiple cysts or lesions formed from lymphatic vessels. Lymphangiosarcoma is a malignant soft tissue tumor, whereas lymphangioma is a benign tumor occurring frequently in association with Turner syndrome. Lymphangioleiomyomatosis is a benign tumor of the smooth muscles of the lymphatics that occurs in the lungs. Lymphoid leukemias and lymphomas are now considered to be tumors of the same type of cell lineage. They are called "leukemia" when in the blood or marrow and "lymphoma" when in lymphatic tissue. They are grouped together under the name "lymphoid malignancy".[]
Lymphatic system
505
Development of lymphatic tissue
Lymphatic tissues begin to develop by the end of the fifth week of embryonic development. Lymphatic vessels develop from lymph sacs that arise from developing veins, which are derived from mesoderm. The first lymph sacs to appear are the paired jugular lymph sacs at the junction of the internal jugular and subclavian veins. From the jugular lymph sacs, lymphatic capillary plexuses spread to the thorax, upper limbs, neck and head. Some of the plexuses enlarge and form lymphatic vessels in their respective regions. Each jugular lymph sac retains at least one connection with its jugular vein, the left one developing into the superior portion of the thoracic duct. The next lymph sac to appear is the unpaired retroperitoneal lymph sac at the root of the mesentery of the intestine. It develops from the primitive vena cava and mesonephric veins. Capillary plexuses and lymphatic vessels spread from the retroperitoneal lymph sac to the abdominal viscera and diaphragm. The sac establishes connections with the cisterna chyli but loses its connections with neighboring veins. The last of the lymph sacs, the paired posterior lymph sacs, develop from the iliac veins. The posterior lymph sacs produce capillary plexuses and lymphatic vessels of the abdominal wall, pelvic region, and lower limbs. The posterior lymph sacs join the cisterna chyli and lose their connections with adjacent veins. With the exception of the anterior part of the sac from which the cisterna chyli develops, all lymph sacs become invaded by mesenchymal cells and are converted into groups of lymph nodes. The spleen develops from mesenchymal cells between layers of the dorsal mesentery of the stomach. The thymus arises as an outgrowth of the third pharyngeal pouch.
Lymphatico-venous communications
Present research has found clues about a lymphatico-venous communication. In mammals, lymphatico-venous communications other than those at the base of the neck are not easy to demonstrate, but described in some experiments.[] The specialists observed that the pulmonary complications following lymphangiography (a test which utilizes X ray technology, along with the injection of a contrast agent, to view lymphatic circulation and lymph nodes for diagnostic purposes) are more often severe in patients with lymphatic obstruction. In these cases, the contrast medium is thought to reach the vascular system via lymphovenous communications which shunt the material directly into the venous stream, bypassing those lymph nodes distal to the communications,[] Because less contrast agent is absorbed in lymph nodes, a greater portion of the injected volume passes into the vascular system. Since pulmonary complications are related to the amount of medium reaching the lungs area, the early recognition of lymphovenous communications is a great significance to the lymphangiographer.[] Another "hint" in proving a lymph-vein communication is offered by a Robert F Dunn experiment. The passage of radioactively tagged tracers, injected at elevated pressure, through the lymph node-venous communications coincides with the increased pressures of injection and subsequent nodal palpation in dogs. The passage of iodinated I 125 serum albumen (ISA) indicates that direct lymph node-venous communications are present, whereas passage of nucleated erythrocytes requires a communication structure the size of a capillary or larger.[9] Moreover, the evidence suggest that in mammals under normal conditions, most of the lymph is returned to the blood stream through the lymphatico-venous communications at the base of the neck. When the thoracic duct-venous communication is blocked, however, the resultant raised intralymphatic pressure will usually cause other normal non-functioning communications to open and thereby allow the return of lymph to the blood stream.[]
Lymphatic system
506
History
Hippocrates was one of the first people to mention the lymphatic system in 5th century BC. In his work On Joints, he briefly mentioned the lymph nodes in one sentence. Rufus of Ephesus, a Roman physician, identified the axillary, inguinal and mesenteric lymph nodes as well as the thymus during the 1st to 2nd century AD.[] The first mention of lymphatic vessels was in 3rd century BC by Herophilos, a Greek anatomist living in Alexandria, who incorrectly concluded that the "absorptive veins of the lymphatics," by which he meant the lacteals (lymph vessels of the intestines), drained into the hepatic portal veins, and thus into the liver.[] Findings of Ruphus and Herophilos findings were further propagated by the Greek physician Galen, who described the lacteals and mesenteric lymph nodes which he observed in his dissection of apes and pigs in the 2nd century AD.[][] In the mid 16th century, Gabriele Falloppio (discoverer of the fallopian tubes), described what are now known as the lacteals as "coursing over the intestines full of yellow matter."[] In about 1563 Bartolomeo Eustachi, a professor of anatomy, described the thoracic duct in horses as vena alba thoracis.[] The next breakthrough came when in 1622 a physician, Gaspare Aselli, identified lymphatic vessels of the intestines in dogs and termed them venae alba et lacteae, which is now known as simply the lacteals. The lacteals were termed the fourth kind of vessels (the other three being the artery, vein and nerve, which was then believed to be a type of vessel), and disproved Galen's assertion that chyle was carried by the veins. But, he still believed that the lacteals carried the chyle to the liver (as taught by Galen).[] He also identified the thoracic duct but failed to notice its connection with the lacteals.[] This connection was established by Jean Pecquet in 1651, who found a white fluid mixing with blood in a dog's heart. He suspected that fluid to be chyle as its flow increased when abdominal pressure was applied. He traced this fluid to the thoracic duct, which he then followed to a chyle-filled sac he called the chyli receptaculum, which is now known as the cisternae chyli; further investigations led him to find that lacteals' contents enter the venous system via the thoracic duct.[][] Thus, it was proven convincingly that the lacteals did not terminate in the liver, thus disproving Galen's second idea: that the chyle flowed to the liver.[] Johann Veslingius drew the earliest sketches of the lacteals in humans in 1647.[] The idea that blood recirculates through the body rather than being produced anew by the liver and the heart was first accepted as a result of works of William Harvey—a work he published in 1628. In 1652, Olaus Rudbeck (1630–1702), a Swede, discovered certain transparent vessels in the liver that contained clear fluid (and not white), and thus named them hepatico-aqueous vessels. He also learned that they emptied into the thoracic duct, and that they had valves.[] He announced his findings in the court of Queen Christina of Sweden, but did not publish his findings for a year,[] and in the interim similar findings were published by Thomas Bartholin, who additionally published that such vessels are present everywhere in the body, and not just the liver. He is also the one to have named them "lymphatic vessels."[] This had resulted in a bitter dispute between one of Bartholin's pupils, Martin Bogdan,[10] and Rudbeck, whom he accused of plagiarism.[] Galen's ideas prevailed in medicine until the 17th century. It was believed that blood was produced by the liver from chyle contaminated with ailments by the intestine and stomach, to which various spirits were added by other organs, and that this blood was consumed by all the organs of the body. This theory required that the blood be consumed and produced many times over. Even in the 17th century, his ideas were defended by some physicians.[]
Lymphatic system
507
"Claude Galien". Lithograph by Pierre Roche Vigneron. (Paris: Lith de Gregoire et Deneux, ca. 1865)
Portrait of Eustachius
Olaus Rudbeck in 1696.
Thomas Bartholin
References
[2] Human Physiology: From Cells to Systems, by Lauralee Sherwood (http:/ / books. google. com/ books?id=I9qH3eZ1pP0C& pg=PT401#v=onepage& q& f=false)
External links
• Lymphatic System (http://www.emc.maricopa.edu/faculty/farabee/BIOBK/BioBookIMMUN.html) • Lymphatic System Overview (http://www.innerbody.com/image/lympov.html) (innerbody.com)
Microglia
508
Microglia
Microglia
Code TH H2.00.06.2.00004 [1]
Microglia are a type of glial cell that are the resident macrophages of the brain and spinal cord, and thus act as the first and main form of active immune defense in the central nervous system (CNS). Microglia constitute 20% of the total glial cell population within the brain.[1] Microglia (and astrocytes) are distributed in large non-overlapping regions throughout the brain and spinal cord.[][] Microglia are constantly scavenging the CNS for plaques, damaged neurons and infectious agents.[] The brain and spinal cord are considered "immune privileged" organs in that they are separated from the rest of the body by a series of endothelial cells known as the blood–brain barrier, which prevents most infections from reaching the vulnerable nervous tissue. In the case where infectious agents are directly introduced to the brain or cross the blood–brain barrier, microglial cells must react quickly to decrease inflammation and destroy the infectious agents before they damage the sensitive neural tissue. Due to the unavailability of antibodies from the rest of the body (few antibodies are small enough to cross the blood brain barrier), microglia must be able to recognize foreign bodies, swallow them, and act as antigen-presenting cells activating T-cells. Since this process must be done quickly to prevent potentially fatal damage, microglia are extremely sensitive to even small pathological changes in the CNS.[] They achieve this sensitivity in part by having unique potassium channels that respond to even small changes in extracellular potassium.[]
Microglia - ramified form from rat cortex after traumatic brain injury (lactins staining with HRP)
Microglia/Macrophage - activated form from rat cortex after traumatic brain injury (lactins staining with HRP)
Origin
Microglial cells differentiate in the bone marrow from hematopoietic stem cells, the progenitors of all blood cells. During hematopoiesis, some of these stem cells differentiate into monocytes and travel from the bone marrow to the brain, where they settle and further differentiate into microglia.[] Monocytes can also differentiate into myeloid dendritic cells and macrophages in the peripheral systems. Like macrophages in the rest of the body, microglia use phagocytic and cytotoxic mechanisms to destroy foreign materials. Microglia and macrophages both contribute to the immune response by acting as antigen presenting cells, as well as promoting inflammation and homeostatic mechanisms within the body by secreting cytokines and other signaling molecules.
Microglia In their downregulated form, microglia lack the MHC class I/MHC class II proteins, IFN-γ cytokines, CD45 antigens, and many other surface receptors required to act in the antigen-presenting, phagocytic, and cytotoxic roles that hallmark normal macrophages. Microglia also differ from macrophages in that they are much more tightly regulated spatially and temporally in order to maintain a precise immune response.[] Another difference between microglia and other cells that differentiate from myeloid progenitor cells is the turnover rate. Macrophages and dendritic cells are constantly being used up and replaced by myeloid progenitor cells which differentiate into the needed type. Due to the blood brain barrier, it would be fairly difficult for the body to constantly replace microglia. Therefore, instead of constantly being replaced with myeloid progenitor cells, the microglia maintain their status quo while in their quiescent state, and then, when they are activated, they rapidly proliferate in order to keep their numbers up. Bone chimera studies have shown, however, that in cases of extreme infection the blood–brain barrier will weaken, and microglia will be replaced with haematogenous, cart-marrow derived cells, namely myeloid progenitor cells and macrophages. Once the infection has decreased the disconnect between peripheral and central systems is reestablished and only microglia are present for the recovery and regrowth period.[]
509
History
The ability to view and characterize different neural cells including microglia began in 1880 when Nissl staining was developed by Franz Nissl. Franz Nissl and F. Robertson first described microglial cells during their histology experiments. The cell staining techniques in the 1880s showed that microglia are related to macrophages. The activation of microglia and formation of ramified microglial clusters was first noted by Victor Babeş while studying a rabies case in 1897. Babeş noted the cells were found in a variety of viral brain infections but did not know what the clusters of microglia he saw were.[] Pío del Río Hortega, a student of Santiago Ramón y Cajal, first called the cells "microglia" around 1920. He went on to characterize microglial response to brain lesions in 1927 and note the "fountains of microglia" present in the corpus callosum and other perinatal white matter areas in 1932. After many years of research Rio-Hortega became generally considered as the "Father of Microglia."[][] For a long period of time little improvement was made in our knowledge of microglia. Then, in 1988, Hickey and Kimura showed that perivascular microglial cells are bone-marrow derived, and express high levels of MHC class II proteins used for antigen presentation. This confirmed Pio Del Rio-Hortega's postulate that microglial cells functioned similarly to macrophages by performing phagocytosis and antigen presentation.
Types
Microglial cells are extremely plastic, and undergo a variety of structural changes based on their location and current role. This level of plasticity is required to fulfill the vast variety of immunological functions that microglia perform, as well as maintaining homeostasis within the brain. If microglia were not capable of this they would need to be replaced on a regular basis like macrophages, and would not be available to the CNS immune defense on extremely short notice without causing immunological imbalance under normal conditions.[]
Amoeboid
This form of microglial cell is found mainly within the perinatal white matter areas in the corpus callosum known as the "Fountains of Microglia." This shape allows the microglial free movement throughout the neural tissue, which allows it to fulfill its role as a scavenger cell. Amoeboid microglia are able to phagocytose debris, but do not fulfill the same antigen-presenting and inflammatory roles as activated microglia. Amoeboid microglia are especially prevalent during the development and rewiring of the brain, when there are large amounts of extracellular debris and apoptotic cells to remove.[][][]
Microglia
510
Ramified
This form of microglial cell is commonly found at specific locations throughout the entire brain and spinal cord in the absence of foreign material or dying cells. This "resting" form of microglia is composed of long branching processes and a small cellular body. Unlike the ameboid forms of microglia, the cell body of the ramified form remains fairly motionless, while its branches are constantly moving and surveying the surrounding area. The branches are very sensitive to small changes in physiological condition and require very specific culture conditions to observe in vitro. Unlike activated or ameboid microglia, ramified microglia are unable to phagocytose cells and display little or no immunomolecules. This includes the MHC class I/II proteins normally used by macrophages and dendritic cells to present antigens to t-cells, and as a result ramified microglia function extremely poorly as antigen presenters. The purpose of this state is to maintain a constant level of available microglia to detect and fight infection, while maintaining an immunologically silent environment.[][]
Activated
Activated microglia can be stained via the marker Iba1, which is upregulated during activation. Microglia are the only cells in the brain to express Iba1. Non-phagocytic This state is actually part of a graded response as microglia move from their ramified form to their fully active phagocytic form. Microglia can be activated by a variety of factors including: glutamate receptor agonists, pro-inflammatory cytokines, cell necrosis factors, lipopolysaccharide, and changes in extracellular potassium (indicative of ruptured cells). Once activated the cells undergo several key morphological changes including the thickening and retraction of branches, uptake of MHC class I/II proteins, expression of immunomolecules, secretion of cytotoxic factors, secretion of recruitment molecules, and secretion of pro-inflammatory signaling molecules (resulting in a pro-inflammation signal cascade). Activated non-phagocytic microglia generally appear as "bushy," "rods," or small ameboids depending on how far along the ramified to full phagocytic transformation continuum they are. In addition, the microglia also undergo rapid proliferation in order to increase their numbers. From a strictly morphological perspective, the variation in microglial form along the continuum is associated with changing morphological complexity and can be quantitated using the methods of fractal analysis, which have proven sensitive to even subtle, visually undetectable changes associated with different morphologies in different pathological states.[][][][] Phagocytic Activated phagocytic microglia are the maximally immune responsive form of microglia. These cells generally take on a large, ameboid shape, although some variance has been observed. In addition to having the antigen presenting, cytotoxic and inflammatory mediating signaling of activated non-phagocytic microglia, they are also able to phagocytose foreign materials and display the resulting immunomolecules for T-cell activation. Phagocytic microglia travel to the site of the injury, engulf the offending material, and secrete pro-inflammatory factors to promote more cells to proliferate and do the same. Activated phagocytic microglia also interact with astrocytes and neural cells to fight off the infection as quickly as possible with minimal damage to the healthy brain cells.[][]
Microglia
511
Gitter cells
Gitter cells are the eventual result of microglial cell's phagocytosis of infectious material. Eventually, after engulfing a certain amount of material, the phagocytic microglia becomes unable to phagocytose any further materials. The resulting cellular mass is known as a granular corpuscle, named for its ‘grainy' appearance. By looking at tissues stained to reveal gitter cells, scientists can see post-infection areas that have healed.[]
Perivascular
Unlike the other types of microglia mentioned above, "perivascular" microglia refers to the location of the cell rather than its form/function. Perivascular microglia are mainly found encased within the walls of the basal lamina. They perform normal microglial functions, but unlike normal microglia they are replaced by bone marrow derived precursor cells on a regular basis and express MHC class II antigens regardless of the outside environment. Perivascular microglia also react strongly to macrophage differentiation antigens.[] These microglia have been shown to be essential to repair of vascular walls, as shown by Ritter's experiments and observations on ischemic retinopathy. Perivascular microglia promote endothelial cell proliferation allowing new vessels to be formed and damaged vessels to be repaired. During repair and development, myeloid recruitment and differentiation into microglial cells is highly accelerated to accomplish these tasks.[]
Juxtavascular
Like perivascular microglia, juxtavascular microglia can be distinguished mainly by their location. Juxtavascular microglia are found making direct contact with the basal lamina wall of blood vessels but are not found within the walls. Like perivascular cells, they express MHC class II proteins even at low levels of inflammatory cytokine activity. Unlike perivascular cells, but similar to resident microglia, juxtavascular microglia do not exhibit rapid turnover or replacement with myeloid precursor cells on a regular basis.[]
Functions
Microglial cells fulfill a variety of different tasks within the CNS mainly related to both immune response and maintaining homeostasis. The following are some of the major known functions carried out by these cells.
Scavenging
In addition to being very sensitive to small changes in their environment, each microglial cell also physically surveys its domain on a regular basis. This action is carried out in the ameboid and resting states. While moving through its set region, if the microglial cell finds any foreign material, damaged cells, apoptotic cells, neural tangles, DNA fragments, or plaques it will activate and phagocytose the material or cell. In this manner microglial cells also act as "housekeepers" cleaning up random cellular debris.[] During developmental wiring of the brain, microglial cells play a large role removing unwanted excess cellular matter. Post development, the majority of dead or apoptotic cells are found in the cerebral cortex and the subcortical white matter. This may explain why the majority of ameboid microglial cells are found within the "fountains of microglia" in the cerebral cortex.[]
Microglia
512
Phagocytosis
The main role of microglia, phagocytosis, involves the engulfing of various materials. Engulfed materials generally consist of cellular debris, lipids, and apoptotic cells in the non-inflamed state, and invading virus, bacteria, or other foreign materials in the inflamed state. Once the microglial cell is "full" it stops phagocytic activity and changes into a relatively non-reactive gitter cell.
Cytotoxicity
In addition to being able to destroy infectious organisms through cell to cell contact via phagocytosis, microglia can also release a variety of cytotoxic substances. Microglia in culture secrete large amounts of H2O2 and NO in a process known as ‘respiratory burst'. Both of these chemicals can directly damage cells and lead to neuronal cell death. Proteases secreted by microglia catabolise specific proteins causing direct cellular damage, while cytokines like IL-1 promote demyelination of neuronal axons. Finally, microglia can injure neurons through NMDA receptor-mediated processes by secreting glutamate and aspartate. Cytotoxic secretion is aimed at destroying infected neurons, virus, and bacteria, but can also cause large amounts of collateral neural damage. As a result, chronic inflammatory response can result in large scale neural damage as the microglia ravage the brain in an attempt to destroy the invading infection.[]
Antigen presentation
As mentioned above, resident non-activated microglia act as poor antigen presenting cells due to their lack of MHC class I/II proteins. Upon activation they rapidly uptake MHC class I/II proteins and quickly become efficient antigen presenters. In some cases, microglia can also be activated by IFN-γ to present antigens, but do not function as effectively as if they had undergone uptake of MHC class I/II proteins. During inflammation, T-cells cross the blood–brain barrier thanks to specialized surface markers and then directly bind to microglia in order to receive antigens. Once they have been presented with antigens, T-cells go on to fulfill a variety of roles including pro-inflammatory recruitment, formation of immunomemories, secretion of cytotoxic materials, and direct attacks on the plasma membranes of foreign cells.[][]
Synaptic stripping
In a phenomenon first noticed in spinal lesions by Blinzinger and Kreutzberg in 1968, post-inflammation microglia remove the branches from nerves near damaged tissue. This helps promote regrowth and remapping of damaged neural circuitry.[]
Promotion of repair
Post-inflammation, microglia undergo several steps to promote regrowth of neural tissue. These include synaptic stripping, secretion of anti-inflammatory cytokines, recruitment of neurons and astrocytes to the damaged area, and formation of gitter cells. Without microglial cells regrowth and remapping would be considerably slower in the resident areas of the CNS and almost impossible in many of the vascular systems surrounding the brain and eyes.[][]
Extracellular signaling
A large part of microglial cell's role in the brain is maintaining homeostasis in non-infected regions and promoting inflammation in infected or damaged tissue. Microglia accomplish this through an extremely complicated series of extracellular signaling molecules which allow them to communicate with other microglia, astrocytes, nerves, T-cells, and myeloid progenitor cells. As mentioned above the cytokine IFN-γ can be used to activate microglial cells. In addition, after becoming activated with IFN-γ, microglia also release more IFN-γ into the extracellular space. This activates more microglia and starts a cytokine induced activation cascade rapidly activating all nearby microglia. Microglia-produced TNF-α causes neural tissue to undergo apoptosis and increases inflammation. IL-8 promotes
Microglia B-cell growth and differentiation, allowing it to assist microglia in fighting infection. Another cytokine, IL-1, inhibits the cytokines IL-10 and TGF-β, which downregulate antigen presentation and pro-inflammatory signaling. Additional dendritic cells and T-cells are recruited to the site of injury through the microglial production of the chemotactic molecules like MDC, IL-8, and MIP-3β. Finally, PGE2 and other prostanoids help prevent chronic inflammation by inhibiting microglial pro-inflammatory response and downregulating Th1 (T-helper cell) response.[]
513
Role in chronic neuroinflammation
The word neuroinflammation has come to stand for chronic, central nervous system (CNS) specific, inflammation-like glial responses that may produce neurodegenerative symptoms such as plaque formation, dystrophic neurite growth, and excessive tau phosphorylation.[] It is important to distinguish between acute and chronic neuroinflammation. Acute neuroinflammation is generally caused by some neuronal injury after which microglia migrate to the injured site engulfing dead cells and debris.[] The term neuroinflammation generally refers to more chronic, sustained injury when the responses of microglial cells contribute to and expand the neurodestructive effects, worsening the disease process.[] When microglia are activated they take on an amoeboid shape and they alter their gene expression. Altered gene expression leads to the production of numerous potentially neurotoxic mediators. These mediators are important in the normal functions of microglia and their production is usually decreased once their task is complete.[] In chronic neuroinflammation, microglia remain activated for an extended period during which the production of mediators is sustained longer than usual.[] This increase in mediators contributes to neuronal death.[] Neuroinflammation is unique from inflammation in other organs, but does include some similar mechanisms such as the localized production of chemoattractant molecules to the site of inflammation.[] The following list contains a few of the numerous substances that are secreted when microglia are activated:
Cytokines
Microglia activate the proinflammatory cytokines IL-1α, IL-1β and TNF-α in the CNS.[] Cytokines play a potential role in neurodegeneration when microglia remain in a sustained activated state.[] Direct injection of the cytokines IL-1α, IL-1β and TNF-α into the CNS result in local inflammatory responses and neuronal degradation.[] This is in contrast with the potential neurotrophic (inducing growth of neurons) actions of these cytokines during acute neuroinflammation.[]
Chemokines
Chemokines are cytokines that stimulate directional migration of inflammatory cells in vitro and in vivo.[] Chemokines are divided into four main subfamilies: C, CC, CXC, and CX3C. Microglial cells are sources of some chemokines and express the monocyte chemoattractant protein-1 (MCP-1) chemokine in particular.[] Other inflammatory cytokines like IL-1β and TNF-α, as well as bacterial-derived lipopolysaccharide (LPS) may stimulate microglia to produce MCP-1, MIP-1α, and MIP-1β.[] Microglia can express CCR3, CCR5, CXCR4, and CX3CR1 in vitro.[] Chemokines are proinflammatory and therefore contribute to the neuroinflammation process.[]
Proteases
When microglia are activated they induce the synthesis and secretion of proteolytic enzymes that are potentially involved in many functions.[] There are a number of proteases that possess the potential to degrade both the extracellular matrix and neuronal cells that are in the neighborhood of the microglia releasing these compounds.[] These proteases include; cathepsins B, L, and S, the matrix metalloproteinases MMP-1, MMP-2, MMP-3, and MMP-9, and the metalloprotease-disintegrin ADAM8 plasminogen which forms outside microglia and degrades the extracellular matrix.[] Both Cathepsin B, MMP-1 and MMP-3 have been found to be increased in Alzheimer's disease (AD) and cathepsin B is increased in multiple sclerosis (MS).[] Elastase, another protease, could have large
Microglia negative effects on the extracellular matrix.[]
514
Amyloid precursor protein
Microglia synthesize amyloid precursor protein (APP) in response to excitotoxic injury.[] Plaques result from abnormal proteolytic cleavage of membrane bound APP.[] Amyloid plaques can stimulate microglia to produce neurotoxic compounds such as cytokines, excitotoxin, nitric oxide and lipophylic amines, which all cause neural damage.[] Plaques in Alzheimer's disease contain activated microglia.[] A study has shown that direct injection of amyloid into brain tissue activates microglia, which reduces the number of neurons.[] Microglia have also been suggested as a possible source of secreted β amyloid.[]
Aging
Microglia undergo a burst of mitotic activity during injury; this proliferation is followed by apoptosis to reduce the cell numbers back to baseline.[] Activation of microglia places a load on the anabolic and catabolic machinery of the cells causing activated microglia to die sooner than non-activated cells.[] To compensate for microglial loss over time, microglia undergo mitosis and bone marrow derived progenitor cells migrate into the brain via the meninges and vasculature.[] Accumulation of minor neuronal damage that occurs during normal aging can transform microglia into enlarged and activated cells.[] These chronic, age-associated increases in microglial activation and IL-1 expression may contribute to increased risk of Alzheimer's disease with advancing age through favoring neuritic plaque formation in susceptible patients.[] DNA damage might contribute to age-associated microglial activation. Another factor might be the accumulation of advanced glycation endproducts, which accumulate with aging.[] These proteins are strongly resistant to proteolytic processes and promote protein cross-linking.[] Research has discovered dystrophic (defective development) human microglia. "These cells are characterized by abnormalities in their cytoplasmic structure, such as deramified, atrophic, fragmented or unusually tortuous processes, frequently bearing spheroidal or bulbous swellings."[] The incidence of dystrophic microglia increases with aging.[] Microglial degeneration and death have been reported in research on Prion disease, Schizophrenia and Alzheimer's disease, indicating that microglial deterioration might be involved in neurodegenerative diseases.[] A complication of this theory is the fact that it is difficult to distinguish between "activated" and "dystrophic" microglia in the human brain.[]
Role of microglia in neurodegeneration
Neurodegenerative disorders are characterized by progressive cell loss in specific neuronal populations.[] "Many of the normal trophic functions of glia may be lost or overwhelmed when the cells become chronically activated in progressive neurodegenerative disorders, for there is abundant evidence that in such disorders, activated glia play destructive roles by direct and indirect inflammatory attack."[] The following are prominent examples of microglial cells' role in neurodegenerative disorders.
Alzheimer's disease
Alzheimer's disease (AD) is a progressive, neurodegenerative disease where the brain develops abnormal clumps (amyloid plaques) and tangled fiber bundles (neurofibrillary tangles).[] There are many activated microglia over-expressing IL-1 in the brains of Alzheimer patients that are distributed with both Aβ plaques and neurofibrillary tangles.[] This over expression of IL-1 leads to excessive tau phosphorylation that is related to tangle development in Alzheimer's disease.[] Many activated microglia are found to be associated with amyloid deposits in the brains of Alzheimer's patients.[] Microglia interact with β-amyloid plaques through cell surface receptors that are linked to tyrosine kinase based
Microglia signaling cascades that induce inflammation.[] When microglia interact with the deposited fibrillar forms of β-amyloid it leads to the conversion of the microglia into an activated cell and results in the synthesis and secretion of cytokines and other proteins that are neurotoxic.[] Treatment Non-steroidal anti-inflammatory drugs (NSAIDs) have proven to be effective in reducing the risk of AD.[] "Sustained treatment with NSAIDs lowers the risk of AD by 55%, delays disease onset, attenuates symptomatic severity and slows the loss of cognitive abilities. The main cellular target for NSAIDs is thought to be microglia. This is supported by the fact that in patients taking NSAIDs the number of activated microglia is decreased by 65%."[]
515
Parkinson's disease
Parkinson's disease is a movement disorder in which the dopamine-producing neurons in the brain do not function as they should, the neurons of the Substantia Nigra become disfunctional and eventually die, leaving a lack of domamine input into the thalamus. This causes the symptoms of Parkinson's disease.[]
Cardiovascular Diseases
Recently microglial activation has been reported in rats with myocardial infarction (Rana et al.,2010). These activation was specific to brain nuclei involved in cardiovascular regulation suggesting possible role of microglial activation in pathogenesis of heart failure.
Role in viral infections
Human immunodeficiency virus
The infection of mononuclear phagocytes with HIV-1 is an important element in the development of HIV-associated dementia complex (HAD).[] The only brain cell type that is "productively" infected with the virus are microglial cells.[] It has also become clear that neurotoxic mediators released from brain microglia play an important role in the pathogenesis of HIV-1.[] "HIV-1 can enter the microglial cell via CD4 receptors and chemokine co-receptors such as CCR3, CCR5, and CXCR4, with CCR5 being the most important of these. Interestingly, humans with double allelic loss of CCR5 are virtually immune to HIV acquired via the sexual route (though can be infected by IV transmission of CXCR4 tropic viruses). IL-4 and IL-10 enhance the entry and replication of HIV-1 in microglia through the up-regulation of CD4 and CCR5 expression, respectively. The chemokines CCL5/RANTES, CCL3/MIP-1α, CCL4/MIP-1β, all of which bind to CCR5, are inhibitory to HIV-1 replication in microglial cells, apparently by their ability to block viral entry."[] Infected microglia contain viral particles intracellularly.[] There is a correlation between the severity of dementia and microglial production of neurotoxins.[] One discrepancy in HAD is the limited number of HIV-1 infected microglia in comparison to the many CNS abnormalities that occur.[] This suggests that chemical factors that are released from microglial cells are contributing to neuronal loss. "It has become more and more apparent that HIV-1 infected microglial cells actively secrete both endogenous neurotoxins such as TNF-α, IL-1β, CXCL8/IL-8, glutamate, quinolinic acid, platelet activating factor, eicosanoids, and NO as well as the neurotoxic viral proteins Tat, gp120, and gp41."[] Microglia are the main target of HIV-1 in the brain. When activated by HIV-1 or viral proteins, they secrete or induce other cells to secrete neurotoxic factors; this process is accompanied by neuronal dysfunction (HAD).[]
Microglia
516
Herpes simplex virus
Herpes simplex virus (HSV) can cause herpes encephalitis in babies and immunocompetent adults. Studies have shown that long-term neuroimmune activation persists after the herpes infection in patients.[] Microglia produce cytokines that are toxic to neurons; this may be a mechanism underlying HSV-related CNS damage.[] It has been found that "active microglial cells in HSV encephalitis patients do persist for more than 12 months after antiviral treatment."[]
Role in bacterial infections
Lipopolysaccharide (LPS) is the major component of the outer membrane of a gram-negative bacterial cell wall. LPS has been shown to activate microglia in vitro and stimulates microglia to produce cytokines, chemokines, and prostaglandins.[] "Although LPS has been used as a classic activating agent, a recent study of rat microglia demonstrated that prolonged LPS exposure induces a distinctly different activated state from that in microglia acutely exposed to LPS."[]
Streptococcus pneumoniae
Streptococcus pneumoniae is the most common cause of bacterial meningitis. It is primarily localized to the subarachnoid space while cytokines and chemokines are produced inside the blood brain barrier.[] Microglia interact with streptococcus via their TLR2 receptor; this interaction then activates microglia to produce nitric oxide which is neurotoxic.[] The inflammatory response, triggered by microglia, may cause intracerebral edema.[]
Role in parasitic infections
Plasmodium falciparum
Plasmodium falciparum is a parasite that causes malaria in humans.[] A serious complication of malaria is cerebral malaria (CM).[] CM occurs when red blood cells break through the blood brain barrier causing microhemorrhages, ischemia and glial cell growth.[] This can lead to microglial aggregates called Durck's granulomas.[] Recent research has indicated that microglia play a major role in the pathogenesis of CM.[]
As a target to treat neuroinflammation
Inhibition of activation
One way to control neuroinflammation is to inhibit microglial activation. Studies on microglia have shown that they are activated by diverse stimuli but they are dependent on activation of mitogen-activated protein kinase (MAPK).[] Previous approaches to down-regulate activated microglia focused on immunosuppressants.[] Recently, minocycline (a tetracycline derivative) has shown down-regulation of microglial MAPK.[] Another promising treatment is CPI-1189, which induces cell death in a TNF α-inhibiting compound that also down-regulates MAPK.[] Recent study shows that nicergoline (Sermion) suppresses the production of proinflammatory cytokines and superoxide anion by activated microglia.[2] Microglial activation can be inhibited by MIF (microglia/macrophage inhibitory factor, tuftsin fragment 1–3, Thr-Lys-Pro). MIF-treated mice showed reduced brain injury and improved neurologic function in a mouse model of collagenase-induced intracerebral hemorrhage. [3][4]
Microglia
517
Regulation of chemokine receptor
The chemokine receptor, CX3CR1, is expressed by microglia in the central nervous system.[5] Fractalkine (CX3CL1) is the exclusive ligand for CX3CR1 and is made as a transmembrane glycoprotein from which a chemokine can be released.[5] Cardona, et al. stated in 2006 that "using three different in vivo models, we show that CX3CR1 deficiency dysregulates microglial responses, resulting in neurotoxicity."[5] Further studies into how CX3CR1 regulates microglial neurotoxicity could lead to new therapeutic strategies for neuroprotection.[5]
Inhibition of amyloid deposition
Inhibitors of amyloid deposition include the enzymes responsible for the production of extracellular amyloid such as β-secretase and γ-secretase inhibitors.[] Currently the γ-secretase inhibitors are in phase II clinical trials as a treatment for Alzheimer's disease but they have immunosuppressive properties, which could limit their use.[] Another strategy involves increasing the antibodies against a fragment of amyloid.[] This treatment is also in phase II clinical trials for the treatment of Alzheimer's disease.[]
Inhibition of cytokine synthesis
Glucocorticosteroids (GCS) are anti-inflammatory steroids that inhibit both central and peripheral cytokine synthesis and action.[] In a study conducted by Kalipada Pahan from the Department of Pediatrics at the Medical University of South Carolina, both lovastatin and sodium phenylacetate were found to inhibit TNF-α, IL-1β, and IL-6 in rat microglia.[] This shows that the mevalonate pathway plays a role in controlling the expression of cytokines in microglia and may be important in developing drugs to treat neurodegenerative diseases.[] Naltrexone may pose a solution to the inflammatory mediators produced by microglia. Although naltrexone's main action is to competitively bind to opioid receptors thereby upregulating the number of receptors; moverover, it is used to help patients with an opioid dependency. New research shows that low-dose naltrexone can inhibit cytokine synthesis of microglia cells. This mechanism is still in its infancy, but it has proven to help some patients suffering from fibromyalgia syndrome. Naltrexone shows more promise than GCSs because the GCSs inhibit immune system function, increase allergic reactions and, as the name implies, increase blood glucose levels.[]
References External links
• Microglia home page (http://www.microglia.net/microglia.htm) at microglia.net • The Role of Microglia in the Central Nervous System (http://cmr.asm.org/cgi/content/full/17/4/942) Clinical Microbiology Reviews October 2004, p. 942-964, Vol. 17, No. 4 • Creeping into your Head - A Brief Introduction to Microglia (http://www.scq.ubc.ca/?p=674) - A Review from the Science Creative Quarterly • "Immune Scavengers Target Alzheimer's Plaques" (http://focus.hms.harvard.edu/2007/040607/neuroscience. shtml). April 6, 2007. Retrieved 2007-05-09. - from Harvard University • The Department of Neuroscience at Wikiversity • NIF Search - Microglial Cell (https://www.neuinfo.org/mynif/search.php?q=Microglial Cell&t=data& s=cover&b=0&r=20) via the Neuroscience Information Framework
Neutrophil granulocyte
518
Neutrophil granulocyte
Neutrophil granulocyte
Neutrophils with a segmented nuclei surrounded by erythrocytes, the intra-cellular granules are visible in the cytoplasm (Giemsa stained) Code TH H2.00.04.1.02012
[1]
Neutrophil granulocytes are the most abundant type of white blood cells in mammals and form an essential part of the innate immune system. In general, they are referred to as either neutrophils or polymorphonuclear neutrophils (or PMNs), and are subdivided into segmented neutrophils (or segs) and banded neutrophils (or bands). They form part of the polymorphonuclear cell family (PMNs) together with basophils and eosinophils.[][][] The name neutrophil derives from staining characteristics on hematoxylin and eosin (H&E) histological or cytological preparations. Whereas basophilic white blood cells stain dark blue and eosinophilic white blood cells stain bright red, neutrophils stain a neutral pink. Normally, neutrophils contain a nucleus divided into 2–5 lobes. Neutrophils are a type of phagocyte and are normally found in the blood stream. During the beginning (acute) phase of inflammation, particularly as a result of bacterial infection, environmental exposure,[] and some cancers,[1][2] neutrophils are one of the first-responders of inflammatory cells to migrate towards the site of inflammation. They migrate through the blood vessels, then through interstitial tissue, following chemical signals such as Interleukin-8 (IL-8), C5a, fMLP and Leukotriene B4 in a process called chemotaxis. They are the predominant cells in pus, accounting for its whitish/yellowish appearance. Neutrophils are recruited to the site of injury within minutes following trauma and are the hallmark of acute inflammation.[3]
Neutrophil granulocyte
519
Characteristics
Neutrophil granulocytes have an average diameter of 12–15 micrometers (µm) in peripheral blood smears. When analyzing a pure neutrophil suspension on an automated cell counter, neutrophils have an average diameter of 8–9 µm. With the eosinophil and the basophil, they form the class of polymorphonuclear cells, named for the nucleus's multilobulated shape (as compared to lymphocytes and monocytes, the other types of white cells). The nucleus has a characteristic lobed appearance, the separate lobes connected by chromatin. The nucleolus disappears as the neutrophil matures, which is something that happens in only a few other types of nucleated cells.[4] In the cytoplasm, the Golgi apparatus is small, mitochondria and ribosomes are sparse, and the rough endoplasmic reticulum is absent.[5] The cytoplasm also contains about 200 granules, of which a third are azurophilic.[5] A minor difference is found between the neutrophils from a male subject and a female subject. The cell nucleus of a neutrophil from a female subject shows a small additional X chromosome structure, known as a "neutrophil drumstick".[6]
Neutrophil granulocyte migrates from the blood vessel to the matrix, sensing proteolytic enzymes, in order to determine intercellular connections (to the improvement of its mobility) and envelop bacteria through phagocytosis.
Neutrophils will show hypersegmentation (many segments of nucleus) in B12 and folate deficiency. Neutrophils are the most abundant white blood cells in humans (approximately 1011 are produced daily); they account for approximately 50-70% of all white blood cells (leukocytes). The stated normal range Reference ranges for blood tests of white blood cells, comparing neutrophil amount for human blood counts varies between (shown in pink) with that of other cells. laboratories, but a neutrophil count of 2.5–7.5 x 109/L is a standard normal range. People of African and Middle Eastern descent may have lower counts, which are still normal. A report may divide neutrophils into segmented neutrophils and bands. When circulating in the bloodstream and unactivated, neutrophils are spherical. Once activated, they change shape and become more amorphous or amoeba-like and can extend pseudopods as they hunt for antigens.[]
Neutrophil granulocyte
520
Life span
The average lifespan of (non-activated human) neutrophils in the circulation is about 5.4 days.[7] Upon activation, they marginate (position themselves adjacent to the blood vessel endothelium), and undergo selectin-dependent capture followed by integrin-dependent adhesion in most cases, after which they migrate into tissues, where they survive for 1–2 days.[] Neutrophils are much more numerous than the longer-lived HSC=Hematopoietic stem cell, Progenitor=Progenitor cell, L-blast=lymphoblast, monocyte/macrophage phagocytes. A Lymphocyte, Mo-blast=Monoblast, Monocyte, Myeloblast, Pro-M=Promyelocyte, pathogen (disease-causing Myelocyte, Meta-M=Metamyelocyte, Neutrophil, Eosinophil, Basophil, microorganism or virus) is likely to Pro-E=Proerythroblast, Baso-E=Basophilic erythroblast, poly-e=Polychromatic first encounter a neutrophil. Some erythroblast, Ortho-E=orthochromatic erythroblast, Erythrocyte, Promegakaryocyte, megakaryocyte, Platlet experts hypothesize that the short lifetime of neutrophils is an evolutionary adaptation. The short lifetime of neutrophils minimizes propagation of those pathogens that parasitize phagocytes because the more time such parasites spend outside a host cell, the more likely they will be destroyed by some component of the body's defenses. Also, because neutrophil antimicrobial products can also damage host tissues, their short life limits damage to the host during inflammation.[] Neutrophils will often be phagocytosed themselves by macrophages after digestion of pathogens. PECAM-1 and phosphatidylserine on the cell surface are involved in this process.
Chemotaxis
Neutrophils undergo a process called chemotaxis, which allows them to migrate toward sites of infection or inflammation. Cell surface receptors allow neutrophils to detect chemical gradients of molecules such as interleukin-8 (IL-8), interferon gamma (IFN-gamma), C5a, and Leukotriene B4, which these cells use to direct the path of their migration. Neutrophils have a variety of specific receptors, including complement receptors, cytokine receptors for interleukins and interferon gamma (IFN-gamma), receptors for chemokines, receptors to detect and adhere to endothelium, receptors for leptins and proteins, and Fc receptors for opsonin.[8]
Anti-microbial function
Being highly motile, neutrophils quickly congregate at a focus of infection, attracted by cytokines expressed by activated endothelium, mast cells, and macrophages. Neutrophils express[9] and release cytokines, which in turn amplify inflammatory reactions by several other cell types. In addition to recruiting and activating other cells of the immune system, neutrophils play a key role in the front-line defence against invading pathogens. Neutrophils have three methods for directly attacking micro-organisms: phagocytosis (ingestion), release of soluble anti-microbials (including granule proteins), and generation of neutrophil
Neutrophil granulocyte extracellular traps (NETs).[]
521
Phagocytosis
Neutrophils are phagocytes, capable of ingesting microorganisms or particles. For targets to be recognised, they must be coated in opsonins—a process known as antibody opsonization.[] They can internalize and kill many microbes, each phagocytic event resulting in the formation of a phagosome into which reactive oxygen species and hydrolytic enzymes are secreted. The consumption of oxygen during the generation of reactive oxygen species has been termed the "respiratory burst", although unrelated to respiration or energy production. The respiratory burst involves the activation of the enzyme NADPH oxidase, which produces large quantities of superoxide, a reactive oxygen species. Superoxide decays spontaneously or is broken down via enzymes known as superoxide dismutases (Cu/ZnSOD and MnSOD), to hydrogen peroxide, which is then converted to hypochlorous acid HClO, by the green heme enzyme myeloperoxidase. It is thought that the bactericidal properties of HClO are enough to kill bacteria phagocytosed by the neutrophil, but this may instead be a step necessary for the activation of proteases. []
Degranulation
Neutrophils also release an assortment of proteins in three types of granules by a process called degranulation. The contents of these granules have antimicrobial properties, and help combat infection.
Granule type azurophilic granules (or "primary granules") specific granules (or "secondary granules") tertiary granules Protein myeloperoxidase, bactericidal/permeability-increasing protein (BPI), Defensins, and the serine proteases neutrophil elastase and cathepsin G alkaline phosphatase, lysozyme, NADPH oxidase, collagenase, Lactoferrin and Cathelicidin
cathepsin and gelatinase
Neutrophil extracellular traps (NETs)
In 2004, Brinkmann and colleagues described a striking observation that activation of neutrophils causes the release of web-like structures of DNA; this represents a third mechanism for killing bacteria.[] These neutrophil extracellular traps (NETs) comprise a web of fibers composed of chromatin and serine proteases that trap and kill microbes extracellularly. It is suggested that NETs provide a high local concentration of antimicrobial components and bind, disarm, and kill microbes independent of phagocytic uptake. In addition to their possible antimicrobial properties, NETs may serve as a physical barrier that prevents further spread of pathogens. Trapping of bacteria may be a particularly important role for NETs in sepsis, where NET are formed within blood vessels.[] Recently, NETs have been shown to play a role in inflammatory diseases, as NETs could be detected in preeclampsia, a pregnancy-related inflammatory disorder in which neutrophils are known to be activated.[] In addition, NETs are known to exhibit pro-thrombotic effects both in vitro [10] and in vivo.[11][12]
Neutrophil granulocyte
522
Role in disease
Low neutrophil counts are termed neutropenia. This can be congenital (genetic disorder) or it can develop later, as in the case of aplastic anemia or some kinds of leukemia. It can also be a side-effect of medication, most prominently chemotherapy. Neutropenia makes an individual highly susceptible to infections. Neutropenia can be the result of colonization by intracellular neutrophilic parasites. In alpha 1-antitrypsin deficiency, the important neutrophil enzyme elastase is not adequately inhibited by alpha 1-antitrypsin, leading to excessive tissue damage in the presence of inflammation – the most prominent one being pulmonary emphysema. In Familial Mediterranean fever (FMF), a mutation in the pyrin (or marenostrin) gene, which is expressed mainly in neutrophil granulocytes, leads to a constitutively active acute-phase response and causes attacks of fever, arthralgia, peritonitis, and – eventually – amyloidosis.[]
Media
A neutrophil can be seen here selectively taking up several Candida yeasts (fluorescently labeled in green) despite several contacts with Aspergillus fumigatus conidia (unlabeled, white/clear) in a 3-D collagen matrix. Imaging time was 2 hours with one frame every 30 seconds.
[13] Neutrophils display highly directional amoeboid motility in infected footpad and phalanges. Intravital imaging was performed in the footpad path of LysM-eGFP mice 20 minutes after infection with LM.[13]
Neutrophil granulocyte
523
Additional images
A scanning electron microscope image of a single neutrophil (yellow), engulfing anthrax bacteria (orange)
Blood cell lineage
More complete lineages (very large)
References
[3] [4] [5] [6] [7] Cohen, Stephen. Burns, Richard C. Pathways of the Pulp, 8th Edition. St. Louis: Mosby, Inc. 2002. page 465. Zucker-Franklin, p. 168. Zucker-Franklin, p. 170. Zucker-Franklin, p. 174. Pillay J, den Braber I, Vrisekoop N, Kwast LM, de Boer RJ, Borghans JA, Tesselaar K, Koenderman L. In vivo labeling with 2H2O reveals a human neutrophil lifespan of 5.4 days (http:/ / bloodjournal. hematologylibrary. org/ cgi/ content/ full/ 116/ 4/ 625) Blood. 2010 Jul 29;116(4):625-7.
Cited text
• Zucker-Franklin, Dorothy; Greaves, M.F.; Grossi, C.E.; Marmont, A.M. (1988). "Neutrophils". Atlas of Blood Cells: Function and Pathology 1 (2nd ed. ed.). Philadelphia: Lea & Ferbiger. ISBN 0-8121-1094-3.
Eosinophil granulocyte
524
Eosinophil granulocyte
Eosinophil granulocyte
Eosinophil under the microscope (400x) from a peripheral blood smear. Red blood cells surround the eosinophil, two platelets at the top left corner. Code TH H2.00.04.1.02017
[1]
Eosinophil granulocytes, usually called eosinophils or eosinophiles (or, less commonly, acidophils), are white blood cells that are one of the immune system components responsible for combating multicellular parasites and certain infections in vertebrates. Along with mast cells, they also control mechanisms associated with allergy and asthma. They are granulocytes that develop during hematopoiesis in the bone marrow before migrating into blood. These cells are eosinophilic or 'acid-loving' as shown by their affinity to coal tar dyes: Normally transparent, it is this affinity that causes them to appear brick-red after staining with eosin, a red dye, using the Romanowsky method. The staining is concentrated in small granules within the cellular cytoplasm, which contain many chemical mediators, such as histamines and proteins such as eosinophil peroxidase, ribonuclease (RNase), deoxyribonucleases, lipase, plasminogen, and major basic protein. These mediators are released by a process called degranulation following activation of the eosinophil, and are toxic to both parasite and host tissues. In normal individuals, eosinophils make up about 1-6% of white blood cells, and are about 12-17 micrometers in size.[1] They are found in the medulla and the junction between the cortex and medulla of the thymus, and, in the lower gastrointestinal tract, ovary, uterus, spleen, and lymph nodes, but not in the lung, skin, esophagus, or some other internal organs Wikipedia:Vagueness under normal conditions. The presence of eosinophils in these latter organs is associated with disease. Eosinophils persist in the circulation for 8–12 hours, and can survive in tissue for an additional 8–12 days in the absence of stimulation.[2] Pioneering work in the 1980s elucidated that eosinophils were unique granulocytes, having the capacity to survive for extended periods of time after their maturation as demonstrated by ex-vivo culture experiments.
Eosinophil development, migration and activation
Eosinophils develop and mature in the bone marrow. They differentiate from myeloid precursor cells in response to the cytokines interleukin 3 (IL-3), interleukin 5 (IL-5), and granulocyte macrophage-colony stimulating factor (GM-CSF).[3][4][5] Eosinophils produce and store many secondary granule proteins prior to their exit from the bone marrow. After maturation, eosinophils circulate in blood and migrate to inflammatory sites in tissues, or to sites of helminth infection in response to chemokines like CCL11 (eotaxin-1), CCL24 (eotaxin-2), CCL5 (RANTES), and certain leukotrienes like leukotriene B4 (LTB4) and MCP1/4. At these infectious sites, eosinophils are activated by Type 2 cytokines released from a specific subset of helper T cells (Th2); IL-5, GM-CSF, and IL-3 are important for eosinophil activation as well as maturation. There is evidence to suggest that eosinophil granule protein expression is regulated by the non-coding RNA EGOT (gene)[]
Eosinophil granulocyte
525
Functions of eosinophils
Following activation, eosinophils effector functions include production of: • cationic granule proteins and their release by degranulation.[6][][] • reactive oxygen species such as superoxide, peroxide, and hypobromite (hypobromous acid, which is preferentially produced by eosinophil peroxidase).[7] • lipid mediators like the eicosanoids from the leukotriene (e.g., LTC4, LTD4, LTE4) and prostaglandin (e.g., PGE2) families.[8] • enzymes, such as elastase. • growth factors such as TGF beta, VEGF, and PDGF.[9][10] • cytokines such as IL-1, IL-2, IL-4, IL-5, IL-6, IL-8, IL-13, and TNF alpha.[][] In addition, eosinophils play a role in fighting viral infections, which is evident from the abundance of RNases they contain within their granules, and in fibrin removal during inflammation. Eosinophils along with basophils and mast cells, are important mediators of allergic responses and asthma pathogenesis and are associated with disease severity. They also fight helminth (worm) colonization and may be slightly elevated in the presence of certain parasites. Eosinophils are also involved in many other biological processes, including postpubertal mammary gland development, oestrus cycling, allograft rejection and neoplasia.[] They have also recently been implicated in antigen presentation to T cells.[11]
Eosinophil granule proteins
Following activation by an immune stimulus, eosinophils degranulate to release an array of cytotoxic granule cationic proteins that are capable of inducing tissue damage and dysfunction.[12] These include: • • • • major basic protein (MBP) eosinophil cationic protein (ECP) eosinophil peroxidase (EPO) eosinophil-derived neurotoxin (EDN)
Major basic protein, eosinophil peroxidase, and eosinophil cationic protein are toxic to many tissues.[] Eosinophil cationic protein and eosinophil-derived neurotoxin are ribonucleases with antiviral activity.[13] Major basic protein induces mast cell and basophil degranulation, and is implicated in peripheral nerve remodelling.[14][15] Eosinophil cationic protein creates toxic pores in the membranes of target cells allowing potential entry of other cytotoxic molecules to the cell,[16] can inhibit proliferation of T cells, suppress antibody production by B cells, induce degranulation by mast cells, and stimulate fibroblast cells to secrete mucus and glycosaminoglycan.[17] Eosinophil peroxidase forms reactive oxygen species and reactive nitrogen intermediates that promote oxidative stress in the target, causing cell death by apoptosis and necrosis.[]
Eosinophilia
An increase in eosinophils, i.e., the presence of more than 500 eosinophils/microlitre of blood is called an eosinophilia, and is typically seen in people with a parasitic infestation of the intestines, a collagen vascular disease (such as rheumatoid arthritis), malignant diseases such as Hodgkin's disease, extensive skin diseases (such as exfoliative dermatitis), Addison's disease, in the squamous epithelium of the esophagus in the case of reflux esophagitis, eosinophilic esophagitis, and with the use of certain drugs such as penicillin. In 1989, contaminated L-tryptophan supplements caused a deadly form of eosinophilia known as eosinophilia-myalgia syndrome, which was reminiscent of the Toxic Oil Syndrome in Spain in 1981.
Eosinophil granulocyte
526
Reference ranges for blood tests of white blood cells, comparing eosinophil granulocyte amount (shown in light red) with other cells.
Treatment
Treatments used to combat autoimmune diseases and conditions caused by eosinophils include: • • • • corticosteroids- promote apoptosis. Numbers of eosinophils in blood are rapidly reduced monoclonal antibody therapy- e.g., mepoluzimab or reslizumab against IL-5, prevents eosinophilopoiesis antagonists of leukotriene synthesis or receptors Gleevec (STI571)- inhibits PDGF-BB in hypereosinophilic leukemia
Additional images
Eosinophil in peripheral blood (Giemsa stain)
Blood cell lineage
Eosinophil
References External links
• eosinophilic+leukocyte (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=eosinophilic+ leukocyte) at eMedicine Dictionary • Bioweb at UWLAX Eosinophil (http://bioweb.uwlax.edu/APlab/Table_of_Contents/Lab_11/Eosinophil/ eosinophil.html) • Histology at ucsf.edu (http://missinglink.ucsf.edu/lm/IDS_101_histo_resource/images/ eosinophil_100x-labelled.jpg) • "What is an eosinophil?" at the Cincinnati Center for Eosinophilic Disorders (http://www.cincinnatichildrens. org/svc/alpha/e/eosinophilic/about/eosinophil.htm)
Basophil granulocyte
527
Basophil granulocyte
Basophil granulocyte
Basophil granulocyte
Basophil Code TH H2.00.04.1.02022 [1]
Basophil granulocytes, mostly referred to as basophils, are the least common of the granulocytes, representing about 0.01% to 0.3% of circulating white blood cells. The name comes from the fact that these leukocytes are basophilic, i.e., they are susceptible to staining by basic dyes, as shown in the picture. Basophils contain large cytoplasmic granules which obscure the cell nucleus under the microscope. However, when unstained, the nucleus is visible and it usually has 2 lobes. The mast cell, a cell in tissues, has many similar characteristics. For example, both cell types store histamine, a chemical that is secreted by the cells when stimulated in certain ways (histamine causes some of the symptoms of an allergic reaction). Like all circulating granulocytes, basophils can be recruited out of the blood into a tissue when needed.
Function
Basophils appear in many specific kinds of inflammatory reactions, particularly those that cause allergic symptoms. Basophils contain anticoagulant heparin, which prevents blood from clotting too quickly. They Reference ranges for blood tests of white blood cells, comparing basophil granulocyte also contain the vasodilator histamine, amount (shown in violet) with other cells. which promotes blood flow to tissues. They can be found in unusually high numbers at sites of ectoparasite infection, e.g., ticks. Like eosinophils, basophils play a role in both parasitic infections and allergies.[1] They are found in tissues where allergic reactions are occurring and probably contribute to the severity of these reactions. Basophils have protein receptors on their cell surface that bind IgE, an immunoglobulin involved in macroparasite defense and allergy. It is the bound IgE antibody that confers a selective response of these cells to environmental substances, for example, pollen proteins or helminth antigens. Recent studies in mice suggest that basophils may also regulate the behavior of T cells and mediate the magnitude of the secondary immune response.[2]
Basophil granulocyte
528
Immunophenotyping of basophils
Basophils of mouse and human have consistent immunophenotypes as follows: FcεRI+, CD123, CD49b(DX-5)+, CD69+, Thy-1.2+, 2B4+, CD11bdull, CD117(c-kit)–, CD24–, CD19–, CD80–, CD14–, CD23–, Ly49c–, CD122–, CD11c–, Gr-1–, NK1.1–, B220–, CD3–, γδTCR–, αβTCR–, α4 and β4-integrin negative.[3] Recently, Heneberg [] proposed that basophils may be defined as the cellular population positive for CD13, CD44, CD54, CD63, CD69, CD107a, CD123, CD164, CD193/ CCR3, CD203c, TLR-4, and FcεRI. When activated, some additional surface markers are known to be upregulated (CD13, CD107a, CD164), or surface-exposed (CD63, and the ectoenzyme CD203c).[]
Secretions
When activated, basophils degranulate to release histamine, proteoglycans (e.g. heparin and chondroitin), and proteolytic enzymes (e.g. elastase and lysophospholipase). They also secrete lipid mediators like leukotrienes, and several cytokines. Histamine and proteoglycans are pre-stored in the cell's granules while the other secreted substances are newly generated. Each of these substances contributes to inflammation. Recent evidence suggests that basophils are an important source of the cytokine, interleukin-4, perhaps more important than T cells. Interleukin-4 is considered one of the critical cytokines in the development of allergies and the production of IgE antibody by the immune system. There are other substances that can activate basophils to secrete which suggests that these cells have other roles in inflammation.[] The degranulation of basophils can be investigated in vitro by using flow cytometry and the so-called basophil-activation-test (BAT). Especially, in the diagnosis of allergies including of drug reactions (e.g. induced by contrast medium), the BAT of is great impact [4]. Basopenia (a low basophil count) is difficult to demonstrate as the normal basophil count is so low; it has been reported in association with autoimmune urticaria[5] (a chronic itching condition). Basophilia is also uncommon but may be seen in some forms of leukaemia or lymphoma.
References
[1] Voehringer D. 2009. Trends in Parasitology. [3] Schroeder JT (2009). "Basophils beyond effector cells of allergic inflammation." Adv Immunol 101:123-161, PMID 19231594, . [4] Böhm I et al. Pilot study on basophil activation induced by contrast medium. Fundam Clin Pharmacol 2011;25:267 - 276
Additional images
Blood cell lineage
Alternate stain of a basophil
Hybridoma technology
529
Hybridoma technology
Hybridoma technology is a technology of forming hybrid cell lines (called hybridomas) by fusing a specific antibody-producing B cell with a myeloma (B cell cancer) cell that is selected for its ability to grow in tissue culture and for an absence of antibody chain synthesis. The antibodies produced by the hybridoma are all of a single specificity and are therefore monoclonal antibodies (in contrast to polyclonal antibodies). The production of monoclonal antibodies was invented by Cesar Milstein and Georges J. F. Köhler in 1975. They shared the Nobel Prize of 1984 for Medicine and Physiology with Niels Kaj Jerne, who made other contributions to immunology. The term hybridoma was coined by Leonard Herzenberg during his sabbatical in Cesar Milstein's laboratory in 1976/1977.[1]
Method
Laboratory animals (mammals, e.g. mice) are first exposed to an antigen to which we are interested in isolating an antibody against. Usually this is done by a series of injections of the antigen in question, over the course of several weeks. Once splenocytes are isolated from the mammal's spleen, the B cells are fused with immortalised myeloma cells. The myeloma cells are selected beforehand to ensure they are not secreting antibody themselves and that they lack the hypoxanthine-guanine phosphoribosyltransferase (HGPRT) gene, making them sensitive to the HAT medium (see below). The fusion is accomplished using polyethylene glycol or the Sendai virus. It is performed by making the cell membranes more permeable.Wikipedia:Please clarify Fused cells are incubated in HAT medium (hypoxanthine-aminopterin-thymidine medium) for roughly 10 to 14 days. Aminopterin blocks the pathway that allows for nucleotide synthesis. Hence, unfused myeloma cells die, as they cannot produce nucleotides by the de novo or salvage pathways because they lack HGPRT. Removal of the unfused myeloma cells is necessary because they have the potential to outgrow other cells, especially weakly established hybridomas. Unfused B cells die as they have a short life span. In this way, only the B cell-myeloma hybrids survive, since the HGPRT gene coming from the B cells is functional. These cells produce antibodies (a property of B cells) and are immortal (a property of myeloma cells). The incubated medium is then diluted into multi-well plates to such an extent that each well
(1) Immunisation of a mouse (2) Isolation of B cells from the spleen (3) Cultivation of myeloma cells (4) Fusion of myeloma and B cells (5) Separation of cell lines (6) Screening of suitable cell lines (7) in vitro (a) or in vivo (b) multiplication (8) Harvesting
Hybridoma technology
530
contains only one cell. Since the antibodies in a well are produced by the same B cell, they will be directed towards the same epitope, and are thus monoclonal antibodies. The next stage is a rapid primary screening process, which identifies and selects only those hybridomas that produce antibodies of appropriate specificity. The hybridoma culture supernatant, secondary enzyme labeled conjugate, and chromogenic substrate, are then incubated, and the formation of a colored product indicates a positive hybridoma. Alternatively, immunocytochemical screening can also be used.[] The B cell that produces the desired antibodies can be cloned to produce many identical daughter clones. Supplemental media containing interleukin-6 (such as briclone) are essential for this step. Once a hybridoma colony is established, it will continually grow in culture medium like RPMI-1640 (with antibiotics and fetal bovine serum) and produce antibodies.[]
Hybridoma cells grown in tissue culture. The image shows a single clone of cells each of which is producing large amounts of a specific monoclonal antibody which the cells secrete and which can be readily purified from the culture media.
Multiwell plates are used initially to grow the hybridomas, and after selection, are changed to larger tissue culture flasks. This maintains the well-being of the hybridomas and provides enough cells for cryopreservation and supernatant for subsequent investigations. The culture supernatant can yield 1 to 60 µg/ml of monoclonal antibody, which is maintained at -20 °C or lower until required.[] By using culture supernatant or a purified immunoglobulin preparation, further analysis of a potential monoclonal antibody producing hybridoma can be made in terms of reactivity, specificity, and cross-reactivity.[]
Applications
The use of monoclonal antibodies is numerous and includes the prevention, diagnosis, and treatment of disease. For example, monoclonal antibodies can distinguish subsets of B cells and T cells, which is helpful in identifying different types of leukaemias. In addition, specific monoclonal antibodies have been used to define cell surface markers on white blood cells and other cell types. This led to the Cluster of differentiation series of markers. These are often referred to as CD markers and define several hundred different cell surface components of cells, each specified by binding of a particular monoclonal antibody. Such antibodies are extremely useful for fluorescence-activated cell sorting, the specific isolation of particular types of cells.
In diagnostic histopathology
With the help of monoclonal antibodies, tissues and organs can be classified based on their expression of certain defined markers, which reflect tissue or cellular genesis. Prostate specific antigen, placental alkaline phosphatase, human chorionic gonadotrophin, α-fetoprotein and others are organ-associated antigens and the production of monoclonal antibodies against these antigens helps in determining the nature of a primary tumor.[] Monoclonal antibodies are especially useful in distinguishing morphologically similar lesions, like pleural and peritoneal mesothelioma, adenocarcinoma, and in the determination of the organ or tissue origin of undifferentiated metastases. Selected monoclonal antibodies help in the detection of occult metastases by immuno-cytological analysis of bone marrow, other tissue aspirates, as well as lymph nodes and other tissues.[]
Hybridoma technology One study[2] performed a sensitive immuno-histochemical assay on bone marrow aspirates of 20 patients with localized prostate cancer. Three monoclonal antibodies (T16, C26, and AE-1), capable of recognizing membrane and cytoskeletal antigens expressed by epithelial cells to detect tumour cells, were used in the assay. Bone marrow aspirates of 22% of patients with localized prostate cancer (stage B, 0/5; Stage C, 2/4), and 36% patients with metastatic prostate cancer (Stage D1, 0/7 patients; Stage D2, 4/4 patients) had antigen-positive cells in their bone marrow. It was concluded that immuno-histochemical staining of bone marrow aspirates are very useful to detect occult bone marrow metastases in patients with apparently localized prostate cancer. Although immuno-cytochemistry using tumor-associated monoclonal antibodies has led to an improved ability to detect occult breast cancer cells in bone marrow aspirates and peripheral blood, further development of this method is necessary before it can be used routinely.[3] One major drawback of immuno-cytochemistry is that only tumor-associated and not tumor-specific monoclonal antibodies are used, and as a result, some cross-reaction with normal cells can occur.[4] The detection of small quantities of invasive or metastatic cells by normal histopathological staining with haematoxylin and eosin is not always sensitive. The use of monoclonal antibodies increases the sensitivity to a large extent. For example, the use of monoclonal antibodies to cytokeratin in the investigation of the sentinel axillary lymph node for metastatic breast cancer increases nodal positivity by up to 10%.[] In order to effectively stage breast cancer and assess the efficacy of purging regimens prior to autologous stem cell infusion, it is important to detect even small quantities of breast cancer cells. Immuno-histochemical methods are ideal for this purpose because they are simple, sensitive, and quite specific. Franklin et al.[5] performed a sensitive immuno-cytochemical assay by using a combination of four monoclonal antibodies (260F9, 520C9, 317G5 and BrE-3) against tumor cell surface glycoproteins to identify breast tumour cells in bone marrow and peripheral blood. They concluded from the results that immuno-cytochemical staining of bone marrow and peripheral blood is a sensitive and simple way to detect and quantify breast cancer cells. One of the main reasons for metastatic relapse in patients with solid tumours is the early dissemination of malignant cells. The use of monoclonal antibodies (mAbs) specific for cytokeratins can identify disseminated individual epithelial tumor cells in the bone marrow. One study[6] reports on having developed an immuno-cytochemical procedure for simultaneous labeling of cytokeratin component no. 18 (CK18) and prostate specific antigen (PSA). This would help in the further characterization of disseminated individual epithelial tumor cells in patients with prostate cancer. The twelve control aspirates from patients with benign prostatic hypertrophy showed negative staining, which further supports the specificity of CK18 in detecting epithelial tumour cells in bone marrow. In most cases of malignant disease complicated by effusion, neoplastic cells can be easily recognized. However, in some cases, malignant cells are not so easily seen or their presence is doubtful to call it a positive report. The use of immuno-cytochemical techniques increases diagnostic accuracy in these cases. Ghosh, Mason and Spriggs[7] analysed 53 samples of pleural or peritoneal fluid from 41 patients with malignant disease. Conventional cytological examination had not revealed any neoplastic cells. Three monoclonal antibodies (anti-CEA, Ca 1 and HMFG-2) were used to search for malignant cells. Immunocytochemical labelling was performed on unstained smears, which had been stored at -20°C up to 18 months. Twelve of the forty-one cases in which immuno-cytochemical staining was performed, revealed malignant cells. The result represented an increase in diagnostic accuracy of approximately 20%. The study concluded that in patients with suspected malignant disease, immuno-cytochemical labeling should be used routinely in the examination of cytologically negative samples and has important implications with respect to patient management. The use of immuno-cytochemical techniques can help to avoid performing procedures, which are painful, uncomfortable and expensive to the patient. It can also help to speed up the start of appropriate treatment.
531
Hybridoma technology Another application of immuno-cytochemical staining is for the detection of two antigens in the same smear. Double staining with light chain antibodies and with T and B cell markers can indicate the neoplastic origin of a lymphoma.[8] One study has reported the isolation of a hybridoma cell line (clone 1E10), which produces a monoclonal antibody (IgM, k isotype). This monoclonal antibody shows specific immuno-cytochemical staining of nucleoli.[9] Tissues and tumours can be classified based on their expression of certain markers, with the help of monoclonal antibodies. They help in distinguishing morphologically similar lesions and in determining the organ or tissue origin of undifferentiated metastases. Immuno-cytological analysis of bone marrow, tissue aspirates, lymph nodes etc. with selected monoclonal antibodies help in the detection of occult metastases. Monoclonal antibodies increase the sensitivity in detecting even small quantities of invasive or metastatic cells. Monoclonal antibodies (mAbs) specific for cytokeratins can detect disseminated individual epithelial tumour cells in the bone marrow. Immuno-cytochemical staining can also detect the presence of two antigens in the same smear.
532
References External links
• Hybridomas (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Hybridomas) at the US National Library of Medicine Medical Subject Headings (MeSH) • "Hybridoma Technology" (http://www.cancer.gov/cancertopics/understandingcancer/immunesystem/ page36). Understanding Cancer Series: The Immune System. National Cancer Institute.
Mast cell
533
Mast cell
Mast cell
Mast cells Latin Code mastocytus TH H2.00.03.0.01010
[1]
A mast cell (also known as mastocyte and labrocyte[1]) is a resident cell of several types of tissues and contains many granules rich in histamine and heparin. Although best known for their role in allergy and anaphylaxis, mast cells play an important protective role as well, being intimately involved in wound healing and defense against pathogens.[] The mast cell is very similar in both appearance and function to the basophil, a type of white blood cell. However, they are not the same, as they arise from different cell lines.[2]
Origin and classification
Mast cells were first described by Paul Ehrlich in his 1878 doctoral thesis on the basis of their unique staining characteristics and large granules. These granules also led him to the mistaken belief that they existed to nourish the surrounding tissue, and he named them "Mastzellen" (from the German: Mast, "fattening" as of animals).[3][4] They are now considered to be part of the immune system.
Mast cell
Mast cells are very similar to basophil granulocytes (a class of white blood cells) in blood. Both are granulated cells that contain histamine and heparin, an anticoagulant. Both cells also release histamine upon binding to immunoglobulin E.[2] These similarities have led many to speculate that mast cells are basophils that have "homed in" on tissues. Furthermore they share a common precursor in bone marrow. Nevertheless, both mast cells and basophils are thought to originate from bone marrow precursors expressing the CD34 molecule. Basophils leave the bone marrow already mature, whereas the mast cell circulates in an immature form, only maturing once in a tissue site. The site an immature mast cell settles in probably determines its precise characteristics.[] The first in vitro differentiation and growth of a pure population of mouse mast cells has been carried out using conditioned medium derived from concanavalin A-stimulated splenocytes.[] Later, it was discovered that T cell-derived interleukin 3 was the component present in the conditioned media that was required for mast cell differentiation and growth.[] Two types of mast cells are recognized, those from connective tissue and a distinct set of mucosal mast cells. The activities of the latter are dependent on T-cells.[] Mast cells are present in most tissues characteristically surrounding blood vessels and nerves, and are especially prominent near the boundaries between the outside world and the internal milieu, such as the skin, mucosa of the lungs and digestive tract, as well as in the mouth, conjunctiva and nose.[]
Mast cell
534
Physiology
Mast cells play a key role in the inflammatory process. When activated, a mast cell rapidly releases its characteristic granules and various hormonal mediators into the interstitium. Mast cells can be stimulated to degranulate by direct injury (e.g. physical or chemical [such as opioids, alcohols, and certain antibiotics such as polymyxins]), cross-linking of Immunoglobulin E (IgE) receptors, or by activated complement proteins.[] Mast cells express a high-affinity receptor (FcεRI) for the Fc region of IgE, the least-abundant member of the antibodies. This receptor is of such high affinity that binding of IgE molecules is essentially irreversible. As a result, mast cells are coated with IgE. IgE is produced by plasma cells (the antibody-producing cells of the immune system). IgE molecules, like all antibodies, are specific to one particular antigen. In allergic reactions, mast cells remain inactive until an allergen binds to IgE already in association with the cell (see above). Other membrane activation events can either prime mast cells for subsequent degranulation or can act in synergy with FceRI signal transduction.[] Allergens are generally proteins or polysaccharides. The allergen binds to the antigen-binding sites, which are situated on the variable regions of the IgE molecules bound to the mast cell surface. It appears that binding of two or more IgE molecules (cross-linking) is required to activate the mast cell. The clustering of the intracellular domains of the cell-bound Fc receptors, which are associated with the cross-linked IgE molecules, causes a complex sequence of reactions inside the mast cell that lead to its activation. Although this reaction is most well understood in terms of allergy, it appears to have evolved as a defense system against intestinal worm infestations (tapeworms, etc.)[citation needed]. The molecules thus released into the extracellular environment include:[] • preformed mediators (from the granules): • serine proteases, such as tryptase • histamine (2-5 pg/cell) • serotonin • proteoglycans, mainly heparin (active as anticoagulant) • newly formed lipid mediators (eicosanoids): • thromboxane • prostaglandin D2 • leukotriene C4 • platelet-activating factor • cytokines • Eosinophil chemotactic factor Histamine dilates post capillary venules, activates the endothelium, and increases blood vessel permeability. This leads to local edema (swelling), warmth, redness, and the attraction of other inflammatory cells to the site of release. It also irritates nerve endings (leading to itching or pain). Cutaneous signs of histamine release are the "flare and wheal"-reaction. The bump and redness immediately following a mosquito bite are a good example of this reaction, which occurs seconds after challenge of the mast cell by an allergen.[]
The role of mast cells in the development of allergy.
Mast cell
535 The other physiologic activities of mast cells are much less well-understood. Several lines of evidence suggest that mast cells may have a fairly fundamental role in innate immunity – they are capable of elaborating a vast array of important cytokines and other inflammatory mediators such as TNFa, they express multiple "pattern recognition receptors" thought to be involved in recognizing broad classes of pathogens, and mice without mast cells seem to be much more susceptible to a variety of infections.[citation needed]
Structure of histamine
Mast cell granules carry a variety of bioactive chemicals. These granules have been found to be transferred to adjacent cells of the immune system and neurons via transgranulation via their pseudopodia.[]
Role in disease
Allergic disease
Many forms of cutaneous and mucosal allergy are mediated for a large part by mast cells; they play a central role in asthma, eczema, itch (from various causes) and allergic rhinitis and allergic conjunctivitis. Antihistamine drugs act by blocking the action of histamine on nerve endings. Cromoglicate-based drugs (sodium cromoglicate, nedocromil) block a calcium channel essential for mast cell degranulation, stabilizing the cell and preventing release of histamine and related mediators. Leukotriene antagonists (such as montelukast and zafirlukast) block the action of leukotriene mediators, and are being used increasingly in allergic diseases.[]
Anaphylaxis
In anaphylaxis (a severe systemic reaction to allergens, such as nuts, bee stings or drugs), body-wide degranulation of mast cells leads to vasodilation and, if severe, symptoms of life-threatening shock.[citation needed]
Autoimmunity
Mast cells are implicated in the pathology associated with the autoimmune disorders rheumatoid arthritis, bullous pemphigoid, and multiple sclerosis. They have been shown to be involved in the recruitment of inflammatory cells to the joints (e.g. rheumatoid arthritis) and skin (e.g. bullous pemphigoid) and this activity is dependent on antibodies and complement components.[5]
Reproductive disorders
Mast cells are present within the endometrium, with increased activation and release of mediators in endometriosis.[] In males, mast cells are present in the testes and are increased in oligo- and azoospermia, with mast cell mediators directly suppressing sperm motility in a potentially reversible manner.[]
Mast cell disorders
Mastocytosis is a rare condition featuring proliferation of mast cells. It exists in a cutaneous and systemic form, with the former being limited to the skin and the latter involving multiple organs.[] Mast cell tumors are often seen in dogs and cats.[6]
Mast cell
536
Histological staining
Toluidine blue - one of the most common stains for acid mucopolysaccharides and glycoaminoglycans, components of mast cells granules.[7] Surface markers - Cell surface markers of mast cells were referred in detail by Heneberg,[] claiming that mast cells may be inadverently included in the stem or progenitor cell isolates since part of them is positive for the CD34 antigen. The classical mast cell markers include the high affinity IgE receptor, CD25 (non-neoplastic mast cells), CD117 (c-Kit), CD23 and CD203c (for most of the mast cell populations). Expression of some molecules may change in course of the mast cell activation.[]
References
[1] http:/ / www. memidex. com/ labrocytes [2] Marieb, Elaine N. & Katja Hoehn. Human Anatomy and Physiology. Seventh edition. San Francisco: Pearson Benjamin Cummings, 2007. pg. 659. [3] Ehrlich P. Beiträge zur Theorie und Praxis der histologischen Färbung. Dissertation at Leipzig University, 1878. [4] (http:/ / www. mondofacto. com/ facts/ dictionary?mastocyte) [5] http:/ / www. sciencemag. org/ cgi/ content/ full/ 297/ 5587/ 1689 [7] http:/ / www. springerlink. com/ content/ n3321437646586h8/
External links
• Mast cells (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Mast+cells) at the US National Library of Medicine Medical Subject Headings (MeSH)
T helper cell
T helper cells (Th cells) are a sub-group of lymphocytes, a type of white blood cell, that play an important role in the immune system, particularly in the adaptive immune system. They help the activity of other immune cells by releasing T cell cytokines. They are essential in B cell antibody class switching, in the activation and growth of cytotoxic T cells, and in maximizing bactericidal activity of phagocytes such as macrophages. Mature Th cells express the surface protein CD4 and are referred to as CD4+ T cells. CD4+ T cells are generally treated as having a pre-defined role as helper T cells within the immune system. For example, when an antigen presenting cell expresses an antigen on MHC class II, a CD4+ cell will aid those cells through a combination of cell to cell interactions (e.g. CD40 and CD40L) and through cytokines. Nevertheless, there are rare exceptions; for example, sub-groups of regulatory T cells, natural killer T cells, and cytotoxic T cells express CD4 (although cytotoxic examples have been observed in extremely low numbers in specific disease states, they are usually considered non-existent). All of the latter CD4+ T cell groups are not considered T helper cells. The importance of helper T cells can be seen from HIV, a virus that infects CD4+ cells. Towards the end of an HIV infection the number of functional CD4+ T cells falls, which leads to the symptomatic stage of infection known as the acquired immunodeficiency syndrome (AIDS). There are also some rare disorders that result in the absence or dysfunction of CD4+ T cells. These disorders produce similar symptoms, and many of these are fatal.
T helper cell
537
Activation of naïve helper T cells
Following T cell development, matured, naïve T cells leave the thymus and begin to spread throughout the body, including the lymph nodes. (Naïve T cells are those T cells that have never been exposed to the antigen that they are programmed to respond to). Like all T cells, they express the T cell receptor-CD3 complex. The T cell receptor (TCR) consists of both constant and variable regions. The variable region determines what antigen the T cell can respond to. CD4+ T cells have TCRs with an affinity for Class II MHC, and CD4 is involved in determining MHC affinity during maturation in the thymus. Class II MHC proteins are generally only found on the surface of specialised antigen-presenting cells (APCs). Specialised antigen presenting cells are primarily dendritic cells, macrophages and B cells, although B cells are the only cell group that expresses MHC Class II constitutively (at all times). Some APCs also bind native (or unprocessed) antigens to their surface, such as follicular dendritic cells, but unprocessed antigens do not interact with T cells and are not involved in their activation. The antigens that bind to MHC proteins are always short peptides, 8-10 amino acids long for MHC Class I, and up to 25 or so for MHC Class II.
Recognition (Signal 1)
During an immune response, professional antigen-presenting cells (APCs) endocytose foreign material (typically bacteria or viruses), which undergoes processing, then travel from the infection site to the lymph nodes. Once at the lymph nodes, the APC begin to present antigen peptides that are bound to Class II MHC, allowing CD4+ T cells that express the specific TCRs against the peptide/MHC complex to activate. When a Th cell encounters and recognises the antigen on an APC, the TCR-CD3 complex binds strongly to the peptide-MHC complex present on the surface of professional APCs. CD4, a co-receptor of the TCR complex, also binds to a different section of the MHC molecule. These interactions bring these proteins closer together, allowing the intracellular kinases present on the TCR, CD3 and CD4 proteins to activate each other via phosphorylation. With the assistance of a phosphatase present on the intracellular section of CD45 (common leukocyte antigen), these molecules activate major Th cell intracellular pathways. These active pathways are known as Signal 1 of T cell activation, as it is the first and primary pro-activation signal in a Th cell. Upon subsequent encounters with a given antigen, memory T cells are re-activated using the same TCR pathways. The binding of the antigen-MHC to the TCR complex and CD4 may also help the APC and the Th cell adhere during Th cell activation, but the integrin protein LFA-1 on the T cell and ICAM on the APC are the primary molecules of adhesion in this cell interaction. It is unknown what role the relatively bulky extracellular region of CD45 plays during cell interactions, but CD45 has various isoforms that change in size depending on the Th cell's activation and maturation status. For example, CD45 shortens in length following Th activation (CD45RA+ to CD45RO+), but whether this change in length influences activation is unknown. It has been proposed that the larger CD45RA+ may decrease the accessibility of the T cell receptor for the antigen-MHC molecule, thereby necessitating an increase in the affinity (and specificity) of the T cell for activation. Once the activation has occurred however, CD45 shortens, allowing easier interactions and activation as an effector T helper cell.[citation needed]
Verification (Signal 2)
Having received the first TCR/CD3 signal, the naïve T cell must activate a second independent biochemical pathway, known as Signal 2. This verification step is a protective measure to ensure that a T cell is responding to a foreign antigen. If this second signal is not present during initial antigen exposure, the T cell presumes that it is auto-reactive. This results in the cell becoming anergic (anergy is generated from the unprotected biochemical changes of Signal 1). Anergic cells will not respond to any antigen in the future, even if both signals are present later on. These cells are generally believed to circulate throughout the body with no value until they undergo apoptosis.
T helper cell The second signal involves an interaction between CD28 on the CD4+ T cell and the proteins CD80 (B7.1) or CD86 (B7.2) on the professional APCs. Both CD80 and CD86 activate the CD28 receptor. These proteins are also known as co-stimulatory molecules. Although the verification stage is necessary for the activation of naïve helper T cells, the importance of this stage is best demonstrated during the similar activation mechanism of CD8+ cytotoxic T cells. As naïve CD8+ T cells have no true bias towards foreign sources, these T cells must rely on the activation of CD28 for confirmation that they recognise a foreign antigen (as CD80/CD86 is only expressed by active APC's). CD28 plays an important role in decreasing the risk of T cell auto-immunity against host antigens. Once the naïve T cell has both pathways activated, the biochemical changes induced by Signal 1 are altered, allowing the cell to activate instead of anergise. The second signal is then obsolete; only the first signal is necessary for future activation. This is also true for memory T cells, which is one example of learned immunity. Faster responses occur upon reinfection because memory T cells have already undergone confirmation and can produce effector cells much sooner.
538
Proliferation
Once the two-signal activation is complete the T helper cell (Th) then allows itself to proliferate. It achieves this by releasing a potent T cell growth factor called interleukin 2 (IL-2) which acts upon itself in an autocrine fashion. Activated T cells also produce the alpha sub-unit of the IL-2 receptor (CD25 or IL-2R), enabling a fully functional receptor that can bind with IL-2, which in turn activates the T cell's proliferation pathways. The autocrine or paracrine secretion of IL-2 can bind that same Th cell or neighboring Th's via the IL-2R thus driving proliferation and clonal expansion. The Th cells receiving both signals of activation will then become Th0 cells (T helper 0) cell that secrete IL-2, IL-4 and interferon gamma (IFN-γ). The Th0 cells will then differentiate into Th1 or Th2 cells depending on cytokine environment. IFN-γ drives Th1 cell production while IL-10 and IL-4 inhibit Th1 cell production. Conversely, IL-4 drives Th2 cell production and IFN-γ inhibits Th2 cells. It should be noted that these cytokines are pleiotropic and carry out many other functions of the immune response.
Maturation
After many cell generations, the Th cell's progenitors differentiate into effector Th cells, memory Th cells, and regulatory Th cells. • Effector Th cells secrete cytokines, proteins or peptides that stimulate or interact with other leukocytes, including Th cells. • Memory Th cells retain the antigen affinity of the originally activated T cell, and are used to act as later effector cells during a second immune response (e.g. if there is re-infection of the host at a later stage). • Regulatory T cells do not promote immune function, but act to decrease it instead. Despite their low numbers during an infection, these cells are believed to play an important role in the self-limitation of the immune system; they have been shown to prevent the development of various auto-immune diseases.
Determination of the effector T cell response
Helper T cells are capable of influencing a variety of immune cells, and the T cell response generated (including the extracellular signals such as cytokines) can be essential for a successful outcome from infection. In order to be effective, helper T cells must determine which cytokines will allow the immune system to be most useful or beneficial for the host. Understanding exactly how helper T cells respond to immune challenges is currently of major interest in immunology, because such knowledge may be very useful in the treatment of disease and in increasing the effectiveness of vaccination.
T helper cell
539
Th1/Th2 Model for helper T cells
Proliferating helper T cells that develop into effector T cells differentiate into two major subtypes of cells known as Th1 and Th2 cells (also known as Type 1 and Type 2 helper T cells, respectively).
Th1/Th2 Model for helper T cells. An antigen is ingested and processed by an APC. It presents fragments from [1] it to T cells. The upper, Th0, is a T helper cell. The fragment is presented to it by MHC2. IFN-γ, interferon γ; TGF-β, transforming growth factor β; mø, macrophage; IL-2, interleukin 2; IL-4, interleukin 4
Type 1/ Th1 Main partner Macrophage cell type Cytokines produced
Type 2/ Th2 B-cell
interferon-γ and TGF-beta. (Interleukin-2 was classically interleukin-4, interleukin-5, interleukin-6, interleukin-10, interleukin-13 associated with Th1 cells, but this association may be misleading; IL-2 is produced by all helper T cells early in their activation.) interleukin-10 production has been [2] shown to be induced in activated Th1 cell Cellular immune system. Maximizes the killing efficacy of the macrophages and the proliferation of cytotoxic CD8+ T cells. Also promotes the production of opsonizing antibodies The Type 1 cytokine IFN-γ increases the production of interleukin-12 by dendritic cells and macrophages, and via positive feedback, IL-12 stimulates the production of IFN-γ in helper T cells, thereby promoting the Th1 profile. IFN-gamma also inhibits the production of cytokines such as interleukin-4, an important cytokine associated with the Type 2 response, and thus it also acts to preserve its own response. Humoral immune system. Stimulates B-cells into proliferation, to induce B-cell antibody class switching, and to increase neutralizing antibody production.
Immune stimulation promoted
Other functions
The Type 2 response promotes its own profile using two different cytokines. Interleukin-4 acts on helper T cells to promote the production of Th2 cytokines (including itself; it is auto-regulatory), while interleukin-10 (IL-10) inhibits a variety of cytokines including interleukin-2 and IFN-γ in helper T cells and IL-12 in dendritic cells and macrophages. The combined action of these two cytokines suggests that once the T cell has decided to produce these cytokines, that decision is preserved (and also encourages other T cells to do the same).
While we know about the types of cytokine patterns helper T cells tend to produce, we understand less about how the patterns themselves are decided. Various evidence suggests that the type of APC presenting the antigen to the T cell
T helper cell has a major influence on its profile. Other evidence suggests that the concentration of antigen presented to the T cell during primary activation influences its choice. The presence of some cytokines (such as the ones mentioned above) will also influence the response that will eventually be generated, but our understanding is nowhere near complete.
540
Limitations to the Th1/Th2 model
The interactions between cytokines from the Th1/Th2 model can be more complicated in some animals. For example, the Th2 cytokine IL-10 inhibits cytokine production of both Th subsets in humans. Human IL-10 (hIL-10) suppresses the proliferation and cytokine production of all T cells and the activity of macrophages, but continues to stimulate plasma cells, ensuring that antibody production still occurs. As such, hIL-10 is not believed to truly promote the Th2 response in humans, but acts to prevent over-stimulation of helper T cells while still maximising the production of antibodies. There are also other types of T cells that can influence the expression and activation of helper T cells, such as natural regulatory T cells, along with less common cytokine profiles such as the Th3 subset of helper T cells. Terms such as "regulatory" and "suppression" have become ambiguous after the discovery that helper CD4+ T cells are also capable of regulating (and suppressing) their own responses outside of dedicated regulatory T cells. One major difference between regulatory T cells and effector T cells is that regulatory T cells typically serve to modulate and deactivate the immune response, while effector T cell groups usually begin with immune-promoting cytokines and then switch to inhibitory cytokines later in their life cycle. The latter is a feature of Th3 cells, which transform into a regulatory subset after its initial activation and cytokine production. Both regulatory T cells and Th3 cells produce the cytokine transforming growth factor-beta (TGF-β) and IL-10. Both cytokines are inhibitory to helper T cells; TGF-β suppresses the activity of most of the immune system. There is evidence to suggest that TGF-β may not suppress activated Th2 cells as effectively as it might suppress naive cells, but it is not typically considered a Th2 cytokine. The characterisation of another novel T helper subtype, T helper 17 cells (Th17)[] has cast further doubt on the basic Th1/Th2 model. These IL-17 producing cells were initially described as a pathogenic population implicated in autoimmunity but are now thought to have their own distinct effector and regulatory functions. Of note, recent evidence suggest that functional plasticity is an intrinsic capacity of T helper cells. Indeed, a study in mice demonstrated that Th17 cells transform into Th1 cells in vivo.[3] A subsequent study furthermore showed that extensive T helper cell plasticity is also prominent in man.[4] Many of the cytokines in this article are also expressed by other immune cells (see individual cytokines for details), and it is becoming clear that while the original Th1/Th2 model is enlightening and gives insight into the functions of helper T cells, it is far too simple to define its entire role or actions. Some immunologists question the model completely, as some in vivo studies suggest that individual helper T cells usually do not match the specific cytokine profiles of the Th model, and many cells express cytokines from both profiles.[5] That said, the Th model has still played an important part in developing our understanding of the roles and behaviour of helper T cells and the cytokines they produce during an immune response. Recent scientific studies by Stockinger et al. revealed that another T helper subset may exist. Th9 cells are claimed to be an IL9 (interleukin 9)–producing T cell subset focused on defending helminth infections.[6]
T helper cell
541
Role of helper T cells in disease
Considering the diverse and important role helper T cells play in the immune system, it is not surprising that these cells often influence the immune response against disease. They also appear to make occasional mistakes, or generate responses that would be politely considered non-beneficial. In the worst case scenario, the helper T cell response could lead to a disaster and the fatality of the host. Fortunately this is a very rare occurrence.
Helper T cells and hypersensitivity
The immune system must achieve a balance of sensitivity in order to respond to foreign antigens without responding to the antigens of the host itself. When the immune system responds to very low levels of antigen that it usually shouldn't respond to, a hypersensitivity response occurs. Hypersensitivity is believed to be the cause of allergy and some auto-immune disease. Hypersensitivity reactions can be divided into four types: • Type 1 hypersensitivity includes common immune disorders such as asthma, allergic rhinitis (hay fever), eczema, urticaria (hives) and anaphylaxis. These reactions all involve IgE antibodies, which require a Th2 response during helper T cell development. Preventive treatments, such as corticosteroids and montelukast, focus on suppressing mast cells or other allergic cells; T cells do not play a primary role during the actual inflammatory response. It's important to note that the numeral allocation of hypersensitivity "types" does not correlate (and is completely unrelated) to the "response" in the Th model. • Type 2 and Type 3 hypersensitivity both involve complications from auto-immune or low affinity antibodies. In both of these reactions, T cells may play an accomplice role in generating these auto-specific antibodies, although some of these reactions under Type 2 hypersensitivity would be considered normal in a healthy immune system (for example, Rhesus factor reactions during child-birth is a normal immune response against child antigens). The understanding of the role of helper T cells in these responses is limited but it is generally thought that Th2 cytokines would promote such disorders. For example, studies have suggested that lupus (SLE) and other auto-immune diseases of similar nature can be linked to the production of Th2 cytokines. • Type 4 hypersensitivity, also known as delayed type hypersensitivity, are caused via the over-stimulation of immune cells, commonly lymphocytes and macrophages, resulting in chronic inflammation and cytokine release. Antibodies do not play a direct role in this allergy type. T cells play an important role in this hypersensitivity, as they activate against the stimulus itself and promote the activation of other cells; particularly macrophages via Th1 cytokines. Other cellular hypersensitivities include cytotoxic T cell mediated auto-immune disease, and a similar phenomenon; transplant rejection. Helper T cells are required to fuel the development of these diseases. In order to create sufficient auto-reactive killer T cells, interleukin-2 must be produced, and this is supplied by CD4+ T cells. CD4+ T cells can also stimulate cells such as natural killer cells and macrophages via cytokines such as interferon-gamma, encouraging these cytotoxic cells to kill host cells in certain circumstances. The mechanism that killer T cells use during auto-immunity is almost identical to their response against viruses, and some viruses have been accused of causing auto-immune diseases such as Type 1 Diabetes mellitus. Cellular auto-immune disease occurs because the host antigen recognition systems fail, and the immune system believes, by mistake, that a host antigen is foreign. As a result, the CD8+ T cells treat the host cell presenting that antigen as infected, and go on to destroy all host cells (or in the case of transplant rejection, transplant organ) that express that antigen. Some of this section is a simplification. Many auto-immune diseases are more complex. A well-known example is rheumatoid arthritis, where both antibodies and immune cells are known to play a role in the pathology. Generally the immunology of most auto-immune diseases is not well understood.
T helper cell
542
HIV infection
Perhaps the best example of the importance of CD4+ T cells is demonstrated with human immunodeficiency virus (HIV) infection. HIV targets cells that express CD4, and can infect macrophages, dendritic cells (both groups express CD4 at low levels) and CD4+ T cells. It has been proposed that during the non-symptomatic phase of HIV infection, the virus has a relatively low affinity towards T cells (and has a higher affinity for macrophages), resulting in a slow kill rate of CD4+ T cells by the immune system [citation needed]. This is initially compensated for via the production of new helper T cells from the thymus (originally from the bone marrow). Once the virus becomes lymphotropic (or T-tropic) however, it begins to infect CD4+ T cells far more efficiently (likely due to a change in the co-receptors it binds to during infection), and the immune system is overwhelmed. At this point, functional CD4+ T cell levels begin to decrease, eventually to a point where the CD4+ T cell population is too small to recognize the full range of antigens that could potentially be detected. The lack of full antigen cover results in the core symptoms of acquired immune deficiency syndrome (AIDS). CD4 T cell depletion during AIDS allows various pathogens to escape T cell recognition, thus allowing opportunistic infections that would normally elicit a helper T cell response to bypass the immune system. While these complete bypass situations only occur when the helper T cell response is absolutely necessary for infection clearance, most infections increase in severity and/or duration because the immune system's helper T cells provide a weaker contribution to a less efficient immune response. Two components of the immune system are particularly affected in AIDS, due to its CD4+ T cell dependency: 1. CD8+ T cells are not stimulated as effectively during the AIDS stage of HIV infection, making AIDS patients very susceptible to most viruses, including HIV itself. This decline in killing of CD4+ T cells results in the virus being produced for a longer period (the infected CD4+ T cells are not killed as quickly), increasing the proliferation of the virus, and accelerating the development of the disease. 2. Antibody class switching declines significantly once helper T cell function fails. The immune system loses its ability to improve the affinity of their antibodies, and are unable to generate B cells that can produce antibody groups such as IgG and IgA. These effects are primarily due to the loss of any helper T cell that can interact with the B lymphocyte correctly. Another symptom of AIDS is the reduction in antibody levels due to a decrease in Th2 cytokines (and less interactions by helper T cells). All of these complications result in an increased susceptibility to aggressive bacterial infections, especially in areas of the body not accessible by IgM antibodies. If the patient does not respond to (or does not receive) HIV treatment they will succumb usually to either cancers or infections; the immune system finally reaches a point where it is no longer coordinated or stimulated enough to deal with the disease. Inhibition of CD4 T-cell expansion during HIV infection is also due to microbial translocation in an IL-10-dependent way. Indeed, triggering PD-1, expressed on monocytes and up-regulated upon monocytes activation, by its ligand PD-L1 induces IL-10 production which inhibits CD4 T-cell function.[7]
T helper cell
543
References
[1] Page 223 [6] (Veldhoen and Stockinger, Dardalhon and Kuchroo both papers from Nature Immunology 2008)
• In SLE patients, T helper type 1 polarisation is more abundant rather than type 2, where the main cytokine profile are Inf gama from T cells and its consequence interferon alpha high range production by DC .
External links
• T-cell Group - Cardiff University (http://www.tcells.org/scientific/helper/)
Regulatory T cell
Regulatory T cells (Treg), formerly known as suppressor T cells (Ts), are a subpopulation of T cells which modulate the immune system, maintain tolerance to self-antigens, and abrogate autoimmune disease. Mouse models have suggested that modulation of Tregs can treat autoimmune disease and cancer, and facilitate organ transplantation.
Regulatory T cell populations
T regulatory cells are a component of the immune system that suppress immune responses of other cells. This is an important "self-check" built into the immune system to prevent excessive reactions. Regulatory T cells come in many forms with the most well-understood being those that express CD4, CD25, and Foxp3 (CD4+CD25+ regulatory T cells, or "Tregs").[1] These cells are involved in shutting down immune responses after they have successfully eliminated invading organisms, and also in preventing autoimmunity.[citation needed] CD4+Foxp3+ regulatory T cells have been called "naturally-occurring" regulatory T cells to distinguish them from "suppressor" T cell populations that are generated in vitro. Additional suppressor T cell populations include Tr1, Th3, CD8+CD28-, and Qa-1 restricted T cells. The contribution of these populations to self-tolerance and immune homeostasis is less well defined. FOXP3 can be used as a good marker for CD4+CD25+ T cells as well as recent studies showing evidence for FOXP3 in CD4+CD25- T cells. An additional regulatory T cell subset, induced regulatory T cells, are also needed for tolerance and suppression.
Development
All T cells come from progenitor cells from the bone marrow, which become committed to their lineage in the thymus. All T cells begin as CD4-CD8-TCR- cells at the DN (double-negative) stage, where an individual cell will rearrange its T cell receptor genes to form a unique, functional molecule, which they, in turn, test against cells in the thymic cortex for a minimal level of interaction with self-MHC. If they receive these signals, they proliferate and express both CD4 and CD8, becoming double-positive cells. The selection of Tregs occurs on radio-resistant haemopoietically-derived MHC class II-expressing cells in the medulla or Hassal’s corpuscles in the thymus. At the DP (double-positive) stage, they are selected by their interaction with the cells within the thymus, begin the transcription of Foxp3, and become Treg cells, although they may not begin to express Foxp3 until the single-positive stage, at which point they are functional Tregs. Treg do not have the limited TCR expression of NKT or γδ T cells; Treg have a larger TCR diversity than effector T cells, biased towards self-peptides. The process of Treg selection is determined by the affinity of interaction with the self-peptide MHC complex. Selection to become a Treg is a “Goldilocks” process; T cell that receives very strong signals will undergo apoptotic death; a cell that receives a weak signal will survive and be selected to become an effector cell. If a T cell receives an intermediate signal, then it will become a regulatory cell. Due to the stochastic nature of the process of T cell
Regulatory T cell activation, all T cell populations with a given TCR will end up with a mixture of Teff and Treg – the relative proportions determined by the affinities of the T cell for the self-peptide-MHC. Even in mouse models with TCR-transgenic cells selected on specific-antigen-secreting stroma, deletion or conversion is not complete. Foxp3+ Treg generation in the thymus is delayed by several days compared to Teff cells and does not reach adult levels in either the thymus or periphery until around three weeks post-partum. Treg cells require CD28 co-stimulation and B7.2 expression is largely restricted to the medulla, the development of which seems to parallel the development of Foxp3+ cells. It has been suggested that the two are linked, but no definitive link between the processes has yet been shown. TGF-β is not required for Treg functionality, in the thymus, as thymic Treg from TGF-β insensitive TGFβRII-DN mice are functional.
544
Function
To function properly, the immune system must discriminate between self and non-self. When self/non-self discrimination fails, the immune system destroys cells and tissues of the body and as a result causes autoimmune diseases. Regulatory T cells actively suppress activation of the immune system and prevent pathological self-reactivity, i.e. autoimmune disease. The critical role regulatory T cells play within the immune system is evidenced by the severe autoimmune syndrome that results from a genetic deficiency in regulatory T cells (IPEX syndrome - see also below). The molecular mechanism by which regulatory T cells exert their suppressor/regulatory activity has not been definitively characterized and is the subject of intense research. In vitro experiments have given mixed results regarding the requirement of cell-to-cell contact with the cell being suppressed. The immunosuppressive cytokines TGF-beta and Interleukin 10 (IL-10) have also been implicated in regulatory T cell function.
Induced Regulatory T cells
Induced Regulatory T (iTreg) cells (CD4+CD25+Foxp3+) are suppressive cells involved in tolerance. iTreg cells have been shown to suppress T cell proliferation and experimental autoimmune diseases. iTreg cells develop from mature CD4+ conventional T cells outside of the thymus: a defining distinction between natural regulatory T (nTreg) cells and iTreg cells. Though iTreg and nTreg cells share a similar function iTreg cells have recently been shown to be "an essential non-redundant regulatory subset that supplements nTreg cells, in part by expanding TCR diversity within regulatory responses".[2] Acute depletion of the iTreg cell pool in mouse models has resulted in inflammation and weight loss. The contribution of nTreg cells versus iTreg cells in maintaining tolerance is unknown, but both are important. Epigenetic differences have been observed between nTreg and iTreg cells, with the former having more stable Foxp3 expression and wider demethylation.
Regulatory T cells and Disease
An important question in the field of immunology is how the immunosuppressive activity of regulatory T cells is modulated during the course of an ongoing immune response. While the immunosuppressive function of regulatory T cells prevents the development of autoimmune disease, it is not desirable during immune responses to infectious microorganisms. Current hypotheses suggest that, upon encounter with infectious microorganisms, the activity of regulatory T cells may be downregulated, either directly or indirectly, by other cells to facilitate elimination of the infection. Experimental evidence from mouse models suggests that some pathogens may have evolved to manipulate regulatory T cells to immunosuppress the host and so potentiate their own survival. For example, regulatory T cell activity has been reported to increase in several infectious contexts, such as retroviral infections (the most well-known of which is HIV), mycobacterial infections (like tuberculosis), and various parasitic infections including Leishmania and malaria.
Regulatory T cell Studies of human subjects with a history of leishmania infection suggest that modulation of CD8+ suppressor T cells is, at least partly, mediated by cytokines. Leishmania specific CD4+ helper T cells predominate in adults with strong protective immunity (skin-test positive with no history of clinical infection). When added to autologous leishmania infected macrophages these T cells cause parasite death and secretion of large amounts of interferon-gamma and lymphotoxin. CD8+ T suppressor cells predominate in patients with no protective immunity (visceral leishmaniasis patients). When added to autologous peripheral blood mononuclear cells isolated after successful treatment, these T cells inhibit interferon-gamma secretion and proliferation and increase interleukin-6 and interleukin-10 secretion. A soluble factor(s) generated by antigen or phytohemagglutinin stimulation of leishmania-specific CD4+ helper T cells from skin-test positive adults killed CD8+ T cells but not CD4+ helper T cells when added to culture media. Soluble factors generated by antigen stimulation of peripheral blood mononuclear cells from skin-test positive adults prevented CD8+ suppressor T cell mediated increases in interleukin-10 secretion. These findings suggest that antigen stimulation of CD4+ helper T cells results in production of cytokines that kill or down regulate CD8+ T suppressor cells. Once the leishmania infection has been eliminated and leishmania antigens are gone, CD8+ T suppressor cells down-regulate CD4+ T helper cells. Isolation of cytokines that inhibit and kill CD8+ T suppressor cells might be useful in treating diseases that involve immune suppression such as leishmaniasis, AIDS, and certain cancers.[3][4] CD4+ Regulatory T cells are often associated with solid tumours in both humans and murine models. Increased numbers of regulatory T cells in breast, colorectal and ovarian cancers is associated with a poorer prognosis.[5] CD70+ non-Hodgkin lymphoma B cells induce Foxp3 expression and regulatory function in intratumoral CD4+CD25− T cells [6]
545
Molecular characterization
Similar to other T cells, regulatory T cells develop in the thymus. The latest research suggests that regulatory T cells are defined by expression of the forkhead family transcription factor FOXP3 (forkhead box p3). Expression of FOXP3 is required for regulatory T cell development and appears to control a genetic program specifying this cell fate.[7] The large majority of Foxp3-expressing regulatory T cells are found within the major histocompatibility complex (MHC) class II restricted CD4-expressing (CD4+) helper T cell population and express high levels of the interleukin-2 receptor alpha chain (CD25). In addition to the Foxp3-expressing CD4+CD25+, there also appears to be a minor population of MHC class I restricted CD8+ Foxp3-expressing regulatory T cells. Unlike conventional T cells, regulatory T cells do not produce IL-2 and are therefore anergic at baseline. A number of different methods are employed in research to identify and monitor Treg cells. Originally, high expression of CD25 and CD4 surface markers was used (CD4+CD25+ cells). This is problematic as CD25 is also expressed on non-regulatory T cells in the setting of immune activation such as during an immune response to a pathogen. As defined by CD4 and CD25 expression, regulatory T cells comprise about 5-10% of the mature CD4+ helper T cell subpopulation in mice and humans, while about 1-2% of Treg can be measured in whole blood. The additional measurement of cellular expression of Foxp3 protein allowed a more specific analysis of Treg cells (CD4+CD25+Foxp3+ cells). However, Foxp3 is also transiently expressed in activated human effector T cells, thus complicating a correct Treg analysis using CD4, CD25 and Foxp3 as markers in humans. Therefore, some research groups use another marker, the absence or low-level expression of the surface protein CD127 in combination with the presence of CD4 and CD25. Several additional markers have been described, e.g., high levels of CTLA-4 (cytotoxic T-lymphocyte associated molecule-4) and GITR (glucocorticoid-induced TNF receptor) are also expressed on regulatory T cells, however the functional significance of this expression remains to be defined. There is a great interest in identifying cell surface markers that are uniquely and specifically expressed on all Foxp3-expressing regulatory T cells. However, to date no such molecule has been identified. In addition to the search for novel protein markers, a different method to analyze and monitor Treg cells more accurately has been described in the literature. This method is based on DNA methylation analysis. Only in Treg cells, but not in any other cell type, including activated effector T cells, a certain region within the foxp3 gene
Regulatory T cell (TSDR, Treg-specific-demthylated region) is found demethylated, which allows to monitor Treg cells through a PCR reaction or other DNA-based analysis methods.[8] Recent evidence suggests that mast cells may be important mediators of Treg-dependent peripheral tolerance.[9]
546
Genetic deficiency
Genetic mutations in the gene encoding Foxp3 have been identified in both humans and mice based on the heritable disease caused by these mutations. This disease provides the most striking evidence that regulatory T cells play a critical role in maintaining normal immune system function. Humans with mutations in Foxp3 suffer from a severe and rapidly fatal autoimmune disorder known as Immune dysregulation, Polyendocrinopathy, Enteropathy X-linked (IPEX) syndrome.[10][11] The IPEX syndrome is characterized by the development of overwhelming systemic autoimmunity in the first year of life, resulting in the commonly observed triad of watery diarrhea, eczematous dermatitis, and endocrinopathy seen most commonly as insulin-dependent diabetes mellitus. Most individuals have other autoimmune phenomena including Coombs-positive hemolytic anemia, autoimmune thrombocytopenia, autoimmune neutropenia, and tubular nephropathy. The majority of affected males die within the first year of life of either metabolic derangements or sepsis. An analogous disease is also observed in a spontaneous Foxp3-mutant mouse known as “scurfy”.
References
[3] Holaday B, Pompeu M, Jeronimo S, Texeira M, Sousa A, Vasconcelos W, Pearson R, Abrams J, Locksley R (1993). “Potential Role for Interleukin-10 in Immunosuppression Associated with Kala Azar”. Journal of Clinical Investigation 92: 2626-2632. PMID 8254019 [4] Holaday B (1999). “Immunotherapy for Visceral Leishm,aniasis: Ability of Factors Produced during Anti_leishmania Responses of Skin Test Positive Adults to Inhibit Peripheral Blood Mononuclear Cell Activities Associated with Visceral Leishmaniasis”. Memorias do Instituto Oswaldo Cruz 94: 55-66. PMID 10029912 [10] Online Mendelian Inheritance in Man IPEX (http:/ / www. ncbi. nlm. nih. gov/ entrez/ dispomim. cgi?id=304790)
Further reading
• Moon C, Kim SH (June 2009). "Use of epigenetic modification to induce FOXP3 expression in naïve T cells". Transplant Proc. 41 (5): 1848–54. doi: 10.1016/j.transproceed.2009.02.101 (http://dx.doi.org/10.1016/j. transproceed.2009.02.101). PMID 19545742 (http://www.ncbi.nlm.nih.gov/pubmed/19545742).
External links
• Regulatory T-Cells (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Regulatory+T-Cells) at the US National Library of Medicine Medical Subject Headings (MeSH)
Cytotoxic T cell
547
Cytotoxic T cell
A cytotoxic T cell (also known as TC, Cytotoxic T Lymphocyte, CTL, T-Killer cell, cytolytic T cell, CD8+ T-cells or killer T cell) is a T lymphocyte (a type of white blood cell) that kills cancer cells, cells that are infected (particularly with viruses), or cells that are damaged in other ways. Most cytotoxic T cells express T-cell receptors (TCRs) that can recognize a specific antigen. An antigen is a molecule capable of stimulating an immune response, and is often produced by cancer cells or viruses. Antigens inside a cell are bound to Antigen presentation stimulates T cells to become either "cytotoxic" CD8+ cells or class I MHC molecules, and brought to the "helper" CD4+ cells. surface of the cell by the class I MHC molecule, where they can be recognized by the T cell. If the TCR is specific for that antigen, it binds to the complex of the class I MHC molecule and the antigen and the T cell destroys the cell. In order for the TCR to bind to the class I MHC molecule, the former must be accompanied by a glycoprotein called CD8, which binds to the constant portion of the class I MHC molecule. Therefore, these T cells are called CD8+ T cells. The affinity between CD8 and the MHC molecule keeps the TC cell and the target cell bound closely together during antigen-specific activation. CD8+ T cells are recognized as TC cells once they become activated and are generally classified as having a pre-defined cytotoxic role within the immune system. However, CD8+ T cells also have the ability to make some cytokines.
Cytotoxic T cell
548
Development
The immune system must recognize millions of potential antigens. There are fewer than 30,000 genes in the human body, so it's impossible to have one gene for every antigen. Instead, the DNA in millions of white blood cells in the bone marrow is shuffled to create cells with unique receptors, each of which can bind to a different antigen. Some receptors bind to tissues in the human body itself, so to prevent the body from attacking itself, those self-reactive white blood cells are destroyed during further development in the thymus. TCRs have two parts, usually an alpha and a beta chain. (Some TCRs have a gamma and a delta chain.) Hematopoietic stem cells in the bone marrow migrate into the thymus, where they undergo VDJ recombination of their beta-chain TCR DNA to form a developmental form of the TCR protein, known as pre-TCR. If that rearrangement is successful, the cells then rearrange their alpha-chain TCR DNA to create a functional alpha-beta TCR complex. This highly-variable Development of single positive T cells in the genetic rearrangement product in the TCR genes helps create millions thymus of different T cells with different TCRs, helping the body's immune system respond to virtually any protein of an invader. The vast majority of T cells express alpha-beta TCRs (αβ T cells), but some T cells in epithelial tissues (like the gut) express gamma-delta TCRs (γδ T cells), which recognize non-protein antigens. T cells with functionally stable TCRs express both the CD4 and CD8 co-receptors and are therefore termed "double-positive" (DP) T cells (CD4+CD8+). The double-positive T cells are exposed to a wide variety of self-antigens in the thymus and undergo two selection criteria: 1. positive selection, in which those double-positive T cells that bind too weakly to MHC-presented self antigens undergo apoptosis because of their inability to recognize MHC-protein complexes. 2. negative selection, in which those double-positive T cells that bind too strongly to MHC-presented self antigens undergo apoptosis because they could otherwise become autoreactive, leading to autoimmunity. Only those T cells that bind to the MHC-self-antigen complexes weakly are positively selected. Those cells that survive positive and negative selection differentiate into single-positive T cells (either CD4+ or CD8+), depending on whether their TCR recognizes an MHC class I-presented antigen (CD8) or an MHC class II-presented antigen (CD4). It is the CD8+ T-cells that will mature and go on to become cytotoxic T cells following their activation with a class I-restricted antigen.
Activation
With an exception of some cell types, such as non-nucleated cells (including erythrocytes), Class I MHC is expressed by all host cells. When these cells are infected with a virus (or another intracellular pathogen), the cells degrade foreign proteins via antigen processing. These result in peptide fragments, some of which are presented by MHC Class I to the T cell antigen receptor (TCR) on CD8+ T cells. The activation of cytotoxic T cells is dependent on several simultaneous interactions between molecules expressed on the surface of the T cell and molecules on the surface of the antigen-presenting cell (APC). For instance, consider the two signal model for TC cell activation.
Cytotoxic T cell
549
Signal First Signal Second Signal
T cell TCR
APC peptide-bound MHC class I molecule either CD80 or CD86 (also called B7-1 and B7-2)
Description There is a second interaction between the CD8 coreceptor and the class I MHC molecule to stabilize this signal. CD80 and CD86 are known as costimulators for T cell activation. This second signal can be assisted (or replaced) by stimulating the TC cell with cytokines released from helper T cells.
CD28 molecule on the T cell
While in most cases activation is dependent on TCR recognition of antigen, alternative pathways for activation have been described. For example, cytotoxic T cells have been shown to become activated when targeted by other CD8 T cells leading to tolerization of the latter.[1] Once activated, the TC cell undergoes clonal expansion with the help of the cytokine Interleukin-2 (IL-2), which is a growth and differentiation factor for T cells. This increases the number of cells specific for the target antigen that can then travel throughout the body in search of antigen-positive somatic cells.
Effector functions
When exposed to infected/dysfunctional somatic cells, TC cells release the cytotoxins perforin, granzymes, and granulysin. Perforin forms pores (aqueous channels) in the target cell's plasma membrane allowing granzymes, types of serine proteases that cleave at aspartate residues in the substrate, to enter the target cell, which then activate a series of cysteine proteases, the caspase cascade, that eventually lead to apoptosis (programed cell death). A second way to induce apoptosis is via cell-surface interactions between the TC and the infected cell. When a TC is activated it starts to express the surface protein FAS ligand (FasL)(Apo1L)(CD95L), which can bind to Fas (Apo1)(CD95) molecules expressed on the target cell. However, this Fas-Fas ligand interaction is thought to be more important to the disposal of unwanted T lymphocytes during their development or to the lytic activity of certain TH cells than it is to the cytolytic activity of TC effector cells. Engagement of Fas with FasL allows for recruitment of the death-induced signaling complex (DISC). The Fas-associated death domain (FADD) translocates with the DISC, allowing recruitment of procaspases 8 and 10. These caspases then activate the effector caspases 3, 6, and 7, leading to cleavage of death substrates such as lamin A, lamin B1, lamin B2, PARP (poly-ADP ribose polymerase), and DNAPK (DNA-activated protein kinase). The final result is apoptosis of the cell that expressed Fas.
Role in disease pathogenesis
During hepatitis B virus (HBV) infection cytotoxic T cells play an important pathogenetic role. They contribute to nearly all of the liver injury associated with HBV infection and, by killing infected cells and by producing antiviral cytokines capable of purging HBV from viable hepatocytes, cytotoxic T cells also eliminate the virus.[2] Recently platelets have been shown to facilitate the accumulation of virus-specific cytotoxic T cells into the infected liver.[3] Recently, cytotoxic T cells have been implicated in the progression of arthritis: depletion of knee joint cartilage macromolecules such as glycosaminoglycans by cytotoxic T cells and macrophages has been observed in a rat model of the disease.[4]
Cytotoxic T cell
550
References
[1] Milstein, O., Hagin, D., Lask, A., Reich-Zeliger, S., Shezan E., Ophir E., Eidelshtein Y., Afik R., Antebi YE., Dustin ML. and Reisner Y. (2011) CTLs respond with activation and granule secretion when serving target for T cell recognition. Blood 117,1042-1052 (http:/ / bloodjournal. hematologylibrary. org/ content/ early/ 2010/ 11/ 02/ blood-2010-05-283770)
External links
• T-cell Group - Cardiff University (http://www.tcells.org/scientific/killer/) • Malaria (http://www.1lecture.com/Immunology/Cytotoxic T Cell/index.html) (Flash Animation)
Natural killer T cell
Natural killer T (NKT) cells are a heterogeneous group of T cells that share properties of both T cells and natural killer (NK) cells. Many of these cells recognize the non-polymorphic CD1d molecule, an antigen-presenting molecule that binds self- and foreign lipids and glycolipids. They constitute only approximately 0.1% of all peripheral blood T cells.[]
Nomenclature
The term “NK T cells” was first used in mice to define a subset of T cells that expressed the natural killer (NK) cell-associated marker NK1.1 (CD161). It is now generally accepted that the term “NKT cells” refers to CD1d-restricted T cells, present in mice and humans, some of which coexpress a heavily biased, semi-invariant T cell receptor (TCR) and NK cell markers.[] Natural killer T (NKT) cells should not be confused with natural killer (NK) cells.
Molecular characterization
NKT cells are a subset of T cells that co-express an αβ T cell receptor (TCR), but also express a variety of molecular markers that are typically associated with NK cells, such as NK1.1. The best known NKT cells differ from conventional αβ T cells in that their TCRs are far more limited in diversity ('invariant' or 'Type 1' NKT). They and other CD1d-restricted T cells ('Type 2' NKT) recognize lipids and glycolipids presented by CD1d molecules, a member of the CD1 family of antigen presenting molecules, rather than peptide-MHC complexes. As such, NKT cells are important in recognizing glycolipids from organisms such as mycobacterium, which cause tuberculosis. NKT cells include both NK1.1+ and NK1.1-, as well as CD4+, CD4-, CD8+ and CD8- cells. Natural Killer T cells can share other features with NK cells as well, such as CD16 and CD56 expression and granzyme production.[][] Invariant Natural Killer T (iNKT) cells express high levels of and are dependent on the transcriptional regulator promyelocytic leukemia zinc finger (PLZF) for their development.[1][2]
Classification
Classification of natural killer T cells into three groups has been proposed.[]
Natural killer T cell
551
Type 1 NKT Other names classical NKT invariant NKT (iNKT) Vα14i NKT (mouse) Vα24i NKT (human) CD1d +
Type 2 NKT non-classical NKT diverse NKT
NKT-like NK1.1+ T cells CD3+ CD56+ T cells
Restriction α-GalCer reactivity TCR repertoire
CD1d -
MHC, other? -
Vα14-Jα18: Vβ8.2, 7, 2 (mouse) Vα24-Jα18: Vβ11 (human)
diverse
diverse
iNKT cells
The best known subset of CD1d-dependent NKT cells expresses an invariant T cell receptor α (TCR-α) chain. These are referred to as type I or invariant NKT cells (iNKT) cells. These cells are conserved between humans and mice and are implicated in many immunological processes. Absence of microbe exposure in early development led to increased iNKT cells and immune morbidity in a mouse model. [3]
Function
Upon activation, NKT cells are able to produce large quantities of interferon-gamma, IL-4, and granulocyte-macrophage colony-stimulating factor, as well as multiple other cytokines and chemokines (such as IL-2, Interleukin-13, Interleukin-17, Interleukin-21 and TNF-alpha).
Significance
NKT cells seem to be essential for several aspects of immunity because their dysfunction or deficiency has been shown to lead to the development of autoimmune diseases (such as diabetes or atherosclerosis) and cancers. NKT cells have recently been implicated in the disease progression of human asthma.[4] The clinical potential of NKT cells lies in the rapid release of cytokines (such as IL-2, IFN-gamma, TNF-alpha, and IL-4) that promote or suppress different immune responses.
References
[4] Cromie, William J. Researchers uncover cause of asthma (http:/ / www. news. harvard. edu/ gazette/ 2006/ 03. 16/ 01-asthma. html) Harvard University Gazette, March 16, 2006.
External links
• NKT cell Journal Screening (http://www.nkcells.info/wiki/index.php?title=NKT_cell#References) • Nature glossary on murine NKT cells (http://www.nature.com/nri/journal/v3/n3/glossary/nri1027_glossary. html#DF2) • Nature Reviews Web Focus on regulatory lymphocytes (http://www.nature.com/nri/focus/reglymph/index. html)
B cell
552
B cell
B cell
The cells of the immune system that make antibodies to invading pathogens such as viruses. They form memory cells that remember the same pathogen for faster antibody production in future infections. Latin Code lymphocytus B TH H2.00.04.1.02005 [1] TH H2.00.04.3.07002
[1]
B cells belong to a group of white blood cells known as lymphocytes, making them a vital part of the immune system -- specifically the humoral immunity branch of the adaptive immune system. B cells can be distinguished from other lymphocytes, such as T cells and natural killer cells (NK cells), by the presence of a protein on the B cell's outer surface known as a B cell receptor (BCR). This specialized receptor protein allows a B cell to bind to a specific antigen. The principal functions of B cells are to make antibodies against antigens, to perform the role of antigen-presenting cells (APCs), and to develop into memory B cells after activation by antigen interaction. Recently, a new, suppressive function of B cells has been discovered.[1] The abbreviation "B", in B cell, comes from the bursa of Fabricius in birds, where they mature. In mammals, immature B cells are formed in the bone marrow, which is used as a backronym for the cells' name.[2]
Development of B cells
Immature B cells are produced in the bone marrow of most mammals. Rabbits are an exception; their B cells develop in the appendix-sacculus rotundus. After reaching the IgM+ immature stage in the bone marrow, these immature B cells migrate to secondary lymphoid tissues (such as the spleen, lymph nodes, Peyer's patches, etc.) where they are called transitional B cells, and some of these cells differentiate into mature B lymphocytes.[] B cell development occurs through several stages, each stage representing a change in the genome content at the antibody loci. An antibody is composed of two identical light (L) and two identical heavy (H) chains, and the genes specifying them are found in the 'V' (Variable) region and the 'C' (Constant) region. In the heavy-chain 'V' region there are three segments; V, D and J, which recombine randomly, in a process called VDJ recombination, to produce a unique variable domain in the immunoglobulin of each individual B cell. Similar rearrangements occur for light-chain 'V' region except there are only two segments involved; V and J. The list below describes the process of immunoglobulin formation at the different stages of B cell development.
B cell
553
Stage
Heavy chain
Light chain
Ig
IL-7 receptor? Yes
CD19?
Progenitor (or pre-pro) B cells Early Pro (or pre-pre)-B cells Late Pro (or pre-pre)-B cells
germline
germline
-
No
undergoes D-J rearrangement
germline
-
Yes
No
undergoes V-DJ rearrangement is VDJ rearranged
germline
-
Yes
Yes [] Yes
[]
Large Pre-B cells
germline
IgM in cytoplasm and surface IgM in cytoplasm and surface IgM on surface IgM and IgD on surface
Yes Yes
Small Pre-B cells
is VDJ rearranged
undergoes V-J rearrangement VJ rearranged VJ rearranged
Yes
Immature B cells Mature B cells
is VDJ rearranged is VDJ rearranged
No No
Yes Yes
When the B cell fails in any step of the maturation process, it will die by a mechanism called apoptosis, here called clonal deletion.[3] B cells are continuously produced in the bone marrow. When the B cell receptor, on the surface of the cell matches the detected antigens present in the body, the B cell proliferates and secretes a free form of those receptors (antibodies) with identical binding sites as the ones on the original cell surface. After activation, the cell proliferates and B memory cells would form to recognise the same antigen. This information would then be used as a part of the adaptive immune system for a more efficient and more powerful immune response for future encounters with that antigen. B cell membrane receptors evolve and change throughout the B cell life span.[] The proteins TACI, BCMA and BAFF-R (B cell activating factor receptor) are present on both immature B cells and mature B cells. Belimumab is a monoclonal inhibitor of the soluble form of B cell activating factor (BAFF), while blisibimod is an inhibitor of both membrane and soluble forms of BAFF. CD20 is expressed on all stages of B cell development except the first and last; it is present from pre-B cells through memory cells, but not on either pre-pro-B cells or plasma cells.[]
Immune tolerance
Like their fellow lymphocytes, the T cells, immature B cells are tested for auto-reactivity by the immune system before leaving the bone marrow. In the bone marrow (the central lymphoid organ), central tolerance is produced. The immature B cells whose B cell receptors (BCRs) bind too strongly to self antigens will not be allowed to mature. If B cells are found to be highly reactive to self, three mechanisms can occur. • Clonal deletion: the removal, usually by apoptosis, of B cells of a particular self antigen specificity. • Receptor editing: the BCRs of self reactive B cells are given an opportunity to rearrange their conformation. This process occurs via the continued expression of the Recombination activating gene (RAG). Through the help of RAG, receptor editing involves light chain gene rearrangement of the B cell receptor. If receptor editing fails to produce a BCR that is less autoreactive, apoptosis will occur. Note that defects in the RAG-1 and RAG-2 genes are implicated in Severe Combined Immunodeficiency (SCID). The inability to recombine and generate new receptors lead to failure of maturity for both B cells and T cells. • Anergy: B cells enter a state of permanent unresponsiveness when they bind with weakly cross-linking self antigens that are small and soluble.
B cell
554
Functions
The human body makes millions of different types of B cells each day that circulate in the blood and lymphatic system performing the role of immune surveillance. They do not produce antibodies until they become fully activated. Each B cell has a unique receptor protein (referred to as the B cell receptor (BCR)) on its surface that will bind to one particular antigen. The BCR is a membrane-bound immunoglobulin, and it is this molecule that allows the distinction of B cells from other types of lymphocyte, as well as being the main protein involved in B cell activation. Once a B cell encounters its cognate antigen and receives an additional signal from a T helper cell, it can further differentiate into one of the two types of B cells listed below (plasma B cells and memory B cells). The B cell may either become one of these cell types directly or it may undergo an intermediate differentiation step, the germinal center reaction, where the B cell will hypermutate the variable region of its immunoglobulin gene ("somatic hypermutation") and possibly undergo class switching. Other functions for B cells include antigen presentation, cytokine production and lymphoid tissue organization.
Clonality
B cells exist as clones. All B cells derive from a particular cell, and thus, the antibodies their differentiated progenies (see below) produce can recognize and/or bind the same specific surface components composed of biological macromolecules (epitope) of a given antigen. Such clonality has important consequences, as immunogenic memory relies on it. The great diversity in immune response comes about because there are up to 109 clones with specificities for recognizing different antigens. A single B cell or a clone of cells with shared specificity, upon encountering its specific antigen, divides to produce many B cells. Most of such B cells differentiate into plasma cells that secrete antibodies into blood that bind the same epitope that elicited proliferation in the first place. A small minority survives as memory cells that can recognize only the same epitope. However, with each cycle, the number of surviving memory cells increases. The increase is accompanied by affinity maturation which induces the survival of B cells that bind to the particular antigen with high affinity. This subsequent amplification with improved specificity of immune response is known as secondary immune response. B cells that have not been activated by antigen are known as naive lymphocytes; those that have met their antigen, become activated, and have differentiated further into fully functional lymphocytes are known as effector B lymphocytes.
B cell types
• Plasma B cells (also known as plasma cells, plasmocytes, and effector B cells) are large B cells that have been exposed to antigen and produce and secrete large amounts of antibodies, which assist in the destruction of microbes by binding to them and making them easier targets for phagocytes and activation of the complement system. They are sometimes referred to as antibody factories. An electron micrograph of these cells reveals large amounts of rough endoplasmic reticulum, responsible for synthesizing the antibody, in the cell's cytoplasm. These are short lived cells and undergo apoptosis when the inciting agent that induced immune response is eliminated. This occurs because of cessation of continuous exposure to various colony-stimulating factors required for survival.
A suspected plasma cell. Plasma cells are normally detected in tissue rather than circulation.
• Memory B cells are formed from activated B cells that are specific to the antigen encountered during the primary immune response. These cells are able to live for a long time, and can respond quickly following a second exposure to the same antigen.
B cell • B-1 cells express IgM in greater quantities than IgG and their receptors show polyspecificity, meaning that they have low affinities for many different antigens. Polyspecific immunoglobulins often have a preference for other immunoglobulins, self antigens and common bacterial polysaccharides. B-1 cells are present in low numbers in the lymph nodes and spleen and are instead found predominantly in the peritoneal and pleural cavities.[4][5] • B-2 cells are the cells intended when using the unqualified "B cell." • Marginal-zone B cells • Follicular B Cells
555
Recognition of antigen by B cells
A critical difference between B cells and T cells is how each lymphocyte recognizes its antigen. B cells recognize their cognate antigen in its native form. They recognize free (soluble) antigen in the blood or lymph using their BCR or membrane bound-immunoglobulin. In contrast, T cells recognize their cognate antigen in a processed form, as a peptide fragment presented by an antigen presenting cell's MHC molecule to the T cell receptor.
Activation of B cells
B cell recognition of antigen is not the only element necessary for B cell activation (a combination of clonal proliferation and terminal differentiation into plasma cells). B cells that have not been exposed to antigen, also known as naïve B cells, can be activated in a T cell-dependent or -independent manner.
T cell-dependent activation
Once a pathogen is ingested by an antigen-presenting cell such as a macrophage or dendritic cell, the pathogen's proteins are then digested to peptides and attached to a Mechanism of action. class II MHC protein. This complex is then moved to the outside of the cell membrane. The macrophage is now activated to deliver multiple signals to a specific T cell that recognizes the peptide presented. The T cell is then stimulated to produce autocrines, resulting in the
B cell
556
proliferation and differentiation to effector and memory T cells. Helper T cells (i.e. CD4+ T cells) then activate specific B cells through a phenomenon known as an Immunological synapse. Activated B cells subsequently produce antibodies which assist in inhibiting pathogens until phagocytes (i.e. macrophages, neutrophils) or the complement system for example clears the host of the pathogen(s). Most antigens are T-dependent, meaning T cell help is required for maximal antibody production. With a T-dependent antigen, the first signal comes from antigen cross linking T cell-dependent B cell activation, showing a TH2-cell (left), B cell (right), and the B cell receptor (BCR) and the second several interaction molecules signal comes from co-stimulation provided by a T cell. T dependent antigens contain proteins that are presented on B cell Class II MHC to a special subtype of T cell called a Th2 cell. When a B cell processes and presents the same antigen to the primed Th cell, the T cell secretes cytokines that activate the B cell. These cytokines trigger B cell proliferation and differentiation into plasma cells. Isotype switching to IgG, IgA, and IgE and memory cell generation occur in response to T-dependent antigens. This isotype switching is known as Class Switch Recombination (CSR). Once this switch has occurred, that particular B cell will usually no longer make the earlier isotypes, IgM or IgD.
T cell-independent activation
Many antigens are T cell-independent in that they can deliver both of the signals to the B cell. Mice without a thymus (nude or athymic mice that do not produce any T cells) can respond to T independent antigens. Many bacteria have repeating carbohydrate epitopes that stimulate B cells, by cross-linking the IgM antigen receptors in the B cell, responding with IgM synthesis in the absence of T cell help. Conjugate vaccines are made to provide a stronger immune response against these foreign molecules. There are two types of T cell independent activation; Type 1 T cell-independent (polyclonal) activation, and type 2 T cell-independent activation (in which macrophages present several of the same antigen in a way that causes cross-linking of antibodies on the surface of B cells). T cell independent activation type 1 is when a B cell binds to an antigen and receives secondary activation by toll-like receptors; type 2 is when the antigen is a molecule with multiple repeating subunits which can simultaneously cross link enough B cell receptors to fully activate the B cell. In 2011, it was discovered that immortalized rhesus monkey B cells may be activated by the binding of monoamine ligands to TAAR1, a recently discovered GPCR. They found that methamphetamine, a potent TAAR1 agonist, signals PKA and PKC activation following ligand binding to TAAR1.[6] Although it is largely recognized as an important regulator of monoaminergic systems, TAAR1 has only recently been characterized as being important for T cell-independent lymphocyte activation.
B cell
557
The ancestral roots of B cells
In an October 2006 issue of Nature Immunology, certain B cells of basal vertebrates (like fish and amphibians) were shown to be capable of phagocytosis, a function usually associated with cells of the innate immune system. The authors postulate that these phagocytic B cells represent the ancestral history shared between macrophages and lymphocytes. B cells may have evolved from macrophage-like cells during the formation of the adaptive immune system.[7] B cells in humans (and other vertebrates) are nevertheless able to endocytose antibody-fixed pathogens, and it is through this route that MHC Class II presentation by B cells is possible, allowing Th2 help and stimulation of B cell proliferation. This is purely for the benefit of MHC Class II presentation, not as a significant method of reducing the pathogen load.
Origin of the term
The abbreviation "B" in B cell originally came from Bursa of Fabricius, an organ in birds in which avian B cells mature.[8] When it was discovered that in most mammals immature B cells are formed in bone marrow, the word B cell continued to be used, although other blood cells also originate from pluripotent stem cells in the bone marrow. The fact that bone and bursa both start with the letter 'B' is a coincidence.
B cell-related pathology
Aberrant antibody production by B cells is implicated in many autoimmune diseases, such as rheumatoid arthritis and systemic lupus erythematosus. B cells are also susceptible to malignant transformation.
Additional image
Figure 1: Schematic diagram to explain mechanisms of clonal selection of B cell, and how secondary immune response is stronger, quicker and more specific in [9] comparison with the primary one.
B cell
558
References
[2] Alberts B, Johnson A, Lewis J, Raff M, Roberts k, Walter P (2002) Molecular Biology of the Cell (http:/ / www. ncbi. nlm. nih. gov/ bookshelf/ br. fcgi?book=mboc4& part=A4422). Garland Science: New York, NY pg 1367. [3] Parham, P. (2005). The Immune System, Garland Science Publishing, New York, NY. [8] Bursa of Fabricius (http:/ / www. nlm. nih. gov/ cgi/ mesh/ 2007/ MB_cgi?mode=& term=Bursa+ of+ Fabricius& field=entry)
Activation of B Lymphocytes by T-Independent Antigens. Gary Kaiser. American Society for Microbiology. July 2005.
External links
• B-Lymphocytes (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=B-Lymphocytes) at the US National Library of Medicine Medical Subject Headings (MeSH) • B Cells and T Cells (http://users.rcn.com/jkimball.ma.ultranet/BiologyPages/B/B_and_Tcells.html) • B Cell Development and Generation of Lymphocyte Diversity (http://www.microvet.arizona.edu/Courses/ MIC419/Secure/CaseNoIg/GODfigs.htm) • Interactive Animation of B Cell Maturation (http://www.bio.davidson.edu/courses/immunology/Flash/ Bcellmat.html) (requires Flash video software) • A Tale of Two SHEPherds (http://beaker.sanfordburnham.org/?p=2357) (from Beaker Blog) • Educational Resource on the Biology of Antibody Cells (http://www.wikilite.com/wiki/index.php/ Biology_of_immunoglobulin_light_chains)
Natural killer cell
Natural killer cells (or NK cells) are a type of cytotoxic lymphocyte critical to the innate immune system. The role NK cells play is analogous to that of cytotoxic T cells in the vertebrate adaptive immune response. NK cells provide rapid responses to virally infected cells and respond to tumor formation, acting at around 3 days after infection. Typically immune cells detect MHC presented on infected cell surfaces, triggering cytokine release causing lysis or apoptosis. NK cells are unique, however, as they have the ability to recognize stressed cells in the absence of antibodies and MHC, allowing for a much faster immune reaction. They were named “natural killers” because of the initial notion that they do not require activation in order to kill cells that are missing “self” markers of major histocompatibility complex (MHC) class 1 .[] NK cells are defined as large granular lymphocytes (LGL) and constitute the third kind of cells differentiated from the common lymphoid progenitor generating B and T lymphocytes.[1] NK cells are known to differentiate and mature in the bone marrow, lymph node, spleen, tonsils and thymus where they then enter into the circulation. .[] NK cells differ from Natural Killer T cells (NKT) phenotypically, by origin and by respective effector functions; often NKT cell activity promotes NK cell activity by secreting IFNγ. In contrast to NKT cells, NK cells do not express T-cell antigen receptors (TCR) or Pan T marker CD3 or surface immunoglobulins (Ig) B cell receptors, but they usually express the surface markers CD16 (FcγRIII) and CD56 in humans, NK1.1 or NK1.2 in C57BL/6 mice. Up to 80% of human NK cells also express CD8. In addition to the knowledge that natural killer cells are effectors of innate immunity, recent research has uncovered information on both activating and inhibitory NK cell receptors which play important function roles including self tolerance and sustaining NK cell activity. NK cell also play a role in adaptive immune response ,[] numerous experiments have worked to demonstrate their ability to readily adjust to the immediate environment and formulate antigen-specific immunological memory, fundamental for responding to secondary infections with the same antigen. The ability for NK cells to act in both the innate and adaptive immune response is becoming increasingly important in research utilizing NK cell activity and potential cancer therapies.
Natural killer cell
559
NK cell receptors
NK cell receptors can also be differentiated based on function. Natural cytotoxicity receptors directly induce apoptosis after binding to ligands that directly indicate infection of a cell. The MHC dependent receptors (described above) use an alternate pathway to induce apoptosis in infected cells. Natural killer cell activation is determined by the balance of inhibitory and activating receptor stimulation i.e. if the inhibitory receptor signaling is more prominent then NK cell activity will be inhibited, similarly if the activating signal is dominant then NK cell activation will result .[]
The HLA ligand for KIR
NK cell receptor types (with inhibitory as well as some activating members) are differentiated by structure, with a couple of examples to follow:
Protein Structure of NKG2D
Activating receptors
• Ly49 (homodimers) — a relatively ancient, C-type lectin family receptor; are of multigenic presence in mice, while humans have only one pseudogenic Ly49; the receptor for classical (polymorphic) MHC I molecules. • NCR (natural cytotoxicity receptors), upon stimulation, mediate NK killing and release of IFNϒ. • CD94 : NKG2 (heterodimers) — a C-type lectin family receptor, conserved in both rodents and primates and identifies non-classical (also non-polymorphic) MHC I molecules like HLA-E. Expression of HLA-E at the cell surface is dependent on the presence of nonamer peptide epitope derived from the signal sequence of classical MHC class I molecules, which is generated by the sequential action of signal peptide peptidase and the proteasome. Though indirect, this is a way to survey the levels of classical (polymorphic) HLA molecules. • CD16 (FcγIIIA) play a role in antibody-dependent cell-mediated cytotoxicity (ADCC), in particular they bind IgG.
Protein Structure of NKp44
Natural killer cell
560
Function
Cytolytic granule mediated cell apoptosis
NK cells are cytotoxic; small granules in their cytoplasm contain proteins such as perforin and proteases known as granzymes. Upon release in close proximity to a cell slated for killing, perforin forms pores in the cell membrane of the target cell, creating an aqueous channel through which the granzymes and associated molecules can enter, inducing either apoptosis or osmotic cell lysis. The distinction between apoptosis and cell lysis is important in immunology: lysing a virus-infected cell could potentially only release the virions, whereas apoptosis leads to destruction of the virus inside. αdefensins, an antimicrobial is also secreted by NK cells, it directly kills bacteria by disrupting their cell walls analogous to neutrophils.[]
Antibody-dependent cell-mediated cytotoxicity (ADCC)
Infected cells are routinely opsonised with antibodies for detection by immune cells. Antibodies that bind to antigens can be recognised by FcϒRIII (CD16) receptors expressed on NK cells resulting in NK activation, release of cytolytic granules and consequent cell apoptosis. This is a major mechanism of killing for some monoclonal antibodies like rituximab (Rituxan), ofatumumab (Azzera) and others. The contribution of ADCC to tumor cell killing can be measured with a specific test that uses NK-92 NK-92 that has been transfected with a high affinity FcR. Results are compared to the "wild type" NK-92 NK-92 that does not express the FcR (www.nk-92.com) NK-92. .[]
Cytokine induced NK and CTL activation
Cytokines play a crucial role in NK cell activation. As these are stress molecules released by cells upon viral infection, they serve to signal to the NK cell the presence of viral pathogens. Cytokines involved in NK activation include IL-12, IL-15, IL-18, IL-2, and CCL5. NK cells are activated in response to interferons or macrophage-derived cytokines. They serve to contain viral infections while the adaptive immune response is generating antigen-specific cytotoxic T cells that can clear the infection. NK cells work to control viral infections by secreting IFNγ and TNFα, IFNγ activates macrophages for phagocytosis and lysis and TNFα acts promote direct NK tumor cells killing. Patients deficient in NK cells prove to be highly susceptible to early phases of herpes virus infection.
Natural killer cell
561
Missing 'self' hypothesis
In order for NK cells to defend the body against viruses and other pathogens, they require mechanisms that enable the determination of whether a cell is infected or not. The exact mechanisms remain the subject of current investigation, but recognition of an "altered self" state is thought to be involved. To control their cytotoxic activity, NK cells possess two types of surface receptors: activating receptors and inhibitory receptors. Most of these receptors are not unique to NK cells and can be present in some T cell subsets as well. These inhibitory receptors recognize MHC class I alleles, which could Schematic diagram indicating the complementary activities of cytotoxic T-cells and NK explain why NK cells kill cells cells. possessing low levels of MHC class I molecules. This inhibition is crucial to the role played by NK cells. MHC class I molecules are the main mechanism by which cells display viral or tumor antigens to cytotoxic T-cells. A common evolutionary adaptation to this seen in both intracellular microbes and tumours, the chronic down-regulation of MHC I molecules, rendering the cell impervious to T-cell mediated immunity. It is believed that NK cells, evolved as an evolutionary response to this adaptation (the loss of the MHC deprives CD4/CD8 action so another immune cell evolved to fulfil the requirement). .[]
Tumor cell surveillance
Natural Killer Cells (NK) often lack antigen specific cell surface receptors and therefore are part of innate immunity i.e. able to react immediately with no prior exposure to the pathogen. In both mice and humans NKs can be seen to play a role in tumor immuno-surveillance by directly inducing the death of tumor cells (NKs act as cytolytic effector lymphocytes) even with the absence of surface adhesion molecules and antigenic peptides, this role of NK cells is critical for immune success particularly because T cells are unable to recognize pathogens in the absence of surface antigens.[] Tumor cell detection results in activation of NK cells and consequent cytokine production and release. If the tumor cells do not cause inflammation they will also be regarded as self and therefore will not induce a T cell response. A number of cytokines are produced by NKs including Tumor Necrosis Factor α (TNFα), IFNγ and Interleukin (IL-10); TNFα and IL-10 act as pro-inflammatory and immuno-suppressors respectively. The activation of NK cells and subsequent production of cytolytic effector cells impacts macrophages, dendritic cells and neutrophils which subsequently affects antigen specific T and B cell responses. Instead of acting via antigen specific receptors, lysis of tumor cells by NK cells is mediated by alternative receptors including NKG2D, NKp44, NKp46, NKp30 and DNAM.[] NKG2D is a disulphide linked homodimer which recognizes a number of ligands, including ULBP and MICA, which are typically expressed on tumor cells. NK cells, along with macrophages and several other cell types, express the Fc receptor (FcR) molecule (FC-gamma-RIII = CD16), an activating biochemical receptor that binds the Fc portion of antibodies. This allows NK cells to target cells against which a humoral response has been mobilized and to lyse cells through
Natural killer cell Antibody-dependent cellular cytotoxicity (ADCC). This response depends on the affinity of the Fc receptor expressed on NK cells which can have high, intermediate and low affinity for the Fc portion of the antibody or IgG. This affinity is determined by the nucleotide status in position 158 of the gene. which can code of Phenylalanine (F allele) or Valine (V allele). Individuals with high affinity FcRgammRIII (158 V/V respond better to antibody therapy. This has been shown for lymphoma patients who received the antibody Rituxan. Patients who express the 158 V/V allele had a better anti-tumor response. Only 15-25% of the population expressed the 158 V/V allele. To determine the ADCC contribution of monoclonal antibodies, NK-92 cells (a "pure" NK cell line) NK-92 has been transfected with the gene for the high affinity expressing FcR.
562
NK cell function in adaptive response
The ability to generate memory cells following a primary infection and the consequent rapid immune activation and response to succeeding infections by the same antigen is fundamental to the role T and B cells play in the adaptive immune response. Despite prior belief that NK cells play no role in the adaptive immune responses, they have since been found to undergo expansion, contraction, memory maintenance and recall .[2]
NK cell function in pregnancy
As the majority of pregnancies involve two parents who are not tissue matched, successful pregnancy requires the mother's immune system to be suppressed. NK cells are thought to be an important cell type in this process.[] These cells are known as "uterine NK cells" (uNK cells) and they differ from peripheral NK cells. They are in the CD56bright NK cell subset, potent at cytokine secretion, but with low cytotoxic ability and relatively similar to peripheral CD56bright NK cells, with a slightly different receptor profile.[] These uNK cells are the most abundant leukocytes present in the uterus in early pregnancy, representing approximately 70% of leukocytes here, however where they originate from remains controversial.[] These NK cells have been shown to have the ability to elicit cell cytotoxicity in vitro, however at a lower level than peripheral NK cells, despite containing perforin.[] Lack of cytotoxicity in vivo may be due to the presence of ligands for their inhibitory receptors. Trophoblast cells downregulate HLA-A and HLA-B in order to defend against cytotoxic T cell-mediated death. This would normally trigger NK cells by missing self recognition, however these cells survive. It is thought that the selective retention of HLA-E (which is a ligand for NK cell inhibitory receptor NKG2A) and HLA-G (which is a ligand for NK cell inhibitory receptor KIR2DL4) by the trophoblast defends it against NK cell-mediated death.[] NK cells secrete a high level of cytokines which help mediate their function. Some important cytokines they secrete include TNF-α, IL-10, IFN-γ and TGF-β, among others.[] For example, IFN-γ dilates and thins the walls of maternal spiral arteries to enhance blood flow to the implantation site.[3]
NK cell evasion by tumor cells
By shedding decoy NKG2D soluble ligands tumor cells have evolved a process by which they are able to avoid immune responses. These soluble NKG2D ligands bind to NK cell NKG2D receptors activating a false NK response and consequently creating competition for the receptor site.[] This method of evasion occurs in prostate cancer. In addition, prostate cancer tumors can evade CD8 cell recognition due to the ability to lose expression of MHC class 1 molecules. This example of immune evasion actually highlights NK cell importance in tumor surveillance and response as CD8 cells can consequently only act on tumor cells in response to NK initiated cytokine production (adaptive immune response) .[4]
Natural killer cell
563
History
In early experiments on cell-mediated cytotoxicity against tumor target cells, both in cancer patients and animal models, investigators consistently observed what was termed a "natural" reactivity, that is, a certain population of cells seemed to be able to lyse tumor cells without having been previously sensitized to them. As these discoveries were incompatible with the established model at the time, many initially considered that these observations were artifacts.[5] However, by 1973, 'natural killing' activity was established across a wide variety of species, and the existence of a separate lineage of cells possessing this ability was postulated. The discovery that a unique type of lymphocyte was responsible for “natural” or spontaneous cytotoxicity was made in the early 1970s by doctoral student Rolf Kiessling and post-doctoral fellow Hugh Pross, in the mouse,[6] and by Hugh Pross and doctoral student Mikael Jondal in the human.[7][8] The mouse and human work was carried out under the supervision of professors Eva Klein and Hans Wigzell, respectively, of the Karolinska Institute, Stockholm. Kiessling’s research involved the well-characterized ability of T-lymphocytes to lyse tumor cells against which they had been previously immunized. Pross and Jondal were studying cell-mediated cytotoxicity in normal human blood and the effect of the removal of various receptor-bearing cells on this cytotoxicity. Later that same year Ronald Herberman published similar data with respect to the unique nature of the mouse effector cell.[9] The human data were confirmed, for the most part, by West et al.[10] using similar techniques and the same erythroleukemic target cell line, K562. K562 is highly sensitive to lysis by human NK cells and, over the decades, the K562 51 Chromium-release assay has become the most commonly used assay to detect human NK functional activity.[11] Its almost universal use has meant that experimental data can be compared easily by different laboratories around the world. Using discontinuous density centrifugation and, later, monoclonal antibodies, natural killing ability was mapped to the subset of large, granular lymphocytes known today as NK cells. The demonstration that density gradient-isolated large granular lymphocytes were responsible for human NK activity, made by Timonen and Saksela in 1980,[12] was the first time that NK cells had been visualized microscopically and was a major breakthrough in the field.
New findings
Anti-cancer therapy
Since NK cells recognize target cells when they express non-self HLA antigens (but not self), autologous (patients' own) NK cell infusions have not shown any anti-tumor effects. Instead investigators are working on using allogeneic cells from peripheral blood which requires that the T-cells are removed before infusion into the patients as they would otherwise cause graft versus host disease (GvHD) which can be fatal. This can be achieved using an immunomagnetic column (CliniMACS). In addition, because of the limited number of NK cells in blood (only 10% of lymphocytes are NK-cells) their number needs to be expanded in culture. This can take a few weeks and the yield is donor dependent. A simpler way to achieve high numbers of pure NK cells is to expand NK-92 cells NK-92 whose cells continuously grow in culture and can be expanded to clinical grade numbers in bags or bioreactors [13]. Clinical studies have shown that it is well tolerated and some anti-tumor responses have been seen in patients with lung cancer, melanoma and lymphoma [14]. Recent studies at Sloan Kettering Cancer Center and UPenn have shown that infusions of T-cells that were engineered to express a chimeric antigen receptor (CAR) recognizing an antigen molecule on leukemia cells could induce remissions in patients with advanced leukemia. There are logistical challenges of expanding T-cells and investigators are working on applying the same technology to peripheral blood NK cells and NK-92 NK-92. NK cells in a study at Children's Hospital Boston in coordination with Dana-Farber Cancer Institute, whereby immunocompromised mice had contracted lymphomas from EBV infection, an NK activating receptor called NKG2D was fused with a stimulatory Fc portion of the EBV antibody. The NKG2D-Fc fusion proved capable of reducing tumor growth and prolonging survival of the recipients.[15]
Natural killer cell
564
Innate resistance to HIV?
Recent research suggests that specific KIR-MHC class 1 gene interactions could control innate genetic resistance to certain viral infections including HIV and its consequent development of AIDS.[] Certain HLA allotypes have been found to determine the progression of HIV to AIDS; an example is the HLA-B57 and HLA-B27 alleles, which have been found to defer progression of HIV to AIDS. This is evident because patients expressing these HLA alleles are observed to have lower viral loads and a more gradual decline in CD4+ T cells numbers. Despite considerable research and data collected measuring the genetic correlation of HLA alleles and KIR allotypes, a firm conclusion has not yet been drawn as to what combination provides decrease HIV and AIDS susceptibility. Future research would aim to pinpoint relevant KIR/HLA interactions with aim to produce a vaccine against HIV/AIDS. NK cells can impose immune pressure on HIV, something that had previously been described only for T cells and antibodies [16] and that HIV mutates to avoid NK cell activity.[16]
Literature
• Cellular and Molecular Immunology by Abbul K. Abbas & Andrew Lichtman Saunders Copyright 2003 • How the Immune System Works, 2nd edition, by Lauren Sompayrac, PhD Blackwell Publishing 2003 • Immunobiology: The Immune System In Health And Disease by Janeway, Travers, Walport & Shlomchik Churchchill Livingstone Copyright 2005 • Kuby Immunology, 6th edition, by Thomas J. Kindt, Richard A. Goldsby,and Barbara A.OsborneW.H. Freeman and Company,New York • Tsuda Y, Cygler M, Gibbs BF, et al. (December 1994). "Design of potent bivalent thrombin inhibitors based on hirudin sequence: incorporation of nonsubstrate-type active site inhibitors". Biochemistry 33 (48): 14443–51. doi:10.1021/bi00252a010 [17]. PMID 7981204 [18].
References
[1] Roitt I, Brostoff J, Male D (2001). Immunology (6th ed.), 480p. St. Louis: Mosby, ISBN 0-7234-3189-2. [3] Ashkar AA, Di Santo JP, Croy BA. Interferon gamma contributes to initiation of uterine vascular modification, decidual integrity, and uterine natural killer cell maturation during normal murine pregnancy. J Exp Med. 2000 Jul 17;192(2):259-70. [13] Gong J, Maki G, Klingemann H. Characterization of a human cell line (NK-92) with phenotypical and functional characteristics of activated natural killer cells. Leukemia 1994; 8: 652-58 [14] Arai S, Meagher R, Swearingen M, et al. Infusion of the allogeneic cell line NK-92 in patients with advanced renal cell cancer or melanoma: a phase I trial. Cytotherapy 2008;10:625-32 ^ Tonn T, Becker S, Esser R, Schwabe D, Seifried E. Cellular immunotherapy of malignancies using the clonal natural killer cell line NK-92. J Hematother Stem Cell Res 2001;10:535-44. [edit] [15] In a transplantation model of LMP1-fueled lymphomas, the NKG2D-Fc fusion proved quite capable of reducing tumor growth and prolonging survival of the recipients [16] http:/ / www. sciencedaily. com/ releases/ 2011/ 08/ 110803133509. htm
External links
• Video of natural killer cell (http://www.youtube.com/watch?v=HNP1EAYLhOs) • CopeWithCytoKines Portal to definitions of NK-Cells and closely related topics (http://www. copewithcytokines.de/cope.cgi?key=NK-cells) • http://www.hfea.gov.uk/fertility-treatment-options-reproductive-immunology.html Reproductive immunology and fertility treatment • http://www.cambridgenetwork.co.uk/news/article/default.aspx?objid=58465 • Binns C (June 19, 2006), Natural Body Guards: How Your Killer Cells Get Motivated (http://www.livescience. com/817-natural-body-guards-killer-cells-motivated.html). Livescience.com. Retrieved on 2007-10-20. • Natural Killer Cells (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Natural+Killer+ Cells) at the US National Library of Medicine Medical Subject Headings (MeSH)
Natural killer cell • Nkcells.info (http://www.nkcells.info) - MediaWiki based information platform specializing on natural killer cells • Large granular lymphocyte (http://www.cancer.gov/dictionary?CdrID=44440) entry in the public domain NCI Dictionary of Cancer Terms
565
Reticulocyte
Reticulocyte
Reticulocyte Latin reticulocytus Code TH H2.00.04.1.01007 [1]
Reticulocytes are immature red blood cells, typically composing about 1% of the red cells in the human body. Reticulocytes develop and mature in the red bone marrow and then circulate for about a day in the blood stream before developing into mature red blood cells. Like mature red blood cells, reticulocytes do not have a cell nucleus. They are called reticulocytes because of a reticular (mesh-like) network of ribosomal RNA that becomes visible under a microscope with certain stains such as new methylene blue.
Erythrocyte
Process
To accurately measure reticulocyte counts, automated counters that use lasers mark cell samples with fluorescent dye that marks RNA and DNA (such as thiazole orange or polymethine).[1] This distinguishes reticulocytes as the middle ground of dye response to laser light, between red blood cells (which have neither RNA nor DNA) and lymphocytes (which have a large amount of DNA, unlike reticulocytes).[2] The specimen requirement for a reticulocyte count is EDTA anti-coagulated whole blood (lavender-top bottle if using the Vacutainer, Vacuette or Monoject systems; red-top if using the S-Monovette system). Reticulocytes appear slightly bluer than other red cells when looked at with the normal Romanowsky stain. Reticulocytes are also slightly larger, which can be picked up as a high MCV (mean corpuscular volume) with a full blood count done by a trained medical scientist, who has specialized in hematology, or a machine. Flowcytometry for mouse reticulocytes: One can use a cell-permeable thiazole orange dye (see above) to stain for reticulocytes' residual RNA in conjunction with DRAQ5 DNA-only dye (reticulocytes have no DNA and are, thus, DRAQ5-negative) and Ter119 (glycophorin-A) that is a marker of erythroid lineage. (Thiazole orange dye binds to nucleic acids of both DNA and RNA).
Reticulocyte
566
Interpretation
The normal range of values for reticulocytes in the blood depends on the clinical situation and the lab but is usually 0.5% to 1.5%. However, if a person has anemia, the reticulocyte percentage should be higher than "normal" if the bone marrow's ability to produce new blood cells remains intact. Thus, calculating the reticulocyte production index is an important step in understanding whether or not the reticulocyte count is appropriate to the situation. This is often a more important question than whether the percentage is in the normal range; for instance, if someone is anemic but has a reticulocyte percentage of only 1%, the bone marrow is likely not producing new blood cells at a rate that will correct the anemia.
The number of reticulocytes is a good indicator of bone marrow activity because it represents recent production. This means that the reticulocyte count and the reticulocyte production index that can be calculated from it can be used to determine whether a production problem is contributing to the anemia and can also be used to monitor the progress of treatment for anemia. When there is an increased production of red blood cells to overcome chronic or severe loss of mature red blood cells, such as in a haemolytic anemia, people often have a markedly high number and percentage of reticulocytes. A very high number of reticulocytes in the blood can be described as reticulocytosis. Abnormally low numbers of reticulocytes can be attributed to chemotherapy, aplastic anemia, pernicious anemia, bone marrow malignancies, problems of erythropoietin production, various vitamin or mineral deficiencies (B9, B12, iron), disease states (anemia of chronic disease) and other causes of anemia due to poor RBC production.
Supravital stain of a smear of human blood from a patient with hemolytic anemia. The reticulocytes are the cells with the dark blue dots and curved linear structures (reticulum) in the cytoplasm.
References
[2] http:/ / www. medicaldesign. com/ articles/ ID/ 532
External links
• For more information on Reticulocyte Count (http://www.diagnostic-medical-tests.com/ hematology-coagulation-tests/reticulocyte-count.htm) • Reticulocyte (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=Reticulocyte) at eMedicine Dictionary • http://www.hxbenefit.com/aplastic-crisis-reticulocytopenia.html
Progenitor cell
567
Progenitor cell
A progenitor cell is a biological cell that, like a stem cell, has a tendency to differentiate into a specific type of cell, but is already more specific than a stem cell and is pushed to differentiate into its "target" cell. The most important difference between stem cells and progenitor cells is that stem cells can replicate indefinitely, whereas progenitor cells can divide only a limited number of times. Controversy about the exact definition remains and the concept is still evolving.[1] The terms "progenitor cell" and "stem cell" are sometimes equated.[2]
Properties
Most progenitors are described as oligopotent. In this point of view, they may be compared to adult stem cells. But progenitors are said to be in a further stage of cell differentiation. They are in the “center” between stem cells and fully differentiated cells. The kind of potency they have depends on the type of their "parent" stem cell and also on their niche. Some progenitor cells were found during research, and were isolated. After their marker was found, it was proven that these progenitor could move through the body and migrate towards the tissue where they are needed. Many properties are shared by adult stem cells and progenitor cells. But still, controversy remains because embryonic stem cells are true stem cells in that they are pluripotent and show unlimited capacity for self-renewal. In contrast, many cells termed adult stem cells would be better defined as progenitor cells, as their capacities for unlimited self-renewal and plasticity have not been comprehensively demonstrated. Progenitor cells are found in adult organisms and they act as a repair system for the body. They replenish special cells, but also maintain the blood, skin and intestinal tissues. They can also be found in developing embryonic pancreatic tissue.
Stem Cell Self-renewal in vivo Self-renewal in vitro Potentiality Unlimited Unlimited Multipotent Limited Limited Unipotent, sometimes oligopotent No Progenitor Cell
Maintenance of self-renewal Yes Population
Reaches maximum number of cells before differentiating Does not reach maximum population
Function
The majority of progenitor cells lie dormant or possess little activity in the tissue in which they reside. They exhibit slow growth and their main role is to replace cells lost by normal attrition. In case of tissue injury, damaged or dead cells, progenitor cells can be activated. Growth factors or cytokines are two substances that trigger the progenitors to mobilize toward the damaged tissue. At the same time, they start to differentiate into the target cells. Not all progenitors are mobile and are situated near the tissue of their target differentiation. When the cytokines, growth factors and other cell division enhancing stimulators take on the progenitors, a higher rate of cell division is introduced. It leads to the recovery of the tissue.
Progenitor cell
568
Examples
The characterization or the defining principle of progenitor cells, in order to separate them from others, is based on the different cell markers rather than their morphological appearance. • Satellite cells found in muscles. They play a major role in muscle cell differentiation and injury recoveries. • Intermediate progenitor cells formed in the subventricular zone.[] Some of these transit amplifying neural progenitors migrate via rostral migratory stream to the olfactory bulb and differentiate further into specific types of neural cells. • Bone marrow stromal cells, basal cell of epidermis have 10% of progenitor cell, although they are often classed as stem cells due to their high plasticity and potential for unlimited capacity for self-renewal. • Periosteum contains progenitor cells that develop into osteoblasts and chondroblasts. • Pancreatic progenitor cells are among the most-studied progenitors.[3] They are used in research to develop a cure against diabetes type-1. • Angioblasts or Endothelial progenitor cells (EPC). These are very important for research on fracture and wounds healing.[4] • Blast cells are involved in generation of B- and T-lymphocytes, which participate in immune responses.[5][6]
Development of the human cerebral cortices
Before E40 (embryonic day 40), progenitor cells generate other progenitor cells; after that period, progenitor cells produce only dissimilar daughters. The cells from a single progenitor cell form a proliferative unit that creates one cortical column; these columns contain a variety of neurons with different shapes.
References
Ovum
569
Ovum
Ovum
A human ovum with corona radiata surrounding it
An ovum (plural ova, from the Latin word ovum meaning egg or egg cell) is a haploid female reproductive cell or gamete. Both animals and embryophytes have ova. The term ovule is used for the young ovum of an animal, as well as the plant structure that carries the female gametophyte and egg cell and develops into a seed after fertilization. In lower plants and algae, the ovum is also often called oosphere.
Ova production
In higher animals, ova are produced by female gonads (sexual glands) called ovaries and all of them are present at birth in mammals and mature via oogenesis.
Human and mammal ova
In the viviparous animals (which include humans and all other placental mammals), the ovum is fertilized inside the female body. Human ovum is a haploid cell still waiting to complete its meosis. And its meosis is completed just after fertilization producing secondary polar body and maternal pro nuclei. The polar body produced is immediately degenarates The human ova grow from primitive germ cells that are embedded in the substance of the ovaries. Each of them divides repeatedly to give rise to several smaller cells, the oogonia. The oogonia then develop via meiosis into the ova, the primary oocytes, and the polar bodies.[1] Once the ovum has been fertilized, it begins to divide over the course of a few hours or days, becoming a morula. The morula enters the uterine cavity where it is immersed in the secretions of the uterine glands, ultimately forming a blastocyst.[2] The ovum is one of the largest cells in the human body, typically visible to the naked eye without the aid of a microscope or other magnification device. The human ovum measures approximately 0.12 mm in diameter.[3]
Ovum and sperm fusing together
The process of fertilizing an ovum (Top to bottom)
Ovum
570
Protist and plant ova
In protists, fungi and many plants, such as bryophytes, ferns, and gymnosperms, ova are produced inside archegonia. Since the archegonium is a haploid structure, egg cells are produced via mitosis. The typical bryophyte archegonium consists of a long neck with a wider base containing the egg cell. Upon maturation, the neck opens to allow sperm cells to swim into the archegonium and fertilize the egg. The resulting zygote then gives rise to an embryo, which will grow out of the archegonium as a young sporophyte.[citation needed] In the flowering plants, the female gametophyte, which usually gives rise to the archegonium, has been reduced to just eight cells referred to as the embryo sac inside the ovule. The gametophyte cell closest to the micropyle opening of the embryo sac develops into the egg cell. Upon pollination, a pollen tube delivers sperm into the embryo sac and one sperm nucleus fuses with the egg nucleus. The resulting zygote develops into an embryo inside the ovule. The ovule in turn develops into a seed and in many cases the plant ovary develops into a fruit to facilitate the dispersal of the seeds. Upon germination, the embryo grows into a seedling.[citation needed] In the moss Physcomitrella patens, the Polycomb protein FIE is expressed in the unfertilised egg cell (Figure, right) as the blue colour after GUS staining reveals. Soon after fertilisation the FIE gene is inactivated (the blue colour is no longer visible, left) in the young embryo. [4]
Ooplasm
Ooplasm (also: oöplasm) is the yolk of the ovum, a cell substance at its center, which contains its nucleus, named the germinal vesicle, and the nucleolus, called the germinal spot.[] The ooplasm consists of the cytoplasm of the ordinary animal cell with its spongioplasm and hyaloplasm, often called the formative yolk; and the nutritive yolk or deutoplasm, made of rounded granules of fatty and albuminoid substances imbedded in the cytoplasm.[] Mammalian ova contain only a tiny amount of the nutritive yolk, for nourishing the embryo in the early stages of its development only. In contrast, bird eggs contain enough to supply the chick with nutriment throughout the whole period of incubation.[]
Ova development in oviparous animals
Gene expression pattern determined by histochemical GUS assays in Physcomitrella patens. The Polycomb gene FIE is expressed (blue) in unfertilised egg cells of the moss Physcomitrella patens (right) and expression ceases after fertilisation in the developing diploid sporophyte (left). In situ GUS staining of two female sex organs (archegonia) of a transgenic plant expressing a translational fusion of FIE-uidA under control of the native FIE promoter
In the oviparous animals (all birds, most fishes, amphibians and reptiles) the ova develop protective layers and pass through the oviduct to the outside of the body. They are fertilized by male sperm either inside the female body (as in birds), or outside (as in many fishes). After fertilization, an embryo develops, nourished by nutrients contained in the egg. It then hatches from the egg, outside the mother's body. See egg (biology) for a discussion of eggs of oviparous animals. The egg cell's cytoplasm and mitochondria (and chloroplasts in plants) are the sole means the egg is able to reproduce by mitosis and eventually form a blastocyst after fertilization.
Ovum
571
Ovoviviparity
There is an intermediate form, the ovoviviparous animals: the embryo develops within and is nourished by an egg as in the oviparous case, but then it hatches inside the mother's body shortly before birth, or just after the egg leaves the mother's body. Some fish, reptiles and many invertebrates use this technique.
References
[1] . [3] Search result of "120 micrometers" in Level O Biology - Google books (http:/ / books. google. ca/ books?id=ca51dWOR8nIC& pg=RA5-PA8-IA2& dq=ovum+ 120+ micrometers& hl=en& ei=sXtjTI6_D4OC8gbZ6rCeCQ& sa=X& oi=book_result& ct=result& resnum=1& ved=0CDAQ6AEwAA#v=onepage& q=120 micrometers& f=false) [4] Assaf Mosquna, Aviva Katz, Eva L. Decker, Stefan A. Rensing, Ralf Reski, Nir Ohad (2009): Regulation of stem cell maintenance by the Polycomb protein FIE has been conserved during land plant evolution. Development 136, 2433-2444.
External links
• The Ovarian Kaleidoscope Database (http://ovary.stanford.edu) description of 1800 genes involved in ovarian functions
Oocyte
572
Oocyte
Oocyte
"Stripped" human oocyte; granulosa cells that had surrounded this oocyte have been removed. Gray's MeSH subject #3 38 Oocytes
[2] [1]
An oocyte (UK: /ˈəʊəsʌɪt/, US: /ˈoʊ.oʊ.saɪt/), oöcyte, ovocyte, or rarely ocyte, is a female gametocyte or germ cell involved in reproduction. In other words, it is an immature ovum, or egg cell. An oocyte is produced in the ovary during female gametogenesis. The female germ cells produce a primordial germ cell (PGC) which undergoes mitosis to form an oogonium. During oogenesis the oogonium becomes a primary oocyte.
Formation
The formation of an oocyte is called oocytogenesis, which is a part of oogenesis.[1] Oogenesis results in the formation of both primary oocytes before birth, and of secondary oocytes after it as part of ovulation.
Diagram showing the reduction in number of the chromosomes in the process of maturation of the ovum; the process is known as meiosis.
Oocyte
573
Cell type Oogonium primary Oocyte
ploidy/chromosomes chromatids Process diploid/46(2N) diploid/46(2N) 4N 4N 2N 1N 1N Oocytogenesis (mitosis)
Time of completion third trimester
Ootidogenesis (meiosis 1) (Folliculogenesis) Dictyate in prophase I for up to 50 years Ootidogenesis (meiosis 2) Ootidogenesis (meiosis 2) Halted in metaphase II until fertilization Minutes after fertilization
secondary Oocyte haploid/23(1N) Ootid Ovum haploid/23(1N) haploid/23(1N)
Characteristics
Cytoplasm
Oocytes are rich in cytoplasm which contains yolk granules to nourish the cell early in development.
Nucleus
During the primary oocyte stage of oogenesis, the nucleus is called a germinal vesicle.[2] The only normal human type of secondary oocyte has the 23rd (sex) chromosome as 23,X (female-determining), whereas sperm can have 23,X (female-determining) or 23,Y (male-determining).
Human oocyte with surrounding granulosa cells
Nest
The space wherein an ovum or immature ovum is located is the cell-nest.[3]
Maternal Contributions
Oocyte
574 Because the fate of an oocyte is to become fertilized and ultimately grow into a fully functioning organism, it must be ready to regulate multiple cellular and developmental processes. The oocyte, a large and complex cell, must be supplied with numerous molecules that will direct the growth of the embryo and control cellular activities. As the oocyte is a product of female gametogenesis, the maternal contribution to the oocyte and consequently the newly fertilized egg is enormous. There are many types of molecules that are maternally supplied to the oocyte which will direct various activities within the growing zygote.
mRNAs and Proteins
During the growth of the oocyte, a variety of maternally transcribed messenger RNAs, or mRNAs, are supplied by maternal cells. These mRNAs can be stored in mRNP (message ribonucleoprotein) complexes and be translated at specific time points, they can be localized within a specific region of the cytoplasm, or they can be homogeneously dispersed within the cytoplasm of the entire oocyte.[4] Oocyte Poles Maternally loaded proteins can also be localized or ubiquitous throughout the cytoplasm. The translated products of the mRNAs and the loaded proteins have multiple functions; from regulation of cellular "house-keeping" such as cell cycle progression and cellular metabolism, to regulation of developmental processes such as fertilization, activation of zygotic transcription, and formation of body axes.[4] Below are some examples of maternally inherited mRNAs and proteins found in Xenopus laevis oocytes.
Name [5] VegT Vg1 [6] [7] Type of Maternal Molecule mRNA mRNA mRNA Protein mRNA Protein mRNA Protein [11] mRNA Protein mRNA Protein [11] Protein mRNA Localization Function
Vegetal Hemisphere Transcription Factor Vegetal Hemisphere Transcription Factor Not Known Ubiquitous Ubiquitous Ubiquitous Ubiquitous Nucleus Not Known Transcription Factor Transcription Factor Transcription Factor Transcription Factor Transcription Factor Not Known FGF Signaling
XXBP-1 CREB
[8] [9]
FoxH1 p53
[10] [11]
Lef/Tcf FGF2
[12]
FGF2, 4, 9 FGFR1 Ectodermin PACE4 [13]
Animal Hemisphere Ubiquitin Ligase Vegetal Hemisphere Proprotein Convertase Not Known Not Known BMP inhibitor BMP/Chordin Bindng Protein
[14]
[15] Coco Twisted Gastrulation fatvg [16]
Vegetal Hemisphere Germ Cell Formation and Cortical Rotation
Oocyte
575
Mitochondria
The oocyte receives mitochondria from maternal cells, which will go on to control embryonic metabolism and apoptotic events.[4] The partitioning of mitochondria is carried out by a system of microtubules which will localize mitochondria throughout the oocyte. In certain organisms, such as mammals, paternal mitochondria brought to the oocyte by the spermatozoon are degraded through the attachment of ubiquitinated proteins. The destruction of paternal mitochondria ensures the strictly maternal inheritance of mitochondria and mitochondrial DNA or mtDNA.[4]
Nucleolus
In mammals, the nucleolus of the oocyte is derived solely from maternal cells.[17] The nucleolus, a structure found within the nucleus, is the location where rRNA is transcribed and assembled into ribosomes. While the nucleolus is dense and inactive in a mature oocyte, it is required for proper development of the embryo.[17]
Maternal Determinants in Xenopus laevis Oocyte
Ribosomes
Maternal cells also synthesize and contribute a store of ribosomes that are required for the translation of proteins before the zygotic genome is activated. In mammalian oocytes, maternally derived ribosomes and some mRNAs are stored in a structure called cytoplasmic lattices. These cytoplasmic lattices, a network of fibrils, protein, and RNAs, have been observed to increase in density as the number of ribosomes decrease within a growing oocyte.[18]
Paternal Contributions
The spermatozoon which fertilizes an oocyte will contribute its pronucleus, the other half of the zygotic genome. In some species, the spermatozoon will also contribute a centriole which will help make up the zygotic centrosome required for the first division. However, in some species, such as in the mouse, the entire centrosome is acquired maternally.[19] Currently under investigation is the possibility of other cytoplasmic contributions made to the embryo by the spermatozoon. During fertilization, the sperm provides three essential parts to the oocyte: (1) a signalling or activating factor, which causes the metabolically dormant oocyte to activate; (2) the haploid paternal genome; (3) the centrosome, which is responsible for maintaining the microtubule system. See anatomy of sperm
Oocyte
576
Abnormalities
• nondisjunction -- a failure of proper homolog separation in meiosis I, or sister chromatid separation in meiosis II can lead to aneuploidy, in which the oocyte has the wrong number of chromosomes, for example 22,X or 24,X. This is the cause of conditions like Down syndrome and Edwards syndrome. It is more likely with advanced maternal age. • Some oocytes have multiple nuclei, although it is thought they never mature.
References
[1] [2] [4] [5] answers.com (http:/ / www. answers. com/ topic/ oogenesis?cat=health) Biology-online (http:/ / www. biology-online. org/ dictionary/ Germinal_vesicle) Mtango N.R., Potireddy S., Latham K.E. (2008). Oocyte quality and maternal control of development. Int. Rev. Cell Mol. Biol. 268, 223-290. Zhang J., King M.L. (1996). Xenopus VegT RNA is localized to the vegetal cortex during oogenesis and encodes a novel T-box transcription factor involved in mesodermal patterning. Development. 12, 4119–29. [6] Heasman J., Wessely O., Langland R., Craig E.J., Kessler D.S. (2001). Vegetal localization of maternal mRNAs is disrupted by VegT depletion. Dev Biol. 240, 377–386. [7] Zhao H., Cao Y., Grunz H. (2003). Xenopus X-box binding protein 1, a leucine zipper transcription factor, is involved in the BMP signaling pathway. Dev Biol. 257, 278–291. [8] Sundaram N., Tao Q., Wylie C., Heasman J. (2003). The role of maternal CREB in early embryogenesis of Xenopus laevis. Dev Biol. 261, 337–352. [9] Kofron M., Puck H., Standley H., Wylie C., Old R., Whitman M., et al. (2004). New roles for FoxH1 in patterning the early embryo. Development. 131, 5065–5078. [10] Takebayashi-Suzuki K., Funami J., Tokumori D., Saito A., Watabe T., Miyazono K., et al. (2003). Interplay between the tumor suppressor p53 and TGF beta signaling shapes embryonic body axes in Xenopus. Development. 130, 3929–3939. [11] Heasman, J. (2006). Maternal determinants of embryonic cell fate. Semin. Cell Dev. Biol. 17, 93-98. [12] Song J., Slack J.M. (1994). Spatial and temporal expression of basic fibroblast growth factor (FGF-2) mRNA and protein in early Xenopus development. Mech Dev. 48, 141–151. [13] Dupont S., Zacchigna L., Cordenonsi M., Soligo S., Adorno M., Rugge M., et al. (2005). Germ-layer specification and control of cell growth by Ectodermin, a Smad4 ubiquitin ligase. Cell. 121, 87–99. [14] Birsoy B., Berg L., Williams P.H., Smith J.C., Wylie C.C., Christian J.L., et al. (2005). XPACE4 is a localized pro-protein convertase required for mesoderm induction and the cleavage of specific TGFbeta proteins in Xenopus development. Development. 132, 591–602. [15] Bell E., Munoz-Sanjuan I., Altmann C.R., Vonica A., Brivanlou A.H. (2003). Cell fate specification and competence by Coco, a maternal BMP, TGFbeta and Wnt inhibitor. Development. 130, 1381–1389. [16] Chan A. P., Kloc M., Larabell C. A., LeGros M., Etkin L.D. (2007). The maternally localized RNA fatvg is required for cortical rotation and germ cell formation. Mech Dev. 124, 350-363. [17] Ogushi S., et al. (2008). The maternal nucleolus is essential for early embryonic development in mammals. Science. 319, 613-616 [18] Vitale A.M., Yurttas P., Fitzhenry R.J., Cohen-Gould, L., Wu W., Gossen J.A., Coonrod S.A. (2009). Role for PADI6 and the CPLs in ribosomal storage in oocytes and translation in the early embryo. Development. 135, 2627-2636. [19] Sutovsky P., Schatten G. (2000). Paternal contributions to the mammalian zygote: fertilization after sperm-egg fusion. Int. Rev. Cytol. 195, 1-65.
Resources
William K. Purves, Gordon H. Orians, David Sadava, H. Craig Heller, Craig Heller (2003). Life: The Science of Biology(7th ed.), pp. 823–824
External links
• Slide (http://it.stlawu.edu/~mtem/devbiol/atlas/ANTRAL1.JPG)
Preceded by none Stages of human development Sperm + Oocyte Succeeded by Zygote
Spermatid
577
Spermatid
Spermatid
Germinal epithelium of the testicle. 1: basal lamina 2: spermatogonia 3: spermatocyte 1st order 4: spermatocyte 2nd order 5: spermatid 6: mature spermatid 7: Sertoli cell 8: tight junction (blood testis barrier)
Transverse section of a tubule of the testis of a rat. × 250. Gray's MeSH subject #258 1243 Spermatids
[1] [1]
The spermatid is the haploid male gametid that results from division of secondary spermatocytes. As a result of meiosis, each spermatid contains only half of the genetic material present in the original primary spermatocyte. Spermatids are connected by cytoplasmic material and have superfluous cytoplasmic material around their nuclei. When formed, early round spermatids must undergo further maturational events to develop into spermatozoa, a process termed spermiogenesis (also termed spermeteliosis). The spermatids begin to grow a living thread, develop a thickened mid-piece where the mitochondria become localised, and form an acrosome. Spermatid DNA also undergoes packaging, becoming highly condensed. The DNA is packaged firstly with specific nuclear basic proteins, which are subsequently replaced with protamines during spermatid elongation. The resultant tightly packed chromatin is transcriptionally inactive.
Spermatid
578
Additional images
Scheme showing analogies in the process of maturation of the ovum and the development of the Genyo spermatids (young spermatozoa).
External links
• BU Histology Learning System: 17804loa [2] - "Male Reproductive System: testis, early spermatids" • BU Histology Learning System: 17805loa [3] - "Male Reproductive System: testis, late spermatids" • Histology at okstate.edu [4]
Sperm
579
Sperm
The term sperm is derived from the Greek word (σπέρμα) sperma (meaning "seed") and refers to the male reproductive cells. In the types of sexual reproduction known as anisogamy and oogamy, there is a marked difference in the size of the gametes with the smaller one being termed the "male" or sperm cell. A uniflagellar sperm cell that is motile is referred to as a spermatozoon, whereas a non-motile sperm cell is referred to as a spermatium. Sperm cells cannot divide and have a limited life span, but after fusion with egg cells during fertilization, a new organism begins developing, starting as a totipotent zygote.[citation needed] The human sperm cell is haploid, so that its 23 chromosomes can join the Diagram of a human sperm cell 23 chromosomes of the female egg to form a diploid cell. In mammals, sperm develops in the testicles and is released from the penis. It is also possible to extract sperm throgh TESE.
Sperm in animals
Anatomy
The mammalian sperm cell consists of a head, a midpiece and a tail. The head contains the nucleus with densely coiled chromatin fibres, surrounded anteriorly by an acrosome, which contains enzymes used for penetrating the female egg. The midpiece has a central filamentous core with many mitochondria spiralled around it, used for ATP production for the journey through the female cervix, uterus and uterine tubes. The tail or "flagellum" executes the lashing movements that propel the spermatocyte.[citation needed] During fertilization, the sperm provides three essential parts to the Sperm and egg fusing oocyte: (1) a signalling or activating factor, which causes the metabolically dormant oocyte to activate; (2) the haploid paternal genome; (3) the centrosome, which is responsible for maintaining the microtubule system.[1]
Sperm
580
Origin
The spermatozoa of animals are produced through spermatogenesis inside the male gonads (testicles) via meiotic division. The initial spermatozoon process takes around 70 days to complete. The spermatid stage is where the sperm develops the familiar tail. The next stage where it becomes fully mature takes around 60 days when its called a spermatozoan.[2] Sperm cells are carried out of the male body in a fluid known as semen. Human sperm cells can survive within the female reproductive tract for more than 5 days post coitus.[3] Semen is produced in the seminal vesicles, prostate gland and urethral glands.
Sperm quality
Sperm quantity and quality are the main parameters in semen quality, which is a measure of the ability of semen to accomplish fertilization. Thus, in humans, it is a measure of fertility in a man. The genetic quality of sperm, as well as its volume and motility, all typically decrease with age.[] (See paternal age effect.)
Market for human sperm
On the global market, Denmark has a well-developed system of human sperm export. This success mainly comes from the Human sperm stained for semen quality testing. reputation of Danish sperm donors for being of high quality[4] and, in contrast with the law in the other Nordic countries, gives donors the choice of being either anonymous or non-anonymous to the receiving couple.[4] Furthermore, Nordic sperm donors tend to be tall and highly educated[5] and have altruistic motives for their donations,[5] partly due to the relatively low monetary compensation in Nordic countries. More than 50 countries worldwide are importers of Danish sperm, including Paraguay, Canada, Kenya, and Hong Kong.[4] However, the Food and Drug Administration (FDA) of the US has banned import of any sperm, motivated by a risk of mad cow disease, although such a risk is insignificant, since artificial insemination is very different from the route of transmission of mad cow disease.[6] The prevalence of mad cow disease is one in a million, probably less for donors. If prevalence was the case, the infectious proteins would then have to cross the blood-testis barrier to make transmission possible.[6]
History
Sperm were first observed in 1677 by Antonie van Leeuwenhoek[7] using a microscope, he described them as being animalcules (little animals), probably due to his belief in preformationism, which thought that each sperm contained a fully formed but small human.[citation needed]
Forensic analysis
Ejaculated fluids are detected by ultraviolet light, irrespective of the structure or colour of the surface.[8] Sperm heads, e.g. from vaginal swabs, are still detected by microscopy using the "Christmas Tree Stain" method, i.e., Kernechtrot-Picroindigocarmine (KPIC) staining.[9][10]
Sperm
581
Sperm in plants
Sperm cells in algal and many plant gametophytes are produced in male gametangia (antheridia) via mitotic division. In flowering plants, sperm nuclei are produced inside pollen.[citation needed]
Motile sperm cells
Motile sperm cells typically move via flagella and require a water medium in order to swim toward the egg for fertilization. In animals most of the energy for sperm motility is derived from the metabolism of fructose carried in the seminal fluid. This takes place in the mitochondria located in the sperm's midpiece (at the base of the sperm head). These cells cannot swim backwards due to the nature of their propulsion. The uniflagellated sperm cells (with one flagellum) of animals are referred to as spermatozoa, and are known to vary in size.[citation needed] Motile sperm are also produced by many protists and the gametophytes of bryophytes, ferns and some gymnosperms such as cycads and ginkgo. The sperm cells are the only flagellated cells in the life cycle of these plants. In many ferns and lycophytes, they are multi-flagellated (carrying more than one flagellum).[] In nematodes, the sperm cells are amoeboid and crawl, rather than swim, towards the egg cell.[]
Non-motile sperm cells
Non-motile sperm cells called spermatia lack flagella and therefore cannot swim. Spermatia are produced in a spermatangium.[]
[] Because spermatia cannot swim, they depend on their environment to Motile sperm cells of algae and seedless plants. carry them to the egg cell. Some red algae, such as Polysiphonia, produce non-motile spermatia that are spread by water currents after their release.[] The spermatia of rust fungi are covered with a sticky substance. They are produced in flask-shaped structures containing nectar, which attract flies that transfer the spermatia to nearby hyphae for fertilization in a mechanism similar to insect pollination in flowering plants.[]
Fungal spermatia (also called pycniospores, especially in the Uredinales) may be confused with conidia. Conidia are spores that germinate independently of fertilization, whereas spermatia are gametes that are required for fertilization. In some fungi, such as Neurospora crassa, spermatia are identical to microconidia as they can perform both functions of fertilization as well as giving rise to new organisms without fertilization.[]
Sperm nuclei
In many land plants, including most gymnosperms and all angiosperms, the male gametophytes (pollen grains) are the primary mode of dispersal, for example via wind or insect pollination, eliminating the need for water to bridge the gap between male and female. Each pollen grain contains a spermatogenous (generative) cell. Once the pollen lands on the stigma of a receptive flower, it germinates and starts growing a pollen tube through the carpel. Before the tube reaches the ovule, the nucleus of the generative cell in the pollen grain divides and gives rise to two sperm nuclei which are then discharged through the tube into the ovule for fertilization.[]
Sperm In some protists, fertilization also involves sperm nuclei, rather than cells, migrating toward the egg cell through a fertilization tube. Oomycetes form sperm nuclei in a syncytical antheridium surrounding the egg cells. The sperm nuclei reach the eggs through fertilization tubes, similar to the pollen tube mechanism in plants.[]
582
References
[2] Semen and sperm quality (http:/ / www. netdoctor. co. uk/ menshealth/ facts/ semenandsperm. htm) [3] Gould JE, Overstreet JW and Hanson FW (1984) Assessment of human sperm function after recovery from the female reproductive tract. Biol Reprod 31,888–894. [4] Assisted Reproduction in the Nordic Countries (http:/ / www. ncbio. org/ NcBioBurrell. pdf) ncbio.org [5] FDA Rules Block Import of Prized Danish Sperm (http:/ / www. newser. com/ story/ 34788/ fda-rules-block-import-of-prized-danish-sperm. html) Posted Aug 13, 08 7:37 AM CDT in World, Science & Health [6] The God of Sperm (http:/ / www. laweekly. com/ news/ news/ the-god-of-sperm/ 17290/ ) By Steven Kotler
External links
• The Great Sperm Race (http://www.channel4.com/microsites/G/TGSR/PDF/Great-Sperm-Race.pdf) pdf • Human Sperm Under a Microscope (http://www.youtube.com/watch?v=vvnEsOaKxuw&NR=1)
Preceded by None Stages of human development Sperm cell + Oocyte Succeeded by Zygote
Spermatogonium
583
Spermatogonium
Spermatogonium
Germinal epithelium of the testicle. 1 basal lamina, 2 spermatogonia, 3 spermatocyte 1st order, 4 spermatocyte 2nd order, 5 spermatid, 6 mature spermatid, 7 Sertoli cell, 8 tight junction (blood testis barrier)
Histological section through testicular parenchyma of a boar. 1 Lumen of Tubulus seminiferus contortus, 2 spermatids, 3 spermatocytes, 4 spermatogonia, 5 Sertoli cell, 6 Myofibroblasts, 7 Leydig cells, 8 capillaries Gray's MeSH subject #258 1243 Spermatogonia
[1] [1]
A spermatogonium (plural: spermatogonia) an undifferentiated male germ cell, originating in a seminiferous tubule and dividing into two primary spermatocytes (a kind of germ cell) in the production of spermatozoa. There are three subtypes: • Type A(d) cells, with dark nuclei. These cells replicate to ensure a constant supply of spermatogonia to fuel spermatogenesis. • Type A(p) cells, with pale nuclei. These cells divide by mitosis to produce Type B cells. • Type B cells, which divide to give rise to primary spermatocytes. Each primary spermatocyte duplicates its DNA and subsequently undergoes meiosis I to produce two haploid secondary spermatocytes. Each of the two secondary spermatocytes further undergo meiosis II to produce two spermatids (haploid). (1 primary spermatocyte => 4 spermatids) The spermatids then undergo spermiogenesis to produce spermatozoa.
Spermatogonium
584
Additional images
Transverse section of a tubule of the testis of a rat. X 250.
Schematic diagram of Spermatocytogenesis
References
Sertoli cell
585
Sertoli cell
Sertoli cell
Germinal epithelium of the testicle. 1: basal lamina 2: spermatogonia 3: spermatocyte 1st order 4: spermatocyte 2nd order 5: spermatid 6: mature spermatid 7: Sertoli cell 8: tight junction (blood testis barrier)
Histological section through testicular parenchyma of a boar. 1 Lumen of Tubulus seminiferus contortus 2 spermatids 3 spermatocytes 4 spermatogonia 5 Sertoli cell 6 Myofibroblasts 7 Leydig cells 8 capillaries Gray's MeSH subject #258 1243 Sertoli+Cells
[1] [1]
A Sertoli cell (a kind of sustentacular cell) is a 'nurse' cell of the testes that is part of a seminiferous tubule. It is activated by follicle-stimulating hormone and has FSH-receptor on its membranes. It is specifically located in the convoluted seminiferous tubules (since this is the only place in the testes where the spermatozoa are produced).
Sertoli cell
586
Functions
Because its main function is to nourish the developing sperm cells through the stages of spermatogenesis, the Sertoli cell has also been called the "mother" or "nurse" cell. Sertoli cells also act as phagocytes, consuming the residual cytoplasm during spermatogenesis. Translocation of germ cells from the base to the lumen of the seminiferous tubules occurs by conformational changes in the lateral margins of the Sertoli cells.
Secretory
Sertoli cells secrete the following substances: • anti-Müllerian hormone (AMH) - secreted during the early stages of fetal life. • inhibin and activins - secreted after puberty, and work together to regulate FSH secretion • androgen binding protein (also called testosterone binding globulin) - increases testosterone concentration in the seminiferous tubules to stimulate spermatogenesis • estradiol - aromatase from Sertoli cells convert testosterone to 17 beta estradiol to direct spermatogenesis • glial cell line-derived neurotrophic factor (GDNF) - has been demonstrated to function in promoting undifferentiating spermatogonia, which ensures stem cell self-renewal during the perinatal period. • the Ets related molecule (ERM transcription factor) - needed for maintenance of the spermatogonial stem cell in the adult testis. • transferrin - a blood plasma protein for iron ion delivery [1]
Structural
The tight junctions of Sertoli cells form the blood-testis barrier, a structure that partitions the interstitial blood compartment of the testis from the adluminal compartment of the seminiferous tubules. Because of the apical progression of the spermatogonia, the tight junctions must be dynamically reformed and broken to allow the immunoidentical spermatogonia to cross through the blood-testis barrier so they can become immunologically unique. Sertoli cells control the entry and exit of nutrients, hormones and other chemicals into the tubules of the testis as well as make the adluminal compartment an immune-privileged site. The cell is also responsible for establishing and maintaining the spermatogonial stem cell niche, which ensures the renewal of stem cells and the differentiation of spermatogonia into mature germ cells that progress stepwise through the long process of spermatogenesis, ending in the release of spermatozoa. Sertoli cells bind to spermatogonial cells via N-cadherins and galctosyltransferase (via carbohydrate residues).
Other functions
During the maturation phase of spermiogenesis, the Sertoli cells consume the unneeded portions of the spermatozoa.
Production of Sertoli cells
Sertoli cells are required for male sexual development. During male development, the gene SRY activates SOX9, which then activates and forms a feedforward loop with FGF9. Sertoli cell proliferation and differentiation is mainly activated by FGF9.[2] The absence of FGF9 tends to cause a female to develop [] Once fully differentiated, the Sertoli cell is unable to proliferate. Therefore, once spermatogenesis has begun, no more Sertoli cells are created. Recently however, some scientists have found a way to grow these cells outside of the body. This gives rise to the possibility of repairing some defects that cause male infertility. It has been suggested that they may derive from mesonephros.[]
Sertoli cell
587
Nomenclature
Sertoli cells are called so because of their eponym Enrico Sertoli, an Italian physiologist who discovered them while studying medicine in the University of Pavia, Italy.[3] He published a description of this cell in 1865. The cell was discovered by Sertoli with a Belthle microscope purchased in 1862, which he used while studying medicine. In the 1865 publication, his first description used the terms "tree-like cell" or "stringy cell" and most importantly he referred to these "mother cells." It was other scientists who used Enrico's family name, Sertoli, to label these cell in publications, starting in 1888. As of 2006, two textbooks that are devoted specifically to the Sertoli cell have been published.
Histology
On slides, using standard staining, it can be easy to confuse the Sertoli cells with the other cells of the germinal epithelium. The most distinctive feature of the Sertoli cells is the dark nucleolus.[4]
Pathology
Sertoli-Leydig cell tumour are part of the sex cord-stromal tumour group of ovarian neoplasms.
Additional images
Transverse section of a tubule of the testis of a rat. X 250.
Sertoli cell
588
References
[4] OSU Center for Veterinary Health Sciences - OSU-CVHS Home (http:/ / www. cvm. okstate. edu/ instruction/ mm_curr/ histology/ MR/ HiMRP4. htm)
External links
• BU Histology Learning System: 17805loa (http://www.bu.edu/histology/p/17805loa.htm) • BU Histology Learning System: 17806loa (http://www.bu.edu/histology/p/17806loa.htm)
Kidney
589
Kidney
Kidney
Human kidneys viewed from behind with spine removed Latin System Artery Vein Nerve MeSH Ren (Greek: nephros) Urinary system and endocrine system Renal artery Renal vein Renal plexus Kidney
[1]
Dorlands/Elsevier Kidney [2]
The kidneys are organs that serve several essential regulatory roles in most animals, including vertebrates and some invertebrates. They are essential in the urinary system and also serve homeostatic functions such as the regulation of electrolytes, maintenance of acid–base balance, and regulation of blood pressure (via maintaining salt and water balance). They serve the body as a natural filter of the blood, and remove wastes which are diverted to the urinary bladder. In producing urine, the kidneys excrete wastes such as urea and ammonium, and they are also responsible for the reabsorption of water, glucose, and amino acids. The kidneys also produce hormones including calcitriol, erythropoietin, and the enzyme renin. Located at the rear of the abdominal cavity in the retroperitoneum, the kidneys receive blood from the paired renal arteries, and drain into the paired renal veins. Each kidney excretes urine into a ureter, itself a paired structure that empties into the urinary bladder. Renal physiology is the study of kidney function, while nephrology is the medical specialty concerned with kidney diseases. Diseases of the kidney are diverse, but individuals with kidney disease frequently display characteristic clinical features. Common clinical conditions involving the kidney include the nephritic and nephrotic syndromes, renal cysts, acute kidney injury, chronic kidney disease, urinary tract infection, nephrolithiasis, and urinary tract obstruction.[] Various cancers of the kidney exist; the most common adult renal cancer is renal cell carcinoma. Cancers, cysts, and some other renal conditions can be managed with removal of the kidney, or nephrectomy. When renal function, measured by glomerular filtration rate, is persistently poor, dialysis and kidney transplantation may be treatment options. Although they are not severely harmful, kidney stones can be painful and a nuisance. The removal of kidney stones involves ultrasound treatment to break up the stones into smaller pieces, which are then passed through the urinary tract. One common symptom of kidney stones is a sharp pain in the medial/lateral segments of the lower back.
Kidney
590
Anatomy
Location
In humans the kidneys are located in the abdominal cavity, more specifically in the paravertebral gutter and lie in a retroperitoneal position at a slightly oblique angle. There are two, one on each side of the spine.[1] The asymmetry within the abdominal cavity caused by the liver typically results in the right kidney being slightly lower than the left, and left kidney being located slightly more medial than the right.[2][3] The left kidney is approximately at the vertebral level T12 to L3,[4] and the right slightly lower. The right kidney sits just below the diaphragm and posterior to the liver, the left below the diaphragm and posterior to the spleen. Resting on top of each kidney is an adrenal gland. The upper (cranial) parts of the kidneys are partially protected by the eleventh and twelfth ribs, and each whole kidney and adrenal gland are surrounded by two layers of fat (the perirenal and pararenal fat) and the renal fascia. Each adult kidney weighs between 125 and 170 grams in males and between 115 and 155 grams in females.[] The left kidney is typically slightly larger than the right kidney.[]
Surface projections of the organs of the trunk, showing kidneys at the level of T12 to L3.
A CT scan in which the kidneys are shown
Kidney
591
Structure
The kidney has a bean-shaped structure; each kidney has a convex and concave surface. The concave surface, the renal hilum, is the point at which the renal artery enters the organ, and the renal vein and ureter leave. The kidney is surrounded by tough fibrous tissue, the renal capsule, which is itself surrounded by perinephric fat, renal fascia (of Gerota) and paranephric fat. The anterior (front) border of these tissues is the peritoneum, while the posterior (rear) border is the transversalis fascia. The superior border of the right kidney is adjacent to the liver; and the spleen, for the left kidney. Therefore, both move down on inhalation. The kidney is approximately 11–14 cm in length, 6 cm wide and 4 cm thick. The substance, or parenchyma, of the kidney is divided into two major structures: superficial is the renal cortex and deep is the renal medulla. Grossly, these structures take the shape of 8 to 18 cone-shaped renal lobes, each containing renal cortex surrounding a portion of [] medulla called a renal pyramid (of Malpighi). Between the renal pyramids are projections of cortex called renal columns (of Bertin). Nephrons, the urine-producing functional structures of the kidney, span the cortex and medulla. The initial filtering portion of a nephron is the renal corpuscle, located in the cortex, which is followed by a renal tubule that passes from the cortex deep into the medullary pyramids. Part of the renal cortex, a medullary ray is a collection of renal tubules that drain into a single collecting duct. The tip, or papilla, of each pyramid empties urine into a minor calyx; minor calyces empty into major calyces, and major calyces empty into the renal pelvis, which becomes the ureter. At the hilum, the ureter and renal vein exit the kidney while the renal artery enters. Surrounding these structures is hilar fat and lymphatic tissue with lymph nodes. The hilar fat is contiguous with a fat-filled cavity called the renal sinus. The renal sinus collectively contains the renal pelvis and calyces and separates these structures from the renal medullary tissue.[5]
1. Renal pyramid • 2. Interlobular artery • 3. Renal artery • 4. Renal vein 5. Renal hilum • 6. Renal pelvis • 7. Ureter • 8. Minor calyx • 9. Renal capsule • 10. Inferior renal capsule • 11. Superior renal capsule • 12. Interlobular vein • 13. Nephron • 14. Minor calyx • 15. Major calyx • 16. Renal papilla 17. Renal column
Blood supply
The kidneys receive blood from the renal arteries, left and right, which branch directly from the abdominal aorta. Despite their relatively small size, the kidneys receive approximately 20% of the cardiac output.[] Each renal artery branches into segmental arteries, dividing further into interlobar arteries which penetrate the renal capsule and extend through the renal columns between the renal pyramids. The interlobar arteries then supply blood to the arcuate arteries that run through the boundary of the cortex and the medulla. Each arcuate artery supplies several interlobular arteries that feed into the afferent arterioles that supply the glomeruli.
3D-rendered computed tomography, showing renal arteries and veins.
Kidney The interstitum (or interstitium) is the functional space in the kidney beneath the individual filters (glomeruli) which are rich in blood vessels. The interstitum absorbs fluid recovered from urine. Various conditions can lead to scarring and congestion of this area, which can cause kidney dysfunction and failure. After filtration occurs the blood moves through a small network of venules that converge into interlobular veins. As with the arteriole distribution the veins follow the same pattern, the interlobular provide blood to the arcuate veins then back to the interlobar veins which come to form the renal vein exiting the kidney for transfusion for blood.
592
Histology
Renal histology studies the structure of the kidney as viewed under a microscope. Various distinct cell types occur in the kidney, including: • • • • • • • • • Kidney glomerulus parietal cell Kidney glomerulus podocyte Kidney proximal tubule brush border cell Loop of Henle thin segment cell Thick ascending limb cell Kidney distal tubule cell Kidney collecting duct cell Interstitial kidney cells Renal arteries and their branches
Microscopic photograph of the renal medulla
The renal artery enters into the kidney at the level of first lumbar vertebra just below the superior mesenteric artery. As it enters the kidney it divides into branches: first the segmental artery, which divides into 2 or 3 lobar arteries, then further divides into interlobar arteries, which further divide into the arcuate artery which leads into the interlobular artery, which form afferent arterioles. The afferent arterioles form the glomerulus (network of capillaries closed in Bowman's capsule). From here, efferent arterioles leaves the glomerulus and divide into peritubular capillaries, which drain into the Microscopic photograph of the renal cortex interlobular veins and then into arcuate vein and then into interlobar vein, which runs into lobar vein, which opens into the segmental vein and which drains into the renal vein, and then from it blood moves into the inferior vena cava.
Innervation
The kidney and nervous system communicate via the renal plexus, whose fibers course along the renal arteries to reach each kidney.[] Input from the sympathetic nervous system triggers vasoconstriction in the kidney, thereby reducing renal blood flow.[] The kidney also receives input from the parasympathetic nervous system, by way of the renal branches of the vagus nerve (cranial nerve X); the function of this is yet unclear.[][6] Sensory input from the kidney travels to the T10-11 levels of the spinal cord and is sensed in the corresponding dermatome.[] Thus, pain in the flank region may be referred from corresponding kidney.[]
Kidney
593
Functions
The kidney participates in whole-body homeostasis, regulating acid-base balance, electrolyte concentrations, extracellular fluid volume, and regulation of blood pressure. The kidney accomplishes these homeostatic functions both independently and in concert with other organs, particularly those of the endocrine system. Various endocrine hormones coordinate these endocrine functions; these include renin, angiotensin II, aldosterone, antidiuretic hormone, and atrial natriuretic peptide, among others. Many of the kidney's functions are accomplished by relatively simple mechanisms of filtration, reabsorption, and secretion, which take place in the nephron. Filtration, which takes place at the renal corpuscle, is the process by which cells and large proteins are filtered from the blood to make an ultrafiltrate that eventually becomes urine. The kidney generates 180 liters of filtrate a day, while reabsorbing a large percentage, allowing for the generation of only approximately 2 liters of urine. Reabsorption is the transport of molecules from this ultrafiltrate and into the blood. Secretion is the reverse process, in which molecules are transported in the opposite direction, from the blood into the urine.
Excretion of wastes
The kidneys excrete a variety of waste products produced by metabolism. These include the nitrogenous wastes called "urea", from protein catabolism, as well as uric acid, from nucleic acid metabolism. Formation of urine is also the function of the kidney. The concentration of nitrogenous wastes, in the urine of mammals and some birds, is dependent on an elaborate countercurrent multiplication system. This requires several independent nephron characteristics to operate: a tight hair pin configuration of the tubules, water and ion permeability in the descending limb of the loop, water impermeability in the ascending loop and active ion transport out of most of the ascending loop. In addition, countercurrent exchange by the vessels carrying the blood supply to the nephron is essential for enabling this function.
Acid-base homeostasis
Two organ systems, the kidneys and lungs, maintain acid-base homeostasis, which is the maintenance of pH around a relatively stable value. The lungs contribute to acid-base homeostasis by regulating carbon dioxide (CO2) concentration. The kidneys have two very important roles in maintaining the acid-base balance: to reabsorb bicarbonate from urine, and to excrete hydrogen ions into urine
Osmolality regulation
Any significant rise in plasma osmolality is detected by the hypothalamus, which communicates directly with the posterior pituitary gland. An increase in osmolality causes the gland to secrete antidiuretic hormone (ADH), resulting in water reabsorption by the kidney and an increase in urine concentration. The two factors work together to return the plasma osmolality to its normal levels. ADH binds to principal cells in the collecting duct that translocate aquaporins to the membrane, allowing water to leave the normally impermeable membrane and be reabsorbed into the body by the vasa recta, thus increasing the plasma volume of the body. There are two systems that create a hyperosmotic medulla and thus increase the body plasma volume: Urea recycling and the 'single effect.' Urea is usually excreted as a waste product from the kidneys. However, when plasma blood volume is low and ADH is released the aquaporins that are opened are also permeable to urea. This allows urea to leave the collecting duct into the medulla creating a hyperosmotic solution that 'attracts' water. Urea can then re-enter the nephron and be excreted or recycled again depending on whether ADH is still present or not.
Kidney The 'Single effect' describes the fact that the ascending thick limb of the loop of Henle is not permeable to water but is permeable to NaCl. This allows for a countercurrent exchange system whereby the medulla becomes increasingly concentrated, but at the same time setting up an osmotic gradient for water to follow should the aquaporins of the collecting duct be opened by ADH.
594
Blood pressure regulation
Although the kidney cannot directly sense blood, long-term regulation of blood pressure predominantly depends upon the kidney. This primarily occurs through maintenance of the extracellular fluid compartment, the size of which depends on the plasma sodium concentration. Renin is the first in a series of important chemical messengers that make up the renin-angiotensin system. Changes in renin ultimately alter the output of this system, principally the hormones angiotensin II and aldosterone. Each hormone acts via multiple mechanisms, but both increase the kidney's absorption of sodium chloride, thereby expanding the extracellular fluid compartment and raising blood pressure. When renin levels are elevated, the concentrations of angiotensin II and aldosterone increase, leading to increased sodium chloride reabsorption, expansion of the extracellular fluid compartment, and an increase in blood pressure. Conversely, when renin levels are low, angiotensin II and aldosterone levels decrease, contracting the extracellular fluid compartment, and decreasing blood pressure.
Hormone secretion
The kidneys secrete a variety of hormones, including erythropoietin, and the enzyme renin. Erythropoietin is released in response to hypoxia (low levels of oxygen at tissue level) in the renal circulation. It stimulates erythropoiesis (production of red blood cells) in the bone marrow. Calcitriol, the activated form of vitamin D, promotes intestinal absorption of calcium and the renal reabsorption of phosphate. Part of the renin-angiotensin-aldosterone system, renin is an enzyme involved in the regulation of aldosterone levels.
Development
The mammalian kidney develops from intermediate mesoderm. Kidney development, also called nephrogenesis, proceeds through a series of three successive phases, each marked by the development of a more advanced pair of kidneys: the pronephros, mesonephros, and metanephros.[7]
Evolutionary adaptation
Kidneys of various animals show evidence of evolutionary adaptation and have long been studied in ecophysiology and comparative physiology. Kidney morphology, often indexed as the relative medullary thickness, is associated with habitat aridity among species of mammals.[]
Kidney
595
Related terms
Medical terms related to the kidneys commonly use terms such as renal and the prefix nephro-. The adjective renal, meaning related to the kidney, is from the Latin rēnēs, meaning kidneys; the prefix nephro- is from the Ancient Greek word for kidney, nephros (νεφρός).[8] For example, surgical removal of the kidney is a nephrectomy, while a reduction in kidney function is called renal dysfunction.
Diseases and disorders
Congenital
• Congenital hydronephrosis • Congenital obstruction of urinary tract • Duplex kidneys, or double kidneys, occur in approximately 1% of the population. This occurrence normally causes no complications, but can occasionally cause urine infections.[9][10] • Duplicated ureter occurs in approximately one in 100 live births • Horseshoe kidney occurs in approximately one in 400 live births • Polycystic kidney disease • Autosomal dominant polycystic kidney disease afflicts patients later in life. Approximately one in 1000 people will develop this condition • Autosomal recessive polycystic kidney disease is far less common, but more severe, than the dominant condition. It is apparent in utero or at birth. Renal agenesis. Failure of one kidney to form occurs in approximately one in 750 live births. Failure of both kidneys to form is invariably fatal. Renal dysplasia Unilateral small kidney Multicystic dysplastic kidney occurs in approximately one in every 2400 live births Ureteropelvic Junction Obstruction or UPJO; although most cases appear congenital, some appear to be an acquired condition[11]
• • • • •
Kidney
596
Acquired
• Diabetic nephropathy • Glomerulonephritis • Hydronephrosis is the enlargement of one or both of the kidneys caused by obstruction of the flow of urine. • Interstitial nephritis • Kidney stones (nephrolithiasis) are a relatively common and particularly painful disorder. • Kidney tumors • Wilms tumor • Renal cell carcinoma • Lupus nephritis • Minimal change disease • In nephrotic syndrome, the glomerulus has been damaged so that a large amount of protein in the blood enters the urine. Other frequent features of the nephrotic syndrome include swelling, low serum albumin, and high cholesterol. • Pyelonephritis is infection of the kidneys and is frequently caused by complication of a urinary tract infection. • Renal failure • Acute renal failure • Stage 5 Chronic Kidney Disease Kidney Failure Generally, humans can live normally with just one kidney, as one has more functioning renal tissue than is needed to survive. Only when the amount of functioning kidney tissue is greatly diminished does one develop chronic kidney disease. Renal replacement therapy, in the form of dialysis or kidney transplantation, is indicated when the glomerular filtration rate has fallen very low or if the renal dysfunction leads to severe symptoms.
Drawing of an enlarged kidney by John Hunter.
Diagnosis
Clinical Many renal diseases are diagnosed on the basis of classical clinical findings. A physician (usually a nephrologist) begins by taking a detailed clinical history and performs a physical examination. In addition to medical history and presenting symptoms, a physician will ask about medication history, family history recent infections, toxic/chemical exposures and other historical factors which may indicate an etiology for the patient's renal disease. Often, some diseases are suggested by clinical history and time course alone. For example, in a formerly healthy child with a recent upper respiratory tract infection and facial/lower limb swelling, findings of proteinuria on urinalysis, a diagnosis of minimal change disease is highly suggested. Similarly, a patient with a history of diabetes who presents with decreased urine output is most likely to be suffering from diabetic nephropathy. Often, such cases do not require extensive workup (such as with renal biopsy). A presumptive diagnosis can be made on the basis of history, physical exam and supportive laboratory studies.
Kidney Laboratory Laboratory studies are an important adjunct to clinical evaluation for assessment of renal function. An initial workup of a patient may include a complete blood count (CBC); serum electrolytes including sodium, potassium, chloride, bicarbonate, calcium, and phosphorus; blood urea, nitrogen and creatinine; blood glucose and glycocylated hemoglobin. Glomerular filtration rate (GFR) can be calculated.[12] Urine studies may include urine electrolytes, creatinine, protein, fractional excretion of sodium (FENA) and other studies to assist in evaluation of the etiology of a patient's renal disease. Urinalysis is used to evaluate urine for its pH, protein, glucose, specific gravity and the presence of blood/hemoglobin. Microscopic analysis can be helpful in the identification of casts, red blood cells, white blood cells and crystals.[12] Imaging studies Imaging studies are important in the evaluation of structural renal disease caused by urinary tract obstruction, renal stones, renal cyst, mass lesions, renal vascular disease, and vesicoureteral reflux.[12] Imaging techniques used most frequently include renal ultrasound and helical CT scan. Patients with suspected vesicoureteral reflux may undergo voiding cystourethrogram (VCUG). Renal biopsy The role of the renal biopsy is to diagnose renal disease in which the etiology is not clear based upon noninvasive means (clinical history, past medical history, medication history, physical exam, laboratory studies, imaging studies). A detailed description of renal biopsy interpretation is beyond the scope of this article. In general- a renal pathologist will perform a detailed morphological evaluation and integrate the morphologic findings with the clinical history and laboratory data, ultimately arriving at a pathological diagnosis. A renal pathologist is a physician who has undergone general training in anatomic pathology and additional specially training in the interpretation of renal biopsy specimens. Ideally, multiple core sections are obtained and evaluated for adequacy (presence of glomeruli) intraoperatively. A pathologist/pathology assistant divides the specimen(s) for submission for light microscopy, immunofluorescence microscopy and electron microscopy. The pathologist will examine the specimen using light microscopy with multiple staining techniques (hematoxylin and eosin/H&E, PAS, trichrome, silver stain) on multiple level sections. Multiple immunofluorescence stains are performed to evaluate for antibody, protein and complement deposition. Finally, ultra-structural examination is performed with electron microscopy and may reveal the presence of electron-dense deposits or other characteristic abnormalities which may suggest an etiology for the patient's renal disease.
597
Kidney
598
In other animals
In the majority of vertebrates, the mesonephros persists into the adult, albeit usually fused with the more advanced metanephros; only in amniotes is the mesonephros restricted to the embryo. The kidneys of fish and amphibians are typically narrow, elongated organs, occupying a significant portion of the trunk. The collecting ducts from each cluster of nephrons usually drain into an archinephric duct, which is homologous with the vas deferens of amniotes. However, the situation is not always so simple; in cartilaginous fish and some amphibians, there is also a shorter duct, similar to the amniote ureter, which drains A pig's kidney opened. the posterior (metanephric) parts of the kidney, and joins with the archinephric duct at the bladder or cloaca. Indeed, in many cartilaginous fish, the anterior portion of the kidney may degenerate or cease to function altogether in the adult.[] In the most primitive vertebrates, the hagfish and lampreys, the kidney is unusually simple: it consists of a row of nephrons, each emptying directly into the archinephric duct. Invertebrates may possess excretory organs that are sometimes referred to as "kidneys", but, even in Amphioxus, these are never homologous with the kidneys of vertebrates, and are more accurately referred to by other names, such as nephridia.[] The kidneys of reptiles consist of a number of lobules arranged in a broadly linear pattern. Each lobule contains a single branch of the ureter in its centre, into which the collecting ducts empty. Reptiles have relatively few nephrons compared with other amniotes of a similar size, possibly because of their lower metabolic rate.[] Birds have relatively large, elongated kidneys, each of which is divided into three or more distinct lobes. The lobes consists of several small, irregularly arranged, lobules, each centred on a branch of the ureter. Birds have small glomeruli, but about twice as many nephrons as similarly sized mammals.[] The human kidney is fairly typical of that of mammals. Distinctive features of the mammalian kidney, in comparison with that of other vertebrates, include the presence of the renal pelvis and renal pyramids, and of a clearly distinguishable cortex and medulla. The latter feature is due to the presence of elongated loops of Henle; these are much shorter in birds, and not truly present in other vertebrates (although the nephron often has a short intermediate segment between the convoluted tubules). It is only in mammals that the kidney takes on its classical "kidney" shape, although there are some exceptions, such as the multilobed reniculate kidneys of cetaceans.[]
History
The Latin term renes is related to the English word "reins", a synonym for the kidneys in Shakespearean English (e.g. Merry Wives of Windsor 3.5), which was also the time the King James Version was translated. Kidneys were once popularly regarded as the seat of the conscience and reflection,[13][14] and a number of verses in the Bible (e.g. Ps. 7:9, Rev. 2:23) state that God searches out and inspects the kidneys, or "reins", of humans. Similarly, the Talmud (Berakhoth 61.a) states that one of the two kidneys counsels what is good, and the other evil.
Kidney
599
Kidneys as food
The kidneys can be cooked and eaten (along with other offal). Kidneys are usually grilled or sautéed, but in more complex dishes they are stewed with a sauce that will improve their flavor. In many preparations, kidneys are combined with pieces of meat or liver, as in mixed grill or meurav Yerushalmi. Dishes include the British steak and kidney pie, the Swedish hökarpanna (pork and kidney stew), the French rognons de veau sauce moutarde (veal kidneys in mustard sauce) and the Spanish riñones al Jerez (kidneys stewed in sherry sauce) .[15]
Hökarpanna, Swedish pork and kidney stew
Additional Images
Right Kidney
Kidney
Right Kidney
Kidney Posterior View
Anterior relation of Left Kidney
Right kidney
Left kidney
Kidneys
Left kidney
Kidney Cross Section
Kidney
600
References
[3] (http:/ / www. bioportfolio. com/ indepth/ Kidney. html) [4] Bålens ytanatomy (Superficial anatomy of the trunk). Anca Dragomir, Mats Hjortberg and Godfried M. Romans. Section for human anatomy at the Department of medical biology, Uppsala university, Sweden. [5] Clapp, WL. Renal Anatomy. In: Zhou XJ, Laszik Z, Nadasdy T, D'Agati VD, Silva FG, eds. Silva's Diagnostic Renal Pathology. New York, NY: Cambridge University Press; 2009. [12] Post TW, Rose BD, auths and Curhan GC, Sheridan AM, eds. Diagnostic Approach to the Patient With Acute Kidney Injury (Acute Renal Failure) or Chronic Kidney Disease. UpToDate.com, Dec. 2012. http:/ / www. uptodate. com. ezproxy2. library. arizona. edu/ contents/ diagnostic-approach-to-the-patient-with-acute-kidney-injury-acute-renal-failure-or-chronic-kidney-disease?source=preview& anchor=H12& selectedTitle=1~150#H12 [13] The Patient as Person: Explorations in Medical Ethics p. 60 by Paul Ramsey, Margaret Farley, Albert Jonsen, William F. May (2002) [14] History of Nephrology 2 p. 235 by International Association for the History of Nephrology Congress, Garabed Eknoyan, Spyros G. Marketos, Natale G. De Santo - 1997; Reprint of American Journal of Nephrology; v. 14, no. 4-6, 1994. [15] Rognons dans les recettes (http:/ / cuisine. notrefamille. com/ recettes-cuisine/ rognons-recette. html)
External links
• The NephCure Foundation offers educational materials on the kidney diseases/conditions Nephrotic Syndrome and FSGS (http://www.nephcure.org) • The Kidney Foundation of Canada (http://www.kidney.ca) • electron microscopic images of the kidney (Dr. Jastrow's EM-Atlas) (http://www.uni-mainz.de/FB/Medizin/ Anatomie/workshop/EM/EMNiereE.html) • European Renal Genome project kidney function tutorial (http://www.euregene.org/euregene/pages/ kidney_tut_e.html) • Kidney Foundation of Canada kidney disease information (http://www.kidneyquebec.ca/ang/kidney_disease/ index.htm) • Renal Fellow Network: Structure & Function of Other Animals' Kidneys (http://renalfellow.blogspot.com/ 2009/06/structure-function-of-other-animals.html) • Kidney Stones (http://symptomsofakidneystone.com) • Kidney Diseases (http://www.kidney-stone.us) • Kidney Information (http://www.redurine.com/urinary_tract/kidney_facts.html) • Animated Presentatin on Kidney Function (http://www.davita.com/kidney_animation/) • CAT Scans of various kidney diseases and conditions (http://www.ctcases.net/ct-cases-database/4 Abdomen And Pelvis/6 Kidneys/) - CT Cases • Kidney Stones; Information and Treatments (http://www.mountsinai.org/patient-care/service-areas/ urological-conditions-and-surgery/areas-of-care/kidney-disease-program)
Article Sources and Contributors
601
Article Sources and Contributors
List of distinct cell types in the adult human body Source: http://en.wikipedia.org/w/index.php?oldid=549416469 Contributors: -Majestic-, ABF, Abc518, Abstraktn, Achowat, AdamRetchless, Aditya, Ahoerstemeier, Aldaron, Allens, Allmightyduck, AnteaterZot, Arcadian, Arthena, Atif.t2, Auntof6, Banus, Belovedfreak, Benesch, Blahblahblah97, Bluemoose, Blurpeace, Bobo192, CWenger, Capricorn42, Carl T, Cflm001, Chris the speller, Christopher Kraus, Chrysaor, Cmcnicoll, Cobi, Conti, CopperKettle, Da best editor, Dbenbenn, DennyColt, Dozenist, Drkarthi, Eikenhein, Epbr123, Excirial, Fieari, Forluvoft, Fraggle81, Franamax, Gongshow, Haymaker, Hello71, Hodja Nasreddin, I dream of horses, Isarra (HG), JZUK, Jackibuddy, Jackson Peebles, Jamoche, Jarradpowell, Jfdwolff, John Abbe, John254, Johntobey, Jomunro, Jordan Yang, Juliancolton, Ka Faraq Gatri, Kevin Rector, Kubigula, Liam Skoda, Lvl, Markjohndaley, Materialscientist, Mathonius, Megaman en m, Mercury, Mikael Häggström, Moe Epsilon, Mporch, My very best wishes, Nathan, Neo139, Nono64, NotWith, Nsaa, Ombudsman, Ozborn, PenguiN42, Pharaoh of the Wizards, Pinkadelica, Puchiko, Pyfan, QuackOfaThousandSuns, R'n'B, Rajah, Revolution1221, Robfbms, Rockpocket, San04, Sayeth, Shanes, Sionus, Smoove Z, Spectrumsaymyname, SpiderJon, Tameeria, The Anome, The Anonymouse, Titodutta, Tohd8BohaithuGh1, Trusilver, Wavelength, West.andrew.g, Wilson44691, Wimt, Wimvandorst, 342 anonymous edits Salivary gland Source: http://en.wikipedia.org/w/index.php?oldid=551178225 Contributors: 10014derek, Aitias, Alex Khimich, Alex.tan, Alfarq, Anaxial, Andrewrp, AnnaP, Arcadian, Ascidian, Avram, Axarus, AxelBoldt, BillC, Bluerasberry, Bomac, Bongwarrior, Breno, BrucePodger, Butko, CSJN, CanadianLinuxUser, Cburnett, Cetaugama, Cmcnicoll, CommonsDelinker, Cshemmerich, DRosenbach, Davidruben, Diberri, Doktor911, Dommyboy7, Don4of4, Draeco, Dravecky, Drmies, Epbr123, Eranb, Eras-mus, Favonian, Fergking, Fisty234, Franamax, Frankster200277, Ghoongta, Greelz, I dream of horses, InverseHypercube, J.delanoy, JVinocur, JaGa, JakobSteenberg, Jayron32, Jfdwolff, Jim1138, JimVC3, Jmarchn, JohnDoran, Juicyboy2k, Jwri7474, Katiedid27, Keilana, Khargas, Kissekatt, Kjkolb, Knutux, Kpjas, Lesion, Lesnail, Li-sung, LuisArmandoRasteletti, Luka Krstulović, Mac Davis, MartinDK, Membender, Metju, Mikael Häggström, Miniyazz, Naddy, Nephron, Nexus 215, Nick Number, Njardarlogar, Nlu, O.Koslowski, Ohnoitsjamie, Pdcook, Pip2andahalf, Pmlineditor, Psbsub, Rb1248, Rlevente, Ryan, Sannab, ScAvenger, Sd31415, Sebastiano venturi, Shell Kinney, Shikexue2, SimonP, Slysplace, Snafflekid, Soap, Some jerk on the Internet, Soulkeeper, Stickee, SuperHamster, Swamp Ig, Symplectic Map, Tachyon01, The Anome, The Thing That Should Not Be, TheEgyptian, Thesis4Eva, Tide rolls, Tjd1, Tommy2010, Tristanb, Vinne2, Vrenator, Wavelength, Welldad, Wereon, WikHead, Wikieditor06, William Avery, Wnme, WojPob, Zzedar, 267 anonymous edits Von Ebner's gland Source: http://en.wikipedia.org/w/index.php?oldid=541485832 Contributors: 04mamich, Arcticcoconut, Black Falcon, Cmcnicoll, Devinburn, Ego White Tray, Facts707, Falcon8765, Gene Nygaard, Gyopi, Isopropyl, Jpogi, Krm232, Materialscientist, Sayanmitra, Snafje, 12 anonymous edits Mammary gland Source: http://en.wikipedia.org/w/index.php?oldid=548828046 Contributors: Ackerman22, Adrian J. Hunter, Alex.tan, AlrightEdits, Andrewmc123, Anthonyhcole, Arcadian, Arthur Rubin, AxelBoldt, Batsnumbereleven, Beth 84, BrainyBabe, Brest39, Brian Crawford, Brow276, BullRangifer, CTho, CWii, CarTick, Carturo222, Caulfieldholden, Ccevo2010, Celllist, Cgingold, Chanlyn, Chaser, Chris G, Chrisn0113, Christian75, CiaPan, ClamDip, Clawed, Clngre, Cointyro, CommonsDelinker, ConfuciusOrnis, Craig Pemberton, Dan100, Daniel Case, Darth Panda, Diberri, Dina, Dynzmoar, ENeville, Ealdgyth, EdC, Emijrp, Eras-mus, Erud, Favonian, Flarn2006, Flewis, Fratrep, Gilliam, Ginsengbomb, Gogo Dodo, Graham87, Grakk, Gvw686, Hans.vmobile, Henrygb, HiEv, HiMyNameIsDick, I liek breasts, Illnab1024, Itai, JackAidley, Jackhynes, Jarble, Jfurr1981, Jlcarter2, Joelmills, Julian Mendez, Jwissick, Karada, Kartano, Keenan Pepper, Keilana, Kerowyn, Khajidha, Latka, LeyteWolfer, Lmbhull, Louis Waweru, Lucy346, Luigifan, MONGO, Materialscientist, Matt26, Mentifisto, Millw001, Mmxx, MrCheeseBasket, My Core Competency is Competency, Naturehead, NawlinWiki, Neelix, Nhsnoboarder17, Nishkid64, NotAnonymous0, Notonegoro, Oneiros, Orlandoturner, Osm agha, Paul Erik, Pecolee, Prof. Squirrel, QueenCake, RNLockwood, Raymondwinn, Rich Farmbrough, Richiez, Rickyrab, Rjwilmsi, Rockpocket, Roleplayer, Rory096, Rune X2, SDC, Salvio giuliano, SchreiberBike, Scottalter, Scottandrewhutchins, Search255, Septegram, SophiePon, Sp3000, Star Trek Man, Steverapaport, SummerWithMorons, Tabletop, Takagi, Techman224, Template namespace initialisation script, The Anome, The Thing That Should Not Be, The Wednesday Island, TimVickers, Timc, Tinman11, Torchiest, Toyalla, Trinanjon, Ulric1313, Ursasapien, Van helsing, WLU, WerewolfHunter65, Westvoja, Why Not A Duck, WinterSpw, Woohookitty, Zigger, 152 anonymous edits Lacrimal gland Source: http://en.wikipedia.org/w/index.php?oldid=548680179 Contributors: AED, Alex.tan, Anatomist90, Andyafire, Arcadian, Argarrett826, Arthena, Aviados, Babedacus, Bluemoose, Chris the speller, Difu Wu, DiverDave, Dj Capricorn, Dr Bilal Alshareef, Editorjohn, ElAmericano, Eyesurgeon, Finlay McWalter, Gail, Greenjeans8888, Hovea, Iloveeragon, ImperatorExercitus, Irisx, Isnow, Jaysmasher, Jfdwolff, Jmarchn, John of Reading, Juliancolton, Kbdank71, L Kensington, ML5, Mandarax, Mikael Häggström, Moagabeeshum, Netizen, Nnh, Nono64, Nuvitauy07, Old Moonraker, Osmodiar, Pacifica007, Persian Poet Gal, PhatRita, Rkvignesh, SF007, Snigbrook, Steveprutz, Teamonits, Themfromspace, Tubantia, Varano, Vikte, 64 anonymous edits Ceruminous gland Source: http://en.wikipedia.org/w/index.php?oldid=526530422 Contributors: Arcadian, AtmanDave, Bobsagat, Eleassar, Kerowyn, Lynntyler, My Core Competency is Competency, ResearchRave, Samyutan, Skela, Spiral5800, Xezbeth, 4 anonymous edits Eccrine sweat gland Source: http://en.wikipedia.org/w/index.php?oldid=541717046 Contributors: Arcadian, Baville, Chris Capoccia, Coolstoryhansel, Docfaust, Drphilharmonic, Edward, Kaxap, Leonard^Bloom, Mike2vil, MisterSheik, My Core Competency is Competency, Nelly4, Prof. Squirrel, ResearchRave, The Anome, Tiphaine800, Zazpot, Zz2, 30 anonymous edits Apocrine sweat gland Source: http://en.wikipedia.org/w/index.php?oldid=551814721 Contributors: AK456, Arcadian, Axeman89, Barticus88, BeardWand, Bejnar, Blueshifter, Closedmouth, Cpl Syx, Craig Pemberton, DaGizza, DannyBoy7783, Diannaa, Draeco, Drphilharmonic, Gould363, Hippietrail, Isopropyl, JakobSteenberg, Jarble, Jason Quinn, Jrmonirian, Lawrence Mayer, Marchije, Mathmo, MisterSheik, Monolemma, My Core Competency is Competency, Neverquick, Penguat, Prof. Squirrel, Queenmomcat, Recurring dreams, Rjwilmsi, Saeidbaki, Samyutan, SchreiberBike, Sgamer1770, Stevegray, Teimu.tm, TenPoundHammer, TheGrimReaper NS, Tiphaine800, Topbanana, Tuckerekcut, Zazpot, 55 anonymous edits Moll's gland Source: http://en.wikipedia.org/w/index.php?oldid=548166562 Contributors: Arcadian, Betacommand, Draeco, Fgegypt, Hovea, My Core Competency is Competency, Prof. Squirrel, Riffle, 3 anonymous edits Sebaceous gland Source: http://en.wikipedia.org/w/index.php?oldid=543059574 Contributors: 1st2Bomb, AED, Abdull, Aitias, Anc sierra, Andycjp, AnnaP, Arcadian, Auntof6, AxelBoldt, Bansp, Bender235, Bobo192, CIS, CerealBabyMilk, Ceyockey, Chris Capoccia, CommonsDelinker, Darklilac, Davewho2, DeadEyeArrow, Divide, Dougluce, Dprady, Dr. Doof, Dreamer.redeemer, Drphilharmonic, Ds13, Edgar181, Eeekster, Eug, Evets21, Fences and windows, Fsotrain09, Fuzzbox, Fuzzy901, Gareth Griffith-Jones, Geni, GorillaWarfare, Gpresearch, Hankwang, Helix84, Hightower 40, Intersofia, Iraqidude, Jchae88, Kajerm, Keala.richardson, Keetanii, Kjkolb, Lando242, Lichee66, Littenberg, Lord EDITS, Majorly, MarcoTolo, Mattygabe, Mctt, Mikael Häggström, Mikekearn, Moshe Constantine Hassan Al-Silverburg, My Core Competency is Competency, Neckoneckonecko, Neilbeach, Niceguyedc, Nono64, Nuno Tavares, Oatmeal batman, Obli, OlEnglish, Pablo X, Peter Ellis, Ph.eyes, Prof. Squirrel, Pwjb, R sirahata, RDBrown, Ratdesh, Rjwilmsi, Rlfb, Rogermw, Rune X2, Saleen1996, Seanmiz, Showvaughan29, Smulthaup, Snow Blizzard, Snowmanradio, SofiaSoGood, Sprostini, Sriharsh1234, Steven Walling, Stratuspower88, Suffusion of Yellow, TLazzo, Taco325i, Telekenesis, That Guy, From That Show!, Tjmayerinsf, UnicornTapestry, Valentij01, Velella, Vojtech.dostal, Vsion, WLU, Waitak, WhatamIdoing, Wike490, Wikid77, Wikijens, Wolfkeeper, Writerite, X-Fi6, Yvwv, Zinnmann, 참, 127 anonymous edits Olfactory glands Source: http://en.wikipedia.org/w/index.php?oldid=544509978 Contributors: Arcadian, LittleWink, Lovelager, Prissi, Rjwilmsi, Romanmb, Torgeirh, Xezbeth, 3 anonymous edits Brunner's glands Source: http://en.wikipedia.org/w/index.php?oldid=543848118 Contributors: Andreas Erick, Arcadian, Blue Danube, Bossair2, Brim, Caerwine, Cherribr, David Kernow, Gastro-en, Graham87, Jag123, JakobSteenberg, Jfdwolff, Jj137, Joehall45, Jpogi, Matan Hemli, Michael Kan, Selket, StuffOfInterest, Thisisborin9, Vogon77, Vojtech.dostal, WhatamIdoing, Ww2censor, Xezbeth, Zanimum, 25 anonymous edits Prostate Source: http://en.wikipedia.org/w/index.php?oldid=551253555 Contributors: A little insignificant, AMK1211, Abstraktn, Abune, Academia salad, Acroterion, Ajp, Alanhay, Alasdair, Alex.tan, AlexR, Alt f in, Anaxial, AndrewWTaylor, Andrij Kursetsky, Androlog, Anomalocaris, Anthony Appleyard, Arcadian, Asarelah, Atlant, AxelBoldt, Azmcs, BBuchbinder, BMF81, Baazandar, Bald Zebra, Beetstra, Before My Ken, Bemoeial, Bgordski, Bigjhoninelcasa28, BillC, Biolog2, Bizflyer, Bleakcomb, Bobo192, Bongwarrior, Bopizzle, Boradis, Bryan Derksen, Bushytails, C.Fred, CMD Beaker, CTF83!, Cairo123, Can't sleep, clown will eat me, CattleGirl, Centrx, Chanlyn, Chris G, Chriswaterguy, Chuunen Baka, Circeus, Cmmuell, Cnjanis, CompliantDrone, Conductcode, Contentmaven, Ctrlfreak13, Cuahl, Daleee, DanielCD, Daveb, Davidruben, Dbfirs, DeadEyeArrow, Deli nk, Delldot, Dennisthe2, DevastatorIIC, Dffgd, Diberri, Digitalh2o, Diotti, Disposableman, Djb217, Djsignal, Dono, Doug, Dragon12597, Drzaphod, ERK, Ebehn, Eleassar, Eleassar777, Emperorbma, Enviromaxinfo, Eog1916, Etan J. Tal, Evo584, Exir Kamalabadi, FT2, Fajar78, FallenAngelII, Fama Clamosa, Fleela, Floppy Tits, Flyer22, Fokklife, Frap, Frecklefoot, Fuzheado, Gareth.ellisthomas, Gfoley4, Gildindaimoth, Gilliam, Giraffedata, Glennwells, GoShow, Googie man, Grafen, GregAsche, Gsarwa, Guanaco, Gugilymugily, Gurch, Gwernol, HJames, HalJor, Hanacy, Hardcorelife, Headbomb, Helix84, Hirpex, Hu12, Hybernizer, Ibanix, Ihealthbuzz, Ilyushka88, Imnotoneofyou, Indon, InvictaHOG, Iridescent, Isfppoet, Ishfaq Khan8, Iwilcox, J.delanoy, JHunterJ, JJHeart, Jammie, Janice Vian, Janko, Jarble, Jayelani, Jerome Charles Potts, Jfdwolff, Jhenderson777, Jmarchn, Jmunroo, Johan1298, Johanname, John robinson, Johnbtv, Joshuas88, Jrsvc, Judgeking, Julesd, Juliancolton, JumpingInSlowMotion, Jun-Dai, Kaobear, KarlFarrell, KaurJmeb, Keenan Pepper, Keldan, Kevin Rector, Kieron a m, King of Hearts, Kntrabssi, Kocio, Kozuch, Kronnang Dunn, Kw0, Laburke, LafinJack, Larryclapp, Leafyplant, Lesouris, Lineslarge, Livajo, Livitup, LonghornDIT, Luckygohappy115, MER-C, Mac, Macedonian, Man It's So Loud In Here, Mariushendrik, Markaci, Materialscientist, Mathew5000, Mav, Maxxicum, Mcstrother, Mczack26, Mghabmw, Mgoodyear, Miami33139, Michael Devore, Michael.Urban, Mikael Häggström, Mike hayes, MishaPan, Miss Tanit, Misslloid, Mkweise, Montrealais, Monty845, Moreau36, Msfishi, Munblog, Mycoderma, Myrealana, Myseda, NapoliRoma, Navy10760, NeilN, Nephron, NerdyScienceDude, Nick, NightFlyer, Nitroshockwave, Nongendered, NotWith, Nufy8, Nuviapalomar, Odedee, Ohnoitsjamie, OldakQuill, Ole E. Sorensen, Openhands, Orange roughie, Orlandoturner, Oxymoron83, Patrick Berry, Patxi lurra, Paulfp, Pbmaise, Pcp111, Pedro, Philip Trueman, Prince Harry of England, Project icecap, Prostatainforma, Psytrist, REscano, Radinruslan, RadioFan, Ratel, Raul654,
Article Sources and Contributors
Raxicoricofallapatorius, Reaper Eternal, Reggy73, Revision17, Rich Farmbrough, RichF, Richardcavell, Rjwilmsi, Roberta F., Roland2, Romanm, Ruy Pugliesi, SCEhardt, Sarbruis, SarekOfVulcan, Scottandrewhutchins, Seaphoto, Serephine, Shellinbox, Sitush, Slashme, Spencer, Spudst3r, Ssetd, Stepheng4, Stevenfruitsmaak, Sultan11, Szquirrel, Tainter, Tameeria, TastyPoutine, Tbsdy lives, Template namespace initialisation script, The Anome, The Thing That Should Not Be, The very model of a minor general, TheLimbicOne, Thebestofall007, Thedeadlypython, ThoHug, Tide rolls, ToNToNi, Todd Vierling, Tomyumgoong, Tpbradbury, Traxs7, TutterMouse, Unit 5, Vanished user giiw8u4ikmfw823foinc2, Velps, Vianello, Vrenator, Vsmith, WJSProwler1, Waggers, Websi7, Weetoddid, Westogent, Whizistic, Wimt, Wmahan, WoodsGnome, Wsiegmund, Ww2censor, Wynler, XfreddytanX, Xoder, Yamamoto Ichiro, ZainAliNawazish, Zigger, Zomno, Zorakoid, ﻋﻠﯽ ﻭﯾﮑﯽ, 495 anonymous edits Bulbourethral gland Source: http://en.wikipedia.org/w/index.php?oldid=539416952 Contributors: Ahmad.ghamdi.24, Ahuskay, Alansohn, AnemoneProjectors, Animeronin, Anonymousphrase, Arcadian, Arent, Brushdrawn, Bryan Derksen, Caiyu, Chanlyn, Den fjättrade ankan, Diberri, DocWatson42, Dpol, Drphilharmonic, Durova, Eras-mus, Fibonacci, Giraffedata, Guanaco, Hede2000, Hovea, James086, Japanese Searobin, Jarble, Jeffro77, Jerry, Jugger90, KDS4444, Karl-Henner, Kauczuk, Keenan Pepper, KellyCoinGuy, Kjkolb, Lexusuns, Macaddict10, Mcstrother, Meco, Montrealais, Myseda, Nick Number, Nuviapalomar, Obradovic Goran, Omicronpersei8, Orlandoturner, Ratel, Raul654, Romanm, Serephine, Sfahey, Stupid6, Szquirrel, Tchaika, Template namespace initialisation script, TheJC, Versus22, 87 anonymous edits Bartholin's gland Source: http://en.wikipedia.org/w/index.php?oldid=539416636 Contributors: AnemoneProjectors, Arcadian, Ask123, AxelBoldt, Betacommand, Blackbyrus, Bryan Derksen, Chanlyn, Clintonboyd, DMacks, Dandelion1, Delldot, Diberri, DocWatson42, Draeco, Drgarden, Eleassar, Eras-mus, Faigl.ladislav, Falcon994, Fangfufu, Hydrargyrum, Igno2, Ionutzmovie, JDobby, JulieADriver, Katydidit, Keenan Pepper, Kelly Martin, Kibi78704, Knutux, Ksanyi, Lexusuns, Lmaxsmith, Malik Shabazz, Miraceti, Nicholasolan, PaddyM, Pigman, Poindexter Propellerhead, Postrach, Qwerty Binary, Rjwilmsi, Rune X2, Saimhe, Sietse Snel, Slightsmile, Someone else, Sonjaaa, Superbeecat, Szquirrel, TakuyaMurata, Template namespace initialisation script, The Anome, Tsiaojian lee, Vaughan, Veck Strack, Wikitanvir, 39 anonymous edits Endometrium Source: http://en.wikipedia.org/w/index.php?oldid=547998992 Contributors: 24.234.70.xxx, Alansohn, Altenmann, Andycjp, Anxietycello, Arcadian, AxelBoldt, BCSWowbagger, Belovedfreak, Bemoeial, Brim, Bryan Derksen, Cbkallen, Clicketyclack, Conversion script, Damian Yerrick, Dasani, Davidruben, Decoy, Delldot, Diberri, Dlohcierekim's sock, Download, Drphilharmonic, Dub8lad1, Ekem, Epingchris, Eras-mus, Erud, Everyking, Floranerolia, Fluffernutter, Flyer22, General Wesc, Gonzonoir, Guidod, Habj, JackSparrow Ninja, Jeijoe, Jeronimo, Jmarchn, Jpogi, Jsherwood0, Kurykh, Mayday 1234, Mikael Häggström, Modify, Monobi, Nephron, Nick Number, Pigman, QuizzicalBee, Redyka94, RexNL, Robert McClenon, Rymanes, Santonellis, Seans Potato Business, Seejyb, Selket, TheEgyptian, Tjmoel, TravisTX, Trosoft, Uwe Gille, Viriditas, Vldscore, Werieth, WhatamIdoing, Wolfmankurd, Yca.zuback, Zephyris, 63 anonymous edits Urethral gland Source: http://en.wikipedia.org/w/index.php?oldid=547331842 Contributors: Animeronin, Anticipation of a New Lover's Arrival, The, Arcadian, Beeswaxcandle, Dcshank, Delldot, Denni, Draeco, Jarble, JeremyA, Joel7687, Richard001, Vldscore, 2 anonymous edits Gastric chief cell Source: http://en.wikipedia.org/w/index.php?oldid=540549394 Contributors: Anirishwoman, Arcadian, Basmoq, Boghog, Comrade stuvak, Crocodilesareforwimps, Delldot, Draeco, Eleassar, Franamax, FrozenMan, Ghirlandajo, Gsibbel, Jpogi, Miguelferig, Neodop, Xquizit.decorum, 4 anonymous edits Pepsin Source: http://en.wikipedia.org/w/index.php?oldid=547172026 Contributors: .V., Alexander sar, Alexbateman, Arcadian, Artichoke-Boy, Astrochemist, Aymatth2, Aziz1005, BQmUB2009002, Bdoc13, Ben211086, Bersl2, Bertolucci18, Boghog, BrettMontgomery, Bubbachuck, CTZMSC3, Chinasaur, ChrisGualtieri, Chrisfow, Christopher Cooper, Chrumps, DARTH SIDIOUS 2, Decembermouse, Derelk, Doriftu, Doulos Christos, Drphilharmonic, EhJJ, Eleassar, Eleassar777, Emerson7, Extransit, Favonian, Fconaway, Feezo, Ferengi, Fordgumballs, Friendlyliz, Frietjes, GAThrawn22, Giftlite, Gogo Dodo, Guðsþegn, Hadal, Haham hanuka, Hede2000, Holyman666, I do not exist, ImperatorExercitus, J Milburn, Jahiegel, Japo, Jcesare, Jlick, John254, Jotomicron, Kaboytes, Karpenm, Kf4bdy, Kjaergaard, Klinckc, Lakers, Liftarn, LightBringer, Lightmouse, Lithpiperpilot, Lotje, Low-frequency internal, MER-C, Maden2204, Magnus Manske, Materialscientist, Mattyjenjen, Mbtran, Mike2vil, Mike5598, Modeha, Nakon, Nashini-Kontan, Nid29ron6, No Guru, Nuujinn, Oxymoron83, Patstuart, Paul-L, Pelirojopajaro, Pne, PurfektWepon, Ragesoss, RelentlessRecusant, Rich Farmbrough, Rickyo, Rjwilmsi, Roadnottaken, Saravask, SkyMachine, Smappy, Snapperman2, Snow Blizzard, Snowbringer, Taka, Teles, Teslamike, Therealsarsi, Thiseye, Tristanb, Tsamuels100, Uthbrian, Velella, Vrenator, Webridge, Wikimachine, WriterHound, Xquizit.decorum, Yath, Yerpo, 192 anonymous edits Parietal cell Source: http://en.wikipedia.org/w/index.php?oldid=542980686 Contributors: Aaronbrick, Arcadian, Axl, Bignoter, Bubbachuck, Clicketyclack, Cmcnicoll, DMY, Delta Tango, Deviator13, Edwin, Eleassar, Fastfission, Fireballfx, Franamax, Gastro-en, Gobonobo, GrahamColm, Hoffmeier, Hooperbloob, Hópur 5, Ianvandriel, Jag123, Jfdwolff, Jpogi, Juoj8, Kanesue, Metalhead94, Nlu, Noxidious, Orlandoturner, Pisanidavid, Rb1248, Rhcastilhos, Rhys, Richardslgc, Rsc227, Skittleys, Spirit365, Sverdrup, Tanthalas39, Temporaluser, Tevildo, Ulric1313, Uwe Gille, Vojtech.dostal, Wedge oli, Welsh, WhatamIdoing, Wikisilki, Xquizit.decorum, Xris0, 86 anonymous edits Hydrochloric acid Source: http://en.wikipedia.org/w/index.php?oldid=551628556 Contributors: 1exec1, 2D, 334a, A concerned reader, Aaeamdar, Abcsoccer4me, Abutorsam007, Acroterion, Adashiel, Addaone, Addshore, Ahoerstemeier, Alan Pascoe, Alansohn, Alanyst, Albedo, Alexander.stohr, Alison, Alkivar, Allen3, Alnokta, Alphachimp, Anand Karia, Andres, Andros 1337, Andy Dingley, Angr, AnonGuy, Anskas, Antandrus, Anti-Semitic Stobie, Antonio Lopez, Anypodetos, Arnobarnard, Art LaPella, Arthena, Athf1234, Atif.t2, Atlant, Atooms, Aussie Alchemist, Averyisland, AvicAWB, Avnjay, AxelBoldt, BD2412, Babahu, Bakasuprman, Barhamd, Beao, Beetstra, Ben Webber, Benjah-bmm27, Benjamindees, Berkay0652, Bfesser, Bignoseman, BillFlis, Blandalison, BlazerKnight, BmikeSci, Bobblewik, Bobo192, Bogey97, Bongwarrior, Boonukem, Boothy443, Brian0918, Brianga, BrightStarSky, Brighterorange, Brockert, Brodriguezmueller, Bryan Derksen, Brycemoody, Btsk8rboi, Bubba hotep, Bucketsofg, Cacycle, Cadwaladr, Caltas, Can't sleep, clown will eat me, CanisRufus, CardinalDan, Carlosp123, Carnildo, Casforty, Casliber, Cedrus-Libani, Charon, Chazzy12345, Chem Lady, Chem-awb, ChemNerd, Chris Henniker, ChrisFollower, ChrisO, Christian75, Christy747, Chromega, Cirt, Colo1115, Colonel Warden, Cometstyles, CoolKoon, Crazytales, Creidieki, Curlymeatball38, Cyclonenim, D, DARTH SIDIOUS 2, DVD R W, DVdm, DanMS, Daniel5127, Darth Panda, Dcteas17, Deglr6328, Dendodge, DerHexer, Discospinster, Dispenser, DizzyLAD6197, Dorgan, DrKiernan, Drphilharmonic, Dsmdgold, DutchUncleDeanLancman, Dynamic1, Dystopos, EarthPerson, Edgar181, Edward, Edward321, Eequor, Egil530, Einstien galilei, Eleassar, Eleassar777, Elliott007kf, Ellisgeek, Eloc Jcg, Emerson7, Emurphy42, Enggmayur, EoGuy, Epbr123, Eric Kvaalen, Eridani, Eugene-elgato, Everyking, Evil saltine, Eyesnore, Faradayplank, Finlay McWalter, Fireswordfight, Foxj, Free Bear, Freestyle-69, Funion987, Fuzzzzzzzz, GCarty, Gadfium, Garyzx, Gaurav1146, Gawaxay, Gemini1980, Gene Nygaard, Geoking66, George Burgess, Giant A+circle, Giftlite, Goatmilkfro, Greatpatton, GreenEyez0815, GreenLocust, GregAsche, GregRM, Grenavitar, Grunt, Gscshoyru, Gurch, H Padleckas, HaItsNotOver, Hadal, Hajor, HalfShadow, Happysailor, Harry491, Heightwatcher, Heron, Hhso60, Histrion, Ho949494, HorsePunchKid, Huey45, Hébus, Iantresman, Icseaturtles, Igotnolife, Im not dead xxx, Insanity Incarnate, Invincible Shield, Itub, Izno, J.delanoy, J8079s, JForget, JRM, JYolkowski, JZNIOSH, Jag123, Jagged, Jagged 85, James086, Jerzy, Jeshii, Jfdwolff, Jfreyre, Jidan, Jkl, JoeSmack, John Quincy Adding Machine, JohnM4402, JohnSRoberts99, Jok2000, Jorge Stolfi, Jose77, Jossi, Joyous!, Jpo, Juliancolton, Jumping cheese, Jynto, K1Bond007, Karlhahn, Kashk, Katalaveno, Katherine, Kbh3rd, KeasbeyMornings, Keith Edkins, Kgrad, Khoikhoi, King of Hearts, Kingpin13, Knight1993, Knowledge Seeker, Kozuch, Kpengboy, Kpjas, KrakatoaKatie, Kramden, Krich, Kristof vt, Kukini, Kuyabribri, Kyoko, LOL, La goutte de pluie, Laberkiste, LeaveSleaves, Lightlowemon, Ligulem, Lilandy45, LittleOldMe, Llull, Louisajb, Luk, Luka Krstulović, Lupin, M archer92, M.Komorniczak, Magic.dominic, Magioladitis, Makecat, Malcolm Farmer, ManiF, Mannafredo, Marek69, Marj Tiefert, Markornikov, Materialscientist, Matthewrbowker, Mav, Mavrisa, Maxim, Mayneframe, Maziar fayaz, Mbeychok, McSly, Mdd4696, Meggar, MementoVivere, Mendaliv, Mentifisto, Mercury, Merope, Michael Hardy, Microtony, Mike V, Mike18xx, Milesma, Mindspillage, Minipie8, Mpa, MsDivagin, Msikma, Munford, Nakon, Nao1958, Nathan2345Rawr, Nergaal, Netkinetic, NeuronExMachina, Neutrality, Neverquick, Newone, Niaz, Nichalp, Nicolae Coman, Nilyad, Nsaa, NuclearVacuum, NuclearWarfare, O.Koslowski, Oblivious, OldakQuill, Oleg Alexandrov, Olessi, Onesspite, Originalrawwr, Ortolan88, Ouishoebean, OverlordQ, Ozuma, Paperblossom, Parhat, Paul August, Pavel Vozenilek, Pb30, Penthouse, Pepito123, PerryTachett, Persian Poet Gal, PeteX, Petswodahs, Pgk, Philip Trueman, Phils, Physchim62, Pikiwedia, Pilotguy, Pinethicket, Pit, Plasmic Physics, PoccilScript, Polyamorph, Puckly, Quadell, Queenmomcat, Qxz, RJASE1, Rangek, RatedAAA, Raul654, Razorflame, Rdsmith4, Recognizance, RedRollerskate, Remember me, Renaissance Man, RexNL, Rich Farmbrough, Rifleman 82, Rjwilmsi, Rknasc, Rmhermen, Roastytoast, Robchurch, Roberdin, RobertG, Romanm, Rozevoeten, Rumping, RyanJones, Ryanaxp, Ryulong, SandyGeorgia, Sceptre, Schicagos, Seaphoto, Securiger, Sftpbr, Shanes, Sherool, Shikhars24, Shindo9Hikaru, Shootbamboo, Shovon76, Shultzc, Sietse Snel, Sintaku, Skyezx, Slakr, Sleigh, Smashanator, Smirriw, Smokefoot, Smurfoid, Snowolf, Some jerk on the Internet, Sophus Bie, Spiffy sperry, Srich32977, Sshagunsharma, Starwiz, Steel, Steinsky, Steven J. Anderson, Stone, StoyanWiki, Suicidalhamster, Supernova366, T3h 1337 b0y, TJEY9988, Ta bu shi da yu, TangentCube, Tarquin, Taxman, Tbhotch, Tech00, Ted H Lourent, The chemistds, The tooth, TheAnarcat, TheTrainEnthusiast, Theresa knott, Thomas.Hedden, Thricecube, Tide rolls, Tim Starling, Tlosk, Toon05, Tranletuhan, Trojan traveler, Tsemii, Tutmosis, Ugen64, Unschool, User27091, Velella, Versageek, Versus22, Vrenator, Vslashg, Vsmith, Vuong Ngan Ha, Wachholder0, Walkerma, Wapcaplet, WatermelonPotion, Wayward, Wikibofh, Wikipedia Administration, WikipedianMarlith, Wimt, Wimvandorst, WmRowan, WolfmanSF, Worldtraveller, X201, Xaosflux, Xiner, XofWiki, Yamamoto Ichiro, Yintan, Yk Yk Yk, Youssefsan, Yuber, Yzmo, Zelmerszoetrop, Zfa808, Zoicon5, Zoz, Zsinj, Јованвб, Ὁ οἶστρος, 912 anonymous edits Human gastrointestinal tract Source: http://en.wikipedia.org/w/index.php?oldid=550984165 Contributors: (aeropagitica), 28421u2232nfenfcenc, 2over0, 83d40m, Aadal, Aaron McDaid, Abcgo7, Aboutmovies, Ace of Spades, Adamlankford, Addshore, Aeluwas, Ahoerstemeier, Aitias, Al B G, Alansohn, Alex.muller, Alex.tan, Alias Flood, Allstarecho, Alucard (Dr.), Anbellofe, Angela, Angr, Animeronin, Animum, Aniten21, Annamacd, Anomalocaris, Antandrus, Anthony Appleyard, Arcadian, Aruton, AscendedAnathema, Asikhi, Askarmuk, Astroboy2013, Asymptote, Aua, Auntof6, Aurista25, Avedomni, AxelBoldt, Az29, Backpackadam, Badagnani, Balcer, BananaFiend, Barry the chopper, Bdesham, Be bbes, Beaumont, Beelaj., Beland, Belovedfreak, Ben Ben, Benatkin, Bencherlite, Bendzh, Bigbluefish, Bihco, Bill.martin, BioAegypti, Bkonrad, Blabberfruit, Blueyoshi321, Bobbias, Bobblewik, Bobo192, Bonadea, Bongwarrior, Bonnief, Boonshoft2013, Boston, Boulaur, Brian Crawford, Brighterorange, Brinerustle, Btm67, Bunyonfire, Burntsauce, CJ, Cactus.man, Caltas, Calvero JP, Calvin 1998, Can't sleep, clown will eat me, CapitalR, Captain Weirdo the Great, Carenab, Carlosforonda, CaseyPenk, ChemNerd, Chetvorno, Chill doubt, ChongDae, Chowbok, CiaPan, Cimex, Citicat, Clicketyclack, Cliff smith, Cmungall, Conheery, Coolbob2422, Cosmic Latte, CosmicWaffles, Countincr, Cpl Syx, Cremepuff222, Csörföly D, Cww, Cyberdemon4, D.c.camero, DBigXray, DCEdwards1966, DO11.10, DVD R W, Daffycrooke12, Dainis, Daleang, Daniel Toth, Daniel.Cardenas, Danish Expert, Dar-Ape, Davewild, Dawn Bard, DeadEyeArrow, DeathbyChiasmus, Debnathsandeep, Deeptrivia, Delldot, Deor, Dgw, Diberri, Digitalme, Dinesh smita, Discospinster, Dolphingeek, Dpol, Drgarden, Dudemeister123, Dumrance, Dureo, Dysepsion, EOBeav, EPO, ESkog, Editorofthewiki, Edward, Ekr, Eliz81, Elliot235funny, Emijrp, Enchanter, EnochBethany, Enric Naval, Entropy, Enuja, Eoghanacht, Epbr123, Epgui, Eribro, Erielhonan, EronMain, Eukesh, Evertype, Everyking, Excirial, Faradayplank, Farosdaughter, Fastfission, Ferretremover, Fictitiouskies, Figma, Finlay McWalter, Finn-Zoltan, Frap, Freakofnurture, GTBacchus, Gaff, Gdo01, GetAgrippa, Giftlite,
602
Article Sources and Contributors
Gilgamesh he, Gman124, Goldom, Gracenotes, Grafen, Graham87, Gtearsg, Gurch, Gzli888, HJ Mitchell, HamburgerRadio, Hard Sin, HaroX, Hasanbay, Headbomb, Headsrfun, Heimstern, Heron, Hhofuentes, Hi i like chocolate, Hotdude155, Hu12, Hut 8.5, IAmAMillionContradictions, II MusLiM HyBRiD II, Iain marcuson, Inter16, Iridescent, Isnow, IvanLanin, Iwilcox, Ixfd64, J.delanoy, JFreeman, JLaTondre, JNW, JR98664, Jacklee, Jacobluver13, Jaknouse, JakobSteenberg, Jamib0y, Jauhienij, Jeffrey O. Gustafson, Jeffreyarthur, Jerryseinfeld, JesseAlanGordon, Jevaughngraham, Jfdwolff, Jfurr1981, Jhgipson211, Jimp, JinJian, Jjalexand, Jketola, Jmundo, JoanneB, Joehall45, John, John Vandenberg, John of Reading, JohnnyB256, Jojhutton, Joseph Solis in Australia, Jossi, Jsphkann, Just plain Bill, KGasso, KJS77, KParks7, Kablammo, Kakofonous, Kandar, Kday, Kdon27, Keilana, Keithwhopkins, Kencomer, Kf4bdy, King of Hearts, Kingdomsingapura, Klundarr, Knowledge Seeker, KnowledgeOfSelf, KrakatoaKatie, Krash, Kreperskater, Kubigula, KuduIO, Kukini, Kungfuadam, Kuru, LOL, LadyofHats, Lamro, Laparaparapa, Laura.Connolly123, Leafyplant, LeaveSleaves, LedgendGamer, Leeannedy, Lemonadeyeti, Lenoxus, Lesion, Lew Zealand XV, Lexi Marie, Lexor, Lights, Lilkadil, Limxzero, Logan, Luk, Luka Krstulović, Luna Santin, MER-C, MK8, Mac, Mackeriv, Madhero88, Majorly, Malcolm Farmer, Mammothm1, Mandarax, Mani1, Manuel Trujillo Berges, Maork, Marek69, MarsRover, Martarius, MartinHarper, Mas 18 dl, Mathonius, Mav, Max Naylor, Maxim, Mayooranathan, McSly, Me Black Cullen, Mendors, Metamagician3000, Metju, Metsavend, Michael93555, Mikael Häggström, Mike Rosoft, Min.neel, Miquonranger03, Miranda, Mishuletz, Mj455972007, MnemosynesMusings, Mnyakaba-GMU, Montie5, Moogle10000, Mooie410, Moyogo, MrBlueSky, Msh210, Mstislavl, Munita Prasad, Music&Medicine, Myanw, Naddy, Natural Val, NawlinWiki, Nbauman, Neelix, Nehrams2020, NellieBly, NeoJustin, Neurolysis, NewEnglandYankee, Nick, NickGorton, Nidht, NightFalcon90909, Nlu, Noah Salzman, Noformation, NotWith, Notinasnaid, Nubiatech, Nxl256, Nzmonkey, Ohnoitsjamie, Ombudsman, Omicronpersei8, OnePt618, Onorem, Opabinia regalis, Ouchitburns, OwenX, Oxymoron83, PFHLai, Paddy Jow, Paiev, Part Deux, Patrick, Patstuart, Paul August, Pax:Vobiscum, Peruvianllama, Peter M Dodge, Phantomsteve, Phasechange, Philip Trueman, Piano non troppo, Pichpich, Pilotguy, Pjvpjv, Plasticup, PoccilScript, Poopoomaniac103, Porterjoh, Prankster nikki, Prashanthns, PrestonH, Quirk, R'n'B, RHB, RJHall, Ragib, Ranveig, Rcsprinter123, Rdsess, Refsworldlee, RenOfHeavens, Rettetast, RexNL, Riana, Rich Farmbrough, Richard New Forest, Riotrocket8676, Robertaedwards, Romanm, Ronz, Rsabbatini, SJP, Sam Korn, Samej71, Sango123, Sasata, Savidan, SchuminWeb, Scientizzle, Scorpionman, Seaphoto, ShajiA, Shanes, Shirulashem, Sirmelle, Sirprojects, Skalskal, Skittleys, Smartdogz123456, Smjg, Sneakerkid1, Snowolf, Snoyes, Some jerk on the Internet, Someone else, Spellcast, Splat, Stardust8212, SteinbDJ, StephenBuxton, Stereotek, Steven Zhang, Stickee, Strafpeloton2, Styrofoam1994, Supermagle, Sylvienguyen, Tarquin, Taylor drake01, Taylortime17, Tdxiang, Tellyaddict, Template namespace initialisation script, Tero, The All-Traq, The Anome, The Rhymesmith, The Thing That Should Not Be, The Utahraptor, The undertow, The unknownEX, TheProject, Thegreencoat, Thehelpfulone, Thehumorous, ThermoNuclearWar, ThreeDee912, Tide rolls, TimVickers, Timir2, Todowd, Tony K10, Toothfish, Travelbird, Trixt, Trusilver, Ubiq, Ukexpat, Ulflarsen, Uncle Dick, Urgos, Vagary, Vary, Vdegroot, Vinceouca, Viriditas, Viskonsas, Vojtech.dostal, Vrenator, Vriullop, Vrymor, WLU, WadeSimMiser, Wakto, Welsh, Wenli, Werdan7, Westendgirl, Wiki alf, WikipedianMarlith, Wikipedsuks, Williamma323, Willotter, Wimt, Wknight94, WojPob, Wolfch, WriterHound, Wtmitchell, Xeno, Xxstertoka99, Yamamoto Ichiro, Yeng-Wang-Yeh, Yidisheryid, Ylem, Youssefsan, Ysheng99, Yuckfoo, Zachary Gibbons, Zimmermanstein, Zinjboss, Zzuuzz, 1190 , יוסיanonymous edits Goblet cell Source: http://en.wikipedia.org/w/index.php?oldid=544935416 Contributors: AK456, Ameliorate!, AndreNatas, Arcadian, Barticus88, Beeswaxcandle, Caerwine, Citizen Premier, Cmcnicoll, Cometstyles, ConCompS, Copysan, Dietzel65, Dkettle, Dramalpaul, Drphilharmonic, Eleassar, Evermorepy, Favonian, Foobar, Franamax, Gobonobo, Halo32007, Hitokirishinji, Hovea, Iameukarya, InvictaHOG, JForget, Jarich, Jeangabin, Jfdwolff, John of Reading, Jonathan.s.kt, Kesal, Kingpin13, La Pianista, Lenrodman, Luna Santin, MPerel, MarkSutton, Mmxx, Monty845, Nephron, Nhandler, Nishio, Nlu, Oxymoron83, Rumpenisse, SABenyunes, Salvadorjo, Serephine, Sses401, TEB728, TheJJJunk, Tide rolls, WikHead, Wikipelli, William Avery, WingateChristopher, 102 anonymous edits Respiratory tract Source: http://en.wikipedia.org/w/index.php?oldid=536084791 Contributors: Alex.tan, Anmats, Barticus88, Bibi Saint-Pol, Bryan Derksen, Cooladoola, CyclePat, DRTllbrg, Danish Expert, Hyarmendacil, J.delanoy, LadyofHats, LiDaobing, Monkeymox, Mseliw, Nlu, Nono64, Olivier, Once111, Petersam, PhatRita, Phil Lu, Rhcastilhos, Robodoc.at, Ryulong, Skittleys, The Thing That Should Not Be, Thegoodguy49, Tristanb, Unara, Xic667, 29 anonymous edits Mucus Source: http://en.wikipedia.org/w/index.php?oldid=551203269 Contributors: (jarbarf), 065211105iscool, 1966batfan, Abce2, Abd, Academic Challenger, Acather96, Actrlvr94Str365, Adashiel, Addict 2006, Addshore, AdjustShift, Adriaan, Adys, Agathoclea, Ahoerstemeier, Ainslieg, Aitias, Aleenf1, Alexandria, Alksentrs, Altenmann, Alterego, Andres, Andrew c, Angela, Anna Frodesiak, Anon969, Anonymous2121kittykittylicklick, Apenrules, Aqwis, Art LaPella, Arwel Parry, Asleep at the Wheel, Avenged Eightfold, Avnjay, Axl, Bakabaka, Bananas Reunited, Basawala, Batchelor, Bejnar, Betterusername, Bharath94, Bibliomaniac15, BigNate37, Blakegripling ph, Bluerasberry, Bobo192, Boing! said Zebedee, Bonadea, Bongwarrior, Boobinhower90, Bree's Block, Btom1993, Bungle, BurritoBazooka, Buster7, CWenger, Cactus.man, CambridgeBayWeather, Canthusus, Capricorn42, Car salesman, Carlthecactus, Catgut, Changer1000, Chester Markel, Chikanamakalaka, Choochootrain2.0, Chovain, Closedmouth, Coffee and TV, Correogsk, Cremepuff222, Crockspot, Cwgh, D. Recorder, DAJF, DJsunkid, Dan D. Ric, Dar-Ape, Darkxpunkygirl, Darth Panda, Dave56789, Deadlightbulb1234, Deli nk, DerBorg, DerHexer, Dgw, Diablorex, Digitalme, Dirac1933, Disciple freak, Discospinster, Djm1279, DlronW, Dnvrfantj, Doctor Procto, Doosky, Download, Dr. Doof, Drphilharmonic, Dweller, Dysepsion, ESkog, Ean5533, EddEdmondson, Edgar181, EditorBobobo, Ekm02001, EmmetCaulfield, Engelmann15, Enigmaman, Epbr123, Eras-mus, Erielhonan, Everyone Dies In the End, Ewlyahoocom, Excirial, Exert, Ezhiki, Falcon8765, Faradayplank, Fcee80, Fiveop, Flewis, Foregone conclusion, Forgetster, Fraggle81, Fremsley, FreplySpang, Froth, Frumbleabumb, Fubar Obfusco, G4rfunkel, Gadfium, Galactor213, Galaxiaad, Galo1969X, Gerrish, Gilgamesh he, Gilliam, GillianHunt, Gimboid13, Glenn, Gluonman, Grunkhead, Gscshoyru, Gurch, Hackerb9, Halo3 homeboy, Hammersoft, Hengsheng120, Henry W. Schmitt, Herbee, Hetar, Holizz, HolyT, Hooperbloob, Huadpe, Hyacinth, Hyperspite, ICAPTCHA, Iiii2333, Inox-art, Insanity Incarnate, InsufficientData, Introductory adverb clause, Invertzoo, Iridescent, IronGargoyle, Ixfd64, J.delanoy, J04n, JaGa, Jacoblawrence32, JamesDumont, Janus Shadowsong, Javsav, Jbamb, Jcwf, Jehan60188, Jfdwolff, Jim1138, Jj is adam, Jj137, Jkoates, Jncraton, Joe5555, JoergenB, John, John Reaves, JohnOw, Jonathan.s.kt, Jooler, Josh murray, Jossi, Junglecat, Kafziel, Kam voo, Karaiyn7157, Katalaveno, Kathryn NicDhàna, KenSharp, Kickus, Kintetsubuffalo, Kku, Kochipoik, Kumioko, Kupojsin, Kurt Shaped Box, Kwertii, Kyorosuke, LAX, LLDMart, LSX, Lacrimosus, Lajohnst, Langhorn, Leibniz, Liaocyed, Lisatwo, LittleT889, LongBay, Lowellian, Luis Felipe Schenone, Luna Santin, M1xmast3r, Magnus Manske, Maharetm, Makurayami, Marklar2007, Materialscientist, Matt Gies, Meaningless, Meelar, Metrowestjp, Mgrollman, Michael Anon, Mike Rosoft, Minimac's Clone, Miniyazz, Minna Sora no Shita, MisfitToys, Mlouns, Moeron, Monty845, Mr Whiteside, Mr. Billion, MrSomeone, Mukadderat, Mystery4you, Nachelavery, Naddy, Nakon, Neil916, Neilbeach, Netsnipe, Neurolysis, Nicci bethel, Nicholan18, NigelR, Ninjatacoshell, Nintendo5000, Nlu, Nn123645, NoMecy071311, Noctibus, Nsteinberg, Nuttycoconut, Nässprejen, Obli, OlEnglish, Onceler, Oren0, Ottawa4ever, Otto2294, Oxymoron83, Pacaro, PaladinWhite, Pandalover1, Paul Barlow, Pepperroni57, Pepperronii57, Perry04061994, Perryperry, Peter Karlsen, Pgk, Philip Trueman, Pinethicket, Pip2andahalf, Plasticup, Poeloq, Polluks, Ppk3000, PrestonH, Professor Fiendish, Prolog, Pstaveley, Puchiko, Purplebigcats, Pyrofork, Pyrospirit, QueenAshley, R, RJFJR, Radon210, Raymondwinn, Recnilgiarc, Redrobin5, Redvers, Reedy, Regulov, Richard001, Rickterp, Rm1271, Rmosler2100, Rodsan18, Rubylover234, RyanCross, Ryoji.kun, S.dedalus, Salvadorjo, Samtheboy, Samwaltz, Sannse, Saraandjenna, Saros136, Sasha Callahan, Scapler, Scetoaux, SchmuckyTheCat, SchuminWeb, ScienceGolfFanatic, Scott S, Scott14, Screwtop, SeekingOne, Seethaki, Shirulashem, Shrieker2k, Sjschen, SkerHawx, Smalljim, Snowyiet, Some jerk on the Internet, Spartan-James, Spcoolbomb, Spike spikeson, SpikeToronto, Spiros01, Spitfire19, Splash, SpuriousQ, Stuffhangin, Super edd, SvartMan, Sven Klemm, Svick, Szczawik, Tanthalas39, Tarret, Tartan, Tbhotch, Tdw, Terik brunson, That can't be right?, The Anome, The Thing That Should Not Be, TheChrisF, TheMightyOrb, ThePenguinStrangler, Thehelpfulone, Thejuanchonater, Thesis4Eva, Thingg, Thomascrapper, Tiddly Tom, Tide rolls, TomGibb, Twinsluv4eva, UglyShirts, Umofomia, Undead warrior, Useight, Utcursch, Vesta, Vsmith, WLU, WadeSimMiser, Waggers, Warcraftfan111, Wavelength, WeniWidiWiki, WesBrandt, Wetman, Why Not A Duck, Willking1979, Wknight94, Wolfdog, Wolfman92, Woohookitty, WormRunner, Wtmitchell, Wyss, X1987x, Xezbeth, Ycyryryry, Ylem, Yoshi032192, Yudiweb, Zachbe, Zack5210, Zapvet, Zargulon, Zoogoo, 805 anonymous edits Enzyme Source: http://en.wikipedia.org/w/index.php?oldid=550081455 Contributors: (3ucky(3all, 01roshay, 10014derek, 10buttz, 13shepht, 168..., 171.65.26.xxx, 1exec1, 209.234.79.xxx, 5ko, 6AND5, 84user, A2-25, A8UDI, AXRL, Aaron Brenneman, Academic Challenger, AdjustShift, Adrian 1001, Aerographer1981, Ahoerstemeier, Aitias, Ajpratt56, Aksi great, Alansohn, Albert109, Alfie66, AlimanRuna, Aljasm, Alsandro, Altermike, AmH2, AmiDaniel, Amren, Anaxial, Anclation, Andre Engels, Androstachys, Anthony Appleyard, Apdang, Apothecia, Arakin, Arbor to SJ, Arcadian, Arjun01, ArmadilloFromHell, Arthena, Articles for analfuckbaggage-!, Artman40, Atif.t2, Atlant, Attilios, Awg usc, AxelBoldt, Ballboy070707, Baoilleach, Barliman Butterbur, Barneycleo, Bassbonerocks, Bcebul, Beastinbman, Beeswaxcandle, Beetstra, Beki Hellens, Bender235, Bensaccount, Benwd, Beta cafe, Bhadani, Bill52270, Bjhiggins, Blabberfruit, Blackprince, Blanchardb, Blehfu, Blue520, Bluerasberry, Bob888, Bobadillo, Bobo192, Bongwarrior, Bookofjude, BorgQueen, BradBeattie, Bradley1545, Brighterorange, Brisvegas, Bryan Derksen, Buzybeez, CBSB, CDN99, Cacycle, Calmer Waters, CalumH93, Can't sleep, clown will eat me, CanisRufus, Canuckian89, Capecodeph, CapitalR, Captain-n00dle, Captaindan, CardinalDan, Carstensen, Casper2k3, Catherine-maguire, Causa sui, CephasE, CharlotteWebb, Chazz88, ChemGardener, ChemNerd, ChicXulub, Chihowa, Chios1127, Chris 73, Chris CII, Chrislk02, Christopher Parham, Chun-hian, Clemwang, Clicketyclack, Clone1, Closedmouth, Cmichael, CommonsDelinker, Conscious, Conversion script, Correctist, Cpeditorial, Cppgx, Crazycomputers, Cst17, Curiousgeorgie, Cwhitt817, Cwkmail, Cybercyclone3993, D, DARTH SIDIOUS 2, DIG, DMacks, DVD R W, Dakarai99, Dalmoz, Dalstadt, Damonchicken, DanMS, Daniel5127, Danny, Danny B-), Dannyboy600, Darth Panda, David D., David Shear, DavidRader, Daycd, Dcflyer, DeadEyeArrow, Debresser, Decltype, Deflective, Delldot, Delta G, Den fjättrade ankan, Denisarona, DennyColt, DerHexer, Derek Ross, Dfrg.msc, Dheenkumar, Dhruvrajgohil, Diberri, Dirac1933, Dirac66, DirkvdM, Dlamming, Dlohcierekim, DocteurCosmos, Doctorcherokee, Donbert, Doniago, Dono, Dpark, Dr. Krishna Prasad Nooralabettu, Dr. St-Amant, DrKiernan, DrNixon, Dreamm, Drphilharmonic, Drummstikk, Dspoel, Duncharris, Dwmyers, EMacG, ESkog, EWikist, Ebuxbaum, EconoPhysicist, Economo, Ed g2s, Edderso, Edgar181, Eequor, Elano, Elassint, Elem3nt, Eleuther, Eltronio, Emhale, Emw, EncycloPetey, Epbr123, Evan57, EvelinaB, Everyking, Evil Monkey, Ewen, Exaton, F. Cosoleto, FF2010, Fabrício Kury, FaerieInGrey, Falcon8765, Fallschirmjäger, FastLizard4, Fedir, Felyza, Fennec, Fieldday-sunday, Fishyfishy, Flannelgraf, Flomenbom, Flugs, Fondls, Forluvoft, Frankenpuppy, FrozenMan, Frymaster, Fuzzform, Fvasconcellos, Fvw, G3pro, GABaker, Gaff, GainLine, Gaius Cornelius, Gdo01, GeneMosher, Geneb1955, Gentgeen, Gfoley4, Ghjfdhgdju, Gianfranco, Giftlite, Gilderien, Gilliam, Gimmetrow, Gingekerr, Giraffedata, GiveItSomeThought, Glen, Glenn, Gn96, Gogo Dodo, Gourgeousladyy, GraemeL, Grafen, Graham, GreatWhiteNortherner, Gregogil, Guiltyspark, Gwernol, Gzuckier, HJ Mitchell, Hadal, Haetmachine, Haham hanuka, Hammer1980, Hans Dunkelberg, HappyCamper, Happylama101, Harlequin2134, Harry491, Harryboyles, Hashar, Hazel77, Hector kevin, Hellfire68, Hello32020, HexaChord, Hezzy140, Hichris, HistoricPandaBear, Hmains, Hobartimus, Holeung, Hu, Huntthetroll, Hut 8.5, Hv, I dream of horses, II MusLiM HyBRiD II, Iamstaurtmayle, Ian Pitchford, Ianblair23, Icelight, Ichbintux, Idontknowmyname, Ike9898, Indy 900, Instantnood, Intelati, Intelligentsium, Intgr, Ioannes Pragensis, Iridescence, Iridescent, IronGargoyle, Ixfd64, J. Finkelstein, J.delanoy, J04n, JForget, JWSchmidt, JaGa, Jab843, Jackol, JacobTrue, Jak123, James086, JamesBWatson, Jamesscottbrown, Jamesters, Jaraalbe, Jauerback, Jauhienij, Jdhowens90, Jebus989, Jedonnelley, Jeff G., Jengod, Jeremyb650, JesseW, Jiddisch, Jitu jain, Jj137, JoanneB, Jobe6, Johan Elisson, John Mackenzie Burke, John NRW, John Quincy Adding Machine, John Riemann Soong, JohnJohn, JohnOwens, JohnnyRush10, Jojhutton, JonHarder, Jonnylyman, Jorwisgar, Jose77, Josh Parris, Jovianeye, Joyous!, Jpbrenna, Jrc2005, Jroenick2797, Jstew87, Jusdafax, Jusjih, Justine Hill, Jwanderson, Jynto, Jyril, K.C. Tang, K1lla abbas, KES47, KGasso, Kasper90, Katalaveno, Katimawan2005, Kbh3rd, Kerivoula, Kheiron, KhoousesWiki, Khukri, Killacoll123, Kingpin13, Kipala, Kjoonlee, Kmdouglass, Knights who say ni, Knowledge Seeker, KnowledgeOfSelf, Kochipoik, Kosigrim, Kozuch, KrakatoaKatie, Krellis, Kukini, Kuru, L Kensington, Lalo1121, Langbein Rise, Lascorz, Lelkesa, Lenticel, Leptictidium, Lexor, Liempt, Lightmouse, Lir, Little Mountain 5, LittleHow, LizardJr8, Loganloganlogand, Low-frequency internal, LtPowers,
603
Article Sources and Contributors
Lugnuts, Luigifan, Lumos3, Luna Santin, Lupo, M412k, MER-C, Maaayowa, MacGyverMagic, Magister Mathematicae, Magnus Manske, Malcolm Farmer, Mani1, Maphyche, MarcoTolo, Marek69, Marj Tiefert, Marxspiro, Materialscientist, Mathel, Mato, Matthew Yeager, Matthiascarrigan, Matty616, Maver1ck, Maxwell754, Mbols, Mboverload, Mcrkramer, Mcy jerry, Mdemian, Mejor Los Indios, Mendaliv, Mets501, Mewilliams95, MiShogun, Michael Devore, Michael Hardy, Michael%Sappir, Michaelas10, Michaeljwilson, Michał Sobkowski, Mikhail Garouznov, Mild Bill Hiccup, MilkMiruku, Miller17CU94, Minna Sora no Shita, Mion, MisfitToys, Mister Matt, Mj455972007, Mmxx, Modulus86, Moguls, Monkeymox, Moshe Constantine Hassan Al-Silverburg, Mouse Nightshirt, Mperkins, MrDrBob, MrOllie, Mrspkapila, Mrt3366, Msikma, Myplace345, N5iln, NCurse, NEUROtiker, Naipicnirp, Nakon, Narsil, NawlinWiki, NellieBly, Neptune5000, Netesq, Neutrality, NewEnglandYankee, Nhandler, Nick123, Nige111, Nihiltres, Nivix, Nk, Nlu, NoahElhardt, Northumbrian, Nunh-huh, Nutiketaiel, Oatmeal batman, OccamzRazor, Olivier, Omicronpersei8, Omnipedian, Onco p53, Opabinia regalis, OverlordQ, Oxymoron83, PDH, PFHLai, PaePae, PandaRepublican, Papapu, Patstuart, Paul venter, Pax deorum, Pdcook, PeaceNT, Petergans, Phantomsteve, Pharaoh of the Wizards, Philip Trueman, Phpham31, Physis, Pietrosperoni, Pilotguy, Pinethicket, Pinkadelica, Pjvpjv, Pkarp11, Plasticup, Pmm530, Pne, Poindexter Propellerhead, PopUpPirate, Popnose, Prolog, Psyche825, Pt, Q3w3e3, Qaz, Quale, Qwfp, Qxz, RB972, RDBrown, Rcjohns1, Reach Out to the Truth, Recurring dreams, Redeemer079, Redvers, Regibox, Rettetast, RexNL, Riana, Rich Farmbrough, Richard001, Rjwilmsi, Rlevse, Rlmrace, Rob Hooft, RobertG, Robertohaas, Rocket71048576, Romanm, Ronhjones, Ronz, Rose090, RoyArnon, Rror, Ruhrfisch, RyanGerbil10, SCEhardt, Saebjorn, Samulili, SandyGeorgia, Sango123, Saravask, Sardanaphalus, Savidan, SchuminWeb, Scimitar, Scottiedog15, Scuzzer, Sean Whitton, Seans Potato Business, Secretlondon, Sefog, Serephine, SergeantBolt, Sfmammamia, Shadowjams, Shane wallmann, ShelfSkewed, Shirik, Shizhao, Shoeofdeath, Shosh3333, Shultzc, Siim, SilkTork, SimBioUSA, Simpler12, Sinharaja2002, Sk741, Skarebo, Skunkboy74, Sky380, Smalljim, Smartsmith, Smellysam524, Snigbrook, Snow storm in Eastern Asia, Some standardized rigour, Sonicology, Sopranosmob781, Squidonius, StaticGull, Steel, Stefano Garibaldi, Stephenb, Stevenfruitsmaak, Stillnotelf, Stone, Stuartmayle, Stuckonempty, Sturm br, Suffusion of Yellow, Suhail174, SupaStarGirl, Superiority, Swpb, Syd Midnight, TAKEN00, THF, TJClark, TKD, TWUChemLS, Tabletop, Takometer, Talktomarie1, Tantal-ja, Taw, Taxman, Tbhotch, Tekks, Tempel, Texasrocks, The Banner Turbo, The Rambling Man, The Thing That Should Not Be, The Wiki ghost, The wub, Theyeti, Think outside the box, Tide rolls, TigerShark, TimBarrel, TimVickers, Timberman, Timflutre, Timhewitt101, Timir2, Tizio, Tkenna, Tlesher, Tomharris, Tommy2010, Tomos ANTIGUA Tomos, TonyClarke, Trevor MacInnis, Tristanb, Trusilver, Ttony21, Tunheim, Turnstep, Tvd12110, Twisted86, Tyler, Typer 525, U+003F, Unyoyega, Useight, User A1, Van helsing, Vanished User 0001, Vanisheduser12345, Vary, Veesicle, Victuallers, Videot43, Vina, Viskonsas, Vojtech.dostal, Vrenator, WDavis1911, Wavelength, Wayne Slam, Wayward, Wdflake, Webridge, Weregerbil, West Brom 4ever, WhatamIdoing, Widr, Wiki alf, WikiDao, Wikiborg, Wikidenizen, Wikidudeman, Wikieditor06, Wikipelli, WillowW, Wknight94, Wmahan, Wmpearl, Wolfgang Kufner, Woohookitty, WookieInHeat, Xdenizen, Xevious, Xxpsycho37xx, Yaksha, Yaser al-Nabriss, Yasitha2, Yelyos, Yikrazuul, Ynhockey, Yoilish, Yorubaspartan, Young Pioneer, Zaijaj, Zephyris, Zero1328, Zidonuke, Zoe, Zondor, ZooFari, Zzuuzz, Ævar Arnfjörð Bjarmason, Саша Стефановић, Սահակ, ﮐﺎﺷﻒ ﻋﻘﯿﻞ, 1995 anonymous edits Paneth cell Source: http://en.wikipedia.org/w/index.php?oldid=550526898 Contributors: Arcadian, Bliyanto, Boonshofter, Bosfeld, C.Carlsbad, Capricorn42, DMG413, Dan Gluck, Darkchun, Deviator13, Diberri, Draeco, Eivind F Øyangen, Eleassar, Finlay McWalter, Fongfongchu, Franamax, Gumruch, Joelpi, JohnCD, Jpogi, Leeearnest, LouisAlain, M dorothy, Mccready, Mcstrother, Mediran, MichaK, Mifam, Mikael Häggström, Paralucent, Pechanga, Pekaje, Quadell, Radzimowski, Robodoc.at, Samir, Serephine, Sun Creator, Tavilis, 24 anonymous edits Intestine Source: http://en.wikipedia.org/w/index.php?oldid=550938207 Contributors: 1ForTheMoney, A. B., Abceasyas, Adashiel, Ageekgal, AkiAkira, Alansohn, Alex.tan, Alexwagner, Alpha Male in the Sunset, Alucard (Dr.), Anakin101, Andy M. Wang, Animum, Anoko moonlight, Apokryltaros, Appleton1324, Aranel, Arcadian, Auxiliary Watchlist, Avoided, B4r4n5k1, BD2412, BWDuncan, Basharh, Bensaccount, Beyond silence, BillyW 1, Blu Aardvark, Blubba112, Boing! said Zebedee, Bongwarrior, Bubba hotep, C6541, CIreland, CaseyPenk, Ceyockey, Chochopk, Chrisjj, Cmh, Crabulon, Craterib, Crithit5000, Crohnie, Csylcox, Ctcl123, CubBC, Cwaug52, D898, DF5GO, DO'Neil, Dammloo, Dan D. Ric, Danjel, Danny, DerHexer, Dffgd, Diberri, Djihinne1, Dominiktesla, Dominus, Draeco, Dumrance, EarthPerson, El estremeñu, Esrob, Fabioli2010, Fieldday-sunday, Flywhc, Fraea, Gadfium, Gahaba, Gail, Gaius Cornelius, Gilliam, Graham87, Grendelkhan, Guyd, Halfalah, Huon, Hvan, Ian Page, Igoldste, Ixfd64, J.delanoy, JForget, JFreeman, JHunterJ, JR98664, JTN, JackPetersen, Jackfork, JakobSteenberg, James086, Japanese Searobin, Jay Litman, Jclemens, Jfdwolff, Jj137, Joele Gilbert, Johntobz, Julian.walters, Jwissick, Kandar, Kappa, Karebear2884, Karen Johnson, Kbbbb, Kehkuansun, Kelly Katula, Knishfaces, Kostisl, Kozuch, LETSskankTHEnightAWAY, Lathyrus100, Laundry, Leslie Mateus, Liamdaly620, Linuxlad, LionMans Account, LjL, Longhair, Lord Pistachio, M dorothy, MBisanz, MC10, MER-C, MadridTeacher, Maralia, Marek69, Master Jay, Maxis ftw, Metagraph, Mikael Häggström, Mineshabadyal, Misza13, Moralis, Morken, Mrhelloilike, Mrs.smithakacheese, Myskills, Nakon, Nihiltres, Nivix, Nthep, Nv8200p, OsamaK, Paxse, PeaceNT, Pearle, Philip Cross, Pinethicket, PoccilScript, Pocketfox, PubliusFL, Pythian Habenero, Qwfp, Radishes, Radonir, Rainbowlori, Rajkiandris, Renaissancee, Rich Farmbrough, Robwingfield, RodC, Rodsan18, Rojomoke, Rrrmmmbbb, Rsabbatini, Sae1962, Salvio giuliano, Sam Korn, ScriptHoward, Sctrojans1112, Shniken, Shoshonna, Smalltalkman, Snowolf, Spaceboss, Srini81, StuHarris, Sun Creator, Surfeited, TedE, Template namespace initialisation script, The Anome, TheAMmollusc, TheJC, Thesnuffla, Tiddly Tom, Tide rolls, Timir2, Tizio, Tocant, Tohd8BohaithuGh1, Tombomp, TommyBoy, Treisijs, Tryptofish, Tvinh, Ukexpat, Una Smith, Useight, Vcohen, Vicki Rosenzweig, Vuo, WAvegetarian, Waggers, WhatamIdoing, WikHead, WikipedianMarlith, Willbyr, Wimt, X201, Xiahou, Yed79, Yidisheryid, Ykvach, आशीष भटनागर, 437 anonymous edits Bicarbonate Source: http://en.wikipedia.org/w/index.php?oldid=539226249 Contributors: 16@r, 17Drew, Adastra1960, Akane700, Albedo, Amirreza, Anlace, Anwar saadat, Arcadian, AstroHurricane001, AxelBoldt, Bart133, Beetstra, Benjah-bmm27, Bennybp, Bensaccount, Buggia, Cajolingwilhelm, Calvin08, Chemicalinterest, Chrislk02, Chrumps, CommonsDelinker, Conversion script, CoyneT, Davemcarlson, DeadEyeArrow, Deli nk, Double sharp, Drnoitall.hello, Drphilharmonic, Dwmyers, Ed g2s, Eug, Faradayplank, GeeJo, Gene Nygaard, Gentgeen, Giftlite, Gilliam, GregorB, Hansonslee, Hellbus, Hugo-cs, Incnis Mrsi, Inkling, J-Kama-Ka-C, JeremyA, Jfdwolff, JimR, Jynto, Kakofonous, Kevin512, KhryssoHeart, Krylonblue83, Ktsquare, Lavateraguy, Linus M., LoyalSoldier, LuigiManiac, Luna Santin, Madgenberyl, Merovingian, Mikael Häggström, Mild Bill Hiccup, Miroku Sanna, Mni9791, N2e, Nergaal, Nurg, P76837, Paul P, Pedrocelli, PenguiN42, Petergans, PioveNevica, Plasmic Physics, Plumbago, Puppy8800, Rcej, Rettetast, Rror, Ryancormack, Salt Yeung, Schizmatic, Shuttlecockfc, Snowmanradio, Stasas, Stepa, Superjoel, The MoUsY spell-checker, The myoclonic jerk, Thricecube, Tikai, Tomgally, Velella, Versus22, WikHead, 132 anonymous edits Lysozyme Source: http://en.wikipedia.org/w/index.php?oldid=547519468 Contributors: A Softer Answer, Agentilini, Alias Flood, AlphaEta, AndiK, Arc de Ciel, Arcadian, Arjayay, Banus, Beemee, Bjsobelmd, Boghog, Brianhe, BurnellShively, CTF83!, Carstensen, Cpelkas, Dejvid, Doctor Procto, Drphilharmonic, Engelenco, Eyal Bairey, Eyu100, Frietjes, Fvasconcellos, Gene Nygaard, Gigemag76, Glida1, Golwengaud, GraemeL, Hadal, Heathmoor, Holeung, IMGrant, Iantresman, Ike9898, J.delanoy, Jag123, Jeppelbaum, Jfdwolff, Jjalexand, K10wnsta, Katharineamy, Kinglz, Kinkreet, Lode (Germany), Logan, LostLucidity, Low-frequency internal, Magioladitis, Magnus Manske, MarcoTolo, Matijap, Maxim Razin, MiPe, MicroBio Hawk, Miniyazz, Mthsmith, Niels Olson, Nneonneo, Nnh, PM Poon, Pierreb24, Precious Roy, Reaper Eternal, Rich Farmbrough, Rjwilmsi, Shaddack, Silasmellor, Spencerw, Squidonius, Squigish, Steveh2000, Strater, Suffusion of Yellow, Teuteul, That Guy, From That Show!, Theresa knott, Traveseru, Vedran12, Webridge, WolfmanSF, Ziphon, 129 anonymous edits Surfactant Source: http://en.wikipedia.org/w/index.php?oldid=551920387 Contributors: 149AFK, 2BeOrNot, AKlilbit, Abdull, Aboalbiss, Adrian J. Hunter, Ahoerstemeier, Alan Liefting, ArnaudContet, Arthena, Ashtonltp, Auntof6, BartlettInteractive, Beetstra, Beland, Bensaccount, Bo Basil, Bssquirrel, Cacycle, Captain-n00dle, Cecile751, Cgsenette, ChemGardener, Chmee2, Choij, Chris Capoccia, Christian75, Church of emacs, Copeland.James.H, Cwage, Cyferz, Cygay, CyrilThePig4, DON 08, Daniele Pugliesi, Darkfred, Deathbypapercutz, Deli nk, Diberri, Discospinster, DocWatson42, DoktorDec, Drat, Drphilharmonic, Dyanega, Eboireau, Edgar181, Efe, Egredior, Elkman, Enviroboy, Evil Monkey, Excirial, Futhark, Fuxx, Glacialfox, Glane23, Golftapsa, Graham87, Ground Zero, Hadal, Haianqutang, Hgrosser, Huhtala, Hulburkj, Ipatrol, Iridescent, Isidore, J.delanoy, JForget, Jaipuria, Jak123, JamesBWatson, Jaubouin, Jcw69, Jeffq, Jeremyb650, Jerome Charles Potts, Jetcrew66, Jhawkinson, Johner, JonRichfield, Joonkimphd, Jstupple7, JustAGal, Jvcarpen, Kevink707, Khaled7stars, Kkmurray, Kpjas, Kupirijo, Kuru, Kwizy, Kymacpherson, Langbein Rise, Latka, Lbeaumont, LedgendGamer, Leuko, Light current, Little hickey, LittleOldMe old, Maderibeyza, Manticore, Mark Arsten, Materialscientist, Maximus Rex, Mcannella, Meister23, Michel Awkal, Mike2vil, Moocha, MrBell, Mxn, NawlinWiki, Ndenison, Newone, Nick Number, Nikevich, Nneonneo, NordicFire, Ojigiri, Oldlaptop321, OllieFury, Orn-luco, Pbsouthwood, Pedrodeigo3, Peterlewis, Pinethicket, PolymerTim, Pumuckl76, Quickone, Quintote, Raucanum, Raymondwinn, Resolute, Rifleman 82, Ringbang, Robert zab, Ryulong, Sandyqun, Scientific29, SebastianHelm, Shaddack, Shmetzler, Shootbamboo, Shrigley, Siawase, Silverchemist, Sjschen, Skittleys, Sloth monkey, Smitz, Smokefoot, Solidpeg, Spectrun, Spiperon, Spiritia, Stacydreis, Struway, Swales, Swyilk, TachikomaAI, Tardigrada2008, The Epopt, Timdew, Tslocum, Tvasailor, Ulflund, Vanished User 1004, Wavelength, Welsh, Xellos, Xris0, YUL89YYZ, Youngbohemian, Zebruh, มือใหม่, 272 anonymous edits Clara cell Source: http://en.wikipedia.org/w/index.php?oldid=540535891 Contributors: 5 albert square, Alex.tan, Animeronin, Arcadian, Axeman89, Axl, Cd830, Ceyockey, DarkArcher25, Daveeroy, Deviator13, Filip em, Franamax, Gaius Cornelius, Gracenotes, Gumruch, J.delanoy, Jclemens, Jesse057, Jfurr1981, Jonathan Drain, Jxs338, Kmg90, Letdemsay, Luke poa, Maristoddard, Mattbartek, MaxEnt, Mcstrother, Mrpark01, Rjwilmsi, Schnurrbart, Scottywong, SharkinthePool, Tagallyat, Thunderboltz, TyA, 32 anonymous edits Somatotropic cell Source: http://en.wikipedia.org/w/index.php?oldid=541164180 Contributors: Alice Mudgarden, Arcadian, ChrisGualtieri, Edward, Ellis2ca, Emeraude, Excentrifuge, Franamax, Fruit.bmp, JonHarder, Jytdog, Mindmatrix, PhiJ, RJFJR, Rich Farmbrough, Template namespace initialisation script, TheParanoidOne, Trevor MacInnis, WikHead, 28 anonymous edits Prolactin cell Source: http://en.wikipedia.org/w/index.php?oldid=547346739 Contributors: Addicted04, Arcadian, Casalinga, Chikiss, Delldot, Feral mage, Franamax, InvictaHOG, Ruutiainen, Steinsky, Template namespace initialisation script, TheParanoidOne, 6 anonymous edits Thyrotropic cell Source: http://en.wikipedia.org/w/index.php?oldid=543564690 Contributors: Arcadian, Franamax, Icairns, Jfdwolff, Template namespace initialisation script, 3 anonymous edits Gonadotropic cell Source: http://en.wikipedia.org/w/index.php?oldid=541162305 Contributors: Arcadian, Drphilharmonic, Druep, Franamax, InvictaHOG, Jarivasell, Mhollida, Template namespace initialisation script, TheParanoidOne, Thecheesykid, 7 anonymous edits Corticotropic cell Source: http://en.wikipedia.org/w/index.php?oldid=543781170 Contributors: Acgator09, Arcadian, Drphilharmonic, Franamax, InvictaHOG, Nmg20, Pascal666, Template namespace initialisation script, TheParanoidOne, TranscendTranslation, 3 anonymous edits
604
Article Sources and Contributors
Melanocyte-stimulating hormone Source: http://en.wikipedia.org/w/index.php?oldid=551576665 Contributors: .Koen, Al bateman, Alex.tan, Anassagora, Anthropodeus, Arcadian, Boghog, Bomac, Cacycle, Centrx, Chaldor, Chemgirl131, Dcirovic, Diberri, Docfaust, Dugwiki, Eras-mus, Gleng, Gustafberg, Hordaland, IMSoP, JWSchmidt, James Crippen, Jezpas, KnightRider, Louisajb, Marc Venot, Meodipt, Netscott, Nmg20, Richardcavell, Rockpocket, Romanc19s, SlothMcCarty, Smily, Sometime-science-editor, Stepa, The Anome, The chemistds, Tristanb, Роман Беккер, 56 anonymous edits Magnocellular neurosecretory cell Source: http://en.wikipedia.org/w/index.php?oldid=540225032 Contributors: Addashaw, Arcadian, Cmcnicoll, Diberri, Drphilharmonic, E=MC^2, Feral mage, Franamax, Gleng, InvictaHOG, RelentlessRecusant, Rettetast, Template namespace initialisation script, 1 anonymous edits Oxytocin Source: http://en.wikipedia.org/w/index.php?oldid=548929574 Contributors: A314268, AbderrahmanNajjar, Achowat, Adolphie, Adomh, Aghochikyan, Ajay5150, AlbertHall, Alertjean, Alex naish, Alex.tan, Alienus, Alousybum, AltiusBimm, Amorymeltzer, Anm28, Anonymous Dissident, AnotherSolipsist, Ansell, Apokrif, Aratuk, Arcadian, Arjayay, Arne Saknussem, Astanton, Athelwulf, Atif.t2, AugustinMa, AxelBoldt, BD2412, Bahkibulle, Barnaby dawson, Beetstra, Before My Ken, Beland, Benbest, Bendav, Bfinn, BigHairRef, Bignoter, Bluerasberry, Bobrayner, Boghog, Bomac, Bongwarrior, Boomur, BorisTM, Boulevardier, Buda118, CDN99, CO, CaliforniaAliBaba, Calton, Carl Wivagg, CarsonsDad, Carusus, Casforty, Cburnett, Cenarium, Cezarika1, Cforrester101, Cgingold, Chemgirl131, Chooserr, Chowbok, Chris Capoccia, Chris Howard, Christian75, Chrysaor, Chuunen Baka, Ciao!derhead, Crystallina, Cspenn, Cybercobra, D, DMacks, Daf, Damian Yerrick, Danalache, David spector, Davidgn, Deflective, Denis tarasov, Deor, Dewatf, Diamondunicorn, Djleslie, Djneufville, Doc.Ian, Dont do drugs, Douglasr007, Download, Dr Bilal Alshareef, Dratman, Drphilharmonic, Duncan.france, Dureo, Dwilletts, ESkog, Edcolins, Edgar181, Egjjones, Eleassar, EllenCT, EmmaEThomas, Eubulides, EugeneZelenko, Everyking, Ewawer, Fangz, Farmacol, Feezo, Feisty.gibbon, Francesfrog, FrozenMan, Fusz432, Fvasconcellos, Gaius Cornelius, Gigemag76, Ginkgo100, Glane23, Glen, Gleng, Gracefool, Guitarmankev1, Gurch, Gz33, Habj, Hazard-SJ, Hazer65, Henk Poley, Henning Makholm, Hobied, Hordaland, Iamcuriousblue, Iapetus, Imsoright, Infrogmation, J.delanoy, JWSchmidt, JamesMLane, Jarble, Jason7825, JasonAQuest, JasonAllen, JaucelynnP, Jeffreyfrench, Jeremy68, Jfdwolff, Jobnikon, Jrockley, Juliecarver, Juntas, Justin Tsay, Justin W Smith, Kaicarver, Kaobear, Karakal, Karl Stas, Keenan Pepper, KnowledgeOfSelf, Kurtan, Kwamikagami, LanceBarber, Leechinyen, Lexi0214, LittleHow, Longhairandabeard, Louisajb, Luke poa, Luonade, Luvsdaheat, Madhero88, Mardus, Marek69, Mark Renier, Materialscientist, Mav, Maxkingesq, May Cause Dizziness, Meanstheatre, Megapanphilos, Mentifisto, Meodipt, Metalloid, Mfourman, Mguttman, Mifter, Mikael Häggström, Mimihitam, MindZiper, Naraht, NeilN, Neoman2026, Nigelj, Nikejulia, Noah Salzman, Nono64, NotAbel, Novangelis, Nrcprm2026, Obscurans, OlEnglish, Ombudsman, Omed2, Originalbigj, Orlandoturner, Osmodiar, OverMyHead, PFHLai, Paine Ellsworth, Pashihiko, Pastiness, Pdcook, Peachypoh, Peryeat, Peteb4, Peterl, Philkon, Philthecow, Pierre-Alain Gouanvic, Platypus222, Poindexter Propellerhead, Postlewaight, Power piglet, Puchiko, Qwerty Binary, RB972, Reaverdrop, Rheez, Rjwilmsi, Rl, Rogermw, RoyGoldsmith, SJFriedl, Salomeya, Sammyj, SarekOfVulcan, Sderose, Seraphimblade, Shadowjams, Shadowlynk, Solidhart, Sondreskarsten, SpLoT, Stevegray, SummerPhD, TBadger, Tameeria, Tarotcards, Tavilis, Tayste, Tb81, Techauthor, The Thing That Should Not Be, Theexamined life, Thelittlegreyman, Themissinglint, Thw1309, Tijmz, TimVickers, Tony Mach, TonyW, Trivialist, Tsiaojian lee, Ultra Venia, Vala M, Vectro, Violetriga, Ward20, Wavelength, Weasel extraordinaire, Weebeman022, Why Not A Duck, WikHead, Wondercow, Wormcast, WriterHound, Wwheaton, Yoninah, Yuubinbako, Zackopacko107, Zakp, Zefryl, Роман Беккер, Ὁ οἶστρος, 神 仙, 444 anonymous edits Vasopressin Source: http://en.wikipedia.org/w/index.php?oldid=546451712 Contributors: A314268, A3camero, AaronM, Abtinb, Adolphie, AlbertHall, Alex.tan, Alousybum, Als022, Amovrvs, Andrux, Antelan, Arcadian, Armando Navarro, Artur Lion, Aude, AxelBoldt, Axl, Aytrus, Backwardtoes, Bensaccount, Blackmarketpenguin, Bobo192, Boghog, Bomac, BorisTM, Bowman, Bwrs, CDN99, Caltas, Caseyisahobo69, Cezarika1, Chaldor, Chemgirl131, Chris the speller, Chymæra, Csobankai Aladar, DRosenbach, Dab2108, Darth Panda, Dcirovic, Denis tarasov, DerHexer, Dhatfield, Diberri, Docfaust, Drphilharmonic, Edgar181, EerieNight, EhJJ, Electric goat, EmlivOlcano, EmmetCaulfield, Epingchris, Eug, Expergefactionist, Feral mage, Forluvoft, FrozenMan, Fvasconcellos, Geetarmainiac, GermanX, Giftlite, Gleng, Guillaume2303, Gurch, Harriv, Hattaway, Hodja Nasreddin, I9606, IO Device, IONTRANSP, Inoculatedcities, Invalidsyntax, InverseHypercube, JForget, James McNally, Javierstroud, JesseAlanGordon, Jfdwolff, Jmoneydizzle, Joel7687, John, John.mapleview, Jonathan.s.kt, Juliecarver, Katoa, Kelson, Kilo-Lima, Krylonblue83, Lepidoptera, M1ss1ontomars2k4, MPerel, ManiF, Mark Knepper, Matdaddy, MauriceTrainer, Mav, Mboverload, Medevo, Medicineman84, Mikael Häggström, Mike2vil, Mimihitam, Minnsurfur2, Misskidney, Mthteh, Nagy, Nathan Johnson, Netopoa, Nishkid64, Nyq, Odoketa, Olegkolesnikov, Osm agha, Philip Trueman, Pit, Pranks16, Prayingmantis78, Puckly, RDBrown, RadicalHarmony, Raghuram.chimata, Rich Farmbrough, Rjwilmsi, RyanGerbil10, SPhotographer, Sammyj, Sgtpepper66, Shrimppesto, Someone else, Spaully, Stepanka, Stismail, Tameeria, Tavilis, Tbhotch, Techfiend, Tgilhou, The Legendary Douglas Butcher, Theodore Kloba, Tide rolls, Tony Mach, Tpjv86b, Uncle G, Vanv2642, Vogelbacherr, Vokesk, Wavelength, Wiki.saeid, WordyGirl90, Xris0, Zain Arshad, Ødipus sic, Роман Беккер, ﻫﻤﺎﻥ, 255 anonymous edits Serotonin Source: http://en.wikipedia.org/w/index.php?oldid=549358753 Contributors: 00AgentBond93, 19.168, 213.253.39.xxx, 2over0, A2-33, A314268, ANGGUN, Abby, Aeluwas, Alalej, Alex.tan, AlexandriNo, Andkore, Andycjp, Apophenic, Arcadian, Arjayay, AshleySt, Astavats, AxelBoldt, BD2412, Badgettrg, Baseball Bugs, Basudhabasu, Beetstra, Belovedfreak, Ben-Zin, BenM, Benjah-bmm27, Besh Saab, Bignoter, Biochemza, Biosthmors, Bluptr, Boghog, Boing! said Zebedee, Bongwarrior, BorisTM, Brandon, Brandon.macuser, Brian0918, Brian1975, Brianherman, Bujatti, Burntsauce, C6541, CDN99, CM Grunge, CMBJ, CWenger, Cacycle, Cantorman, Captain Infinity, Casforty, Catch-fly, Causa sui, Ccroberts, Cedders, Celestialpillow, Ceyockey, Charles Gaudette, Chem-awb, Chemgirl131, Chris Rocen, Chunky Rice, Claud1234, Colinmcc, Conversion script, Correogsk, Corti, Crusadeonilliteracy, Csörföly D, Cue the Strings, CustardJack, Cyberfay, DARTH SIDIOUS 2, DJBarney24, DM4242, DMacks, DVdm, DaGizza, Daksya, Dancter, Danelo, DarkSword, DavidH, Dbtfz, Deepkamal, Deflective, Deli nk, Delta G, Diberri, Docfaust, DonIncognito, DopeChicken, DrSparticle, Drakarst, Dreviscerator, Drphilharmonic, Edgar181, Eequor, El Mariachi, ElaineRitter, Eleassar, Eloil, Epipelagic, Eric-Albert, Escp11, Esperant, Euloiix, EvelinaB, Evercat, Everyking, EvilResident, Ex nihil, Eykanal, Facts707, Falcon8765, Fedayee, Felinefox, Felipe Aira, Ffirehorse, FinnBjork, Firebird9, Flockmeal, Florescent, Fners, Fnielsen, Forthnoggin, Fox816, Fuzheado, Fuzzform, Fvasconcellos, G2star, GABaker, GBronson, GabeIglesia, Gadgit7, Gaius Cornelius, Gastro guy, Geneffects, Genie, Gerriet42, Giftlite, Gigemag76, Gioto, Googie man, Guitarmankev1, Haakenlid, Hadal, Hairy Dude, Hamiltondaniel, Harbinary, Hazard-SJ, Heah, HomicidalWorms, Hon-3s-T, Hordaland, Hpyoup, Hreid11, I dream of horses, IRP, Ianvitro, Immunize, Impossiblepolis, Iothiania, Ipatrol, Iris lorain, IstvanWolf, It Is Me Here, Iwilcox, Izecksohn, JGM73, Jake.knaub, Jarrydn, Jartur, Jauhienij, Jayunderscorezero, Jcw69, Jennavecia, JeremyA, Jfdwolff, Jmh649, Joe Decker, John Vandenberg, JohnInDC, Johner, Jojit fb, Jonathan Drain, Joonhon, Jorgelopest, JorisvS, Joseph11h, Josh Cherry, Joyous!, Julesd, Jynto, Karonaway, Keenan Pepper, Kelvlam, Ken Gillman, Kgrevstad, Kilom691, Kingpin13, Klonimus, KonradG, Ksj123, Kst447, Ksyrie, Kubigula, Kwamikagami, Lehacarpenter, Lenisc, Liangxiao, Liaocyed, Light current, LittleHow, Looie496, Looxix, Louisajb, Luckydhaliwal, Lunakeet, Lyod, M1ss1ontomars2k4, Madacs, Magister Mathematicae, Malljaja, MarXidad, MarcK, Mark PEA, Martynd, Materialscientist, Mathchem271828, Matthew Kornya, Mav, Mazi, McSly, Mcduf01, Meekywiki, MegaHasher, Mentifisto, Mfourman, MiPe, MichaelSHoffman, Mikael Häggström, Mikespedia, Moe Epsilon, Mogism, Mr.alhuwaykim, MrPMonday, Mshake3, Muriel Gottrop, N5iln, Nono64, Northfox, Notjim, Nubb38, Nucleophilic, Ohnoitsjamie, Oliverlyc, Orlandoturner, Ott2, PFHLai, Paul D. Anderson, Paul Drye, Pengortm, Persephone12, Perussi Incendia, PetWolverine, Petey Parrot, Pgk, Philip Trueman, Philopedia, Phlep-phlep, Physchim62, PianoSpleen, Pikiwyn, Pine (usurped), Pinethicket, Pocopocopocopoco, Pol430, Polarbearbabies, Povmcdov, PratzStrike, Prelate Zeratul, ProxyChemist, Purinebug, R'n'B, R.O.C, RDBrown, RadicalHarmony, Rajrajmarley, RatnimSnave, Raybechard, Rcsprinter123, Rehanz1, Reinyday, Renamed user 39932kk3, Reo On, ResearchRave, Reubzz, Rhetth, Rich Farmbrough, Rjanag, Rjwilmsi, Rmky87, Rob Hooft, RohypnolFTW, Rojogrande, Ronhjones, RossBoss, Rossmcd, Rousfo, Rovership27, RoyBoy, Rursus, Russell E, Rünno, SD5, Sadaphal, Samuel Blanning, SandyGeorgia, Sausagerooster, Saxifrage, Sbharris, Sburke, Schauf, Seb144, Senaiboy, Sequoyah, Serotin, Shakajo, Shanedidona, Shisock, Silverxxx, Singlelaw, Sleuth21, Smalljim, Snag99, Socialservice, Sockettome, Sophie means wisdom, Soulthriller, Starcross, StaticGull, Stephenb, Stephensuleeman, Stevertigo, Stijn Calle, StradivariusTV, Sudeshna Chandrashekhar, Suisui, SummerPhD, Sven Jähnichen, Sweikart, TTile, TYelliot, Tabletop, Tal Avigdory, Tarotcards, Tea with toast, Techelf, Teemu08, Teol, The Agitator333, The Anome, The chemistds, TheBaur, Thricecube, Tim Long, TomCerul, Tree Biting Conspiracy, Twaz, Ukexpat, Urhixidur, VI, Varuna, Vaughan, Velvetron, Versus22, Victoria'sSeeker, Vijay2101, Vladaig, Vokesk, Vzambrano, WLU, Walker959, Walkerma, Wapcaplet, Where next Columbus?, Wiki alf, Wikiborg, Willking1979, Wisdom89, Wjejskenewr, Wnissen, Woohookitty, Wormald, Wrfrancis, WriterHound, X1987x, Xabian40409, Xdisaster911, Xris0, XsHoa10pSogRcAVgjAxsVMs1C1BbYUspRh, Xtinacuila, Yamamoto Ichiro, Zoomcake, Åkebråke, Роман Беккер, ﺃﺣﻤﺪ.ﻏﺎﻣﺪﻱ.24, ﮐﺎﺷﻒ ﻋﻘﯿﻞ, 742 anonymous edits Endorphins Source: http://en.wikipedia.org/w/index.php?oldid=549508923 Contributors: A314268, A8UDI, Acather96, Acdx, Ademkader, Aguabranca, Alexander Iwaschkin, Allmightyduck, Allowother, Amakuha, Amcbride, Analoguedragon, Ancos, AndrewHowse, Anthony Appleyard, Apparition11, Arcadian, Armeria, Arpingstone, Arvindn, Ashdog137, Auric, Awien, Beland, Benbread, BigbossSNK, Bizso, Bk0, Bobo192, Bodnotbod, Boghog, BuickCenturyDriver, Bunchofgrapes, C6541, Cameronpb, Camw, Can't sleep, clown will eat me, Celeron, Chill doubt, Chitarrista, Chumchum7, Chuq, Church of emacs, Cimon Avaro, Cntras, Cometstyles, Corpx, Crazz bug 5, Crispytd13, Crywalt, Cybercobra, Cyrus XIII, Czego szukasz, Davidgindelberger, Dcfleck, DeathByNukes, Defenestration, Dennis714, Derek Andrews, Dereleased, Diblidabliduu, DocWatson42, DoubleUTT, Doug-e-fresh74, Dreadstar, Drphilharmonic, Ducducpham, Dweissma, E Wing, Edgar181, Eemton, Eequor, Efege, Ehn, Elaborate, Elbreapoly, Eliz81, Elmer92413, Epbr123, Eraserhead72, Esrogs, Face, FerralMoonrender, Fieldday-sunday, Firewave11, Firien, Francis Tyers, FrancoGG, Furrykef, Gaff, Giftlite, Gleng, Gogo Dodo, Grace Note, Gracefool, GregW, Gveret Tered, Hazard-SJ, Hch2, Headbomb, Healingkid, Hede2000, Hodja Nasreddin, Hosterweis, Huji, Hydrargyrum, Hz.tiang, Ianmathwiz7, InternetMeme, Ipsingh, Ivan Bajlo, Ixfd64, J. Van Meter, J.delanoy, J04n, JForget, Jahiegel, James086, Japanese Searobin, Jasper Cirkel, Jimmy, Jinma, Jisatsusha, Jittat, Jmcq1, Jojhutton, Jonathan Drain, Jose Ramos, Jsjunkie, Jtyson3202, Judzillah, Juliancolton, Junkers0900, Karada, Karl Stas, Katalaveno, Kbh3rd, Killiondude, Klimintine, Kst447, Ksyrie, Ladder222, Lajos.rozsa, Lerikson, Lkinkade, Looxix, Lova Falk, Lovecz, Luna Santin, MagneticFlux, Martian375, MartinRobinson, Mashford, Materialscientist, Matt121, Mfwnoface, Mgiganteus1, Michael Hardy, Michaelbusch, Miknight, Mleonard85032, Mrs.meganmmc, Myanw, Narssarssuaq, Nathan Johnson, Naturalmotion, NickCatal, Noloop, NotAnonymous0, OGoncho, Obsessivelanguagelearner, Oda Mari, OlEnglish, Orlandoturner, OwenBlacker, Ozrician, PFHLai, Paine Ellsworth, Paranoid, Paul Drye, Pearle, Philip Trueman, Phlegat, PkScary, Playadom, Pro bug catcher, Profstandwellback, Quendus, R'n'B, RJASE1, Rajah, Raquel Baranow, Rasd, Rbmj, Rffreq, Rgaddipa, Rjwilmsi, Ronocdh, Rosskey711, Ryanaxp, Saint91, Saman1212a, Schaefer, Search4Lancer, Shatteredshards, Silverxxx, SiobhanHansa, Skew-t, Skihtg12, Smegal723, Snoyes, Sockr44e, Spalding, Sparklegurl32, Spiff, St3vo, Steevven1, Stiang, Sticky Parkin, Stpcreepstp, Subzero Ray, Sunray, Superbeecat, Supernatent, Sylvain Mielot, Szaszicska, Tavilis, Techelf, TeresaTeng, Terriblefish, Teutonic Tamer, Tgeairn, The Anome, The Epopt, TheGerm, TheRasIsBack, Tide rolls, Tntdj, Tomyumgoong, Triggtay, Tyciol, Uthbrian, VI, Versus22, Vrenator, WOLfan112, Wik, Will Beback, WriterHound, X!, X3qt0r, Ylem, Yms, Yorick8080, Zenomax, ﺷﻤﺎﻝ ﺑﺰﺭﮒ, 533 anonymous edits Somatostatin Source: http://en.wikipedia.org/w/index.php?oldid=547887868 Contributors: Alansohn, Aleator, Alex.tan, Amisten, Anthonyhcole, Arcadian, AvicAWB, Banus, Betswiki, Boghog, CDN99, Ccevo2010, Ceyockey, Cezarika1, Chemgirl131, Chrysaor, Cy21, Delldot, Dextrosity, Dr.fuchs, Drphilharmonic, ESCapade, Edgar181, Epingchris, Epolk, Franklinjefferson, GHe, Gelu Ignisque, Gleng, Guidod, Hodja Nasreddin, Jalan z, Japanese Searobin, Jjohnsonwbc, Jonathan.s.kt, Jujutacular, Korey Pesicka, Kpjas, Magioladitis, Mattinbgn, Maumugnel, Miaow Miaow, Mikael Häggström, Minesweeper.007, MsHyde, Nonantum, Phoebus87, Prakashmalshe, Richardcavell, Rjwilmsi, RuED, Seanmpeterson, Snecked, Temporaluser, Terrace4, Tgilhou, TomSands, Tomjc, Trabelsiismail, TranscendTranslation, TylerDurden8823, Vedran12, Wavelength, Westin, Wik, Xerxesgrinder, Xris0, Yerpo, Yobol, Zoicon5, Роман Беккер, 68 anonymous
605
Article Sources and Contributors
edits Gastrin Source: http://en.wikipedia.org/w/index.php?oldid=547268797 Contributors: 21655, A.s, Adamlankford, Alex.tan, Andrew Su, Arcadian, Atlant, Atlantia, Bignoter, Boghog, Bogwhistle, Borgx, Brim, Caltas, CanadianLinuxUser, Carstensen, Chem Lady, CiaranAnthony, Curb Chain, Danierrr, Dcirovic, Diberri, Dlaat, Doctorcherokee, Duncan.Hull, Edwin, Emilymg, Epingchris, FrozenMan, Gaius Cornelius, Guidod, Hodja Nasreddin, Horiavulpe, InverseHypercube, Japanese Searobin, Jfdwolff, KC Panchal, Kiral, LowLifer, Majkinetor, Meodipt, Mike2vil, MindZiper, Mira Gambolputty, Ms1702, Naraht, Naranoth, Nickwilkie, Puppy8800, Raymondwinn, Rb1248, Rich Farmbrough, Rjwilmsi, RyanGerbil10, Sgpsaros, Szalzala, Temporaluser, Theespuja, Trbdavies, Vedran12, Vldscore, Wlodzimierz, WriterHound, Yms, Yongwang100, Роман Беккер, 79 anonymous edits Secretin Source: http://en.wikipedia.org/w/index.php?oldid=549491271 Contributors: Alex.tan, AmyNelson, Arcadian, Bender235, Bignoter, Boghog, Brim, CMBJ, Calvero JP, Dawn Bard, Delirium, Diberri, Dr.Wink, Eleassar, Flower-gmu, Gabeframe, Guidod, Imagine-GMU, InverseHypercube, Jwinius, Kallimachus, Kim De Gelder, Km2452-GMU, LittleHow, LowLifer, Maork, Mcstrother, MichaelJanich, Mike2vil, MindZiper, Naj-GMU, Naniwako, Nephron, Niels Olson, Ohconfucius, Paul D. Anderson, Pitabread640, Quirk, R'n'B, Rb1248, Red58bill, Rjwilmsi, Rrburke, STanwir MD, Simon Kilpin, Sjakkalle, Stepa, Steveking 89, Stone, Swithrow2546, Vedran12, Vogon77, WLU, Wlodzimierz, Yehudamalul, Роман Беккер, 61 anonymous edits Cholecystokinin Source: http://en.wikipedia.org/w/index.php?oldid=548995917 Contributors: A314268, Alex.tan, Arcadian, Aylaf, Bissinger, Boghog, CDN99, Captain-n00dle, Chrisvanlang, Corblimeywot, Corinne68, Cossy, Daranz, Dcirovic, Diberri, Dr Bilal Alshareef, Drphilharmonic, Edgar181, EerieNight, Emanueru, Falkonry, Flopster2, Gikü, Harbinary, Healthwise, Horiavulpe, Hreid11, Immunize, JHunterJ, JesseAlanGordon, JohnnyCashIsNotDead, Jrtayloriv, Kpjas, Maork, Meodipt, Mgdurand, Mike2vil, NatusRoma, Nick Number, PCHS-NJROTC, Petersam, Probios, Rb1248, Rjwilmsi, Rsabbatini, Snapperman2, Sreerup, Tony1, Vedran12, Vogon77, Wlodzimierz, Yeast2Hybrid, Yongwang100, Роман Беккер, 12יעלד, ﺣﺴﻦ ﻋﻠﻲ ﺍﻟﺒﻂ, 70 anonymous edits Insulin Source: http://en.wikipedia.org/w/index.php?oldid=551722783 Contributors: (榮), - ), 1297, 217.99.96.xxx, 5 albert square, 7, 75th Trombone, A hilton johnson, A.R., A314268, A3r0, ACEOREVIVED, AMackenzie, Aa77zz, Aboros, Acroterion, Addshore, Aelleth, Afil, Ahoerstemeier, Ajd, Ajh16, Akinoame, Alandeus, Ale jrb, Alex.tan, Alexithymia, Alexius08, Alexville, AltheaJ, Andre Engels, Andres, Andrew Su, Andrew73, Andybellenie, Antandrus, AntonioMartin, Anwar saadat, Aphenry, Appraiser, Arcadian, ArchonMagnus, Arielco, Ash, Aswang, Atreid3s, AxelBoldt, Axlq, B.d.mills, BDD, Bachrach44, Badgettrg, Baltimore00, Ben-Zin, Bender235, Benweatherhead, Bernfarr, BeteNoir, Bethenco, BlackTerror, Blake's Star, Bob horn, Bobblewik, Bobdewhirst, Boccobrock, Boghog, BokicaK, Bollar, Bongwarrior, BorgQueen, Bravekermit, Brian Crawford, Brianga, BrightStarSky, Btstuff, Bubba73, Bubeck, Bucephalus, Buchanan-Hermit, Bwhack, C0nanPayne, CLGroup1, Cacycle, Calabraxthis, Callacatacat, Can't sleep, clown will eat me, Canis Lupus, Carbuncle, Carcharoth, CardinalDan, Carpaticus, Carturo222, Ceyockey, Chi 271, Chickenfocker, Chowbok, Chris the speller, Christian List, Chrysaor, Citicat, Clarince63, Cless Alvein, CliffC, Cliffradz, Cmcnicoll, Conversion script, Corpx, Cottingham, Cpyder, Crazypaco, Crecy99, Crimsonarcher, Cybercobra, Cybergoth, DGG, DMS, DVdm, Dachannien, Daevatgl, Dale Arnett, Damian Yerrick, Danny beaudoin, Dararivera, Darentig, Darkwind, Darrell Greenwood, David Underdown, DavidSchooley, Davidruben, Dawn Bard, Db099221, Dcoetzee, Deans-nl, Deelkar, Deepakpurang, Delta G, Denni, DennisDaniels, Deviathan, Dgee15, Diberri, Digital infinity, Ding.xk, Discospinster, Discoveryofinsulin, DocWatson42, Donarreiskoffer, Donfbreed, Douglas Bradford Oliver, Dougofborg, DownUnder555, Download, Dratman, Drphilharmonic, Drz1627, Dullhunk, Dutai68, Dwmyers, EMahony34, ERcheck, East718, Eddideigel, Edward, Eingangskontrolle, Ekem, Eleassar, Eleassar777, Elenaschifirnet, Eliazar, Elyelu, EmadIV, EoGuy, Epolk, FF2010, Fabiform, Fantumphool, Farmacol, Fattyjwoods, Ferrarinimi, Feydey, Fieldday-sunday, Flamingspinach, Fluppy, Foo1942, Foobar, Foregone conclusion, Fram, FreeBird, Frietjes, Fromthevaults, G2star, GAThrawn22, Gabi S., Gadfium, Gbrizey, Gene Nygaard, Geraldshields11, Giftlite, Gigemag76, Gilliam, Gioto, Gleng, Glenn Magus Harvey, Glittergaia101, Googie man, Gorgiogo, Goto Dengo, Grika, Gunnernett, Gutza, Guy Harris, Gwrightnyc, HJ Mitchell, Habbit, Habj, Hadal, Hapticfever, Harry Raffan, Healthabetic, Hebrides, Hellbus, Henkeldg, Hichris, Hmmwhatsthisdo, Hokeman, Holme053, Howcheng, Hu12, Hunter1084, Husky141, Hylian Auree, Hzh, Ibbn, In actu, Iridescent, Isnow, Ita3aai, Itub, IvanTheRussian, Iyantha, Jack Daw, Jackfork, Jackol, Jakob Suckale, Jamesontai, Jantaro, Jarble, Jared81, Jeronimo, Jerryseinfeld, JessieTech, Jfdwolff, Jihadcola, Jim1138, Jnrubenstein, Joao Xavier, JoeSmack, Johansosa, Johnlogic, Johnteslade, Johnuniq, Jon Harald Søby, JonHarder, Joseph Spadaro, Jovianeye, Julesd, Juliancolton, Jwissick, Jyril, Jóna Þórunn, Kaiba, Kanags, Kandar, Karen Johnson, Katalaveno, Katieh5584, Keerthi78, Kenyon, Kingpin13, KittenMya, Kkpatel1, Konman72, Kostisl, Kowey, Koyaanis Qatsi, Kozuch, Kpjas, Krauss, Krenair, Kristof vt, Kungfuadam, Lexington50, Lightmouse, Lilac Soul, LittleHow, Lizwalk, Llull, LoneRifle, Looxix, LovePatsyCline, Low-frequency internal, LtPowers, Lucid, Lzjwhu, M3I5K7E, Magnus Manske, Malcolm Farmer, Mallanox, ManVhv, Mardochaios, Mark Arsten, MarkSutton, Martg76, MartinezMD, MauriceTrainer, Maury Markowitz, Mav, Maxim, Mbbradford, Mcvmccarty, Meiquer, Mergneed, MetsFan76, Mhjb, Michael Devore, Michael Ross, Michaelas10, Mifter, Mig11, Mihaiam, Mikael Häggström, Mildly odd, Mindmatrix, Miss Madeline, Misza13, Mitchthest, Mj455972007, Mlaffs, Mortene, MrFish, Mrcoldfire, Mss01, Muhandes, Munita Prasad, Nakon, Naniwako, Naohiro19 revertvandal, Nbauman, Neet nl, NellieBly, Neparis, NewEnglandYankee, Nhandler, Nicksterlingtek, Nikkimaria, Nk, NobelSturegatan 14, Nosh321, Nutriveg, Nxtid, Nysalor, Oaktree b, Ohnoitsjamie, Olahus, OldakQuill, Oliverdl, Oszillodrom, PFHLai, Paine Ellsworth, Panoramix303, Patricia Meadows, Paul20070, Pedantic of Purley, Pegasus1138, Pelirojopajaro, PericlesofAthens, Peter Ellis, Pfranson, Pharaoh of the Wizards, Philip Trueman, PhilipO, PicNick, Piledhigheranddeeper, Pilotguy, Pinethicket, Pmcmeans, Pmd, Pmm530, Porsche997SBS, Princess LJ, Prisonblues, Psychonaut, Quantpole, Quelsen, Quintote, Qwyrxian, R3m0t, RBBrittain, RJaguar3, RXPhd, Radagast83, Ragesoss, Rajrajmarley, Ratza, Raul654, Realdeal21, RedWolf, Regulov, Renato Caniatti, RexNL, Rich Farmbrough, Richard Arthur Norton (1958- ), Richardcavell, Rillian, Rjwilmsi, Rmky87, Rob Hurt, Roberta F., Roberthistoria, Robinhaw, Robma, Rogerd, Romanm, Ronk01, Royalguard11, Rsabbatini, RudolfRed, Ruy Pugliesi, Rwflammang, RyanCross, Saddhiyama, Saganaki-, Sakkura, Sakura black, Sango123, Sara Howland, SaraPulis, Sasuke Sarutobi, Sbledsoe, Schmausschmaus, Scray, Serketan, Set theorist, Shadowjams, Shifan84, Shobhitha, Shoeofdeath, Silver Edge, Silverchemist, Sjakkalle, Smileh, Smobri, Smyth, Snacks, Snowolf, Solled1, Someone else, Songrit, Soosed, Sorenostergaard, Sourabh.khot, Specs112, SpencerThiel, Spike.robinson, Sstrumello, Starfirewind, Staylor71, Stenemo, Steve03Mills, Steve10345, SteveChervitzTrutane, Stevenscollege, Stevertigo, Strider yellow, Subsolar, Sun Creator, Surfeited, Susan118, T g7, TBloemink, Tabletop, Takometer, Tangsonghe, Tarquin, Tasc, Tasos Serbis, Tassedethe, Tatiparti.katyayani, Taw, Tedickey, Teh Untouchable, TenOfAllTrades, Testosterone vs diabetes, Tevildo, The Anome, The wub, Thingg, Tide rolls, Tobby72, Tobesbmx, Tobias Hoevekamp, Tommy2010, TonyW, Triona, Triplemaya, TwoTwoHello, Tyciol, TylerDurden8823, Ultimus, Universityavegangsta, Unofficialeditor, Unyoyega, User27091, Uthbrian, Uzbad, Valerij, Vanderesch, Veevek, Veinor, Vipinhari, Vsmith, WLU, Wackymacs, Waggers, Wasell, Wavelength, We hope, Webaj, Wik, WikHead, Wiki Raja, Wikipedia brown, Will Beback Auto, Wimt, Wojichek, Woohookitty, WriterHound, Ww, Xjevx, Yamamoto Ichiro, Yash manu, Yava e, Ybbor, Yerpo, Ymwang42, Youssefsan, Ypomichelle, Yurivict, Yyy, Zad68, Zain Ebrahim111, Zesty3, Zigger, Ziva David, Роман Беккер, ﺣﺴﻦ ﻋﻠﻲ ﺍﻟﺒﻂ, 1187 anonymous edits Glucagon Source: http://en.wikipedia.org/w/index.php?oldid=550825528 Contributors: 4twenty42o, Alex.tan, All knowing69, Andrea105, Andrew Su, Arbitrarily0, Arcadian, Autoerrant, AxelBoldt, Bahar101, Beetstra, Bobsagat, Boghog, Bomac, Borgx, Brazucs, Breadified, Brian0918, Brinerustle, Bryan Derksen, Centenarian, Cezarika1, Chowbok, Clicketyclack, Cntras, Craig Pemberton, Dancraggs, Darked, Deltawarrior60, Deryck Chan, Diberri, Don4of4, Drphilharmonic, Dws, Elb2000, Elipongo, Em Mitchell, Ephrone, Eric-Wester, Erud, Giftlite, Gigemag76, Glane23, Guidod, Hanfuzzy, Hede2000, Heron, HexaChord, Hichris, Hodja Nasreddin, Hroðulf, Hylian Auree, Ibrmrn3000, Immunize, Iohannes Animosus, It Is Me Here, J.delanoy, Jasont47, Jfdwolff, Jmh649, Jonathan.s.kt, Jóna Þórunn, KBi, Karl-Henner, Keron Cyst, Kpjas, Kvasi, Leoadec, Lightmouse, Louisajb, Lportil, MONGO, Mattis, Mdh8b, Meegs, Mhaitham.shammaa, Miaow Miaow, Mintleaf, Msraia, Nbauman, Netalarm, Nicksterlingtek, Nk, NotALizard, Nutriveg, Oreo Priest, Peryeat, Purplewowies, R3m0t, RFerreira, RXPhd, RadioFan, Reub2000, Richardcavell, Rjwilmsi, Robinhaw, Rsabbatini, Ruslik0, Sbmehta, Sixpence, Skaaii, Some jerk on the Internet, Stevertigo, StrangeAesculapian, Supergeneraliast, TBloemink, TPK, Techman224, Thumperward, Tra, Vedran12, VenomousConcept, Vogon77, Wavelength, Wiccan Quagga, Wikibofh, Willking1979, Writ Keeper, Yerpo, Yintan, Yk Yk Yk, ZnFinger, Роман Беккер, 160 anonymous edits Bombesin Source: http://en.wikipedia.org/w/index.php?oldid=540380323 Contributors: Aranel, Arcadian, CDN99, Cewvero, Chem-awb, Dcirovic, Deviator13, Drphilharmonic, Edgar181, EncycloPetey, Fuzzform, Howrealisreal, Jesse V., Jfdwolff, Kaarel, Louisajb, Megac7, Ntsimp, Rhys, Robodoc.at, Stepa, The chemistds, Vogon77, WriterHound, Zanimum, ﺣﺴﻦ ﻋﻠﻲ ﺍﻟﺒﻂ, 17 anonymous edits Follicular cell Source: http://en.wikipedia.org/w/index.php?oldid=541154323 Contributors: Arcadian, Brian Crawford, Diberri, Drphilharmonic, Franamax, Garion96, GlassCobra, Jwdietrich2, Kktor, Mikael Häggström, Mike Rosoft, Rogermw, Template namespace initialisation script, TheParanoidOne, Vojtech.dostal, 26 anonymous edits Parafollicular cell Source: http://en.wikipedia.org/w/index.php?oldid=543230436 Contributors: Arcadian, Ayacop, Cajolingwilhelm, Diberri, Feral mage, Franamax, Greensburger, Hurricane767b, InvictaHOG, Jgalt23, Jwdietrich2, Mauvila, Petrb, Rfgagel, Selket, Shunju-kun, Speiererg, Tameamseo, Template namespace initialisation script, TheParanoidOne, WhatamIdoing, 13 anonymous edits Parathyroid gland Source: http://en.wikipedia.org/w/index.php?oldid=551740818 Contributors: Acdx, Alex.tan, Anaxial, Andrux, Anthonyhcole, Arcadian, B2322858, Badgermilk5518, Bamyers99, BetaCentauri, Binky, Bomac, Bookandcoffee, Bprash, Bryan Derksen, Chowbok, Cooladoola, Courcelles, Dan Polansky, Davidruben, Dede2008, Delirium, Diberri, Dnunn27, Drguttler, Drphilharmonic, Drptl, E rulez, Emperorbma, Eog1916, Exemplar72, Facts707, Fdsafdsa, Freekozak, Garion96, GetAgrippa, Giftlite, Google.co, Greensburger, Gveret Tered, Haricotvert10612, Hexane2000, Icairns, Icmac, Igiffin, InvictaHOG, J.delanoy, Jag123, Jfdwolff, Jmarchn, Johner, Keenan Pepper, Kelovy, Kozuch, Lanternix, Larrybob, Limulus, M1ss1ontomars2k4, Magnus Manske, Martin S Taylor, Michael Patrick, Mikael Häggström, MrOllie, Nephron, Otiose315, PKT, Paul August, Pustelnik, RJASE1, Rhys, Richard D. LeCour, Ronhjones, RupertMillard, Rvflyboy, Ryanbibler, Saif husam, Salvadorjo, Schneelocke, Scoresby, Sct72, Shaaaheeen, ShakingSpirit, Squids and Chips, TastyPoutine, Template namespace initialisation script, The Thing That Should Not Be, TheLimbicOne, Themrpotatohead, Truthflux, Tuac, Vedran12, Vincentmirabueno, Wfeidt, Wisdom89, YUL89YYZ, Zenlax, 152 ,יוסי anonymous edits Parathyroid chief cell Source: http://en.wikipedia.org/w/index.php?oldid=541156214 Contributors: Annandale, Arcadian, Ceyockey, Dreadstar, Franamax, Garion96, Gon-no-suke, Grendelkhan, Im.a.lumberjack, Mikael Häggström, Neodop, Nephron, Richardsur, Template namespace initialisation script, YUL89YYZ, 5 anonymous edits Oxyphil cell (parathyroid) Source: http://en.wikipedia.org/w/index.php?oldid=542521918 Contributors: Arcadian, Arfy900, Deviator13, Franamax, Grutness, King of Hearts (old account 1), Knandor, Lenny Kaufman, Markjohndaley, Master of Puppets, Neilymon, Nephron, NeuroE, Rdenu, Template namespace initialisation script, 3 anonymous edits
606
Article Sources and Contributors
Chromaffin cell Source: http://en.wikipedia.org/w/index.php?oldid=550769376 Contributors: Arcadian, Bdekker, Bender235, CopperKettle, Creidieki, Diberri, DragonflySixtyseven, Drphilharmonic, Eleassar, EoGuy, Falconerd, Feral mage, Franamax, InvictaHOG, Jamesscottbrown, Jesse V., Johnhfst, Lenrodman, Mcardlester, T52nd, Tameeria, Template namespace initialisation script, TheParanoidOne, 34 anonymous edits Steroid hormone Source: http://en.wikipedia.org/w/index.php?oldid=539821098 Contributors: AMRDeuce, Aeternitatis, Alteripse, Antandrus, Apers0n, Appleseed, Arcadian, Art LaPella, Bongwarrior, Chemgirl131, Col.Kiwi, Dasani, Dcirovic, Diberri, Drphilharmonic, Dycedarg, Edgar181, Eleassar, Eras-mus, Extransit, Fconaway, Fletcher809, Foobaz, Foogleplex, Freshmeister, Giftlite, Habj, InverseHypercube, JBancroftBrown, Jfdwolff, Jmarchn, JoeSmack, Kimiko, Lova Falk, LowLifer, MER-C, Marc Venot, Memphis88, Mikael Häggström, Mike2vil, Milanannmathew, MindZiper, Mkot390, NBS, Nono64, Novangelis, Parasympathy, Pretzelpaws, RA0808, Rhys, Rjwilmsi, Ron Ritzman, RyanGerbil10, Slashme, Some jerk on the Internet, SpikeToronto, Takowl, TangParadise, Tgeairn, Toddfreitag, Voidxor, Wickey-nl, Wtmitchell, Xavier6984, 95 anonymous edits Mineralocorticoid Source: http://en.wikipedia.org/w/index.php?oldid=539757517 Contributors: Acbdyho, Alex.tan, AlexandriNo, Alexrexpvt, Aranel, Arcadian, Axelaxelj, Bemoeial, Bomac, Ceyockey, Chemgirl131, Chowbok, Cmcnicoll, Docfaust, Edgar181, EivindEklund, Eleassar, Eras-mus, Farmacol, GeeJo, Isoptera, Jack B108, Jezpas, Jfdwolff, Jmarchn, King Pickle, Korg, LeadSongDog, Michael Devore, Middayexpress, Mikael Häggström, Mike2vil, Mild Bill Hiccup, Mrezai, Ph.eyes, Rich Farmbrough, Settersr, SilkTork, Stepa, Su-no-G, Takowl, Tarek, Woohookitty, Yikrazuul, 33 anonymous edits Glucocorticoid Source: http://en.wikipedia.org/w/index.php?oldid=546586582 Contributors: AXRL, Aangari, AaronM, Ahmpaz2010, Alex.tan, Alexrexpvt, Alteripse, Anypodetos, Arcadian, Av01d, Axl, Bahar101, Before My Ken, Boghog, Bonnie Dixon, Chanoyu, Chemgirl131, Chris the speller, Chrisgj, Chrisscrewball, Cpiral, Dan100, Diberri, Dirk Gently, Doritopr, Doworks000, Dr.liuchao, Drphilharmonic, Edgar181, EivindEklund, Eleassar, Eleassar777, Fluffernutter, GeeJo, Huckfinne, Janek78, Jeepday, Jeff G., Jfdwolff, Jmarchn, JoanneB, JohnCD, Jyavner, KBi, KX36, Kangell, Kelson, Kevyn, Kgrad, Klghrt5487, Kman543210, Ksaraf, Kyba274, LSD, Lab-oratory, LovelyLillith, LowLifer, MarkusQ, Mefatpenguin, Michael Shields, Mikael Häggström, Miniyazz, Nabel619, Natazavrik, Nbauman, Nirmos, Ntsimp, NuclearWarfare, Nutriveg, Orlandoturner, Porejide, Princhemi, Pro crast in a tor, RelentlessRecusant, Romanfall, Rose Irmersh, Rror, Salvadorjo, Sbmehta, Seans Potato Business, Selket, Settersr, Sorensen ru, T.vanschaik, Unyoyega, Uthbrian, Vldscore, Wavelength, Wham Bam Rock II, Woohookitty, Wwallacee, Yid, Zertron, 100 anonymous edits Leydig cell Source: http://en.wikipedia.org/w/index.php?oldid=551738900 Contributors: Abstraktn, Adrian.benko, Andreas Erick, Arcadian, Cezarika1, Chopin-Ate-Liszt!, Coldbringer, Coolstoryhansel, CopperKettle, Craig Pemberton, Diberri, Drphilharmonic, ELLusKa 86, Fct, Franamax, GoingBatty, Greid, Hadal, InvictaHOG, Jarble, Jpogi, KnightRider, Lji1942, M1ss1ontomars2k4, Magnus Manske, MaxEnt, Mikael Häggström, Nephron, Pearle, Pengortm, Rjwilmsi, Scohoust, Template namespace initialisation script, TheParanoidOne, Tim hole, Uriel8, Vogon77, 39 anonymous edits Folliculogenesis Source: http://en.wikipedia.org/w/index.php?oldid=547725290 Contributors: After Midnight, Arcadian, Avkrules, Bachrach44, Bobblewik, Bobjgalindo, Breadified, CKCortez, Cacycle, Chemgirl131, CommonsDelinker, D. Wu, DabMachine, Drisar, Epingchris, Faradayplank, Franamax, Geremia, GoShow, Gustavocarra, Headbomb, JLaTondre, Janette.quennell, JeffreyN, John of Reading, Jpogi, Lottamiata, Lyrl, MER-C, Madhero88, Micemug, Mikael Häggström, Moreschi, Rjwilmsi, SDC, Scienceeditor, Shenme, Terrasque, TimBentley, 40 anonymous edits Progesterone Source: http://en.wikipedia.org/w/index.php?oldid=550042315 Contributors: 101scientist21, 16445970cl, 21655, AirBa, Airplaneman, Alexiusnovius, Alison, Alisonmcallister, Altenmann, Ambix, Andrew c, Angr, Ansell, Arcadian, AxelBoldt, AzadMashari, Beetstra, Beland, Beneluxboy, Benith, Benjah-bmm27, Benjamintchip, Benlisquare, Benslaststand, Bluegreen, Boghog, BrightStarSky, Bubbachuck, Bwhack, C6541, CarinaT, Chaser, Chem-awb, Chemgirl131, Christian75, Cindery, Col.Kiwi, CommonsDelinker, CopperKettle, Coppertwig, Crazytales, Cvwdev, Dadsweet, Dandoodle, Darth Panda, David Hedlund, Davidruben, Dcirovic, Debresser, Deli nk, Denisarona, Diberri, Dina, Dinosaurdarrell, Dkeithley, Dmullery, Drphilharmonic, Earl Moss, Edgar181, Edward, Ekem, Eleassar, Elisabeth Rieping, Eras-mus, Eric Kvaalen, Eric22, Evil Monkey, Excesses, Fightindaman, Flghtmstr1, Fuhghettaboutit, Fvasconcellos, GirlForLife, Gits (Neo), Graham87, HJ Mitchell, Hcysweet, Horiavulpe, IceCreamAntisocial, JCKB, JWSchmidt, Jag123, Jason Quinn, Jayunderscorezero, Jdoelder, Jedidan747, Jjsimpsn, JoanneB, Joel.geerling, John of Reading, Jphekman, Juliecarver, Karada, Karen Johnson, Keenan Pepper, Kellyprice, Khalismatic, Kosmotheoria, Kpjas, Kukini, Lance1949, Lemccan, Lifewhyse, LilHelpa, Louisajb, Lupin, Lynn4, Lyrl, MER-C, Magister Mathematicae, Mbilezikjian, Mcstrother, Metalloid, Mikael Häggström, MrADHD, Mumonkan, Mwanner, NameIsRon, Natalya, Naugyanks, Neelie nibor, Nephron, Nick Taylor1, Nirmos, Oaktree b, Officiallyover, Olivier, Osterluzei, Oxymoron83, Pearle, Photouploaded, Physchim62, R'n'B, REACHist, Radagast, Rainbowofknowledge, Rhombus, Rhys, Rich Farmbrough, Richardcavell, Richiez, Rjwilmsi, Robodoc.at, Sam Hocevar, Sander123, Saravask, Selket, Settersr, Seven of Nine, Silume, Skingski, Skpearman, Staceymg, Stannered, Supten, Svick, Tapir Terrific, TedE, The Anome, The Brain, Thecell, Thehoneykitten, TimBentley, Tristanb, Troykyo, Tsemii, UGAcodon, Unschool, Vala M, WLU, Wavelength, Whkoh, WiccaIrish, Wikipaddn, WriterHound, Wtmitchell, Yikrazuul, Zhuuu, ZooFari, Zzyzx11, 236 anonymous edits Corpus luteum cell Source: http://en.wikipedia.org/w/index.php?oldid=186256845 Contributors: Carlossuarez46, Mikael Häggström Corpus luteum Source: http://en.wikipedia.org/w/index.php?oldid=547725267 Contributors: Arcadian, Bgwhite, Boghog, Bomac, Bryan Derksen, Bubbachuck, CDN99, CanisRufus, Chilian51, CommonsDelinker, DerHexer, Diberri, Drphilharmonic, Dudewheresmywallet, Earlypsychosis, Eleassar, Epeefleche, Eras-mus, Erud, Esufer, Fieldday-sunday, Gdarin, Gjbbms640, Gnowor, Grenadine, Habj, Hoffmeier, Imprint007, Ivan.Lt, Jackfork, Jag123, Jarble, Jfurr1981, Jmh649, Jmjanzen, Jsherwood0, Kelly Martin, Kero584, Klingoncowboy4, Lab-oratory, Lyzzis, M1ss1ontomars2k4, Mark Lundquist, Markjohndaley, Materialscientist, Matt26, Mgutierrezyach, Miert, Mikael Häggström, NcSchu, NellieBly, Nephron, Omegawp, Oreobrine, Pigman, Prashanthns, Psquared2, Ricksakti, Robodoc.at, Rytyho usa, Sbharris, Schaaftin, Seejyb, Siebrand, Sky Attacker, Stylese, Template namespace initialisation script, Vldscore, Vokesk, Winderful1, Woohookitty, Wtmitchell, 125 anonymous edits Juxtaglomerular cell Source: http://en.wikipedia.org/w/index.php?oldid=540575536 Contributors: Arcadian, Beeswaxcandle, Diberri, Dr Bilal Alshareef, Franamax, Jpogi, Loganberry, NikeTenis, Onthevirge, Scottalter, Spaully, Timothydavie, 24 anonymous edits Renin Source: http://en.wikipedia.org/w/index.php?oldid=547344242 Contributors: -Midorihana-, 99 Willys on Wheels on the wall, 99 Willys on Wheels..., A3camero, Adh30, Agibso02, Alex.tan, Andrew.e.gibson, Anthonyhcole, Arcadian, Austinlarson, Banano03, Bemoeial, Bensaccount, Boghog, BorisTM, Brighterorange, Bunnyhop11, Cajolingwilhelm, Carlossuarez46, Chaheel Riens, Chemya, Ciar, Clayboy, Cmcnicoll, Colonies Chris, Creidieki, Curb Chain, D6, Dauddarseno, Dawkeye, Defactocomms, Deflective, Diberri, Drphilharmonic, Edgar181, Esprit15d, FrozenMan, GAThrawn22, GJeffery, Gaius Cornelius, Gene Nygaard, GermanX, Gikü, Groovenstein, Haisook, Hodja Nasreddin, Hroychow, Iamgangsta, Icairns, Imiousse, InverseHypercube, Itub, Jag123, Jamesscottbrown, Jco7, Jfdwolff, Jo3sampl, [email protected], Kpjas, Krash, Kwamikagami, Larsjo, Liangxiao, Lights, Looxix, Mattyjenjen, Megaman en m, Mikael Häggström, MiyagiDO, Modeha, Mr. Billion, Ndrawlings, Nephron, Ondewelle, PFHLai, Peak, Ppgardne, RDBrown, Rich Farmbrough, RickDC, Rjwilmsi, Rockpocket, Rorro, Rpseal, Rrten00, S3000, Saravask, Sarindam7, Schzmo, Shakiestone, Snowmanradio, Spaully, Temporaluser, Terkwoizebloo, Tpjv86b, Tristanb, Una Smith, Wavelength, Who, WikHead, Wisdom89, Роман Беккер, 105 anonymous edits Macula densa Source: http://en.wikipedia.org/w/index.php?oldid=546480822 Contributors: Alex.tan, Arcadian, Avaron676, Aytrus, Beeswaxcandle, CopperKettle, Dreaded Walrus, Ekotkie, Eyesighter, Franamax, GermanX, Hydro, Icairns, Jaapinholland, Jag123, Jenistranslucent, Jfdwolff, Lacrimosa, Lamro, M.Komorniczak, MC10, Mikael Häggström, Mrwalliekat, Nfstein, PFHLai, Paul August, Peco15, Quartertone, Rocaveli, Scottalter, Spaully, The Anome, YUL89YYZ, 43 anonymous edits Mesangial cell Source: http://en.wikipedia.org/w/index.php?oldid=543489891 Contributors: Alsocal, Arcadian, Bearcat, Beeblebrox, Ceyockey, Drphilharmonic, Faduart, Inkypaws, Lynntyler, Nlu, PFHLai, 8 anonymous edits Keratinocyte Source: http://en.wikipedia.org/w/index.php?oldid=540490959 Contributors: Alan Liefting, Arcadian, Auriol, Bissinger, Brambleclawx, Buzybeez, DutchDevil, ElAmericano, Evil saltine, Fconaway, Fraggle81, Franamax, Gerriet42, Gurch, Ithunn, Jag123, JayC, Jfdwolff, Kjkolb, KrakatoaKatie, Luquimi, Marek69, My Core Competency is Competency, Nodar95, Nono64, ResearchRave, Rjwilmsi, Scottalter, Shinryuu, Soptsai, SuperHamster, Swpb, Topbanana, Vojtech.dostal, Wnt, 44 anonymous edits Epidermis (skin) Source: http://en.wikipedia.org/w/index.php?oldid=550387026 Contributors: Abrech, Adhanali, Alansohn, Albert109, Anduril171, Antandrus, Arcadian, Arctic Kangaroo, Atlantia, Atura, BTLizard, Bpeps, Buzybeez, Capricorn42, Chamonix2010, Chowbok, ChrisGualtieri, Circeus, Closedmouth, Cocoaguy, Coffeepusher, Cybercobra, DRosenbach, Discospinster, DivineBurner, Dlae, Docfaust, Docta247, Dorianrea, Dprady, Dreg743, Epbr123, Espetkov, Eubanks718, Fama Clamosa, Flightx52, Fluffernutter, Franamax, Froggo Zijgeb, Gail, Gareth Griffith-Jones, Geovani.s, Gerriet42, Giftlite, Graham87, GrahamAsher, HarlandQPitt, Hbent, Hellbus, Ironbam7, JFreeman, JakobSteenberg, Jon186, Joshua Scott, Justanotheralias, KJS77, Kazkaskazkasako, Keilana, Krushdiva, L Kensington, LOL, Liaocyed, Life of Riley, Locogato, Lunchscale, Luxor, Mark Arsten, Masaqui, Maximillion Pegasus, McDutchie, Mcstrother, Microdoctor, Mikael Häggström, Mike Rosoft, Minghong, Mocs56, My Core Competency is Competency, Mysdaao, Nicke L, NikNaks, Nn123645, Nodar95, Notmyhandle, Nutsofthemutt, Omegatron, Peirigill, Prof. Squirrel, Pseudomonas, Recurve7, Rjwilmsi, Rocket000, Ronz, SFK2, SSM93, SchfiftyThree, SchreiberBike, Scottalter, ShakataGaNai, Shanes, Someguy1221, SuddenFrost, Surfspecz, SweetNightmares, Tad Lincoln, Tenacious.Genius, The Rambling Man, The Ultimate Koopa, Tide rolls, Tiggerjay, Tim Q. Wells, Tktktk, Tommy2010, Trax247, Troytsm98, Trr82, Trusilver, UninvitedCompany, Vojtech.dostal, VolatileChemical, WLU, Walrustree, Whateveryousaysir, Wikipelli, Woohookitty, Xoid, Zigger, 305 anonymous edits Stem cell Source: http://en.wikipedia.org/w/index.php?oldid=551818881 Contributors: 041744, 04spicerc, 203.170.3.xxx, 217.99.96.xxx, 2602:304:5D60:9499:293F:1DF9:B733:C105, 5 albert square, 9Nak, A.V., A930913, AHands, AVM, Aaron Schulz, Aaron charles, Abb615, Abbaroodle, Abbasbeyli, Aberdam, Accuruss, Acgator09, Adam.douggie, AdamJacobMuller, AdamRetchless, Adashiel, Adenosine, Adraeus, Adrian, Aeon221, Aetheling, AgadaUrbanit, Agathman, Agricolae, Aircorn, Ajournaleditor, Alakey2010, Alan Liefting, Alanliddell, Alansohn, Alasdair.g1998, Alchewizzard, Aldux, Alenshrew, Alex.tan, Alexei Kouprianov, AlexiusHoratius, Alextill95, Alienus, Allen4names, Allmightyduck, AllyUnion, Alphachimp, Altenmann, Altonbr, Amaury, AmiDaniel, Andcarne, Andre Engels, Andres, Andrewbadr, Andrewdekamp, Androstachys, Anetode, Angus Lepper, Anonymous Dissident, Antandrus, Anthonyhcole,
607
Article Sources and Contributors
Antonrojo, Arcadian, Arcus, Argon233, Arkantosstevius, Arkrishna, ArneLH, Arthena, Artichoker, Arx Fortis, Astoman, AstroHurricane001, Astronaut, Astronautics, Atrix20, AuroraReloaded, Austinbond, Autonova, Avb, Averross, Avoided, AxelBoldt, Axl, Aymatth2, Bachrach44, Badanagram, Badarkace, Banman1004, Bartimaeus666, Baughnie, BballJones, Benbread, Bender235, Bento00, Berlickshane, BesigedB, Betacommand, Bethelizebeth, Bfiggis, Bgpaulus, Big Smooth, Big iron, Bigal78, Bigminisachin1231, Bill52270, Bioinformin, Bisyork, Blake-, Blankfaction.tk, Blazersguy, Blkpowernig2, Blonde chik819, Blunub, Bob Wiyadabebe-Iytsaboi, Bobblewik, Bobbyus, Bobo192, Boghog, Bomac, Bongwarrior, Bookandcoffee, Boothy443, Boots bklyn, Boredzo, BorgHunter, BorgQueen, Borisblue, Bradeos Graphon, Braincricket, Brainfood, Brainhell, BreeRobinson, Brendan Moody, Brendanconway, Brian Crawford, Brian Kendig, Brian0918, Brim, Brossow, Brown boi5, Bryan Derksen, Bubbles3, Bucaro1975, Bucketsofg, Buhuzu, Bushytails, Butros, Byornski, C45207, CBFan, CMacMillan, CRUCIFYKEVIN, Cabodoc, Caelarch, Calliopejen1, Caltas, CambridgeBayWeather, Can't sleep, clown will eat me, Canderson7, Capecodeph, Captain-n00dle, Cassivs, Cburnett, Cellmedsociety, Centrx, Change93, Chimera16, ChipsAhoya, Choach, Chocolatelana, Chodorkovskiy, Cholerashot, Chowbok, Chris 73, ChrisGlew, ChrisGualtieri, Chrisdale92, Chrislk02, Chrismeehan, Christopher Parham, Circeus, ClockworkSoul, Closedmouth, Cntras, CoJaBo, Cobi, Cohesion, Colin marks, Conversion script, Corporate.legal, Corvus cornix, Cosmic Latte, Courcelles, Cpt.squeaky, Cquan, Crazycomputers, Crazydog115, Crazynas, Cryptic, CyrilleDunant, Cyrus Andiron, D. Wu, D3monicVeng3ance, DARTH SIDIOUS 2, DGG, DMacks, DVdm, Dabomb87, Dan100, Danandlollie, Daniel5127, DanielCD, Danny, Dantheman531, Darena mipt, Dark.ranger, Darqcyde, Dave Nelson, Davejohnsan, Davewho2, Davfoster88, David Peacham, David Shankbone, DavidCary, Daycd, Dbsteve100, Dbtfz, DeadEyeArrow, Debatesensei, Decumanus, Deepakpurang, Defunkt, Delldot, Demong, DerHexer, Derek Ross, Deselliers, Deving, Dharmabum420, Dimitmant, Discospinster, DividedByNegativeZero, Dlh-stablelights, Dmitry Dzhagarov, Dobett, DocWatson42, DonSiano, Dougofborg, Dr Aaron, Dr d12, Dr.enh, Draeco, Dragostanasie, Drbohlav, Drianmcniece, Drphilharmonic, Drumman91, Drunken Whale, Duckzilla2000, Dusti, Dwayne, ERcheck, ESkog, Ed Poor, EdBever, EdJ343, Edgar181, Egandrews, ElKevbo, Elektrik Shoos, Ellmist, Ellwyn, Eloquence, EncMstr, Encephalon, Epbr123, Epeefleche, Espetkov, Esprit15d, Etparle, Eubanks718, Eurobas, Europa284, Everard Proudfoot, Evercat, Everyking, Everyone Dies In the End, Evil Monkey, Evil saltine, Excirial, Extro, FF2010, Fama Clamosa, Fang Aili, Fatalityduff, Favonian, Fenice, Feverinlove, Fic-in, Fingerz, Flatterworld, Fleminra, Florentino floro, Fluffernutter, Flux.books, Flyingdream, Forluvoft, Frankie, Frazzydee, Fredrik, Free Bear, Freeze42084, FreplySpang, Freshyill, FrozenUmbrella, Fstorino, Funky Monkey, G.-M. Cupertino, GSlicer, Gabbe, Gadfium, Gail, Garion96, Garywest1111, Gatewaycat, Gavin300, Gazpacho, Gdo01, Geoff.green, George100, Getaway, Getwood, Gilabrand, Gimboid13, Ginkgo100, Glagolev, Glimz, Glisteringwaters, Gmaxwell, Goethean, Gogglecollector, Goododa, GraemeL, Graft, Graham87, Green88en, Greenbough, Gregbrak, Grendelkhan, Grika, Grm wnr, Ground Zero, Grunt, Gscshoyru, Gurch, Guyonthesubway, Gwen-chan, Gwilym84, Gyll, Gyrofrog, H2g2bob, HJ Mitchell, HRED, Habj, Hadal, Haham hanuka, Hamiltonstone, HandyAndy, Hank Ramsey, Harrisd5917, Harry, Haukurth, Hdynes, Healthwise, Hede2000, Helixblue, Hendog456, Henrygb, Herb West, Heybbyy, Heyhombre, Hfastedge, Hikoto, Hirenism, Hockey87, Holdek, Holyone2, Howcheng, Howdy, Huangcjz, Huon, Hurricane111, Husond, Hut 8.5, I c linguist, I80and, Iced Kola, Id711, Idont Havaname, Iknows, Ilaiho, Immunize, Impact red, InaMaka, Incitatus4, Independovirus, Inthend9, InvisibleK, Iohannes Animosus, Ipscellmate, Irishboy5, Irishguy, Isaacsurh, Isarra (HG), Isgsimeng, Ishikawa Minoru, Iwilcox, Ixfd64, J.delanoy, JForget, JFreeman, JONJONAUG, JWSchmidt, JYolkowski, Jag123, JakobSteenberg, James cudahy, James301294, JamesMLane, Jamintime, Jan1nad, Jarash, Jauerback, JavaJawaUK, Javeryt, Jaysonlam, Jblatt, Jdm64, Jeanettephair, Jeff G., JeremyA, Jersyko, Jezhotwells, Jfdwolff, Jgwlaw, Jh51681, Jim Douglas, Jim hoerner, Jimmybass, Jinkbl0t, Jivecat, Jkelly, Jkp44, Jmabel, Jmh649, Jncraton, Joecool94, John of Reading, Johnstone, Johntex, Jonathan.s.kt, Jonny-mt, Josh.K.Poole, Jossi, Joyous!, Jpkoester1, Jprg1966, Jsan, Juansidious, Jusdafax, Jv9mmm, Jvbishop, Jwalte04, K8bigelow, K955301, KF, Kagome 85, Kamker, Kamocsai, Karafias, Karch, Kbdank71, Keegan, Keesiewonder, Keetoowah, Key45, Kfor, KillZOne, Kim Bruning, Kimiko, KinStrategy, Kingpin13, Kjveeley, KnowledgeOfSelf, Konstable, Korinkami, Korovin2, Krohon, Ksargent, Kungfuadam, Kuru, Kuzaar, Kyphe, L Kensington, Langston, Lankenau, Larba200, Lawilkin, Lazydaisy, Lbuckler, LeaHazel, LeadSongDog, Leafyplant, Leevanjackson, Lelestopme, Leo181, Les boys, Lethaniol, Levtchenkov, Lexor, Lgirard, Lightmouse, LilHelpa, Lilblackmc, LizardJr8, Llull, Logan, Logiboy123, LordRM, Lova Falk, Luddite, Luk, Lukey jones, Lulurascal, Luna Santin, Lupin, M0s6p, MBCF, MDChanderson, MHGinTN, MIT Trekkie, MOF, MONGO, MPS, MZMcBride, Magicnxnja, Magioladitis, Magister Mathematicae, MagneticFlux, Magnus Manske, Maha ts, Malleus Fatuorum, Malo, Mandarax, Manogamez, Marcogreguzzoni, Marcos987, Marek69, Mark Lewis, Martinp23, Martyman, Masonian, MastCell, Master of Puppets, Materialscientist, Mathprog777, MatthewJS, Matty j, Mattythewhite, Maurauth, Mav, Max boettcher, Mbm124verizon, Meaghan, Mediaworker, Megalaser, Meghaljani, Mel Etitis, Melah Hashamaim, MeltBanana, Mfoti610, MiamiDolphins3, Michael Hardy, Michael3180, Michaelas10, Michaelll, Mikael Häggström, Mike Rosoft, Mike6271, MikeF, MikeSar, Milnivlek, Mindspillage, Minimac, Mirabellen, Mirceat, Mishmash8, Mister Congeniality, Misza13, Mjharrison, Mjmurphyjr, Mlaffs, Mlpearc, Mmxx, Mocirne, Modemac, Moe Epsilon, Moeron, Moink, Monty845, Moop stick, Moosepers, Moriori, Mpt, Mr Stephen, MrOllie, Mu5ti, Mullagatawny, Munna.alerts, Mwanner, Myanw, N5iln, NYCJosh, Nadejla, Nadyes, Nakon, Nanpae, Narayanese, Nashpaul, Natgoo, Naturespace, Naudefj, Naus, NawlinWiki, Ncrm, Nectarflowed, NetRolller 3D, Netsnipe, NeuronExMachina, Neutrality, NewEnglandYankee, Nichefinder, Nicholas Cimini, Nick123, Nickst, Nicolae Coman, Niels, Nightscream, Nihiltres, Nina, Nishkid64, Nivix, Nobleeagle, Nohat, Nonerds2, Noq, Notreallydavid, Nouseforaname312, NuclearWarfare, Numbo3, O.Koslowski, OOODDD, Oarih, Obesegypsi, Oblivious, Obradovic Goran, Octane, Ohio34895, Ojigiri, OlEnglish, Olbrich, Oliverdl, Omhafeieio, OnlyWayne, Orange Suede Sofa, Ormers, Oskar Sigvardsson, Otvaltak, Owen, OwenX, Oxfordwang, Oxymoron83, PDH, PFHLai, Pakraw, Paleorthid, Paranoid, Parijata, Parkyk219, PatrickFisher, Paul August, Pegasus1138, Perfectblue97, Peter Chastain, Peter Ellis, Peter Znamenskiy, Peterish, Peyton20, Pflueger, Pgan002, Pgk, Phidauex, Philg88, Philip Trueman, Phizzy, PhuryPrime, PiMaster3, PinchasC, Pinethicket, Pingveno, Plain jack, Plastikspork, PochWiki, Poetnk, Polyparadigm, Poothebob, Potionism, Pramod Vora, Prasadmalladi, Prestonmcconkie, Previously ScienceApologist, Prince wiki thai, Private Butcher, Provider uk, Prowler08, Pschemp, Pugetbill, Pvosta, Quiddity, Quizkajer, Qwyrxian, R'n'B, RDBrown, RJII, RMann, RadioFan, RadioKirk, Raekwon, Ralphxcrunner, Raul654, Ravenswood, Ravidreams, Rdsmith4, Realm of Shadows, Regener, Reinyday, RelentlessRecusant, RenamedUser01302013, RenamedUser2, RexNL, Rfl, Rhobite, Ricardogpn, Rich Farmbrough, Richard Taylor, Richiekim, Rjwilmsi, Rkevins, Rmosler2100, Roadghost, RobM, Robert Happelberg, Rod57, Rogen123, Ronabop, Ronhjones, RoyBoy, Royalguard11, Rrburke, Rtdrury, Ruha9, Ruineye, RunOrDie, Runningamok, Ruud Koot, RyanGerbil10, Ryanjunk, Ryddragyn, SJK, SMC23, Sailer247, Sam Korn, SamMichaels, Samsara, Sango123, Sankalpdravid, Sasha Kopf, Savant13, Savidan, Scapermoya, Scarian, Scemers, Schzmo, Scohoust, Scottttttt, Seahorseruler, Sean Whitton, Sean William, Sean.hoyland, Seans Potato Business, Seaphoto, Searchme, SearedIce, Selkem, Seriv, Seth Ilys, Seth brady, Shafei, Shanes, Shangrilaista, Shibby970, Shorthoped again, Shrinkshooter, Sigma77, Sil3nt4ss4sin, Silicon Beach Comber, Silver seren, Simetrical, Siroxo, Sjakkalle, Skier Dude, Skittle, SkyWalker, Slakr, Slowking Man, Smackerlacker, Smalljim, Snap Davies, Snek01, Snoop a la boop, Snow Blizzard, Snowbord60, Snowmanradio, So cool, Soccerkid1212, Sodium, Solitude, Some jerk on the Internet, Someoneinmyheadbutit'snotme, Sonare, Sonic3KMaster, Spalding, Speimer, Spicywiener123, SpikeToronto, Spoon!, Sriram sh, Srlasky, Stable attractor, StaticGull, Stbalbach, Steinsky, Stemcell2, Stemcellhub, Stemcellmafia, Stemscientist, Stephen Compall, Stephenb, Stevenfruitsmaak, Stocx, Strangethingintheland, Sundar, Sunshine4921, Svick, Svm2, Switchercat, SylviaStanley, Systemfolder, Sziegler, T-woo22, THEN WHO WAS PHONE?, TMLutas, Tabletop, Tangotango, Tapir Terrific, Tasc, Taw, Tawker, Tbhotch, Ted4d7, Tedwardo2, Teflon Don, TenOfAllTrades, Terence, Tero, TestPilot, TexasAndroid, The Anome, The Haunted Angel, The High Fin Sperm Whale, The Librarian, The Rambling Man, The Thing That Should Not Be, The colledge teacher, The7thmagus, TheAxeGrinder, TheFourFreedoms, TheLimbicOne, TheMidnighters, ThePointblank, Theglockner, Theredbanana, Thestonesfieldmonster, Thethird33, ThomWatson, Thunder365, Thunderboltz, Tide rolls, TimVickers, Timwi, Tintin1107, Tish18, Tizio, Tlotoxl, Tobby72, Tobias Hoevekamp, Tobymanchee, Todderk, Todobo, Tolly4bolly, Tom Morris, Tom harrison, Tombomp, Tomgally, Tommy2010, Tony Sidaway, Tooto, Topmec, Toughpigs, Toyokuni3, Toytoy, Tpbradbury, Tpikonen, Tregoweth, Trekphiler, Triscomn1, Truejim, Trusilver, Tslocum, TubularWorld, TwoTwoHello, TyA, Tycho, UBERxL33T, UConn Multimedia, Ucanlookitup, Uncle Dick, Uncle G, Usbdriver, Useight, User27091, Userdce, Vague Rant, Vanished user 19794758563875, Vanished user 39948282, Vanished user svinet8j3ogifm98wjfgoi3tjosfg, Vedranf, Velella, Versus22, Viewtiful Zoidberg, Vikkidly, Vin9, Vindicata, Vinegarfod, Violetriga, Vir, VirtualSteve, Visual Basic 5.0, Vogon77, Vrenator, WLU, Walik, Warren.cheung, Wavelength, Wayne Slam, Wayward, Webclient101, Werdna, Who, Wi-king, Widr, Wik, Wiki alf, Wiki emma johnson, Wikiborg, Wikipelli, Wikitavanti, Will314159, Wimt, Wjfox2005, Wmahan, Wojcz, Wolf ODonnell, Wolfkeeper, Woohookitty, Wordwhiz, Wykis, Wywin, Xanchester, Xaosflux, Xcrunner29, Xenonice, Xiahou, Xnuala, YELKENN, Yadmat, Yamaguchi先 生, Yamamoto Ichiro, Yansa, Yeah nit, Yegorka, Yolo12348, Yossarian, Youssefa, Youssefsan, Zachfdog, Zachlipton, Zanter, Zeamays, ZimZalaBim, Zsinj, Ztrawhcs, ТимофейЛееСуда, आशीष भटनागर, 上 野 彦 馬, 2350 anonymous edits Huxley's layer Source: http://en.wikipedia.org/w/index.php?oldid=544474708 Contributors: Arcadian, Garion96, Human anatomy, Lavateraguy, My Core Competency is Competency, Scottalter, WhatamIdoing Henle's layer Source: http://en.wikipedia.org/w/index.php?oldid=544474808 Contributors: Arcadian, Flowingaa, Garion96, Human anatomy, JakobSteenberg, Lavateraguy, MZMcBride, Scottalter Trichocyte (human) Source: http://en.wikipedia.org/w/index.php?oldid=546651822 Contributors: Arcadian, Barneca, Eleassar, Franamax, GregorB, Irwin McLean, JoeVector, RDBrown, Smith609, Xp54321, 2 anonymous edits Epithelium Source: http://en.wikipedia.org/w/index.php?oldid=549046203 Contributors: 16@r, 777sms, A01chtra, ABF, AS, Accurizer, Addihockey10, Adrian J. Hunter, Adrian.benko, Aeon1006, Agstf, Alansohn, Alex S, Alex.tan, Andreas Erick, Animeronin, Anoddgirl, Antandrus, Anthonyhcole, Arakunem, Arbitrarily0, Arcadian, Arctic Kangaroo, Arthena, AshLin, Avoided, AxelBoldt, Axl, Az29, Barticus88, Belovedfreak, Bensaccount, Black Kite, Bobo192, Bobomarch, BrightStarSky, Brighterorange, Britney901, Brww, CWii, CambridgeBayWeather, CanadianLinuxUser, Capricorn42, Carlifenkm, Caue.cm.rego, Cbbjch, Choess, Christian75, Chzz, ClockworkSoul, CopperKettle, Crazymonkeyfred, Crimson30, Cyrius, Czar, D. Recorder, Dancingteen, DarkProdigy, Darth Panda, Davidlwinkler, Dcfleck, DeadEyeArrow, Delldot, Diberri, Dipsitenikhil, Dirkbb, Discospinster, DivineAlpha, Djlafu22, Doulos Christos, Dprust, Dr Bilal Alshareef, Drphilharmonic, ESkog, Eeekster, Ekko, EncycloPetey, Epbr123, Everyking, EvilResident, Excirial, Fenkys, Fongus5555, Frammo, Freshlysqueezedorangejuice, Frycow, Geoffrey Gibson, Gilliam, GoShow, Gogo Dodo, Gongoozler123, Graham87, GreatWhiteNortherner, Gurch, Gwynnet, Hadal, Hexane2000, Higbvuyb, Hima.1234, Hroychow, Hu12, Ihope127, ImmortalAl, Immunize, Iune, Ixfd64, JPaestpreornJeolhlna, Jabronimus, Jag123, JakobSteenberg, Jcmo, Jcwf, JeffreyN, Jennes83, Jesanj, Jfdwolff, Jfingers88, Joehall45, JoeyC1313, John Elson, Jonathan.s.kt, Josephingraffia, Juliancolton, Kaiwhakahaere, Kazkaskazkasako, Kbdank71, Keithonearth, Kewpid, Kfogel, Kibi78704, Kku, Knutux, Krawi, L Kensington, LLDMart, Lfoley123, Lifeguard79, Lir, Lkc159, Llywrch, Lmatt, LoonyLuke, Lotje, LovesMacs, Lovesick, Lriley47, Maork, Mark Arsten, Masterpjz9, Mateuszica, Maxis ftw, Maxviwe, Mayur, Meredyth, Mesoderm, Midozx, Miguel.mateo, Mikael Häggström, Millermk, Minna Sora no Shita, Mstislavl, Mushin, N2e, Naudefj, NewEnglandYankee, Nguyen Thanh Quang, Nikai, Nilsonne, Nimish17102000, Nirakka, Nixeagle, Nonagonal Spider, Northamerica1000, Nsaa, Orenburg1, Paste, Pdcook, PeaceNT, Peony Muds, Peter G Werner, Peter.C, Philip Trueman, Piano non troppo, Pinethicket, Plasticup, Pozytyv, Pro crast in a tor, Pstoker, Putney Bridge, Quirk, R. S. Shaw, RDBrown, Radiant chains, Rajah, Rakaha, Ravenbrand, Rdnewman, Renato Caniatti, Rettetast, RexNL, Richiez, Rjwilmsi, Rockhurst singer, Rolando555, Romanm, Rsmn, Rubybrian, Samarqandi, Sardanaphalus, Sbbeef, ScAvenger lv, Scottrainey, Scumbagdog, Scyldscefing, Sfmammamia, Shuanang, SimonP, Sionus, Sir Nicholas de Mimsy-Porpington, Sirshane13, Sky380, Sree.korrapati, Steve2011, Sxoa, THEN WHO WAS PHONE?, Tarotcards, Techdawg667, Tempodivalse, Thatguyflint, The Thing That Should Not Be, The cattr, This lousy T-shirt, Tide rolls, Tristanb, Triwbe, Unknown0801, VanessaLylithe, Vinnievinz06, Vinvik420, Vogon77, Vsion, Wavelength, WereSpielChequers, Widr, WikHead, WingateChristopher, Wisebridge, Wtmitchell, Wysdom, Yserarau, Zarius, ZimZalaBim, 577 anonymous edits
608
Article Sources and Contributors
Squamous epithelial cell Source: http://en.wikipedia.org/w/index.php?oldid=540784155 Contributors: Arcadian, AxelBoldt, Bensaccount, CanadianCaesar, ClockworkSoul, DasBub, Diberri, Dougluce, Drphilharmonic, Epbr123, Fanatix, Fratrep, Gilliam, Gimboid13, Hmwith, InvictaHOG, Jfdwolff, Joehall45, KDS4444, Karlthegreat, Kdavidk, Kgibs, Killiondude, Kjkolb, Korg, Largoplazo, LeaveSleaves, LilHelpa, M1ss1ontomars2k4, Mesoderm, Michael Hardy, Mike2vil, Myr heille, Naranoth, Nephron, Northerncedar, Novangelis, Pajz, Riana, S3000, Saebjorn, Scapermoya, Serephine, The RedBurn, The Thing That Should Not Be, TheGerm, Thstehle, Tide rolls, Tommy2010, Triplepoint217, 91 anonymous edits Hair cell Source: http://en.wikipedia.org/w/index.php?oldid=551502709 Contributors: A314268, Aaron north, Abhishkeghsh8, Anthonyhcole, Arcadian, Auntof6, Beansweet99, Bexxyboop, BillC, Bingme2001, Bobjgalindo, Caitlinmayhew, Christoffer von Schwerin, Clicketyclack, CopperKettle, Cpl Syx, DARTH SIDIOUS 2, Delldot, DiMare, Diberri, Dicklyon, Dinisoe, Dirac1933, EJF, Fences and windows, Gfoley4, Gobeirne, Hart9bay, Hodja Nasreddin, Hooperbloob, Ibderm, Iroewer, JWSchmidt, Jasmin Ros, KRibble, Katieh5584, Kauczuk, Kgrad, LeadSongDog, Legion fi, Lexor, Lylz jenny, Madhero88, Marcel31, Marek69, Martin451, Mikael Häggström, NawlinWiki, NifCurator1, Nrets, Nunh-huh, Owen, Paul venter, Pauli133, Pinethicket, Rhys, Rich Farmbrough, Rjwilmsi, Robert P. O'Shea, Robertinventor, SDC, SQGibbon, ST47, Sanguinity, Sean William, Selket, Selmo, Skarebo, Smith609, SoundAdvise, St3vo, THEN WHO WAS PHONE?, Tameamseo, Thue, Tiara021, Trusilver, Tycho, Warut, WookieInHeat, Zvar, 120 anonymous edits Sensory neuron Source: http://en.wikipedia.org/w/index.php?oldid=549342412 Contributors: A.Ou, Andymc, Antandrus, Anthonyhcole, Arcadian, CAPS LOCK, CambGrad, Can't sleep, clown will eat me, Carbonix, Ciar, CommonsDelinker, Courcelles, DVdm, Diberri, Dolfrog, Dunedain2558, Eouw0o83hf, Fama Clamosa, Fuzzform, Hodja Nasreddin, Intelati, Ipsenaut, J.delanoy, Jerryseinfeld, JoannaCini, Joshschr, Juzeris, Kauczuk, Kku, Lexor, Looie496, Lova Falk, Magioladitis, Martarius, MaxSem, Metricopolus, Mikael Häggström, Mike2vil, Nepenthes, Nick Number, OLLIEJACKSON, Patstuart, Qxz, R'n'B, Raystorm, Reyk, Robert Daoust, Ronhjones, ShaunES, Slon02, Snowolf, Stantia3, Technopat, Tufflaw, Uncle Dick, Unused0030, Welsh, Wikitavanti, WillowW, ﭘﺎﻣﻔﯿﮕﻮﺱ, 114 anonymous edits Merkel cell Source: http://en.wikipedia.org/w/index.php?oldid=551190471 Contributors: Andreahaws, Arcadian, Beeswaxcandle, Beliar, CarrieVS, Clicketyclack, DeCaux, Dicklyon, Dinisoe, Eleassar, Eoghanacht, Fama Clamosa, Fratrep, Jh51681, Joaquin008, Jonathani1, Juicy-one, LittleHow, Margaret52, Merkelcell, Michael Hardy, Motyka, My Core Competency is Competency, NifCurator1, Rjwilmsi, Rubybrian, Scapermoya, Spaully, Tomas e, Vojtech.dostal, Zixaq, 28 anonymous edits Olfactory receptor neuron Source: http://en.wikipedia.org/w/index.php?oldid=550901612 Contributors: Aboalbiss, Aicchalmers, Arcadian, Archelon, Armen Enikolopov, Boghog, Clicketyclack, Cowbert, Daniel Mietchen, Delldot, Dicklyon, Dinisoe, Fantomdrives, Fredrik, Gobonobo, Hcaldwell, MJ94, MarXidad, MelForbes, NifCurator1, Nihiltres, Nono64, Nrets, Pekaje, PlaMarky, Sachio340, Sarenne, Sayeth, Selket, Sluox, Template namespace initialisation script, Vrenator, Xbcj0843hck3, 45 anonymous edits Photoreceptor cell Source: http://en.wikipedia.org/w/index.php?oldid=550892341 Contributors: AED, Ambitiousboy, Appraiser, Arcadian, AxelBoldt, BD2412, Bensaccount, BobbyBoulders, Bomac, CDN99, Cam27, Canley, Chris the speller, Citotoxico, ClockworkSoul, Closedmouth, CommonsDelinker, Cybercobra, Dcirovic, Delldot, Denis tarasov, Dicklyon, Dinisoe, Download, Drphilharmonic, Drybittermelon, Dual Freq, Excirial, Fangfufu, Fantomdrives, Giftlite, GoingBatty, H2g2bob, Hodja Nasreddin, Hordaland, Horuskemwer, Icairns, Indolering, Iste Praetor, Jag123, JessTobin, Jjron, Jonkerz, Just plain Bill, Kaihsu, Kim Darby, KnightRider, Kosigrim, L Kensington, Lessato, Livick75, Lovemuffin333, Magioladitis, Magister Mathematicae, MartinSpacek, Materialscientist, Mikael Häggström, Mild Bill Hiccup, MollyNYC, Nbhatla, NifCurator1, Nono64, Nrets, Nuno Tavares, Nuvitauy07, Nxtid, Nymf, Old Moonraker, Ost316, Panek, Paskari, PhilKnight, Phtalo, R'n'B, Rayman60, Rbarreira, Rettetast, Rich257, Richard001, Rjwilmsi, Robert P. O'Shea, Sakurambo, Sayeth, Sbierwagen, Science Study, Scott Coleman, Serpent's Choice, Sfgrieco, Slmader, Srleffler, Stemonitis, Steveprutz, Stillnotelf, Tameeria, Tevildo, Theshadow27, Thue, Tipiac, Tjerman, TomViza, Trekphiler, Tyluma, Wickey-nl, Xhin, YUL89YYZ, Yuckfoo, 108 anonymous edits Rod cell Source: http://en.wikipedia.org/w/index.php?oldid=551190660 Contributors: 2405:B000:703:2:90E5:DDCD:1981:2AF9, 777sms, AED, Abmac, Accius, Amplitude101, Arcadian, BenduKiwi, Bensaccount, BillFlis, BirdValiant, CardinalDan, Chris the speller, Darkwind, Davidlwinkler, Dcarney, Dcirovic, Deglr6328, Delldot, Denis tarasov, Dhanish007, Dinisoe, Dinty121, Discospinster, DrBob, Dreviscerator, Duoduoduo, Dureo, Edgar181, Editor randy, Eequor, Eliptis, Emperorbma, Epbr123, Esbboston, Fangfufu, Felisopus, Ghfrisbee, Giftlite, Helix84, HendrixEesti, Heron, Hodja Nasreddin, Hordaland, I dream of horses, Iamthecheese44, Irisx, Ironholds, JTN, Japanese Searobin, Jhfortier, Jjron, Jklin, Jmlk17, Kpjas, La goutte de pluie, Lambyte, Levineps, Ligulem, Lilmike121, Lovemuffin333, Lysdexia, Macy, MadCow257, Madhero88, MaiCall, Mannafredo, Martarius, Materialscientist, MathFacts, Mdsam2, Mitchdarcy, Moe Epsilon, NifCurator1, Noetica, Nono64, Npho, Nuvitauy07, Odie5533, Oxymoron83, PartyDude!, Ph.eyes, Philbradley, Pikiwyn, Qaddosh, Ramaksoud2000, Richard001, Robert P. O'Shea, RodC, Sayeth, Sean.hoyland, Selket, Sgpsaros, Slmader, Smullangi, Spudtater, Stefan.loska, Stephenb, Stillnotelf, Template namespace initialisation script, Teodor605, TokyoJunkie, Unionhawk, Vojtech.dostal, Wapcaplet, Widr, Wikipete, XPTO, Yanij, Zachcoggin, 164 , נטע, ליאורanonymous edits Cone cell Source: http://en.wikipedia.org/w/index.php?oldid=551195039 Contributors: 1F025, 5 albert square, AED, Abmac, Aboalbiss, Ace of Clubs and Spades, Adamantios, Adoniscik, Akulo, Alamnagh, Ale jrb, Alexf, Allens, Amber.mccallum, Anetta773, Anusan.rasalingam, Arcadian, Arno Matthias, Beetstra, Blitterbug, Cacycle, Chagai, Chelmite, Christopherlin, ClanCC, Clopsywiki12, DVdm, Da5nsy, Daniel5127, Dcirovic, Delldot, Deltabeignet, Dicklyon, Dinisoe, Diomidis Spinellis, Discospinster, Dr.enh, DrBob, Drzank, Emperorbma, EncMstr, Epbr123, Fangfufu, FisherQueen, Fred Hsu, GcSwRhIc, GideonMarkCabanban, Gobonobo, Helix84, Hellbus, HendrixEesti, Hodja Nasreddin, Iluvcapra, InternetMeme, JTN, Jacobolus, Janet13, Japanese Searobin, Jeltz, Jfdwolff, Jimfbleak, JinJ, JohnOwens, Jwmillerusa, Kgreer, Kittyblue101, Kpjas, KrakatoaKatie, L'œuf, La goutte de pluie, Ligulem, Loladee91, Lucas718, Lysdexia, MXVN, MadCow257, Madhero88, Materialscientist, Meaghan, Metalman94, Mfc, Michał Sobkowski, Nagualdesign, NawlinWiki, NifCurator1, Nisar.a.shaik, Nn123645, Nono64, Notch, PAntoni, Paskari, Pekaje, Peter Karlsen, Ph.eyes, Phynicen, Quiddity, Quota, RedWolf, ReddyVarun, RexNL, Richard001, Rjwilmsi, SMA2012, Sander123, Shawn81, Shehal, ShelllbyF, Slmader, Sluzzelin, Soccer1818, Srleffler, Stbruton, Stefan.loska, Stillnotelf, Tameeria, Tanthalas39, Template namespace initialisation script, The359, Thirumaran13, Tide rolls, Tideflat, TimBentley, Tyw7, UTSCholar, Vanessaezekowitz, Vojtech.dostal, WereSpielChequers, Wikianon, Wikipelli, Xiaoxuey, Yossofz, Youragain, 193 anonymous edits Carotid body Source: http://en.wikipedia.org/w/index.php?oldid=549094927 Contributors: Alansohn, Alex.tan, Arcadian, Bdmed, Bensaccount, Bomac, Brim, Davidhaha, Edward, EncycloPetey, Feral mage, JackWasey, Jag123, Keb ch, LittleHow, MHillyard, Michael Devore, Micol bode, Mikael Häggström, Morleymonkey, Nbauman, Nephron, Nick Number, Pbergson, PizzaofDoom, Rich Farmbrough, Richardcavell, Rutigor, Stevecalloway, Stone, TheAMmollusc, ThinkerThoughts, Trice2010, Vojtech.dostal, Volantares, Washburnmav, Wjeck, ﺯﻳﺎﺩ, 47 anonymous edits Taste bud Source: http://en.wikipedia.org/w/index.php?oldid=551853855 Contributors: 2A01:E35:2EF8:92E0:A0FC:7F0E:79C4:3D2A, A Raider Like Indiana, A. Parrot, Acole5, Aeonx, Ajaxfiore, Akcarver, Alansohn, Alex nadiger, Alexman1713, Allens, Allycat, Anaxial, AndreniW, Aquilosion, Arcadian, ArchonMagnus, Arthena, Aude, Azazyel, Badgernet, Bathysphere, Bazzargh, Belg4mit, Bn, BoomerAB, Brenont, Bucephalus, CWY2190, CWii, Canadian-Bacon, Catherineroxs1, Charlesbridge, Chris G, Christian75, Craptree, DOHC Holiday, Daedalus969, Debresser, DerHexer, Dicklyon, Doit!, Dontkillme, Download, Drewdesouza, EJF, Eclectic hippie, El Pollo Diablo, Electron9, Epbr123, EvanHarper, Eyrian, Faigl.ladislav, Filovirus, FisherQueen, Gaius Cornelius, Garyzx, Geravago, Gilgamesh he, Gilliam, Gongshow, Graham87, Greenwise1025, Habanero-tan, Hajatvrc, Hanumhartanto, Harpi711, Hu, IGeMiNix, Ianthegecko, Igoldste, Isbelja, IvanLanin, J.delanoy, JEB90, Jblavit, Jebba, Jitterro, Jive Dadson, John254, Johnelson, Johnkarp, Jojhutton, Judithreiter, Jutta, Kane61991, Katalaveno, Keenan Pepper, Lazulilasher, LedgendGamer, Lisatwo, Little Mountain 5, Marek69, Mastercampbell, Meaghan, Mendaliv, Mhsia, Miquonranger03, MnSteve, Moe Epsilon, Molerat, Mononomic, Morel, Mr. Anon515, Mr. Wheely Guy, Mycroft.Holmes, NEUROtiker, Natalie Erin, NawlinWiki, Neurograd, NewEnglandYankee, Nick Number, Niente21, NifCurator1, Nihonjoe, Nono64, NotWith, Novangelis, Nrets, Nsaum75, Nuggetmuncher, Omegatron, Orpheo, Parkerjohnson1234567, Pdauwe, Peter Karlsen, PhilKnight, Philip Trueman, Piano non troppo, Pinethicket, Plumbago, Radon210, Raymondwinn, RedWolf, Reedzupancic, Reverend Loki, Rich Farmbrough, Romanm, Ruittenb, Rumilofaniel, Sarrus, Sayeth, Scott182, Scott5834, Sheled Umlal, Silenceisgod, SilkTork, Smalljim, Stephenb, Sulforaphane, Swerdnaneb, TAKASUGI Shinji, TJ09, TYelliot, Tamorlan, Tanbircdq, Template namespace initialisation script, TheCatalyst31, TheKMan, TheRanger, Thingg, Tide rolls, Tim1988, Tinctorius, Tony Fox, Tonyng84, Tristanb, Tsumaru, Ulcha, Utcursch, Velella, W.stanovsky, WikHead, Wikih101, Williamborg, X!, Yowikiiou, 502 anonymous edits Schwann cell Source: http://en.wikipedia.org/w/index.php?oldid=543678692 Contributors: A.Ou, AHMartin, Ahoerstemeier, Amccloy01, Antandrus, Arcadian, Atif.t2, Bender235, Boing! said Zebedee, Brady8, Brainmachine, [email protected], Capricorn42, Carmichael, Carwil, Chalwalk, Chong Lim, Chris Capoccia, Chris53516, Clicketyclack, DanielCD, Delta G, Diberri, Dino, Discworldian, DocWatson42, Drew1515, Edelhart, Edward Vielmetti, Epbr123, Eras-mus, Erxnmedia, FFMG, Faigl.ladislav, Fantumphool, Flowerpotman, Freederick, Funkysapien, Fyrael, Gaius Cornelius, Galmicmi, Giftlite, Gikü, Graham87, Gurch, Hbdgaz, Heatheralleen, Heikolocher, Ian.thomson, Imoen, Interiot, InternetMeme, Iqzaquezzs, J.delanoy, JForget, Jabronimus, Jag123, Jay Litman, Jfdwolff, KasugaHuang, Kauczuk, Kithira, Kmoraros, Kubigula, Kung Midas, Lightmouse, Looie496, MBVECO, Mego'brien, Moreschi, Nbauman, NorkNork, Philip Trueman, RBJ, ResearchRave, Rettetast, Salvadorjo, SchfiftyThree, Selket, Solomonthepornactor, Sryshti, Sub-life, T.M.M. Dowd, TWIXMIX, Taylorjs, Tb81, The Sailor Poet, Topbanana, Tpk5010, Trevor MacInnis, Ucbtbej, Unyoyega, Wayward, WolfmanSF, Woohookitty, Xanzzibar, Xxxx00, 132 anonymous edits Satellite glial cell Source: http://en.wikipedia.org/w/index.php?oldid=549595869 Contributors: Aircorn, Arcadian, Bueller 007, Burgart, Delldot, Drewlew, Garion96, Garrondo, Gdusing12315, Hazard-SJ, ITasteLikePaint, LaurenMalishchak, Manfi, ManfromButtonwillow, Marc Gabriel Schmid, Muhandes, NeuroJoe, NotWith, Rjwilmsi, Serephine, Ytpete, 23 anonymous edits Neuroglia Source: http://en.wikipedia.org/w/index.php?oldid=550288381 Contributors: 2001:18E8:3:1278:E949:89BF:FE91:62E8, 2D, A purple wikiuser, A5, ABF, AJVincelli, AThing, Abanima, Abhishek727, AfroBrazilian, Alansohn, Amry, Angelic Wraith, Angelito7, Anthonyhcole, Arcadian, Arctic Night, Ardonik, ArizonaLifeScience, Atlantia, Bananastalktome, Bashirshir, Bensh, Biocon, Boomtown90, Bruno Pascal, CardinalDan, Christopherlin, Clicketyclack, Consumed Crustacean, CopperKettle, Cory Kohn, Crohnie, Cwbvb13, DARTH SIDIOUS 2, DRosenbach, Dalibor Bosits, DavidBKinnear, DeadEyeArrow, Delldot, Delta G, Dertilman, Detectivefirstgradesamspade1, Diberri, DocWatson42, Drphilharmonic, Dwaipayanc, Dylan2106, Emiellaiendiay, Epingchris, Ewlyahoocom, Faigl.ladislav, Farqual100, Felicipnzln, Feral mage, FireBrandon, Fizzlebug81, Former user, Furmanj, Gilliam, GlialStudent, Hadal, Hazard-SJ, Hu12, Icairns, Idh0854, Ijustam, Izvora, Jag123, James Pioneer, Janakatechno, Jfdwolff, Jo3sampl, JohnDillon, Johnwprior, JordanDeLong, Joseph Solis in Australia, Jrtayloriv, Jutiphan, Kboor, Khmir2467, KnightRider, Knotnic, Kwamikagami, La comadreja, Lightmouse, LittleHow, Looie496, Luke13579, Mac Davis, Marc Venot, Mark Marathon, Marnoldm, MartinPoulter, Mbartz, Meelar, Mercurywoodrose, Merlion444, Michaelbusch, Mikael Häggström, MrADHD, Mrducks122, Mrs.meganmmc, NBeale, NeoNeuroGeek, Nephron, NifCurator1, Nikai, Nikpapag,
609
Article Sources and Contributors
Northamerica1000, Nrets, Omnipaedista, Oobopshark, Pcu123456789, Pianoplonkers, Rjwilmsi, Rodago, Rojypala, RoyBoy, Sayeth, Sbisolo, Seans Potato Business, Seijihyouronka, Setanta747 (locked), Sir48, Skyezx, Slawojarek, Smithbrenon, Snakesteuben, Son0fHobs, Sparkym3, Steiger, Sunnymedia11, TTile, Tarotcards, Tblackma222, Tdc204, TheLimbicOne, ThePI, Thesis4Eva, Three-quarter-ten, ThreeFt, Tiddly Tom, TonyClarke, Trnj2000, Uthbrian, VernoWhitney, Virtual Loïc, Ward20, Wareh, Whitepaw, William Avery, Xris0, Zsinj, Zubachi, ﻣﺎﻧﻲ, Ὁ οἶστρος, 236 anonymous edits Astrocyte Source: http://en.wikipedia.org/w/index.php?oldid=551191836 Contributors: A purple wikiuser, AManWithNoPlan, Abenedik, AnOddName, Anthonyhcole, Arcadian, Auntof6, AxelBoldt, Betacommand, Biologist2001, Blueshirts, Bruno Pascal, Bunnyhop11, Consumed Crustacean, CopperKettle, Danger, DanielCD, Danny lost, Delldot, Diberri, Dicklyon, Dinisoe, Discospinster, Dr.saptarshi, Drphilharmonic, EhJJ, Eleassar, Eleschinski2000, Eng101, Etrielle, Faigl.ladislav, Feral mage, Franamax, Fuzbaby, Helix84, IONTRANSP, Immunize, Iqzaquezzs, Isnow, Jackol, Jag123, Jeffq, John of Reading, Jonathanischoice, Kauczuk, Kernsters, KevinTR, Klemen Kocjancic, Kso3713, La comadreja, Leokhi, Lerion, Liaocyed, LilHelpa, Litanss, Looie496, Lova Falk, Luke poa, M1ss1ontomars2k4, MER-C, Maralia, MarcoTolo, Marnoldm, MaynardClark, Mhisted, MrADHD, MrDomino, Muhandes, Narayanese, Nephron, NeuroWikiProject, Neurorocker, NifCurator1, Nopedia, Northamerica1000, OldakQuill, Overand, PDH, Pdewilde, Philgoetz, Piltech, PlasmaDragon, Probios, Radagast83, Reactiveastrocyte, Rich Farmbrough, Richi, Rjwilmsi, Rob Hurt, Robodoc.at, Rodago, SDC, SKK123, Sameerbau, Sjschen, Sriram sh, Tea with toast, The Banner, ThinkerThoughts, Timur lenk, Tony1, Truthflux, Txdoc13, VMHman, Vogon77, Wavelength, WereSpielChequers, Whitepaw, Wiki emma johnson, Wikipendant, Wikitavanti, Ww2censor, Wynand.winterbach, Xasodfuih, 174 anonymous edits Neuron Source: http://en.wikipedia.org/w/index.php?oldid=550893151 Contributors: .:Ajvol:., 168..., 2A02:2F02:2021:F00A:0:0:4F77:1AB4, A314268, A8UDI, Absinf, Acalamari, Accurizer, Achowat, Acroterion, Adashiel, Addihockey10, AdjustShift, Adrian CZ, Ae77, Aengus, Ahoerstemeier, Alansohn, Alessandro f2001, Alex.tan, Alexandria, Alexrexpvt, Amazedsaint, Amorymeltzer, Amp71, Amry, Anaxial, Andonic, AndreasPDemetriou, Andres, AndresGottlieb, Animalresearcher, Anmats, Anoop2000, Anthere, Anthonyhcole, Appleseed, Arakunem, Arathald, Arcadian, Arvindn, Ascorbic, Ashv3524, Asianguy48, AugPi, AuroraReloaded, AxelBoldt, AzumayaKoyuki, BJEG5, Babybluepearls08, Bandrow, Barthe7ruth, Bcjordan, Bdesham, Beefman, Belinrahs, Benholter:D, Bensaccount, Bentogoa, Bethnim, Bilz0r, BioProfessor2.0, Biology2k, Birdman1, Blajbal, Bobblewik, Bobo192, Bobosse, Bonadea, Bongwarrior, Brackpedia, Bradeos Graphon, Bradv, Brain-mapper, Brandmeister (old), Branka France, Brendan Moody, Brentor, Brianga, BrotherGeorge, Bryan Derksen, Buzzybirdbrain, C-gold, CSS2013, Callisto2091, Caltas, Can't sleep, clown will eat me, CanadianLinuxUser, Canyouhearmenow, Capricorn42, CarsonsDad, Cburnett, Celestra, Cerealkiller13, Chaojoker, Chizeng, ChrisGualtieri, Chrislk02, Chrispounds, Christian75, Cinnamonsticks, Ciphers, Ckatz, Clement Cherlin, Clicketyclack, ClubOranje, CommonsDelinker, Conversion script, Corinne68, Corvana, Courcelles, Cpiral, Crazytales, Crohnie, Ctbolt, Cureden, CursedKiller95, Cyberman, DARTH SIDIOUS 2, Dan East, Dancter, Danger, Daonguyen95, Darkmeerkat, Darkwind, Darth Panda, David Martland, DavidRader, Dbenbenn, DeadEyeArrow, Deflective, Delldot, Delta G, Deor, DerHexer, Desalato, Dettydet, Diberri, Dicklyon, Digfarenough, Dinisoe, Discospinster, Diza, Djayjp, Dolda2000, Dr.Kane, Drakestail, Dreamafter, Dreish, Drifter3, Driftwoodzebulin, Dry dust, Dysepsion, E23, ESkog, Edan Starforth, Edison, Edward Z. Yang, Emilk, Entropy, Epbr123, Evanherk, Excirial, Eykanal, FMRI, Fastily, Feweria, Flami72, Flashn00b, Fletcher, Floating Boat, Former user 6, Foscoe, Frenchman113, Frozin ice, Furmanj, Furrykef, Fuzheado, Gail, Garydino, Gene Nygaard, Geneb1955, Ghidorah221, Giftlite, Gilliam, Gillyweed, Giraffedata, Gkandlikar, Gleng, GoShow, Goldenrowley, Gordyandramsey, Graminophile, GranBianconero, Gregkaye, Gunjan verma81, Gypsydoctor, Hadal, HaeB, Hagerman, Haham hanuka, Hajenso, HamburgerRadio, Hanacy, Hardyplants, Harland1, Headbomb, Helix84, Hellhound overblood, Hempfel, Henrycranfield, Heyyy123, Hithereifixedurblinds, Hm0ngLauj, Hmrox, Holcombea, Hskwk, Hu, Hullaballoo Wolfowitz, I'm really Sweet, II MusLiM HyBRiD II, Iamthedeus, Ian Pitchford, Immunize, Imoeng, Info wrecker, Info wrecker2, Inkling, Interiot, Intranetusa, InverseHypercube, Invinciblegavin, Ioeth, Ipatrol, Iridescent, Ixfd64, J.delanoy, JForget, JPaestpreornJeolhlna, JWSchmidt, JaGa, Jackhynes, Jackibuddy, Jahayes, Jakeiyounis2, Jakejakejake1313, Jameshfisher, Jauhienij, Jawnpiece, Jaxl, Jayden54, Jcbutler, Jdyachimec, Jeff G., JeffreyN, Jenks, Jeroje, Jimgawn, Jncraton, Jo3sampl, John Price, JohnCD, JonathanWilliford, Jschnur, Jumping cheese, Junglecat, Just Another Dan, JustVisiting, Jutta, Jvr725, KCinDC, Kalexander, Kamilvlcek, Karl-Henner, Kashmiri, Katieh5584, Keenan Pepper, Kevin B12, Kghose, Khargas, Khukri, Kingofslackrs, Kingpin13, Kirkus M, Knight1993, Koavf, Kosigrim, Krashlandon, Kuspyder, Kwamikagami, Kwekubo, L Kensington, La Pianista, La comadreja, Lachlan12345, Ladii artiste, Lam Kin Keung, Laracoode, LeadSongDog, LedgendGamer, Leomessi1094, Lexor, Lightmouse, LilHelpa, LindsayH, Linnell, LittleHow, Lji1942, Looie496, Looxix, Lova Falk, Lradrama, Luccas, Lugia2453, Luna Santin, MER-C, MJ94, Macsking, MadScientistMatt, Magnus Manske, Mailforsid4585, Makeemlighter, Male1979, Marc Venot, MarkEchidna, Markan, Martarius, Martian.knight, Maryamjoon, Massimo Macconi, Materialscientist, Mato, Matt Crypto, Matt Hutson, Mav, Maxis ftw, Maz640, Mccready, Mchcopl, Me020, Medlat, Meduz, Memenen, MemoriesFade, Mendaliv, Mentifisto, Meswallen, Mgiganteus1, Michael Hardy, Mikael Häggström, Mikaey, Mike2vil, MikeX, Mikeo, Mikespedia, Miltonkeynes, Mindstalk, Minimac, Miquonranger03, Miserlou, Mitch Cumberworth, Mod.torrentrealm, Mohd. Toukir Hamid, Monotonehell, Moreschi, Moxfyre, Mpatel, Mphi03, MrFish, Mydrian, Mygerardromance, Mütze, NCurse, NPalmius, NaLalina, NawlinWiki, Neurophilia, Neutrality, NewEnglandYankee, NifCurator1, Nihiltres, Nk, Nlu, No1lakersfan, No3, Nolelover, Nomad2u001, Nono64, Northfox, Nposs, Nrets, NuclearWarfare, Numbo3, Odie5533, OldakQuill, Ombudsman, Orangemarlin, Otisjimmy1, OverlordQ, Oxymoron83, PahaOlo, Panoramix303, Panscient, Parker007, Pedroshin, Penwhale, Persian Poet Gal, Pharaoh of the Wizards, PhilKnight, Philip Trueman, PhineasG, Pie Man 360, Pinethicket, Pkatz, Pnkrockr, Pontificalibus, Pr495du, ProBonoPublicoA90, Proofreader77, Pseudomonas, Ptrf, R'n'B, RUL3R, RadioFan, RainbowOfLight, Ramaksoud2000, Randompedia, Rberlow, Redbo, Rettetast, RexNL, Reyk, Rhetth, Rib0fl4vin, Rich Farmbrough, Richwil, Ridge Runner, Rjstott, Rjwilmsi, Robin klein, Robinatron, Robma, Rrichhart, Rror, Rsabbatini, Rukuruku, RussellMcKenzie, Russfrohardt, Ruy Lopez, S.cheese, SJFriedl, SJP, Sabre23t, Saganaki-, Sarah Cherlin, Savant13, Scarian, SchfiftyThree, Schumi555, Schwartz1011, Scott5114, Sel0003, Selket, Setanta747 (locked), Seyet, SgtThroat, Shadowjams, Shame On You, Shattered, Shawdogg12, Shenme, Shock an awe, Silas S. Brown, Silverxxx, Sjschen, Skizzik, Slarson, Smalljim, Snehalshekatkar, Snow Blizzard, Snow.blizzard, Some jerk on the Internet, Someone else, South Bay, SpNeo, SpaceFlight89, SpyMagician, SriMesh, Stain, Stephendcole, Sternthinker, Storm Rider, Strzelczyk, Studentne, Sunray, SuperHamster, SvenGodo, Sverdrup, Synaptidude, Tahome, Tarotcards, Tbhotch, Teles, Terence, Thanhluan001, The Recycling Troll, The Thing That Should Not Be, The.Filsouf, TheEgyptian, TheKMan, TheTechMaester, Theirishpianist, Thingg, Thtraddles, Tide rolls, Tilo1111, Tlork Thunderhead, Tom harrison, Tomwsulcer, Tony Fox, Treisijs, Tryptofish, Twilight Realm, Tylerttts, UA1high, Undercovervision, Varuna, Vetty123, Vina, Vrenator, Vyn, Vyroglyph, Wakebrdkid, Wanderingpeanut, Wavelength, Wdfarmer, Wegener1406, West.andrew.g, Wik, WikiPuppies, Wikicallen, Wikipediawikipedia123, Wikipelli, Williamemersonwood, Wimt, WissensDürster, Woohookitty, Wouterstomp, Wranadu2, Wyoun2, Xargque, Xiahou, Yamamoto Ichiro, Yath, Yerpo, Yettie0711, Yidisheryid, Youandme, Youre dreaming eh?, Yuriy Kolodin, Yvwv, Zach425, Zfaulkes, 1154 anonymous edits Oligodendrocyte Source: http://en.wikipedia.org/w/index.php?oldid=550872701 Contributors: Angela, Anthonyhcole, Anypodetos, Arcadian, Bobblewik, Boghog, BonsaiViking, [email protected], CDN99, Captain-n00dle, Cbsmall1, CecilWard, Clicketyclack, Dabomb87, Delta G, Deltaecho, Deviator13, Diberri, Dicklyon, Dinisoe, Drphilharmonic, EncycloPetey, Faigl.ladislav, Iqzaquezzs, Jag123, Jfdwolff, Jrockit24, Juraska, Kauczuk, Koavf, La comadreja, Ligulem, Looie496, Lova Falk, Lundse, Maria.Kukley, Matthew Kelly, Methoxyroxy, Nbauman, NifCurator1, Nihiltres, OldakQuill, Parker007, R'n'B, RJFJR, Rjwilmsi, Rōnin, Skiron, Smallman12q, That Guy, From That Show!, TheJJJunk, TogetherinParis, Uman1916, Vasiľ, Wiki emma johnson, Wvangeit, Xris0, 77 anonymous edits Spindle neuron Source: http://en.wikipedia.org/w/index.php?oldid=551849656 Contributors: 1000Faces, Acsantis, Aempinc, Aleixalix, Alfio, Armarshall, BD2412, Beckydornon, Bob, Bryan Derksen, Cberry01, CopperKettle, Dr.enh, Efb18, Envygreen333, Ettrig, Eubulides, Gwnucha, Igiffin, Iztwoz, J.delanoy, Javidjamae, Jcarnelian, JoeSperrazza, Joel7687, Jogloran, John Bessa, JorisvS, KenyaSong, Kghose, Khazar2, LittleHow, Lostart, Lotje, Malangthon, Mandarax, Moe33, Neil916, Nephron, NeuronExMachina, Nsnyder, Ombudsman, Pluto888, Pluto988, RDBrown, Rich Farmbrough, Rjwilmsi, SCEhardt, Selket, Southclh, T Long, TedPavlic, Vokesk, Woohookitty, 65 anonymous edits Hepatocyte Source: http://en.wikipedia.org/w/index.php?oldid=549384842 Contributors: Alee2000, AmiDaniel, AndreasJS, Arcadian, Bensaccount, Bentogoa, Bobo192, Bomac, Casliber, Chemya, CommonsDelinker, CopperKettle, Crazysane, Dcirovic, Eleassar, Florian Huber, Franamax, Gibbja, Gogo Dodo, Ilke71, J.delanoy, JackWasey, Jag123, January, Jeffq, Jfdwolff, Jimmyvet, Johncartmell, Kaarel, Kristenq, Ksero, Leuko, MZMcBride, Maelstromm, Mikael Häggström, Mike2vil, Mindmatrix, Nereocystis, Neznanec, NotWith, Ntsimp, Optichan, Pepper, Pinkysnowbunnyco, Quadell, Reo On, ResearchRave, Rhcastilhos, Riana, Rich Farmbrough, Rror, Rsabbatini, SchreiberBike, Sclohr, Scottalter, Seaphoto, Skizzik, StacyMGA, Tarek, Tide rolls, ToNToNi, 97 anonymous edits Adipocyte Source: http://en.wikipedia.org/w/index.php?oldid=542220303 Contributors: AThing, Adipocytes, Agibso02, Alansohn, Arcadian, AvicAWB, BeardWand, Celuici, Ceyockey, Chris Capoccia, Chris b shanks, ChrisGualtieri, Dagilson, Dan Polansky, Dan Wylie-Sears 2, David from Downunder, Devilanna, Dgiroux, Discospinster, Dr R Bowri, Drphilharmonic, Enigma55, Erich gasboy, Essam Sharaf, FallingGravity, Farosdaughter, Franamax, Gadfium, Glacialfox, Godfinger, Golgi, Htniawiki, Ianml, Jag123, Jfdwolff, Jmh649, Kanesue, Kenguest, Kibbles5724, Kj29, Kummi, Lenschulwitz, Livingston7, Lugia2453, Man pl, MarcoTolo, Marek Wagner, Mattimals, Mattisse, Mgiganteus1, Mikael Häggström, Mikeo, Mushin, Offiikart, OlliffeObscurity, Pekaje, RainbowOfLight, Rjwilmsi, Rmky87, SchreiberBike, Senator Palpatine, Settersr, Shmike1, The Anome, Trevinci, Uncle Milty, Useight, Wtmitchell, Xochiyotl, Zephalis, ﺭﺍﻣﻰ ﻣﺤﻤﺪ ﻓﺆﺍﺩ, 98 anonymous edits White adipose tissue Source: http://en.wikipedia.org/w/index.php?oldid=550685173 Contributors: Ageekgal, Annalise, Arcadian, Davebridges, Dikteren, Greensburger, J.delanoy, Jennes83, Lenschulwitz, Locos epraix, MER-C, Marek69, MedicRoo, Smallman12q, The Anome, TheBlueFlamingo, Uncle Dick, WhatamIdoing, 24 anonymous edits Brown adipose tissue Source: http://en.wikipedia.org/w/index.php?oldid=547226098 Contributors: Ageekgal, Aiken drum, Albmont, Alex.tan, Amaury, Apoyon, Aragorn2, Arcadian, Arolla, Auric, Boligoma33, Btwied, Bundas, Choij, Christopherlin, CyborgTosser, Daycd, Dogcow, Drphilharmonic, Edgar181, Eteq, Fat7926, Fredrik, Froggo Zijgeb, Fuzbaby, Gaijin42, Georgexu316, GhBatt, Ghosts&empties, Hanacy, Hg6996, Iceanimal, Islam Ezzat, Jag123, Jennes83, Kompas, Kroonepedia, Lenschulwitz, Lijnema, Macetw, Mcstrother, Middayexpress, Mikael Häggström, Mindmatrix, Mr.Rocks, Nbauman, Neil916, Nephron, Pmj, RDBrown, Ricky81682, Riley Huntley, Rjwilmsi, Ruakh, Sanbeg, SharkinthePool, Shingij2, Solvig, StN, Sumo.fatty, Susan118, TastyPoutine, The Anome, Thetrick, TimVickers, Trevinci, Tristanb, Triwbe, Uriel8, Wik, Williamb, Wknight94, Wkrocek, Wouterstomp, Xaosflux, Yamamoto Ichiro, Zer0faults, 111 anonymous edits Hepatic stellate cell Source: http://en.wikipedia.org/w/index.php?oldid=540453653 Contributors: Arcadian, Aukbc, CHARGERLEVANI, Cmcnicoll, CopperKettle, Hodja Nasreddin, Luckydhaliwal, Micga, Rjwilmsi, Temporaluser, Wikielwikingo, Xbcj0843hck3, 3 anonymous edits Podocyte Source: http://en.wikipedia.org/w/index.php?oldid=540670355 Contributors: Adeez, Alperen, Arcadian, Broississy, CheekyMonkey, CopperKettle, Delldot, Diberri, Dpyeon, Eleassar, Franamax, Ganymead, Hadal, IONTRANSP, Iwilcox, Jared81, Jestr, Jorvik29, KC Panchal, Kerowyn, M.Komorniczak, Merfles, Nbauman, Nephron, Papa November, Rhcastilhos, SchreiberBike, Scottalter, Spaully, Swaq, 25 anonymous edits
610
Article Sources and Contributors
Proximal convoluted tubule Source: http://en.wikipedia.org/w/index.php?oldid=550412524 Contributors: A2Kafir, Animeronin, Arcadian, Arthena, Bensaccount, Clicketyclack, Diberri, Drphilharmonic, Evox777, Figma, Fullstop, Gangsterls, GermanX, HeavyQuark, Insorak, Kar.ma, Leolaursen, Mark Richards, Mba123, Mcstrother, Mfwitten, Mikael Häggström, Nephron, Nerdseeksblonde, Pearle, Petesmif, Ph.eyes, R'n'B, Rjwilmsi, Robert.Allen, Scottalter, Skittleys, Spaully, Vwslee, 34 anonymous edits Thin segment Source: http://en.wikipedia.org/w/index.php?oldid=504694966 Contributors: Beeswaxcandle, ChrisGualtieri, Haruth, Ju97les, LilHelpa, Mikael Häggström, Neo1738, 1 anonymous edits Distal convoluted tubule Source: http://en.wikipedia.org/w/index.php?oldid=540846268 Contributors: Aaron Schulz, Alex.tan, Arcadian, Axl, Barefootguy, Beeswaxcandle, Bensaccount, Betacommand, Diberri, GermanX, ImmortalWombat, Jfdwolff, Kuebi, Mcstrother, Mikael Häggström, Mild Bill Hiccup, Nick Number, Nlu, Platysma, PneumaShack, R'n'B, Scottalter, Selket, Spaully, Szalzala, Topbanana, UberMD, WhatamIdoing, 34 , יונה בנדלאקanonymous edits Kidney collecting duct cell Source: http://en.wikipedia.org/w/index.php?oldid=197597645 Contributors: Carlossuarez46, Mikael Häggström, TexasAndroid Pneumocyte Source: http://en.wikipedia.org/w/index.php?oldid=544226953 Contributors: 5-HT8, AkashAD, Alynna Kasmira, Arcadian, Audry2, Bissinger, BubNorr, Caerwine, Can't sleep, clown will eat me, Delldot, Eras-mus, Franamax, Justin.ere, Kilopi, Mj455972007, Mkdw, Nlu, Samith senadeera, Tomas e, Uncle G, Unused0026, Vkotelnik, Vojtech.dostal, Waldmas, 20 anonymous edits Centroacinar cell Source: http://en.wikipedia.org/w/index.php?oldid=544575160 Contributors: Arcadian, Beeswaxcandle, Caerwine, Eikenhein, Franamax, Jebus989, Kazkaskazkasako, Mcstrother, Mikael Häggström, Oxynthes, 5 anonymous edits Collecting duct system Source: http://en.wikipedia.org/w/index.php?oldid=551047419 Contributors: Alex.tan, Arakin, Arcadian, Bensaccount, Bloodshedder, Bogwhistle, Camrn86, Diberri, Drphilharmonic, Drpickem, Eighty8s finest, Enqueror, Enviroboy, Eug, Faduart, Felix-felix, Hoverflysmiles, Hpswimmer, Jfdwolff, Ksaraf, Luckydhaliwal, Materialscientist, Mcstrother, Mikael Häggström, NeilN, Nlu, OldakQuill, Rswarbrick, Ryan Roos, SchreiberBike, Scottalter, Some jerk on the Internet, Spaully, Temporaluser, Welsh, Wikid77, Xionbox, 28 anonymous edits Microvillus Source: http://en.wikipedia.org/w/index.php?oldid=549393530 Contributors: AK456, Alansohn, Angela, Arcadian, AxelBoldt, Belasd, Bensaccount, Bobblewik, Bruinleth, Capricorn42, D, Daf, Dan Gluck, Defwheezer, Deryck Chan, Diberri, Dromioofephesus, Droseratron, Elassint, Frby, Gobonobo, Grover cleveland, Hac13, HandGrenadePins, Hyungjoo98, Hégésippe Cormier, Jag123, Kaarel, Lavateraguy, Maaayowa, Madkayaker, Magnus Manske, Martious, Mh, MrBeeAreWhy, PFHLai, Penghaiyanwiki, RShorty30, Razor Sharp Wisdom, Reyk, Rhys, Robin S, Sarefo, THExGunsliner, Taketa, Thewikipopo, Vojtech.dostal, Wavehunter, Wbensmith, William Avery, Zchangu, 94 anonymous edits Epididymis Source: http://en.wikipedia.org/w/index.php?oldid=551506291 Contributors: 78.26, Abstraktn, AdaronKentano, Anatomist90, Anaxial, Arc Orion, Arcadian, Arjun01, BarkingFish, Biglovinb, Chanlyn, Chevapdva, Chinux, Chris the speller, Cmungall, Deflective, Diberri, Drphilharmonic, Dungodung, Ekem, Flyer22, Fredwerner, Freedomlinux, Fui in terra aliena, Georgette2, Giancoli, Guaca, Guanaco, Hadal, HexaChord, Hkarim19, Hyperborea13, Jabaway, Jag123, JakobSteenberg, Jauerback, Jim1138, Jmarchn, Jpogi, KDS4444, Kauczuk, Keith D, Kwamikagami, LeCire, Lexusuns, LilHelpa, Magioladitis, Mani1, Matt Gies, Mcstrother, Minimac, Naturehead, Nbarth, Nephron, Nsaa, Osnimf, PaddyM, Paul venter, Porcher, Pwjb, Ramurf, Raul654, Red Act, Remember the dot, Robodoc.at, Romanm, RupertMillard, Rushbugled13, Snalwibma, Squids and Chips, Stevenfruitsmaak, Szquirrel, Tameeria, Template namespace initialisation script, The Anome, Vedran12, WLU, Whkoh, Yefi, 100 anonymous edits Ameloblast Source: http://en.wikipedia.org/w/index.php?oldid=540323911 Contributors: Acroterion, Adamlankford, Arcadian, Billyb, Chris Capoccia, DRosenbach, El guanaquito, ElfQrin, Enochlau, Footballfan190, Franamax, Headbomb, InvictaHOG, Jacek FH, Jfraser, Michael Hardy, Nuck3lz, Prasun Dubey, RandomP, Sn0wflake, Zocky, 21 anonymous edits Organ of Corti Source: http://en.wikipedia.org/w/index.php?oldid=539772168 Contributors: A314268, Ahoerstemeier, Albacore, Anlace, Arcadian, Arco de Rayne, Bensaccount, Bobbyphysics, CDN99, Chinasaur, DiMare, Dicklyon, DreamGuy, Eleassar, Fred the Oyster, Granito diaz, Guidod, Gyll, Hashem sfarim, Iqzaquezzs, Jabencarsey, Jmarchn, KnightRider, LeadSongDog, Madhero88, Mangoe, Mgrati, Myocastor, Oarih, OldakQuill, Owen, Paul venter, Peytonio, Plindenbaum, R oshea, RelentlessRecusant, Sweetpoet, Template namespace initialisation script, Was a bee, 38 , ליאורanonymous edits Corneal keratocyte Source: http://en.wikipedia.org/w/index.php?oldid=543868054 Contributors: Arcadian, BD2412, CopperKettle, Ringbang, Rjwilmsi, 2 anonymous edits Tendon cell Source: http://en.wikipedia.org/w/index.php?oldid=488310503 Contributors: A412, Arcadian, Barisal, Chris the speller, Ka Faraq Gatri, Te pukapuka, 2 anonymous edits Bone marrow Source: http://en.wikipedia.org/w/index.php?oldid=551927095 Contributors: AThing, Acdx, Airplaneman, Aitias, Alansohn, Alex.tan, Alexwcovington, Allycat0527, Amroc, AnakngAraw, Angela, Angelito7, Angryshot, Arakunem, Arcadian, Ashadeofgrey, Ashcraft, Astanhope, Aveekbh, AxelBoldt, B9 hummingbird hovering, Baylaurel, Before My Ken, Bejnar, Biomed10, Bjb, Blanchardb, BlueDevil, Blueronin, Bme206timewasting, Bobjgalindo, Bobo192, Bogey97, Boing! said Zebedee, Borbrav, Bz2, COMPFUNK2, CapitalLetterBeginning, CatherineMunro, Catongue, Cburnett, Ceclaeys, Ched, Cholerashot, Chris G, Clarkcj12, Cliff smith, Connormah, Corti, Courcelles, Cpl Syx, Crystallina, Curb Chain, Cxz111, Cybermaniac sachit, Cyrus XIII, DARTH SIDIOUS 2, Danno uk, Deor, Diberri, Discospinster, DiverDave, Diyar se, Dr Aaron, Dr d12, Draalles, Dreadstar, Drphilharmonic, Dysprosia, ERK, Enviroboy, Eras-mus, Erkcan, Erlenmayr, Everard Proudfoot, Excirial, Falcon8765, Fbarw, Fernando S. Aldado, Flowerpotman, Freekozak, Friginator, Funnyfarmofdoom, Fvasconcellos, G Clark, GT5162, Gadriel, Gaff, Gareth Griffith-Jones, Gaurav1146, GehfREE8, Germet, Giftlite, Gigemag76, Gimboid13, Glimz, Gongoozler123, Gregorius Pilosus, Gronky, Gsp8181, Gunkarta, Guðsþegn, Hadal, Hanacy, Haydnaston, HendrixEesti, HexaChord, Hobartimus, IRP, Ifrit, Igoldste, Immunize, Iph, Isfisk, Ish ishwar, IvanLanin, J.delanoy, JMD, Ja 62, JackWasey, Jackfork, Jag123, Jauhienij, Jbergste, Jcbvsn, Jctcool1, Jean.artegui, Jengod, Jfdwolff, Jncraton, Joehall45, Joewright, Johan1298, John, JohnCD, Jordan117, Julesd, Jóna Þórunn, Kandar, Katalaveno, KateSelik, Keilana, Keith Lehwald, Kerowyn, Kim298, King Pickle, Kinotgell, Kukini, L Kensington, Larsobrien, Lateg, LeaveSleaves, Les boys, Lesgles, LiDaobing, Lightmouse, LindsayH, Linzhoo2u, Little Mountain 5, Logan, LordCo Centre, LorenzoB, MER-C, Mad Max, Majorly, Malcolm Farmer, Malvineous, Maralia, Marek69, Marimberito, MarsRover, MastCell, Matthew Yeager, McSly, Michaelmas1957, Mikael Häggström, Mintleaf, Missionary, Monedula, Mononomic, Mr.Z-man, Mysid, Naddy, Nagy, Namayan, Natpowning, NellieBly, Newyowker, Niceguyedc, Nihiltres, Nono64, Notheruser, Nunh-huh, Occono, Oda Mari, Ohnoitsjamie, OliverHovmand, OohBunnies!, Optimist on the run, Otend, OverlordQ, Pacifist, Papercliper, Parent5446, Park3r, Pascal666, Patxi lurra, Persian Poet Gal, Peruvianllama, Phantomsteve, Pharaoh of the Wizards, Philip Trueman, Pinethicket, Polyamorph, Prashanthns, Pyrrhus16, RA0808, RJaguar3, Rachgia, Radon210, Raidon Kane, RandomAct, Registrar, Renato Caniatti, Res2216firestar, Rexbobo, Rklawton, Rkoiym, Roadmr, Robert M. Hunt, Rpm099, Russianplayer, Ryan032, SMC, Satarnion, Sceptre, Schrödinger's Cake, Scruffymmh, Seforadev, ShadowRangerRIT, Shadowjams, Shendar, SimonD, Sjones23, Slakr, Smartse, Smith11v, Socialmediarox, SohanDsouza, Sokching, SonicAD, Splatg, Stevencho, Stevenfruitsmaak, Svick, Syrthiss, TallNapoleon, Teles, Template namespace initialisation script, Tetracube, Tgeairn, Thatguyflint, The High Fin Sperm Whale, The Thing That Should Not Be, Theda, Thehelpfulone, Themfromspace, Thumperward, Tide rolls, Tired time, Tombliboo, Tombomp, Trusilver, U+003F, Uncle G, Venkatesh, Versus22, Vina, Vivio Testarossa, Vldscore, Vulturejoe, Wackjum, Waggers, Washburnmav, Wayiran, WhisperToMe, WhyBeNormal, Wiki13, Workster, Wouterstomp, Wtmitchell, Xxpor, Yidisheryid, Zack325, Zahakiel, Zenwhat, Zoe, Zuky79, Žiedas, Дарко Максимовић, 663 anonymous edits Reticular connective tissue Source: http://en.wikipedia.org/w/index.php?oldid=548534937 Contributors: Arcadian, Beyond My Ken, Bobjgalindo, C.man8, CIreland, CarolP52, Cst17, Darkness Shines, Drahcir, Garion96, Guthrie, Jennes83, Jfdwolff, Kushpatel141289, Macholl, Magairlin, Malcolma, Mgiganteus1, Mikael Häggström, R. S. Shaw, Robert M. Hunt, The cattr, Widefox, Zrenneh, 37 anonymous edits Fibroblast Source: http://en.wikipedia.org/w/index.php?oldid=550367186 Contributors: -- April, Altenmann, Andre Engels, Appraiser, Aqua112233, Arcadian, ArionVII, Asdasder, AxelBoldt, Bensaccount, Biologist2001, Bomac, CTF83!, Cacycle, CardinalDan, Cerealkiller13, Chibi.akutenshi, Ciar, Colin, Corvus cornix, Darked, Dfrg.msc, Dr.saptarshi, Dravecky, El C, EnglishEfternamn, Epolk, Essam Sharaf, FBW, Franamax, Godering, Hendrik Fuß, Holme053, Ibrmrn3000, IvanLanin, J.delanoy, Jag123, Jhfortier, Jitterro, JohnnyCalifornia, Jsc83, Ka Faraq Gatri, Keegscee, KnightRider, Kubigula, Lab-oratory, Leeearnest, Light current, Lir, Mbarden, Mikael Häggström, MithrandirAgain, MuffledThud, Mygerardromance, Nilmerg, Professor marginalia, Robert M. Hunt, Roidroid, Ryddragyn, Sbisolo, Seans Potato Business, Shadowjams, Splette, SubtleGuest, Temporaluser, The Wordsmith, TheLimbicOne, Tide rolls, Tijmz, Tinz, Trevor MacInnis, Wavelength, Wedian, WhatamIdoing, 123 anonymous edits Pericyte Source: http://en.wikipedia.org/w/index.php?oldid=545715839 Contributors: AS, Arcadian, Artw, BD2412, Bloomingdedalus, CarolinaBookHound, Choino, Chrysaor, CommonsDelinker, Dietzel65, Dr Aaron, Drphilharmonic, Eperotao, Eug, Franamax, GSMcL, Hazard-SJ, Jamesdalton67, Jfdwolff, John of Reading, JorisvS, Kuebi, Leeafe, Leeearnest, LewisCS13, LightBringer, MBob, Meneswa, Mild Bill Hiccup, Mistamoneill, Musicmojo, NeuroJoe, PathGrad, Pdauwe, PhiJ, Qetuth, RDBrown, RJFJR, RNAlovesDNA, Rhcastilhos, Rjwilmsi, Robert M. Hunt, Rod57, SchreiberBike, Stepa, TimBentley, Vegaswikian, 50 anonymous edits Nucleus pulposus Source: http://en.wikipedia.org/w/index.php?oldid=542550199 Contributors: A314268, Arcadian, BullRangifer, Cmcnicoll, Cyberknife, EncycloPetey, Fuzheado, Greensburger, JakobSteenberg, Mmrruugg, Sci0x, Spiegelberg88, Wouterstomp, 5 anonymous edits Cementoblast Source: http://en.wikipedia.org/w/index.php?oldid=550436489 Contributors: Ano-User, Arcadian, Brim, Daniel Mietchen, Dozenist, Franamax, Gsingh, Iridescent, Jeffq, Logical2u, Nicolas1981, Serephine, Susesisa, WTucker, 8 anonymous edits Odontoblast Source: http://en.wikipedia.org/w/index.php?oldid=540254983 Contributors: 2004-12-29T22:45Z, Arcadian, BD2412, Bemoeial, Chikiss, CopperKettle, DRosenbach, Doulos Christos, Dozenist, Drano, ElfQrin, EncycloPetey, Gsingh, He Takes A Whiskey Drink He Takes A Cider Drink, Icelight, JamesAM, KMT, Kaarel, Khukri, Mac2664, Mentifisto, Rjwilmsi, Smith609, Supten, Thomas Willerich, TimBentley, WhisperToMe, Wiki alf, 24 anonymous edits
611
Article Sources and Contributors
Hyaline cartilage Source: http://en.wikipedia.org/w/index.php?oldid=551818782 Contributors: Anatomist90, Anthonyhcole, Arcadian, Barticus88, Calaka, Ck lostsword, Credema, Cyrius, Darklilac, Discospinster, Drmies, Epbr123, Fama Clamosa, Footprintx, Ganímedes, Ghirlandajo, Ibrmrn3000, Jagun, Jeff G., JeffreyN, Jennes83, Jmh649, Joshua Scott, Ka Faraq Gatri, MaxSem, Mcstrother, Millermk, Milton Stanley, Mr.Atoz, Mrfordsclass, Name5555, NickCT, Quique H., RainbowOfLight, Riana, Robert M. Hunt, Slysplace, Tgxstudent, Tormentwriter, Who then was a gentleman?, Wikiuser100, 52 anonymous edits Fibrocartilage Source: http://en.wikipedia.org/w/index.php?oldid=546967169 Contributors: Arcadian, ArinArin, Caerwine, Caps tiki, Docfaust, ELLusKa 86, Gobonobo, Jag123, Jennes83, John of Reading, Lir, Mehmet Karatay, Naraht, Nephron, Niceguyedc, RainbowOfLight, River1791, SchreiberBike, Sovbeos, Sxoa, 春 秋 君, 26 anonymous edits Chondrocyte Source: http://en.wikipedia.org/w/index.php?oldid=539671091 Contributors: 2004-12-29T22:45Z, Apers0n, Arcadian, Arostron, Ceyockey, ChadyWady, Cquan, Davidhaha, Eras-mus, Faldizzle, Figma, Franamax, GB fan, Htniawiki, Icairns, Iridescent, Jag123, Ka Faraq Gatri, Kerrigm, Lauranrg, Lemchesvej, Lystrablue, Ncirillopenn, Nibbs06, Nonantum, Robert M. Hunt, Suraj514, The Anome, ThisIsAce, Vojtech.dostal, Ydriuf, 29 anonymous edits Osteoblast Source: http://en.wikipedia.org/w/index.php?oldid=542955391 Contributors: AS, Adrian J. Hunter, Ajlimroen, Arcadian, Astaroth5, Bme206timewasting, Bpat, Brghntr, Cellpath, Checkenpox, Chris 73, Cquan, DRosenbach, Daa89563, Danfa1971, Dawibo, Dr Aaron, Dr. Matteo, Eeekster, Evenios, Fama Clamosa, Firien, Fluffybun, Flute138, Franamax, Freshlysqueezedorangejuice, GAThrawn22, Gabbe, Gabriel Caponetti, Gadfium, H Padleckas, Igoldste, Infrogmation, J36miles, Jag123, Jeff G., Jesanj, Jfraser, Joehall45, Jonemerson, Kinaro, Lemchesvej, Lir, Lockeownzj00, Manuel Anastácio, MasterOfThePuppets, Materialscientist, Moe Epsilon, NawlinWiki, Ncirillopenn, Nephron, Nicke L, Nuttycoconut, Paul 012, Paulkappelle, Peterjanbroomans, Remuel, ResearchRave, Robert M. Hunt, Roboy600, Shibboleth, Stillnotelf, Tameamseo, TheAMmollusc, Tjc, Utcursch, Vojtech.dostal, Wbensmith, Wireddevin, Yacine lil, 116 anonymous edits Osteocyte Source: http://en.wikipedia.org/w/index.php?oldid=543869916 Contributors: Aleashisa, Arcadian, Bluedustmite, Bomac, Brim, Bubbachuck, Bueller 007, Buxtor, Carre, Cellpath, Ceyockey, Coemgenus, DarkFalls, DroEsperanto, Elassint, Epbr123, ForcaForte, Franamax, Fryed-peach, Gadfium, Giftlite, Glane23, Grendelkhan, IRP, InsufficientData, Irbisgreif, Jag123, James McNally, JamesAM, Jameswcheng, Jll, Katychatel, Kdammers, Lbbzman, Lesnail, Lexor, Mcshadypl, Pal5017, Pinar, SchreiberBike, Skicavs, Tameamseo, Tide rolls, Tox, Zink53, 98 anonymous edits Stellate cell Source: http://en.wikipedia.org/w/index.php?oldid=551185417 Contributors: A314268, Arcadian, Bilz0r, Cmcnicoll, Dicklyon, Dinisoe, Franamax, Histomaster, Jaysunn, Minghong, Niceguyedc, NifCurator1, Nikopoley, Roadnottaken, Temporaluser, 11 anonymous edits Skeletal striated muscle Source: http://en.wikipedia.org/w/index.php?oldid=550383579 Contributors: 5 albert square, AHands, Abmac, Acgator09, AerobicFox, Alanstorph, Alphachimp, Amalas, Amalva, Andycjp, Animum, Anthonyhcole, Antiuser, Arcadian, Armin123321, Asenine, Autocracy, Bc789, Ben Ben, Bender235, Bhadani, Biolady101, Bluerasberry, Bms766, Bobo192, Bogey97, Boijunk, Butko, Caltas, Capricorn42, Ccouper, Centurioncode, Chris the speller, Cinkapp, Corruptcopper, Csari, Cumulus Clouds, Cutler, D. Webb, DJ Creature, DRosenbach, DVD R W, DVdm, Dannyyyyyyy, Dante Alighieri, DeadEyeArrow, Delldot, Deon, DerHexer, Diberri, Discospinster, Djinn112, Doug4, Download, Dsyme, Ekren, ElKevbo, EncycloPetey, Enviroboy, Epbr123, Excirial, Flyer22, Foxj, Frankdushantha, Frigotoni, Fyyer, Fæ, Gacggt, Gautehuus, Gciriani, Gcm, Gogo Dodo, Gongoozler123, Gökhan, HCA, Hadal, Hayabusa future, Hectorthebat, Henry W. Schmitt, Horiavulpe, Ingridmfgjelstad, J.delanoy, JDP90, Ja 62, JakobSteenberg, Jan eissfeldt, Jannelliburganduli, Jennes83, Jeremykemp, Jewk, Jjron, Joe Jarvis, Joec456, Juliancolton, Junglecat, Jy, KBworker, Kalaiarasy, Kam012069, Kbdank71, Keilana, Kevin12xd, Kingturtle, Klilidiplomus, Knass097, Kupirijo, Kwertii, L Kensington, Lamaybe, Leeearnest, LimoWreck, Lir, Lowhp1995, Luigifan, Lunettes, MacGyverMagic, Maghnus, Mandarax, Massobusa, Mayur, McSly, Mdecha pup, Measly Swan, Mentifisto, Michbich, Mike Rosoft, MikeJ9919, Mintleaf, Mondeen, N5iln, Nagara373, Naonaonao, NawlinWiki, Neptune5000, Nic tan33, NightFalcon90909, Nightenbelle, Nlu, Nutriveg, O, Oldelpaso, OllieFury, Orphan Wiki, Osm agha, Passw0rd, Patriarch, Pdcook, Peaceduck, Physicistjedi, Physta, Pietaster, Postglock, PranksterTurtle, Profipix, Quailman, RDBrown, RJaguar3, Raul654, Razorflame, Rcf86, Rdsmith4, Reaper Eternal, Redrvm, Rinasoetanto, Robinrhysjones, Rsrikanth05, Rudolf.hellmuth, Ryulong, Sarah sofía, Satellizer, SchnitzelMannGreek, Seaphoto, Segv11, Shanmugamp7, Shin a imai shin, Shira Ronen, Shirulashem, Shreyas4tejas, Shyran, SimonP, Sisyphustkd, Skittleys, Smajie, Smettems, Smr1, Snillet, Someguydude, Spitfire ch, Squire of the Infernal Knight-Lord of Penguins, StAnselm, Stephenb, Storm Hawk, Swid, T456, Template namespace initialisation script, Tempodivalse, Temporaluser, The Haunted Angel, The Thing That Should Not Be, TheTrojanHought, Thingg, Tideflat, Titodutta, Topbanana, Tskuzzy, Ukuk, Uncle Dick, Useight, Vanished user 2340rujowierfj08234irjwfw4, Versus22, Vojtech.dostal, Vrenator, WLU, WOSlinker, Weregerbil, Wik, WikHead, Wikidudeman, Wikipelli, William Avery, Wisdom89, Wknight94, World, XaosBits, Xolom, Y12J, Yahia.barie, Zalgo, 547 anonymous edits Nuclear bag fiber Source: http://en.wikipedia.org/w/index.php?oldid=430772631 Contributors: Arcadian, Dryman, EncycloPetey, FvdP, Livetolearn, Murdochious, Riana, RxS, Some standardized rigour, WikHead, 4 anonymous edits Nuclear chain cell Source: http://en.wikipedia.org/w/index.php?oldid=455015428 Contributors: 1ForTheMoney, Abhih, Chase me ladies, I'm the Cavalry, Franamax, Kel71194, Martijn Hoekstra, Tony1 Myosatellite cell Source: http://en.wikipedia.org/w/index.php?oldid=550903959 Contributors: Arcadian, Asafdar, Bueller 007, Bunnyhop11, Denni, Dilbert2000, Dinisoe, Dr Aaron, EoGuy, Ettrig, Kenmcl2, Mandarax, Manfi, MaxEnt, NifCurator1, Nospamboz, Pandnh4, RDBrown, Rich Farmbrough, Rjwilmsi, StanfordProgrammer, Thomasehall, 54 anonymous edits Cardiac muscle Source: http://en.wikipedia.org/w/index.php?oldid=550669283 Contributors: 2001:558:6045:A0:391F:B005:179D:8DD9, 2602:306:32C3:3430:81D0:82CA:40FD:54ED, 890bhuiop, ABF, Abanima, Achowat, Adh30, Ahoerstemeier, Allstarecho, Altaïr, AnOddName, Andre Engels, Arcadian, Bananastalktome, Bazza1971, Ben Ben, BigPimpinBrah, Bill37212, Binary TSO, Bmord, Bongwarrior, Bubbachuck, Butterfly reflections, Caltas, Carioca, Carlwfbird, Cbass007, Cburnett, Ckatz, Codetiger, Crinoidgirl, CrookedAsterisk, DRosenbach, DVdm, Daniel Mietchen, Danielil, Daonguyen95, Diberri, Discospinster, DjMD, Dreadstar, Drgarden, Drphilharmonic, Dudefromlastnight, Duncharris, Dycedarg, DéRahier, Eeekster, EhJJ, Enlil Ninlil, Epbr123, Eric-Wester, Excirial, Fieldday-sunday, Figma, Frammo, Freedomlinux, Fumitol, G.Kiruthikan, GVOLTT, GeneralCheese, Gfoley4, GgKfc, Gimmetrow, Gisse, Glenusa, Gobonobo, Grade4, Greensburger, Gurch, Guybrush007, Hasha100, Headbomb, Henrik, Hob, Ibrmrn3000, Innkeeper7, Island Monkey, J.delanoy, J04n, Ja 62, JackWasey, Jag123, Jake Wartenberg, Jakob Theorell, JamesBWatson, Jannelliburganduli, Jcaraballo, Jeangabin, Jennes83, Jess Milonaw, Jholman, Jkl, Joehall45, John Elson, JohnJohn, JohnWheater, Johnelson, Jojhutton, Jonah22, JoostyBoy, Joshmo4, Kadellar, Kaitlinnicoleholland, Kayleebabygrl, Keegan, Keilana, Kevin Dorner, Ksheka, Kukini, Kyoko, Latka, Laurasaccount, Lbeben, LedgendGamer, Lir, Lupin, Lynntyler, MER-C, MITBeaverRocks, Madhero88, Manticore, Marek69, MarkkuP, Marshmellis, Mbcannell, McGeddon, Mentisock, Meters, Michbich, Mininbettyinthelrc2k3, Mkikkawa, Movyn, Mr.kornrow, Mschel, Mygerardromance, Nilfanion, Nlu, Optichan, Oscopz, Osnimf, PFHLai, Persian Poet Gal, Peter Fleet, Peter.C, Philip Trueman, Physicistjedi, Pinethicket, PlaydohIsSalty, Ppntori, QuiteUnusual, RDBrown, Rawrr-becky, Red Director, Relleh22hctac, RexNL, Richhead, Rjwilmsi, Rob Hurt, RodC, Ronhjones, Ronz, SV Resolution, Sadads, Schzmo, SciGuy013, Shakiestone, Skizzik, Smajie, Snoyes, Spitfire ch, Stifle, Studerby, Supernovvva, Teenboi001, Template namespace initialisation script, TerraFrost, Tgeairn, The Deviant, The Thing That Should Not Be, TheKMan, TheProject, Thine Antique Pen, Thingg, Tiggerjay, Tijuana Brass, Tropboy, Ttony21, Ukexpat, Verbum Veritas, Vericuester, Versus22, Vinsfan368, Vrenator, W guice, Wavelength, William Avery, Wimt, Wisdom89, Woohookitty, Wtmitchell, Zad68, 533 anonymous edits Purkinje fibers Source: http://en.wikipedia.org/w/index.php?oldid=551464161 Contributors: Acgator09, Arcadian, Captain-n00dle, ChrisGualtieri, CommonsDelinker, Dcfleck, DocElisa, Downtowngal, Drphilharmonic, Edward, EerieNight, Emilyrader, Giftlite, Hadal, Hojasmuertas, Iohannes Animosus, Jusdafax, Jusses2, Kauczuk, Ksheka, Kums, Lbeben, Madhero88, Mikael Häggström, Nathanael, PFHLai, PaddyM, Qertis, Raghith, Rich Farmbrough, Rich257, Rob Hurt, Snek01, Some standardized rigour, Suffusion of Yellow, Synchronism, Template namespace initialisation script, Tevildo, Tracylau1223, West.andrew.g, Whitepowa69, 52 anonymous edits Smooth muscle tissue Source: http://en.wikipedia.org/w/index.php?oldid=551607493 Contributors: 28421u2232nfenfcenc, AManWithNoPlan, Abce2, Acalamari, Acroterion, Alansohn, Alex.tan, Alias Flood, Allens, Anarchivist, Andres, Andycjp, Animum, Anna Lincoln, ApocryphalAuthor, Arcadian, Axfangli, Axl, Backslash Forwardslash, BananaFiend, Blethering Scot, Bluemonkey33, Bobo192, Bogey97, Bolipapel, Boonshoft2013, BozoTC, Brianga, Bryan Derksen, Calaka, CanadianLinuxUser, Carlos T. Blackburn, Cburnett, Chaldor, Chip123456, Choess, Chris 100487, Chris the speller, Cleanupman, Clicketyclack, Cpl Syx, Cremepuff222, Cyfal, DARTH SIDIOUS 2, DRosenbach, DanielRigal, Dark Lord of the Sith, Dark Tea, Daven200520, David D., Decembermouse, DerHexer, Diberri, Discospinster, Download, Drphilharmonic, Dysepsion, EPM, Edgar181, Eivind F Øyangen, Elassint, Eleassar777, Emperorbma, EncycloPetey, Enigmaman, EoGuy, Epingchris, Epothes, Escape Orbit, Falcon8765, Fieldday-sunday, Finlay McWalter, Fishnet37222, Floria L, Frankenpuppy, GetAgrippa, Giftlite, Gz33, HamburgerRadio, Hamiltondaniel, HexaChord, Hey112, Hgcoolz23, IceDragon64, Ilyushka88, Indosauros, Ita3aai, Ivan.vukovic, J.delanoy, JWSchmidt, Jake Wartenberg, Jakob Theorell, JakobSteenberg, Jamesooders, Jamesters, Javawizard, Jennes83, Jeoth, Jfdwolff, Joehall45, John of Reading, Johnelson, Jojhutton, Joshuagross, Kbh3rd, Kevin Rector, Kyoko, LLDMart, Laggard, Lateg, Laug, Leeearnest, LilHelpa, Liorkaplan, Lir, Loyalgadfly, Lrunge, MTKKirkcaldie, Maayaah, Marek69, Mean as custard, Michael Hardy, Mig174, Mikael Häggström, Mkweise, Moilleadóir, Mttcmbs, Mudiej10, NawlinWiki, Nekitsune, NellieBly, NewEnglandYankee, NotWith, Nothingmore Nevermore, Notmanning, Numbo3, Ocaasi, Off2riorob, Oliphaunt, OllieFury, Omicronpersei8, Oxymoron83, PHNX22, PaddyM, Pdavis24, Persian Poet Gal, PeterSymonds, Pharaoh of the Wizards, Phil Boswell, Philip Trueman, Physicistjedi, Polarlys, QVanillaQ, Qooth, R'n'B, Ready, Redpriest187, RexNL, Rhetth, Riana, Richard0612, Rjwilmsi, Robodoc.at, Robvanvee, Ronz, Rspanton, Ryulong, S.O.S66100, Sampi, Sasquatch, Seraphim, Sfmammamia, Shell Kinney, Shirulashem, Sleepy yuci, Slightsmile, Smellsofbikes, Stephenb, Stewartadcock, Suffusion of Yellow, Tahmmo, Teenboi001, Template namespace initialisation script, Tgeairn, The Rambling Man, Thingg, Tom Morris, Trabelsiismail, Tremello, Tresiden, Tristanb, Typing monkey, WLU, Welsh, Widr, Wikipelli, William Avery, Wisdom89, Wknight94, Woggwogg, Work permit, Zandperl, 569 anonymous edits Myoepithelial cell Source: http://en.wikipedia.org/w/index.php?oldid=541269878 Contributors: Arcadian, Bearcat, Caerwine, Delldot, Dr.saptarshi, Enviroboy, Finlay McWalter, JackSparrow Ninja, Jennes83, Malcolma, Noclevername, Prof. Squirrel, Shunju-kun, Uwe Gille, Vojtech.dostal, White Shadows, Woohookitty, 14 anonymous edits Red blood cell Source: http://en.wikipedia.org/w/index.php?oldid=551605912 Contributors: (jarbarf), -df-, 03lausmi, 28421u2232nfenfcenc, AJim, ASEEMASEEM, Academic Challenger, Adambro, Addshore, Adhib, AdjustShift, Ahoerstemeier, Alansohn, Alec - U.K., Alfie66, Ali, Alksub, Alpha Quadrant, Amaher, Andre Engels, Andres, Andrew Delong, AndrewWTaylor,
612
Article Sources and Contributors
Andypandy.UK, Angelic Wraith, Angrycrustacean, Ann Stouter, Anoko moonlight, Anupam, Apers0n, Arcadian, Arisa, Arjun01, ArnoLagrange, Arvind0602, ArwinJ, Asparagirl, AssistantX, Atlantia, Aviad2001, Avoided, AxelBoldt, Baa, Bassbonerocks, Bbb2007, Beaumont, Benjamin.friedrich, Bensaccount, Bfigura, Bidabadi, Bignoter, Bobblewik, Bobo192, Bomac, Bongwarrior, Borgx, Boud, Brantonli, Brianski, BrightStarSky, BryanD, Burek, CIreland, Caeruleancentaur, Caltas, Can't sleep, clown will eat me, Carturo222, Caseydyck, Causa sui, Ccvic2, Chaldor, Chanting Fox, ChongDae, Chris Capoccia, ClockworkSoul, Closedmouth, Corinne68, Corvus cornix, Countincr, Countmike, Cpl Syx, Crack98, Craig Pemberton, Craigmillar94, Crohnie, DARTH SIDIOUS 2, DRosenbach, Dabomb87, Dan Gluck, Daniel5127, Danrudd, Darth Panda, Darthanakin, Davewild, DeadEyeArrow, Debresser, Deus Ex, Dictabeard, Dietzel65, Discospinster, Dogcow, Dogposter, Dominus, DoubleBlue, Download, Dr.Kane, DrMicro, Drmies, Dungodung, E Wing, ESkog, Eaefremov, Ed, Edcgooner, Egmontaz, Ego White Tray, Ekko, Ellywa, Emilyalbinoman, Epbr123, Everyking, Excirial, Ferkelparade, Fieldday-sunday, Fishyghost, Flamingspinach, Fr34k, Fraggle81, Franamax, Fratter, Fredil Yupigo, Fritzlein, Fryed-peach, Frymaster, Funnybunny, Fuzheado, Fvasconcellos, Gabbe, Gawaxay, Gene Nygaard, Giftlite, Gimboid13, Gobonobo, Golfandme, Gouerouz, Grafen, GraybeardBiochemist, Greentryst, GregorB, Grim23, Guest9999, Guy Peters, Hadal, HaeB, Haham hanuka, HalfShadow, HamburgerRadio, Harthacnut, Haza-w, Hellbus, Hempelmann, Hodja Nasreddin, Honette, Hu, Hunterd, Hydrogen Iodide, II MusLiM HyBRiD II, Ihope127, Immortal0king, ImplyingAuthority, Iridescent, J.delanoy, J04n, JNW, JWSchmidt, JaGa, Jakejakejake1313, Jaknouse, James Crippen, JamesTseng, JamillyM, JediLofty, Jeffq, Jfdwolff, Jfurr1981, Jnquach, JoanneB, John254, Johnbrownsbody, Jon salisbury, JonLS, Jordell 000, Josh3580, Jossi, Jsfouche, Juju Power, Jusdafax, Jyril, KC0ZHQ, Kander, Kariteh, Kassal, Katimawan2005, KaySL, Kazrak, Kbir1, Kennycub, Kerfern, Killerkris88, Kineticman, KingTT, Kingpin13, KnowledgeOfSelf, Kpjas, Kriptyk, Krylonblue83, Kubra, Kusma, KyraVixen, L Kensington, L33th4x0rguy, La goutte de pluie, Lahiru k, Landon1980, Lars Washington, LeaveSleaves, Lectonar, Lightdarkness, Lilfti332, Linas, Linzhoo2u, Little Mountain 5, LittleOldMe old, LizardJr8, Looper5920, Lord of the Pit, Lotje, Luckydhaliwal, MC MasterChef, MZMcBride, Mad Max, Madhero88, Magister Mathematicae, Maias, Mailer diablo, Mandarax, Mangal.anukriti, Marek69, Markacohen, MartinGugino, Massimo Macconi, Masterjamie, Masur, Matt Deres, Mav, McSly, Mdw123, Meewam, Mexinadian, Mfero, Michael Devore, Mikael Häggström, Mike2vil, Mindspillage, Minna Sora no Shita, Mintleaf, Miquonranger03, Moe Epsilon, Monkey.invasion, Mrfickle, Mwilso24, Nakon, Natty1991, NeilN, Nemesis of Reason, Netalarm, NewEnglandYankee, Nifky?, Nlu, Norman21, NotWith, Novalincoln, Nsaa, Nscheffey, Nunh-huh, Omnipaedista, Orkybash, Oscarthecat, Oxymoron83, PDH, Pablo-flores, Paul 012, Pb30, Peak, Perspeculum, Peter Karlsen, Phantomsteve, Philip Trueman, Piano non troppo, PierreAbbat, Pinethicket, Pinkadelica, Policarp, Prari, Priyanath, Prolog, Prowster, Prvc, Pschwarzbaum, Puchiko, RUL3R, RainbowOfLight, Razimantv, Rcingham, Reaper X, Recognizance, Reconsider the static, RenamedUser01302013, Rettetast, Rgracesmyrna, Riana, Rich Farmbrough, Rjwilmsi, Rob Maguire, Robo-rory, Rogeriopfm, Roshan baladhanvi, Roux, Rrburke, Rsabbatini, Ryulong, SDY, SGGH, SJP, Sakkura, Salgueiro, Samuel, Samwb123, Santoshpath, Sceptre, Schoolscienceteacher, Scootdive, Scottalter, Scwlong, Ser Amantio di Nicolao, SetRochelewsad, Sfmammamia, Shadowjams, Shanel, Sheitan, Sheogorath, Shirik, Shoeofdeath, Shyamdash, Siegele, Sir Vicious, SkepticalRaptor, Sky Attacker, Slashme, Slowking Man, Smitz, Snowmanradio, Someone else, Spartan, Specs112, Spliffy, SquidSK, Squidnchips, StaticGull, Stephenb, Stevenfruitsmaak, Sundar, SuperHamster, SuperStingray, Sverdrup, SwammerBAM, THEN WHO WAS PHONE?, TYelliot, Talu42, Tanthalas39, Tarquin, Taxman, Tchite, Template namespace initialisation script, Tempodivalse, The Bushranger, The Moose, The Rambling Man, The Thing That Should Not Be, TheEgyptian, Theroadislong, Tide rolls, TimVickers, Tiptoety, Torchwoodwho, Tosta Dojen, Traderjohn, Trevor Wennblom, Treygdor, Trojancowboy, Tsange, Turnstep, Tuspm, Tweetlebeetle367, Tyw7, Umheisman20, Uncle Dick, Valenciano, Vegfarandi, Vipinhari, Vrenator, WDM27, Wardface, Wars, Wavelength, Wayne Slam, Wayward, Wham Bam Rock II, Wiki alf, WikipedianMarlith, Willking1979, Wimt, Wisdom89, Wknight94, WolfmanSF, Woohookitty, Xenobiologista, Yamaguchi先 生, YetiSSM, Yuckfoo, Yurik, Zephyris, Zoomlines, ﺃﺣﻤﺪ.ﻏﺎﻣﺪﻱ.24, ﺳﻤﺮﻗﻨﺪﯼ, 901 anonymous edits Megakaryocyte Source: http://en.wikipedia.org/w/index.php?oldid=543767460 Contributors: A2Kafir, Akradecki, Arcadian, Brightguy88, Bush gem, Ciar, Coldbringer, DO11.10, Darklilac, Eras-mus, EryZ, Franamax, Funandtrvl, Island, JWSchmidt, Jag123, Jdalton308, Jfdwolff, Jordanawell, Kubra, Lennert B, Linzhoo2u, Mcstrother, Meganaos, Mikael Häggström, NCurse, Niceguyedc, Nihiltres, Pauli133, Rampart, Renata3, Rich Farmbrough, Rjwilmsi, Sedmic, Shell Kinney, Smartyhall, Snowmanradio, Thue, Topbanana, TractorDan, Vanishedlight, Vojtech.dostal, Vokesk, Wbensmith, Windwardside, 43 anonymous edits Monocyte Source: http://en.wikipedia.org/w/index.php?oldid=543384906 Contributors: Acetylcholinesterase, Adrian.benko, Alex.tan, Andy Rosenthal, Angesee, Arcadian, Arcturus, Ariconte, Audrius u, Audriusa, Auenfeld, Auntof6, Banan14kab, Barkeep, Bazzargh, Besieged, Bobblewik, Bobjgalindo, CS99, Camw, Ciar, CommonsDelinker, DO11.10, DoubleUnderscore, Download, Drjames1, ELLusKa 86, Eras-mus, Facts707, Fawcett5, Fluffernutter, Franamax, Friedo, GrahamColm, Jduffner, Jfdwolff, Joehall45, JohnJohn, JorisvS, Kaiba, Karl Dickman, Ksyrie, Kubra, Kumold, Linzhoo2u, LittleHow, Luigifan, Mattert, Mgiganteus1, Michael Devore, MichaelJanich, Mikael Häggström, Mike2vil, Mild Bill Hiccup, Mm1972, MuanN, Octahedron80, Osm agha, Palanq, Paul Klenk, Pissant, PornAndPrawnExtravaganza, RelentlessRecusant, Rjwilmsi, Rlmorgan, Rmarik, Rod57, Scien801, Seans Potato Business, Skittleys, Snowmanradio, Spark.bisht, TerraFrost, Varlaam, Veganfanatic, Wikijens, Yamla, 104 anonymous edits Langerhans cell Source: http://en.wikipedia.org/w/index.php?oldid=539736855 Contributors: AlphaEta, Arcadian, Artw, Beyond My Ken, Bobby70, Bstandley, Bus stop, Ceyockey, Chris Capoccia, Chris the speller, Chris53516, CopperKettle, Countincr, DRosenbach, Diberri, Docfaust, Dr. F.C. Turner, Drjames1, Fatphil, Fratrep, Glucose6phosphate, GregorB, Haymanj, Hovea, Ianbrettcooper, Jakew, Jarble, Juicy-one, Junkyardprince, Kauczuk, Kerowyn, Koene, Kogejoe, Lambiam, M.M, MaxEnt, Mikael Häggström, Millueradfa, Mion, NetRolller 3D, Nicke.me, Pinethicket, Pixie, Plasticup, Rich Farmbrough, Schneedrache, Scottalter, Snowmanradio, Studiodan, Szlevi, Timberframe, Tremello, Uthbrian, Vojtech.dostal, Woohookitty, Xwdl, Zandrous, Ziusudra, 38 anonymous edits Platelet Source: http://en.wikipedia.org/w/index.php?oldid=546736053 Contributors: .:Ajvol:., A.j.perrin, ABF, AZDub, Adeez, Adrenalinehound, Aesculap, Alekseyenko av, Allergist, Anders.Warga, Andreas Toth, Anto217, Apers0n, Arcadian, Arstchnca, BadCannstatt, Ben.roham, Bensaccount, Bigdumbdinosaur, Bignoter, Bjb, Bmecoli, Bobblewik, Bobjgalindo, Bomac, Brianski, Bryan Derksen, C.Fred, COMPFUNK2, Calmer Waters, Caltas, Capricorn42, CatherineMunro, Ceyockey, Chris the speller, Ciar, CommonsDelinker, Costis pap, Damian Yerrick, Davewild, Davorian, Dawn Bard, Deagle AP, DerHexer, Diberri, Dietzel65, Dlovinger, Double positive, Dr. Doof, Dr.michael.benjamin, Dr.saptarshi, DrMicro, Draeco, Dreviscerator, Drphilharmonic, Dungodung, Edward321, EerieNight, Egmontaz, Eleassar, Electrosaurus, Ellywa, Eog1916, Eras-mus, Erich gasboy, FeatherPluma, Ferengi, Franamax, Frecklefoot, FrozenMan, Fusionmix, Fuzheado, Gaius Cornelius, Galmicmi, Garffreak, Geldart, Gimboid13, Gnusmas, Gor n bein, GrahamColm, Grantgw, Grstain, Habj, Hadal, Haham hanuka, Hazmat2, Headbomb, Hede2000, HexaChord, Hgrosser, Hovea, Hroðulf, Huzzah for the Shopkeep, ILike2BeAnonymous, Iamstronghaha, Iice74, InverseHypercube, Iridescent, Ironsman, Iroony, Isabel123456, It Is Me Here, Itub, IvanLanin, J.Dong820, JamesAM, JamesTseng, Jauerback, Jeepday, Jeffq, Jfdwolff, Jitse Niesen, Jjhmccarty, Jprawn, Justme89, Jwilty, Jyril, KBi, Ka Faraq Gatri, Karaschultz, Kcordina, King of Hearts, Kungfuadam, Lauri195, Lazyday1397, Leslie Mateus, Linzhoo2u, Lrunge, M7, MAlvis, MER-C, Marek69, Markjohndaley, Maryhannah, Master Conjurer, Matanya (renamed), Materialscientist, Miannacone, MichaK, Michael Snow, Michi zh, Mikael Häggström, Mikeylane, Mj455972007, Mmxx, Modeha, Mogg, MrSomeone, Mrezai, Muhandes, NCurse, Naddy, NawlinWiki, Nbauman, Ndkartik, NerdyScienceDude, Nick Boulevard, Niteowlneils, Nmg20, Notheruser, Nunh-huh, Oblivious, Omicronpersei8, Oroboros, Orphan Wiki, Oxymoron83, PFHLai, PREMIS2010, Paul August, Peipei, Phil Wardle, PhilGaskill, Philip Trueman, Phlebas, Piano non troppo, Pinethicket, Poo9dle, Puglet, R.O.C, RDBrown, Radon210, Ravensky, Rb1248, Rbethune, Reedy, ResearchRave, Rewster, Rich Farmbrough, Rjwilmsi, Rkohin, Rlhutton, Robchurch, Rod57, SWAdair, Sahands, Salsa Shark, Scorpian ad, Sergei Gutnikov, Shadowjams, SimDarthMaul, Slconnor uk, Slightsmile, Smartse, Snowmanradio, Sophus Bie, SpK, Spaully, Spidey104, Sport woman, Spril4, Stereotek, Sun Creator, TAKEN00, Taucetiman, Template namespace initialisation script, Tevildo, The Universe1, Thecheesykid, Thingg, Tide rolls, Tim1357, Tleonardi, Topbanana, Toytoy, Tpb, TransUtopian, Trevor MacInnis, Tristanb, Unara, Uusitunnus, Vertigo35, Vogon77, WadeSimMiser, Ward20, Wavelength, Whig, Whkoh, Wik2kassa, WikipedianMarlith, Wikipelli, Wouterstomp, Wsloand, Yishubin, Yuckfoo, Zefr, Zeimusu, パ タ ゴ ニ ア, 483 anonymous edits Osteoclast Source: http://en.wikipedia.org/w/index.php?oldid=551048746 Contributors: 0304984r, Abalinson, Abe (or Abraham), Adapter, Aljullu, Arcadian, Ashley Payne, CalicoCatLover, Cape ryano, Cellpath, Cepacia, Chaldor, ChrisGualtieri, Chuunen Baka, Ciar, Cquan, DO11.10, Danfa1971, DerHexer, Diberri, DragonflySixtyseven, Eixo, Eleassar, Ellusion, Franamax, Frederickjeanguerin, Gadfium, Giftlite, Giraffedata, Greensburger, Homosinthemedow, J04n, JLCA, Jaded2, Jag123, Jared81, Joehall45, John of Reading, Josh Parris, Ketiltrout, Kungfuadam, Kyleca, Leia, MDoube, Matt.breeden, Meredyth, MichaK, Mobius, Mrich, Nicke L, Nono64, Nsaa, Orlandoturner, Polartysken, Rjwilmsi, Robert M. Hunt, Ryanrs, Salam32, Schneedrache, StatAustin, Tameamseo, Thegreenj, Totto6627, Vibitz, Vojtech.dostal, Vokesk, Wsussman, ﻣﺎﻧﻲ, 86 anonymous edits Dendritic cell Source: http://en.wikipedia.org/w/index.php?oldid=547135080 Contributors: AaronM, Acegikmo1, Aqua112233, Arcadian, Auenfeld, AxelBoldt, Axl, Bbh112, Bendzh, Bibiniki, Biggus Dictus, Blacklegendx, Brim, CLW, CanisRufus, Chaldor, Ciar, Circusgod, CrzyMke, DO11.10, Danaman5, Danfreak, Demiurge, Dirac1933, Doctorsclinic, Dominicanpapi82, DragonflySixtyseven, Drjames1, Dryman, Dysmorodrepanis, Ectoplasmical, Ediacara, Electric goat, Everyking, Feddegroot, Fhayashi, Franamax, GeeJo, Guess007, Hop12009, Horatio, Hugo Dufort, Itub, JWSchmidt, Jessemoya, Johnwalton, Jon the Geek, JorisvS, Jsnir, Juicy-one, JustAGal, Kalaiarasy, Kazvorpal, Kimjw7, Knuckles, Leptictidium, Lexor, Linzhoo2u, Marcelin0, Michael Greiner, Mimihitam, Nico KG, Nono64, Ohconfucius, Peisapooran, Petri Krohn, R'n'B, Reo On, Rich Farmbrough, Rjwilmsi, Rummy666, Rutigor, Sarah Morwood, Scray, Seans Potato Business, Sedmic, Shalinnaik, Skyelorien, Smirkster, Snowmanradio, Stepa, SteveChervitzTrutane, Strike Eagle, Sylvie.Lesage, Thumperward, Tony1, Trooper26 26, Urban.gecko, Vietbio, WLU, Wavelength, Wedic, WereSpielChequers, WhatamIdoing, XcepticZP, Yupik, 135 anonymous edits Lymphatic system Source: http://en.wikipedia.org/w/index.php?oldid=551697196 Contributors: 1dragon, 3dscience, 5Celcious, 879(CoDe), 9258fahsflkh917fas, Acroterion, Adi4094, Adriennefgnht23bgv33gbf32gn3g, Aetkin, Aeusoes1, Akerbeltz, Al Silonov, Alansohn, Alex.tan, Alexandermiller, Alexh3791, Allens, Allmightyduck, Alphachimp, Alteripse, Andrewman327, AndyA55555, Andyras, Angst7, Anna Karolina Heinrich, Anna Lincoln, Anthonyhcole, Arcadian, Ariedartin, ArielGold, Arsony, Aruton, Ashcraft, Astronautics, Atropos235, Attys, AxelBoldt, Axl, BathTub, Beantwo, Bender235, Betacommand, Bibliomaniac15, Blanchardb, BlueDevil, Bomac, BorgHunter, Brettz9, Brianski, Brim, Bryan Derksen, Burzmali, C933103, Cammomile, Can't sleep, clown will eat me, CanisRufus, CapitalR, Capricorn42, Carps, CaseyPenk, Cburnett, CesarB, Cflm001, ChrisGualtieri, Chrishel, Christian75, Ciotog, Clattuc, Closedmouth, Cmcnicoll, Coasterlover1994, CommonsDelinker, CoolKoon, Cpl Syx, Cuahl, Cyclonenim, DO11.10, DVD R W, Danny252, Darkdrakey2000, Darkfight, Darkwater657, DebC123, Decltype, DerHexer, DesertAngel, Dexter prog, Dfrg.msc, Diberri, Diomidis Spinellis, Dipankan001, Diza, DocElisa, DocWatson42, Dr.pompo, Dragos101, Drdcarlz, Dreadstar, Dungodung, Dustin Dewynne, Dysprosia, EWikist, Egghead06, Epbr123, Equendil, Eras-mus, Erich gasboy, Erielhonan, Exert, EyebrowOnVacation, Faradayplank, Feydey, Figma, Finlay McWalter, Flewis, FrankCostanza, GFHandel, GHe, Gareth Griffith-Jones, Gatster 04, Gensanders, Giftlite, Gilliam, Glane23, Goffrie, Gurch, Gwernol, Gyrobo, HYC, Habj, Haemo, HalfShadow, Harrisd5917, Harryboyles, Hfastedge, Hmains, Hughcharlesparker, Husond, Hydrogen Iodide, Iammisc, Ibnsina786, Igoldste, Iohannes Animosus, Ipwnzors, Iridescent, Ixfd64, Izvora, J.delanoy, JASpencer, JForget, JaGa, Jack Holt, Jackomos, Jaispeed, JakobSteenberg, JamesBWatson, Jamiejackson, Jauhienij, Jc86035, Jeff G., Jfdwolff, Jhenderson777, Jmcw37, Joehall45, John254, Johnanth, Jordan Yang, Jordanmif, Jose Jethro L. Villaverde, Jrodor, Julesd, Julietwhite, Jusdafax, Just plain Bill, JustinForce, KC Panchal, KaiAdin, Katalaveno, Kazubon, Kdavidk, Keilana, Kip R. S., KnowledgeOfSelf, Kosebamse, Krashlandon, Krawi, Kubigula, Larry Dunn, LearnAnatomy, Lennert B, Lepetitvagabond, LilHelpa, Little Mountain 5, LittleOldMe, Littlealien182, Lord Anubis,
613
Article Sources and Contributors
LuK3, Luk, Luna Santin, Lymphoma, MER-C, MPerel, Maralia, MarcoTolo, Marcus Qwertyus, Marek69, Mark Arsten, MarkRose, Marshallsumter, Martinp, Materialscientist, Maxmaxb, McDogm, Mcmillin24, Mecil, Meegs, Merope, MetsFan76, Mifter, MightyWarrior, Mikael Häggström, Mike Rosoft, Mike2vil, Mikebar, Mild Bill Hiccup, Min.neel, Momo san, Mr Peanuts, Msi09222, Mwanner, NJPharris, Nastajus, Natpal, Neolog, Nick, Nina Gerlach, Nishkid64, Nivix, Nlu, Nn123645, Now is relative, Nuno Tavares, Nurg, Orangemike, Orphan Wiki, Otisjimmy1, Oxymoron83, PDH, PFHLai, Panoptical, Paperfork, Paul August, Perryperry, Peter bertok, PeterSymonds, Phnk, Phogg2, Piano non troppo, Pinethicket, Polly, Postglock, Ppyo, PseudoSudo, Puchiko, RadioKirk, RaminusFalcon, Rannyfash, RastNim, Raven in Orbit, Razorflame, Rduddington, Realdog, Redhookesb, Renato Caniatti, RexNL, Richard75, Rintrah, Rjwilmsi, Robertdench, Rodsan18, Ronhjones, Rowan Moore, RoyBoy, Rumiton, S3000, SDY, Salt Yeung, Salvor, Samir, Satellizer, Sdumont, Seans Potato Business, Seelefant, Seventh Holy Scripture, Shalom Yechiel, Sharkface217, Shinkolobwe, Simonwilms, SiobhanHansa, Skittleys, Slartibartfast1992, Slightsmile, Snowmanradio, SoWhy, Social tamarisk, Splash, SpuriousQ, Srushe, Steven Luo, Stevenmitchell, Stollerdj, Superbeecat, Tarnas, Tartan, Tatrgel, Tcncv, Template namespace initialisation script, The Anome, The Emirr, The Red, The Thing That Should Not Be, Thejerm, Theopolisme, Thgang, TiCPU, Tide rolls, Tirkfl, Tony K10, Tossh eng, Trailspark, TruthbringerToronto, Tvarnoe, Ulflarsen, Urashimataro, Urwrongstud, UtherSRG, Vokesk, Vuo, WBardwin, WE.WE.WE.WE, WLU, Wainwra, Warcraftfan111, Werdan7, West.andrew.g, WhatamIdoing, WhyBeNormal, Wiccan Quagga, Wikigenevan, Willking1979, Wongm, Wouterstomp, Writ Keeper, Xil, Yidisheryid, Yvwv, Zalgo, Zaxius, Zeitgeist24, Ziphon, Zloyvolsheb, ﺳﻤﺮﻗﻨﺪﯼ, 837 anonymous edits Microglia Source: http://en.wikipedia.org/w/index.php?oldid=550893374 Contributors: AHands, AManWithNoPlan, Arcadian, Audreykarperien, Bogwhistle, Calerc, Camerong, Ciar, ClockworkSoul, CopperKettle, CraigTheBrit, D6, Dafunk, Delldot, Diberri, Dinisoe, Drdaveng, Filip em, Franamax, Fredweis, Gauss01, Guy M, Gzkn, Hazard-SJ, Headbomb, Helge Skjeveland, Iqzaquezzs, Joehall45, Jorvis, Kauczuk, Kilom691, La comadreja, Lkf0919, Manabeast333, Martious, Materialscientist, Metropolitan90, Michael Devore, Miguelferig, Mikael Häggström, Mike2vil, Mimihitam, MollyNYC, MrADHD, Mrbigtoe, Nbauman, NifCurator1, Nono64, PaddyM, Paolo.dL, Papovik, Pcu123456789, PhnomPencil, Pmokeefe, Pol098, Probios, RDBrown, Rich Farmbrough, RichardGautney, Rjwilmsi, Robertmuil, Sgpsaros, Sjbarrett, Snowmanradio, Time9, Tmangray, Vojtech.dostal, WereSpielChequers, Wiki emma johnson, ^demon, יונה 87 , בנדלאקanonymous edits Neutrophil granulocyte Source: http://en.wikipedia.org/w/index.php?oldid=546586763 Contributors: 2over0, A-wal16, Abstraktn, AdjustShift, Alansohn, Albondigas123, Arcadian, Axelregens, Bahoxu, Banano03, Bender235, Bob Blaylock, Borgx, Boxandice8, Branwall, Casliber, CasualVisitor, Chimeira, Ciar, Clark SR, DO11.10, DRosenbach, Davince, Dbabbitt, Dbroadwell, Delldot, Dexterreneer, Diberri, Drphilharmonic, E Pluribus Anthony, El Mariachi, Elliotgoodrich, Emsta88, Epingchris, Eribro, Evands, FearlessRahul, Flumignan, Franamax, Gabe20770, Garion96, GeeJo, Gene Nygaard, Geniac, Giraffedata, Gnusmas, GrahamColm, Greensburger, Hlangeveld, Hydrargyrum, IGeMiNix, Iwilcox, Janesh1980, Janesh2323, Jayden54, Jdlambert, Jfdwolff, Jloftus22, Joanjoc, Johnuniq, Julian.ilcheff, Just Susan, JustAnotherKinase, Kalaiarasy, Karl Dickman, Kazikameuk, Kehrbykid, Kirper, Kosebamse, Kww, Kyukyu18, La goutte de pluie, Lars Washington, Leeearnest, Leolaursen, Linzhoo2u, Llnoba, Lombroso, Looie496, Luigifan, Luk, M1ss1ontomars2k4, MER-C, Majkinetor, Malerin, Martarius, MaseRayL, Maximus Rex, Mhking, Michaeloqu, Mikael Häggström, Mike2vil, Minnsurfur2, Miracle Pen, MisfitToys, Nbauman, NighthawkJ, Nk, Noctibus, Nrsmoll, O18, Opsuty, Pointpride, Primmuno2, Prolog, Randyoo, RexNL, Rhode Island Red, Rich Farmbrough, Rjwilmsi, Rlmorgan, Rogiervw, SFSingleton, Salih, Schizmatic, SchreiberBike, Scwlong, Shadowlynk, StephenBuxton, SystemBuilder, Tabletop, Thumperward, Tinngo, Tleonardi, Triesault, Trolleymusic, Useight, Wavelength, Wedian, Wiki emma johnson, Yashgaroth, パ タ ゴ ニ ア, 202 anonymous edits Eosinophil granulocyte Source: http://en.wikipedia.org/w/index.php?oldid=543702007 Contributors: Ahoerstemeier, Alex.tan, Andromeda, Arcadian, Bobblewik, Bobjgalindo, Borglife, Boxandice8, Branwall, CDN99, CS99, CarlESundberg, Cburnett, Ceyockey, CharlesClarkson, Cheaposgrungy, Ciar, Clicketyclack, Dan McScience, Dathomp1, Davidruben, Dcirovic, Diberri, Donaldal, Drphilharmonic, E Pluribus Anthony, Emperorbma, Eosinophil7, Eosinophils99, Feral mage, Franamax, Frumpel, Gene Nygaard, Glenn Magus Harvey, GrahamColm, Hairy Dude, Husond, Jackol, Jeffq, Jfdwolff, Jkhamlin, Joanjoc, Josh Parris, Jsjsjs1111, Kalaiarasy, Karl Dickman, Khanna06, Kkmurray, Knuckles, Kristenq, Kubra, Linzhoo2u, Lombroso, Martpol, Mikael Häggström, Misty7, Mjbat7, Nono64, Nunh-huh, Oliverdl, Ppgardne, Pro Grape, R'n'B, Rex Manning, Rob.bastholm, Rockfang, Rrenner, Saimhe, Sbharris, Schtigy, Sciwred, Seans Potato Business, Skittleys, Snowmanradio, Someone else, Thaurisil, Thranduil, Timferno, Tracylau1223, Tristanb, Una Smith, Unara, WhatamIdoing, WillFinnigan, 101 anonymous edits Basophil granulocyte Source: http://en.wikipedia.org/w/index.php?oldid=551695867 Contributors: Algumacoisaqq, Ameyadkr, Arcadian, Bela Bartoszek, Bencherlite, Benmd, Bloodcancerguy, Bob Blaylock, Bobomarch, Branwall, CDN99, CS99, Ciar, Cyberman, DO11.10, Delldot, Donmacglashan, ESCapade, Elbonia, Elboy99, Epgui, Epingchris, Franamax, Frazzydee, Graham87, GrahamColm, Hephaestos, Ht9150, Infinitys 7th, Iwilcox, Jfdwolff, Joanjoc, Karl Dickman, Kauczuk, Kerowyn, KnightRider, Kubra, Linzhoo2u, M1ss1ontomars2k4, MastCell, Menue, Mikael Häggström, Mike2vil, Murdochious, Natkeeran, Onco p53, Oxymoron83, Pearle, Piano non troppo, Pingveno, Porqin, Prolog, RB972, RDBrown, RelentlessRecusant, RenamedUser01302013, Rich Farmbrough, Shirik, Sligocki, Snowmanradio, Thue, Timurite, Tossh eng, Voxii, Wandering Raleighite, Wood Thrush, Þjóðólfr, パ タ ゴ ニ ア, 67 anonymous edits Hybridoma technology Source: http://en.wikipedia.org/w/index.php?oldid=548151808 Contributors: Aetkin, Ahoerstemeier, Anypodetos, Arcadian, Arup Acharjee, Autoerrant, AxelBoldt, Bejnar, Biotec ha, DoctorKubla, Friendlyliz, GerryShaw, Janetyler, Joeyzhu123, JonHarder, Jonathanfu, Joseph pepito, Miguel Andrade, Movses, NewEnglandYankee, NickPenguin, OrbitSoldier, Playtime, Prazwol, Proquence, R'n'B, Rich Farmbrough, SMasters, Seans Potato Business, Shadowjams, SlothMcCarty, Someguy1221, Tonipares, Tyranitar Man, Wedian, WikHead, Wsmith202, 48 anonymous edits Mast cell Source: http://en.wikipedia.org/w/index.php?oldid=543707550 Contributors: Aleichem, Alex motzik, Arcadian, Arthena, Begoon, Bender235, Benjah-bmm27, Boghog, Bogwhistle, Bomac, Casliber, Chikantikka, Ciar, DO11.10, DRE, DarkFalls, Davidruben, Dr U, ESCapade, Electric goat, Essam Sharaf, Franamax, Fsiebenh, Goodnightmush, Graham87, Greenleaf87, Hadal, Harrisd5917, Hede2000, Hotcrocodile, Hvyhiter, Höyhens, Jastrow, Jfdwolff, Joehall45, Joelmills, JohnnyCalifornia, Julesd, Kauczuk, Kiran Gopi, Kku, Kyukyu18, Lekeebler, Lidabet, Linzhoo2u, Ludisia, Mandarax, Mikael Häggström, Mike2vil, Nbauman, Neverquick, Nono64, Nrets, NunoAgostinho, Omnipaedista, Orlandoturner, PFHLai, Petersam, Philbradley, R. S. Shaw, Rafiqr, RedDrag0n, Reza luke, Rjwilmsi, Russot1, Ryddragyn, SLATE, Seans Potato Business, SgtThroat, Sharanth, Snowmanradio, Stino v, Tristanb, Unara, Vokesk, Volantares, WLU, Woohookitty, Xetxo, 110 anonymous edits T helper cell Source: http://en.wikipedia.org/w/index.php?oldid=549148820 Contributors: Abramsonj, Adr11iano, Allens, Anupam, Aqua112233, Arcadian, Avaron676, AxelBoldt, Beland, Benjamin.haley, Bob247, Bobo192, Bogwhistle, Borgx, Brendan19, Brendanconway, Brentdax, Bullhaddha, Bwwhite, Charles Matthews, Chris the speller, Cmdrjameson, ComfyKem, CopperKettle, Davekcole, David Johnson, Dcirovic, Diberri, Dirac1933, DoktorDec, Eleassar777, Elliotgoodrich, Essexmutant, Ettrig, Finalius, Franamax, Frycow, Gamingmaster125, Gbleem, Gikü, GiollaUidir, Gurch, Happiness4ever, Immunoboy, JLaTondre, JackWasey, Jakob Theorell, James McNally, JamesBWatson, Jbarin, JeffreyN, JorisvS, Jotomicron, Julianonions, Kantokano, Ketiltrout, Koavf, Lanka007, Larryisgood, Leptictidium, Lexor, Mala76, Mboverload, Mikael Häggström, Mike2vil, Mimihitam, Mohawkjohn, MrPMonday, MuanN, Nbauman, Niels Olson, Nina, Nonpareility, Nuno Tavares, Oda Mari, Ohnoitsjamie, Optigan13, Orderinchaos, Orlandoturner, Owenhyfryd, Philbradley, Pro bug catcher, Promelior, Prometheus, RelentlessRecusant, Rich Farmbrough, Rjwilmsi, Rod57, Samuel, Scien801, Seans Potato Business, Serephine, Sfahey, Shawnnph, SimonPerera, Sk741, Slashme, Smalerie, Snigbrook, Snowmanradio, Sophie means wisdom, Sxim, TKD, Template namespace initialisation script, TenOfAllTrades, Tide rolls, Tommy2010, Triggtay, Tristanb, Tycho, Utcursch, Volantares, Vyn, WhatamIdoing, Wikid77, Wikitoov, Yamamoto Ichiro, Youkai-kun, ZayZayEM, 239 , דגיגanonymous edits Regulatory T cell Source: http://en.wikipedia.org/w/index.php?oldid=543039170 Contributors: Adr11iano, Anupam, Arcadian, AxelBoldt, BettieHoladay, Biohacker, Boghog, Bryolith, Chrisch, Chupacabras, Danierrr, Davidruben, Drphilharmonic, El C, Emersoni, Escobar2, FCAlive, Fnielsen, Franamax, GAThrawn22, Gearoidmm, Geuss, Ioeth, Iridescent, JLaTondre, JackWasey, Jakob Theorell, Jbarin, JohnnyBxo, Kantokano, Karawaque, Kinkreet, Kirbymaur, Lbruegge, MastCell, Mauvila, Mboverload, Nbauman, Negarci, Nina, Onco p53, Oxymoron83, Perencake, Pion, Ramujana, Rich Farmbrough, Rjwilmsi, Schroding79, Science4us, Southernwayfarer, Sunjongko, TaeSaBiAe, Tretcher, Twas Now, Twooars, Univer, Who, Wiccan Quagga, Wiki Katie, Zeearend, 81 anonymous edits Cytotoxic T cell Source: http://en.wikipedia.org/w/index.php?oldid=548082771 Contributors: Adrian J. Hunter, Anupam, Arcadian, Cd8tcell, Chris Capoccia, Christian75, Ciar, Crazysane, Davekcole, Davin, Diberri, Drphilharmonic, DéRahier, Ebmat, Ediacara, Eras-mus, Excirial, Fabiform, Franamax, Gaius Cornelius, Gikü, Habj, Heero Kirashami, Heero@Yuy, IvanLanin, J.delanoy, J04n, JaGa, Jbarin, Jfdwolff, Lenrodman, Leptictidium, Lexor, Lockley, Miannacone, Mild Bill Hiccup, Nbauman, Nina, Petri Krohn, Prometheus, RelentlessRecusant, Rich Farmbrough, Rich257, Richwil, Rotatoria, RyanGerbil10, Rünno, S88136738, Seans Potato Business, Serephine, Sfahey, SimonPerera, Slashme, Snowmanradio, Template namespace initialisation script, TheTito, Thepunisher22, Theroachman, Volantares, Wavelength, Zklaus40, 79 anonymous edits Natural killer T cell Source: http://en.wikipedia.org/w/index.php?oldid=540624257 Contributors: Adams5400, Anthony Appleyard, Anupam, Arcadian, Brim, Cplatt, DIG1964, DO11.10, Dalf, Figma, Franamax, Jeffq, Karasunoko, Ketiltrout, Loopback007, Mattert, Monterey Bay, Nz101, RelentlessRecusant, Rjwilmsi, Schneedrache, Snowmanradio, SocratesJedi, Timetraveler3.14, Vesriram, Wbm1058, 34 anonymous edits B cell Source: http://en.wikipedia.org/w/index.php?oldid=550542105 Contributors: 069952497a, Abramsonj, AdjustShift, After Midnight, Alansohn, Allens, Altaileopard, Anypodetos, Arcadian, BD2412, Banano03, Bcmyangx, Bearpiggoreman, Blitzmut, Butterfly reflections, CUSENZA Mario, Calvinchong, Cburnett, CesarB, Chefyingi, Chris Capoccia, Chrumps, Chucky123456789, Ciar, Cockers1987, Coemgenus, DO11.10, Dana boomer, Daniel, Darkfrog24, Davidazus, Davlag, Dcooper, Delentye, Diberri, Docfaust, DragonSlayer210, Dwight666, Eleassar777, Eras-mus, Eric-Wester, Falcon8765, Franamax, GargleBlaster, Geuss, Giftlite, Ginkgo100, Greensburger, Greggp42, Gremmer, Grey ham22, Hamham1012, Hamjue, Hazmat2, Healthvalue, Helper100, Herrpoon, Hotncool123, Hqb, I dream of horses, Ian Glenn, Igoldste, Ilyushka88, InverseHypercube, Iohannes Animosus, Iridescent, JBellis, JMiall, JackWasey, Jacuzzijo, Jeffq, Jj137, Jojousa, Jonathan.s.kt, JorisvS, Jotomicron, Juliamweiss, KC Panchal, KCinDC, Kinkydoc22, Knowledge keen, L Kensington, Leptictidium, Lexor, Liidiie, Ling.Nut, M1ss1ontomars2k4, Mac Davis, MastCell, Maxí, Mikael Häggström, Mimihitam, Mj455972007, N4nojohn, Niels Olson, Nina Gerlach, Nonagonal Spider, Novangelis, Oasisbob, Palpalpalpal, Paulasb, Peisapooran, Pgallert, Ph.eyes, Phil Boswell, Postglock, Prometheus, Quirk, RandomP, RelentlessRecusant, Reverting, Rey lcm, Rgoodermote, Rjwilmsi, RobinHood70, Ronincyberpunk, Sagefoole, Sayeth, SchfiftyThree, Schtigy, Silveramini, Simonmoore, Skittleys, Smoe, Snoeleopard, Some jerk on the Internet, Srlasky, Stevereichh, Stmoran, Sun Creator, TKD, Taoster, Teamfido, Template namespace initialisation script, Thorncrag, Tide rolls, Timemutt, Tristanb, Tycho, VMS Mosaic, Vokesk, Warden99, WhatamIdoing, Wknight94, Woohookitty, Wpktsfs, Youssefsan, Yurei-eggtart, 258 anonymous edits
614
Article Sources and Contributors
Natural killer cell Source: http://en.wikipedia.org/w/index.php?oldid=551164749 Contributors: Acoury, Adr11iano, Aesopos, Alansohn, Alejocn5, Ali ahmadzada, Alksentrs, AlphaEta, Andrew73, Apocalypse Now, Arcadian, Ary29, Bisc import, Bluemoose, CIreland, Cab.jones, Cacofonie, Calmer Waters, Capricorn42, Chamal N, ChrisGualtieri, Chrumps, Conkwest, Cph3992, Cyberman, DRMJNY, Dbollard99, Delldot, Diberri, Doctor medicine, DougsTech, Download, Dr.saptarshi, Draeco, Drchazz, Drphilharmonic, Durova, Enviroboy, Epingchris, Franamax, Furrykef, Gibson Flying V, Giftlite, Gjbbms640, Harriemkali, Icedemon, Jakob Theorell, Jaranda, JeffreyN, Jfdwolff, JorisvS, Kazkaskazkasako, Kenmcl2, Kittty08, Kubra, Kupirijo, LeeHunter, Leptictidium, Lexor, Lockley, LoneSeeker, Lycurgus, MPerel, Mattert, Matthewmazurek, MicroBio Hawk, Mikael Häggström, NetRolller 3D, Nmajdan, Nunh-huh, PAStheLoD, Park4223, Pgrote, Phfred, PhnomPencil, Pixie, Prometheus, Rdsmith4, Regford, RelentlessRecusant, Rickjpelleg, Rjwilmsi, Roastytoast, Rod57, Schneedrache, SchreiberBike, Seans Potato Business, Serephine, Smithbrenon, Snapperman2, Snowmanradio, Songrit, Squidilicious, Stemscientist, Supergroover, Tamarkapterian, TheTito, Timemutt, Tjoneslo, Tlabshier, Tmangray, Tossh eng, Unga Khan, Varbas, Volker Huppert, Wavelength, Wedgeoli, Wjejskenewr, Wo0dstock79, XavierEverett, YouRang?, Zach the Wanderer, 129 anonymous edits Reticulocyte Source: http://en.wikipedia.org/w/index.php?oldid=549064794 Contributors: 2001:468:C80:4340:DAA2:5EFF:FE91:F41E, AaronM, Alex.tan, Arcadian, Arthena, AxelBoldt, Brinerustle, Chowbok, Diberri, Drphilharmonic, Franamax, Gaius Cornelius, Gak, Gobonobo, Happy B., Hoverflysmiles, Ian Pitchford, Jeffq, Jmarchn, Joewright, Kubra, MiloszD, Monkeyontheloose, NewEnglandYankee, Niroby, Ozmaweezer, Patch101, Randyoo, Romanm, Sedmic, Seforadev, Snowmanradio, Some standardized rigour, Tiptoety, Tristanb, Wouterstomp, 43 , דניאל צביanonymous edits Progenitor cell Source: http://en.wikipedia.org/w/index.php?oldid=551063018 Contributors: Alaa al-Otaibi, Amaher, Arcadian, Bagatelle, Bihawang, Canadian hockey1, CardinalDan, Christian75, CopperKettle, DVdm, Discospinster, Dr Aaron, Drphilharmonic, EOZyo, EWikist, Eumolpo, Jeff G., Kerribergeron7197, Kerrio, Lenticel, Lijealso, Mild Bill Hiccup, Obaid221, Peter Znamenskiy, Pgan002, Philip Trueman, Poojans, Rob Hurt, Robert M. Hunt, Rod57, StanfordProgrammer, Stansz, Stepa, Susan Carley, The High Fin Sperm Whale, TheChymera, Tinlv7, VUBio Pieterjan, Volodymyr Stetsyuk, ﺗﺮﺟﻤﺎﻥ05, 32 anonymous edits Ovum Source: http://en.wikipedia.org/w/index.php?oldid=550501112 Contributors: 165.123.179.xxx, 2004-12-29T22:45Z, 22232222vb, 24.234.70.xxx, Abstraktn, Achven, Addshore, Adrian J. Hunter, Adrigon, Alansohn, Ale jrb, Alfonso Márquez, Allens, Amatulic, Andrei Stroe, Andrewa, Anthonyhcole, Arcadian, Arjun G. Menon, Arkuat, AxelBoldt, Bagatelle, Bcorr, Beano, Bhojanimihir, BiT, BigPimpinBrah, Bkrosnov, BlueGoose, Bomac, Bongwarrior, Brandmeister (old), Btd, C.Logan, CallumN, Caltas, Capricorn42, Carlossuarez46, Carpenter aka, Cesiumfrog, Chanlyn, Christiangrimm84, Closedmouth, Cmichael, CommonsDelinker, Conscious, Conversion script, Dasani, David.Gaya, DavidRader, Dbfirs, DerHexer, Eatingbrunch, Eewild, Ehn, Ekem, Eleassar777, Empty Buffer, Epbr123, Epipelagic, Fabiform, Finlay McWalter, Finn-Zoltan, Fixstamac, Flockmeal, Franamax, Francs2000, Freemarket, Furbinator, G026r, Gajanandjha, Gblaz, Gbnogkfs, Gleader9, GoingBatty, Grafic, Gwernol, Haham hanuka, Hall Monitor, IW.HG, IceDragon64, IronChris, Isnow, Itai, J.delanoy, Jakejakejake1313, Jiddisch, Jj137, JoanneB, Jonathan.s.kt, Joshbuddy, Josq, Jovianeye, Jrockley, Judygreenberg, Jusdafax, Kandar, Katieh5584, Keegscee, Knowz, Kudpung, Kwakpwns, Kyng, L Kensington, La goutte de pluie, Leevclarke, Legend II, LemonTwinkle, Lexor, LilHelpa, Lilyv129, Lobstercake1, Lokicarbis, Lottamiata, Lugia2453, Lugnuts, MBisanz, MCRfan911, Magnus Manske, MarsRover, Maxí, Meiskam, Menchi, Mesoderm, Mgiganteus1, Mike5193, MilborneOne, Minimac, Modify, Mr. Lefty, Nadiatalent, NerdyScienceDude, Netoholic, Nifky?, Nilmerg, Nkayesmith, Nuno Tavares, Ochloese, Orphan Wiki, Osmodiar, Patrick0Moran, Patrickk112, Patxi lurra, Philip Trueman, Pigman, Plantguy, Pollinator, Radagast83, Rainy888, Ratherthanflesh, RebekahThorn, RenniePet, Rep07, Riotrocket8676, Rm1271, Rob Hooft, Robin Chen, Romarin, Rune X2, RxS, Sabisteb, Samsara, Sean.hoyland, Sharkb, Shirulashem, Shoombooly, Skizzik, Slakr, Soupforone, Steven Zhang, Swid, Tameeria, Taranet, Tarquin, Tbhotch, The Anome, The Rambling Man, The Thing That Should Not Be, ThePirate, Tide rolls, TigerShark, Tjoms12, Tmshates, Toddy1, Treisijs, Tresiden, Trijnstel, Tsca, Tyrol5, Ulric1313, Vanished User 1004, Victoriagirl, Victormdc10, Vojtech.dostal, Voyevoda, Waggers, Wavelength, Werieth, Wipfeln, Youssefsan, Zfr, Àlex, כל יכול,יוסי, आशीष भटनागर, 朝 彦, 252 anonymous edits Oocyte Source: http://en.wikipedia.org/w/index.php?oldid=546452397 Contributors: 2004-12-29T22:45Z, Abstraktn, Addit, Amaury, Arcadian, Arkuat, Basilicofresco, Bobjgalindo, Cameron Nedland, Catcasillas, Cburnett, Ceyockey, Chris the speller, Crazycomputers, Curb Chain, Db099221, EagleFan, EamonnPKeane, Edward, Erianna, Face, Former user, Furrykef, Gabbe, Glimz, Hgrosser, InverseSubstance, Kaobear, Kbusdriver, Kerfern, Leeannedy, Lexor, Lymanbellows, MarcosR, Mgiganteus1, Microinjection, Mikael Häggström, Minna Sora no Shita, Modify, Mysid, Nkmosley, Nmg20, Oliver202, PauAmma, Phuzion, Poissonbreaker, Rasbak, RedWolf, Remuel, Riana, Sdou, Shano85, Skizzik, Snek01, Snoyes, Stephenb, Stylese, Sugemax, Tameeria, Thomas 564312, Tmshates, Tour86rocker, Trovatore, Vanished User 1004, Vojtech.dostal, 82 , ברוקוליanonymous edits Spermatid Source: http://en.wikipedia.org/w/index.php?oldid=540782500 Contributors: 2004-12-29T22:45Z, Abstraktn, AdmiralHood, Alsbluegoat, Arcadian, Chowbok, Diligent, Gilliam, Kaobear, Wikielwikingo, 12 anonymous edits Sperm Source: http://en.wikipedia.org/w/index.php?oldid=551477424 Contributors: 123456789101121cccccc, 2004-12-29T22:45Z, 21655, AB, AaronM, Accurizer, Acdx, Acroterion, Addit, Adrigon, Agateller, Ahmad.ghamdi.24, Ahmed32 UK, Aitias, Al tally, Aleenf1, Alexandre Bouthors, AlexiusHoratius, Andrei Anghelov, Andrewjlockley, Andrewpmk, Avaya1, Avnjay, Bakerccm, Baosheng, Bass fishing physicist, Beeftheboss, Beland, Benfranklinlover, Bhojanimihir, Bility, Blairbob, Blehfu, Bobo192, Bob™, Bongwarrior, Briefblowtothehead(dick), Brougham96, Bytenik, CIreland, CWii, Caltas, Calvin 1998, CambridgeBayWeather, Camelface123, CanadianLinuxUser, CapitalR, Chamal N, Chris Bainbridge, Chris the speller, Coffee, ColinBoylett, Cometstyles, Commander Keane, Cornchips, D, D1536, Dantheman216, Darth Mike, Dasani, DeadEyeArrow, Deconstructhis, Dekisugi, Delldot, DerHexer, Dgw, Dickneck99, Dikteren, Dikwad1, Discospinster, Dominus Vobisdu, Dreadstar, Dreby14, Drsocc, Dumbnuts, Dust Filter, Dycedarg, EJF, Eaglesiegle, Edison, Epbr123, Esc2003, Excirial, Extransit, Face, Feezo, Fess56, Fieldday-sunday, Filelakeshoe, Fl, Florentyna, Foxj, Francs2000, Frederikfederspiel, FrozenMan, Ftwklg, FunPika, GB fan, Gadha, Gail, Gekaap, Gggh, Gilliam, Gjuny, Gonzo fan2007, GoodDamon, Gregfitzy, Greystoke35, GrooveDog, Grstain, Gspinoza, Gtva1234, GuffasBorgz8, Guldenat, Guntiur983, Gurch, Gurchzilla, Gurukkal, HaeB, HeirloomGardener, Hiberniantears, Hiddekel, HisSpaceResearch, Hogyn Lleol, Horny t, HotHistoryBuff69, Hu12, Hyacinth, I.r.ande.t.a, INazi, Indon, IndulgentReader, Insanity Incarnate, Instinct, InverseHypercube, Iridescent, J.delanoy, Jackol, JammydodgerUK, Jarble, JayFS89, Jcaliguy, Jclemens, Joannyluteman534, John Doe42, Jonadin93, Joost de Kleine, Jtknowles, Julesd, Juliancolton, Jumbawumba, Kaobear, Katdye123, Keilana, Keith D, Kelovy, Ketsuekigata, Kewsss, Kiyi-chan, KnowledgeOfSelf, Kuru, Kyleeberle, LadyofShalott, Lec CRP1, Lenticel, Lindentree, LittleOldMe, LizardWizard, Lomis, Longhorngirl 5284, Luna Santin, Mack2, Madhero88, Mairi, MarcoTolo, Markbenecke, MarsRover, Martarius, MartinezMD, Mesoderm, Mihalis, Mikael Häggström, Mike-shearer92, MikeNicho231, MikesPlant, Miquonranger03, MoogleEXE, Mschel, NHRHS2010, Nakon, Nattycan, Neverquick, Newlyteeth, Nicolae Coman, Nihiltres, Nintendude, Nivix, Nnemo, Nosolution182, Notedgrant, Novjunulo, Nwbeeson, Ocatecir, Octahedron80, Oda Mari, Ohnoitsjamie, Ohyababy1, Osborne, Ospalh, OverlordQ, OwenX, Oxymoron83, P-squad4251, Pass a Method, Patrick, Pb30, Pcarter7, Phil havercroft, Philip Trueman, Piano non troppo, Pimpboy, Poindexter Propellerhead, Press Start, Private Butcher, PubLife, Rafael MC, RainbowOfLight, Rami radwan, RandomXYZb, Rangek, Raquel PWNZ, Rawfact, Razorflame, Revancher, Rey101011, Rglong, Richard001, Richardedgerton, Rodsan18, Rohitrrrrr, Rrburke, Rror, Rsmn, RucasHost, Ryan Postlethwaite, SU Linguist, Sam Korn, Sam nead, Sceptre, SeanBBSc, Sexworms, Shadiac, Shawtyrockmi, Shibby970, Sidasta, Silly rabbit, Skier Dude, Slushy9, Smartse, Smashingpumkin, Smithy998877665544332211, Sohelpme, Spencer, Stephenb, Steven Zhang, Stone, Storch6308, Supersixfour, Surfeited, Svetovid, THEN WHO WAS PHONE?, Tameeria, Telcourbanio, Tessmac9708, The Thing That Should Not Be, TheBilly, TheNoise, Thedjatclubrock, Theguy14, TheiGuard, Thincat, Thine Antique Pen, This deserves inclusion, Tiddly Tom, TimVickers, Tmshates, Torc2, Transcendence, Treisijs, Twinsday, Twooars, TyrS, Ukexpat, Uravjjfaceandvjjarms, Urthogie, Useight, Vikoula5, Vsmith, WCFrancis, WadeSimMiser, Waterloocook, Wavelength, Werdan7, Wervo, WikipedianMarlith, Wingschlong, Wirbelwind, Wisdom89, Wknight94, Wlmg, Womblejonny, Wootwootlmaoftw, Wowcamj, X!, Xavcam, Xhellxringerx, Xymmax, Y12J, YKWSG, Yamamoto Ichiro, YourEyesOnly, Zsinj, Zzuuzz, ﺃﺣﻤﺪ.ﻏﺎﻣﺪﻱ.24, ဇာမဏီ, 白 布 飘 扬, 487 anonymous edits Spermatogonium Source: http://en.wikipedia.org/w/index.php?oldid=544013232 Contributors: 2004-12-29T22:45Z, Aelamass, Arcadian, Bensisko95, Craig Pemberton, Demax hemed, DoriSmith, Easixy5, Espresso Addict, Kaobear, Kappa, Lab-oratory, Lachaume, Mat8989, PDH, Peter Grey, Rich Farmbrough, SCEhardt, Sovbeos, Squirrels2nuts, Transposagen, 18 anonymous edits Sertoli cell Source: http://en.wikipedia.org/w/index.php?oldid=549673146 Contributors: 2004-12-29T22:45Z, A3camero, Abstraktn, Arcadian, Beno1000, Creol, DannyWilde, Dr.queso, ELLusKa 86, Fisher4.wemo, Franamax, France3470, Fyrael, Good Olfactory, Grutness, Gurch, Horiavulpe, Kanabekobaton, MaxEnt, Mgiganteus1, Mikael Häggström, Mild Bill Hiccup, Nephron, Nick Number, Optigan13, Pres27, Rayc, Rexhess, Rjwilmsi, Sababutt, Salam32, Selket, Serephine, Snalwibma, Sovbeos, Tjmayerinsf, Tony Makhlouf, Vespristiano, ViktorWettergren, Vogon77, Vojtech.dostal, Vokesk, 59 anonymous edits Kidney Source: http://en.wikipedia.org/w/index.php?oldid=551560920 Contributors: 03141119, 1607m4dsk1llz, 16clumsyandshy, 62.253.64.xxx, A3RO, AGodofIrony, AS, Abrech, Accurizer, Acd1208, Acroterion, Adashiel, AdjustShift, Agentmoose, Agüeybaná, Ahoerstemeier, Alansohn, Albert Tellier, Aldenrw, Aldis90, Alex.tan, AlexiusHoratius, Allens, Alperen, Alphachimp, AnakngAraw, Anatomist90, Anaxial, Anclation, Andre Engels, Andrea.gf, Andreas Toth, Andy Dingley, Angela, Animum, Anmats, Antandrus, Antennaman, Anthony, Anthonyhcole, Apparition11, Aravindk editing, Arcadian, ArcticFrog, ArielGold, Ascidian, Askari Mark, Athar shams, Austinpow, AxelBoldt, B'er Rabbit, B-rat, Babajobu, Back ache, Badger Drink, Basharh, Bass fishing physicist, Beetstra, Bell cheese jk, BenBreen2003, Bensaccount, Bertinho, Bgwhite, Big iron, Big.tuna1515, BigDogRufus, BillpSea, Blac8, Blah987654, Blast Ulna, Bloodshedder, Blueman1878, BobKawanaka, Bobblewik, Bobsmith040689, Bogey97, Boing! said Zebedee, Bomac, Bongwarrior, Bonhomie, Boofs, Brainmouse, Broderick, Brother Jonathan, Bryan Aldea, Bryan Derksen, Bryan121, Bunchofgrapes, C.Fred, CE, CFCF, CIreland, Can't sleep, clown will eat me, CanDo, CanadianLinuxUser, Canuckle, Capricorn42, CardinalDan, Carpentc, Caryw123, CaseyPenk, Catgut, Ceccomaster, Ceoil, Chaldor, Chaojoker, Charltonasmith, Chaveso, Cheesemongerbumcheese, Chris Roy, Chrislk02, Ckatz, Closedmouth, Clovis Sangrail, Cmdrjameson, Common Good, CommonsDelinker, Consequencefree, Conversion script, Corvus cornix, Cpsoper, Craig Pemberton, CrazyChemGuy, CrazyTerabyte, Cremepuff222, DARTH SIDIOUS 2, DDima, DVD R W, DVdm, Dah Supa Panda, Dale013, DanMS, DanaCake, Dandonkey, DanielCD, Darth Pejka, DavidTanCool, Davidjk, Davidruben, Dawnseeker2000, Dbouillo, Dduck, Delirium, Delldot, Deor, DerHexer, Derpidness123, Diberri, Discospinster, Diyako, Diyar se, DjMD, Doc.mari, Doddy Wuid, Dooky, Doops, DoriSchatell, Dougofborg, Dpwkbw, DrBethersMD, Drsupermikey, Drunken Pirate, Duagloth, Dublinflorg231, ERcheck, Earthengine, Echothegecko, Ecopley, Edgar181, Edward, Eeekster, Eekerz, Ejdjr, El C, EliasAlucard, Ely1, Epbr123, Eperotao, Eras-mus, Eribro, Erudecorp, Euniceespiritu, Evaa, Ewen, Ewulp, Excirial, Exciter1001, FJPB, Falcon8765, Fama Clamosa, Fantasticarlo, Faradayplank, Fastily, Favonian, FelisLeo, Felix-felix, Fieldday-sunday, Fluffernutter, Forschung, Fratter, Freecat, FreplySpang, Furrykef, Fæ, GB fan, Gabbe, Gaff, Gaia Octavia Agrippa, Gail, Galactor213, Gareth Griffith-Jones, Garik, Garion96, Gary King, Gaseous Snake, Gciriani, Geeoharee, Gekritzl, Geneb1955, GermanX, Giftlite, Gilgamesh he, Gilliam, Gillyweed, Ginger555, Ginsengbomb, Glacious, Gludwiczak, Goalie1998, Gogo Dodo, Googie man, Gouerouz, GraemeL, Grafikm fr, Graham87, Greeney, GregorB, Grundle, Gtstricky, Gurch, Gurchzilla, Gwernol, Hadal, Hagerman, Hancong, Hannabee,
615
Article Sources and Contributors
Hannes Hirzel, Haoie, Harej, Harris7, Harry, Hauberg, Hawaiian717, Headwes, Hede2000, HendrixEesti, HenryLi, Hermant patel, Hersfold, HiDrNick, Hmsedit, Hoplophile, HowiAuckland, Huckfinne, HumbleGod, Husond, I dream of horses, Icarus, Icarus3, IceCreamAntisocial, Iggy402, Indiajal, Inoculatedcities, InverseHypercube, Iridescent, Ivan Bajlo, J.delanoy, JForget, JPalonus, JWSchmidt, JaGa, JackPetersen, Jahnavisatyan, Jakob Theorell, JakobSteenberg, James McNally, Jamoche, January, Jaranda, Jauhienij, Jazzbeer27, Jbeans, Jbelker, Jclemens, Jeff G., Jerryseinfeld, Jessdro, Jfdwolff, Jhelton, Jhenderson777, Jidanni, Jim Douglas, JimVC3, Jlautier, Jmjanzen, John, Johndarrington, Johnleemk, Johnny235, Jojhutton, Joliefille, Jonathan.s.kt, Jose Ramos, Jose77, Joseph Solis in Australia, Joshays, Jovianeye, Jpkb24, Jpogi, JuJube, Julia823, JulieADriver, Juliusceaser101, Jumbo Snails, JustinMullins, [email protected], Jwkpiano1, Jyril, KC Panchal, Ka Faraq Gatri, Kabeman1001, Kajasudhakarababu, Kappa, Karada, Karlhahn, Karolfranks, Kartano, Katalaveno, Keegscee, Keenan Pepper, Keilana, Kelly Katula, Kevin Rector, Khazar, Kibi78704, KidneyQuest, King steal7, Kingpin13, Kirrages, Kku, Kleptosquirrel, Knutux, Kochipoik, KokomoNYC, Korg, Kozuch, Kpjas, Kubigula, Kukini, Kungfuadam, Kuru, L Kensington, LPJamesBond007, Lamro, LearnAnatomy, Leevclarke, Legaldeath, Leonard^Bloom, Leslie Mateus, Lexor, Liam Skoda, Linkinparkdawg, Lisatwo, Littlealien182, Lordofthe9, Lova Falk, Luckas Blade, Luk, Luka Krstulović, Luna Santin, Lycurgus, MC10, MER-C, MONGO, Maartentje, Madskile, Magister Mathematicae, Makeemlighter, Manderso, Mani1, Mansavian, Maork, Marcatz18, Marcsin, Marek69, Marnanel, Maroux, Marshman, Martin S Taylor, Massimo Catarinella, Matt Deres, Mav, Max Naylor, Maxxicum, McGeddon, McSly, Mentifisto, Michael H 34, MichaelMaggs, Michig, Mikael Häggström, Mike Rosoft, Mikefadock, Milanlan, Mintleaf, Miquonranger03, Moonriddengirl, Mooquackwooftweetmeow, Mothpit, Motmit, MrDarcy, MrTroy, Mridhula, Mseliw, MuanN, Mulder416, Mushroom, Myanw, N5iln, NCurse, Nahum Reduta, Nakon, Nathan B. Kitchen, NawlinWiki, Ndkartik, Nepenthes, Nephron, NerdyScienceDude, NewEnglandYankee, Nezzadar, Ngantengyuen, Ni1997, NickGorton, NickW557, Nightenbelle, Nihiltres, Nikkislayer7, Niteowlneils, No madol, Noommos, Northumbrian, NotWith, Nthngb, Nubiatech, NuclearWarfare, Numbo3, Nv8200p, O.Koslowski, Oda Mari, Ohnoitsjamie, OldakQuill, Onceonthisisland, Onlyemarie, Orangepoobumapple, Oxymoron83, Ozgod, PFHLai, Pan narrans, Pancreas eater303, Pashute, Patrick, Patxi lurra, Pb30, Pdcook, Pekinensis, Pepper, Peytons, Philpossett, Phrasont, Piano non troppo, Picpower13, Pilotguy, Pinethicket, Pinko1977, Planet88 co .uk, Polskigirl16, Prashanthns, PrincessofLlyr, Prodego, Puffin, QFlyer, Quintote, Qxz, RAlbert NIDDK, RGshredfox, Radiant chains, RadioFan, Rajkiandris, Random Nonsense, RandomAct, Ranveig, Ratarsed, Ratemonth, RattusMaximus, RealGrouchy, Regulov, RenamedUser01302013, RexNL, RhiannonAmelie, Rhomboid, Riana, Richard001, Rje, Rjwilmsi, Rock mechanics, Rodhullandemu, Ronhjones, Ronnoc6655, Ronz, Rossj81, Rossumcapek, Routerone, Roux, RoyBoy, Rror, RubberDuckyMan, Rumping, Ryan032, SC Young Republican, SJP, SPUI, Saavedro300, Salguy, Salvio giuliano, Sam42, Sandgem Addict, Sannse, Sayeth, Sbblr0803, Sceptre, Schafferm, Schmancy47, SchreiberBike, Schzmo, Scorpian ad, Scottalter, Scotty mctotty, Secretlondon, Sephiroth BCR, Serephine, Shadowbeast656, ShakingSpirit, Shanes, Shawn in Montreal, Shoeofdeath, Shoessss, SimonMayer, Sjakkalle, Sjö, Smalljim, Smooth O, Snek01, Soakologist, Soap, Softlavender, Sonjaaa, Soosed, Sophos II, Sougato, Sovereignscience, SpaceFlight89, Spaully, Spongefrog, Spoonaway, Squids and Chips, Squirepants101, Staffwaterboy, StephenBuxton, Stephenb, Stitchmniac123, Sugarcolt, Summer Song, Sun Creator, Sunlei431, Supapuerco, Sven Manguard, Swiley1983, Syth, Tam83, Tangent747, Tapir Terrific, Tarquin, Tassedethe, Tatterfly, Tdb 32, Techman224, Terry Vaserum, The Evil Spartan, The JPS, The Magnificent Clean-keeper, The Thing That Should Not Be, TheAMmollusc, TheWeakWilled, Theresa knott, Thesnuffla, Think outside the box, Thumperward, Thurinym, Tide rolls, Til Eulenspiegel, Timc, Tlsnyder, Tnabtaf, Tnxman307, Tomcowley, Tommy2010, Top.Squark, Toreau, Tpbradbury, TranscendTranslation, Travelbird, Trevor MacInnis, Trevor Wennblom, Tristanb, Trumpy, Tsemii, Tubular, Tweetlebeetle367, Twix617, Tyrol5, Ubiq, Ucucha, Uhai, Unckc, Unschool, Unveiled, Unyoyega, V.narsikar, Vadith, Vanished user 39948282, Vary, Versageek, Versus22, ViciousPotato, Vihsadas, Vishnava, Vivio Testarossa, Vrenator, WadeSimMiser, Walter2cobb, Wavelength, Wayne Slam, Webclient101, Wham Bam Rock II, Whatiguana, Whkoh, Widr, Wikid77, WikipedianMarlith, Wikipelli, Will Beback, Wimt, WinContro, Woohookitty, World, Worldedixor, Woudloper, Wouterstomp, Wronghumor67, Wtmitchell, Xanchester, Xcentaur, Xufanc, Yanamad, YauTou, Ybbor, Yboord028, Yojimbo9102, Yurei-eggtart, Zackkelly, Zannah, Zefr, Zuzuu, ﺃﺣﻤﺪ.ﻏﺎﻣﺪﻱ.24, आशीष भटनागर, 1599 anonymous edits
616
Image Sources, Licenses and Contributors
617
Image Sources, Licenses and Contributors
Image:Illu_quiz_hn_02.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_quiz_hn_02.jpg License: Public Domain Contributors: Arcadian, Flappiefh, It Is Me Here, Petrus Adamus, 3 anonymous edits Image:Digestive system diagram en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Digestive_system_diagram_en.svg License: Public Domain Contributors: Mariana Ruiz Villarreal(LadyofHats) Image:chronic sialadenitis.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Chronic_sialadenitis.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron File:Ebner's gland.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Ebner's_gland.JPG License: Creative Commons Zero Contributors: Pawelolek1991 Image:illu_breast_anatomy.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_breast_anatomy.jpg License: Public Domain Contributors: user:Maksim Image:Dissected lactating breast gray1172.png Source: http://en.wikipedia.org/w/index.php?title=File:Dissected_lactating_breast_gray1172.png License: Public Domain Contributors: AxelBoldt, The Honorable Image:Bezerro mamando REFON .jpg Source: http://en.wikipedia.org/w/index.php?title=File:Bezerro_mamando_REFON_.jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: José Reynaldo da Fonseca (user Reynaldo) Image:White Cat Nursing Four Kittens HQ.jpg Source: http://en.wikipedia.org/w/index.php?title=File:White_Cat_Nursing_Four_Kittens_HQ.jpg License: GNU Free Documentation License Contributors: Ardfern, Kilom691, Pitke, Rune X2, 1 anonymous edits Image:Piglets1.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Piglets1.jpg License: Creative Commons Attribution 2.0 Contributors: FlickrLickr, FlickreviewR, Juiced lemon, Kersti Nebelsiek, Para, Ranveig Image:Baby sheep feeding.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Baby_sheep_feeding.JPG License: Creative Commons Attribution 2.5 Contributors: Gabriel Pollard Image:Kid feeding on mothers milk.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Kid_feeding_on_mothers_milk.jpg License: unknown Contributors: Fir0002 Image:Elephant_breastfeading.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Elephant_breastfeading.jpg License: Creative Commons Attribution-Sharealike 2.0 Contributors: rkimpeljr Image:Breastfeeding_infant.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Breastfeeding_infant.jpg License: Public Domain Contributors: Ken Hammond () Image:Gray896.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray896.png License: Public Domain Contributors: Arcadian, Str4nd, Was a bee, 3 anonymous edits Image:Tear system.svg Source: http://en.wikipedia.org/w/index.php?title=File:Tear_system.svg License: Creative Commons Attribution-Sharealike 2.5 Contributors: User:Erin_Silversmith, User:FML Image:Gray514.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray514.png License: Public Domain Contributors: Arcadian, Lipothymia, Was a bee, 1 anonymous edits Image:Gray776.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray776.png License: Public Domain Contributors: Athaenara, FAEP, Foroa, Kersti Nebelsiek, Lipothymia, Torsch, Was a bee, 2 anonymous edits Image:Gray841.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray841.png License: Public Domain Contributors: Jacklee, Magnus Manske Image:Gray895.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray895.png License: Public Domain Contributors: Arcadian, Was a bee Image:Gray897.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray897.png License: Public Domain Contributors: Arcadian File:Slide3abab.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide3abab.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide4abab.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide4abab.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide5abab.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide5abab.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide6abab.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide6abab.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide7abab.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide7abab.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 Image:Gray940 - sweat gland.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray940_-_sweat_gland.png License: Public Domain Contributors: Prof. Squirrel Image:HairFollicle.png Source: http://en.wikipedia.org/w/index.php?title=File:HairFollicle.png License: Public domain Contributors: User:Helix84 Image:Skin.png Source: http://en.wikipedia.org/w/index.php?title=File:Skin.png License: Public Domain Contributors: US-Gov Image:Haarbalgmilbe.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Haarbalgmilbe.jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: Blauerauerhahn, Eusebius, Liné1 Image:Pilosebaceous_Unit_4x.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Pilosebaceous_Unit_4x.JPG License: unknown Contributors: Kilbad Image:Base of Pilosebaceous Unit 10x.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Base_of_Pilosebaceous_Unit_10x.JPG License: Public Domain Contributors: Kilbad Image:Insertion_of_sebaceous_glands_into_hair_shaft_x10.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Insertion_of_sebaceous_glands_into_hair_shaft_x10.jpg License: Public Domain Contributors: Kilbad Image:Gray893.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray893.png License: Public Domain Contributors: Arcadian, Eug, 1 anonymous edits Image:Gray944.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray944.png License: Public Domain Contributors: Keenan Pepper, Lennert B, Man vyi, Omegatron Image:Gray857.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray857.png License: Public Domain Contributors: Arcadian, Magnus Manske, OldakQuill Image:gray1058.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1058.png License: Public Domain Contributors: Arcadian, Magnus Manske, Origamiemensch File:Duodenum-brunner's glands.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Duodenum-brunner's_glands.JPG License: Public Domain Contributors: Jpogi at en.wikipedia Image:Prostatelead.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Prostatelead.jpg License: Public Domain Contributors: Created by US government agency National Cancer Institute Image:Gray1160.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1160.png License: Public Domain Contributors: Arcadian, Lennert B, Mdangers Image:Corpora amylacea intermed mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Corpora_amylacea_intermed_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:UltrasoundBPH.jpg Source: http://en.wikipedia.org/w/index.php?title=File:UltrasoundBPH.jpg License: Creative Commons Attribution 3.0 Contributors: Etan J. Tal Image:Prostate middle lobe orig.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Prostate_middle_lobe_orig.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Steven Fruitsmaak Image:Inflammation of prostate.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Inflammation_of_prostate.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Prostate adenocarcinoma 2 high mag hps.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Prostate_adenocarcinoma_2_high_mag_hps.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Illu bladder.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_bladder.jpg License: Public Domain Contributors: U.S. National Cancer Institute's Surveillance, Epidemiology and End Results (SEER) Program Image:Illu penis.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_penis.jpg License: Public Domain Contributors: Arcadian, Ephraim33, Hu Totya, Origamiemensch Image:Illu prostate lobes.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_prostate_lobes.jpg License: Public Domain Contributors: Arcadian, Ephraim33 Image:Illu prostate zones.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_prostate_zones.jpg License: Public Domain Contributors: Arcadian, Nevit Image:Illu quiz prostate01.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_quiz_prostate01.jpg License: Public Domain Contributors: Arcadian Image:Prostatehistology.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Prostatehistology.jpg License: Public Domain Contributors: Original: NIH, Explanation: en:User:InvictaHOG Image:male anatomy.png Source: http://en.wikipedia.org/w/index.php?title=File:Male_anatomy.png License: GNU Free Documentation License Contributors: Ephraim33, Frank C. Müller, Lennert B, Odedee, Ranveig, Saperaud, Stephanie, Tsaitgaist, Xiong Chiamiov Image:Gray543.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray543.png License: Public Domain Contributors: Arcadian, Ephraim33 Image:Gray619.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray619.png License: Public Domain Contributors: Arcadian
Image Sources, Licenses and Contributors
Image:Gray1152.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1152.png License: Public Domain Contributors: Arcadian, Origamiemensch Image:Gray1153.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1153.png License: Public Domain Contributors: Arcadian, Ephraim33 Image:Gray1156.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1156.png License: Public Domain Contributors: Arcadian, Ephraim33, Origamiemensch, Yestadae Image:Prostatic urethra.svg Source: http://en.wikipedia.org/w/index.php?title=File:Prostatic_urethra.svg License: Creative Commons Attribution 3.0 Contributors: User:Mcstrother File:Prostatic urethra.svg Source: http://en.wikipedia.org/w/index.php?title=File:Prostatic_urethra.svg License: Creative Commons Attribution 3.0 Contributors: User:Mcstrother Image:Gray1136.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1136.png License: Public Domain Contributors: Arcadian, Ephraim33, Magnus Manske, Origamiemensch Image:Skenes gland.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Skenes_gland.jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: Original uploader was Nicholasolan at en.wikipedia Image:Illu cervix.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_cervix.jpg License: Public Domain Contributors: Arcadian, LERK, M1ss1ontomars2k4, MichaelFrey, Nevit, Speck-Made, Waldir File:Endometrium ocp use3.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Endometrium_ocp_use3.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron File:Endometrium ocp use0.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Endometrium_ocp_use0.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron File:HumanEmbryogenesis.svg Source: http://en.wikipedia.org/w/index.php?title=File:HumanEmbryogenesis.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Zephyris Image:Gray1169.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1169.png License: Public Domain Contributors: Arcadian Image:Endometrial adenocarcinoma (1).jpg Source: http://en.wikipedia.org/w/index.php?title=File:Endometrial_adenocarcinoma_(1).jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: Ares.it, Dam, KGH Image:Uterus (endometrium).JPG Source: http://en.wikipedia.org/w/index.php?title=File:Uterus_(endometrium).JPG License: Public Domain Contributors: Jpogi Image:Endometrium_ocp_use2.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Endometrium_ocp_use2.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Endometrium_ocp_use1.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Endometrium_ocp_use1.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Endometrial stromal condensation high mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Endometrial_stromal_condensation_high_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Fundic gland polyp (1).jpg Source: http://en.wikipedia.org/w/index.php?title=File:Fundic_gland_polyp_(1).jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: Alex brollo, Ares.it, Dam, KGH, 1 anonymous edits Image:Gray1055.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1055.png License: Public Domain Contributors: Arcadian, Magnus Manske, Origamiemensch Image:Chief cells.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Chief_cells.JPG License: GNU Free Documentation License Contributors: en:User:Jpogi Image:Parietal cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Parietal_cells.jpg License: Public Domain Contributors: Original uploader was Jpogi at en.wikipedia Image:Control-of-stomach-acid-sec.png Source: http://en.wikipedia.org/w/index.php?title=File:Control-of-stomach-acid-sec.png License: Creative Commons Attribution-ShareAlike 1.0 Generic Contributors: Haabet, Jacklee, Julia W, Perhelion, Psychonaut, Saperaud, Sophus Bie File:GASTRIC PARIETAL CELL ANTIBODIES.jpg Source: http://en.wikipedia.org/w/index.php?title=File:GASTRIC_PARIETAL_CELL_ANTIBODIES.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Simoncaulton Image:Hydrochloric acid 30 percent.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Hydrochloric_acid_30_percent.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Chemicalinterest, Materialscientist, Woelen, 2 anonymous edits File:Yes check.svg Source: http://en.wikipedia.org/w/index.php?title=File:Yes_check.svg License: Public Domain Contributors: Anomie File:X mark.svg Source: http://en.wikipedia.org/w/index.php?title=File:X_mark.svg License: Public Domain Contributors: User:Gmaxwell File:Phase diagram HCl H2O s l.PNG Source: http://en.wikipedia.org/w/index.php?title=File:Phase_diagram_HCl_H2O_s_l.PNG License: Public Domain Contributors: Steffen 962 File:Stomach mucosal layer labeled.svg Source: http://en.wikipedia.org/w/index.php?title=File:Stomach_mucosal_layer_labeled.svg License: Creative Commons Attribution 3.0 Contributors: M•Komorniczak -talk- 11:43, 23 April 2011 (UTC) File:UN transport pictogram - 8.svg Source: http://en.wikipedia.org/w/index.php?title=File:UN_transport_pictogram_-_8.svg License: Public Domain Contributors: United Nations Economic Commsion for Europe File:Hazard C.svg Source: http://en.wikipedia.org/w/index.php?title=File:Hazard_C.svg License: Public Domain Contributors: Amishaa, Augiasstallputzer, BLueFiSH.as, Bangin, Cosmo1976, Cäsium137, Herbythyme, MarianSigler, Matthias M., Pavel92, Phrood, W!B:, ﺭﻫﮕﺬﺭ ﻏﺮﯾﺐ, 12 anonymous edits Image:Stomach colon rectum diagram.svg Source: http://en.wikipedia.org/w/index.php?title=File:Stomach_colon_rectum_diagram.svg License: Public Domain Contributors: Indolences created it on the English Wikipedia. Image:Digestive system diagram edit.svg Source: http://en.wikipedia.org/w/index.php?title=File:Digestive_system_diagram_edit.svg License: Public Domain Contributors: Mariana RuizLadyofHats, edited by Joaquim Alves Gaspar File:Gut wall.svg Source: http://en.wikipedia.org/w/index.php?title=File:Gut_wall.svg License: Creative Commons Attribution 3.0 Contributors: Original uploader was Auawise at en.wikipedia (Original text : Λua∫Wise (Operibus anteire)) Image:Gray1053.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1053.png License: Public Domain Contributors: Arcadian, DO11.10, Haabet, Jacklee, Magnus Manske, Origamiemensch Image:Gray1060.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1060.png License: Public Domain Contributors: Arcadian, Magnus Manske, Origamiemensch Image:Gray1062.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1062.png License: Public Domain Contributors: Arcadian, Magnus Manske, Origamiemensch Image:Gobletcel.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Gobletcel.jpg License: Copyrighted free use Contributors: Arcadian, JMCC1, Theoteryi File:MultiPhotonExcitation-Fig10-doi10.1186slash1475-925X-5-36.JPEG Source: http://en.wikipedia.org/w/index.php?title=File:MultiPhotonExcitation-Fig10-doi10.1186slash1475-925X-5-36.JPEG License: Creative Commons Attribution 2.0 Contributors: Alberto Diaspro, Paolo Bianchini, Giuseppe Vicidomini, Mario Faretta, Paola Ramoino and Cesare Usai Image:Respiratory system complete numbered.svg Source: http://en.wikipedia.org/w/index.php?title=File:Respiratory_system_complete_numbered.svg License: Public Domain Contributors: LadyofHats File:Respiratory Tract Histological Differences.png Source: http://en.wikipedia.org/w/index.php?title=File:Respiratory_Tract_Histological_Differences.png License: Creative Commons Attribution 3.0 Contributors: Anmats, Dmalicke, Trijnstel File:Mucus cells.png Source: http://en.wikipedia.org/w/index.php?title=File:Mucus_cells.png License: Creative Commons Attribution 2.5 Contributors: see source Image:GLO1 Homo sapiens small fast.gif Source: http://en.wikipedia.org/w/index.php?title=File:GLO1_Homo_sapiens_small_fast.gif License: Creative Commons Attribution 3.0 Contributors: WillowW Image:Carbonic anhydrase.png Source: http://en.wikipedia.org/w/index.php?title=File:Carbonic_anhydrase.png License: Public Domain Contributors: Labrador2 Image:Induced fit diagram.svg Source: http://en.wikipedia.org/w/index.php?title=File:Induced_fit_diagram.svg License: Public Domain Contributors: Created by TimVickers, vectorized by Fvasconcellos Image:Enzyme allostery en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Enzyme_allostery_en.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: File:Enzyme allostery es.svg: File:Enzyme allostery es.png: File:Enzyme allostery.png: Allostery.png: Nicolas Le Novere (talk). Original uploader was Lenov at en.wikipedia derivative work: TimVickers (talk) derivative work: Retama (talk) derivative work: KES47 (talk) derivative work: KES47 (talk) Image:NADH-3D-vdW.png Source: http://en.wikipedia.org/w/index.php?title=File:NADH-3D-vdW.png License: Public Domain Contributors: Benjah-bmm27 Image:Carbonic anhydrase reaction in tissue.svg Source: http://en.wikipedia.org/w/index.php?title=File:Carbonic_anhydrase_reaction_in_tissue.svg License: GNU Free Documentation License Contributors: Fvasconcellos Image:Simple mechanism.svg Source: http://en.wikipedia.org/w/index.php?title=File:Simple_mechanism.svg License: Public domain Contributors: TimVickers at en.wikipedia
618
Image Sources, Licenses and Contributors
Image:Michaelis-Menten saturation curve of an enzyme reaction.svg Source: http://en.wikipedia.org/w/index.php?title=File:Michaelis-Menten_saturation_curve_of_an_enzyme_reaction.svg License: Public Domain Contributors: fullofstars Image:Competitive inhibition.svg Source: http://en.wikipedia.org/w/index.php?title=File:Competitive_inhibition.svg License: Public Domain Contributors: Authored by Jerry Crimson Mann, modified by TimVickers, vectorized by Fvasconcellos Image:Types of inhibition en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Types_of_inhibition_en.svg License: Public Domain Contributors: fullofstars Image:Methotrexate and folic acid compared.png Source: http://en.wikipedia.org/w/index.php?title=File:Methotrexate_and_folic_acid_compared.png License: Public domain Contributors: TimVickers Image:Glycolysis.svg Source: http://en.wikipedia.org/w/index.php?title=File:Glycolysis.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: WYassineMrabetTalk ✉ Image:Phenylalanine hydroxylase brighter.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Phenylalanine_hydroxylase_brighter.jpg License: Public domain Contributors: TimVickers Image:Amylose.svg Source: http://en.wikipedia.org/w/index.php?title=File:Amylose.svg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: HenkvD, Jan Homann, Sunridin, Yarl, 2 anonymous edits Image:Sjb whiskey malt.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Sjb_whiskey_malt.jpg License: GNU Free Documentation License Contributors: Finlay_McWalter's friend SJB Image:Roquefort cheese.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Roquefort_cheese.jpg License: GNU Free Documentation License Contributors: HenkvD, Lionel Allorge, Mercurywoodrose, Olivier2, Quadell, Ranveig, Yosri, Zerohund Image:Alpha-D-Glucopyranose.svg Source: http://en.wikipedia.org/w/index.php?title=File:Alpha-D-Glucopyranose.svg License: Public Domain Contributors: NEUROtiker Image:Alpha-D-Fructofuranose.svg Source: http://en.wikipedia.org/w/index.php?title=File:Alpha-D-Fructofuranose.svg License: Public Domain Contributors: NEUROtiker Image:InternationalPaper6413.jpg Source: http://en.wikipedia.org/w/index.php?title=File:InternationalPaper6413.jpg License: GNU Free Documentation License Contributors: Pollinator Image:Cellulose-Ibeta-from-xtal-2002-3D-balls.png Source: http://en.wikipedia.org/w/index.php?title=File:Cellulose-Ibeta-from-xtal-2002-3D-balls.png License: Public Domain Contributors: Ben Mills Image:DNA123 rotated.png Source: http://en.wikipedia.org/w/index.php?title=File:DNA123_rotated.png License: Public Domain Contributors: DNA Image:Human Paneth cells.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Human_Paneth_cells.JPG License: Public Domain Contributors: en:Jpogi Image:Bicarbonate-resonance.png Source: http://en.wikipedia.org/w/index.php?title=File:Bicarbonate-resonance.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: Hellbus Image:Bicarbonate-ion-3D-balls.png Source: http://en.wikipedia.org/w/index.php?title=File:Bicarbonate-ion-3D-balls.png License: Public Domain Contributors: Ben Mills and Jynto Image:Equilibrium.svg Source: http://en.wikipedia.org/w/index.php?title=File:Equilibrium.svg License: Public Domain Contributors: L'Aquatique File:Riassorbimento bicarbonati e respirazione cellulare.svg Source: http://en.wikipedia.org/w/index.php?title=File:Riassorbimento_bicarbonati_e_respirazione_cellulare.svg License: Public Domain Contributors: Riassorbimento_bicarbonati_e_respirazione_cellulare.jpg: Gianreali derivative work: Luigi Chiesa (talk) File:Reference ranges for blood tests - by molarity.png Source: http://en.wikipedia.org/w/index.php?title=File:Reference_ranges_for_blood_tests_-_by_molarity.png License: Public Domain Contributors: Mikael Häggström File:lysozyme crystal1.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Lysozyme_crystal1.JPG License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: Chrumps, Kruusamägi, Lode, Perditax file:Lysozyme.png Source: http://en.wikipedia.org/w/index.php?title=File:Lysozyme.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: Yikrazuul file:PBB_GE_LYZ_213975_s_at_tn.png Source: http://en.wikipedia.org/w/index.php?title=File:PBB_GE_LYZ_213975_s_at_tn.png License: GNU Free Documentation License Contributors: File:Mecanism of action for Lysozyme.svg Source: http://en.wikipedia.org/w/index.php?title=File:Mecanism_of_action_for_Lysozyme.svg License: Creative Commons Zero Contributors: User:Pierreb24 File:Micelle.png Source: http://en.wikipedia.org/w/index.php?title=File:Micelle.png License: GNU Free Documentation License Contributors: User:Onco p53 Image:Micelle scheme-en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Micelle_scheme-en.svg License: Creative Commons Attribution-Sharealike 3.0,2.5,2.0,1.0 Contributors: SuperManu File:TensideHyrophilHydrophob.png Source: http://en.wikipedia.org/w/index.php?title=File:TensideHyrophilHydrophob.png License: GNU Free Documentation License Contributors: Roland.chem Original uploader was Roland.chem at de.wikipedia file:Oxytocin with labels.png Source: http://en.wikipedia.org/w/index.php?title=File:Oxytocin_with_labels.png License: Public Domain Contributors: Edgar181 file:OxitocinaCPK3D.png Source: http://en.wikipedia.org/w/index.php?title=File:OxitocinaCPK3D.png License: Creative Commons Zero Contributors: MindZiper File:Oxytocin-neurophysin.png Source: http://en.wikipedia.org/w/index.php?title=File:Oxytocin-neurophysin.png License: Public Domain Contributors: Edgar181 file:Arginine vasopressin3d.png Source: http://en.wikipedia.org/w/index.php?title=File:Arginine_vasopressin3d.png License: Public Domain Contributors: Fvasconcellos file:PBB_GE_AVP_207848_at_tn.png Source: http://en.wikipedia.org/w/index.php?title=File:PBB_GE_AVP_207848_at_tn.png License: GNU Free Documentation License Contributors: File:AVP, ISH, periventricular region of the hypothalamus, adult mouse.jpg Source: http://en.wikipedia.org/w/index.php?title=File:AVP,_ISH,_periventricular_region_of_the_hypothalamus,_adult_mouse.jpg License: Creative Commons Attribution 1.0 Generic Contributors: Allen Institute for Brain Science File:vasopressin labeled.png Source: http://en.wikipedia.org/w/index.php?title=File:Vasopressin_labeled.png License: Public Domain Contributors: Edgar181 File:Oxytocin with labels.png Source: http://en.wikipedia.org/w/index.php?title=File:Oxytocin_with_labels.png License: Public Domain Contributors: Edgar181 Image:Serotonin-2D-skeletal.svg Source: http://en.wikipedia.org/w/index.php?title=File:Serotonin-2D-skeletal.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Liaocyed Image:Serotonin-Spartan-HF-based-on-xtal-3D-balls-web.png Source: http://en.wikipedia.org/w/index.php?title=File:Serotonin-Spartan-HF-based-on-xtal-3D-balls-web.png License: Public Domain Contributors: Ben Mills Image:Serotonin-Spartan-HF-based-on-xtal-3D-sf-web.png Source: http://en.wikipedia.org/w/index.php?title=File:Serotonin-Spartan-HF-based-on-xtal-3D-sf-web.png License: Public Domain Contributors: Ben Mills File:Dopamineseratonin.png Source: http://en.wikipedia.org/w/index.php?title=File:Dopamineseratonin.png License: Public Domain Contributors: A3 nm, Fuzzform, MithrandirMage, Monkeybait, Åkebråke, 1 anonymous edits File:Serotonin biosynthesis.svg Source: http://en.wikipedia.org/w/index.php?title=File:Serotonin_biosynthesis.svg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: NEUROtiker Image:Alpha-neoendorphin.svg Source: http://en.wikipedia.org/w/index.php?title=File:Alpha-neoendorphin.svg License: Public Domain Contributors: Ed (Edgar181) Image:Beta-endorphin.png Source: http://en.wikipedia.org/w/index.php?title=File:Beta-endorphin.png License: Public Domain Contributors: Edgar181 (talk) file:Somatostatin.svg Source: http://en.wikipedia.org/w/index.php?title=File:Somatostatin.svg License: Public Domain Contributors: Ed (Edgar181) file:PBB_GE_SST_213921_at_tn.png Source: http://en.wikipedia.org/w/index.php?title=File:PBB_GE_SST_213921_at_tn.png License: GNU Free Documentation License Contributors: File:Sst, ISH, E15.5, telencephalon.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Sst,_ISH,_E15.5,_telencephalon.jpg License: Creative Commons Attribution 1.0 Generic Contributors: Allen Institute for Brain Science File:Sst, ISH, p56 mouse.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Sst,_ISH,_p56_mouse.jpg License: Creative Commons Attribution 1.0 Generic Contributors: Allen Institute for Brain Science file:PBB_GE_GAST_208138_at_tn.png Source: http://en.wikipedia.org/w/index.php?title=File:PBB_GE_GAST_208138_at_tn.png License: GNU Free Documentation License Contributors: file:PBB_GE_CCK_205827_at_tn.png Source: http://en.wikipedia.org/w/index.php?title=File:PBB_GE_CCK_205827_at_tn.png License: GNU Free Documentation License Contributors: file:InsulinHexamer.jpg Source: http://en.wikipedia.org/w/index.php?title=File:InsulinHexamer.jpg License: Creative Commons Attribution 2.5 Contributors: Original uploader was Takometer at en.wikipedia file:PBB_GE_INS_206598_at_tn.png Source: http://en.wikipedia.org/w/index.php?title=File:PBB_GE_INS_206598_at_tn.png License: GNU Free Documentation License Contributors: -
619
Image Sources, Licenses and Contributors
Image:Insulinpath.png Source: http://en.wikipedia.org/w/index.php?title=File:Insulinpath.png License: Creative Commons Attribution 2.5 Contributors: Original uploader was Takometer at en.wikipedia Image:Pancreas insulin oscillations.svg Source: http://en.wikipedia.org/w/index.php?title=File:Pancreas_insulin_oscillations.svg License: Public Domain Contributors: Made with inkscape, for the sake of free knowledge to all mankind, by Mikael Häggström (User:Mikael Häggström) Image:Suckale08 fig3 glucose insulin day.png Source: http://en.wikipedia.org/w/index.php?title=File:Suckale08_fig3_glucose_insulin_day.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: Jakob Suckale, Michele Solimena File:Insulin glucose metabolism ZP.svg Source: http://en.wikipedia.org/w/index.php?title=File:Insulin_glucose_metabolism_ZP.svg License: Public domain Contributors: XcepticZP at en.wikipedia File:Inzulín.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Inzulín.jpg License: Public Domain Contributors: Original uploader was Mr Hyde at cs.wikipedia (Original text : moje foto) Image:InsulinMonomer.jpg Source: http://en.wikipedia.org/w/index.php?title=File:InsulinMonomer.jpg License: Creative Commons Attribution 2.5 Contributors: Isaac Yonemoto. File:C. H. Best and F. G. Banting ca. 1924.png Source: http://en.wikipedia.org/w/index.php?title=File:C._H._Best_and_F._G._Banting_ca._1924.png License: Public Domain Contributors: YUL89YYZ Image:Nicolae Paulescu - Foto03.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Nicolae_Paulescu_-_Foto03.jpg License: Public Domain Contributors: FSII, Mvelam file:Glucagon- 1GCN.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Glucagon-_1GCN.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Truthortruth file:PBB_GE_GCG_206422_at_tn.png Source: http://en.wikipedia.org/w/index.php?title=File:PBB_GE_GCG_206422_at_tn.png License: GNU Free Documentation License Contributors: Image:Glucagon rednblue.png Source: http://en.wikipedia.org/w/index.php?title=File:Glucagon_rednblue.png License: Public domain Contributors: Original uploader was Brazucs at en.wikipedia file:Glucagon.png Source: http://en.wikipedia.org/w/index.php?title=File:Glucagon.png License: Public Domain Contributors: User:Brian0918 Image:Bombesin_full.png Source: http://en.wikipedia.org/w/index.php?title=File:Bombesin_full.png License: Attribution Contributors: Megac7 Image:Gray1176.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1176.png License: Public Domain Contributors: Arcadian, Materialscientist, Quibik File:Thyroid hormone synthesis.png Source: http://en.wikipedia.org/w/index.php?title=File:Thyroid_hormone_synthesis.png License: Creative Commons Zero Contributors: Mikael Häggström Image:illu_endocrine_system.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_endocrine_system.jpg License: Public Domain Contributors: Kam Solusar, Kilom691, Truthflux, Was a bee, 2 anonymous edits Image:Illu thyroid parathyroid.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_thyroid_parathyroid.jpg License: Public Domain Contributors: Bemoeial1, Kulmalukko, Lennert B, 2 anonymous edits Image:Parathyroid gland high mag cropped.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Parathyroid_gland_high_mag_cropped.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Parathyroid gland high mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Parathyroid_gland_high_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Parathyroid gland intermed mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Parathyroid_gland_intermed_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Parathyroid gland low mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Parathyroid_gland_low_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Gray1175.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1175.png License: Public Domain Contributors: Arcadian image:Gray1177.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1177.png License: Public Domain Contributors: Arcadian, Tsca Image:Gray1185.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1185.png License: Public Domain Contributors: Dodo File:Adrenaline.svg Source: http://en.wikipedia.org/w/index.php?title=File:Adrenaline.svg License: Public Domain Contributors: Harbin File:Norepinephrine structure.png Source: http://en.wikipedia.org/w/index.php?title=File:Norepinephrine_structure.png License: Public Domain Contributors: Original uploader was Edgar181 at en.wikipedia File:Steroidogenesis.svg Source: http://en.wikipedia.org/w/index.php?title=File:Steroidogenesis.svg License: GNU Free Documentation License Contributors: David Richfield (User:Slashme) and Mikael Häggström Derived from previous version by Hoffmeier and Settersr. Image:Aldosterone-2D-skeletal.svg Source: http://en.wikipedia.org/w/index.php?title=File:Aldosterone-2D-skeletal.svg License: Public Domain Contributors: Image:Aldosterone-2D-skeletal.png by Ben Mills, vectorized by Image:11-Deoxycorticosterone.svg Source: http://en.wikipedia.org/w/index.php?title=File:11-Deoxycorticosterone.svg License: Public Domain Contributors: Ed (Edgar181) Image:Fludrocortisone structure.png Source: http://en.wikipedia.org/w/index.php?title=File:Fludrocortisone_structure.png License: Public Domain Contributors: Edgar181 Image:Cortisol2.svg Source: http://en.wikipedia.org/w/index.php?title=File:Cortisol2.svg License: Public Domain Contributors: Calvero. Image:Dexamethasone structure.svg Source: http://en.wikipedia.org/w/index.php?title=File:Dexamethasone_structure.svg License: Public Domain Contributors: Ed (Edgar181) Image:YerkesDodsonLawGraph.png Source: http://en.wikipedia.org/w/index.php?title=File:YerkesDodsonLawGraph.png License: Public Domain Contributors: User:Vaughan File:Cortisone acetate.png Source: http://en.wikipedia.org/w/index.php?title=File:Cortisone_acetate.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: Yid (talk). Original uploader was Yid at en.wikipedia Image:Leydig cells - very high mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Leydig_cells_-_very_high_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Testicle-histology-boar-2.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Testicle-histology-boar-2.jpg License: Creative Commons Attribution-Sharealike 2.5 Contributors: Original uploader was Mikael Häggström at en.wikipedia Image:Leydig cell tumour3.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Leydig_cell_tumour3.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Gray1114.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1114.png License: Public Domain Contributors: Arcadian, Ephraim33, Magnus Manske, Origamiemensch Image:Leydig cell tumour2.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Leydig_cell_tumour2.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image: Leydig cells.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Leydig_cells.JPG License: Public Domain Contributors: Jpogi File:Order of changes in ovary.svg Source: http://en.wikipedia.org/w/index.php?title=File:Order_of_changes_in_ovary.svg License: GNU Free Documentation License Contributors: user:Shazz File:Folliculogenesis chart.gif Source: http://en.wikipedia.org/w/index.php?title=File:Folliculogenesis_chart.gif License: Public domain Contributors: Original uploader was D. Wu at en.wikipedia File:Non-Growing Follicles.png Source: http://en.wikipedia.org/w/index.php?title=File:Non-Growing_Follicles.png License: Creative Commons Attribution 3.0 Contributors: Geremia, Rjwilmsi Image:Gray1163.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1163.png License: Public Domain Contributors: Arcadian, Mdangers, Origamiemensch File:Primary follicle (transition).jpg Source: http://en.wikipedia.org/w/index.php?title=File:Primary_follicle_(transition).jpg License: Public Domain Contributors: Original uploader was Jpogi at en.wikipedia file:Progesteron.svg Source: http://en.wikipedia.org/w/index.php?title=File:Progesteron.svg License: Public Domain Contributors: NEUROtiker file:Progesterone-3D-vdW.png Source: http://en.wikipedia.org/w/index.php?title=File:Progesterone-3D-vdW.png License: Public Domain Contributors: Benjah-bmm27, Edgar181, MindZiper Image:Progesterone biosynthesis.png Source: http://en.wikipedia.org/w/index.php?title=File:Progesterone_biosynthesis.png License: Public Domain Contributors: Boghog2 Image:Marker snythesis.png Source: http://en.wikipedia.org/w/index.php?title=File:Marker_snythesis.png License: Public Domain Contributors: Boghog2 Image:Progesterone Synthesis.png Source: http://en.wikipedia.org/w/index.php?title=File:Progesterone_Synthesis.png License: Public Domain Contributors: Johnson, W. S. File:Progesterone during menstrual cycle.png Source: http://en.wikipedia.org/w/index.php?title=File:Progesterone_during_menstrual_cycle.png License: Public Domain Contributors: Mikael Häggström
620
Image Sources, Licenses and Contributors
Image:Endometrium ocp use3.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Endometrium_ocp_use3.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron File:000527lg Prometrium 100 MG Oral Capsule.jpg Source: http://en.wikipedia.org/w/index.php?title=File:000527lg_Prometrium_100_MG_Oral_Capsule.jpg License: Public domain Contributors: NLM Image:Pregnenolone.svg Source: http://en.wikipedia.org/w/index.php?title=File:Pregnenolone.svg License: Public Domain Contributors: Ed (Edgar181) Image:Order_of_changes_in_ovary.svg Source: http://en.wikipedia.org/w/index.php?title=File:Order_of_changes_in_ovary.svg License: GNU Free Documentation License Contributors: user:Shazz Image:Human Ovary with Fully Developed Corpus Luteum.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Human_Ovary_with_Fully_Developed_Corpus_Luteum.jpg License: Creative Commons Attribution-Sharealike 2.0 Contributors: Ed Uthman Image:Luteinized follicular cyst.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Luteinized_follicular_cyst.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Juxtaglomerular cells.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Juxtaglomerular_cells.JPG License: Public Domain Contributors: Jpogi Image:Renal corpuscle.svg Source: http://en.wikipedia.org/w/index.php?title=File:Renal_corpuscle.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: M•Komorniczak -talk- (polish Wikipedist) file:PDB_2ren_EBI.jpg Source: http://en.wikipedia.org/w/index.php?title=File:PDB_2ren_EBI.jpg License: unknown Contributors: File:Renin-angiotensin system in man shadow.svg Source: http://en.wikipedia.org/w/index.php?title=File:Renin-angiotensin_system_in_man_shadow.svg License: Public Domain Contributors: Mikael Häggström Image:Renin-angiotensin-aldosterone system.png Source: http://en.wikipedia.org/w/index.php?title=File:Renin-angiotensin-aldosterone_system.png License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: A. Rad, Joey-das-WBF, Kallerna, Rillke, 4 anonymous edits Image:Epidermis-delimited.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Epidermis-delimited.JPG License: Public Domain Contributors: Normal_Epidermis_and_Dermis_with_Intradermal_Nevus_10x.JPG: Kilbad Cropped and labeled by Fama Clamosa (talk) and Mikael Häggström, respectively Image:Epidermal layers.png Source: http://en.wikipedia.org/w/index.php?title=File:Epidermal_layers.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: Mikael Häggström, based on work by Wbensmith Image:Skinlayers.png Source: http://en.wikipedia.org/w/index.php?title=File:Skinlayers.png License: Public Domain Contributors: Serephine, 1 anonymous edits Image:Normal Epidermis and Dermis with Intradermal Nevus 10x.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Normal_Epidermis_and_Dermis_with_Intradermal_Nevus_10x.JPG License: Public Domain Contributors: Kilbad Image:HautFingerspitzeOCT.gif Source: http://en.wikipedia.org/w/index.php?title=File:HautFingerspitzeOCT.gif License: Creative Commons Attribution-Sharealike 2.0 Contributors: User:BoP, Supplied by the medOCT group, Medical University Vienna, Austria Image:Mouse embryonic stem cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Mouse_embryonic_stem_cells.jpg License: Public Domain Contributors: ChongDae, Salix, The Evil IP address, 1 anonymous edits Image:Human embryonic stem cell colony phase.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Human_embryonic_stem_cell_colony_phase.jpg License: Public Domain Contributors: Original uploader was Id711 at en.wikipedia Image:Stem cells diagram.png Source: http://en.wikipedia.org/w/index.php?title=File:Stem_cells_diagram.png License: Creative Commons Attribution-Sharealike 2.5 Contributors: Mike Jones Image:Human embryonic stem cells.png Source: http://en.wikipedia.org/w/index.php?title=File:Human_embryonic_stem_cells.png License: Creative Commons Attribution 2.5 Contributors: (Images: Nissim Benvenisty) Image:Stem cell division and differentiation.svg Source: http://en.wikipedia.org/w/index.php?title=File:Stem_cell_division_and_differentiation.svg License: Public Domain Contributors: User:Wykis File:Stem cell treatments.svg Source: http://en.wikipedia.org/w/index.php?title=File:Stem_cell_treatments.svg License: Public Domain Contributors: Mikael Häggström File:Yong Zhao smiling Portrait.png Source: http://en.wikipedia.org/w/index.php?title=File:Yong_Zhao_smiling_Portrait.png License: Creative Commons Attribution 3.0 Contributors: Leo181 File:Martin Evans Nobel Prize.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Martin_Evans_Nobel_Prize.jpg License: Creative Commons Attribution 3.0 Contributors: Cardiff University Image:Gray945.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray945.png License: Public Domain Contributors: Arcadian, Jacklee, Kersti Nebelsiek, Lamiot, Magnus Manske File:Illu epithelium.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_epithelium.jpg License: Public Domain Contributors: Arcadian, BenFrantzDale, Incnis Mrsi, Origamiemensch, Romanm, 3 anonymous edits Image:Dogsquamos100x.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Dogsquamos100x.jpg License: Creative Commons Attribution-Share Alike Contributors: John Alan Elson Image:Cheekcells stained.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Cheekcells_stained.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Mulletsrokk Image:Illu epithelium.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_epithelium.jpg License: Public Domain Contributors: Arcadian, BenFrantzDale, Incnis Mrsi, Origamiemensch, Romanm, 3 anonymous edits File:Gray931.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray931.png License: Public Domain Contributors: Arcadian, Iainf, Jacklee, Jmarchn, Magnus Manske, Mike.lifeguard, Was a bee File:Organ of corti.svg Source: http://en.wikipedia.org/w/index.php?title=File:Organ_of_corti.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Madhero88 File:Gray932.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray932.png License: Public Domain Contributors: Gray's Anatomy File:Vestibular system's semicircular canal- a cross-section.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Vestibular_system's_semicircular_canal-_a_cross-section.jpg License: Public Domain Contributors: United States government File:Stereocilia of frog inner ear.01.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Stereocilia_of_frog_inner_ear.01.jpg License: Public Domain Contributors: Bechara Kachar File:Diagram of human skin.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Diagram_of_human_skin.jpg License: GNU Free Documentation License Contributors: Ngb, 1 anonymous edits File:Riechschleimhaut.svg Source: http://en.wikipedia.org/w/index.php?title=File:Riechschleimhaut.svg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: User:MarianSigler Image:Gray772.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray772.png License: Public Domain Contributors: Arcadian, Lipothymia, Magnus Manske, OldakQuill, Túrelio, Was a bee, 1 anonymous edits Image:Rod&Cone.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Rod&Cone.jpg License: Public Domain Contributors: Kosigrim Image:Cone-response.svg Source: http://en.wikipedia.org/w/index.php?title=File:Cone-response.svg License: GNU Free Documentation License Contributors: User:Maxim Razin File:Fig retine.png Source: http://en.wikipedia.org/w/index.php?title=File:Fig_retine.png License: Public Domain Contributors: Chrkl, Diego UFCG, Drahkrub, Jarry1250, Lipothymia, 1 anonymous edits Image:Cone2.svg Source: http://en.wikipedia.org/w/index.php?title=File:Cone2.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Madhero88 File:Cones SMJ2 E.svg Source: http://en.wikipedia.org/w/index.php?title=File:Cones_SMJ2_E.svg License: Creative Commons Attribution-Sharealike 3.0,2.5,2.0,1.0 Contributors: Vanessaezekowitz at en.wikipedia / Later version uploaded by BenRG. Image:Cone cell en.png Source: http://en.wikipedia.org/w/index.php?title=File:Cone_cell_en.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: Ivo Kruusamägi Image:BirdCone.png Source: http://en.wikipedia.org/w/index.php?title=File:BirdCone.png License: Public Domain Contributors: Jimfbleak Image:Gray1186.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1186.png License: Public Domain Contributors: Arcadian Image:Gray474.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray474.png License: Public Domain Contributors: Arcadian, Lipothymia Image:Carotid body tumour 2 intermed mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Carotid_body_tumour_2_intermed_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Gray1018.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1018.png License: Public Domain Contributors: Arcadian, Magnus Manske
621
Image Sources, Licenses and Contributors
Image:Taste bud.svg Source: http://en.wikipedia.org/w/index.php?title=File:Taste_bud.svg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: NEUROtiker Image:Smagsloeg.png Source: http://en.wikipedia.org/w/index.php?title=File:Smagsloeg.png License: unknown Contributors: User:Sjoehest Image:Neuron Hand-tuned.svg Source: http://en.wikipedia.org/w/index.php?title=File:Neuron_Hand-tuned.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Original uploader was Quasar Jarosz at en.wikipedia Image:Cultured schwann cell.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Cultured_schwann_cell.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Ucbtbej File:Gray839.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray839.png License: Public Domain Contributors: Gray's Anatomy File:SchematicP2XRsubunitJPG.jpg Source: http://en.wikipedia.org/w/index.php?title=File:SchematicP2XRsubunitJPG.jpg License: Public Domain Contributors: Subcellular File:Herpes simplex virions, TEM.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Herpes_simplex_virions,_TEM.jpg License: Public Domain Contributors: CDC/ Dr. Fred Murphy File:Neuroglia.png Source: http://en.wikipedia.org/w/index.php?title=File:Neuroglia.png License: Public Domain Contributors: Original uploader was Diberri at en.wikipedia File:Gfapastr5.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Gfapastr5.jpg License: Public Domain Contributors: Jacopo Werther, Maksim, Uwe Gille File:2010-3-15 rGFAP 1-4000 1-200 Hip 20x(4).jpg Source: http://en.wikipedia.org/w/index.php?title=File:2010-3-15_rGFAP_1-4000_1-200_Hip_20x(4).jpg License: Public Domain Contributors: ArizonaLifeScience File:Human astrocyte.png Source: http://en.wikipedia.org/w/index.php?title=File:Human_astrocyte.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Bruno Pascal File:Anaplastic astrocytoma - gfap - very high mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Anaplastic_astrocytoma_-_gfap_-_very_high_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Oligodendrocyte.png Source: http://en.wikipedia.org/w/index.php?title=File:Oligodendrocyte.png License: Public Domain Contributors: CopperKettle, Kluka, Methoxyroxy, NEON ja, Sultan11 Image:Gray667.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray667.png License: Public Domain Contributors: Arcadian Image:Gray706.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray706.png License: Public Domain Contributors: Arcadian, Lipothymia, Origamiemensch Image:Astrocytre.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Astrocytre.jpg License: Creative Commons Attribution 3.0 Contributors: Original uploader was Neurorocker at en.wikipedia Image:Astrocyte - cultutures - GFAP.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Astrocyte_-_cultutures_-_GFAP.jpg License: GNU Free Documentation License Contributors: Original uploader was GrzegorzWicher at pl.wikipedia Image:Astrocyte - rat spinal cord - GFAP.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Astrocyte_-_rat_spinal_cord_-_GFAP.jpg License: GNU Free Documentation License Contributors: Original uploader was GrzegorzWicher at pl.wikipedia Image:astrocytes-mouse-cortex.png Source: http://en.wikipedia.org/w/index.php?title=File:Astrocytes-mouse-cortex.png License: Creative Commons Attribution-Share Alike Contributors: Mhisted File:Metabolic interactions between astrocytes and neurons with major reactions.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Metabolic_interactions_between_astrocytes_and_neurons_with_major_reactions.jpg License: Creative Commons Attribution 2.0 Contributors: Tunahan Çakιr, Selma Alsan, Hale Saybaş, Ata Akιn and Kutlu Ö Ülgen Image:Slcla3 in Bergmann Glia.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Slcla3_in_Bergmann_Glia.jpg License: Public Domain Contributors: The Gene Expression Nervous System Atlas (GENSAT) Project, NINDS Contract # N01NS02331 to The Rockefeller University (New York, NY) File:PurkinjeCell.jpg Source: http://en.wikipedia.org/w/index.php?title=File:PurkinjeCell.jpg License: Public Domain Contributors: Chrislb, Feezil, Hystrix, Interpretix, Jacklee, SriMesh, 1 anonymous edits Image:Complete neuron cell diagram en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Complete_neuron_cell_diagram_en.svg License: Public Domain Contributors: LadyofHats Image:Gyrus Dentatus 40x.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Gyrus_Dentatus_40x.jpg License: Creative Commons Attribution-Sharealike 2.5 Contributors: MethoxyRoxy Image:GFPneuron.png Source: http://en.wikipedia.org/w/index.php?title=File:GFPneuron.png License: Creative Commons Attribution 2.5 Contributors: Original uploader was Nrets at en.wikipedia Image:smi32neuron.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Smi32neuron.jpg License: Creative Commons Attribution 3.0 Contributors: UC Regents Davis campus File:Neurons uni bi multi pseudouni.svg Source: http://en.wikipedia.org/w/index.php?title=File:Neurons_uni_bi_multi_pseudouni.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Pseudounipolar_bipolar_neurons.svg: Juoj8 derivative work: Jonathan Haas (talk) Image:Chemical synapse schema cropped.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Chemical_synapse_schema_cropped.jpg License: Public Domain Contributors: user:Looie496 created file, US National Institutes of Health, National Institute on Aging created original Image:Golgi Hippocampus.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Golgi_Hippocampus.jpg License: Public Domain Contributors: Ephraim33, Marc Gabriel Schmid, Methoxyroxy, Rory096, Was a bee, 2 anonymous edits Image:Purkinje cell by Cajal.png Source: http://en.wikipedia.org/w/index.php?title=File:Purkinje_cell_by_Cajal.png License: Public Domain Contributors: Original uploader was PNG crusade bot at en.wikipedia Image:Neuron with oligodendrocyte and myelin sheath.svg Source: http://en.wikipedia.org/w/index.php?title=File:Neuron_with_oligodendrocyte_and_myelin_sheath.svg License: Public Domain Contributors: Neuron_with_oligodendrocyte_and_myelin_sheath.svg: *Complete_neuron_cell_diagram_en.svg: LadyofHats derivative work: Andrew c (talk) File:Oligodendrocyte illustration.png Source: http://en.wikipedia.org/w/index.php?title=File:Oligodendrocyte_illustration.png License: Creative Commons Attribution 3.0 Contributors: Anmats, Dmalicke, Smallman12q, Trijnstel File:Spindle-cell.png Source: http://en.wikipedia.org/w/index.php?title=File:Spindle-cell.png License: Creative Commons Attribution-Sharealike 2.5 Contributors: Selket, 1 anonymous edits Image:Spindle neurons - very high mag - cropped.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Spindle_neurons_-_very_high_mag_-_cropped.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Sinusoid.jpeg Source: http://en.wikipedia.org/w/index.php?title=File:Sinusoid.jpeg License: Public Domain Contributors: AndreasJS, Jacopo Werther, Lamiot, Quietbritishjim, 1 anonymous edits Image:Human liver.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Human_liver.jpg License: GNU Free Documentation License Contributors: Jacklee, Jacopo Werther, Reytan, Túrelio, 1 anonymous edits Image:Hepato-biliary.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Hepato-biliary.jpg License: Public Domain Contributors: Drriad Image:Yellow adipose tissue in paraffin section - lipids washed out.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Yellow_adipose_tissue_in_paraffin_section_-_lipids_washed_out.jpg License: GNU Free Documentation License Contributors: Jacklee, Reytan File:White adipose distribution in the body..jpg Source: http://en.wikipedia.org/w/index.php?title=File:White_adipose_distribution_in_the_body..jpg License: Creative Commons Attribution 3.0 Contributors: Smallman12q Image:Brownfat PETCT.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Brownfat_PETCT.jpg License: Public Domain Contributors: Hg6996 Image:Hibernoma2.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Hibernoma2.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Hepatic stellate cell (ito cell) 1476-5926-6-7-3-l.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Hepatic_stellate_cell_(ito_cell)_1476-5926-6-7-3-l.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Gressner et al. Comparative Hepatology 2007 6:7 doi:10.1186/1476-5926-6-7 Image:Hepatic structure2.svg Source: http://en.wikipedia.org/w/index.php?title=File:Hepatic_structure2.svg License: Creative Commons Attribution 2.5 Contributors: Originally by Frevert U, Engelmann S, Zougbédé S, Stange J, Ng B, et al. Converted to SVG by Viacheslav Vtyurin who was hired to do so by User:Eug. Image:PhysiologieGlomérulaire.png Source: http://en.wikipedia.org/w/index.php?title=File:PhysiologieGlomérulaire.png License: Creative Commons Attribution-ShareAlike 1.0 Generic Contributors: Tieum at fr.wikipedia Image:Filtration barrier.svg Source: http://en.wikipedia.org/w/index.php?title=File:Filtration_barrier.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: M•Komorniczak -talk-, polish wikipedist.
622
Image Sources, Licenses and Contributors
Image:Gray1128.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1128.png License: Public Domain Contributors: Arcadian, German, Jmarchn, Magnus Manske, Origamiemensch Image:Histology-kidney.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Histology-kidney.jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: --Uwe Gille 13:16, 13 May 2006 (UTC) File:Kidney cd10 ihc.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Kidney_cd10_ihc.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Gray1129.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1129.png License: Public Domain Contributors: Arcadian, German, Jmarchn, Magnus Manske, 1 anonymous edits Image:Tight_junction_blowup.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Tight_junction_blowup.jpg License: Creative Commons Attribution-Sharealike 2.5 Contributors: Original uploader was DrEricYH at en.wikipedia Image:Kidney nephron molar transport diagram.svg Source: http://en.wikipedia.org/w/index.php?title=File:Kidney_nephron_molar_transport_diagram.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron-urine.svg: M•Komorniczak -talk-, polish wikipedist. Kidney_nephron_molar_transport_diagram.png: *Nephron-urine.svg: M•Komorniczak -talk-, polish wikipedist. derivative work: Juvo415 (talk) derivative work: Mcstrother (talk) Image:Kidney_nephron.png Source: http://en.wikipedia.org/w/index.php?title=File:Kidney_nephron.png License: Public Domain Contributors: Henry Gray Image:Gray1132.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1132.png License: Public Domain Contributors: Arcadian, German, Jmarchn, Magnus Manske, Origamiemensch Image:Gray1133.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1133.png License: Public Domain Contributors: Arcadian, German, Jmarchn, Magnus Manske, Origamiemensch, 1 anonymous edits Image:centroacinar cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Centroacinar_cells.jpg License: Public Domain Contributors: User:Mortsggah Image:Alpha Intercalated Cell Cartoon.svg Source: http://en.wikipedia.org/w/index.php?title=File:Alpha_Intercalated_Cell_Cartoon.svg License: Creative Commons Attribution 3.0 Contributors: Rswarbrick Image:Human jejunum microvilli 2 - TEM.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Human_jejunum_microvilli_2_-_TEM.jpg License: Public Domain Contributors: Louisa Howard, Katherine Connollly Image:Epididymis-KDS.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Epididymis-KDS.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:KDS444 Image:Gray1148.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1148.png License: Public Domain Contributors: Arcadian, Ephraim33, Magnus Manske, Origamiemensch Image:Illu repdt male.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_repdt_male.jpg License: Public Domain Contributors: US Federal Government/National Cancer Institute. Image:Illu testis 1b.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_testis_1b.jpg License: Public Domain Contributors: Arcadian, Ephraim33, Origamiemensch Image:Mesorchium.svg Source: http://en.wikipedia.org/w/index.php?title=File:Mesorchium.svg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: User:Uwe Gille Image:Epididymis high mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Epididymis_high_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Epididymis.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Epididymis.JPG License: Public Domain Contributors: Jpogi Image:Enamelmineralization11-17-05.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Enamelmineralization11-17-05.jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: user:Dozenist Image:Cervical-loop.png Source: http://en.wikipedia.org/w/index.php?title=File:Cervical-loop.png License: Public Domain Contributors: Original uploader was Tummers at en.wikipedia Image:Cochlea-crosssection.svg Source: http://en.wikipedia.org/w/index.php?title=File:Cochlea-crosssection.svg License: GNU Free Documentation License Contributors: Cochlea-crosssection.png: Original uploader was Oarih at en.wikipedia derivative work: Fred the Oyster Image:Organ of corti.svg Source: http://en.wikipedia.org/w/index.php?title=File:Organ_of_corti.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Madhero88 File:Gray903.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray903.png License: Public Domain Contributors: Arcadian, Iainf, Jacklee File:Gray928.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray928.png License: Public Domain Contributors: Arcadian, Iainf, Jacklee, Magnus Manske, Mike.lifeguard File:Gray929.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray929.png License: Public Domain Contributors: Arcadian, Iainf, Jacklee, Jmarchn, Magnus Manske, Mike.lifeguard File:Gray930.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray930.png License: Public Domain Contributors: Arcadian, Dicklyon, Iainf, Jacklee, Jmarchn, Magnus Manske, Mike.lifeguard, Was a bee File:Keratoconus keratocytes alcohol dehydrogenase 3.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Keratoconus_keratocytes_alcohol_dehydrogenase_3.jpg License: Creative Commons Attribution 3.0 Contributors: V.V. Mootha, J.M. Kanoff, J. Shankardas, and S. Dimitrijevich Image:Gray72-en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Gray72-en.svg License: Public Domain Contributors: Mysid Image:Caput femoris cortex medulla.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Caput_femoris_cortex_medulla.jpg License: Public Domain Contributors: Stevenfruitsmaak File:Bone marrow WBC.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Bone_marrow_WBC.JPG License: Creative Commons Attribution-Share Alike Contributors: Bobjgalindo Image:acute leukemia-ALL.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Acute_leukemia-ALL.jpg License: GNU Free Documentation License Contributors: Original uploader was VashiDonsk at en.wikipedia Image:Bone marrow biopsy.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Bone_marrow_biopsy.jpg License: Public Domain Contributors: Photographer’s Mate 2nd Class Chad McNeeley Image:Markkloesschensuppe.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Markkloesschensuppe.jpg License: Public Domain Contributors: 1029man, AlexanderDreyer, Monstourz Image:NIH 3T3.jpg Source: http://en.wikipedia.org/w/index.php?title=File:NIH_3T3.jpg License: Creative Commons Attribution 2.5 Contributors: Didym, Kruusamägi, Magog the Ogre Image:Microvessel.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Microvessel.jpg License: Creative Commons Attribution 3.0 Contributors: Robert M. Hunt File:Gap_cell_junction-en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Gap_cell_junction-en.svg License: Public Domain Contributors: Mariana Ruiz LadyofHats File:Solitary fibrous tumour intermed mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Solitary_fibrous_tumour_intermed_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Cervical vertebra english.png Source: http://en.wikipedia.org/w/index.php?title=File:Cervical_vertebra_english.png License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: user:debivort Image:Disc Herniation.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Disc_Herniation.JPG License: Public Domain Contributors: Dematt Image:Gray66.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray66.png License: Public Domain Contributors: User Magnus Manske on en.wikipedia Image:Hypertrophic Zone of Epiphyseal Plate.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Hypertrophic_Zone_of_Epiphyseal_Plate.jpg License: Public Domain Contributors: Robert M. Hunt File:Slide6VVVVVV.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide6VVVVVV.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Gray300.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray300.png License: Public Domain Contributors: User Magnus Manske on en.wikipedia File:Slide1xzxzx.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide1xzxzx.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide2xzxzxz.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide2xzxzxz.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 Image:Gray295.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray295.png License: Public Domain Contributors: User Magnus Manske on en.wikipedia Image:Gray321.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray321.png License: Public Domain Contributors: Hellerhoff, Mats Halldin, Nono64, Phyzome, Was a bee Image:Degenerative disc disease - high mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Degenerative_disc_disease_-_high_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Cartilage polarised.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Cartilage_polarised.jpg License: Creative Commons Attribution 3.0 Contributors: Emmanuelm at en.wikipedia
623
Image Sources, Licenses and Contributors
Image:Chondrocyte- calcium stain.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Chondrocyte-_calcium_stain.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Robert M. Hunt Image:Bone hypercalcemia - cropped - very high mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Bone_hypercalcemia_-_cropped_-_very_high_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Osteoblast.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Osteoblast.jpg License: Creative Commons Attribution 3.0 Contributors: User:Gabriel Caponetti Image:Active osteoblasts.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Active_osteoblasts.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Robert M. Hunt Image:Bony_nidus_2.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Bony_nidus_2.jpg License: Creative Commons Attribution 3.0 Contributors: Robert M. Hunt Image:Bony_nidus_3.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Bony_nidus_3.jpg License: Creative Commons Attribution 3.0 Contributors: Robert M. Hunt Image:Bone_hypercalcemia_-_2_-_very_high_mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Bone_hypercalcemia_-_2_-_very_high_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:WVSOM Osteoblast.JPG Source: http://en.wikipedia.org/w/index.php?title=File:WVSOM_Osteoblast.JPG License: Creative Commons Attribution 3.0 Contributors: Wbensmith Image:Transverse Section Of Bone.png Source: http://en.wikipedia.org/w/index.php?title=File:Transverse_Section_Of_Bone.png License: Creative Commons Attribution-Sharealike 2.5 Contributors: BDB Image:Osteocyte 2.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Osteocyte_2.jpg License: Public Domain Contributors: Alexraw, Marek Mazurkiewicz, 1 anonymous edits File:CerebCircuit.png Source: http://en.wikipedia.org/w/index.php?title=File:CerebCircuit.png License: unknown Contributors: en:User:Nrets Image:Pyramsdal-and-Spiny-stellate-cell.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Pyramsdal-and-Spiny-stellate-cell.JPG License: Creative Commons Attribution 2.5 Contributors: Bilz0r Image:Skeletal muscle.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Skeletal_muscle.jpg License: GNU Free Documentation License Contributors: Deadstar, Jacklee, Noca2plus, Rama, Raul654, Splette, 2 anonymous edits File:Muscle pathways.svg Source: http://en.wikipedia.org/w/index.php?title=File:Muscle_pathways.svg License: Public Domain Contributors: Indolences Image:Glanzstreifen.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Glanzstreifen.jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: Dr. S. Girod, Anton Becker Image:Dogcardiacmuscle400.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Dogcardiacmuscle400.jpg License: Creative Commons Attribution-Share Alike Contributors: John Alan Elson File:A single cardiomyocyte beating, five days after purification from cell culture.ogv Source: http://en.wikipedia.org/w/index.php?title=File:A_single_cardiomyocyte_beating,_five_days_after_purification_from_cell_culture.ogv License: Creative Commons Attribution 2.5 Contributors: Uosaki H, Fukushima H, Takeuchi A, Matsuoka S, Nakatsuji N, Yamanaka S, Yamashita J Image:ConductionsystemoftheheartwithouttheHeart.png Source: http://en.wikipedia.org/w/index.php?title=File:ConductionsystemoftheheartwithouttheHeart.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: Madhero88 Image:ECG_Principle_fast.gif Source: http://en.wikipedia.org/w/index.php?title=File:ECG_Principle_fast.gif License: GNU Free Documentation License Contributors: Kalumet Image:Glatte Muskelzellen.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Glatte_Muskelzellen.jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: User:Polarlys Image:Illu esophageal layers.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_esophageal_layers.jpg License: Public Domain Contributors: Arcadian, Origamiemensch, 2 anonymous edits File:Actin myosin filaments.png Source: http://en.wikipedia.org/w/index.php?title=File:Actin_myosin_filaments.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: Boumphreyfr Image:redbloodcells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Redbloodcells.jpg License: Public domain Contributors: Dietzel65, Habj, Ranveig, Shizhao, Simon Shek, Solon, Sundar, Thuresson Image:Erythrocytes in vertebrates.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Erythrocytes_in_vertebrates.jpg License: Public Domain Contributors: G Gulliver - Proceedings of the Royal Society of London Image:Gray453.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray453.png License: Public Domain Contributors: Henry Gray Image:Red White Blood cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Red_White_Blood_cells.jpg License: Public Domain Contributors: Electron Microscopy Facility at The National Cancer Institute at Frederick (NCI-Frederick) Image:NIK 3232-Drops of blood medium.JPG Source: http://en.wikipedia.org/w/index.php?title=File:NIK_3232-Drops_of_blood_medium.JPG License: Creative Commons Attribution 3.0 Contributors: unkown Image:Erytrocyte deoxy to oxy v0.7.gif Source: http://en.wikipedia.org/w/index.php?title=File:Erytrocyte_deoxy_to_oxy_v0.7.gif License: Creative Commons Attribution-Sharealike 3.0 Contributors: Rogeriopfm Image:Erythrocyte Membrane lipids.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Erythrocyte_Membrane_lipids.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Cholesterol.svg: BorisTM Phosphatidylcholine.png: Likeitsmyjob Sphingomyelin.png: Original uploader was Jag123 at en.wikipedia Phosphatidyl-Inositol.png: Original uploader was Jag123 at en.wikipedia Phosphatidyl-Serine.png: Original uploader was Jag123 at en.wikipedia Phosphatidyl-Ethanolamine.png: Original uploader was Jag123 at en.wikipedia derivative work: Rogeriopfm (talk) File:RBC Membrane Proteins SDS-PAGE gel.jpg Source: http://en.wikipedia.org/w/index.php?title=File:RBC_Membrane_Proteins_SDS-PAGE_gel.jpg License: Creative Commons Zero Contributors: Ernst Hempelmann File:RBC membrane major proteins.png Source: http://en.wikipedia.org/w/index.php?title=File:RBC_membrane_major_proteins.png License: Public Domain Contributors: RBC_membrane_major_proteins.jpg: Author is Ernst Hempelmann derivative work: TimVickers (talk) Image:Sicklecells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Sicklecells.jpg License: Public Domain Contributors: NIDDK Image:Osmotic pressure on blood cells diagram.svg Source: http://en.wikipedia.org/w/index.php?title=File:Osmotic_pressure_on_blood_cells_diagram.svg License: Public Domain Contributors: LadyofHats File:Human Erythrocytes OsmoticPressure PhaseContrast Plain.svg Source: http://en.wikipedia.org/w/index.php?title=File:Human_Erythrocytes_OsmoticPressure_PhaseContrast_Plain.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Zephyris Image:WVSOM Megakaryocytes.JPG Source: http://en.wikipedia.org/w/index.php?title=File:WVSOM_Megakaryocytes.JPG License: Creative Commons Attribution 3.0 Contributors: Wbensmith Image:Illu blood cell lineage.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_blood_cell_lineage.jpg License: Public Domain Contributors: Arcadian, Bestiasonica, Cristobal carrasco, DO11.10, MichaelFrey, 5 anonymous edits Image:Monocytes, a type of white blood cell (Giemsa stained).jpg Source: http://en.wikipedia.org/w/index.php?title=File:Monocytes,_a_type_of_white_blood_cell_(Giemsa_stained).jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:GrahamColm Image:SEM blood cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:SEM_blood_cells.jpg License: Public Domain Contributors: Bruce Wetzel (photographer). Harry Schaefer (photographer) Image:Reference ranges for blood tests - white blood cells.png Source: http://en.wikipedia.org/w/index.php?title=File:Reference_ranges_for_blood_tests_-_white_blood_cells.png License: Public Domain Contributors: Mikael Häggström File:Dendritic cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Dendritic_cells.jpg License: Public Domain Contributors: Haymanj File:The representation of Langerhans cells in the Cell Ontology.jpg Source: http://en.wikipedia.org/w/index.php?title=File:The_representation_of_Langerhans_cells_in_the_Cell_Ontology.jpg License: Creative Commons Attribution 2.0 Contributors: Masci AM, Arighi CN, Diehl AD, Lieberman AE, Mungall C, Scheuermann RH, Smith B, Cowell LG Image:Giant platelets.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Giant_platelets.JPG License: Creative Commons Attribution-Share Alike Contributors: Bobjgalindo File:Blood cells differentiation chart.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Blood_cells_differentiation_chart.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: パ タ ゴ ニ ア
624
Image Sources, Licenses and Contributors
File:Thrombocyteaggregation.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Thrombocyteaggregation.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Dietzel65, Steffen Dietzel File:Red White Blood cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Red_White_Blood_cells.jpg License: Public Domain Contributors: Electron Microscopy Facility at The National Cancer Institute at Frederick (NCI-Frederick) File:Platelets.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Platelets.jpg License: Creative Commons Attribution 3.0 Contributors: Tleonardi File:Platelet structure.png Source: http://en.wikipedia.org/w/index.php?title=File:Platelet_structure.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:GrahamColm File:Platelet blood bag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Platelet_blood_bag.jpg License: Public Domain Contributors: Bobjgalindo, DO11.10, Gveret Tered, Pfctdayelise, PhilippN, Sundar, 1 anonymous edits Image:Osteoclast.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Osteoclast.jpg License: Public Domain Contributors: Original uploader was Robert M. Hunt at en.wikipedia File:TRAPosteoclastculture.jpg Source: http://en.wikipedia.org/w/index.php?title=File:TRAPosteoclastculture.jpg License: GNU Free Documentation License Contributors: Original uploader was Cellpath at en.wikipedia File:osteoclast1.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Osteoclast1.jpg License: GNU Free Documentation License Contributors: Cellpath (talk) Image:Dendritic cell.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Dendritic_cell.JPG License: Creative Commons Attribution 2.5 Contributors: Judith Behnsen, Priyanka Narang, Mike Hasenberg, Frank Gunzer, Ursula Bilitewski, Nina Klippel, Manfred Rohde, Matthias Brock, Axel A. Brakhage, Matthias Gunzer Image:Dendritic cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Dendritic_cells.jpg License: Public Domain Contributors: Haymanj Image:S6-Dendritic Cells with Conidia in Collagen.ogg Source: http://en.wikipedia.org/w/index.php?title=File:S6-Dendritic_Cells_with_Conidia_in_Collagen.ogg License: Creative Commons Attribution 2.5 Contributors: Judith Behnsen, Priyanka Narang, Mike Hasenberg, Frank Gunzer, Ursula Bilitewski, Nina Klippel, Manfred Rohde, Matthias Brock, Axel A. Brakhage, Matthias Gunzer Image:Lymphatic system.png Source: http://en.wikipedia.org/w/index.php?title=File:Lymphatic_system.png License: Public Domain Contributors: NIH File:Illu lymph node structure.png Source: http://en.wikipedia.org/w/index.php?title=File:Illu_lymph_node_structure.png License: Public Domain Contributors: SEER File:DH lymphatic system.jpg Source: http://en.wikipedia.org/w/index.php?title=File:DH_lymphatic_system.jpg License: Creative Commons Attribution 3.0 Contributors: LearnAnatomy (talk) Image:Galen detail.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Galen_detail.jpg License: Public Domain Contributors: NLM Image:Bartolomeus Eustachius.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Bartolomeus_Eustachius.jpg License: Public Domain Contributors: Unknown (not specified); possibly from one of Eustachius' books. File:Olaus Rudbeck Sr (portrait by Martin Mijtens Sr, 1696).jpg Source: http://en.wikipedia.org/w/index.php?title=File:Olaus_Rudbeck_Sr_(portrait_by_Martin_Mijtens_Sr,_1696).jpg License: Public Domain Contributors: Martin Mijtens the Elder (1548-1736), Dutch-Swedish painter. File:Thomas bartholin.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Thomas_bartholin.jpg License: Public Domain Contributors: Nico File:Mikroglej 1.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Mikroglej_1.jpg License: Public Domain Contributors: GrzegorzWicher File:Makrofagi 2.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Makrofagi_2.jpg License: Public Domain Contributors: GrzegorzWicher Image:Neutrophils.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Neutrophils.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:GrahamColm Image:NeutrophilerAktion.png Source: http://en.wikipedia.org/w/index.php?title=File:NeutrophilerAktion.png License: GNU Free Documentation License Contributors: Uwe Thormann (http://de.wikipedia.org/wiki/Benutzer:Uwe_Thormann) Image:Hematopoiesis simple.svg Source: http://en.wikipedia.org/w/index.php?title=File:Hematopoiesis_simple.svg License: GNU Free Documentation License Contributors: Mikael Häggström (no attribution required), from original by A. Rad (requires attribution) Image:S15-Competitive Phagocytosis Assay in Collagen.ogg Source: http://en.wikipedia.org/w/index.php?title=File:S15-Competitive_Phagocytosis_Assay_in_Collagen.ogg License: Creative Commons Attribution 2.5 Contributors: Judith Behnsen, Priyanka Narang, Mike Hasenberg, Frank Gunzer, Ursula Bilitewski, Nina Klippel, Manfred Rohde, Matthias Brock, Axel A. Brakhage, Matthias Gunzer Image:Neutrophil with anthrax copy.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Neutrophil_with_anthrax_copy.jpg License: Creative Commons Attribution 2.5 Contributors: Volker Brinkmann Image:Hematopoiesis (human) diagram.png Source: http://en.wikipedia.org/w/index.php?title=File:Hematopoiesis_(human)_diagram.png License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: A. Rad Image:Eosinophil blood smear.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Eosinophil_blood_smear.JPG License: Creative Commons Attribution-Share Alike Contributors: Bobjgalindo Image:Eosinophil 2.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Eosinophil_2.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:GrahamColm image:Eosinophil2.png Source: http://en.wikipedia.org/w/index.php?title=File:Eosinophil2.png License: GNU Free Documentation License Contributors: Arcadian, Cwbm (commons), Joey-das-WBF, Marek Mazurkiewicz, TimVickers, Väsk Image:pBBasophil.jpg Source: http://en.wikipedia.org/w/index.php?title=File:PBBasophil.jpg License: Public Domain Contributors: Dirk Hünniger, Elboy99, Lennert B, MichaelFrey, Santosga, 2 anonymous edits Image:Baso-hemo.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Baso-hemo.JPG License: Copyrighted free use Contributors: パ タ ゴ ニ ア Image:Basophil.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Basophil.jpg License: GNU Free Documentation License Contributors: Bestiasonica, Elboy99, Origamiemensch, Reytan, Santosga File:Hybridoma technology.png Source: http://en.wikipedia.org/w/index.php?title=File:Hybridoma_technology.png License: Creative Commons Attribution-Sharealike 2.5 Contributors: Hybridomtechnik.png: Martin Brändli derivative work: ἀνυπόδητος (talk) File:Hybridoma cells grown in tissue culture.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Hybridoma_cells_grown_in_tissue_culture.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: GerryShaw Image:SMCpolyhydroxysmall.jpg Source: http://en.wikipedia.org/w/index.php?title=File:SMCpolyhydroxysmall.jpg License: Copyrighted free use Contributors: Kauczuk Image:Mast cell.png Source: http://en.wikipedia.org/w/index.php?title=File:Mast_cell.png License: GNU Free Documentation License Contributors: Arcadian, Cwbm (commons), Väsk Image:Mast cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Mast_cells.jpg License: Public Domain Contributors: Template drawing from "The Immune System", any modifications, made by myself are released into the public domain. Image:histamine.png Source: http://en.wikipedia.org/w/index.php?title=File:Histamine.png License: Public Domain Contributors: Ayacop, Benjah-bmm27, BorisTM, Edgar181, Jean-no, Mixtures, Mrgreen71, Роман Беккер Image:Lymphocyte activation.png Source: http://en.wikipedia.org/w/index.php?title=File:Lymphocyte_activation.png License: Public Domain Contributors: Made in Inkscape by Mikael Häggström (User:Mikael Häggström) Image:Antigen presentation.svg Source: http://en.wikipedia.org/w/index.php?title=File:Antigen_presentation.svg License: GNU Free Documentation License Contributors: user:Sjef Image:Intrathymic T Cell Differentiation.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Intrathymic_T_Cell_Differentiation.JPG License: Creative Commons Attribution 2.5 Contributors: Wilson Savino is at the Laboratory on Thymus Research, Department of Immunology, Oswaldo Cruz Institute, Inserm-Fiocruz Associated Laboratory of Immunology, Oswaldo Cruz Foundation, Rio de Janeiro, RJ, Brazil. E-mail: [email protected] Image:Original antigenic sin.svg Source: http://en.wikipedia.org/w/index.php?title=File:Original_antigenic_sin.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Original_antigenic_sin.png: User:DO11.10 derivative work: Hazmat2 (talk) Image:Plasmacell.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Plasmacell.jpg License: Public Domain Contributors: Original uploader was CS99 at de.wikipedia Image:B cell activation.png Source: http://en.wikipedia.org/w/index.php?title=File:B_cell_activation.png License: Public Domain Contributors: Template drawing and caption from "The Immune System". Any modifcations, made by myself are released into the public domain. Image:T-dependent B cell activation.png Source: http://en.wikipedia.org/w/index.php?title=File:T-dependent_B_cell_activation.png License: Public Domain Contributors: Altaileopard Image:Stimulation of specific clone of B cells and its proliferation.PNG Source: http://en.wikipedia.org/w/index.php?title=File:Stimulation_of_specific_clone_of_B_cells_and_its_proliferation.PNG License: Public Domain Contributors: Ketan Panchal, MBBS (talk) at en.wikipedia
625
Image Sources, Licenses and Contributors
File:HLA-Cw4.png Source: http://en.wikipedia.org/w/index.php?title=File:HLA-Cw4.png License: Public Domain Contributors: Pdeitiker File:PDB 1hq8 EBI.jpg Source: http://en.wikipedia.org/w/index.php?title=File:PDB_1hq8_EBI.jpg License: unknown Contributors: File:PDB 1hkf EBI.jpg Source: http://en.wikipedia.org/w/index.php?title=File:PDB_1hkf_EBI.jpg License: unknown Contributors: Image:Missingself.svg Source: http://en.wikipedia.org/w/index.php?title=File:Missingself.svg License: GNU Free Documentation License Contributors: Cacofonie, Slashme Image:Polychromatic erythrocyte.png Source: http://en.wikipedia.org/w/index.php?title=File:Polychromatic_erythrocyte.png License: GNU Free Documentation License Contributors: Arcadian, Cycneavox, Dietzel65, Tano4595 Image:Erythrocyte.png Source: http://en.wikipedia.org/w/index.php?title=File:Erythrocyte.png License: GNU Free Documentation License Contributors: =g b r=, Arcadian, Dietzel65 File:Reticulocytes Human Blood Supravital Stain.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Reticulocytes_Human_Blood_Supravital_Stain.jpg License: Creative Commons Attribution 3.0 Contributors: Ed Uthman, MD, pathologist, Houston, Texas, USA Image:Gray9.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray9.png License: Public Domain Contributors: User Magnus Manske on en.wikipedia File:Sperm-egg.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Sperm-egg.jpg License: Public Domain Contributors: Blurpeace, Conscious, EugeneZelenko, Giggy, Gourami Watcher, GrawpSock, Herbythyme, Ies, Jacklee, Kameraad Pjotr, Manuelt15, Mattes, Myself488, Noddy93, Pi@k, Platonides, Techman224, The Evil IP address, Tronicum, 14 anonymous edits File:Acrosome reaction diagram en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Acrosome_reaction_diagram_en.svg License: Public Domain Contributors: LadyofHats. File:DEV035048A.jpg Source: http://en.wikipedia.org/w/index.php?title=File:DEV035048A.jpg License: Public Domain Contributors: Sabisteb Image:Oocyte.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Oocyte.jpg License: Public Domain Contributors: Original uploader was Ekem at en.wikipedia File:Gray5.svg Source: http://en.wikipedia.org/w/index.php?title=File:Gray5.svg License: Public Domain Contributors: Mysid File:Oocyte granulosa cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Oocyte_granulosa_cells.jpg License: Public Domain Contributors: Original uploader was Ekem at en.wikipedia Image:Oocyte Poles.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Oocyte_Poles.jpg License: Creative Commons Attribution 3.0 Contributors: Catcasillas21 Image:Oocyte Determinants.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Oocyte_Determinants.jpg License: Creative Commons Attribution 3.0 Contributors: Catcasillas21 Image:Germinal_epithelium_testicle.svg Source: http://en.wikipedia.org/w/index.php?title=File:Germinal_epithelium_testicle.svg License: Creative Commons Attribution 2.5 Contributors: User:Uwe Gille Image:Gray1150.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1150.png License: Public Domain Contributors: Arcadian, Ephraim33, Origamiemensch Image:Gray7.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray7.png License: Public Domain Contributors: User Magnus Manske on en.wikipedia File:Complete diagram of a human spermatozoa en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Complete_diagram_of_a_human_spermatozoa_en.svg License: Public Domain Contributors: Mariana Ruiz Villarreal File:Sperm stained.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Sperm_stained.JPG License: Creative Commons Attribution-Share Alike Contributors: Bobjgalindo File:Plant sperm.png Source: http://en.wikipedia.org/w/index.php?title=File:Plant_sperm.png License: Public Domain Contributors: Original uploader was Tameeria at en.wikipedia Image:Testicle-histology-boar.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Testicle-histology-boar.jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: User:Uwe Gille Image:Spermatocytogenesis.png Source: http://en.wikipedia.org/w/index.php?title=File:Spermatocytogenesis.png License: Public Domain Contributors: Ies, Serephine, 1 anonymous edits Image:Gray1123.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1123.png License: Public Domain Contributors: Arcadian, German, Magnus Manske File:Surface projections of the organs of the trunk.png Source: http://en.wikipedia.org/w/index.php?title=File:Surface_projections_of_the_organs_of_the_trunk.png License: Public Domain Contributors: Mikael Häggström File:CTscankidney.jpg Source: http://en.wikipedia.org/w/index.php?title=File:CTscankidney.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: RGshredfox File:KidneyStructures PioM.svg Source: http://en.wikipedia.org/w/index.php?title=File:KidneyStructures_PioM.svg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: Piotr Michał Jaworski; PioM EN DE PL File:3D rendered CT of abdominal aortic branches and kidneys.svg Source: http://en.wikipedia.org/w/index.php?title=File:3D_rendered_CT_of_abdominal_aortic_branches_and_kidneys.svg License: GNU Free Documentation License Contributors: Mikael Häggström from original image created and uploaded by by Dr. I-Chen Tsai () File:Kidney-medulla.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Kidney-medulla.JPG License: Public Domain Contributors: File:Kidney-Cortex.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Kidney-Cortex.JPG License: Public Domain Contributors: File:Hunter enlarged kidney.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Hunter_enlarged_kidney.jpg License: Public Domain Contributors: McLeod File:Kidney.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Kidney.JPG License: Creative Commons Attribution 3.0 Contributors: Pöllö File:1407871818 5c7f215934 o.jpg Source: http://en.wikipedia.org/w/index.php?title=File:1407871818_5c7f215934_o.jpg License: Creative Commons Attribution-Sharealike 3.0,2.5,2.0,1.0 Contributors: Jonathan Koertge File:Slide4nn.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide4nn.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide5pp.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide5pp.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide3ppp.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide3ppp.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide22222.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide22222.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide42222.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide42222.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Right kidney.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Right_kidney.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Left kidneys.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Left_kidneys.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Kidneys.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Kidneys.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Left kidney.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Left_kidney.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Kidney Cross Section.png Source: http://en.wikipedia.org/w/index.php?title=File:Kidney_Cross_Section.png License: Creative Commons Attribution 3.0 Contributors: Anmats, Dmalicke, Trijnstel
626
License
627
License
Creative Commons Attribution-Share Alike 3.0 Unported //creativecommons.org/licenses/by-sa/3.0/
PDF generated using the open source mwlib toolkit. See http://code.pediapress.com/ for more information. PDF generated at: Wed, 24 Apr 2013 09:08:34 UTC
Contents
List of distinct cell types in the adult human body Salivary gland Von Ebner's gland Mammary gland Lacrimal gland Ceruminous gland Eccrine sweat gland Apocrine sweat gland Moll's gland Sebaceous gland Olfactory glands Brunner's glands Prostate Bulbourethral gland Bartholin's gland Endometrium Urethral gland Gastric chief cell Pepsin Parietal cell Hydrochloric acid Human gastrointestinal tract Goblet cell Respiratory tract Mucus Enzyme Paneth cell Intestine Bicarbonate Lysozyme Surfactant Clara cell Somatotropic cell Prolactin cell Thyrotropic cell Gonadotropic cell 1 7 10 11 16 19 20 21 24 25 29 30 31 41 43 45 48 49 51 57 60 67 73 76 77 79 97 99 102 105 110 117 119 120 121 122
Corticotropic cell Melanocyte-stimulating hormone Magnocellular neurosecretory cell Oxytocin Vasopressin Serotonin Endorphins Somatostatin Gastrin Secretin Cholecystokinin Insulin Glucagon Bombesin Follicular cell Parafollicular cell Parathyroid gland Parathyroid chief cell Oxyphil cell (parathyroid) Chromaffin cell Steroid hormone Mineralocorticoid Glucocorticoid Leydig cell Folliculogenesis Progesterone Corpus luteum cell Corpus luteum Juxtaglomerular cell Renin Macula densa Mesangial cell Keratinocyte Epidermis (skin) Stem cell Huxley's layer Henle's layer Trichocyte (human)
123 123 126 127 138 148 158 162 168 174 179 182 192 199 200 202 203 207 208 209 211 213 215 226 228 235 246 247 250 251 257 259 259 262 267 279 280 280
Epithelium Squamous epithelial cell Hair cell Sensory neuron Merkel cell Olfactory receptor neuron Photoreceptor cell Rod cell Cone cell Carotid body Taste bud Schwann cell Satellite glial cell Neuroglia Astrocyte Neuron Oligodendrocyte Spindle neuron Hepatocyte Adipocyte White adipose tissue Brown adipose tissue Hepatic stellate cell Podocyte Proximal convoluted tubule Thin segment Distal convoluted tubule Kidney collecting duct cell Pneumocyte Centroacinar cell Collecting duct system Microvillus Epididymis Ameloblast Organ of Corti Corneal keratocyte Tendon cell Bone marrow
281 287 288 292 296 298 300 308 312 316 319 321 324 330 336 344 357 361 365 369 371 372 375 377 380 384 385 387 387 388 389 393 396 399 401 403 405 406
Reticular connective tissue Fibroblast Pericyte Nucleus pulposus Cementoblast Odontoblast Hyaline cartilage Fibrocartilage Chondrocyte Osteoblast Osteocyte Stellate cell Skeletal striated muscle Nuclear bag fiber Nuclear chain cell Myosatellite cell Cardiac muscle Purkinje fibers Smooth muscle tissue Myoepithelial cell Red blood cell Megakaryocyte Monocyte Langerhans cell Platelet Osteoclast Dendritic cell Lymphatic system Microglia Neutrophil granulocyte Eosinophil granulocyte Basophil granulocyte Hybridoma technology Mast cell T helper cell Regulatory T cell Cytotoxic T cell Natural killer T cell
412 413 415 420 422 423 425 427 429 431 433 437 438 445 445 446 450 453 455 463 464 475 478 481 484 492 496 501 508 518 524 527 529 533 536 543 547 550
B cell Natural killer cell Reticulocyte Progenitor cell Ovum Oocyte Spermatid Sperm Spermatogonium Sertoli cell Kidney
552 558 565 567 569 572 577 579 583 585 589
References
Article Sources and Contributors Image Sources, Licenses and Contributors 601 617
Article Licenses
License 627
List of distinct cell types in the adult human body
1
List of distinct cell types in the adult human body
Cells that are derived primarily from endoderm
Exocrine secretory epithelial cells
300 different cell types in the human body • • • • • • • • • • • • • • • • • • • • • • • • • • • Salivary gland mucous cell (polysaccharide-rich secretion) Salivary gland serous cell (glycoprotein enzyme-rich secretion) Von Ebner's gland cell in tongue (washes taste buds) Mammary gland cell (milk secretion) Lacrimal gland cell (tear secretion) Ceruminous gland cell in ear (earwax secretion) Eccrine sweat gland dark cell (glycoprotein secretion) Eccrine sweat gland clear cell (small molecule secretion) Apocrine sweat gland cell (odoriferous secretion, sex-hormone sensitive) Gland of Moll cell in eyelid (specialized sweat gland) Sebaceous gland cell (lipid-rich sebum secretion) Bowman's gland cell in nose (washes olfactory epithelium) Brunner's gland cell in duodenum (enzymes and alkaline mucus) Seminal vesicle cell (secretes seminal fluid components, including fructose for swimming sperm) Prostate gland cell (secretes seminal fluid components) Bulbourethral gland cell (mucus secretion) Bartholin's gland cell (vaginal lubricant section) Gland of Littre cell (mucus secretion) Uterus endometrium cell (carbohydrate secretion) Isolated goblet cell of respiratory and digestive tracts (mucus secretion) Stomach lining mucous cell (mucus secretion) Gastric gland zymogenic cell (pepsinogen secretion) Gastric gland oxyntic cell (hydrochloric acid secretion) Pancreatic acinar cell (bicarbonate and digestive enzyme secretion Paneth cell of small intestine (lysozyme secretion) Type II pneumocyte of lung (surfactant secretion) Clara cell of lung
Hormone secreting cells
• Anterior pituitary cells • Somatotropes • Lactotropes • Thyrotropes • Gonadotropes • Corticotropes • Intermediate pituitary cell, secreting melanocyte-stimulating hormone • Magnocellular neurosecretory cells • secreting oxytocin • secreting vasopressin
List of distinct cell types in the adult human body • Gut and respiratory tract cells • secreting serotonin • secreting endorphin • secreting somatostatin • secreting gastrin • secreting secretin • secreting cholecystokinin • secreting insulin • secreting glucagon • secreting bombesin • Thyroid gland cells • thyroid epithelial cell • parafollicular cell • Parathyroid gland cells • Parathyroid chief cell • Oxyphil cell • Adrenal gland cells • chromaffin cells • secreting steroid hormones (mineralcorticoids and gluco corticoids) • Leydig cell of testes secreting testosterone • Theca interna cell of ovarian follicle secreting estrogen • Corpus luteum cell of ruptured ovarian follicle secreting progesterone • Granulosa lutein cells • Theca lutein cells Juxtaglomerular cell (renin secretion) Macula densa cell of kidney Peripolar cell of kidney Mesangial cell of kidney
2
• • • •
Derived primarily from ectoderm
Integumentary system
Keratinizing epithelial cells • • • • • • • • • • Epidermal keratinocyte (differentiating epidermal cell) Epidermal basal cell (stem cell) Keratinocyte of fingernails and toenails Nail bed basal cell (stem cell) Medullary hair shaft cell Cortical hair shaft cell Cuticular hair shaft cell Cuticular hair root sheath cell Hair root sheath cell of Huxley's layer Hair root sheath cell of Henle's layer
• External hair root sheath cell • Hair matrix cell (stem cell)
List of distinct cell types in the adult human body Wet stratified barrier epithelial cells • Surface epithelial cell of stratified squamous epithelium of cornea, tongue, oral cavity, esophagus, anal canal, distal urethra and vagina • basal cell (stem cell) of epithelia of cornea, tongue, oral cavity, esophagus, anal canal, distal urethra and vagina • Urinary epithelium cell (lining urinary bladder and urinary ducts)
3
Nervous system
Sensory transducer cells • • • • • • • • Auditory inner hair cell of organ of Corti Auditory outer hair cell of organ of Corti Basal cell of olfactory epithelium (stem cell for olfactory neurons) Cold-sensitive primary sensory neurons Heat-sensitive primary sensory neurons Merkel cell of epidermis (touch sensor) Olfactory receptor neuron Pain-sensitive primary sensory neurons (various types) • Photoreceptor rod cells • Photoreceptor blue-sensitive cone cell of eye • Photoreceptor green-sensitive cone cell of eye • Photoreceptor red-sensitive cone cell of eye Proprioceptive primary sensory neurons (various types) Touch-sensitive primary sensory neurons (various types) Type I carotid body cell (blood pH sensor) Type II carotid body cell (blood pH sensor) Type I hair cell of vestibular apparatus of ear (acceleration and gravity) Type II hair cell of vestibular apparatus of ear (acceleration and gravity) Type I taste bud cell
• Photoreceptor cells of retina in eye:
• • • • • • •
Autonomic neuron cells • Cholinergic neural cell (various types) • Adrenergic neural cell (various types) • Peptidergic neural cell (various types) Sense organ and peripheral neuron supporting cells • • • • • • • • • Inner pillar cell of organ of Corti Outer pillar cell of organ of Corti Inner phalangeal cell of organ of Corti Outer phalangeal cell of organ of Corti Border cell of organ of Corti Hensen cell of organ of Corti Vestibular apparatus supporting cell Taste bud supporting cell Olfactory epithelium supporting cell
• Schwann cell • Satellite glial cell (encapsulating peripheral nerve cell bodies)
List of distinct cell types in the adult human body • Enteric glial cell Central nervous system neurons and glial cells • • • • Astrocyte (various types) Neuron cells (large variety of types, still poorly classified) Oligodendrocyte Spindle neuron
4
Lens cells • Anterior lens epithelial cell • Crystallin-containing lens fiber cell
Derived primarily from mesoderm
Metabolism and storage cells
• Hepatocyte (liver cell) • Adipocytes: • White fat cell • Brown fat cell • Liver lipocyte
Barrier function cells (lung, gut, exocrine glands and urogenital tract)
Kidney • • • • • • • • • Kidney parietal cell Kidney glomerulus podocyte Kidney proximal tubule brush border cell Loop of Henle thin segment cell Kidney distal tubule cell Kidney collecting duct cell Type I pneumocyte (lining air space of lung cell) Pancreatic duct cell (centroacinar cell) Nonstriated duct cell (of sweat gland, salivary gland, mammary gland, etc.) • principal cell • Intercalated cell Duct cell (of seminal vesicle, prostate gland, etc.) Intestinal brush border cell (with microvilli) Exocrine gland striated duct cell Gall bladder epithelial cell Ductulus efferens nonciliated cell Epididymal principal cell Epididymal basal cell
• • • • • • •
List of distinct cell types in the adult human body
5
Extracellular matrix cells
• • • • • • • • • • • • • • • • • • • • • Ameloblast epithelial cell (tooth enamel secretion) Planum semilunatum epithelial cell of vestibular apparatus of ear (proteoglycan secretion) Organ of Corti interdental epithelial cell (secreting tectorial membrane covering hair cells) Loose connective tissue fibroblasts Corneal fibroblasts (corneal keratocytes) Tendon fibroblasts Bone marrow reticular tissue fibroblasts Other nonepithelial fibroblasts Pericyte Nucleus pulposus cell of intervertebral disc Cementoblast/cementocyte (tooth root bonelike cementum secretion) Odontoblast/odontocyte (tooth dentin secretion) Hyaline cartilage chondrocyte Fibrocartilage chondrocyte Elastic cartilage chondrocyte Osteoblast/osteocyte Osteoprogenitor cell (stem cell of osteoblasts) Hyalocyte of vitreous body of eye Stellate cell of perilymphatic space of ear Hepatic stellate cell (Ito cell) Pancreatic stelle cell
Contractile cells
• Skeletalex muscle cells • Red skeletal muscle cell (slow) • White skeletal muscle cell (fast) • Intermediate skeletal muscle cell • nuclear bag cell of muscle spindle • nuclear chain cell of muscle spindle • Satellite cell (stem cell) • Heart muscle cells • Ordinary heart muscle cell • Nodal heart muscle cell • Purkinje fiber cell • Smooth muscle cell (various types) • Myoepithelial cell of iris • Myoepithelial cell of exocrine glands
List of distinct cell types in the adult human body
6
Blood and immune system cells
• • • • • • • • • • • • • • • • • • • • • Erythrocyte (red blood cell) Megakaryocyte (platelet precursor) Monocyte Connective tissue macrophage (various types) Epidermal Langerhans cell Osteoclast (in bone) Dendritic cell (in lymphoid tissues) Microglial cell (in central nervous system) Neutrophil granulocyte Eosinophil granulocyte Basophil granulocyte Hybridoma cell Mast cell Helper T cell Suppressor T cell Cytotoxic T cell Natural Killer T cell B cell Natural killer cell Reticulocyte Stem cells and committed progenitors for the blood and immune system (various types)
Germ cells
• • • • • Oogonium/Oocyte Spermatid Spermatocyte Spermatogonium cell (stem cell for spermatocyte) Spermatozoon
Nurse cells
• Ovarian follicle cell • Sertoli cell (in testis) • Thymus epithelial cell
Interstitial cells
• Interstitial kidney cells
References External links
• Types of neurons from NeuroLex (http://neurolex.org/wiki/Cell_Types_With_Definitions) • Eukaryotic cell types in COPE database (http://www.copewithcytokines.de/cope.cgi?key=cell types).
Salivary gland
7
Salivary gland
Salivary gland
Salivary glands: #1 is Parotid gland, #2 is Submandibular gland, #3 is Sublingual gland Latin glandulae salivariae
The salivary glands in mammals are exocrine glands, glands with ducts, that produce saliva. They also secrete amylase, an enzyme that breaks down starch into maltose. In other organisms such as insects, salivary glands are often used to produce biologically important proteins like silk or glues, and fly salivary glands contain polytene chromosomes that have been useful in genetic research.
Histology
The gland is internally divided into lobules. Blood vessels and nerves enter the glands at the hilum and gradually branch out into the lobules.
Ducts
In the duct system, the lumina are formed by intercalated ducts, which in turn join to form striated ducts. These drain into ducts situated between the lobes of the gland (called interlobar ducts or secretory ducts). All of the human salivary glands terminate in the mouth, where the saliva proceeds to aid in digestion. The saliva that salivary glands release is quickly inactivated in the stomach by the acid that is present there but the saliva also contains enzymes that are actually activated by the acid.
Salivary gland
8
Anatomy
Parotid glands
The parotid gland is a salivary gland wrapped around the mandibular ramus in humans. It is one of a pair being the largest of the salivary glands, it secretes saliva through Stensen's ducts into the oral cavity, to facilitate mastication and swallowing and to begin the digestion of starches. The secretion produced is mainly serous in nature and enters the oral cavity via Stensen's duct. It is located posterior to the mandibular ramus and in front of the mastoid process of temporal bone. This gland is clinically relevant in dissections of facial nerve branches while exposing the different lobes of it since any iatrogenic lesion will result in either loss of action or strength of muscles involved in facial expression.
Submandibular glands
The submandibular glands are a pair of glands located beneath the The salivary glands are situated at the entrance to lower jaws, superior to the digastric muscles. The secretion produced is the gastrointestinal system to help begin the a mixture of both serous fluid and mucus, and enters the oral cavity via process of digestion. Wharton's ducts. Approximately 70% of saliva in the oral cavity is produced by the submandibular glands, even though they are much smaller than the parotid glands.You can usually feel this gland, as it is in the upper neck and feels like a rounded ball. It is located about two fingers above the Adam's apple (on a man) and about two inches apart under the chin.
Sublingual glands
The sublingual glands are a pair of glands located beneath the tongue, anterior to the submandibular glands. The secretion produced is mainly mucus in nature, however it is categorized as a mixed gland. Unlike the other two major glands, the ductal system of the sublingual glands do not have striated ducts, and exit from 8-20 excretory ducts. Approximately 5% of saliva entering the oral cavity come from these glands.
Minor salivary glands
There are 800-1000 minor salivary glands located throughout the oral cavity within the submucosa[1] of the oral mucosa, apart from areas including the anterior third of the hard palate, the attached gingivaand the anterior third of the dorsal surface of the tongue.[] They are 1-2mm in diameter and unlike the other glands, they are not encapsulated by connective tissue only surrounded by it. The gland is usually a number of acini connected in a tiny lobule. A minor salivary gland may have a common excretory duct with another gland, or may have its own excretory duct. Their secretion is mainly mucous in nature (except for Von Ebner's glands) and have many functions such as coating the oral cavity with saliva. Problems with dentures are sometimes associated with minor salivary glands.[1]
Salivary gland Von Ebner's glands Von Ebner's glands are glands found in circumvallate papillae of the tongue. They secrete a serous fluid that begin lipid hydrolysis. They facilitate the perception of taste.
9
Innervation
Salivary glands are innervated, either directly or indirectly, by the parasympathetic and sympathetic arms of the autonomic nervous system. Both result in increased amylase output and volume flow. • Parasympathetic innervation to the salivary glands is carried via cranial nerves. The parotid gland receives its parasympathetic input from the glossopharyngeal nerve (CN IX) via the otic ganglion, while the submandibular and sublingual glands receive their parasympathetic input from the facial nerve (CN VII) via the submandibular ganglion. These nerves release acetylcholine and substance P, which activate the IP3 and DAG pathways respectively. • Direct sympathetic innervation of the salivary glands takes place via preganglionic nerves in the thoracic segments T1-T3 which synapse in the superior cervical ganglion with postganglionic neurons that release norepinephrine, which is then received by β-adrenergic receptors on the acinar and ductal cells of the salivary glands, leading to an increase in cyclic adenosine monophosphate (cAMP) levels and the corresponding increase of saliva secretion. Note that in this regard both parasympathetic and sympathetic stimuli result in an increase in salivary gland secretions.[2] The sympathetic nervous system also affects salivary gland secretions indirectly by innervating the blood vessels that supply the glands.
Role in disease
See mumps (parotiditis epidemica), Sjögren's syndrome, Mucocele, Graft versus host disease and Salivary gland neoplasm. Salivary duct calculus may cause blockage of the ducts, causing pain and swelling of the gland because of cysts. Many anti-cancer treatments may impair salivary flow. Radiation therapy may cause permanent xerostomia, whereas chemotherapy may cause only temporary salivary impairment. Graft versus host disease after allogeneic bone marrow transplantation may manifest as dry mouth and many small mucoceles. Tumors of the salivary glands may occur. A sialogram is a radiocontrast study of a salivary duct. Saliva production may be pharmacologically stimulated by so-called sialagogues (e.g., pilocarpin, cevimeline). It can also be suppressed by so-called antisialagogues (e.g., tricyclic antidepressants, SSRI, antihypertensives, polypharmacy). [] The salivary glands of some species, however, are modified to produce enzymes; salivary amylase is found in many, but by no means all, bird and mammal species (including humans, as noted above). Furthermore, the venom glands of poisonous snakes, Gila monsters, and some shrews, are modified salivary glands.[]
Micrograph of chronic inflammation of the salivary gland sialadenitis).
Salivary gland
10
References
[1] A.R TEN CATE, "Oral histology. Development, structure, and function".(1998), 2003, 2008|page=3|Edition=5thISBN=0-8151-2952-1
External links
• Salivary Gland Disorders at intelihealth.com (http://www.intelihealth.com/IH/ihtIH/WSIHW000/9339/9658. html) • Illustration at merck.com (http://www.merck.com/media/mmhe2/figures/fg111_1.gif) • Illustration at .washington.edu (http://www.orthop.washington.edu/_Rainbow/Album/ 10357m26b8e09e-6490-41ab-8955-725a7a75ec05.gif) • plastic/371 (http://www.emedicine.com/plastic/topic371.htm#) at eMedicine - "Parotid Tumors, Benign" • Medical Encyclopedia Medline Plus: Salivary gland (http://vsearch.nlm.nih.gov/vivisimo/cgi-bin/ query-meta?v:project=medlineplus&query=Salivary+Gland+&x=25&y=14)
Von Ebner's gland
Ebner's glands, also Von Ebner's glands are exocrine glands found in the mouth. More specifically, they are serous salivary glands which reside adjacent to the moats surrounding the circumvallate papillae in the posterior one-third of the tongue, anterior to the terminal sulcus. Von Ebner's glands (also called gustatory glands) are named after Anton Gilbert Victor von Ebner, Ritter von Rosenstein, who was an Austrian histologist. These glands are located around circumvallate and foliate papillae in the tongue, and they secrete lingual lipase, beginning the process of Human Von Ebner's Gland. lipid hydrolysis in the mouth. These glands empty their serous secretion into the base of the moats located around the foliate and circumvallate papillae. This secretion presumably flushes material from the moat to enable the taste buds to respond rapidly to changing stimuli. The Von Ebner glands are innervated by Cranial Nerve IX, the glossopharyngeal nerve. It secretes lingual lipase.[1]
References External links
• Anton Gilbert Viktor Ebner, Ritter von Rofenstein entry @ whonamedit.com (http://www.whonamedit.com/ doctor.cfm/2269.html) • pubmed/16859632 (http://www.ncbi.nlm.nih.gov/pubmed/16859632) • synd/2602 (http://www.whonamedit.com/synd.cfm/2602.html) at Who Named It? • BU Histology Learning System: 09503loa (http://www.bu.edu/histology/p/09503loa.htm) • Histology at OU 126_05 (http://w3.ouhsc.edu/histology/Glass slides/126_05.jpg) • Dental histology at usc.edu (http://www.usc.edu/hsc/dental/ohisto/Cards/muc/57_bb.html)
Mammary gland
11
Mammary gland
Mammary gland in a human female
Cross section of the breast of a human female
Dissection of a lactating breast. 1 – Fat 2 – Lactiferous duct/lobule 3 – Lobule 4 – Connective tissue 5 – Sinus of lactiferous duct 6 – Lactiferous duct Latin Gray's Artery glandula mammaria subject #271 1267
[1]
Internal thoracic artery [] Lateral thoracic artery Internal thoracic vein [] Axillary vein Supraclavicular nerves [1] Intercostal nerves (lateral and medial branches) Pectoral axillary lymph nodes
[]
Vein
Nerve
Lymph
Precursor Mesoderm (blood vessels and connective tissue) [2] Ectoderm (cellular elements) MeSH A01.236.249
[4]
Mammary gland A mammary gland is an organ in female mammals that produces milk to feed young offspring. Mammals get their name from the word "mammary." In humans, the mammary glands are situated in the breasts. In ruminants such as cows, goats, and deer, the mammary glands are contained in the udders. The mammary glands of mammals having more than two breasts, such as dogs and cats, are sometimes called dugs.
12
Humans
Histology
A mammary gland is a specific type of apocrine gland specialized for manufacture of colostrum when giving birth. Mammary glands can be identified as apocrine because they exhibit striking "decapitation" secretion. Many sources assert that mammary glands are modified sweat glands.[3][4][] Some authors dispute that and argue instead that they are sebaceous glands.[3]
Structure
The basic components of a mature mammary gland are the alveoli (hollow cavities, a few millimeters large) lined with milk-secreting cuboidal cells and surrounded by myoepithelial cells. These alveoli join to form groups known as lobules. Each lobule has a lactiferous duct that drains into openings in the nipple. The myoepithelial cells contract under the stimulation of oxytocin, excreting the milk secreted by alveolar units into the lobule lumen toward the nipple. As the infant begins to suck, the oxytocin-mediated "let down reflex" ensues and the mother's milk is secreted – not sucked from the gland – into the baby's mouth. All the milk-secreting tissue leading to a single lactiferous duct is called a "simple mammary gland"; in a "complex mammary gland" all the simple mammary glands serve one nipple. Humans normally have two complex mammary glands, one in each breast, and each complex mammary gland consists of 10–20 simple glands. The presence of more than two nipples is known as polythelia and the presence of more than two complex mammary glands as polymastia. Maintaining the correct polarized morphology of the lactiferous duct tree requires another essential component – mammary epithelial cells extracellular matrix (ECM) which, together with adipocytes, fibroblast, inflammatory cells, and others, constitute mammary stroma. [] Mammary epithelial ECM mainly contains myoepithelial basement membrane and the connective tissue. They not only help to support mammary basic structure, but also serve as a communicating bridge between mammary epithelia and their local and global environment throughout this organ's development.[][]
Development and hormonal control
Mammary glands develop during different growth cycles. They exist in both sexes during embryonic stage, forming only a rudimentary duct tree at birth. In this stage, mammary gland development depends on systemic (and maternal) hormones,[] but is also under the (local) regulation of paracrine communication between neighboring epithelial and mesenchymal cells by parathyroid hormone-related protein(PTHrP).[5] This locally secreted factor gives rise to a series of outside-in and inside-out positive feedback between these two types of cells, so that mammary bud epithelial cells can proliferate and sprout down into the mesenchymal layer until they reach the fat pad to begin the first round of branching.[] At the same time, the embryonic mesenchymal cells around the epithelial bud receive secreting factors activated by PTHrP, such as BMP4. These mesenchymal cells can transform into a dense, mammary-specific mesenchyme, which later develop into connective tissue with fibrous threads, forming blood vessels and the lymph system.[6] A basement membrane, mainly containing laminin and collagen, formed afterward by differentiated myoepithelial cells, keeps the polarity of this primary duct tree. Lactiferous duct development occurs in females in response to circulating hormones. First development is frequently seen during pre- and postnatal stages, and later during puberty. Estrogen promotes branching differentiation,[7]
Mammary gland whereas in males testosterone inhibits it. A mature duct tree reaching the limit of the fat pad of the mammary gland comes into being by bifurcation of duct terminal end buds (TEB), secondary branches sprouting from primary ducts[][8] and proper duct lumen formation. These processes are tightly modulated by components of mammary epithelial ECM interacting with systemic hormones and local secreting factors. However, for each mechanism the epithelial cells' "niche" can be delicately unique with different membrane receptor profiles and basement membrane thickness from specific branching area to area, so as to regulate cell growth or differentiation sub-locally.[9] Important players include beta-1 integrin, epidermal growth factor receptor (EGFR), laminin-1/5, collagen-IV, matrix metalloproteinase(MMPs), heparan sulfate proteoglycans, and others. Elevated circulating level of growth hormone and estrogen get to multipotent cap cells on TEB tips through a thin, leaky layer of basement membrane. These hormones promote specific gene expression. Hence cap cells can differentiate into myoepithelial and luminal (duct) epithelial cells, and the increased amount of activated MMPs can degrade surrounding ECM helping duct buds to reach further in the fat pads.[10][11] On the other hand, basement membrane along the mature mammary ducts is thicker, with strong adhesion to epithelial cells via binding to integrin and non-integrin receptors. When side branches develop, it is a much more “pushing-forward” working process including extending through myoepithelial cells, degrading basement membrane and then invading into a periductal layer of fibrous stromal tissue.[] Degraded basement membrane fragments (laminin-5) roles to lead the way of mammary epithelial cells migration.[12] Whereas, laminin-1 interacts with non-integrin receptor dystroglycan negatively regulates this side branching process in case of cancer.[13] These complex "Yin-yang" balancing crosstalks between mammary ECM and epithelial cells "instruct" healthy mammary gland development until adult. Secretory alveoli develop mainly in pregnancy, when rising levels of prolactin, estrogen, and progesterone cause further branching, together with an increase in adipose tissue and a richer blood flow. In gestation, serum progesterone remains at a stably high concentration so signaling through its receptor is continuously activated. As one of the transcribed genes, Wnts secreted from mammary epithelial cells act paracrinely to induce more neighboring cells' branching.[14][15] When the lactiferous duct tree is almost ready, "leaves" alveoli are differentiated from luminal epithelial cells and added at the end of each branch. In late pregnancy and for the first few days after giving birth, colostrum is secreted. Milk secretion (lactation) begins a few days later due to reduction in circulating progesterone and the presence of another important hormone prolactin, which mediates further alveologenesis, milk protein production, and regulates osmotic balance and tight junction function. Laminin and collagen in myoepithelial basement membrane interacting with beta-1 integrin on epithelial surface again, is essential in this process.[][] Their binding ensures correct placement of prolactin receptors on the basal lateral side of alveoli cells and directional secretion of milk into lactiferous ducts.[][] Suckling of the baby causes release of the hormone oxytocin, which stimulates contraction of the myoepithelial cells. In this combined control from ECM and systemic hormones, milk secretion can be reciprocally amplified so as to provide enough nutrition for the baby. During weaning, decreased prolactin, missing mechanical stimulation (baby suckling), and changes in osmotic balance caused by milk stasis and leaking of tight junctions cause cessation of milk production. In some species there is complete or partial involution of alveolar structures after weaning, in humans there is only partial involution and the level of involution in humans appears to be highly individual. In some other species (such as cows), all alveoli and secretory duct structures collapse by programmed cell death (apoptosis) and autophagy for lack of growth promoting factors either from the ECM or circulating hormones.[16][17] At the same time, apoptosis of blood capillary endothelial cells speeds up the regression of lactation ductal beds. Shrinkage of the mammary duct tree and ECM remodeling by various proteinase is under the control of somatostatin and other growth inhibiting hormones and local factors.[18] This major structural change leads loose fat tissue to fill the empty space afterward. But a functional lactiferous duct tree can be formed again when a female is pregnant again.
13
Mammary gland
14
Breast cancer
Tumorigenesis in mammary glands can be induced biochemically by abnormal expression level of circulating hormones or local ECM components,[19] or from a mechanical change in the tension of mammary stroma.[20] Under either of the two circumstances, mammary epithelial cells would grow out of control and eventually result in cancer. Almost all instances of breast cancer originate in the lobules or ducts of the mammary glands.
Other mammals
The constantly protruding breasts of the adult human female, unusually large relative to body size, are a unique evolutionary development whose purpose is not yet fully known (see breasts); other mammals tend to have less conspicuous mammary glands that protrude only while actually filling with milk. The number and positioning of complex and simple mammary glands varies widely in different mammals. The nipples and glands can occur anywhere along the two milk lines, two nearly parallel lines along the ventral aspect of the body. In general most mammals develop mammary glands in pairs along these lines, with a number approximating the number of young typically birthed at a time. The number of nipples varies from 2 (in most primates) to 18 (in pigs). The Virginia Opossum has 13, one of the few mammals with an odd number.[21][22] The following table lists the number and position of glands normally found in a range of mammals:
Species [23] Anterior Intermediate Posterior (thoracic) (abdominal) (inguinal) 0 0 2 Total
Goat, sheep, horse guinea pig Cattle Cat Dog [24]
2
0 2 4 6 6 6 2
0 2 2 0 2 6 0
4 4 2 or 4 4 4 6 0
4 8 8 or 10 10 12 18 2
Mouse Rat Pig proboscideans, primates
Male mammals typically have rudimentary mammary glands and nipples, with a few exceptions: male mice do not have nipples, and male horses lack nipples and mammary glands.[citation needed] The male Dayak fruit bat has lactating mammary glands.[25] Male lactation occurs infrequently in some species, including humans. Mammary glands are true protein factories, and several labs have constructed transgenic animals, mainly goats and cows, to produce proteins for pharmaceutical use.[26] Complex glycoproteins such as monoclonal antibodies or antithrombin cannot be produced by genetically engineered bacteria, and the production in live mammals is much cheaper than the use of mammalian cell cultures.
Evolution
The evolution of the mammary gland is difficult to explain; this is because mammary glands are typically required by mammals to feed their young. There are many theories on how mammary glands evolved, for example, it is believed that the mammary gland is a transformed sweat gland, more closely related to apocrine sweat glands.[27] Since mammary glands do not fossilize well, supporting such theories with fossil evidence is difficult. Many of the current theories are based on comparisons between lines of living mammals – monotremes, marsupials and eutherians. One theory proposes that mammary glands evolved from glands that were used to keep the eggs of early mammals moist[28][29] and free from infection[30][31] (monotremes still lay eggs). Other theories suggest that early
Mammary gland secretions were used directly by hatched young,[32] or that the secretions were used by young to help them orient to their mothers.[33] Lactation is assumed to have developed long before the evolution of the mammary gland and mammals; see evolution of lactation.
15
Gallery
Cattle
Cat
Pig
Sheep
Goat
Elephant
Human
References
[3] Ackerman (2005) ch.1 Apocrine Units (http:/ / www. derm101. com/ content/ 13501) [4] Moore (2010) ch.1 Thorax, p. 99 [22] Stockard, Mary (2005) Raising Orphaned Baby Opossums (http:/ / web. archive. org/ web/ 20100701012225/ http:/ / www. awrc. org/ Baby Opossums. htm). Alabama Wildlife Center. [24] Dog breeds vary in the number of mammary glands: larger breeds tend to have 5 pairs, smaller breeds have 4 pairs. [28] Lactating on Eggs (http:/ / web. archive. org/ web/ 20090419024229/ http:/ / nationalzoo. si. edu/ ConservationAndScience/ SpotlightOnScience/ oftedalolav20030714. cfm). Smithsonian National Zoo, July 14, 2003. [30] Breast beginnings (http:/ / web. archive. org/ web/ 20070312005054/ http:/ / scienceblogs. com/ pharyngula/ 2006/ 05/ breast_beginnings. php). scienceblogs.com
Bibliography
• Ackerman, A. Bernard; Almut Böer, Bruce Bennin, and Geoffrey J. Gottlieb (2005). Histologic Diagnosis of Inflammatory Skin Diseases An Algorithmic Method Based on Pattern Analysis (http://www.derm101.com/ content/13501). ISBN 978-1-893357-25-9. • Moore, Keith L. et al. (2010) Clinically Oriented Anatomy 6th Ed
External links
• Comparative Mammary Gland Anatomy (http://web.archive.org/web/20051201011719/http://classes.aces. uiuc.edu/AnSci308/anatomycompar.html) by W. L. Hurley • On the anatomy of the breast (http://jdc.jefferson.edu/cooper/61/) by Sir Astley Paston Cooper (1840). Numerous drawings, in the public domain. • mammary+gland (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=mammary+gland) at eMedicine Dictionary
Lacrimal gland
16
Lacrimal gland
Lacrimal gland
Lacrimal apparatus of the right eye. The lacrimal gland is to the upper left. The right side of the picture is towards the nose.
Tear system. a = lacrimal gland b = superior lacrimal punctum c = superior lacrimal canal d = lacrimal sac e = inferior lacrimal punctum f = inferior lacrimal canal g = nasolacrimal canal Latin Gray's Artery Nerve glandula lacrimalis subject #227 1028 lacrimal artery lacrimal nerve, Zygomatic nerve via Communicating branch
[1]
The lacrimal glands are paired almond-shaped glands, one for each eye, that secrete the aqueous layer of the tear film. They are situated in the upper, outer portion of each orbit, in the lacrimal fossa of the orbit formed by the frontal bone.[1] Inflammation of the lacrimal glands is called dacryoadenitis. The lacriminal gland produces tears which then flow into canals that lead to the lacriminal sac. From this sac, the tears drain through a passage into the nose. [citation needed] Anatomists divide the gland into two sections. The smaller palpebral portion, lies close to the eye, along the inner surface of the eyelid; if the upper eyelid is everted, the palpebral portion can be seen. The orbital portion contains fine interlobular ducts that unite to form 3 - 5 main excretory ducts, joining 5 - 7 ducts in the palpebral portion before the secreted fluid may enter on the surface of the eye. Tears secreted collect in the fornix conjunctiva of the upper lid, and pass over the eye surface to the lacrimal puncta, small holes found at the inner corner of the eyelids. These pass the tears on to the lacrimal sac, in turn to the nasolacrimal duct, which dumps them out into the nose.[2]
Lacrimal gland
17
Microanatomy
The lacrimal gland is a compound tubuloacinar gland, it is made up of many lobules separated by connective tissue, each lobule contains many acini. The acini contain only serous cells and produce a watery serous secretion. Each acinus consists of a grape-like mass of lacrimal gland cells with their apices pointed to a central lumen. The central lumen of many of the units converge to form intralobular ducts, and then unite to from interlobular ducts. The gland lacks striated ducts.
Innervation
The parasympathetic nerve supply originates from the lacrimal nucleus of the facial nerve in the pons. Just distal to the geniculate ganglion, the facial nerve gives off the greater petrosal nerve. This nerve carries the parasympathetic secretomotor fibers through the pterygoid canal, where it joins the deep petrosal nerve (containing postganglionic sympathetic fibers from the superior cervical ganglion) to form the nerve of the pterygoid canal (vidian nerve). This nerve travels through the pterygoid canal to the pterygopalatine ganglion. Here the fibers synapse and postganglionic fibers join the fibers of the maxillary nerve, which travels through the inferior orbital fissure. Once it has traversed this opening, the parasympathetic secretomotor fibers branch off with the zygomatic nerve and then branch off again, joining with the lacrimal branch of the ophthalmic division of CN V, which supplies sensory innervation to the lacrimal gland along with the eyelid and conjunctiva. The sympathetic postganglionic fibers originate from the superior cervical ganglion. They travel as a periarteriolar plexus with the middle meningeal artery, before they merge and form the deep petrosal nerve, which joins the greater petrosal nerve in the pterygoid canal. Together, greater petrosal and deep petrosal nerves form the nerve of the pterygoid canal (vidian nerve) and reach the pterygopalatine ganglion in the pterygopalatine fossa. In contrast to their parasympathetic counterparts, sympathetic fibers do not synapse in the pterygopalatine ganglion, having done so already in the sympathetic trunk. However, they continue to course with the parasympathetic fibers innervating the lacrimal gland.
Blood supply
The lacrimal artery, derived from the ophthalmic artery supplies the lacrimal gland. Venous blood returns via the superior ophthalmic vein.
Nerve supply
The lacrimal nerve, derived from the ophthalmic nerve supplies the lacrimal gland
Applied anatomy
• The upper part of the lacrimal sac is covered by the medial palpabral ligament. Hence the abscesses within the sac bulge below the medial palpabrel ligament, where it should be incised for letting out the pus. • The angular vein is in front of the sac and it should be take care during incising the sac. Between the lacrimal sac and the fascia coverning the sac there is the collection of venous plexus present hence the incising causes considerable bleeding. • Around the nasolacrimal duct there is the rich plexus of veins, in the form of an erectile tissue, which may engorge and cause obstruction to the duct.
Lacrimal gland
18
Pathology
• Dacryoadenitis • Sjögren's syndrome
Additional images
The ophthalmic artery and its branches.
Nerves of the orbit. Seen from above.
Sympathetic connections of the sphenopalatine and superior cervical ganglia.
The tarsal glands, etc., seen from the inner surface of the eyelids.
Alveoli of lacrimal gland.
Extrinsic eye muscle. Nerves of orbita. Deep dissection.
Extrinsic eye muscle. Nerves of orbita. Deep dissection.
Extrinsic eye muscle. Nerves of orbita. Deep dissection.
Extrinsic eye muscle. Nerves of orbita. Deep dissection.
Extrinsic eye muscle. Nerves of orbita. Deep dissection.
References
[1] Clinically Oriented Anatomy (http:/ / www. amazon. com/ dp/ 0781775256), Moore, Dalley & Agur. [2] "eye, human."Encyclopædia Britannica. 2010. Encyclopædia Britannica 2010 Ultimate Reference Suite DVD 2010
External links
• Lacrimal+gland (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=Lacrimal+gland) at eMedicine Dictionary • lesson3 (http://mywebpages.comcast.net/wnor/lesson3.htm) at The Anatomy Lesson (http://home.comcast. net/~wnor/homepage.htm) by Wesley Norman (Georgetown University) ( orbit2 (http://mywebpages.comcast. net/wnor/orbit2.jpg))
Ceruminous gland
19
Ceruminous gland
Ceruminous glands are specialized sudoriferous glands (sweat glands) located subcutaneously in the external auditory canal. Ceruminous glands are simple, coiled, tubular glands made up of an inner secretory layer of cells and an outer myoepithelial layer of cells.[1] The glands drain into larger ducts, which then drain into the guard hairs that reside in the external auditory canal.[2] Here they produce cerumen, or earwax, by mixing their secretion with sebum and dead epidermal cells. Cerumen keeps the eardrum pliable, lubricates and cleans the external auditory canal, waterproofs the canal, kills bacteria, and serves as a barrier to trap foreign particles (dust, fungal spores, etc.) by coating the guard hairs of the ear, making them sticky.[1] These glands are capable of developing both benign and malignant tumors. The benign tumors include ceruminous adenoma, ceruminous pleomorphic adenoma, and ceruminous syringocystadenoma papilliferum. The Malignant tumors include ceruminous adenocarcinoma, adenoid cystic carcinoma, and mucoepidermoid carcinoma.[2]
References
[1] Saladin,Kenneth. Anatomy & Physiology: The Unity of Form and Function, Fifth Edition. McGraw-Hill. 2010 [2] http:/ / emedicine. medscape. com/ article/ 1960501-overview
External links
• http://www.anatomyatlases.org/MicroscopicAnatomy/Section07/Plate07142.shtml • http://emedicine.medscape.com/article/1960501-overview
Eccrine sweat gland
20
Eccrine sweat gland
Eccrine sweat gland
A sectional view of the skin (magnified), with eccrine glands highlighted. Latin System Nerve Precursor MeSH Code Glandula sudorifera merocrina; Glandula sudorifera eccrina Integumentary
[] []
Cholinergic sympathetic nerves Ectoderm
[] [1]
Eccrine+Glands
TH H3.12.00.3.03009
Eccrine glands (/ˈɛkrən/, /ˈɛˌkraɪn/, or /ˈɛˌkrin/; from ekkrinein "secrete";[1] sometimes called merocrine glands) are the major sweat glands of the human body, found in virtually all skin.[1] They produce a clear, odorless substance, consisting primarily of water and NaCl (note that the odor from sweat is due to bacterial activity on the secretions of the apocrine glands). NaCl is reabsorbed in the duct to reduce salt loss.[2] They are active in thermoregulation and emotional sweating (induced by anxiety, fear, stress, and pain).[]:170 Eccrine glands are composed of an intreaepidermal spiral duct, the "acrosyringium"; a dermal duct, comprising a straight and coiled portion; and a secretory tubule, coiled deep in the dermis or hypodermis.[]:172 Eccrine glands are innervated by the sympathetic nervous system, primarily by cholinergic fibers, but by adrenergic fibers as well.[3] Dermcidin is a newly isolated antimicrobial peptide produced by the eccrine sweat glands.[4]
References External links
• American Academy of Dermatology – Eccrine and Apocrine Glands (http://www.aad.org/education/students/ glands.htm)
Apocrine sweat gland
21
Apocrine sweat gland
Apocrine sweat gland
Latin System Nerve Glandula sudorifera apocrina Integumentary system Adrenergic nerves
[1] [] []
Precursor Primary epithelial germ[2] MeSH Code Apocrine+Glands
[3]
TH H3.12.00.3.03002
An apocrine sweat gland (/ˈæpəkrən/, /ˈæpəˌkraɪn/, or /ˈæpəˌkrin/, from Greek apo– "away" and krinein "to separate")[3][4] is a sweat gland composed of a coiled secretory portion located at the junction of the dermis and subcutaneous fat, from which a straight portion inserts and secretes into the infundibular portion of the hair follicle.[1] In humans, apocrine sweat glands are found only in certain locations of the body: the axillae (armpits), areola and nipples of the breast, ear canal, eyelids, wings of the nostril, perianal region, and some parts of the external genitalia.[5] Modified apocrine glands include the ciliary glands in the eyelids; the ceruminous glands, which produce ear wax; and the mammary glands, which produce milk.[1] The rest of the body is covered by eccrine sweat glands.[] Most non-primate mammals, however, have apocrine sweat glands over the greater part of their body.[5] Domestic animals such as dogs and cats have apocrine glands at each hair follicle but eccrine glands only in foot pads and snout. Their apocrine glands, like those in humans, produce an odorless, oily, opaque secretion[] that gains its characteristic odor upon bacterial decomposition.[6] Eccrine glands on their paws increase friction and prevent them from slipping when fleeing from danger.[7]
Structure
The apocrine gland comprises a glomerulus of secretory tubules and an excretory duct that opens into hair follicle;[8] on occasion, an excretory duct opens to the skin surface next to the hair.[9] The gland is large and spongy, located in the subcutaneous fat deep in the dermis,[][10] and has a larger overall structure and lumen diameter than the eccrine sweat gland.[11][5] Unlike eccrine secretory tubules, secretory tubules of the apocrine gland are single-layered (lacking ductal cells),[10] vary in diameter from place to place, and sometimes branch off into multiple ducts. The tubules are wrapped in myoepithelial cells, which are more developed than their eccrine gland counterparts.[12][13]
Sweating
In hoofed animals and marsupials, apocrine glands act as the main thermoregulator, secreting watery sweat.[] For most mammals, however, apocrine sweat glands secrete an oily (and eventually smelly) compound that acts as a pheromone,[] territorial marker, and warning signal.[][14][15] Being sensitive to adrenaline, apocrine sweat glands are involved in emotional sweating in humans (induced by anxiety, stress, fear, sexual stimulation, and pain).[14] In a five-month-old human fetus, apocrine glands are distributed all over the body; after a few weeks, they exist in only restricted areas,[] including the armpits and external genitalia.[5] They are inactive until stimulated by hormonal changes in puberty.[14]
Apocrine sweat gland
22
Mechanism
The apocrine gland secretes an oily fluid with proteins, lipids, and steroids that is odorless before microbial activity. It appears on the skin surface mixed with sebum, as sebaceous glands open into the same hair follicle.[16] Unlike eccrine sweat glands, which secrete continuously, the apocrine glands secrete in periodic spurts.[] Apocrine sweat glands were originally thought use only apocrine secretion: vesicles pinch off the secretory cells, then degrade in the secretory lumen, releasing their product.[] More recent research has also shown that merocrine secretion takes place.[] Myoepithelial cells form a smooth muscle lining around the secretory cells; when the muscle contracts, they squeeze the secretory ducts and push out the accumulated fluid into the hair follicle.[][] Sweat and sebum are mixed in the hair follicle and arrive mixed at the epidermal surface.[] The apocrine sweat is cloudy, viscous, initially odorless, and at a pH of 6–7.5. It contains water, protein, carbohydrate waste material, and NaCl.[] The sweat only attains its characteristic odor upon being degraded by bacteria, which releases volatile odor molecules.[16] More bacteria (especially corynebacteria) leads to stronger odor. The presence of axillary hair also makes the odor worse, as secretions, debris, keratin, and bacteria accumulate on the hairs.[10]
Prevalence
Non-primate mammals have usually apocrine sweat glands over most of their bodies.[5] Horses use them as a thermoregulatory device, as they are regulated by adrenaline and more widely distributed on equines than on other groups.[] Skunks, on the other hand, use the glands to release a stench that acts as a defense mechanism.[] The "axillary organs", limited regions with equal numbers of apocrine and eccrine sweat glands, only exist in humans, gorillas, and chimpanzees.[] In humans, the apocrine glands in this region are the most developed (with the most complex glomeruli).[12] Men have fewer apocrine sweat glands than women in all axillary regions.[17][18] East Asians have fewer such glands than Europeans and people of African descent, which decreases their susceptibility to body odor.[17][19] Individuals of African ancestry have the largest and most active apocrine glands.[20] Racial differences also exist in the cerumen glands: apocrine sweat glands which produce earwax.[1] East Asians have predominantly dry earwax, as opposed to sticky; the gene encoding for this is strongly linked to reduced body odor, whereas those with wet, sticky earwax (Europeans and Africans) are prone to more body odor.[21]
Notes
[1] Krstic 2004, p. 466. [2] Tsai 2006, p. 496. [5] Kurosumi, Shibasaki & Ito 1984, p. 255. [6] Eroschenko 2008, pp. 228–229. [7] Wilke et al. 2007, p. 170. [8] Kurosumi, Shibasaki & Ito 1984, pp. 255–256. [9] Tsai 2006, pp. 496–497. [10] Tsai 2006, p. 497. [11] Krstic 2004, p. 468. [12] Kurosumi, Shibasaki & Ito 1984, p. 256. [13] Eroschenko 2008, p. 226. [14] Wilke et al. 2007, p. 171. [16] Wilke et al. 2007, p. 175. [17] Wilke et al. 2007, p. 174. [18] Stoddart 1990, p. 60. [19] Stoddart 1990, p. 61.
Apocrine sweat gland
23
References
• Eroschenko, Victor P. (2008). "Integumentary System". DiFiore's Atlas of Histology with Functional Correlations. Lippincott Williams & Wilkins. pp. 212–234. ISBN 9780781770576. • Krstic, Radivoj V. (18 March 2004). Human Microscopic Anatomy: An Atlas for Students of Medicine and Biology. Springer. pp. 464, 466–469. ISBN 9783540536666. • Kurosumi, Kazumasa; Shibasaki, Susumu; Ito, Toshiho (1984). "Cytology of the Secretion in Mammalian Sweat Glands". In Bourne, Geoffrey H.; Danielli, James F. Protein Diffusion in Cell Membranes: Some Biological Implications. Orlando, Florida: Academic Press. pp. 253–330. ISBN 9780123644879. • Stoddart, D. Michael (1990). The scented ape: The biology and culture of human odour. Cambridge: Cambridge University Press. pp. 60–61. ISBN 0521375118. • Tsai, Ren-Yu (1 January 2006). "Treatment of Excessive Axillary Sweat Syndrome (Hyperhidrosis, Osmidrosis, Bromhidrosis) with Liposuction". In Shiffman, Melvin A.; Di Giuseppe, Alberto. Liposuction: Non-Cosmetic Applications. Germany: Springer. pp. 496–497. ISBN 9783540280439. • Wilke, K.; Martin, A.; Terstegen, L.; Biel, S. S. (June 2007). "A short history of sweat gland biology" (http:// onlinelibrary.wiley.com/doi/10.1111/j.1467-2494.2007.00387.x/pdf) (pdf). International journal of cosmetic science 29 (3): 169–179. doi: 10.1111/j.1467-2494.2007.00387.x (http://dx.doi.org/10.1111/j. 1467-2494.2007.00387.x). ISSN 1468-2494 (http://www.worldcat.org/issn/1468-2494).
External links
• Diagram of eccrine and apocrine sweat glands (http://www.mayoclinic.com/health/medical/IM00027) from Mayo Clinic
Moll's gland
24
Moll's gland
Gland of Moll
Latin glandulae ciliares conjunctivales Gray's subject #227 1025 [1]
Glands of Moll, also known as ciliary glands, are modified apocrine sweat glands that are found on the margin of the eyelid. They are next to the base of the eyelashes, and anterior to the Meibomian glands within the distal eyelid margin. These glands are relatively large and tubular-shaped. The glands of Moll are named after Dutch oculist Jacob Anton Moll (1832–1914). Glands of Moll empty into the adjacent lashes. Glands of Moll and Zeis secrete lipid that adds to the superficial layer of the tear film, retarding evaporation. The glands of Moll are prone to infection and blockage of its duct with sebum and cell debris. Blockage of the gland's duct causes swelling which can manifest itself as a stye.
References
• American Family Physician, Eyelid Disorders: Diagnosis and Management [2] • Anatomy of the Human Eyelid [3]
Sebaceous gland
25
Sebaceous gland
Sebaceous gland
Schematic view of hair follicle & sebaceous gland.
Cross-section of all skin layers. A hair follicle with associated structures. (Sebaceous glands labeled at center left.) Latin Gray's MeSH glandula sebacea subject #234 1069
[1] [2]
Sebaceous+glands
The sebaceous glands are microscopic glands in the skin that secrete an oily/waxy matter, called sebum, to lubricate and waterproof the skin and hair of mammals.[1] In humans, they are found in greatest abundance on the face and scalp, though they are distributed throughout all skin sites except the palms and soles.[1] In the eyelids, meibomian sebaceous glands secrete a special type of sebum into tears. There are several related medical conditions, including acne, sebaceous cysts, hyperplasia, sebaceous adenoma and sebaceous gland carcinoma (see section below: Pathology).
Locations and morphology
A branched type of acinar gland, the sebaceous glands exist in humans throughout the skin except in the palms of the hands and soles of the feet. Sebaceous glands can usually be found in hair-covered areas, where they are connected to hair follicles (see image at top). The glands deposit sebum on the hairs, and bring it to the skin surface along the hair shaft. The structure consisting of hair, hair follicle, arrector pili muscle, and sebaceous gland is known as a pilosebaceous unit. Sebaceous glands are also found in non-haired areas (glabrous skin) of eyelids, nose, penis, labia minora and nipples. Here, the sebum traverses ducts that terminate in sweat pores on the surface of the skin.[citation needed] At the rim of the eyelids, meibomian glands are a specialized form of sebaceous gland. They secrete a form of sebum (called (meibum)) onto the eye, slowing the evaporation of tears.
Sebaceous gland
26
Sebum
Sebaceous glands secrete the oily, waxy substance called sebum (Latin, meaning fat or tallow) that is made of triglyceride oils, wax, squalene, and metabolytes of fat-producing cells.[2][3] In the glands, sebum is produced within specialized cells and is released as these cells burst; sebaceous glands are thus classified as holocrine glands. Seborrhoea is the name for the condition of greasy skin caused by excess sebum.[4] Sebum keeps hair and skin supple. Sebum is odorless, but its bacterial breakdown can produce odors. Sebum is the cause of some people's experiencing "oily" hair,[5] as in hot weather or if not washed for several days. Earwax is partly composed of sebum.
Function
All of the sebaceous glands in humans have been demonstrated to show similarity in structure and secrete sebum by a holocrine process. Sebum excreted by the sebaceous gland is primarily composed of tryglycerides, wax esters, and squalene.[6] Wax esters, like squalene, are unique to sebum and not produced anywhere else in the body.[7] Sebum also contains 45% water-insoluble fatty acids known to have broad antimicrobial activity.[][8] Additionally, sebaceous gland secretion provides Vitamin E to the upper layers of facial skin.[9] Sebaceous lipids contribute to maintaining the integrity of the skin barrier, and express pro-inflammatory and anti-inflammatory properties.[10][][] Recent research suggests that sebum may represent a delivery system for antioxidants, antimicrobial lipids, pheromones, and hydration of stratum corneum.[] During the last gestation trimester, it is known that sebaceous glands produce vernix caseosa which protects the embryonic skin from amniotic water.[11] Sebaceous secretions in conjunction with apocrine glands also play an important thermoregulatory role. In hot conditions, the secretions emulsify and foment formation of and prevent the loss of sweat drops from the skin. In colder conditions, sebum repels rain from skin and hair.[] Increased facial surface sebum secretion is also associated with the development of acne.[]
Composition
The composition of sebum varies across species. In humans, the lipid content is as follows:[12]
Percent composition Substance 25% 41% 16% 12% wax monoesters triglycerides free fatty acids squalene
Sapienic acid is a sebum fatty acid that is unique to humans.
Sebaceous gland
27
Control
The following treatments have been shown to reduce sebum secretion rates: • Isotretinoin[13] • SMT D002[14] • Spironolactone[15] (suitable for females only)
Changes during development
The sebaceous glands of a human fetus in utero secrete a substance called Vernix caseosa, a "waxy" or "cheesy" white substance coating the skin of newborns. The activity of the sebaceous glands increases during puberty because of heightened levels of androgens, producing smegma. In males, sebaceous glands begin to appear predominantly on the penis, on the shaft and around the rim of the penile head during and after puberty. This is however normal, not to be confused with an STD. In females, they appear predominantly in the labia minora.
Pathology
Sebaceous glands are involved in skin problems such as acne and keratosis pilaris. In the skin pores, sebum and keratin can create a hyperkeratotic plug called a "microcomedone". The prescription drug isotretinoin significantly reduces the amount of sebum produced by the sebaceous glands, and is used to treat acne. The extreme use (up to 10 times doctor-prescribed amounts) of anabolic steroids by bodybuilders, for muscle gain can cause acne. The sebaceous gland is stimulated due to some steroids conversion into dihydrotestosterone. This may cause serious acne on the face, neck, chest, back and shoulders. It is a common misconception that a blocked sebaceous gland is known as a sebaceous cyst. Cysts that are commonly called sebaceous cysts actually do not involve a sebaceous gland. Instead, they are collection of keratin and dead keratinocytes which develop within the epidermal skin layer. These cysts are called Epidermal Cysts. A condition involving enlarged sebaceous glands is known as sebaceous hyperplasia. Sebaceous gland carcinoma is a rare and aggressive form of cancer involving the sebaceous glands; sebaceous adenoma is a more benign neoplasm of the sebaceous glands. Sebum can also build up around body piercings.[16]
Importance to other animals
Certain species of Demodex mites feed on sebum and are commonly found in the sebaceous glands of mammals, including those of humans. The preputial glands of mice and rats are large modified sebaceous glands that produce pheromones.
Demodex mite
Sebaceous gland
28
Additional images
Pilosebaceous unit
Base of pilosebaceous unit
Insertion of sebaceous glands into hair shaft
Sagittal section through the upper eyelid.
A hair follicle with associated structures.
References
[1] Dellmann's textbook of veterinary histology (405 pages), Jo Ann Coers Eurell, Brian L. Frappier, 2006, p.29, weblink: Books-Google-RTOC (http:/ / books. google. com/ books?id=FnS4uiOlRT0C& pg=PA29& lpg=PA29). [2] "Exercise 15: Hair", VT.edu, 2008, webpage: Vetmed-lab15 (http:/ / education. vetmed. vt. edu/ Curriculum/ VM8054/ Labs/ Lab15/ Lab15. htm). [5] "Hair Care: An Illustrated Dermatologic Handbook", Zoe Diana Draelos, Zoe Kececioglu Draelos, 2005, p.26, web: Books-Google-5QC (http:/ / books. google. com/ books?id=Z2rHHGQc-5QC& pg=PA26& lpg=PA26): oily hair & detergents. [14] http:/ / www. summitplc. com/ uploads/ RNSSeborrhoeatrialFINAL. pdf
External links
• BU Histology Learning System: 08801loa (http://www.bu.edu/histology/p/08801loa.htm) - "Integument: scalp" • Sebaceous Glands (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Sebaceous+Glands) at the US National Library of Medicine Medical Subject Headings (MeSH)
Olfactory glands
29
Olfactory glands
Olfactory glands
Section of the olfactory mucous membrane. Latin Gray's Code glandulae olfactoriae subject #223 996
[1] [2]
TH H3.05.00.0.00026
Bowman's glands (a.k.a. olfactory glands, glands of Bowman) are situated in the olfactory mucosa, beneath the olfactory epithelium, in the lamina propria, a connective tissue also containing fibroblasts, blood vessels, and bundles of fine axons from the olfactory neurons.[1] The structure of the Bowman's glands consists of an acinus in the lamina propria and a secretory duct going out through the olfactory epithelium. Electron microscopy studies show that Bowman's glands contain cells with large secretory vesicles.[2] Bowman's glands might secrete proteins such as Lysozyme, amylase and IgA similarly to serous glands. The exact composition of the secretions from Bowman's glands is unclear, but there is evidence that Bowman's glands do not produce odorant binding protein.[3]
References External links
• Slide at ouhsc.edu (http://w3.ouhsc.edu/histology/Glass slides/11_07.jpg) This article incorporates text from a public domain edition of Gray's Anatomy.
Brunner's glands
30
Brunner's glands
Brunner's glands
Section of duodenum. (Duodenal glands in submucosa are labeled at right, fourth from the top.) Latin Gray's glandulae duodenales subject #248 1176
[1]
Brunner's glands (or duodenal glands) are compound tubular submucosal glands found in that portion of the duodenum which is above the hepatopancreatic sphincter (Sphincter of Oddi). The main function of these glands is to produce a mucus-rich alkaline secretion (containing bicarbonate) in order to: • protect the duodenum from the acidic content of chyme (which is introduced into the duodenum from the stomach); • provide an alkaline condition for the intestinal enzymes to be active, thus enabling absorption to take place; • lubricate the intestinal walls. They also secrete urogastrone, which inhibits parietal and chief cells of the stomach from secreting acid and their digestive enzymes. This is another form of protection for the duodenum. They are the distinguishing feature of the duodenum, and are named for the Swiss physician who first described them, Johann Conrad Brunner.
External links
• duodenal+glands [2] at eMedicine Dictionary • BU Histology Learning System: 11504loa [3] - "Digestive System: Alimentary Canal: pyloro/duodenal junction, duodenum" • BU Histology Learning System: 11513loa [4] - "Digestive System: Alimentary Canal: pyloro/duodenal junction" • BU Histology Learning System: 11609loa [5] - "Digestive System: Alimentary Canal: duodenum, plicae circularis"
Human brunner's gland
Prostate
31
Prostate
Prostate
Male Anatomy
Prostate with seminal vesicles and seminal ducts, viewed from in front and above. Latin Gray's Artery Vein Nerve Lymph Precursor MeSH prostata subject #263 1251
[1]
internal pudendal artery, inferior vesical artery, and middle rectal artery prostatic venous plexus, pudendal plexus, vesicle plexus, internal iliac vein inferior hypogastric plexus external iliac lymph nodes, internal iliac lymph nodes, sacral lymph nodes Endodermic evaginations of the urethra Prostate
[2]
Dorlands/Elsevier Prostate [3]
The prostate (from Greek προστάτης – prostates, literally "one who stands before", "protector", "guardian"[1]) is a compound tubuloalveolar exocrine gland of the male reproductive system in most mammals.[][2] It differs considerably among species anatomically, chemically, and physiologically. In 2002, female paraurethral glands, or Skene's glands, were officially renamed the female prostate by the Federative International Committee on Anatomical Terminology.[3]
Prostate
32
Function
The function of the prostate is to secrete a slightly alkaline fluid, milky or white in appearance,[] that usually constitutes 50–75% of the volume of the semen along with spermatozoa and seminal vesicle fluid.[] Semen is made alkaline overall with the secretions from the other contributing glands, including, at least, the seminal vesicle fluid. The alkalinity of semen helps neutralize the acidity of the vaginal tract, prolonging the lifespan of sperm. The alkalinization of semen is primarily accomplished through secretion from the seminal vesicles.[4] The prostatic fluid is expelled in the first ejaculate fractions, together with most of the spermatozoa. In comparison with the few spermatozoa expelled together with mainly seminal vesicular fluid, those expelled in prostatic fluid have better motility, longer survival and better protection of the genetic material. The prostate also contains some smooth muscles that help expel semen during ejaculation.
Secretions
Prostatic secretions vary among species. They are generally composed of simple sugars and are often slightly acidic. In human prostatic secretions, the protein content is less than 1% and includes proteolytic enzymes, prostatic acid phosphatase, beta-microseminoprotein, and prostate-specific antigen. The secretions also contain zinc with a concentration 500–1,000 times the concentration in blood.
Regulation
To work properly, the prostate needs male hormones (testosterones), which are responsible for male sex characteristics. The main male hormone is testosterone, which is produced mainly by the testicles. Some male hormones are produced in small amounts by the adrenal glands. However, it is dihydrotestosterone that regulates the prostate.
Development
The prostatic part of the urethra develops from the pelvic (middle) part of the urogenital sinus (endodermal origin). Endodermal outgrowths arise from the prostatic part of the urethra and grow into the surrounding mesenchyme. The glandular epithelium of the prostate differentiates from these endodermal cells, and the associated mesenchyme differentiates into the dense stroma and the smooth muscle of the prostate.[5] The prostate glands represent the modified wall of the proximal portion of the male urethra and arises by the 9th week of embryonic life in the development of the reproductive system. Condensation of mesenchyme, urethra and Wolffian ducts gives rise to the adult prostate gland, a composite organ made up of several glandular and non-glandular components tightly fused.
Female prostate gland
The Skene's gland, also known as the paraurethral gland, found in females, is homologous to the prostate gland in males. However, anatomically, the uterus is in the same position as the prostate gland. In 2002 the Skene's gland was officially renamed to female prostate by the Federative International Committee on Anatomical Terminology.[6] The female prostate, like the male prostate, secretes PSA and levels of this antigen rise in the presence of carcinoma of the gland. The gland also expels fluid, like the male prostate, during orgasm.[]
Prostate
33
Structure
A healthy human prostate is classically said to be slightly larger than a walnut. The mean weight of the "normal" prostate in adult males is about 11 grams, usually ranging between 7 and 16 grams.[7] It surrounds the urethra just below the urinary bladder and can be felt during a rectal exam. It is the only exocrine organ located in the midline in humans and similar animals. The secretory epithelium is mainly pseudostratified, comprising tall columnar cells and basal cells which are supported by a fibroelastic stroma containing randomly orientated smooth muscle bundles. The epithelium is highly variable and areas of low cuboidal or squamous epithelium are also present, with transitional epithelium in the distal regions of the longer ducts.[] Within the prostate, the urethra coming from the bladder is called the prostatic urethra and merges with the two ejaculatory ducts. The prostate can be divided in two ways: by zone, or by lobe.[] It does not have a capsule, rather an integral fibromuscular band surrounds it.[8] It is sheathed in the muscles of the pelvic floor, which contract during the ejaculatory process.
Micrograph of benign prostatic glands with corpora amylacea. H&E stain.
Zones
The "zone" classification is more often used in pathology. The idea of "zones" was first proposed by McNeal in 1968. McNeal found that the relatively homogeneous cut surface of an adult prostate in no way resembled "lobes" and thus led to the description of "zones."[9] The prostate gland has four distinct glandular regions, two of which arise from different segments of the prostatic urethra:
Urinary bladder (black butterfly-like shape) and hyperplastic prostate (BPH) visualized by Medical ultrasonography technique
Name Peripheral zone (PZ)
Fraction of gland
Description
Up to 70% in young The sub-capsular portion of the posterior aspect of the prostate gland that surrounds the distal [10][11] men urethra. It is from this portion of the gland that ~70–80% of prostatic cancers originate. Approximately 25% This zone surrounds the ejaculatory ducts. The central zone accounts for roughly 2.5% of prostate normally cancers although these cancers tend to be more aggressive and more likely to invade the seminal [] vesicles. 5% at puberty ~10–20% of prostate cancers originate in this zone. The transition zone surrounds the proximal urethra and is the region of the prostate gland that grows throughout life and is responsible for the [10][11] disease of benign prostatic enlargement. (2) This zone is usually devoid of glandular components, and composed only, as its name suggests, of muscle and fibrous tissue.
Central zone (CZ)
Transition zone (TZ)
Anterior fibro-muscular Approximately 5% zone (or stroma)
Prostate
34
Lobes
The "lobe" classification is more often used in anatomy.
Prostate with a large median lobe bulging upwards. A metal instrument is placed in the urethra which passes through the prostate. This specimen was almost 7 centimeters long with a volume of about 60 cubic centimetres on transrectal ultrasound and was removed during a Hryntschak procedure or transvesical prostatectomy (removal of the prostate through the bladder) for benign prostatic hyperplasia.
Anterior lobe (or isthmus) Posterior lobe Lateral lobes
roughly corresponds to part of transitional zone roughly corresponds to peripheral zone spans all zones
Median lobe (or middle lobe) roughly corresponds to part of central zone
Prostate
35
Prostate disorders
Prostatitis
Prostatitis is inflammation of the prostate gland. There are primarily four different forms of prostatitis, each with different causes and outcomes. Two relatively uncommon forms, acute prostatitis and chronic bacterial prostatitis, are treated with antibiotics (category I and II, respectively). Chronic non-bacterial prostatitis or male chronic pelvic pain syndrome (category III), which comprises about 95% of prostatitis diagnoses, is treated by a large variety of modalities including alpha blockers, phytotherapy, physical therapy, psychotherapy, antihistamines, anxiolytics, nerve modulators, surgery,[12] and more.[] More recently, a combination of trigger point and psychological therapy has proved effective for category III prostatitis as well.[] Category IV prostatitis, relatively uncommon in the general population, is a type of leukocytosis.
Micrograph showing an inflamed prostate gland, the histologic correlate of prostatitis. A normal non-inflamed prostatic gland is seen on the left of the image. H&E stain.
Benign prostatic hyperplasia
Benign prostatic hyperplasia (BPH) occurs in older men;[] the prostate often enlarges to the point where urination becomes difficult. Symptoms include needing to urinate often (frequency) or taking a while to get started (hesitancy). If the prostate grows too large, it may constrict the urethra and impede the flow of urine, making urination difficult and painful and, in extreme cases, completely impossible. BPH can be treated with medication, a minimally invasive procedure or, in extreme cases, surgery that removes the prostate. Minimally invasive procedures include transurethral needle ablation of the prostate (TUNA) and transurethral microwave thermotherapy (TUMT).[13] These outpatient procedures may be followed by the insertion of a temporary prostatic stent, to allow normal voluntary urination, without exacerbating irritative symptoms.[] The surgery most often used in such cases is called transurethral resection of the prostate (TURP or TUR). In TURP, an instrument is inserted through the urethra to remove prostate tissue that is pressing against the upper part of the urethra and restricting the flow of urine. TURP results in the removal of mostly transitional zone tissue in a patient with BPH. Older men often have corpora amylacea[14] (amyloid), dense accumulations of calcified proteinaceous material, in the ducts of their prostates. The corpora amylacea may obstruct the lumens of the prostatic ducts, and may underlie some cases of BPH. Urinary frequency due to bladder spasm, common in older men, may be confused with prostatic hyperplasia. Statistical observations suggest that a diet low in fat and red meat and high in protein and vegetables, as well as regular alcohol consumption, could protect against BPH.[]
Prostate
36
Prostate cancer
Prostate cancer is one of the most common cancers affecting older men in developed countries and a significant cause of death for elderly men (estimated by some specialists at 3%). Despite this, the American Cancer Society's position regarding early detection is "Research has not yet proven that the potential benefits of testing outweigh the harms of testing and treatment" and that they believe "that men should not be tested without learning about what we know and don’t know about the risks and possible benefits of testing and treatment. Starting at age 50 Micrograph showing normal prostatic glands and (age 45 if you are of Black race or if your father or brother acquired glands of prostate cancer (prostate prostate cancer before age 65), talk to your doctor about the pros and adenocarcinoma) – right upper aspect of image. cons of testing so you can decide if testing is the right choice for HPS stain. Prostate biopsy. you".[15] If checks are performed, they can be in the form of a physical rectal exam, measurement of prostate specific antigen (PSA) level in the blood, or checking for the presence of the protein Engrailed-2 (EN2) in the urine. Co-researchers Hardev Pandha and Richard Morgan published their findings regarding checking for EN2 in urine in the 1 March 2011 issue of the journal Clinical Cancer Research.[16] A laboratory test currently identifies EN2 in urine, and a home test kit is envisioned similar to a home pregnancy test strip. According to Morgan, "We are preparing several large studies in the UK and in the US and although the EN2 test is not yet available, several companies have expressed interest in taking it forward."[17]
Male sexual response
During male ejaculation, sperm is transmitted from the ductus deferens into the male urethra via the ejaculatory ducts, which lie within the prostate gland. It is possible for men to achieve orgasm solely through stimulation of the prostate gland, such as prostate massage or receptive anal intercourse.[][][]
Vasectomy and risk of prostate cancer
In 1983, the Journal of the American Medical Association reported a connection between vasectomy and an increased risk of prostate cancer. Reported studies of 48,000 and 29,000 men who had vasectomies showed 66 percent and 56 percent higher rates of prostate cancer, respectively. The risk increased with age and the number of years since the vasectomy was performed. However, in March of the same year, the National Institute of Child Health and Human Development held a conference cosponsored by the National Cancer Institute and others to review the available data and information on the link between prostate cancer and vasectomies. It was determined that an association between the two was very weak at best, and even if having a vasectomy increased one's risk, the risk was relatively small. In 1997, the NCI held a conference with the prostate cancer Progressive Review Group (a committee of scientists, medical personnel, and others). Their final report, published in 1998 stated that evidence that vasectomies help to develop prostate cancer was weak at best.[18]
Prostate
37
Unclogging a prostate
A surgeon can unclog a blocked prostate by inserting an artificial 'tube' called a stent. Stents can be temporary or permanent. They are inserted into the urethra. This is mostly done on an outpatient basis under local or spinal anesthesia and takes about 30 minutes.
Additional images
Urinary bladder
Structure of the penis
Lobes of prostate
Zones of prostate
Prostate
38
Prostate
Microscopic glands of the prostate
Male Anatomy
The deeper branches of the internal pudendal artery.
Prostate
39
Lymphatics of the prostate.
Fundus of the bladder with the vesiculæ seminales.
Vesiculae seminales and ampullae of ductus deferentes, front view.
Vertical section of bladder, penis, and urethra.
Prostate
40
Dissection of prostate showing prostatic urethra.
References
The text of this article was originally taken from NIH Publication No. 02-4806, a public domain resource.[19]
[5] Moore, Keith L.; Persaud, T. V. N. and Torchia, Mark G. (2008) Before We Are Born, Essentials of Embryology and Birth Defects, 7th edition, Saunders Elsevier, ISBN 978-1-4160-3705-7 [10] "Basic Principals: Prostate Anatomy" (http:/ / www. urologymatch. com/ ProstateAnatomy. htm). Urology Match. Www.urologymatch.com. Web. 14 June 2010. [11] "Prostate Cancer Information from the Foundation of the Prostate Gland." (http:/ / www. prostate-cancer. com/ prostate-cancer-treatment-overview/ overview-prostate-anatomy. html) Prostate Cancer Treatment Guide. Web. 14 June 2010. [15] American Cancer Society American Cancer Society Guidelines for the early detection of cancer Cited: September 2011 (http:/ / www. cancer. org/ Healthy/ FindCancerEarly/ CancerScreeningGuidelines/ american-cancer-society-guidelines-for-the-early-detection-of-cancer). Cancer.org. Retrieved on 2013-01-21. [17] New prostate cancer twice as effective as a PSA test could be available by next year (http:/ / www. medicinechest. co. uk/ index. php?option=com_content& view=article& id=543). medicinechest.co.uk (2 March 2011)
Bulbourethral gland
41
Bulbourethral gland
Bulbourethral gland
Male Anatomy
The deeper branches of the internal pudendal artery. (Bulbourethral gland labeled at center left.) Latin Gray's Artery Precursor MeSH glandulæ bulbourethrales subject #264 1253
[1]
Artery of the urethral bulb Urogenital sinus Bulbourethral+Glands
[2]
A bulbourethral gland, also called a Cowper's gland for anatomist William Cowper, is one of two small exocrine glands present in the reproductive system of male mammals (including humans). They are homologous to Bartholin's glands in females.
Bulbourethral gland
42
Location
Bulbourethral glands are located posterior and lateral to the membranous portion of the urethra at the base of the penis, between the two layers of the fascia of the urogenital diaphragm, in the deep perineal pouch. They are enclosed by transverse fibers of the sphincter urethrae membranaceae muscle.
Structure
The bulbourethral glands are compound tubulo-alveolar glands, each approximately the size of a pea. They are composed of several lobules held together by a fibrous covering. Each lobule consists of a number of acini, lined by columnar epithelial cells, opening into a duct that joins with the ducts of other lobules to form a single excretory duct. This duct is approximately 2.5 cm long and opens into the urethra at the base of the penis. The glands gradually diminish in size with advancing age.[1] Wikipedia:Identifying reliable sources
Function
During sexual arousal each gland produces a clear, salty, viscous secretion known as pre-ejaculate. This fluid helps to lubricate the urethra for spermatozoa to pass through, neutralizing traces of acidic urine in the urethra,[2] and helps flush out any residual urine or foreign matter. It is possible for this fluid to pick up sperm, remaining in the urethral bulb from previous ejaculations, and carry them out prior to the next ejaculation. The Dissection of prostate showing the bulbourethral glands within the fibers of the external urethral sphincter just underneath the prostate. Cowper's gland also produces some amount of prostate-specific antigen (PSA), and Cowper's tumors may increase PSA to a level that makes prostate cancer suspected.[citation needed]
Gallery
Structure of the penis
Male pelvic organs seen from right side.
Vertical section of bladder, penis, and urethra.
Bulbourethral gland
43
Notes
[1] Gray's Anatomy, 38th edn, p 1861.
Bartholin's gland
Bartholin's gland
Genital organs of female. Latin Gray's Artery Nerve Lymph Precursor MeSH glandula vestibularis major subject #270 1266
[1] [1]
external pudendal artery ilioinguinal nerve
[1]
superficial inguinal lymph nodes Urogenital sinus Bartholin's+Glands
[3]
Dorlands/Elsevier Bartholin gland [4]
The Bartholin's glands (also called Bartholin glands or greater vestibular glands) are two glands located slightly posterior and to the left and right of the opening of the vagina. They secrete mucus to lubricate the vagina and are homologous to bulbourethral glands in males. However, while Bartholin's glands are located in the superficial perineal pouch in females, bulbourethral glands are located in the deep perineal pouch in males.
Function
They secrete mucus to provide vaginal lubrication.[2][3] Bartholin's glands secrete relatively minute amounts (one or two drops) of fluid when a woman is sexually aroused.[] The minute droplets of fluid were once believed to be important for lubricating the vagina, but research from Masters and Johnson demonstrated that vaginal lubrication comes from deeper within the vagina.[] The fluid may slightly moisten the labial opening of the vagina, serving to make contact with this sensitive area more comfortable for the woman.[]
Bartholin's gland
44
Pathology
Although unusual, it is possible for the Bartholin's glands to become irritated or infected, resulting in pain.[] If the duct becomes obstructed, a Bartholin's cyst can develop, and a Bartholin's cyst in turn can become infected and form an abscess. Adenocarcinoma of the gland is rare, but benign tumors and hyperplasia are even more rare.[4]
Eponym
Bartholin's glands were first described in the 17th century by the Danish anatomist Caspar Bartholin the Younger (1655–1738).[5] Some sources mistakenly ascribe their discovery to his grandfather, theologian and anatomist Caspar Bartholin the Elder (1585–1629).[6]
References
[1] Greater Vestibular (Bartholin) gland (http:/ / summit. stanford. edu/ ourwork/ PROJECTS/ LUCY/ lucywebsite/ vestib_gl. html) [6] C. C. Gillispie (ed.): Dictionary of Scientific Biography, New York 1970. See the article on Thomas Bartholin.
External links
• SUNY Labs 41:11-0200 (http://ect.downstate.edu/courseware/haonline/labs/l41/110200.htm)—"The Female Perineum: Muscles of the Superficial Perineal Pouch" • SUNY Anatomy Image 9243 (http://ect.downstate.edu/courseware/haonline/imgs/00000/9000/200/9243. jpg) • SUNY Anatomy Image 9694 (http://ect.downstate.edu/courseware/haonline/imgs/00000/9000/600/9694. jpg)—opening • greater+vestibular+gland (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=greater+ vestibular+gland) at eMedicine Dictionary
Endometrium
45
Endometrium
Endometrium
Uterus and uterine tubes. (Endometrium labeled at center right.) Latin Gray's MeSH Dorlands/Elsevier tunica mucosa uteri subject #268 1262 Endometrium Endometrium
[2] [3] [1]
The endometrium is the inner mucous membrane of the mammalian uterus.
Function
The endometrium is the innermost glandular layer and functions as a lining for the uterus, preventing adhesions between the opposed walls of the myometrium, thereby maintaining the patency of the uterine cavity. During the menstrual cycle or estrous cycle, the endometrium grows to a thick, blood vessel-rich, glandular tissue layer. This represents an optimal environment for the implantation of a blastocyst upon its arrival in the uterus. The endometrium is central, echogenic (detectable using ultrasound scanners), and has an average thickness of 6.7 mm. During pregnancy, the glands and blood vessels in the endometrium further increase in size and number. Vascular spaces fuse and become interconnected, forming the placenta, which supplies oxygen and nutrition to the embryo and foetus.
Cycle
The endometrial lining undergoes cyclic regeneration. Humans and the great apes display the menstrual cycle, whereas most other mammals are subject to an estrous cycle. In both cases, the endometrium initially proliferates under the influence of estrogen. However, once ovulation occurs, in addition to estrogen, the ovary will also start to produce progesterone. This changes the proliferative pattern of the endometrium to a secretory lining. Eventually, the secretory lining provides a hospitable environment for one or more blastocysts. If a blastocyst implants, then the lining remains as decidua. The decidua becomes part of the placenta; it provides support and protection for the gestation. If there is inadequate stimulation of the lining, due to lack of hormones, the endometrium remains thin and inactive. In humans, this will result in amenorrhea, or the absence of a menstrual period. After menopause, the lining is often described as being atrophic. In contrast, endometrium that is chronically exposed to estrogens, but not to progesterone, may become hyperplastic. Long-term use of oral contraceptives with highly potent progestins can also induce endometrial atrophy.[1][2] In humans, the cycle of building and shedding the endometrial lining lasts an average of 28 days. The endometrium develops at different rates in different mammals. Its formation is sometimes affected by seasons, climate, stress, and other factors. The endometrium itself produces certain hormones at different points along the cycle. This affects
Endometrium other portions of the reproductive system.
46
Histology
The endometrium consists of a single layer of columnar epithelium resting on the stroma, a layer of connective tissue that varies in thickness according to hormonal influences. Simple tubular uterine glands reach from the endometrial surface through to the base of the stroma, which also carries a rich blood supply of spiral arteries. In a woman of reproductive age, two layers of endometrium can be distinguished. These two layers occur only in endometrium lining the cavity of the uterus, not in the lining of the Fallopian tubes:[3] • The functional layer is adjacent to the uterine cavity. This layer is built up after the end of menstruation during the first part of the previous menstrual cycle. Proliferation is induced by estrogen (follicular phase of menstrual cycle), and later changes in this layer are engendered by progestrone from the corpus luteum (luteal phase). It is adapted to provide an optimum environment for the implantation and growth of the embryo. This layer is completely shed during menstruation. • The basal layer, adjacent to the myometrium and below the functional layer, is not shed at any time during the menstrual cycle, and from it the functional layer develops. In the absence of progesterone, the arteries supplying blood to the functional layer constrict, so that cells in that layer become ischaemic and die, leading to menstruation. It is possible to identify the phase of the menstrual cycle by observing histological differences at each phase:
Phase Menstrual phase Days 1–4 Thickness Thin Absent Epithelium High magnification micrograph of decidualized endometrium due to exogenous progesterone (oral contraceptive pill). H&E stain.
Low magnification micrograph of decidualized endometrium. H&E stain.
Proliferative phase 4–14 Secretory phase
Intermediate Columnar Columnar. Also visible are helicine branches of uterine artery
15–28 Thick
Chorionic tissue can result in marked endometrial changes, known as an Arias-Stella reaction, that have an appearance similar to cancer.[] Historically, this change was diagnosed as endometrial cancer and it is important only in so far as it should not be misdiagnosed as cancer.
Endometrium
47
Pathological conditions
Adenomyosis is the growth of the endometrium into the muscle layer of the uterus (the myometrium). Endometriosis is the growth of endometrial tissue outside the uterus. Endometrial cancer is the most common cancer of the human female genital tract. Asherman's syndrome, also known as intrauterine adhesions occurs when the basal layer of the endometrium is damaged by instrumentation (e.g., D&C) or infection (e.g., endometrial tuberculosis) resulting in endometrial sclerosis and adhesion formation partially or completely obliterating the uterine cavity. Thin endometrium may be defined as an endometrial thickness of less than 8 mm. It usually occurs after menopause. Treatments that can improve endometrial thickness include Vitamin E, L-arginine and sildenafil citrate.[4] Gene expression profiling using cDNA microarray can be used for the diagnosis of endometrial disorders.[5]
Additional images
The initial stages of human embryogenesis
Vertical section of mucous membrane of human uterus.
Endometrioid adenocarcinoma from biopsy. H&E stain.
Micrograph of the endometrium.
Micrograph of decidualized endometrium due to exogenous progesterone. H&E stain.
Micrograph of decidualized endometrium due to exogenous progesterone. H&E stain.
Micrograph showing endometrial stromal condensation, a finding seen in menses.
References
[1] Effects of hormone therapy on the endometrium, http:/ / www. ncbi. nlm. nih. gov/ pubmed/ 8426860 [2] William's Gynecology, McGraw 2008, Chapter 8, Abnormal Uterine Bleeding [3] Blue Histology - Female Reproductive System. School of Anatomy and Human Biology - The University of Western Australia http:/ / www. lab. anhb. uwa. edu. au/ mb140/ CorePages/ FemaleRepro/ FemaleRepro. htm Accessed 20061228 20:35
External links
• SUNY Figs 43:05-15 (http://ect.downstate.edu/courseware/haonline/figs/l43/430515.htm) - "The uterus, uterine tubes and ovary with associated structures." • BU Histology Learning System: 18902loa (http://www.bu.edu/histology/p/18902loa.htm) - "Female Reproductive System uterus, endometrium" • Swiss embryology (from UL, UB, and UF) gnidation/role02 (http://www.embryology.ch/anglais/gnidation/ role02.html)
Endometrium • Histology at OU 20_01 (http://w3.ouhsc.edu/histology/Glass slides/20_01.jpg) • Histology at utah.edu. Slide is proliferative phase - click forward to see secretory phase (http://medlib.med. utah.edu/WebPath/FEMHTML/FEM017.html)
48
Urethral gland
Urethral gland
Latin glandulae urethrales urethrae masculinae Gray's subject #262 1250 [1]
The urethral or periurethral glands (also Littre glands after Alexis Littré)[] are glands that branch off the wall of the urethra of male mammals. The glands secrete mucus[1] and are most numerous in the section of the urethra that runs through the penis. Urethral glands produce a colloid secretion containing glycosaminoglycans; this secretion protects the epithelium against urine.[2] Unsafe sex can lead to urethritis. Untreated, this can lead to infection of the urethral glands, which can cause the urethra to be impeded by strictures.
References
[2] Human Microscopic Anatomy: An Atlas for Students of Medicine and Biology By Radivoj V. Krstić, page 382
External links
• Slide at uottawa.ca (http://courseweb.edteched.uottawa.ca/Medicine-histology/English/Reproduction/male/ fig22malerepro.htm) • glands+of+the+male+urethra (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=glands+ of+the+male+urethra) at eMedicine Dictionary
Gastric chief cell
49
Gastric chief cell
Chief cell
H&E stain of fundic gland polyp showing shortening of the gastric pits with cystic dilatation
A fundus gland. A. Transverse section of gland. Latin Code exocrinocytus principalis TH H3.04.02.1.00031
A gastric chief cell (or peptic cell, or gastric zymogenic cell) is a cell in the stomach that releases pepsinogen, gastric lipase and chymosin.[1] The cell stains basophilic upon H&E prep due to the large proportion of rough endoplasmic reticulum in its cytoplasm. Chief cells release the zymogen (enzyme precursor) pepsinogen when stimulated by a variety of factors including cholinergic activity from the vagus nerve and acidic condition in the stomach. Gastrin and secretin may also act as secretagogues.[2] It works in conjunction with the parietal cell, which releases gastric acid, converting the pepsinogen into pepsin.
Gastric chief cell
50
Nomenclature
The terms "chief cell" and "zymogenic cell" are often used without the word "gastric" to name this type of cell. However those terms can also be used to describe other cell types (for example, parathyroid chief cells.) Chief cells are also known as peptic cells.
References
[2] Johnson. Gastrointestinal Physiology 6th Edition. Mosby. 2001
External links
• Anatomy Atlases - Microscopic Anatomy, plate 01.05 (http:// www.anatomyatlases.org/MicroscopicAnatomy/Section01/ Plate0105.shtml) • BU Histology Learning System: 22201loa (http://www.bu. edu/histology/p/22201loa.htm) - "Ultrastructure of the Cell: chief cells and enteroendocrine cell"
human chief cells
• BU Histology Learning System: 11304loa (http://www.bu.edu/histology/p/11304loa.htm) - "Digestive System: Alimentary Canal: fundic stomach, gastric glands, base" • " chief cell (http://web.archive.org/web/20090616022448/http://www.mercksource.com/pp/us/cns/ cns_hl_dorlands_split.jsp?pg=/ppdocs/us/common/dorlands/dorland/two/000018589.htm)" at Dorland's Medical Dictionary • Physiology at MCG 6/6ch4/s6ch4_8 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section6/6ch4/s6ch4_8.htm)
Pepsin
51
Pepsin
pepsin B
Identifiers EC number CAS number 3.4.23.2 [1] [2]
9025-48-3
Databases IntEnz BRENDA ExPASy KEGG MetaCyc PRIAM PDB structures IntEnz view [3] [4] [5]
BRENDA entry NiceZyme view KEGG entry [6]
metabolic pathway profile [8] [9]
[7]
RCSB PDB
PDBe
[10]
PDBsum
[11]
Search PMC articles [12]
PubMed articles [13] NCBI proteins [14]
pepsin C (gastricsin)
Identifiers EC number CAS number 3.4.23.3 [15] [16]
9012-71-9
Databases IntEnz BRENDA ExPASy KEGG MetaCyc PRIAM PDB structures IntEnz view [17] [18] [19]
BRENDA entry NiceZyme view KEGG entry
[20] [21]
metabolic pathway profile [22] [23]
RCSB PDB
PDBe
[24]
PDBsum
[25]
Pepsin
52
Search PMC articles [26]
PubMed articles [27] NCBI proteins [28]
Pepsin is an enzyme whose zymogen (pepsinogen) is released by the chief cells in the stomach and that degrades food proteins into peptides. It was discovered in 1836 by Theodor Schwann who also coined its name from the Greek word pepsis, meaning digestion (peptein: to digest).[][] It was the first enzyme to be discovered, and, in 1929, it became one of the first enzymes to be crystallized, by John H. Northrop.[] Pepsin is a digestive protease, a member of the aspartate protease family.[1] Pepsin is one of three principal protein-degrading, or proteolytic, enzymes in the digestive system, the other two being chymotrypsin and trypsin. The three enzymes were among the first to be isolated in crystalline form. During the process of digestion, these enzymes, each of which is specialized in severing links between particular types of amino acids, collaborate to break down dietary proteins into their components, i.e., peptides and amino acids, which can be readily absorbed by the intestinal lining. Pepsin is most efficient in cleaving peptide bonds between hydrophobic and preferably aromatic amino acids such as phenylalanine, tryptophan, and tyrosine.[]
History
The term "pepsin" was first coined by Theodor Schwann in the early 19th century. Scientists around this time began discovering many biochemical compounds that play a significant role in biological processes and pepsin was one of them. It was with the identification of a chemical agent found in the stomachs of animals, that scientists began looking into the digestive properties of organisms. This acidic substance that was able to convert nitrogen based foods into water soluble material was determined to be pepsin.[]
Precursor
Pepsin is expressed as a pro-form zymogen, pepsinogen, whose primary structure has an additional 44 amino acids. In the stomach, chief cells release pepsinogen. This zymogen is activated by hydrochloric acid (HCl), which is released from parietal cells in the stomach lining. The hormone gastrin and the vagus nerve trigger the release of both pepsinogen and HCl from the stomach lining when food is ingested. Hydrochloric acid creates an acidic environment, which allows pepsinogen to unfold and cleave itself in an autocatalytic fashion, thereby generating pepsin (the active form). Pepsin cleaves the 44 amino acids from pepsinogen to create more pepsin. Pepsin will digest up to 20% of ingested amide bonds by cleaving preferentially after the N-terminal[]:96 of aromatic amino acids such as phenylalanine, tryptophan, and tyrosine.[]:675 Pepsin exhibits preferential cleavage for hydrophobic, preferably aromatic, residues in P1 and P1' positions. Increased susceptibility to hydrolysis occurs if there is a sulfur-containing amino acid close to the peptide bond, which has an aromatic amino acid. Pepsin cleaves Phe1Val, Gln4His, Glu13Ala, Ala14Leu, Leu15Tyr, Tyr16Leu, Gly23Phe, Phe24Phe and Phe25Tyr bonds in the B chain of insulin.[2] Peptides may be further digested by other proteases (in the duodenum) and eventually absorbed by the body. Pepsin is stored as pepsinogen so it will only be released when needed, and does not digest the body's own proteins in the stomach's lining.
Pepsin
53
Activity and stability
Pepsin is most active in acidic environments between 37°C and 42°C.[3][4] Accordingly, its primary site of synthesis and activity is the stomach (pH 1.5 to 2). Pepsin exhibits maximal activity at pH 2.0 and is inactive at pH 6.5 and above, however pepsin is not fully denatured or irreversibly inactivated until pH 8.0.[] Therefore pepsin in solution of up to pH 8.0 can be reactivated upon re-acidification. The stability of pepsin at high pH has significant implications on disease attributed to laryngopharyngeal reflux. Pepsin remains in the larynx following a gastric reflux event.[][] At the mean pH of the laryngopharynx (pH = 6.8) pepsin would be inactive but could be reactivated upon subsequent acid reflux events resulting in damage to local tissues.
In laryngopharyngeal reflux
Pepsin is one of the primary causes of mucosal damage during laryngopharyngeal reflux.[][] Pepsin remains in the larynx (pH 6.8) following a gastric reflux event.[][] While enzymatically inactive in this environment, pepsin would remain stable and could be reactivated upon subsequent acid reflux events.[] Exposure of laryngeal mucosa to enzymatically active pepsin, but not irreversibly inactivated pepsin or acid, results in reduced expression of protective proteins and thereby increases laryngeal susceptibility to damage.[][][] Pepsin may also cause mucosal damage during weakly acidic or non-acid gastric reflux. Weak or non-acid reflux is correlated with reflux symptoms and mucosal injury.[][][5][] Under non-acid conditions (neutral pH), pepsin is internalized by cells of the upper airways such as the larynx and hypopharynx by a process known as receptor-mediated endocytosis.[] The receptor by which pepsin is endocytosed is currently unknown. Upon cellular uptake, pepsin is stored in intracellular vesicles of low pH at which its enzymatic activity would be restored. Pepsin is retained within the cell for up to 24 hours.[] Such exposure to pepsin at neutral pH and endoyctosis of pepsin causes changes in gene expression associated with inflammation, which underlies signs and symptoms of reflux,[] and tumor progression.[] This and other research[] implicates pepsin in carcinogenesis attributed to gastric reflux. Pepsin in airway specimens is considered to be a sensitive and specific marker for laryngopharyngeal reflux.[][] Research to develop new pepsin-targeted therapeutic and diagnostic tools for gastric reflux is ongoing.
Storage
Pepsins should be stored at very cold temperatures (between −80 °C and −20 °C) to prevent autolysis (self-cleavage).
Inhibitors
Pepsin may be inhibited by high pH (see "Activity" and "Stability", above) or by inhibitor compounds. Pepstatin is a low molecular weight compound and potent inhibitor specific for acid proteases with a Ki of about 10−10 M for pepsin. The statyl residue of pepstatin is thought to be responsible for pepstatin inhibition of pepsin; statine is a potential analog of the transition state for catalysis by pepsin and other acid proteases. Pepstatin does not covalently bind pepsin and inhibition of pepsin by pepstatin is therefore reversible.[] 1-bis(diazoacetyl)-2-penylethane reversibly inactivates pepsin at pH 5, a reaction which is accelerated by the presence of Cu(II).[] Pepsin also undergoes feedback inhibition; a product of protein digestion slows down the reaction by inhibiting pepsin.[][]
Pepsin
54
Applications
Commercial pepsin is extracted from the glandular layer of hog stomachs. It is a component of rennet used to curdle milk during the manufacture of cheese. Pepsin is used for a variety of applications in food manufacturing: to modify and provide whipping qualities soy protein and gelatin,[] to modify vegetable proteins for use in nondairy snack items, to make precooked cereals into instant hot cereals[] and to prepare animal and vegetable protein hydrolysates for use in flavoring foods and beverages. It is used in the leather industry to remove hair and residual tissue from hides and in the recovery of silver from discarded photographic films by digesting the gelatin layer that holds the silver.[] Pepsin was historically an additive of Beemans gum brand chewing gum by Dr. Edward E. Beeman. It also gave name to Pepsi-Cola, originally formulated with pepsin and cola nuts. Pepsin is commonly used in the preparation of F(ab')2 fragments from antibodies. In some assays, it is preferable to use only the antigen-binding (Fab) portion of the antibody. For these applications, antibodies may be enzymatically digested to produce either an Fab or an F(ab')2 fragment of the antibody. To produce an F(ab')2 fragment, IgG is digested with pepsin, which cleaves the heavy chains near the hinge region. One or more of the disulfide bonds that join the heavy chains in the hinge region are preserved, so the two Fab regions of the antibody remain joined together, yielding a divalent molecule (containing two antibody binding sites), hence the designation F(ab')2. The light chains remain intact and attached to the heavy chain. The Fc fragment is digested into small peptides. Fab fragments are generated by cleavage of IgG with papain instead of pepsin. Papain cleaves IgG above the hinge region containing the disulfide bonds that join the heavy chains, but below the site of the disulfide bond between the light chain and heavy chain. This generates two separate monovalent (containing a single antibody binding site) Fab fragments and an intact Fc fragment. The fragments can be purified by gel filtration, ion exchange, or affinity chromatography.[] Fab and F(ab')2 antibody fragments are used in assay systems where the presence of the Fc region may cause problems. In tissues such as lymph nodes or spleen, or in peripheral blood preparations, cells with Fc receptors (macrophages, monocytes, B lymphocytes, and natural killer cells) are present which can bind the Fc region of intact antibodies, causing background staining in areas that do not contain the target antigen. Use of F(ab')2 or Fab fragments ensures that the antibodies are binding to the antigen and not Fc receptors. These fragments may also be desirable for staining cell preparations in the presence of plasma, because they are not able to bind complement, which could lyse the cells. F(ab')2, and to a greater extent Fab, fragments allow more exact localization of the target antigen, i.e., in staining tissue for electron microscopy. The divalency of the F(ab')2 fragment enables it to cross-link antigens, allowing use for precipitation assays, cellular aggregation via surface antigens, or rosetting assays.[]
Genes
The following three genes encode identical human pepsinogen A enyzmes:
pepsinogen 3, group I (pepsinogen A)
Identifiers Symbol Entrez HUGO OMIM RefSeq UniProt PGA3 643834 8885 [34]
[35] [36] [37]
169710
NM_001079807 P00790 [38]
Pepsin
55
Other data EC number Locus 3.4.23.1 [39] [40]
Chr. 11 q13
pepsinogen 4, group I (pepsinogen A)
Identifiers Symbol Entrez HUGO OMIM RefSeq UniProt PGA4 643847 8886 [41]
[42] [43] [44]
169720
NM_001079808 P00790 Other data [38]
EC number Locus
3.4.23.1
[39] [40]
Chr. 11 q13
pepsinogen 5, group I (pepsinogen A)
Identifiers Symbol Entrez HUGO OMIM RefSeq UniProt PGA5 5222 8887 [45] [46] [47] [48]
169730
NM_014224 P00790 Other data [38]
EC number Locus
3.4.23.1
[39] [40]
Chr. 11 q13
A fourth human gene encodes gastricsin also known as pepsinogen C:
Pepsin
56
progastricsin (pepsinogen C)
Identifiers Symbol Entrez HUGO OMIM RefSeq UniProt PGC 5225 8890 [49] [50] [51] [52]
169740
NM_001166424 P20142 [53]
Other data EC number 3.4.23.3 [54] Locus Chr. 6 pter-p21.1 [55]
References
[2] IUBMB Enzyme Nomenclature: http:/ / www. chem. qmul. ac. uk/ iubmb/ enzyme/ EC3/ 4/ 23/ 1. html [4] "Brenda-enzymes: Entry of pepsin A (EC-Number 3.4.23.1 )". Retrieved 2008-12-14 [5] Oelschlager BK, Quiroga E, Isch JA, et al. Gastroesophageal and pharyngeal reflux detection using impedance and 24-hour pH monitoring in asymptomatic subjects: defining the normal environment. J Gastrointest Surg 2006;10:54–62.
External links
• The MEROPS online database for peptidases and their inhibitors: Pepsin A A01.001 (http://merops.sanger.ac. uk/cgi-bin/merops.cgi?id=A01.001), Pepsin B A01.002 (http://merops.sanger.ac.uk/cgi-bin/merops. cgi?id=A01.002), Pepsin C (Gastricsin) A01.003 (http://merops.sanger.ac.uk/cgi-bin/merops.cgi?id=A01. 003) • Pepsin A (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Pepsin+A) at the US National Library of Medicine Medical Subject Headings (MeSH) • Pepsinogens (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Pepsinogens) at the US National Library of Medicine Medical Subject Headings (MeSH) • Pepsinogen A (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Pepsinogen+A) at the US National Library of Medicine Medical Subject Headings (MeSH) • Pepsinogen C (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Pepsinogen+C) at the US National Library of Medicine Medical Subject Headings (MeSH) • Beemans Gum (http://beemansgum.org) • Pepsin: Molecule of the Month (http://www.rcsb.org/pdb/101/motm.do?momID=12), by David Goodsell, RCSB Protein Data Bank
Parietal cell
57
Parietal cell
Parietal cell
Human parietal cells (pink staining) - stomach
Control of stomach acid Latin MeSH Code exocrinocytus parietalis Gastric+Parietal+Cells TH H3.04.02.1.00033
[1]
Parietal cells, or oxyntic cells, are the stomach epithelium cells that secrete gastric acid (HCl) and intrinsic factor in response to histamine (H2 receptor), acetylcholine (M3 receptors[]) and gastrin (CCK2 receptors). The histamine receptors act by increasing intracellular cAMP, whereas the muscarinic and gastrin receptors increase intracellular Ca2+ levels. Both cAMP and Ca2+ act via protein kinases to increase the transport of acid into the stomach. Gastrin is more important indirectly by increasing histamine synthesis in ECL cells,[1] as gastrin has no effect on the maximum histamine-stimulated gastric acid secretion.[2] Parietal cells contain an extensive secretory network (called canaliculi) from which the HCl is secreted by active transport into the stomach. The enzyme hydrogen potassium ATPase (H+/K+ ATPase) is unique to the parietal cells and transports the H+ against a concentration gradient of about 3 million to 1, which is the steepest ion gradient formed in the human body. Hydrochloric acid is formed in the following manner: • Hydrogen ions are formed from the dissociation of water molecules. The enzyme carbonic anhydrase converts one molecule of carbon dioxide and one molecule of water indirectly into a bicarbonate ion (HCO3-) and a hydrogen ion (H+). • The bicarbonate ion (HCO3-) is exchanged for a chloride ion (Cl-) on the basal side of the cell and the bicarbonate diffuses into the venous blood, leading to an alkaline tide. • Potassium (K+) and chloride (Cl-) ions diffuse into the canaliculi. • Hydrogen ions are pumped out of the cell into the canaliculi in exchange for potassium ions, via the H+/K+ ATPase.
Parietal cell The resulting highly-acidic environment causes proteins from food to unfold (or denature), exposing the peptide bonds that link together amino acids. HCl also activates pepsinogen, an endopeptidase, allowing it to help digestion by breaking specific peptide bonds, a process known as proteolysis. Furthermore, the sudden increase in gastric acid secretion following a meal can cause a physiological phenomenon called an alkaline tide, which is due to the production and export of bicarbonate from parietal cells. The alkaline tide is neutralized by the action of the pancreatic duct which produces a bicarbonate secretion that is deposited into the lumen of the duct while the byproduct, hydrogen ions, are pumped out the basal membrane into the portal blood stream, thereby neutralizing the bicarbonate from the stomach. Parietal cells secrete acid in response to three types of stimuli:[3] • H2 histamine receptors (most significant contribution) • Acetylcholine from parasympathetic activity via the vagus nerve and enteric nervous system • gastrin (least significant contribution, but note that histamine secretion by ECL cells is due in part to gastrin) Upon stimulation, adenylate cyclase is activated within the parietal cells. This increases intracellular cyclic AMP, which leads to activation of protein kinase A. Protein kinase A phosphorylates proteins involved in the transport of H+/K+ ATPase from the cytoplasm to the cell membrane. This causes resorption of K+ ions and secretion of H+ ions. The pH of the secreted fluid can fall by 0.8.
58
Intrinsic factor
Parietal cells also produce intrinsic factor. Intrinsic factor is required for the absorption of Vitamin B12 in the diet. A long-term deficiency in vitamin B12 can lead to megaloblastic anemia, characterized by large fragile erythrocytes. Pernicious anemia is a condition where intrinsic factor is not produced and leads to the same type of anemia. Atrophic gastritis, particularly in the elderly, will cause an inability to absorb B12 and can lead to deficiencies such as decreased DNA synthesis and nucleotide metabolism in the bone marrow.
Canaliculus
A canaliculus is an adaptation found on gastric parietal cells. It is a deep infolding, or little channel, which serves to increase the surface area, e.g. for secretion. The membrane of parietal cells is dynamic; the numbers of canaliculi rise and fall according to secretory need. This is accomplished by the fusion of canalicular precursors, or "tubulovesicles", with the membrane to increase surface area, and the reciprocal endocytosis of the canaliculi (reforming the tubulovesicles) to decrease it.
Diseases of parietal cells
• Peptic ulcers can result from over-acidity in the stomach. Antacids can be used to enhance the natural tolerance of the gastric lining. Antimuscarinic drugs such as pirenzepine or H2 antihistamines can reduce acid secretion. Proton pump inhibitors are more potent at reducing gastric acid production since that is the final common pathway of all stimulation of acid production. • In pernicious anemia, autoantibodies directed against parietal cells or intrinsic factor cause a reduction in vitamin B12 absorption. It can be treated with injections of replacement vitamin B12 (methylcobalamin, hydroxocobalamin or cyanocobalamin).
Immunofluorescence staining pattern of gastric parietal antibodies on a stomach section
• Achlorhydria is another autoimmune disease of the parietal cells. The damaged parietal cells are unable to produce the required amount of gastric acid. This leads to an increase in gastric pH, impaired digestion of food and increased risk of gastroenteritis.
Parietal cell
59
References
[1] Waldum, Helge L., Kleveland, Per M., et al. (2009)'Interactions between gastric acid secretagogues and the localization of the gastrin receptor',Scandinavian Journal of Gastroenterology,44:4,390 — 393 [2] Kleveland PM, Waldum HL, Larsson M. Gastric acid secretion in the totally isolated, vascularly perfused rat stomach. A selective muscarinic-1 agent does, whereas gastrin does not, augment maximal histamine-stimulated acid secretion. Scand J Gastroenterol 1987;/22:/705�13.
External links
• Illustration of Chief cells and Parietal cells at anatomyatlases.org (http://www.anatomyatlases.org/ MicroscopicAnatomy/Section01/Plate0105.shtml) • The Parietal Cell: Mechanism of Acid Secretion at vivo.colostate.edu (http://www.vivo.colostate.edu/hbooks/ pathphys/digestion/stomach/parietal.html) • BU Histology Learning System: 11303loa (http://www.bu.edu/histology/p/11303loa.htm) - Digestive System: Alimentary Canal: fundic stomach, gastric glands, lumen" • Physiology at MCG 6/6ch4/s6ch4_8 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section6/6ch4/s6ch4_8.htm) • Physiology at MCG 6/6ch4/s6ch4_14 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section6/6ch4/s6ch4_14.htm) • Parietal cell antibody (http://www.antibodypatterns.com/gpc.php) • Antibody to GPC (http://www.ii.bham.ac.uk/clinicalimmunology/CISimagelibrary/GPC.htm)
Hydrochloric acid
60
Hydrochloric acid
Hydrochloric acid
Identifiers CAS number ChemSpider UNII EC number ChEMBL ATC code 7647-01-0 10633809
[1] [2] [3]
QTT17582CB 231-595-7
[4]
CHEMBL1231821 A09 AB03 Properties
[6]
[5] [7]
,B05 XA13
Appearance
Colourless, transparent liquid Hazards
MSDS EU Index R-phrases S-phrases
External MSDS 017-002-01-X R34, R37 (S1/2), S26, S45 Related compounds
Related compounds
• • •
Hydrofluoric acid Hydrobromic acid Hydroiodic acid
Supplementary data page Structure and properties Thermodynamic data Spectral data
(verify) [8]
n, ε , etc.
r
Phase behaviour Solid, liquid, gas UV, IR, NMR, MS
(what is: / ?) Except where noted otherwise, data are given for materials in their standard state (at 25 °C, 100 kPa)
Infobox references
Hydrochloric acid Hydrochloric acid is a clear, colourless solution of hydrogen chloride (H Cl) in water. It is a highly corrosive, strong mineral acid with many industrial uses. Hydrochloric acid is found naturally in gastric acid. Historically called muriatic acid, and spirits of salt, hydrochloric acid was produced from vitriol (sulfuric acid) and common salt. It first appeared during the Renaissance, Wikipedia:Verifiability and then it was used by chemists such as Glauber, Priestley and Davy in their scientific research. With major production starting in the Industrial Revolution, hydrochloric acid is used in the chemical industry as a chemical reagent in the large-scale production of vinyl chloride for PVC plastic, and MDI/TDI for polyurethane. It has numerous smaller-scale applications, including household cleaning, production of gelatin and other food additives, descaling, and leather processing. About 20 million tonnes of hydrochloric acid are produced annually.
61
Etymology
Hydrochloric acid was known to European alchemists as spirits of salt or acidum salis (salt acid). Both names are still used, especially in non-English languages, such as German: Salzsäure and Dutch: Zoutzuur. Gaseous HCl was called marine acid air. The old (pre-systematic) name muriatic acid has the same origin (muriatic means "pertaining to brine or salt"), and this name is still sometimes used.[][1]
History
Aqua regia, a mixture consisting of hydrochloric acid and nitric acid, prepared by dissolving sal ammoniac in nitric acid, was described in the works of Pseudo-Geber, the 13th-century European alchemist.[2][][][3][4] Other references suggest that the first mention of aqua regia is in Byzantine manuscripts dating to the end of the thirteenth century.[][5][6][7] Free hydrochloric acid was first formally described in the 16th century by Libavius, who prepared it by heating salt in clay crucibles.[] Other authors claim that pure hydrochloric acid was first discovered by the German benedictine monk Basil Valentine in the 15th century,[8] by heating common salt and green vitriol,[9] whereas others claim that there is no clear reference to the preparation of pure hydrochloric acid until the end of the sixteenth century.[] In the seventeenth century, Johann Rudolf Glauber from Karlstadt am Main, Germany used sodium chloride salt and sulfuric acid for the preparation of sodium sulfate in the Mannheim process, releasing hydrogen chloride gas. Joseph Priestley of Leeds, England prepared pure hydrogen chloride in 1772, and in 1818 Humphry Davy of Penzance, England proved that the chemical composition included hydrogen and chlorine.[] During the Industrial Revolution in Europe, demand for alkaline substances increased. A new industrial process by Nicolas Leblanc (Issoundun, France) enabled cheap large-scale production of sodium carbonate (soda ash). In this Leblanc process, common salt is converted to soda ash, using sulfuric acid, limestone, and coal, releasing hydrogen chloride as a by-product. Until the British Alkali Act 1863 and similar legislation in other countries, the excess HCl was vented to air. After the passage of the act, soda ash producers were obliged to absorb the waste gas in water, producing hydrochloric acid on an industrial scale.[][] In the twentieth century, the Leblanc process was effectively replaced by the Solvay process without a hydrochloric acid by-product. Since hydrochloric acid was already fully settled as an important chemical in numerous applications, the commercial interest initiated other production methods, some of which are still used today. After the year 2000, hydrochloric acid is mostly made by absorbing by-product hydrogen chloride from industrial organic compounds production.[][][] Since 1988, hydrochloric acid has been listed as a Table II precursor under the 1988 United Nations Convention Against Illicit Traffic in Narcotic Drugs and Psychotropic Substances because of its use in the production of heroin, cocaine, and methamphetamine.[]
Hydrochloric acid
62
Chemical properties and reactions
Hydrogen chloride (HCl) is a monoprotic acid, which means it can dissociate (i.e., ionize) only once to give up one H+ ion (a single proton). In aqueous hydrochloric acid, the H+ joins a water molecule to form a hydronium ion, H3O+:[][] The other ion formed is Cl−, the chloride ion. Hydrochloric acid can therefore be used to prepare salts called chlorides, such as sodium chloride. Hydrochloric acid is a strong acid, since it is essentially completely dissociated in water.[][] Monoprotic acids have one acid dissociation constant, Ka, which indicates the level of dissociation in water. For a strong acid like HCl, the Ka is large. Theoretical attempts to assign a Ka to HCl have been made.[] When chloride salts such as NaCl are added to aqueous HCl they have practically no effect on pH, indicating that Cl− is an exceedingly weak conjugate base and that HCl is fully dissociated in aqueous solution. For intermediate to strong solutions of hydrochloric acid, the assumption that H+ molarity (a unit of concentration) equals HCl molarity is excellent, agreeing to four significant digits.[][] Of the six common strong mineral acids in chemistry, hydrochloric acid is the monoprotic acid least likely to undergo an interfering oxidation-reduction reaction. It is one of the least hazardous strong acids to handle; despite its acidity, it consists of the non-reactive and non-toxic chloride ion. Intermediate-strength hydrochloric acid solutions are quite stable upon storage, maintaining their concentrations over time. These attributes, plus the fact that it is available as a pure reagent, make hydrochloric acid an excellent acidifying reagent. Hydrochloric acid is the preferred acid in titration for determining the amount of bases. Strong acid titrants give more precise results due to a more distinct endpoint. Azeotropic or "constant-boiling" hydrochloric acid (roughly 20.2%) can be used as a primary standard in quantitative analysis, although its exact concentration depends on the atmospheric pressure when it is prepared.[10] Hydrochloric acid is frequently used in chemical analysis to prepare ("digest") samples for analysis. Concentrated hydrochloric acid dissolves many metals and forms oxidized metal chlorides and hydrogen gas, and it reacts with basic compounds such as calcium carbonate or copper(II) oxide, forming the dissolved chlorides that can be analyzed.[][] HCl + H2O → H3O+ + Cl−
Physical properties
Concentration Density Molarity pH Viscosity Specific heat kJ/(kg·K) 3.47 2.99 2.60 2.55 2.50 2.46 2.43 Vapour pressure kPa 1.95 1.40 2.13 3.73 7.24 14.5 28.3 Boiling point °C 103 108 90 84 71 61 48 Melting point °C −18 −59 −52 −43 −36 −30 −26
kg HCl/kg 10% 20% 30% 32% 34% 36% 38%
kg HCl/m3 Baumé 104.80 219.60 344.70 370.88 397.46 424.44 451.82 6.6 13 19 20 21 22 23
kg/L 1.048 1.098 1.149 1.159 1.169 1.179 1.189
mol/dm3 2.87 6.02 9.45 10.17 10.90 11.64 12.39 −0.5 −0.8 −1.0 −1.0 −1.0 −1.1 −1.1
mPa·s 1.16 1.37 1.70 1.80 1.90 1.99 2.10
The reference temperature and pressure for the above table are 20 °C and 1 atmosphere (101.325 kPa). Vapour pressure values are taken from the International Critical Tables, and refer to the total vapour pressure of the solution.
Hydrochloric acid
63
Physical properties of hydrochloric acid, such as boiling and melting points, density, and pH, depend on the concentration or molarity of HCl in the aqueous solution. They range from those of water at very low concentrations approaching 0% HCl to values for fuming hydrochloric acid at over 40% HCl.[][][] Hydrochloric acid as the binary (two-component) mixture of HCl and H2O has a constant-boiling azeotrope at 20.2% HCl and 108.6 °C (227 °F). There are four constant-crystallization eutectic points for hydrochloric acid, between the crystal form of HCl·H2O (68% HCl), HCl·2H2O (51% HCl), HCl·3H2O (41% HCl), HCl·6H2O (25% HCl), and ice (0% HCl). There is also a metastable eutectic point at 24.8% between ice and the HCl·3H2O crystallization.[]
Melting temperature as a function of HCl [11][12] concentration in water.
Production
Hydrochloric acid is prepared by dissolving hydrogen chloride in water. Hydrogen chloride can be generated in many ways, and thus several precursors to hydrochloric acid exist. The large-scale production of hydrochloric acid is almost always integrated with the industrial scale production of other chemicals.
Industrial market
Hydrochloric acid is produced in solutions up to 38% HCl (concentrated grade). Higher concentrations up to just over 40% are chemically possible, but the evaporation rate is then so high that storage and handling need extra precautions, such as pressure and low temperature. Bulk industrial-grade is therefore 30% to 34%, optimized for effective transport and limited product loss by HCl vapors. Solutions for household purposes in the US, mostly cleaning, are typically 10% to 12%, with strong recommendations to dilute before use. In the United Kingdom, where it is sold as "Spirits of Salt" for domestic cleaning, the potency is the same as the US industrial grade.[] Major producers worldwide include Dow Chemical at 2 million metric tons annually (2 Mt/year), calculated as HCl gas, and FMC, Georgia Gulf Corporation, Tosoh Corporation, Akzo Nobel, and Tessenderlo at 0.5 to 1.5 Mt/year each. Total world production, for comparison purposes expressed as HCl, is estimated at 20 Mt/year, with 3 Mt/year from direct synthesis, and the rest as secondary product from organic and similar syntheses. By far, most hydrochloric acid is consumed captively by the producer. The open world market size is estimated at 5 Mt/year.[]
Applications
Hydrochloric acid is a strong inorganic acid that is used in many industrial processes. The application often determines the required product quality.[]
Pickling of steel
One of the most important applications of hydrochloric acid is in the pickling of steel, to remove rust or iron oxide scale from iron or steel before subsequent processing, such as extrusion, rolling, galvanizing, and other techniques.[][] Technical quality HCl at typically 18% concentration is the most commonly used pickling agent for the pickling of carbon steel grades. Fe2O3 + Fe + 6 HCl → 3 FeCl2 + 3 H2O The spent acid has long been re-used as iron(II) chloride (also known as ferrous chloride) solutions, but high heavy-metal levels in the pickling liquor have decreased this practice.
Hydrochloric acid The steel pickling industry has developed hydrochloric acid regeneration processes, such as the spray roaster or the fluidized bed HCl regeneration process, which allow the recovery of HCl from spent pickling liquor. The most common regeneration process is the pyrohydrolysis process, applying the following formula:[] By recuperation of the spent acid, a closed acid loop is established.[] The iron(III) oxide by-product of the regeneration process is valuable, used in a variety of secondary industries.[] 4 FeCl2 + 4 H2O + O2 → 8 HCl+ 2 Fe2O3
64
Production of organic compounds
Another major use of hydrochloric acid is in the production of organic compounds, such as vinyl chloride and dichloroethane for PVC. This is often captive use, consuming locally produced hydrochloric acid that never actually reaches the open market. Other organic compounds produced with hydrochloric acid include bisphenol A for polycarbonate, activated carbon, and ascorbic acid, as well as numerous pharmaceutical products.[] 2 CH2=CH2 + 4 HCl + O2 → 2 ClCH2CH2Cl + 2 H2O (dichloroethane by oxychlorination) wood + HCl + heat → activated carbon (chemical activation)
Production of inorganic compounds
Numerous products can be produced with hydrochloric acid in normal acid-base reactions, resulting in inorganic compounds. These include water treatment chemicals such as iron(III) chloride and polyaluminium chloride (PAC). Fe2O3 + 6 HCl → 2 FeCl3 + 3 H2O (iron(III) chloride from magnetite) Both iron(III) chloride and PAC are used as flocculation and coagulation agents in sewage treatment, drinking water production, and paper production. Other inorganic compounds produced with hydrochloric acid include road application salt calcium chloride, nickel(II) chloride for electroplating, and zinc chloride for the galvanizing industry and battery production.[] CaCO3 + 2 HCl → CaCl2 + CO2 + H2O (calcium chloride from limestone)
pH Control and neutralization
Hydrochloric acid can be used to regulate the acidity (pH) of solutions. OH− + HCl → H2O + Cl− In industry demanding purity (food, pharmaceutical, drinking water), high-quality hydrochloric acid is used to control the pH of process water streams. In less-demanding industry, technical quality hydrochloric acid suffices for neutralizing waste streams and swimming pool treatment.[]
Regeneration of ion exchangers
High-quality hydrochloric acid is used in the regeneration of ion exchange resins. Cation exchange is widely used to remove ions such as Na+ and Ca2+ from aqueous solutions, producing demineralized water. The acid is used to rinse the cations from the resins.[] Na+ is replaced with H+ and Ca2+ with 2 H+. Ion exchangers and demineralized water are used in all chemical industries, drinking water production, and many food industries.[]
Hydrochloric acid
65
Other
Hydrochloric acid is used for a large number of small-scale applications, such as leather processing, purification of common salt, household cleaning,[13] and building construction.[] Oil production may be stimulated by injecting hydrochloric acid into the rock formation of an oil well, dissolving a portion of the rock, and creating a large-pore structure. Oil well acidizing is a common process in the North Sea oil production industry.[] Many chemical reactions involving hydrochloric acid are applied in the production of food, food ingredients, and food additives. Typical products include aspartame, fructose, citric acid, lysine, hydrolyzed vegetable protein as food enhancer, and in gelatin production. Food-grade (extra-pure) hydrochloric acid can be applied when needed for the final product.[][]
Presence in living organisms
Gastric acid is one of the main secretions of the stomach. It consists mainly of hydrochloric acid and acidifies the stomach content to a pH of 1 to 2.[] [14] Chloride (Cl−) and hydrogen (H+) ions are secreted separately in the stomach fundus region at the top of the stomach by parietal cells of the gastric mucosa into a secretory network called canaliculi before it enters the stomach lumen.[] Gastric acid acts as a barrier against microorganisms to prevent infections and is important for the digestion of food. Its low pH denatures proteins and thereby makes them susceptible to degradation by digestive enzymes such as pepsin. The low pH also activates the enzyme precursor pepsinogen into the active enzyme pepsin by self-cleavage. After leaving the stomach, the hydrochloric acid of the chyme is neutralized in the duodenum by sodium bicarbonate.[]
Diagram of alkaline mucous layer in stomach with mucosal defense mechanisms
The stomach itself is protected from the strong acid by the secretion of a thick mucus layer, and by secretin induced buffering with sodium bicarbonate. Heartburn or peptic ulcers can develop when these mechanisms fail. Drugs of the antihistaminic and proton pump inhibitor classes can inhibit the production of acid in the stomach, and antacids are used to neutralize existing acid.[][15]
Safety
Hydrochloric acid
66
Concentration Classification[] R-Phrases by weight 10–25% > 25% Irritant (Xi) Corrosive (C) R36/37/38 R34 R37
Concentrated hydrochloric acid (fuming hydrochloric acid) forms acidic mists. Both the mist and the solution have a corrosive effect on human tissue, with the potential to damage respiratory organs, eyes, skin, and intestines irreversibly. Upon mixing hydrochloric acid with common oxidizing chemicals, such as sodium hypochlorite (bleach, NaClO) or potassium permanganate (KMnO4), the toxic gas chlorine is produced. NaClO + 2 HCl → H2O + NaCl + Cl2 2 KMnO4 + 16 HCl → 2 MnCl2 + 8 H2O + 2 KCl + 5 Cl2 Personal protective equipment such as rubber or PVC gloves, protective eye goggles, and chemical-resistant clothing and shoes are used to minimize risks when handling hydrochloric acid. The United States Environmental Protection Agency rates and regulates hydrochloric acid as a toxic substance.[16] The UN number or DOT number is 1789. This number will be displayed on a placard on the container.
References External links
• NIST WebBook, general link (http://webbook.nist.gov/) • Hydrochloric Acid – Part One (http://www.periodicvideos.com/videos/mv_HCl1.htm) and Hydrochloric Acid – Part Two (http://www.periodicvideos.com/videos/mv_HCl2.htm) at The Periodic Table of Videos (University of Nottingham) General safety information • EPA Hazard Summary (http://www.epa.gov/ttn/atw/hlthef/hydrochl.html) • Hydrochloric acid MSDS by Georgia Institute of Technology (http://grover.mirc.gatech.edu/data/msds/50. html) • NIOSH Pocket Guide to Chemical Hazards (http://www.cdc.gov/niosh/npg/npgd0332.html) Pollution information • National Pollutant Inventory – Hydrochloric Acid Fact Sheet (http://www.npi.gov.au/substances/ hydrochloric-acid/index.html)
Human gastrointestinal tract
67
Human gastrointestinal tract
Human gastrointestinal tract (Digestive System)
Stomach colon rectum diagram Latin Tractus digestorius (mouth to anus), canalis alimentarius (esophagus to large Intestine), canalis gastrointestinales (stomach to large Intestine]
System Digestive system
The human gastrointestinal tract is the stomach and intestine,[1] sometimes including all the structures from the mouth to the anus.[2] (The "digestive system" is a broader term that includes other structures, including the accessory organs of digestion).[3] In an adult male human, the gastrointestinal (GI) tract is 5 metres (20 ft) long in a live subject, or up to 9 metres (30 ft) without the effect of muscle tone, and consists of the upper and lower GI tracts. The tract may also be divided into foregut, midgut, and hindgut, reflecting the embryological origin of each segment of the tract. The GI tract always releases hormones to help regulate the digestive process. These hormones, including gastrin, secretin, cholecystokinin, and grehlin, are mediated through either intracrine or autocrine mechanisms, indicating that the cells releasing these hormones are conserved structures throughout evolution.[4]
Human gastrointestinal tract
68
Upper gastrointestinal tract
The upper gastrointestinal tract consists of the esophagus, stomach, and duodenum.[5] The exact demarcation between "upper" and "lower" can vary. Upon dissection, the duodenum may appear to be a unified organ, but it is often divided into two parts based upon function, arterial supply, or embryology.
Lower gastrointestinal tract
The lower gastrointestinal tract includes most of the small intestine and all of the large intestine.[6] According to some sources, it also includes the anus.[citation needed] • Bowel or intestine • Small Intestine: Has three parts: • Duodenum: Here the digestive juices from the pancreas (digestive enzymes) and hormones and the gall bladder (bile) mix. The digestive enzymes break down proteins and bile and emulsify fats into micelles. The duodenum contains Brunner's glands which produce bicarbonate. In combination with bicarbonate from pancreatic juice, this neutralizes HCl of the stomach.
Upper and Lower human gastrointestinal tract
• Jejunum: This is the midsection of the intestine, connecting the duodenum to the ileum. It contains the plicae circulares, and villi to increase the surface area of that part of the GI Tract. Products of digestion (sugars, amino acids, fatty acids) are absorbed into the bloodstream. • Ileum: Has villi and absorbs mainly vitamin B12 and bile acids, as well as any other remaining nutrients. • Large Intestine: Has three parts: • Caecum: The Vermiform appendix is attached to the caecum. • Colon: Includes the ascending colon, transverse colon, descending colon and sigmoid Flexure: The main function of the Colon is to absorb water, but it also contains bacteria that produce beneficial vitamins like vitamin K. • Rectum • Anus: Passes fecal matter from the body. The Ligament of Treitz is sometimes used to divide the upper and lower GI tracts.[]
Human gastrointestinal tract
69
Embryology
The gut is an endoderm-derived structure. At approximately the sixteenth day of human development, the embryo begins to fold ventrally (with the embryo's ventral surface becoming concave) in two directions: the sides of the embryo fold in on each other and the head and tail fold toward one another. The result is that a piece of the yolk sac, an endoderm-lined structure in contact with the ventral aspect of the embryo, begins to be pinched off to become the primitive gut. The yolk sac remains connected to the gut tube via the vitelline duct. Usually this structure regresses during development; in cases where it does not, it is known as Meckel's diverticulum. During fetal life, the primitive gut can be divided into three segments: foregut, midgut, and hindgut. Although these terms are often used in reference to segments of the primitive gut, they are also used regularly to describe components of the definitive gut as well. Each segment of the gut gives rise to specific gut and gut-related structures in later development. Components derived from the gut proper, including the stomach and colon, develop as swellings or dilatations of the primitive gut. In contrast, gut-related derivatives — that is, those structures that derive from the primitive gut but are not part of the gut proper, in general develop as out-pouchings of the primitive gut. The blood vessels supplying these structures remain constant throughout development.[7]
Part Part in adult Gives rise to Esophagus, Stomach, Duodenum (1st and 2nd parts), Liver, Gallbladder, Pancreas, Superior portion of pancreas (Note that though the Spleen is supplied by the celiac trunk, it is derived from dorsal mesentery and therefore not a foregut derivative) lower duodenum, jejunum, ileum, cecum, appendix, ascending colon, and first two-third of the transverse colon last third of the transverse colon, descending colon, rectum, and upper part of the anal canal Arterial supply celiac trunk
Foregut Esophagus to first 2 sections of the duodenum
Midgut
lower duodenum, to the first two-thirds of the transverse colon
branches of the superior mesenteric artery branches of the inferior mesenteric artery
Hindgut last third of the transverse colon, to the upper part of the anal canal
Transit time
The time taken for food or other ingested objects to transit through the gastrointestinal tract varies depending on many factors, but roughly, it takes less than an hour after a meal for 50% of stomach contents to empty into the intestines and total emptying of the stomach takes around 2 hours. Subsequently, 50% emptying of the small intestine takes 1 to 2 hours. Finally, transit through the colon takes 12 to 50 hours with wide variation between individuals.[8] [9]
Pathology
There are a number of diseases and conditions affecting the gastrointestinal system, including: • • • • • • • • • • Appendicitis Cancer Celiac Disease Cholera Colorectal cancer Diarrhoea Diverticulitis Enteric duplication cyst Gastroenteritis, also known as "stomach flu"; an inflammation of the stomach and intestines Giardiasis
Human gastrointestinal tract • • • • • Inflammatory bowel disease (including Crohn's disease and ulcerative colitis) Irritable bowel syndrome Pancreatitis Peptic ulcer disease Yellow Fever
70
Immune function
The gastrointestinal tract is also a prominent part of the immune system.[10] The surface area of the digestive tract is estimated to be the surface area of a football field. With such a large exposure, the immune system must work hard to prevent pathogens from entering into blood and lymph.[11] The low pH (ranging from 1 to 4) of the stomach is fatal for many microorganisms that enter it. Similarly, mucus (containing IgA antibodies) neutralizes many of these microorganisms. Other factors in the GI tract help with immune function as well, including enzymes in saliva and bile. Enzymes such as Cyp3A4, along with the antiporter activities, also are instrumental in the intestine's role of detoxification of antigens and xenobiotics, such as drugs, involved in first pass metabolism. Health-enhancing intestinal bacteria serve to prevent the overgrowth of potentially harmful bacteria in the gut. These two types of bacteria compete for space and "food," as there are limited resources within the intestinal tract. A ratio of 80-85% beneficial to 15-20% potentially harmful bacteria generally is considered normal within the intestines. Microorganisms also are kept at bay by an extensive immune system comprising the gut-associated lymphoid tissue (GALT).
Histology
The gastrointestinal tract has a form of general histology with some differences that reflect the specialization in functional anatomy.[12] The GI tract can be divided into four concentric layers in the following order: • Mucosa • Submucosa • Muscularis externa (the external muscular layer) • Adventitia or serosa
Mucosa
General structure of the gut wall The mucosa is the innermost layer of the gastrointestinal tract. that is surrounding the lumen, or open space within the tube. This layer comes in direct contact with digested food (chyme),
The mucosa is made up of three layers: • Epithelium - innermost layer. Responsible for most digestive, absorptive and secretory processes. • Lamina propria - a layer of connective tissue. Unusually cellular compared to most connective tissue • Muscularis mucosae - a thin layer of smooth muscle. Function is still under debate The mucosae are highly specialized in each organ of the gastrointestinal tract to deal with the different conditions. The most variation is seen in the epithelium. In the esophagus, the epithelium is stratified, squamous and non-keratinising, for protective purposes.
Human gastrointestinal tract In the stomach it is simple columnar, and is organised into gastric pits and glands to deal with secretion. The gastro-oesophageal junction is extremely abrupt. The small intestine epithelium (particularly the ileum) is specialised for absorption; it is organised into plicae circulares and villi, and the enterocytes have microvilli. This creates a brush border which greatly increases the surface area for absoption. The epithelium is simple columnar with microvilli. In the ileum there are occasionally Peyer's patches in the lamina propria. The colon has simple columnar epithelium with no villi. There are goblet cells. The appendix has a mucosa resembling the colon but is heavily infiltrated with lymphocytes. The ano-rectal junction (at the pectinate line) is again very abrupt; there is a transition from simple columnar to stratified squamous non-keratinising epithelium (as in the oesophagus) for protective purposes.
71
Submucosa
The submucosa consists of a dense irregular layer of connective tissue with large blood vessels, lymphatics, and nerves branching into the mucosa and muscularis externa. It contains Meissner's plexus, an enteric nervous plexus, situated on the inner surface of the muscularis externa.
Muscularis externa
The muscularis externa consists of an inner circular layer and a longitudinal outer muscular layer. The circular muscle layer prevents food from traveling backward and the longitudinal layer shortens the tract. The layers are not truly longitudinal or circular, rather the layers of muscle are helical with different pitches. The inner circular is helical with a steep pitch and the outer longitudinal is helical with a much shallower pitch. The coordinated contractions of these layers is called peristalsis and propels the food through the tract. Food in the GI tract is called a bolus (ball of food) from the mouth down to the stomach. After the stomach, the food is partially digested and semi-liquid, and is referred to as chyme. In the large intestine the remaining semi-solid substance is referred to as faeces. Between the two muscle layers are the myenteric or Auerbach's plexus. This controls peristalsis. Activity is initiated by the pacemaker cells (interstitial cells of Cajal). The gut has intrinsic peristaltic activity (basal electrical rhythm) due to its self-contained enteric nervous system. The rate can of course be modulated by the rest of the autonomic nervous system. The thickness of muscularis externa varies in each part of the tract. In the colon, for example, the muscularis externa is much thicker because the faeces are large and heavy, and require more force to push along. The outer longitudinal layer of the colon thins out into 3 discontinuous longitudinal bands, known as tiniae coli (bands of the colon). This is one of the 3 features helping to distinguish between the large and small intestine. Occasionally in the large intestine (2-3 times a day) there will be mass contraction of certain segments, moving a lot of faeces along. This is generally when one gets the urge to defecate. The pylorus of the stomach has a thickened portion of the inner circular layer: the pyloric sphincter. Alone among the GI tract, the stomach has a third layer of muscularis externa. This is the inner oblique layer, and helps churn the chyme in the stomach.
Human gastrointestinal tract
72
Adventitia/serosa
The outermost layer of the GI tract consists of several layers of connective tissue. Intraperitoneal parts of the GI tract are covered with serosa. These include most of the stomach, first part of the duodenum, all of the small intestine, caecum and appendix, transverse colon, sigmoid colon and rectum. In these sections of the gut there is clear boundary between the gut and the surrounding tissue. These parts of the tract have a mesentery. Retroperitoneal parts are covered with adventitia. They blend in to the surrounding tissue and are fixed in position. For example, the retroperitoneal section of the duodenum usually passes through the transpyloric plane. These include the oesophagus, pylorus of the stomach, distal duodenum, ascending colon, descending colon and anal canal. In addition, the oral cavity has adventitia.
References
[4] Nelson RJ. 2005. Introduction to Behavioral Endocrinology. Sinauer Associates: Massachusetts. p 57. [8] Kim SK. Small intestine transit time in the normal small bowel study. American Journal of Roentgenology 1968; 104(3):522-524. [9] (http:/ / www. ncbi. nlm. nih. gov/ pmc/ articles/ PMC3325313/ ) Uday C Ghoshal, Vikas Sengar, and Deepakshi Srivastava. Colonic Transit Study Technique and Interpretation: Can These Be Uniform Globally in Different Populations With Non-uniform Colon Transit Time? J Neurogastroenterol Motil. 2012 April; 18(2): 227–228. [11] Animal Physiology textbook
External links
• • • • Pediatric Overview of Human Digestive System (http://www.pediatricfeeding.org/gi_anatomy.html) Anatomy atlas of the Digestive System (http://www.innerbody.com/image/digeov.html) Overview (http://www.vivo.colostate.edu/hbooks/pathphys/digestion/) at Colorado State University Your Digestive System and How It Works at National Institutes of Health (http://digestive.niddk.nih.gov/ ddiseases/pubs/yrdd/)
Goblet cell
73
Goblet cell
Goblet cell
Section of mucus membrane of human stomach, near the cardiac orifice. X 45. c. Cardiac glands. d. Their ducts. cr. Gland similar to the intestinal glands, with goblet cells. mm. Mucous membrane. m. Muscularis mucosae. m’. Muscular tissue within the mucous membrane.
Transverse section of a villus, from the human intestine. X 350. a. Basement membrane, here somewhat shrunken away from the epithelium. b. Lacteal. c. Columnar epithelium. d. Its striated border. e. Goblet cells. f. Leucocytes in epithelium. f’. Leucocytes below epithelium. g. Blood vessels. h. Muscle cells cut across. Latin Code exocrimohsinocytus caliciformis TH H3.04.03.0.00009; H3.04.03.0.00016 H3.05.00.0.00006
Goblet cells are glandular simple columnar epithelial cells whose function is to secrete mucin, which dissolves in water to form mucus. They use both apocrine and merocrine methods for secretion. The majority of the cell's cytoplasm is occupied by mucinogen granules, except at the bottom. Rough endoplasmic reticulum, mitochondria, the nucleus, and other organelles are concentrated in the basal portion. The apical plasma membrane projects microvilli to increase surface area for secretion. Recent study suggests that glycoprotein is
Goblet cell located inside goblet cells. It is an organ-specific antigen in the gut.
74
Locations
They are found scattered among the epithelial lining of organs, such as the intestinal and respiratory tracts.[1] They are found inside the trachea, bronchus, and larger bronchioles in respiratory tract, small intestines, the colon, and conjunctiva in the upper eyelid.(Goblet cells are the chief source of tear mucus. These occur throughout the conjunctiva, especially the plica semilunaris. These are most dense in nasal conjunctiva, least dense in upper temporal fornix and absent in palpebral mucocutaneous junction and limbus.) They may be an indication of metaplasia, such as in Barrett's esophagus.
Histology
In mucicarmine stains, deep red mucin found within goblet cell bodies. The nuclei of goblet cells tend to be displaced toward the basal end of the cell body, leading to intense basophilic staining.
Etymology
The term goblet refers to these cells' goblet-like shape. The apical portion is shaped like a cup, as it is distended by abundant mucinogen granules; its basal portion is shaped like a stem, as it is narrow for lack of these granules. There are other cells that secrete mucus (as in the foveolar cells of the stomach[2]), but they are not usually called "goblet cells" because they do not have this distinctive shape.
Basal secretion
This is the normal base level secretion of mucus, which is accomplished by cytoskeletal movement of secretory granules.
Stimulated secretion
Secretion may be stimulated by dust, smoke, etc. Other stimuli include viruses, bacteria, etc.
Role in Oral Tolerance
Oral tolerance is the proccess by which the immune system is prevented from responding to antigen derived from food products, as peptides from food may pass into the bloodstream via the gut, which would in theory lead to an immune response. A recent paper published in Nature, has shed some light on the process and implicated goblet cells as having a role in the process.[] It was known that CD103 expressing dendritic cells of the lamina propria had a role to play in the induction of oral tolerance (potentially by inducing the differentiation of regulatory T cells), and this paper suggests that the goblet cells act to preferentially deliver antigen to these CD103+ dendritic cells.[]
Goblet cell
75
References
[2] - Digestive System: Alimentary Canal: fundic stomach, gastric glands, lumen"
Additional images
An intestinal gland from the human intestine.
Goblet cell in ileum
section of mouse intestine. Mucus of goblet cells in blue.
External links
• Histology at KUMC epithel-epith08 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/epithel/ epith08.htm) "Slide 8: Trachea" • Goblet+cell (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=Goblet+cell) at eMedicine Dictionary • Goblet Cells at cvmbs.colostate.edu (http://arbl.cvmbs.colostate.edu/hbooks/pathphys/misc_topics/goblets. html) • Diagram at uwlax.edu (http://bioweb.uwlax.edu/) • Bioweb at UWLAX Zoolab (http://bioweb.uwlax.edu/zoolab/Table_of_Contents/Lab-1b/ Cross_section_of_the_small_int/Goblet_cells/goblet_cells.htm)
Respiratory tract
76
Respiratory tract
In humans the respiratory tract is the part of the anatomy involved with the process of respiration. The respiratory tract is divided into 3 segments: • Upper respiratory tract: nose and nasal passages, paranasal sinuses, and throat or pharynx • Respiratory airways: voice box or larynx, trachea, bronchi, and bronchioles • Lungs: respiratory bronchioles, alveolar ducts, alveolar sacs, and alveoli The respiratory tract is a common site for infections. Upper respiratory tract infections are probably the most common infections in the world. Most of the respiratory tract exists merely as a piping system for air to travel in the lungs, and alveoli are the only part of the lung that exchanges oxygen and carbon dioxide with the blood. Moving down the respiratory tract starting at the trachea, the tubes get smaller and divide into more and more tubes. There are estimated to be about 20 to 23 divisions, ending up at an alveolus. Even though the cross-sectional area of each bronchus or bronchiole is smaller, because there are so many, the total surface area is larger. This means there is less resistance at the terminal bronchioles. (Most resistance is around the 3-4 division from the trachea due to turbulence.)
General histology
The respiratory tract is covered in an epithelium, the type of which varies down the tract. There are glands and mucus produced by goblet cells in parts, as well as smooth muscle, elastin or cartilage. Most of the epithelium (from the nose to the bronchi) is covered in pseudostratified columnar ciliated epithelial cells, commonly called respiratory epithelium. The cilia beat in one direction, moving mucus towards the throat where it is swallowed. Moving down the bronchioles, the cells get more cuboidal in shape but are still ciliated. Cartilage is present until the small bronchi. In the trachea they are C-shaped rings, whereas in the bronchi they are interspersed plates.
This image compares the histological differences along the respiratory tract.
Glands are abundant in the upper respiratory tract, but there are fewer lower down and they are absent starting at the bronchioles. The same goes for goblet cells, although there are scattered ones in the first bronchioles. Smooth muscle starts in the trachea, where it joins the C-shaped rings of cartilage. It continues down the bronchi and bronchioles, which it completely encircles. Instead of hard cartilage, the bronchi and bronchioles are composed of elastic tissue.
Respiratory tract
77
References
• Syllabus: Infectious Diseases (http://www.kcom.edu/faculty/chamberlain/Website/lectures/syllabi3.htm) see Respiratory Tract Infections by Neal Chamberlain, PhD. Kirksville College of Osteopathic Medicine, Missouri, USA
Mucus
In vertebrates, mucus (adjectival form: "mucous") is a slippery secretion produced by, and covering, mucous membranes. Mucous fluid is typically produced from cells found in mucous glands. Mucous cells secrete products that are rich in glycoproteins and water. Mucous fluid may also originate from mixed glands, which contain both serous and mucous cells. It is a viscous colloid containing antiseptic enzymes (such as lysozyme), immunoglobulins, inorganic salts, proteins such as lactoferrin,[1] and glycoproteins known as mucins that are produced by goblet cells in the mucous membranes and submucosal glands. This mucus serves to protect epithelial cells (the lining of the tubes) in the respiratory, gastrointestinal, urogenital, visual, and auditory systems in mammals; the epidermis in amphibians; and the gills in fish. A major Mucous cells on the stomach lining function of this mucus is to protect against infectious agents such as fungi, bacteria and viruses. The average human body produces about a litre of mucus per day.[2] Bony fish, hagfish, snails, slugs, and some other invertebrates also produce external mucus. In addition to serving a protective function against infectious agents, such mucus provides protection against toxins produced by predators, can facilitate movement and may play a role in communication. The rest of this article is devoted entirely to mucus production and function in humans.
Respiratory system
In the human respiratory system, mucus aids in the protection of the lungs by trapping foreign particles that enter it, in particular, through the nose, during normal breathing. "Phlegm" is a specialized term for mucus that is restricted to the respiratory tract, whereas the term "nasal mucus" describes secretions of the nasal passages. Nasal mucus is produced by the nasal mucosa; and mucosal tissues lining the airways (trachea, bronchus, bronchioles) is produced by specialized airway epithelial cells (goblet cells) and submucosal glands. Small particles such as dust, particulate pollutants, and allergens, as well as infectious agents bacteria are caught in the viscous nasal or airway mucus and prevented from entering the system. This event along with the continual movement of the respiratory mucus layer toward the oropharynx, helps prevent foreign objects from entering the lungs during breathing. This explains why coughing often occurs in those who smoke filtered cigarettes. The body's natural reaction is to increase mucus production. In addition, mucus aids in moisturizing the inhaled air and prevents tissues such as the nasal and airway epithelia from drying out.[] Nasal and airway mucus is produced continuously, with most of it swallowed unconsciously, even when it is dried.[] Increased mucus production in the respiratory tract is a symptom of many common illnesses, such as the common cold and influenza. Hypersecretion of mucus can occur in inflammatory respiratory diseases such as respiratory allergies, asthma, and chronic bronchitis.[] The presence of mucus in the nose and throat is normal, but increased quantities can impede comfortable breathing and must be cleared by blowing the nose or expectorating phlegm from the throat.
Mucus
78
Diseases involving mucus
In general, nasal mucus is clear and thin, serving to filter air during inhalation. During times of infection, mucus can change color to yellow or green either as a result of trapped bacteria[3] or due to the body's reaction to viral infection.[4] The green color of mucus comes from the heme group in the iron-containing enzyme myeloperoxidase secreted by white blood cells as a cytotoxic defense during a respiratory burst. In the case of bacterial infection, the bacterium becomes trapped in already-clogged sinuses, breeding in the moist, nutrient-rich environment. Sinusitis is an uncomfortable condition which may include congestion of mucus. A bacterial infection in sinusitis will cause discolored mucus and would respond to antibiotic treatment; viral infections typically resolve without treatment.[5] Almost all sinusitis infections are viral and antibiotics are ineffective and not recommended for treating typical cases.[6] In the case of a viral infection such as cold or flu, the first stage and also the last stage of the infection cause the production of a clear, thin mucus in the nose or back of the throat. As the body begins to react to the virus (generally one to three days), mucus thickens and may turn yellow or green. Viral infections cannot be treated with antibiotics, and are a major avenue for their misuse. Treatment is generally symptom-based; often it is sufficient to allow the immune system to fight off the virus over time.[7] Cystic fibrosis Cystic fibrosis is an inherited disease that affects the entire body, but symptoms begin mostly in the lungs with extremely viscous (thick) production of mucus that is difficult to expel. Mucus as a medical symptom Increased mucus production in the upper respiratory tract is a symptom of many common ailments, such as the common cold. Nasal mucus may be removed by blowing the nose or by using nasal irrigation. Excess nasal mucus, as with a cold or allergies may be treated cautiously with decongestant medications. Excess mucus production in the bronchi and bronchioles, as may occur in asthma, bronchitis or influenza, may be treated with anti-inflammatory medications as a means of reducing the airway inflammation, which triggers mucus over-production. Thickening of mucus as a "rebound" effect following overuse of decongestants may produce nasal or sinus drainage problems and circumstances that promote infection.
Cold weather and mucus
During cold weather, the cilia, which normally sweep mucus away from the nostrils and toward the back of the throat (see respiratory epithelium), become sluggish or completely cease functioning. This results in mucus running down the nose and dripping (a runny nose).Template:Citation neeeded Mucus also thickens in cold weather; when an individual comes in from the cold, the mucus thaws and begins to run before the cilia begin to work again.Template:Citation neeeded
Mucus
79
Digestive system
In the human digestive system, mucus is used as a lubricant for materials that must pass over membranes, e.g., food passing down the esophagus. A layer of mucus along the inner walls of the stomach is vital to protect the cell linings of that organ from the highly acidic environment within it.[] Mucus is not digested in the intestinal tract. Mucus is also secreted from glands within the rectum due to stimulation of the mucous membrane within. [citation needed]
Reproductive system
In the human female reproductive system, cervical mucus prevents infection. The consistency of cervical mucus varies depending on the stage of a woman's menstrual cycle. At ovulation cervical mucus is clear, runny, and conducive to sperm; post-ovulation, mucus becomes thicker and is more likely to block sperm.[citation needed] In the human male reproductive system, the seminal vesicles contribute up to 100% of the total volume of the semen and contain mucus, amino acids, prostaglandins, vitamin C, and fructose as the main energy source for the sperm.[citation needed]
Notes References
Enzyme
Enzymes (pron.: /ˈɛnzaɪmz/) are large biological molecules responsible for the thousands of chemical interconversions that sustain life.[1][2] They are highly selective catalysts, greatly accelerating both the rate and specificity of metabolic reactions, from the digestion of food to the synthesis of DNA. Most enzymes are proteins, although some catalytic RNA molecules have been identified. Enzymes adopt a specific three-dimensional structure, and may employ organic (e.g. biotin) and inorganic (e.g. magnesium ion) cofactors to assist in catalysis. In enzymatic reactions, the molecules at the beginning of the process, called substrates, Human glyoxalase I. Two zinc ions that are needed for the enzyme to catalyze its are converted into different molecules, reaction are shown as purple spheres, and an enzyme inhibitor called called products. Almost all chemical S-hexylglutathione is shown as a space-filling model, filling the two active sites. reactions in a biological cell need enzymes in order to occur at rates sufficient for life. Since enzymes are selective for their substrates and speed up only a few reactions from among many possibilities, the set of enzymes made in a cell determines which metabolic pathways occur in that cell.
Enzyme Like all catalysts, enzymes work by lowering the activation energy (Ea‡) for a reaction, thus dramatically increasing the rate of the reaction. As a result, products are formed faster and reactions reach their equilibrium state more rapidly. Most enzyme reaction rates are millions of times faster than those of comparable un-catalyzed reactions. As with all catalysts, enzymes are not consumed by the reactions they catalyze, nor do they alter the equilibrium of these reactions. However, enzymes do differ from most other catalysts in that they are highly specific for their substrates. Enzymes are known to catalyze about 4,000 biochemical reactions.[3] A few RNA molecules called ribozymes also catalyze reactions, with an important example being some parts of the ribosome.[4][5] Synthetic molecules called artificial enzymes also display enzyme-like catalysis.[6] Enzyme activity can be affected by other molecules. Inhibitors are molecules that decrease enzyme activity; activators are molecules that increase activity. Many drugs and poisons are enzyme inhibitors. Activity is also affected by temperature, pressure, chemical environment (e.g., pH), and the concentration of substrate. Some enzymes are used commercially, for example, in the synthesis of antibiotics. In addition, some household products use enzymes to speed up biochemical reactions (e.g., enzymes in biological washing powders break down protein or fat stains on clothes; enzymes in meat tenderizers break down proteins into smaller molecules, making the meat easier to chew).
80
Etymology and history
As early as the late 17th and early 18th centuries, the digestion of meat by stomach secretions[] and the conversion of starch to sugars by plant extracts and saliva were known. However, the mechanism by which this occurred had not been identified.[7] In 1833, French chemist Anselme Payen discovered the first enzyme, diastase. A few decades later, when studying the fermentation of sugar to alcohol by yeast, Louis Pasteur came to the conclusion that this fermentation was catalyzed by a vital force contained within the yeast cells called "ferments", which were thought to function only within living organisms. He wrote that "alcoholic fermentation is an act correlated with the life and organization of the yeast cells, not with the death or putrefaction of the cells."[8] In 1877, German physiologist Wilhelm Kühne (1837–1900) first used the term enzyme, which comes from Greek ενζυμον, "in leaven", to describe this process.[9] The word enzyme was used later to refer to nonliving substances such as pepsin, and the word ferment was used to refer to chemical activity produced by living organisms. In 1897, Eduard Buchner submitted his first paper on the ability of yeast extracts that lacked any living yeast cells to ferment sugar. In a series of experiments at the University of Berlin, he found that the sugar was fermented even when there were no living yeast cells in the mixture.[10] He named the enzyme that brought about the fermentation of sucrose "zymase".[11] In 1907, he received the Nobel Prize in Chemistry "for his biochemical research and his discovery of cell-free fermentation". Following Buchner's example, enzymes are usually named according to the reaction they carry out. Typically, to generate the name of an enzyme, the suffix -ase is added to the name of its substrate (e.g., lactase is the enzyme that cleaves lactose) or the type of reaction (e.g., DNA polymerase forms DNA polymers).[12] Having shown that enzymes could function outside a living cell, the next step was to determine their biochemical nature. Many early workers noted that enzymatic activity was associated with proteins, but several scientists (such as Nobel laureate Richard Willstätter) argued that proteins were merely carriers for the true enzymes and that proteins per se were incapable of catalysis.[13] However, in 1926, James B. Sumner showed that the enzyme urease was a pure protein and crystallized it; Sumner did likewise for the enzyme catalase in 1937. The conclusion that pure proteins can be enzymes was definitively proved by Northrop and Stanley, who worked on the digestive enzymes pepsin (1930), trypsin and chymotrypsin. These three scientists were awarded the 1946 Nobel Prize in Chemistry.[14] This discovery that enzymes could be crystallized eventually allowed their structures to be solved by x-ray crystallography. This was first done for lysozyme, an enzyme found in tears, saliva and egg whites that digests the coating of some bacteria; the structure was solved by a group led by David Chilton Phillips and published in
Enzyme 1965.[15] This high-resolution structure of lysozyme marked the beginning of the field of structural biology and the effort to understand how enzymes work at an atomic level of detail.
81
Structures and mechanisms
Enzymes are in general globular proteins and range from just 62 amino acid residues in size, for the monomer of 4-oxalocrotonate tautomerase,[16] to over 2,500 residues in the animal fatty acid synthase.[17] A small number of RNA-based biological catalysts exist, with the most common being the ribosome; these are referred to as either RNA-enzymes or ribozymes. The activities of enzymes are determined by their three-dimensional structure.[18] However, although structure does determine function, predicting a novel enzyme's activity just from its structure is a very difficult problem that has not yet been solved.[19] Most enzymes are much larger than the substrates they act on, and only a small Ribbon diagram showing human carbonic anhydrase II. The grey sphere is the zinc [16] portion of the enzyme (around 2–4 amino cofactor in the active site. Diagram drawn from PDB 1MOO . [20] acids) is directly involved in catalysis. The region that contains these catalytic residues, binds the substrate, and then carries out the reaction is known as the active site. Enzymes can also contain sites that bind cofactors, which are needed for catalysis. Some enzymes also have binding sites for small molecules, which are often direct or indirect products or substrates of the reaction catalyzed. This binding can serve to increase or decrease the enzyme's activity, providing a means for feedback regulation. Like all proteins, enzymes are long, linear chains of amino acids that fold to produce a three-dimensional product. Each unique amino acid sequence produces a specific structure, which has unique properties. Individual protein chains may sometimes group together to form a protein complex. Most enzymes can be denatured—that is, unfolded and inactivated—by heating or chemical denaturants, which disrupt the three-dimensional structure of the protein. Depending on the enzyme, denaturation may be reversible or irreversible. Structures of enzymes with substrates or substrate analogs during a reaction may be obtained using Time resolved crystallography methods.
Enzyme
82
Specificity
Enzymes are usually very specific as to which reactions they catalyze and the substrates that are involved in these reactions. Complementary shape, charge and hydrophilic/hydrophobic characteristics of enzymes and substrates are responsible for this specificity. Enzymes can also show impressive levels of stereospecificity, regioselectivity and chemoselectivity.[21] Some of the enzymes showing the highest specificity and accuracy are involved in the copying and expression of the genome. These enzymes have "proof-reading" mechanisms. Here, an enzyme such as DNA polymerase catalyzes a reaction in a first step and then checks that the product is correct in a second step.[22] This two-step process results in average error rates of less than 1 error in 100 million reactions in high-fidelity mammalian polymerases.[23] Similar proofreading mechanisms are also found in RNA polymerase,[24] aminoacyl tRNA synthetases[25] and ribosomes.[26] Some enzymes that produce secondary metabolites are described as promiscuous, as they can act on a relatively broad range of different substrates. It has been suggested that this broad substrate specificity is important for the evolution of new biosynthetic pathways.[27] "Lock and key" model Enzymes are very specific, and it was suggested by the Nobel laureate organic chemist Emil Fischer in 1894 that this was because both the enzyme and the substrate possess specific complementary geometric shapes that fit exactly into one another.[28] This is often referred to as "the lock and key" model. However, while this model explains enzyme specificity, it fails to explain the stabilization of the transition state that enzymes achieve. In 1958, Daniel Koshland suggested a modification to the lock and key model: since enzymes are rather flexible structures, the active site is continuously reshaped by interactions with the substrate as the substrate interacts with the enzyme.[29] As a result, the substrate does not simply bind to a rigid active site; the amino Diagrams to show the induced fit hypothesis of enzyme action acid side-chains that make up the active site are molded into the precise positions that enable the enzyme to perform its catalytic function. In some cases, such as glycosidases, the substrate molecule also changes shape slightly as it enters the active site.[30] The active site continues to change until the substrate is completely bound, at which point the final shape and charge is determined.[31] Induced fit may enhance the fidelity of molecular recognition in the presence of competition and noise via the conformational proofreading mechanism.[32]
Mechanisms
Enzymes can act in several ways, all of which lower ΔG‡ (Gibbs energy):[33] • Lowering the activation energy by creating an environment in which the transition state is stabilized (e.g. straining the shape of a substrate—by binding the transition-state conformation of the substrate/product molecules, the enzyme distorts the bound substrate(s) into their transition state form, thereby reducing the amount of energy required to complete the transition). • Lowering the energy of the transition state, but without distorting the substrate, by creating an environment with the opposite charge distribution to that of the transition state. • Providing an alternative pathway. For example, temporarily reacting with the substrate to form an intermediate ES complex, which would be impossible in the absence of the enzyme.
Enzyme • Reducing the reaction entropy change by bringing substrates together in the correct orientation to react. Considering ΔH‡ alone overlooks this effect. • Increases in temperatures speed up reactions. Thus, temperature increases help the enzyme function and develop the end product even faster. However, if heated too much, the enzyme's shape deteriorates and the enzyme becomes denatured. Some enzymes like thermolabile enzymes work best at low temperatures. It is interesting that this entropic effect involves destabilization of the ground state,[34] and its contribution to catalysis is relatively small.[35] Transition state stabilization The understanding of the origin of the reduction of ΔG‡ requires one to find out how the enzymes can stabilize its transition state more than the transition state of the uncatalyzed reaction. It seems that the most effective way for reaching large stabilization is the use of electrostatic effects, in particular, when having a relatively fixed polar environment that is oriented toward the charge distribution of the transition state.[36] Such an environment does not exist in the uncatalyzed reaction in water. Dynamics and function The internal dynamics of enzymes has been suggested to be linked with their mechanism of catalysis.[37][38][39] Internal dynamics are the movement of parts of the enzyme's structure, such as individual amino acid residues, a group of amino acids, or even an entire protein domain. These movements occur at various time-scales ranging from femtoseconds to seconds. Networks of protein residues throughout an enzyme's structure can contribute to catalysis through dynamic motions.[40][41][42][43] This is simply seen in the kinetic scheme of the combined process, enzymatic activity and dynamics; this scheme can have several independent Michaelis-Menten-like reaction pathways that are connected through fluctuation rates.[][][] Protein motions are vital to many enzymes, but whether small and fast vibrations, or larger and slower conformational movements are more important depends on the type of reaction involved. However, although these movements are important in binding and releasing substrates and products, it is not clear if protein movements help to accelerate the chemical steps in enzymatic reactions.[44] These new insights also have implications in understanding allosteric effects and developing new medicines.
83
Allosteric modulation
Allosteric sites are sites on the enzyme that bind to molecules in the cellular environment. The sites form weak, noncovalent bonds with these molecules, causing a change in the conformation of the enzyme. This change in conformation translates to the active site, which then affects the reaction rate of the enzyme.[45] Allosteric interactions can both inhibit and activate enzymes and are a common way that enzymes are controlled in the body.[46]
Allosteric transition of an enzyme between R and T states, stabilized by an agonist, an inhibitor and a substrate (the MWC model)
Cofactors and coenzymes
Enzyme
84
Cofactors
Some enzymes do not need any additional components to show full activity. However, others require non-protein molecules called cofactors to be bound for activity.[47] Cofactors can be either inorganic (e.g., metal ions and iron-sulfur clusters) or organic compounds (e.g., flavin and heme). Organic cofactors can be either prosthetic groups, which are tightly bound to an enzyme, or coenzymes, which are released from the enzyme's active site during the reaction. Coenzymes include NADH, NADPH and adenosine triphosphate. These molecules transfer chemical groups between enzymes.[48] An example of an enzyme that contains a cofactor is carbonic anhydrase, and is shown in the ribbon diagram above with a zinc cofactor bound as part of its active site.[49] These tightly bound molecules are usually found in the active site and are involved in catalysis. For example, flavin and heme cofactors are often involved in redox reactions. Enzymes that require a cofactor but do not have one bound are called apoenzymes or apoproteins. An apoenzyme together with its cofactor(s) is called a holoenzyme (this is the active form). Most cofactors are not covalently attached to an enzyme, but are very tightly bound. However, organic prosthetic groups can be covalently bound (e.g., biotin in the enzyme pyruvate carboxylase). The term "holoenzyme" can also be applied to enzymes that contain multiple protein subunits, such as the DNA polymerases; here the holoenzyme is the complete complex containing all the subunits needed for activity.
Coenzymes
Coenzymes are small organic molecules that can be loosely or tightly bound to an enzyme. Tightly bound coenzymes can be called prosthetic groups. Coenzymes transport chemical groups from one enzyme to another.[50] Some of these chemicals such as riboflavin, thiamine and folic acid are vitamins (compounds that cannot be synthesized by the body and must be acquired from the diet). The chemical groups carried include the hydride ion (H-) carried by NAD or NADP+, the phosphate group carried by adenosine triphosphate, the acetyl group carried by coenzyme A, formyl, methenyl or methyl groups carried by folic acid and the methyl group carried by S-adenosylmethionine. Since coenzymes are chemically changed as a consequence of enzyme action, it is useful to consider coenzymes to be a special class of substrates, or second substrates, which are common to many different enzymes. For example, about 700 enzymes are known to use the coenzyme NADH.[51]
Space-filling model of the coenzyme NADH
Coenzymes are usually continuously regenerated and their concentrations maintained at a steady level inside the cell: for example, NADPH is regenerated through the pentose phosphate pathway and S-adenosylmethionine by methionine adenosyltransferase. This continuous regeneration means that even small amounts of coenzymes are used very intensively. For example, the human body turns over its own weight in ATP each day.[52]
Enzyme
85
Thermodynamics
As all catalysts, enzymes do not alter the position of the chemical equilibrium of the reaction. Usually, in the presence of an enzyme, the reaction runs in the same direction as it would without the enzyme, just more quickly. However, in the absence of the enzyme, other possible uncatalyzed, "spontaneous" reactions might lead to different products, because in those conditions this different product is formed faster. Furthermore, enzymes can couple two or more reactions, so that a thermodynamically favorable reaction can be used to "drive" a thermodynamically unfavorable one. For example, the hydrolysis of ATP is often used to drive other chemical reactions.[]
The energies of the stages of a chemical reaction. Substrates need a lot of potential energy to reach a transition state, which then decays into products. The enzyme stabilizes the transition state, reducing the energy needed to form products.
Enzymes catalyze the forward and backward reactions equally. They do not alter the equilibrium itself, but only the speed at which it is reached. For example, carbonic anhydrase catalyzes its reaction in either direction depending on the concentration of its reactants. (in tissues; high CO2 concentration) (in lungs; low CO2 concentration) Nevertheless, if the equilibrium is greatly displaced in one direction, that is, in a very exergonic reaction, the reaction is in effect irreversible. Under these conditions, the enzyme will, in fact, catalyze the reaction only in the thermodynamically allowed direction.
Kinetics
Enzyme kinetics is the investigation of how enzymes bind substrates and turn them into products. The rate data used in kinetic analyses are commonly obtained from enzyme assays, where since the 90s, the dynamics of many enzymes are studied on the level of individual molecules. In 1902 Victor Henri proposed a quantitative theory of enzyme kinetics,[53] but his experimental data were not useful because the significance of the hydrogen ion concentration was not yet appreciated. After Peter Lauritz Sørensen had defined the logarithmic pH-scale and introduced the concept of buffering in 1909[54] the German chemist Leonor Michaelis and his Canadian postdoc Maud Leonora Menten repeated Henri's experiments and confirmed his equation, which is referred to as Henri-Michaelis-Menten kinetics (termed also Michaelis-Menten kinetics).[55] Their work was further developed by G. E. Briggs and J. B. S. Haldane, who derived kinetic equations that are still widely considered today a starting point in solving enzymatic activity.[56]
Mechanism for a single substrate enzyme catalyzed reaction. The enzyme (E) binds a substrate (S) and produces a product (P).
Enzyme The major contribution of Henri was to think of enzyme reactions in two stages. In the first, the substrate binds reversibly to the enzyme, forming the enzyme-substrate complex. This is sometimes called the Michaelis complex. The enzyme then catalyzes the chemical step in the reaction and releases the product. Note that the simple Michaelis Menten mechanism for the enzymatic activity is considered today a basic idea, where many examples show that the enzymatic activity involves structural dynamics. This is incorporated in the enzymatic mechanism while introducing several Michaelis Menten pathways that are connected with fluctuating rates.[][][] Nevertheless, there is a mathematical relation connecting the behavior obtained from the basic Michaelis Menten mechanism (that was indeed proved correct in many experiments) with the generalized Michaelis Menten mechanisms involving dynamics and activity; [] this means that the measured activity of enzymes on the level of many enzymes may be explained with the simple Michaelis-Menten equation, yet, the actual activity of enzymes is richer and involves structural dynamics. Enzymes can catalyze up to several million reactions per second. For example, the uncatalyzed decarboxylation of orotidine 5'-monophosphate has a half life of 78 million years. However, when the enzyme orotidine 5'-phosphate decarboxylase is added, the same process takes just 25 milliseconds.[57] Enzyme rates depend on solution conditions and substrate concentration. Conditions that denature the protein abolish enzyme activity, such as high temperatures, extremes of pH or high salt concentrations, while raising substrate concentration tends to increase activity Saturation curve for an enzyme reaction showing the relation between the substrate concentration (S) and rate (v) when [S] is low. To find the maximum speed of an enzymatic reaction, the substrate concentration is increased until a constant rate of product formation is seen. This is shown in the saturation curve on the right. Saturation happens because, as substrate concentration increases, more and more of the free enzyme is converted into the substrate-bound ES form. At the maximum reaction rate (Vmax) of the enzyme, all the enzyme active sites are bound to substrate, and the amount of ES complex is the same as the total amount of enzyme. However, Vmax is only one kinetic constant of enzymes. The amount of substrate needed to achieve a given rate of reaction is also important. This is given by the Michaelis-Menten constant (Km), which is the substrate concentration required for an enzyme to reach one-half its maximum reaction rate. Each enzyme has a characteristic Km for a given substrate, and this can show how tight the binding of the substrate is to the enzyme. Another useful constant is kcat, which is the number of substrate molecules handled by one active site per second. The efficiency of an enzyme can be expressed in terms of kcat/Km. This is also called the specificity constant and incorporates the rate constants for all steps in the reaction. Because the specificity constant reflects both affinity and catalytic ability, it is useful for comparing different enzymes against each other, or the same enzyme with different substrates. The theoretical maximum for the specificity constant is called the diffusion limit and is about 108 to 109 (M−1 s−1). At this point every collision of the enzyme with its substrate will result in catalysis, and the rate of product formation is not limited by the reaction rate but by the diffusion rate. Enzymes with this property are called catalytically perfect or kinetically perfect. Example of such enzymes are triose-phosphate isomerase, carbonic anhydrase, acetylcholinesterase, catalase, fumarase, β-lactamase, and superoxide dismutase. Michaelis-Menten kinetics relies on the law of mass action, which is derived from the assumptions of free diffusion and thermodynamically driven random collision. However, many biochemical or cellular processes deviate
86
Enzyme significantly from these conditions, because of macromolecular crowding, phase-separation of the enzyme/substrate/product, or one or two-dimensional molecular movement.[58] In these situations, a fractal Michaelis-Menten kinetics may be applied.[59][60][61][62] Some enzymes operate with kinetics, which are faster than diffusion rates, which would seem to be impossible. Several mechanisms have been invoked to explain this phenomenon. Some proteins are believed to accelerate catalysis by drawing their substrate in and pre-orienting them by using dipolar electric fields. Other models invoke a quantum-mechanical tunneling explanation, whereby a proton or an electron can tunnel through activation barriers, although for proton tunneling this model remains somewhat controversial.[63][64] Quantum tunneling for protons has been observed in tryptamine.[65] This suggests that enzyme catalysis may be more accurately characterized as "through the barrier" rather than the traditional model, which requires substrates to go "over" a lowered energy barrier.
87
Inhibition
Enzyme reaction rates can be decreased by various types of enzyme inhibitors. Competitive inhibition In competitive inhibition, the inhibitor and substrate compete for the enzyme (i.e., they can not bind at the same time).[67] Often competitive inhibitors strongly resemble the real substrate of the enzyme. For example, methotrexate is a competitive inhibitor of the enzyme dihydrofolate reductase, which catalyzes the reduction of dihydrofolate to tetrahydrofolate. The Competitive inhibitors bind reversibly to the enzyme, preventing the binding of substrate. similarity between the structures of On the other hand, binding of substrate prevents binding of the inhibitor. Substrate and folic acid and this drug are shown in inhibitor compete for the enzyme. the figure to the right bottom. In some cases, the inhibitor can bind to a site other than the binding-site of the usual substrate and exert an allosteric effect to change the shape of the usual binding-site. For example, strychnine acts as an allosteric inhibitor of the glycine receptor in the mammalian spinal cord and brain stem. Glycine is a major post-synaptic inhibitory neurotransmitter with a specific receptor site. Strychnine binds to an alternate site that reduces the affinity of the glycine receptor for glycine, resulting in convulsions due to
Enzyme lessened inhibition by the glycine.[68] In competitive inhibition the maximal rate of the reaction is not changed, but higher substrate concentrations are required to reach a given maximum rate, increasing the apparent Km. Uncompetitive inhibition In uncompetitive inhibition, the inhibitor cannot bind to the free enzyme, only to the ES-complex. The EIS-complex thus formed is enzymatically inactive. This type of inhibition is rare, but may occur in multimeric enzymes. Non-competitive inhibition Non-competitive inhibitors can bind to the enzyme at the binding site at the same time as the substrate,but not to the active site. Both the EI and EIS complexes are enzymatically inactive. Because the inhibitor can not be driven from the enzyme by higher substrate concentration (in contrast to competitive inhibition), the apparent Vmax changes. But because the substrate can still bind to the enzyme, the Km stays the same.
88
Types of inhibition. This classification was introduced by W.W. Cleland.
[66]
Mixed inhibition This type of inhibition resembles the non-competitive, except that the EIS-complex has residual enzymatic activity.This type of inhibitor does not follow Michaelis-Menten equation. In many organisms, inhibitors may act as part of a feedback mechanism. If an enzyme produces too much of one substance in the organism, that substance may act as an inhibitor for the enzyme at the beginning of the pathway that produces it, causing production of the substance to slow down or stop when there is sufficient amount. This is a form of negative feedback. Enzymes that are subject to this form of regulation are often multimeric and have allosteric binding sites for regulatory substances. Their substrate/velocity plots are not hyperbolar, but sigmoidal (S-shaped). Irreversible inhibitors react with the enzyme and form a covalent adduct with the protein. The inactivation is irreversible. These compounds include eflornithine a drug used to treat the parasitic disease sleeping sickness.[] Penicillin and Aspirin also act in this The coenzyme folic acid (left) and the anti-cancer drug methotrexate (right) are very manner. With these drugs, the similar in structure. As a result, methotrexate is a competitive inhibitor of many enzymes that use folates. compound is bound in the active site and the enzyme then converts the inhibitor into an activated form that reacts irreversibly with one or more amino acid residues. Uses of inhibitors
Enzyme Since inhibitors modulate the function of enzymes they are often used as drugs. A common example of an inhibitor that is used as a drug is aspirin, which inhibits the COX-1 and COX-2 enzymes that produce the inflammation messenger prostaglandin, thus suppressing pain and inflammation. However, other enzyme inhibitors are poisons. For example, the poison cyanide is an irreversible enzyme inhibitor that combines with the copper and iron in the active site of the enzyme cytochrome c oxidase and blocks cellular respiration.[69]
89
Biological function
Enzymes serve a wide variety of functions inside living organisms. They are indispensable for signal transduction and cell regulation, often via kinases and phosphatases.[70] They also generate movement, with myosin hydrolyzing ATP to generate muscle contraction and also moving cargo around the cell as part of the cytoskeleton.[71] Other ATPases in the cell membrane are ion pumps involved in active transport. Enzymes are also involved in more exotic functions, such as luciferase generating light in fireflies.[72] Viruses can also contain enzymes for infecting cells, such as the HIV integrase and reverse transcriptase, or for viral release from cells, like the influenza virus neuraminidase. An important function of enzymes is in the digestive systems of animals. Enzymes such as amylases and proteases break down large molecules (starch or proteins, respectively) into smaller ones, so they can be absorbed by the intestines. Starch molecules, for example, are too large to be absorbed from the intestine, but enzymes hydrolyze the starch chains into smaller molecules such as maltose and eventually glucose, which can then be absorbed. Different enzymes digest different food substances. In ruminants, which have herbivorous diets, microorganisms in the gut produce another enzyme, cellulase, to break down the cellulose cell walls of plant fiber.[73] Several enzymes can work together in a specific order, creating metabolic pathways. In a metabolic pathway, one enzyme takes the product of another enzyme as a substrate. After the catalytic reaction, the product is then passed on to another enzyme. Sometimes more than one enzyme can catalyze the same reaction in parallel; this can allow more complex regulation: with, for example, a low constant activity provided by one
Glycolytic enzymes and their functions in the metabolic pathway of glycolysis
enzyme but an inducible high activity from a second enzyme. Enzymes determine what steps occur in these pathways. Without enzymes, metabolism would neither progress through the same steps nor be fast enough to serve the needs of the cell. Indeed, a metabolic pathway such as glycolysis could not exist independently of enzymes. Glucose, for example, can react directly with ATP to become phosphorylated at one or more of its carbons. In the absence of enzymes, this occurs so slowly as to be insignificant. However, if hexokinase is added, these slow reactions continue to take place except that phosphorylation at carbon 6 occurs so rapidly that, if the mixture is tested a short time later, glucose-6-phosphate is found to be the only significant product. As a consequence, the network of metabolic pathways within each cell depends on the set of functional enzymes that are present.
Enzyme
90
Control of activity
There are five main ways that enzyme activity is controlled in the cell. 1. Enzyme production (transcription and translation of enzyme genes) can be enhanced or diminished by a cell in response to changes in the cell's environment. This form of gene regulation is called enzyme induction and inhibition. For example, bacteria may become resistant to antibiotics such as penicillin because enzymes called beta-lactamases are induced that hydrolyze the crucial beta-lactam ring within the penicillin molecule. Another example are enzymes in the liver called cytochrome P450 oxidases, which are important in drug metabolism. Induction or inhibition of these enzymes can cause drug interactions. 2. Enzymes can be compartmentalized, with different metabolic pathways occurring in different cellular compartments. For example, fatty acids are synthesized by one set of enzymes in the cytosol, endoplasmic reticulum and the Golgi apparatus and used by a different set of enzymes as a source of energy in the mitochondrion, through β-oxidation.[74] 3. Enzymes can be regulated by inhibitors and activators. For example, the end product(s) of a metabolic pathway are often inhibitors for one of the first enzymes of the pathway (usually the first irreversible step, called committed step), thus regulating the amount of end product made by the pathways. Such a regulatory mechanism is called a negative feedback mechanism, because the amount of the end product produced is regulated by its own concentration. Negative feedback mechanism can effectively adjust the rate of synthesis of intermediate metabolites according to the demands of the cells. This helps allocate materials and energy economically, and prevents the manufacture of excess end products. The control of enzymatic action helps to maintain a stable internal environment in living organisms. 4. Enzymes can be regulated through post-translational modification. This can include phosphorylation, myristoylation and glycosylation. For example, in the response to insulin, the phosphorylation of multiple enzymes, including glycogen synthase, helps control the synthesis or degradation of glycogen and allows the cell to respond to changes in blood sugar.[75] Another example of post-translational modification is the cleavage of the polypeptide chain. Chymotrypsin, a digestive protease, is produced in inactive form as chymotrypsinogen in the pancreas and transported in this form to the stomach where it is activated. This stops the enzyme from digesting the pancreas or other tissues before it enters the gut. This type of inactive precursor to an enzyme is known as a zymogen. 5. Some enzymes may become activated when localized to a different environment (e.g., from a reducing (cytoplasm) to an oxidizing (periplasm) environment, high pH to low pH, etc.). For example, hemagglutinin in the influenza virus is activated by a conformational change caused by the acidic conditions, these occur when it is taken up inside its host cell and enters the lysosome.[76]
Enzyme
91
Involvement in disease
Since the tight control of enzyme activity is essential for homeostasis, any malfunction (mutation, overproduction, underproduction or deletion) of a single critical enzyme can lead to a genetic disease. The importance of enzymes is shown by the fact that a lethal illness can be caused by the malfunction of just one type of enzyme out of the thousands of types present in our bodies. One example is the most common type of phenylketonuria. A mutation of a single amino acid in the enzyme phenylalanine hydroxylase, which catalyzes the first step in the degradation of phenylalanine, results in build-up of phenylalanine and related products. This can lead to mental retardation if the disease is untreated.[77] Another example of enzyme deficiency is pseudocholinesterase, in which there is slow metabolic degradation of exogenous choline.[citation needed]
Phenylalanine hydroxylase. Created from PDB 1KW0 [78]
Another example is when germline mutations in genes coding for DNA repair enzymes cause hereditary cancer syndromes such as xeroderma pigmentosum. Defects in these enzymes cause cancer since the body is less able to repair mutations in the genome. This causes a slow accumulation of mutations and results in the development of many types of cancer in the sufferer. Oral administration of enzymes can be used to treat several diseases (e.g. pancreatic insufficiency and lactose intolerance). Since enzymes are proteins themselves they are potentially subject to inactivation and digestion in the gastrointestinal environment. Therefore a non-invasive imaging assay was developed to monitor gastrointestinal activity of exogenous enzymes (prolyl endopeptidase as potential adjuvant therapy for celiac disease) in vivo.[78]
Naming conventions
An enzyme's name is often derived from its substrate or the chemical reaction it catalyzes, with the word ending in -ase. Examples are lactase, alcohol dehydrogenase and DNA polymerase. This may result in different enzymes, called isozymes, with the same function having the same basic name. Isoenzymes have a different amino acid sequence and might be distinguished by their optimal pH, kinetic properties or immunologically. Isoenzyme and isozyme are homologous proteins. Furthermore, the normal physiological reaction an enzyme catalyzes may not be the same as under artificial conditions. This can result in the same enzyme being identified with two different names. For example, glucose isomerase, which is used industrially to convert glucose into the sweetener fructose, is a xylose isomerase in vivo (within the body). The International Union of Biochemistry and Molecular Biology have developed a nomenclature for enzymes, the EC numbers; each enzyme is described by a sequence of four numbers preceded by "EC". The first number broadly classifies the enzyme based on its mechanism. The top-level classification is[79] • EC 1 Oxidoreductases: catalyze oxidation/reduction reactions • EC 2 Transferases: transfer a functional group (e.g. a methyl or phosphate group) • EC 3 Hydrolases: catalyze the hydrolysis of various bonds • EC 4 Lyases: cleave various bonds by means other than hydrolysis and oxidation • EC 5 Isomerases: catalyze isomerization changes within a single molecule
Enzyme • EC 6 Ligases: join two molecules with covalent bonds. According to the naming conventions, enzymes are generally classified into six main family classes and many sub-family classes. Some web-servers, e.g., EzyPred [82] [80] and bioinformatics tools have been developed to predict which main family class [81] and sub-family class [82] [83] an enzyme molecule belongs to according to its sequence information alone via the pseudo amino acid composition.
92
Industrial applications
Enzymes are used in the chemical industry and other industrial applications when extremely specific catalysts are required. However, enzymes in general are limited in the number of reactions they have evolved to catalyze and also by their lack of stability in organic solvents and at high temperatures. As a consequence, protein engineering is an active area of research and involves attempts to create new enzymes with novel properties, either through rational design or in vitro evolution.[84][85] These efforts have begun to be successful, and a few enzymes have now been designed "from scratch" to catalyze reactions that do not occur in nature.[86]
Application Food processing Enzymes used Amylases from fungi and plants Uses Production of sugars from starch, such as in making [87] high-fructose corn syrup. In baking, catalyze breakdown of starch in the flour to sugar. Yeast fermentation of sugar produces the carbon dioxide that raises the dough.
Amylases catalyze the release of simple sugars from starch. Baby foods Brewing industry
Proteases
Biscuit manufacturers use them to lower the protein level of flour.
Trypsin Enzymes from barley are released during the mashing stage of beer production. Industrially produced barley enzymes Amylase, glucanases, proteases Betaglucanases and arabinoxylanases Amyloglucosidase and pullulanases
To predigest baby foods They degrade starch and proteins to produce simple sugar, amino acids and peptides that are used by yeast for fermentation. Widely used in the brewing process to substitute for the natural enzymes found in barley. Split polysaccharides and proteins in the malt. Improve the wort and beer filtration characteristics.
Low-calorie beer and adjustment of fermentability.
Germinating barley used for malt
Proteases Acetolactatedecarboxylase (ALDC)
Remove cloudiness produced during storage of beers. Increases fermentation efficiency by reducing diacetyl [88] formation. Clarify fruit juices.
Fruit juices
Cellulases, pectinases
Enzyme
93
Rennin, derived from the stomachs Manufacture of cheese, used to hydrolyze protein of young ruminant animals (like calves and lambs)
Dairy industry
Microbially produced enzyme
Now finding increasing use in the dairy industry
Lipases
Is implemented during the production of Roquefort cheese to enhance the ripening of the blue-mold cheese.
Roquefort cheese Meat tenderizers Starch industry
Lactases
Break down lactose to glucose and galactose.
Papain
To soften meat for cooking
Amylases, amyloglucosideases and Converts starch into glucose and various syrups. glucoamylases Glucose isomerase Converts glucose into fructose in production of high-fructose syrups from starchy materials. These syrups have enhanced sweetening properties and lower calorific values than sucrose for the same level of sweetness. Degrade starch to lower viscosity, aiding sizing and coating paper. Xylanases reduce bleach required for decolorizing; cellulases smooth fibers, enhance water drainage, and promote ink removal; lipases reduce pitch and lignin-degrading enzymes remove lignin to soften paper.
Glucose
Fructose
Paper industry
Amylases, Xylanases, Cellulases and ligninases
A paper mill in South Carolina Biofuel industry Cellulases Used to break down cellulose into sugars that can be fermented (see cellulosic ethanol)
Ligninases
Use of lignin waste
Cellulose in 3D Biological detergent Primarily proteases, produced in an Used for presoak conditions and direct liquid extracellular form from bacteria applications helping with removal of protein stains from clothes Amylases Detergents for machine dish washing to remove resistant starch residues Used to assist in the removal of fatty and oily stains Used in biological fabric conditioners
Lipases Cellulases
Enzyme
94
Proteases To remove proteins on contact lens to prevent infections To generate oxygen from peroxide to convert latex into foam rubber Dissolve gelatin off scrap film, allowing recovery of its silver content. Used to manipulate DNA in genetic engineering, important in pharmacology, agriculture and medicine. Essential for restriction digestion and the polymerase chain reaction. Molecular biology is also important in forensic science.
Contact lens cleaners
Rubber industry
Catalase
Photographic industry
Protease (ficin)
Molecular biology
Restriction enzymes, DNA ligase and polymerases
Part of the DNA double helix
References
[7] Williams, H. S. (1904) A History of Science: in Five Volumes. Volume IV: Modern Development of the Chemical and Biological Sciences (http:/ / etext. lib. virginia. edu/ toc/ modeng/ public/ Wil4Sci. html) Harper and Brothers (New York) Accessed 4 April 2007 [9] Kühne coined the word "enzyme" in: W. Kühne (1877) " Über das Verhalten verschiedener organisirter und sog. ungeformter Fermente (http:/ / books. google. com/ books?id=jzdMAAAAYAAJ& pg=PA190& ie=ISO-8859-1& output=html)" (On the behavior of various organized and so-called unformed ferments), Verhandlungen des naturhistorisch-medicinischen Vereins zu Heidelberg, new series, vol. 1, no. 3, pages 190–193. The relevant passage occurs on page 190: "Um Missverständnissen vorzubeugen und lästige Umschreibungen zu vermeiden schlägt Vortragender vor, die ungeformten oder nicht organisirten Fermente, deren Wirkung ohne Anwesenheit von Organismen und ausserhalb derselben erfolgen kann, als Enzyme zu bezeichnen." (Translation: In order to obviate misunderstandings and avoid cumbersome periphrases, [the author, a university lecturer] suggests designating as "enzymes" the unformed or not organized ferments, whose action can occur without the presence of organisms and outside of the same.) [10] Nobel Laureate Biography of Eduard Buchner at http:/ / nobelprize. org (http:/ / nobelprize. org/ nobel_prizes/ chemistry/ laureates/ 1907/ buchner-bio. html). Retrieved 4 April 2007. [11] Text of Eduard Buchner's 1907 Nobel lecture at http:/ / nobelprize. org (http:/ / nobelprize. org/ nobel_prizes/ chemistry/ laureates/ 1907/ buchner-lecture. html). Retrieved 4 April 2007. [12] The naming of enzymes by adding the suffix "-ase" to the substrate on which the enzyme acts, has been traced to French scientist Émile Duclaux (1840–1904), who intended to honor the discoverers of diastase – the first enzyme to be isolated – by introducing this practice in his book Traité de Microbiologie (http:/ / books. google. com/ books?id=Kp9EAAAAQAAJ& printsec=frontcover), vol. 2 (Paris, France: Masson and Co., 1899). See Chapter 1, especially page 9. [13] Willstätter, R. (1927). Problems and Methods in Enzyme Research. Cornell University Press, Ithaca. quoted in [14] 1946 Nobel prize for Chemistry laureates at http:/ / nobelprize. org (http:/ / nobelprize. org/ nobel_prizes/ chemistry/ laureates/ 1946/ ). Retrieved 4 April 2007. [20] The Catalytic Site Atlas at The European Bioinformatics Institute (http:/ / www. ebi. ac. uk/ thornton-srv/ databases/ CSA/ ). Retrieved 4 April 2007. [51] BRENDA The Comprehensive Enzyme Information System (http:/ / www. brenda. uni-koeln. de/ ). Retrieved 4 April 2007. [55] English translation (http:/ / web. lemoyne. edu/ ~giunta/ menten. html). Retrieved 6 April 2007. [77] Phenylketonuria: NCBI Genes and Disease (http:/ / www. ncbi. nlm. nih. gov/ books/ bv. fcgi?call=bv. View. . ShowSection& rid=gnd. section. 234). Retrieved 4 April 2007. [79] The complete nomenclature can be browsed at Enzyme Nomenclature (http:/ / www. chem. qmul. ac. uk/ iubmb/ enzyme/ ). Recommendations of the Nomenclature Committee of the International Union of Biochemistry and Molecular Biology on the Nomenclature and Classification of Enzymes by the Reactions they Catalyse. Nomenclature Committee of the International Union of Biochemistry and Molecular Biology (NC-IUBMB)
Enzyme
95
Further reading
Etymology and history • "New Beer in an Old Bottle: Eduard Buchner and the Growth of Biochemical Knowledge, edited by Athel Cornish-Bowden and published by Universitat de València (1997): ISBN 84-370-3328-4" (http:/ / web. archive. org/ web/ 20080207101706/ http:/ / bip. cnrs-mrs. fr/ bip10/ buchner. htm). Archived from the original (http:/ / bip. cnrs-mrs. fr/ bip10/ buchner. htm) on 7 February 2008., A history of early enzymology. Williams, Henry Smith, 1863–1943. A History of Science: in Five Volumes. Volume IV: Modern Development of the Chemical and Biological Sciences (http:/ / etext. lib. virginia. edu/ toc/ modeng/ public/ Wil4Sci. html), A textbook from the 19th century. Kleyn J, Hough J (1971). "The microbiology of brewing". Annu. Rev. Microbiol. 25: 583–608. doi: 10.1146/annurev.mi.25.100171.003055 (http:/ / dx. doi. org/ 10. 1146/ annurev. mi. 25. 100171. 003055). PMID 4949040 (http:/ / www. ncbi. nlm. nih. gov/ pubmed/ 4949040). Kinetics and inhibition • Cornish-Bowden, Athel. Fundamentals of Enzyme Kinetics. (3rd edition), Portland Press, 2004. ISBN 1-85578-158-1. Segel Irwin H. Enzyme Kinetics: Behavior and Analysis of Rapid Equilibrium and Steady-State Enzyme Systems. (New Ed edition), Wiley-Interscience, 1993. ISBN 0-471-30309-7. Baynes, John W. Medical Biochemistry. (2nd edition), Elsevier-Mosby, 2005. ISBN 0-7234-3341-0, p. 57.
•
•
•
•
Function and control of enzymes in the cell • Price, N. and Stevens, L. Fundamentals of Enzymology: Cell and Molecular Biology of Catalytic Proteins. Oxford University Press, 1999. ISBN 0-19-850229-X. "Nutritional and Metabolic Diseases" (http:/ / www. ncbi. nlm. nih. gov/ books/ bv. fcgi?rid=gnd. chapter. 86). Chapter of the on-line textbook Introduction to Genes and Disease from the NCBI.
Enzyme structure and mechanism • • • • • Fersht, Alan (1999). Structure and mechanism in protein science: a guide to enzyme catalysis and protein folding. San Francisco: W.H. Freeman. ISBN 0-7167-3268-8. Walsh C (1979). Enzymatic reaction mechanisms. San Francisco: W. H. Freeman. ISBN 0-7167-0070-0. Page, M. I., and Williams, A. (Eds.). Enzyme Mechanisms. Royal Society of Chemistry, 1987. ISBN 0-85186-947-5. Bugg, T. Introduction to Enzyme and Coenzyme Chemistry. (2nd edition), Blackwell Publishing Limited, 2004. ISBN 1-4051-1452-5. Warshel, A. Computer Modeling of Chemical Reactions in enzymes and Solutions. John Wiley & Sons Inc., 1991. ISBN 0-471-18440-3.
•
Enzyme-naming conventions • Enzyme Nomenclature (http:/ / www. chem. qmul. ac. uk/ iubmb/ enzyme/ ), Recommendations for enzyme names from the Nomenclature Committee of the International Union of Biochemistry and Molecular Biology. Koshland, D. The Enzymes, v. I, ch. 7. Acad. Press, New York, 1959.
Thermodynamics • "Reactions and Enzymes" (http:/ / www. emc. maricopa. edu/ faculty/ farabee/ BIOBK/ BioBookEnzym. html) Chapter 10 of on-line biology book at Estrella Mountain Community College. •
Industrial applications • "History of industrial enzymes" (http:/ / www. mapsenzymes. com/ History_of_Enzymes. asp), Article about the history of industrial enzymes from the late 1900s to the present times.
External links
• Structure/Function of Enzymes (http://mcdb-webarchive.mcdb.ucsb.edu/sears/biochemistry/), Web tutorial on enzyme structure and function. • Enzymes in diagnosis (http://www.science2day.info/2008/02/enzyme-test-or-cpk-test-what-is-it.html) Role of enzymes in diagnosis of diseases. • Enzyme spotlight (http://www.ebi.ac.uk/intenz/spotlight.jsp) Monthly feature at the European Bioinformatics Institute on a selected enzyme. • AMFEP (http://www.amfep.org/), Association of Manufacturers and Formulators of Enzyme Products • BRENDA (http://www.brenda-enzymes.org/) database, a comprehensive compilation of information and literature references about all known enzymes; requires payment by commercial users. • Enzyme Structures (http://pdbe.org/ec) Explore 3-D structure data of enzymes in the Protein Data Bank. • Enzyme Structures Database (http://www.ebi.ac.uk/thornton-srv/databases/enzymes/) links to the known 3-D structure data of enzymes in the Protein Data Bank.
Enzyme • ExPASy enzyme (http://us.expasy.org/enzyme/) database, links to Swiss-Prot sequence data, entries in other databases and to related literature searches. • KEGG: Kyoto Encyclopedia of Genes and Genomes (http://www.genome.jp/kegg/) Graphical and hypertext-based information on biochemical pathways and enzymes. • (http://www.enzyme-database.org/) enzyme database • MACiE (http://www.ebi.ac.uk/thornton-srv/databases/MACiE/) database of enzyme reaction mechanisms. • MetaCyc database of enzymes and metabolic pathways • Face-to-Face Interview with Sir John Cornforth who was awarded a Nobel Prize for work on stereochemistry of enzyme-catalyzed reactions (http://www.vega.org.uk/video/programme/19) Freeview video by the Vega Science Trust • Sigma Aldrich Enzyme Assays by Enzyme Name (http://www.sigmaaldrich.com/life-science/metabolomics/ enzyme-explorer.html)—Hundreds of assays sorted by enzyme name. • Bugg TD (2001). "The development of mechanistic enzymology in the 20th century". Nat Prod Rep 18 (5): 465–93. doi: 10.1039/b009205n (http://dx.doi.org/10.1039/b009205n). PMID 11699881 (http://www.ncbi. nlm.nih.gov/pubmed/11699881).
96
Paneth cell
97
Paneth cell
Paneth cell
Paneth cells Latin MeSH Code cellula panethensis Paneth+Cells
[1]
TH H3.04.03.0.00017
Paneth cells, along with goblet cells, enterocytes, and enteroendocrine cells, represent the principal cell types of the epithelium of the small intestine.[1] (A few may also be found sporadically in the cecum and appendix.) They are identified microscopically by their location just below the intestinal stem cells in the intestinal glands (AKA crypts of Lieberkühn) and the large eosinophilic refractile granules that occupy most of their cytoplasm. These granules consist of several anti-microbial compounds and other compounds that are known to be important in immunity and host-defense. When exposed to bacteria or bacterial antigens, Paneth cells secrete some of these compounds into the lumen of the intestinal gland, thereby contributing to maintenance of the gastrointestinal barrier. Paneth cells are named after Joseph Paneth (1857–1890), an Austrian physician.
Location
Paneth cells are found throughout the small intestine and the appendix at the base of the intestinal glands.[2] The Paneth cell numbers demonstrate an ascending trend with highest numbers towards the distal end of the small intestine. Like the other epithelial cell lineages in the small intestine, paneth cells originate at the stem cell region near the bottom of the gland.[3] However, unlike the other epithelial cell types, paneth cells migrate downward from the stem cell region and settle just adjacent to it.[3] This close relationship to the stem cell region is thought to suggest that Paneth cells are important in defending the gland stem cells from microbial damage,[3] although their function is not entirely known.[2] Furthermore, among the four aforementioned intestinal cell lineages, the Paneth cells live the longest (18-23 days).
Function
Small intestinal crypts house stem cells that serve to constantly replenish epithelial cells that die and are lost from the villi. Protection of these stem cells is essential for long-term maintenance of the intestinal epithelium, and the location of Paneth cells adjacent to stem cells suggests that they play a critical role in defending epithelial cell renewal.
Sensing microbiota
Paneth cells sense bacteria via MyD88-dependent toll-like receptor (TLR) activation which then triggers antimicrobial action.[4]
Paneth cell
98
Secretions
Defensins
The principal defense molecules secreted by Paneth cells are alpha-defensins, which are known as cryptdins in mice.[5] These peptides have hydrophobic and positively-charged domains that can interact with phospholipids in cell membranes. This structure allows defensins to insert into membranes, where they interact with one another to form pores that disrupt membrane function, leading to cell lysis. Due to the higher concentration of negatively-charged phospholipids in bacterial than vertebrate cell membranes, defensins preferentially bind to and disrupt bacterial cells, sparing the cells they are functioning to protect.[6] Paneth cells are stimulated to secrete defensins when exposed to bacteria (both Gram positive and negative types) or such bacterial products as lipopolysaccharide, muramyl dipeptide and lipid A.
Other secretions
In addition to defensins, Paneth cells secrete lysozyme,[] tumor necrosis factor-alpha,[] and phospholipase A2.[citation needed] Lysozyme and phospholipase A2 both have clear antimicrobial activity. This battery of secretory molecules gives Paneth cells a potent arsenal against a broad spectrum of agents, including bacteria, fungi and even some enveloped viruses.
References
[1] http:/ / www. copewithcytokines. org/ cope. cgi?key=Paneth%20cells [2] http:/ / www. britannica. com/ EBchecked/ topic/ 441200/ Paneths-cell [3] http:/ / books. google. com/ books?id=wSTISCdSIosC& pg=PA244& lpg=PA244& dq=paneth+ cell& source=vrt& ots=KZ4tH-wh4s& sig=mMRz3PETnVY9URDkCDyjoIGkLM8& hl=en& ei=fOR-TeW2BInagQeSyoGgCA& sa=X& oi=book_result& ct=result& resnum=13& ved=0CHkQ6AEwDA#v=onepage& q=paneth%20cell& f=false
Further reading
• Ganz T (1999). "Defensins and host defense.". Science 286 (5439): 420–1. doi: 10.1126/science.286.5439.420 (http://dx.doi.org/10.1126/science.286.5439.420). PMID 10577203 (http://www.ncbi.nlm.nih.gov/ pubmed/10577203). • Ganz T (2000). "Paneth cells--guardians of the gut cell hatchery.". Nat Immunol 1 (2): 99–100. doi: 10.1038/77884 (http://dx.doi.org/10.1038/77884). PMID 11248797 (http://www.ncbi.nlm.nih.gov/ pubmed/11248797).
External links
• BU Histology Learning System: 11604loa (http://www.bu.edu/histology/p/11604loa.htm) - "Endocrine System: duodenum, enteroendocrine cells" • BU Histology Learning System: 11606loa (http://www.bu.edu/histology/p/11606loa.htm) - "Digestive System: Alimentary Canal - duodenum, paneth cells" • Overview and diagram at colostate.edu (http://www.vivo.colostate.edu/hbooks/pathphys/digestion/smallgut/ paneth.html) • Histology at ucsd.edu (http://meded.ucsd.edu/hist-img-bank/chapter_6/Slide_94_crypts_duodenum/pages/b. 6.94.1.5.htm)
Intestine
99
Intestine
In human anatomy, the intestine (or bowel, hose or gut) is the segment of the alimentary canal extending from the pyloric sphincter of the stomach to the anus and, in humans and other mammals, consists of two segments, the small intestine and the large intestine. In humans, the small intestine is further subdivided into the duodenum, jejunum and ileum while the large intestine is subdivided into the cecum and colon.[1]
Structure and function
The structure and function can be described both as gross anatomy and at a microscopic level. The intestinal tract can be broadly divided into two different parts, the small and large intestine.[2] People will have different sized intestines according to their size and age. The intestine is divided into two parts: The Small Intestine and the Large Intestine. The lumen is the cavity where digested food passes through and from where nutrients are absorbed. Both intestines share a general structure with the whole gut, and are composed of several layers. Going from inside the lumen radially outwards, one passes the mucosa (glandular epithelium and muscularis mucosa), sub mucosa, muscularis externa (made up of inner circular and outer longitudinal), and lastly serosa.
• Along the whole length of the gut in the glandular epithelium are goblet cells. These secrete mucus which lubricates the passage of food along and protects it from digestive enzymes. In the small intestine, villi are vaginations (folds) of the mucosa and increase the overall surface area of the intestine while also containing a lacteal, which is connected to the lymph system and aids in the removal of lipids and tissue fluid from the blood supply. Micro villi are present on the epithelium of a villus and further increase the surface area over which The general structure of the intestinal wall absorption can take place. Pocket-like invaginations into the underlying tissue are termed Crypts of Lieberkühn. In the large intestines, villi are absent and a flat surface with thousands of crypts is observed. • Underlying the epithelium is the lamina propria, which contains myofibroblasts, blood vessels, nerves, and several different immune cells. • The next layer is the muscularis mucosa which is a layer of smooth muscle that aids in the action of continued peristalsis and catastalsis along the gut. The sub mucosa contains nerves (e.g. Meissner's plexus), blood vessels and elastic fibre with collagen that stretches with increased capacity but maintains the shape of the intestine.
Intestine • Surrounding this is the muscularis externa which comprises longitudinal and circular smooth muscle that again helps with continued peristalsis and the movement of digested material out of and along the gut. In between the two layers of muscle lies Auerbach's plexus. • Lastly there is the serosa which is made up of loose connective tissue and coated in mucus so as to prevent friction damage from the intestine rubbing against other tissue. Holding all this in place are the mesenteries which suspend the intestine in the abdominal cavity and stop it being disturbed when a person is physically active. The large intestine hosts several kinds of bacteria that deal with molecules the human body is not able to break down itself.[citation needed] This is an example of symbiosis. These bacteria also account for the production of gases inside our intestine (this gas is released as flatulence when eliminated through the anus). However the large intestine is mainly concerned with the absorption of water from digested material (which is regulated by the hypothalamus) and the re absorption of sodium, as well as any nutrients that may have escaped primary digestion in the ileum.
100
Diseases and disorders
• • • • Gastroenteritis is an inflammation of the intestines. It is the most common disease of all the intestines. Ileus is a blockage of the intestines. Ileitis is an inflammation of the ileum. Colitis is an inflammation of the large intestine.
• Appendicitis is inflammation of the vermiform appendix located at the caecum. This is a potentially fatal disease if left untreated; most cases of appendicitis require surgical intervention. • Coeliac disease is a common form of malabsorption, affecting up to 1% of people of northern European descent. An autoimmune response is triggered in intestinal cells by digestion of gluten proteins. Ingestion of proteins found in wheat, barley and rye, causes villous atrophy in the small intestine. Lifelong dietary avoidance of these foodstuffs in a gluten-free diet is the only treatment. • Crohn's disease and ulcerative colitis are examples of inflammatory bowel disease. While Crohn's can affect the entire gastrointestinal tract, ulcerative colitis is limited to the large intestine. Crohn's disease is widely regarded as an autoimmune disease. Although ulcerative colitis is often treated as though it were an autoimmune disease, there is no consensus that it actually is such. (See List of autoimmune diseases). • Enteroviruses are named by their transmission-route through the intestine (enteric meaning intestinal), but their symptoms aren't mainly associated with the intestine. • Irritable bowel syndrome (IBS) is the most common functional disorder of the intestine. Functional constipation and chronic functional abdominal pain are other disorders of the intestine that have physiological causes, but do not have identifiable structural, chemical, or infectious pathologies. They are aberrations of normal bowel function but not diseases.[3] • Diverticular disease is a condition that is very common in older people in industrialized countries. It usually affects the large intestine but has been known to affect the small intestine as well. Diverticulosis occurs when pouches form on the intestinal wall. Once the pouches become inflamed it is known as diverticulitis. • Endometriosis can affect the intestines, with similar symptoms to IBS. • Bowel twist (or similarly, bowel strangulation) is a comparatively rare event (usually developing sometime after major bowel surgery). It is, however, hard to diagnose correctly, and if left uncorrected can lead to bowel infarction and death. (The singer Maurice Gibb is understood to have died from this.) • Angiodysplasia of the colon • Chronic functional abdominal pain • Colorectal cancer • Constipation • Diarrhea • Hirschsprung's disease (aganglionosis) • Intussusception
Intestine • Polyp (medicine) (see also Colorectal polyp) • Pseudomembranous colitis • Ulcerative colitis and toxic megacolon
101
In non-human animals
Animal intestines have multiple uses. From each species of livestock that is a source of milk, a corresponding rennet is obtained from the intestines of milk-fed calves. Pig and calf intestines are eaten, and pig intestines are used as sausage casings. Calf intestines supply Calf Intestinal Alkaline Phosphatase (CIP), and are used to make Goldbeater's skin.
References
[3] http:/ / www. irregularbowelsyndrome. info
• Encyclopædia Britannica article on intestine (http://www.britannica.com/eb/article-9002491/intestine) retrieved on 2007-03-27
Bicarbonate
102
Bicarbonate
Bicarbonate
Identifiers CAS number PubChem ChemSpider KEGG ChEBI ChEMBL Beilstein Reference Gmelin Reference 3DMet Jmol-3D images 71-52-3 769 749
[2] [3] [4] [5] [6] [1]
C00288
CHEBI:17544
CHEMBL363707 3903504 49249 B00080
[7] [8]
Image 1 [9] Image 2 Properties
Molecular formula Molar mass log P Acidity (pK )
a
CHO− 3 61.0168 g mol-1 -0.82 10.3 3.7
Basicity (pK )
b
Except where noted otherwise, data are given for materials in their standard state (at 25 °C, 100 kPa) Infobox references
In inorganic chemistry, bicarbonate (IUPAC-recommended nomenclature: hydrogencarbonate[1]) is an intermediate form in the deprotonation of carbonic acid. It is an anion with the chemical formula HCO3−. Bicarbonate serves a crucial biochemical role in the physiological pH buffering system.[]
Bicarbonate
103
Chemical properties
The bicarbonate ion (hydrogen carbonate ion) is an anion with the empirical formula HCO3− and a molecular mass of 61.01 daltons; it consists of one central carbon atom surrounded by three oxygen atoms in a trigonal planar arrangement, with a hydrogen atom attached to one of the oxygens. It is isoelectronic with nitric acid HNO3. The bicarbonate ion carries a negative one formal charge and is the conjugate base of carbonic acid H2CO3; it is the conjugate acid of CO2− 3, the carbonate ion, as shown by these equilibrium reactions. CO32− + 2 H2O H2CO3 + 2 H2O HCO3− + H2O + OH− HCO3− + H3O+ + H2O H2CO3 +2 OH− CO32− + 2 H3O+
A bicarbonate salt forms when a positively charged ion attaches to the negatively charged oxygen atoms of the ion, forming an ionic compound. Many bicarbonates are soluble in water at standard temperature and pressure, in particular sodium bicarbonate contributes to total dissolved solids, a common parameter for assessing water quality.[citation needed]
Biochemical role
Bicarbonate is alkaline, and a vital component of the pH buffering system[] of the human body (maintaining acid-base homeostasis). 70-75% of CO2 in the body is converted into carbonic acid (H2CO3), which can quickly turn into bicarbonate (HCO3−). With carbonic acid as the central intermediate species, bicarbonate – in conjunction with water, hydrogen ions, and carbon dioxide – forms this buffering system, which is maintained at the volatile equilibrium[] required to provide prompt resistance to drastic pH changes in both the acidic and basic directions. This is especially important for protecting tissues of the central nervous system, where pH changes too far outside of the normal range in either direction could prove disastrous (see acidosis or alkalosis). Bicarbonate also acts to regulate pH in the small intestine. It is released from the pancreas in response to the hormone secretin to neutralize the acidic chyme entering the duodenum from the stomach.[2]
Bicarbonate
104
Bicarbonate in the environment
In freshwater ecology, strong photosynthetic activity by freshwater plants in daylight releases gaseous oxygen into the water and at the same time produces bicarbonate ions. These shift the pH upward until in certain circumstances the degree of alkalinity can become toxic to some organisms or can make other chemical constituents such as ammonia toxic. In darkness, when no photosynthesis occurs, respiration processes release carbon dioxide, and no new bicarbonate ions are produced, resulting in a rapid fall in pH.
Other uses
The most common salt of the bicarbonate ion is sodium bicarbonate, NaHCO3, which is commonly known as baking soda. When heated or exposed to an acid such as acetic acid (vinegar), sodium bicarbonate releases carbon dioxide. This is used as a leavening agent in baking. The flow of bicarbonate ions from rocks weathered by the carbonic acid in rainwater is an important part of the carbon cycle. Bicarbonate also serves much in the digestive system. It raises the internal pH of the stomach, after highly acidic digestive juices have finished in their digestion of food. Ammonium bicarbonate is used in digestive biscuit manufacture.
Diagnostics
In diagnostic medicine, the blood value of bicarbonate is one of several indicators of the state of acid-base physiology in the body. The parameter standard bicarbonate concentration (SBCe) is the bicarbonate concentration in the blood at a PaCO2 of 40 mmHg (5.33 kPa), full oxygen saturation and 36 °C.[3]
Reference ranges for blood tests, comparing blood content of bicarbonate (shown in blue at right) with other constituents.
Bicarbonate compounds
• • • • • Sodium bicarbonate Potassium bicarbonate Calcium bicarbonate Ammonium bicarbonate Carbonic acid
References
[2] Berne & Levy, Principles of Physiology [3] Acid Base Balance (page 3) (http:/ / www. nda. ox. ac. uk/ wfsa/ html/ u13/ u1312_03. htm)
External links
• Bicarbonates (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Bicarbonates) at the US National Library of Medicine Medical Subject Headings (MeSH)
Lysozyme
105
Lysozyme
Lysozyme
Lysozyme single crystal Identifiers EC number CAS number 3.2.1.17 [1] [2]
9001-63-2
Databases IntEnz BRENDA ExPASy KEGG MetaCyc PRIAM PDB structures Gene Ontology IntEnz view [3] [4] [5]
BRENDA entry NiceZyme view KEGG entry [6]
metabolic pathway profile [8] [9]
[7]
RCSB PDB AmiGO
PDBe
[10]
PDBsum
[11]
[12]
/ EGO
[13]
Search PMC articles [14]
PubMed articles [15] NCBI proteins [16]
Lysozyme
106
Lysozyme
PDB rendering based on 132l. Available structures PDB Ortholog search: PDBe [17], RCSB [18] List of PDB id codes 133L , 134L , 1B5U , 1B5V , 1B5W , 1B5X , 1B5Y , 1B5Z , 1B7L , 1B7M , 1B7N [29] [30] [31] [32] [33] [34] [35] [36] [37] [38] [39] , 1B7O , 1B7P , 1B7Q , 1B7R , 1B7S , 1BB3 , 1BB4 , 1BB5 , 1C43 , 1C45 , 1C46 [40] [41] [42] [43] [44] [45] [46] [47] [48] [49] [50] , 1C7P , 1CJ6 , 1CJ7 , 1CJ8 , 1CJ9 , 1CKC , 1CKD , 1CKF , 1CKG , 1CKH , [51] [52] [53] [54] [55] [56] [57] [58] [59] [60] 1D6P , 1D6Q , 1DI3 , 1DI4 , 1DI5 , 1EQ4 , 1EQ5 , 1EQE , 1GAY , 1GAZ , 1GB0 [61] [62] [63] [64] [65] [66] [67] [68] [69] [70] [71] , 1GB2 , 1GB3 , 1GB5 , 1GB6 , 1GB7 , 1GB8 , 1GB9 , 1GBO , 1GBW , 1GBX , [72] [73] [74] [75] [76] [77] [78] [79] [80] [81] 1GBY , 1GBZ , 1GDW , 1GDX , 1GE0 , 1GE1 , 1GE2 , 1GE3 , 1GE4 , 1GEV , 1GEZ [82] [83] [84] [85] [86] [87] [88] [89] [90] [91] [92] , 1GF0 , 1GF3 , 1GF4 , 1GF5 , 1GF6 , 1GF7 , 1GF8 , 1GF9 , 1GFA , 1GFE , [93] [94] [95] [96] [97] [98] [99] [100] [101] [102] 1GFG , 1GFH , 1GFJ , 1GFK , 1GFR , 1GFT , 1GFU , 1GFV , 1HNL , 1I1Z , 1I20 [103] [104] [105] [106] [107] [108] [109] [110] [111] [112] [113] , 1I22 , 1INU , 1IOC , 1IP1 , 1IP2 , 1IP3 , 1IP4 , 1IP5 , 1IP6 , 1IP7 , [114] [115] [116] [117] [118] [119] [120] [121] [122] 1IWT , 1IWU , 1IWV , 1IWW , 1IWX , 1IWY , 1IWZ , 1IX0 , 1IY3 , 1IY4 [123] [124] [125] [126] [127] [128] [129] [130] [131] [132] , 1JKA , 1JKB , 1JKC , 1JKD , 1JSF , 1JWR , 1LAA , 1LHH , 1LHI , [133] [134] [135] [136] [137] [138] [139] [140] [141] 1LHJ , 1LHK , 1LHL , 1LHM , 1LMT , 1LOZ , 1LYY , 1LZ1 , 1LZ4 , 1LZ5 [142] [143] [144] [145] [146] [147] [148] [149] [150] [151] , 1LZ6 , 1LZR , 1LZS , 1OP9 , 1OUA , 1OUB , 1OUC , 1OUD , 1OUE , [152] [153] [154] [155] [156] [157] [158] [159] [160] 1OUF , 1OUG , 1OUH , 1OUI , 1OUJ , 1QSW , 1RE2 , 1REM , 1REX , 1REY [161] [162] [163] [164] [165] [166] [167] [168] [169] , 1REZ , 1TAY , 1TBY , 1TCY , 1TDY , 1UBZ , 1W08 , 1WQM , 1WQN [170] [171] [172] [173] [174] [175] [176] [177] [178] , 1WQO , 1WQP , 1WQQ , 1WQR , 1YAM , 1YAN , 1YAO , 1YAP , 1YAQ [179] [180] [181] [182] [183] [184] [185] [186] [187] [188] , 207L , 208L , 2BQA , 2BQB , 2BQC , 2BQD , 2BQE , 2BQF , 2BQG , [189] [190] [191] [192] [193] [194] [195] [196] [197] 2BQH , 2BQI , 2BQJ , 2BQK , 2BQL , 2BQM , 2BQN , 2BQO , 2HEA , 2HEB [198] [199] [200] [201] [202] [203] [204] [205] [206] , 2HEC , 2HED , 2HEE , 2HEF , 2LHM , 2MEA , 2MEB , 2MEC , 2MED [207] [208] [209] [210] [211] [212] [213] [214] [215] [216] , 2MEE , 2MEF , 2MEG , 2MEH , 2MEI , 2NWD , 2ZIJ , 2ZIK , 2ZIL , [217] [218] [219] [220] [221] 2ZWB , 3EBA , 3FE0 , 3LHM , 3LN2
[19] [20] [21] [22] [23] [24] [25] [26] [27] [28]
Identifiers Symbols External IDs EC number LYZ
[222]
; LZM
[223]
OMIM: 153450 3.2.1.17
[227]
MGI: 96897
[224]
HomoloGene: 121490
[225]
GeneCards: LYZ Gene
[226]
Lysozyme
107
Gene Ontology Molecular function • lysozyme activity [228] Cellular component • extracellular region [229] [230] • extracellular space Biological process • inflammatory response • cell wall macromolecule catabolic process
[232] [231]
• cytolysis [234] • defense response to bacterium Sources: Amigo
[235]
[233]
/ QuickGO
[236]
RNA expression pattern
More reference expression data Orthologs Species Entrez Ensembl UniProt RefSeq (mRNA) RefSeq (protein) Location (UCSC) Human 4069
[238] [240]
[237]
Mouse 17105
[239] [241]
ENSG00000090382 P61626
[242] [244]
ENSMUSG00000069516 Q3TXG2
[243] [245]
NM_000239 NP_000230
NM_017372 NP_059068
[246]
[247]
Chr 12: [248] 69.74 – 69.75 Mb
[250]
Chr 10: [249] 116.68 – 116.69 Mb
[251]
PubMed search
Lysozymes, also known as muramidase or N-acetylmuramide glycanhydrolase, are glycoside hydrolases. These are enzymes (EC 3.2.1.17 [252]) that damage bacterial cell walls by catalyzing hydrolysis of 1,4-beta-linkages between N-acetylmuramic acid and N-acetyl-D-glucosamine residues in a peptidoglycan and between N-acetyl-D-glucosamine residues in chitodextrins. Lysozyme is abundant in a number of secretions, such as tears, saliva, human milk, and mucus. It is also present in cytoplasmic granules of the polymorphonuclear neutrophils (PMN). Large amounts of lysozyme can be found in egg white. C-type lysozymes are closely related to alpha-lactalbumin in sequence and structure, making them part of the same family. In humans, the lysozyme enzyme is encoded by the LYZ gene.[][]
Lysozyme
108
Function
The enzyme functions by attacking peptidoglycans (found in the cell walls of bacteria, especially Gram-positive bacteria) and hydrolyzing the glycosidic bond that connects N-acetylmuramic acid with the fourth carbon atom of N-acetylglucosamine. It does this by binding to the peptidoglycan molecule in the binding site within the prominent cleft between its two domains. This causes the substrate molecule to adopt a strained conformation similar to that of the transition state.[] According to Phillips-Mechanism, the lysozyme binds to a hexasaccharide. The lysozyme then distorts the fourth sugar in hexasaccharide (the D ring) into a half-chair conformation. In this stressed state, the glycosidic bond is easily broken.
Overview of the reaction
The amino acid side-chains glutamic acid 35 (Glu35) and aspartate 52 (Asp52) have been found to be critical to the activity of this enzyme. Glu35 acts as a proton donor to the glycosidic bond, cleaving the C-O bond in the substrate, whereas Asp52 acts as a nucleophile to generate a glycosyl enzyme intermediate. The glycosyl enzyme intermediate then reacts with a water molecule, to give the product of hydrolysis and leaving the enzyme unchanged.[]
Role in disease
Lysozyme is part of the innate immune system. Reduced lysozyme levels have been associated with bronchopulmonary dysplasia in newborns.[] Children fed infant formula lacking lysozyme in their diet have three times the rate of diarrheal disease.[] Since lysozyme is a natural form of protection from gram-positive pathogens like Bacillus and Streptococcus,[1] a deficiency due to infant formula feeding can lead to increased incidence of disease. Whereas the skin is a protective barrier due to its dryness and acidity, the conjunctiva (membrane covering the eye) is, instead, protected by secreted enzymes, mainly lysozyme and defensin. However, when these protective barriers fail, conjunctivitis results. In certain cancers (especially myelomonocytic leukemia) excessive production of lysozyme by cancer cells can lead to toxic levels of lysozyme in the blood. High lysozyme blood levels can lead to kidney failure and low blood potassium, conditions that may improve or resolve with treatment of the primary malignancy.
Lysozyme
109
History
The antibacterial property of hen egg white, due to the lysozyme it contains, was first observed by Laschtschenko in 1909,[] although it was not until 1922 that the name 'lysozyme' was coined, by Alexander Fleming (1881–1955), the discoverer of penicillin.[] Fleming first observed the antibacterial action of lysozyme when he treated bacterial cultures with nasal mucus from a patient suffering from a head cold.[] The three-dimensional structure of hen egg white lysozyme was described by David Chilton Phillips (1924–1999) in 1965, when he obtained the first 2-Ångström (200 pm) resolution model via X-ray crystallography.[2][3] The structure was publicly presented at a Royal Institution lecture in 1965.[] Lysozyme was the second protein structure and the first enzyme structure to be solved via X-ray diffraction methods, and the first enzyme to be fully sequenced that contains all twenty common amino acids.[] As a result of Phillips' elucidation of the structure of lysozyme, it was also the first enzyme to have a detailed, specific mechanism suggested for its method of catalytic action.[] This work led Phillips to provide an explanation for how enzymes speed up a chemical reaction in terms of its physical structures. The original mechanism proposed by Phillips was more recently revised.[4] Howard Florey (1898–1968) and Ernst B. Chain (1906–1979) also investigated lysozymes. Although they never made much progress in this field, they, along with Fleming, developed penicillin.
References
[1] Microbiology: A human perspective. Nester, Anderson, Roberts, Nester. 5th Ed. 2007
External links
• Muramidase (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Muramidase) at the US National Library of Medicine Medical Subject Headings (MeSH) • "Lysozyme: enzyme, sequence, crystallization, structure" (http://lysozyme.co.uk/). lysozyme.co.uk. Retrieved 2009-01-04. • Proteopedia.org HEW Lysozyme (http://www.proteopedia.org/wiki/index.php/ Hen_Egg-White_(HEW)_Lysozyme) • JBdirectory: Lysozyme chloride (http://health.jbdirectory.com/Lysozyme_chloride)
Surfactant
110
Surfactant
Surfactants are compounds that lower the surface tension of a liquid, the interfacial tension between two liquids, or that between a liquid and a solid. Surfactants may act as detergents, wetting agents, emulsifiers, foaming agents, and dispersants.
Etymology and definition
The term surfactant/surfactants is a blend of surface active agents.[] In Index Medicus and the United States National Library of Medicine, surfactant/surfactants is reserved for the meaning pulmonary surfactant. For the more general meaning, surface active agent/s is the heading.
Micelle in aqueous solution
Composition and structure
Surfactants are usually organic compounds that are amphiphilic, meaning they contain both hydrophobic groups (their tails) and hydrophilic groups (their heads).[] Therefore, a surfactant contains both a water insoluble (or oil soluble) component and a water soluble component. Surfactants will diffuse in water and adsorb at interfaces between air and water or at the interface between oil and water, in the case where water is mixed with oil. The insoluble hydrophobic group may extend out of the bulk water phase, into the air or into the oil phase, while the water soluble head group remains in the water phase. This alignment of surfactants at the surface modifies the surface properties of water at the water/air or water/oil interface. World production of surfactants is estimated at 15 Mton/y, of which about half are soaps. Other surfactants produced on a particularly large scale are linear alkylbenzenesulfonates (1700 kton/y), lignin sulfonates (600 kton/y), fatty alcohol ethoxylates (700 ktons/y), and alkylphenol ethoxylates (500 kton/y).[1]
A micelle—the lipophilic tails of the surfactant ions remain on the inside of the micelle due to unfavourable interactions. The polar "heads" of the micelle, due to favourable interactions with water, form a hydrophilic outer layer that in effect protects the hydrophobic core of the micelle. The compounds that make up a micelle are typically amphiphilic in nature, meaning that micelles are soluble not only in protic solvents such as water but also in aprotic solvents as a reverse micelle.
Structure of surfactant phases in water
In the bulk aqueous phase, surfactants form aggregates, such as micelles, where the hydrophobic tails form the core of the aggregate and the hydrophilic heads are in contact with the surrounding liquid. Other types of aggregates such as spherical or cylindrical micelles or bilayers can be formed. The shape of the aggregates depends on the chemical
Surfactant structure of the surfactants, depending on the balance of the sizes of the hydrophobic tail and hydrophilic head. This is known as the HLB, Hydrophilic-lipophilic balance. Surfactants reduce the surface tension of water by adsorbing at the liquid-gas interface. The relation that links the surface tension and the surface excess is known as the Gibbs isotherm.
111
Dynamics of surfactants at interfaces
The dynamics of adsorption of surfactants is of great importance for practical applications such as foaming, emulsifying or coating processes, where bubbles or drops are rapidly generated and need to be stabilized. The dynamics of adsorption depends on the diffusion coefficient of the surfactants. Indeed, as the interface is created, the adsorption is limited by the diffusion of the surfactants to the interface. In some cases, there exists a barrier of energy for the adsorption or the desorption of the surfactants, then the adsorption dynamics is known as ‘kinetically limited'. Such energy barrier can be due to steric or electrostatic repulsions. The surface rheology of surfactant layers, including the elasticity and viscosity of the surfactant layers plays a very important role in foam or emulsion stability.
Characterization of interfaces and surfactant layers
Interfacial and surface tension can be characterized by classical methods such as the -pendant or spinning drop method Dynamic surface tensions, i.e. surface tension as a function of time, can be obtained by the Maximum Bubble Pressure apparatus The structure of surfactant layers can be studied by ellipsometry or X-Ray reflectivity. Surface rheology can be characterized by the oscillating drop method or shear surface rheometers such as double-cone, double-ring or magnetic rod shear surface rheometer.
Detergents in biochemistry and biotechnology
In solution, detergents help solubilize a variety of chemical species by dissociating aggregates and unfolding proteins. Popular surfactants in the biochemistry laboratory are SDS and CTAB. Detergents are key reagents to extract protein by lysis of the cells and tissues: They disorganize the membrane's lipidic bilayer (SDS, Triton X-100, X-114, CHAPS, DOC, and NP-40), and solubilize proteins. Milder detergents such as (OctylThioGlucosides) are used to solubilize sensible proteins (enzymes, receptors). Non-solubilized material is harvested by centrifugation or other means. For electrophoresis, for example, proteins are classically treated with SDS to denature the native tertiary and quaternary structures, allowing the separation of proteins according to their molecular weight. Detergents have also been used to decellularise organs. This process maintains a matrix of proteins that preserves the structure of the organ and often the microvascular network. The process has been successfully used to prepare organs such as the liver and heart for transplant in rats.[2] Pulmonary surfactants are also naturally secreted by type II cells of the lung alveoli in mammals.
Classification of surfactants
The "tail" of most surfactants are fairly similar, consisting of a hydrocarbon chain, which can be branch, linear, or aromatic. Fluorosurfactants have fluorocarbon chains. Siloxane surfactants have siloxane chains. Many important surfactants include a polyether chain terminating in a highly polar anionic group. The polyether groups often comprise ethoxylated (polyethylene oxide-like) sequences inserted to increase the hydrophilic character of a surfactant. Polypropylene oxides conversely, may be inserted to increase the lipophilic character of a surfactant. Surfactant molecules have either one tail or two; those with two tails are said to be double-chained.
Surfactant
112
Most commonly, surfactants are classified according to polar head group. A non-ionic surfactant has no charge groups in its head. The head of an ionic surfactant carries a net charge. If the charge is negative, the surfactant is more specifically called anionic; if the charge is positive, it is called cationic. If a surfactant contains a head with two oppositely charged groups, it is termed zwitterionic. Commonly encountered surfactants of each type include:
Anionic
Sulfate, sulfonate, and phosphate esters
Surfactant classification according to the composition of their head: nonionic, anionic, cationic, amphoteric.
Anionic surfactants contain anionic functional groups at their head, such as sulfate, sulfonate, phosphate, and carboxylates. Prominent alkyl sulfates include ammonium lauryl sulfate, sodium lauryl sulfate (SDS, sodium dodecyl sulfate, another name for the compound) and the related alkyl-ether sulfates sodium laureth sulfate, also known as sodium lauryl ether sulfate (SLES), and sodium myreth sulfate. Docusates: dioctyl sodium sulfosuccinate, perfluorooctanesulfonate (PFOS), perfluorobutanesulfonate, linear alkylbenzene sulfonates (LABs). These include alkyl-aryl ether phosphates and the alkyl ether phosphate Carboxylates These are the most common surfactants and comprise the alkyl carboxylates (soaps), such as sodium stearate. More specialized species include sodium lauroyl sarcosinate and carboxylate-based fluorosurfactants such as perfluorononanoate, perfluorooctanoate (PFOA or PFO).
Cationic head groups
• pH-dependent primary, secondary, or tertiary amines: Primary and secondary amines become positively charged at pH < 10:[3] • Octenidine dihydrochloride; • Permanently charged quaternary ammonium cation: • Alkyltrimethylammonium salts: cetyl trimethylammonium bromide (CTAB) a.k.a. hexadecyl trimethyl ammonium bromide, cetyl trimethylammonium chloride (CTAC • Cetylpyridinium chloride (CPC) • Benzalkonium chloride (BAC) • Benzethonium chloride (BZT) • 5-Bromo-5-nitro-1,3-dioxane • Dimethyldioctadecylammonium chloride • Cetrimonium bromide • Dioctadecyldimethylammonium bromide (DODAB)
Surfactant
113
Zwitterionic surfactants
Zwitterionic (amphoteric) surfactants have both cationic and anionic centers attached to the same molecule. The cationic part is based on primary, secondary, or tertiary amines or quaternary ammonium cations. The anionic part can be more variable and include sulfonates, as in CHAPS (3-[(3-Cholamidopropyl)dimethylammonio]-1-propanesulfonate). Other anionic groups are sultaines illustrated by cocamidopropyl hydroxysultaine. Betaines, e.g., cocamidopropyl betaine. Phosphates: lecithin
Nonionic surfactant
Many long chain alcohols exhibit some surfactant properties. Prominent among these are the fatty alcohols cetyl alcohol, stearyl alcohol, and cetostearyl alcohol (consisting predominantly of cetyl and stearyl alcohols), and oleyl alcohol. • Polyoxyethylene glycol alkyl ethers (Brij): CH3–(CH2)10–16–(O-C2H4)1–25–OH: • Octaethylene glycol monododecyl ether • Pentaethylene glycol monododecyl ether • Polyoxypropylene glycol alkyl ethers: CH3–(CH2)10–16–(O-C3H6)1–25–O • Glucoside alkyl ethers: CH3–(CH2)10–16–(O-Glucoside)1–3–OH: • Decyl glucoside, • Lauryl glucoside • Octyl glucoside • Polyoxyethylene glycol octylphenol ethers: C8H17–(C6H4)–(O-C2H4)1–25–OH: • Triton X-100 • Polyoxyethylene glycol alkylphenol ethers: C9H19–(C6H4)–(O-C2H4)1–25–OH: • Nonoxynol-9 • Glycerol alkyl esters: • • • • • • • Glyceryl laurate Polyoxyethylene glycol sorbitan alkyl esters: Polysorbate Sorbitan alkyl esters: Spans Cocamide MEA, cocamide DEA Dodecyldimethylamine oxide Block copolymers of polyethylene glycol and polypropylene glycol: Poloxamers Polyethoxylated tallow amine (POEA).
According to the composition of their counter-ion
In the case of ionic surfactants, the counter-ion can be: • Monoatomic / Inorganic: • Cations: metals : alkali metal, alkaline earth metal, transition metal • Anions: halides: chloride (Cl−), bromide (Br−), iodide (I−) • Polyatomic / Organic: • Cations: ammonium, pyridinium, triethanolamine (TEA) • Anions: tosyls, trifluoromethanesulfonates, methylsulfate
Surfactant
114
Current market and forecast
The annual global production of surfactants was 13 million metric tons in 2008, and the annual turnover reached US$24.33 billion in 2009, nearly 2% up from the previous year. The market is expected to experience quite healthy growth by 2.8% annually to 2012 and by 3.5 – 4% thereafter.[4][] Specialists expect the global surfactant market to generate revenues of more than US$41 billion in 2018 – translating to an average annual growth of 4.5%[5]
Health and environmental controversy
Surfactants are routinely deposited in numerous ways on land and into water systems, whether as part of an intended process or as industrial and household waste. Some of them are known to be toxic to animals, ecosystems, and humans, and can increase the diffusion of other environmental contaminants.[][][] As a result, there are proposed or voluntary restrictions on the use of some surfactants. For example, PFOS is a persistent organic pollutant as judged by the Stockholm Convention. Additionally, PFOA has been subject to a voluntary agreement by the U.S. Environmental Protection Agency and eight chemical companies to reduce and eliminate emissions of the chemical and its precursors.[6] The two major surfactants used in the year 2000 were linear alkylbenzene sulfonates (LAS) and the alkyl phenol ethoxylates (APE). They break down in the aerobic conditions found in sewage treatment plants and in soil.[] Ordinary dishwashing detergent, for example, will promote water penetration in soil, but the effect would last only a few days (many standard laundry detergent powders contain levels of chemicals such as alkali and chelating agents that can be damaging to plants and should not be applied to soils). Commercial soil wetting agents will continue to work for a considerable period, but they will eventually be degraded by soil micro-organisms. Some can, however, interfere with the life-cycles of some aquatic organisms, so care should be taken to prevent run-off of these products into streams, and excess product should not be washed down.[citation needed] Anionic surfactants can be found in soils as the result of sludge application, wastewater irrigation, and remediation processes. Relatively high concentrations of surfactants together with multimetals can represent an environmental risk. At low concentrations, surfactant application is unlikely to have a significant effect on trace metal mobility.[7][8]
Biosurfactants
Biosurfactants are surface-active substances synthesised by living cells.[citation needed] Interest in microbial surfactants has been steadily increasing in recent years due to their diversity, environmentally friendly nature, possibility of large-scale production, selectivity, performance under extreme conditions, and potential applications in environmental protection.[][] Biosurfactants enhance the emulsification of hydrocarbons, have the potential to solubilise hydrocarbon contaminants and increase their availability for microbial degradation. The use of chemicals for the treatment of a hydrocarbon polluted site may contaminate the environment with their by-products, whereas biological treatment may efficiently destroy pollutants, while being biodegradable themselves. Hence, biosurfactant-producing microorganisms may play an important role in the accelerated bioremediation of hydrocarbon-contaminated sites.[9][10][] These compounds can also be used in enhanced oil recovery and may be considered for other potential applications in environmental protection.[][11] Other applications include herbicides and pesticides formulations, detergents, healthcare and cosmetics, pulp and paper, coal, textiles, ceramic processing and food industries, uranium ore-processing, and mechanical dewatering of peat.[][][12] Several microorganisms are known to synthesise surface-active agents; most of them are bacteria and yeasts.[13][14] When grown on hydrocarbon substrate as the carbon source, these microorganisms synthesise a wide range of chemicals with surface activity, such as glycolipid, phospholipid, and others.[15][16] These chemicals are synthesised to emulsify the hydrocarbon substrate and facilitate its transport into the cells. In some bacterial species such as Pseudomonas aeruginosa, biosurfactants are also involved in a group motility behavior called swarming motility.
Surfactant
115
Safety and environmental risks
Most anionic and nonionic surfactants are nontoxic, having LD50 comparable to sodium chloride. The situation for cationic surfactants is more diverse. Dialkyldimethylammonium chlorides have very low LD50's (5 g/kg) but alkylbenzyldimethylammonium chloride has an LD50 of 0.35 g/kg. Prolonged exposure of skin to surfactants can cause chaffing because surfactants (e.g., soap) disrupts the lipid coating that protects skin (and other) cells.[1]
Biosurfactants and Deepwater Horizon
The use of biosurfactants as a way to remove petroleum from contaminated sites has been questioned, and criticized as environmentally unsafe. Biosurfactants were not used by BP after the Deepwater Horizon oil spill. However, unprecedented amounts of Corexit (active ingredient: Tween-80), were sprayed directly into the ocean at the leak and on the sea-water's surface, the theory being that the surfactants isolate droplets of oil, making it easier for petroleum-consuming microbes to digest the oil.
Applications
Surfactants play an important role as cleaning, wetting, dispersing, emulsifying, foaming and anti-foaming agents in many practical applications and products, including: • • • • • • • • • • • Detergents Fabric softeners Emulsions Paints Adhesives Inks Anti-fogs Ski waxes, snowboard wax Deinking of recycled papers, in flotation, washing and enzymatic processes Laxatives Agrochemical formulations
• Herbicides (some) • Insecticides • Quantum dot coatings • Biocides (sanitizers) • Cosmetics: • Shampoos • Hair conditioners (after shampoo) • Toothpastes Spermicides (nonoxynol-9) Firefighting Pipelines, liquid drag reducing agent Alkali Surfactant Polymers (used to mobilize oil in oil wells) Ferrofluids Leak Detectors
• • • • • •
Surfactant
116
References
[1] Kurt Kosswig "Surfactants" in Ullmann's Encyclopedia of Industrial Chemistry, Wiley-VCH, 2005, Weinheim. [5] Market Study on Surfactants by Ceresana Research (http:/ / www. ceresana. com/ en/ market-studies/ chemicals/ surfactants) [6] USEPA: "2010/15 PFOA Stewardship Program" (http:/ / www. epa. gov/ opptintr/ pfoa/ pubs/ pfoastewardship. htm) Accessed October 26, 2008.
External links
• Surfactants explained for parents (http://www.curoservice.com/parents_visitors/surfactant/ surfactant_composition_action.asp) • Identification of Surfactants Using Liquid Chromatography-Mass Spectrometry (LC-MS) (http:// littlemsandsailing.wordpress.com/2011/05/01/ identification-of-surfactants-in-commercial-products-by-mass-spectrometry/)
Clara cell
117
Clara cell
Clara cell
Latin exocrinocytus bronchiolaris Code TH H3.05.02.0.00008 [2]
Clara cells are dome-shaped cells with short microvilli found in the small airways (bronchioles) of the lungs.[] Clara cells are found in the ciliated simple epithelium. These cells may secrete glycosaminoglycans to protect the bronchiole lining. Bronchiolar cells gradually increase in number as the number of goblet cells decrease. They are also known as "bronchiolar exocrine cells".[]
Name
"Clara cells" were originally described by their namesake, Max Clara in 1937. Clara was born in South Tyrol in 1899 and died in 1966. He was a Nazi doctor who used tissue from executed victims of the Third Reich for his research at Leipzig, including the work that led to his discovery of Clara cells.[1] Some scholars believe that the eponymous name of these cells should be changed because of the ethical controversy surrounding the discovery of the cells but other scholars disagree and think that the name should remain because it is a testament to a time when medicine crossed an ethical line.[2]
Function
One of the main functions of Clara cells is to protect the bronchiolar epithelium. They do this by secreting a small variety of products, including Clara cell secretory protein (CCSP) and a solution similar to the component of the lung surfactant. They are also responsible for detoxifying harmful substances inhaled into the lungs. Clara cells accomplish this with cytochrome P450 enzymes found in their smooth endoplasmic reticulum. Clara cells also act as a stem cell and multiply and differentiate into ciliated cells to regenerate the bronchiolar epithelium.[3]
Mechanism
The respiratory bronchioles represent the transition from the conducting portion to the respiratory portion of the respiratory system. The narrow channels are usually less than 2 mm in diameter and they are lined by a simple cuboidal epithelium, consisting of ciliated cells and non-ciliated Clara cells, which are unique to bronchioles. In addition to being structurally diverse, Clara cells are also functionally variable. One major function they carry out is the synthesis and secretion of the material lining the bronchiolar lumen. This material includes glycosaminoglycans, proteins such as lysozymes, and conjugation of the secretory portion of IgA antibodies. These play an important defensive role, and they also contribute to the degradation of the mucus produced by the upper airways. The heterogeneous nature of the dense granules within the Clara cell's cytoplasm suggests that they may not all have a secretory function. Some of them may contain lysosomal enzymes, which carry out a digestive role, either in defense: Clara cells engulf airborne toxins and break them down via their cytochrome P-450 enzymes (particularly CYP4B1, which is only present in the clara cells) present in their smooth endoplasmic reticulum; or in the recycling of secretory products. Clara cells are mitotically active cells. They divide and differentiate to form both ciliated and non-ciliated epithelial cells.
Clara cell
118
Role in disease
Clara cells contain Tryptase clara, which is believed to be responsible for cleaving the hemagglutinin surface protein of influenza A virus, thereby activating it and causing the symptoms of flu.[] When the l7Rn6 protein is disrupted in mice, these mice display severe emphysema at birth as a result of disorganization of the Golgi apparatus and formation of aberrant vesicular structures within clara cells.[]
References
[3] http:/ / medical-dictionary. thefreedictionary. com/ Clara+ cell
External links
• • • • BU Histology Learning System: 13805loa (http://www.bu.edu/histology/p/13805loa.htm) -415956935 (http://www.gpnotebook.co.uk/simplepage.cfm?ID=-415956935) at GPnotebook UIUC Histology Subject 1385 (https://histo.life.illinois.edu/histo/atlas/oimages.php?oid=1385) Histology at ucsf.edu (http://pathhsw5m54.ucsf.edu/case24/image245.html)
Somatotropic cell
119
Somatotropic cell
Somatotropic cell
Code TH H3.08.02.2.00021 [1]
Somatotropes are cells in the anterior pituitary that produce growth hormone.
Description
Somatotropic cells constitute 30-40% of anterior pituitary cells. They release growth hormone (GH) in response to Growth hormone releasing hormone (GHRH, or somatocrinin) or are inhibited by GHIH (somatostatin), both received from the hypothalamus via the hypophyseal portal system vein and the secondary plexus. Somatotrope cells are classified as acidophilic cells. These cells take years to grow and mature very slowly. If these cells grow large enough they can impair vision, cause headaches or damage other pituitary functions.
Hormone Deficiency
When levels of somatotropin are low in the body, a physican may prescribe human growth hormone as a drug—see Growth hormone treatment. Deficiency in somatotrope secretion before puberty, or before the end of new bone tissue growth, can lead to pituitary dwarfism. When growth hormone is deficient, blood sugar is low because insulin is not opposed by normal amount of growth hormone. Dwarfs are usually well proportioned, but sometimes have a large head compared to the body.
Hormone Excess
If there is an excess of growth hormone it is usually because of over-secretion of somatotrope cells in the anterior pituitary gland. A significant amount of excess somatotrope secretion before puberty, or before the end of new bone tissue growth, can lead to gigantism. Gigantism is a disease that causes excess growth of body (e.g. being over 7 ft. tall) and unusually long limbs. An excess of secretion of growth hormone after puberty can lead to acromegaly. This is a disease that causes abnormal growth in the hands, head, jaw, and tongue. Some symptoms associated with acromegaly include heavy sweating, oily skin, improper processing of sugars in the diet (diabetes), high blood pressure, increased calcium in urine and swelling of the thyroid gland and arthritis
Bovine
Bovine somatotropin occurs in the pituitary of cattle and differs in structure from human pituitary growth hormone and is biologically inactive in the human being. Bovine somatotropin aids in regulating the amount of milk produced. Recombinant bovine somatotropin (rBST) is a hormone that is injected in cows that increases milk production.
References
• "E-Study Guide For: Human Anatomy" by By Cram101 Reviews, Michael OLoughlin
Prolactin cell
120
Prolactin cell
Prolactin cell
Code TH H3.08.02.2.00022 [1]
Prolactin cell (also known as epsilon acidophil, lactotrope, lactotropic cell, lactotroph, mammatroph, mammotroph) is a cell in the anterior pituitary which produces prolactin in response to hormonal signals including dopamine which is inhibitory and thyrotropin-releasing hormone which is secretagogue. Other regulators include oxytocin, estrogen and progesterone. Prolactin is involved in the maturation of mammary glands and their secretion of milk in association with oxytocin, estrogen, progesterone, glucocorticoids, and others. Prolactin has numerous other effects in both sexes. Prolactin cell are acidophilic by H&E stains and comprise about 20% of all cells in the anterior pituitary gland. If these cells undergo neoplastic transformation, they will give rise to a prolactinoma, a prolactin-secreting pituitary adenoma.
External links
• "Lactotroph [1]" at Dorland's Medical Dictionary
Thyrotropic cell
121
Thyrotropic cell
Thyrotropic cell
Code TH H3.08.02.2.00005 [1]
Thyrotropes (also called thyrotrophs) are endocrine cells in the anterior pituitary which produce thyroid stimulating hormone (TSH) in response to thyrotropin releasing hormone (TRH). Thyrotropes appear basophilic in histological preparations.
Gonadotropic cell
122
Gonadotropic cell
Gonadotropic cell
Code TH H3.08.02.2.00004 [1]
Gonadotropes are endocrine cells in the anterior pituitary that produce the gonadotropins, such as the follicle-stimulating hormone (FSH) and luteinizing hormone (LH). Release of FSH and LH by gonadotrophs is regulated by gonadotropin-releasing hormone (GnRH) from the hypothalamus.[1] Gonadotropes appear basophilic in histological preparations. Gonadotropes have insulin receptors, which can be overstimulated by too high insulin levels. This may lead to infertility as hormone release levels are disrupted. [][2]
References
[1] Ganong, William F.: "Review of Medical Physiology", page 248. Lange, 2005.
Corticotropic cell
123
Corticotropic cell
Corticotropic cell
Code TH H3.08.02.2.00009 [1]
Corticotropes (or corticotrophs) are basophilic cells in the anterior pituitary that produce melanocyte-stimulating hormone, adrenocorticotropic hormone (ACTH) and lipotropin. The cells produce pro-opiomelanocortin (POMC) which undergoes cleavage to ACTH and β-lipotropin (β-LPH). These cells respond to corticotropin releasing hormone (CRH) and make up about 20% of the cells in the anterior pituitary.
Melanocyte-stimulating hormone
pro-opiomelanocortin
Identifiers Symbol POMC Entrez HUGO OMIM RefSeq 5443 9201 [1] [2] [3] [4]
176830
NM_000939
UniProt P01189 [5] Other data Locus Chr. 2 p23 [6]
Melanocyte-stimulating hormone
Clinical data Pregnancy cat. ? Legal status ? Identifiers ATC code ChEMBL ? CHEMBL214332 [7]
Chemical data Formula ? [8]
(what is this?) (verify)
The melanocyte-stimulating hormones (collectively referred to as MSH or intermedins) are a class of peptide hormones that are produced by cells in the intermediate lobe of the pituitary gland. Synthetic analogs of these naturally occurring hormones have also been developed and researched.
Melanocyte-stimulating hormone
124
Function
They stimulate the production and release of melanin (melanogenesis) by melanocytes in skin and hair. MSH signals to the brain have effects on appetite and sexual arousal.
In amphibians
In some animals (such as the claw-toed frog Xenopus laevis) production of MSH is increased when the animal is in a dark location. This causes pigment to be dispersed in pigment cells in the toad's skin, making it become darker, and harder for predators to spot. The pigment cells are called melanophores and therefore, in amphibians, the hormone is often called melanophore-stimulating hormone.
In humans
An increase in MSH will cause a darkening in humans too. Melanocyte-stimulating hormone increases in humans during pregnancy. This, along with increased estrogens, causes increased pigmentation in pregnant women. Cushing's syndrome due to excess adrenocorticotropic hormone (ACTH) may also result in hyperpigmentation, such as acanthosis nigricans in the axilla. Most people with primary Addison's have darkening (hyperpigmentation) of the skin, including areas not exposed to the sun; characteristic sites are skin creases (e.g. of the hands), nipple, and the inside of the cheek (buccal mucosa), new scars become hyperpigmented, whereas older ones do not darken. This occurs because melanocyte-stimulating hormone (MSH) and adrenocorticotropic hormone (ACTH) share the same precursor molecule, Pro-opiomelanocortin (POMC). Different levels of MSH are not the major cause of racial variation in skin colour. However, in many red headed people, and other people who do not tan well, there are variations in their hormone receptors, causing them to not respond to MSH in the blood. See melanocortin receptor for more information.
Structure of MSH
proopiomelanocortin derivatives POMC γ-MSH ACTH α-MSH CLIP β-lipotropin γ-lipotropin β-MSH β-endorphin
Melanocyte-stimulating hormone belongs to a group called the melanocortins. This group includes ACTH, alpha-melanocyte-stimulating hormone (α-MSH), beta-melanocyte-stimulating hormone (β-MSH) and gamma-melanocyte-stimulating hormone (γ-MSH); these peptides are all cleavage products of a large precursor peptide called pro-opiomelanocortin (POMC). α-MSH is the most important melanocortin for pigmentation. The different melanocyte-stimulating hormones have the following amino acid sequences:
Melanocyte-stimulating hormone
125
α-MSH: β-MSH (human):
Ac-Ser-Tyr-Ser-Met-Glu-His-Phe-Arg-Trp-Gly-Lys-Pro-Val Ala-Glu-Lys-Lys-Asp-Glu-Gly-Pro-Tyr-Arg-Met-Glu-His-Phe-Arg-Trp-Gly-Ser-Pro-Pro-Lys-Asp
β-MSH (porcine): Asp-Glu-Gly-Pro-Tyr-Lys-Met-Glu-His-Phe-Arg-Trp-Gly-Ser-Pro-Pro-Lys-Asp γ-MSH: Tyr-Val-Met-Gly-His-Phe-Arg-Trp-Asp-Arg-Phe-Gly
Synthetic MSH
Synthetic analogs of α-MSH have been developed for human use. Two of the better known are afamelanotide (melanotan-1) in testing by Clinuvel Pharmaceuticals in Australia and bremelanotide by Palatin Technologies, a New Jersey company. • Afamelanotide (formerly CUV1647) is being investigated as a method of photoprotection in patients with erythropoietic protoporphyria, polymorphous light eruption, actinic keratosis and squamous cell carcinoma (a form of skin cancer).[1] • An additional analog called Melanotan II causes enhanced libido and erections in most male test subject and arousal with corresponding genital involvement in most female test subjects.[] Bremelanotide (formerly PT-141) which stemmed from Melanotan II research was previously under development by the New Jersey company for its aphrodisiac effects. These effects are mediated by actions in the hypothalamus on neurons that express MC3R and MC4R receptors.
References
[1] Clinuvel FAQs (http:/ / www. clinuvel. com/ en/ faqs/ )
Further reading
• Millington GW (May 2006). "Proopiomelanocortin (POMC): the cutaneous roles of its melanocortin products and receptors". Clin. Exp. Dermatol. 31 (3): 407–12. doi: 10.1111/j.1365-2230.2006.02128.x (http://dx.doi.org/10. 1111/j.1365-2230.2006.02128.x). PMID 16681590 (http://www.ncbi.nlm.nih.gov/pubmed/16681590). • Millington GW (2007). "The role of proopiomelanocortin (POMC) neurones in feeding behaviour" (http://www. ncbi.nlm.nih.gov/pmc/articles/PMC2018708). Nutr Metab (Lond) 4: 18. doi: 10.1186/1743-7075-4-18 (http:// dx.doi.org/10.1186/1743-7075-4-18). PMC 2018708 (http://www.ncbi.nlm.nih.gov/pmc/articles/ PMC2018708). PMID 17764572 (http://www.ncbi.nlm.nih.gov/pubmed/17764572).
External links
• Melanocyte-Stimulating Hormones (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=& term=Melanocyte-Stimulating+Hormones) at the US National Library of Medicine Medical Subject Headings (MeSH) • Clinuvel Pharmaceuticals (http://www.clinuvel.com) • Palatin Technologies (http://www.palatin.com/)
Magnocellular neurosecretory cell
126
Magnocellular neurosecretory cell
Magnocellular neurosecretory cells are large neuroendocrine cells within the supraoptic nucleus and paraventricular nucleus of the hypothalamus. They are also found in smaller numbers in accessory cell groups between these two nuclei, the largest one being the nucleus circularis. There are two types of magnocellular neurosecretory cells, oxytocin-producing cells and vasopressin-producing cells, but a small number can produce both hormones. These cells are neuroendocrine neurons, are electrically excitable, and generate action potentials in response to afferent stimulation.[1] Magnocellular neurosecretory cells in the rat (where these neurons have been most extensively studied) in general have a single long varicose axon, which projects to the posterior pituitary. Each axon gives rise to about 10,000 neurosecretory terminals and many axon swellings that store very large numbers of hormone-containing vesicles.[2] These vesicles are released from the axon swellings and nerve terminals by exocytosis in response to calcium entry through voltage-gated channels, which occurs when action potentials are propagated down the axons.[3] The cells typically have two or three long dendrites, which also contain large dilations, and which also contain a very high density of hormone-containing vesicles. Oxytocin and vasopressin can, thus, be released within the brain from these dendrites, as well as into the blood from the terminals in the posterior pituitary gland.[4] However, the release of oxytocin and vasopressin from dendrites is not consistently accompanied by peripheral secretion, as dendritic release is regulated differently. Dendritic release can be triggered by depolarisation, but can also be triggered by the mobilisation of intracellular calcium stores. The dendrites receive most of the synaptic inputs from afferent neurons that regulate the magnocellular neurons; typically a magnocellular neuron receives about 10,000 synapses from afferent neurons.
References
Oxytocin
127
Oxytocin
Oxytocin
Systematic (IUPAC) name
1-({(4R,7S,10S,13S,16S,19R)-19-amino- 7-(2-amino-2-oxoethyl)- 10-(3-amino-3-oxopropyl)- 16-(4-hydroxybenzoyl)13-[(1S)-1-methylpropyl]- 6,9,12,15,18-pentaoxo- 1,2-dithia- 5,8,11,14,17-pentaazacycloicosan-4-yl}carbonyl)- L-prolylL-leucylglycinamide
Clinical data Trade names AHFS/Drugs.com Pregnancy cat. Legal status Routes Pitocin monograph A (AU) POM (UK) ℞-only (US) Intranasal, IV, IM Pharmacokinetic data Bioavailability Protein binding Metabolism Half-life Excretion nil 30% hepatic oxytocinases 1–6 min Biliary and renal Identifiers CAS number ATC code PubChem IUPHAR ligand 50-56-6 [2] [1]
H01BB02
[3] [4]
CID 439302 2174 [5]
Oxytocin
[6] [8]
128
DrugBank ChemSpider UNII KEGG ChEBI ChEMBL
DB00107 388434
[7]
1JQS135EYN D00089 [9]
CHEBI:7872
[10]
[11]
CHEMBL265640 Chemical data
Formula Mol. mass
C43H66N12O12S2 1007.19 g/mol
(what is this?) (verify)
[12]
Oxytocin (Oxt) (pron.: /ˌɒksɨˈtoʊsɪn/) is a mammalian neurohypophysial hormone that acts primarily as a neuromodulator in the brain. Oxytocin plays roles in sexual reproduction, in particular during and after childbirth. It is released in large amounts after distension of the cervix and uterus during labor, facilitating birth, maternal bonding, and, after stimulation of the nipples, breastfeeding. Both childbirth and milk ejection result from positive feedback mechanisms.[1] Recent studies have begun to investigate oxytocin's role in various behaviors, including orgasm, social recognition, pair bonding, anxiety, and maternal behaviors.[] For this reason, it is sometimes referred to as the "love hormone". There is some evidence that oxytocin promotes ethnocentric behavior, incorporating the trust and empathy of in-groups with their suspicion and rejection of outsiders.[] Furthermore, genetic differences in the oxytocin receptor gene (OXTR) have been associated with maladaptive social traits such as aggressive behaviour.[]
Discovery
The word oxytocin was derived from Greek ὀξύς, oxys, and τόκος, tokos, meaning "quick birth", after its uterine-contracting properties were discovered by British pharmacologist Sir Henry Hallett Dale in 1906.[] The milk ejection property of oxytocin was described by Ott and Scott in 1910[2] and by Schafer and Mackenzie in 1911.[] The nine amino acid sequence of oxytocin was elucidated by Vincent du Vigneaud et al. and by Tuppy in 1953[] and synthesized biochemically soon after by du Vigneaud et al. in 1953.[3][] Oxytocin was the first polypeptide hormone to be sequenced and synthesized.[]
Structure and relation to vasopressin
Oxytocin is a peptide of nine amino acids (a nonapeptide). Its systematic name is cysteine-tyrosine-isoleucine-glutamine-asparagine-cysteine-proline-leucine-glycine-amine (cys – tyr – ile – gln – asn – cys – pro – leu – gly – NH2, or CYIQNCPLG-NH2). Oxytocin has a molecular mass of 1007 daltons. One international unit (IU) of oxytocin is the equivalent of about 2 micrograms of pure peptide. While the structure of oxytocin is highly conserved in placental mammals, a novel structure of oxytocin was recently reported in marmosets, tamarins, and other new world primates. Genomic sequencing of the gene for oxytocin revealed a single in-frame mutation(thymine for cytosine) which results in a single amino acid substitution at the 8-position (proline for leucine).[] The biologically active form of oxytocin, commonly measured by RIA and/or HPLC techniques, is also known as the octapeptide "oxytocin disulfide" (oxidized form), but oxytocin also exists as a reduced dithiol nonapeptide called
Oxytocin oxytoceine.[4] It has been theorized that open chain oxytoceine (the reduced form of oxytocin) may also act as a free radical scavenger (by donating an electron to a free radical); oxytoceine may then be oxidized back to oxytocin via the redox potential of dehydroascorbate <---> ascorbate.[] The structure of oxytocin is very similar to that of vasopressin (cys – tyr – phe – gln – asn – cys – pro – arg – gly – NH2), also a nonapeptide with a sulfur bridge, whose sequence differs from oxytocin by two amino acids. A table showing the sequences of members of the vasopressin/oxytocin superfamily and the species expressing them is present in the vasopressin article. Oxytocin and vasopressin were isolated and synthesized by Vincent du Vigneaud in 1953, work for which he received the Nobel Prize in Chemistry in 1955. Oxytocin and vasopressin are the only known hormones released by the human posterior pituitary gland to act at a distance. However, oxytocin neurons make other Oxytocin (ball-and-stick) bound to its carrier protein neurophysin peptides, including corticotropin-releasing hormone and (ribbons) dynorphin, for example, that act locally. The magnocellular neurons that make oxytocin are adjacent to magnocellular neurons that make vasopressin, and are similar in many respects.
129
Actions
Oxytocin has peripheral (hormonal) actions, and also has actions in the brain. Its actions are mediated by specific, high-affinity oxytocin receptors. The oxytocin receptor is a G-protein-coupled receptor that requires Mg2+ and cholesterol. It belongs to the rhodopsin-type (class I) group of G-protein-coupled receptors.
Peripheral (hormonal) actions
The peripheral actions of oxytocin mainly reflect secretion from the pituitary gland. (See oxytocin receptor for more detail on its action.) • Letdown reflex: In lactating (breastfeeding) mothers, oxytocin acts at the mammary glands, causing milk to be 'let down' into subareolar sinuses, from where it can be excreted via the nipple.[5] Suckling by the infant at the nipple is relayed by spinal nerves to the hypothalamus. The stimulation causes neurons that make oxytocin to fire action potentials in intermittent bursts; these bursts result in the secretion of pulses of oxytocin from the neurosecretory nerve terminals of the pituitary gland. • Uterine contraction: Important for cervical dilation before birth, oxytocin causes contractions during the second and third stages of labor. Oxytocin release during breastfeeding causes mild but often painful contractions during the first few weeks of lactation. This also serves to assist the uterus in clotting the placental attachment point postpartum. However, in knockout mice lacking the oxytocin receptor, reproductive behavior and parturition are normal.[] • Social behavior and wound healing: Oxytocin is also thought to modulate inflammation by decreasing certain cytokines. Thus, the increased release in oxytocin following positive social interactions has the potential to improve wound healing. A study by Marazziti and colleagues used heterosexual couples to address this possibility. They found increases in plasma oxytocin following a social interaction were correlated with faster wound healing. They hypothesized this was due to oxytocin reducing inflammation, thus allowing the wound to heal faster. This study provides preliminary evidence that positive social interactions may directly impact aspects
Oxytocin of health.[6] • The relationship between oxytocin and human sexual response is unclear. At least two uncontrolled studies have found increases in plasma oxytocin at orgasm – in both men and women.[][] Plasma oxytocin levels are notably increased around the time of self-stimulated orgasm and are still higher than baseline when measured five minutes after self arousal.[] The authors of one of these studies speculated that oxytocin's effects on muscle contractibility may facilitate sperm and egg transport.[] In a study measuring oxytocin serum levels in women before and after sexual stimulation, the author suggests it serves an important role in sexual arousal. This study found genital tract stimulation resulted in increased oxytocin immediately after orgasm.[] Another study reported increases of oxytocin during sexual arousal could be in response to nipple/areola, genital, and/or genital tract stimulation as confirmed in other mammals.[] Murphy et al. (1987), studying men, found oxytocin levels were raised throughout sexual arousal with no acute increase at orgasm.[] A more recent study of men found an increase in plasma oxytocin immediately after orgasm, but only in a portion of their sample that did not reach statistical significance. The authors noted these changes "may simply reflect contractile properties on reproductive tissue".[] Oxytocin evokes feelings of contentment, reductions in anxiety, and feelings of calmness and security around the mate.[] This suggests oxytocin may be important for the inhibition of the brain regions associated with behavioral control, fear, and anxiety, thus allowing orgasm to occur. Oxytocin also functions to protect against stress. Meta-analyses conducted in 2003 demonstrated that oxytocin can alleviate mood and reduce stress with a good efficiency.[7] • Due to its similarity to vasopressin, it can reduce the excretion of urine slightly. In several species, oxytocin can stimulate sodium excretion from the kidneys (natriuresis), and, in humans, high doses can result in hyponatremia. • Oxytocin and oxytocin receptors are also found in the heart in some rodents, and the hormone may play a role in the embryonal development of the heart by promoting cardiomyocyte differentiation.[][] However, the absence of either oxytocin or its receptor in knockout mice has not been reported to produce cardiac insufficiencies.[] • Modulation of hypothalamic-pituitary-adrenal axis activity: Oxytocin, under certain circumstances, indirectly inhibits release of adrenocorticotropic hormone and cortisol and, in those situations, may be considered an antagonist of vasopressin.[] • Autism: Oxytocin may play a role in autism and may be an effective treatment for autism's repetitive and affiliative behaviors.[8] Oxytocin treatments also resulted in an increased retention of affective speech in adults with autism.[] Two related studies in adults, in 2003 and 2007, found oxytocin decreased repetitive behaviors and improved interpretation of emotions. More recently, intranasal administration of oxytocin was found to increase emotion recognition in children as young as 12 who are diagnosed with autism spectrum disorders [] Oxytocin has also been implicated in the etiology of autism, with one report suggesting autism is correlated with genomic deletion of the gene containing the oxytocin receptor gene (OXTR). Studies involving Caucasian and Finnish samples and Chinese Han families provide support for the relationship of OXTR with autism.[][] Autism may also be associated with an aberrant methylation of OXTR.[] After treatment with inhaled oxytocin, autistic patients exhibit more appropriate social behavior.[] While this research suggests some promise, further clinical trials of oxytocin are required to demonstrate potential benefit and side effects in the treatment of autism. As such, researchers do not recommend use of oxytocin as a treatment for autism outside of clinical trials. • Increasing trust and reducing fear: In a risky investment game, experimental subjects given nasally administered oxytocin displayed "the highest level of trust" twice as often as the control group. Subjects who were told they were interacting with a computer showed no such reaction, leading to the conclusion that oxytocin was not merely affecting risk-aversion.[] Nasally administered oxytocin has also been reported to reduce fear, possibly by inhibiting the amygdala (which is thought to be responsible for fear responses).[] Indeed, studies in rodents have shown oxytocin can efficiently inhibit fear responses by activating an inhibitory circuit within the amygdala. Some researchers have argued oxytocin has a general enhancing effect on all social emotions, since intranasal
130
Oxytocin administration of oxytocin also increases envy and Schadenfreude.[9] • Oxytocin effects social distance between adult males and females, and may be responsible at least in part for romantic attraction and subsequent monogamous pair bonding. An oxytocin nasal spray caused men in a monogamous relationship, but not single men, to increase the distance between themselves and an attractive woman during a first encounter by 10 to 15 centimeters. The researchers suggested that oxytocin may help promote fidelity within monogamous relationships.[] • Affecting generosity by increasing empathy during perspective taking: In a neuroeconomics experiment, intranasal oxytocin increased generosity in the Ultimatum Game by 80%, but has no effect in the Dictator Game that measures altruism. Perspective-taking is not required in the Dictator Game, but the researchers in this experiment explicitly induced perspective-taking in the Ultimatum Game by not identifying to participants into which role they would be placed.[] Serious methodological questions have arisen, however, with regard to the role of oxytocin in trust and generosity.[10] Empathy in healthy males has been shown to be increased after intranasal oxytocin[][] This is most likely due to the effect of oxytocin in enhancing eye gaze.[] There is some discussion about which aspect of empathy oxytocin might alter – for example, cognitive vs. emotional empathy.[] • Cognitive function: Certain learning and memory functions are impaired by centrally administered oxytocin.[] Also, systemic oxytocin administration can impair memory retrieval in certain aversive memory tasks.[] Interestingly, oxytocin does seem to facilitate learning and memory specifically for social information. Healthy males administered intranasal oxytocin show improved memory for human faces, in particular happy faces.[][] They also show improved recognition for positive social cues over threatening social cues [][] and improved recognition of fear.[11]
131
Actions within the brain
Oxytocin secreted from the pituitary gland cannot re-enter the brain because of the blood–brain barrier. Instead, the behavioral effects of oxytocin are thought to reflect release from centrally projecting oxytocin neurons, different from those that project to the pituitary gland, or that are collaterals from them.[] Oxytocin receptors are expressed by neurons in many parts of the brain and spinal cord, including the amygdala, ventromedial hypothalamus, septum, nucleus accumbens, and brainstem. • Sexual arousal: Oxytocin injected into the cerebrospinal fluid causes spontaneous erections in rats,[] reflecting actions in the hypothalamus and spinal cord. Centrally administrated oxytocin receptor antagonists can prevent noncontact erections, which is a measure of sexual arousal. Studies using oxytocin antagonists in female rats provide data that oxytocin increases lordosis behavior, indicating an increase in sexual receptivity.[] • Bonding: In the prairie vole, oxytocin released into the brain of the female during sexual activity is important for forming a monogamous pair bond with her sexual partner. Vasopressin appears to have a similar effect in males.[12] Oxytocin has a role in social behaviors in many species, so it likely also does in humans. In a 2003 study, both humans and dog oxytocin levels in the blood rose after five to 24 minutes of a petting session. This possibly plays a role in the emotional bonding between humans and dogs.[13] • Maternal behavior: Female rats given oxytocin antagonists after giving birth do not exhibit typical maternal behavior.[] By contrast, virgin female sheep show maternal behavior toward foreign lambs upon cerebrospinal fluid infusion of oxytocin, which they would not do otherwise.[] Oxytocin is involved in the initiation of maternal behavior, not its maintenance; for example, it is higher in mothers after they interact with unfamiliar children rather than their own.[] • Drug interactions: According to some studies in animals, oxytocin inhibits the development of tolerance to various addictive drugs (opiates, cocaine, alcohol), and reduces withdrawal symptoms.[] MDMA (ecstasy) may increase feelings of love, empathy, and connection to others by stimulating oxytocin activity via activation of
Oxytocin serotonin 5-HT1A receptors, if initial studies in animals apply to humans.[] The anxiolytic Buspar (buspirone) also appears to produce some or all of its effect via 5-HT1A receptor-induced oxytocin stimulation.[][] • Preparing fetal neurons for delivery: Crossing the placenta, maternal oxytocin reaches the fetal brain and induces a switch in the action of neurotransmitter GABA from excitatory to inhibitory on fetal cortical neurons. This silences the fetal brain for the period of delivery and reduces its vulnerability to hypoxic damage.[] • Romantic attachment: In some studies, high levels of plasma oxytocin have been correlated with romantic attachment. For example, if a couple is separated for a long period of time, anxiety can increase due to the lack of physical affection. Oxytocin may aid romantically attached couples by decreasing their feelings of anxiety when they are separated.[]
132
Drug forms
Synthetic oxytocin is sold as proprietary medication under the trade names Pitocin and Syntocinon, and as generic oxytocin. Oxytocin is destroyed in the gastrointestinal tract, so must be administered by injection or as nasal spray. It has a half-life of typically about three minutes in the blood, and given intravenously does not enter the brain in significant quantities – it is excluded from the brain by the blood–brain barrier. Evidence in rhesus macaques indicates oxytocin by nasal spray does enter the brain.[] Oxytocin nasal sprays have been used to stimulate breastfeeding, but the efficacy of this approach is doubtful.[] Injected oxytocin analogues are used for labor induction and to support labor in case of difficult parturition. It has largely replaced ergometrine as the principal agent to increase uterine tone in acute postpartum hemorrhage. Oxytocin is also used in veterinary medicine to facilitate birth and to stimulate milk release. The tocolytic agent atosiban (Tractocile) acts as an antagonist of oxytocin receptors; this drug is registered in many countries to suppress premature labor between 24 and 33 weeks of gestation. It has fewer side effects than drugs previously used for this purpose (ritodrine, salbutamol, and terbutaline). The trust-inducing property of oxytocin might help those who suffer from social anxieties and mood disorders,[] but with the potential for abuse with confidence tricks[][] and military applications.[]
Potential adverse reactions
Oxytocin is relatively safe when used at recommended doses, and side effects are uncommon.[] The following maternal events have been reported:[] • • • • • • • • • Subarachnoid hemorrhage Increased heart rate Decreased blood pressure Cardiac arrhythmia and premature ventricular contraction Impaired uterine blood flow Pelvic hematoma Afibrinogenonemia, which can lead to hemorrhage and death Anaphylaxis Nausea and vomiting
Excessive dosage or long-term administration (over a period of 24 hours or longer) have been known to result in tetanic uterine contractions, uterine rupture, postpartum hemorrhage, and water intoxication, sometimes fatal. Increased uterine motility has led to the following complications in the fetus/neonate:[] • Decreased heart rate or heart rate decelerations • Cardiac arrhythmia • Brain damage • Seizures
Oxytocin • Death
133
Synthesis, storage, and release
Oxytocin/neurophysin I prepropeptide
Identifiers Symbols External IDs OXT
[26]
; OT; OT-NPI; OXT-NPI
[27]
OMIM: 167050
MGI: 97453
[28]
HomoloGene: 55494
[29]
GeneCards: OXT Gene
[30]
Oxytocin
134
Gene Ontology Molecular function • neurohypophyseal hormone activity [31] [32] • oxytocin receptor binding Cellular component • extracellular region [229] [230] • extracellular space [33] • secretory granule [34] • terminal button Biological process • response to amphetamine [36] • regulation of heart rate [37] • maternal aggressive behavior [38] • signal transduction [39] • elevation of cytosolic calcium ion concentration [40] • heart development [41] • female pregnancy [42] • memory [43] • grooming behavior [44] • response to sucrose stimulus [45] • positive regulation of norepinephrine secretion [46] • response to activity [47] • sleep [48] • positive regulation of prostaglandin secretion [49] • response to estradiol stimulus [50] • response to retinoic acid [51] • response to progesterone stimulus [52] • response to prostaglandin E stimulus [53] • social behavior [54] • negative regulation of urine volume [55] • positive regulation of renal sodium excretion [56] • response to cocaine [57] • hyperosmotic salinity response [58] • maternal behavior [59] • sperm ejaculation [60] • eating behavior [61] • drinking behavior [62] • response to peptide hormone stimulus [63] • response to ether [64] • negative regulation of blood pressure [65] • positive regulation of blood pressure [66] • positive regulation of ossification [67] • positive regulation of female receptivity [68] • positive regulation of synaptic transmission [69] • response to glucocorticoid stimulus [70] • response to cAMP [71] • response to electrical stimulus [72] • regulation of sensory perception of pain [73] • positive regulation of synapse assembly [74] • male mating behavior [75] • positive regulation of penile erection [76] • positive regulation of hindgut contraction [77] • negative regulation of gastric acid secretion [78] • positive regulation of uterine smooth muscle contraction Sources: Amigo
[79] [35]
/ QuickGO
[80]
Orthologs
Oxytocin
135
Species Entrez Ensembl UniProt RefSeq (mRNA) RefSeq (protein) Human 5020
[81] [83]
Mouse 18429
[82] [84]
ENSG00000101405 P01178
[85] [87]
ENSMUSG00000027301 P35454
[86] [88]
NM_000915 NP_000906
NM_011025 NP_035155
[89]
[90]
Location (UCSC) Chr 20: [91] 3.05 – 3.05 Mb PubMed search
[93]
Chr 2: [92] 130.58 – 130.58 Mb
[94]
The oxytocin peptide is synthesized as an inactive precursor protein from the OXT gene.[][][] This precursor protein also includes the oxytocin carrier protein neurophysin I.[] The inactive precursor protein is progressively hydrolyzed into smaller fragments (one of which is neurophysin I) via a series of enzymes. The last hydrolysis that releases the active oxytocin nonapeptide is catalyzed by peptidylglycine alpha-amidating monooxygenase (PAM).[] The activity of the PAM enzyme system is dependent upon vitamin C (ascorbate), which is a necessary vitamin cofactor. By chance, sodium ascorbate by itself was found to stimulate the production of oxytocin from ovarian tissue over a range of concentrations in a dose-dependent manner.[] Many of the same tissues (e.g. ovaries, testes, eyes, adrenals, placenta, thymus, pancreas) where PAM (and oxytocin by default) is found are also known to store higher concentrations of vitamin C.[]
Neural sources
In the hypothalamus, oxytocin is made in magnocellular neurosecretory cells of the supraoptic and paraventricular nuclei, and is stored in Herring bodies at the axon terminals in the posterior pituitary. It is then released into the blood from the posterior lobe (neurohypophysis) of the pituitary gland. These axons (likely, but dendrites have not been ruled out) have collaterals that innervate oxytocin receptors in the nucleus accumbens.[] The peripheral hormonal and behavioral brain effects of oxytocin are thought to be coordinated through its common release through these collaterals.[] Oxytocin is also made by some neurons in the paraventricular nucleus that project to other parts of the brain and to the spinal cord.[14] Depending on the species, oxytocin receptor-expressing cells are located in other areas, including the amygdala and bed nucleus of the stria terminalis. In the pituitary gland, oxytocin is packaged in large, dense-core vesicles, where it is bound to neurophysin I as shown in the inset of the figure; neurophysin is a large peptide fragment of the larger precursor protein molecule from which oxytocin is derived by enzymatic cleavage. Secretion of oxytocin from the neurosecretory nerve endings is regulated by the electrical activity of the oxytocin cells in the hypothalamus. These cells generate action potentials that propagate down axons to the nerve endings in the pituitary; the endings contain large numbers of oxytocin-containing vesicles, which are released by exocytosis when the nerve terminals are depolarised.
Oxytocin
136
Non-neural sources
Outside the brain, oxytocin-containing cells have been identified in several diverse tissues, including the corpus luteum,[][] the interstitial cells of Leydig,[] the retina,[] the adrenal medulla,[] the placenta,[] the thymus[] and the pancreas.[] The finding of significant amounts of this classically "neurohypophysial" hormone outside the central nervous system raises many questions regarding its possible importance in these different tissues. Female Oxytocin is synthesized by corpora lutea of several species, including ruminants and primates. Along with estrogen, it is involved in inducing the endometrial synthesis of prostaglandin F2α to cause regression of the corpus luteum. Male The Leydig cells in some species have also been shown to possess the biosynthetic machinery to manufacture testicular oxytocin de novo, to be specific, in rats (which can synthesize vitamin C endogenously), and in guinea pigs, which, like humans, require an exogenous source of vitamin C (ascorbate) in their diets.[]
Oxytocin receptor polymorphism
The oxytocin receptor in humans has several alleles, which differ in their effectiveness. For example, at one particular marker, individuals homozygous for the "G" allele, when compared to carriers of the "A" allele, show higher empathy and lower stress response,[15] as well as lower prevalence of autism and of poor parenting skills.[16]
Evolution
Virtually all vertebrates have an oxytocin-like nonapeptide hormone that supports reproductive functions and a vasopressin-like nonapeptide hormone involved in water regulation. The two genes are usually located close to each other (less than 15,000 bases apart) on the same chromosome, and are transcribed in opposite directions (however, in fugu,[] the homologs are further apart and transcribed in the same direction). The two genes are believed to result from a gene duplication event; the ancestral gene is estimated to be about 500 million years old and is found in cyclostomata (modern members of the Agnatha).[]
References
[1] Marieb Human Anatomy & Physiology 9th edition, chapter:16, page:599 [2] Ott I, Scott JC. The Action of Infundibulum upon Mammary Secretion. Proc Soc Exp Biol. (1910) p.8:48–49. [5] http:/ / emedicine. medscape. com/ article/ 976504-overview [12] Vacek M, High on Fidelity. What can voles teach us about monogamy? (http:/ / www. americanscientist. org/ issues/ pub/ high-on-fidelity) [13] Kuchinskas Susan, The Chemistry of Connection: How the Oxytocin Response Can Help You Find Trust, Intimacy, and Love p65 (http:/ / books. google. com/ books?hl=en& lr=& id=VO6dp52RxnQC& oi=fnd& pg=PR5& dq=oxytocin+ petting+ dog& ots=mTRRd4zj_9& sig=5xIdHdfrvmOOmZJh0Eak_KgYl2w#v=onepage& q= petting dog& f=false)
Further reading
• Lee HJ, Macbeth AH, Pagani JH, Young WS (June 2009). "Oxytocin: the Great Facilitator of Life" (http://www. ncbi.nlm.nih.gov/pmc/articles/PMC2689929). Progress in Neurobiology 88 (2): 127–51. doi: 10.1016/j.pneurobio.2009.04.001 (http://dx.doi.org/10.1016/j.pneurobio.2009.04.001). PMC 2689929 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2689929). PMID 19482229 (http://www.ncbi.nlm.nih. gov/pubmed/19482229). • Caldwell HK, Young WS III (2006). "Oxytocin and Vasopressin: Genetics and Behavioral Implications" (http:// refworks.springer.com/mrw/fileadmin/pdf/Neurochemistry/0387303480C25.PDF). In Abel L, Lim R. Handbook of neurochemistry and molecular neurobiology. Berlin: Springer. pp. 573–607. ISBN 0-387-30348-0.
Oxytocin
137
External links
• Hug the Monkey (http://kuchinskas.typepad.com/hug_the_monkey/) – A weblog devoted entirely to oxytocin • The Soft Machine (http://tijmz.files.wordpress.com/2011/06/softmachine4.pdf) – Review of oxytocin and bonding in animal and human research (.pdf) • A Neurophysiologic Model of the Circuitry of Oxytocin in Arousal, Female Distress and Depression – Rainer K. Liedtke, MD (http://www.rkliedtke.de/oxytocin2_us.html) (2004) • Oxytocin.org (http://www.oxytocin.org/oxytoc/love-science.html) – 'I get a kick out of you: Scientists are finding that, after all, love really is down to a chemical addiction between people', The Economist (February 12, 2004) • NewScientist.com (http://www.newscientist.com/channel/sex/mg18925365.500) – 'Release of Oxytocin due to penetrative sex reduces stress and neurotic tendencies', New Scientist (January 26, 2006) • SMH.com.au (http://smh.com.au/news/mind-matters/to-sniff-at-danger/2006/01/12/1136956247384.html) – 'To sniff at danger: Inhalable oxytocin could become a cure for social fears', Boston Globe (January 12, 2006) • 'Cuddle chemical' could treat mental illness (http://www.newscientist.com/channel/being-human/ mg19826561.900-cuddle-chemical-could-treat-mental-illness.html) (14 May 2008) New Scientist • Molecular neurobiology of social bonding: Implications for autism spectrum disorders (http://videocast.nih. gov/Summary.asp?File=15521) a lecture by Prof. Larry Young, Jan. 4, 2010. • A TED talk by Prof.Paul Zak on Trust,Morality & Oxytocin (http://www.ted.com/talks/ paul_zak_trust_morality_and_oxytocin.html)
Vasopressin
138
Vasopressin
Arginine vasopressin
Space-filling model of arginine vasopressin Available structures PDB Ortholog search: PDBe [1], RCSB [2] List of PDB id codes 1jk4
[3]
, 1jk6
[4]
, 1npo
[5]
, 2bn2
[6]
Identifiers Symbols External IDs AVP
[7]
; ADH; ARVP; AVP-NPII; AVRP; VP
[8]
OMIM: 192340
MGI: 88121
[9]
HomoloGene: 417
[10]
GeneCards: AVP Gene
[11]
Vasopressin
139
Gene Ontology Molecular function • protein kinase activity [12] [13] • signal transducer activity [14] • receptor binding [15] • neuropeptide hormone activity [31] • neurohypophyseal hormone activity [16] • V1A vasopressin receptor binding [17] • V1B vasopressin receptor binding [18] • cysteine-type endopeptidase inhibitor activity involved in apoptotic process Cellular component • extracellular region [229] [230] • extracellular space [19] • cytosol [33] • secretory granule [20] • dendrite Biological process • maternal aggressive behavior [21] • positive regulation of systemic arterial blood pressure [22] • generation of precursor metabolites and energy [23] • protein phosphorylation [24] • water transport [38] • signal transduction [39] • elevation of cytosolic calcium ion concentration [25] • cell-cell signaling [26] • negative regulation of female receptivity [43] • grooming behavior [27] • locomotory behavior [28] • positive regulation of cell proliferation [29] • positive regulation of gene expression [30] • positive regulation of glutamate secretion [31] • positive regulation of cell growth [32] • positive regulation of cAMP biosynthetic process [33] • positive regulation of prostaglandin biosynthetic process [34] • positive regulation of cellular pH reduction [35] • positive regulation of peptidyl-serine phosphorylation [36] • response to nicotine [53] • social behavior [37] • regulation of renal sodium excretion [38] • vasoconstriction [57] • hyperosmotic salinity response [58] • maternal behavior [39] • negative regulation of apoptotic process [40] • penile erection • negative regulation of cysteine-type endopeptidase activity involved in apoptotic process
[41] [37]
• sodium-independent organic anion transport [43] • response to ethanol [44] • positive regulation of vasoconstriction [45] • multicellular organismal water homeostasis [46] • negative regulation of transmission of nerve impulse [47] • transmembrane transport [48] • ERK1 and ERK2 cascade [49] • protein kinase C signaling cascade [50] • negative regulation of release of cytochrome c from mitochondria Sources: Amigo
[51]
[42]
/ QuickGO
[52]
Vasopressin
140
RNA expression pattern
More reference expression data Orthologs Species Entrez Ensembl UniProt RefSeq (mRNA) RefSeq (protein) Location (UCSC) Human 551
[54] [56]
[53]
Mouse 11998
[55] [57]
ENSG00000101200 P01185
[58] [60]
ENSMUSG00000037727 P35455
[59] [61]
NM_000490 NP_000481
NM_009732 NP_033862
[62]
[63]
Chr 20: [64] 3.06 – 3.07 Mb
[66]
Chr 2: [65] 130.58 – 130.58 Mb
[67]
PubMed search
Arginine vasopressin (AVP), also known as vasopressin, argipressin or antidiuretic hormone (ADH), is a neurohypophysial hormone found in most mammals. Its two primary functions are to retain water in the body and to constrict blood vessels. Vasopressin regulates the body's retention of water by acting to increase water absorption in the collecting ducts of the kidney nephron.[] Vasopressin increases water permeability of the kidney's collecting duct and distal convoluted tubule by inducing translocation of aquaporin-CD water channels in the kidney nephron collecting duct plasma membrane.[] Vasopressin is a peptide hormone that controls the reabsorption of molecules in the tubules of the kidneys by affecting the tissue's permeability. It also increases peripheral vascular resistance, which in turn increases arterial blood pressure. It plays a key role in homeostasis, by the regulation of water, glucose, and salts in the blood. It is derived from a preprohormone precursor that is synthesized in the hypothalamus and stored in vesicles at the posterior pituitary. Most of it is stored in the posterior pituitary to be released into the bloodstream. However, some AVP may also be released directly into the brain, and accumulating evidence suggests it plays an important role in social behavior, sexual motivation and bonding, and maternal responses to stress.
Physiology
Function
One of the most important roles of AVP is to regulate the body's retention of water; it is released when the body is dehydrated and causes the kidneys to conserve water, thus concentrating the urine and reducing urine volume. At high concentrations, it also raises blood pressure by inducing moderate vasoconstriction. In addition, it has a variety of neurological effects on the brain, having been found, for example, to influence pair-bonding in voles. The high-density distributions of vasopressin receptor AVPr1a in prairie vole ventral forebrain regions have been shown to facilitate and coordinate reward circuits during partner preference formation, critical for pair bond formation.[] A very similar substance, lysine vasopressin (LVP) or lypressin, has the same function in pigs and is often used in human therapy.
Vasopressin Kidney Vasopressin has two effects by which it contributes to increased urine osmolarity (increased concentration) and decreased water excretion. These are: 1. Increasing the water permeability of distal tubule and collecting duct cells in the kidney, thus allowing water reabsorption and excretion of more concentrated urine, i.e., antidiuresis. This occurs through insertion of water channels (Aquaporin-2) into the apical membrane of distal tubule and collecting duct epithelial cells. Aquaporins allow water to move down their osmotic gradient and out of the nephron, increasing the amount of water re-absorbed from the filtrate (forming urine) back into the bloodstream. V2 receptors, which are G protein-coupled receptors on the basolateral plasma membrane of the epithelial cells, couple to the heterotrimeric G-protein Gs, which activates adenylyl cyclases III and VI to convert ATP into cAMP, plus 2 inorganic phosphates. The rise in cAMP then triggers the insertion of aquaporin-2 water channels by exocytosis of intracellular vesicles, recycling endosomes. Vasopressin also increases the concentration of calcium in the collecting duct cells, by episodic release from intracellular stores. Vasopressin, acting through cAMP, also increases transcription of the aquaporin-2 gene, thus increasing the total number of aquaporin-2 molecules in collecting duct cells. Cyclic-AMP activates protein kinase A (PKA) by binding to its regulatory subunits and allowing them to detach from the catalytic subunits. Detachment exposes the catalytic site in the enzyme, allowing it to add phosphate groups to proteins (including the aquaporin-2 protein), which alters their functions. 2. Increasing permeability of the inner medullary portion of the collecting duct to urea by regulating the cell surface expression of urea transporters,[] which facilitates its reabsorption into the medullary interstitium as it travels down the concentration gradient created by removing water from the connecting tubule, cortical collecting duct, and outer medullary collecting duct. Cardiovascular system Vasopressin increases peripheral vascular resistance (vasoconstriction) and thus increases arterial blood pressure. This effect appears small in healthy individuals; however it becomes an important compensatory mechanism for restoring blood pressure in hypovolemic shock such as that which occurs during hemorrhage. Central nervous system Vasopressin released within the brain has many actions: • It has been implicated in memory formation, including delayed reflexes, image, short- and long-term memory, though the mechanism remains unknown; these findings are controversial. However, the synthetic vasopressin analogue desmopressin has come to interest as a likely nootropic.
[68] Avp is expressed in the periventricular [] region of the hypothalamus in the adult mouse. Allen Brain Atlases
141
• Vasopressin is released into the brain in a circadian rhythm by neurons of the supraoptic nucleus. • Vasopressin released from centrally projecting hypothalamic neurons is involved in aggression, blood pressure regulation and
temperature regulation. • It is likely that vasopressin acts in conjunction with corticotropin-releasing hormone to modulate the release of corticosteroids from the adrenal gland in response to stress, particularly during pregnancy and lactation in mammals.[][][] • Selective AVPr1a blockade in the ventral pallidum has been shown to prevent partner preference in prairie voles, suggesting that these receptors in this ventral forebrain region are crucial for pair bonding.[]
Vasopressin • Recent evidence suggests that vasopressin may have analgesic effects. The analgesia effects of vasopressin were found to be dependent on both stress and gender.[] Evidence for this comes from experimental studies in several species, which indicate that the precise distribution of vasopressin and vasopressin receptors in the brain is associated with species-typical patterns of social behavior. In particular, there are consistent differences between monogamous species and promiscuous species in the distribution of AVP receptors, and sometimes in the distribution of vasopressin-containing axons, even when closely related species are compared.[] Moreover, studies involving either injecting AVP agonists into the brain or blocking the actions of AVP support the hypothesis that vasopressin is involved in aggression toward other males. There is also evidence that differences in the AVP receptor gene between individual members of a species might be predictive of differences in social behavior. One study has suggested that genetic variation in male humans affects pair-bonding behavior. The brain of males uses vasopressin as a reward for forming lasting bonds with a mate, and men with one or two of the genetic alleles are more likely to experience marital discord. The partners of the men with two of the alleles affecting vasopressin reception state disappointing levels of satisfaction, affection, and cohesion.[] Vasopressin receptors distributed along the reward circuit pathway, to be specific in the ventral pallidum, are activated when AVP is released during social interactions such as mating, in monogamous prairie voles. The activation of the reward circuitry reinforces this behavior, leading to conditioned partner preference, and thereby initiates the formation of a pair bond.[]
142
Control
Vasopressin is secreted from the posterior pituitary gland in response to reductions in plasma volume, in response to increases in the plasma osmolality, and in response to cholecystokinin (CCK) secreted by the small intestine: • Secretion in response to reduced plasma volume is activated by pressure receptors in the veins, atria, and carotids. • Secretion in response to increases in plasma osmotic pressure is mediated by osmoreceptors in the hypothalamus. • Secretion in response to increases in plasma CCK is mediated by an unknown pathway. The neurons that make AVP, in the hypothalamic supraoptic nuclei (SON) and paraventricular nuclei (PVN), are themselves osmoreceptors, but they also receive synaptic input from other osmoreceptors located in regions adjacent to the anterior wall of the third ventricle. These regions include the organum vasculosum of the lamina terminalis and the subfornical organ. Many factors influence the secretion of vasopressin: • Ethanol (alcohol) reduces the calcium-dependent secretion of AVP by blocking voltage-gated calcium channels in neurohypophyseal nerve terminals.[1] • Angiotensin II stimulates AVP secretion, in keeping with its general pressor and pro-volumic effects on the body.[] • Atrial natriuretic peptide inhibits AVP secretion, in part by inhibiting Angiotensin II-induced stimulation of AVP secretion.[]
Secretion
The main stimulus for secretion of vasopressin is increased osmolality of plasma. Reduced volume of extracellular fluid also has this effect, but is a less sensitive mechanism. The AVP that is measured in peripheral blood is almost all derived from secretion from the posterior pituitary gland (except in cases of AVP-secreting tumours). Vasopressin is produced by magnocellular neurosecretory neurons in the Paraventricular nucleus of hypothalamus (PVN) and Supraoptic nucleus (SON). It then travels down the axon through the infundibulum within neurosecretory granules that are found within Herring bodies, localized swellings of the axons and nerve terminals. These carry the peptide directly to the posterior pituitary gland, where it is stored until released into the blood. However there are two other sources of AVP with important local effects:
Vasopressin • AVP is also synthesized by parvocellular neurosecretory neurons at the PVN, transported and released at the median eminence, which then travels through the hypophyseal portal system to the anterior pituitary where it stimulates corticotropic cells synergistically with CRH to produce ACTH (by itself it is a weak secretagogue).[] • Vasopressin is also released into the brain by several different populations of smaller neurons.
143
Receptors
Below is a table summarizing some of the actions of AVP at its four receptors, differently expressed in different tissues and exerting different actions:
Type AVPR1A Second messenger system Locations Actions Vasoconstriction, gluconeogenesis, platelet aggregation, and release [] of factor VIII and von Willebrand factor; social recognition, [] circadian tau Adrenocorticotropic hormone secretion in response to stress; [] social interpretation of olfactory cues []
Phosphatidylinositol/calcium Liver, kidney, peripheral vasculature, brain
AVPR1B or AVPR3 AVPR2
Phosphatidylinositol/calcium Pituitary gland, brain
Adenylate cyclase/cAMP
Basolateral membrane of the cells lining the collecting ducts of the kidneys (especially the cortical and outer medullary collecting ducts)
Insertion of aquaporin-2 (AQP2) channels (water channels). This allows water to be reabsorbed down an osmotic gradient, and so the urine is more concentrated. Release of von Willebrand factor and surface expression of P-selectin through exocytosis of [][] Weibel-Palade bodies from endothelial cells Increases cytosolic calcium and acts as an inverse agonist of cAMP [] accumulation
VACM-1
Phosphatidylinositol/calcium Vascular endothelium and renal collecting tubules
Structure and relation to oxytocin
The vasopressins are peptides consisting of nine amino acids (nonapeptides). (NB: the value in the table above of 164 amino acids is that obtained before the hormone is activated by cleavage). The amino acid sequence of arginine vasopressin is Cys-Tyr-Phe-Gln-Asn-Cys-Pro-Arg-Gly, with the cysteine residues forming a disulfide bond. Lysine vasopressin has a lysine in place of the arginine. The structure of oxytocin is very similar to that of the vasopressins: It is also a nonapeptide with a disulfide bridge and its amino acid sequence differs at only two positions (see table below). The two genes are located on the same chromosome separated by a relatively small distance of less than 15,000 bases in most species. The magnocellular neurons that make vasopressin are adjacent to magnocellular neurons that make oxytocin, and are similar in many respects. The similarity of the two peptides can cause some cross-reactions: oxytocin has a slight antidiuretic function, and high levels of AVP can cause uterine contractions.[][] Below is a table showing the superfamily of vasopressin and oxytocin neuropeptides:
Chemical structure of the argipressin (indicating that this compound is of the vasopressin family with an arginine at the 8th amino acid position.
Chemical structure of oxytocin
Vasopressin
144
Vertebrate Vasopressin Family Cys-Tyr-Phe-Gln-Asn-Cys-Pro-Arg-Gly-NH2 Argipressin (AVP, ADH) Lypressin (LVP) Phenypressin Vasotocin† Most mammals
Cys-Tyr-Phe-Gln-Asn-Cys-Pro-Lys-Gly-NH2 Cys-Phe-Phe-Gln-Asn-Cys-Pro-Arg-Gly-NH2 Cys-Tyr-Ile-Gln-Asn-Cys-Pro-Arg-Gly-NH2
Pigs, hippos, warthogs, some marsupials Some marsupials Non-mammals
Vertebrate Oxytocin Family Cys-Tyr-Ile-Gln-Asn-Cys-Pro-Leu-Gly-NH2 Cys-Tyr-Ile-Gln-Asn-Cys-Pro-Pro-Gly-NH2 Cys-Tyr-Ile-Gln-Asn-Cys-Pro-Ile-Gly-NH2 Oxytocin (OXT) Prol-Oxytocin Mesotocin Most mammals, ratfish Some New World monkeys, northern tree shrews Most marsupials, all birds, reptiles, amphibians, lungfishes, coelacanths Frogs Bony fishes Skates Sharks
Cys-Tyr-Ile-Gln-Ser-Cys-Pro-Ile-Gly-NH2 Cys-Tyr-Ile-Ser-Asn-Cys-Pro-Ile-Gly-NH2 Cys-Tyr-Ile-Ser-Asn-Cys-Pro-Gln-Gly-NH2
Seritocin Isotocin Glumitocin
Cys-Tyr-Ile-Asn/Gln-Asn-Cys-Pro-Leu/Val-Gly-NH2 Various tocins
Invertebrate VP/OT Superfamily Cys-Leu-Ile-Thr-Asn-Cys-Pro-Arg-Gly-NH2 Cys-Phe-Val-Arg-Asn-Cys-Pro-Thr-Gly-NH2 Cys-Phe-Ile-Arg-Asn-Cys-Pro-Lys-Gly-NH2 Cys-Ile-Ile-Arg-Asn-Cys-Pro-Arg-Gly-NH2 Cys-Tyr-Phe-Arg-Asn-Cys-Pro-Ile-Gly-NH2 Cys-Phe-Trp-Thr-Ser-Cys-Pro-Ile-Gly-NH2 Diuretic Hormone Annetocin Lys-Connopressin Arg-Connopressin Cephalotocin Octopressin Locust Earthworm Geography & imperial cone snail, pond snail, sea hare, leech Striped cone snail Octopus Octopus [2]
†Vasotocin is the evolutionary progenitor of all the vertebrate neurohypophysial hormones.
Role in disease
Lack of AVP
Decreased AVP release or decreased renal sensitivity to AVP leads to diabetes insipidus, a condition featuring hypernatremia (increased blood sodium concentration), polyuria (excess urine production), and polydipsia (thirst).
Excess AVP
High levels of AVP secretion may lead to hyponatremia. In many cases, the AVP secretion is appropriate (due to severe hypovolemia), and the state is labelled "hypovolemic hyponatremia". In certain disease states (heart failure, nephrotic syndrome) the body fluid volume is increased but AVP production is not suppressed for various reasons; this state is labelled "hypervolemic hyponatremia". A proportion of cases of hyponatremia feature neither hyper- nor hypovolemia. In this group (labelled "euvolemic hyponatremia"), AVP secretion is either driven by a lack of cortisol or thyroxine (hypoadrenalism and hypothyroidism, respectively) or a very low level of urinary solute excretion (potomania, low-protein diet), or it is entirely inappropriate. This last category is classified as the syndrome of inappropriate antidiuretic hormone (SIADH).[] SIADH in turn can be caused by a number of problems. Some forms of cancer can cause SIADH, particularly small cell lung carcinoma but also a number of other tumors. A variety of diseases affecting the brain or the lung
Vasopressin (infections, bleeding) can be the driver behind SIADH. A number of drugs has been associated with SIADH, such as certain antidepressants (serotonin reuptake inhibitors and tricyclic antidepressants), the anticonvulsant carbamazepine, oxytocin (used to induce and stimulate labor), and the chemotherapy drug vincristine. Finally, it can occur without a clear explanation.[] Hyponatremia can be treated pharmaceutically through the use of vasopressin receptor antagonists.[]
145
Pharmacology
Vasopressin analogues
Vasopressin agonists are used therapeutically in various conditions, and its long-acting synthetic analogue desmopressin is used in conditions featuring low vasopressin secretion, as well as for control of bleeding (in some forms of von Willebrand disease and in mild haemophilia A) and in extreme cases of bedwetting by children. Terlipressin and related analogues are used as vasoconstrictors in certain conditions. Use of vasopressin analogues for esophageal varices commenced in 1970.[] Vasopressin infusion has also been used as a second line of management in septic shock patients not responding to high dose of inotropes (e.g., dopamine or norepinephrine).
The role of vasopressin analogues in cardiac arrest
Injection of vasopressors for the treatment of cardiac arrest was first suggested in the literature in 1896 when Austrian scientist Dr. R. Gottlieb described the vasopressor epinephrine as an "infusion of a solution of suprarenal extract [that] would restore circulation when the blood pressure had been lowered to unrecordable levels by chloral hydrate."[] Modern interest in vasopressors as a treatment for cardiac arrest stem mostly from canine studies performed in the 1960s by anesthesiologists Dr. John W. Pearson and Dr. Joseph Stafford Redding in which they demonstrated improved outcomes with the use of adjunct intracardiac epinephrine injection during resuscitation attempts after induced cardiac arrest.[] Also contributing to the idea that vasopressors may be useful treatments in cardiac arrest are studies performed in the early to mid 1990's that found significantly higher levels of endogenous serum vasopressin in adults after successful resuscitation from out-of-hospital cardiac arrest compared to those who did not live.[][] Results of animal models have supported the use of either vasopressin or epinephrine in cardiac arrest resuscitation attempts, showing improved coronary perfusion pressure[] and overall improvement in short-term survival as well as neurological outcomes.[] Vasopressin vs. epinephrine
Table 1. Meta-analysis of outcomes for patients treated with vasopressin versus epinephrine[]
RR (95% CI) Failure of ROSC Death before hospital admission Death within 24 hours Death before hospital discharge 0.81 (0.58-1.12) 0.72 (0.38-1.39) 0.74 (0.38-1.43) 0.96 (0.87-1.05)
Number of deaths and neurologically impaired survivors 1.00 (0.94-1.07)
Although both vasopressors, vasopressin and epinephrine differ in that vasopressin does not have direct effects on cardiac contractility as epinephrine does.[] Thus, vasopressin is theorized to be of increased benefit over epinephrine in cardiac arrest due to its properties of not increasing myocardial and cerebral oxygen demands.[] This idea has led
Vasopressin to the advent of several studies searching for the presence of a clinical difference in benefit of these two treatment choices. Initial small studies demonstrated improved outcomes with vasopressin in comparison to epinephrine.[] However, subsequent studies have not all been in agreement. Several randomized controlled trials have been unable to reproduce positive results with vasopressin treatment in both return of spontaneous circulation (ROSC) and survival to hospital discharge,[][][][] including a systematic review and meta-analysis completed in 2005 that found no evidence of a significant difference with vasopressin in five studied outcomes (see Table 1).[] Vasopressin and epinephrine vs. epinephrine alone
146
Table 2. Significant outcomes for combined vasopressin and epinephrine treatment
RR (95% CI) [] ROSC Survival to hospital admission [] In subgroup: PEA [] 1.42 (1.14-1.77) 1.42 (1.02-2.04) 0.05 1.30 (0.90-2.06) 0.02 p value
[] In subgroup: Collapse to ED arrival time of 15–30 minutes 1.22 (1.01-1.49) 0.05 [] In subgroup: Collapse to ED arrival time of 30–45 minutes 1.11 (1.00-1.24) 0.05 Survival to hospital discharge [] 3.69 (1.52-8.95)
There is no current evidence of significant survival benefit with improved neurological outcomes in patients given combinations of both epinephrine and vasopressin during cardiac arrest.[][][3][] A systematic review from 2008 did, however, find one study that showed a statistically significant improvement in ROSC and survival to hospital discharge with this combination treatment; unfortunately, those patients that survived to hospital discharge had overall poor outcomes and many suffered permanent, severe neurological damage.[][] A more recently published clinical trial out of Singapore has shown similar results, finding combination treatment to only improve the rate of survival to hospital admission, especially in the subgroup analysis of patients with longer "collapse to emergency department" arrival times of 15 to 45 minutes.[] Table 2 lists all statistically significant findings of a correlation between combined treatment and positive outcomes found in these two studies. 2010 American Heart Association Guidelines The 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care recommend the consideration of vasopressor treatment in the form of epinephrine in adults with cardiac arrest (Class IIb, LOE A recommendation).[] Due to the absence of evidence that vasopressin administered instead of or in addition to epinephrine has significant positive outcomes, the guidelines do not currently contain vasopressin as a part of the cardiac arrest algorithms.[] It does, however, allow for one dose of vasopressin to replace either the first or second dose of epinephrine in the treatment of cardiac arrest (Class IIb, LOE A recommendation).[]
Vasopressin
147
Vasopressin receptor inhibition
A vasopressin receptor antagonist is an agent that interferes with action at the vasopressin receptors. They can be used in the treatment of hyponatremia.[]
References Further reading
• Rector, Floyd C.; Brenner, Barry M. (2004). Brenner & Rector's the kidney (http://home.mdconsult.com/das/ search/openres/56203699-5?searchisbn=460046813) (7th ed.). Philadelphia: Saunders. ISBN 0-7216-0164-2.
External links
• Molecular neurobiology of social bonding: Implications for autism spectrum disorders (http://videocast.nih. gov/Summary.asp?File=15521) a lecture by Prof. Larry Young, Jan. 4, 2010.
Serotonin
148
Serotonin
Serotonin
Identifiers CAS number PubChem ChemSpider UNII KEGG MeSH ChEBI ChEMBL IUPHAR ligand Jmol-3D images 50-67-9 5202 5013
[2] [3] [4] [1]
333DO1RDJY C00780
[5]
Serotonin
[6] [7]
CHEBI:28790 CHEMBL39 5
[9] [10]
[8]
Image 1
Properties Molecular formula C H N O
10 12 2
Molar mass Appearance
176.215 g/mol White powder
Serotonin
[1] [2]
149
Melting point Boiling point
121–122°C (ligroin)
416 ±30.0°C (at 760 Torr)
Solubility in water slightly soluble Dipole moment 2.98 D Hazards MSDS LD50 External MSDS
[13] [] []
750 mg/kg (subcutaneous, rat), 4500 mg/kg (intraperitoneal, rat), 60 mg/kg (oral, rat)
(verify) [14]
(what is: / ?) Except where noted otherwise, data are given for materials in their standard state (at 25 °C, 100 kPa)
Infobox references
Serotonin (pron.: /ˌsɛrəˈtoʊnɨn/) or 5-hydroxytryptamine (5-HT) is a monoamine neurotransmitter. Biochemically derived from tryptophan, serotonin is primarily found in the gastrointestinal (GI) tract, platelets, and in the central nervous system (CNS) of animals including humans. It is popularly thought to be a contributor to feelings of well-being and happiness.[3] Approximately 90% of the human body's total serotonin is located in the enterochromaffin cells in the alimentary canal (gut), where it is used to regulate intestinal movements.[][] The remainder is synthesized in serotonergic neurons of the CNS, where it has various functions. These include the regulation of mood, appetite, and sleep. Serotonin also has some cognitive functions, including memory and learning. Modulation of serotonin at synapses is thought to be a major action of several classes of pharmacological antidepressants. Serotonin secreted from the enterochromaffin cells eventually finds its way out of tissues into the blood. There, it is actively taken up by blood platelets, which store it. When the platelets bind to a clot, they disgorge serotonin, where it serves as a vasoconstrictor and helps to regulate hemostasis and blood clotting. Serotonin also is a growth factor for some types of cells, which may give it a role in wound healing. Serotonin is mainly metabolized to 5-HIAA, chiefly by the liver. Metabolism involves first oxidation by monoamine oxidase to the corresponding aldehyde. This is followed by oxidation by aldehyde dehydrogenase to 5-HIAA, the indole acetic acid derivative. The latter is then excreted by the kidneys. One type of tumor, called carcinoid, sometimes secretes large amounts of serotonin into the blood, which causes various forms of the carcinoid syndrome of flushing, diarrhea, and heart problems. Because of serotonin's growth-promoting effect on cardiac myocytes, persons with serotonin-secreting carcinoid may suffer a right heart (tricuspid) valve disease syndrome, caused by proliferation of myocytes onto the valve. In addition to animals, serotonin is found in fungi and plants.[] Serotonin's presence in insect venoms and plant spines serves to cause pain, which is a side effect of serotonin injection. Serotonin is produced by pathogenic amoebae, and its effect on the gut causes diarrhea. Its widespread presence in many seeds and fruits may serve to stimulate the digestive tract into expelling the seeds.
Functions
Serotonin is a neurotransmitter, and is found in all bilateral animals [citation needed], where it mediates gut movements and the animals' perceptions of resource availability. In the simplest animals, resources are equivalent with food, but in advanced animals, such as arthropods and vertebrates, resources also can mean social dominance. In response to the perceived abundance or scarcity of resources, an animal's growth, reproduction or mood may be elevated or lowered[citation needed].
Serotonin
150
Gauge of food availability (appetite)
Serotonin functions as a neurotransmitter in the nervous systems of simple, as well as complex, animals. For example, in the roundworm Caenorhabditis elegans, which feeds on bacteria, serotonin is released as a signal in response to positive events, e.g., finding a new source of food or in male animals finding a female with which to mate[citation needed]. When a well-fed worm feels bacteria on its cuticle, dopamine is released, which slows it down; if it is starved, serotonin also is released, which slows the animal down further. This mechanism increases the amount of time animals spend in the presence of food.[] The released serotonin activates the muscles used for feeding, while octopamine suppresses them.[] Serotonin diffuses to serotonin-sensitive neurons, which control the animal's perception of nutrient availability. When humans smell food, dopamine is released to increase the appetite. But unlike in worms, serotonin does not increase anticipatory behaviour in humans; instead, the serotonin released while consuming activates 5-HT2C receptors on dopamine-producing cells. This halts their dopamine release, and thereby serotonin decreases appetite. Drugs which block 5-HT2C receptors make the body unable to shut off appetite, and are associated with increased weight gain,[] especially in people who have a low number of receptors.[] The expression of 5-HT2C receptors in the hippocampus follows a diurnal rhythm,[] just as the serotonin release in the ventromedial nucleus, which is characterised by a peak at morning when the motivation to eat is strongest.[] Effects of food content In humans, serotonin levels are affected by diet. An increase in the ratio of tryptophan to phenylalanine and leucine will increase serotonin levels. Fruits with a good ratio include dates, papayas and bananas. Foods with a lower ratio inhibit the production of serotonin. [citation needed] Research also suggests eating a diet rich in carbohydrates and low in protein will increase serotonin by secreting insulin, which helps in amino acid competition.[] However, increasing insulin for a long period may trigger the onset of insulin resistance, obesity, type 2 diabetes, and lower serotonin levels.[4][5] Muscles use many of the amino acids except tryptophan, allowing more muscular individuals to produce more serotonin.[] Myoinositol, a carbocyclic polyol present in many foods, is known to play a role in serotonin modulation.[] In the digestive tract (emetic) The gut is surrounded by enterochromaffin cells, which release serotonin in response to food in the lumen. This makes the gut contract around the food. Platelets in the veins draining the gut collect excess serotonin. If irritants are present in the food, the enterochromaffin cells release more serotonin to make the gut move faster, i.e., to cause diarrhea, so the gut is emptied of the noxious substance. If serotonin is released in the blood faster than the platelets can absorb it, the level of free serotonin in the blood is increased. This activates 5HT3 receptors in the chemoreceptor trigger zone that stimulate vomiting.[6] The enterochromaffin cells not only react to bad food, but they are also very sensitive to irradiation and cancer chemotherapy. Drugs that block 5HT3 are very effective in controlling the nausea and vomiting produced by cancer treatment, and are considered the gold standard for this purpose.[7] Gauge of social situation How much food an animal gets not only depends on the abundance of food, but also on the animal's ability to compete with others. This is especially true for social animals, where the stronger individuals might steal food from the weaker. Thus, serotonin is not only involved in the perception of food availability, but also of social rank. If a lobster is injected with serotonin, it behaves like a dominant animal, while octopamine causes subordinate behavior.[] A frightened crayfish flips its tail to flee, and the effect of serotonin on this behavior depends on the animal's social status. Serotonin inhibits the fleeing reaction in subordinates, but enhances it in socially dominant or isolated individuals. The reason for this is social experience alters the proportion between serotonin receptors (5-HT receptors) that have opposing effects on the fight-or-flight response.Wikipedia:Please clarify The effect of 5-HT1 receptors predominates in subordinate animals, while 5-HT2 receptors predominates in dominants.[] In humans,
Serotonin levels of 5-HT1A receptor activation in the brain show negative correlation with aggression,[8] and a mutation in the gene that codes for the 5-HT2A receptor may double the risk of suicide for those with that genotype.[] Most of the brain serotonin is not degraded after use, but is collected by serotonergic neurons by serotonin transporters on their cell surfaces. Studies have revealed nearly 10% of total variance in anxiety-related personality depends on variations in the description of where, when and how many serotonin transporters the neurons should deploy.[]
151
Growth and reproduction
In C. elegans, artificial depletion of serotonin or increase of octopamine cues behavior typical of a low-food environment: C. elegans becomes more active, and mating and egg-laying are suppressed, while the opposite occurs if serotonin is increased or octopamine is decreased in this animal.[] Serotonin is necessary for normal nematode male mating behavior,[] and the inclination to leave food to search for a mate.[] The serotonergic signaling used to adapt the worm's behaviour to fast changes in the environment affects insulin-like signaling and the TGF beta signaling pathway,[9] which control long-term adaption.
Aging and age-related phenotypes
Serotonin is known to regulate aging, learning and memory. The first evidence comes from the study of longevity in C. elegans.[10] During early phase of aging, the level of serotonin increases, which alters locomotory behaviors and associative memory.[11] The effect is restored by mutations and drugs (including mianserin and methiothepin) that inhibit serotonin receptors. The observation does not contradict with the notion that the serotonin level goes down in mammals and humans, which is typically seen in late but not early phase of aging.
Bone metabolism
In mice and humans, alterations in serotonin levels and signalling have been shown to regulate bone mass.[][][][] Mice that lack brain serotonin have osteopenia, while mice that lack gut serotonin have high bone density. In humans, increased blood serotonin levels have been shown to be significant negative predictor of low bone density. Serotonin can also be synthesized, albeit at very low levels, in the bone cells. It mediates its actions on bone cells using three different receptors. Through Htr1b receptors, it negatively regulates bone mass, while it does so positively through Htr2b and Htr2c. There is very delicate balance between physiological role of gut serotonin and its pathology. Increase in the extracellular content of serotonin results in a complex relay of signals in the osteoblasts culminating in FoxO1/ Creb and ATF4 dependent transcriptional events.[] These studies have opened a new area of research in bone metabolism that can be potentially harnessed to treat bone mass disorders.[]
Behavior
In the fruitfly, where insulin both regulates blood sugar and acts as a growth factor, serotonergic neurons regulate the adult body size by affecting insulin secretion.[][] Serotonin has also been identified as the trigger for swarm behavior in locusts.[] In humans, though insulin regulates blood sugar and IGF regulates growth, serotonin controls the release of both hormones, so serotonin suppresses insulin release from the beta cells in the pancreas,[] and exposure to SSRIs reduces fetal growth.[] Human serotonin can also act as a growth factor directly. Liver damage increases cellular expression of 5-HT2A and 5-HT2B receptors.[] Serotonin present in the blood then stimulates cellular growth to repair liver damage.[] 5HT2B receptors also activate osteocytes, which build up bone[] However, serotonin also inhibits osteoblasts, through 5-HT1B receptors.[]
Serotonin
152
Cardiovascular growth factor
Serotonin, in addition, evokes endothelial nitric oxide synthase activation and stimulates, through a 5-HT1B receptor-mediated mechanism, the phosphorylation of p44/p42 mitogen-activated protein kinase activation in bovine aortic endothelial cell cultures.[] In blood, serotonin is collected from plasma by platelets, which store it. It is thus active wherever platelets bind in damaged tissue, as a vasoconstrictor to stop bleeding, and also as a fibrocyte mitotic (growth factor), to aid healing.[] Some serotonergic agonist drugs also cause fibrosis anywhere in the body, particularly the syndrome of retroperitoneal fibrosis, as well as cardiac valve fibrosis.[] In the past, three groups of serotonergic drugs have been epidemiologically linked with these syndromes. They are the serotonergic vasoconstrictive antimigraine drugs (ergotamine and methysergide),[] the serotonergic appetite suppressant drugs (fenfluramine, chlorphentermine, and aminorex), and certain anti-Parkinsonian dopaminergic agonists, which also stimulate serotonergic 5-HT2B receptors. These include pergolide and cabergoline, but not the more dopamine-specific lisuride.[] As with fenfluramine, some of these drugs have been withdrawn from the market after groups taking them showed a statistical increase of one or more of the side effects described. An example is pergolide. The drug was declining in use since reported in 2003 to be associated with cardiac fibrosis.[12] Two independent studies published in the New England Journal of Medicine in January 2007, implicated pergolide, along with cabergoline, in causing valvular heart disease.[][] As a result of this, the FDA removed pergolide from the U.S. market in March, 2007.[13] (Since cabergoline is not approved in the U.S. for Parkinson's Disease, but for hyperprolactinemia, the drug remains on the market. Treatment for hyperprolactinemia requires lower doses than that for Parkinson's Disease, diminishing the risk of valvular heart disease).[] Local effects of injection: venoms and pain Since serotonin is an indicator of bleeding, a sudden large increase in peripheral levels causes pain. The reason wasps and deathstalker scorpions have serotonin in their venom [][] may be to increase the pain of their stings on large animals, and also to cause lethal vasoconstriction in smaller prey.
Deficiency
Genetically altered C. elegans worms that lack serotonin have an increased reproductive lifespan, may become obese, and sometimes present with arrested development at a dormant larval state.[][] Serotonin in mammals is made by two different tryptophan hydroxylases: TPH1 produces serotonin in the pineal gland[citation needed] and the enterochromaffin cells, while TPH2 produces it in the raphe nuclei and in the myenteric plexus. Genetically altered mice lacking TPH1 develop progressive loss of heart strength early on. They have pale skin and breathing difficulties, are easily tired, and eventually die of heart failure.[] Genetically altered mice that lack TPH2 are normal when they are born. However, after three days, they appear to be smaller and weaker, and have softer skin than their siblings. In a purebred strain, 50% of the mutants died during the first four weeks, but in a mixed strain, 90% survived. Normally, the mother weans the litter after three weeks, but the mutant animals needed five weeks. After that, they caught up in growth and had normal mortality rates. Subtle changes in the autonomic nervous system are present, but the most obvious difference from normal mice is the increased aggressiveness and impairment in maternal care of young.[] Despite the blood–brain barrier, the loss of serotonin production in the brain is partially compensated by intestinal serotonin. The behavioural changes become greatly enhanced if one crosses TPH1- with TPH2-lacking mice and gets animals that lack TPH entirely.[] In humans, defective signaling of serotonin in the brain may be the root cause of sudden infant death syndrome (SIDS). Scientists from the European Molecular Biology Laboratory in Monterotondo, Italy[14] genetically modified lab mice to produce low levels of the neurotransmitter serotonin. The results showed the mice suffered drops in heart rate and other symptoms of SIDS, and many of the animals died at an early age. Researchers now believe low levels of serotonin in the animals' brainstems, which control heartbeat and breathing, may have caused sudden death, they
Serotonin said in the July 4, 2008 issue of Science.[] If neurons that make serotonin — serotonergic neurons — are abnormal in infants, there is a risk of sudden infant death syndrome (SIDS).[] Recent research conducted at Rockefeller University shows, in both patients who suffer from depression and mice that model the disorder, levels of the p11 protein are decreased. This protein is related to serotonin transmission within the brain.[]
153
In the brain
Gross anatomy
The neurons of the raphe nuclei are the principal source of 5-HT release in the brain.[15] There are 7 or 8 raphe nuclei (some scientists chose to group the raphe linearis nuclei into one nucleus), all of which are located along the midline of the brainstem, and centered around the reticular formation.[16] Axons from the neurons of the raphe nuclei form a neurotransmitter system, reaching almost every part of the central nervous system. Axons of neurons in the lower raphe nuclei terminate in the cerebellum and spinal cord, while the axons of the higher nuclei spread out in the entire brain.
Serotonin system, contrasted with the dopamine system
Microanatomy
Serotonin is released into the space between neurons, and diffuses over a relatively wide gap (>20 µm) to activate 5-HT receptors located on the dendrites, cell bodies and presynaptic terminals of adjacent neurons. Receptors The 5-HT receptors, the receptors for serotonin, are located on the cell membrane of nerve cells and other cell types in animals, and mediate the effects of serotonin as the endogenous ligand and of a broad range of pharmaceutical and hallucinogenic drugs. With the exception of the 5-HT3 receptor, a ligand-gated ion channel, all other 5-HT receptors are G protein-coupled, seven transmembrane (or heptahelical) receptors that activate an intracellular second messenger cascade.[] Termination Serotonergic action is terminated primarily via uptake of 5-HT from the synapse. This is accomplished through the specific monoamine transporter for 5-HT, SERT, on the presynaptic neuron. Various agents can inhibit 5-HT reuptake, including MDMA (ecstasy), amphetamine, cocaine, dextromethorphan (an antitussive), tricyclic antidepressants and selective serotonin reuptake inhibitors (SSRIs). Interestingly, a 2006 study conducted by the University of Washington suggested a newly discovered monoamine transporter, known as PMAT, may account for "a significant percentage of 5-HT clearance".[] Contrasting with the high-affinity SERT, the PMAT has been identified as a low-affinity transporter, with an apparent Km of 114 micromoles/l for serotonin; approximately 230 times higher than that of SERT. However, the PMAT, despite its relatively low serotonergic affinity, has a considerably higher transport 'capacity' than SERT, "..resulting in roughly comparable uptake efficiencies to SERT in heterologous expression systems." The study also suggests some SSRIs, such as fluoxetine and sertraline, inhibit PMAT but at IC50 values which surpass the therapeutic plasma concentrations by up to four orders of magnitude; therefore, SSRI monotherapy is "ineffective" in PMAT inhibition. At present, no known pharmaceuticals are known to appreciably inhibit PMAT at normal therapeutic doses. The PMAT also suggestively transports dopamine and
Serotonin norepinephrine, albeit at Km values even higher than that of 5-HT (330–15,000 μmoles/L). Serotonylation Serotonin can also signal through a nonreceptor mechanism called serotonylation, in which serotonin modifies proteins.[] This process underlies serotonin effects upon platelet-forming cells (thrombocytes) in which it links to the modification of signaling enzymes called GTPases that then trigger the release of vesicle contents by exocytosis.[] A similar process underlies the pancreatic release of insulin.[] The effects of serotonin upon vascular smooth muscle "tone" (this is the biological function from which serotonin originally got its name) depend upon the serotonylation of proteins involved in the contractile apparatus of muscle cells.[]
154
Biosynthesis
In animals including humans, serotonin is synthesized from the amino acid L-tryptophan by a short metabolic pathway consisting of two enzymes: tryptophan hydroxylase (TPH) and amino acid decarboxylase (DDC). The TPH-mediated reaction is the rate-limiting step in the pathway. TPH has been shown to exist in two forms: TPH1, found in several tissues, and TPH2, which is a neuron-specific isoform.[] Serotonin can be synthesized from tryptophan in the lab using Aspergillus niger and Psilocybe coprophila as catalysts. The first phase to 5-hydroxytryptophan would require letting tryptophan sit in ethanol and water for 7 days, then mixing in enough HCl (or other acid) to bring the pH to 3, and then adding NaOH to make a pH of 13 for 1 hour. Asperigillus niger would be the catalyst for this first phase. The second phase to synthesizing tryptophan itself from the 5-hydroxytryptophan intermediate would require adding ethanol and water, and letting sit for 30 days this time. The next two steps would be the same as the first phase: adding HCl to make the pH = 3, and then adding NaOH to make the pH very basic at 13 for 1 hour. This phase uses the Psilocybe coprophila as the catalyst for the reaction. [17] Serotonin taken orally does not pass into the serotonergic The pathway for the synthesis of serotonin from pathways of the central nervous system, because it does not tryptophan. cross the blood–brain barrier. However, tryptophan and its metabolite 5-hydroxytryptophan (5-HTP), from which serotonin is synthesized, can and do cross the blood–brain barrier. These agents are available as dietary supplements, and may be effective serotonergic agents. One product of serotonin breakdown is 5-hydroxyindoleacetic acid (5-HIAA), which is excreted in the urine. Serotonin and 5-HIAA are sometimes produced in excess amounts by certain tumors or cancers, and levels of these substances may be measured in the urine to test for these tumors.
Serotonin
155
Drugs targeting the 5-HT system
Several classes of drugs target the 5-HT system, including some antidepressants, antipsychotics, anxiolytics, antiemetics, and antimigraine drugs, as well as the psychedelic drugs and empathogens.
Psychedelic drugs
The psychedelic drugs psilocin/psilocybin, DMT, mescaline, and LSD are agonists, primarily at 5HT2A/2C receptors.[][] The empathogen-entactogen MDMA releases serotonin from synaptic vesicles of neurons.[]
Antidepressants
Drugs which alter serotonin levels are used in depression, generalized anxiety disorder and social phobia. Monoamine oxidase inhibitors (MAOIs) prevent the breakdown of monoamine neurotransmitters (including serotonin), and therefore increase concentrations of the neurotransmitter in the brain. MAOI therapy is associated with many adverse drug reactions, and patients are at risk of hypertensive emergency triggered by foods with high tyramine content, and certain drugs. Some drugs inhibit the reuptake of serotonin, making it stay in the synaptic cleft longer. The tricyclic antidepressants (TCAs) inhibit the reuptake of both serotonin and norepinephrine. The newer selective serotonin reuptake inhibitors (SSRIs) have fewer side effects and fewer interactions with other drugs. The side effects that have become apparent recently include a decrease in bone mass in elderly and increased risk for osteoporosis. However, it is not yet clear whether it is due to SSRI action on peripheral serotonin production and or action in the gut or in the brain.[] Certain SSRI medications have been shown to lower serotonin levels below the baseline after chronic use, despite initial increases. This has been connected to the observation that the benefit of SSRIs may decrease in selected patients after a long-term treatment. A switch in medication will usually resolve this issue (up to 70% of the time).[] The novel antidepressant tianeptine, a selective serotonin reuptake "enhancer", has mood-elevating effects. This provides evidence for the theory that serotonin is most likely used to regulate the extent or intensity of moods, rather than level directly correlating with mood. In fact, the 5-HTTLPR gene codes for the number of serotonin transporters in the brain, with more serotonin transporters causing decreased duration and magnitude of serotonergic signaling.[18] The 5-HTTLPR polymorphism (l/l) causing more serotonin transporters to be formed is also found to be more resilient against depression and anxiety.[19][20] Therefore, increasing levels of extracellular serotonin may be associated with increased affect, for good or for worse. Although phobias and depression might be attenuated by serotonin-altering drugs, this does not mean the individual's situation has been improved, but only the individual's perception of the environment. Sometimes, a lower serotonin level might be beneficial, for example in the ultimatum game, where players with normal serotonin levels are more prone to accept unfair offers than participants whose serotonin levels have been artificially lowered.[] Serotonin syndrome Extremely high levels of serotonin can cause a condition known as serotonin syndrome, with toxic and potentially fatal effects. In practice, such toxic levels are essentially impossible to reach through an overdose of a single antidepressant drug, but require a combination of serotonergic agents, such as an SSRI with an MAOI.[21] The intensity of the symptoms of serotonin syndrome vary over a wide spectrum, and the milder forms are seen even at nontoxic levels.[]
Antiemetics
Some 5-HT3 antagonists, such as ondansetron, granisetron, and tropisetron, are important antiemetic agents. They are particularly important in treating the nausea and vomiting that occur during anticancer chemotherapy using cytotoxic drugs. Another application is in the treatment of postoperative nausea and vomiting.
Serotonin
156
In unicellular organisms
Serotonin is used by a variety of single-cell organisms for various purposes. SSRIs have been found to be toxic to algae.[] The gastrointestinal parasite Entamoeba histolytica secretes serotonin, causing a sustained secretory diarrhea in some patients.[][] Patients infected with E. histolytica have been found to have highly elevated serum serotonin levels which returned to normal following resolution of the infection.[] E. histolytica also responds to the presence of serotonin by becoming more virulent.[] This means serotonin secretion not only serves to increase the spread of enteamoebas by giving the host diarrhea, but also to coordinate their behaviour according to their population density, a phenomenon known as quorum sensing. Outside a host, the density of entoamoebas is low, hence also the serotonin concentration. Low serotonin signals to the entoamoebas they are outside a host and they become less virulent to conserve energy. When they enter a new host, they multiply in the gut, and become more virulent as the serotonin concentration increases.
In plants
In drying seeds, serotonin production is a way to get rid of the buildup of poisonous ammonia. The ammonia is collected and placed in the indole part of L-tryptophan, which is then decarboxylated by tryptophan decarboxylase to give tryptamine, which is then hydroxylated by a cytochrome P450 monooxygenase, yielding serotonin.[] However, since serotonin is a major gastrointestinal tract modulator, it may be produced by plants in fruits as a way of speeding the passage of seeds through the digestive tract, in the same way as many well-known seed and fruit associated laxatives. Serotonin is found in mushrooms, fruits and vegetables. The highest values of 25–400 mg/kg have been found in nuts of the walnut (Juglans) and hickory (Carya) genera. Serotonin concentrations of 3–30 mg/kg have been found in plantains, pineapples, banana, kiwifruit, plums, and tomatoes. Moderate levels from 0.1–3 mg/kg have been found in a wide range of tested vegetables.[22] Serotonin is one compound of the poison contained in stinging nettles (Urtica dioica), where it causes pain on injection in the same manner as its presence in insect venoms (see above). It is also naturally found in Paramuricea clavata, or the Red Sea Fan.[23] Serotonin and tryptophan have been found in chocolate with varying cocoa contents. The highest serotonin content (2.93 ug g-1) was found in chocolate with 85% cocoa, and the highest tryptophan content (13.27-13.34 ug g-1) was found in 70-85% cocoa. The intermediate in the synthesis from tryptophan to serotonin, 5-hydroxytryptophan, was not found.[24] Unlike its precursors, 5-HTP and tryptophan, serotonin does not cross the blood–brain barrier, which means ingesting serotonin in the diet has no effect on brain serotonin levels.
Methyl-tryptamines and hallucinogens
Several plants contain serotonin together with a family of related tryptamines that are methylated at the amino (NH2) and (OH) groups, are N-oxides, or miss the OH group. These compounds do reach the brain, although some portion of them are metabolized by MAO-B enzymes in the liver. Examples are plants from the Anadenanthera genus that are used in the hallucinogenic yopo snuff. These compounds are widely present in the leaves of many plants, and may serve as deterrents for animal ingestion. Serotonin occurs in several mushrooms of the genus Panaeolus.[25] Serotonin is also naturally occurring in toad venom.[26]
Serotonin
157
History
In 1935, Italian Vittorio Erspamer showed an extract from enterochromaffin cells made intestines contract. Some believed it contained adrenaline, but two years later, Erspamer was able to show it was a previously unknown amine, which he named "enteramine".[] In 1948, Maurice M. Rapport, Arda Green, and Irvine Page of the Cleveland Clinic discovered a vasoconstrictor substance in blood serum, and since it was a serum agent affecting vascular tone, they named it serotonin.[] In 1952, enteramine was shown to be the same substance as serotonin, and as the broad range of physiological roles was elucidated, the abbreviation 5-HT of the proper chemical name 5-hydroxytryptamine became the preferred name in the pharmacological field.[] Synonyms of serotonin include: 5-hydroxytriptamine, thrombotin, enteramin, substance DS, and 3-(β-Aminoethyl)-5-hydroxyindole.[27]
References
[1] Pietra, S.;Farmaco, Edizione Scientifica 1958, Vol. 13, pp. 75–9. [2] Calculated using Advanced Chemistry Development (ACD/Labs) Software V11.02 (©1994–2011 ACD/Labs) [9] Murakami H, Bessinger K, Hellmann J, Murakami S. Aging-dependent and -independent modulation of associative learning behavior by insulin/insulin-like growth factor-1 signal in Caenorhabditis elegans. J Neurosci. 2005 Nov 23;25(47):10894-904. PMID 16306402 (http:/ / www. ncbi. nlm. nih. gov/ pubmed/ 17559503) [12] Free full text (http:/ / www. tga. gov. au/ adr/ aadrb/ aadr0408. htm) from the Australian Therapeutic Goods Administration [16] The Raphe nuclei group of neurons are located along the brain stem from the labels 'Mid Brain' to 'Oblongata', centered on the pons. (See relevant image.) [17] Alarcon, J. Biotransformation of indole derivatives by mycelial cultures. Zeitschrift für Naturforschung.C, A journal of biosciences 2008, 63, 82. [23] Penez, N.; Culioli, G.; Briand, J.; Blache, Y.; Perez, T.; Thomas, O. P. Antifouling Properties of Simple Indole and Purine Alkaloids from the Mediterranean Gorgonian Paramuricea clavata. J. Nat. Prod. 2011, 74, 2304-2308. [24] Guillen-Casla, V.; Rosales-Conrado, N.; Leon-Gonzalez, M. E.; Perez-Arribas, L. V.; Polo-Diez, L. M. Determination ofserotonin and its precursors in chocolate samples by capillary liquid chromatography with mass spectrometry detection. J. Chromatogr. A. 2012, 1232, 158-165. [26] Zhang, P.; Cui, Z.; Liu, Y.; Wang, D.; Liu, N.; Yoshikawa, M. Quality Evaluation of Drug Toad Venom fromDifferent Origins through a Simultaneous Determination of Bufogeninsand Indole Alkaloids by HPLC. Chem. Pharm. Bull. 2005, 53, 1582-1586. [27] SciFinder – Serotonin Substance Detail. Accessed (4-11-2012).
External links
• Serotonin bound to proteins (http://www.ebi.ac.uk/pdbe-srv/PDBeXplore/ligand/?ligand=SRO) in the PDB • PsychoTropicalResearch (http://www.psychotropical.com/) Extensive reviews on serotonergic drugs and Serotonin Syndrome. • Molecule of the Month: Serotonin (http://www.chm.bris.ac.uk/motm/serotonin/home1.htm) at University of Bristol • 60-Second Psych: No Fair! My Serotonin Level Is Low (http://www.sciam.com/podcast/episode. cfm?id=68FC98F1-E48A-251D-8F65277181DB9A4E), Scientific American • Serotonin Test Interpretation on ClinLab Navigator (http://www.clinlabnavigator.com/Tests/Serotonin.html). • Tryptophan hydroxylase-2 gene variation influences personality traits and disorders related to emotional dysregulation (http://www.ncbi.nlm.nih.gov/pubmed/17176492) at the National Center for Biotechnology Information.
Endorphins
158
Endorphins
Endorphins ("endogenous morphine") are endogenous opioid peptides that function as neurotransmitters.[1] They are produced by the pituitary gland and the hypothalamus in vertebrates during exercise,[] excitement, pain, consumption of spicy food, love and orgasm,[][] and they resemble the opiates in their abilities to produce analgesia and a feeling of well-being.
Chemical structure of alpha-Neoendorphin (α-Neoendorphin)
The term implies a pharmacological activity (analogous to the activity of the corticosteroid category of biochemicals) as opposed to a specific chemical formulation. It consists of two parts: endo- and -orphin; these are short forms of the words endogenous and morphine, intended to mean "a morphine-like substance originating from within the body."[] The term "endorphin rush" has been adopted in popular speech to refer to feelings of exhilaration brought on by pain, danger, or other forms of stress,[] supposedly due to the influence of endorphins. When a nerve impulse reaches the spinal cord, endorphins that prevent nerve cells from releasing more pain signals are released.
History
Opioid neuropeptides were first discovered in 1974 by two independent groups of investigators: • John Hughes and Hans Kosterlitz of Scotland isolated — from the brain of a pig — what some called enkephalins (from the Greek εγκέφαλος, cerebrum).[][2] • Around the same time, in the calf brain, Rabi Simantov and Solomon H. Snyder of the United States found[3] what Eric Simon (who independently discovered opioid receptors in the brain) later termed "endorphin" by an abbreviation of "endogenous morphine", meaning "morphine produced naturally in the body".[] Importantly, recent studies have demonstrated that diverse animal and human tissues are in fact capable of producing morphine itself, which is not a peptide.[][]
Mechanism of action
Beta-endorphin (β-Endorphin) is released into blood from the pituitary gland and into the spinal cord and brain from hypothalamic neurons. The β-endorphin that is released into the blood cannot enter the brain in large quantities because of the blood–brain barrier, so the physiological Chemical structure of beta-endorphin importance of the β-endorphin that can be measured in the blood is far from clear. β-Endorphin is a cleavage product of pro-opiomelanocortin (POMC), which is also the precursor hormone for adrenocorticotrophic hormone (ACTH). The behavioural effects of β-endorphin are exerted by its actions in the brain and spinal cord, and it is presumed that the hypothalamic neurons are the major source of β-endorphin at these sites.
Endorphins In situations where the level of ACTH is increased (e.g., Cushing’s Syndrome), the level of endorphins also increases slightly. β-Endorphin has the highest affinity for the μ1 opioid receptor, slightly lower affinity for the μ2 and δ opioid receptors, and low affinity for the κ1 opioid receptors. μ-Opioid receptors are the main receptor through which morphine acts. In the classical sense, μ opioid receptors are presynaptic, and inhibit neurotransmitter release; through this mechanism, they inhibit the release of the inhibitory neurotransmitter GABA, and disinhibit the dopamine pathways, causing more dopamine to be released. By hijacking this process, exogenous opioids cause inappropriate dopamine release, and lead to aberrant synaptic plasticity, which causes dependency. Opioid receptors have many other and more important roles in the brain and periphery however, modulating pain, cardiac, gastric and vascular function as well as possibly panic and satiation, and receptors are often found at postsynaptic locations as well as presynaptically.
159
Activity
Scientists sometimes debate whether specific activities release measurable levels of endorphins. Much of the current data comes from animal models which may not be relevant to humans. The studies that do involve humans often measure endorphin plasma levels, which do not necessarily correlate with levels in the central nervous system. Other studies use a blanket opioid antagonist (usually naloxone) to indirectly measure the release of endorphins by observing the changes that occur when any endorphin activity that might be present is blocked.
Runner's high
A publicized effect of endorphin production is the so-called "runner's high", which is said to occur when strenuous exercise takes a person over a threshold that activates endorphin production. Endorphins are released during long, continuous workouts, when the level of intensity is between moderate and high, and breathing is difficult. This also corresponds with the time that muscles use up their stored glycogen. During a release of endorphins, the person may be exposed to bodily harm from strenuous bodily functions after going past his or her body's physical limit. This means that runners can keep running despite pain, continuously surpassing what they otherwise would consider to be their limit. Runner's high has also been known to create feelings of euphoria and happiness. Altough it is called runners high, the effect occurs to strenous exercise in general, and not just running. Runner's high has been suggested to have evolutionary roots based on the theory that it helped with the survival of early humans. Current African tribes make use of runner's high when conducting persistence hunting (a method in which tribesman hunt an animal and track it for miles, eventually killing the animal due to its vulnerability brought on by exhaustion[4]). In 2008, researchers in Germany reported on the mechanisms that cause the runner's high. Using PET scans combined with recently available chemicals that reveal endorphins in the brain, they were able to compare runners’ brains before and after a run.[] Previous research on the role of endorphins in producing runner's high questioned the mechanisms at work, their data possibly demonstrated that the "high" comes from completing a challenge rather than as a result of exertion.[5] Studies in the early 1980s cast doubt on the relationship between endorphins and the runner's high for several reasons: • The first was that when an antagonist (pharmacological agent that blocks the action for the substance under study) was infused (e.g., naloxone) or ingested (naltrexone) the same changes in mood state occurred as when the person exercised with no blocker. • A study in 2003 by the Georgia Institute of Technology found that runner's high might be caused by the release of another naturally produced chemical, anandamide.[][] The authors suggest that the body produces this chemical to deal with prolonged stress and pain from strenuous exercise, similar to the original theory involving endorphins.
Endorphins However, the release of anandamide was not reported with the cognitive effects of the runner's high; this suggests that anandamide release may not be significantly related to runner's high.[] • A study at the University of Arizona, published in April 2012, argues implicitly that endocannabinoids are, most likely, the causative agent in runner's high, while also arguing this to be a result of the evolutionary advantage endocannabinoids provide to endurance-based cursorial species. This largely refers to quadruped mammals, but also to biped hominids, such as humans. The study shows that both humans and dogs show significantly increased endocannabinoid signaling following high intensity running, but not low-intensity walking. The study does not, however, ever address the potential contribution of endorphins to runner's high.[6] However, in other research that has focused on the blood–brain barrier, it has been shown that endorphin molecules are too large to pass freely, thus very unlikely to be the cause of the runner's high feeling of euphoria.[7] It has been suggested that apart from endorphins, other chemicals can contribute to runner's high; candidates include epinephrine, serotonin, and dopamine.[citation needed]
160
Depersonalization disorder
Endorphins are known to play a role in depersonalization disorder. The opioid antagonists naloxone and naltrexone have both been proven to be successful in treating depersonalization.[][8] To quote a 2001 naloxone study, "In three of 14 patients, depersonalization symptoms disappeared entirely and seven patients showed a marked improvement. The therapeutic effect of naloxone provides evidence for the role of the endogenous opioid system in the pathogenesis of depersonalization."
Relaxation
In 2003, clinical researchers reported that profound relaxation in a float tank triggers the production of endorphins.[9] This explains the pain relief experienced during float sessions.[10]
Acupuncture
In 1999, clinical researchers reported that inserting acupuncture needles into specific body points triggers the production of endorphins.[][] In another study, higher levels of endorphins were found in cerebrospinal fluid after patients underwent acupuncture.[11] In addition, naloxone appeared to block acupuncture’s pain-relieving effects.
Pregnancy
A placental tissue of fetal origin — i.e., the syncytiotrophoblast — excretes beta-endorphins into the maternal blood system from the 3rd month of pregnancy. A recent study[] proposes an adaptive background for this phenomenon. The authors argue that fetuses make their mothers endorphin-dependent then manipulate them to increase nutrient allocation to the placenta. Their hypothesis predicts that: (1) anatomic position of endorphin production should mirror its presumed role in foetal-maternal conflict; (2) endorphin levels should co-vary positively with nutrient carrying capacity of maternal blood system; (3) postpartum psychological symptoms (such as postpartum blues, depression, and psychosis) in humans are side-effects of this mechanism that can be interpreted as endorphin-deprivation symptoms; (4) shortly after parturition, placentophagy could play an adaptive role in decreasing the negative side-effects of foetal manipulation; (5) later, breast-feeding-induced endorphin excretion of the maternal pituitary saves the mother from further deprivation symptoms. These predictions appear to be supported by empirical data.[]
Endorphins
161
Etymology
From the Greek: word endo ενδο meaning "within" (endogenous, Greek: ενδογενής, "proceeding from within") and morphine, from Morpheus, Greek: Μορφέας, the god of sleep in the Greek mythology, thus 'endo(genous) (mo)rphine’.
References
[1] Oswald Steward: Functional neuroscience (2000), page 116. Preview at: Google books. (http:/ / books. google. com/ books?id=nNH3p29wjK4C& pg=PA116& dq=endorphins+ neurotransmitter& hl=en& ei=IwwlTKfzHMr-_Aa-w6zGBA& sa=X& oi=book_result& ct=result& resnum=10& ved=0CFMQ6AEwCTgK#v=onepage& q=endorphins neurotransmitter& f=false) [4] http:/ / www. youtube. com/ watch?v=826HMLoiE_o [9] Anette Kjellgren, 2003, The experience of floatation REST (restricted Environmental stimulation technique), subjective stress and pain, Goteborg University Sweden,
External links
• Endorphins (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Endorphins) at the US National Library of Medicine Medical Subject Headings (MeSH) • "A genetic influence on alcohol addiction found - lack of endorphin" (http://www.news-medical.net/ ?id=33701#). News-Medical.Net. Dec-2007-12-21. Retrieved 2008-10-15.
Somatostatin
162
Somatostatin
Somatostatin
Available structures PDB Ortholog search: PDBe [1], RCSB [2] List of PDB id codes 1P2W
[3]
Identifiers Symbols External IDs SST
[4]
; SMST
[5]
OMIM: 182450
MGI: 98326
[6]
HomoloGene: 819
[7]
ChEMBL: 1795130
[8]
GeneCards: SST Gene
[9]
Gene Ontology Molecular function • hormone activity [10] Cellular component • extracellular region [229] [230] • extracellular space [11] • neuronal cell body Biological process • hyperosmotic response [13] • cell surface receptor signaling pathway [14] • G-protein coupled receptor signaling pathway [25] • cell-cell signaling [15] • synaptic transmission [16] • response to nutrient [17] • digestion [18] • negative regulation of cell proliferation • hormone-mediated apoptotic signaling pathway
[19] [12]
• response to heat [21] • regulation of cell migration [22] • response to drug [23] • response to amino acid stimulus [24] • response to steroid hormone stimulus Sources: Amigo
[25]
[20]
/ QuickGO
[26]
RNA expression pattern
Somatostatin
163
More reference expression data Orthologs Species Entrez Ensembl UniProt RefSeq (mRNA) RefSeq (protein) Human 6750
[28] [30]
[27]
Mouse 20604
[29] [31]
ENSG00000157005 P61278
[32] [34]
ENSMUSG00000004366 P60041
[33] [35]
NM_001048 NP_001039
NM_009215 NP_033241
[36]
[37]
Location (UCSC) Chr 3: [38] 187.39 – 187.39 Mb PubMed search
[40]
Chr 16: [39] 23.89 – 23.89 Mb
[41]
Somatostatin (also known as growth hormone-inhibiting hormone (GHIH) or somatotropin release-inhibiting factor (SRIF)) or somatotropin release-inhibiting hormone[citation needed] is a peptide hormone that regulates the endocrine system and affects neurotransmission and cell proliferation via interaction with G protein-coupled somatostatin receptors and inhibition of the release of numerous secondary hormones. Somatostatin has two active forms produced by alternative cleavage of a single preproprotein: one of 14 amino acids, the other of 28 amino acids.[] In all vertebrates, there exists six different somatostatin genes that have been named SS1, SS2, SS3, SS4, SS5, and SS6.[] The six different genes along with the five different somatostatin receptors allows somatostatin to possess a large range of functions.[] Humans have only one somatostatin gene, SST.[][][]
Somatostatin
164
Production
Digestive system
Somatostatin is secreted in several locations in the digestive system: • stomach • intestine • delta cells of the pancreas[]
Brain
[42] Sst is expressed in interneurons in the telencephalon of the embryonic day 15.5 mouse. Allen Brain Atlases Sst [43] expression in the adult mouse. Allen Brain Atlases
Somatostatin is produced by neuroendocrine neurons of the periventricular nucleus of the hypothalamus. These neurons project to the median eminence, where somatostatin is released from neurosecretory nerve endings into the hypothalamo-hypophysial system through neuron axons. Somatostatin is then carried to the anterior pituitary gland, where it inhibits the secretion of growth hormone from somatotrope cells. The somatostatin neurons in the periventricular nucleus mediate negative feedback effects of growth hormone on its own release; the somatostatin neurons respond to high circulating concentrations of growth hormone and somatomedins by increasing the release of somatostatin, so reducing the rate of secretion of growth hormone. Somatostatin is also produced by several other populations that project centrally, i.e., to other areas of the brain, and somatostatin receptors are expressed at many different sites in the brain. In particular, there are populations of somatostatin neurons in the arcuate nucleus,[citation needed] the hippocampus,[citation needed] and the brainstem nucleus of the solitary tract.[citation needed]
Somatostatin
165
Actions
Somatostatin is classified as an inhibitory hormone,[] whose actions are spread to different parts of the body:
Anterior pituitary
In the anterior pituitary gland, the effects of somatostatin are: • Inhibit the release of growth hormone (GH)[] (thus opposing the effects of Growth Hormone-Releasing Hormone (GHRH)) • Inhibit the release of thyroid-stimulating hormone (TSH)[1] • It is induced by low pH. • Inhibit adenylyl cyclase in parietal cells.
Gastrointestinal system
• Somatostatin is homologous with cortistatin (see somatostatin family) and suppresses the release of gastrointestinal hormones • Gastrin • Cholecystokinin (CCK) • Secretin • Motilin • Vasoactive intestinal peptide (VIP) • Gastric inhibitory polypeptide (GIP) • Enteroglucagon • Decrease rate of gastric emptying, and reduces smooth muscle contractions and blood flow within the intestine[] • Suppresses the release of pancreatic hormones • Inhibits insulin release when somatostatin is released from delta cells of pancreas[] • Inhibits the release of glucagon[] • Suppresses the exocrine secretory action of pancreas.
D cell is visible at upper-right, and somatostatin is represented by middle arrow pointing left
Synthetic substitutes
Octreotide (brand name Sandostatin, Novartis Pharmaceuticals) is an octapeptide that mimics natural somatostatin pharmacologically, though is a more potent inhibitor of growth hormone, glucagon, and insulin than the natural hormone and has a much longer half-life (approximately 90 minutes, compared to 2–3 minutes for somatostatin). Since it is absorbed poorly from the gut, it is administered parenterally (subcutaneously, intramuscularly, or intravenously). It is indicated for symptomatic treatment of carcinoid syndrome and acromegaly. It is also finding increased use in polycystic diseases of the liver and kidney. Lanreotide (INN) is a medication used in the management of acromegaly and symptoms caused by neuroendocrine tumors, most notably carcinoid syndrome. It is a long-acting analogue of somatostatin, like octreotide.
Somatostatin Lanreotide (as lanreotide acetate) is manufactured by Ipsen and marketed under the trade name Somatuline. It is available in several countries, including the United Kingdom, Australia, and Canada, and was approved for sale in the United States by the Food and Drug Administration (FDA) on August 30, 2007.
166
Evolutionary history
There are six somatostatin genes that have been discovered in vertebrates. The current proposed history as to how these six genes arose is based on the three whole-genome duplication events that took place in vertebrate evolution along with local duplications in teleost fish. An ancestral somatostatin gene was duplicated during the first whole-genome duplication event (1R) to create SS1 and SS2. These two genes were duplicated during the second whole-genome duplication event (2R) to create four new somatostatin genes: SS1, SS2, SS3, and one gene that was lost during the evolution of vertebrates. Tetrapods retained SS1 (also known as SS-14 and SS-28) and SS2 (also known as cortistatin) after the split in the sarcopterygii and actinopterygii lineage split. In teleost fish, SS1, SS2, and SS3 were duplicated during the third whole-genome duplication event (3R) to create SS1, SS2, SS4, SS5, and two genes that were lost during the evolution of teleost fish. SS1 and SS2 went through local duplications to give rise to SS6 and SS3.[]
References
[1] First Aid for the USMLE Step 1, 2010. Page 286.
Further reading
• Florio T, Schettini G (2002). "[Somatostatin and its receptors. Role in the control of cell proliferation]". Minerva Endocrinol. 26 (3): 91–102. PMID 11753230 (http://www.ncbi.nlm.nih.gov/pubmed/11753230). • Yamada Y, Reisine T, Law SF, et al. (1993). "Somatostatin receptors, an expanding gene family: cloning and functional characterization of human SSTR3, a protein coupled to adenylyl cyclase". Mol. Endocrinol. 6 (12): 2136–42. doi: 10.1210/me.6.12.2136 (http://dx.doi.org/10.1210/me.6.12.2136). PMID 1337145 (http:// www.ncbi.nlm.nih.gov/pubmed/1337145). • Yamada Y, Post SR, Wang K, et al. (1992). "Cloning and functional characterization of a family of human and mouse somatostatin receptors expressed in brain, gastrointestinal tract, and kidney" (http://www.ncbi.nlm.nih. gov/pmc/articles/PMC48214). Proc. Natl. Acad. Sci. U.S.A. 89 (1): 251–5. doi: 10.1073/pnas.89.1.251 (http:// dx.doi.org/10.1073/pnas.89.1.251). PMC 48214 (http://www.ncbi.nlm.nih.gov/pmc/articles/ PMC48214). PMID 1346068 (http://www.ncbi.nlm.nih.gov/pubmed/1346068). • Brazeau P, Vale W, Burgus R, et al. (1973). "Hypothalamic polypeptide that inhibits the secretion of immunoreactive pituitary growth hormone". Science 179 (4068): 77–9. doi: 10.1126/science.179.4068.77 (http:// dx.doi.org/10.1126/science.179.4068.77). PMID 4682131 (http://www.ncbi.nlm.nih.gov/pubmed/ 4682131). • Shen LP, Pictet RL, Rutter WJ (1982). "Human somatostatin I: sequence of the cDNA" (http://www.ncbi.nlm. nih.gov/pmc/articles/PMC346717). Proc. Natl. Acad. Sci. U.S.A. 79 (15): 4575–9. doi: 10.1073/pnas.79.15.4575 (http://dx.doi.org/10.1073/pnas.79.15.4575). PMC 346717 (http://www.ncbi. nlm.nih.gov/pmc/articles/PMC346717). PMID 6126875 (http://www.ncbi.nlm.nih.gov/pubmed/ 6126875). • Shen LP, Rutter WJ (1984). "Sequence of the human somatostatin I gene". Science 224 (4645): 168–71. doi: 10.1126/science.6142531 (http://dx.doi.org/10.1126/science.6142531). PMID 6142531 (http://www.ncbi. nlm.nih.gov/pubmed/6142531). • Montminy MR, Goodman RH, Horovitch SJ, Habener JF (1984). "Primary structure of the gene encoding rat preprosomatostatin" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC345502). Proc. Natl. Acad. Sci. U.S.A. 81 (11): 3337–40. doi: 10.1073/pnas.81.11.3337 (http://dx.doi.org/10.1073/pnas.81.11.3337). PMC
Somatostatin 345502 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC345502). PMID 6145156 (http://www.ncbi.nlm. nih.gov/pubmed/6145156). • Zabel BU, Naylor SL, Sakaguchi AY, et al. (1984). "High-resolution chromosomal localization of human genes for amylase, proopiomelanocortin, somatostatin, and a DNA fragment (D3S1) by in situ hybridization" (http:// www.ncbi.nlm.nih.gov/pmc/articles/PMC390100). Proc. Natl. Acad. Sci. U.S.A. 80 (22): 6932–6. doi: 10.1073/pnas.80.22.6932 (http://dx.doi.org/10.1073/pnas.80.22.6932). PMC 390100 (http://www.ncbi. nlm.nih.gov/pmc/articles/PMC390100). PMID 6196780 (http://www.ncbi.nlm.nih.gov/pubmed/ 6196780). • Panetta R, Greenwood MT, Warszynska A, et al. (1994). "Molecular cloning, functional characterization, and chromosomal localization of a human somatostatin receptor (somatostatin receptor type 5) with preferential affinity for somatostatin-28". Mol. Pharmacol. 45 (3): 417–27. PMID 7908405 (http://www.ncbi.nlm.nih. gov/pubmed/7908405). • Demchyshyn LL, Srikant CB, Sunahara RK, et al. (1993). "Cloning and expression of a human somatostatin-14-selective receptor variant (somatostatin receptor 4) located on chromosome 20". Mol. Pharmacol. 43 (6): 894–901. PMID 8100352 (http://www.ncbi.nlm.nih.gov/pubmed/8100352). • Kaupmann K, Bruns C, Hoyer D, et al. (1993). "Distribution and second messenger coupling of four somatostatin receptor subtypes expressed in brain". FEBS Lett. 331 (1–2): 53–9. doi: 10.1016/0014-5793(93)80296-7 (http:// dx.doi.org/10.1016/0014-5793(93)80296-7). PMID 8405411 (http://www.ncbi.nlm.nih.gov/pubmed/ 8405411). • Aguila MC, Rodriguez AM, Aguila-Mansilla HN, Lee WT (1996). "Somatostatin antisense oligodeoxynucleotide-mediated stimulation of lymphocyte proliferation in culture". Endocrinology 137 (5): 1585–90. doi: 10.1210/en.137.5.1585 (http://dx.doi.org/10.1210/en.137.5.1585). PMID 8612489 (http:// www.ncbi.nlm.nih.gov/pubmed/8612489). • Sharma K, Patel YC, Srikant CB (1997). "Subtype-selective induction of wild-type p53 and apoptosis, but not cell cycle arrest, by human somatostatin receptor 3". Mol. Endocrinol. 10 (12): 1688–96. doi: 10.1210/me.10.12.1688 (http://dx.doi.org/10.1210/me.10.12.1688). PMID 8961277 (http://www.ncbi.nlm.nih.gov/pubmed/ 8961277). • Dournaud P, Boudin H, Schonbrunn A, et al. (1998). "Interrelationships between somatostatin sst2A receptors and somatostatin-containing axons in rat brain: evidence for regulation of cell surface receptors by endogenous somatostatin". J. Neurosci. 18 (3): 1056–71. PMID 9437026 (http://www.ncbi.nlm.nih.gov/pubmed/ 9437026). • Barnea A, Roberts J, Ho RH (1999). "Evidence for a synergistic effect of the HIV-1 envelope protein gp120 and brain-derived neurotrophic factor (BDNF) leading to enhanced expression of somatostatin neurons in aggregate cultures derived from the human fetal cortex". Brain Res. 815 (2): 349–57. doi: 10.1016/S0006-8993(98)01098-1 (http://dx.doi.org/10.1016/S0006-8993(98)01098-1). PMID 9878821 (http://www.ncbi.nlm.nih.gov/ pubmed/9878821). • Ferone D, van Hagen PM, van Koetsveld PM, et al. (1999). "In vitro characterization of somatostatin receptors in the human thymus and effects of somatostatin and octreotide on cultured thymic epithelial cells". Endocrinology 140 (1): 373–80. doi: 10.1210/en.140.1.373 (http://dx.doi.org/10.1210/en.140.1.373). PMID 9886848 (http://www.ncbi.nlm.nih.gov/pubmed/9886848). • Brakch N, Lazar N, Panchal M, et al. (2002). "The somatostatin-28(1-12)-NPAMAP sequence: an essential helical-promoting motif governing prosomatostatin processing at mono- and dibasic sites". Biochemistry 41 (5): 1630–9. doi: 10.1021/bi011928m (http://dx.doi.org/10.1021/bi011928m). PMID 11814357 (http://www. ncbi.nlm.nih.gov/pubmed/11814357). • Oomen SP, van Hennik PB, Antonissen C, et al. (2002). "Somatostatin is a selective chemoattractant for primitive (CD34(+)) hematopoietic progenitor cells". Exp. Hematol. 30 (2): 116–25. doi: 10.1016/S0301-472X(01)00772-X (http://dx.doi.org/10.1016/S0301-472X(01)00772-X). PMID 11823046 (http://www.ncbi.nlm.nih.gov/
167
Somatostatin pubmed/11823046). • Simonetti M, Di BC (2002). "Structural motifs in the maturation process of peptide hormones. The somatostatin precursor. I. A CD conformational study". J. Pept. Sci. 8 (2): 66–79. doi: 10.1002/psc.370 (http://dx.doi.org/ 10.1002/psc.370). PMID 11860030 (http://www.ncbi.nlm.nih.gov/pubmed/11860030).
168
Gastrin
Gastrin
Identifiers Symbol Pfam InterPro PROSITE Gastrin PF00918 [1] [2] [3]
IPR001651
PDOC00232
Available protein structures: Pfam PDB structures [4] [5] ; PDBe [6]
RCSB PDB
PDBsum structure summary [7]
Gastrin
Identifiers Symbols External IDs GAST
[8]
; GAS
[9]
OMIM: 137250
MGI: 104768
[10]
HomoloGene: 628
[11]
GeneCards: GAST Gene
[12]
Gene Ontology Molecular function • hormone activity [10] Cellular component • extracellular region [229] Biological process • signal transduction [14] • G-protein coupled receptor signaling pathway
[13] [38]
Sources: Amigo
/ QuickGO
[14]
RNA expression pattern
More reference expression data
[15]
Gastrin
169
Orthologs Species Entrez Ensembl UniProt RefSeq (mRNA) RefSeq (protein) Human 2520
[16] [18]
Mouse 14459
[17] [19]
ENSG00000184502 P01350
[20] [22]
ENSMUSG00000017165 P48757
[21] [23]
NM_000805 NP_000796
NM_010257 NP_034387
[24]
[25]
Location (UCSC) Chr 17: [26] 39.87 – 39.87 Mb PubMed search
[28]
Chr 11: [27] 100.33 – 100.34 Mb
[29]
In humans, gastrin is a peptide hormone that stimulates secretion of gastric acid (HCl) by the parietal cells of the stomach and aids in gastric motility. It is released by G cells in the antrum of the stomach (the portion of the stomach adjacent the pyloric valve), duodenum, and the pancreas. It binds to cholecystokinin B receptors to stimulate the release of histamines in enterochromaffin-like cells, and it induces the insertion of K+/H+ ATPase pumps into the apical membrane of parietal cells (which in turn increases H+ release into the stomach cavity). Its release is stimulated by peptides in the lumen of the stomach.
History
Its existence was first suggested in 1905 by the British physiologist John Sydney Edkins,[1][2] and gastrins were isolated in 1964 by Roderic Alfred Gregory at the University of Liverpool.[3] In 1964 the structure of Gastrin was determined.[4]
G cell is visible near bottom left, and gastrin is labeled as the two black arrows leading from it. Note: this diagram does not illustrate gastrin's stimulatory effect on ECL cells.
Physiology
Genetics
The GAS gene is located on the long arm of the seventeenth chromosome (17q21).[5]
Gastrin
170
Synthesis
Gastrin is a linear peptide hormone produced by G cells of the duodenum and in the pyloric antrum of the stomach. It is secreted into the bloodstream. Gastrin is found primarily in three forms: • gastrin-34 ("big gastrin") • gastrin-17 ("little gastrin") • gastrin-14 ("minigastrin") Also, pentagastrin is an artificially synthesized, five amino acid sequence identical to the last five amino acid sequence at the C-terminus end of gastrin. The numbers refer to the amino acid count.
Release
Gastrin is released in response to certain stimuli. These include: • • • • stomach distension vagal stimulation (mediated by the neurocrine bombesin, or GRP in humans) the presence of partially digested proteins especially amino acids hypercalcemia
Gastrin release is inhibited by:[6][7] • The presence of acid (primarily the secreted HCl) in the stomach (a case of negative feedback). • Somatostatin also inhibits the release of gastrin, along with secretin, GIP (gastroinhibitory peptide), VIP (vasoactive intestinal peptide), glucagon and calcitonin.
Function
The presence of gastrin stimulates parietal cells of the stomach to secrete hydrochloric acid (HCl)/gastric acid. This is done both directly on the parietal cell and indirectly via binding onto CCK2/gastrin receptors on ECL cells in the stomach, which then responds by releasing histamine, which in turn acts in a paracrine manner on parietal cells stimulating them to secrete H+ ions. This is the major stimulus for acid secretion by parietal cells. Along with the above mentioned function, gastrin has been shown to have additional functions as well: • • • • Stimulates parietal cell maturation and fundal growth. Causes chief cells to secrete pepsinogen, the zymogen (inactive) form of the digestive enzyme pepsin. Increases antral muscle mobility and promotes stomach contractions. Strengthens antral contractions against the pylorus, and relaxes the pyloric sphincter, which stimulates gastric emptying. • Plays a role in the relaxation of the ileocecal valve.[] • Induces pancreatic secretions and gallbladder emptying.[] • Impacts lower esophageal sphincter (LES) tone, causing it to contract.[]
Gastrin
171
Factors influencing secretion
Gastric lumen • Stimulatory factors: dietary protein and amino acids (meat), hypercalcemia. (i.e. during the gastric phase) • Inhibitory factor: acidity (pH below 3) - a negative feedback mechanism, exerted via the release of somatostatin from δ cells in the stomach, which inhibits gastrin and histamine release. Paracrine • Stimulatory factor: bombesin • Inhibitory factor: somatostatin - acts on somatostatin-2 receptors on G cells. in a paracrine manner via local diffusion in the intercellular spaces, but also systemically through its release into the local mucosal blood circulation; it inhibits acid secretion by acting on parietal cells. Nervous • Stimulatory factors: Beta-adrenergic agents, cholinergic agents, gastrin-releasing peptide (GRP) • Inhibitory factor: Enterogastric reflex Circulation • Stimulatory factor: epinephrine • Inhibitory factors:gastric inhibitory peptide (GIP), secretin, somatostatin, glucagon, calcitonin
Role in disease
In the Zollinger-Ellison syndrome, gastrin is produced at excessive levels, often by a gastrinoma (gastrin-producing tumor, mostly benign) of the duodenum or the pancreas. To investigate for hypergastrinemia (high blood levels of gastrin), a "pentagastrin test" can be performed. In autoimmune gastritis, the immune system attacks the parietal cells leading to hypochlorhydria (low stomach acidity). This results in an elevated gastrin level in an attempt to compensate for increased pH in the stomach. Eventually, all the parietal cells are lost and achlorhydria results leading to a loss of negative feedback on gastrin secretion. Plasma gastrin concentration is elevated in virtually all individuals with mucolipidosis type IV (mean 1507 pg/mL; range 400-4100 pg/mL) (normal 0-200 pg/mL) secondary to a constitutive achlorhydria. This finding facilitates the diagnosis of patients with this neurogenetic disorder.[]
References Further reading
• Rozengurt E, Walsh JH (2001). "Gastrin, CCK, signaling, and cancer". Annu. Rev. Physiol. 63: 49–76. doi: 10.1146/annurev.physiol.63.1.49 (http://dx.doi.org/10.1146/annurev.physiol.63.1.49). PMID 11181948 (http://www.ncbi.nlm.nih.gov/pubmed/11181948). • Dockray GJ (2005). "Clinical endocrinology and metabolism. Gastrin". Best Pract. Res. Clin. Endocrinol. Metab. 18 (4): 555–68. doi: 10.1016/j.beem.2004.07.003 (http://dx.doi.org/10.1016/j.beem.2004.07.003). PMID 15533775 (http://www.ncbi.nlm.nih.gov/pubmed/15533775). • Anlauf M, Garbrecht N, Henopp T, et al. (2006). "Sporadic versus hereditary gastrinomas of the duodenum and pancreas: distinct clinico-pathological and epidemiological features". World J. Gastroenterol. 12 (34): 5440–6. PMID 17006979 (http://www.ncbi.nlm.nih.gov/pubmed/17006979). • Polosatov MV, Klimov PK, Masevich CG, et al. (1979). "Interaction of synthetic human big gastrin with blood proteins of man and animals". Acta hepato-gastroenterologica 26 (2): 154–9. PMID 463490 (http://www.ncbi.
Gastrin nlm.nih.gov/pubmed/463490). Fritsch WP, Hausamen TU, Scholten T (1977). "[Gastrointestinal hormones. I. Hormones of the gastrin group]". Zeitschrift für Gastroenterologie 15 (4): 264–76. PMID 871064 (http://www.ncbi.nlm.nih.gov/pubmed/ 871064). Higashimoto Y, Himeno S, Shinomura Y, et al. (1989). "Purification and structural determination of urinary NH2-terminal big gastrin fragments". Biochem. Biophys. Res. Commun. 160 (3): 1364–70. doi: 10.1016/S0006-291X(89)80154-8 (http://dx.doi.org/10.1016/S0006-291X(89)80154-8). PMID 2730647 (http://www.ncbi.nlm.nih.gov/pubmed/2730647). Pauwels S, Najdovski T, Dimaline R, et al. (1989). "Degradation of human gastrin and CCK by endopeptidase 24.11: differential behaviour of the sulphated and unsulphated peptides". Biochim. Biophys. Acta 996 (1–2): 82–8. doi: 10.1016/0167-4838(89)90098-8 (http://dx.doi.org/10.1016/0167-4838(89)90098-8). PMID 2736261 (http://www.ncbi.nlm.nih.gov/pubmed/2736261). Lund T, Geurts van Kessel AH, Haun S, Dixon JE (1986). "The genes for human gastrin and cholecystokinin are located on different chromosomes". Hum. Genet. 73 (1): 77–80. doi: 10.1007/BF00292669 (http://dx.doi.org/ 10.1007/BF00292669). PMID 3011648 (http://www.ncbi.nlm.nih.gov/pubmed/3011648).
172
•
•
•
•
• Kariya Y, Kato K, Hayashizaki Y, et al. (1987). "Expression of human gastrin gene in normal and gastrinoma tissues". Gene 50 (1–3): 345–52. doi: 10.1016/0378-1119(86)90338-0 (http://dx.doi.org/10.1016/ 0378-1119(86)90338-0). PMID 3034736 (http://www.ncbi.nlm.nih.gov/pubmed/3034736). • Gregory RA, Tracy HJ, Agarwal KL, Grossman MI (1969). "Aminoacid constitution of two gastrins isolated from Zollinger-Ellison tumour tissue" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1552899). Gut 10 (8): 603–8. doi: 10.1136/gut.10.8.603 (http://dx.doi.org/10.1136/gut.10.8.603). PMC 1552899 (http://www. ncbi.nlm.nih.gov/pmc/articles/PMC1552899). PMID 5822140 (http://www.ncbi.nlm.nih.gov/pubmed/ 5822140). • Bentley PH, Kenner GW, Sheppard RC (1967). "Structures of human gastrins I and II". Nature 209 (5023): 583–5. doi: 10.1038/209583b0 (http://dx.doi.org/10.1038/209583b0). PMID 5921183 (http://www.ncbi. nlm.nih.gov/pubmed/5921183). • Ito R, Sato K, Helmer T, et al. (1984). "Structural analysis of the gene encoding human gastrin: the large intron contains an Alu sequence" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC391550). Proc. Natl. Acad. Sci. U.S.A. 81 (15): 4662–6. doi: 10.1073/pnas.81.15.4662 (http://dx.doi.org/10.1073/pnas.81.15.4662). PMC 391550 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC391550). PMID 6087340 (http://www.ncbi.nlm. nih.gov/pubmed/6087340). • Wiborg O, Berglund L, Boel E, et al. (1984). "Structure of a human gastrin gene" (http://www.ncbi.nlm.nih. gov/pmc/articles/PMC344765). Proc. Natl. Acad. Sci. U.S.A. 81 (4): 1067–9. doi: 10.1073/pnas.81.4.1067 (http://dx.doi.org/10.1073/pnas.81.4.1067). PMC 344765 (http://www.ncbi.nlm.nih.gov/pmc/articles/ PMC344765). PMID 6322186 (http://www.ncbi.nlm.nih.gov/pubmed/6322186). • Kato K, Hayashizaki Y, Takahashi Y, et al. (1984). "Molecular cloning of the human gastrin gene" (http://www. ncbi.nlm.nih.gov/pmc/articles/PMC326575). Nucleic Acids Res. 11 (23): 8197–203. doi: 10.1093/nar/11.23.8197 (http://dx.doi.org/10.1093/nar/11.23.8197). PMC 326575 (http://www.ncbi.nlm. nih.gov/pmc/articles/PMC326575). PMID 6324077 (http://www.ncbi.nlm.nih.gov/pubmed/6324077). • Boel E, Vuust J, Norris F, et al. (1983). "Molecular cloning of human gastrin cDNA: evidence for evolution of gastrin by gene duplication" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC393933). Proc. Natl. Acad. Sci. U.S.A. 80 (10): 2866–9. doi: 10.1073/pnas.80.10.2866 (http://dx.doi.org/10.1073/pnas.80.10.2866). PMC 393933 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC393933). PMID 6574456 (http://www.ncbi.nlm. nih.gov/pubmed/6574456). • Kato K, Himeno S, Takahashi Y, et al. (1984). "Molecular cloning of human gastrin precursor cDNA". Gene 26 (1): 53–7. doi: 10.1016/0378-1119(83)90035-5 (http://dx.doi.org/10.1016/0378-1119(83)90035-5). PMID 6689486 (http://www.ncbi.nlm.nih.gov/pubmed/6689486).
Gastrin • Koh TJ, Wang TC (1995). "Molecular cloning and sequencing of the murine gastrin gene". Biochem. Biophys. Res. Commun. 216 (1): 34–41. doi: 10.1006/bbrc.1995.2588 (http://dx.doi.org/10.1006/bbrc.1995.2588). PMID 7488110 (http://www.ncbi.nlm.nih.gov/pubmed/7488110). • Rehfeld JF, Hansen CP, Johnsen AH (1995). "Post-poly(Glu) cleavage and degradation modified by O-sulfated tyrosine: a novel post-translational processing mechanism" (http://www.ncbi.nlm.nih.gov/pmc/articles/ PMC398093). EMBO J. 14 (2): 389–96. PMC 398093 (http://www.ncbi.nlm.nih.gov/pmc/articles/ PMC398093). PMID 7530658 (http://www.ncbi.nlm.nih.gov/pubmed/7530658). • Rehfeld JF, Johnsen AH (1994). "Identification of gastrin component I as gastrin-71. The largest possible bioactive progastrin product". Eur. J. Biochem. 223 (3): 765–73. doi: 10.1111/j.1432-1033.1994.tb19051.x (http:/ /dx.doi.org/10.1111/j.1432-1033.1994.tb19051.x). PMID 8055952 (http://www.ncbi.nlm.nih.gov/ pubmed/8055952). • Varro A, Dockray GJ (1993). "Post-translational processing of progastrin: inhibition of cleavage, phosphorylation and sulphation by brefeldin A" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1134634). Biochem. J. 295 (Pt 3): 813–9. PMC 1134634 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1134634). PMID 8240296 (http://www.ncbi.nlm.nih.gov/pubmed/8240296).
173
External links
• Overview at colostate.edu (http://www.vivo.colostate.edu/hbooks/pathphys/endocrine/gi/gastrin.html) • Physiology at MCG 6/6ch4/s6ch4_14 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section6/6ch4/s6ch4_14.htm)
Secretin
174
Secretin
Secretin
Identifiers Symbol External IDs SCT
[1] [2]
OMIM: 182099 Gene Ontology
MGI: 99466
[3]
HomoloGene: 7928
[4]
GeneCards: SCT Gene
[5]
Molecular function • hormone activity [10] Cellular component • cellular_component [6] [229] • extracellular region Biological process • pancreatic juice secretion
[8] [7]
Sources: Amigo
/ QuickGO
[9]
Orthologs Species Entrez Ensembl UniProt RefSeq (mRNA) RefSeq (protein) Human 6343
[10] [12]
Mouse 20287
[11] [13]
ENSG00000070031 P09683
[14] [16]
ENSMUSG00000038580 Q08535
[15] [17]
NM_021920 NP_068739
NM_011328 NP_035458
[18]
[19]
Location (UCSC) Chr 11: [20] 0.63 – 0.63 Mb PubMed search
[22]
Chr 7: [21] 141.28 – 141.28 Mb
[23]
Secretin is a hormone that both controls the environment in the duodenum by regulating secretions of the stomach and pancreas, and regulates water homeostasis throughout the body. It is produced in the S cells of the duodenum, which are located in the crypts of Lieberkühn.[] In humans, the secretin peptide is encoded by the SCT gene.[] Secretin was also the first hormone to be identified.[1] Secretin regulates the pH within the duodenum by inhibiting gastric acid secretion by the parietal cells of the stomach, and by stimulating bicarbonate production by the centroacinar cells and intercalated ducts of the pancreas.
[]
In 2007, secretin was discovered to play a role in osmoregulation by acting on the hypothalamus, pituitary, and kidney.[][]
Secretin
175
Discovery
In 1902, William Bayliss and Ernest Starling were studying how the nervous system controls the process of digestion.[] It was known that the pancreas secreted digestive juices in response to the passage of food (chyme) through the pyloric sphincter into the duodenum. They discovered (by cutting all the nerves to the pancreas in their experimental animals) that this process was not, in fact, governed by the nervous system. They determined that a substance secreted by the intestinal lining stimulates the pancreas after being transported via the bloodstream. They named this intestinal secretion secretin. Secretin was the first such "chemical messenger" identified. This type of substance is now called a hormone, a term coined by Bayliss in 1905.
Structure
Secretin is initially synthesized as a 120 amino acid precursor protein known as prosecretin. This precursor contains an N-terminal signal peptide, spacer, secretin itself (residues 28–54), and a 72-amino acid C-terminal peptide.[] The mature secretin peptide is a linear peptide hormone, which is composed of 27 amino acids and has a molecular weight of 3055. A helix is formed in the amino acids between positions 5 and 13. The amino acids sequences of secretin have some similarities to that of glucagon, vasoactive intestinal peptide (VIP), and gastric inhibitory peptide (GIP). Fourteen of 27 amino acids of secretin reside in the same positions as in glucagon, 7 the same as in VIP, and 10 the same as in GIP.[]
Secretin also has an amidated carboxyl-terminal amino acid which is valine.[] The sequence of amino acids in secretin is H2N–His-Ser-Asp-Gly-Thr-Phe-Thr-Ser-Glu-Leu-Ser-Arg-Leu-Arg-Asp-Ser-Ala-Arg-Leu-Gln-Arg-Leu-Leu-Gln-Gly-Leu-Val–CO
Physiology
Production
Secretin is synthesized in cytoplasmic secretory granules of S-cells, which are found mainly in the mucosa of the duodenum, and in smaller numbers in the jejunum of the small intestine.[]
Stimulus
Secretin is released into circulation and/or intestinal lumen in response to low duodenal pH that ranges between 2 and 4.5 depending on species.[] Also, the secretion of secretin is increased by the products of protein digestion bathing the mucosa of the upper small intestine.[] The acidity is due to hydrochloric acid in the chyme that enters the duodenum from the stomach via the pyloric sphincter. Secretin targets the pancreas, which causes the organ to secrete a bicarbonate-rich fluid that flows into the intestine. Bicarbonate ion is a base that neutralizes the acid, thus establishing a pH favorable to the action of other digestive enzymes in the small intestine and preventing acid burns.[2] Other factors are involved in the release of secretin such as bile salts and fatty acids, which result in additional bicarbonates being added to the small intestine.[] Secretin release is inhibited by H2 antagonists, which reduce gastric acid secretion. As a result, if the pH in the duodenum increases above 4.5, secretin cannot be released.[]
Function
Secretin increases watery bicarbonate solution from pancreatic and bile duct epithelium. Pancreatic centroacinar cells have secretin receptors in their plasma membrane. As secretin binds to these receptors, it stimulates adenylate cyclase activity and converts ATP to cyclic AMP.[] Cyclic AMP acts as second messenger in intracellular signal transduction and leads to increase in release of watery carbonate. It is known to promote the normal growth and maintenance of the pancreas.
Secretin Secretin increases water and bicarbonate secretion from duodenal Brunner's glands to buffer the incoming protons of the acidic chyme.[] It also enhances the effects of cholecystokinin to induce the secretion of digestive enzymes and bile from pancreas and gallbladder, respectively. It counteracts blood glucose concentration spikes by triggering increased insulin release from pancreas, following oral glucose intake.[] Although secretin releases gastrin from gastrinomas, it inhibits gastrin release from the normal stomach. It reduces acid secretion from the stomach by inhibiting gastrin release from G cells.[]:844 This helps neutralize the pH of the digestive products entering the duodenum from the stomach, as digestive enzymes from the pancreas (e.g., pancreatic amylase and pancreatic lipase) function optimally at slightly basic pH.[citation needed] In addition, secretin stimulates pepsin secretion from chief cells, which can help break down proteins in food digestion. It stimulates release of glucagon, pancreatic polypeptide and somatostatin.[]
176
Uses
Secretin has been widely used in medical field especially in pancreatic functioning test because it increases pancreatic secretions. Secretin is either injected[3] or given through a tube that is inserted through nose, stomach then duodenum.[] This test can provide information about whether there are any abnormalities in pancreas which can be gastrinoma, pancreatitis or pancreatic cancer. Secretin has been proposed as a possible treatment for autism based on a hypothetical gut-brain connection; as yet there is no evidence to support it as effective.[]
Osmoregulation
Secretin modulates water and electrolyte transport in pancreatic duct cells,[] liver cholangiocytes,[] and epididymis epithelial cells.[] It is found[] to play a role in the vasopressin-independent regulation of renal water reabsorption.[] Secretin is found in the magnocellular neurons of the paraventricular and supraoptic nuclei of the hypothalamus and along the neurohypophysial tract to neurohypophysis. During increased osmolality, it is released from the posterior pituitary. In the hypothalamus, it activates vasopressin release.[] It is also needed to carry out the central effects of angiotensin II. In the absence of secretin or its receptor in the gene knockout animals, central injection of angiotensin II was unable to stimulate water intake and vasopressin release.[] It has been suggested that abnormalities in such secretin release could explain the abnormalities underlying type D syndrome of inappropriate antidiuretic hormone hypersecretion (SIADH).[] In these individuals, vasopressin release and response are normal, although abnormal renal expression, translocation of aquaporin 2, or both are found.[] It has been suggested that "Secretin as a neurosecretory hormone from the posterior pituitary, therefore, could be the long-sought vasopressin independent mechanism to solve the riddle that has puzzled clinicians and physiologists for decades."[]
Secretin
177
Food intake
Secretin and its receptor are found in discrete nuclei of the hypothalamus, including the paraventricular nucleus and the arcuate nucleus, which are the primary brain sites for regulating body energy homeostasis. It was found that both central and peripheral injection of Sct reduce food intake in mouse, indicating a anorectic role of the peptide. This function of the peptide is mediated by the central melanocortin system.[]
References
[1] http:/ / www. ncbi. nlm. nih. gov/ pubmed/ 11816326 [2] http:/ / www. vivo. colostate. edu/ hbooks/ pathphys/ endocrine/ gi/ secretin. html
Further reading
• Saus E, Brunet A, Armengol L et al. (2010). "Comprehensive copy number variant (CNV) analysis of neuronal pathways genes in psychiatric disorders identifies rare variants within patients". Journal of Psychiatric Research 44 (14): 971–978. doi: 10.1016/j.jpsychires.2010.03.007 (http://dx.doi.org/10.1016/j.jpsychires.2010.03. 007). PMID 20398908 (http://www.ncbi.nlm.nih.gov/pubmed/20398908). • Bertenshaw GP, Turk BE, Hubbard SJ et al. (2001). "Marked differences between metalloproteases meprin A and B in substrate and peptide bond specificity". J. Biol. Chem. 276 (16): 13248–13255. doi: 10.1074/jbc.M011414200 (http://dx.doi.org/10.1074/jbc.M011414200). PMID 11278902 (http://www. ncbi.nlm.nih.gov/pubmed/11278902). • Lee LT, Lam IP, Chow BK (2008). "A functional variable number of tandem repeats is located at the 5' flanking region of the human secretin gene plays a downregulatory role in expression". J. Mol. Neurosci. 36 (1–3): 125–131. doi: 10.1007/s12031-008-9083-5 (http://dx.doi.org/10.1007/s12031-008-9083-5). PMID 18566919 (http://www.ncbi.nlm.nih.gov/pubmed/18566919). • Nussdorfer GG, Bahçelioglu M, Neri G, Malendowicz LK (2000). "Secretin, glucagon, gastric inhibitory polypeptide, parathyroid hormone, and related peptides in the regulation of the hypothalamus- pituitary-adrenal axis". Peptides 21 (2): 309–324. doi: 10.1016/S0196-9781(99)00193-X (http://dx.doi.org/10.1016/ S0196-9781(99)00193-X). PMID 10764961 (http://www.ncbi.nlm.nih.gov/pubmed/10764961). • Lossi L, Bottarelli L, Candusso ME et al. (2004). "Transient expression of secretin in serotoninergic neurons of mouse brain during development". Eur. J. Neurosci. 20 (12): 3259–3269. doi: 10.1111/j.1460-9568.2004.03816.x (http://dx.doi.org/10.1111/j.1460-9568.2004.03816.x). PMID 15610158 (http://www.ncbi.nlm.nih. gov/pubmed/15610158). • Lee SM, Yung WH, Chen L, Chow BK (2005). "Expression and spatial distribution of secretin and secretin receptor in human cerebellum". NeuroReport 16 (3): 219–222. doi: 10.1097/00001756-200502280-00003 (http:// dx.doi.org/10.1097/00001756-200502280-00003). PMID 15706223 (http://www.ncbi.nlm.nih.gov/ pubmed/15706223). • Lam IP, Lee LT, Choi HS et al. (2009). "Bile acids inhibit duodenal secretin expression via orphan nuclear receptor small heterodimer partner (SHP)" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2711755). Am. J. Physiol. Gastrointest. Liver Physiol. 297 (1): G90–G97. doi: 10.1152/ajpgi.00094.2009 (http://dx.doi.org/ 10.1152/ajpgi.00094.2009). PMC 2711755 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2711755). PMID 19372104 (http://www.ncbi.nlm.nih.gov/pubmed/19372104). • Yamagata T, Aradhya S, Mori M et al. (2002). "The human secretin gene: fine structure in 11p15.5 and sequence variation in patients with autism". Genomics 80 (2): 185–194. doi: 10.1006/geno.2002.6814 (http://dx.doi.org/ 10.1006/geno.2002.6814). PMID 12160732 (http://www.ncbi.nlm.nih.gov/pubmed/12160732). • Lee LT, Tan-Un KC, Chow BK (2006). "Retinoic acid-induced human secretin gene expression in neuronal cells is mediated by cyclin-dependent kinase 1". Ann. N. Y. Acad. Sci. 1070: 393–398. doi: 10.1196/annals.1317.051 (http://dx.doi.org/10.1196/annals.1317.051). PMID 16888198 (http://www.ncbi.nlm.nih.gov/pubmed/
Secretin 16888198). • Onori P, Wise C, Gaudio E et al. (2010). "Secretin inhibits cholangiocarcinoma growth via dysregulation of the cAMP-dependent signaling mechanisms of secretin receptor". Int. J. Cancer 127 (1): NA–NA. doi: 10.1002/ijc.25028 (http://dx.doi.org/10.1002/ijc.25028). PMID 19904746 (http://www.ncbi.nlm.nih.gov/ pubmed/19904746). • Lee LT, Tan-Un KC, Pang RT et al. (2004). "Regulation of the human secretin gene is controlled by the combined effects of CpG methylation, Sp1/Sp3 ratio, and the E-box element". Mol. Endocrinol. 18 (7): 1740–1755. doi: 10.1210/me.2003-0461 (http://dx.doi.org/10.1210/me.2003-0461). PMID 15118068 (http:/ /www.ncbi.nlm.nih.gov/pubmed/15118068). • Lu Y, Owyang C (2009). "Secretin-induced gastric relaxation is mediated by vasoactive intestinal polypeptide and prostaglandin pathways" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2743409). Neurogastroenterol. Motil. 21 (7): 754–e47. doi: 10.1111/j.1365-2982.2009.01271.x (http://dx.doi.org/10. 1111/j.1365-2982.2009.01271.x). PMC 2743409 (http://www.ncbi.nlm.nih.gov/pmc/articles/ PMC2743409). PMID 19239625 (http://www.ncbi.nlm.nih.gov/pubmed/19239625). • Gandhi S, Rubinstein I, Tsueshita T, Onyuksel H (2002). "Secretin self-assembles and interacts spontaneously with phospholipids in vitro". Peptides 23 (1): 201–204. doi: 10.1016/S0196-9781(01)00596-4 (http://dx.doi. org/10.1016/S0196-9781(01)00596-4). PMID 11814635 (http://www.ncbi.nlm.nih.gov/pubmed/ 11814635). • Love JW (2008). "Peptic ulceration may be a hormonal deficiency disease". Med. Hypotheses 70 (6): 1103–1107. doi: 10.1016/j.mehy.2007.12.011 (http://dx.doi.org/10.1016/j.mehy.2007.12.011). PMID 18280672 (http:/ /www.ncbi.nlm.nih.gov/pubmed/18280672). • Lam IP, Lee LT, Choi HS, Chow BK (2006). "Localization of small heterodimer partner (SHP) and secretin in mouse duodenal cells". Ann. N. Y. Acad. Sci. 1070: 371–375. doi: 10.1196/annals.1317.047 (http://dx.doi.org/ 10.1196/annals.1317.047). PMID 16888194 (http://www.ncbi.nlm.nih.gov/pubmed/16888194). • Luttrell LM (2008). "Reviews in molecular biology and biotechnology: transmembrane signaling by G protein-coupled receptors". Mol. Biotechnol. 39 (3): 239–264. doi: 10.1007/s12033-008-9031-1 (http://dx.doi. org/10.1007/s12033-008-9031-1). PMID 18240029 (http://www.ncbi.nlm.nih.gov/pubmed/18240029). • Du K, Couvineau A, Rouyer-Fessard C et al. (2002). "Human VPAC1 receptor selectivity filter. Identification of a critical domain for restricting secretin binding". J. Biol. Chem. 277 (40): 37016–37022. doi: 10.1074/jbc.M203049200 (http://dx.doi.org/10.1074/jbc.M203049200). PMID 12133828 (http://www. ncbi.nlm.nih.gov/pubmed/12133828). • Portela-Gomes GM, Johansson H, Olding L, Grimelius L (1999). "Co-localization of neuroendocrine hormones in the human fetal pancreas". Eur. J. Endocrinol. 141 (5): 526–533. doi: 10.1530/eje.0.1410526 (http://dx.doi.org/ 10.1530/eje.0.1410526). PMID 10576771 (http://www.ncbi.nlm.nih.gov/pubmed/10576771). • Mutoh H, Ratineau C, Ray S, Leiter AB (2000). "Review article: transcriptional events controlling the terminal differentiation of intestinal endocrine cells". Aliment. Pharmacol. Ther. 14 Suppl 1: 170–5. PMID 10807420 (http://www.ncbi.nlm.nih.gov/pubmed/10807420).
178
External links
• Overview at colostate.edu (http://www.vivo.colostate.edu/hbooks/pathphys/endocrine/gi/secretin.html) • Secretin (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Secretin) at the US National Library of Medicine Medical Subject Headings (MeSH) • Physiology at MCG 6/6ch2/s6ch2_17 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section6/6ch2/s6ch2_17.htm)
Cholecystokinin
179
Cholecystokinin
Cholecystokinin
Identifiers Symbols External IDs CCK
[1]
; MGC117187
[2]
OMIM: 118440
MGI: 88297
[3]
HomoloGene: 583
[4]
ChEMBL: 1649050
[5]
GeneCards: CCK Gene
[6]
Gene Ontology Molecular function • hormone activity [10] [15] • neuropeptide hormone activity Cellular component • extracellular region [229] [230] • extracellular space [7] • axon [20] • dendrite [8] • axon initial segment [34] • terminal button [9] • axon hillock [10] • perikaryon Biological process • behavioral fear response [12] • neuron migration [13] • release of cytochrome c from mitochondria • activation of cysteine-type endopeptidase activity involved in apoptotic process
[14] [11]
• signal transduction [15] • protein kinase C-activating G-protein coupled receptor signaling pathway [16] • axonogenesis [28] • positive regulation of cell proliferation [17] • negative regulation of appetite [18] • positive regulation of protein oligomerization [60] • eating behavior [19] • positive regulation of apoptotic process [20] • positive regulation of peptidyl-tyrosine phosphorylation [21] • positive regulation of mitochondrial depolarization [72] • regulation of sensory perception of pain Sources: Amigo
[22]
[38]
/ QuickGO
[23]
RNA expression pattern
More reference expression data Orthologs Species Entrez Human 885
[25]
[24]
Mouse 12424
[26]
Cholecystokinin
[27] [28]
180
Ensembl UniProt RefSeq (mRNA) RefSeq (protein)
ENSG00000187094 P06307
[29] [31]
ENSMUSG00000032532 P09240
[30] [32]
NM_000729 NP_000720
NM_031161 NP_112438
[33]
[34]
Location (UCSC) Chr 3: [35] 42.3 – 42.31 Mb PubMed search
[37]
Chr 9: [36] 121.49 – 121.5 Mb
[38]
Cholecystokinin (CCK or CCK-PZ; from Greek chole, "bile"; cysto, "sac"; kinin, "move"; hence, move the bile-sac (gallbladder)) is a peptide hormone of the gastrointestinal system responsible for stimulating the digestion of fat and protein. Cholecystokinin, previously called pancreozymin, is synthesized by I-cells in the mucosal epithelium of the small intestine and secreted in the duodenum, the first segment of the small intestine, and causes the release of digestive enzymes and bile from the pancreas and gallbladder, respectively. It also acts as a hunger suppressant. Recent evidence has suggested that it also plays a major role in inducing drug tolerance to opioids like morphine and heroin, and is partly implicated in experiences of pain hypersensitivity during opioid withdrawal.[][]
Structure
CCK identified at bottom right.
CCK is composed of varying numbers of amino acids depending on post-translational modification of the CCK gene product, preprocholecystokinin. Thus CCK is actually a family of hormones identified by number of amino acids, e.g., CCK58, CCK33, and CCK8. CCK58 assumes a helix-turn-helix configuration.[] Its existence was first suggested in 1905 by the British physiologist Joy Simcha Cohen. CCK is very similar in structure to gastrin, another of the gastrointestinal hormones. CCK and gastrin share the same five amino acids at their C-termini.
Functions
CCK mediates a number of physiological processes, including digestion and satiety. It is released by I cells located in the mucosal epithelium of the small intestine (mostly in the duodenum and jejunum), neurons of the enteric nervous system and neurons in the brain. Release of CCK is stimulated by monitor peptide released by pancreatic acinar cells as well as CCK-releasing protein, a paracrine factor secreted by enterocytes in the gastrointestinal mucosa. In addition, release of acetylcholine by the parasympathetic nerve fibers of the vagus nerve also stimulate its secretion. The presence of fatty acids and/or certain amino acids in the chyme entering the duodenum is the greatest stimulator of CCK release. CCK mediates digestion in the small intestine by inhibiting gastric emptying and gastric acid secretion. It stimulates the acinar cells of the pancreas to release digestive enzymes and stimulates the secretion of a juice rich in pancreatic digestive enzymes, hence the old name pancreozymin. Together these enzymes catalyze the digestion of fat, protein, and carbohydrates. Thus, as the levels of the substances that stimulated the release of CCK drop, the concentration of the hormone drops as well. The release of CCK is also inhibited by somatostatin. Trypsin, a protease released by pancreatic acinar cells hydrolyzes CCK-releasing peptide and monitor peptide effectively turning off the additional
Cholecystokinin signals to secrete CCK. CCK also causes the increased production of hepatic bile, and stimulates the contraction of the gall bladder and the relaxation of the Sphincter of Oddi (Glisson's sphincter), resulting in the delivery of bile into the duodenal part of the small intestine. Bile salts form amphipathic micelles that emulsify fats, aiding in their digestion and absorption.
181
Neurobiology
As a neuropeptide, CCK mediates satiety by acting on the CCK receptors distributed widely throughout the central nervous system. In humans, it has been suggested that CCK administration causes nausea and anxiety, and induces a satiating effect. CCK-4 is routinely used to induce anxiety in humans though certainly different forms of CCK are being shown to have highly variable effects.[] The mechanism for this hunger suppression is thought to be a decrease in the rate of gastric emptying.[] CCK also has stimulatory effects on the vagus nerve, effects that can be inhibited by capsaicin.[] The stimulatory effects of CCK oppose those of ghrelin, which has been shown to inhibit the vagus nerve.[] The CCK tetrapeptide fragment CCK-4 (Trp-Met-Asp-Phe-NH2) reliably causes anxiety when administered to humans, and is commonly used in scientific research to induce panic attacks for the purpose of testing new anxiolytic drugs.[] The effects of CCK vary between individuals. For example, in rats, CCK administration significantly reduces hunger in young males, but is slightly less effective in older subjects, and even slightly less effective in females. The hunger-suppressive effects of CCK also are reduced in obese rats.[]
Interactions
Cholecystokinin has been shown to interact with the Cholecystokinin A receptor located mainly on pancreatic acinar cells and Cholecystokinin B receptor mostly in the brain and stomach. CCKB receptor also binds gastrin, a gastrointestinal hormone involved in stimulating gastric acid release and growth of the gastric mucosa.[][][] CCK has also been shown to interact with calcineurin in the pancreas. Calcineurin will go on to activate the transcription factors NFAT 1–3, which will stimulate hypertrophy and growth of the pancreas. CCK can be stimulated by a diet high in protein, or by protease inhibitors.[] Cholecystokinin has been shown to interact with orexin neurons which control appetite and wakefulness (sleep).[] Cholecystokinin can have indirect effects on sleep regulation.[1] Cholecystokinin in the body cannot cross the blood brain barrier, but certain parts of the hypothalamus and brainstem aren't protected by the barrier. In the hypothalamus, CCK8 injection excites CRF neurosecretory neurons in par ventricular nucleus that is different cell responsive to pain stimulation:They show slow a 1 sec-hyperpolarizaiton with subsequent long (30min) depolarization to CCK8 injection (psychological stress), whereas tail pinch (physical stress), transient excitation. Consistently, in the cerebellum, Golgi cells express c-fos mRNA to CCK8 injection, whereas granule cells express junD mRNA to capsaicin injection to the limb skin. Thus, psychological and physical stress excite different neural path.
References External links
• Cholecystokinin (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Cholecystokinin) at the US National Library of Medicine Medical Subject Headings (MeSH)
Insulin
182
Insulin
WARNING: Article could not be rendered - ouputting plain text. Potential causes of the problem are: (a) a bug in the pdf-writer software (b) problematic Mediawiki markup (c) table is too wide InsulinComputer-generated image of six insulin molecules assembled in a hexamer, highlighting the threefold symmetry, the zinc ions holding it together, and the histidine residues involved in zinc binding. Insulin is stored in the body as a hexamer, while the active form is the monomer. ; Available structuresProtein Data BankPDB Ortholog search: PDBe, RCSBList of PDB id codes 1A7F, 1AI0, 1AIY, 1B9E, 1BEN, 1EFE, 1EV3, 1EV6, 1EVR, 1FU2, 1FUB, 1G7A, 1G7B, 1GUJ, 1HIQ, 1HIS, 1HIT, 1HLS, 1HTV, 1HUI, 1IOG, 1IOH, 1J73, 1JCA, 1JCO, 1K3M, 1KMF, 1LKQ, 1LPH, 1MHI, 1MHJ, 1MSO, 1OS3, 1OS4, 1Q4V, 1QIY, 1QIZ, 1QJ0, 1RWE, 1SF1, 1SJT, 1SJU, 1T0C, 1T1K, 1T1P, 1T1Q, 1TRZ, 1TYL, 1TYM, 1UZ9, 1VKT, 1W8P, 1XDA, 1XGL, 1XW7, 1ZEG, 1ZEH, 1ZNJ, 2AIY, 2C8Q, 2C8R, 2CEU, 2G54, 2G56, 2H67, 2HH4, 2HHO, 2HIU, 2JMN, 2JUM, 2JUU, 2JUV, 2JV1, 2JZQ, 2K91, 2K9R, 2KJJ, 2KJU, 2KQP, 2KQQ, 2KXK, 2L1Y, 2L1Z, 2LGB, 2M1D, 2M1E, 2M2M, 2M2N, 2M2O, 2M2P, 2OLY, 2OLZ, 2OM0, 2OM1, 2OMG, 2OMH, 2OMI, 2QIU, 2R34, 2R35, 2R36, 2RN5, 2VJZ, 2VK0, 2W44, 2WBY, 2WC0, 2WRU, 2WRV, 2WRW, 2WRX, 2WS0, 2WS1, 2WS4, 2WS6, 2WS7, 3AIY, 3BRR, 3BXQ, 3E7Y, 3E7Z, 3EXX, 3FQ9, 3HYD, 3I3Z, 3I40, 3ILG, 3INC, 3IR0, 3JSD, 3KQ6, 3P2X, 3P33, 3Q6E, 3ROV, 3TT8, 3U4N, 3UTQ, 3UTS, 3UTT, 3V19, 3V1G, 3W11, 3W12, 3W13, 3ZI3, 3ZQR, 3ZS2, 3ZU1, 4AIY, 4AJX, 4AJZ, 4AK0, 4AKJ, 4EFX, 4FKA, 4IUZ, 5AIYIdentifiersHuman Genome OrganisationSymbols INS; IDDM2; ILPR; IRDN; MODY10External IDsMendelian Inheritance in ManOMIM: 176730 Mouse Genome InformaticsMGI: 96573 HomoloGene: 173 ChEMBL: 5881 GeneCards: INS GeneGene OntologyMolecular function• protease binding• insulin receptor binding• insulin-like growth factor receptor binding• hormone activity• protein bindingCellular component• extracellular region• extracellular space• endoplasmic reticulum lumen• Golgi lumen• secretory granule• endosome lumenBiological process• MAPK cascade• negative regulation of acute inflammatory response• glucose metabolic process• energy reserve metabolic process• regulation of transcription, DNA-dependent• regulation of cellular amino acid metabolic process• acute-phase response• G-protein coupled receptor signaling pathway• cell-cell signaling• positive regulation of cell proliferation• insulin receptor signaling pathway• positive regulation of phosphatidylinositol 3-kinase cascade• glucose transport• regulation of transmembrane transporter activity• positive regulation of cell growth• positive regulation of cell migration• endocrine pancreas development• positive regulation of protein autophosphorylation• activation of protein kinase B activity• positive regulation of cellular protein metabolic process• negative regulation of protein oligomerization• regulation of protein localization• negative regulation of NAD(P)H oxidase activity• wound healing• negative regulation of protein catabolic process• glucose homeostasis• negative regulation of apoptotic process• positive regulation of MAPK cascade• small molecule metabolic process• positive regulation of nitric oxide biosynthetic process• positive regulation of cell differentiation• negative regulation of gluconeogenesis• positive regulation of glycogen biosynthetic process• positive regulation of DNA replication• negative regulation of glycogen catabolic process• positive regulation of glycolysis• positive regulation of mitosis• negative regulation of proteolysis• negative regulation of vasodilation• positive regulation of vasodilation• negative regulation of fatty acid metabolic process• positive regulation of glucose import• positive regulation of insulin receptor signaling pathway• alpha-beta T cell activation• positive regulation of lipid biosynthetic process• regulation of protein secretion• negative regulation of protein secretion• positive regulation of cytokine secretion• positive regulation of peptidyl-tyrosine phosphorylation• regulation of insulin secretion• negative regulation of lipid catabolic process• positive regulation of nitric-oxide synthase activity• positive regulation of
Insulin NF-kappaB transcription factor activity• positive regulation of protein kinase B signaling cascade• fatty acid homeostasis• negative regulation of respiratory burst involved in inflammatory response• positive regulation of respiratory burst• positive regulation of peptide hormone secretion• positive regulation of brown fat cell differentiation• negative regulation of feeding behaviorSources: Amigo / QuickGORNA expression pattern More reference expression dataOrthologsSpeciesHumanMouseEntrez 3630 16334Ensembl ENSG00000254647 ENSMUSG00000000215UniProt P01308 P01326RefSeq (mRNA) NM_000207 NM_001185083RefSeq (protein) NP_000198 NP_001172012Location (UCSC) Chr 11:2.18 – 2.18 Mb Chr 7:142.68 – 142.7 MbPubMed searchInsulin is a peptide hormone, produced by beta cells of the pancreas, and is central to regulating carbohydrate and fat metabolism in the body. Insulin causes cells in the liver, skeletal muscles, and fat cellfat tissue to absorb glucose from the blood. In the liver and skeletal muscles, glucose is stored as glycogen, and in fat cells (adipocytes) it is stored as triglycerides.Insulin stops the use of fat as an energy source by inhibiting the release of glucagon. With the exception of the metabolic disorder diabetes mellitus and metabolic syndrome, insulin is provided within the body in a constant proportion to remove excess glucose from the blood, which otherwise would be toxic. When blood glucose levels fall below a certain level, the body begins to use stored sugar as an energy source through glycogenolysis, which breaks down the glycogen stored in the liver and muscles into glucose, which can then be utilized as an energy source. As a central metabolic control mechanism, its status is also used as a control signal to other body systems (such as amino acid uptake by body cells). In addition, it has several other anabolismanabolic effects throughout the body. When control of insulin levels fails, diabetes mellitus can result. As a consequence, insulin is used medically to treat some forms of diabetes mellitus. Patients with Diabetes mellitus type 1type 1 diabetes depend on external insulin (most commonly Subcutaneous injectioninjected subcutaneously) for their survival because the hormone is no longer produced internally. Patients with Diabetes mellitus type 2type 2 diabetes are often insulin resistanceinsulin resistant and, because of such resistance, may suffer from a "relative" insulin deficiency. Some patients with type 2 diabetes may eventually require insulin if other medications fail to control blood glucose levels adequately. Over 40% of those with Type 2 diabetes require insulin as part of their diabetes management plan. The human insulin protein is composed of 51 amino acids, and has a molecular weight of 5808 Dalton (unit)Da. It is a protein dimerdimer of an A-chain and a B-chain, which are linked together by disulfide bonds. Insulin's name is derived from the Latin insula for "island". Insulin's structure varies slightly between species of animals. Insulin from animal sources differs somewhat in "strength" (in carbohydrate metabolism control effects) in humans because of those variations. pigPorcine insulin is especially close to the human version.Gene The preproinsulin precursor of insulin is encoded by the INS gene.Alleles A variety of mutant alleles with changes in the coding region have been identified. A Conjoined generead-through gene, INS-IGF2, overlaps with this gene at the 5' region and with the IGF2 gene at the 3' region.Regulation Several regulatory sequences in the Promoter (biology)promoter region of the human insulin gene bind to transcription factors. In general, the A-boxes bind to Pdx1 factors, E-boxes bind to NeuroD, C-boxes bind to MafA, and cAMP response elements to CREB. There are also silencer (genetics)silencers that inhibit transcription. Regulatory sequences and their transcription factors for the insulin gene.Regulatory sequence binding transcription factorsILPRDBP (gene)Par1A-box 5 of insulin geneA5Pdx1negative regulatory element (NRE)glucocorticoid receptor, POU2F1Oct1Z-box of insulin geneZ (overlapping NRE and C2) ISF (transcription factor)ISFC2 regulatory sequenceC2Pax4, MafA(?) E-box 2 of insulin geneE2USF1/USF2A-box 3 of insulin geneA3Pdx1CAMP response elementCREB RE - CAMP response elementCREB RECREB, CREMA-box 2 of insulin geneA2 - CAAT enhancer binding (CEB) (partly overlapping A2 and C1) - C-box 1 of insulin geneC1 - E-box 1 of insulin geneE1E2A, NeuroD1, TCF12HEBA-box 1 of insulin geneA1Pdx1G-box 1 of insulin geneG1 - Protein structure Within vertebrates, the amino acid sequence of insulin is conserved_sequencestrongly conserved. CowBovine insulin differs from human in only three amino acid residues, and Pigporcine insulin in one. Even insulin from some species of fish is similar enough to human to be clinically effective in humans. Insulin in some invertebrates is quite similar in sequence to human insulin, and has similar physiological effects. The strong homology seen in the insulin sequence of diverse species suggests that it has been conserved across much of animal evolutionary history. The C-peptide of proinsulin (discussed later), however,
183
Insulin differs much more among species; it is also a hormone, but a secondary one. The primary structure of bovine insulin was first determined by Frederick Sanger in 1951.; ; ; After that, this polypeptide was synthesized independently by several groups.Insulin is produced and stored in the body as a hexamer (a unit of six insulin molecules), while the active form is the monomer. The hexamer is an inactive form with long-term stability, which serves as a way to keep the highly reactive insulin protected, yet readily available. The hexamer-monomer conversion is one of the central aspects of insulin formulations for injection. The hexamer is far more stable than the monomer, which is desirable for practical reasons; however, the monomer is a much faster-reacting drug because diffusion rate is inversely related to particle size. A fast-reacting drug means insulin injections do not have to precede mealtimes by hours, which in turn gives diabetics more flexibility in their daily schedules. Insulin can aggregate and form fibrillar interdigitated beta-sheets. This can cause injection amyloidosis, and prevents the storage of insulin for long periods.Synthesis, physiological effects, and degradation Synthesis Insulin is produced in the pancreas and released when any of several stimuli are detected. These stimuli include ingested protein and glucose in the blood produced from digested food.[citation needed] Carbohydrates can be polymers of simple sugars or the simple sugars themselves. If the carbohydrates include glucose, then that glucose will be absorbed into the bloodstream and blood glucose level will begin to rise. In target cells, insulin initiates a signal transduction, which has the effect of increasing glucose uptake and storage. Finally, insulin is degraded, terminating the response. Insulin undergoes extensive posttranslational modification along the production pathway. Production and secretion are largely independent; prepared insulin is stored awaiting secretion. Both C-peptide and mature insulin are biologically active. Cell components and proteins in this image are not to scale.In mammals, insulin is synthesized in the pancreas within the beta cellβ-cells of the islets of Langerhans. One million to three million islets of Langerhans (pancreatic islets) form the endocrine part of the pancreas, which is primarily an exocrine gland. The endocrine portion accounts for only 2% of the total mass of the pancreas. Within the islets of Langerhans, beta cells constitute 65–80% of all the cells. Insulin consists of two polypeptide chains, the A- and B- chains, linked together by disulfide bonds. It is however first synthesized as a single polypeptide called preproinsulin in pancreatic beta cellβ-cells. Preproinsulin contains a 24-residue signal peptide which directs the nascent polypeptide chain to the rough endoplasmic reticulum (RER). The signal peptide is cleaved as the polypeptide is translocated into lumen of the RER, forming proinsulin. In the RER the proinsulin folds into the correct conformation and 3 disulfide bonds are formed. About 5–10 min after its assembly in the endoplasmic reticulum, proinsulin is transported to the trans-Golgi network (TGN) where immature granules are formed. Transport to the TGN may take about 30 min. Proinsulin undergoes maturation into active insulin through the action of cellular endopeptidases known as prohormone convertases (Proprotein convertase 1PC1 and proprotein convertase 2PC2), as well as the exoprotease carboxypeptidase E. The endopeptidases cleave at 2 positions, releasing a fragment called the C-peptide, and leaving 2 peptide chains, the B- and A- chains, linked by 2 disulfide bonds. The cleavage sites are each located after a pair of basic residues (lysine-64 and arginine-65, and arginine-31 and -32), and after cleavage these 2 pairs of basic residues are removed by the carboxypeptidase. The C-peptide is the central portion of proinsulin, and the primary sequence of proinsulin goes in the order "B-C-A" (the B and A chains were identified on the basis of mass and the C-peptide was discovered later). The resulting mature insulin is packaged inside mature granules waiting for metabolic signals (such as leucine, arginine, glucose and mannose) and vagal nerve stimulation to be exocytosed from the cell into the circulation.The endogenous production of insulin is regulated in several steps along the synthesis pathway: At DNA transcriptiontranscription from the insulin gene In mRNA stability At the mRNA translation In the posttranslational modifications Insulin and its related proteins have been shown to be produced inside the brain, and reduced levels of these proteins are linked to Alzheimer's disease.Release Beta CellBeta cells in the islets of Langerhans release insulin in two phases. The first phase release is rapidly triggered in response to increased blood glucose levels. The second phase is a sustained, slow release of newly formed vesicles triggered independently of sugar. The description of first phase release is as follows: Glucose enters the β-cells through the glucose transporter, GLUT2. Glucose goes into glycolysis and the respiratory cycle, where multiple, high-energy adenosine triphosphateATP molecules are produced by oxidation, leading to a rise in the ATP:ADP ratio within the cell. An increased intracellular ATP:ADP ratio closes the ATP-sensitive SUR1/Kir6.2
184
Insulin potassium channel (see sulfonylurea receptor). This prevents potassium ions (K+) from leaving the cell by facilitated diffusion, leading to a build up of potassium ions. As a result, the inside of the cell becomes more positive with respect to the outside, leading to the depolarisation of the cell surface membrane. On depolarizationdepolarisation, voltage-gated calcium channelscalcium ion (Ca2+) channels open which allows calcium ions to move into the cells by facilitated diffusion. An increased intracellular calcium ion concentration causes the activation of phospholipasephospholipase C, which cleaves the membrane phospholipid phosphatidyl inositol 4,5-bisphosphate into inositol 1,4,5-trisphosphate and diglyceridediacylglycerol. Inositol 1,4,5-trisphosphate (IP3) binds to receptor proteins in the plasma membrane of the endoplasmic reticulum (ER). This allows the release of Ca2+ ions from the ER via IP3-gated channels, and further raises the intracellular concentration of calcium ions. Significantly increased amounts of calcium ions in the cells causes the release of previously synthesized insulin, which has been stored in secretionsecretory vesicle (biology)vesicles. This is the primary mechanism for release of insulin. Other substances known to stimulate insulin release include the amino acids arginine and leucine, parasympathetic release of acetylcholine (via phospholipase C), sulfonylurea, cholecystokinin (CCK, via phospholipase C), and the gastrointestinally derived incretins glucagon-like peptide-1 (GLP-1) and glucose-dependent insulinotropic peptide (GIP). Release of insulin is strongly inhibited by the stress hormone norepinephrine (noradrenaline), which leads to increased blood glucose levels during stress. It appears that release of catecholamines by the sympathetic nervous system has conflicting influences on insulin release by beta cells, because insulin release is inhibited by α2-adrenergic receptors and stimulated by β2-adrenergic receptors. The net effect of norepinephrine from sympathetic nerves and epinephrine from adrenal glands on insulin release is inhibition due to dominance of the α-adrenergic receptors.When the glucose level comes down to the usual physiologic value, insulin release from the β-cells slows or stops. If blood glucose levels drop lower than this, especially to dangerously low levels, release of hyperglycemic hormones (most prominently glucagon from islet of Langerhans alpha cells) forces release of glucose into the blood from cellular stores, primarily liver cell stores of glycogen. By increasing blood glucose, the hyperglycemic hormones prevent or correct life-threatening hypoglycemia. Evidence of impaired first-phase insulin release can be seen in the glucose tolerance test, demonstrated by a substantially elevated blood glucose level at 30 minutes, a marked drop by 60 minutes, and a steady climb back to baseline levels over the following hourly time points. Oscillations Insulin release from pancreas oscillates with a period of 3–6 minutes.Even during digestion, in general, one or two hours following a meal, insulin release from the pancreas is not continuous, but oscillates with a period of 3–6 minutes, changing from generating a blood insulin concentration more than about 800 pico-punit molemol/l to less than 100 pmol/l. This is thought to avoid receptor downregulationdownregulation of insulin receptors in target cells, and to assist the liver in extracting insulin from the blood. This oscillation is important to consider when administering insulin-stimulating medication, since it is the oscillating blood concentration of insulin release, which should, ideally, be achieved, not a constant high concentration. This may be achieved by delivering insulin rhythmically to the portal vein or by islet cell transplantation to the liver. Future insulin pumps hope to address this characteristic. (See also Pulsatile Insulin.) Blood content The idealized diagram shows the fluctuation of blood sugar (red) and the sugar-lowering hormone insulin (blue) in humans during the course of a day containing three meals. In addition, the effect of a sucrosesugar-rich versus a starch-rich meal is highlighted. The blood content of insulin can be measured in international units, such as µIU/mL or in molar concentration, such as pmol/L, where 1 µIU/mL equals 6.945 pmol/L. A Dictionary of Units of Measurement By Russ Rowlett, the University of North Carolina at Chapel Hill. June 13, 2001 A typical blood level between meals is 8–11 μIU/mL (57–79 pmol/L).Signal transduction Special transporter proteins in cell membranes allow glucose from the blood to enter a cell. These transporters are, indirectly, under blood insulin's control in certain body cell types (e.g., muscle cells). Low levels of circulating insulin, or its absence, will prevent glucose from entering those cells (e.g., in type 1 diabetes). More commonly, however, there is a decrease in the sensitivity of cells to insulin (e.g., the reduced insulin sensitivity characteristic of type 2 diabetes), resulting in decreased glucose absorption. In either case, there is 'cell starvation' and weight loss, sometimes extreme. In a few cases, there is a defect in the release of insulin from the pancreas. Either way, the effect is the same: elevated blood glucose levels. Activation of insulin receptors leads to internal
185
Insulin cellular mechanisms that directly affect glucose uptake by regulating the number and operation of protein molecules in the cell membrane that transport glucose into the cell. The genes that specify the proteins that make up the insulin receptor in cell membranes have been identified, and the structures of the interior, transmembrane section, and the extra-membrane section of receptor have been solved. Two types of tissues are most strongly influenced by insulin, as far as the stimulation of glucose uptake is concerned: muscle cells (myocytes) and fat cells (adipocytes). The former are important because of their central role in movement, breathing, circulation, etc., and the latter because they accumulate excess food energy against future needs. Together, they account for about two-thirds of all cells in a typical human body. Insulin binds to the extracellular portion of the alpha subunits of the insulin receptor. This, in turn, causes a conformational change in the insulin receptor that activates the kinase domain residing on the intracellular portion of the beta subunits. The activated kinase domain autophosphorylates tyrosine residues on the C-terminus of the receptor as well as tyrosine residues in the IRS-1 protein. phosphorylated IRS-1, in turn, binds to and activates phosphoinositol 3 kinase (phosphoinositide 3-kinasePI3K) PI3K catalyzes the reaction phosphatidylinositol 4,5-bisphosphatePIP2 + Adenosine triphosphateATP → Phosphatidylinositol (3,4,5)-trisphosphatePIP3 + Adenosine diphosphateADP PIP3 activates protein kinase B (AKTPKB) PKB phosphorylates glycogen synthase kinase (GSK-3GSK) and thereby inactivates GSK GSK can no longer phosphorylate glycogen synthase (glycogen synthaseGS) unphosphorylated GS makes more glycogen PKB also facilitates vesicle fusion, resulting in an increase in GLUT4 transporters in the plasma membraneAfter the signal has been produced, termination of signaling is then needed. As mentioned below in the section on degradation, endocytosis and degradation of the receptor bound to insulin is a main mechanism to end signaling. In addition, signaling can be terminated by dephosphorylation of the tyrosine residues by tyrosine phosphatases. Serine/Threonine kinases are also known to reduce the activity of insulin. Finally, with insulin action being associated with the number of receptors on the plasma membrane, a decrease in the amount of receptors also leads to termination of insulin signaling.The structure of the insulin–insulin receptor complex has been determined using the techniques of X-ray crystallography.Physiological effects Effect of insulin on glucose uptake and metabolism. Insulin binds to its receptor (1), which starts many protein activation cascades (2). These include translocation of Glut-4 transporter to the plasma membrane and influx of glucose (3), glycogen synthesis (4), glycolysis (5) and triglyceride (6).The actions of insulin on the global human metabolism level include: Control of cellular intake of certain substances, most prominently glucose in muscle and adipose tissue (about two-thirds of body cells) Increase of DNA replication and protein synthesis via control of amino acid uptake Modification of the activity of numerous enzymes. The actions of insulin (indirect and direct) on cells include: Increased glycogen synthesis – insulin forces storage of glucose in liver (and muscle) cells in the form of glycogen; lowered levels of insulin cause liver cells to convert glycogen to glucose and excrete it into the blood. This is the clinical action of insulin, which is directly useful in reducing high blood glucose levels as in diabetes. Increased lipid synthesis – insulin forces fat cells to take in blood lipids, which are converted to triglycerides; lack of insulin causes the reverse. Increased esterification of fatty acids – forces adipose tissue to make fats (i.e., triglycerides) from fatty acid esters; lack of insulin causes the reverse. Decreased proteolysis – decreasing the breakdown of protein Decreased lipolysis – forces reduction in conversion of fat cell lipid stores into blood fatty acids; lack of insulin causes the reverse. Decreased gluconeogenesis – decreases production of glucose from nonsugar substrates, primarily in the liver (the vast majority of endogenous insulin arriving at the liver never leaves the liver); lack of insulin causes glucose production from assorted substrates in the liver and elsewhere. Decreased Autophagy (cellular)autophagy - decreased level of degradation of damaged organelles. Postprandial levels inhibit autophagy completely. Increased amino acid uptake – forces cells to absorb circulating amino acids; lack of insulin inhibits absorption. Increased potassium uptake – forces cells to absorb serum potassium; lack of insulin inhibits absorption. Insulin's increase in cellular potassium uptake lowers potassium levels in blood. This possibly occurs via insulin-induced translocation of the Na+/K+-ATPase to the surface of skeletal muscle cells. Arterial muscle tone – forces arterial wall muscle to relax, increasing blood flow, especially in microarteries; lack of insulin reduces flow by allowing these muscles to contract. Increase in the secretion of hydrochloric acid by parietal cells in the stomach Decreased renal sodium
186
Insulin excretion.Insulin also influences other body functions, such as compliance (physiology)#Blood vesselsvascular compliance and cognition. Once insulin enters the human brain, it enhances learning and memory and benefits verbal memory in particular. Enhancing brain insulin signaling by means of intranasal insulin administration also enhances the acute thermoregulatory and glucoregulatory response to food intake, suggesting that central nervous insulin contributes to the control of whole-body energy homeostasis in humans.Degradation Once an insulin molecule has docked onto the receptor and effected its action, it may be released back into the extracellular environment, or it may be degraded by the cell. The two primary sites for insulin clearance are the liver and the kidney. The liver clears most insulin during first-pass transit, whereas the kidney clears most of the insulin in systemic circulation. Degradation normally involves endocytosis of the insulin-receptor complex, followed by the action of insulin-degrading enzyme. An insulin molecule produced endogenously by the pancreatic beta cells is estimated to be degraded within about one hour after its initial release into circulation (insulin biological half-lifehalf-life ~ 4–6 minutes).Hypoglycemia Although other cells can use other fuels (most prominently fatty acids), neurons depend on glucose as a source of energy in the nonstarving human. They do not require insulin to absorb glucose, unlike muscle and adipose tissue, and they have very small internal stores of glycogen. Glycogen stored in liver cells (unlike glycogen stored in muscle cells) can be converted to glucose, and released into the blood, when glucose from digestion is low or absent, and the glycerol backbone in triglycerides can also be used to produce blood glucose. Sufficient lack of glucose and scarcity of these sources of glucose can dramatically make itself manifest in the impaired functioning of the central nervous system: dizziness, speech problems, and even loss of consciousness. Low blood glucose level is known as hypoglycemia or, in cases producing unconsciousness, "hypoglycemic coma" (sometimes termed "insulin shock" from the most common causative agent). Endogenous causes of insulin excess (such as an insulinoma) are very rare, and the overwhelming majority of insulin excess-induced hypoglycemia cases are Iatrogenesisiatrogenic and usually accidental. A few cases of murder, attempted murder, or suicide using insulin overdoses have been reported, but most insulin shocks appear to be due to errors in dosage of insulin (e.g., 20 units instead of 2) or other unanticipated factors (did not eat as much as anticipated, or exercised more than expected, or unpredicted kinetics of the subcutaneously injected insulin itself). Possible causes of hypoglycemia include: External insulin (usually injected subcutaneously) Oral hypoglycemic agents (e.g., any of the sulfonylureas, or similar drugs, which increase insulin release from β-cells in response to a particular blood glucose level) Ingestion of low-carbohydrate sugar substitutes in people without diabetes or with type 2 diabetes. Animal studies show these can trigger insulin release, albeit in much smaller quantities than sugar, according to a report in Discover magazine, August 2004, p 18. (This can never be a cause of hypoglycemia in patients with type 1 diabetes, since there is no endogenous insulin production to stimulate.)Diseases and syndromes There are several conditions in which insulin disturbance is pathologic: Diabetes mellitus – general term referring to all states characterized by hyperglycemia Diabetes mellitus type 1Type 1 – autoimmune-mediated destruction of insulin-producing β-cells in the pancreas, resulting in absolute insulin deficiency Diabetes mellitus type 2Type 2 – multifactoral syndrome with combined influence of genetic susceptibility and influence of environmental factors, the best known being obesity, age, and physical inactivity, resulting in insulin resistance in cells requiring insulin for glucose absorption. This form of diabetes is strongly inherited. Other types of impaired glucose tolerance (see the Diabetes) Insulinoma - a tumor of pancreatic β-cells producing excess insulin or reactive hypoglycemia. Metabolic syndrome – a poorly understood condition first called Syndrome X by Gerald Reaven, Reaven's Syndrome after Reaven, CHAOS in Australia (from the signs that seem to travel together). It is currently not clear whether these signs have a single, treatable cause, or are the result of body changes leading to type 2 diabetes. It is characterized by elevated blood pressure, dyslipidemia (disturbances in blood cholesterol forms and other blood lipids), and increased waist circumference (at least in populations in much of the developed world). The basic underlying cause may be the insulin resistance that precedes type 2 diabetes, which is a diminished capacity for Insulin#Physiological effectsinsulin response in some tissues (e.g., muscle, fat). It is common that morbidities, such as essential hypertension, obesity, type 2 diabetes, and cardiovascular disease (CVD) develop. Polycystic ovary syndrome – a complex syndrome in women in the reproductive years where anovulation and androgen excess are commonly displayed as hirsutism. In many cases of
187
Insulin PCOS, insulin resistance is present. As a medication Insulin vial Biosynthetic "human" insulin is now manufactured for widespread clinical use using Recombinant DNA#Synthetic insulin production using recombinant DNArecombinant DNA technology. More recently, researchers have succeeded in introducing the gene for human insulin into plants and in producing insulin in them, to be specific safflower. From SemBiosys, A New Kind Of Insulin INSIDE WALL STREET By Gene G. Marcial(AUGUST 13, 2007) This technique is anticipated to reduce production costs. Several of these slightly modified versions of human insulin, while having a clinical effect on blood glucose levels as though they were exact copies, have been designed to have somewhat different absorption or duration of action characteristics. They are usually referred to as "insulin analogues". For instance, the first one available, Humalog (insulin lispro), does not exhibit a delayed absorption effect found in regular insulin, and begins to have an effect in as little as 15 minutes. Other rapid-acting analogues are NovoRapid and Apidra, with similar profiles. All are rapidly absorbed due to a mutation in the sequence that prevents the insulin analogue from forming dimers and hexamers. Instead, the insulin molecule is a monomer, which is more rapidly absorbed. Using it, therefore, does not require the planning required for other insulins that begin to take effect much later (up to many hours) after administration. Another type is extended-release insulin; the first of these was Lantus (insulin glargine). These have a steady effect for the entire time they are active, without the peak and drop off effect in other insulins; typically, they continue to have an insulin effect for an extended period from 18 to 24 hours. Likewise, another protracted insulin analogue (Levemir) is based on a fatty acid acylation approach. A myristyric acid molecule is attached to this analogue, which in turn associates the insulin molecule to the abundant serum albumin, which in turn extends the effect and reduces the risk of hypoglycemia. Both protracted analogues need to be taken only once-daily, and are very much used in the type 1 diabetes market as the basal insulin. A combination of a rapid acting and a protracted insulin is also available for the patients, making it more likely for them to achieve an insulin profile that mimics that of the body´s own insulin release. Insulin is usually taken as subcutaneous Injection (medicine)injections by single-use syringes with hypodermic needleneedles, via an insulin pump, or by repeated-use insulin pens with needles. Unlike many medicines, insulin currently cannot be taken orally because, like nearly all other proteins introduced into the gastrointestinal tract, it is reduced to fragments (even single amino acid components), whereupon all activity is lost. There has been some research into ways to protect insulin from the digestive tract, so that it can be administered orally or sublingually. While experimental, several companies now have various formulations in human clinical trials, and one, the India-based Biocon, has formed an agreement with Bristol-MyersBMS to produce an oral-insulin alternative. NDTV Profit – November 16, 2012 – Biocon in pact with Bristol-Myers for oral insulin. Retrieved 2013-04-22.History Discovery In 1869 Paul Langerhans, a medical student in Berlin, was studying the structure of the pancreas under a microscope when he identified some previously unnoticed tissue clumps scattered throughout the bulk of the pancreas. The function of the "little heaps of cells", later eponymknown as the islets of Langerhans, was unknown, but Edouard Laguesse later suggested they might produce secretions that play a regulatory role in digestion. Paul Langerhans' son, Archibald, also helped to understand this regulatory role. The term "insulin" originates from insula, the Latin word for islet/island.In 1889, the Poles in GermanyPolish-German physician Oscar Minkowski, in collaboration with Joseph von Mering, removed the pancreas from a healthy dog to test its assumed role in digestion. Several days after the dog's pancreas was removed, Minkowski's animal keeper noticed a swarm of flies feeding on the dog's urine. On testing the urine, they found there was sugar in the dog's urine, establishing for the first time a relationship between the pancreas and diabetes. In 1901, another major step was taken by Eugene Opie, when he clearly established the link between the islets of Langerhans and diabetes: "Diabetes mellitus . . . is caused by destruction of the islets of Langerhans and occurs only when these bodies are in part or wholly destroyed." Before his work, the link between the pancreas and diabetes was clear, but not the specific role of the islets. The structure of insulin. The left side is a space-filling model of the insulin monomer, believed to be biologically active. Carbon is green, hydrogen white, oxygen red, and nitrogen blue. On the right side is a ribbon diagram of the insulin hexamer, believed to be the stored form. A monomer unit is highlighted with the A chain in blue and the B chain in cyan. Yellow denotes disulfide bonds, and magenta spheres are zinc ions.Over the next two decades, several attempts were made to isolate whatever it was the islets produced as a potential treatment. In 1906,
188
Insulin George Ludwig Zuelzer was partially successful treating dogs with pancreatic extract, but was unable to continue his work. Between 1911 and 1912, E.L. Scott at the University of Chicago used aqueous pancreatic extracts, and noted "a slight diminution of glycosuria", but was unable to convince his director of his work's value; it was shut down. Israel Kleiner (biochemist)Israel Kleiner demonstrated similar effects at Rockefeller University in 1915, but his work was interrupted by World War I, and he did not return to it.In 1916 Nicolae Paulescu, a RomaniansRomanian professor of physiology at the Carol Davila University of Medicine and PharmacyUniversity of Medicine and Pharmacy in Bucharest, developed an aqueous Pancreaspancreatic extract which, when injected into a Diabetesdiabetic dog, had a normalizing effect on blood sugar levels. He had to interrupt his experiments because of World War I, and in 1921 he wrote four papers about his work carried out in Bucharest and his tests on a diabetic dog. Later that year, he published "Research on the Role of the Pancreas in Food Assimilation".Extraction and purification In October 1920, Canadian Frederick Banting was reading one of Minkowski's papers and concluded that it was the very digestive secretions that Minkowski had originally studied that were breaking down the islet secretion(s), thereby making it impossible to extract successfully. He jotted a note to himself: "Ligate pancreatic ducts of the dog. Keep dogs alive till acini degenerate leaving islets. Try to isolate internal secretion of these and relieve glycosurea." The idea was the pancreas's internal secretion, which, it was supposed, regulates sugar in the bloodstream, might hold the key to the treatment of diabetes. A surgeon by training, Banting knew certain arteries could be tied off that would lead to atrophy of most of the pancreas, while leaving the islets of Langerhans intact. He theorized a relatively pure extract could be made from the islets once most of the rest of pancreas was gone. In the spring of 1921, Banting traveled to Toronto to explain his idea to John James Rickard MacleodJ.J.R. Macleod, who was Professor of Physiology at the University of Toronto, and asked Macleod if he could use his lab space to test the idea. Macleod was initially skeptical, but eventually agreed to let Banting use his lab space while he was on holiday for the summer. He also supplied Banting with ten dogs on which to experiment, and two medical students, Charles Herbert BestCharles Best and Clark Noble, to use as lab assistants, before leaving for Scotland. Since Banting required only one lab assistant, Best and Noble flipped a coin to see which would assist Banting for the first half of the summer. Best won the coin toss, and took the first shift as Banting's assistant. Loss of the coin toss may have proved unfortunate for Noble, given that Banting decided to keep Best for the entire summer, and eventually shared half his Nobel Prize money and a large part of the credit for the discovery of insulin with the winner of the toss. Had Noble won the toss, his career might have taken a different path. Banting's method was to tie a ligature (medicine)ligature around the pancreatic duct; when examined several weeks later, the pancreatic digestive cells had died and been absorbed by the immune system, leaving thousands of islets. They then isolated an extract from these islets, producing what they called "isletin" (what we now know as insulin), and tested this extract on the dogs starting July 27. Banting and Best were then able to keep a pancreatectomized dog named Marjorie alive for the rest of the summer by injecting her with the crude extract they had prepared. Removal of the pancreas in test animals in essence mimics diabetes, leading to elevated blood glucose levels. Marjorie was able to remain alive because the extracts, containing isletin, were able to lower her blood glucose levels. Banting and Best presented their results to Macleod on his return to Toronto in the fall of 1921, but Macleod pointed out flaws with the experimental design, and suggested the experiments be repeated with more dogs and better equipment. He then supplied Banting and Best with a better laboratory, and began paying Banting a salary from his research grants. Several weeks later, the second round of experiments was also a success; and Macleod helped publish their results privately in Toronto that November. However, they needed six weeks to extract the isletin, which forced considerable delays. Banting suggested they try to use fetal calf pancreas, which had not yet developed digestive glands; he was relieved to find this method worked well. With the supply problem solved, the next major effort was to purify the extract. In December 1921, Macleod invited the biochemist James Collip to help with this task, and, within a month, the team felt ready for a clinical test. On January 11, 1922, Leonard Thompson (diabetic)Leonard Thompson, a 14-year-old diabetic who lay dying at the Toronto General Hospital, was given the first injection of insulin. However, the extract was so impure, Thompson suffered a severe anaphylaxisallergic reaction, and further injections were canceled. Over the next 12 days, Collip worked day and night to improve the ox-pancreas extract, and a second dose was injected on
189
Insulin January 23. This was completely successful, not only in having no obvious side-effects but also in completely eliminating the glycosuria sign of diabetes. The first American patient was Elizabeth Hughes Gossett, the daughter of the governor of New York. The first patient treated in the U.S. was future woodcut artist James D. Havens; Dr. John Ralston Williams imported insulin from Toronto to Rochester, New York, to treat Havens.Children dying from diabetic ketoacidosis were kept in large wards, often with 50 or more patients in a ward, mostly comatose. Grieving family members were often in attendance, awaiting the (until then, inevitable) death. In one of medicine's more dramatic moments, Banting, Best, and Collip went from bed to bed, injecting an entire ward with the new purified extract. Before they had reached the last dying child, the first few were awakening from their coma, to the joyous exclamations of their families.Banting and Best never worked well with Collip, regarding him as something of an interloper, and Collip left the project soon after. Over the spring of 1922, Best managed to improve his techniques to the point where large quantities of insulin could be extracted on demand, but the preparation remained impure. The drug firm Eli Lilly and Company had offered assistance not long after the first publications in 1921, and they took Lilly up on the offer in April. In November, Lilly made a major breakthrough and was able to produce large quantities of highly refined insulin. Insulin was offered for sale shortly thereafter. Synthesis Purified animal-sourced insulin was the only type of insulin available to diabetics until genetic advances occurred later with medical research. The amino acid structure of insulin was characterized in the early 1950s by Frederick Sanger#Sequencing insulinFrederick Sanger, and the first synthetic insulin was produced simultaneously in the labs of Panayotis Katsoyannis at the University of Pittsburgh and Helmut Zahn at RWTH Aachen University in the early 1960s.The first genetically engineered, synthetic "human" insulin was produced in a laboratory in 1977 by Arthur Riggs, PhD, Keiichi Itakura, PhD, and Herbert Boyer using Escherichia coliE. coli. Partnering with Genentech founded by Swanson, Boyer and Eli Lilly and Company went on in 1982 to sell the first commercially available biosynthetic human insulin under the brand name Humulin. The vast majority of insulin currently used worldwide is now biosynthetic recombinant "human" insulin or its analogues.Recombinant insulin is produced either in yeast (usually baker's yeastsaccharomyces cerevisiae) or E. coli. In yeast, insulin may be engineered as a single-chain protein with a KexII endoprotease (a yeast homolog of PCI/PCII) site that separates the insulin A chain from a c-terminally truncated insulin B chain. A chemically synthesized c-terminal tail is then grafted onto insulin by reverse proteolysis using the inexpensive protease trypsin; typically the lysine on the c-terminal tail is protected with a chemical protecting group to prevent proteolysis. The ease of modular synthesis and the relative safety of modifications in that region accounts for common insulin analogs with c-terminal modifications (e.g. lispro, aspart, glulisine). The Genentech synthesis and completely chemical synthesis such as that by Bruce Merrifield are not preferred because the efficiency of recombining the two insulin chains is low, primarily due to competition with the precipitation of insulin B chain.Nobel Prizes Frederick Banting joined by Charles Best in office, 1924 The Nobel Prize committee in 1923 credited the practical extraction of insulin to a team at the University of Toronto and awarded the Nobel Prize to two men: Frederick Banting and John James Rickard MacleodJ.J.R. Macleod. They were awarded the Nobel Prize in Physiology or Medicine in 1923 for the discovery of insulin. Banting, insulted that Best was not mentioned, shared his prize with him, and Macleod immediately shared his with James Collip. The patent for insulin was sold to the University of Toronto for one half-dollar. The primary structure of insulin was determined by British molecular biologist Frederick Sanger. It was the first protein to have its sequence be determined. He was awarded the 1958 Nobel Prize in Chemistry for this work. In 1969, after decades of work, Dorothy Hodgkin determined the spatial conformation of the molecule, the so-called tertiary structure, by means of X-ray diffraction studies. She had been awarded a Nobel Prize in Chemistry in 1964 for the development of crystallography. Rosalyn Sussman Yalow received the 1977 Nobel Prize in Medicine for the development of the radioimmunoassay for insulin. George Minot, co-recipient of the 1934 Nobel Prize for the development of the first effective treatment for pernicious anemia, had diabetes mellitus. Dr. William Bosworth CastleWilliam Castle observed that the 1921 discovery of insulin, arriving in time to keep Minot alive, was therefore also responsible for the discovery of a cure for pernicious anemia.Nobel Prize controversy Nicolae PaulescuThe work published by Banting, Best, Collip and Macleod represented the preparation of purified insulin extract suitable for use on human patients. Although Paulescu discovered the
190
Insulin principles of the treatment his saline extract could not be used on humans, and he was not mentioned in the 1923 Nobel Prize. Professor Ian Murray was particularly active in working to correct "the historical wrong" against Nicolae Paulescu. Murray was a professor of physiology at the Anderson College of Medicine in Glasgow, Scotland, the head of the department of Metabolic Diseases at a leading Glasgow hospital, vice-president of the British Association of Diabetes, and a founding member of the International Diabetes Federation. Murray wrote: Insufficient recognition has been given to Paulesco, the distinguished RomaniaRoumanian scientist, who at the time when the Toronto team were commencing their research had already succeeded in extracting the antidiabetic hormone of the pancreas and proving its efficacy in reducing the hyperglycaemia in diabetic dogs.In a recent private communication Professor Arne TiseliusTiselius, head of the Nobel Institute, has expressed his personal opinion that Paulescu was equally worthy of the award in 1923.References Further reading Reaven, Gerald M.; Ami Laws (ed.) (1999--04-15). Insulin Resistance: The Metabolic Syndrome X (1st ed.). Totowa, New Jersey: Humana Press. Digital object identifierdoi: 10.1226/0896035883. International Standard Book NumberISBN 0-89603-588-3.Leahy, Jack L.; William T. Cefalu (ed.) (2002-03-22). Insulin Therapy (1st ed.). New York: Marcel Dekker. International Standard Book NumberISBN 0-8247-0711-7.Kumar, Sudhesh; Stephen O'Rahilly (ed.) (2005-01-14). Insulin Resistance: Insulin Action and Its Disturbances in Disease. Chichester, England: Wiley. International Standard Book NumberISBN 0-470-85008-6.Ehrlich, Ann; Carol L. Schroeder (2000-06-16). Medical Terminology for Health Professions (4th ed.). Thomson Delmar Learning. International Standard Book NumberISBN 0-7668-1297-9.Draznin, Boris; Derek LeRoith (September 1994). Molecular Biology of Diabetes: Autoimmunity and Genetics; Insulin Synthesis and Secretion. Totowa, New Jersey: Humana Press. Digital object identifierdoi: 10.1226/0896032868. International Standard Book NumberISBN 0-89603-286-8. Famous Canadian Physicians: Sir Frederick Banting at Library and Archives Canada McKeage K, Goa KL (2001). "Insulin glargine: a review of its therapeutic use as a long-acting agent for the management of type 1 and 2 diabetes mellitus". Drugs 61 (11): 1599–624. Digital object identifierdoi: 10.2165/00003495-200161110-00007. PubMed IdentifierPMID 11577797.External links The Insulin Protein Inspired by Insulin article by parent of a diabetic child Frederick Sanger, Nobel Prize for sequencing Insulin Freeview video with John Sanger and John Walker by the Vega Science Trust. Insulin: entry from protein databank The History of Insulin Insulin Lispro CBC Digital Archives - Banting, Best, Macleod, Collip: Chasing a Cure for Diabetes GeneReviews/NCBI/NIH/UW entry on Permanent Neonatal Diabetes Mellitus Cosmos Magazine: Insulin mystery cracked after 20 years National Diabetes Information Clearinghouse Discovery and Early Development of Insulin, 1920–1925 Secretion of Insulin and Glucagon Insulin Types Comparison Chart Insulin hormone dosage and side effects The True Discoverer of Insulin - Nicolae Paulescu Insulin signaling pathway Molecular Physiology of Signalling Proteins Animations of insulin's action in the body at AboutKidsHealth.ca
191
Glucagon
192
Glucagon
Glucagon
PDB rendering based on 1GCN. Available structures PDB Ortholog search: PDBe [1], RCSB [2] List of PDB id codes 1BH0
[3]
, 1D0R
[4]
, 1NAU
[5]
, 2G49
[6]
, 2L63
[7]
, 2L64
[8]
, 2M5P
[9]
, 2M5Q
[10]
, 3IOL
[11]
Identifiers Symbols External IDs GCG
[12]
; GLP1; GLP2; GRPP
[13]
OMIM: 138030 [17] Gene
MGI: 95674
[14]
HomoloGene: 1553
[15]
ChEMBL: 5736
[16]
GeneCards: GCG
Glucagon
193
Gene Ontology Molecular function • receptor binding [14] [10] • hormone activity [18] • glucagon receptor binding Cellular component • extracellular region [229] [230] • extracellular space [172] • endoplasmic reticulum lumen [19] • plasma membrane [33] • secretory granule Biological process • energy reserve metabolic process [38] • signal transduction [14] • G-protein coupled receptor signaling pathway [20] • adenylate cyclase-modulating G-protein coupled receptor signaling pathway [21] • feeding behavior [22] • cell proliferation [23] • protein kinase A signaling cascade [24] • positive regulation of peptidyl-threonine phosphorylation [32] • positive regulation of cAMP biosynthetic process [25] • positive regulation of protein binding [17] • negative regulation of appetite [35] • positive regulation of peptidyl-serine phosphorylation • positive regulation of insulin secretion involved in cellular response to glucose stimulus
[26] [178]
• negative regulation of apoptotic process [198] • small molecule metabolic process [27] • positive regulation of protein kinase activity [218] • regulation of insulin secretion [28] • positive regulation of ERK1 and ERK2 cascade [29] • cellular response to glucagon stimulus [30] • positive regulation of calcium ion import Sources: Amigo
[31]
[39]
/ QuickGO
[32]
RNA expression pattern
More reference expression data Orthologs Species Entrez Ensembl UniProt RefSeq (mRNA) RefSeq (protein) Human 2641
[34] [36]
[33]
Mouse 14526
[35] [37]
ENSG00000115263 P01275
[38] [40]
ENSMUSG00000000394 P55095
[39] [41]
NM_002054 NP_002045
NM_008100 NP_032126
[42]
[43]
Glucagon
194
Location (UCSC)
Chr 2: [44] 163 – 163.01 Mb
[46]
Chr 2: [45] 62.47 – 62.48 Mb
[47]
PubMed search
Glucagon, a peptide hormone secreted by the pancreas, raises blood glucose levels. Its effect is opposite that of insulin, which lowers blood glucose levels.[] The pancreas releases glucagon when blood sugar (glucose) levels fall too low. Glucagon causes the liver to convert stored glycogen into glucose, which is released into the bloodstream. High blood glucose levels stimulate the release of insulin. Insulin allows glucose to be taken up and used by insulin-dependent tissues. Thus, glucagon and insulin are part of a feedback system that keeps blood glucose levels at a stable level. Glucagon belongs to a family of several other related hormones.
Physiology
Production
The hormone is synthesized and secreted from alpha cells (α-cells) of the islets of Langerhans, which are located in the endocrine portion of the pancreas. In rodents, the alpha cells are located in the outer rim of the islet. Human islet structure is much less segregated, and alpha cells are distributed throughout the islet.
Regulation
Secretion of glucagon is stimulated by: • • • • • • Hypoglycemia Epinephrine (via β2, α2,[] and α1[] adrenergic receptors) Arginine Alanine (often from muscle-derived pyruvate/glutamate transamination (see alanine transaminase reaction). Acetylcholine[] Cholecystokinin
Secretion of glucagon is inhibited by: • • • • Somatostatin Insulin (via GABA)[] Increased free fatty acids and keto acids into the blood Increased urea production
Function
Glucagon generally elevates the amount of glucose in the blood by promoting gluconeogenesis and glycogenolysis.
A microscopic image stained for glucagon
Glucagon
195
Glucagon
Clinical data Pregnancy cat. Legal status ? ? Identifiers ATC code PubChem ? CID 16186314 [48]
IUPHAR ligand 1136 [49] ChemSpider UNII ChEMBL 10481928 [50]
76LA80IG2G
[51]
CHEMBL266481 Chemical data
[52]
Formula
? [53]
(what is this?) (verify)
Glucose is stored in the liver in the form of glycogen, which is a starch-like polymer chain made up of glucose molecules. Liver cells (hepatocytes) have glucagon receptors. When glucagon binds to the glucagon receptors, the liver cells convert the glycogen polymer into individual glucose molecules, and release them into the bloodstream, in a process known as glycogenolysis. As these stores become depleted, glucagon then encourages the liver and kidney to synthesize additional glucose by gluconeogenesis. Glucagon turns off glycolysis in the liver, causing glycolytic intermediates to be shuttled to gluconeogenesis. Glucagon also regulates the rate of glucose production through lipolysis. Glucagon has a minimal effect on lipolysis in humans. Glucagon production appears to be dependent on the central nervous system through pathways yet to be defined. In invertebrate animals, eyestalk removal has been reported to affect glucagon production. Excising the eyestalk in young crayfish produces glucagon-induced hyperglycemia.[]
Glucagon
196
Mechanism of action
Glucagon binds to the glucagon receptor, a G protein-coupled receptor, located in the plasma membrane. The conformation change in the receptor activates G proteins, a heterotrimeric protein with α, β, and γ subunits. When the G protein interacts with the receptor, it undergoes a conformational change that results in the replacement of the GDP molecule that was bound to the α subunit with a GTP molecule. This substitution results in the releasing of the α subunit from the β and γ subunits. The alpha subunit specifically activates the next enzyme in the cascade, adenylate cyclase. Adenylate cyclase manufactures cyclic adenosine monophosphate (cyclic AMP or cAMP), which activates protein kinase A (cAMP-dependent protein kinase). This enzyme, in turn, activates phosphorylase kinase, which, in turn, phosphorylates glycogen phosphorylase, converting into the active form called phosphorylase A. Phosphorylase A is the enzyme responsible for the release of glucose-1-phosphate from glycogen polymers.
History
In the 1920s, Kimball and Murlin studied pancreatic extracts, and found an additional substance with hyperglycemic properties. They described glucagon in 1923.[] The amino acid sequence of glucagon was described in the late 1950s.[] A more complete understanding of its role in physiology and disease was not established until the 1970s, when a specific radioimmunoassay was developed.
Etymology
Glucagon was named in 1923, probably from the Greek γλυκός sweet, and ἄγειν to lead.[1]
Structure
Glucagon is a 29-amino acid polypeptide. Its primary structure in humans is: NH2-His-Ser-Gln-Gly-Thr-Phe-Thr-Ser-Asp-Tyr-Ser-Lys-Tyr-Leu-Asp-Ser-Arg-Arg-Ala-Gln-Asp-Phe-Val-Gln-Trp-Leu-Met-Asn-T The polypeptide has a molecular weight of 3485 daltons. Glucagon is a peptide (nonsteroid) hormone. Glucagon is generated from the cleavage of proglucagon secreted by pancreatic islet α cells. In intestinal L cells, proglucagon is cleaved to the alternate products glicentin, GLP-1 (an incretin), IP-2, and GLP-2 (promotes intestinal growth).
Pathology
Abnormally elevated levels of glucagon may be caused by pancreatic tumors, such as glucagonoma, symptoms of which include necrolytic migratory erythema, reduced amino acids, and hyperglycemia. It may occur alone or in the context of multiple endocrine neoplasia type 1.
Uses and contraindications
Hypoglycemia
An injectable form of glucagon is vital first aid in cases of severe hypoglycemia when the victim is unconscious or for other reasons cannot take glucose orally. The dose for an adult is typically 1 milligram, and the glucagon is given by intramuscular, intravenous or subcutaneous injection, and quickly raises blood glucose levels. Glucagon can also be administered intravenously at 0.25 - 0.5 unit. To use the injectable form, it must be reconstituted prior to use, a step that requires a sterile diluent to be injected into a vial containing powdered glucagon, because the hormone is highly unstable when dissolved in solution. When dissolved in a fluid state, glucagon can form amyloid fibrils, or tightly woven chains of proteins made up of the individual glucagon peptides, and once glucagon begins to fibrilize,
Glucagon it becomes useless when injected, as the glucagon cannot be absorbed and used by the body. The reconstitution process makes using glucagon cumbersome, although there are a number of products now in development from a number of companies that aim to make the product easier to use.
197
Beta blocker overdose
Anecdotal evidence suggests a benefit of higher doses of glucagon in the treatment of overdose with beta blockers; the likely mechanism of action is the increase of cAMP in the myocardium, in effect bypassing the β-adrenergic second messenger system.[]
Impacted food bolus
Glucagon relaxes the lower esophageal sphincter and is used in emergencies involving an impacted food bolus in the esophagus.[]
Side-effects and interactions
Glucagon acts very quickly; common side-effects include headache and nausea. Drug interactions: Glucagon interacts only with oral anticoagulants, increasing the tendency to bleed.
Contraindications
While glucagon can be used clinically to treat various forms of hypoglycemia, it is severely contraindicated in patients with pheochromocytoma, as the drug interaction with elevated levels of adrenaline produced by the tumor may produce an exponential increase in blood sugar levels, leading to a hyperglycemic state, which may incur a fatal elevation in blood pressure.[] Likewise, glucagon is contraindicated in patients with an insulinoma, as its use may lead to rebound hypoglycemia.[]
Media References
[1] glucagon (http:/ / dictionary. reference. com/ browse/ glucagon) on dictionary.com
Further reading
• Kieffer TJ, Habener JF (2000). "The glucagon-like peptides". Endocr. Rev. 20 (6): 876–913. doi: 10.1210/er.20.6.876 (http://dx.doi.org/10.1210/er.20.6.876). PMID 10605628 (http://www.ncbi.nlm.nih. gov/pubmed/10605628). • Drucker DJ (2003). "Glucagon-like peptides: regulators of cell proliferation, differentiation, and apoptosis". Mol. Endocrinol. 17 (2): 161–71. doi: 10.1210/me.2002-0306 (http://dx.doi.org/10.1210/me.2002-0306). PMID 12554744 (http://www.ncbi.nlm.nih.gov/pubmed/12554744). • Jeppesen PB (2004). "Clinical significance of GLP-2 in short-bowel syndrome". J. Nutr. 133 (11): 3721–4. PMID 14608103 (http://www.ncbi.nlm.nih.gov/pubmed/14608103). • Brubaker PL, Anini Y (2004). "Direct and indirect mechanisms regulating secretion of glucagon-like peptide-1 and glucagon-like peptide-2". Can. J. Physiol. Pharmacol. 81 (11): 1005–12. doi: 10.1139/y03-107 (http://dx. doi.org/10.1139/y03-107). PMID 14719035 (http://www.ncbi.nlm.nih.gov/pubmed/14719035). • Baggio LL, Drucker DJ (2005). "Clinical endocrinology and metabolism. Glucagon-like peptide-1 and glucagon-like peptide-2". Best Pract. Res. Clin. Endocrinol. Metab. 18 (4): 531–54. doi: 10.1016/j.beem.2004.08.001 (http://dx.doi.org/10.1016/j.beem.2004.08.001). PMID 15533774 (http:// www.ncbi.nlm.nih.gov/pubmed/15533774).
Glucagon • Holz GG, Chepurny OG (2006). "Diabetes Outfoxed by GLP-1?" (http://www.ncbi.nlm.nih.gov/pmc/ articles/PMC2909599). Sci. STKE 2005 (268): pe2. doi: 10.1126/stke.2682005pe2 (http://dx.doi.org/10.1126/ stke.2682005pe2). PMC 2909599 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2909599). PMID 15671479 (http://www.ncbi.nlm.nih.gov/pubmed/15671479). • Dunning BE, Foley JE, Ahrén B (2006). "Alpha cell function in health and disease: influence of glucagon-like peptide-1". Diabetologia 48 (9): 1700–13. doi: 10.1007/s00125-005-1878-0 (http://dx.doi.org/10.1007/ s00125-005-1878-0). PMID 16132964 (http://www.ncbi.nlm.nih.gov/pubmed/16132964). • Gautier JF, Fetita S, Sobngwi E, Salaün-Martin C (2005). "Biological actions of the incretins GIP and GLP-1 and therapeutic perspectives in patients with type 2 diabetes". Diabetes Metab. 31 (3 Pt 1): 233–42. doi: 10.1016/S1262-3636(07)70190-8 (http://dx.doi.org/10.1016/S1262-3636(07)70190-8). PMID 16142014 (http://www.ncbi.nlm.nih.gov/pubmed/16142014). • De León DD, Crutchlow MF, Ham JY, Stoffers DA (2006). "Role of glucagon-like peptide-1 in the pathogenesis and treatment of diabetes mellitus". Int. J. Biochem. Cell Biol. 38 (5–6): 845–59. doi: 10.1016/j.biocel.2005.07.011 (http://dx.doi.org/10.1016/j.biocel.2005.07.011). PMID 16202636 (http:// www.ncbi.nlm.nih.gov/pubmed/16202636). • Beglinger C, Degen L (2007). "Gastrointestinal satiety signals in humans--physiologic roles for GLP-1 and PYY?". Physiol. Behav. 89 (4): 460–4. doi: 10.1016/j.physbeh.2006.05.048 (http://dx.doi.org/10.1016/j. physbeh.2006.05.048). PMID 16828127 (http://www.ncbi.nlm.nih.gov/pubmed/16828127). • Stephens JW, Bain SC (2007). "Safety and adverse effects associated with GLP-1 analogues". Expert opinion on drug safety 6 (4): 417–22. doi: 10.1517/14740338.6.4.417 (http://dx.doi.org/10.1517/14740338.6.4.417). PMID 17688385 (http://www.ncbi.nlm.nih.gov/pubmed/17688385). • Orskov C, Bersani M, Johnsen AH et al. (1989). "Complete sequences of glucagon-like peptide-1 from human and pig small intestine". J. Biol. Chem. 264 (22): 12826–9. PMID 2753890 (http://www.ncbi.nlm.nih.gov/ pubmed/2753890). • Drucker DJ, Asa S (1988). "Glucagon gene expression in vertebrate brain". J. Biol. Chem. 263 (27): 13475–8. PMID 2901414 (http://www.ncbi.nlm.nih.gov/pubmed/2901414). • Novak U, Wilks A, Buell G, McEwen S (1987). "Identical mRNA for preproglucagon in pancreas and gut". Eur. J. Biochem. 164 (3): 553–8. doi: 10.1111/j.1432-1033.1987.tb11162.x (http://dx.doi.org/10.1111/j. 1432-1033.1987.tb11162.x). PMID 3569278 (http://www.ncbi.nlm.nih.gov/pubmed/3569278). • White JW, Saunders GF (1986). "Structure of the human glucagon gene" (http://www.ncbi.nlm.nih.gov/pmc/ articles/PMC311486). Nucleic Acids Res. 14 (12): 4719–30. doi: 10.1093/nar/14.12.4719 (http://dx.doi.org/ 10.1093/nar/14.12.4719). PMC 311486 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC311486). PMID 3725587 (http://www.ncbi.nlm.nih.gov/pubmed/3725587). • Schroeder WT, Lopez LC, Harper ME, Saunders GF (1984). "Localization of the human glucagon gene (GCG) to chromosome segment 2q36----37". Cytogenet. Cell Genet. 38 (1): 76–9. doi: 10.1159/000132034 (http://dx.doi. org/10.1159/000132034). PMID 6546710 (http://www.ncbi.nlm.nih.gov/pubmed/6546710). • Bell GI, Sanchez-Pescador R, Laybourn PJ, Najarian RC (1983). "Exon duplication and divergence in the human preproglucagon gene". Nature 304 (5924): 368–71. doi: 10.1038/304368a0 (http://dx.doi.org/10.1038/ 304368a0). PMID 6877358 (http://www.ncbi.nlm.nih.gov/pubmed/6877358). • Kärgel HJ, Dettmer R, Etzold G et al. (1982). "Action of rat liver cathepsin L on glucagon". Acta Biol. Med. Ger. 40 (9): 1139–43. PMID 7340337 (http://www.ncbi.nlm.nih.gov/pubmed/7340337). • Wayman GA, Impey S, Wu Z et al. (1994). "Synergistic activation of the type I adenylyl cyclase by Ca2+ and Gs-coupled receptors in vivo". J. Biol. Chem. 269 (41): 25400–5. PMID 7929237 (http://www.ncbi.nlm.nih. gov/pubmed/7929237). • Unson CG, Macdonald D, Merrifield RB (1993). "The role of histidine-1 in glucagon action". Arch. Biochem. Biophys. 300 (2): 747–50. doi: 10.1006/abbi.1993.1103 (http://dx.doi.org/10.1006/abbi.1993.1103). PMID 8382034 (http://www.ncbi.nlm.nih.gov/pubmed/8382034).
198
Bombesin
199
Bombesin
Bombesin
Identifiers CAS number PubChem ChemSpider ChEMBL IUPHAR ligand Jmol-3D images 31362-50-2 16133891 26286924
[1]
[2] [3] [4]
CHEMBL437027 616
[5] [6]
Image 1 Properties
Molecular formula Molar mass
(verify) [7]
C71H110N24O18S 1619.85
(what is: / ?) Except where noted otherwise, data are given for materials in their standard state (at 25 °C, 100 kPa)
Infobox references
Bombesin is a 14-amino acid peptide[] originally isolated from the skin of the oriental fire-bellied toad (Bombina orientalis). It has two known homologs in mammals called neuromedin B and gastrin-releasing peptide. It stimulates gastrin release from G cells. It activates three different G-protein-coupled receptors known as BBR1, -2, and -3.[] It also activates these receptors in the brain. Together with cholecystokinin, it is the second major source of negative feedback signals that stop eating behaviour.[] Bombesin is also a tumor marker for small cell carcinoma of lung, gastric cancer, and neuroblastoma.[]
References
Follicular cell
200
Follicular cell
Follicular cell
Section of thyroid gland of sheep. X 160. ("Cubical epithelium" labeled at center left.) Code TH H3.08.02.4.00007
[1]
Thyroid epithelial cells (also called follicular cells or principal cells) are cells in the thyroid gland that are responsible for the production and secretion of thyroid hormones, that is, thyroxine (T4) and triiodothyronine (T3).
Function
The thyroid epithelial cells take up iodine and amino acids from the blood circulation on the basolateral side, synthesize thyroglobulin and thyroperoxidase from amino acids and secrete these into the thyroid follicles together with iodine. The thyroid epithelial cells can subsequently take up iodinated thyroglobulin from the follicles by endocytosis, extract thyroid hormones from it with the help of proteases and subsequently release thyroid hormones to the blood.
Thyroid hormone synthesis.
[1]
These thyroid hormones are transported throughout the body where they control metabolism (which is the conversion of oxygen and calories to energy). Every cell in the body depends upon thyroid hormones for regulation of their metabolism. The normal thyroid gland produces about 80% T4 and about 20% T3, however, T3 is about four times as potent as T4.
Follicular cell
201
Iodine transport
Iodine is taken up on the basolateral side of the thyroid epithelial cells by sodium-iodide symporters.[2] It is secreted into the follicle through the chloride/iodide transporter pendrin on the apical side.
Structure and development
They are simple cuboidal epithelium and are arranged in spherical follicles surrounding colloid. The interiors of one of these follicles is known as the follicular lumen. They have thyrotropin receptors on their surface, which respond to thyroid-stimulating hormone. Embryologic origin is from a median endodermal mass in the region of the tongue (foramen cecum) in contrast to the parafollicular (C) cells that arise from the 4th branchial pouch.
Relationship to other cell types
Calcitonin-producing parafollicular cells (C cells) can be found scattered along the basement membrane of the thyroid epithelium. Embryologic origin of these C-cells is neural crest, from the ultimobranchial body (4th pharyngeal pouch).
References External links
• Anatomy Atlases - Microscopic Anatomy, plate 15.287 (http://www.anatomyatlases.org/MicroscopicAnatomy/ Section15/Plate15287.shtml) • BU Histology Learning System: 14302loa (http://www.bu.edu/histology/p/14302loa.htm)
Parafollicular cell
202
Parafollicular cell
Parafollicular cell
Code TH H3.08.02.4.00009 [1]
Parafollicular cells (also called C cells) are neuroendocrine cells in the thyroid with primary function to secrete calcitonin. They are located adjacent to the thyroid follicles and reside in the connective tissue. These cells are large and have a pale stain compared with the follicular cells or colloid. In teleost and avian species these cells occupy a structure outside of the thyroid gland named the ultimobranchial body. Parafollicular cells themselves are derived from neural crest cells. Embryologically, they associate with the ultimobranchial body, which itself is a ventral derivative of the fourth (or fifth) pharyngeal pouch. In a series of experiments, Nicole LeDouarin transplanted neural crest cells from quail, with unique and easily identified nuclei, into non-quail neural crest. She subsequently demonstrated the presence of cells with quail nuclei populating the ultimobranchial body and concluded that C cells migrate during embryologic development from the neural crest.[1][2] They are not numerous in the thyroid and are typically situated basally in the epithelium, without direct contact with the follicular lumen. They are always situated within the basement membrane, which surrounds the entire follicle. Parafollicular cell are also known to secrete in smaller quantities several neuroendocrine peptides such as serotonin, somatostatin or CGRP.[3][4][5] They may also have a paracrine role in regulating thyroid hormones production, as they express TRH.[6][7] When parafollicular cells become cancerous, they lead to medullary carcinoma of the thyroid.
Literature
• Baber EC: Contributions to the minute anatomy of the thyroid gland of the dog. Phil Trans R Soc 166 (1876) 557-568 (full text)
References External links
• Histology at OU 42_04 (http://w3.ouhsc.edu/histology/Glass slides/42_04.jpg) • BU Histology Learning System: 14302loa (http://www.bu.edu/histology/p/14302loa.htm) • Histology at KUMC endo-/endo10 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/endo// endo10.htm) • Anatomy Atlases - Microscopic Anatomy, plate 15.287 (http://www.anatomyatlases.org/MicroscopicAnatomy/ Section15/Plate15287.shtml)
Parathyroid gland
203
Parathyroid gland
Parathyroid glands
Endocrine system. (Parathyroid gland not pictured, but are present on surface of thyroid gland, as shown below.)
Thyroid and parathyroid. Latin Gray's System Artery Vein Nerve Lymph Precursor MeSH glandula parathyroidea inferior, glandula parathyroidea superior subject #273 1271 Endocrine superior thyroid artery, inferior thyroid artery, superior thyroid vein, middle thyroid vein, inferior thyroid vein, middle cervical ganglion, inferior cervical ganglion pretracheal, prelaryngeal, jugulo-diagastric,and lympahtics of thymus neural crest mesenchyme and third and fourth pharyngeal pouch endoderm Parathyroid+Glands
[2] [1]
The parathyroid glands are small endocrine glands in the neck that produce parathyroid hormone. Humans usually have four parathyroid glands, which are usually located on the rear surface of the thyroid gland, or, in rare cases, within the thyroid gland itself or in the chest. Parathyroid glands control the amount of calcium in the blood and within the bones.
Parathyroid gland
204
Anatomy
The parathyroid glands are four or more small glands, about the size of a grain of rice, located on the posterior surface (back side) of the thyroid gland. The parathyroid glands usually weigh between 25 mg and 40 mg in humans. There are typically four parathyroid glands. The two parathyroid glands on each side which are positioned higher (closer to the head) are called the superior parathyroid glands, while the lower two are called the inferior parathyroid glands. Occasionally, some individuals may have six, eight, or even more parathyroid glands. The parathyroid glands are named for their proximity to the thyroid but serve a completely different role than the thyroid gland. The parathyroid glands are quite easily recognizable from the thyroid as they have densely packed cells, in contrast with the follicle structure of the thyroid.[1][2] However, at surgery, they are harder to differentiate from the thyroid or fat. Because the inferior thyroid arteries provide the primary blood supply to the posterior aspect of the thyroid gland where the parathyroid glands are located, branches of these arteries usually supply the parathyroid glands. However they may also be supplied by the branches of the superior thyroid arteries; the thyroid ima artery; or the laryngeal, tracheal and esophageal artery. Parathyroid veins drain into thyroid plexus of veins of the thyroid gland. Lymphatic vessels from the parathyroid glands drain into deep cervical lymph nodes and paratracheal lymph nodes. In the histological sense, they distinguish themselves from the thyroid gland, as they contain two types of cells:[3]
Name Staining Quantity Size many few Function Micrograph of a parathyroid gland. H&E stain.
parathyroid chief cells darker oxyphil cells lighter
smaller manufacture PTH (see below). larger function unknown. [4]
History
The parathyroid glands were first discovered in the Indian Rhinoceros by Richard Owen in 1850.[] The glands were first discovered in humans by Ivar Viktor Sandström (1852-1889), a Swedish medical student, in 1880 at Uppsala University.[] It is the last major organ to be recognized in humans so far.
Physiology
The major function of the parathyroid glands is to maintain the body's calcium level within a very narrow range, so that the nervous and muscular systems can function properly. Parathyroid hormone (PTH, also known as parathormone) is a small protein that takes part in the control of calcium and phosphate homeostasis, as well as bone physiology. Parathyroid hormone has effects antagonistic to those of calcitonin. Calcium PTH increases blood calcium levels by stimulating osteoclasts to break down bone and release calcium. PTH also increases gastrointestinal calcium absorption by activating vitamin D, and promotes calcium conservation (reabsorption) by the kidneys. Phosphate
Parathyroid gland PTH is the major regulator of serum phosphate concentrations via actions on the kidney. It is an inhibitor of proximal and also distal tubular reabsorption of phosphorus. Through activation of Vitamin D the absorption of Phosphate is increased.
205
Role in disease
Many conditions are associated with disorders of parathyroid function. These can be divided into those causing hyperparathyroidism, and those causing hypoparathyroidism.
Embryology and evolution
The parathyroid glands originate from the interaction of neural crest mesenchyme and third and fourth branchial pouch endoderm. Eya-1 (transcripitonal co-activator), Six-1 (a homeobox transcription factor), and Gcm-2 (a transcription factor) have been associated with the development of the parathyroid gland, and alterations in these genes alters parathyroid gland development. The superior parathyroids arise from the fourth pharyngeal pouch, and the inferior parathyroids arise from the third pharyngeal pouch. They are vertically transposed during embryogenesis. This is significant in function-preserving parathyroidectomy, because both the superior and the inferior parathyroids are supplied by the inferior thyroid artery. If the surgeon is to leave a single functional parathyroid for the patient, he/she must preserve the appropriate blood supply.
In other animals
Parathyroid glands are found in all adult tetrapods, although they vary in their number, and in their exact position. Mammals typically have four parathyroids, while other groups typically have six. Fish do not possess parathyroid glands, although the ultimobranchial glands, which are found close to the oesophagus, may have a similar function and could even be homologous with the tetrapod parathyroids. Even these glands are absent in the most primitive vertebrates, the jawless fish, but as these species have no bone in their skeletons, only cartilage, it may be that they have less need to regulate calcium metabolism. The conserved homology of genes and calcium-sensing receptors in fish gills with those in the parathryroid glands of birds and mammals is recognized by evolutionary developmental biology as evolution-using genes and gene networks in novel ways to generate new structures with some similar functions and novel functions.
Additional images
High magnification micrograph of a parathyroid gland. H&E stain.
Intermediate magnification micrograph of a parathyroid gland. H&E stain.
Low magnification micrograph of a parathyroid gland and parathyroid adenoma (bottom left). H&E stain.
Scheme showing development of branchial epithelial bodies. I, II, III, IV. Branchial pouches.
Parathyroid gland
206
Human parathyroid glands
References External links
• Endocrine Web at endocrineweb.com (http://www.endocrineweb.com/parathyroid.html) • The origin of the parathyroid gland at pnas.org (http://www.pnas.org/cgi/content/full/101/51/17716) • Parathyroid+gland (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=Parathyroid+ gland) at eMedicine Dictionary • Virtual Slidebox at Univ. Iowa Slide 149 (http://www.path.uiowa.edu/cgi-bin-pub/vs/fpx_gen. cgi?slide=149&viewer=java&view=0&lay=nlm)
Parathyroid chief cell
207
Parathyroid chief cell
Parathyroid chief cell
Micrograph of a parathyroid gland. H&E stain. Code TH H3.08.02.5.00002
[1]
Parathyroid chief cells (also called parathyroid principal cells or simply parathyroid cells) are cells in the parathyroid glands which produce parathyroid hormone. The end result of increased secretion by the chief cells of a parathyroid gland is an increase in the serum level of Calcium. Parathyroid chief cells constitute one of the few cell types of the body that regulate intracellular calcium levels as a consequence of extracellular (or serum) changes in calcium concentration. The calcium-sensing receptor (CaSR) is sensitive to an increase in serum calcium, and stimulates the uptake of calcium by the parathyroid chief cell. This mechanism is critically important, as it describes a physiological feed-back loop by which parathyroid hormone secretion is down-regulated in response to a restoration of serum calcium.
External links
• BU Histology Learning System: 15002loa [1]
Oxyphil cell (parathyroid)
208
Oxyphil cell (parathyroid)
Oxyphil cell (parathyroid)
Micrograph of a parathyroid gland. H&E stain. MeSH Code Oxyphil+Cells
[1] [1]
TH H3.08.02.5.00005
In the parathyroid gland, the parathyroid oxyphil cell is larger and paler than the parathyroid chief cell.[1] These cells can be found in clusters in the center of the section and at the periphery.[2][3][4][5] Oxyphil cells appear at the onset of puberty, but have no known function. With nuclear medicine scans, they selectively take up the Technetium-sestamibi complex radiotracer dye to allow delineation of glandular anatomy.[6] Oxyphil cells have been shown to express parathyroid-relevant genes found in the chief cells and have the potential to produce additional autocrine/paracrine factors, such as Parathyroid hormone-related protein (PTHrP) and calcitriol.[7] More work needs to be done to fully understand the functions of these cells and their secretions.
References
[2] [3] [4] [5] [6] Gartner, p. 208, Fig. 3 Ross, p. 628, Fig. 1 DiFiore, pp. 270 - 271 Wheater, pp. 312 - 313 "Minimally Invasive Radio-guided Surgery for Primary Hyperparathyroidism," Annals of Surgical Oncology 12/07 14(12) pp 3401-3402
Chromaffin cell
209
Chromaffin cell
Medullary chromaffin cell
Adrenal gland. (Medulla labeled at bottom right.) Latin Code endocrinocytus medullaris TH H3.08.02.6.00015
[1]
Chromaffin cells are neuroendocrine cells found mostly in the medulla of the adrenal glands (located above the kidneys) in mammals. They are in close proximity to pre-synaptic sympathetic ganglia of the sympathetic nervous system, with which they communicate, and structurally they are similar to post-synaptic sympathetic neurons. They release catecholamines: ~80% of Epinephrine (Adrenaline) and ~20% of Norepinephrine (Noradrenaline) into systemic circulation for systemic effects on multiple organs (similarly to secretory neurons of the hypothalamus), and can also send paracrine signals. Hence they are called neuroendocrine cells. In the mammalian fetal development (fourth to fifth week in humans), neuroblast cells migrate from the neural crest to form the sympathetic chain and preaortic ganglia. The cells migrate a second time to the adrenal medulla.[1] Chromaffin cells also settle near the sympathetic ganglia, vagus nerve, paraganglia, and carotid arteries. The largest extra-adrenal cluster of chromaffin cells in mammals is the organ of Zuckerkandl.[2] In lower concentrations, extra-adrenal chromaffin cells also reside in the bladder wall, prostate, and behind the liver. In non-mammals, chromaffin cells are found in a variety of places, generally not organized as an individual organ, and may be without innervation, relying only on endocrine or paracrine signals for secretion.[3][4]
Function
Chromaffin cells of the adrenal medulla are innervated by the splanchnic nerve and secrete adrenaline (epinephrine), noradrenaline (norepinephrine), a little dopamine, enkephalin and enkephalin-containing peptides, and a few other hormones into the blood stream. The secreted adrenaline and noradrenaline play an important role in the fight-or-flight response. The enkephalins and enkephalin-containing peptides are related to, but distinct from Epinephrine endogenous peptides named endorphins (which are secreted from the pituitary); all of these peptides bind to opioid receptors and produce analgesic (and other) responses. The hormones are secreted from chromaffin granules; this is where the enzyme dopamine
Chromaffin cell
210
β-hydroxylase catalyzes the conversion of dopamine to noradrenaline.[5] Distinct N and E cell forms exist (also Na and A cells in British nomenclature - noradrenaline and adrenaline); the former produce norepinephrine, the latter arise out of N cells through interaction with glucocorticoids, and convert norepinephrine into epinephrine.[6]
Nomenclature
Norepinephrine
The word 'Chromaffin' comes from a portmanteau of chromium and affinity. They are named as such because they can be visualized by staining with chromium salts. Chromium salts oxidize and polymerize catecholamines to form a brown color, most strongly in the cells secreting noradrenaline. Chromaffin cells are also called pheochromocytes. The enterochromaffin cells are so named because of their histological similarity to chromaffin cells (they also stain yellow when treated with chromium salts), but their function is quite different and they are not derivatives of the neural crest. Paraganglia are clusters of either chromaffin cells of glomus cells near sympathetic ganglia.
Pathology
Neoplasms arising from these cells are pheochromocytomas (also called chromaffin or sympathetic paragangliomas, in contrast to non-chromaffin or parasympathetic paragangliomas of glomus cells). Sometimes only neoplasms of adrenal origin are named pheochromocytomas, while others are named extra-adrenal paragangliomas.
References External links
• BU Histology Learning System: 14507loa (http://www.bu.edu/histology/p/14507loa.htm) - "Endocrine System: adrenal gland, reticularis and medulla" • Secretion Control in Adrenal Chromaffin Cells (http://www.mpibpc.gwdg.de/abteilungen/140/projects/ Chromaffin.html) • UC-San Diego Chromaffin Cell and Hypertension Research (http://hypertension.ucsd.edu) • A Primer on Chromaffin Cells (http://webpages.ull.es/users/isccb12/ChromaffinCell/Primer.html) • Rat Chromaffin cells primary cultures: Standardization and quality assessment for single-cell assays (a protocol) (http://www.natureprotocols.com/2006/09/29/rat_chromaffin_cells_primary_c.php)
Steroid hormone
211
Steroid hormone
A steroid hormone (abbreviated as sterone)[1] is a steroid that acts as a hormone. Steroid hormones can be grouped into five groups by the receptors to which they bind: glucocorticoids, mineralocorticoids, androgens, estrogens, and progestogens. Vitamin D derivatives are a sixth closely related hormone system with homologous receptors, though they are technically sterols rather than steroids. Steroid hormones help control metabolism, inflammation, immune functions, salt and water balance, development of sexual characteristics, and the ability to withstand illness and injury. The term steroid describes both hormones produced by the body and artificially produced medications that duplicate the action for the naturally occurring steroids.
Synthesis
The natural steroid hormones are generally synthesized from cholesterol in the gonads and adrenal glands. These forms of hormones are lipids. They can pass through the cell membrane[] as they are fat-soluble, and then bind to steroid hormone receptors which may be nuclear or cytosolic depending on the steroid hormone, to bring about changes within the cell. Steroid hormones are generally carried in the blood bound to specific carrier proteins such as sex hormone-binding globulin or corticosteroid-binding globulin. Further conversions and catabolism occurs in the liver, in other "peripheral" tissues, and in the target tissues.
Steroidogenesis with enzymes and intermediates
Synthetic steroids and sterols
A variety of synthetic steroids and sterols have also been contrived. Most are steroids, but some non-steroidal molecules can interact with the steroid receptors because of a similarity of shape. Some synthetic steroids are weaker, and some much stronger, than the natural steroids whose receptors they activate. Some examples of synthetic steroid hormones: • • • • • • Glucocorticoids: prednisone, dexamethasone, triamcinolone Mineralocorticoid: fludrocortisone Vitamin D: dihydrotachysterol Androgens: oxandrolone, testosterone, nandrolone (also known as anabolic steroids) Oestrogens: diethylstilbestrol (DES) Progestins: norethindrone, medroxyprogesterone acetate.
Steroid hormone
212
Effects
Steroids exert a wide variety of effects mediated by slow genomic as well as by rapid nongenomic mechanisms. They bind to nuclear receptors in the cell nucleus for genomic actions. Membrane-associated steroid receptors activate intracellular signaling cascades involved in nongenomic actions. Because steroids and sterols are lipid-soluble, they can diffuse fairly freely from the blood through the cell membrane and into the cytoplasm of target cells. In the cytoplasm, the steroid may or may not undergo an enzyme-mediated alteration such as reduction, hydroxylation, or aromatization. In the cytoplasm, the steroid binds to the specific receptor, a large metalloprotein. Upon steroid binding, many kinds of steroid receptor dimerize: Two receptor subunits join together to form one functional DNA-binding unit that can enter the cell nucleus. In some of the hormone systems known, the receptor is associated with a heat shock protein, which is released on the binding of the ligand, the hormone. Once in the nucleus, the steroid-receptor ligand complex binds to specific DNA sequences and induces transcription of its target genes.
References
[1] Definition @ Merriam-Webster online: -sterone (http:/ / mw1. m-w. com/ dictionary/ -sterone)
• Brook CG. Mechanism of puberty. Horm Res. 1999;51 Suppl 3:52–4. Review.PMID 10592444 • Holmes SJ, Shalet SM. Role of growth hormone and sex steroids in achieving and maintaining normal bone mass. Horm Res. 1996;45(1–2):86–93. Review. PMID 8742125 • Ottolenghi C, Uda M, Crisponi L, Omari S, Cao A, Forabosco A, Schlessinger D. Determination and stability of sex. Bioessays. 2007 Jan;29(1):15–25. Review. PMID 17187356 • Couse JF, Korach KS. Exploring the role of sex steroids through studies of receptor deficient mice. J Mol Med. 1998 Jun;76(7):497–511. Review. PMID 9660168 • McEwen BS. Steroid hormones: effect on brain development and function. Horm Res. 1992;37 Suppl 3:1–10. Review. PMID 1330863 • Simons SS Jr. What goes on behind closed doors: physiological versus pharmacological steroid hormone actions. Bioessays. 2008 Aug;30(8):744–56. PMID 18623071
External links
• An animated and narrated tutorial about nuclear receptor signaling (http://www.nursa.org/template. cfm?threadId=11320)
Mineralocorticoid
213
Mineralocorticoid
Mineralocorticoids are a class of steroid hormones characterized by their influence on salt and water balances. The primary mineralocorticoid is aldosterone.
Physiology
The name mineralocorticoid derives from early observations that these hormones were involved in the retention of sodium, a mineral. The primary endogenous mineralocorticoid is aldosterone, although a number of other endogenous hormones (including progesterone and deoxycorticosterone) have mineralocorticoid function. Aldosterone acts on the kidneys to provide active reabsorption of sodium and an associated passive reabsorption of water, as well as the active secretion of potassium in the principal cells of the cortical collecting tubule and active secretion of protons via proton ATPases in the lumenal membrane of the intercalated cells of the collecting tubule. This in turn results in an increase of blood pressure and blood volume. Aldosterone is produced in the cortex of the adrenal gland and its secretion is mediated principally by angiotensin II but also by adrenocorticotrophic hormone (ACTH) and local potassium levels.
Aldosterone
Deoxycorticosterone
Mode of action
The effects of mineralocorticoids are mediated by slow genomic mechanisms through nuclear receptors as well as by fast nongenomic mechanisms through membrane-associated receptors and signaling cascades.
Fludrocortisone
Mineralocorticoid
214
Genomic mechanisms
Mineralocorticoids bind to the cytosolic mineralocorticoid receptor. This type of receptor gets activated upon ligand binding. After a hormone binds to the corresponding receptor, the newly formed receptor-ligand complex translocates itself into the cell nucleus, where it binds to many hormone response elements (HREs) in the promoter region of the target genes in the DNA. The opposite mechanism is called transrepression. The hormone receptor without ligand binding interacts with heat shock proteins and prevents the transcription of targeted genes.
Steroidogenesis, showing mineralocorticoids in ellipse at top right. Note that it is not a
Aldosterone and cortisol (a strictly bounded group, but a continuum of structures with increasing mineralocorticoid effect, with the primary example aldosterone at top. glucosteroid) have similar affinity for the mineralocorticoid receptor; however, glucocorticoids circulate at roughly 100 times the level of mineralocorticoids. An enzyme exists in mineralocorticoid target tissues to prevent overstimulation by glucocorticoids. This enzyme, 11-beta hydroxysteroid dehydrogenase type II (Protein:HSD11B2), catalyzes the deactivation of glucocorticoids to 11-dehydro metabolites. Licorice is known to be an inhibitor of this enzyme and chronic consumption can result in a condition known as pseudohyperaldosteronism.
Pathophysiology
Hyperaldosteronism (the syndrome caused by elevated aldosterone) generally results from adrenal cancers. The two main resulting problems: 1. Hypertension and edema due to excessive Na+ and water retention. 2. Accelerated excretion of potassium ions (K+). With extreme K+ loss there is muscle weakness and eventually paralysis. Underproduction, or hypoaldosteronism, leads to the salt-wasting state associated with Addison's disease, although classical congenital adrenal hyperplasia and other disease states may also cause this situation.
Mineralocorticoid
215
Pharmacology
An example of a synthetic mineralocorticoid is fludrocortisone (Florinef). Important mineralocorticoid inhibitors are spironolactone and eplerenone.
References
• Stewart P (2008): "The Adrenal Cortex " In: Kronenberg, Melmed, Polonsky, Larsen (eds.) Williams Textbook of Endocrinology (11 ed)., Saunders Elsevier, Philadelphia, pp.445-504. • Bennett PN and Brown MJ (2008) “Adrenal corticosteroids, antagonists, corticotropin”, in Clinical Pharmacology (10ed), Churchill Livingstone Elsevier, Publ. pp. 593-607. • Hu X, Funder JW (2006) The evolution of mineralocorticoid receptors. Mol Endocrinol. 20(7):1471-8. • McKay L, Renoir JM, Weigel NL, Wilson EM, McDonnell DP, Cidlowski JA. (2006) International Union of Pharmacology. LXV. The pharmacology and classification of the nuclear receptor superfamily: glucocorticoid, mineralocorticoid, progesterone, and androgen receptors. Pharmacol Rev. Dec;58(4):782-97. • Pippal JB, Fuller PJ. (2008) Structure-function relationships in the mineralocorticoid receptor. J Mol Endocrinol. 41(6):405-13.
Glucocorticoid
Glucocorticoids (GC) are a class of steroid hormones that bind to the glucocorticoid receptor (GR), which is present in almost every vertebrate animal cell. The name glucocorticoid (pertaining to glucose + cortex ) derives from its role in the regulation of the metabolism of glucose, its synthesis in the adrenal cortex, and its steroidal structure (see structure to the right). GCs are part of the feedback mechanism in the immune system that turns immune activity (inflammation) down. They are therefore used in medicine to treat diseases caused by an overactive immune system, such Chemical structure of cortisol, a glucocorticoid as allergies, asthma, autoimmune diseases and sepsis. GCs have many diverse (pleiotropic) effects, including potentially harmful side effects, and as a result are rarely sold over the counter.[] They also interfere with some of the abnormal mechanisms in cancer cells, so they are used in high doses to treat cancer. This includes mainly inhibitory effects on lymphocyte proliferation (treatment of lymphomas and leukaemias) and mitigation of side effects of anticancer drugs. GCs cause their effects by binding to the glucocorticoid receptor (GR). The activated GR complex, in turn, up-regulates the expression of anti-inflammatory proteins in the nucleus (a process known as
Glucocorticoid
216
transactivation) and represses the expression of proinflammatory proteins in the cytosol by preventing the translocation of other transcription factors from the cytosol into the nucleus (transrepression).[] Glucocorticoids are distinguished from mineralocorticoids and sex steroids by their specific receptors, target cells, and effects. In technical terms, "corticosteroid" refers to both glucocorticoids and mineralocorticoids (as both are mimics of hormones produced by the adrenal cortex), but is often used as a synonym for "glucocorticoid". Cortisol (or hydrocortisone) is the most important Dexamethasone binds more powerfully to the glucocorticoid receptor human glucocorticoid. It is essential for life, and it than cortisol does. Dexamethasone is based on the cortisol structure regulates or supports a variety of important but differs in three positions (extra double bond in the A-ring cardiovascular, metabolic, immunologic, and between carbons 1 and 2 and addition of a 9-α-fluoro group and a 16-α-methyl substituent). homeostatic functions. Various synthetic glucocorticoids are available; these are used either as replacement therapy in glucocorticoid deficiency or to suppress the immune system.
Effects
Glucocorticoid effects may be broadly classified into two major categories: immunological and metabolic. In addition, glucocorticoids play important roles in fetal development and body fluid homeostasis.
Immune
As discussed in more detail below, glucocorticoids function through interaction with the glucocorticoid receptor: • up-regulate the expression of anti-inflammatory proteins. • down-regulate the expression of proinflammatory proteins. Glucocorticoids are also shown to play Steroidogenesis showing glucocorticoids in green ellipse at right - it is not a strictly a role in the development and bounded group, but a continuum of structures with increasing glucocorticoid effect, with homeostasis of T lymphocytes. This the primary example being cortisol. has been shown in transgenic mice with either increased or decreased sensitivity of T cell lineage to glucocorticoids.[]
Metabolic
Glucocorticoid The name "glucocorticoid" derives from early observations that these hormones were involved in glucose metabolism. In the fasted state, cortisol stimulates several processes that collectively serve to increase and maintain normal concentrations of glucose in blood. Metabolic effects: • Stimulation of gluconeogenesis, in particular, in the liver: This pathway results in the synthesis of glucose from nonhexose substrates, such as amino acids and glycerol from triglyceride breakdown, and is particularly important in carnivores and certain herbivores. Enhancing the expression of enzymes involved in gluconeogenesis is probably the best-known metabolic function of glucocorticoids. • Mobilization of amino acids from extrahepatic tissues: These serve as substrates for gluconeogenesis. • Inhibition of glucose uptake in muscle and adipose tissue: A mechanism to conserve glucose • Stimulation of fat breakdown in adipose tissue: The fatty acids released by lipolysis are used for production of energy in tissues like muscle, and the released glycerol provide another substrate for gluconeogenesis. Excessive glucocorticoid levels resulting from administration as a drug or hyperadrenocorticism have effects on many systems. Some examples include inhibition of bone formation, suppression of calcium absorption (both of which can lead to osteoporosis), delayed wound healing, muscle weakness, and increased risk of infection. These observations suggest a multitude of less-dramatic physiologic roles for glucocorticoids.[]
217
Developmental
Glucocorticoids have multiple effects on fetal development. An important example is their role in promoting maturation of the lung and production of the surfactant necessary for extrauterine lung function. Mice with homozygous disruptions in the corticotropin-releasing hormone gene (see below) die at birth due to pulmonary immaturity. In addition, glucocorticoids are necessary for normal brain development, by initiating terminal maturation, remodeling axons and dendrites, and affecting cell survival.[]
Arousal and cognition
Glucocorticoids act on the hippocampus, amygdala, and frontal lobes. Along with adrenaline, these enhance the formation of flashbulb memories of events associated with strong emotions, both positive and negative.[1] This has been confirmed in studies, whereby blockade of either glucocorticoids or noradrenaline activity impaired the recall of emotionally relevant information. Additional sources have shown subjects whose fear learning was accompanied by high cortisol levels had better consolidation of this memory (this effect was more important in men). Glucocorticoids have also been shown to have a significant impact on vigilance and cognitive performance. This A graphical representation of the Yerkes-Dodson curve appears to follow the Yerkes-Dodson curve, as studies have shown circulating levels of glucocorticoids vs. memory performance follow an upside-down U pattern, much like the Yerkes-Dodson curve. For example, long-term potentiation (the process of forming long-term memories) is optimal when glucocorticoid levels are mildly elevated, whereas significant decreases of LTP are observed after adrenalectomy (low-GC state) or after exogenous glucocorticoid administration (high-GC state). Elevated levels of glucocorticoids enhance memory for emotionally arousing events, but lead more often than not to poor memory for material unrelated to the source of stress/emotional arousal.[2] In contrast to the dose-dependent enhancing effects of glucocorticoids on memory consolidation, these stress hormones have been shown to inhibit the retrieval of already stored information.[3][4]
Glucocorticoid
218
Body fluid homeostasis
Glucocorticoids could act centrally, as well as peripherally, to assist in the normalization of extracellular fluid volume by regulating body’s action to atrial natriuretic peptide (ANP). Centrally, glucocorticoids could inhibit dehydration induced water intake;[] peripherally, glucocorticoids could induce a potent diuresis.[] The overall effect of glucocorticoids is to keep the body from volume overload.
Mechanism of action
Transactivation
Glucocorticoids bind to the cytosolic glucocorticoid receptor (GR). This type of receptor is activated by ligand binding. After a hormone binds to the corresponding receptor, the newly formed receptor-ligand complex translocates itself into the cell nucleus, where it binds to glucocorticoid response elements (GRE) in the promoter region of the target genes resulting in the regulation of gene expression. This process is commonly referred to as transactivation.[] The proteins encoded by these up-regulated genes have a wide range of effects, including, for example:[] • anti-inflammatory – lipocortin I, p11/calpactin binding protein and secretory leukoprotease inhibitor 1 (SLPI) • increased gluconeogenesis – glucose-6-phosphatase and tyrosine aminotransferase
Transrepression
The opposite mechanism is called transrepression. The activated hormone receptor interacts with specific transcription factors (such as AP-1 and NF-κB) and prevents the transcription of targeted genes. Glucocorticoids are able to prevent the transcription of proinflammatory genes, including interleukins IL-1B, IL-4, IL-5, and IL-8, chemokines, cytokines, GM-CSF, and TNFA genes.[]
Dissociation
The ordinary glucocorticoids do not distinguish among transactivation and transrepression and influence both the "wanted" immune and the "unwanted" genes regulating the metabolic and cardiovascular functions. Intensive research is aimed at discovering selectively acting glucocorticoids that will be able to repress only the immune system.[][] Genetically modified mice that express a modified GR incapable of DNA binding are still responsive to the anti-inflammatory effects of glucocorticoids, while the stimulation of gluconeogenesis by glucocorticoids is blocked.[] This result strongly suggests most of the desirable anti-inflammatory effects are due to transrepression, while the undesirable metabolic effects arise from transactivation, a hypothesis also underlying the development of selective glucocorticoid receptor agonists.
Nongenomic
Glucocorticoids have been shown to exert a number of rapid actions that are independent of the regulations of gene transcription. Binding of corticosteroids to the glucocorticoid receptor (GR) stimulates phosphatidylinositol 3-kinase and protein kinase AKT, leading to endothelial nitric oxide synthase (eNOS) activation and nitric oxide-dependent vasorelaxation.[] Membrane associated GR has been shown to mediate lymphocytolysis.[][][] In addition, some glucocorticoids have been shown to rapidly inhibit the release of the inflammatory prostaglandin PGE2, this effect is blocked by the glucocorticoid receptor antagonist mifepristone (RU-486) and is not affected by protein synthesis inhibitors. These data together suggest a nongenomic mechanism of action.[][]
Glucocorticoid
219
Glucocorticoid-induced neutrophilia
Acute or chronic administration of corticosteroids causes neutrophilia,[5] suggesting the enhanced release of PMNs from the bone marrow is an important mechanism of the glucocorticoid-induced granulocytosis. An alternative mechanism for the granulocytosis induced by glucocorticoids is an influx of PMNs from the intravascular marginated PMN pools.[6] The response is caused by a shift of cells from the marginal to the circulating pool; hence, it frequently is referred to as demargination.[7] Some of the immunosuppressive effects of glucocorticoids are mediated by nongenomic signalling involving the glucocortiocid receptor (GR). A multiprotein complex composed of the unliganded glucocorticoid receptor, Hsp90, and the tyrosine kinases LCK and FYN is recruited to the antigen-activated T cell receptor (TCR) in T cells. This GR complex is necessary for TCR signalling. On binding of glucocorticoids to GR, this complex dissociates, thus blocking TCR signalling.[]
Glucocorticoid-induced diuresis
Glucocorticoids could mediate the gene expression of ANP and its primary receptor, natriuretic peptide receptor A (NPR-A). It is well documented that glucocorticoids could up-regulate the expression of ANP gene in the cardiomyocytes in vitro and stimulated ANP release in vivo without negative effects on renal sodium and water excretion.[8][9] Additionally, glucocorticoids could up-regulate NPR-A expression in the kidney and hypothalamus. In the kidney, glucocorticoids improve renal responsiveness to ANP by upregulating NPR-A expression in the renal inner medullary collecting duct, inducing a potent diuresis.[] In hypothalamus, glucocorticoids inhibited dehydration or angiotensin II induced water intake by potentiating hypothalamic response to ANP.[] They work in concert to keep the body fluid volume in homeostasis.
Pharmacology
A variety of synthetic glucocorticoids, some far more potent than cortisol, have been created for therapeutic use. They differ in both pharmacokinetics (absorption factor, half-life, volume of distribution, clearance) and pharmacodynamics (for example the capacity of mineralocorticoid activity: retention of sodium (Na+) and water; renal physiology). Because they permeate the intestines easily, they are administered primarily per os (by mouth), but also by other methods, such as topically on skin. More than 90% of them bind different plasma proteins, though with a different binding specificity. Endogenous glucocorticoids and some synthetic corticoids have high affinity to the protein transcortin (also called corticosteroid-binding globulin), whereas all of them bind albumin. In the liver, they quickly metabolize by conjugation with a sulfate or glucuronic acid, and are secreted in the urine. Glucocorticoid potency, duration of effect, and overlapping mineralocorticoid potency varies. Cortisol (hydrocortisone) is the standard of comparison for glucocorticoid potency. Hydrocortisone is the name used for pharmaceutical preparations of cortisol. Data refer to oral dosing, except when mentioned. Oral potency may be less than parenteral potency because significant amounts (up to 50% in some cases) may not be absorbed from the intestine. Fludrocortisone, DOCA (Deoxycorticosterone acetate), and aldosterone are, by definition, not considered glucocorticoids, although they may have minor glucocorticoid potency, and are included in this table to provide perspective on mineralocorticoid potency.
Glucocorticoid
220
Comparative steroid potencies
Name Glucocorticoid potency Mineralocorticoid potency 1 0.8 0.8 0.8 0.5 0 0 0 Duration of action (t1/2 in hours) 8 oral 8, intramuscular 18+ 16-36 16-36 18-40 36-54 36-54 12-36 -
Hydrocortisone (cortisol) Cortisone Prednisone Prednisolone Methylprednisolone Dexamethasone Betamethasone Triamcinolone Beclometasone
1 0.8 3.5-5 4 5-7.5 25-80 25-30 5 8 puffs 4 times a day equals 14 mg oral prednisone once a dayWikipedia:Please clarify 15 0
Fludrocortisone acetate Deoxycorticosterone acetate (DOCA) Aldosterone
200 20
24 -
0.3
200-1000
-
Therapeutic use
Glucocorticoids may be used in low doses in adrenal insufficiency. In much higher doses, oral or inhaled glucocorticoids are used to suppress various allergic, inflammatory, and autoimmune disorders. Inhaled glucocorticoids are the second-line treatment for asthma. They are also administered as post-transplantory immunosuppressants to prevent the acute transplant rejection and the graft-versus-host disease. Nevertheless, they do not prevent an infection and also inhibit later reparative processes. Newly emerging evidence showed that glucocorticoids could be used in the treatment of heart failure to increase the renal responsiveness to diuretics and natriuretic peptides.
Physiological replacement
Any glucocorticoid can be given in a dose that provides approximately the same glucocorticoid effects as normal cortisol production; this is referred to as physiologic, replacement, or maintenance dosing. This is approximately 6–12 mg/m²/day (m² refers to body surface area (BSA), and is a measure of body size; an average man's BSA is 1.7 m²).
Therapeutic immunosuppression
Glucocorticoids cause immunosuppression, and the therapeutic component of this effect is mainly the decreases in the function and numbers of lymphocytes, including both B cells and T cells. The major mechanism for this immunosuppression through inhibition of nuclear factor kappa-light-chain-enhancer of activated B cells(NF-κB). NF-κB is a critical transcription factor involved in the synthesis of many mediators (i.e., cytokines) and proteins (i.e., adhesion proteins) that promote the immune response. Inhibition of this transcription factor, therefore, blunts the capacity of the immune system to mount a response.[]
Glucocorticoid Glucocorticoids suppress cell-mediated immunity by inhibiting genes that code for the cytokines IL-1, IL-2, IL-3, IL-4, IL-5, IL-6, IL-8 and IFN-γ, the most important of which is IL-2. Smaller cytokine production reduces the T cell proliferation.[] Glucocorticoids, however, not only reduce T cell proliferation, but also lead to another well known effect glucocorticoid-induced apoptosis. The effect is more prominent in immature T cells still inside in the thymus, but peripheral T cells are also affected. The exact mechanism underlying this glucocorticoid sensitivity still remains to be elucidated.[citation needed] Glucocorticoids also suppress the humoral immunity, thereby causing a humoral immune deficiency. Glucocorticoids cause B cells to express smaller amounts of IL-2 and of IL-2 receptors. This diminishes both B cell clone expansion and antibody synthesis. The diminished amounts of IL-2 also cause fewer T lymphocyte cells to be activated. Since glucocorticoid is a steroid, it regulates transcription factors; another factor it down-regulates is the expression of Fc receptors on macrophages, so there is a decreased phagocytosis of opsonised cells.[citation needed]
221
Anti-inflammatory
Glucocorticoids are potent anti-inflammatories, regardless of the inflammation's cause; their primary anti-inflammatory mechanism is lipocortin-1 (annexin-1) synthesis. Lipocortin-1 both suppresses phospholipase A2, thereby blocking eicosanoid production, and inhibits various leukocyte inflammatory events (epithelial adhesion, emigration, chemotaxis, phagocytosis, respiratory burst, etc.). In other words, glucocorticoids not only suppress immune response, but also inhibit the two main products of inflammation, prostaglandins and leukotrienes. They inhibit prostaglandin synthesis at the level of phospholipase A2 as well as at the level of cyclooxygenase/PGE isomerase (COX-1 and COX-2),[10] the latter effect being much like that of NSAIDs, potentiating the anti-inflammatory effect. In addition, glucocorticoids also suppress cyclooxygenase expression. Glucocorticoids marketed as anti-inflammatories are often topical formulations, such as nasal sprays for rhinitis or inhalers for asthma. These preparations have the advantage of only affecting the targeted area, thereby reducing side effects or potential interactions. In this case, the main compounds used are beclometasone, budesonide, fluticasone, mometasone and ciclesonide. In rhinitis, sprays are used. For asthma, glucocorticoids are administered as inhalants with a metered-dose or dry powder inhaler.[]
Hyperaldosteronism
Glucocorticoids can be used in the management of familial hyperaldosteronism type 1. They are not effective, however, for use in the type 2 condition.
Resistance
Resistance to the therapeutic uses of glucocorticoids can present difficulty; for instance, 25% of cases of severe asthma may be unresponsive to steroids. This may be the result of genetic predisposition, ongoing exposure to the cause of the inflammation (such as allergens), immunological phenomena that bypass glucocorticoids, and pharmacokinetic disturbances (incomplete absorption or accelerated excretion or metabolism).[]
Glucocorticoid
222
Heart failure
Glucocorticoids could be used in the treatment of decompensated heart failure to potentiate renal responsiveness to diuretics, especially in heart failure patients with refractory diuretic resistance with large dose of loop diuretics.[11][12][13][14][15][16][17]
Side effects
Glucocorticoid drugs currently being used act nonselectively, so in the long run they may impair many healthy anabolic processes. To prevent this, much research has been focused recently on the elaboration of selectively acting glucocorticoid drugs. Side effects include: • immunodeficiency (see separate section below) • hyperglycemia due to increased gluconeogenesis, insulin resistance, and impaired glucose tolerance ("steroid diabetes"); caution in those with diabetes mellitus • increased skin fragility, easy bruising • negative calcium balance due to reduced intestinal calcium absorption[18] • steroid-induced osteoporosis: reduced bone density (osteoporosis, osteonecrosis, higher fracture risk, slower fracture repair) • • • • • • • • • • weight gain due to increased visceral and truncal fat deposition (central obesity) and appetite stimulation adrenal insufficiency (if used for long time and stopped suddenly without a taper) muscle breakdown (proteolysis), weakness, reduced muscle mass and repair expansion of malar fat pads and dilation of small blood vessels in skin anovulation, irregularity of menstrual periods growth failure, delayed puberty increased plasma amino acids, increased urea formation, negative nitrogen balance excitatory effect on central nervous system (euphoria, psychosis) glaucoma due to increased cranial pressure cataracts
In high doses, hydrocortisone (cortisol) and those glucocorticoids with appreciable mineralocorticoid potency can exert a mineralocorticoid effect as well, although in physiologic doses this is prevented by rapid degradation of cortisol by 11β-hydroxysteroid dehydrogenase isoenzyme 2 (11β-HSD2) in mineralocorticoid target tissues. Mineralocorticoid effects can include salt and water retention, extracellular fluid volume expansion, hypertension, potassium depletion, and metabolic alkalosis. The combination of clinical problems produced by prolonged, excess glucocorticoids, whether synthetic or endogenous, is termed Cushing's syndrome.
Glucocorticoid
223
Immunodeficiency
Glucocorticoids cause immunosuppression, decreasing the function and/or numbers of neutrophils, lymphocytes (including both B cells and T cells), monocytes, macrophages, and the anatomical barrier function of the skin.[] This suppression, if large enough, can cause manifestations of immunodeficiency, including T cell deficiency, humoral immune deficiency and neutropenia.
Main pathogens of concern in glucocorticoid-induced immunodeficiency:[]
Bacteria • • • • • • • • • • Fungi • • • • • • • • • • Enterobacteriaceae Legionella micdadei Listeria monocytogenes Mycobacterium tuberculosis Nontuberculous mycobacteria Nocardia asteroides Rhodococcus equi Salmonella species Staphylococcus aureus Streptococci Aspergillus Blastomyces Candida albicans and nonalbicans species Coccidioides immitis Cryptococcus neoformans Fusarium species Histoplasma capsulatum Penicillium marneffei Pseudallescheria boydii Zygomycosis Adenovirus Cytomegalovirus Herpes simplex virus Human papillomavirus Influenza/parainfluenza Respiratory syncytial virus Varicella zoster Cryptosporidiosis/lsospora belli Pneumocystis carinii Strongyloides stercoralis Toxoplasma gondii
Viruses • • • • • • • Other • • • •
Withdrawal
In addition to the effects listed above, use of high-dose steroids for more than a week begins to produce suppression of the patient's adrenal glands because the exogenous glucocorticoids suppress hypothalamic corticotropin-releasing hormone and pituitary adrenocorticotropic hormone. With prolonged suppression, the adrenal glands atrophy (physically shrink), and can take months to recover full function after discontinuation of the exogenous glucocorticoid. During this recovery time, the patient is vulnerable to adrenal insufficiency during times of stress, such as illness. While suppressive dose and time for adrenal recovery vary widely, clinical guidelines have been devised to estimate potential adrenal suppression and recovery, to reduce risk to the patient. The following is one example, but many variations exist or may be appropriate in individual circumstances.[citation needed]
Glucocorticoid • If patients have been receiving daily high doses for five days or less, they can be abruptly stopped (or reduced to physiologic replacement if patients are adrenal-deficient). Full adrenal recovery can be assumed to occur by a week afterward. • If high doses were used for six to 10 days, reduce to replacement dose immediately and taper over four more days. Adrenal recovery can be assumed to occur within two to four weeks of completion of steroids. • If high doses were used for 11–30 days, cut immediately to twice replacement, and then by 25% every four days. Stop entirely when dose is less than half of replacement. Full adrenal recovery should occur within one to three months of completion of withdrawal. • If high doses were used more than 30 days, cut dose immediately to twice replacement, and reduce by 25% each week until replacement is reached. Then change to oral hydrocortisone or cortisone as a single morning dose, and gradually decrease by 2.5 mg each week. When the morning dose is less than replacement, the return of normal basal adrenal function may be documented by checking 0800 cortisol levels prior to the morning dose; stop drugs when 0800 cortisol is 10 μg/dl. Predicting the time to full adrenal recovery after prolonged suppressive exogenous steroids is difficult; some people may take nearly a year. • Flare-up of the underlying condition for which steroids are given may require a more gradual taper than outlined above.
224
Chemical synthesis
Hogg, J. A.; Beal, P. F.; Nathan, A. H.; Lincoln, F. H.; Schneider, W. P.; Magerlein, B. J.; Hanze, A. R.; Jackson, R. W. (1955). Journal of the American Chemical Society 77 (16): 4436. doi:10.1021/ja01621a092 [19].
Glucocorticoid
225
References
[3] de Quervain, D et al., Stress and glucocorticoids impair retrieval of long-term spatial memory. Nature, 394, 787-790 (1998) [4] de Quervain, D et al., Acute cortisone administration impairs retrieval of long-term declarative memory in humans. Nature Neuroscience, 3, 313-314 (2000) [5] http:/ / emedicine. medscape. com/ article/ 208576-overview#showall [6] http:/ / circ. ahajournals. org/ content/ 98/ 21/ 2307. full. pdf+ html [7] Williams Hematology, 8ed, Ch.65, Neutropenia and Neutrophylia
External links
• Glucocorticoids (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Glucocorticoids) at the US National Library of Medicine Medical Subject Headings (MeSH) • R. Bowen (2006-05-26). "Glucocorticoids" (http://www.vivo.colostate.edu/hbooks/pathphys/endocrine/ adrenal/gluco.html). Colorado State University. Retrieved 2008-05-11.
Leydig cell
226
Leydig cell
Leydig cell
Micrograph showing a cluster of Leydig cells (center of image). H&E stain.
Histological section through testicular parenchyma of a boar. 1 Lumen of convoluted part of the seminiferous tubules, 2 spermatids, 3 spermatocytes, 4 spermatogonia, 5 Sertoli cell, 6 myofibroblasts, 7 Leydig cells, 8 capillaries Gray's MeSH subject #258 1243 Leydig+cells
[2] [1]
Leydig cells, also known as interstitial cells of Leydig, are found adjacent to the seminiferous tubules in the testicle. They produce testosterone in the presence of luteinizing hormone (LH). Leydig cells are polyhedral in shape, display a large prominent nucleus, an eosinophilic cytoplasm and numerous lipid-filled vesicles.
Nomenclature
Leydig cells are named after the German anatomist Franz Leydig, who discovered them in 1850.[1]
Functions
Leydig cells release a class of hormones called androgens (19-carbon steroids). They secrete testosterone, androstenedione and dehydroepiandrosterone (DHEA), when stimulated by the pituitary hormone luteinizing hormone (LH). LH increases cholesterol desmolase activity (an enzyme associated with the conversion of cholesterol to pregnenolone), leading to testosterone synthesis and secretion by Leydig cells. Prolactin (PRL) increases the response of Leydig cells to LH by increasing the number of LH receptors expressed on Leydig cells.
Leydig cell
227
Ultrastructure
The mammalian Leydig cell is a polyhedral epithelioid cell with a single eccentrically located ovoid nucleus. The nucleus contains one to three prominent nucleoli and large amounts of dark-staining peripheral heterochromatin. The acidophilic cytoplasm usually contains numerous membrane-bound lipid droplets and large amounts of smooth endoplasmic reticulum (SER). Besides the obvious abundance of SER with scattered patches of rough endoplasmic reticulum, several mitochondria are also prominent within the cytoplasm. Frequently, lipofuscin pigment and rod-shaped crystal-like structures 3 to 20 micrometres in diameter (Reinke's crystals) are found. These inclusions have no known function.[][2] No other interstitial cell within the testes has a nucleus or cytoplasm with these characteristics, making identification relatively easy.
Development
'Adult'-type Leydig cells differentiate in the post-natal testis and are quiescent until puberty. They are preceded in the testis by a population of 'fetal'-type Leydig cells from the 8th to the 20th week of gestation, which produce enough testosterone for masculinisation of a male fetus.[]
Pathology
Leydig cells may grow uncontrollably and form a Leydig cell tumour. These tumours are usually benign. They may be hormonally active, i.e. secrete testosterone. Adrenomyeloneuropathy is another example of a disease affecting the Leydig cell: the patient's testosterone may fall despite higher-than-normal levels of LH and FSH. Electrostimulation therapy has been found to induce destruction of Leydig cells.[]
Micrograph of a Leydig cell tumour. H&E stain.
Additional images
Section of a genital cord of the testis of a human embryo 3.5 cm. long.
Intermediate magnification micrograph of a Leydig cell tumour. H&E stain.
High magnification micrograph of a Leydig cell tumour. H&E stain.
Cross-section of seminiferous tubules. Arrows indicate location of Leydig cells.
Leydig cell
228
References External links
• BU Histology Learning System: 16907loa (http://www.bu.edu/histology/p/16907loa.htm) • Reproductive Physiology (http://www2.ufp.pt/~pedros/qfisio/reproduction.htm) • Diagram at umassmed.edu (http://www.umassmed.edu/faculty/graphics/700/Leefig1.jpg)
Folliculogenesis
Note: Although the process is similar in many animals, this article will deal exclusively with human folliculogenesis. In biology, folliculogenesis is the maturation of the ovarian follicle, a densely-packed shell of somatic cells that contains an immature oocyte. Folliculogenesis describes the progression of a number of small primordial follicles into large preovulatory follicles that enter the menstrual cycle. Contrary to male spermatogenesis, which can last indefinitely, folliculogenesis ends when the remaining follicles in the ovaries are incapable of responding to the hormonal cues that previously recruited some follicles to mature. This depletion in follicle supply signals the beginning of menopause.
Overview
The primary role of the follicle is oocyte support. From birth, the ovaries of the human female contain a number of immature, primordial follicles. These follicles each contain a similarly immature primary oocyte. After puberty and commencing with the first menstruation, a clutch of follicles begins folliculogenesis, entering a growth pattern that will end in death or in ovulation (the process where the oocyte leaves the follicle). During post-pubescent follicular development, and over the course of roughly a year, primordial follicles that have begun development undergo a series of critical changes in character, both histologically and hormonally. Two-thirds of the way through this process, the follicles have transitioned to tertiary, or antral, follicles. At this stage in development, they become dependent on hormones emanating from the host body, causing a substantial increase in their growth rate. With a little more than ten days until the end of the period of follicular development, most of the original group of follicles have died (a process known as atresia). The remaining cohort of follicles enter the menstrual cycle,
Order of changes in ovary. 1 - Menstruation 2 - Developing follicle 3 - Mature follicle 4 - Ovulation 5 - Corpus luteum 6 - Deterioration of corpus luteum
Folliculogenesis competing with each other until only one follicle is left. This remaining follicle, the late tertiary or pre-ovulatory follicle, ruptures and discharges the oocyte (that has since grown into a secondary oocyte), ending folliculogenesis.
229
Diagram of folliculogenesis, starting from pre-antral (late secondary), courtesy NCBI
Phases of development
Folliculogenesis lasts for approximately 375 days. It coincides with thirteen menstrual cycles. The process begins continuously, meaning that at any time the ovary contains follicles in all stages of development, and ends when a mature oocyte departs from the preovulatory follicle in a process called ovulation. The growing follicle passes through the following distinct stages that are defined by certain structural characteristics (unfamiliar terms will be defined in their respective sections): In a larger perspective, the whole folliculogenesis, from primordial to preovulatory follicle, belongs to the stage of ootidogenesis of oogenesis.
Stage Primordial Description Dormant, small, only one layer of flat granulosa cells Mitotic cells, cuboidal granulosa cells Presence of theca cells, multiple layers of granulosa cells Size Primordial follicles are about 0.03-0.05 mm in diameter.
Primary Secondary
Almost 0.1 mm in diameter The follicle is now 0.2 mm in diameter
Early tertiary
The early tertiary follicle is arbitrarily divided into five classes. Class 1 follicles are 0.2 mm in diameter, class 2 about 0.4 mm, class 3 about 0.9 mm, class 4 about 2 mm, and class 5 about 5 mm. Fully formed antrum, no further cytodifferentiation, no novel progress Class 6 follicles are about 10 mm in diameter, class 7 about 16 mm, and class 8 about 20 mm. It is common for non-dominant follicles to grow beyond class 5, but rarely is there more than one class 8 follicle.
Late tertiary
Preovulatory Building growth in estrogen concentration, all other follicles atretic or dead
In addition, follicles that have formed an antrum are called antral follicles or Graafian follicles. Definitions differ in where this shift occurs in the staging given above, with some stating that it occurs when entering the secondary stage,[1] and others stating that it occurs when entering the tertiary stage.[2] Until the preovulatory stage, the follicle contains a primary oocyte that is arrested in prophase of meiosis I. During the late preovulatory stage, the oocyte continues meiosis and becomes a secondary oocyte, arrested in metaphase II.
Folliculogenesis
230
Primordial
At 18–22 weeks post-conception, the cortex of the female ovary contains its peak number of follicles (about 300,000 in the average case, but individual peak populations range from 35,000 to 2.5 million[3]). These primordial follicles contain immature oocytes surrounded by flat, squamous granulosa cells (the support cells) that are segregated from the oocyte's environment by the basal lamina. They are quiescent, showing little to no biological activity. Because primordial follicles can be dormant for up to 50 years in the human, the length of the ovarian cycle does not include this time. The supply of follicles decreases slightly before birth, and to 180,000 by puberty for the average case (populations at puberty range from 25,000 to 1.5 million).[3] By virtue of the "inefficient" nature of folliculogenesis (discussed later), only 400 of these follicles will ever reach the preovulatory stage. At menopause, only 1,000 follicles remain. It seems likely that early menopause occurs for women with low populations at birth, and late menopause occurs for women with high populations at birth, but there is as yet no clinical evidence for this.[3] The process by which primordial cells wake up is known as initial recruitment. Research has shown that initial recruitment is mediated by the counterbalance of various stimulatory and inhibitory hormones and locally produced growth factors.[4]
Primary
The granulosa cells of these primordial follicles change from a flat to a cuboidal structure, marking the beginning of the primary follicle. The oocyte genome is activated and genes become transcribed. Rudimentary paracrine signalling pathways that are vital for communication between the follicle and oocyte are formed. Both the oocyte and the follicle grow dramatically, increasing to almost 0.1 mm in diameter. Primary follicles develop receptors to follicle stimulating hormone (FSH) at this time, but they are gonadotropin-independent until the antral stage. Research has shown, however, that the presence of FSH accelerates follicle growth in vitro. A glycoprotein polymer capsule called the zona pellucida forms around the oocyte, separating it from the surrounding granulosa cells. The zona pellucida, which remains with the oocyte after ovulation, contains enzymes that catalyze with sperm to allow penetration.
Secondary
Stroma-like theca cells are recruited by oocyte-secreted signals. They surround the follicle's outermost layer, the basal lamina, and undergo cytodifferentiation to become the theca externa and theca interna. An intricate network of capillary vessels forms between these two thecal layers and begins to circulate blood to and from the follicle. The late-term secondary follicle is marked histologically by a fully grown oocyte surrounded by a zona pellucida, approximately nine layers of granulosa cells, a basal lamina, a theca interna, a capillary net, and a theca externa. 290 days have lapsed since recruitment.
Folliculogenesis
231
Antrum formation
The formation of a fluid-filled cavity adjacent to the oocyte called the antrum designates the follicle as an antral follicle, in contrast to so a called preantral follicle that still lacks an antrum. An antral follicle is also called a Graafian follicle. Definitions differ in which stage this shift occurs, with some designating follicles in the secondary stage as antral,[1] and others designating them as preantral.[2]
Early tertiary
In the tertiary follicle, the basic structure of the mature follicle has formed and no novel cells are detectable. Granulosa and theca cells continue to undergo mitotis concomitant with an increase in antrum volume. Tertiary follicles can attain a tremendous size that is hampered only by the availability of FSH, which it is now dependent on. Under action of an oocyte-secreted morphogenic gradient, the granulosa cells of the tertiary follicle undergo differentiation into four distinct subtypes: corona radiata, surrounding the zona pellucida; membrana, interior to the basal lamina; periantral, adjacent to the antrum and cumulus oophorous, which connects the membrana and corona radiata granulosa cells together. Each type of cell behaves differently in response to FSH. Theca cells express receptors for luteinizing hormone (LH). LH induces the production of androgens by the theca cells, most notably androstendione, which are aromatized by granulosa cells to produce estrogens, primarily estradiol. Consequently, estrogen levels begin to rise.
Late tertiary and preovulatory (the follicular phase of the menstrual cycle)
At this point, the majority of the group of follicles that started growth 360 days ago have already died. This process of follicle death is known as atresia, and it is characterized by radical apoptosis of all constituent cells and the oocyte. Although it is not known what causes atresia, the presence of high concentrations of FSH has been shown to prevent it. A rise in pituitary FSH caused by the disintegration of the corpus luteum at the conclusion of the twelfth menstrual cycle precipitates the selection of five to seven class 5 follicles to participate in the thirteenth. These follicles enter the end of the twelfth menstrual cycle and transition into the follicular phase of the thirteenth cycle. The selected follicles, called antral follicles, compete with each other for growth-inducing FSH. In response to the rise of FSH, the antral follicles begin to secrete estrogen and inhibin, which have a negative feedback effect on FSH.[5] Follicles that have fewer FSH-receptors will not be able to develop further; they will show retardation of their growth rate and become atretic. Eventually, only one follicle will be viable. This remaining follicle, called the dominant follicle, will grow quickly and dramatically—up to 20 mm in diameter—to become the preovulatory follicle. Note: Many sources misrepresent the pace of follicle growth, some even suggesting that it takes only fourteen days for a primordial follicle to become preovulatory. In all cases, the follicular phase of the menstrual cycle means the time between selection of a tertiary follicle and its subsequent growth into a preovulatory follicle.
Ovulation and the corpus luteum
By the end of the follicular, or proliferative, phase of the thirteenth day of the menstrual cycle, the cumulus oophorus layer of the preovulatory follicle will develop an opening, or stigma, and excrete the oocyte with a complement of cumulus cells in a process called ovulation. The oocyte is now called the ovum and is competent to undergo fertilization. The ovum will now travel down one of the fallopian tubes to eventually be discharged through menstruation, if not fertilized by a sperm cell, or implanted in the uterus, if previously fertilized. The fully developed oocyte (gamete) is now at the behest of the menstrual cycle.
Folliculogenesis The ruptured follicle will undergo a dramatic transformation into the corpus luteum, a steroidiogenic cluster of cells that maintains the endometrium of the uterus by the secretion of large amounts of progesterone and minor amounts of estrogen. These two steps, while not part of folliculogenesis, are included for completeness. They are discussed in their entirety by their respective articles, and placed into perspective by the menstrual cycle article. It is recommended that these three topics be reviewed.
232
Hormone function
As with most things related to the reproductive system, folliculogenesis is controlled by the endocrine system. Five hormones participate in an intricate process of positive and negative feedback to regulate folliculogenesis. They are: • gonadotropin-releasing hormone (GnRH) secreted by the hypothalamus • two gonadotropins: • follicle-stimulating hormone (FSH) • luteinizing hormone (LH) • estrogen • progesterone GnRH stimulates the release of FSH and LH from the anterior pituitary gland that will later have a stimulatory effect on follicle growth (not immediately, however, because only antral follicles are dependent on FSH and LH). When theca cells form in the tertiary follicle the amount of estrogen increases sharply (theca-derived androgen is aromatized into estrogen by the granulosa cells). At low concentration, estrogen inhibits gonadotropins, but high concentration of estrogen stimulates them. In addition, as more estrogen is secreted, more LH receptors are made by the theca cells, inciting theca cells to create more androgen that will become estrogen downstream. This positive feedback loop causes LH to spike sharply, and it is this spike that causes ovulation. Following ovulation, LH stimulates the formation of the corpus luteum. Estrogen has since dropped to negative stimulatory levels after ovulation and therefore serves to maintain the concentration of FSH and LH. Inhibin, which is also secreted by the corpus luteum, contributes to FSH inhibition. The endocrine system coincides with the menstrual cycle and goes through thirteen cycles (and thus thirteen LH spikes) during the course of normal folliculogenesis. However, coordinated enzyme signalling and the time-specific expression of hormonal receptors ensures that follicle growth does not become disregulated during these premature spikes.
Folliculogenesis
233
Number of follicles
Recently, two publications have challenged the idea that a finite number of follicles are set around the time of birth.[6][7] Renewal of ovarian follicles from germline stem cells (originating from bone marrow and peripheral blood) was reported in the postnatal mouse ovary. Studies attempting to replicate these results are underway, but a study of populations in 325 human ovaries found no supporting evidence for follicular replenishment.[3] In 2010, researchers at the University of Edinburgh determined that by the time women are 30 years old, only 10% of their non-growing follicles (NGFs) remain.[] At birth, women have all their follicles for folliculogenesis, and they steadily decline until menopause.
"Percentage of ovarian reserve related to increasing age. The curve describes the percentage of ovarian reserve remaining at ages from birth to 55 years, based on the ADC model. 100% is taken to be the maximum ovarian reserve, occurring at 18–22 weeks post-conception. The percentages apply to all women whose ovarian reserve declines in line with our model (i.e. late and early menopause are associated with high and low peak NGF populations, respectively). We estimate that for 95% of women by the age of 30 years only 12% of their maximum pre-birth NGF population is present and by the age of [6] [] 40 years only 3% remains. doi:10.1371/journal.pone.0008772.g005 "
Additional images
Section of the ovary. (#5 through #9 represent stages of folliculogenesis)
transitional primary follicle.
Folliculogenesis
234
References
[1] Page 769 (http:/ / books. google. com/ books?id=gOmpysGBC90C& pg=PT797), section "formation of the antrum" in: [2] Page 76 in: [3] Wallace WHB and Kelsey TW (2010) Human Ovarian Reserve from Conception to the Menopause. (http:/ / dx. plos. org/ 10. 1371/ journal. pone. 0008772) PLoS ONE 5(1):e8772. [5] de Ziegler D (2007), "Roles of FSH and LH during the follicular phase: insight into the natural cycle IVF", RBM Online volume 15 No. 5, page 508
• Caglar G, Asimakopoulos B, Nikolettos N, Diedrich K, Al-Hasani S (2005). "Recombinant LH in ovarian stimulation.". Reprod Biomed Online 10 (6): 774–85. doi: 10.1016/S1472-6483(10)61123-6 (http://dx.doi.org/ 10.1016/S1472-6483(10)61123-6). PMID 15970010 (http://www.ncbi.nlm.nih.gov/pubmed/15970010). • Gougeon A (1996). "Regulation of ovarian follicular development in primates: facts and hypotheses.". Endocr Rev 17 (2): 121–55. doi: 10.1210/er.17.2.121 (http://dx.doi.org/10.1210/er.17.2.121). PMID 8706629 (http://www.ncbi.nlm.nih.gov/pubmed/8706629). • Gougeon A (1986). "Dynamics of follicular growth in the human: a model from preliminary results.". Hum Reprod 1 (2): 81–7. PMID 3558758 (http://www.ncbi.nlm.nih.gov/pubmed/3558758). • van den Hurk R, Zhao J (2005). "Formation of mammalian oocytes and their growth, differentiation and maturation within ovarian follicles.". Theriogenology 63 (6): 1717–51. doi: 10.1016/j.theriogenology.2004.08.005 (http://dx.doi.org/10.1016/j.theriogenology.2004.08.005). PMID 15763114 (http://www.ncbi.nlm.nih. gov/pubmed/15763114).
External links
• Morphology and Physiology of the Ovary at endotext.org (http://www.endotext.org/female/female1/ femaleframe1.htm) • The ovary - folliculogenesis and oogenesis at nlm.nih.gov (http://www.ncbi.nlm.nih.gov/books/bv. fcgi?db=Books&rid=endocrin.section.1229) • Folliculogenesis and Ovulation at gfmer.ch (http://www.gfmer.ch/Books/Reproductive_health/ Folliculogenesis_and_ovulation.html) • Reproductive Physiology at ufp.pt (http://www2.ufp.pt/~pedros/qfisio/reproduction.htm)
Progesterone
235
Progesterone
Progesterone
Systematic (IUPAC) name
Pregn-4-ene-3,20-dione
Clinical data Trade names Crinone, Endometrin
AHFS/Drugs.com monograph [1] MedlinePlus Pregnancy cat. Legal status Routes a604017 B (USA) ? oral, implant, transdermal Pharmacokinetic data Bioavailability Protein binding Metabolism Half-life Excretion prolonged absorption, half-life approx 25-50 hours 96%-99% hepatic to pregnanediols and pregnanolones 34.8-55.13 hours renal Identifiers CAS number ATC code PubChem IUPHAR ligand DrugBank ChemSpider 57-83-0 [3] [2]
G03DA04 CID 5994 2377 [6]
[4] [5]
DB00396 5773 [8]
[7]
Progesterone
[9]
236
UNII KEGG ChEBI ChEMBL Synonyms
4G7DS2Q64Y D00066 [10]
CHEBI:17026 CHEMBL103
[11] [12]
4-pregnene-3,20-dione Chemical data
Formula Mol. mass
C21H30O2 314.46
Physical data Melt. point Spec. rot 126 °C (259 °F) [α]D (what is this?) (verify) [13]
Progesterone also known as P4 (pregn-4-ene-3,20-dione) is a C-21 steroid hormone involved in the female menstrual cycle, pregnancy (supports gestation) and embryogenesis of humans and other species. Progesterone belongs to a class of hormones called progestogens, and is the major naturally occurring human progestogen.
Chemistry
Progesterone was independently discovered by four research groups.[][][][] Willard Myron Allen co-discovered progesterone with his anatomy professor George Washington Corner at the University of Rochester Medical School in 1933. Allen first determined its melting point, molecular weight, and partial molecular structure. He also gave it the name Progesterone derived from Progestational Steroidal ketone.[] Like other steroids, progesterone consists of four interconnected cyclic hydrocarbons. Progesterone contains ketone and oxygenated functional groups, as well as two methyl branches. Like all steroid hormones, it is hydrophobic.
Sources
Animal
Progesterone is produced in the ovaries (by the corpus luteum), the adrenal glands (near the kidney), and, during pregnancy, in the placenta. Progesterone is also stored in adipose (fat) tissue. In humans, increasing amounts of progesterone are produced during pregnancy: • At first, the source is the corpus luteum that has been "rescued" by the presence of human chorionic gonadotropins (hCG) from the conceptus. • However, after the 8th week, production of progesterone shifts to the placenta. The placenta utilizes maternal cholesterol as the initial substrate, and most of the produced progesterone enters the maternal circulation, but some is picked up by the fetal circulation and used as substrate for fetal corticosteroids. At term the placenta produces about 250 mg progesterone per day. • An additional source of progesterone is milk products. After consumption of milk products the level of bioavailable progesterone goes up.[]
Progesterone
237
Plants
In at least one plant, Juglans regia, progesterone has been detected.[] In addition, progesterone-like steroids are found in Dioscorea mexicana. Dioscorea mexicana is a plant that is part of the yam family native to Mexico.[] It contains a steroid called diosgenin that is taken from the plant and is converted into progesterone.[] Diosgenin and progesterone are found in other Dioscorea species as well. Another plant that contains substances readily convertible to progesterone is Dioscorea pseudojaponica native to Taiwan. Research has shown that the Taiwanese yam contains saponins — steroids that can be converted to diosgenin and thence to progesterone.[] Many other Dioscorea species of the yam family contain steroidal substances from which progesterone can be produced. Among the more notable of these are Dioscorea villosa and Dioscorea polygonoides. One study showed that the Dioscorea villosa contains 3.5% diosgenin.[] Dioscorea polygonoides has been found to contain 2.64% diosgenin as shown by gas chromatography-mass spectrometry.[1] Many of the Dioscorea species that originate from the yam family grow in countries that have tropical and subtropical climates.[2]
Synthesis
Biosynthesis
In mammals, progesterone (6), like all other steroid hormones, is synthesized from pregnenolone (3), which in turn is derived from cholesterol (1) (see the upper half of the figure to the right). Cholesterol (1) undergoes double oxidation to produce 20,22-dihydroxycholesterol (2). This vicinal diol is then further oxidized with loss of the side chain starting at position C-22 to produce pregnenolone (3). This reaction is catalyzed by cytochrome P450scc. The conversion Top: Conversion of cholesterol (1) into pregnenolone (3) to progesterone (6). of pregnenolone to progesterone takes Bottom: Progesterone is important for aldosterone (mineralocorticoid) synthesis, as 17-hydroxyprogesterone is for cortisol (glucocorticoid), and androstenedione for sex place in two steps. First, the steroids. 3-hydroxyl group is oxidized to a keto group (4) and second, the double bond is moved to C-4, from C-5 through a keto/enol tautomerization reaction.[] This reaction is catalyzed by 3beta-hydroxysteroid dehydrogenase/delta(5)-delta(4)isomerase. Progesterone in turn (see lower half of figure to the right) is the precursor of the mineralocorticoid aldosterone, and after conversion to 17-hydroxyprogesterone (another natural progestogen) of cortisol and androstenedione. Androstenedione can be converted to testosterone, estrone and estradiol. Pregenolone and progesterone can also be synthesized by yeast.[]
Progesterone
238
Laboratory
An economical semisynthesis of progesterone from the plant steroid diosgenin isolated from yams was developed by Russell Marker in 1940 for the Parke-Davis pharmaceutical company (see figure to the right).[] This synthesis is known as the Marker degradation. Additional semisyntheses of progesterone have also been reported starting from a variety of [] The Marker semisynthesis of progesterone from diosgenin. steroids. For the example, cortisone can be simultaneously deoxygenated at the C-17 and C-21 position by treatment with iodotrimethylsilane in chloroform to produce 11-keto-progesterone (ketogestin), which in turn can be reduced at position-11 to yield progesterone.[] A total synthesis of progesterone was reported in 1971 by W.S. Johnson (see figure to the right).[] The synthesis begins with reacting the phosphonium salt 7 with phenyl lithium to produce the phosphonium ylide 8. The ylide 8 is reacted with an aldehyde to produce the alkene 9. The ketal protecting groups of 9 are hydrolyzed to produce the diketone 10, which in turn is cyclized to form the cyclopentenone 11. The ketone of 11 is reacted with methyl lithium to yield the tertiary alcohol 12, which in turn is treated with acid to produce the tertiary cation 13. The key step of the synthesis is the π-cation cyclization of 13 in which the B-, C-, and D-rings of the steroid are simultaneously formed to produce 14. This step resembles the cationic cyclization reaction used in the biosynthesis of steroids and hence is referred to as biomimetic. In the next step the enol orthoester is hydrolyzed to produce the ketone 15. The cyclopentene A-ring is then opened by oxidizing with ozone to produce 16. Finally, the diketone 17 undergoes an intramolecular aldol condensation by treating with aqueous potassium hydroxide to produce progesterone.[]
Levels
In women, progesterone levels are relatively low during the [] preovulatory phase of the menstrual cycle, rise after ovulation, and The Johnson total synthesis of progesterone. are elevated during the luteal phase, as shown in diagram below. Progesterone levels tend to be < 2 ng/ml prior to ovulation, and > 5 ng/ml after ovulation. If pregnancy occurs, human chorionic gonadotropin is released maintaining the corpus leuteum allowing it to maintain levels of progesterone. At around 12 weeks the placenta begins to produce progesterone in place of the corpus leuteum, this process is named the luteal-placental shift. After the luteal-placental shift progesterone levels start to rise further and may reach 100-200 ng/ml at term. Whether a decrease in progesterone levels is critical for the initiation of labor has been argued and may be species-specific. After delivery of the placenta and during lactation, progesterone levels are very low.
Progesterone Progesterone levels are relatively low in children and postmenopausal women.[] Adult males have levels similar to those in women during the follicular phase of the menstrual cycle.
Person type Reference range for blood test Lower limit Female - menstrual cycle Female - postmenopausal Upper limit Unit
239
(see diagram below) <0.2 <0,6 [3] [4] 1 3 [3] [4] [3] ng/mL nmol/L ng/mL nmol/L ng/mL nmol/L or 4.5 [3] ng/mL nmol/L
Female on oral contraceptives 0.34[3] 1.1 Males ≥16 years [4] [3] [4]
0.92 2.9 0.9 2.9 4.1 13
[4] [3] [4] [3]
0.27 0.86
Female or male 1–9 years
0.1 0.3
[3] [4]
[4]
[5] Progesterone levels during the menstrual cycle. - The ranges denoted By biological stage may be used in closely monitored menstrual cycles in regard to other markers of its biological progression, with the time scale being compressed or stretched to how much faster or slower, respectively, the cycle progresses compared to an average cycle.- The ranges denoted Inter-cycle variability are more appropriate to use in non-monitored cycles with only the beginning of menstruation known, but where the woman accurately knows her average cycle lengths and time of ovulation, and that they are somewhat averagely regular, with the time scale being compressed or stretched to how much a woman's average cycle length is shorter or longer, respectively, than the average of the population.- The ranges denoted Inter-woman variability are more appropriate to use when the average cycle lengths and time of ovulation are unknown, but only the beginning of menstruation is given.
Progesterone
240
Effects
Progesterone exerts its primary action through the intracellular progesterone receptor although a distinct, membrane bound progesterone receptor has also been postulated.[][] In addition, progesterone is a highly potent antagonist of the mineralocorticoid receptor (MR, the receptor for aldosterone and other mineralocorticosteroids). It prevents MR activation by binding to this receptor with an affinity exceeding even those of aldosterone and other corticosteroids such as cortisol and corticosterone.[] Progesterone has a number of physiological effects that are amplified Micrograph showing changes to the endometrium in the presence of estrogen. Estrogen through estrogen receptors due to progesterone (decidualization) H&E stain. upregulates the expression of progesterone receptors.[] Also, elevated levels of progesterone potently reduce the sodium-retaining activity of aldosterone, resulting in natriuresis and a reduction in extracellular fluid volume. Progesterone withdrawal, on the other hand, is associated with a temporary increase in sodium retention (reduced natriuresis, with an increase in extracellular fluid volume) due to the compensatory increase in aldosterone production, which combats the blockade of the mineralocorticoid receptor by the previously elevated level of progesterone.[]
Reproductive system
Progesterone has key effects via non-genomic signalling on human sperm as they migrate through the female tract before fertilization occurs, though the receptor(s) as yet remain unidentified.[] Detailed characterisation of the events occurring in sperm in response to progesterone has elucidated certain events including intracellular calcium transients and maintained changes,[] slow calcium oscillations,[] now thought to possibly regulate motility.[] Interestingly progesterone has also been shown to demonstrate effects on octopus spermatozoa.[] Progesterone modulates the activity of CatSper (cation channels of sperm) voltage-gated Ca2+ channels. Since eggs release progesterone, sperm may use progesterone as a homing signal to swim toward eggs (chemotaxis). Hence substances that block the progesterone binding site on CatSper channels could potentially be used in male contraception.[][] Progesterone is sometimes called the "hormone of pregnancy",[] and it has many roles relating to the development of the fetus: • Progesterone converts the endometrium to its secretory stage to prepare the uterus for implantation. At the same time progesterone affects the vaginal epithelium and cervical mucus, making it thick and impenetrable to sperm. If pregnancy does not occur, progesterone levels will decrease, leading, in the human, to menstruation. Normal menstrual bleeding is progesterone-withdrawal bleeding. If ovulation does not occur and the corpus luteum does not develop, levels of progesterone may be low, leading to anovulatory dysfunctional uterine bleeding. • During implantation and gestation, progesterone appears to decrease the maternal immune response to allow for the acceptance of the pregnancy. • Progesterone decreases contractility of the uterine smooth muscle.[] • In addition progesterone inhibits lactation during pregnancy. The fall in progesterone levels following delivery is one of the triggers for milk production. • A drop in progesterone levels is possibly one step that facilitates the onset of labor. The fetus metabolizes placental progesterone in the production of adrenal steroids.
Progesterone
241
Nervous system
Progesterone, like pregnenolone and dehydroepiandrosterone, belongs to the group of neurosteroids. It can be synthesized within the central nervous system and also serves as a precursor to another major neurosteroid, allopregnanolone. Neurosteroids affect synaptic functioning, are neuroprotective, and affect myelination.[] They are investigated for their potential to improve memory and cognitive ability. Progesterone affects regulation of apoptotic genes. Its effect as a neurosteroid works predominantly through the GSK-3 beta pathway, as an inhibitor. (Other GSK-3 beta inhibitors include bipolar mood stabilizers, lithium and valproic acid.)
Other effects
• It raises epidermal growth factor-1 levels, a factor often used to induce proliferation, and used to sustain cultures, of stem cells. • It increases core temperature (thermogenic function) during ovulation.[] • It reduces spasm and relaxes smooth muscle. Bronchi are widened and mucus regulated. (Progesterone receptors are widely present in submucosal tissue.) • It acts as an antiinflammatory agent and regulates the immune response. • It reduces gall-bladder activity.[] • It normalizes blood clotting and vascular tone, zinc and copper levels, cell oxygen levels, and use of fat stores for energy. • It may affect gum health, increasing risk of gingivitis (gum inflammation) and tooth decay.[citation needed] • It appears to prevent endometrial cancer (involving the uterine lining) by regulating the effects of estrogen. • Progesterone plays an important role in the signaling of insulin release and pancreatic function, and may affect the susceptibility to diabetes or gestational diabetes.[6][7]
Medical applications
The use of progesterone and its analogues have many medical applications, both to address acute situations and to address the long-term decline of natural progesterone levels. Because of the poor bioavailability of progesterone when taken orally, many synthetic progestins have been designed with improved oral bioavailability and have been used long before progesterone formulations became available.[] Progesterone was approved by the United States Food and Drug Administration as vaginal gel on July 31, 1997,[8] an oral capsule on May 14, 1998[9] in an injection form on April 25, 2001[10] and as a vaginal insert on June 21, 2007.[11] In Italy and Spain, Progesterone is sold under the trademark Progeffik.
Prometrium 100 mg Oral Capsule
Progesterone
242
Bioavailability
The route of administration impacts the effect of the drug. Given orally, progesterone has a wide person-to-person variability in absorption and bioavailability while synthetic progestins are rapidly absorbed with a longer half-life than progesterone and maintain stable levels in the blood.[12] Progesterone does not dissolve in water and is poorly absorbed when taken orally unless micronized in oil. Products are often sold as capsules containing micronised progesterone in oil. Progesterone can also be administered through vaginal or rectal suppositories or pessaries, transdermally through a gel or cream,[] or via injection (though the latter has a short half-life requiring daily administration). Transdermal "natural progesterone" products made with Progesterone USP do not require a prescription. Some of these products also contain "wild yam extract" derived from Dioscorea villosa, but there is no evidence that the human body can convert its active ingredient (diosgenin, the plant steroid that is chemically converted to produce progesterone industrially[]) into progesterone.[][]
Prevention of preterm birth
Vaginally dosed progesterone is being investigated as potentially beneficial in preventing preterm birth in women at risk for preterm birth. The initial study by Fonseca suggested that vaginal progesterone could prevent preterm birth in women with a history of preterm birth.[] According to a recent study, women with a short cervix that received hormonal treatment with a progesterone gel had their risk of prematurely giving birth reduced. The hormone treatment was administered vaginally every day during the second half of a pregnancy.[13] A subsequent and larger study showed that vaginal progesterone was no better than placebo in preventing recurrent preterm birth in women with a history of a previous preterm birth,[] but a planned secondary analysis of the data in this trial showed that women with a short cervix at baseline in the trial had benefit in two ways: a reduction in births less than 32 weeks and a reduction in both the frequency and the time their babies were in intensive care.[] In another trial, vaginal progesterone was shown to be better than placebo in reducing preterm birth prior to 34 weeks in women with an extremely short cervix at baseline.[] An editorial by Roberto Romero discusses the role of sonographic cervical length in identifying patients who may benefit from progesterone treatment.[] A meta-analysis published in 2011 found that vaginal progesterone cut the risk of premature births by 42 percent in women with short cervixes.[] The meta-analysis, which pooled published results of five large clinical trials, also found that the treatment cut the rate of breathing problems and reduced the need for placing a baby on a ventilator.[]
Other specific uses
• Progesterone is used for luteal support in Assisted Reproductive Technology (ART) cycles such as In-vitro Fertilization (IVF). • Progesterone is used to control persistent anovulatory bleeding. It is also used to prepare uterine lining in infertility therapy and to support early pregnancy. Patients with recurrent pregnancy loss due to inadequate progesterone production may receive progesterone. • Progesterone is also used in nonpregnant women with a delayed menstruation of one or more weeks, in order to allow the thickened endometrial lining to slough off. This process is termed a progesterone withdrawal bleed. The progesterone is taken orally for a short time (usually one week), after which the progesterone is discontinued and bleeding should occur.[citation needed] • Progesterone is being investigated as potentially beneficial in treating multiple sclerosis, since the characteristic deterioration of nerve myelin insulation halts during pregnancy, when progesterone levels are raised; deterioration commences again when the levels drop. • Progesterone also has a role in skin elasticity and bone strength, in respiration, in nerve tissue and in female sexuality, and the presence of progesterone receptors in certain muscle and fat tissue may hint at a role in sexually dimorphic proportions of those.[]WP:COPYLINK
Progesterone • Progesterone receptor antagonists, or selective progesterone receptor modulators (SPRM)s, such as RU-486 (Mifepristone), can be used to prevent conception or induce medical abortions (Note that methods of hormonal contraception do not contain progesterone but a progestin). • Progesterone may affect male behavior.[] • Progesterone is starting to be used in the treatment of the skin condition hidradenitis suppurativa.[citation needed]
243
Role in aging
Since most progesterone in males is created during testicular production of testosterone, and most in females by the ovaries, the shutting down (whether by natural or chemical means), or removal, of those inevitably causes a considerable reduction in progesterone levels. Previous concentration upon the role of progestogens (progesterone and molecules with similar effects) in female reproduction, when progesterone was simply considered a "female hormone", obscured the significance of progesterone elsewhere in both sexes. The tendency for progesterone to have a regulatory effect, the presence of progesterone receptors in many types of body tissue, and the pattern of deterioration (or tumor formation) in many of those increasing in later years when progesterone levels have dropped, is prompting widespread research into the potential value of maintaining progesterone levels in both males and females.
Role in brain damage
Studies as far back as 1987 show that female sex hormones have an effect on the recovery of traumatic brain injury.[] In these studies, it was first observed that pseudopregnant female rats had reduced edema after traumatic brain injury. Recent clinical trials have shown that among patients that have suffered moderate traumatic brain injury, those that have been treated with progesterone are more likely to have a better outcome than those who have not.[] Previous studies have shown that progesterone supports the normal development of neurons in the brain, and that the hormone has a protective effect on damaged brain tissue. It has been observed in animal models that females have reduced susceptibility to traumatic brain injury and this protective effect has been hypothesized to be caused by increased circulating levels of estrogen and progesterone in females.[] A number of additional animal studies have confirmed that progesterone has neuroprotective effects when administered shortly after traumatic brain injury.[] Encouraging results have also been reported in human clinical trials.[][]
Proposed mechanism
The mechanism of progesterone protective effects may be the reduction of inflammation that follows brain trauma.[] Damage incurred by traumatic brain injury is believed to be caused in part by mass depolarization leading to excitotoxicity. One way in which progesterone helps to alleviate some of this excitotoxicity is by blocking the voltage-dependent calcium channels that trigger neurotransmitter release.[] It does so by manipulating the signaling pathways of transcription factors involved in this release. Another method for reducing the excitotoxicity is by up-regulating the inhibitory neurotransmitter receptor, GABAA.[] Progesterone has also been shown to prevent apoptosis in neurons, a common consequence of brain injury.[] It does so by inhibiting enzymes involved in the apoptosis pathway specifically concerning the mitochondria, such as activated caspase 3 and cytochrome c. Not only does progesterone help prevent further damage, it has also been shown to aid in neuroregeneration. One of the serious effects of traumatic brain injury includes edema. Animal studies show that progesterone treatment leads to a decrease in edema levels by increasing the concentration of macrophages and microglia sent to the injured tissue.[][] This was observed in the form of reduced leakage from the blood brain barrier in secondary recovery in progesterone treated rats. In addition, progesterone was observed to have antioxidant properties, reducing the concentration of oxygen free radicals faster than without.[] There is also evidence that the addition of progesterone
Progesterone can also help remyelinate damaged axons due to trauma, restoring some lost neural signal conduction.[] Another way progesterone aids in regeneration includes increasing the circulation of endothelial progenitor cells in the brain.[] This helps new vasculature to grow around scar tissue which helps repair the area of insult.
244
Combination treatments
Vitamin D and progesterone separately have neuroprotective effects after traumatic brain injury, but when combined their effects are synergistic.[] When used at their optimal respective concentrations, the two combined have been shown to reduce cell death more than when alone. One study looks at a combination of progesterone with estrogen. Both progesterone and estrogen are known to have antioxidant-like qualities and are shown to reduce edema without injuring the blood-brain barrier. In this study, when the two hormones are administered alone it does reduce edema, but the combination of the two increases the water content, thereby increasing edema.[]
Clinical trials
The clinical trials for progesterone as a treatment for traumatic brain injury have only recently begun. ProTECT, a phase II trial conducted in Atlanta at Grady Memorial Hospital in 2007, the first to show that progesterone reduces edema in humans. Since then, trials have moved on to phase III. The National Institute of Health began conducting a nationwide phase III trial in 2011 led by Emory University.[] A global phase III initiative called SyNAPSe®, initiated in June 2010, is run by a U.S.-based private pharmaceutical company, BHR Pharma, and is being conducted in the United States, Argentina, Europe, Israel and Asia.[][14] Approximately 1,200 patients with severe (Glasgow Coma Scale scores of 3-8), closed-head TBI will be enrolled in the study at nearly 150 medical centers.
Progesterone
245
References
[3] Progesterone Reference Ranges (http:/ / cclnprod. cc. nih. gov/ dlm/ testguide. nsf/ 0/ CB26894E1EB28DEF85256BA5005B000E?OpenDocument), Performed at the Clinical Center at the National Institutes of Health, Bethesda MD, 03Feb09 [4] Converted from mass values using molar mass of 314.46 g/mol [5] References and further description of values are given in image page in Wikimedia Commons at Commons:File:Progesterone during menstrual cycle.png.
Additional images
Steroidogenesis, showing progesterone among the progestogens in yellow area.
Pregnenolone
Progesterone
246
Deoxycorticosterone
External links
• Progesterone (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Progesterone) at the US National Library of Medicine Medical Subject Headings (MeSH) • Kimball JW (2007-05-27). "Progesterone" (http://users.rcn.com/jkimball.ma.ultranet/BiologyPages/P/ Progesterone.html). Kimball's Biology Pages. Retrieved 2008-06-18. • "Progesterone Resource Center" (http://www.pms-menopause-progesterone.org/progesterone/). PMS, Menopause, and Progesterone Resource Center. Oasis Advanced Wellness, Inc. Retrieved 2008-06-18. • General discussion document on Progesterone, its uses and applications (http://www.lawleybasecamp.com/ media/pdf/condition-booklets/Progesterone_Booklet.pdf)
Corpus luteum cell
Corpus luteum cell may refer to: • Granulosa lutein cell • Theca lutein cell
Corpus luteum
247
Corpus luteum
Corpus luteum
Section of the ovary. 1. Outer covering. 1’. Attached border. 2. Central stroma. 3. Peripheral stroma. 4. Bloodvessels. 5. Vesicular follicles in their earliest stage. 6, 7, 8. More advanced follicles. 9. An almost mature follicle. 9’. Follicle from which the ovum has escaped. 10. Corpus luteum. Gray's subject #266 1256
[1]
The corpus luteum (Latin for "yellow body") (plural corpora lutea) is a temporary endocrine structure in female mammals that is involved in the production of relatively high levels of progesterone and moderate levels of estradiol and inhibin A. It is colored as a result of concentrating carotenoids from the diet and secretes a moderate amount of estrogen to inhibit further release of Gonadotropin-releasing hormone (GnRH) and thus secretion of Luteinizing hormone (LH) and Follicle-stimulating hormone (FSH).
Development and structure
The corpus luteum develops from an ovarian follicle during the luteal phase of the menstrual cycle or estrous cycle, following the release of a secondary oocyte from the follicle during ovulation. The follicle first forms a corpus hemorrhagicum before it becomes a corpus luteum, but the term refers to the visible collection of blood left after rupture of the follicle that secretes progesterone. While the oocyte (later the zygote if fertilization occurs) traverses the Fallopian tube into the uterus, the corpus luteum remains in the ovary. The corpus luteum is typically very large relative to the size of the ovary; in humans, the size of the structure ranges from under 2 cm to 5 cm in diameter.[][] Its cells develop from the follicular cells surrounding the ovarian follicle.[1] The follicular theca cells luteinize into small luteal cells, (thecal-lutein cells) and follicular granulosa cells (granulosal-lutein cells), luteinize into large luteal cells forming the corpus luteum. Progesterone is synthesized from cholesterol by both the large and small luteal cells upon luteal maturation. Cholesterol-LDL complexes bind to receptors on the plasma membrane of luteal cells and are internalized. Cholesterol is released and stored within the cell as cholesterol ester. LDL is recycled for further cholesterol transport. Large luteal cells produce more progesterone due to uninhibited/basal levels of PKA activity within the cell. Small luteal cells have LH receptors that regulate PKA activity within the cell. PKA actively phosphorylates StAR (steroidogenic acute regulatory protein) and PBR (peripheral benzodiazepine receptors) to transport cholesterol from the outer mitochondrial membrane to the inner mitochondrial membrane.[] The development of the corpus luteum is accompanied by an increase in the level of the steroidogenic enzyme P450scc that converts cholesterol to pregnenolone in the mitochondria.[] Pregnenolone is then converted to
Corpus luteum progesterone that is secreted out of the cell and into the blood stream. During the bovine estrous cycle, plasma levels of progesterone increase in parallel to the levels of P450scc and its electron donor adrenodoxin, indicating that progesterone secretion is a result of enhanced expression of P450scc in the corpus luteum.[] The mitochondrial P450 system electron transport chain including adrenodoxin reductase and adrenodoxin has been shown to leak electrons leading to the formation of superoxide radical.[][] Apparently to cope with the radicals produced by this system and by enhanced mitochondrial metabolism, the levels of antioxidant enzymes catalase and superoxide dismutase also increase in parallel with the enhanced steroidogenesis in the corpus luteum.[]
Follicular structure Luteal structure Theca cells Granulosa cells Theca lutein cells Secretion androgens, [2] estrogen [1] , and progesterone [2]
248
Granulosa lutein cells progesterone [1]), estrogen(majority),[1] and inhibin A[1][2]
Like the previous theca cells, the theca lutein cells lack the aromatase enzyme that is necessary to produce estrogen, so they can only perform steroidogenesis until formation of androgens.[3] The granulosa lutein cells do have aromatase, and use it to produce estrogens, using the androgens previously synthesized by the theca lutein cells, as the granulosa lutein cells in themselves do not have the 17α-hydroxylase or 17,20 lyase to produce androgens.[3] Once the corpus luteum regressed the remnant is known as corpus albicans.[4]
Function
The corpus luteum is essential for establishing and maintaining pregnancy in females. The corpus luteum secretes progesterone, which is a steroid hormone responsible for the decidualization of the endometrium (its development) and maintenance, respectively.
Steroidogenesis, with progesterone in yellow field at upper center. The androgens are shown in blue field, and aromatase at lower center - the enzyme present in granulosa lutein cells that convert androgens into estrogens (shown in pink triangle).
When egg is not fertilized
If the egg is not fertilized, the corpus luteum stops secreting progesterone and decays (after approximately 14 days in humans). It then degenerates into a corpus albicans, which is a mass of fibrous scar tissue. The uterine lining sloughs off without progesterone and is expelled through the vagina (in humans and some great apes, which go through a menstrual cycle). In an estrous cycle, the lining degenerates back to normal size.
When egg is fertilized
If the egg is fertilized and implantation occurs, the syncytiotrophoblast (derived from trophoblast) cells of the blastocyst secrete the hormone human chorionic gonadotropin (hCG, or a similar hormone in other species) by day 9 post-fertilization. Human chorionic gonadotropin signals the corpus luteum to continue progesterone secretion, thereby maintaining the thick lining (endometrium) of the uterus and providing an area rich in blood vessels in which the zygote(s) can develop. From this point on, the corpus luteum is called the corpus luteum graviditatis. The introduction of prostaglandins at this point causes the degeneration of the corpus luteum and the abortion of the fetus. However, in placental animals such as humans, the placenta eventually takes over progesterone production and the corpus luteum degrades into a corpus albicans without embryo/fetus loss.
Corpus luteum Luteal support refers to the administration of medication (generally progestins) for the purpose of increasing the success of implantation and early embryogenesis, thereby complementing the function of the corpus luteum.
249
Content of carotenoids
The yellow color and name of the corpus luteum, like that of the macula lutea of the retina, is due to its concentration of certain carotenoids, especially lutein. In 1968, a report indicated that beta-carotene was synthesized in laboratory conditions in slices of corpus luteum from cows. However, attempts have been made to replicate these findings, but have not succeeded. The idea is not presently accepted by the scientific community.[5] Rather, the corpus luteum concentrates carotenoids from the diet of the mammal.
Additional images
Order of changes in ovary
Human ovary with fully developed corpus luteum
Luteinized follicular cyst. H&E stain.
External links
• BU Histology Learning System: 18201loa [7] • SUNY Labs 43:05-0106 [8] – "The Female Pelvis: The Ovary"
References
[1] Page 1159 in: [2] The IUPS Physiome Project --> Female Reproductive System – Cells (http:/ / www. bioeng. auckland. ac. nz/ physiome/ ontologies/ female_repro_system/ cells. php) Retrieved on Nov 9, 2009 [3] Chapter 54, The Female Reproductive System > THE OVARIAN STEROIDS, in: [4] (http:/ / www. jstor. org/ pss/ 1563350) [5] Brian Davis. Carotenoid metabolism as a preparation for function. Pure & Applied Chemistry, Vol. 63, No. 1, pp. 131–140, 1991. available online. (http:/ / media. iupac. org/ publications/ pac/ 1991/ pdf/ 6301x0131. pdf) Accessed April 30, 2010.
Juxtaglomerular cell
250
Juxtaglomerular cell
The juxtaglomerular cells (JG cells, or granular cells) are cells in the kidney that synthesize, store, and secrete the enzyme renin. They are specialized smooth muscle cells in the wall of the afferent arteriole (and sometimes the efferent arteriole) that delivers blood to the glomerulus. In synthesizing renin, they play a critical role in the renin-angiotensin system and thus in renal autoregulation, the self-governance of the kidney. They secrete renin in response to the detection of low Na by the macula densa cells located on the distal convoluted tubule which has direct contact with its own afferent arterioles. In appropriately stained slides, juxtaglomerular cells are distinguished by their granulated cytoplasm. Similar to cardiac tissue, juxtaglomerular cells harbor β1 adrenergic receptors. When stimulated by epinephrine or norepinephrine, these receptors induce the secretion of renin. These cells also respond directly to a decrease in systemic blood pressure which is manifested as a lower renal perfusion pressure.
JG cells
Renal corpuscle. Juxtaglomerular cells are #6.
External links
• BU Histology Learning System: 16010loa [1] • juxtaglomerular+cells [2] at eMedicine Dictionary
Renin
251
Renin
Renin
PDB rendering based on 2ren Available structures PDB Ortholog search: PDBe [1], RCSB [2] List of PDB id codes 1BBS , 1BIL , 1BIM , 1HRN , 1RNE , 2BKS , 2BKT , 2FS4 , 2G1N , 2G1O , 2G1R , [14] [15] [16] [17] [18] [19] [20] [21] [22] [23] 2G1S , 2G1Y , 2G20 , 2G21 , 2G22 , 2G24 , 2G26 , 2G27 , 2I4Q , 2IKO , 2IKU [24] [25] [26] [27] [28] [29] [30] [31] [32] [33] [34] , 2IL2 , 2REN , 2V0Z , 2V10 , 2V11 , 2V12 , 2V13 , 2V16 , 2X0B , 3D91 , [35] [36] [37] [38] [39] [40] [41] [42] [43] [44] 3G6Z , 3G70 , 3G72 , 3GW5 , 3K1W , 3KM4 , 3O9L , 3OAD , 3OAG , 3OOT , [45] [46] [47] [48] [49] [50] [51] [52] [53] [54] 3OQF , 3OQK , 3OWN , 3Q3T , 3Q4B , 3Q5H , 3SFC , 3VCM , 3VSW , 3VSX , [55] [56] [57] [58] [59] [60] [61] [62] [63] [64] 3VYD , 3VYE , 3VYF , 4AMT , 4GJ5 , 4GJ6 , 4GJ7 , 4GJ8 , 4GJ9 , 4GJA , [65] [66] [67] 4GJB , 4GJC , 4GJD
[3] [4] [5] [6] [7] [8] [9] [10] [11] [12] [13]
Identifiers Symbols External IDs REN
[68]
; HNFJ2
[69]
OMIM: 179820 [73] Gene 3.4.23.15
[74]
MGI: 97898
[70]
HomoloGene: 20151
[71]
ChEMBL: 286
[72]
GeneCards: REN
EC number
Renin
252
Gene Ontology Molecular function • aspartic-type endopeptidase activity [75] [14] • receptor binding [170] • insulin-like growth factor receptor binding [76] • peptidase activity Cellular component • extracellular space [230] [77] • membrane [78] • cytoplasmic part Biological process • kidney development [80] • mesonephros development [81] • angiotensin maturation • renin-angiotensin regulation of aldosterone production
[82] [79]
• proteolysis [84] • response to stress [85] • regulation of blood pressure [86] • male gonad development [87] • hormone-mediated signaling pathway [22] • response to drug [61] • drinking behavior [88] • regulation of MAPK cascade [89] • cell maturation [70] • response to cAMP [90] • response to cGMP Sources: Amigo
[91]
[83]
/ QuickGO
[92]
Orthologs Species Entrez Ensembl UniProt RefSeq (mRNA) RefSeq (protein) Location (UCSC) Human 5972
[93] [95]
Mouse 19701
[94] [96]
ENSG00000143839 P00797
[97] [99]
ENSMUSG00000070645 P06281
[98] [100]
NM_000537 NP_000528
NM_031192 NP_112469
[101]
[102]
Chr 1: [103] 204.12 – 204.14 Mb
[105]
Chr 1: [104] 133.35 – 133.36 Mb
[106]
PubMed search
Renin
253
renin
Identifiers EC number CAS number 3.4.23.15 [107] [108]
9015-94-5
Databases IntEnz BRENDA ExPASy KEGG MetaCyc PRIAM PDB structures Gene Ontology IntEnz view [109] [110] [111]
BRENDA entry NiceZyme view KEGG entry
[112] [113]
metabolic pathway profile [114] [115]
RCSB PDB AmiGO
PDBe
[116]
PDBsum
[117]
[118]
/ EGO
[119]
Search PMC articles [120]
PubMed articles [121] NCBI proteins [122]
Renin (pron.: /ˈriːnɨn/ REE-nin), also known as an angiotensinogenase, is an enzyme that participates in the body's renin-angiotensin system (RAS)—also known as the renin-angiotensin-aldosterone axis—that mediates extracellular volume (i.e., that of the blood plasma, lymph and interstitial fluid), and arterial vasoconstriction. Thus, it regulates the body's mean arterial blood pressure.
Biochemistry and physiology
Structure
The primary structure of renin precursor consists of 406 amino acids with a pre- and a pro-segment carrying 20 and 46 amino acids, respectively. Mature renin contains 340 amino acids and has a mass of 37 kDa.[]
Secretion
The enzyme renin is secreted by the kidney from specialized cells called granular cells of the juxtaglomerular apparatus via 3 responses: 1. A decrease in arterial blood pressure (that could be related to a decrease in blood volume) as detected by baroreceptors (pressure-sensitive cells). This is the most direct causal link between blood pressure and renin secretion (the other two methods operate via longer pathways). 2. A decrease in sodium chloride levels in the ultra-filtrate of the nephron. This flow is measured by the macula densa of the juxtaglomerular apparatus.
Renin 3. Sympathetic nervous system activity, which also controls blood pressure, acting through the beta1 adrenergic receptors. Human renin is secreted by at least 2 cellular pathways: a constitutive pathway for the secretion of prorenin and a regulated pathway for the secretion of mature renin.[]
254
Renin-angiotensin system
The renin enzyme circulates in the blood stream and breaks down (hydrolyzes) angiotensinogen secreted from the liver into the peptide angiotensin I. Angiotensin I is further cleaved in the lungs by endothelial-bound angiotensin-converting enzyme (ACE) into angiotensin II, the most vasoactive peptide.[][2] Angiotensin II is a potent constrictor of all blood vessels. It acts on the smooth muscle and, therefore, raises the resistance posed by these arteries to the heart. The heart, trying to overcome this increase in its 'load', works more vigorously, causing the blood pressure to rise. Angiotensin II also acts on the adrenal glands and releases Aldosterone, which stimulates the epithelial cells in the distal tubule and collecting ducts of the kidneys to increase re-absorption of sodium and water, leading to raised blood volume and raised blood pressure. The RAS also acts on the CNS to increase water intake by stimulating thirst, as well as conserving blood volume, by reducing urinary loss through the secretion of Vasopressin from the posterior pituitary gland.
The renin-angiotensin system, showing role of renin at [1] bottom.
The normal concentration of renin in adult human plasma is 1.98-24.6 ng/L in the upright position.[3]
Function
Renin activates the renin-angiotensin system by cleaving angiotensinogen, produced by the liver, to yield angiotensin I, which is further converted into angiotensin II by ACE, the angiotensin-converting enzyme primarily within the capillaries of the lungs. Angiotensin II then constricts blood vessels, increases the secretion of ADH and aldosterone, and stimulates the hypothalamus to activate the thirst reflex, each leading to an increase in blood pressure. Renin is secreted from kidney cells, which are activated via signaling from the macula densa, which responds to the rate of fluid flow through the distal tubule, by decreases in renal perfusion pressure (through stretch receptors in the vascular wall), and by sympathetic nervous stimulation, mainly through beta-1 adrenoceptor activation. A drop in the rate of flow past the macula densa implies a drop in renal filtration pressure. Renin's primary function is therefore to eventually cause an increase in blood pressure, leading to restoration of perfusion pressure in the kidneys. Renin can bind to ATP6AP2, which results in a fourfold increase in the conversion of angiotensinogen to angiotensin I over that shown by soluble renin. In addition, renin binding results in phosphorylation of serine and tyrosine residues of ATP6AP2.[] The level of renin mRNA appears to be modulated by the binding of HADHB, HuR and CP1 to a regulatory region in the 3' UTR.[]
Renin
255
Genetics
The gene for renin, REN, spans 12 kb of DNA and contains 8 introns.[] It produces several mRNA that encode different REN isoforms.
Model organisms Ren1 knockout mouse phenotype
Characteristic Homozygote viability Fertility Body weight Anxiety Neurological assessment Grip strength Hot plate Dysmorphology Phenotype Normal Normal Normal Normal Normal Normal Normal Normal
Non-Invasive Blood Pressure Abnormal[] Indirect calorimetry Glucose tolerance test Normal Normal
Auditory brainstem response Normal DEXA Radiography Body temperature Eye morphology Clinical chemistry Haematology Micronucleus test Heart weight Skin Histopathology Brain histopathology Salmonella infection Citrobacter infection Normal Normal Normal Normal Normal Normal Normal Normal Normal Normal Normal [] []
Abnormal [][4]
All tests and analysis from
Model organisms have been used in the study of REN function. A knockout mouse line, called Ren1Ren-1c Enhancer KO was generated.[5] Male and female animals underwent a standardized phenotypic screen to determine the effects of deletion.[][6] Twenty four tests were carried out on mutant mice and two significant abnormalities were observed. Homozygous mutant animals had a decreased heart rate and an increased susceptibility to bacterial infection.[] A more detailed analysis of this line indicated plasma creatinine was also increased and males had lower mean arterial pressure than controls.[5]
Renin
256
Clinical applications
An over-active renin-angiotension system leads to vasoconstriction and retention of sodium and water. These effects lead to hypertension. Therefore, renin inhibitors can be used for the treatment of hypertension.[7][] This is measured by the plasma renin activity (PRA). In current medical practice, the renin-angiotensin-aldosterone-System's overactivity (and resultant hypertension) is more commonly reduced using either ACE inhibitors (such as ramipril and perindopril) or angiotensin II receptor blockers (ARBs, such as losartan, irbesartan or candesartan) rather than a direct oral renin inhibitor. ACE inhibitors or ARBs are also part of the standard treatment after a heart attack. The differential diagnosis of kidney cancer in a young patient with hypertension includes juxtaglomerular cell tumor (reninoma), Wilms' tumor, and renal cell carcinoma, all of which may produce renin.[]
Measurement
Renin is usually measured as the plasma renin activity (PRA). PRA is measured specially in case of certain diseases that present with hypertension or hypotension. PRA is also raised in certain tumors.[8] A PRA measurement may be compared to a plasma aldosterone concentration (PAC) as a PAC/PRA ratio.
Discovery
Renin was discovered, characterized, and named in 1898 by Robert Tigerstedt, Professor of Physiology and his student, Per Bergman, at the Karolinska Institute in Stockholm.[][9]
References
[1] Page 866-867 (Integration of Salt and Water Balance) and 1059 (The Adrenal Gland) in: [2] Brenner & Rector's The Kidney, 7th ed., Saunders, 2004. pp.2118-2119. Full Text with MDConsult subscription (http:/ / home. mdconsult. com/ das/ book/ 56203699-6/ view/ 1201?sid=460067115) [3] Hamilton Regional Laboratory Medicine Program - Laboratory Reference Centre Manual. [deadlink] [4] Mouse Resources Portal (http:/ / www. sanger. ac. uk/ mouseportal/ ), Wellcome Trust Sanger Institute. [7] Presentation on Direct Renin Inhibitors as Antihypertensive Drugs (http:/ / pharmaxchange. info/ presentations/ dri. html) [8] Hamilton Regional Laboratory Medicine Program - Laboratory Reference Centre Manual. Renin Direct.
External links
• GeneReviews/NCBI/NIH/UW entry on Familial Juvenile Hyperuricemic Nephropathy Type 2 (http://www. ncbi.nlm.nih.gov/books/NBK53700/) • OMIM entries on Familial Juvenile Hyperuricemic Nephropathy Type 2 (http://www.ncbi.nlm.nih.gov/omim/ 179820,613092) • The MEROPS online database for peptidases and their inhibitors: A01.007 (http://merops.sanger.ac.uk/ cgi-bin/merops.cgi?id=A01.007) • Renin (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Renin) at the US National Library of Medicine Medical Subject Headings (MeSH) • renin (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=renin) at eMedicine Dictionary
Macula densa
257
Macula densa
In the kidney, the macula densa is an area of closely packed specialized cells lining the wall of the distal tubule at the point of return of the nephron to the vascular pole of its parent glomerulus, (glomerular vascular pole). The cells of the macula densa are sensitive to the concentration of sodium chloride in the distal convoluted tubule. A decrease in sodium chloride concentration initiates a signal from the macula densa that has two effects: (1) it decreases resistance to blood flow in the afferent arterioles, which increases glomerular hydrostatic pressure Renal corpuscle. Macula densa is #7. and helps return glomerulus filtration rate (GFR) toward normal, and (2) it increases renin release from the juxtaglomerular cells of the afferent and efferent arterioles, which are the major storage sites for renin.[1] The release of renin is an essential component of the renin-angiotensin-aldosterone system (RAAS), which regulates blood pressure and volume.
Histology
The cells of the macula densa are taller and have more prominent nuclei than surrounding cells of the distal straight tubule (cortical thick ascending limb). The close proximity and prominence of the nuclei cause this segment of the distal tubule wall to appear darker in microscopic preparations,[2] hence the name macula densa.
Function
A decrease in blood pressure causes a decrease in the GFR (glomerular filtration rate) which causes more reabsorption, resulting in a decreased concentration of sodium and chloride ions in the filtrate and/or decreased filtrate flow rate. The macula densa can sense this decrease and trigger an autoregulatory response to further increase reabsorption of ions and water in order to return blood pressure to normal. Reduced blood pressure means
Schematic depicting how the RAAS works. Here, activation of the RAAS is initiated by a low perfusion pressure in the juxtaglomerular apparatus
Macula densa decreased venous pressure and hence a decreased peritubular capillary pressure. This causes a smaller capillary hydrostatic pressure which causes an increased absorption of sodium ions into the vasa recta at the proximal tubule. Because of this increased absorption, less NaCl is present at the distal tubule where the macula densa is located. The macula densa senses this drop in salt concentration and responds through two mechanisms: first, it triggers dilation of the renal afferent arteriole, decreasing afferent arteriole resistance and thus offsetting the decrease in glomerular hydrostatic pressure caused by the drop in blood pressure. Second, macula densa cells release prostaglandins, which triggers granular juxtaglomerular cells lining the afferent arterioles to release renin into the bloodstream. (The juxtaglomerular cells can also release renin independently of the macula densa, as they are also triggered by baroreceptors lining the arterioles, and release renin if a fall in blood pressure in the arterioles is detected.) Furthermore, activation of the sympathetic nervous system stimulates renin release through activation of beta-1 receptors. The process triggered by the Macula densa helps keep the glomerular filtration rate (GFR) fairly steady in response to varying artery pressure, due to dilation of the afferent arterioles and the action of Renin, which triggers constriction of the efferent arterioles, both of which increase hydrostatic pressure in the glomerulus.
258
References
[1] Guyton & Hall Textbook Of Physiology, 11th Edition 2006 - pg 324
External links
• Organology at UC Davis Urinary/mammal/cortex1/cortex5 (http://trc.ucdavis.edu/mjguinan/apc100/modules/ Urinary/mammal/cortex1/cortex5.html) - "Mammal, kidney cortex (LM, Medium)" • Physiology at MCG 7/7ch03/7ch03p17 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section7/7ch03/7ch03p17.htm) - "The Nephron: Juxtaglomerular Apparatus"
Mesangial cell
259
Mesangial cell
Mesangial cells are specialized cells around blood vessels in the kidneys, at the mesangium. They are specialized smooth muscle cells that function to regulate blood flow through the capillaries, usually divided into two types, each having a very distinct function and location: • Extraglomerular mesangial cells • Intraglomerular mesangial cells
Keratinocyte
Keratinocyte is the predominant cell type in the epidermis, the outermost layer of the skin, constituting 90% of the cells found there.[1] Those keratinocytes found in the basal layer (Stratum germinativum) of the skin are sometimes referred to as "basal cells" or "basal keratinocytes".[1]
Function
The primary function of keratinocytes is the formation of a barrier against environmental damage such as pathogens (bacteria, fungi, parasites, viruses), heat, UV radiation and water loss. Once pathogens start to invade the upper layers of the epidermis, keratinocytes can react with the production of proinflammatory mediators and in particular chemokines such as CXCL10, CCL2 which attract leukocytes to the site of pathogen invasion. [citation needed]
Structure
A number of structural proteins (filaggrin, keratin), enzymes (proteases), lipids and antimicrobial peptides (defensins) contribute to maintain the important barrier function of the skin. Keratinization is part of the physical barrier formation (cornification), in which the keratinocytes produce more and more keratin and eventually undergo programmed cell death. The fully cornified keratinocytes that form the outermost layer are constantly shed off and replaced by new cells. [citation needed]
Cell differentiation
Keratinocytes are formed first by differentiation from epidermal stem cells (transit amplifying cells), residing in the lower part of the stratum basale of the epidermis, attached to the basement membrane through hemidesmosomes.[2] Those stem cells and their differentiated progeny are organized into columns named epidermal proliferation units.[3][4] Keratinocytes in the stratum basale layer of the epidermis are attached together through desmosomes and will proliferate through a few rounds of cell divisions within the stratum basale before moving up through the epidermis as they differentiate. During this differentiation process, keratinocytes permanently withdraw from the cell cycle, initiate expression of epidermal differentiation markers, and move suprabasally as they become part of the stratum spinosum, stratum granulosum and eventually become corneocytes in the stratum corneum. Corneocytes are keratinocytes that have completed their differentiation program and have lost their nucleus and cytoplasmic organelles.[5] Corneocytes will eventually be shed off through desquamation as new one come in. At each stage of differentiation, keratinocytes express specific keratins, such as keratin 1, keratin 5, keratin 10 and keratin 14, but also other markers such as involucrin, loricrin, transglutaminase, filaggrin and caspase 14. In humans, it is estimated that keratinocytes turnover from stem cells to desquamation every 40–56 days[6] whereas in mice the estimated turnover time is 8–10 days.[7]
Keratinocyte Factors promoting keratinocyte differentiation: • A calcium gradient, with the lowest concentration in the stratum basale and increasing concentrations until the outer stratum granulosum, where it reaches its maximum. Calcium concentration in the stratum corneum is very low in part because those relatively dry cells are not able to dissolve the ions.[] Those elevations of extracellular calcium concentrations induces an increase in intracellular free calcium concentrations in keratinocyte.[8] Part of that intracellular calcium increase comes from calcium released from intracellular stores[9] and another part comes from transmembrane calcium influx,[10] through both calcium-sensitive chloride channels[11] and voltage-independent cation channels permeable to calcium.[12] Moreover, it has been suggested that an extracellular calcium-sensing receptor (CaSR) also contributes to the rise in intracellular calcium concentration.[13] • Vitamin D3 (cholecalciferol) regulates keratinocyte proliferation and differentiation mostly by modulating calcium concentrations and regulating the expression of genes involved in keratinocytes differentiation.[14][15] Keratinocytes are the only cells in the body with the entire vitamin D metabolic pathway from vitamin D production to catabolism and Vitamin D receptor expression.[16] • Cathepsin E.[17] • TALE homeodomain transcription factors.[18] • Hydrocortisone.[] Since keratinocyte differentiation stops keratinocyte proliferation, factors that promote keratinocyte proliferation should be considered as preventing differentiation, such as: • • • • • The transcription factor p63, by preventing epidermal stem cells to differentiate into keratinocytes.[19] Vitamin A and its analogues.[20] Epidermal growth factor.[21] Tumor growth factor alpha.[22] Cholera toxin[]
260
Interaction with other cells
Within the epidermis keratinocytes are associated with other cell types such as melanocytes and Langerhans cells. Keratinocytes form tight junctions with the nerves of the skin and hold the Langerhans cells and intra-dermal lymphocytes in position within the epidermis. Keratinocytes also modulate the immune system: apart from the above mentioned antimicrobial peptides and chemokines they are also potent producers of anti-inflammatory mediators such as IL-10 and TGF-β. When activated, they can stimulate cutaneous inflammation and Langerhans cell activation via TNFα and IL-1β secretion.[citation needed] Keratinocytes contribute to protecting the body from ultraviolet radiation (UVR) by taking up melanosomes, vesicles containing the endogenous photoprotectant melanin, from epidermal melanocytes. Each melanocyte in the epidermis has several dendrites that stretch out to connect it with many keratinocytes. The melanin is then stored within keratinocytes and melanocytes in the perinuclear area as supranuclear “caps”, where it protects the DNA from UVR-induced damage.[23]
Keratinocyte
261
Role in wound healing
Wounds to the skin will be repaired in part by the migration of keratinocytes to fill in the gap created by the wound. The first set of keratinocytes to participate in that repair come from the bulge region of the hair follicle and will only survive transiently. Within the healed epidermis they will be replaced by keratinocytes originating from the epidermis.[24][25] At the opposite, epidermal keratinocytes, can contribute to de novo hair follicle formation during the healing of large wounds.[26] Keratinocytes migrate with a rolling motion during the process of wound healing.[27][28] Functional keratinocytes are needed for tympanic perforation healing. [29]
Sunburn cells
A sunburn cell is a keratinocyte with a pyknotic nucleus and eosinophilic cytoplasm that appears after exposure to UVC or UVB radiation or UVA in the presence of psoralens. It shows premature and abnormal keratinization, and has been described as an example of apoptosis.[30][31]
References
[29] Y Shen, Y Guo, C Du, M Wilczynska, S Hellström, T Ny, Mice Deficient in Urokinase-Type Plasminogen Activator Have Delayed Healing of Tympanic Membrane Perforations, PLOS ONE, 2012
External links
• L. Tang1, J.J. Wu2, Q. Ma1, T. Cui1, F.M. Andreopoulos3, J. Gil1, J. Valdes1, S.C. Davis1, J. Li1,4 "Human lactoferrin stimulates skin keratinocyte function and wound re-epithelialization", British Journal of Dermatology Volume 163, Issue 1, pages 38–47 (July 2010). Article first published online: 6 MAR 2010. (http://www3. interscience.wiley.com/journal/123313996/abstract) doi: 10.1111/j.1365-2133.2010.09748.x (http://dx.doi. org/10.1111/j.1365-2133.2010.09748.x)
Epidermis (skin)
262
Epidermis (skin)
Epidermis
Histologic image of epidermis, delimited by white bar.
Histologic image detailing epidermal layers. Stratum corneum appears more compact in this image than above because of different sample preparation. Latin Code Epidermis TH H13.12.00.1.01001 TA A16.0.00.009
The epidermis is composed of the outermost layers of cells in the skin,[1] "epi" in Greek meaning "over" or "upon", which together with the dermis forms the cutis. The epidermis is a stratified squamous epithelium,[1] composed of proliferating basal and differentiated suprabasal keratinocytes which acts as the body's major barrier against an inhospitable environment, by preventing pathogens from entering, making the skin a natural barrier to infection.[] It also regulates the amount of water released from the body into the atmosphere through transepidermal water loss (TEWL).[] In humans, it is thinnest on the eyelids at 0.05 mm (0.0020 in) and thickest on the palms and soles at 1.5 mm (0.059 in).[] It is ectodermal in origin.
Structure
Cellular components
The epidermis is avascular, nourished by diffusion from the dermis, constituted at 95% of keratinocytes[1] but also containing melanocytes, Langerhans cells, Merkel cells,[1] and inflammatory cells. Rete ridges ("rete tips"[2]) are epidermal thickenings that extend downward between dermal papillae.[3] Blood capillaries are found beneath the epidermis, and are linked to an arteriole and a venule. Arterial shunt vessels may bypass the network in ears, the nose and fingertips.[citation needed]
Epidermis (skin)
263
Layers
The epidermis is composed of 4 or 5 layers depending on the region of skin being considered.[4] Those layers in descending order are[]: • cornified layer (stratum corneum) Composed of 10 to 30 layers of polyhedral, anucleated corneocytes (final step of keratinocyte differentiation), with the palms and soles having the most layers. Corneocytes are surrounded by a protein envelope (cornified envelope proteins), filled with water-retaining keratin proteins, attached together through corneodesmosomes and surrounded in the extracellular space by stacked layers of lipids.[5] Most of the barrier functions of the epidermis localize to this layer.[] • clear/translucent layer (stratum lucidum, only in palms and soles) • granular layer (stratum granulosum) Keratinocytes lose their nuclei and their cytoplasm appears granular. Lipids, contained into those keratinocytes within lamellar bodies, are released into the extracellular space through exocytosis to form a lipid barrier. Those polar lipids are then converted into non-polar lipids and arranged parallel to the cell surface. For example glycosphingolipids become ceramides and phospholipids become free fatty acids.[5] • spinous layer (stratum spinosum) Keratinocytes become connected through desmosomes and start produce lamellar bodies, from within the Golgi, enriched in polar lipids, glycosphingolipids, free sterols, phospholipids and catabolic enzymes.[] Langerhans cells, immunologically active cells, are located in the middle of this layer.[5] • basal/germinal layer (stratum basale/germinativum). Composed mainly of proliferating and non-proliferating keratinocytes, attached to the basement membrane by hemidesmosomes. Melanocytes are present, connected to numerous keratinocytes in this and other strata through dendrites. Merkel cells are also found in the stratum basale with large numbers in touch-sensitive sites such as the fingertips and lips. They are closely associated with cutaneous nerves and seem to be involved in light touch sensation.[5] The term Malpighian layer (stratum malpighi) is usually defined as both the stratum basale and stratum spinosum.[1] The epidermis is separated from the dermis, its underlying tissue, by a basement membrane.
Schematic image showing a section of epidermis with epidermal layers labeled.
Cellular kinyotics
Cell division The stratified squamous epithelium is maintained by cell division within the stratum basale. Differentiating cell delaminate from the basement membrane and are displaced outwards through the epidermal layers, undergoing multiple stages of differentiation until, in the stratum corneum, losing their nucleus and fusing to squamous sheets, which are eventually shed from the surface (desquamation). Differentiated keratinocytes secrete keratin proteins which contribute to the formation of an extracellular matrix and is an integral part of the skin barrier function. In normal skin, the rate of keratinocyte production equals the rate of loss,[1] taking about two weeks for a cell to journey from the stratum basale to the top of the stratum granulosum, and an additional four weeks to cross the stratum corneum.[] The entire epidermis is replaced by new cell growth over a period of about 48 days.[]
Epidermis (skin) Calcium concentration Keratinocyte differentiation throughout the epidermis is in part mediated by a calcium gradient, increasing from the stratum basale until the outer stratum granulosum, where it reaches its maximum, and decreasing in the stratum corneum. Calcium concentration in the stratum corneum is very low in part because those relatively dry cells are not able to dissolve the ions. This calcium gradient parallels keratinocyte differentiation and as such is considered a key regulator in the formation of the epidermal layers.[] Elevation of extracellular calcium concentrations induces an increase in intracellular free calcium concentrations.[6] Part of that intracellular increase comes from calcium released from intracellular stores[7] and another part comes from transmembrane calcium influx,[8] through both calcium-sensitive chloride channels[9] and voltage-independent cation channels permeable to calcium.[10] Moreover, it has been suggested that an extracellular calcium-sensing receptor (CaSR) also contributes to the rise in intracellular calcium concentration.[11]
264
Organogenesis
Epidermal organogenesis, the formation of the epidermis, begins in the cells covering the embryo after neurulation, the formation of the central nervous system. In most vertebrates, this original one-layered structure quickly transforms into a two-layered tissue; a temporary outer layer, the periderm, which is disposed once the inner basal layer or stratum germinativum has formed. [] This inner layer is a germinal epithelium that give rise to all epidermal cells. It divides to form the outer spinous layer (stratum spinosum). The cells of these two layers, together called the Malpighian layer(s) after Marcello Malpighi, divide to form the superficial granular layer (Stratum granulosum) of the epidermis. [] The cells in the stratum granulosum do not divide, but instead form skin cells called keratinocytes from the granules of keratin. These skin cells finally become the cornified layer (stratum corneum), the outermost epidermal layer, where the cells become flattened sacks with their nuclei located at one end of the cell. After birth these outermost cells are replaced by new cells from the stratum granulosum and throughout life they are shed at a rate of 1.5 g (0.053 oz) per day. [] Epidermal development is a product of several growth factors, two of which are:[] • Transforming growth factor Alpha (TGFα) is an autocrine growth factor by which basal cells stimulate their own division. • Keratinocyte growth factor (KGF or FGF7) is a paracrine growth factor produced by the underlying dermal fibroblasts in which the proliferation of basal cells is regulated.
Function
Barrier
The epidermis serves as a barrier to protect the body against microbial pathogens, oxidant stress (UV light) and chemical compounds and provides mechanical resistance. Most of that function is played by the stratum corneum.[] Characteristics of the barrier • Physical barrier through keratinocytes attached together via cell–cell junctions and associated to cytoskeletal proteins, which gives the epidermis its mechanical strength.[] • Chemical barrier through the presence of highly organized lipids, acids, hydrolytic enzymes and antimicrobial peptides.[] • Immunologically active barrier through humoral and cellular constituents of the immune system.[] • Water content of the stratum corneum drops towards the surface, creating hostile conditions for pathogenic microorganism growth.[]
Epidermis (skin) • An acidic pH (around 5.0) and low amounts of water make it hostile to many microorganic pathogens.[] • The presence of non-pathogenic microorganism on the epidermis surface help defend against pathogenic one by limiting food availability and through chemical secretions.[] Factors that will alter the barrier • Psychological stress, through an increase in glucocorticoids, compromises the stratum corneum and thus the barrier function.[12] • Sudden and large shifts in humidity alter stratum corneum hydration in a way that could allow entry of pathogenic microorganisms.[13]
265
Skin hydration
The ability of the skin to hold water is primarily due to the stratum corneum and is critical for maintaining healthy skin.[14] Lipids arranged through a gradient and in an organized manner between the cells of the stratum corneum form a barrier to transepidermal water loss.[15][16]
Skin color
The amount and distribution of melanin pigment in the epidermis is the main reason for variation in skin color in Homo sapiens. Melanin is found in the small melanosomes, particles formed in melanocytes from where they are transferred to the surrounding keratinocytes. The size, number, and arrangement of the melanosomes varies between racial groups, but while the number of melanocytes can vary between different body regions, their numbers remain the same in individual body regions in all human beings. In white and oriental skin the melanosomes are packed in "aggregates", but in black skin they are larger and distributed more evenly. The number of melanosomes in the keratinocytes increases with UV radiation exposure, while their distribution remain largely unaffected. [17]
Culture
Laboratory culture of keratinocytes to form a 3D structure (artificial skin) recapitulating most of the properties of the epidermis is routinely used as a tool for drug development and testing.
Additional images
Epidermis and dermis of human skin
Epidermis (skin)
266
Cross-section of all skin layers
Optical coherence tomography of fingertip
References
[1] James, William; Berger, Timothy; Elston, Dirk (2005) Andrews' Diseases of the Skin: Clinical Dermatology (10th ed.). Saunders. Page 2-3. ISBN 0-7216-2921-0. [2] http:/ / archderm. ama-assn. org/ cgi/ reprint/ 120/ 3/ 324. pdf [3] TheFreeDictionary > rete ridge (http:/ / medical-dictionary. thefreedictionary. com/ rete+ ridge) Citing: The American Heritage Medical Dictionary Copyright 2007, 2004 [4] The Ageing Skin - Structure (http:/ / pharmaxchange. info/ press/ 2011/ 03/ the-ageing-skin-part-1-structure-of-skin-and-introduction/ ) [5] http:/ / www. radcliffe-oxford. com/ books/ samplechapter/ 7750/ 01_bensouillah-241a6c80rdz. pdf [13] http:/ / onlinelibrary. wiley. com/ doi/ 10. 1021/ js950219p/ abstract
Stem cell
267
Stem cell
Stem cell
Mouse embryonic stem cells with fluorescent marker
Human embryonic stem cell colony on mouse embryonic fibroblast feeder layer Latin Code cellula precursoria TH H2.00.01.0.00001
Stem cells are biological cells found in all multicellular organisms, that can divide (through mitosis) and differentiate into diverse specialized cell types and can self-renew to produce more stem cells. In mammals, there are two broad types of stem cells: embryonic stem cells, which are isolated from the inner cell mass of blastocysts, and adult stem cells, which are found in various tissues. In adult organisms, stem cells and progenitor cells act as a repair system for the body, replenishing adult tissues. In a developing embryo, stem cells can differentiate into all the specialized cells (these are called pluripotent cells), but also maintain the normal turnover of regenerative organs, such as blood, skin, or intestinal tissues. There are three accessible sources of autologous adult stem cells in humans: 1. Bone marrow, which requires extraction by harvesting, that is, drilling into bone (typically the femur or iliac crest), 2. Adipose tissue (lipid cells), which requires extraction by liposuction, and 3. Blood, which requires extraction through pheresis, wherein blood is drawn from the donor (similar to a blood donation), passed through a machine that extracts the stem cells and returns other portions of the blood to the donor. Stem cells can also be taken from umbilical cord blood just after birth. Of all stem cell types, autologous harvesting involves the least risk. By definition, autologous cells are obtained from one's own body, just as one may bank his or her own blood for elective surgical procedures. Highly plastic adult stem cells are routinely used in medical therapies, for example in bone marrow transplantation. Stem cells can now be artificially grown and transformed (differentiated) into specialized cell types with
Stem cell characteristics consistent with cells of various tissues such as muscles or nerves through cell culture. Embryonic cell lines and autologous embryonic stem cells generated through therapeutic cloning have also been proposed as promising candidates for future therapies.[1] Research into stem cells grew out of findings by Ernest A. McCulloch and James E. Till at the University of Toronto in the 1960s.[2][3]
268
Properties
The classical definition of a stem cell requires that it possess two properties: • Self-renewal: the ability to go through numerous cycles of cell division while maintaining the undifferentiated state. • Potency: the capacity to differentiate into specialized cell types. In the strictest sense, this requires stem cells to be either totipotent or pluripotent—to be able to give rise to any mature cell type, although multipotent or unipotent progenitor cells are sometimes referred to as stem cells. Apart from this it is said that stem cell function is regulated in a feed back mechanism.
Self-renewal
Two mechanisms exist to ensure that a stem cell population is maintained: 1. Obligatory asymmetric replication: a stem cell divides into one father cell that is identical to the original stem cell, and another daughter cell that is differentiated 2. Stochastic differentiation: when one stem cell develops into two differentiated daughter cells, another stem cell undergoes mitosis and produces two stem cells identical to the original.
Potency definitions
Potency specifies the differentiation potential (the potential to differentiate into different cell types) of the stem cell.[] • Totipotent (a.k.a. omnipotent) stem cells can differentiate into embryonic and extraembryonic cell types. Such cells can construct a complete, viable organism.[] These cells are produced from the fusion of an egg and sperm cell. Cells produced by the first few divisions of the fertilized egg are also totipotent.[4] • Pluripotent stem cells are the descendants of totipotent cells and can differentiate into nearly all cells,[] i.e. cells derived from any of the three germ layers.[5] • Multipotent stem cells can differentiate into a number of cells, but only those of a closely related family of cells.[]
Pluripotent, embryonic stem cells originate as inner cell mass (ICM) cells within a blastocyst. These stem cells can become any tissue in the body, excluding a placenta. Only cells from an earlier stage of the embryo, known as the morula, are totipotent, able to become all tissues in the body and the extraembryonic placenta.
Stem cell • Oligopotent stem cells can differentiate into only a few cells, such as lymphoid or myeloid stem cells.[] • Unipotent cells can produce only one cell type, their own,[] but have the property of self-renewal, which distinguishes them from non-stem cells (e.g., muscle stem cells).
269
Identification
The practical definition of a stem cell is the functional definition—a cell that has the potential to regenerate tissue over a lifetime. For example, the defining test for a bone marrow or hematopoietic stem cell (HSC) is the ability to transplant one cell and save an individual without HSCs. In this case, a stem cell must be able to produce new blood cells and immune cells over a long term, demonstrating potency. It should also be possible to isolate stem cells from the transplanted individual, which can themselves be transplanted into another individual without HSCs, demonstrating that the stem cell was able to self-renew. Properties of stem cells can be illustrated in vitro, using methods such as clonogenic assays, in which single cells are assessed for their ability to differentiate and self-renew.[6][7] Stem cells can also be isolated by their possession of a distinctive set of cell surface markers. However, in vitro culture conditions can alter the behavior of cells, making it unclear whether the cells will behave in a similar manner in vivo. There is considerable debate as to whether some proposed adult cell populations are truly stem cells.
Human embryonic stem cells A: Cell colonies that are not yet differentiated. B: Nerve cell
Embryonic
Embryonic stem (ES) cell lines are cultures of cells derived from the epiblast tissue of the inner cell mass (ICM) of a blastocyst or earlier morula stage embryos.[8] A blastocyst is an early stage embryo—approximately four to five days old in humans and consisting of 50–150 cells. ES cells are pluripotent and give rise during development to all derivatives of the three primary germ layers: ectoderm, endoderm and mesoderm. In other words, they can develop into each of the more than 200 cell types of the adult body when given sufficient and necessary stimulation for a specific cell type. They do not contribute to the extra-embryonic membranes or the placenta. The endoderm is composed of the entire gut tube and the lungs, the ectoderm gives rise to the nervous system and skin, and the mesoderm gives rise to muscle, bone, blood—in essence, everything else that connects the endoderm to the ectoderm. Nearly all research to date has made use of mouse embryonic stem cells (mES) or human embryonic stem cells (hES). Both have the essential stem cell characteristics, yet they require very different environments in order to maintain an undifferentiated state. Mouse ES cells are grown on a layer of gelatin as an extracellular matrix (for support) and require the presence of leukemia inhibitory factor (LIF).[9] Human ES cells are grown on a feeder layer of mouse embryonic fibroblasts (MEFs) and require the presence of basic fibroblast growth factor (bFGF or FGF-2).[10] Without optimal culture conditions or genetic manipulation,[11] embryonic stem cells will rapidly differentiate. A human embryonic stem cell is also defined by the expression of several transcription factors and cell surface proteins. The transcription factors Oct-4, Nanog, and Sox2 form the core regulatory network that ensures the
Stem cell suppression of genes that lead to differentiation and the maintenance of pluripotency.[12] The cell surface antigens most commonly used to identify hES cells are the glycolipids stage specific embryonic antigen 3 and 4 and the keratan sulfate antigens Tra-1-60 and Tra-1-81. The molecular definition of a stem cell includes many more proteins and continues to be a topic of research.[13] There are currently no approved treatments using embryonic stem cells. The first human trial was approved by the US Food and Drug Administration in January 2009.[14] However, the human trial was not initiated until October 13, 2010 in Atlanta for spinal injury victims. On November 14, 2011 the company conducting the trial announced that it will discontinue further development of its stem cell programs.[15] ES cells, being pluripotent cells, require specific signals for correct differentiation—if injected directly into another body, ES cells will differentiate into many different types of cells, causing a teratoma. Differentiating ES cells into usable cells while avoiding transplant rejection are just a few of the hurdles that embryonic stem cell researchers still face.[16] Many nations currently have moratoria on either ES cell research or the production of new ES cell lines. Because of their combined abilities of unlimited expansion and pluripotency, embryonic stem cells remain a theoretically potential source for regenerative medicine and tissue replacement after injury or disease.
270
Fetal
The primitive stem cells located in the organs of fetuses are referred to as fetal stem cells.[]
Adult
Stem cell
271
Also known as somatic (from Greek Σωματικóς, "of the body") stem cells and germline (giving rise to gametes) stem cells, they can be found in children, as well as adults.[17] Pluripotent adult stem cells are rare and generally small in number but can be found in a number of tissues including umbilical cord blood.[18] Bone marrow has been found to be one of the rich sources of adult stem cells [19] which have been used in treating several conditions including Spinal cord injury,[20] Liver Cirrhosis,[21] Chronic Limb Ischemia [22] and Endstage heart failure.[23] The bone marrow stem cell quantity has been found to be declining with age and in reproductive age group of females it is relatively lesser than in males of same age group.[24] A great deal of adult stem cell research to date has had the aim of characterizing the capacity of the cells to divide or self-renew indefinitely and their differentiation potential.[25] In mice, pluripotent stem cells are directly generated from adult fibroblast cultures. Unfortunately, many mice do not live long with stem cell organs.[] Most adult stem cells are lineage-restricted (multipotent) and are generally referred to by their tissue origin (mesenchymal stem cell, adipose-derived stem cell, endothelial stem cell, dental pulp stem cell, etc.).[26][27] Adult stem cell treatments have been successfully used for many years to treat leukemia and related bone/blood cancers through bone marrow transplants.[28] Adult stem cells are also used in veterinary medicine to treat tendon and ligament injuries in horses.[29]
Stem cell division and differentiation. A: stem cell; B: progenitor cell; C: differentiated cell; 1: symmetric stem cell division; 2: asymmetric stem cell division; 3: progenitor division; 4: terminal differentiation
The use of adult stem cells in research and therapy is not as controversial as the use of embryonic stem cells, because the production of adult stem cells does not require the destruction of an embryo. Additionally, in instances where adult stem cells are obtained from the intended recipient (an autograft), the risk of rejection is essentially non-existent. Consequently, more US government funding is being provided for adult stem cell research.[30] An extremely rich source for adult mesenchymal stem cells is the developing tooth bud of the mandibular third molar.[31] The stem cells eventually form enamel (ectoderm), dentin, periodontal ligament, blood vessels, dental pulp, nervous tissues, and a minimum of 29 different end organs. Because of extreme ease in collection at 8–10 years of age before calcification and minimal to no morbidity, these will probably constitute a major source of cells for personal banking, research and current or future therapies. These stem cells have been shown capable of producing hepatocytes.[citation needed]
Amniotic
Multipotent stem cells are also found in amniotic fluid. These stem cells are very active, expand extensively without feeders and are not tumorigenic. Amniotic stem cells are multipotent and can differentiate in cells of adipogenic, osteogenic, myogenic, endothelial, hepatic and also neuronal lines.[32] All over the world, universities and research institutes are studying amniotic fluid to discover all the qualities of amniotic stem cells, and scientists such as Anthony Atala[33][34] and Giuseppe Simoni [35][36] have discovered important results. Use of stem cells from amniotic fluid overcomes the ethical objections to using human embryos as a source of cells. Roman Catholic teaching forbids the use of embryonic stem cells in experimentation; accordingly, the Vatican newspaper "Osservatore Romano" called amniotic stem cells "the future of medicine".[37]
Stem cell It is possible to collect amniotic stem cells for donors or for autologuous use: the first US amniotic stem cells bank [38][39] was opened in 2009 in Medford, MA, by Biocell Center Corporation[40][41][42] and collaborates with various hospitals and universities all over the world.[43]
272
Cord blood
A certain kind of cord blood stem cell (CB-SC) is multipotent and displays embryonic and hematopoietic characteristics. Phenotypic characterization demonstrates that (CB-SCs) display embryonic cell markers (e.g., transcription factors OCT-4 and Nanog, stage-specific embryonic antigen (SSEA)-3, and SSEA-4) and leukocyte common antigen CD45, but that they are negative for blood cell lineage markers (e.g., CD1a, CD3, CD4, CD8, CD11b, CD11c, CD13, CD14, CD19, CD20, CD34, CD41a, CD41b, CD83, CD90, CD105, and CD133).[44][] Additionally, CB-SCs display very low immunogenicity as indicated by expression of a very low level of major histocompatibility complex (MHC) antigens and failure to stimulate the proliferation of allogeneic lymphocytes.[44][45] They can give rise to three embryonic layer-derived cells in the presence of different inducers.[44][] More specifically, CB-SCs tightly adhere to culture dishes with a large rounded morphology and are resistant to common detaching methods (trypsin/EDTA).[44][45][] CB-SCs are the active agent in stem cell educator therapy, which has therapeutic potential against autoimmune diseases like type 1 diabetes according to studies by Yong Zhao et al.[][46][47][48]Wikipedia:Identifying reliable sources (medicine)
Induced pluripotent
These are not adult stem cells, but rather adult cells (e.g. epithelial cells) reprogrammed to give rise to pluripotent capabilities. Using genetic reprogramming with protein transcription factors, pluripotent stem cells equivalent to embryonic stem cells have been derived from human adult skin tissue.[][49][50] Shinya Yamanaka and his colleagues at Kyoto University used the transcription factors Oct3/4, Sox2, c-Myc, and Klf4[] in their experiments on cells from human faces. Junying Yu, James Thomson, and their colleagues at the University of Wisconsin–Madison used a different set of factors, Oct4, Sox2, Nanog and Lin28,[] and carried out their experiments using cells from human foreskin. As a result of the success of these experiments, Ian Wilmut, who helped create the first cloned animal Dolly the Sheep, has announced that he will abandon somatic cell nuclear transfer as an avenue of research.[51] Frozen blood samples can be used as a source of induced pluripotent stem cells, opening a new avenue for obtaining the valued cells.[52]
Lineage
To ensure self-renewal, stem cells undergo two types of cell division (see Stem cell division and differentiation diagram). Symmetric division gives rise to two identical daughter cells both endowed with stem cell properties. Asymmetric division, on the other hand, produces only one stem cell and a progenitor cell with limited self-renewal potential. Progenitors can go through several rounds of cell division before terminally differentiating into a mature cell. It is possible that the molecular distinction between symmetric and asymmetric divisions lies in differential segregation of cell membrane proteins (such as receptors) between the daughter cells.[53] An alternative theory is that stem cells remain undifferentiated due to environmental cues in their particular niche. Stem cells differentiate when they leave that niche or no longer receive those signals. Studies in Drosophila germarium have identified the signals decapentaplegic and adherens junctions that prevent germarium stem cells from differentiating.[54][55]
Stem cell The signals that lead to reprogramming of cells to an embryonic-like state are also being investigated. These signal pathways include several transcription factors including the oncogene c-Myc. Initial studies indicate that transformation of mice cells with a combination of these anti-differentiation signals can reverse differentiation and may allow adult cells to become pluripotent.[] However, the need to transform these cells with an oncogene may prevent the use of this approach in therapy. Challenging the terminal nature of cellular differentiation and the integrity of lineage commitment, it was recently determined that the somatic expression of combined transcription factors can directly induce other defined somatic cell fates; researchers identified three neural-lineage-specific transcription factors that could directly convert mouse fibroblasts (skin cells) into fully functional neurons. This "induced neurons" (iN) cell research inspires the researchers to induce other cell types. It implies that all cells are totipotent: with the proper tools, all cells may form all kinds of tissue.[56]
273
Treatments
Medical researchers believe that stem cell therapy has the potential to dramatically change the treatment of human disease. A number of adult stem cell therapies already exist, particularly bone marrow transplants that are used to treat leukemia.[58] In the future, medical researchers anticipate being able to use technologies derived from stem cell research to treat a wider variety of diseases including cancer, Parkinson's disease, spinal cord injuries, Amyotrophic lateral sclerosis, multiple sclerosis, and muscle damage, amongst a number of other impairments and conditions.[59][60] However, there still [57] Diseases and conditions where stem cell treatment is promising or emerging. Bone exists a great deal of social and marrow transplantation is, as of 2009, the only established use of stem cells. scientific uncertainty surrounding stem cell research, which could possibly be overcome through public debate and future research, and further education of the public. One concern of treatment is the risk that transplanted stem cells could form tumors and become cancerous if cell division continues uncontrollably.[61] Stem cells are widely studied, for their potential therapeutic use and for their inherent interest.[62] Supporters of embryonic stem cell research argue that such research should be pursued because the resultant treatments could have significant medical potential. It has been proposed that surplus embryos created for in vitro fertilization could be donated with consent and used for the research. The recent development of iPS cells has been called a bypass of the legal controversy. Laws limiting the destruction of human embryos have been credited for being the reason for development of iPS cells, but it is still not completely clear whether hiPS cells are equivalent to hES cells. Recent work demonstrates hotspots of aberrant epigenomic reprogramming in hiPS cells (Lister, R., et al., 2011).
Stem cell
274
Toxicity screening
Hepatotoxicity and drug-induced liver injury account for a substantial number of failures of new drugs in development and market withdrawal, highlighting the need for screening assays such as stem cell-derived hepatocyte-like cells, that are capable of detecting toxicity early in the drug development process.[]
Research patents
The patents covering a lot of work on human embryonic stem cells are owned by the Wisconsin Alumni Research Foundation (WARF). WARF does not charge academics to study human stem cells but does charge commercial users. WARF sold Geron Corp. exclusive rights to work on human stem cells but later sued Geron Corp. to recover some of the previously sold rights. The two sides agreed that Geron Corp. would keep the rights to only three cell types. In 2001, WARF came under public pressure to widen access to human stem-cell technology.[63] A request for reviewing the WARF patents 5,843,780; 6,200,806; 7,029,913 US Patent and Trademark Office were filed by non-profit patent-watchdogs The Foundation for Taxpayer & Consumer Rights [64], and the Public Patent Foundation as well as molecular biologist Jeanne Loring of the Burnham Institute. According to them, two of the patents granted to WARF are invalid because they cover a technique published in 1993 for which a patent had already been granted to an Australian researcher. Another part of the challenge states that these techniques, developed by James A. Thomson, are rendered obvious by a 1990 paper and two textbooks. Based on this challenge, patent 7,029,913 was rejected in 2010. The two remaining hES WARF patents are due to expire in 2015. The outcome of this legal challenge is particularly relevant to the Geron Corp. as it can only license patents that are upheld.[64]
Key research events
• 1908: The term "stem cell" was proposed for scientific use by the Russian histologist Alexander Maksimov (1874–1928) at congress of hematologic society in Berlin. It postulated existence of haematopoietic stem cells. • 1960s: Joseph Altman and Gopal Das present scientific evidence of adult neurogenesis, ongoing stem cell activity in the brain; their reports contradict Cajal's "no new neurons" dogma and are largely ignored. • 1963: McCulloch and Till illustrate the presence of self-renewing cells in mouse bone marrow. • 1968: Bone marrow transplant between two siblings successfully treats SCID. • 1978: Haematopoietic stem cells are discovered in human cord blood. • 1981: Mouse embryonic stem cells are derived from the inner cell mass by scientists Martin Evans, Matthew Kaufman, and Gail R. Martin. Gail Martin is attributed for coining the term "Embryonic Stem Cell". • 1992: Neural stem cells are cultured in vitro as neurospheres. • 1997: Leukemia is shown to originate from a haematopoietic stem cell, the first direct evidence for cancer stem cells. • 1998: James Thomson and coworkers derive the first human embryonic stem cell line at the University of Wisconsin–Madison.[] • 1998: John Gearhart (Johns Hopkins University) extracted germ cells from fetal gonadal tissue (primordial germ cells) before developing pluripotent stem cell lines from the original extract. • 2000s: Several reports of adult stem cell plasticity are published. • 2001: Scientists at Advanced Cell Technology clone first early (four- to six-cell stage) human embryos for the purpose of generating embryonic stem cells.[65] • 2003: Dr. Songtao Shi of NIH discovers new source of adult stem cells in children's primary teeth.[66] • 2004–2005: Korean researcher Hwang Woo-Suk claims to have created several human embryonic stem cell lines from unfertilised human oocytes. The lines were later shown to be fabricated.
Stem cell • 2005: Researchers at Kingston University in England claim to have discovered a third category of stem cell, dubbed cord-blood-derived embryonic-like stem cells (CBEs), derived from umbilical cord blood. The group claims these cells are able to differentiate into more types of tissue than adult stem cells. • 2005: Researchers at UC Irvine's Reeve-Irvine Research Center are able to partially restore the ability of rats with paralyzed spines to walk through the injection of human neural stem cells.[67] • April 2006 Scientists at the University of Illinois at Chicago identified novel stem cells from the umbilical cord blood with embryonic and hematopoietic characteristics.[44] • August 2006: Mouse Induced pluripotent stem cells: the journal Cell publishes Kazutoshi Takahashi and Shinya Yamanaka.[68] • November 2006: Yong Zhao et al. revealed the immune regulation of T lymphocytes by Cord Blood-Derived Multipotent Stem Cells (CB-SCs).[45] • October 2006: Scientists at Newcastle University in England create the first ever artificial liver cells using umbilical cord blood stem cells.[69][70]
275
• January 2007: Scientists at Wake Forest University led by Dr. Anthony Atala and Harvard University report discovery of a new type of stem cell in amniotic fluid.[71] This may potentially provide an alternative to embryonic stem cells for use in research and therapy.[72]
Yong Zhao, University of Illinois at Chicago
• June 2007: Research reported by three different groups shows that normal skin cells can be reprogrammed to an embryonic state in mice.[73] In the same month, scientist Shoukhrat Mitalipov reports the first successful creation of a primate stem cell line through somatic cell nuclear transfer[74] • October 2007: Mario Capecchi, Martin Evans, and Oliver Smithies win the 2007 Nobel Prize for Physiology or Medicine for their work on embryonic stem cells from mice using gene targeting strategies producing genetically engineered mice (known as knockout mice) for gene research.[] • November 2007: Human induced pluripotent stem cells: Two similar papers released by their respective journals prior to formal publication: in Cell by Kazutoshi Takahashi and Shinya Yamanaka, "Induction of pluripotent stem cells from adult human fibroblasts by defined factors",[75] and in Science by Junying Yu, et al., from the research group of James Thomson, "Induced pluripotent stem cell lines derived from human somatic cells":[76] pluripotent stem cells generated from mature human fibroblasts. It is possible now to produce a stem cell from almost any other human cell instead of using embryos as needed previously, albeit the risk of tumorigenesis due to c-myc and retroviral gene transfer remains to be determined. • January 2008: Robert Lanza and colleagues at Advanced Cell Technology and UCSF create the first human embryonic stem cells without destruction of the embryo[77]
Martin Evans, a co-winner of the Nobel Prize in recognition of his gene targeting work.
• January 2008: Development of human cloned blastocysts following somatic cell nuclear transfer with adult fibroblasts[78] • February 2008: Generation of pluripotent stem cells from adult mouse liver and stomach: these iPS cells seem to be more similar to embryonic stem cells than the previously developed iPS cells and not tumorigenic, moreover genes that are required for iPS cells do not need to be inserted into specific sites, which encourages the development of non-viral reprogramming techniques.[79]
Stem cell • March 2008-The first published study of successful cartilage regeneration in the human knee using autologous adult mesenchymal stem cells is published by clinicians from Regenerative Sciences[80] • October 2008: Sabine Conrad and colleagues at Tübingen, Germany generate pluripotent stem cells from spermatogonial cells of adult human testis by culturing the cells in vitro under leukemia inhibitory factor (LIF) supplementation.[81] • 30 October 2008: Embryonic-like stem cells from a single human hair.[82] • January 2009: Yong Zhao and colleagues confirmed the reversal of autoimmune-caused type 1 diabetes by Cord Blood-Derived Multipotent Stem Cells (CB-SCs) in an animal experiment.[][46] • 1 March 2009: Andras Nagy, Keisuke Kaji, et al. discover a way to produce embryonic-like stem cells from normal adult cells by using a novel "wrapping" procedure to deliver specific genes to adult cells to reprogram them into stem cells without the risks of using a virus to make the change.[83][84][85] The use of electroporation is said to allow for the temporary insertion of genes into the cell.[86][87][88][89] • 28 May 2009 Kim et al. announced that they had devised a way to manipulate skin cells to create patient specific "induced pluripotent stem cells" (iPS), claiming it to be the 'ultimate stem cell solution'.[90] • 11 October 2010 First trial of embryonic stem cells in humans.[91] • 25 October 2010: Ishikawa et al. write in the Journal of Experimental Medicine that research shows that transplanted cells that contain their new host's nuclear DNA could still be rejected by the invidual's immune system due to foreign mitochondrial DNA. Tissues made from a person's stem cells could therefore be rejected, because mitochondrial genomes tend to accumulate mutations.[92] • 2011: Israeli scientist Inbar Friedrich Ben-Nun led a team which produced the first stem cells from endangered species, a breakthrough that could save animals in danger of extinction.[93] • January 2012: The human clinical trial of treating type 1 diabetes with lymphocyte modification using Cord Blood-Derived Multipotent Stem Cells (CB-SCs) achieved an improvement of C-peptide levels, reduced the median glycated hemoglobin A1C (HbA1c) values, and decreased the median daily dose of insulin in both human patient groups with and without residual beta cell function.[47][48] Yong Zhao's Stem Cell Educator Therapy appears "so simple and so safe"[94] • 2012: Katsuhiko Hayashi et al. reported in the Journal Science that they used mouse skin cells to create stem cells and then used these stem cells to create mouse eggs. These eggs were then fertilized and produced healthy baby offspring. These latter mice were able to have their own babies.[95]
276
References
[51] "His inspiration comes from the research by Prof Shinya Yamanaka at Kyoto University, which suggests a way to create human embryo stem cells without the need for human eggs, which are in extremely short supply, and without the need to create and destroy human cloned embryos, which is bitterly opposed by the pro life movement." [52] Frozen blood a source of stem cells, study finds (http:/ / web. archive. org/ web/ 20100703175036/ http:/ / www. newsdaily. com/ stories/ tre6604si-us-stemcells-frozen/ ). newsdaily.com (2010-07-01) [57] Diabetes, rheumatoid arthritis, Parkinson's, Alzheimer's disease, osteoarthritis: • Cell Basics: What are the potential uses of human stem cells and the obstacles that must be overcome before these potential uses will be realized? (http:/ / stemcells. nih. gov/ info/ basics/ basics6Stem). In Stem Cell Information World Wide Web site. Bethesda, MD: National Institutes of Health, U.S. Department of Health and Human Services, 2009. cited Sunday, April 26, 2009
Stroke and traumatic brain injury repair:
• Stem Cells Tapped to Replenish Organs (http:/ / www. mult-sclerosis. org/ news/ Dec2000/ StemCellDebatePartII. html) thescientist.com, Nov 2000. By Douglas Steinberg
Learning defects:
• ISRAEL21c: Israeli scientists reverse brain birth defects using stem cells (http:/ / www. israel21c. org/ health/ israeli-scientists-reverse-brain-birth-defects-using-stem-cells) December 25, 2008. (Researchers from the Hebrew University of Jerusalem-Hadassah Medical led by Prof. Joseph Yanai)
Spinal cord injury repair:
Stem cell Heart infarction: Anti-cancer:
• thescientist.com, Nov 2000. By Douglas Steinberg
277
Baldness:
• Hair Cloning Nears Reality as Baldness Cure (http:/ / web. archive. org/ web/ 20080530042215rn_3/ www. webmd. com/ skin-problems-and-treatments/ hair-loss/ news/ 20041104/ hair-cloning-nears-reality-as-baldness-cure) WebMD November 2004
Replace missing teeth: Repair hearing:
• Gene therapy is first deafness 'cure' – health – 14 February 2005 – New Scientist (http:/ / www. newscientist. com/ article/ dn7003)
Restore vision:
• BBC NEWS | England | Southern Counties | Stem cells used to restore vision (http:/ / news. bbc. co. uk/ 1/ hi/ england/ southern_counties/ 4495419. stm)
Amyotrophic lateral sclerosis:
• Drs. Gearhart and Kerr of Johns Hopkins University. April 4, 2001 edition of JAMA (Vol. 285, 1691–1693)
Crohn's disease: Wound healing:
[61] "Stem-cell therapy: Promise and reality." Consumer Reports on Health 17.6 (2005): 8–9. Academic Search Premier. EBSCO. Web. 5 Apr. 2010. [63] Regalado, Antonio, David P. Hamilton (July 2006). "How a University's Patents May Limit Stem-Cell Researcher." (http:/ / www. geneticsandsociety. org/ article. php?id=1896) The Wall Street Journal. Retrieved on July 24, 2006. [64] Kintisch, Eli (2006-07-18) "Groups Target Stem Cell Patents." (http:/ / news. sciencemag. org/ sciencenow/ 2006/ 07/ 18-02. html) ScienceNOW Daily News. Retrieved August 15, 2006. [90] (cited in lay summary, not read) [93] Shtull-Trauring, Asaf (2011-09-06) Israeli scientist leads breakthrough stem cell research on endangered species (http:/ / www. haaretz. com/ print-edition/ news/ israeli-scientist-leads-breakthrough-stem-cell-research-on-endangered-species-1. 382754)
External links
General • Stem Cell Basics (http://stemcells.nih.gov/info/basics/) • Nature Reports Stem Cells: Introductory material, research advances and debates concerning stem cell research. (http://www.nature.com/stemcells) • Understanding Stem Cells: A View of the Science and Issues from the National Academies (http://dels.nas.edu/ bls/stemcells/booklet.shtml) • Scientific American Magazine (June 2004 Issue) The Stem Cell Challenge (http://www.scientificamerican. com/article.cfm?id=the-stem-cell-challenge) • Scientific American Magazine (July 2006 Issue) Stem Cells: The Real Culprits in Cancer? (http://www. scientificamerican.com/article.cfm?id=stem-cells-the-real-culpr-2006-07) • Ethics of Stem Cell Research (http://plato.stanford.edu/entries/stem-cells) entry by Andrew Siegel in the Stanford Encyclopedia of Philosophy • Isolation of amniotic stem cell lines with potential for therapy (http://www.nature.com/nbt/journal/v25/n1/ abs/nbt1274.html) • Children's Hospital Stem Cell Research (http://stemcell.childrenshospital.org) • Stem Cell Research and Industry Directory (http://stemcelllist.com) • Corneal endothelial and epithelial stem cell research and application (http://www.cesbank.org) • Stem Cell Consumer Progress and Research (http://www.stemcelltelevision.com) Peer-reviewed journals • Cytotherapy (http://www.tandf.co.uk/journals/titles/14653249.asp)
Stem cell • • • • • Cloning and Stem Cells (http://www.liebertpub.com/products/product.aspx?pid=9) Journal of Stem Cells and Regenerative Medicine (http://www.pubstemcell.com) Stem Cells and Development (http://www.liebertpub.com/products/product.aspx?pid=125) Regenerative Medicine (http://www.futuremedicine.com/loi/rme) Stem Cell Research (http://www.elsevier.com/wps/find/journaldescription.cws_home/711630/ description#description) • StemBook (http://www.stembook.org)
278
Huxley's layer
279
Huxley's layer
Huxley's layer
Transverse section of hair follicle. Gray's subject #234 1068
[1]
The second layer of the inner root sheath of the hair consists of one or two layers of horny, flattened, nucleated cells, known as Huxley's layer.
Henle's layer
280
Henle's layer
Henle's layer
Transverse section of hair follicle. Gray's subject #234 1068
[1]
Henle's layer is the third layer of the inner root sheath of the hair, consisting of a single layer of cubical cells with clear flattened nuclei. It is named after German physician, pathologist and anatomist Friedrich Gustav Jakob Henle.
External links
• synd/649 [1] at Who Named It? This article incorporates text from a public domain edition of Gray's Anatomy.
Trichocyte (human)
In mammals, trichocytes are the specialized epithelial cells from which the highly mechanically resilient tissues hair and nails are formed. They can be identified by the fact that they express "hard", "trichocyte" or "hair" keratin proteins.[1] These are modified keratins containing large amounts of the amino acid cysteine, which facilitates chemical cross-linking of these proteins to form the tough material from which hair and nail is composed. These cells give rise to non-hair non-keratinized IRSC (inner root sheath cell) as well.
References
Epithelium
281
Epithelium
Epithelium
Latin Epithelium Code TH H2.00.02.0.00001 [1]
Epithelium is one of the four basic types of animal tissue, along with connective tissue, muscle tissue and nervous tissue. Epithelial tissues line the cavities and surfaces of structures throughout the body, and also form many glands. Functions of epithelial cells include secretion, selective absorption, protection, transcellular transport and detection of sensation. In Greek "ἐπί" ("epi") means "on" or "upon", and "θηλή" ("thēlē") means "nipple".[1] Epithelial layers are avascular, so they must receive nourishment via diffusion of substances from the underlying connective tissue, through the basement membrane.[][2] Epithelia can also be organized into clusters of cells that function as exocrine and endocrine glands.
Structure
Cells in epithelium are very densely packed together like bricks in a wall, leaving very little intercellular space. The cells can form continuous sheets which are attached to each other at many locations by adherens junctions, tight junctions and desmosomes.[]
Basement membrane
All epithelial cells rest on a basement membrane, which acts as a scaffolding on which epithelium can grow and regenerate after injuries.[3] Epithelial tissue is innervated, but avascular. This epithelial tissue must be nourished by substances diffusing from the blood vessels in the underlying tissue, but they don't have their own blood supply. The basement membrane acts as a selectively permeable membrane that determines which substances will be able to enter the epithelium.[][2]
Cell junctions
Cell junctions are especially abundant in epithelial tissues. They consist of protein complexes and provide contact between neighbouring cells, between a cell and the extracellular matrix, or they build up the paracellular barrier of epithelia and control the paracellular transport.[citation needed] Cell junctions are the contact points between plasma membrane and tissue cells. There are mainly 5 different types of cell junctions. They are tight junctions, adherens junctions, desmosomes, hemidesmosomes, and gap junctions. Tight junctions are a pair of trans-membranar protein fused on outer plasma membrane. Adherens junctions are a plaque (protein layer on the inside plasma membrane) which attaches both cells' microfilaments. Desmosomes attach to the microfilaments of cytoskeleton made up of keratin protein. Hemidesmosomes resemble desmosomes on a section. They are made up of the integrin (a transmembraner protein) instead of cadherin. They attach the epithelial cell to the basement membrane. Gap junctions connect the cytoplasm of two cells and are made up of proteins called connexins (six of which come together to make a connexon).
Epithelium
282
Classification
Tissues are generally classified by the morphology of their cells, and the number of layers they are composed of.[][][4] Epithelial tissue that is only one cell thick is known as simple epithelium.[5] If it is two or more cells thick, it is known as stratified epithelium.[6] However, when taller simple epithelial cells (see columnar, Types of epithelium below) are viewed in cross section with several nuclei appearing at different heights, they can be confused with stratified epithelia. This kind of epithelium is therefore described as "pseudostratified" epithelium.[7] There are three principal morphologies associated with epithelial cells. Squamous epithelium has cells which are wider than they are tall (flat and scale-like). Cuboidal epithelium has cells whose height and width are approximately the same (cube shaped). Columnar epithelium has cells taller than they are wide (column shaped). In addition, the morphology of the cells in transitional epithelium may vary from squamous to cuboidal, depending on the amount of tension on the epithelium.[8]
Simple epithelium
Simple epithelium is one cell thick, that is, every cell is in direct contact with the underlying basement membrane. It is generally found where absorption and filtration occur. The thinness of the epithelial barrier facilitates these processes.[] Simple epithelial tissues are generally classified by the shape of their cells. The four major classes of simple epithelium are: (1) simple squamous; (2) simple cuboidal; (3) simple columnar; (4) pseudostratified.[] Simple squamous epithelium is found lining areas where passive diffusion of gases occur, including the walls of capillaries, the linings of the alveoli of the lungs, and the linings of the pericardial, pleural, and peritoneal cavities.
Functions
The primary functions of epithelial tissues are: (1) to protect the tissues that lie beneath it from radiation, desiccation, toxins, invasion by pathogens, and physical trauma; (2) the regulation and exchange of chemicals between the underlying tissues and a body cavity; (3) the secretion of hormones into the blood vascular system, and/or the secretion of sweat, mucus, enzymes, and other products that are delivered by ducts glandular epithelium;[9] (4) to provide sensation [11].
Secretory epithelia
As stated above, secretion is one major function of epithelial cells. Glands are formed from the invagination / infolding of epithelial cells and subsequent growth in the underlying connective tissue. There are two major classifications of glands: endocrine glands and exocrine glands. Endocrine glands secrete their product into the extracellular space where it is rapidly taken up by the blood vascular system. The exocrine glands secrete their products into a duct that then delivers the product to the lumen of an organ or onto the free surface of the epithelium. In arthropods, the integument, or external "skin", consists of a single layer of epithelial ectoderm from which arises the cuticle,[] an outer covering of chitin the rigidity of which varies as per its chemical composition.
Epithelium
283
Sensing the extracellular environment
"Some epithelial cells are ciliated, and they commonly exist as a sheet of polarised cells forming a tube or tubule with cilia projecting into the lumen." Primary cilia on epithelial cells provide chemosensation, thermosensation and mechanosensation of the extracellular environment by playing "a sensory role mediating specific signalling cues, including soluble factors in the external cell environment, a secretory role in which a soluble protein is released to have an effect downstream of the fluid flow, and mediation of fluid flow if the cilia are motile."[]
Embryological development
In general, there are epithelial tissues deriving from all of the embryological germ layers[citation needed]: • from ectoderm (e.g., the epidermis); • from endoderm (e.g., the lining of the gastrointestinal tract); • from mesoderm (e.g., the inner linings of body cavities). However, it is important to note that pathologists do not consider endothelium and mesothelium (both derived from mesoderm) to be true epithelium. This is because such tissues present very different pathology. For that reason, pathologists label cancers in endothelium and mesothelium sarcomas, whereas true epithelial cancers are called carcinomas. Also, the filaments that support these mesoderm-derived tissues are very distinct. Outside of the field of pathology, it is, in general, accepted that the epithelium arises from all three germ layers.[citation needed]
Growing in culture
When growing epithelium in culture, one can determine whether or not a particular cell is epithelial by examining its morphological characteristics. Epithelial cells tend to cluster together, and have a "characteristic tight pavementlike appearance". But this is not always the case, such as when the cells are derived from a tumor. In these cases, it is often necessary to use certain biochemical markers to make a positive identification. The intermediate filament proteins in the cytokeratin group are almost exclusively found in epithelial cells, and so are often used for this purpose.[10]
Location
Epithelium lines both the outside (skin) and the inside cavities and lumen of bodies. The outermost layer of our skin is composed of dead stratified squamous, keratinized epithelial cells.[citation needed] Tissues that line the inside of the mouth, the esophagus and part of the rectum are composed of nonkeratinized stratified squamous epithelium. Other surfaces that separate body cavities from the outside environment are lined by simple squamous, columnar, or pseudostratified epithelial cells. Other epithelial cells line the insides of the lungs, the gastrointestinal tract, the reproductive and urinary tracts, and make up the exocrine and endocrine glands. The outer surface of the cornea is covered with fast-growing, easily regenerated epithelial cells. Endothelium (the inner lining of blood vessels, the heart, and lymphatic vessels) is a specialized form of epithelium. Another type, mesothelium, forms the walls of the pericardium, pleurae, and peritoneum.[citation needed]
Epithelium
284
System circulatory digestive digestive digestive digestive digestive digestive digestive digestive digestive digestive
Tissue blood vessels ducts of submandibular glands attached gingiva dorsum of tongue hard palate oesophagus stomach small intestine large intestine rectum anus Simple squamous Stratified columnar
Epithelium
Subtype endothelium gastric epithelium intestinal epithelium intestinal epithelium -
Stratified squamous, keratinized Stratified squamous, keratinized Stratified squamous, keratinized Stratified squamous, non-keratinized Simple columnar, non-ciliated Simple columnar, non-ciliated Simple columnar, non-ciliated Simple columnar, non-ciliated Stratified squamous, non-keratinized superior to Hilton's white line Stratified squamous, keratinized inferior to Hilton's white line Simple columnar, non-ciliated Simple cuboidal Simple cuboidal Simple squamous Stratified squamous, keratinized Stratified cuboidal Simple squamous Simple cuboidal
digestive endocrine nervous lymphatic integumentary integumentary integumentary reproductive - female
gallbladder thyroid follicles ependyma lymph vessel skin - dead superficial layer sweat gland ducts mesothelium of body cavities ovaries
endothelium mesothelium germinal epithelium (female) germinal epithelium (male) -
reproductive - female reproductive - female reproductive - female reproductive - female reproductive - female reproductive - female reproductive - male
Fallopian tubes endometrium (uterus) cervix (endocervix) cervix (ectocervix) vagina labia majora tubuli recti
Simple columnar, ciliated Simple columnar, ciliated Simple columnar Stratified squamous, non-keratinized Stratified squamous, non-keratinized Stratified squamous, keratinized Simple cuboidal
reproductive - male reproductive - male reproductive - male reproductive - male reproductive - male reproductive - male (gland) reproductive - male (gland)
rete testis ductuli efferentes epididymis vas deferens ejaculatory duct bulbourethral glands
Simple cuboidal Pseudostratified columnar Pseudostratified columnar, with stereocilia Pseudostratified columnar Simple columnar Simple columnar
seminal vesicle
Pseudostratified columnar
-
Epithelium
285
oropharynx larynx larynx - True vocal cords trachea respiratory bronchioles cornea nose kidney - proximal convoluted tubule kidney - ascending thin limb Stratified squamous, non-keratinized Pseudostratified columnar, ciliated Stratified squamous, non-keratinized Pseudostratified columnar, ciliated Simple cuboidal Stratified squamous, non-keratinized Pseudostratified columnar Simple cuboidal, with microvilli respiratory epithelium respiratory epithelium corneal epithelium olfactory epithelium -
respiratory respiratory respiratory respiratory respiratory sensory sensory urinary
urinary urinary urinary urinary urinary urinary urinary urinary urinary urinary
Simple squamous
urothelium urothelium urothelium urothelium -
kidney - distal convoluted tubule Simple cuboidal, without microvilli kidney - collecting duct renal pelvis ureter urinary bladder prostatic urethra membranous urethra penile urethra external urethral orifice Simple cuboidal Transitional Transitional Transitional Transitional Pseudostratified columnar, non-ciliated Pseudostratified columnar, non-ciliated Stratified squamous
Additional images
Squamous Epithelium 100x
Human cheek cells (Nonkeratinized stratified squamous epithelium) 500x
Epithelium
286
References
Notes
[1] Epitheium at Wiktionary (http:/ / en. wiktionary. org/ wiki/ epithelium) [2] Freshney, 2002: p. 3 (http:/ / books. google. com/ books?id=KqKNxeWlU6MC& pg=PA3) [5] van Lommel, 2002: p. 94 (http:/ / books. google. com/ books?id=EvYjLNKLu9sC& pg=PA94) [6] van Lommel, 2002: p. 97 (http:/ / books. google. com/ books?id=EvYjLNKLu9sC& pg=PA97) [9] van Lommel, 2002: p. 91 (http:/ / books. google. com/ books?id=EvYjLNKLu9sC& pg=PA91) [10] Freshney, 2002: p. 9 (http:/ / books. google. com/ books?id=KqKNxeWlU6MC& pg=PA9)
Bibliography
• Freshney, R.I. (2002). "Introduction" (http://books.google.com/books?id=KqKNxeWlU6MC&pg=PA1). In Freshney, R. Ian & Freshney, Mary. Culture of epithelial cells. John Wiley & Sons. ISBN 978-0-471-40121-6. • van Lommel, Alfons T.L. (2002). From cells to organs: a histology textbook and atlas (http://books.google. com/books?id=EvYjLNKLu9sC). Springer. ISBN 978-1-4020-7257-4.
Further reading
• Green H (September 2008). "The birth of therapy with cultured cells". BioEssays 30 (9): 897–903. doi: 10.1002/bies.20797 (http://dx.doi.org/10.1002/bies.20797). PMID 18693268 (http://www.ncbi.nlm.nih. gov/pubmed/18693268). • Kefalides, Nicholas A. & Borel, Jacques P., ed. (2005). Basement membranes: cell and molecular biology (http:// books.google.com/books?id=RM-FVY47NEgC). Gulf Professional Publishing. ISBN 978-0-12-153356-4. • Nagpal R, Patel A, Gibson MC (March 2008). "Epithelial topology". BioEssays 30 (3): 260–6. doi: 10.1002/bies.20722 (http://dx.doi.org/10.1002/bies.20722). PMID 18293365 (http://www.ncbi.nlm.nih. gov/pubmed/18293365). • Yamaguchi Y, Brenner M, Hearing VJ (September 2007). "The regulation of skin pigmentation" (http://www. jbc.org/cgi/pmidlookup?view=long&pmid=17635904) (Review). J. Biol. Chem. 282 (38): 27557–61. doi: 10.1074/jbc.R700026200 (http://dx.doi.org/10.1074/jbc.R700026200). PMID 17635904 (http://www.ncbi. nlm.nih.gov/pubmed/17635904).
Squamous epithelial cell
287
Squamous epithelial cell
Squamous epithelial cell
Squamous epithelium is one of several types of epithelia. Code TH H2.00.02.0.01027
[1]
In anatomy, squamous epithelium (from Latin squama, "scale") is an epithelium characterised by its most superficial layer consisting of flat, scale-like cells called squamous epithelial cells. Epithelium may be composed of one layer of these cells, in which case it is referred to as simple squamous epithelium, or it may possess multiple layers, referred to then as stratified squamous epithelium. Both types perform differing functions, ranging from nutrient exchange to protection.[citation needed] Cancers of the squamous epithelium include squamous cell carcinoma, basal cell carcinoma, and other adnexal tumors.[citation needed] Squamous epithelial cells have a polygonal appearance when viewed from above.[1]
References External links
• Histology at KUMC epithel-epith02 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/epithel/ epith02.htm) Simple squamous epithelium of the glomerulus (kidney) • Diagrams of simple squamous epithelium (http://www.lima.ohio-state.edu/academics/biology/images/ anatomy/Simple Squamous Epithelium 400X.jpg) • Histology at KUMC epithel-epith12 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/epithel/ epith12.htm) Stratified squamous epithelium of the vagina • Histology at KUMC epithel-epith14 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/epithel/ epith14.htm) Stratified squamous epithelium of the skin (thin skin) • Histology at KUMC epithel-epith15 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/epithel/ epith15.htm) Stratified squamous epithelium of the skin (thick skin) • Stratified squamous epithelium of the esophagus (http://bioweb.uwlax.edu/zoolab/Table_of_Contents/ Lab-1b/Cross_section_of_the_esophagou/Stratified_squamous_epithelium/stratified_squamous_epithelium. htm) • Research News about Squamous Cell (http://www.ningishzida.com/classifieds/Squamous_Cell.html)
Hair cell
288
Hair cell
Neuron: PswiandfSW
Section through the spiral organ of Corti. Magnified. ("Outer hair cells" labeled near top; "inner hair cells" labeled near center). Location Function Morphology Presynaptic connections Postsynaptic connections Gray's NeuroLex ID Cochlea Amplify sound waves and transduce auditory information to the Brain Stem Unique (see text) None Via auditory nerve to vestibulocochlear nerve to inferior colliculus subject #232 1057 nifext_61 [2] [1]
Hair cells are the sensory receptors of both the auditory system and the vestibular system in all vertebrates. In mammals, the auditory hair cells are located within the organ of Corti on a thin basilar membrane in the cochlea of the inner ear. They derive their name from the tufts of stereocilia that protrude from the apical surface of the cell, a structure known as the hair bundle, into the scala media, a fluid-filled tube within the cochlea. Mammalian cochlear hair cells come in two anatomically and functionally distinct types: the outer and inner hair cells. Damage to these hair cells results in decreased hearing sensitivity, i.e. sensorineural hearing loss.
Hair bundles as sound detectors and amplifiers
Research of the past decades has shown that outer hair cells do not send neural signals to the brain, but that they mechanically amplify low-level sound that enters the cochlea. The amplification may be powered by movement of their hair bundles, or by an electrically driven motility of their cell bodies. The inner hair cells transform the sound vibrations in the fluids of the cochlea into electrical signals that are then relayed via the auditory nerve to the auditory brainstem and to the auditory cortex. Results in recent years further indicate that mammals apparently have conserved an evolutionarily earlier type of hair-cell motility. This so-called hair-bundle motility amplifies sound in all non-mammalian land vertebrates. It is affected by the closing mechanism of the mechanical sensory ion channels at the tips of the hair bundles. Thus, the same hair-bundle mechanism that detects sound vibrations also actively "vibrates back" and thereby mechanically amplifies weak incoming sound.
Hair cell
289
Inner hair cells – from sound to nerve signal
The deflection of the hair-cell stereocilia opens mechanically gated ion channels that allow any small, positively charged ions (primarily potassium and calcium) to enter the cell.[1] Unlike many other electrically active cells, the hair cell itself does not fire an action potential. Instead, the influx of positive ions from the endolymph in Scala media depolarizes the cell, resulting in a receptor potential. This receptor potential opens voltage gated calcium channels; calcium ions then enter the cell and trigger the release of neurotransmitters at the basal end of the cell. The neurotransmitters diffuse across the narrow space between the hair cell and a nerve terminal, where they then bind to receptors and thus trigger action Section through the organ of corti, showing inner and outer hair cells potentials in the nerve. In this way, the mechanical sound signal is converted into an electrical nerve signal. The repolarization in the hair cell is done in a special manner. The Perilymph in Scala tympani has a very low concentration of positive ions. The electrochemical gradient makes the positive ions flow through channels to the Perilymph. Hair cells chronically leak Ca2+. This leakage causes a tonic release of neurotransmitter to the synapses. It is thought that this tonic release is what allows the hair cells to respond so quickly in response to mechanical stimuli. The quickness of the hair cell response may also be due to that fact that it can increase the amount of neurotransmitter release in response to a change as little as 100 μV in membrane potential.[2]
Outer hair cells – acoustical pre-amplifiers
In mammalian outer hair cells, the receptor potential triggers active vibrations of the cell body. This mechanical response to electrical signals is termed somatic electromotility[3] and drives oscillations in the cell’s length, which occur at the frequency of the incoming sound and provide mechanical feedback amplification. A movie clip showing an isolated outer hair cell moving in response to electrical stimulation can be seen here. [6] Outer hair cells have evolved only in mammals. While hearing sensitivity of mammals is similar to that of other classes of vertebrates, without functioning outer hair cells, the sensitivity decreases by approximately 50 dB. Outer hair cells extend the hearing range to about 200 kHz in some marine mammals.[4] They have also improved frequency selectivity (frequency discrimination), which is of particular benefit for humans, because it enabled sophisticated speech and music. The effect of this system is to non-linearly amplify quiet sounds more than large ones, so that a wide range of sound pressures can be reduced to a much smaller range of hair displacements.[] This property of amplification is called the cochlear amplifier. The molecular biology of hair cells has seen considerable progress in recent years, with the identification of the motor protein (prestin) that underlies somatic electromotility in the outer hair cells. Santos-Sacchi et al. have shown that prestin's function is dependent on chloride channel signalling and that it is compromised by the common marine pesticide tributyltin (TBT). Because this class of pollutant bioconcentrates up the food chain, the effect is pronounced in top marine predators such as orcas and toothed whales.[5]
Hair cell
290
Neural connection
Neurons of the auditory or vestibulocochlear nerve (the VIIIth cranial nerve) innervate cochlear and vestibular hair cells.[6] The neurotransmitter released by hair cells to stimulate the dendrites of afferent neurons is thought to be glutamate. At the presynaptic juncture, there is a distinct presynaptic dense body or ribbon. This dense body is surrounded by synaptic vesicles and is thought to aid in the fast release of neurotransmitter. Nerve fiber innervation is much denser for inner hair cells than for outer hair cells. A single inner hair cell is innervated by numerous nerve fibers, whereas a single nerve fiber innervates many outer hair cells. Inner hair cell nerve fibers are also very heavily myelinated, which is in contrast to the unmyelinated outer hair cell nerve fibers. The region of the basilar membrane supplying the inputs to a particular afferent nerve fibre can be considered to be its receptive field. Efferent projections from the brain to the cochlea also play a role in the perception of sound. Efferent synapses occur on outer hair cells and on afferent (towards the brain) dendrites under inner hair cells. The presynaptic terminal bouton is filled with vesicles containing acetylcholine and a neuropeptide called Calcitonin gene-related peptide (CGRP). The effects of these compounds varies, in some hair cells the acetylcholine hyperpolarized the cell, which reduces the sensitivity of the cochlea locally.
Regrowth
Research on the regrowth of cochlea cells may lead to medical treatments that restore hearing. Unlike fish, birds, and reptiles, post-birth humans and other mammals are normally unable to regrow the cells of the inner ear that convert sound into neural signals when those cells are damaged by age or disease.[7] There is some contradictory information regarding the possibility of hair cell regeneration in mature mammals.[8][9][10] Researchers are making progress toward gene and stem-cell therapies that may allow the damaged cells to be regenerated.[11] Researchers have identified a mammalian gene that normally acts as a molecular switch to block the regrowth of cochlear hair cells in adults.[12] The Rb1 gene encodes the retinoblastoma protein that performs several physiological functions.[13] Not only do hair cells in a culture dish regenerate when the Rb1 gene is deleted, but mice bred to be missing the gene grow more hair cells than control mice that have the gene. The cell cycle inhibitor p27kip1 has also been shown to allow regrowth of cochlear hair cells in mice following genetic deletion or knock down with siRNA targeting p27.[14][15][16]
Additional images
The lamina reticularis and subjacent structures.
Inner ear illustration showing semicircular canal, hair cells, ampulla, cupula, vestibular nerve, & fluid
Stereocilia of frog inner ear
Hair cell
291
Notes
[14] (primary source) [15] (primary source)
References
• Coffin A, Kelley M, Manley GA, Popper AN. "Evolution of sensory hair cells". pp. 55–94. in Manley et al. (2004) • Fettiplace R, Hackney CM (2006). "The sensory and motor roles of auditory hair cells". Nature Reviews. Neuroscience 7 (1): 19–29. doi: 10.1038/nrn1828 (http://dx.doi.org/10.1038/nrn1828). PMID 16371947 (http://www.ncbi.nlm.nih.gov/pubmed/16371947). • Kandel ER, Schwartz JH, Jessell TM (2000). Principles of Neural Science (4th ed.). New York: McGraw-Hill. pp. 590–594. ISBN 0-8385-7701-6. • Manley GA, Popper AN, Fay RR (2004). Evolution of the Vertebrate Auditory System. New York: Springer-Verlag. ISBN 0-387-21093-8. • Manley GA. "Advances and perspectives in the study of the evolution of the vertebrate auditory system". pp. 360–368. in Manley et al. (2004) • Rabbitt RD, Boyle B, Highstein SM (1–5 February 2010). "Mechanical amplification by hair cells in the semicircular canals" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2840494). Proceedings of the National Academy of Sciences 107 (8): 3864–9. doi: 10.1073/pnas0906765107 (http://dx.doi.org/10.1073/ pnas0906765107). PMC 2840494 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2840494). PMID 20133682 (http://www.ncbi.nlm.nih.gov/pubmed/20133682). Lay summary (http://www.physorg.com/ news184935465.html). • Breneman KD, Brownell WE, Rabbitt RD (22 April 2009). "Hair cell bundles: flexoelectric motors of the inner ear" (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2668172). In Brezina, Vladimir. PLOS One 4 (4): e5201. doi: 10.1371/journal.pone.0005201 (http://dx.doi.org/10.1371/journal.pone.0005201). PMC 2668172 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2668172). PMID 19384413 (http://www.ncbi. nlm.nih.gov/pubmed/19384413). Lay summary (http://www.physorg.com/news159599814.html).
External links
• Molecular Basis of Hearing (http://www.ks.uiuc.edu/Research/hearing/) • Hair Cells at the University of Montpellier (http://www.iurc.montp.inserm.fr/cric51/audition/english/corti/ hcells/fhcells.htm) • Dancing OHC (http://www.yaleearlab.org/) video Yale Ear Lab • NIF Search - Hair Cell (https://www.neuinfo.org/mynif/search.php?q=Hair Cell&t=data&s=cover&b=0& r=20) via the Neuroscience Information Framework • Hair-Tuning-Sound-Sensor (http://www.scribd.com/doc/96781099/Hair-Tuning-Sound-Sensor) A concise report on the recent development of sound sensors based on hair tuning by students of SMMEE, IIT Ropar (http:/ /www.iitrpr.ac.in/)
Sensory neuron
292
Sensory neuron
Sensory neurons are neurons responsible for converting various external stimuli that come from the environment into corresponding internal stimuli. They are activated by sensory input (vision, touch, hearing, etc.), and send projections to other elements of nervous system, ultimately conveying sensory information to the brain or spinal cord. Unlike neurons of the central nervous system, whose inputs come from other neurons, sensory neurons are activated by physical modalities such as light, sound, and temperature. In complex organisms, the central nervous system is the destination to which sensory neurons transmit their data; in the case of less complex organisms, such as the hydra, sensory neurons send their data to motor neurons and sensory neurons can also send data via electrical impulses to the brain. At the molecular level, sensory receptors located on the cell membrane of sensory neurons are responsible for the conversion of stimuli into electrical impulses. The type of receptor employed by a given sensory neuron determines the type of stimulus it will be sensitive to. For example, neurons containing mechanoreceptors are sensitive to tactile stimuli, while olfactory receptors make a cell sensitive to odors.[1]
Types and function
Somatic sensory system
The somatic sensory system includes the sensations of touch, pressure, vibration, limb position, heat, cold, and pain. The cell bodies of somatic sensory afferent fibers lie in ganglia throughout the spine. These neurons are responsible for relaying information about the body to the central nervous system. Neurons residing in ganglia of the head and body supply the central nervous system with information about the aforementioned external stimuli occurring to the body. Pseudounipolar neurons are located in the dorsal root ganglia (the head).[2] Mechanoreceptors Specialized receptor cells called mechanoreceptors often encapsulate afferent fibers to help tune the afferent fibers to the different types of somatic stimulation. Mechanoreceptors also help lower thresholds for action potential generation in afferent fibers and thus make them more likely to fire in the presence of sensory stimulation.[3] Proprioceptors are another type of mechanoreceptors which literally means "receptors for self." These receptors provide spatial information about limbs and other body parts.[4] Nociceptors are responsible for processing pain and temperature changes. The burning pain and irritation experienced after eating a chili pepper (due to its main ingredient, capsaicin), the cold sensation experienced after ingesting a chemical such as menthol or icillin, as well as the common sensation of pain are all a result of neurons with these receptors.[5] Problems with mechanoreceptors lead to disorders such as: • Neuropathic pain - a severe pain condition resulting from a damaged sensory nerve [6] • Hyperalgesia - an increased sensitivity to pain caused by sensory ion channel, TRPM8, which is typically responds to temperatures between 23 and 26 degrees, and provides the cooling sensation associated with menthol and icillin [7] • Phantom limb syndrome - a sensory system disorder where pain or movement is experienced in a limb that does not exist [8]
Sensory neuron
293
Vision
Vision is one of the most complex sensory systems. The eye has to first "see" via refraction of light. Then, light energy has to be converted to electrical signals by photoreceptor cells and finally these signals have to be refined and controlled by the synaptic interactions within the neurons of the retina. The five basic classes of neurons within the retina are photoreceptor cells, bipolar cells, ganglion cells, horizontal cells, and amacrine cells. The basic circuitry of the retina incorporates a three-neuron chain consisting of the photoreceptor (either a rod or cone), bipolar cell, and the ganglion cell. The first action potential occurs in the retinal ganglion cell. This pathway is the most direct way for transmitting visual information to the brain. Problems and decay of sensory neurons associated with vision lead to disorders such as: • Macular degeneration – degeneration of the central visual field due to either cellular debris or blood vessels accumulating between the retina and the choroid, thereby disturbing and/or destroying the complex interplay of neurons that are present there.[9] • Glaucoma – loss of retinal ganglion cells which causes some loss of vision to blindness.[10] • Diabetic retinopathy – poor blood sugar control due to diabetes damages the tiny blood vessels in the retina.[11]
Auditory
The auditory system is responsible for converting pressure waves generated by vibrating air molecules or sound into signals that can be interpreted by the brain. This mechanoelectrical transduction is mediated with hair cells within the ear. Depending on the movement, the hair cell can either hyperpolarize or depolarize. When the movement is towards the tallest stereocilia, the K+ cation channels open allowing K+ to flow into cell and the resulting depolarization causes the Ca2+ channels to open, thus releasing its neurotransmitter into the afferent auditory nerve. There are two types of hair cells: inner and outer. The inner hair cells are the sensory receptors while the outer hair cells are usually from efferent axons originating from cells in the superior olivary complex[12] Problems with sensory neurons associated with the auditory system leads to disorders such as: • Auditory Processing Disorder – auditory information in the brain is processed in an abnormal way. Patients with auditory processing disorder can usually gain the information normally, but their brain cannot process it properly, leading to hearing disability.[13] • Auditory verbal agnosia – comprehension of speech is lost but hearing, speaking, reading, and writing ability is retained. This is caused by damage to the posterior superior temporal lobes, again not allowing the brain to process auditory input correctly.[14]
Drugs
There are many drugs currently on the market that are used to manipulate or treat sensory system disorders. For instance, Gabapentin is a drug that is used to treat neuropathic pain by interacting with one of the voltage-dependent calcium channels present on non-receptive neurons.[15] Some drugs may be used to combat other health problems, but can have unintended side effects on the sensory system. Ototoxic drugs are drugs which affect the cochlea through the use of a toxin like aminoglycoside antibiotics, which poison hair cells. Through the use of these toxins, the K+ pumping hair cells cease their function. Thus, the energy generated by the endocochlear potential which drives the auditory signal transduction process is lost, leading to hearing loss.[16]
Sensory neuron
294
Plasticity (Neuroplasticity)
Ever since scientists observed cortical remapping in the brain of Taub’s Silver Spring monkeys, there has been a lot of research into sensory system plasticity. Huge strides have been made in treating disorders of the sensory system. Techniques such as constraint-induced movement therapy developed by Taub have helped patients with paralyzed limbs regain use of their limbs by forcing the sensory system to grow new neural pathways.[17] Phantom limb syndrome is a sensory system disorder in which amputees perceive that their amputated limb still exists and they may still be experiencing pain in it. The mirror box developed by V.S. Ramachandran, has enabled patients with phantom limb syndrome to realign their body map, the somatosensory system’s perception of where the body is in space with physical reality. It is a simple device which uses a mirror in a box to create an illusion in which the sensory system perceives that it is seeing two hands instead of one, therefore allowing the sensory system to control the "phantom limb". By doing this, the sensory system can gradually get acclimated to the amputated limb, and thus alleviate this syndrome.[18]
Fiber types
Peripheral nerve fibers can be classified based on axonal conduction velocity, mylenation, fiber size etc. For example, there are slow-conducting unmyelinated C fibers and faster-conducting myelinated Aδ fibers. These nerve fibers work with neurons to form the nervous system
Footnotes
[1] Purves et al., 207-392 [2] Purves et al., pg 207 [3] Purves et al., 209 [4] Purves et al., 215-216 [5] Lee 2005 [6] Lee 2005 [7] Lee 2005 [8] Halligan 1999 [9] de Jong 2006 [10] Alguire 1990 [11] Diabetic retinopathy 2005 [12] Purves et al., pg 327-330 [13] Auditory processing disorder, 2004 [14] Stefanatos et al., 2005 [15] Lee 2005 [16] Priuska and Schact 1997 [17] Schwartz and Begley 2002 [18] Ramachandran 1998
References
• Alguire P (1990). "The Eye Chapter 118 Tonometry>Basic Science". in Walker HK, Hall WD, Hurst JW. Clinical methods: the history, physical, and laboratory examinations (3rd ed.). London: Butterworths. ISBN 0-409-90077-X. http://www.ncbi.nlm.nih.gov/bookshelf/br.fcgi?book=cm&partid=222#A3607. • "Auditory Processing Disorder (APD). Pamphlet, (2004).". British Society of Audiology APD Special Interest Group. MRC Institute of Hearing Research. http://www.ihr.mrc.ac.uk/research/apd.php/apd. php?page=apd_docs. • De Jong, Ptvm. "Mechanisms of Disease: Age-Related Macular Degeneration." New England Journal of Medicine 355 14 (2006): 1474-85. Print. • Halligan, P. W., A. Zeman, and A. Berger. "Phantoms in the Brain - Question the Assumption That the Adult Brain Is "Hard Wired"." British Medical Journal 319 7210 (1999): 587-88. Print.
Sensory neuron • Lee, Y., Lee, C. H., & Oh, U. (2005). Painful channels in sensory neurons. [Review]. Molecules and Cells, 20(3), 315-324. Print. • "NIHSeniorHealth: Diabetic Retinopathy - Causes and Risk Factors". Diabetic Retinopathy. NIHSenior Health. 2005. http://nihseniorhealth.gov/diabeticretinopathy/causesandriskfactors/02.html. • Priuska, E.M. and J. Schact (1997) Mechanism and prevention of aminoglycoside ototoxicity: Outer hair cells as targets and tools. Ear, Nose, Throat J. 76: 164-171. • Purves, D., Augustine, G.J., Fitzpatrick, D., Hall, W.C., LaMantia, A., McNamara, J.O., White, L.E. Neuroscience. Fourth edition. (2008). Sinauer Associates, Sunderland, Mass. Print. • Ramachandran, V. S. and S. Blakeslee (1998), Phantoms in the brain: Probing the mysteries of the human mind., William Morrow & Company, ISBN 0-688-15247-3. Print. • Schwartz and Begley 2002, p. 160; "Constraint-Induced Movement Therapy", excerpted from "A Rehab Revolution," Stroke Connection Magazine, September/October 2004. Print. • Stefanatos GA, Gershkoff A, Madigan S (2005). "On pure word deafness, temporal processing, and the left hemisphere". Journal of the International Neuropsychological Society : JINS 11 (4): 456–70; discussion 455.
295
Merkel cell
296
Merkel cell
Neuron: Merkel cell
Diagram of human skin. In humans, Merkel cells (yellow dot) are found clustered beneath the epidermal ridges (aka fingerprints). NeuroLex ID nifext_87 [1]
Merkel cells or Merkel-Ranvier cells are oval receptor cells found in the skin of vertebrates that have synaptic contacts with somatosensory afferents. They are associated with the sense of light touch discrimination of shapes and textures. They can turn malignant and form the skin tumor known as Merkel cell carcinoma. There is evidence that they are derived from neural crest.[] More recent experiments in mammals have indicated that they are in fact epithelial in origin.[1]
Location
Merkel cells are found in the skin and some parts of the mucosa of all vertebrates. In mammalian skin, they are clear cells found in the stratum basale (at the bottom of sweat duct ridges) of the epidermis approximately 10 µm in diameter. They also occur in epidermal invaginations of the plantar foot surface called rete ridges.[2] Most often, they are associated with sensory nerve endings, when they are known as Merkel nerve endings (also called a Merkel cell-neurite complex). They are associated with slowly adapting (SA1) somatosensory nerve fibers.
Function
Friedrich Sigmund Merkel referred to these cells as Tastzellen or "touch cells" but this proposed function has been controversial as it has been hard to prove. However, genetic knockout mice have recently shown that Merkel cells are essential for the specialized coding by which afferent nerves resolve fine spatial details.[3] Merkel cells are sometimes considered APUD cells (an older definition. More commonly classified as a part of dispersed neuroendocrine system) because they contain dense core granules, and thus may also have a neuroendocrine function.
Merkel cell
297
Developmental origin
The origin of Merkel cells has been debated for over 20 years. Evidence from skin graft experiments in birds implies that they are neural crest derived, but experiments in mammals now demonstrate an epidermal origin.[4][5]
References External links
• MeSH A08.800.550.700.500.425 (http://www.nlm.nih.gov/cgi/mesh/2012/MB_cgi?mode=&term=Merkel+ Cells&field=entry#TreeA08.800.550.700.500.425) • NIF Search - Merckel Disc Cell (https://www.neuinfo.org/mynif/search.php?q=Merkel Cell&t=data& s=cover&b=0&r=20) via the Neuroscience Information Framework
Olfactory receptor neuron
298
Olfactory receptor neuron
Neuron: Olfactory receptor neuron
Labels in German. "Zellen" = "cell","riech" = "smell", "Riechnerv" = olfactory nerve, "cillien" = cilia. Location Function Neurotransmitter Morphology Presynaptic connections Postsynaptic connections Gray's NeuroLex ID Code olfactory epithelium in the nose Detect traces of chemicals in inhaled air (sense of smell) Glutamate Bipolar sensory receptor None Olfactory bulb subject #223 996 nifext_116 [1] [2] [1]
TH H3.11.07.0.01003
An olfactory receptor neuron (ORN), also called an olfactory sensory neuron (OSN), is a transduction cell within the olfactory system.[1]
Vertebrates
Humans have about 40 million olfactory receptors that detect up to 10,000 different odors. In vertebrates, ORNs are bipolar neurons with dendrites facing the inferior space of the nasal cavity and an axon that passes through the cribiform plate then travels along the olfactory nerve to the olfactory bulb. The ORNs are located in the olfactory epithelium in the nasal cavity. The cell bodies of the ORNs are distributed among all three of the stratified layers of the olfactory epithelium.[2]
Plan of olfactory neurons.
Structure
Many tiny hair-like cilia protrude from the olfactory receptor cell's dendrite into the mucus covering the surface of the olfactory epithelium. The surface of these cilia is covered with olfactory receptors, a type of G protein-coupled receptor. Each olfactory receptor cell expresses only one type of olfactory receptor (OR), but many separate olfactory receptor cells express ORs which bind the same set of odors. The axons of olfactory receptor cells which express the same OR converge to form glomeruli in the olfactory bulb.
Olfactory receptor neuron
299
Function
ORs, which are located on the membranes of the cilia have been classified as a complex type of ligand-gated metabotropic channels.[3] There are approximately 1000 different genes that code for the ORs, making them the largest gene family. An odorant will dissolve into the mucus of the olfactory epithelium and then bind to an OR. ORs can bind to a variety of odor molecules, with varying affinities. The difference in affinities causes differences in activation patterns resulting in unique odorant profiles.[4] [5] The activated OR in turn activates the intracellular G-protein, GOLF (GNAL), adenylate cyclase and production of cyclic AMP (cAMP) opens ion channels in the cell membrane, resulting in an influx of sodium and calcium ions into the cell, and an efflux of chloride ions. This influx of positive ions and efflux of negative ions causes the neuron to depolarize, generating an action potential.
Insects
In insects, olfactory receptor neurons typically reside on the antenna. Much like in vertebrates, axons from the sensory neurons converge into glomeruli in the antennal lobe.
References
[1] J. Rospars, (1998) Dendritic integration in olfactory sensory neurons: a steady-state analysis of how the neuron structure and neuron environment influence the coding of odor intensity. J Comput Neurosci. 5: 243-266. PMID 9663551 [2] A. Cunningham, P. Manis, P. Reed, G. Ronnett, (1999) Olfactory receptor neurons exist as distinct subclasses of immature and mature cells in primary culture. Neuroscience 93(4): 1301-1312. PMID 10501454 [3] K. Touhara, (2009) Insect olfactory receptor complex functions as a ligand-gated ionotropic channel 1170 International Symposium on Olfaction and Taste: Ann. N.Y. Acad. Sci. 177-180 PMID 19686133 [4] S. Bieri, K. Monastyrskaia, B. Schilling, (2004) Olfactory receptor neuron profiling using sandalwood odorants. Chem. Senses 29:483-487 PMID 15269120 [5] J. Fan and J. Ngai, (2001) Onset of odorant receptor gene expression during olfactory sensory neuron regeneration. Dev Biol. 229: 119-127 PMID 11133158
External links
• olfactory+receptor+cells (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=olfactory+ receptor+cells) at eMedicine Dictionary • NIF Search - Olfactory receptor neuron (https://www.neuinfo.org/mynif/search.php?q=Olfactory Receptor Neuron&t=data&s=cover&b=0&r=20) via the Neuroscience Information Framework • (http://www.olfacts.nl) Insect olfaction
Photoreceptor cell
300
Photoreceptor cell
Neuron: Photoreceptor Cell
NeuroLex ID sao1233810115 [1]
A photoreceptor cell is a specialized type of neuron found in the retina that is capable of phototransduction. The great biological importance of photoreceptors is that they convert light (visible electromagnetic radiation) into signals that can stimulate biological processes. To be more specific, photoreceptor proteins in the cell absorb photons, triggering a change in the cell's membrane potential. The two classic photoreceptor cells are rods and cones, each contributing information used by the visual system to form a representation of the visual world, sight. The rods are narrower than the cones and distributed differently across the retina, but the chemical process in each that supports phototransduction is similar.[1] A third class of photoreceptor cells was discovered during the 1990s:[] the photosensitive ganglion cells. These cells do not contribute to sight directly, but are thought to support circadian rhythms and pupillary reflex. There are major functional differences between the rods and cones. Rods are extremely sensitive, and can be triggered by as few as 6 photons.[] At very low light levels, visual experience is based solely on the rod signal. This explains why colors cannot be seen at low light levels: only one type of photoreceptor cell is active. Cones require significantly brighter light (i.e., a larger numbers of photons) in order to produce a signal. In humans, there are three different types of cone cell, distinguished by their pattern of response to different wavelengths of light. Color experience is calculated from these three distinct signals, perhaps via an opponent process.[] The three types of cone cell respond (roughly) to light of short, medium, and long wavelengths. Note that, due to the principle of univariance, the firing of the cell depends upon only the number of photons absorbed. The different responses of the three types of cone cells are determined by the likelihoods that their respective photoreceptor proteins will absorb photons of different wavelengths. So, for example, an L cone cell contains a photoreceptor protein that more readily absorbs long wavelengths of light (i.e., more "red"). Light of a shorter wavelength can also produce the same response, but it must be much brighter to do so. The human retina contains about 120 million rod cells and 6 million cone cells. The number and ratio of rods to cones varies among species, dependent on whether an animal is primarily diurnal or nocturnal. Certain owls, such as the tawny owl,[2] have a tremendous number of rods in their retinae. In addition, there are about 1.5 million ganglion cells in the human visual system, 1 to 2% of them photosensitive. Described here are vertebrate photoreceptors. Invertebrate photoreceptors in organisms such as insects and molluscs are different in both their morphological organization and their underlying biochemical pathways.
Photoreceptor cell
301
Histology
Rod and cone photoreceptors are found on the outermost layer of the retina; they both have the same basic structure. Closest to the visual field (and farthest from the brain) is the axon terminal, which releases a neurotransmitter called glutamate to bipolar cells. Farther back is the cell body, which contains the cell's organelles. Farther back still is the inner segment, a specialized part of the cell full of mitochondria. The chief function of the inner segment is to provide ATP (energy) for the sodium-potassium pump. Finally, closest to the brain (and farthest from the field of view) is the outer segment, the part of the photoreceptor that absorbs light. Outer segments are actually modified cilia [][] that contain disks filled with opsin, the molecule that absorbs photons, as well as voltage-gated sodium channels. The membranous photoreceptor protein opsin contains a pigment molecule called retinal. In rod cells, these together are called rhodopsin. In cone cells, there are different types of opsins that combine with retinal to form pigments called photopsins. Three different classes of photopsins in the cones react to different ranges of light frequency, a differentiation that allows the visual system to calculate color. The function of the photoreceptor cell is to convert the light energy of the photon into a form of energy communicable to the nervous system and readily usable to the organism: This conversion is called signal transduction.
Anatomy of a Rod Cell
[3]
The opsin found in the photosensitive ganglion cells of the retina that are involved in various reflexive responses of the brain and body to the presence of (day)light, such as the regulation of circadian rhythms, pupillary reflex and other non-visual responses to light, is called melanopsin. Atypical in vertebrates, melanopsin functionally resembles invertebrate opsins. In structure, it is an opsin, a retinylidene protein variety of G-protein-coupled receptor. When light activates the melanopsin signaling system, the melanopsin-containing ganglion cells discharge nerve impulses that are conducted through their axons to specific brain targets. These targets include the olivary pretectal nucleus (a center responsible for controlling the pupil of the eye), the LGN, and, through the retinohypothalamic tract (RHT), the suprachiasmatic nucleus of the hypothalamus (the master pacemaker of circadian rhythms). Melanopsin-containing ganglion cells are thought to influence these targets by releasing from their axon terminals the neurotransmitters glutamate and pituitary adenylate cyclase activating polypeptide (PACAP).
Photoreceptor cell
302
Humans
The human retina has approximately 6 million cones and 120 million rods.[] Signals from the rods and cones converge on ganglion and bipolar cells for preprocessing before they are sent to the lateral geniculate nucleus. At the "center" of the retina (the point directly behind the lens) is the fovea, which contains only cone photoreceptor cells; this is the region capable of producing the highest visual acuity. Across the rest of the retina, rods and cones are intermingled. No photoreceptors are found at the blind spot, the area where ganglion cell fibers are collected into the optic nerve and leave the eye.[]
Normalized human photoreceptor absorbances for different wavelengths of light
[4]
The photoreceptor proteins in the three types of cones differ in their sensitivity to photons of different wavelengths (see graph). Since cones respond to both the wavelength and intensity of light, the cone's sensitivity to wavelength is measured in terms of its relative rate of response if the intensity of a stimulus is held fixed, while the wavelength is varied. From this, in turn, is inferred the absorbance.[] The graph normalizes the degree of absorbance on a hundred point scale. For example, the S cone's relative response peaks around 420 nm (nanometers, a measure of wavelength). This tells us that an S cone is more likely to absorb a photon at 420 nm than at any other wavelength. If light of a different wavelength to which it is less sensitive, say 480 nm, is increased in brightness appropriately, however, it will produce exactly the same response in the S cone. So, the colors of the curves are misleading. Cones cannot detect color by themselves; rather, color vision requires comparison of the signal across different cone types.
Phototransduction
The process of phototransduction occurs in the retina.[5] The retina is thick with cells.[6] The photoreceptor cells (rods and cones) form the innermost layer.[7] The middle layer contains bipolar cells, which collect neural signals from the rods and the cones and then transmit them to the outermost layer of the retina[8] where the neurons called retinal ganglion cells (RGCs) organize the signals and send them to the brain.[9] The bundled RGC axons form the optic nerve, which leaves the eye through a hole in the retina creating the blind spot.[10] Activation of rods and cones is actually hyperpolarization; when they are not being stimulated, they depolarize and release glutamate continuously. In the dark, cells have a relatively high concentration of cyclic guanosine 3'-5' monophosphate (cGMP), which opens ion channels (largely sodium channels, though calcium can enter through these channels as well). The positive charges of the ions that enter the cell down its electrochemical gradient change the cell's membrane potential, cause depolarization, and lead to the release of the neurotransmitter glutamate. Glutamate can depolarize some neurons and hyperpolarize others. When light hits a photoreceptive pigment within the photoreceptor cell, the pigment changes shape. The pigment, called iodopsin or rhodopsin, consists of large proteins called opsin (situated in the plasma membrane), attached to a covalently bound prosthetic group: an organic molecule called retinal (a derivative of vitamin A). The retinal exists in the 11-cis-retinal form when in the dark, and stimulation by light causes its structure to change to all-trans-retinal. This structural change causes it to activate a regulatory protein called transducin, which leads to the activation of cGMP phosphodiesterase, which breaks cGMP down into 5'-GMP. Reduction in cGMP allows the ion channels to close, preventing the influx of positive ions, hyperpolarizing the cell, and stopping the release of neurotransmitters.[3]
Photoreceptor cell The entire process by which light initiates a sensory response is called visual phototransduction.
303
Dark current
Unstimulated (in the dark), cyclic-nucleotide gated channels in the outer segment are open because cyclic GMP (cGMP) is bound to them. Hence, positively charged ions (namely sodium ions) enter the photoreceptor, depolarizing it to about −40 mV (resting potential in other nerve cells is usually −65 mV). This depolarizing current is often known as dark current.
Signal transduction pathway
The signal transduction pathway is the mechanism by which the energy of a photon signals a mechanism in the cell that leads to its electrical polarization. This polarization ultimately leads to either the transmittance or inhibition of a neural signal that will be fed to the brain via the optic nerve. The steps, or signal transduction pathway, in the vertebrate eye's rod and cone photoreceptors are then: 1. The rhodopsin or iodopsin in the disc membrane of the outer segment absorbs a photon, changing the configuration of a retinal Schiff base cofactor inside the protein from the cis-form to the trans-form, causing the retinal to change shape. 2. This results in a series of unstable intermediates, the last of which binds stronger to the G protein in the membrane and activates transducin, a protein inside the cell. This is the first amplification step – each photoactivated rhodopsin triggers activation of about 100 transducins. (The shape change in the opsin activates a G protein called transducin.) 3. Each transducin then activates the enzyme cGMP-specific phosphodiesterase (PDE). 4. PDE then catalyzes the hydrolysis of cGMP to 5' GMP. This is the second amplification step, where a single PDE hydrolyses about 1000 cGMP molecules. 5. The net concentration of intracellular cGMP is reduced (due to its conversion to 5' GMP via PDE), resulting in the closure of cyclic nucleotide-gated Na+ ion channels located in the photoreceptor outer segment membrane. 6. As a result, sodium ions can no longer enter the cell, and the photoreceptor outer segment membrane becomes hyperpolarized, due to the charge inside the membrane becoming more negative. 7. This change in the cell's membrane potential causes voltage-gated calcium channels to close. This leads to a decrease in the influx of calcium ions into the cell and thus the intracellular calcium ion concentration falls. 8. A decrease in the intracellular calcium concentration means that less glutamate is released via calcium-induced exocytosis to the bipolar cell (see below). (The decreased calcium level slows the release of the neurotransmitter glutamate, which can either excite or inhibit the postsynaptic bipolar cells.) 9. Reduction in the release of glutamate means one population of bipolar cells will be depolarized and a separate population of bipolar cells will be hyperpolarized, depending on the nature of receptors (ionotropic or metabotropic) in the postsynaptic terminal (see receptive field). Thus, a rod or cone photoreceptor actually releases less neurotransmitter when stimulated by light. Less neurotransmitter could either stimulate (depolarize) or inhibit (hyperpolarize) the bi-polar cell it synapses with, dependent on the nature of the receptor on the bipolar cell. This ability is integral to the center on/off mapping of visual units.[citation needed] ATP provided by the inner segment powers the sodium-potassium pump. This pump is necessary to reset the initial state of the outer segment by taking the sodium ions that are entering the cell and pumping them back out. Although photoreceptors are neurons, they do not conduct action potentials with the exception of the photosensitive ganglion cell – which are involved mainly in the regulation of circadian rhythms, melatonin, and pupil dilation.
Photoreceptor cell
304
Advantages
Phototransduction in rods and cones is unique in that the stimulus (in this case, light) actually reduces the cell's response or firing rate, which is unusual for a sensory system where the stimulus usually increases the cell's response or firing rate. However, this system offers several key advantages. First, the classic (rod or cone) photoreceptor is depolarized in the dark, which means many sodium ions are flowing into the cell. Thus, the random opening or closing of sodium channels will not affect the membrane potential of the cell; only the closing of a large number of channels, through absorption of a photon, will affect it and signal that light is in the visual field. Hence, the system is noiseless. Second, there is a lot of amplification in two stages of classic phototransduction: one pigment will activate many molecules of transducin, and one PDE will cleave many cGMPs. This amplification means that even the absorption of one photon will affect membrane potential and signal to the brain that light is in the visual field. This is the main feature that differentiates rod photoreceptors from cone photoreceptors. Rods are extremely sensitive and have the capacity of registering a single photon of light, unlike cones. On the other hand, cones are known to have very fast kinetics in terms of rate of amplification of phototransduction, unlike rods.
Difference between rods and cones
Comparison of human rod and cone cells, from Eric Kandel et al. in Principles of Neural Science.[3]
Rods Used for scotopic vision (vision under low light conditions) Very light sensitive; sensitive to scattered light Loss causes night blindness Low visual acuity Not present in fovea Slow response to light, stimuli added over time Have more pigment than cones, so can detect lower light levels Cones Used for photopic vision (vision under high light conditions) Not very light sensitive; sensitive to only direct light Loss causes legal blindness High visual acuity; better spatial resolution Concentrated in fovea Fast response to light, can perceive more rapid changes in stimuli Have less pigment than rods, require more light to detect images
Stacks of membrane-enclosed disks are unattached to cell membrane directly Disks are attached to outer membrane About 120 million rods distributed around the retina One type of photosensitive pigment Confer achromatic vision [11] [12] About 6 million cones distributed in each retina Three types of photosensitive pigment in humans Confer color vision
Function
Photoreceptors do not signal color; they only signal the presence of light in the visual field. A given photoreceptor responds to both the wavelength and intensity of a light source. For example, red light at a certain intensity can produce the same exact response in a photoreceptor as green light of a different intensity. Therefore, the response of a single photoreceptor is ambiguous when it comes to color. To determine color, the visual system compares responses across a population of photoreceptors (specifically, the three different cones with differing absorption spectra). To determine intensity, the visual system computes how many photoreceptors are responding. This is the mechanism that allows trichromatic color vision in humans and some other animals.
Photoreceptor cell
305
Development
The key events mediating rod versus S cone versus M cone differentiation are induced by several transcription factors, including RORbeta, OTX2, NRL, CRX, NR2E3 and TRbeta2. The S cone fate represents the default photoreceptor program, however differential transcriptional activity can bring about rod or M cone generation. L cones are present in primates, however there is not much known for their developmental program due to use of rodents in research. There are five steps to developing photoreceptors: proliferation of multi-potent retinal progenitor cells (RPCs); restriction of competence of RPCs; cell fate specification; photoreceptor gene expression; and lastly axonal growth, synapse formation and outer segment growth. Early Notch signaling maintains progenitor cycling. Photoreceptor precursors come about through inhibition of Notch signaling and increased activity of various factors including achaete-scute homologue 1. OTX2 activity commits cells to the photoreceptor fate. CRX further defines the photoreceptor specific panel of genes being expressed. NRL expression leads to the rod fate. NR2E3 further restricts cells to the rod fate by repressing cone genes. RORbeta is needed for both rod and cone development. TRbeta2 mediates the M cone fate. If any of the previously mentioned factors' functions are ablated, the default photoreceptor is a S cone. These events take place at different time periods for different species and include a complex pattern of activities that bring about a spectrum of phenotypes. If these regulatory networks are disrupted, retinitis pigmentosa, macular degeneration or other visual deficits may result.[13]
Signaling
The rod and cone photoreceptors signal their absorption of photons via a decrease in the release of the neurotransmitter glutamate to bipolar cells at its axon terminal. Since the photoreceptor is depolarized in the dark, a high amount of glutamate is being released to bipolar cells in the dark. Absorption of a photon will hyperpolarize the photoreceptor and therefore result in the release of less glutamate at the presynaptic terminal to the bipolar cell. Every rod or cone photoreceptor releases the same neurotransmitter, glutamate. However, the effect of glutamate differs in the bipolar cells, depending upon the type of receptor imbedded in that cell's membrane. When glutamate binds to an ionotropic receptor, the bipolar cell will depolarize (and therefore will hyperpolarize with light as less glutamate is released). On the other hand, binding of glutamate to a metabotropic receptor results in a hyperpolarization, so this bipolar cell will depolarize to light as less glutamate is released. In essence, this property allows for one population of bipolar cells that gets excited by light and another population that gets inhibited by it, even though all photoreceptors show the same response to light. This complexity becomes both important and necessary for detecting color, contrast, edges, etc. Further complexity arises from the various interconnections among bipolar cells, horizontal cells, and amacrine cells in the retina. The final result is differing populations of ganglion cells in the retina, a sub-population of which is also intrinsically photosensitive, using the photopigment melanopsin.
Ganglion cell (non-rod non-cone) photoreceptors
A non-rod non-cone photoreceptor in the eyes of mice, which was shown to mediate circadian rhythms, was discovered in 1991 by Foster et al.[] These neuronal cells, called intrinsically photosensitive retinal ganglion cells (ipRGC), are a small subset (~1–3%) of the retinal ganglion cells located in the inner retina, that is, in front[14] of the rods and cones located in the outer retina. These light sensitive neurons contain a photopigment, melanopsin,[15][][16][17][] which has an absorption peak of the light at a different wavelength (~480 nm[]) than rods and cones. Beside circadian / behavioral functions, ipRGCs have a role in initiating the pupillary light reflex.[] Dennis Dacey with colleagues showed in a species of Old World monkey that giant ganglion cells expressing melanopsin projected to the lateral geniculate nucleus (LGN).[18] Previously only projections to the midbrain (pre-tectal nucleus) and hypothalamus (suprachiasmatic nucleus) had been shown. However a visual role for the
Photoreceptor cell receptor was still unsuspected and unproven. In 2007, Farhan H. Zaidi and colleagues published pioneering work using rodless coneless humans. Current Biology subsequently announced in their 2008 editorial, commentary and despatches to scientists and ophthalmologists, that the non-rod non-cone photoreceptor had been conclusively discovered in humans using landmark experiments on rodless coneless humans by Zaidi and colleagues[][19][20][21] As had been found in other mammals, the identity of the non-rod non-cone photoreceptor in humans was found to be a ganglion cell in the inner retina. The workers had tracked down patients with rare diseases wiping out classic rod and cone photoreceptor function but preserving ganglion cell function.[19][20][21] Despite having no rods or cones the patients continued to exhibit circadian photoentrainment, circadian behavioural patterns, melanopsin suppression, and pupil reactions, with peak spectral sensitivities to environmental and experimental light matching that for the melanopsin photopigment. Their brains could also associate vision with light of this frequency. In humans the retinal ganglion cell photoreceptor contributes to conscious sight as well as to non-image-forming functions like circadian rhythms, behaviour and pupil reactions.[] Since these cells respond mostly to blue light, it has been suggested that they have a role in mesopic vision.[citation needed] Zaidi and colleagues' work with rodless coneless human subjects hence also opened the door into image-forming (visual) roles for the ganglion cell photoreceptor. It was discovered that there are parallel pathways for vision – one classic rod and cone-based pathway arising from the outer retina, and the other a rudimentary visual brightness detector pathway arising from the inner retina, which seems to be activated by light before the other.[] Classic photoreceptors also feed into the novel photoreceptor system, and colour constancy may be an important role as suggested by Foster. The receptor could be instrumental in understanding many diseases including major causes of blindness worldwide like glaucoma, a disease that affects ganglion cells, and the study of the receptor offered potential as a new avenue to explore in trying to find treatments for blindness. It is in these discoveries of the novel photoreceptor in humans and in the receptors role in vision, rather than its non-image-forming functions, where the receptor may have the greatest impact on society as a whole, though the impact of disturbed circadian rhythms is another area of relevance to clinical medicine. Most work suggests that the peak spectral sensitivity of the receptor is between 460 and 482 nm. Steven Lockley et al. in 2003 showed that 460 nm wavelengths of light suppress melatonin twice as much as longer 555 nm light. However, in more recent work by Farhan Zaidi et al., using rodless coneless humans, it was found that what consciously led to light perception was a very intense 481 nm stimulus; this means that the receptor, in visual terms, enables some rudimentary vision maximally for blue light.[]
306
References
[1] "eye, human." Encyclopædia Britannica. Encyclopaedia Britannica Ultimate Reference Suite. Chicago: Encyclopædia Britannica, 2010. [2] "Owl Eyesight" (http:/ / www. owls. org/ Information/ eyesight. htm) at owls.org [3] Human Physiology and Mechanisms of Disease by Arthur C. Guyton (1992) ISBN 0-7216-3299-8 p. 373 [11] Schacter, Daniel L., Daniel T. Gilbert, and Daniel M. Wegner. "Sensation and Perception, Phototransduction in the Retina." Psychology. ; Second Edition. New York: Worth, Incorporated, 2011. 136-37. Print. [12] Schacter, Daniel L., Daniel T. Gilbert, and Daniel M. Wegner. "Sensation and Perception, Phototransduction in the Retina." Psychology. ; Second Edition. New York: Worth, Incorporated, 2011. 136-37. Print. [14] See retina for information on the retinal layer structure. [19] Genova, Cathleen, Blind humans lacking rods and cones retain normal responses to nonvisual effects of light (http:/ / www. eurekalert. org/ pub_releases/ 2007-12/ cp-bhl121307. php). Cell Press, December 13, 2007. [20] Coghlan A. Blind people 'see' sunrise and sunset (http:/ / www. newscientist. com/ article/ mg19626354. 100-blind-people-see-sunrise-and-sunset. html). New Scientist, 26 December 2007, issue 2635. [21] Medical News Today. Normal Responses To Non-visual Effects Of Light Retained By Blind Humans Lacking Rods And Cones (http:/ / www. medicalnewstoday. com/ articles/ 91836. php). 14 December 2007.
Photoreceptor cell
307
Bibliography
• Campbell, Neil A., and Reece, Jane B. (2002). Biology. San Francisco: Benjamin Cummings. pp. 1064–1067. ISBN 0-8053-6624-5. • Freeman, Scott (2002). Biological Science (2nd Edition). Englewood Cliffs, N.J: Prentice Hall. pp. 835–837. ISBN 0-13-140941-7.
External links
• NIF Search – Photoreceptor Cell (https://www.neuinfo.org/mynif/search.php?q=Photoreceptor Cell& t=data&s=cover&b=0&r=20) via the Neuroscience Information Framework
Rod cell
308
Rod cell
Neuron: Rod cell
Cross section of the retina. Rods are visible at far right. Location Function Morphology Presynaptic connections Retina Low light photoreceptor rod shaped None
Postsynaptic connections Bipolar Cells and Horizontal cells NeuroLex ID Code sao1458938856 [1] [2]
TH H3.11.08.3.01030
Rod cells, or rods, are photoreceptor cells in the retina of the eye that can function in less intense light than the other type of visual photoreceptor, cone cells. Rods are concentrated at the outer edges of the retina and are used in peripheral vision. On average, there are approximately 125 million rod cells in the human retina.[1] More sensitive than cone cells, rod cells are almost entirely responsible for night vision.
Structure and function
Rods are a little longer and leaner than cones but have the same structural basis. The pigment is on the outer side, lying on the pigment epithelium, completing the cell's homeostasis. This epithelium end contains many stacked disks. Rods have a high area for visual pigment and thus substantial efficiency of light absorption. Because they have only one type of light-sensitive pigment, rather than the three types that human cone cells have, rods have little, if any, role in colored vision. Like cones, rod cells have a synaptic terminal, an inner segment, and an outer segment. The synaptic terminal forms a synapse with another neuron, for example a bipolar cell. The inner and outer segments are connected by a cilium,[2] which lines the distal segment.[3] The inner segment contains organelles and the cell's nucleus, while the rod outer segment (abbreviated to ROS), which is pointed toward the back of the eye, contains the light-absorbing materials.[2]
Sensitivity
A rod cell is sensitive enough to respond to a single photon of light[] and is about 100 times more sensitive to a single photon than cones. Since rods require less light to function than cones, they are the primary source of visual information at night (scotopic vision). Cone cells, on the other hand, require tens to hundreds of photons to become activated. Additionally, multiple rod cells converge on a single interneuron, collecting and amplifying the signals. However, this convergence comes at a cost to visual acuity (or image resolution) because the pooled information from multiple cells is less distinct than it would be if the visual system received information from each rod cell individually.
Rod cell
309
Rod cells also respond slower to light than cones and the stimuli they receive are added over roughly 100 milliseconds. While this makes rods more sensitive to smaller amounts of light, it also means that their ability to sense temporal changes, such as quickly changing images, is less accurate than that of cones.[2] Experiments by George Wald and others showed that rods are most sensitive to wavelengths of light around 498 nm (green-blue), and insensitive to wavelengths Wavelength responsiveness of rods compared to that of three types of cones. The [4] longer than about 640 nm (red). This fact is dashed gray curve is for rods. responsible for the Purkinje effect: as intensity dims at twilight, the rods take over, and before color disappears completely, peak sensitivity of vision shifts towards the rods' peak sensitivity (blue-green).
Response to light
In vertebrates, activation of a photoreceptor cell is actually a hyperpolarization (inhibition) of the cell. When they are not being stimulated, such as in the dark, rod cells and cone cells depolarize and release a neurotransmitter spontaneously. This neurotransmitter hyperpolarizes the bipolar cell. Bipolar cells exist between photoreceptors and ganglion cells and act to transmit signals from the photoreceptors to the ganglion cells. As a result of the bipolar cell being hyperpolarized, it does not release its transmitter at the bipolar-ganglion synapse and the synapse is not excited. Activation of photopigments by light sends a signal by hyperpolarizing the rod cell, leading to the rod cell not sending its neurotransmitter, which leads to the bipolar cell then releasing its transmitter at the bipolar-ganglion synapse and exciting the synapse.
Anatomy of a Rod Cell
[5]
Depolarization of rod cells (causing release of their neurotransmitter) occurs because in the dark, cells have a relatively high concentration of cyclic guanosine 3'-5' monophosphate (cGMP), which opens ion channels (largely sodium channels, though calcium can enter through these channels as well). The positive charges of the ions that enter the cell down its electrochemical gradient change the cell's membrane potential, cause depolarization, and lead to the release of the neurotransmitter glutamate. Glutamate can depolarize some neurons and hyperpolarize others, allowing photoreceptors to interact in an antagonistic manner. When light hits photoreceptive pigments within the photoreceptor cell, the pigment changes shape. The pigment, called rhodopsin (photopsin is found in cone cells) comprises a large protein called opsin (situated in the plasma membrane), attached to which is a covalently bound prosthetic group: an organic molecule called retinal (a derivative of vitamin A). The retinal exists in the 11-cis-retinal form when in the dark, and stimulation by light causes its structure to change to all-trans-retinal. This structural change causes a series of changes in the opsin that
Rod cell ultimately lead it to activate a regulatory protein called transducin (a type of G protein), which leads to the activation of cGMP phosphodiesterase, which breaks cGMP down into 5'-GMP. Reduction in cGMP allows the ion channels to close, preventing the influx of positive ions, hyperpolarizing the cell, and stopping the release of neurotransmitters (Kandel et al., 2000). Though cone cells primarily use the neurotransmitter substance acetylcholine, rod cells use a variety. The entire process by which light initiates a sensory response is called visual phototransduction. Activation of a single unit of rhodopsin, the photosensitive pigment in rods, can lead to a large reaction in the cell because the signal is amplified. Once activated, rhodopsin can activate hundreds of transducin molecules, each of which in turn activates a phosphodiesterase molecule, which can break down over a thousand cGMP molecules per second (Kandel et al. 2000). Thus, rods can have a large response to a small amount of light. As the retinal component of rhodopsin is derived from vitamin A, a deficiency of vitamin A causes a deficit in the pigment needed by rod cells. Consequently, fewer rod cells are able to sufficiently respond in darker conditions, and as the cone cells are poorly adapted for sight in the dark, blindness can result. This is night-blindness.
310
Revert to the resting state
Rods make use of three inhibitory mechanisms (negative feedback mechanisms) to allow a rapid revert to the resting state after a flash of light. Firstly, there exists a rhodopsin kinase (RK) which would phosphorylate the cytosolic tail of the activated rhodopsin on the multiple serines, partially inhibiting the activation of transducin. Also, an inhibitory protein - arrestin then binds to the phosphorylated rhodopsins to further inhibit the rhodopsin's activity. While arrestin shuts off rhodopsin, an RGS protein (functioning as a GTPase-activating proteins(GAPs)) drives the transducin (G-protein) into an "off" state by increasing the rate of hydrolysis of the bounded GTP to GDP. Also as the cGMP sensitive channels allow not only the influx of sodium ions, but also calcium ions, with the decrease in concentration of cGMP, cGMP sensitive channels are then closed and reducing the normal influx of calcium ions. The decrease in the concentration of calcium ions stimulates the calcium ion-sensitive proteins, which would then activate the guanylyl cyclase to replenish the cGMP, rapidly restoring its original concentration. The restoration opens the cGMP sensitive channels and causes a depolarization of the plasma membrane.[6]
Desensitization
When the rods are exposed to a high concentration of photons for a prolonged period, they become desensitized (adapted) to the environment. As rhodopsin is phosphorylated by rhodopsin kinase (a member of the GPCR kinases(GRKs)), it binds with high affinity to the arrestin. The bound arrestin can contribute to the desensitization process in at least two ways. First, it prevents the interaction between the G protein and the activated receptor. Second, it serves as an adaptor protein to aid the receptor to the clathrin-dependent endocytosis machinery (to induce receptor-mediated endocytosis).[6]
Rod cell
311
References
[1] [2] [3] [5] [6] Curcio, C. A., K. R. Sloan, et al. (1990). "Human photoreceptor topography." The Journal of Comparative Neurology 292(4): 497-523. Kandel E.R., Schwartz, J.H., Jessell, T.M. (2000). Principles of Neural Science, 4th ed., pp.507-513. McGraw-Hill, New York. "Photoreception" McGraw-Hill Encyclopedia of Science & Technology, vol. 13, p.460 2007 Human Physiology and Mechanisms of Disease by Arthur C. Guyton (1992) p.373 Bruce Alberts, Alexander Johnson, Julian Lewis, Martin Raff, Keith Roberts, Peter Walter (2008). Molecular Biology of The Cell, 5th ed., pp.919-921. Garland Science.
External links
• NIF Search - Rod Cell (https://www.neuinfo.org/mynif/search.php?q=Rod Cell&t=data&s=cover&b=0& r=20) via the Neuroscience Information Framework
Cone cell
312
Cone cell
Neuron: Cone cell
Normalized responsivity spectra of human cone cells, S, M, and L types Function NeuroLex ID Code Color vision sao1103104164 [1] [2]
TH H3.11.08.3.01046
Cone cells, or cones, are one of the two types of photoreceptor cells that are in the retina of the eye which are responsible for color vision as well as eye color sensitivity; they function best in relatively bright light, as opposed to rod cells that work better in dim light. Cone cells are densely packed in the fovea centralis a 0.3 mm diameter rod-free area with very thin, densely packed cones, but quickly reduce in number towards the periphery of the retina. There are about six to seven million cones in a human eye and are most concentrated towards the macula. [1] A commonly cited figure of six million in the human eye was found by Osterberg in 1935.[2] Oyster's textbook (1999)[3] cites work by Curcio et al. (1990) indicating an average close to 4.5 million cone cells and 90 million rod cells in the human retina.[4] Cones are less sensitive to light than the rod cells in the retina (which support vision at low light levels), but allow the perception of colour. Cone cell structure They are also able to perceive finer detail and more rapid changes in images, because their response times to stimuli are faster than those of rods.[2] As opposed to rods, cones consist one of the three types of pigment namely: S-cones (absorbs blue), M-cones (absorbs green) and L-cones (absorbs red). Each cone is therefore sensitive to visible wavelengths of light that correspond to red (long-wavelength), green (medium-wavelength), or blue (short-wavelength) light.[5] Because humans usually have three kinds of cones with different photopsins, which have different response curves and thus respond to variation in colour in different ways, we have trichromatic vision. Being colour blind can change this, and there have been some unverified reports of people with four or more types of cones, giving them tetrachromatic vision.[6][7][8] Destruction to the cone cells from disease would result in blindness.
Cone cell
313
Types
Humans normally have three kinds of cones. The first responds the most to light of long wavelengths, peaking at a reddish colour; this type is sometimes designated L for long. The second type responds the most to light of medium-wavelength, peaking at a green colour, and is abbreviated M for medium. The third type responds the most to short-wavelength light, of a bluish colour, and is designated S for short. The three types have peak wavelengths near 564–580 nm, 534–545 nm, and 420–440 nm, respectively.[][9] The difference in the signals received from the three cone types allows the brain to perceive all possible colours, through the opponent process of colour vision. (Rod cells have a peak sensitivity at 498 nm, roughly halfway between the peak sensitivities of the S and M cones.) All of the receptors contain the pigment photopsin, with variations in its conformation causing differences in the optimum wavelengths absorbed. The colour yellow, for example, is perceived when the L cones are stimulated slightly more than the M cones, and the colour red is perceived when the L cones are stimulated significantly more than the M cones. Similarly, blue and violet hues are perceived when the S receptor is stimulated more than the other two. The S cones are most sensitive to light at wavelengths around 420 nm. However, the lens and cornea of the human eye are increasingly absorptive to shorter wavelengths, and this sets the short wavelength limit of human-visible light to approximately 380 nm, which is therefore called 'ultraviolet' light. People with aphakia, a condition where the eye lacks a lens, sometimes report the ability to see into the ultraviolet range.[10] At moderate to bright light levels where the cones function, the eye is more sensitive to yellowish-green light than other colors because this stimulates the two most common (M and L) of the three kinds of cones almost equally. At lower light levels, where only the rod cells function, the sensitivity is greatest at a blueish-green wavelength. Cones also tend to possess a significantly elevated visual acuity because each cone cell has a lone connection to the optic nerve, therefore, the cones have an easier time telling that two stimuli are isolated. Separate connectivity is established in the inner plexiform layer so that each connection is parallel. [11] While it has been discovered that there exists a mixed type of bipolar cells that bind to both rod and cone cells, bipolar cells still predominantly receive their input from cone cells.[12]
Structure
Cone cells are somewhat shorter than rods, but wider and tapered, and are much less numerous than rods in most parts of the retina, but greatly outnumber rods in the fovea. Structurally, cone cells have a cone-like shape at one end where a pigment filters incoming light, giving them their different response curves. They are typically 40–50 µm long, and their diameter varies from 0.5 to 4.0 µm, being smallest and most tightly packed at the center of the eye at the fovea. The S cones are a little larger than the others.[citation needed] Photobleaching can be used to determine cone arrangement. This is done by exposing dark-adapted retina to a certain wavelength of light that paralyzes the particular type of cone sensitive to that wavelength for up to thirty minutes from being able to dark-adapt making it appear white in contrast to the grey dark-adapted cones when a picture of the retina is taken. The results illustrate that S cones are randomly placed and appear much less frequently than the M and L cones. The ratio of M and L cones varies greatly among different people with regular
Bird, reptilian, and monotreme cone cells.
Cone cell vision (e.g. values of 75.8% L with 20.0% M versus 50.6% L with 44.2% M in two male subjects).[13] Like rods, each cone cell has a synaptic terminal, an inner segment, and an outer segment as well as an interior nucleus and various mitochondria. The synaptic terminal forms a synapse with a neuron such as a bipolar cell. The inner and outer segments are connected by a cilium.[2] The inner segment contains organelles and the cell's nucleus, while the outer segment, which is pointed toward the back of the eye, contains the light-absorbing materials.[2] Like rods, the outer segments of cones have invaginations of their cell membranes that create stacks of membranous disks. Photopigments exist as transmembrane proteins within these disks, which provide more surface area for light to affect the pigments. In cones, these disks are attached to the outer membrane, whereas they are pinched off and exist separately in rods. Neither rods nor cones divide, but their membranous disks wear out and are worn off at the end of the outer segment, to be consumed and recycled by phagocytic cells. The response of cone cells to light is also directionally nonuniform, peaking at a direction that receives light from the center of the pupil; this effect is known as the Stiles–Crawford effect.
314
Diseases
One of the diseases related to cone cells present in retina is retinoblastoma. Retinoblastoma is a rare cancer of the retina, caused by the mutation of both copies of retinoblastoma genes (RB1). Most cases of Retinablastoma occur during early childhood, because it is commonly found in children.[14] One or both eyes may be affected. The protein encoded by RB1 regulates a signal transduction pathway while controlling the cell cycle progression as normally. Retinoblastoma seems to originate in cone precursor cells present in the retina that consist of natural signalling networks which restrict cell death and promote cell survival after losing the RB1, or having both the RB1 copies mutated. It has been found that TRβ2 which is a transcription factor specifically affiliated with cones is essential for rapid reproduction and existence of the retinoblastoma cell.[] A drug that can be useful in the treatment of this disease is MDM2 (murine double minute 2) gene. Knockdown studies have shown that the MDM2 gene silences ARF-induced apoptosis in retinoblastoma cells and that MDM2 is necessary for the survival of cone cells.[] Although research and scientist have been able to discover a lot about this type of disease, there is still much to understand. It is unclear at this point why the retinoblastoma in humans is sensitive to RB1 inactivation. [15] The pupil may appear white or have white spots. A white glow in the eye is often seen in photographs taken with a flash, instead of the typical "red eye" from the flash, and the pupil may appear white or distorted. Other symptoms can include crossed eyes, double vision, eyes that do not align, eye pain and redness, poor vision or differing iris colours in each eye. If the cancer has spread, bone pain and other symptoms may occur.[][]
Color Afterimage
Sensitivity to a prolonged stimulation tends to decline over time, leading to neural adaptation. An interesting effect occurs when staring at a particular color for too long. Such action leads to an exhaustion of the cone cells that respond to that color - resulting in the afterimage. This vivid color aftereffect can last for a minute or more. [16]
References
[2] G. Osterberg (1935). “Topography of the layer of rods and cones in the human retina,” Acta Ophthalmol., Suppl. 13:6, pp. 1–102. [5] Schacter,Gilbert, Wegner, "Psychology", New York: Worth Publishers,2009. [10] Let the light shine in: You don't have to come from another planet to see ultraviolet light (http:/ / education. guardian. co. uk/ higher/ medicalscience/ story/ 0,9837,724257,00. html) EducationGuardian.co.uk, David Hambling (May 30, 2002) [11] Strettoi, E., et all; Complexity of retinal cone bipolar cells. Progress in Retinal and Eye Research (2010), 29 (4), pg. 272-283 [12] Strettoi et al. (2010), "Complexity of retinal cone bipolar cells", Progress in Retinal and Eye Research, 29 (4), pg. 272–283. [15] http:/ / www. nature. com. myaccess. library. utoronto. ca/ nrc/ index. html [16] Schacter, Daniel L. Psychology: the second edition. Chapter 4.9.
Cone cell
315
External links
• Cell Centered Database – Cone cell (http://ccdb.ucsd.edu/sand/main?stype=lite&keyword=cone& Submit=Go&event=display&start=1) • Webvision's Photoreceptors (http://webvision.umh.es/webvision/photo1.html) • NIF Search – Cone Cell (https://www.neuinfo.org/mynif/search.php?q=Cone Cell&t=data&s=cover&b=0& r=20) via the Neuroscience Information Framework • Model and image of cone cell (http://www.nanobotmodels.com/node/33)
Carotid body
316
Carotid body
Carotid body
Section of part of human glomus caroticum. Highly magnified. Numerous blood vessels are seen in section among the gland cells.
Diagram showing the origins of the main branches of the carotid arteries. Latin Gray's glomus caroticum subject #277 1281
[1]
The carotid body (carotid glomus or glomus caroticum) is a small cluster of chemoreceptors and supporting cells located near the fork (bifurcation) of the carotid artery (which runs along both sides of the throat). The carotid body detects changes in the composition of arterial blood flowing through it, mainly the partial pressure of oxygen, but also of carbon dioxide. Furthermore, it is also sensitive to changes in pH and temperature.
Composition
The carotid body is made up of two types of cells, called glomus cells: glomus type I (chief) cells, and glomus type II (sustentacular) cells. • Glomus type I/chief cells are derived from neural crest,[] which, in turn are derived from neuroectoderm. They release a variety of neurotransmitters, including acetylcholine, ATP, and dopamine that trigger EPSPs in synapsed neurons leading to the respiratory center. • Glomus type II/sustentacular cells resemble glia, express the glial marker S100 and act as supporting cells. The carotid body contains the most vascular tissue in the human body. The thyroid gland is very vascular, but not quite as much as the carotid body.
Carotid body
317
Function
The carotid body functions as a sensor: it responds to a stimulus, primarily O2 partial pressure, which is detected by the type I (glomus) cells, and triggers an action potential through the afferent fibers of the glossopharyngeal nerve, which relays the information to the central nervous system.
Stimulus
While the central chemoreceptors in the brainstem are highly sensitive to CO2 the carotid body is a peripheral chemoreceptor that mainly provides afferent input to the respiratory center that is highly O2 dependent. However, the carotid body also senses increases in CO2 partial pressure and decreases in arterial pH, but to a lesser degree than for O2 The output of the carotid bodies is low at an oxygen partial pressure above about 100 mmHg (13,3 kPa) (at normal physiological pH), but below this the activity of the type I (glomus) cells increases rapidly.
Detection
The mechanism for detecting reductions in PO2 has yet to be identified, there may be multiple mechanisms[] and could vary between species. Hypoxia detection has been shown to depend upon increased Hydrogen sulfide generation produced by cystathionine gamma-lyase as hypoxia detection is reduced in mice in which this enzyme is knocked out or pharmacologically inhibited. The process of detection involves the interaction of cystathionine gamma-lyase with hemeoxygenase-2 and the production of carbon monoxide.[1] Other theories suggest it may involve mitochondrial oxygen sensors and the haem-containing cytochromes that undergo reversible one-electron reduction during oxidative-phosphorylation. Haem reversibly binds O2 with an affinity similar to that of the carotid body, suggesting that haem containing proteins may have a role in O2, potentially this could be one of the complexes involved in oxidative-phosphorylation. This leads to increases in reactive oxygen species and rises in intracellular Ca2+. However, whether hypoxia leads to an increase or decrease in reactive oxygen species is unknown. The role of reactive oxygen species in hypoxia sensing is also under question.[] The oxygen dependent enzyme haem-oxidase has also been put forward as a hypoxia sensor. In normoxia, haem-oxygenase generates carbon monoxide (CO), CO activates the large conductance calcium-activated potassium channel, BK. Falls in CO that occur as a consequence of hypoxia would lead to closure of this potassium channel and this would lead to membrane depolarisation and consequence activation of the carotid body.[] A role for the "energy sensor" AMP-activated protein kinase (AMPK) has also been proposed in hypoxia sensing. This enzyme is activated during times of net energy usage and metabolic stress, including hypoxia. AMPK has a number of targets and it appears that, in the carotid body, when AMPK is activated by hypoxia, it leads to downstream potassium channel closure of both O2-sentive TASK-like and BK channels [] An increased PCO2 is detected because the CO2 diffuses into the cell, where it increases the concentration of carbonic acid and thus protons. The precise mechanism of CO2 sensing is unknown, however it has been demonstrated that CO2 and low pH inhibit a TASK-like potassium conductance, reducing potassium current. This leads to depolarisation of the cell membrane which leads to Ca2+ entry, excitation of glomus cells and consequent neurotransmitter release.[] Arterial acidosis (either metabolic or from altered PCO2) inhibits acid-base transporters (e.g. Na+-H+) which raise intracellular pH, and activates transporters (e.g. Cl--HCO3-) which decrease it. Changes in proton concentration caused by acidosis (or the opposite from alkalosis) inside the cell stimulates the same pathways involved in PCO2 sensing. Another mechanism is through oxygen sensitive potassium channels. A drop in dissolved oxygen lead to closing of these channels which results in depolarization. This leads to release of the neurotransmitter dopamine in the glossopharengeal and vagus afferente to the vasomotor area.
Carotid body
318
Action potential
The type I (glomus) cells in the carotid (and aortic bodies) are derived from neuroectoderm and are thus electrically excitable. A decrease in oxygen partial pressure, an increase in carbon dioxide partial pressure, and a decrease in arterial pH can all cause depolarization of the cell membrane, and they affect this by blocking potassium currents. This reduction in the membrane potential opens voltage-gated calcium channels, which causes a rise in intracellular calcium concentration. This causes exocytosis of vesicles containing a variety of neurotransmitters, including acetylcholine, noradrenaline, dopamine, adenosine, ATP, substance P, and met-enkephalin. These act on receptors on the afferent nerve fibres which lie in apposition to the glomus cell to cause an action potential.
Relay
The feedback from the carotid body is sent to the cardiorespiratory centers in the medulla oblongata via the afferent branches of the Glossopharyngeal nerve. The efferent fibres of the aortic body chemoreceptors are relayed by the Vagus nerve. These centers, in turn, regulate breathing and blood pressure.
Disorders
A paraganglioma is a tumor that may involve the carotid body and is usually benign. Rarely, a malignant neuroblastoma may originate from the carotid body.
References
[1] Peng Y-J, Nanduri J, Raghuraman G, Souvannakitti D, Gadalla M.M, Kumar GK, Snyder SH, Prabhakar NR. (2010). H2S mediates O2 sensing in the carotid body PNAS 107 (23) 10719-10724.
Micrograph of a carotid body tumor.
External links
• Carotid+body (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=Carotid+body) at eMedicine Dictionary
Taste bud
319
Taste bud
Taste buds
Semidiagrammatic view of a portion of the mucous membrane of the tongue. Two fungiform papillæ are shown. On some of the filiform papillæ the epithelial prolongations stand erect, in one they are spread out, and in three they are folded in. Latin Gray's MeSH Code caliculus gustatorius subject #222 991 Taste+Buds
[2] [3] [1]
TH H3.04.01.0.02116 [3] TH H3.04.01.0.03013
Taste buds contain the receptors for taste. They are located around the small structures on the upper surface of the tongue, soft palate, upper esophagus and epiglottis, which are called papillae.[1] These structures are involved in detecting the five (known) elements of taste perception: salty, sour, bitter, sweet, and umami. Via small openings in the tongue epithelium, called taste pores, parts of the food dissolved in saliva come into contact with taste receptors. These are located on top of the taste receptor cells that constitute the taste buds. The taste receptor cells send information detected by clusters of various receptors and ion channels to the gustatory areas of the brain via the seventh, ninth and tenth cranial nerves. On average, the human tongue has 2,000–8,000 taste buds.[2]
Types of papillae
The majority of taste buds on the tongue sit on raised protrusions of the tongue surface called papillae. There are four types of papillae present in the human tongue: • Fungiform papillae - as the name suggests, these are slightly mushroom-shaped if looked at in longitudinal section. These are present mostly at the dorsal surface of the tongue, as well as at the sides. Innervated by facial nerve. • Filiform papillae - these are thin, long papillae "V"-shaped cones that don't contain taste buds but are the most numerous. These papillae are mechanical and not involved in gustation. They are characterized by increased keratinization. • Foliate papillae - these are ridges and grooves towards the posterior part of the tongue found at the lateral borders. Innervated by facial nerve (anterior papillae) and glossopharyngeal nerve (posterior papillae). • Circumvallate papillae - there are only about 10 to 14 of these papillae on most people, and they are present at the back of the oral part of the tongue. They are arranged in a circular-shaped row just in front of the sulcus terminalis of the tongue. They are he associated with ducts of Von Ebner's glands, and are innervated by the glossopharyngeal nerve.
Taste bud Salts, sweet, sour and umami tastes causes depolarization of the taste cells, although different mechanisms are applied. Bitter causes an internal release of Ca2+, no external Ca2+ is required. The bud is formed by two kinds of cells: supporting cells and gustatory cells. The supporting (sustentacular) cells are mostly arranged like the staves of a cask, and form an outer envelope for the bud. Some, however, are found in the interior of the bud between the gustatory cells. The gustatory (taste) cells, a chemoreceptor, occupy the central portion of the bud; they are spindle-shaped, and each possesses a large spherical nucleus near the middle of the cell. The peripheral end of the cell terminates at the gustatory pore in a fine hair filament, the gustatory hair. The central process passes toward the deep extremity of the bud, and there ends in single or bifurcated varicosities. The nerve fibrils after losing their medullary sheaths enter the taste bud, and end in fine extremities between the gustatory cells; other nerve fibrils ramify between the supporting cells and terminate in fine extremities; these, however, are believed to be nerves of ordinary sensation and not gustatory. The average life of a taste bud is 10 days.
320
Additional images
schematic drawing of a taste bud
taste bud (nerve missing)
References
[1] Discovery News, October 26, 2010 (http:/ / news. discovery. com/ human/ taste-buds-found-in-lungs. ) [2] Encyclopædia Britannica. 2009. Encyclopædia Britannica Online. (http:/ / www. britannica. com/ EBchecked/ topic/ 584034/ taste-bud)
External links
• Taste Perception: Cracking the Code (http://biology.plosjournals.org/perlserv/?request=get-document& doi=10.1371/journal.pbio.0020064) • Scientists Explore the Workings of Taste Buds (http://www.npr.org/templates/story/story. php?storyId=4766647) from National Public Radio's Talk of the Nation, July 22, 2005 • http://kidshealth.org/kid/talk/qa/taste_buds.html For kids about taste buds! • http://www.newser.com/story/103744/your-lungs-have-their-own-taste-buds.html
Schwann cell
321
Schwann cell
Structure of a typical neuron
Schwann cells wrapped around an axon
Schwann cells (named after physiologist Theodor Schwann) or neurolemmocytes are the principal glia of the peripheral nervous system (PNS). Glial cells function to support neurons and in the PNS, also include satellite cells, olfactory ensheathing cells, enteric glia and glia that reside at sensory nerve endings, such as the Pacinian corpuscle. There are two types of Schwann cell, myelinating and nonmyelinating. Myelinating Schwann cells wrap around axons of motor and sensory neurons to form the myelin sheath. Schwann cells are involved in many important aspects of peripheral nerve biology—the conduction of nervous impulses along axons, nerve development and regeneration, trophic support for neurons, production of the nerve extracellular matrix, modulation of neuromuscular synaptic activity, and presentation of antigens to T-lymphocytes. Charcot-Marie-Tooth disease (CMT), Guillain-Barré syndrome (GBS), schwannomatosis and chronic inflammatory demyelinating polyneuropathy (CIDP) are all neuropathies involving Schwann cells.
Schwann cell
322
Description
Named after the German physiologist Theodor Schwann, Schwann cells are a variety of glial cell that keep peripheral nerve fibres (both myelinated and unmyelinated) alive. In myelinated axons, Schwann cells form the myelin sheath (see above). The sheath is not continuous. Individual myelinating Schwann cells cover about 100 micrometres of an axon—equating to approximately 10,000 Schwann cells along a 1 metre length of the axon—which can be up to a metre or more in length. The gaps between adjacent Schwann cells are called nodes of Ranvier (see above). The vertebrate nervous system relies on the myelin sheath for insulation and as a method of decreasing membrane capacitance in the axon. The action potential jumps from node to node, in a process called saltatory conduction, which can increase conduction velocity up to ten times, without an increase in axonal diameter. In this sense, Schwann cells are the peripheral nervous system's analogues of the central nervous system's oligodendrocytes. However, unlike oligodendrocytes, each myelinating Schwann cell provides insulation to only one axon (see image). This arrangement permits saltatory conduction of action potentials with repropagation at the nodes of Ranvier. In this way, myelination greatly increases speed of conduction and saves energy.[1] Non-myelinating Schwann cells are involved in maintenance of axons and are crucial for neuronal survival. Some group around smaller axons (External image here [2]) and form Remak bundles.[2] Myelinating Schwann cells begin to form the myelin sheath in mammals during fetal development and work by spiraling around the axon, sometimes with as many A Schwann cell in culture. as 100 revolutions. A well-developed Schwann cell is shaped like a rolled-up sheet of paper, with layers of myelin in between each coil. The inner layers of the wrapping, which are predominantly membrane material, form the myelin sheath while the outermost layer of nucleated cytoplasm forms the neurolemma. Only a small volume of residual cytoplasm communicates the inner from the outer layers. This is seen histologically as the Schmidt-Lantermann incisure. A number of experimental studies since 2001 have implanted Schwann cells in an attempt to induce remyelination in multiple sclerosis-afflicted patients.[3] In the past two decades, many studies have demonstrated positive results and potential for Schwann cell transplantation as a therapy for spinal cord injury, both in aiding regrowth and myelination of damaged CNS axons.[4] Indeed, Schwann cells are known for their roles in supporting nerve regeneration.[5] Nerves in the PNS consist of many axons myelinated by Schwann cells. If damage occurs to a nerve, the Schwann cells will aid in digestion of its axons (phagocytosis). Following this process, the Schwann cells can guide regeneration by forming a type of tunnel that leads toward the target neurons. The stump of the damaged axon is able to sprout, and those sprouts that grow through the Schwann-cell “tunnel” do so at the rate of approximately 1mm/day in good conditions. The rate of regeneration decreases with time. Successful axons can therefore reconnect with the muscles or organs they previously controlled with the help of Schwann cells, however, specificity is not maintained and errors are frequent, especially when long distances are involved.[6] If Schwann cells are prevented from associating with axons, the axons die. Regenerating axons will not reach any target unless Schwann cells are there to support them and guide them. They have been shown to be in advance of the growth cones. Schwann cells are essential for the maintenance of healthy axons. They produce a variety of factors, including neurotrophins, and also transfer essential molecules across to axons.
Schwann cell
323
Schwann cell lineage
Schwann cells are of neural crest origin. During mouse embryonic development, neural crest cells first differentiate into Schwann cell precursors (SCPs) at around embryonic day (E) 12–13. These precursor cells subsequently differentiate into immature Schwann cells at approximately E15–16, persisting until birth. The postnatal fate of the immature Schwann cell depends on its random association with axons. In a process called radial sorting, whereby Schwann cells segregate axons by extending processes into axon bundles, the Schwann cells that happen to associate with a large diameter axon (>1 μm) will develop into myelinating Schwann cells. Small diameter axons become entrenched in the invaginations of non-myelinating Schwann cells, also called Remak bundles. A key regulator of this process is the axonally-derived signal Neuregulin-1, which binds to cell surface receptors on the Schwann cell and promotes myelination of large diameter axons and sorting of small diameter axons in Remak bundles, dependent on the activity of the β-secretase BACE1 ([7][8][9][10][11]). A further class of non-myelinating Schwann cell, the terminal (or perisynaptic) Schwann cell, exists at the neuromuscular junction, in close proximity to the neuron-muscle synapse. The transition from immature Schwann cell to myelinating/non-myelinating Schwann cell is reversible. When the nerve is injured, Schwann cells can dedifferentiate to form a cell type resembling the immature Schwann cell, often referred to as a denervated or dedifferentiated Schwann cell. This allows them to re-enter the cell cycle in order to proliferate and aid nerve regeneration.[12]
Immunoreactivity
The different classes of Schwann cells express characteristic antigenic markers that can be targeted with antibodies. Myelinating Schwann cells can be visualised by immunohistochemistry using antibodies against the proteins S-100, Myelin protein zero (P-Zero) and Myelin basic protein (MBP). Non-myelinating Schwann cells such as those that form Remak bundles and terminal Schwann cells are positive for S-100 and Glial fibrillary acidic protein (GFAP).
References
[1] Kalat, James W. Biological Psychology, 9th ed. USA: Thompson Learning, 2007. [2] "Medical Student Named Rhodes Scholar" (http:/ / focus. hms. harvard. edu/ 2003/ Oct24_2003/ neurology. html) - FOCUS - News from Harvard Medical, Dental and Public Health Schools - Copyright © 2010 President and Fellows of Harvard College. [6] Carlson, Neil R. Physiology of Behavior, 9th ed. USA: Pearson Education, Inc., 2007.
External links
• Diagram at clc.uc.edu (http://biology.clc.uc.edu/courses/bio105/nervous.htm) • BU Histology Learning System: 21301loa (http://www.bu.edu/histology/p/21301loa.htm)—"Ultrastructure of the Cell: myelinated axon and Schwann cell" • Cell Centered Database - Schwann cell (http://ccdb.ucsd.edu/sand/main?stype=lite&keyword=schwann& Submit=Go&event=display&start=1)
Satellite glial cell
324
Satellite glial cell
Neuron: Satellite Cell
NeuroLex ID sao792373294 [1] Code Latin TH H2.00.06.2.02002 gliocytus ganglionicus [1]
Satellite glial cells are a type of glial cell that line the exterior surface of neurons in the peripheral nervous system (PNS). Satellite glial cells (SGCs) also surround neuron cell bodies within ganglia.[][] They are of a similar embryological origin to Schwann cells of the PNS, as they are both derived from the neural crest of the embryo during development.[] SGCs have been found to hold a variety of roles, including control over the microenvironment of sympathetic ganglia.[] They are thought to have a similar role to astrocytes in the central nervous system (CNS).[] They supply nutrients to the surrounding neurons and also have some structural function. Satellite cells also act as protective, cushioning cells. Additionally, they express a variety of receptors that allow for a range of interactions with neuroactive chemicals.[] Many of these receptors and other ion channels have recently been implicated in health issues including chronic pain[] and herpes simplex.[] There is much more to be learned about these cells, and research surrounding additional properties and roles of the SGCs is ongoing.[]
Anatomy
Satellite glial cells are the principle glial cells found in the peripheral nervous system, specifically in sensory,[] sympathetic, and parasympathetic ganglia.[] They compose the thin cellular sheaths that surround the individual neurons in these ganglia. In an SGC, the cell body is denoted by the region containing the single, relatively large nucleus. Each side of the cell body extends outward, forming perineuronal processes. The region containing the nucleus has the largest volume of cytoplasm, making this region of the SGC sheath thicker.[] The sheath can be even thicker if multiple SGCs are layered on top of one another, each measuring 0.1 micrometres (3.9×10−6 in).[] Despite their flattened shape, satellite glial cells contain all common organelles necessary to make cellular products and to maintain the homeostatic environment of the cell. The plasma membrane of SGCs is thin and not very dense,[] and it is associated with adhesion molecules,[] receptors for neurotransmitters and other molecules,[] and ion channels, specifically potassium ion channels.[] Within individual Satellite glial cells are expressed throughout the SGCs, there is both rough endoplasmic reticulum[] and smooth sympathetic and parasympathetic ganglia in their [] endoplasmic reticulum, but the latter is much less abundant.[] Most respective nervous system divisions. often the Golgi apparatus and the centrioles in an SGC are found in a region very close to the cell’s nucleus. On the other hand, mitochondria are found throughout the cytoplasm[] along with the organelles involved in autophagy and other forms of catabolic degradation, such as lysosomes, lipofuscin granules, and peroxisomes.[] Both microtubules and intermediate filaments can be seen throughout the cytoplasm, and most often they lie parallel to the SGC sheath. These filaments are found in greater concentrations at the axon
Satellite glial cell hillock and at the beginning portion of an axon in an SGC of the sympathetic ganglia.[] In some SGCs of the sensory ganglia researchers have seen a single cilium that extends outward from the cell surface near the nucleus and into the extracellular space of a deep indentation in the plasma membrane.[] The cilium, however, only has the nine pairs of peripheral microtubules while it lacks the axial pair of microtubules, making its structure very similar to the cilia of neurons, Schwann cells, and astrocytes of the CNS.[]
325
In sensory ganglia
Satellite glial cells in sensory ganglia are laminar cells that most often lack any true processes extending from the cell body. In general an envelope of multiple SGCs completely surrounds each sensory neuron.[] The number of SGCs that make up the sheath increases proportionately with the volume of the neuron which it surrounds. Additionally, the volume of the sheath itself increases proportionately with the volume and surface area of the neuron’s somata. The distance of extracellular space between the sheath and the neuronal plasma membrane measures 20 nanometres (7.9×10−7 in), allowing the neuron and its SGC sheath to form a single anatomical and functional unit.[] These individual units are separated by areas of connective tissue. However, there are some sensory neurons that occupy the same space within connective tissue and are therefore grouped together in a “cluster” of two or three neurons. Most often each individual neuron in a cluster is still surrounded by its own SGC sheath, but in some cases it is missing.[] Some sensory neurons have small projections called microvilli that extend outward from their cell surfaces. Due to their close proximity to the SGC sheath, these microvilli of the neuronal plasma membrane reach into the grooves of the sheath, allowing for possible exchange of materials between the cells.[]
In sympathetic ganglia
In the sympathetic ganglia, satellite glial cells are one of three main types of cells, the other two being the sympathetic ganglion neurons and small intensely fluorescent (SIF) cells.[] SIF cells of sympathetic ganglia are separated into groups, each of which is surrounded by an SGC sheath.[] The SGCs of the sympathetic ganglia come from the neural crest and do not proliferate during embryonic development until the neurons are present and mature, indicating that the neurons signal the division and maturation of the SGCs.[] The SGCs of sympathetic ganglia follow the same basic structure as the SGCs of sensory ganglia, except that sympathetic ganglia also receive synapses. Therefore, the SGC sheath of sympathetic neurons must extend even further to cover the axon hillock near the somata.[] Like the regions of the sheath near the glial nucleus, the regions of the sheath at the axon hillocks are thicker than those surrounding the rest of the neuron. This indicates that the SGCs play a role in the synaptic environment, thereby influencing synaptic transmission.
Differences from other glial cells
Many people liken SGCs to the astrocytes of the CNS because they share certain anatomical and physiological properties, such as the presence of neurotransmitter transporters and the expression of glutamine synthetase.[] However, there are distinguishing factors that put SGCs in their own distinct category of glial cells. SGCs most often surround individual sensory and parasympathetic neurons with a complete, unbroken sheath while most neurons of sympathetic ganglia lack a completely continuous SGC sheath, allowing for limited direct exchange of materials between the extracellular space of the neuron and the space within the connective tissue where the SGCs are situated.[] Furthermore, gap junctions exist between SGCs in the sheaths of adjacent neurons as well as between SGCs in the same sheath (reflexive gap junctions).[] These gap junctions have been identified through the use of electron microscopy and weight tracer markers, such as Lucifer yellow or neurobiotin. The degree to which SGCs are coupled to SGCs of another sheath or to SGCs of the same sheath is dependent on the pH of the cellular environment.[] From studies on rats and mice, researchers have found that satellite glial cells express many neurotransmitter receptors, such as muscarinic acetylcholine and erythropoietin receptors.[] In order to differentiate between SGCs
Satellite glial cell and other glial cells researchers have used markers to identify which proteins are found in different cells. Although SGCs express glial fibrillary acidic protein (GFAP)[]and different S-100 proteins,[] the most useful marker available today for SGC identification is glutamine synthetase (GS). The levels of GS are relatively low at rest, but they greatly increase if the neuron undergoes axonal damage.[] Furthermore, SGCs also possess mechanisms to release cytokines, adenosine triphosphate (ATP), and other chemical messengers.[]
326
Function
Research is currently ongoing in determining the physiological role of satellite glial cells. Current theories suggest that SGCs have a significant role in controlling the microenvironment of the sympathetic ganglia. This is based on the observation that SGCs almost completely envelop the neuron and can regulate the diffusion of molecules across the cell membrane.[] It has been previously shown that when fluorescent protein tracers are injected into the cervical ganglion in order to bypass the circulatory system, they are not found on the neuron surface. This suggests that the SGCs can regulate the extracellular space of individual neurons.[] Some speculate that SGCs in the autonomic ganglia have a similar role to the blood–brain barrier as a functional barrier to large molecules.[] SGCs role as a regulator of neuronal microenvironment is further characterized by its electrical properties which are very similar to that of astrocytes.[] Astrocytes have a well studied and defined role in controlling the microenvironment within the brain, therefore researchers are investigating any homologous role of SGCs within the sympathetic ganglia. An established mode of controlling the microenvironment in sensory ganglia is the uptake of substances by specialized transporters which carry neurotransmitters into cells when coupled with Na+ and Cl−.[] Transporters for glutamate and gamma-Aminobutyric acid (GABA)[] have been found in SGCs. They appear to be actively engaged in the control of the composition of the extracellular space of the ganglia. The enzyme glutamine synthetase, which catalyzes the conversion of glutamate into glutamine, is found in large amounts in SGCs.[] Additionally, SGCs contain the glutamate related enzymes glutamate dehydrogenase and pyruvate carboxylase, and thus can supply the neurons not only with glutamine, but also with malate and lactate.[]
Molecular properties
Unlike their adjacent neurons, SGCs do not have synapses but are equipped with receptors for a variety of neuroactive substances that are analogous to those found in neurons.[] Axon terminals as well as other parts of the neuron carry receptors to substances such as acetylcholine (ACh), GABA, glutamate, ATP, noradrenaline, substance P, and capsaicin that directly affect the physiology of these cells.[] Current research is revealing that SGCs are also able to respond to some of the same chemical stimuli as neurons. The research is ongoing and SGCs role in injury repair mechanisms is not yet fully understood. Molecular characteristics of SGCs
Molecule [] Type of Ganglia Method of Detection Comments
Glutamine synthetase Mouse TG GFAP Rat DRG, TG Rat DRG Rat, rabbit DRG Rat DRG
IHC IHC
Catalyzes the condensation of glutamate and ammonia to form glutamine Upregulated by nerve damage
S100 Endothelin ETB receptor Bradykinin B2 receptor P2Y receptor
IHC IHC, autoradiography
Upregulated by nerve damage Blockers of ETs are shown to alleviate pain in animal models
Electrophysiology
Involved in the inflammatory process
Mouse TG
Ca2+ imaging, IHC
Contributes to nociception
Satellite glial cell
327
Rat DRG IHC, mRNA (ISH) Role not well defined in sensory ganglia
ACh muscarinic receptor NGF trkA receptor TGFα Erythropoietin receptor TNF-α
Rat DRG Rat DRG Rat DRG
Immuno-EM mRNA (ISH), IHC IHC
May play a role in response to neuronal injury Stimulates neural proliferation after injury
Mouse DRG, IHC TG Mouse TG Rat DRG Rat DRG Rat DRG IHC IHC IHC IHC
Inflammatory mediator increased by nerve crush, herpes simplex activation
IL-6 ERK JAK2 Somatostatin sst1 receptor GABA transporter Glutamate transporter Guanylate cyclase
Cytokine released during inflammation, increased by UV irradiation Involved in functions including the regulation of meiosis, and mitosis Signaling protein apart of the type II cytokine receptor family Somatostatin inhibits the release of many hormones and other secretory proteins
Rat DRG Rat DRG
Autoradiography mRNA (ISH), IHC, Autoradiography IHC for cGMP Terminates the excitatory neurotransmitter signal by removal (uptake) of glutamate Second messenger that internalizes the message carried by intercellular messengers such as peptide hormones and NO Known to function as a neuromodulator as well as a trophic factor in the central nervous system
Rat DRG, TG Chick DRG
PGD synthase
IHC
Roles in health issues
Chronic pain
Glial cells, including SGCs, have long been recognized for their roles in response to neuronal damage and injury. SCGs have specifically been implicated in a new role involving the creation and persistence of chronic pain, which may involve hyperalgesia and other forms of spontaneous pain.[] Secretion of bioactive molecules SGCs have the ability to release cytokines and other bioactive molecules that transmit pain neuronally.[] Neurotrophins and tumor necrosis factor α (TNFα) are other cellular factors that work to sensitize neurons to pain.[] SGCs are present in the PNS in fewer numbers than other more well-known types of glial cells, like astrocytes, but have been determined to have an impact on nociception because of some of their physiological and pharmacological properties.[] In fact, just like astrocytes, SGCs have the ability to sense and regulate neighboring neuronal activity.[] First, after a period of nerve cell injury, SGCs are known to up-regulate GFAP and to undergo cell division. They have the ability to release chemoattractants, which are analogous to those released by Schwann cells and contribute to the recruitment and proliferation of macrophages. Additionally, several research groups have found that SGC coupling increases after nerve damage, which has an effect on the perception of pain, likely for several reasons. Normally, the gap junctions between SGCs are used in order to redistribute potassium ions between adjacent cells. However, in coupling of SGCs, the number of gap junctions greatly increases. This may possibly be to deal with larger amounts of ATP and glutamate, which eventually leads to increased recycling of the glutamate. The increased levels of glutamate lead to over excitation and an increase in nociception.[]
Satellite glial cell Expression of receptors and ion channels Various neuronal receptors present on SGCs have been named as participants in ATP-evoked pain signals, particularly the homomultimer P2X3 and the heteromultimer P2X2/3 purinoceptors. In general, the P2X family of receptors responds to neuronally released ATP. Each of the P2X subtypes are found in sensory neurons with the exception of the P2X7 receptor, which is selectively expressed by glial cells, including SGCs. The receptor has been implicated in the release of interleukin IL-1β from macrophages or microglia and astrocytes. The receptor likely has a part in the cascade of events that end with inflammation and neuropathic pain. It has been discovered that this receptor has an antagonist in the form of A-317491, which, when present, has the ability to reduce both the evoked and unprompted firing of various classes of spinal neurons, as well as to inhibit release of IL-1β. However, the outside influences of receptors P2X3 and P2Y1 are believed to complicate the interactions between P2X7 and its antagonist, making it a non-ideal target when using pharmacological strategy.[]
328
Representation of a typical P2X receptor subunit associated with the plasma membrane.
P2Y receptors are also found on both neurons and glial cells. Their role is less clear than that of the P2X receptors, but it has been noted they have several conflicting functions. In some cases, these receptors act as analgesics, as P2Y1 has the ability to inhibit the action of P2X3. In other cases, the receptors contribute to nociception through the modulation of the extracellular concentration of calcitonin gene related peptide (CGRP). These conflicting roles are being researched further so that they may serve as potential targets for the development of a variety of therapeutic drugs.[] SGCs also express a specific type of channel, the Kir4.1 channel, which works to maintain the desired low extracellular K+ concentration in order to control hyperexcitability, which is known to cause migraines. Additionally, extracellular K+ concentration has been found to be controlled by guanine nucleoside guanosine (Guo). Guo, which may be involved in neuron-to-SGC communication and interaction in sensory ganglia, is also a potential target that could control the alterations of extracellular K+ concentration associated with chronic pain.[]
Satellite glial cell
329
Herpes simplex
Sensory ganglia have been associated with infections from viruses like herpes simplex, which can exist in a dormant state within the ganglia for decades after the primary infection.[] When the virus becomes reactivated, blisters on the skin and mucous membranes appear. During the latent stage of the virus, the viruses are rarely located in the SGCs within the sensory ganglia, but the SGCs may still play an important role within the disease.[] It has been proposed that SGCs act to create walls to prevent the spread of the virus from infected to uninfected neurons.[][] If this wall of protection was to break down, then the infection could become more widespread.[] This property may be explained by looking at the location and arrangement of the SGCs, as they are centered on the neurons, allowing them to protect the neurons. It has also been proposed that SGCs may have a job in ridding the ganglia of the virus and in protecting and repairing the nervous system after the virus has left the dormant stage.[]
Herpes simplex virions.
Research directions
The majority of the information available on the subject of SGCs comes from research which was focused on the sensory neurons that the SGCs surround rather than the SGCs themselves. In the future, researchers plan to give more time and attention to the SGCs, which have many supportive and protective functions essential for life.[] Neurotransmitter and hormone receptors on SGCs in situ rather than in culture will likely be explored and definitively characterized.[] Changes in the receptors caused by various mutations and diseases will also be explored in order to determine the impact of these conditions.[] Additionally, the mechanisms behind neuronal-SGC communication is essentially unidentified, though it is likely that the various receptors both the neurons and SGCs have are used for chemical signaling, perhaps with P2Y.[] Ca2+ and NO and their impacts must also be observed to gain further understanding of interactions between the two types of cells.[] Finally, the possibility of an influence of SGCs on synaptic transmission within autonomic ganglia provides another direction for future research.[]
References
Neuroglia
330
Neuroglia
Glia
MeSH Glia [1] Code TA A14.0.00.005 [1] TH H2.00.06.2.00001
[2]
Glial cells, sometimes called neuroglia or simply glia (Greek γλία, γλοία "glue"; pronounced in English as either /ˈɡliːə/ or /ˈɡlaɪə/), are non-neuronal cells that maintain homeostasis, form myelin, and provide support and protection for neurons in the brain, and for neurons in other parts of the nervous system such as in the autonomic nervous system.[1] As the Greek name implies, glia are commonly known as the glue of the nervous system; however, this is not fully accurate. Neuroscience currently identifies four main functions of glial cells: 1. To surround neurons and hold them in place, 2. To supply nutrients and oxygen to neurons, 3. To insulate one neuron from another, 4. To destroy pathogens and remove dead neurons. For over a century, it was believed that they did not play any role in neurotransmission. That idea is now discredited;[] they do modulate neurotransmission, although the mechanisms are not yet well understood.[][][]
Neuroglia of the brain shown by Golgi's method.
Functions
Astrocytes can be identified in culture because, unlike other mature
glia, they express glial fibrillary acidic protein. Some glial cells function primarily as the physical support for neurons. Others regulate the internal environment of the brain, especially the fluid surrounding neurons and their synapses, and nutrify neurons. During early embryogenesis glial cells direct the migration of neurons and produce molecules that modify the growth of axons and dendrites. Recent researchWikipedia:Avoid weasel words indicates that glial cells of the hippocampus and cerebellum participate in synaptic transmission, regulate the clearance of neurotransmitters from the synaptic cleft, and release gliotransmitters such as ATP, which modulate synaptic function.
Neuroglia
331
Glial cells are known to be capable of mitosis. By contrast, scientific understanding of whether neurons are permanently post-mitotic,[2] or capable of mitosis,[3] is still developing. In the past, glia had been consideredWikipedia:Avoid weasel words to lack certain features of neurons. For example, glial cells were not believed to have chemical synapses or to release transmitters. They were considered to be the passive bystanders of neural transmission. However, recent studies have shown this to be untrue.[4] For example, astrocytes are crucial in clearance of neurotransmitters from within the synaptic cleft, which provides distinction between arrival of action potentials and prevents toxic build-up of certain neurotransmitters such as glutamate (excitotoxicity). It is also thought that glia play a role in many neurological diseases, including Alzheimer's disease. Furthermore, at least in vitro, astrocytes can release gliotransmitter glutamate in response to certain stimulation. Another unique type of glial cell, the oligodendrocyte precursor cells or OPCs, have very well-defined and functional synapses from at least two major groups of neurons.[citation needed] The only notable differences between neurons and glial cells are neurons' possession of axons and dendrites, and capacity to generate action potentials.
Glial cells in a rat brain stained with an antibody against GFAP.
23 week fetal brain culture astrocyte
Glia ought not to be regarded as "glue" in the nervous system as the name implies; rather, they are more of a partner to neurons.[5] They are also crucial in the development of the nervous system and in processes such as synaptic plasticity and synaptogenesis. Glia have a role in the regulation of repair of neurons after injury. In the CNS (Central Nervous System), glia suppress repair. Glial cells known as astrocytes enlarge and proliferate to form a scar and produce inhibitory molecules that inhibit regrowth of a damaged or Neoplastic glial cells stained with an antibody against GFAP severed axon. In the PNS (Peripheral Nervous System), (brown). Brain biopsy. glial cells known as Schwann cells promote repair. After axonal injury, Schwann cells regress to an earlier developmental state to encourage regrowth of the axon. This difference between PNS and CNS raises hopes for the regeneration of nervous tissue in the CNS. For example a spinal cord may be able to be repaired following injury or severance.
Neuroglia
332
Types
Microglia
Microglia are specialized macrophages capable of phagocytosis that protect neurons of the central nervous system.[6] They are derived from hematopoietic precursors rather than ectodermal tissue; they are commonly categorized as such because of their supportive role to neurons. These cells are found in all regions of the brain and spinal cord. Microglial cells are small relative to macroglial cells, with changing shapes and oblong nuclei. They are mobile within the brain and multiply when the brain is damaged. In the healthy central nervous system, microglia processes constantly sample all aspects of their environment (neurons, macroglia and blood vessels).
Macroglia
Location Name CNS Astrocytes Description The most abundant type of macroglial cell, astrocytes (also called astroglia) have numerous projections that anchor neurons to their blood supply. They regulate the external chemical environment of neurons by removing excess ions, notably potassium, and recycling neurotransmitters released during synaptic transmission. The current theory suggests that astrocytes may be the predominant "building blocks" of the blood–brain barrier. Astrocytes may regulate vasoconstriction and vasodilation by producing substances such as arachidonic acid, whose metabolites are vasoactive. Astrocytes signal each other using calcium. The gap junctions (also known as electrical synapses) between astrocytes allow the messenger molecule IP3 to diffuse from one astrocyte to another. IP3 activates calcium channels on cellular organelles, releasing calcium into the cytoplasm. This calcium may stimulate the production of more IP3. The net effect is a calcium wave that propagates from cell to cell. Extracellular release of ATP, and consequent activation of purinergic receptors on other astrocytes, may also mediate calcium waves in some cases. In general, there are two types of astrocytes, protoplasmic and fibrous, similar in function but distinct in morphology and distribution. Protoplasmic astrocytes have short, thick, highly branched processes and are typically found in gray matter. Fibrous astrocytes have long, thin, less branched processes and are more commonly found in white matter. It has recently been shown that astrocyte activity is linked to blood flow in the brain, and that this is what is actually [7] being measured in fMRI. They also have been involved in neuronal circuits playing an inhibitory role after [8] sensing changes in extracellular calcium. CNS Oligodendrocytes Oligodendrocytes are cells that coat axons in the central nervous system (CNS) with their cell membrane forming a specialized membrane differentiation called myelin, producing the so-called myelin sheath. The myelin sheath [9] provides insulation to the axon that allows electrical signals to propagate more efficiently. Ependymal cells Ependymal cells, also named ependymocytes, line the cavities of the CNS and make up the walls of the ventricles. These cells create and secrete cerebrospinal fluid(CSF) and beat their cilia to help circulate the CSF and make up the [10] Blood-CSF barrier. They are also thought to act as neural stem cells. Radial glia cells arise from neuroepithelial cells after the onset of neurogenesis. Their differentiation abilities are more restricted than those of neuroepithelial cells. In the developing nervous system, radial glia function both as neuronal progenitors and as a scaffold upon which newborn neurons migrate. In the mature brain, the cerebellum and retina retain characteristic radial glial cells. In the cerebellum, these are Bergmann glia, which regulate synaptic plasticity. In the retina, the radial Müller cell is the principal glial cell, and participates in a bidirectional [11] communication with neurons. Similar in function to oligodendrocytes, Schwann cells provide myelination to axons in the peripheral nervous system (PNS). They also have phagocytotic activity and clear cellular debris that allows for regrowth of PNS [12] neurons.
CNS
CNS
Radial glia
PNS
Schwann cells
Neuroglia
[13] Satellite glial cells are small cells that surround neurons in sensory, sympathetic and parasympathetic ganglia. These cells help regulate the external chemical environment. Like astrocytes, they are interconnected by gap junctions and respond to ATP by elevating intracellular concentration of calcium ions. They are highly sensitive to [14] injury and inflammation, and appear to contribute to pathological states, such as chronic pain.
333
Satellite cells
PNS
PNS
Enteric glial cells Are found in the intrinsic ganglia of the digestive system.They are thought to have many roles in the enteric system, [15] some related to homeostasis and muscular digestive processes.
Other
Pituicytes from the posterior pituitary are glia cells with characteristics in common to astrocytes.[16] Tanycytes from the hypothalamus descend from radial glia.[17]
Capacity to divide
Glia retain the ability to undergo cell division in adulthood, whereas most neurons cannot. The view is based on the general deficiency of the mature nervous system in replacing neurons after an injury, such as a stroke or trauma, while very often there is a profound proliferation of glia, or gliosis near or at the site of damage. However, detailed studies found no evidence that 'mature' glia, such as astrocytes or oligodendrocytes, retain the ability of mitosis. Only the resident oligodendrocyte precursor cells seem to keep this ability after the nervous system matures. On the other hand, there are a few regions in the mature nervous system, such as the dentate gyrus of the hippocampus and the subventricular zone, where generation of new neurons can be observed.[18]
Embryonic development
Most glia are derived from ectodermal tissue of the developing embryo, in particular the neural tube and crest. The exception is microglia, which are derived from hemopoietic stem cells. In the adult, microglia are largely a self-renewing population and are distinct from macrophages and monocytes, which infiltrate the injured and diseased CNS. In the central nervous system, glia develop from the ventricular zone of the neural tube. These glia include the oligodendrocytes, ependymal cells, and astrocytes. In the peripheral nervous system, glia derive from the neural crest. These PNS glia include Schwann cells in nerves and satellite glial cells in ganglia.
History
Glia were first described in 1856 by the pathologist Rudolf Virchow in a comment to his 1846 publication on connective tissue. In his 1858 publication `Cellularpathology´, he described glial cells in more detail. [19]
Numbers
Neuroglial cells are generally smaller than neurons and outnumber them by five to ten times; they comprise about half the total volume of the brain and spinal cord.(Clinical Neuro-Anatomy, Richard S. Snell, 7th edition) [] The ratio differs from one part of the brain to another. The glia/neuron ratio in the cerebral cortex is 3.72 (60.84 billion glia; 16.34 billion neurons) while that of the cerebellum is only 0.23 (16.04 billion glia; 69.03 billion neurons). The ratio in the cerebral cortex gray matter is 1.48 (the white matter part has few neurons). The ratio of the basal ganglia, diencephalon and brainstem combined is 11.35.[] Most cerebral cortex glia are oligodendrocytes (75.6%); astrocytes account for 17.3% and microglia (6.5%)[20] The amount of brain tissue that is made up of glial cells increases with brain size: the nematode brain contains only a few glia; a fruitfly's brain is 25% glia; that of a mouse, 65%; a human, 90%; and an elephant, 97%.Wikipedia:Please clarify[21]
Neuroglia
334
Additional images
Oligodendrocyte
Section of central canal of medulla spinalis, showing ependymal and neuroglial cells.
Transverse section of a cerebellar folium.
References
Notes
[1] Jessen, Kristjan R. & Mirsky, Rhona Glial cells in the enteric nervous system contain glial fibrillary acidic protein Nature 286, 736–737 (14 August 1980); [2] Nature Reviews Neuroscience 8, 368–378 (May 2007) | [3] ; ; . [4] The Other Brain, by R. Douglas Fields, Ph. D. Simon & Schuster, 2009 [5] The Root of Thought: Unlocking Glia, by Andrew Koob, FT Science Press, 2009 [6] Brodal, 2010: p. 19 (http:/ / books. google. com/ books?id=iJjI6yDNmr8C& pg=PA19) [9] Baumann, Nicole; Pham-Dinh, Danielle (2001), "Biology of Oligodendrocyte and Myelin in the Mammalian Central Nervous System", Physiological Reviews 18 (2): 871–927 [12] Jessen, K. R. & Mirsky, R. (2005), "The origin and development of glial cells in peripheral nerves", Nature Reviews Neuroscience 6 (9): 671–682 [13] Hanani, M. Satellite glial cells in sensory ganglia: from form to function. Brain Res. Rev. 48:457–476, 2005 [14] Ohara PT et al., Evidence for a role of connexin 43 in trigeminal pain using RNA interference in vivo. J Neurophysiol 2008;100:3064–3073 [15] Bassotti, G. et al, Laboratory Investigation (2007) 87, 628–632 [18] David R. Kornack*, Pasko Rakic (2008). Continuation of neurogenesis in the hippocampus of the adult macaque monkey Section of Neurobiology, Yale University School of Medicine, New Haven, CT 06510- (http:/ / www. pnas. org/ content/ 96/ 10/ 5768. abstract) [20] (figures given are those for females)
Bibliography
• Brodal, Per (2010). "Glia" (http://books.google.com/books?id=iJjI6yDNmr8C&pg=PA19). The central nervous system: structure and function. Oxford University Press. p. 19. ISBN 978-0-19-538115-3. • Kettenmann and Ransom, Neuroglia, Oxford University Press, 2012, ISBN13: 9780199794591 |http:// ukcatalogue.oup.com/product/9780199794591.do#.UVcswaD3Ay4|
Further reading
• "The Mystery and Magic of Glia: A Perspective on Their Roles in Health and Disease." (http://download.cell. com/images/edimages/neuron/pdf/barres.pdf) Neuron 60, November 6, 2008 by Ben Barres • Role of glia in synapse development (http://pfrieger.gmxhome.de/work/publications/pfrieger_2002.pdf) • Overstreet L (2005). "Quantal transmission: not just for neurons". Trends Neurosci 28 (2): 59–62. doi: 10.1016/j.tins.2004.11.010 (http://dx.doi.org/10.1016/j.tins.2004.11.010). PMID 15667925 (http://www. ncbi.nlm.nih.gov/pubmed/15667925). article (http://www.sciencedirect.com/science?_ob=ArticleURL&
Neuroglia _udi=B6T0V-4F05G3W-1&_coverDate=02/01/2005&_alid=242540802&_rdoc=1&_fmt=&_orig=search& _qd=1&_cdi=4872&_sort=d&view=c&_acct=C000006078&_version=1&_urlVersion=0&_userid=75682& md5=a6462b73c196ee912e6ea3407462f0b3) Peters A (2004). "A fourth type of neuroglial cell in the adult central nervous system". J Neurocytol 33 (3): 345–57. doi: 10.1023/B:NEUR.0000044195.64009.27 (http://dx.doi.org/10.1023/B:NEUR.0000044195. 64009.27). PMID 15475689 (http://www.ncbi.nlm.nih.gov/pubmed/15475689). Volterra A, Steinhäuser C (2004). "Glial modulation of synaptic transmission in the hippocampus". Glia 47 (3): 249–57. doi: 10.1002/glia.20080 (http://dx.doi.org/10.1002/glia.20080). PMID 15252814 (http://www. ncbi.nlm.nih.gov/pubmed/15252814). Huang Y, Bergles D (2004). "Glutamate transporters bring competition to the synapse". Curr Opin Neurobiol 14 (3): 346–52. doi: 10.1016/j.conb.2004.05.007 (http://dx.doi.org/10.1016/j.conb.2004.05.007). PMID 15194115 (http://www.ncbi.nlm.nih.gov/pubmed/15194115). Artist ADSkyler (http://www.anioman.com/Profile.php?viewedArtistID=1793201250&gallery=&page=1& back=1)(uses concepts of neuroscience and found inspiration from Glia)
335
•
•
•
•
External links
Audio • "The Other Brain" (http://www.wnyc.org/shows/lopate/2010/jan/22/the-other-brain/)—The Leonard Lopate Show (WNYC) "Neuroscientist Douglas Field, explains how glia, which make up approximately 85 percent of the cells in the brain, work. In The Other Brain: From Dementia to Schizophrenia, How New Discoveries about the Brain Are Revolutionizing Medicine and Science, he explains recent discoveries in glia research and looks at what breakthroughs in brain science and medicine are likely to come." • "Network Glia" (http://www.networkglia.eu/en/) A homepage devoted to glial cells
Astrocyte
336
Astrocyte
For the cell in the gastrointestinal tract, see Interstitial cell of Cajal.
Neuron: Astrocyte
Immunocytochemical staining of Astrocytes in culture using an antibody against glial fibrillary acidic protein. NeuroLex ID Dorlands/Elsevier sao1394521419 12165688 [2] [1]
Astrocytes (etymology: astron gk. star, cyte gk. cell), also known collectively as astroglia, are characteristic star-shaped glial cells in the brain and spinal cord. They are the most abundant cell of the human brain. They perform many functions, including biochemical support of endothelial cells that form the blood–brain barrier, provision of nutrients to the nervous tissue, maintenance of extracellular ion balance, and a role in the repair and scarring process of the brain and spinal cord following traumatic injuries. Research since the mid-1990s has shown that astrocytes propagate intercellular Ca2+ waves over long distances in response to stimulation, and, similar to neurons, release transmitters (called gliotransmitters) in a Ca2+-dependent manner. Data suggest that astrocytes also signal to neurons through Ca2+-dependent release of glutamate.[] Such discoveries have made astrocytes an important area of research within the field of neuroscience.
Description
Astrocytes are a sub-type of glial cells in the central nervous system. They are also known as astrocytic glial cells. Star-shaped, their many processes envelope synapses made by neurons. Astrocytes are classically identified using histological analysis; many of these cells express the intermediate filament glial fibrillary acidic protein (GFAP). Several forms of astrocytes exist in the Central Nervous System including fibrous (in white matter), protoplasmic (in grey matter), and radial. The fibrous glia are usually located within white matter, have relatively few organelles, and exhibit long unbranched cellular processes. This type often has "vascular feet" that physically connect the cells to the outside of capillary walls when they are in close proximity to them. The protoplasmic glia are the most prevalent and are found in grey matter tissue, possess a
Isolated Astrocyte shown with confocal microscopy. Image: Nathan S. Ivey and Andrew G. MacLean
Astrocyte
337
larger quantity of organelles, and exhibit short and highly branched tertiary processes. The radial glia are disposed in a plane perpendicular to axis of ventricles. One of their processes about the pia mater, while the other is deeply buried in gray matter. Radial glia are mostly present during development, playing a role in neuron migration. Mueller cells of retina and Bergmann glia cells of cerebellar cortex represent an exception, being present still during adulthood. When in proximity to the pia mater, all three forms of astrocytes send out processes to form the pia-glial membrane.
Astrocyte - rodent cell culture stained for GFAP (red)
23 weeks fetal brain culture human astrocyte
Astrocytes - rat spinal cord stained for GFAP (green)
Astrocytes (red) among neurons in the living cerebral cortex
Astrocyte
338
Functions
Previously in medical science, the neuronal network was considered the only important one, and astrocytes were looked upon as gap fillers. More recently, the function of astrocytes has been reconsidered,[1] and are now thought to play a number of active roles in the brain, including the secretion or absorption of neural transmitters and maintenance of the blood–brain barrier.[2] Following on this idea the concept of a "tripartite synapse" has been proposed, referring to the tight relationship occurring at synapses among a presynaptic element, a postsynaptic element and a glial element.[3]
• Structural: They are involved in the physical structuring of the brain. Astrocytes get their name because they are "star-shaped". They are the most abundant glial cells in the brain that are closely associated with neuronal synapses. They regulate the transmission of electrical impulses within the brain. • Glycogen fuel reserve buffer: Astrocytes contain glycogen and are capable of glycogenesis. The astrocytes next to neurons in the frontal cortex and hippocampus store and release glycogen. Thus, Astrocytes can fuel neurons with glucose during periods of high rate of glucose consumption and glucose shortage. Recent research suggests there may be a connection between this activity and exercise. [4] • Metabolic support: They provide neurons with nutrients such as lactate. • Blood–brain barrier: The astrocyte end-feet encircling endothelial cells were thought to aid in the maintenance of the blood–brain barrier, but recent research indicates that they do not play a substantial role; instead, it is the tight junctions and basal lamina of the cerebral endothelial cells that play the most substantial role in maintaining the barrier.[5] However, it has recently been shown that astrocyte activity is linked to blood flow in the brain, and that this is what is actually being measured in fMRI.[6] [7] • Transmitter uptake and release: Astrocytes express plasma membrane transporters such as glutamate transporters for several neurotransmitters, including glutamate, ATP, and GABA. More recently, astrocytes were shown to release glutamate or ATP in a vesicular, Ca2+-dependent manner.[8] (This has been disputed for hippocampal astrocytes.)[9] • Regulation of ion concentration in the extracellular space: Astrocytes express potassium channels at a high density. When neurons are active, they release potassium, increasing the local extracellular concentration. Because astrocytes are highly permeable to potassium, they rapidly clear the excess accumulation in the extracellular space.[10] If this function is interfered with, the extracellular concentration of potassium will rise, leading to neuronal depolarization by the Goldman equation. Abnormal accumulation of extracellular potassium is well known to result in epileptic neuronal activity.[citation needed] • Modulation of synaptic transmission: In the supraoptic nucleus of the hypothalamus, rapid changes in astrocyte morphology have been shown to affect heterosynaptic transmission between neurons.[11] In the hippocampus, astrocytes suppress synaptic transmission by releasing ATP, which is hydrolyzed by ectonucliotidases to yield adenosine. Adenosine acts on neuronal adenosine receptors to inhibit synaptic transmission, thereby increasing the dynamic range available for LTP.[12] • Vasomodulation: Astrocytes may serve as intermediaries in neuronal regulation of blood flow.[13]
Metabolic interactions between astrocytes and neurons. From a computational study by Çakιr et al., 2007.
Astrocyte • Promotion of the myelinating activity of oligodendrocytes: Electrical activity in neurons causes them to release ATP, which serves as an important stimulus for myelin to form. However, the ATP does not act directly on oligodendrocytes. Instead, it causes astrocytes to secrete cytokine leukemia inhibitory factor (LIF), a regulatory protein that promotes the myelinating activity of oligodendrocytes. This suggest that astrocytes have an executive-coordinating role in the brain.[14] • Nervous system repair: Upon injury to nerve cells within the central nervous system, astrocytes fill up the space to form a glial scar, repairing the area and replacing the CNS cells that cannot regenerate.[citation needed] • Long-term potentiation: Scientists continue to argue back and forth as to whether or not astrocytes integrate learning and memory in the hippocampus. It is known that glial cells are included in neuronal synapses, but many of the LTP studies are performed on slices, so scientists disagree on whether or not astrocytes have a direct role of modulating synaptic plasticity.
339
Recent studies
A recent study, done in November 2010 and published March 2011, was done by a team of scientists from the University of Rochester and University of Colorado School of Medicine They did an experiment to attempt to repair trauma to the Central Nervous System of an adult rat by replacing the glial cells. When the glial cells were injected into the injury of the adult rat’s spinal cord, astrocytes were generated by exposing human glial precursor cells to bone morphogenetic protein (Bone morphogenetic protein is important because it is considered to create tissue architecture throughout the body). So, with the bone protein and human glial cells combined, they promoted significant recovery of conscious foot placement, axonal growth, and obvious increases in neuronal survival in the spinal cord laminae. On the other hand, human glial precursor cells and astrocytes generated from these cells by being in contact with ciliary neurotrophic factors, failed to promote neuronal survival and support of axonal growth at the spot of the injury.[] One study done in Shanghai had two types of hippocampal neuronal cultures: In one culture, the neuron was grown from a layer of astrocytes and the other culture was not in contact with any astrocytes, but they were instead fed a Glial Conditioned Medium (GCM), which inhibits the rapid growth of cultured astrocytes in the brains of rats in most cases. In their results they were able to see that astrocytes had a direct role in Long-term potentiation with the mixed culture (which is the culture that was grown from a layer of astrocytes) but not in GCM cultures.[] Recent studies have shown that astrocytes play an important function in the regulation of neural stem cells. Research from the Schepens Eye Research Institute at Harvard shows the human brain to abound in neural stem cells, which are kept in a dormant state by chemical signals (ephrin-A2 and ephrin-A3) from the astrocytes. The astrocytes are able to activate the stem cells to transform into working neurons by dampening the release of ephrin-A2 and ephrin-A3.[citation needed] Furthermore, studies are underway to determine whether astroglia play an instrumental role in depression, based on the link between diabetes and depression. Altered CNS glucose metabolism is seen in both these conditions, and the astroglial cells are the only cells with insulin receptors in the brain. In a study published in a 2011 issue of Nature Biotechnology[15] and reported in lay science article,[16] a group of researchers from the University of Wisconsin reports that it has been able to direct embryonic and induced human stem cells to become astrocytes. A 2012 study[17] of the effects of marijuana on short term memories found that THC activates CB1 receptors of astrocytes which cause receptors for AMPA to be removed from the membranes of associated neurons.
Astrocyte
340
Calcium waves
Astrocytes are linked by gap junctions, creating an electrically coupled (functional) syncytium.[18] Because of this ability of astrocytes to communicate with their neighbors, changes in the activity of one astrocyte can have repercussions on the activities of others that are quite distant from the original astrocyte. An influx of Ca2+ ions into astrocytes is the essential change that ultimately generates calcium waves. Because this influx is directly caused by an increase in blood flow to the brain, calcium waves are said to be a kind of hemodynamic response function. An increase in intracellular calcium concentration can propagate outwards through this functional syncytium. Mechanisms of calcium wave propagation include diffusion of calcium ions and IP3 through gap junctions and extracellular ATP signalling.[19] Calcium elevations are the primary known axis of activation in astrocytes, and are necessary and sufficient for some types of astrocytic glutamate release.[20]
Development
Astrocytes are macroglial cells in the central nervous system. Astrocytes are derived from heterogeneous populations of progenitor cells in the neuroepithelium of the developing central nervous system. Recent works, summarized in a review by Rowitch and Kriegstein,[21] indicate that there is remarkable similarity between the well known genetic mechanisms that specify the lineage of diverse neuron subtypes and that of macroglial cells. Just as with neuronal cell specification, canonical signaling factors like Sonic hedgehog (SHH), Fibroblast growth factor (FGFs), WNTs and bone morphogenetic proteins (BMPs), provide positional information to developing macroglial cells through morphogen gradients along the dorsal–ventral, anterior–posterior and medial–lateral axes. The resultant patterning along the neuraxis leads to segmentation of the neuroepithelium into progenitor domains (p0, p1 p2, p3 and pMN) for distinct neuron types in the developing spinal cord. On the basis of several studies it is now believed that that this model also applies to macroglial cell specification. Studies carried out by Hochstim and colleagues have demonstrated that three distinct populations of astrocytes arise from the p1, p2 and p3 domains.[22] These subtypes of astrocytes can be identified on the basis of their expression of different transcription factors (PAX6, NKX6.1) and cell surface markers (reelin and SLIT1). The three populations of astrocyte subtypes which have been identified are 1) dorsally located VA1 astrocytes, derived from p1 domain, express PAX6 and reelin 2) ventrally located VA3 astrocytes, derived from p3, express NKX6.1 and SLIT1 and 3) and intermediate white-matter located VA2 astrocyte, derived from the p2 domain, which express PAX6, NKX6.1, reelin and SLIT1.[23] After astrocyte specification has occurred in the developing CNS, it is believed that astrocyte precursors migrate to their final positions within the nervous system before the process of terminal differentiation occurs.
Classification
There are several different ways to classify astrocytes.
Lineage and antigenic phenotype
These have been established by classic work by Raff et al. in early 1980s on Rat optic nerves. • Type 1: Antigenically Ran2+, GFAP+, FGFR3+, A2B5-, thus resembling the "type 1 astrocyte" of the postnatal day 7 rat optic nerve. These can arise from the tripotential glial restricted precursor cells (GRP), but not from the bipotential O2A/OPC (oligodendrocyte, type 2 astrocyte precursor, also called Oligodendrocyte progenitor cell) cells. • Type 2: Antigenically A2B5+, GFAP+, FGFR3-, Ran 2-. These cells can develop in vitro from the either tripotential GRP (probably via O2A stage) or from bipotential O2A cells (which some peopleWikipedia:Avoid weasel words think may in turn have been derived from the GRP) or in vivo when these progenitor cells are transplanted into lesion sites (but probably not in normal development, at least not in the rat optic nerve). Type-2 astrocytes are the major astrocytic component in postnatal optic nerve cultures that are generated by O2A
Astrocyte cells grown in the presence of fetal calf serum but are not thought to exist in vivo (Fulton et al., 1992).
341
Anatomical classification
• Protoplasmic: found in grey matter and have many branching processes whose end-feet envelop synapses. Some protoplasmic astrocytes are generated by multipotent subventricular zone progenitor cells.[][] • Gömöri-positive astrocytes. These are a subset of protoplasmic astrocytes that contain numerous cytoplasmic inclusions, or granules, that stain positively with Gömöri's chrome-alum hematoxylin stain. It is now known that these granules are formed from the remnants of degenerating mitochondria engulfed within lysosomes,[24] Some type of oxidative stress appears to be responsible for the mitochondrial damage within these specialized astrocytes. Gömöri-positive astrocytes are much more abundant within the arcuate nucleus of the hypothalamus and in the hippocampus than in other brain regions. They may have a role in regulating the response of the hypothalamus to glucose.[25][26] • Fibrous: found in white matter and have long thin unbranched processes whose end-feet envelop nodes of Ranvier.[27] Some fibrous astrocytes are generated by radial glia.[][][][][]
Transporter/receptor classification
• GluT type: express glutamate transporters (EAAT1/ SLC1A3 [30] and EAAT2/ SLC1A2 [31]) and respond to synaptic release of glutamate by transporter currents • GluR type: express glutamate receptors (mostly mGluR and AMPA type) and respond to synaptic release of glutamate by channel-mediated currents and IP3-dependent Ca2+ transients
Bergmann glia
Bergmann glia, a type of glia[28][29] also known as radial epithelial cells (as named by Camillo Golgi) or Golgi epithelial cells (GCEs; not to be mixed up with Golgi cells), are astrocytes in the cerebellum that have their cell bodies in the Purkinje cell layer and processes that extend into the molecular layer, terminating with bulbous endfeet at the pial surface. Bergmann glia express high densities of glutamate transporters that limit diffusion of the neurotransmitter glutamate during its release from synaptic terminals. Besides their role in early development of the cerebellum, Bergmann glia are also required for the pruning or addition of synapses.[citation needed]
Pathology
SLC1A3 expression highlights Bergmann glia in the brain of a mouse at 7th postnatal day, sagittal section.
Astrocytomas are primary intracranial tumors derived from astrocytes cells of the brain. It is also possible that glial progenitors or neural stem cells give rise to astrocytomas. Astrocytomas are brain tumors that develop from astrocytes. They may occur in many parts of the brain and sometimes in the spinal cord. They can occur at any age but they primarily occur in males. Astrocytomas are divided into two categories: Low grade (I and II) and High Grade (III and IV). Low grade tumors are more common in children and high grade tumors are more common in adults.[30] Pilocytic Astrocytoma are Grade I tumors. They are considered benign and slow growing tumors. Pilocytic Astrocytomas frequently have cystic portions filled with fluid and a nodule, which is the solid portion. Most are located in the cerebellum. Therefore, most symptoms are related to balance or coordination difficulties.[30] They also
Astrocyte occur more frequently in children and teens.[31] Grade II Tumors grow relatively slow but invade surrounding healthy tissue. Usually considered benign but can grow into malignant tumors. Other names that are used are Fibrillary or Protoplasmic astrocytomas. They are prevalent in younger people who are often present with seizures.[31] Anaplastic astrocytoma is classified as grade III and are malignant tumors. They grow more rapidly than lower grade tumors and tend to invade nearby healthy tissue. Anaplastic astrocytomas recur more frequently than lower grade tumors because of their tendency to spread into surrounding tissue makes them difficult to completely remove surgically.[30] Glioblastoma Multiforme is also a malignant tumor and classified as a grade IV. Glioblastomas can contain more than one cell type (i.e., astrocytes, oligondroctyes). Also, while one cell type may die off in response to a particular treatment, the other cell types may continue to multiply. Glioblastomas are the most invasive type of glial tumors. Grows rapidly and spreads to nearby tissue. Approximately 50% of astrocytomas are glioblastomas and are very difficult to treat.[30]
342
Tripartite synapse
Within the dorsal horn of the spinal cord, activated astrocytes have the ability to respond to almost all neurotransmitters (Haydon, 2001) and, upon activation, release a multitude of neuroactive molecules such as glutamate, ATP, nitric oxide (NO), prostaglandins (PG), and D-serine, which in turn influences neuronal excitability. The close association between astrocytes and presynaptic and postsynaptic terminals as well as their ability to integrate synaptic activity and release neuromodulators has been termed the "tripartite synapse" (Araque et al., 1999). Synaptic modulation by astrocytes takes place because of this 3-part association.
Astrocytes in chronic pain sensitization
Under normal conditions, pain conduction begins with some noxious signal followed by an action potential carried by nociceptive (pain sensing) afferent neurons, which elicit excitatory postsynaptic potentials (EPSP) in the dorsal horn of the spinal cord. That message is then relayed to the cerebral cortex, where we translate those EPSPs into "pain". Since the discovery of astrocytic influence, our understanding of the conduction of pain has been dramatically complicated. Pain processing is no longer seen as a repetitive relay of signals from body to brain, but as a complex system that can be up- and down-regulated by a number of different factors. One factor at the forefront of recent research is in the pain-potentiating synapse located in the dorsal horn of the spinal cord and the role of astrocytes in encapsulating these synapses. Garrison and co-workers (Garrison, 1991)Wikipedia:Citing sources#What information to include were the first to suggest association when they found a correlation between astrocyte hypertrophy in the dorsal horn of the spinal cord and hypersensitivity to pain after peripheral nerve injury, typically considered an indicator of glial activation after injury. Astrocytes detect neuronal activity and can release chemical transmitters, which in turn control synaptic activity (Volters and Meldolesi, 2005; Haydon, 2001; Fellin, et al., 2006). In the past, hyperalgesia was thought to be modulated by the release of substance P and excitatory amino acids (EAA), such as glutamate, from the presynaptic afferent nerve terminals in the spinal cord dorsal horn. Subsequent activation of AMPA (α-amino-3-hydroxy-5-methyl-4-isoxazole proprionic acid), NMDA (N-methyl-D-aspartate) and kainate subtypes of ionotropic glutamate receptors follows. It is the activation of these receptors that potentiates the pain signal up the spinal cord. This idea, although true, is an oversimplification of pain transduction. A litany of other neurotransmitter and neuromodulators, such as calcitonin gene-related peptide (CGRP), adenosine triphosphate (ATP), brain-derived neurotrophic factor (BDNF), somatostatin, vasoactive intestinal peptide (VIP), galanin, and vasopressin are all synthesized and released in response to noxious stimuli. In addition to each of these regulatory factors, several other interactions between pain-transmitting neurons and other neurons in the dorsal horn have added impact on pain pathways.
Astrocyte
343
Two states of persistent pain
After persistent peripheral tissue damage there is a release of several factors from the injured tissue as well as in the spinal dorsal horn. These factors increase the responsiveness of the dorsal horn pain-projection neurons to ensuing stimuli, termed "spinal sensitization," thus amplifying the pain impulse to the brain. Release of glutamate, substance P, and calcitonin gene-related peptide (CGRP) mediates NMDAR activation (originally silent because it is plugged by Mg2+), thus aiding in depolarization of the postsynaptic pain-transmitting neurons (PTN). In addition, activation of IP3 signaling and MAPKs (mitogen-activated protein kinases) such as ERK and JNK, bring about an increase in the synthesis of inflammatory factors that alter glutamate transporter function. ERK also further activates AMPARs and NMDARs in neurons. Nociception is further sensitized by the association of ATP and substance P with their respective receptors, P<sub>2</sub>X<sub>3</sub>, and neurokinin 1 receptor (NK1R), as well as activation of metabotropic glutamate receptors and release of BDNF. Persistent presence of glutamate in the synapse eventually results in dysregulation of GLT1 and GLAST, crucial transporters of glutamate into astrocytes. Ongoing excitation can also induce ERK and JNK activation, resulting in release of several inflammatory factors. As noxious pain is sustained, spinal sensitization creates transcriptional changes in the neurons of the dorsal horn that lead to altered function for extended periods. Mobilization of Ca2+ from internal stores results from persistent synaptic activity and leads to the release of glutamate, ATP, tumor necrosis factor-α (TNF-α), interleukin 1β (IL-1β), IL-6, nitric oxide (NO), and prostaglandin E2 (PGE2). Activated astrocytes are also a source of matrix metalloproteinase 2 (MMP2), which induces pro-IL-1β cleavage and sustains astrocyte activation. In this chronic signaling pathway, p38 is activated as a result of IL-1β signaling, and there is a presence of chemokines that trigger their receptors to become active. In response to nerve damage, heat shock proteins (HSP) are released and can bind to their respective TLRs, leading to further activation.
References
[2] Kolb & Whishaw: Fundamentals of Human Neuropsychology, 2008 [15] http:/ / www. nature. com/ nbt/ journal/ vaop/ ncurrent/ abs/ nbt. 1877. html [16] http:/ / www. sciencedebate. com/ science-blog/ human-astrocytes-cultivated-stem-cells-lab-dish-u-wisconsin-researchers [19] Newman, EA.(2001) "Propagation of intercellular calcium waves in retinal astrocytes and Müller cells." (http:/ / www. pubmedcentral. nih. gov/ articlerender. fcgi?tool=pubmed& pubmedid=11264297)J Neurosci. 21(7):2215-23 [25] Young JK, McKenzie JC (2004) " GLUT2 immunoreactivity in Gömöri-positive astrocytes of the hypothalamus (http:/ / www. jhc. org/ cgi/ content/ full/ 52/ 11/ 1519)."J. Histochemistry & Cytochemistry 52: 1519-1524 PMID [30] Astrocytomas. (2010). Retrieved 2011, from IRSA: http:/ / www. irsa. org/ astrocytoma. html [31] Astrocytoma Tumors (2005, August). Retrieved 2011, from American Association of Neurological Surgeons: http:/ / www. aans. org/ Patient%20Information/ Conditions%20and%20Treatments/ Astrocytoma%20Tumors. aspx.
• Halassa, M.M., Fellin, T., and Haydon, P.G. (2006). "The tripartite synapse: roles for gliotransmission in health and disease". Trends in Mol. Sci 13 (2): 54–63. doi: 10.1016/j.molmed.2006.12.005 (http://dx.doi.org/10. 1016/j.molmed.2006.12.005). PMID 17207662 (http://www.ncbi.nlm.nih.gov/pubmed/17207662). • White, F.A., Jung, H. and Miller, R.J. (2007). "Chemokines and the pathophysiology of neuropathic pain" (http:// www.ncbi.nlm.nih.gov/pmc/articles/PMC2154400). Proc. Natl Acad. Sci. USA 104 (51): 20151–20158. doi: 10.1073/pnas.0709250104 (http://dx.doi.org/10.1073/pnas.0709250104). PMC 2154400 (http://www.ncbi. nlm.nih.gov/pmc/articles/PMC2154400). PMID 18083844 (http://www.ncbi.nlm.nih.gov/pubmed/ 18083844). • Milligan, E.D. and Watson, L.R. (2009). "Pathological and protective roles of glia in chronic pain". Neuron-Glia Interactions 10: 23–36. • Watkins, L.R., Milligan, E.D. and Maier, S.F. (2001). "Glial activation: a driving force for pathological pain". Trends in Neurosci. 24 (8): 450–455. doi: 10.1016/S0166-2236(00)01854-3 (http://dx.doi.org/10.1016/ S0166-2236(00)01854-3). • Volterra, A. and Meldolesi, J. (2005). "Astrocytes, from brain glue to communication elements: the revolution continues". Nat. Rev Neurosci. 6 (8): 626–640. doi: 10.1038/nrn1722 (http://dx.doi.org/10.1038/nrn1722).
Astrocyte PMID 16025096 (http://www.ncbi.nlm.nih.gov/pubmed/16025096). • Freeman, M. R. (2010). "Specification and Morphogenesis of Astrocytes". Science 330 (6005): 774–8. doi: 10.1126/science.1190928 (http://dx.doi.org/10.1126/science.1190928). PMID 21051628 (http://www.ncbi. nlm.nih.gov/pubmed/21051628).
344
External links
• Cell Centered Database - Astrocyte (http://ccdb.ucsd.edu/sand/main?stype=lite&keyword=protoplasmic astrocyte&Submit=Go&event=display&start=1) • UIUC Histology Subject 57 (https://histo.life.illinois.edu/histo/atlas/oimages.php?oid=57) • "Astrocytes" (http://www.sfn.org/index.cfm?pagename=brainBriefings_astrocytes) at Society for Neuroscience • The Department of Neuroscience at Wikiversity • NIF Search - Astrocyte (https://www.neuinfo.org/mynif/search.php?q=Astrocyte&t=data&s=cover&b=0& r=20) via the Neuroscience Information Framework
Neuron
Neuron: nerve cell
Drawing by Santiago Ramón y Cajal of neurons in the pigeon cerebellum. (A) Denotes Purkinje cells, an example of a multipolar neuron. (B) Denotes granule cells, which are also multipolar. NeuroLex ID sao1417703748 [1]
A neuron (pron.: /ˈnjʊərɒn/ NYEWR-on or pron.: /ˈnʊərɒn/ NEWR-on; also known as a neurone or nerve cell) is an electrically excitable cell that processes and transmits information through electrical and chemical signals. A chemical signal occurs via a synapse, a specialized connection with other cells. Neurons connect to each other to form neural networks. Neurons are the core components of the nervous system, which includes the brain, spinal cord, and peripheral ganglia. A number of specialized types of neurons exist: sensory neurons respond to touch, sound, light and numerous other stimuli affecting cells of the sensory organs that then send signals to the spinal cord and brain. Motor neurons receive signals from the brain and spinal cord, cause muscle contractions, and affect glands. Interneurons connect neurons to other neurons within the same region of the brain or spinal cord. A typical neuron possesses a cell body (often called the soma), dendrites, and an axon. Dendrites are thin structures that arise from the cell body, often extending for hundreds of micrometres and branching multiple times, giving rise to a complex "dendritic tree". An axon is a special cellular extension that arises from the cell body at a site called the axon hillock and travels for a distance, as far as 1 meter in humans or even more in other species. The cell body of a neuron frequently gives rise to multiple dendrites, but never to more than one axon, although the axon may branch hundreds of times before it terminates. At the majority of synapses, signals are sent from the axon of one neuron to a
Neuron dendrite of another. There are, however, many exceptions to these rules: neurons that lack dendrites, neurons that have no axon, synapses that connect an axon to another axon or a dendrite to another dendrite, etc. All neurons are electrically excitable, maintaining voltage gradients across their membranes by means of metabolically driven ion pumps, which combine with ion channels embedded in the membrane to generate intracellular-versus-extracellular concentration differences of ions such as sodium, potassium, chloride, and calcium. Changes in the cross-membrane voltage can alter the function of voltage-dependent ion channels. If the voltage changes by a large enough amount, an all-or-none electrochemical pulse called an action potential is generated, which travels rapidly along the cell's axon, and activates synaptic connections with other cells when it arrives. Neurons do not undergo cell division. In most cases, neurons are generated by special types of stem cells. Astrocytes, a type of glial cell, have also been observed to turn into neurons by virtue of the stem cell characteristic pluripotency. In humans, neurogenesis largely ceases during adulthood—but in two brain areas, the hippocampus and olfactory bulb, there is strong evidence for generation of substantial numbers of new neurons.[1][]
345
Overview
Structure of a typical neuron
Neuron (peripheral nervous system)
A neuron is a specialized type of cell found in the bodies of most animals (all members of the group Eumetazoa). Only sponges and a few other simpler animals have no neurons. The features that define a neuron are electrical excitability and the presence of synapses, which are complex membrane junctions that transmit signals to other cells. The body's neurons, plus the glial cells that give them structural and metabolic support, together constitute the nervous system. In vertebrates, the majority of neurons belong to the central nervous system, but some reside in peripheral ganglia, and many sensory neurons are situated in sensory organs such as the retina and cochlea. Although neurons are very diverse and there are exceptions to nearly every rule, it is convenient to begin with a schematic description of the structure and function of a "typical" neuron. A typical neuron is divided into three parts: the soma or cell body, dendrites, and axon. The soma is usually compact; the axon and dendrites are filaments that extrude from it. Dendrites typically branch profusely, getting thinner with each branching, and extending their farthest branches a few hundred micrometres from the soma. The axon leaves the soma at a swelling called the axon hillock, and can extend for great distances, giving rise to hundreds of branches. Unlike dendrites, an axon usually maintains the same diameter as it extends. The soma may give rise to numerous dendrites, but never to more than one axon. Synaptic signals from other neurons are received by the soma and dendrites; signals to other neurons are transmitted by the axon. A typical synapse, then, is a contact between the axon of one neuron and a dendrite or soma of another. Synaptic signals may be excitatory or inhibitory. If the net excitation received by a neuron over a short
Neuron period of time is large enough, the neuron generates a brief pulse called an action potential, which originates at the soma and propagates rapidly along the axon, activating synapses onto other neurons as it goes. Many neurons fit the foregoing schema in every respect, but there are also exceptions to most parts of it. There are no neurons that lack a soma, but there are neurons that lack dendrites, and others that lack an axon. Furthermore, in addition to the typical axodendritic and axosomatic synapses, there are axoaxonic (axon-to-axon) and dendrodendritic (dendrite-to-dendrite) synapses. The key to neural function is the synaptic signaling process, which is partly electrical and partly chemical. The electrical aspect depends on properties of the neuron's membrane. Like all animal cells, every neuron is surrounded by a plasma membrane, a bilayer of lipid molecules with many types of protein structures embedded in it. A lipid bilayer is a powerful electrical insulator, but in neurons, many of the protein structures embedded in the membrane are electrically active. These include ion channels that permit electrically charged ions to flow across the membrane, and ion pumps that actively transport ions from one side of the membrane to the other. Most ion channels are permeable only to specific types of ions. Some ion channels are voltage gated, meaning that they can be switched between open and closed states by altering the voltage difference across the membrane. Others are chemically gated, meaning that they can be switched between open and closed states by interactions with chemicals that diffuse through the extracellular fluid. The interactions between ion channels and ion pumps produce a voltage difference across the membrane, typically a bit less than 1/10 of a volt at baseline. This voltage has two functions: first, it provides a power source for an assortment of voltage-dependent protein machinery that is embedded in the membrane; second, it provides a basis for electrical signal transmission between different parts of the membrane. Neurons communicate by chemical and electrical synapses in a process known as synaptic transmission. The fundamental process that triggers synaptic transmission is the action potential, a propagating electrical signal that is generated by exploiting the electrically excitable membrane of the neuron. This is also known as a wave of depolarization.
346
Anatomy and histology
Neurons are highly specialized for the processing and transmission of cellular signals. Given the diversity of functions performed by neurons in different parts of the nervous system, there is, as expected, a wide variety in the shape, size, and electrochemical properties of neurons. For instance, the soma of a neuron can vary from 4 to 100 micrometers in diameter.[2] • The soma is the central part of the neuron. It contains the nucleus of the cell, and therefore is where most protein synthesis occurs. The nucleus ranges from 3 to 18 micrometers in diameter.[3]
Diagram of a typical myelinated vertebrate motoneuron
• The dendrites of a neuron are cellular extensions with many branches, and metaphorically this overall shape and structure is referred to as a dendritic tree. This is where the majority of input to the neuron occurs via the dendritic spine.
Neuron • The axon is a finer, cable-like projection that can extend tens, hundreds, or even tens of thousands of times the diameter of the soma in length. The axon carries nerve signals away from the soma (and also carries some types of information back to it). Many neurons have only one axon, but this axon may—and usually will—undergo extensive branching, enabling communication with many target cells. The part of the axon where it emerges from the soma is called the axon hillock. Besides being an anatomical structure, the axon hillock is also the part of the neuron that has the greatest density of voltage-dependent sodium channels. This makes it the most easily excited part of the neuron and the spike initiation zone for the axon: in electrophysiological terms it has the most negative action potential threshold. While the axon and axon hillock are generally involved in information outflow, this region can also receive input from other neurons. • The axon terminal contains synapses, specialized structures where neurotransmitter chemicals are released to communicate with target neurons. Although the canonical view of the neuron attributes dedicated functions to its various anatomical components, dendrites and axons often act in ways contrary to their so-called main function. Axons and dendrites in the central nervous system are typically only about one micrometer thick, while some in the peripheral nervous system are much thicker. The soma is usually about 10–25 micrometers in diameter and often is not much larger than the cell nucleus it contains. The longest axon of a human motoneuron can be over a meter long, reaching from the base of the spine to the toes. Sensory neurons have axons that run from the toes to the dorsal columns, over 1.5 meters in adults. Giraffes have single axons several meters in length running along the entire length of their necks. Much of what is known about axonal function comes from studying the squid giant axon, an ideal experimental preparation because of its relatively immense size (0.5–1 millimeters thick, several centimeters long). Fully differentiated neurons are permanently postmitotic;[4] however, recent research shows that additional neurons throughout the brain can originate from neural stem cells found throughout the brain but in particularly high concentrations in the subventricular zone and subgranular zone through the process of neurogenesis.[5]
347
Histology and internal structure
Nerve cell bodies stained with basophilic dyes show numerous microscopic clumps of Nissl substance (named after German psychiatrist and neuropathologist Franz Nissl, 1860–1919), which consists of rough endoplasmic reticulum and associated ribosomal RNA. The prominence of the Nissl substance can be explained by the fact that nerve cells are metabolically very active, and hence are involved in large amounts of protein synthesis. The cell body of a neuron is supported by a complex meshwork of structural proteins called neurofilaments, which are assembled into larger neurofibrils. Some Golgi-stained neurons in human hippocampal tissue neurons also contain pigment granules, such as neuromelanin (a brownish-black pigment, byproduct of synthesis of catecholamines) and lipofuscin (yellowish-brown pigment that accumulates with age). There are different internal structural characteristics between axons and dendrites. Typical axons almost never contain ribosomes, except some in the initial segment. Dendrites contain granular endoplasmic reticulum or ribosomes, with diminishing amounts with distance from the cell body.
Neuron
348
Classes
Neurons exist in a number of different shapes and sizes and can be classified by their morphology and function. The anatomist Camillo Golgi grouped neurons into two types; type I with long axons used to move signals over long distances and type II with short axons, which can often be confused with dendrites. Type I cells can be further divided by where the cell body or soma is located. The basic morphology of type I neurons, represented by spinal motor neurons, consists of a cell body called the soma and a long thin axon covered by the myelin sheath. Around the cell body is a branching dendritic tree that receives signals from other neurons. The end of the axon has branching terminals (axon terminal) that release neurotransmitters into a gap called the synaptic cleft between the terminals and the dendrites of the next neuron.
Image of pyramidal neurons in mouse cerebral cortex expressing green fluorescent protein. The red staining indicates GABAergic [6] interneurons.
Structural classification
SMI32-stained pyramidal neurons in cerebral cortex
Neuron Polarity Most neurons can be anatomically characterized as: • Unipolar or pseudounipolar: dendrite and axon emerging from same process. • Bipolar: axon and single dendrite on opposite ends of the soma. • Multipolar: more than two dendrites: • Golgi I: neurons with long-projecting axonal processes; examples are pyramidal cells, Purkinje cells, and anterior horn cells. • Golgi II: neurons whose axonal process projects locally; the best example is the granule cell. Other Furthermore, some unique neuronal types can be identified according to their location in the nervous system and distinct shape. Some examples are: • Basket cells, interneurons that form a dense plexus of terminals around the soma of target cells, found in the cortex and cerebellum. • Betz cells, large motor neurons. • Medium spiny neurons, most neurons in the corpus striatum. • Purkinje cells, huge neurons in the cerebellum, a type of Golgi I multipolar neuron. • Pyramidal cells, neurons with triangular soma, a type of Golgi I. • Renshaw cells, neurons with both ends linked to alpha motor neurons. • Granule cells, a type of Golgi II neuron. • Anterior horn cells, motoneurons located in the spinal cord. • Spindle cells, interneurons that connect widely separated areas of the brain
Different kinds of neurons: 1 Unipolar neuron 2 Bipolar neuron 3 Multipolar neuron 4 Pseudounipolar neuron
349
Functional classification
Direction • Afferent neurons convey information from tissues and organs into the central nervous system and are sometimes also called sensory neurons. • Efferent neurons transmit signals from the central nervous system to the effector cells and are sometimes called motor neurons. • Interneurons connect neurons within specific regions of the central nervous system. Afferent and efferent also refer generally to neurons that, respectively, bring information to or send information from the brain region. Action on other neurons A neuron affects other neurons by releasing a neurotransmitter that binds to chemical receptors. The effect upon the postsynaptic neuron is determined not by the presynaptic neuron or by the neurotransmitter, but by the type of receptor that is activated. A neurotransmitter can be thought of as a key, and a receptor as a lock: the same type of key can here be used to open many different types of locks. Receptors can be classified broadly as excitatory (causing an increase in firing rate), inhibitory (causing a decrease in firing rate), or modulatory (causing long-lasting effects not directly related to firing rate).
Neuron The two most common neurotransmitters in the brain, glutamate and GABA, have actions that are largely consistent. Glutamate acts on several different types of receptors, and have effects that are excitatory at ionotropic receptors and a modulatory effect at metabotropic receptors. Similarly GABA acts on several different types of receptors, but all of them have effects (in adult animals, at least) that are inhibitory. Because of this consistency, it is common for neuroscientists to simplify the terminology by referring to cells that release glutamate as "excitatory neurons," and cells that release GABA as "inhibitory neurons." Since over 90% of the neurons in the brain release either glutamate or GABA, these labels encompass the great majority of neurons. There are also other types of neurons that have consistent effects on their targets, for example "excitatory" motor neurons in the spinal cord that release acetylcholine, and "inhibitory" spinal neurons that release glycine. The distinction between excitatory and inhibitory neurotransmitters is not absolute, however. Rather, it depends on the class of chemical receptors present on the postsynaptic neuron. In principle, a single neuron, releasing a single neurotransmitter, can have excitatory effects on some targets, inhibitory effects on others, and modulatory effects on others still. For example, photoreceptor cells in the retina constantly release the neurotransmitter glutamate in the absence of light. So-called OFF bipolar cells are, like most neurons, excited by the released glutamate. However, neighboring target neurons called ON bipolar cells are instead inhibited by glutamate, because they lack the typical ionotropic glutamate receptors and instead express a class of inhibitory metabotropic glutamate receptors.[7] When light is present, the photoreceptors cease releasing glutamate, which relieves the ON bipolar cells from inhibition, activating them; this simultaneously removes the excitation from the OFF bipolar cells, silencing them. It is possible to identify the type of inhibitory effect a presynaptic neuron will have on a postsynaptic neuron, based on the proteins the presynaptic neuron expresses. Parvalbumin-expressing neurons typically dampen the output signal of the postsynaptic neuron in the visual cortex, whereas somatostatin-expressing neurons typically block dendritic inputs to the postsynaptic neuron.[8] Discharge patterns Neurons can be classified according to their electrophysiological characteristics: • Tonic or regular spiking. Some neurons are typically constantly (or tonically) active. Example: interneurons in neurostriatum. • Phasic or bursting. Neurons that fire in bursts are called phasic. • Fast spiking. Some neurons are notable for their high firing rates, for example some types of cortical inhibitory interneurons, cells in globus pallidus, retinal ganglion cells.[9][10] Classification by neurotransmitter production Neurons differ in the type of neurotransmitter they manufacture. Some examples are: • Cholinergic neurons—acetylcholine. Acetylcholine is released from presynaptic neurons into the synaptic cleft. It acts as a ligand for both ligand-gated ion channels and metabotropic (GPCRs) muscarinic receptors. Nicotinic receptors, are pentameric ligand-gated ion channels composed of alpha and beta subunits that bind nicotine. Ligand binding opens the channel causing influx of Na+ depolarization and increases the probability of presynaptic neurotransmitter release. • GABAergic neurons—gamma aminobutyric acid. GABA is one of two neuroinhibitors in the CNS, the other being Glycine. GABA has a homologous function to ACh, gating anion channels that allow Cl- ions to enter the post synaptic neuron. Cl- causes hyperpolarization within the neuron, decreasing the probability of an action potential firing as the voltage becomes more negative (recall that for an action potential to fire, a positive voltage threshold must be reached). • Glutamatergic neurons—glutamate. Glutamate is one of two primary excitatory amino acids, the other being Aspartate. Glutamate receptors are one of four categories, three of which are ligand-gated ion channels and one of which is a G-protein coupled receptor (often referred to as GPCR).
350
Neuron 1. AMPA and Kainate receptors both function as cation channels permeable to Na+ cation channels mediating fast excitatory synaptic transmission 2. NMDA receptors are another cation channel that is more permeable to Ca2+. The function of NMDA receptors is dependant on Glycine receptor binding as a co-agonist within the channel pore. NMDA receptors do not function without both ligands present. 3. Metabotropic receptors, GPCRs modulate synaptic transmission and postsynaptic excitability. Glutamate can cause excitotoxicity when blood flow to the brain is interrupted, resulting in brain damage. When blood flow is suppressed, glutamate is released from presynaptic neurons causing NMDA and AMPA receptor activation moreso than would normally be the case outside of stress conditions, leading to elevated Ca2+ and Na+ entering the post synaptic neuron and cell damage. • Dopaminergic neurons—dopamine. Dopamine is a neurotransmitter that acts on D1 type (D1 and D5) Gs coupled receptors, which increase cAMP and PKA, and D2 type (D2, D3, and D4) receptors, which activate Gi-coupled receptors that decrease cAMP and PKA. Dopamine is connected to mood and behavior, and modulates both pre and post synaptic neurotransmission. Loss of dopamine neurons in the substantia nigra has been linked to Parkinson's disease. • Serotonergic neurons—serotonin. Serotonin,(5-Hydroxytryptamine, 5-HT), can act as excitatory or inhibitory. Of the four 5-HT receptor classes, 3 are GPCR and 1 is ligand gated cation channel. Serotonin is synthesized from tryptophan by tryptophan hydroxylase, and then further by aromatic acid decarboxylase. A lack of 5-HT at postsynaptic neurons has been linked to depression. Drugs that block the presynaptic serotonin transporter are used for treatment, such as Prozac and Zoloft.
351
Connectivity
Neurons communicate with one another via synapses, where the axon terminal or en passant boutons (terminals located along the length of the axon) of one cell impinges upon another neuron's dendrite, soma or, less commonly, axon. Neurons such as Purkinje cells in the cerebellum can have over 1000 dendritic branches, making connections with tens of thousands of other cells; other neurons, such as the magnocellular neurons of the supraoptic nucleus, have only one or two dendrites, each of which receives thousands of synapses. Synapses can be excitatory or inhibitory and either increase or decrease activity in the target neuron. Some neurons also communicate via electrical synapses, which are direct, electrically conductive junctions between cells. In a chemical synapse, the process of synaptic transmission is as follows: when an action potential reaches the axon terminal, it opens voltage-gated calcium channels, allowing calcium ions to enter the terminal. Calcium causes synaptic vesicles filled with neurotransmitter molecules to fuse with the membrane, releasing their contents into the synaptic cleft. The neurotransmitters diffuse across the synaptic cleft and activate receptors on the postsynaptic neuron. The human brain has a huge number of synapses. Each of the 1011 (one hundred billion) neurons has on average 7,000 synaptic connections to other neurons. It has been estimated that the brain of a three-year-old child has about 1015 synapses (1 quadrillion). This number declines with age, stabilizing by adulthood. Estimates vary for an adult, ranging from 1014 to 5 x 1014 synapses (100 to 500 trillion).[11]
Neuron
352
Mechanisms for propagating action potentials
In 1937, John Zachary Young suggested that the squid giant axon could be used to study neuronal electrical properties.[12] Being larger than but similar in nature to human neurons, squid cells were easier to study. By inserting electrodes into the giant squid axons, accurate measurements were made of the membrane potential. The cell membrane of the axon and soma contain voltage-gated ion channels that allow the neuron to generate and propagate an electrical signal (an action potential). These signals are generated and propagated by charge-carrying ions including sodium (Na+), potassium (K+), chloride (Cl-), and calcium (Ca2+). There are several stimuli that can activate a neuron leading to electrical activity, including pressure, stretch, chemical transmitters, and changes of the electric potential across the cell membrane.[13] Stimuli cause specific ion-channels within the cell membrane to open, leading to a flow of ions through the cell membrane, changing the membrane potential.
A signal propagating down an axon to the cell body and dendrites of the next cell
Thin neurons and axons require less metabolic expense to produce and carry action potentials, but thicker axons convey impulses more rapidly. To minimize metabolic expense while maintaining rapid conduction, many neurons have insulating sheaths of myelin around their axons. The sheaths are formed by glial cells: oligodendrocytes in the central nervous system and Schwann cells in the peripheral nervous system. The sheath enables action potentials to travel faster than in unmyelinated axons of the same diameter, whilst using less energy. The myelin sheath in peripheral nerves normally runs along the axon in sections about 1 mm long, punctuated by unsheathed nodes of Ranvier, which contain a high density of voltage-gated ion channels. Multiple sclerosis is a neurological disorder that results from demyelination of axons in the central nervous system. Some neurons do not generate action potentials, but instead generate a graded electrical signal, which in turn causes graded neurotransmitter release. Such nonspiking neurons tend to be sensory neurons or interneurons, because they cannot carry signals long distances.
Neuron
353
Neural coding
Neural coding is concerned with how sensory and other information is represented in the brain by neurons. The main goal of studying neural coding is to characterize the relationship between the stimulus and the individual or ensemble neuronal responses, and the relationships amongst the electrical activities of the neurons within the ensemble.[] It is thought that neurons can encode both digital and analog information.[14]
All-or-none principle
The conduction of nerve impulses is an example of an all-or-none response. In other words, if a neuron responds at all, then it must respond completely. Greater intensity of stimulation does not produce a stronger signal but can produce a higher frequency of firing. There are different types of receptor response to stimulus, slowly adapting or tonic receptors respond to steady stimulus and produce a steady rate of firing. These tonic receptors most often respond to increased intensity of stimulus by increasing their firing frequency, usually as a power function of stimulus plotted against impulses per second. This can be likened to an intrinsic property of light where to get greater intensity of a specific frequency (color) there have to be more photons, as the photons can't become "stronger" for a specific frequency. There are a number of other receptor types that are called quickly adapting or phasic receptors, where firing decreases or stops with steady stimulus; examples include: skin when touched by an object causes the neurons to fire, but if the object maintains even pressure against the skin, the neurons stop firing. The neurons of the skin and muscles that are responsive to pressure and vibration have filtering accessory structures that aid their function. The pacinian corpuscle is one such structure. It has concentric layers like an onion, which form around the axon terminal. When pressure is applied and the corpuscle is deformed, mechanical stimulus is transferred to the axon, which fires. If the pressure is steady, there is no more stimulus; thus, typically these neurons respond with a transient depolarization during the initial deformation and again when the pressure is removed, which causes the corpuscle to change shape again. Other types of adaptation are important in extending the function of a number of other neurons.[15]
History
The term neuron was coined by the German anatomist Heinrich Wilhelm Waldeyer. The neuron's place as the primary functional unit of the nervous system was first recognized in the early 20th century through the work of the Spanish anatomist Santiago Ramón y Cajal.[] Ramón y Cajal proposed that neurons were discrete cells that communicated with each other via specialized junctions, or spaces, between cells.[] This became known as the neuron doctrine, one of the central tenets of modern neuroscience.[] To observe the structure of individual neurons, Ramón y Cajal improved a silver staining process Drawing by Camillo Golgi of a hippocampus stained with the silver nitrate method known as Golgi's method, which had been developed by his rival, Camillo Golgi.[] Cajal's improvement, which involved a technique he called "double impregnation", is still in use. The silver impregnation stains are an extremely useful method for neuroanatomical investigations because, for reasons unknown, it stains a very small percentage of cells in a tissue, so one is able to see the complete micro structure of individual neurons without much overlap from other cells in the densely packed brain.[]
Neuron
354
The neuron doctrine
The neuron doctrine is the now fundamental idea that neurons are the basic structural and functional units of the nervous system. The theory was put forward by Santiago Ramón y Cajal in the late 19th century. It held that neurons are discrete cells (not connected in a meshwork), acting as metabolically distinct units. Later discoveries yielded a few refinements to the simplest form of the doctrine. For example, glial cells, which are not considered neurons, play an essential role in information processing.[16] Also, electrical synapses are more common than previously thought,[17] meaning that there are direct, cytoplasmic connections between neurons. In fact, there are examples of neurons forming even tighter coupling: the squid giant axon arises from the fusion of multiple axons.[18] Ramón y Cajal also postulated the Law of Dynamic Polarization, which states that a neuron receives signals at its dendrites and cell body and transmits them, as action potentials, along the axon in one direction: away from the cell body.[19] The Law of Dynamic Polarization has important exceptions; dendrites can serve as synaptic output sites of neurons[20] and axons can receive synaptic inputs.[21]
Drawing of a Purkinje cell in the cerebellar cortex done by Santiago Ramón y Cajal, demonstrating the ability of Golgi's staining method to reveal fine detail
Neurons in the brain
The number of neurons in the brain varies dramatically from species to species.[] One estimate puts the human brain at about 100 billion (1011) neurons and 100 trillion (1014) synapses.[] A lower 2012 estimate is 86 billion neurons, of which 16.3 billion are in the cerebral cortex, and 69 billion in the cerebellum.[] By contrast, the nematode worm Caenorhabditis elegans has just 302 neurons, making it an ideal experimental subject as scientists have been able to map all of the organism's neurons. The fruit fly Drosophila melanogaster, a common subject in biological experiments, has around 100,000 neurons and exhibits many complex behaviors. Many properties of neurons, from the type of neurotransmitters used to ion channel composition, are maintained across species, allowing scientists to study processes occurring in more complex organisms in much simpler experimental systems.
Neurological disorders
Charcot–Marie–Tooth disease (CMT), also known as hereditary motor and sensory neuropathy (HMSN), hereditary sensorimotor neuropathy and peroneal muscular atrophy, is a heterogeneous inherited disorder of nerves (neuropathy) that is characterized by loss of muscle tissue and touch sensation, predominantly in the feet and legs but also in the hands and arms in the advanced stages of disease. Presently incurable, this disease is one of the most common inherited neurological disorders, with 37 in 100,000 affected. Alzheimer's disease (AD), also known simply as Alzheimer's, is a neurodegenerative disease characterized by progressive cognitive deterioration together with declining activities of daily living and neuropsychiatric symptoms or behavioral changes. The most striking early symptom is loss of short-term memory (amnesia), which usually manifests as minor forgetfulness that becomes steadily more pronounced with illness progression, with relative preservation of older memories. As the disorder progresses, cognitive (intellectual) impairment extends to the domains of language (aphasia), skilled movements (apraxia), and recognition (agnosia), and functions such as decision-making and planning become impaired.
Neuron Parkinson's disease (PD), also known as Parkinson disease, is a degenerative disorder of the central nervous system that often impairs the sufferer's motor skills and speech. Parkinson's disease belongs to a group of conditions called movement disorders. It is characterized by muscle rigidity, tremor, a slowing of physical movement (bradykinesia), and in extreme cases, a loss of physical movement (akinesia). The primary symptoms are the results of decreased stimulation of the motor cortex by the basal ganglia, normally caused by the insufficient formation and action of dopamine, which is produced in the dopaminergic neurons of the brain. Secondary symptoms may include high level cognitive dysfunction and subtle language problems. PD is both chronic and progressive. Myasthenia gravis is a neuromuscular disease leading to fluctuating muscle weakness and fatigability during simple activities. Weakness is typically caused by circulating antibodies that block acetylcholine receptors at the post-synaptic neuromuscular junction, inhibiting the stimulative effect of the neurotransmitter acetylcholine. Myasthenia is treated with immunosuppressants, cholinesterase inhibitors and, in selected cases, thymectomy.
355
Demyelination
Demyelination is the act of demyelinating, or the loss of the myelin sheath insulating the nerves. When myelin degrades, conduction of signals along the nerve can be impaired or lost, and the nerve eventually withers. This leads to certain neurodegenerative disorders like multiple sclerosis and chronic inflammatory demyelinating polyneuropathy.
Axonal degeneration
Although most injury responses include a calcium influx signaling to promote resealing of severed parts, axonal injuries initially lead to acute axonal degeneration (AAD), which is rapid separation of the proximal and distal ends within 30 minutes of injury. Degeneration follows with swelling of the axolemma, and eventually leads to bead like formation. Granular disintegration of the axonal cytoskeleton and inner organelles occurs after axolemma degradation. Early changes include accumulation of mitochondria in the paranodal regions at the site of injury. Endoplasmic reticulum degrades and mitochondria swell up and eventually disintegrate. The disintegration is dependent on Ubiquitin and Calpain proteases (caused by influx of calcium ion), suggesting that axonal degeneration is an active process. Thus the axon undergoes complete fragmentation. The process takes about roughly 24 hrs in the PNS, and longer in the CNS. The signaling pathways leading to axolemma degeneration are currently unknown.
Nerve regeneration
It has been demonstrated that neurogenesis can sometimes occur in the adult vertebrate brain, a finding that led to controversy in 1999.[22] However, more recent studies of the age of human neurons suggest that this process occurs only for a minority of cells, and the overwhelming majority of neurons comprising the neocortex were formed before birth and persist without replacement.[] It is often possible for peripheral axons to regrow if they are severed. A report in Nature suggested that researchers had found a way to transform human skin cells into working nerve cells using a process called transdifferentiation in which "cells are forced to adopt new identities."[]
Neuron
356
References
[14] Thorpe, SJ (1990) Spike arrival times: A highly efficient coding scheme for neural networks (http:/ / web. archive. org/ web/ 20120215151304/ http:/ / pop. cerco. ups-tlse. fr/ fr_vers/ documents/ thorpe_sj_90_91. pdf). In R. Eckmiller, G. Hartmann, & G. Hauske (Eds.) Parallel processing in neural systems, Elsevier, pp. 91–94 ISBN 0444883908 [19] Sabbatini R.M.E. April–July 2003. Neurons and Synapses: The History of Its Discovery (http:/ / www. cerebromente. org. br/ n17/ history/ neurons3_i. htm). Brain & Mind Magazine, 17. Retrieved on March 19, 2007.
Further reading
• Kandel E.R., Schwartz, J.H., Jessell, T.M. 2000. Principles of Neural Science, 4th ed., McGraw-Hill, New York. • Bullock, T.H., Bennett, M.V.L., Johnston, D., Josephson, R., Marder, E., Fields R.D. 2005. The Neuron Doctrine, Redux, Science, V.310, p. 791–793. • Ramón y Cajal, S. 1933 Histology, 10th ed., Wood, Baltimore. • Richard S. Snell: Clinical neuroanatomy (Lippincott Williams & Wilkins, Ed.6th 2006) Philadelphia, Baltimore, New York, London. ISBN 978-963-226-293-2 • Roberts A., Bush B.M.H. 1981. Neurones Without Impulses. Cambridge University Press, Cambridge. • Peters, A., Palay, S.L., Webster, H, D., 1991 The Fine Structure of the Nervous System, 3rd ed., Oxford, New York
External links
• IBRO (International Brain Research Organization) (http://www.ibro.info). Fostering neuroscience research especially in less well-funded countries. • NeuronBank (http://NeuronBank.org) an online neuromics tool for cataloging neuronal types and synaptic connectivity. • High Resolution Neuroanatomical Images of Primate and Non-Primate Brains (http://brainmaps.org). • The Department of Neuroscience at Wikiversity, which presently offers two courses: Fundamentals of Neuroscience and Comparative Neuroscience. • NIF Search – Neuron (https://www.neuinfo.org/mynif/search.php?q=Neuron&t=data&s=cover&b=0& r=20) via the Neuroscience Information Framework • Cell Centered Database – Neuron (http://ccdb.ucsd.edu/sand/main?event=showMPByType&typeid=0& start=1&pl=y) • Complete list of neuron types (http://neurolex.org/wiki/Category:Neuron) according to the Petilla convention, at NeuroLex. • NeuroMorpho.Org (http://NeuroMorpho.org) an online database of digital reconstructions of neuronal morphology. • Immunohistochemistry Image Gallery: Neuron (http://www.immunoportal.com/modules. php?name=gallery2&g2_view=keyalbum.KeywordAlbum&g2_keyword=Neuron)
Oligodendrocyte
357
Oligodendrocyte
Oligodendrocyte
Oligodendrocyte
Oligodendrocytes form the electrical insulation around the axons of CNS nerve cells. Latin Code oligodendrocytus TH H2.00.06.2.01018
[1]
Oligodendrocytes (from Greek, meaning cells with a few branches), or oligodendroglia (Greek, few tree glue),[1] are a type of brain cell. They are a variety of neuroglia. Their main functions are to provide support and to insulate the axons (the long projection of nerve cells) in the central nervous system (the brain and spinal cord) of some vertebrates. (The same function is performed by Schwann cells in the peripheral nervous system.) Oligodendrocytes do this by creating the myelin sheath, which is 80% lipid and 20% protein.[2] A single oligodendrocyte can extend its processes to 50 axons, wrapping approximately 1 μm of myelin sheath around each axon; Schwann cells, on the other hand, can wrap around only 1 axon. Each oligodendrocyte forms one segment of myelin for several adjacent axons.[2]
Origin
Oligodendroglia, types of glial cells, arise during development from oligodendrocyte precursor cells, which can be identified by their expression of a number of antigens, including the ganglioside GD3,[3] the NG2 chondroitin sulfate proteoglycan,[4] and the platelet-derived growth factor-alpha receptor subunit PDGF-alphaR.[5] Most oligodendrocytes develop during embryogenesis and early postnatal life from restricted periventricular germinal regions.[6] They are the last cell type to be generated in the CNS.[7] Myelination is only prevalent in a few brain regions at birth and continues into adulthood. The entire process is not complete until about 25–30 years of age.[8] Oligodendrocyte formation in the adult brain is associated with glial-restricted progenitors cells, known as oligodendrocyte progenitor cells (OPCs).[9] SVZ cells migrate away from germinal[10] zones to populate both developing white and gray matter, where they differentiate and mature into myelin-forming oligodendroglia.[11]
Oligodendrocyte However, it is not clear whether all oligodendroglial progenitors undergo this sequence of events. It has been suggested that some undergo apoptosis [12] and others fail to differentiate into mature oligodendroglia but persist as adult oligodendroglial progenitors.[13]
358
Function
As part of the nervous system, oligodendrocytes are closely related to nerve cells, and, like all other glial cells, oligodendrocytes provide a supporting role for neurons. In addition, the nervous system of mammals depends crucially on myelin sheaths, which reduce ion leakage and decrease the capacitance of the cell membrane.[14] Myelin also increases impulse speed, as saltatory propagation of action potentials occurs at the nodes of Ranvier in between Schwann cells (of the PNS) and oligodendrocytes (of the CNS). Oligodendrocytes provide the same functionality as the insulation on a household electrical wire (with the rather large difference that, while household An oligodendrocyte seen myelinating several axons. electrical wires are in a non-conducting medium - air - the axons run in a solution of water and ions, which conducts electrical current well). Furthermore, impulse speed of myelinated axons increases linearly with the axon diameter, whereas the impulse speed of unmyelinated cells increases only with the square root of the diameter. The insulation must be proportional to the diameter of the fiber inside. The optimal ratio of axon diameter divided by the total fiber diameter (which includes the myelin) is 0.6.[8] In contrast, Satellite oligodendrocytes are functionally distinct from most oligodendrocytes. They are not attached to neurons and, therefore, do not serve an insulating role. They remain apposed to neurons and regulate the extracellular fluid.[15] Satellite oligodendrocytes are considered to be a part of the gray matter whereas myelinating oligodendrocytes are a part of the white matter. Myelination is an important component of intelligence. Neuroscientist Vincent J. Schmithorst found that there is a correlation with white matter and intelligence. People with greater white matter had higher IQ's.[8] A study done with rats by Janice M Juraska showed that rats that were raised in an enriched environment had more myelination in their corpus callosum.[16]
Pathology
Diseases that result in injury to the oligodendroglial cells include demyelinating diseases such as multiple sclerosis and leukodystrophies. Trauma to the body, e.g. spinal cord injury, can also cause demyelination. Cerebral palsy (periventricular leukomalacia) is caused by damage to developing oligodendrocytes in the brain areas around the cerebral ventricles. In cerebral palsy, spinal cord injury, stroke and possibly multiple sclerosis, oligodendrocytes are thought to be damaged by excessive release of the neurotransmitter glutamate.[17] Damage has also been shown to be mediated by N-methyl-d-aspartate receptors.[17] Oligodendrocyte dysfunction may also be implicated in the pathophysiology of schizophrenia and bipolar disorder.[18] Oligodendroglia are also susceptible to infection by the JC virus, which causes progressive multifocal leukoencephalopathy (PML), a condition that specifically affects white matter, typically in immunocompromised patients. Tumors of oligodendroglia are called oligodendrogliomas. The chemotherapy agent Fluorouracil (5-FU) causes damage to the oligodendrocytes in mice, leading to both acute central nervous system (CNS) damage and progressively worsening delayed degeneration of the CNS.[19]
Oligodendrocyte
359
Notes
[1] . [2] Carlson, Physiology of Behavior, 2010 [3] Curtis et al., 1988; LeVine and Goldman, 1988; Hardy and Reynolds, 1991; Levine et al., 1993 [4] Levine et al., 1993 [5] Pringle et al., 1992 [6] Vallstedt et al., 2004 [7] Thomas et al., Spatiotemporal development of oligodendrocytes in the embryonic brain., 2000 [8] Fields, 2008 [9] Menn, et al., Origin of Oligodendrocytes in the Subventricular Zone of the Adult Brain, 2006 [10] Menn, et al., 2006 [11] Hardy and Reynolds, 1991; Levison and Goldman, 1993 [12] Barres et al., 1992 [13] Wren et al., 1992 [14] Sokol, 2009 [15] Baumann and Pham-Dinh, 2001 [17] Káradóttir et al., 2007 [18] Tkachev et al., 2003 [19] "Chemotherapy-induced Damage to the CNS as a Precursor Cell Disease" (http:/ / www. urmc. rochester. edu/ biomedical-genetics/ faculty/ chemotherapy-induced-damage-to-cns. cfm) by Dr. Mark D. Noble, University of Rochester
References
• Baumann, N; Pham-Dinh, D (2001). "Biology of Oligodendrocyte and Myelin in the Mammalian Central Nervous System" (http://physrev.physiology.org/cgi/content/full/81/2/871). Physiological Reviews 18 (2): 871–927. PMID 11274346 (http://www.ncbi.nlm.nih.gov/pubmed/11274346). Retrieved 2007-07-13 More than one of |surname1= and |last1= specified (help); More than one of |given1= and |first1= specified (help); More than one of |surname2= and |last2= specified (help); More than one of |given2= and |first2= specified (help) • Ragheb, Fadi (1999). The M3 Muscarinic Acetylcholine Receptor Mediates p42mapk Activation and c-fos mRNA Expression in Oligodendrocyte Progenitors (http://www.collectionscanada.ca/obj/s4/f2/dsk1/tape9/ PQDD_0025/MQ50862.pdf). Ottawa: National Library of Canada. Retrieved 2006-03-07 • Raine, C.S. (1991). Oligodendrocytes and central nervous system myelin. In Textbook of Neuropathology, second edition, R.L. Davis and D.M. Robertson, eds. (Baltimore, Maryland: Williams and Wilkins), pp. 115–141. • Tkachev D, Mimmack ML, Ryan MM, et al. (September 2003). "Oligodendrocyte dysfunction in schizophrenia and bipolar disorder". Lancet 362 (9386): 798–805. doi: 10.1016/S0140-6736(03)14289-4 (http://dx.doi.org/ 10.1016/S0140-6736(03)14289-4). PMID 13678875 (http://www.ncbi.nlm.nih.gov/pubmed/13678875). • Káradóttir, R.; D. Attwell (14). "Neurotransmiter receptors in the life and death of oligodendrocytes" (http:// www.ncbi.nlm.nih.gov/pmc/articles/PMC2173944). Neuroscience 145 (4): 1426–1438. doi: 10.1038/bjc.1990.391 (http://dx.doi.org/10.1038/bjc.1990.391). PMC 2173944 (http://www.ncbi.nlm. nih.gov/pmc/articles/PMC2173944). PMID 2173944 (http://www.ncbi.nlm.nih.gov/pubmed/2173944). • Carlson, Neil (2010). Physiology of Behavior. Boston, MA: Allyn & Bacon. pp. 38–39. ISBN 0-205-66627-2. • Sokol, Stacey. "The Physiology and Pathophysiology of Multiple Sclerosis" (http://mylifehealthandprosperity. com/index.php?option=com_content&view=article&id=65&Itemid=160). Multiple Sclerosis: Physiological Tutorial. Retrieved 2012-04-29. • Fields, Douglas (18). "White Matter Matters" (http://www.scientificamerican.com/article. cfm?id=white-matter-matters). Scientific American 298 (March 2008): 54–61. Bibcode: 2008SciAm.298c..54D (http://adsabs.harvard.edu/abs/2008SciAm.298c..54D). doi: 10.1038/scientificamerican0308-54 (http://dx. doi.org/10.1038/scientificamerican0308-54). Retrieved 2012-04-29.
Oligodendrocyte • Menn, Benedicte; Jose Manuel Garcia-Verdugo, Cynthia Yaschine, Oscar Gonzalez-Perez, David Rowitch, Arturo Alvarez-Buylla (26). "Origin of Oligodendrocytes in the Subventricular Zone of the Adult Brain" (http:// www.jneurosci.org/content/26/30/7907.full). The Journal of Neuroscience 26 (30): 7907–7918. doi: 10.1523/JNEUROSCI.1299-06.2006 (http://dx.doi.org/10.1523/JNEUROSCI.1299-06.2006). PMID 16870736 (http://www.ncbi.nlm.nih.gov/pubmed/16870736). Retrieved 2012-04-29. • Vallstedt, A; Klos JM, Ericson F (6). "Multiple dorsoventral origins of oligodendrocyte generation in the spinal cord and hindbrain". Neuron. 1 45 (1): 55–67. doi: 10.1016/j.neuron.2004.12.026 (http://dx.doi.org/10.1016/j. neuron.2004.12.026). PMID 15629702 (http://www.ncbi.nlm.nih.gov/pubmed/15629702). • Thomas, JL; Spassky N, Perez Villegas EM, Olivier C, Cobos I, Goujet-Zalc C, Martínez S, Zalc B. (15). "Spatiotemporal development of oligodendrocytes in the embryonic brain" (http://www.ncbi.nlm.nih.gov/ pubmed/10679785). Journal of Neuroscience Research 59 (4): 471–476. doi: 10.1002/(SICI)1097-4547(20000215)59:4<471::AID-JNR1>3.0.CO;2-3 (http://dx.doi.org/10.1002/ (SICI)1097-4547(20000215)59:4<471::AID-JNR1>3.0.CO;2-3). PMID 10679785 (http://www.ncbi.nlm.nih. gov/pubmed/10679785). Retrieved 2012-04-29.
360
External links
• The Department of Neuroscience at Wikiversity • NIF Search - Oligodendrocyte (https://www.neuinfo.org/mynif/search.php?q="Oligodendrocyte"&t=data& s=cover&b=0&r=20) via the Neuroscience Information Framework
Spindle neuron
361
Spindle neuron
Neuron: Spindle neuron
Cartoon of a spindle cell (right) compared to a normal pyramidal cell (left). Location Function Morphology Presynaptic connections Anterior cingulate cortex and Fronto-insular cortex Global firing rate regulation and regulation of emotional state Unique spindle-shaped projection neuron Local input to ACC and FI
Postsynaptic connections Frontal and temporal cortex.
Spindle neurons, also called von Economo neurons (VENs), are a specific class of neurons that are characterized by a large spindle-shaped soma, gradually tapering into a single apical axon in one direction, with only a single dendrite facing opposite. Whereas other types of cells tend to have many dendrites, the polar shaped morphology of spindle neurons is unique. They are found in two very restricted regions in the brains of hominids – the family of species comprising humans and other great apes – the anterior cingulate cortex (ACC) and the fronto-insular cortex (FI). Recently they have been Micrograph showing a spindle neuron of the discovered in the dorsolateral prefrontal cortex of humans.[] Spindle cingulate. HE-LFB stain. cells are also found in the brains of the humpback whales, fin whales, killer whales, sperm whales,[1][] bottlenose dolphin, Risso’s dolphin, beluga whales,[] and the African and Asian elephants.[] The name von Economo neuron comes from their discoverer, Constantin von Economo (1876–1931) who described them in 1929.[2]
Function of spindle neurons
Spindle neurons are relatively enormous cells that may allow rapid communication across the relatively large brains of great apes, Elephantidaes, and Cetacea. Spindle neurons have been implicated by scientists as having an important role in many cognitive abilities and disabilities generally unique to humans, ranging from savant perceptiveness and perfect pitch to dyslexia and autism. While rare in comparison to other neurons, spindle neurons are abundant, and large, in humans. However, the concentration of spindle cells has been measured to be three times higher in Cetaceans in comparison to humans.[][3] They have only been found thus far in the anterior cingulate cortex (ACC), fronto-insular cortex (FI), and the dorsolateral prefrontal cortex.
Spindle neuron
362
Evolutionary significance
The observation that spindle neurons only occur in a highly significant group of animals (from a human point of view) has led to speculation that they are of great importance in human evolution and/or brain function. Their restriction (among the primates) to great apes leads to the hypothesis that they developed no earlier than 15-20 million years ago, prior to the divergence of orangutans from the African great apes. The discovery of spindle neurons in diverse whale species[][] has led to the suggestion that they are "a possible obligatory neuronal adaptation in very large brains, permitting fast information processing and transfer along highly specific projections and that evolved in relation to emerging social behaviors."[]p. 254 Their presence in the brains of these species supports this theory, pointing towards the existence of these specialized neurons only in highly intelligent mammals, and may be an example of convergent evolution.[4] Recently, primitive forms of spindle neurons have also been discovered in macaque monkey brains.[5]
ACC spindle neurons
In 1999, Professor John Allman, a neuroscientist, and colleagues at the California Institute of Technology first published a report on spindle neurons found in the anterior cingulate cortex (ACC) of hominids, but not in any other species. Neuronal volumes of ACC spindle neurons were larger in humans and the gracile (slender) chimpanzees than the spindle neurons of the robust gorillas and orangutans. Allman and his colleagues have delved beyond the level of brain infrastructure to investigate how spindle neurons function at the superstructural level, focusing on their role as 'air traffic controllers' for emotions. Allman's team reports that spindle neurons help channel neural signals from deep within the cortex to relatively distant parts of the brain. Specifically, Allman's team found signals from the ACC are received in Brodmann's area 10, in the frontal polar cortex, where regulation of cognitive dissonance (disambiguation between alternatives) is thought to occur. According to Allman, this neural relay appears to convey motivation to act, and concerns the recognition of error. Self-control – and avoidance of error – is thus facilitated by the executive gatekeeping function of the ACC, as it regulates the interference patterns of neural signals between these two brain regions. In humans, intense emotion activates the anterior cingulate cortex, as it relays neural signals transmitted from the amygdala (a primary processing center for emotions) to the frontal cortex, perhaps by functioning as a sort of lens to focus the complex texture of neural signal interference patterns. The ACC is also active during demanding tasks requiring judgment and discrimination, and when errors are detected by an individual. During difficult tasks, or when experiencing intense love, anger, or lust, activation of the ACC increases. In brain imaging studies, the ACC has specifically been found to be active when mothers hear infants cry, underscoring its role in affording a heightened degree of social sensitivity. The ACC is a relatively ancient cortical region, and is involved with many autonomic functions, including motor and digestive functions, while also playing a role in the regulation of blood pressure and heart rate. Significant olfactory and gustatory capabilities of the ACC and fronto-insular cortex appear to have been usurped, during recent evolution, to serve enhanced roles related to higher cognition – ranging from planning and self-awareness to role playing and deception. The diminished olfactory function of humans, compared to other primates, may be related to the fact that spindle cells located at crucial neural network hubs have only two dendrites rather than many, resulting in reduced neurological integration.
Spindle neuron
363
Fronto-insular spindle neurons
At a Society for Neuroscience meeting in 2003, Allman reported on spindle cells his team found in another brain region, the fronto-insular cortex, a region which appears to have undergone significant evolutionary adaptations in mankind – perhaps as recently as 100,000 years ago. This fronto-insular cortex is closely connected to the insula, a region that is roughly the size of a thumb in each hemisphere of the human brain. The insula and fronto-insular cortex are part of the orbitofrontal cortex, wherein the elaborate circuitry associated with spatial awareness and the sense of touch are found, and where self awareness and the complexities of emotion are thought to be generated and experienced. Moreover, this region of the right hemisphere is crucial to navigation and perception of three dimensional rotations.
Spindle neuron concentrations
ACC
The largest number of ACC spindle neurons are found in humans, fewer in the gracile great apes, and fewest in the robust great apes. In both humans and bonobos they are often found in clusters of 3 to 6 neurons. They are found in humans, bonobos, common chimpanzees, gorillas, orangutans, some cetaceans, and elephants.[6]:245 While total quantities of ACC spindle neurons were not reported by Allman in his seminal research report (as they were in a later report describing their presence in the frontoinsular cortex, below), his team's initial analysis of the ACC layer V in hominids revealed an average of ~9 spindle neurons per section for orangutans (rare, 0.6% of section cells), ~22 for gorillas (frequent, 2.3%), ~37 for chimpanzees (abundant, 3.8%), ~68 for bonobos (abundant/clusters, 4.8%), ~89 for humans (abundant/clusters, 5.6%).[7]
Fronto-insula
All of the primates examined had more spindle cells in the fronto-insula of the right hemisphere than in the left. In contrast to the higher number of spindle cells found in the ACC of the gracile bonobos and chimpanzees, the number of fronto-insular spindle cells was far higher in the cortex of robust gorillas (no data for Orangutans was given). An adult human had 82,855 such cells, a gorilla had 16,710, a bonobo had 2,159, and a chimpanzee had a mere 1,808 – despite the fact that chimpanzees and bonobos are great apes most closely related to humans.
Dorsolateral PFC
Von Economo neurons have been located in the Dorsolateral prefrontal cortex of humans[] and elephants.[] In humans they have been observed in higher concentration in Brodmann area 9 (BA9) – mostly isolated or in clusters of 2, while in Brodmann area 24 (BA24) they have been found mostly in clusters of 2-4.[]
Related pathologies
Abnormal spindle neuron development may be linked to several psychotic disorders, typically those characterized by distortions of reality, disturbances of thought, disturbances of language, and withdrawal from social contact. Altered spindle neuron states have been implicated in both schizophrenia and autism, but research into these correlations remains at a very early stage. An initial study suggested that Alzheimer's disease specifically targeted Von Economo neurons, however, this study was performed with end-stage Alzheimer brains in which cell destruction was widespread. Later, it was found that Alzheimer's disease doesn't affect the VENS, but behavioral variant frontotemporal lobe degeneration specifically targets these cell populations in the anterior cingulate cortex and the anterior insula early in the disease. [8]
Spindle neuron
364
References
[2] von Economo, C., & Koskinas, G. N. (1929). The cytoarchitectonics of the human cerebral cortex. London: Oxford University Press [5] http:/ / www. sciencedaily. com/ releases/ 2012/ 05/ 120521115353. htm
General References
• Allman J, Hakeem A, Watson K (Aug 2002). "Two phylogenetic specializations in the human brain" (http://nro. sagepub.com/cgi/pmidlookup?view=long&pmid=12194502). Neuroscientist 8 (4): 335–46. doi: 10.1177/107385840200800409 (http://dx.doi.org/10.1177/107385840200800409). PMID 12194502 (http:// www.ncbi.nlm.nih.gov/pubmed/12194502).
External links
• TaipeiTimes.com (http://www.taipeitimes.com/News/feat/archives/2003/12/10/2003079090/ print)Wikipedia:Link rot – Know Thyself and Others • "Well-wired whales" (http://sciencenow.sciencemag.org/cgi/content/full/2006/1127/1) Michael Balter (2006) ScienceNOW Daily News. 27 November • "Brain Cells for Socializing" (http://www.smithsonianmag.com/science-nature/The-Social-Brain.html?c=y& story=fullstory) Smithsonian, June 2009
Hepatocyte
365
Hepatocyte
Template:PAGE,n kgmkjNAME
Hepatocyte and sinusoid (blood vessel) in a rat liver with fenestrated endothelial cells. Fenestration are approx 100 nm diameter, and the sinusoidal width 5 µm.
Cross-section of the human liver. Latin Code hepatocytus TH H3.04.05.0.00006
A hepatocyte is a cell of the main tissue of the liver. Hepatocytes make up 70-85% of the liver's cytoplasmic mass. These cells are involved in: • • • • • Protein synthesis Protein storage Transformation of carbohydrates Synthesis of cholesterol, bile salts and phospholipids Detoxification, modification, and excretion of exogenous and endogenous substances
The hepatocyte also initiates formation and secretion of bile.
Hepatocyte
366
Structure
The typical hepatocyte forms a cubical cell of 15 µm sides (in comparison, a human hair has a diameter of 17 to 180 µm). The typical volume of a hepatocyte is 3.4 x 10-9 cm3. [1] The smooth endoplasmic reticulum (Smooth ER) is an abundant organelle in hepatocytes, whereas most cells in the body have small amounts of smooth ER. [2]
Histology
Hepatocytes display an eosinophilic cytoplasm, reflecting numerous mitochondria, and basophilic stippling due to large amounts of rough endoplasmic reticulum and free ribosomes. Brown lipofuscin granules are also observed (with increasing age) together with irregular unstained areas of cytoplasm; these correspond to cytoplasmic glycogen and lipid stores removed during histological preparation. The average life span of the hepatocyte is 5 months; they are able to regenerate. Hepatocyte nuclei are round with dispersed chromatin and prominent nucleoli. Anisokaryosis is common and often reflects tetraploidy and other degrees of polyploidy, a normal feature of 30-40% of hepatocytes in adult human liver.[3] Binucleate cells are also common. Hepatocytes are organised into plates separated by vascular channels (sinusoids), an arrangement supported by a reticulin (collagen type III) network. The hepatocyte plates are one cell thick in mammals and two cells thick in the chicken. Sinusoids display a discontinuous, fenestrated endothelial cell lining. The endothelial cells have no basement membrane and are separated from the hepatocytes by the space of Disse, which drains lymph into the portal tract lymphatics. Kupffer cells are scattered between endothelial cells; they are part of the reticuloendothelial system and phagocytose spent erythrocytes. Stellate (Ito) cells store vitamin A and produce extracellular matrix and collagen; they are also distributed amongst endothelial cells but are difficult to visualise by light microscopy. Hepatocytes are an important physiological example for evalutation of both biological and metabolic effects of xenobiotics. They are separated from the liver by collagenase digestion, which is a two step process. In the first step, the liver is placed in an isotonic solution, in which calcium is removed to disrupt cell-cell tight junctions by the use of a calcium chelating agent. Next, a solution containing collagenase is added to separate the hepatocytes from the liver stroma. This process creates a suspension of hepatocytes, which can be cultured and plated on 96 well plates for immediate use, or cryopreserved by freezing.[4] They do not proliferate in culture. Hepatocytes are intensely sensitive to damage during the cycles of cryopreservation including freezing and thawing. Even after the addition of classical cryoprotectants there is still damage done while being cryopreserved. [5]
Protein synthesis
The hepatocyte is a cell in the body that manufactures serum albumin, fibrinogen, and the prothrombin group of clotting factors (except for Factors 3 and 4). It is the main site for the synthesis of lipoproteins, ceruloplasmin, transferrin, complement, and glycoproteins. Hepatocytes manufacture their own structural proteins and intracellular enzymes. Synthesis of proteins is by the rough endoplasmic reticulum (RER), and both the rough and smooth endoplasmic reticulum (SER) are involved in secretion of the proteins formed. The endoplasmic reticulum (ER) is involved in conjugation of proteins to lipid and carbohydrate moieties synthesized by, or modified within, the hepatocytes.
Hepatocyte
367
Carbohydrate metabolism
The liver forms fatty acids from carbohydrates and synthesizes triglycerides from fatty acids and glycerol. Hepatocytes also synthesize apoproteins with which they then assemble and export lipoproteins (VLDL, HDL). The liver is also the main site in the body for gluconeogenesis, the formation of carbohydrates from precursors such as alanine, glycerol, and oxaloacetate.
Lipid metabolism
The liver receives many lipids from the systemic circulation and metabolizes chylomicron remnants. It also synthesizes cholesterol from acetate and further synthesizes bile salts. The liver is the sole site of bile salts formation.
Detoxification
Hepatocytes have the ability to metabolize, detoxify, and inactivate exogenous compounds such as drugs, (drug metabolism), and insecticides, and endogenous compounds such as steroids. The drainage of the intestinal venous blood into the liver requires efficient detoxification of miscellaneous absorbed substances to maintain homeostasis and protect the body against ingested toxins. One of the detoxifying functions of hepatocytes is to modify ammonia into urea for excretion. The most abundant organelle in liver cell is the smooth endoplasmic reticulum.
Additional images
Schemic diagram of Biliary system
Hepatocyte
368
References
[1] Lodish, H., Berk, A., Zipursky, S. L., Matsudaira, P., Baltimore, D., Darnell, J. E. Molecular Cell Biology (Fifth Edition). W. H. Freeman and Company. New York, 2000, pp 10. [2] Lodish, H., Berk, A., Zipursky, S. L., Matsudaira, P., Baltimore, D., Darnell, J. E. Molecular Cell Biology (Fifth Edition). W. H. Freeman and Company. New York, 2000, pp 168. [4] Li, Albert P.; "Screening for human ADME/Tox drug properties in Drug Discovery": Drug Discovery Today, Vol. 6, No. 7, April 2001, pp. 357-366 [5] Hamel et al.; "Wheat Extracts as an Efficient Cryoprotective Agent for Primary Cultures of Rat Hepatocytes": published online 21 Aug 2006 in Wiley Interscience www.interscience.wiley.com. Department des sciences bogiques, Montreal University.
External links
• BU Histology Learning System: 22101ooa (http://www.bu.edu/histology/p/22101ooa.htm) - "Ultrastructure of the Cell: hepatocytes and sinusoids" • Hepatic Histology: Hepatocytes (Colorado State University (http://www.vivo.colostate.edu/hbooks/pathphys/ digestion/liver/histo_hcytes.html) • The use of hepatocytes to measure clearance (http://www.cyprotex.com/admepk/in-vitro-metabolism/ hepatocyte-stability/) The performance of in vitro hepatic clearance studies including analysis of the data.
Adipocyte
369
Adipocyte
Adipocyte
Yellow adipose tissue in paraffin section Latin Code adipocytus TH H2.00.03.0.01005
[1]
Adipocytes, also known as lipocytes and fat cells, are the cells that primarily compose adipose tissue, specialized in storing energy as fat. There are two types of adipose tissue, white adipose tissue (WAT) and brown adipose tissue (BAT), which are also known as white fat and brown fat, respectively, and comprise two types of fat cells. Most recently presence of beige adipocytes with gene expression pattern distinct from either white or brown adipocytes has been described.[1]
White fat cells (unilocular cells)
White fat cells or monovacuolar cells contain a large lipid droplet surrounded by a layer of cytoplasm. The nucleus is flattened and located on the periphery. A typical fat cell is 0.1mm in diameter with some being twice that size and others half that size. The fat stored is in a semi-liquid state, and is composed primarily of triglycerides and cholesteryl ester. White fat cells secrete many proteins acting as adipokines such as resistin, adiponectin, leptin and Apelin. An average adult has 30 billion fat cells with a weight of 30 lbs or 13.5 kg. If excess weight is gained as an adult, fat cells increase in size about fourfold before dividing and increasing the absolute number of fat cells present.[2]
Brown fat cells (multilocular cells)
Brown fat cells or plurivacuolar cells are polygonal in shape. Unlike white fat cells, these cells have considerable cytoplasm, with lipid droplets scattered throughout. The nucleus is round, and, although eccentrically located, it is not in the periphery of the cell. The brown color comes from the large quantity of mitochondria. Brown fat, also known as "baby fat," is used to generate heat.
Lineage
Although the lineage of adipocytes is still unclear, pre-adipocytes are undifferentiated fibroblasts that can be stimulated to form adipocytes. Mesenchymal stem cells can differentiate into adipocytes, connective tissue, muscle or bone. Areolar connective tissue is composed of adipocytes. The term "lipoblast" is used to describe the precursor of the adult cell. The term "lipoblastoma" is used to describe a tumor of this cell type.[]
Adipocyte
370
Cell turnover
After marked weight loss the number of fat cells does not decrease (the cells contain less fat). Fat cells swell or shrink but remain constant in number. However, the number of fat cells may increase once existing fat cells are sufficiently full. Adult rats of various strains became obese when they were fed a highly palatable diet for several months. Analysis of their adipose tissue morphology revealed increases in both adipocyte size and number in most depots. Reintroduction of an ordinary chow diet to such animals precipitated a period of weight loss during which only mean adipocyte size returned to normal. Adipocyte number remained at the elevated level achieved during the period of weight gain.[3] However, in some reports and textbooks, the number of fat cell (adipocytes) increased in childhood and adolescence. The total number is constant in both obese and lean adult. Individuals who become obese as adults have no more fat cell than they had before.[] People who have been fat since childhood generally have an inflated number of fat cells. People who become fat as adults may have no more fat cells than their lean peers, but their fat cells are larger. In general, people with an excess of fat cells find it harder to lose weight and keep it off than the obese who simply have enlarged fat cells.[4] According to a research by Tchoukalova et al., 2010, it has been reported that the body fat cells could have regional responses to the overfeeding studied in adult subjects. In upper body, an increasing of the adipocyte size was correlated with upper-body fat gain; however, the total fat cells were not significantly changed. In contrast to the upper body fat cell responses, a number of lower-body adipocytes were significantly increased during the course of experiment but there was no change in the cell size.[5] Approximately 10% of fat cells are renewed annually at all adult ages and levels of body mass index without a significant increase in the overall number of adipocytes in adulthood.[]
Endocrine functions
Adipocytes can synthesize estrogens from androgens,[6] potentially being the reason why being underweight or overweight are risk factors for infertility.[7] Additionally, adipocytes are responsible for the production of the hormone leptin. Leptin is important in regulation of appetite and acts as a satiety factor.[8]
References
[1] Wu J, Bostrom P, Sparks LM, Ye L, Choi JH, Giang AH, et al. Beige adipocytes are a distinct type of thermogenic fat cell in mouse and human. Cell 2012; 150:366-76. [7] UNIQ-nowiki-0-b868a355cd8ea4cc-QINU FERTILITY FACT > Female Risks By the American Society for Reproductive Medicine (ASRM). Retrieved on Jan 4, 2009
External links
• BU Histology Learning System: 08201loa (http://www.bu.edu/histology/p/08201loa.htm) - "Connective Tissue: unilocular (white) adipocytes " • BU Histology Learning System: 04901lob (http://www.bu.edu/histology/p/04901lob.htm) - "Connective Tissue: multilocular (brown) adipocytes"
White adipose tissue
371
White adipose tissue
White adipose tissue
Latin textus adiposus albus Code TH H2.00.04.0.0002 [1]
White adipose tissue (WAT) or white fat is one of the two types of adipose tissue found in mammals. The other kind of adipose tissue is brown adipose tissue. In healthy, non-overweight humans, white adipose tissue composes as much as 20% of the body weight in men and 25% of the body weight in women. Its cells contain a single large fat droplet, which forces the nucleus to be squeezed into a thin rim at the periphery. They have receptors for insulin, growth hormones, norepinephrine and glucocorticoids. White adipose tissue is used as a store of energy. Upon release of insulin from the pancreas, white adipose cells' insulin receptors cause a Distribution of white adipose tissue in the human dephosphorylation cascade that lead to the inactivation of body. hormone-sensitive lipase. It was previously thought that upon release of glucagon from the pancreas, glucagon receptors cause a phosphorylation cascade that activates hormone-sensitive lipase, causing the breakdown of the stored fat to fatty acids, which are exported into the blood and bound to albumin, and glycerol, which is exported into the blood freely.There is actually no evidence at present that glucagon has any effect on white adipose tissue.[1] Glucagon is now thought to act exclusively on the liver to trigger glycogenolysis and gluconeogenesis.[] The trigger for this process in white adipose tissue is instead now thought to be adrenocorticotropic hormone (ACTH), adrenaline and noradrenaline[citation needed]. Fatty acids are taken up by muscle and cardiac tissue as a fuel source, and glycerol is taken up by the liver for gluconeogenesis. White adipose tissue also acts as a thermal insulator, helping to maintain body temperature. The hormone leptin is primarily manufactured in the adipocytes of white adipose tissue.
References
Brown adipose tissue
372
Brown adipose tissue
Brown adipose tissue
Brown adipose tissue in a woman shown in a PET/CT exam Latin Code textus adiposus fuscus TH H2.00.04.0.0004
[1]
Brown adipose tissue (BAT) or brown fat is one of two types of fat or adipose tissue (the other being white adipose tissue) found in mammals. It is especially abundant in newborns and in hibernating mammals.[] Its primary function is to generate body heat in animals or newborns that do not shiver. In contrast to white adipocytes (fat cells), which contain a single lipid droplet, brown adipocytes contain numerous smaller droplets and a much higher number of (iron containing) mitochondria, which make it brown.[] Brown fat also contains more capillaries than white fat, since it has a greater need for oxygen than most tissues.
Biochemistry
The mitochondria in a eukaryotic cell utilize fuels to produce energy (in the form of ATP). This process involves storing energy as a proton gradient, also known as the proton motive force (PMF), across the mitochondrial inner membrane. This energy is used to synthesize ATP when the protons flow across the membrane (down their concentration gradient) through the ATP synthase enzyme; this is known as chemiosmosis. In warm-blooded animals, body heat is maintained by signaling the mitochondria to allow protons to run back along the gradient without producing ATP.[citation needed] This can occur since an alternative return route for the protons exists through an uncoupling protein in the inner membrane. This protein, known as uncoupling protein 1 (thermogenin), facilitates the return of the protons after they have been actively pumped out of the mitochondria by the electron transport chain. This alternative route for protons uncouples oxidative phosphorylation and the energy in the PMF is instead released as heat. To some degree, all cells of endotherms give off heat, especially when body temperature is below a regulatory threshold. However, brown adipose tissue is highly specialized for this non-shivering thermogenesis. First, each cell has a higher number of mitochondria compared to more typical cells. Second, these mitochondria have a higher-than-normal concentration of thermogenin in the inner membrane.
Brown adipose tissue
373
Function in infants
In neonates (newborn infants), brown fat, which then makes up about 5% of the body mass and is located on the back, along the upper half of the spine and toward the shoulders, is of great importance to avoid lethal cold (hypothermia is a major death risk for premature neonates). Numerous factors make infants more susceptible to cold than adults: • • • • • • The higher ratio of body surface (proportional to heat loss) to body volume (proportional to heat production) The higher proportional surface area of the head The low amount of musculature and the inability or reluctance to shiver A lack of thermal insulation, e.g., subcutaneous fat and fine body hair (especially in prematurely born children) The inability to move away from cold areas, air currents or heat-draining materials The inability to use additional ways of keeping warm (e.g., drying their skin, putting on clothing, moving into warmer areas, or performing physical exercise) • The nervous system is not fully developed and does not respond quickly and/or properly to cold (e.g., by contracting blood vessels in and just below the skin; vasoconstriction). Heat production in brown fat provides an infant with an alternative means of heat regulation.
Presence in adults
It was believed that after infants grow up, most of the mitochondria (which are responsible for the brown color) in brown adipose tissue disappear, and the tissue becomes similar in function and appearance to white fat. However, more recent research has shown that brown fat is related not to white fat, but to skeletal muscle.[][1][2] Further, recent studies using Positron Emission Tomography scanning of adult humans have shown that it is still present in adults in the upper chest and neck. The remaining deposits become more visible Micrograph of a hibernoma, a benign tumour (increasing tracer uptake, that is, more metabolically active) with cold thought to arise from brown fat. H&E stain. exposure, and less visible if an adrenergic beta blocker is given before the scan. The recent study could lead to a new method of weight loss, since brown fat takes calories from normal fat and burns it. Scientists were able to stimulate brown fat growth in mice, but human trials have not yet begun.[3][4] In rare cases, brown fat continues to grow, rather than involuting; this leads to a tumour known as a hibernoma.
Embryology
Brown fat cells and muscle cells both seem to be derived from the same stem cells in the embryo. Both have the same marker on their surface (Myf5, myogenic factor), which white fat cells do not have.[] Brown fat cells and muscle cells both come from the middle embryo layer. The three layers of the embryo during the gastrulation stage are ectoderm, mesoderm, endoderm. Mesoderm is the source of myocytes (muscle cells), adipocytes, and chondrocytes (cartilage cells). Adipocytes give rise to white fat cells and brown fat cells. Researchers found that both muscle and brown fat cells expressed the same muscle factor Myf5, whereas white fat cells did not. This suggested that muscle cells and brown fat cells were both derived from the same stem cell. Furthermore, muscle cells that were cultured with the transcription factor PRDM16 were converted into brown fat cells, and brown fat cells without PRDM16 were converted into muscle cells.[] However, there may be two types of brown fat cells—with and without Myf5. The other type, without Myf5, may share the same origin as white fat cells. They both seem to be derived from pericytes, the cells which surround the blood vessels that run through white fat tissue.[]
Brown adipose tissue
374
References
[1] Brown adipose tissue -- when it pays to be inefficient, Francesco S. Celi, N Engl J Med, 360:1553, Apr. 9, 2009 [4] Scientists Create Energy-burning Brown Fat In Mice (http:/ / www. sciencedaily. com/ releases/ 2009/ 07/ 090729132109. htm) Science Daily, July 30, 2009
External links
• BU Histology Learning System: 04901lob (http://www.bu.edu/histology/p/04901lob.htm) - "Connective Tissue: multilocular (brown) adipocytes"
Hepatic stellate cell
375
Hepatic stellate cell
Hepatic stellate cell
Schematic presentation of hepatic stellate cells (HSC) located in the vicinity of adjacent hepatocytes (PC) beneath the sinusoidal endothelial cells (EC). S – liver sinusoids; KC – Kupffer cells. Down left shows cultured HSC at light-microscopy, whereas at down right electron microscopy (EM) illustrates numerous fat vacuoles (L) in a HSC, in which retinoids are stored.
Basic liver structure Latin Code cellula perisinusoidalis; cellula accumulans adipem TH H3.04.05.0.00013
Hepatic stellate cells (here HSC), also known as perisinusoidal cells or Ito cells (earlier lipocytes or fat-storing cells), are pericytes found in the perisinusoidal space (a small area between the sinusoids and hepatocytes) of the liver also known as the space of Disse. The stellate cell is the major cell type involved in liver fibrosis, which is the formation of scar tissue in response to liver damage.
Staining
Ito cells can be selectively stained with gold chloride, but their distinguishing feature in routine histological preparations is the presence of multiple lipid droplets in their cytoplasm.[] Reelin expressed by Ito cells has been shown to be a reliable marker in discerning them from other myofibroblasts.[1] The expression of reelin is increased after liver injury.
Function
In normal liver, stellate cells are described as being in a quiescent state. Quiescent stellate cells represent 5-8% of the total number of liver cells.[2] Each cell has several long protrusions that extend from the cell body and wrap around the sinusoids. The lipid droplets in the cell body store vitamin A as retinol ester. The function and role of quiescent hepatic stellate cells is unclear. Recent evidence suggests a role as a liver-resident antigen-presenting cell, presenting lipid antigens to and stimulating proliferation of NKT cells.[] When the liver is damaged, stellate cells can change into an activated state. The activated stellate cell is characterized by proliferation, contractility, and chemotaxis. The amount of stored vitamin A decreases progressively in liver injury.[] The activated stellate cell is also responsible for secreting collagen scar tissue, which can lead to cirrhosis. More recent studies have also shown that in vivo activation of hepatic stellate cells by agents
Hepatic stellate cell causing liver fibrosis can eventually lead to senescence of these cells, marked by increased SA-beta-galactosidase staining, as well as p53 accumulation and activation of Rb–hallmarks of cellular senescence. The senescent hepatic stellate cells have been demonstrated to limit liver fibrosis by activating the immune system by activating interactions with the NK cells.[]
376
Eponym
The cells of Ito were named for Toshio Ito, a twentieth century Japanese physician.[3]
References External links
• MedEd at Loyola orfpath/murali2.htm (http://www.meddean.luc.edu/Lumen/MedEd/orfpath/murali2.htm) • Liver Research at AU-KBC Stellate cell biology (http://bio.au-kbc.org/faculty/suvro/liver.php?go=hepatic)
Podocyte
377
Podocyte
Podocyte
Renal corpuscle structure Blood flows in the afferent arteriole (9) at the top, and out the efferent arteriole (11) at the bottom. Blood flows through the capillaries of the glomerulus (10), where it is filtered by pressure. The podocytes (3a and 3b, green) are wrapped around the capillaries. Blood is filtered through the slit diaphragm (or filtration slit), between the feet or processes of the podocytes. The filtered urine passes out the proximal tubule (B, yellow) on the right. A - Renal corpuscle B - Proximal tubule C - Distal convoluted tubule D - Juxtaglomerular apparatus 1. Basement membrane (Basal lamina) 2. Bowman's capsule - parietal layer) 3. Bowman's capsule - visceral layer 3a. Podocyte 3b. Pedicels (podocyte processes) 4. Bowman's space (urinary space) 5a. Mesangium - Intraglomerular cell 5b. Mesangium - Extraglomerular cell 6. Granular cells (Juxtaglomerular cells) 7. Macula densa 8. Myocytes (smooth muscle) 9. Afferent arteriole 10. Glomerulus capillaries 11. Efferent arteriole
Glomerulus. (Diagram in French, but "Membrane basale glomerulaire et ses podocytes" labeled near center.) Latin Dorlands/Elsevier podocytus Podocyte
[1]
Podocytes (or visceral epithelial cells) are cells in the Bowman's capsule in the kidneys that wrap around the capillaries of the glomerulus.[1] The Bowman's capsule filters blood, holding back large molecules such as proteins, and passing through small molecules such as water, salts, and sugar, as the first step in forming urine. The long processes, or "foot projections," of the podocytes wrap around the capillaries, and leave slits between them. Blood is filtered through these slits, each known as a slit diaphragm or filtration slit. Several proteins are required for the foot projections to wrap around the capillaries and function. When infants are born with certain defects in these proteins, such as nephrin and CD2AP, their kidneys cannot function. People have variations in these proteins, and
Podocyte some variations may predispose them to kidney failure later in life. Nephrin is a zipper-like protein that forms the slit diaphragm, with spaces between the teeth of the zipper, big enough to allow sugar and water through, but too small to allow proteins through. Nephron defects are responsible for congenital kidney failure. CD2AP regulates the podocyte cytoskeleton and stabilizes the slit diaphragm.[2][3]
378
Function
Adjacent podocytes interdigitate to cover the basal lamina which is intimately associated with the glomerular capillaries, but the podocytes leave gaps or thin filtration slits. The slits are covered by slit diaphragms which are composed of a number of cell-surface proteins including nephrin, podocalyxin, and P-cadherin, which ensure that large macromolecules such as serum albumin and gamma globulin remain in the bloodstream. Small molecules such as water, glucose, and ionic salts are able to pass through the slit diaphragms and form an ultrafiltrate[4] which is further processed by the nephron to produce urine. Podocytes are also involved in regulation of glomerular filtration rate (GFR). When podocytes contract, they cause closure of filtration slits. This decreases the GFR by reducing the surface area available for filtration.
Structure features
Structural features of podocytes indicate a high rate of vesicular traffic in these cells. Many coated vesicles and coated pits can be seen along the basolateral domain of the podocytes. In their cell bodies, podocytes possess a well-developed endoplasmic reticulum and a large Golgi apparatus, indicative of a high capacity for protein synthesis and post-translational modifications. There is also growing evidence of a large number of multivesicular bodies and other lysosomal components seen in these cells, indicating a high endocytic activity. "Pedicels" (or "foot processes") extend from the podocyte and increase the surface area which is crucial for the efficiency of ultrafiltration.[5]
Pathology
Disruption of the slit diaphragms or destruction of the podocytes can lead to massive proteinuria where large amounts of protein are lost from the blood. An example of this occurs in the congenital disorder Finnish-type nephrosis, which is characterised by neonatal proteinuria leading to end-stage renal failure. This disease has been found to be caused by a mutation in the nephrin gene.
Podocyte
379
Additional images
Filtration barrier
References
[2] First components found for key kidney filter, Ingrid Wickelgren, Science, 8 October 1999, 286:225
External links
• Organology at UC Davis Urinary/mammal/vasc1/vasc1 (http://trc.ucdavis.edu/mjguinan/apc100/modules/ Urinary/mammal/vasc1/vasc1.html) - "Mammal, renal vasculature (EM, High) • BU Histology Learning System: 22401loa (http://www.bu.edu/histology/p/22401loa.htm) - ". Ultrastructure of the Cell: podocytes and glomerular capillaries" • UIUC Histology Subject 1400 (https://histo.life.illinois.edu/histo/atlas/oimages.php?oid=1400) • podocyte.ca (http://www.podocyte.ca/) at Samuel Lunenfeld Research Institute
Proximal convoluted tubule
380
Proximal convoluted tubule
Proximal Convoluted Tubule
Scheme of renal tubule and its vascular supply. (1st convoluted tubule labeled at center top.)
1 Glomerulus, 2 proximal tubule, 3 distal tubule Latin Gray's Precursor tubulus contortus proximalis subject #253 1223
[1]
Metanephric blastema
The proximal tubule is the portion of the duct system of the nephron of the kidney which leads from Bowman's capsule to the loop of Henle.
Structure and appearance
The most distinctive characteristic of the proximal tubule is its brush border (or "striated border").
Brush border cell
The luminal surface of the epithelial cells of this segment of the nephron is covered with densely packed microvilli forming a border readily visible under the light microscope giving the brush border cell its name. The microvilli greatly increase the luminal surface area of the cells, presumably facilitating their resorptive function as well as putative flow sensing within the lumen.[1] The cytoplasm of the cells is densely packed with mitochondria, which are largely found in the basal region within the infoldings of the basal plasma membrane. The high quantity of mitochondria gives the cells an acidophilic appearance. The mitochondria are needed in order to supply the energy for the active transport of sodium ions out of the proximal tubule. Water passively follows the sodium out of the cell along its concentration gradient. Cuboidal epithelial cells lining the proximal tubule have extensive lateral interdigitations between neighboring cells, which lend an appearance of having no discrete cell margins when viewed with a light microscope.
Proximal convoluted tubule Agonal resorption of the proximal tubular contents after interruption of circulation in the capillaries surrounding the tubule often leads to disturbance of the cellular morphology of the proximal tubule cells, including the ejection of cell nuclei into the tubule lumen. This has led some observers to describe the lumen of proximal tubules as occluded or "dirty-looking," in contrast to the "clean" appearance of distal tubules, which have quite different properties.
381
Divisions
The proximal tubule as a part of the nephron can be divided into two sections, pars convoluta and pars recta. Differences in cell outlines exist between these segments, and therefore presumably in function too. Regarding ultrastructure, it can be divided into three segments, S1, S2, and S3:
Segment Gross divisions Ultrastructure divisions Description S1 S2 S3 [2] [2] [2] Lower cell complexity [2] Higher cell complexity [2]
Proximal tubule convoluted
straight
Pars convoluta
The "Pars convoluta" is the initial convoluted portion. In relation to the morphology of the kidney as a whole, the convoluted segments of the proximal tubules are confined entirely to the renal cortex. Some investigators on the basis of particular functional differences have divided the convoluted part into two segments designated S1 and S2.
Pars recta
The "Pars recta" is the following straight (descending) portion. Straight segments descend into the outer medulla. They terminate at a remarkably uniform level and it is their line of termination that establishes the boundary between the inner and outer stripes of the outer zone of the renal medulla. As a logical extension of the nomenclature described above, this segment is sometimes designated as S3.
Absorption
The proximal tubule regulates the pH of the filtrate by exchanging hydrogen ions in the interstitium for bicarbonate ions in the filtrate; it is also responsible for secreting organic acids, such as creatinine and other bases, into the filtrate. Fluid in the filtrate entering the proximal convoluted tubule is reabsorbed into the peritubular capillaries. This is driven by sodium transport from the lumen into the blood by the Na+/K+ ATPase in the basolateral membrane of the epithelial cells. Sodium reabsorption is primarily driven by this P-type ATPase. This is the most important transport mechanism in the PCT.
Proximal convoluted tubule
382
Substance
% of filtrate reabsorbed approximately two-thirds
Comments
salt and water
Much of the mass movement of water and solutes occurs through the cells, passively across the lumenal membrane via transcellular transport, which is then actively resorbed across the basolateral membrane via the Na/K/ATPase pump. The solutes are absorbed isotonically, in that the osmotic potential of the fluid leaving the proximal tubule is the same as that of the initial glomerular filtrate. Glucose, amino acids, inorganic phosphate, and some other solutes are reabsorbed via secondary active transport through cotransport channels driven by the sodium gradient out of the nephron.
organic solutes (primarily glucose and amino acids) potassium
100%
approximately 65% approximately 50% approximately 80%
Most of the filtered potassium is reabsorbed by two paracellular mechanisms - solvent drag and simple [3] diffusion. Paracellular fluid reabsorption sweeps some urea with it via solvent drag. As water leaves the lumen, the [4] concentration of urea increases, which facilitates diffusion in the late proximal tubule. Parathyroid hormone reduces reabsorption of phosphate in the proximal tubules, but, because it also enhances the uptake of phosphate from the intestine and bones into the blood, the responses to PTH cancel each other out, and the serum concentration of phosphate remains approximately the same. Acidosis increases absorption. Alkalosis decreases absorption.
urea
phosphate
citrate
70%–90%
[5]
Secretion
Many types of medications are secreted in the proximal tubule. Further reading: Table of medication secreted in kidney Most of the ammonium that is excreted in the urine is formed in the proximal tubule via the breakdown of glutamine to alpha-ketoglutarate.[] This takes place in two steps, each of which generates an ammonium anion: the conversion of glutamine to glutamate and the conversion of glutamate to alpha-ketoglutarate. [] The alpha-ketoglutarate generated in this process is then further broken down to form two bicarbonate anions,[] which are pumped out of the basolateral portion of the tubule cell by cotransport with sodium ions.
Pathophysiology in kidney disease
Proximal tubular epithelial cells (PTECs) have a pivotal role in kidney disease.
Malignant
Most renal cell carcinoma, the most common form of kidney cancer, arises from the convoluted tubules.[6]
Non-malignant
Acute tubular necrosis occurs when PTECs are directly damaged by Immunohistochemical staining of the convoluted toxins such as antibiotics (e.g., gentamicin), pigments (e.g., myoglobin tubules and glomeruli with CD10. and sepsis (e.g., mediated by lipopolysaccharide from gram-negative bacteria). Renal tubular acidosis (proximal type) (Fanconi syndrome) occurs when the PTECs are unable to properly reabsorb glomerular filtrate so that there is increased loss of bicarbonate, glucose, amino acids, and phosphate. PTECs also participate in the progression of tubulointerstitial injury due to glomerulonephritis, ischemia, interstitial nephritis, vascular injury, and diabetic nephropathy. In these situations, PTECs may be directly affected by protein
Proximal convoluted tubule (e.g., proteinuria in glomerulonephritis), glucose (in diabetes mellitus), or cytokines (e.g., interferon-γ and tumor necrosis factors). There are several ways in which PTECs may respond: producing cytokines, chemokines, and collagen; undergoing epithelial mesenchymal trans-differentiation; necrosis or apoptosis.
383
Additional images
Distribution of blood vessels in cortex of kidney.
Glomerulus.
TEM of negatively stained proximal convoluted tubule of Rat kidney tissue at a magnification of ~55,000x and 80KV with Tight junction.
Renal corpuscle
Diagram outlining movement of ions in nephron.
References
[2] Page 743 [3] Boron & Boulpaep. Medical Physiology. Updated Edition. 2005. [4] Boron & Boulpaep. Medical Physiology. Updated Edition. 2005.
External links
• 1771700264 (http://www.gpnotebook.co.uk/simplepage.cfm?ID=1771700264) at GPnotebook • Organology at UC Davis Urinary/mammal/cortex1/cortex6 (http://trc.ucdavis.edu/mjguinan/apc100/modules/ Urinary/mammal/cortex1/cortex6.html) - "Mammal, kidney cortex (LM, Medium)" • Physiology at MCG 7/7ch03/7ch03p14 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section7/7ch03/7ch03p14.htm) - "The Nephron: Proximal Tubule, Pars Convoluta & Pars Recta" • Swiss embryology (from UL, UB, and UF) turinary/urinhaute02 (http://www.embryology.ch/anglais/turinary/ urinhaute02.html) This article incorporates text from a public domain edition of Gray's Anatomy.
Thin segment
384
Thin segment
The thin segment is a segment of the nephron, which consists of: • thin descending limb of loop of Henle • thin ascending limb of loop of Henle
Histology
The basement membrane of the thin limb in humans has very uniform nodular thickenings that form a network that surrounds the tubule and acts as a support structure that is homologous to the collenchyma in plants. Smith, RA et al. (Arch Pathol Lab Med Vol 108, May 1984) have designated these nodules "Belliveau Bodies" after Robert Belliveau the pathologist who originally described these structures. The epithelium is Simple squamous epithelium.[1]
References
[1] - "University of Illinois College of Medicine"
Distal convoluted tubule
385
Distal convoluted tubule
Distal convoluted tubule
Kidney nephron ("1st proximal convoluted tubule", "2nd distal convoluted tubule")
Section of cortex of human kidney. Latin Gray's Precursor MeSH tubulus contortus distalis subject #253 1223
[1]
Metanephric blastema Distal+Kidney+Tubule
[1]
The distal convoluted tubule (DCT) is a portion of kidney nephron between the loop of Henle and the collecting duct system.
Physiology
It is partly responsible for the regulation of potassium, sodium, calcium, and pH. It is the primary site for the kidneys' hormone based regulation of calcium (Ca). On its apical surface (lumen side), cells of the DCT have a thiazide-sensitive Na-Cl cotransporter and are permeable to Ca, via TRPV5 channel. On the basolateral surface (blood) there is an ATP dependent Na/K antiport pump, a secondary active Na/Ca transporter-- antiport, and an ATP dependent Ca transporter. The basolateral ATP dependent Na/K pump produces the gradient for Na to be absorbed from the apical surface via the Na/Cl synport and for Ca to be reclaimed into the blood by the Na/Ca basolateral antiport. • It regulates pH by absorbing bicarbonate and secreting protons (H+) into the filtrate, or by absorbing protons and secreting bicarbonate into the filtrate. • Sodium and potassium levels are controlled by secreting K+ and absorbing Na+. Sodium absorption by the distal tubule is mediated by the hormone aldosterone. Aldosterone increases sodium reabsorption. Sodium and chloride (salt) reabsorption is also mediated by a group of kinases called WNK kinases. There are 4 different WNK
Distal convoluted tubule kinases, WNK1 [2], WNK2 [3], WNK3 [4], and WNK4 [5]. • It also participates in calcium regulation by reabsorbing Ca2+ in response to parathyroid hormone. [1] PTH effect is mediated through phosphorylation of regulatory proteins and enhancing the synthesis of all transporters within the distal convoluted tubule. • Arginine vasopressin receptor 2 is also expressed in the DCT.
386
Clinical significance
Thiazide diuretics inhibit Na+/Cl- reabsorption from the DCT by blocking the thiazide-sensitive Na-Cl cotransporter. By inhibiting the cotransporter, thiazide diuretics increase the gradient potential for Na. This increases the activity of the basolateral Na/Ca antiport and causes the increase in calcium reclamation associated with thiazide diuretics.
Histology
The DCT is lined with simple cuboidal cells that are shorter than those of the proximal convoluted tubule (PCT). The lumen appears larger in DCT than the PCT lumen because the PCT has a brush border (microvilli). DCT can be recognized by its numerous mitochondria, basal infoldings and lateral membrane interdigitations with neighboring cells. The point where DCT contacts afferent arteriole of renal corpuscle is called macula densa. It has tightly packed columnar cells which display reversed polarity and may monitor the osmolarity of blood. Histologically, cells of the DCT can be differentiated from cells of the proximal convoluted tubule:
Characteristic Apical brush border Eosinophilicity Cytoplasm PCT DCT
Usually present Not present More More Less Less More likely
Readily discernible nuclei Less likely
Additional images
1 Glomerulus, 2 proximal tubule, 3 distal tubule
Transverse section of pyramidal substance of kidney of pig, the bloodvessels of which are injected.
Renal corpuscle
Diagram outlining movement of ions in nephron.
Distal convoluted tubule
387
References External links
• Histology at OU 35_19 (http://w3.ouhsc.edu/histology/Glass slides/35_19.jpg) • Physiology at MCG 7/7ch03/7ch03p18 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section7/7ch03/7ch03p18.htm) • Physiology at MCG 7/7ch07/7ch07p14 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section7/7ch07/7ch07p14.htm) • BU Histology Learning System: 16004loa (http://www.bu.edu/histology/p/16004loa.htm) • BU Histology Learning System: 16007loa (http://www.bu.edu/histology/p/16007loa.htm)
Kidney collecting duct cell
A kidney collecting duct cell can be of two different cell types: • principal cells • Intercalated cells
Pneumocyte
Two types of pneumocytes (also named pneumonocyte) contribute to the maintenance of the alveoli of the lungs: Type I pneumocytes and Type II pneumocytes. These cells function to aid in gas exchange, secretion of pulmonary surfactant, and self-regeneration
External links
• Histology at KUMC resp-resp17 [1] • BU Histology Learning System: 13905loa [2] • Electron micrograph at luc.edu [3]
Centroacinar cell
388
Centroacinar cell
Centroacinar cell
Latin Gray's Code
cellula centroacinosa subject #251 1204
[1]
TH H3.04.07.0.00008
Centroacinar cells are spindle-shaped cells in the exocrine pancreas. Centroacinar cells are an extension of the intercalated duct cells into each pancreatic acinus.[] The intercalated ducts take the bicarbonate to intralobular ducts which become lobular ducts. These lobular ducts finally converge to form the main pancreatic duct.[] These cells are commonly known as duct cells, and secrete an aqueous bicarbonate solution under stimulation by the hormone secretin. They also secrete mucin.
References External links
• Anatomy Atlases - Microscopic Anatomy, plate 10.213 (http://www.anatomyatlases.org/MicroscopicAnatomy/ Section10/Plate10213.shtml) - "Pancreas" • BU Histology Learning System: 10406loa (http://www.bu.edu/histology/p/10406loa.htm) - "Liver, Gall Bladder, and Pancreas: pancreas, centroacinar cells" • UIUC Histology Subject 870 (https://histo.life.illinois.edu/histo/atlas/oimages.php?oid=870) This article incorporates text from a public domain edition of Gray's Anatomy.
Collecting duct system
389
Collecting duct system
Collecting duct system
Scheme of renal tubule and its vascular supply. Latin Gray's MeSH tubulus renalis colligens subject #253 1223
[1] [1]
Kidney+Collecting+Ducts
The collecting duct system of the kidney consists of a series of tubules and ducts that connect the nephrons to the ureter. It participates in electrolyte and fluid balance through reabsorption and excretion, processes regulated by the hormones aldosterone and antidiuretic hormone. There are several components of the collecting duct system, including the connecting tubules, cortical collecting ducts, and medullary collecting ducts.
Function
The collecting duct system is the final component of the kidney to influence the body's electrolyte and fluid balance. In humans, the system accounts for 4–5% of the kidney's reabsorption of sodium and 5% of the kidney's reabsorption of water. At times of extreme dehydration, over 24% of the filtered water may be reabsorbed in the collecting duct system. The wide variation in water reabsorption levels for the collecting duct system reflects its dependence on hormonal activation. The collecting ducts, in particular, the outer medullary and cortical collecting ducts, are largely impermeable to water without the presence of antidiuretic hormone (ADH, or vasopressin). • In the absence of ADH, water in the renal filtrate is left alone to enter the urine, promoting diuresis. • When ADH is present, aquaporins allow for the reabsorption of this water, thereby inhibiting diuresis. The collecting duct system participates in the regulation of other electrolytes, including chloride, potassium, hydrogen ions, and bicarbonate.
Anatomy
The segments of the system are as follows:
Collecting duct system
390
Segment connecting tubule initial collecting tubule cortical collecting ducts medullary collecting ducts papillary ducts, also known as duct of Bellini
Description
Before convergence of nephrons
Connecting tubule
With respect to the renal corpuscle, the "connecting tubule" is the most proximal part of the collecting duct system. It is adjacent to the distal convoluted tubule, the most distal segment of the renal tubule. Connecting tubules from several adjacent nephrons merge to form cortical collecting tubules, and these may join to form cortical collecting ducts. Connecting tubules of some juxtamedullary nephrons may arch upward, forming an arcade. The connecting tubule derives from the metanephric blastema, but the rest of the system derives from the ureteric bud. Because of this, some sources group the connecting tubule as part of the nephron, rather than grouping it with the collecting duct system.
Initial collecting tubule
The initial collecting tubule is a segment with a constitution similar as the collecting duct, but before the convergence with other tubules.[1]Wikipedia:Citing sources
Cortical collecting duct
The "cortical collecting ducts" receive filtrate from multiple initial collecting tubules and descend into the renal medulla to form medullary collecting ducts.
Medullary collecting duct
"Medullary collecting ducts" are divided into outer and inner segments, the latter reaching more deeply into the medulla. The variable reabsorption of water and, depending on fluid balances and hormonal influences, the reabsorption or secretion of sodium, potassium, hydrogen and bicarbonate ion continues here. Urea passively transports out of duct here and creates 500mOsm gradient. Outer segment The outer segment of the medullary collecting duct follows the cortical collecting duct. It reaches the level of the renal medulla where the thick ascending limb of loop of Henle borders with the thin ascending limb of loop of Henle[2] Inner segment The inner segment is the part of the collecting duct system between the outer segment and the papillary ducts.
Papillary duct
The terminal portions of the medullary collecting ducts are the "papillary ducts", which end at the renal papilla and empty into a minor calyx. It is also called duct of Bellini.
Collecting duct system
391
Cell types
Each component of the collecting duct system contains two cell types, intercalated cells and a segment-specific cell type: • For the connecting tubules, this specific cell type is the connecting tubule cell • For the collecting ducts, it is the principal cell. The inner medullary collecting ducts contain an additional cell type, called the inner medullary collecting duct cell.
Principal cells
The principal cell mediates the collecting duct's influence on sodium and potassium balance via sodium channels and potassium channels located on the cell's apical membrane. Aldosterone determines expression of sodium channels with increased aldosterone causing increased expression of luminal sodium channels[3]Wikipedia:Verifiability. Aldosterone increases the number of Na⁺/K⁺-ATPase pumps[4] that allow increased sodium reabsorption and potassium secretion.[5] Vasopressin determines the expression of aquaporin channels on the cell surface.[6] Together, aldosterone and vasopressin let the principal cell control the quantity of water that is reabsorbed.
Intercalated cells
Intercalated cells come in α and β varieties and participate in acid-base homeostasis.
Type of cell α-intercalated cells β-intercalated cells Secretes acid (via an apical H+-ATPase and H+/K+ exchanger) in the form of hydrogen ions bicarbonate (via pendrin a specialised apical Cl-/HCO3-) Reabsorbs bicarbonate (via band 3, a basolateral Cl-/HCO3[7] exchanger) acid (via a basal H+-ATPase)
For their contribution to acid-base homeostasis, the intercalated cells play important roles in the kidney's response to acidosis and alkalosis. Damage to the α-intercalated cell's ability to secrete acid can result in distal renal tubular acidosis (RTA type I, classical RTA).
Additional images
Transverse section of pyramidal substance of kidney of pig, the blood vessels of which are injected.
Alpha intercalated cell cartoon
Diagram outlining movement of ions in nephron.
Collecting duct system
392
References
[1] [2] [3] [4] [5] [7] Boron Boron, p. 837. – "The Nephron: Collecting Duct" Guyton 2006, p. 949. Guyton 2006, p. 336. – "Intercalated Cells"
• Boron, Walter F. (2005). Medical Physiology: A Cellular and Molecular Approach (updated ed.). Philadelphia: Elsevier/Saunders. ISBN 1-4160-2328-3. • Guyton, Arthur C.; John E. Hall (2006). Textbook of Medical Physiology (11 ed.). Philadelphia: Elsevier Saunders. ISBN 0-7216-0240-1.
External links
• Histology at KUMC epithel-epith04 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/epithel/ epith04.htm) "Collecting Duct (Kidney)" • BU Histology Learning System: 15803loa (http://www.bu.edu/histology/p/15803loa.htm) – "Urinary System: kidney, medulla, collecting duct and ascending tubule" • BU Histology Learning System: 16013loa (http://www.bu.edu/histology/p/16013loa.htm) – "Urinary System: kidney, H&E, collecting duct and ascending tubule"
Microvillus
393
Microvillus
Microvillus
Enterocytes with microvilli Code TH H1.00.01.1.01011
[1]
Microvilli (singular: microvillus) are microscopic cellular membrane protrusions that increase the surface area of cells,[] and are involved in a wide variety of functions, including absorption, secretion, cellular adhesion, and mechanotransduction.
Locations
Thousands of microvilli form a structure called the brush border that is found on the apical surface of some epithelial cells, such as the small intestinal. Microvilli are observed on the plasma surface of eggs, aiding in the anchoring of sperm cells that have penetrated the extracellular coat of egg cells. Clustering of elongated microtubules around a sperm allows for it to be drawn closer and held firmly so fusion can occur. Microvilli are also of importance on the cell surface of white blood cells, as they aid in the migration of white blood cells.
Structure
Microvilli are covered in plasma membrane, which encloses cytoplasm and microfilaments. Though these are cellular extensions, there are little or no cellular organelles present in the microvilli. Each microvillus has a dense bundle of cross-linked actin filaments, which serves as its structural core. 20 to 30 tightly bundled actin filaments are cross-linked by bundling proteins fimbrin and villin to form the core of the microvilli. In the enterocyte microvillus, the structural core is attached to the plasma membrane along its length by lateral arms made of myosin 1a and Ca2+ binding protein calmodulin. Myosin 1a functions through a binding site for filamentous actin on one end and a lipid binding domain on the other. The plus ends of the actin filaments are located at the tip of the microvillus and are capped, possibly by capZ proteins,[1] while the minus ends are anchored in the terminal web composed of a complicated set of proteins including spectrin and myosin II.
Microvillus
394
Function
Microvilli can act as mechanosensors in kidney proximal tubule.[2] They sense the fluid flow in the tubule lumen and convert this information via biochemical responses into reabsorption. Microvilli are also of importance on the cell surface of white blood cells, as they aid in the migration of white blood cells.[citation needed]
Relationship to cell
As mentioned, microvilli are formed as cell extensions from the plasma membrane surface. Actin filaments, present in the cytosol, are most abundant near the cell surface. These filaments are thought to determine the shape and movement of the plasma membrane. The nucleation of actin fibers occurs as a response to external stimuli, allowing a cell to alter its shape to suit a particular situation. This could account for the uniformity of the microvilli, which are observed to be of equal length and diameter. This nucleation process occurs from the minus end, allowing rapid growth from the plus end. Interestingly, though the length and composition of microvilli is consistent within a certain group of homogenous cells, it can differ slightly in a different part of the same organism. For example, the microvilli in the small and large intestines in mice are slightly different in length and amount of surface coat covering.[3] the microvilli of on the cell membrane differs in terms shape
Enzymes
Microvilli function as the primary surface of nutrient absorption in the gastrointestinal tract. Because of this vital function, the microvillar membrane is packed with enzymes that aid in the breakdown of complex nutrients into simpler compounds that are more easily absorbed. For example, enzymes that digest carbohydrates called glycosidases are present at high concentrations on the surface of enterocyte microvilli. Thus, microvilli not only increase the cellular surface area for absorption, they also increase the number of digestive enzymes that can be present on the cell surface.
Glycocalyx
The microvilli are covered with glycocalyx, consisting of peripheral glycoproteins that can attach themselves to a plasma membrane via transmembrane proteins. This layer may be used to aid binding of substances needed for uptake, to adhere nutrients or as protection against harmful elements. It can be another location for functional enzymes to be localized.
Destruction of microvilli
The destruction of microvilli can occur in certain diseases because of the rearrangement of cytoskeleton in host cells. This can lead to malabsorption of nutrients and persistent osmotic diarrhea, often accompanied by fever. This is seen in infections caused by EPEC subgroup Escherichia coli, in Celiac disease, and Microvillus Inclusion Disease[4] (an inherited disease characterized by defective microvilli and presence of cytoplasmic inclusions of the cell membrane other than the apical surface). The destruction of microvilli can actually be beneficial sometimes, as in the case of elimination of microvilli on white blood cells which can be used to combat auto immune diseases.[5] Congenital lack of microvilli in the intestinal tract causes microvillous atrophy, a rare, usually fatal condition found in new-born babies.
Microvillus
395
References
[1] The Cytoskeleton: Cytoskeleton in specialized tissues and in pathological states, edited by JE Hesketh and IF Pryme, Elsevier 1996 ,ISBN 1559386894, 9781559386890. Vol3, pp371, (http:/ / books. google. co. il/ books?id=lyrFRieEw-EC& pg=PA371& lpg=PA371& dq=actin+ filaments+ capping+ in+ microvilli+ tips& source=bl& ots=q7Pn83HgrA& sig=ZIOtFM0qPGS-ysoi0GQicqzYjQ8& hl=iw& ei=-VQeStPgNcTDsgbdpe3KCg& sa=X& oi=book_result& ct=result& resnum=4#PPP1,M1) [2] Guo P, Weinstein A, and Weinbaum S. A hydrodynamic mechanosensory hypothesis for brush border microvilli. Am. J. Physiol.: Renal Physiol., 279:F698-F712, 2000 [3] link (http:/ / www. jcb. org/ cgi/ reprint/ 34/ 2/ 447. pdf) [4] Malathy Kapali, MD, Ronald Jaffe, MD and Rocco M Agostini Jr. B.Sc. Final Diagnosis: Microvillus Inclusion Disease. http:/ / path. upmc. edu/ cases/ case163/ dx. html [5] Shattuck, T. (2004) Cells studied for immune function. http:/ / www. dartmouth. edu/ ~vox/ 0405/ 0927/ cells. html.
External links
• Organology at UC Davis TermsCells&Tissues/structures/microvilli (http://trc.ucdavis.edu/mjguinan/apc100/ modules/TermsCells&Tissues/structures/microvilli.html) • BU Histology Learning System: 21904loa (http://www.bu.edu/histology/p/21904loa.htm) - "Ultrastructure of the Cell: microvilli and basal enfoldings, endocytic vesicles" • BU Histology Learning System: 20601loa (http://www.bu.edu/histology/p/20601loa.htm) - "Ultrastructure of the Cell: microvillous border and Junctional Complex, oblique section" • Microvillus (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=Microvillus) at eMedicine Dictionary
Epididymis
396
Epididymis
Epididymis
Adult human testicle with epididymis: A. Head of epididymis, B. Body of epididymis, C. Tail of epididymis, and D. Vas deferens
The right testis, exposed by laying open the tunica vaginalis. Latin Gray's Vein Precursor MeSH Epididymis subject #258 1242
[1]
Pampiniform plexus Wolffian duct Epididymis
[2]
The epididymis (pron.: /ɛpɨˈdɪdɨmɪs/; plural: epididymides /ɛpɨˌdɪdɨˈmiːdiːz/) is part of the male reproductive system and is present in all male amniotes. It is a single, narrow, tightly-coiled tube (in adult humans, six to seven meters in length[1]) connecting the efferent ducts from the rear of each testicle to its vas deferens. A similar, but probably non-homologous, structure is found in cartilaginous fishes[citation needed].
Regions
The epididymis can be divided into three main regions: • The head (Caput). The head of the epididymis receives spermatozoa via the efferent ducts of the mediastinum of the testis. It is characterized histologically by a thin myoepithelium. The concentration of the sperm here is dilute. • The body (Corpus) • The tail (Cauda). This has a thicker myoepithelium than the head region, as it is involved in absorbing fluid to make the sperm more concentrated. In reptiles, there is an additional canal between the testis and the head of the epididymis and which receives the various efferent ducts. This is, however, absent in all birds and mammals.[]
Epididymis
397
Histology
The epididymis is covered by a two layered pseudostratified epithelium. The epithelium is separated by a basement membrane from the connective tissue wall which has smooth muscle cells. The major cell types in the epithelium are: • Principal cells: columnar cells that, with the basal cells, form the majority of the epithelium. These cells extend from the lumen to the basal lamina,[] They also have non-motile stereocilia, which are long and branching in the head region and shorter in the tail region.[] They also secrete carnitine, sialic acid, glycoproteins, and glycerylphosphorylcholine into the lumen. • Basal cells: shorter, pyramid-shaped cells which contact the basal lamina but taper off before their apical surfaces reach the lumen.[] These are thought to be undifferentiated precursors of principal cells.[] • Apical cells: predominantly found in the head region[] • Clear cells: predominant in the tail region[] • Intraepithelial lymphocytes: distributed throughout the tissue.[]
Role in storage of sperm and ejaculant
Spermatozoa formed in the testis enter the caput epididymis, progress to the corpus, and finally reach the cauda region, where they are stored. Sperm entering the caput epididymis are incomplete - they lack the ability to swim forward (motility) and to fertilize an egg. It stores the sperm for 2–3 months. During their transit in the epididymis, sperm undergo maturation processes necessary for them to acquire these functions.[2] Final maturation is completed in the female reproductive tract (capacitation). During ejaculation, sperm flow from the lower portion of the epididymis (which functions as a storage reservoir). They have not been activated by products from the prostate gland, and they are unable to swim, but are transported via the peristaltic action of muscle layers within the vas deferens, and are mixed with the diluting fluids of the seminal vesicles and other accessory glands prior to ejaculation (forming semen). The epithelial cells of the epididymis possess numerous apical modifications that are often referred to as stereocilia, as under the light microscope they look like cilia. However, as electron microscopy has revealed them to be structurally and functionally more similar to microvilli, some now refer to them as stereovilli.[3]
Pathology
An inflammation of the epididymis is called epididymitis. It is much more common than testicular inflammation, termed orchitis.
Embryology and vestigial structures
A Gartner's duct is a homologous remnant in the female. In the embryo, the epididymis develops from tissue that once formed the mesonephros, a primitive kidney found in many aquatic vertebrates. Persistence of the cranial end of the mesonephric duct will leave behind a remnant called the appendix of the epididymis. In addition, some mesonephric tubules can persist as the paradidymis, a small body caudal to the efferent ductules.
Epididymis
398
Epididymectomy
Epididymectomy is the surgical removal of the epididymis sometimes performed for post-vasectomy pain syndrome.
Gallery
Human Male reproductive system.
Testis
Schematic drawing of a cross-section through a testicle.
Micrograph of an epididymis. H&E stain.
Microscopic shot.
Notes
[2] abstract (http:/ / www. ingentaconnect. com/ search/ expand?pub=infobike:/ / bsc/ ija/ 1999/ 00000022/ 00000002/ art00151)
External links
• BU Histology Learning System: 16903loa (http://www.bu.edu/histology/p/16903loa.htm) • inguinalregion (http://mywebpages.comcast.net/wnor/inguinalregion.htm) at The Anatomy Lesson (http:// home.comcast.net/~wnor/homepage.htm) by Wesley Norman (Georgetown University) ( testes (http:// mywebpages.comcast.net/wnor/testes.jpg))
Ameloblast
399
Ameloblast
Ameloblast
A developing tooth with odontoblasts marked.
The cervical loop area: (1) dental follicle cells, (2) dental mesenchyme, (3) Odontoblasts, (4) Dentin, (5) stellate reticulum, (6) outer enamel epithelium, (7)inner enamel epithelium, (8) ameloblasts, (9) enamel. Latin Code ameloblastus TE E05.04.1.1.2.3.20
[1]
Ameloblasts are cells, present only during tooth development, that deposit tooth enamel, the hard outermost layer of the tooth that forms the chewing surface. Ameloblasts are cells which secrete the enamel proteins enamelin and amelogenin which will later mineralize to form enamel on teeth, the hardest substance in the human body.[1] Each ameloblast is approximately 4 micrometers in diameter, 40 micrometers in length and has a hexagonal cross section. The secretory end of the ameloblast ends in a six-sided pyramid-like projection known as the Tomes' process. The angulation of the Tomes' process is significant in the orientation of enamel rods. Ameloblasts are derived from oral epithelium tissue of ectodermal origin. Their differentiation from preameloblasts is a result of signaling from the ectomesenchymal cells of the dental papilla. The ameloblasts will only become fully functional after the first layer of dentine has been formed by odontoblasts. Ameloblasts control ionic and organic compositions of enamel. They adjust their secretory and resorptive activities to maintain favorable conditions for biomineralization. The murine ALC cell line is of ameloblastic origin.[2]
Ameloblast
400
Life cycle of ameloblasts
The life cycle of ameloblasts consists of six stages : 1. 2. 3. 4. 5. 6. Morphogenic stage Organizing stage Formative (secretory) stage (Tome's processes appear in secretory stage) Maturative stage Protective stage Desmolytic stage
References
Organ of Corti
401
Organ of Corti
Organ of Corti
A cross section of the cochlea illustrating the organ of Corti.
Section through the spiral organ of Corti. Magnified. Latin Gray's MeSH organum spirale subject #232 1056 Organ+of+Corti
[1]
[2]
The organ of Corti, found only in mammals, is part of the cochlea of the inner ear and is provided with hair cells or auditory sensory cells. [1] It evolved from the basilar papilla found in all tetrapods, except for a few derived species that have lost it. [2] The organ was named after the Italian anatomist Marquis Alfonso Giacomo Gaspare Corti (1822–1876), who conducted microscopic research of the mammalian auditory system.
Structure and functions
The organ of Corti has highly specialized structures that respond to fluid-borne vibrations in the cochlea with a shearing vector in the hairs of some cochlear hair cells. It contains between 15,000-20,000 auditory nerve receptors. Each receptor has its own hair cell. The shear on the hairs opens non-selective transduction ion channels that are permeable to potassium and calcium, leading to hair cell plasma membrane depolarization, activation of voltage-dependent calcium channels at the synaptic basolateral pole of the cells which triggers vesicle exocytosis and liberation of glutamate neurotransmitter to the synaptic cleft and electrical signaling to the auditory cortex via spiral ganglion neurons. The pinna and middle ear act as mechanical transformers and amplifiers, so that by the time sound waves reach the organ of Corti, their pressure amplitude is 22 times that of the air impinging on the pinna. The organ of Corti can be damaged by excessive sound levels, leading to noise-induced health effects. The organ of Corti is the structure that transduces pressure waves to action potentials. The organ of Corti sits inside the cochlear duct, between the scala vestibuli and the scala tympani. The basilar membrane on the scala tympani presses against the
Organ of Corti hair cells of the organ as perilymphatic pressure waves pass.
402
Hearing loss
The most common kind of hearing impairment, sensorineural hearing loss, includes as one major cause the reduction of function in the organ of Corti. Specifically, the active amplification function of the outer hair cells is very sensitive to damage from exposure to trauma from overly-loud sounds or to certain ototoxic drugs. Once outer hair cells are damaged, they do not regenerate, and the result is a loss of sensitivity and an abnormally large growth of loudness (known as recruitment) in the part of the spectrum that the damaged cells serve.[3] While hearing loss has always been considered irreversible in mammals, fish and birds routinely repair such damage. A recent study has shown that the use of particular drugs may reactivate genes normally expressed only during hair cell development. The research was carried out at Harvard Medical School, the Massachusetts Eye and Ear Infirmary, and the Keio University School of Medicine in Japan.[4]
Additional images
Transverse section of the cochlear duct of a fetal cat.
Diagrammatic longitudinal section of the cochlea.
Floor of ductus cochlearis.
Limbus laminæ spiralis and membrana basilaris.
Section through the spiral organ of Corti. Magnified.
Notes
[1] Definition of Organ of Corti (http:/ / www. merriam-webster. com/ medical/ organ of corti) - Merriam Webster - Retrieved 30 April 2012. [2] Dissecting the molecular basis of organ of Corti development (http:/ / pubmedcentralcanada. ca/ pmcc/ articles/ PMC3097286/ ) [4] Drug Induces Hearing Restoration in Rodents (http:/ / beyondthedish. wordpress. com/ tag/ cochlear-hair-cells/ )
References
• Corti A (1851) "Recherches sur l'organe de Corti de l'ouïe des mammifères". Z wiss Zool 3: 1-106. • Pritchard U. "On the organ of Corti in mammals". 2 March 1876, Proceedings of the Royal Society of London, volume 24, pp. 346–52 OCLC 1778190 (http://www.worldcat.org/oclc/1778190)
Organ of Corti
403
External links
• Dissecting the molecular basis of organ of Corti development (http://pubmedcentralcanada.ca/pmcc/articles/ PMC3097286/) • Organ of Corti 3D animation (http://www.youtube.com/watch?v=1JE8WduJKV4&feature=related) • http://lobe.ibme.utoronto.ca/presentations/OHC_Electromotility/sld005.htm Diagram at University of Toronto • http://mayoresearch.mayo.edu/mayo/research/ent_research/images/image02.gif Diagram at Mayo • http://www.iurc.montp.inserm.fr/cric51/audition/english/corti/fcorti.htm at University of Montpellier 1
Corneal keratocyte
Corneal keratocytes (corneal fibroblasts) are specialized fibroblasts residing in the stroma. This corneal layer, representing about 85-90% of corneal thickness, is built up from highly regular collagenous lamellae and extracellular matrix components. Keratocytes play the major role in keeping it transparent, healing its wounds, and synthesizing its components. In the unperturbed cornea keratocytes stay dormant, coming into action after any kind of injury or inflammation. Some keratocytes underlying the site of injury, even a light one, undergo apoptosis immediately after the injury.[] Any glitch in the precisely orchestrated process of healing may cloud the cornea, while excessive keratocyte apoptosis may be a part of the pathological process in the degenerative corneal disorders such as keratoconus, and these considerations prompt the ongoing research into the function of these cells.
Origin and functions
Keratocytes are developmentally derived from the cranial population of neural crest cells, from whence they migrate to settle in the mesenchyme. In some species the migration from neural crest comes in two waves, with the first giving birth to the corneal epithelium and the second invading the epithelium-secreted stromal anlage devoid of cells; in other species both populations come from a single wave of migration. Once settled in the stroma, keratocytes start synthesizing collagen molecules of different types (I, V, VI) and keratan sulfate. By the moment of eye opening after birth the proliferation of keratocytes is all but finished and most of them are in the quiescent state.[] By the end of eye development an interconnected keratocyte network is established in the cornea, with dendrites of neighbouring cells contacting each over.[] Quiescent keratocytes synthesize the so-called crystallins, known primarily for their role in the lens. Corneal crystallins, like the lens ones, are thought to help maintain the transparency and optimal refraction.[] They are also part of corneal antioxidant defense.[] Crystallins expressed by human keratocytes are ALDH1A1, ALDH3A1,[] ALDH2 and TKT. Different sets of crystallins are typical to distinct species.[] Keratan sulfate produced by keratocytes is thought to help maintain optimal corneal hydration;[] genetic disruption of its synthesis leads to the macular corneal dystrophy.[1] According to one study, average keratocyte density in the human stroma is about 20500 cells per mm3, or 9600 in a column of 1 mm2 in section. The highest density is observed in the upper 10% of the stroma. The number of keratocytes declines with age, at a rate approximately 0.45% per year.[] After an injury to the cornea, some keratocytes undergo apoptosis, prompted by the signaling molecules secreted by the upper layers, such as IL1 alpha and TNF-alpha. Other neighbouring keratocytes, when acted upon by the same molecules, become active, proliferate and start synthesizing matrix metalloproteinases that cause tissue remodeling. These activated cells are designated in different sources either as "active keratocytes" or "fibroblasts" or are said to assume a "repair phenotype". After heavier injuries or at the advanced stages of healing process a number of keratocytes transforms into myofibroblasts actively secreting ECM components; this transformation is thought to be caused by TGF-beta. As soon as the basement membrane of corneal epithelium is restored, TGF beta inflow into the stroma drastically decreases and myofibroblasts disappear, after which the remaining activated keratocytes continue
Corneal keratocyte for some time to reshape the extracellular matrix, secreting IL1-alpha in order to maintain their "repair phenotype".[] Apoptosis of keratocytes, either in quiescent or active state, is a process that attracts special attention. In a healthy cornea the programmed cell death is a rare occasion, but immediately after an injury to the uppermost layer keratocytes directly under the injury site commit apoptosis.[] One hypothesis explains such rapid reaction by the need to stem the possible infection from spreading into the cornea, because due to the limitations of ocular immune system the immune cells take up to several hours to arrive at the site of injury.[] In a normal course of events, the lack of keratocytes in gradually replenished by the mitosis of the adjacent cells.[] Apoptosis is observed after eye operations, including keratotomy and laser surgery,[] and may play a role in the development of post-surgery complications.
404
Clinical significance
Keratocytes may play a role in different corneal disorders. According to comparative research, their functions drastically diverge from the norm in keratoconus, the most frequent form of corneal dystrophy. In keratoconic corneas they have been shown to commit apoptosis far away from any epithelial injury; a hypothesis exists that presents excessive keratocyte apoptosis as a major pathological event in keratoconus.[] According to one study, patient's keratocytes have decreased levels of one of the alcohol dehydrogenase subforms,[] they secrete significantly less superoxide dismutase 3, according to another.[]
References
[1] MACULAR DYSTROPHY, CORNEAL, 1; MCDC1 (http:/ / www. ncbi. nlm. nih. gov/ entrez/ dispomim. cgi?id=217800) - OMIM.
External links
• Nigel Brookes (http://www.chimaera.co.nz/proto/pages/science. html) - researcher
Alcohol dehydrogenase immunoreactivity in a healthy cornea (top), in Fuchs' dystrophy and keratoconic cornea. Diaminobenzidine stains keratocytes in the cross-section of cornea. [] From Mootha et al., 2009.
Tendon cell
405
Tendon cell
Tendon cell
Latin Tendinocytus Code TH H3.03.00.0.00024 [1]
Vertebrates
Tendon cells, or tenocytes, are elongated fibroblast type cells. The cytoplasm is stretched between the collagen fibres of the tendon. They have a central cell nucleus with a prominent nucleolus. Tendon cells have a well-developed rough endoplasmic reticulum and they are responsible for synthesis and turnover of tendon fibres and ground substance.
Invertebrates
Tendon cells form a connecting epithelial layer between the muscle and shell in molluscs. In gastropods, for example, the retractor muscles connect to the shell via tendon cells. Muscle cells are attached to the collagenous myo-tendon space via hemidesmosomes. The myo-tendon space is then attached to the base of the tendon cells via basal hemidesmosomes, while apical hemidesmosomes, which sit atop microvilli, attach the tendon cells to a thin layer of collagen. This is in turn attached to the shell via organic fibres which insert into the shell. Molluscan tendon cells appear columnar and contain a large basal cell nucleus. The cytoplasm is filled with granular endoplasmic reticulum and sparse golgi. Dense bundles of microfilaments run the length of the cell connecting the basal to the apical hemidesmosomes.
References
Krstić, R. V. (1984) Illustrated Encyclopedia of Human Histology, Springer Verlag, Berlin Tompa, A. S. and Watabe, N. (1976). "Ultrastructural investigation of the mechanism of muscle attachment to the gastropod shell.". Journal of Morphology 149 (3): 339–351. doi:10.1002/jmor.1051490304 [2]. PMID 957445 [3].
Bone marrow
406
Bone marrow
Bone marrow
A simplified illustration of cells in bone marrow Latin MeSH Code Medulla ossium Bone+Marrow
[1] [2]
TA A13.1.01.001
Bone marrow is the flexible tissue found in the interior of bones. In humans, red blood cells are produced in the heads of long bones, in a process known as hematopoesis. On average, bone marrow constitutes 4% of the total body mass of humans; in an adult weighing 65 kilograms (140 lb), bone marrow accounts for approximately 2.6 kilograms (5.7 lb). The hematopoietic compartment of bone marrow produces approximately 500 billion blood cells per day, which use the bone marrow vasculature as a conduit to the body's systemic circulation.[1] Bone marrow is also a key component of the lymphatic system, producing the lymphocytes that support the body's immune system.[2] Bone marrow transplants can be conducted to treat severe diseases of the bone marrow, including certain forms of cancer. Additionally, bone marrow stem cells have been successfully transformed into functional neural cells,[] and can also potentially be used to treat illnesses such as inflammatory bowel disease.[3]
Marrow types
The two types of bone marrow are medulla ossium rubra (red marrow), which consists mainly of hematopoietic tissue, and medulla ossium flava (yellow marrow), which is mainly made up of fat cells. Red blood cells, platelets and most white blood cells arise in red marrow. Both types of bone marrow contain numerous blood vessels and capillaries. At birth, all bone marrow is red. With age, more and more of it is converted to the yellow type; only around half of adult bone marrow is red. Red marrow is found mainly in the flat bones, such as the pelvis, sternum, cranium, ribs, vertebrae and scapulae, and in the cancellous ("spongy") material at the epiphyseal ends of long bones such as the femur and humerus. Yellow marrow is found in the medullary cavity, the hollow interior of the middle portion of long bones. In cases of severe blood loss, the body can convert yellow marrow back to red marrow to increase blood cell production.
A femoral head with a cortex of cortical bone and medulla of trabecular bone. Both red bone marrow and a focus of yellow bone marrow are visible.
Stroma
Bone marrow The stroma of the bone marrow is all tissue not directly involved in the primary function of hematopoiesis. Yellow bone marrow makes up the majority of bone marrow stroma, in addition to smaller concentrations of stromal cells located in the red bone marrow. Though not as active as parenchymal red marrow, stroma is indirectly involved in hematopoiesis, since it provides the hematopoietic microenvironment that facilitates hematopoiesis by the parenchymal cells. For instance, they generate colony stimulating factors, which have a significant effect on hematopoiesis. Cells that constitute the bone marrow stroma are: • • • • • • fibroblasts (reticular connective tissue) macrophages adipocytes osteoblasts osteoclasts endothelial cells, which form the sinusoids. These derive from endothelial stem cells, which are also present in the bone marrow.[]
407
Macrophages contribute especially to red blood cell production, as they deliver iron for hemoglobin production.
Bone marrow barrier
The blood vessels of the bone marrow constitute a barrier, inhibiting immature blood cells from leaving the marrow. Only mature blood cells contain the membrane proteins required to attach to and pass the blood vessel endothelium. Hematopoietic stem cells may also cross the bone marrow barrier, and may thus be harvested from blood.
Mesenchymal stem cells
The bone marrow stroma contains mesenchymal stem cells (MSCs),[] also known as marrow stromal cells. These are multipotent stem cells that can differentiate into a variety of cell types. MSCs have been shown to differentiate, in vitro or in vivo, into osteoblasts, chondrocytes, myocytes, adipocytes and beta-pancreatic islets cells. MSCs can also transdifferentiate into neuronal cells.[]
Red marrow parenchyma
Cellular components
Hematopoietic precursor cells: promyelocyte in the center, two metamyelocytes next to it and band cells from a bone marrow aspirate.
Bone marrow
408
Cellular constitution of the red bone marrow parenchyma[4]
Group Cell type Average Reference fraction range 0.9% 3.3% 12.7% 0.8% 15.9% 1.2% 12.4% 0.9% 7.4% 0.5% 0.2-1.5 2.1-4.1 8.2-15.7 0.2-1.3 9.6-24.6 0.4-2.2 9.5-15.3 0.2-2.4 6.0-12.0 0.0-1.3 0.0-0.2 0.2-1.3 0.5-2.4 17.9-29.2 0.4-4.6 0.0-0.4 0.4-3.9 0.0-0.9 11.1-23.2 0.0-0.8
Cells of myelopoiesis
Myeloblasts Promyelocytes Neutrophilic myelocytes Eosinophilic myelocytes Neutrophilic metamyelocytes Eosinophilic metamyelocytes Neutrophilic band cells Eosinophilic band cells Segmented neutrophils Segmented eosinophils
Segmented basophils and mast cells 0.1% Cells of erythropoiesis Pronormoblasts Basophilic normoblasts Polychromatic normoblasts Orthochromatic normoblast Other cell types Megakaryocytes Plasma cells Reticular cells Lymphocytes Monocytes 0.6% 1.4% 21.6% 2.0% < 0.1% 1.3% 0.3% 16.2% 0.3%
In addition, the bone marrow contains hematopoietic stem cells, which give rise to the three classes of blood cells that are found in the circulation: white blood cells (leukocytes), red blood cells (erythrocytes), and platelets (thrombocytes).[]
Compartmentalization
Biological compartmentalization is evident within the bone marrow, in that certain cell types tend to aggregate in specific areas. For instance, erythrocytes, macrophages, and their precursors tend to gather around blood vessels, while granulocytes gather at the borders of the bone marrow.
Lymphatic role
The red bone marrow is a key element of the lymphatic system, being one of the primary lymphoid organs that generate lymphocytes from immature hematopoietic progenitor cells.[2] The bone marrow and thymus constitute the primary lymphoid tissues involved in the production and early selection of lymphocytes. Furthermore, bone marrow performs a valve-like function to prevent the backflow of lymphatic fluid in the lymphatic system.
Bone marrow
409
Diseases of the bone marrow
The normal bone marrow architecture can be damaged or displaced by aplastic anemia, malignancies such as multiple myeloma, or infections such as tuberculosis, leading to a decrease in the production of blood cells and blood platelets. The bone marrow can also be affected by various forms of leukemia, which attacks its hematologic progenitor cells.[5] Furthermore, exposure to radiation or chemotherapy will kill many of the rapidly dividing cells of the bone marrow, and will therefore result in a depressed immune system. Many of the symptoms of radiation sickness are due to damage sustained by the bone marrow cells. To diagnose diseases involving the bone marrow, a bone marrow aspiration is sometimes performed. This typically involves using a hollow needle to acquire a sample of red bone marrow from the crest of the ilium under general or local anesthesia.
Examination
Bone marrow examination is the pathologic analysis of samples of bone marrow obtained via biopsy and bone marrow aspiration. Bone marrow examination is used in the diagnosis of a number of conditions, including leukemia, multiple myeloma, anemia, and pancytopenia. The bone marrow produces the cellular elements of the blood, including platelets, red blood cells and white blood cells. While much information can be gleaned by testing the blood itself (drawn from a vein by phlebotomy), it is sometimes necessary to examine the source of the blood cells in the bone marrow to obtain more information on hematopoiesis; this is the role of bone marrow aspiration and biopsy. The ratio between myeloid series and erythroid cells is relevant to bone marrow function, and also to diseases of the bone marrow and peripheral blood, such as leukemia and anemia. The normal myeloid-to-erythroid ratio is around 3:1; this ratio may increase in myelogenous leukemias, decrease in polycythemias, and reverse in cases of thalassemia.[6]
A Wright's-stained bone marrow aspirate smear from a patient with leukemia.
Donation and transplantation
In a bone marrow transplant, hematopoietic stem cells are removed from a person and infused into another person (allogenic) or into the same person at a later time (autologous). If the donor and recipient are compatible, these infused cells will then travel to the bone marrow and initiate blood cell production. Transplantation from one person to another is conducted for the treatment of severe bone marrow diseases, such as congenital defects, autoimmune diseases or malignancies. The patient's own marrow is first killed off with drugs or radiation, and then A bone marrow harvest in progress. the new stem cells are introduced. Before radiation therapy or chemotherapy in cases of cancer, some of the patient's hematopoietic stem cells are sometimes harvested and later infused back when the therapy is finished to restore the immune system. In addition, bone marrow stem cells can be induced to become neural cells to treat neurological illnesses,[] and can also potentially be used for the treatment of other illnesses, such as inflammatory bowel disease.[7]
Bone marrow
410
Harvesting
The stem cells are typically harvested directly from the red marrow in the iliac crest, often under general anesthesia. The procedure is minimally invasive and does not require stitches afterwards. Depending on the donor's health and reaction to the procedure, the actual harvesting can be an outpatient procedure, or can require 1–2 days of recovery in the hospital.[8] Another option is to administer certain drugs that stimulate the release of stem cells from the bone marrow into circulating blood.[9] An IV is inserted into the donor's arm, and the stem cells are filtered out of the blood. This procedure is similar to donating blood or platelets. In adults, bone marrow may also be taken from the sternum, while the tibia is often used when taking samples from infants.[] In newborns, stem cells may be retrieved from the umbilical cord.[10]
Bone marrow in cuisine
Many cultures have used bone marrow as food throughout history. Some anthropologists believe that early humans were scavengers rather than hunters in some regions of the world. Marrow would have been a useful food source (largely due to its fat content) for tool-using hominids, who were able to crack open the bones of carcasses left by apex predators such as lions.[11] European diners in the 18th century often used a marrow scoop (or marrow spoon), often of silver and with a long, thin bowl, as a table implement for removing marrow from a bone. Bone marrow was also used in various preparations, such as pemmican. Bone marrow's popularity as a food is now relatively limited in the western world, but it remains in use in some gourmet restaurants, and is popular among food enthusiasts.[12]
In some parts of Germany, beef soup is served with Markklößchen (bone marrow balls).
In Vietnam, beef bone marrow is used as the soup base for the national staple dish, phở, while in the Philippines, the soup bulalo is made primarily of beef stock and marrow bones, seasoned with vegetables and boiled meat; a similar soup in the Philippines is called kansi.[13] In Indonesia, bone marrow is called sumsum and can be found especially in Minangkabau cuisine. Sumsum is often cooked as soup or as gulai (a curry-like dish). In India and Pakistan, slow-cooked marrow is the core ingredient of the dish nalli nihari. In Hungary, tibia is a main ingredient of beef soup; the bone is chopped into 10–15 cm pieces, and the ends are covered with salt to prevent the marrow from leaking from the bone while cooking. Upon serving the soup, the marrow is usually spread on toast. Beef bone marrow is also the main ingredient in Italian dish ossobuco (braised veal shanks), and beef marrow bones are often included in the French pot-au-feu broth, the cooked marrow being traditionally eaten on toasted bread with sprinkled coarse sea salt. In Iranian cuisine, lamb shanks are usually broken before cooking to allow diners to suck out and eat the marrow when the dish is served. Similar practices are also common in Pakistani cuisine. Some Native Alaskans eat the bone marrow of caribou and moose.
Bone marrow
411
References
[1] "Challenges in Cardiac Tissue Engineering"; Gordana Vunjak-Novakovic, Ph.D.,Nina Tandon, Ph.D., Amandine Godier, B.S.,1 Robert Maidhof, M.S.,Anna Marsano, Ph.D., Timothy P. Martens, M.D., Ph.D., and Milica Radisic, Ph.D. Tissue Engineering: Part B; Volume 16, Number 2 (2010). [2] The Lymphatic System (http:/ / allonhealth. com/ health-news/ par-lymphatic-system. htm). Allonhealth.com. Retrieved 5 December 2011. [4] Appendix A:IV (http:/ / www. msd. com. mx/ secure/ ebooks/ WintrobesClinicalHematology/ sid4266054. html) in Wintrobe's clinical hematology (9th edition). Philadelphia: Lea & Febiger (1993). [8] National Marrow Donor Program Donor Guide (http:/ / www. marrow. org/ DONOR/ When_You_re_Asked_to_Donate_fo/ index. html). Marrow.org. Retrieved 5 November 2012. [9] Mayo Clinic: Bone marrow donation: What to expect when you donate (http:/ / www. mayoclinic. com/ health/ bone-marrow/ CA00047). Mayo Clinic. Retrieved 16 February 2013. [10] "Production of stem cells with embryonic characteristics from human umbilical cord blood" (http:/ / www3. interscience. wiley. com/ journal/ 118705649/ abstract). Wiley Online Library. 11 August 2005. Retrieved 29 January 2012. [11] Bruce Bower. "Hunting ancient scavengers – some anthropologists say early humans were scavengers, not hunters" (http:/ / findarticles. com/ p/ articles/ mi_m1200/ is_v127/ ai_3677563). Science News. 9 March 1985. Retrieved 16 February 2013. [12] La Petite Bouche (Food Blog): Roasted Bone Marrow (http:/ / lapetitebouche. blogspot. com/ 2010/ 08/ roasted-bone-marrow. html). 30 August 2010. Retrieved 5 December 2011. [13] "Kansi" (http:/ / www. flickr. com/ photos/ kamums/ 4378949248/ ). Flickr. 22 February 2010. Retrieved 26 November 2012.
Further reading
• Nature Bone Marrow Transplantation (http://www.nature.com/bmt/index.html) (Nature Publishing Group) – specialist scientific journal with articles on bone marrow biology and clinical uses. • Cooper, B (2011). "The origins of bone marrow as the seedbed of our blood: from antiquity to the time of Osler" (http://baylorhealth.edu/proceedings/24_2/24_2_Cooper.pdf). Baylor University Medical Center Proceedings 24 (2): 115–8. PMC 3069519 (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3069519). PMID 21566758 (http://www.ncbi.nlm.nih.gov/pubmed/21566758).
Reticular connective tissue
412
Reticular connective tissue
Reticular connective tissue is a type of connective tissue.[1] It has a network of reticular fibers, made of type III collagen.[] Reticular fibers are not unique to reticular connective tissue, but only in this type are they dominant.[] Reticular fibers are synthesized by special fibroblasts called reticular cells. The fibers are thin branching structures.
Location
Reticular connective tissue is found around the liver, the kidney, the spleen, and lymph nodes, as well as in bone marrow.[2]
Function
The fibers form a soft skeleton (stroma) to support the lymphoid organs (lymph nodes, red bone marrow, and spleen). Adipose tissue is held together by reticular fibers.
Staining
They can be identified in histology by staining with a heavy metal like silver or the PAS stain that stains carbohydrates.
Appearance
Reticular connective tissue resembles areolar connective tissue, but the only fibers in its matrix are reticular fibers, which form a delicate network along which fibroblasts called reticular cells lie scattered. Although reticular fibers are widely distributed in the body, reticular tissue is limited to certain sites. It forms a labyrinth-like stroma (literally, "bed or "mattress"), or internal framework, that can support many free blood cells (large lymphocytes) in lymph nodes, the spleen, and red bone marrow.
Classification
There are more than 20 types of reticular fibers. In Reticular Connective Tissue type III collagen/reticular fiber (100-150 nm in diameter) is the major fiber component. It forms the architectural framework of; liver, adipose tissue, bone marrow, spleen, basement membrane to name a few
References
Notes
[2] Martini, Frederic H. Fundamentals of Anatomy and Physiology. Seventh Edition. Pearson Benjamin Cummings. United States. 2006.
External links
• Organology at UC Davis TermsCells&Tissues/connective/reticular/reticular1 (http://trc.ucdavis.edu/mjguinan/ apc100/modules/TermsCells&Tissues/connective/reticular/reticular1.html) - "Connective tissue, reticular (LM, Medium)" • Histology at uwa.edu.au (http://www.lab.anhb.uwa.edu.au/mb140/CorePages/Connective/Connect. htm#labreticular)
Fibroblast
413
Fibroblast
Fibroblast
NIH/3T3 Fibroblasts in cell culture Latin Code fibroblastus TH H2.00.03.0.01002
[1]
A fibroblast is a type of cell that synthesizes the extracellular matrix and collagen,[1] the structural framework (stroma) for animal tissues, and plays a critical role in wound healing. Fibroblasts are the most common cells of connective tissue in animals.
Background information
Fibroblasts and fibrocytes are two states of the same cells, the former being the activated state, the latter the less active state, concerned with maintenance and tissue metabolism. Currently, there is a tendency to call both forms fibroblasts. The suffix "blast" is used in cellular biology to denote a stem cell or a cell in an activated state of metabolism. Fibroblasts are morphologically heterogeneous with diverse appearances depending on their location and activity. Though morphologically inconspicuous, ectopically transplanted fibroblasts can often retain positional memory of the location and tissue context where they had previously resided, at least over a few generations. This remarkable behavior may lead to discomfortWikipedia:Please clarify in the rare event that they stagnate there excessively.
Embryologic origin
The main function of fibroblasts is to maintain the structural integrity of connective tissues by continuously secreting precursors of the extracellular matrix. Fibroblasts secrete the precursors of all the components of the extracellular matrix, primarily the ground substance and a variety of fibers. The composition of the extracellular matrix determines the physical properties of connective tissues. Like other cells of connective tissue, fibroblasts are derived from primitive mesenchyme. Thus they express the intermediate filament protein vimentin, a feature used as a marker to distinguish their mesodermal origin. However, this test is not specific as epithelial cells cultured in vitro on adherent substratum may also express vimentin after some time. In certain situations epithelial cells can give rise to fibroblasts, a process called epithelial-mesenchymal transition (EMT). Conversely, fibroblasts in some situations may give rise to epithelia by undergoing a mesenchymal to epithelial transition (MET) and organizing into a condensed, polarized, laterally connected true epithelial sheet. This process is seen in many developmental situations (e.g. nephron and notocord development), as well as in wound healing and tumorigenesis.
Fibroblast
414
Structure and function
Fibroblasts have a branched cytoplasm surrounding an elliptical, speckled nucleus having two or more nucleoli. Active fibroblasts can be recognized by their abundant rough endoplasmic reticulum. Inactive fibroblasts, which are also called fibrocytes[citation needed], are smaller and spindle shaped. They have a reduced rough endoplasmic reticulum. Although disjointed and scattered when they have to cover a large space, fibroblasts when crowded often locally align in parallel clusters. Fibroblasts make collagens, glycosaminoglycans, reticular and elastic fibers, glycoproteins found in the extracellular matrix and cytokine TSLP. Growing individuals' fibroblasts are dividing and synthesizing ground substance. Tissue damage stimulates fibrocytes and induces the mitosis of fibroblasts. Unlike the epithelial cells lining the body structures, fibroblasts do not form flat monolayers and are not restricted by a polarizing attachment to a basal lamina on one side, although they may contribute to basal lamina components in some situations (e.g. subepithelial myofibroblasts in intestine may secrete the α-2 chain carrying component of the laminin which is absent only in regions of follicle associated epithelia which lack the myofibroblast lining). Fibroblasts can also migrate slowly over substratum as individual cells, again in contrast to epithelial cells. While epithelial cells form the lining of body structures, it is fibroblasts and related connective tissues which sculpt the "bulk" of an organism. The life span of a fibroblast, as measured in chick embryos, is 57 ± 3 days.[2]
Secondary actions
Mouse embryonic fibroblasts (MEFs) are often used as "feeder cells" in human embryonic stem cell research. However, many researchers are gradually phasing out MEFs in favor of culture media with precisely defined ingredients of exclusively human derivation[citation needed]. Further, the difficulty of exclusively using human derivation for media supplements is most often solved by the use of "defined media" where the supplements are synthetic and achieve the primary goal of eliminating the chance of contamination from derivative sources.
References
[1] http:/ / ghr. nlm. nih. gov/ glossary=fibroblast
External links
• UIUC Histology Subject 240 (https://histo.life.illinois.edu/histo/atlas/oimages.php?oid=240) • MedEd at Loyola Histo/practical/ctproper/hp3-15.html (http://www.meddean.luc.edu/Lumen/MedEd/Histo/ practical/ctproper/hp3-15.html)
Pericyte
415
Pericyte
Pericyte
Pericytes characteristically lining the outer surface of endothelial cells which encircle an erythrocyte (E). Latin Code pericytus TH H3.09.02.0.02006
[1]
Pericytes are contractile cells that wrap around the endothelial cells of capillaries and venules throughout the body. Also known as Rouget cells or mural cells, pericytes are embedded in basement membrane where they communicate with endothelial cells of the body's smallest blood vessels by means of both direct physical contact and paracrine signaling.[1] In the brain, pericytes help sustain the blood–brain barrier as well as several other homeostatic and hemostatic functions of the brain.[] These cells are also a key component of the neurovascular unit, which includes endothelial cells, astrocytes, and neurons.[] Pericytes regulate capillary blood flow, the clearance and phagocytosis of cellular debris, and the permeability of the blood–brain barrier. Pericytes stabilize and monitor the maturation of endothelial cells by means of direct communication between the cell membrane as well as through paracrine signaling.[] A deficiency of pericytes in the central nervous system can cause the blood–brain barrier to break down.[]
Morphology
In the central nervous system, pericytes wrap around the endothelial cells that line the outside of the capillary. These two types of cells can be easily distinguished from one another based on the presence of the prominent round nucleus of the pericyte compared to the flat elongated nucleus of the endothelial cells.[] Pericytes also project finger-like extensions that wrap around the capillary wall, allowing the cells to regulate capillary blood flow.[] Both pericytes and endothelial cells share a basement membrane where a variety of intercellular connections are made. Many types of integrin molecules facilitate Gap cell junction created between two neighboring cells by connexin. communication between pericytes and endothelial cells separated by [] the basement membrane. Pericytes can also form direct connections with neighboring cells by forming peg and socket arrangements in which parts of the cells interlock, similar to the gears of a clock. At these interlocking sites, gap junctions can be formed which allow the pericytes and neighboring cells to exchange ions and other small molecules.[] Important molecules in these intercellular connections include N-cadherin, fibronectin, connexin and various integrins.[] In some regions of the basement membrane, adhesion
Pericyte plaques composed of fibronectin can be found. These plaques facilitate the connection of the basement membrane to the cytoskeletal structure composed of actin, and the plasma membrane of the pericytes and endothelial cells.[]
416
Function
Blood–brain barrier
Pericytes play a crucial role in the formation and functionality of the selective permeable space between the circulatory system and central nervous system. This space is known as the blood–brain barrier. This barrier is composed of endothelial cells and assures the protection and functionality of the brain and central nervous system. Although it had been theorized that astrocytes were crucial to the postnatal formation of this barrier, it has been found that pericytes are now largely responsible for this role. Pericytes are responsible for tight junction formation and vesicle trafficking amongst endothelial cells. Furthermore, they allow the formation of the blood–brain barrier by inhibiting the effects of CNS immune cells (which can damage the formation of the barrier) and by reducing the expression of molecules that increase vascular permeability.[2] Aside from blood–brain barrier formation, pericytes also play an active role in its functionality by controlling the flow within blood vessels and between blood vessels and the brain. As contractile cells, they can open or close a given amount to allow (or disallow) certain sized particles to flow through the vessel. Such regulation of blood flow is beneficial to neuronal function because it prevents certain particles in the blood from entering the brain. When pericytes are not present, a process known as transcytosis occurs in the blood–brain barrier. This essentially allows particles of varying sizes, including large plasma proteins, to easily enter the brain with little to no regulation. This process is peculiar because the blood–brain barrier is highly regulatory under normal conditions. Therefore, such may confer a dysfunction of pericytes in the blood–brain barrier.[3] Thus, pericytes play a critical role in assuring that harmful chemicals do not enter the brain and disrupt neurological function. Pericyte functionality (or dysfunctionality) is also theorized to contribute to neurodegenerative diseases such as Alzheimer’s, Parkinson’s and ALS (Lou Gehrig's Disease). Furthermore, the elasticity of pericyte is beneficial because they can expand to reduce inflammation and allow harmful substances to diffuse out of the brain.[4] These cells also play a key role in increasing microcirculation and reducing the effects of brain aging. In a study involving adult pericyte-deficient mice, the absence of such cells in the brain had been found to lead to vascular damage from loss of microcirculation and cerebral blood flow. Such blood flow is imperative to mediate the effects caused by stress, hypoxia and several other conditions which may alter homeostasis. In addition, when pericytes are not present, the blood–brain barrier does not degrade certain neurotoxic and vasculotoxic serum proteins which thus bolsters degenerative changes. Such changes include inflammation as well as learning and memory impairment.[5]
Angiogenesis and the survival of endothelial cells
Pericytes are also associated with allowing endothelial cells to differentiate, multiply, form vascular branches (Angiogenesis), survive apoptotic signals and travel throughout the body. Certain pericytes, known as microvascular pericytes develop around the walls of capillaries and help to serve this function. Microvascular pericytes may not be contractile cells because they lack alpha-actin isoforms; structures that are common amongst other contractile cells. These cells communicate with endothelial cells via gap junctions and in turn cause endothelial cells to proliferate or be selectively inhibited. If this process did not occur, hyperplasia and abnormal vascular morphogenesis could occur. These types of pericyte can also phagocytose exogenous proteins. This suggests that the cell type might have been derived from microglia.[6] It is also important to note that pericytes maintain plasticity and thus can differentiate into various other cell types including, smooth muscle cells as well as fibroblasts and other mesenchymal stem cells. Such versatility is conducive because they actively remodel blood vessels throughout the body and can thereby blend homogeneously with the local tissue environment .[7]
Pericyte Aside from creating and remodeling blood vessels in a viable fashion, pericytes have been found to protect endothelial cells from death via apoptosis or cytotoxic elements. It has been studied in vivo that pericytes release a hormone known as pericytic aminopeptidase N/pAPN that may help to promote angiogenesis. When this hormone was mixed with cerebral endothelial cells as well as astrocytes, the pericytes grouped into structures that resembled capillaries. Furthermore, if experimental group contained all of the following with the exception of pericytes, the endothelial cells would undergo apoptosis. That being said, it was concluded that pericytes must be present to assure the proper function of endothelial cells and astrocytes must be present to assure that both remain in contact. If not, then proper angiogenesis cannot occur.[8] In addition, it has been found that pericytes contribute to the survival of endothelial cells because they secrete the protein Bcl-w during cellular crosstalk. Bcl-w is an instrumental protein in the pathway that enforces VEGF-A expression and discourages apoptosis.[9] Although there is some speculation as to why VEGF is directly responsible for preventing apoptosis, it is believed to be responsible for modulating apoptotic signal transduction pathways and inhibiting activation of apoptosis inducing enzymes. Two biochemical mechanisms utilized by VEGF to accomplish such would be phosphorylation of extracellular regulatory kinase 1 (ERK-1) which sustains cell survival over time and inhibition of stress-activated protein kinase/c-jun-NH2 kinase which also promotes apoptosis.[10]
417
Pathologies
Because of their crucial role in maintaining and regulating endothelial cell structure and blood flow, abnormalities in pericyte function are seen in many pathologies. They may either be present in excess, leading to diseases such as hypertension and tumor formation, or in deficiency, leading to neurodegenerative diseases.
Hemangiopericytoma
Hemangiopericytoma is a rare vascular neoplasm, or abnormal growth, that may either be benign or malignant. In its malignant form, metastasis to the lungs, liver, brain, and extremities may occur. It most commonly manifests itself in the femur and proximal tibia as a bone sarcoma, and is usually found in older individuals, though cases have been found in children. Hemangiopericytoma is caused by the excessive layering of sheets of pericytes around improperly formed blood vessels. Diagnosis of this tumor is difficult because of the inability to distinguish pericytes from other types of cells using light microscopy. Treatment may involve surgical removal and radiation therapy, depending on the level of bone penetration and stage in the tumor's development.[11]
Image of a solitary fibrous tumour that is most likely a hemangiopericytoma. It surrounds a staghorn-shaped blood vessel, which results from the arrangement of pericytes around the vessel
Diabetic retinopathy
The retina of diabetic individuals often exhibits loss of pericytes, and this loss is a characteristic factor of the early stages of diabetic retinopathy. Studies have found that pericytes are essential in diabetic individuals to protect the endothelial cells of retinal capillaries. With the loss of pericytes, microaneuryisms form in the capillaries. In response, the retina either increases its vascular permeability, leading to swelling of the eye through a macular edema, or forms new vessels that permeate into the vitreous membrane of the eye. The end result is reduction or loss of vision.[] While it is unclear why pericytes are lost in diabetic patients, one hypothesis is that toxic sorbitol and advanced glycation end products (AGE) accumulate in the pericytes. Because of the build-up of glucose, the polyol pathway increases its flux, and intracellular sorbitol and fructose accumulate. This leads to osmotic imbalance,which results in cellular damage. The presence of high glucose levels also leads to the buildup of AGE's, which also
Pericyte damage cells. []
418
Neurodegenerative diseases
Studies have found that pericyte loss in the adult and aging brain leads to the disruption of proper cerebral perfusion and maintenance of the blood–brain barrier, which causes neurodegeneration and neuroinflammation. The apoptosis of pericytes in the aging brain may be the result of a failure in communication between growth factors and receptors on pericytes. Platelet-derived growth factor B (PDGF-B)is released from endothelial cells in brain vasculature and binds to the receptor PDGFR-Beta on pericytes, initiating their proliferation and migration for proper vasculature maintenance. When this signalling is disrupted, pericytes undergo apoptosis, leading to many neurodegenerative diseases including Alzheimer's disease and Multiple Sclerosis.[12]
Current research
Endothelial and pericyte interactions
Endothelial cell and pericytes are interdependent, so failure of proper communication between the two cells can lead to numerous human pathologies, such as the ones listed above.[] There are several pathways of communication between the endothelial cells and pericytes. The first is transforming growth factor (TGF) signaling, which is mediated by endothelial cells. This is important for pericyte differentiation.[][] Angiopoietin 1 and Tie-2 signaling is essential for maturation and stabilization of endothelial cells.[] Platelet-derived growth factor (PDGF) pathway signaling from endothelial cells recruit pericytes, so that pericytes can migrate to growing vessels. If this pathway is blocked, it leads to pericyte deficiency.[] Sphingosine-1-phosphate (S1P) signaling also aides in pericyte recruitment by communication through G protein-coupled receptors. S1P signals through GTPases that promote N-cadherin trafficking to endothelial membranes. This trafficking strengthens contacts with pericytes.[] Communication between endothelial cells and pericytes are important. Inhibiting the PDGF pathway leads to pericyte deficiency. This causes endothelial hyperplasia, abnormal junctions, and diabetic retinotropy.[] A lack of pericytes also causes an upregulation of vascular endothelial growth factor (VEGF), leading to vascular leakage and hemorrhage.[] Also, angiopoietin 2 can act as an antagonist to Tie-2.[] This destabilizes the endothelial cells, which accounts for less endothelial cell and pericyte interaction. This can actually lead to the formation of tumors.[] Similar to the inhibition of the PDGF pathway, angiopoietin 2 reduces levels of pericyte, leading to diabetic retinopathy.[]
Scarring
After an injury in the CNS, scarring occurs to preserve the integrity of surrounding cells. Usually, astrocytes are associated with the scarring and are called glial scars. However, there is a stromal or nonglial component of the scarring, and there is evidence that perivascular pericytes play a critical role in assisting scar formation.[] An experiment was conducted on mice that have been genetically labeled using glutamate aspartate transporter (Glast). They found two different subtypes of pericytes and termed them subtype A and B. Subtype A accounts for about 10% of the pericytes in the adult spinal cord and plays a critical role in scarring. Subtype B accounts for the rest of the pericytes and has desmin and alpha smooth muscles. After the two subtypes were isolated and labeled, an incision was made to the dorsal part of the brain. Typically in an uninjured spinal cord there are ten times as many astrocytes than subtype A pericytes.[] However, two weeks after the injury, the number of pericytes were double that of the astrocytes. Subtype A were three times more prevalent than subtype B. The main difference in prevalence arises from the fact that subtype A is able to detach from blood vessel walls and can send tiny projections to nearby cells and deposit extracellular matrix proteins. The scarring is highly compartmentalized. The pericytes form the core of the scar, while ependymal cells form a second layer around the core, followed by another layer of astrocytes that originated through self-duplication.[]
Pericyte Inhibition of subtype A pericyte generation caused improper closing of spinal cord incisions, which supports the idea that pericytes are important for scarring.
419
References
[1] http:/ / www. ncbi. nlm. nih. gov/ pmc/ articles/ PMC1871727/ [2] Daneman, Richard et al. (2010) Pericytes are required for blood–brain barrier integrity during embryogenesis. "nature" 468, 562-566 [3] Investigators Reveal Key to Blood-Brain Barrier. This passage of particles can be adverse to brain function because many of such can are toxic or harmful to some extent."GEN" (2010)http:/ / www. genengnews. com/ gen-news-highlights/ investigators-reveal-key-to-blood-brain-barrier/ 81244067/ [4] Pericytes regulate blood–brain barrier (2010) (http:/ / www. news-medical. net/ news/ 20101015/ Pericytes-regulate-blood-brain-barrier. aspx) [5] Bell, Robert D. et al. Pericytes Control Key Neurovascular Functions and Neuronal Phenotype in the Adult Brain and during Brain Aging. "Cell" 68 Vol 3 409-427 (2010) http:/ / www. cell. com/ neuron/ abstract/ S0896-6273(10)00824-X [6] Pericyte, Astrocyte and Basal Lamina Association with the Blood Brain Barrier (BBB) http:/ / davislab. med. arizona. edu/ content/ pericyte-astrocyte-and-basal-lamina-association-blood-brain-barrier-bbb [7] Gerhardt H, Betsholtz C.(2003) Endothelial-pericyte interactions in angiogenesis. "Cell Tissue Res." 314(1), 15-23 http:/ / www. ncbi. nlm. nih. gov/ pubmed/ 12883993 [8] Ramsauer, Markus et. al. (2002) Angiogenesis of the blood–brain barrier in vitro and the function of cerebral pericytes "The FASEB Journal" 10.1096/fj.01-0814fje http:/ / www. fasebj. org/ content/ early/ 2002/ 08/ 02/ fj. 01-0814fje. full. pdf [9] Franco, Marcela et al. (2011) Pericytes promote endothelial cell survival through induction of autocrine VEGF-A signaling and Bcl-w expression "Blood" http:/ / bloodjournal. hematologylibrary. org/ content/ 118/ 10/ 2906 [10] VEGF prevents apoptosis of human microvascular endothelial cells via opposing effects on MAPK/ERK and SAPK/JNK signaling. Exp Cell Res. 1999 Mar 15;247(2):495-504. http:/ / www. ncbi. nlm. nih. gov/ pubmed/ 10066377 [12] http:/ / www. cell. com/ neuron/ abstract/ S0896-6273(10)00824-X
External links
• Pericytes (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Pericytes) at the US National Library of Medicine Medical Subject Headings (MeSH) • Diagram at udel.edu (http://www.udel.edu/Biology/Wags/histopage/illuspage/icv/icv17.gif)
Nucleus pulposus
420
Nucleus pulposus
Nucleus pulposus
Cervical vertebra with intervertebral disc. (Nucleus pulposus labeled at center right, and is visible at center in light blue.)
Stages of Spinal Disc Herniation Latin Gray's Precursor Nucleus pulposus subject #17 82 notochord
[1]
Nucleus pulposus is the jelly-like substance in the middle of the spinal disc. It is the remnant of the notochord.[1] It functions to distribute hydraulic pressure in all directions within each disc under compressive loads. The nucleus pulposus consists of chondrocyte-like cells, collagen fibrils, and proteoglycan aggrecans that aggregate through hyaluronic chains. Attached to each aggrecan molecule are the glycosaminoglycan (GAG) chains of chondroitin sulfate and keratan sulfate.[2] Aggrecan is negatively charged and hydrophilic. This property allows it to draw water into the Nucleus Pulposus.
Nucleus pulposus
421
Additional images
Sagittal section through an intervertebral fibrocartilage and adjacent parts of two vertebræ of an advanced sheep’s embryo.
References
[3] [2] See Figure 1 in US patent application 2007/0003525. [3] Link to referenced patent application. (http:/ / www. google. com/ patents?id=csSXAAAAEBAJ& printsec=abstract& zoom=4& dq=2007/ 0003525#PPA2,M1)
External links
• Image at spinesource.com (http://www.spinesource.com/images/Anatomy3.jpg) • Presentation on synthetic nucleus pulposus (http://www.campoly.com/documents/presentation/nucleus.pdf)
Cementoblast
422
Cementoblast
Cementoblast
Latin cementoblastus Code TE E05.041.1.2.3.36 [1]
A cementoblast is a biological cell that forms from the follicular cells around the root of a tooth, and whose biological function is cementogenesis, which is the creation of cementum (the hard tissue that covers the root of the tooth). Cementoblasts lay down the organic matrix of cementum which later gets mineralized by minerals from oral fluids. Thus the cementoblasts lay down collagen and secrete osteocalcin and sialoprotein. They possess all the organelles associated with protein synthesis such as RER and Golgi apparatus. The mechanism of differentiation of the cementoblasts is controversial but circumstantial evidence suggests that an epithelium or epithelial component may cause dental follicle cells to differentiate into cementoblasts, characterised by an increase in length. The initially formed cementum in coronal two-thirds of the root is acellular, but when the cementoblasts get trapped in lacunae in their own matrix like bone cells, the cementum is called cellular or secondary cementum and is present only in the apical third of the root. Once in this situation, the cementoblasts lose their secretory activity and become cementocytes.
Odontoblast
423
Odontoblast
Odontoblast
A developing tooth with odontoblasts marked.
The cervical loop area: (1) dental follicle cells, (2) dental mesenchyme, (3) Odontoblasts, (4) Dentin, (5) stellate reticulum, (6) outer enamel epithelium, (7)inner enamel epithelium, (8) ameloblasts, (9) enamel. Latin Code odontoblastus TE E04.0.3.3.1.0.13
[1]
In vertebrates, an odontoblast is a biological cell of neural crest origin that is part of the outer surface of the dental pulp, and whose biological function is dentinogenesis, which is the creation of dentin, the substance under the tooth enamel. Teeth in the molluscan radula are also produced by cells termed "odontoblasts".
Origin and differentiation
Odontoblasts first appear at sites of tooth development at 17–18 weeks in utero and remain present until death unless killed by bacterial or chemical attack, or indirectly through other means (e.g. being aspirated into dentinal tubules by the use of a turbine handpiece on tooth tissue above). The odontoblasts secrete dentin throughout life (secondary dentin, once root formation is complete), which may be an attempt to compensate for natural wear of the enamel. Odontoblasts also secrete tertiary dentin when irritated. Tertiary dentin secreted by odontoblasts is often due to chemical attack, either by chemicals diffusing through the dentin and insulting the odontoblasts, or by diffusion of toxic bacterial metabolites down the dentinal tubules in the instance of a carious attack. This tertiary dentin is called reactionary dentin. This is an attempt to slow down the progress of the caries so that it does not reach the pulp. In the case of an infection breaching the dentin to or very near the pulp, or in the instance of odontoblast death due to other attack (e.g. chemical or physical), Pulpal Stem Cells can differentiate into odontoblast-like cells which then secrete the other kind of tertiary dentin, reparative dentin, underneath the site of attack. This is not only to slow the progress of the attack, but also to prevent the diffusion of bacteria and their metabolites into the pulp, reducing the probability
Odontoblast of partial pulp necrosis. The distinction of the two kinds of tertiary dentin is important, because they are secreted by different cells for different reasons. Reactionary dentine is secreted at varying speeds, dependant on the speed of progression of caries above. Histologically, it is easily distinguishable by its disordered tube structure, its local secretion (causing it to protrude into the pulpal cavity) and its slightly lower degree of mineralisation than normal. The tooth is often able to be saved by a simple restoration. Reparative dentine is secreted when the tooth's situation is dire. The odontoblasts are dead, forcing the differentiation of pulpal stem cells into odontoblast-like cells that try desperately to avoid pulpitis.
424
Morphology
Odontoblasts are large columnar cells arranged in an epithelioid sheet along the junction between dentin and pulp, all the way down to the root apex. It is rich in endoplasmic reticulum and golgi apparatus, especially during primary dentin formation, to give it a high secretory capacity (firstly collagenous matrix to form predentine, then mineral to form the complete dentine). Its nucleus is aligned away from the dentine, with its golgi and ER above it (towards the dentine) reflecting its unidirectional secretion. On initial dentine formation it moves pulpally, away from the primitive amelodentinal junction (then Inner Enamel Epithelium/dental papillary junction) leaving behind a tubular structure known as the odontoblast process. This keeps its tapered structure with cytoskeletal fibres, mainly intermediate filaments. A pulpal A-delta (noxious, short sharp pain) nerve fibre is wrapped around the base of this process, or travels a short way into the dentinal tubule with the odontoblast process (max ~0.1mm) This process lies in a tubule, known simply as a dentinal tubule. In a complete tooth, this process rarely extends beyond 1/3 the depth of the dentine, which is why the odontoblast transduction theory of dentin sensitivity is unlikely. The functions of the odontoblast process are as follows: 1. To aid in the secretion of tubular dentin (dentin surrounding tubule) which further organises and strengthens the dentine as a whole tissue 2. General maintenance of the dentinal tubule and dentinal fluid (ion/protein content etc.) 3. To secrete sclerotic dentin upon carious attack to block off dentinal tubules, slowing the progress of the attack (air space above blockage is known as a dead tract) 4. To channel signals of attack to the odontoblast cell body, initiating reactionary dentin secretion 5. To channel hydrokinetic forces of water movement to the A delta fibre wrapped around its base, maintaining dentine sensitivity The biological tissue formed by odontoblasts is a type of hard tissue. It has been shown that odontoblasts secrete the extracellular matrix protein reelin.[][][]
References External links
• Odontoblasts (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Odontoblasts) at the US National Library of Medicine Medical Subject Headings (MeSH)
Hyaline cartilage
425
Hyaline cartilage
Hyaline cartilage
Hyaline cartilage showing microanatomy of chondrocytes and organelles, lacunae and matrix. Code TH H2.00.03.5.00015
[1]
Hyaline cartilage is a type of cartilage found on many joint surfaces. It is pearly bluish in color with firm consistency and considerable collagen. It contains no nerves or blood vessels, and its structure is relatively simple.
Description
Hyaline cartilage is covered externally by a fibrous membrane, called the perichondrium, except at the articular ends of bones and also where it is found directly under the skin, i.e. ears and nose. This membrane contains vessels that provide the cartilage with nutrition. If a thin slice is examined under the microscope, it will be found to consist of cells of a rounded or bluntly angular form, lying in groups of two or more in a granular or almost homogeneous matrix. The cells, when arranged in groups of two or more, have generally straight outlines where they are in contact with each other, and in the rest of their circumference are rounded. They consist of clear translucent protoplasm in which fine interlacing filaments and minute granules are sometimes present; embedded in this are one or two round nuclei, having the usual intranuclear network. The cells are contained in cavities in the matrix, called cartilage lacunae; these are actually artificial gaps formed by the shrinking of the cells during the staining and setting of the tissue for observation. The interterritorial space between the isogenous cell groups contains relatively more collagen fibers, causing it to maintain its shape while the actual cells shrink, creating the lacunae. This constitutes the so-called capsule of the space. Each lacuna is generally occupied by a single cell, but during the division of the cells it may contain two, four, or eight cells. (see isogenous group) Hyaline cartilage also contains chondrocytes which are cartilage cells that produce the matrix. Hyaline cartilage matrix is mostly made up of type II collagen and Chondroitin sulfate, both of which are also found in elastic cartilage. Hyaline cartilage exists on the ventral ends of ribs; in the larynx, trachea, and bronchi; and on the articular surface of bones.
Hyaline cartilage
426
Articular cartilage
Articular cartilage refers to hyaline cartilage on the articular[1] surfaces of bones.[1] Though it is often found in close contact with menisci and articular disks, articular cartilage is not considered a part of either of these structures, which are made entirely of fibrocartilage.
Images
Articular cartilage of the elbow joint as seen in dissection
A synovial joint with bone, articular cartilage, and articular disc shown.
Elbow joint. Deep dissection. Anterior view.
Elbow joint. Deep dissection. Anterior view.
External links
• Hyaline+cartilage [3] at eMedicine Dictionary • UIUC Histology Subject 331 [4] • BU Histology Learning System: 03301lba [5]
References
[1] http:/ / www. wheelessonline. com/ ortho/ articular_cartilage
Fibrocartilage
427
Fibrocartilage
Fibrocartilage
White fibrocartilage from an intervertebral fibrocartilage.
Symphysis pubis exposed by a coronal section. (Pubic symphysis visible at center left.) Gray's Code subject #68 281
[1] [1]
TH H2.00.03.5.00017
White fibrocartilage consists of a mixture of white fibrous tissue and cartilaginous tissue in various proportions. It owes its flexibility and toughness to the former of these constituents, and its elasticity to the latter. It is the only type of cartilage that contains type I collagen in addition to the normal type II. Fibrocartilage is found in the pubic symphysis, the annulus fibrosus of intervertebral discs, menisci, and the TMJ. During labor, relaxin loosens the pubic symphysis to aid in delivery, but this can lead to later joint problems.
Formation as a repair mechanism
If hyaline cartilage is torn all the way down to the bone, the blood supply from inside the bone is sometimes enough to start some healing inside the lesion. In cases like this, the body will form a scar in the area using a special type of cartilage called fibrocartilage. Fibrocartilage is a tough, dense, fibrous material that helps fill in the torn part of the cartilage; however, it is not an ideal replacement for the smooth, glassy articular cartilage that normally covers the surface of the knee joint.
Fibrocartilage
428
Pathology
Degeneration of fibrocartilage is seen in degenerative disc disease.
External links
• Fibrocartilage [2] at eMedicine Dictionary • BU Histology Learning System: 03201loa [3] This article incorporates text from a public domain edition of Gray's Anatomy.
Micrograph showing a fragment of an intervertebral disc demonstrating degenerative fibrocartilage with loss of nuclei and nests of chondrocytes, as seen in degenerative disc disease. HPS stain.
Chondrocyte
429
Chondrocyte
Chondrocyte
Chondrocytes of hyaline cartilage showing organelles, lacunae and matrix. Latin Code chondrocytus TH H2.00.03.5.00003
[1]
Chondrocytes (from Greek chondros cartilage + kytos cell) are the only cells found in healthy cartilage. They produce and maintain the cartilaginous matrix, which consists mainly of collagen and proteoglycans. Although chondroblast is still commonly used to describe an immature chondrocyte, use of the term is discouraged, for it is technically inaccurate since the progenitor of chondrocytes (which are mesenchymal stem cells) can also differentiate into several cell types including osteoblasts. The organization of chondrocytes within cartilage differs depending upon the type of cartilage and where in the tissue they are found.
Differentiation
From least- to terminally-differentiated, the chondrocytic lineage is: 1. 2. 3. 4. Colony-forming unit-fibroblast (CFU-F) Mesenchymal stem cell / marrow stromal cell (MSC) Chondrocyte Hypertrophic chondrocyte
When referring to bone or cartilage, mesenchymal stem cell (mesoderm origin) are undifferentiated meaning they can differentiate into different variance of generative cells (MSC) are commonly known as osteochondrogenic (or osteogenic, chondrogenic, osteoprogenitor, etc.) cell. Undifferentiated mesenchymal stem cell lose their process, proliferate and crowd together in a dense aggregate of chondrogenic cells(cartilage) at the center of chondrification. These condrogenic cells will then differentiate to chondroblasts which will then to synthesize the cartilage ECM(extra cellular matrix). Which consists of ground substance(proteoglycans, glycosaminoglycans for low osmotic potential) and fibers. The chondroblasts then trap themselves in a small space that is no longer in contact with the newly created matrix called lacunae which contain extracellular fluid. The chondroblast is now a chondrocyte, which is usually inactive but can still secrete and degrade matrix depending on the conditions. The majority of the cartilage that has been built has been synthesized from the chondroblast which are much more inactive at a late age (adult hood) compared to earlier years (pre-pubesence) BMP4 and FGF2 have been experimentally shown to increase chondrocyte differentiation.[1] Chondrocytes undergo terminal differentiation when they become hypertrophic during endochondral ossification. This last stage is characterized by major phenotypic changes in the cell.
Chondrocyte
430
Gallery
Chondrocytes in hyaline cartilage
Chondrocyte, stained for calcium, showing nucleus (N) and mitochondria (M)
References
• Dominici M, Hofmann T, Horwitz E (2001). "Bone marrow mesenchymal cells: biological properties and clinical applications". J Biol Regul Homeost Agents 15 (1): 28–37. PMID 11388742 (http://www.ncbi.nlm.nih.gov/ pubmed/11388742). • Bianco P, Riminucci M, Gronthos S, Robey P (2001). "Bone marrow stromal stem cells: nature, biology, and potential applications". Stem Cells 19 (3): 180–92. doi: 10.1634/stemcells.19-3-180 (http://dx.doi.org/10. 1634/stemcells.19-3-180). PMID 11359943 (http://www.ncbi.nlm.nih.gov/pubmed/11359943). • Stem cell information (http://stemcells.nih.gov/info/scireport/appendixE.asp)
External links
• BU Histology Learning System: 03317loa (http://www.bu.edu/histology/p/03317loa.htm) • Chondrocytes (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Chondrocytes) at the US National Library of Medicine Medical Subject Headings (MeSH)
Osteoblast
431
Osteoblast
Osteoblast
Osteoblasts (blue) rimming a bony spicule (pink - on diagonal of image). H&E stain. Latin Code osteoblastus TH H2.00.03.7.00002
[1]
Osteoblasts (from the Greek words for "bone" and "germ" or embryonic) are mononucleate cells that are responsible for bone formation; in essence, osteoblasts are specialized fibroblasts that in addition to fibroblastic products, express bone sialoprotein and osteocalcin.[1] Osteoblasts produce a matrix of osteoid, which is composed mainly of Type I collagen. Osteoblasts are also responsible for mineralization of this matrix. Zinc, copper and sodium are some of the minerals required in this process. Bone is a dynamic tissue that is constantly being reshaped by osteoblasts, which are in charge of production of matrix and mineral, and osteoclasts, which break down the tissue. The number of osteoblasts tends to decrease with age, affecting the balance of formation and resorption in the bone tissue,[] and potentially leading to osteoporosis.
Osteogenesis
Osteoblasts arise from osteoprogenitor cells located in the deeper layer of periosteum and the bone marrow. Osteoprogenitors are immature progenitor cells that express the master regulatory transcription factor Cbfa1/Runx2. Osteoprogenitors are induced to differentiate under the influence of growth factors, in particular the bone morphogenetic proteins (BMPs).[] Aside from BMPs, other growth factors including fibroblast growth factor (FGF),[] platelet-derived growth factor (PDGF) and transforming growth factor beta (TGF-β) may promote the division of osteoprogenitors and potentially increase osteogenesis.BMP4 and FGF2 have been experimentally shown to increase osteoblast differentiation.[2] Once osteoprogenitors start to differentiate into osteoblasts, they begin to express a range of genetic markers including Osterix, Col1,[] BSP, M-CSF, ALP,[3] osteocalcin,[] osteopontin, and osteonectin. Although the term osteoblast implies an immature cell type, osteoblasts are in fact the mature bone cells entirely responsible for generating bone tissue in animals and humans.
Osteoblast
432
Morphology and histological staining
Hematoxylin and eosin staining, or H&E staining, reveals that the cytoplasm of osteoblasts is basophilic due to the presence of a large amount of rough endoplasmic reticulum. The nucleus is spherical and large. An active osteoblast is characterized morphologically by a prominent Golgi apparatus that appears histologically as a clear zone adjacent to the nucleus. Active osteoblasts synthesize, and stain positively for, Type-I collagen and alkaline phosphatase.
Osteoblast (Wright Giemsa stain, 100x)
Osteoblasts lining bone (bottom) and actively synthesizing osteoid, containing two osteocytes.
Osteoblasts actively synthesizing osteoid (center).
Osteoblasts actively synthesizing rudimentary bone tissue (center).
Osteoblasts lining bone (H&E stain).
Osteoblasts (pointer) lining bone (H&E stain).
Osteoblasts and osteocytes
Osteoblasts that become trapped in the bone matrix and remain isolated in lacunae become osteocytes. They cease to generate osteoid and mineralized matrix, and instead act in a paracrine manner on active osteoblasts. They are believed to respond to mechanosensory stimuli.[][]
References
[1] Salentijn, L. Biology of Mineralized Tissues: Cartilage and Bone, Columbia University College of Dental Medicine post-graduate dental lecture series, 2007
Further reading
• Netter, Frank H. (1987). Musculoskeletal system: anatomy, physiology, and metabolic disorders. Summit, New Jersey: Ciba-Geigy Corporation ISBN 0-914168-88-6.
External links
• MedEd at Loyola Histo/practical/cartilage/hp9-49.html (http://www.meddean.luc.edu/Lumen/MedEd/Histo/ practical/cartilage/hp9-49.html)
Osteocyte
433
Osteocyte
Osteocyte
Transverse Section Of Bone Latin Code osteocytus TH H2.00.03.7.00003
[1]
An osteocyte, a star shaped cell, is the most commonly found cell in mature bone, and can live as long as the organism itself.[1] Osteocytes have an average half life of 25 years(Full life of 50 years), they do not divide, and they are derived from osteoprogenitors, some of which differentiate into active osteoblasts.[1] In mature bone, osteocytes and their processes reside inside spaces called lacunae and canaliculi, respectively.[1] Cells contain a nucleus and a thin ring piece of cytoplasm. When osteoblasts become trapped in the matrix that they secrete, they become osteocytes. Osteocytes are networked to each other via long cytoplasmic extensions that occupy tiny canals called canaliculi, which are used for exchange of nutrients and waste through gap junctions. The space that an osteocyte occupies is called a lacuna (Latin for a pit). Although osteocytes have reduced synthetic activity and, like osteoblasts are not capable of mitotic division, they are actively involved in the routine turnover of bony matrix, through various mechanosensory mechanisms. They destroy bone through a rapid, transient (relative to osteoclasts) mechanism called osteocytic osteolysis. Osteoblasts/osteocytes develop in mesenchyme. Hydroxyapatite, calcium carbonate and calcium phosphate is deposited around the cell.
Morphology
Osteocytes have a stellate shape, and in humans they are approximately 9 micrometers long in the short axis by 20 micrometers long in the long axis.[2] The cell body varies in size from 5-20micrometers in diameter and contain 40-60 cell processes per cell,[3] with a cell to cell distance between 20-30 micrometers.[4] A mature osteocyte contains a single nucleus that is located toward the vascular side and has one or two nucleoli and a membrane.[5] The cell also exhibits a reduced size endoplasmic reticulum, Golgi apparatus and mitochondria, and cell processes that radiate towards the mineralizing matrix.[5] Osteocytes form an extensive connecting syncitial network via small cytoplasmic/dendritic processes in canaliculi.[6]
Osteocyte
Osteocyte
434
Origin
Osteocytes are derived from Osteoblasts.[6] The fossil record shows that osteocytes were present in bones of jawless fish 400-250 million years ago, and dinosaurs 80 million years old.[7] Therefore, osteocytes have been used to estimate the size of the genome of extinct species.[6] During bone formation, an osteoblast is left behind and buried in the bone matrix as an "osteoid osteocyte", which maintains contact with the osteoblasts through extending cellular processes.[8] The process of osteocytogenesis is largely unknown, but the following molecules have been shown to play a crucial role in the production of healthy osteocytes, either in correct numbers or specific distributions: Matrix Metalloproteinases (MMPs), Dentin Matrix Protein 1 (DMP-1), Osteoblast/Osteocyte factor 45 (OF45), Klotho gene, TGF Beta inducile factor (TIEG), Lysophosphatidic acid (LPA), E11 antigen, and Oxygen.[6] The transformation from motile osteoblast to entraped osteocyte takes about three days, and during this time, the cell produces a volume of extracellular matrix three times its own cellular volume, which results in 70% volume reduction in the mature osteocyte cell body compared to the original osteoblast volume.[9] 10-20% of osteoblasts differentiate into osteocytes.[6] The cell undergoes a dramatic transformation from a polygonal shape to a cell that extends dendrites toward the mineralizing front, followed by dendrites that extend to either the vascular space or bone surface.[10] The embedded "osteoid-osteocyte" must do two functions simultaneously: regulate mineralization and form connective dendritic processes, which requires cleavage of collagen and other matrix molecules.[10] As the osteoblast transitions to an osteocyte, alkaline phosphatase is reduced, and casein kinase II is elevated, as is osteocalcin.[10] Those osteoblasts on the bone surface that are destined for burial as osteocytes slow down matrix production, and are buried by neighboring osteoblasts that continue to produce matrix actively.[11] Palumbo et al.(1990) distinguish three cell types from osteoblast to mature osteocyte: type I preosteocyte (osteoblastic osteocyte), type II preosteocyte (osteoid osteocyte), and type III preosteocyte (partially surrounded by mineral matrix.[11] Osteocytes appear to be enriched in proteins that are resistant to hypoxia, which appears to be due to their embedded location and restricted oxygen supply[12] Oxygen tension may regulate the differentiation of osteoblasts into osteocytes, and osteocyte hypoxia may play a role in disuse-mediated bone resorption.[12]
Function
Although osteocytes are relatively inert cells, they are capable of molecular synthesis and modification, as well as transmission of signals over long distances, in a way similar to the nervous system.[6] They are the most common cell type in bone (31,900 mm-3 in bovine bone to 93,200 mm-3 in rat bone).[6] Most of the receptor activities that play an important role in bone function are present in the mature osteocyte.[6] Osteocytes contain glutamate transporters that produce nerve growth factors after bone fracture, which provides evidence of a sensing and information transfer system.[6] When osteocytes were experimentally destroyed, the bones showed a significant increase in bone resorption, decreased bone formation, trabecular bone loss, and loss of response to unloading.[6] Osteocytes are thought to be mechanosensor cells that control the activity of osteoblasts and osteoclasts within a basic multicellular unit (BMU), a temporary anatomic structure where bone remodeling occurs.[13] Osteocytes generate an inhibitory signal that is passed through their cell processes to osteoblasts for recruitment to enable bone formation.[14] Osteocyte specific proteins such as sclerostin have been shown to function in mineral metabolism, as well as other molecules such as PHEX, DMP-1, MEPE, and FGF-23, which are highly expressed by osteocytes and regulate phosphate and biomineralization.[10] The osteocyte is an important regulator of bone mass and a key endocrine regulator of phosphate metabolism.[12]
Osteocyte
435
Sclerostin
Osteocytes synthesize sclerostin, a secreted protein that inhibits bone formation by binding to LRP5/LRP6 coreceptors and blunting Wnt signaling.[7] Sclerostin, the product of the SOST gene, is the first mediator of communication between osteocytes, bone forming osteoblasts and bone resorbing osteoclasts, critical for bone remodeling.[15] Only osteocytes express sclerostin, which acts in a paracrine fashion to inhibit bone formation.[15] Sclerostin is inhibited by parathyroid hormone (PTH) and mechanical loading.[15] Sclerostin anatagonizes the activity of BMP (bone morphogenetic protein),a citokine that induces bone and cartilage formation.[13]
Osteocyte Apoptosis and Associated Pathologies
Osteocytes die as a consequence of senescence, degeneration/necrosis, apoptosis(programmed cell death), and/or osteoclastic engulfment.[1] The percentage of dead osteocytes in bone increases with age from less than 1% at birth to 75% after age 80.[16] Osteocyte apoptosis is thought to be related to decreased mecanotransduction, which possibly leads to the development of osteoporosis.[17] Apoptotic osteocytes release apoptotic bodies expressing RANKL to recruit osteoclasts.[10] Mechanical loading increases osteocyte viability in vitro, and contributes to solute transport through the lacuno-canalicular system in bone, which enhances oxygen and nutrient exchange and diffusion to osteocytes.[17] Skeletal unloading has been shown to induce osteocyte hypoxia in vivo, this is when osteocytes undergo apoptosis and recruit osteoclasts to resorb bone.[17] Microdamage in bone occurs as the result of repetitive events of cycling loading, and appears to be associated with osteocyte death by apoptosis, which appear to secrete a signal to target osteoclasts to perform remodeling at a damaged site.[17] Under normal conditions, osteocytes express high amounts of TGF-β and thus repress bone resorption, but when bone grows old, the expression levels of TGF-β decrease, and the expression of osteoclast-stimulatory factors, such as RANKL and M-CSF increases, bone resorption is then enhanced, leading to net bone loss.[17] Mechanical stimulation of osteocytes results in opening of hemichannels to release PGE2 and ATP, among other biochemical signaling molecules, which play a crucial role in maintaining the balance between bone formation and resorption.[18] Osteocyte cell death can occur in association with pathologic conditions such as osteoporosis and osteoarthritis, which leads to increased skeletal fragility, linked to the loss of ability to sense microdamage and/or signal repair.[10][19] Oxygen deprivation that occurs as the result of immobilization (bed rest), glucocorticoid treatment, and withdrawal of oxygen have all been shown to promote osteocyte apoptosis.[10]
References
[1] Tate ML, Adamson JR, Tami AE, Bauer TW, (2004). "Cells in Focus, The osteocyte". The International Journal of Biochemistry and Cell Biology (36), 1-8. [2] Mullender,MG, van deer Meer, DD, Huiskes, R,Lips, P,(1996). Bone18(2):109-113. [3] Tanaka-Kamioka,K, Kamioka H, Ris, H, Lim, SS, (1998). "Osteocyte shape is dependant on actin filaments and osteocyte processes are unique actin-rich projections". J. Bone Miner. Res. 13(10):1555-68. [4] Sugawara, Y, Kamioka, H, Honjo, T, Tezuka, K, Takano-Yamamoto, T, (2005). "Three dimensional reconstruction of chick calvarial osteocytes and their cell processes using confocal microscopy". Bone 36(5):877-83. [5] Dudley, HR,and Spiro, D, (1961). "The fine structure of bone cells". The Journal of Biophysical and Biochemical Cytology 11, 627-649. [6] Noble,SN (2008). "The osteocyte lineage". Archives of Biochemistry and Biophysics 473, 106-111. [7] Divieti Pajevic P,(2009). "Regulation of Bone Resorption and Mineral Homeostasis by Osteocytes". IBMS BoneKEy 6(2):63-70. [8] Palumbo,C, Pallazini,D, Zaffe,D, Marotti,G, (1990). Acta Anat.(Basel) 137(4):350-358. [9] Palumbo,C (1986) "A three dimensional ultrastructural study of osteoid-osteocytes in the tibia of chick embryos." Cell Tissue Research, 246:125-131. [10] Bonewald L, (2011). "The Amazing Osteocyte" Journal of Bone and Mineral Research 26(2):229-238. [11] Franz-Odendaal T, Hall B, Witten PE, (2006). "Buried Alive: How Osteoblasts Become Osteocytes" Developmental Dynamics 235:176-190. [12] Dallas SL, Bonewald L, (2010). "Dynamics of the Transition from Osteoblast to Osteocyte" Ann N Y Acad. Sci. 1192:437-443. [13] ran Bezooijen Rl, Papapoulos SE, Hamdy NA, ten Dijke P, Lowik C (2005) "Control of Bone Formation by Osteocytes." BoneKEy-Osteovision, 2(12):33-38.
Osteocyte
[14] Marotti G, Ferretti M, Muglia MA, Palumbo C, Palazzani SA (1992) "A quantitative evaluation of osteoblast-osteocyte relationships on growing endosteal surface of rabbit tibiae." Bone, 13(5):363-368. [15] Bellido, T (2007) "Osteocyte Apoptosis Induces Bone Resorption and Impairs the Skeletal Response to Weighlessness." BoneKEy-Osteovision 4(9):252-256. [16] Tomkinson A, Reeve J, Shaw RW, Noble BS (1997) "The death of osteocytes via apoptosis accompanies estrogen withdrawal in human bone." The Journal of Clinical Endocrinology and Metabolism, 82(9):3128-3135. [17] Heino TJ, Kurata K, Higaki H, Vaananen K, (2009). "Evidence of the role of osteocytes in the initiation of targeted remodeling." Technology and Healthcare 17:49-56. [18] Burra S, Nicolella DP, Jiang JX, (2011). "Dark horse in osteocyte biology" Communicative and Integrative Biology 4(1)48-50. [19] Carpentier VT, Wong J, Yeap Y, Gan C, Sutton-Smith P, Badiei A, Fazzalari NL, Kuliwaba JS, (2012). "Increased proportion of hypermineralized osteocyte lacunae in osteoporotic and osteoarthritic human trabecular bone: Implications for bone remodeling" Bone 50 (3): 688–694
436
External links
• BU Histology Learning System: 02003loa (http://www.bu.edu/histology/p/02003loa.htm) - "Cartilage and Bone and Bone Histogenesis: cells of* BU Histology Learning System: 02705loa (http://www.bu.edu/ histology/p/02705loa.htm) - "Cartilage and Bone and Bone Histogenesis: compact bone"* =D Histology at ou.edu (http://casweb.cas.ou.edu/pbell/Histology/Captions/Bone/osteocyte.2.html)
Stellate cell
437
Stellate cell
Neuron: Stellate cell
Microcircuitry of the cerebellum. Excitatory synapses are denoted by (+) and inhibitory synapses by (-). MF: Mossy fiber. DCN: Deep cerebellar nuclei. IO: Inferior olive. CF: Climbing fiber. GC: Granule cell. PF: Parallel fiber. PC: Purkinje cell. GgC: Golgi cell. SC: Stellate cell. BC: Basket cell. NeuroLex ID Dorlands/Elsevier sao2046525601 12225156 [2] [1]
In neuroscience, stellate cells are neurons with several dendrites radiating from the cell body giving them a star shape. The three most common stellate cells are the inhibitory interneurons found within the molecular layer of the cerebellum, excitatory spiny stellate interneurons and inhibitory aspiny stellate interneurons. Cerebellar stellate cells synapse onto the dendritic arbors of Purkinje cells. Cortical spiny stellate cells are found in layer IVC of the V1 region in the visual cortex. They receive excitatory synaptic fibres from the thalamus and process feed forward excitation to 2/3 layer of V1 visual cortex to pyramidal cells. Cortical Spiny Stellate cells have a 'regular' firing pattern.
Golgi stained cortical neurons A) Layer II/IIIpyramidal cell B) layer IV spiny stellate cell
External links
• NIF Search - Stellate Cell [3] via the Neuroscience Information
Framework
Skeletal striated muscle
438
Skeletal striated muscle
Skeletal striated muscle
A top-down view of skeletal muscle Latin Code textus muscularis striatus skeletalis TH H2.00.05.2.00002
[1]
Skeletal muscle is a form of striated muscle tissue which is under the control of the somatic nervous system; that is to say, it is voluntarily controlled. It is one of three major muscle types, the others being cardiac and smooth muscle. As their name suggests, most skeletal muscles are attached to bones by bundles of collagen fibers known as tendons. Skeletal muscle is made up of individual components known as myocytes, or "muscle cells", sometimes colloquially called "muscle fibers". They are formed from the fusion of developmental myoblasts (a type of embryonic progenitor cell that gives rise to a muscle cell). These long, cylindrical, multinucleated cells are also called myofibers. The myofibers are in turn composed of myofibrils. The myofibrils are composed of actin and myosin filaments repeated as a sarcomere, the basic functional unit of the muscle fiber and responsible for skeletal muscle's striated appearance and forming the basic machinery necessary for muscle contraction. The term muscle refers to multiple bundles of muscle fibers held together by connective tissue.
Muscle fibers
Individual muscle fibers are formed during development from the fusion of several undifferentiated immature cells known as myoblasts into long, cylindrical, multi-nucleated cells. Differentiation into this state is primarily completed before birth with the cells continuing to grow in size thereafter. Skeletal muscle exhibits a distinctive banding pattern when viewed under the microscope due to the arrangement of cytoskeletal elements in the cytoplasm of the muscle fibers. The principal cytoplasmic proteins are myosin and actin (also known as "thick" and "thin" filaments, respectively) which are arranged in a repeating unit called a sarcomere. The interaction of myosin and actin is responsible for muscle contraction. There are two principal ways to categorize muscle fibers: the type of myosin (fast or slow) present, and the degree of oxidative phosphorylation that the fiber undergoes. Skeletal muscle can thus be broken down into two broad categories: Type I and Type II. Type I fibers appear red due to the presence of the oxygen binding protein myoglobin. These fibers are suited for endurance and are slow to fatigue because they use oxidative metabolism to generate ATP. Type II fibers are white due to the absence of myoglobin and a reliance on glycolytic enzymes. These fibers are efficient for short bursts of speed and power and use both oxidative metabolism and anaerobic metabolism depending on the particular sub-type. These fibers are quicker to fatigue.
Skeletal striated muscle
439
Type I fibers (red) Contraction time Size of motor neuron Resistance to fatigue Activity Used for Maximum duration of use Power produced Mitochondrial density Capillary density Oxidative capacity Glycolytic capacity Major storage fuel Slow Small High Aerobic Hours
Type II a fibers (red)
Type II x fibers
Type II b fibers (white)
Moderately Fast Medium Fairly high Long-term anaerobic <30 minutes
Fast Large Intermediate Short-term anaerobic <5 minutes
Very fast Very large Low Short-term anaerobic <1 minute
Low Very High High High Low Triglycerides
Medium High Intermediate High High Creatine phosphate, glycogen
High Medium Low Intermediate High
Very high Low Low Low High
ATP, Creatine phosphate, glycogen ATP, Creatine (little) phosphate Consume Creatine phosphate Consume Creatine phosphate MYH4 [1]
Note
Consume lactic acid MYH7
Produce lactic acid and Creatine phosphate MYH2
Myosin heavy chain, human genes
MYH1
Skeletal muscle fibers are not all the same. Traditionally, they were categorized depending on their varying color, which is a reflection of myoglobin content. Red Fibers: Those containing high levels of myoglobin and oxygen storing proteins had a red appearance. Red muscle fibers tend to have more mitochondria and greater local capillary density. White Fibers: Those with a low content had a white appearance. As more was learned about the functional differences between skeletal muscle fibers, they were also classified, depending on their twitch capabilities, into fast and slow twitch, traits that largely, but not completely, overlap the previous classification based on color. Fast Twitch: Some authors define a fast twitch fiber as one in which the myosin can split ATP very quickly. However, fast twitch fibers also demonstrate a higher capability for electrochemical transmission of action potentials and a rapid level of calcium release and uptake by the sarcoplasmic reticulum. The fast twitch fibers rely on a well-developed, short term, glycolytic system for energy transfer and can contract and develop tension at 2-3 times the rate of slow twitch fibers. Slow Twitch: The slow twitch fibers generate energy for ATP re-synthesis by means of a long term system of aerobic energy transfer. They tend to have a low activity level of ATPase, a slower speed of contraction with a less well developed glycolytic capacity. They contain large and numerous mitochondria and with the high levels of myoglobin that gives them a red pigmentation. They have been demonstrated to have high concentration of mitochondrial enzymes, thus they are fatigue resistant. The 2 main categories of muscle fibers become several, when further differentiating type II into several subtypes, based on myosin isoforms and denoted with letters of the alphabet. In humans the two subtypes are IIa and IIx; IIx is often referred to as IIb because earlier classification had clumped together two different types. Later on, further research recognized these subtypes as distinct, but the use of the name IIb remained entrenched.[1] Non human fiber types include true IIb fibers, IIc, IId and so on. Type I Red fibers. Slow oxidative (also called slow twitch or fatigue resistant fibers). Contain:
Skeletal striated muscle • • • • • • • • • Large amounts of myoglobin. Many mitochondria. Many blood capillaries. Generate ATP by the aerobic system, hence the term oxidative fibers. Split ATP at a slow rate. Slow contraction velocity. Resistant to fatigue. Found in large numbers in postural muscles. Needed for aerobic activities like long distance running.
440
Type IIa Red fibers. Fast oxidative (also called fast twitch A or fatigue resistant fibers). Contain: • • • • • Large amounts of myoglobin. Many mitochondria. Many blood capillaries. Large amount of glycogen. High capacity for generating ATP by oxidation. Split ATP at a very rapid rate and, hence, high contraction velocity • Resistant to fatigue but not as much as slow oxidative fibers. • Needed for sports such as middle distance running and swimming. Type IIx / IIb (dependent upon species) White. Fast glycolytic (also called fast twitch B or fatigable fibers). Contain: • • • • • • • Low myoglobin content. Few mitochondria. Few blood capillaries. Large amount of Creatine phosphate. Split ATP very quickly. Fatigue easily. Needed for sports like sprinting.
Individual muscles are a mixture of 3 types of muscle fibers (type 1, type 2a and type 2b), but their proportions vary depending on the action of that muscle. It must be remembered that skeletal muscles, although a mixture, can only have one type of muscle fiber within a motor unit. This is demonstrated if we look at contractions. E.g. If a weak contraction is needed only the type 1 motor units will be activated. These fibers are used mainly for endurance activities. If a stronger contraction is required the type 2a fibers will be activated or used to assist the type 1 fibers. Maximal contractions facilitate the use of type 2b fibers which are always activated last. These fibers are used during ballistic activities but tire easily. With advanced EMG techniques it is possible to look at which muscle fibers are recruited when performing an exercise/test. The total number of skeletal muscle fibers has traditionally been thought not to change. It is believed there are no sex or age differences in fiber distribution, however, relative fiber types vary considerably from muscle to muscle and person to person. Sedentary men and women (as well as young children) have 45% type 2 and 55% type 1 fibers.[citation needed] People at the higher end of any sport tend to demonstrate patterns of fiber distribution e.g. endurance athletes show a higher level of type 1 fibers. Sprint athletes, on the other hand, require large numbers of type 2 b fibers. Middle distance event athletes show approximately equal distribution of the 2 types. This is also often the case for power athletes such as throwers and jumpers. It has been suggested that various types of exercise can induce changes in the fibers of a skeletal muscle.[2] It is thought that if you perform endurance type events for a sustained period of time, some of the type 2b fibers transform into type 2a fibers. However, there is no consensus on the subject. It may well be that the type 2b fibers show enhancements of the oxidative capacity after high intensity endurance training which brings them to a level at which they are able to perform oxidative metabolism as effectively as slow twitch fibers of untrained subjects. This would be brought about
Skeletal striated muscle by an increase in mitochondrial size and number and the associated related changes not a change in fiber type.
441
Structure of skeletal muscle fiber
Every organelle and macromolecule of a muscle fiber are arranged to ensure form meets function. The plasma membrane is called the sarcolemma with the cytoplasm known as the sarcoplasm. In the sarcoplasm are the myofibrils. The myofibrils are long protein bundles about 1 micrometer in diameter each containing myofilaments. Pressed against the inside of the sarcolemma are the unusual flattened nuclei. Between the myofibrils are the mitochondria. While the muscle fiber does not have a smooth endoplasmic reticulum, it contains a sarcoplasmic reticulum. The sarcoplasmic reticulum surrounds the myofibrils and holds a reserve of the calcium ions needed to cause a muscle contraction. Periodically, it has dilated end sacs known as terminal cisternae. These cross the muscle fiber from one side to the other. In between two terminal cisternae is a tubular infoldings called a transverse tubule (T tubule). The T tubule are the pathway for the action potential to signal the sarcoplasmic reticulum to release calcium causing a muscle contraction. Together, two terminal cisternae and a transverse tubule form a triad.[3]
Organization of skeletal muscle fibers
While the muscle fibers of the fascicles lie parallel to one another, the fascicles themselves can vary in their relationship to one another and to their tendons.[] The different patterns of arrangement of the fasciles produce four different types of skeletal muscles: parallel muscles, convergent muscles, pennate muscles, and sphincter muscles.[] Parallel muscles The fascicles of parallel muscles run parallel to the direction of the muscle, thus these muscles on a whole function similarly to a single muscle fiber.[] Most skeletal muscles in the body are parallel muscles; although they can be seen in a variety of shapes such as flat bands, spindle shaped, and some can have large protrusions in their middle known as the belly of the muscle.[] ex: Triceps, biceps Convergent muscles The fibers in convergent muscles fan out from a common point of attachment.[] Covering a broad surface these fibers allow for more versatile types of movement.[] These muscles do not pull as hard on their corresponding tendons as their parallel muscle counterparts however due to the fibers not all pulling in the same direction, even pulling in different directions at opposite ends.[] ex: Pectoralis muscles Pennate muscles In a pennate muscle one or more tendons run through the body of the muscle with the fascicles forming an oblique angle to the tendons.[] Because the fascicles pull on the tendons at an angle they do not move the tendon as far as their parallel muscle counterparts. Despite this they generate greater tension due to their possessing a greater amount of muscle fibers than similarly sized parallel muscles.[] ex: Rectus femoris Sphincter muscles The fibers of the sphincter or circular muscles are arranged concentrically around an opening or recess.[] As the muscle contracts, the opening it circumvents gets smaller, for this reason these muscles are often found at the entrances and exits of external and internal passage ways.[] ex: Orbicularis oris
Skeletal striated muscle
442
Cellular physiology and contraction
In addition to the actin and myosin components that constitute the sarcomere, skeletal muscle fibers also contain two other important regulatory proteins, troponin and tropomyosin, that are necessary for muscle contraction to occur. These proteins are associated with actin and cooperate to prevent its interaction with myosin. Skeletal muscle cells are excitable and are subject to depolarization by the neurotransmitter acetylcholine, released at the neuromuscular junction by motor neurons.[4] Once a cell is sufficiently stimulated, the cell's sarcoplasmic reticulum releases ionic calcium (Ca2+), which then interacts with the regulatory protein troponin. Calcium-bound troponin undergoes a conformational change that leads to the movement of tropomyosin, subsequently exposing the myosin-binding sites on actin. This allows for myosin and actin ATP-dependent cross-bridge cycling and shortening of the muscle.
Physics
Muscle force is proportional to physiologic cross-sectional area (PCSA), and muscle velocity is proportional to muscle fiber length.[5] The strength of a joint, however, is determined by a number of biomechanical parameters, including the distance between muscle insertions and pivot points and muscle size. Muscles are normally arranged in opposition so that as one group of muscles contract, another group relaxes or lengthens. Antagonism in the transmission of nerve impulses to the muscles means that it is impossible to fully stimulate the contraction of two antagonistic muscles at any one time. During ballistic motions such as throwing, the antagonist muscles act to 'brake' the agonist muscles throughout the contraction, particularly at the end of the motion. In the example of throwing, the chest and front of the shoulder (anterior Deltoid) contract to pull the arm forward, while the muscles in the back and rear of the shoulder (posterior Deltoid) also contract and undergo eccentric contraction to slow the motion down to avoid injury. Part of the training process is learning to relax the antagonist muscles to increase the force input of the chest and anterior shoulder. Contracting muscles produce vibration and sound.[6] Slow twitch fibers produce 10 to 30 contractions per second (10 to 30 Hz). Fast twitch fibers produce 30 to 70 contractions per second (30 to 70 Hz).[7] The vibration can be witnessed and felt by highly tensing one's muscles, as when making a firm fist. The sound can be heard by pressing a highly tensed muscle against the ear, again a firm fist is a good example. The sound is usually described as a rumbling sound. Some individuals can voluntarily produce this rumbling sound by contracting the tensor tympani muscle of the middle ear. The rumbling sound can also be heard when the neck or jaw muscles are highly tensed.
Signal transduction pathways
Skeletal muscle fiber-type phenotype in adult animals is regulated by several independent signaling pathways. These include pathways involved with the Ras/mitogen-activated protein kinase (MAPK), calcineurin, calcium/calmodulin-dependent protein kinase IV, and the peroxisome proliferator γ coactivator 1 (PGC-1). The Ras/MAPK signaling pathway links the motor neurons and signaling systems, coupling excitation and transcription regulation to promote the nerve-dependent induction of the slow program in regenerating muscle. Calcineurin, a Ca2+/calmodulin-activated phosphatase implicated in nerve activity-dependent fiber-type specification in skeletal muscle, directly controls the phosphorylation state of the transcription factor NFAT, allowing for its translocation to the nucleus and leading to the activation of slow-type muscle proteins in cooperation with myocyte enhancer factor 2 (MEF2) proteins and other regulatory proteins. Calcium-dependent Ca2+/calmodulin kinase activity is also upregulated by slow motor neuron activity, possibly because it amplifies the slow-type calcineurin-generated responses by promoting MEF2 transactivator functions and enhancing oxidative capacity through stimulation of mitochondrial biogenesis. Contraction-induced changes in intracellular calcium or reactive oxygen species provide signals to diverse pathways that include the MAPKs, calcineurin and calcium/calmodulin-dependent protein kinase IV to activate transcription
Skeletal striated muscle factors that regulate gene expression and enzyme activity in skeletal muscle. PGC1-α (PPARGC1A), a transcriptional coactivator of nuclear receptors important to the regulation of a number of mitochondrial genes involved in oxidative metabolism, directly interacts with MEF2 to synergistically activate selective ST muscle genes and also serves as a target for calcineurin signaling. A peroxisome proliferator-activated receptor δ (PPARδ)-mediated Exercise-Included Signaling Pathways in Skeletal Muscle That Determine Specialized Characteristics of ST and FT Muscle Fibers transcriptional pathway is involved in the regulation of the skeletal musclefiber phenotype. Mice that harbor an activated form of PPARd display an “endurance” phenotype, with a coordinated increase in oxidative enzymes and mitochondrial biogenesis and an increased proportion of ST fibers. Thus—through functional genomics—calcineurin, calmodulin-dependent kinase, PGC-1α, and activated PPARδ form the basis of a signaling network that controls skeletal muscle fiber-type transformation and metabolic profiles that protect against insulin resistance and obesity. The transition from aerobic to anaerobic metabolism during intense work requires that several systems are rapidly activated to ensure a constant supply of ATP for the working muscles. These include a switch from fat-based to carbohydrate-based fuels, a redistribution of blood flow from nonworking to exercising muscles, and the removal of several of the by-products of anaerobic metabolism, such as carbon dioxide and lactic acid. Some of these responses are governed by transcriptional control of the FT glycolytic phenotype. For example, skeletal muscle reprogramming from an ST glycolytic phenotype to an FT glycolytic phenotype involves the Six1/Eya1 complex, composed of members of the Six protein family. Moreover, the Hypoxia Inducible Factor-1α (HIF-1α) has been identified as a master regulator for the expression of genes involved in essential hypoxic responses that maintain ATP levels in cells. Ablation of HIF-1α in skeletal muscle was associated with an increase in the activity of rate-limiting enzymes of the mitochondria, indicating that the citric acid cycle and increased fatty acid oxidation may be compensating for decreased flow through the glycolytic pathway in these animals. However, hypoxia-mediated HIF-1α responses are also linked to the regulation of mitochondrial dysfunction through the formation of excessive reactive oxygen species in mitochondria. Other pathways also influence adult muscle character. For example, physical force inside a muscle fiber may release the transcription factor Serum Response Factor (SRF) from the structural protein titin, leading to altered muscle growth.
443
Skeletal striated muscle
444
Research
Research on skeletal muscle properties uses many techniques. Electrical muscle stimulation is used to determine force and contraction speed at different stimulation frequencies, which are related to fiber-type composition and mix within an individual muscle group. In vitro muscle testing is used for more complete characterization of muscle properties.
References
[5] Quoted from National Skeletal Muscle Research Center; UCSD, Muscle Physiology Home Page - Skeletal Muscle Architecture (http:/ / muscle. ucsd. edu/ musintro/ arch. shtml), Effect of Muscle Architecture on Muscle Function [7] (http:/ / www. pponline. co. uk/ encyc/ endurance-training-understanding-your-slow-twitch-muscle-fibres-will-boost-performance-41374), Peak Performance - Endurance training: understanding your slow twitch muscle fibres will boost performance
Nuclear bag fiber
445
Nuclear bag fiber
Nuclear bag fiber
Latin myofibra sacculiformis Code TH H3.03.00.0.00013 [1]
A nuclear bag fiber is a type of intrafusal muscle fiber that lies in the center of a muscle spindle. Each has a large number of nuclei concentrated in bags and they cause excitation of both the primary and secondary nerve fibers. There are 2 kinds of bag fibers based upon contraction speed and motor innervation. 1) Bag2 fibers - are the largest. They have no striations in middle region and swell to enclose nuclei (hence their name) 2) Bag1 fibers - are smaller than bag2. Both bag types extend beyond the spindle capsule.
External links
• http://www.unmc.edu/Physiology/Mann/mann11.html
Nuclear chain cell
A nuclear chain cell is a type of cell that is found in the human body.
References
Myosatellite cell
446
Myosatellite cell
Myosatellite cell
Latin myosatellitocytus Code TH H2.00.05.2.01020 [1]
Myosatellite cells or satellite cells are small mononuclear progenitor cells with virtually no cytoplasm found in mature muscle. Satellite cells are precursors to skeletal muscle cells, able to give rise to satellite cells or differentiated skeletal muscle cells.[1] They have the potential to generate new muscle fibers, provide additional myonuclei to their parent muscle fiber, or return to a quiescent state.[2] More specifically, upon activation, satellite cells can re-enter the cell cycle to proliferate and differentiate into myoblasts.[3] Myosatellite cells are located between the basal lamina and sarcolemma of muscle fibers, and can lie in grooves either parallel or transversely to the longitudinal axis of the fiber. Their distribution across the fiber can vary significantly. Non-proliferative, quiescent myosatellite cells, which adjoin resting skeletal muscles, can be identified by their distinct location between sarcolemma and basal lamina, a high nuclear-to-cytoplasmic volume ratio, few organelles (e.g. ribosomes, endoplasmic reticulum, mitochondia, golgi complexes), small nuclear size, and a large quantity of nuclear heterochromatin relative to myonuclei. On the other hand, activated satellite cells have an increased number of caveolae, cytoplasmic organelles, and decreased levels of heterochromatin.[1] Satellite cells are able to differentiate and fuse to augment existing muscle fibers and to form new fibers. These cells represent the oldest known adult stem cell niche, and are involved in the normal growth of muscle, as well as regeneration following injury or disease. In undamaged muscle, the majority of satellite cells are quiescent; they neither differentiate nor undergo cell division. In response to mechanical strain, satellite cells become activated. Activated satellite cells initially proliferate as skeletal myoblasts before undergoing myogenic differentiation.
Genetic markers of satellite cells
Satellite cells express a number of distinctive genetic markers. Current thinking is that all satellite cells express PAX7 and PAX3[4] Moreover, both quiescent and activated human satellite cells can be identified by the membrane-bound neural cell adhesion molecule (N-CAM/CD56/Leu-19), a cell-surface glycoprotein. Myocyte nuclear factor (MNF), and c-met proto-oncogene (receptor for hepatocyte growth factor (HGF)) are less commonly used markers. [1] CD34 and Myf5 markers specifically define the majority of quiescent satellite cells.[5] Activated satellite cells prove problematic to identify, especially as their markers change with the degree of activation; for example, greater activation results in the progressive loss of Pax7 expression as the they enter the proliferative stage. However, Pax7 is expressed prominently after satellite cell differentiation.[6] Greater activation also results in increased expression of myogenic basic helix-loop-helix transcription factors MyoD, myogenin, and MRF4 - all responsible for the induction of myocyte-specific genes.[7] HGF testing is also used to identify active satellite cells.[1] Activated satellite cells also begin expressing muscle-specific filament proteins such as desmin as they differentiate. The field of satellite cell biology suffers from the same technical difficulties as other stem cell fields. Studies rely almost exclusively on Flow cytometry and Fluorescence Activated Cell Sorting (FACS) analysis, which gives no information about cell lineage or behaviour. As such, the satellite cell niche is relatively ill-defined and it is likely that it consists of multiple sub-populations.
Myosatellite cell
447
Function in muscle repair
When muscle cells undergo injury, quiescent satellite cells are released from beneath the basement membrane. They become activated and re-enter the cell cycle. These dividing cells are known as the "transit amplifying pool" before undergoing myogenic differentiation to form new (post-mitotic) myotubes. There is also evidence suggesting that these cells are capable of fusing with existing myofibers to facilitate growth and repair. The process of muscle regeneration involves considerable remodeling of extracellular matrix and, where extensive damage occurs, is incomplete. Fibroblasts within the muscle deposit scar tissue, which can impair muscle function, and is a significant part of the pathology of muscular dystrophies. Satellite cells proliferate following muscle trauma[8] and form new myofibers through a process similar to foetal muscle development.[] After several cell divisions, the satellite cells begin to fuse with the damaged myotubes and undergo further differentiations and maturation, with peripheral nuclei as in hallmark.[] One of the first roles described for IGF-1 was its involvement in the proliferation and differentiation of satellite cells. In addition, IGF-1 expression in skeletal muscle extends the capacity to activate satellite cell proliferation (Charkravarthy, et al., 2000), increasing and prolonging the beneficial effects to the aging muscle. [9] [10]
Effects of Exercise on Satellite Cell Activity
Satellite cell activation is measured by the extent of proliferation and differentiation. Typically, satellite cell content is expressed per muscle fiber or as a percentage of total nuclear content, the sum of satellite cell nuclei and myonuclei. While the adaptive response to exercise largely varies on an individual basis on factors such as genetics, age, diet, acclimatization to exercise, and exercise volume, human studies have demonstrated general trends.[1] It is suggested that exercise triggers the release of signaling molecules including inflammatory substances, cytokines and growth factors from surrounding connective tissues and active skeletal muscles.[1] Notably, HGF, a cytokine, is transferred from the extracellular matrix into muscles through the nitric-oxide dependent pathway. It is thought that HGF activates satellite cells, while insulin growth factor-I (IGF-1) and fibroblast growth factor (FGF) enhance satellite cell proliferation rate following activation.[11] Studies have demonstrated that intense exercise generally increases IGF-1 production, though individual responses vary significantly.[12] [13] More specifically, IGF-1 exists in two isoforms: mechano growth factor (MGF) and IGF-IEa.[14] While the former induces activation and proliferation, the latter causes differentiation of proliferating satellite cells.[14] Human studies have shown that both high resistance training and endurance training have yielded an increased number of satellite cells.[15] [6] These results suggest that a light, endurance training regimen may be useful to counteract the age-correlated satellite cell decrease.[1] In high-resistance training, activation and proliferation of satellite cells are evidenced by increased cyclinD1 mRNA, and p21 mRNA levels. This is consistent with the fact that cyclinD1 and p21 upregulation correlates to division and differentiation of cells. [2] Satellite cell activation has also been demonstrated on an ultrastructural level following exercise. Aerobic exercise has been shown to significantly increase granular endoplasmic reticulum, free ribosomes, and mitochondria of the stimulated muscle groups. Additionally, satellite cells have been shown to fuse with muscle fibers, developing new muscle fibers.[16] Other ultrastructural evidence for activated satellite cells include increased concentration of Golgi apparatus and pinocytotic vesicles.[17]
Myosatellite cell
448
Plasticity and therapeutic applications
Upon minimal stimulation, satellite cells in vitro or in vivo will undergo a myogenic differentiation program. Unfortunately, it seems that transplanted satellite cells have a limited capacity for migration, and are only able to regenerate muscle in the region of the delivery site. As such systemic treatments or even the treatment of an entire muscle in this way is not possible. However, other cells in the body such as pericytes and hematopoietic stem cells have all been shown to be able to contribute to muscle repair in a similar manner to the endogenous satellite cell. The advantage of using these cell types for therapy in muscle diseases is that they can be systemically delivered, autonomously migrating to the site of injury. Particularly successful recently has been the delivery of mesoangioblast cells into the Golden Retriever dog model of Duchenne muscular dystrophy, which effectively cured the disease.[18] However, the sample size used was relatively small and the study has since been criticized for a lack of appropriate controls for the use of immunosuppressive drugs. Recently, it has been reported that Pax7 expressing cells contribute to dermal wound repair by adopting a fibrotic phenotype through a Wnt/β-catenin mediated process.[19]
Regulation
Little is known of the regulation of satellite cells. Whilst together PAX3 and PAX7 currently form the definitive satellite markers, Pax genes are notoriously poor transcriptional activators. The dynamics of activation and quiesence and the induction of the myogenic program through the myogenic regulatory factors, Myf5, MyoD, myogenin, and MRF4 remains to be determined. There is some research indicating that satellite cells are negatively regulated by a protein called myostatin. Increased levels of myostatin up-regulate a cyclin-dependent kinase inhibitor called p21 and thereby induce the differentiation of satellite cells.[20]
References
[1] Kadi F, Charifi N, Denis C, Lexell J, Andersen JL, Schjerling P, Olsen S, Kjaer M. “The behaviour of satellite cells in response to exercise: what have we learned from human studies?” Pflugers Arch 2005; 451:319-27. [2] Kadi F, Schjerling P, Andersen LL, Charifi N, Madsen JL, Christensen LR, Andersen JL. “The effects of heavy resistance training and detraining on satellite cells in human skeletal muscles.” J Physiol 2004; 558:1005-12. [3] Siegel AL, Kuhlmann PK, Cornelison DD. “Muscle satellite cell proliferation and association: new insights from myofiber time-lapse imaging.” Skelet Muscle 2011; 1:7. [5] Beauchamp JR, Heslop L, Yu DS, Tajbakhsh S, Kelly RG, Wernig A, Buckingham ME, Partridge TA, Zammit PS. “Expression of CD34 and Myf5 defines the majority of quiescent adult skeletal muscle satellite cells.” J Cell Biol 2000; 151:1221-34 [6] Crameri R, Aagaard P, Qvortrup K, Kjaer M. “N-CAM and Pax7 immunoreactive cells are expressed differently in the human vastus lateralis after a single bout of exhaustive eccentric exercise.” J Physiol 2004; 565:165. [7] Marchildon F, Lala N, Li G, St-Louis C, Lamothe D, Keller C, Wiper-Bergeron N. “CCAAT/Enhancer Binding Protein Beta is Expressed in Satellite Cells and Controls Myogenesis.” Stem Cells 2012 [Epub ahead of print] [11] Anderson JE, Wozniak AC. “Satellite cell activation on fibers: modeling events in vivo—an invited review.” Can J Physiol Pharmacol 2004; 82:300–10. [12] Bamman MM, Shipp JR, Jiang J, Gower BA, Hunter GR, Goodman A, McLafferty CL, Urban RJ. “Mechanical load increases muscle IGF-I and androgen receptor mRNA concentrations in humans.” Am J Physiol 2001; 280:383–90. [13] Hellsten Y, Hansson HA, Johnson L, Frandsen U, Sjodin B. “Increased expression of xanthine oxidase and insulin-like growth factor I (IGF-I) immunoreactivity in skeletal muscle after strenuous exercise in humans.” Acta Physiol Scand 1996; 157:191–97. [14] Yang SY, Goldspink G. “Different roles of the IGF-I Ec peptide (MGF) and mature IGF-I in myoblast proliferation and differentiation.” FEBS Lett 2002; 522:156–60. [15] Charifi N, Kadi F, Feasson L, Denis C. “Effects of endurance training on satellite cell frequency in skeletal muscle of old men.” Muscle Nerve 2003; 28:87–92. [16] Appell HJ, Forsberg S, Hollmann W. “Satellite cell activation in human skeletal muscle after training: evidence for muscle fiber neoformation.” Int J Sports Med 1988; 9:297–99. [17] Roth SM, Martel GF, Ivey FM, Lemmer JT, Tracy BL, Metter EJ, Hurley BF, Rogers MA. “Skeletal muscle satellite cell characteristics in young and older men and women after heavy resistance strength training.” J Gerontol A Biol Sci Med Sci 2001; 56:240–47.
Myosatellite cell
449
External links
• Image at neuro.wustl.edu (http://www.neuro.wustl.edu/neuromuscular/mother/myogenesis.html#satcell) • Overview at brown.edu (http://www.brown.edu/Courses/BI0032/adltstem/sc.htm) • NIF Search - Satellite Cell (https://www.neuinfo.org/mynif/search.php?q=Satellite Cell&t=data&s=cover& b=0&r=20) via the Neuroscience Information Framework
Cardiac muscle
450
Cardiac muscle
Cardiac muscle
Cardiac muscle
Dog Cardiac Muscle 400X Latin Code textus muscularis striatus cardiacus TH H2.00.05.2.02001
[1]
Cardiac muscle (heart muscle) is a type of involuntary striated muscle found in the walls and histological foundation of the heart, specifically the myocardium. Cardiac muscle is one of three major types of muscle, the others being skeletal and smooth muscle. The cells that comprise cardiac muscle, called cardiomyocytes or myocardiocytes, only contain one, unique nucleus.[1][2] Coordinated contractions of cardiac muscle cells in the heart propel blood out of the atria and ventricles to the blood vessels of the left/body/systemic and right/lungs/pulmonary circulatory systems. This complex of actions makes up the systole of the heart.
An isolated cardiac muscle cell, beating.
Cardiac muscle cells, like all tissues in the body, rely on an ample blood supply to deliver oxygen and nutrients and to remove waste products such as carbon dioxide. The coronary arteries fulfill this function.
Metabolism
Cardiac muscle is adapted to be highly resistant to fatigue: it has a large number of mitochondria, enabling continuous aerobic respiration via oxidative phosphorylation, numerous myoglobins (oxygen-storing pigment) and a good blood supply, which provides nutrients and oxygen. The heart is so tuned to aerobic metabolism that it is unable to pump sufficiently in ischaemic conditions. At basal metabolic rates, about 1% of energy is derived from anaerobic metabolism. This can increase to 10% under moderately hypoxic conditions, but, under more severe hypoxic conditions, not enough energy can be liberated by lactate production to sustain ventricular contractions.[3]
Cardiac muscle Under basal aerobic conditions, 60% of energy comes from fat (free fatty acids and triglycerides), 35% from carbohydrates (primarily as glucose), and 5% from amino acids and ketone bodies. However, these proportions vary widely according to nutritional state. For example, during starvation, lactate can be recycled by the heart. This is very energy efficient, because one NAD+ is reduced to NADH and H+ (equal to 2.5 or 3 ATP) when lactate is oxidized to pyruvate, which can then be burned aerobically in the TCA cycle, liberating much more energy (ca 14 ATP per cycle). In the condition of diabetes, more fat and less carbohydrate is used due to the reduced induction of GLUT4 glucose transporters to the cell surfaces. However, contraction itself plays a part in bringing GLUT4 transporters to the surface.[4] This is true of skeletal muscle as well, but relevant in particular to cardiac muscle due to its continuous contractions.
451
Appearance
Striation
Cardiac muscle exhibits cross striations formed by alternating segments of thick and thin protein filaments. Like skeletal muscle, the primary structural proteins of cardiac muscle are actin and myosin. The actin filaments are thin causing the lighter appearance of the I bands in striated muscle, while the myosin filament is thicker lending a darker appearance to the alternating A bands as observed with electron microscopy. However, in contrast to skeletal muscle, cardiac muscle cells may be branched instead of linear and longitudinal.
T-Tubules
Another histological difference between cardiac muscle and skeletal muscle is that the T-tubules in the cardiac muscle are larger, broader and run along the Z-Discs. There are fewer T-tubules in comparison with skeletal muscle. Additionally, cardiac muscle forms diads instead of the triads formed between the T-tubules and the sarcoplasmic reticulum in skeletal muscle. T-tubules play critical role in excitation-contraction coupling (ECC). Recently, the action potentials of T-tubules were recorded optically by Guixue Bu et al.[5]
Intercalated discs
Intercalated discs (IDs) are complex adhering structures which connect single cardiac myocytes to an electrochemical syncytium (in contrast to the skeletal muscle, which becomes a multicellular syncytium during mammalian embryonic development) and are mainly responsible for force transmission during muscle contraction. Intercalated discs also support the rapid spread of action potentials and the synchronized contraction of the myocardium. IDs are described to consist of three different types of cell-cell junctions: the actin filament anchoring adherens junctions (fascia adherens), the intermediate filament anchoring desmosomes (macula adherens) and gap junctions. Gap junctions are responsible for electrochemical and metabolic coupling. They allow action potentials to spread between cardiac cells by permitting the passage of ions between cells, producing depolarization of the heart muscle. However, novel molecular biological and comprehensive studies unequivocally showed that IDs consist for the most part of mixed type adhering junctions named area composita (pl. areae compositae) representing an amalgamation of typical desmosomal and fascia adhaerens proteins (in contrast to various epithelia).[6][7][8] The authors discuss the high importance of these findings for the understanding of inherited cardiomyopathies (such as Arrhythmogenic Right Ventricular Cardiomyopathy, ARVC). Under light microscopy, intercalated discs appear as thin, typically dark-staining lines dividing adjacent cardiac muscle cells. The intercalated discs run perpendicular to the direction of muscle fibers. Under electron microscopy, an intercalated disc's path appears more complex. At low magnification, this may appear as a convoluted electron dense structure overlying the location of the obscured Z-line. At high magnification, the intercalated disc's path appears even more convoluted, with both longitudinal and transverse areas appearing in longitudinal section.[9]
Cardiac muscle
452
Role of calcium in contraction
In contrast to skeletal muscle, cardiac muscle requires extracellular calcium ions for contraction to occur. Like skeletal muscle, the initiation and upshoot of the action potential in ventricular muscle cells is derived from the entry of sodium ions across the sarcolemma in a regenerative process. However, an inward flux of extracellular calcium ions through L-type calcium channels sustains the depolarization of cardiac muscle cells for a longer duration. The reason for the calcium dependence is due to the mechanism of calcium-induced calcium release (CICR) from the sarcoplasmic reticulum that must occur under normal excitation-contraction (EC) coupling to cause contraction. Once the intracellular concentration of calcium increases, calcium ions bind to the protein troponin, which initiate extracellular fluid and intracellular stores, and skeletal muscle, which is only activated by calcium stored in the sarcoplasmic reticulum.
Regeneration of heart muscle cells
Until recently, it was commonly believed that cardiac muscle cells could not be regenerated. However, a study reported in the April 3, 2009 issue of Science contradicts that belief.[10] Olaf Bergmann and his colleagues at the Karolinska Institute in Stockholm tested samples of heart muscle from people born before 1955 when nuclear bomb testing caused elevated levels of radioactive carbon 14 in the Earth's atmosphere. They found that samples from people born before 1955 did have elevated carbon 14 in their heart muscle cell DNA, indicating that the cells had divided after the person's birth. By using DNA samples from many hearts, the researchers estimated that a 20-year-old renews about 1% of heart muscle cells per year and about 45 percent of the heart muscle cells of a 50-year-old were generated after he or she was born.
References
[1] Pollard, Thomas D. and Earnshaw, William. C., "Cell Biology". Philadelphia: Saunders. 2007. [3] Ganong, Review of Medical Physiology, 22nd Edition.Specialized form of muscle that is peculiar to the vertebrate heart.p81
External links
• Indiana State University, Muscle action (http://web.indstate.edu/thcme/mwking/muscle.html) • Physiology at MCG 2/2ch7/2ch7line (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section2/2ch7/2ch7line.htm)
Purkinje fibers
453
Purkinje fibers
Purkinje fibres
Isolated Heart conduction system showing purkinje fibers
The QRS complex is the large peak.
For the nervous cells, see Purkinje cell The Purkinje fibres (Purkyne tissue or subendocardial branches) are located in the inner ventricular walls of the heart, just beneath the endocardium. These fibers consist of specialized cardiomyocytes that are able to conduct cardiac action potentials more quickly and efficiently than any other cells in the heart. Purkinje fibres allow the heart's conduction system to create synchronized contractions of its ventricles, and are therefore essential for maintaining a consistent heart rhythm.
Histology
Purkinje fibers are a unique cardiac end-organ. Further histologic examination reveals that these fibers are split in atria and ventricles walls. The electrical origin of atrial Purkinje fibres arrives from the sinoatrial node. Given no aberrant channels, the atrial and ventricular Purkinje fibres are distinctly shielded from each other by collagen or the cardiac skeleton. The Purkinje fibres are further specialized to rapidly conduct impulses (numerous fast voltage-gated sodium channels and mitochondria, fewer myofibrils than the surrounding muscle tissue). Purkinje fibres take up stain differently from the surrounding muscle cells, and, on a slide, they often appear lighter and larger than their neighbors. They are binucleated.
Purkinje fibers
454
Function
Heart rate is governed by many influences from the Autonomic Nervous System. The Purkinje Fibers do not have any known role in setting heart rate, but are influenced by electrical discharge from the Sinoatrial node. During the ventricular contraction portion of the cardiac cycle, the Purkinje fibres carry the contraction impulse from both the left and right bundle branch to the myocardium of the ventricles. This causes the muscle tissue of the ventricles to contract, thus enabling a force to eject blood out of the heart; either to the Pulmonary circulation from the right ventricle or to the Systemic circulation from the left ventricle. Purkinje fibers also have the ability of automaticity,[1] firing at a rate of 15-40 beats per minute if left to their own devices. In contrast, the SA node in normal state can fire at 60-100 beats per minute. - in short, they generate action potentials, but at a slower rate than sinoatrial node. Thus they serve as the last resort when other pacemakers fail. When a Purkinje fibre does fire, it is called a premature ventricular contraction or PVC, or in other situations can be a ventricular escape. It plays a vital role in the circulatory system.
Etymology
They were discovered in 1839 by Jan Evangelista Purkyně, who gave them his name.
References
[1] [biomed.engr.sc.edu/bme_lab/lab%20reports/36)%20ECG%20I.pdf ]
External links
• subendocardial+branches+of+atrioventricular+bundles (http://www.emedicinehealth.com/script/main/ srchcont_dict.asp?src=subendocardial+branches+of+atrioventricular+bundles) at eMedicine Dictionary • Organology at UC Davis Circulatory/heart/purkinje/purkinje1 (http://trc.ucdavis.edu/mjguinan/apc100/ modules/Circulatory/heart/purkinje/purkinje1.html) - "Mammal heart, purkinje fibers (LM, Medium)" • Anatomy Atlases - Microscopic Anatomy, plate 05.78 (http://www.anatomyatlases.org/MicroscopicAnatomy/ Section05/Plate0578.shtml) • MedEd at Loyola Histo/practical/cardio/hp8-21.html (http://www.meddean.luc.edu/Lumen/MedEd/Histo/ practical/cardio/hp8-21.html) • Histology at ucsd.edu (http://meded.ucsd.edu/hist-img-bank/chapter_3/Slides_43_44_45_cardiac/pages/d.2. 44.1.2.htm) • Histology at nhmccd.edu (http://science.nhmccd.edu/Biol/cardio/purkinje.htm)
Smooth muscle tissue
455
Smooth muscle tissue
Smooth muscle tissue
Smooth muscle
Layers of Esophageal Wall: 1. Mucosa 2. Submucosa 3. Muscularis 4. Adventitia 5. Striated muscle 6. Striated and smooth 7. Smooth muscle 8. Lamina muscularis mucosae 9. Esophageal glands Latin textus muscularis levis; textus muscularis nonstriatus Code TH H2.00.05.1.00001 [1]
Smooth muscle is an involuntary non-striated muscle. It is divided into two sub-groups; the single-unit (unitary) and multiunit smooth muscle. Within single-unit smooth muscle tissues, the autonomic nervous system innervates a single cell within a sheet or bundle and the action potential is propagated by gap junctions to neighboring cells such that the whole bundle or sheet contracts as a syncytium (i.e., a multinucleate mass of cytoplasm that is not separated into cells). Multiunit smooth muscle tissues innervate individual cells; as such, they allow for fine control and gradual responses, much like motor unit recruitment in skeletal muscle. Smooth muscle is found within the walls of blood vessels (such smooth muscle specifically being termed vascular smooth muscle) such as in the tunica media layer of large (aorta) and small arteries, arterioles and veins. Smooth muscle is also found in lymphatic vessels, the urinary bladder, uterus (termed uterine smooth muscle), male and female reproductive tracts, gastrointestinal tract, respiratory tract, arrector pili of skin, the ciliary muscle, and iris of the eye. The structure and function is basically the same in smooth muscle cells in different organs, but the inducing stimuli differ substantially, in order to perform individual effects in the body at individual times. In addition, the
Smooth muscle tissue glomeruli of the kidneys contain smooth muscle-like cells called mesangial cells.
456
Structure
Most smooth muscle is of the single-unit variety, that is, either the whole muscle contracts or the whole muscle relaxes, but there is multiunit smooth muscle in the trachea, the large elastic arteries, and the iris of the eye. Single unit smooth muscle, however, is most common and lines blood vessels (except large elastic arteries), the urinary tract, and the digestive tract. Smooth muscle is fundamentally different from skeletal muscle and cardiac muscle in terms of structure, function, regulation of contraction, and excitation-contraction coupling. Smooth muscle fibers have a fusiform shape and, like striated muscle, can tense and relax. However, smooth muscle containing tissue tend to demonstrate greater elasticity and function within a larger length-tension curve than striated muscle. This ability to stretch and still maintain contractility is important in organs like the intestines and urinary bladder. In the relaxed state, each cell is spindle-shaped, 20-500 micrometers in length.
Molecular structure
A substantial portion of the volume of the cytoplasm of smooth muscle cells are taken up by the molecules myosin and actin,[1] which together have the capability to contract, and, through a chain of tensile structures, make the entire smooth muscle tissue contract with them. Myosin Myosin is primarily of class II in smooth muscle.[] • Myosin II contains two heavy chains which constitute the head and tail domains. Each of these heavy chains contains the N-terminal head domain, while the C-terminal tails take on a coiled-coil morphology, holding the two heavy chains together (imagine two snakes wrapped around each other, such as in a caduceus). Thus, myosin II has two heads. In smooth muscle, there is a single gene (MYH11[2]) that codes for the heavy chains myosin II, but there are splice variants of this gene that result in four distinct isoforms.[] Also, smooth muscle may contain MHC that is not involved in contraction, and that can arise from multiple genes.[] • Myosin II also contains 4 light chains, resulting in 2 per head, weighing 20 (MLC20) and 17 (MLC17) kDa.[] These bind the heavy chains in the "neck" region between the head and tail. • The MLC20 is also known as the regulatory light chain and actively participates in muscle contraction.[] Two MLC20 isoforms are found in smooth muscle, and they are encoded by different genes, but only one isoform participates in contractility.[] • The MLC17 is also known as the essential light chain.[] Its exact function is unclear, but it's believed that it contributes to the structural stability of the myosin head along with MLC20.[] Two variants of MLC17 (MLC17a/b) exist as a result of alternate splicing at the MLC17 gene.[] Different combinations of heavy and light chains allow for up to hundreds of different types of myosin structures, but it is unlikely that more than a few such combinations are actually used or permitted within a specific smooth muscle bed.[] In the uterus, a shift in myosin expression has been hypothesized to avail for changes in the directions
Smooth muscle tissue of uterine contractions that are seen during the menstrual cycle.[] Actin The thin filaments that form part of the contractile machinery are predominantly composed of α- and γ-actin.[] Smooth muscle α-actin (alpha actin) is the predominate isoform within smooth muscle. There are also lots of actin (mainly β-actin) that does not take part in contraction, but that polymerizes just below the plasma membrane in the presence of a contractile stimulant and may thereby assist in mechanical tension.[] Alpha actin is also expressed as distinct genetic isoforms such there is smooth muscle, cardiac muscle and skeletal muscle specific isoforms of alpha actin. (ref The actin gene family: function follows isoform.Perrin BJ, Ervasti JM.Cytoskeleton (Hoboken). 2010 Oct;67(10):630-4. Review.) The ratio of actin to myosin is between 2:1[] and 10:1[] in smooth muscle, compared to ~6:1 in skeletal muscle and 4:1 in cardiac muscle. Other proteins of the contractile apparatus Smooth muscle does not contain the protein troponin; instead calmodulin (which takes on the regulatory role in smooth muscle), caldesmon and calponin are significant proteins expressed within smooth muscle. • Tropomyosin is present in smooth muscle, spanning seven actin monomers and is laid out end to end over the entire length of the thin filaments. In striated muscle, tropomyosin serves to enhance actin–myosin interactions, but in smooth muscle, its function is unknown.[] • Calponin molecules may exist in equal number as actin, and has been proposed to be a load-bearing protein.[] • Caldesmon has been suggested to be involved in tethering actin, myosin and tropomyosin, and thereby enhance the ability of smooth muscle to maintain tension.[] Also, all three of these proteins may have a role in inhibiting the ATPase activity of the myosin complex that otherwise provides energy to fuel muscle contraction.[] Other tensile structures The myosin and actin are the contractile parts of continuous chains of tensile structures that stretch both across and between smooth muscle cells. The actin filaments of contractile units are attached to dense bodies. Dense bodies are rich in α-actinin,[] and also attach intermediate filaments (consisting largely of vimentin and desmin), and thereby appear to serve as anchors from which the thin filaments can exert force.[] Dense bodies also are associated with β-actin, which is the type found in the cytoskeleton, suggesting that dense bodies may coordinate tensions from both the contractile machinery and the cytoskeleton.[] The intermediate filaments are connected to other intermediate filaments via dense bodies, which eventually are attached to adherens junctions (also called focal adhesions) in the cell membrane of the smooth muscle cell, called the sarcolemma. The adherens junctions consist of large number of proteins including α-actinin, vinculin and cytoskeletal actin.[] The adherens junctions are scattered around dense bands that are circumfering the smooth muscle cell in a rib-like pattern.[1] The dense band (or dense plaques) areas alternate with regions of membrane containing numerous caveolae. When complexes of actin and myosin contract, force is transduced to the sarcolemma through intermediate filaments attaching to such dense bands. During contraction, there is a spatial reorganization of the contractile machinery to optimize force development.[] part of this reorganization consists of vimentin being phosphorylated at Ser56 by a p21 activated kinase, resulting in some disassembly of vimentin polymers.[] Also, the number of myosin filaments is dynamic between the relaxed and contracted state in some tissues as the ratio of actin to myosin changes, and the length and number of myosin filaments change.
457
Smooth muscle tissue Smooth muscle cells have been observed contracting in a spiral corkscrew fashion, and contractile proteins have been observed organizing into zones of actin and myosin along the axis of the cell. Smooth muscle-containing tissue needs to be stretched often, so elasticity is an important attribute of smooth muscle. Smooth muscle cells may secrete a complex extracellular matrix containing collagen (predominantly types I and III), elastin, glycoproteins, and proteoglycans. Smooth muscle also has specific elastin and collagen receptors to interact with these proteins of the extracellular matrix. These fibers with their extracellular matrices contribute to the viscoelasticity of these tissues. For example, the great arteries are viscolelastic vessels that act like a Windkessel, propagating ventricular contraction and smoothing out the pulsatile flow, and the smooth muscle within the tunica media contributes to this property. Caveolae The sarcolemma also contains caveolae, which are microdomains of lipid rafts specialized to cell-signaling events and ion channels. These invaginations in the sarcoplasma contain a host of receptors (prostacyclin, endothelin, serotonin, muscarinic receptors, adrenergic receptors), second messenger generators (adenylate cyclase, Phospholipase C), G proteins (RhoA, G alpha), kinases (rho kinase-ROCK, Protein kinase C, Protein Kinase A), ion channels (L type Calcium channels, ATP sensitive Potassium channels, Calcium sensitive Potassium channels) in close proximity. The caveolae are often close to sarcoplasmic reticulum or mitochondria, and have been proposed to organize signaling molecules in the membrane.
458
Excitation-contraction coupling
A smooth muscle is excited by external stimuli, which causes contraction. Each step is further detailed below.
Inducing stimuli and factors
Smooth muscle may contract spontaneously (via ionic channel dynamics) or as in the gut special pacemakers cells interstitial cells of Cajal produce rhythmic contractions. Also, contraction, as well as relaxation, can be induced by a number of physiochemical agents (e.g., hormones, drugs, neurotransmitters - particularly from the autonomic nervous system). Smooth muscle in various regions of the vascular tree, the airway and lungs, kidneys and vagina is different in their expression of ionic channels, hormone receptors, cell-signaling pathways, and other proteins that determine function. External substances For instance, most blood vessels respond to norepinephrine and epinephrine (from sympathetic stimulation or the adrenal medulla) by producing vasoconstriction (this response is mediated through alpha 1-adrenergic receptors). Blood vessels in skeletal muscle and cardiac muscle respond to these catecholamines producing vasodilation because the smooth muscle possess beta-adrenergic receptors. Generally, arterial smooth muscle responds to carbon dioxide by producing vasodilation, and responds to oxygen by producing vasoconstriction. Pulmonary blood vessels within the lung are unique as they vasodilate to high oxygen tension and vasoconstrict when it falls. Bronchiole, smooth muscle that line the airways of the lung, respond to high carbon dioxide producing vasodilation and vasoconstrict when carbon dioxide is low. These responses to carbon dioxide and oxygen by pulmonary blood vessels and bronchiole airway smooth muscle aid in matching perfusion and ventilation within the lungs. Further different smooth muscle tissues display extremes of abundant to little sarcoplasmic reticulum so excitation-contraction coupling varies with its dependence on intracellular or extracellular calcium. Recent research indicates that sphingosine-1-phosphate (S1P) signaling is an important regulator of vascular smooth muscle contraction. When transmural pressure increases, sphingosine kinase 1 phosphorylates sphingosine to S1P, which binds to the S1P2 receptor in plasma membrane of cells. This leads to a transient increase in intracellular
Smooth muscle tissue calcium, and activates Rac and Rhoa signaling pathways. Collectively, these serve to increase MLCK activity and decrease MLCP activity, promoting muscle contraction. This allows arterioles to increase resistance in response to increased blood pressure and thus maintain constant blood flow. The Rhoa and Rac portion of the signaling pathway provides a calcium-independent way to regulate resistance artery tone.[3]
459
Spread of impulse
To maintain organ dimensions against force, cells are fastened to one another by adherens junctions. As a consequence, cells are mechanically coupled to one another such that contraction of one cell invokes some degree of contraction in an adjoining cell. Gap junctions couple adjacent cells chemically and electrically, facilitating the spread of chemicals (e.g., calcium) or action potentials between smooth muscle cells. Single unit smooth muscle displays numerous gap junctions and these tissues often organize into sheets or bundles which contract in bulk.
Contraction
Smooth muscle contraction is caused by the sliding of myosin and actin filaments (a sliding filament mechanism) over each other. The energy for this to happen is provided by the hydrolysis of ATP. Myosin functions as an ATPase utilizing ATP to produce a molecular conformational change of part of the myosin and produces movement. Movement of the filaments over each other happens when the globular heads protruding from myosin filaments attach and interact with actin filaments to form crossbridges. The myosin heads tilt and drag along the actin filament a small distance (10-12 nm). The heads then release the actin filament and then changes angle to relocate to another site on the actin filament a further distance (10-12 nm) away. They can then re-bind to the actin molecule and drag it along further. This process is called crossbridge cycling and is the same for all muscles (see muscle contraction). Unlike cardiac and skeletal muscle, smooth muscle does not contain the calcium-binding protein troponin. Contraction is initiated by a calcium-regulated phosphorylation of myosin, rather than a calcium-activated troponin system. Crossbridge cycling causes contraction of myosin and actin complexes, in turn causing increased tension along the entire chains of tensile structures, ultimately resulting in contraction of the entire smooth muscle tissue. Phasic or tonic Smooth muscle may contract phasically with rapid contraction and relaxation, or tonically with slow and sustained contraction. The reproductive, digestive, respiratory, and urinary tracts, skin, eye, and vasculature all contain this tonic muscle type. This type of smooth muscle can maintain force for prolonged time with only little energy utilization. There are differences in the myosin heavy and light chains that also correlate with these differences in contractile patterns and kinetics of contraction between tonic and phasic smooth muscle. Activation of myosin heads Crossbridge cycling cannot occur until the myosin heads have been activated to allow crossbridges to form. When the light chains are phosphorylated, they become active and will allow contraction to occur. The enzyme that phosphorylates the light chains is called myosin light-chain kinase (MLCK), also called MLC20 kinase.[] In order to control contraction, MLCK will work only when the muscle is stimulated to contract. Stimulation will increase the intracellular concentration of calcium ions. These bind to a molecule called calmodulin, and form a calcium-calmodulin complex. It is this complex that will bind to MLCK to activate it, allowing the chain of reactions for contraction to occur. Activation consists of phosphorylation of a serine on position 19 (Ser19) on the MLC20 light chain, which causes a conformational change that increases the angle in the neck domain of the myosin heavy chain,[] which corresponds to the part of the cross-bridge cycle where the myosin head is unattached to the actin filament and relocates to another site on it. After attachment of the myosin head to the actin filament, this serine phosphorylation also activates the
Smooth muscle tissue ATPase activity of the myosin head region to provide the energy to fuel the subsequent contraction.[] Phosphorylation of a threonine on position 18 (Thr18) on MLC20 is also possible and may further increase the ATPase activity of the myosin complex.[] Sustained maintenance Phosphorylation of the MLC20 myosin light chains correlates well with the shortening velocity of smooth muscle. During this period there is a rapid burst of energy utilization as measured by oxygen consumption. Within a few minutes of initiation the calcium level markedly decrease, MLC20 myosin light chains phosphorylation decreases, and energy utilization decreases and the muscle can relax. Still, smooth muscle has the ability of sustained maintenance of force in this situation as well. This sustained phase has been attributed to certain myosin crossbridges, termed latch-bridges, that are cycling very slowly, notably slowing the progression to the cycle stage whereby dephosphorylated myosin detaches from the actin, thereby maintaining the force at low energy costs.[] This phenomenon is of great value especially for tonically active smooth muscle.[] Isolated preparations of vascular and visceral smooth muscle contract with depolarizing high potassium balanced saline generating a certain amount of contractile force. The same preparation stimulated in normal balanced saline with an agonist such as endothelin or serotonin will generate more contractile force. This increase in force is termed calcium sensitization. The myosin light chain phosphatase is inhibited to increase the gain or sensitivity of myosin light chain kinase to calcium. There are number of cell signalling pathways believed to regulate this decrease in myosin light chain phosphatase: a RhoA-Rock kinase pathway, a Protein kinase C-Protein kinase C potentiation inhibitor protein 17 (CPI-17) pathway, telokin, and a Zip kinase pathway. Further Rock kinase and Zip kinase have been implicated to directly phosphorylate the 20kd myosin light chains. Other contractile mechanisms Other cell signaling pathways and protein kinases (Protein kinase C, Rho kinase, Zip kinase, Focal adhesion kinases) have been implicated as well and actin polymerization dynamics plays a role in force maintenance. While myosin light chain phosphorylation correlates well with shortening velocity, other cell signaling pathways have been implicated in the development of force and maintenance of force. Notably the phosphorylation of specific tyrosine residues on the focal adhesion adapter protein-paxillin by specific tyrosine kinases has been demonstrated to be essential to force development and maintenance. For example, cyclic nucleotides can relax arterial smooth muscle without reductions in crossbridge phosphorylation, a process termed force suppression. This process is mediated by the phosphorylation of the small heat shock protein, hsp20, and may prevent phosphorylated myosin heads from interacting with actin.
460
Relaxation
The phosphorylation of the light chains by MLCK is countered by a myosin light-chain phosphatase, which dephosphorylates the MLC20 myosin light chains and thereby inhibits contraction.[] Other signaling pathways have also been implicated in the regulation actin and myosin dynamics. In general, the relaxation of smooth muscle is by cell-signaling pathways that increase the myosin phosphatase activity, decrease the intracellular calcium levels, hyperpolarize the smooth muscle, and/or regulate actin and myosin dynamics. Relaxation-inducing factors The relaxation of smooth muscle can be mediated by the endothelium-derived relaxing factor-nitric oxide, endothelial derived hyperpolarizing factor (either an endogenous cannabinoid, cytochrome P450 metabolite, or hydrogen peroxide), or prostacyclin (PGI2). Nitric oxide and PGI2 stimulate soluble guanylate cyclase and membrane bound adenylate cyclase, respectively. The cyclic nucleotides (cGMP and cAMP) produced by these cyclases activate Protein Kinase G and Proten Kinase A and phosphorylate a number of proteins. The phosphorylation events lead to a decrease in intracelluar calcium (inhibit L type Calcium channels, inhibits IP3
Smooth muscle tissue receptor channels, stimulates sarcoplasmic reticulum Calcium pump ATPase), a decrease in the 20kd myosin light chain phosphorylation by altering calcium sensitization and increasing myosin light chain phosphatase activity, a stimulation of calcium sensitive potassium channels which hyperpolarize the cell, and the phosphorylation of amino acid residue serine 16 on the small heat shock protein (hsp20)by Protein Kinases A and G. The phosphorylation of hsp20 appears to alter actin and focal adhesion dynamics and actin-myosin interaction, and recent evidence indicates that hsp20 binding to 14-3-3 protein is involved in this process. An alternative hypothesis is that phosphorylated Hsp20 may also alter the affinity of phosphorylated myosin with actin and inhibit contractility by interfering with crossbridge formation. The endothelium derived hyperpolarizing factor stimulates calcium sensitive potassium channels and/or ATP sensitive potassium channels and stimulate potassium efflux which hyperpolarizes the cell and produces relaxation.
461
Invertebrate smooth muscle
In invertebrate smooth muscle, contraction is initiated with the binding of calcium directly to myosin and then rapidly cycling cross-bridges, generating force. Similar to the mechanism of vertebrate smooth muscle, there is a low calcium and low energy utilization catch phase. This sustained phase or catch phase has been attributed to a catch protein that has similarities to myosin light-chain kinase and the elastic protein-titin called twitchin. Clams and other bivalve mollusks use this catch phase of smooth muscle to keep their shell closed for prolonged periods with little energy usage.
Specific effects
Although the structure and function is basically the same in smooth muscle cells in different organs, their specific effects or end-functions differ. Smooth muscle forms precapillary sphincters in blood vessels in metarterioles which regulates the blood flow in capillary beds of various organs and tissues. The contractile function of vascular smooth muscle also regulates the lumenal diameter of the small arteries-arterioles called resistance vessels, thereby contributing significantly to setting the level of blood pressure. Smooth muscle contracts slowly and may maintain the contraction (tonically) for prolonged periods in blood vessels, bronchioles, and some sphincters. Activating arteriole smooth muscle can decrease the lumenal diameter 1/3 of resting so it drastically alters blood flow and resistance. Activation of aortic smooth muscle doesn't significantly alter the lumenal diameter but serves to increase the viscoelasticity of the vascular wall. In the digestive tract, smooth muscle contracts in a rhythmic peristaltic fashion, rhythmically forcing foodstuffs through the digestive tract as the result of phasic contraction. A non-contractile function is seen in specialized smooth muscle within the afferent arteriole of the juxtaglomerular apparatus, which secretes renin in response to osmotic and pressure changes, and also it is believed to secrete ATP in tubuloglomerular regulation of glomerular filtration rate. Renin in turn activates the renin-angiotensin system to regulate blood pressure.
Smooth muscle tissue
462
Growth and rearrangement
The mechanism in which external factors stimulate growth and rearrangement is not yet fully understood. A number of growth factors and neurohumoral agents influence smooth muscle growth and differentiation. The Notch receptor and cell-signaling pathway have been demonstrated to be essential to vasculogenesis and the formation of arteries and veins. The proliferation is implicated in the pathogenesis of atherosclerosis and is inhibited by nitric oxide. The embryological origin of smooth muscle is usually of mesodermal origin. However, the smooth muscle within the Aorta and Pulmonary arteries (the Great Arteries of the heart) is derived from ectomesenchyme of neural crest origin, although coronary artery smooth muscle is of mesodermal origin.
Related diseases
"Smooth muscle condition" is a condition in which the body of a developing embryo does not create enough smooth muscle for the gastrointestinal system. This condition is fatal. Anti-smooth muscle antibodies (ASMA) can be a symptom of an auto-immune disorder, such as hepatitis, cirrhosis, or lupus. Vascular smooth muscle tumors are very rare. They can be malignant or benign, and morbidity can be significant with either type. Intravascular leiomyomatosis is a benign neoplasm that extends through the veins; angioleiomyoma is a benign neoplasm of the extremities; vascular leiomyosarcomas is a malignant neoplasm that can be found in the inferior vena cava, pulmonary arteries and veins, and other peripheral vessels. See Atherosclerosis.
References
[1] Page 174 (http:/ / books. google. com/ books?id=iOEQWGfiurYC& pg=PA175& lpg=PA174) in: The vascular smooth muscle cell: molecular and biological responses to the extracellular matrix. Authors: Stephen M. Schwartz, Robert P. Mecham. Editors: Stephen M. Schwartz, Robert P. Mecham. Contributors: Stephen M. Schwartz, Robert P. Mecham. Publisher: Academic Press, 1995. ISBN 0-12-632310-0, ISBN 978-0-12-632310-8 [3] Scherer EQ et al. Sphingosine-1-phosphate modulates spiral modiolar artery tone: A potential role in vascular-based inner ear pathologies? Cardiovasc Res. 2006 Apr 1;70(1):79–87.
External links
• BBC (http://news.bbc.co.uk/2/hi/health/3549285.stm) - baby born with smooth muscle condition has 8 organs transplanted • Smooth muscle antibody (http://www.ii.bham.ac.uk/clinicalimmunology/CISimagelibrary/smoothmuscle. htm) • Stomach smooth muscle identified using antibody (http://www.antibodypatterns.com/smoothmuscle.php) • UIUC Histology Subject 265 (https://histo.life.illinois.edu/histo/atlas/oimages.php?oid=265) • Histology at KUMC muscular-muscle08 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/ muscular/muscle08.htm) "Smooth Muscle" • BU Histology Learning System: 21701ooa (http://www.bu.edu/histology/p/21701ooa.htm)
Myoepithelial cell
463
Myoepithelial cell
Myoepithelial cell
Latin myoepitheliocytus Code TH H2.00.02.0.03059 [1]
Myoepithelial cells (sometimes referred to as myoepithelium) are cells usually found in glandular epithelium as a thin layer above the basement membrane but generally beneath the luminal cells. These may be positive for alpha smooth muscle actin and can contract and expel the secretions of exocrine glands. They are found in the sweat glands, mammary glands, lacrimal glands, and salivary glands. Myoepithelial cells in these cases constitute the basal cell layer of an epithelium that harbors the epithelial progenitor. In the case of wound healing, myoepithelial cells reactively proliferate. Presence of myoepithelial cells in a hyperplastic tissue proves the benignity of the gland and, when absent, indicates cancer. Only rare cancers like adenoid cystic carcinomas contains myoepithelial cells as one of the malignant components. It can be found in endoderm or ectoderm.[]
Markers
Myoepithelial cells are true epithelial cells positive for keratins, not to be confused with myofibroblasts which are true mesenchymal cells positive for vimentin. These cells are generally positive for alpha smooth muscle actin (αSMA), cytokeratin 5/6 and other high molecular weight cytokeratins, p63 and caldesmon. Myoepithelial cells are stellate in shape an are also known as basket cells. They lie between the basement membrane and glandular epithelium. Each cell consists of a cell body from which 4-8 processes radiate and embrace the secretory unit. Myoepithelial cells have contractile functions. They help in expelling secretions from the lumen of secretory units and facilitate the movement of saliva in salivary ducts.
References External links
• Myoepithelium (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=Myoepithelium) at eMedicine Dictionary • Anatomy Atlases - Microscopic Anatomy, plate 07.141 (http://www.anatomyatlases.org/MicroscopicAnatomy/ Section07/Plate07141.shtml) - "Axillary Sweat Gland: Myoepithelium" • Histology at OU 43_13 (http://w3.ouhsc.edu/histology/Glass slides/43_13.jpg) - "thick skin" • Histology at KUMC glands-glands09 (http://www.kumc.edu/instruction/medicine/anatomy/histoweb/ glands/glands09.htm) "Simple Tubular Coiled" • Physiology at MCG 6/6ch4/s6ch4_4 (http://web.archive.org/web/20080401093403/http://www.lib.mcg. edu/edu/eshuphysio/program/section6/6ch4/s6ch4_4.htm)
Red blood cell
464
Red blood cell
Red blood cells, or erythrocytes, are the most common type of blood cell and the vertebrate organism's principal means of delivering oxygen (O2) to the body tissues via the blood flow through the circulatory system.[1] They take up oxygen in the lungs or gills and release it while squeezing through the body's capillaries. These cells' cytoplasm is rich in haemoglobin, an iron-containing biomolecule that can bind oxygen and is responsible for the blood's red color. In humans, mature red blood cells are oval and flexible biconcave disks. They lack a cell nucleus and most organelles to accommodate maximum space for haemoglobin. 2.4 million new erythrocytes are produced per second.[2] The cells develop in the bone marrow and circulate for about 100–120 days in the body before their components are recycled by macrophages. Each circulation takes about 20 seconds. Approximately a quarter of the cells in the human body are red blood cells.[3][]
Scanning electron micrograph of human red blood cells (size approximately 6-8 μm; artificial colors)
Red blood cells are also known as RBCs, red cells,[4] red blood corpuscles (an archaic term), haematids, erythroid cells or erythrocytes (from Greek erythros for "red" and kytos for "hollow vessel", with -cyte translated as "cell" in modern usage).
History
The first person to describe red blood cells was the young Dutch biologist Jan Swammerdam, who had used an early microscope in 1658 to study the blood of a frog.[5] Unaware of this work, Anton van Leeuwenhoek provided another microscopic description in 1674, this time providing a more precise description of red blood cells, even approximating their size, "25,000 times smaller than a fine grain of sand". In 1901, Karl Landsteiner published his discovery of the three main blood groups—A, B, and C (which he later renamed to O). Landsteiner described the regular patterns in which reactions occurred when serum was mixed with red blood cells, thus identifying compatible and conflicting combinations between these blood groups. A year later Alfred von Decastello and Adriano Sturli, two colleagues of Landsteiner, identified a fourth blood group—AB. In 1959, by use of X-ray crystallography, Dr. Max Perutz was able to unravel the structure of hemoglobin, the red blood cell protein that carries oxygen.[6] The oldest intact red blood cells ever discovered were found in Ötzi the Iceman, a natural mummy of a man who died around 3255 BCE. These cells were discovered in May 2012.[7]
Red blood cell
465
Vertebrate erythrocytes
Erythrocytes consist mainly of hemoglobin, a complex metalloprotein containing heme groups whose iron atoms temporarily bind to oxygen molecules (O2) in the lungs or gills and release them throughout the body. Oxygen can easily diffuse through the red blood cell's cell membrane. Hemoglobin in the erythrocytes also carries some of the waste product carbon dioxide back from the tissues; most waste carbon dioxide, however, is transported back to the pulmonary capillaries of the lungs as bicarbonate (HCO3-) dissolved in the blood plasma. Myoglobin, a compound related to hemoglobin, acts to store oxygen in muscle cells.[8] The color of erythrocytes is due to the heme group of hemoglobin. The blood plasma alone is straw-colored, but the red blood cells change color depending on the state of the hemoglobin: when combined with oxygen the resulting oxyhemoglobin is scarlet, and when oxygen has been released the resulting deoxyhemoglobin is of a dark red burgundy color, appearing bluish through the vessel wall and skin. Pulse oximetry takes advantage of this color change to directly measure the arterial blood oxygen saturation using colorimetric techniques. The sequestration of oxygen-carrying proteins inside specialized There is an immense size variation in vertebrate cells (rather than having them dissolved in body fluid) was an erythrocytes, as well as a correlation between cell and important step in the evolution of vertebrates as it allows for less nucleus size. Mammalian erythrocytes, which do not viscous blood, higher concentrations of oxygen, and better contain nuclei, are considerably smaller than those of [] most other vertebrates. diffusion of oxygen from the blood to the tissues. The size of erythrocytes varies widely among vertebrate species; erythrocyte width is on average about 25% larger than capillary diameter, and it has been hypothesized that this improves the oxygen transfer from erythrocytes to tissues.[] The only known vertebrates without erythrocytes are the crocodile icefishes (family Channichthyidae); they live in very oxygen-rich cold water and transport oxygen freely dissolved in their blood.[9] While they do not use hemoglobin anymore, remnants of hemoglobin genes can be found in their genome.[10]
Nucleus
Erythrocytes in mammals are anucleate when mature, meaning that they lack a cell nucleus. In comparison, the erythrocytes of other vertebrates have nuclei; the only known exceptions are salamanders of the Batrachoseps genus and fish of the Maurolicus genus with closely related species.[11][12]
Secondary functions
When erythrocytes undergo shear stress in constricted vessels, they release ATP, which causes the vessel walls to relax and dilate so as to promote normal blood flow.[13] When their hemoglobin molecules are deoxygenated, erythrocytes release S-nitrosothiols, which also acts to dilate vessels,[14] thus directing more blood to areas of the body depleted of oxygen.
Red blood cell It has been recently demonstrated that erythrocytes can also synthesize nitric oxide enzymatically, using L-arginine as substrate, just like endothelial cells.[15] Exposure of erythrocytes to physiological levels of shear stress activates nitric oxide synthase and export of nitric oxide,[16] which may contribute to the regulation of vascular tonus. Erythrocytes can also produce hydrogen sulfide, a signalling gas that acts to relax vessel walls. It is believed that the cardioprotective effects of garlic are due to erythrocytes converting its sulfur compounds into hydrogen sulfide.[17] Erythrocytes also play a part in the body's immune response: when lysed by pathogens such as bacteria, their hemoglobin releases free radicals, which break down the pathogen's cell wall and membrane, killing it.[18][19]
466
Mammalian erythrocytes
Mammalian erythrocytes are unique among the vertebrates as they are non-nucleated cells in their mature form. These cells have nuclei during early phases of erythropoiesis, but extrude them during development as they mature in order to provide more space for hemoglobin. In mammals, erythrocytes also lose all other cellular organelles such as their mitochondria, Golgi apparatus and endoplasmic reticulum. As a result of not containing mitochondria, these cells use none of the oxygen they transport; instead they produce the energy carrier ATP by the glycolysis of glucose and lactic acid fermentation on the resulting pyruvate.
Typical mammalian erythrocytes: (a) seen from surface; (b) in profile, forming rouleaux; (c) rendered spherical by water; (d) rendered crenate by salt. (c) and (d) do not normally occur in the body.
Because of the lack of nuclei and organelles, mature red blood cells do not contain DNA and cannot synthesize any RNA, and consequently cannot divide and have limited repair capabilities.[] This also ensures that no virus can evolve to target mammalian red blood cells.[20] Mammalian erythrocytes are typically shaped as biconcave disks: flattened and depressed in the center, with a dumbbell-shaped cross section, and a torus-shaped rim on the edge of the disk. This distinctive biconcave shape optimises the flow properties of blood in the large vessels, such as maximization of laminar flow and minimization of platelet scatter, which suppresses their atherogenic activity in those large vessels.[21] However, there are some exceptions concerning shape in the artiodactyl order (even-toed ungulates including cattle, deer, and their relatives), which displays a wide variety of bizarre erythrocyte morphologies: small and highly ovaloid cells in llamas and camels (family Camelidae), tiny spherical cells in mouse deer (family Tragulidae), and cells which assume fusiform, lanceolate, crescentic, and irregularly polygonal and other angular forms in red deer and wapiti (family Cervidae). Members of this order have clearly evolved a mode of red blood cell development substantially different from the mammalian norm.[][22] Overall, mammalian erythrocytes are remarkably flexible and deformable so as to squeeze through tiny capillaries, as well as to maximize their apposing surface by assuming a cigar shape, where they efficiently release their oxygen load.[23] In large blood vessels, red blood cells sometimes occur as a stack, flat side next to flat side. This is known as rouleaux formation, and it occurs more often if the levels of certain serum proteins are elevated, as for instance during inflammation. The spleen acts as a reservoir of red blood cells, but this effect is somewhat limited in humans. In some other mammals such as dogs and horses, the spleen sequesters large numbers of red blood cells which are dumped into the
Red blood cell blood during times of exertion stress, yielding a higher oxygen transport capacity.
467
Scanning electron micrograph of blood cells. From left to right: human erythrocyte, thrombocyte (platelet), leukocyte.
Human erythrocytes
A typical human erythrocyte has a disk diameter of approximately 6.2-8.2 µm[24] and a thickness at the thickest point of 2-2.5 µm and a minimum thickness in the centre of 0.8-1 µm, being much smaller than most other human cells. These cells have an average volume of about 90 fL[25] with a surface of about 136 μm2, and can swell up to a sphere shape containing 150 fL, without membrane distension. Adult humans have roughly 2–3 × 1013 (20-30 trillion) red blood cells at any given time, comprising approximately one quarter of the total human body cell number (women have about 4 to 5 million erythrocytes per microliter (cubic millimeter) of blood and men about 5 to 6 million; people living at high altitudes with low oxygen tension will have more). Red blood cells are thus much more common than the other blood particles: there are about 4,000–11,000 white blood cells and about 150,000–400,000 platelets in each microliter of human blood. Human red blood cells take on average 20 seconds to complete one cycle of circulation.[3][][26] As red blood cells contain no nucleus, protein biosynthesis is currently assumed to be absent in these cells, although a recent study indicates the presence of all the necessary biomachinery in the cells to do so.[]
Two drops of blood are shown with a bright red oxygenated drop on the left and a deoxygenated drop on the right.
The blood's red color is due to the spectral properties of the hemic iron ions in hemoglobin. Each human red blood cell contains approximately 270 million of these hemoglobin biomolecules, each carrying four heme groups; hemoglobin comprises about a third of the total cell volume. This protein is responsible for the transport of more than 98% of the oxygen (the remaining oxygen is carried dissolved in the blood plasma). The red blood cells of an average adult human male store collectively about 2.5 grams of iron, representing about 65% of the total iron contained in the body.[27][28] (See Human iron metabolism.)
An animation of a typical human red blood cell cycle in the circulatory system. This animation occurs at real time (20 seconds of cycle) and shows the red blood cell deform as it enters capillaries, as well as changing color as it alternates in states of oxygenation along the circulatory system.
Red blood cell
468
Life cycle
Human erythrocytes are produced through a process named erythropoiesis, developing from committed stem cells to mature erythrocytes in about 7 days. When matured, these cells live in blood circulation for about 100 to 120 days (and 80 to 90 days in a full term infant).[29] At the end of their lifespan, they become senescent, and are removed from circulation. Erythropoiesis Erythropoiesis is the development process by which new erythrocytes are produced; it lasts about 7 days. Through this process erythrocytes are continuously produced in the red bone marrow of large bones, at a rate of about 2 million per second in a healthy adult. (In the embryo, the liver is the main site of red blood cell production.) The production can be stimulated by the hormone erythropoietin (EPO), synthesised by the kidney. Just before and after leaving the bone marrow, the developing cells are known as reticulocytes; these comprise about 1% of circulating red blood cells. Functional lifetime The functional lifetime of an erythrocyte is about 100–120 days, during which time the erythrocytes are continually moved by the blood flow push (in arteries), pull (in veins) and a combination of the two as they squeeze through microvessels such as capillaries. Senescence The aging erythrocyte undergoes changes in its plasma membrane, making it susceptible to selective recognition by macrophages and subsequent phagocytosis in the reticuloendothelial system (spleen, liver and bone marrow), thus removing old and defective cells and continually purging the blood. This process is termed eryptosis, erythrocyte programmed cell death. This process normally occurs at the same rate of production by erythropoiesis, balancing the total circulating red blood cell count. Eryptosis is increased in a wide variety of diseases including sepsis, haemolytic uremic syndrome, malaria, sickle cell anemia, beta-thalassemia, glucose-6-phosphate dehydrogenase deficiency, phosphate depletion, iron deficiency and Wilson's disease. Eryptosis can be elicited by osmotic shock, oxidative stress, energy depletion as well as a wide variety of endogenous mediators and xenobiotics. Excessive eryptosis is observed in erythrocytes lacking the cGMP-dependent protein kinase type I or the AMP-activated protein kinase AMPK. Inhibitors of eryptosis include erythropoietin, nitric oxide, catecholamines and high concentrations of urea. Much of the resulting breakdown products are recirculated in the body. The heme constituent of hemoglobin are broken down into Fe3+ and biliverdin. The biliverdin is reduced to bilirubin, which is released into the plasma and recirculated to the liver bound to albumin. The iron is released into the plasma to be recirculated by a carrier protein called transferrin. Almost all erythrocytes are removed in this manner from the circulation before they are old enough to hemolyze. Hemolyzed hemoglobin is bound to a protein in plasma called haptoglobin which is not excreted by the kidney.[30]
Membrane composition
The membrane of the red blood cell plays many roles that aid in regulating their surface deformability, flexibility, adhesion to other cells and immune recognition. These functions are highly dependent on its composition, which defines its properties. The red blood cell membrane is composed of 3 layers: the glycocalyx on the exterior, which is rich in carbohydrates; the lipid bilayer which contains many transmembrane proteins, besides its lipidic main constituents; and the membrane skeleton, a structural network of proteins located on the inner surface of the lipid bilayer. Half of the membrane mass in human and most mammalian erythrocytes are proteins. The other half are lipids, namely phospholipids and cholesterol.[]
Red blood cell Membrane lipids The erythrocyte cell membrane comprises a typical lipid bilayer, similar to what can be found in virtually all human cells. Simply put, this lipid bilayer is composed of cholesterol and phospholipids in equal proportions by weight. The lipid composition is important as it defines many physical properties such as membrane permeability and fluidity. Additionally, the activity of many membrane proteins is regulated by interactions with lipids in the bilayer. Unlike cholesterol which is evenly distributed between the inner and outer leaflets, the 5 major phospholipids are asymmetrically disposed, as shown below: Outer monolayer • Phosphatidylcholine (PC); • Sphingomyelin (SM). Inner monolayer • Phosphatidylethanolamine (PE); • Phosphoinositol (PI) (small amounts). • Phosphatidylserine (PS); This asymmetric phospholipid distribution among the The most common erythrocyte cell membrane lipids, schematically bilayer is the result of the function of several disposed as they are distributed on the bilayer. Relative abundances energy-dependent and energy-independent are not at scale. phospholipid transport proteins. Proteins called “Flippases” move phospholipids from the outer to the inner monolayer while others called “floppases” do the opposite operation, against a concentration gradient in an energy dependent manner. Additionally, there are also “scramblase” proteins that move phospholipids in both directions at the same time, down their concentration gradients in an energy independent manner. There is still considerable debate ongoing regarding the identity of these membrane maintenance proteins in the red cell membrane. The maintenance of an asymmetric phospholipid distribution in the bilayer (such as an exclusive localization of PS and PIs in the inner monolayer) is critical for the cell integrity and function due to several reasons: • Macrophages recognize and phagocytose red cells that expose PS at their outer surface. Thus the confinement of PS in the inner monolayer is essential if the cell is to survive its frequent encounters with macrophages of the reticuloendothelial system, especially in the spleen. • Premature destruction of thallassemic and sickle red cells has been linked to disruptions of lipid asymmetry leading to exposure of PS on the outer monolayer. • An exposure of PS can potentiate adhesion of red cells to vascular endothelial cells, effectively preventing normal transit through the microvasculature. Thus it is important that PS is maintained only in the inner leaflet of the bilayer to ensure normal blood flow in microcirculation. • Both PS and phosphatidylinositol-4,5-bisphosphate (PIP2) can regulate membrane mechanical function, due to their interactions with skeletal proteins such as spectrin and protein 4.1R. Recent studies have shown that binding of spectrin to PS promotes membrane mechanical stability. PIP2 enhances the binding of protein band 4.1R to glycophorin C but decreases its interaction with protein band 3, and thereby may modulate the linkage of the
469
Red blood cell bilayer to the membrane skeleton. The presence of specialized structures named "lipid rafts" in the erythrocyte membrane have been described by recent studies. These are structures enriched in cholesterol and sphingolipids associated with specific membrane proteins, namely flotillins, stomatins (band 7), G-proteins, and β-adrenergic receptors. Lipid rafts that have been implicated in cell signaling events in nonerythroid cells have been shown in erythroid cells to mediate β2-adregenic receptor signaling and increase cAMP levels, and thus regulating entry of malarial parasites into normal red cells.[][31] Membrane proteins The proteins of the membrane skeleton are responsible for the deformability, flexibility and durability of the red blood cell, enabling it to squeeze through capillaries less than half the diameter of the erythrocyte (7-8 μm) and recovering the discoid shape as soon as these cells stop receiving compressive forces, in a similar fashion to an object made of rubber. There are currently more than 50 known membrane proteins, which can exist in a few hundred up to a million copies per erythrocyte. Approximately 25 of these membrane proteins carry the various blood group antigens, such as the A, B and Rh antigens, among many others. These membrane proteins can perform a wide diversity of functions, such as transporting ions and molecules across the red cell membrane, adhesion and interaction with other cells such as endothelial cells, as Red blood cell membrane proteins separated by signaling receptors, as well as other currently unknown functions. The [32] SDS-Page and silverstained blood types of humans are due to variations in surface glycoproteins of erythrocytes. Disorders of the proteins in these membranes are associated with many disorders, such as hereditary spherocytosis, hereditary elliptocytosis, hereditary stomatocytosis, and paroxysmal nocturnal hemoglobinuria.[][] The red blood cell membrane proteins organized according to their function: Transport • Band 3 - Anion transporter, also an important structural component of the erythrocyte cell membrane, makes up to 25% of the cell membrane surface, each red cell contains approximately one million copies. Defines the Diego Blood Group;[33] • Aquaporin 1 - water transporter, defines the Colton Blood Group; • Glut1 - glucose and L-dehydroascorbic acid transporter; • Kidd antigen protein - urea transporter; • RhAG - gas transporter, probably of carbon dioxide, defines Rh Blood Group and the associated unusual blood group phenotype Rhnull; • • • • • Na+/K+ - ATPase; Ca2+ - ATPase; Na+ K+ 2Cl- - cotransporter; Na+-Cl- - cotransporter; Na-H exchanger;
Red Blood Cell membrane major proteins
470
• K-Cl - cotransporter; • Gardos Channel.
Red blood cell Cell adhesion • ICAM-4 - interacts with integrins; • BCAM - a glycoprotein that defines the Lutheran blood group and also known as Lu or laminin-binding protein. Structural role - The following membrane proteins establish linkages with skeletal proteins and may play an important role in regulating cohesion between the lipid bilayer and membrane skeleton, likely enabling the red cell to maintain its favorable membrane surface area by preventing the membrane from collapsing (vesiculating). • Ankyrin-based macromolecular complex - proteins linking the bilayer to the membrane skeleton through the interaction of their cytoplasmic domains with Ankyrin. • Band 3 - also assembles various glycolytic enzymes, the presumptive CO2 transporter, and carbonic anhydrase into a macromolecular complex termed a “metabolon,” which may play a key role in regulating red cell metabolism and ion and gas transport function); • RhAG - also involved in transport, defines associated unusual blood group phenotype Rhmod. • Protein 4.1R-based macromolecular complex - proteins interacting with Protein 4.1R. • Protein 4.1R - weak expression of Gerbich antigens; • Glycophorin C and D - glycoprotein, defines Gerbich Blood Group; • XK - defines the Kell Blood Group and the Mcleod unusual phenotype (lack of Kx antigen and greatly reduced expression of Kell antigens); • RhD/RhCE - defines Rh Blood Group and the associated unusual blood group phenotype Rhnull; • Duffy protein - has been proposed to be associated with chemokine clearance;[34] • Adducin - interaction with band 3; • Dematin- interaction with the Glut1 glucose transporter.
[][]
471
Surface electrostatic potential
The zeta potential is an electrochemical property of cell surfaces that is determined by the net electrical charge of molecules exposed at the surface of cell membranes of the cell. The normal zeta potential of the erythrocyte is -15.7 millivolts (mV).[35] Much of this potential appears to be contributed by the exposed sialic acid residues in the membrane: their removal results in zeta potential of -6.06 mV.
Clinical notes
Separation and blood doping
Red blood cells can be obtained from whole blood by centrifugation, which separates the cells from the blood plasma in a process known as blood fractionation. Packed red blood cells, which are made in this way from whole blood with the plasma removed, are used in transfusion medicine.[36] During plasma donation, the red blood cells are pumped back into the body right away and only the plasma is collected. Some athletes have tried to improve their performance by blood doping: first about 1 litre of their blood is extracted, then the red blood cells are isolated, frozen and stored, to be reinjected shortly before the competition. (Red blood cells can be conserved for 5 weeks at −79 °C.) This practice is hard to detect but may endanger the human cardiovascular system which is not equipped to deal with blood of the resulting higher viscosity. Another method of blood doping involves injection with erythropoietin in order to stimulate production of red blood cells.
Red blood cell
472
Artificially grown red blood cells
In 2008 it was reported that human embryonic stem cells had been successfully coaxed into becoming erythrocytes in the lab. The difficult step was to induce the cells to eject their nucleus; this was achieved by growing the cells on stromal cells from the bone marrow. It is hoped that these artificial erythrocytes can eventually be used for blood transfusions.[37]
Diseases and diagnostic tools
Blood diseases involving the red blood cells include: • Anemias (or anaemias) are diseases characterized by low oxygen transport capacity of the blood, because of low red cell count or some abnormality of the red blood cells or the hemoglobin. • Iron deficiency anemia is the most common anemia; it occurs when the dietary intake or absorption of iron is insufficient, and hemoglobin, which contains iron, cannot be formed • Sickle-cell disease is a genetic disease that results in abnormal hemoglobin molecules. When these release their oxygen load in the tissues, they become insoluble, leading to mis-shaped red blood cells. These sickle shaped red cells are less deformable and viscoelastic meaning that they have become rigid and can cause blood vessel blockage, pain, strokes, and other tissue damage. • Thalassemia is a genetic disease that results in the production of an abnormal ratio of hemoglobin subunits. • Spherocytosis is a genetic disease that causes a defect in the red blood cell's cytoskeleton, causing the red blood cells to be small, sphere-shaped, and fragile instead of donut-shaped and flexible. • Pernicious anemia is an autoimmune disease wherein the body lacks intrinsic factor, required to absorb vitamin B12 from food. Vitamin B12 is needed for the production of hemoglobin. • Aplastic anemia is caused by the inability of the bone marrow to produce blood cells. • Pure red cell aplasia is caused by the inability of the bone marrow to produce only red blood cells. • Hemolysis is the general term for excessive breakdown of red blood cells. It can have several causes and can result in hemolytic anemia. • The malaria parasite spends part of its life-cycle in red blood cells, feeds on their hemoglobin and then breaks them apart, causing fever. Both sickle-cell disease and thalassemia are more common in malaria areas, because these mutations convey some protection against the parasite.
Affected by Sickle-cell disease, red blood cells alter shape and threaten to damage internal organs.
Effect of osmotic pressure on blood cells
• Polycythemias (or erythrocytoses) are diseases characterized by a surplus of red blood cells. The increased viscosity of the blood can cause a number of symptoms. • In polycythemia vera the increased number of red blood cells results from an abnormality in the bone marrow.
Red blood cell
473
• Several microangiopathic diseases, including disseminated intravascular coagulation and thrombotic microangiopathies, present with pathognomonic (diagnostic) red blood cell fragments called schistocytes. These pathologies generate fibrin strands that sever red blood cells as they try to move past a thrombus.
Micrographs of the effects of osmotic pressure
• Inherited hemolytic anemias caused by abnormalities of the erythrocyte membrane comprise an important group of inherited disorders. These disorders are characterized by clinical and biochemical heterogeneity and also genetic heterogeneity, as evidenced by recent molecular studies. • The Hereditary spherocytosis (HS) syndromes are a group of inherited disorders characterized by the presence of spherical-shaped erythrocytes on the peripheral blood smear. HS is found worldwide. It is the most common inherited anemia in individuals of northern European descent, affecting approximately 1 in 1000-2500 individuals depending on the diagnostic criteria. The primary defect in hereditary spherocytosis is a deficiency of membrane surface area. Decreased surface area may produced by two different mechanisms: 1) Defects of spectrin, ankyrin, or protein 4.2 lead to reduced density of the membrane skeleton, destabilizing the overlying lipid bilayer and releasing band 3-containing microvesicles. 2) Defects of band 3 lead to band 3 deficiency and loss of its lipid-stabilizing effect. This results in the loss of band 3-free microvesicles. Both pathways result in membrane loss, decreased surface area, and formation of spherocytes with decreased deformability. These deformed erythrocytes become trapped in the hostile environment of the spleen where splenic conditioning inflicts further membrane damage, amplifying the cycle of membrane injury. • Hereditary elliptocytosis • Hereditary pyropoikilocytosis • Hereditary stomatocytosis[38] • Hemolytic transfusion reaction is the destruction of donated red blood cells after a transfusion, mediated by host antibodies, often as a result of a blood type mismatch. Several blood tests involve red blood cells, including the RBC count (the number of red blood cells per volume of blood), the hematocrit (percentage of blood volume occupied by red blood cells), and the erythrocyte sedimentation rate. The blood type needs to be determined to prepare for a blood transfusion or an organ transplantation.
References
[2] Erich Sackmann, Biological Membranes Architecture and Function., Handbook of Biological Physics, (ed. R.Lipowsky and E.Sackmann, vol.1, Elsevier, 1995 [3] Laura Dean. Blood Groups and Red Cell Antigens (http:/ / www. ncbi. nlm. nih. gov/ books/ bv. fcgi?call=bv. View. . ShowTOC& rid=rbcantigen. TOC& depth=2) [5] "Swammerdam, Jan (1637–1680)", McGraw Hill AccessScience, 2007. Accessed 27 December 2007. [6] Red Gold - Blood History Timeline (http:/ / www. pbs. org/ wnet/ redgold), PBS 2002. Accessed 27 December 2007. [27] Iron Metabolism (http:/ / www. med-ed. virginia. edu/ courses/ path/ innes/ nh/ iron. cfm), University of Virginia Pathology. Accessed 22 September 2007. [28] Iron Transport and Cellular Uptake (http:/ / sickle. bwh. harvard. edu/ iron_transport. html) by Kenneth R. Bridges, Information Center for Sickle Cell and Thalassemic Disorders. Accessed 22 September 2007. [35] Tokumasu F, Ostera GR, Amaratunga C, Fairhurst RM (2012) Modifications in erythrocyte membrane zeta potential by Plasmodium falciparum infection. Exp Parasitol [37] First red blood cells grown in the lab (http:/ / www. newscientist. com/ article/ dn14565-first-red-blood-cells-grown-in-the-lab. html), New Scientist News, 19 August 2008
Red blood cell
474
External links
• Blood Groups and Red Cell Antigens (http://www.ncbi.nlm.nih.gov/books/bv.fcgi?call=bv.View.. ShowTOC&rid=rbcantigen.TOC&depth=2) by Laura Dean. Searchable and downloadable online textbook in the public domain. • Database of vertebrate erythrocyte sizes (http://www.genomesize.com/cellsize/). • Red Gold (http://www.pbs.org/wnet/redgold), PBS site containing facts and history
Megakaryocyte
475
Megakaryocyte
Megakaryocyte
two megakaryocytes in bone marrow, slightly below centre Latin Code megakaryocytus TH H2.00.04.3.05003
[1]
The megakaryocyte is a bone marrow cell responsible for the production of blood thrombocytes (platelets), which are necessary for normal blood clotting. Megakaryocytes normally account for 1 out of 10,000 bone marrow cells but can increase in number nearly 10-fold during the course of certain diseases.[]
Structure
In general, megakaryocytes are 10 to 15 times larger than a typical red blood cell, averaging 50-100 μm in diameter. During its maturation, the megakaryocyte grows in size and replicates its DNA without cytokinesis in a process called endomitosis. As a result, the nucleus of the megakaryocyte can become very large and lobulated, which, under a light microscope, can give the false impression that there are several nuclei. In some cases, the nucleus may contain up to 64N DNA, or 32 copies of the normal complement of DNA in a human cell. The cytoplasm, just as the platelets that bud off from it, contains α-granula and Dense bodies.
Megakaryocyte development
Megakaryocytes are derived from hematopoietic stem cell precursor cells in the bone marrow. They are primarily produced by the liver, kidney, spleen, and bone marrow. These multipotent stem cells live in the marrow sinusoids and are capable of producing all types of blood cells depending on the signals they receive. The primary signal for megakaryocyte production is thrombopoietin or TPO. TPO is sufficient but not absolutely necessary[] for inducing differentiation of progenitor cells in the bone marrow towards a final megakaryocyte phenotype. Other molecular signals for megakaryocyte differentiation include GM-CSF, IL-3, IL-6, IL-11, chemokines (SDF-1 ; FGF-4),[] and [] erythropoietin. The megakaryocyte develops through the following lineage: CFU-Me (pluripotential hemopoietic stem cell or hemocytoblast) -> megakaryoblast -> promegakaryocyte -> megakaryocyte. J
Megakaryocyte The cell eventually reaches megakaryocyte stage and loses its ability to divide. However, it is still able to replicate its DNA and continue development, becoming polyploid.[] The cytoplasm continues to expand and the DNA complement can increase up to 64N.
476
Platelet release
Once the cell has completed differentiation and become a mature megakaryocyte, it begins the process of producing platelets. The maturation process occurs via endomitotic synchronous replication whereby the cytoplasmic volume enlarges as the number of nuclei multiplies without cellular division. The cell ceases its growth at 4N, 8N or 16N, becomes granular, and begins to produce platelets.[1] Thrombopoietin plays a role in inducing the megakaryocyte to form small proto-platelet processes. Platelets are held within these internal membranes within the cytoplasm of megakaryocytes. There are two proposed mechanisms for platelet release. In one scenario, these proto-platelet processes break up explosively to become platelets.[] Alternatively, the cell may form platelet ribbons into blood vessels. The ribbons are formed via pseudopodia and they are able to continuously emit platelets into circulation. In either scenario, each of these proto-platelet processes can give rise to 2000-5000 new platelets upon breakup. Overall, 2/3 of these newly-produced platelets will remain in circulation while 1/3 will be sequestered by the spleen. After budding off platelets, what remains is mainly the cell nucleus. This crosses the bone marrow barrier to the blood and is consumed in the lung by alveolar macrophages.
Effects of cytokines
Cytokines are signals used in the immune system for intercellular communication. There are many cytokines which affect megakaryocytes. Certain cytokines such as IL-3, IL-6, IL-11, LIF, erythropoietin, and thrombopoietin all stimulate the maturation of megakaryocytic progenitor cells.[] Other signals such as PF4, CXCL5, CXCL7, and CCL5 inhibit platelet formation.[]
Thrombopoietin
Thrombopoietin (TPO) is a 353-amino acid protein located on chromosome 3p27. TPO is primarily synthesized in the liver[] but can be made by kidneys, testes, brain, and even bone marrow stromal cells. It has high homology with erythropoietin. It is essential for the formation of an adequate quantity of platelets. Mice lacking TPO or the TPO receptor (Mpl) have a 90% reduction in circulating platelet number, although the platelets are normal in morphology and function.[]
Disorders involving megakaryocytes
Megakaryocytes are directly responsible for producing platelets which are needed for the formation of a thrombus, or blood clot. There are several diseases which are directly attributable to abnormal megakaryocyte function or abnormal platelet function.[]
Essential Thrombocythemia
Essential thrombocytosis (ET-Also known as Essential thrombocythemia) is a disorder characterized by extremely high numbers of circulating platelets. The disease occurs in 1-2 per 100,000 people. The current WHO requirements for diagnosis include > 600,000 platelets/μL of blood (normal 150,000-400,000) and a bone marrow biopsy. Some of the consequences of having such high numbers of platelets include thrombosis or clots throughout the body. Thrombi form more frequently in arteries than veins. Ironically, having platelet counts above 1,000,000 platelets/μL can lead to hemorrhagic events.[] Recent evidence suggests that the majority of ET cases are due to a mutation in the JAK2 protein, a member of the JAK-STAT pathway.[] Evidence suggests this mutation renders the megakaryocyte hypersensitive to thrombopoietin and causes clonal proliferation of megakaryocytes. There is a significant risk of
Megakaryocyte transformation to leukemia with this disorder. The primary treatment consists of anagrelide or hydroxyurea to lower platelet levels.
477
Congenital amegakaryocytic thrombocytopenia (CAMT)
Congenital amegakaryocytic thrombocytopenia (CAMT) is a rare inherited disorder. The primary manifestations are thrombocytopenia and megakaryocytopenia, i.e. low numbers of platelets and megakaryocytes. There is an absence of megakaryocytes in the bone marrow with no associated physical abnormalities.[] The cause for this disorder appears to be a mutation in the gene for the TPO receptor, c-mpl, despite high levels of serum TPO.[][] In addition, there may be abnormalities with the central nervous system including the cerebrum and cerebellum which could cause symptoms.[] The primary treatment for CAMT is bone marrow transplantation. Bone marrow/stem cell transplant is the only remedy for this genetic disease. Frequent platelet transfusions are required to keep the patient from bleeding to death until transplant has been completed, although this is not always the case. One of the few non-medical research related sources on the web with some information on CAMT is: • CAMT Specific Infant Bone Marrow Transplant Journal [2] There appears to be no generic resource for CAMT patients on the web and this is potentially due to the rariety of the disease.
External links
• Megakaryocytes: Mature [3] Many microscopic images of mature megakaryocytes including in disease settings. • Cell size comparison [4] • CAMT Specific Infant Bone Marrow Transplant Journal [2]
References
Monocyte
478
Monocyte
Monocyte
Monocytes under a light microscope from a peripheral blood smear surrounded by red blood cells. Latin Code monocytus TH H2.00.04.1.02010
[1]
Monocytes are a type of white blood cell and are part of the innate immune system of vertebrates including all mammals (humans included), birds, reptiles, and fish. Monocytes play multiple roles in immune function. Such roles include: (1) replenish resident macrophages and dendritic cells under normal states, and (2) in response to inflammation signals, monocytes can move quickly (approx. 8–12 hours) to sites of infection in the tissues and divide/differentiate into macrophages and dendritic cells to elicit an immune response. Half of them are stored in the spleen.[1] Monocytes are usually identified in stained smears by their large kidney shaped or notched nucleus.
Physiology
Monocytes are produced by the bone marrow from hematopoietic stem cell precursors called monoblasts. Monocytes circulate in the bloodstream for about one to three days and then typically move into tissues throughout the body. They constitute between three to eight percent of the leukocytes in the blood. Half of them are stored as a reserve in the spleen in clusters in the red pulp's Cords of Billroth.[1] In the tissues, monocytes mature into different types of macrophages at different anatomical locations. Monocytes are the largest corpuscles in the blood. Monocytes which migrate from the bloodstream to other tissues will then differentiate into tissue resident macrophages or dendritic cells. Macrophages are responsible for protecting tissues from foreign substances, but are also suspected to be important in the formation of important organs like the heart and brain. They are cells that possess a large smooth nucleus, a large area of cytoplasm, and many internal vesicles for processing foreign material. Monocytes and their macrophage and dendritic-cell progeny serve three main functions in the immune system. These are phagocytosis, antigen presentation, and cytokine production. Phagocytosis is the process of uptake of microbes and particles followed by digestion and destruction of this material. Monocytes can perform phagocytosis using intermediary (opsonising) proteins such as antibodies or complement that coat the pathogen, as well as by binding to the microbe directly via pattern-recognition receptors that recognize pathogens. Monocytes are also capable of killing infected host cells via antibody, termed antibody-mediated cellular cytotoxicity. Vacuolization may be present in a cell that has recently phagocytized foreign matter. Microbial fragments that remain after such digestion can serve as antigen. The fragments can be incorporated into MHC molecules and then traffic to the cell surface of monocytes (and macrophages and dendritic cells). This process is called antigen presentation and it leads to activation of T lymphocytes, which then mount a specific immune response against the antigen.
Monocyte Other microbial products can directly activate monocytes and this leads to production of pro-inflammatory and with some delay of anti-inflammatory cytokines. Typical cytokines produced by monocytes are TNF, IL-1, and IL-12.
479
Monocyte subpopulations
There are at least three types of monocytes in human blood:[2] a) the classical monocyte is characterized by high level expression of the CD14 cell surface receptor (CD14++ CD16- monocyte) b) the non-classical monocyte shows low level expression of CD14 and with additional co-expression of the CD16 receptor (CD14+CD16++ monocyte).[3] c) the intermediate monocyte with high level expression of CD14 and low level expression of CD16 (CD14++CD16+ monocytes). There appears to be a developmental relationship in that the classical monocytes develop into the intermediate monocytes to then become the non-classical CD14+CD16++ monocytes. Hence the non-classical monocytes may represent a more mature version. After stimulation with microbial products the CD14+CD16++ monocytes produce high amounts of pro-inflammatory cytokines like tumor necrosis factor and interleukin-12. Said et al. showed that activated monocytes express high levels of PD-1 which might explain the higher expression of PD-1 in CD14+CD16++ monocytes as compared to CD14++CD16- monocytes. Triggering monocytes-expressed PD-1 by its ligand PD-L1 induces IL-10 production which activates CD4 Th2-cells and inhibits CD4 Th1-cell function.[4]
Diagnostic use
A monocyte count is part of a complete blood count and is expressed either as a ratio of monocytes to the total number of white blood cells counted, or by absolute numbers. Both may be useful in determining or refuting a possible diagnosis.
Monocytosis
Monocytosis is the state of excess monocytes in the peripheral blood. It may be indicative of various disease states. Examples of processes that can increase a monocyte count include: • chronic inflammation • stress response • • • • • hyperadrenocorticism immune-mediated disease pyogranulomatous disease necrosis red cell regeneration
• Viral Fever • sarcoidosis
A scanning electron microscope (SEM) image of normal circulating human blood. One can see red blood cells, several knobby white blood cells including lymphocytes, a monocyte, a neutrophil, and many small disc-shaped platelets.
A high count of CD14+CD16++ monocytes is found in severe infection (sepsis)[5] and a very low count of these cells is found after therapy with immuno-suppressive glucocorticoids[6]
Monocyte
480
Monocytopenia
Monocytopenia is a form of leukopenia associated with a deficiency of monocytes.
Dendritic cells
Monocytes can be used to generate dendritic cells in vitro by adding cytokines like Granulocyte Monocyte Colony Stimulating Factor (GMCSF) and IL-4.[]
Blood content
Reference ranges for blood tests of white blood cells, comparing monocyte amount (shown in green) with other cells.
References
[1] Swirski FK, Nahrendorf M, Etzrodt M, Wildgruber M, Cortez-Retamozo V, Panizzi P, Figueiredo J-L, Kohler RH, Chudnovskiy A, Waterman P, Aikawa E, Mempel TR, Libby P, Weissleder R, Pittet MJ. (2009). Identification of Splenic Reservoir Monocytes and Their Deployment to Inflammatory Sites. Science, 325: 612-616. PMID 19644120 [2] Ziegler-Heitbrock, L et al (2010): Nomenclature of monocytes and dendritic cells in blood. Blood,116 (16): e74-e80. PMID 20628149 [3] Ziegler-Heitbrock, L: The CD14+ CD16+ Blood Monocytes: their Role in Infection and Inflammation, Review. J Leukocyte Biology, 81:584, 2007 PMID 17135573 [4] Elias A. Said et al. 2009, PD-1 Induced IL10 Production by Monocytes Impairs T-cell Activation in a Reversible Fashion. Nature Medicine. 2010; 452-9. [5] Fingerle, G., Pforte, A., Passlick, B., Blumenstein, M., Ströbel, M., Ziegler-Heitbrock, H.W.L.: The novel subset of CD14+ CD16+ blood monocytes is expanded in sepsis patients. Blood, 82: 3170-3176, 1993 PMID 7693040 [6] Fingerle-Rowson, G., Angstwurm, M., Andreesen, R., Ziegler-Heitbrock, H.W.L.:Selective depletion of CD14+ CD16+ monocytes by glucocorticoid therapy.Clin. Exp. Immunol., 112: 501-506, 1998 PMID 9649222
External links
• BU Histology Learning System: 01702ooa (http://www.bu.edu/histology/p/01702ooa.htm) • Human Monocytes - Prof. Dr. Ziegler-Heitbrock (http://www.monocyte.eu/) • Circulation of Body Fluids (http://www.simplylearnt.com/topic/Circulation-of-Body-Fluids)
Langerhans cell
481
Langerhans cell
Not to be confused with the cells of the islets of Langerhans, found in the pancreas, or Langhans giant cell. Langerhans cells are dendritic cells (antigen-presenting immune cells) of the skin and mucosa, and contain large granules called Birbeck granules. They are present in all layers of the epidermis, but are most prominent in the stratum spinosum.[] They also occur in the papillary dermis, particularly around blood vessels,[] as well as in the mucosa of the mouth, foreskin, and vagina.[] They can be found in other tissues, such as lymph nodes, particularly in association with the condition Langerhans cell histiocytosis (LCH).
Section of skin showing large numbers of dendritic cells (Langerhans cells) in the epidermis. (M. ulcerans infection, S100 immunoperoxidase stain.)
History
The Langerhans cell is named after Paul Langerhans, a German physician and anatomist, who discovered the cells at the age of 21 while he was a medical student.[1] Because of their dendritic nature, he mistakenly identified the cells as part of the nervous system.[]
Function
In skin infections, the local Langerhans cells take up and process microbial antigens to become fully functional antigen-presenting cells. Generally, dendritic cells in tissue are active in the capture, uptake and processing of antigens. Once dendritic cells arrive in secondary lymphoid tissue, however, they lose these properties while gaining the capacity to interact with naive T-cells. Langerhans cells derive from the cellular differentiation of monocytes with the marker "Gr-1" (also known as "Ly-6G/Ly-6C"). This differentiation requires stimulation by colony stimulating factor (CSF)-1.[2] They are similar in morphology and function to macrophages.
Langerhans cell Langerin is a protein found in Langerhans cells,[] and other types of dendritic cells.[]
482
Clinical significance
LCH
In the rare disease Langerhans cell histiocytosis (LCH), an excess of these cells is produced. This can cause damage to skin, bone and other organs.
HIV
Langerhans cells may be initial cellular targets in the sexual transmission of HIV,[3] and may be a target, reservoir, and vector of dissemination.[4] Langerhans cells have been observed in foreskin, vaginal, and oral mucosa of humans; the lower concentrations in oral mucosa suggest that it is not a likely source of HIV infection relative to foreskin and vaginal mucosa.[]
The representation of Langerhans cells in the Cell Ontology. A portion of the Cell Ontology is shown with ovals corresponding to cell types defined in the ontology and arrows corresponding to relations between those cell types. Langerhans cell is represented by a yellow oval; blue arrows correspond to is_a relations, and orange arrows correspond to develops_from relations. Only a subset of [] Langerhans cell parent types are included in the figure.
On March 4, 2007 the online Nature Medicine magazine published the letter "Langerin is a natural barrier to HIV-1 transmission by Langerhans cells."[5] One of the authors of the study, Teunis Geijtenbeek, said that "Langerin is able to scavenge viruses from the surrounding environment, thereby preventing infection" and "since generally all tissues on the outside of our bodies have Langerhans cells, we think that the human body is equipped with an antiviral defense mechanism, destroying incoming viruses."[6]
Langerhans cell
483
References External links
• Langerhans Cell Histiocytosis (http://www.emedicine.com/derm/topic216.htm#) at eMedicine • http://www.trinity.edu/rblyston/MicroA/Lectures/L34-html/img018.jpgWikipedia:Link rot Illustration at trinity.edu • Brun, Scott C.; Rubin, Peter A. D. (1997). "25 year old kickboxer with progressive proptosis" (http://www.djo. harvard.edu/site.php?url=/physicians/gr/356). Digital Journal of Ophthalmology 3 (26). • Langerhans Cells (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Langerhans+Cells) at the US National Library of Medicine Medical Subject Headings (MeSH)
Platelet
484
Platelet
Platelet
Image from a light microscope (40×) from a peripheral blood smear surrounded by red blood cells. One normal platelet can be seen in the upper left side of the image (purple) and is significantly smaller in size than the red blood cells (stained pink). Two giant platelets (stained purple) are also visible. Latin Code thrombocytes TH H2.00.04.1.03001
[1]
Platelets, or thrombocytes (from Greek θρόμβος, "clot" and κύτος, "cell"), are small, disk shaped clear cell fragments (i.e. cells that do not have a nucleus), 2–3 µm in diameter,[1] which are derived from fragmentation of precursor megakaryocytes. The average lifespan of a platelet is normally just 5 to 9 days. Platelets are a natural source of growth factors. They circulate in the blood of mammals and are involved in hemostasis, leading to the formation of blood clots. If the number of platelets is too low, excessive bleeding can occur. However, if the number of platelets is too high, blood clots can form (thrombosis), which may obstruct blood vessels and result in such events as a stroke, myocardial infarction, pulmonary embolism or the blockage of blood vessels to other parts of the body, such as the extremities of the arms or legs. An abnormality or disease of the platelets is called a thrombocytopathy,[2] which could be either a low number of platelets (thrombocytopenia), a decrease in function of platelets (thrombasthenia), or an increase in the number of platelets (thrombocytosis). There are disorders that reduce the number of platelets, such as heparin-induced thrombocytopenia (HIT) or thrombotic thrombocytopenic purpura (TTP) that typically cause thromboses, or clots, instead of bleeding. Platelets release a multitude of growth factors including platelet-derived growth factor (PDGF), a potent chemotactic agent, and TGF beta, which stimulates the deposition of extracellular matrix. Both of these growth factors have been shown to play a significant role in the repair and regeneration of connective tissues. Other healing-associated growth factors produced by platelets include basic fibroblast growth factor, insulin-like growth factor 1, platelet-derived epidermal growth factor, and vascular endothelial growth factor. Local application of these factors in increased concentrations through Platelet-rich plasma (PRP) has been used as an adjunct to wound healing for several decades.[3][4][5][6][7][8][9]
Platelet
485
Kinetics
• The physiological range for platelets is (150 – 400) × 103 per mm3. • Platelets are produced in blood cell formation (thrombopoiesis) in bone marrow, by budding off from megakaryocytes. • Megakaryocyte and platelet production is regulated by thrombopoietin, a hormone usually produced by the liver and kidneys. • Each megakaryocyte produces between 5,000 and 10,000 platelets. • Around 1011 platelets are produced each day by an average healthy adult.
• Reserve platelets are stored in the spleen, and are released when needed by sympathetically induced splenic contraction. • The lifespan of circulating platelets is 5 to 9 days. • Old platelets are destroyed by phagocytosis in the spleen and by Kupffer cells in the liver.
HSC=hematopoietic stem cell, Progenitor=progenitor cell, L-blast=lymphoblast, lymphocyte, Mo-blast=monoblast, monocyte, myeloblast, Pro-M=promyelocyte, myelocyte, Meta-M=metamyelocyte, neutrophil, eosinophil, basophil, Pro-E=proerythroblast, Baso-E=basophilic erythroblast, poly-E=polychromatic erythroblast, Ortho-E=Orthochromatic erythroblast, erythrocyte, promegakaryocyte, megakaryocyte, platelet.
Thrombus formation
The function of platelets is the maintenance of hemostasis. This is achieved primarily by the formation of thrombi, when damage to the endothelium of blood vessels occurs. On the converse, thrombus formation must be inhibited at times when there is no damage to the endothelium.
Activation
The inner surface of blood vessels is lined with a thin layer of endothelial cells that, in normal hemostasis, acts to inhibit platelet activation by producing nitric oxide, endothelial-ADPase, and PGI2. Endothelial-ADPase clears away the platelet activator, ADP. Endothelial cells produce a protein called von Willebrand factor (vWF), a cell adhesion ligand, which helps endothelial cells adhere to collagen in the basement membrane. Under physiological conditions, collagen is not exposed to the bloodstream. vWF is secreted constitutively into the plasma by the endothelial cells, and is stored in granules within the endothelial cell and in platelets.
Aggregation of platelets. Platelet rich human blood plasma (left vial) is a turbid liquid. Upon addition of ADP, platelets are activated and start to aggregate, forming white flakes (right vial).
Platelet When the endothelial layer is injured, collagen, vWF and tissue factor from the subendothelium is exposed to the bloodstream. When the platelets contact collagen or vWF, they are activated (e.g. to clump together). They are also activated by thrombin (formed with the help of tissue factor). They can also be activated by a negatively charged surface, such as glass. Non-physiological flow conditions (especially high values of shear stress) caused by arterial stenosis or artificial devices (Mechanical Heart Valves, blood pumps etc) can also lead to platelet activation.[10] Platelet activation further results in the scramblase-mediated transport of negatively charged phospholipids to the platelet surface. These phospholipids provide a catalytic surface (with the charge provided by phosphatidylserine and phosphatidylethanolamine) for the tenase and prothrombinase complexes. Calcium ions are essential for binding of these coagulation factors. Shape change Activated platelets change in shape to become more spherical, and pseudopods form on their surface. Thus they assume a stellate shape. Granule secretion Platelets contain alpha and dense granules. Activated platelets excrete the contents of these granules into their canalicular systems and into surrounding blood. There are three types of granules: • dense (or delta) granules (containing ADP or ATP, calcium, and serotonin) • lambda granules – similar to lysosomes and contain several hydrolytic enzymes.
Scanning electron micrograph of blood cells. From left to right: human erythrocyte, activated thrombocyte (platelet), leukocyte.
486
• Alpha granules (containing P-selectin, platelet factor 4, transforming growth factor-β1, platelet-derived growth factor, fibronectin, B-thromboglobulin, vWF, fibrinogen, and coagulation factors V and XIII). Thromboxane A2 synthesis Platelet activation initiates the arachidonic acid pathway to produce TXA2. TXA2 is involved in activating other platelets and its formation is inhibited by COX inhibitors, such as aspirin.
Adhesion and aggregation
Platelets aggregate, or clump together, using fibrinogen and von Willebrand factor (vWF) as a connecting agent. The most abundant platelet aggregation receptor is glycoprotein IIb/IIIa (gpIIb/IIIa); this is a calcium-dependent receptor for fibrinogen, fibronectin, vitronectin, thrombospondin, and vWF. Other receptors include GPIb-V-IX complex (vWF) and GPVI (collagen). Activated platelets will adhere, via glycoprotein (GP) Ia, to the collagen that is exposed by endothelial damage. Aggregation and adhesion act together to form the platelet plug. Myosin and actin filaments in platelets are stimulated to contract during aggregation, further reinforcing the plug.
Platelets clumping from a blood smear. May Grunwald-Giemsa. Light Microscopy, oil immersion 100x.
Platelet aggregation is stimulated by ADP, thromboxane, and α2 receptor-activation, but inhibited by other inflammatory products like PGI2 and PGD2. Platelet aggregation is enhanced by exogenous administration of anabolic steroids.
Platelet
487
Wound repair
The blood clot is only a temporary solution to stop bleeding; vessel repair is therefore needed. The aggregated platelets help this process by secreting chemicals that promote the invasion of fibroblasts from surrounding connective tissue into the wounded area to completely heal the wound or form a scar. The obstructing clot is slowly dissolved by the fibrinolytic enzyme, plasmin, and the platelets are cleared by phagocytosis.
ADP (purinergic/P2) receptors
Human platelets have three types of P2 receptors: P2X(1), P2Y(1) and P2Y(12). Although abnormalities in all three genes have been documented, but clinical correlation is available only for P2Y(12).[11] Patients with P2Y(12) defects have a mild to moderate bleeding diathesis, characterized by mucocutaneous bleeding and excessive post-surgical and post-traumatic blood loss. A defects in P2Y(12) should be suspected when ADP, even at concentrations ≥10 micro molar, is unable to induce full, irreversible platelet aggregation. Confirmation of the diagnosis is with tests that evaluate the degree of inhibition of adenylyl cyclase by ADP.
Other functions
• Clot retraction • • • • Procoagulant Inflammation Cytokine signalling Phagocytosis[12]
Cytokine signaling
In addition to being the chief cellular effector of hemostasis, platelets are rapidly deployed to sites of injury or infection, and potentially modulate inflammatory processes by interacting with leukocytes and by secreting cytokines, chemokines, and other inflammatory mediators.[13][14][15][16] Platelets also secrete platelet-derived growth factor (PDGF).
Role in disease
High and low counts
A normal platelet count in a healthy individual is between 150,000 and 450,000 per μL (microlitre) of blood ((150–450)×109/L).[] Ninety-five percent of healthy people will have platelet counts in this range. Some will have statistically abnormal platelet counts while having no demonstrable abnormality. However, if it is either very low or very high, the likelihood of an abnormality being present is higher. Both thrombocytopenia and thrombocytosis may present with Diagram of the internal structure of a platelet coagulation problems. In general, low platelet counts increase bleeding risks; however there are exceptions (such as immune-mediated heparin-induced thrombocytopenia or paroxysmal nocturnal hemoglobinuria). High counts may lead to thrombosis, although this is mainly when the elevated count is due to myeloproliferative disorder. Transfusion is generally used only to correct unusually low platelet counts (typically below (10–15)×109/L). Transfusion is contraindicated in thrombotic thrombocytopenic purpura (TTP), as it fuels the coagulopathy. In patients undergoing surgery, a level below 50×109/L is associated with abnormal surgical bleeding, and regional
Platelet anaesthetic procedures such as epidurals are avoided for levels below 80×109/L.[17] Normal platelet counts are not a guarantee of adequate function. In some states, the platelets, while being adequate in number, are dysfunctional. For instance, aspirin irreversibly disrupts platelet function by inhibiting cyclooxygenase-1 (COX1), and hence normal hemostasis. The resulting platelets are unable to produce new cyclooxygenase because they have no DNA. Normal platelet function will not return until the use of aspirin has ceased and enough of the affected platelets have been replaced by new ones, which can take over a week. Ibuprofen, another NSAID, does not have such a long duration effect, with platelet function usually returning within 24 hours,[18] and taking ibuprofen before aspirin sometimes may prevent the irreversible effects of aspirin.[19] Uremia, a consequence of renal failure, leads to platelet dysfunction that may be ameliorated by the administration of desmopressin.
488
Medications
Oral agents often used to alter/suppress platelet function include aspirin, clopidogrel, cilostazol, ticlopidine, ticagrelor and prasugrel. Intravenous agents often used to alter/suppress platelet function include: abciximab, eptifibatide, tirofiban. In addition to platelet transfusion, hematopoetic agents such as Oprelvekin, Romiplostim, and Eltrombopag can be used to increase platelet counts.
Diseases
Disorders leading to a reduced platelet count: • Thrombocytopenia • Idiopathic thrombocytopenic purpura – also known as immune thrombocytopenic purpura (ITP) • Thrombotic thrombocytopenic purpura • Drug-induced thrombocytopenic purpura (for example heparin-induced thrombocytopenia (HIT)) • Gaucher's disease • Aplastic anemia • Onyalai Alloimmune disorders • Fetomaternal alloimmune thrombocytopenia • Some transfusion reactions Disorders leading to platelet dysfunction or reduced count: • • • • HELLP syndrome Hemolytic-uremic syndrome Chemotherapy Dengue
Disorders featuring an elevated count: • Thrombocytosis, including essential thrombocytosis (elevated counts, either reactive or as an expression of myeloproliferative disease); may feature dysfunctional platelets Disorders of platelet adhesion or aggregation: • Bernard-Soulier syndrome • Glanzmann thrombasthenia Disorders of platelet granule amount or release • Hermansky-Pudlak Syndrome • Gray platelet syndrome
Platelet Disorders of platelet metabolism • Decreased cyclooxygenase activity, induced or congenital • Storage pool defects, acquired or congenital Disorders that compromise platelet signaling: • Wiskott–Aldrich syndrome Disorders in which platelets play a key role: • • • • • • • • Atherosclerosis Coronary artery disease, CAD and myocardial infarction, MI Cerebrovascular disease and Stroke, CVA (cerebrovascular accident) Peripheral artery occlusive disease (PAOD) Cancer[20] Malaria[21] Asthma[22][23] Samter’s Triad (Aspirin Exacerbated Respiratory Disease/AERD)[24][25]
489
Laboratory findings in various platelet and coagulation disorders (V - T)
Condition Vitamin K deficiency or warfarin Disseminated intravascular coagulation Von Willebrand disease Hemophilia Aspirin Thrombocytopenia Liver failure, early Liver failure, end-stage Uremia Congenital afibrinogenemia Factor V deficiency Prothrombin time Partial thromboplastin time Bleeding time Prolonged Prolonged Unaffected Unaffected Unaffected Unaffected Prolonged Prolonged Unaffected Prolonged Prolonged Normal or mildly prolonged Unaffected Prolonged Prolonged Prolonged Unaffected Unaffected Unaffected Prolonged Unaffected Prolonged Prolonged Prolonged Unaffected Unaffected Prolonged Shortened Prolonged Prolonged Unaffected Prolonged Prolonged Unaffected Prolonged Prolonged Prolonged Unaffected Unaffected Prolonged Prolonged Unaffected Unaffected Platelet count Unaffected Decreased Unaffected Unaffected Unaffected Decreased Unaffected Decreased Unaffected Unaffected Unaffected Unaffected Unaffected Decreased or unaffected Unaffected Unaffected
Factor X deficiency as seen in amyloid purpura Prolonged Glanzmann's thrombasthenia Bernard-Soulier syndrome Factor XII deficiency C1INH deficiency Unaffected Unaffected Unaffected Unaffected
Platelet
490
Discovery
Although red blood cells had been known since van Leeuwenhoek (1632–1723), the German anatomist Max Schultze (1825–1874) was the first to describe platelets.[][] He described "spherules" that were much smaller than red blood cells and that occasionally clumped and were found in collections of fibrous material. Giulio Bizzozero (1846–1901), building on Schultze's findings, used "living circulation" to study blood cells of amphibians microscopically in vivo. He is especially noted for discovering that platelets clump at the site of blood vessel injury, a process that precedes the formation of a blood clot. This observation confirmed the role of platelets in coagulation.[]
In transfusion medicine
Platelets are either isolated from collected units of whole blood and pooled to make a therapeutic dose or collected by apheresis, sometimes concurrently with plasma or red blood cells. The industry standard is for platelets to be tested for bacteria before transfusion to avoid septic reactions, which can be fatal. Recently the AABB Industry Standards for Blood Banks and Transfusion Services (5.1.5.1) has allowed for use of pathogen reduction technology as an alternative to bacterial screenings in platelets.[26] Pooled whole-blood platelets, sometimes called “random” platelets, are made primarily by two methods.[27] In the US, a unit of whole blood is placed into a large centrifuge in what is referred to as a “soft spin.” At these settings, the platelets remain suspended in the plasma. The platelet-rich plasma (PRP) is removed from the RBCs, then centrifuged at a faster setting to harvest the platelets from the plasma. In other Platelet concentrate. regions of the world, the unit of whole blood is centrifuged using settings that cause the platelets to become suspended in the “buffy coat” layer, which includes the platelets and the white blood cells. The “buffy coat” is isolated in a sterile bag, suspended in a small amount of red blood cells and plasma, then centrifuged again to separate the platelets and plasma from the red and white blood cells. Regardless of the initial method of preparation, multiple donations may be combined into one container using a sterile connection device to manufacture a single product with the desired therapeutic dose. Apheresis platelets are collected using a mechanical device that draws blood from the donor and centrifuges the collected blood to separate out the platelets and other components to be collected. The remaining blood is returned to the donor. The advantage to this method is that a single donation provides at least one therapeutic dose, as opposed to the multiple donations for whole-blood platelets. This means that a recipient is not exposed to as many different donors and has less risk of transfusion-transmitted disease and other complications. Sometimes a person such as a cancer patient who requires routine transfusions of platelets will receive repeated donations from a specific donor to further minimize the risk. Pathogen reduction of platelets using for example, riboflavin and UV light treatments can also be carried out to reduce the infectious load of pathogens contained in donated blood products, thereby reducing the risk of transmission of transfusion transmitted diseases.[28][29] Platelets are not cross-matched unless they contain a significant amount of red blood cells (RBCs), which results in a reddish-orange color to the product. This is usually associated with whole-blood platelets, as apheresis methods are more efficient than “soft spin” centrifugation at isolating the specific components of blood. An effort is usually made to issue type specific platelets, but this is not as critical as it is with RBCs. Platelets collected by either method have a very short shelf life, typically five days. This results in frequent problems with short supply, as testing the donations often requires up to a full day. Since there are no effective preservative
Platelet solutions for platelets, they lose potency quickly and are best when fresh. Platelets are stored under constant agitation at 20–24 °C. Storage at room temperature provides an environment where any bacteria that are introduced to the blood component during the collection process may proliferate and subsequently cause bacteremia in the patient. Regulations are in place in the United States that require products to be tested for the presence of bacterial contamination before transfusion.[30] Platelets, either apheresis or random-donor platelets, can be processed through a volume reduction process. In this process, the platelets are spun in a centrifuge and the excess plasma is removed, leaving 10 to 100 mL of platelet concentrate. Volume-reduced platelets are normally transfused only to neonatal and pediatric patients when a large volume of plasma could overload the child's small circulatory system. The lower volume of plasma also reduces the chances of an adverse transfusion reaction to plasma proteins.[] Volume reduced platelets have a shelf life of only four hours.[31]
491
Other species
Nucleated thrombocytes of nonmammalian vertebrates differ from the mammalian thrombocytes not only in having a nucleus and resembling B lymphocytes, but also these nucleated thrombocytes do not aggregate in response to ADP, serotonin and adrenaline (although they do aggregate with thrombin).[citation needed]
References
[10] Kroll, M., J. Hellums, et al. (1996). "Platelets and shear stress." Blood 88(5): 1525-1541 [11] Cattaneo M (2011) Molecular defects of the platelet P2 receptors.Purinergic Signal [22] Kornerup KN, Page CP. The role of platelets in the pathophysiology of asthma. Platelets. 2007 Aug 18(5):319-28. [23] http:/ / www. ncbi. nlm. nih. gov/ pubmed/ 17654302 [24] Laidlaw TM, Kidder MS, Bhattacharyya N, Xing W, Shen S, Milne GL, Castells MC, Chhay H, Boyce JA. Cysteinyl leukotriene overproduction in aspirin exacerbated respiratory disease is driven by platelet-adherent leukocytes. Blood. 2012 Jan 18. [25] http:/ / www. ncbi. nlm. nih. gov/ pubmed/ 22262771 [26] American Association of Blood Banks Standards for Blood Banks and Transfusion Services, Bethesda, MD: 22rd ed, AABB, 2003, Section 5.1.5.1. [30] AABB Standards for Blood Banks and Transfusion Services 26th Edition Bethesda, MD: AABB, 2009. [31] CBBS: Washed and volume-reduced Plateletpheresis units (http:/ / www. cbbsweb. org/ enf/ 2001/ pltwashvol. html). Cbbsweb.org (2001-10-25). Retrieved on 2011-11-14.
Osteoclast
492
Osteoclast
Osteoclast
Osteoclast, with bone below it, showing typical distinguishing characteristics: a large cell with multiple nuclei and a "foamy" cytosol. Latin Code osteoclastus TH H2.00.03.7.00005
[1]
An osteoclast (from the Greek words for "bone" (Οστό) and "broken" (κλαστός)) is a type of bone cell that removes bone tissue by removing its mineralized matrix and breaking up the organic bone (organic dry weight is 90% collagen). This process is known as bone resorption. Osteoclasts were discovered by Kolliker in 1873.[] Osteoclasts and osteoblasts are instrumental in controlling the amount of bone tissue: osteoblasts form bone, osteoclasts resorb bone. Osteoclasts are formed by the fusion of cells of the monocyte-macrophage cell line.[1] Osteoclasts are characterized by high expression of tartrate resistant acid phosphatase (TRAP) and cathepsin K.
Morphology
An osteoclast is a large cell that is 40 micrometer in diameter. It contains 15-20 closely packed oval-shaped nuclei. Osteoclasts are found in pits in the bone surface which are called resorption bays, or Howship's Lacunae. Osteoclasts are characterized by a cytoplasm with a homogeneous, "foamy" appearance. This appearance is due to a high concentration of vesicles and vacuoles. These vacuoles are lysosomes filled with acid phophatase. Osteoclast rough endoplasmic reticulum is sparse, and the Golgi complex is extensive.[2][3][4] At a site of active bone resorption, the osteoclast forms a specialized cell membrane, the "ruffled border," that touches the surface of the bone tissue.[1] The ruffled border, which facilitates removal of the
Tartrate resistant acid phosphatase positive osteoclast in cell culture
bony
matrix,
Osteoclast
493
is a morphologic characteristic of an osteoclast that is actively resorbing bone. The ruffled border increases surface area interface for bone resorption. The mineral portion of the matrix (called hydroxyapatite) includes calcium and phosphate ions. These ions are absorbed into small vesicles (see endocytosis), which move across the cell and eventually are released into the extracellular fluid, thus increasing levels of the ions in the blood.
Illustrated cross-section of an activated osteoclast
Origin
Since their discovery in 1873 there has been considerable debate about their origin. Three theories were dominant: from 1949 to 1970 the connective tissue origin was popular, which stated that osteoclasts and osteoblasts are of the same lineage, and ostoblasts fuse together to form osteoclasts. At certain times osteoclasts dissociate into osteoblasts, which finally form osteocytes. In the 1970s the biphyletic theory became popular; it states that osteoblasts and osteoclasts are of different lineage. It was in the beginning of 1980 that the monocyte phagocytic system was recognized as precursor of osteoclasts.[] Osteoclast formation requires the presence of RANKL (receptor activator of nuclear factor κβ ligand) and M-CSF (Macrophage colony-stimulating factor). These membrane bound proteins are produced by neighbouring stromal cells and osteoblasts, thus requiring direct contact between these cells and osteoclast [Precursor (chemistry)[precursors. M-CSF acts through its receptor on the osteoclast, c-fms (colony-stimulating factor 1 receptor), a transmembrane tyrosine kinase-receptor, leading to secondary messenger activation of tyrosine kinase Src. Both of these molecules are necessary for osteoclastogenesis and are widely involved in the differentiation of monocyte/macrophage derived cells. RANKL is a member of the tumour necrosis family (TNF), and is essential in osteoclastogenesis. RANKL knockout mice exhibit a phenotype of osteopetrosis and defects of tooth eruption, along with an absence or deficiency of osteoclasts. RANKL activates NF-κβ (nuclear factor-κβ) and NFATc1 (nuclear factor of activated t cells, cytoplasmic, calcineurin-dependent 1) through RANK. NF-κβ activation is stimulated almost immediately after RANKL-RANK interaction occurs, and is not upregulated. NFATc1 stimulation, however, begins ~24–48 hours after binding occurs and its expression has been shown to be RANKL dependent. Osteoclast differentiation is inhibited by osteoprotegerin (OPG), which is produced by osteoblasts and binds to RANKL thereby preventing interaction with RANK.
Osteoclast
494
Function
Once activated, osteoclasts move to areas of microfracture in the bone by chemotaxis. Osteoclasts lie in a small cavity called Howship's lacunae, formed from the digestion of the underlying bone. The sealing zone is the attachment of the osteoclast's plasma membrane to the underlying bone. Sealing zones are bounded by belts of specialized adhesion structures called podosomes. Attachment to the bone matrix is facilitated by integrin receptors, such as αvβ3, via the specific amino acid motif Arg-Gly-Asp in bone matrix proteins, such as osteopontin. The osteoclast releases hydrogen ions through the action of carbonic anhydrase (H2O + CO2 → HCO3- + H+) through the ruffled border into the resorptive cavity, acidifying and aiding dissolution of the mineralized bone matrix into Ca2+, H3PO4, H2CO3, water and other substances. Dysfunction of the carbonic anhydrase has been documented to cause some forms of osteopetrosis. Hydrogen ions are pumped against a high concentration gradient by proton pumps, specifically a unique vacuolar-ATPase. This enzyme has been targeted in the prevention of osteoporosis. In addition, several hydrolytic enzymes, such as members of the cathepsin and matrix metalloprotease(MMP) groups, are released to digest the organic components of the matrix. These enzymes are released into the compartment by lysosomes. Of these hydrolytic enzymes, cathepsin K is of most importance.
Cathepsin K and other cathepsins
Cathepsin K is a collagenolytic, papain-like, cysteine protease that is mainly expressed in osteoclasts, and is secreted into the resorptive pit. Cathepsin K is the major protease involved in the degradation of type I collagen and other noncollagenous proteins. Mutations in the cathepsin K gene are associated with pycnodysostosis, a hereditary osteopetrotic disease, characterised by lack of functional cathepsin K expression. Knockout studies of cathepsin K in mice lead to an osteopetrotic phenotype, which, is partially compensated by increased expression of proteases other that cathepsin K and enhanced osteoclastogenesis. Cathepsin K has an optimal enzymatic activity in acidic conditions. It is synthesized as a proenzyme with a molecular weight of 37kDa, and upon activation by autocatalytic cleavage, is transformed into the mature, active form with a molecular weight of ~27kDa. Upon polarization of the osteoclast over the site of resorption, cathepsin K is secreted from the ruffled border into the resorptive pit. Cathepsin K transmigrates across the ruffled border by intercellular vesicles and is then released by the functional secretory domain. Within these intercellular vesicles, cathepsin K, along with reactive oxygen species generated by TRAP, further degrades the bone extracellular matrix. Numerous other cathepsins are expressed in osteoclasts. These include cathepsin B, C, D, E, G, and L. The function of these cysteine and aspartic proteases is generally unknown within bone, and they are expressed at much lower levels than cathepsin K. Studies on cathepsin L knockout mice have been mixed, with a report of reduced trabecular bone in homozygous and heterozygous cathepsin L knockout mice compared to wild-type and another report finding no skeletal abnormalities.
Matrix metalloproteinases
The matrix metalloproteinases (MMPs) comprise a family of more than 20 zinc-dependent endopeptidases. The role of matrix metalloproteinases (MMPs) in osteoclast biology is ill-defined, but in other tissue they have been linked with tumor promoting activities, such as activation of growth factors and are required for tumor metastasis and angiogenesis. MMP-9 is associated with the bone microenvironment. It is expressed by osteoclasts, and is known to be required for osteoclast migration and is a powerful gelatinase. Transgenic mice lacking MMP-9 develop defects in bone development, intraosseous angiogenesis, and fracture repair. MMP-13 is believed to be involved in bone resorption and in osteoclast differentiation, as knockout mice revealed decreased osteoclast numbers, osteopetrosis, and decreased bone resorption.
Osteoclast MMPs expressed by the osteoclast include MMP-9, -10, -12, and -14. apart from MMP-9, little is known about their relevance to the osteoclast, however, high levels of MMP-14 are found at the sealing zone.
495
Regulation
Osteoclasts are regulated by several hormones, including parathyroid hormone (PTH) from the parathyroid gland, calcitonin from the thyroid gland, and growth factor interleukin 6 (IL-6). This last hormone, IL-6, is one of the factors in the disease osteoporosis, which is an imbalance between bone resorption and bone formation. Osteoclast activity is also mediated by the interaction of two molecules produced by osteoblasts, namely osteoprotegerin and RANK ligand. Note that these molecules also regulate differentiation of the osteoclast.[5]
Alternate use of term
An osteoclast can also be an instrument used to fracture and reset bones (the origin is Greek osteon:bone and klastos:broken). To avoid confusion, the cell was originally termed osotoclast. When the surgical instrument went out of use, the cell became known by its present name.
References
[1] Netter, Frank H. (1987), Musculoskeletal system: anatomy, physiology, and metabolic disorders. Summit, New Jersey: Ciba-Geigy Corporation ISBN 0-914168-88-6, p. 169 [2] Standring S., Ed. Gray's Anatomy. 39th ed. 2005, Elsevier [4] p. 378
External links
• MedicineNet (http://www.medterms.com/script/main/art.asp?articlekey=11794) • Osteoclasts (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Osteoclasts) at the US National Library of Medicine Medical Subject Headings (MeSH) • The Life of Osteoclast (http://www.youtube.com/watch?v=6Cn4uusbGk8) • Animation by Random42 Medical Animation on the role of osteoclasts in bone remodeling (http://www. random42.com/bone-biology-osteoblasts-and-osteoclasts)
Dendritic cell
496
Dendritic cell
Dendritic cells (DCs) are immune cells forming part of the mammalian immune system. Their main function is to process antigen material and present it on the surface to other cells of the immune system. That is, dendritic cells function as antigen-presenting cells. They act as messengers between the innate and adaptive immunity. Dendritic cells are present in tissues in contact with the external environment, such as the skin (where there is a specialized dendritic cell type called Langerhans cells) and the inner lining of the nose, lungs, stomach and intestines. They can also be found in an immature state in the blood. Once activated, they migrate to the lymph nodes where they interact with T cells and B cells to initiate and shape the adaptive immune response. At certain development stages they grow branched projections, the dendrites that give the cell its name (δένδρον or déndron being Greek for "tree"). While similar in appearance, these are distinct structures from the dendrites of neurons. Immature dendritic cells are also called veiled cells, as they possess large cytoplasmic 'veils' rather than dendrites.
A dendritic cell
History
Dendritic cells were first described by Paul Langerhans (hence "Langerhans cells") in the late nineteenth century. It wasn't until 1973, however, that the term "dendritic cells" was coined by Ralph M. Steinman and Zanvil A. Cohn.[] For discovering the central role of dendritic cells in the adaptive immune response,[] Steinman was awarded the Albert Lasker Award for Basic Medical Research in 2007[] and the Nobel Prize in Physiology or Medicine in 2011.[]
Dendritic cells in skin
Types of dendritic cells
In all dendritic cells, the similar morphology results in a very large contact surface to their surroundings compared to overall cell volume.
In vivo – primate
The most common division of dendritic cells is "myeloid" vs. "plasmacytoid":
Dendritic cell
497
Name
Description
Secretion
Toll-like [1] receptors TLR 2, TLR 4
Myeloid dendritic cell (mDC)
Most similar to monocytes. mDC are IL-12 made up of at least two subsets: (1) the more common mDC-1, which is a major stimulator of T cells (2) the extremely rare mDC-2, which may have a function in fighting wound infection
[] Plasmacytoid Look like plasma cells, but have certain Can produce high amounts of interferon-alpha and thus became dendritic cell (pDC) characteristics similar to myeloid known as IPC (interferon-producing cells) before their dendritic [2] [3] dendritic cells. cell nature was revealed.
TLR 7, TLR 9
The markers BDCA-2, BDCA-3, and BDCA-4 can be used to discriminate among the types.[4] Lymphoid and myeloid DCs evolve from lymphoid or myeloid precursors respectively and thus are of hematopoietic origin. By contrast, follicular dendritic cells (FDC) are probably of mesenchymal rather than hematopoietic origin and do not express MHC class II, but are so named because they are located in lymphoid follicles and have long "dendritic" processes.
Dendritic cells in blood
The blood DCs are typically identified and enumerated in flow cytometry. Three types of DCs have been defined in human blood and these are the CD11c+ myeloid DCs, the CD141+ myeloid DCs and the CD303+ plasmacytoid DCs. This represents the nomenclature proposed by the respective IUIS nomenclature committee [5] Dendritic cells that circulate in blood do not have all the typical features of their counterparts in tissue, i.e. they are less mature and have no dendrites. Still, they can perform complex functions including chemokine-production in CD11c+ myeloid DCs, cross-presentation in CD141+ myeloid DCs and IFNalpha production in CD303+ plasmacytoid DCs.
In vitro
In some respects, dendritic cells cultured in vitro do not show the same behaviour or capability as dendritic cells isolated ex vivo. Nonetheless, they are often used for research as they are still much more readily available than genuine DCs. • Mo-DC or MDDC refers to cells matured from monocytes[6] • HP-DC refers to cells derived from hematopoietic progenitor cells.
Nonprimate
While humans and non-human primates such as Rhesus macaques appear to have DCs divided into these groups, other species (such as the mouse) have different subdivisions of DCs.
Life cycle
Formation of immature cells
Dendritic cells are derived from hematopoietic bone marrow progenitor cells. These progenitor cells initially transform into immature dendritic cells. These cells are characterized by high endocytic activity and low T-cell activation potential. Immature dendritic cells constantly sample the surrounding environment for pathogens such as viruses and bacteria. This is done through pattern recognition receptors (PRRs) such as the toll-like receptors (TLRs). TLRs recognize specific chemical signatures found on subsets of pathogens. Immature dendritic cells may
Dendritic cell also phagocytize small quantities of membrane from live own cells, in a process called nibbling. Once they have come into contact with a presentable antigen, they become activated into mature dendritic cells and begin to migrate to the lymph node. Immature dendritic cells phagocytose pathogens and degrade their proteins into small pieces and upon maturation present those fragments at their cell surface using MHC molecules. Simultaneously, they upregulate cell-surface receptors that act as co-receptors in T-cell activation such as CD80 (B7.1), CD86 (B7.2), and CD40 greatly enhancing their ability to activate T-cells. They also upregulate CCR7, a chemotactic receptor that induces the dendritic cell to travel through the blood stream to the spleen or through the lymphatic system to a lymph node. Here they act as antigen-presenting cells: they activate helper T-cells and killer T-cells as well as B-cells by presenting them with antigens derived from the pathogen, alongside non-antigen specific costimulatory signals Every helper T-cell is specific to one particular antigen. Only professional antigen-presenting cells (macrophages, B lymphocytes, and dendritic cells) are able to activate a resting helper T-cell when the matching antigen is presented. However, macrophages and B cells can only activate memory T cells[citation needed] whereas dendritic cells can activate both memory and naive T cells, and are the most potent of all the antigen-presenting cells. As mentioned above, mDC probably arise from monocytes, white blood cells which circulate in the body and, depending on the right signal, can turn into either dendritic cells or macrophages. The monocytes in turn are formed from stem cells in the bone marrow. Monocyte-derived dendritic cells can be generated in vitro from peripheral blood mononuclear cells (PBMCs). Plating of PBMCs in a tissue culture flask permits adherence of monocytes. Treatment of these monocytes with interleukin 4 (IL-4) and granulocyte-macrophage colony stimulating factor (GM-CSF) leads to differentiation to immature dendritic cells (iDCs) in about a week. Subsequent treatment with tumor necrosis factor (TNF) further differentiates the iDCs into mature dendritic cells.
498
Life span of dendritic cells
Activated macrophages have a lifespan of only a few days though new evidence suggest that it could be extended to weeks rather than days.[citation needed] The lifespan of activated dendritic cells, while somewhat varying according to type and origin, is of a similar order of magnitude, but immature dendritic cells seem to be able to exist in an inactivated state for much longer.
Research challenges
The exact genesis and development of the different types and subsets of dendritic cells and their interrelationship is only marginally understood at the moment, as dendritic cells are so rare and difficult to isolate that only in recent years they have become subject of focused research. Distinct surface antigens that characterize dendritic cells have only become known from 2000 on; before that, researchers had to work with a 'cocktail' of several antigens which, used in combination, result in isolation of cells with characteristics unique to DCs.
Dendritic cells and cytokines
The dendritic cells are constantly in communication with other cells in the body. This communication can take the form of direct cell–cell contact based on the interaction of cell-surface proteins. An example of this includes the interaction of the membrane proteins of the B7 family of the dendritic cell with CD28 present on the lymphocyte. However, the cell–cell interaction can also take place at a distance via cytokines. For example, stimulating dendritic cells in vivo with microbial extracts causes the dendritic cells to rapidly begin producing IL-12.[] IL-12 is a signal that helps send naive CD4 T cells towards a Th1 phenotype. The ultimate consequence is priming and activation of the immune system for attack against the antigens which the dendritic cell presents on its surface. However, there are differences in the cytokines produced depending on the type of dendritic cell. The plasmacytoid DC has the ability to produce huge amounts of type-1 IFN's, which recruit more activated macrophages to allow phagocytosis.[]
Dendritic cell
499
Disease
HIV infection
HIV, which causes AIDS, can bind to dendritic cells via various receptors expressed on the cell. The best studied example is DC-SIGN (usually on MDC subset 1, but also on other subsets under certain conditions; since not all dendritic cell subsets express DC-SIGN, its exact role in sexual HIV-1 transmission is not clear)[citation needed]. When the dendritic cell takes up HIV and then travels to the lymph node, the virus can be transferred to helper CD4+ T-cells, contributing to the developing infection. This infection of dendritic cells by HIV explains one mechanism by which the virus could persist after prolonged HAART[citation needed]. Many other viruses, such as the SARS virus seems to use DC-SIGN to 'hitchhike' to its target cells.[7] However, most work with virus binding to DC-SIGN expressing cells has been conducted using in vitro derived cells such as moDCs. The physiological role of DC-SIGN in vivo is more difficult to ascertain.
Autoimmunity
Altered function of dendritic cells is also known to play a major or even key role in allergy and autoimmune diseases like lupus erythematosus and inflammatory bowel diseases (Crohn's disease and ulcerative colitis).[][][]
Dendritic cells in animals other than humans
The above applies to humans. In other organisms, the function of dendritic cells can differ slightly. For example, in brown rats (but not mice), a subset of dendritic cells exists that displays pronounced killer cell-like activity, apparently through its entire lifespan[citation needed]. However, the principal function of dendritic cells as known to date is always to act as an immune sentinel. They survey the body and collect information relevant to the immune system, they are then able to instruct and direct the adaptive arms to respond to challenges. In addition, an immediate precursor to myeloid and lymphoid dendritic cells of the spleen has been identified.[] This precursor, termed pre-DC, lacks MHC class II surface expression, and is distinct from monocytes, which primarily give rise to DCs in non-lymphoid tissues. Although typically described in mammals, dendritic cells have also been found in chickens[8] and turtles.[9]
Dendritic cell
500
Media
A single dendritic cell can be seen here efficiently taking up at least four conidia in its vicinity.
References
[5] Ziegler-Heitbrock, L et al (2010): Nomenclature of monocytes and dendritic cells in blood. Blood,116 (16): e74-e80. PMID 20628149
External links
• (http://u1019.lille.inserm.fr/research-activities/?lang=en), Website of the Center for Infection and Immunity of Lille contains information on DCs and their study in research • Dendritic Cells (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Dendritic+Cells) at the US National Library of Medicine Medical Subject Headings (MeSH) • www.dc2007.eu : 5th International Meeting on Dendritic Cell Vaccination and other Strategies to tip the Balance of the Immune System (http://www.dc2007.eu) • Website of Dr. Ralph M. Steinman at The Rockefeller University (http://www.rockefeller.edu/labheads/ steinman/steinman-lab.php) contains information on DCs, links to articles, pictures and videos • Cancer 'danger receptor' found (http://news.bbc.co.uk/2/hi/health/7888042.stm), BBC News, 15 February 2009
Lymphatic system
501
Lymphatic system
Lymphatic System
Human lymphatic system Latin systema lymphoideum
The lymphatic system is part of the circulatory system, comprising a network of conduits called lymphatic vessels that carry a clear fluid called lymph (from Latin lympha "water goddess"[1]) directionally towards the heart. The lymphatic system was first described in the seventeenth century independently by Olaus Rudbeck and Thomas Bartholin. The lymph system is not a closed system. The circulatory system processes an average of 20 liters of blood per day through capillary filtration which removes plasma while leaving the blood cells. Roughly 17 liters of the filtered plasma actually get reabsorbed directly into the blood vessels, while the remaining 3 liters are left behind in the interstitial fluid. The primary function of the lymph system is to provide an accessory route for these excess 3 liters per day to get returned to the blood.[2] Lymph is essentially recycled blood plasma. Lymphatic organs play an important part in the immune system, having a considerable overlap with the lymphoid system. Lymphoid tissue is found in many organs, particularly the lymph nodes, and in the lymphoid follicles associated with the digestive system such as the tonsils. Lymphoid tissues contain lymphocytes, but they also contain other types of cells for support.[] The system also includes all the structures dedicated to the circulation and production of lymphocytes (the primary cellular component of lymph), which includes the spleen, thymus, bone marrow, and the lymphoid tissue associated with the digestive system.[] The blood does not directly come in contact with the parenchymal cells and tissues in the body, but constituents of the blood first exit the microvascular exchange blood vessels to become interstitial fluid, which comes into contact with the parenchymal cells of the body. Lymph is the fluid that is formed when interstitial fluid enters the initial lymphatic vessels of the lymphatic system. The lymph is then moved along the lymphatic vessel network by either intrinsic contractions of the lymphatic passages or by extrinsic compression of the lymphatic vessels via external tissue forces (e.g. the contractions of skeletal muscles). The organization of lymph nodes and drainage follows the organization of the body into external and internal regions; therefore, the lymphatic drainage of the head, limbs, and body cavity walls follows an external route, and the lymphatic drainage of the thorax, abdomen, and pelvic cavities follows an internal route.[3] Eventually, the lymph vessels empty into the lymphatic ducts, which drain into one of the two subclavian veins (near the junctions of the subclavian veins with the internal jugular veins).
Lymphatic system
502
Terminology
The adjective used for the lymph-transporting system is "lymphatic." The adjective used for the tissues where lymphocytes are formed is "lymphoid." Lymphatic comes from the Latin word lymphaticus, meaning "connected to water."
Functions
The lymphatic system has multiple interrelated functions:[4] • • • • It is responsible for the removal of interstitial fluid from tissues It absorbs and transports fatty acids and fats as chyle from the digestive system It transports white blood cells to and from the lymph nodes into the bones The lymph transports antigen-presenting cells (APCs), such as dendritic cells, to the lymph nodes where an immune response is stimulated.
Clinical significance
The study of lymphatic drainage of various organs is important in diagnosis, prognosis, and treatment of cancer. The lymphatic system, because of its physical proximity to many tissues of the body, is responsible for carrying cancerous cells between the various parts of the body in a process called metastasis. The intervening lymph nodes can trap the cancer cells. If they are not successful in destroying the cancer cells the nodes may become sites of secondary tumors.
Organization
The lymphatic system can be broadly divided into the conducting system and the lymphoid tissue. • The conducting system carries the lymph and consists of tubular vessels that include the lymph capillaries, the lymph vessels, and the right and left thoracic ducts. • The lymphoid tissue is primarily involved in immune responses and consists of lymphocytes[5] and other white blood cells enmeshed in connective tissue through which the lymph passes. Regions of the lymphoid tissue that are densely packed with lymphocytes are known as lymphoid follicles. Lymphoid tissue can either be structurally well organized as lymph nodes or may consist of loosely organized lymphoid follicles known as the mucosa-associated lymphoid tissue (MALT).
Lymphoid tissue
Lymphoid tissue associated with the lymphatic system is concerned with immune functions in defending the body against the infections and spread of tumors. It consists of connective tissue with various types of white blood cells enmeshed in it, most numerous being the lymphocytes. The lymphoid tissue may be primary, secondary, or tertiary depending upon the stage of lymphocyte development and maturation it is involved in. (The tertiary lymphoid tissue typically contains far fewer lymphocytes, and assumes an immune role only when challenged with antigens that result in inflammation. It achieves this by importing the lymphocytes from blood and lymph.[])
Lymphatic system
503
Primary lymphoid organs
The central or primary lymphoid organs generate lymphocytes from immature progenitor cells. The thymus and the bone marrow constitute the primary lymphoid tissues involved in the production and early selection of lymphocytes.
Secondary lymphoid organs
Secondary or peripheral lymphoid organs maintain mature naive lymphocytes and initiate an adaptive immune response. The peripheral lymphoid organs are the sites of lymphocyte activation by antigen. Activation leads to clonal expansion and affinity maturation. Mature lymphocytes recirculate between the blood and the peripheral lymphoid organs until they encounter their specific antigen. Secondary lymphoid tissue provides the environment for the foreign or altered native molecules (antigens) to interact with the lymphocytes. It is exemplified by the lymph nodes, and the lymphoid follicles in tonsils, Peyer's patches, spleen, adenoids, skin, etc. that are associated with the mucosa-associated lymphoid tissue (MALT). Lymph nodes A lymph node is an organized collection of lymphoid tissue, through which the lymph passes on its way to returning to the blood. Lymph nodes are located at intervals along the lymphatic system. Several afferent lymph vessels bring in lymph, which percolates through the substance of the lymph node, and is drained out by an efferent lymph vessel. The substance of a lymph node consists of lymphoid follicles in the A lymph node showing afferent and efferent lymphatic vessels outer portion called the "cortex," which contains the lymphoid follicles, and an inner portion called "medulla," which is surrounded by the cortex on all sides except for a portion known as the "hilum." The hilum presents as a depression on the surface of the lymph node, which makes the otherwise spherical or ovoid lymph node bean-shaped. The efferent lymph vessel directly emerges from the lymph node here. The arteries and veins supplying the lymph node with blood enter and exit through the hilum. Lymph follicles are a dense collection of lymphocytes, the number, size and configuration of which change in accordance with the functional state of the lymph node. For example, the follicles expand significantly upon encountering a foreign antigen. The selection of B cells occurs in the germinal center of the lymph nodes. Lymph nodes are particularly numerous in the mediastinum in the chest, neck, pelvis, axilla (armpit), inguinal (groin) region, and in association with the blood vessels of the intestines.[]
Lymphatic system
504
Lymphatics
Tubular vessels transport back lymph to the blood ultimately replacing the volume lost from the blood during the formation of the interstitial fluid. These channels are the lymphatic channels or simply called lymphatics.[6]
Function of the fatty acid transport system
Lymph vessels called lacteals are present in the lining of the gastrointestinal tract, predominantly in the small intestine. While most lymphatic system other nutrients absorbed by the small intestine are passed on to the portal venous system to drain via the portal vein into the liver for processing, fats (lipids) are passed on to the lymphatic system to be transported to the blood circulation via the thoracic duct. (There are exceptions, for example medium-chain triglycerides (MCTs) are fatty acid esters of glycerol that passively diffuse from the GI tract to the portal system.) The enriched lymph originating in the lymphatics of the small intestine is called chyle. The nutrients that are released to the circulatory system are processed by the liver, having passed through the systemic circulation.
Diseases of the lymphatic system
Lymphedema is the swelling caused by the accumulation of lymph fluid, which may occur if the lymphatic system is damaged or has malformations. It usually affects limbs, though face, neck and abdomen may also be affected. In an extreme state the edema progresses. Skin becomes thicken with an appearance similar to elephant limbs. Is called elephantiasis.[7] Causes are unknown in most of cases but sometimes the patient have a previous history of severe infection most commonly caused by a parasitic disease, like the lymphatic filariasis for example. Some common causes of swollen lymph nodes include infections, infectious mononucleosis, and cancer, e.g. Hodgkin's and non-Hodgkin lymphoma, and metastasis of cancerous cells via the lymphatic system. Hodgkin's lymphoma is a type of cancer. This type of cancer usually results from the white blood cells in the body becoming diseased or damaged. Nowadays, this kind of cancer is easily controlled [8] Lymphangiomatosis is a disease involving multiple cysts or lesions formed from lymphatic vessels. Lymphangiosarcoma is a malignant soft tissue tumor, whereas lymphangioma is a benign tumor occurring frequently in association with Turner syndrome. Lymphangioleiomyomatosis is a benign tumor of the smooth muscles of the lymphatics that occurs in the lungs. Lymphoid leukemias and lymphomas are now considered to be tumors of the same type of cell lineage. They are called "leukemia" when in the blood or marrow and "lymphoma" when in lymphatic tissue. They are grouped together under the name "lymphoid malignancy".[]
Lymphatic system
505
Development of lymphatic tissue
Lymphatic tissues begin to develop by the end of the fifth week of embryonic development. Lymphatic vessels develop from lymph sacs that arise from developing veins, which are derived from mesoderm. The first lymph sacs to appear are the paired jugular lymph sacs at the junction of the internal jugular and subclavian veins. From the jugular lymph sacs, lymphatic capillary plexuses spread to the thorax, upper limbs, neck and head. Some of the plexuses enlarge and form lymphatic vessels in their respective regions. Each jugular lymph sac retains at least one connection with its jugular vein, the left one developing into the superior portion of the thoracic duct. The next lymph sac to appear is the unpaired retroperitoneal lymph sac at the root of the mesentery of the intestine. It develops from the primitive vena cava and mesonephric veins. Capillary plexuses and lymphatic vessels spread from the retroperitoneal lymph sac to the abdominal viscera and diaphragm. The sac establishes connections with the cisterna chyli but loses its connections with neighboring veins. The last of the lymph sacs, the paired posterior lymph sacs, develop from the iliac veins. The posterior lymph sacs produce capillary plexuses and lymphatic vessels of the abdominal wall, pelvic region, and lower limbs. The posterior lymph sacs join the cisterna chyli and lose their connections with adjacent veins. With the exception of the anterior part of the sac from which the cisterna chyli develops, all lymph sacs become invaded by mesenchymal cells and are converted into groups of lymph nodes. The spleen develops from mesenchymal cells between layers of the dorsal mesentery of the stomach. The thymus arises as an outgrowth of the third pharyngeal pouch.
Lymphatico-venous communications
Present research has found clues about a lymphatico-venous communication. In mammals, lymphatico-venous communications other than those at the base of the neck are not easy to demonstrate, but described in some experiments.[] The specialists observed that the pulmonary complications following lymphangiography (a test which utilizes X ray technology, along with the injection of a contrast agent, to view lymphatic circulation and lymph nodes for diagnostic purposes) are more often severe in patients with lymphatic obstruction. In these cases, the contrast medium is thought to reach the vascular system via lymphovenous communications which shunt the material directly into the venous stream, bypassing those lymph nodes distal to the communications,[] Because less contrast agent is absorbed in lymph nodes, a greater portion of the injected volume passes into the vascular system. Since pulmonary complications are related to the amount of medium reaching the lungs area, the early recognition of lymphovenous communications is a great significance to the lymphangiographer.[] Another "hint" in proving a lymph-vein communication is offered by a Robert F Dunn experiment. The passage of radioactively tagged tracers, injected at elevated pressure, through the lymph node-venous communications coincides with the increased pressures of injection and subsequent nodal palpation in dogs. The passage of iodinated I 125 serum albumen (ISA) indicates that direct lymph node-venous communications are present, whereas passage of nucleated erythrocytes requires a communication structure the size of a capillary or larger.[9] Moreover, the evidence suggest that in mammals under normal conditions, most of the lymph is returned to the blood stream through the lymphatico-venous communications at the base of the neck. When the thoracic duct-venous communication is blocked, however, the resultant raised intralymphatic pressure will usually cause other normal non-functioning communications to open and thereby allow the return of lymph to the blood stream.[]
Lymphatic system
506
History
Hippocrates was one of the first people to mention the lymphatic system in 5th century BC. In his work On Joints, he briefly mentioned the lymph nodes in one sentence. Rufus of Ephesus, a Roman physician, identified the axillary, inguinal and mesenteric lymph nodes as well as the thymus during the 1st to 2nd century AD.[] The first mention of lymphatic vessels was in 3rd century BC by Herophilos, a Greek anatomist living in Alexandria, who incorrectly concluded that the "absorptive veins of the lymphatics," by which he meant the lacteals (lymph vessels of the intestines), drained into the hepatic portal veins, and thus into the liver.[] Findings of Ruphus and Herophilos findings were further propagated by the Greek physician Galen, who described the lacteals and mesenteric lymph nodes which he observed in his dissection of apes and pigs in the 2nd century AD.[][] In the mid 16th century, Gabriele Falloppio (discoverer of the fallopian tubes), described what are now known as the lacteals as "coursing over the intestines full of yellow matter."[] In about 1563 Bartolomeo Eustachi, a professor of anatomy, described the thoracic duct in horses as vena alba thoracis.[] The next breakthrough came when in 1622 a physician, Gaspare Aselli, identified lymphatic vessels of the intestines in dogs and termed them venae alba et lacteae, which is now known as simply the lacteals. The lacteals were termed the fourth kind of vessels (the other three being the artery, vein and nerve, which was then believed to be a type of vessel), and disproved Galen's assertion that chyle was carried by the veins. But, he still believed that the lacteals carried the chyle to the liver (as taught by Galen).[] He also identified the thoracic duct but failed to notice its connection with the lacteals.[] This connection was established by Jean Pecquet in 1651, who found a white fluid mixing with blood in a dog's heart. He suspected that fluid to be chyle as its flow increased when abdominal pressure was applied. He traced this fluid to the thoracic duct, which he then followed to a chyle-filled sac he called the chyli receptaculum, which is now known as the cisternae chyli; further investigations led him to find that lacteals' contents enter the venous system via the thoracic duct.[][] Thus, it was proven convincingly that the lacteals did not terminate in the liver, thus disproving Galen's second idea: that the chyle flowed to the liver.[] Johann Veslingius drew the earliest sketches of the lacteals in humans in 1647.[] The idea that blood recirculates through the body rather than being produced anew by the liver and the heart was first accepted as a result of works of William Harvey—a work he published in 1628. In 1652, Olaus Rudbeck (1630–1702), a Swede, discovered certain transparent vessels in the liver that contained clear fluid (and not white), and thus named them hepatico-aqueous vessels. He also learned that they emptied into the thoracic duct, and that they had valves.[] He announced his findings in the court of Queen Christina of Sweden, but did not publish his findings for a year,[] and in the interim similar findings were published by Thomas Bartholin, who additionally published that such vessels are present everywhere in the body, and not just the liver. He is also the one to have named them "lymphatic vessels."[] This had resulted in a bitter dispute between one of Bartholin's pupils, Martin Bogdan,[10] and Rudbeck, whom he accused of plagiarism.[] Galen's ideas prevailed in medicine until the 17th century. It was believed that blood was produced by the liver from chyle contaminated with ailments by the intestine and stomach, to which various spirits were added by other organs, and that this blood was consumed by all the organs of the body. This theory required that the blood be consumed and produced many times over. Even in the 17th century, his ideas were defended by some physicians.[]
Lymphatic system
507
"Claude Galien". Lithograph by Pierre Roche Vigneron. (Paris: Lith de Gregoire et Deneux, ca. 1865)
Portrait of Eustachius
Olaus Rudbeck in 1696.
Thomas Bartholin
References
[2] Human Physiology: From Cells to Systems, by Lauralee Sherwood (http:/ / books. google. com/ books?id=I9qH3eZ1pP0C& pg=PT401#v=onepage& q& f=false)
External links
• Lymphatic System (http://www.emc.maricopa.edu/faculty/farabee/BIOBK/BioBookIMMUN.html) • Lymphatic System Overview (http://www.innerbody.com/image/lympov.html) (innerbody.com)
Microglia
508
Microglia
Microglia
Code TH H2.00.06.2.00004 [1]
Microglia are a type of glial cell that are the resident macrophages of the brain and spinal cord, and thus act as the first and main form of active immune defense in the central nervous system (CNS). Microglia constitute 20% of the total glial cell population within the brain.[1] Microglia (and astrocytes) are distributed in large non-overlapping regions throughout the brain and spinal cord.[][] Microglia are constantly scavenging the CNS for plaques, damaged neurons and infectious agents.[] The brain and spinal cord are considered "immune privileged" organs in that they are separated from the rest of the body by a series of endothelial cells known as the blood–brain barrier, which prevents most infections from reaching the vulnerable nervous tissue. In the case where infectious agents are directly introduced to the brain or cross the blood–brain barrier, microglial cells must react quickly to decrease inflammation and destroy the infectious agents before they damage the sensitive neural tissue. Due to the unavailability of antibodies from the rest of the body (few antibodies are small enough to cross the blood brain barrier), microglia must be able to recognize foreign bodies, swallow them, and act as antigen-presenting cells activating T-cells. Since this process must be done quickly to prevent potentially fatal damage, microglia are extremely sensitive to even small pathological changes in the CNS.[] They achieve this sensitivity in part by having unique potassium channels that respond to even small changes in extracellular potassium.[]
Microglia - ramified form from rat cortex after traumatic brain injury (lactins staining with HRP)
Microglia/Macrophage - activated form from rat cortex after traumatic brain injury (lactins staining with HRP)
Origin
Microglial cells differentiate in the bone marrow from hematopoietic stem cells, the progenitors of all blood cells. During hematopoiesis, some of these stem cells differentiate into monocytes and travel from the bone marrow to the brain, where they settle and further differentiate into microglia.[] Monocytes can also differentiate into myeloid dendritic cells and macrophages in the peripheral systems. Like macrophages in the rest of the body, microglia use phagocytic and cytotoxic mechanisms to destroy foreign materials. Microglia and macrophages both contribute to the immune response by acting as antigen presenting cells, as well as promoting inflammation and homeostatic mechanisms within the body by secreting cytokines and other signaling molecules.
Microglia In their downregulated form, microglia lack the MHC class I/MHC class II proteins, IFN-γ cytokines, CD45 antigens, and many other surface receptors required to act in the antigen-presenting, phagocytic, and cytotoxic roles that hallmark normal macrophages. Microglia also differ from macrophages in that they are much more tightly regulated spatially and temporally in order to maintain a precise immune response.[] Another difference between microglia and other cells that differentiate from myeloid progenitor cells is the turnover rate. Macrophages and dendritic cells are constantly being used up and replaced by myeloid progenitor cells which differentiate into the needed type. Due to the blood brain barrier, it would be fairly difficult for the body to constantly replace microglia. Therefore, instead of constantly being replaced with myeloid progenitor cells, the microglia maintain their status quo while in their quiescent state, and then, when they are activated, they rapidly proliferate in order to keep their numbers up. Bone chimera studies have shown, however, that in cases of extreme infection the blood–brain barrier will weaken, and microglia will be replaced with haematogenous, cart-marrow derived cells, namely myeloid progenitor cells and macrophages. Once the infection has decreased the disconnect between peripheral and central systems is reestablished and only microglia are present for the recovery and regrowth period.[]
509
History
The ability to view and characterize different neural cells including microglia began in 1880 when Nissl staining was developed by Franz Nissl. Franz Nissl and F. Robertson first described microglial cells during their histology experiments. The cell staining techniques in the 1880s showed that microglia are related to macrophages. The activation of microglia and formation of ramified microglial clusters was first noted by Victor Babeş while studying a rabies case in 1897. Babeş noted the cells were found in a variety of viral brain infections but did not know what the clusters of microglia he saw were.[] Pío del Río Hortega, a student of Santiago Ramón y Cajal, first called the cells "microglia" around 1920. He went on to characterize microglial response to brain lesions in 1927 and note the "fountains of microglia" present in the corpus callosum and other perinatal white matter areas in 1932. After many years of research Rio-Hortega became generally considered as the "Father of Microglia."[][] For a long period of time little improvement was made in our knowledge of microglia. Then, in 1988, Hickey and Kimura showed that perivascular microglial cells are bone-marrow derived, and express high levels of MHC class II proteins used for antigen presentation. This confirmed Pio Del Rio-Hortega's postulate that microglial cells functioned similarly to macrophages by performing phagocytosis and antigen presentation.
Types
Microglial cells are extremely plastic, and undergo a variety of structural changes based on their location and current role. This level of plasticity is required to fulfill the vast variety of immunological functions that microglia perform, as well as maintaining homeostasis within the brain. If microglia were not capable of this they would need to be replaced on a regular basis like macrophages, and would not be available to the CNS immune defense on extremely short notice without causing immunological imbalance under normal conditions.[]
Amoeboid
This form of microglial cell is found mainly within the perinatal white matter areas in the corpus callosum known as the "Fountains of Microglia." This shape allows the microglial free movement throughout the neural tissue, which allows it to fulfill its role as a scavenger cell. Amoeboid microglia are able to phagocytose debris, but do not fulfill the same antigen-presenting and inflammatory roles as activated microglia. Amoeboid microglia are especially prevalent during the development and rewiring of the brain, when there are large amounts of extracellular debris and apoptotic cells to remove.[][][]
Microglia
510
Ramified
This form of microglial cell is commonly found at specific locations throughout the entire brain and spinal cord in the absence of foreign material or dying cells. This "resting" form of microglia is composed of long branching processes and a small cellular body. Unlike the ameboid forms of microglia, the cell body of the ramified form remains fairly motionless, while its branches are constantly moving and surveying the surrounding area. The branches are very sensitive to small changes in physiological condition and require very specific culture conditions to observe in vitro. Unlike activated or ameboid microglia, ramified microglia are unable to phagocytose cells and display little or no immunomolecules. This includes the MHC class I/II proteins normally used by macrophages and dendritic cells to present antigens to t-cells, and as a result ramified microglia function extremely poorly as antigen presenters. The purpose of this state is to maintain a constant level of available microglia to detect and fight infection, while maintaining an immunologically silent environment.[][]
Activated
Activated microglia can be stained via the marker Iba1, which is upregulated during activation. Microglia are the only cells in the brain to express Iba1. Non-phagocytic This state is actually part of a graded response as microglia move from their ramified form to their fully active phagocytic form. Microglia can be activated by a variety of factors including: glutamate receptor agonists, pro-inflammatory cytokines, cell necrosis factors, lipopolysaccharide, and changes in extracellular potassium (indicative of ruptured cells). Once activated the cells undergo several key morphological changes including the thickening and retraction of branches, uptake of MHC class I/II proteins, expression of immunomolecules, secretion of cytotoxic factors, secretion of recruitment molecules, and secretion of pro-inflammatory signaling molecules (resulting in a pro-inflammation signal cascade). Activated non-phagocytic microglia generally appear as "bushy," "rods," or small ameboids depending on how far along the ramified to full phagocytic transformation continuum they are. In addition, the microglia also undergo rapid proliferation in order to increase their numbers. From a strictly morphological perspective, the variation in microglial form along the continuum is associated with changing morphological complexity and can be quantitated using the methods of fractal analysis, which have proven sensitive to even subtle, visually undetectable changes associated with different morphologies in different pathological states.[][][][] Phagocytic Activated phagocytic microglia are the maximally immune responsive form of microglia. These cells generally take on a large, ameboid shape, although some variance has been observed. In addition to having the antigen presenting, cytotoxic and inflammatory mediating signaling of activated non-phagocytic microglia, they are also able to phagocytose foreign materials and display the resulting immunomolecules for T-cell activation. Phagocytic microglia travel to the site of the injury, engulf the offending material, and secrete pro-inflammatory factors to promote more cells to proliferate and do the same. Activated phagocytic microglia also interact with astrocytes and neural cells to fight off the infection as quickly as possible with minimal damage to the healthy brain cells.[][]
Microglia
511
Gitter cells
Gitter cells are the eventual result of microglial cell's phagocytosis of infectious material. Eventually, after engulfing a certain amount of material, the phagocytic microglia becomes unable to phagocytose any further materials. The resulting cellular mass is known as a granular corpuscle, named for its ‘grainy' appearance. By looking at tissues stained to reveal gitter cells, scientists can see post-infection areas that have healed.[]
Perivascular
Unlike the other types of microglia mentioned above, "perivascular" microglia refers to the location of the cell rather than its form/function. Perivascular microglia are mainly found encased within the walls of the basal lamina. They perform normal microglial functions, but unlike normal microglia they are replaced by bone marrow derived precursor cells on a regular basis and express MHC class II antigens regardless of the outside environment. Perivascular microglia also react strongly to macrophage differentiation antigens.[] These microglia have been shown to be essential to repair of vascular walls, as shown by Ritter's experiments and observations on ischemic retinopathy. Perivascular microglia promote endothelial cell proliferation allowing new vessels to be formed and damaged vessels to be repaired. During repair and development, myeloid recruitment and differentiation into microglial cells is highly accelerated to accomplish these tasks.[]
Juxtavascular
Like perivascular microglia, juxtavascular microglia can be distinguished mainly by their location. Juxtavascular microglia are found making direct contact with the basal lamina wall of blood vessels but are not found within the walls. Like perivascular cells, they express MHC class II proteins even at low levels of inflammatory cytokine activity. Unlike perivascular cells, but similar to resident microglia, juxtavascular microglia do not exhibit rapid turnover or replacement with myeloid precursor cells on a regular basis.[]
Functions
Microglial cells fulfill a variety of different tasks within the CNS mainly related to both immune response and maintaining homeostasis. The following are some of the major known functions carried out by these cells.
Scavenging
In addition to being very sensitive to small changes in their environment, each microglial cell also physically surveys its domain on a regular basis. This action is carried out in the ameboid and resting states. While moving through its set region, if the microglial cell finds any foreign material, damaged cells, apoptotic cells, neural tangles, DNA fragments, or plaques it will activate and phagocytose the material or cell. In this manner microglial cells also act as "housekeepers" cleaning up random cellular debris.[] During developmental wiring of the brain, microglial cells play a large role removing unwanted excess cellular matter. Post development, the majority of dead or apoptotic cells are found in the cerebral cortex and the subcortical white matter. This may explain why the majority of ameboid microglial cells are found within the "fountains of microglia" in the cerebral cortex.[]
Microglia
512
Phagocytosis
The main role of microglia, phagocytosis, involves the engulfing of various materials. Engulfed materials generally consist of cellular debris, lipids, and apoptotic cells in the non-inflamed state, and invading virus, bacteria, or other foreign materials in the inflamed state. Once the microglial cell is "full" it stops phagocytic activity and changes into a relatively non-reactive gitter cell.
Cytotoxicity
In addition to being able to destroy infectious organisms through cell to cell contact via phagocytosis, microglia can also release a variety of cytotoxic substances. Microglia in culture secrete large amounts of H2O2 and NO in a process known as ‘respiratory burst'. Both of these chemicals can directly damage cells and lead to neuronal cell death. Proteases secreted by microglia catabolise specific proteins causing direct cellular damage, while cytokines like IL-1 promote demyelination of neuronal axons. Finally, microglia can injure neurons through NMDA receptor-mediated processes by secreting glutamate and aspartate. Cytotoxic secretion is aimed at destroying infected neurons, virus, and bacteria, but can also cause large amounts of collateral neural damage. As a result, chronic inflammatory response can result in large scale neural damage as the microglia ravage the brain in an attempt to destroy the invading infection.[]
Antigen presentation
As mentioned above, resident non-activated microglia act as poor antigen presenting cells due to their lack of MHC class I/II proteins. Upon activation they rapidly uptake MHC class I/II proteins and quickly become efficient antigen presenters. In some cases, microglia can also be activated by IFN-γ to present antigens, but do not function as effectively as if they had undergone uptake of MHC class I/II proteins. During inflammation, T-cells cross the blood–brain barrier thanks to specialized surface markers and then directly bind to microglia in order to receive antigens. Once they have been presented with antigens, T-cells go on to fulfill a variety of roles including pro-inflammatory recruitment, formation of immunomemories, secretion of cytotoxic materials, and direct attacks on the plasma membranes of foreign cells.[][]
Synaptic stripping
In a phenomenon first noticed in spinal lesions by Blinzinger and Kreutzberg in 1968, post-inflammation microglia remove the branches from nerves near damaged tissue. This helps promote regrowth and remapping of damaged neural circuitry.[]
Promotion of repair
Post-inflammation, microglia undergo several steps to promote regrowth of neural tissue. These include synaptic stripping, secretion of anti-inflammatory cytokines, recruitment of neurons and astrocytes to the damaged area, and formation of gitter cells. Without microglial cells regrowth and remapping would be considerably slower in the resident areas of the CNS and almost impossible in many of the vascular systems surrounding the brain and eyes.[][]
Extracellular signaling
A large part of microglial cell's role in the brain is maintaining homeostasis in non-infected regions and promoting inflammation in infected or damaged tissue. Microglia accomplish this through an extremely complicated series of extracellular signaling molecules which allow them to communicate with other microglia, astrocytes, nerves, T-cells, and myeloid progenitor cells. As mentioned above the cytokine IFN-γ can be used to activate microglial cells. In addition, after becoming activated with IFN-γ, microglia also release more IFN-γ into the extracellular space. This activates more microglia and starts a cytokine induced activation cascade rapidly activating all nearby microglia. Microglia-produced TNF-α causes neural tissue to undergo apoptosis and increases inflammation. IL-8 promotes
Microglia B-cell growth and differentiation, allowing it to assist microglia in fighting infection. Another cytokine, IL-1, inhibits the cytokines IL-10 and TGF-β, which downregulate antigen presentation and pro-inflammatory signaling. Additional dendritic cells and T-cells are recruited to the site of injury through the microglial production of the chemotactic molecules like MDC, IL-8, and MIP-3β. Finally, PGE2 and other prostanoids help prevent chronic inflammation by inhibiting microglial pro-inflammatory response and downregulating Th1 (T-helper cell) response.[]
513
Role in chronic neuroinflammation
The word neuroinflammation has come to stand for chronic, central nervous system (CNS) specific, inflammation-like glial responses that may produce neurodegenerative symptoms such as plaque formation, dystrophic neurite growth, and excessive tau phosphorylation.[] It is important to distinguish between acute and chronic neuroinflammation. Acute neuroinflammation is generally caused by some neuronal injury after which microglia migrate to the injured site engulfing dead cells and debris.[] The term neuroinflammation generally refers to more chronic, sustained injury when the responses of microglial cells contribute to and expand the neurodestructive effects, worsening the disease process.[] When microglia are activated they take on an amoeboid shape and they alter their gene expression. Altered gene expression leads to the production of numerous potentially neurotoxic mediators. These mediators are important in the normal functions of microglia and their production is usually decreased once their task is complete.[] In chronic neuroinflammation, microglia remain activated for an extended period during which the production of mediators is sustained longer than usual.[] This increase in mediators contributes to neuronal death.[] Neuroinflammation is unique from inflammation in other organs, but does include some similar mechanisms such as the localized production of chemoattractant molecules to the site of inflammation.[] The following list contains a few of the numerous substances that are secreted when microglia are activated:
Cytokines
Microglia activate the proinflammatory cytokines IL-1α, IL-1β and TNF-α in the CNS.[] Cytokines play a potential role in neurodegeneration when microglia remain in a sustained activated state.[] Direct injection of the cytokines IL-1α, IL-1β and TNF-α into the CNS result in local inflammatory responses and neuronal degradation.[] This is in contrast with the potential neurotrophic (inducing growth of neurons) actions of these cytokines during acute neuroinflammation.[]
Chemokines
Chemokines are cytokines that stimulate directional migration of inflammatory cells in vitro and in vivo.[] Chemokines are divided into four main subfamilies: C, CC, CXC, and CX3C. Microglial cells are sources of some chemokines and express the monocyte chemoattractant protein-1 (MCP-1) chemokine in particular.[] Other inflammatory cytokines like IL-1β and TNF-α, as well as bacterial-derived lipopolysaccharide (LPS) may stimulate microglia to produce MCP-1, MIP-1α, and MIP-1β.[] Microglia can express CCR3, CCR5, CXCR4, and CX3CR1 in vitro.[] Chemokines are proinflammatory and therefore contribute to the neuroinflammation process.[]
Proteases
When microglia are activated they induce the synthesis and secretion of proteolytic enzymes that are potentially involved in many functions.[] There are a number of proteases that possess the potential to degrade both the extracellular matrix and neuronal cells that are in the neighborhood of the microglia releasing these compounds.[] These proteases include; cathepsins B, L, and S, the matrix metalloproteinases MMP-1, MMP-2, MMP-3, and MMP-9, and the metalloprotease-disintegrin ADAM8 plasminogen which forms outside microglia and degrades the extracellular matrix.[] Both Cathepsin B, MMP-1 and MMP-3 have been found to be increased in Alzheimer's disease (AD) and cathepsin B is increased in multiple sclerosis (MS).[] Elastase, another protease, could have large
Microglia negative effects on the extracellular matrix.[]
514
Amyloid precursor protein
Microglia synthesize amyloid precursor protein (APP) in response to excitotoxic injury.[] Plaques result from abnormal proteolytic cleavage of membrane bound APP.[] Amyloid plaques can stimulate microglia to produce neurotoxic compounds such as cytokines, excitotoxin, nitric oxide and lipophylic amines, which all cause neural damage.[] Plaques in Alzheimer's disease contain activated microglia.[] A study has shown that direct injection of amyloid into brain tissue activates microglia, which reduces the number of neurons.[] Microglia have also been suggested as a possible source of secreted β amyloid.[]
Aging
Microglia undergo a burst of mitotic activity during injury; this proliferation is followed by apoptosis to reduce the cell numbers back to baseline.[] Activation of microglia places a load on the anabolic and catabolic machinery of the cells causing activated microglia to die sooner than non-activated cells.[] To compensate for microglial loss over time, microglia undergo mitosis and bone marrow derived progenitor cells migrate into the brain via the meninges and vasculature.[] Accumulation of minor neuronal damage that occurs during normal aging can transform microglia into enlarged and activated cells.[] These chronic, age-associated increases in microglial activation and IL-1 expression may contribute to increased risk of Alzheimer's disease with advancing age through favoring neuritic plaque formation in susceptible patients.[] DNA damage might contribute to age-associated microglial activation. Another factor might be the accumulation of advanced glycation endproducts, which accumulate with aging.[] These proteins are strongly resistant to proteolytic processes and promote protein cross-linking.[] Research has discovered dystrophic (defective development) human microglia. "These cells are characterized by abnormalities in their cytoplasmic structure, such as deramified, atrophic, fragmented or unusually tortuous processes, frequently bearing spheroidal or bulbous swellings."[] The incidence of dystrophic microglia increases with aging.[] Microglial degeneration and death have been reported in research on Prion disease, Schizophrenia and Alzheimer's disease, indicating that microglial deterioration might be involved in neurodegenerative diseases.[] A complication of this theory is the fact that it is difficult to distinguish between "activated" and "dystrophic" microglia in the human brain.[]
Role of microglia in neurodegeneration
Neurodegenerative disorders are characterized by progressive cell loss in specific neuronal populations.[] "Many of the normal trophic functions of glia may be lost or overwhelmed when the cells become chronically activated in progressive neurodegenerative disorders, for there is abundant evidence that in such disorders, activated glia play destructive roles by direct and indirect inflammatory attack."[] The following are prominent examples of microglial cells' role in neurodegenerative disorders.
Alzheimer's disease
Alzheimer's disease (AD) is a progressive, neurodegenerative disease where the brain develops abnormal clumps (amyloid plaques) and tangled fiber bundles (neurofibrillary tangles).[] There are many activated microglia over-expressing IL-1 in the brains of Alzheimer patients that are distributed with both Aβ plaques and neurofibrillary tangles.[] This over expression of IL-1 leads to excessive tau phosphorylation that is related to tangle development in Alzheimer's disease.[] Many activated microglia are found to be associated with amyloid deposits in the brains of Alzheimer's patients.[] Microglia interact with β-amyloid plaques through cell surface receptors that are linked to tyrosine kinase based
Microglia signaling cascades that induce inflammation.[] When microglia interact with the deposited fibrillar forms of β-amyloid it leads to the conversion of the microglia into an activated cell and results in the synthesis and secretion of cytokines and other proteins that are neurotoxic.[] Treatment Non-steroidal anti-inflammatory drugs (NSAIDs) have proven to be effective in reducing the risk of AD.[] "Sustained treatment with NSAIDs lowers the risk of AD by 55%, delays disease onset, attenuates symptomatic severity and slows the loss of cognitive abilities. The main cellular target for NSAIDs is thought to be microglia. This is supported by the fact that in patients taking NSAIDs the number of activated microglia is decreased by 65%."[]
515
Parkinson's disease
Parkinson's disease is a movement disorder in which the dopamine-producing neurons in the brain do not function as they should, the neurons of the Substantia Nigra become disfunctional and eventually die, leaving a lack of domamine input into the thalamus. This causes the symptoms of Parkinson's disease.[]
Cardiovascular Diseases
Recently microglial activation has been reported in rats with myocardial infarction (Rana et al.,2010). These activation was specific to brain nuclei involved in cardiovascular regulation suggesting possible role of microglial activation in pathogenesis of heart failure.
Role in viral infections
Human immunodeficiency virus
The infection of mononuclear phagocytes with HIV-1 is an important element in the development of HIV-associated dementia complex (HAD).[] The only brain cell type that is "productively" infected with the virus are microglial cells.[] It has also become clear that neurotoxic mediators released from brain microglia play an important role in the pathogenesis of HIV-1.[] "HIV-1 can enter the microglial cell via CD4 receptors and chemokine co-receptors such as CCR3, CCR5, and CXCR4, with CCR5 being the most important of these. Interestingly, humans with double allelic loss of CCR5 are virtually immune to HIV acquired via the sexual route (though can be infected by IV transmission of CXCR4 tropic viruses). IL-4 and IL-10 enhance the entry and replication of HIV-1 in microglia through the up-regulation of CD4 and CCR5 expression, respectively. The chemokines CCL5/RANTES, CCL3/MIP-1α, CCL4/MIP-1β, all of which bind to CCR5, are inhibitory to HIV-1 replication in microglial cells, apparently by their ability to block viral entry."[] Infected microglia contain viral particles intracellularly.[] There is a correlation between the severity of dementia and microglial production of neurotoxins.[] One discrepancy in HAD is the limited number of HIV-1 infected microglia in comparison to the many CNS abnormalities that occur.[] This suggests that chemical factors that are released from microglial cells are contributing to neuronal loss. "It has become more and more apparent that HIV-1 infected microglial cells actively secrete both endogenous neurotoxins such as TNF-α, IL-1β, CXCL8/IL-8, glutamate, quinolinic acid, platelet activating factor, eicosanoids, and NO as well as the neurotoxic viral proteins Tat, gp120, and gp41."[] Microglia are the main target of HIV-1 in the brain. When activated by HIV-1 or viral proteins, they secrete or induce other cells to secrete neurotoxic factors; this process is accompanied by neuronal dysfunction (HAD).[]
Microglia
516
Herpes simplex virus
Herpes simplex virus (HSV) can cause herpes encephalitis in babies and immunocompetent adults. Studies have shown that long-term neuroimmune activation persists after the herpes infection in patients.[] Microglia produce cytokines that are toxic to neurons; this may be a mechanism underlying HSV-related CNS damage.[] It has been found that "active microglial cells in HSV encephalitis patients do persist for more than 12 months after antiviral treatment."[]
Role in bacterial infections
Lipopolysaccharide (LPS) is the major component of the outer membrane of a gram-negative bacterial cell wall. LPS has been shown to activate microglia in vitro and stimulates microglia to produce cytokines, chemokines, and prostaglandins.[] "Although LPS has been used as a classic activating agent, a recent study of rat microglia demonstrated that prolonged LPS exposure induces a distinctly different activated state from that in microglia acutely exposed to LPS."[]
Streptococcus pneumoniae
Streptococcus pneumoniae is the most common cause of bacterial meningitis. It is primarily localized to the subarachnoid space while cytokines and chemokines are produced inside the blood brain barrier.[] Microglia interact with streptococcus via their TLR2 receptor; this interaction then activates microglia to produce nitric oxide which is neurotoxic.[] The inflammatory response, triggered by microglia, may cause intracerebral edema.[]
Role in parasitic infections
Plasmodium falciparum
Plasmodium falciparum is a parasite that causes malaria in humans.[] A serious complication of malaria is cerebral malaria (CM).[] CM occurs when red blood cells break through the blood brain barrier causing microhemorrhages, ischemia and glial cell growth.[] This can lead to microglial aggregates called Durck's granulomas.[] Recent research has indicated that microglia play a major role in the pathogenesis of CM.[]
As a target to treat neuroinflammation
Inhibition of activation
One way to control neuroinflammation is to inhibit microglial activation. Studies on microglia have shown that they are activated by diverse stimuli but they are dependent on activation of mitogen-activated protein kinase (MAPK).[] Previous approaches to down-regulate activated microglia focused on immunosuppressants.[] Recently, minocycline (a tetracycline derivative) has shown down-regulation of microglial MAPK.[] Another promising treatment is CPI-1189, which induces cell death in a TNF α-inhibiting compound that also down-regulates MAPK.[] Recent study shows that nicergoline (Sermion) suppresses the production of proinflammatory cytokines and superoxide anion by activated microglia.[2] Microglial activation can be inhibited by MIF (microglia/macrophage inhibitory factor, tuftsin fragment 1–3, Thr-Lys-Pro). MIF-treated mice showed reduced brain injury and improved neurologic function in a mouse model of collagenase-induced intracerebral hemorrhage. [3][4]
Microglia
517
Regulation of chemokine receptor
The chemokine receptor, CX3CR1, is expressed by microglia in the central nervous system.[5] Fractalkine (CX3CL1) is the exclusive ligand for CX3CR1 and is made as a transmembrane glycoprotein from which a chemokine can be released.[5] Cardona, et al. stated in 2006 that "using three different in vivo models, we show that CX3CR1 deficiency dysregulates microglial responses, resulting in neurotoxicity."[5] Further studies into how CX3CR1 regulates microglial neurotoxicity could lead to new therapeutic strategies for neuroprotection.[5]
Inhibition of amyloid deposition
Inhibitors of amyloid deposition include the enzymes responsible for the production of extracellular amyloid such as β-secretase and γ-secretase inhibitors.[] Currently the γ-secretase inhibitors are in phase II clinical trials as a treatment for Alzheimer's disease but they have immunosuppressive properties, which could limit their use.[] Another strategy involves increasing the antibodies against a fragment of amyloid.[] This treatment is also in phase II clinical trials for the treatment of Alzheimer's disease.[]
Inhibition of cytokine synthesis
Glucocorticosteroids (GCS) are anti-inflammatory steroids that inhibit both central and peripheral cytokine synthesis and action.[] In a study conducted by Kalipada Pahan from the Department of Pediatrics at the Medical University of South Carolina, both lovastatin and sodium phenylacetate were found to inhibit TNF-α, IL-1β, and IL-6 in rat microglia.[] This shows that the mevalonate pathway plays a role in controlling the expression of cytokines in microglia and may be important in developing drugs to treat neurodegenerative diseases.[] Naltrexone may pose a solution to the inflammatory mediators produced by microglia. Although naltrexone's main action is to competitively bind to opioid receptors thereby upregulating the number of receptors; moverover, it is used to help patients with an opioid dependency. New research shows that low-dose naltrexone can inhibit cytokine synthesis of microglia cells. This mechanism is still in its infancy, but it has proven to help some patients suffering from fibromyalgia syndrome. Naltrexone shows more promise than GCSs because the GCSs inhibit immune system function, increase allergic reactions and, as the name implies, increase blood glucose levels.[]
References External links
• Microglia home page (http://www.microglia.net/microglia.htm) at microglia.net • The Role of Microglia in the Central Nervous System (http://cmr.asm.org/cgi/content/full/17/4/942) Clinical Microbiology Reviews October 2004, p. 942-964, Vol. 17, No. 4 • Creeping into your Head - A Brief Introduction to Microglia (http://www.scq.ubc.ca/?p=674) - A Review from the Science Creative Quarterly • "Immune Scavengers Target Alzheimer's Plaques" (http://focus.hms.harvard.edu/2007/040607/neuroscience. shtml). April 6, 2007. Retrieved 2007-05-09. - from Harvard University • The Department of Neuroscience at Wikiversity • NIF Search - Microglial Cell (https://www.neuinfo.org/mynif/search.php?q=Microglial Cell&t=data& s=cover&b=0&r=20) via the Neuroscience Information Framework
Neutrophil granulocyte
518
Neutrophil granulocyte
Neutrophil granulocyte
Neutrophils with a segmented nuclei surrounded by erythrocytes, the intra-cellular granules are visible in the cytoplasm (Giemsa stained) Code TH H2.00.04.1.02012
[1]
Neutrophil granulocytes are the most abundant type of white blood cells in mammals and form an essential part of the innate immune system. In general, they are referred to as either neutrophils or polymorphonuclear neutrophils (or PMNs), and are subdivided into segmented neutrophils (or segs) and banded neutrophils (or bands). They form part of the polymorphonuclear cell family (PMNs) together with basophils and eosinophils.[][][] The name neutrophil derives from staining characteristics on hematoxylin and eosin (H&E) histological or cytological preparations. Whereas basophilic white blood cells stain dark blue and eosinophilic white blood cells stain bright red, neutrophils stain a neutral pink. Normally, neutrophils contain a nucleus divided into 2–5 lobes. Neutrophils are a type of phagocyte and are normally found in the blood stream. During the beginning (acute) phase of inflammation, particularly as a result of bacterial infection, environmental exposure,[] and some cancers,[1][2] neutrophils are one of the first-responders of inflammatory cells to migrate towards the site of inflammation. They migrate through the blood vessels, then through interstitial tissue, following chemical signals such as Interleukin-8 (IL-8), C5a, fMLP and Leukotriene B4 in a process called chemotaxis. They are the predominant cells in pus, accounting for its whitish/yellowish appearance. Neutrophils are recruited to the site of injury within minutes following trauma and are the hallmark of acute inflammation.[3]
Neutrophil granulocyte
519
Characteristics
Neutrophil granulocytes have an average diameter of 12–15 micrometers (µm) in peripheral blood smears. When analyzing a pure neutrophil suspension on an automated cell counter, neutrophils have an average diameter of 8–9 µm. With the eosinophil and the basophil, they form the class of polymorphonuclear cells, named for the nucleus's multilobulated shape (as compared to lymphocytes and monocytes, the other types of white cells). The nucleus has a characteristic lobed appearance, the separate lobes connected by chromatin. The nucleolus disappears as the neutrophil matures, which is something that happens in only a few other types of nucleated cells.[4] In the cytoplasm, the Golgi apparatus is small, mitochondria and ribosomes are sparse, and the rough endoplasmic reticulum is absent.[5] The cytoplasm also contains about 200 granules, of which a third are azurophilic.[5] A minor difference is found between the neutrophils from a male subject and a female subject. The cell nucleus of a neutrophil from a female subject shows a small additional X chromosome structure, known as a "neutrophil drumstick".[6]
Neutrophil granulocyte migrates from the blood vessel to the matrix, sensing proteolytic enzymes, in order to determine intercellular connections (to the improvement of its mobility) and envelop bacteria through phagocytosis.
Neutrophils will show hypersegmentation (many segments of nucleus) in B12 and folate deficiency. Neutrophils are the most abundant white blood cells in humans (approximately 1011 are produced daily); they account for approximately 50-70% of all white blood cells (leukocytes). The stated normal range Reference ranges for blood tests of white blood cells, comparing neutrophil amount for human blood counts varies between (shown in pink) with that of other cells. laboratories, but a neutrophil count of 2.5–7.5 x 109/L is a standard normal range. People of African and Middle Eastern descent may have lower counts, which are still normal. A report may divide neutrophils into segmented neutrophils and bands. When circulating in the bloodstream and unactivated, neutrophils are spherical. Once activated, they change shape and become more amorphous or amoeba-like and can extend pseudopods as they hunt for antigens.[]
Neutrophil granulocyte
520
Life span
The average lifespan of (non-activated human) neutrophils in the circulation is about 5.4 days.[7] Upon activation, they marginate (position themselves adjacent to the blood vessel endothelium), and undergo selectin-dependent capture followed by integrin-dependent adhesion in most cases, after which they migrate into tissues, where they survive for 1–2 days.[] Neutrophils are much more numerous than the longer-lived HSC=Hematopoietic stem cell, Progenitor=Progenitor cell, L-blast=lymphoblast, monocyte/macrophage phagocytes. A Lymphocyte, Mo-blast=Monoblast, Monocyte, Myeloblast, Pro-M=Promyelocyte, pathogen (disease-causing Myelocyte, Meta-M=Metamyelocyte, Neutrophil, Eosinophil, Basophil, microorganism or virus) is likely to Pro-E=Proerythroblast, Baso-E=Basophilic erythroblast, poly-e=Polychromatic first encounter a neutrophil. Some erythroblast, Ortho-E=orthochromatic erythroblast, Erythrocyte, Promegakaryocyte, megakaryocyte, Platlet experts hypothesize that the short lifetime of neutrophils is an evolutionary adaptation. The short lifetime of neutrophils minimizes propagation of those pathogens that parasitize phagocytes because the more time such parasites spend outside a host cell, the more likely they will be destroyed by some component of the body's defenses. Also, because neutrophil antimicrobial products can also damage host tissues, their short life limits damage to the host during inflammation.[] Neutrophils will often be phagocytosed themselves by macrophages after digestion of pathogens. PECAM-1 and phosphatidylserine on the cell surface are involved in this process.
Chemotaxis
Neutrophils undergo a process called chemotaxis, which allows them to migrate toward sites of infection or inflammation. Cell surface receptors allow neutrophils to detect chemical gradients of molecules such as interleukin-8 (IL-8), interferon gamma (IFN-gamma), C5a, and Leukotriene B4, which these cells use to direct the path of their migration. Neutrophils have a variety of specific receptors, including complement receptors, cytokine receptors for interleukins and interferon gamma (IFN-gamma), receptors for chemokines, receptors to detect and adhere to endothelium, receptors for leptins and proteins, and Fc receptors for opsonin.[8]
Anti-microbial function
Being highly motile, neutrophils quickly congregate at a focus of infection, attracted by cytokines expressed by activated endothelium, mast cells, and macrophages. Neutrophils express[9] and release cytokines, which in turn amplify inflammatory reactions by several other cell types. In addition to recruiting and activating other cells of the immune system, neutrophils play a key role in the front-line defence against invading pathogens. Neutrophils have three methods for directly attacking micro-organisms: phagocytosis (ingestion), release of soluble anti-microbials (including granule proteins), and generation of neutrophil
Neutrophil granulocyte extracellular traps (NETs).[]
521
Phagocytosis
Neutrophils are phagocytes, capable of ingesting microorganisms or particles. For targets to be recognised, they must be coated in opsonins—a process known as antibody opsonization.[] They can internalize and kill many microbes, each phagocytic event resulting in the formation of a phagosome into which reactive oxygen species and hydrolytic enzymes are secreted. The consumption of oxygen during the generation of reactive oxygen species has been termed the "respiratory burst", although unrelated to respiration or energy production. The respiratory burst involves the activation of the enzyme NADPH oxidase, which produces large quantities of superoxide, a reactive oxygen species. Superoxide decays spontaneously or is broken down via enzymes known as superoxide dismutases (Cu/ZnSOD and MnSOD), to hydrogen peroxide, which is then converted to hypochlorous acid HClO, by the green heme enzyme myeloperoxidase. It is thought that the bactericidal properties of HClO are enough to kill bacteria phagocytosed by the neutrophil, but this may instead be a step necessary for the activation of proteases. []
Degranulation
Neutrophils also release an assortment of proteins in three types of granules by a process called degranulation. The contents of these granules have antimicrobial properties, and help combat infection.
Granule type azurophilic granules (or "primary granules") specific granules (or "secondary granules") tertiary granules Protein myeloperoxidase, bactericidal/permeability-increasing protein (BPI), Defensins, and the serine proteases neutrophil elastase and cathepsin G alkaline phosphatase, lysozyme, NADPH oxidase, collagenase, Lactoferrin and Cathelicidin
cathepsin and gelatinase
Neutrophil extracellular traps (NETs)
In 2004, Brinkmann and colleagues described a striking observation that activation of neutrophils causes the release of web-like structures of DNA; this represents a third mechanism for killing bacteria.[] These neutrophil extracellular traps (NETs) comprise a web of fibers composed of chromatin and serine proteases that trap and kill microbes extracellularly. It is suggested that NETs provide a high local concentration of antimicrobial components and bind, disarm, and kill microbes independent of phagocytic uptake. In addition to their possible antimicrobial properties, NETs may serve as a physical barrier that prevents further spread of pathogens. Trapping of bacteria may be a particularly important role for NETs in sepsis, where NET are formed within blood vessels.[] Recently, NETs have been shown to play a role in inflammatory diseases, as NETs could be detected in preeclampsia, a pregnancy-related inflammatory disorder in which neutrophils are known to be activated.[] In addition, NETs are known to exhibit pro-thrombotic effects both in vitro [10] and in vivo.[11][12]
Neutrophil granulocyte
522
Role in disease
Low neutrophil counts are termed neutropenia. This can be congenital (genetic disorder) or it can develop later, as in the case of aplastic anemia or some kinds of leukemia. It can also be a side-effect of medication, most prominently chemotherapy. Neutropenia makes an individual highly susceptible to infections. Neutropenia can be the result of colonization by intracellular neutrophilic parasites. In alpha 1-antitrypsin deficiency, the important neutrophil enzyme elastase is not adequately inhibited by alpha 1-antitrypsin, leading to excessive tissue damage in the presence of inflammation – the most prominent one being pulmonary emphysema. In Familial Mediterranean fever (FMF), a mutation in the pyrin (or marenostrin) gene, which is expressed mainly in neutrophil granulocytes, leads to a constitutively active acute-phase response and causes attacks of fever, arthralgia, peritonitis, and – eventually – amyloidosis.[]
Media
A neutrophil can be seen here selectively taking up several Candida yeasts (fluorescently labeled in green) despite several contacts with Aspergillus fumigatus conidia (unlabeled, white/clear) in a 3-D collagen matrix. Imaging time was 2 hours with one frame every 30 seconds.
[13] Neutrophils display highly directional amoeboid motility in infected footpad and phalanges. Intravital imaging was performed in the footpad path of LysM-eGFP mice 20 minutes after infection with LM.[13]
Neutrophil granulocyte
523
Additional images
A scanning electron microscope image of a single neutrophil (yellow), engulfing anthrax bacteria (orange)
Blood cell lineage
More complete lineages (very large)
References
[3] [4] [5] [6] [7] Cohen, Stephen. Burns, Richard C. Pathways of the Pulp, 8th Edition. St. Louis: Mosby, Inc. 2002. page 465. Zucker-Franklin, p. 168. Zucker-Franklin, p. 170. Zucker-Franklin, p. 174. Pillay J, den Braber I, Vrisekoop N, Kwast LM, de Boer RJ, Borghans JA, Tesselaar K, Koenderman L. In vivo labeling with 2H2O reveals a human neutrophil lifespan of 5.4 days (http:/ / bloodjournal. hematologylibrary. org/ cgi/ content/ full/ 116/ 4/ 625) Blood. 2010 Jul 29;116(4):625-7.
Cited text
• Zucker-Franklin, Dorothy; Greaves, M.F.; Grossi, C.E.; Marmont, A.M. (1988). "Neutrophils". Atlas of Blood Cells: Function and Pathology 1 (2nd ed. ed.). Philadelphia: Lea & Ferbiger. ISBN 0-8121-1094-3.
Eosinophil granulocyte
524
Eosinophil granulocyte
Eosinophil granulocyte
Eosinophil under the microscope (400x) from a peripheral blood smear. Red blood cells surround the eosinophil, two platelets at the top left corner. Code TH H2.00.04.1.02017
[1]
Eosinophil granulocytes, usually called eosinophils or eosinophiles (or, less commonly, acidophils), are white blood cells that are one of the immune system components responsible for combating multicellular parasites and certain infections in vertebrates. Along with mast cells, they also control mechanisms associated with allergy and asthma. They are granulocytes that develop during hematopoiesis in the bone marrow before migrating into blood. These cells are eosinophilic or 'acid-loving' as shown by their affinity to coal tar dyes: Normally transparent, it is this affinity that causes them to appear brick-red after staining with eosin, a red dye, using the Romanowsky method. The staining is concentrated in small granules within the cellular cytoplasm, which contain many chemical mediators, such as histamines and proteins such as eosinophil peroxidase, ribonuclease (RNase), deoxyribonucleases, lipase, plasminogen, and major basic protein. These mediators are released by a process called degranulation following activation of the eosinophil, and are toxic to both parasite and host tissues. In normal individuals, eosinophils make up about 1-6% of white blood cells, and are about 12-17 micrometers in size.[1] They are found in the medulla and the junction between the cortex and medulla of the thymus, and, in the lower gastrointestinal tract, ovary, uterus, spleen, and lymph nodes, but not in the lung, skin, esophagus, or some other internal organs Wikipedia:Vagueness under normal conditions. The presence of eosinophils in these latter organs is associated with disease. Eosinophils persist in the circulation for 8–12 hours, and can survive in tissue for an additional 8–12 days in the absence of stimulation.[2] Pioneering work in the 1980s elucidated that eosinophils were unique granulocytes, having the capacity to survive for extended periods of time after their maturation as demonstrated by ex-vivo culture experiments.
Eosinophil development, migration and activation
Eosinophils develop and mature in the bone marrow. They differentiate from myeloid precursor cells in response to the cytokines interleukin 3 (IL-3), interleukin 5 (IL-5), and granulocyte macrophage-colony stimulating factor (GM-CSF).[3][4][5] Eosinophils produce and store many secondary granule proteins prior to their exit from the bone marrow. After maturation, eosinophils circulate in blood and migrate to inflammatory sites in tissues, or to sites of helminth infection in response to chemokines like CCL11 (eotaxin-1), CCL24 (eotaxin-2), CCL5 (RANTES), and certain leukotrienes like leukotriene B4 (LTB4) and MCP1/4. At these infectious sites, eosinophils are activated by Type 2 cytokines released from a specific subset of helper T cells (Th2); IL-5, GM-CSF, and IL-3 are important for eosinophil activation as well as maturation. There is evidence to suggest that eosinophil granule protein expression is regulated by the non-coding RNA EGOT (gene)[]
Eosinophil granulocyte
525
Functions of eosinophils
Following activation, eosinophils effector functions include production of: • cationic granule proteins and their release by degranulation.[6][][] • reactive oxygen species such as superoxide, peroxide, and hypobromite (hypobromous acid, which is preferentially produced by eosinophil peroxidase).[7] • lipid mediators like the eicosanoids from the leukotriene (e.g., LTC4, LTD4, LTE4) and prostaglandin (e.g., PGE2) families.[8] • enzymes, such as elastase. • growth factors such as TGF beta, VEGF, and PDGF.[9][10] • cytokines such as IL-1, IL-2, IL-4, IL-5, IL-6, IL-8, IL-13, and TNF alpha.[][] In addition, eosinophils play a role in fighting viral infections, which is evident from the abundance of RNases they contain within their granules, and in fibrin removal during inflammation. Eosinophils along with basophils and mast cells, are important mediators of allergic responses and asthma pathogenesis and are associated with disease severity. They also fight helminth (worm) colonization and may be slightly elevated in the presence of certain parasites. Eosinophils are also involved in many other biological processes, including postpubertal mammary gland development, oestrus cycling, allograft rejection and neoplasia.[] They have also recently been implicated in antigen presentation to T cells.[11]
Eosinophil granule proteins
Following activation by an immune stimulus, eosinophils degranulate to release an array of cytotoxic granule cationic proteins that are capable of inducing tissue damage and dysfunction.[12] These include: • • • • major basic protein (MBP) eosinophil cationic protein (ECP) eosinophil peroxidase (EPO) eosinophil-derived neurotoxin (EDN)
Major basic protein, eosinophil peroxidase, and eosinophil cationic protein are toxic to many tissues.[] Eosinophil cationic protein and eosinophil-derived neurotoxin are ribonucleases with antiviral activity.[13] Major basic protein induces mast cell and basophil degranulation, and is implicated in peripheral nerve remodelling.[14][15] Eosinophil cationic protein creates toxic pores in the membranes of target cells allowing potential entry of other cytotoxic molecules to the cell,[16] can inhibit proliferation of T cells, suppress antibody production by B cells, induce degranulation by mast cells, and stimulate fibroblast cells to secrete mucus and glycosaminoglycan.[17] Eosinophil peroxidase forms reactive oxygen species and reactive nitrogen intermediates that promote oxidative stress in the target, causing cell death by apoptosis and necrosis.[]
Eosinophilia
An increase in eosinophils, i.e., the presence of more than 500 eosinophils/microlitre of blood is called an eosinophilia, and is typically seen in people with a parasitic infestation of the intestines, a collagen vascular disease (such as rheumatoid arthritis), malignant diseases such as Hodgkin's disease, extensive skin diseases (such as exfoliative dermatitis), Addison's disease, in the squamous epithelium of the esophagus in the case of reflux esophagitis, eosinophilic esophagitis, and with the use of certain drugs such as penicillin. In 1989, contaminated L-tryptophan supplements caused a deadly form of eosinophilia known as eosinophilia-myalgia syndrome, which was reminiscent of the Toxic Oil Syndrome in Spain in 1981.
Eosinophil granulocyte
526
Reference ranges for blood tests of white blood cells, comparing eosinophil granulocyte amount (shown in light red) with other cells.
Treatment
Treatments used to combat autoimmune diseases and conditions caused by eosinophils include: • • • • corticosteroids- promote apoptosis. Numbers of eosinophils in blood are rapidly reduced monoclonal antibody therapy- e.g., mepoluzimab or reslizumab against IL-5, prevents eosinophilopoiesis antagonists of leukotriene synthesis or receptors Gleevec (STI571)- inhibits PDGF-BB in hypereosinophilic leukemia
Additional images
Eosinophil in peripheral blood (Giemsa stain)
Blood cell lineage
Eosinophil
References External links
• eosinophilic+leukocyte (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=eosinophilic+ leukocyte) at eMedicine Dictionary • Bioweb at UWLAX Eosinophil (http://bioweb.uwlax.edu/APlab/Table_of_Contents/Lab_11/Eosinophil/ eosinophil.html) • Histology at ucsf.edu (http://missinglink.ucsf.edu/lm/IDS_101_histo_resource/images/ eosinophil_100x-labelled.jpg) • "What is an eosinophil?" at the Cincinnati Center for Eosinophilic Disorders (http://www.cincinnatichildrens. org/svc/alpha/e/eosinophilic/about/eosinophil.htm)
Basophil granulocyte
527
Basophil granulocyte
Basophil granulocyte
Basophil granulocyte
Basophil Code TH H2.00.04.1.02022 [1]
Basophil granulocytes, mostly referred to as basophils, are the least common of the granulocytes, representing about 0.01% to 0.3% of circulating white blood cells. The name comes from the fact that these leukocytes are basophilic, i.e., they are susceptible to staining by basic dyes, as shown in the picture. Basophils contain large cytoplasmic granules which obscure the cell nucleus under the microscope. However, when unstained, the nucleus is visible and it usually has 2 lobes. The mast cell, a cell in tissues, has many similar characteristics. For example, both cell types store histamine, a chemical that is secreted by the cells when stimulated in certain ways (histamine causes some of the symptoms of an allergic reaction). Like all circulating granulocytes, basophils can be recruited out of the blood into a tissue when needed.
Function
Basophils appear in many specific kinds of inflammatory reactions, particularly those that cause allergic symptoms. Basophils contain anticoagulant heparin, which prevents blood from clotting too quickly. They Reference ranges for blood tests of white blood cells, comparing basophil granulocyte also contain the vasodilator histamine, amount (shown in violet) with other cells. which promotes blood flow to tissues. They can be found in unusually high numbers at sites of ectoparasite infection, e.g., ticks. Like eosinophils, basophils play a role in both parasitic infections and allergies.[1] They are found in tissues where allergic reactions are occurring and probably contribute to the severity of these reactions. Basophils have protein receptors on their cell surface that bind IgE, an immunoglobulin involved in macroparasite defense and allergy. It is the bound IgE antibody that confers a selective response of these cells to environmental substances, for example, pollen proteins or helminth antigens. Recent studies in mice suggest that basophils may also regulate the behavior of T cells and mediate the magnitude of the secondary immune response.[2]
Basophil granulocyte
528
Immunophenotyping of basophils
Basophils of mouse and human have consistent immunophenotypes as follows: FcεRI+, CD123, CD49b(DX-5)+, CD69+, Thy-1.2+, 2B4+, CD11bdull, CD117(c-kit)–, CD24–, CD19–, CD80–, CD14–, CD23–, Ly49c–, CD122–, CD11c–, Gr-1–, NK1.1–, B220–, CD3–, γδTCR–, αβTCR–, α4 and β4-integrin negative.[3] Recently, Heneberg [] proposed that basophils may be defined as the cellular population positive for CD13, CD44, CD54, CD63, CD69, CD107a, CD123, CD164, CD193/ CCR3, CD203c, TLR-4, and FcεRI. When activated, some additional surface markers are known to be upregulated (CD13, CD107a, CD164), or surface-exposed (CD63, and the ectoenzyme CD203c).[]
Secretions
When activated, basophils degranulate to release histamine, proteoglycans (e.g. heparin and chondroitin), and proteolytic enzymes (e.g. elastase and lysophospholipase). They also secrete lipid mediators like leukotrienes, and several cytokines. Histamine and proteoglycans are pre-stored in the cell's granules while the other secreted substances are newly generated. Each of these substances contributes to inflammation. Recent evidence suggests that basophils are an important source of the cytokine, interleukin-4, perhaps more important than T cells. Interleukin-4 is considered one of the critical cytokines in the development of allergies and the production of IgE antibody by the immune system. There are other substances that can activate basophils to secrete which suggests that these cells have other roles in inflammation.[] The degranulation of basophils can be investigated in vitro by using flow cytometry and the so-called basophil-activation-test (BAT). Especially, in the diagnosis of allergies including of drug reactions (e.g. induced by contrast medium), the BAT of is great impact [4]. Basopenia (a low basophil count) is difficult to demonstrate as the normal basophil count is so low; it has been reported in association with autoimmune urticaria[5] (a chronic itching condition). Basophilia is also uncommon but may be seen in some forms of leukaemia or lymphoma.
References
[1] Voehringer D. 2009. Trends in Parasitology. [3] Schroeder JT (2009). "Basophils beyond effector cells of allergic inflammation." Adv Immunol 101:123-161, PMID 19231594, . [4] Böhm I et al. Pilot study on basophil activation induced by contrast medium. Fundam Clin Pharmacol 2011;25:267 - 276
Additional images
Blood cell lineage
Alternate stain of a basophil
Hybridoma technology
529
Hybridoma technology
Hybridoma technology is a technology of forming hybrid cell lines (called hybridomas) by fusing a specific antibody-producing B cell with a myeloma (B cell cancer) cell that is selected for its ability to grow in tissue culture and for an absence of antibody chain synthesis. The antibodies produced by the hybridoma are all of a single specificity and are therefore monoclonal antibodies (in contrast to polyclonal antibodies). The production of monoclonal antibodies was invented by Cesar Milstein and Georges J. F. Köhler in 1975. They shared the Nobel Prize of 1984 for Medicine and Physiology with Niels Kaj Jerne, who made other contributions to immunology. The term hybridoma was coined by Leonard Herzenberg during his sabbatical in Cesar Milstein's laboratory in 1976/1977.[1]
Method
Laboratory animals (mammals, e.g. mice) are first exposed to an antigen to which we are interested in isolating an antibody against. Usually this is done by a series of injections of the antigen in question, over the course of several weeks. Once splenocytes are isolated from the mammal's spleen, the B cells are fused with immortalised myeloma cells. The myeloma cells are selected beforehand to ensure they are not secreting antibody themselves and that they lack the hypoxanthine-guanine phosphoribosyltransferase (HGPRT) gene, making them sensitive to the HAT medium (see below). The fusion is accomplished using polyethylene glycol or the Sendai virus. It is performed by making the cell membranes more permeable.Wikipedia:Please clarify Fused cells are incubated in HAT medium (hypoxanthine-aminopterin-thymidine medium) for roughly 10 to 14 days. Aminopterin blocks the pathway that allows for nucleotide synthesis. Hence, unfused myeloma cells die, as they cannot produce nucleotides by the de novo or salvage pathways because they lack HGPRT. Removal of the unfused myeloma cells is necessary because they have the potential to outgrow other cells, especially weakly established hybridomas. Unfused B cells die as they have a short life span. In this way, only the B cell-myeloma hybrids survive, since the HGPRT gene coming from the B cells is functional. These cells produce antibodies (a property of B cells) and are immortal (a property of myeloma cells). The incubated medium is then diluted into multi-well plates to such an extent that each well
(1) Immunisation of a mouse (2) Isolation of B cells from the spleen (3) Cultivation of myeloma cells (4) Fusion of myeloma and B cells (5) Separation of cell lines (6) Screening of suitable cell lines (7) in vitro (a) or in vivo (b) multiplication (8) Harvesting
Hybridoma technology
530
contains only one cell. Since the antibodies in a well are produced by the same B cell, they will be directed towards the same epitope, and are thus monoclonal antibodies. The next stage is a rapid primary screening process, which identifies and selects only those hybridomas that produce antibodies of appropriate specificity. The hybridoma culture supernatant, secondary enzyme labeled conjugate, and chromogenic substrate, are then incubated, and the formation of a colored product indicates a positive hybridoma. Alternatively, immunocytochemical screening can also be used.[] The B cell that produces the desired antibodies can be cloned to produce many identical daughter clones. Supplemental media containing interleukin-6 (such as briclone) are essential for this step. Once a hybridoma colony is established, it will continually grow in culture medium like RPMI-1640 (with antibiotics and fetal bovine serum) and produce antibodies.[]
Hybridoma cells grown in tissue culture. The image shows a single clone of cells each of which is producing large amounts of a specific monoclonal antibody which the cells secrete and which can be readily purified from the culture media.
Multiwell plates are used initially to grow the hybridomas, and after selection, are changed to larger tissue culture flasks. This maintains the well-being of the hybridomas and provides enough cells for cryopreservation and supernatant for subsequent investigations. The culture supernatant can yield 1 to 60 µg/ml of monoclonal antibody, which is maintained at -20 °C or lower until required.[] By using culture supernatant or a purified immunoglobulin preparation, further analysis of a potential monoclonal antibody producing hybridoma can be made in terms of reactivity, specificity, and cross-reactivity.[]
Applications
The use of monoclonal antibodies is numerous and includes the prevention, diagnosis, and treatment of disease. For example, monoclonal antibodies can distinguish subsets of B cells and T cells, which is helpful in identifying different types of leukaemias. In addition, specific monoclonal antibodies have been used to define cell surface markers on white blood cells and other cell types. This led to the Cluster of differentiation series of markers. These are often referred to as CD markers and define several hundred different cell surface components of cells, each specified by binding of a particular monoclonal antibody. Such antibodies are extremely useful for fluorescence-activated cell sorting, the specific isolation of particular types of cells.
In diagnostic histopathology
With the help of monoclonal antibodies, tissues and organs can be classified based on their expression of certain defined markers, which reflect tissue or cellular genesis. Prostate specific antigen, placental alkaline phosphatase, human chorionic gonadotrophin, α-fetoprotein and others are organ-associated antigens and the production of monoclonal antibodies against these antigens helps in determining the nature of a primary tumor.[] Monoclonal antibodies are especially useful in distinguishing morphologically similar lesions, like pleural and peritoneal mesothelioma, adenocarcinoma, and in the determination of the organ or tissue origin of undifferentiated metastases. Selected monoclonal antibodies help in the detection of occult metastases by immuno-cytological analysis of bone marrow, other tissue aspirates, as well as lymph nodes and other tissues.[]
Hybridoma technology One study[2] performed a sensitive immuno-histochemical assay on bone marrow aspirates of 20 patients with localized prostate cancer. Three monoclonal antibodies (T16, C26, and AE-1), capable of recognizing membrane and cytoskeletal antigens expressed by epithelial cells to detect tumour cells, were used in the assay. Bone marrow aspirates of 22% of patients with localized prostate cancer (stage B, 0/5; Stage C, 2/4), and 36% patients with metastatic prostate cancer (Stage D1, 0/7 patients; Stage D2, 4/4 patients) had antigen-positive cells in their bone marrow. It was concluded that immuno-histochemical staining of bone marrow aspirates are very useful to detect occult bone marrow metastases in patients with apparently localized prostate cancer. Although immuno-cytochemistry using tumor-associated monoclonal antibodies has led to an improved ability to detect occult breast cancer cells in bone marrow aspirates and peripheral blood, further development of this method is necessary before it can be used routinely.[3] One major drawback of immuno-cytochemistry is that only tumor-associated and not tumor-specific monoclonal antibodies are used, and as a result, some cross-reaction with normal cells can occur.[4] The detection of small quantities of invasive or metastatic cells by normal histopathological staining with haematoxylin and eosin is not always sensitive. The use of monoclonal antibodies increases the sensitivity to a large extent. For example, the use of monoclonal antibodies to cytokeratin in the investigation of the sentinel axillary lymph node for metastatic breast cancer increases nodal positivity by up to 10%.[] In order to effectively stage breast cancer and assess the efficacy of purging regimens prior to autologous stem cell infusion, it is important to detect even small quantities of breast cancer cells. Immuno-histochemical methods are ideal for this purpose because they are simple, sensitive, and quite specific. Franklin et al.[5] performed a sensitive immuno-cytochemical assay by using a combination of four monoclonal antibodies (260F9, 520C9, 317G5 and BrE-3) against tumor cell surface glycoproteins to identify breast tumour cells in bone marrow and peripheral blood. They concluded from the results that immuno-cytochemical staining of bone marrow and peripheral blood is a sensitive and simple way to detect and quantify breast cancer cells. One of the main reasons for metastatic relapse in patients with solid tumours is the early dissemination of malignant cells. The use of monoclonal antibodies (mAbs) specific for cytokeratins can identify disseminated individual epithelial tumor cells in the bone marrow. One study[6] reports on having developed an immuno-cytochemical procedure for simultaneous labeling of cytokeratin component no. 18 (CK18) and prostate specific antigen (PSA). This would help in the further characterization of disseminated individual epithelial tumor cells in patients with prostate cancer. The twelve control aspirates from patients with benign prostatic hypertrophy showed negative staining, which further supports the specificity of CK18 in detecting epithelial tumour cells in bone marrow. In most cases of malignant disease complicated by effusion, neoplastic cells can be easily recognized. However, in some cases, malignant cells are not so easily seen or their presence is doubtful to call it a positive report. The use of immuno-cytochemical techniques increases diagnostic accuracy in these cases. Ghosh, Mason and Spriggs[7] analysed 53 samples of pleural or peritoneal fluid from 41 patients with malignant disease. Conventional cytological examination had not revealed any neoplastic cells. Three monoclonal antibodies (anti-CEA, Ca 1 and HMFG-2) were used to search for malignant cells. Immunocytochemical labelling was performed on unstained smears, which had been stored at -20°C up to 18 months. Twelve of the forty-one cases in which immuno-cytochemical staining was performed, revealed malignant cells. The result represented an increase in diagnostic accuracy of approximately 20%. The study concluded that in patients with suspected malignant disease, immuno-cytochemical labeling should be used routinely in the examination of cytologically negative samples and has important implications with respect to patient management. The use of immuno-cytochemical techniques can help to avoid performing procedures, which are painful, uncomfortable and expensive to the patient. It can also help to speed up the start of appropriate treatment.
531
Hybridoma technology Another application of immuno-cytochemical staining is for the detection of two antigens in the same smear. Double staining with light chain antibodies and with T and B cell markers can indicate the neoplastic origin of a lymphoma.[8] One study has reported the isolation of a hybridoma cell line (clone 1E10), which produces a monoclonal antibody (IgM, k isotype). This monoclonal antibody shows specific immuno-cytochemical staining of nucleoli.[9] Tissues and tumours can be classified based on their expression of certain markers, with the help of monoclonal antibodies. They help in distinguishing morphologically similar lesions and in determining the organ or tissue origin of undifferentiated metastases. Immuno-cytological analysis of bone marrow, tissue aspirates, lymph nodes etc. with selected monoclonal antibodies help in the detection of occult metastases. Monoclonal antibodies increase the sensitivity in detecting even small quantities of invasive or metastatic cells. Monoclonal antibodies (mAbs) specific for cytokeratins can detect disseminated individual epithelial tumour cells in the bone marrow. Immuno-cytochemical staining can also detect the presence of two antigens in the same smear.
532
References External links
• Hybridomas (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Hybridomas) at the US National Library of Medicine Medical Subject Headings (MeSH) • "Hybridoma Technology" (http://www.cancer.gov/cancertopics/understandingcancer/immunesystem/ page36). Understanding Cancer Series: The Immune System. National Cancer Institute.
Mast cell
533
Mast cell
Mast cell
Mast cells Latin Code mastocytus TH H2.00.03.0.01010
[1]
A mast cell (also known as mastocyte and labrocyte[1]) is a resident cell of several types of tissues and contains many granules rich in histamine and heparin. Although best known for their role in allergy and anaphylaxis, mast cells play an important protective role as well, being intimately involved in wound healing and defense against pathogens.[] The mast cell is very similar in both appearance and function to the basophil, a type of white blood cell. However, they are not the same, as they arise from different cell lines.[2]
Origin and classification
Mast cells were first described by Paul Ehrlich in his 1878 doctoral thesis on the basis of their unique staining characteristics and large granules. These granules also led him to the mistaken belief that they existed to nourish the surrounding tissue, and he named them "Mastzellen" (from the German: Mast, "fattening" as of animals).[3][4] They are now considered to be part of the immune system.
Mast cell
Mast cells are very similar to basophil granulocytes (a class of white blood cells) in blood. Both are granulated cells that contain histamine and heparin, an anticoagulant. Both cells also release histamine upon binding to immunoglobulin E.[2] These similarities have led many to speculate that mast cells are basophils that have "homed in" on tissues. Furthermore they share a common precursor in bone marrow. Nevertheless, both mast cells and basophils are thought to originate from bone marrow precursors expressing the CD34 molecule. Basophils leave the bone marrow already mature, whereas the mast cell circulates in an immature form, only maturing once in a tissue site. The site an immature mast cell settles in probably determines its precise characteristics.[] The first in vitro differentiation and growth of a pure population of mouse mast cells has been carried out using conditioned medium derived from concanavalin A-stimulated splenocytes.[] Later, it was discovered that T cell-derived interleukin 3 was the component present in the conditioned media that was required for mast cell differentiation and growth.[] Two types of mast cells are recognized, those from connective tissue and a distinct set of mucosal mast cells. The activities of the latter are dependent on T-cells.[] Mast cells are present in most tissues characteristically surrounding blood vessels and nerves, and are especially prominent near the boundaries between the outside world and the internal milieu, such as the skin, mucosa of the lungs and digestive tract, as well as in the mouth, conjunctiva and nose.[]
Mast cell
534
Physiology
Mast cells play a key role in the inflammatory process. When activated, a mast cell rapidly releases its characteristic granules and various hormonal mediators into the interstitium. Mast cells can be stimulated to degranulate by direct injury (e.g. physical or chemical [such as opioids, alcohols, and certain antibiotics such as polymyxins]), cross-linking of Immunoglobulin E (IgE) receptors, or by activated complement proteins.[] Mast cells express a high-affinity receptor (FcεRI) for the Fc region of IgE, the least-abundant member of the antibodies. This receptor is of such high affinity that binding of IgE molecules is essentially irreversible. As a result, mast cells are coated with IgE. IgE is produced by plasma cells (the antibody-producing cells of the immune system). IgE molecules, like all antibodies, are specific to one particular antigen. In allergic reactions, mast cells remain inactive until an allergen binds to IgE already in association with the cell (see above). Other membrane activation events can either prime mast cells for subsequent degranulation or can act in synergy with FceRI signal transduction.[] Allergens are generally proteins or polysaccharides. The allergen binds to the antigen-binding sites, which are situated on the variable regions of the IgE molecules bound to the mast cell surface. It appears that binding of two or more IgE molecules (cross-linking) is required to activate the mast cell. The clustering of the intracellular domains of the cell-bound Fc receptors, which are associated with the cross-linked IgE molecules, causes a complex sequence of reactions inside the mast cell that lead to its activation. Although this reaction is most well understood in terms of allergy, it appears to have evolved as a defense system against intestinal worm infestations (tapeworms, etc.)[citation needed]. The molecules thus released into the extracellular environment include:[] • preformed mediators (from the granules): • serine proteases, such as tryptase • histamine (2-5 pg/cell) • serotonin • proteoglycans, mainly heparin (active as anticoagulant) • newly formed lipid mediators (eicosanoids): • thromboxane • prostaglandin D2 • leukotriene C4 • platelet-activating factor • cytokines • Eosinophil chemotactic factor Histamine dilates post capillary venules, activates the endothelium, and increases blood vessel permeability. This leads to local edema (swelling), warmth, redness, and the attraction of other inflammatory cells to the site of release. It also irritates nerve endings (leading to itching or pain). Cutaneous signs of histamine release are the "flare and wheal"-reaction. The bump and redness immediately following a mosquito bite are a good example of this reaction, which occurs seconds after challenge of the mast cell by an allergen.[]
The role of mast cells in the development of allergy.
Mast cell
535 The other physiologic activities of mast cells are much less well-understood. Several lines of evidence suggest that mast cells may have a fairly fundamental role in innate immunity – they are capable of elaborating a vast array of important cytokines and other inflammatory mediators such as TNFa, they express multiple "pattern recognition receptors" thought to be involved in recognizing broad classes of pathogens, and mice without mast cells seem to be much more susceptible to a variety of infections.[citation needed]
Structure of histamine
Mast cell granules carry a variety of bioactive chemicals. These granules have been found to be transferred to adjacent cells of the immune system and neurons via transgranulation via their pseudopodia.[]
Role in disease
Allergic disease
Many forms of cutaneous and mucosal allergy are mediated for a large part by mast cells; they play a central role in asthma, eczema, itch (from various causes) and allergic rhinitis and allergic conjunctivitis. Antihistamine drugs act by blocking the action of histamine on nerve endings. Cromoglicate-based drugs (sodium cromoglicate, nedocromil) block a calcium channel essential for mast cell degranulation, stabilizing the cell and preventing release of histamine and related mediators. Leukotriene antagonists (such as montelukast and zafirlukast) block the action of leukotriene mediators, and are being used increasingly in allergic diseases.[]
Anaphylaxis
In anaphylaxis (a severe systemic reaction to allergens, such as nuts, bee stings or drugs), body-wide degranulation of mast cells leads to vasodilation and, if severe, symptoms of life-threatening shock.[citation needed]
Autoimmunity
Mast cells are implicated in the pathology associated with the autoimmune disorders rheumatoid arthritis, bullous pemphigoid, and multiple sclerosis. They have been shown to be involved in the recruitment of inflammatory cells to the joints (e.g. rheumatoid arthritis) and skin (e.g. bullous pemphigoid) and this activity is dependent on antibodies and complement components.[5]
Reproductive disorders
Mast cells are present within the endometrium, with increased activation and release of mediators in endometriosis.[] In males, mast cells are present in the testes and are increased in oligo- and azoospermia, with mast cell mediators directly suppressing sperm motility in a potentially reversible manner.[]
Mast cell disorders
Mastocytosis is a rare condition featuring proliferation of mast cells. It exists in a cutaneous and systemic form, with the former being limited to the skin and the latter involving multiple organs.[] Mast cell tumors are often seen in dogs and cats.[6]
Mast cell
536
Histological staining
Toluidine blue - one of the most common stains for acid mucopolysaccharides and glycoaminoglycans, components of mast cells granules.[7] Surface markers - Cell surface markers of mast cells were referred in detail by Heneberg,[] claiming that mast cells may be inadverently included in the stem or progenitor cell isolates since part of them is positive for the CD34 antigen. The classical mast cell markers include the high affinity IgE receptor, CD25 (non-neoplastic mast cells), CD117 (c-Kit), CD23 and CD203c (for most of the mast cell populations). Expression of some molecules may change in course of the mast cell activation.[]
References
[1] http:/ / www. memidex. com/ labrocytes [2] Marieb, Elaine N. & Katja Hoehn. Human Anatomy and Physiology. Seventh edition. San Francisco: Pearson Benjamin Cummings, 2007. pg. 659. [3] Ehrlich P. Beiträge zur Theorie und Praxis der histologischen Färbung. Dissertation at Leipzig University, 1878. [4] (http:/ / www. mondofacto. com/ facts/ dictionary?mastocyte) [5] http:/ / www. sciencemag. org/ cgi/ content/ full/ 297/ 5587/ 1689 [7] http:/ / www. springerlink. com/ content/ n3321437646586h8/
External links
• Mast cells (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Mast+cells) at the US National Library of Medicine Medical Subject Headings (MeSH)
T helper cell
T helper cells (Th cells) are a sub-group of lymphocytes, a type of white blood cell, that play an important role in the immune system, particularly in the adaptive immune system. They help the activity of other immune cells by releasing T cell cytokines. They are essential in B cell antibody class switching, in the activation and growth of cytotoxic T cells, and in maximizing bactericidal activity of phagocytes such as macrophages. Mature Th cells express the surface protein CD4 and are referred to as CD4+ T cells. CD4+ T cells are generally treated as having a pre-defined role as helper T cells within the immune system. For example, when an antigen presenting cell expresses an antigen on MHC class II, a CD4+ cell will aid those cells through a combination of cell to cell interactions (e.g. CD40 and CD40L) and through cytokines. Nevertheless, there are rare exceptions; for example, sub-groups of regulatory T cells, natural killer T cells, and cytotoxic T cells express CD4 (although cytotoxic examples have been observed in extremely low numbers in specific disease states, they are usually considered non-existent). All of the latter CD4+ T cell groups are not considered T helper cells. The importance of helper T cells can be seen from HIV, a virus that infects CD4+ cells. Towards the end of an HIV infection the number of functional CD4+ T cells falls, which leads to the symptomatic stage of infection known as the acquired immunodeficiency syndrome (AIDS). There are also some rare disorders that result in the absence or dysfunction of CD4+ T cells. These disorders produce similar symptoms, and many of these are fatal.
T helper cell
537
Activation of naïve helper T cells
Following T cell development, matured, naïve T cells leave the thymus and begin to spread throughout the body, including the lymph nodes. (Naïve T cells are those T cells that have never been exposed to the antigen that they are programmed to respond to). Like all T cells, they express the T cell receptor-CD3 complex. The T cell receptor (TCR) consists of both constant and variable regions. The variable region determines what antigen the T cell can respond to. CD4+ T cells have TCRs with an affinity for Class II MHC, and CD4 is involved in determining MHC affinity during maturation in the thymus. Class II MHC proteins are generally only found on the surface of specialised antigen-presenting cells (APCs). Specialised antigen presenting cells are primarily dendritic cells, macrophages and B cells, although B cells are the only cell group that expresses MHC Class II constitutively (at all times). Some APCs also bind native (or unprocessed) antigens to their surface, such as follicular dendritic cells, but unprocessed antigens do not interact with T cells and are not involved in their activation. The antigens that bind to MHC proteins are always short peptides, 8-10 amino acids long for MHC Class I, and up to 25 or so for MHC Class II.
Recognition (Signal 1)
During an immune response, professional antigen-presenting cells (APCs) endocytose foreign material (typically bacteria or viruses), which undergoes processing, then travel from the infection site to the lymph nodes. Once at the lymph nodes, the APC begin to present antigen peptides that are bound to Class II MHC, allowing CD4+ T cells that express the specific TCRs against the peptide/MHC complex to activate. When a Th cell encounters and recognises the antigen on an APC, the TCR-CD3 complex binds strongly to the peptide-MHC complex present on the surface of professional APCs. CD4, a co-receptor of the TCR complex, also binds to a different section of the MHC molecule. These interactions bring these proteins closer together, allowing the intracellular kinases present on the TCR, CD3 and CD4 proteins to activate each other via phosphorylation. With the assistance of a phosphatase present on the intracellular section of CD45 (common leukocyte antigen), these molecules activate major Th cell intracellular pathways. These active pathways are known as Signal 1 of T cell activation, as it is the first and primary pro-activation signal in a Th cell. Upon subsequent encounters with a given antigen, memory T cells are re-activated using the same TCR pathways. The binding of the antigen-MHC to the TCR complex and CD4 may also help the APC and the Th cell adhere during Th cell activation, but the integrin protein LFA-1 on the T cell and ICAM on the APC are the primary molecules of adhesion in this cell interaction. It is unknown what role the relatively bulky extracellular region of CD45 plays during cell interactions, but CD45 has various isoforms that change in size depending on the Th cell's activation and maturation status. For example, CD45 shortens in length following Th activation (CD45RA+ to CD45RO+), but whether this change in length influences activation is unknown. It has been proposed that the larger CD45RA+ may decrease the accessibility of the T cell receptor for the antigen-MHC molecule, thereby necessitating an increase in the affinity (and specificity) of the T cell for activation. Once the activation has occurred however, CD45 shortens, allowing easier interactions and activation as an effector T helper cell.[citation needed]
Verification (Signal 2)
Having received the first TCR/CD3 signal, the naïve T cell must activate a second independent biochemical pathway, known as Signal 2. This verification step is a protective measure to ensure that a T cell is responding to a foreign antigen. If this second signal is not present during initial antigen exposure, the T cell presumes that it is auto-reactive. This results in the cell becoming anergic (anergy is generated from the unprotected biochemical changes of Signal 1). Anergic cells will not respond to any antigen in the future, even if both signals are present later on. These cells are generally believed to circulate throughout the body with no value until they undergo apoptosis.
T helper cell The second signal involves an interaction between CD28 on the CD4+ T cell and the proteins CD80 (B7.1) or CD86 (B7.2) on the professional APCs. Both CD80 and CD86 activate the CD28 receptor. These proteins are also known as co-stimulatory molecules. Although the verification stage is necessary for the activation of naïve helper T cells, the importance of this stage is best demonstrated during the similar activation mechanism of CD8+ cytotoxic T cells. As naïve CD8+ T cells have no true bias towards foreign sources, these T cells must rely on the activation of CD28 for confirmation that they recognise a foreign antigen (as CD80/CD86 is only expressed by active APC's). CD28 plays an important role in decreasing the risk of T cell auto-immunity against host antigens. Once the naïve T cell has both pathways activated, the biochemical changes induced by Signal 1 are altered, allowing the cell to activate instead of anergise. The second signal is then obsolete; only the first signal is necessary for future activation. This is also true for memory T cells, which is one example of learned immunity. Faster responses occur upon reinfection because memory T cells have already undergone confirmation and can produce effector cells much sooner.
538
Proliferation
Once the two-signal activation is complete the T helper cell (Th) then allows itself to proliferate. It achieves this by releasing a potent T cell growth factor called interleukin 2 (IL-2) which acts upon itself in an autocrine fashion. Activated T cells also produce the alpha sub-unit of the IL-2 receptor (CD25 or IL-2R), enabling a fully functional receptor that can bind with IL-2, which in turn activates the T cell's proliferation pathways. The autocrine or paracrine secretion of IL-2 can bind that same Th cell or neighboring Th's via the IL-2R thus driving proliferation and clonal expansion. The Th cells receiving both signals of activation will then become Th0 cells (T helper 0) cell that secrete IL-2, IL-4 and interferon gamma (IFN-γ). The Th0 cells will then differentiate into Th1 or Th2 cells depending on cytokine environment. IFN-γ drives Th1 cell production while IL-10 and IL-4 inhibit Th1 cell production. Conversely, IL-4 drives Th2 cell production and IFN-γ inhibits Th2 cells. It should be noted that these cytokines are pleiotropic and carry out many other functions of the immune response.
Maturation
After many cell generations, the Th cell's progenitors differentiate into effector Th cells, memory Th cells, and regulatory Th cells. • Effector Th cells secrete cytokines, proteins or peptides that stimulate or interact with other leukocytes, including Th cells. • Memory Th cells retain the antigen affinity of the originally activated T cell, and are used to act as later effector cells during a second immune response (e.g. if there is re-infection of the host at a later stage). • Regulatory T cells do not promote immune function, but act to decrease it instead. Despite their low numbers during an infection, these cells are believed to play an important role in the self-limitation of the immune system; they have been shown to prevent the development of various auto-immune diseases.
Determination of the effector T cell response
Helper T cells are capable of influencing a variety of immune cells, and the T cell response generated (including the extracellular signals such as cytokines) can be essential for a successful outcome from infection. In order to be effective, helper T cells must determine which cytokines will allow the immune system to be most useful or beneficial for the host. Understanding exactly how helper T cells respond to immune challenges is currently of major interest in immunology, because such knowledge may be very useful in the treatment of disease and in increasing the effectiveness of vaccination.
T helper cell
539
Th1/Th2 Model for helper T cells
Proliferating helper T cells that develop into effector T cells differentiate into two major subtypes of cells known as Th1 and Th2 cells (also known as Type 1 and Type 2 helper T cells, respectively).
Th1/Th2 Model for helper T cells. An antigen is ingested and processed by an APC. It presents fragments from [1] it to T cells. The upper, Th0, is a T helper cell. The fragment is presented to it by MHC2. IFN-γ, interferon γ; TGF-β, transforming growth factor β; mø, macrophage; IL-2, interleukin 2; IL-4, interleukin 4
Type 1/ Th1 Main partner Macrophage cell type Cytokines produced
Type 2/ Th2 B-cell
interferon-γ and TGF-beta. (Interleukin-2 was classically interleukin-4, interleukin-5, interleukin-6, interleukin-10, interleukin-13 associated with Th1 cells, but this association may be misleading; IL-2 is produced by all helper T cells early in their activation.) interleukin-10 production has been [2] shown to be induced in activated Th1 cell Cellular immune system. Maximizes the killing efficacy of the macrophages and the proliferation of cytotoxic CD8+ T cells. Also promotes the production of opsonizing antibodies The Type 1 cytokine IFN-γ increases the production of interleukin-12 by dendritic cells and macrophages, and via positive feedback, IL-12 stimulates the production of IFN-γ in helper T cells, thereby promoting the Th1 profile. IFN-gamma also inhibits the production of cytokines such as interleukin-4, an important cytokine associated with the Type 2 response, and thus it also acts to preserve its own response. Humoral immune system. Stimulates B-cells into proliferation, to induce B-cell antibody class switching, and to increase neutralizing antibody production.
Immune stimulation promoted
Other functions
The Type 2 response promotes its own profile using two different cytokines. Interleukin-4 acts on helper T cells to promote the production of Th2 cytokines (including itself; it is auto-regulatory), while interleukin-10 (IL-10) inhibits a variety of cytokines including interleukin-2 and IFN-γ in helper T cells and IL-12 in dendritic cells and macrophages. The combined action of these two cytokines suggests that once the T cell has decided to produce these cytokines, that decision is preserved (and also encourages other T cells to do the same).
While we know about the types of cytokine patterns helper T cells tend to produce, we understand less about how the patterns themselves are decided. Various evidence suggests that the type of APC presenting the antigen to the T cell
T helper cell has a major influence on its profile. Other evidence suggests that the concentration of antigen presented to the T cell during primary activation influences its choice. The presence of some cytokines (such as the ones mentioned above) will also influence the response that will eventually be generated, but our understanding is nowhere near complete.
540
Limitations to the Th1/Th2 model
The interactions between cytokines from the Th1/Th2 model can be more complicated in some animals. For example, the Th2 cytokine IL-10 inhibits cytokine production of both Th subsets in humans. Human IL-10 (hIL-10) suppresses the proliferation and cytokine production of all T cells and the activity of macrophages, but continues to stimulate plasma cells, ensuring that antibody production still occurs. As such, hIL-10 is not believed to truly promote the Th2 response in humans, but acts to prevent over-stimulation of helper T cells while still maximising the production of antibodies. There are also other types of T cells that can influence the expression and activation of helper T cells, such as natural regulatory T cells, along with less common cytokine profiles such as the Th3 subset of helper T cells. Terms such as "regulatory" and "suppression" have become ambiguous after the discovery that helper CD4+ T cells are also capable of regulating (and suppressing) their own responses outside of dedicated regulatory T cells. One major difference between regulatory T cells and effector T cells is that regulatory T cells typically serve to modulate and deactivate the immune response, while effector T cell groups usually begin with immune-promoting cytokines and then switch to inhibitory cytokines later in their life cycle. The latter is a feature of Th3 cells, which transform into a regulatory subset after its initial activation and cytokine production. Both regulatory T cells and Th3 cells produce the cytokine transforming growth factor-beta (TGF-β) and IL-10. Both cytokines are inhibitory to helper T cells; TGF-β suppresses the activity of most of the immune system. There is evidence to suggest that TGF-β may not suppress activated Th2 cells as effectively as it might suppress naive cells, but it is not typically considered a Th2 cytokine. The characterisation of another novel T helper subtype, T helper 17 cells (Th17)[] has cast further doubt on the basic Th1/Th2 model. These IL-17 producing cells were initially described as a pathogenic population implicated in autoimmunity but are now thought to have their own distinct effector and regulatory functions. Of note, recent evidence suggest that functional plasticity is an intrinsic capacity of T helper cells. Indeed, a study in mice demonstrated that Th17 cells transform into Th1 cells in vivo.[3] A subsequent study furthermore showed that extensive T helper cell plasticity is also prominent in man.[4] Many of the cytokines in this article are also expressed by other immune cells (see individual cytokines for details), and it is becoming clear that while the original Th1/Th2 model is enlightening and gives insight into the functions of helper T cells, it is far too simple to define its entire role or actions. Some immunologists question the model completely, as some in vivo studies suggest that individual helper T cells usually do not match the specific cytokine profiles of the Th model, and many cells express cytokines from both profiles.[5] That said, the Th model has still played an important part in developing our understanding of the roles and behaviour of helper T cells and the cytokines they produce during an immune response. Recent scientific studies by Stockinger et al. revealed that another T helper subset may exist. Th9 cells are claimed to be an IL9 (interleukin 9)–producing T cell subset focused on defending helminth infections.[6]
T helper cell
541
Role of helper T cells in disease
Considering the diverse and important role helper T cells play in the immune system, it is not surprising that these cells often influence the immune response against disease. They also appear to make occasional mistakes, or generate responses that would be politely considered non-beneficial. In the worst case scenario, the helper T cell response could lead to a disaster and the fatality of the host. Fortunately this is a very rare occurrence.
Helper T cells and hypersensitivity
The immune system must achieve a balance of sensitivity in order to respond to foreign antigens without responding to the antigens of the host itself. When the immune system responds to very low levels of antigen that it usually shouldn't respond to, a hypersensitivity response occurs. Hypersensitivity is believed to be the cause of allergy and some auto-immune disease. Hypersensitivity reactions can be divided into four types: • Type 1 hypersensitivity includes common immune disorders such as asthma, allergic rhinitis (hay fever), eczema, urticaria (hives) and anaphylaxis. These reactions all involve IgE antibodies, which require a Th2 response during helper T cell development. Preventive treatments, such as corticosteroids and montelukast, focus on suppressing mast cells or other allergic cells; T cells do not play a primary role during the actual inflammatory response. It's important to note that the numeral allocation of hypersensitivity "types" does not correlate (and is completely unrelated) to the "response" in the Th model. • Type 2 and Type 3 hypersensitivity both involve complications from auto-immune or low affinity antibodies. In both of these reactions, T cells may play an accomplice role in generating these auto-specific antibodies, although some of these reactions under Type 2 hypersensitivity would be considered normal in a healthy immune system (for example, Rhesus factor reactions during child-birth is a normal immune response against child antigens). The understanding of the role of helper T cells in these responses is limited but it is generally thought that Th2 cytokines would promote such disorders. For example, studies have suggested that lupus (SLE) and other auto-immune diseases of similar nature can be linked to the production of Th2 cytokines. • Type 4 hypersensitivity, also known as delayed type hypersensitivity, are caused via the over-stimulation of immune cells, commonly lymphocytes and macrophages, resulting in chronic inflammation and cytokine release. Antibodies do not play a direct role in this allergy type. T cells play an important role in this hypersensitivity, as they activate against the stimulus itself and promote the activation of other cells; particularly macrophages via Th1 cytokines. Other cellular hypersensitivities include cytotoxic T cell mediated auto-immune disease, and a similar phenomenon; transplant rejection. Helper T cells are required to fuel the development of these diseases. In order to create sufficient auto-reactive killer T cells, interleukin-2 must be produced, and this is supplied by CD4+ T cells. CD4+ T cells can also stimulate cells such as natural killer cells and macrophages via cytokines such as interferon-gamma, encouraging these cytotoxic cells to kill host cells in certain circumstances. The mechanism that killer T cells use during auto-immunity is almost identical to their response against viruses, and some viruses have been accused of causing auto-immune diseases such as Type 1 Diabetes mellitus. Cellular auto-immune disease occurs because the host antigen recognition systems fail, and the immune system believes, by mistake, that a host antigen is foreign. As a result, the CD8+ T cells treat the host cell presenting that antigen as infected, and go on to destroy all host cells (or in the case of transplant rejection, transplant organ) that express that antigen. Some of this section is a simplification. Many auto-immune diseases are more complex. A well-known example is rheumatoid arthritis, where both antibodies and immune cells are known to play a role in the pathology. Generally the immunology of most auto-immune diseases is not well understood.
T helper cell
542
HIV infection
Perhaps the best example of the importance of CD4+ T cells is demonstrated with human immunodeficiency virus (HIV) infection. HIV targets cells that express CD4, and can infect macrophages, dendritic cells (both groups express CD4 at low levels) and CD4+ T cells. It has been proposed that during the non-symptomatic phase of HIV infection, the virus has a relatively low affinity towards T cells (and has a higher affinity for macrophages), resulting in a slow kill rate of CD4+ T cells by the immune system [citation needed]. This is initially compensated for via the production of new helper T cells from the thymus (originally from the bone marrow). Once the virus becomes lymphotropic (or T-tropic) however, it begins to infect CD4+ T cells far more efficiently (likely due to a change in the co-receptors it binds to during infection), and the immune system is overwhelmed. At this point, functional CD4+ T cell levels begin to decrease, eventually to a point where the CD4+ T cell population is too small to recognize the full range of antigens that could potentially be detected. The lack of full antigen cover results in the core symptoms of acquired immune deficiency syndrome (AIDS). CD4 T cell depletion during AIDS allows various pathogens to escape T cell recognition, thus allowing opportunistic infections that would normally elicit a helper T cell response to bypass the immune system. While these complete bypass situations only occur when the helper T cell response is absolutely necessary for infection clearance, most infections increase in severity and/or duration because the immune system's helper T cells provide a weaker contribution to a less efficient immune response. Two components of the immune system are particularly affected in AIDS, due to its CD4+ T cell dependency: 1. CD8+ T cells are not stimulated as effectively during the AIDS stage of HIV infection, making AIDS patients very susceptible to most viruses, including HIV itself. This decline in killing of CD4+ T cells results in the virus being produced for a longer period (the infected CD4+ T cells are not killed as quickly), increasing the proliferation of the virus, and accelerating the development of the disease. 2. Antibody class switching declines significantly once helper T cell function fails. The immune system loses its ability to improve the affinity of their antibodies, and are unable to generate B cells that can produce antibody groups such as IgG and IgA. These effects are primarily due to the loss of any helper T cell that can interact with the B lymphocyte correctly. Another symptom of AIDS is the reduction in antibody levels due to a decrease in Th2 cytokines (and less interactions by helper T cells). All of these complications result in an increased susceptibility to aggressive bacterial infections, especially in areas of the body not accessible by IgM antibodies. If the patient does not respond to (or does not receive) HIV treatment they will succumb usually to either cancers or infections; the immune system finally reaches a point where it is no longer coordinated or stimulated enough to deal with the disease. Inhibition of CD4 T-cell expansion during HIV infection is also due to microbial translocation in an IL-10-dependent way. Indeed, triggering PD-1, expressed on monocytes and up-regulated upon monocytes activation, by its ligand PD-L1 induces IL-10 production which inhibits CD4 T-cell function.[7]
T helper cell
543
References
[1] Page 223 [6] (Veldhoen and Stockinger, Dardalhon and Kuchroo both papers from Nature Immunology 2008)
• In SLE patients, T helper type 1 polarisation is more abundant rather than type 2, where the main cytokine profile are Inf gama from T cells and its consequence interferon alpha high range production by DC .
External links
• T-cell Group - Cardiff University (http://www.tcells.org/scientific/helper/)
Regulatory T cell
Regulatory T cells (Treg), formerly known as suppressor T cells (Ts), are a subpopulation of T cells which modulate the immune system, maintain tolerance to self-antigens, and abrogate autoimmune disease. Mouse models have suggested that modulation of Tregs can treat autoimmune disease and cancer, and facilitate organ transplantation.
Regulatory T cell populations
T regulatory cells are a component of the immune system that suppress immune responses of other cells. This is an important "self-check" built into the immune system to prevent excessive reactions. Regulatory T cells come in many forms with the most well-understood being those that express CD4, CD25, and Foxp3 (CD4+CD25+ regulatory T cells, or "Tregs").[1] These cells are involved in shutting down immune responses after they have successfully eliminated invading organisms, and also in preventing autoimmunity.[citation needed] CD4+Foxp3+ regulatory T cells have been called "naturally-occurring" regulatory T cells to distinguish them from "suppressor" T cell populations that are generated in vitro. Additional suppressor T cell populations include Tr1, Th3, CD8+CD28-, and Qa-1 restricted T cells. The contribution of these populations to self-tolerance and immune homeostasis is less well defined. FOXP3 can be used as a good marker for CD4+CD25+ T cells as well as recent studies showing evidence for FOXP3 in CD4+CD25- T cells. An additional regulatory T cell subset, induced regulatory T cells, are also needed for tolerance and suppression.
Development
All T cells come from progenitor cells from the bone marrow, which become committed to their lineage in the thymus. All T cells begin as CD4-CD8-TCR- cells at the DN (double-negative) stage, where an individual cell will rearrange its T cell receptor genes to form a unique, functional molecule, which they, in turn, test against cells in the thymic cortex for a minimal level of interaction with self-MHC. If they receive these signals, they proliferate and express both CD4 and CD8, becoming double-positive cells. The selection of Tregs occurs on radio-resistant haemopoietically-derived MHC class II-expressing cells in the medulla or Hassal’s corpuscles in the thymus. At the DP (double-positive) stage, they are selected by their interaction with the cells within the thymus, begin the transcription of Foxp3, and become Treg cells, although they may not begin to express Foxp3 until the single-positive stage, at which point they are functional Tregs. Treg do not have the limited TCR expression of NKT or γδ T cells; Treg have a larger TCR diversity than effector T cells, biased towards self-peptides. The process of Treg selection is determined by the affinity of interaction with the self-peptide MHC complex. Selection to become a Treg is a “Goldilocks” process; T cell that receives very strong signals will undergo apoptotic death; a cell that receives a weak signal will survive and be selected to become an effector cell. If a T cell receives an intermediate signal, then it will become a regulatory cell. Due to the stochastic nature of the process of T cell
Regulatory T cell activation, all T cell populations with a given TCR will end up with a mixture of Teff and Treg – the relative proportions determined by the affinities of the T cell for the self-peptide-MHC. Even in mouse models with TCR-transgenic cells selected on specific-antigen-secreting stroma, deletion or conversion is not complete. Foxp3+ Treg generation in the thymus is delayed by several days compared to Teff cells and does not reach adult levels in either the thymus or periphery until around three weeks post-partum. Treg cells require CD28 co-stimulation and B7.2 expression is largely restricted to the medulla, the development of which seems to parallel the development of Foxp3+ cells. It has been suggested that the two are linked, but no definitive link between the processes has yet been shown. TGF-β is not required for Treg functionality, in the thymus, as thymic Treg from TGF-β insensitive TGFβRII-DN mice are functional.
544
Function
To function properly, the immune system must discriminate between self and non-self. When self/non-self discrimination fails, the immune system destroys cells and tissues of the body and as a result causes autoimmune diseases. Regulatory T cells actively suppress activation of the immune system and prevent pathological self-reactivity, i.e. autoimmune disease. The critical role regulatory T cells play within the immune system is evidenced by the severe autoimmune syndrome that results from a genetic deficiency in regulatory T cells (IPEX syndrome - see also below). The molecular mechanism by which regulatory T cells exert their suppressor/regulatory activity has not been definitively characterized and is the subject of intense research. In vitro experiments have given mixed results regarding the requirement of cell-to-cell contact with the cell being suppressed. The immunosuppressive cytokines TGF-beta and Interleukin 10 (IL-10) have also been implicated in regulatory T cell function.
Induced Regulatory T cells
Induced Regulatory T (iTreg) cells (CD4+CD25+Foxp3+) are suppressive cells involved in tolerance. iTreg cells have been shown to suppress T cell proliferation and experimental autoimmune diseases. iTreg cells develop from mature CD4+ conventional T cells outside of the thymus: a defining distinction between natural regulatory T (nTreg) cells and iTreg cells. Though iTreg and nTreg cells share a similar function iTreg cells have recently been shown to be "an essential non-redundant regulatory subset that supplements nTreg cells, in part by expanding TCR diversity within regulatory responses".[2] Acute depletion of the iTreg cell pool in mouse models has resulted in inflammation and weight loss. The contribution of nTreg cells versus iTreg cells in maintaining tolerance is unknown, but both are important. Epigenetic differences have been observed between nTreg and iTreg cells, with the former having more stable Foxp3 expression and wider demethylation.
Regulatory T cells and Disease
An important question in the field of immunology is how the immunosuppressive activity of regulatory T cells is modulated during the course of an ongoing immune response. While the immunosuppressive function of regulatory T cells prevents the development of autoimmune disease, it is not desirable during immune responses to infectious microorganisms. Current hypotheses suggest that, upon encounter with infectious microorganisms, the activity of regulatory T cells may be downregulated, either directly or indirectly, by other cells to facilitate elimination of the infection. Experimental evidence from mouse models suggests that some pathogens may have evolved to manipulate regulatory T cells to immunosuppress the host and so potentiate their own survival. For example, regulatory T cell activity has been reported to increase in several infectious contexts, such as retroviral infections (the most well-known of which is HIV), mycobacterial infections (like tuberculosis), and various parasitic infections including Leishmania and malaria.
Regulatory T cell Studies of human subjects with a history of leishmania infection suggest that modulation of CD8+ suppressor T cells is, at least partly, mediated by cytokines. Leishmania specific CD4+ helper T cells predominate in adults with strong protective immunity (skin-test positive with no history of clinical infection). When added to autologous leishmania infected macrophages these T cells cause parasite death and secretion of large amounts of interferon-gamma and lymphotoxin. CD8+ T suppressor cells predominate in patients with no protective immunity (visceral leishmaniasis patients). When added to autologous peripheral blood mononuclear cells isolated after successful treatment, these T cells inhibit interferon-gamma secretion and proliferation and increase interleukin-6 and interleukin-10 secretion. A soluble factor(s) generated by antigen or phytohemagglutinin stimulation of leishmania-specific CD4+ helper T cells from skin-test positive adults killed CD8+ T cells but not CD4+ helper T cells when added to culture media. Soluble factors generated by antigen stimulation of peripheral blood mononuclear cells from skin-test positive adults prevented CD8+ suppressor T cell mediated increases in interleukin-10 secretion. These findings suggest that antigen stimulation of CD4+ helper T cells results in production of cytokines that kill or down regulate CD8+ T suppressor cells. Once the leishmania infection has been eliminated and leishmania antigens are gone, CD8+ T suppressor cells down-regulate CD4+ T helper cells. Isolation of cytokines that inhibit and kill CD8+ T suppressor cells might be useful in treating diseases that involve immune suppression such as leishmaniasis, AIDS, and certain cancers.[3][4] CD4+ Regulatory T cells are often associated with solid tumours in both humans and murine models. Increased numbers of regulatory T cells in breast, colorectal and ovarian cancers is associated with a poorer prognosis.[5] CD70+ non-Hodgkin lymphoma B cells induce Foxp3 expression and regulatory function in intratumoral CD4+CD25− T cells [6]
545
Molecular characterization
Similar to other T cells, regulatory T cells develop in the thymus. The latest research suggests that regulatory T cells are defined by expression of the forkhead family transcription factor FOXP3 (forkhead box p3). Expression of FOXP3 is required for regulatory T cell development and appears to control a genetic program specifying this cell fate.[7] The large majority of Foxp3-expressing regulatory T cells are found within the major histocompatibility complex (MHC) class II restricted CD4-expressing (CD4+) helper T cell population and express high levels of the interleukin-2 receptor alpha chain (CD25). In addition to the Foxp3-expressing CD4+CD25+, there also appears to be a minor population of MHC class I restricted CD8+ Foxp3-expressing regulatory T cells. Unlike conventional T cells, regulatory T cells do not produce IL-2 and are therefore anergic at baseline. A number of different methods are employed in research to identify and monitor Treg cells. Originally, high expression of CD25 and CD4 surface markers was used (CD4+CD25+ cells). This is problematic as CD25 is also expressed on non-regulatory T cells in the setting of immune activation such as during an immune response to a pathogen. As defined by CD4 and CD25 expression, regulatory T cells comprise about 5-10% of the mature CD4+ helper T cell subpopulation in mice and humans, while about 1-2% of Treg can be measured in whole blood. The additional measurement of cellular expression of Foxp3 protein allowed a more specific analysis of Treg cells (CD4+CD25+Foxp3+ cells). However, Foxp3 is also transiently expressed in activated human effector T cells, thus complicating a correct Treg analysis using CD4, CD25 and Foxp3 as markers in humans. Therefore, some research groups use another marker, the absence or low-level expression of the surface protein CD127 in combination with the presence of CD4 and CD25. Several additional markers have been described, e.g., high levels of CTLA-4 (cytotoxic T-lymphocyte associated molecule-4) and GITR (glucocorticoid-induced TNF receptor) are also expressed on regulatory T cells, however the functional significance of this expression remains to be defined. There is a great interest in identifying cell surface markers that are uniquely and specifically expressed on all Foxp3-expressing regulatory T cells. However, to date no such molecule has been identified. In addition to the search for novel protein markers, a different method to analyze and monitor Treg cells more accurately has been described in the literature. This method is based on DNA methylation analysis. Only in Treg cells, but not in any other cell type, including activated effector T cells, a certain region within the foxp3 gene
Regulatory T cell (TSDR, Treg-specific-demthylated region) is found demethylated, which allows to monitor Treg cells through a PCR reaction or other DNA-based analysis methods.[8] Recent evidence suggests that mast cells may be important mediators of Treg-dependent peripheral tolerance.[9]
546
Genetic deficiency
Genetic mutations in the gene encoding Foxp3 have been identified in both humans and mice based on the heritable disease caused by these mutations. This disease provides the most striking evidence that regulatory T cells play a critical role in maintaining normal immune system function. Humans with mutations in Foxp3 suffer from a severe and rapidly fatal autoimmune disorder known as Immune dysregulation, Polyendocrinopathy, Enteropathy X-linked (IPEX) syndrome.[10][11] The IPEX syndrome is characterized by the development of overwhelming systemic autoimmunity in the first year of life, resulting in the commonly observed triad of watery diarrhea, eczematous dermatitis, and endocrinopathy seen most commonly as insulin-dependent diabetes mellitus. Most individuals have other autoimmune phenomena including Coombs-positive hemolytic anemia, autoimmune thrombocytopenia, autoimmune neutropenia, and tubular nephropathy. The majority of affected males die within the first year of life of either metabolic derangements or sepsis. An analogous disease is also observed in a spontaneous Foxp3-mutant mouse known as “scurfy”.
References
[3] Holaday B, Pompeu M, Jeronimo S, Texeira M, Sousa A, Vasconcelos W, Pearson R, Abrams J, Locksley R (1993). “Potential Role for Interleukin-10 in Immunosuppression Associated with Kala Azar”. Journal of Clinical Investigation 92: 2626-2632. PMID 8254019 [4] Holaday B (1999). “Immunotherapy for Visceral Leishm,aniasis: Ability of Factors Produced during Anti_leishmania Responses of Skin Test Positive Adults to Inhibit Peripheral Blood Mononuclear Cell Activities Associated with Visceral Leishmaniasis”. Memorias do Instituto Oswaldo Cruz 94: 55-66. PMID 10029912 [10] Online Mendelian Inheritance in Man IPEX (http:/ / www. ncbi. nlm. nih. gov/ entrez/ dispomim. cgi?id=304790)
Further reading
• Moon C, Kim SH (June 2009). "Use of epigenetic modification to induce FOXP3 expression in naïve T cells". Transplant Proc. 41 (5): 1848–54. doi: 10.1016/j.transproceed.2009.02.101 (http://dx.doi.org/10.1016/j. transproceed.2009.02.101). PMID 19545742 (http://www.ncbi.nlm.nih.gov/pubmed/19545742).
External links
• Regulatory T-Cells (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Regulatory+T-Cells) at the US National Library of Medicine Medical Subject Headings (MeSH)
Cytotoxic T cell
547
Cytotoxic T cell
A cytotoxic T cell (also known as TC, Cytotoxic T Lymphocyte, CTL, T-Killer cell, cytolytic T cell, CD8+ T-cells or killer T cell) is a T lymphocyte (a type of white blood cell) that kills cancer cells, cells that are infected (particularly with viruses), or cells that are damaged in other ways. Most cytotoxic T cells express T-cell receptors (TCRs) that can recognize a specific antigen. An antigen is a molecule capable of stimulating an immune response, and is often produced by cancer cells or viruses. Antigens inside a cell are bound to Antigen presentation stimulates T cells to become either "cytotoxic" CD8+ cells or class I MHC molecules, and brought to the "helper" CD4+ cells. surface of the cell by the class I MHC molecule, where they can be recognized by the T cell. If the TCR is specific for that antigen, it binds to the complex of the class I MHC molecule and the antigen and the T cell destroys the cell. In order for the TCR to bind to the class I MHC molecule, the former must be accompanied by a glycoprotein called CD8, which binds to the constant portion of the class I MHC molecule. Therefore, these T cells are called CD8+ T cells. The affinity between CD8 and the MHC molecule keeps the TC cell and the target cell bound closely together during antigen-specific activation. CD8+ T cells are recognized as TC cells once they become activated and are generally classified as having a pre-defined cytotoxic role within the immune system. However, CD8+ T cells also have the ability to make some cytokines.
Cytotoxic T cell
548
Development
The immune system must recognize millions of potential antigens. There are fewer than 30,000 genes in the human body, so it's impossible to have one gene for every antigen. Instead, the DNA in millions of white blood cells in the bone marrow is shuffled to create cells with unique receptors, each of which can bind to a different antigen. Some receptors bind to tissues in the human body itself, so to prevent the body from attacking itself, those self-reactive white blood cells are destroyed during further development in the thymus. TCRs have two parts, usually an alpha and a beta chain. (Some TCRs have a gamma and a delta chain.) Hematopoietic stem cells in the bone marrow migrate into the thymus, where they undergo VDJ recombination of their beta-chain TCR DNA to form a developmental form of the TCR protein, known as pre-TCR. If that rearrangement is successful, the cells then rearrange their alpha-chain TCR DNA to create a functional alpha-beta TCR complex. This highly-variable Development of single positive T cells in the genetic rearrangement product in the TCR genes helps create millions thymus of different T cells with different TCRs, helping the body's immune system respond to virtually any protein of an invader. The vast majority of T cells express alpha-beta TCRs (αβ T cells), but some T cells in epithelial tissues (like the gut) express gamma-delta TCRs (γδ T cells), which recognize non-protein antigens. T cells with functionally stable TCRs express both the CD4 and CD8 co-receptors and are therefore termed "double-positive" (DP) T cells (CD4+CD8+). The double-positive T cells are exposed to a wide variety of self-antigens in the thymus and undergo two selection criteria: 1. positive selection, in which those double-positive T cells that bind too weakly to MHC-presented self antigens undergo apoptosis because of their inability to recognize MHC-protein complexes. 2. negative selection, in which those double-positive T cells that bind too strongly to MHC-presented self antigens undergo apoptosis because they could otherwise become autoreactive, leading to autoimmunity. Only those T cells that bind to the MHC-self-antigen complexes weakly are positively selected. Those cells that survive positive and negative selection differentiate into single-positive T cells (either CD4+ or CD8+), depending on whether their TCR recognizes an MHC class I-presented antigen (CD8) or an MHC class II-presented antigen (CD4). It is the CD8+ T-cells that will mature and go on to become cytotoxic T cells following their activation with a class I-restricted antigen.
Activation
With an exception of some cell types, such as non-nucleated cells (including erythrocytes), Class I MHC is expressed by all host cells. When these cells are infected with a virus (or another intracellular pathogen), the cells degrade foreign proteins via antigen processing. These result in peptide fragments, some of which are presented by MHC Class I to the T cell antigen receptor (TCR) on CD8+ T cells. The activation of cytotoxic T cells is dependent on several simultaneous interactions between molecules expressed on the surface of the T cell and molecules on the surface of the antigen-presenting cell (APC). For instance, consider the two signal model for TC cell activation.
Cytotoxic T cell
549
Signal First Signal Second Signal
T cell TCR
APC peptide-bound MHC class I molecule either CD80 or CD86 (also called B7-1 and B7-2)
Description There is a second interaction between the CD8 coreceptor and the class I MHC molecule to stabilize this signal. CD80 and CD86 are known as costimulators for T cell activation. This second signal can be assisted (or replaced) by stimulating the TC cell with cytokines released from helper T cells.
CD28 molecule on the T cell
While in most cases activation is dependent on TCR recognition of antigen, alternative pathways for activation have been described. For example, cytotoxic T cells have been shown to become activated when targeted by other CD8 T cells leading to tolerization of the latter.[1] Once activated, the TC cell undergoes clonal expansion with the help of the cytokine Interleukin-2 (IL-2), which is a growth and differentiation factor for T cells. This increases the number of cells specific for the target antigen that can then travel throughout the body in search of antigen-positive somatic cells.
Effector functions
When exposed to infected/dysfunctional somatic cells, TC cells release the cytotoxins perforin, granzymes, and granulysin. Perforin forms pores (aqueous channels) in the target cell's plasma membrane allowing granzymes, types of serine proteases that cleave at aspartate residues in the substrate, to enter the target cell, which then activate a series of cysteine proteases, the caspase cascade, that eventually lead to apoptosis (programed cell death). A second way to induce apoptosis is via cell-surface interactions between the TC and the infected cell. When a TC is activated it starts to express the surface protein FAS ligand (FasL)(Apo1L)(CD95L), which can bind to Fas (Apo1)(CD95) molecules expressed on the target cell. However, this Fas-Fas ligand interaction is thought to be more important to the disposal of unwanted T lymphocytes during their development or to the lytic activity of certain TH cells than it is to the cytolytic activity of TC effector cells. Engagement of Fas with FasL allows for recruitment of the death-induced signaling complex (DISC). The Fas-associated death domain (FADD) translocates with the DISC, allowing recruitment of procaspases 8 and 10. These caspases then activate the effector caspases 3, 6, and 7, leading to cleavage of death substrates such as lamin A, lamin B1, lamin B2, PARP (poly-ADP ribose polymerase), and DNAPK (DNA-activated protein kinase). The final result is apoptosis of the cell that expressed Fas.
Role in disease pathogenesis
During hepatitis B virus (HBV) infection cytotoxic T cells play an important pathogenetic role. They contribute to nearly all of the liver injury associated with HBV infection and, by killing infected cells and by producing antiviral cytokines capable of purging HBV from viable hepatocytes, cytotoxic T cells also eliminate the virus.[2] Recently platelets have been shown to facilitate the accumulation of virus-specific cytotoxic T cells into the infected liver.[3] Recently, cytotoxic T cells have been implicated in the progression of arthritis: depletion of knee joint cartilage macromolecules such as glycosaminoglycans by cytotoxic T cells and macrophages has been observed in a rat model of the disease.[4]
Cytotoxic T cell
550
References
[1] Milstein, O., Hagin, D., Lask, A., Reich-Zeliger, S., Shezan E., Ophir E., Eidelshtein Y., Afik R., Antebi YE., Dustin ML. and Reisner Y. (2011) CTLs respond with activation and granule secretion when serving target for T cell recognition. Blood 117,1042-1052 (http:/ / bloodjournal. hematologylibrary. org/ content/ early/ 2010/ 11/ 02/ blood-2010-05-283770)
External links
• T-cell Group - Cardiff University (http://www.tcells.org/scientific/killer/) • Malaria (http://www.1lecture.com/Immunology/Cytotoxic T Cell/index.html) (Flash Animation)
Natural killer T cell
Natural killer T (NKT) cells are a heterogeneous group of T cells that share properties of both T cells and natural killer (NK) cells. Many of these cells recognize the non-polymorphic CD1d molecule, an antigen-presenting molecule that binds self- and foreign lipids and glycolipids. They constitute only approximately 0.1% of all peripheral blood T cells.[]
Nomenclature
The term “NK T cells” was first used in mice to define a subset of T cells that expressed the natural killer (NK) cell-associated marker NK1.1 (CD161). It is now generally accepted that the term “NKT cells” refers to CD1d-restricted T cells, present in mice and humans, some of which coexpress a heavily biased, semi-invariant T cell receptor (TCR) and NK cell markers.[] Natural killer T (NKT) cells should not be confused with natural killer (NK) cells.
Molecular characterization
NKT cells are a subset of T cells that co-express an αβ T cell receptor (TCR), but also express a variety of molecular markers that are typically associated with NK cells, such as NK1.1. The best known NKT cells differ from conventional αβ T cells in that their TCRs are far more limited in diversity ('invariant' or 'Type 1' NKT). They and other CD1d-restricted T cells ('Type 2' NKT) recognize lipids and glycolipids presented by CD1d molecules, a member of the CD1 family of antigen presenting molecules, rather than peptide-MHC complexes. As such, NKT cells are important in recognizing glycolipids from organisms such as mycobacterium, which cause tuberculosis. NKT cells include both NK1.1+ and NK1.1-, as well as CD4+, CD4-, CD8+ and CD8- cells. Natural Killer T cells can share other features with NK cells as well, such as CD16 and CD56 expression and granzyme production.[][] Invariant Natural Killer T (iNKT) cells express high levels of and are dependent on the transcriptional regulator promyelocytic leukemia zinc finger (PLZF) for their development.[1][2]
Classification
Classification of natural killer T cells into three groups has been proposed.[]
Natural killer T cell
551
Type 1 NKT Other names classical NKT invariant NKT (iNKT) Vα14i NKT (mouse) Vα24i NKT (human) CD1d +
Type 2 NKT non-classical NKT diverse NKT
NKT-like NK1.1+ T cells CD3+ CD56+ T cells
Restriction α-GalCer reactivity TCR repertoire
CD1d -
MHC, other? -
Vα14-Jα18: Vβ8.2, 7, 2 (mouse) Vα24-Jα18: Vβ11 (human)
diverse
diverse
iNKT cells
The best known subset of CD1d-dependent NKT cells expresses an invariant T cell receptor α (TCR-α) chain. These are referred to as type I or invariant NKT cells (iNKT) cells. These cells are conserved between humans and mice and are implicated in many immunological processes. Absence of microbe exposure in early development led to increased iNKT cells and immune morbidity in a mouse model. [3]
Function
Upon activation, NKT cells are able to produce large quantities of interferon-gamma, IL-4, and granulocyte-macrophage colony-stimulating factor, as well as multiple other cytokines and chemokines (such as IL-2, Interleukin-13, Interleukin-17, Interleukin-21 and TNF-alpha).
Significance
NKT cells seem to be essential for several aspects of immunity because their dysfunction or deficiency has been shown to lead to the development of autoimmune diseases (such as diabetes or atherosclerosis) and cancers. NKT cells have recently been implicated in the disease progression of human asthma.[4] The clinical potential of NKT cells lies in the rapid release of cytokines (such as IL-2, IFN-gamma, TNF-alpha, and IL-4) that promote or suppress different immune responses.
References
[4] Cromie, William J. Researchers uncover cause of asthma (http:/ / www. news. harvard. edu/ gazette/ 2006/ 03. 16/ 01-asthma. html) Harvard University Gazette, March 16, 2006.
External links
• NKT cell Journal Screening (http://www.nkcells.info/wiki/index.php?title=NKT_cell#References) • Nature glossary on murine NKT cells (http://www.nature.com/nri/journal/v3/n3/glossary/nri1027_glossary. html#DF2) • Nature Reviews Web Focus on regulatory lymphocytes (http://www.nature.com/nri/focus/reglymph/index. html)
B cell
552
B cell
B cell
The cells of the immune system that make antibodies to invading pathogens such as viruses. They form memory cells that remember the same pathogen for faster antibody production in future infections. Latin Code lymphocytus B TH H2.00.04.1.02005 [1] TH H2.00.04.3.07002
[1]
B cells belong to a group of white blood cells known as lymphocytes, making them a vital part of the immune system -- specifically the humoral immunity branch of the adaptive immune system. B cells can be distinguished from other lymphocytes, such as T cells and natural killer cells (NK cells), by the presence of a protein on the B cell's outer surface known as a B cell receptor (BCR). This specialized receptor protein allows a B cell to bind to a specific antigen. The principal functions of B cells are to make antibodies against antigens, to perform the role of antigen-presenting cells (APCs), and to develop into memory B cells after activation by antigen interaction. Recently, a new, suppressive function of B cells has been discovered.[1] The abbreviation "B", in B cell, comes from the bursa of Fabricius in birds, where they mature. In mammals, immature B cells are formed in the bone marrow, which is used as a backronym for the cells' name.[2]
Development of B cells
Immature B cells are produced in the bone marrow of most mammals. Rabbits are an exception; their B cells develop in the appendix-sacculus rotundus. After reaching the IgM+ immature stage in the bone marrow, these immature B cells migrate to secondary lymphoid tissues (such as the spleen, lymph nodes, Peyer's patches, etc.) where they are called transitional B cells, and some of these cells differentiate into mature B lymphocytes.[] B cell development occurs through several stages, each stage representing a change in the genome content at the antibody loci. An antibody is composed of two identical light (L) and two identical heavy (H) chains, and the genes specifying them are found in the 'V' (Variable) region and the 'C' (Constant) region. In the heavy-chain 'V' region there are three segments; V, D and J, which recombine randomly, in a process called VDJ recombination, to produce a unique variable domain in the immunoglobulin of each individual B cell. Similar rearrangements occur for light-chain 'V' region except there are only two segments involved; V and J. The list below describes the process of immunoglobulin formation at the different stages of B cell development.
B cell
553
Stage
Heavy chain
Light chain
Ig
IL-7 receptor? Yes
CD19?
Progenitor (or pre-pro) B cells Early Pro (or pre-pre)-B cells Late Pro (or pre-pre)-B cells
germline
germline
-
No
undergoes D-J rearrangement
germline
-
Yes
No
undergoes V-DJ rearrangement is VDJ rearranged
germline
-
Yes
Yes [] Yes
[]
Large Pre-B cells
germline
IgM in cytoplasm and surface IgM in cytoplasm and surface IgM on surface IgM and IgD on surface
Yes Yes
Small Pre-B cells
is VDJ rearranged
undergoes V-J rearrangement VJ rearranged VJ rearranged
Yes
Immature B cells Mature B cells
is VDJ rearranged is VDJ rearranged
No No
Yes Yes
When the B cell fails in any step of the maturation process, it will die by a mechanism called apoptosis, here called clonal deletion.[3] B cells are continuously produced in the bone marrow. When the B cell receptor, on the surface of the cell matches the detected antigens present in the body, the B cell proliferates and secretes a free form of those receptors (antibodies) with identical binding sites as the ones on the original cell surface. After activation, the cell proliferates and B memory cells would form to recognise the same antigen. This information would then be used as a part of the adaptive immune system for a more efficient and more powerful immune response for future encounters with that antigen. B cell membrane receptors evolve and change throughout the B cell life span.[] The proteins TACI, BCMA and BAFF-R (B cell activating factor receptor) are present on both immature B cells and mature B cells. Belimumab is a monoclonal inhibitor of the soluble form of B cell activating factor (BAFF), while blisibimod is an inhibitor of both membrane and soluble forms of BAFF. CD20 is expressed on all stages of B cell development except the first and last; it is present from pre-B cells through memory cells, but not on either pre-pro-B cells or plasma cells.[]
Immune tolerance
Like their fellow lymphocytes, the T cells, immature B cells are tested for auto-reactivity by the immune system before leaving the bone marrow. In the bone marrow (the central lymphoid organ), central tolerance is produced. The immature B cells whose B cell receptors (BCRs) bind too strongly to self antigens will not be allowed to mature. If B cells are found to be highly reactive to self, three mechanisms can occur. • Clonal deletion: the removal, usually by apoptosis, of B cells of a particular self antigen specificity. • Receptor editing: the BCRs of self reactive B cells are given an opportunity to rearrange their conformation. This process occurs via the continued expression of the Recombination activating gene (RAG). Through the help of RAG, receptor editing involves light chain gene rearrangement of the B cell receptor. If receptor editing fails to produce a BCR that is less autoreactive, apoptosis will occur. Note that defects in the RAG-1 and RAG-2 genes are implicated in Severe Combined Immunodeficiency (SCID). The inability to recombine and generate new receptors lead to failure of maturity for both B cells and T cells. • Anergy: B cells enter a state of permanent unresponsiveness when they bind with weakly cross-linking self antigens that are small and soluble.
B cell
554
Functions
The human body makes millions of different types of B cells each day that circulate in the blood and lymphatic system performing the role of immune surveillance. They do not produce antibodies until they become fully activated. Each B cell has a unique receptor protein (referred to as the B cell receptor (BCR)) on its surface that will bind to one particular antigen. The BCR is a membrane-bound immunoglobulin, and it is this molecule that allows the distinction of B cells from other types of lymphocyte, as well as being the main protein involved in B cell activation. Once a B cell encounters its cognate antigen and receives an additional signal from a T helper cell, it can further differentiate into one of the two types of B cells listed below (plasma B cells and memory B cells). The B cell may either become one of these cell types directly or it may undergo an intermediate differentiation step, the germinal center reaction, where the B cell will hypermutate the variable region of its immunoglobulin gene ("somatic hypermutation") and possibly undergo class switching. Other functions for B cells include antigen presentation, cytokine production and lymphoid tissue organization.
Clonality
B cells exist as clones. All B cells derive from a particular cell, and thus, the antibodies their differentiated progenies (see below) produce can recognize and/or bind the same specific surface components composed of biological macromolecules (epitope) of a given antigen. Such clonality has important consequences, as immunogenic memory relies on it. The great diversity in immune response comes about because there are up to 109 clones with specificities for recognizing different antigens. A single B cell or a clone of cells with shared specificity, upon encountering its specific antigen, divides to produce many B cells. Most of such B cells differentiate into plasma cells that secrete antibodies into blood that bind the same epitope that elicited proliferation in the first place. A small minority survives as memory cells that can recognize only the same epitope. However, with each cycle, the number of surviving memory cells increases. The increase is accompanied by affinity maturation which induces the survival of B cells that bind to the particular antigen with high affinity. This subsequent amplification with improved specificity of immune response is known as secondary immune response. B cells that have not been activated by antigen are known as naive lymphocytes; those that have met their antigen, become activated, and have differentiated further into fully functional lymphocytes are known as effector B lymphocytes.
B cell types
• Plasma B cells (also known as plasma cells, plasmocytes, and effector B cells) are large B cells that have been exposed to antigen and produce and secrete large amounts of antibodies, which assist in the destruction of microbes by binding to them and making them easier targets for phagocytes and activation of the complement system. They are sometimes referred to as antibody factories. An electron micrograph of these cells reveals large amounts of rough endoplasmic reticulum, responsible for synthesizing the antibody, in the cell's cytoplasm. These are short lived cells and undergo apoptosis when the inciting agent that induced immune response is eliminated. This occurs because of cessation of continuous exposure to various colony-stimulating factors required for survival.
A suspected plasma cell. Plasma cells are normally detected in tissue rather than circulation.
• Memory B cells are formed from activated B cells that are specific to the antigen encountered during the primary immune response. These cells are able to live for a long time, and can respond quickly following a second exposure to the same antigen.
B cell • B-1 cells express IgM in greater quantities than IgG and their receptors show polyspecificity, meaning that they have low affinities for many different antigens. Polyspecific immunoglobulins often have a preference for other immunoglobulins, self antigens and common bacterial polysaccharides. B-1 cells are present in low numbers in the lymph nodes and spleen and are instead found predominantly in the peritoneal and pleural cavities.[4][5] • B-2 cells are the cells intended when using the unqualified "B cell." • Marginal-zone B cells • Follicular B Cells
555
Recognition of antigen by B cells
A critical difference between B cells and T cells is how each lymphocyte recognizes its antigen. B cells recognize their cognate antigen in its native form. They recognize free (soluble) antigen in the blood or lymph using their BCR or membrane bound-immunoglobulin. In contrast, T cells recognize their cognate antigen in a processed form, as a peptide fragment presented by an antigen presenting cell's MHC molecule to the T cell receptor.
Activation of B cells
B cell recognition of antigen is not the only element necessary for B cell activation (a combination of clonal proliferation and terminal differentiation into plasma cells). B cells that have not been exposed to antigen, also known as naïve B cells, can be activated in a T cell-dependent or -independent manner.
T cell-dependent activation
Once a pathogen is ingested by an antigen-presenting cell such as a macrophage or dendritic cell, the pathogen's proteins are then digested to peptides and attached to a Mechanism of action. class II MHC protein. This complex is then moved to the outside of the cell membrane. The macrophage is now activated to deliver multiple signals to a specific T cell that recognizes the peptide presented. The T cell is then stimulated to produce autocrines, resulting in the
B cell
556
proliferation and differentiation to effector and memory T cells. Helper T cells (i.e. CD4+ T cells) then activate specific B cells through a phenomenon known as an Immunological synapse. Activated B cells subsequently produce antibodies which assist in inhibiting pathogens until phagocytes (i.e. macrophages, neutrophils) or the complement system for example clears the host of the pathogen(s). Most antigens are T-dependent, meaning T cell help is required for maximal antibody production. With a T-dependent antigen, the first signal comes from antigen cross linking T cell-dependent B cell activation, showing a TH2-cell (left), B cell (right), and the B cell receptor (BCR) and the second several interaction molecules signal comes from co-stimulation provided by a T cell. T dependent antigens contain proteins that are presented on B cell Class II MHC to a special subtype of T cell called a Th2 cell. When a B cell processes and presents the same antigen to the primed Th cell, the T cell secretes cytokines that activate the B cell. These cytokines trigger B cell proliferation and differentiation into plasma cells. Isotype switching to IgG, IgA, and IgE and memory cell generation occur in response to T-dependent antigens. This isotype switching is known as Class Switch Recombination (CSR). Once this switch has occurred, that particular B cell will usually no longer make the earlier isotypes, IgM or IgD.
T cell-independent activation
Many antigens are T cell-independent in that they can deliver both of the signals to the B cell. Mice without a thymus (nude or athymic mice that do not produce any T cells) can respond to T independent antigens. Many bacteria have repeating carbohydrate epitopes that stimulate B cells, by cross-linking the IgM antigen receptors in the B cell, responding with IgM synthesis in the absence of T cell help. Conjugate vaccines are made to provide a stronger immune response against these foreign molecules. There are two types of T cell independent activation; Type 1 T cell-independent (polyclonal) activation, and type 2 T cell-independent activation (in which macrophages present several of the same antigen in a way that causes cross-linking of antibodies on the surface of B cells). T cell independent activation type 1 is when a B cell binds to an antigen and receives secondary activation by toll-like receptors; type 2 is when the antigen is a molecule with multiple repeating subunits which can simultaneously cross link enough B cell receptors to fully activate the B cell. In 2011, it was discovered that immortalized rhesus monkey B cells may be activated by the binding of monoamine ligands to TAAR1, a recently discovered GPCR. They found that methamphetamine, a potent TAAR1 agonist, signals PKA and PKC activation following ligand binding to TAAR1.[6] Although it is largely recognized as an important regulator of monoaminergic systems, TAAR1 has only recently been characterized as being important for T cell-independent lymphocyte activation.
B cell
557
The ancestral roots of B cells
In an October 2006 issue of Nature Immunology, certain B cells of basal vertebrates (like fish and amphibians) were shown to be capable of phagocytosis, a function usually associated with cells of the innate immune system. The authors postulate that these phagocytic B cells represent the ancestral history shared between macrophages and lymphocytes. B cells may have evolved from macrophage-like cells during the formation of the adaptive immune system.[7] B cells in humans (and other vertebrates) are nevertheless able to endocytose antibody-fixed pathogens, and it is through this route that MHC Class II presentation by B cells is possible, allowing Th2 help and stimulation of B cell proliferation. This is purely for the benefit of MHC Class II presentation, not as a significant method of reducing the pathogen load.
Origin of the term
The abbreviation "B" in B cell originally came from Bursa of Fabricius, an organ in birds in which avian B cells mature.[8] When it was discovered that in most mammals immature B cells are formed in bone marrow, the word B cell continued to be used, although other blood cells also originate from pluripotent stem cells in the bone marrow. The fact that bone and bursa both start with the letter 'B' is a coincidence.
B cell-related pathology
Aberrant antibody production by B cells is implicated in many autoimmune diseases, such as rheumatoid arthritis and systemic lupus erythematosus. B cells are also susceptible to malignant transformation.
Additional image
Figure 1: Schematic diagram to explain mechanisms of clonal selection of B cell, and how secondary immune response is stronger, quicker and more specific in [9] comparison with the primary one.
B cell
558
References
[2] Alberts B, Johnson A, Lewis J, Raff M, Roberts k, Walter P (2002) Molecular Biology of the Cell (http:/ / www. ncbi. nlm. nih. gov/ bookshelf/ br. fcgi?book=mboc4& part=A4422). Garland Science: New York, NY pg 1367. [3] Parham, P. (2005). The Immune System, Garland Science Publishing, New York, NY. [8] Bursa of Fabricius (http:/ / www. nlm. nih. gov/ cgi/ mesh/ 2007/ MB_cgi?mode=& term=Bursa+ of+ Fabricius& field=entry)
Activation of B Lymphocytes by T-Independent Antigens. Gary Kaiser. American Society for Microbiology. July 2005.
External links
• B-Lymphocytes (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=B-Lymphocytes) at the US National Library of Medicine Medical Subject Headings (MeSH) • B Cells and T Cells (http://users.rcn.com/jkimball.ma.ultranet/BiologyPages/B/B_and_Tcells.html) • B Cell Development and Generation of Lymphocyte Diversity (http://www.microvet.arizona.edu/Courses/ MIC419/Secure/CaseNoIg/GODfigs.htm) • Interactive Animation of B Cell Maturation (http://www.bio.davidson.edu/courses/immunology/Flash/ Bcellmat.html) (requires Flash video software) • A Tale of Two SHEPherds (http://beaker.sanfordburnham.org/?p=2357) (from Beaker Blog) • Educational Resource on the Biology of Antibody Cells (http://www.wikilite.com/wiki/index.php/ Biology_of_immunoglobulin_light_chains)
Natural killer cell
Natural killer cells (or NK cells) are a type of cytotoxic lymphocyte critical to the innate immune system. The role NK cells play is analogous to that of cytotoxic T cells in the vertebrate adaptive immune response. NK cells provide rapid responses to virally infected cells and respond to tumor formation, acting at around 3 days after infection. Typically immune cells detect MHC presented on infected cell surfaces, triggering cytokine release causing lysis or apoptosis. NK cells are unique, however, as they have the ability to recognize stressed cells in the absence of antibodies and MHC, allowing for a much faster immune reaction. They were named “natural killers” because of the initial notion that they do not require activation in order to kill cells that are missing “self” markers of major histocompatibility complex (MHC) class 1 .[] NK cells are defined as large granular lymphocytes (LGL) and constitute the third kind of cells differentiated from the common lymphoid progenitor generating B and T lymphocytes.[1] NK cells are known to differentiate and mature in the bone marrow, lymph node, spleen, tonsils and thymus where they then enter into the circulation. .[] NK cells differ from Natural Killer T cells (NKT) phenotypically, by origin and by respective effector functions; often NKT cell activity promotes NK cell activity by secreting IFNγ. In contrast to NKT cells, NK cells do not express T-cell antigen receptors (TCR) or Pan T marker CD3 or surface immunoglobulins (Ig) B cell receptors, but they usually express the surface markers CD16 (FcγRIII) and CD56 in humans, NK1.1 or NK1.2 in C57BL/6 mice. Up to 80% of human NK cells also express CD8. In addition to the knowledge that natural killer cells are effectors of innate immunity, recent research has uncovered information on both activating and inhibitory NK cell receptors which play important function roles including self tolerance and sustaining NK cell activity. NK cell also play a role in adaptive immune response ,[] numerous experiments have worked to demonstrate their ability to readily adjust to the immediate environment and formulate antigen-specific immunological memory, fundamental for responding to secondary infections with the same antigen. The ability for NK cells to act in both the innate and adaptive immune response is becoming increasingly important in research utilizing NK cell activity and potential cancer therapies.
Natural killer cell
559
NK cell receptors
NK cell receptors can also be differentiated based on function. Natural cytotoxicity receptors directly induce apoptosis after binding to ligands that directly indicate infection of a cell. The MHC dependent receptors (described above) use an alternate pathway to induce apoptosis in infected cells. Natural killer cell activation is determined by the balance of inhibitory and activating receptor stimulation i.e. if the inhibitory receptor signaling is more prominent then NK cell activity will be inhibited, similarly if the activating signal is dominant then NK cell activation will result .[]
The HLA ligand for KIR
NK cell receptor types (with inhibitory as well as some activating members) are differentiated by structure, with a couple of examples to follow:
Protein Structure of NKG2D
Activating receptors
• Ly49 (homodimers) — a relatively ancient, C-type lectin family receptor; are of multigenic presence in mice, while humans have only one pseudogenic Ly49; the receptor for classical (polymorphic) MHC I molecules. • NCR (natural cytotoxicity receptors), upon stimulation, mediate NK killing and release of IFNϒ. • CD94 : NKG2 (heterodimers) — a C-type lectin family receptor, conserved in both rodents and primates and identifies non-classical (also non-polymorphic) MHC I molecules like HLA-E. Expression of HLA-E at the cell surface is dependent on the presence of nonamer peptide epitope derived from the signal sequence of classical MHC class I molecules, which is generated by the sequential action of signal peptide peptidase and the proteasome. Though indirect, this is a way to survey the levels of classical (polymorphic) HLA molecules. • CD16 (FcγIIIA) play a role in antibody-dependent cell-mediated cytotoxicity (ADCC), in particular they bind IgG.
Protein Structure of NKp44
Natural killer cell
560
Function
Cytolytic granule mediated cell apoptosis
NK cells are cytotoxic; small granules in their cytoplasm contain proteins such as perforin and proteases known as granzymes. Upon release in close proximity to a cell slated for killing, perforin forms pores in the cell membrane of the target cell, creating an aqueous channel through which the granzymes and associated molecules can enter, inducing either apoptosis or osmotic cell lysis. The distinction between apoptosis and cell lysis is important in immunology: lysing a virus-infected cell could potentially only release the virions, whereas apoptosis leads to destruction of the virus inside. αdefensins, an antimicrobial is also secreted by NK cells, it directly kills bacteria by disrupting their cell walls analogous to neutrophils.[]
Antibody-dependent cell-mediated cytotoxicity (ADCC)
Infected cells are routinely opsonised with antibodies for detection by immune cells. Antibodies that bind to antigens can be recognised by FcϒRIII (CD16) receptors expressed on NK cells resulting in NK activation, release of cytolytic granules and consequent cell apoptosis. This is a major mechanism of killing for some monoclonal antibodies like rituximab (Rituxan), ofatumumab (Azzera) and others. The contribution of ADCC to tumor cell killing can be measured with a specific test that uses NK-92 NK-92 that has been transfected with a high affinity FcR. Results are compared to the "wild type" NK-92 NK-92 that does not express the FcR (www.nk-92.com) NK-92. .[]
Cytokine induced NK and CTL activation
Cytokines play a crucial role in NK cell activation. As these are stress molecules released by cells upon viral infection, they serve to signal to the NK cell the presence of viral pathogens. Cytokines involved in NK activation include IL-12, IL-15, IL-18, IL-2, and CCL5. NK cells are activated in response to interferons or macrophage-derived cytokines. They serve to contain viral infections while the adaptive immune response is generating antigen-specific cytotoxic T cells that can clear the infection. NK cells work to control viral infections by secreting IFNγ and TNFα, IFNγ activates macrophages for phagocytosis and lysis and TNFα acts promote direct NK tumor cells killing. Patients deficient in NK cells prove to be highly susceptible to early phases of herpes virus infection.
Natural killer cell
561
Missing 'self' hypothesis
In order for NK cells to defend the body against viruses and other pathogens, they require mechanisms that enable the determination of whether a cell is infected or not. The exact mechanisms remain the subject of current investigation, but recognition of an "altered self" state is thought to be involved. To control their cytotoxic activity, NK cells possess two types of surface receptors: activating receptors and inhibitory receptors. Most of these receptors are not unique to NK cells and can be present in some T cell subsets as well. These inhibitory receptors recognize MHC class I alleles, which could Schematic diagram indicating the complementary activities of cytotoxic T-cells and NK explain why NK cells kill cells cells. possessing low levels of MHC class I molecules. This inhibition is crucial to the role played by NK cells. MHC class I molecules are the main mechanism by which cells display viral or tumor antigens to cytotoxic T-cells. A common evolutionary adaptation to this seen in both intracellular microbes and tumours, the chronic down-regulation of MHC I molecules, rendering the cell impervious to T-cell mediated immunity. It is believed that NK cells, evolved as an evolutionary response to this adaptation (the loss of the MHC deprives CD4/CD8 action so another immune cell evolved to fulfil the requirement). .[]
Tumor cell surveillance
Natural Killer Cells (NK) often lack antigen specific cell surface receptors and therefore are part of innate immunity i.e. able to react immediately with no prior exposure to the pathogen. In both mice and humans NKs can be seen to play a role in tumor immuno-surveillance by directly inducing the death of tumor cells (NKs act as cytolytic effector lymphocytes) even with the absence of surface adhesion molecules and antigenic peptides, this role of NK cells is critical for immune success particularly because T cells are unable to recognize pathogens in the absence of surface antigens.[] Tumor cell detection results in activation of NK cells and consequent cytokine production and release. If the tumor cells do not cause inflammation they will also be regarded as self and therefore will not induce a T cell response. A number of cytokines are produced by NKs including Tumor Necrosis Factor α (TNFα), IFNγ and Interleukin (IL-10); TNFα and IL-10 act as pro-inflammatory and immuno-suppressors respectively. The activation of NK cells and subsequent production of cytolytic effector cells impacts macrophages, dendritic cells and neutrophils which subsequently affects antigen specific T and B cell responses. Instead of acting via antigen specific receptors, lysis of tumor cells by NK cells is mediated by alternative receptors including NKG2D, NKp44, NKp46, NKp30 and DNAM.[] NKG2D is a disulphide linked homodimer which recognizes a number of ligands, including ULBP and MICA, which are typically expressed on tumor cells. NK cells, along with macrophages and several other cell types, express the Fc receptor (FcR) molecule (FC-gamma-RIII = CD16), an activating biochemical receptor that binds the Fc portion of antibodies. This allows NK cells to target cells against which a humoral response has been mobilized and to lyse cells through
Natural killer cell Antibody-dependent cellular cytotoxicity (ADCC). This response depends on the affinity of the Fc receptor expressed on NK cells which can have high, intermediate and low affinity for the Fc portion of the antibody or IgG. This affinity is determined by the nucleotide status in position 158 of the gene. which can code of Phenylalanine (F allele) or Valine (V allele). Individuals with high affinity FcRgammRIII (158 V/V respond better to antibody therapy. This has been shown for lymphoma patients who received the antibody Rituxan. Patients who express the 158 V/V allele had a better anti-tumor response. Only 15-25% of the population expressed the 158 V/V allele. To determine the ADCC contribution of monoclonal antibodies, NK-92 cells (a "pure" NK cell line) NK-92 has been transfected with the gene for the high affinity expressing FcR.
562
NK cell function in adaptive response
The ability to generate memory cells following a primary infection and the consequent rapid immune activation and response to succeeding infections by the same antigen is fundamental to the role T and B cells play in the adaptive immune response. Despite prior belief that NK cells play no role in the adaptive immune responses, they have since been found to undergo expansion, contraction, memory maintenance and recall .[2]
NK cell function in pregnancy
As the majority of pregnancies involve two parents who are not tissue matched, successful pregnancy requires the mother's immune system to be suppressed. NK cells are thought to be an important cell type in this process.[] These cells are known as "uterine NK cells" (uNK cells) and they differ from peripheral NK cells. They are in the CD56bright NK cell subset, potent at cytokine secretion, but with low cytotoxic ability and relatively similar to peripheral CD56bright NK cells, with a slightly different receptor profile.[] These uNK cells are the most abundant leukocytes present in the uterus in early pregnancy, representing approximately 70% of leukocytes here, however where they originate from remains controversial.[] These NK cells have been shown to have the ability to elicit cell cytotoxicity in vitro, however at a lower level than peripheral NK cells, despite containing perforin.[] Lack of cytotoxicity in vivo may be due to the presence of ligands for their inhibitory receptors. Trophoblast cells downregulate HLA-A and HLA-B in order to defend against cytotoxic T cell-mediated death. This would normally trigger NK cells by missing self recognition, however these cells survive. It is thought that the selective retention of HLA-E (which is a ligand for NK cell inhibitory receptor NKG2A) and HLA-G (which is a ligand for NK cell inhibitory receptor KIR2DL4) by the trophoblast defends it against NK cell-mediated death.[] NK cells secrete a high level of cytokines which help mediate their function. Some important cytokines they secrete include TNF-α, IL-10, IFN-γ and TGF-β, among others.[] For example, IFN-γ dilates and thins the walls of maternal spiral arteries to enhance blood flow to the implantation site.[3]
NK cell evasion by tumor cells
By shedding decoy NKG2D soluble ligands tumor cells have evolved a process by which they are able to avoid immune responses. These soluble NKG2D ligands bind to NK cell NKG2D receptors activating a false NK response and consequently creating competition for the receptor site.[] This method of evasion occurs in prostate cancer. In addition, prostate cancer tumors can evade CD8 cell recognition due to the ability to lose expression of MHC class 1 molecules. This example of immune evasion actually highlights NK cell importance in tumor surveillance and response as CD8 cells can consequently only act on tumor cells in response to NK initiated cytokine production (adaptive immune response) .[4]
Natural killer cell
563
History
In early experiments on cell-mediated cytotoxicity against tumor target cells, both in cancer patients and animal models, investigators consistently observed what was termed a "natural" reactivity, that is, a certain population of cells seemed to be able to lyse tumor cells without having been previously sensitized to them. As these discoveries were incompatible with the established model at the time, many initially considered that these observations were artifacts.[5] However, by 1973, 'natural killing' activity was established across a wide variety of species, and the existence of a separate lineage of cells possessing this ability was postulated. The discovery that a unique type of lymphocyte was responsible for “natural” or spontaneous cytotoxicity was made in the early 1970s by doctoral student Rolf Kiessling and post-doctoral fellow Hugh Pross, in the mouse,[6] and by Hugh Pross and doctoral student Mikael Jondal in the human.[7][8] The mouse and human work was carried out under the supervision of professors Eva Klein and Hans Wigzell, respectively, of the Karolinska Institute, Stockholm. Kiessling’s research involved the well-characterized ability of T-lymphocytes to lyse tumor cells against which they had been previously immunized. Pross and Jondal were studying cell-mediated cytotoxicity in normal human blood and the effect of the removal of various receptor-bearing cells on this cytotoxicity. Later that same year Ronald Herberman published similar data with respect to the unique nature of the mouse effector cell.[9] The human data were confirmed, for the most part, by West et al.[10] using similar techniques and the same erythroleukemic target cell line, K562. K562 is highly sensitive to lysis by human NK cells and, over the decades, the K562 51 Chromium-release assay has become the most commonly used assay to detect human NK functional activity.[11] Its almost universal use has meant that experimental data can be compared easily by different laboratories around the world. Using discontinuous density centrifugation and, later, monoclonal antibodies, natural killing ability was mapped to the subset of large, granular lymphocytes known today as NK cells. The demonstration that density gradient-isolated large granular lymphocytes were responsible for human NK activity, made by Timonen and Saksela in 1980,[12] was the first time that NK cells had been visualized microscopically and was a major breakthrough in the field.
New findings
Anti-cancer therapy
Since NK cells recognize target cells when they express non-self HLA antigens (but not self), autologous (patients' own) NK cell infusions have not shown any anti-tumor effects. Instead investigators are working on using allogeneic cells from peripheral blood which requires that the T-cells are removed before infusion into the patients as they would otherwise cause graft versus host disease (GvHD) which can be fatal. This can be achieved using an immunomagnetic column (CliniMACS). In addition, because of the limited number of NK cells in blood (only 10% of lymphocytes are NK-cells) their number needs to be expanded in culture. This can take a few weeks and the yield is donor dependent. A simpler way to achieve high numbers of pure NK cells is to expand NK-92 cells NK-92 whose cells continuously grow in culture and can be expanded to clinical grade numbers in bags or bioreactors [13]. Clinical studies have shown that it is well tolerated and some anti-tumor responses have been seen in patients with lung cancer, melanoma and lymphoma [14]. Recent studies at Sloan Kettering Cancer Center and UPenn have shown that infusions of T-cells that were engineered to express a chimeric antigen receptor (CAR) recognizing an antigen molecule on leukemia cells could induce remissions in patients with advanced leukemia. There are logistical challenges of expanding T-cells and investigators are working on applying the same technology to peripheral blood NK cells and NK-92 NK-92. NK cells in a study at Children's Hospital Boston in coordination with Dana-Farber Cancer Institute, whereby immunocompromised mice had contracted lymphomas from EBV infection, an NK activating receptor called NKG2D was fused with a stimulatory Fc portion of the EBV antibody. The NKG2D-Fc fusion proved capable of reducing tumor growth and prolonging survival of the recipients.[15]
Natural killer cell
564
Innate resistance to HIV?
Recent research suggests that specific KIR-MHC class 1 gene interactions could control innate genetic resistance to certain viral infections including HIV and its consequent development of AIDS.[] Certain HLA allotypes have been found to determine the progression of HIV to AIDS; an example is the HLA-B57 and HLA-B27 alleles, which have been found to defer progression of HIV to AIDS. This is evident because patients expressing these HLA alleles are observed to have lower viral loads and a more gradual decline in CD4+ T cells numbers. Despite considerable research and data collected measuring the genetic correlation of HLA alleles and KIR allotypes, a firm conclusion has not yet been drawn as to what combination provides decrease HIV and AIDS susceptibility. Future research would aim to pinpoint relevant KIR/HLA interactions with aim to produce a vaccine against HIV/AIDS. NK cells can impose immune pressure on HIV, something that had previously been described only for T cells and antibodies [16] and that HIV mutates to avoid NK cell activity.[16]
Literature
• Cellular and Molecular Immunology by Abbul K. Abbas & Andrew Lichtman Saunders Copyright 2003 • How the Immune System Works, 2nd edition, by Lauren Sompayrac, PhD Blackwell Publishing 2003 • Immunobiology: The Immune System In Health And Disease by Janeway, Travers, Walport & Shlomchik Churchchill Livingstone Copyright 2005 • Kuby Immunology, 6th edition, by Thomas J. Kindt, Richard A. Goldsby,and Barbara A.OsborneW.H. Freeman and Company,New York • Tsuda Y, Cygler M, Gibbs BF, et al. (December 1994). "Design of potent bivalent thrombin inhibitors based on hirudin sequence: incorporation of nonsubstrate-type active site inhibitors". Biochemistry 33 (48): 14443–51. doi:10.1021/bi00252a010 [17]. PMID 7981204 [18].
References
[1] Roitt I, Brostoff J, Male D (2001). Immunology (6th ed.), 480p. St. Louis: Mosby, ISBN 0-7234-3189-2. [3] Ashkar AA, Di Santo JP, Croy BA. Interferon gamma contributes to initiation of uterine vascular modification, decidual integrity, and uterine natural killer cell maturation during normal murine pregnancy. J Exp Med. 2000 Jul 17;192(2):259-70. [13] Gong J, Maki G, Klingemann H. Characterization of a human cell line (NK-92) with phenotypical and functional characteristics of activated natural killer cells. Leukemia 1994; 8: 652-58 [14] Arai S, Meagher R, Swearingen M, et al. Infusion of the allogeneic cell line NK-92 in patients with advanced renal cell cancer or melanoma: a phase I trial. Cytotherapy 2008;10:625-32 ^ Tonn T, Becker S, Esser R, Schwabe D, Seifried E. Cellular immunotherapy of malignancies using the clonal natural killer cell line NK-92. J Hematother Stem Cell Res 2001;10:535-44. [edit] [15] In a transplantation model of LMP1-fueled lymphomas, the NKG2D-Fc fusion proved quite capable of reducing tumor growth and prolonging survival of the recipients [16] http:/ / www. sciencedaily. com/ releases/ 2011/ 08/ 110803133509. htm
External links
• Video of natural killer cell (http://www.youtube.com/watch?v=HNP1EAYLhOs) • CopeWithCytoKines Portal to definitions of NK-Cells and closely related topics (http://www. copewithcytokines.de/cope.cgi?key=NK-cells) • http://www.hfea.gov.uk/fertility-treatment-options-reproductive-immunology.html Reproductive immunology and fertility treatment • http://www.cambridgenetwork.co.uk/news/article/default.aspx?objid=58465 • Binns C (June 19, 2006), Natural Body Guards: How Your Killer Cells Get Motivated (http://www.livescience. com/817-natural-body-guards-killer-cells-motivated.html). Livescience.com. Retrieved on 2007-10-20. • Natural Killer Cells (http://www.nlm.nih.gov/cgi/mesh/2011/MB_cgi?mode=&term=Natural+Killer+ Cells) at the US National Library of Medicine Medical Subject Headings (MeSH)
Natural killer cell • Nkcells.info (http://www.nkcells.info) - MediaWiki based information platform specializing on natural killer cells • Large granular lymphocyte (http://www.cancer.gov/dictionary?CdrID=44440) entry in the public domain NCI Dictionary of Cancer Terms
565
Reticulocyte
Reticulocyte
Reticulocyte Latin reticulocytus Code TH H2.00.04.1.01007 [1]
Reticulocytes are immature red blood cells, typically composing about 1% of the red cells in the human body. Reticulocytes develop and mature in the red bone marrow and then circulate for about a day in the blood stream before developing into mature red blood cells. Like mature red blood cells, reticulocytes do not have a cell nucleus. They are called reticulocytes because of a reticular (mesh-like) network of ribosomal RNA that becomes visible under a microscope with certain stains such as new methylene blue.
Erythrocyte
Process
To accurately measure reticulocyte counts, automated counters that use lasers mark cell samples with fluorescent dye that marks RNA and DNA (such as thiazole orange or polymethine).[1] This distinguishes reticulocytes as the middle ground of dye response to laser light, between red blood cells (which have neither RNA nor DNA) and lymphocytes (which have a large amount of DNA, unlike reticulocytes).[2] The specimen requirement for a reticulocyte count is EDTA anti-coagulated whole blood (lavender-top bottle if using the Vacutainer, Vacuette or Monoject systems; red-top if using the S-Monovette system). Reticulocytes appear slightly bluer than other red cells when looked at with the normal Romanowsky stain. Reticulocytes are also slightly larger, which can be picked up as a high MCV (mean corpuscular volume) with a full blood count done by a trained medical scientist, who has specialized in hematology, or a machine. Flowcytometry for mouse reticulocytes: One can use a cell-permeable thiazole orange dye (see above) to stain for reticulocytes' residual RNA in conjunction with DRAQ5 DNA-only dye (reticulocytes have no DNA and are, thus, DRAQ5-negative) and Ter119 (glycophorin-A) that is a marker of erythroid lineage. (Thiazole orange dye binds to nucleic acids of both DNA and RNA).
Reticulocyte
566
Interpretation
The normal range of values for reticulocytes in the blood depends on the clinical situation and the lab but is usually 0.5% to 1.5%. However, if a person has anemia, the reticulocyte percentage should be higher than "normal" if the bone marrow's ability to produce new blood cells remains intact. Thus, calculating the reticulocyte production index is an important step in understanding whether or not the reticulocyte count is appropriate to the situation. This is often a more important question than whether the percentage is in the normal range; for instance, if someone is anemic but has a reticulocyte percentage of only 1%, the bone marrow is likely not producing new blood cells at a rate that will correct the anemia.
The number of reticulocytes is a good indicator of bone marrow activity because it represents recent production. This means that the reticulocyte count and the reticulocyte production index that can be calculated from it can be used to determine whether a production problem is contributing to the anemia and can also be used to monitor the progress of treatment for anemia. When there is an increased production of red blood cells to overcome chronic or severe loss of mature red blood cells, such as in a haemolytic anemia, people often have a markedly high number and percentage of reticulocytes. A very high number of reticulocytes in the blood can be described as reticulocytosis. Abnormally low numbers of reticulocytes can be attributed to chemotherapy, aplastic anemia, pernicious anemia, bone marrow malignancies, problems of erythropoietin production, various vitamin or mineral deficiencies (B9, B12, iron), disease states (anemia of chronic disease) and other causes of anemia due to poor RBC production.
Supravital stain of a smear of human blood from a patient with hemolytic anemia. The reticulocytes are the cells with the dark blue dots and curved linear structures (reticulum) in the cytoplasm.
References
[2] http:/ / www. medicaldesign. com/ articles/ ID/ 532
External links
• For more information on Reticulocyte Count (http://www.diagnostic-medical-tests.com/ hematology-coagulation-tests/reticulocyte-count.htm) • Reticulocyte (http://www.emedicinehealth.com/script/main/srchcont_dict.asp?src=Reticulocyte) at eMedicine Dictionary • http://www.hxbenefit.com/aplastic-crisis-reticulocytopenia.html
Progenitor cell
567
Progenitor cell
A progenitor cell is a biological cell that, like a stem cell, has a tendency to differentiate into a specific type of cell, but is already more specific than a stem cell and is pushed to differentiate into its "target" cell. The most important difference between stem cells and progenitor cells is that stem cells can replicate indefinitely, whereas progenitor cells can divide only a limited number of times. Controversy about the exact definition remains and the concept is still evolving.[1] The terms "progenitor cell" and "stem cell" are sometimes equated.[2]
Properties
Most progenitors are described as oligopotent. In this point of view, they may be compared to adult stem cells. But progenitors are said to be in a further stage of cell differentiation. They are in the “center” between stem cells and fully differentiated cells. The kind of potency they have depends on the type of their "parent" stem cell and also on their niche. Some progenitor cells were found during research, and were isolated. After their marker was found, it was proven that these progenitor could move through the body and migrate towards the tissue where they are needed. Many properties are shared by adult stem cells and progenitor cells. But still, controversy remains because embryonic stem cells are true stem cells in that they are pluripotent and show unlimited capacity for self-renewal. In contrast, many cells termed adult stem cells would be better defined as progenitor cells, as their capacities for unlimited self-renewal and plasticity have not been comprehensively demonstrated. Progenitor cells are found in adult organisms and they act as a repair system for the body. They replenish special cells, but also maintain the blood, skin and intestinal tissues. They can also be found in developing embryonic pancreatic tissue.
Stem Cell Self-renewal in vivo Self-renewal in vitro Potentiality Unlimited Unlimited Multipotent Limited Limited Unipotent, sometimes oligopotent No Progenitor Cell
Maintenance of self-renewal Yes Population
Reaches maximum number of cells before differentiating Does not reach maximum population
Function
The majority of progenitor cells lie dormant or possess little activity in the tissue in which they reside. They exhibit slow growth and their main role is to replace cells lost by normal attrition. In case of tissue injury, damaged or dead cells, progenitor cells can be activated. Growth factors or cytokines are two substances that trigger the progenitors to mobilize toward the damaged tissue. At the same time, they start to differentiate into the target cells. Not all progenitors are mobile and are situated near the tissue of their target differentiation. When the cytokines, growth factors and other cell division enhancing stimulators take on the progenitors, a higher rate of cell division is introduced. It leads to the recovery of the tissue.
Progenitor cell
568
Examples
The characterization or the defining principle of progenitor cells, in order to separate them from others, is based on the different cell markers rather than their morphological appearance. • Satellite cells found in muscles. They play a major role in muscle cell differentiation and injury recoveries. • Intermediate progenitor cells formed in the subventricular zone.[] Some of these transit amplifying neural progenitors migrate via rostral migratory stream to the olfactory bulb and differentiate further into specific types of neural cells. • Bone marrow stromal cells, basal cell of epidermis have 10% of progenitor cell, although they are often classed as stem cells due to their high plasticity and potential for unlimited capacity for self-renewal. • Periosteum contains progenitor cells that develop into osteoblasts and chondroblasts. • Pancreatic progenitor cells are among the most-studied progenitors.[3] They are used in research to develop a cure against diabetes type-1. • Angioblasts or Endothelial progenitor cells (EPC). These are very important for research on fracture and wounds healing.[4] • Blast cells are involved in generation of B- and T-lymphocytes, which participate in immune responses.[5][6]
Development of the human cerebral cortices
Before E40 (embryonic day 40), progenitor cells generate other progenitor cells; after that period, progenitor cells produce only dissimilar daughters. The cells from a single progenitor cell form a proliferative unit that creates one cortical column; these columns contain a variety of neurons with different shapes.
References
Ovum
569
Ovum
Ovum
A human ovum with corona radiata surrounding it
An ovum (plural ova, from the Latin word ovum meaning egg or egg cell) is a haploid female reproductive cell or gamete. Both animals and embryophytes have ova. The term ovule is used for the young ovum of an animal, as well as the plant structure that carries the female gametophyte and egg cell and develops into a seed after fertilization. In lower plants and algae, the ovum is also often called oosphere.
Ova production
In higher animals, ova are produced by female gonads (sexual glands) called ovaries and all of them are present at birth in mammals and mature via oogenesis.
Human and mammal ova
In the viviparous animals (which include humans and all other placental mammals), the ovum is fertilized inside the female body. Human ovum is a haploid cell still waiting to complete its meosis. And its meosis is completed just after fertilization producing secondary polar body and maternal pro nuclei. The polar body produced is immediately degenarates The human ova grow from primitive germ cells that are embedded in the substance of the ovaries. Each of them divides repeatedly to give rise to several smaller cells, the oogonia. The oogonia then develop via meiosis into the ova, the primary oocytes, and the polar bodies.[1] Once the ovum has been fertilized, it begins to divide over the course of a few hours or days, becoming a morula. The morula enters the uterine cavity where it is immersed in the secretions of the uterine glands, ultimately forming a blastocyst.[2] The ovum is one of the largest cells in the human body, typically visible to the naked eye without the aid of a microscope or other magnification device. The human ovum measures approximately 0.12 mm in diameter.[3]
Ovum and sperm fusing together
The process of fertilizing an ovum (Top to bottom)
Ovum
570
Protist and plant ova
In protists, fungi and many plants, such as bryophytes, ferns, and gymnosperms, ova are produced inside archegonia. Since the archegonium is a haploid structure, egg cells are produced via mitosis. The typical bryophyte archegonium consists of a long neck with a wider base containing the egg cell. Upon maturation, the neck opens to allow sperm cells to swim into the archegonium and fertilize the egg. The resulting zygote then gives rise to an embryo, which will grow out of the archegonium as a young sporophyte.[citation needed] In the flowering plants, the female gametophyte, which usually gives rise to the archegonium, has been reduced to just eight cells referred to as the embryo sac inside the ovule. The gametophyte cell closest to the micropyle opening of the embryo sac develops into the egg cell. Upon pollination, a pollen tube delivers sperm into the embryo sac and one sperm nucleus fuses with the egg nucleus. The resulting zygote develops into an embryo inside the ovule. The ovule in turn develops into a seed and in many cases the plant ovary develops into a fruit to facilitate the dispersal of the seeds. Upon germination, the embryo grows into a seedling.[citation needed] In the moss Physcomitrella patens, the Polycomb protein FIE is expressed in the unfertilised egg cell (Figure, right) as the blue colour after GUS staining reveals. Soon after fertilisation the FIE gene is inactivated (the blue colour is no longer visible, left) in the young embryo. [4]
Ooplasm
Ooplasm (also: oöplasm) is the yolk of the ovum, a cell substance at its center, which contains its nucleus, named the germinal vesicle, and the nucleolus, called the germinal spot.[] The ooplasm consists of the cytoplasm of the ordinary animal cell with its spongioplasm and hyaloplasm, often called the formative yolk; and the nutritive yolk or deutoplasm, made of rounded granules of fatty and albuminoid substances imbedded in the cytoplasm.[] Mammalian ova contain only a tiny amount of the nutritive yolk, for nourishing the embryo in the early stages of its development only. In contrast, bird eggs contain enough to supply the chick with nutriment throughout the whole period of incubation.[]
Ova development in oviparous animals
Gene expression pattern determined by histochemical GUS assays in Physcomitrella patens. The Polycomb gene FIE is expressed (blue) in unfertilised egg cells of the moss Physcomitrella patens (right) and expression ceases after fertilisation in the developing diploid sporophyte (left). In situ GUS staining of two female sex organs (archegonia) of a transgenic plant expressing a translational fusion of FIE-uidA under control of the native FIE promoter
In the oviparous animals (all birds, most fishes, amphibians and reptiles) the ova develop protective layers and pass through the oviduct to the outside of the body. They are fertilized by male sperm either inside the female body (as in birds), or outside (as in many fishes). After fertilization, an embryo develops, nourished by nutrients contained in the egg. It then hatches from the egg, outside the mother's body. See egg (biology) for a discussion of eggs of oviparous animals. The egg cell's cytoplasm and mitochondria (and chloroplasts in plants) are the sole means the egg is able to reproduce by mitosis and eventually form a blastocyst after fertilization.
Ovum
571
Ovoviviparity
There is an intermediate form, the ovoviviparous animals: the embryo develops within and is nourished by an egg as in the oviparous case, but then it hatches inside the mother's body shortly before birth, or just after the egg leaves the mother's body. Some fish, reptiles and many invertebrates use this technique.
References
[1] . [3] Search result of "120 micrometers" in Level O Biology - Google books (http:/ / books. google. ca/ books?id=ca51dWOR8nIC& pg=RA5-PA8-IA2& dq=ovum+ 120+ micrometers& hl=en& ei=sXtjTI6_D4OC8gbZ6rCeCQ& sa=X& oi=book_result& ct=result& resnum=1& ved=0CDAQ6AEwAA#v=onepage& q=120 micrometers& f=false) [4] Assaf Mosquna, Aviva Katz, Eva L. Decker, Stefan A. Rensing, Ralf Reski, Nir Ohad (2009): Regulation of stem cell maintenance by the Polycomb protein FIE has been conserved during land plant evolution. Development 136, 2433-2444.
External links
• The Ovarian Kaleidoscope Database (http://ovary.stanford.edu) description of 1800 genes involved in ovarian functions
Oocyte
572
Oocyte
Oocyte
"Stripped" human oocyte; granulosa cells that had surrounded this oocyte have been removed. Gray's MeSH subject #3 38 Oocytes
[2] [1]
An oocyte (UK: /ˈəʊəsʌɪt/, US: /ˈoʊ.oʊ.saɪt/), oöcyte, ovocyte, or rarely ocyte, is a female gametocyte or germ cell involved in reproduction. In other words, it is an immature ovum, or egg cell. An oocyte is produced in the ovary during female gametogenesis. The female germ cells produce a primordial germ cell (PGC) which undergoes mitosis to form an oogonium. During oogenesis the oogonium becomes a primary oocyte.
Formation
The formation of an oocyte is called oocytogenesis, which is a part of oogenesis.[1] Oogenesis results in the formation of both primary oocytes before birth, and of secondary oocytes after it as part of ovulation.
Diagram showing the reduction in number of the chromosomes in the process of maturation of the ovum; the process is known as meiosis.
Oocyte
573
Cell type Oogonium primary Oocyte
ploidy/chromosomes chromatids Process diploid/46(2N) diploid/46(2N) 4N 4N 2N 1N 1N Oocytogenesis (mitosis)
Time of completion third trimester
Ootidogenesis (meiosis 1) (Folliculogenesis) Dictyate in prophase I for up to 50 years Ootidogenesis (meiosis 2) Ootidogenesis (meiosis 2) Halted in metaphase II until fertilization Minutes after fertilization
secondary Oocyte haploid/23(1N) Ootid Ovum haploid/23(1N) haploid/23(1N)
Characteristics
Cytoplasm
Oocytes are rich in cytoplasm which contains yolk granules to nourish the cell early in development.
Nucleus
During the primary oocyte stage of oogenesis, the nucleus is called a germinal vesicle.[2] The only normal human type of secondary oocyte has the 23rd (sex) chromosome as 23,X (female-determining), whereas sperm can have 23,X (female-determining) or 23,Y (male-determining).
Human oocyte with surrounding granulosa cells
Nest
The space wherein an ovum or immature ovum is located is the cell-nest.[3]
Maternal Contributions
Oocyte
574 Because the fate of an oocyte is to become fertilized and ultimately grow into a fully functioning organism, it must be ready to regulate multiple cellular and developmental processes. The oocyte, a large and complex cell, must be supplied with numerous molecules that will direct the growth of the embryo and control cellular activities. As the oocyte is a product of female gametogenesis, the maternal contribution to the oocyte and consequently the newly fertilized egg is enormous. There are many types of molecules that are maternally supplied to the oocyte which will direct various activities within the growing zygote.
mRNAs and Proteins
During the growth of the oocyte, a variety of maternally transcribed messenger RNAs, or mRNAs, are supplied by maternal cells. These mRNAs can be stored in mRNP (message ribonucleoprotein) complexes and be translated at specific time points, they can be localized within a specific region of the cytoplasm, or they can be homogeneously dispersed within the cytoplasm of the entire oocyte.[4] Oocyte Poles Maternally loaded proteins can also be localized or ubiquitous throughout the cytoplasm. The translated products of the mRNAs and the loaded proteins have multiple functions; from regulation of cellular "house-keeping" such as cell cycle progression and cellular metabolism, to regulation of developmental processes such as fertilization, activation of zygotic transcription, and formation of body axes.[4] Below are some examples of maternally inherited mRNAs and proteins found in Xenopus laevis oocytes.
Name [5] VegT Vg1 [6] [7] Type of Maternal Molecule mRNA mRNA mRNA Protein mRNA Protein mRNA Protein [11] mRNA Protein mRNA Protein [11] Protein mRNA Localization Function
Vegetal Hemisphere Transcription Factor Vegetal Hemisphere Transcription Factor Not Known Ubiquitous Ubiquitous Ubiquitous Ubiquitous Nucleus Not Known Transcription Factor Transcription Factor Transcription Factor Transcription Factor Transcription Factor Not Known FGF Signaling
XXBP-1 CREB
[8] [9]
FoxH1 p53
[10] [11]
Lef/Tcf FGF2
[12]
FGF2, 4, 9 FGFR1 Ectodermin PACE4 [13]
Animal Hemisphere Ubiquitin Ligase Vegetal Hemisphere Proprotein Convertase Not Known Not Known BMP inhibitor BMP/Chordin Bindng Protein
[14]
[15] Coco Twisted Gastrulation fatvg [16]
Vegetal Hemisphere Germ Cell Formation and Cortical Rotation
Oocyte
575
Mitochondria
The oocyte receives mitochondria from maternal cells, which will go on to control embryonic metabolism and apoptotic events.[4] The partitioning of mitochondria is carried out by a system of microtubules which will localize mitochondria throughout the oocyte. In certain organisms, such as mammals, paternal mitochondria brought to the oocyte by the spermatozoon are degraded through the attachment of ubiquitinated proteins. The destruction of paternal mitochondria ensures the strictly maternal inheritance of mitochondria and mitochondrial DNA or mtDNA.[4]
Nucleolus
In mammals, the nucleolus of the oocyte is derived solely from maternal cells.[17] The nucleolus, a structure found within the nucleus, is the location where rRNA is transcribed and assembled into ribosomes. While the nucleolus is dense and inactive in a mature oocyte, it is required for proper development of the embryo.[17]
Maternal Determinants in Xenopus laevis Oocyte
Ribosomes
Maternal cells also synthesize and contribute a store of ribosomes that are required for the translation of proteins before the zygotic genome is activated. In mammalian oocytes, maternally derived ribosomes and some mRNAs are stored in a structure called cytoplasmic lattices. These cytoplasmic lattices, a network of fibrils, protein, and RNAs, have been observed to increase in density as the number of ribosomes decrease within a growing oocyte.[18]
Paternal Contributions
The spermatozoon which fertilizes an oocyte will contribute its pronucleus, the other half of the zygotic genome. In some species, the spermatozoon will also contribute a centriole which will help make up the zygotic centrosome required for the first division. However, in some species, such as in the mouse, the entire centrosome is acquired maternally.[19] Currently under investigation is the possibility of other cytoplasmic contributions made to the embryo by the spermatozoon. During fertilization, the sperm provides three essential parts to the oocyte: (1) a signalling or activating factor, which causes the metabolically dormant oocyte to activate; (2) the haploid paternal genome; (3) the centrosome, which is responsible for maintaining the microtubule system. See anatomy of sperm
Oocyte
576
Abnormalities
• nondisjunction -- a failure of proper homolog separation in meiosis I, or sister chromatid separation in meiosis II can lead to aneuploidy, in which the oocyte has the wrong number of chromosomes, for example 22,X or 24,X. This is the cause of conditions like Down syndrome and Edwards syndrome. It is more likely with advanced maternal age. • Some oocytes have multiple nuclei, although it is thought they never mature.
References
[1] [2] [4] [5] answers.com (http:/ / www. answers. com/ topic/ oogenesis?cat=health) Biology-online (http:/ / www. biology-online. org/ dictionary/ Germinal_vesicle) Mtango N.R., Potireddy S., Latham K.E. (2008). Oocyte quality and maternal control of development. Int. Rev. Cell Mol. Biol. 268, 223-290. Zhang J., King M.L. (1996). Xenopus VegT RNA is localized to the vegetal cortex during oogenesis and encodes a novel T-box transcription factor involved in mesodermal patterning. Development. 12, 4119–29. [6] Heasman J., Wessely O., Langland R., Craig E.J., Kessler D.S. (2001). Vegetal localization of maternal mRNAs is disrupted by VegT depletion. Dev Biol. 240, 377–386. [7] Zhao H., Cao Y., Grunz H. (2003). Xenopus X-box binding protein 1, a leucine zipper transcription factor, is involved in the BMP signaling pathway. Dev Biol. 257, 278–291. [8] Sundaram N., Tao Q., Wylie C., Heasman J. (2003). The role of maternal CREB in early embryogenesis of Xenopus laevis. Dev Biol. 261, 337–352. [9] Kofron M., Puck H., Standley H., Wylie C., Old R., Whitman M., et al. (2004). New roles for FoxH1 in patterning the early embryo. Development. 131, 5065–5078. [10] Takebayashi-Suzuki K., Funami J., Tokumori D., Saito A., Watabe T., Miyazono K., et al. (2003). Interplay between the tumor suppressor p53 and TGF beta signaling shapes embryonic body axes in Xenopus. Development. 130, 3929–3939. [11] Heasman, J. (2006). Maternal determinants of embryonic cell fate. Semin. Cell Dev. Biol. 17, 93-98. [12] Song J., Slack J.M. (1994). Spatial and temporal expression of basic fibroblast growth factor (FGF-2) mRNA and protein in early Xenopus development. Mech Dev. 48, 141–151. [13] Dupont S., Zacchigna L., Cordenonsi M., Soligo S., Adorno M., Rugge M., et al. (2005). Germ-layer specification and control of cell growth by Ectodermin, a Smad4 ubiquitin ligase. Cell. 121, 87–99. [14] Birsoy B., Berg L., Williams P.H., Smith J.C., Wylie C.C., Christian J.L., et al. (2005). XPACE4 is a localized pro-protein convertase required for mesoderm induction and the cleavage of specific TGFbeta proteins in Xenopus development. Development. 132, 591–602. [15] Bell E., Munoz-Sanjuan I., Altmann C.R., Vonica A., Brivanlou A.H. (2003). Cell fate specification and competence by Coco, a maternal BMP, TGFbeta and Wnt inhibitor. Development. 130, 1381–1389. [16] Chan A. P., Kloc M., Larabell C. A., LeGros M., Etkin L.D. (2007). The maternally localized RNA fatvg is required for cortical rotation and germ cell formation. Mech Dev. 124, 350-363. [17] Ogushi S., et al. (2008). The maternal nucleolus is essential for early embryonic development in mammals. Science. 319, 613-616 [18] Vitale A.M., Yurttas P., Fitzhenry R.J., Cohen-Gould, L., Wu W., Gossen J.A., Coonrod S.A. (2009). Role for PADI6 and the CPLs in ribosomal storage in oocytes and translation in the early embryo. Development. 135, 2627-2636. [19] Sutovsky P., Schatten G. (2000). Paternal contributions to the mammalian zygote: fertilization after sperm-egg fusion. Int. Rev. Cytol. 195, 1-65.
Resources
William K. Purves, Gordon H. Orians, David Sadava, H. Craig Heller, Craig Heller (2003). Life: The Science of Biology(7th ed.), pp. 823–824
External links
• Slide (http://it.stlawu.edu/~mtem/devbiol/atlas/ANTRAL1.JPG)
Preceded by none Stages of human development Sperm + Oocyte Succeeded by Zygote
Spermatid
577
Spermatid
Spermatid
Germinal epithelium of the testicle. 1: basal lamina 2: spermatogonia 3: spermatocyte 1st order 4: spermatocyte 2nd order 5: spermatid 6: mature spermatid 7: Sertoli cell 8: tight junction (blood testis barrier)
Transverse section of a tubule of the testis of a rat. × 250. Gray's MeSH subject #258 1243 Spermatids
[1] [1]
The spermatid is the haploid male gametid that results from division of secondary spermatocytes. As a result of meiosis, each spermatid contains only half of the genetic material present in the original primary spermatocyte. Spermatids are connected by cytoplasmic material and have superfluous cytoplasmic material around their nuclei. When formed, early round spermatids must undergo further maturational events to develop into spermatozoa, a process termed spermiogenesis (also termed spermeteliosis). The spermatids begin to grow a living thread, develop a thickened mid-piece where the mitochondria become localised, and form an acrosome. Spermatid DNA also undergoes packaging, becoming highly condensed. The DNA is packaged firstly with specific nuclear basic proteins, which are subsequently replaced with protamines during spermatid elongation. The resultant tightly packed chromatin is transcriptionally inactive.
Spermatid
578
Additional images
Scheme showing analogies in the process of maturation of the ovum and the development of the Genyo spermatids (young spermatozoa).
External links
• BU Histology Learning System: 17804loa [2] - "Male Reproductive System: testis, early spermatids" • BU Histology Learning System: 17805loa [3] - "Male Reproductive System: testis, late spermatids" • Histology at okstate.edu [4]
Sperm
579
Sperm
The term sperm is derived from the Greek word (σπέρμα) sperma (meaning "seed") and refers to the male reproductive cells. In the types of sexual reproduction known as anisogamy and oogamy, there is a marked difference in the size of the gametes with the smaller one being termed the "male" or sperm cell. A uniflagellar sperm cell that is motile is referred to as a spermatozoon, whereas a non-motile sperm cell is referred to as a spermatium. Sperm cells cannot divide and have a limited life span, but after fusion with egg cells during fertilization, a new organism begins developing, starting as a totipotent zygote.[citation needed] The human sperm cell is haploid, so that its 23 chromosomes can join the Diagram of a human sperm cell 23 chromosomes of the female egg to form a diploid cell. In mammals, sperm develops in the testicles and is released from the penis. It is also possible to extract sperm throgh TESE.
Sperm in animals
Anatomy
The mammalian sperm cell consists of a head, a midpiece and a tail. The head contains the nucleus with densely coiled chromatin fibres, surrounded anteriorly by an acrosome, which contains enzymes used for penetrating the female egg. The midpiece has a central filamentous core with many mitochondria spiralled around it, used for ATP production for the journey through the female cervix, uterus and uterine tubes. The tail or "flagellum" executes the lashing movements that propel the spermatocyte.[citation needed] During fertilization, the sperm provides three essential parts to the Sperm and egg fusing oocyte: (1) a signalling or activating factor, which causes the metabolically dormant oocyte to activate; (2) the haploid paternal genome; (3) the centrosome, which is responsible for maintaining the microtubule system.[1]
Sperm
580
Origin
The spermatozoa of animals are produced through spermatogenesis inside the male gonads (testicles) via meiotic division. The initial spermatozoon process takes around 70 days to complete. The spermatid stage is where the sperm develops the familiar tail. The next stage where it becomes fully mature takes around 60 days when its called a spermatozoan.[2] Sperm cells are carried out of the male body in a fluid known as semen. Human sperm cells can survive within the female reproductive tract for more than 5 days post coitus.[3] Semen is produced in the seminal vesicles, prostate gland and urethral glands.
Sperm quality
Sperm quantity and quality are the main parameters in semen quality, which is a measure of the ability of semen to accomplish fertilization. Thus, in humans, it is a measure of fertility in a man. The genetic quality of sperm, as well as its volume and motility, all typically decrease with age.[] (See paternal age effect.)
Market for human sperm
On the global market, Denmark has a well-developed system of human sperm export. This success mainly comes from the Human sperm stained for semen quality testing. reputation of Danish sperm donors for being of high quality[4] and, in contrast with the law in the other Nordic countries, gives donors the choice of being either anonymous or non-anonymous to the receiving couple.[4] Furthermore, Nordic sperm donors tend to be tall and highly educated[5] and have altruistic motives for their donations,[5] partly due to the relatively low monetary compensation in Nordic countries. More than 50 countries worldwide are importers of Danish sperm, including Paraguay, Canada, Kenya, and Hong Kong.[4] However, the Food and Drug Administration (FDA) of the US has banned import of any sperm, motivated by a risk of mad cow disease, although such a risk is insignificant, since artificial insemination is very different from the route of transmission of mad cow disease.[6] The prevalence of mad cow disease is one in a million, probably less for donors. If prevalence was the case, the infectious proteins would then have to cross the blood-testis barrier to make transmission possible.[6]
History
Sperm were first observed in 1677 by Antonie van Leeuwenhoek[7] using a microscope, he described them as being animalcules (little animals), probably due to his belief in preformationism, which thought that each sperm contained a fully formed but small human.[citation needed]
Forensic analysis
Ejaculated fluids are detected by ultraviolet light, irrespective of the structure or colour of the surface.[8] Sperm heads, e.g. from vaginal swabs, are still detected by microscopy using the "Christmas Tree Stain" method, i.e., Kernechtrot-Picroindigocarmine (KPIC) staining.[9][10]
Sperm
581
Sperm in plants
Sperm cells in algal and many plant gametophytes are produced in male gametangia (antheridia) via mitotic division. In flowering plants, sperm nuclei are produced inside pollen.[citation needed]
Motile sperm cells
Motile sperm cells typically move via flagella and require a water medium in order to swim toward the egg for fertilization. In animals most of the energy for sperm motility is derived from the metabolism of fructose carried in the seminal fluid. This takes place in the mitochondria located in the sperm's midpiece (at the base of the sperm head). These cells cannot swim backwards due to the nature of their propulsion. The uniflagellated sperm cells (with one flagellum) of animals are referred to as spermatozoa, and are known to vary in size.[citation needed] Motile sperm are also produced by many protists and the gametophytes of bryophytes, ferns and some gymnosperms such as cycads and ginkgo. The sperm cells are the only flagellated cells in the life cycle of these plants. In many ferns and lycophytes, they are multi-flagellated (carrying more than one flagellum).[] In nematodes, the sperm cells are amoeboid and crawl, rather than swim, towards the egg cell.[]
Non-motile sperm cells
Non-motile sperm cells called spermatia lack flagella and therefore cannot swim. Spermatia are produced in a spermatangium.[]
[] Because spermatia cannot swim, they depend on their environment to Motile sperm cells of algae and seedless plants. carry them to the egg cell. Some red algae, such as Polysiphonia, produce non-motile spermatia that are spread by water currents after their release.[] The spermatia of rust fungi are covered with a sticky substance. They are produced in flask-shaped structures containing nectar, which attract flies that transfer the spermatia to nearby hyphae for fertilization in a mechanism similar to insect pollination in flowering plants.[]
Fungal spermatia (also called pycniospores, especially in the Uredinales) may be confused with conidia. Conidia are spores that germinate independently of fertilization, whereas spermatia are gametes that are required for fertilization. In some fungi, such as Neurospora crassa, spermatia are identical to microconidia as they can perform both functions of fertilization as well as giving rise to new organisms without fertilization.[]
Sperm nuclei
In many land plants, including most gymnosperms and all angiosperms, the male gametophytes (pollen grains) are the primary mode of dispersal, for example via wind or insect pollination, eliminating the need for water to bridge the gap between male and female. Each pollen grain contains a spermatogenous (generative) cell. Once the pollen lands on the stigma of a receptive flower, it germinates and starts growing a pollen tube through the carpel. Before the tube reaches the ovule, the nucleus of the generative cell in the pollen grain divides and gives rise to two sperm nuclei which are then discharged through the tube into the ovule for fertilization.[]
Sperm In some protists, fertilization also involves sperm nuclei, rather than cells, migrating toward the egg cell through a fertilization tube. Oomycetes form sperm nuclei in a syncytical antheridium surrounding the egg cells. The sperm nuclei reach the eggs through fertilization tubes, similar to the pollen tube mechanism in plants.[]
582
References
[2] Semen and sperm quality (http:/ / www. netdoctor. co. uk/ menshealth/ facts/ semenandsperm. htm) [3] Gould JE, Overstreet JW and Hanson FW (1984) Assessment of human sperm function after recovery from the female reproductive tract. Biol Reprod 31,888–894. [4] Assisted Reproduction in the Nordic Countries (http:/ / www. ncbio. org/ NcBioBurrell. pdf) ncbio.org [5] FDA Rules Block Import of Prized Danish Sperm (http:/ / www. newser. com/ story/ 34788/ fda-rules-block-import-of-prized-danish-sperm. html) Posted Aug 13, 08 7:37 AM CDT in World, Science & Health [6] The God of Sperm (http:/ / www. laweekly. com/ news/ news/ the-god-of-sperm/ 17290/ ) By Steven Kotler
External links
• The Great Sperm Race (http://www.channel4.com/microsites/G/TGSR/PDF/Great-Sperm-Race.pdf) pdf • Human Sperm Under a Microscope (http://www.youtube.com/watch?v=vvnEsOaKxuw&NR=1)
Preceded by None Stages of human development Sperm cell + Oocyte Succeeded by Zygote
Spermatogonium
583
Spermatogonium
Spermatogonium
Germinal epithelium of the testicle. 1 basal lamina, 2 spermatogonia, 3 spermatocyte 1st order, 4 spermatocyte 2nd order, 5 spermatid, 6 mature spermatid, 7 Sertoli cell, 8 tight junction (blood testis barrier)
Histological section through testicular parenchyma of a boar. 1 Lumen of Tubulus seminiferus contortus, 2 spermatids, 3 spermatocytes, 4 spermatogonia, 5 Sertoli cell, 6 Myofibroblasts, 7 Leydig cells, 8 capillaries Gray's MeSH subject #258 1243 Spermatogonia
[1] [1]
A spermatogonium (plural: spermatogonia) an undifferentiated male germ cell, originating in a seminiferous tubule and dividing into two primary spermatocytes (a kind of germ cell) in the production of spermatozoa. There are three subtypes: • Type A(d) cells, with dark nuclei. These cells replicate to ensure a constant supply of spermatogonia to fuel spermatogenesis. • Type A(p) cells, with pale nuclei. These cells divide by mitosis to produce Type B cells. • Type B cells, which divide to give rise to primary spermatocytes. Each primary spermatocyte duplicates its DNA and subsequently undergoes meiosis I to produce two haploid secondary spermatocytes. Each of the two secondary spermatocytes further undergo meiosis II to produce two spermatids (haploid). (1 primary spermatocyte => 4 spermatids) The spermatids then undergo spermiogenesis to produce spermatozoa.
Spermatogonium
584
Additional images
Transverse section of a tubule of the testis of a rat. X 250.
Schematic diagram of Spermatocytogenesis
References
Sertoli cell
585
Sertoli cell
Sertoli cell
Germinal epithelium of the testicle. 1: basal lamina 2: spermatogonia 3: spermatocyte 1st order 4: spermatocyte 2nd order 5: spermatid 6: mature spermatid 7: Sertoli cell 8: tight junction (blood testis barrier)
Histological section through testicular parenchyma of a boar. 1 Lumen of Tubulus seminiferus contortus 2 spermatids 3 spermatocytes 4 spermatogonia 5 Sertoli cell 6 Myofibroblasts 7 Leydig cells 8 capillaries Gray's MeSH subject #258 1243 Sertoli+Cells
[1] [1]
A Sertoli cell (a kind of sustentacular cell) is a 'nurse' cell of the testes that is part of a seminiferous tubule. It is activated by follicle-stimulating hormone and has FSH-receptor on its membranes. It is specifically located in the convoluted seminiferous tubules (since this is the only place in the testes where the spermatozoa are produced).
Sertoli cell
586
Functions
Because its main function is to nourish the developing sperm cells through the stages of spermatogenesis, the Sertoli cell has also been called the "mother" or "nurse" cell. Sertoli cells also act as phagocytes, consuming the residual cytoplasm during spermatogenesis. Translocation of germ cells from the base to the lumen of the seminiferous tubules occurs by conformational changes in the lateral margins of the Sertoli cells.
Secretory
Sertoli cells secrete the following substances: • anti-Müllerian hormone (AMH) - secreted during the early stages of fetal life. • inhibin and activins - secreted after puberty, and work together to regulate FSH secretion • androgen binding protein (also called testosterone binding globulin) - increases testosterone concentration in the seminiferous tubules to stimulate spermatogenesis • estradiol - aromatase from Sertoli cells convert testosterone to 17 beta estradiol to direct spermatogenesis • glial cell line-derived neurotrophic factor (GDNF) - has been demonstrated to function in promoting undifferentiating spermatogonia, which ensures stem cell self-renewal during the perinatal period. • the Ets related molecule (ERM transcription factor) - needed for maintenance of the spermatogonial stem cell in the adult testis. • transferrin - a blood plasma protein for iron ion delivery [1]
Structural
The tight junctions of Sertoli cells form the blood-testis barrier, a structure that partitions the interstitial blood compartment of the testis from the adluminal compartment of the seminiferous tubules. Because of the apical progression of the spermatogonia, the tight junctions must be dynamically reformed and broken to allow the immunoidentical spermatogonia to cross through the blood-testis barrier so they can become immunologically unique. Sertoli cells control the entry and exit of nutrients, hormones and other chemicals into the tubules of the testis as well as make the adluminal compartment an immune-privileged site. The cell is also responsible for establishing and maintaining the spermatogonial stem cell niche, which ensures the renewal of stem cells and the differentiation of spermatogonia into mature germ cells that progress stepwise through the long process of spermatogenesis, ending in the release of spermatozoa. Sertoli cells bind to spermatogonial cells via N-cadherins and galctosyltransferase (via carbohydrate residues).
Other functions
During the maturation phase of spermiogenesis, the Sertoli cells consume the unneeded portions of the spermatozoa.
Production of Sertoli cells
Sertoli cells are required for male sexual development. During male development, the gene SRY activates SOX9, which then activates and forms a feedforward loop with FGF9. Sertoli cell proliferation and differentiation is mainly activated by FGF9.[2] The absence of FGF9 tends to cause a female to develop [] Once fully differentiated, the Sertoli cell is unable to proliferate. Therefore, once spermatogenesis has begun, no more Sertoli cells are created. Recently however, some scientists have found a way to grow these cells outside of the body. This gives rise to the possibility of repairing some defects that cause male infertility. It has been suggested that they may derive from mesonephros.[]
Sertoli cell
587
Nomenclature
Sertoli cells are called so because of their eponym Enrico Sertoli, an Italian physiologist who discovered them while studying medicine in the University of Pavia, Italy.[3] He published a description of this cell in 1865. The cell was discovered by Sertoli with a Belthle microscope purchased in 1862, which he used while studying medicine. In the 1865 publication, his first description used the terms "tree-like cell" or "stringy cell" and most importantly he referred to these "mother cells." It was other scientists who used Enrico's family name, Sertoli, to label these cell in publications, starting in 1888. As of 2006, two textbooks that are devoted specifically to the Sertoli cell have been published.
Histology
On slides, using standard staining, it can be easy to confuse the Sertoli cells with the other cells of the germinal epithelium. The most distinctive feature of the Sertoli cells is the dark nucleolus.[4]
Pathology
Sertoli-Leydig cell tumour are part of the sex cord-stromal tumour group of ovarian neoplasms.
Additional images
Transverse section of a tubule of the testis of a rat. X 250.
Sertoli cell
588
References
[4] OSU Center for Veterinary Health Sciences - OSU-CVHS Home (http:/ / www. cvm. okstate. edu/ instruction/ mm_curr/ histology/ MR/ HiMRP4. htm)
External links
• BU Histology Learning System: 17805loa (http://www.bu.edu/histology/p/17805loa.htm) • BU Histology Learning System: 17806loa (http://www.bu.edu/histology/p/17806loa.htm)
Kidney
589
Kidney
Kidney
Human kidneys viewed from behind with spine removed Latin System Artery Vein Nerve MeSH Ren (Greek: nephros) Urinary system and endocrine system Renal artery Renal vein Renal plexus Kidney
[1]
Dorlands/Elsevier Kidney [2]
The kidneys are organs that serve several essential regulatory roles in most animals, including vertebrates and some invertebrates. They are essential in the urinary system and also serve homeostatic functions such as the regulation of electrolytes, maintenance of acid–base balance, and regulation of blood pressure (via maintaining salt and water balance). They serve the body as a natural filter of the blood, and remove wastes which are diverted to the urinary bladder. In producing urine, the kidneys excrete wastes such as urea and ammonium, and they are also responsible for the reabsorption of water, glucose, and amino acids. The kidneys also produce hormones including calcitriol, erythropoietin, and the enzyme renin. Located at the rear of the abdominal cavity in the retroperitoneum, the kidneys receive blood from the paired renal arteries, and drain into the paired renal veins. Each kidney excretes urine into a ureter, itself a paired structure that empties into the urinary bladder. Renal physiology is the study of kidney function, while nephrology is the medical specialty concerned with kidney diseases. Diseases of the kidney are diverse, but individuals with kidney disease frequently display characteristic clinical features. Common clinical conditions involving the kidney include the nephritic and nephrotic syndromes, renal cysts, acute kidney injury, chronic kidney disease, urinary tract infection, nephrolithiasis, and urinary tract obstruction.[] Various cancers of the kidney exist; the most common adult renal cancer is renal cell carcinoma. Cancers, cysts, and some other renal conditions can be managed with removal of the kidney, or nephrectomy. When renal function, measured by glomerular filtration rate, is persistently poor, dialysis and kidney transplantation may be treatment options. Although they are not severely harmful, kidney stones can be painful and a nuisance. The removal of kidney stones involves ultrasound treatment to break up the stones into smaller pieces, which are then passed through the urinary tract. One common symptom of kidney stones is a sharp pain in the medial/lateral segments of the lower back.
Kidney
590
Anatomy
Location
In humans the kidneys are located in the abdominal cavity, more specifically in the paravertebral gutter and lie in a retroperitoneal position at a slightly oblique angle. There are two, one on each side of the spine.[1] The asymmetry within the abdominal cavity caused by the liver typically results in the right kidney being slightly lower than the left, and left kidney being located slightly more medial than the right.[2][3] The left kidney is approximately at the vertebral level T12 to L3,[4] and the right slightly lower. The right kidney sits just below the diaphragm and posterior to the liver, the left below the diaphragm and posterior to the spleen. Resting on top of each kidney is an adrenal gland. The upper (cranial) parts of the kidneys are partially protected by the eleventh and twelfth ribs, and each whole kidney and adrenal gland are surrounded by two layers of fat (the perirenal and pararenal fat) and the renal fascia. Each adult kidney weighs between 125 and 170 grams in males and between 115 and 155 grams in females.[] The left kidney is typically slightly larger than the right kidney.[]
Surface projections of the organs of the trunk, showing kidneys at the level of T12 to L3.
A CT scan in which the kidneys are shown
Kidney
591
Structure
The kidney has a bean-shaped structure; each kidney has a convex and concave surface. The concave surface, the renal hilum, is the point at which the renal artery enters the organ, and the renal vein and ureter leave. The kidney is surrounded by tough fibrous tissue, the renal capsule, which is itself surrounded by perinephric fat, renal fascia (of Gerota) and paranephric fat. The anterior (front) border of these tissues is the peritoneum, while the posterior (rear) border is the transversalis fascia. The superior border of the right kidney is adjacent to the liver; and the spleen, for the left kidney. Therefore, both move down on inhalation. The kidney is approximately 11–14 cm in length, 6 cm wide and 4 cm thick. The substance, or parenchyma, of the kidney is divided into two major structures: superficial is the renal cortex and deep is the renal medulla. Grossly, these structures take the shape of 8 to 18 cone-shaped renal lobes, each containing renal cortex surrounding a portion of [] medulla called a renal pyramid (of Malpighi). Between the renal pyramids are projections of cortex called renal columns (of Bertin). Nephrons, the urine-producing functional structures of the kidney, span the cortex and medulla. The initial filtering portion of a nephron is the renal corpuscle, located in the cortex, which is followed by a renal tubule that passes from the cortex deep into the medullary pyramids. Part of the renal cortex, a medullary ray is a collection of renal tubules that drain into a single collecting duct. The tip, or papilla, of each pyramid empties urine into a minor calyx; minor calyces empty into major calyces, and major calyces empty into the renal pelvis, which becomes the ureter. At the hilum, the ureter and renal vein exit the kidney while the renal artery enters. Surrounding these structures is hilar fat and lymphatic tissue with lymph nodes. The hilar fat is contiguous with a fat-filled cavity called the renal sinus. The renal sinus collectively contains the renal pelvis and calyces and separates these structures from the renal medullary tissue.[5]
1. Renal pyramid • 2. Interlobular artery • 3. Renal artery • 4. Renal vein 5. Renal hilum • 6. Renal pelvis • 7. Ureter • 8. Minor calyx • 9. Renal capsule • 10. Inferior renal capsule • 11. Superior renal capsule • 12. Interlobular vein • 13. Nephron • 14. Minor calyx • 15. Major calyx • 16. Renal papilla 17. Renal column
Blood supply
The kidneys receive blood from the renal arteries, left and right, which branch directly from the abdominal aorta. Despite their relatively small size, the kidneys receive approximately 20% of the cardiac output.[] Each renal artery branches into segmental arteries, dividing further into interlobar arteries which penetrate the renal capsule and extend through the renal columns between the renal pyramids. The interlobar arteries then supply blood to the arcuate arteries that run through the boundary of the cortex and the medulla. Each arcuate artery supplies several interlobular arteries that feed into the afferent arterioles that supply the glomeruli.
3D-rendered computed tomography, showing renal arteries and veins.
Kidney The interstitum (or interstitium) is the functional space in the kidney beneath the individual filters (glomeruli) which are rich in blood vessels. The interstitum absorbs fluid recovered from urine. Various conditions can lead to scarring and congestion of this area, which can cause kidney dysfunction and failure. After filtration occurs the blood moves through a small network of venules that converge into interlobular veins. As with the arteriole distribution the veins follow the same pattern, the interlobular provide blood to the arcuate veins then back to the interlobar veins which come to form the renal vein exiting the kidney for transfusion for blood.
592
Histology
Renal histology studies the structure of the kidney as viewed under a microscope. Various distinct cell types occur in the kidney, including: • • • • • • • • • Kidney glomerulus parietal cell Kidney glomerulus podocyte Kidney proximal tubule brush border cell Loop of Henle thin segment cell Thick ascending limb cell Kidney distal tubule cell Kidney collecting duct cell Interstitial kidney cells Renal arteries and their branches
Microscopic photograph of the renal medulla
The renal artery enters into the kidney at the level of first lumbar vertebra just below the superior mesenteric artery. As it enters the kidney it divides into branches: first the segmental artery, which divides into 2 or 3 lobar arteries, then further divides into interlobar arteries, which further divide into the arcuate artery which leads into the interlobular artery, which form afferent arterioles. The afferent arterioles form the glomerulus (network of capillaries closed in Bowman's capsule). From here, efferent arterioles leaves the glomerulus and divide into peritubular capillaries, which drain into the Microscopic photograph of the renal cortex interlobular veins and then into arcuate vein and then into interlobar vein, which runs into lobar vein, which opens into the segmental vein and which drains into the renal vein, and then from it blood moves into the inferior vena cava.
Innervation
The kidney and nervous system communicate via the renal plexus, whose fibers course along the renal arteries to reach each kidney.[] Input from the sympathetic nervous system triggers vasoconstriction in the kidney, thereby reducing renal blood flow.[] The kidney also receives input from the parasympathetic nervous system, by way of the renal branches of the vagus nerve (cranial nerve X); the function of this is yet unclear.[][6] Sensory input from the kidney travels to the T10-11 levels of the spinal cord and is sensed in the corresponding dermatome.[] Thus, pain in the flank region may be referred from corresponding kidney.[]
Kidney
593
Functions
The kidney participates in whole-body homeostasis, regulating acid-base balance, electrolyte concentrations, extracellular fluid volume, and regulation of blood pressure. The kidney accomplishes these homeostatic functions both independently and in concert with other organs, particularly those of the endocrine system. Various endocrine hormones coordinate these endocrine functions; these include renin, angiotensin II, aldosterone, antidiuretic hormone, and atrial natriuretic peptide, among others. Many of the kidney's functions are accomplished by relatively simple mechanisms of filtration, reabsorption, and secretion, which take place in the nephron. Filtration, which takes place at the renal corpuscle, is the process by which cells and large proteins are filtered from the blood to make an ultrafiltrate that eventually becomes urine. The kidney generates 180 liters of filtrate a day, while reabsorbing a large percentage, allowing for the generation of only approximately 2 liters of urine. Reabsorption is the transport of molecules from this ultrafiltrate and into the blood. Secretion is the reverse process, in which molecules are transported in the opposite direction, from the blood into the urine.
Excretion of wastes
The kidneys excrete a variety of waste products produced by metabolism. These include the nitrogenous wastes called "urea", from protein catabolism, as well as uric acid, from nucleic acid metabolism. Formation of urine is also the function of the kidney. The concentration of nitrogenous wastes, in the urine of mammals and some birds, is dependent on an elaborate countercurrent multiplication system. This requires several independent nephron characteristics to operate: a tight hair pin configuration of the tubules, water and ion permeability in the descending limb of the loop, water impermeability in the ascending loop and active ion transport out of most of the ascending loop. In addition, countercurrent exchange by the vessels carrying the blood supply to the nephron is essential for enabling this function.
Acid-base homeostasis
Two organ systems, the kidneys and lungs, maintain acid-base homeostasis, which is the maintenance of pH around a relatively stable value. The lungs contribute to acid-base homeostasis by regulating carbon dioxide (CO2) concentration. The kidneys have two very important roles in maintaining the acid-base balance: to reabsorb bicarbonate from urine, and to excrete hydrogen ions into urine
Osmolality regulation
Any significant rise in plasma osmolality is detected by the hypothalamus, which communicates directly with the posterior pituitary gland. An increase in osmolality causes the gland to secrete antidiuretic hormone (ADH), resulting in water reabsorption by the kidney and an increase in urine concentration. The two factors work together to return the plasma osmolality to its normal levels. ADH binds to principal cells in the collecting duct that translocate aquaporins to the membrane, allowing water to leave the normally impermeable membrane and be reabsorbed into the body by the vasa recta, thus increasing the plasma volume of the body. There are two systems that create a hyperosmotic medulla and thus increase the body plasma volume: Urea recycling and the 'single effect.' Urea is usually excreted as a waste product from the kidneys. However, when plasma blood volume is low and ADH is released the aquaporins that are opened are also permeable to urea. This allows urea to leave the collecting duct into the medulla creating a hyperosmotic solution that 'attracts' water. Urea can then re-enter the nephron and be excreted or recycled again depending on whether ADH is still present or not.
Kidney The 'Single effect' describes the fact that the ascending thick limb of the loop of Henle is not permeable to water but is permeable to NaCl. This allows for a countercurrent exchange system whereby the medulla becomes increasingly concentrated, but at the same time setting up an osmotic gradient for water to follow should the aquaporins of the collecting duct be opened by ADH.
594
Blood pressure regulation
Although the kidney cannot directly sense blood, long-term regulation of blood pressure predominantly depends upon the kidney. This primarily occurs through maintenance of the extracellular fluid compartment, the size of which depends on the plasma sodium concentration. Renin is the first in a series of important chemical messengers that make up the renin-angiotensin system. Changes in renin ultimately alter the output of this system, principally the hormones angiotensin II and aldosterone. Each hormone acts via multiple mechanisms, but both increase the kidney's absorption of sodium chloride, thereby expanding the extracellular fluid compartment and raising blood pressure. When renin levels are elevated, the concentrations of angiotensin II and aldosterone increase, leading to increased sodium chloride reabsorption, expansion of the extracellular fluid compartment, and an increase in blood pressure. Conversely, when renin levels are low, angiotensin II and aldosterone levels decrease, contracting the extracellular fluid compartment, and decreasing blood pressure.
Hormone secretion
The kidneys secrete a variety of hormones, including erythropoietin, and the enzyme renin. Erythropoietin is released in response to hypoxia (low levels of oxygen at tissue level) in the renal circulation. It stimulates erythropoiesis (production of red blood cells) in the bone marrow. Calcitriol, the activated form of vitamin D, promotes intestinal absorption of calcium and the renal reabsorption of phosphate. Part of the renin-angiotensin-aldosterone system, renin is an enzyme involved in the regulation of aldosterone levels.
Development
The mammalian kidney develops from intermediate mesoderm. Kidney development, also called nephrogenesis, proceeds through a series of three successive phases, each marked by the development of a more advanced pair of kidneys: the pronephros, mesonephros, and metanephros.[7]
Evolutionary adaptation
Kidneys of various animals show evidence of evolutionary adaptation and have long been studied in ecophysiology and comparative physiology. Kidney morphology, often indexed as the relative medullary thickness, is associated with habitat aridity among species of mammals.[]
Kidney
595
Related terms
Medical terms related to the kidneys commonly use terms such as renal and the prefix nephro-. The adjective renal, meaning related to the kidney, is from the Latin rēnēs, meaning kidneys; the prefix nephro- is from the Ancient Greek word for kidney, nephros (νεφρός).[8] For example, surgical removal of the kidney is a nephrectomy, while a reduction in kidney function is called renal dysfunction.
Diseases and disorders
Congenital
• Congenital hydronephrosis • Congenital obstruction of urinary tract • Duplex kidneys, or double kidneys, occur in approximately 1% of the population. This occurrence normally causes no complications, but can occasionally cause urine infections.[9][10] • Duplicated ureter occurs in approximately one in 100 live births • Horseshoe kidney occurs in approximately one in 400 live births • Polycystic kidney disease • Autosomal dominant polycystic kidney disease afflicts patients later in life. Approximately one in 1000 people will develop this condition • Autosomal recessive polycystic kidney disease is far less common, but more severe, than the dominant condition. It is apparent in utero or at birth. Renal agenesis. Failure of one kidney to form occurs in approximately one in 750 live births. Failure of both kidneys to form is invariably fatal. Renal dysplasia Unilateral small kidney Multicystic dysplastic kidney occurs in approximately one in every 2400 live births Ureteropelvic Junction Obstruction or UPJO; although most cases appear congenital, some appear to be an acquired condition[11]
• • • • •
Kidney
596
Acquired
• Diabetic nephropathy • Glomerulonephritis • Hydronephrosis is the enlargement of one or both of the kidneys caused by obstruction of the flow of urine. • Interstitial nephritis • Kidney stones (nephrolithiasis) are a relatively common and particularly painful disorder. • Kidney tumors • Wilms tumor • Renal cell carcinoma • Lupus nephritis • Minimal change disease • In nephrotic syndrome, the glomerulus has been damaged so that a large amount of protein in the blood enters the urine. Other frequent features of the nephrotic syndrome include swelling, low serum albumin, and high cholesterol. • Pyelonephritis is infection of the kidneys and is frequently caused by complication of a urinary tract infection. • Renal failure • Acute renal failure • Stage 5 Chronic Kidney Disease Kidney Failure Generally, humans can live normally with just one kidney, as one has more functioning renal tissue than is needed to survive. Only when the amount of functioning kidney tissue is greatly diminished does one develop chronic kidney disease. Renal replacement therapy, in the form of dialysis or kidney transplantation, is indicated when the glomerular filtration rate has fallen very low or if the renal dysfunction leads to severe symptoms.
Drawing of an enlarged kidney by John Hunter.
Diagnosis
Clinical Many renal diseases are diagnosed on the basis of classical clinical findings. A physician (usually a nephrologist) begins by taking a detailed clinical history and performs a physical examination. In addition to medical history and presenting symptoms, a physician will ask about medication history, family history recent infections, toxic/chemical exposures and other historical factors which may indicate an etiology for the patient's renal disease. Often, some diseases are suggested by clinical history and time course alone. For example, in a formerly healthy child with a recent upper respiratory tract infection and facial/lower limb swelling, findings of proteinuria on urinalysis, a diagnosis of minimal change disease is highly suggested. Similarly, a patient with a history of diabetes who presents with decreased urine output is most likely to be suffering from diabetic nephropathy. Often, such cases do not require extensive workup (such as with renal biopsy). A presumptive diagnosis can be made on the basis of history, physical exam and supportive laboratory studies.
Kidney Laboratory Laboratory studies are an important adjunct to clinical evaluation for assessment of renal function. An initial workup of a patient may include a complete blood count (CBC); serum electrolytes including sodium, potassium, chloride, bicarbonate, calcium, and phosphorus; blood urea, nitrogen and creatinine; blood glucose and glycocylated hemoglobin. Glomerular filtration rate (GFR) can be calculated.[12] Urine studies may include urine electrolytes, creatinine, protein, fractional excretion of sodium (FENA) and other studies to assist in evaluation of the etiology of a patient's renal disease. Urinalysis is used to evaluate urine for its pH, protein, glucose, specific gravity and the presence of blood/hemoglobin. Microscopic analysis can be helpful in the identification of casts, red blood cells, white blood cells and crystals.[12] Imaging studies Imaging studies are important in the evaluation of structural renal disease caused by urinary tract obstruction, renal stones, renal cyst, mass lesions, renal vascular disease, and vesicoureteral reflux.[12] Imaging techniques used most frequently include renal ultrasound and helical CT scan. Patients with suspected vesicoureteral reflux may undergo voiding cystourethrogram (VCUG). Renal biopsy The role of the renal biopsy is to diagnose renal disease in which the etiology is not clear based upon noninvasive means (clinical history, past medical history, medication history, physical exam, laboratory studies, imaging studies). A detailed description of renal biopsy interpretation is beyond the scope of this article. In general- a renal pathologist will perform a detailed morphological evaluation and integrate the morphologic findings with the clinical history and laboratory data, ultimately arriving at a pathological diagnosis. A renal pathologist is a physician who has undergone general training in anatomic pathology and additional specially training in the interpretation of renal biopsy specimens. Ideally, multiple core sections are obtained and evaluated for adequacy (presence of glomeruli) intraoperatively. A pathologist/pathology assistant divides the specimen(s) for submission for light microscopy, immunofluorescence microscopy and electron microscopy. The pathologist will examine the specimen using light microscopy with multiple staining techniques (hematoxylin and eosin/H&E, PAS, trichrome, silver stain) on multiple level sections. Multiple immunofluorescence stains are performed to evaluate for antibody, protein and complement deposition. Finally, ultra-structural examination is performed with electron microscopy and may reveal the presence of electron-dense deposits or other characteristic abnormalities which may suggest an etiology for the patient's renal disease.
597
Kidney
598
In other animals
In the majority of vertebrates, the mesonephros persists into the adult, albeit usually fused with the more advanced metanephros; only in amniotes is the mesonephros restricted to the embryo. The kidneys of fish and amphibians are typically narrow, elongated organs, occupying a significant portion of the trunk. The collecting ducts from each cluster of nephrons usually drain into an archinephric duct, which is homologous with the vas deferens of amniotes. However, the situation is not always so simple; in cartilaginous fish and some amphibians, there is also a shorter duct, similar to the amniote ureter, which drains A pig's kidney opened. the posterior (metanephric) parts of the kidney, and joins with the archinephric duct at the bladder or cloaca. Indeed, in many cartilaginous fish, the anterior portion of the kidney may degenerate or cease to function altogether in the adult.[] In the most primitive vertebrates, the hagfish and lampreys, the kidney is unusually simple: it consists of a row of nephrons, each emptying directly into the archinephric duct. Invertebrates may possess excretory organs that are sometimes referred to as "kidneys", but, even in Amphioxus, these are never homologous with the kidneys of vertebrates, and are more accurately referred to by other names, such as nephridia.[] The kidneys of reptiles consist of a number of lobules arranged in a broadly linear pattern. Each lobule contains a single branch of the ureter in its centre, into which the collecting ducts empty. Reptiles have relatively few nephrons compared with other amniotes of a similar size, possibly because of their lower metabolic rate.[] Birds have relatively large, elongated kidneys, each of which is divided into three or more distinct lobes. The lobes consists of several small, irregularly arranged, lobules, each centred on a branch of the ureter. Birds have small glomeruli, but about twice as many nephrons as similarly sized mammals.[] The human kidney is fairly typical of that of mammals. Distinctive features of the mammalian kidney, in comparison with that of other vertebrates, include the presence of the renal pelvis and renal pyramids, and of a clearly distinguishable cortex and medulla. The latter feature is due to the presence of elongated loops of Henle; these are much shorter in birds, and not truly present in other vertebrates (although the nephron often has a short intermediate segment between the convoluted tubules). It is only in mammals that the kidney takes on its classical "kidney" shape, although there are some exceptions, such as the multilobed reniculate kidneys of cetaceans.[]
History
The Latin term renes is related to the English word "reins", a synonym for the kidneys in Shakespearean English (e.g. Merry Wives of Windsor 3.5), which was also the time the King James Version was translated. Kidneys were once popularly regarded as the seat of the conscience and reflection,[13][14] and a number of verses in the Bible (e.g. Ps. 7:9, Rev. 2:23) state that God searches out and inspects the kidneys, or "reins", of humans. Similarly, the Talmud (Berakhoth 61.a) states that one of the two kidneys counsels what is good, and the other evil.
Kidney
599
Kidneys as food
The kidneys can be cooked and eaten (along with other offal). Kidneys are usually grilled or sautéed, but in more complex dishes they are stewed with a sauce that will improve their flavor. In many preparations, kidneys are combined with pieces of meat or liver, as in mixed grill or meurav Yerushalmi. Dishes include the British steak and kidney pie, the Swedish hökarpanna (pork and kidney stew), the French rognons de veau sauce moutarde (veal kidneys in mustard sauce) and the Spanish riñones al Jerez (kidneys stewed in sherry sauce) .[15]
Hökarpanna, Swedish pork and kidney stew
Additional Images
Right Kidney
Kidney
Right Kidney
Kidney Posterior View
Anterior relation of Left Kidney
Right kidney
Left kidney
Kidneys
Left kidney
Kidney Cross Section
Kidney
600
References
[3] (http:/ / www. bioportfolio. com/ indepth/ Kidney. html) [4] Bålens ytanatomy (Superficial anatomy of the trunk). Anca Dragomir, Mats Hjortberg and Godfried M. Romans. Section for human anatomy at the Department of medical biology, Uppsala university, Sweden. [5] Clapp, WL. Renal Anatomy. In: Zhou XJ, Laszik Z, Nadasdy T, D'Agati VD, Silva FG, eds. Silva's Diagnostic Renal Pathology. New York, NY: Cambridge University Press; 2009. [12] Post TW, Rose BD, auths and Curhan GC, Sheridan AM, eds. Diagnostic Approach to the Patient With Acute Kidney Injury (Acute Renal Failure) or Chronic Kidney Disease. UpToDate.com, Dec. 2012. http:/ / www. uptodate. com. ezproxy2. library. arizona. edu/ contents/ diagnostic-approach-to-the-patient-with-acute-kidney-injury-acute-renal-failure-or-chronic-kidney-disease?source=preview& anchor=H12& selectedTitle=1~150#H12 [13] The Patient as Person: Explorations in Medical Ethics p. 60 by Paul Ramsey, Margaret Farley, Albert Jonsen, William F. May (2002) [14] History of Nephrology 2 p. 235 by International Association for the History of Nephrology Congress, Garabed Eknoyan, Spyros G. Marketos, Natale G. De Santo - 1997; Reprint of American Journal of Nephrology; v. 14, no. 4-6, 1994. [15] Rognons dans les recettes (http:/ / cuisine. notrefamille. com/ recettes-cuisine/ rognons-recette. html)
External links
• The NephCure Foundation offers educational materials on the kidney diseases/conditions Nephrotic Syndrome and FSGS (http://www.nephcure.org) • The Kidney Foundation of Canada (http://www.kidney.ca) • electron microscopic images of the kidney (Dr. Jastrow's EM-Atlas) (http://www.uni-mainz.de/FB/Medizin/ Anatomie/workshop/EM/EMNiereE.html) • European Renal Genome project kidney function tutorial (http://www.euregene.org/euregene/pages/ kidney_tut_e.html) • Kidney Foundation of Canada kidney disease information (http://www.kidneyquebec.ca/ang/kidney_disease/ index.htm) • Renal Fellow Network: Structure & Function of Other Animals' Kidneys (http://renalfellow.blogspot.com/ 2009/06/structure-function-of-other-animals.html) • Kidney Stones (http://symptomsofakidneystone.com) • Kidney Diseases (http://www.kidney-stone.us) • Kidney Information (http://www.redurine.com/urinary_tract/kidney_facts.html) • Animated Presentatin on Kidney Function (http://www.davita.com/kidney_animation/) • CAT Scans of various kidney diseases and conditions (http://www.ctcases.net/ct-cases-database/4 Abdomen And Pelvis/6 Kidneys/) - CT Cases • Kidney Stones; Information and Treatments (http://www.mountsinai.org/patient-care/service-areas/ urological-conditions-and-surgery/areas-of-care/kidney-disease-program)
Article Sources and Contributors
601
Article Sources and Contributors
List of distinct cell types in the adult human body Source: http://en.wikipedia.org/w/index.php?oldid=549416469 Contributors: -Majestic-, ABF, Abc518, Abstraktn, Achowat, AdamRetchless, Aditya, Ahoerstemeier, Aldaron, Allens, Allmightyduck, AnteaterZot, Arcadian, Arthena, Atif.t2, Auntof6, Banus, Belovedfreak, Benesch, Blahblahblah97, Bluemoose, Blurpeace, Bobo192, CWenger, Capricorn42, Carl T, Cflm001, Chris the speller, Christopher Kraus, Chrysaor, Cmcnicoll, Cobi, Conti, CopperKettle, Da best editor, Dbenbenn, DennyColt, Dozenist, Drkarthi, Eikenhein, Epbr123, Excirial, Fieari, Forluvoft, Fraggle81, Franamax, Gongshow, Haymaker, Hello71, Hodja Nasreddin, I dream of horses, Isarra (HG), JZUK, Jackibuddy, Jackson Peebles, Jamoche, Jarradpowell, Jfdwolff, John Abbe, John254, Johntobey, Jomunro, Jordan Yang, Juliancolton, Ka Faraq Gatri, Kevin Rector, Kubigula, Liam Skoda, Lvl, Markjohndaley, Materialscientist, Mathonius, Megaman en m, Mercury, Mikael Häggström, Moe Epsilon, Mporch, My very best wishes, Nathan, Neo139, Nono64, NotWith, Nsaa, Ombudsman, Ozborn, PenguiN42, Pharaoh of the Wizards, Pinkadelica, Puchiko, Pyfan, QuackOfaThousandSuns, R'n'B, Rajah, Revolution1221, Robfbms, Rockpocket, San04, Sayeth, Shanes, Sionus, Smoove Z, Spectrumsaymyname, SpiderJon, Tameeria, The Anome, The Anonymouse, Titodutta, Tohd8BohaithuGh1, Trusilver, Wavelength, West.andrew.g, Wilson44691, Wimt, Wimvandorst, 342 anonymous edits Salivary gland Source: http://en.wikipedia.org/w/index.php?oldid=551178225 Contributors: 10014derek, Aitias, Alex Khimich, Alex.tan, Alfarq, Anaxial, Andrewrp, AnnaP, Arcadian, Ascidian, Avram, Axarus, AxelBoldt, BillC, Bluerasberry, Bomac, Bongwarrior, Breno, BrucePodger, Butko, CSJN, CanadianLinuxUser, Cburnett, Cetaugama, Cmcnicoll, CommonsDelinker, Cshemmerich, DRosenbach, Davidruben, Diberri, Doktor911, Dommyboy7, Don4of4, Draeco, Dravecky, Drmies, Epbr123, Eranb, Eras-mus, Favonian, Fergking, Fisty234, Franamax, Frankster200277, Ghoongta, Greelz, I dream of horses, InverseHypercube, J.delanoy, JVinocur, JaGa, JakobSteenberg, Jayron32, Jfdwolff, Jim1138, JimVC3, Jmarchn, JohnDoran, Juicyboy2k, Jwri7474, Katiedid27, Keilana, Khargas, Kissekatt, Kjkolb, Knutux, Kpjas, Lesion, Lesnail, Li-sung, LuisArmandoRasteletti, Luka Krstulović, Mac Davis, MartinDK, Membender, Metju, Mikael Häggström, Miniyazz, Naddy, Nephron, Nexus 215, Nick Number, Njardarlogar, Nlu, O.Koslowski, Ohnoitsjamie, Pdcook, Pip2andahalf, Pmlineditor, Psbsub, Rb1248, Rlevente, Ryan, Sannab, ScAvenger, Sd31415, Sebastiano venturi, Shell Kinney, Shikexue2, SimonP, Slysplace, Snafflekid, Soap, Some jerk on the Internet, Soulkeeper, Stickee, SuperHamster, Swamp Ig, Symplectic Map, Tachyon01, The Anome, The Thing That Should Not Be, TheEgyptian, Thesis4Eva, Tide rolls, Tjd1, Tommy2010, Tristanb, Vinne2, Vrenator, Wavelength, Welldad, Wereon, WikHead, Wikieditor06, William Avery, Wnme, WojPob, Zzedar, 267 anonymous edits Von Ebner's gland Source: http://en.wikipedia.org/w/index.php?oldid=541485832 Contributors: 04mamich, Arcticcoconut, Black Falcon, Cmcnicoll, Devinburn, Ego White Tray, Facts707, Falcon8765, Gene Nygaard, Gyopi, Isopropyl, Jpogi, Krm232, Materialscientist, Sayanmitra, Snafje, 12 anonymous edits Mammary gland Source: http://en.wikipedia.org/w/index.php?oldid=548828046 Contributors: Ackerman22, Adrian J. Hunter, Alex.tan, AlrightEdits, Andrewmc123, Anthonyhcole, Arcadian, Arthur Rubin, AxelBoldt, Batsnumbereleven, Beth 84, BrainyBabe, Brest39, Brian Crawford, Brow276, BullRangifer, CTho, CWii, CarTick, Carturo222, Caulfieldholden, Ccevo2010, Celllist, Cgingold, Chanlyn, Chaser, Chris G, Chrisn0113, Christian75, CiaPan, ClamDip, Clawed, Clngre, Cointyro, CommonsDelinker, ConfuciusOrnis, Craig Pemberton, Dan100, Daniel Case, Darth Panda, Diberri, Dina, Dynzmoar, ENeville, Ealdgyth, EdC, Emijrp, Eras-mus, Erud, Favonian, Flarn2006, Flewis, Fratrep, Gilliam, Ginsengbomb, Gogo Dodo, Graham87, Grakk, Gvw686, Hans.vmobile, Henrygb, HiEv, HiMyNameIsDick, I liek breasts, Illnab1024, Itai, JackAidley, Jackhynes, Jarble, Jfurr1981, Jlcarter2, Joelmills, Julian Mendez, Jwissick, Karada, Kartano, Keenan Pepper, Keilana, Kerowyn, Khajidha, Latka, LeyteWolfer, Lmbhull, Louis Waweru, Lucy346, Luigifan, MONGO, Materialscientist, Matt26, Mentifisto, Millw001, Mmxx, MrCheeseBasket, My Core Competency is Competency, Naturehead, NawlinWiki, Neelix, Nhsnoboarder17, Nishkid64, NotAnonymous0, Notonegoro, Oneiros, Orlandoturner, Osm agha, Paul Erik, Pecolee, Prof. Squirrel, QueenCake, RNLockwood, Raymondwinn, Rich Farmbrough, Richiez, Rickyrab, Rjwilmsi, Rockpocket, Roleplayer, Rory096, Rune X2, SDC, Salvio giuliano, SchreiberBike, Scottalter, Scottandrewhutchins, Search255, Septegram, SophiePon, Sp3000, Star Trek Man, Steverapaport, SummerWithMorons, Tabletop, Takagi, Techman224, Template namespace initialisation script, The Anome, The Thing That Should Not Be, The Wednesday Island, TimVickers, Timc, Tinman11, Torchiest, Toyalla, Trinanjon, Ulric1313, Ursasapien, Van helsing, WLU, WerewolfHunter65, Westvoja, Why Not A Duck, WinterSpw, Woohookitty, Zigger, 152 anonymous edits Lacrimal gland Source: http://en.wikipedia.org/w/index.php?oldid=548680179 Contributors: AED, Alex.tan, Anatomist90, Andyafire, Arcadian, Argarrett826, Arthena, Aviados, Babedacus, Bluemoose, Chris the speller, Difu Wu, DiverDave, Dj Capricorn, Dr Bilal Alshareef, Editorjohn, ElAmericano, Eyesurgeon, Finlay McWalter, Gail, Greenjeans8888, Hovea, Iloveeragon, ImperatorExercitus, Irisx, Isnow, Jaysmasher, Jfdwolff, Jmarchn, John of Reading, Juliancolton, Kbdank71, L Kensington, ML5, Mandarax, Mikael Häggström, Moagabeeshum, Netizen, Nnh, Nono64, Nuvitauy07, Old Moonraker, Osmodiar, Pacifica007, Persian Poet Gal, PhatRita, Rkvignesh, SF007, Snigbrook, Steveprutz, Teamonits, Themfromspace, Tubantia, Varano, Vikte, 64 anonymous edits Ceruminous gland Source: http://en.wikipedia.org/w/index.php?oldid=526530422 Contributors: Arcadian, AtmanDave, Bobsagat, Eleassar, Kerowyn, Lynntyler, My Core Competency is Competency, ResearchRave, Samyutan, Skela, Spiral5800, Xezbeth, 4 anonymous edits Eccrine sweat gland Source: http://en.wikipedia.org/w/index.php?oldid=541717046 Contributors: Arcadian, Baville, Chris Capoccia, Coolstoryhansel, Docfaust, Drphilharmonic, Edward, Kaxap, Leonard^Bloom, Mike2vil, MisterSheik, My Core Competency is Competency, Nelly4, Prof. Squirrel, ResearchRave, The Anome, Tiphaine800, Zazpot, Zz2, 30 anonymous edits Apocrine sweat gland Source: http://en.wikipedia.org/w/index.php?oldid=551814721 Contributors: AK456, Arcadian, Axeman89, Barticus88, BeardWand, Bejnar, Blueshifter, Closedmouth, Cpl Syx, Craig Pemberton, DaGizza, DannyBoy7783, Diannaa, Draeco, Drphilharmonic, Gould363, Hippietrail, Isopropyl, JakobSteenberg, Jarble, Jason Quinn, Jrmonirian, Lawrence Mayer, Marchije, Mathmo, MisterSheik, Monolemma, My Core Competency is Competency, Neverquick, Penguat, Prof. Squirrel, Queenmomcat, Recurring dreams, Rjwilmsi, Saeidbaki, Samyutan, SchreiberBike, Sgamer1770, Stevegray, Teimu.tm, TenPoundHammer, TheGrimReaper NS, Tiphaine800, Topbanana, Tuckerekcut, Zazpot, 55 anonymous edits Moll's gland Source: http://en.wikipedia.org/w/index.php?oldid=548166562 Contributors: Arcadian, Betacommand, Draeco, Fgegypt, Hovea, My Core Competency is Competency, Prof. Squirrel, Riffle, 3 anonymous edits Sebaceous gland Source: http://en.wikipedia.org/w/index.php?oldid=543059574 Contributors: 1st2Bomb, AED, Abdull, Aitias, Anc sierra, Andycjp, AnnaP, Arcadian, Auntof6, AxelBoldt, Bansp, Bender235, Bobo192, CIS, CerealBabyMilk, Ceyockey, Chris Capoccia, CommonsDelinker, Darklilac, Davewho2, DeadEyeArrow, Divide, Dougluce, Dprady, Dr. Doof, Dreamer.redeemer, Drphilharmonic, Ds13, Edgar181, Eeekster, Eug, Evets21, Fences and windows, Fsotrain09, Fuzzbox, Fuzzy901, Gareth Griffith-Jones, Geni, GorillaWarfare, Gpresearch, Hankwang, Helix84, Hightower 40, Intersofia, Iraqidude, Jchae88, Kajerm, Keala.richardson, Keetanii, Kjkolb, Lando242, Lichee66, Littenberg, Lord EDITS, Majorly, MarcoTolo, Mattygabe, Mctt, Mikael Häggström, Mikekearn, Moshe Constantine Hassan Al-Silverburg, My Core Competency is Competency, Neckoneckonecko, Neilbeach, Niceguyedc, Nono64, Nuno Tavares, Oatmeal batman, Obli, OlEnglish, Pablo X, Peter Ellis, Ph.eyes, Prof. Squirrel, Pwjb, R sirahata, RDBrown, Ratdesh, Rjwilmsi, Rlfb, Rogermw, Rune X2, Saleen1996, Seanmiz, Showvaughan29, Smulthaup, Snow Blizzard, Snowmanradio, SofiaSoGood, Sprostini, Sriharsh1234, Steven Walling, Stratuspower88, Suffusion of Yellow, TLazzo, Taco325i, Telekenesis, That Guy, From That Show!, Tjmayerinsf, UnicornTapestry, Valentij01, Velella, Vojtech.dostal, Vsion, WLU, Waitak, WhatamIdoing, Wike490, Wikid77, Wikijens, Wolfkeeper, Writerite, X-Fi6, Yvwv, Zinnmann, 참, 127 anonymous edits Olfactory glands Source: http://en.wikipedia.org/w/index.php?oldid=544509978 Contributors: Arcadian, LittleWink, Lovelager, Prissi, Rjwilmsi, Romanmb, Torgeirh, Xezbeth, 3 anonymous edits Brunner's glands Source: http://en.wikipedia.org/w/index.php?oldid=543848118 Contributors: Andreas Erick, Arcadian, Blue Danube, Bossair2, Brim, Caerwine, Cherribr, David Kernow, Gastro-en, Graham87, Jag123, JakobSteenberg, Jfdwolff, Jj137, Joehall45, Jpogi, Matan Hemli, Michael Kan, Selket, StuffOfInterest, Thisisborin9, Vogon77, Vojtech.dostal, WhatamIdoing, Ww2censor, Xezbeth, Zanimum, 25 anonymous edits Prostate Source: http://en.wikipedia.org/w/index.php?oldid=551253555 Contributors: A little insignificant, AMK1211, Abstraktn, Abune, Academia salad, Acroterion, Ajp, Alanhay, Alasdair, Alex.tan, AlexR, Alt f in, Anaxial, AndrewWTaylor, Andrij Kursetsky, Androlog, Anomalocaris, Anthony Appleyard, Arcadian, Asarelah, Atlant, AxelBoldt, Azmcs, BBuchbinder, BMF81, Baazandar, Bald Zebra, Beetstra, Before My Ken, Bemoeial, Bgordski, Bigjhoninelcasa28, BillC, Biolog2, Bizflyer, Bleakcomb, Bobo192, Bongwarrior, Bopizzle, Boradis, Bryan Derksen, Bushytails, C.Fred, CMD Beaker, CTF83!, Cairo123, Can't sleep, clown will eat me, CattleGirl, Centrx, Chanlyn, Chris G, Chriswaterguy, Chuunen Baka, Circeus, Cmmuell, Cnjanis, CompliantDrone, Conductcode, Contentmaven, Ctrlfreak13, Cuahl, Daleee, DanielCD, Daveb, Davidruben, Dbfirs, DeadEyeArrow, Deli nk, Delldot, Dennisthe2, DevastatorIIC, Dffgd, Diberri, Digitalh2o, Diotti, Disposableman, Djb217, Djsignal, Dono, Doug, Dragon12597, Drzaphod, ERK, Ebehn, Eleassar, Eleassar777, Emperorbma, Enviromaxinfo, Eog1916, Etan J. Tal, Evo584, Exir Kamalabadi, FT2, Fajar78, FallenAngelII, Fama Clamosa, Fleela, Floppy Tits, Flyer22, Fokklife, Frap, Frecklefoot, Fuzheado, Gareth.ellisthomas, Gfoley4, Gildindaimoth, Gilliam, Giraffedata, Glennwells, GoShow, Googie man, Grafen, GregAsche, Gsarwa, Guanaco, Gugilymugily, Gurch, Gwernol, HJames, HalJor, Hanacy, Hardcorelife, Headbomb, Helix84, Hirpex, Hu12, Hybernizer, Ibanix, Ihealthbuzz, Ilyushka88, Imnotoneofyou, Indon, InvictaHOG, Iridescent, Isfppoet, Ishfaq Khan8, Iwilcox, J.delanoy, JHunterJ, JJHeart, Jammie, Janice Vian, Janko, Jarble, Jayelani, Jerome Charles Potts, Jfdwolff, Jhenderson777, Jmarchn, Jmunroo, Johan1298, Johanname, John robinson, Johnbtv, Joshuas88, Jrsvc, Judgeking, Julesd, Juliancolton, JumpingInSlowMotion, Jun-Dai, Kaobear, KarlFarrell, KaurJmeb, Keenan Pepper, Keldan, Kevin Rector, Kieron a m, King of Hearts, Kntrabssi, Kocio, Kozuch, Kronnang Dunn, Kw0, Laburke, LafinJack, Larryclapp, Leafyplant, Lesouris, Lineslarge, Livajo, Livitup, LonghornDIT, Luckygohappy115, MER-C, Mac, Macedonian, Man It's So Loud In Here, Mariushendrik, Markaci, Materialscientist, Mathew5000, Mav, Maxxicum, Mcstrother, Mczack26, Mghabmw, Mgoodyear, Miami33139, Michael Devore, Michael.Urban, Mikael Häggström, Mike hayes, MishaPan, Miss Tanit, Misslloid, Mkweise, Montrealais, Monty845, Moreau36, Msfishi, Munblog, Mycoderma, Myrealana, Myseda, NapoliRoma, Navy10760, NeilN, Nephron, NerdyScienceDude, Nick, NightFlyer, Nitroshockwave, Nongendered, NotWith, Nufy8, Nuviapalomar, Odedee, Ohnoitsjamie, OldakQuill, Ole E. Sorensen, Openhands, Orange roughie, Orlandoturner, Oxymoron83, Patrick Berry, Patxi lurra, Paulfp, Pbmaise, Pcp111, Pedro, Philip Trueman, Prince Harry of England, Project icecap, Prostatainforma, Psytrist, REscano, Radinruslan, RadioFan, Ratel, Raul654,
Article Sources and Contributors
Raxicoricofallapatorius, Reaper Eternal, Reggy73, Revision17, Rich Farmbrough, RichF, Richardcavell, Rjwilmsi, Roberta F., Roland2, Romanm, Ruy Pugliesi, SCEhardt, Sarbruis, SarekOfVulcan, Scottandrewhutchins, Seaphoto, Serephine, Shellinbox, Sitush, Slashme, Spencer, Spudst3r, Ssetd, Stepheng4, Stevenfruitsmaak, Sultan11, Szquirrel, Tainter, Tameeria, TastyPoutine, Tbsdy lives, Template namespace initialisation script, The Anome, The Thing That Should Not Be, The very model of a minor general, TheLimbicOne, Thebestofall007, Thedeadlypython, ThoHug, Tide rolls, ToNToNi, Todd Vierling, Tomyumgoong, Tpbradbury, Traxs7, TutterMouse, Unit 5, Vanished user giiw8u4ikmfw823foinc2, Velps, Vianello, Vrenator, Vsmith, WJSProwler1, Waggers, Websi7, Weetoddid, Westogent, Whizistic, Wimt, Wmahan, WoodsGnome, Wsiegmund, Ww2censor, Wynler, XfreddytanX, Xoder, Yamamoto Ichiro, ZainAliNawazish, Zigger, Zomno, Zorakoid, ﻋﻠﯽ ﻭﯾﮑﯽ, 495 anonymous edits Bulbourethral gland Source: http://en.wikipedia.org/w/index.php?oldid=539416952 Contributors: Ahmad.ghamdi.24, Ahuskay, Alansohn, AnemoneProjectors, Animeronin, Anonymousphrase, Arcadian, Arent, Brushdrawn, Bryan Derksen, Caiyu, Chanlyn, Den fjättrade ankan, Diberri, DocWatson42, Dpol, Drphilharmonic, Durova, Eras-mus, Fibonacci, Giraffedata, Guanaco, Hede2000, Hovea, James086, Japanese Searobin, Jarble, Jeffro77, Jerry, Jugger90, KDS4444, Karl-Henner, Kauczuk, Keenan Pepper, KellyCoinGuy, Kjkolb, Lexusuns, Macaddict10, Mcstrother, Meco, Montrealais, Myseda, Nick Number, Nuviapalomar, Obradovic Goran, Omicronpersei8, Orlandoturner, Ratel, Raul654, Romanm, Serephine, Sfahey, Stupid6, Szquirrel, Tchaika, Template namespace initialisation script, TheJC, Versus22, 87 anonymous edits Bartholin's gland Source: http://en.wikipedia.org/w/index.php?oldid=539416636 Contributors: AnemoneProjectors, Arcadian, Ask123, AxelBoldt, Betacommand, Blackbyrus, Bryan Derksen, Chanlyn, Clintonboyd, DMacks, Dandelion1, Delldot, Diberri, DocWatson42, Draeco, Drgarden, Eleassar, Eras-mus, Faigl.ladislav, Falcon994, Fangfufu, Hydrargyrum, Igno2, Ionutzmovie, JDobby, JulieADriver, Katydidit, Keenan Pepper, Kelly Martin, Kibi78704, Knutux, Ksanyi, Lexusuns, Lmaxsmith, Malik Shabazz, Miraceti, Nicholasolan, PaddyM, Pigman, Poindexter Propellerhead, Postrach, Qwerty Binary, Rjwilmsi, Rune X2, Saimhe, Sietse Snel, Slightsmile, Someone else, Sonjaaa, Superbeecat, Szquirrel, TakuyaMurata, Template namespace initialisation script, The Anome, Tsiaojian lee, Vaughan, Veck Strack, Wikitanvir, 39 anonymous edits Endometrium Source: http://en.wikipedia.org/w/index.php?oldid=547998992 Contributors: 24.234.70.xxx, Alansohn, Altenmann, Andycjp, Anxietycello, Arcadian, AxelBoldt, BCSWowbagger, Belovedfreak, Bemoeial, Brim, Bryan Derksen, Cbkallen, Clicketyclack, Conversion script, Damian Yerrick, Dasani, Davidruben, Decoy, Delldot, Diberri, Dlohcierekim's sock, Download, Drphilharmonic, Dub8lad1, Ekem, Epingchris, Eras-mus, Erud, Everyking, Floranerolia, Fluffernutter, Flyer22, General Wesc, Gonzonoir, Guidod, Habj, JackSparrow Ninja, Jeijoe, Jeronimo, Jmarchn, Jpogi, Jsherwood0, Kurykh, Mayday 1234, Mikael Häggström, Modify, Monobi, Nephron, Nick Number, Pigman, QuizzicalBee, Redyka94, RexNL, Robert McClenon, Rymanes, Santonellis, Seans Potato Business, Seejyb, Selket, TheEgyptian, Tjmoel, TravisTX, Trosoft, Uwe Gille, Viriditas, Vldscore, Werieth, WhatamIdoing, Wolfmankurd, Yca.zuback, Zephyris, 63 anonymous edits Urethral gland Source: http://en.wikipedia.org/w/index.php?oldid=547331842 Contributors: Animeronin, Anticipation of a New Lover's Arrival, The, Arcadian, Beeswaxcandle, Dcshank, Delldot, Denni, Draeco, Jarble, JeremyA, Joel7687, Richard001, Vldscore, 2 anonymous edits Gastric chief cell Source: http://en.wikipedia.org/w/index.php?oldid=540549394 Contributors: Anirishwoman, Arcadian, Basmoq, Boghog, Comrade stuvak, Crocodilesareforwimps, Delldot, Draeco, Eleassar, Franamax, FrozenMan, Ghirlandajo, Gsibbel, Jpogi, Miguelferig, Neodop, Xquizit.decorum, 4 anonymous edits Pepsin Source: http://en.wikipedia.org/w/index.php?oldid=547172026 Contributors: .V., Alexander sar, Alexbateman, Arcadian, Artichoke-Boy, Astrochemist, Aymatth2, Aziz1005, BQmUB2009002, Bdoc13, Ben211086, Bersl2, Bertolucci18, Boghog, BrettMontgomery, Bubbachuck, CTZMSC3, Chinasaur, ChrisGualtieri, Chrisfow, Christopher Cooper, Chrumps, DARTH SIDIOUS 2, Decembermouse, Derelk, Doriftu, Doulos Christos, Drphilharmonic, EhJJ, Eleassar, Eleassar777, Emerson7, Extransit, Favonian, Fconaway, Feezo, Ferengi, Fordgumballs, Friendlyliz, Frietjes, GAThrawn22, Giftlite, Gogo Dodo, Guðsþegn, Hadal, Haham hanuka, Hede2000, Holyman666, I do not exist, ImperatorExercitus, J Milburn, Jahiegel, Japo, Jcesare, Jlick, John254, Jotomicron, Kaboytes, Karpenm, Kf4bdy, Kjaergaard, Klinckc, Lakers, Liftarn, LightBringer, Lightmouse, Lithpiperpilot, Lotje, Low-frequency internal, MER-C, Maden2204, Magnus Manske, Materialscientist, Mattyjenjen, Mbtran, Mike2vil, Mike5598, Modeha, Nakon, Nashini-Kontan, Nid29ron6, No Guru, Nuujinn, Oxymoron83, Patstuart, Paul-L, Pelirojopajaro, Pne, PurfektWepon, Ragesoss, RelentlessRecusant, Rich Farmbrough, Rickyo, Rjwilmsi, Roadnottaken, Saravask, SkyMachine, Smappy, Snapperman2, Snow Blizzard, Snowbringer, Taka, Teles, Teslamike, Therealsarsi, Thiseye, Tristanb, Tsamuels100, Uthbrian, Velella, Vrenator, Webridge, Wikimachine, WriterHound, Xquizit.decorum, Yath, Yerpo, 192 anonymous edits Parietal cell Source: http://en.wikipedia.org/w/index.php?oldid=542980686 Contributors: Aaronbrick, Arcadian, Axl, Bignoter, Bubbachuck, Clicketyclack, Cmcnicoll, DMY, Delta Tango, Deviator13, Edwin, Eleassar, Fastfission, Fireballfx, Franamax, Gastro-en, Gobonobo, GrahamColm, Hoffmeier, Hooperbloob, Hópur 5, Ianvandriel, Jag123, Jfdwolff, Jpogi, Juoj8, Kanesue, Metalhead94, Nlu, Noxidious, Orlandoturner, Pisanidavid, Rb1248, Rhcastilhos, Rhys, Richardslgc, Rsc227, Skittleys, Spirit365, Sverdrup, Tanthalas39, Temporaluser, Tevildo, Ulric1313, Uwe Gille, Vojtech.dostal, Wedge oli, Welsh, WhatamIdoing, Wikisilki, Xquizit.decorum, Xris0, 86 anonymous edits Hydrochloric acid Source: http://en.wikipedia.org/w/index.php?oldid=551628556 Contributors: 1exec1, 2D, 334a, A concerned reader, Aaeamdar, Abcsoccer4me, Abutorsam007, Acroterion, Adashiel, Addaone, Addshore, Ahoerstemeier, Alan Pascoe, Alansohn, Alanyst, Albedo, Alexander.stohr, Alison, Alkivar, Allen3, Alnokta, Alphachimp, Anand Karia, Andres, Andros 1337, Andy Dingley, Angr, AnonGuy, Anskas, Antandrus, Anti-Semitic Stobie, Antonio Lopez, Anypodetos, Arnobarnard, Art LaPella, Arthena, Athf1234, Atif.t2, Atlant, Atooms, Aussie Alchemist, Averyisland, AvicAWB, Avnjay, AxelBoldt, BD2412, Babahu, Bakasuprman, Barhamd, Beao, Beetstra, Ben Webber, Benjah-bmm27, Benjamindees, Berkay0652, Bfesser, Bignoseman, BillFlis, Blandalison, BlazerKnight, BmikeSci, Bobblewik, Bobo192, Bogey97, Bongwarrior, Boonukem, Boothy443, Brian0918, Brianga, BrightStarSky, Brighterorange, Brockert, Brodriguezmueller, Bryan Derksen, Brycemoody, Btsk8rboi, Bubba hotep, Bucketsofg, Cacycle, Cadwaladr, Caltas, Can't sleep, clown will eat me, CanisRufus, CardinalDan, Carlosp123, Carnildo, Casforty, Casliber, Cedrus-Libani, Charon, Chazzy12345, Chem Lady, Chem-awb, ChemNerd, Chris Henniker, ChrisFollower, ChrisO, Christian75, Christy747, Chromega, Cirt, Colo1115, Colonel Warden, Cometstyles, CoolKoon, Crazytales, Creidieki, Curlymeatball38, Cyclonenim, D, DARTH SIDIOUS 2, DVD R W, DVdm, DanMS, Daniel5127, Darth Panda, Dcteas17, Deglr6328, Dendodge, DerHexer, Discospinster, Dispenser, DizzyLAD6197, Dorgan, DrKiernan, Drphilharmonic, Dsmdgold, DutchUncleDeanLancman, Dynamic1, Dystopos, EarthPerson, Edgar181, Edward, Edward321, Eequor, Egil530, Einstien galilei, Eleassar, Eleassar777, Elliott007kf, Ellisgeek, Eloc Jcg, Emerson7, Emurphy42, Enggmayur, EoGuy, Epbr123, Eric Kvaalen, Eridani, Eugene-elgato, Everyking, Evil saltine, Eyesnore, Faradayplank, Finlay McWalter, Fireswordfight, Foxj, Free Bear, Freestyle-69, Funion987, Fuzzzzzzzz, GCarty, Gadfium, Garyzx, Gaurav1146, Gawaxay, Gemini1980, Gene Nygaard, Geoking66, George Burgess, Giant A+circle, Giftlite, Goatmilkfro, Greatpatton, GreenEyez0815, GreenLocust, GregAsche, GregRM, Grenavitar, Grunt, Gscshoyru, Gurch, H Padleckas, HaItsNotOver, Hadal, Hajor, HalfShadow, Happysailor, Harry491, Heightwatcher, Heron, Hhso60, Histrion, Ho949494, HorsePunchKid, Huey45, Hébus, Iantresman, Icseaturtles, Igotnolife, Im not dead xxx, Insanity Incarnate, Invincible Shield, Itub, Izno, J.delanoy, J8079s, JForget, JRM, JYolkowski, JZNIOSH, Jag123, Jagged, Jagged 85, James086, Jerzy, Jeshii, Jfdwolff, Jfreyre, Jidan, Jkl, JoeSmack, John Quincy Adding Machine, JohnM4402, JohnSRoberts99, Jok2000, Jorge Stolfi, Jose77, Jossi, Joyous!, Jpo, Juliancolton, Jumping cheese, Jynto, K1Bond007, Karlhahn, Kashk, Katalaveno, Katherine, Kbh3rd, KeasbeyMornings, Keith Edkins, Kgrad, Khoikhoi, King of Hearts, Kingpin13, Knight1993, Knowledge Seeker, Kozuch, Kpengboy, Kpjas, KrakatoaKatie, Kramden, Krich, Kristof vt, Kukini, Kuyabribri, Kyoko, LOL, La goutte de pluie, Laberkiste, LeaveSleaves, Lightlowemon, Ligulem, Lilandy45, LittleOldMe, Llull, Louisajb, Luk, Luka Krstulović, Lupin, M archer92, M.Komorniczak, Magic.dominic, Magioladitis, Makecat, Malcolm Farmer, ManiF, Mannafredo, Marek69, Marj Tiefert, Markornikov, Materialscientist, Matthewrbowker, Mav, Mavrisa, Maxim, Mayneframe, Maziar fayaz, Mbeychok, McSly, Mdd4696, Meggar, MementoVivere, Mendaliv, Mentifisto, Mercury, Merope, Michael Hardy, Microtony, Mike V, Mike18xx, Milesma, Mindspillage, Minipie8, Mpa, MsDivagin, Msikma, Munford, Nakon, Nao1958, Nathan2345Rawr, Nergaal, Netkinetic, NeuronExMachina, Neutrality, Neverquick, Newone, Niaz, Nichalp, Nicolae Coman, Nilyad, Nsaa, NuclearVacuum, NuclearWarfare, O.Koslowski, Oblivious, OldakQuill, Oleg Alexandrov, Olessi, Onesspite, Originalrawwr, Ortolan88, Ouishoebean, OverlordQ, Ozuma, Paperblossom, Parhat, Paul August, Pavel Vozenilek, Pb30, Penthouse, Pepito123, PerryTachett, Persian Poet Gal, PeteX, Petswodahs, Pgk, Philip Trueman, Phils, Physchim62, Pikiwedia, Pilotguy, Pinethicket, Pit, Plasmic Physics, PoccilScript, Polyamorph, Puckly, Quadell, Queenmomcat, Qxz, RJASE1, Rangek, RatedAAA, Raul654, Razorflame, Rdsmith4, Recognizance, RedRollerskate, Remember me, Renaissance Man, RexNL, Rich Farmbrough, Rifleman 82, Rjwilmsi, Rknasc, Rmhermen, Roastytoast, Robchurch, Roberdin, RobertG, Romanm, Rozevoeten, Rumping, RyanJones, Ryanaxp, Ryulong, SandyGeorgia, Sceptre, Schicagos, Seaphoto, Securiger, Sftpbr, Shanes, Sherool, Shikhars24, Shindo9Hikaru, Shootbamboo, Shovon76, Shultzc, Sietse Snel, Sintaku, Skyezx, Slakr, Sleigh, Smashanator, Smirriw, Smokefoot, Smurfoid, Snowolf, Some jerk on the Internet, Sophus Bie, Spiffy sperry, Srich32977, Sshagunsharma, Starwiz, Steel, Steinsky, Steven J. Anderson, Stone, StoyanWiki, Suicidalhamster, Supernova366, T3h 1337 b0y, TJEY9988, Ta bu shi da yu, TangentCube, Tarquin, Taxman, Tbhotch, Tech00, Ted H Lourent, The chemistds, The tooth, TheAnarcat, TheTrainEnthusiast, Theresa knott, Thomas.Hedden, Thricecube, Tide rolls, Tim Starling, Tlosk, Toon05, Tranletuhan, Trojan traveler, Tsemii, Tutmosis, Ugen64, Unschool, User27091, Velella, Versageek, Versus22, Vrenator, Vslashg, Vsmith, Vuong Ngan Ha, Wachholder0, Walkerma, Wapcaplet, WatermelonPotion, Wayward, Wikibofh, Wikipedia Administration, WikipedianMarlith, Wimt, Wimvandorst, WmRowan, WolfmanSF, Worldtraveller, X201, Xaosflux, Xiner, XofWiki, Yamamoto Ichiro, Yintan, Yk Yk Yk, Youssefsan, Yuber, Yzmo, Zelmerszoetrop, Zfa808, Zoicon5, Zoz, Zsinj, Јованвб, Ὁ οἶστρος, 912 anonymous edits Human gastrointestinal tract Source: http://en.wikipedia.org/w/index.php?oldid=550984165 Contributors: (aeropagitica), 28421u2232nfenfcenc, 2over0, 83d40m, Aadal, Aaron McDaid, Abcgo7, Aboutmovies, Ace of Spades, Adamlankford, Addshore, Aeluwas, Ahoerstemeier, Aitias, Al B G, Alansohn, Alex.muller, Alex.tan, Alias Flood, Allstarecho, Alucard (Dr.), Anbellofe, Angela, Angr, Animeronin, Animum, Aniten21, Annamacd, Anomalocaris, Antandrus, Anthony Appleyard, Arcadian, Aruton, AscendedAnathema, Asikhi, Askarmuk, Astroboy2013, Asymptote, Aua, Auntof6, Aurista25, Avedomni, AxelBoldt, Az29, Backpackadam, Badagnani, Balcer, BananaFiend, Barry the chopper, Bdesham, Be bbes, Beaumont, Beelaj., Beland, Belovedfreak, Ben Ben, Benatkin, Bencherlite, Bendzh, Bigbluefish, Bihco, Bill.martin, BioAegypti, Bkonrad, Blabberfruit, Blueyoshi321, Bobbias, Bobblewik, Bobo192, Bonadea, Bongwarrior, Bonnief, Boonshoft2013, Boston, Boulaur, Brian Crawford, Brighterorange, Brinerustle, Btm67, Bunyonfire, Burntsauce, CJ, Cactus.man, Caltas, Calvero JP, Calvin 1998, Can't sleep, clown will eat me, CapitalR, Captain Weirdo the Great, Carenab, Carlosforonda, CaseyPenk, ChemNerd, Chetvorno, Chill doubt, ChongDae, Chowbok, CiaPan, Cimex, Citicat, Clicketyclack, Cliff smith, Cmungall, Conheery, Coolbob2422, Cosmic Latte, CosmicWaffles, Countincr, Cpl Syx, Cremepuff222, Csörföly D, Cww, Cyberdemon4, D.c.camero, DBigXray, DCEdwards1966, DO11.10, DVD R W, Daffycrooke12, Dainis, Daleang, Daniel Toth, Daniel.Cardenas, Danish Expert, Dar-Ape, Davewild, Dawn Bard, DeadEyeArrow, DeathbyChiasmus, Debnathsandeep, Deeptrivia, Delldot, Deor, Dgw, Diberri, Digitalme, Dinesh smita, Discospinster, Dolphingeek, Dpol, Drgarden, Dudemeister123, Dumrance, Dureo, Dysepsion, EOBeav, EPO, ESkog, Editorofthewiki, Edward, Ekr, Eliz81, Elliot235funny, Emijrp, Enchanter, EnochBethany, Enric Naval, Entropy, Enuja, Eoghanacht, Epbr123, Epgui, Eribro, Erielhonan, EronMain, Eukesh, Evertype, Everyking, Excirial, Faradayplank, Farosdaughter, Fastfission, Ferretremover, Fictitiouskies, Figma, Finlay McWalter, Finn-Zoltan, Frap, Freakofnurture, GTBacchus, Gaff, Gdo01, GetAgrippa, Giftlite,
602
Article Sources and Contributors
Gilgamesh he, Gman124, Goldom, Gracenotes, Grafen, Graham87, Gtearsg, Gurch, Gzli888, HJ Mitchell, HamburgerRadio, Hard Sin, HaroX, Hasanbay, Headbomb, Headsrfun, Heimstern, Heron, Hhofuentes, Hi i like chocolate, Hotdude155, Hu12, Hut 8.5, IAmAMillionContradictions, II MusLiM HyBRiD II, Iain marcuson, Inter16, Iridescent, Isnow, IvanLanin, Iwilcox, Ixfd64, J.delanoy, JFreeman, JLaTondre, JNW, JR98664, Jacklee, Jacobluver13, Jaknouse, JakobSteenberg, Jamib0y, Jauhienij, Jeffrey O. Gustafson, Jeffreyarthur, Jerryseinfeld, JesseAlanGordon, Jevaughngraham, Jfdwolff, Jfurr1981, Jhgipson211, Jimp, JinJian, Jjalexand, Jketola, Jmundo, JoanneB, Joehall45, John, John Vandenberg, John of Reading, JohnnyB256, Jojhutton, Joseph Solis in Australia, Jossi, Jsphkann, Just plain Bill, KGasso, KJS77, KParks7, Kablammo, Kakofonous, Kandar, Kday, Kdon27, Keilana, Keithwhopkins, Kencomer, Kf4bdy, King of Hearts, Kingdomsingapura, Klundarr, Knowledge Seeker, KnowledgeOfSelf, KrakatoaKatie, Krash, Kreperskater, Kubigula, KuduIO, Kukini, Kungfuadam, Kuru, LOL, LadyofHats, Lamro, Laparaparapa, Laura.Connolly123, Leafyplant, LeaveSleaves, LedgendGamer, Leeannedy, Lemonadeyeti, Lenoxus, Lesion, Lew Zealand XV, Lexi Marie, Lexor, Lights, Lilkadil, Limxzero, Logan, Luk, Luka Krstulović, Luna Santin, MER-C, MK8, Mac, Mackeriv, Madhero88, Majorly, Malcolm Farmer, Mammothm1, Mandarax, Mani1, Manuel Trujillo Berges, Maork, Marek69, MarsRover, Martarius, MartinHarper, Mas 18 dl, Mathonius, Mav, Max Naylor, Maxim, Mayooranathan, McSly, Me Black Cullen, Mendors, Metamagician3000, Metju, Metsavend, Michael93555, Mikael Häggström, Mike Rosoft, Min.neel, Miquonranger03, Miranda, Mishuletz, Mj455972007, MnemosynesMusings, Mnyakaba-GMU, Montie5, Moogle10000, Mooie410, Moyogo, MrBlueSky, Msh210, Mstislavl, Munita Prasad, Music&Medicine, Myanw, Naddy, Natural Val, NawlinWiki, Nbauman, Neelix, Nehrams2020, NellieBly, NeoJustin, Neurolysis, NewEnglandYankee, Nick, NickGorton, Nidht, NightFalcon90909, Nlu, Noah Salzman, Noformation, NotWith, Notinasnaid, Nubiatech, Nxl256, Nzmonkey, Ohnoitsjamie, Ombudsman, Omicronpersei8, OnePt618, Onorem, Opabinia regalis, Ouchitburns, OwenX, Oxymoron83, PFHLai, Paddy Jow, Paiev, Part Deux, Patrick, Patstuart, Paul August, Pax:Vobiscum, Peruvianllama, Peter M Dodge, Phantomsteve, Phasechange, Philip Trueman, Piano non troppo, Pichpich, Pilotguy, Pjvpjv, Plasticup, PoccilScript, Poopoomaniac103, Porterjoh, Prankster nikki, Prashanthns, PrestonH, Quirk, R'n'B, RHB, RJHall, Ragib, Ranveig, Rcsprinter123, Rdsess, Refsworldlee, RenOfHeavens, Rettetast, RexNL, Riana, Rich Farmbrough, Richard New Forest, Riotrocket8676, Robertaedwards, Romanm, Ronz, Rsabbatini, SJP, Sam Korn, Samej71, Sango123, Sasata, Savidan, SchuminWeb, Scientizzle, Scorpionman, Seaphoto, ShajiA, Shanes, Shirulashem, Sirmelle, Sirprojects, Skalskal, Skittleys, Smartdogz123456, Smjg, Sneakerkid1, Snowolf, Snoyes, Some jerk on the Internet, Someone else, Spellcast, Splat, Stardust8212, SteinbDJ, StephenBuxton, Stereotek, Steven Zhang, Stickee, Strafpeloton2, Styrofoam1994, Supermagle, Sylvienguyen, Tarquin, Taylor drake01, Taylortime17, Tdxiang, Tellyaddict, Template namespace initialisation script, Tero, The All-Traq, The Anome, The Rhymesmith, The Thing That Should Not Be, The Utahraptor, The undertow, The unknownEX, TheProject, Thegreencoat, Thehelpfulone, Thehumorous, ThermoNuclearWar, ThreeDee912, Tide rolls, TimVickers, Timir2, Todowd, Tony K10, Toothfish, Travelbird, Trixt, Trusilver, Ubiq, Ukexpat, Ulflarsen, Uncle Dick, Urgos, Vagary, Vary, Vdegroot, Vinceouca, Viriditas, Viskonsas, Vojtech.dostal, Vrenator, Vriullop, Vrymor, WLU, WadeSimMiser, Wakto, Welsh, Wenli, Werdan7, Westendgirl, Wiki alf, WikipedianMarlith, Wikipedsuks, Williamma323, Willotter, Wimt, Wknight94, WojPob, Wolfch, WriterHound, Wtmitchell, Xeno, Xxstertoka99, Yamamoto Ichiro, Yeng-Wang-Yeh, Yidisheryid, Ylem, Youssefsan, Ysheng99, Yuckfoo, Zachary Gibbons, Zimmermanstein, Zinjboss, Zzuuzz, 1190 , יוסיanonymous edits Goblet cell Source: http://en.wikipedia.org/w/index.php?oldid=544935416 Contributors: AK456, Ameliorate!, AndreNatas, Arcadian, Barticus88, Beeswaxcandle, Caerwine, Citizen Premier, Cmcnicoll, Cometstyles, ConCompS, Copysan, Dietzel65, Dkettle, Dramalpaul, Drphilharmonic, Eleassar, Evermorepy, Favonian, Foobar, Franamax, Gobonobo, Halo32007, Hitokirishinji, Hovea, Iameukarya, InvictaHOG, JForget, Jarich, Jeangabin, Jfdwolff, John of Reading, Jonathan.s.kt, Kesal, Kingpin13, La Pianista, Lenrodman, Luna Santin, MPerel, MarkSutton, Mmxx, Monty845, Nephron, Nhandler, Nishio, Nlu, Oxymoron83, Rumpenisse, SABenyunes, Salvadorjo, Serephine, Sses401, TEB728, TheJJJunk, Tide rolls, WikHead, Wikipelli, William Avery, WingateChristopher, 102 anonymous edits Respiratory tract Source: http://en.wikipedia.org/w/index.php?oldid=536084791 Contributors: Alex.tan, Anmats, Barticus88, Bibi Saint-Pol, Bryan Derksen, Cooladoola, CyclePat, DRTllbrg, Danish Expert, Hyarmendacil, J.delanoy, LadyofHats, LiDaobing, Monkeymox, Mseliw, Nlu, Nono64, Olivier, Once111, Petersam, PhatRita, Phil Lu, Rhcastilhos, Robodoc.at, Ryulong, Skittleys, The Thing That Should Not Be, Thegoodguy49, Tristanb, Unara, Xic667, 29 anonymous edits Mucus Source: http://en.wikipedia.org/w/index.php?oldid=551203269 Contributors: (jarbarf), 065211105iscool, 1966batfan, Abce2, Abd, Academic Challenger, Acather96, Actrlvr94Str365, Adashiel, Addict 2006, Addshore, AdjustShift, Adriaan, Adys, Agathoclea, Ahoerstemeier, Ainslieg, Aitias, Aleenf1, Alexandria, Alksentrs, Altenmann, Alterego, Andres, Andrew c, Angela, Anna Frodesiak, Anon969, Anonymous2121kittykittylicklick, Apenrules, Aqwis, Art LaPella, Arwel Parry, Asleep at the Wheel, Avenged Eightfold, Avnjay, Axl, Bakabaka, Bananas Reunited, Basawala, Batchelor, Bejnar, Betterusername, Bharath94, Bibliomaniac15, BigNate37, Blakegripling ph, Bluerasberry, Bobo192, Boing! said Zebedee, Bonadea, Bongwarrior, Boobinhower90, Bree's Block, Btom1993, Bungle, BurritoBazooka, Buster7, CWenger, Cactus.man, CambridgeBayWeather, Canthusus, Capricorn42, Car salesman, Carlthecactus, Catgut, Changer1000, Chester Markel, Chikanamakalaka, Choochootrain2.0, Chovain, Closedmouth, Coffee and TV, Correogsk, Cremepuff222, Crockspot, Cwgh, D. Recorder, DAJF, DJsunkid, Dan D. Ric, Dar-Ape, Darkxpunkygirl, Darth Panda, Dave56789, Deadlightbulb1234, Deli nk, DerBorg, DerHexer, Dgw, Diablorex, Digitalme, Dirac1933, Disciple freak, Discospinster, Djm1279, DlronW, Dnvrfantj, Doctor Procto, Doosky, Download, Dr. Doof, Drphilharmonic, Dweller, Dysepsion, ESkog, Ean5533, EddEdmondson, Edgar181, EditorBobobo, Ekm02001, EmmetCaulfield, Engelmann15, Enigmaman, Epbr123, Eras-mus, Erielhonan, Everyone Dies In the End, Ewlyahoocom, Excirial, Exert, Ezhiki, Falcon8765, Faradayplank, Fcee80, Fiveop, Flewis, Foregone conclusion, Forgetster, Fraggle81, Fremsley, FreplySpang, Froth, Frumbleabumb, Fubar Obfusco, G4rfunkel, Gadfium, Galactor213, Galaxiaad, Galo1969X, Gerrish, Gilgamesh he, Gilliam, GillianHunt, Gimboid13, Glenn, Gluonman, Grunkhead, Gscshoyru, Gurch, Hackerb9, Halo3 homeboy, Hammersoft, Hengsheng120, Henry W. Schmitt, Herbee, Hetar, Holizz, HolyT, Hooperbloob, Huadpe, Hyacinth, Hyperspite, ICAPTCHA, Iiii2333, Inox-art, Insanity Incarnate, InsufficientData, Introductory adverb clause, Invertzoo, Iridescent, IronGargoyle, Ixfd64, J.delanoy, J04n, JaGa, Jacoblawrence32, JamesDumont, Janus Shadowsong, Javsav, Jbamb, Jcwf, Jehan60188, Jfdwolff, Jim1138, Jj is adam, Jj137, Jkoates, Jncraton, Joe5555, JoergenB, John, John Reaves, JohnOw, Jonathan.s.kt, Jooler, Josh murray, Jossi, Junglecat, Kafziel, Kam voo, Karaiyn7157, Katalaveno, Kathryn NicDhàna, KenSharp, Kickus, Kintetsubuffalo, Kku, Kochipoik, Kumioko, Kupojsin, Kurt Shaped Box, Kwertii, Kyorosuke, LAX, LLDMart, LSX, Lacrimosus, Lajohnst, Langhorn, Leibniz, Liaocyed, Lisatwo, LittleT889, LongBay, Lowellian, Luis Felipe Schenone, Luna Santin, M1xmast3r, Magnus Manske, Maharetm, Makurayami, Marklar2007, Materialscientist, Matt Gies, Meaningless, Meelar, Metrowestjp, Mgrollman, Michael Anon, Mike Rosoft, Minimac's Clone, Miniyazz, Minna Sora no Shita, MisfitToys, Mlouns, Moeron, Monty845, Mr Whiteside, Mr. Billion, MrSomeone, Mukadderat, Mystery4you, Nachelavery, Naddy, Nakon, Neil916, Neilbeach, Netsnipe, Neurolysis, Nicci bethel, Nicholan18, NigelR, Ninjatacoshell, Nintendo5000, Nlu, Nn123645, NoMecy071311, Noctibus, Nsteinberg, Nuttycoconut, Nässprejen, Obli, OlEnglish, Onceler, Oren0, Ottawa4ever, Otto2294, Oxymoron83, Pacaro, PaladinWhite, Pandalover1, Paul Barlow, Pepperroni57, Pepperronii57, Perry04061994, Perryperry, Peter Karlsen, Pgk, Philip Trueman, Pinethicket, Pip2andahalf, Plasticup, Poeloq, Polluks, Ppk3000, PrestonH, Professor Fiendish, Prolog, Pstaveley, Puchiko, Purplebigcats, Pyrofork, Pyrospirit, QueenAshley, R, RJFJR, Radon210, Raymondwinn, Recnilgiarc, Redrobin5, Redvers, Reedy, Regulov, Richard001, Rickterp, Rm1271, Rmosler2100, Rodsan18, Rubylover234, RyanCross, Ryoji.kun, S.dedalus, Salvadorjo, Samtheboy, Samwaltz, Sannse, Saraandjenna, Saros136, Sasha Callahan, Scapler, Scetoaux, SchmuckyTheCat, SchuminWeb, ScienceGolfFanatic, Scott S, Scott14, Screwtop, SeekingOne, Seethaki, Shirulashem, Shrieker2k, Sjschen, SkerHawx, Smalljim, Snowyiet, Some jerk on the Internet, Spartan-James, Spcoolbomb, Spike spikeson, SpikeToronto, Spiros01, Spitfire19, Splash, SpuriousQ, Stuffhangin, Super edd, SvartMan, Sven Klemm, Svick, Szczawik, Tanthalas39, Tarret, Tartan, Tbhotch, Tdw, Terik brunson, That can't be right?, The Anome, The Thing That Should Not Be, TheChrisF, TheMightyOrb, ThePenguinStrangler, Thehelpfulone, Thejuanchonater, Thesis4Eva, Thingg, Thomascrapper, Tiddly Tom, Tide rolls, TomGibb, Twinsluv4eva, UglyShirts, Umofomia, Undead warrior, Useight, Utcursch, Vesta, Vsmith, WLU, WadeSimMiser, Waggers, Warcraftfan111, Wavelength, WeniWidiWiki, WesBrandt, Wetman, Why Not A Duck, Willking1979, Wknight94, Wolfdog, Wolfman92, Woohookitty, WormRunner, Wtmitchell, Wyss, X1987x, Xezbeth, Ycyryryry, Ylem, Yoshi032192, Yudiweb, Zachbe, Zack5210, Zapvet, Zargulon, Zoogoo, 805 anonymous edits Enzyme Source: http://en.wikipedia.org/w/index.php?oldid=550081455 Contributors: (3ucky(3all, 01roshay, 10014derek, 10buttz, 13shepht, 168..., 171.65.26.xxx, 1exec1, 209.234.79.xxx, 5ko, 6AND5, 84user, A2-25, A8UDI, AXRL, Aaron Brenneman, Academic Challenger, AdjustShift, Adrian 1001, Aerographer1981, Ahoerstemeier, Aitias, Ajpratt56, Aksi great, Alansohn, Albert109, Alfie66, AlimanRuna, Aljasm, Alsandro, Altermike, AmH2, AmiDaniel, Amren, Anaxial, Anclation, Andre Engels, Androstachys, Anthony Appleyard, Apdang, Apothecia, Arakin, Arbor to SJ, Arcadian, Arjun01, ArmadilloFromHell, Arthena, Articles for analfuckbaggage-!, Artman40, Atif.t2, Atlant, Attilios, Awg usc, AxelBoldt, Ballboy070707, Baoilleach, Barliman Butterbur, Barneycleo, Bassbonerocks, Bcebul, Beastinbman, Beeswaxcandle, Beetstra, Beki Hellens, Bender235, Bensaccount, Benwd, Beta cafe, Bhadani, Bill52270, Bjhiggins, Blabberfruit, Blackprince, Blanchardb, Blehfu, Blue520, Bluerasberry, Bob888, Bobadillo, Bobo192, Bongwarrior, Bookofjude, BorgQueen, BradBeattie, Bradley1545, Brighterorange, Brisvegas, Bryan Derksen, Buzybeez, CBSB, CDN99, Cacycle, Calmer Waters, CalumH93, Can't sleep, clown will eat me, CanisRufus, Canuckian89, Capecodeph, CapitalR, Captain-n00dle, Captaindan, CardinalDan, Carstensen, Casper2k3, Catherine-maguire, Causa sui, CephasE, CharlotteWebb, Chazz88, ChemGardener, ChemNerd, ChicXulub, Chihowa, Chios1127, Chris 73, Chris CII, Chrislk02, Christopher Parham, Chun-hian, Clemwang, Clicketyclack, Clone1, Closedmouth, Cmichael, CommonsDelinker, Conscious, Conversion script, Correctist, Cpeditorial, Cppgx, Crazycomputers, Cst17, Curiousgeorgie, Cwhitt817, Cwkmail, Cybercyclone3993, D, DARTH SIDIOUS 2, DIG, DMacks, DVD R W, Dakarai99, Dalmoz, Dalstadt, Damonchicken, DanMS, Daniel5127, Danny, Danny B-), Dannyboy600, Darth Panda, David D., David Shear, DavidRader, Daycd, Dcflyer, DeadEyeArrow, Debresser, Decltype, Deflective, Delldot, Delta G, Den fjättrade ankan, Denisarona, DennyColt, DerHexer, Derek Ross, Dfrg.msc, Dheenkumar, Dhruvrajgohil, Diberri, Dirac1933, Dirac66, DirkvdM, Dlamming, Dlohcierekim, DocteurCosmos, Doctorcherokee, Donbert, Doniago, Dono, Dpark, Dr. Krishna Prasad Nooralabettu, Dr. St-Amant, DrKiernan, DrNixon, Dreamm, Drphilharmonic, Drummstikk, Dspoel, Duncharris, Dwmyers, EMacG, ESkog, EWikist, Ebuxbaum, EconoPhysicist, Economo, Ed g2s, Edderso, Edgar181, Eequor, Elano, Elassint, Elem3nt, Eleuther, Eltronio, Emhale, Emw, EncycloPetey, Epbr123, Evan57, EvelinaB, Everyking, Evil Monkey, Ewen, Exaton, F. Cosoleto, FF2010, Fabrício Kury, FaerieInGrey, Falcon8765, Fallschirmjäger, FastLizard4, Fedir, Felyza, Fennec, Fieldday-sunday, Fishyfishy, Flannelgraf, Flomenbom, Flugs, Fondls, Forluvoft, Frankenpuppy, FrozenMan, Frymaster, Fuzzform, Fvasconcellos, Fvw, G3pro, GABaker, Gaff, GainLine, Gaius Cornelius, Gdo01, GeneMosher, Geneb1955, Gentgeen, Gfoley4, Ghjfdhgdju, Gianfranco, Giftlite, Gilderien, Gilliam, Gimmetrow, Gingekerr, Giraffedata, GiveItSomeThought, Glen, Glenn, Gn96, Gogo Dodo, Gourgeousladyy, GraemeL, Grafen, Graham, GreatWhiteNortherner, Gregogil, Guiltyspark, Gwernol, Gzuckier, HJ Mitchell, Hadal, Haetmachine, Haham hanuka, Hammer1980, Hans Dunkelberg, HappyCamper, Happylama101, Harlequin2134, Harry491, Harryboyles, Hashar, Hazel77, Hector kevin, Hellfire68, Hello32020, HexaChord, Hezzy140, Hichris, HistoricPandaBear, Hmains, Hobartimus, Holeung, Hu, Huntthetroll, Hut 8.5, Hv, I dream of horses, II MusLiM HyBRiD II, Iamstaurtmayle, Ian Pitchford, Ianblair23, Icelight, Ichbintux, Idontknowmyname, Ike9898, Indy 900, Instantnood, Intelati, Intelligentsium, Intgr, Ioannes Pragensis, Iridescence, Iridescent, IronGargoyle, Ixfd64, J. Finkelstein, J.delanoy, J04n, JForget, JWSchmidt, JaGa, Jab843, Jackol, JacobTrue, Jak123, James086, JamesBWatson, Jamesscottbrown, Jamesters, Jaraalbe, Jauerback, Jauhienij, Jdhowens90, Jebus989, Jedonnelley, Jeff G., Jengod, Jeremyb650, JesseW, Jiddisch, Jitu jain, Jj137, JoanneB, Jobe6, Johan Elisson, John Mackenzie Burke, John NRW, John Quincy Adding Machine, John Riemann Soong, JohnJohn, JohnOwens, JohnnyRush10, Jojhutton, JonHarder, Jonnylyman, Jorwisgar, Jose77, Josh Parris, Jovianeye, Joyous!, Jpbrenna, Jrc2005, Jroenick2797, Jstew87, Jusdafax, Jusjih, Justine Hill, Jwanderson, Jynto, Jyril, K.C. Tang, K1lla abbas, KES47, KGasso, Kasper90, Katalaveno, Katimawan2005, Kbh3rd, Kerivoula, Kheiron, KhoousesWiki, Khukri, Killacoll123, Kingpin13, Kipala, Kjoonlee, Kmdouglass, Knights who say ni, Knowledge Seeker, KnowledgeOfSelf, Kochipoik, Kosigrim, Kozuch, KrakatoaKatie, Krellis, Kukini, Kuru, L Kensington, Lalo1121, Langbein Rise, Lascorz, Lelkesa, Lenticel, Leptictidium, Lexor, Liempt, Lightmouse, Lir, Little Mountain 5, LittleHow, LizardJr8, Loganloganlogand, Low-frequency internal, LtPowers,
603
Article Sources and Contributors
Lugnuts, Luigifan, Lumos3, Luna Santin, Lupo, M412k, MER-C, Maaayowa, MacGyverMagic, Magister Mathematicae, Magnus Manske, Malcolm Farmer, Mani1, Maphyche, MarcoTolo, Marek69, Marj Tiefert, Marxspiro, Materialscientist, Mathel, Mato, Matthew Yeager, Matthiascarrigan, Matty616, Maver1ck, Maxwell754, Mbols, Mboverload, Mcrkramer, Mcy jerry, Mdemian, Mejor Los Indios, Mendaliv, Mets501, Mewilliams95, MiShogun, Michael Devore, Michael Hardy, Michael%Sappir, Michaelas10, Michaeljwilson, Michał Sobkowski, Mikhail Garouznov, Mild Bill Hiccup, MilkMiruku, Miller17CU94, Minna Sora no Shita, Mion, MisfitToys, Mister Matt, Mj455972007, Mmxx, Modulus86, Moguls, Monkeymox, Moshe Constantine Hassan Al-Silverburg, Mouse Nightshirt, Mperkins, MrDrBob, MrOllie, Mrspkapila, Mrt3366, Msikma, Myplace345, N5iln, NCurse, NEUROtiker, Naipicnirp, Nakon, Narsil, NawlinWiki, NellieBly, Neptune5000, Netesq, Neutrality, NewEnglandYankee, Nhandler, Nick123, Nige111, Nihiltres, Nivix, Nk, Nlu, NoahElhardt, Northumbrian, Nunh-huh, Nutiketaiel, Oatmeal batman, OccamzRazor, Olivier, Omicronpersei8, Omnipedian, Onco p53, Opabinia regalis, OverlordQ, Oxymoron83, PDH, PFHLai, PaePae, PandaRepublican, Papapu, Patstuart, Paul venter, Pax deorum, Pdcook, PeaceNT, Petergans, Phantomsteve, Pharaoh of the Wizards, Philip Trueman, Phpham31, Physis, Pietrosperoni, Pilotguy, Pinethicket, Pinkadelica, Pjvpjv, Pkarp11, Plasticup, Pmm530, Pne, Poindexter Propellerhead, PopUpPirate, Popnose, Prolog, Psyche825, Pt, Q3w3e3, Qaz, Quale, Qwfp, Qxz, RB972, RDBrown, Rcjohns1, Reach Out to the Truth, Recurring dreams, Redeemer079, Redvers, Regibox, Rettetast, RexNL, Riana, Rich Farmbrough, Richard001, Rjwilmsi, Rlevse, Rlmrace, Rob Hooft, RobertG, Robertohaas, Rocket71048576, Romanm, Ronhjones, Ronz, Rose090, RoyArnon, Rror, Ruhrfisch, RyanGerbil10, SCEhardt, Saebjorn, Samulili, SandyGeorgia, Sango123, Saravask, Sardanaphalus, Savidan, SchuminWeb, Scimitar, Scottiedog15, Scuzzer, Sean Whitton, Seans Potato Business, Secretlondon, Sefog, Serephine, SergeantBolt, Sfmammamia, Shadowjams, Shane wallmann, ShelfSkewed, Shirik, Shizhao, Shoeofdeath, Shosh3333, Shultzc, Siim, SilkTork, SimBioUSA, Simpler12, Sinharaja2002, Sk741, Skarebo, Skunkboy74, Sky380, Smalljim, Smartsmith, Smellysam524, Snigbrook, Snow storm in Eastern Asia, Some standardized rigour, Sonicology, Sopranosmob781, Squidonius, StaticGull, Steel, Stefano Garibaldi, Stephenb, Stevenfruitsmaak, Stillnotelf, Stone, Stuartmayle, Stuckonempty, Sturm br, Suffusion of Yellow, Suhail174, SupaStarGirl, Superiority, Swpb, Syd Midnight, TAKEN00, THF, TJClark, TKD, TWUChemLS, Tabletop, Takometer, Talktomarie1, Tantal-ja, Taw, Taxman, Tbhotch, Tekks, Tempel, Texasrocks, The Banner Turbo, The Rambling Man, The Thing That Should Not Be, The Wiki ghost, The wub, Theyeti, Think outside the box, Tide rolls, TigerShark, TimBarrel, TimVickers, Timberman, Timflutre, Timhewitt101, Timir2, Tizio, Tkenna, Tlesher, Tomharris, Tommy2010, Tomos ANTIGUA Tomos, TonyClarke, Trevor MacInnis, Tristanb, Trusilver, Ttony21, Tunheim, Turnstep, Tvd12110, Twisted86, Tyler, Typer 525, U+003F, Unyoyega, Useight, User A1, Van helsing, Vanished User 0001, Vanisheduser12345, Vary, Veesicle, Victuallers, Videot43, Vina, Viskonsas, Vojtech.dostal, Vrenator, WDavis1911, Wavelength, Wayne Slam, Wayward, Wdflake, Webridge, Weregerbil, West Brom 4ever, WhatamIdoing, Widr, Wiki alf, WikiDao, Wikiborg, Wikidenizen, Wikidudeman, Wikieditor06, Wikipelli, WillowW, Wknight94, Wmahan, Wmpearl, Wolfgang Kufner, Woohookitty, WookieInHeat, Xdenizen, Xevious, Xxpsycho37xx, Yaksha, Yaser al-Nabriss, Yasitha2, Yelyos, Yikrazuul, Ynhockey, Yoilish, Yorubaspartan, Young Pioneer, Zaijaj, Zephyris, Zero1328, Zidonuke, Zoe, Zondor, ZooFari, Zzuuzz, Ævar Arnfjörð Bjarmason, Саша Стефановић, Սահակ, ﮐﺎﺷﻒ ﻋﻘﯿﻞ, 1995 anonymous edits Paneth cell Source: http://en.wikipedia.org/w/index.php?oldid=550526898 Contributors: Arcadian, Bliyanto, Boonshofter, Bosfeld, C.Carlsbad, Capricorn42, DMG413, Dan Gluck, Darkchun, Deviator13, Diberri, Draeco, Eivind F Øyangen, Eleassar, Finlay McWalter, Fongfongchu, Franamax, Gumruch, Joelpi, JohnCD, Jpogi, Leeearnest, LouisAlain, M dorothy, Mccready, Mcstrother, Mediran, MichaK, Mifam, Mikael Häggström, Paralucent, Pechanga, Pekaje, Quadell, Radzimowski, Robodoc.at, Samir, Serephine, Sun Creator, Tavilis, 24 anonymous edits Intestine Source: http://en.wikipedia.org/w/index.php?oldid=550938207 Contributors: 1ForTheMoney, A. B., Abceasyas, Adashiel, Ageekgal, AkiAkira, Alansohn, Alex.tan, Alexwagner, Alpha Male in the Sunset, Alucard (Dr.), Anakin101, Andy M. Wang, Animum, Anoko moonlight, Apokryltaros, Appleton1324, Aranel, Arcadian, Auxiliary Watchlist, Avoided, B4r4n5k1, BD2412, BWDuncan, Basharh, Bensaccount, Beyond silence, BillyW 1, Blu Aardvark, Blubba112, Boing! said Zebedee, Bongwarrior, Bubba hotep, C6541, CIreland, CaseyPenk, Ceyockey, Chochopk, Chrisjj, Cmh, Crabulon, Craterib, Crithit5000, Crohnie, Csylcox, Ctcl123, CubBC, Cwaug52, D898, DF5GO, DO'Neil, Dammloo, Dan D. Ric, Danjel, Danny, DerHexer, Dffgd, Diberri, Djihinne1, Dominiktesla, Dominus, Draeco, Dumrance, EarthPerson, El estremeñu, Esrob, Fabioli2010, Fieldday-sunday, Flywhc, Fraea, Gadfium, Gahaba, Gail, Gaius Cornelius, Gilliam, Graham87, Grendelkhan, Guyd, Halfalah, Huon, Hvan, Ian Page, Igoldste, Ixfd64, J.delanoy, JForget, JFreeman, JHunterJ, JR98664, JTN, JackPetersen, Jackfork, JakobSteenberg, James086, Japanese Searobin, Jay Litman, Jclemens, Jfdwolff, Jj137, Joele Gilbert, Johntobz, Julian.walters, Jwissick, Kandar, Kappa, Karebear2884, Karen Johnson, Kbbbb, Kehkuansun, Kelly Katula, Knishfaces, Kostisl, Kozuch, LETSskankTHEnightAWAY, Lathyrus100, Laundry, Leslie Mateus, Liamdaly620, Linuxlad, LionMans Account, LjL, Longhair, Lord Pistachio, M dorothy, MBisanz, MC10, MER-C, MadridTeacher, Maralia, Marek69, Master Jay, Maxis ftw, Metagraph, Mikael Häggström, Mineshabadyal, Misza13, Moralis, Morken, Mrhelloilike, Mrs.smithakacheese, Myskills, Nakon, Nihiltres, Nivix, Nthep, Nv8200p, OsamaK, Paxse, PeaceNT, Pearle, Philip Cross, Pinethicket, PoccilScript, Pocketfox, PubliusFL, Pythian Habenero, Qwfp, Radishes, Radonir, Rainbowlori, Rajkiandris, Renaissancee, Rich Farmbrough, Robwingfield, RodC, Rodsan18, Rojomoke, Rrrmmmbbb, Rsabbatini, Sae1962, Salvio giuliano, Sam Korn, ScriptHoward, Sctrojans1112, Shniken, Shoshonna, Smalltalkman, Snowolf, Spaceboss, Srini81, StuHarris, Sun Creator, Surfeited, TedE, Template namespace initialisation script, The Anome, TheAMmollusc, TheJC, Thesnuffla, Tiddly Tom, Tide rolls, Timir2, Tizio, Tocant, Tohd8BohaithuGh1, Tombomp, TommyBoy, Treisijs, Tryptofish, Tvinh, Ukexpat, Una Smith, Useight, Vcohen, Vicki Rosenzweig, Vuo, WAvegetarian, Waggers, WhatamIdoing, WikHead, WikipedianMarlith, Willbyr, Wimt, X201, Xiahou, Yed79, Yidisheryid, Ykvach, आशीष भटनागर, 437 anonymous edits Bicarbonate Source: http://en.wikipedia.org/w/index.php?oldid=539226249 Contributors: 16@r, 17Drew, Adastra1960, Akane700, Albedo, Amirreza, Anlace, Anwar saadat, Arcadian, AstroHurricane001, AxelBoldt, Bart133, Beetstra, Benjah-bmm27, Bennybp, Bensaccount, Buggia, Cajolingwilhelm, Calvin08, Chemicalinterest, Chrislk02, Chrumps, CommonsDelinker, Conversion script, CoyneT, Davemcarlson, DeadEyeArrow, Deli nk, Double sharp, Drnoitall.hello, Drphilharmonic, Dwmyers, Ed g2s, Eug, Faradayplank, GeeJo, Gene Nygaard, Gentgeen, Giftlite, Gilliam, GregorB, Hansonslee, Hellbus, Hugo-cs, Incnis Mrsi, Inkling, J-Kama-Ka-C, JeremyA, Jfdwolff, JimR, Jynto, Kakofonous, Kevin512, KhryssoHeart, Krylonblue83, Ktsquare, Lavateraguy, Linus M., LoyalSoldier, LuigiManiac, Luna Santin, Madgenberyl, Merovingian, Mikael Häggström, Mild Bill Hiccup, Miroku Sanna, Mni9791, N2e, Nergaal, Nurg, P76837, Paul P, Pedrocelli, PenguiN42, Petergans, PioveNevica, Plasmic Physics, Plumbago, Puppy8800, Rcej, Rettetast, Rror, Ryancormack, Salt Yeung, Schizmatic, Shuttlecockfc, Snowmanradio, Stasas, Stepa, Superjoel, The MoUsY spell-checker, The myoclonic jerk, Thricecube, Tikai, Tomgally, Velella, Versus22, WikHead, 132 anonymous edits Lysozyme Source: http://en.wikipedia.org/w/index.php?oldid=547519468 Contributors: A Softer Answer, Agentilini, Alias Flood, AlphaEta, AndiK, Arc de Ciel, Arcadian, Arjayay, Banus, Beemee, Bjsobelmd, Boghog, Brianhe, BurnellShively, CTF83!, Carstensen, Cpelkas, Dejvid, Doctor Procto, Drphilharmonic, Engelenco, Eyal Bairey, Eyu100, Frietjes, Fvasconcellos, Gene Nygaard, Gigemag76, Glida1, Golwengaud, GraemeL, Hadal, Heathmoor, Holeung, IMGrant, Iantresman, Ike9898, J.delanoy, Jag123, Jeppelbaum, Jfdwolff, Jjalexand, K10wnsta, Katharineamy, Kinglz, Kinkreet, Lode (Germany), Logan, LostLucidity, Low-frequency internal, Magioladitis, Magnus Manske, MarcoTolo, Matijap, Maxim Razin, MiPe, MicroBio Hawk, Miniyazz, Mthsmith, Niels Olson, Nneonneo, Nnh, PM Poon, Pierreb24, Precious Roy, Reaper Eternal, Rich Farmbrough, Rjwilmsi, Shaddack, Silasmellor, Spencerw, Squidonius, Squigish, Steveh2000, Strater, Suffusion of Yellow, Teuteul, That Guy, From That Show!, Theresa knott, Traveseru, Vedran12, Webridge, WolfmanSF, Ziphon, 129 anonymous edits Surfactant Source: http://en.wikipedia.org/w/index.php?oldid=551920387 Contributors: 149AFK, 2BeOrNot, AKlilbit, Abdull, Aboalbiss, Adrian J. Hunter, Ahoerstemeier, Alan Liefting, ArnaudContet, Arthena, Ashtonltp, Auntof6, BartlettInteractive, Beetstra, Beland, Bensaccount, Bo Basil, Bssquirrel, Cacycle, Captain-n00dle, Cecile751, Cgsenette, ChemGardener, Chmee2, Choij, Chris Capoccia, Christian75, Church of emacs, Copeland.James.H, Cwage, Cyferz, Cygay, CyrilThePig4, DON 08, Daniele Pugliesi, Darkfred, Deathbypapercutz, Deli nk, Diberri, Discospinster, DocWatson42, DoktorDec, Drat, Drphilharmonic, Dyanega, Eboireau, Edgar181, Efe, Egredior, Elkman, Enviroboy, Evil Monkey, Excirial, Futhark, Fuxx, Glacialfox, Glane23, Golftapsa, Graham87, Ground Zero, Hadal, Haianqutang, Hgrosser, Huhtala, Hulburkj, Ipatrol, Iridescent, Isidore, J.delanoy, JForget, Jaipuria, Jak123, JamesBWatson, Jaubouin, Jcw69, Jeffq, Jeremyb650, Jerome Charles Potts, Jetcrew66, Jhawkinson, Johner, JonRichfield, Joonkimphd, Jstupple7, JustAGal, Jvcarpen, Kevink707, Khaled7stars, Kkmurray, Kpjas, Kupirijo, Kuru, Kwizy, Kymacpherson, Langbein Rise, Latka, Lbeaumont, LedgendGamer, Leuko, Light current, Little hickey, LittleOldMe old, Maderibeyza, Manticore, Mark Arsten, Materialscientist, Maximus Rex, Mcannella, Meister23, Michel Awkal, Mike2vil, Moocha, MrBell, Mxn, NawlinWiki, Ndenison, Newone, Nick Number, Nikevich, Nneonneo, NordicFire, Ojigiri, Oldlaptop321, OllieFury, Orn-luco, Pbsouthwood, Pedrodeigo3, Peterlewis, Pinethicket, PolymerTim, Pumuckl76, Quickone, Quintote, Raucanum, Raymondwinn, Resolute, Rifleman 82, Ringbang, Robert zab, Ryulong, Sandyqun, Scientific29, SebastianHelm, Shaddack, Shmetzler, Shootbamboo, Shrigley, Siawase, Silverchemist, Sjschen, Skittleys, Sloth monkey, Smitz, Smokefoot, Solidpeg, Spectrun, Spiperon, Spiritia, Stacydreis, Struway, Swales, Swyilk, TachikomaAI, Tardigrada2008, The Epopt, Timdew, Tslocum, Tvasailor, Ulflund, Vanished User 1004, Wavelength, Welsh, Xellos, Xris0, YUL89YYZ, Youngbohemian, Zebruh, มือใหม่, 272 anonymous edits Clara cell Source: http://en.wikipedia.org/w/index.php?oldid=540535891 Contributors: 5 albert square, Alex.tan, Animeronin, Arcadian, Axeman89, Axl, Cd830, Ceyockey, DarkArcher25, Daveeroy, Deviator13, Filip em, Franamax, Gaius Cornelius, Gracenotes, Gumruch, J.delanoy, Jclemens, Jesse057, Jfurr1981, Jonathan Drain, Jxs338, Kmg90, Letdemsay, Luke poa, Maristoddard, Mattbartek, MaxEnt, Mcstrother, Mrpark01, Rjwilmsi, Schnurrbart, Scottywong, SharkinthePool, Tagallyat, Thunderboltz, TyA, 32 anonymous edits Somatotropic cell Source: http://en.wikipedia.org/w/index.php?oldid=541164180 Contributors: Alice Mudgarden, Arcadian, ChrisGualtieri, Edward, Ellis2ca, Emeraude, Excentrifuge, Franamax, Fruit.bmp, JonHarder, Jytdog, Mindmatrix, PhiJ, RJFJR, Rich Farmbrough, Template namespace initialisation script, TheParanoidOne, Trevor MacInnis, WikHead, 28 anonymous edits Prolactin cell Source: http://en.wikipedia.org/w/index.php?oldid=547346739 Contributors: Addicted04, Arcadian, Casalinga, Chikiss, Delldot, Feral mage, Franamax, InvictaHOG, Ruutiainen, Steinsky, Template namespace initialisation script, TheParanoidOne, 6 anonymous edits Thyrotropic cell Source: http://en.wikipedia.org/w/index.php?oldid=543564690 Contributors: Arcadian, Franamax, Icairns, Jfdwolff, Template namespace initialisation script, 3 anonymous edits Gonadotropic cell Source: http://en.wikipedia.org/w/index.php?oldid=541162305 Contributors: Arcadian, Drphilharmonic, Druep, Franamax, InvictaHOG, Jarivasell, Mhollida, Template namespace initialisation script, TheParanoidOne, Thecheesykid, 7 anonymous edits Corticotropic cell Source: http://en.wikipedia.org/w/index.php?oldid=543781170 Contributors: Acgator09, Arcadian, Drphilharmonic, Franamax, InvictaHOG, Nmg20, Pascal666, Template namespace initialisation script, TheParanoidOne, TranscendTranslation, 3 anonymous edits
604
Article Sources and Contributors
Melanocyte-stimulating hormone Source: http://en.wikipedia.org/w/index.php?oldid=551576665 Contributors: .Koen, Al bateman, Alex.tan, Anassagora, Anthropodeus, Arcadian, Boghog, Bomac, Cacycle, Centrx, Chaldor, Chemgirl131, Dcirovic, Diberri, Docfaust, Dugwiki, Eras-mus, Gleng, Gustafberg, Hordaland, IMSoP, JWSchmidt, James Crippen, Jezpas, KnightRider, Louisajb, Marc Venot, Meodipt, Netscott, Nmg20, Richardcavell, Rockpocket, Romanc19s, SlothMcCarty, Smily, Sometime-science-editor, Stepa, The Anome, The chemistds, Tristanb, Роман Беккер, 56 anonymous edits Magnocellular neurosecretory cell Source: http://en.wikipedia.org/w/index.php?oldid=540225032 Contributors: Addashaw, Arcadian, Cmcnicoll, Diberri, Drphilharmonic, E=MC^2, Feral mage, Franamax, Gleng, InvictaHOG, RelentlessRecusant, Rettetast, Template namespace initialisation script, 1 anonymous edits Oxytocin Source: http://en.wikipedia.org/w/index.php?oldid=548929574 Contributors: A314268, AbderrahmanNajjar, Achowat, Adolphie, Adomh, Aghochikyan, Ajay5150, AlbertHall, Alertjean, Alex naish, Alex.tan, Alienus, Alousybum, AltiusBimm, Amorymeltzer, Anm28, Anonymous Dissident, AnotherSolipsist, Ansell, Apokrif, Aratuk, Arcadian, Arjayay, Arne Saknussem, Astanton, Athelwulf, Atif.t2, AugustinMa, AxelBoldt, BD2412, Bahkibulle, Barnaby dawson, Beetstra, Before My Ken, Beland, Benbest, Bendav, Bfinn, BigHairRef, Bignoter, Bluerasberry, Bobrayner, Boghog, Bomac, Bongwarrior, Boomur, BorisTM, Boulevardier, Buda118, CDN99, CO, CaliforniaAliBaba, Calton, Carl Wivagg, CarsonsDad, Carusus, Casforty, Cburnett, Cenarium, Cezarika1, Cforrester101, Cgingold, Chemgirl131, Chooserr, Chowbok, Chris Capoccia, Chris Howard, Christian75, Chrysaor, Chuunen Baka, Ciao!derhead, Crystallina, Cspenn, Cybercobra, D, DMacks, Daf, Damian Yerrick, Danalache, David spector, Davidgn, Deflective, Denis tarasov, Deor, Dewatf, Diamondunicorn, Djleslie, Djneufville, Doc.Ian, Dont do drugs, Douglasr007, Download, Dr Bilal Alshareef, Dratman, Drphilharmonic, Duncan.france, Dureo, Dwilletts, ESkog, Edcolins, Edgar181, Egjjones, Eleassar, EllenCT, EmmaEThomas, Eubulides, EugeneZelenko, Everyking, Ewawer, Fangz, Farmacol, Feezo, Feisty.gibbon, Francesfrog, FrozenMan, Fusz432, Fvasconcellos, Gaius Cornelius, Gigemag76, Ginkgo100, Glane23, Glen, Gleng, Gracefool, Guitarmankev1, Gurch, Gz33, Habj, Hazard-SJ, Hazer65, Henk Poley, Henning Makholm, Hobied, Hordaland, Iamcuriousblue, Iapetus, Imsoright, Infrogmation, J.delanoy, JWSchmidt, JamesMLane, Jarble, Jason7825, JasonAQuest, JasonAllen, JaucelynnP, Jeffreyfrench, Jeremy68, Jfdwolff, Jobnikon, Jrockley, Juliecarver, Juntas, Justin Tsay, Justin W Smith, Kaicarver, Kaobear, Karakal, Karl Stas, Keenan Pepper, KnowledgeOfSelf, Kurtan, Kwamikagami, LanceBarber, Leechinyen, Lexi0214, LittleHow, Longhairandabeard, Louisajb, Luke poa, Luonade, Luvsdaheat, Madhero88, Mardus, Marek69, Mark Renier, Materialscientist, Mav, Maxkingesq, May Cause Dizziness, Meanstheatre, Megapanphilos, Mentifisto, Meodipt, Metalloid, Mfourman, Mguttman, Mifter, Mikael Häggström, Mimihitam, MindZiper, Naraht, NeilN, Neoman2026, Nigelj, Nikejulia, Noah Salzman, Nono64, NotAbel, Novangelis, Nrcprm2026, Obscurans, OlEnglish, Ombudsman, Omed2, Originalbigj, Orlandoturner, Osmodiar, OverMyHead, PFHLai, Paine Ellsworth, Pashihiko, Pastiness, Pdcook, Peachypoh, Peryeat, Peteb4, Peterl, Philkon, Philthecow, Pierre-Alain Gouanvic, Platypus222, Poindexter Propellerhead, Postlewaight, Power piglet, Puchiko, Qwerty Binary, RB972, Reaverdrop, Rheez, Rjwilmsi, Rl, Rogermw, RoyGoldsmith, SJFriedl, Salomeya, Sammyj, SarekOfVulcan, Sderose, Seraphimblade, Shadowjams, Shadowlynk, Solidhart, Sondreskarsten, SpLoT, Stevegray, SummerPhD, TBadger, Tameeria, Tarotcards, Tavilis, Tayste, Tb81, Techauthor, The Thing That Should Not Be, Theexamined life, Thelittlegreyman, Themissinglint, Thw1309, Tijmz, TimVickers, Tony Mach, TonyW, Trivialist, Tsiaojian lee, Ultra Venia, Vala M, Vectro, Violetriga, Ward20, Wavelength, Weasel extraordinaire, Weebeman022, Why Not A Duck, WikHead, Wondercow, Wormcast, WriterHound, Wwheaton, Yoninah, Yuubinbako, Zackopacko107, Zakp, Zefryl, Роман Беккер, Ὁ οἶστρος, 神 仙, 444 anonymous edits Vasopressin Source: http://en.wikipedia.org/w/index.php?oldid=546451712 Contributors: A314268, A3camero, AaronM, Abtinb, Adolphie, AlbertHall, Alex.tan, Alousybum, Als022, Amovrvs, Andrux, Antelan, Arcadian, Armando Navarro, Artur Lion, Aude, AxelBoldt, Axl, Aytrus, Backwardtoes, Bensaccount, Blackmarketpenguin, Bobo192, Boghog, Bomac, BorisTM, Bowman, Bwrs, CDN99, Caltas, Caseyisahobo69, Cezarika1, Chaldor, Chemgirl131, Chris the speller, Chymæra, Csobankai Aladar, DRosenbach, Dab2108, Darth Panda, Dcirovic, Denis tarasov, DerHexer, Dhatfield, Diberri, Docfaust, Drphilharmonic, Edgar181, EerieNight, EhJJ, Electric goat, EmlivOlcano, EmmetCaulfield, Epingchris, Eug, Expergefactionist, Feral mage, Forluvoft, FrozenMan, Fvasconcellos, Geetarmainiac, GermanX, Giftlite, Gleng, Guillaume2303, Gurch, Harriv, Hattaway, Hodja Nasreddin, I9606, IO Device, IONTRANSP, Inoculatedcities, Invalidsyntax, InverseHypercube, JForget, James McNally, Javierstroud, JesseAlanGordon, Jfdwolff, Jmoneydizzle, Joel7687, John, John.mapleview, Jonathan.s.kt, Juliecarver, Katoa, Kelson, Kilo-Lima, Krylonblue83, Lepidoptera, M1ss1ontomars2k4, MPerel, ManiF, Mark Knepper, Matdaddy, MauriceTrainer, Mav, Mboverload, Medevo, Medicineman84, Mikael Häggström, Mike2vil, Mimihitam, Minnsurfur2, Misskidney, Mthteh, Nagy, Nathan Johnson, Netopoa, Nishkid64, Nyq, Odoketa, Olegkolesnikov, Osm agha, Philip Trueman, Pit, Pranks16, Prayingmantis78, Puckly, RDBrown, RadicalHarmony, Raghuram.chimata, Rich Farmbrough, Rjwilmsi, RyanGerbil10, SPhotographer, Sammyj, Sgtpepper66, Shrimppesto, Someone else, Spaully, Stepanka, Stismail, Tameeria, Tavilis, Tbhotch, Techfiend, Tgilhou, The Legendary Douglas Butcher, Theodore Kloba, Tide rolls, Tony Mach, Tpjv86b, Uncle G, Vanv2642, Vogelbacherr, Vokesk, Wavelength, Wiki.saeid, WordyGirl90, Xris0, Zain Arshad, Ødipus sic, Роман Беккер, ﻫﻤﺎﻥ, 255 anonymous edits Serotonin Source: http://en.wikipedia.org/w/index.php?oldid=549358753 Contributors: 00AgentBond93, 19.168, 213.253.39.xxx, 2over0, A2-33, A314268, ANGGUN, Abby, Aeluwas, Alalej, Alex.tan, AlexandriNo, Andkore, Andycjp, Apophenic, Arcadian, Arjayay, AshleySt, Astavats, AxelBoldt, BD2412, Badgettrg, Baseball Bugs, Basudhabasu, Beetstra, Belovedfreak, Ben-Zin, BenM, Benjah-bmm27, Besh Saab, Bignoter, Biochemza, Biosthmors, Bluptr, Boghog, Boing! said Zebedee, Bongwarrior, BorisTM, Brandon, Brandon.macuser, Brian0918, Brian1975, Brianherman, Bujatti, Burntsauce, C6541, CDN99, CM Grunge, CMBJ, CWenger, Cacycle, Cantorman, Captain Infinity, Casforty, Catch-fly, Causa sui, Ccroberts, Cedders, Celestialpillow, Ceyockey, Charles Gaudette, Chem-awb, Chemgirl131, Chris Rocen, Chunky Rice, Claud1234, Colinmcc, Conversion script, Correogsk, Corti, Crusadeonilliteracy, Csörföly D, Cue the Strings, CustardJack, Cyberfay, DARTH SIDIOUS 2, DJBarney24, DM4242, DMacks, DVdm, DaGizza, Daksya, Dancter, Danelo, DarkSword, DavidH, Dbtfz, Deepkamal, Deflective, Deli nk, Delta G, Diberri, Docfaust, DonIncognito, DopeChicken, DrSparticle, Drakarst, Dreviscerator, Drphilharmonic, Edgar181, Eequor, El Mariachi, ElaineRitter, Eleassar, Eloil, Epipelagic, Eric-Albert, Escp11, Esperant, Euloiix, EvelinaB, Evercat, Everyking, EvilResident, Ex nihil, Eykanal, Facts707, Falcon8765, Fedayee, Felinefox, Felipe Aira, Ffirehorse, FinnBjork, Firebird9, Flockmeal, Florescent, Fners, Fnielsen, Forthnoggin, Fox816, Fuzheado, Fuzzform, Fvasconcellos, G2star, GABaker, GBronson, GabeIglesia, Gadgit7, Gaius Cornelius, Gastro guy, Geneffects, Genie, Gerriet42, Giftlite, Gigemag76, Gioto, Googie man, Guitarmankev1, Haakenlid, Hadal, Hairy Dude, Hamiltondaniel, Harbinary, Hazard-SJ, Heah, HomicidalWorms, Hon-3s-T, Hordaland, Hpyoup, Hreid11, I dream of horses, IRP, Ianvitro, Immunize, Impossiblepolis, Iothiania, Ipatrol, Iris lorain, IstvanWolf, It Is Me Here, Iwilcox, Izecksohn, JGM73, Jake.knaub, Jarrydn, Jartur, Jauhienij, Jayunderscorezero, Jcw69, Jennavecia, JeremyA, Jfdwolff, Jmh649, Joe Decker, John Vandenberg, JohnInDC, Johner, Jojit fb, Jonathan Drain, Joonhon, Jorgelopest, JorisvS, Joseph11h, Josh Cherry, Joyous!, Julesd, Jynto, Karonaway, Keenan Pepper, Kelvlam, Ken Gillman, Kgrevstad, Kilom691, Kingpin13, Klonimus, KonradG, Ksj123, Kst447, Ksyrie, Kubigula, Kwamikagami, Lehacarpenter, Lenisc, Liangxiao, Liaocyed, Light current, LittleHow, Looie496, Looxix, Louisajb, Luckydhaliwal, Lunakeet, Lyod, M1ss1ontomars2k4, Madacs, Magister Mathematicae, Malljaja, MarXidad, MarcK, Mark PEA, Martynd, Materialscientist, Mathchem271828, Matthew Kornya, Mav, Mazi, McSly, Mcduf01, Meekywiki, MegaHasher, Mentifisto, Mfourman, MiPe, MichaelSHoffman, Mikael Häggström, Mikespedia, Moe Epsilon, Mogism, Mr.alhuwaykim, MrPMonday, Mshake3, Muriel Gottrop, N5iln, Nono64, Northfox, Notjim, Nubb38, Nucleophilic, Ohnoitsjamie, Oliverlyc, Orlandoturner, Ott2, PFHLai, Paul D. Anderson, Paul Drye, Pengortm, Persephone12, Perussi Incendia, PetWolverine, Petey Parrot, Pgk, Philip Trueman, Philopedia, Phlep-phlep, Physchim62, PianoSpleen, Pikiwyn, Pine (usurped), Pinethicket, Pocopocopocopoco, Pol430, Polarbearbabies, Povmcdov, PratzStrike, Prelate Zeratul, ProxyChemist, Purinebug, R'n'B, R.O.C, RDBrown, RadicalHarmony, Rajrajmarley, RatnimSnave, Raybechard, Rcsprinter123, Rehanz1, Reinyday, Renamed user 39932kk3, Reo On, ResearchRave, Reubzz, Rhetth, Rich Farmbrough, Rjanag, Rjwilmsi, Rmky87, Rob Hooft, RohypnolFTW, Rojogrande, Ronhjones, RossBoss, Rossmcd, Rousfo, Rovership27, RoyBoy, Rursus, Russell E, Rünno, SD5, Sadaphal, Samuel Blanning, SandyGeorgia, Sausagerooster, Saxifrage, Sbharris, Sburke, Schauf, Seb144, Senaiboy, Sequoyah, Serotin, Shakajo, Shanedidona, Shisock, Silverxxx, Singlelaw, Sleuth21, Smalljim, Snag99, Socialservice, Sockettome, Sophie means wisdom, Soulthriller, Starcross, StaticGull, Stephenb, Stephensuleeman, Stevertigo, Stijn Calle, StradivariusTV, Sudeshna Chandrashekhar, Suisui, SummerPhD, Sven Jähnichen, Sweikart, TTile, TYelliot, Tabletop, Tal Avigdory, Tarotcards, Tea with toast, Techelf, Teemu08, Teol, The Agitator333, The Anome, The chemistds, TheBaur, Thricecube, Tim Long, TomCerul, Tree Biting Conspiracy, Twaz, Ukexpat, Urhixidur, VI, Varuna, Vaughan, Velvetron, Versus22, Victoria'sSeeker, Vijay2101, Vladaig, Vokesk, Vzambrano, WLU, Walker959, Walkerma, Wapcaplet, Where next Columbus?, Wiki alf, Wikiborg, Willking1979, Wisdom89, Wjejskenewr, Wnissen, Woohookitty, Wormald, Wrfrancis, WriterHound, X1987x, Xabian40409, Xdisaster911, Xris0, XsHoa10pSogRcAVgjAxsVMs1C1BbYUspRh, Xtinacuila, Yamamoto Ichiro, Zoomcake, Åkebråke, Роман Беккер, ﺃﺣﻤﺪ.ﻏﺎﻣﺪﻱ.24, ﮐﺎﺷﻒ ﻋﻘﯿﻞ, 742 anonymous edits Endorphins Source: http://en.wikipedia.org/w/index.php?oldid=549508923 Contributors: A314268, A8UDI, Acather96, Acdx, Ademkader, Aguabranca, Alexander Iwaschkin, Allmightyduck, Allowother, Amakuha, Amcbride, Analoguedragon, Ancos, AndrewHowse, Anthony Appleyard, Apparition11, Arcadian, Armeria, Arpingstone, Arvindn, Ashdog137, Auric, Awien, Beland, Benbread, BigbossSNK, Bizso, Bk0, Bobo192, Bodnotbod, Boghog, BuickCenturyDriver, Bunchofgrapes, C6541, Cameronpb, Camw, Can't sleep, clown will eat me, Celeron, Chill doubt, Chitarrista, Chumchum7, Chuq, Church of emacs, Cimon Avaro, Cntras, Cometstyles, Corpx, Crazz bug 5, Crispytd13, Crywalt, Cybercobra, Cyrus XIII, Czego szukasz, Davidgindelberger, Dcfleck, DeathByNukes, Defenestration, Dennis714, Derek Andrews, Dereleased, Diblidabliduu, DocWatson42, DoubleUTT, Doug-e-fresh74, Dreadstar, Drphilharmonic, Ducducpham, Dweissma, E Wing, Edgar181, Eemton, Eequor, Efege, Ehn, Elaborate, Elbreapoly, Eliz81, Elmer92413, Epbr123, Eraserhead72, Esrogs, Face, FerralMoonrender, Fieldday-sunday, Firewave11, Firien, Francis Tyers, FrancoGG, Furrykef, Gaff, Giftlite, Gleng, Gogo Dodo, Grace Note, Gracefool, GregW, Gveret Tered, Hazard-SJ, Hch2, Headbomb, Healingkid, Hede2000, Hodja Nasreddin, Hosterweis, Huji, Hydrargyrum, Hz.tiang, Ianmathwiz7, InternetMeme, Ipsingh, Ivan Bajlo, Ixfd64, J. Van Meter, J.delanoy, J04n, JForget, Jahiegel, James086, Japanese Searobin, Jasper Cirkel, Jimmy, Jinma, Jisatsusha, Jittat, Jmcq1, Jojhutton, Jonathan Drain, Jose Ramos, Jsjunkie, Jtyson3202, Judzillah, Juliancolton, Junkers0900, Karada, Karl Stas, Katalaveno, Kbh3rd, Killiondude, Klimintine, Kst447, Ksyrie, Ladder222, Lajos.rozsa, Lerikson, Lkinkade, Looxix, Lova Falk, Lovecz, Luna Santin, MagneticFlux, Martian375, MartinRobinson, Mashford, Materialscientist, Matt121, Mfwnoface, Mgiganteus1, Michael Hardy, Michaelbusch, Miknight, Mleonard85032, Mrs.meganmmc, Myanw, Narssarssuaq, Nathan Johnson, Naturalmotion, NickCatal, Noloop, NotAnonymous0, OGoncho, Obsessivelanguagelearner, Oda Mari, OlEnglish, Orlandoturner, OwenBlacker, Ozrician, PFHLai, Paine Ellsworth, Paranoid, Paul Drye, Pearle, Philip Trueman, Phlegat, PkScary, Playadom, Pro bug catcher, Profstandwellback, Quendus, R'n'B, RJASE1, Rajah, Raquel Baranow, Rasd, Rbmj, Rffreq, Rgaddipa, Rjwilmsi, Ronocdh, Rosskey711, Ryanaxp, Saint91, Saman1212a, Schaefer, Search4Lancer, Shatteredshards, Silverxxx, SiobhanHansa, Skew-t, Skihtg12, Smegal723, Snoyes, Sockr44e, Spalding, Sparklegurl32, Spiff, St3vo, Steevven1, Stiang, Sticky Parkin, Stpcreepstp, Subzero Ray, Sunray, Superbeecat, Supernatent, Sylvain Mielot, Szaszicska, Tavilis, Techelf, TeresaTeng, Terriblefish, Teutonic Tamer, Tgeairn, The Anome, The Epopt, TheGerm, TheRasIsBack, Tide rolls, Tntdj, Tomyumgoong, Triggtay, Tyciol, Uthbrian, VI, Versus22, Vrenator, WOLfan112, Wik, Will Beback, WriterHound, X!, X3qt0r, Ylem, Yms, Yorick8080, Zenomax, ﺷﻤﺎﻝ ﺑﺰﺭﮒ, 533 anonymous edits Somatostatin Source: http://en.wikipedia.org/w/index.php?oldid=547887868 Contributors: Alansohn, Aleator, Alex.tan, Amisten, Anthonyhcole, Arcadian, AvicAWB, Banus, Betswiki, Boghog, CDN99, Ccevo2010, Ceyockey, Cezarika1, Chemgirl131, Chrysaor, Cy21, Delldot, Dextrosity, Dr.fuchs, Drphilharmonic, ESCapade, Edgar181, Epingchris, Epolk, Franklinjefferson, GHe, Gelu Ignisque, Gleng, Guidod, Hodja Nasreddin, Jalan z, Japanese Searobin, Jjohnsonwbc, Jonathan.s.kt, Jujutacular, Korey Pesicka, Kpjas, Magioladitis, Mattinbgn, Maumugnel, Miaow Miaow, Mikael Häggström, Minesweeper.007, MsHyde, Nonantum, Phoebus87, Prakashmalshe, Richardcavell, Rjwilmsi, RuED, Seanmpeterson, Snecked, Temporaluser, Terrace4, Tgilhou, TomSands, Tomjc, Trabelsiismail, TranscendTranslation, TylerDurden8823, Vedran12, Wavelength, Westin, Wik, Xerxesgrinder, Xris0, Yerpo, Yobol, Zoicon5, Роман Беккер, 68 anonymous
605
Article Sources and Contributors
edits Gastrin Source: http://en.wikipedia.org/w/index.php?oldid=547268797 Contributors: 21655, A.s, Adamlankford, Alex.tan, Andrew Su, Arcadian, Atlant, Atlantia, Bignoter, Boghog, Bogwhistle, Borgx, Brim, Caltas, CanadianLinuxUser, Carstensen, Chem Lady, CiaranAnthony, Curb Chain, Danierrr, Dcirovic, Diberri, Dlaat, Doctorcherokee, Duncan.Hull, Edwin, Emilymg, Epingchris, FrozenMan, Gaius Cornelius, Guidod, Hodja Nasreddin, Horiavulpe, InverseHypercube, Japanese Searobin, Jfdwolff, KC Panchal, Kiral, LowLifer, Majkinetor, Meodipt, Mike2vil, MindZiper, Mira Gambolputty, Ms1702, Naraht, Naranoth, Nickwilkie, Puppy8800, Raymondwinn, Rb1248, Rich Farmbrough, Rjwilmsi, RyanGerbil10, Sgpsaros, Szalzala, Temporaluser, Theespuja, Trbdavies, Vedran12, Vldscore, Wlodzimierz, WriterHound, Yms, Yongwang100, Роман Беккер, 79 anonymous edits Secretin Source: http://en.wikipedia.org/w/index.php?oldid=549491271 Contributors: Alex.tan, AmyNelson, Arcadian, Bender235, Bignoter, Boghog, Brim, CMBJ, Calvero JP, Dawn Bard, Delirium, Diberri, Dr.Wink, Eleassar, Flower-gmu, Gabeframe, Guidod, Imagine-GMU, InverseHypercube, Jwinius, Kallimachus, Kim De Gelder, Km2452-GMU, LittleHow, LowLifer, Maork, Mcstrother, MichaelJanich, Mike2vil, MindZiper, Naj-GMU, Naniwako, Nephron, Niels Olson, Ohconfucius, Paul D. Anderson, Pitabread640, Quirk, R'n'B, Rb1248, Red58bill, Rjwilmsi, Rrburke, STanwir MD, Simon Kilpin, Sjakkalle, Stepa, Steveking 89, Stone, Swithrow2546, Vedran12, Vogon77, WLU, Wlodzimierz, Yehudamalul, Роман Беккер, 61 anonymous edits Cholecystokinin Source: http://en.wikipedia.org/w/index.php?oldid=548995917 Contributors: A314268, Alex.tan, Arcadian, Aylaf, Bissinger, Boghog, CDN99, Captain-n00dle, Chrisvanlang, Corblimeywot, Corinne68, Cossy, Daranz, Dcirovic, Diberri, Dr Bilal Alshareef, Drphilharmonic, Edgar181, EerieNight, Emanueru, Falkonry, Flopster2, Gikü, Harbinary, Healthwise, Horiavulpe, Hreid11, Immunize, JHunterJ, JesseAlanGordon, JohnnyCashIsNotDead, Jrtayloriv, Kpjas, Maork, Meodipt, Mgdurand, Mike2vil, NatusRoma, Nick Number, PCHS-NJROTC, Petersam, Probios, Rb1248, Rjwilmsi, Rsabbatini, Snapperman2, Sreerup, Tony1, Vedran12, Vogon77, Wlodzimierz, Yeast2Hybrid, Yongwang100, Роман Беккер, 12יעלד, ﺣﺴﻦ ﻋﻠﻲ ﺍﻟﺒﻂ, 70 anonymous edits Insulin Source: http://en.wikipedia.org/w/index.php?oldid=551722783 Contributors: (榮), - ), 1297, 217.99.96.xxx, 5 albert square, 7, 75th Trombone, A hilton johnson, A.R., A314268, A3r0, ACEOREVIVED, AMackenzie, Aa77zz, Aboros, Acroterion, Addshore, Aelleth, Afil, Ahoerstemeier, Ajd, Ajh16, Akinoame, Alandeus, Ale jrb, Alex.tan, Alexithymia, Alexius08, Alexville, AltheaJ, Andre Engels, Andres, Andrew Su, Andrew73, Andybellenie, Antandrus, AntonioMartin, Anwar saadat, Aphenry, Appraiser, Arcadian, ArchonMagnus, Arielco, Ash, Aswang, Atreid3s, AxelBoldt, Axlq, B.d.mills, BDD, Bachrach44, Badgettrg, Baltimore00, Ben-Zin, Bender235, Benweatherhead, Bernfarr, BeteNoir, Bethenco, BlackTerror, Blake's Star, Bob horn, Bobblewik, Bobdewhirst, Boccobrock, Boghog, BokicaK, Bollar, Bongwarrior, BorgQueen, Bravekermit, Brian Crawford, Brianga, BrightStarSky, Btstuff, Bubba73, Bubeck, Bucephalus, Buchanan-Hermit, Bwhack, C0nanPayne, CLGroup1, Cacycle, Calabraxthis, Callacatacat, Can't sleep, clown will eat me, Canis Lupus, Carbuncle, Carcharoth, CardinalDan, Carpaticus, Carturo222, Ceyockey, Chi 271, Chickenfocker, Chowbok, Chris the speller, Christian List, Chrysaor, Citicat, Clarince63, Cless Alvein, CliffC, Cliffradz, Cmcnicoll, Conversion script, Corpx, Cottingham, Cpyder, Crazypaco, Crecy99, Crimsonarcher, Cybercobra, Cybergoth, DGG, DMS, DVdm, Dachannien, Daevatgl, Dale Arnett, Damian Yerrick, Danny beaudoin, Dararivera, Darentig, Darkwind, Darrell Greenwood, David Underdown, DavidSchooley, Davidruben, Dawn Bard, Db099221, Dcoetzee, Deans-nl, Deelkar, Deepakpurang, Delta G, Denni, DennisDaniels, Deviathan, Dgee15, Diberri, Digital infinity, Ding.xk, Discospinster, Discoveryofinsulin, DocWatson42, Donarreiskoffer, Donfbreed, Douglas Bradford Oliver, Dougofborg, DownUnder555, Download, Dratman, Drphilharmonic, Drz1627, Dullhunk, Dutai68, Dwmyers, EMahony34, ERcheck, East718, Eddideigel, Edward, Eingangskontrolle, Ekem, Eleassar, Eleassar777, Elenaschifirnet, Eliazar, Elyelu, EmadIV, EoGuy, Epolk, FF2010, Fabiform, Fantumphool, Farmacol, Fattyjwoods, Ferrarinimi, Feydey, Fieldday-sunday, Flamingspinach, Fluppy, Foo1942, Foobar, Foregone conclusion, Fram, FreeBird, Frietjes, Fromthevaults, G2star, GAThrawn22, Gabi S., Gadfium, Gbrizey, Gene Nygaard, Geraldshields11, Giftlite, Gigemag76, Gilliam, Gioto, Gleng, Glenn Magus Harvey, Glittergaia101, Googie man, Gorgiogo, Goto Dengo, Grika, Gunnernett, Gutza, Guy Harris, Gwrightnyc, HJ Mitchell, Habbit, Habj, Hadal, Hapticfever, Harry Raffan, Healthabetic, Hebrides, Hellbus, Henkeldg, Hichris, Hmmwhatsthisdo, Hokeman, Holme053, Howcheng, Hu12, Hunter1084, Husky141, Hylian Auree, Hzh, Ibbn, In actu, Iridescent, Isnow, Ita3aai, Itub, IvanTheRussian, Iyantha, Jack Daw, Jackfork, Jackol, Jakob Suckale, Jamesontai, Jantaro, Jarble, Jared81, Jeronimo, Jerryseinfeld, JessieTech, Jfdwolff, Jihadcola, Jim1138, Jnrubenstein, Joao Xavier, JoeSmack, Johansosa, Johnlogic, Johnteslade, Johnuniq, Jon Harald Søby, JonHarder, Joseph Spadaro, Jovianeye, Julesd, Juliancolton, Jwissick, Jyril, Jóna Þórunn, Kaiba, Kanags, Kandar, Karen Johnson, Katalaveno, Katieh5584, Keerthi78, Kenyon, Kingpin13, KittenMya, Kkpatel1, Konman72, Kostisl, Kowey, Koyaanis Qatsi, Kozuch, Kpjas, Krauss, Krenair, Kristof vt, Kungfuadam, Lexington50, Lightmouse, Lilac Soul, LittleHow, Lizwalk, Llull, LoneRifle, Looxix, LovePatsyCline, Low-frequency internal, LtPowers, Lucid, Lzjwhu, M3I5K7E, Magnus Manske, Malcolm Farmer, Mallanox, ManVhv, Mardochaios, Mark Arsten, MarkSutton, Martg76, MartinezMD, MauriceTrainer, Maury Markowitz, Mav, Maxim, Mbbradford, Mcvmccarty, Meiquer, Mergneed, MetsFan76, Mhjb, Michael Devore, Michael Ross, Michaelas10, Mifter, Mig11, Mihaiam, Mikael Häggström, Mildly odd, Mindmatrix, Miss Madeline, Misza13, Mitchthest, Mj455972007, Mlaffs, Mortene, MrFish, Mrcoldfire, Mss01, Muhandes, Munita Prasad, Nakon, Naniwako, Naohiro19 revertvandal, Nbauman, Neet nl, NellieBly, Neparis, NewEnglandYankee, Nhandler, Nicksterlingtek, Nikkimaria, Nk, NobelSturegatan 14, Nosh321, Nutriveg, Nxtid, Nysalor, Oaktree b, Ohnoitsjamie, Olahus, OldakQuill, Oliverdl, Oszillodrom, PFHLai, Paine Ellsworth, Panoramix303, Patricia Meadows, Paul20070, Pedantic of Purley, Pegasus1138, Pelirojopajaro, PericlesofAthens, Peter Ellis, Pfranson, Pharaoh of the Wizards, Philip Trueman, PhilipO, PicNick, Piledhigheranddeeper, Pilotguy, Pinethicket, Pmcmeans, Pmd, Pmm530, Porsche997SBS, Princess LJ, Prisonblues, Psychonaut, Quantpole, Quelsen, Quintote, Qwyrxian, R3m0t, RBBrittain, RJaguar3, RXPhd, Radagast83, Ragesoss, Rajrajmarley, Ratza, Raul654, Realdeal21, RedWolf, Regulov, Renato Caniatti, RexNL, Rich Farmbrough, Richard Arthur Norton (1958- ), Richardcavell, Rillian, Rjwilmsi, Rmky87, Rob Hurt, Roberta F., Roberthistoria, Robinhaw, Robma, Rogerd, Romanm, Ronk01, Royalguard11, Rsabbatini, RudolfRed, Ruy Pugliesi, Rwflammang, RyanCross, Saddhiyama, Saganaki-, Sakkura, Sakura black, Sango123, Sara Howland, SaraPulis, Sasuke Sarutobi, Sbledsoe, Schmausschmaus, Scray, Serketan, Set theorist, Shadowjams, Shifan84, Shobhitha, Shoeofdeath, Silver Edge, Silverchemist, Sjakkalle, Smileh, Smobri, Smyth, Snacks, Snowolf, Solled1, Someone else, Songrit, Soosed, Sorenostergaard, Sourabh.khot, Specs112, SpencerThiel, Spike.robinson, Sstrumello, Starfirewind, Staylor71, Stenemo, Steve03Mills, Steve10345, SteveChervitzTrutane, Stevenscollege, Stevertigo, Strider yellow, Subsolar, Sun Creator, Surfeited, Susan118, T g7, TBloemink, Tabletop, Takometer, Tangsonghe, Tarquin, Tasc, Tasos Serbis, Tassedethe, Tatiparti.katyayani, Taw, Tedickey, Teh Untouchable, TenOfAllTrades, Testosterone vs diabetes, Tevildo, The Anome, The wub, Thingg, Tide rolls, Tobby72, Tobesbmx, Tobias Hoevekamp, Tommy2010, TonyW, Triona, Triplemaya, TwoTwoHello, Tyciol, TylerDurden8823, Ultimus, Universityavegangsta, Unofficialeditor, Unyoyega, User27091, Uthbrian, Uzbad, Valerij, Vanderesch, Veevek, Veinor, Vipinhari, Vsmith, WLU, Wackymacs, Waggers, Wasell, Wavelength, We hope, Webaj, Wik, WikHead, Wiki Raja, Wikipedia brown, Will Beback Auto, Wimt, Wojichek, Woohookitty, WriterHound, Ww, Xjevx, Yamamoto Ichiro, Yash manu, Yava e, Ybbor, Yerpo, Ymwang42, Youssefsan, Ypomichelle, Yurivict, Yyy, Zad68, Zain Ebrahim111, Zesty3, Zigger, Ziva David, Роман Беккер, ﺣﺴﻦ ﻋﻠﻲ ﺍﻟﺒﻂ, 1187 anonymous edits Glucagon Source: http://en.wikipedia.org/w/index.php?oldid=550825528 Contributors: 4twenty42o, Alex.tan, All knowing69, Andrea105, Andrew Su, Arbitrarily0, Arcadian, Autoerrant, AxelBoldt, Bahar101, Beetstra, Bobsagat, Boghog, Bomac, Borgx, Brazucs, Breadified, Brian0918, Brinerustle, Bryan Derksen, Centenarian, Cezarika1, Chowbok, Clicketyclack, Cntras, Craig Pemberton, Dancraggs, Darked, Deltawarrior60, Deryck Chan, Diberri, Don4of4, Drphilharmonic, Dws, Elb2000, Elipongo, Em Mitchell, Ephrone, Eric-Wester, Erud, Giftlite, Gigemag76, Glane23, Guidod, Hanfuzzy, Hede2000, Heron, HexaChord, Hichris, Hodja Nasreddin, Hroðulf, Hylian Auree, Ibrmrn3000, Immunize, Iohannes Animosus, It Is Me Here, J.delanoy, Jasont47, Jfdwolff, Jmh649, Jonathan.s.kt, Jóna Þórunn, KBi, Karl-Henner, Keron Cyst, Kpjas, Kvasi, Leoadec, Lightmouse, Louisajb, Lportil, MONGO, Mattis, Mdh8b, Meegs, Mhaitham.shammaa, Miaow Miaow, Mintleaf, Msraia, Nbauman, Netalarm, Nicksterlingtek, Nk, NotALizard, Nutriveg, Oreo Priest, Peryeat, Purplewowies, R3m0t, RFerreira, RXPhd, RadioFan, Reub2000, Richardcavell, Rjwilmsi, Robinhaw, Rsabbatini, Ruslik0, Sbmehta, Sixpence, Skaaii, Some jerk on the Internet, Stevertigo, StrangeAesculapian, Supergeneraliast, TBloemink, TPK, Techman224, Thumperward, Tra, Vedran12, VenomousConcept, Vogon77, Wavelength, Wiccan Quagga, Wikibofh, Willking1979, Writ Keeper, Yerpo, Yintan, Yk Yk Yk, ZnFinger, Роман Беккер, 160 anonymous edits Bombesin Source: http://en.wikipedia.org/w/index.php?oldid=540380323 Contributors: Aranel, Arcadian, CDN99, Cewvero, Chem-awb, Dcirovic, Deviator13, Drphilharmonic, Edgar181, EncycloPetey, Fuzzform, Howrealisreal, Jesse V., Jfdwolff, Kaarel, Louisajb, Megac7, Ntsimp, Rhys, Robodoc.at, Stepa, The chemistds, Vogon77, WriterHound, Zanimum, ﺣﺴﻦ ﻋﻠﻲ ﺍﻟﺒﻂ, 17 anonymous edits Follicular cell Source: http://en.wikipedia.org/w/index.php?oldid=541154323 Contributors: Arcadian, Brian Crawford, Diberri, Drphilharmonic, Franamax, Garion96, GlassCobra, Jwdietrich2, Kktor, Mikael Häggström, Mike Rosoft, Rogermw, Template namespace initialisation script, TheParanoidOne, Vojtech.dostal, 26 anonymous edits Parafollicular cell Source: http://en.wikipedia.org/w/index.php?oldid=543230436 Contributors: Arcadian, Ayacop, Cajolingwilhelm, Diberri, Feral mage, Franamax, Greensburger, Hurricane767b, InvictaHOG, Jgalt23, Jwdietrich2, Mauvila, Petrb, Rfgagel, Selket, Shunju-kun, Speiererg, Tameamseo, Template namespace initialisation script, TheParanoidOne, WhatamIdoing, 13 anonymous edits Parathyroid gland Source: http://en.wikipedia.org/w/index.php?oldid=551740818 Contributors: Acdx, Alex.tan, Anaxial, Andrux, Anthonyhcole, Arcadian, B2322858, Badgermilk5518, Bamyers99, BetaCentauri, Binky, Bomac, Bookandcoffee, Bprash, Bryan Derksen, Chowbok, Cooladoola, Courcelles, Dan Polansky, Davidruben, Dede2008, Delirium, Diberri, Dnunn27, Drguttler, Drphilharmonic, Drptl, E rulez, Emperorbma, Eog1916, Exemplar72, Facts707, Fdsafdsa, Freekozak, Garion96, GetAgrippa, Giftlite, Google.co, Greensburger, Gveret Tered, Haricotvert10612, Hexane2000, Icairns, Icmac, Igiffin, InvictaHOG, J.delanoy, Jag123, Jfdwolff, Jmarchn, Johner, Keenan Pepper, Kelovy, Kozuch, Lanternix, Larrybob, Limulus, M1ss1ontomars2k4, Magnus Manske, Martin S Taylor, Michael Patrick, Mikael Häggström, MrOllie, Nephron, Otiose315, PKT, Paul August, Pustelnik, RJASE1, Rhys, Richard D. LeCour, Ronhjones, RupertMillard, Rvflyboy, Ryanbibler, Saif husam, Salvadorjo, Schneelocke, Scoresby, Sct72, Shaaaheeen, ShakingSpirit, Squids and Chips, TastyPoutine, Template namespace initialisation script, The Thing That Should Not Be, TheLimbicOne, Themrpotatohead, Truthflux, Tuac, Vedran12, Vincentmirabueno, Wfeidt, Wisdom89, YUL89YYZ, Zenlax, 152 ,יוסי anonymous edits Parathyroid chief cell Source: http://en.wikipedia.org/w/index.php?oldid=541156214 Contributors: Annandale, Arcadian, Ceyockey, Dreadstar, Franamax, Garion96, Gon-no-suke, Grendelkhan, Im.a.lumberjack, Mikael Häggström, Neodop, Nephron, Richardsur, Template namespace initialisation script, YUL89YYZ, 5 anonymous edits Oxyphil cell (parathyroid) Source: http://en.wikipedia.org/w/index.php?oldid=542521918 Contributors: Arcadian, Arfy900, Deviator13, Franamax, Grutness, King of Hearts (old account 1), Knandor, Lenny Kaufman, Markjohndaley, Master of Puppets, Neilymon, Nephron, NeuroE, Rdenu, Template namespace initialisation script, 3 anonymous edits
606
Article Sources and Contributors
Chromaffin cell Source: http://en.wikipedia.org/w/index.php?oldid=550769376 Contributors: Arcadian, Bdekker, Bender235, CopperKettle, Creidieki, Diberri, DragonflySixtyseven, Drphilharmonic, Eleassar, EoGuy, Falconerd, Feral mage, Franamax, InvictaHOG, Jamesscottbrown, Jesse V., Johnhfst, Lenrodman, Mcardlester, T52nd, Tameeria, Template namespace initialisation script, TheParanoidOne, 34 anonymous edits Steroid hormone Source: http://en.wikipedia.org/w/index.php?oldid=539821098 Contributors: AMRDeuce, Aeternitatis, Alteripse, Antandrus, Apers0n, Appleseed, Arcadian, Art LaPella, Bongwarrior, Chemgirl131, Col.Kiwi, Dasani, Dcirovic, Diberri, Drphilharmonic, Dycedarg, Edgar181, Eleassar, Eras-mus, Extransit, Fconaway, Fletcher809, Foobaz, Foogleplex, Freshmeister, Giftlite, Habj, InverseHypercube, JBancroftBrown, Jfdwolff, Jmarchn, JoeSmack, Kimiko, Lova Falk, LowLifer, MER-C, Marc Venot, Memphis88, Mikael Häggström, Mike2vil, Milanannmathew, MindZiper, Mkot390, NBS, Nono64, Novangelis, Parasympathy, Pretzelpaws, RA0808, Rhys, Rjwilmsi, Ron Ritzman, RyanGerbil10, Slashme, Some jerk on the Internet, SpikeToronto, Takowl, TangParadise, Tgeairn, Toddfreitag, Voidxor, Wickey-nl, Wtmitchell, Xavier6984, 95 anonymous edits Mineralocorticoid Source: http://en.wikipedia.org/w/index.php?oldid=539757517 Contributors: Acbdyho, Alex.tan, AlexandriNo, Alexrexpvt, Aranel, Arcadian, Axelaxelj, Bemoeial, Bomac, Ceyockey, Chemgirl131, Chowbok, Cmcnicoll, Docfaust, Edgar181, EivindEklund, Eleassar, Eras-mus, Farmacol, GeeJo, Isoptera, Jack B108, Jezpas, Jfdwolff, Jmarchn, King Pickle, Korg, LeadSongDog, Michael Devore, Middayexpress, Mikael Häggström, Mike2vil, Mild Bill Hiccup, Mrezai, Ph.eyes, Rich Farmbrough, Settersr, SilkTork, Stepa, Su-no-G, Takowl, Tarek, Woohookitty, Yikrazuul, 33 anonymous edits Glucocorticoid Source: http://en.wikipedia.org/w/index.php?oldid=546586582 Contributors: AXRL, Aangari, AaronM, Ahmpaz2010, Alex.tan, Alexrexpvt, Alteripse, Anypodetos, Arcadian, Av01d, Axl, Bahar101, Before My Ken, Boghog, Bonnie Dixon, Chanoyu, Chemgirl131, Chris the speller, Chrisgj, Chrisscrewball, Cpiral, Dan100, Diberri, Dirk Gently, Doritopr, Doworks000, Dr.liuchao, Drphilharmonic, Edgar181, EivindEklund, Eleassar, Eleassar777, Fluffernutter, GeeJo, Huckfinne, Janek78, Jeepday, Jeff G., Jfdwolff, Jmarchn, JoanneB, JohnCD, Jyavner, KBi, KX36, Kangell, Kelson, Kevyn, Kgrad, Klghrt5487, Kman543210, Ksaraf, Kyba274, LSD, Lab-oratory, LovelyLillith, LowLifer, MarkusQ, Mefatpenguin, Michael Shields, Mikael Häggström, Miniyazz, Nabel619, Natazavrik, Nbauman, Nirmos, Ntsimp, NuclearWarfare, Nutriveg, Orlandoturner, Porejide, Princhemi, Pro crast in a tor, RelentlessRecusant, Romanfall, Rose Irmersh, Rror, Salvadorjo, Sbmehta, Seans Potato Business, Selket, Settersr, Sorensen ru, T.vanschaik, Unyoyega, Uthbrian, Vldscore, Wavelength, Wham Bam Rock II, Woohookitty, Wwallacee, Yid, Zertron, 100 anonymous edits Leydig cell Source: http://en.wikipedia.org/w/index.php?oldid=551738900 Contributors: Abstraktn, Adrian.benko, Andreas Erick, Arcadian, Cezarika1, Chopin-Ate-Liszt!, Coldbringer, Coolstoryhansel, CopperKettle, Craig Pemberton, Diberri, Drphilharmonic, ELLusKa 86, Fct, Franamax, GoingBatty, Greid, Hadal, InvictaHOG, Jarble, Jpogi, KnightRider, Lji1942, M1ss1ontomars2k4, Magnus Manske, MaxEnt, Mikael Häggström, Nephron, Pearle, Pengortm, Rjwilmsi, Scohoust, Template namespace initialisation script, TheParanoidOne, Tim hole, Uriel8, Vogon77, 39 anonymous edits Folliculogenesis Source: http://en.wikipedia.org/w/index.php?oldid=547725290 Contributors: After Midnight, Arcadian, Avkrules, Bachrach44, Bobblewik, Bobjgalindo, Breadified, CKCortez, Cacycle, Chemgirl131, CommonsDelinker, D. Wu, DabMachine, Drisar, Epingchris, Faradayplank, Franamax, Geremia, GoShow, Gustavocarra, Headbomb, JLaTondre, Janette.quennell, JeffreyN, John of Reading, Jpogi, Lottamiata, Lyrl, MER-C, Madhero88, Micemug, Mikael Häggström, Moreschi, Rjwilmsi, SDC, Scienceeditor, Shenme, Terrasque, TimBentley, 40 anonymous edits Progesterone Source: http://en.wikipedia.org/w/index.php?oldid=550042315 Contributors: 101scientist21, 16445970cl, 21655, AirBa, Airplaneman, Alexiusnovius, Alison, Alisonmcallister, Altenmann, Ambix, Andrew c, Angr, Ansell, Arcadian, AxelBoldt, AzadMashari, Beetstra, Beland, Beneluxboy, Benith, Benjah-bmm27, Benjamintchip, Benlisquare, Benslaststand, Bluegreen, Boghog, BrightStarSky, Bubbachuck, Bwhack, C6541, CarinaT, Chaser, Chem-awb, Chemgirl131, Christian75, Cindery, Col.Kiwi, CommonsDelinker, CopperKettle, Coppertwig, Crazytales, Cvwdev, Dadsweet, Dandoodle, Darth Panda, David Hedlund, Davidruben, Dcirovic, Debresser, Deli nk, Denisarona, Diberri, Dina, Dinosaurdarrell, Dkeithley, Dmullery, Drphilharmonic, Earl Moss, Edgar181, Edward, Ekem, Eleassar, Elisabeth Rieping, Eras-mus, Eric Kvaalen, Eric22, Evil Monkey, Excesses, Fightindaman, Flghtmstr1, Fuhghettaboutit, Fvasconcellos, GirlForLife, Gits (Neo), Graham87, HJ Mitchell, Hcysweet, Horiavulpe, IceCreamAntisocial, JCKB, JWSchmidt, Jag123, Jason Quinn, Jayunderscorezero, Jdoelder, Jedidan747, Jjsimpsn, JoanneB, Joel.geerling, John of Reading, Jphekman, Juliecarver, Karada, Karen Johnson, Keenan Pepper, Kellyprice, Khalismatic, Kosmotheoria, Kpjas, Kukini, Lance1949, Lemccan, Lifewhyse, LilHelpa, Louisajb, Lupin, Lynn4, Lyrl, MER-C, Magister Mathematicae, Mbilezikjian, Mcstrother, Metalloid, Mikael Häggström, MrADHD, Mumonkan, Mwanner, NameIsRon, Natalya, Naugyanks, Neelie nibor, Nephron, Nick Taylor1, Nirmos, Oaktree b, Officiallyover, Olivier, Osterluzei, Oxymoron83, Pearle, Photouploaded, Physchim62, R'n'B, REACHist, Radagast, Rainbowofknowledge, Rhombus, Rhys, Rich Farmbrough, Richardcavell, Richiez, Rjwilmsi, Robodoc.at, Sam Hocevar, Sander123, Saravask, Selket, Settersr, Seven of Nine, Silume, Skingski, Skpearman, Staceymg, Stannered, Supten, Svick, Tapir Terrific, TedE, The Anome, The Brain, Thecell, Thehoneykitten, TimBentley, Tristanb, Troykyo, Tsemii, UGAcodon, Unschool, Vala M, WLU, Wavelength, Whkoh, WiccaIrish, Wikipaddn, WriterHound, Wtmitchell, Yikrazuul, Zhuuu, ZooFari, Zzyzx11, 236 anonymous edits Corpus luteum cell Source: http://en.wikipedia.org/w/index.php?oldid=186256845 Contributors: Carlossuarez46, Mikael Häggström Corpus luteum Source: http://en.wikipedia.org/w/index.php?oldid=547725267 Contributors: Arcadian, Bgwhite, Boghog, Bomac, Bryan Derksen, Bubbachuck, CDN99, CanisRufus, Chilian51, CommonsDelinker, DerHexer, Diberri, Drphilharmonic, Dudewheresmywallet, Earlypsychosis, Eleassar, Epeefleche, Eras-mus, Erud, Esufer, Fieldday-sunday, Gdarin, Gjbbms640, Gnowor, Grenadine, Habj, Hoffmeier, Imprint007, Ivan.Lt, Jackfork, Jag123, Jarble, Jfurr1981, Jmh649, Jmjanzen, Jsherwood0, Kelly Martin, Kero584, Klingoncowboy4, Lab-oratory, Lyzzis, M1ss1ontomars2k4, Mark Lundquist, Markjohndaley, Materialscientist, Matt26, Mgutierrezyach, Miert, Mikael Häggström, NcSchu, NellieBly, Nephron, Omegawp, Oreobrine, Pigman, Prashanthns, Psquared2, Ricksakti, Robodoc.at, Rytyho usa, Sbharris, Schaaftin, Seejyb, Siebrand, Sky Attacker, Stylese, Template namespace initialisation script, Vldscore, Vokesk, Winderful1, Woohookitty, Wtmitchell, 125 anonymous edits Juxtaglomerular cell Source: http://en.wikipedia.org/w/index.php?oldid=540575536 Contributors: Arcadian, Beeswaxcandle, Diberri, Dr Bilal Alshareef, Franamax, Jpogi, Loganberry, NikeTenis, Onthevirge, Scottalter, Spaully, Timothydavie, 24 anonymous edits Renin Source: http://en.wikipedia.org/w/index.php?oldid=547344242 Contributors: -Midorihana-, 99 Willys on Wheels on the wall, 99 Willys on Wheels..., A3camero, Adh30, Agibso02, Alex.tan, Andrew.e.gibson, Anthonyhcole, Arcadian, Austinlarson, Banano03, Bemoeial, Bensaccount, Boghog, BorisTM, Brighterorange, Bunnyhop11, Cajolingwilhelm, Carlossuarez46, Chaheel Riens, Chemya, Ciar, Clayboy, Cmcnicoll, Colonies Chris, Creidieki, Curb Chain, D6, Dauddarseno, Dawkeye, Defactocomms, Deflective, Diberri, Drphilharmonic, Edgar181, Esprit15d, FrozenMan, GAThrawn22, GJeffery, Gaius Cornelius, Gene Nygaard, GermanX, Gikü, Groovenstein, Haisook, Hodja Nasreddin, Hroychow, Iamgangsta, Icairns, Imiousse, InverseHypercube, Itub, Jag123, Jamesscottbrown, Jco7, Jfdwolff, Jo3sampl, [email protected], Kpjas, Krash, Kwamikagami, Larsjo, Liangxiao, Lights, Looxix, Mattyjenjen, Megaman en m, Mikael Häggström, MiyagiDO, Modeha, Mr. Billion, Ndrawlings, Nephron, Ondewelle, PFHLai, Peak, Ppgardne, RDBrown, Rich Farmbrough, RickDC, Rjwilmsi, Rockpocket, Rorro, Rpseal, Rrten00, S3000, Saravask, Sarindam7, Schzmo, Shakiestone, Snowmanradio, Spaully, Temporaluser, Terkwoizebloo, Tpjv86b, Tristanb, Una Smith, Wavelength, Who, WikHead, Wisdom89, Роман Беккер, 105 anonymous edits Macula densa Source: http://en.wikipedia.org/w/index.php?oldid=546480822 Contributors: Alex.tan, Arcadian, Avaron676, Aytrus, Beeswaxcandle, CopperKettle, Dreaded Walrus, Ekotkie, Eyesighter, Franamax, GermanX, Hydro, Icairns, Jaapinholland, Jag123, Jenistranslucent, Jfdwolff, Lacrimosa, Lamro, M.Komorniczak, MC10, Mikael Häggström, Mrwalliekat, Nfstein, PFHLai, Paul August, Peco15, Quartertone, Rocaveli, Scottalter, Spaully, The Anome, YUL89YYZ, 43 anonymous edits Mesangial cell Source: http://en.wikipedia.org/w/index.php?oldid=543489891 Contributors: Alsocal, Arcadian, Bearcat, Beeblebrox, Ceyockey, Drphilharmonic, Faduart, Inkypaws, Lynntyler, Nlu, PFHLai, 8 anonymous edits Keratinocyte Source: http://en.wikipedia.org/w/index.php?oldid=540490959 Contributors: Alan Liefting, Arcadian, Auriol, Bissinger, Brambleclawx, Buzybeez, DutchDevil, ElAmericano, Evil saltine, Fconaway, Fraggle81, Franamax, Gerriet42, Gurch, Ithunn, Jag123, JayC, Jfdwolff, Kjkolb, KrakatoaKatie, Luquimi, Marek69, My Core Competency is Competency, Nodar95, Nono64, ResearchRave, Rjwilmsi, Scottalter, Shinryuu, Soptsai, SuperHamster, Swpb, Topbanana, Vojtech.dostal, Wnt, 44 anonymous edits Epidermis (skin) Source: http://en.wikipedia.org/w/index.php?oldid=550387026 Contributors: Abrech, Adhanali, Alansohn, Albert109, Anduril171, Antandrus, Arcadian, Arctic Kangaroo, Atlantia, Atura, BTLizard, Bpeps, Buzybeez, Capricorn42, Chamonix2010, Chowbok, ChrisGualtieri, Circeus, Closedmouth, Cocoaguy, Coffeepusher, Cybercobra, DRosenbach, Discospinster, DivineBurner, Dlae, Docfaust, Docta247, Dorianrea, Dprady, Dreg743, Epbr123, Espetkov, Eubanks718, Fama Clamosa, Flightx52, Fluffernutter, Franamax, Froggo Zijgeb, Gail, Gareth Griffith-Jones, Geovani.s, Gerriet42, Giftlite, Graham87, GrahamAsher, HarlandQPitt, Hbent, Hellbus, Ironbam7, JFreeman, JakobSteenberg, Jon186, Joshua Scott, Justanotheralias, KJS77, Kazkaskazkasako, Keilana, Krushdiva, L Kensington, LOL, Liaocyed, Life of Riley, Locogato, Lunchscale, Luxor, Mark Arsten, Masaqui, Maximillion Pegasus, McDutchie, Mcstrother, Microdoctor, Mikael Häggström, Mike Rosoft, Minghong, Mocs56, My Core Competency is Competency, Mysdaao, Nicke L, NikNaks, Nn123645, Nodar95, Notmyhandle, Nutsofthemutt, Omegatron, Peirigill, Prof. Squirrel, Pseudomonas, Recurve7, Rjwilmsi, Rocket000, Ronz, SFK2, SSM93, SchfiftyThree, SchreiberBike, Scottalter, ShakataGaNai, Shanes, Someguy1221, SuddenFrost, Surfspecz, SweetNightmares, Tad Lincoln, Tenacious.Genius, The Rambling Man, The Ultimate Koopa, Tide rolls, Tiggerjay, Tim Q. Wells, Tktktk, Tommy2010, Trax247, Troytsm98, Trr82, Trusilver, UninvitedCompany, Vojtech.dostal, VolatileChemical, WLU, Walrustree, Whateveryousaysir, Wikipelli, Woohookitty, Xoid, Zigger, 305 anonymous edits Stem cell Source: http://en.wikipedia.org/w/index.php?oldid=551818881 Contributors: 041744, 04spicerc, 203.170.3.xxx, 217.99.96.xxx, 2602:304:5D60:9499:293F:1DF9:B733:C105, 5 albert square, 9Nak, A.V., A930913, AHands, AVM, Aaron Schulz, Aaron charles, Abb615, Abbaroodle, Abbasbeyli, Aberdam, Accuruss, Acgator09, Adam.douggie, AdamJacobMuller, AdamRetchless, Adashiel, Adenosine, Adraeus, Adrian, Aeon221, Aetheling, AgadaUrbanit, Agathman, Agricolae, Aircorn, Ajournaleditor, Alakey2010, Alan Liefting, Alanliddell, Alansohn, Alasdair.g1998, Alchewizzard, Aldux, Alenshrew, Alex.tan, Alexei Kouprianov, AlexiusHoratius, Alextill95, Alienus, Allen4names, Allmightyduck, AllyUnion, Alphachimp, Altenmann, Altonbr, Amaury, AmiDaniel, Andcarne, Andre Engels, Andres, Andrewbadr, Andrewdekamp, Androstachys, Anetode, Angus Lepper, Anonymous Dissident, Antandrus, Anthonyhcole,
607
Article Sources and Contributors
Antonrojo, Arcadian, Arcus, Argon233, Arkantosstevius, Arkrishna, ArneLH, Arthena, Artichoker, Arx Fortis, Astoman, AstroHurricane001, Astronaut, Astronautics, Atrix20, AuroraReloaded, Austinbond, Autonova, Avb, Averross, Avoided, AxelBoldt, Axl, Aymatth2, Bachrach44, Badanagram, Badarkace, Banman1004, Bartimaeus666, Baughnie, BballJones, Benbread, Bender235, Bento00, Berlickshane, BesigedB, Betacommand, Bethelizebeth, Bfiggis, Bgpaulus, Big Smooth, Big iron, Bigal78, Bigminisachin1231, Bill52270, Bioinformin, Bisyork, Blake-, Blankfaction.tk, Blazersguy, Blkpowernig2, Blonde chik819, Blunub, Bob Wiyadabebe-Iytsaboi, Bobblewik, Bobbyus, Bobo192, Boghog, Bomac, Bongwarrior, Bookandcoffee, Boothy443, Boots bklyn, Boredzo, BorgHunter, BorgQueen, Borisblue, Bradeos Graphon, Braincricket, Brainfood, Brainhell, BreeRobinson, Brendan Moody, Brendanconway, Brian Crawford, Brian Kendig, Brian0918, Brim, Brossow, Brown boi5, Bryan Derksen, Bubbles3, Bucaro1975, Bucketsofg, Buhuzu, Bushytails, Butros, Byornski, C45207, CBFan, CMacMillan, CRUCIFYKEVIN, Cabodoc, Caelarch, Calliopejen1, Caltas, CambridgeBayWeather, Can't sleep, clown will eat me, Canderson7, Capecodeph, Captain-n00dle, Cassivs, Cburnett, Cellmedsociety, Centrx, Change93, Chimera16, ChipsAhoya, Choach, Chocolatelana, Chodorkovskiy, Cholerashot, Chowbok, Chris 73, ChrisGlew, ChrisGualtieri, Chrisdale92, Chrislk02, Chrismeehan, Christopher Parham, Circeus, ClockworkSoul, Closedmouth, Cntras, CoJaBo, Cobi, Cohesion, Colin marks, Conversion script, Corporate.legal, Corvus cornix, Cosmic Latte, Courcelles, Cpt.squeaky, Cquan, Crazycomputers, Crazydog115, Crazynas, Cryptic, CyrilleDunant, Cyrus Andiron, D. Wu, D3monicVeng3ance, DARTH SIDIOUS 2, DGG, DMacks, DVdm, Dabomb87, Dan100, Danandlollie, Daniel5127, DanielCD, Danny, Dantheman531, Darena mipt, Dark.ranger, Darqcyde, Dave Nelson, Davejohnsan, Davewho2, Davfoster88, David Peacham, David Shankbone, DavidCary, Daycd, Dbsteve100, Dbtfz, DeadEyeArrow, Debatesensei, Decumanus, Deepakpurang, Defunkt, Delldot, Demong, DerHexer, Derek Ross, Deselliers, Deving, Dharmabum420, Dimitmant, Discospinster, DividedByNegativeZero, Dlh-stablelights, Dmitry Dzhagarov, Dobett, DocWatson42, DonSiano, Dougofborg, Dr Aaron, Dr d12, Dr.enh, Draeco, Dragostanasie, Drbohlav, Drianmcniece, Drphilharmonic, Drumman91, Drunken Whale, Duckzilla2000, Dusti, Dwayne, ERcheck, ESkog, Ed Poor, EdBever, EdJ343, Edgar181, Egandrews, ElKevbo, Elektrik Shoos, Ellmist, Ellwyn, Eloquence, EncMstr, Encephalon, Epbr123, Epeefleche, Espetkov, Esprit15d, Etparle, Eubanks718, Eurobas, Europa284, Everard Proudfoot, Evercat, Everyking, Everyone Dies In the End, Evil Monkey, Evil saltine, Excirial, Extro, FF2010, Fama Clamosa, Fang Aili, Fatalityduff, Favonian, Fenice, Feverinlove, Fic-in, Fingerz, Flatterworld, Fleminra, Florentino floro, Fluffernutter, Flux.books, Flyingdream, Forluvoft, Frankie, Frazzydee, Fredrik, Free Bear, Freeze42084, FreplySpang, Freshyill, FrozenUmbrella, Fstorino, Funky Monkey, G.-M. Cupertino, GSlicer, Gabbe, Gadfium, Gail, Garion96, Garywest1111, Gatewaycat, Gavin300, Gazpacho, Gdo01, Geoff.green, George100, Getaway, Getwood, Gilabrand, Gimboid13, Ginkgo100, Glagolev, Glimz, Glisteringwaters, Gmaxwell, Goethean, Gogglecollector, Goododa, GraemeL, Graft, Graham87, Green88en, Greenbough, Gregbrak, Grendelkhan, Grika, Grm wnr, Ground Zero, Grunt, Gscshoyru, Gurch, Guyonthesubway, Gwen-chan, Gwilym84, Gyll, Gyrofrog, H2g2bob, HJ Mitchell, HRED, Habj, Hadal, Haham hanuka, Hamiltonstone, HandyAndy, Hank Ramsey, Harrisd5917, Harry, Haukurth, Hdynes, Healthwise, Hede2000, Helixblue, Hendog456, Henrygb, Herb West, Heybbyy, Heyhombre, Hfastedge, Hikoto, Hirenism, Hockey87, Holdek, Holyone2, Howcheng, Howdy, Huangcjz, Huon, Hurricane111, Husond, Hut 8.5, I c linguist, I80and, Iced Kola, Id711, Idont Havaname, Iknows, Ilaiho, Immunize, Impact red, InaMaka, Incitatus4, Independovirus, Inthend9, InvisibleK, Iohannes Animosus, Ipscellmate, Irishboy5, Irishguy, Isaacsurh, Isarra (HG), Isgsimeng, Ishikawa Minoru, Iwilcox, Ixfd64, J.delanoy, JForget, JFreeman, JONJONAUG, JWSchmidt, JYolkowski, Jag123, JakobSteenberg, James cudahy, James301294, JamesMLane, Jamintime, Jan1nad, Jarash, Jauerback, JavaJawaUK, Javeryt, Jaysonlam, Jblatt, Jdm64, Jeanettephair, Jeff G., JeremyA, Jersyko, Jezhotwells, Jfdwolff, Jgwlaw, Jh51681, Jim Douglas, Jim hoerner, Jimmybass, Jinkbl0t, Jivecat, Jkelly, Jkp44, Jmabel, Jmh649, Jncraton, Joecool94, John of Reading, Johnstone, Johntex, Jonathan.s.kt, Jonny-mt, Josh.K.Poole, Jossi, Joyous!, Jpkoester1, Jprg1966, Jsan, Juansidious, Jusdafax, Jv9mmm, Jvbishop, Jwalte04, K8bigelow, K955301, KF, Kagome 85, Kamker, Kamocsai, Karafias, Karch, Kbdank71, Keegan, Keesiewonder, Keetoowah, Key45, Kfor, KillZOne, Kim Bruning, Kimiko, KinStrategy, Kingpin13, Kjveeley, KnowledgeOfSelf, Konstable, Korinkami, Korovin2, Krohon, Ksargent, Kungfuadam, Kuru, Kuzaar, Kyphe, L Kensington, Langston, Lankenau, Larba200, Lawilkin, Lazydaisy, Lbuckler, LeaHazel, LeadSongDog, Leafyplant, Leevanjackson, Lelestopme, Leo181, Les boys, Lethaniol, Levtchenkov, Lexor, Lgirard, Lightmouse, LilHelpa, Lilblackmc, LizardJr8, Llull, Logan, Logiboy123, LordRM, Lova Falk, Luddite, Luk, Lukey jones, Lulurascal, Luna Santin, Lupin, M0s6p, MBCF, MDChanderson, MHGinTN, MIT Trekkie, MOF, MONGO, MPS, MZMcBride, Magicnxnja, Magioladitis, Magister Mathematicae, MagneticFlux, Magnus Manske, Maha ts, Malleus Fatuorum, Malo, Mandarax, Manogamez, Marcogreguzzoni, Marcos987, Marek69, Mark Lewis, Martinp23, Martyman, Masonian, MastCell, Master of Puppets, Materialscientist, Mathprog777, MatthewJS, Matty j, Mattythewhite, Maurauth, Mav, Max boettcher, Mbm124verizon, Meaghan, Mediaworker, Megalaser, Meghaljani, Mel Etitis, Melah Hashamaim, MeltBanana, Mfoti610, MiamiDolphins3, Michael Hardy, Michael3180, Michaelas10, Michaelll, Mikael Häggström, Mike Rosoft, Mike6271, MikeF, MikeSar, Milnivlek, Mindspillage, Minimac, Mirabellen, Mirceat, Mishmash8, Mister Congeniality, Misza13, Mjharrison, Mjmurphyjr, Mlaffs, Mlpearc, Mmxx, Mocirne, Modemac, Moe Epsilon, Moeron, Moink, Monty845, Moop stick, Moosepers, Moriori, Mpt, Mr Stephen, MrOllie, Mu5ti, Mullagatawny, Munna.alerts, Mwanner, Myanw, N5iln, NYCJosh, Nadejla, Nadyes, Nakon, Nanpae, Narayanese, Nashpaul, Natgoo, Naturespace, Naudefj, Naus, NawlinWiki, Ncrm, Nectarflowed, NetRolller 3D, Netsnipe, NeuronExMachina, Neutrality, NewEnglandYankee, Nichefinder, Nicholas Cimini, Nick123, Nickst, Nicolae Coman, Niels, Nightscream, Nihiltres, Nina, Nishkid64, Nivix, Nobleeagle, Nohat, Nonerds2, Noq, Notreallydavid, Nouseforaname312, NuclearWarfare, Numbo3, O.Koslowski, OOODDD, Oarih, Obesegypsi, Oblivious, Obradovic Goran, Octane, Ohio34895, Ojigiri, OlEnglish, Olbrich, Oliverdl, Omhafeieio, OnlyWayne, Orange Suede Sofa, Ormers, Oskar Sigvardsson, Otvaltak, Owen, OwenX, Oxfordwang, Oxymoron83, PDH, PFHLai, Pakraw, Paleorthid, Paranoid, Parijata, Parkyk219, PatrickFisher, Paul August, Pegasus1138, Perfectblue97, Peter Chastain, Peter Ellis, Peter Znamenskiy, Peterish, Peyton20, Pflueger, Pgan002, Pgk, Phidauex, Philg88, Philip Trueman, Phizzy, PhuryPrime, PiMaster3, PinchasC, Pinethicket, Pingveno, Plain jack, Plastikspork, PochWiki, Poetnk, Polyparadigm, Poothebob, Potionism, Pramod Vora, Prasadmalladi, Prestonmcconkie, Previously ScienceApologist, Prince wiki thai, Private Butcher, Provider uk, Prowler08, Pschemp, Pugetbill, Pvosta, Quiddity, Quizkajer, Qwyrxian, R'n'B, RDBrown, RJII, RMann, RadioFan, RadioKirk, Raekwon, Ralphxcrunner, Raul654, Ravenswood, Ravidreams, Rdsmith4, Realm of Shadows, Regener, Reinyday, RelentlessRecusant, RenamedUser01302013, RenamedUser2, RexNL, Rfl, Rhobite, Ricardogpn, Rich Farmbrough, Richard Taylor, Richiekim, Rjwilmsi, Rkevins, Rmosler2100, Roadghost, RobM, Robert Happelberg, Rod57, Rogen123, Ronabop, Ronhjones, RoyBoy, Royalguard11, Rrburke, Rtdrury, Ruha9, Ruineye, RunOrDie, Runningamok, Ruud Koot, RyanGerbil10, Ryanjunk, Ryddragyn, SJK, SMC23, Sailer247, Sam Korn, SamMichaels, Samsara, Sango123, Sankalpdravid, Sasha Kopf, Savant13, Savidan, Scapermoya, Scarian, Scemers, Schzmo, Scohoust, Scottttttt, Seahorseruler, Sean Whitton, Sean William, Sean.hoyland, Seans Potato Business, Seaphoto, Searchme, SearedIce, Selkem, Seriv, Seth Ilys, Seth brady, Shafei, Shanes, Shangrilaista, Shibby970, Shorthoped again, Shrinkshooter, Sigma77, Sil3nt4ss4sin, Silicon Beach Comber, Silver seren, Simetrical, Siroxo, Sjakkalle, Skier Dude, Skittle, SkyWalker, Slakr, Slowking Man, Smackerlacker, Smalljim, Snap Davies, Snek01, Snoop a la boop, Snow Blizzard, Snowbord60, Snowmanradio, So cool, Soccerkid1212, Sodium, Solitude, Some jerk on the Internet, Someoneinmyheadbutit'snotme, Sonare, Sonic3KMaster, Spalding, Speimer, Spicywiener123, SpikeToronto, Spoon!, Sriram sh, Srlasky, Stable attractor, StaticGull, Stbalbach, Steinsky, Stemcell2, Stemcellhub, Stemcellmafia, Stemscientist, Stephen Compall, Stephenb, Stevenfruitsmaak, Stocx, Strangethingintheland, Sundar, Sunshine4921, Svick, Svm2, Switchercat, SylviaStanley, Systemfolder, Sziegler, T-woo22, THEN WHO WAS PHONE?, TMLutas, Tabletop, Tangotango, Tapir Terrific, Tasc, Taw, Tawker, Tbhotch, Ted4d7, Tedwardo2, Teflon Don, TenOfAllTrades, Terence, Tero, TestPilot, TexasAndroid, The Anome, The Haunted Angel, The High Fin Sperm Whale, The Librarian, The Rambling Man, The Thing That Should Not Be, The colledge teacher, The7thmagus, TheAxeGrinder, TheFourFreedoms, TheLimbicOne, TheMidnighters, ThePointblank, Theglockner, Theredbanana, Thestonesfieldmonster, Thethird33, ThomWatson, Thunder365, Thunderboltz, Tide rolls, TimVickers, Timwi, Tintin1107, Tish18, Tizio, Tlotoxl, Tobby72, Tobias Hoevekamp, Tobymanchee, Todderk, Todobo, Tolly4bolly, Tom Morris, Tom harrison, Tombomp, Tomgally, Tommy2010, Tony Sidaway, Tooto, Topmec, Toughpigs, Toyokuni3, Toytoy, Tpbradbury, Tpikonen, Tregoweth, Trekphiler, Triscomn1, Truejim, Trusilver, Tslocum, TubularWorld, TwoTwoHello, TyA, Tycho, UBERxL33T, UConn Multimedia, Ucanlookitup, Uncle Dick, Uncle G, Usbdriver, Useight, User27091, Userdce, Vague Rant, Vanished user 19794758563875, Vanished user 39948282, Vanished user svinet8j3ogifm98wjfgoi3tjosfg, Vedranf, Velella, Versus22, Viewtiful Zoidberg, Vikkidly, Vin9, Vindicata, Vinegarfod, Violetriga, Vir, VirtualSteve, Visual Basic 5.0, Vogon77, Vrenator, WLU, Walik, Warren.cheung, Wavelength, Wayne Slam, Wayward, Webclient101, Werdna, Who, Wi-king, Widr, Wik, Wiki alf, Wiki emma johnson, Wikiborg, Wikipelli, Wikitavanti, Will314159, Wimt, Wjfox2005, Wmahan, Wojcz, Wolf ODonnell, Wolfkeeper, Woohookitty, Wordwhiz, Wykis, Wywin, Xanchester, Xaosflux, Xcrunner29, Xenonice, Xiahou, Xnuala, YELKENN, Yadmat, Yamaguchi先 生, Yamamoto Ichiro, Yansa, Yeah nit, Yegorka, Yolo12348, Yossarian, Youssefa, Youssefsan, Zachfdog, Zachlipton, Zanter, Zeamays, ZimZalaBim, Zsinj, Ztrawhcs, ТимофейЛееСуда, आशीष भटनागर, 上 野 彦 馬, 2350 anonymous edits Huxley's layer Source: http://en.wikipedia.org/w/index.php?oldid=544474708 Contributors: Arcadian, Garion96, Human anatomy, Lavateraguy, My Core Competency is Competency, Scottalter, WhatamIdoing Henle's layer Source: http://en.wikipedia.org/w/index.php?oldid=544474808 Contributors: Arcadian, Flowingaa, Garion96, Human anatomy, JakobSteenberg, Lavateraguy, MZMcBride, Scottalter Trichocyte (human) Source: http://en.wikipedia.org/w/index.php?oldid=546651822 Contributors: Arcadian, Barneca, Eleassar, Franamax, GregorB, Irwin McLean, JoeVector, RDBrown, Smith609, Xp54321, 2 anonymous edits Epithelium Source: http://en.wikipedia.org/w/index.php?oldid=549046203 Contributors: 16@r, 777sms, A01chtra, ABF, AS, Accurizer, Addihockey10, Adrian J. Hunter, Adrian.benko, Aeon1006, Agstf, Alansohn, Alex S, Alex.tan, Andreas Erick, Animeronin, Anoddgirl, Antandrus, Anthonyhcole, Arakunem, Arbitrarily0, Arcadian, Arctic Kangaroo, Arthena, AshLin, Avoided, AxelBoldt, Axl, Az29, Barticus88, Belovedfreak, Bensaccount, Black Kite, Bobo192, Bobomarch, BrightStarSky, Brighterorange, Britney901, Brww, CWii, CambridgeBayWeather, CanadianLinuxUser, Capricorn42, Carlifenkm, Caue.cm.rego, Cbbjch, Choess, Christian75, Chzz, ClockworkSoul, CopperKettle, Crazymonkeyfred, Crimson30, Cyrius, Czar, D. Recorder, Dancingteen, DarkProdigy, Darth Panda, Davidlwinkler, Dcfleck, DeadEyeArrow, Delldot, Diberri, Dipsitenikhil, Dirkbb, Discospinster, DivineAlpha, Djlafu22, Doulos Christos, Dprust, Dr Bilal Alshareef, Drphilharmonic, ESkog, Eeekster, Ekko, EncycloPetey, Epbr123, Everyking, EvilResident, Excirial, Fenkys, Fongus5555, Frammo, Freshlysqueezedorangejuice, Frycow, Geoffrey Gibson, Gilliam, GoShow, Gogo Dodo, Gongoozler123, Graham87, GreatWhiteNortherner, Gurch, Gwynnet, Hadal, Hexane2000, Higbvuyb, Hima.1234, Hroychow, Hu12, Ihope127, ImmortalAl, Immunize, Iune, Ixfd64, JPaestpreornJeolhlna, Jabronimus, Jag123, JakobSteenberg, Jcmo, Jcwf, JeffreyN, Jennes83, Jesanj, Jfdwolff, Jfingers88, Joehall45, JoeyC1313, John Elson, Jonathan.s.kt, Josephingraffia, Juliancolton, Kaiwhakahaere, Kazkaskazkasako, Kbdank71, Keithonearth, Kewpid, Kfogel, Kibi78704, Kku, Knutux, Krawi, L Kensington, LLDMart, Lfoley123, Lifeguard79, Lir, Lkc159, Llywrch, Lmatt, LoonyLuke, Lotje, LovesMacs, Lovesick, Lriley47, Maork, Mark Arsten, Masterpjz9, Mateuszica, Maxis ftw, Maxviwe, Mayur, Meredyth, Mesoderm, Midozx, Miguel.mateo, Mikael Häggström, Millermk, Minna Sora no Shita, Mstislavl, Mushin, N2e, Naudefj, NewEnglandYankee, Nguyen Thanh Quang, Nikai, Nilsonne, Nimish17102000, Nirakka, Nixeagle, Nonagonal Spider, Northamerica1000, Nsaa, Orenburg1, Paste, Pdcook, PeaceNT, Peony Muds, Peter G Werner, Peter.C, Philip Trueman, Piano non troppo, Pinethicket, Plasticup, Pozytyv, Pro crast in a tor, Pstoker, Putney Bridge, Quirk, R. S. Shaw, RDBrown, Radiant chains, Rajah, Rakaha, Ravenbrand, Rdnewman, Renato Caniatti, Rettetast, RexNL, Richiez, Rjwilmsi, Rockhurst singer, Rolando555, Romanm, Rsmn, Rubybrian, Samarqandi, Sardanaphalus, Sbbeef, ScAvenger lv, Scottrainey, Scumbagdog, Scyldscefing, Sfmammamia, Shuanang, SimonP, Sionus, Sir Nicholas de Mimsy-Porpington, Sirshane13, Sky380, Sree.korrapati, Steve2011, Sxoa, THEN WHO WAS PHONE?, Tarotcards, Techdawg667, Tempodivalse, Thatguyflint, The Thing That Should Not Be, The cattr, This lousy T-shirt, Tide rolls, Tristanb, Triwbe, Unknown0801, VanessaLylithe, Vinnievinz06, Vinvik420, Vogon77, Vsion, Wavelength, WereSpielChequers, Widr, WikHead, WingateChristopher, Wisebridge, Wtmitchell, Wysdom, Yserarau, Zarius, ZimZalaBim, 577 anonymous edits
608
Article Sources and Contributors
Squamous epithelial cell Source: http://en.wikipedia.org/w/index.php?oldid=540784155 Contributors: Arcadian, AxelBoldt, Bensaccount, CanadianCaesar, ClockworkSoul, DasBub, Diberri, Dougluce, Drphilharmonic, Epbr123, Fanatix, Fratrep, Gilliam, Gimboid13, Hmwith, InvictaHOG, Jfdwolff, Joehall45, KDS4444, Karlthegreat, Kdavidk, Kgibs, Killiondude, Kjkolb, Korg, Largoplazo, LeaveSleaves, LilHelpa, M1ss1ontomars2k4, Mesoderm, Michael Hardy, Mike2vil, Myr heille, Naranoth, Nephron, Northerncedar, Novangelis, Pajz, Riana, S3000, Saebjorn, Scapermoya, Serephine, The RedBurn, The Thing That Should Not Be, TheGerm, Thstehle, Tide rolls, Tommy2010, Triplepoint217, 91 anonymous edits Hair cell Source: http://en.wikipedia.org/w/index.php?oldid=551502709 Contributors: A314268, Aaron north, Abhishkeghsh8, Anthonyhcole, Arcadian, Auntof6, Beansweet99, Bexxyboop, BillC, Bingme2001, Bobjgalindo, Caitlinmayhew, Christoffer von Schwerin, Clicketyclack, CopperKettle, Cpl Syx, DARTH SIDIOUS 2, Delldot, DiMare, Diberri, Dicklyon, Dinisoe, Dirac1933, EJF, Fences and windows, Gfoley4, Gobeirne, Hart9bay, Hodja Nasreddin, Hooperbloob, Ibderm, Iroewer, JWSchmidt, Jasmin Ros, KRibble, Katieh5584, Kauczuk, Kgrad, LeadSongDog, Legion fi, Lexor, Lylz jenny, Madhero88, Marcel31, Marek69, Martin451, Mikael Häggström, NawlinWiki, NifCurator1, Nrets, Nunh-huh, Owen, Paul venter, Pauli133, Pinethicket, Rhys, Rich Farmbrough, Rjwilmsi, Robert P. O'Shea, Robertinventor, SDC, SQGibbon, ST47, Sanguinity, Sean William, Selket, Selmo, Skarebo, Smith609, SoundAdvise, St3vo, THEN WHO WAS PHONE?, Tameamseo, Thue, Tiara021, Trusilver, Tycho, Warut, WookieInHeat, Zvar, 120 anonymous edits Sensory neuron Source: http://en.wikipedia.org/w/index.php?oldid=549342412 Contributors: A.Ou, Andymc, Antandrus, Anthonyhcole, Arcadian, CAPS LOCK, CambGrad, Can't sleep, clown will eat me, Carbonix, Ciar, CommonsDelinker, Courcelles, DVdm, Diberri, Dolfrog, Dunedain2558, Eouw0o83hf, Fama Clamosa, Fuzzform, Hodja Nasreddin, Intelati, Ipsenaut, J.delanoy, Jerryseinfeld, JoannaCini, Joshschr, Juzeris, Kauczuk, Kku, Lexor, Looie496, Lova Falk, Magioladitis, Martarius, MaxSem, Metricopolus, Mikael Häggström, Mike2vil, Nepenthes, Nick Number, OLLIEJACKSON, Patstuart, Qxz, R'n'B, Raystorm, Reyk, Robert Daoust, Ronhjones, ShaunES, Slon02, Snowolf, Stantia3, Technopat, Tufflaw, Uncle Dick, Unused0030, Welsh, Wikitavanti, WillowW, ﭘﺎﻣﻔﯿﮕﻮﺱ, 114 anonymous edits Merkel cell Source: http://en.wikipedia.org/w/index.php?oldid=551190471 Contributors: Andreahaws, Arcadian, Beeswaxcandle, Beliar, CarrieVS, Clicketyclack, DeCaux, Dicklyon, Dinisoe, Eleassar, Eoghanacht, Fama Clamosa, Fratrep, Jh51681, Joaquin008, Jonathani1, Juicy-one, LittleHow, Margaret52, Merkelcell, Michael Hardy, Motyka, My Core Competency is Competency, NifCurator1, Rjwilmsi, Rubybrian, Scapermoya, Spaully, Tomas e, Vojtech.dostal, Zixaq, 28 anonymous edits Olfactory receptor neuron Source: http://en.wikipedia.org/w/index.php?oldid=550901612 Contributors: Aboalbiss, Aicchalmers, Arcadian, Archelon, Armen Enikolopov, Boghog, Clicketyclack, Cowbert, Daniel Mietchen, Delldot, Dicklyon, Dinisoe, Fantomdrives, Fredrik, Gobonobo, Hcaldwell, MJ94, MarXidad, MelForbes, NifCurator1, Nihiltres, Nono64, Nrets, Pekaje, PlaMarky, Sachio340, Sarenne, Sayeth, Selket, Sluox, Template namespace initialisation script, Vrenator, Xbcj0843hck3, 45 anonymous edits Photoreceptor cell Source: http://en.wikipedia.org/w/index.php?oldid=550892341 Contributors: AED, Ambitiousboy, Appraiser, Arcadian, AxelBoldt, BD2412, Bensaccount, BobbyBoulders, Bomac, CDN99, Cam27, Canley, Chris the speller, Citotoxico, ClockworkSoul, Closedmouth, CommonsDelinker, Cybercobra, Dcirovic, Delldot, Denis tarasov, Dicklyon, Dinisoe, Download, Drphilharmonic, Drybittermelon, Dual Freq, Excirial, Fangfufu, Fantomdrives, Giftlite, GoingBatty, H2g2bob, Hodja Nasreddin, Hordaland, Horuskemwer, Icairns, Indolering, Iste Praetor, Jag123, JessTobin, Jjron, Jonkerz, Just plain Bill, Kaihsu, Kim Darby, KnightRider, Kosigrim, L Kensington, Lessato, Livick75, Lovemuffin333, Magioladitis, Magister Mathematicae, MartinSpacek, Materialscientist, Mikael Häggström, Mild Bill Hiccup, MollyNYC, Nbhatla, NifCurator1, Nono64, Nrets, Nuno Tavares, Nuvitauy07, Nxtid, Nymf, Old Moonraker, Ost316, Panek, Paskari, PhilKnight, Phtalo, R'n'B, Rayman60, Rbarreira, Rettetast, Rich257, Richard001, Rjwilmsi, Robert P. O'Shea, Sakurambo, Sayeth, Sbierwagen, Science Study, Scott Coleman, Serpent's Choice, Sfgrieco, Slmader, Srleffler, Stemonitis, Steveprutz, Stillnotelf, Tameeria, Tevildo, Theshadow27, Thue, Tipiac, Tjerman, TomViza, Trekphiler, Tyluma, Wickey-nl, Xhin, YUL89YYZ, Yuckfoo, 108 anonymous edits Rod cell Source: http://en.wikipedia.org/w/index.php?oldid=551190660 Contributors: 2405:B000:703:2:90E5:DDCD:1981:2AF9, 777sms, AED, Abmac, Accius, Amplitude101, Arcadian, BenduKiwi, Bensaccount, BillFlis, BirdValiant, CardinalDan, Chris the speller, Darkwind, Davidlwinkler, Dcarney, Dcirovic, Deglr6328, Delldot, Denis tarasov, Dhanish007, Dinisoe, Dinty121, Discospinster, DrBob, Dreviscerator, Duoduoduo, Dureo, Edgar181, Editor randy, Eequor, Eliptis, Emperorbma, Epbr123, Esbboston, Fangfufu, Felisopus, Ghfrisbee, Giftlite, Helix84, HendrixEesti, Heron, Hodja Nasreddin, Hordaland, I dream of horses, Iamthecheese44, Irisx, Ironholds, JTN, Japanese Searobin, Jhfortier, Jjron, Jklin, Jmlk17, Kpjas, La goutte de pluie, Lambyte, Levineps, Ligulem, Lilmike121, Lovemuffin333, Lysdexia, Macy, MadCow257, Madhero88, MaiCall, Mannafredo, Martarius, Materialscientist, MathFacts, Mdsam2, Mitchdarcy, Moe Epsilon, NifCurator1, Noetica, Nono64, Npho, Nuvitauy07, Odie5533, Oxymoron83, PartyDude!, Ph.eyes, Philbradley, Pikiwyn, Qaddosh, Ramaksoud2000, Richard001, Robert P. O'Shea, RodC, Sayeth, Sean.hoyland, Selket, Sgpsaros, Slmader, Smullangi, Spudtater, Stefan.loska, Stephenb, Stillnotelf, Template namespace initialisation script, Teodor605, TokyoJunkie, Unionhawk, Vojtech.dostal, Wapcaplet, Widr, Wikipete, XPTO, Yanij, Zachcoggin, 164 , נטע, ליאורanonymous edits Cone cell Source: http://en.wikipedia.org/w/index.php?oldid=551195039 Contributors: 1F025, 5 albert square, AED, Abmac, Aboalbiss, Ace of Clubs and Spades, Adamantios, Adoniscik, Akulo, Alamnagh, Ale jrb, Alexf, Allens, Amber.mccallum, Anetta773, Anusan.rasalingam, Arcadian, Arno Matthias, Beetstra, Blitterbug, Cacycle, Chagai, Chelmite, Christopherlin, ClanCC, Clopsywiki12, DVdm, Da5nsy, Daniel5127, Dcirovic, Delldot, Deltabeignet, Dicklyon, Dinisoe, Diomidis Spinellis, Discospinster, Dr.enh, DrBob, Drzank, Emperorbma, EncMstr, Epbr123, Fangfufu, FisherQueen, Fred Hsu, GcSwRhIc, GideonMarkCabanban, Gobonobo, Helix84, Hellbus, HendrixEesti, Hodja Nasreddin, Iluvcapra, InternetMeme, JTN, Jacobolus, Janet13, Japanese Searobin, Jeltz, Jfdwolff, Jimfbleak, JinJ, JohnOwens, Jwmillerusa, Kgreer, Kittyblue101, Kpjas, KrakatoaKatie, L'œuf, La goutte de pluie, Ligulem, Loladee91, Lucas718, Lysdexia, MXVN, MadCow257, Madhero88, Materialscientist, Meaghan, Metalman94, Mfc, Michał Sobkowski, Nagualdesign, NawlinWiki, NifCurator1, Nisar.a.shaik, Nn123645, Nono64, Notch, PAntoni, Paskari, Pekaje, Peter Karlsen, Ph.eyes, Phynicen, Quiddity, Quota, RedWolf, ReddyVarun, RexNL, Richard001, Rjwilmsi, SMA2012, Sander123, Shawn81, Shehal, ShelllbyF, Slmader, Sluzzelin, Soccer1818, Srleffler, Stbruton, Stefan.loska, Stillnotelf, Tameeria, Tanthalas39, Template namespace initialisation script, The359, Thirumaran13, Tide rolls, Tideflat, TimBentley, Tyw7, UTSCholar, Vanessaezekowitz, Vojtech.dostal, WereSpielChequers, Wikianon, Wikipelli, Xiaoxuey, Yossofz, Youragain, 193 anonymous edits Carotid body Source: http://en.wikipedia.org/w/index.php?oldid=549094927 Contributors: Alansohn, Alex.tan, Arcadian, Bdmed, Bensaccount, Bomac, Brim, Davidhaha, Edward, EncycloPetey, Feral mage, JackWasey, Jag123, Keb ch, LittleHow, MHillyard, Michael Devore, Micol bode, Mikael Häggström, Morleymonkey, Nbauman, Nephron, Nick Number, Pbergson, PizzaofDoom, Rich Farmbrough, Richardcavell, Rutigor, Stevecalloway, Stone, TheAMmollusc, ThinkerThoughts, Trice2010, Vojtech.dostal, Volantares, Washburnmav, Wjeck, ﺯﻳﺎﺩ, 47 anonymous edits Taste bud Source: http://en.wikipedia.org/w/index.php?oldid=551853855 Contributors: 2A01:E35:2EF8:92E0:A0FC:7F0E:79C4:3D2A, A Raider Like Indiana, A. Parrot, Acole5, Aeonx, Ajaxfiore, Akcarver, Alansohn, Alex nadiger, Alexman1713, Allens, Allycat, Anaxial, AndreniW, Aquilosion, Arcadian, ArchonMagnus, Arthena, Aude, Azazyel, Badgernet, Bathysphere, Bazzargh, Belg4mit, Bn, BoomerAB, Brenont, Bucephalus, CWY2190, CWii, Canadian-Bacon, Catherineroxs1, Charlesbridge, Chris G, Christian75, Craptree, DOHC Holiday, Daedalus969, Debresser, DerHexer, Dicklyon, Doit!, Dontkillme, Download, Drewdesouza, EJF, Eclectic hippie, El Pollo Diablo, Electron9, Epbr123, EvanHarper, Eyrian, Faigl.ladislav, Filovirus, FisherQueen, Gaius Cornelius, Garyzx, Geravago, Gilgamesh he, Gilliam, Gongshow, Graham87, Greenwise1025, Habanero-tan, Hajatvrc, Hanumhartanto, Harpi711, Hu, IGeMiNix, Ianthegecko, Igoldste, Isbelja, IvanLanin, J.delanoy, JEB90, Jblavit, Jebba, Jitterro, Jive Dadson, John254, Johnelson, Johnkarp, Jojhutton, Judithreiter, Jutta, Kane61991, Katalaveno, Keenan Pepper, Lazulilasher, LedgendGamer, Lisatwo, Little Mountain 5, Marek69, Mastercampbell, Meaghan, Mendaliv, Mhsia, Miquonranger03, MnSteve, Moe Epsilon, Molerat, Mononomic, Morel, Mr. Anon515, Mr. Wheely Guy, Mycroft.Holmes, NEUROtiker, Natalie Erin, NawlinWiki, Neurograd, NewEnglandYankee, Nick Number, Niente21, NifCurator1, Nihonjoe, Nono64, NotWith, Novangelis, Nrets, Nsaum75, Nuggetmuncher, Omegatron, Orpheo, Parkerjohnson1234567, Pdauwe, Peter Karlsen, PhilKnight, Philip Trueman, Piano non troppo, Pinethicket, Plumbago, Radon210, Raymondwinn, RedWolf, Reedzupancic, Reverend Loki, Rich Farmbrough, Romanm, Ruittenb, Rumilofaniel, Sarrus, Sayeth, Scott182, Scott5834, Sheled Umlal, Silenceisgod, SilkTork, Smalljim, Stephenb, Sulforaphane, Swerdnaneb, TAKASUGI Shinji, TJ09, TYelliot, Tamorlan, Tanbircdq, Template namespace initialisation script, TheCatalyst31, TheKMan, TheRanger, Thingg, Tide rolls, Tim1988, Tinctorius, Tony Fox, Tonyng84, Tristanb, Tsumaru, Ulcha, Utcursch, Velella, W.stanovsky, WikHead, Wikih101, Williamborg, X!, Yowikiiou, 502 anonymous edits Schwann cell Source: http://en.wikipedia.org/w/index.php?oldid=543678692 Contributors: A.Ou, AHMartin, Ahoerstemeier, Amccloy01, Antandrus, Arcadian, Atif.t2, Bender235, Boing! said Zebedee, Brady8, Brainmachine, [email protected], Capricorn42, Carmichael, Carwil, Chalwalk, Chong Lim, Chris Capoccia, Chris53516, Clicketyclack, DanielCD, Delta G, Diberri, Dino, Discworldian, DocWatson42, Drew1515, Edelhart, Edward Vielmetti, Epbr123, Eras-mus, Erxnmedia, FFMG, Faigl.ladislav, Fantumphool, Flowerpotman, Freederick, Funkysapien, Fyrael, Gaius Cornelius, Galmicmi, Giftlite, Gikü, Graham87, Gurch, Hbdgaz, Heatheralleen, Heikolocher, Ian.thomson, Imoen, Interiot, InternetMeme, Iqzaquezzs, J.delanoy, JForget, Jabronimus, Jag123, Jay Litman, Jfdwolff, KasugaHuang, Kauczuk, Kithira, Kmoraros, Kubigula, Kung Midas, Lightmouse, Looie496, MBVECO, Mego'brien, Moreschi, Nbauman, NorkNork, Philip Trueman, RBJ, ResearchRave, Rettetast, Salvadorjo, SchfiftyThree, Selket, Solomonthepornactor, Sryshti, Sub-life, T.M.M. Dowd, TWIXMIX, Taylorjs, Tb81, The Sailor Poet, Topbanana, Tpk5010, Trevor MacInnis, Ucbtbej, Unyoyega, Wayward, WolfmanSF, Woohookitty, Xanzzibar, Xxxx00, 132 anonymous edits Satellite glial cell Source: http://en.wikipedia.org/w/index.php?oldid=549595869 Contributors: Aircorn, Arcadian, Bueller 007, Burgart, Delldot, Drewlew, Garion96, Garrondo, Gdusing12315, Hazard-SJ, ITasteLikePaint, LaurenMalishchak, Manfi, ManfromButtonwillow, Marc Gabriel Schmid, Muhandes, NeuroJoe, NotWith, Rjwilmsi, Serephine, Ytpete, 23 anonymous edits Neuroglia Source: http://en.wikipedia.org/w/index.php?oldid=550288381 Contributors: 2001:18E8:3:1278:E949:89BF:FE91:62E8, 2D, A purple wikiuser, A5, ABF, AJVincelli, AThing, Abanima, Abhishek727, AfroBrazilian, Alansohn, Amry, Angelic Wraith, Angelito7, Anthonyhcole, Arcadian, Arctic Night, Ardonik, ArizonaLifeScience, Atlantia, Bananastalktome, Bashirshir, Bensh, Biocon, Boomtown90, Bruno Pascal, CardinalDan, Christopherlin, Clicketyclack, Consumed Crustacean, CopperKettle, Cory Kohn, Crohnie, Cwbvb13, DARTH SIDIOUS 2, DRosenbach, Dalibor Bosits, DavidBKinnear, DeadEyeArrow, Delldot, Delta G, Dertilman, Detectivefirstgradesamspade1, Diberri, DocWatson42, Drphilharmonic, Dwaipayanc, Dylan2106, Emiellaiendiay, Epingchris, Ewlyahoocom, Faigl.ladislav, Farqual100, Felicipnzln, Feral mage, FireBrandon, Fizzlebug81, Former user, Furmanj, Gilliam, GlialStudent, Hadal, Hazard-SJ, Hu12, Icairns, Idh0854, Ijustam, Izvora, Jag123, James Pioneer, Janakatechno, Jfdwolff, Jo3sampl, JohnDillon, Johnwprior, JordanDeLong, Joseph Solis in Australia, Jrtayloriv, Jutiphan, Kboor, Khmir2467, KnightRider, Knotnic, Kwamikagami, La comadreja, Lightmouse, LittleHow, Looie496, Luke13579, Mac Davis, Marc Venot, Mark Marathon, Marnoldm, MartinPoulter, Mbartz, Meelar, Mercurywoodrose, Merlion444, Michaelbusch, Mikael Häggström, MrADHD, Mrducks122, Mrs.meganmmc, NBeale, NeoNeuroGeek, Nephron, NifCurator1, Nikai, Nikpapag,
609
Article Sources and Contributors
Northamerica1000, Nrets, Omnipaedista, Oobopshark, Pcu123456789, Pianoplonkers, Rjwilmsi, Rodago, Rojypala, RoyBoy, Sayeth, Sbisolo, Seans Potato Business, Seijihyouronka, Setanta747 (locked), Sir48, Skyezx, Slawojarek, Smithbrenon, Snakesteuben, Son0fHobs, Sparkym3, Steiger, Sunnymedia11, TTile, Tarotcards, Tblackma222, Tdc204, TheLimbicOne, ThePI, Thesis4Eva, Three-quarter-ten, ThreeFt, Tiddly Tom, TonyClarke, Trnj2000, Uthbrian, VernoWhitney, Virtual Loïc, Ward20, Wareh, Whitepaw, William Avery, Xris0, Zsinj, Zubachi, ﻣﺎﻧﻲ, Ὁ οἶστρος, 236 anonymous edits Astrocyte Source: http://en.wikipedia.org/w/index.php?oldid=551191836 Contributors: A purple wikiuser, AManWithNoPlan, Abenedik, AnOddName, Anthonyhcole, Arcadian, Auntof6, AxelBoldt, Betacommand, Biologist2001, Blueshirts, Bruno Pascal, Bunnyhop11, Consumed Crustacean, CopperKettle, Danger, DanielCD, Danny lost, Delldot, Diberri, Dicklyon, Dinisoe, Discospinster, Dr.saptarshi, Drphilharmonic, EhJJ, Eleassar, Eleschinski2000, Eng101, Etrielle, Faigl.ladislav, Feral mage, Franamax, Fuzbaby, Helix84, IONTRANSP, Immunize, Iqzaquezzs, Isnow, Jackol, Jag123, Jeffq, John of Reading, Jonathanischoice, Kauczuk, Kernsters, KevinTR, Klemen Kocjancic, Kso3713, La comadreja, Leokhi, Lerion, Liaocyed, LilHelpa, Litanss, Looie496, Lova Falk, Luke poa, M1ss1ontomars2k4, MER-C, Maralia, MarcoTolo, Marnoldm, MaynardClark, Mhisted, MrADHD, MrDomino, Muhandes, Narayanese, Nephron, NeuroWikiProject, Neurorocker, NifCurator1, Nopedia, Northamerica1000, OldakQuill, Overand, PDH, Pdewilde, Philgoetz, Piltech, PlasmaDragon, Probios, Radagast83, Reactiveastrocyte, Rich Farmbrough, Richi, Rjwilmsi, Rob Hurt, Robodoc.at, Rodago, SDC, SKK123, Sameerbau, Sjschen, Sriram sh, Tea with toast, The Banner, ThinkerThoughts, Timur lenk, Tony1, Truthflux, Txdoc13, VMHman, Vogon77, Wavelength, WereSpielChequers, Whitepaw, Wiki emma johnson, Wikipendant, Wikitavanti, Ww2censor, Wynand.winterbach, Xasodfuih, 174 anonymous edits Neuron Source: http://en.wikipedia.org/w/index.php?oldid=550893151 Contributors: .:Ajvol:., 168..., 2A02:2F02:2021:F00A:0:0:4F77:1AB4, A314268, A8UDI, Absinf, Acalamari, Accurizer, Achowat, Acroterion, Adashiel, Addihockey10, AdjustShift, Adrian CZ, Ae77, Aengus, Ahoerstemeier, Alansohn, Alessandro f2001, Alex.tan, Alexandria, Alexrexpvt, Amazedsaint, Amorymeltzer, Amp71, Amry, Anaxial, Andonic, AndreasPDemetriou, Andres, AndresGottlieb, Animalresearcher, Anmats, Anoop2000, Anthere, Anthonyhcole, Appleseed, Arakunem, Arathald, Arcadian, Arvindn, Ascorbic, Ashv3524, Asianguy48, AugPi, AuroraReloaded, AxelBoldt, AzumayaKoyuki, BJEG5, Babybluepearls08, Bandrow, Barthe7ruth, Bcjordan, Bdesham, Beefman, Belinrahs, Benholter:D, Bensaccount, Bentogoa, Bethnim, Bilz0r, BioProfessor2.0, Biology2k, Birdman1, Blajbal, Bobblewik, Bobo192, Bobosse, Bonadea, Bongwarrior, Brackpedia, Bradeos Graphon, Bradv, Brain-mapper, Brandmeister (old), Branka France, Brendan Moody, Brentor, Brianga, BrotherGeorge, Bryan Derksen, Buzzybirdbrain, C-gold, CSS2013, Callisto2091, Caltas, Can't sleep, clown will eat me, CanadianLinuxUser, Canyouhearmenow, Capricorn42, CarsonsDad, Cburnett, Celestra, Cerealkiller13, Chaojoker, Chizeng, ChrisGualtieri, Chrislk02, Chrispounds, Christian75, Cinnamonsticks, Ciphers, Ckatz, Clement Cherlin, Clicketyclack, ClubOranje, CommonsDelinker, Conversion script, Corinne68, Corvana, Courcelles, Cpiral, Crazytales, Crohnie, Ctbolt, Cureden, CursedKiller95, Cyberman, DARTH SIDIOUS 2, Dan East, Dancter, Danger, Daonguyen95, Darkmeerkat, Darkwind, Darth Panda, David Martland, DavidRader, Dbenbenn, DeadEyeArrow, Deflective, Delldot, Delta G, Deor, DerHexer, Desalato, Dettydet, Diberri, Dicklyon, Digfarenough, Dinisoe, Discospinster, Diza, Djayjp, Dolda2000, Dr.Kane, Drakestail, Dreamafter, Dreish, Drifter3, Driftwoodzebulin, Dry dust, Dysepsion, E23, ESkog, Edan Starforth, Edison, Edward Z. Yang, Emilk, Entropy, Epbr123, Evanherk, Excirial, Eykanal, FMRI, Fastily, Feweria, Flami72, Flashn00b, Fletcher, Floating Boat, Former user 6, Foscoe, Frenchman113, Frozin ice, Furmanj, Furrykef, Fuzheado, Gail, Garydino, Gene Nygaard, Geneb1955, Ghidorah221, Giftlite, Gilliam, Gillyweed, Giraffedata, Gkandlikar, Gleng, GoShow, Goldenrowley, Gordyandramsey, Graminophile, GranBianconero, Gregkaye, Gunjan verma81, Gypsydoctor, Hadal, HaeB, Hagerman, Haham hanuka, Hajenso, HamburgerRadio, Hanacy, Hardyplants, Harland1, Headbomb, Helix84, Hellhound overblood, Hempfel, Henrycranfield, Heyyy123, Hithereifixedurblinds, Hm0ngLauj, Hmrox, Holcombea, Hskwk, Hu, Hullaballoo Wolfowitz, I'm really Sweet, II MusLiM HyBRiD II, Iamthedeus, Ian Pitchford, Immunize, Imoeng, Info wrecker, Info wrecker2, Inkling, Interiot, Intranetusa, InverseHypercube, Invinciblegavin, Ioeth, Ipatrol, Iridescent, Ixfd64, J.delanoy, JForget, JPaestpreornJeolhlna, JWSchmidt, JaGa, Jackhynes, Jackibuddy, Jahayes, Jakeiyounis2, Jakejakejake1313, Jameshfisher, Jauhienij, Jawnpiece, Jaxl, Jayden54, Jcbutler, Jdyachimec, Jeff G., JeffreyN, Jenks, Jeroje, Jimgawn, Jncraton, Jo3sampl, John Price, JohnCD, JonathanWilliford, Jschnur, Jumping cheese, Junglecat, Just Another Dan, JustVisiting, Jutta, Jvr725, KCinDC, Kalexander, Kamilvlcek, Karl-Henner, Kashmiri, Katieh5584, Keenan Pepper, Kevin B12, Kghose, Khargas, Khukri, Kingofslackrs, Kingpin13, Kirkus M, Knight1993, Koavf, Kosigrim, Krashlandon, Kuspyder, Kwamikagami, Kwekubo, L Kensington, La Pianista, La comadreja, Lachlan12345, Ladii artiste, Lam Kin Keung, Laracoode, LeadSongDog, LedgendGamer, Leomessi1094, Lexor, Lightmouse, LilHelpa, LindsayH, Linnell, LittleHow, Lji1942, Looie496, Looxix, Lova Falk, Lradrama, Luccas, Lugia2453, Luna Santin, MER-C, MJ94, Macsking, MadScientistMatt, Magnus Manske, Mailforsid4585, Makeemlighter, Male1979, Marc Venot, MarkEchidna, Markan, Martarius, Martian.knight, Maryamjoon, Massimo Macconi, Materialscientist, Mato, Matt Crypto, Matt Hutson, Mav, Maxis ftw, Maz640, Mccready, Mchcopl, Me020, Medlat, Meduz, Memenen, MemoriesFade, Mendaliv, Mentifisto, Meswallen, Mgiganteus1, Michael Hardy, Mikael Häggström, Mikaey, Mike2vil, MikeX, Mikeo, Mikespedia, Miltonkeynes, Mindstalk, Minimac, Miquonranger03, Miserlou, Mitch Cumberworth, Mod.torrentrealm, Mohd. Toukir Hamid, Monotonehell, Moreschi, Moxfyre, Mpatel, Mphi03, MrFish, Mydrian, Mygerardromance, Mütze, NCurse, NPalmius, NaLalina, NawlinWiki, Neurophilia, Neutrality, NewEnglandYankee, NifCurator1, Nihiltres, Nk, Nlu, No1lakersfan, No3, Nolelover, Nomad2u001, Nono64, Northfox, Nposs, Nrets, NuclearWarfare, Numbo3, Odie5533, OldakQuill, Ombudsman, Orangemarlin, Otisjimmy1, OverlordQ, Oxymoron83, PahaOlo, Panoramix303, Panscient, Parker007, Pedroshin, Penwhale, Persian Poet Gal, Pharaoh of the Wizards, PhilKnight, Philip Trueman, PhineasG, Pie Man 360, Pinethicket, Pkatz, Pnkrockr, Pontificalibus, Pr495du, ProBonoPublicoA90, Proofreader77, Pseudomonas, Ptrf, R'n'B, RUL3R, RadioFan, RainbowOfLight, Ramaksoud2000, Randompedia, Rberlow, Redbo, Rettetast, RexNL, Reyk, Rhetth, Rib0fl4vin, Rich Farmbrough, Richwil, Ridge Runner, Rjstott, Rjwilmsi, Robin klein, Robinatron, Robma, Rrichhart, Rror, Rsabbatini, Rukuruku, RussellMcKenzie, Russfrohardt, Ruy Lopez, S.cheese, SJFriedl, SJP, Sabre23t, Saganaki-, Sarah Cherlin, Savant13, Scarian, SchfiftyThree, Schumi555, Schwartz1011, Scott5114, Sel0003, Selket, Setanta747 (locked), Seyet, SgtThroat, Shadowjams, Shame On You, Shattered, Shawdogg12, Shenme, Shock an awe, Silas S. Brown, Silverxxx, Sjschen, Skizzik, Slarson, Smalljim, Snehalshekatkar, Snow Blizzard, Snow.blizzard, Some jerk on the Internet, Someone else, South Bay, SpNeo, SpaceFlight89, SpyMagician, SriMesh, Stain, Stephendcole, Sternthinker, Storm Rider, Strzelczyk, Studentne, Sunray, SuperHamster, SvenGodo, Sverdrup, Synaptidude, Tahome, Tarotcards, Tbhotch, Teles, Terence, Thanhluan001, The Recycling Troll, The Thing That Should Not Be, The.Filsouf, TheEgyptian, TheKMan, TheTechMaester, Theirishpianist, Thingg, Thtraddles, Tide rolls, Tilo1111, Tlork Thunderhead, Tom harrison, Tomwsulcer, Tony Fox, Treisijs, Tryptofish, Twilight Realm, Tylerttts, UA1high, Undercovervision, Varuna, Vetty123, Vina, Vrenator, Vyn, Vyroglyph, Wakebrdkid, Wanderingpeanut, Wavelength, Wdfarmer, Wegener1406, West.andrew.g, Wik, WikiPuppies, Wikicallen, Wikipediawikipedia123, Wikipelli, Williamemersonwood, Wimt, WissensDürster, Woohookitty, Wouterstomp, Wranadu2, Wyoun2, Xargque, Xiahou, Yamamoto Ichiro, Yath, Yerpo, Yettie0711, Yidisheryid, Youandme, Youre dreaming eh?, Yuriy Kolodin, Yvwv, Zach425, Zfaulkes, 1154 anonymous edits Oligodendrocyte Source: http://en.wikipedia.org/w/index.php?oldid=550872701 Contributors: Angela, Anthonyhcole, Anypodetos, Arcadian, Bobblewik, Boghog, BonsaiViking, [email protected], CDN99, Captain-n00dle, Cbsmall1, CecilWard, Clicketyclack, Dabomb87, Delta G, Deltaecho, Deviator13, Diberri, Dicklyon, Dinisoe, Drphilharmonic, EncycloPetey, Faigl.ladislav, Iqzaquezzs, Jag123, Jfdwolff, Jrockit24, Juraska, Kauczuk, Koavf, La comadreja, Ligulem, Looie496, Lova Falk, Lundse, Maria.Kukley, Matthew Kelly, Methoxyroxy, Nbauman, NifCurator1, Nihiltres, OldakQuill, Parker007, R'n'B, RJFJR, Rjwilmsi, Rōnin, Skiron, Smallman12q, That Guy, From That Show!, TheJJJunk, TogetherinParis, Uman1916, Vasiľ, Wiki emma johnson, Wvangeit, Xris0, 77 anonymous edits Spindle neuron Source: http://en.wikipedia.org/w/index.php?oldid=551849656 Contributors: 1000Faces, Acsantis, Aempinc, Aleixalix, Alfio, Armarshall, BD2412, Beckydornon, Bob, Bryan Derksen, Cberry01, CopperKettle, Dr.enh, Efb18, Envygreen333, Ettrig, Eubulides, Gwnucha, Igiffin, Iztwoz, J.delanoy, Javidjamae, Jcarnelian, JoeSperrazza, Joel7687, Jogloran, John Bessa, JorisvS, KenyaSong, Kghose, Khazar2, LittleHow, Lostart, Lotje, Malangthon, Mandarax, Moe33, Neil916, Nephron, NeuronExMachina, Nsnyder, Ombudsman, Pluto888, Pluto988, RDBrown, Rich Farmbrough, Rjwilmsi, SCEhardt, Selket, Southclh, T Long, TedPavlic, Vokesk, Woohookitty, 65 anonymous edits Hepatocyte Source: http://en.wikipedia.org/w/index.php?oldid=549384842 Contributors: Alee2000, AmiDaniel, AndreasJS, Arcadian, Bensaccount, Bentogoa, Bobo192, Bomac, Casliber, Chemya, CommonsDelinker, CopperKettle, Crazysane, Dcirovic, Eleassar, Florian Huber, Franamax, Gibbja, Gogo Dodo, Ilke71, J.delanoy, JackWasey, Jag123, January, Jeffq, Jfdwolff, Jimmyvet, Johncartmell, Kaarel, Kristenq, Ksero, Leuko, MZMcBride, Maelstromm, Mikael Häggström, Mike2vil, Mindmatrix, Nereocystis, Neznanec, NotWith, Ntsimp, Optichan, Pepper, Pinkysnowbunnyco, Quadell, Reo On, ResearchRave, Rhcastilhos, Riana, Rich Farmbrough, Rror, Rsabbatini, SchreiberBike, Sclohr, Scottalter, Seaphoto, Skizzik, StacyMGA, Tarek, Tide rolls, ToNToNi, 97 anonymous edits Adipocyte Source: http://en.wikipedia.org/w/index.php?oldid=542220303 Contributors: AThing, Adipocytes, Agibso02, Alansohn, Arcadian, AvicAWB, BeardWand, Celuici, Ceyockey, Chris Capoccia, Chris b shanks, ChrisGualtieri, Dagilson, Dan Polansky, Dan Wylie-Sears 2, David from Downunder, Devilanna, Dgiroux, Discospinster, Dr R Bowri, Drphilharmonic, Enigma55, Erich gasboy, Essam Sharaf, FallingGravity, Farosdaughter, Franamax, Gadfium, Glacialfox, Godfinger, Golgi, Htniawiki, Ianml, Jag123, Jfdwolff, Jmh649, Kanesue, Kenguest, Kibbles5724, Kj29, Kummi, Lenschulwitz, Livingston7, Lugia2453, Man pl, MarcoTolo, Marek Wagner, Mattimals, Mattisse, Mgiganteus1, Mikael Häggström, Mikeo, Mushin, Offiikart, OlliffeObscurity, Pekaje, RainbowOfLight, Rjwilmsi, Rmky87, SchreiberBike, Senator Palpatine, Settersr, Shmike1, The Anome, Trevinci, Uncle Milty, Useight, Wtmitchell, Xochiyotl, Zephalis, ﺭﺍﻣﻰ ﻣﺤﻤﺪ ﻓﺆﺍﺩ, 98 anonymous edits White adipose tissue Source: http://en.wikipedia.org/w/index.php?oldid=550685173 Contributors: Ageekgal, Annalise, Arcadian, Davebridges, Dikteren, Greensburger, J.delanoy, Jennes83, Lenschulwitz, Locos epraix, MER-C, Marek69, MedicRoo, Smallman12q, The Anome, TheBlueFlamingo, Uncle Dick, WhatamIdoing, 24 anonymous edits Brown adipose tissue Source: http://en.wikipedia.org/w/index.php?oldid=547226098 Contributors: Ageekgal, Aiken drum, Albmont, Alex.tan, Amaury, Apoyon, Aragorn2, Arcadian, Arolla, Auric, Boligoma33, Btwied, Bundas, Choij, Christopherlin, CyborgTosser, Daycd, Dogcow, Drphilharmonic, Edgar181, Eteq, Fat7926, Fredrik, Froggo Zijgeb, Fuzbaby, Gaijin42, Georgexu316, GhBatt, Ghosts&empties, Hanacy, Hg6996, Iceanimal, Islam Ezzat, Jag123, Jennes83, Kompas, Kroonepedia, Lenschulwitz, Lijnema, Macetw, Mcstrother, Middayexpress, Mikael Häggström, Mindmatrix, Mr.Rocks, Nbauman, Neil916, Nephron, Pmj, RDBrown, Ricky81682, Riley Huntley, Rjwilmsi, Ruakh, Sanbeg, SharkinthePool, Shingij2, Solvig, StN, Sumo.fatty, Susan118, TastyPoutine, The Anome, Thetrick, TimVickers, Trevinci, Tristanb, Triwbe, Uriel8, Wik, Williamb, Wknight94, Wkrocek, Wouterstomp, Xaosflux, Yamamoto Ichiro, Zer0faults, 111 anonymous edits Hepatic stellate cell Source: http://en.wikipedia.org/w/index.php?oldid=540453653 Contributors: Arcadian, Aukbc, CHARGERLEVANI, Cmcnicoll, CopperKettle, Hodja Nasreddin, Luckydhaliwal, Micga, Rjwilmsi, Temporaluser, Wikielwikingo, Xbcj0843hck3, 3 anonymous edits Podocyte Source: http://en.wikipedia.org/w/index.php?oldid=540670355 Contributors: Adeez, Alperen, Arcadian, Broississy, CheekyMonkey, CopperKettle, Delldot, Diberri, Dpyeon, Eleassar, Franamax, Ganymead, Hadal, IONTRANSP, Iwilcox, Jared81, Jestr, Jorvik29, KC Panchal, Kerowyn, M.Komorniczak, Merfles, Nbauman, Nephron, Papa November, Rhcastilhos, SchreiberBike, Scottalter, Spaully, Swaq, 25 anonymous edits
610
Article Sources and Contributors
Proximal convoluted tubule Source: http://en.wikipedia.org/w/index.php?oldid=550412524 Contributors: A2Kafir, Animeronin, Arcadian, Arthena, Bensaccount, Clicketyclack, Diberri, Drphilharmonic, Evox777, Figma, Fullstop, Gangsterls, GermanX, HeavyQuark, Insorak, Kar.ma, Leolaursen, Mark Richards, Mba123, Mcstrother, Mfwitten, Mikael Häggström, Nephron, Nerdseeksblonde, Pearle, Petesmif, Ph.eyes, R'n'B, Rjwilmsi, Robert.Allen, Scottalter, Skittleys, Spaully, Vwslee, 34 anonymous edits Thin segment Source: http://en.wikipedia.org/w/index.php?oldid=504694966 Contributors: Beeswaxcandle, ChrisGualtieri, Haruth, Ju97les, LilHelpa, Mikael Häggström, Neo1738, 1 anonymous edits Distal convoluted tubule Source: http://en.wikipedia.org/w/index.php?oldid=540846268 Contributors: Aaron Schulz, Alex.tan, Arcadian, Axl, Barefootguy, Beeswaxcandle, Bensaccount, Betacommand, Diberri, GermanX, ImmortalWombat, Jfdwolff, Kuebi, Mcstrother, Mikael Häggström, Mild Bill Hiccup, Nick Number, Nlu, Platysma, PneumaShack, R'n'B, Scottalter, Selket, Spaully, Szalzala, Topbanana, UberMD, WhatamIdoing, 34 , יונה בנדלאקanonymous edits Kidney collecting duct cell Source: http://en.wikipedia.org/w/index.php?oldid=197597645 Contributors: Carlossuarez46, Mikael Häggström, TexasAndroid Pneumocyte Source: http://en.wikipedia.org/w/index.php?oldid=544226953 Contributors: 5-HT8, AkashAD, Alynna Kasmira, Arcadian, Audry2, Bissinger, BubNorr, Caerwine, Can't sleep, clown will eat me, Delldot, Eras-mus, Franamax, Justin.ere, Kilopi, Mj455972007, Mkdw, Nlu, Samith senadeera, Tomas e, Uncle G, Unused0026, Vkotelnik, Vojtech.dostal, Waldmas, 20 anonymous edits Centroacinar cell Source: http://en.wikipedia.org/w/index.php?oldid=544575160 Contributors: Arcadian, Beeswaxcandle, Caerwine, Eikenhein, Franamax, Jebus989, Kazkaskazkasako, Mcstrother, Mikael Häggström, Oxynthes, 5 anonymous edits Collecting duct system Source: http://en.wikipedia.org/w/index.php?oldid=551047419 Contributors: Alex.tan, Arakin, Arcadian, Bensaccount, Bloodshedder, Bogwhistle, Camrn86, Diberri, Drphilharmonic, Drpickem, Eighty8s finest, Enqueror, Enviroboy, Eug, Faduart, Felix-felix, Hoverflysmiles, Hpswimmer, Jfdwolff, Ksaraf, Luckydhaliwal, Materialscientist, Mcstrother, Mikael Häggström, NeilN, Nlu, OldakQuill, Rswarbrick, Ryan Roos, SchreiberBike, Scottalter, Some jerk on the Internet, Spaully, Temporaluser, Welsh, Wikid77, Xionbox, 28 anonymous edits Microvillus Source: http://en.wikipedia.org/w/index.php?oldid=549393530 Contributors: AK456, Alansohn, Angela, Arcadian, AxelBoldt, Belasd, Bensaccount, Bobblewik, Bruinleth, Capricorn42, D, Daf, Dan Gluck, Defwheezer, Deryck Chan, Diberri, Dromioofephesus, Droseratron, Elassint, Frby, Gobonobo, Grover cleveland, Hac13, HandGrenadePins, Hyungjoo98, Hégésippe Cormier, Jag123, Kaarel, Lavateraguy, Maaayowa, Madkayaker, Magnus Manske, Martious, Mh, MrBeeAreWhy, PFHLai, Penghaiyanwiki, RShorty30, Razor Sharp Wisdom, Reyk, Rhys, Robin S, Sarefo, THExGunsliner, Taketa, Thewikipopo, Vojtech.dostal, Wavehunter, Wbensmith, William Avery, Zchangu, 94 anonymous edits Epididymis Source: http://en.wikipedia.org/w/index.php?oldid=551506291 Contributors: 78.26, Abstraktn, AdaronKentano, Anatomist90, Anaxial, Arc Orion, Arcadian, Arjun01, BarkingFish, Biglovinb, Chanlyn, Chevapdva, Chinux, Chris the speller, Cmungall, Deflective, Diberri, Drphilharmonic, Dungodung, Ekem, Flyer22, Fredwerner, Freedomlinux, Fui in terra aliena, Georgette2, Giancoli, Guaca, Guanaco, Hadal, HexaChord, Hkarim19, Hyperborea13, Jabaway, Jag123, JakobSteenberg, Jauerback, Jim1138, Jmarchn, Jpogi, KDS4444, Kauczuk, Keith D, Kwamikagami, LeCire, Lexusuns, LilHelpa, Magioladitis, Mani1, Matt Gies, Mcstrother, Minimac, Naturehead, Nbarth, Nephron, Nsaa, Osnimf, PaddyM, Paul venter, Porcher, Pwjb, Ramurf, Raul654, Red Act, Remember the dot, Robodoc.at, Romanm, RupertMillard, Rushbugled13, Snalwibma, Squids and Chips, Stevenfruitsmaak, Szquirrel, Tameeria, Template namespace initialisation script, The Anome, Vedran12, WLU, Whkoh, Yefi, 100 anonymous edits Ameloblast Source: http://en.wikipedia.org/w/index.php?oldid=540323911 Contributors: Acroterion, Adamlankford, Arcadian, Billyb, Chris Capoccia, DRosenbach, El guanaquito, ElfQrin, Enochlau, Footballfan190, Franamax, Headbomb, InvictaHOG, Jacek FH, Jfraser, Michael Hardy, Nuck3lz, Prasun Dubey, RandomP, Sn0wflake, Zocky, 21 anonymous edits Organ of Corti Source: http://en.wikipedia.org/w/index.php?oldid=539772168 Contributors: A314268, Ahoerstemeier, Albacore, Anlace, Arcadian, Arco de Rayne, Bensaccount, Bobbyphysics, CDN99, Chinasaur, DiMare, Dicklyon, DreamGuy, Eleassar, Fred the Oyster, Granito diaz, Guidod, Gyll, Hashem sfarim, Iqzaquezzs, Jabencarsey, Jmarchn, KnightRider, LeadSongDog, Madhero88, Mangoe, Mgrati, Myocastor, Oarih, OldakQuill, Owen, Paul venter, Peytonio, Plindenbaum, R oshea, RelentlessRecusant, Sweetpoet, Template namespace initialisation script, Was a bee, 38 , ליאורanonymous edits Corneal keratocyte Source: http://en.wikipedia.org/w/index.php?oldid=543868054 Contributors: Arcadian, BD2412, CopperKettle, Ringbang, Rjwilmsi, 2 anonymous edits Tendon cell Source: http://en.wikipedia.org/w/index.php?oldid=488310503 Contributors: A412, Arcadian, Barisal, Chris the speller, Ka Faraq Gatri, Te pukapuka, 2 anonymous edits Bone marrow Source: http://en.wikipedia.org/w/index.php?oldid=551927095 Contributors: AThing, Acdx, Airplaneman, Aitias, Alansohn, Alex.tan, Alexwcovington, Allycat0527, Amroc, AnakngAraw, Angela, Angelito7, Angryshot, Arakunem, Arcadian, Ashadeofgrey, Ashcraft, Astanhope, Aveekbh, AxelBoldt, B9 hummingbird hovering, Baylaurel, Before My Ken, Bejnar, Biomed10, Bjb, Blanchardb, BlueDevil, Blueronin, Bme206timewasting, Bobjgalindo, Bobo192, Bogey97, Boing! said Zebedee, Borbrav, Bz2, COMPFUNK2, CapitalLetterBeginning, CatherineMunro, Catongue, Cburnett, Ceclaeys, Ched, Cholerashot, Chris G, Clarkcj12, Cliff smith, Connormah, Corti, Courcelles, Cpl Syx, Crystallina, Curb Chain, Cxz111, Cybermaniac sachit, Cyrus XIII, DARTH SIDIOUS 2, Danno uk, Deor, Diberri, Discospinster, DiverDave, Diyar se, Dr Aaron, Dr d12, Draalles, Dreadstar, Drphilharmonic, Dysprosia, ERK, Enviroboy, Eras-mus, Erkcan, Erlenmayr, Everard Proudfoot, Excirial, Falcon8765, Fbarw, Fernando S. Aldado, Flowerpotman, Freekozak, Friginator, Funnyfarmofdoom, Fvasconcellos, G Clark, GT5162, Gadriel, Gaff, Gareth Griffith-Jones, Gaurav1146, GehfREE8, Germet, Giftlite, Gigemag76, Gimboid13, Glimz, Gongoozler123, Gregorius Pilosus, Gronky, Gsp8181, Gunkarta, Guðsþegn, Hadal, Hanacy, Haydnaston, HendrixEesti, HexaChord, Hobartimus, IRP, Ifrit, Igoldste, Immunize, Iph, Isfisk, Ish ishwar, IvanLanin, J.delanoy, JMD, Ja 62, JackWasey, Jackfork, Jag123, Jauhienij, Jbergste, Jcbvsn, Jctcool1, Jean.artegui, Jengod, Jfdwolff, Jncraton, Joehall45, Joewright, Johan1298, John, JohnCD, Jordan117, Julesd, Jóna Þórunn, Kandar, Katalaveno, KateSelik, Keilana, Keith Lehwald, Kerowyn, Kim298, King Pickle, Kinotgell, Kukini, L Kensington, Larsobrien, Lateg, LeaveSleaves, Les boys, Lesgles, LiDaobing, Lightmouse, LindsayH, Linzhoo2u, Little Mountain 5, Logan, LordCo Centre, LorenzoB, MER-C, Mad Max, Majorly, Malcolm Farmer, Malvineous, Maralia, Marek69, Marimberito, MarsRover, MastCell, Matthew Yeager, McSly, Michaelmas1957, Mikael Häggström, Mintleaf, Missionary, Monedula, Mononomic, Mr.Z-man, Mysid, Naddy, Nagy, Namayan, Natpowning, NellieBly, Newyowker, Niceguyedc, Nihiltres, Nono64, Notheruser, Nunh-huh, Occono, Oda Mari, Ohnoitsjamie, OliverHovmand, OohBunnies!, Optimist on the run, Otend, OverlordQ, Pacifist, Papercliper, Parent5446, Park3r, Pascal666, Patxi lurra, Persian Poet Gal, Peruvianllama, Phantomsteve, Pharaoh of the Wizards, Philip Trueman, Pinethicket, Polyamorph, Prashanthns, Pyrrhus16, RA0808, RJaguar3, Rachgia, Radon210, Raidon Kane, RandomAct, Registrar, Renato Caniatti, Res2216firestar, Rexbobo, Rklawton, Rkoiym, Roadmr, Robert M. Hunt, Rpm099, Russianplayer, Ryan032, SMC, Satarnion, Sceptre, Schrödinger's Cake, Scruffymmh, Seforadev, ShadowRangerRIT, Shadowjams, Shendar, SimonD, Sjones23, Slakr, Smartse, Smith11v, Socialmediarox, SohanDsouza, Sokching, SonicAD, Splatg, Stevencho, Stevenfruitsmaak, Svick, Syrthiss, TallNapoleon, Teles, Template namespace initialisation script, Tetracube, Tgeairn, Thatguyflint, The High Fin Sperm Whale, The Thing That Should Not Be, Theda, Thehelpfulone, Themfromspace, Thumperward, Tide rolls, Tired time, Tombliboo, Tombomp, Trusilver, U+003F, Uncle G, Venkatesh, Versus22, Vina, Vivio Testarossa, Vldscore, Vulturejoe, Wackjum, Waggers, Washburnmav, Wayiran, WhisperToMe, WhyBeNormal, Wiki13, Workster, Wouterstomp, Wtmitchell, Xxpor, Yidisheryid, Zack325, Zahakiel, Zenwhat, Zoe, Zuky79, Žiedas, Дарко Максимовић, 663 anonymous edits Reticular connective tissue Source: http://en.wikipedia.org/w/index.php?oldid=548534937 Contributors: Arcadian, Beyond My Ken, Bobjgalindo, C.man8, CIreland, CarolP52, Cst17, Darkness Shines, Drahcir, Garion96, Guthrie, Jennes83, Jfdwolff, Kushpatel141289, Macholl, Magairlin, Malcolma, Mgiganteus1, Mikael Häggström, R. S. Shaw, Robert M. Hunt, The cattr, Widefox, Zrenneh, 37 anonymous edits Fibroblast Source: http://en.wikipedia.org/w/index.php?oldid=550367186 Contributors: -- April, Altenmann, Andre Engels, Appraiser, Aqua112233, Arcadian, ArionVII, Asdasder, AxelBoldt, Bensaccount, Biologist2001, Bomac, CTF83!, Cacycle, CardinalDan, Cerealkiller13, Chibi.akutenshi, Ciar, Colin, Corvus cornix, Darked, Dfrg.msc, Dr.saptarshi, Dravecky, El C, EnglishEfternamn, Epolk, Essam Sharaf, FBW, Franamax, Godering, Hendrik Fuß, Holme053, Ibrmrn3000, IvanLanin, J.delanoy, Jag123, Jhfortier, Jitterro, JohnnyCalifornia, Jsc83, Ka Faraq Gatri, Keegscee, KnightRider, Kubigula, Lab-oratory, Leeearnest, Light current, Lir, Mbarden, Mikael Häggström, MithrandirAgain, MuffledThud, Mygerardromance, Nilmerg, Professor marginalia, Robert M. Hunt, Roidroid, Ryddragyn, Sbisolo, Seans Potato Business, Shadowjams, Splette, SubtleGuest, Temporaluser, The Wordsmith, TheLimbicOne, Tide rolls, Tijmz, Tinz, Trevor MacInnis, Wavelength, Wedian, WhatamIdoing, 123 anonymous edits Pericyte Source: http://en.wikipedia.org/w/index.php?oldid=545715839 Contributors: AS, Arcadian, Artw, BD2412, Bloomingdedalus, CarolinaBookHound, Choino, Chrysaor, CommonsDelinker, Dietzel65, Dr Aaron, Drphilharmonic, Eperotao, Eug, Franamax, GSMcL, Hazard-SJ, Jamesdalton67, Jfdwolff, John of Reading, JorisvS, Kuebi, Leeafe, Leeearnest, LewisCS13, LightBringer, MBob, Meneswa, Mild Bill Hiccup, Mistamoneill, Musicmojo, NeuroJoe, PathGrad, Pdauwe, PhiJ, Qetuth, RDBrown, RJFJR, RNAlovesDNA, Rhcastilhos, Rjwilmsi, Robert M. Hunt, Rod57, SchreiberBike, Stepa, TimBentley, Vegaswikian, 50 anonymous edits Nucleus pulposus Source: http://en.wikipedia.org/w/index.php?oldid=542550199 Contributors: A314268, Arcadian, BullRangifer, Cmcnicoll, Cyberknife, EncycloPetey, Fuzheado, Greensburger, JakobSteenberg, Mmrruugg, Sci0x, Spiegelberg88, Wouterstomp, 5 anonymous edits Cementoblast Source: http://en.wikipedia.org/w/index.php?oldid=550436489 Contributors: Ano-User, Arcadian, Brim, Daniel Mietchen, Dozenist, Franamax, Gsingh, Iridescent, Jeffq, Logical2u, Nicolas1981, Serephine, Susesisa, WTucker, 8 anonymous edits Odontoblast Source: http://en.wikipedia.org/w/index.php?oldid=540254983 Contributors: 2004-12-29T22:45Z, Arcadian, BD2412, Bemoeial, Chikiss, CopperKettle, DRosenbach, Doulos Christos, Dozenist, Drano, ElfQrin, EncycloPetey, Gsingh, He Takes A Whiskey Drink He Takes A Cider Drink, Icelight, JamesAM, KMT, Kaarel, Khukri, Mac2664, Mentifisto, Rjwilmsi, Smith609, Supten, Thomas Willerich, TimBentley, WhisperToMe, Wiki alf, 24 anonymous edits
611
Article Sources and Contributors
Hyaline cartilage Source: http://en.wikipedia.org/w/index.php?oldid=551818782 Contributors: Anatomist90, Anthonyhcole, Arcadian, Barticus88, Calaka, Ck lostsword, Credema, Cyrius, Darklilac, Discospinster, Drmies, Epbr123, Fama Clamosa, Footprintx, Ganímedes, Ghirlandajo, Ibrmrn3000, Jagun, Jeff G., JeffreyN, Jennes83, Jmh649, Joshua Scott, Ka Faraq Gatri, MaxSem, Mcstrother, Millermk, Milton Stanley, Mr.Atoz, Mrfordsclass, Name5555, NickCT, Quique H., RainbowOfLight, Riana, Robert M. Hunt, Slysplace, Tgxstudent, Tormentwriter, Who then was a gentleman?, Wikiuser100, 52 anonymous edits Fibrocartilage Source: http://en.wikipedia.org/w/index.php?oldid=546967169 Contributors: Arcadian, ArinArin, Caerwine, Caps tiki, Docfaust, ELLusKa 86, Gobonobo, Jag123, Jennes83, John of Reading, Lir, Mehmet Karatay, Naraht, Nephron, Niceguyedc, RainbowOfLight, River1791, SchreiberBike, Sovbeos, Sxoa, 春 秋 君, 26 anonymous edits Chondrocyte Source: http://en.wikipedia.org/w/index.php?oldid=539671091 Contributors: 2004-12-29T22:45Z, Apers0n, Arcadian, Arostron, Ceyockey, ChadyWady, Cquan, Davidhaha, Eras-mus, Faldizzle, Figma, Franamax, GB fan, Htniawiki, Icairns, Iridescent, Jag123, Ka Faraq Gatri, Kerrigm, Lauranrg, Lemchesvej, Lystrablue, Ncirillopenn, Nibbs06, Nonantum, Robert M. Hunt, Suraj514, The Anome, ThisIsAce, Vojtech.dostal, Ydriuf, 29 anonymous edits Osteoblast Source: http://en.wikipedia.org/w/index.php?oldid=542955391 Contributors: AS, Adrian J. Hunter, Ajlimroen, Arcadian, Astaroth5, Bme206timewasting, Bpat, Brghntr, Cellpath, Checkenpox, Chris 73, Cquan, DRosenbach, Daa89563, Danfa1971, Dawibo, Dr Aaron, Dr. Matteo, Eeekster, Evenios, Fama Clamosa, Firien, Fluffybun, Flute138, Franamax, Freshlysqueezedorangejuice, GAThrawn22, Gabbe, Gabriel Caponetti, Gadfium, H Padleckas, Igoldste, Infrogmation, J36miles, Jag123, Jeff G., Jesanj, Jfraser, Joehall45, Jonemerson, Kinaro, Lemchesvej, Lir, Lockeownzj00, Manuel Anastácio, MasterOfThePuppets, Materialscientist, Moe Epsilon, NawlinWiki, Ncirillopenn, Nephron, Nicke L, Nuttycoconut, Paul 012, Paulkappelle, Peterjanbroomans, Remuel, ResearchRave, Robert M. Hunt, Roboy600, Shibboleth, Stillnotelf, Tameamseo, TheAMmollusc, Tjc, Utcursch, Vojtech.dostal, Wbensmith, Wireddevin, Yacine lil, 116 anonymous edits Osteocyte Source: http://en.wikipedia.org/w/index.php?oldid=543869916 Contributors: Aleashisa, Arcadian, Bluedustmite, Bomac, Brim, Bubbachuck, Bueller 007, Buxtor, Carre, Cellpath, Ceyockey, Coemgenus, DarkFalls, DroEsperanto, Elassint, Epbr123, ForcaForte, Franamax, Fryed-peach, Gadfium, Giftlite, Glane23, Grendelkhan, IRP, InsufficientData, Irbisgreif, Jag123, James McNally, JamesAM, Jameswcheng, Jll, Katychatel, Kdammers, Lbbzman, Lesnail, Lexor, Mcshadypl, Pal5017, Pinar, SchreiberBike, Skicavs, Tameamseo, Tide rolls, Tox, Zink53, 98 anonymous edits Stellate cell Source: http://en.wikipedia.org/w/index.php?oldid=551185417 Contributors: A314268, Arcadian, Bilz0r, Cmcnicoll, Dicklyon, Dinisoe, Franamax, Histomaster, Jaysunn, Minghong, Niceguyedc, NifCurator1, Nikopoley, Roadnottaken, Temporaluser, 11 anonymous edits Skeletal striated muscle Source: http://en.wikipedia.org/w/index.php?oldid=550383579 Contributors: 5 albert square, AHands, Abmac, Acgator09, AerobicFox, Alanstorph, Alphachimp, Amalas, Amalva, Andycjp, Animum, Anthonyhcole, Antiuser, Arcadian, Armin123321, Asenine, Autocracy, Bc789, Ben Ben, Bender235, Bhadani, Biolady101, Bluerasberry, Bms766, Bobo192, Bogey97, Boijunk, Butko, Caltas, Capricorn42, Ccouper, Centurioncode, Chris the speller, Cinkapp, Corruptcopper, Csari, Cumulus Clouds, Cutler, D. Webb, DJ Creature, DRosenbach, DVD R W, DVdm, Dannyyyyyyy, Dante Alighieri, DeadEyeArrow, Delldot, Deon, DerHexer, Diberri, Discospinster, Djinn112, Doug4, Download, Dsyme, Ekren, ElKevbo, EncycloPetey, Enviroboy, Epbr123, Excirial, Flyer22, Foxj, Frankdushantha, Frigotoni, Fyyer, Fæ, Gacggt, Gautehuus, Gciriani, Gcm, Gogo Dodo, Gongoozler123, Gökhan, HCA, Hadal, Hayabusa future, Hectorthebat, Henry W. Schmitt, Horiavulpe, Ingridmfgjelstad, J.delanoy, JDP90, Ja 62, JakobSteenberg, Jan eissfeldt, Jannelliburganduli, Jennes83, Jeremykemp, Jewk, Jjron, Joe Jarvis, Joec456, Juliancolton, Junglecat, Jy, KBworker, Kalaiarasy, Kam012069, Kbdank71, Keilana, Kevin12xd, Kingturtle, Klilidiplomus, Knass097, Kupirijo, Kwertii, L Kensington, Lamaybe, Leeearnest, LimoWreck, Lir, Lowhp1995, Luigifan, Lunettes, MacGyverMagic, Maghnus, Mandarax, Massobusa, Mayur, McSly, Mdecha pup, Measly Swan, Mentifisto, Michbich, Mike Rosoft, MikeJ9919, Mintleaf, Mondeen, N5iln, Nagara373, Naonaonao, NawlinWiki, Neptune5000, Nic tan33, NightFalcon90909, Nightenbelle, Nlu, Nutriveg, O, Oldelpaso, OllieFury, Orphan Wiki, Osm agha, Passw0rd, Patriarch, Pdcook, Peaceduck, Physicistjedi, Physta, Pietaster, Postglock, PranksterTurtle, Profipix, Quailman, RDBrown, RJaguar3, Raul654, Razorflame, Rcf86, Rdsmith4, Reaper Eternal, Redrvm, Rinasoetanto, Robinrhysjones, Rsrikanth05, Rudolf.hellmuth, Ryulong, Sarah sofía, Satellizer, SchnitzelMannGreek, Seaphoto, Segv11, Shanmugamp7, Shin a imai shin, Shira Ronen, Shirulashem, Shreyas4tejas, Shyran, SimonP, Sisyphustkd, Skittleys, Smajie, Smettems, Smr1, Snillet, Someguydude, Spitfire ch, Squire of the Infernal Knight-Lord of Penguins, StAnselm, Stephenb, Storm Hawk, Swid, T456, Template namespace initialisation script, Tempodivalse, Temporaluser, The Haunted Angel, The Thing That Should Not Be, TheTrojanHought, Thingg, Tideflat, Titodutta, Topbanana, Tskuzzy, Ukuk, Uncle Dick, Useight, Vanished user 2340rujowierfj08234irjwfw4, Versus22, Vojtech.dostal, Vrenator, WLU, WOSlinker, Weregerbil, Wik, WikHead, Wikidudeman, Wikipelli, William Avery, Wisdom89, Wknight94, World, XaosBits, Xolom, Y12J, Yahia.barie, Zalgo, 547 anonymous edits Nuclear bag fiber Source: http://en.wikipedia.org/w/index.php?oldid=430772631 Contributors: Arcadian, Dryman, EncycloPetey, FvdP, Livetolearn, Murdochious, Riana, RxS, Some standardized rigour, WikHead, 4 anonymous edits Nuclear chain cell Source: http://en.wikipedia.org/w/index.php?oldid=455015428 Contributors: 1ForTheMoney, Abhih, Chase me ladies, I'm the Cavalry, Franamax, Kel71194, Martijn Hoekstra, Tony1 Myosatellite cell Source: http://en.wikipedia.org/w/index.php?oldid=550903959 Contributors: Arcadian, Asafdar, Bueller 007, Bunnyhop11, Denni, Dilbert2000, Dinisoe, Dr Aaron, EoGuy, Ettrig, Kenmcl2, Mandarax, Manfi, MaxEnt, NifCurator1, Nospamboz, Pandnh4, RDBrown, Rich Farmbrough, Rjwilmsi, StanfordProgrammer, Thomasehall, 54 anonymous edits Cardiac muscle Source: http://en.wikipedia.org/w/index.php?oldid=550669283 Contributors: 2001:558:6045:A0:391F:B005:179D:8DD9, 2602:306:32C3:3430:81D0:82CA:40FD:54ED, 890bhuiop, ABF, Abanima, Achowat, Adh30, Ahoerstemeier, Allstarecho, Altaïr, AnOddName, Andre Engels, Arcadian, Bananastalktome, Bazza1971, Ben Ben, BigPimpinBrah, Bill37212, Binary TSO, Bmord, Bongwarrior, Bubbachuck, Butterfly reflections, Caltas, Carioca, Carlwfbird, Cbass007, Cburnett, Ckatz, Codetiger, Crinoidgirl, CrookedAsterisk, DRosenbach, DVdm, Daniel Mietchen, Danielil, Daonguyen95, Diberri, Discospinster, DjMD, Dreadstar, Drgarden, Drphilharmonic, Dudefromlastnight, Duncharris, Dycedarg, DéRahier, Eeekster, EhJJ, Enlil Ninlil, Epbr123, Eric-Wester, Excirial, Fieldday-sunday, Figma, Frammo, Freedomlinux, Fumitol, G.Kiruthikan, GVOLTT, GeneralCheese, Gfoley4, GgKfc, Gimmetrow, Gisse, Glenusa, Gobonobo, Grade4, Greensburger, Gurch, Guybrush007, Hasha100, Headbomb, Henrik, Hob, Ibrmrn3000, Innkeeper7, Island Monkey, J.delanoy, J04n, Ja 62, JackWasey, Jag123, Jake Wartenberg, Jakob Theorell, JamesBWatson, Jannelliburganduli, Jcaraballo, Jeangabin, Jennes83, Jess Milonaw, Jholman, Jkl, Joehall45, John Elson, JohnJohn, JohnWheater, Johnelson, Jojhutton, Jonah22, JoostyBoy, Joshmo4, Kadellar, Kaitlinnicoleholland, Kayleebabygrl, Keegan, Keilana, Kevin Dorner, Ksheka, Kukini, Kyoko, Latka, Laurasaccount, Lbeben, LedgendGamer, Lir, Lupin, Lynntyler, MER-C, MITBeaverRocks, Madhero88, Manticore, Marek69, MarkkuP, Marshmellis, Mbcannell, McGeddon, Mentisock, Meters, Michbich, Mininbettyinthelrc2k3, Mkikkawa, Movyn, Mr.kornrow, Mschel, Mygerardromance, Nilfanion, Nlu, Optichan, Oscopz, Osnimf, PFHLai, Persian Poet Gal, Peter Fleet, Peter.C, Philip Trueman, Physicistjedi, Pinethicket, PlaydohIsSalty, Ppntori, QuiteUnusual, RDBrown, Rawrr-becky, Red Director, Relleh22hctac, RexNL, Richhead, Rjwilmsi, Rob Hurt, RodC, Ronhjones, Ronz, SV Resolution, Sadads, Schzmo, SciGuy013, Shakiestone, Skizzik, Smajie, Snoyes, Spitfire ch, Stifle, Studerby, Supernovvva, Teenboi001, Template namespace initialisation script, TerraFrost, Tgeairn, The Deviant, The Thing That Should Not Be, TheKMan, TheProject, Thine Antique Pen, Thingg, Tiggerjay, Tijuana Brass, Tropboy, Ttony21, Ukexpat, Verbum Veritas, Vericuester, Versus22, Vinsfan368, Vrenator, W guice, Wavelength, William Avery, Wimt, Wisdom89, Woohookitty, Wtmitchell, Zad68, 533 anonymous edits Purkinje fibers Source: http://en.wikipedia.org/w/index.php?oldid=551464161 Contributors: Acgator09, Arcadian, Captain-n00dle, ChrisGualtieri, CommonsDelinker, Dcfleck, DocElisa, Downtowngal, Drphilharmonic, Edward, EerieNight, Emilyrader, Giftlite, Hadal, Hojasmuertas, Iohannes Animosus, Jusdafax, Jusses2, Kauczuk, Ksheka, Kums, Lbeben, Madhero88, Mikael Häggström, Nathanael, PFHLai, PaddyM, Qertis, Raghith, Rich Farmbrough, Rich257, Rob Hurt, Snek01, Some standardized rigour, Suffusion of Yellow, Synchronism, Template namespace initialisation script, Tevildo, Tracylau1223, West.andrew.g, Whitepowa69, 52 anonymous edits Smooth muscle tissue Source: http://en.wikipedia.org/w/index.php?oldid=551607493 Contributors: 28421u2232nfenfcenc, AManWithNoPlan, Abce2, Acalamari, Acroterion, Alansohn, Alex.tan, Alias Flood, Allens, Anarchivist, Andres, Andycjp, Animum, Anna Lincoln, ApocryphalAuthor, Arcadian, Axfangli, Axl, Backslash Forwardslash, BananaFiend, Blethering Scot, Bluemonkey33, Bobo192, Bogey97, Bolipapel, Boonshoft2013, BozoTC, Brianga, Bryan Derksen, Calaka, CanadianLinuxUser, Carlos T. Blackburn, Cburnett, Chaldor, Chip123456, Choess, Chris 100487, Chris the speller, Cleanupman, Clicketyclack, Cpl Syx, Cremepuff222, Cyfal, DARTH SIDIOUS 2, DRosenbach, DanielRigal, Dark Lord of the Sith, Dark Tea, Daven200520, David D., Decembermouse, DerHexer, Diberri, Discospinster, Download, Drphilharmonic, Dysepsion, EPM, Edgar181, Eivind F Øyangen, Elassint, Eleassar777, Emperorbma, EncycloPetey, Enigmaman, EoGuy, Epingchris, Epothes, Escape Orbit, Falcon8765, Fieldday-sunday, Finlay McWalter, Fishnet37222, Floria L, Frankenpuppy, GetAgrippa, Giftlite, Gz33, HamburgerRadio, Hamiltondaniel, HexaChord, Hey112, Hgcoolz23, IceDragon64, Ilyushka88, Indosauros, Ita3aai, Ivan.vukovic, J.delanoy, JWSchmidt, Jake Wartenberg, Jakob Theorell, JakobSteenberg, Jamesooders, Jamesters, Javawizard, Jennes83, Jeoth, Jfdwolff, Joehall45, John of Reading, Johnelson, Jojhutton, Joshuagross, Kbh3rd, Kevin Rector, Kyoko, LLDMart, Laggard, Lateg, Laug, Leeearnest, LilHelpa, Liorkaplan, Lir, Loyalgadfly, Lrunge, MTKKirkcaldie, Maayaah, Marek69, Mean as custard, Michael Hardy, Mig174, Mikael Häggström, Mkweise, Moilleadóir, Mttcmbs, Mudiej10, NawlinWiki, Nekitsune, NellieBly, NewEnglandYankee, NotWith, Nothingmore Nevermore, Notmanning, Numbo3, Ocaasi, Off2riorob, Oliphaunt, OllieFury, Omicronpersei8, Oxymoron83, PHNX22, PaddyM, Pdavis24, Persian Poet Gal, PeterSymonds, Pharaoh of the Wizards, Phil Boswell, Philip Trueman, Physicistjedi, Polarlys, QVanillaQ, Qooth, R'n'B, Ready, Redpriest187, RexNL, Rhetth, Riana, Richard0612, Rjwilmsi, Robodoc.at, Robvanvee, Ronz, Rspanton, Ryulong, S.O.S66100, Sampi, Sasquatch, Seraphim, Sfmammamia, Shell Kinney, Shirulashem, Sleepy yuci, Slightsmile, Smellsofbikes, Stephenb, Stewartadcock, Suffusion of Yellow, Tahmmo, Teenboi001, Template namespace initialisation script, Tgeairn, The Rambling Man, Thingg, Tom Morris, Trabelsiismail, Tremello, Tresiden, Tristanb, Typing monkey, WLU, Welsh, Widr, Wikipelli, William Avery, Wisdom89, Wknight94, Woggwogg, Work permit, Zandperl, 569 anonymous edits Myoepithelial cell Source: http://en.wikipedia.org/w/index.php?oldid=541269878 Contributors: Arcadian, Bearcat, Caerwine, Delldot, Dr.saptarshi, Enviroboy, Finlay McWalter, JackSparrow Ninja, Jennes83, Malcolma, Noclevername, Prof. Squirrel, Shunju-kun, Uwe Gille, Vojtech.dostal, White Shadows, Woohookitty, 14 anonymous edits Red blood cell Source: http://en.wikipedia.org/w/index.php?oldid=551605912 Contributors: (jarbarf), -df-, 03lausmi, 28421u2232nfenfcenc, AJim, ASEEMASEEM, Academic Challenger, Adambro, Addshore, Adhib, AdjustShift, Ahoerstemeier, Alansohn, Alec - U.K., Alfie66, Ali, Alksub, Alpha Quadrant, Amaher, Andre Engels, Andres, Andrew Delong, AndrewWTaylor,
612
Article Sources and Contributors
Andypandy.UK, Angelic Wraith, Angrycrustacean, Ann Stouter, Anoko moonlight, Anupam, Apers0n, Arcadian, Arisa, Arjun01, ArnoLagrange, Arvind0602, ArwinJ, Asparagirl, AssistantX, Atlantia, Aviad2001, Avoided, AxelBoldt, Baa, Bassbonerocks, Bbb2007, Beaumont, Benjamin.friedrich, Bensaccount, Bfigura, Bidabadi, Bignoter, Bobblewik, Bobo192, Bomac, Bongwarrior, Borgx, Boud, Brantonli, Brianski, BrightStarSky, BryanD, Burek, CIreland, Caeruleancentaur, Caltas, Can't sleep, clown will eat me, Carturo222, Caseydyck, Causa sui, Ccvic2, Chaldor, Chanting Fox, ChongDae, Chris Capoccia, ClockworkSoul, Closedmouth, Corinne68, Corvus cornix, Countincr, Countmike, Cpl Syx, Crack98, Craig Pemberton, Craigmillar94, Crohnie, DARTH SIDIOUS 2, DRosenbach, Dabomb87, Dan Gluck, Daniel5127, Danrudd, Darth Panda, Darthanakin, Davewild, DeadEyeArrow, Debresser, Deus Ex, Dictabeard, Dietzel65, Discospinster, Dogcow, Dogposter, Dominus, DoubleBlue, Download, Dr.Kane, DrMicro, Drmies, Dungodung, E Wing, ESkog, Eaefremov, Ed, Edcgooner, Egmontaz, Ego White Tray, Ekko, Ellywa, Emilyalbinoman, Epbr123, Everyking, Excirial, Ferkelparade, Fieldday-sunday, Fishyghost, Flamingspinach, Fr34k, Fraggle81, Franamax, Fratter, Fredil Yupigo, Fritzlein, Fryed-peach, Frymaster, Funnybunny, Fuzheado, Fvasconcellos, Gabbe, Gawaxay, Gene Nygaard, Giftlite, Gimboid13, Gobonobo, Golfandme, Gouerouz, Grafen, GraybeardBiochemist, Greentryst, GregorB, Grim23, Guest9999, Guy Peters, Hadal, HaeB, Haham hanuka, HalfShadow, HamburgerRadio, Harthacnut, Haza-w, Hellbus, Hempelmann, Hodja Nasreddin, Honette, Hu, Hunterd, Hydrogen Iodide, II MusLiM HyBRiD II, Ihope127, Immortal0king, ImplyingAuthority, Iridescent, J.delanoy, J04n, JNW, JWSchmidt, JaGa, Jakejakejake1313, Jaknouse, James Crippen, JamesTseng, JamillyM, JediLofty, Jeffq, Jfdwolff, Jfurr1981, Jnquach, JoanneB, John254, Johnbrownsbody, Jon salisbury, JonLS, Jordell 000, Josh3580, Jossi, Jsfouche, Juju Power, Jusdafax, Jyril, KC0ZHQ, Kander, Kariteh, Kassal, Katimawan2005, KaySL, Kazrak, Kbir1, Kennycub, Kerfern, Killerkris88, Kineticman, KingTT, Kingpin13, KnowledgeOfSelf, Kpjas, Kriptyk, Krylonblue83, Kubra, Kusma, KyraVixen, L Kensington, L33th4x0rguy, La goutte de pluie, Lahiru k, Landon1980, Lars Washington, LeaveSleaves, Lectonar, Lightdarkness, Lilfti332, Linas, Linzhoo2u, Little Mountain 5, LittleOldMe old, LizardJr8, Looper5920, Lord of the Pit, Lotje, Luckydhaliwal, MC MasterChef, MZMcBride, Mad Max, Madhero88, Magister Mathematicae, Maias, Mailer diablo, Mandarax, Mangal.anukriti, Marek69, Markacohen, MartinGugino, Massimo Macconi, Masterjamie, Masur, Matt Deres, Mav, McSly, Mdw123, Meewam, Mexinadian, Mfero, Michael Devore, Mikael Häggström, Mike2vil, Mindspillage, Minna Sora no Shita, Mintleaf, Miquonranger03, Moe Epsilon, Monkey.invasion, Mrfickle, Mwilso24, Nakon, Natty1991, NeilN, Nemesis of Reason, Netalarm, NewEnglandYankee, Nifky?, Nlu, Norman21, NotWith, Novalincoln, Nsaa, Nscheffey, Nunh-huh, Omnipaedista, Orkybash, Oscarthecat, Oxymoron83, PDH, Pablo-flores, Paul 012, Pb30, Peak, Perspeculum, Peter Karlsen, Phantomsteve, Philip Trueman, Piano non troppo, PierreAbbat, Pinethicket, Pinkadelica, Policarp, Prari, Priyanath, Prolog, Prowster, Prvc, Pschwarzbaum, Puchiko, RUL3R, RainbowOfLight, Razimantv, Rcingham, Reaper X, Recognizance, Reconsider the static, RenamedUser01302013, Rettetast, Rgracesmyrna, Riana, Rich Farmbrough, Rjwilmsi, Rob Maguire, Robo-rory, Rogeriopfm, Roshan baladhanvi, Roux, Rrburke, Rsabbatini, Ryulong, SDY, SGGH, SJP, Sakkura, Salgueiro, Samuel, Samwb123, Santoshpath, Sceptre, Schoolscienceteacher, Scootdive, Scottalter, Scwlong, Ser Amantio di Nicolao, SetRochelewsad, Sfmammamia, Shadowjams, Shanel, Sheitan, Sheogorath, Shirik, Shoeofdeath, Shyamdash, Siegele, Sir Vicious, SkepticalRaptor, Sky Attacker, Slashme, Slowking Man, Smitz, Snowmanradio, Someone else, Spartan, Specs112, Spliffy, SquidSK, Squidnchips, StaticGull, Stephenb, Stevenfruitsmaak, Sundar, SuperHamster, SuperStingray, Sverdrup, SwammerBAM, THEN WHO WAS PHONE?, TYelliot, Talu42, Tanthalas39, Tarquin, Taxman, Tchite, Template namespace initialisation script, Tempodivalse, The Bushranger, The Moose, The Rambling Man, The Thing That Should Not Be, TheEgyptian, Theroadislong, Tide rolls, TimVickers, Tiptoety, Torchwoodwho, Tosta Dojen, Traderjohn, Trevor Wennblom, Treygdor, Trojancowboy, Tsange, Turnstep, Tuspm, Tweetlebeetle367, Tyw7, Umheisman20, Uncle Dick, Valenciano, Vegfarandi, Vipinhari, Vrenator, WDM27, Wardface, Wars, Wavelength, Wayne Slam, Wayward, Wham Bam Rock II, Wiki alf, WikipedianMarlith, Willking1979, Wimt, Wisdom89, Wknight94, WolfmanSF, Woohookitty, Xenobiologista, Yamaguchi先 生, YetiSSM, Yuckfoo, Yurik, Zephyris, Zoomlines, ﺃﺣﻤﺪ.ﻏﺎﻣﺪﻱ.24, ﺳﻤﺮﻗﻨﺪﯼ, 901 anonymous edits Megakaryocyte Source: http://en.wikipedia.org/w/index.php?oldid=543767460 Contributors: A2Kafir, Akradecki, Arcadian, Brightguy88, Bush gem, Ciar, Coldbringer, DO11.10, Darklilac, Eras-mus, EryZ, Franamax, Funandtrvl, Island, JWSchmidt, Jag123, Jdalton308, Jfdwolff, Jordanawell, Kubra, Lennert B, Linzhoo2u, Mcstrother, Meganaos, Mikael Häggström, NCurse, Niceguyedc, Nihiltres, Pauli133, Rampart, Renata3, Rich Farmbrough, Rjwilmsi, Sedmic, Shell Kinney, Smartyhall, Snowmanradio, Thue, Topbanana, TractorDan, Vanishedlight, Vojtech.dostal, Vokesk, Wbensmith, Windwardside, 43 anonymous edits Monocyte Source: http://en.wikipedia.org/w/index.php?oldid=543384906 Contributors: Acetylcholinesterase, Adrian.benko, Alex.tan, Andy Rosenthal, Angesee, Arcadian, Arcturus, Ariconte, Audrius u, Audriusa, Auenfeld, Auntof6, Banan14kab, Barkeep, Bazzargh, Besieged, Bobblewik, Bobjgalindo, CS99, Camw, Ciar, CommonsDelinker, DO11.10, DoubleUnderscore, Download, Drjames1, ELLusKa 86, Eras-mus, Facts707, Fawcett5, Fluffernutter, Franamax, Friedo, GrahamColm, Jduffner, Jfdwolff, Joehall45, JohnJohn, JorisvS, Kaiba, Karl Dickman, Ksyrie, Kubra, Kumold, Linzhoo2u, LittleHow, Luigifan, Mattert, Mgiganteus1, Michael Devore, MichaelJanich, Mikael Häggström, Mike2vil, Mild Bill Hiccup, Mm1972, MuanN, Octahedron80, Osm agha, Palanq, Paul Klenk, Pissant, PornAndPrawnExtravaganza, RelentlessRecusant, Rjwilmsi, Rlmorgan, Rmarik, Rod57, Scien801, Seans Potato Business, Skittleys, Snowmanradio, Spark.bisht, TerraFrost, Varlaam, Veganfanatic, Wikijens, Yamla, 104 anonymous edits Langerhans cell Source: http://en.wikipedia.org/w/index.php?oldid=539736855 Contributors: AlphaEta, Arcadian, Artw, Beyond My Ken, Bobby70, Bstandley, Bus stop, Ceyockey, Chris Capoccia, Chris the speller, Chris53516, CopperKettle, Countincr, DRosenbach, Diberri, Docfaust, Dr. F.C. Turner, Drjames1, Fatphil, Fratrep, Glucose6phosphate, GregorB, Haymanj, Hovea, Ianbrettcooper, Jakew, Jarble, Juicy-one, Junkyardprince, Kauczuk, Kerowyn, Koene, Kogejoe, Lambiam, M.M, MaxEnt, Mikael Häggström, Millueradfa, Mion, NetRolller 3D, Nicke.me, Pinethicket, Pixie, Plasticup, Rich Farmbrough, Schneedrache, Scottalter, Snowmanradio, Studiodan, Szlevi, Timberframe, Tremello, Uthbrian, Vojtech.dostal, Woohookitty, Xwdl, Zandrous, Ziusudra, 38 anonymous edits Platelet Source: http://en.wikipedia.org/w/index.php?oldid=546736053 Contributors: .:Ajvol:., A.j.perrin, ABF, AZDub, Adeez, Adrenalinehound, Aesculap, Alekseyenko av, Allergist, Anders.Warga, Andreas Toth, Anto217, Apers0n, Arcadian, Arstchnca, BadCannstatt, Ben.roham, Bensaccount, Bigdumbdinosaur, Bignoter, Bjb, Bmecoli, Bobblewik, Bobjgalindo, Bomac, Brianski, Bryan Derksen, C.Fred, COMPFUNK2, Calmer Waters, Caltas, Capricorn42, CatherineMunro, Ceyockey, Chris the speller, Ciar, CommonsDelinker, Costis pap, Damian Yerrick, Davewild, Davorian, Dawn Bard, Deagle AP, DerHexer, Diberri, Dietzel65, Dlovinger, Double positive, Dr. Doof, Dr.michael.benjamin, Dr.saptarshi, DrMicro, Draeco, Dreviscerator, Drphilharmonic, Dungodung, Edward321, EerieNight, Egmontaz, Eleassar, Electrosaurus, Ellywa, Eog1916, Eras-mus, Erich gasboy, FeatherPluma, Ferengi, Franamax, Frecklefoot, FrozenMan, Fusionmix, Fuzheado, Gaius Cornelius, Galmicmi, Garffreak, Geldart, Gimboid13, Gnusmas, Gor n bein, GrahamColm, Grantgw, Grstain, Habj, Hadal, Haham hanuka, Hazmat2, Headbomb, Hede2000, HexaChord, Hgrosser, Hovea, Hroðulf, Huzzah for the Shopkeep, ILike2BeAnonymous, Iamstronghaha, Iice74, InverseHypercube, Iridescent, Ironsman, Iroony, Isabel123456, It Is Me Here, Itub, IvanLanin, J.Dong820, JamesAM, JamesTseng, Jauerback, Jeepday, Jeffq, Jfdwolff, Jitse Niesen, Jjhmccarty, Jprawn, Justme89, Jwilty, Jyril, KBi, Ka Faraq Gatri, Karaschultz, Kcordina, King of Hearts, Kungfuadam, Lauri195, Lazyday1397, Leslie Mateus, Linzhoo2u, Lrunge, M7, MAlvis, MER-C, Marek69, Markjohndaley, Maryhannah, Master Conjurer, Matanya (renamed), Materialscientist, Miannacone, MichaK, Michael Snow, Michi zh, Mikael Häggström, Mikeylane, Mj455972007, Mmxx, Modeha, Mogg, MrSomeone, Mrezai, Muhandes, NCurse, Naddy, NawlinWiki, Nbauman, Ndkartik, NerdyScienceDude, Nick Boulevard, Niteowlneils, Nmg20, Notheruser, Nunh-huh, Oblivious, Omicronpersei8, Oroboros, Orphan Wiki, Oxymoron83, PFHLai, PREMIS2010, Paul August, Peipei, Phil Wardle, PhilGaskill, Philip Trueman, Phlebas, Piano non troppo, Pinethicket, Poo9dle, Puglet, R.O.C, RDBrown, Radon210, Ravensky, Rb1248, Rbethune, Reedy, ResearchRave, Rewster, Rich Farmbrough, Rjwilmsi, Rkohin, Rlhutton, Robchurch, Rod57, SWAdair, Sahands, Salsa Shark, Scorpian ad, Sergei Gutnikov, Shadowjams, SimDarthMaul, Slconnor uk, Slightsmile, Smartse, Snowmanradio, Sophus Bie, SpK, Spaully, Spidey104, Sport woman, Spril4, Stereotek, Sun Creator, TAKEN00, Taucetiman, Template namespace initialisation script, Tevildo, The Universe1, Thecheesykid, Thingg, Tide rolls, Tim1357, Tleonardi, Topbanana, Toytoy, Tpb, TransUtopian, Trevor MacInnis, Tristanb, Unara, Uusitunnus, Vertigo35, Vogon77, WadeSimMiser, Ward20, Wavelength, Whig, Whkoh, Wik2kassa, WikipedianMarlith, Wikipelli, Wouterstomp, Wsloand, Yishubin, Yuckfoo, Zefr, Zeimusu, パ タ ゴ ニ ア, 483 anonymous edits Osteoclast Source: http://en.wikipedia.org/w/index.php?oldid=551048746 Contributors: 0304984r, Abalinson, Abe (or Abraham), Adapter, Aljullu, Arcadian, Ashley Payne, CalicoCatLover, Cape ryano, Cellpath, Cepacia, Chaldor, ChrisGualtieri, Chuunen Baka, Ciar, Cquan, DO11.10, Danfa1971, DerHexer, Diberri, DragonflySixtyseven, Eixo, Eleassar, Ellusion, Franamax, Frederickjeanguerin, Gadfium, Giftlite, Giraffedata, Greensburger, Homosinthemedow, J04n, JLCA, Jaded2, Jag123, Jared81, Joehall45, John of Reading, Josh Parris, Ketiltrout, Kungfuadam, Kyleca, Leia, MDoube, Matt.breeden, Meredyth, MichaK, Mobius, Mrich, Nicke L, Nono64, Nsaa, Orlandoturner, Polartysken, Rjwilmsi, Robert M. Hunt, Ryanrs, Salam32, Schneedrache, StatAustin, Tameamseo, Thegreenj, Totto6627, Vibitz, Vojtech.dostal, Vokesk, Wsussman, ﻣﺎﻧﻲ, 86 anonymous edits Dendritic cell Source: http://en.wikipedia.org/w/index.php?oldid=547135080 Contributors: AaronM, Acegikmo1, Aqua112233, Arcadian, Auenfeld, AxelBoldt, Axl, Bbh112, Bendzh, Bibiniki, Biggus Dictus, Blacklegendx, Brim, CLW, CanisRufus, Chaldor, Ciar, Circusgod, CrzyMke, DO11.10, Danaman5, Danfreak, Demiurge, Dirac1933, Doctorsclinic, Dominicanpapi82, DragonflySixtyseven, Drjames1, Dryman, Dysmorodrepanis, Ectoplasmical, Ediacara, Electric goat, Everyking, Feddegroot, Fhayashi, Franamax, GeeJo, Guess007, Hop12009, Horatio, Hugo Dufort, Itub, JWSchmidt, Jessemoya, Johnwalton, Jon the Geek, JorisvS, Jsnir, Juicy-one, JustAGal, Kalaiarasy, Kazvorpal, Kimjw7, Knuckles, Leptictidium, Lexor, Linzhoo2u, Marcelin0, Michael Greiner, Mimihitam, Nico KG, Nono64, Ohconfucius, Peisapooran, Petri Krohn, R'n'B, Reo On, Rich Farmbrough, Rjwilmsi, Rummy666, Rutigor, Sarah Morwood, Scray, Seans Potato Business, Sedmic, Shalinnaik, Skyelorien, Smirkster, Snowmanradio, Stepa, SteveChervitzTrutane, Strike Eagle, Sylvie.Lesage, Thumperward, Tony1, Trooper26 26, Urban.gecko, Vietbio, WLU, Wavelength, Wedic, WereSpielChequers, WhatamIdoing, XcepticZP, Yupik, 135 anonymous edits Lymphatic system Source: http://en.wikipedia.org/w/index.php?oldid=551697196 Contributors: 1dragon, 3dscience, 5Celcious, 879(CoDe), 9258fahsflkh917fas, Acroterion, Adi4094, Adriennefgnht23bgv33gbf32gn3g, Aetkin, Aeusoes1, Akerbeltz, Al Silonov, Alansohn, Alex.tan, Alexandermiller, Alexh3791, Allens, Allmightyduck, Alphachimp, Alteripse, Andrewman327, AndyA55555, Andyras, Angst7, Anna Karolina Heinrich, Anna Lincoln, Anthonyhcole, Arcadian, Ariedartin, ArielGold, Arsony, Aruton, Ashcraft, Astronautics, Atropos235, Attys, AxelBoldt, Axl, BathTub, Beantwo, Bender235, Betacommand, Bibliomaniac15, Blanchardb, BlueDevil, Bomac, BorgHunter, Brettz9, Brianski, Brim, Bryan Derksen, Burzmali, C933103, Cammomile, Can't sleep, clown will eat me, CanisRufus, CapitalR, Capricorn42, Carps, CaseyPenk, Cburnett, CesarB, Cflm001, ChrisGualtieri, Chrishel, Christian75, Ciotog, Clattuc, Closedmouth, Cmcnicoll, Coasterlover1994, CommonsDelinker, CoolKoon, Cpl Syx, Cuahl, Cyclonenim, DO11.10, DVD R W, Danny252, Darkdrakey2000, Darkfight, Darkwater657, DebC123, Decltype, DerHexer, DesertAngel, Dexter prog, Dfrg.msc, Diberri, Diomidis Spinellis, Dipankan001, Diza, DocElisa, DocWatson42, Dr.pompo, Dragos101, Drdcarlz, Dreadstar, Dungodung, Dustin Dewynne, Dysprosia, EWikist, Egghead06, Epbr123, Equendil, Eras-mus, Erich gasboy, Erielhonan, Exert, EyebrowOnVacation, Faradayplank, Feydey, Figma, Finlay McWalter, Flewis, FrankCostanza, GFHandel, GHe, Gareth Griffith-Jones, Gatster 04, Gensanders, Giftlite, Gilliam, Glane23, Goffrie, Gurch, Gwernol, Gyrobo, HYC, Habj, Haemo, HalfShadow, Harrisd5917, Harryboyles, Hfastedge, Hmains, Hughcharlesparker, Husond, Hydrogen Iodide, Iammisc, Ibnsina786, Igoldste, Iohannes Animosus, Ipwnzors, Iridescent, Ixfd64, Izvora, J.delanoy, JASpencer, JForget, JaGa, Jack Holt, Jackomos, Jaispeed, JakobSteenberg, JamesBWatson, Jamiejackson, Jauhienij, Jc86035, Jeff G., Jfdwolff, Jhenderson777, Jmcw37, Joehall45, John254, Johnanth, Jordan Yang, Jordanmif, Jose Jethro L. Villaverde, Jrodor, Julesd, Julietwhite, Jusdafax, Just plain Bill, JustinForce, KC Panchal, KaiAdin, Katalaveno, Kazubon, Kdavidk, Keilana, Kip R. S., KnowledgeOfSelf, Kosebamse, Krashlandon, Krawi, Kubigula, Larry Dunn, LearnAnatomy, Lennert B, Lepetitvagabond, LilHelpa, Little Mountain 5, LittleOldMe, Littlealien182, Lord Anubis,
613
Article Sources and Contributors
LuK3, Luk, Luna Santin, Lymphoma, MER-C, MPerel, Maralia, MarcoTolo, Marcus Qwertyus, Marek69, Mark Arsten, MarkRose, Marshallsumter, Martinp, Materialscientist, Maxmaxb, McDogm, Mcmillin24, Mecil, Meegs, Merope, MetsFan76, Mifter, MightyWarrior, Mikael Häggström, Mike Rosoft, Mike2vil, Mikebar, Mild Bill Hiccup, Min.neel, Momo san, Mr Peanuts, Msi09222, Mwanner, NJPharris, Nastajus, Natpal, Neolog, Nick, Nina Gerlach, Nishkid64, Nivix, Nlu, Nn123645, Now is relative, Nuno Tavares, Nurg, Orangemike, Orphan Wiki, Otisjimmy1, Oxymoron83, PDH, PFHLai, Panoptical, Paperfork, Paul August, Perryperry, Peter bertok, PeterSymonds, Phnk, Phogg2, Piano non troppo, Pinethicket, Polly, Postglock, Ppyo, PseudoSudo, Puchiko, RadioKirk, RaminusFalcon, Rannyfash, RastNim, Raven in Orbit, Razorflame, Rduddington, Realdog, Redhookesb, Renato Caniatti, RexNL, Richard75, Rintrah, Rjwilmsi, Robertdench, Rodsan18, Ronhjones, Rowan Moore, RoyBoy, Rumiton, S3000, SDY, Salt Yeung, Salvor, Samir, Satellizer, Sdumont, Seans Potato Business, Seelefant, Seventh Holy Scripture, Shalom Yechiel, Sharkface217, Shinkolobwe, Simonwilms, SiobhanHansa, Skittleys, Slartibartfast1992, Slightsmile, Snowmanradio, SoWhy, Social tamarisk, Splash, SpuriousQ, Srushe, Steven Luo, Stevenmitchell, Stollerdj, Superbeecat, Tarnas, Tartan, Tatrgel, Tcncv, Template namespace initialisation script, The Anome, The Emirr, The Red, The Thing That Should Not Be, Thejerm, Theopolisme, Thgang, TiCPU, Tide rolls, Tirkfl, Tony K10, Tossh eng, Trailspark, TruthbringerToronto, Tvarnoe, Ulflarsen, Urashimataro, Urwrongstud, UtherSRG, Vokesk, Vuo, WBardwin, WE.WE.WE.WE, WLU, Wainwra, Warcraftfan111, Werdan7, West.andrew.g, WhatamIdoing, WhyBeNormal, Wiccan Quagga, Wikigenevan, Willking1979, Wongm, Wouterstomp, Writ Keeper, Xil, Yidisheryid, Yvwv, Zalgo, Zaxius, Zeitgeist24, Ziphon, Zloyvolsheb, ﺳﻤﺮﻗﻨﺪﯼ, 837 anonymous edits Microglia Source: http://en.wikipedia.org/w/index.php?oldid=550893374 Contributors: AHands, AManWithNoPlan, Arcadian, Audreykarperien, Bogwhistle, Calerc, Camerong, Ciar, ClockworkSoul, CopperKettle, CraigTheBrit, D6, Dafunk, Delldot, Diberri, Dinisoe, Drdaveng, Filip em, Franamax, Fredweis, Gauss01, Guy M, Gzkn, Hazard-SJ, Headbomb, Helge Skjeveland, Iqzaquezzs, Joehall45, Jorvis, Kauczuk, Kilom691, La comadreja, Lkf0919, Manabeast333, Martious, Materialscientist, Metropolitan90, Michael Devore, Miguelferig, Mikael Häggström, Mike2vil, Mimihitam, MollyNYC, MrADHD, Mrbigtoe, Nbauman, NifCurator1, Nono64, PaddyM, Paolo.dL, Papovik, Pcu123456789, PhnomPencil, Pmokeefe, Pol098, Probios, RDBrown, Rich Farmbrough, RichardGautney, Rjwilmsi, Robertmuil, Sgpsaros, Sjbarrett, Snowmanradio, Time9, Tmangray, Vojtech.dostal, WereSpielChequers, Wiki emma johnson, ^demon, יונה 87 , בנדלאקanonymous edits Neutrophil granulocyte Source: http://en.wikipedia.org/w/index.php?oldid=546586763 Contributors: 2over0, A-wal16, Abstraktn, AdjustShift, Alansohn, Albondigas123, Arcadian, Axelregens, Bahoxu, Banano03, Bender235, Bob Blaylock, Borgx, Boxandice8, Branwall, Casliber, CasualVisitor, Chimeira, Ciar, Clark SR, DO11.10, DRosenbach, Davince, Dbabbitt, Dbroadwell, Delldot, Dexterreneer, Diberri, Drphilharmonic, E Pluribus Anthony, El Mariachi, Elliotgoodrich, Emsta88, Epingchris, Eribro, Evands, FearlessRahul, Flumignan, Franamax, Gabe20770, Garion96, GeeJo, Gene Nygaard, Geniac, Giraffedata, Gnusmas, GrahamColm, Greensburger, Hlangeveld, Hydrargyrum, IGeMiNix, Iwilcox, Janesh1980, Janesh2323, Jayden54, Jdlambert, Jfdwolff, Jloftus22, Joanjoc, Johnuniq, Julian.ilcheff, Just Susan, JustAnotherKinase, Kalaiarasy, Karl Dickman, Kazikameuk, Kehrbykid, Kirper, Kosebamse, Kww, Kyukyu18, La goutte de pluie, Lars Washington, Leeearnest, Leolaursen, Linzhoo2u, Llnoba, Lombroso, Looie496, Luigifan, Luk, M1ss1ontomars2k4, MER-C, Majkinetor, Malerin, Martarius, MaseRayL, Maximus Rex, Mhking, Michaeloqu, Mikael Häggström, Mike2vil, Minnsurfur2, Miracle Pen, MisfitToys, Nbauman, NighthawkJ, Nk, Noctibus, Nrsmoll, O18, Opsuty, Pointpride, Primmuno2, Prolog, Randyoo, RexNL, Rhode Island Red, Rich Farmbrough, Rjwilmsi, Rlmorgan, Rogiervw, SFSingleton, Salih, Schizmatic, SchreiberBike, Scwlong, Shadowlynk, StephenBuxton, SystemBuilder, Tabletop, Thumperward, Tinngo, Tleonardi, Triesault, Trolleymusic, Useight, Wavelength, Wedian, Wiki emma johnson, Yashgaroth, パ タ ゴ ニ ア, 202 anonymous edits Eosinophil granulocyte Source: http://en.wikipedia.org/w/index.php?oldid=543702007 Contributors: Ahoerstemeier, Alex.tan, Andromeda, Arcadian, Bobblewik, Bobjgalindo, Borglife, Boxandice8, Branwall, CDN99, CS99, CarlESundberg, Cburnett, Ceyockey, CharlesClarkson, Cheaposgrungy, Ciar, Clicketyclack, Dan McScience, Dathomp1, Davidruben, Dcirovic, Diberri, Donaldal, Drphilharmonic, E Pluribus Anthony, Emperorbma, Eosinophil7, Eosinophils99, Feral mage, Franamax, Frumpel, Gene Nygaard, Glenn Magus Harvey, GrahamColm, Hairy Dude, Husond, Jackol, Jeffq, Jfdwolff, Jkhamlin, Joanjoc, Josh Parris, Jsjsjs1111, Kalaiarasy, Karl Dickman, Khanna06, Kkmurray, Knuckles, Kristenq, Kubra, Linzhoo2u, Lombroso, Martpol, Mikael Häggström, Misty7, Mjbat7, Nono64, Nunh-huh, Oliverdl, Ppgardne, Pro Grape, R'n'B, Rex Manning, Rob.bastholm, Rockfang, Rrenner, Saimhe, Sbharris, Schtigy, Sciwred, Seans Potato Business, Skittleys, Snowmanradio, Someone else, Thaurisil, Thranduil, Timferno, Tracylau1223, Tristanb, Una Smith, Unara, WhatamIdoing, WillFinnigan, 101 anonymous edits Basophil granulocyte Source: http://en.wikipedia.org/w/index.php?oldid=551695867 Contributors: Algumacoisaqq, Ameyadkr, Arcadian, Bela Bartoszek, Bencherlite, Benmd, Bloodcancerguy, Bob Blaylock, Bobomarch, Branwall, CDN99, CS99, Ciar, Cyberman, DO11.10, Delldot, Donmacglashan, ESCapade, Elbonia, Elboy99, Epgui, Epingchris, Franamax, Frazzydee, Graham87, GrahamColm, Hephaestos, Ht9150, Infinitys 7th, Iwilcox, Jfdwolff, Joanjoc, Karl Dickman, Kauczuk, Kerowyn, KnightRider, Kubra, Linzhoo2u, M1ss1ontomars2k4, MastCell, Menue, Mikael Häggström, Mike2vil, Murdochious, Natkeeran, Onco p53, Oxymoron83, Pearle, Piano non troppo, Pingveno, Porqin, Prolog, RB972, RDBrown, RelentlessRecusant, RenamedUser01302013, Rich Farmbrough, Shirik, Sligocki, Snowmanradio, Thue, Timurite, Tossh eng, Voxii, Wandering Raleighite, Wood Thrush, Þjóðólfr, パ タ ゴ ニ ア, 67 anonymous edits Hybridoma technology Source: http://en.wikipedia.org/w/index.php?oldid=548151808 Contributors: Aetkin, Ahoerstemeier, Anypodetos, Arcadian, Arup Acharjee, Autoerrant, AxelBoldt, Bejnar, Biotec ha, DoctorKubla, Friendlyliz, GerryShaw, Janetyler, Joeyzhu123, JonHarder, Jonathanfu, Joseph pepito, Miguel Andrade, Movses, NewEnglandYankee, NickPenguin, OrbitSoldier, Playtime, Prazwol, Proquence, R'n'B, Rich Farmbrough, SMasters, Seans Potato Business, Shadowjams, SlothMcCarty, Someguy1221, Tonipares, Tyranitar Man, Wedian, WikHead, Wsmith202, 48 anonymous edits Mast cell Source: http://en.wikipedia.org/w/index.php?oldid=543707550 Contributors: Aleichem, Alex motzik, Arcadian, Arthena, Begoon, Bender235, Benjah-bmm27, Boghog, Bogwhistle, Bomac, Casliber, Chikantikka, Ciar, DO11.10, DRE, DarkFalls, Davidruben, Dr U, ESCapade, Electric goat, Essam Sharaf, Franamax, Fsiebenh, Goodnightmush, Graham87, Greenleaf87, Hadal, Harrisd5917, Hede2000, Hotcrocodile, Hvyhiter, Höyhens, Jastrow, Jfdwolff, Joehall45, Joelmills, JohnnyCalifornia, Julesd, Kauczuk, Kiran Gopi, Kku, Kyukyu18, Lekeebler, Lidabet, Linzhoo2u, Ludisia, Mandarax, Mikael Häggström, Mike2vil, Nbauman, Neverquick, Nono64, Nrets, NunoAgostinho, Omnipaedista, Orlandoturner, PFHLai, Petersam, Philbradley, R. S. Shaw, Rafiqr, RedDrag0n, Reza luke, Rjwilmsi, Russot1, Ryddragyn, SLATE, Seans Potato Business, SgtThroat, Sharanth, Snowmanradio, Stino v, Tristanb, Unara, Vokesk, Volantares, WLU, Woohookitty, Xetxo, 110 anonymous edits T helper cell Source: http://en.wikipedia.org/w/index.php?oldid=549148820 Contributors: Abramsonj, Adr11iano, Allens, Anupam, Aqua112233, Arcadian, Avaron676, AxelBoldt, Beland, Benjamin.haley, Bob247, Bobo192, Bogwhistle, Borgx, Brendan19, Brendanconway, Brentdax, Bullhaddha, Bwwhite, Charles Matthews, Chris the speller, Cmdrjameson, ComfyKem, CopperKettle, Davekcole, David Johnson, Dcirovic, Diberri, Dirac1933, DoktorDec, Eleassar777, Elliotgoodrich, Essexmutant, Ettrig, Finalius, Franamax, Frycow, Gamingmaster125, Gbleem, Gikü, GiollaUidir, Gurch, Happiness4ever, Immunoboy, JLaTondre, JackWasey, Jakob Theorell, James McNally, JamesBWatson, Jbarin, JeffreyN, JorisvS, Jotomicron, Julianonions, Kantokano, Ketiltrout, Koavf, Lanka007, Larryisgood, Leptictidium, Lexor, Mala76, Mboverload, Mikael Häggström, Mike2vil, Mimihitam, Mohawkjohn, MrPMonday, MuanN, Nbauman, Niels Olson, Nina, Nonpareility, Nuno Tavares, Oda Mari, Ohnoitsjamie, Optigan13, Orderinchaos, Orlandoturner, Owenhyfryd, Philbradley, Pro bug catcher, Promelior, Prometheus, RelentlessRecusant, Rich Farmbrough, Rjwilmsi, Rod57, Samuel, Scien801, Seans Potato Business, Serephine, Sfahey, Shawnnph, SimonPerera, Sk741, Slashme, Smalerie, Snigbrook, Snowmanradio, Sophie means wisdom, Sxim, TKD, Template namespace initialisation script, TenOfAllTrades, Tide rolls, Tommy2010, Triggtay, Tristanb, Tycho, Utcursch, Volantares, Vyn, WhatamIdoing, Wikid77, Wikitoov, Yamamoto Ichiro, Youkai-kun, ZayZayEM, 239 , דגיגanonymous edits Regulatory T cell Source: http://en.wikipedia.org/w/index.php?oldid=543039170 Contributors: Adr11iano, Anupam, Arcadian, AxelBoldt, BettieHoladay, Biohacker, Boghog, Bryolith, Chrisch, Chupacabras, Danierrr, Davidruben, Drphilharmonic, El C, Emersoni, Escobar2, FCAlive, Fnielsen, Franamax, GAThrawn22, Gearoidmm, Geuss, Ioeth, Iridescent, JLaTondre, JackWasey, Jakob Theorell, Jbarin, JohnnyBxo, Kantokano, Karawaque, Kinkreet, Kirbymaur, Lbruegge, MastCell, Mauvila, Mboverload, Nbauman, Negarci, Nina, Onco p53, Oxymoron83, Perencake, Pion, Ramujana, Rich Farmbrough, Rjwilmsi, Schroding79, Science4us, Southernwayfarer, Sunjongko, TaeSaBiAe, Tretcher, Twas Now, Twooars, Univer, Who, Wiccan Quagga, Wiki Katie, Zeearend, 81 anonymous edits Cytotoxic T cell Source: http://en.wikipedia.org/w/index.php?oldid=548082771 Contributors: Adrian J. Hunter, Anupam, Arcadian, Cd8tcell, Chris Capoccia, Christian75, Ciar, Crazysane, Davekcole, Davin, Diberri, Drphilharmonic, DéRahier, Ebmat, Ediacara, Eras-mus, Excirial, Fabiform, Franamax, Gaius Cornelius, Gikü, Habj, Heero Kirashami, Heero@Yuy, IvanLanin, J.delanoy, J04n, JaGa, Jbarin, Jfdwolff, Lenrodman, Leptictidium, Lexor, Lockley, Miannacone, Mild Bill Hiccup, Nbauman, Nina, Petri Krohn, Prometheus, RelentlessRecusant, Rich Farmbrough, Rich257, Richwil, Rotatoria, RyanGerbil10, Rünno, S88136738, Seans Potato Business, Serephine, Sfahey, SimonPerera, Slashme, Snowmanradio, Template namespace initialisation script, TheTito, Thepunisher22, Theroachman, Volantares, Wavelength, Zklaus40, 79 anonymous edits Natural killer T cell Source: http://en.wikipedia.org/w/index.php?oldid=540624257 Contributors: Adams5400, Anthony Appleyard, Anupam, Arcadian, Brim, Cplatt, DIG1964, DO11.10, Dalf, Figma, Franamax, Jeffq, Karasunoko, Ketiltrout, Loopback007, Mattert, Monterey Bay, Nz101, RelentlessRecusant, Rjwilmsi, Schneedrache, Snowmanradio, SocratesJedi, Timetraveler3.14, Vesriram, Wbm1058, 34 anonymous edits B cell Source: http://en.wikipedia.org/w/index.php?oldid=550542105 Contributors: 069952497a, Abramsonj, AdjustShift, After Midnight, Alansohn, Allens, Altaileopard, Anypodetos, Arcadian, BD2412, Banano03, Bcmyangx, Bearpiggoreman, Blitzmut, Butterfly reflections, CUSENZA Mario, Calvinchong, Cburnett, CesarB, Chefyingi, Chris Capoccia, Chrumps, Chucky123456789, Ciar, Cockers1987, Coemgenus, DO11.10, Dana boomer, Daniel, Darkfrog24, Davidazus, Davlag, Dcooper, Delentye, Diberri, Docfaust, DragonSlayer210, Dwight666, Eleassar777, Eras-mus, Eric-Wester, Falcon8765, Franamax, GargleBlaster, Geuss, Giftlite, Ginkgo100, Greensburger, Greggp42, Gremmer, Grey ham22, Hamham1012, Hamjue, Hazmat2, Healthvalue, Helper100, Herrpoon, Hotncool123, Hqb, I dream of horses, Ian Glenn, Igoldste, Ilyushka88, InverseHypercube, Iohannes Animosus, Iridescent, JBellis, JMiall, JackWasey, Jacuzzijo, Jeffq, Jj137, Jojousa, Jonathan.s.kt, JorisvS, Jotomicron, Juliamweiss, KC Panchal, KCinDC, Kinkydoc22, Knowledge keen, L Kensington, Leptictidium, Lexor, Liidiie, Ling.Nut, M1ss1ontomars2k4, Mac Davis, MastCell, Maxí, Mikael Häggström, Mimihitam, Mj455972007, N4nojohn, Niels Olson, Nina Gerlach, Nonagonal Spider, Novangelis, Oasisbob, Palpalpalpal, Paulasb, Peisapooran, Pgallert, Ph.eyes, Phil Boswell, Postglock, Prometheus, Quirk, RandomP, RelentlessRecusant, Reverting, Rey lcm, Rgoodermote, Rjwilmsi, RobinHood70, Ronincyberpunk, Sagefoole, Sayeth, SchfiftyThree, Schtigy, Silveramini, Simonmoore, Skittleys, Smoe, Snoeleopard, Some jerk on the Internet, Srlasky, Stevereichh, Stmoran, Sun Creator, TKD, Taoster, Teamfido, Template namespace initialisation script, Thorncrag, Tide rolls, Timemutt, Tristanb, Tycho, VMS Mosaic, Vokesk, Warden99, WhatamIdoing, Wknight94, Woohookitty, Wpktsfs, Youssefsan, Yurei-eggtart, 258 anonymous edits
614
Article Sources and Contributors
Natural killer cell Source: http://en.wikipedia.org/w/index.php?oldid=551164749 Contributors: Acoury, Adr11iano, Aesopos, Alansohn, Alejocn5, Ali ahmadzada, Alksentrs, AlphaEta, Andrew73, Apocalypse Now, Arcadian, Ary29, Bisc import, Bluemoose, CIreland, Cab.jones, Cacofonie, Calmer Waters, Capricorn42, Chamal N, ChrisGualtieri, Chrumps, Conkwest, Cph3992, Cyberman, DRMJNY, Dbollard99, Delldot, Diberri, Doctor medicine, DougsTech, Download, Dr.saptarshi, Draeco, Drchazz, Drphilharmonic, Durova, Enviroboy, Epingchris, Franamax, Furrykef, Gibson Flying V, Giftlite, Gjbbms640, Harriemkali, Icedemon, Jakob Theorell, Jaranda, JeffreyN, Jfdwolff, JorisvS, Kazkaskazkasako, Kenmcl2, Kittty08, Kubra, Kupirijo, LeeHunter, Leptictidium, Lexor, Lockley, LoneSeeker, Lycurgus, MPerel, Mattert, Matthewmazurek, MicroBio Hawk, Mikael Häggström, NetRolller 3D, Nmajdan, Nunh-huh, PAStheLoD, Park4223, Pgrote, Phfred, PhnomPencil, Pixie, Prometheus, Rdsmith4, Regford, RelentlessRecusant, Rickjpelleg, Rjwilmsi, Roastytoast, Rod57, Schneedrache, SchreiberBike, Seans Potato Business, Serephine, Smithbrenon, Snapperman2, Snowmanradio, Songrit, Squidilicious, Stemscientist, Supergroover, Tamarkapterian, TheTito, Timemutt, Tjoneslo, Tlabshier, Tmangray, Tossh eng, Unga Khan, Varbas, Volker Huppert, Wavelength, Wedgeoli, Wjejskenewr, Wo0dstock79, XavierEverett, YouRang?, Zach the Wanderer, 129 anonymous edits Reticulocyte Source: http://en.wikipedia.org/w/index.php?oldid=549064794 Contributors: 2001:468:C80:4340:DAA2:5EFF:FE91:F41E, AaronM, Alex.tan, Arcadian, Arthena, AxelBoldt, Brinerustle, Chowbok, Diberri, Drphilharmonic, Franamax, Gaius Cornelius, Gak, Gobonobo, Happy B., Hoverflysmiles, Ian Pitchford, Jeffq, Jmarchn, Joewright, Kubra, MiloszD, Monkeyontheloose, NewEnglandYankee, Niroby, Ozmaweezer, Patch101, Randyoo, Romanm, Sedmic, Seforadev, Snowmanradio, Some standardized rigour, Tiptoety, Tristanb, Wouterstomp, 43 , דניאל צביanonymous edits Progenitor cell Source: http://en.wikipedia.org/w/index.php?oldid=551063018 Contributors: Alaa al-Otaibi, Amaher, Arcadian, Bagatelle, Bihawang, Canadian hockey1, CardinalDan, Christian75, CopperKettle, DVdm, Discospinster, Dr Aaron, Drphilharmonic, EOZyo, EWikist, Eumolpo, Jeff G., Kerribergeron7197, Kerrio, Lenticel, Lijealso, Mild Bill Hiccup, Obaid221, Peter Znamenskiy, Pgan002, Philip Trueman, Poojans, Rob Hurt, Robert M. Hunt, Rod57, StanfordProgrammer, Stansz, Stepa, Susan Carley, The High Fin Sperm Whale, TheChymera, Tinlv7, VUBio Pieterjan, Volodymyr Stetsyuk, ﺗﺮﺟﻤﺎﻥ05, 32 anonymous edits Ovum Source: http://en.wikipedia.org/w/index.php?oldid=550501112 Contributors: 165.123.179.xxx, 2004-12-29T22:45Z, 22232222vb, 24.234.70.xxx, Abstraktn, Achven, Addshore, Adrian J. Hunter, Adrigon, Alansohn, Ale jrb, Alfonso Márquez, Allens, Amatulic, Andrei Stroe, Andrewa, Anthonyhcole, Arcadian, Arjun G. Menon, Arkuat, AxelBoldt, Bagatelle, Bcorr, Beano, Bhojanimihir, BiT, BigPimpinBrah, Bkrosnov, BlueGoose, Bomac, Bongwarrior, Brandmeister (old), Btd, C.Logan, CallumN, Caltas, Capricorn42, Carlossuarez46, Carpenter aka, Cesiumfrog, Chanlyn, Christiangrimm84, Closedmouth, Cmichael, CommonsDelinker, Conscious, Conversion script, Dasani, David.Gaya, DavidRader, Dbfirs, DerHexer, Eatingbrunch, Eewild, Ehn, Ekem, Eleassar777, Empty Buffer, Epbr123, Epipelagic, Fabiform, Finlay McWalter, Finn-Zoltan, Fixstamac, Flockmeal, Franamax, Francs2000, Freemarket, Furbinator, G026r, Gajanandjha, Gblaz, Gbnogkfs, Gleader9, GoingBatty, Grafic, Gwernol, Haham hanuka, Hall Monitor, IW.HG, IceDragon64, IronChris, Isnow, Itai, J.delanoy, Jakejakejake1313, Jiddisch, Jj137, JoanneB, Jonathan.s.kt, Joshbuddy, Josq, Jovianeye, Jrockley, Judygreenberg, Jusdafax, Kandar, Katieh5584, Keegscee, Knowz, Kudpung, Kwakpwns, Kyng, L Kensington, La goutte de pluie, Leevclarke, Legend II, LemonTwinkle, Lexor, LilHelpa, Lilyv129, Lobstercake1, Lokicarbis, Lottamiata, Lugia2453, Lugnuts, MBisanz, MCRfan911, Magnus Manske, MarsRover, Maxí, Meiskam, Menchi, Mesoderm, Mgiganteus1, Mike5193, MilborneOne, Minimac, Modify, Mr. Lefty, Nadiatalent, NerdyScienceDude, Netoholic, Nifky?, Nilmerg, Nkayesmith, Nuno Tavares, Ochloese, Orphan Wiki, Osmodiar, Patrick0Moran, Patrickk112, Patxi lurra, Philip Trueman, Pigman, Plantguy, Pollinator, Radagast83, Rainy888, Ratherthanflesh, RebekahThorn, RenniePet, Rep07, Riotrocket8676, Rm1271, Rob Hooft, Robin Chen, Romarin, Rune X2, RxS, Sabisteb, Samsara, Sean.hoyland, Sharkb, Shirulashem, Shoombooly, Skizzik, Slakr, Soupforone, Steven Zhang, Swid, Tameeria, Taranet, Tarquin, Tbhotch, The Anome, The Rambling Man, The Thing That Should Not Be, ThePirate, Tide rolls, TigerShark, Tjoms12, Tmshates, Toddy1, Treisijs, Tresiden, Trijnstel, Tsca, Tyrol5, Ulric1313, Vanished User 1004, Victoriagirl, Victormdc10, Vojtech.dostal, Voyevoda, Waggers, Wavelength, Werieth, Wipfeln, Youssefsan, Zfr, Àlex, כל יכול,יוסי, आशीष भटनागर, 朝 彦, 252 anonymous edits Oocyte Source: http://en.wikipedia.org/w/index.php?oldid=546452397 Contributors: 2004-12-29T22:45Z, Abstraktn, Addit, Amaury, Arcadian, Arkuat, Basilicofresco, Bobjgalindo, Cameron Nedland, Catcasillas, Cburnett, Ceyockey, Chris the speller, Crazycomputers, Curb Chain, Db099221, EagleFan, EamonnPKeane, Edward, Erianna, Face, Former user, Furrykef, Gabbe, Glimz, Hgrosser, InverseSubstance, Kaobear, Kbusdriver, Kerfern, Leeannedy, Lexor, Lymanbellows, MarcosR, Mgiganteus1, Microinjection, Mikael Häggström, Minna Sora no Shita, Modify, Mysid, Nkmosley, Nmg20, Oliver202, PauAmma, Phuzion, Poissonbreaker, Rasbak, RedWolf, Remuel, Riana, Sdou, Shano85, Skizzik, Snek01, Snoyes, Stephenb, Stylese, Sugemax, Tameeria, Thomas 564312, Tmshates, Tour86rocker, Trovatore, Vanished User 1004, Vojtech.dostal, 82 , ברוקוליanonymous edits Spermatid Source: http://en.wikipedia.org/w/index.php?oldid=540782500 Contributors: 2004-12-29T22:45Z, Abstraktn, AdmiralHood, Alsbluegoat, Arcadian, Chowbok, Diligent, Gilliam, Kaobear, Wikielwikingo, 12 anonymous edits Sperm Source: http://en.wikipedia.org/w/index.php?oldid=551477424 Contributors: 123456789101121cccccc, 2004-12-29T22:45Z, 21655, AB, AaronM, Accurizer, Acdx, Acroterion, Addit, Adrigon, Agateller, Ahmad.ghamdi.24, Ahmed32 UK, Aitias, Al tally, Aleenf1, Alexandre Bouthors, AlexiusHoratius, Andrei Anghelov, Andrewjlockley, Andrewpmk, Avaya1, Avnjay, Bakerccm, Baosheng, Bass fishing physicist, Beeftheboss, Beland, Benfranklinlover, Bhojanimihir, Bility, Blairbob, Blehfu, Bobo192, Bob™, Bongwarrior, Briefblowtothehead(dick), Brougham96, Bytenik, CIreland, CWii, Caltas, Calvin 1998, CambridgeBayWeather, Camelface123, CanadianLinuxUser, CapitalR, Chamal N, Chris Bainbridge, Chris the speller, Coffee, ColinBoylett, Cometstyles, Commander Keane, Cornchips, D, D1536, Dantheman216, Darth Mike, Dasani, DeadEyeArrow, Deconstructhis, Dekisugi, Delldot, DerHexer, Dgw, Dickneck99, Dikteren, Dikwad1, Discospinster, Dominus Vobisdu, Dreadstar, Dreby14, Drsocc, Dumbnuts, Dust Filter, Dycedarg, EJF, Eaglesiegle, Edison, Epbr123, Esc2003, Excirial, Extransit, Face, Feezo, Fess56, Fieldday-sunday, Filelakeshoe, Fl, Florentyna, Foxj, Francs2000, Frederikfederspiel, FrozenMan, Ftwklg, FunPika, GB fan, Gadha, Gail, Gekaap, Gggh, Gilliam, Gjuny, Gonzo fan2007, GoodDamon, Gregfitzy, Greystoke35, GrooveDog, Grstain, Gspinoza, Gtva1234, GuffasBorgz8, Guldenat, Guntiur983, Gurch, Gurchzilla, Gurukkal, HaeB, HeirloomGardener, Hiberniantears, Hiddekel, HisSpaceResearch, Hogyn Lleol, Horny t, HotHistoryBuff69, Hu12, Hyacinth, I.r.ande.t.a, INazi, Indon, IndulgentReader, Insanity Incarnate, Instinct, InverseHypercube, Iridescent, J.delanoy, Jackol, JammydodgerUK, Jarble, JayFS89, Jcaliguy, Jclemens, Joannyluteman534, John Doe42, Jonadin93, Joost de Kleine, Jtknowles, Julesd, Juliancolton, Jumbawumba, Kaobear, Katdye123, Keilana, Keith D, Kelovy, Ketsuekigata, Kewsss, Kiyi-chan, KnowledgeOfSelf, Kuru, Kyleeberle, LadyofShalott, Lec CRP1, Lenticel, Lindentree, LittleOldMe, LizardWizard, Lomis, Longhorngirl 5284, Luna Santin, Mack2, Madhero88, Mairi, MarcoTolo, Markbenecke, MarsRover, Martarius, MartinezMD, Mesoderm, Mihalis, Mikael Häggström, Mike-shearer92, MikeNicho231, MikesPlant, Miquonranger03, MoogleEXE, Mschel, NHRHS2010, Nakon, Nattycan, Neverquick, Newlyteeth, Nicolae Coman, Nihiltres, Nintendude, Nivix, Nnemo, Nosolution182, Notedgrant, Novjunulo, Nwbeeson, Ocatecir, Octahedron80, Oda Mari, Ohnoitsjamie, Ohyababy1, Osborne, Ospalh, OverlordQ, OwenX, Oxymoron83, P-squad4251, Pass a Method, Patrick, Pb30, Pcarter7, Phil havercroft, Philip Trueman, Piano non troppo, Pimpboy, Poindexter Propellerhead, Press Start, Private Butcher, PubLife, Rafael MC, RainbowOfLight, Rami radwan, RandomXYZb, Rangek, Raquel PWNZ, Rawfact, Razorflame, Revancher, Rey101011, Rglong, Richard001, Richardedgerton, Rodsan18, Rohitrrrrr, Rrburke, Rror, Rsmn, RucasHost, Ryan Postlethwaite, SU Linguist, Sam Korn, Sam nead, Sceptre, SeanBBSc, Sexworms, Shadiac, Shawtyrockmi, Shibby970, Sidasta, Silly rabbit, Skier Dude, Slushy9, Smartse, Smashingpumkin, Smithy998877665544332211, Sohelpme, Spencer, Stephenb, Steven Zhang, Stone, Storch6308, Supersixfour, Surfeited, Svetovid, THEN WHO WAS PHONE?, Tameeria, Telcourbanio, Tessmac9708, The Thing That Should Not Be, TheBilly, TheNoise, Thedjatclubrock, Theguy14, TheiGuard, Thincat, Thine Antique Pen, This deserves inclusion, Tiddly Tom, TimVickers, Tmshates, Torc2, Transcendence, Treisijs, Twinsday, Twooars, TyrS, Ukexpat, Uravjjfaceandvjjarms, Urthogie, Useight, Vikoula5, Vsmith, WCFrancis, WadeSimMiser, Waterloocook, Wavelength, Werdan7, Wervo, WikipedianMarlith, Wingschlong, Wirbelwind, Wisdom89, Wknight94, Wlmg, Womblejonny, Wootwootlmaoftw, Wowcamj, X!, Xavcam, Xhellxringerx, Xymmax, Y12J, YKWSG, Yamamoto Ichiro, YourEyesOnly, Zsinj, Zzuuzz, ﺃﺣﻤﺪ.ﻏﺎﻣﺪﻱ.24, ဇာမဏီ, 白 布 飘 扬, 487 anonymous edits Spermatogonium Source: http://en.wikipedia.org/w/index.php?oldid=544013232 Contributors: 2004-12-29T22:45Z, Aelamass, Arcadian, Bensisko95, Craig Pemberton, Demax hemed, DoriSmith, Easixy5, Espresso Addict, Kaobear, Kappa, Lab-oratory, Lachaume, Mat8989, PDH, Peter Grey, Rich Farmbrough, SCEhardt, Sovbeos, Squirrels2nuts, Transposagen, 18 anonymous edits Sertoli cell Source: http://en.wikipedia.org/w/index.php?oldid=549673146 Contributors: 2004-12-29T22:45Z, A3camero, Abstraktn, Arcadian, Beno1000, Creol, DannyWilde, Dr.queso, ELLusKa 86, Fisher4.wemo, Franamax, France3470, Fyrael, Good Olfactory, Grutness, Gurch, Horiavulpe, Kanabekobaton, MaxEnt, Mgiganteus1, Mikael Häggström, Mild Bill Hiccup, Nephron, Nick Number, Optigan13, Pres27, Rayc, Rexhess, Rjwilmsi, Sababutt, Salam32, Selket, Serephine, Snalwibma, Sovbeos, Tjmayerinsf, Tony Makhlouf, Vespristiano, ViktorWettergren, Vogon77, Vojtech.dostal, Vokesk, 59 anonymous edits Kidney Source: http://en.wikipedia.org/w/index.php?oldid=551560920 Contributors: 03141119, 1607m4dsk1llz, 16clumsyandshy, 62.253.64.xxx, A3RO, AGodofIrony, AS, Abrech, Accurizer, Acd1208, Acroterion, Adashiel, AdjustShift, Agentmoose, Agüeybaná, Ahoerstemeier, Alansohn, Albert Tellier, Aldenrw, Aldis90, Alex.tan, AlexiusHoratius, Allens, Alperen, Alphachimp, AnakngAraw, Anatomist90, Anaxial, Anclation, Andre Engels, Andrea.gf, Andreas Toth, Andy Dingley, Angela, Animum, Anmats, Antandrus, Antennaman, Anthony, Anthonyhcole, Apparition11, Aravindk editing, Arcadian, ArcticFrog, ArielGold, Ascidian, Askari Mark, Athar shams, Austinpow, AxelBoldt, B'er Rabbit, B-rat, Babajobu, Back ache, Badger Drink, Basharh, Bass fishing physicist, Beetstra, Bell cheese jk, BenBreen2003, Bensaccount, Bertinho, Bgwhite, Big iron, Big.tuna1515, BigDogRufus, BillpSea, Blac8, Blah987654, Blast Ulna, Bloodshedder, Blueman1878, BobKawanaka, Bobblewik, Bobsmith040689, Bogey97, Boing! said Zebedee, Bomac, Bongwarrior, Bonhomie, Boofs, Brainmouse, Broderick, Brother Jonathan, Bryan Aldea, Bryan Derksen, Bryan121, Bunchofgrapes, C.Fred, CE, CFCF, CIreland, Can't sleep, clown will eat me, CanDo, CanadianLinuxUser, Canuckle, Capricorn42, CardinalDan, Carpentc, Caryw123, CaseyPenk, Catgut, Ceccomaster, Ceoil, Chaldor, Chaojoker, Charltonasmith, Chaveso, Cheesemongerbumcheese, Chris Roy, Chrislk02, Ckatz, Closedmouth, Clovis Sangrail, Cmdrjameson, Common Good, CommonsDelinker, Consequencefree, Conversion script, Corvus cornix, Cpsoper, Craig Pemberton, CrazyChemGuy, CrazyTerabyte, Cremepuff222, DARTH SIDIOUS 2, DDima, DVD R W, DVdm, Dah Supa Panda, Dale013, DanMS, DanaCake, Dandonkey, DanielCD, Darth Pejka, DavidTanCool, Davidjk, Davidruben, Dawnseeker2000, Dbouillo, Dduck, Delirium, Delldot, Deor, DerHexer, Derpidness123, Diberri, Discospinster, Diyako, Diyar se, DjMD, Doc.mari, Doddy Wuid, Dooky, Doops, DoriSchatell, Dougofborg, Dpwkbw, DrBethersMD, Drsupermikey, Drunken Pirate, Duagloth, Dublinflorg231, ERcheck, Earthengine, Echothegecko, Ecopley, Edgar181, Edward, Eeekster, Eekerz, Ejdjr, El C, EliasAlucard, Ely1, Epbr123, Eperotao, Eras-mus, Eribro, Erudecorp, Euniceespiritu, Evaa, Ewen, Ewulp, Excirial, Exciter1001, FJPB, Falcon8765, Fama Clamosa, Fantasticarlo, Faradayplank, Fastily, Favonian, FelisLeo, Felix-felix, Fieldday-sunday, Fluffernutter, Forschung, Fratter, Freecat, FreplySpang, Furrykef, Fæ, GB fan, Gabbe, Gaff, Gaia Octavia Agrippa, Gail, Galactor213, Gareth Griffith-Jones, Garik, Garion96, Gary King, Gaseous Snake, Gciriani, Geeoharee, Gekritzl, Geneb1955, GermanX, Giftlite, Gilgamesh he, Gilliam, Gillyweed, Ginger555, Ginsengbomb, Glacious, Gludwiczak, Goalie1998, Gogo Dodo, Googie man, Gouerouz, GraemeL, Grafikm fr, Graham87, Greeney, GregorB, Grundle, Gtstricky, Gurch, Gurchzilla, Gwernol, Hadal, Hagerman, Hancong, Hannabee,
615
Article Sources and Contributors
Hannes Hirzel, Haoie, Harej, Harris7, Harry, Hauberg, Hawaiian717, Headwes, Hede2000, HendrixEesti, HenryLi, Hermant patel, Hersfold, HiDrNick, Hmsedit, Hoplophile, HowiAuckland, Huckfinne, HumbleGod, Husond, I dream of horses, Icarus, Icarus3, IceCreamAntisocial, Iggy402, Indiajal, Inoculatedcities, InverseHypercube, Iridescent, Ivan Bajlo, J.delanoy, JForget, JPalonus, JWSchmidt, JaGa, JackPetersen, Jahnavisatyan, Jakob Theorell, JakobSteenberg, James McNally, Jamoche, January, Jaranda, Jauhienij, Jazzbeer27, Jbeans, Jbelker, Jclemens, Jeff G., Jerryseinfeld, Jessdro, Jfdwolff, Jhelton, Jhenderson777, Jidanni, Jim Douglas, JimVC3, Jlautier, Jmjanzen, John, Johndarrington, Johnleemk, Johnny235, Jojhutton, Joliefille, Jonathan.s.kt, Jose Ramos, Jose77, Joseph Solis in Australia, Joshays, Jovianeye, Jpkb24, Jpogi, JuJube, Julia823, JulieADriver, Juliusceaser101, Jumbo Snails, JustinMullins, [email protected], Jwkpiano1, Jyril, KC Panchal, Ka Faraq Gatri, Kabeman1001, Kajasudhakarababu, Kappa, Karada, Karlhahn, Karolfranks, Kartano, Katalaveno, Keegscee, Keenan Pepper, Keilana, Kelly Katula, Kevin Rector, Khazar, Kibi78704, KidneyQuest, King steal7, Kingpin13, Kirrages, Kku, Kleptosquirrel, Knutux, Kochipoik, KokomoNYC, Korg, Kozuch, Kpjas, Kubigula, Kukini, Kungfuadam, Kuru, L Kensington, LPJamesBond007, Lamro, LearnAnatomy, Leevclarke, Legaldeath, Leonard^Bloom, Leslie Mateus, Lexor, Liam Skoda, Linkinparkdawg, Lisatwo, Littlealien182, Lordofthe9, Lova Falk, Luckas Blade, Luk, Luka Krstulović, Luna Santin, Lycurgus, MC10, MER-C, MONGO, Maartentje, Madskile, Magister Mathematicae, Makeemlighter, Manderso, Mani1, Mansavian, Maork, Marcatz18, Marcsin, Marek69, Marnanel, Maroux, Marshman, Martin S Taylor, Massimo Catarinella, Matt Deres, Mav, Max Naylor, Maxxicum, McGeddon, McSly, Mentifisto, Michael H 34, MichaelMaggs, Michig, Mikael Häggström, Mike Rosoft, Mikefadock, Milanlan, Mintleaf, Miquonranger03, Moonriddengirl, Mooquackwooftweetmeow, Mothpit, Motmit, MrDarcy, MrTroy, Mridhula, Mseliw, MuanN, Mulder416, Mushroom, Myanw, N5iln, NCurse, Nahum Reduta, Nakon, Nathan B. Kitchen, NawlinWiki, Ndkartik, Nepenthes, Nephron, NerdyScienceDude, NewEnglandYankee, Nezzadar, Ngantengyuen, Ni1997, NickGorton, NickW557, Nightenbelle, Nihiltres, Nikkislayer7, Niteowlneils, No madol, Noommos, Northumbrian, NotWith, Nthngb, Nubiatech, NuclearWarfare, Numbo3, Nv8200p, O.Koslowski, Oda Mari, Ohnoitsjamie, OldakQuill, Onceonthisisland, Onlyemarie, Orangepoobumapple, Oxymoron83, Ozgod, PFHLai, Pan narrans, Pancreas eater303, Pashute, Patrick, Patxi lurra, Pb30, Pdcook, Pekinensis, Pepper, Peytons, Philpossett, Phrasont, Piano non troppo, Picpower13, Pilotguy, Pinethicket, Pinko1977, Planet88 co .uk, Polskigirl16, Prashanthns, PrincessofLlyr, Prodego, Puffin, QFlyer, Quintote, Qxz, RAlbert NIDDK, RGshredfox, Radiant chains, RadioFan, Rajkiandris, Random Nonsense, RandomAct, Ranveig, Ratarsed, Ratemonth, RattusMaximus, RealGrouchy, Regulov, RenamedUser01302013, RexNL, RhiannonAmelie, Rhomboid, Riana, Richard001, Rje, Rjwilmsi, Rock mechanics, Rodhullandemu, Ronhjones, Ronnoc6655, Ronz, Rossj81, Rossumcapek, Routerone, Roux, RoyBoy, Rror, RubberDuckyMan, Rumping, Ryan032, SC Young Republican, SJP, SPUI, Saavedro300, Salguy, Salvio giuliano, Sam42, Sandgem Addict, Sannse, Sayeth, Sbblr0803, Sceptre, Schafferm, Schmancy47, SchreiberBike, Schzmo, Scorpian ad, Scottalter, Scotty mctotty, Secretlondon, Sephiroth BCR, Serephine, Shadowbeast656, ShakingSpirit, Shanes, Shawn in Montreal, Shoeofdeath, Shoessss, SimonMayer, Sjakkalle, Sjö, Smalljim, Smooth O, Snek01, Soakologist, Soap, Softlavender, Sonjaaa, Soosed, Sophos II, Sougato, Sovereignscience, SpaceFlight89, Spaully, Spongefrog, Spoonaway, Squids and Chips, Squirepants101, Staffwaterboy, StephenBuxton, Stephenb, Stitchmniac123, Sugarcolt, Summer Song, Sun Creator, Sunlei431, Supapuerco, Sven Manguard, Swiley1983, Syth, Tam83, Tangent747, Tapir Terrific, Tarquin, Tassedethe, Tatterfly, Tdb 32, Techman224, Terry Vaserum, The Evil Spartan, The JPS, The Magnificent Clean-keeper, The Thing That Should Not Be, TheAMmollusc, TheWeakWilled, Theresa knott, Thesnuffla, Think outside the box, Thumperward, Thurinym, Tide rolls, Til Eulenspiegel, Timc, Tlsnyder, Tnabtaf, Tnxman307, Tomcowley, Tommy2010, Top.Squark, Toreau, Tpbradbury, TranscendTranslation, Travelbird, Trevor MacInnis, Trevor Wennblom, Tristanb, Trumpy, Tsemii, Tubular, Tweetlebeetle367, Twix617, Tyrol5, Ubiq, Ucucha, Uhai, Unckc, Unschool, Unveiled, Unyoyega, V.narsikar, Vadith, Vanished user 39948282, Vary, Versageek, Versus22, ViciousPotato, Vihsadas, Vishnava, Vivio Testarossa, Vrenator, WadeSimMiser, Walter2cobb, Wavelength, Wayne Slam, Webclient101, Wham Bam Rock II, Whatiguana, Whkoh, Widr, Wikid77, WikipedianMarlith, Wikipelli, Will Beback, Wimt, WinContro, Woohookitty, World, Worldedixor, Woudloper, Wouterstomp, Wronghumor67, Wtmitchell, Xanchester, Xcentaur, Xufanc, Yanamad, YauTou, Ybbor, Yboord028, Yojimbo9102, Yurei-eggtart, Zackkelly, Zannah, Zefr, Zuzuu, ﺃﺣﻤﺪ.ﻏﺎﻣﺪﻱ.24, आशीष भटनागर, 1599 anonymous edits
616
Image Sources, Licenses and Contributors
617
Image Sources, Licenses and Contributors
Image:Illu_quiz_hn_02.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_quiz_hn_02.jpg License: Public Domain Contributors: Arcadian, Flappiefh, It Is Me Here, Petrus Adamus, 3 anonymous edits Image:Digestive system diagram en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Digestive_system_diagram_en.svg License: Public Domain Contributors: Mariana Ruiz Villarreal(LadyofHats) Image:chronic sialadenitis.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Chronic_sialadenitis.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron File:Ebner's gland.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Ebner's_gland.JPG License: Creative Commons Zero Contributors: Pawelolek1991 Image:illu_breast_anatomy.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_breast_anatomy.jpg License: Public Domain Contributors: user:Maksim Image:Dissected lactating breast gray1172.png Source: http://en.wikipedia.org/w/index.php?title=File:Dissected_lactating_breast_gray1172.png License: Public Domain Contributors: AxelBoldt, The Honorable Image:Bezerro mamando REFON .jpg Source: http://en.wikipedia.org/w/index.php?title=File:Bezerro_mamando_REFON_.jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: José Reynaldo da Fonseca (user Reynaldo) Image:White Cat Nursing Four Kittens HQ.jpg Source: http://en.wikipedia.org/w/index.php?title=File:White_Cat_Nursing_Four_Kittens_HQ.jpg License: GNU Free Documentation License Contributors: Ardfern, Kilom691, Pitke, Rune X2, 1 anonymous edits Image:Piglets1.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Piglets1.jpg License: Creative Commons Attribution 2.0 Contributors: FlickrLickr, FlickreviewR, Juiced lemon, Kersti Nebelsiek, Para, Ranveig Image:Baby sheep feeding.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Baby_sheep_feeding.JPG License: Creative Commons Attribution 2.5 Contributors: Gabriel Pollard Image:Kid feeding on mothers milk.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Kid_feeding_on_mothers_milk.jpg License: unknown Contributors: Fir0002 Image:Elephant_breastfeading.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Elephant_breastfeading.jpg License: Creative Commons Attribution-Sharealike 2.0 Contributors: rkimpeljr Image:Breastfeeding_infant.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Breastfeeding_infant.jpg License: Public Domain Contributors: Ken Hammond () Image:Gray896.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray896.png License: Public Domain Contributors: Arcadian, Str4nd, Was a bee, 3 anonymous edits Image:Tear system.svg Source: http://en.wikipedia.org/w/index.php?title=File:Tear_system.svg License: Creative Commons Attribution-Sharealike 2.5 Contributors: User:Erin_Silversmith, User:FML Image:Gray514.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray514.png License: Public Domain Contributors: Arcadian, Lipothymia, Was a bee, 1 anonymous edits Image:Gray776.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray776.png License: Public Domain Contributors: Athaenara, FAEP, Foroa, Kersti Nebelsiek, Lipothymia, Torsch, Was a bee, 2 anonymous edits Image:Gray841.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray841.png License: Public Domain Contributors: Jacklee, Magnus Manske Image:Gray895.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray895.png License: Public Domain Contributors: Arcadian, Was a bee Image:Gray897.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray897.png License: Public Domain Contributors: Arcadian File:Slide3abab.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide3abab.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide4abab.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide4abab.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide5abab.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide5abab.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide6abab.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide6abab.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide7abab.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide7abab.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 Image:Gray940 - sweat gland.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray940_-_sweat_gland.png License: Public Domain Contributors: Prof. Squirrel Image:HairFollicle.png Source: http://en.wikipedia.org/w/index.php?title=File:HairFollicle.png License: Public domain Contributors: User:Helix84 Image:Skin.png Source: http://en.wikipedia.org/w/index.php?title=File:Skin.png License: Public Domain Contributors: US-Gov Image:Haarbalgmilbe.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Haarbalgmilbe.jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: Blauerauerhahn, Eusebius, Liné1 Image:Pilosebaceous_Unit_4x.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Pilosebaceous_Unit_4x.JPG License: unknown Contributors: Kilbad Image:Base of Pilosebaceous Unit 10x.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Base_of_Pilosebaceous_Unit_10x.JPG License: Public Domain Contributors: Kilbad Image:Insertion_of_sebaceous_glands_into_hair_shaft_x10.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Insertion_of_sebaceous_glands_into_hair_shaft_x10.jpg License: Public Domain Contributors: Kilbad Image:Gray893.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray893.png License: Public Domain Contributors: Arcadian, Eug, 1 anonymous edits Image:Gray944.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray944.png License: Public Domain Contributors: Keenan Pepper, Lennert B, Man vyi, Omegatron Image:Gray857.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray857.png License: Public Domain Contributors: Arcadian, Magnus Manske, OldakQuill Image:gray1058.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1058.png License: Public Domain Contributors: Arcadian, Magnus Manske, Origamiemensch File:Duodenum-brunner's glands.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Duodenum-brunner's_glands.JPG License: Public Domain Contributors: Jpogi at en.wikipedia Image:Prostatelead.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Prostatelead.jpg License: Public Domain Contributors: Created by US government agency National Cancer Institute Image:Gray1160.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1160.png License: Public Domain Contributors: Arcadian, Lennert B, Mdangers Image:Corpora amylacea intermed mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Corpora_amylacea_intermed_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:UltrasoundBPH.jpg Source: http://en.wikipedia.org/w/index.php?title=File:UltrasoundBPH.jpg License: Creative Commons Attribution 3.0 Contributors: Etan J. Tal Image:Prostate middle lobe orig.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Prostate_middle_lobe_orig.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Steven Fruitsmaak Image:Inflammation of prostate.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Inflammation_of_prostate.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Prostate adenocarcinoma 2 high mag hps.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Prostate_adenocarcinoma_2_high_mag_hps.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Illu bladder.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_bladder.jpg License: Public Domain Contributors: U.S. National Cancer Institute's Surveillance, Epidemiology and End Results (SEER) Program Image:Illu penis.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_penis.jpg License: Public Domain Contributors: Arcadian, Ephraim33, Hu Totya, Origamiemensch Image:Illu prostate lobes.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_prostate_lobes.jpg License: Public Domain Contributors: Arcadian, Ephraim33 Image:Illu prostate zones.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_prostate_zones.jpg License: Public Domain Contributors: Arcadian, Nevit Image:Illu quiz prostate01.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_quiz_prostate01.jpg License: Public Domain Contributors: Arcadian Image:Prostatehistology.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Prostatehistology.jpg License: Public Domain Contributors: Original: NIH, Explanation: en:User:InvictaHOG Image:male anatomy.png Source: http://en.wikipedia.org/w/index.php?title=File:Male_anatomy.png License: GNU Free Documentation License Contributors: Ephraim33, Frank C. Müller, Lennert B, Odedee, Ranveig, Saperaud, Stephanie, Tsaitgaist, Xiong Chiamiov Image:Gray543.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray543.png License: Public Domain Contributors: Arcadian, Ephraim33 Image:Gray619.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray619.png License: Public Domain Contributors: Arcadian
Image Sources, Licenses and Contributors
Image:Gray1152.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1152.png License: Public Domain Contributors: Arcadian, Origamiemensch Image:Gray1153.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1153.png License: Public Domain Contributors: Arcadian, Ephraim33 Image:Gray1156.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1156.png License: Public Domain Contributors: Arcadian, Ephraim33, Origamiemensch, Yestadae Image:Prostatic urethra.svg Source: http://en.wikipedia.org/w/index.php?title=File:Prostatic_urethra.svg License: Creative Commons Attribution 3.0 Contributors: User:Mcstrother File:Prostatic urethra.svg Source: http://en.wikipedia.org/w/index.php?title=File:Prostatic_urethra.svg License: Creative Commons Attribution 3.0 Contributors: User:Mcstrother Image:Gray1136.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1136.png License: Public Domain Contributors: Arcadian, Ephraim33, Magnus Manske, Origamiemensch Image:Skenes gland.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Skenes_gland.jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: Original uploader was Nicholasolan at en.wikipedia Image:Illu cervix.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_cervix.jpg License: Public Domain Contributors: Arcadian, LERK, M1ss1ontomars2k4, MichaelFrey, Nevit, Speck-Made, Waldir File:Endometrium ocp use3.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Endometrium_ocp_use3.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron File:Endometrium ocp use0.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Endometrium_ocp_use0.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron File:HumanEmbryogenesis.svg Source: http://en.wikipedia.org/w/index.php?title=File:HumanEmbryogenesis.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Zephyris Image:Gray1169.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1169.png License: Public Domain Contributors: Arcadian Image:Endometrial adenocarcinoma (1).jpg Source: http://en.wikipedia.org/w/index.php?title=File:Endometrial_adenocarcinoma_(1).jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: Ares.it, Dam, KGH Image:Uterus (endometrium).JPG Source: http://en.wikipedia.org/w/index.php?title=File:Uterus_(endometrium).JPG License: Public Domain Contributors: Jpogi Image:Endometrium_ocp_use2.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Endometrium_ocp_use2.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Endometrium_ocp_use1.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Endometrium_ocp_use1.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Endometrial stromal condensation high mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Endometrial_stromal_condensation_high_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Fundic gland polyp (1).jpg Source: http://en.wikipedia.org/w/index.php?title=File:Fundic_gland_polyp_(1).jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: Alex brollo, Ares.it, Dam, KGH, 1 anonymous edits Image:Gray1055.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1055.png License: Public Domain Contributors: Arcadian, Magnus Manske, Origamiemensch Image:Chief cells.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Chief_cells.JPG License: GNU Free Documentation License Contributors: en:User:Jpogi Image:Parietal cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Parietal_cells.jpg License: Public Domain Contributors: Original uploader was Jpogi at en.wikipedia Image:Control-of-stomach-acid-sec.png Source: http://en.wikipedia.org/w/index.php?title=File:Control-of-stomach-acid-sec.png License: Creative Commons Attribution-ShareAlike 1.0 Generic Contributors: Haabet, Jacklee, Julia W, Perhelion, Psychonaut, Saperaud, Sophus Bie File:GASTRIC PARIETAL CELL ANTIBODIES.jpg Source: http://en.wikipedia.org/w/index.php?title=File:GASTRIC_PARIETAL_CELL_ANTIBODIES.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Simoncaulton Image:Hydrochloric acid 30 percent.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Hydrochloric_acid_30_percent.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Chemicalinterest, Materialscientist, Woelen, 2 anonymous edits File:Yes check.svg Source: http://en.wikipedia.org/w/index.php?title=File:Yes_check.svg License: Public Domain Contributors: Anomie File:X mark.svg Source: http://en.wikipedia.org/w/index.php?title=File:X_mark.svg License: Public Domain Contributors: User:Gmaxwell File:Phase diagram HCl H2O s l.PNG Source: http://en.wikipedia.org/w/index.php?title=File:Phase_diagram_HCl_H2O_s_l.PNG License: Public Domain Contributors: Steffen 962 File:Stomach mucosal layer labeled.svg Source: http://en.wikipedia.org/w/index.php?title=File:Stomach_mucosal_layer_labeled.svg License: Creative Commons Attribution 3.0 Contributors: M•Komorniczak -talk- 11:43, 23 April 2011 (UTC) File:UN transport pictogram - 8.svg Source: http://en.wikipedia.org/w/index.php?title=File:UN_transport_pictogram_-_8.svg License: Public Domain Contributors: United Nations Economic Commsion for Europe File:Hazard C.svg Source: http://en.wikipedia.org/w/index.php?title=File:Hazard_C.svg License: Public Domain Contributors: Amishaa, Augiasstallputzer, BLueFiSH.as, Bangin, Cosmo1976, Cäsium137, Herbythyme, MarianSigler, Matthias M., Pavel92, Phrood, W!B:, ﺭﻫﮕﺬﺭ ﻏﺮﯾﺐ, 12 anonymous edits Image:Stomach colon rectum diagram.svg Source: http://en.wikipedia.org/w/index.php?title=File:Stomach_colon_rectum_diagram.svg License: Public Domain Contributors: Indolences created it on the English Wikipedia. Image:Digestive system diagram edit.svg Source: http://en.wikipedia.org/w/index.php?title=File:Digestive_system_diagram_edit.svg License: Public Domain Contributors: Mariana RuizLadyofHats, edited by Joaquim Alves Gaspar File:Gut wall.svg Source: http://en.wikipedia.org/w/index.php?title=File:Gut_wall.svg License: Creative Commons Attribution 3.0 Contributors: Original uploader was Auawise at en.wikipedia (Original text : Λua∫Wise (Operibus anteire)) Image:Gray1053.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1053.png License: Public Domain Contributors: Arcadian, DO11.10, Haabet, Jacklee, Magnus Manske, Origamiemensch Image:Gray1060.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1060.png License: Public Domain Contributors: Arcadian, Magnus Manske, Origamiemensch Image:Gray1062.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1062.png License: Public Domain Contributors: Arcadian, Magnus Manske, Origamiemensch Image:Gobletcel.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Gobletcel.jpg License: Copyrighted free use Contributors: Arcadian, JMCC1, Theoteryi File:MultiPhotonExcitation-Fig10-doi10.1186slash1475-925X-5-36.JPEG Source: http://en.wikipedia.org/w/index.php?title=File:MultiPhotonExcitation-Fig10-doi10.1186slash1475-925X-5-36.JPEG License: Creative Commons Attribution 2.0 Contributors: Alberto Diaspro, Paolo Bianchini, Giuseppe Vicidomini, Mario Faretta, Paola Ramoino and Cesare Usai Image:Respiratory system complete numbered.svg Source: http://en.wikipedia.org/w/index.php?title=File:Respiratory_system_complete_numbered.svg License: Public Domain Contributors: LadyofHats File:Respiratory Tract Histological Differences.png Source: http://en.wikipedia.org/w/index.php?title=File:Respiratory_Tract_Histological_Differences.png License: Creative Commons Attribution 3.0 Contributors: Anmats, Dmalicke, Trijnstel File:Mucus cells.png Source: http://en.wikipedia.org/w/index.php?title=File:Mucus_cells.png License: Creative Commons Attribution 2.5 Contributors: see source Image:GLO1 Homo sapiens small fast.gif Source: http://en.wikipedia.org/w/index.php?title=File:GLO1_Homo_sapiens_small_fast.gif License: Creative Commons Attribution 3.0 Contributors: WillowW Image:Carbonic anhydrase.png Source: http://en.wikipedia.org/w/index.php?title=File:Carbonic_anhydrase.png License: Public Domain Contributors: Labrador2 Image:Induced fit diagram.svg Source: http://en.wikipedia.org/w/index.php?title=File:Induced_fit_diagram.svg License: Public Domain Contributors: Created by TimVickers, vectorized by Fvasconcellos Image:Enzyme allostery en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Enzyme_allostery_en.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: File:Enzyme allostery es.svg: File:Enzyme allostery es.png: File:Enzyme allostery.png: Allostery.png: Nicolas Le Novere (talk). Original uploader was Lenov at en.wikipedia derivative work: TimVickers (talk) derivative work: Retama (talk) derivative work: KES47 (talk) derivative work: KES47 (talk) Image:NADH-3D-vdW.png Source: http://en.wikipedia.org/w/index.php?title=File:NADH-3D-vdW.png License: Public Domain Contributors: Benjah-bmm27 Image:Carbonic anhydrase reaction in tissue.svg Source: http://en.wikipedia.org/w/index.php?title=File:Carbonic_anhydrase_reaction_in_tissue.svg License: GNU Free Documentation License Contributors: Fvasconcellos Image:Simple mechanism.svg Source: http://en.wikipedia.org/w/index.php?title=File:Simple_mechanism.svg License: Public domain Contributors: TimVickers at en.wikipedia
618
Image Sources, Licenses and Contributors
Image:Michaelis-Menten saturation curve of an enzyme reaction.svg Source: http://en.wikipedia.org/w/index.php?title=File:Michaelis-Menten_saturation_curve_of_an_enzyme_reaction.svg License: Public Domain Contributors: fullofstars Image:Competitive inhibition.svg Source: http://en.wikipedia.org/w/index.php?title=File:Competitive_inhibition.svg License: Public Domain Contributors: Authored by Jerry Crimson Mann, modified by TimVickers, vectorized by Fvasconcellos Image:Types of inhibition en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Types_of_inhibition_en.svg License: Public Domain Contributors: fullofstars Image:Methotrexate and folic acid compared.png Source: http://en.wikipedia.org/w/index.php?title=File:Methotrexate_and_folic_acid_compared.png License: Public domain Contributors: TimVickers Image:Glycolysis.svg Source: http://en.wikipedia.org/w/index.php?title=File:Glycolysis.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: WYassineMrabetTalk ✉ Image:Phenylalanine hydroxylase brighter.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Phenylalanine_hydroxylase_brighter.jpg License: Public domain Contributors: TimVickers Image:Amylose.svg Source: http://en.wikipedia.org/w/index.php?title=File:Amylose.svg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: HenkvD, Jan Homann, Sunridin, Yarl, 2 anonymous edits Image:Sjb whiskey malt.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Sjb_whiskey_malt.jpg License: GNU Free Documentation License Contributors: Finlay_McWalter's friend SJB Image:Roquefort cheese.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Roquefort_cheese.jpg License: GNU Free Documentation License Contributors: HenkvD, Lionel Allorge, Mercurywoodrose, Olivier2, Quadell, Ranveig, Yosri, Zerohund Image:Alpha-D-Glucopyranose.svg Source: http://en.wikipedia.org/w/index.php?title=File:Alpha-D-Glucopyranose.svg License: Public Domain Contributors: NEUROtiker Image:Alpha-D-Fructofuranose.svg Source: http://en.wikipedia.org/w/index.php?title=File:Alpha-D-Fructofuranose.svg License: Public Domain Contributors: NEUROtiker Image:InternationalPaper6413.jpg Source: http://en.wikipedia.org/w/index.php?title=File:InternationalPaper6413.jpg License: GNU Free Documentation License Contributors: Pollinator Image:Cellulose-Ibeta-from-xtal-2002-3D-balls.png Source: http://en.wikipedia.org/w/index.php?title=File:Cellulose-Ibeta-from-xtal-2002-3D-balls.png License: Public Domain Contributors: Ben Mills Image:DNA123 rotated.png Source: http://en.wikipedia.org/w/index.php?title=File:DNA123_rotated.png License: Public Domain Contributors: DNA Image:Human Paneth cells.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Human_Paneth_cells.JPG License: Public Domain Contributors: en:Jpogi Image:Bicarbonate-resonance.png Source: http://en.wikipedia.org/w/index.php?title=File:Bicarbonate-resonance.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: Hellbus Image:Bicarbonate-ion-3D-balls.png Source: http://en.wikipedia.org/w/index.php?title=File:Bicarbonate-ion-3D-balls.png License: Public Domain Contributors: Ben Mills and Jynto Image:Equilibrium.svg Source: http://en.wikipedia.org/w/index.php?title=File:Equilibrium.svg License: Public Domain Contributors: L'Aquatique File:Riassorbimento bicarbonati e respirazione cellulare.svg Source: http://en.wikipedia.org/w/index.php?title=File:Riassorbimento_bicarbonati_e_respirazione_cellulare.svg License: Public Domain Contributors: Riassorbimento_bicarbonati_e_respirazione_cellulare.jpg: Gianreali derivative work: Luigi Chiesa (talk) File:Reference ranges for blood tests - by molarity.png Source: http://en.wikipedia.org/w/index.php?title=File:Reference_ranges_for_blood_tests_-_by_molarity.png License: Public Domain Contributors: Mikael Häggström File:lysozyme crystal1.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Lysozyme_crystal1.JPG License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: Chrumps, Kruusamägi, Lode, Perditax file:Lysozyme.png Source: http://en.wikipedia.org/w/index.php?title=File:Lysozyme.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: Yikrazuul file:PBB_GE_LYZ_213975_s_at_tn.png Source: http://en.wikipedia.org/w/index.php?title=File:PBB_GE_LYZ_213975_s_at_tn.png License: GNU Free Documentation License Contributors: File:Mecanism of action for Lysozyme.svg Source: http://en.wikipedia.org/w/index.php?title=File:Mecanism_of_action_for_Lysozyme.svg License: Creative Commons Zero Contributors: User:Pierreb24 File:Micelle.png Source: http://en.wikipedia.org/w/index.php?title=File:Micelle.png License: GNU Free Documentation License Contributors: User:Onco p53 Image:Micelle scheme-en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Micelle_scheme-en.svg License: Creative Commons Attribution-Sharealike 3.0,2.5,2.0,1.0 Contributors: SuperManu File:TensideHyrophilHydrophob.png Source: http://en.wikipedia.org/w/index.php?title=File:TensideHyrophilHydrophob.png License: GNU Free Documentation License Contributors: Roland.chem Original uploader was Roland.chem at de.wikipedia file:Oxytocin with labels.png Source: http://en.wikipedia.org/w/index.php?title=File:Oxytocin_with_labels.png License: Public Domain Contributors: Edgar181 file:OxitocinaCPK3D.png Source: http://en.wikipedia.org/w/index.php?title=File:OxitocinaCPK3D.png License: Creative Commons Zero Contributors: MindZiper File:Oxytocin-neurophysin.png Source: http://en.wikipedia.org/w/index.php?title=File:Oxytocin-neurophysin.png License: Public Domain Contributors: Edgar181 file:Arginine vasopressin3d.png Source: http://en.wikipedia.org/w/index.php?title=File:Arginine_vasopressin3d.png License: Public Domain Contributors: Fvasconcellos file:PBB_GE_AVP_207848_at_tn.png Source: http://en.wikipedia.org/w/index.php?title=File:PBB_GE_AVP_207848_at_tn.png License: GNU Free Documentation License Contributors: File:AVP, ISH, periventricular region of the hypothalamus, adult mouse.jpg Source: http://en.wikipedia.org/w/index.php?title=File:AVP,_ISH,_periventricular_region_of_the_hypothalamus,_adult_mouse.jpg License: Creative Commons Attribution 1.0 Generic Contributors: Allen Institute for Brain Science File:vasopressin labeled.png Source: http://en.wikipedia.org/w/index.php?title=File:Vasopressin_labeled.png License: Public Domain Contributors: Edgar181 File:Oxytocin with labels.png Source: http://en.wikipedia.org/w/index.php?title=File:Oxytocin_with_labels.png License: Public Domain Contributors: Edgar181 Image:Serotonin-2D-skeletal.svg Source: http://en.wikipedia.org/w/index.php?title=File:Serotonin-2D-skeletal.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Liaocyed Image:Serotonin-Spartan-HF-based-on-xtal-3D-balls-web.png Source: http://en.wikipedia.org/w/index.php?title=File:Serotonin-Spartan-HF-based-on-xtal-3D-balls-web.png License: Public Domain Contributors: Ben Mills Image:Serotonin-Spartan-HF-based-on-xtal-3D-sf-web.png Source: http://en.wikipedia.org/w/index.php?title=File:Serotonin-Spartan-HF-based-on-xtal-3D-sf-web.png License: Public Domain Contributors: Ben Mills File:Dopamineseratonin.png Source: http://en.wikipedia.org/w/index.php?title=File:Dopamineseratonin.png License: Public Domain Contributors: A3 nm, Fuzzform, MithrandirMage, Monkeybait, Åkebråke, 1 anonymous edits File:Serotonin biosynthesis.svg Source: http://en.wikipedia.org/w/index.php?title=File:Serotonin_biosynthesis.svg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: NEUROtiker Image:Alpha-neoendorphin.svg Source: http://en.wikipedia.org/w/index.php?title=File:Alpha-neoendorphin.svg License: Public Domain Contributors: Ed (Edgar181) Image:Beta-endorphin.png Source: http://en.wikipedia.org/w/index.php?title=File:Beta-endorphin.png License: Public Domain Contributors: Edgar181 (talk) file:Somatostatin.svg Source: http://en.wikipedia.org/w/index.php?title=File:Somatostatin.svg License: Public Domain Contributors: Ed (Edgar181) file:PBB_GE_SST_213921_at_tn.png Source: http://en.wikipedia.org/w/index.php?title=File:PBB_GE_SST_213921_at_tn.png License: GNU Free Documentation License Contributors: File:Sst, ISH, E15.5, telencephalon.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Sst,_ISH,_E15.5,_telencephalon.jpg License: Creative Commons Attribution 1.0 Generic Contributors: Allen Institute for Brain Science File:Sst, ISH, p56 mouse.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Sst,_ISH,_p56_mouse.jpg License: Creative Commons Attribution 1.0 Generic Contributors: Allen Institute for Brain Science file:PBB_GE_GAST_208138_at_tn.png Source: http://en.wikipedia.org/w/index.php?title=File:PBB_GE_GAST_208138_at_tn.png License: GNU Free Documentation License Contributors: file:PBB_GE_CCK_205827_at_tn.png Source: http://en.wikipedia.org/w/index.php?title=File:PBB_GE_CCK_205827_at_tn.png License: GNU Free Documentation License Contributors: file:InsulinHexamer.jpg Source: http://en.wikipedia.org/w/index.php?title=File:InsulinHexamer.jpg License: Creative Commons Attribution 2.5 Contributors: Original uploader was Takometer at en.wikipedia file:PBB_GE_INS_206598_at_tn.png Source: http://en.wikipedia.org/w/index.php?title=File:PBB_GE_INS_206598_at_tn.png License: GNU Free Documentation License Contributors: -
619
Image Sources, Licenses and Contributors
Image:Insulinpath.png Source: http://en.wikipedia.org/w/index.php?title=File:Insulinpath.png License: Creative Commons Attribution 2.5 Contributors: Original uploader was Takometer at en.wikipedia Image:Pancreas insulin oscillations.svg Source: http://en.wikipedia.org/w/index.php?title=File:Pancreas_insulin_oscillations.svg License: Public Domain Contributors: Made with inkscape, for the sake of free knowledge to all mankind, by Mikael Häggström (User:Mikael Häggström) Image:Suckale08 fig3 glucose insulin day.png Source: http://en.wikipedia.org/w/index.php?title=File:Suckale08_fig3_glucose_insulin_day.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: Jakob Suckale, Michele Solimena File:Insulin glucose metabolism ZP.svg Source: http://en.wikipedia.org/w/index.php?title=File:Insulin_glucose_metabolism_ZP.svg License: Public domain Contributors: XcepticZP at en.wikipedia File:Inzulín.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Inzulín.jpg License: Public Domain Contributors: Original uploader was Mr Hyde at cs.wikipedia (Original text : moje foto) Image:InsulinMonomer.jpg Source: http://en.wikipedia.org/w/index.php?title=File:InsulinMonomer.jpg License: Creative Commons Attribution 2.5 Contributors: Isaac Yonemoto. File:C. H. Best and F. G. Banting ca. 1924.png Source: http://en.wikipedia.org/w/index.php?title=File:C._H._Best_and_F._G._Banting_ca._1924.png License: Public Domain Contributors: YUL89YYZ Image:Nicolae Paulescu - Foto03.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Nicolae_Paulescu_-_Foto03.jpg License: Public Domain Contributors: FSII, Mvelam file:Glucagon- 1GCN.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Glucagon-_1GCN.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Truthortruth file:PBB_GE_GCG_206422_at_tn.png Source: http://en.wikipedia.org/w/index.php?title=File:PBB_GE_GCG_206422_at_tn.png License: GNU Free Documentation License Contributors: Image:Glucagon rednblue.png Source: http://en.wikipedia.org/w/index.php?title=File:Glucagon_rednblue.png License: Public domain Contributors: Original uploader was Brazucs at en.wikipedia file:Glucagon.png Source: http://en.wikipedia.org/w/index.php?title=File:Glucagon.png License: Public Domain Contributors: User:Brian0918 Image:Bombesin_full.png Source: http://en.wikipedia.org/w/index.php?title=File:Bombesin_full.png License: Attribution Contributors: Megac7 Image:Gray1176.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1176.png License: Public Domain Contributors: Arcadian, Materialscientist, Quibik File:Thyroid hormone synthesis.png Source: http://en.wikipedia.org/w/index.php?title=File:Thyroid_hormone_synthesis.png License: Creative Commons Zero Contributors: Mikael Häggström Image:illu_endocrine_system.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_endocrine_system.jpg License: Public Domain Contributors: Kam Solusar, Kilom691, Truthflux, Was a bee, 2 anonymous edits Image:Illu thyroid parathyroid.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_thyroid_parathyroid.jpg License: Public Domain Contributors: Bemoeial1, Kulmalukko, Lennert B, 2 anonymous edits Image:Parathyroid gland high mag cropped.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Parathyroid_gland_high_mag_cropped.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Parathyroid gland high mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Parathyroid_gland_high_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Parathyroid gland intermed mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Parathyroid_gland_intermed_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Parathyroid gland low mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Parathyroid_gland_low_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Gray1175.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1175.png License: Public Domain Contributors: Arcadian image:Gray1177.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1177.png License: Public Domain Contributors: Arcadian, Tsca Image:Gray1185.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1185.png License: Public Domain Contributors: Dodo File:Adrenaline.svg Source: http://en.wikipedia.org/w/index.php?title=File:Adrenaline.svg License: Public Domain Contributors: Harbin File:Norepinephrine structure.png Source: http://en.wikipedia.org/w/index.php?title=File:Norepinephrine_structure.png License: Public Domain Contributors: Original uploader was Edgar181 at en.wikipedia File:Steroidogenesis.svg Source: http://en.wikipedia.org/w/index.php?title=File:Steroidogenesis.svg License: GNU Free Documentation License Contributors: David Richfield (User:Slashme) and Mikael Häggström Derived from previous version by Hoffmeier and Settersr. Image:Aldosterone-2D-skeletal.svg Source: http://en.wikipedia.org/w/index.php?title=File:Aldosterone-2D-skeletal.svg License: Public Domain Contributors: Image:Aldosterone-2D-skeletal.png by Ben Mills, vectorized by Image:11-Deoxycorticosterone.svg Source: http://en.wikipedia.org/w/index.php?title=File:11-Deoxycorticosterone.svg License: Public Domain Contributors: Ed (Edgar181) Image:Fludrocortisone structure.png Source: http://en.wikipedia.org/w/index.php?title=File:Fludrocortisone_structure.png License: Public Domain Contributors: Edgar181 Image:Cortisol2.svg Source: http://en.wikipedia.org/w/index.php?title=File:Cortisol2.svg License: Public Domain Contributors: Calvero. Image:Dexamethasone structure.svg Source: http://en.wikipedia.org/w/index.php?title=File:Dexamethasone_structure.svg License: Public Domain Contributors: Ed (Edgar181) Image:YerkesDodsonLawGraph.png Source: http://en.wikipedia.org/w/index.php?title=File:YerkesDodsonLawGraph.png License: Public Domain Contributors: User:Vaughan File:Cortisone acetate.png Source: http://en.wikipedia.org/w/index.php?title=File:Cortisone_acetate.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: Yid (talk). Original uploader was Yid at en.wikipedia Image:Leydig cells - very high mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Leydig_cells_-_very_high_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Testicle-histology-boar-2.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Testicle-histology-boar-2.jpg License: Creative Commons Attribution-Sharealike 2.5 Contributors: Original uploader was Mikael Häggström at en.wikipedia Image:Leydig cell tumour3.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Leydig_cell_tumour3.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Gray1114.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1114.png License: Public Domain Contributors: Arcadian, Ephraim33, Magnus Manske, Origamiemensch Image:Leydig cell tumour2.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Leydig_cell_tumour2.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image: Leydig cells.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Leydig_cells.JPG License: Public Domain Contributors: Jpogi File:Order of changes in ovary.svg Source: http://en.wikipedia.org/w/index.php?title=File:Order_of_changes_in_ovary.svg License: GNU Free Documentation License Contributors: user:Shazz File:Folliculogenesis chart.gif Source: http://en.wikipedia.org/w/index.php?title=File:Folliculogenesis_chart.gif License: Public domain Contributors: Original uploader was D. Wu at en.wikipedia File:Non-Growing Follicles.png Source: http://en.wikipedia.org/w/index.php?title=File:Non-Growing_Follicles.png License: Creative Commons Attribution 3.0 Contributors: Geremia, Rjwilmsi Image:Gray1163.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1163.png License: Public Domain Contributors: Arcadian, Mdangers, Origamiemensch File:Primary follicle (transition).jpg Source: http://en.wikipedia.org/w/index.php?title=File:Primary_follicle_(transition).jpg License: Public Domain Contributors: Original uploader was Jpogi at en.wikipedia file:Progesteron.svg Source: http://en.wikipedia.org/w/index.php?title=File:Progesteron.svg License: Public Domain Contributors: NEUROtiker file:Progesterone-3D-vdW.png Source: http://en.wikipedia.org/w/index.php?title=File:Progesterone-3D-vdW.png License: Public Domain Contributors: Benjah-bmm27, Edgar181, MindZiper Image:Progesterone biosynthesis.png Source: http://en.wikipedia.org/w/index.php?title=File:Progesterone_biosynthesis.png License: Public Domain Contributors: Boghog2 Image:Marker snythesis.png Source: http://en.wikipedia.org/w/index.php?title=File:Marker_snythesis.png License: Public Domain Contributors: Boghog2 Image:Progesterone Synthesis.png Source: http://en.wikipedia.org/w/index.php?title=File:Progesterone_Synthesis.png License: Public Domain Contributors: Johnson, W. S. File:Progesterone during menstrual cycle.png Source: http://en.wikipedia.org/w/index.php?title=File:Progesterone_during_menstrual_cycle.png License: Public Domain Contributors: Mikael Häggström
620
Image Sources, Licenses and Contributors
Image:Endometrium ocp use3.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Endometrium_ocp_use3.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron File:000527lg Prometrium 100 MG Oral Capsule.jpg Source: http://en.wikipedia.org/w/index.php?title=File:000527lg_Prometrium_100_MG_Oral_Capsule.jpg License: Public domain Contributors: NLM Image:Pregnenolone.svg Source: http://en.wikipedia.org/w/index.php?title=File:Pregnenolone.svg License: Public Domain Contributors: Ed (Edgar181) Image:Order_of_changes_in_ovary.svg Source: http://en.wikipedia.org/w/index.php?title=File:Order_of_changes_in_ovary.svg License: GNU Free Documentation License Contributors: user:Shazz Image:Human Ovary with Fully Developed Corpus Luteum.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Human_Ovary_with_Fully_Developed_Corpus_Luteum.jpg License: Creative Commons Attribution-Sharealike 2.0 Contributors: Ed Uthman Image:Luteinized follicular cyst.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Luteinized_follicular_cyst.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Juxtaglomerular cells.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Juxtaglomerular_cells.JPG License: Public Domain Contributors: Jpogi Image:Renal corpuscle.svg Source: http://en.wikipedia.org/w/index.php?title=File:Renal_corpuscle.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: M•Komorniczak -talk- (polish Wikipedist) file:PDB_2ren_EBI.jpg Source: http://en.wikipedia.org/w/index.php?title=File:PDB_2ren_EBI.jpg License: unknown Contributors: File:Renin-angiotensin system in man shadow.svg Source: http://en.wikipedia.org/w/index.php?title=File:Renin-angiotensin_system_in_man_shadow.svg License: Public Domain Contributors: Mikael Häggström Image:Renin-angiotensin-aldosterone system.png Source: http://en.wikipedia.org/w/index.php?title=File:Renin-angiotensin-aldosterone_system.png License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: A. Rad, Joey-das-WBF, Kallerna, Rillke, 4 anonymous edits Image:Epidermis-delimited.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Epidermis-delimited.JPG License: Public Domain Contributors: Normal_Epidermis_and_Dermis_with_Intradermal_Nevus_10x.JPG: Kilbad Cropped and labeled by Fama Clamosa (talk) and Mikael Häggström, respectively Image:Epidermal layers.png Source: http://en.wikipedia.org/w/index.php?title=File:Epidermal_layers.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: Mikael Häggström, based on work by Wbensmith Image:Skinlayers.png Source: http://en.wikipedia.org/w/index.php?title=File:Skinlayers.png License: Public Domain Contributors: Serephine, 1 anonymous edits Image:Normal Epidermis and Dermis with Intradermal Nevus 10x.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Normal_Epidermis_and_Dermis_with_Intradermal_Nevus_10x.JPG License: Public Domain Contributors: Kilbad Image:HautFingerspitzeOCT.gif Source: http://en.wikipedia.org/w/index.php?title=File:HautFingerspitzeOCT.gif License: Creative Commons Attribution-Sharealike 2.0 Contributors: User:BoP, Supplied by the medOCT group, Medical University Vienna, Austria Image:Mouse embryonic stem cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Mouse_embryonic_stem_cells.jpg License: Public Domain Contributors: ChongDae, Salix, The Evil IP address, 1 anonymous edits Image:Human embryonic stem cell colony phase.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Human_embryonic_stem_cell_colony_phase.jpg License: Public Domain Contributors: Original uploader was Id711 at en.wikipedia Image:Stem cells diagram.png Source: http://en.wikipedia.org/w/index.php?title=File:Stem_cells_diagram.png License: Creative Commons Attribution-Sharealike 2.5 Contributors: Mike Jones Image:Human embryonic stem cells.png Source: http://en.wikipedia.org/w/index.php?title=File:Human_embryonic_stem_cells.png License: Creative Commons Attribution 2.5 Contributors: (Images: Nissim Benvenisty) Image:Stem cell division and differentiation.svg Source: http://en.wikipedia.org/w/index.php?title=File:Stem_cell_division_and_differentiation.svg License: Public Domain Contributors: User:Wykis File:Stem cell treatments.svg Source: http://en.wikipedia.org/w/index.php?title=File:Stem_cell_treatments.svg License: Public Domain Contributors: Mikael Häggström File:Yong Zhao smiling Portrait.png Source: http://en.wikipedia.org/w/index.php?title=File:Yong_Zhao_smiling_Portrait.png License: Creative Commons Attribution 3.0 Contributors: Leo181 File:Martin Evans Nobel Prize.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Martin_Evans_Nobel_Prize.jpg License: Creative Commons Attribution 3.0 Contributors: Cardiff University Image:Gray945.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray945.png License: Public Domain Contributors: Arcadian, Jacklee, Kersti Nebelsiek, Lamiot, Magnus Manske File:Illu epithelium.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_epithelium.jpg License: Public Domain Contributors: Arcadian, BenFrantzDale, Incnis Mrsi, Origamiemensch, Romanm, 3 anonymous edits Image:Dogsquamos100x.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Dogsquamos100x.jpg License: Creative Commons Attribution-Share Alike Contributors: John Alan Elson Image:Cheekcells stained.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Cheekcells_stained.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Mulletsrokk Image:Illu epithelium.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_epithelium.jpg License: Public Domain Contributors: Arcadian, BenFrantzDale, Incnis Mrsi, Origamiemensch, Romanm, 3 anonymous edits File:Gray931.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray931.png License: Public Domain Contributors: Arcadian, Iainf, Jacklee, Jmarchn, Magnus Manske, Mike.lifeguard, Was a bee File:Organ of corti.svg Source: http://en.wikipedia.org/w/index.php?title=File:Organ_of_corti.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Madhero88 File:Gray932.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray932.png License: Public Domain Contributors: Gray's Anatomy File:Vestibular system's semicircular canal- a cross-section.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Vestibular_system's_semicircular_canal-_a_cross-section.jpg License: Public Domain Contributors: United States government File:Stereocilia of frog inner ear.01.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Stereocilia_of_frog_inner_ear.01.jpg License: Public Domain Contributors: Bechara Kachar File:Diagram of human skin.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Diagram_of_human_skin.jpg License: GNU Free Documentation License Contributors: Ngb, 1 anonymous edits File:Riechschleimhaut.svg Source: http://en.wikipedia.org/w/index.php?title=File:Riechschleimhaut.svg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: User:MarianSigler Image:Gray772.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray772.png License: Public Domain Contributors: Arcadian, Lipothymia, Magnus Manske, OldakQuill, Túrelio, Was a bee, 1 anonymous edits Image:Rod&Cone.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Rod&Cone.jpg License: Public Domain Contributors: Kosigrim Image:Cone-response.svg Source: http://en.wikipedia.org/w/index.php?title=File:Cone-response.svg License: GNU Free Documentation License Contributors: User:Maxim Razin File:Fig retine.png Source: http://en.wikipedia.org/w/index.php?title=File:Fig_retine.png License: Public Domain Contributors: Chrkl, Diego UFCG, Drahkrub, Jarry1250, Lipothymia, 1 anonymous edits Image:Cone2.svg Source: http://en.wikipedia.org/w/index.php?title=File:Cone2.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Madhero88 File:Cones SMJ2 E.svg Source: http://en.wikipedia.org/w/index.php?title=File:Cones_SMJ2_E.svg License: Creative Commons Attribution-Sharealike 3.0,2.5,2.0,1.0 Contributors: Vanessaezekowitz at en.wikipedia / Later version uploaded by BenRG. Image:Cone cell en.png Source: http://en.wikipedia.org/w/index.php?title=File:Cone_cell_en.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: Ivo Kruusamägi Image:BirdCone.png Source: http://en.wikipedia.org/w/index.php?title=File:BirdCone.png License: Public Domain Contributors: Jimfbleak Image:Gray1186.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1186.png License: Public Domain Contributors: Arcadian Image:Gray474.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray474.png License: Public Domain Contributors: Arcadian, Lipothymia Image:Carotid body tumour 2 intermed mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Carotid_body_tumour_2_intermed_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Gray1018.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1018.png License: Public Domain Contributors: Arcadian, Magnus Manske
621
Image Sources, Licenses and Contributors
Image:Taste bud.svg Source: http://en.wikipedia.org/w/index.php?title=File:Taste_bud.svg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: NEUROtiker Image:Smagsloeg.png Source: http://en.wikipedia.org/w/index.php?title=File:Smagsloeg.png License: unknown Contributors: User:Sjoehest Image:Neuron Hand-tuned.svg Source: http://en.wikipedia.org/w/index.php?title=File:Neuron_Hand-tuned.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Original uploader was Quasar Jarosz at en.wikipedia Image:Cultured schwann cell.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Cultured_schwann_cell.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Ucbtbej File:Gray839.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray839.png License: Public Domain Contributors: Gray's Anatomy File:SchematicP2XRsubunitJPG.jpg Source: http://en.wikipedia.org/w/index.php?title=File:SchematicP2XRsubunitJPG.jpg License: Public Domain Contributors: Subcellular File:Herpes simplex virions, TEM.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Herpes_simplex_virions,_TEM.jpg License: Public Domain Contributors: CDC/ Dr. Fred Murphy File:Neuroglia.png Source: http://en.wikipedia.org/w/index.php?title=File:Neuroglia.png License: Public Domain Contributors: Original uploader was Diberri at en.wikipedia File:Gfapastr5.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Gfapastr5.jpg License: Public Domain Contributors: Jacopo Werther, Maksim, Uwe Gille File:2010-3-15 rGFAP 1-4000 1-200 Hip 20x(4).jpg Source: http://en.wikipedia.org/w/index.php?title=File:2010-3-15_rGFAP_1-4000_1-200_Hip_20x(4).jpg License: Public Domain Contributors: ArizonaLifeScience File:Human astrocyte.png Source: http://en.wikipedia.org/w/index.php?title=File:Human_astrocyte.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Bruno Pascal File:Anaplastic astrocytoma - gfap - very high mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Anaplastic_astrocytoma_-_gfap_-_very_high_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Oligodendrocyte.png Source: http://en.wikipedia.org/w/index.php?title=File:Oligodendrocyte.png License: Public Domain Contributors: CopperKettle, Kluka, Methoxyroxy, NEON ja, Sultan11 Image:Gray667.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray667.png License: Public Domain Contributors: Arcadian Image:Gray706.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray706.png License: Public Domain Contributors: Arcadian, Lipothymia, Origamiemensch Image:Astrocytre.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Astrocytre.jpg License: Creative Commons Attribution 3.0 Contributors: Original uploader was Neurorocker at en.wikipedia Image:Astrocyte - cultutures - GFAP.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Astrocyte_-_cultutures_-_GFAP.jpg License: GNU Free Documentation License Contributors: Original uploader was GrzegorzWicher at pl.wikipedia Image:Astrocyte - rat spinal cord - GFAP.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Astrocyte_-_rat_spinal_cord_-_GFAP.jpg License: GNU Free Documentation License Contributors: Original uploader was GrzegorzWicher at pl.wikipedia Image:astrocytes-mouse-cortex.png Source: http://en.wikipedia.org/w/index.php?title=File:Astrocytes-mouse-cortex.png License: Creative Commons Attribution-Share Alike Contributors: Mhisted File:Metabolic interactions between astrocytes and neurons with major reactions.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Metabolic_interactions_between_astrocytes_and_neurons_with_major_reactions.jpg License: Creative Commons Attribution 2.0 Contributors: Tunahan Çakιr, Selma Alsan, Hale Saybaş, Ata Akιn and Kutlu Ö Ülgen Image:Slcla3 in Bergmann Glia.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Slcla3_in_Bergmann_Glia.jpg License: Public Domain Contributors: The Gene Expression Nervous System Atlas (GENSAT) Project, NINDS Contract # N01NS02331 to The Rockefeller University (New York, NY) File:PurkinjeCell.jpg Source: http://en.wikipedia.org/w/index.php?title=File:PurkinjeCell.jpg License: Public Domain Contributors: Chrislb, Feezil, Hystrix, Interpretix, Jacklee, SriMesh, 1 anonymous edits Image:Complete neuron cell diagram en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Complete_neuron_cell_diagram_en.svg License: Public Domain Contributors: LadyofHats Image:Gyrus Dentatus 40x.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Gyrus_Dentatus_40x.jpg License: Creative Commons Attribution-Sharealike 2.5 Contributors: MethoxyRoxy Image:GFPneuron.png Source: http://en.wikipedia.org/w/index.php?title=File:GFPneuron.png License: Creative Commons Attribution 2.5 Contributors: Original uploader was Nrets at en.wikipedia Image:smi32neuron.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Smi32neuron.jpg License: Creative Commons Attribution 3.0 Contributors: UC Regents Davis campus File:Neurons uni bi multi pseudouni.svg Source: http://en.wikipedia.org/w/index.php?title=File:Neurons_uni_bi_multi_pseudouni.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Pseudounipolar_bipolar_neurons.svg: Juoj8 derivative work: Jonathan Haas (talk) Image:Chemical synapse schema cropped.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Chemical_synapse_schema_cropped.jpg License: Public Domain Contributors: user:Looie496 created file, US National Institutes of Health, National Institute on Aging created original Image:Golgi Hippocampus.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Golgi_Hippocampus.jpg License: Public Domain Contributors: Ephraim33, Marc Gabriel Schmid, Methoxyroxy, Rory096, Was a bee, 2 anonymous edits Image:Purkinje cell by Cajal.png Source: http://en.wikipedia.org/w/index.php?title=File:Purkinje_cell_by_Cajal.png License: Public Domain Contributors: Original uploader was PNG crusade bot at en.wikipedia Image:Neuron with oligodendrocyte and myelin sheath.svg Source: http://en.wikipedia.org/w/index.php?title=File:Neuron_with_oligodendrocyte_and_myelin_sheath.svg License: Public Domain Contributors: Neuron_with_oligodendrocyte_and_myelin_sheath.svg: *Complete_neuron_cell_diagram_en.svg: LadyofHats derivative work: Andrew c (talk) File:Oligodendrocyte illustration.png Source: http://en.wikipedia.org/w/index.php?title=File:Oligodendrocyte_illustration.png License: Creative Commons Attribution 3.0 Contributors: Anmats, Dmalicke, Smallman12q, Trijnstel File:Spindle-cell.png Source: http://en.wikipedia.org/w/index.php?title=File:Spindle-cell.png License: Creative Commons Attribution-Sharealike 2.5 Contributors: Selket, 1 anonymous edits Image:Spindle neurons - very high mag - cropped.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Spindle_neurons_-_very_high_mag_-_cropped.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Sinusoid.jpeg Source: http://en.wikipedia.org/w/index.php?title=File:Sinusoid.jpeg License: Public Domain Contributors: AndreasJS, Jacopo Werther, Lamiot, Quietbritishjim, 1 anonymous edits Image:Human liver.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Human_liver.jpg License: GNU Free Documentation License Contributors: Jacklee, Jacopo Werther, Reytan, Túrelio, 1 anonymous edits Image:Hepato-biliary.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Hepato-biliary.jpg License: Public Domain Contributors: Drriad Image:Yellow adipose tissue in paraffin section - lipids washed out.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Yellow_adipose_tissue_in_paraffin_section_-_lipids_washed_out.jpg License: GNU Free Documentation License Contributors: Jacklee, Reytan File:White adipose distribution in the body..jpg Source: http://en.wikipedia.org/w/index.php?title=File:White_adipose_distribution_in_the_body..jpg License: Creative Commons Attribution 3.0 Contributors: Smallman12q Image:Brownfat PETCT.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Brownfat_PETCT.jpg License: Public Domain Contributors: Hg6996 Image:Hibernoma2.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Hibernoma2.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Hepatic stellate cell (ito cell) 1476-5926-6-7-3-l.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Hepatic_stellate_cell_(ito_cell)_1476-5926-6-7-3-l.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Gressner et al. Comparative Hepatology 2007 6:7 doi:10.1186/1476-5926-6-7 Image:Hepatic structure2.svg Source: http://en.wikipedia.org/w/index.php?title=File:Hepatic_structure2.svg License: Creative Commons Attribution 2.5 Contributors: Originally by Frevert U, Engelmann S, Zougbédé S, Stange J, Ng B, et al. Converted to SVG by Viacheslav Vtyurin who was hired to do so by User:Eug. Image:PhysiologieGlomérulaire.png Source: http://en.wikipedia.org/w/index.php?title=File:PhysiologieGlomérulaire.png License: Creative Commons Attribution-ShareAlike 1.0 Generic Contributors: Tieum at fr.wikipedia Image:Filtration barrier.svg Source: http://en.wikipedia.org/w/index.php?title=File:Filtration_barrier.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: M•Komorniczak -talk-, polish wikipedist.
622
Image Sources, Licenses and Contributors
Image:Gray1128.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1128.png License: Public Domain Contributors: Arcadian, German, Jmarchn, Magnus Manske, Origamiemensch Image:Histology-kidney.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Histology-kidney.jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: --Uwe Gille 13:16, 13 May 2006 (UTC) File:Kidney cd10 ihc.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Kidney_cd10_ihc.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Gray1129.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1129.png License: Public Domain Contributors: Arcadian, German, Jmarchn, Magnus Manske, 1 anonymous edits Image:Tight_junction_blowup.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Tight_junction_blowup.jpg License: Creative Commons Attribution-Sharealike 2.5 Contributors: Original uploader was DrEricYH at en.wikipedia Image:Kidney nephron molar transport diagram.svg Source: http://en.wikipedia.org/w/index.php?title=File:Kidney_nephron_molar_transport_diagram.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron-urine.svg: M•Komorniczak -talk-, polish wikipedist. Kidney_nephron_molar_transport_diagram.png: *Nephron-urine.svg: M•Komorniczak -talk-, polish wikipedist. derivative work: Juvo415 (talk) derivative work: Mcstrother (talk) Image:Kidney_nephron.png Source: http://en.wikipedia.org/w/index.php?title=File:Kidney_nephron.png License: Public Domain Contributors: Henry Gray Image:Gray1132.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1132.png License: Public Domain Contributors: Arcadian, German, Jmarchn, Magnus Manske, Origamiemensch Image:Gray1133.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1133.png License: Public Domain Contributors: Arcadian, German, Jmarchn, Magnus Manske, Origamiemensch, 1 anonymous edits Image:centroacinar cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Centroacinar_cells.jpg License: Public Domain Contributors: User:Mortsggah Image:Alpha Intercalated Cell Cartoon.svg Source: http://en.wikipedia.org/w/index.php?title=File:Alpha_Intercalated_Cell_Cartoon.svg License: Creative Commons Attribution 3.0 Contributors: Rswarbrick Image:Human jejunum microvilli 2 - TEM.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Human_jejunum_microvilli_2_-_TEM.jpg License: Public Domain Contributors: Louisa Howard, Katherine Connollly Image:Epididymis-KDS.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Epididymis-KDS.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:KDS444 Image:Gray1148.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1148.png License: Public Domain Contributors: Arcadian, Ephraim33, Magnus Manske, Origamiemensch Image:Illu repdt male.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_repdt_male.jpg License: Public Domain Contributors: US Federal Government/National Cancer Institute. Image:Illu testis 1b.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_testis_1b.jpg License: Public Domain Contributors: Arcadian, Ephraim33, Origamiemensch Image:Mesorchium.svg Source: http://en.wikipedia.org/w/index.php?title=File:Mesorchium.svg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: User:Uwe Gille Image:Epididymis high mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Epididymis_high_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Epididymis.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Epididymis.JPG License: Public Domain Contributors: Jpogi Image:Enamelmineralization11-17-05.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Enamelmineralization11-17-05.jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: user:Dozenist Image:Cervical-loop.png Source: http://en.wikipedia.org/w/index.php?title=File:Cervical-loop.png License: Public Domain Contributors: Original uploader was Tummers at en.wikipedia Image:Cochlea-crosssection.svg Source: http://en.wikipedia.org/w/index.php?title=File:Cochlea-crosssection.svg License: GNU Free Documentation License Contributors: Cochlea-crosssection.png: Original uploader was Oarih at en.wikipedia derivative work: Fred the Oyster Image:Organ of corti.svg Source: http://en.wikipedia.org/w/index.php?title=File:Organ_of_corti.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Madhero88 File:Gray903.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray903.png License: Public Domain Contributors: Arcadian, Iainf, Jacklee File:Gray928.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray928.png License: Public Domain Contributors: Arcadian, Iainf, Jacklee, Magnus Manske, Mike.lifeguard File:Gray929.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray929.png License: Public Domain Contributors: Arcadian, Iainf, Jacklee, Jmarchn, Magnus Manske, Mike.lifeguard File:Gray930.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray930.png License: Public Domain Contributors: Arcadian, Dicklyon, Iainf, Jacklee, Jmarchn, Magnus Manske, Mike.lifeguard, Was a bee File:Keratoconus keratocytes alcohol dehydrogenase 3.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Keratoconus_keratocytes_alcohol_dehydrogenase_3.jpg License: Creative Commons Attribution 3.0 Contributors: V.V. Mootha, J.M. Kanoff, J. Shankardas, and S. Dimitrijevich Image:Gray72-en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Gray72-en.svg License: Public Domain Contributors: Mysid Image:Caput femoris cortex medulla.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Caput_femoris_cortex_medulla.jpg License: Public Domain Contributors: Stevenfruitsmaak File:Bone marrow WBC.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Bone_marrow_WBC.JPG License: Creative Commons Attribution-Share Alike Contributors: Bobjgalindo Image:acute leukemia-ALL.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Acute_leukemia-ALL.jpg License: GNU Free Documentation License Contributors: Original uploader was VashiDonsk at en.wikipedia Image:Bone marrow biopsy.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Bone_marrow_biopsy.jpg License: Public Domain Contributors: Photographer’s Mate 2nd Class Chad McNeeley Image:Markkloesschensuppe.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Markkloesschensuppe.jpg License: Public Domain Contributors: 1029man, AlexanderDreyer, Monstourz Image:NIH 3T3.jpg Source: http://en.wikipedia.org/w/index.php?title=File:NIH_3T3.jpg License: Creative Commons Attribution 2.5 Contributors: Didym, Kruusamägi, Magog the Ogre Image:Microvessel.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Microvessel.jpg License: Creative Commons Attribution 3.0 Contributors: Robert M. Hunt File:Gap_cell_junction-en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Gap_cell_junction-en.svg License: Public Domain Contributors: Mariana Ruiz LadyofHats File:Solitary fibrous tumour intermed mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Solitary_fibrous_tumour_intermed_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Cervical vertebra english.png Source: http://en.wikipedia.org/w/index.php?title=File:Cervical_vertebra_english.png License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: user:debivort Image:Disc Herniation.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Disc_Herniation.JPG License: Public Domain Contributors: Dematt Image:Gray66.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray66.png License: Public Domain Contributors: User Magnus Manske on en.wikipedia Image:Hypertrophic Zone of Epiphyseal Plate.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Hypertrophic_Zone_of_Epiphyseal_Plate.jpg License: Public Domain Contributors: Robert M. Hunt File:Slide6VVVVVV.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide6VVVVVV.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Gray300.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray300.png License: Public Domain Contributors: User Magnus Manske on en.wikipedia File:Slide1xzxzx.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide1xzxzx.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide2xzxzxz.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide2xzxzxz.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 Image:Gray295.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray295.png License: Public Domain Contributors: User Magnus Manske on en.wikipedia Image:Gray321.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray321.png License: Public Domain Contributors: Hellerhoff, Mats Halldin, Nono64, Phyzome, Was a bee Image:Degenerative disc disease - high mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Degenerative_disc_disease_-_high_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Cartilage polarised.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Cartilage_polarised.jpg License: Creative Commons Attribution 3.0 Contributors: Emmanuelm at en.wikipedia
623
Image Sources, Licenses and Contributors
Image:Chondrocyte- calcium stain.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Chondrocyte-_calcium_stain.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Robert M. Hunt Image:Bone hypercalcemia - cropped - very high mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Bone_hypercalcemia_-_cropped_-_very_high_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:Osteoblast.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Osteoblast.jpg License: Creative Commons Attribution 3.0 Contributors: User:Gabriel Caponetti Image:Active osteoblasts.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Active_osteoblasts.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Robert M. Hunt Image:Bony_nidus_2.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Bony_nidus_2.jpg License: Creative Commons Attribution 3.0 Contributors: Robert M. Hunt Image:Bony_nidus_3.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Bony_nidus_3.jpg License: Creative Commons Attribution 3.0 Contributors: Robert M. Hunt Image:Bone_hypercalcemia_-_2_-_very_high_mag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Bone_hypercalcemia_-_2_-_very_high_mag.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Nephron Image:WVSOM Osteoblast.JPG Source: http://en.wikipedia.org/w/index.php?title=File:WVSOM_Osteoblast.JPG License: Creative Commons Attribution 3.0 Contributors: Wbensmith Image:Transverse Section Of Bone.png Source: http://en.wikipedia.org/w/index.php?title=File:Transverse_Section_Of_Bone.png License: Creative Commons Attribution-Sharealike 2.5 Contributors: BDB Image:Osteocyte 2.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Osteocyte_2.jpg License: Public Domain Contributors: Alexraw, Marek Mazurkiewicz, 1 anonymous edits File:CerebCircuit.png Source: http://en.wikipedia.org/w/index.php?title=File:CerebCircuit.png License: unknown Contributors: en:User:Nrets Image:Pyramsdal-and-Spiny-stellate-cell.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Pyramsdal-and-Spiny-stellate-cell.JPG License: Creative Commons Attribution 2.5 Contributors: Bilz0r Image:Skeletal muscle.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Skeletal_muscle.jpg License: GNU Free Documentation License Contributors: Deadstar, Jacklee, Noca2plus, Rama, Raul654, Splette, 2 anonymous edits File:Muscle pathways.svg Source: http://en.wikipedia.org/w/index.php?title=File:Muscle_pathways.svg License: Public Domain Contributors: Indolences Image:Glanzstreifen.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Glanzstreifen.jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: Dr. S. Girod, Anton Becker Image:Dogcardiacmuscle400.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Dogcardiacmuscle400.jpg License: Creative Commons Attribution-Share Alike Contributors: John Alan Elson File:A single cardiomyocyte beating, five days after purification from cell culture.ogv Source: http://en.wikipedia.org/w/index.php?title=File:A_single_cardiomyocyte_beating,_five_days_after_purification_from_cell_culture.ogv License: Creative Commons Attribution 2.5 Contributors: Uosaki H, Fukushima H, Takeuchi A, Matsuoka S, Nakatsuji N, Yamanaka S, Yamashita J Image:ConductionsystemoftheheartwithouttheHeart.png Source: http://en.wikipedia.org/w/index.php?title=File:ConductionsystemoftheheartwithouttheHeart.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: Madhero88 Image:ECG_Principle_fast.gif Source: http://en.wikipedia.org/w/index.php?title=File:ECG_Principle_fast.gif License: GNU Free Documentation License Contributors: Kalumet Image:Glatte Muskelzellen.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Glatte_Muskelzellen.jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: User:Polarlys Image:Illu esophageal layers.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_esophageal_layers.jpg License: Public Domain Contributors: Arcadian, Origamiemensch, 2 anonymous edits File:Actin myosin filaments.png Source: http://en.wikipedia.org/w/index.php?title=File:Actin_myosin_filaments.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: Boumphreyfr Image:redbloodcells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Redbloodcells.jpg License: Public domain Contributors: Dietzel65, Habj, Ranveig, Shizhao, Simon Shek, Solon, Sundar, Thuresson Image:Erythrocytes in vertebrates.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Erythrocytes_in_vertebrates.jpg License: Public Domain Contributors: G Gulliver - Proceedings of the Royal Society of London Image:Gray453.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray453.png License: Public Domain Contributors: Henry Gray Image:Red White Blood cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Red_White_Blood_cells.jpg License: Public Domain Contributors: Electron Microscopy Facility at The National Cancer Institute at Frederick (NCI-Frederick) Image:NIK 3232-Drops of blood medium.JPG Source: http://en.wikipedia.org/w/index.php?title=File:NIK_3232-Drops_of_blood_medium.JPG License: Creative Commons Attribution 3.0 Contributors: unkown Image:Erytrocyte deoxy to oxy v0.7.gif Source: http://en.wikipedia.org/w/index.php?title=File:Erytrocyte_deoxy_to_oxy_v0.7.gif License: Creative Commons Attribution-Sharealike 3.0 Contributors: Rogeriopfm Image:Erythrocyte Membrane lipids.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Erythrocyte_Membrane_lipids.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Cholesterol.svg: BorisTM Phosphatidylcholine.png: Likeitsmyjob Sphingomyelin.png: Original uploader was Jag123 at en.wikipedia Phosphatidyl-Inositol.png: Original uploader was Jag123 at en.wikipedia Phosphatidyl-Serine.png: Original uploader was Jag123 at en.wikipedia Phosphatidyl-Ethanolamine.png: Original uploader was Jag123 at en.wikipedia derivative work: Rogeriopfm (talk) File:RBC Membrane Proteins SDS-PAGE gel.jpg Source: http://en.wikipedia.org/w/index.php?title=File:RBC_Membrane_Proteins_SDS-PAGE_gel.jpg License: Creative Commons Zero Contributors: Ernst Hempelmann File:RBC membrane major proteins.png Source: http://en.wikipedia.org/w/index.php?title=File:RBC_membrane_major_proteins.png License: Public Domain Contributors: RBC_membrane_major_proteins.jpg: Author is Ernst Hempelmann derivative work: TimVickers (talk) Image:Sicklecells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Sicklecells.jpg License: Public Domain Contributors: NIDDK Image:Osmotic pressure on blood cells diagram.svg Source: http://en.wikipedia.org/w/index.php?title=File:Osmotic_pressure_on_blood_cells_diagram.svg License: Public Domain Contributors: LadyofHats File:Human Erythrocytes OsmoticPressure PhaseContrast Plain.svg Source: http://en.wikipedia.org/w/index.php?title=File:Human_Erythrocytes_OsmoticPressure_PhaseContrast_Plain.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Zephyris Image:WVSOM Megakaryocytes.JPG Source: http://en.wikipedia.org/w/index.php?title=File:WVSOM_Megakaryocytes.JPG License: Creative Commons Attribution 3.0 Contributors: Wbensmith Image:Illu blood cell lineage.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Illu_blood_cell_lineage.jpg License: Public Domain Contributors: Arcadian, Bestiasonica, Cristobal carrasco, DO11.10, MichaelFrey, 5 anonymous edits Image:Monocytes, a type of white blood cell (Giemsa stained).jpg Source: http://en.wikipedia.org/w/index.php?title=File:Monocytes,_a_type_of_white_blood_cell_(Giemsa_stained).jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:GrahamColm Image:SEM blood cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:SEM_blood_cells.jpg License: Public Domain Contributors: Bruce Wetzel (photographer). Harry Schaefer (photographer) Image:Reference ranges for blood tests - white blood cells.png Source: http://en.wikipedia.org/w/index.php?title=File:Reference_ranges_for_blood_tests_-_white_blood_cells.png License: Public Domain Contributors: Mikael Häggström File:Dendritic cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Dendritic_cells.jpg License: Public Domain Contributors: Haymanj File:The representation of Langerhans cells in the Cell Ontology.jpg Source: http://en.wikipedia.org/w/index.php?title=File:The_representation_of_Langerhans_cells_in_the_Cell_Ontology.jpg License: Creative Commons Attribution 2.0 Contributors: Masci AM, Arighi CN, Diehl AD, Lieberman AE, Mungall C, Scheuermann RH, Smith B, Cowell LG Image:Giant platelets.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Giant_platelets.JPG License: Creative Commons Attribution-Share Alike Contributors: Bobjgalindo File:Blood cells differentiation chart.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Blood_cells_differentiation_chart.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: パ タ ゴ ニ ア
624
Image Sources, Licenses and Contributors
File:Thrombocyteaggregation.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Thrombocyteaggregation.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Dietzel65, Steffen Dietzel File:Red White Blood cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Red_White_Blood_cells.jpg License: Public Domain Contributors: Electron Microscopy Facility at The National Cancer Institute at Frederick (NCI-Frederick) File:Platelets.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Platelets.jpg License: Creative Commons Attribution 3.0 Contributors: Tleonardi File:Platelet structure.png Source: http://en.wikipedia.org/w/index.php?title=File:Platelet_structure.png License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:GrahamColm File:Platelet blood bag.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Platelet_blood_bag.jpg License: Public Domain Contributors: Bobjgalindo, DO11.10, Gveret Tered, Pfctdayelise, PhilippN, Sundar, 1 anonymous edits Image:Osteoclast.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Osteoclast.jpg License: Public Domain Contributors: Original uploader was Robert M. Hunt at en.wikipedia File:TRAPosteoclastculture.jpg Source: http://en.wikipedia.org/w/index.php?title=File:TRAPosteoclastculture.jpg License: GNU Free Documentation License Contributors: Original uploader was Cellpath at en.wikipedia File:osteoclast1.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Osteoclast1.jpg License: GNU Free Documentation License Contributors: Cellpath (talk) Image:Dendritic cell.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Dendritic_cell.JPG License: Creative Commons Attribution 2.5 Contributors: Judith Behnsen, Priyanka Narang, Mike Hasenberg, Frank Gunzer, Ursula Bilitewski, Nina Klippel, Manfred Rohde, Matthias Brock, Axel A. Brakhage, Matthias Gunzer Image:Dendritic cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Dendritic_cells.jpg License: Public Domain Contributors: Haymanj Image:S6-Dendritic Cells with Conidia in Collagen.ogg Source: http://en.wikipedia.org/w/index.php?title=File:S6-Dendritic_Cells_with_Conidia_in_Collagen.ogg License: Creative Commons Attribution 2.5 Contributors: Judith Behnsen, Priyanka Narang, Mike Hasenberg, Frank Gunzer, Ursula Bilitewski, Nina Klippel, Manfred Rohde, Matthias Brock, Axel A. Brakhage, Matthias Gunzer Image:Lymphatic system.png Source: http://en.wikipedia.org/w/index.php?title=File:Lymphatic_system.png License: Public Domain Contributors: NIH File:Illu lymph node structure.png Source: http://en.wikipedia.org/w/index.php?title=File:Illu_lymph_node_structure.png License: Public Domain Contributors: SEER File:DH lymphatic system.jpg Source: http://en.wikipedia.org/w/index.php?title=File:DH_lymphatic_system.jpg License: Creative Commons Attribution 3.0 Contributors: LearnAnatomy (talk) Image:Galen detail.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Galen_detail.jpg License: Public Domain Contributors: NLM Image:Bartolomeus Eustachius.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Bartolomeus_Eustachius.jpg License: Public Domain Contributors: Unknown (not specified); possibly from one of Eustachius' books. File:Olaus Rudbeck Sr (portrait by Martin Mijtens Sr, 1696).jpg Source: http://en.wikipedia.org/w/index.php?title=File:Olaus_Rudbeck_Sr_(portrait_by_Martin_Mijtens_Sr,_1696).jpg License: Public Domain Contributors: Martin Mijtens the Elder (1548-1736), Dutch-Swedish painter. File:Thomas bartholin.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Thomas_bartholin.jpg License: Public Domain Contributors: Nico File:Mikroglej 1.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Mikroglej_1.jpg License: Public Domain Contributors: GrzegorzWicher File:Makrofagi 2.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Makrofagi_2.jpg License: Public Domain Contributors: GrzegorzWicher Image:Neutrophils.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Neutrophils.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:GrahamColm Image:NeutrophilerAktion.png Source: http://en.wikipedia.org/w/index.php?title=File:NeutrophilerAktion.png License: GNU Free Documentation License Contributors: Uwe Thormann (http://de.wikipedia.org/wiki/Benutzer:Uwe_Thormann) Image:Hematopoiesis simple.svg Source: http://en.wikipedia.org/w/index.php?title=File:Hematopoiesis_simple.svg License: GNU Free Documentation License Contributors: Mikael Häggström (no attribution required), from original by A. Rad (requires attribution) Image:S15-Competitive Phagocytosis Assay in Collagen.ogg Source: http://en.wikipedia.org/w/index.php?title=File:S15-Competitive_Phagocytosis_Assay_in_Collagen.ogg License: Creative Commons Attribution 2.5 Contributors: Judith Behnsen, Priyanka Narang, Mike Hasenberg, Frank Gunzer, Ursula Bilitewski, Nina Klippel, Manfred Rohde, Matthias Brock, Axel A. Brakhage, Matthias Gunzer Image:Neutrophil with anthrax copy.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Neutrophil_with_anthrax_copy.jpg License: Creative Commons Attribution 2.5 Contributors: Volker Brinkmann Image:Hematopoiesis (human) diagram.png Source: http://en.wikipedia.org/w/index.php?title=File:Hematopoiesis_(human)_diagram.png License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: A. Rad Image:Eosinophil blood smear.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Eosinophil_blood_smear.JPG License: Creative Commons Attribution-Share Alike Contributors: Bobjgalindo Image:Eosinophil 2.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Eosinophil_2.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:GrahamColm image:Eosinophil2.png Source: http://en.wikipedia.org/w/index.php?title=File:Eosinophil2.png License: GNU Free Documentation License Contributors: Arcadian, Cwbm (commons), Joey-das-WBF, Marek Mazurkiewicz, TimVickers, Väsk Image:pBBasophil.jpg Source: http://en.wikipedia.org/w/index.php?title=File:PBBasophil.jpg License: Public Domain Contributors: Dirk Hünniger, Elboy99, Lennert B, MichaelFrey, Santosga, 2 anonymous edits Image:Baso-hemo.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Baso-hemo.JPG License: Copyrighted free use Contributors: パ タ ゴ ニ ア Image:Basophil.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Basophil.jpg License: GNU Free Documentation License Contributors: Bestiasonica, Elboy99, Origamiemensch, Reytan, Santosga File:Hybridoma technology.png Source: http://en.wikipedia.org/w/index.php?title=File:Hybridoma_technology.png License: Creative Commons Attribution-Sharealike 2.5 Contributors: Hybridomtechnik.png: Martin Brändli derivative work: ἀνυπόδητος (talk) File:Hybridoma cells grown in tissue culture.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Hybridoma_cells_grown_in_tissue_culture.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: GerryShaw Image:SMCpolyhydroxysmall.jpg Source: http://en.wikipedia.org/w/index.php?title=File:SMCpolyhydroxysmall.jpg License: Copyrighted free use Contributors: Kauczuk Image:Mast cell.png Source: http://en.wikipedia.org/w/index.php?title=File:Mast_cell.png License: GNU Free Documentation License Contributors: Arcadian, Cwbm (commons), Väsk Image:Mast cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Mast_cells.jpg License: Public Domain Contributors: Template drawing from "The Immune System", any modifications, made by myself are released into the public domain. Image:histamine.png Source: http://en.wikipedia.org/w/index.php?title=File:Histamine.png License: Public Domain Contributors: Ayacop, Benjah-bmm27, BorisTM, Edgar181, Jean-no, Mixtures, Mrgreen71, Роман Беккер Image:Lymphocyte activation.png Source: http://en.wikipedia.org/w/index.php?title=File:Lymphocyte_activation.png License: Public Domain Contributors: Made in Inkscape by Mikael Häggström (User:Mikael Häggström) Image:Antigen presentation.svg Source: http://en.wikipedia.org/w/index.php?title=File:Antigen_presentation.svg License: GNU Free Documentation License Contributors: user:Sjef Image:Intrathymic T Cell Differentiation.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Intrathymic_T_Cell_Differentiation.JPG License: Creative Commons Attribution 2.5 Contributors: Wilson Savino is at the Laboratory on Thymus Research, Department of Immunology, Oswaldo Cruz Institute, Inserm-Fiocruz Associated Laboratory of Immunology, Oswaldo Cruz Foundation, Rio de Janeiro, RJ, Brazil. E-mail: [email protected] Image:Original antigenic sin.svg Source: http://en.wikipedia.org/w/index.php?title=File:Original_antigenic_sin.svg License: Creative Commons Attribution-Sharealike 3.0 Contributors: Original_antigenic_sin.png: User:DO11.10 derivative work: Hazmat2 (talk) Image:Plasmacell.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Plasmacell.jpg License: Public Domain Contributors: Original uploader was CS99 at de.wikipedia Image:B cell activation.png Source: http://en.wikipedia.org/w/index.php?title=File:B_cell_activation.png License: Public Domain Contributors: Template drawing and caption from "The Immune System". Any modifcations, made by myself are released into the public domain. Image:T-dependent B cell activation.png Source: http://en.wikipedia.org/w/index.php?title=File:T-dependent_B_cell_activation.png License: Public Domain Contributors: Altaileopard Image:Stimulation of specific clone of B cells and its proliferation.PNG Source: http://en.wikipedia.org/w/index.php?title=File:Stimulation_of_specific_clone_of_B_cells_and_its_proliferation.PNG License: Public Domain Contributors: Ketan Panchal, MBBS (talk) at en.wikipedia
625
Image Sources, Licenses and Contributors
File:HLA-Cw4.png Source: http://en.wikipedia.org/w/index.php?title=File:HLA-Cw4.png License: Public Domain Contributors: Pdeitiker File:PDB 1hq8 EBI.jpg Source: http://en.wikipedia.org/w/index.php?title=File:PDB_1hq8_EBI.jpg License: unknown Contributors: File:PDB 1hkf EBI.jpg Source: http://en.wikipedia.org/w/index.php?title=File:PDB_1hkf_EBI.jpg License: unknown Contributors: Image:Missingself.svg Source: http://en.wikipedia.org/w/index.php?title=File:Missingself.svg License: GNU Free Documentation License Contributors: Cacofonie, Slashme Image:Polychromatic erythrocyte.png Source: http://en.wikipedia.org/w/index.php?title=File:Polychromatic_erythrocyte.png License: GNU Free Documentation License Contributors: Arcadian, Cycneavox, Dietzel65, Tano4595 Image:Erythrocyte.png Source: http://en.wikipedia.org/w/index.php?title=File:Erythrocyte.png License: GNU Free Documentation License Contributors: =g b r=, Arcadian, Dietzel65 File:Reticulocytes Human Blood Supravital Stain.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Reticulocytes_Human_Blood_Supravital_Stain.jpg License: Creative Commons Attribution 3.0 Contributors: Ed Uthman, MD, pathologist, Houston, Texas, USA Image:Gray9.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray9.png License: Public Domain Contributors: User Magnus Manske on en.wikipedia File:Sperm-egg.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Sperm-egg.jpg License: Public Domain Contributors: Blurpeace, Conscious, EugeneZelenko, Giggy, Gourami Watcher, GrawpSock, Herbythyme, Ies, Jacklee, Kameraad Pjotr, Manuelt15, Mattes, Myself488, Noddy93, Pi@k, Platonides, Techman224, The Evil IP address, Tronicum, 14 anonymous edits File:Acrosome reaction diagram en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Acrosome_reaction_diagram_en.svg License: Public Domain Contributors: LadyofHats. File:DEV035048A.jpg Source: http://en.wikipedia.org/w/index.php?title=File:DEV035048A.jpg License: Public Domain Contributors: Sabisteb Image:Oocyte.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Oocyte.jpg License: Public Domain Contributors: Original uploader was Ekem at en.wikipedia File:Gray5.svg Source: http://en.wikipedia.org/w/index.php?title=File:Gray5.svg License: Public Domain Contributors: Mysid File:Oocyte granulosa cells.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Oocyte_granulosa_cells.jpg License: Public Domain Contributors: Original uploader was Ekem at en.wikipedia Image:Oocyte Poles.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Oocyte_Poles.jpg License: Creative Commons Attribution 3.0 Contributors: Catcasillas21 Image:Oocyte Determinants.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Oocyte_Determinants.jpg License: Creative Commons Attribution 3.0 Contributors: Catcasillas21 Image:Germinal_epithelium_testicle.svg Source: http://en.wikipedia.org/w/index.php?title=File:Germinal_epithelium_testicle.svg License: Creative Commons Attribution 2.5 Contributors: User:Uwe Gille Image:Gray1150.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1150.png License: Public Domain Contributors: Arcadian, Ephraim33, Origamiemensch Image:Gray7.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray7.png License: Public Domain Contributors: User Magnus Manske on en.wikipedia File:Complete diagram of a human spermatozoa en.svg Source: http://en.wikipedia.org/w/index.php?title=File:Complete_diagram_of_a_human_spermatozoa_en.svg License: Public Domain Contributors: Mariana Ruiz Villarreal File:Sperm stained.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Sperm_stained.JPG License: Creative Commons Attribution-Share Alike Contributors: Bobjgalindo File:Plant sperm.png Source: http://en.wikipedia.org/w/index.php?title=File:Plant_sperm.png License: Public Domain Contributors: Original uploader was Tameeria at en.wikipedia Image:Testicle-histology-boar.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Testicle-histology-boar.jpg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: User:Uwe Gille Image:Spermatocytogenesis.png Source: http://en.wikipedia.org/w/index.php?title=File:Spermatocytogenesis.png License: Public Domain Contributors: Ies, Serephine, 1 anonymous edits Image:Gray1123.png Source: http://en.wikipedia.org/w/index.php?title=File:Gray1123.png License: Public Domain Contributors: Arcadian, German, Magnus Manske File:Surface projections of the organs of the trunk.png Source: http://en.wikipedia.org/w/index.php?title=File:Surface_projections_of_the_organs_of_the_trunk.png License: Public Domain Contributors: Mikael Häggström File:CTscankidney.jpg Source: http://en.wikipedia.org/w/index.php?title=File:CTscankidney.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: RGshredfox File:KidneyStructures PioM.svg Source: http://en.wikipedia.org/w/index.php?title=File:KidneyStructures_PioM.svg License: Creative Commons Attribution-ShareAlike 3.0 Unported Contributors: Piotr Michał Jaworski; PioM EN DE PL File:3D rendered CT of abdominal aortic branches and kidneys.svg Source: http://en.wikipedia.org/w/index.php?title=File:3D_rendered_CT_of_abdominal_aortic_branches_and_kidneys.svg License: GNU Free Documentation License Contributors: Mikael Häggström from original image created and uploaded by by Dr. I-Chen Tsai () File:Kidney-medulla.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Kidney-medulla.JPG License: Public Domain Contributors: File:Kidney-Cortex.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Kidney-Cortex.JPG License: Public Domain Contributors: File:Hunter enlarged kidney.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Hunter_enlarged_kidney.jpg License: Public Domain Contributors: McLeod File:Kidney.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Kidney.JPG License: Creative Commons Attribution 3.0 Contributors: Pöllö File:1407871818 5c7f215934 o.jpg Source: http://en.wikipedia.org/w/index.php?title=File:1407871818_5c7f215934_o.jpg License: Creative Commons Attribution-Sharealike 3.0,2.5,2.0,1.0 Contributors: Jonathan Koertge File:Slide4nn.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide4nn.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide5pp.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide5pp.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide3ppp.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide3ppp.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide22222.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide22222.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Slide42222.JPG Source: http://en.wikipedia.org/w/index.php?title=File:Slide42222.JPG License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Right kidney.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Right_kidney.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Left kidneys.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Left_kidneys.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Kidneys.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Kidneys.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Left kidney.jpg Source: http://en.wikipedia.org/w/index.php?title=File:Left_kidney.jpg License: Creative Commons Attribution-Sharealike 3.0 Contributors: User:Anatomist90 File:Kidney Cross Section.png Source: http://en.wikipedia.org/w/index.php?title=File:Kidney_Cross_Section.png License: Creative Commons Attribution 3.0 Contributors: Anmats, Dmalicke, Trijnstel
626
License
627
License
Creative Commons Attribution-Share Alike 3.0 Unported //creativecommons.org/licenses/by-sa/3.0/